User login
Cancer Data Trends 2024: Colorectal Cancer
1. May FP, Yano EM, Provenzale D, et al. Barriers to follow-up colonoscopies for patients with positive results from fecal immunochemical tests during colorectal cancer screening. Clin Gastroenterol Hepatol. 2019;17(3):469-476. doi:10.1016/j.cgh.2018.05.022
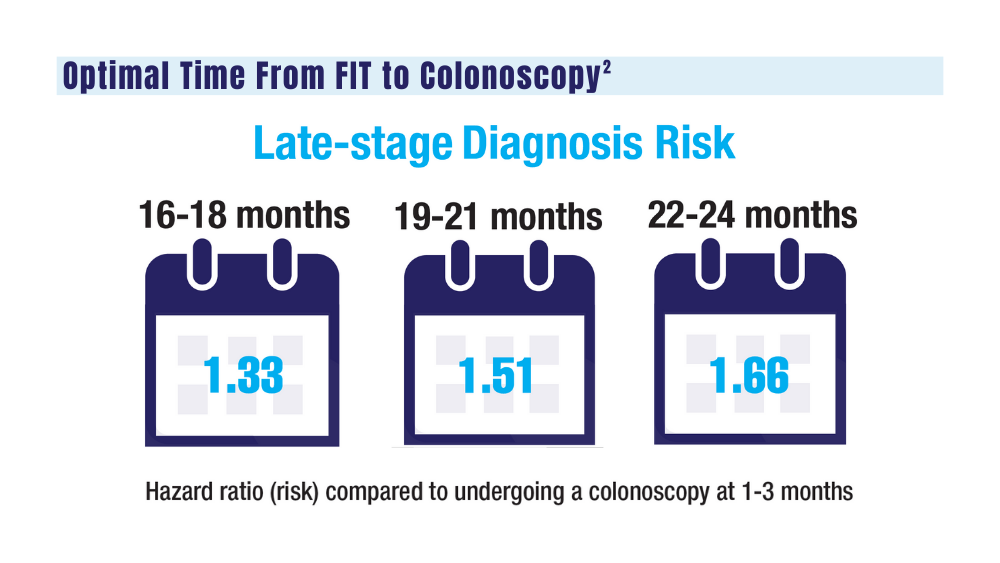
2. San Miguel Y, Demb J, Martinez ME, Gupta S, May FP. Time to colonoscopy after abnormal stool-based screening and risk for colorectal cancer incidence and mortality. Gastroenterology. 2021;160(6):1997-2005.e3. doi:10.1053/j.gastro.2021.01.219
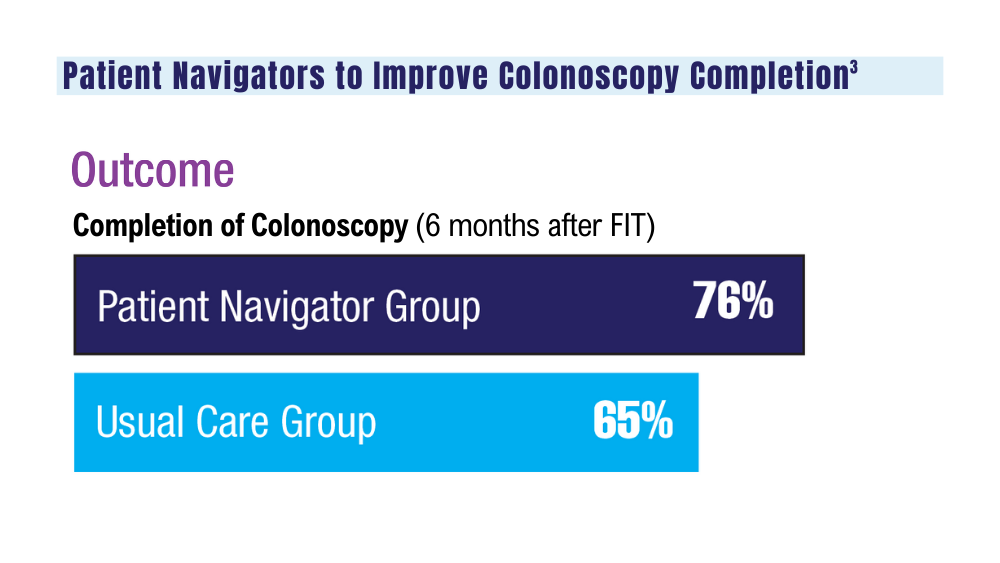
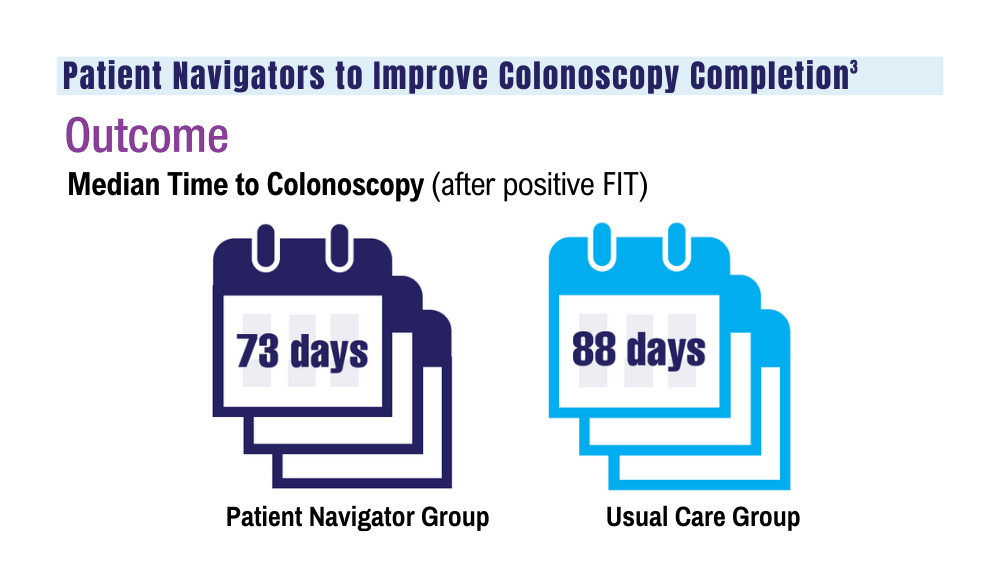
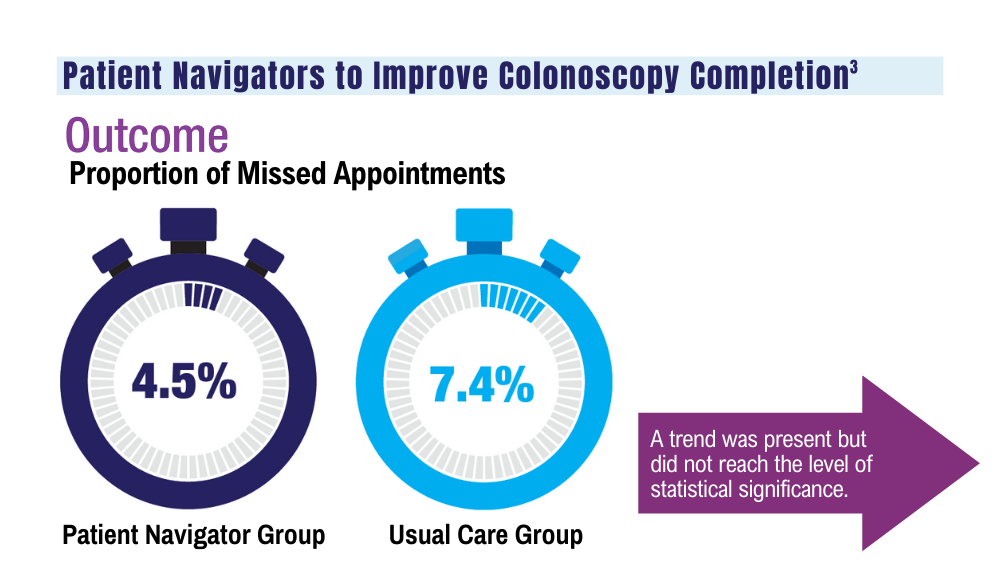
3. Coronado GD, Rawlings AM, Petrik AF, et al. Precision patient navigation to improve rates of follow-up colonoscopy, an individual randomized effectiveness trial. Cancer Epidemiol Biomarkers Prev. 2021;30(12):2327-2333. doi:10.1158/1055-9965.EPI-20-1793
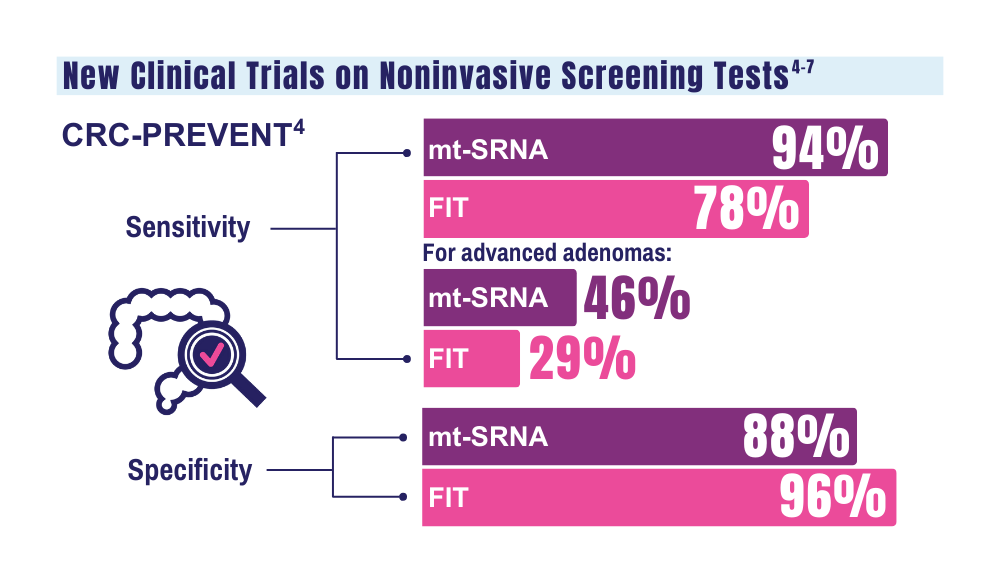
4. Barnell EK, Wurtzler EM, La Rocca J, et al. Multitarget stool RNA test for colorectal cancer screening. JAMA. 2023;330(18):1760- 1768. doi:10.1001/jama.2023.22231
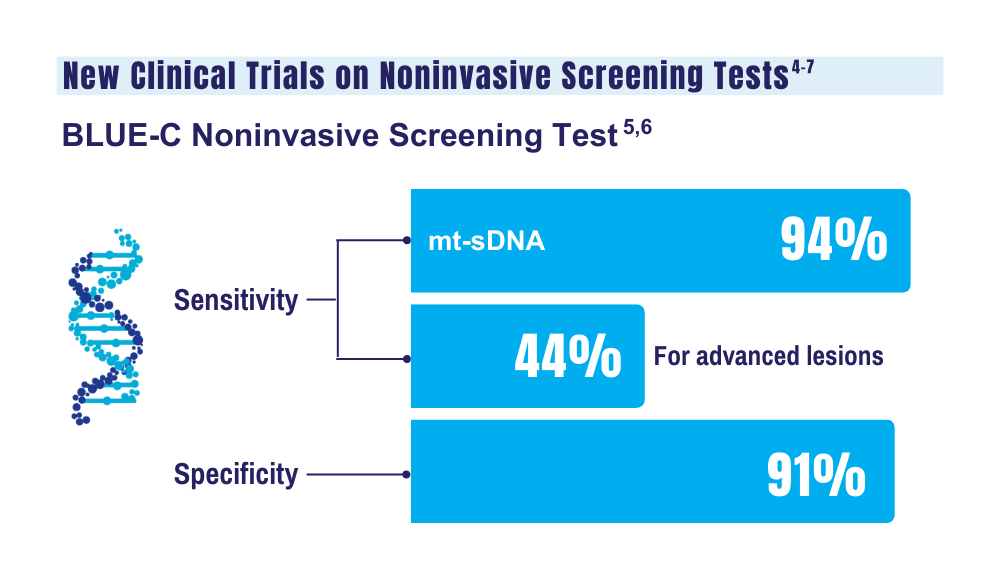
5. McNamara D. Two multitarget stool tests show promise for CRC screening: studies. Medscape. Published October 22, 2023. Accessed December 20, 2023. https://www.medscape.com/viewarticle/997609#vp_1
6. Clinical validation of an optimized multi-target stool DNA (Mt-sDNA 2.0) test, for colorectal cancer screening “BLUE-C.” ClinicalTrials. gov identifier: NCT04144738. Updated September 1, 2023. Accessed December 20, 2023. https://www.clinicaltrials.gov/study/ NCT04144738
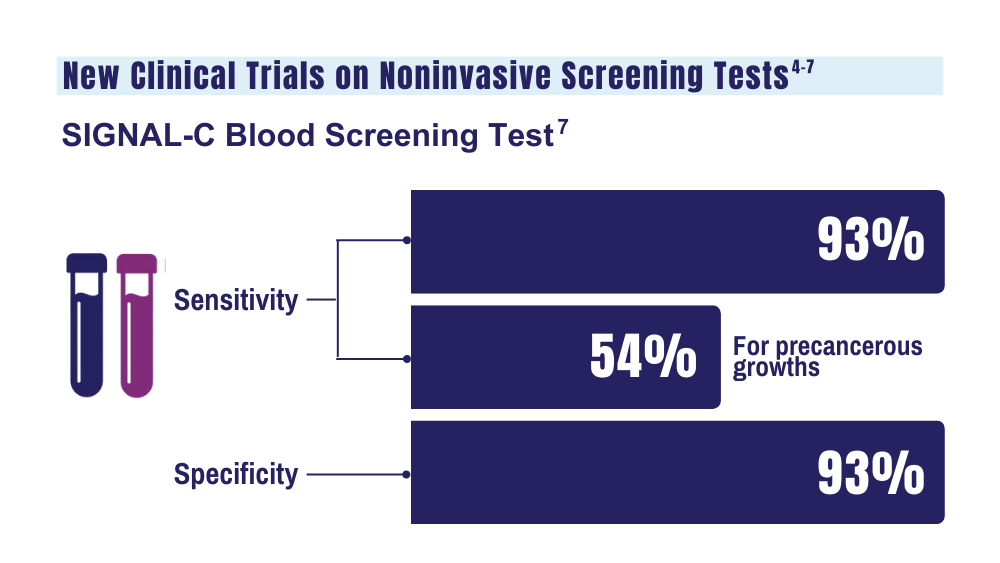
7. Universal Diagnostics. Universal DX Presents Data from Large, 1,000-patient, Multi-Cohort Study Proving 93% Sensitivity for Colorectal Cancer and 54% Sensitivity for Advanced Adenoma at 92% Specificity. Press Release. Published May 2023. Accessed January 26. 2024.
1. May FP, Yano EM, Provenzale D, et al. Barriers to follow-up colonoscopies for patients with positive results from fecal immunochemical tests during colorectal cancer screening. Clin Gastroenterol Hepatol. 2019;17(3):469-476. doi:10.1016/j.cgh.2018.05.022
2. San Miguel Y, Demb J, Martinez ME, Gupta S, May FP. Time to colonoscopy after abnormal stool-based screening and risk for colorectal cancer incidence and mortality. Gastroenterology. 2021;160(6):1997-2005.e3. doi:10.1053/j.gastro.2021.01.219
3. Coronado GD, Rawlings AM, Petrik AF, et al. Precision patient navigation to improve rates of follow-up colonoscopy, an individual randomized effectiveness trial. Cancer Epidemiol Biomarkers Prev. 2021;30(12):2327-2333. doi:10.1158/1055-9965.EPI-20-1793
4. Barnell EK, Wurtzler EM, La Rocca J, et al. Multitarget stool RNA test for colorectal cancer screening. JAMA. 2023;330(18):1760- 1768. doi:10.1001/jama.2023.22231
5. McNamara D. Two multitarget stool tests show promise for CRC screening: studies. Medscape. Published October 22, 2023. Accessed December 20, 2023. https://www.medscape.com/viewarticle/997609#vp_1
6. Clinical validation of an optimized multi-target stool DNA (Mt-sDNA 2.0) test, for colorectal cancer screening “BLUE-C.” ClinicalTrials. gov identifier: NCT04144738. Updated September 1, 2023. Accessed December 20, 2023. https://www.clinicaltrials.gov/study/ NCT04144738
7. Universal Diagnostics. Universal DX Presents Data from Large, 1,000-patient, Multi-Cohort Study Proving 93% Sensitivity for Colorectal Cancer and 54% Sensitivity for Advanced Adenoma at 92% Specificity. Press Release. Published May 2023. Accessed January 26. 2024.
