User login
Understanding properties of fentanyl, other opioids key to treatment
Naloxone increasingly coming up short, expert says
BONITA SPRINGS, FLA. – Treating disorders tied to the use of highly potent synthetic opioids (HPSO), such as fentanyl, is challenging at best, an expert said at the annual meeting of the American Academy of Addiction Psychiatry.
“We have essentially no data to guide pharmacotherapy management decisions for the leading cause of fatal overdose deaths in the U.S.,” said John J. Mariani, MD, associate professor of clinical psychiatry at Columbia University, New York. “In the absence of data to make evidence-based recommendations, we still need to treat patients.”
That means taking what is known about the properties of those drugs into account when making treatment decisions, he said. Fentanyl quickly crosses the blood-brain barrier and is rapidly distributed to peripheral tissue. It has a short duration of action, but its duration can be extended with multiple injections or an infusion, he said. Research suggests that it has opioid receptor affinity similar to that of morphine, and it’s not known why it is up to 100 times more potent than morphine.
From his own experience, he offered some suggestions on treating patients who use HPSOs:
- Buprenorphine: Clinicians using buprenorphine as induction treatment have to wait longer from the last use to the first dose because of its longer effective half-life, and other medications might be needed to manage withdrawal. For maintenance, higher doses possibly should be considered to prevent HPSO override and to maintain opioid tolerance.
- Extended-release naltrexone: This involves a more difficult induction, and there is a question of whether inpatient treatment is better than outpatient, he said. For maintenance, more frequent administration should be considered, with closer monitoring for the risk of override and more urine toxicology testing.
- Methadone: For induction, methadone could offer an advantage over buprenorphine, because there is no risk of precipitated withdrawal. For maintenance, Dr. Mariani said, it’s not known whether standard doses protect against raising tolerance out of the reach of HPSOs’ effects.
- Naloxone: He said there have been increasing reports of multiple doses being needed to reverse an overdose. Because of the shorter time between substance use and death with fentanyl, more reports have been filed on unsuccessful attempts to revive people with naloxone despite multiple doses or stronger doses. Some naloxone programs have been giving more than two standard doses or using devices that give higher doses, he said. Also, , he said.
Addiction psychiatrists “need to educate patients, families, and other clinicians of this new risk of using opioids,” he said.
Meanwhile, in another talk, Thomas Kosten, MD, described progress in the efforts to develop a vaccine against fentanyl addiction, in the hopes of preventing overdoses. Researchers are taking cues from the failed attempt to develop a cocaine vaccine a few years ago, in which not enough antibodies were produced in about half the patients.
This time, researchers are using toll-like receptor agonists to boost the effects of the main vaccine component, known as norcocaine. Those agonists can more than double the antibody increase that is seen without them, said Dr. Kosten, professor of psychiatry at Baylor College of Medicine, Houston.
So far, researchers have found that the vaccine produces blockade of fentanyl analgesia and respiratory depression in rats. Dr. Kosten said his lab is looking for funding to continue the research. “It looks like we’re going to have some money in February to start making the vaccine,” he said.
Dr. Mariani and Dr. Kosten reported no relevant disclosures.
Naloxone increasingly coming up short, expert says
Naloxone increasingly coming up short, expert says
BONITA SPRINGS, FLA. – Treating disorders tied to the use of highly potent synthetic opioids (HPSO), such as fentanyl, is challenging at best, an expert said at the annual meeting of the American Academy of Addiction Psychiatry.
“We have essentially no data to guide pharmacotherapy management decisions for the leading cause of fatal overdose deaths in the U.S.,” said John J. Mariani, MD, associate professor of clinical psychiatry at Columbia University, New York. “In the absence of data to make evidence-based recommendations, we still need to treat patients.”
That means taking what is known about the properties of those drugs into account when making treatment decisions, he said. Fentanyl quickly crosses the blood-brain barrier and is rapidly distributed to peripheral tissue. It has a short duration of action, but its duration can be extended with multiple injections or an infusion, he said. Research suggests that it has opioid receptor affinity similar to that of morphine, and it’s not known why it is up to 100 times more potent than morphine.
From his own experience, he offered some suggestions on treating patients who use HPSOs:
- Buprenorphine: Clinicians using buprenorphine as induction treatment have to wait longer from the last use to the first dose because of its longer effective half-life, and other medications might be needed to manage withdrawal. For maintenance, higher doses possibly should be considered to prevent HPSO override and to maintain opioid tolerance.
- Extended-release naltrexone: This involves a more difficult induction, and there is a question of whether inpatient treatment is better than outpatient, he said. For maintenance, more frequent administration should be considered, with closer monitoring for the risk of override and more urine toxicology testing.
- Methadone: For induction, methadone could offer an advantage over buprenorphine, because there is no risk of precipitated withdrawal. For maintenance, Dr. Mariani said, it’s not known whether standard doses protect against raising tolerance out of the reach of HPSOs’ effects.
- Naloxone: He said there have been increasing reports of multiple doses being needed to reverse an overdose. Because of the shorter time between substance use and death with fentanyl, more reports have been filed on unsuccessful attempts to revive people with naloxone despite multiple doses or stronger doses. Some naloxone programs have been giving more than two standard doses or using devices that give higher doses, he said. Also, , he said.
Addiction psychiatrists “need to educate patients, families, and other clinicians of this new risk of using opioids,” he said.
Meanwhile, in another talk, Thomas Kosten, MD, described progress in the efforts to develop a vaccine against fentanyl addiction, in the hopes of preventing overdoses. Researchers are taking cues from the failed attempt to develop a cocaine vaccine a few years ago, in which not enough antibodies were produced in about half the patients.
This time, researchers are using toll-like receptor agonists to boost the effects of the main vaccine component, known as norcocaine. Those agonists can more than double the antibody increase that is seen without them, said Dr. Kosten, professor of psychiatry at Baylor College of Medicine, Houston.
So far, researchers have found that the vaccine produces blockade of fentanyl analgesia and respiratory depression in rats. Dr. Kosten said his lab is looking for funding to continue the research. “It looks like we’re going to have some money in February to start making the vaccine,” he said.
Dr. Mariani and Dr. Kosten reported no relevant disclosures.
BONITA SPRINGS, FLA. – Treating disorders tied to the use of highly potent synthetic opioids (HPSO), such as fentanyl, is challenging at best, an expert said at the annual meeting of the American Academy of Addiction Psychiatry.
“We have essentially no data to guide pharmacotherapy management decisions for the leading cause of fatal overdose deaths in the U.S.,” said John J. Mariani, MD, associate professor of clinical psychiatry at Columbia University, New York. “In the absence of data to make evidence-based recommendations, we still need to treat patients.”
That means taking what is known about the properties of those drugs into account when making treatment decisions, he said. Fentanyl quickly crosses the blood-brain barrier and is rapidly distributed to peripheral tissue. It has a short duration of action, but its duration can be extended with multiple injections or an infusion, he said. Research suggests that it has opioid receptor affinity similar to that of morphine, and it’s not known why it is up to 100 times more potent than morphine.
From his own experience, he offered some suggestions on treating patients who use HPSOs:
- Buprenorphine: Clinicians using buprenorphine as induction treatment have to wait longer from the last use to the first dose because of its longer effective half-life, and other medications might be needed to manage withdrawal. For maintenance, higher doses possibly should be considered to prevent HPSO override and to maintain opioid tolerance.
- Extended-release naltrexone: This involves a more difficult induction, and there is a question of whether inpatient treatment is better than outpatient, he said. For maintenance, more frequent administration should be considered, with closer monitoring for the risk of override and more urine toxicology testing.
- Methadone: For induction, methadone could offer an advantage over buprenorphine, because there is no risk of precipitated withdrawal. For maintenance, Dr. Mariani said, it’s not known whether standard doses protect against raising tolerance out of the reach of HPSOs’ effects.
- Naloxone: He said there have been increasing reports of multiple doses being needed to reverse an overdose. Because of the shorter time between substance use and death with fentanyl, more reports have been filed on unsuccessful attempts to revive people with naloxone despite multiple doses or stronger doses. Some naloxone programs have been giving more than two standard doses or using devices that give higher doses, he said. Also, , he said.
Addiction psychiatrists “need to educate patients, families, and other clinicians of this new risk of using opioids,” he said.
Meanwhile, in another talk, Thomas Kosten, MD, described progress in the efforts to develop a vaccine against fentanyl addiction, in the hopes of preventing overdoses. Researchers are taking cues from the failed attempt to develop a cocaine vaccine a few years ago, in which not enough antibodies were produced in about half the patients.
This time, researchers are using toll-like receptor agonists to boost the effects of the main vaccine component, known as norcocaine. Those agonists can more than double the antibody increase that is seen without them, said Dr. Kosten, professor of psychiatry at Baylor College of Medicine, Houston.
So far, researchers have found that the vaccine produces blockade of fentanyl analgesia and respiratory depression in rats. Dr. Kosten said his lab is looking for funding to continue the research. “It looks like we’re going to have some money in February to start making the vaccine,” he said.
Dr. Mariani and Dr. Kosten reported no relevant disclosures.
REPORTING FROM AAAP 2018
Novel SSc classification scheme aims to improve risk stratification
CHICAGO – A simple new classification scheme that combines autoantibody specificity and extent of skin involvement could improve risk stratification of patients with systemic sclerosis, according to researchers at University College London.
“The Le Roy et al. classification of SSc [systemic sclerosis] into limited and diffuse cutaneous subtype remains the most commonly used classification system for systemic sclerosis, but autoantibodies are much better predictors of organ involvement, and while more sophisticated approaches exist, this proposed simple classification using antibodies and skin subset is relevant to clinical practice and could help risk stratification,” Svetlana I. Nihtyanova, MD, said at the annual meeting of the American College of Rheumatology.
Dr. Nihtyanova, a clinical research fellow at University College London, reported how she and her colleagues at UCL divided 1,025 SSc patients into 12 subgroups based on skin subset and autoantibodies and then conducted Kaplan-Meier estimates of survival and cumulative incidence of organ complications to rank these 12 subgroups by endpoint estimates. They merged subgroups with similar ranking in multiple endpoints, ending up with seven groups in the final classification.
Group 1 comprised anti–centromere antibody–positive limited cutaneous SSc (lcSSc) patients and accounted for 29% of patients.
