User login
Blog: Top Five Most Watched Dermatology Videos
What were dermatologists watching from Skin & Allergy News in 2011? Here's the top five countdown.
5. New Drugs Help Melanoma Patients Live Longer: Dr. Lynn Schuchter puts the studies, which were presented at the 2011 ASCO Annual Meeting in Chicago, in perspective and offers advice to physicians.
4. Laviv May Offer Longer-Term Acne Scarring Tx: Azficel-T, an autologous cellular product, produced significant improvement in acne scarring, compared with placebo, according to study results reported at the annual meeting of the American Society for Dermatologic Surgery. Laviv was approved by the FDA earlier this year for treating wrinkles. We interviewed Dr. Girish Munavalli, a study investigator, at the meeting.
3. How to ID and Treat Fire Ant Bites: Dr. Ronald Rapini offered advice on recognizing and treating fire ant bites at the American Academy of Dermatology's Summer Academy meeting in New York.
2. Eczema and Food Allergies Often Go Hand and Hand: Dr. Lawrence Eichenfield talked about atopic dermatitis, food allergies, and national guidelines at the American Academy of Dermatology's Summer Academy meeting in New York.
Drum roll please…
1. Gel Nail Polish: The Painted Truth: Dr. Richard K. Scher discussed the dangers of gel nail polish, and also gave tips to share with patients on how to have a safe experience at the nail salon at the American Academy of Dermatology's Summer Academy meeting in New York.
What were dermatologists watching from Skin & Allergy News in 2011? Here's the top five countdown.
5. New Drugs Help Melanoma Patients Live Longer: Dr. Lynn Schuchter puts the studies, which were presented at the 2011 ASCO Annual Meeting in Chicago, in perspective and offers advice to physicians.
4. Laviv May Offer Longer-Term Acne Scarring Tx: Azficel-T, an autologous cellular product, produced significant improvement in acne scarring, compared with placebo, according to study results reported at the annual meeting of the American Society for Dermatologic Surgery. Laviv was approved by the FDA earlier this year for treating wrinkles. We interviewed Dr. Girish Munavalli, a study investigator, at the meeting.
3. How to ID and Treat Fire Ant Bites: Dr. Ronald Rapini offered advice on recognizing and treating fire ant bites at the American Academy of Dermatology's Summer Academy meeting in New York.
2. Eczema and Food Allergies Often Go Hand and Hand: Dr. Lawrence Eichenfield talked about atopic dermatitis, food allergies, and national guidelines at the American Academy of Dermatology's Summer Academy meeting in New York.
Drum roll please…
1. Gel Nail Polish: The Painted Truth: Dr. Richard K. Scher discussed the dangers of gel nail polish, and also gave tips to share with patients on how to have a safe experience at the nail salon at the American Academy of Dermatology's Summer Academy meeting in New York.
What were dermatologists watching from Skin & Allergy News in 2011? Here's the top five countdown.
5. New Drugs Help Melanoma Patients Live Longer: Dr. Lynn Schuchter puts the studies, which were presented at the 2011 ASCO Annual Meeting in Chicago, in perspective and offers advice to physicians.
4. Laviv May Offer Longer-Term Acne Scarring Tx: Azficel-T, an autologous cellular product, produced significant improvement in acne scarring, compared with placebo, according to study results reported at the annual meeting of the American Society for Dermatologic Surgery. Laviv was approved by the FDA earlier this year for treating wrinkles. We interviewed Dr. Girish Munavalli, a study investigator, at the meeting.
3. How to ID and Treat Fire Ant Bites: Dr. Ronald Rapini offered advice on recognizing and treating fire ant bites at the American Academy of Dermatology's Summer Academy meeting in New York.
2. Eczema and Food Allergies Often Go Hand and Hand: Dr. Lawrence Eichenfield talked about atopic dermatitis, food allergies, and national guidelines at the American Academy of Dermatology's Summer Academy meeting in New York.
Drum roll please…
1. Gel Nail Polish: The Painted Truth: Dr. Richard K. Scher discussed the dangers of gel nail polish, and also gave tips to share with patients on how to have a safe experience at the nail salon at the American Academy of Dermatology's Summer Academy meeting in New York.
The Top 10 Stories on OncologyReport.com in 2011
Catch up with what you missed as we count down the 10 most-read stories on OncologyReport.com last year.
10. Everolimus Posts Big Win in ER-Positive Breast Cancer By Patrice Wendling
This first report of the BOLERO-2 trial -- a potential practice changer -- came out of the European Multidisciplinary Cancer Congress in Stockholm.
9. Multimodal DCIS Therapy, Tamoxifen Cuts Breast Cancer Deaths By Neil Osterweil
A meta-analysis from Australia found that adding radiotherapy and tamoxifen to breast-conserving surgery significantly reduces the local recurrence rate and the breast cancer–specific death rate in women with ductal carcinoma in situ. It was presented at the American Society of Radiation Oncology (ASTRO) meeitng in Miami Beach.
8. Crizotinib Approval Personalizes Lung Cancer Therapy By Miriam E. Tucker
The swift approval of crizotinib capsules by the Food and Drug Administration as the first and only targeted therapy for locally advanced or metastatic ALK-positive non–small cell lung cancer represented another milestone in biomarker-driven, personalized medicine. Crizotinib was approved, along with a companion diagnostic test, Abbott Molecular’s Vysis ALK Break Apart FISH Probe Kit, which identifies the anaplastic lymphoma kinase (ALK) fusion gene that the drug targets.
7. Clinicians Slow to Embrace Sipuleucel-T for Prostate Cancer By Diana Mahoney
Most physicians have strong opinions on sipuleucel-T, including dubbing its approval "a milestone in the history of oncology," but many of them refused to speak about it on the record. Our persistent reporter found the reasons for their reluctance to use the first cancer vaccine went beyond reimbursement issues belabored in the financial press.
6. Drug Shortages Increasingly Take Toll on Care By Elizabeth Mechcatie
With their increasing prevalence, drug shortages in the United States have led to delays in treatment, forced the use of less effective alternatives, and encouraged a burgeoning gray market that sells tough-to-obtain medications at highly inflated prices, according to stakeholders gathered at a recent Food and Drug Administration meeting.
5. Practice Changers Expected at San Antonio Breast Cancer Symposium By Jane Salodof MacNeil
The 2011 San Antonio Breast Cancer Symposium featured a hefty number of studies that could change clinical practice. One of the most exciting SABCS meetings in recent years, it featured the phase III BOLERO-2 and CLEOPATRA trials, a new Oncotype DX assay for ductal carcinoma in situ, reports from four bisphosphonate trials, and a controversial brachytherapy study.
4. FDA Approves Brentuximab for Two Lymphomas By Elizabeth Mechcatie
The Food and Drug Administration on Aug. 19 gave an accelerated approval to brentuximab, a CD30-directed antibody drug-conjugate, for the treatment of Hodgkin’s lymphoma and systemic anaplastic large-cell lymphoma, after other treatments have failed.
3. FDA Approves Vemurafenib for Advanced Melanoma By Jane Salodof MacNeil
The Food and Drug Administration announced on August 17 the approval of vemurafenib, a highly anticipated metastatic melanoma therapy that targets the BRAF V600E mutation found in 40%-60% of patients. It also approved the cobas 4800 BRAF V600 Mutation Test, a companion diagnostic test designed to help determine whether a patient’s melanoma cells carry the BRAF V600E mutation.
2. Novel Therapies Put Multiple Myeloma 'On the Ropes' By Susan London
A sweep of new agents are poised to deliver what could be a knock-out blow to multiple myeloma, according to the director of the myeloma program at the University of California, San Francisco. Some are second- or third-generation agents in a mainstay class that appear to have less toxicity than and/or overcome resistance to their predecessors, Dr. Jeffrey L. Wolf said at the annual Oncology Congress in San Francisco. Others come from classes not previously used in this disease.
1. NICE Rejects Ipilimumab by Jennie Smith
A drug considered a breakthrough treatment for advanced melanoma was turned down by England’s clinical and cost-effectiveness agency. The National Institute for Health and Clinical Excellence, which makes recommendations to the National Health Service in England and Wales, said that it was not likely to recommend ipilimumab (Bristol-Myers Squibb’s Yervoy). The agency cited cost concerns and what it called insufficient follow-up results from a manufacturer-sponsored, phase III, randomized, placebo-controlled trial of ipilimumab.
Did you miss any of last year's top reads in oncology? Click here to receive our weekly e-newsletter.
Catch up with what you missed as we count down the 10 most-read stories on OncologyReport.com last year.
10. Everolimus Posts Big Win in ER-Positive Breast Cancer By Patrice Wendling
This first report of the BOLERO-2 trial -- a potential practice changer -- came out of the European Multidisciplinary Cancer Congress in Stockholm.
9. Multimodal DCIS Therapy, Tamoxifen Cuts Breast Cancer Deaths By Neil Osterweil
A meta-analysis from Australia found that adding radiotherapy and tamoxifen to breast-conserving surgery significantly reduces the local recurrence rate and the breast cancer–specific death rate in women with ductal carcinoma in situ. It was presented at the American Society of Radiation Oncology (ASTRO) meeitng in Miami Beach.