1. May FP, Yano EM, Provenzale D, et al. Barriers to follow-up colonoscopies for patients with positive results from fecal immunochemical tests during colorectal cancer screening. Clin Gastroenterol Hepatol. 2019;17(3):469-476. doi:10.1016/j.cgh.2018.05.022
2. San Miguel Y, Demb J, Martinez ME, Gupta S, May FP. Time to colonoscopy after abnormal stool-based screening and risk for colorectal cancer incidence and mortality. Gastroenterology. 2021;160(6):1997-2005.e3. doi:10.1053/j.gastro.2021.01.219
3. Coronado GD, Rawlings AM, Petrik AF, et al. Precision patient navigation to improve rates of follow-up colonoscopy, an individual randomized effectiveness trial. Cancer Epidemiol Biomarkers Prev. 2021;30(12):2327-2333. doi:10.1158/1055-9965.EPI-20-1793
4. Barnell EK, Wurtzler EM, La Rocca J, et al. Multitarget stool RNA test for colorectal cancer screening. JAMA. 2023;330(18):1760- 1768. doi:10.1001/jama.2023.22231
5. McNamara D. Two multitarget stool tests show promise for CRC screening: studies. Medscape. Published October 22, 2023. Accessed December 20, 2023. https://www.medscape.com/viewarticle/997609#vp_1
6. Clinical validation of an optimized multi-target stool DNA (Mt-sDNA 2.0) test, for colorectal cancer screening “BLUE-C.” ClinicalTrials. gov identifier: NCT04144738. Updated September 1, 2023. Accessed December 20, 2023. https://www.clinicaltrials.gov/study/ NCT04144738
7. Universal Diagnostics. Universal DX Presents Data from Large, 1,000-patient, Multi-Cohort Study Proving 93% Sensitivity for Colorectal Cancer and 54% Sensitivity for Advanced Adenoma at 92% Specificity. Press Release. Published May 2023. Accessed January 26. 2024.
Cancer Data Trends 2024
The annual issue of Cancer Data Trends, produced in collaboration with the Association of VA Hematology/Oncology (AVAHO), highlights the latest research in some of the top cancers impacting US veterans.
Click to view the Digital Edition.
In this issue:
Hepatocellular Carcinoma
Special care for veterans, changes in staging, and biomarkers for early diagnosis
Lung Cancer
Guideline updates and racial disparities in veterans
Multiple Myeloma
Improving survival in the VA
Colorectal Cancer
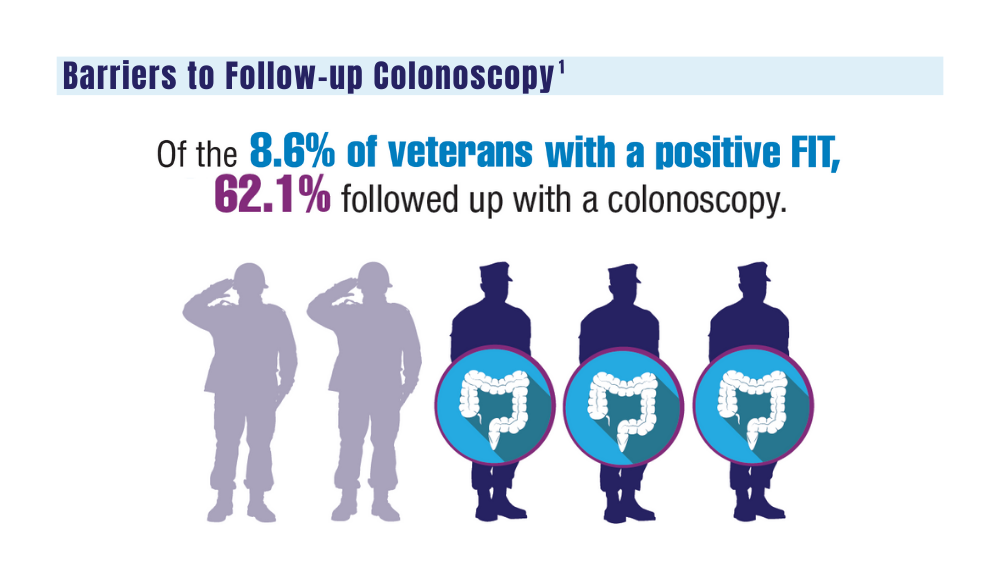
Barriers to follow-up colonoscopies after FIT testing
B-Cell Lymphomas
Findings from the VA's National TeleOncology Program and recent therapy updates
Breast Cancer
A look at the VA's Risk Assessment Pipeline and incidence among veterans vs the general population
Genitourinary Cancers
Molecular testing in prostate cancer, improving survival for metastatic RCC, and links between bladder cancer and Agent Orange exposure
The annual issue of Cancer Data Trends, produced in collaboration with the Association of VA Hematology/Oncology (AVAHO), highlights the latest research in some of the top cancers impacting US veterans.
Click to view the Digital Edition.
In this issue:
Hepatocellular Carcinoma
Special care for veterans, changes in staging, and biomarkers for early diagnosis
Lung Cancer
Guideline updates and racial disparities in veterans
Multiple Myeloma
Improving survival in the VA
Colorectal Cancer
Barriers to follow-up colonoscopies after FIT testing
B-Cell Lymphomas
Findings from the VA's National TeleOncology Program and recent therapy updates
Breast Cancer
A look at the VA's Risk Assessment Pipeline and incidence among veterans vs the general population
Genitourinary Cancers
Molecular testing in prostate cancer, improving survival for metastatic RCC, and links between bladder cancer and Agent Orange exposure
The annual issue of Cancer Data Trends, produced in collaboration with the Association of VA Hematology/Oncology (AVAHO), highlights the latest research in some of the top cancers impacting US veterans.