“This was the subgroup with the highest survival (72%) and the lowest incidence of pulmonary fibrosis (13%) and scleroderma renal crisis (no cases) at 20 years from onset,” she said, noting that the incidence of pulmonary hypertension in this group was similar to the average for the whole cohort.
Group 2 comprised all anti–RNA polymerase antibody–positive subjects and accounted for 11% of patients. This group had the highest incidence of scleroderma renal crisis (SRC; 32% at 20 years), but other organ complications and survival were similar to the cohort average.
Group 3 comprised Scl-70–positive lcSSc patients, and accounted for 11% of patients.
“Although incidence of pulmonary fibrosis in this group was the second highest (69% at 20 years), other complications were rare,” Dr. Nihtyanova said, adding that this group had the lowest incidence of pulmonary hypertension (6%) and the second lowest incidence of SRC (3%) at 20 years.
Group 4, conversely, included Scl-70–positive dcSSc patients and accounted for 11% of patients, who had a very poor prognosis; they had the highest incidence of pulmonary fibrosis (91%) and cardiac scleroderma (14%), and the worst survival (41%) at 20 years, she said.
Group 5 included all U3 RNP–positive patients, accounting for 5% of patients.
“Although survival in this group was not bad (70% at 20 years), the group had the highest pulmonary hypertension incidence (40%) and the second highest incidence of cardiac SSc (11%) at 20 years,” she noted.
Groups 6 and 7 (comprising 22% and 11% of study subjects, respectively) included lcSSc and diffuse cutaneous SSc (dcSSc) patients with other antibody specificities. Group 6 had low overall SRC and cardiac SSc risk, while other outcomes were similar to the cohort average. Group 7, however, had poor prognosis, with the second lowest survival (42% at 20 years) and above average rates of organ disease, particularly pulmonary fibrosis and SRC, she said.
Overall, estimated survival for the entire cohort was 60% at 20 years from onset, and in that time frame 44% developed significant pulmonary fibrosis, 25% pulmonary hypertension, 7% SRC, and 6% cardiac SSc. The patients had a mean age of 47 years at disease onset, and 16% were men. Diffuse cutaneous SSc was diagnosed in 35% of the subjects, she noted.
Dr. Nihtyanova reported having no disclosures.
SOURCE: Nihtyanova S et al. Arthritis Rheumatol. 2018;70(Suppl 10): Abstract 2935.
CHICAGO – A simple new classification scheme that combines autoantibody specificity and extent of skin involvement could improve risk stratification of patients with systemic sclerosis, according to researchers at University College London.
“The Le Roy et al. classification of SSc [systemic sclerosis] into limited and diffuse cutaneous subtype remains the most commonly used classification system for systemic sclerosis, but autoantibodies are much better predictors of organ involvement, and while more sophisticated approaches exist, this proposed simple classification using antibodies and skin subset is relevant to clinical practice and could help risk stratification,” Svetlana I. Nihtyanova, MD, said at the annual meeting of the American College of Rheumatology.
Dr. Nihtyanova, a clinical research fellow at University College London, reported how she and her colleagues at UCL divided 1,025 SSc patients into 12 subgroups based on skin subset and autoantibodies and then conducted Kaplan-Meier estimates of survival and cumulative incidence of organ complications to rank these 12 subgroups by endpoint estimates. They merged subgroups with similar ranking in multiple endpoints, ending up with seven groups in the final classification.
Group 1 comprised anti–centromere antibody–positive limited cutaneous SSc (lcSSc) patients and accounted for 29% of patients.
“This was the subgroup with the highest survival (72%) and the lowest incidence of pulmonary fibrosis (13%) and scleroderma renal crisis (no cases) at 20 years from onset,” she said, noting that the incidence of pulmonary hypertension in this group was similar to the average for the whole cohort.
Group 2 comprised all anti–RNA polymerase antibody–positive subjects and accounted for 11% of patients. This group had the highest incidence of scleroderma renal crisis (SRC; 32% at 20 years), but other organ complications and survival were similar to the cohort average.
Group 3 comprised Scl-70–positive lcSSc patients, and accounted for 11% of patients.
“Although incidence of pulmonary fibrosis in this group was the second highest (69% at 20 years), other complications were rare,” Dr. Nihtyanova said, adding that this group had the lowest incidence of pulmonary hypertension (6%) and the second lowest incidence of SRC (3%) at 20 years.
Group 4, conversely, included Scl-70–positive dcSSc patients and accounted for 11% of patients, who had a very poor prognosis; they had the highest incidence of pulmonary fibrosis (91%) and cardiac scleroderma (14%), and the worst survival (41%) at 20 years, she said.
Group 5 included all U3 RNP–positive patients, accounting for 5% of patients.
“Although survival in this group was not bad (70% at 20 years), the group had the highest pulmonary hypertension incidence (40%) and the second highest incidence of cardiac SSc (11%) at 20 years,” she noted.
Groups 6 and 7 (comprising 22% and 11% of study subjects, respectively) included lcSSc and diffuse cutaneous SSc (dcSSc) patients with other antibody specificities. Group 6 had low overall SRC and cardiac SSc risk, while other outcomes were similar to the cohort average. Group 7, however, had poor prognosis, with the second lowest survival (42% at 20 years) and above average rates of organ disease, particularly pulmonary fibrosis and SRC, she said.
Overall, estimated survival for the entire cohort was 60% at 20 years from onset, and in that time frame 44% developed significant pulmonary fibrosis, 25% pulmonary hypertension, 7% SRC, and 6% cardiac SSc. The patients had a mean age of 47 years at disease onset, and 16% were men. Diffuse cutaneous SSc was diagnosed in 35% of the subjects, she noted.
Dr. Nihtyanova reported having no disclosures.
SOURCE: Nihtyanova S et al. Arthritis Rheumatol. 2018;70(Suppl 10): Abstract 2935.
CHICAGO – A simple new classification scheme that combines autoantibody specificity and extent of skin involvement could improve risk stratification of patients with systemic sclerosis, according to researchers at University College London.
“The Le Roy et al. classification of SSc [systemic sclerosis] into limited and diffuse cutaneous subtype remains the most commonly used classification system for systemic sclerosis, but autoantibodies are much better predictors of organ involvement, and while more sophisticated approaches exist, this proposed simple classification using antibodies and skin subset is relevant to clinical practice and could help risk stratification,” Svetlana I. Nihtyanova, MD, said at the annual meeting of the American College of Rheumatology.
Dr. Nihtyanova, a clinical research fellow at University College London, reported how she and her colleagues at UCL divided 1,025 SSc patients into 12 subgroups based on skin subset and autoantibodies and then conducted Kaplan-Meier estimates of survival and cumulative incidence of organ complications to rank these 12 subgroups by endpoint estimates. They merged subgroups with similar ranking in multiple endpoints, ending up with seven groups in the final classification.
Group 1 comprised anti–centromere antibody–positive limited cutaneous SSc (lcSSc) patients and accounted for 29% of patients.
“This was the subgroup with the highest survival (72%) and the lowest incidence of pulmonary fibrosis (13%) and scleroderma renal crisis (no cases) at 20 years from onset,” she said, noting that the incidence of pulmonary hypertension in this group was similar to the average for the whole cohort.
Group 2 comprised all anti–RNA polymerase antibody–positive subjects and accounted for 11% of patients. This group had the highest incidence of scleroderma renal crisis (SRC; 32% at 20 years), but other organ complications and survival were similar to the cohort average.
Group 3 comprised Scl-70–positive lcSSc patients, and accounted for 11% of patients.
“Although incidence of pulmonary fibrosis in this group was the second highest (69% at 20 years), other complications were rare,” Dr. Nihtyanova said, adding that this group had the lowest incidence of pulmonary hypertension (6%) and the second lowest incidence of SRC (3%) at 20 years.
Group 4, conversely, included Scl-70–positive dcSSc patients and accounted for 11% of patients, who had a very poor prognosis; they had the highest incidence of pulmonary fibrosis (91%) and cardiac scleroderma (14%), and the worst survival (41%) at 20 years, she said.
Group 5 included all U3 RNP–positive patients, accounting for 5% of patients.
“Although survival in this group was not bad (70% at 20 years), the group had the highest pulmonary hypertension incidence (40%) and the second highest incidence of cardiac SSc (11%) at 20 years,” she noted.
Groups 6 and 7 (comprising 22% and 11% of study subjects, respectively) included lcSSc and diffuse cutaneous SSc (dcSSc) patients with other antibody specificities. Group 6 had low overall SRC and cardiac SSc risk, while other outcomes were similar to the cohort average. Group 7, however, had poor prognosis, with the second lowest survival (42% at 20 years) and above average rates of organ disease, particularly pulmonary fibrosis and SRC, she said.
Overall, estimated survival for the entire cohort was 60% at 20 years from onset, and in that time frame 44% developed significant pulmonary fibrosis, 25% pulmonary hypertension, 7% SRC, and 6% cardiac SSc. The patients had a mean age of 47 years at disease onset, and 16% were men. Diffuse cutaneous SSc was diagnosed in 35% of the subjects, she noted.
Dr. Nihtyanova reported having no disclosures.
SOURCE: Nihtyanova S et al. Arthritis Rheumatol. 2018;70(Suppl 10): Abstract 2935.
REPORTING FROM THE ACR ANNUAL MEETING
Key clinical point:
Major finding: The classification scheme for SSc risk stratification identified seven distinct SSc subgroups.
Study details: Development and testing of a novel risk classification scheme in 1,025 SSc patients.
Disclosures: Dr. Nihtyanova reported having no disclosures.
Source: Nihtyanova S et al. Arthritis Rheumatol. 2018;70(Suppl 10):Abstract 2935.
Increased cancer risk in dermatomyositis has temporal limits
The increased risk of cancer associated with anti-TIF1-Ab-positive dermatomyositis is limited almost exclusively to 3 years on either side of the onset of dermatomyositis, new research suggests.
Idiopathic inflammatory myopathy have been associated with malignancy, in particular dermatomyositis (DM) and the DM-specific antitranscriptional intermediary factor 1 antibody (anti-TIF1-Ab).
Around one-fifth of the 236 patients diagnosed with DM in the current study, published online Dec. 7 in Rheumatology, were anti-TIF1-Ab positive, and these patients had a more than threefold higher risk of developing cancer comapared with patients who were anti-TIF1-Ab negative (hazard ratio = 3.4, 95% confidence interval, 2.2-5.4; P less than .01).