8. Crizotinib Approval Personalizes Lung Cancer Therapy By Miriam E. Tucker
The swift approval of crizotinib capsules by the Food and Drug Administration as the first and only targeted therapy for locally advanced or metastatic ALK-positive non–small cell lung cancer represented another milestone in biomarker-driven, personalized medicine. Crizotinib was approved, along with a companion diagnostic test, Abbott Molecular’s Vysis ALK Break Apart FISH Probe Kit, which identifies the anaplastic lymphoma kinase (ALK) fusion gene that the drug targets.
7. Clinicians Slow to Embrace Sipuleucel-T for Prostate Cancer By Diana Mahoney
Most physicians have strong opinions on sipuleucel-T, including dubbing its approval "a milestone in the history of oncology," but many of them refused to speak about it on the record. Our persistent reporter found the reasons for their reluctance to use the first cancer vaccine went beyond reimbursement issues belabored in the financial press.
6. Drug Shortages Increasingly Take Toll on Care By Elizabeth Mechcatie
With their increasing prevalence, drug shortages in the United States have led to delays in treatment, forced the use of less effective alternatives, and encouraged a burgeoning gray market that sells tough-to-obtain medications at highly inflated prices, according to stakeholders gathered at a recent Food and Drug Administration meeting.
5. Practice Changers Expected at San Antonio Breast Cancer Symposium By Jane Salodof MacNeil
The 2011 San Antonio Breast Cancer Symposium featured a hefty number of studies that could change clinical practice. One of the most exciting SABCS meetings in recent years, it featured the phase III BOLERO-2 and CLEOPATRA trials, a new Oncotype DX assay for ductal carcinoma in situ, reports from four bisphosphonate trials, and a controversial brachytherapy study.
4. FDA Approves Brentuximab for Two Lymphomas By Elizabeth Mechcatie
The Food and Drug Administration on Aug. 19 gave an accelerated approval to brentuximab, a CD30-directed antibody drug-conjugate, for the treatment of Hodgkin’s lymphoma and systemic anaplastic large-cell lymphoma, after other treatments have failed.
3. FDA Approves Vemurafenib for Advanced Melanoma By Jane Salodof MacNeil
The Food and Drug Administration announced on August 17 the approval of vemurafenib, a highly anticipated metastatic melanoma therapy that targets the BRAF V600E mutation found in 40%-60% of patients. It also approved the cobas 4800 BRAF V600 Mutation Test, a companion diagnostic test designed to help determine whether a patient’s melanoma cells carry the BRAF V600E mutation.
2. Novel Therapies Put Multiple Myeloma 'On the Ropes' By Susan London
A sweep of new agents are poised to deliver what could be a knock-out blow to multiple myeloma, according to the director of the myeloma program at the University of California, San Francisco. Some are second- or third-generation agents in a mainstay class that appear to have less toxicity than and/or overcome resistance to their predecessors, Dr. Jeffrey L. Wolf said at the annual Oncology Congress in San Francisco. Others come from classes not previously used in this disease.
1. NICE Rejects Ipilimumab by Jennie Smith
A drug considered a breakthrough treatment for advanced melanoma was turned down by England’s clinical and cost-effectiveness agency. The National Institute for Health and Clinical Excellence, which makes recommendations to the National Health Service in England and Wales, said that it was not likely to recommend ipilimumab (Bristol-Myers Squibb’s Yervoy). The agency cited cost concerns and what it called insufficient follow-up results from a manufacturer-sponsored, phase III, randomized, placebo-controlled trial of ipilimumab.
Did you miss any of last year's top reads in oncology? Click here to receive our weekly e-newsletter.
Catch up with what you missed as we count down the 10 most-read stories on OncologyReport.com last year.
10. Everolimus Posts Big Win in ER-Positive Breast Cancer By Patrice Wendling
This first report of the BOLERO-2 trial -- a potential practice changer -- came out of the European Multidisciplinary Cancer Congress in Stockholm.
9. Multimodal DCIS Therapy, Tamoxifen Cuts Breast Cancer Deaths By Neil Osterweil
A meta-analysis from Australia found that adding radiotherapy and tamoxifen to breast-conserving surgery significantly reduces the local recurrence rate and the breast cancer–specific death rate in women with ductal carcinoma in situ. It was presented at the American Society of Radiation Oncology (ASTRO) meeitng in Miami Beach.
8. Crizotinib Approval Personalizes Lung Cancer Therapy By Miriam E. Tucker
The swift approval of crizotinib capsules by the Food and Drug Administration as the first and only targeted therapy for locally advanced or metastatic ALK-positive non–small cell lung cancer represented another milestone in biomarker-driven, personalized medicine. Crizotinib was approved, along with a companion diagnostic test, Abbott Molecular’s Vysis ALK Break Apart FISH Probe Kit, which identifies the anaplastic lymphoma kinase (ALK) fusion gene that the drug targets.
7. Clinicians Slow to Embrace Sipuleucel-T for Prostate Cancer By Diana Mahoney
Most physicians have strong opinions on sipuleucel-T, including dubbing its approval "a milestone in the history of oncology," but many of them refused to speak about it on the record. Our persistent reporter found the reasons for their reluctance to use the first cancer vaccine went beyond reimbursement issues belabored in the financial press.
6. Drug Shortages Increasingly Take Toll on Care By Elizabeth Mechcatie
With their increasing prevalence, drug shortages in the United States have led to delays in treatment, forced the use of less effective alternatives, and encouraged a burgeoning gray market that sells tough-to-obtain medications at highly inflated prices, according to stakeholders gathered at a recent Food and Drug Administration meeting.
5. Practice Changers Expected at San Antonio Breast Cancer Symposium By Jane Salodof MacNeil
The 2011 San Antonio Breast Cancer Symposium featured a hefty number of studies that could change clinical practice. One of the most exciting SABCS meetings in recent years, it featured the phase III BOLERO-2 and CLEOPATRA trials, a new Oncotype DX assay for ductal carcinoma in situ, reports from four bisphosphonate trials, and a controversial brachytherapy study.
4. FDA Approves Brentuximab for Two Lymphomas By Elizabeth Mechcatie
The Food and Drug Administration on Aug. 19 gave an accelerated approval to brentuximab, a CD30-directed antibody drug-conjugate, for the treatment of Hodgkin’s lymphoma and systemic anaplastic large-cell lymphoma, after other treatments have failed.
3. FDA Approves Vemurafenib for Advanced Melanoma By Jane Salodof MacNeil
The Food and Drug Administration announced on August 17 the approval of vemurafenib, a highly anticipated metastatic melanoma therapy that targets the BRAF V600E mutation found in 40%-60% of patients. It also approved the cobas 4800 BRAF V600 Mutation Test, a companion diagnostic test designed to help determine whether a patient’s melanoma cells carry the BRAF V600E mutation.
2. Novel Therapies Put Multiple Myeloma 'On the Ropes' By Susan London
A sweep of new agents are poised to deliver what could be a knock-out blow to multiple myeloma, according to the director of the myeloma program at the University of California, San Francisco. Some are second- or third-generation agents in a mainstay class that appear to have less toxicity than and/or overcome resistance to their predecessors, Dr. Jeffrey L. Wolf said at the annual Oncology Congress in San Francisco. Others come from classes not previously used in this disease.
1. NICE Rejects Ipilimumab by Jennie Smith
A drug considered a breakthrough treatment for advanced melanoma was turned down by England’s clinical and cost-effectiveness agency. The National Institute for Health and Clinical Excellence, which makes recommendations to the National Health Service in England and Wales, said that it was not likely to recommend ipilimumab (Bristol-Myers Squibb’s Yervoy). The agency cited cost concerns and what it called insufficient follow-up results from a manufacturer-sponsored, phase III, randomized, placebo-controlled trial of ipilimumab.
Did you miss any of last year's top reads in oncology? Click here to receive our weekly e-newsletter.
Blog: Cosmeceutical Experts Agree on Best Anti-Aging Product
Three of the top experts on cosmeceuticals agreed that the best over-the-counter, anti-aging products come down to two simple words: "moisturizer" and "sunscreen."
There is oh, so much more out there being sold in the $9 billion/year skin care market, much of which are anti-aging products. But the skin regimen that provides the biggest bang for the buck: moisturizer and sunscreen. Spend $100 on a product, and chances are its moisturizer and sunscreen anyway.
Speaking in separate presentations at the annual meeting of the American Society of Cosmetic Dermatology and Aesthetic Surgery (ASCDAS), Dr. Zoe D. Draelos, Dr. Ellen S. Marmur and Dr. Michael H. Gold agreed that there is little science to back up claims made by cosmeceutical companies.
Cosmeceuticals fall somewhere between cosmetics and pharmaceuticals; therefore, they are not regulated, and manufacturers are not required to show evidence of anti-aging effectiveness. When evidence does exist, it generally points back to – you guessed it – moisturizer and sunscreen.
Dr. Draelos a dermatologist in High Point, N.C., and a consulting professor of dermatology at Duke University, studied the ingredients in over-the-counter skin care products. She found that 80% of products are moisturizers that serve as a vehicle to deliver whichever high-profile ingredient is being touted by the manufacturer (Plast. Reconst. Surg. 2010;125:719-24).
"Hands down, it's the moisturizer" that's the most important cosmeceutical choice, she said. "All the products that make anti-aging claims are making moisturizer claims," and most anti-aging products also have sunscreen ingredients in them.
When Dr. Gold first spoke at a medical conference many years ago about selling cosmeceutical products in his practice, most dermatologists frowned on the idea. He said he has been dispensing cosmeceuticals for 22 years and has seen the market explode. "There is now a $700 moisturizer," he said. "There may be no difference" between that and a $10 moisturizer, "but some people will pay the $700 because it's $700."