Click to view the Digital Edition.
In this issue:
Hepatocellular Carcinoma
Special care for veterans, changes in staging, and biomarkers for early diagnosis
Lung Cancer
Guideline updates and racial disparities in veterans
Multiple Myeloma
Improving survival in the VA
Colorectal Cancer
Barriers to follow-up colonoscopies after FIT testing
B-Cell Lymphomas
Findings from the VA's National TeleOncology Program and recent therapy updates
Breast Cancer
A look at the VA's Risk Assessment Pipeline and incidence among veterans vs the general population
Genitourinary Cancers
Molecular testing in prostate cancer, improving survival for metastatic RCC, and links between bladder cancer and Agent Orange exposure
Is Primary Tumor Resection Beneficial in Stage IV CRC?
TOPLINE:
not amenable to curative therapy, new data showed.
METHODOLOGY:
- Chemotherapy is the primary treatment in patients with stage IV (CRC) and unresectable metastases. It’s unclear whether primary tumor resection before chemotherapy prolongs survival.
- Among 393 patients with stage IV colon cancer and unresectable metastases enrolled in the and trials, 187 were randomly allocated to undergo primary tumor resection and 206 to upfront chemotherapy.
- The chemotherapy regimen was left up to the treating physician. Overall survival was the primary endpoint. Median follow-up time was 36.7 months.
TAKEAWAY:
- Median overall survival was 16.7 months with primary tumor resection and 18.6 months with upfront chemotherapy (P = .191).
- Comparable overall survival between the study groups was further confirmed on multivariate analysis (hazard ratio, 0.944; P = .65) and across all subgroups.
- Serious adverse events were more common with upfront chemo than surgery (18% vs 10%; P = .027), due mainly to a significantly higher incidence of GI-related events (11% vs 5%; P = .031).
- Overall, 24% of the primary tumor resection group did not receive any chemotherapy.
IN PRACTICE:
“The results of our study provide compelling data that upfront primary tumor resection in treatment-naive stage IV CRC not amenable for curative treatment does not prolong [overall survival]. A relatively low incidence of serious adverse events in patients with an intact primary tumor together with a considerable number of patients who did not receive any chemotherapy in the primary tumor resection group provides further arguments against resection of the primary tumor in this group of patients,” the authors of the combined analysis concluded.
SOURCE:
The study, with first author Nuh N. Rahbari, MD, University of Ulm, Ulm, Germany, was published online in the Journal of Clinical Oncology.
LIMITATIONS:
Neither study completed their planned patient accrual. Although both trials are nearly identical, differences in the individual study cohorts and trial implementation could have introduced bias. Tumor molecular profiling was not performed.
DISCLOSURES:
The study had no commercial funding. Disclosures for authors are available with the original article.
A version of this article appeared on Medscape.com.
TOPLINE:
not amenable to curative therapy, new data showed.
METHODOLOGY:
- Chemotherapy is the primary treatment in patients with stage IV (CRC) and unresectable metastases. It’s unclear whether primary tumor resection before chemotherapy prolongs survival.
- Among 393 patients with stage IV colon cancer and unresectable metastases enrolled in the and trials, 187 were randomly allocated to undergo primary tumor resection and 206 to upfront chemotherapy.
- The chemotherapy regimen was left up to the treating physician. Overall survival was the primary endpoint. Median follow-up time was 36.7 months.
TAKEAWAY:
- Median overall survival was 16.7 months with primary tumor resection and 18.6 months with upfront chemotherapy (P = .191).
- Comparable overall survival between the study groups was further confirmed on multivariate analysis (hazard ratio, 0.944; P = .65) and across all subgroups.
- Serious adverse events were more common with upfront chemo than surgery (18% vs 10%; P = .027), due mainly to a significantly higher incidence of GI-related events (11% vs 5%; P = .031).
- Overall, 24% of the primary tumor resection group did not receive any chemotherapy.
IN PRACTICE:
“The results of our study provide compelling data that upfront primary tumor resection in treatment-naive stage IV CRC not amenable for curative treatment does not prolong [overall survival]. A relatively low incidence of serious adverse events in patients with an intact primary tumor together with a considerable number of patients who did not receive any chemotherapy in the primary tumor resection group provides further arguments against resection of the primary tumor in this group of patients,” the authors of the combined analysis concluded.
SOURCE:
The study, with first author Nuh N. Rahbari, MD, University of Ulm, Ulm, Germany, was published online in the Journal of Clinical Oncology.
LIMITATIONS:
Neither study completed their planned patient accrual. Although both trials are nearly identical, differences in the individual study cohorts and trial implementation could have introduced bias. Tumor molecular profiling was not performed.
DISCLOSURES:
The study had no commercial funding. Disclosures for authors are available with the original article.
A version of this article appeared on Medscape.com.
TOPLINE:
not amenable to curative therapy, new data showed.
METHODOLOGY:
- Chemotherapy is the primary treatment in patients with stage IV (CRC) and unresectable metastases. It’s unclear whether primary tumor resection before chemotherapy prolongs survival.
- Among 393 patients with stage IV colon cancer and unresectable metastases enrolled in the and trials, 187 were randomly allocated to undergo primary tumor resection and 206 to upfront chemotherapy.
- The chemotherapy regimen was left up to the treating physician. Overall survival was the primary endpoint. Median follow-up time was 36.7 months.
TAKEAWAY:
- Median overall survival was 16.7 months with primary tumor resection and 18.6 months with upfront chemotherapy (P = .191).
- Comparable overall survival between the study groups was further confirmed on multivariate analysis (hazard ratio, 0.944; P = .65) and across all subgroups.
- Serious adverse events were more common with upfront chemo than surgery (18% vs 10%; P = .027), due mainly to a significantly higher incidence of GI-related events (11% vs 5%; P = .031).
- Overall, 24% of the primary tumor resection group did not receive any chemotherapy.
IN PRACTICE:
“The results of our study provide compelling data that upfront primary tumor resection in treatment-naive stage IV CRC not amenable for curative treatment does not prolong [overall survival]. A relatively low incidence of serious adverse events in patients with an intact primary tumor together with a considerable number of patients who did not receive any chemotherapy in the primary tumor resection group provides further arguments against resection of the primary tumor in this group of patients,” the authors of the combined analysis concluded.
SOURCE:
The study, with first author Nuh N. Rahbari, MD, University of Ulm, Ulm, Germany, was published online in the Journal of Clinical Oncology.
LIMITATIONS:
Neither study completed their planned patient accrual. Although both trials are nearly identical, differences in the individual study cohorts and trial implementation could have introduced bias. Tumor molecular profiling was not performed.
DISCLOSURES:
The study had no commercial funding. Disclosures for authors are available with the original article.
A version of this article appeared on Medscape.com.
Low-Dose Aspirin Associated With Reduced CRC Risk
TOPLINE:
Low-dose aspirin use is associated with a reduced risk for colorectal cancer (CRC), confirms a large-scale cohort study, which also suggests that the risk reduction is greatest for metastatic disease and in individuals who take the drug for at least 5 years.
METHODOLOGY:
- Researchers used several population-based registries to identify individuals aged ≥ 50 years living in Norway between 2014 and 2018, excluding those with a prior history of invasive cancer or who had lived in Norway for less than 6 months before study commencement.
- Sociodemographic information was obtained, as well as low-dose aspirin prescription data to determine the prescription date, number of dispensed packages, and defined daily dose.
- Follow-up began 6 months after entering the cohort and continued until CRC diagnosis, another cancer diagnosis, death, emigration, or the end of follow-up on December 31, 2018.
- CRC cases were categorized by site as well as by clinical stage.
TAKEAWAY:
- Of 2,186,390 individuals included, 38,577 (1.8%) were diagnosed with CRC after a median follow-up of 10.9 years. Low-dose aspirin was used at least once by 579,196 (26.5%) individuals.
- Low-dose aspirin use was more common among males, older individuals, those with a lower education or lower income, those of Norwegian origin, and individuals using other medications, including those targeting cardiovascular conditions.
- Duration of current aspirin use was also associated with the degree of CRC risk, at HRs of 0.91 for < 3 years, 0.85 for ≥ 3 and < 5 years, and 0.84 for ≥ 5 years.
- It was estimated that aspirin use averted 1073 cases of CRC over the study period.
IN PRACTICE:
“We believe that new randomized controlled trials are urgently needed to confirm the potential protective effect of aspirin against CRC and to identify subgroups in the population who might benefit the most from the use of aspirin,” the authors wrote.
SOURCE:
The research, led by Edoardo Botteri, PhD, Department of Research, Cancer Registry of Norway, National Institute of Public Health, Oslo, Norway, was published online in The American Journal of Gastroenterology.
LIMITATIONS:
This study is limited by its observational nature. Users and nonusers are also “incomparable,” as aspirin is used for the primary prevention of cardiovascular events. Moreover, information was lacking in the registries about “several known risk factors for CRC,” and so the link between aspirin and CRC risk could have been over- or underestimated. Finally, the defined daily dose may not necessarily reflect the dose actually taken by the individual or how often it was taken.
DISCLOSURES:
No relevant financial relationships were declared. The study was funded by the Norwegian Research Council.
A version of this article appeared on Medscape.com.
TOPLINE:
Low-dose aspirin use is associated with a reduced risk for colorectal cancer (CRC), confirms a large-scale cohort study, which also suggests that the risk reduction is greatest for metastatic disease and in individuals who take the drug for at least 5 years.
METHODOLOGY:
- Researchers used several population-based registries to identify individuals aged ≥ 50 years living in Norway between 2014 and 2018, excluding those with a prior history of invasive cancer or who had lived in Norway for less than 6 months before study commencement.
- Sociodemographic information was obtained, as well as low-dose aspirin prescription data to determine the prescription date, number of dispensed packages, and defined daily dose.
- Follow-up began 6 months after entering the cohort and continued until CRC diagnosis, another cancer diagnosis, death, emigration, or the end of follow-up on December 31, 2018.
- CRC cases were categorized by site as well as by clinical stage.
TAKEAWAY:
- Of 2,186,390 individuals included, 38,577 (1.8%) were diagnosed with CRC after a median follow-up of 10.9 years. Low-dose aspirin was used at least once by 579,196 (26.5%) individuals.
- Low-dose aspirin use was more common among males, older individuals, those with a lower education or lower income, those of Norwegian origin, and individuals using other medications, including those targeting cardiovascular conditions.
- Duration of current aspirin use was also associated with the degree of CRC risk, at HRs of 0.91 for < 3 years, 0.85 for ≥ 3 and < 5 years, and 0.84 for ≥ 5 years.
- It was estimated that aspirin use averted 1073 cases of CRC over the study period.
IN PRACTICE:
“We believe that new randomized controlled trials are urgently needed to confirm the potential protective effect of aspirin against CRC and to identify subgroups in the population who might benefit the most from the use of aspirin,” the authors wrote.
SOURCE:
The research, led by Edoardo Botteri, PhD, Department of Research, Cancer Registry of Norway, National Institute of Public Health, Oslo, Norway, was published online in The American Journal of Gastroenterology.
