User login
Alzheimer’s and Comorbidities: Implications for Patient Care
Alzheimer’s disease (AD), the most common cause of dementia, is the fifth leading cause of death in the United States. An estimated 6.9 million Americans aged 65 years or older have AD. Comorbid conditions in AD may exacerbate the progression of dementia and negatively affect overall health.
Although the exact mechanisms remain unclear, systemic inflammation is thought to play a significant role in the development of many common comorbidities associated with AD. Among the most frequently observed comorbid conditions are hypertension, diabetes, and depression. The presence of these comorbidities affects the treatment and management of AD, underscoring the need to understand the mechanisms of their interrelationship and develop effective management strategies.
Hypertension
Hypertension is a well-established risk factor for numerous health conditions, including AD. A comprehensive review of five meta-analyses and 52 primary studies revealed that elevated systolic blood pressure (SBP) correlates with an 11 % increased risk of developing AD, raising the question of whether early intervention and control of blood pressure would mitigate the risk for AD later in life.
Findings from the Northern Manhattan Study suggest that although elevated SBP contributes to cognitive decline in older patients, the use of antihypertensive medications can neutralize the effects of high SBP on certain cognitive functions. Furthermore, a systematic review and meta-analysis comprising 12 trials (92,135 participants) demonstrated a significant reduction in the risk for dementia and cognitive impairment with antihypertensive treatment.
Notably, a retrospective cohort study involving 69,081 participants treated with beta-blockers for hypertension found that beta-blockers with high blood-brain barrier permeability were associated with a reduced risk for AD compared with those with low blood-brain barrier permeability. Additionally, a secondary analysis of the SPRINT trial found antihypertensive medications that stimulate vs inhibit type 2 and 4 angiotensin II receptors were associated with a lower incidence of cognitive impairment. Although further clinical trials are necessary to directly assess specific medications, these findings emphasize the potential of antihypertensive treatment as a strategic approach to reduce the risk for AD.
Type 2 Diabetes
The connection between AD and type 2 diabetes is such that AD is sometimes referred to as “type 3 diabetes.” Both diseases share some of the same underlying pathophysiologic mechanisms, particularly the development of insulin resistance and oxidative stress. A prospective cohort study of 10,095 participants showed that diabetes was significantly associated with a higher risk of developing dementia; this risk is even greater in patients who develop diabetes at an earlier age.
In an interview with this news organization, Alvaro Pascual-Leone, MD, PhD, a professor of neurology at Harvard Medical School, Boston, said, “In addition to being a comorbidity factor, diabetes appears to be a predisposing risk factor for AD.” This is supported by a comprehensive literature review showing an increased progression from mild cognitive impairment (MCI) to dementia in patients with diabetes, prediabetes, or metabolic syndrome, with a pooled odds ratio for dementia progression in individuals with diabetes of 1.53.
Owing to the overlapping pathophysiologic mechanisms in AD and diabetes, treating one condition may have beneficial effects on the other. A systematic umbrella review and meta-analysis that included 10 meta-analyses across nine classes of diabetes drugs found a protective effect against dementia with the use of metformin, thiazolidinediones (including pioglitazone), glucagon-like peptide 1 receptor agonists, and sodium-glucose cotransporter 2 inhibitors. Moreover, a cohort study of 12,220 patients who discontinued metformin early (ie, stopped using metformin without a prior history of abnormal kidney function) and 29,126 patients considered routine users found an increased risk for dementia in the early terminator group. Although further research is warranted, the concurrent treatment of AD and diabetes with antidiabetic agents holds considerable promise.
Depression and Anxiety
Anxiety and depression are significant risk factors for AD, and conversely, AD increases the likelihood of developing these psychiatric conditions. A systematic review of 14,760 studies showed dysthymia often emerges during the early stages of AD as an emotional response to cognitive decline.
Data from the Australian Imaging Biomarkers and Lifestyle study showed a markedly elevated risk for AD and MCI among individuals with preexisting anxiety or depression. This study also found that age, sex, and marital status are important determinants, with men and single individuals with depression being particularly susceptible to developing AD. Conversely, a cohort study of 129,410 AD patients with AD, 390,088 patients with all-cause dementia, and 3,900,880 age-matched controls without a history of depression showed a cumulative incidence of depression of 13% in the AD group vs 3% in the control group, suggesting a heightened risk for depression following an AD diagnosis.
These findings underscore the importance of targeted screening and assessment for patients with anxiety and depression who may be at risk for AD or those diagnosed with AD who are at risk for subsequent depression and anxiety. Although antidepressants are effective in treating depression in general, their efficacy in AD-related depression is of variable quality, probably owing to differing pathophysiologic mechanisms of the disease. Further research is necessary to explore both pharmacologic and nonpharmacologic interventions for treating depression in AD patients. Some studies have found that cognitive behavioral-therapy can be effective in improving depression in patients with AD.
Sleep Disorders
Research has shown a strong correlation between AD and sleep disorders, particularly obstructive sleep apnea, insomnia, and circadian rhythm disruptions. Additionally, studies suggest that insomnia and sleep deprivation contribute to increased amyloid beta production and tau pathology, hallmark features of AD. A scoping review of 70 studies proposed that this relationship is mediated by the glymphatic system (glial-dependent waste clearance pathway in the central nervous system), and that sleep deprivation disrupts its function, leading to protein accumulation and subsequent neurologic symptoms of AD. Another study showed that sleep deprivation triggers glial cell activation, initiating an inflammatory cascade that accelerates AD progression.
Given that the gold standard treatment for obstructive sleep apnea is continuous positive airway pressure (CPAP), it has been hypothesized that CPAP could also alleviate AD symptoms owing to shared pathophysiologic mechanisms of these conditions. A large systemic review found that CPAP use improved AD symptoms in patients with mild AD or MCI, though other sleep interventions, such as cognitive-behavioral therapy and melatonin supplementation, have yielded mixed outcomes. However, most studies in this area are small in scale, and there remains a paucity of research on treating sleep disorders in AD patients, indicating a need for further investigation.
Musculoskeletal Disorders
Although no direct causative link has been established, research indicates an association between osteoarthritis (OA) and dementia, likely because of similar pathophysiologic mechanisms, including systemic inflammation. Longitudinal analyses of data from the Alzheimer’s Disease Neuroimaging Initiative study found cognitively normal older individuals with OA experience more rapid declines in hippocampal volumes compared to those without OA, suggesting that OA may elevate the risk of cognitive impairment. Current treatments for OA, such as nonsteroidal anti-inflammatory drugs, glucocorticoids, and disease-modifying OA drugs, might also help alleviate AD symptoms related to inflammation, though the research in this area is limited.
AD has also been linked to osteoporosis. In a longitudinal follow-up study involving 78,994 patients with osteoporosis and 78,994 controls, AD developed in 5856 patients with osteoporosis compared with 3761 patients in the control group. These findings represent a 1.27-fold higher incidence of AD in patients with osteoporosis than in the control group, suggesting that osteoporosis might be a risk factor for AD.
Additionally, research has identified a relationship between AD and increased fracture risk and decreased bone mineral density, with AD patients exhibiting a significantly higher likelihood of bone fractures compared with those without AD. “Falls and fractures, aside from the risk they pose in all geriatric patients, in individuals with cognitive impairment — whether due to AD or another cause — have higher risk to cause delirium and that can result in greater morbidity and mortality and a lasting increase in cognitive disability,” stated Dr. Pascual-Leone. Current recommendations emphasize exercise and fall prevention strategies to reduce fracture risk in patients with AD, but there is a lack of comprehensive research on the safety and efficacy of osteoporosis medications in this population.
Implications for Clinical Practice
The intricate interplay between AD and its comorbidities highlights the need for a comprehensive and integrated approach to patient care. The overlapping pathophysiologic mechanisms suggest that these comorbidities can contribute to the evolution and progression of AD. Likewise, AD can exacerbate comorbid conditions. As such, a holistic assessment strategy that prioritizes early detection and management of comorbid conditions to mitigate their impact on AD progression would be beneficial. Dr. Pascual-Leone added, “The presence of any of these comorbidities suggests a need to screen for MCI earlier than might otherwise be indicated or as part of the treatment for the comorbid condition. In many cases, patients can make lifestyle modifications that improve not only the comorbid condition but also reduce its effect on dementia.” In doing so, healthcare providers can help improve patient outcomes and enhance the overall quality of life for individuals living with AD.
Alissa Hershberger, Professor of Nursing, University of Central Missouri, Lee’s Summit, Missouri, has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Alzheimer’s disease (AD), the most common cause of dementia, is the fifth leading cause of death in the United States. An estimated 6.9 million Americans aged 65 years or older have AD. Comorbid conditions in AD may exacerbate the progression of dementia and negatively affect overall health.
Although the exact mechanisms remain unclear, systemic inflammation is thought to play a significant role in the development of many common comorbidities associated with AD. Among the most frequently observed comorbid conditions are hypertension, diabetes, and depression. The presence of these comorbidities affects the treatment and management of AD, underscoring the need to understand the mechanisms of their interrelationship and develop effective management strategies.
Hypertension
Hypertension is a well-established risk factor for numerous health conditions, including AD. A comprehensive review of five meta-analyses and 52 primary studies revealed that elevated systolic blood pressure (SBP) correlates with an 11 % increased risk of developing AD, raising the question of whether early intervention and control of blood pressure would mitigate the risk for AD later in life.
Findings from the Northern Manhattan Study suggest that although elevated SBP contributes to cognitive decline in older patients, the use of antihypertensive medications can neutralize the effects of high SBP on certain cognitive functions. Furthermore, a systematic review and meta-analysis comprising 12 trials (92,135 participants) demonstrated a significant reduction in the risk for dementia and cognitive impairment with antihypertensive treatment.
Notably, a retrospective cohort study involving 69,081 participants treated with beta-blockers for hypertension found that beta-blockers with high blood-brain barrier permeability were associated with a reduced risk for AD compared with those with low blood-brain barrier permeability. Additionally, a secondary analysis of the SPRINT trial found antihypertensive medications that stimulate vs inhibit type 2 and 4 angiotensin II receptors were associated with a lower incidence of cognitive impairment. Although further clinical trials are necessary to directly assess specific medications, these findings emphasize the potential of antihypertensive treatment as a strategic approach to reduce the risk for AD.
Type 2 Diabetes
The connection between AD and type 2 diabetes is such that AD is sometimes referred to as “type 3 diabetes.” Both diseases share some of the same underlying pathophysiologic mechanisms, particularly the development of insulin resistance and oxidative stress. A prospective cohort study of 10,095 participants showed that diabetes was significantly associated with a higher risk of developing dementia; this risk is even greater in patients who develop diabetes at an earlier age.
In an interview with this news organization, Alvaro Pascual-Leone, MD, PhD, a professor of neurology at Harvard Medical School, Boston, said, “In addition to being a comorbidity factor, diabetes appears to be a predisposing risk factor for AD.” This is supported by a comprehensive literature review showing an increased progression from mild cognitive impairment (MCI) to dementia in patients with diabetes, prediabetes, or metabolic syndrome, with a pooled odds ratio for dementia progression in individuals with diabetes of 1.53.
Owing to the overlapping pathophysiologic mechanisms in AD and diabetes, treating one condition may have beneficial effects on the other. A systematic umbrella review and meta-analysis that included 10 meta-analyses across nine classes of diabetes drugs found a protective effect against dementia with the use of metformin, thiazolidinediones (including pioglitazone), glucagon-like peptide 1 receptor agonists, and sodium-glucose cotransporter 2 inhibitors. Moreover, a cohort study of 12,220 patients who discontinued metformin early (ie, stopped using metformin without a prior history of abnormal kidney function) and 29,126 patients considered routine users found an increased risk for dementia in the early terminator group. Although further research is warranted, the concurrent treatment of AD and diabetes with antidiabetic agents holds considerable promise.
Depression and Anxiety
Anxiety and depression are significant risk factors for AD, and conversely, AD increases the likelihood of developing these psychiatric conditions. A systematic review of 14,760 studies showed dysthymia often emerges during the early stages of AD as an emotional response to cognitive decline.
Data from the Australian Imaging Biomarkers and Lifestyle study showed a markedly elevated risk for AD and MCI among individuals with preexisting anxiety or depression. This study also found that age, sex, and marital status are important determinants, with men and single individuals with depression being particularly susceptible to developing AD. Conversely, a cohort study of 129,410 AD patients with AD, 390,088 patients with all-cause dementia, and 3,900,880 age-matched controls without a history of depression showed a cumulative incidence of depression of 13% in the AD group vs 3% in the control group, suggesting a heightened risk for depression following an AD diagnosis.
These findings underscore the importance of targeted screening and assessment for patients with anxiety and depression who may be at risk for AD or those diagnosed with AD who are at risk for subsequent depression and anxiety. Although antidepressants are effective in treating depression in general, their efficacy in AD-related depression is of variable quality, probably owing to differing pathophysiologic mechanisms of the disease. Further research is necessary to explore both pharmacologic and nonpharmacologic interventions for treating depression in AD patients. Some studies have found that cognitive behavioral-therapy can be effective in improving depression in patients with AD.
Sleep Disorders
Research has shown a strong correlation between AD and sleep disorders, particularly obstructive sleep apnea, insomnia, and circadian rhythm disruptions. Additionally, studies suggest that insomnia and sleep deprivation contribute to increased amyloid beta production and tau pathology, hallmark features of AD. A scoping review of 70 studies proposed that this relationship is mediated by the glymphatic system (glial-dependent waste clearance pathway in the central nervous system), and that sleep deprivation disrupts its function, leading to protein accumulation and subsequent neurologic symptoms of AD. Another study showed that sleep deprivation triggers glial cell activation, initiating an inflammatory cascade that accelerates AD progression.
Given that the gold standard treatment for obstructive sleep apnea is continuous positive airway pressure (CPAP), it has been hypothesized that CPAP could also alleviate AD symptoms owing to shared pathophysiologic mechanisms of these conditions. A large systemic review found that CPAP use improved AD symptoms in patients with mild AD or MCI, though other sleep interventions, such as cognitive-behavioral therapy and melatonin supplementation, have yielded mixed outcomes. However, most studies in this area are small in scale, and there remains a paucity of research on treating sleep disorders in AD patients, indicating a need for further investigation.
Musculoskeletal Disorders
Although no direct causative link has been established, research indicates an association between osteoarthritis (OA) and dementia, likely because of similar pathophysiologic mechanisms, including systemic inflammation. Longitudinal analyses of data from the Alzheimer’s Disease Neuroimaging Initiative study found cognitively normal older individuals with OA experience more rapid declines in hippocampal volumes compared to those without OA, suggesting that OA may elevate the risk of cognitive impairment. Current treatments for OA, such as nonsteroidal anti-inflammatory drugs, glucocorticoids, and disease-modifying OA drugs, might also help alleviate AD symptoms related to inflammation, though the research in this area is limited.
AD has also been linked to osteoporosis. In a longitudinal follow-up study involving 78,994 patients with osteoporosis and 78,994 controls, AD developed in 5856 patients with osteoporosis compared with 3761 patients in the control group. These findings represent a 1.27-fold higher incidence of AD in patients with osteoporosis than in the control group, suggesting that osteoporosis might be a risk factor for AD.
Additionally, research has identified a relationship between AD and increased fracture risk and decreased bone mineral density, with AD patients exhibiting a significantly higher likelihood of bone fractures compared with those without AD. “Falls and fractures, aside from the risk they pose in all geriatric patients, in individuals with cognitive impairment — whether due to AD or another cause — have higher risk to cause delirium and that can result in greater morbidity and mortality and a lasting increase in cognitive disability,” stated Dr. Pascual-Leone. Current recommendations emphasize exercise and fall prevention strategies to reduce fracture risk in patients with AD, but there is a lack of comprehensive research on the safety and efficacy of osteoporosis medications in this population.
Implications for Clinical Practice
The intricate interplay between AD and its comorbidities highlights the need for a comprehensive and integrated approach to patient care. The overlapping pathophysiologic mechanisms suggest that these comorbidities can contribute to the evolution and progression of AD. Likewise, AD can exacerbate comorbid conditions. As such, a holistic assessment strategy that prioritizes early detection and management of comorbid conditions to mitigate their impact on AD progression would be beneficial. Dr. Pascual-Leone added, “The presence of any of these comorbidities suggests a need to screen for MCI earlier than might otherwise be indicated or as part of the treatment for the comorbid condition. In many cases, patients can make lifestyle modifications that improve not only the comorbid condition but also reduce its effect on dementia.” In doing so, healthcare providers can help improve patient outcomes and enhance the overall quality of life for individuals living with AD.
Alissa Hershberger, Professor of Nursing, University of Central Missouri, Lee’s Summit, Missouri, has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Alzheimer’s disease (AD), the most common cause of dementia, is the fifth leading cause of death in the United States. An estimated 6.9 million Americans aged 65 years or older have AD. Comorbid conditions in AD may exacerbate the progression of dementia and negatively affect overall health.
Although the exact mechanisms remain unclear, systemic inflammation is thought to play a significant role in the development of many common comorbidities associated with AD. Among the most frequently observed comorbid conditions are hypertension, diabetes, and depression. The presence of these comorbidities affects the treatment and management of AD, underscoring the need to understand the mechanisms of their interrelationship and develop effective management strategies.
Hypertension
Hypertension is a well-established risk factor for numerous health conditions, including AD. A comprehensive review of five meta-analyses and 52 primary studies revealed that elevated systolic blood pressure (SBP) correlates with an 11 % increased risk of developing AD, raising the question of whether early intervention and control of blood pressure would mitigate the risk for AD later in life.
Findings from the Northern Manhattan Study suggest that although elevated SBP contributes to cognitive decline in older patients, the use of antihypertensive medications can neutralize the effects of high SBP on certain cognitive functions. Furthermore, a systematic review and meta-analysis comprising 12 trials (92,135 participants) demonstrated a significant reduction in the risk for dementia and cognitive impairment with antihypertensive treatment.
Notably, a retrospective cohort study involving 69,081 participants treated with beta-blockers for hypertension found that beta-blockers with high blood-brain barrier permeability were associated with a reduced risk for AD compared with those with low blood-brain barrier permeability. Additionally, a secondary analysis of the SPRINT trial found antihypertensive medications that stimulate vs inhibit type 2 and 4 angiotensin II receptors were associated with a lower incidence of cognitive impairment. Although further clinical trials are necessary to directly assess specific medications, these findings emphasize the potential of antihypertensive treatment as a strategic approach to reduce the risk for AD.
Type 2 Diabetes
The connection between AD and type 2 diabetes is such that AD is sometimes referred to as “type 3 diabetes.” Both diseases share some of the same underlying pathophysiologic mechanisms, particularly the development of insulin resistance and oxidative stress. A prospective cohort study of 10,095 participants showed that diabetes was significantly associated with a higher risk of developing dementia; this risk is even greater in patients who develop diabetes at an earlier age.
In an interview with this news organization, Alvaro Pascual-Leone, MD, PhD, a professor of neurology at Harvard Medical School, Boston, said, “In addition to being a comorbidity factor, diabetes appears to be a predisposing risk factor for AD.” This is supported by a comprehensive literature review showing an increased progression from mild cognitive impairment (MCI) to dementia in patients with diabetes, prediabetes, or metabolic syndrome, with a pooled odds ratio for dementia progression in individuals with diabetes of 1.53.
Owing to the overlapping pathophysiologic mechanisms in AD and diabetes, treating one condition may have beneficial effects on the other. A systematic umbrella review and meta-analysis that included 10 meta-analyses across nine classes of diabetes drugs found a protective effect against dementia with the use of metformin, thiazolidinediones (including pioglitazone), glucagon-like peptide 1 receptor agonists, and sodium-glucose cotransporter 2 inhibitors. Moreover, a cohort study of 12,220 patients who discontinued metformin early (ie, stopped using metformin without a prior history of abnormal kidney function) and 29,126 patients considered routine users found an increased risk for dementia in the early terminator group. Although further research is warranted, the concurrent treatment of AD and diabetes with antidiabetic agents holds considerable promise.
Depression and Anxiety
Anxiety and depression are significant risk factors for AD, and conversely, AD increases the likelihood of developing these psychiatric conditions. A systematic review of 14,760 studies showed dysthymia often emerges during the early stages of AD as an emotional response to cognitive decline.
Data from the Australian Imaging Biomarkers and Lifestyle study showed a markedly elevated risk for AD and MCI among individuals with preexisting anxiety or depression. This study also found that age, sex, and marital status are important determinants, with men and single individuals with depression being particularly susceptible to developing AD. Conversely, a cohort study of 129,410 AD patients with AD, 390,088 patients with all-cause dementia, and 3,900,880 age-matched controls without a history of depression showed a cumulative incidence of depression of 13% in the AD group vs 3% in the control group, suggesting a heightened risk for depression following an AD diagnosis.
These findings underscore the importance of targeted screening and assessment for patients with anxiety and depression who may be at risk for AD or those diagnosed with AD who are at risk for subsequent depression and anxiety. Although antidepressants are effective in treating depression in general, their efficacy in AD-related depression is of variable quality, probably owing to differing pathophysiologic mechanisms of the disease. Further research is necessary to explore both pharmacologic and nonpharmacologic interventions for treating depression in AD patients. Some studies have found that cognitive behavioral-therapy can be effective in improving depression in patients with AD.
Sleep Disorders
Research has shown a strong correlation between AD and sleep disorders, particularly obstructive sleep apnea, insomnia, and circadian rhythm disruptions. Additionally, studies suggest that insomnia and sleep deprivation contribute to increased amyloid beta production and tau pathology, hallmark features of AD. A scoping review of 70 studies proposed that this relationship is mediated by the glymphatic system (glial-dependent waste clearance pathway in the central nervous system), and that sleep deprivation disrupts its function, leading to protein accumulation and subsequent neurologic symptoms of AD. Another study showed that sleep deprivation triggers glial cell activation, initiating an inflammatory cascade that accelerates AD progression.
Given that the gold standard treatment for obstructive sleep apnea is continuous positive airway pressure (CPAP), it has been hypothesized that CPAP could also alleviate AD symptoms owing to shared pathophysiologic mechanisms of these conditions. A large systemic review found that CPAP use improved AD symptoms in patients with mild AD or MCI, though other sleep interventions, such as cognitive-behavioral therapy and melatonin supplementation, have yielded mixed outcomes. However, most studies in this area are small in scale, and there remains a paucity of research on treating sleep disorders in AD patients, indicating a need for further investigation.
Musculoskeletal Disorders
Although no direct causative link has been established, research indicates an association between osteoarthritis (OA) and dementia, likely because of similar pathophysiologic mechanisms, including systemic inflammation. Longitudinal analyses of data from the Alzheimer’s Disease Neuroimaging Initiative study found cognitively normal older individuals with OA experience more rapid declines in hippocampal volumes compared to those without OA, suggesting that OA may elevate the risk of cognitive impairment. Current treatments for OA, such as nonsteroidal anti-inflammatory drugs, glucocorticoids, and disease-modifying OA drugs, might also help alleviate AD symptoms related to inflammation, though the research in this area is limited.
AD has also been linked to osteoporosis. In a longitudinal follow-up study involving 78,994 patients with osteoporosis and 78,994 controls, AD developed in 5856 patients with osteoporosis compared with 3761 patients in the control group. These findings represent a 1.27-fold higher incidence of AD in patients with osteoporosis than in the control group, suggesting that osteoporosis might be a risk factor for AD.
Additionally, research has identified a relationship between AD and increased fracture risk and decreased bone mineral density, with AD patients exhibiting a significantly higher likelihood of bone fractures compared with those without AD. “Falls and fractures, aside from the risk they pose in all geriatric patients, in individuals with cognitive impairment — whether due to AD or another cause — have higher risk to cause delirium and that can result in greater morbidity and mortality and a lasting increase in cognitive disability,” stated Dr. Pascual-Leone. Current recommendations emphasize exercise and fall prevention strategies to reduce fracture risk in patients with AD, but there is a lack of comprehensive research on the safety and efficacy of osteoporosis medications in this population.
Implications for Clinical Practice
The intricate interplay between AD and its comorbidities highlights the need for a comprehensive and integrated approach to patient care. The overlapping pathophysiologic mechanisms suggest that these comorbidities can contribute to the evolution and progression of AD. Likewise, AD can exacerbate comorbid conditions. As such, a holistic assessment strategy that prioritizes early detection and management of comorbid conditions to mitigate their impact on AD progression would be beneficial. Dr. Pascual-Leone added, “The presence of any of these comorbidities suggests a need to screen for MCI earlier than might otherwise be indicated or as part of the treatment for the comorbid condition. In many cases, patients can make lifestyle modifications that improve not only the comorbid condition but also reduce its effect on dementia.” In doing so, healthcare providers can help improve patient outcomes and enhance the overall quality of life for individuals living with AD.