Overall, 38% of patients in the anti-TIF1-Ab-positive group developed cancer during the 10-year follow-up, compared with 15% of patients with anti-TIF1-Ab-negative DM.
However, all the cancers in the anti-TIF1-Ab-positive group occurred within the 3 years before the onset of DM or within 2.5 years after onset. No anti-TIF1-Ab-positive patients developed cancers after this time, but some patients in the anti-TIF1-Ab-negative group did.
“This finding is not likely to be due to a disparity in follow-up time between anti-TIF1-Ab-positive and -negative cases, as the median follow-up times were similar for both groups: 10 years and 12 years, respectively,” wrote Alexander Oldroyd, MBChB, a clinical research fellow in the Centre for Musculoskeletal Research at the University of Manchester (England), and his coauthors. “Further, this finding is unlikely to be due to differences in cancer detection methods, as both cohorts’ cancer diagnoses were identified through HSCIC [U.K. Health and Social Care Information Centre] data, ensuring capture of all incident cancers during the follow-up period.”
Anti-TIF1-Ab-positive patients were more likely to develop cancer if they were older. None of the 15 anti-TIF1-Ab-positive patients who were aged under 39 when they developed DM went on to develop cancer. But cancer developed in around half of the anti-TIF1-Ab-positive patients who were aged 39 years or older when their DM began.
The anti-TIF1 antibody is commonly found in juvenile DM, but previous research has not found an association with an increased risk of cancer in this younger patient population.
“Our findings add strength to the hypothesis that there exists a subset of young adult anti-TIF1-Ab-positive cases who do not have a discernible increased risk of cancer, similar to that observed in TIF1-Ab-positive juvenile DM,” the authors wrote. They suggested that given the increased risk of malignancy in older patients who were anti-TIF1-Ab positive, this group should be subject to more detailed cancer screening.
Breast cancer was the most common malignancy among both anti-TIF1-Ab-positive and anti-TIF1-Ab-negative patients (33% and 25%, respectively). However, ovarian cancer was significantly more common among the anti-TIF1-Ab-positive patients than among the anti-TIF1-Ab-negative patients (19% vs. 2%; P less than .05); four of the five ovarian cancers in the entire cohort occurred in the anti-TIF1-Ab-positive group.
The authors noted that this confirmed the finding of a number of previous studies suggesting an increased risk of ovarian cancer with DM.
“However, this is the first large study to identify that ovarian cancer is overrepresented in anti-TIF1-Ab-positive individuals, suggesting that the true association between DM and ovarian cancer may be through possession of anti-TIF1-Abs,” they noted.
The authors wrote that they had aimed to inform cancer screening strategies among patients with DM.
“It may be that a focus on screening for cancer within the first 3 years after DM onset and particularly screening for ovarian cancer in anti-TIF1-Ab-positive female patients may be required,” they wrote. “Our findings also strengthen the hypothesis that inflammatory myopathies represent a paraneoplastic reaction initiated by attempted immune-mediated clearance of a cancer.”
The study was supported by Arthritis Research UK, Myositis UK, the European Science Foundation for EuMyoNet, Association Francaise Contre Les Myopathies, the Medical Research Council, and the Manchester Academic Health Science Centre. No conflicts of interest were declared.
SOURCE: Oldroyd A et al. Rheumatology. 2018 Dec 7. doi: 10.1093/rheumatology/key357.
The increased risk of cancer associated with anti-TIF1-Ab-positive dermatomyositis is limited almost exclusively to 3 years on either side of the onset of dermatomyositis, new research suggests.
Idiopathic inflammatory myopathy have been associated with malignancy, in particular dermatomyositis (DM) and the DM-specific antitranscriptional intermediary factor 1 antibody (anti-TIF1-Ab).
Around one-fifth of the 236 patients diagnosed with DM in the current study, published online Dec. 7 in Rheumatology, were anti-TIF1-Ab positive, and these patients had a more than threefold higher risk of developing cancer comapared with patients who were anti-TIF1-Ab negative (hazard ratio = 3.4, 95% confidence interval, 2.2-5.4; P less than .01).
Overall, 38% of patients in the anti-TIF1-Ab-positive group developed cancer during the 10-year follow-up, compared with 15% of patients with anti-TIF1-Ab-negative DM.
However, all the cancers in the anti-TIF1-Ab-positive group occurred within the 3 years before the onset of DM or within 2.5 years after onset. No anti-TIF1-Ab-positive patients developed cancers after this time, but some patients in the anti-TIF1-Ab-negative group did.
“This finding is not likely to be due to a disparity in follow-up time between anti-TIF1-Ab-positive and -negative cases, as the median follow-up times were similar for both groups: 10 years and 12 years, respectively,” wrote Alexander Oldroyd, MBChB, a clinical research fellow in the Centre for Musculoskeletal Research at the University of Manchester (England), and his coauthors. “Further, this finding is unlikely to be due to differences in cancer detection methods, as both cohorts’ cancer diagnoses were identified through HSCIC [U.K. Health and Social Care Information Centre] data, ensuring capture of all incident cancers during the follow-up period.”
Anti-TIF1-Ab-positive patients were more likely to develop cancer if they were older. None of the 15 anti-TIF1-Ab-positive patients who were aged under 39 when they developed DM went on to develop cancer. But cancer developed in around half of the anti-TIF1-Ab-positive patients who were aged 39 years or older when their DM began.
The anti-TIF1 antibody is commonly found in juvenile DM, but previous research has not found an association with an increased risk of cancer in this younger patient population.
“Our findings add strength to the hypothesis that there exists a subset of young adult anti-TIF1-Ab-positive cases who do not have a discernible increased risk of cancer, similar to that observed in TIF1-Ab-positive juvenile DM,” the authors wrote. They suggested that given the increased risk of malignancy in older patients who were anti-TIF1-Ab positive, this group should be subject to more detailed cancer screening.
Breast cancer was the most common malignancy among both anti-TIF1-Ab-positive and anti-TIF1-Ab-negative patients (33% and 25%, respectively). However, ovarian cancer was significantly more common among the anti-TIF1-Ab-positive patients than among the anti-TIF1-Ab-negative patients (19% vs. 2%; P less than .05); four of the five ovarian cancers in the entire cohort occurred in the anti-TIF1-Ab-positive group.
The authors noted that this confirmed the finding of a number of previous studies suggesting an increased risk of ovarian cancer with DM.
“However, this is the first large study to identify that ovarian cancer is overrepresented in anti-TIF1-Ab-positive individuals, suggesting that the true association between DM and ovarian cancer may be through possession of anti-TIF1-Abs,” they noted.
The authors wrote that they had aimed to inform cancer screening strategies among patients with DM.
“It may be that a focus on screening for cancer within the first 3 years after DM onset and particularly screening for ovarian cancer in anti-TIF1-Ab-positive female patients may be required,” they wrote. “Our findings also strengthen the hypothesis that inflammatory myopathies represent a paraneoplastic reaction initiated by attempted immune-mediated clearance of a cancer.”
The study was supported by Arthritis Research UK, Myositis UK, the European Science Foundation for EuMyoNet, Association Francaise Contre Les Myopathies, the Medical Research Council, and the Manchester Academic Health Science Centre. No conflicts of interest were declared.
SOURCE: Oldroyd A et al. Rheumatology. 2018 Dec 7. doi: 10.1093/rheumatology/key357.
The increased risk of cancer associated with anti-TIF1-Ab-positive dermatomyositis is limited almost exclusively to 3 years on either side of the onset of dermatomyositis, new research suggests.
Idiopathic inflammatory myopathy have been associated with malignancy, in particular dermatomyositis (DM) and the DM-specific antitranscriptional intermediary factor 1 antibody (anti-TIF1-Ab).
Around one-fifth of the 236 patients diagnosed with DM in the current study, published online Dec. 7 in Rheumatology, were anti-TIF1-Ab positive, and these patients had a more than threefold higher risk of developing cancer comapared with patients who were anti-TIF1-Ab negative (hazard ratio = 3.4, 95% confidence interval, 2.2-5.4; P less than .01).
Overall, 38% of patients in the anti-TIF1-Ab-positive group developed cancer during the 10-year follow-up, compared with 15% of patients with anti-TIF1-Ab-negative DM.
However, all the cancers in the anti-TIF1-Ab-positive group occurred within the 3 years before the onset of DM or within 2.5 years after onset. No anti-TIF1-Ab-positive patients developed cancers after this time, but some patients in the anti-TIF1-Ab-negative group did.
“This finding is not likely to be due to a disparity in follow-up time between anti-TIF1-Ab-positive and -negative cases, as the median follow-up times were similar for both groups: 10 years and 12 years, respectively,” wrote Alexander Oldroyd, MBChB, a clinical research fellow in the Centre for Musculoskeletal Research at the University of Manchester (England), and his coauthors. “Further, this finding is unlikely to be due to differences in cancer detection methods, as both cohorts’ cancer diagnoses were identified through HSCIC [U.K. Health and Social Care Information Centre] data, ensuring capture of all incident cancers during the follow-up period.”
Anti-TIF1-Ab-positive patients were more likely to develop cancer if they were older. None of the 15 anti-TIF1-Ab-positive patients who were aged under 39 when they developed DM went on to develop cancer. But cancer developed in around half of the anti-TIF1-Ab-positive patients who were aged 39 years or older when their DM began.
The anti-TIF1 antibody is commonly found in juvenile DM, but previous research has not found an association with an increased risk of cancer in this younger patient population.
“Our findings add strength to the hypothesis that there exists a subset of young adult anti-TIF1-Ab-positive cases who do not have a discernible increased risk of cancer, similar to that observed in TIF1-Ab-positive juvenile DM,” the authors wrote. They suggested that given the increased risk of malignancy in older patients who were anti-TIF1-Ab positive, this group should be subject to more detailed cancer screening.
Breast cancer was the most common malignancy among both anti-TIF1-Ab-positive and anti-TIF1-Ab-negative patients (33% and 25%, respectively). However, ovarian cancer was significantly more common among the anti-TIF1-Ab-positive patients than among the anti-TIF1-Ab-negative patients (19% vs. 2%; P less than .05); four of the five ovarian cancers in the entire cohort occurred in the anti-TIF1-Ab-positive group.