LIMITATIONS:
This study is limited by its observational nature. Users and nonusers are also “incomparable,” as aspirin is used for the primary prevention of cardiovascular events. Moreover, information was lacking in the registries about “several known risk factors for CRC,” and so the link between aspirin and CRC risk could have been over- or underestimated. Finally, the defined daily dose may not necessarily reflect the dose actually taken by the individual or how often it was taken.
DISCLOSURES:
No relevant financial relationships were declared. The study was funded by the Norwegian Research Council.
A version of this article appeared on Medscape.com.
TOPLINE:
Low-dose aspirin use is associated with a reduced risk for colorectal cancer (CRC), confirms a large-scale cohort study, which also suggests that the risk reduction is greatest for metastatic disease and in individuals who take the drug for at least 5 years.
METHODOLOGY:
- Researchers used several population-based registries to identify individuals aged ≥ 50 years living in Norway between 2014 and 2018, excluding those with a prior history of invasive cancer or who had lived in Norway for less than 6 months before study commencement.
- Sociodemographic information was obtained, as well as low-dose aspirin prescription data to determine the prescription date, number of dispensed packages, and defined daily dose.
- Follow-up began 6 months after entering the cohort and continued until CRC diagnosis, another cancer diagnosis, death, emigration, or the end of follow-up on December 31, 2018.
- CRC cases were categorized by site as well as by clinical stage.
TAKEAWAY:
- Of 2,186,390 individuals included, 38,577 (1.8%) were diagnosed with CRC after a median follow-up of 10.9 years. Low-dose aspirin was used at least once by 579,196 (26.5%) individuals.
- Low-dose aspirin use was more common among males, older individuals, those with a lower education or lower income, those of Norwegian origin, and individuals using other medications, including those targeting cardiovascular conditions.
- Duration of current aspirin use was also associated with the degree of CRC risk, at HRs of 0.91 for < 3 years, 0.85 for ≥ 3 and < 5 years, and 0.84 for ≥ 5 years.
- It was estimated that aspirin use averted 1073 cases of CRC over the study period.
IN PRACTICE:
“We believe that new randomized controlled trials are urgently needed to confirm the potential protective effect of aspirin against CRC and to identify subgroups in the population who might benefit the most from the use of aspirin,” the authors wrote.
SOURCE:
The research, led by Edoardo Botteri, PhD, Department of Research, Cancer Registry of Norway, National Institute of Public Health, Oslo, Norway, was published online in The American Journal of Gastroenterology.
LIMITATIONS:
This study is limited by its observational nature. Users and nonusers are also “incomparable,” as aspirin is used for the primary prevention of cardiovascular events. Moreover, information was lacking in the registries about “several known risk factors for CRC,” and so the link between aspirin and CRC risk could have been over- or underestimated. Finally, the defined daily dose may not necessarily reflect the dose actually taken by the individual or how often it was taken.
DISCLOSURES:
No relevant financial relationships were declared. The study was funded by the Norwegian Research Council.
A version of this article appeared on Medscape.com.
Does Bariatric Surgery Increase or Decrease Cancer Risk? It Depends.
Bariatric surgery appears to decrease the risk for some cancers, but it may increase the risk for others, particularly colorectal cancer (CRC), according to a synthesis of current evidence.
“There has been a recent burst of studies examining the association between bariatric surgery and the longitudinal risks of developing cancer,” corresponding author Zhi Ven Fong, MD, MPH, DrPH, surgical oncologist, Mayo Clinic Arizona, Phoenix, said in an interview. “However, there has not been a rigorous and critical analysis of the data published to date.”
In evaluating research showing an association between bariatric surgery and longitudinal cancer risk, the investigators found that the quality of the studies and their findings are “heterogeneous and might be susceptible to bias,” Dr. Fong said.
Bariatric surgery appears to have the strongest and most consistent association with the reduction of breast, ovarian, and endometrial cancer risk, first author Pei-Wen Lim, MD, MS, bariatric surgeon at Mayo Clinic Arizona, Phoenix, told this news organization. “However, there have been concerning signals from preclinical and epidemiological studies that bariatric surgery may be associated with a higher risk of developing colorectal cancers,” she added.
The authors cautioned against certain changes in clinical management.
“First, cancer surveillance frequency should not be altered after bariatric surgery because of any assumed reduction in longitudinal cancer risk, and surveillance strategy should mirror that of an average-risk individual,” they wrote. “Secondly, the indications for bariatric surgery should not be expanded for the purpose of cancer-risk mitigation.”
The review was published online in JAMA Surgery.
Protection Against Hormone-Related Cancers
The authors pointed to several studies that appear to support the association between bariatric surgery and decreased risk for hormone-related cancers.
Among them is an observational study of 6781 patients in Canada that showed a significant reduction in breast cancer risk at a median follow-up of 5 years in those who had bariatric surgery vs those who did not (P = .01).
The largest study to date on risk for hormone-related cancer after bariatric surgery was conducted using New York State data for 302,883 women.
It showed a lower rate of breast, endometrial, and ovarian cancers after bariatric surgery (hazard ratio [HR], 0.78; P < .001), with Roux-en-Y gastric bypass conferring the greatest benefit compared with laparoscopic sleeve gastrectomy (HR, 0.66; P = .006) and laparoscopic adjustable gastric banding (HR, 0.83; P = .006).
Beyond the shared mechanisms explaining obesity and cancer risk, a proposed explanation for the strong, consistent association between bariatric surgery and hormone-sensitive cancers is the role obesity-related changes in estrogen stimulation play in development of such cancers, the authors noted.
Association With GI Cancers
The association between bariatric surgery and development of esophageal, gastric, liver, and pancreas cancers is less clear. The data are heterogeneous, with studies showing either no association or decreased longitudinal incidence, the authors reported.
The data are also mixed when it comes to CRC. Epidemiological studies have demonstrated decreased longitudinal incidence of colon and rectal cancer after bariatric surgery; however, two studies have suggested an increased CRC risk after bariatric surgery, the authors noted.
A 15-year study from England that matched 8794 patients with obesity who underwent bariatric surgery with 8794 patients with obesity who did not have the surgery showed that gastric bypass (but not gastric banding or sleeve gastrectomy) was associated with a greater than twofold increased risk of developing colon and rectal cancer (odds ratio, 2.63).
These findings were corroborated in a Swedish cohort study with more than 10 years of follow-up data.
One potential explanation for the heterogeneous findings is that “present studies do not discriminate the sub-types of colon and rectal cancer, with bariatric surgery possibly increasing the incidence of colitis-associated cancers but not hereditary cancers,” the authors wrote.
“The mechanism by which gastric bypass may increase the risk of colorectal cancer is through changes in the gut’s microbiome. These changes in gut flora may triumph the protective effect of weight loss on the development of colorectal cancers,” Dr. Fong said.
Prospective studies are necessary to better delineate CRC risk after bariatric surgery, the authors wrote.
Benefits Outweigh Risk
“Ultimately, it has been proven that bariatric surgery saves lives by improving the metabolic profile of patients with obesity through reduction in cardiovascular risk factors such as hypertension, diabetes, and nonalcoholic fatty liver disease,” Dr. Lim said.
“If patients qualify for bariatric surgery on the basis of their BMI or comorbidities, they should pursue it for its metabolic benefits, but perhaps consider timely or closer-interval screening colonoscopies to monitor for potential colorectal cancer development,” Dr. Lim added.
When asked to comment on the review, Marina Kurian, MD, president, American Society for Metabolic and Bariatric Surgery, also pointed to the advantages of bariatric surgery in reducing major adverse cardiovascular events and improving hypertension, hyperlipidemia, and diabetes.
Bariatric surgery reduces many types of cancers, although the data specific to CRC risk with bariatric surgery are mixed, she added.
“The jury is still out,” said Dr. Kurian, clinical professor of surgery at NYU Langone Health in New York, who was not involved in the review. “There are papers and meta-analyses that show benefit even in colorectal cancer, but then there are a couple of papers out there that suggest a risk that seems to be specific to men.
“It could just be a numbers game, where we may not have enough data. We need more granular data that will help address these nuances and really determine what is the actual risk,” Dr. Kurian said. “But overall, for cancer, bariatric surgery is a win.”
This research had no specific funding. Dr. Fong and Dr. Lim had no relevant disclosures. Dr. Kurian disclosed relationships with Allergan, Allurion, CineMed, CSATS, Ezisurg Medical, Hernon, Johnson & Johnson, Medtronic, Novo, Stryker, and Vivus.
A version of this article appeared on Medscape.com.
Bariatric surgery appears to decrease the risk for some cancers, but it may increase the risk for others, particularly colorectal cancer (CRC), according to a synthesis of current evidence.
“There has been a recent burst of studies examining the association between bariatric surgery and the longitudinal risks of developing cancer,” corresponding author Zhi Ven Fong, MD, MPH, DrPH, surgical oncologist, Mayo Clinic Arizona, Phoenix, said in an interview. “However, there has not been a rigorous and critical analysis of the data published to date.”
In evaluating research showing an association between bariatric surgery and longitudinal cancer risk, the investigators found that the quality of the studies and their findings are “heterogeneous and might be susceptible to bias,” Dr. Fong said.
Bariatric surgery appears to have the strongest and most consistent association with the reduction of breast, ovarian, and endometrial cancer risk, first author Pei-Wen Lim, MD, MS, bariatric surgeon at Mayo Clinic Arizona, Phoenix, told this news organization. “However, there have been concerning signals from preclinical and epidemiological studies that bariatric surgery may be associated with a higher risk of developing colorectal cancers,” she added.
The authors cautioned against certain changes in clinical management.
“First, cancer surveillance frequency should not be altered after bariatric surgery because of any assumed reduction in longitudinal cancer risk, and surveillance strategy should mirror that of an average-risk individual,” they wrote. “Secondly, the indications for bariatric surgery should not be expanded for the purpose of cancer-risk mitigation.”
The review was published online in JAMA Surgery.
Protection Against Hormone-Related Cancers
The authors pointed to several studies that appear to support the association between bariatric surgery and decreased risk for hormone-related cancers.
Among them is an observational study of 6781 patients in Canada that showed a significant reduction in breast cancer risk at a median follow-up of 5 years in those who had bariatric surgery vs those who did not (P = .01).
The largest study to date on risk for hormone-related cancer after bariatric surgery was conducted using New York State data for 302,883 women.
It showed a lower rate of breast, endometrial, and ovarian cancers after bariatric surgery (hazard ratio [HR], 0.78; P < .001), with Roux-en-Y gastric bypass conferring the greatest benefit compared with laparoscopic sleeve gastrectomy (HR, 0.66; P = .006) and laparoscopic adjustable gastric banding (HR, 0.83; P = .006).
Beyond the shared mechanisms explaining obesity and cancer risk, a proposed explanation for the strong, consistent association between bariatric surgery and hormone-sensitive cancers is the role obesity-related changes in estrogen stimulation play in development of such cancers, the authors noted.
Association With GI Cancers
The association between bariatric surgery and development of esophageal, gastric, liver, and pancreas cancers is less clear. The data are heterogeneous, with studies showing either no association or decreased longitudinal incidence, the authors reported.
The data are also mixed when it comes to CRC. Epidemiological studies have demonstrated decreased longitudinal incidence of colon and rectal cancer after bariatric surgery; however, two studies have suggested an increased CRC risk after bariatric surgery, the authors noted.