Alissa Hershberger, Professor of Nursing, University of Central Missouri, Lee’s Summit, Missouri, has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Pediatric Melanoma Outcomes by Race and Socioeconomic Factors
To the Editor:
Skin cancers are extremely common worldwide. Malignant melanomas comprise approximately 1 in 5 of these cancers. Exposure to UV radiation is postulated to be responsible for a global rise in melanoma cases over the past 50 years.1 Pediatric melanoma is a particularly rare condition that affects approximately 6 in every 1 million children.2 Melanoma incidence in children ranges by age, increasing by approximately 10-fold from age 1 to 4 years to age 15 to 19 years. Tumor ulceration is a feature more commonly seen among children younger than 10 years and is associated with worse outcomes. Tumor thickness and ulceration strongly predict sentinel lymph node metastases among children, which also is associated with a poor prognosis.3
A recent study evaluating stage IV melanoma survival rates in adolescents and young adults (AYAs) vs older adults found that survival is much worse among AYAs. Thicker tumors and public health insurance also were associated with worse survival rates for AYAs, while early detection was associated with better survival rates.4
Health disparities and their role in the prognosis of pediatric melanoma is another important factor. One study analyzed this relationship at the state level using Texas Cancer Registry data (1995-2009).5 Patients’ socioeconomic status (SES) and driving distance to the nearest pediatric cancer care center were included in the analysis. Hispanic children were found to be 3 times more likely to present with advanced disease than non-Hispanic White children. Although SES and distance to the nearest treatment center were not found to affect the melanoma stage at presentation, Hispanic ethnicity or being in the lowest SES quartile were correlated with a higher mortality risk.5
When considering specific subtypes of melanoma, acral lentiginous melanoma (ALM) is known to develop in patients with skin of color. A 2023 study by Holman et al6 reported that the percentage of melanomas that were ALMs ranged from 0.8% in non-Hispanic White individuals to 19.1% in Hispanic Black, American Indian/Alaska Native, and Asian/Pacific Islander individuals. However, ALM is rare in children. In a pooled cohort study with patient information retrieved from the nationwide Dutch Pathology Registry, only 1 child and 1 adolescent were found to have ALM across a total of 514 patients.7 We sought to analyze pediatric melanoma outcomes based on race and other barriers to appropriate care.
We conducted a search of the Surveillance, Epidemiology, and End Results (SEER) database from January 1995 to December 2016 for patients aged 21 years and younger with a primary melanoma diagnosis. The primary outcome was the 5-year survival rate. County-level SES variables were used to calculate a prosperity index. Kaplan-Meier analysis and Cox proportional hazards model were used to compare 5-year survival rates among the different racial/ethnic groups.
A sample of 2742 patients was identified during the study period and followed for 5 years. Eighty-two percent were White, 6% Hispanic, 2% Asian, 1% Black, and 5% classified as other/unknown race (data were missing for 4%). The cohort was predominantly female (61%). White patients were more likely to present with localized disease than any other race/ethnicity (83% vs 65% in Hispanic, 60% in Asian/Pacific Islander, and 45% in Black patients [P<.05]).
Black and Hispanic patients had the worst 5-year survival rates on bivariate analysis. On multivariate analysis, this finding remained significant for Hispanic patients when compared with White patients (hazard ratio, 2.37 [P<.05]). Increasing age, male sex, advanced stage at diagnosis, and failure to receive surgery were associated with increased odds of mortality.
Patients with regionalized and disseminated disease had increased odds of mortality (6.16 and 64.45, respectively; P<.05) compared with patients with localized disease. Socioeconomic status and urbanization were not found to influence 5-year survival rates.
Pediatric melanoma often presents a clinical challenge with special considerations. Pediatric-specific predisposing risk factors for melanoma and an atypical clinical presentation are some of the major concerns that necessitate a tailored approach to this malignancy, especially among different age groups, skin types, and racial and socioeconomic groups.5
Standard ABCDE criteria often are inadequate for accurate detection of pediatric melanomas. Initial lesions often manifest as raised, red, amelanotic lesions mimicking pyogenic granulomas. Lesions tend to be very small (<6 mm in diameter) and can be uniform in color, thereby making the melanoma more difficult to detect compared to the characteristic findings in adults.5 Bleeding or ulceration often can be a warning sign during physical examination.
With regard to incidence, pediatric melanoma is relatively rare. Since the 1970s, the incidence of pediatric melanoma has been increasing; however, a recent analysis of the SEER database showed a decreasing trend from 2000 to 2010.4
Our analysis of the SEER data showed an increased risk for pediatric melanoma in older adolescents. In addition, the incidence of pediatric melanoma was higher in females of all racial groups except Asian/Pacific Islander individuals. However, SES was not found to significantly influence the 5-year survival rate in pediatric melanoma.
White pediatric patients were more likely to present with localized disease compared with other races. Pediatric melanoma patients with regional disease had a 6-fold increase in mortality rate vs those with localized disease; those with disseminated disease had a 65-fold higher risk. Consistent with this, Black and Hispanic patients had the worst 5-year survival rates on bivariate analysis.
These findings suggest a relationship between race, melanoma spread, and disease severity. Patient education programs need to be directed specifically to minority groups to improve their knowledge on evolving skin lesions and sun protection practices. Physicians also need to have heightened suspicion and better knowledge of the unique traits of pediatric melanoma.5
Given the considerable influence these disparities can have on melanoma outcomes, further research is needed to characterize outcomes based on race and determine obstacles to appropriate care. Improved public outreach initiatives that accommodate specific cultural barriers (eg, language, traditional patterns of behavior) also are required to improve current circumstances.
- Arnold M, Singh D, Laversanne M, et al. Global burden of cutaneous melanoma in 2020 and projections to 2040. JAMA Dermatol. 2022;158:495-503.
- McCormack L, Hawryluk EB. Pediatric melanoma update. G Ital Dermatol Venereol. 2018;153:707-715.
- Saiyed FK, Hamilton EC, Austin MT. Pediatric melanoma: incidence, treatment, and prognosis. Pediatric Health Med Ther. 2017;8:39-45.
- Wojcik KY, Hawkins M, Anderson-Mellies A, et al. Melanoma survival by age group: population-based disparities for adolescent and young adult patients by stage, tumor thickness, and insurance type. J Am Acad Dermatol. 2023;88:831-840.
- Hamilton EC, Nguyen HT, Chang YC, et al. Health disparities influence childhood melanoma stage at diagnosis and outcome. J Pediatr. 2016;175:182-187.
- Holman DM, King JB, White A, et al. Acral lentiginous melanoma incidence by sex, race, ethnicity, and stage in the United States, 2010-2019. Prev Med. 2023;175:107692. doi:10.1016/j.ypmed.2023.107692
- El Sharouni MA, Rawson RV, Potter AJ, et al. Melanomas in children and adolescents: clinicopathologic features and survival outcomes. J Am Acad Dermatol. 2023;88:609-616. doi:10.1016/j.jaad.2022.08.067
To the Editor:
Skin cancers are extremely common worldwide. Malignant melanomas comprise approximately 1 in 5 of these cancers. Exposure to UV radiation is postulated to be responsible for a global rise in melanoma cases over the past 50 years.1 Pediatric melanoma is a particularly rare condition that affects approximately 6 in every 1 million children.2 Melanoma incidence in children ranges by age, increasing by approximately 10-fold from age 1 to 4 years to age 15 to 19 years. Tumor ulceration is a feature more commonly seen among children younger than 10 years and is associated with worse outcomes. Tumor thickness and ulceration strongly predict sentinel lymph node metastases among children, which also is associated with a poor prognosis.3
A recent study evaluating stage IV melanoma survival rates in adolescents and young adults (AYAs) vs older adults found that survival is much worse among AYAs. Thicker tumors and public health insurance also were associated with worse survival rates for AYAs, while early detection was associated with better survival rates.4
Health disparities and their role in the prognosis of pediatric melanoma is another important factor. One study analyzed this relationship at the state level using Texas Cancer Registry data (1995-2009).5 Patients’ socioeconomic status (SES) and driving distance to the nearest pediatric cancer care center were included in the analysis. Hispanic children were found to be 3 times more likely to present with advanced disease than non-Hispanic White children. Although SES and distance to the nearest treatment center were not found to affect the melanoma stage at presentation, Hispanic ethnicity or being in the lowest SES quartile were correlated with a higher mortality risk.5
When considering specific subtypes of melanoma, acral lentiginous melanoma (ALM) is known to develop in patients with skin of color. A 2023 study by Holman et al6 reported that the percentage of melanomas that were ALMs ranged from 0.8% in non-Hispanic White individuals to 19.1% in Hispanic Black, American Indian/Alaska Native, and Asian/Pacific Islander individuals. However, ALM is rare in children. In a pooled cohort study with patient information retrieved from the nationwide Dutch Pathology Registry, only 1 child and 1 adolescent were found to have ALM across a total of 514 patients.7 We sought to analyze pediatric melanoma outcomes based on race and other barriers to appropriate care.
We conducted a search of the Surveillance, Epidemiology, and End Results (SEER) database from January 1995 to December 2016 for patients aged 21 years and younger with a primary melanoma diagnosis. The primary outcome was the 5-year survival rate. County-level SES variables were used to calculate a prosperity index. Kaplan-Meier analysis and Cox proportional hazards model were used to compare 5-year survival rates among the different racial/ethnic groups.
A sample of 2742 patients was identified during the study period and followed for 5 years. Eighty-two percent were White, 6% Hispanic, 2% Asian, 1% Black, and 5% classified as other/unknown race (data were missing for 4%). The cohort was predominantly female (61%). White patients were more likely to present with localized disease than any other race/ethnicity (83% vs 65% in Hispanic, 60% in Asian/Pacific Islander, and 45% in Black patients [P<.05]).
Black and Hispanic patients had the worst 5-year survival rates on bivariate analysis. On multivariate analysis, this finding remained significant for Hispanic patients when compared with White patients (hazard ratio, 2.37 [P<.05]). Increasing age, male sex, advanced stage at diagnosis, and failure to receive surgery were associated with increased odds of mortality.
Patients with regionalized and disseminated disease had increased odds of mortality (6.16 and 64.45, respectively; P<.05) compared with patients with localized disease. Socioeconomic status and urbanization were not found to influence 5-year survival rates.
Pediatric melanoma often presents a clinical challenge with special considerations. Pediatric-specific predisposing risk factors for melanoma and an atypical clinical presentation are some of the major concerns that necessitate a tailored approach to this malignancy, especially among different age groups, skin types, and racial and socioeconomic groups.5
Standard ABCDE criteria often are inadequate for accurate detection of pediatric melanomas. Initial lesions often manifest as raised, red, amelanotic lesions mimicking pyogenic granulomas. Lesions tend to be very small (<6 mm in diameter) and can be uniform in color, thereby making the melanoma more difficult to detect compared to the characteristic findings in adults.5 Bleeding or ulceration often can be a warning sign during physical examination.
With regard to incidence, pediatric melanoma is relatively rare. Since the 1970s, the incidence of pediatric melanoma has been increasing; however, a recent analysis of the SEER database showed a decreasing trend from 2000 to 2010.4
Our analysis of the SEER data showed an increased risk for pediatric melanoma in older adolescents. In addition, the incidence of pediatric melanoma was higher in females of all racial groups except Asian/Pacific Islander individuals. However, SES was not found to significantly influence the 5-year survival rate in pediatric melanoma.
White pediatric patients were more likely to present with localized disease compared with other races. Pediatric melanoma patients with regional disease had a 6-fold increase in mortality rate vs those with localized disease; those with disseminated disease had a 65-fold higher risk. Consistent with this, Black and Hispanic patients had the worst 5-year survival rates on bivariate analysis.
These findings suggest a relationship between race, melanoma spread, and disease severity. Patient education programs need to be directed specifically to minority groups to improve their knowledge on evolving skin lesions and sun protection practices. Physicians also need to have heightened suspicion and better knowledge of the unique traits of pediatric melanoma.5
Given the considerable influence these disparities can have on melanoma outcomes, further research is needed to characterize outcomes based on race and determine obstacles to appropriate care. Improved public outreach initiatives that accommodate specific cultural barriers (eg, language, traditional patterns of behavior) also are required to improve current circumstances.
To the Editor:
Skin cancers are extremely common worldwide. Malignant melanomas comprise approximately 1 in 5 of these cancers. Exposure to UV radiation is postulated to be responsible for a global rise in melanoma cases over the past 50 years.1 Pediatric melanoma is a particularly rare condition that affects approximately 6 in every 1 million children.2 Melanoma incidence in children ranges by age, increasing by approximately 10-fold from age 1 to 4 years to age 15 to 19 years. Tumor ulceration is a feature more commonly seen among children younger than 10 years and is associated with worse outcomes. Tumor thickness and ulceration strongly predict sentinel lymph node metastases among children, which also is associated with a poor prognosis.3
A recent study evaluating stage IV melanoma survival rates in adolescents and young adults (AYAs) vs older adults found that survival is much worse among AYAs. Thicker tumors and public health insurance also were associated with worse survival rates for AYAs, while early detection was associated with better survival rates.4
Health disparities and their role in the prognosis of pediatric melanoma is another important factor. One study analyzed this relationship at the state level using Texas Cancer Registry data (1995-2009).5 Patients’ socioeconomic status (SES) and driving distance to the nearest pediatric cancer care center were included in the analysis. Hispanic children were found to be 3 times more likely to present with advanced disease than non-Hispanic White children. Although SES and distance to the nearest treatment center were not found to affect the melanoma stage at presentation, Hispanic ethnicity or being in the lowest SES quartile were correlated with a higher mortality risk.5
When considering specific subtypes of melanoma, acral lentiginous melanoma (ALM) is known to develop in patients with skin of color. A 2023 study by Holman et al6 reported that the percentage of melanomas that were ALMs ranged from 0.8% in non-Hispanic White individuals to 19.1% in Hispanic Black, American Indian/Alaska Native, and Asian/Pacific Islander individuals. However, ALM is rare in children. In a pooled cohort study with patient information retrieved from the nationwide Dutch Pathology Registry, only 1 child and 1 adolescent were found to have ALM across a total of 514 patients.7 We sought to analyze pediatric melanoma outcomes based on race and other barriers to appropriate care.
We conducted a search of the Surveillance, Epidemiology, and End Results (SEER) database from January 1995 to December 2016 for patients aged 21 years and younger with a primary melanoma diagnosis. The primary outcome was the 5-year survival rate. County-level SES variables were used to calculate a prosperity index. Kaplan-Meier analysis and Cox proportional hazards model were used to compare 5-year survival rates among the different racial/ethnic groups.
A sample of 2742 patients was identified during the study period and followed for 5 years. Eighty-two percent were White, 6% Hispanic, 2% Asian, 1% Black, and 5% classified as other/unknown race (data were missing for 4%). The cohort was predominantly female (61%). White patients were more likely to present with localized disease than any other race/ethnicity (83% vs 65% in Hispanic, 60% in Asian/Pacific Islander, and 45% in Black patients [P<.05]).
Black and Hispanic patients had the worst 5-year survival rates on bivariate analysis. On multivariate analysis, this finding remained significant for Hispanic patients when compared with White patients (hazard ratio, 2.37 [P<.05]). Increasing age, male sex, advanced stage at diagnosis, and failure to receive surgery were associated with increased odds of mortality.
Patients with regionalized and disseminated disease had increased odds of mortality (6.16 and 64.45, respectively; P<.05) compared with patients with localized disease. Socioeconomic status and urbanization were not found to influence 5-year survival rates.
Pediatric melanoma often presents a clinical challenge with special considerations. Pediatric-specific predisposing risk factors for melanoma and an atypical clinical presentation are some of the major concerns that necessitate a tailored approach to this malignancy, especially among different age groups, skin types, and racial and socioeconomic groups.5
Standard ABCDE criteria often are inadequate for accurate detection of pediatric melanomas. Initial lesions often manifest as raised, red, amelanotic lesions mimicking pyogenic granulomas. Lesions tend to be very small (<6 mm in diameter) and can be uniform in color, thereby making the melanoma more difficult to detect compared to the characteristic findings in adults.5 Bleeding or ulceration often can be a warning sign during physical examination.
With regard to incidence, pediatric melanoma is relatively rare. Since the 1970s, the incidence of pediatric melanoma has been increasing; however, a recent analysis of the SEER database showed a decreasing trend from 2000 to 2010.4
Our analysis of the SEER data showed an increased risk for pediatric melanoma in older adolescents. In addition, the incidence of pediatric melanoma was higher in females of all racial groups except Asian/Pacific Islander individuals. However, SES was not found to significantly influence the 5-year survival rate in pediatric melanoma.
White pediatric patients were more likely to present with localized disease compared with other races. Pediatric melanoma patients with regional disease had a 6-fold increase in mortality rate vs those with localized disease; those with disseminated disease had a 65-fold higher risk. Consistent with this, Black and Hispanic patients had the worst 5-year survival rates on bivariate analysis.
These findings suggest a relationship between race, melanoma spread, and disease severity. Patient education programs need to be directed specifically to minority groups to improve their knowledge on evolving skin lesions and sun protection practices. Physicians also need to have heightened suspicion and better knowledge of the unique traits of pediatric melanoma.5
Given the considerable influence these disparities can have on melanoma outcomes, further research is needed to characterize outcomes based on race and determine obstacles to appropriate care. Improved public outreach initiatives that accommodate specific cultural barriers (eg, language, traditional patterns of behavior) also are required to improve current circumstances.
- Arnold M, Singh D, Laversanne M, et al. Global burden of cutaneous melanoma in 2020 and projections to 2040. JAMA Dermatol. 2022;158:495-503.
- McCormack L, Hawryluk EB. Pediatric melanoma update. G Ital Dermatol Venereol. 2018;153:707-715.
- Saiyed FK, Hamilton EC, Austin MT. Pediatric melanoma: incidence, treatment, and prognosis. Pediatric Health Med Ther. 2017;8:39-45.
- Wojcik KY, Hawkins M, Anderson-Mellies A, et al. Melanoma survival by age group: population-based disparities for adolescent and young adult patients by stage, tumor thickness, and insurance type. J Am Acad Dermatol. 2023;88:831-840.
- Hamilton EC, Nguyen HT, Chang YC, et al. Health disparities influence childhood melanoma stage at diagnosis and outcome. J Pediatr. 2016;175:182-187.
- Holman DM, King JB, White A, et al. Acral lentiginous melanoma incidence by sex, race, ethnicity, and stage in the United States, 2010-2019. Prev Med. 2023;175:107692. doi:10.1016/j.ypmed.2023.107692
- El Sharouni MA, Rawson RV, Potter AJ, et al. Melanomas in children and adolescents: clinicopathologic features and survival outcomes. J Am Acad Dermatol. 2023;88:609-616. doi:10.1016/j.jaad.2022.08.067
- Arnold M, Singh D, Laversanne M, et al. Global burden of cutaneous melanoma in 2020 and projections to 2040. JAMA Dermatol. 2022;158:495-503.
- McCormack L, Hawryluk EB. Pediatric melanoma update. G Ital Dermatol Venereol. 2018;153:707-715.
- Saiyed FK, Hamilton EC, Austin MT. Pediatric melanoma: incidence, treatment, and prognosis. Pediatric Health Med Ther. 2017;8:39-45.
- Wojcik KY, Hawkins M, Anderson-Mellies A, et al. Melanoma survival by age group: population-based disparities for adolescent and young adult patients by stage, tumor thickness, and insurance type. J Am Acad Dermatol. 2023;88:831-840.
- Hamilton EC, Nguyen HT, Chang YC, et al. Health disparities influence childhood melanoma stage at diagnosis and outcome. J Pediatr. 2016;175:182-187.
- Holman DM, King JB, White A, et al. Acral lentiginous melanoma incidence by sex, race, ethnicity, and stage in the United States, 2010-2019. Prev Med. 2023;175:107692. doi:10.1016/j.ypmed.2023.107692
- El Sharouni MA, Rawson RV, Potter AJ, et al. Melanomas in children and adolescents: clinicopathologic features and survival outcomes. J Am Acad Dermatol. 2023;88:609-616. doi:10.1016/j.jaad.2022.08.067
Practice Points
- Pediatric melanoma is a unique clinical entity with a different clinical presentation than in adults.
- Thicker tumors and disseminated disease are associated with a worse prognosis, and these factors are more commonly seen in Black and Hispanic patients.
New Research Consortium on Quest to Improve Male Infertility Treatment
A study by researchers at two academic medical centers determined which infertile men may benefit from treatment with anastrozole. They found that those with azoospermia (no sperm in their ejaculate) rarely respond to the drug while those with baseline nonazoospermia, lower levels of luteinizing hormone and follicle-stimulating hormone, and higher levels of testosterone are more likely to obtain improvement in semen parameters.
The retrospective cohort study of 90 infertile men, published in the October 2023 issue of Fertility and Sterility, was conducted by researchers at Cleveland Clinic and the University of California Los Angeles. It is the first project of Male Organ Biology Yielding United Science (MOBYUS), a new, multi-institutional research consortium seeking to better understand male infertility and expand treatment options.
Launched last year, MOBYUS now includes investigators from 14 large US-based academic medical centers. They select research topics and search their patient population for eligible participants and share resulting deidentified data for analysis and publication.
Members of the consortium conducted another study which found that combination therapy with clomiphene citrate and anastrozole was associated with modest benefits on semen parameters, including volume, concentration, and motility after treatment, compared with anastrozole monotherapy. That retrospective cohort analysis of 21 men was published online in Translational Andrology and Urology in February.
“We know that if we treat the right men with these medications, about 40% will improve their fertility, but only if we choose the right population. These studies identified those groups,” Scott Lundy, MD, PhD, section head of male infertility at Cleveland Clinic’s Glickman Urological and Kidney Institute in Cleveland, and director of the clinic’s andrology lab, told Medscape Medical News.
Dr. Lundy, a coauthor of both papers, conceived MOBYUS to overcome constraints in research into male infertility. Many studies in the field are limited by small numbers of patients and retrospective designs, he said. “I sought to develop a collaborative network of reproductive urologists and hospitals like ours, so that we can combine our data and generate large series of data, even for rare patient groups, so that we can improve their patient outcomes,” he said.
“Our treatments are in the stone age in many ways. We are far behind other types of treatment for other conditions, including female infertility,” Dr. Lundy added. “And so, our goal is to identify new and data-driven ways to help these men become fathers, whether those are medications or surgeries or combinations of treatments.”
Moving the Field Forward
The name of the consortium is a cheeky play on Moby Dick, the most famous sperm whale. MOBYUS investigators conveyed the challenges that patients, doctors, and researchers experience in an article published last December in the Journal of Urology.
They noted that 1 in 6 couples will have difficulty conceiving a child, with male-factor infertility contributing to at least half of such cases. The lead author, Catherine Nam, MD, a principal investigator for MOBYUS at the University of Michigan, in Ann Arbor, said the paper is unusual for a medical journal, as it provides personal accounts of the psychological and emotional aspects of infertility as well as factors that have led to a global decline in sperm counts among men and the financial costs of treatment.
Dr. Nam said infertility is a sensitive topic for couples and families to talk about and there is less conversation about male infertility than female infertility. “I think the only way that we can be able to make headway, both in terms of protocol and policy outcomes, is to really start to raise awareness,” said Dr. Nam, who is doing a fellowship in clinical andrology at Northwestern University, in Chicago.
Dr. Nam said the collaborative environment of MOBYUS has enabled her to learn about different practice patterns across different institutions. “For someone like me just starting off my professional career in male infertility, an opportunity like this is incredibly exciting and makes me very hopeful about the kinds of collaboration and scientific discovery that we’re able to do together as a group,” she said.
Robert E. Brannigan, MD, vice chair of clinical urology at Northwestern University Feinberg School of Medicine, Chicago, said the consortium is drawing on the strength of many individual centers and allowing them to study critical issues in the field. The group’s outstanding clinicians and scientists “are looking to move the field forward, and I applaud them and I’m eager to watch things unfold,” said Dr. Brannigan, who is not a member of the group.
Dr. Brannigan noted that for a large percentage of patients, clinicians cannot identify the root cause of their impaired reproductive potential. Some people may have a recognizable decline in semen parameters over time without clear lifestyle issues or clear hormonal imbalances or anatomical problems.
“And the question is, what’s causing that? Is there some as yet unrecognized environmental exposure? Is there some underlying genetic issue that’s predisposing to decline in semen parameters over time? We see this, and we don’t have answers,” Dr. Brannigan said.
“This is where I think the potential power of a large group like MOBYUS comes into play,” he added. “When you’ve got large datasets and very granular information about your patients, sometimes that can provide the opportunity for insights that can then answer the question, ‘What is the root cause of my patient’s challenges?’ ”
Dr. Brannigan was part of a previous group, the Andrology Research Consortium, which collected data on patient history and treatment through a standardized questionnaire. The consortium was founded in 2013 by the Society for the Study of Male Reproduction, a specialty section of the American Urological Association, to obtain data on the demographics, clinical characteristics, and fertility histories and therapies of men referred for a male infertility investigation at clinics across North America.
Clinicians analyzed data from the questionnaires, which a team in Toronto collected and stored, in a series of studies, including a comparison of fertility characteristics between men in the United States and Canada. Dr. Brannigan said MOBYUS is poised to produce a large dataset that can address retrospective questions and potentially prospectively collect data to answer prospective questions.
Clinical Implications
Dr. Lundy said between 100 and 200 practicing reproductive urologists across the country regularly communicate with each other. He first raised the idea of creating a consortium with friends and colleagues and then discussed it at scientific meetings. The network steadily gained traction and is continuing to add institutions. “There’s a great deal of excitement in our community about this,” Dr. Lundy said.
MOBYUS, which is IRB approved, has a database with data from more than 4000 patients. The consortium has not received any industry funding but plans to pursue grant applications in the future.
The MOBYUS website includes a list of its member institutions and leading investigators and its three proof-of-principle manuscripts published to date. The team identifies new research projects at monthly virtual meetings.
Dr. Lundy said MOBYUS’ main goal is to identify a treatment that will change the avenue available for a couple to get pregnant. For example, he said, if a man has zero sperm in his semen, he often requires surgery to find and remove sperm from the testicle. If medications can produce low sperm counts, sperm found in the ejaculate can be frozen and surgery can be avoided.
Dr. Lundy said MOBYUS’ two publications on medical therapies have changed clinical practice, as he and many others have begun to provide the treatments on more carefully selected patients with good outcomes.