Dr. Gold, who is based in Nashville, urged his colleagues, "If you dispense, do it ethically."
Dermatologists have an important role to play by not just listening to marketing claims of cosmeceuticals, but assessing them. "Even though we don't have a lot of good research right now, patients want something their doctor feels good about," said Dr. Marmur of Mount Sinai School of Medicine, New York, and president of the ASCDAS.
She took that approach in her book, written with Gina Way, Simple Skin Beauty: Every Woman’s Guide to a Lifetime of Healthy, Gorgeous Skin (Atria Books, 2009).
The book "perhaps put me at odds with some of the industry, but we're challenging them to produce better science," she said.
Dr. Marmur and her associates are conducting the first randomized, controlled trial comparing over-the-counter anti-aging creams. With more than 130 subjects enrolled, the study will evaluate 28 biomarkers in seven lines of products, with the patients who apply the products blinded to the product being used.
Not all anti-aging cream manufacturers are included, however. "Some brands refused to participate," perhaps because they were afraid that the study would show that their product is effective but is a pharmaceutical, she said.
Dr. Draelos echoed that idea during the question-and-answer session: "The industry doesn't want closer scrutiny," she said.
I also heard Dr. Draelos speak recently at the Skin Disease and Education Foundation's Women's and Pediatric Dermatology Seminar. Her recommendations for cosmeceuticals include starting with a moisturizer containing dimethicone, glycerin, and/or petrolatum. "The most robust moisturizer known to man has these three ingredients," she said. For anti-aging, she suggests a sunscreen containing avobenzone, oxybenzone, octocrylene, reflecting spheres, or antioxidant botanicals.
How does that translate into over-the-counter products? For hands, Dr. Draelos favors Neutrogena Norwegian Formula Hand Cream. For the face, she recommends Johnson & Johnson's Aveeno Positively Radiant Daily Moisturizer SPF 30. And for the body, Galderma's Cetaphil cream.
Dr. Draelos has been a consultant and researcher for Johnson & Johnson, L'Oreal, Procter & Gamble, Nu Skin, Avon, Stiefel, and Dial Corp. Dr. Marmur disclosed financial relationships with Allergan, DUSA Pharmaceuticals, Genentech, Medicis, Merz, and Sanofi Aventis. Dr. Gold has been a consultant or researcher for Allergan, Medicis, Mentor (Johnson & Johnson), Merz, Galderma, and numerous other companies.
SDEF and this news organization are owned by Elsevier.
Three of the top experts on cosmeceuticals agreed that the best over-the-counter, anti-aging products come down to two simple words: "moisturizer" and "sunscreen."
There is oh, so much more out there being sold in the $9 billion/year skin care market, much of which are anti-aging products. But the skin regimen that provides the biggest bang for the buck: moisturizer and sunscreen. Spend $100 on a product, and chances are its moisturizer and sunscreen anyway.
Speaking in separate presentations at the annual meeting of the American Society of Cosmetic Dermatology and Aesthetic Surgery (ASCDAS), Dr. Zoe D. Draelos, Dr. Ellen S. Marmur and Dr. Michael H. Gold agreed that there is little science to back up claims made by cosmeceutical companies.
Cosmeceuticals fall somewhere between cosmetics and pharmaceuticals; therefore, they are not regulated, and manufacturers are not required to show evidence of anti-aging effectiveness. When evidence does exist, it generally points back to – you guessed it – moisturizer and sunscreen.
Dr. Draelos a dermatologist in High Point, N.C., and a consulting professor of dermatology at Duke University, studied the ingredients in over-the-counter skin care products. She found that 80% of products are moisturizers that serve as a vehicle to deliver whichever high-profile ingredient is being touted by the manufacturer (Plast. Reconst. Surg. 2010;125:719-24).
"Hands down, it's the moisturizer" that's the most important cosmeceutical choice, she said. "All the products that make anti-aging claims are making moisturizer claims," and most anti-aging products also have sunscreen ingredients in them.
When Dr. Gold first spoke at a medical conference many years ago about selling cosmeceutical products in his practice, most dermatologists frowned on the idea. He said he has been dispensing cosmeceuticals for 22 years and has seen the market explode. "There is now a $700 moisturizer," he said. "There may be no difference" between that and a $10 moisturizer, "but some people will pay the $700 because it's $700."
Dr. Gold, who is based in Nashville, urged his colleagues, "If you dispense, do it ethically."
Dermatologists have an important role to play by not just listening to marketing claims of cosmeceuticals, but assessing them. "Even though we don't have a lot of good research right now, patients want something their doctor feels good about," said Dr. Marmur of Mount Sinai School of Medicine, New York, and president of the ASCDAS.
She took that approach in her book, written with Gina Way, Simple Skin Beauty: Every Woman’s Guide to a Lifetime of Healthy, Gorgeous Skin (Atria Books, 2009).
The book "perhaps put me at odds with some of the industry, but we're challenging them to produce better science," she said.
Dr. Marmur and her associates are conducting the first randomized, controlled trial comparing over-the-counter anti-aging creams. With more than 130 subjects enrolled, the study will evaluate 28 biomarkers in seven lines of products, with the patients who apply the products blinded to the product being used.
Not all anti-aging cream manufacturers are included, however. "Some brands refused to participate," perhaps because they were afraid that the study would show that their product is effective but is a pharmaceutical, she said.
Dr. Draelos echoed that idea during the question-and-answer session: "The industry doesn't want closer scrutiny," she said.
I also heard Dr. Draelos speak recently at the Skin Disease and Education Foundation's Women's and Pediatric Dermatology Seminar. Her recommendations for cosmeceuticals include starting with a moisturizer containing dimethicone, glycerin, and/or petrolatum. "The most robust moisturizer known to man has these three ingredients," she said. For anti-aging, she suggests a sunscreen containing avobenzone, oxybenzone, octocrylene, reflecting spheres, or antioxidant botanicals.
How does that translate into over-the-counter products? For hands, Dr. Draelos favors Neutrogena Norwegian Formula Hand Cream. For the face, she recommends Johnson & Johnson's Aveeno Positively Radiant Daily Moisturizer SPF 30. And for the body, Galderma's Cetaphil cream.
Dr. Draelos has been a consultant and researcher for Johnson & Johnson, L'Oreal, Procter & Gamble, Nu Skin, Avon, Stiefel, and Dial Corp. Dr. Marmur disclosed financial relationships with Allergan, DUSA Pharmaceuticals, Genentech, Medicis, Merz, and Sanofi Aventis. Dr. Gold has been a consultant or researcher for Allergan, Medicis, Mentor (Johnson & Johnson), Merz, Galderma, and numerous other companies.
SDEF and this news organization are owned by Elsevier.
Three of the top experts on cosmeceuticals agreed that the best over-the-counter, anti-aging products come down to two simple words: "moisturizer" and "sunscreen."
There is oh, so much more out there being sold in the $9 billion/year skin care market, much of which are anti-aging products. But the skin regimen that provides the biggest bang for the buck: moisturizer and sunscreen. Spend $100 on a product, and chances are its moisturizer and sunscreen anyway.
Speaking in separate presentations at the annual meeting of the American Society of Cosmetic Dermatology and Aesthetic Surgery (ASCDAS), Dr. Zoe D. Draelos, Dr. Ellen S. Marmur and Dr. Michael H. Gold agreed that there is little science to back up claims made by cosmeceutical companies.
Cosmeceuticals fall somewhere between cosmetics and pharmaceuticals; therefore, they are not regulated, and manufacturers are not required to show evidence of anti-aging effectiveness. When evidence does exist, it generally points back to – you guessed it – moisturizer and sunscreen.
Dr. Draelos a dermatologist in High Point, N.C., and a consulting professor of dermatology at Duke University, studied the ingredients in over-the-counter skin care products. She found that 80% of products are moisturizers that serve as a vehicle to deliver whichever high-profile ingredient is being touted by the manufacturer (Plast. Reconst. Surg. 2010;125:719-24).
"Hands down, it's the moisturizer" that's the most important cosmeceutical choice, she said. "All the products that make anti-aging claims are making moisturizer claims," and most anti-aging products also have sunscreen ingredients in them.
When Dr. Gold first spoke at a medical conference many years ago about selling cosmeceutical products in his practice, most dermatologists frowned on the idea. He said he has been dispensing cosmeceuticals for 22 years and has seen the market explode. "There is now a $700 moisturizer," he said. "There may be no difference" between that and a $10 moisturizer, "but some people will pay the $700 because it's $700."
Dr. Gold, who is based in Nashville, urged his colleagues, "If you dispense, do it ethically."
Dermatologists have an important role to play by not just listening to marketing claims of cosmeceuticals, but assessing them. "Even though we don't have a lot of good research right now, patients want something their doctor feels good about," said Dr. Marmur of Mount Sinai School of Medicine, New York, and president of the ASCDAS.
She took that approach in her book, written with Gina Way, Simple Skin Beauty: Every Woman’s Guide to a Lifetime of Healthy, Gorgeous Skin (Atria Books, 2009).
The book "perhaps put me at odds with some of the industry, but we're challenging them to produce better science," she said.