The authors noted that this confirmed the finding of a number of previous studies suggesting an increased risk of ovarian cancer with DM.
“However, this is the first large study to identify that ovarian cancer is overrepresented in anti-TIF1-Ab-positive individuals, suggesting that the true association between DM and ovarian cancer may be through possession of anti-TIF1-Abs,” they noted.
The authors wrote that they had aimed to inform cancer screening strategies among patients with DM.
“It may be that a focus on screening for cancer within the first 3 years after DM onset and particularly screening for ovarian cancer in anti-TIF1-Ab-positive female patients may be required,” they wrote. “Our findings also strengthen the hypothesis that inflammatory myopathies represent a paraneoplastic reaction initiated by attempted immune-mediated clearance of a cancer.”
The study was supported by Arthritis Research UK, Myositis UK, the European Science Foundation for EuMyoNet, Association Francaise Contre Les Myopathies, the Medical Research Council, and the Manchester Academic Health Science Centre. No conflicts of interest were declared.
SOURCE: Oldroyd A et al. Rheumatology. 2018 Dec 7. doi: 10.1093/rheumatology/key357.
FROM RHEUMATOLOGY
Key clinical point: Patients with dermatomyositis are at increased risk of cancer only in the 3-year periods before and after the onset of dermatomyositis.
Major finding: Overall, 38% of patients in the anti-TIF1-Ab-positive group developed cancer during the 10-year follow-up, compared with 15% of patients with anti-TIF1-Ab-negative DM.
Study details: Cohort study of 236 people with dermatomyositis.
Disclosures: The study was supported by Arthritis Research UK, Myositis UK, the European Science Foundation for EuMyoNet, Association Francaise Contre Les Myopathies, the Medical Research Council, and the Manchester Academic Health Science Centre. No conflicts of interest were declared.
Source: Oldroyd A et al. Rheumatology. 2018 Dec 7. doi: 10.1093/rheumatology/key357.
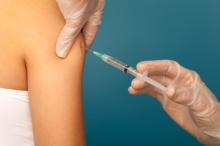
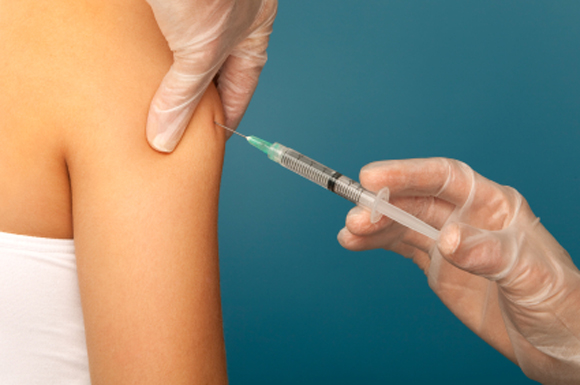
Flu vaccine effectiveness drops by half after 6 months
The , according to 5 years of data from approximately 15,000 children in Hong Kong.
The vaccine is known to last less than a year, but the findings support the need for more vaccine availability in areas where influenza activity occurs year-round, wrote Shuo Feng, PhD, and Susan S. Chiu, MD, of the University of Hong Kong, and their colleagues.
In a study published in the Lancet Respiratory Medicine, the researchers reviewed how vaccine effectiveness changed over time by analyzing data from children aged 6 months to 17 years admitted to a Hong Kong hospital between 2012 and 2017. The study population involved 15,695 children hospitalized for respiratory infections, including 2,500 who were positive for influenza A or B and 13,195 who were negative. Of these, 6.4% of the positive patients and 11% of the negative patients had been vaccinated; 70% to 80% of the vaccinations occurred before the end of December of a given year.
Overall, the vaccination effectiveness rate was 79% for 0.5 to 2 months after vaccination, then dropped to 60% at 2-4 months, 57% at 4-6 months, and 45% at 6-9 months.
The researchers estimated vaccine effectiveness by three time periods: September to December, January to April, and May to August. Across seasons, vaccine effectiveness for all age groups was 79% for September to December, 67% for January to April, and 43% for May to August.
The study results were strengthened by the inclusion of year-round activity, but limited by several factors including lack of data on patients’ vaccination history and the specifics of each year’s flu virus, and lack of generalizability to an adult population, the researchers said.
However, the findings support data from previous studies on the effectiveness of annual vaccination, with the optimal timing from October to December in Hong Kong, they said. “Improved influenza vaccines are needed to provide year-round protection for children, particularly in subtropical and tropical locations,” they added.
The study was supported by the Health and Medical Research Fund and the Research Grants Council, Hong Kong. The lead authors had no financial conflicts to disclose.
SOURCE: Feng S et al. Lancet Respir Med. 2018;6:925-34.
The , according to 5 years of data from approximately 15,000 children in Hong Kong.
The vaccine is known to last less than a year, but the findings support the need for more vaccine availability in areas where influenza activity occurs year-round, wrote Shuo Feng, PhD, and Susan S. Chiu, MD, of the University of Hong Kong, and their colleagues.
In a study published in the Lancet Respiratory Medicine, the researchers reviewed how vaccine effectiveness changed over time by analyzing data from children aged 6 months to 17 years admitted to a Hong Kong hospital between 2012 and 2017. The study population involved 15,695 children hospitalized for respiratory infections, including 2,500 who were positive for influenza A or B and 13,195 who were negative. Of these, 6.4% of the positive patients and 11% of the negative patients had been vaccinated; 70% to 80% of the vaccinations occurred before the end of December of a given year.
Overall, the vaccination effectiveness rate was 79% for 0.5 to 2 months after vaccination, then dropped to 60% at 2-4 months, 57% at 4-6 months, and 45% at 6-9 months.
The researchers estimated vaccine effectiveness by three time periods: September to December, January to April, and May to August. Across seasons, vaccine effectiveness for all age groups was 79% for September to December, 67% for January to April, and 43% for May to August.
The study results were strengthened by the inclusion of year-round activity, but limited by several factors including lack of data on patients’ vaccination history and the specifics of each year’s flu virus, and lack of generalizability to an adult population, the researchers said.
However, the findings support data from previous studies on the effectiveness of annual vaccination, with the optimal timing from October to December in Hong Kong, they said. “Improved influenza vaccines are needed to provide year-round protection for children, particularly in subtropical and tropical locations,” they added.
The study was supported by the Health and Medical Research Fund and the Research Grants Council, Hong Kong. The lead authors had no financial conflicts to disclose.
SOURCE: Feng S et al. Lancet Respir Med. 2018;6:925-34.
The , according to 5 years of data from approximately 15,000 children in Hong Kong.
The vaccine is known to last less than a year, but the findings support the need for more vaccine availability in areas where influenza activity occurs year-round, wrote Shuo Feng, PhD, and Susan S. Chiu, MD, of the University of Hong Kong, and their colleagues.
In a study published in the Lancet Respiratory Medicine, the researchers reviewed how vaccine effectiveness changed over time by analyzing data from children aged 6 months to 17 years admitted to a Hong Kong hospital between 2012 and 2017. The study population involved 15,695 children hospitalized for respiratory infections, including 2,500 who were positive for influenza A or B and 13,195 who were negative. Of these, 6.4% of the positive patients and 11% of the negative patients had been vaccinated; 70% to 80% of the vaccinations occurred before the end of December of a given year.
Overall, the vaccination effectiveness rate was 79% for 0.5 to 2 months after vaccination, then dropped to 60% at 2-4 months, 57% at 4-6 months, and 45% at 6-9 months.
The researchers estimated vaccine effectiveness by three time periods: September to December, January to April, and May to August. Across seasons, vaccine effectiveness for all age groups was 79% for September to December, 67% for January to April, and 43% for May to August.
The study results were strengthened by the inclusion of year-round activity, but limited by several factors including lack of data on patients’ vaccination history and the specifics of each year’s flu virus, and lack of generalizability to an adult population, the researchers said.
However, the findings support data from previous studies on the effectiveness of annual vaccination, with the optimal timing from October to December in Hong Kong, they said. “Improved influenza vaccines are needed to provide year-round protection for children, particularly in subtropical and tropical locations,” they added.
The study was supported by the Health and Medical Research Fund and the Research Grants Council, Hong Kong. The lead authors had no financial conflicts to disclose.
SOURCE: Feng S et al. Lancet Respir Med. 2018;6:925-34.
FROM THE LANCET RESPIRATORY MEDICINE
Key clinical point: The effectiveness of the influenza vaccine decreased after 9 months in a cohort of children in Hong Kong.
Major finding: Vaccine effectiveness was 79% from 0.5 to 2 months after vaccination, but dropped to 45% within 6-9 months.
Study details: The data come from a review of 15,695 children aged 6 months to 17 years hospitalized for influenza in Hong Kong.
Disclosures: The study was supported by the Health and Medical Research Fund and the Research Grants Council, Hong Kong.
Source: Feng S et al. Lancet Respir Med. 2018;6:925-34.
Carol Bernstein Part II
Telemedicine not widely used
Also today, you ought to be judicious with empiric antibiotics for febrile neutropenia, home-based exercise is better than supervised treadmill exercise for peripheral arterial disease, and brain injury in sickle cell merits more attention.
Amazon Alexa
Apple Podcasts
Google Podcasts
Spotify
Also today, you ought to be judicious with empiric antibiotics for febrile neutropenia, home-based exercise is better than supervised treadmill exercise for peripheral arterial disease, and brain injury in sickle cell merits more attention.
Amazon Alexa
Apple Podcasts
Google Podcasts
Spotify
Also today, you ought to be judicious with empiric antibiotics for febrile neutropenia, home-based exercise is better than supervised treadmill exercise for peripheral arterial disease, and brain injury in sickle cell merits more attention.
Amazon Alexa
Apple Podcasts
Google Podcasts
Spotify
Test proves accurate for sickle cell screening
SAN DIEGO—An inexpensive, rapid, and easy-to-use blood test accurately detected sickle cell disease in young children in Uganda, according to a speaker at the 2018 ASH Annual Meeting.
The test, called HemoTypeSC, uses monoclonal antibodies to detect hemoglobins A, S, and C in a drop of whole blood.
HemoTypeSC costs less than $2 to the end user and delivers results in about 10 minutes.
“This is ideal for use in resource-constrained regions of high prevalence, such as Africa and central India,” said Erik Serrao, PhD, of Silver Lake Research in Azusa, California.