Dr. Nam said patients want to know what they can expect from therapies and these research findings will have “a lot of clinical implications” in counseling them.
The MOBYUS team will be describing the consortium and its goals in an abstract presentation at the American Society for Reproductive Medicine Scientific Congress & Expo, to be held October 19-23 in Denver, Colorado, and in an oral presentation at the Sexual Medicine Society of North America’s annual fall scientific meeting, to be held October 17-20 in Scottsdale, Arizona.
The sources in this story reported no relevant financial conflicts of interest.
A version of this article first appeared on Medscape.com.
A study by researchers at two academic medical centers determined which infertile men may benefit from treatment with anastrozole. They found that those with azoospermia (no sperm in their ejaculate) rarely respond to the drug while those with baseline nonazoospermia, lower levels of luteinizing hormone and follicle-stimulating hormone, and higher levels of testosterone are more likely to obtain improvement in semen parameters.
The retrospective cohort study of 90 infertile men, published in the October 2023 issue of Fertility and Sterility, was conducted by researchers at Cleveland Clinic and the University of California Los Angeles. It is the first project of Male Organ Biology Yielding United Science (MOBYUS), a new, multi-institutional research consortium seeking to better understand male infertility and expand treatment options.
Launched last year, MOBYUS now includes investigators from 14 large US-based academic medical centers. They select research topics and search their patient population for eligible participants and share resulting deidentified data for analysis and publication.
Members of the consortium conducted another study which found that combination therapy with clomiphene citrate and anastrozole was associated with modest benefits on semen parameters, including volume, concentration, and motility after treatment, compared with anastrozole monotherapy. That retrospective cohort analysis of 21 men was published online in Translational Andrology and Urology in February.
“We know that if we treat the right men with these medications, about 40% will improve their fertility, but only if we choose the right population. These studies identified those groups,” Scott Lundy, MD, PhD, section head of male infertility at Cleveland Clinic’s Glickman Urological and Kidney Institute in Cleveland, and director of the clinic’s andrology lab, told Medscape Medical News.
Dr. Lundy, a coauthor of both papers, conceived MOBYUS to overcome constraints in research into male infertility. Many studies in the field are limited by small numbers of patients and retrospective designs, he said. “I sought to develop a collaborative network of reproductive urologists and hospitals like ours, so that we can combine our data and generate large series of data, even for rare patient groups, so that we can improve their patient outcomes,” he said.
“Our treatments are in the stone age in many ways. We are far behind other types of treatment for other conditions, including female infertility,” Dr. Lundy added. “And so, our goal is to identify new and data-driven ways to help these men become fathers, whether those are medications or surgeries or combinations of treatments.”
Moving the Field Forward
The name of the consortium is a cheeky play on Moby Dick, the most famous sperm whale. MOBYUS investigators conveyed the challenges that patients, doctors, and researchers experience in an article published last December in the Journal of Urology.
They noted that 1 in 6 couples will have difficulty conceiving a child, with male-factor infertility contributing to at least half of such cases. The lead author, Catherine Nam, MD, a principal investigator for MOBYUS at the University of Michigan, in Ann Arbor, said the paper is unusual for a medical journal, as it provides personal accounts of the psychological and emotional aspects of infertility as well as factors that have led to a global decline in sperm counts among men and the financial costs of treatment.
Dr. Nam said infertility is a sensitive topic for couples and families to talk about and there is less conversation about male infertility than female infertility. “I think the only way that we can be able to make headway, both in terms of protocol and policy outcomes, is to really start to raise awareness,” said Dr. Nam, who is doing a fellowship in clinical andrology at Northwestern University, in Chicago.
Dr. Nam said the collaborative environment of MOBYUS has enabled her to learn about different practice patterns across different institutions. “For someone like me just starting off my professional career in male infertility, an opportunity like this is incredibly exciting and makes me very hopeful about the kinds of collaboration and scientific discovery that we’re able to do together as a group,” she said.
Robert E. Brannigan, MD, vice chair of clinical urology at Northwestern University Feinberg School of Medicine, Chicago, said the consortium is drawing on the strength of many individual centers and allowing them to study critical issues in the field. The group’s outstanding clinicians and scientists “are looking to move the field forward, and I applaud them and I’m eager to watch things unfold,” said Dr. Brannigan, who is not a member of the group.
Dr. Brannigan noted that for a large percentage of patients, clinicians cannot identify the root cause of their impaired reproductive potential. Some people may have a recognizable decline in semen parameters over time without clear lifestyle issues or clear hormonal imbalances or anatomical problems.
“And the question is, what’s causing that? Is there some as yet unrecognized environmental exposure? Is there some underlying genetic issue that’s predisposing to decline in semen parameters over time? We see this, and we don’t have answers,” Dr. Brannigan said.
“This is where I think the potential power of a large group like MOBYUS comes into play,” he added. “When you’ve got large datasets and very granular information about your patients, sometimes that can provide the opportunity for insights that can then answer the question, ‘What is the root cause of my patient’s challenges?’ ”
Dr. Brannigan was part of a previous group, the Andrology Research Consortium, which collected data on patient history and treatment through a standardized questionnaire. The consortium was founded in 2013 by the Society for the Study of Male Reproduction, a specialty section of the American Urological Association, to obtain data on the demographics, clinical characteristics, and fertility histories and therapies of men referred for a male infertility investigation at clinics across North America.
Clinicians analyzed data from the questionnaires, which a team in Toronto collected and stored, in a series of studies, including a comparison of fertility characteristics between men in the United States and Canada. Dr. Brannigan said MOBYUS is poised to produce a large dataset that can address retrospective questions and potentially prospectively collect data to answer prospective questions.
Clinical Implications
Dr. Lundy said between 100 and 200 practicing reproductive urologists across the country regularly communicate with each other. He first raised the idea of creating a consortium with friends and colleagues and then discussed it at scientific meetings. The network steadily gained traction and is continuing to add institutions. “There’s a great deal of excitement in our community about this,” Dr. Lundy said.
MOBYUS, which is IRB approved, has a database with data from more than 4000 patients. The consortium has not received any industry funding but plans to pursue grant applications in the future.
The MOBYUS website includes a list of its member institutions and leading investigators and its three proof-of-principle manuscripts published to date. The team identifies new research projects at monthly virtual meetings.
Dr. Lundy said MOBYUS’ main goal is to identify a treatment that will change the avenue available for a couple to get pregnant. For example, he said, if a man has zero sperm in his semen, he often requires surgery to find and remove sperm from the testicle. If medications can produce low sperm counts, sperm found in the ejaculate can be frozen and surgery can be avoided.
Dr. Lundy said MOBYUS’ two publications on medical therapies have changed clinical practice, as he and many others have begun to provide the treatments on more carefully selected patients with good outcomes.
Dr. Nam said patients want to know what they can expect from therapies and these research findings will have “a lot of clinical implications” in counseling them.
The MOBYUS team will be describing the consortium and its goals in an abstract presentation at the American Society for Reproductive Medicine Scientific Congress & Expo, to be held October 19-23 in Denver, Colorado, and in an oral presentation at the Sexual Medicine Society of North America’s annual fall scientific meeting, to be held October 17-20 in Scottsdale, Arizona.
The sources in this story reported no relevant financial conflicts of interest.
A version of this article first appeared on Medscape.com.
A study by researchers at two academic medical centers determined which infertile men may benefit from treatment with anastrozole. They found that those with azoospermia (no sperm in their ejaculate) rarely respond to the drug while those with baseline nonazoospermia, lower levels of luteinizing hormone and follicle-stimulating hormone, and higher levels of testosterone are more likely to obtain improvement in semen parameters.
The retrospective cohort study of 90 infertile men, published in the October 2023 issue of Fertility and Sterility, was conducted by researchers at Cleveland Clinic and the University of California Los Angeles. It is the first project of Male Organ Biology Yielding United Science (MOBYUS), a new, multi-institutional research consortium seeking to better understand male infertility and expand treatment options.
Launched last year, MOBYUS now includes investigators from 14 large US-based academic medical centers. They select research topics and search their patient population for eligible participants and share resulting deidentified data for analysis and publication.
Members of the consortium conducted another study which found that combination therapy with clomiphene citrate and anastrozole was associated with modest benefits on semen parameters, including volume, concentration, and motility after treatment, compared with anastrozole monotherapy. That retrospective cohort analysis of 21 men was published online in Translational Andrology and Urology in February.
“We know that if we treat the right men with these medications, about 40% will improve their fertility, but only if we choose the right population. These studies identified those groups,” Scott Lundy, MD, PhD, section head of male infertility at Cleveland Clinic’s Glickman Urological and Kidney Institute in Cleveland, and director of the clinic’s andrology lab, told Medscape Medical News.
Dr. Lundy, a coauthor of both papers, conceived MOBYUS to overcome constraints in research into male infertility. Many studies in the field are limited by small numbers of patients and retrospective designs, he said. “I sought to develop a collaborative network of reproductive urologists and hospitals like ours, so that we can combine our data and generate large series of data, even for rare patient groups, so that we can improve their patient outcomes,” he said.
“Our treatments are in the stone age in many ways. We are far behind other types of treatment for other conditions, including female infertility,” Dr. Lundy added. “And so, our goal is to identify new and data-driven ways to help these men become fathers, whether those are medications or surgeries or combinations of treatments.”
Moving the Field Forward
The name of the consortium is a cheeky play on Moby Dick, the most famous sperm whale. MOBYUS investigators conveyed the challenges that patients, doctors, and researchers experience in an article published last December in the Journal of Urology.
They noted that 1 in 6 couples will have difficulty conceiving a child, with male-factor infertility contributing to at least half of such cases. The lead author, Catherine Nam, MD, a principal investigator for MOBYUS at the University of Michigan, in Ann Arbor, said the paper is unusual for a medical journal, as it provides personal accounts of the psychological and emotional aspects of infertility as well as factors that have led to a global decline in sperm counts among men and the financial costs of treatment.
Dr. Nam said infertility is a sensitive topic for couples and families to talk about and there is less conversation about male infertility than female infertility. “I think the only way that we can be able to make headway, both in terms of protocol and policy outcomes, is to really start to raise awareness,” said Dr. Nam, who is doing a fellowship in clinical andrology at Northwestern University, in Chicago.
Dr. Nam said the collaborative environment of MOBYUS has enabled her to learn about different practice patterns across different institutions. “For someone like me just starting off my professional career in male infertility, an opportunity like this is incredibly exciting and makes me very hopeful about the kinds of collaboration and scientific discovery that we’re able to do together as a group,” she said.
Robert E. Brannigan, MD, vice chair of clinical urology at Northwestern University Feinberg School of Medicine, Chicago, said the consortium is drawing on the strength of many individual centers and allowing them to study critical issues in the field. The group’s outstanding clinicians and scientists “are looking to move the field forward, and I applaud them and I’m eager to watch things unfold,” said Dr. Brannigan, who is not a member of the group.
Dr. Brannigan noted that for a large percentage of patients, clinicians cannot identify the root cause of their impaired reproductive potential. Some people may have a recognizable decline in semen parameters over time without clear lifestyle issues or clear hormonal imbalances or anatomical problems.
“And the question is, what’s causing that? Is there some as yet unrecognized environmental exposure? Is there some underlying genetic issue that’s predisposing to decline in semen parameters over time? We see this, and we don’t have answers,” Dr. Brannigan said.
“This is where I think the potential power of a large group like MOBYUS comes into play,” he added. “When you’ve got large datasets and very granular information about your patients, sometimes that can provide the opportunity for insights that can then answer the question, ‘What is the root cause of my patient’s challenges?’ ”
Dr. Brannigan was part of a previous group, the Andrology Research Consortium, which collected data on patient history and treatment through a standardized questionnaire. The consortium was founded in 2013 by the Society for the Study of Male Reproduction, a specialty section of the American Urological Association, to obtain data on the demographics, clinical characteristics, and fertility histories and therapies of men referred for a male infertility investigation at clinics across North America.
Clinicians analyzed data from the questionnaires, which a team in Toronto collected and stored, in a series of studies, including a comparison of fertility characteristics between men in the United States and Canada. Dr. Brannigan said MOBYUS is poised to produce a large dataset that can address retrospective questions and potentially prospectively collect data to answer prospective questions.
Clinical Implications
Dr. Lundy said between 100 and 200 practicing reproductive urologists across the country regularly communicate with each other. He first raised the idea of creating a consortium with friends and colleagues and then discussed it at scientific meetings. The network steadily gained traction and is continuing to add institutions. “There’s a great deal of excitement in our community about this,” Dr. Lundy said.
MOBYUS, which is IRB approved, has a database with data from more than 4000 patients. The consortium has not received any industry funding but plans to pursue grant applications in the future.
The MOBYUS website includes a list of its member institutions and leading investigators and its three proof-of-principle manuscripts published to date. The team identifies new research projects at monthly virtual meetings.
Dr. Lundy said MOBYUS’ main goal is to identify a treatment that will change the avenue available for a couple to get pregnant. For example, he said, if a man has zero sperm in his semen, he often requires surgery to find and remove sperm from the testicle. If medications can produce low sperm counts, sperm found in the ejaculate can be frozen and surgery can be avoided.
Dr. Lundy said MOBYUS’ two publications on medical therapies have changed clinical practice, as he and many others have begun to provide the treatments on more carefully selected patients with good outcomes.
Dr. Nam said patients want to know what they can expect from therapies and these research findings will have “a lot of clinical implications” in counseling them.
The MOBYUS team will be describing the consortium and its goals in an abstract presentation at the American Society for Reproductive Medicine Scientific Congress & Expo, to be held October 19-23 in Denver, Colorado, and in an oral presentation at the Sexual Medicine Society of North America’s annual fall scientific meeting, to be held October 17-20 in Scottsdale, Arizona.
The sources in this story reported no relevant financial conflicts of interest.
A version of this article first appeared on Medscape.com.
Eyelid Dermatitis: Common Patterns and Contact Allergens
Eyelid dermatitis is a common dermatologic concern representing a broad group of inflammatory dermatoses and typically presenting as eczematous lesions on the eyelids.1 One of the most common causes of eyelid dermatitis is thought to be allergic contact dermatitis (ACD), a type IV delayed hypersensitivity reaction caused by exposure to external allergens.2 Although ACD can occur anywhere on the body, dermatitis on the face and eyelids is quite common.1,2 This article aims to explore the clinical manifestation, evaluation, and management of eyelid ACD.
Pathophysiology of Eyelid ACD
Studies have shown that ACD is the most common cause of eyelid dermatitis, estimated to account for 46% to 72% of cases worldwide.3-6 Allergic contact dermatitis is a T cell–mediated type IV hypersensitivity reaction to external antigens that manifests as eczematous lesions at the site of contact with the allergen that may spread.7 Allergic contact dermatitis is a common condition, and it is estimated that at least 20% of the general worldwide population has a contact allergy.8,9 Histologically, ACD manifests as spongiotic dermatitis, though this is not unique and also may be seen in atopic dermatitis (AD) and irritant contact dermatitis.2 Allergic contact dermatitis is diagnosed via epicutaneous patch testing, and treatment involves allergen avoidance with or without adjuvant topical and/or systemic immunomodulatory treatments.7
The eyelids are uniquely prone to the development of ACD given their thinner epidermis and increased susceptibility to irritation. They frequently are exposed to allergens through the direct topical route as well as indirectly via airborne exposure, rinse-down products (eg, shampoos), and substances transferred from an individual’s own hands. The occluded skin folds of the eyelids facilitate increased exposure to trapped allergens.10,11 Additionally, the skin of the eyelids is thin, flexible, highly vascularized, and lacking in subcutaneous tissue, making this area more susceptible to antigen penetration than other locations on the body.1,2,10,12,13
Clinical Manifestations
Eyelid ACD is more common in females than males, which is thought to be related to increased use of cosmetics and fragrances.1,3,12,14-16 Clinical manifestations may resemble eczematous papules and plaques.1 Eyelid ACD commonly spreads beyond the eyelid margin, which helps to differentiate it from AD and irritant contact dermatitis. Symptoms of ACD on the eyelids typically include pruritus, redness, swelling, tearing, scaling, and pain.2 Persistent untreated eyelid dermatitis can lead to eyelash loss, damage to meibomian glands, and hyperpigmentation.2,17,18
Patterns of Eyelid ACD
Allergic contact dermatitis on the eyelids can occur due to direct application of allergens onto the skin of the eyelids, runoff of products from the hair/scalp (eg, shampoo), transfer of allergens from the hands, or contact with airborne allergens.1,2,11,12 Some reports have suggested that eyelid ACD more often is caused by products applied to the scalp or face rather than those applied directly to the eyelids.11 Because the scalp and face are less reactive to contact allergens, in some cases the eyelids may be the only affected site.10,12,13
The specific pattern of dermatitis on or around the eyelids can provide clues to the allergenic source. Dermatitis present around the eyelids and periorbital region with involvement of the bilateral upper and lower eyelids suggests direct exposure to a contact allergen, such as makeup or other cosmetic products.1 Unilateral involvement of only 1 eyelid can occur with ectopic transfer of allergens from the hands or nails.1,19 Involvement of the fingers or nails in addition to the eyelids may further suggest ectopic transfer, such as from allergens in nail polish.10 Unilateral eyelid dermatitis also could be caused by unique exposures such as a microscope or camera eyepiece.19 Distribution around the lower eyelids and upper cheeks is indicative of a drip or runoff pattern, which may result from an ophthalmic solution such as eye drops or contact lens solution.1,19 Finally, dermatitis affecting the upper eyelids along with the nasolabial folds and upper chest may suggest airborne contact dermatitis to fragrances or household cleaning products.1,11
Common Culprits of Eyelid ACD
Common causes of eyelid ACD include cosmetic products, ophthalmic medications, nail lacquers, and jewelry.10,13,20 Within the broader category of cosmetics, allergens may be found in makeup and makeup removers, cosmetic applicators and brushes, soaps and cleansers, creams and sunscreens, antiaging products, hair products, nail polish and files, and hair removal products, among many others.10,13,16,20 Additionally, ophthalmologic and topical medications are common sources of ACD, including eyedrops, contact lens solution, and topical antibiotics.10,13,21 Costume jewelry commonly contains allergenic metals, which also can be found in eyelash curlers, eyeglasses, toys, and other household items.22,23 Finally, contact allergens can be found in items such as goggles, gloves, textiles, and a variety of other occupational and household exposures.
Allergic contact dermatitis of the eyelids occurs predominantly—but not exclusively—in females.16,20,24 This finding has been attributed to the traditionally greater use of cosmetics and fragrances among women; however, the use of skin care products among men is increasing, and recent studies have shown the eyelids to be a common location of facial contact dermatitis among men.16,24 Although eyelid dermatitis has not been specifically analyzed by sex, a retrospective analysis of 1332 male patients with facial dermatitis found the most common sites to be the face (not otherwise specified)(48.9%), eyelids (23.5%), and lips (12.6%). In this cohort, the most common allergens were surfactants in shampoos and paraphenylenediamine in hair dyes.24
Common Allergens
Common contact allergens among patients with ACD of the eyelids include metals, fragrances, preservatives, acrylates, and topical medications.3,10,16,20,25-27 Sources of common contact allergens are reviewed in Table 1.
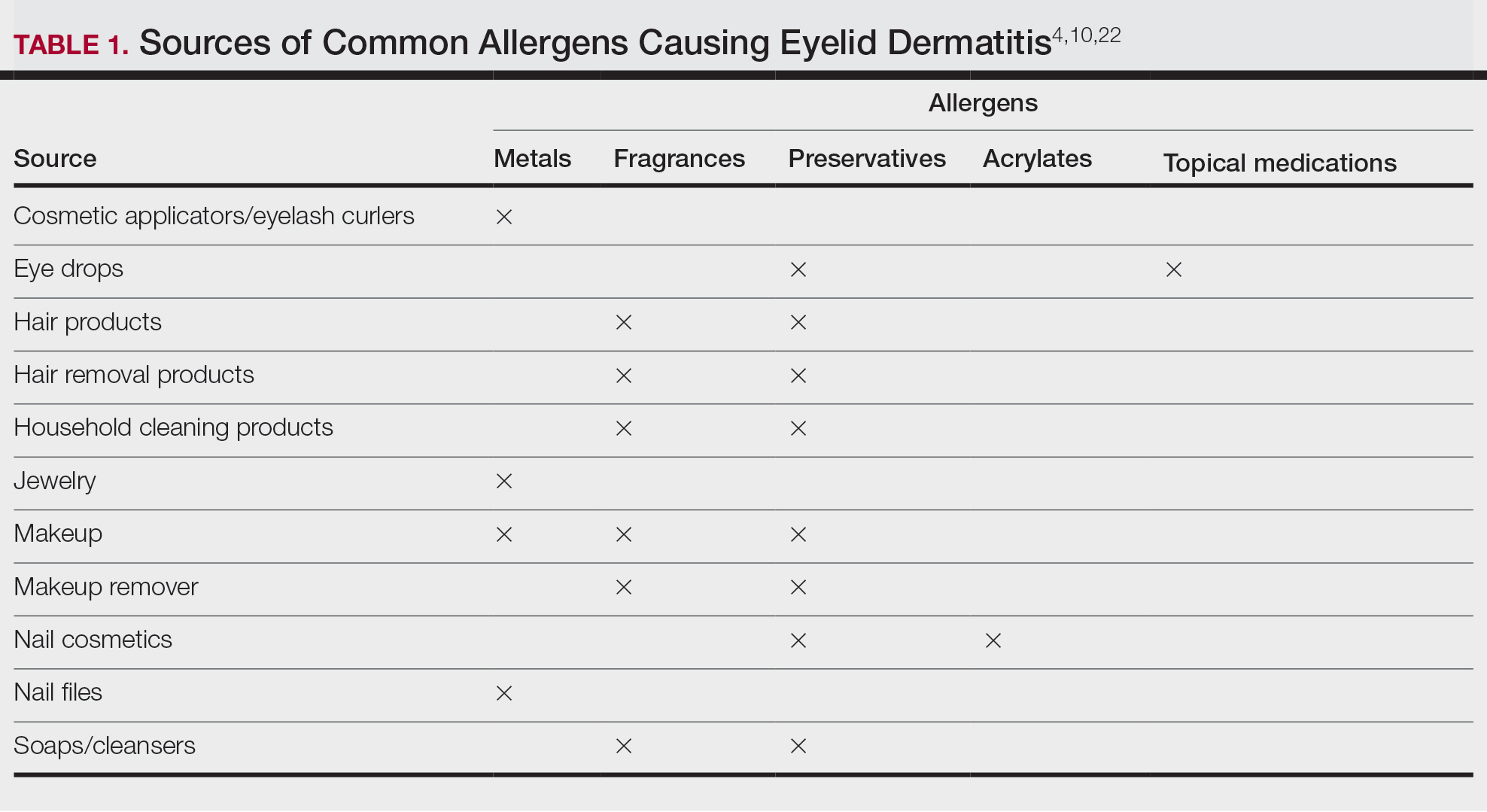
Metals—Metals are among the most common causes of ACD overall, and nickel frequently is reported as one of the top contact allergens in patients with eyelid dermatitis.16,27 A retrospective analysis of 2332 patients with eyelid dermatitis patch tested by the North American Contact Dermatitis Group from 1994 to 2016 found that 18.6% of patients with eyelid ACD had a clinically relevant nickel allergy. Sources of nickel exposure include jewelry, grooming devices, makeup and makeup applicators, and eyelash curlers, as well as direct transfer from the hands after contact with consumer products.16
Other metals that can cause ACD include cobalt (found in similar products to nickel) and gold. Gold often is associated with eyelid dermatitis, though its clinical relevance has been debated, as gold is a relatively inert metal that rarely is present in eye cosmetics and its ions are not displaced from objects and deposited on the skin via sweat in the same way as nickel.4,16,20,28-30 Despite this, studies have shown that gold is a common positive patch test reaction among patients with eyelid dermatitis, even in patients with no dermatitis at the site of contact with gold jewelry.20,29,31 Gold has been reported to be the most common allergen causing unilateral eyelid dermatitis via ectopic transfer.16,19,20,29 It has been proposed that titanium dioxide, present in many cosmetics and sunscreens, displaces gold allowing its release from jewelry, thereby liberating the fine gold ions and allowing them to desposit on the face and eyelids.30,31 Given the uncertain clinical relevance of positive patch test reactions to gold, Warshaw at al16 recommend a 2- to 3-month trial of gold jewelry avoidance to establish relevance, and Ehrlich and Gold29 noted that avoidance of gold leads to improvement.