Dr. Marmur and her associates are conducting the first randomized, controlled trial comparing over-the-counter anti-aging creams. With more than 130 subjects enrolled, the study will evaluate 28 biomarkers in seven lines of products, with the patients who apply the products blinded to the product being used.
Not all anti-aging cream manufacturers are included, however. "Some brands refused to participate," perhaps because they were afraid that the study would show that their product is effective but is a pharmaceutical, she said.
Dr. Draelos echoed that idea during the question-and-answer session: "The industry doesn't want closer scrutiny," she said.
I also heard Dr. Draelos speak recently at the Skin Disease and Education Foundation's Women's and Pediatric Dermatology Seminar. Her recommendations for cosmeceuticals include starting with a moisturizer containing dimethicone, glycerin, and/or petrolatum. "The most robust moisturizer known to man has these three ingredients," she said. For anti-aging, she suggests a sunscreen containing avobenzone, oxybenzone, octocrylene, reflecting spheres, or antioxidant botanicals.
How does that translate into over-the-counter products? For hands, Dr. Draelos favors Neutrogena Norwegian Formula Hand Cream. For the face, she recommends Johnson & Johnson's Aveeno Positively Radiant Daily Moisturizer SPF 30. And for the body, Galderma's Cetaphil cream.
Dr. Draelos has been a consultant and researcher for Johnson & Johnson, L'Oreal, Procter & Gamble, Nu Skin, Avon, Stiefel, and Dial Corp. Dr. Marmur disclosed financial relationships with Allergan, DUSA Pharmaceuticals, Genentech, Medicis, Merz, and Sanofi Aventis. Dr. Gold has been a consultant or researcher for Allergan, Medicis, Mentor (Johnson & Johnson), Merz, Galderma, and numerous other companies.
SDEF and this news organization are owned by Elsevier.
Less Than Half of Melanoma Survivors Regularly Use Sunscreen
Melanoma survivors are more likely to regularly use sunscreen, when compared with individuals who have never had cancer, but only 46.2% of survivors report frequent use, according to a new study published online.
Among 156 melanoma survivors who took part in the 2005 and 2007 Health Information National Trends Survey, 25% reported always using sunscreen and 21.2% reported often using sunscreen when outdoors for more than an hour on a warm, sunny day. Frequent use among those who reported never having cancer (n = 11,408) was 32.4% (14.5% always/17.9% often), reported Deborah Mayer, Ph.D., and her associates at the University of North Carolina, Chapel Hill.
The rate of frequent use of protective clothing was 70.5% among melanoma survivors and 65.8% for cancer-free control subjects. Frequent use of shade was 41% for melanoma survivors and 35.5% for controls (J. Am. Acad. Dermatol. 2012;66;e9-10).
"Given the high risk for new skin cancers, one would expect higher adherence," wrote Dr. Mayer and her associates, who noted that "10 melanoma survivors reported using tanning beds after their cancer diagnosis."
The study was supported by the National Cancer Institute. The investigators did not report any conflicts of interest.
Note: 2005 and 2007 Health Information National Trends Survey data.
Source: J. Am. Acad. Dermatol. 2012;66;e9-10
Melanoma survivors are more likely to regularly use sunscreen, when compared with individuals who have never had cancer, but only 46.2% of survivors report frequent use, according to a new study published online.
Among 156 melanoma survivors who took part in the 2005 and 2007 Health Information National Trends Survey, 25% reported always using sunscreen and 21.2% reported often using sunscreen when outdoors for more than an hour on a warm, sunny day. Frequent use among those who reported never having cancer (n = 11,408) was 32.4% (14.5% always/17.9% often), reported Deborah Mayer, Ph.D., and her associates at the University of North Carolina, Chapel Hill.
The rate of frequent use of protective clothing was 70.5% among melanoma survivors and 65.8% for cancer-free control subjects. Frequent use of shade was 41% for melanoma survivors and 35.5% for controls (J. Am. Acad. Dermatol. 2012;66;e9-10).
"Given the high risk for new skin cancers, one would expect higher adherence," wrote Dr. Mayer and her associates, who noted that "10 melanoma survivors reported using tanning beds after their cancer diagnosis."
The study was supported by the National Cancer Institute. The investigators did not report any conflicts of interest.
Note: 2005 and 2007 Health Information National Trends Survey data.
Source: J. Am. Acad. Dermatol. 2012;66;e9-10
Melanoma survivors are more likely to regularly use sunscreen, when compared with individuals who have never had cancer, but only 46.2% of survivors report frequent use, according to a new study published online.
Among 156 melanoma survivors who took part in the 2005 and 2007 Health Information National Trends Survey, 25% reported always using sunscreen and 21.2% reported often using sunscreen when outdoors for more than an hour on a warm, sunny day. Frequent use among those who reported never having cancer (n = 11,408) was 32.4% (14.5% always/17.9% often), reported Deborah Mayer, Ph.D., and her associates at the University of North Carolina, Chapel Hill.
The rate of frequent use of protective clothing was 70.5% among melanoma survivors and 65.8% for cancer-free control subjects. Frequent use of shade was 41% for melanoma survivors and 35.5% for controls (J. Am. Acad. Dermatol. 2012;66;e9-10).
"Given the high risk for new skin cancers, one would expect higher adherence," wrote Dr. Mayer and her associates, who noted that "10 melanoma survivors reported using tanning beds after their cancer diagnosis."
The study was supported by the National Cancer Institute. The investigators did not report any conflicts of interest.
Note: 2005 and 2007 Health Information National Trends Survey data.
Source: J. Am. Acad. Dermatol. 2012;66;e9-10
Blog: Top 10 Stories of 2011
For those of you who have had a busy year and haven't had the chance to regularly read the latest dermatology news on Skin and Allergy News Digital Network, we have you covered. As we ring in the new year, here's a rundown of last year's most-viewed stories:
10. Experts: Medical Dermatology Is Losing Ground, By Bruce Jancin: Experts in medical dermatology predicted the specialty will become narrower and less medically oriented by 2020. As we enter 2012, some experts said they were concerned about the emphasis on aesthetic dermatology and dermatologic surgery.
9. Mohs Surgery in Medicare Patients Skyrocketing, By Sherry Boschert: Several Mohs surgery experts found that the rate of Mohs surgery per 1,000 Medicare beneficiaries increased by 236% between 1999 and 2009. Dr. Matthew Donaldson and his associates presented the data at the annual meeting of the American College of Mohs Surgery.
8. Blog: New Isotretinoin Drug May Address Safety Concerns, By Amy Pfeiffer: This much-viewed blog post highlighted an investigational isotretinoin drug that may eliminate safety concerns associated with the drug, like IBD and depression. The gelatin capsules of CIP-iisotretinoin help reduce GI irritation and the drug is less food dependent.
7. Dosing Isotretinoin: Go Big to Avoid Second Course, By Jeffrey Eisenberg: In another isotretinoin study, investigators found that patients receiving a higher cumulative dose of the drug were no less likely to experience an acne relapse than those who received a lower cumulative dose. However, the investigators found that patients treated with a higher dose were less likely to need a second course of treatment.
6. Knifelike Vulvar Ulcers May Signal Crohn's Disease, By Kate Johnson: Knifelike vulvar ulcers could be a sign of Crohn's disease in women, according to experts at a conference on vulvovaginal diseases. For some patients, ulcers may be the only manifestation of the disorder.
5. Biologics Up Cardiovascular Risk, New Analysis Finds, By Sherry Boschert: Biologic therapies used to treat psoriasis have been linked to an increase in major cardiovascular events, according to researchers. One patient on placebo developed a major cardiovascular event in a study of etanercept. Five patients on ustekinumab, five on briakinumab, and one on adalimumab also developed major cardiovascular events.
4. Future Technologies Hold Promise for Hair Restoration, By Damian McNamara: At an annual meeting of dermatologic surgeons, Dr. Ricardo Mejia discussed technological advancements in hair restoration. He said the future for hair restoration could include technologies like robotic hair transfer, hair cloning, and technologies to optimize new growth.
3. AAD: Potential Doxycycline, IBD Link Considered Worrisome, By Bruce Jancin: In more acne news, a retrospective cohort study linked tetracycline-class antibiotics with an increase in inflammatory bowel disease. The highly controversial findings were one of the hottest topics at the annual meeting of the American Academy of Dermatology and on this website.
2. Bimatoprost Repigments Vitiligo Patient Skin, By Bruce Jancin: A topical bimatoprost ophthalmic solution could serve as treatment for focal vitiligo, according to a pilot study presented at the World Congress of Dermatology. Researchers said 7 out of 10 patients exhibited pronounced repigmentation after 2 months of treatment.
1. Marijuana Allergies "Fairly Common," Expert Says, By M. Alexander Otto: A heads up to physicians: allergy experts said marijuana allergies are more common than most people think. Patients with with a marijuana allergy exhibit symptoms including wheezing, sinusitis, throat swelling, and inhalation issues.
Best wishes for 2012!
-- Frances Correa (FMCReporting)
For those of you who have had a busy year and haven't had the chance to regularly read the latest dermatology news on Skin and Allergy News Digital Network, we have you covered. As we ring in the new year, here's a rundown of last year's most-viewed stories:
10. Experts: Medical Dermatology Is Losing Ground, By Bruce Jancin: Experts in medical dermatology predicted the specialty will become narrower and less medically oriented by 2020. As we enter 2012, some experts said they were concerned about the emphasis on aesthetic dermatology and dermatologic surgery.