“Early screening plus treatment plus counseling equals saving millions of lives over the coming decades, and we believe HemoTypeSC can form an integral part of the initial part of this equation.”
Dr. Serrao reported results from a study of HemoTypeSC during the late-breaking abstracts session at ASH (abstract LBA-3).
He and his colleagues compared results with the HemoTypeSC test to results with hemoglobin electrophoresis for detection of the phenotypes HbAA (normal), HbAS (sickle cell trait), and HbSS (sickle cell disease).
The investigators compared these two testing methods in 1,000 children between the ages of 1 month and 5 years who were prospectively recruited from hospital wards and outpatient clinics in Uganda.
Results
The initial analysis suggested HemoTypeSC had an overall accuracy of 99.8%, correctly identifying 998 of 1,000 phenotypes as initially determined by electrophoresis.
HemoTypeSC correctly identified 100% of the 720 HbAA specimens and 100% of 182 HbAS specimens.
HemoTypeSC identified as HbSS 98% (96/98) of specimens that were identified as HbSS by electrophoresis. This left two discordant samples, both of which HemoTypeSC identified as HbAS.
Investigators subsequently discovered that both individuals with the discordant samples had previously been diagnosed with sickle cell disease and had received recent transfusions with HbAA blood.
“Therefore, the true phenotype at the time of testing for these samples was HbAS, as hemoglobin A and S were both in the blood,” Dr. Serrao said.
This brought the accuracy rate of HemoTypeSC up to 100%.
Dr. Serrao noted that this study excluded newborns. However, a different study of HemoTypeSC, recently published in the American Journal of Hematology, demonstrated 100% accuracy across multiple phenotypes in the setting of newborn screening.
Implications
Of all the late-breaking abstracts at ASH this year, the study by Dr. Serrao and his colleagues is the one with the potential to save the most lives, according to Mark Crowther, MD, of McMaster University in Hamilton, Ontario, Canada.
He said using current gold-standard methods for diagnosing sickle cell disease is, at minimum, challenging and “frankly impossible” in many low-resource settings because of the cost and the requirement for sophisticated equipment and reliable electricity.
However, he believes HemoTypeSC could change that.
“The ability to diagnose sickle cell disease early and intervene early will result in potentially thousands of infants, who would otherwise die in infancy or early childhood, surviving into adulthood,” Dr. Crowther said.
Dr. Serrao noted that sickle cell disease screening programs have been projected to be cost-effective in Africa. Such programs could even save money for governments over time as budgets are reallocated toward screening, with less money needed for treatment of patients presenting with severe complications in hospitals.
Dr. Serrao reported that he is an employee of Silver Lake Research, which funded this study, approved the study design, and donated HemoTypeSC tests.
SAN DIEGO—An inexpensive, rapid, and easy-to-use blood test accurately detected sickle cell disease in young children in Uganda, according to a speaker at the 2018 ASH Annual Meeting.
The test, called HemoTypeSC, uses monoclonal antibodies to detect hemoglobins A, S, and C in a drop of whole blood.
HemoTypeSC costs less than $2 to the end user and delivers results in about 10 minutes.
“This is ideal for use in resource-constrained regions of high prevalence, such as Africa and central India,” said Erik Serrao, PhD, of Silver Lake Research in Azusa, California.
“Early screening plus treatment plus counseling equals saving millions of lives over the coming decades, and we believe HemoTypeSC can form an integral part of the initial part of this equation.”
Dr. Serrao reported results from a study of HemoTypeSC during the late-breaking abstracts session at ASH (abstract LBA-3).
He and his colleagues compared results with the HemoTypeSC test to results with hemoglobin electrophoresis for detection of the phenotypes HbAA (normal), HbAS (sickle cell trait), and HbSS (sickle cell disease).
The investigators compared these two testing methods in 1,000 children between the ages of 1 month and 5 years who were prospectively recruited from hospital wards and outpatient clinics in Uganda.
Results
The initial analysis suggested HemoTypeSC had an overall accuracy of 99.8%, correctly identifying 998 of 1,000 phenotypes as initially determined by electrophoresis.
HemoTypeSC correctly identified 100% of the 720 HbAA specimens and 100% of 182 HbAS specimens.
HemoTypeSC identified as HbSS 98% (96/98) of specimens that were identified as HbSS by electrophoresis. This left two discordant samples, both of which HemoTypeSC identified as HbAS.
Investigators subsequently discovered that both individuals with the discordant samples had previously been diagnosed with sickle cell disease and had received recent transfusions with HbAA blood.
“Therefore, the true phenotype at the time of testing for these samples was HbAS, as hemoglobin A and S were both in the blood,” Dr. Serrao said.
This brought the accuracy rate of HemoTypeSC up to 100%.
Dr. Serrao noted that this study excluded newborns. However, a different study of HemoTypeSC, recently published in the American Journal of Hematology, demonstrated 100% accuracy across multiple phenotypes in the setting of newborn screening.
Implications
Of all the late-breaking abstracts at ASH this year, the study by Dr. Serrao and his colleagues is the one with the potential to save the most lives, according to Mark Crowther, MD, of McMaster University in Hamilton, Ontario, Canada.
He said using current gold-standard methods for diagnosing sickle cell disease is, at minimum, challenging and “frankly impossible” in many low-resource settings because of the cost and the requirement for sophisticated equipment and reliable electricity.
However, he believes HemoTypeSC could change that.
“The ability to diagnose sickle cell disease early and intervene early will result in potentially thousands of infants, who would otherwise die in infancy or early childhood, surviving into adulthood,” Dr. Crowther said.
Dr. Serrao noted that sickle cell disease screening programs have been projected to be cost-effective in Africa. Such programs could even save money for governments over time as budgets are reallocated toward screening, with less money needed for treatment of patients presenting with severe complications in hospitals.
Dr. Serrao reported that he is an employee of Silver Lake Research, which funded this study, approved the study design, and donated HemoTypeSC tests.
SAN DIEGO—An inexpensive, rapid, and easy-to-use blood test accurately detected sickle cell disease in young children in Uganda, according to a speaker at the 2018 ASH Annual Meeting.
The test, called HemoTypeSC, uses monoclonal antibodies to detect hemoglobins A, S, and C in a drop of whole blood.
HemoTypeSC costs less than $2 to the end user and delivers results in about 10 minutes.
“This is ideal for use in resource-constrained regions of high prevalence, such as Africa and central India,” said Erik Serrao, PhD, of Silver Lake Research in Azusa, California.
“Early screening plus treatment plus counseling equals saving millions of lives over the coming decades, and we believe HemoTypeSC can form an integral part of the initial part of this equation.”
Dr. Serrao reported results from a study of HemoTypeSC during the late-breaking abstracts session at ASH (abstract LBA-3).
He and his colleagues compared results with the HemoTypeSC test to results with hemoglobin electrophoresis for detection of the phenotypes HbAA (normal), HbAS (sickle cell trait), and HbSS (sickle cell disease).
The investigators compared these two testing methods in 1,000 children between the ages of 1 month and 5 years who were prospectively recruited from hospital wards and outpatient clinics in Uganda.
Results
The initial analysis suggested HemoTypeSC had an overall accuracy of 99.8%, correctly identifying 998 of 1,000 phenotypes as initially determined by electrophoresis.
HemoTypeSC correctly identified 100% of the 720 HbAA specimens and 100% of 182 HbAS specimens.
HemoTypeSC identified as HbSS 98% (96/98) of specimens that were identified as HbSS by electrophoresis. This left two discordant samples, both of which HemoTypeSC identified as HbAS.
Investigators subsequently discovered that both individuals with the discordant samples had previously been diagnosed with sickle cell disease and had received recent transfusions with HbAA blood.
“Therefore, the true phenotype at the time of testing for these samples was HbAS, as hemoglobin A and S were both in the blood,” Dr. Serrao said.
This brought the accuracy rate of HemoTypeSC up to 100%.
Dr. Serrao noted that this study excluded newborns. However, a different study of HemoTypeSC, recently published in the American Journal of Hematology, demonstrated 100% accuracy across multiple phenotypes in the setting of newborn screening.
Implications
Of all the late-breaking abstracts at ASH this year, the study by Dr. Serrao and his colleagues is the one with the potential to save the most lives, according to Mark Crowther, MD, of McMaster University in Hamilton, Ontario, Canada.
He said using current gold-standard methods for diagnosing sickle cell disease is, at minimum, challenging and “frankly impossible” in many low-resource settings because of the cost and the requirement for sophisticated equipment and reliable electricity.
However, he believes HemoTypeSC could change that.
“The ability to diagnose sickle cell disease early and intervene early will result in potentially thousands of infants, who would otherwise die in infancy or early childhood, surviving into adulthood,” Dr. Crowther said.
Dr. Serrao noted that sickle cell disease screening programs have been projected to be cost-effective in Africa. Such programs could even save money for governments over time as budgets are reallocated toward screening, with less money needed for treatment of patients presenting with severe complications in hospitals.
Dr. Serrao reported that he is an employee of Silver Lake Research, which funded this study, approved the study design, and donated HemoTypeSC tests.
ACS Academy of Master Surgeon Educators admits inaugural class of members
A total of 91 surgeons from seven countries comprised the inaugural class of esteemed surgeon educators who were admitted into the new American College of Surgeons (ACS) Academy of Master Surgeon Educators™ as Members or Associate Members. The Academy’s inaugural induction ceremony occurred on October 3 at the John B. Murphy Memorial Auditorium in Chicago, IL. Academy Members and Associate Members in attendance were publicly recognized at the annual Convocation Sunday, October 21, at the ACS Clinical Congress 2018 in Boston, MA.
Developed under the auspices of the ACS Division of Education, the Academy recognizes surgeon educators who have devoted their careers to surgical education. Individuals are selected as Members or Associate Members following stringent peer review. The Academy’s mission is to play a leadership role in advancing the science and practice of education across all surgical specialties, promoting the highest achievements in the lifetimes of surgeons. Academy membership carries an obligation for commitment to the Academy’s goals, which are to identify, recognize, and recruit innovators and thought leaders committed to advancing lifelong surgical education; translate innovation into actions; offer mentorship to surgeon educators; foster exchange of creative ideas; disseminate advances in surgical education; and positively impact the quality of surgical care and patient safety.