Fragrances—Fragrances represent a broad category of naturally occurring and man-made components that often are combined to produce a desired scent in personal care products.32 Essential oils and botanicals are both examples of natural fragrances.33 Fragrances are found in numerous products including makeup, hair products, and household cleaning supplies and represent some of the most common contact allergens.32 Common fragrance allergens include fragrance mixes I and II, hydroperoxides of linalool, and balsam of Peru.12,32,34 Allergic contact dermatitis to fragrances typically manifests on the eyelids, face, or hands.33 Several studies have found fragrances to be among the top contact allergens in patients with eyelid dermatitis.3,12,20,25,34 Patch testing for fragrance allergy may include baseline series, supplemental fragrance series, and personal care products.32,35
Preservatives—Preservatives, including formaldehyde and formaldehyde releasers (eg, quaternium-15 and bronopol) and methylchloroisothiazolinone/methylisothiazolinone, may be found in personal care products such as makeup, makeup removers, emollients, shampoos, hair care products, and ophthalmologic solutions and are among the most common cosmetic sources of ACD.13,36-39 Preservatives are among the top allergens causing eyelid dermatitis.20 In particular, patch test positivity rates to methylchloroisothiazolinone/methylisothiazolinone have been increasing in North America.40 Sensitization to preservatives may occur through direct skin contact or transfer from the hands.41
Acrylates—Acrylates are compounds derived from acrylic acid that may be found in acrylic and gel nails, eyelash extensions, and other adhesives and are frequent causes of eyelid ACD.4,10,42 Acrylate exposure may be cosmetic among consumers or occupational (eg, aestheticians).42,43 Acrylates on the nails may cause eyelid dermatitis via ectopic transfer from the hands and also may cause periungual dermatitis manifesting as nail bed erythema.10 Hydroxyethyl methacrylate is one of the more common eyelid ACD allergens, and studies have shown increasing prevalence of positive reaction rates to hydroxyethylmethacrylate.10,44Topical Medications—Contact allergies to topical medications are quite common, estimated to occur in 10% to 17% of patients undergoing patch testing.45 Both active and inactive ingredients of topical medications may be culprits in eyelid ACD. The most common topical medication allergens include antibiotics, steroids, local anesthetics, and nonsteroidal anti-inflammatory drugs.45 Topical antibiotics such as neomycin and bacitracin represent some of the most common causes of eyelid dermatitis4,10 and may be found in a variety of products, including antibacterial ointments and eye drops.1 Many ophthalmologic medications also contain corticosteroids, with the most common allergenic steroids being tixocortol pivalate (a marker for hydrocortisone allergy) and budesonide.10,20 Topical steroids pose a particular dilemma, as they can be either the source of or a treatment for ACD.10 Eye drops also may contain anesthetics, β-blockers, and antihistamines, as well as the preservative benzalkonium chloride, all of which may be contact allergens.21,39
Differential Diagnosis of Eyelid Dermatitis
Although ACD is reported to be the most common cause of eyelid dermatitis, the differential diagnosis is broad, including endogenous inflammatory dermatoses and exogenous exposures (Table 2). Symptoms of eyelid ACD can be nonspecific (eg, erythema, pruritus), making diagnosis challenging.46

Atopic dermatitis represents another common cause of eyelid dermatitis, accounting for 14% to 39.5% of cases.3-5,49 Atopic dermatitis of the eyelids classically manifests with lichenification of the medial aspects of the eyelids.50 Atopic dermatitis and ACD may be difficult to distinguish, as the 2 conditions appear clinically similar and can develop concomitantly.51 Additionally, atopic patients are likely to have comorbid allergic rhinitis and sensitivity to environmental allergens, which may lead to chronic eye scratching and lichenification.1,51 Clinical features of eyelid dermatitis suggesting allergic rhinitis and likely comorbid AD include creases in the lower eyelids (Dennie-Morgan lines) and periorbital hyperpigmentation (known as the allergic shiner) due to venous congestion.1,52
Seborrheic dermatitis is an inflammatory reaction to Malassezia yeast that occurs in sebaceous areas such as the groin, scalp, eyebrows, eyelids, and nasolabial folds.1,53,54
Irritant contact dermatitis, a nonspecific inflammatory reaction caused by direct cell damage from external irritants, also may affect the eyelids and appear similar to ACD.1 It typically manifests with a burning or stinging sensation, as opposed to pruritus, and generally develops and resolves more rapidly than ACD.1 Personal care products are common causes of eyelid irritant contact dermatitis.16
Patch Testing for Eyelid ACD
The gold standard for diagnosis of ACD is patch testing, outlined by the International Contact Dermatitis Research Group.55-57 Patch testing generally is performed with standardized panels of allergens and can be customized either with supplemental panels based on unique exposures or with the patient’s own personal care products to increase the sensitivity of testing. Therefore, a thorough history is crucial to identifying potential allergens in a patient’s environment.
False negatives are possible, as the skin on the back may be thicker and less sensitive than the skin at the location of dermatitis.2,58 This is particularly relevant when using patch testing to diagnose ACD of the eyelids, where the skin is particularly thin and sensitive.2 Additionally, ingredients of ophthalmic medications are known to have an especially high false-negative rate with standard patch testing and may require repeated testing with higher drug concentrations or modified patch testing procedures (eg, open testing, scratch-patch testing).1,59
Treatment
Management of ACD involves allergen avoidance, typically dictated by patch test results.10 Allergen avoidance may be facilitated using online resources such as the Contact Allergen Management Program (https://www.acdscamp.org/) created by the American Contact Dermatitis Society.10,18 Patient counseling following patch testing is crucial to educating patients about sources of potential allergen exposures and strategies for avoidance. In the case of eyelid dermatitis, it is particularly important to consider exposure to airborne allergens such as fragrances.16 Fragrance avoidance is uniquely difficult, as labelling standards in the United States currently do not require disclosure of specific fragrance components.33 Additionally, products labelled as unscented may still contain fragrances. As such, some patients with fragrance allergy may need to carefully avoid all products containing fragrances.33
In addition to allergen avoidance, eyelid ACD may be treated with topical medications (eg, steroids, calcineurin inhibitors, Janus kinase inhibitors); however, these same topical medications also can cause ACD due to some ingredients such as propylene glycol.10 Topical steroids should be used with caution on the eyelids given the risk for atrophy, cataracts, and glaucoma.1
Final Interpretation
Eyelid dermatitis is a common dermatologic condition most frequently caused by ACD due to exposure to allergens in cosmetic products, ophthalmic medications, nail lacquers, and jewelry, among many other potential sources. The most common allergens causing eyelid dermatitis include metals (particularly nickel), fragrances, preservatives, acrylates, and topical medications. Eyelid ACD is diagnosed via patch testing, and the mainstay of treatment is strict allergen avoidance. Patient counseling is vital for successful allergen avoidance and resolution of eyelid ACD.
- Hine AM, Waldman RA, Grzybowski A, et al. Allergic disorders of the eyelid. Clin Dermatol. 2023;41:476-480. doi:10.1016/j.clindermatol.2023.08.002
- Turkiewicz M, Shah A, Yang YW, et al. Allergic contact dermatitis of the eyelids: an interdisciplinary review. Ocul Surf. 2023;28:124-130. doi:10.1016/j.jtos.2023.03.001
- Valsecchi R, Imberti G, Martino D, et al. Eyelid dermatitis: an evaluation of 150 patients. Contact Dermatitis. 1992;27:143-147. doi:10.1111/j.1600-0536.1992.tb05242.x
- Guin JD. Eyelid dermatitis: experience in 203 cases. J Am Acad Dermatol. 2002;47:755-765. doi:10.1067/mjd.2002.122736
- Nethercott JR, Nield G, Holness DL. A review of 79 cases of eyelid dermatitis. J Am Acad Dermatol. 1989;21(2 pt 1):223-230. doi:10.1016/s0190-9622(89)70165-1
- Shah M, Lewis FM, Gawkrodger DJ. Facial dermatitis and eyelid dermatitis: a comparison of patch test results and final diagnoses. Contact Dermatitis. 1996;34:140-141. doi:10.1111/j.1600-0536.1996.tb02148.x
- Brites GS, Ferreira I, Sebastião AI, et al. Allergic contact dermatitis: from pathophysiology to development of new preventive strategies. Pharmacol Res. 2020;162:105282. doi:10.1016/j.phrs.2020.105282
- Alinaghi F, Bennike NH, Egeberg A, et al. Prevalence of contact allergy in the general population: a systematic review and meta-analysis. Contact Dermatitis. 2019;80:77-85. doi:10.1111/cod.13119
- Adler BL, DeLeo VA. Allergic contact dermatitis. JAMA Dermatol. 2021;157:364. doi:10.1001/jamadermatol.2020.5639
- Huang CX, Yiannias JA, Killian JM, et al. Seven common allergen groups causing eyelid dermatitis: education and avoidance strategies. Clin Ophthalmol Auckl NZ. 2021;15:1477-1490. doi:10.2147/OPTH.S297754
- Rozas-Muñoz E, Gamé D, Serra-Baldrich E. Allergic contact dermatitis by anatomical regions: diagnostic clues. Actas Dermo-Sifiliográficas Engl Ed. 2018;109:485-507. doi:10.1016/j.adengl.2018.05.016
- Amin KA, Belsito DV. The aetiology of eyelid dermatitis: a 10-year retrospective analysis. Contact Dermatitis. 2006;55:280-285. doi:10.1111/j.1600-0536.2006.00927.x
- Wolf R, Orion E, Tüzün Y. Periorbital (eyelid) dermatides. Clin Dermatol. 2014;32:131-140. doi:10.1016/j.clindermatol.2013.05.035
- Ockenfels HM, Seemann U, Goos M. Contact allergy in patients with periorbital eczema: an analysis of allergens. data recorded by the Information Network of the Departments of Dermatology. Dermatol Basel Switz. 1997;195:119-124. doi:10.1159/000245712
- Landeck L, John SM, Geier J. Periorbital dermatitis in 4779 patients—patch test results during a 10-year period. Contact Dermatitis. 2014;70:205-212. doi:10.1111/cod.12157
- Warshaw EM, Voller LM, Maibach HI, et al. Eyelid dermatitis in patients referred for patch testing: retrospective analysis of North American Contact Dermatitis Group data, 1994-2016. J Am Acad Dermatol. 2021;84:953-964. doi:10.1016/j.jaad.2020.07.020
- McMonnies CW. Management of chronic habits of abnormal eye rubbing. Contact Lens Anterior Eye. 2008;31:95-102. doi:10.1016/j.clae.2007.07.008
- Chisholm SAM, Couch SM, Custer PL. Etiology and management of allergic eyelid dermatitis. Ophthal Plast Reconstr Surg. 2017;33:248-250. doi:10.1097/IOP.0000000000000723
- Lewallen R, Feldman S, eds. Regional atlas of contact dermatitis. The Dermatologist. Accessed April 22, 2024. https://s3.amazonaws.com/HMP/hmp_ln/imported/Regional%20Atlas%20of%20Contact%20Dermatitis%20Book_lr.pdf
- Rietschel RL, Warshaw EM, Sasseville D, et al. Common contact allergens associated with eyelid dermatitis: data from the North American Contact Dermatitis Group 2003-2004 study period. Dermat Contact Atopic Occup Drug. 2007;18:78-81. doi:10.2310/6620.2007.06041
- Mughal AA, Kalavala M. Contact dermatitis to ophthalmic solutions. Clin Exp Dermatol. 2012;37:593-597; quiz 597-598. doi:10.1111/j.1365-2230.2012.04398.x
- Goossens A. Contact allergic reactions on the eyes and eyelids. Bull Soc Belge Ophtalmol. 2004;292:11-17.
- Silverberg NB, Pelletier JL, Jacob SE, et al. Nickel allergic contact dermatitis: identification, treatment, and prevention. Pediatrics. 2020;145:E20200628. doi:10.1542/peds.2020-0628
- Warshaw EM, Schlarbaum JP, Maibach HI, et al. Facial dermatitis in male patients referred for patch testing. JAMA Dermatol. 2020;156:79-84. doi:10.1001/jamadermatol.2019.3531
- Wenk KS, Ehrlich A. Fragrance series testing in eyelid dermatitis. Dermatitis. 2012;23:22-26. doi:10.1097/DER.0b013e31823d180f
- Crouse L, Ziemer C, Ziemer C, et al. Trends in eyelid dermatitis. Dermat Contact Atopic Occup Drug. 2018;29:96-97. doi:10.1097/DER.0000000000000338
- Yazdanparast T, Nassiri Kashani M, Shamsipour M, et al. Contact allergens responsible for eyelid dermatitis in adults. J Dermatol. 2024;51:691-695. doi:10.1111/1346-8138.17140
- Fowler J, Taylor J, Storrs F, et al. Gold allergy in North America. Am J Contact Dermat. 2001;12:3-5.
- Ehrlich A, Belsito DV. Allergic contact dermatitis to gold. Cutis. 2000;65:323-326.
- Danesh M, Murase JE. Titanium dioxide induces eyelid dermatitis in patients allergic to gold. J Am Acad Dermatol. 2015;73:E21. doi:10.1016/j.jaad.2015.03.046
- Katta R. Common misconceptions in contact dermatitis counseling. Dermatol Online J. 2008;14:2.
- De Groot AC. Fragrances: contact allergy and other adverse effects. Dermatitis. 2020;31:13-35. doi:10.1097/DER.0000000000000463
- Reeder MJ. Allergic contact dermatitis to fragrances. Dermatol Clin. 2020;38:371-377. doi:10.1016/j.det.2020.02.009
- Warshaw EM, Zhang AJ, DeKoven JG, et al. Epidemiology of nickel sensitivity: retrospective cross-sectional analysis of North American Contact Dermatitis Group data 1994-2014. J Am Acad Dermatol. 2019;80:701-713. doi:10.1016/j.jaad.2018.09.058
- Schalock PC, Dunnick CA, Nedorost S, et al. American Contact Dermatitis Society core allergen series: 2020 update. Dermatitis. 2020;31:279-282. doi:10.1097/DER.0000000000000621
- Yim E, Baquerizo Nole KL, Tosti A. Contact dermatitis caused by preservatives. Dermatitis. 2014;25:215-231. doi:10.1097/DER.0000000000000061
- Alani JI, Davis MDP, Yiannias JA. Allergy to cosmetics. Dermatitis. 2013;24:283-290. doi:10.1097/DER.0b013e3182a5d8bc
- Hamilton T, de Gannes GC. Allergic contact dermatitis to preservatives and fragrances in cosmetics. Skin Ther Lett. 2011;16:1-4.
- Ashton SJ, Mughal AA. Contact dermatitis to ophthalmic solutions: an update. Dermat Contact Atopic Occup Drug. 2023;34:480-483. doi:10.1089/derm.2023.0033
- Reeder MJ, Warshaw E, Aravamuthan S, et al. Trends in the prevalence of methylchloroisothiazolinone/methylisothiazolinone contact allergy in North America and Europe. JAMA Dermatol. 2023;159:267-274. doi:10.1001/jamadermatol.2022.5991
- Herro EM, Elsaie ML, Nijhawan RI, et al. Recommendations for a screening series for allergic contact eyelid dermatitis. Dermatitis. 2012;23:17-21. doi:10.1097/DER.0b013e31823d191f
- Kucharczyk M, Słowik-Rylska M, Cyran-Stemplewska S, et al. Acrylates as a significant cause of allergic contact dermatitis: new sources of exposure. Adv Dermatol Allergol Dermatol Alergol. 2021;38:555-560. doi:10.5114/ada.2020.95848
- Rodriguez I, George SE, Yu J, et al. Tackling acrylate allergy: the sticky truth. Cutis. 2023;112:282-286. doi:10.12788/cutis.0909
- DeKoven JG, Warshaw EM, Reeder MJ, et al. North American Contact Dermatitis Group Patch Test Results: 2019–2020. Dermatitis. 2023;34:90-104. doi:10.1089/derm.2022.29017.jdk
- de Groot A. Allergic contact dermatitis from topical drugs: an overview. Dermatitis. 2021;32:197-213. doi:10.1097/DER.0000000000000737
- Zug KA, Palay DA, Rock B. Dermatologic diagnosis and treatment of itchy red eyelids. Surv Ophthalmol. 1996;40:293-306. doi:10.1016/s0039-6257(96)82004-2
- Beltrani VS. Eyelid dermatitis. Curr Allergy Asthma Rep. 2001;1:380-388. doi:10.1007/s11882-001-0052-0
- Hirji SH, Maeng MM, Tran AQ, et al. Cutaneous T-cell lymphoma of the eyelid masquerading as dermatitis. Orbit Amst Neth. 2021;40:75-78. doi:10.1080/01676830.2020.1739080
- Svensson A, Möller H. Eyelid dermatitis: the role of atopy and contact allergy. Contact Dermatitis. 1986;15:178-182. doi:10.1111/j.1600-0536.1986.tb01321.x
- Papier A, Tuttle DJ, Mahar TJ. Differential diagnosis of the swollen red eyelid. Am Fam Physician. 2007;76:1815-1824.
- Johnson H, Novack DE, Adler BL, et al. Can atopic dermatitis and allergic contact dermatitis coexist? Cutis. 2022;110:139-142. doi:10.12788cutis.0599
- Berger WE. Allergic rhinitis in children: diagnosis and management strategies. Paediatr Drugs. 2004;6:233-250. doi:10.2165/00148581-200406040-00003
- Singh A, Kansal NK, Kumawat D, et al. Ophthalmic manifestations of seborrheic dermatitis. Skinmed. 2023;21:397-401.
- Clark GW, Pope SM, Jaboori KA. Diagnosis and treatment of seborrheic dermatitis. Am Fam Physician. 2015;91:185-190.
- Lachapelle JM, Maibach HI. Patch Testing and Prick Testing. Springer; 2012.
- Fregert S. Manual of Contact Dermatitis: On Behalf of the International Contact Dermatitis Research Group. Munksgaard; 1974.
- Reeder M, Reck Atwater A. Patch testing 101, part 1: performing the test. Cutis. 2020;106:165-167. doi:10.12788/cutis.0093
- Wolf R, Perluk H. Failure of routine patch test results to detect eyelid dermatitis. Cutis. 1992;49:133-134.
- Grey KR, Warshaw EM. Allergic contact dermatitis to ophthalmic medications: relevant allergens and alternative testing methods. Dermat Contact Atopic Occup Drug. 2016;27:333-347. doi:10.1097/DER.0000000000000224
Eyelid dermatitis is a common dermatologic concern representing a broad group of inflammatory dermatoses and typically presenting as eczematous lesions on the eyelids.1 One of the most common causes of eyelid dermatitis is thought to be allergic contact dermatitis (ACD), a type IV delayed hypersensitivity reaction caused by exposure to external allergens.2 Although ACD can occur anywhere on the body, dermatitis on the face and eyelids is quite common.1,2 This article aims to explore the clinical manifestation, evaluation, and management of eyelid ACD.
Pathophysiology of Eyelid ACD
Studies have shown that ACD is the most common cause of eyelid dermatitis, estimated to account for 46% to 72% of cases worldwide.3-6 Allergic contact dermatitis is a T cell–mediated type IV hypersensitivity reaction to external antigens that manifests as eczematous lesions at the site of contact with the allergen that may spread.7 Allergic contact dermatitis is a common condition, and it is estimated that at least 20% of the general worldwide population has a contact allergy.8,9 Histologically, ACD manifests as spongiotic dermatitis, though this is not unique and also may be seen in atopic dermatitis (AD) and irritant contact dermatitis.2 Allergic contact dermatitis is diagnosed via epicutaneous patch testing, and treatment involves allergen avoidance with or without adjuvant topical and/or systemic immunomodulatory treatments.7
The eyelids are uniquely prone to the development of ACD given their thinner epidermis and increased susceptibility to irritation. They frequently are exposed to allergens through the direct topical route as well as indirectly via airborne exposure, rinse-down products (eg, shampoos), and substances transferred from an individual’s own hands. The occluded skin folds of the eyelids facilitate increased exposure to trapped allergens.10,11 Additionally, the skin of the eyelids is thin, flexible, highly vascularized, and lacking in subcutaneous tissue, making this area more susceptible to antigen penetration than other locations on the body.1,2,10,12,13
Clinical Manifestations
Eyelid ACD is more common in females than males, which is thought to be related to increased use of cosmetics and fragrances.1,3,12,14-16 Clinical manifestations may resemble eczematous papules and plaques.1 Eyelid ACD commonly spreads beyond the eyelid margin, which helps to differentiate it from AD and irritant contact dermatitis. Symptoms of ACD on the eyelids typically include pruritus, redness, swelling, tearing, scaling, and pain.2 Persistent untreated eyelid dermatitis can lead to eyelash loss, damage to meibomian glands, and hyperpigmentation.2,17,18
Patterns of Eyelid ACD
Allergic contact dermatitis on the eyelids can occur due to direct application of allergens onto the skin of the eyelids, runoff of products from the hair/scalp (eg, shampoo), transfer of allergens from the hands, or contact with airborne allergens.1,2,11,12 Some reports have suggested that eyelid ACD more often is caused by products applied to the scalp or face rather than those applied directly to the eyelids.11 Because the scalp and face are less reactive to contact allergens, in some cases the eyelids may be the only affected site.10,12,13
The specific pattern of dermatitis on or around the eyelids can provide clues to the allergenic source. Dermatitis present around the eyelids and periorbital region with involvement of the bilateral upper and lower eyelids suggests direct exposure to a contact allergen, such as makeup or other cosmetic products.1 Unilateral involvement of only 1 eyelid can occur with ectopic transfer of allergens from the hands or nails.1,19 Involvement of the fingers or nails in addition to the eyelids may further suggest ectopic transfer, such as from allergens in nail polish.10 Unilateral eyelid dermatitis also could be caused by unique exposures such as a microscope or camera eyepiece.19 Distribution around the lower eyelids and upper cheeks is indicative of a drip or runoff pattern, which may result from an ophthalmic solution such as eye drops or contact lens solution.1,19 Finally, dermatitis affecting the upper eyelids along with the nasolabial folds and upper chest may suggest airborne contact dermatitis to fragrances or household cleaning products.1,11
Common Culprits of Eyelid ACD
Common causes of eyelid ACD include cosmetic products, ophthalmic medications, nail lacquers, and jewelry.10,13,20 Within the broader category of cosmetics, allergens may be found in makeup and makeup removers, cosmetic applicators and brushes, soaps and cleansers, creams and sunscreens, antiaging products, hair products, nail polish and files, and hair removal products, among many others.10,13,16,20 Additionally, ophthalmologic and topical medications are common sources of ACD, including eyedrops, contact lens solution, and topical antibiotics.10,13,21 Costume jewelry commonly contains allergenic metals, which also can be found in eyelash curlers, eyeglasses, toys, and other household items.22,23 Finally, contact allergens can be found in items such as goggles, gloves, textiles, and a variety of other occupational and household exposures.
Allergic contact dermatitis of the eyelids occurs predominantly—but not exclusively—in females.16,20,24 This finding has been attributed to the traditionally greater use of cosmetics and fragrances among women; however, the use of skin care products among men is increasing, and recent studies have shown the eyelids to be a common location of facial contact dermatitis among men.16,24 Although eyelid dermatitis has not been specifically analyzed by sex, a retrospective analysis of 1332 male patients with facial dermatitis found the most common sites to be the face (not otherwise specified)(48.9%), eyelids (23.5%), and lips (12.6%). In this cohort, the most common allergens were surfactants in shampoos and paraphenylenediamine in hair dyes.24
Common Allergens
Common contact allergens among patients with ACD of the eyelids include metals, fragrances, preservatives, acrylates, and topical medications.3,10,16,20,25-27 Sources of common contact allergens are reviewed in Table 1.

Metals—Metals are among the most common causes of ACD overall, and nickel frequently is reported as one of the top contact allergens in patients with eyelid dermatitis.16,27 A retrospective analysis of 2332 patients with eyelid dermatitis patch tested by the North American Contact Dermatitis Group from 1994 to 2016 found that 18.6% of patients with eyelid ACD had a clinically relevant nickel allergy. Sources of nickel exposure include jewelry, grooming devices, makeup and makeup applicators, and eyelash curlers, as well as direct transfer from the hands after contact with consumer products.16
Other metals that can cause ACD include cobalt (found in similar products to nickel) and gold. Gold often is associated with eyelid dermatitis, though its clinical relevance has been debated, as gold is a relatively inert metal that rarely is present in eye cosmetics and its ions are not displaced from objects and deposited on the skin via sweat in the same way as nickel.4,16,20,28-30 Despite this, studies have shown that gold is a common positive patch test reaction among patients with eyelid dermatitis, even in patients with no dermatitis at the site of contact with gold jewelry.20,29,31 Gold has been reported to be the most common allergen causing unilateral eyelid dermatitis via ectopic transfer.16,19,20,29 It has been proposed that titanium dioxide, present in many cosmetics and sunscreens, displaces gold allowing its release from jewelry, thereby liberating the fine gold ions and allowing them to desposit on the face and eyelids.30,31 Given the uncertain clinical relevance of positive patch test reactions to gold, Warshaw at al16 recommend a 2- to 3-month trial of gold jewelry avoidance to establish relevance, and Ehrlich and Gold29 noted that avoidance of gold leads to improvement.