9. Mohs Surgery in Medicare Patients Skyrocketing, By Sherry Boschert: Several Mohs surgery experts found that the rate of Mohs surgery per 1,000 Medicare beneficiaries increased by 236% between 1999 and 2009. Dr. Matthew Donaldson and his associates presented the data at the annual meeting of the American College of Mohs Surgery.
8. Blog: New Isotretinoin Drug May Address Safety Concerns, By Amy Pfeiffer: This much-viewed blog post highlighted an investigational isotretinoin drug that may eliminate safety concerns associated with the drug, like IBD and depression. The gelatin capsules of CIP-iisotretinoin help reduce GI irritation and the drug is less food dependent.
7. Dosing Isotretinoin: Go Big to Avoid Second Course, By Jeffrey Eisenberg: In another isotretinoin study, investigators found that patients receiving a higher cumulative dose of the drug were no less likely to experience an acne relapse than those who received a lower cumulative dose. However, the investigators found that patients treated with a higher dose were less likely to need a second course of treatment.
6. Knifelike Vulvar Ulcers May Signal Crohn's Disease, By Kate Johnson: Knifelike vulvar ulcers could be a sign of Crohn's disease in women, according to experts at a conference on vulvovaginal diseases. For some patients, ulcers may be the only manifestation of the disorder.
5. Biologics Up Cardiovascular Risk, New Analysis Finds, By Sherry Boschert: Biologic therapies used to treat psoriasis have been linked to an increase in major cardiovascular events, according to researchers. One patient on placebo developed a major cardiovascular event in a study of etanercept. Five patients on ustekinumab, five on briakinumab, and one on adalimumab also developed major cardiovascular events.
4. Future Technologies Hold Promise for Hair Restoration, By Damian McNamara: At an annual meeting of dermatologic surgeons, Dr. Ricardo Mejia discussed technological advancements in hair restoration. He said the future for hair restoration could include technologies like robotic hair transfer, hair cloning, and technologies to optimize new growth.
3. AAD: Potential Doxycycline, IBD Link Considered Worrisome, By Bruce Jancin: In more acne news, a retrospective cohort study linked tetracycline-class antibiotics with an increase in inflammatory bowel disease. The highly controversial findings were one of the hottest topics at the annual meeting of the American Academy of Dermatology and on this website.
2. Bimatoprost Repigments Vitiligo Patient Skin, By Bruce Jancin: A topical bimatoprost ophthalmic solution could serve as treatment for focal vitiligo, according to a pilot study presented at the World Congress of Dermatology. Researchers said 7 out of 10 patients exhibited pronounced repigmentation after 2 months of treatment.
1. Marijuana Allergies "Fairly Common," Expert Says, By M. Alexander Otto: A heads up to physicians: allergy experts said marijuana allergies are more common than most people think. Patients with with a marijuana allergy exhibit symptoms including wheezing, sinusitis, throat swelling, and inhalation issues.
Best wishes for 2012!
-- Frances Correa (FMCReporting)
For those of you who have had a busy year and haven't had the chance to regularly read the latest dermatology news on Skin and Allergy News Digital Network, we have you covered. As we ring in the new year, here's a rundown of last year's most-viewed stories:
10. Experts: Medical Dermatology Is Losing Ground, By Bruce Jancin: Experts in medical dermatology predicted the specialty will become narrower and less medically oriented by 2020. As we enter 2012, some experts said they were concerned about the emphasis on aesthetic dermatology and dermatologic surgery.
9. Mohs Surgery in Medicare Patients Skyrocketing, By Sherry Boschert: Several Mohs surgery experts found that the rate of Mohs surgery per 1,000 Medicare beneficiaries increased by 236% between 1999 and 2009. Dr. Matthew Donaldson and his associates presented the data at the annual meeting of the American College of Mohs Surgery.
8. Blog: New Isotretinoin Drug May Address Safety Concerns, By Amy Pfeiffer: This much-viewed blog post highlighted an investigational isotretinoin drug that may eliminate safety concerns associated with the drug, like IBD and depression. The gelatin capsules of CIP-iisotretinoin help reduce GI irritation and the drug is less food dependent.
7. Dosing Isotretinoin: Go Big to Avoid Second Course, By Jeffrey Eisenberg: In another isotretinoin study, investigators found that patients receiving a higher cumulative dose of the drug were no less likely to experience an acne relapse than those who received a lower cumulative dose. However, the investigators found that patients treated with a higher dose were less likely to need a second course of treatment.
6. Knifelike Vulvar Ulcers May Signal Crohn's Disease, By Kate Johnson: Knifelike vulvar ulcers could be a sign of Crohn's disease in women, according to experts at a conference on vulvovaginal diseases. For some patients, ulcers may be the only manifestation of the disorder.
5. Biologics Up Cardiovascular Risk, New Analysis Finds, By Sherry Boschert: Biologic therapies used to treat psoriasis have been linked to an increase in major cardiovascular events, according to researchers. One patient on placebo developed a major cardiovascular event in a study of etanercept. Five patients on ustekinumab, five on briakinumab, and one on adalimumab also developed major cardiovascular events.
4. Future Technologies Hold Promise for Hair Restoration, By Damian McNamara: At an annual meeting of dermatologic surgeons, Dr. Ricardo Mejia discussed technological advancements in hair restoration. He said the future for hair restoration could include technologies like robotic hair transfer, hair cloning, and technologies to optimize new growth.
3. AAD: Potential Doxycycline, IBD Link Considered Worrisome, By Bruce Jancin: In more acne news, a retrospective cohort study linked tetracycline-class antibiotics with an increase in inflammatory bowel disease. The highly controversial findings were one of the hottest topics at the annual meeting of the American Academy of Dermatology and on this website.
2. Bimatoprost Repigments Vitiligo Patient Skin, By Bruce Jancin: A topical bimatoprost ophthalmic solution could serve as treatment for focal vitiligo, according to a pilot study presented at the World Congress of Dermatology. Researchers said 7 out of 10 patients exhibited pronounced repigmentation after 2 months of treatment.
1. Marijuana Allergies "Fairly Common," Expert Says, By M. Alexander Otto: A heads up to physicians: allergy experts said marijuana allergies are more common than most people think. Patients with with a marijuana allergy exhibit symptoms including wheezing, sinusitis, throat swelling, and inhalation issues.
Best wishes for 2012!
-- Frances Correa (FMCReporting)
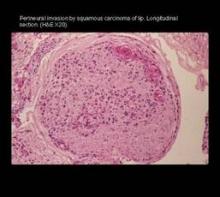
Chronic Inflammation Implies Perineural Invasion
SAN DIEGO – Evidence of chronic inflammation noted during Mohs surgery is a telltale sign of perineural invasion.
"If you see chronic inflammatory infiltrate within or proximal to a neurovascular bundle, look for perineural tumor," said Dr. Alexander Miller, a dermatologic surgeon in private practice in Yorba Linda, Calif. Histologically, that means abundant lymphocytes and perhaps histiocytes.
An abundance of neutrophils, however, is likely indicative of an acute inflammatory response. Perhaps even a response resulting from electrocautery during a Mohs procedure.
Neutrophils might also be present if a keratinizing tumor has ruptured into stroma, generating a microabscess. "But then it’s pretty darned obvious what you have," said Dr. Miller at a meeting sponsored by the American Society for Mohs Surgery.
Finding perineural tumor cells within a cluster of inflammatory cells can be like hunting for the proverbial needle in a haystack. A low-power view might miss them, he said. On medium or higher power views, tumor cells may appear as minute dots, a tiny stripe, or a sliver along one edge of a nerve.
To demonstrate, Dr. Miller displayed a slide depicting voluminous chronic inflammation surrounding an artery, vessel, and nerve.
"No tumor," he said.
"But if one looks carefully, two sections down, same slide, same patient, lo and behold there’s the tumor. Complacency should not be had here. One has to ensure that particularly when there’s inflammation, one needs to look very carefully at all sections of the slide."
Dr. Miller reported having no financial disclosures relevant to his talk.
SAN DIEGO – Evidence of chronic inflammation noted during Mohs surgery is a telltale sign of perineural invasion.
"If you see chronic inflammatory infiltrate within or proximal to a neurovascular bundle, look for perineural tumor," said Dr. Alexander Miller, a dermatologic surgeon in private practice in Yorba Linda, Calif. Histologically, that means abundant lymphocytes and perhaps histiocytes.
An abundance of neutrophils, however, is likely indicative of an acute inflammatory response. Perhaps even a response resulting from electrocautery during a Mohs procedure.
Neutrophils might also be present if a keratinizing tumor has ruptured into stroma, generating a microabscess. "But then it’s pretty darned obvious what you have," said Dr. Miller at a meeting sponsored by the American Society for Mohs Surgery.
Finding perineural tumor cells within a cluster of inflammatory cells can be like hunting for the proverbial needle in a haystack. A low-power view might miss them, he said. On medium or higher power views, tumor cells may appear as minute dots, a tiny stripe, or a sliver along one edge of a nerve.
To demonstrate, Dr. Miller displayed a slide depicting voluminous chronic inflammation surrounding an artery, vessel, and nerve.
"No tumor," he said.
"But if one looks carefully, two sections down, same slide, same patient, lo and behold there’s the tumor. Complacency should not be had here. One has to ensure that particularly when there’s inflammation, one needs to look very carefully at all sections of the slide."
Dr. Miller reported having no financial disclosures relevant to his talk.