In addition to supporting the mission and goals of the Academy, members must actively participate in Academy programs and activities. “To start, small groups of Members and Associate Members will be assembled to work on addressing these goals. We also plan to publish an annual publication, Proceedings of the American College of Surgeons Academy of Master Surgeon Educators, which will be launched in late 2019,” said Ajit K. Sachdeva, MD, FACS, FRCSC, FSACME, Director of the ACS Division of Education and Co-Chair of the Steering Committee of the Academy.
“With highest quality patient care through education being the paramount theme of the American College of Surgeons, the establishment of the Academy of Master Surgeon Educators is an important new chapter for the ACS, the world’s largest organization for surgeons,” explained L.D. Britt, MD, MPH, DSc(Hon), FACS, FCCM, FRCSEng(Hon), FRCSEd(Hon), FWACS(Hon), FRCSI(Hon), FCS(SA)(Hon), FRCSGlasg(Hon), Past-President of the ACS and Co-Chair of the Steering Committee of the Academy.
A complete list of selected Members and Associate Members is available at www.facs.org/education/academy/2018selection.
A total of 91 surgeons from seven countries comprised the inaugural class of esteemed surgeon educators who were admitted into the new American College of Surgeons (ACS) Academy of Master Surgeon Educators™ as Members or Associate Members. The Academy’s inaugural induction ceremony occurred on October 3 at the John B. Murphy Memorial Auditorium in Chicago, IL. Academy Members and Associate Members in attendance were publicly recognized at the annual Convocation Sunday, October 21, at the ACS Clinical Congress 2018 in Boston, MA.
Developed under the auspices of the ACS Division of Education, the Academy recognizes surgeon educators who have devoted their careers to surgical education. Individuals are selected as Members or Associate Members following stringent peer review. The Academy’s mission is to play a leadership role in advancing the science and practice of education across all surgical specialties, promoting the highest achievements in the lifetimes of surgeons. Academy membership carries an obligation for commitment to the Academy’s goals, which are to identify, recognize, and recruit innovators and thought leaders committed to advancing lifelong surgical education; translate innovation into actions; offer mentorship to surgeon educators; foster exchange of creative ideas; disseminate advances in surgical education; and positively impact the quality of surgical care and patient safety.
In addition to supporting the mission and goals of the Academy, members must actively participate in Academy programs and activities. “To start, small groups of Members and Associate Members will be assembled to work on addressing these goals. We also plan to publish an annual publication, Proceedings of the American College of Surgeons Academy of Master Surgeon Educators, which will be launched in late 2019,” said Ajit K. Sachdeva, MD, FACS, FRCSC, FSACME, Director of the ACS Division of Education and Co-Chair of the Steering Committee of the Academy.
“With highest quality patient care through education being the paramount theme of the American College of Surgeons, the establishment of the Academy of Master Surgeon Educators is an important new chapter for the ACS, the world’s largest organization for surgeons,” explained L.D. Britt, MD, MPH, DSc(Hon), FACS, FCCM, FRCSEng(Hon), FRCSEd(Hon), FWACS(Hon), FRCSI(Hon), FCS(SA)(Hon), FRCSGlasg(Hon), Past-President of the ACS and Co-Chair of the Steering Committee of the Academy.
A complete list of selected Members and Associate Members is available at www.facs.org/education/academy/2018selection.
A total of 91 surgeons from seven countries comprised the inaugural class of esteemed surgeon educators who were admitted into the new American College of Surgeons (ACS) Academy of Master Surgeon Educators™ as Members or Associate Members. The Academy’s inaugural induction ceremony occurred on October 3 at the John B. Murphy Memorial Auditorium in Chicago, IL. Academy Members and Associate Members in attendance were publicly recognized at the annual Convocation Sunday, October 21, at the ACS Clinical Congress 2018 in Boston, MA.
Developed under the auspices of the ACS Division of Education, the Academy recognizes surgeon educators who have devoted their careers to surgical education. Individuals are selected as Members or Associate Members following stringent peer review. The Academy’s mission is to play a leadership role in advancing the science and practice of education across all surgical specialties, promoting the highest achievements in the lifetimes of surgeons. Academy membership carries an obligation for commitment to the Academy’s goals, which are to identify, recognize, and recruit innovators and thought leaders committed to advancing lifelong surgical education; translate innovation into actions; offer mentorship to surgeon educators; foster exchange of creative ideas; disseminate advances in surgical education; and positively impact the quality of surgical care and patient safety.
In addition to supporting the mission and goals of the Academy, members must actively participate in Academy programs and activities. “To start, small groups of Members and Associate Members will be assembled to work on addressing these goals. We also plan to publish an annual publication, Proceedings of the American College of Surgeons Academy of Master Surgeon Educators, which will be launched in late 2019,” said Ajit K. Sachdeva, MD, FACS, FRCSC, FSACME, Director of the ACS Division of Education and Co-Chair of the Steering Committee of the Academy.
“With highest quality patient care through education being the paramount theme of the American College of Surgeons, the establishment of the Academy of Master Surgeon Educators is an important new chapter for the ACS, the world’s largest organization for surgeons,” explained L.D. Britt, MD, MPH, DSc(Hon), FACS, FCCM, FRCSEng(Hon), FRCSEd(Hon), FWACS(Hon), FRCSI(Hon), FCS(SA)(Hon), FRCSGlasg(Hon), Past-President of the ACS and Co-Chair of the Steering Committee of the Academy.
A complete list of selected Members and Associate Members is available at www.facs.org/education/academy/2018selection.
Letter to the Editor: Strengthening the relationships between transferring and accepting surgeons
“Nobody is happy when a patient needs to be transferred.” As the general surgery group who receives requests for transfer of patients to our tertiary care hospital, we understand and sympathize with many of the issues raised in Dr. Puls’ article (“Rural Surgery – A view from the front lines” ‘I need to transfer this patient,” ACS Surgery News, September 2018, p. 7).
There is no doubt that sometimes patients benefit from support only available at a tertiary care center. The need can be for subspeciality surgical expertise, but many times it is driven by other available hospital-level support (critical care, interventional radiology, etc.).
Transfers are time consuming for physicians on both ends – while referring physicians have the responsibility of reaching out, accepting physicians have the responsibility of timely response to a request, regardless of other demands on their time and attention. We agree wholeheartedly with Dr. Puls’s argument that the phone call process “should not be delegated to the hospitalist or anyone else.” The benefit of speaking directly to the surgeon who has personally evaluated the patient cannot be overemphasized. When referrals for surgical care are initiated by the hospitalist or emergency department physician caring for a patient, there is almost always a lack of clarity around the surgical history, reason for transfer, and ongoing needs of the patient. It is our practice to request to speak to the surgeon who has evaluated and cared for the patient so we can fully understand the clinical course. It is the rare, typically life-threatening, situation in which we transfer patients without this crucial conversation.
Another crucial conversation, one in which the receiving physicians have room for improvement, is that of closing the loop after transfer. Dr. Puls recommended that there be periodic communication between the referring physician and the accepting physician, as well as closing the loop at the time the patient is discharged. There is a lack of “best practice” and infrastructure to support this work in many institutions, including ours, in part complicated by the variable EHRs utilized by individual hospitals. We believe the burden of this communication is shared by both parties and critical to optimal patient outcomes. At our hospital, we are currently working on standardizing this process and hope it will continue to strengthen the relationships we are building with our community surgeons.
At the end of the day, referring physicians and accepting physicians should function as team members with a shared goal – to always provide excellent surgical care to patients, by optimally matching patient needs with appropriate resources. or this reason, we disagree with Dr. Puls’ statement that “accepting physicians at larger hospitals should be treated like gold.” The work of “networking” should not be placed solely on the shoulders of rural surgeons. We believe it is best practice for the tertiary care hospital team to visit their community hospitals to better understand their resources, rather than the other way around. The Atrium Health National Surgical Quality Improvement Program Collaborative has been a valuable platform for making these connections for hospitals within our system and provides infrastructure for ongoing collaboration. Surgeons at tertiary care centers should also make themselves available for phone consultation for the complicated patient for whom a surgeon may simply need a second opinion. Not all “transfer calls” result in a transfer, and if both parties agree that the patient can continue to receive the same care at the local hospital that is often in his or her best interest.
Strengthening relationships with our community surgeons will allow surgeons at tertiary care centers to partner with them to optimally match patient needs to available resources. We truly appreciate our referring surgeons and thank them for the incredible work they do in serving our communities. Without their care on the front lines, we would not be able to provide the complex care and support to patients who need it most.
I very much appreciate the comments made by Drs. Reinke, Matthews, Paton, and Schiffern of the Carolinas Medical Center, Atrium Health, regarding my commentary on a rural surgeon’s take on transferring patients. They have provided the important perspective of the surgeon at a tertiary care center accepting a transferred patient. They also point out some of the important responsibilities that accepting surgeons have regarding the patient transfer process. If all tertiary facilities had the philosophy described by Drs. Reinke, Matthews, Paton, and Schiffern regarding patient transfers, many more patients would benefit
I agree that more easily arranged phone consultations between a rural surgeon and a tertiary surgeon regarding the need for a potential patient transfer would be helpful. Sometimes the simple reassurance from a tertiary care surgeon that the rural surgeon is doing the right thing, and the comfort the patient and his/her family derives from knowing that their surgeon has spoken with a surgeon at a tertiary care center, can be enough to prevent the need for an immediate transfer.
I also agree that “closing the loop” after a transfer is an important responsibility of both the transferring surgeon and the accepting surgeon. This is difficult partly because everyone is busy, but also because of factors such as the incompatibility of EHRs. Perhaps if part of the transfer process involved the transferring surgeon and accepting surgeon exchanging cell phone numbers and email addresses, then a quick phone call, text, or email every couple of days could help to “close the loop.
I accept their mild criticism of my statement that “accepting physicians at larger hospitals should be treated like gold” since they really are saying that there is a shared responsibility between tertiary care surgeons and rural surgeons to develop relationships that allow for the optimal care of transferred patients. I couldn’t agree more with their statement that “referring physicians and accepting physicians should function as team members with a shared goal – to always provide excellent surgical care to patients.” When we do this, we are treating the patient like gold, which is our ultimate objective.