Fragrances—Fragrances represent a broad category of naturally occurring and man-made components that often are combined to produce a desired scent in personal care products.32 Essential oils and botanicals are both examples of natural fragrances.33 Fragrances are found in numerous products including makeup, hair products, and household cleaning supplies and represent some of the most common contact allergens.32 Common fragrance allergens include fragrance mixes I and II, hydroperoxides of linalool, and balsam of Peru.12,32,34 Allergic contact dermatitis to fragrances typically manifests on the eyelids, face, or hands.33 Several studies have found fragrances to be among the top contact allergens in patients with eyelid dermatitis.3,12,20,25,34 Patch testing for fragrance allergy may include baseline series, supplemental fragrance series, and personal care products.32,35
Preservatives—Preservatives, including formaldehyde and formaldehyde releasers (eg, quaternium-15 and bronopol) and methylchloroisothiazolinone/methylisothiazolinone, may be found in personal care products such as makeup, makeup removers, emollients, shampoos, hair care products, and ophthalmologic solutions and are among the most common cosmetic sources of ACD.13,36-39 Preservatives are among the top allergens causing eyelid dermatitis.20 In particular, patch test positivity rates to methylchloroisothiazolinone/methylisothiazolinone have been increasing in North America.40 Sensitization to preservatives may occur through direct skin contact or transfer from the hands.41
Acrylates—Acrylates are compounds derived from acrylic acid that may be found in acrylic and gel nails, eyelash extensions, and other adhesives and are frequent causes of eyelid ACD.4,10,42 Acrylate exposure may be cosmetic among consumers or occupational (eg, aestheticians).42,43 Acrylates on the nails may cause eyelid dermatitis via ectopic transfer from the hands and also may cause periungual dermatitis manifesting as nail bed erythema.10 Hydroxyethyl methacrylate is one of the more common eyelid ACD allergens, and studies have shown increasing prevalence of positive reaction rates to hydroxyethylmethacrylate.10,44Topical Medications—Contact allergies to topical medications are quite common, estimated to occur in 10% to 17% of patients undergoing patch testing.45 Both active and inactive ingredients of topical medications may be culprits in eyelid ACD. The most common topical medication allergens include antibiotics, steroids, local anesthetics, and nonsteroidal anti-inflammatory drugs.45 Topical antibiotics such as neomycin and bacitracin represent some of the most common causes of eyelid dermatitis4,10 and may be found in a variety of products, including antibacterial ointments and eye drops.1 Many ophthalmologic medications also contain corticosteroids, with the most common allergenic steroids being tixocortol pivalate (a marker for hydrocortisone allergy) and budesonide.10,20 Topical steroids pose a particular dilemma, as they can be either the source of or a treatment for ACD.10 Eye drops also may contain anesthetics, β-blockers, and antihistamines, as well as the preservative benzalkonium chloride, all of which may be contact allergens.21,39
Differential Diagnosis of Eyelid Dermatitis
Although ACD is reported to be the most common cause of eyelid dermatitis, the differential diagnosis is broad, including endogenous inflammatory dermatoses and exogenous exposures (Table 2). Symptoms of eyelid ACD can be nonspecific (eg, erythema, pruritus), making diagnosis challenging.46

Atopic dermatitis represents another common cause of eyelid dermatitis, accounting for 14% to 39.5% of cases.3-5,49 Atopic dermatitis of the eyelids classically manifests with lichenification of the medial aspects of the eyelids.50 Atopic dermatitis and ACD may be difficult to distinguish, as the 2 conditions appear clinically similar and can develop concomitantly.51 Additionally, atopic patients are likely to have comorbid allergic rhinitis and sensitivity to environmental allergens, which may lead to chronic eye scratching and lichenification.1,51 Clinical features of eyelid dermatitis suggesting allergic rhinitis and likely comorbid AD include creases in the lower eyelids (Dennie-Morgan lines) and periorbital hyperpigmentation (known as the allergic shiner) due to venous congestion.1,52
Seborrheic dermatitis is an inflammatory reaction to Malassezia yeast that occurs in sebaceous areas such as the groin, scalp, eyebrows, eyelids, and nasolabial folds.1,53,54
Irritant contact dermatitis, a nonspecific inflammatory reaction caused by direct cell damage from external irritants, also may affect the eyelids and appear similar to ACD.1 It typically manifests with a burning or stinging sensation, as opposed to pruritus, and generally develops and resolves more rapidly than ACD.1 Personal care products are common causes of eyelid irritant contact dermatitis.16
Patch Testing for Eyelid ACD
The gold standard for diagnosis of ACD is patch testing, outlined by the International Contact Dermatitis Research Group.55-57 Patch testing generally is performed with standardized panels of allergens and can be customized either with supplemental panels based on unique exposures or with the patient’s own personal care products to increase the sensitivity of testing. Therefore, a thorough history is crucial to identifying potential allergens in a patient’s environment.
False negatives are possible, as the skin on the back may be thicker and less sensitive than the skin at the location of dermatitis.2,58 This is particularly relevant when using patch testing to diagnose ACD of the eyelids, where the skin is particularly thin and sensitive.2 Additionally, ingredients of ophthalmic medications are known to have an especially high false-negative rate with standard patch testing and may require repeated testing with higher drug concentrations or modified patch testing procedures (eg, open testing, scratch-patch testing).1,59
Treatment
Management of ACD involves allergen avoidance, typically dictated by patch test results.10 Allergen avoidance may be facilitated using online resources such as the Contact Allergen Management Program (https://www.acdscamp.org/) created by the American Contact Dermatitis Society.10,18 Patient counseling following patch testing is crucial to educating patients about sources of potential allergen exposures and strategies for avoidance. In the case of eyelid dermatitis, it is particularly important to consider exposure to airborne allergens such as fragrances.16 Fragrance avoidance is uniquely difficult, as labelling standards in the United States currently do not require disclosure of specific fragrance components.33 Additionally, products labelled as unscented may still contain fragrances. As such, some patients with fragrance allergy may need to carefully avoid all products containing fragrances.33
In addition to allergen avoidance, eyelid ACD may be treated with topical medications (eg, steroids, calcineurin inhibitors, Janus kinase inhibitors); however, these same topical medications also can cause ACD due to some ingredients such as propylene glycol.10 Topical steroids should be used with caution on the eyelids given the risk for atrophy, cataracts, and glaucoma.1
Final Interpretation
Eyelid dermatitis is a common dermatologic condition most frequently caused by ACD due to exposure to allergens in cosmetic products, ophthalmic medications, nail lacquers, and jewelry, among many other potential sources. The most common allergens causing eyelid dermatitis include metals (particularly nickel), fragrances, preservatives, acrylates, and topical medications. Eyelid ACD is diagnosed via patch testing, and the mainstay of treatment is strict allergen avoidance. Patient counseling is vital for successful allergen avoidance and resolution of eyelid ACD.
Eyelid dermatitis is a common dermatologic concern representing a broad group of inflammatory dermatoses and typically presenting as eczematous lesions on the eyelids.1 One of the most common causes of eyelid dermatitis is thought to be allergic contact dermatitis (ACD), a type IV delayed hypersensitivity reaction caused by exposure to external allergens.2 Although ACD can occur anywhere on the body, dermatitis on the face and eyelids is quite common.1,2 This article aims to explore the clinical manifestation, evaluation, and management of eyelid ACD.
Pathophysiology of Eyelid ACD
Studies have shown that ACD is the most common cause of eyelid dermatitis, estimated to account for 46% to 72% of cases worldwide.3-6 Allergic contact dermatitis is a T cell–mediated type IV hypersensitivity reaction to external antigens that manifests as eczematous lesions at the site of contact with the allergen that may spread.7 Allergic contact dermatitis is a common condition, and it is estimated that at least 20% of the general worldwide population has a contact allergy.8,9 Histologically, ACD manifests as spongiotic dermatitis, though this is not unique and also may be seen in atopic dermatitis (AD) and irritant contact dermatitis.2 Allergic contact dermatitis is diagnosed via epicutaneous patch testing, and treatment involves allergen avoidance with or without adjuvant topical and/or systemic immunomodulatory treatments.7
The eyelids are uniquely prone to the development of ACD given their thinner epidermis and increased susceptibility to irritation. They frequently are exposed to allergens through the direct topical route as well as indirectly via airborne exposure, rinse-down products (eg, shampoos), and substances transferred from an individual’s own hands. The occluded skin folds of the eyelids facilitate increased exposure to trapped allergens.10,11 Additionally, the skin of the eyelids is thin, flexible, highly vascularized, and lacking in subcutaneous tissue, making this area more susceptible to antigen penetration than other locations on the body.1,2,10,12,13
Clinical Manifestations
Eyelid ACD is more common in females than males, which is thought to be related to increased use of cosmetics and fragrances.1,3,12,14-16 Clinical manifestations may resemble eczematous papules and plaques.1 Eyelid ACD commonly spreads beyond the eyelid margin, which helps to differentiate it from AD and irritant contact dermatitis. Symptoms of ACD on the eyelids typically include pruritus, redness, swelling, tearing, scaling, and pain.2 Persistent untreated eyelid dermatitis can lead to eyelash loss, damage to meibomian glands, and hyperpigmentation.2,17,18
Patterns of Eyelid ACD
Allergic contact dermatitis on the eyelids can occur due to direct application of allergens onto the skin of the eyelids, runoff of products from the hair/scalp (eg, shampoo), transfer of allergens from the hands, or contact with airborne allergens.1,2,11,12 Some reports have suggested that eyelid ACD more often is caused by products applied to the scalp or face rather than those applied directly to the eyelids.11 Because the scalp and face are less reactive to contact allergens, in some cases the eyelids may be the only affected site.10,12,13
The specific pattern of dermatitis on or around the eyelids can provide clues to the allergenic source. Dermatitis present around the eyelids and periorbital region with involvement of the bilateral upper and lower eyelids suggests direct exposure to a contact allergen, such as makeup or other cosmetic products.1 Unilateral involvement of only 1 eyelid can occur with ectopic transfer of allergens from the hands or nails.1,19 Involvement of the fingers or nails in addition to the eyelids may further suggest ectopic transfer, such as from allergens in nail polish.10 Unilateral eyelid dermatitis also could be caused by unique exposures such as a microscope or camera eyepiece.19 Distribution around the lower eyelids and upper cheeks is indicative of a drip or runoff pattern, which may result from an ophthalmic solution such as eye drops or contact lens solution.1,19 Finally, dermatitis affecting the upper eyelids along with the nasolabial folds and upper chest may suggest airborne contact dermatitis to fragrances or household cleaning products.1,11
Common Culprits of Eyelid ACD
Common causes of eyelid ACD include cosmetic products, ophthalmic medications, nail lacquers, and jewelry.10,13,20 Within the broader category of cosmetics, allergens may be found in makeup and makeup removers, cosmetic applicators and brushes, soaps and cleansers, creams and sunscreens, antiaging products, hair products, nail polish and files, and hair removal products, among many others.10,13,16,20 Additionally, ophthalmologic and topical medications are common sources of ACD, including eyedrops, contact lens solution, and topical antibiotics.10,13,21 Costume jewelry commonly contains allergenic metals, which also can be found in eyelash curlers, eyeglasses, toys, and other household items.22,23 Finally, contact allergens can be found in items such as goggles, gloves, textiles, and a variety of other occupational and household exposures.
Allergic contact dermatitis of the eyelids occurs predominantly—but not exclusively—in females.16,20,24 This finding has been attributed to the traditionally greater use of cosmetics and fragrances among women; however, the use of skin care products among men is increasing, and recent studies have shown the eyelids to be a common location of facial contact dermatitis among men.16,24 Although eyelid dermatitis has not been specifically analyzed by sex, a retrospective analysis of 1332 male patients with facial dermatitis found the most common sites to be the face (not otherwise specified)(48.9%), eyelids (23.5%), and lips (12.6%). In this cohort, the most common allergens were surfactants in shampoos and paraphenylenediamine in hair dyes.24
Common Allergens
Common contact allergens among patients with ACD of the eyelids include metals, fragrances, preservatives, acrylates, and topical medications.3,10,16,20,25-27 Sources of common contact allergens are reviewed in Table 1.

Metals—Metals are among the most common causes of ACD overall, and nickel frequently is reported as one of the top contact allergens in patients with eyelid dermatitis.16,27 A retrospective analysis of 2332 patients with eyelid dermatitis patch tested by the North American Contact Dermatitis Group from 1994 to 2016 found that 18.6% of patients with eyelid ACD had a clinically relevant nickel allergy. Sources of nickel exposure include jewelry, grooming devices, makeup and makeup applicators, and eyelash curlers, as well as direct transfer from the hands after contact with consumer products.16
Other metals that can cause ACD include cobalt (found in similar products to nickel) and gold. Gold often is associated with eyelid dermatitis, though its clinical relevance has been debated, as gold is a relatively inert metal that rarely is present in eye cosmetics and its ions are not displaced from objects and deposited on the skin via sweat in the same way as nickel.4,16,20,28-30 Despite this, studies have shown that gold is a common positive patch test reaction among patients with eyelid dermatitis, even in patients with no dermatitis at the site of contact with gold jewelry.20,29,31 Gold has been reported to be the most common allergen causing unilateral eyelid dermatitis via ectopic transfer.16,19,20,29 It has been proposed that titanium dioxide, present in many cosmetics and sunscreens, displaces gold allowing its release from jewelry, thereby liberating the fine gold ions and allowing them to desposit on the face and eyelids.30,31 Given the uncertain clinical relevance of positive patch test reactions to gold, Warshaw at al16 recommend a 2- to 3-month trial of gold jewelry avoidance to establish relevance, and Ehrlich and Gold29 noted that avoidance of gold leads to improvement.
Fragrances—Fragrances represent a broad category of naturally occurring and man-made components that often are combined to produce a desired scent in personal care products.32 Essential oils and botanicals are both examples of natural fragrances.33 Fragrances are found in numerous products including makeup, hair products, and household cleaning supplies and represent some of the most common contact allergens.32 Common fragrance allergens include fragrance mixes I and II, hydroperoxides of linalool, and balsam of Peru.12,32,34 Allergic contact dermatitis to fragrances typically manifests on the eyelids, face, or hands.33 Several studies have found fragrances to be among the top contact allergens in patients with eyelid dermatitis.3,12,20,25,34 Patch testing for fragrance allergy may include baseline series, supplemental fragrance series, and personal care products.32,35
Preservatives—Preservatives, including formaldehyde and formaldehyde releasers (eg, quaternium-15 and bronopol) and methylchloroisothiazolinone/methylisothiazolinone, may be found in personal care products such as makeup, makeup removers, emollients, shampoos, hair care products, and ophthalmologic solutions and are among the most common cosmetic sources of ACD.13,36-39 Preservatives are among the top allergens causing eyelid dermatitis.20 In particular, patch test positivity rates to methylchloroisothiazolinone/methylisothiazolinone have been increasing in North America.40 Sensitization to preservatives may occur through direct skin contact or transfer from the hands.41
Acrylates—Acrylates are compounds derived from acrylic acid that may be found in acrylic and gel nails, eyelash extensions, and other adhesives and are frequent causes of eyelid ACD.4,10,42 Acrylate exposure may be cosmetic among consumers or occupational (eg, aestheticians).42,43 Acrylates on the nails may cause eyelid dermatitis via ectopic transfer from the hands and also may cause periungual dermatitis manifesting as nail bed erythema.10 Hydroxyethyl methacrylate is one of the more common eyelid ACD allergens, and studies have shown increasing prevalence of positive reaction rates to hydroxyethylmethacrylate.10,44Topical Medications—Contact allergies to topical medications are quite common, estimated to occur in 10% to 17% of patients undergoing patch testing.45 Both active and inactive ingredients of topical medications may be culprits in eyelid ACD. The most common topical medication allergens include antibiotics, steroids, local anesthetics, and nonsteroidal anti-inflammatory drugs.45 Topical antibiotics such as neomycin and bacitracin represent some of the most common causes of eyelid dermatitis4,10 and may be found in a variety of products, including antibacterial ointments and eye drops.1 Many ophthalmologic medications also contain corticosteroids, with the most common allergenic steroids being tixocortol pivalate (a marker for hydrocortisone allergy) and budesonide.10,20 Topical steroids pose a particular dilemma, as they can be either the source of or a treatment for ACD.10 Eye drops also may contain anesthetics, β-blockers, and antihistamines, as well as the preservative benzalkonium chloride, all of which may be contact allergens.21,39
Differential Diagnosis of Eyelid Dermatitis
Although ACD is reported to be the most common cause of eyelid dermatitis, the differential diagnosis is broad, including endogenous inflammatory dermatoses and exogenous exposures (Table 2). Symptoms of eyelid ACD can be nonspecific (eg, erythema, pruritus), making diagnosis challenging.46

Atopic dermatitis represents another common cause of eyelid dermatitis, accounting for 14% to 39.5% of cases.3-5,49 Atopic dermatitis of the eyelids classically manifests with lichenification of the medial aspects of the eyelids.50 Atopic dermatitis and ACD may be difficult to distinguish, as the 2 conditions appear clinically similar and can develop concomitantly.51 Additionally, atopic patients are likely to have comorbid allergic rhinitis and sensitivity to environmental allergens, which may lead to chronic eye scratching and lichenification.1,51 Clinical features of eyelid dermatitis suggesting allergic rhinitis and likely comorbid AD include creases in the lower eyelids (Dennie-Morgan lines) and periorbital hyperpigmentation (known as the allergic shiner) due to venous congestion.1,52
Seborrheic dermatitis is an inflammatory reaction to Malassezia yeast that occurs in sebaceous areas such as the groin, scalp, eyebrows, eyelids, and nasolabial folds.1,53,54
Irritant contact dermatitis, a nonspecific inflammatory reaction caused by direct cell damage from external irritants, also may affect the eyelids and appear similar to ACD.1 It typically manifests with a burning or stinging sensation, as opposed to pruritus, and generally develops and resolves more rapidly than ACD.1 Personal care products are common causes of eyelid irritant contact dermatitis.16
Patch Testing for Eyelid ACD
The gold standard for diagnosis of ACD is patch testing, outlined by the International Contact Dermatitis Research Group.55-57 Patch testing generally is performed with standardized panels of allergens and can be customized either with supplemental panels based on unique exposures or with the patient’s own personal care products to increase the sensitivity of testing. Therefore, a thorough history is crucial to identifying potential allergens in a patient’s environment.
False negatives are possible, as the skin on the back may be thicker and less sensitive than the skin at the location of dermatitis.2,58 This is particularly relevant when using patch testing to diagnose ACD of the eyelids, where the skin is particularly thin and sensitive.2 Additionally, ingredients of ophthalmic medications are known to have an especially high false-negative rate with standard patch testing and may require repeated testing with higher drug concentrations or modified patch testing procedures (eg, open testing, scratch-patch testing).1,59
Treatment
Management of ACD involves allergen avoidance, typically dictated by patch test results.10 Allergen avoidance may be facilitated using online resources such as the Contact Allergen Management Program (https://www.acdscamp.org/) created by the American Contact Dermatitis Society.10,18 Patient counseling following patch testing is crucial to educating patients about sources of potential allergen exposures and strategies for avoidance. In the case of eyelid dermatitis, it is particularly important to consider exposure to airborne allergens such as fragrances.16 Fragrance avoidance is uniquely difficult, as labelling standards in the United States currently do not require disclosure of specific fragrance components.33 Additionally, products labelled as unscented may still contain fragrances. As such, some patients with fragrance allergy may need to carefully avoid all products containing fragrances.33
In addition to allergen avoidance, eyelid ACD may be treated with topical medications (eg, steroids, calcineurin inhibitors, Janus kinase inhibitors); however, these same topical medications also can cause ACD due to some ingredients such as propylene glycol.10 Topical steroids should be used with caution on the eyelids given the risk for atrophy, cataracts, and glaucoma.1
Final Interpretation
Eyelid dermatitis is a common dermatologic condition most frequently caused by ACD due to exposure to allergens in cosmetic products, ophthalmic medications, nail lacquers, and jewelry, among many other potential sources. The most common allergens causing eyelid dermatitis include metals (particularly nickel), fragrances, preservatives, acrylates, and topical medications. Eyelid ACD is diagnosed via patch testing, and the mainstay of treatment is strict allergen avoidance. Patient counseling is vital for successful allergen avoidance and resolution of eyelid ACD.
- Hine AM, Waldman RA, Grzybowski A, et al. Allergic disorders of the eyelid. Clin Dermatol. 2023;41:476-480. doi:10.1016/j.clindermatol.2023.08.002
- Turkiewicz M, Shah A, Yang YW, et al. Allergic contact dermatitis of the eyelids: an interdisciplinary review. Ocul Surf. 2023;28:124-130. doi:10.1016/j.jtos.2023.03.001
- Valsecchi R, Imberti G, Martino D, et al. Eyelid dermatitis: an evaluation of 150 patients. Contact Dermatitis. 1992;27:143-147. doi:10.1111/j.1600-0536.1992.tb05242.x
- Guin JD. Eyelid dermatitis: experience in 203 cases. J Am Acad Dermatol. 2002;47:755-765. doi:10.1067/mjd.2002.122736
- Nethercott JR, Nield G, Holness DL. A review of 79 cases of eyelid dermatitis. J Am Acad Dermatol. 1989;21(2 pt 1):223-230. doi:10.1016/s0190-9622(89)70165-1
- Shah M, Lewis FM, Gawkrodger DJ. Facial dermatitis and eyelid dermatitis: a comparison of patch test results and final diagnoses. Contact Dermatitis. 1996;34:140-141. doi:10.1111/j.1600-0536.1996.tb02148.x
- Brites GS, Ferreira I, Sebastião AI, et al. Allergic contact dermatitis: from pathophysiology to development of new preventive strategies. Pharmacol Res. 2020;162:105282. doi:10.1016/j.phrs.2020.105282
- Alinaghi F, Bennike NH, Egeberg A, et al. Prevalence of contact allergy in the general population: a systematic review and meta-analysis. Contact Dermatitis. 2019;80:77-85. doi:10.1111/cod.13119
- Adler BL, DeLeo VA. Allergic contact dermatitis. JAMA Dermatol. 2021;157:364. doi:10.1001/jamadermatol.2020.5639
- Huang CX, Yiannias JA, Killian JM, et al. Seven common allergen groups causing eyelid dermatitis: education and avoidance strategies. Clin Ophthalmol Auckl NZ. 2021;15:1477-1490. doi:10.2147/OPTH.S297754
- Rozas-Muñoz E, Gamé D, Serra-Baldrich E. Allergic contact dermatitis by anatomical regions: diagnostic clues. Actas Dermo-Sifiliográficas Engl Ed. 2018;109:485-507. doi:10.1016/j.adengl.2018.05.016
- Amin KA, Belsito DV. The aetiology of eyelid dermatitis: a 10-year retrospective analysis. Contact Dermatitis. 2006;55:280-285. doi:10.1111/j.1600-0536.2006.00927.x
- Wolf R, Orion E, Tüzün Y. Periorbital (eyelid) dermatides. Clin Dermatol. 2014;32:131-140. doi:10.1016/j.clindermatol.2013.05.035
- Ockenfels HM, Seemann U, Goos M. Contact allergy in patients with periorbital eczema: an analysis of allergens. data recorded by the Information Network of the Departments of Dermatology. Dermatol Basel Switz. 1997;195:119-124. doi:10.1159/000245712
- Landeck L, John SM, Geier J. Periorbital dermatitis in 4779 patients—patch test results during a 10-year period. Contact Dermatitis. 2014;70:205-212. doi:10.1111/cod.12157
- Warshaw EM, Voller LM, Maibach HI, et al. Eyelid dermatitis in patients referred for patch testing: retrospective analysis of North American Contact Dermatitis Group data, 1994-2016. J Am Acad Dermatol. 2021;84:953-964. doi:10.1016/j.jaad.2020.07.020
- McMonnies CW. Management of chronic habits of abnormal eye rubbing. Contact Lens Anterior Eye. 2008;31:95-102. doi:10.1016/j.clae.2007.07.008
- Chisholm SAM, Couch SM, Custer PL. Etiology and management of allergic eyelid dermatitis. Ophthal Plast Reconstr Surg. 2017;33:248-250. doi:10.1097/IOP.0000000000000723
- Lewallen R, Feldman S, eds. Regional atlas of contact dermatitis. The Dermatologist. Accessed April 22, 2024. https://s3.amazonaws.com/HMP/hmp_ln/imported/Regional%20Atlas%20of%20Contact%20Dermatitis%20Book_lr.pdf
- Rietschel RL, Warshaw EM, Sasseville D, et al. Common contact allergens associated with eyelid dermatitis: data from the North American Contact Dermatitis Group 2003-2004 study period. Dermat Contact Atopic Occup Drug. 2007;18:78-81. doi:10.2310/6620.2007.06041
- Mughal AA, Kalavala M. Contact dermatitis to ophthalmic solutions. Clin Exp Dermatol. 2012;37:593-597; quiz 597-598. doi:10.1111/j.1365-2230.2012.04398.x
- Goossens A. Contact allergic reactions on the eyes and eyelids. Bull Soc Belge Ophtalmol. 2004;292:11-17.
- Silverberg NB, Pelletier JL, Jacob SE, et al. Nickel allergic contact dermatitis: identification, treatment, and prevention. Pediatrics. 2020;145:E20200628. doi:10.1542/peds.2020-0628
- Warshaw EM, Schlarbaum JP, Maibach HI, et al. Facial dermatitis in male patients referred for patch testing. JAMA Dermatol. 2020;156:79-84. doi:10.1001/jamadermatol.2019.3531
- Wenk KS, Ehrlich A. Fragrance series testing in eyelid dermatitis. Dermatitis. 2012;23:22-26. doi:10.1097/DER.0b013e31823d180f
- Crouse L, Ziemer C, Ziemer C, et al. Trends in eyelid dermatitis. Dermat Contact Atopic Occup Drug. 2018;29:96-97. doi:10.1097/DER.0000000000000338
- Yazdanparast T, Nassiri Kashani M, Shamsipour M, et al. Contact allergens responsible for eyelid dermatitis in adults. J Dermatol. 2024;51:691-695. doi:10.1111/1346-8138.17140
- Fowler J, Taylor J, Storrs F, et al. Gold allergy in North America. Am J Contact Dermat. 2001;12:3-5.
- Ehrlich A, Belsito DV. Allergic contact dermatitis to gold. Cutis. 2000;65:323-326.
- Danesh M, Murase JE. Titanium dioxide induces eyelid dermatitis in patients allergic to gold. J Am Acad Dermatol. 2015;73:E21. doi:10.1016/j.jaad.2015.03.046
- Katta R. Common misconceptions in contact dermatitis counseling. Dermatol Online J. 2008;14:2.