SAN DIEGO – Evidence of chronic inflammation noted during Mohs surgery is a telltale sign of perineural invasion.
"If you see chronic inflammatory infiltrate within or proximal to a neurovascular bundle, look for perineural tumor," said Dr. Alexander Miller, a dermatologic surgeon in private practice in Yorba Linda, Calif. Histologically, that means abundant lymphocytes and perhaps histiocytes.
An abundance of neutrophils, however, is likely indicative of an acute inflammatory response. Perhaps even a response resulting from electrocautery during a Mohs procedure.
Neutrophils might also be present if a keratinizing tumor has ruptured into stroma, generating a microabscess. "But then it’s pretty darned obvious what you have," said Dr. Miller at a meeting sponsored by the American Society for Mohs Surgery.
Finding perineural tumor cells within a cluster of inflammatory cells can be like hunting for the proverbial needle in a haystack. A low-power view might miss them, he said. On medium or higher power views, tumor cells may appear as minute dots, a tiny stripe, or a sliver along one edge of a nerve.
To demonstrate, Dr. Miller displayed a slide depicting voluminous chronic inflammation surrounding an artery, vessel, and nerve.
"No tumor," he said.
"But if one looks carefully, two sections down, same slide, same patient, lo and behold there’s the tumor. Complacency should not be had here. One has to ensure that particularly when there’s inflammation, one needs to look very carefully at all sections of the slide."
Dr. Miller reported having no financial disclosures relevant to his talk.
EXPERT ANALYSIS FROM A MEETING SPONSORED BY THE AMERICAN SOCIETY FOR MOHS SURGERY
Basic Dermoscopy for the Resident
Most Lymphomatoid Papulosis Has Benign Course
LAS VEGAS – Although certain characteristics of lymphomatoid papulosis appear be associated with progression to lymphoma, the majority of patients will have a benign course of disease.
The recurrent papulonodular skin eruption lymphomatoid papulosis (LyP) can be a confusing dermatologic entity because it appears malignant histologically, but it usually follows a clinically benign and indolent course (Arch. Dermatol. 1968;97:23-30). And even the 10%-20% of patients who do progress to lymphoma tend to have less aggressive disease, said Dr. Lawrence E. Gibson, professor of dermatology at the Mayo Clinic in Rochester, Minn. The reasons for this disconnect are not yet known.
"Patients with LyP look like lymphoma under the microscope but have clinically indolent cutaneous disease. ... It is an example of a very important clinical-pathological relationship that really needs to be made to help us understand how to treat patients better," he said.
"The bottom line is most of our patients who have LyP do not go on to have aggressive lymphomas."
To identify which LyP patients are more likely to progress to lymphoma, Dr. Gibson, Dr. Rokea A. el-Azhary, Dr. Aieska de Souza, and their associates conducted a retrospective analysis of 123 patients seen at the Mayo Clinic between 1991 and 2008. The patients were followed for a mean of 4 years (range, 2 months to 14 years). The 65 males and 58 females had a mean age of 47 years (range, 1-83 years), and a mean of 14 lesions (range, 1-100). Most (88%) of the lesions were papules, with a reported mean duration of 5.5 weeks. Pruritis was present in 38% and scar formation in 58%, the researchers reported (J. Am. Acad. Dermatol. 2011 [doi:10.1016/j.jaad.2011.07.012]).
Hematologic malignancies were present in 17 patients (14%). Of those, 10 were cutaneous lymphomas – 8 mycosis fungoides (MF) and 2 anaplastic large-cell lymphomas (ALCL). Hodgkin lymphoma was present in three patients (including the two with ALCL), multiple myeloma or monoclonal gammopathy in three, and myelodysplastic syndrome in one.
"The bottom line is most of our patients who have LyP do not go on to have aggressive lymphomas. They certainly don’t have cytotoxic lymphomas. And if they have lymphoma, they usually have MF. I think that’s somewhat reassuring to us. And for the most part, most of the patients don’t have anything. They have a normal life," Dr. Gibson said at the seminar sponsored by Skin Disease Education Foundation (SDEF).
Of 97 LyP patients for whom original biopsy slides were available, the majority (69) had World Health Organization/European Organization for Research and Treatment of Cancer histologic classification type A, including 35 with immunophenotypic subtype CD8 and 34 with subtype CD4. Another 13 patients had type B lesions (8 CD4, 5 CD8), and 6 had type C, all of which were CD4. The other 9 patients had more than one histologic type (A, B, or C), and/or more than one immunophenotypic subtype (CD4 or CD8). They were designated mixed type.
Clinically, there were no distinguishing features among the subtypes. This finding contrasts with some previous reports that the CD8 subtype might predispose to worse disease outcome (Am. J. Pathol. 1999;155:483-92).
"Our findings indicated that the LyP subtype CD8 does not signify more aggressive disease, a poor prognosis, or an association with malignancy," Dr. Gibson and his colleagues wrote.
Hematologic malignancies were present in 5 of the 9 mixed-type patients (55.5%), compared with 4 of the 34 with A/CD4 (12%), 4 of the 35 A/CD8 (11.5%), 1 of the 8 B/CD4 patients (12.5%), and 1 of the 5 B/CD8 patients (20%). (Two of the 17 malignancies were excluded from analysis because original slides were not available.) The odds ratio for malignancy for the patients with mixed-type LyP versus all other types was a statistically significant 4.33 (P = .03).
In a molecular genetics substudy of 84 LyP lesions from 76 patients, 42 (50%) were positive for clonal T-cell receptor gene rearrangement (TCRGR), 34 (40%) were negative, and 8 (10%) showed equivocal results or had insufficient DNA for analysis. Among the LyP patients who had a hematologic malignancy, 9 of 11 (82%) had positive TCRGR, compared with 30 of 68 (44%) LyP patients without malignancy. That association was also significant, with an odds ratio of 5.7 (P = .02), noted the investigators.
"A positive T-cell receptor gene rearrangement or having more than one type of LyP may have a higher risk of progression to lymphoma, but the evidence is not hard and fast. ... The take-home message is most of these patients do just fine," Dr. Gibson said.
Dr. Gibson stated that he had no relevant financial disclosures or conflicts of interest. SDEF and this news organization are owned by Elsevier.
LAS VEGAS – Although certain characteristics of lymphomatoid papulosis appear be associated with progression to lymphoma, the majority of patients will have a benign course of disease.
The recurrent papulonodular skin eruption lymphomatoid papulosis (LyP) can be a confusing dermatologic entity because it appears malignant histologically, but it usually follows a clinically benign and indolent course (Arch. Dermatol. 1968;97:23-30). And even the 10%-20% of patients who do progress to lymphoma tend to have less aggressive disease, said Dr. Lawrence E. Gibson, professor of dermatology at the Mayo Clinic in Rochester, Minn. The reasons for this disconnect are not yet known.
"Patients with LyP look like lymphoma under the microscope but have clinically indolent cutaneous disease. ... It is an example of a very important clinical-pathological relationship that really needs to be made to help us understand how to treat patients better," he said.
"The bottom line is most of our patients who have LyP do not go on to have aggressive lymphomas."
To identify which LyP patients are more likely to progress to lymphoma, Dr. Gibson, Dr. Rokea A. el-Azhary, Dr. Aieska de Souza, and their associates conducted a retrospective analysis of 123 patients seen at the Mayo Clinic between 1991 and 2008. The patients were followed for a mean of 4 years (range, 2 months to 14 years). The 65 males and 58 females had a mean age of 47 years (range, 1-83 years), and a mean of 14 lesions (range, 1-100). Most (88%) of the lesions were papules, with a reported mean duration of 5.5 weeks. Pruritis was present in 38% and scar formation in 58%, the researchers reported (J. Am. Acad. Dermatol. 2011 [doi:10.1016/j.jaad.2011.07.012]).
Hematologic malignancies were present in 17 patients (14%). Of those, 10 were cutaneous lymphomas – 8 mycosis fungoides (MF) and 2 anaplastic large-cell lymphomas (ALCL). Hodgkin lymphoma was present in three patients (including the two with ALCL), multiple myeloma or monoclonal gammopathy in three, and myelodysplastic syndrome in one.
"The bottom line is most of our patients who have LyP do not go on to have aggressive lymphomas. They certainly don’t have cytotoxic lymphomas. And if they have lymphoma, they usually have MF. I think that’s somewhat reassuring to us. And for the most part, most of the patients don’t have anything. They have a normal life," Dr. Gibson said at the seminar sponsored by Skin Disease Education Foundation (SDEF).
Of 97 LyP patients for whom original biopsy slides were available, the majority (69) had World Health Organization/European Organization for Research and Treatment of Cancer histologic classification type A, including 35 with immunophenotypic subtype CD8 and 34 with subtype CD4. Another 13 patients had type B lesions (8 CD4, 5 CD8), and 6 had type C, all of which were CD4. The other 9 patients had more than one histologic type (A, B, or C), and/or more than one immunophenotypic subtype (CD4 or CD8). They were designated mixed type.
Clinically, there were no distinguishing features among the subtypes. This finding contrasts with some previous reports that the CD8 subtype might predispose to worse disease outcome (Am. J. Pathol. 1999;155:483-92).
"Our findings indicated that the LyP subtype CD8 does not signify more aggressive disease, a poor prognosis, or an association with malignancy," Dr. Gibson and his colleagues wrote.