A 15-year study from England that matched 8794 patients with obesity who underwent bariatric surgery with 8794 patients with obesity who did not have the surgery showed that gastric bypass (but not gastric banding or sleeve gastrectomy) was associated with a greater than twofold increased risk of developing colon and rectal cancer (odds ratio, 2.63).
These findings were corroborated in a Swedish cohort study with more than 10 years of follow-up data.
One potential explanation for the heterogeneous findings is that “present studies do not discriminate the sub-types of colon and rectal cancer, with bariatric surgery possibly increasing the incidence of colitis-associated cancers but not hereditary cancers,” the authors wrote.
“The mechanism by which gastric bypass may increase the risk of colorectal cancer is through changes in the gut’s microbiome. These changes in gut flora may triumph the protective effect of weight loss on the development of colorectal cancers,” Dr. Fong said.
Prospective studies are necessary to better delineate CRC risk after bariatric surgery, the authors wrote.
Benefits Outweigh Risk
“Ultimately, it has been proven that bariatric surgery saves lives by improving the metabolic profile of patients with obesity through reduction in cardiovascular risk factors such as hypertension, diabetes, and nonalcoholic fatty liver disease,” Dr. Lim said.
“If patients qualify for bariatric surgery on the basis of their BMI or comorbidities, they should pursue it for its metabolic benefits, but perhaps consider timely or closer-interval screening colonoscopies to monitor for potential colorectal cancer development,” Dr. Lim added.
When asked to comment on the review, Marina Kurian, MD, president, American Society for Metabolic and Bariatric Surgery, also pointed to the advantages of bariatric surgery in reducing major adverse cardiovascular events and improving hypertension, hyperlipidemia, and diabetes.
Bariatric surgery reduces many types of cancers, although the data specific to CRC risk with bariatric surgery are mixed, she added.
“The jury is still out,” said Dr. Kurian, clinical professor of surgery at NYU Langone Health in New York, who was not involved in the review. “There are papers and meta-analyses that show benefit even in colorectal cancer, but then there are a couple of papers out there that suggest a risk that seems to be specific to men.
“It could just be a numbers game, where we may not have enough data. We need more granular data that will help address these nuances and really determine what is the actual risk,” Dr. Kurian said. “But overall, for cancer, bariatric surgery is a win.”
This research had no specific funding. Dr. Fong and Dr. Lim had no relevant disclosures. Dr. Kurian disclosed relationships with Allergan, Allurion, CineMed, CSATS, Ezisurg Medical, Hernon, Johnson & Johnson, Medtronic, Novo, Stryker, and Vivus.
A version of this article appeared on Medscape.com.
Bariatric surgery appears to decrease the risk for some cancers, but it may increase the risk for others, particularly colorectal cancer (CRC), according to a synthesis of current evidence.
“There has been a recent burst of studies examining the association between bariatric surgery and the longitudinal risks of developing cancer,” corresponding author Zhi Ven Fong, MD, MPH, DrPH, surgical oncologist, Mayo Clinic Arizona, Phoenix, said in an interview. “However, there has not been a rigorous and critical analysis of the data published to date.”
In evaluating research showing an association between bariatric surgery and longitudinal cancer risk, the investigators found that the quality of the studies and their findings are “heterogeneous and might be susceptible to bias,” Dr. Fong said.
Bariatric surgery appears to have the strongest and most consistent association with the reduction of breast, ovarian, and endometrial cancer risk, first author Pei-Wen Lim, MD, MS, bariatric surgeon at Mayo Clinic Arizona, Phoenix, told this news organization. “However, there have been concerning signals from preclinical and epidemiological studies that bariatric surgery may be associated with a higher risk of developing colorectal cancers,” she added.
The authors cautioned against certain changes in clinical management.
“First, cancer surveillance frequency should not be altered after bariatric surgery because of any assumed reduction in longitudinal cancer risk, and surveillance strategy should mirror that of an average-risk individual,” they wrote. “Secondly, the indications for bariatric surgery should not be expanded for the purpose of cancer-risk mitigation.”
The review was published online in JAMA Surgery.
Protection Against Hormone-Related Cancers
The authors pointed to several studies that appear to support the association between bariatric surgery and decreased risk for hormone-related cancers.
Among them is an observational study of 6781 patients in Canada that showed a significant reduction in breast cancer risk at a median follow-up of 5 years in those who had bariatric surgery vs those who did not (P = .01).
The largest study to date on risk for hormone-related cancer after bariatric surgery was conducted using New York State data for 302,883 women.
It showed a lower rate of breast, endometrial, and ovarian cancers after bariatric surgery (hazard ratio [HR], 0.78; P < .001), with Roux-en-Y gastric bypass conferring the greatest benefit compared with laparoscopic sleeve gastrectomy (HR, 0.66; P = .006) and laparoscopic adjustable gastric banding (HR, 0.83; P = .006).
Beyond the shared mechanisms explaining obesity and cancer risk, a proposed explanation for the strong, consistent association between bariatric surgery and hormone-sensitive cancers is the role obesity-related changes in estrogen stimulation play in development of such cancers, the authors noted.
Association With GI Cancers
The association between bariatric surgery and development of esophageal, gastric, liver, and pancreas cancers is less clear. The data are heterogeneous, with studies showing either no association or decreased longitudinal incidence, the authors reported.
The data are also mixed when it comes to CRC. Epidemiological studies have demonstrated decreased longitudinal incidence of colon and rectal cancer after bariatric surgery; however, two studies have suggested an increased CRC risk after bariatric surgery, the authors noted.
A 15-year study from England that matched 8794 patients with obesity who underwent bariatric surgery with 8794 patients with obesity who did not have the surgery showed that gastric bypass (but not gastric banding or sleeve gastrectomy) was associated with a greater than twofold increased risk of developing colon and rectal cancer (odds ratio, 2.63).
These findings were corroborated in a Swedish cohort study with more than 10 years of follow-up data.
One potential explanation for the heterogeneous findings is that “present studies do not discriminate the sub-types of colon and rectal cancer, with bariatric surgery possibly increasing the incidence of colitis-associated cancers but not hereditary cancers,” the authors wrote.
“The mechanism by which gastric bypass may increase the risk of colorectal cancer is through changes in the gut’s microbiome. These changes in gut flora may triumph the protective effect of weight loss on the development of colorectal cancers,” Dr. Fong said.
Prospective studies are necessary to better delineate CRC risk after bariatric surgery, the authors wrote.
Benefits Outweigh Risk
“Ultimately, it has been proven that bariatric surgery saves lives by improving the metabolic profile of patients with obesity through reduction in cardiovascular risk factors such as hypertension, diabetes, and nonalcoholic fatty liver disease,” Dr. Lim said.
“If patients qualify for bariatric surgery on the basis of their BMI or comorbidities, they should pursue it for its metabolic benefits, but perhaps consider timely or closer-interval screening colonoscopies to monitor for potential colorectal cancer development,” Dr. Lim added.
When asked to comment on the review, Marina Kurian, MD, president, American Society for Metabolic and Bariatric Surgery, also pointed to the advantages of bariatric surgery in reducing major adverse cardiovascular events and improving hypertension, hyperlipidemia, and diabetes.
Bariatric surgery reduces many types of cancers, although the data specific to CRC risk with bariatric surgery are mixed, she added.
“The jury is still out,” said Dr. Kurian, clinical professor of surgery at NYU Langone Health in New York, who was not involved in the review. “There are papers and meta-analyses that show benefit even in colorectal cancer, but then there are a couple of papers out there that suggest a risk that seems to be specific to men.
“It could just be a numbers game, where we may not have enough data. We need more granular data that will help address these nuances and really determine what is the actual risk,” Dr. Kurian said. “But overall, for cancer, bariatric surgery is a win.”
This research had no specific funding. Dr. Fong and Dr. Lim had no relevant disclosures. Dr. Kurian disclosed relationships with Allergan, Allurion, CineMed, CSATS, Ezisurg Medical, Hernon, Johnson & Johnson, Medtronic, Novo, Stryker, and Vivus.
A version of this article appeared on Medscape.com.
Oxaliplatin in Older Adults With Resected Colorectal Cancer: Is There a Benefit?
This transcript has been edited for clarity.
Our group, the QUASAR Group, made a very significant contribution in terms of trials and knowledge in this field. One of the things that we still need to discuss and think about in our wider community is the impact of adjuvant chemotherapy in older patients.
Colorectal cancer is a disease of the elderly, with the median age of presentation around 72. We know that, at presentation, more than 50% of patients are aged 65 or over and one third of patients are 75 or over. It’s a disease predominantly of the elderly. Are we justified in giving combination chemotherapy with oxaliplatin to high-risk resected colorectal cancer patients?
There’s a very nice report of a meta-analysis by Dottorini and colleagues that came out recently in the Journal of Clinical Oncology. It’s an excellent group. They did their meta-analytical work according to a strict, rational protocol. Their statistical analyses were on point, and they collected data from all the relevant trials.
According to the results of their study, it could be concluded that the addition of oxaliplatin to adjuvant therapy for resected high-risk colorectal cancer in older patients — patients older than 70 — doesn’t result in any statistically significant gain in terms of preventing recurrences or saving lives.
When we did our QUASAR trials, initially we were looking at control vs fluoropyrimidine chemotherapy. Although there was an overall impact on survival of the whole trial group (the 5000 patients in our study), when we looked by decile, there was a significant diminution of benefit even to fluoropyrimidine therapy in our trial in patients aged 70 or above. I think this careful meta-analysis must make us question the use of oxaliplatin in elderly patients.
What could the explanation be? Why could the well-known and described benefits of oxaliplatin, particularly for stage III disease, attenuate in older people? It may be to do with reduction in dose intensity. Older people have more side effects; therefore, the chemotherapy isn’t completed as planned. Although, increasingly these days, we tend only to be giving 3 months of treatment.
Is there something biologically in terms of the biology or the somatic mutational landscape of the tumor in older people? I don’t think so. Certainly, in terms of their capacity, in terms of stem cell reserve to be as resistant to the side effects of chemotherapy as younger people, we know that does attenuate with age.
Food for thought: The majority of patients I see in the clinic for the adjuvant treatment are elderly. The majority are coming these days with high-risk stage II or stage III disease. There is a real question mark about whether we should be using oxaliplatin at all.
Clearly, one would say that we need more trials of chemotherapy in older folk to see if the addition of drugs like oxaliplatin to a fluoropyrimidine backbone really does make a difference. I’ve said many times before that we, the medical community recommending adjuvant treatment, need to have better risk stratifiers. We need to have better prognostic markers. We need to have better indices that would allow us to perhaps consider these combination treatments in a more focused group of patients who may have a higher risk for recurrence.
Have a look at the paper and see what you think. I think it’s well done. It’s certainly given me pause for thought about the treatment that we will offer our elderly patients.
Have a think about it. Let me know if there are any comments that you’d like to make. For the time being, over and out.
Dr. Kerr is Professor, Nuffield Department of Clinical Laboratory Science, University of Oxford; Professor of Cancer Medicine, Oxford Cancer Centre, Oxford, United Kingdom. He disclosed ties with Celleron Therapeutics, Oxford Cancer Biomarkers, Afrox, GlaxoSmithKline, Bayer HealthCare Pharmaceuticals, Genomic Health, Merck Serono, and Roche.