- De Groot AC. Fragrances: contact allergy and other adverse effects. Dermatitis. 2020;31:13-35. doi:10.1097/DER.0000000000000463
- Reeder MJ. Allergic contact dermatitis to fragrances. Dermatol Clin. 2020;38:371-377. doi:10.1016/j.det.2020.02.009
- Warshaw EM, Zhang AJ, DeKoven JG, et al. Epidemiology of nickel sensitivity: retrospective cross-sectional analysis of North American Contact Dermatitis Group data 1994-2014. J Am Acad Dermatol. 2019;80:701-713. doi:10.1016/j.jaad.2018.09.058
- Schalock PC, Dunnick CA, Nedorost S, et al. American Contact Dermatitis Society core allergen series: 2020 update. Dermatitis. 2020;31:279-282. doi:10.1097/DER.0000000000000621
- Yim E, Baquerizo Nole KL, Tosti A. Contact dermatitis caused by preservatives. Dermatitis. 2014;25:215-231. doi:10.1097/DER.0000000000000061
- Alani JI, Davis MDP, Yiannias JA. Allergy to cosmetics. Dermatitis. 2013;24:283-290. doi:10.1097/DER.0b013e3182a5d8bc
- Hamilton T, de Gannes GC. Allergic contact dermatitis to preservatives and fragrances in cosmetics. Skin Ther Lett. 2011;16:1-4.
- Ashton SJ, Mughal AA. Contact dermatitis to ophthalmic solutions: an update. Dermat Contact Atopic Occup Drug. 2023;34:480-483. doi:10.1089/derm.2023.0033
- Reeder MJ, Warshaw E, Aravamuthan S, et al. Trends in the prevalence of methylchloroisothiazolinone/methylisothiazolinone contact allergy in North America and Europe. JAMA Dermatol. 2023;159:267-274. doi:10.1001/jamadermatol.2022.5991
- Herro EM, Elsaie ML, Nijhawan RI, et al. Recommendations for a screening series for allergic contact eyelid dermatitis. Dermatitis. 2012;23:17-21. doi:10.1097/DER.0b013e31823d191f
- Kucharczyk M, Słowik-Rylska M, Cyran-Stemplewska S, et al. Acrylates as a significant cause of allergic contact dermatitis: new sources of exposure. Adv Dermatol Allergol Dermatol Alergol. 2021;38:555-560. doi:10.5114/ada.2020.95848
- Rodriguez I, George SE, Yu J, et al. Tackling acrylate allergy: the sticky truth. Cutis. 2023;112:282-286. doi:10.12788/cutis.0909
- DeKoven JG, Warshaw EM, Reeder MJ, et al. North American Contact Dermatitis Group Patch Test Results: 2019–2020. Dermatitis. 2023;34:90-104. doi:10.1089/derm.2022.29017.jdk
- de Groot A. Allergic contact dermatitis from topical drugs: an overview. Dermatitis. 2021;32:197-213. doi:10.1097/DER.0000000000000737
- Zug KA, Palay DA, Rock B. Dermatologic diagnosis and treatment of itchy red eyelids. Surv Ophthalmol. 1996;40:293-306. doi:10.1016/s0039-6257(96)82004-2
- Beltrani VS. Eyelid dermatitis. Curr Allergy Asthma Rep. 2001;1:380-388. doi:10.1007/s11882-001-0052-0
- Hirji SH, Maeng MM, Tran AQ, et al. Cutaneous T-cell lymphoma of the eyelid masquerading as dermatitis. Orbit Amst Neth. 2021;40:75-78. doi:10.1080/01676830.2020.1739080
- Svensson A, Möller H. Eyelid dermatitis: the role of atopy and contact allergy. Contact Dermatitis. 1986;15:178-182. doi:10.1111/j.1600-0536.1986.tb01321.x
- Papier A, Tuttle DJ, Mahar TJ. Differential diagnosis of the swollen red eyelid. Am Fam Physician. 2007;76:1815-1824.
- Johnson H, Novack DE, Adler BL, et al. Can atopic dermatitis and allergic contact dermatitis coexist? Cutis. 2022;110:139-142. doi:10.12788cutis.0599
- Berger WE. Allergic rhinitis in children: diagnosis and management strategies. Paediatr Drugs. 2004;6:233-250. doi:10.2165/00148581-200406040-00003
- Singh A, Kansal NK, Kumawat D, et al. Ophthalmic manifestations of seborrheic dermatitis. Skinmed. 2023;21:397-401.
- Clark GW, Pope SM, Jaboori KA. Diagnosis and treatment of seborrheic dermatitis. Am Fam Physician. 2015;91:185-190.
- Lachapelle JM, Maibach HI. Patch Testing and Prick Testing. Springer; 2012.
- Fregert S. Manual of Contact Dermatitis: On Behalf of the International Contact Dermatitis Research Group. Munksgaard; 1974.
- Reeder M, Reck Atwater A. Patch testing 101, part 1: performing the test. Cutis. 2020;106:165-167. doi:10.12788/cutis.0093
- Wolf R, Perluk H. Failure of routine patch test results to detect eyelid dermatitis. Cutis. 1992;49:133-134.
- Grey KR, Warshaw EM. Allergic contact dermatitis to ophthalmic medications: relevant allergens and alternative testing methods. Dermat Contact Atopic Occup Drug. 2016;27:333-347. doi:10.1097/DER.0000000000000224
- Hine AM, Waldman RA, Grzybowski A, et al. Allergic disorders of the eyelid. Clin Dermatol. 2023;41:476-480. doi:10.1016/j.clindermatol.2023.08.002
- Turkiewicz M, Shah A, Yang YW, et al. Allergic contact dermatitis of the eyelids: an interdisciplinary review. Ocul Surf. 2023;28:124-130. doi:10.1016/j.jtos.2023.03.001
- Valsecchi R, Imberti G, Martino D, et al. Eyelid dermatitis: an evaluation of 150 patients. Contact Dermatitis. 1992;27:143-147. doi:10.1111/j.1600-0536.1992.tb05242.x
- Guin JD. Eyelid dermatitis: experience in 203 cases. J Am Acad Dermatol. 2002;47:755-765. doi:10.1067/mjd.2002.122736
- Nethercott JR, Nield G, Holness DL. A review of 79 cases of eyelid dermatitis. J Am Acad Dermatol. 1989;21(2 pt 1):223-230. doi:10.1016/s0190-9622(89)70165-1
- Shah M, Lewis FM, Gawkrodger DJ. Facial dermatitis and eyelid dermatitis: a comparison of patch test results and final diagnoses. Contact Dermatitis. 1996;34:140-141. doi:10.1111/j.1600-0536.1996.tb02148.x
- Brites GS, Ferreira I, Sebastião AI, et al. Allergic contact dermatitis: from pathophysiology to development of new preventive strategies. Pharmacol Res. 2020;162:105282. doi:10.1016/j.phrs.2020.105282
- Alinaghi F, Bennike NH, Egeberg A, et al. Prevalence of contact allergy in the general population: a systematic review and meta-analysis. Contact Dermatitis. 2019;80:77-85. doi:10.1111/cod.13119
- Adler BL, DeLeo VA. Allergic contact dermatitis. JAMA Dermatol. 2021;157:364. doi:10.1001/jamadermatol.2020.5639
- Huang CX, Yiannias JA, Killian JM, et al. Seven common allergen groups causing eyelid dermatitis: education and avoidance strategies. Clin Ophthalmol Auckl NZ. 2021;15:1477-1490. doi:10.2147/OPTH.S297754
- Rozas-Muñoz E, Gamé D, Serra-Baldrich E. Allergic contact dermatitis by anatomical regions: diagnostic clues. Actas Dermo-Sifiliográficas Engl Ed. 2018;109:485-507. doi:10.1016/j.adengl.2018.05.016
- Amin KA, Belsito DV. The aetiology of eyelid dermatitis: a 10-year retrospective analysis. Contact Dermatitis. 2006;55:280-285. doi:10.1111/j.1600-0536.2006.00927.x
- Wolf R, Orion E, Tüzün Y. Periorbital (eyelid) dermatides. Clin Dermatol. 2014;32:131-140. doi:10.1016/j.clindermatol.2013.05.035
- Ockenfels HM, Seemann U, Goos M. Contact allergy in patients with periorbital eczema: an analysis of allergens. data recorded by the Information Network of the Departments of Dermatology. Dermatol Basel Switz. 1997;195:119-124. doi:10.1159/000245712
- Landeck L, John SM, Geier J. Periorbital dermatitis in 4779 patients—patch test results during a 10-year period. Contact Dermatitis. 2014;70:205-212. doi:10.1111/cod.12157
- Warshaw EM, Voller LM, Maibach HI, et al. Eyelid dermatitis in patients referred for patch testing: retrospective analysis of North American Contact Dermatitis Group data, 1994-2016. J Am Acad Dermatol. 2021;84:953-964. doi:10.1016/j.jaad.2020.07.020
- McMonnies CW. Management of chronic habits of abnormal eye rubbing. Contact Lens Anterior Eye. 2008;31:95-102. doi:10.1016/j.clae.2007.07.008
- Chisholm SAM, Couch SM, Custer PL. Etiology and management of allergic eyelid dermatitis. Ophthal Plast Reconstr Surg. 2017;33:248-250. doi:10.1097/IOP.0000000000000723
- Lewallen R, Feldman S, eds. Regional atlas of contact dermatitis. The Dermatologist. Accessed April 22, 2024. https://s3.amazonaws.com/HMP/hmp_ln/imported/Regional%20Atlas%20of%20Contact%20Dermatitis%20Book_lr.pdf
- Rietschel RL, Warshaw EM, Sasseville D, et al. Common contact allergens associated with eyelid dermatitis: data from the North American Contact Dermatitis Group 2003-2004 study period. Dermat Contact Atopic Occup Drug. 2007;18:78-81. doi:10.2310/6620.2007.06041
- Mughal AA, Kalavala M. Contact dermatitis to ophthalmic solutions. Clin Exp Dermatol. 2012;37:593-597; quiz 597-598. doi:10.1111/j.1365-2230.2012.04398.x
- Goossens A. Contact allergic reactions on the eyes and eyelids. Bull Soc Belge Ophtalmol. 2004;292:11-17.
- Silverberg NB, Pelletier JL, Jacob SE, et al. Nickel allergic contact dermatitis: identification, treatment, and prevention. Pediatrics. 2020;145:E20200628. doi:10.1542/peds.2020-0628
- Warshaw EM, Schlarbaum JP, Maibach HI, et al. Facial dermatitis in male patients referred for patch testing. JAMA Dermatol. 2020;156:79-84. doi:10.1001/jamadermatol.2019.3531
- Wenk KS, Ehrlich A. Fragrance series testing in eyelid dermatitis. Dermatitis. 2012;23:22-26. doi:10.1097/DER.0b013e31823d180f
- Crouse L, Ziemer C, Ziemer C, et al. Trends in eyelid dermatitis. Dermat Contact Atopic Occup Drug. 2018;29:96-97. doi:10.1097/DER.0000000000000338
- Yazdanparast T, Nassiri Kashani M, Shamsipour M, et al. Contact allergens responsible for eyelid dermatitis in adults. J Dermatol. 2024;51:691-695. doi:10.1111/1346-8138.17140
- Fowler J, Taylor J, Storrs F, et al. Gold allergy in North America. Am J Contact Dermat. 2001;12:3-5.
- Ehrlich A, Belsito DV. Allergic contact dermatitis to gold. Cutis. 2000;65:323-326.
- Danesh M, Murase JE. Titanium dioxide induces eyelid dermatitis in patients allergic to gold. J Am Acad Dermatol. 2015;73:E21. doi:10.1016/j.jaad.2015.03.046
- Katta R. Common misconceptions in contact dermatitis counseling. Dermatol Online J. 2008;14:2.
- De Groot AC. Fragrances: contact allergy and other adverse effects. Dermatitis. 2020;31:13-35. doi:10.1097/DER.0000000000000463
- Reeder MJ. Allergic contact dermatitis to fragrances. Dermatol Clin. 2020;38:371-377. doi:10.1016/j.det.2020.02.009
- Warshaw EM, Zhang AJ, DeKoven JG, et al. Epidemiology of nickel sensitivity: retrospective cross-sectional analysis of North American Contact Dermatitis Group data 1994-2014. J Am Acad Dermatol. 2019;80:701-713. doi:10.1016/j.jaad.2018.09.058
- Schalock PC, Dunnick CA, Nedorost S, et al. American Contact Dermatitis Society core allergen series: 2020 update. Dermatitis. 2020;31:279-282. doi:10.1097/DER.0000000000000621
- Yim E, Baquerizo Nole KL, Tosti A. Contact dermatitis caused by preservatives. Dermatitis. 2014;25:215-231. doi:10.1097/DER.0000000000000061
- Alani JI, Davis MDP, Yiannias JA. Allergy to cosmetics. Dermatitis. 2013;24:283-290. doi:10.1097/DER.0b013e3182a5d8bc
- Hamilton T, de Gannes GC. Allergic contact dermatitis to preservatives and fragrances in cosmetics. Skin Ther Lett. 2011;16:1-4.
- Ashton SJ, Mughal AA. Contact dermatitis to ophthalmic solutions: an update. Dermat Contact Atopic Occup Drug. 2023;34:480-483. doi:10.1089/derm.2023.0033
- Reeder MJ, Warshaw E, Aravamuthan S, et al. Trends in the prevalence of methylchloroisothiazolinone/methylisothiazolinone contact allergy in North America and Europe. JAMA Dermatol. 2023;159:267-274. doi:10.1001/jamadermatol.2022.5991
- Herro EM, Elsaie ML, Nijhawan RI, et al. Recommendations for a screening series for allergic contact eyelid dermatitis. Dermatitis. 2012;23:17-21. doi:10.1097/DER.0b013e31823d191f
- Kucharczyk M, Słowik-Rylska M, Cyran-Stemplewska S, et al. Acrylates as a significant cause of allergic contact dermatitis: new sources of exposure. Adv Dermatol Allergol Dermatol Alergol. 2021;38:555-560. doi:10.5114/ada.2020.95848
- Rodriguez I, George SE, Yu J, et al. Tackling acrylate allergy: the sticky truth. Cutis. 2023;112:282-286. doi:10.12788/cutis.0909
- DeKoven JG, Warshaw EM, Reeder MJ, et al. North American Contact Dermatitis Group Patch Test Results: 2019–2020. Dermatitis. 2023;34:90-104. doi:10.1089/derm.2022.29017.jdk
- de Groot A. Allergic contact dermatitis from topical drugs: an overview. Dermatitis. 2021;32:197-213. doi:10.1097/DER.0000000000000737
- Zug KA, Palay DA, Rock B. Dermatologic diagnosis and treatment of itchy red eyelids. Surv Ophthalmol. 1996;40:293-306. doi:10.1016/s0039-6257(96)82004-2
- Beltrani VS. Eyelid dermatitis. Curr Allergy Asthma Rep. 2001;1:380-388. doi:10.1007/s11882-001-0052-0
- Hirji SH, Maeng MM, Tran AQ, et al. Cutaneous T-cell lymphoma of the eyelid masquerading as dermatitis. Orbit Amst Neth. 2021;40:75-78. doi:10.1080/01676830.2020.1739080
- Svensson A, Möller H. Eyelid dermatitis: the role of atopy and contact allergy. Contact Dermatitis. 1986;15:178-182. doi:10.1111/j.1600-0536.1986.tb01321.x
- Papier A, Tuttle DJ, Mahar TJ. Differential diagnosis of the swollen red eyelid. Am Fam Physician. 2007;76:1815-1824.
- Johnson H, Novack DE, Adler BL, et al. Can atopic dermatitis and allergic contact dermatitis coexist? Cutis. 2022;110:139-142. doi:10.12788cutis.0599
- Berger WE. Allergic rhinitis in children: diagnosis and management strategies. Paediatr Drugs. 2004;6:233-250. doi:10.2165/00148581-200406040-00003
- Singh A, Kansal NK, Kumawat D, et al. Ophthalmic manifestations of seborrheic dermatitis. Skinmed. 2023;21:397-401.
- Clark GW, Pope SM, Jaboori KA. Diagnosis and treatment of seborrheic dermatitis. Am Fam Physician. 2015;91:185-190.
- Lachapelle JM, Maibach HI. Patch Testing and Prick Testing. Springer; 2012.
- Fregert S. Manual of Contact Dermatitis: On Behalf of the International Contact Dermatitis Research Group. Munksgaard; 1974.
- Reeder M, Reck Atwater A. Patch testing 101, part 1: performing the test. Cutis. 2020;106:165-167. doi:10.12788/cutis.0093
- Wolf R, Perluk H. Failure of routine patch test results to detect eyelid dermatitis. Cutis. 1992;49:133-134.
- Grey KR, Warshaw EM. Allergic contact dermatitis to ophthalmic medications: relevant allergens and alternative testing methods. Dermat Contact Atopic Occup Drug. 2016;27:333-347. doi:10.1097/DER.0000000000000224
Practice Points
- Eyelid dermatitis is a common dermatologic concern representing a broad range of inflammatory dermatoses, most often caused by allergic contact dermatitis (ACD).
- The most common contact allergens associated with eyelid dermatitis are metals (particularly nickel), fragrances, preservatives, acrylates, and topical medications, which may be found in a variety of sources, including cosmetics, ophthalmic medications, nail lacquers, and jewelry.
- Eyelid ACD is diagnosed via patch testing, and management involves strict allergen avoidance.
Hyperandrogenic PCOS Linked to Lower Pregnancy and Live Birth Rates
TOPLINE:
Women with hyperandrogenic polycystic ovary syndrome (PCOS) have lower pregnancy (29.9%) and live birth rates (20.1%) than those with nonhyperandrogenic PCOS (40.2% and 33.1%, respectively).
METHODOLOGY:
- Researchers conducted a retrospective cohort study of 1376 participants from the PPCOS I and II trials, all meeting National Institutes of Health diagnostic criteria for PCOS.
- Participants were categorized into hyperandrogenic (A and B) and nonhyperandrogenic (D) PCOS phenotypes on the basis of medical interviews, demographics, physical examinations, and laboratory data.
- Outcomes of interest included clinical pregnancy, pregnancy loss, live birth, obstetric complications, and neonatal outcomes.
- Fasting blood samples were analyzed for hormonal assays, and Homeostatic Model Assessment for Insulin Resistance scores were calculated using fasting glucose and insulin values.
TAKEAWAY:
- Participants with hyperandrogenic PCOS had higher body mass index (35.5 ± 8.9 vs 31.9 ± 9.3; P < .001) and fasting insulin levels (21.6 ± 27.7 vs 14.7 ± 15.0 μIU/mL; P < .001) than those with nonhyperandrogenic PCOS.
- Participants with hyperandrogenic PCOS had lower odds of achieving pregnancy (odds ratio [OR], 0.63; 95% CI, 0.44-0.92) and live birth (OR, 0.51; 95% CI, 0.34-0.76) than those with nonhyperandrogenic PCOS.
- No significant differences were found in pregnancy loss rates (23.9% vs 32.3%, P = .06) or neonatal outcomes between the two groups.
- The study lacked the power to detect differences in neonatal outcomes because of the low prevalence of these outcomes.
IN PRACTICE:
“Patients with nonhyperandrogenic PCOS may represent a different disease process with unique morbidities and outcomes and could be counseled differently than hyperandrogenic PCOS,” wrote the authors of the study.
SOURCE:
The study was led by Jessica L. Chan, MD, MSCE, Cedars-Sinai Medical Center in Los Angeles, California. It was published online in Obstetrics & Gynecology.
LIMITATIONS:
The primary limitation of this study was that it is a secondary analysis of previously collected randomized controlled trial data, which may affect the availability of certain information. Additionally, the lower number of participants in the nonhyperandrogenic PCOS group could affect the power of the results. The study was underpowered to detect statistically significant differences in neonatal outcomes because of their low prevalence.
DISCLOSURES:
The study was supported by a grant from the ASRM/NICHD/Duke Clinical Research/Reproductive Scientist Training Program. One coauthor disclosed receiving payments from Celmatix, Ferring Pharmaceuticals, Exeltis, Organon, and Monsanto; another disclosed receiving payments from Ferring Pharmaceuticals. Additional disclosures are noted in the original article.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
Women with hyperandrogenic polycystic ovary syndrome (PCOS) have lower pregnancy (29.9%) and live birth rates (20.1%) than those with nonhyperandrogenic PCOS (40.2% and 33.1%, respectively).
METHODOLOGY:
- Researchers conducted a retrospective cohort study of 1376 participants from the PPCOS I and II trials, all meeting National Institutes of Health diagnostic criteria for PCOS.
- Participants were categorized into hyperandrogenic (A and B) and nonhyperandrogenic (D) PCOS phenotypes on the basis of medical interviews, demographics, physical examinations, and laboratory data.
- Outcomes of interest included clinical pregnancy, pregnancy loss, live birth, obstetric complications, and neonatal outcomes.
- Fasting blood samples were analyzed for hormonal assays, and Homeostatic Model Assessment for Insulin Resistance scores were calculated using fasting glucose and insulin values.
TAKEAWAY:
- Participants with hyperandrogenic PCOS had higher body mass index (35.5 ± 8.9 vs 31.9 ± 9.3; P < .001) and fasting insulin levels (21.6 ± 27.7 vs 14.7 ± 15.0 μIU/mL; P < .001) than those with nonhyperandrogenic PCOS.
- Participants with hyperandrogenic PCOS had lower odds of achieving pregnancy (odds ratio [OR], 0.63; 95% CI, 0.44-0.92) and live birth (OR, 0.51; 95% CI, 0.34-0.76) than those with nonhyperandrogenic PCOS.
- No significant differences were found in pregnancy loss rates (23.9% vs 32.3%, P = .06) or neonatal outcomes between the two groups.
- The study lacked the power to detect differences in neonatal outcomes because of the low prevalence of these outcomes.
IN PRACTICE:
“Patients with nonhyperandrogenic PCOS may represent a different disease process with unique morbidities and outcomes and could be counseled differently than hyperandrogenic PCOS,” wrote the authors of the study.
SOURCE:
The study was led by Jessica L. Chan, MD, MSCE, Cedars-Sinai Medical Center in Los Angeles, California. It was published online in Obstetrics & Gynecology.
LIMITATIONS:
The primary limitation of this study was that it is a secondary analysis of previously collected randomized controlled trial data, which may affect the availability of certain information. Additionally, the lower number of participants in the nonhyperandrogenic PCOS group could affect the power of the results. The study was underpowered to detect statistically significant differences in neonatal outcomes because of their low prevalence.
DISCLOSURES:
The study was supported by a grant from the ASRM/NICHD/Duke Clinical Research/Reproductive Scientist Training Program. One coauthor disclosed receiving payments from Celmatix, Ferring Pharmaceuticals, Exeltis, Organon, and Monsanto; another disclosed receiving payments from Ferring Pharmaceuticals. Additional disclosures are noted in the original article.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
Women with hyperandrogenic polycystic ovary syndrome (PCOS) have lower pregnancy (29.9%) and live birth rates (20.1%) than those with nonhyperandrogenic PCOS (40.2% and 33.1%, respectively).
METHODOLOGY:
- Researchers conducted a retrospective cohort study of 1376 participants from the PPCOS I and II trials, all meeting National Institutes of Health diagnostic criteria for PCOS.
- Participants were categorized into hyperandrogenic (A and B) and nonhyperandrogenic (D) PCOS phenotypes on the basis of medical interviews, demographics, physical examinations, and laboratory data.
- Outcomes of interest included clinical pregnancy, pregnancy loss, live birth, obstetric complications, and neonatal outcomes.
- Fasting blood samples were analyzed for hormonal assays, and Homeostatic Model Assessment for Insulin Resistance scores were calculated using fasting glucose and insulin values.
TAKEAWAY:
- Participants with hyperandrogenic PCOS had higher body mass index (35.5 ± 8.9 vs 31.9 ± 9.3; P < .001) and fasting insulin levels (21.6 ± 27.7 vs 14.7 ± 15.0 μIU/mL; P < .001) than those with nonhyperandrogenic PCOS.
- Participants with hyperandrogenic PCOS had lower odds of achieving pregnancy (odds ratio [OR], 0.63; 95% CI, 0.44-0.92) and live birth (OR, 0.51; 95% CI, 0.34-0.76) than those with nonhyperandrogenic PCOS.
- No significant differences were found in pregnancy loss rates (23.9% vs 32.3%, P = .06) or neonatal outcomes between the two groups.
- The study lacked the power to detect differences in neonatal outcomes because of the low prevalence of these outcomes.
IN PRACTICE:
“Patients with nonhyperandrogenic PCOS may represent a different disease process with unique morbidities and outcomes and could be counseled differently than hyperandrogenic PCOS,” wrote the authors of the study.
SOURCE:
The study was led by Jessica L. Chan, MD, MSCE, Cedars-Sinai Medical Center in Los Angeles, California. It was published online in Obstetrics & Gynecology.
LIMITATIONS:
The primary limitation of this study was that it is a secondary analysis of previously collected randomized controlled trial data, which may affect the availability of certain information. Additionally, the lower number of participants in the nonhyperandrogenic PCOS group could affect the power of the results. The study was underpowered to detect statistically significant differences in neonatal outcomes because of their low prevalence.
DISCLOSURES:
The study was supported by a grant from the ASRM/NICHD/Duke Clinical Research/Reproductive Scientist Training Program. One coauthor disclosed receiving payments from Celmatix, Ferring Pharmaceuticals, Exeltis, Organon, and Monsanto; another disclosed receiving payments from Ferring Pharmaceuticals. Additional disclosures are noted in the original article.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
Race Adjustments in Algorithms Boost CRC Risk Prediction
TOPLINE:
Accounting for racial disparities, including in the quality of family history data, enhanced the predictive performance of a colorectal cancer (CRC) risk prediction model.