Mark Puls, MD, FACS, is a general surgeon in Alpena, Mich. He serves as vice chair of the ACS Advisory Council for Rural Surgery. octor’s Name and Bio
I very much appreciate the comments made by Drs. Reinke, Matthews, Paton, and Schiffern of the Carolinas Medical Center, Atrium Health, regarding my commentary on a rural surgeon’s take on transferring patients. They have provided the important perspective of the surgeon at a tertiary care center accepting a transferred patient. They also point out some of the important responsibilities that accepting surgeons have regarding the patient transfer process. If all tertiary facilities had the philosophy described by Drs. Reinke, Matthews, Paton, and Schiffern regarding patient transfers, many more patients would benefit
I agree that more easily arranged phone consultations between a rural surgeon and a tertiary surgeon regarding the need for a potential patient transfer would be helpful. Sometimes the simple reassurance from a tertiary care surgeon that the rural surgeon is doing the right thing, and the comfort the patient and his/her family derives from knowing that their surgeon has spoken with a surgeon at a tertiary care center, can be enough to prevent the need for an immediate transfer.
I also agree that “closing the loop” after a transfer is an important responsibility of both the transferring surgeon and the accepting surgeon. This is difficult partly because everyone is busy, but also because of factors such as the incompatibility of EHRs. Perhaps if part of the transfer process involved the transferring surgeon and accepting surgeon exchanging cell phone numbers and email addresses, then a quick phone call, text, or email every couple of days could help to “close the loop.
I accept their mild criticism of my statement that “accepting physicians at larger hospitals should be treated like gold” since they really are saying that there is a shared responsibility between tertiary care surgeons and rural surgeons to develop relationships that allow for the optimal care of transferred patients. I couldn’t agree more with their statement that “referring physicians and accepting physicians should function as team members with a shared goal – to always provide excellent surgical care to patients.” When we do this, we are treating the patient like gold, which is our ultimate objective.
Mark Puls, MD, FACS, is a general surgeon in Alpena, Mich. He serves as vice chair of the ACS Advisory Council for Rural Surgery. octor’s Name and Bio
I very much appreciate the comments made by Drs. Reinke, Matthews, Paton, and Schiffern of the Carolinas Medical Center, Atrium Health, regarding my commentary on a rural surgeon’s take on transferring patients. They have provided the important perspective of the surgeon at a tertiary care center accepting a transferred patient. They also point out some of the important responsibilities that accepting surgeons have regarding the patient transfer process. If all tertiary facilities had the philosophy described by Drs. Reinke, Matthews, Paton, and Schiffern regarding patient transfers, many more patients would benefit
I agree that more easily arranged phone consultations between a rural surgeon and a tertiary surgeon regarding the need for a potential patient transfer would be helpful. Sometimes the simple reassurance from a tertiary care surgeon that the rural surgeon is doing the right thing, and the comfort the patient and his/her family derives from knowing that their surgeon has spoken with a surgeon at a tertiary care center, can be enough to prevent the need for an immediate transfer.
I also agree that “closing the loop” after a transfer is an important responsibility of both the transferring surgeon and the accepting surgeon. This is difficult partly because everyone is busy, but also because of factors such as the incompatibility of EHRs. Perhaps if part of the transfer process involved the transferring surgeon and accepting surgeon exchanging cell phone numbers and email addresses, then a quick phone call, text, or email every couple of days could help to “close the loop.
I accept their mild criticism of my statement that “accepting physicians at larger hospitals should be treated like gold” since they really are saying that there is a shared responsibility between tertiary care surgeons and rural surgeons to develop relationships that allow for the optimal care of transferred patients. I couldn’t agree more with their statement that “referring physicians and accepting physicians should function as team members with a shared goal – to always provide excellent surgical care to patients.” When we do this, we are treating the patient like gold, which is our ultimate objective.
Mark Puls, MD, FACS, is a general surgeon in Alpena, Mich. He serves as vice chair of the ACS Advisory Council for Rural Surgery. octor’s Name and Bio
“Nobody is happy when a patient needs to be transferred.” As the general surgery group who receives requests for transfer of patients to our tertiary care hospital, we understand and sympathize with many of the issues raised in Dr. Puls’ article (“Rural Surgery – A view from the front lines” ‘I need to transfer this patient,” ACS Surgery News, September 2018, p. 7).
There is no doubt that sometimes patients benefit from support only available at a tertiary care center. The need can be for subspeciality surgical expertise, but many times it is driven by other available hospital-level support (critical care, interventional radiology, etc.).
Transfers are time consuming for physicians on both ends – while referring physicians have the responsibility of reaching out, accepting physicians have the responsibility of timely response to a request, regardless of other demands on their time and attention. We agree wholeheartedly with Dr. Puls’s argument that the phone call process “should not be delegated to the hospitalist or anyone else.” The benefit of speaking directly to the surgeon who has personally evaluated the patient cannot be overemphasized. When referrals for surgical care are initiated by the hospitalist or emergency department physician caring for a patient, there is almost always a lack of clarity around the surgical history, reason for transfer, and ongoing needs of the patient. It is our practice to request to speak to the surgeon who has evaluated and cared for the patient so we can fully understand the clinical course. It is the rare, typically life-threatening, situation in which we transfer patients without this crucial conversation.
Another crucial conversation, one in which the receiving physicians have room for improvement, is that of closing the loop after transfer. Dr. Puls recommended that there be periodic communication between the referring physician and the accepting physician, as well as closing the loop at the time the patient is discharged. There is a lack of “best practice” and infrastructure to support this work in many institutions, including ours, in part complicated by the variable EHRs utilized by individual hospitals. We believe the burden of this communication is shared by both parties and critical to optimal patient outcomes. At our hospital, we are currently working on standardizing this process and hope it will continue to strengthen the relationships we are building with our community surgeons.
At the end of the day, referring physicians and accepting physicians should function as team members with a shared goal – to always provide excellent surgical care to patients, by optimally matching patient needs with appropriate resources. or this reason, we disagree with Dr. Puls’ statement that “accepting physicians at larger hospitals should be treated like gold.” The work of “networking” should not be placed solely on the shoulders of rural surgeons. We believe it is best practice for the tertiary care hospital team to visit their community hospitals to better understand their resources, rather than the other way around. The Atrium Health National Surgical Quality Improvement Program Collaborative has been a valuable platform for making these connections for hospitals within our system and provides infrastructure for ongoing collaboration. Surgeons at tertiary care centers should also make themselves available for phone consultation for the complicated patient for whom a surgeon may simply need a second opinion. Not all “transfer calls” result in a transfer, and if both parties agree that the patient can continue to receive the same care at the local hospital that is often in his or her best interest.
Strengthening relationships with our community surgeons will allow surgeons at tertiary care centers to partner with them to optimally match patient needs to available resources. We truly appreciate our referring surgeons and thank them for the incredible work they do in serving our communities. Without their care on the front lines, we would not be able to provide the complex care and support to patients who need it most.
“Nobody is happy when a patient needs to be transferred.” As the general surgery group who receives requests for transfer of patients to our tertiary care hospital, we understand and sympathize with many of the issues raised in Dr. Puls’ article (“Rural Surgery – A view from the front lines” ‘I need to transfer this patient,” ACS Surgery News, September 2018, p. 7).
There is no doubt that sometimes patients benefit from support only available at a tertiary care center. The need can be for subspeciality surgical expertise, but many times it is driven by other available hospital-level support (critical care, interventional radiology, etc.).
Transfers are time consuming for physicians on both ends – while referring physicians have the responsibility of reaching out, accepting physicians have the responsibility of timely response to a request, regardless of other demands on their time and attention. We agree wholeheartedly with Dr. Puls’s argument that the phone call process “should not be delegated to the hospitalist or anyone else.” The benefit of speaking directly to the surgeon who has personally evaluated the patient cannot be overemphasized. When referrals for surgical care are initiated by the hospitalist or emergency department physician caring for a patient, there is almost always a lack of clarity around the surgical history, reason for transfer, and ongoing needs of the patient. It is our practice to request to speak to the surgeon who has evaluated and cared for the patient so we can fully understand the clinical course. It is the rare, typically life-threatening, situation in which we transfer patients without this crucial conversation.
Another crucial conversation, one in which the receiving physicians have room for improvement, is that of closing the loop after transfer. Dr. Puls recommended that there be periodic communication between the referring physician and the accepting physician, as well as closing the loop at the time the patient is discharged. There is a lack of “best practice” and infrastructure to support this work in many institutions, including ours, in part complicated by the variable EHRs utilized by individual hospitals. We believe the burden of this communication is shared by both parties and critical to optimal patient outcomes. At our hospital, we are currently working on standardizing this process and hope it will continue to strengthen the relationships we are building with our community surgeons.
At the end of the day, referring physicians and accepting physicians should function as team members with a shared goal – to always provide excellent surgical care to patients, by optimally matching patient needs with appropriate resources. or this reason, we disagree with Dr. Puls’ statement that “accepting physicians at larger hospitals should be treated like gold.” The work of “networking” should not be placed solely on the shoulders of rural surgeons. We believe it is best practice for the tertiary care hospital team to visit their community hospitals to better understand their resources, rather than the other way around. The Atrium Health National Surgical Quality Improvement Program Collaborative has been a valuable platform for making these connections for hospitals within our system and provides infrastructure for ongoing collaboration. Surgeons at tertiary care centers should also make themselves available for phone consultation for the complicated patient for whom a surgeon may simply need a second opinion. Not all “transfer calls” result in a transfer, and if both parties agree that the patient can continue to receive the same care at the local hospital that is often in his or her best interest.
Strengthening relationships with our community surgeons will allow surgeons at tertiary care centers to partner with them to optimally match patient needs to available resources. We truly appreciate our referring surgeons and thank them for the incredible work they do in serving our communities. Without their care on the front lines, we would not be able to provide the complex care and support to patients who need it most.
The Right Choice? A New Chapter
As I write this last installment of “The Right Choice?” for ACS Surgery News, a number of different emotions are going through my mind all at the same time. I am surprised at how quickly the time has passed since I wrote my first surgical ethics column for SN in 2011. In the 33 columns that I have written since then, I have tried to focus on aspects of surgical practice that emphasize the ethical dimension. I have tried to write columns that would be of interest to practicing surgeons in any setting and not only to academic surgeons that practice in urban environments such as I practice in. This is the last column and thus the end of a chapter of my life and the beginning of a new one.