Hematologic malignancies were present in 5 of the 9 mixed-type patients (55.5%), compared with 4 of the 34 with A/CD4 (12%), 4 of the 35 A/CD8 (11.5%), 1 of the 8 B/CD4 patients (12.5%), and 1 of the 5 B/CD8 patients (20%). (Two of the 17 malignancies were excluded from analysis because original slides were not available.) The odds ratio for malignancy for the patients with mixed-type LyP versus all other types was a statistically significant 4.33 (P = .03).
In a molecular genetics substudy of 84 LyP lesions from 76 patients, 42 (50%) were positive for clonal T-cell receptor gene rearrangement (TCRGR), 34 (40%) were negative, and 8 (10%) showed equivocal results or had insufficient DNA for analysis. Among the LyP patients who had a hematologic malignancy, 9 of 11 (82%) had positive TCRGR, compared with 30 of 68 (44%) LyP patients without malignancy. That association was also significant, with an odds ratio of 5.7 (P = .02), noted the investigators.
"A positive T-cell receptor gene rearrangement or having more than one type of LyP may have a higher risk of progression to lymphoma, but the evidence is not hard and fast. ... The take-home message is most of these patients do just fine," Dr. Gibson said.
Dr. Gibson stated that he had no relevant financial disclosures or conflicts of interest. SDEF and this news organization are owned by Elsevier.
LAS VEGAS – Although certain characteristics of lymphomatoid papulosis appear be associated with progression to lymphoma, the majority of patients will have a benign course of disease.
The recurrent papulonodular skin eruption lymphomatoid papulosis (LyP) can be a confusing dermatologic entity because it appears malignant histologically, but it usually follows a clinically benign and indolent course (Arch. Dermatol. 1968;97:23-30). And even the 10%-20% of patients who do progress to lymphoma tend to have less aggressive disease, said Dr. Lawrence E. Gibson, professor of dermatology at the Mayo Clinic in Rochester, Minn. The reasons for this disconnect are not yet known.
"Patients with LyP look like lymphoma under the microscope but have clinically indolent cutaneous disease. ... It is an example of a very important clinical-pathological relationship that really needs to be made to help us understand how to treat patients better," he said.
"The bottom line is most of our patients who have LyP do not go on to have aggressive lymphomas."
To identify which LyP patients are more likely to progress to lymphoma, Dr. Gibson, Dr. Rokea A. el-Azhary, Dr. Aieska de Souza, and their associates conducted a retrospective analysis of 123 patients seen at the Mayo Clinic between 1991 and 2008. The patients were followed for a mean of 4 years (range, 2 months to 14 years). The 65 males and 58 females had a mean age of 47 years (range, 1-83 years), and a mean of 14 lesions (range, 1-100). Most (88%) of the lesions were papules, with a reported mean duration of 5.5 weeks. Pruritis was present in 38% and scar formation in 58%, the researchers reported (J. Am. Acad. Dermatol. 2011 [doi:10.1016/j.jaad.2011.07.012]).
Hematologic malignancies were present in 17 patients (14%). Of those, 10 were cutaneous lymphomas – 8 mycosis fungoides (MF) and 2 anaplastic large-cell lymphomas (ALCL). Hodgkin lymphoma was present in three patients (including the two with ALCL), multiple myeloma or monoclonal gammopathy in three, and myelodysplastic syndrome in one.
"The bottom line is most of our patients who have LyP do not go on to have aggressive lymphomas. They certainly don’t have cytotoxic lymphomas. And if they have lymphoma, they usually have MF. I think that’s somewhat reassuring to us. And for the most part, most of the patients don’t have anything. They have a normal life," Dr. Gibson said at the seminar sponsored by Skin Disease Education Foundation (SDEF).
Of 97 LyP patients for whom original biopsy slides were available, the majority (69) had World Health Organization/European Organization for Research and Treatment of Cancer histologic classification type A, including 35 with immunophenotypic subtype CD8 and 34 with subtype CD4. Another 13 patients had type B lesions (8 CD4, 5 CD8), and 6 had type C, all of which were CD4. The other 9 patients had more than one histologic type (A, B, or C), and/or more than one immunophenotypic subtype (CD4 or CD8). They were designated mixed type.
Clinically, there were no distinguishing features among the subtypes. This finding contrasts with some previous reports that the CD8 subtype might predispose to worse disease outcome (Am. J. Pathol. 1999;155:483-92).
"Our findings indicated that the LyP subtype CD8 does not signify more aggressive disease, a poor prognosis, or an association with malignancy," Dr. Gibson and his colleagues wrote.
Hematologic malignancies were present in 5 of the 9 mixed-type patients (55.5%), compared with 4 of the 34 with A/CD4 (12%), 4 of the 35 A/CD8 (11.5%), 1 of the 8 B/CD4 patients (12.5%), and 1 of the 5 B/CD8 patients (20%). (Two of the 17 malignancies were excluded from analysis because original slides were not available.) The odds ratio for malignancy for the patients with mixed-type LyP versus all other types was a statistically significant 4.33 (P = .03).
In a molecular genetics substudy of 84 LyP lesions from 76 patients, 42 (50%) were positive for clonal T-cell receptor gene rearrangement (TCRGR), 34 (40%) were negative, and 8 (10%) showed equivocal results or had insufficient DNA for analysis. Among the LyP patients who had a hematologic malignancy, 9 of 11 (82%) had positive TCRGR, compared with 30 of 68 (44%) LyP patients without malignancy. That association was also significant, with an odds ratio of 5.7 (P = .02), noted the investigators.
"A positive T-cell receptor gene rearrangement or having more than one type of LyP may have a higher risk of progression to lymphoma, but the evidence is not hard and fast. ... The take-home message is most of these patients do just fine," Dr. Gibson said.
Dr. Gibson stated that he had no relevant financial disclosures or conflicts of interest. SDEF and this news organization are owned by Elsevier.
FROM THE SDEF LAS VEGAS DERMATOLOGY SEMINAR
Major Finding: Hematologic malignancies were present in 17 patients (14%).
Data Source: Retrospective analysis of 123 LyP patients seen at the Mayo Clinic between 1991 and 2008.
Disclosures: Dr. Gibson has no relevant financial disclosures or conflicts of interest. SDEF and this news organization are owned by Elsevier.
Are At-Home Devices a Threat?: The Skinny Podcast
In this month's podcast, Reporter Naseem Miller interviews Dr. Ashley Wysong, a former six-time NCAA All-American and national champion in middle distance running, about a recent survey that found nearly half of collegiate athletes don't use sunscreen.
Dr. Sheila Fallon Friedlander discusses who should be receiving vitamin D supplementation, and Dr. Ilona Frieden says that growing evidence suggests propranolol is a "remarkably effective treatment in shrinking hemangioma growth, even in children whose hemangiomas are already fully grown in some cases."
In this month's Cosmetic Counter segment, Dr. Lily Talakoub discusses what at-home devices are worth your patient's investment. And last but not least, Dr. Alan Rockoff shares more patient-story humor.
Don't miss another episode of The Skinny Podcast; subscribe on iTunes!
In this month's podcast, Reporter Naseem Miller interviews Dr. Ashley Wysong, a former six-time NCAA All-American and national champion in middle distance running, about a recent survey that found nearly half of collegiate athletes don't use sunscreen.
Dr. Sheila Fallon Friedlander discusses who should be receiving vitamin D supplementation, and Dr. Ilona Frieden says that growing evidence suggests propranolol is a "remarkably effective treatment in shrinking hemangioma growth, even in children whose hemangiomas are already fully grown in some cases."
In this month's Cosmetic Counter segment, Dr. Lily Talakoub discusses what at-home devices are worth your patient's investment. And last but not least, Dr. Alan Rockoff shares more patient-story humor.
Don't miss another episode of The Skinny Podcast; subscribe on iTunes!
In this month's podcast, Reporter Naseem Miller interviews Dr. Ashley Wysong, a former six-time NCAA All-American and national champion in middle distance running, about a recent survey that found nearly half of collegiate athletes don't use sunscreen.
Dr. Sheila Fallon Friedlander discusses who should be receiving vitamin D supplementation, and Dr. Ilona Frieden says that growing evidence suggests propranolol is a "remarkably effective treatment in shrinking hemangioma growth, even in children whose hemangiomas are already fully grown in some cases."
In this month's Cosmetic Counter segment, Dr. Lily Talakoub discusses what at-home devices are worth your patient's investment. And last but not least, Dr. Alan Rockoff shares more patient-story humor.
Don't miss another episode of The Skinny Podcast; subscribe on iTunes!
Hospital Setting May Pose Collegial Challenges in Mohs
SAN DIEGO – It would be somewhat of an understatement to say that Mohs surgery was not particularly welcomed at hospitals where Dr. Rainer Sachse used to practice.
As a plastic and reconstructive surgeon, he had hoped to utilize the technique to treat extensive, high-stage tumors in high-risk patients within a hospital setting, believing that the literature convincingly suggested that Mohs offered the best hope for cancer control in such patients.
Nurses, he recalled, considered Mohs a "slow, mutilating, expensive" procedure. Surgeons felt it was unnecessary. Pathologists thought their traditional methods "worked perfectly well."
Dermatologists seemed preoccupied by turf battles between the American Society for Mohs Surgery (ASMS) and the American College of Mohs Surgery. Dermatology residents had no time, and plastic surgery residents were uninterested, Dr. Sachse said at the meeting sponsored by the ASMS.