METHODOLOGY:
- The medical community is reevaluating the use of race adjustments in clinical algorithms due to concerns about the exacerbation of health disparities, especially as reported family history data are known to vary by race.
- To understand how adjusting for race affects the accuracy of CRC prediction algorithms, researchers studied data from community health centers across 12 states as part of the Southern Community Cohort Study.
- Researchers compared two screening algorithms that modeled 10-year CRC risk: A race-blind algorithm and a race-adjusted algorithm that included Black race as a main effect and an interaction with family history.
- The primary outcome was the development of CRC within 10 years of enrollment, assessed using data collected from surveys at enrollment and follow-ups, cancer registry data, and National Death Index reports.
- The researchers compared the algorithms’ predictive performance using such measures as area under the receiver operating characteristic curve (AUC) and calibration and also assessed how adjusting for race changed the proportion of Black participants identified as being at high risk for CRC.
TAKEAWAY:
- The study sample included 77,836 adults aged 40-74 years with no history of CRC at baseline.
- Despite having higher cancer rates, Black participants were more likely to report unknown family history (odds ratio [OR], 1.69; P < .001) and less likely to report known positive family history (OR, 0.68; P < .001) than White participants.
- The interaction term between race and family history was 0.56, indicating that reported family history was less predictive of CRC risk in Black participants than in White participants (P = .010).
- Compared with the race-blinded algorithm, the race-adjusted algorithm increased the fraction of Black participants among the predicted high-risk group (66.1% vs 74.4%; P < .001), potentially enhancing access to screening.
- The race-adjusted algorithm improved the goodness of fit (P < .001) and showed a small improvement in AUC among Black participants (0.611 vs 0.608; P = .006).
IN PRACTICE:
“Our analysis found that removing race from colorectal screening predictors could reduce the number of Black patients recommended for screening, which would work against efforts to reduce disparities in colorectal cancer screening and outcomes,” the authors wrote.
SOURCE:
The study, led by Anna Zink, PhD, the University of Chicago Booth School of Business, Chicago, was published online in Proceedings of the National Academy of Sciences of the USA .
LIMITATIONS:
The study did not report any limitations.
DISCLOSURES:
The study was supported by the National Cancer Institute of the National Institutes of Health. The authors declared no conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
Accounting for racial disparities, including in the quality of family history data, enhanced the predictive performance of a colorectal cancer (CRC) risk prediction model.
METHODOLOGY:
- The medical community is reevaluating the use of race adjustments in clinical algorithms due to concerns about the exacerbation of health disparities, especially as reported family history data are known to vary by race.
- To understand how adjusting for race affects the accuracy of CRC prediction algorithms, researchers studied data from community health centers across 12 states as part of the Southern Community Cohort Study.
- Researchers compared two screening algorithms that modeled 10-year CRC risk: A race-blind algorithm and a race-adjusted algorithm that included Black race as a main effect and an interaction with family history.
- The primary outcome was the development of CRC within 10 years of enrollment, assessed using data collected from surveys at enrollment and follow-ups, cancer registry data, and National Death Index reports.
- The researchers compared the algorithms’ predictive performance using such measures as area under the receiver operating characteristic curve (AUC) and calibration and also assessed how adjusting for race changed the proportion of Black participants identified as being at high risk for CRC.
TAKEAWAY:
- The study sample included 77,836 adults aged 40-74 years with no history of CRC at baseline.
- Despite having higher cancer rates, Black participants were more likely to report unknown family history (odds ratio [OR], 1.69; P < .001) and less likely to report known positive family history (OR, 0.68; P < .001) than White participants.
- The interaction term between race and family history was 0.56, indicating that reported family history was less predictive of CRC risk in Black participants than in White participants (P = .010).
- Compared with the race-blinded algorithm, the race-adjusted algorithm increased the fraction of Black participants among the predicted high-risk group (66.1% vs 74.4%; P < .001), potentially enhancing access to screening.
- The race-adjusted algorithm improved the goodness of fit (P < .001) and showed a small improvement in AUC among Black participants (0.611 vs 0.608; P = .006).
IN PRACTICE:
“Our analysis found that removing race from colorectal screening predictors could reduce the number of Black patients recommended for screening, which would work against efforts to reduce disparities in colorectal cancer screening and outcomes,” the authors wrote.
SOURCE:
The study, led by Anna Zink, PhD, the University of Chicago Booth School of Business, Chicago, was published online in Proceedings of the National Academy of Sciences of the USA .
LIMITATIONS:
The study did not report any limitations.
DISCLOSURES:
The study was supported by the National Cancer Institute of the National Institutes of Health. The authors declared no conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
Accounting for racial disparities, including in the quality of family history data, enhanced the predictive performance of a colorectal cancer (CRC) risk prediction model.
METHODOLOGY:
- The medical community is reevaluating the use of race adjustments in clinical algorithms due to concerns about the exacerbation of health disparities, especially as reported family history data are known to vary by race.
- To understand how adjusting for race affects the accuracy of CRC prediction algorithms, researchers studied data from community health centers across 12 states as part of the Southern Community Cohort Study.
- Researchers compared two screening algorithms that modeled 10-year CRC risk: A race-blind algorithm and a race-adjusted algorithm that included Black race as a main effect and an interaction with family history.
- The primary outcome was the development of CRC within 10 years of enrollment, assessed using data collected from surveys at enrollment and follow-ups, cancer registry data, and National Death Index reports.
- The researchers compared the algorithms’ predictive performance using such measures as area under the receiver operating characteristic curve (AUC) and calibration and also assessed how adjusting for race changed the proportion of Black participants identified as being at high risk for CRC.
TAKEAWAY:
- The study sample included 77,836 adults aged 40-74 years with no history of CRC at baseline.
- Despite having higher cancer rates, Black participants were more likely to report unknown family history (odds ratio [OR], 1.69; P < .001) and less likely to report known positive family history (OR, 0.68; P < .001) than White participants.
- The interaction term between race and family history was 0.56, indicating that reported family history was less predictive of CRC risk in Black participants than in White participants (P = .010).
- Compared with the race-blinded algorithm, the race-adjusted algorithm increased the fraction of Black participants among the predicted high-risk group (66.1% vs 74.4%; P < .001), potentially enhancing access to screening.
- The race-adjusted algorithm improved the goodness of fit (P < .001) and showed a small improvement in AUC among Black participants (0.611 vs 0.608; P = .006).
IN PRACTICE:
“Our analysis found that removing race from colorectal screening predictors could reduce the number of Black patients recommended for screening, which would work against efforts to reduce disparities in colorectal cancer screening and outcomes,” the authors wrote.
SOURCE:
The study, led by Anna Zink, PhD, the University of Chicago Booth School of Business, Chicago, was published online in Proceedings of the National Academy of Sciences of the USA .
LIMITATIONS:
The study did not report any limitations.
DISCLOSURES:
The study was supported by the National Cancer Institute of the National Institutes of Health. The authors declared no conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
A Few Rural Towns Are Bucking the Trend and Building New Hospitals
There’s a new morning ritual in Pinedale, Wyoming, a town of about 2000, nestled against the Wind River Mountains.
Friends and neighbors in the oil- and gas-rich community “take their morning coffee and pull up” to watch workers building the county’s first hospital, said Kari DeWitt, the project’s public relations director.
“I think it’s just gratitude,” Ms. DeWitt said.
Sublette County is the only one in Wyoming — where counties span thousands of square miles — without a hospital. The 10-bed, 40,000-square-foot hospital, with a similarly sized attached long-term care facility, is slated to open by the summer of 2025.
Ms. DeWitt, who also is executive director of the Sublette County Health Foundation, has an office at the town’s health clinic with a window view of the construction.
Pinedale’s residents have good reason to be excited. New full-service hospitals with inpatient beds are rare in rural America, where declining population has spurred decades of downsizing and closures. Yet, a few communities in Wyoming and others in Kansas and Georgia are defying the trend.
“To be honest with you, it even seems strange to me,” said Wyoming Hospital Association President Eric Boley. Small rural “hospitals are really struggling all across the country,” he said.
There is no official tally of new hospitals being built in rural America, but industry experts such as Mr. Boley said they’re rare. Typically, health-related construction projects in rural areas are for smaller urgent care centers or stand-alone emergency facilities or are replacements for old hospitals.
About half of rural hospitals lost money in the prior year, according to Chartis, a health analytics and consulting firm. And nearly 150 rural hospitals have closed or converted to smaller operations since 2010, according to data collected by the University of North Carolina’s Cecil G. Sheps Center for Health Services Research.
To stem the tide of closures, Congress created a new rural emergency hospital designation that allowed struggling hospitals to close their inpatient units and provide only outpatient and emergency services. Since January 2023, when the program took effect, 32 of the more than 1700 eligible rural hospitals — from Georgia to New Mexico — have joined the program, according to data from the Centers for Medicare & Medicaid Services.
Tony Breitlow is healthcare studio director for EUA, which has extensive experience working for rural health care systems. Mr. Breitlow said his national architecture and engineering firm’s work expands, replaces, or revamps older buildings, many of which were constructed during the middle of the last century.
The work, Mr. Breitlow said, is part of health care “systems figuring out how to remain robust and viable.”
Freeman Health System, based in Joplin, Missouri, announced plans last year to build a new 50-bed hospital across the state line in Kansas. Paula Baker, Freeman’s president and chief executive, said the system is building for patients in the southeastern corner of the state who travel 45 minutes or more to its bigger Joplin facilities for care.
Freeman’s new hospital, with construction on the building expected to begin in the spring, will be less than 10 miles away from an older, 64-bed hospital that has existed for decades. Kansas is one of more than a dozen states with no “certificate of need” law that would require health providers to obtain approval from the state before offering new services or building or expanding facilities.
Ms. Baker also said Freeman plans to operate emergency services and a small 10-bed outpost in Fort Scott, Kansas, opening early next year in a corner of a hospital that closed in late 2018. Residents there “cried, they cheered, they hugged me,” Ms. Baker said, adding that the “level of appreciation and gratitude that they felt and they displayed was overwhelming to me.”
Michael Topchik, executive director of the Chartis Center for Rural Health, said regional healthcare systems in the Upper Midwest have been particularly active in competing for patients by, among other things, building new hospitals.
And while private corporate money can drive construction, many rural hospital projects tap government programs, especially those supported by the US Department of Agriculture, Mr. Topchik said. That, he said, “surprises a lot of people.”
Since 2021, the USDA’s rural Community Facilities Programs have awarded $2.24 billion in loans and grants to 68 rural hospitals for work that was not related to an emergency or disaster, according to data analyzed by KFF Health News and confirmed by the agency. The federal program is funded through what is often known as the farm bill, which faces a September congressional renewal deadline.
Nearly all the projects are replacements or expansions and updates of older facilities.
The USDA confirmed that three new or planned Wyoming hospitals received federal funding. Hospital projects in Riverton and Saratoga received loans of $37.2 million and $18.3 million, respectively. Pinedale’s hospital received a $29.2 million loan from the agency.
Wyoming’s new construction is rare in a state where more than 80% of rural hospitals reported losses in the third quarter of 2023, according to Chartis. The state association’s Mr. Boley said he worries about several hospitals that have less than 10 days’ cash on hand “day and night.”
Pinedale’s project loan was approved after the community submitted a feasibility study to the USDA that included local clinics and a long-term care facility. “It’s pretty remote and right up in the mountains,” Mr. Boley said.
Pinedale’s Ms. DeWitt said the community was missing key services, such as blood transfusions, which are often necessary when there is a trauma like a car crash or if a pregnant woman faces severe complications. Local ambulances drove 94,000 miles last year, she said.
Ms. DeWitt began working to raise support for the new hospital after her own pregnancy-related trauma in 2014. She was bleeding heavily and arrived at the local health clinic believing it operated like a hospital.
“It was shocking to hear, ‘No, we’re not a hospital. We can’t do blood transfusions. We’re just going to have to pray you live for the next 45 minutes,’ ” Ms. DeWitt said.
Ms. DeWitt had to be airlifted to Idaho, where she delivered a few minutes after landing. When the hospital financing went on the ballot in 2020, Ms. DeWitt — fully recovered, with healthy grade-schoolers at home — began making five calls a night to rally support for a county tax increase to help fund the hospital.
“By improving health care, I think we improve everybody’s chances of survival. You know, it’s pretty basic,” Ms. DeWitt said.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
There’s a new morning ritual in Pinedale, Wyoming, a town of about 2000, nestled against the Wind River Mountains.
Friends and neighbors in the oil- and gas-rich community “take their morning coffee and pull up” to watch workers building the county’s first hospital, said Kari DeWitt, the project’s public relations director.
“I think it’s just gratitude,” Ms. DeWitt said.
Sublette County is the only one in Wyoming — where counties span thousands of square miles — without a hospital. The 10-bed, 40,000-square-foot hospital, with a similarly sized attached long-term care facility, is slated to open by the summer of 2025.
Ms. DeWitt, who also is executive director of the Sublette County Health Foundation, has an office at the town’s health clinic with a window view of the construction.
Pinedale’s residents have good reason to be excited. New full-service hospitals with inpatient beds are rare in rural America, where declining population has spurred decades of downsizing and closures. Yet, a few communities in Wyoming and others in Kansas and Georgia are defying the trend.
“To be honest with you, it even seems strange to me,” said Wyoming Hospital Association President Eric Boley. Small rural “hospitals are really struggling all across the country,” he said.
There is no official tally of new hospitals being built in rural America, but industry experts such as Mr. Boley said they’re rare. Typically, health-related construction projects in rural areas are for smaller urgent care centers or stand-alone emergency facilities or are replacements for old hospitals.
About half of rural hospitals lost money in the prior year, according to Chartis, a health analytics and consulting firm. And nearly 150 rural hospitals have closed or converted to smaller operations since 2010, according to data collected by the University of North Carolina’s Cecil G. Sheps Center for Health Services Research.
To stem the tide of closures, Congress created a new rural emergency hospital designation that allowed struggling hospitals to close their inpatient units and provide only outpatient and emergency services. Since January 2023, when the program took effect, 32 of the more than 1700 eligible rural hospitals — from Georgia to New Mexico — have joined the program, according to data from the Centers for Medicare & Medicaid Services.
Tony Breitlow is healthcare studio director for EUA, which has extensive experience working for rural health care systems. Mr. Breitlow said his national architecture and engineering firm’s work expands, replaces, or revamps older buildings, many of which were constructed during the middle of the last century.
The work, Mr. Breitlow said, is part of health care “systems figuring out how to remain robust and viable.”
Freeman Health System, based in Joplin, Missouri, announced plans last year to build a new 50-bed hospital across the state line in Kansas. Paula Baker, Freeman’s president and chief executive, said the system is building for patients in the southeastern corner of the state who travel 45 minutes or more to its bigger Joplin facilities for care.
Freeman’s new hospital, with construction on the building expected to begin in the spring, will be less than 10 miles away from an older, 64-bed hospital that has existed for decades. Kansas is one of more than a dozen states with no “certificate of need” law that would require health providers to obtain approval from the state before offering new services or building or expanding facilities.
Ms. Baker also said Freeman plans to operate emergency services and a small 10-bed outpost in Fort Scott, Kansas, opening early next year in a corner of a hospital that closed in late 2018. Residents there “cried, they cheered, they hugged me,” Ms. Baker said, adding that the “level of appreciation and gratitude that they felt and they displayed was overwhelming to me.”
Michael Topchik, executive director of the Chartis Center for Rural Health, said regional healthcare systems in the Upper Midwest have been particularly active in competing for patients by, among other things, building new hospitals.
And while private corporate money can drive construction, many rural hospital projects tap government programs, especially those supported by the US Department of Agriculture, Mr. Topchik said. That, he said, “surprises a lot of people.”
Since 2021, the USDA’s rural Community Facilities Programs have awarded $2.24 billion in loans and grants to 68 rural hospitals for work that was not related to an emergency or disaster, according to data analyzed by KFF Health News and confirmed by the agency. The federal program is funded through what is often known as the farm bill, which faces a September congressional renewal deadline.
Nearly all the projects are replacements or expansions and updates of older facilities.
The USDA confirmed that three new or planned Wyoming hospitals received federal funding. Hospital projects in Riverton and Saratoga received loans of $37.2 million and $18.3 million, respectively. Pinedale’s hospital received a $29.2 million loan from the agency.
Wyoming’s new construction is rare in a state where more than 80% of rural hospitals reported losses in the third quarter of 2023, according to Chartis. The state association’s Mr. Boley said he worries about several hospitals that have less than 10 days’ cash on hand “day and night.”
Pinedale’s project loan was approved after the community submitted a feasibility study to the USDA that included local clinics and a long-term care facility. “It’s pretty remote and right up in the mountains,” Mr. Boley said.
Pinedale’s Ms. DeWitt said the community was missing key services, such as blood transfusions, which are often necessary when there is a trauma like a car crash or if a pregnant woman faces severe complications. Local ambulances drove 94,000 miles last year, she said.
Ms. DeWitt began working to raise support for the new hospital after her own pregnancy-related trauma in 2014. She was bleeding heavily and arrived at the local health clinic believing it operated like a hospital.
“It was shocking to hear, ‘No, we’re not a hospital. We can’t do blood transfusions. We’re just going to have to pray you live for the next 45 minutes,’ ” Ms. DeWitt said.
Ms. DeWitt had to be airlifted to Idaho, where she delivered a few minutes after landing. When the hospital financing went on the ballot in 2020, Ms. DeWitt — fully recovered, with healthy grade-schoolers at home — began making five calls a night to rally support for a county tax increase to help fund the hospital.
“By improving health care, I think we improve everybody’s chances of survival. You know, it’s pretty basic,” Ms. DeWitt said.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
There’s a new morning ritual in Pinedale, Wyoming, a town of about 2000, nestled against the Wind River Mountains.
Friends and neighbors in the oil- and gas-rich community “take their morning coffee and pull up” to watch workers building the county’s first hospital, said Kari DeWitt, the project’s public relations director.
“I think it’s just gratitude,” Ms. DeWitt said.
Sublette County is the only one in Wyoming — where counties span thousands of square miles — without a hospital. The 10-bed, 40,000-square-foot hospital, with a similarly sized attached long-term care facility, is slated to open by the summer of 2025.
Ms. DeWitt, who also is executive director of the Sublette County Health Foundation, has an office at the town’s health clinic with a window view of the construction.
Pinedale’s residents have good reason to be excited. New full-service hospitals with inpatient beds are rare in rural America, where declining population has spurred decades of downsizing and closures. Yet, a few communities in Wyoming and others in Kansas and Georgia are defying the trend.
“To be honest with you, it even seems strange to me,” said Wyoming Hospital Association President Eric Boley. Small rural “hospitals are really struggling all across the country,” he said.
There is no official tally of new hospitals being built in rural America, but industry experts such as Mr. Boley said they’re rare. Typically, health-related construction projects in rural areas are for smaller urgent care centers or stand-alone emergency facilities or are replacements for old hospitals.
About half of rural hospitals lost money in the prior year, according to Chartis, a health analytics and consulting firm. And nearly 150 rural hospitals have closed or converted to smaller operations since 2010, according to data collected by the University of North Carolina’s Cecil G. Sheps Center for Health Services Research.
To stem the tide of closures, Congress created a new rural emergency hospital designation that allowed struggling hospitals to close their inpatient units and provide only outpatient and emergency services. Since January 2023, when the program took effect, 32 of the more than 1700 eligible rural hospitals — from Georgia to New Mexico — have joined the program, according to data from the Centers for Medicare & Medicaid Services.
Tony Breitlow is healthcare studio director for EUA, which has extensive experience working for rural health care systems. Mr. Breitlow said his national architecture and engineering firm’s work expands, replaces, or revamps older buildings, many of which were constructed during the middle of the last century.
The work, Mr. Breitlow said, is part of health care “systems figuring out how to remain robust and viable.”
Freeman Health System, based in Joplin, Missouri, announced plans last year to build a new 50-bed hospital across the state line in Kansas. Paula Baker, Freeman’s president and chief executive, said the system is building for patients in the southeastern corner of the state who travel 45 minutes or more to its bigger Joplin facilities for care.
Freeman’s new hospital, with construction on the building expected to begin in the spring, will be less than 10 miles away from an older, 64-bed hospital that has existed for decades. Kansas is one of more than a dozen states with no “certificate of need” law that would require health providers to obtain approval from the state before offering new services or building or expanding facilities.
Ms. Baker also said Freeman plans to operate emergency services and a small 10-bed outpost in Fort Scott, Kansas, opening early next year in a corner of a hospital that closed in late 2018. Residents there “cried, they cheered, they hugged me,” Ms. Baker said, adding that the “level of appreciation and gratitude that they felt and they displayed was overwhelming to me.”
Michael Topchik, executive director of the Chartis Center for Rural Health, said regional healthcare systems in the Upper Midwest have been particularly active in competing for patients by, among other things, building new hospitals.
And while private corporate money can drive construction, many rural hospital projects tap government programs, especially those supported by the US Department of Agriculture, Mr. Topchik said. That, he said, “surprises a lot of people.”
Since 2021, the USDA’s rural Community Facilities Programs have awarded $2.24 billion in loans and grants to 68 rural hospitals for work that was not related to an emergency or disaster, according to data analyzed by KFF Health News and confirmed by the agency. The federal program is funded through what is often known as the farm bill, which faces a September congressional renewal deadline.
Nearly all the projects are replacements or expansions and updates of older facilities.
The USDA confirmed that three new or planned Wyoming hospitals received federal funding. Hospital projects in Riverton and Saratoga received loans of $37.2 million and $18.3 million, respectively. Pinedale’s hospital received a $29.2 million loan from the agency.
Wyoming’s new construction is rare in a state where more than 80% of rural hospitals reported losses in the third quarter of 2023, according to Chartis. The state association’s Mr. Boley said he worries about several hospitals that have less than 10 days’ cash on hand “day and night.”
Pinedale’s project loan was approved after the community submitted a feasibility study to the USDA that included local clinics and a long-term care facility. “It’s pretty remote and right up in the mountains,” Mr. Boley said.
Pinedale’s Ms. DeWitt said the community was missing key services, such as blood transfusions, which are often necessary when there is a trauma like a car crash or if a pregnant woman faces severe complications. Local ambulances drove 94,000 miles last year, she said.
Ms. DeWitt began working to raise support for the new hospital after her own pregnancy-related trauma in 2014. She was bleeding heavily and arrived at the local health clinic believing it operated like a hospital.
“It was shocking to hear, ‘No, we’re not a hospital. We can’t do blood transfusions. We’re just going to have to pray you live for the next 45 minutes,’ ” Ms. DeWitt said.
Ms. DeWitt had to be airlifted to Idaho, where she delivered a few minutes after landing. When the hospital financing went on the ballot in 2020, Ms. DeWitt — fully recovered, with healthy grade-schoolers at home — began making five calls a night to rally support for a county tax increase to help fund the hospital.
“By improving health care, I think we improve everybody’s chances of survival. You know, it’s pretty basic,” Ms. DeWitt said.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Top reads from the CHEST journal portfolio
Explore articles on PAP adherence, plasma biomarkers in ARDS, and airways disorders hospitalizations during wildfire season
Journal CHEST®
Association Between Healthy Behaviors and Health Care Resource Use With Subsequent Positive Airway Pressure Therapy Adherence in OSA
By Launois, MD, PhD, and colleagues
One of the pitfalls in the interpretation of the effect of treatment adherence on health outcomes is the healthy-adherer effect (HAE) bias. Healthy-adherer bias occurs when patients who are treatment-adherent tend to actively seek out preventative care and engage in other healthy behaviors. Incomplete adjustment for such behaviors can lead to spurious inferences regarding study outcomes because healthy behaviors are associated with a reduced risk of many poor health outcomes.
This study demonstrates that HAE proxies (adherence to CV active drugs, no history of smoking, or sleepiness-related car accidents) were associated with subsequent PAP adherence after adjustment for confounders. PAP-adherent patients used less health care resources before PAP initiation. Unfortunately, the study did not measure other healthy behaviors (nutrition, physical activity, psychosocial support) that could also potentially explain HAE. Until the HAE associated with PAP adherence is better understood, clinicians should use caution when interpreting the association of PAP adherence with CV health outcomes and health care resource use.
– Commentary by Sai Venkateshiah, MD, FCCP, Member of the CHEST Physician Editorial Board
CHEST® Critical Care
Circulating Biomarkers of Endothelial Dysfunction Associated With Ventilatory Ratio and Mortality in ARDS Resulting From SARS-CoV-2 Infection Treated With Anti-inflammatory Therapies
By Alladina, MD, and colleagues
Practitioners in the intensive care unit have become increasingly aware that the population of patients with ARDS is highly heterogenous not only in terms of the inciting factors of their condition but also in terms of their respiratory physiology. Calfee and co-workers opened new horizons for us with their 2014 descriptions of two phenotypes of ARDS based upon biological markers that had different clinical outcome profiles. The work by Alladina et al adds to this body of knowledge by studying biomarkers from patients with COVID-ARDS who were receiving anti-inflammatory therapies. These researchers demonstrated that in such patients, endothelial biomarkers, particularly NEDD9, were associated with 60-day mortality. Increased understanding of biologic phenotypes in ARDS patients may facilitate the application of precision medicine to patients with this condition, improving outcome prediction and allowing practitioners to target specific treatments to selected patients.