A version of this article appeared on Medscape.com.
This transcript has been edited for clarity.
Our group, the QUASAR Group, made a very significant contribution in terms of trials and knowledge in this field. One of the things that we still need to discuss and think about in our wider community is the impact of adjuvant chemotherapy in older patients.
Colorectal cancer is a disease of the elderly, with the median age of presentation around 72. We know that, at presentation, more than 50% of patients are aged 65 or over and one third of patients are 75 or over. It’s a disease predominantly of the elderly. Are we justified in giving combination chemotherapy with oxaliplatin to high-risk resected colorectal cancer patients?
There’s a very nice report of a meta-analysis by Dottorini and colleagues that came out recently in the Journal of Clinical Oncology. It’s an excellent group. They did their meta-analytical work according to a strict, rational protocol. Their statistical analyses were on point, and they collected data from all the relevant trials.
According to the results of their study, it could be concluded that the addition of oxaliplatin to adjuvant therapy for resected high-risk colorectal cancer in older patients — patients older than 70 — doesn’t result in any statistically significant gain in terms of preventing recurrences or saving lives.
When we did our QUASAR trials, initially we were looking at control vs fluoropyrimidine chemotherapy. Although there was an overall impact on survival of the whole trial group (the 5000 patients in our study), when we looked by decile, there was a significant diminution of benefit even to fluoropyrimidine therapy in our trial in patients aged 70 or above. I think this careful meta-analysis must make us question the use of oxaliplatin in elderly patients.
What could the explanation be? Why could the well-known and described benefits of oxaliplatin, particularly for stage III disease, attenuate in older people? It may be to do with reduction in dose intensity. Older people have more side effects; therefore, the chemotherapy isn’t completed as planned. Although, increasingly these days, we tend only to be giving 3 months of treatment.
Is there something biologically in terms of the biology or the somatic mutational landscape of the tumor in older people? I don’t think so. Certainly, in terms of their capacity, in terms of stem cell reserve to be as resistant to the side effects of chemotherapy as younger people, we know that does attenuate with age.
Food for thought: The majority of patients I see in the clinic for the adjuvant treatment are elderly. The majority are coming these days with high-risk stage II or stage III disease. There is a real question mark about whether we should be using oxaliplatin at all.
Clearly, one would say that we need more trials of chemotherapy in older folk to see if the addition of drugs like oxaliplatin to a fluoropyrimidine backbone really does make a difference. I’ve said many times before that we, the medical community recommending adjuvant treatment, need to have better risk stratifiers. We need to have better prognostic markers. We need to have better indices that would allow us to perhaps consider these combination treatments in a more focused group of patients who may have a higher risk for recurrence.
Have a look at the paper and see what you think. I think it’s well done. It’s certainly given me pause for thought about the treatment that we will offer our elderly patients.
Have a think about it. Let me know if there are any comments that you’d like to make. For the time being, over and out.
Dr. Kerr is Professor, Nuffield Department of Clinical Laboratory Science, University of Oxford; Professor of Cancer Medicine, Oxford Cancer Centre, Oxford, United Kingdom. He disclosed ties with Celleron Therapeutics, Oxford Cancer Biomarkers, Afrox, GlaxoSmithKline, Bayer HealthCare Pharmaceuticals, Genomic Health, Merck Serono, and Roche.
A version of this article appeared on Medscape.com.
This transcript has been edited for clarity.
Our group, the QUASAR Group, made a very significant contribution in terms of trials and knowledge in this field. One of the things that we still need to discuss and think about in our wider community is the impact of adjuvant chemotherapy in older patients.
Colorectal cancer is a disease of the elderly, with the median age of presentation around 72. We know that, at presentation, more than 50% of patients are aged 65 or over and one third of patients are 75 or over. It’s a disease predominantly of the elderly. Are we justified in giving combination chemotherapy with oxaliplatin to high-risk resected colorectal cancer patients?
There’s a very nice report of a meta-analysis by Dottorini and colleagues that came out recently in the Journal of Clinical Oncology. It’s an excellent group. They did their meta-analytical work according to a strict, rational protocol. Their statistical analyses were on point, and they collected data from all the relevant trials.
According to the results of their study, it could be concluded that the addition of oxaliplatin to adjuvant therapy for resected high-risk colorectal cancer in older patients — patients older than 70 — doesn’t result in any statistically significant gain in terms of preventing recurrences or saving lives.
When we did our QUASAR trials, initially we were looking at control vs fluoropyrimidine chemotherapy. Although there was an overall impact on survival of the whole trial group (the 5000 patients in our study), when we looked by decile, there was a significant diminution of benefit even to fluoropyrimidine therapy in our trial in patients aged 70 or above. I think this careful meta-analysis must make us question the use of oxaliplatin in elderly patients.
What could the explanation be? Why could the well-known and described benefits of oxaliplatin, particularly for stage III disease, attenuate in older people? It may be to do with reduction in dose intensity. Older people have more side effects; therefore, the chemotherapy isn’t completed as planned. Although, increasingly these days, we tend only to be giving 3 months of treatment.
Is there something biologically in terms of the biology or the somatic mutational landscape of the tumor in older people? I don’t think so. Certainly, in terms of their capacity, in terms of stem cell reserve to be as resistant to the side effects of chemotherapy as younger people, we know that does attenuate with age.
Food for thought: The majority of patients I see in the clinic for the adjuvant treatment are elderly. The majority are coming these days with high-risk stage II or stage III disease. There is a real question mark about whether we should be using oxaliplatin at all.
Clearly, one would say that we need more trials of chemotherapy in older folk to see if the addition of drugs like oxaliplatin to a fluoropyrimidine backbone really does make a difference. I’ve said many times before that we, the medical community recommending adjuvant treatment, need to have better risk stratifiers. We need to have better prognostic markers. We need to have better indices that would allow us to perhaps consider these combination treatments in a more focused group of patients who may have a higher risk for recurrence.
Have a look at the paper and see what you think. I think it’s well done. It’s certainly given me pause for thought about the treatment that we will offer our elderly patients.
Have a think about it. Let me know if there are any comments that you’d like to make. For the time being, over and out.
Dr. Kerr is Professor, Nuffield Department of Clinical Laboratory Science, University of Oxford; Professor of Cancer Medicine, Oxford Cancer Centre, Oxford, United Kingdom. He disclosed ties with Celleron Therapeutics, Oxford Cancer Biomarkers, Afrox, GlaxoSmithKline, Bayer HealthCare Pharmaceuticals, Genomic Health, Merck Serono, and Roche.
A version of this article appeared on Medscape.com.
Transcatheter Arterial Chemoembolization for Rectal Tumors?
TOPLINE:
METHODOLOGY:
- The combination of neoadjuvant chemoradiotherapy, total mesorectal excision, and postoperative adjuvant chemotherapy is the current standard of care for locally advanced rectal cancer. But with pathological complete response rates of only 10%-15% and more than 30% of patients developing distant metastases within 3 years, outcomes remain suboptimal.
- Chinese investigators took a step to improve the situation, applying TACE — a standard treatment for colorectal liver metastases — to rectal tumors, dubbing the approach transcatheter rectal arterial chemoembolization (TRACE).
- As in TACE, TRACE uses precisely injected chemotherapeutic and vaso-occlusive agents to shut down blood flow to tumors, starving them of oxygen and nutrients.
- The research team tried the approach in 111 patients with stage II or III rectal tumors and performance status scores of 0-1.
- TRACE was delivered with oxaliplatin and followed by radiotherapy and S1 chemotherapy (tegafur, gimeracil, and potassium oteracil). Total mesorectal excisions were performed 4-8 weeks later, followed by mFOLFOX6 (5-fluorouracil, leucovorin, and oxaliplatin) or CAPOX (oxaliplatin and capecitabine) chemotherapy for 4-6 months.
TAKEAWAY:
- Overall, 20.7% of patients undergoing TRACE had a pathological complete response, and almost half (48.65%) had a major pathological response.
- Nearly 62% of patients were disease-free at 5 years, and almost 75% were alive at 5 years.
- No serious surgical complications occurred, but 21.6% of patients had postoperative complications. Overall, about 26% of patients (29 of 111) had grade 3/4 toxicities.
IN PRACTICE:
“The addition of transcatheter rectal arterial chemoembolisation to the neoadjuvant therapy can improve the pathological remission rate and prognosis in patients with locally advanced rectal cancer, without increasing the incidence of preoperative adverse events and postoperative complications,” the researchers concluded. “Given its promising effectiveness and safe profile, incorporating TRACE into the standard treatment strategy for patients with [locally advanced rectal cancer] should be considered.”
SOURCE:
The work, led by W. Yang of the Army Medical University in Chongqing, China, was published in Clinical Oncology.
LIMITATIONS:
The study was performed at a single center with no control arm in a Chinese population.
DISCLOSURES:
The work was funded by the Third Military Medical University in China. The investigators had no conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- The combination of neoadjuvant chemoradiotherapy, total mesorectal excision, and postoperative adjuvant chemotherapy is the current standard of care for locally advanced rectal cancer. But with pathological complete response rates of only 10%-15% and more than 30% of patients developing distant metastases within 3 years, outcomes remain suboptimal.
- Chinese investigators took a step to improve the situation, applying TACE — a standard treatment for colorectal liver metastases — to rectal tumors, dubbing the approach transcatheter rectal arterial chemoembolization (TRACE).
- As in TACE, TRACE uses precisely injected chemotherapeutic and vaso-occlusive agents to shut down blood flow to tumors, starving them of oxygen and nutrients.
- The research team tried the approach in 111 patients with stage II or III rectal tumors and performance status scores of 0-1.
- TRACE was delivered with oxaliplatin and followed by radiotherapy and S1 chemotherapy (tegafur, gimeracil, and potassium oteracil). Total mesorectal excisions were performed 4-8 weeks later, followed by mFOLFOX6 (5-fluorouracil, leucovorin, and oxaliplatin) or CAPOX (oxaliplatin and capecitabine) chemotherapy for 4-6 months.
TAKEAWAY:
- Overall, 20.7% of patients undergoing TRACE had a pathological complete response, and almost half (48.65%) had a major pathological response.
- Nearly 62% of patients were disease-free at 5 years, and almost 75% were alive at 5 years.
- No serious surgical complications occurred, but 21.6% of patients had postoperative complications. Overall, about 26% of patients (29 of 111) had grade 3/4 toxicities.
IN PRACTICE:
“The addition of transcatheter rectal arterial chemoembolisation to the neoadjuvant therapy can improve the pathological remission rate and prognosis in patients with locally advanced rectal cancer, without increasing the incidence of preoperative adverse events and postoperative complications,” the researchers concluded. “Given its promising effectiveness and safe profile, incorporating TRACE into the standard treatment strategy for patients with [locally advanced rectal cancer] should be considered.”
SOURCE:
The work, led by W. Yang of the Army Medical University in Chongqing, China, was published in Clinical Oncology.
LIMITATIONS:
The study was performed at a single center with no control arm in a Chinese population.