He pressed on, though, inspired by cases in which conventional excisions and standard therapy mutilated patients or led to their untimely deaths from tumors with continuous growth patterns.
He observed colleagues and sought out preceptorships, pored over the literature, and took a Mohs surgery course before beginning to try small cases with a pathologist who had received dermatopathology training. Finally, he began to change minds and take on more challenging cases.
Seeing the results, "a pathologist who was initially very skeptical eventually became a strong supporter," said Dr. Sachse, who is in private practice in Fort Lauderdale, Fla.
Hospital-based Mohs surgery has a role in the treatment of "psychologically problematic" patients, including those with severe anxiety and/or dementia; patients with high-risk medical conditions, including ischemic heart disease, severe arrhythmias, significant pulmonary insufficiencies, or coagulopathies; the physical handicapped; and the morbidly obese, he said.
Additionally, some hospitalized patients require urgent care, what Dr. Sachse terms "emergency Mohs surgery." He offered, as an example, a leukemia patient with skin necrosis of the scalp that was doubling in size every 24 hours. A biopsy revealed that the patient had a zygomycete fungal infection.
Mohs micrographic surgery was followed by topical and oral antifungal therapy and, after a delay, a skin graft, for a clinically and aesthetically acceptable result, he said.
With unusual and complex cases, it is important to build teamwork within the hospital since a multispecialty approach is necessary for cases that invade multiple structures of the head and neck, said Dr. Sachse.
In such cases, the concept of complete margin control must be emphasized, since many colleagues in otolaryngology, plastic surgery, and pathology will be unfamiliar with the basic tenets of the approach and the precision required to achieving those goals, he noted.
He learned to counter perceptions of Mohs surgery as tedious and slow by using careful planning and documentation of results in patients who might have been previously considered inoperable.
Education helps, as does realistic scheduling of operating rooms for the time required for extensive debridement, meticulous staging, excision, and repair.
Presenting Mohs cases to a hospital tumor board can be illuminating to the uninitiated, and the cases themselves are "very rewarding," he said.
Dr. Sachse cautioned that surgeons taking on highly complex cases should "be prepared to meet a patient you may not be able to cure." That said, "Mohs is a surgical tool which can and should be used for very extensive tumors. The complexity of the margins may increase exponentially, but you can always cut quicker than any tumor can grow."
Dr. Sachse said that he had no relevant disclosures.
plastic and reconstructive surgeon, high-stage tumors, high-risk patients, hospital setting, cancer control, Dermatologists, American Society for Mohs Surgery, ASMS, the American College of Mohs Surgery,
SAN DIEGO – It would be somewhat of an understatement to say that Mohs surgery was not particularly welcomed at hospitals where Dr. Rainer Sachse used to practice.
As a plastic and reconstructive surgeon, he had hoped to utilize the technique to treat extensive, high-stage tumors in high-risk patients within a hospital setting, believing that the literature convincingly suggested that Mohs offered the best hope for cancer control in such patients.
Nurses, he recalled, considered Mohs a "slow, mutilating, expensive" procedure. Surgeons felt it was unnecessary. Pathologists thought their traditional methods "worked perfectly well."
Dermatologists seemed preoccupied by turf battles between the American Society for Mohs Surgery (ASMS) and the American College of Mohs Surgery. Dermatology residents had no time, and plastic surgery residents were uninterested, Dr. Sachse said at the meeting sponsored by the ASMS.
He pressed on, though, inspired by cases in which conventional excisions and standard therapy mutilated patients or led to their untimely deaths from tumors with continuous growth patterns.
He observed colleagues and sought out preceptorships, pored over the literature, and took a Mohs surgery course before beginning to try small cases with a pathologist who had received dermatopathology training. Finally, he began to change minds and take on more challenging cases.
Seeing the results, "a pathologist who was initially very skeptical eventually became a strong supporter," said Dr. Sachse, who is in private practice in Fort Lauderdale, Fla.
Hospital-based Mohs surgery has a role in the treatment of "psychologically problematic" patients, including those with severe anxiety and/or dementia; patients with high-risk medical conditions, including ischemic heart disease, severe arrhythmias, significant pulmonary insufficiencies, or coagulopathies; the physical handicapped; and the morbidly obese, he said.
Additionally, some hospitalized patients require urgent care, what Dr. Sachse terms "emergency Mohs surgery." He offered, as an example, a leukemia patient with skin necrosis of the scalp that was doubling in size every 24 hours. A biopsy revealed that the patient had a zygomycete fungal infection.
Mohs micrographic surgery was followed by topical and oral antifungal therapy and, after a delay, a skin graft, for a clinically and aesthetically acceptable result, he said.
With unusual and complex cases, it is important to build teamwork within the hospital since a multispecialty approach is necessary for cases that invade multiple structures of the head and neck, said Dr. Sachse.
In such cases, the concept of complete margin control must be emphasized, since many colleagues in otolaryngology, plastic surgery, and pathology will be unfamiliar with the basic tenets of the approach and the precision required to achieving those goals, he noted.
He learned to counter perceptions of Mohs surgery as tedious and slow by using careful planning and documentation of results in patients who might have been previously considered inoperable.
Education helps, as does realistic scheduling of operating rooms for the time required for extensive debridement, meticulous staging, excision, and repair.
Presenting Mohs cases to a hospital tumor board can be illuminating to the uninitiated, and the cases themselves are "very rewarding," he said.
Dr. Sachse cautioned that surgeons taking on highly complex cases should "be prepared to meet a patient you may not be able to cure." That said, "Mohs is a surgical tool which can and should be used for very extensive tumors. The complexity of the margins may increase exponentially, but you can always cut quicker than any tumor can grow."
Dr. Sachse said that he had no relevant disclosures.
SAN DIEGO – It would be somewhat of an understatement to say that Mohs surgery was not particularly welcomed at hospitals where Dr. Rainer Sachse used to practice.
As a plastic and reconstructive surgeon, he had hoped to utilize the technique to treat extensive, high-stage tumors in high-risk patients within a hospital setting, believing that the literature convincingly suggested that Mohs offered the best hope for cancer control in such patients.
Nurses, he recalled, considered Mohs a "slow, mutilating, expensive" procedure. Surgeons felt it was unnecessary. Pathologists thought their traditional methods "worked perfectly well."
Dermatologists seemed preoccupied by turf battles between the American Society for Mohs Surgery (ASMS) and the American College of Mohs Surgery. Dermatology residents had no time, and plastic surgery residents were uninterested, Dr. Sachse said at the meeting sponsored by the ASMS.
He pressed on, though, inspired by cases in which conventional excisions and standard therapy mutilated patients or led to their untimely deaths from tumors with continuous growth patterns.
He observed colleagues and sought out preceptorships, pored over the literature, and took a Mohs surgery course before beginning to try small cases with a pathologist who had received dermatopathology training. Finally, he began to change minds and take on more challenging cases.
Seeing the results, "a pathologist who was initially very skeptical eventually became a strong supporter," said Dr. Sachse, who is in private practice in Fort Lauderdale, Fla.
Hospital-based Mohs surgery has a role in the treatment of "psychologically problematic" patients, including those with severe anxiety and/or dementia; patients with high-risk medical conditions, including ischemic heart disease, severe arrhythmias, significant pulmonary insufficiencies, or coagulopathies; the physical handicapped; and the morbidly obese, he said.
Additionally, some hospitalized patients require urgent care, what Dr. Sachse terms "emergency Mohs surgery." He offered, as an example, a leukemia patient with skin necrosis of the scalp that was doubling in size every 24 hours. A biopsy revealed that the patient had a zygomycete fungal infection.
Mohs micrographic surgery was followed by topical and oral antifungal therapy and, after a delay, a skin graft, for a clinically and aesthetically acceptable result, he said.
With unusual and complex cases, it is important to build teamwork within the hospital since a multispecialty approach is necessary for cases that invade multiple structures of the head and neck, said Dr. Sachse.
In such cases, the concept of complete margin control must be emphasized, since many colleagues in otolaryngology, plastic surgery, and pathology will be unfamiliar with the basic tenets of the approach and the precision required to achieving those goals, he noted.
He learned to counter perceptions of Mohs surgery as tedious and slow by using careful planning and documentation of results in patients who might have been previously considered inoperable.
Education helps, as does realistic scheduling of operating rooms for the time required for extensive debridement, meticulous staging, excision, and repair.
Presenting Mohs cases to a hospital tumor board can be illuminating to the uninitiated, and the cases themselves are "very rewarding," he said.
Dr. Sachse cautioned that surgeons taking on highly complex cases should "be prepared to meet a patient you may not be able to cure." That said, "Mohs is a surgical tool which can and should be used for very extensive tumors. The complexity of the margins may increase exponentially, but you can always cut quicker than any tumor can grow."
Dr. Sachse said that he had no relevant disclosures.
plastic and reconstructive surgeon, high-stage tumors, high-risk patients, hospital setting, cancer control, Dermatologists, American Society for Mohs Surgery, ASMS, the American College of Mohs Surgery,
plastic and reconstructive surgeon, high-stage tumors, high-risk patients, hospital setting, cancer control, Dermatologists, American Society for Mohs Surgery, ASMS, the American College of Mohs Surgery,
EXPERT ANALYSIS FROM A MEETING SPONSORED BY THE AMERICAN SOCIETY FOR MOHS SURGERY