Over the last 7 years, I have been flattered by the comments from fellow surgeons who report that they actually read the column. I have always said that I wrote this column with the expectation that no one would actually read them. I have to confess that this is not completely true. As I wrote each column, I did so as though I was writing them for my father to read. My father, S. Peter Angelos, MD, FACS, was a general surgeon who spent his entire career practicing in the town of Plattsburgh, N.Y., where he grew up. My father’s practice was very different from mine. I work at an urban academic medical center where I have a very narrow subspecialty practice in endocrine surgery. My father had a small-town community practice of “bread and butter” general surgery. Yet, when he and I would talk about patients, the commonality of the relationship between a surgeon and a patient transcended these differences. I realize that in many ways, I wrote this column as a way of organizing my own thoughts and then presenting them to my father in the hopes that he would find them of some value.
For several years, I would send drafts of my column to my parents, and both my father and mother would read them and give me suggestions. Many of the earlier columns were changed for the better by their comments. In recent years, my father’s health declined and he was no longer able to give me comments. Nevertheless, I continued to compose them as though writing for him. Approximately 6 weeks ago, my father passed away. It has been sad for my mother and my entire family. We all realized that it was the end of one chapter of our lives and the start of a new one without my father.
I find the concept of “beginning a new chapter” to be an important one for surgeons to reflect upon. There are certain events, such as the death of a parent, that force us to think about the end of one phase of life and the beginning of another phase. However, the division of one’s experience into phases or chapters, is somewhat arbitrary. This past summer I became a patient and had surgery myself for the first time. I cannot help but think of that operation as the start of a new chapter for me. I am convinced that although all patients may not reflect upon surgery in the same way that I did, nevertheless, an operation is a dramatic event that most people remember for a long time. In this context, many people will see their interactions with their surgeon and their operation as the end of one chapter and the beginning of a new one.
In this context, it is critical for surgeons to be fully cognizant of the great impact that we may have on our patient’s internal narratives of their lives. When we operate on someone, we run the risk of that person’s functional status changing forever. We may be the means by which our patient is cured of cancer or suffers a debilitating complication. As surgeons, we therefore, occupy a potentially significant role in the trajectory of our patients’ lives. I believe that the relationship between a surgeon and a patient is distinctive and central in the narrative that so many patients create about their lives. It is essential that surgeons continue to appreciate the value of the quality of that relationship with our patients and the impact—potentially positive or negative—that it can have upon our patients.
Throughout medicine, in general, and in surgery in particular, one cannot go a week without hearing about the problem of burnout. Although there is no single cure for burnout, I do believe that paying attention to the ethical dimension of our interactions with our patients and the impact that surgery can have on their lives will go a long way to reducing the risks of burnout among surgeons.
In an era in which we are often pushed to increase RVUs at the expense of spending time with individual patients, we must not forget how significant our relationships with our patients can be. I believe that attention to this relationship will be beneficial to patients and also to us as we help our patients start new chapters in their lives.
Dr. Angelos is the Linda Kohler Anderson Professor of Surgery and Surgical Ethics, chief of endocrine surgery, and associate director of the MacLean Center for Clinical Medical Ethics at the University of Chicago.
As I write this last installment of “The Right Choice?” for ACS Surgery News, a number of different emotions are going through my mind all at the same time. I am surprised at how quickly the time has passed since I wrote my first surgical ethics column for SN in 2011. In the 33 columns that I have written since then, I have tried to focus on aspects of surgical practice that emphasize the ethical dimension. I have tried to write columns that would be of interest to practicing surgeons in any setting and not only to academic surgeons that practice in urban environments such as I practice in. This is the last column and thus the end of a chapter of my life and the beginning of a new one.
Over the last 7 years, I have been flattered by the comments from fellow surgeons who report that they actually read the column. I have always said that I wrote this column with the expectation that no one would actually read them. I have to confess that this is not completely true. As I wrote each column, I did so as though I was writing them for my father to read. My father, S. Peter Angelos, MD, FACS, was a general surgeon who spent his entire career practicing in the town of Plattsburgh, N.Y., where he grew up. My father’s practice was very different from mine. I work at an urban academic medical center where I have a very narrow subspecialty practice in endocrine surgery. My father had a small-town community practice of “bread and butter” general surgery. Yet, when he and I would talk about patients, the commonality of the relationship between a surgeon and a patient transcended these differences. I realize that in many ways, I wrote this column as a way of organizing my own thoughts and then presenting them to my father in the hopes that he would find them of some value.
For several years, I would send drafts of my column to my parents, and both my father and mother would read them and give me suggestions. Many of the earlier columns were changed for the better by their comments. In recent years, my father’s health declined and he was no longer able to give me comments. Nevertheless, I continued to compose them as though writing for him. Approximately 6 weeks ago, my father passed away. It has been sad for my mother and my entire family. We all realized that it was the end of one chapter of our lives and the start of a new one without my father.
I find the concept of “beginning a new chapter” to be an important one for surgeons to reflect upon. There are certain events, such as the death of a parent, that force us to think about the end of one phase of life and the beginning of another phase. However, the division of one’s experience into phases or chapters, is somewhat arbitrary. This past summer I became a patient and had surgery myself for the first time. I cannot help but think of that operation as the start of a new chapter for me. I am convinced that although all patients may not reflect upon surgery in the same way that I did, nevertheless, an operation is a dramatic event that most people remember for a long time. In this context, many people will see their interactions with their surgeon and their operation as the end of one chapter and the beginning of a new one.
In this context, it is critical for surgeons to be fully cognizant of the great impact that we may have on our patient’s internal narratives of their lives. When we operate on someone, we run the risk of that person’s functional status changing forever. We may be the means by which our patient is cured of cancer or suffers a debilitating complication. As surgeons, we therefore, occupy a potentially significant role in the trajectory of our patients’ lives. I believe that the relationship between a surgeon and a patient is distinctive and central in the narrative that so many patients create about their lives. It is essential that surgeons continue to appreciate the value of the quality of that relationship with our patients and the impact—potentially positive or negative—that it can have upon our patients.
Throughout medicine, in general, and in surgery in particular, one cannot go a week without hearing about the problem of burnout. Although there is no single cure for burnout, I do believe that paying attention to the ethical dimension of our interactions with our patients and the impact that surgery can have on their lives will go a long way to reducing the risks of burnout among surgeons.
In an era in which we are often pushed to increase RVUs at the expense of spending time with individual patients, we must not forget how significant our relationships with our patients can be. I believe that attention to this relationship will be beneficial to patients and also to us as we help our patients start new chapters in their lives.
Dr. Angelos is the Linda Kohler Anderson Professor of Surgery and Surgical Ethics, chief of endocrine surgery, and associate director of the MacLean Center for Clinical Medical Ethics at the University of Chicago.
As I write this last installment of “The Right Choice?” for ACS Surgery News, a number of different emotions are going through my mind all at the same time. I am surprised at how quickly the time has passed since I wrote my first surgical ethics column for SN in 2011. In the 33 columns that I have written since then, I have tried to focus on aspects of surgical practice that emphasize the ethical dimension. I have tried to write columns that would be of interest to practicing surgeons in any setting and not only to academic surgeons that practice in urban environments such as I practice in. This is the last column and thus the end of a chapter of my life and the beginning of a new one.
Over the last 7 years, I have been flattered by the comments from fellow surgeons who report that they actually read the column. I have always said that I wrote this column with the expectation that no one would actually read them. I have to confess that this is not completely true. As I wrote each column, I did so as though I was writing them for my father to read. My father, S. Peter Angelos, MD, FACS, was a general surgeon who spent his entire career practicing in the town of Plattsburgh, N.Y., where he grew up. My father’s practice was very different from mine. I work at an urban academic medical center where I have a very narrow subspecialty practice in endocrine surgery. My father had a small-town community practice of “bread and butter” general surgery. Yet, when he and I would talk about patients, the commonality of the relationship between a surgeon and a patient transcended these differences. I realize that in many ways, I wrote this column as a way of organizing my own thoughts and then presenting them to my father in the hopes that he would find them of some value.
For several years, I would send drafts of my column to my parents, and both my father and mother would read them and give me suggestions. Many of the earlier columns were changed for the better by their comments. In recent years, my father’s health declined and he was no longer able to give me comments. Nevertheless, I continued to compose them as though writing for him. Approximately 6 weeks ago, my father passed away. It has been sad for my mother and my entire family. We all realized that it was the end of one chapter of our lives and the start of a new one without my father.
I find the concept of “beginning a new chapter” to be an important one for surgeons to reflect upon. There are certain events, such as the death of a parent, that force us to think about the end of one phase of life and the beginning of another phase. However, the division of one’s experience into phases or chapters, is somewhat arbitrary. This past summer I became a patient and had surgery myself for the first time. I cannot help but think of that operation as the start of a new chapter for me. I am convinced that although all patients may not reflect upon surgery in the same way that I did, nevertheless, an operation is a dramatic event that most people remember for a long time. In this context, many people will see their interactions with their surgeon and their operation as the end of one chapter and the beginning of a new one.
In this context, it is critical for surgeons to be fully cognizant of the great impact that we may have on our patient’s internal narratives of their lives. When we operate on someone, we run the risk of that person’s functional status changing forever. We may be the means by which our patient is cured of cancer or suffers a debilitating complication. As surgeons, we therefore, occupy a potentially significant role in the trajectory of our patients’ lives. I believe that the relationship between a surgeon and a patient is distinctive and central in the narrative that so many patients create about their lives. It is essential that surgeons continue to appreciate the value of the quality of that relationship with our patients and the impact—potentially positive or negative—that it can have upon our patients.
Throughout medicine, in general, and in surgery in particular, one cannot go a week without hearing about the problem of burnout. Although there is no single cure for burnout, I do believe that paying attention to the ethical dimension of our interactions with our patients and the impact that surgery can have on their lives will go a long way to reducing the risks of burnout among surgeons.
In an era in which we are often pushed to increase RVUs at the expense of spending time with individual patients, we must not forget how significant our relationships with our patients can be. I believe that attention to this relationship will be beneficial to patients and also to us as we help our patients start new chapters in their lives.
Dr. Angelos is the Linda Kohler Anderson Professor of Surgery and Surgical Ethics, chief of endocrine surgery, and associate director of the MacLean Center for Clinical Medical Ethics at the University of Chicago.