DISCLOSURES:
The work was funded by the Third Military Medical University in China. The investigators had no conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- The combination of neoadjuvant chemoradiotherapy, total mesorectal excision, and postoperative adjuvant chemotherapy is the current standard of care for locally advanced rectal cancer. But with pathological complete response rates of only 10%-15% and more than 30% of patients developing distant metastases within 3 years, outcomes remain suboptimal.
- Chinese investigators took a step to improve the situation, applying TACE — a standard treatment for colorectal liver metastases — to rectal tumors, dubbing the approach transcatheter rectal arterial chemoembolization (TRACE).
- As in TACE, TRACE uses precisely injected chemotherapeutic and vaso-occlusive agents to shut down blood flow to tumors, starving them of oxygen and nutrients.
- The research team tried the approach in 111 patients with stage II or III rectal tumors and performance status scores of 0-1.
- TRACE was delivered with oxaliplatin and followed by radiotherapy and S1 chemotherapy (tegafur, gimeracil, and potassium oteracil). Total mesorectal excisions were performed 4-8 weeks later, followed by mFOLFOX6 (5-fluorouracil, leucovorin, and oxaliplatin) or CAPOX (oxaliplatin and capecitabine) chemotherapy for 4-6 months.
TAKEAWAY:
- Overall, 20.7% of patients undergoing TRACE had a pathological complete response, and almost half (48.65%) had a major pathological response.
- Nearly 62% of patients were disease-free at 5 years, and almost 75% were alive at 5 years.
- No serious surgical complications occurred, but 21.6% of patients had postoperative complications. Overall, about 26% of patients (29 of 111) had grade 3/4 toxicities.
IN PRACTICE:
“The addition of transcatheter rectal arterial chemoembolisation to the neoadjuvant therapy can improve the pathological remission rate and prognosis in patients with locally advanced rectal cancer, without increasing the incidence of preoperative adverse events and postoperative complications,” the researchers concluded. “Given its promising effectiveness and safe profile, incorporating TRACE into the standard treatment strategy for patients with [locally advanced rectal cancer] should be considered.”
SOURCE:
The work, led by W. Yang of the Army Medical University in Chongqing, China, was published in Clinical Oncology.
LIMITATIONS:
The study was performed at a single center with no control arm in a Chinese population.
DISCLOSURES:
The work was funded by the Third Military Medical University in China. The investigators had no conflicts of interest.
A version of this article appeared on Medscape.com.
Is ChatGPT Reliable for CRC Screening/Surveillance Advice?
TOPLINE:
ChatGPT (version 3.5) provides relatively poor and inconsistent responses when asked about appropriate colorectal cancer (CRC) screening and surveillance, a new study showed.
METHODOLOGY:
- Three board-certified gastroenterologists with 10+ years of clinical experience developed five CRC screening and five CRC surveillance clinical vignettes (with multiple choice answers), which were fed to ChatGPT version 3.5.
- ChatGPT’s responses were recorded over four separate sessions and screened for accuracy to determine reliability of the tool.
- The average number of correct answers was compared to that of 238 gastroenterologists and colorectal surgeons answering the same questions with and without the help of a previously validated CRC screening mobile app.
TAKEAWAY:
- ChatGPT’s average overall performance was 45%; the average number of correct answers was 2.75 for screening and 1.75 for surveillance.
- ChatGPT’s responses were inconsistent in a large proportion of questions; the tool gave a different answer in four questions among the different sessions.
- The average number of total correct answers of ChatGPT was significantly lower (P < .001) than that of physicians with and without the mobile app (7.71 and 5.62 correct answers, respectively).
IN PRACTICE:
“The use of validated mobile apps with decision-making algorithms could serve as more reliable assistants until large language models developed with AI are further refined,” the authors concluded.
SOURCE:
The study, with first author Lisandro Pereyra, MD, Department of Gastroenterology, Hospital Alemán of Buenos Aires, Argentina, was published online on February 7, 2024, in the Journal of Clinical Gastroenterology.
LIMITATIONS:
The 10 clinical vignettes represented a relatively small sample size to assess accuracy. The study did not use the latest version of ChatGPT. No “fine-tuning” attempts with inputs of diverse prompts, instructions, or relevant data were performed, which could potentially improve the performance of the chatbot.
DISCLOSURES:
The study had no specific funding. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
ChatGPT (version 3.5) provides relatively poor and inconsistent responses when asked about appropriate colorectal cancer (CRC) screening and surveillance, a new study showed.
METHODOLOGY:
- Three board-certified gastroenterologists with 10+ years of clinical experience developed five CRC screening and five CRC surveillance clinical vignettes (with multiple choice answers), which were fed to ChatGPT version 3.5.
- ChatGPT’s responses were recorded over four separate sessions and screened for accuracy to determine reliability of the tool.
- The average number of correct answers was compared to that of 238 gastroenterologists and colorectal surgeons answering the same questions with and without the help of a previously validated CRC screening mobile app.
TAKEAWAY:
- ChatGPT’s average overall performance was 45%; the average number of correct answers was 2.75 for screening and 1.75 for surveillance.
- ChatGPT’s responses were inconsistent in a large proportion of questions; the tool gave a different answer in four questions among the different sessions.
- The average number of total correct answers of ChatGPT was significantly lower (P < .001) than that of physicians with and without the mobile app (7.71 and 5.62 correct answers, respectively).
IN PRACTICE:
“The use of validated mobile apps with decision-making algorithms could serve as more reliable assistants until large language models developed with AI are further refined,” the authors concluded.
SOURCE:
The study, with first author Lisandro Pereyra, MD, Department of Gastroenterology, Hospital Alemán of Buenos Aires, Argentina, was published online on February 7, 2024, in the Journal of Clinical Gastroenterology.
LIMITATIONS:
The 10 clinical vignettes represented a relatively small sample size to assess accuracy. The study did not use the latest version of ChatGPT. No “fine-tuning” attempts with inputs of diverse prompts, instructions, or relevant data were performed, which could potentially improve the performance of the chatbot.
DISCLOSURES:
The study had no specific funding. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
ChatGPT (version 3.5) provides relatively poor and inconsistent responses when asked about appropriate colorectal cancer (CRC) screening and surveillance, a new study showed.
METHODOLOGY:
- Three board-certified gastroenterologists with 10+ years of clinical experience developed five CRC screening and five CRC surveillance clinical vignettes (with multiple choice answers), which were fed to ChatGPT version 3.5.
- ChatGPT’s responses were recorded over four separate sessions and screened for accuracy to determine reliability of the tool.
- The average number of correct answers was compared to that of 238 gastroenterologists and colorectal surgeons answering the same questions with and without the help of a previously validated CRC screening mobile app.
TAKEAWAY:
- ChatGPT’s average overall performance was 45%; the average number of correct answers was 2.75 for screening and 1.75 for surveillance.
- ChatGPT’s responses were inconsistent in a large proportion of questions; the tool gave a different answer in four questions among the different sessions.
- The average number of total correct answers of ChatGPT was significantly lower (P < .001) than that of physicians with and without the mobile app (7.71 and 5.62 correct answers, respectively).
IN PRACTICE:
“The use of validated mobile apps with decision-making algorithms could serve as more reliable assistants until large language models developed with AI are further refined,” the authors concluded.
SOURCE:
The study, with first author Lisandro Pereyra, MD, Department of Gastroenterology, Hospital Alemán of Buenos Aires, Argentina, was published online on February 7, 2024, in the Journal of Clinical Gastroenterology.
LIMITATIONS:
The 10 clinical vignettes represented a relatively small sample size to assess accuracy. The study did not use the latest version of ChatGPT. No “fine-tuning” attempts with inputs of diverse prompts, instructions, or relevant data were performed, which could potentially improve the performance of the chatbot.
DISCLOSURES:
The study had no specific funding. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
Should CRC Surveillance Extend Beyond 5 Years Post Surgery?
TOPLINE:
In patients with stages I-III colorectal cancer (CRC) who are cancer-free 5 years after surgery, the incidence of late recurrence or metachronous disease after 5 years is low and has decreased over time, new data showed.
METHODOLOGY:
- Recent treatment advances in CRC have reduced the likelihood that patients with nonmetastatic disease will recur or develop a second primary cancer more than 6 months after the first. Although late recurrences and metachronous CRC remain infrequent, it’s not clear if patients might benefit from longer term surveillance.
- To investigate whether extending surveillance beyond the recommended 5 years is beneficial, researchers assessed the incidence of late recurrence, metachronous CRC, and second primary cancers 5 years after surgical resection with curative intent.
- The researchers identified patients with stages I-III CRC, under age 80 years, from Danish healthcare registries who underwent surgical resection between January 2004 and December 2013.
- A total of 8883 patients were followed from 5 years after primary surgery until the date of recurrence, metachronous CRC, or second non-CRC primary cancer.
TAKEAWAY:
- Between 5 and 10 years after surgery, 370 survivors developed late recurrence (4.16%), 270 developed metachronous disease (3.0%), and 635 were diagnosed with a second primary cancer (7.15%).
- During 2009-2013 and 2004-2008, the risk for late recurrence decreased by 48% (5.6% vs 2.9%; subdistribution hazard ratio [sHR], 0.52) and the risk for metachronous disease decreased by 50% (4.1% vs 2.1%; sHR, 0.50).
- During the same timeframe, the risk for second non-CRC primary cancer remained unchanged (7.1% vs 7.1%; sHR, 0.98).
- Compared with patients diagnosed with late recurrences (46%), 5-year overall survival was higher for patients with metachronous CRC (72%; adjusted HR, 0.37) and slightly higher for those with second primary cancers (48%; adjusted HR, 0.78).
IN PRACTICE:
Because the incidences of late recurrence and metachronous CRC are low and decreased between 2004 and 2013, the data do not support extending CRC-specific surveillance beyond 5 years, the authors concluded. “Symptoms or suspicion of a cancer occurring 5-10 years from primary CRC treatment, is more likely to represent a non-CRC cancer (7.1%).”
SOURCE:
This study, led by Jesper Nors from Aarhus University Hospital, Aarhus, Denmark, was published on February 7, 2024, in the International Journal of Cancer.
LIMITATIONS:
Misclassification of a late recurrence or metachronous CRC could have affected the findings.
DISCLOSURES:
This work was funded by Institute of Clinical Medicine, Aarhus University, Denmark, Novo Nordisk Foundation, Innovation Fund Denmark, and the Danish Cancer Society. The authors reported no conflict of interests.
A version of this article appeared on Medscape.com.
TOPLINE:
In patients with stages I-III colorectal cancer (CRC) who are cancer-free 5 years after surgery, the incidence of late recurrence or metachronous disease after 5 years is low and has decreased over time, new data showed.
METHODOLOGY:
- Recent treatment advances in CRC have reduced the likelihood that patients with nonmetastatic disease will recur or develop a second primary cancer more than 6 months after the first. Although late recurrences and metachronous CRC remain infrequent, it’s not clear if patients might benefit from longer term surveillance.
- To investigate whether extending surveillance beyond the recommended 5 years is beneficial, researchers assessed the incidence of late recurrence, metachronous CRC, and second primary cancers 5 years after surgical resection with curative intent.
- The researchers identified patients with stages I-III CRC, under age 80 years, from Danish healthcare registries who underwent surgical resection between January 2004 and December 2013.
- A total of 8883 patients were followed from 5 years after primary surgery until the date of recurrence, metachronous CRC, or second non-CRC primary cancer.
TAKEAWAY:
- Between 5 and 10 years after surgery, 370 survivors developed late recurrence (4.16%), 270 developed metachronous disease (3.0%), and 635 were diagnosed with a second primary cancer (7.15%).
- During 2009-2013 and 2004-2008, the risk for late recurrence decreased by 48% (5.6% vs 2.9%; subdistribution hazard ratio [sHR], 0.52) and the risk for metachronous disease decreased by 50% (4.1% vs 2.1%; sHR, 0.50).
- During the same timeframe, the risk for second non-CRC primary cancer remained unchanged (7.1% vs 7.1%; sHR, 0.98).
- Compared with patients diagnosed with late recurrences (46%), 5-year overall survival was higher for patients with metachronous CRC (72%; adjusted HR, 0.37) and slightly higher for those with second primary cancers (48%; adjusted HR, 0.78).
IN PRACTICE:
Because the incidences of late recurrence and metachronous CRC are low and decreased between 2004 and 2013, the data do not support extending CRC-specific surveillance beyond 5 years, the authors concluded. “Symptoms or suspicion of a cancer occurring 5-10 years from primary CRC treatment, is more likely to represent a non-CRC cancer (7.1%).”
SOURCE:
This study, led by Jesper Nors from Aarhus University Hospital, Aarhus, Denmark, was published on February 7, 2024, in the International Journal of Cancer.
LIMITATIONS:
Misclassification of a late recurrence or metachronous CRC could have affected the findings.
DISCLOSURES:
This work was funded by Institute of Clinical Medicine, Aarhus University, Denmark, Novo Nordisk Foundation, Innovation Fund Denmark, and the Danish Cancer Society. The authors reported no conflict of interests.
A version of this article appeared on Medscape.com.
TOPLINE:
In patients with stages I-III colorectal cancer (CRC) who are cancer-free 5 years after surgery, the incidence of late recurrence or metachronous disease after 5 years is low and has decreased over time, new data showed.
METHODOLOGY:
- Recent treatment advances in CRC have reduced the likelihood that patients with nonmetastatic disease will recur or develop a second primary cancer more than 6 months after the first. Although late recurrences and metachronous CRC remain infrequent, it’s not clear if patients might benefit from longer term surveillance.
- To investigate whether extending surveillance beyond the recommended 5 years is beneficial, researchers assessed the incidence of late recurrence, metachronous CRC, and second primary cancers 5 years after surgical resection with curative intent.
- The researchers identified patients with stages I-III CRC, under age 80 years, from Danish healthcare registries who underwent surgical resection between January 2004 and December 2013.
- A total of 8883 patients were followed from 5 years after primary surgery until the date of recurrence, metachronous CRC, or second non-CRC primary cancer.
TAKEAWAY:
- Between 5 and 10 years after surgery, 370 survivors developed late recurrence (4.16%), 270 developed metachronous disease (3.0%), and 635 were diagnosed with a second primary cancer (7.15%).
- During 2009-2013 and 2004-2008, the risk for late recurrence decreased by 48% (5.6% vs 2.9%; subdistribution hazard ratio [sHR], 0.52) and the risk for metachronous disease decreased by 50% (4.1% vs 2.1%; sHR, 0.50).
- During the same timeframe, the risk for second non-CRC primary cancer remained unchanged (7.1% vs 7.1%; sHR, 0.98).
- Compared with patients diagnosed with late recurrences (46%), 5-year overall survival was higher for patients with metachronous CRC (72%; adjusted HR, 0.37) and slightly higher for those with second primary cancers (48%; adjusted HR, 0.78).
IN PRACTICE:
Because the incidences of late recurrence and metachronous CRC are low and decreased between 2004 and 2013, the data do not support extending CRC-specific surveillance beyond 5 years, the authors concluded. “Symptoms or suspicion of a cancer occurring 5-10 years from primary CRC treatment, is more likely to represent a non-CRC cancer (7.1%).”
SOURCE:
This study, led by Jesper Nors from Aarhus University Hospital, Aarhus, Denmark, was published on February 7, 2024, in the International Journal of Cancer.
LIMITATIONS:
Misclassification of a late recurrence or metachronous CRC could have affected the findings.
DISCLOSURES:
This work was funded by Institute of Clinical Medicine, Aarhus University, Denmark, Novo Nordisk Foundation, Innovation Fund Denmark, and the Danish Cancer Society. The authors reported no conflict of interests.
A version of this article appeared on Medscape.com.
Do Multivitamin Supplements Lower Mortality Risk in CRC?
TOPLINE:
METHODOLOGY:
- Some studies suggest that multivitamin supplements might increase a person’s risk for CRC, and other research indicates that certain components of multivitamins, such as vitamins C and D, may have anti-CRC properties.
- Because as many as half of CRC survivors take a multivitamin, researchers wanted to assess whether multivitamin use affects overall survival among people with CRC.
- In the current prospective cohort study, researchers evaluated the use and dose of multivitamin supplements in 2424 patients with stages I-III CRC, using detailed information from patients in the Nurses’ Health Study and Health Professionals Follow‐Up Study.
- The participants completed a mailed questionnaire every 2 years, which included questions about the current use of multivitamin supplements as well as doses per week (0, 1-2, 3-5, 6-9, and ≥ 10 tablets).
- The researchers assessed the potential association between multivitamin use and CRC-related as well as all‐cause mortality.
TAKEAWAY:
- Over a median follow-up period of 11 years, 1512 deaths and 343 cancer-specific deaths occurred.
- For patients diagnosed with CRC, a moderate dose of multivitamins (three to five tablets per week) vs no multivitamin use was associated with a 45% lower risk for cancer-related mortality (adjusted hazard ratio [aHR], 0.55; P = .005).
- Moderate multivitamin use was also associated with a lower risk for all-cause mortality (aHR, 0.81; P = .04) as was a higher dose of six to nine tablets per week (aHR, 0.79; P < .001).
- However, high doses of 10 or more tablets per week were associated with a 60% higher risk for cancer-related mortality (aHR, 1.60; P = .02).
IN PRACTICE:
The study findings suggested that moderate multivitamin supplement use may come with a survival benefit in patients with CRC, while high doses may not, but “further studies are needed before making clinical recommendations for multivitamin use in patients with CRC,” the authors said.
SOURCE:
This work, led by Ming‐ming He of Sun Yat‐sen University Cancer Center, Guangzhou, China, was published in Cancer.
LIMITATIONS:
Given the study’s observational design, residual confounding may be possible. Reverse causation and recall bias are also possible limitations.
DISCLOSURES:
This study was funded by the National Institutes of Health, American Institute for Cancer Research, Wellesley College, Dana‐Farber Cancer Institute, and the Entertainment Industry Foundation. Three study authors reported financial relationships outside this work.
A version of this article appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Some studies suggest that multivitamin supplements might increase a person’s risk for CRC, and other research indicates that certain components of multivitamins, such as vitamins C and D, may have anti-CRC properties.
- Because as many as half of CRC survivors take a multivitamin, researchers wanted to assess whether multivitamin use affects overall survival among people with CRC.
- In the current prospective cohort study, researchers evaluated the use and dose of multivitamin supplements in 2424 patients with stages I-III CRC, using detailed information from patients in the Nurses’ Health Study and Health Professionals Follow‐Up Study.
- The participants completed a mailed questionnaire every 2 years, which included questions about the current use of multivitamin supplements as well as doses per week (0, 1-2, 3-5, 6-9, and ≥ 10 tablets).
- The researchers assessed the potential association between multivitamin use and CRC-related as well as all‐cause mortality.
TAKEAWAY:
- Over a median follow-up period of 11 years, 1512 deaths and 343 cancer-specific deaths occurred.
- For patients diagnosed with CRC, a moderate dose of multivitamins (three to five tablets per week) vs no multivitamin use was associated with a 45% lower risk for cancer-related mortality (adjusted hazard ratio [aHR], 0.55; P = .005).
- Moderate multivitamin use was also associated with a lower risk for all-cause mortality (aHR, 0.81; P = .04) as was a higher dose of six to nine tablets per week (aHR, 0.79; P < .001).
- However, high doses of 10 or more tablets per week were associated with a 60% higher risk for cancer-related mortality (aHR, 1.60; P = .02).
IN PRACTICE:
The study findings suggested that moderate multivitamin supplement use may come with a survival benefit in patients with CRC, while high doses may not, but “further studies are needed before making clinical recommendations for multivitamin use in patients with CRC,” the authors said.
SOURCE:
This work, led by Ming‐ming He of Sun Yat‐sen University Cancer Center, Guangzhou, China, was published in Cancer.
LIMITATIONS:
Given the study’s observational design, residual confounding may be possible. Reverse causation and recall bias are also possible limitations.
DISCLOSURES:
This study was funded by the National Institutes of Health, American Institute for Cancer Research, Wellesley College, Dana‐Farber Cancer Institute, and the Entertainment Industry Foundation. Three study authors reported financial relationships outside this work.
A version of this article appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Some studies suggest that multivitamin supplements might increase a person’s risk for CRC, and other research indicates that certain components of multivitamins, such as vitamins C and D, may have anti-CRC properties.
- Because as many as half of CRC survivors take a multivitamin, researchers wanted to assess whether multivitamin use affects overall survival among people with CRC.
- In the current prospective cohort study, researchers evaluated the use and dose of multivitamin supplements in 2424 patients with stages I-III CRC, using detailed information from patients in the Nurses’ Health Study and Health Professionals Follow‐Up Study.
- The participants completed a mailed questionnaire every 2 years, which included questions about the current use of multivitamin supplements as well as doses per week (0, 1-2, 3-5, 6-9, and ≥ 10 tablets).
- The researchers assessed the potential association between multivitamin use and CRC-related as well as all‐cause mortality.
TAKEAWAY:
- Over a median follow-up period of 11 years, 1512 deaths and 343 cancer-specific deaths occurred.
- For patients diagnosed with CRC, a moderate dose of multivitamins (three to five tablets per week) vs no multivitamin use was associated with a 45% lower risk for cancer-related mortality (adjusted hazard ratio [aHR], 0.55; P = .005).
- Moderate multivitamin use was also associated with a lower risk for all-cause mortality (aHR, 0.81; P = .04) as was a higher dose of six to nine tablets per week (aHR, 0.79; P < .001).
- However, high doses of 10 or more tablets per week were associated with a 60% higher risk for cancer-related mortality (aHR, 1.60; P = .02).
IN PRACTICE:
The study findings suggested that moderate multivitamin supplement use may come with a survival benefit in patients with CRC, while high doses may not, but “further studies are needed before making clinical recommendations for multivitamin use in patients with CRC,” the authors said.
SOURCE:
This work, led by Ming‐ming He of Sun Yat‐sen University Cancer Center, Guangzhou, China, was published in Cancer.
LIMITATIONS:
Given the study’s observational design, residual confounding may be possible. Reverse causation and recall bias are also possible limitations.
DISCLOSURES:
This study was funded by the National Institutes of Health, American Institute for Cancer Research, Wellesley College, Dana‐Farber Cancer Institute, and the Entertainment Industry Foundation. Three study authors reported financial relationships outside this work.
A version of this article appeared on Medscape.com.