– Commentary by Daniel R. Ouellette, MD, FCCP, Critical Care Commentary Editor of CHEST Physician
CHEST® Pulmonary
Association of Short-Term Increases in Ambient Fine Particulate Matter With Hospitalization for Asthma or COPD During Wildfire Season and Other Time Periods
By Horne, PhD, MStat, MPH, and colleagues
Trigger avoidance is one the most important interventions in the control of symptoms and prevention of exacerbations in chronic airways diseases. Nevertheless, trigger avoidance is at times not possible. This is the case with wildfire smoke and other environmental irritants—an increasing global health problem. Using data from 11 hospitals along the Utah’s Wasatch Front, the study by Horne and colleagues shows a clear association between a short-term increase in ambient fine particulate matter exposure resulting from wildfires and a surge in asthma exacerbations. This effect was also seen in patients with COPD but to a lesser degree. The study is limited by its observational design and because measurements of pollution levels were performed regionally and not at individual patient level. Yet this study offers valuable insights on the effects of environmental exposures in patients with chronic airways diseases and the consequences to our health care systems. Futures studies are still needed to assess the long-term consequences of sustained exposures to these irritants in patients with respiratory conditions.
– Commentary by Diego J. Maselli, MD, FCCP, Member of the CHEST Physician Editorial Board
Explore articles on PAP adherence, plasma biomarkers in ARDS, and airways disorders hospitalizations during wildfire season
Explore articles on PAP adherence, plasma biomarkers in ARDS, and airways disorders hospitalizations during wildfire season
Journal CHEST®
Association Between Healthy Behaviors and Health Care Resource Use With Subsequent Positive Airway Pressure Therapy Adherence in OSA
By Launois, MD, PhD, and colleagues
One of the pitfalls in the interpretation of the effect of treatment adherence on health outcomes is the healthy-adherer effect (HAE) bias. Healthy-adherer bias occurs when patients who are treatment-adherent tend to actively seek out preventative care and engage in other healthy behaviors. Incomplete adjustment for such behaviors can lead to spurious inferences regarding study outcomes because healthy behaviors are associated with a reduced risk of many poor health outcomes.
This study demonstrates that HAE proxies (adherence to CV active drugs, no history of smoking, or sleepiness-related car accidents) were associated with subsequent PAP adherence after adjustment for confounders. PAP-adherent patients used less health care resources before PAP initiation. Unfortunately, the study did not measure other healthy behaviors (nutrition, physical activity, psychosocial support) that could also potentially explain HAE. Until the HAE associated with PAP adherence is better understood, clinicians should use caution when interpreting the association of PAP adherence with CV health outcomes and health care resource use.
– Commentary by Sai Venkateshiah, MD, FCCP, Member of the CHEST Physician Editorial Board
CHEST® Critical Care
Circulating Biomarkers of Endothelial Dysfunction Associated With Ventilatory Ratio and Mortality in ARDS Resulting From SARS-CoV-2 Infection Treated With Anti-inflammatory Therapies
By Alladina, MD, and colleagues
Practitioners in the intensive care unit have become increasingly aware that the population of patients with ARDS is highly heterogenous not only in terms of the inciting factors of their condition but also in terms of their respiratory physiology. Calfee and co-workers opened new horizons for us with their 2014 descriptions of two phenotypes of ARDS based upon biological markers that had different clinical outcome profiles. The work by Alladina et al adds to this body of knowledge by studying biomarkers from patients with COVID-ARDS who were receiving anti-inflammatory therapies. These researchers demonstrated that in such patients, endothelial biomarkers, particularly NEDD9, were associated with 60-day mortality. Increased understanding of biologic phenotypes in ARDS patients may facilitate the application of precision medicine to patients with this condition, improving outcome prediction and allowing practitioners to target specific treatments to selected patients.
– Commentary by Daniel R. Ouellette, MD, FCCP, Critical Care Commentary Editor of CHEST Physician
CHEST® Pulmonary
Association of Short-Term Increases in Ambient Fine Particulate Matter With Hospitalization for Asthma or COPD During Wildfire Season and Other Time Periods
By Horne, PhD, MStat, MPH, and colleagues
Trigger avoidance is one the most important interventions in the control of symptoms and prevention of exacerbations in chronic airways diseases. Nevertheless, trigger avoidance is at times not possible. This is the case with wildfire smoke and other environmental irritants—an increasing global health problem. Using data from 11 hospitals along the Utah’s Wasatch Front, the study by Horne and colleagues shows a clear association between a short-term increase in ambient fine particulate matter exposure resulting from wildfires and a surge in asthma exacerbations. This effect was also seen in patients with COPD but to a lesser degree. The study is limited by its observational design and because measurements of pollution levels were performed regionally and not at individual patient level. Yet this study offers valuable insights on the effects of environmental exposures in patients with chronic airways diseases and the consequences to our health care systems. Futures studies are still needed to assess the long-term consequences of sustained exposures to these irritants in patients with respiratory conditions.
– Commentary by Diego J. Maselli, MD, FCCP, Member of the CHEST Physician Editorial Board
Journal CHEST®
Association Between Healthy Behaviors and Health Care Resource Use With Subsequent Positive Airway Pressure Therapy Adherence in OSA
By Launois, MD, PhD, and colleagues
One of the pitfalls in the interpretation of the effect of treatment adherence on health outcomes is the healthy-adherer effect (HAE) bias. Healthy-adherer bias occurs when patients who are treatment-adherent tend to actively seek out preventative care and engage in other healthy behaviors. Incomplete adjustment for such behaviors can lead to spurious inferences regarding study outcomes because healthy behaviors are associated with a reduced risk of many poor health outcomes.
This study demonstrates that HAE proxies (adherence to CV active drugs, no history of smoking, or sleepiness-related car accidents) were associated with subsequent PAP adherence after adjustment for confounders. PAP-adherent patients used less health care resources before PAP initiation. Unfortunately, the study did not measure other healthy behaviors (nutrition, physical activity, psychosocial support) that could also potentially explain HAE. Until the HAE associated with PAP adherence is better understood, clinicians should use caution when interpreting the association of PAP adherence with CV health outcomes and health care resource use.
– Commentary by Sai Venkateshiah, MD, FCCP, Member of the CHEST Physician Editorial Board
CHEST® Critical Care
Circulating Biomarkers of Endothelial Dysfunction Associated With Ventilatory Ratio and Mortality in ARDS Resulting From SARS-CoV-2 Infection Treated With Anti-inflammatory Therapies
By Alladina, MD, and colleagues
Practitioners in the intensive care unit have become increasingly aware that the population of patients with ARDS is highly heterogenous not only in terms of the inciting factors of their condition but also in terms of their respiratory physiology. Calfee and co-workers opened new horizons for us with their 2014 descriptions of two phenotypes of ARDS based upon biological markers that had different clinical outcome profiles. The work by Alladina et al adds to this body of knowledge by studying biomarkers from patients with COVID-ARDS who were receiving anti-inflammatory therapies. These researchers demonstrated that in such patients, endothelial biomarkers, particularly NEDD9, were associated with 60-day mortality. Increased understanding of biologic phenotypes in ARDS patients may facilitate the application of precision medicine to patients with this condition, improving outcome prediction and allowing practitioners to target specific treatments to selected patients.
– Commentary by Daniel R. Ouellette, MD, FCCP, Critical Care Commentary Editor of CHEST Physician
CHEST® Pulmonary
Association of Short-Term Increases in Ambient Fine Particulate Matter With Hospitalization for Asthma or COPD During Wildfire Season and Other Time Periods
By Horne, PhD, MStat, MPH, and colleagues
Trigger avoidance is one the most important interventions in the control of symptoms and prevention of exacerbations in chronic airways diseases. Nevertheless, trigger avoidance is at times not possible. This is the case with wildfire smoke and other environmental irritants—an increasing global health problem. Using data from 11 hospitals along the Utah’s Wasatch Front, the study by Horne and colleagues shows a clear association between a short-term increase in ambient fine particulate matter exposure resulting from wildfires and a surge in asthma exacerbations. This effect was also seen in patients with COPD but to a lesser degree. The study is limited by its observational design and because measurements of pollution levels were performed regionally and not at individual patient level. Yet this study offers valuable insights on the effects of environmental exposures in patients with chronic airways diseases and the consequences to our health care systems. Futures studies are still needed to assess the long-term consequences of sustained exposures to these irritants in patients with respiratory conditions.
– Commentary by Diego J. Maselli, MD, FCCP, Member of the CHEST Physician Editorial Board
Advocating for diversity in medical education
Earlier this year,
If enacted, the EDUCATE Act would cut off federal funding to medical schools that force students or faculty to adopt specific beliefs; discriminate based on race or ethnicity; or have diversity, equity, and inclusion (DEI) offices or any functional equivalent. The bill would also require accreditation agencies to check that their standards do not push these practices, while still allowing instruction about health issues tied to race or collecting data for research.
In response to the introduction of this act, CHEST published a statement in support of DEI practices and their necessary role within the practice of health care and medical training programs.
It is our belief that health care requires a solid patient-provider therapeutic alliance to achieve successful outcomes, and decades of scientific research have shown that a lack of clinician diversity worsens health disparities. For patients from historically underserved communities, having clinicians who share similar lived experiences almost always leads to significant improvements in patient outcomes. If identity concordance is not feasible, clinicians with considerable exposure to diverse patient populations, equitable approaches to care, and inclusive perspectives on health gained through continuing, comprehensive medical education and professional training can also positively impact outcomes.
Research indicates that a diverse medical workforce improves cultural competence and can help clinicians better meet the needs of patients from diverse backgrounds and ethnicities and that the benefits of diverse learning environments enhance the educational experience of all participants. Racial and ethnic health inequities illuminate the greatest gaps and worst patient outcomes, especially when compounded by disparities related to gender identity, ability, language, immigration status, sexual orientation, age, socioeconomics, and other social drivers of health. Research also shows that nearly one-fifth of Latine Americans avoid medical care due to concern about experiencing discrimination, Black Americans have significantly lower life expectancies, and Asian Americans are the only racial group to experience cancer as a leading cause of death. It is also well documented that communities experiencing disproportionately high rates of COVID-19 infection, hospitalization, and mortality when compared with White Americans include Black, Latine, Asian, Native Hawaiian, and Native Americans.
“In 2023, the CHEST organization shared its organizational values: community, inclusivity, innovation, advocacy, and integrity,” said CHEST President, Jack D. Buckley, MD, MPH, FCCP. “In strong accordance with these values and with our mission to champion the prevention, diagnosis, and treatment of chest diseases and advance the best patient outcomes, CHEST is firmly committed to the necessity of diversity, equity, and inclusion in health care research, education, and delivery.”
Guided by our core values, CHEST is relentlessly committed to improving the professional’s experience and patient outcomes equally. This commitment compels us to work toward eliminating disparities in the medical field. According to the most recent US Census projections, by 2045, White Americans will no longer be considered a racial majority, with Black, Latine, and Asian Americans continuing to rise. It is incumbent upon us to ensure that our clinician workforce reflects the diversity of its local and national communities.
The underrepresentation of physicians from racially diverse backgrounds is factually clear. Black physicians comprise 5% of the current physician workforce despite Black Americans representing 13% of the population.1 Similarly, while Native Americans comprise 3% of the United States population, Native American physicians account for less than 1% of the physician workforce, with less than 10% of medical schools reporting total enrollment of more than four Native American students.2 Where gender is concerned, women make up about 36% of the physician workforce, a professional disparity that is further exacerbated given the intersections of race and gender, resulting in a significant impact on the current workforce.3 Allowing disinformation to influence the future of medical education and patient care directly contradicts our mission as clinicians dedicated to improving the health of all people.
If physician representation and patient outcomes are linked, as research shows, the lack of diverse medical school representation has dire consequences for matriculation, job recruitment, retention, and promotion. Without supportive policies, programs, and equity-focused curriculums in medical education, we will never close the gap on professional disparities, which means we will similarly never close the gap on health disparities.
Our commitment to our members, all health care professionals, and the field of medicine means that we will stand firm in our defense of DEI today and every day until we have achieved optimal, equitable health for all people in all places. CHEST is committed to an intersectional approach to equitable health care education and delivery. We strive to design solutions that center the most impacted and radiate support outward, ensuring our interventions benefit all others experiencing discrimination.
Read more about CHEST’s commitment to diversity and other advocacy work on the CHEST website.
References
1. AAMC. Figure 18. Percentage of all active physicians by race/ethnicity, 2018. AAMC; 2019. https://www.aamc.org/data-reports/workforce/data/figure-18-percentage-all-active-physicians-race/ethnicity-2018#:~:text=Diversity%20in%20Medicine%3A%20Facts%20and%20Figures%202019,-Diversity%20in%20Medicine&text=Among%20active%20physicians%2C%2056.2%25%20identified,as%20Black%20or%20African%20American
2. Murphy B. New effort to help Native American pre-meds pursue physician dreams. AMA. January 13, 2022. https://www.ama-assn.org/education/medical-school-diversity/new-effort-help-native-american-pre-meds-pursue-physician-dreams
3. AAMC. U.S. Physician Workforce Data Dashboard. AAMC; 2023. https://www.aamc.org/data-reports/report/us-physician-workforce-data-dashboard
Earlier this year,
If enacted, the EDUCATE Act would cut off federal funding to medical schools that force students or faculty to adopt specific beliefs; discriminate based on race or ethnicity; or have diversity, equity, and inclusion (DEI) offices or any functional equivalent. The bill would also require accreditation agencies to check that their standards do not push these practices, while still allowing instruction about health issues tied to race or collecting data for research.
In response to the introduction of this act, CHEST published a statement in support of DEI practices and their necessary role within the practice of health care and medical training programs.
It is our belief that health care requires a solid patient-provider therapeutic alliance to achieve successful outcomes, and decades of scientific research have shown that a lack of clinician diversity worsens health disparities. For patients from historically underserved communities, having clinicians who share similar lived experiences almost always leads to significant improvements in patient outcomes. If identity concordance is not feasible, clinicians with considerable exposure to diverse patient populations, equitable approaches to care, and inclusive perspectives on health gained through continuing, comprehensive medical education and professional training can also positively impact outcomes.
Research indicates that a diverse medical workforce improves cultural competence and can help clinicians better meet the needs of patients from diverse backgrounds and ethnicities and that the benefits of diverse learning environments enhance the educational experience of all participants. Racial and ethnic health inequities illuminate the greatest gaps and worst patient outcomes, especially when compounded by disparities related to gender identity, ability, language, immigration status, sexual orientation, age, socioeconomics, and other social drivers of health. Research also shows that nearly one-fifth of Latine Americans avoid medical care due to concern about experiencing discrimination, Black Americans have significantly lower life expectancies, and Asian Americans are the only racial group to experience cancer as a leading cause of death. It is also well documented that communities experiencing disproportionately high rates of COVID-19 infection, hospitalization, and mortality when compared with White Americans include Black, Latine, Asian, Native Hawaiian, and Native Americans.
“In 2023, the CHEST organization shared its organizational values: community, inclusivity, innovation, advocacy, and integrity,” said CHEST President, Jack D. Buckley, MD, MPH, FCCP. “In strong accordance with these values and with our mission to champion the prevention, diagnosis, and treatment of chest diseases and advance the best patient outcomes, CHEST is firmly committed to the necessity of diversity, equity, and inclusion in health care research, education, and delivery.”
Guided by our core values, CHEST is relentlessly committed to improving the professional’s experience and patient outcomes equally. This commitment compels us to work toward eliminating disparities in the medical field. According to the most recent US Census projections, by 2045, White Americans will no longer be considered a racial majority, with Black, Latine, and Asian Americans continuing to rise. It is incumbent upon us to ensure that our clinician workforce reflects the diversity of its local and national communities.
The underrepresentation of physicians from racially diverse backgrounds is factually clear. Black physicians comprise 5% of the current physician workforce despite Black Americans representing 13% of the population.1 Similarly, while Native Americans comprise 3% of the United States population, Native American physicians account for less than 1% of the physician workforce, with less than 10% of medical schools reporting total enrollment of more than four Native American students.2 Where gender is concerned, women make up about 36% of the physician workforce, a professional disparity that is further exacerbated given the intersections of race and gender, resulting in a significant impact on the current workforce.3 Allowing disinformation to influence the future of medical education and patient care directly contradicts our mission as clinicians dedicated to improving the health of all people.
If physician representation and patient outcomes are linked, as research shows, the lack of diverse medical school representation has dire consequences for matriculation, job recruitment, retention, and promotion. Without supportive policies, programs, and equity-focused curriculums in medical education, we will never close the gap on professional disparities, which means we will similarly never close the gap on health disparities.
Our commitment to our members, all health care professionals, and the field of medicine means that we will stand firm in our defense of DEI today and every day until we have achieved optimal, equitable health for all people in all places. CHEST is committed to an intersectional approach to equitable health care education and delivery. We strive to design solutions that center the most impacted and radiate support outward, ensuring our interventions benefit all others experiencing discrimination.
Read more about CHEST’s commitment to diversity and other advocacy work on the CHEST website.
References
1. AAMC. Figure 18. Percentage of all active physicians by race/ethnicity, 2018. AAMC; 2019. https://www.aamc.org/data-reports/workforce/data/figure-18-percentage-all-active-physicians-race/ethnicity-2018#:~:text=Diversity%20in%20Medicine%3A%20Facts%20and%20Figures%202019,-Diversity%20in%20Medicine&text=Among%20active%20physicians%2C%2056.2%25%20identified,as%20Black%20or%20African%20American
2. Murphy B. New effort to help Native American pre-meds pursue physician dreams. AMA. January 13, 2022. https://www.ama-assn.org/education/medical-school-diversity/new-effort-help-native-american-pre-meds-pursue-physician-dreams
3. AAMC. U.S. Physician Workforce Data Dashboard. AAMC; 2023. https://www.aamc.org/data-reports/report/us-physician-workforce-data-dashboard
Earlier this year,
If enacted, the EDUCATE Act would cut off federal funding to medical schools that force students or faculty to adopt specific beliefs; discriminate based on race or ethnicity; or have diversity, equity, and inclusion (DEI) offices or any functional equivalent. The bill would also require accreditation agencies to check that their standards do not push these practices, while still allowing instruction about health issues tied to race or collecting data for research.
In response to the introduction of this act, CHEST published a statement in support of DEI practices and their necessary role within the practice of health care and medical training programs.
It is our belief that health care requires a solid patient-provider therapeutic alliance to achieve successful outcomes, and decades of scientific research have shown that a lack of clinician diversity worsens health disparities. For patients from historically underserved communities, having clinicians who share similar lived experiences almost always leads to significant improvements in patient outcomes. If identity concordance is not feasible, clinicians with considerable exposure to diverse patient populations, equitable approaches to care, and inclusive perspectives on health gained through continuing, comprehensive medical education and professional training can also positively impact outcomes.
Research indicates that a diverse medical workforce improves cultural competence and can help clinicians better meet the needs of patients from diverse backgrounds and ethnicities and that the benefits of diverse learning environments enhance the educational experience of all participants. Racial and ethnic health inequities illuminate the greatest gaps and worst patient outcomes, especially when compounded by disparities related to gender identity, ability, language, immigration status, sexual orientation, age, socioeconomics, and other social drivers of health. Research also shows that nearly one-fifth of Latine Americans avoid medical care due to concern about experiencing discrimination, Black Americans have significantly lower life expectancies, and Asian Americans are the only racial group to experience cancer as a leading cause of death. It is also well documented that communities experiencing disproportionately high rates of COVID-19 infection, hospitalization, and mortality when compared with White Americans include Black, Latine, Asian, Native Hawaiian, and Native Americans.
“In 2023, the CHEST organization shared its organizational values: community, inclusivity, innovation, advocacy, and integrity,” said CHEST President, Jack D. Buckley, MD, MPH, FCCP. “In strong accordance with these values and with our mission to champion the prevention, diagnosis, and treatment of chest diseases and advance the best patient outcomes, CHEST is firmly committed to the necessity of diversity, equity, and inclusion in health care research, education, and delivery.”
Guided by our core values, CHEST is relentlessly committed to improving the professional’s experience and patient outcomes equally. This commitment compels us to work toward eliminating disparities in the medical field. According to the most recent US Census projections, by 2045, White Americans will no longer be considered a racial majority, with Black, Latine, and Asian Americans continuing to rise. It is incumbent upon us to ensure that our clinician workforce reflects the diversity of its local and national communities.
The underrepresentation of physicians from racially diverse backgrounds is factually clear. Black physicians comprise 5% of the current physician workforce despite Black Americans representing 13% of the population.1 Similarly, while Native Americans comprise 3% of the United States population, Native American physicians account for less than 1% of the physician workforce, with less than 10% of medical schools reporting total enrollment of more than four Native American students.2 Where gender is concerned, women make up about 36% of the physician workforce, a professional disparity that is further exacerbated given the intersections of race and gender, resulting in a significant impact on the current workforce.3 Allowing disinformation to influence the future of medical education and patient care directly contradicts our mission as clinicians dedicated to improving the health of all people.
If physician representation and patient outcomes are linked, as research shows, the lack of diverse medical school representation has dire consequences for matriculation, job recruitment, retention, and promotion. Without supportive policies, programs, and equity-focused curriculums in medical education, we will never close the gap on professional disparities, which means we will similarly never close the gap on health disparities.
Our commitment to our members, all health care professionals, and the field of medicine means that we will stand firm in our defense of DEI today and every day until we have achieved optimal, equitable health for all people in all places. CHEST is committed to an intersectional approach to equitable health care education and delivery. We strive to design solutions that center the most impacted and radiate support outward, ensuring our interventions benefit all others experiencing discrimination.
Read more about CHEST’s commitment to diversity and other advocacy work on the CHEST website.
References
1. AAMC. Figure 18. Percentage of all active physicians by race/ethnicity, 2018. AAMC; 2019. https://www.aamc.org/data-reports/workforce/data/figure-18-percentage-all-active-physicians-race/ethnicity-2018#:~:text=Diversity%20in%20Medicine%3A%20Facts%20and%20Figures%202019,-Diversity%20in%20Medicine&text=Among%20active%20physicians%2C%2056.2%25%20identified,as%20Black%20or%20African%20American
2. Murphy B. New effort to help Native American pre-meds pursue physician dreams. AMA. January 13, 2022. https://www.ama-assn.org/education/medical-school-diversity/new-effort-help-native-american-pre-meds-pursue-physician-dreams
3. AAMC. U.S. Physician Workforce Data Dashboard. AAMC; 2023. https://www.aamc.org/data-reports/report/us-physician-workforce-data-dashboard
Pseudomonas infection in patients with noncystic fibrosis bronchiectasis
Pseudomonas aeruginosa is a clinically important organism that infects patients with noncystic fibrosis bronchiectasis (NCFB). In the United States, the estimated prevalence of NCFB is 213 per 100,000 across all age groups and 813 per 100,000 in the over 65 age group.1 A retrospective cohort study suggests the incidence of NCFB as ascertained from International Classification of Diseases codes may significantly underestimate its true prevalence.2
As the incidence of patients with NCFB continues to increase, the impact of the Pseudomonas infection is expected to grow. A recent retrospective cohort study of commercial claims from IQVIA’s PharMetrics Plus database for the period 2006 to 2020 showed that patients with NCFB and Pseudomonas infection had on average 2.58 hospital admissions per year, with a mean length of stay of 9.94 (± 11.06) days, compared with 1.18 admissions per year, with a mean length of stay of 6.5 (± 8.42) days, in patients with Pseudomonas-negative NCFB. The same trend applied to 30-day readmissions and ICU admissions, 1.32 (± 2.51 days) vs 0.47 (± 1.30 days) and 0.95 (± 1.62 days) vs 0.33 (± 0.76 days), respectively. The differential cost of care per patient per year between patients with NCFB with and without Pseudomonas infection ranged from $55,225 to $315,901.3
Recent data from the United States Bronchiectasis Registry showed the probability of acquiring Pseudomonas aeruginosa was 3% annually.4 The prevalence of Pseudomonas infection in a large, geographically diverse cohort in the United States was quoted at 15%.5 A retrospective analysis of the European Bronchiectasis Registry database showed Pseudomonas infection was the most commonly isolated pathogen (21.8%).6
Given the high incidence and prevalence of NCFB, the high prevalence of Pseudomonas infection in patients with NCFB, and the associated costs and morbidity from infection, identifying effective treatments has become a priority. The British, Spanish (SEPAR), South African, and European bronchiectasis guidelines outline several antibiotic regimens meant to achieve eradication. Generally, there is induction with a (1) quinolone, (2) β-lactam + aminoglycoside, or (3) quinolone with an inhaled antibiotic followed by three months of maintenance inhaled antibiotics.7-10 SEPAR allows for retreatment for recurrence at any time during the first year with any regimen.
For chronic Pseudomonas infection, SEPAR recommends treatment with inhaled antibiotics for patients with more than two exacerbations or one hospitalization, while the threshold in the British and European guidelines is more than three exacerbations. Azithromycin may be used for those who are intolerant or allergic to the nebulized antibiotics. It is worth noting that in the United States, the antibiotics colistin, ciprofloxacin, aztreonam, gentamicin, and tobramycin are administered off label for this indication. A systematic review found a 10% rate of bronchospasm in the treated group compared with 2.3% in the control group, and premedication with albuterol is often needed.11
Unfortunately, the data supporting the listed eradication and suppressive regimens are weak. A systematic review and meta-analysis of six observational studies including 289 patients showed a 12-month eradication rate of only 40% (95% CI, 34-45; P < 0.00001; I2 = 0).12 These results are disappointing and identify a need for further research into the manner in which Pseudomonas infection interacts with the host lung.
We currently know Pseudomonas infection evades antibiotics and host defenses by accumulating mutations and deletions. These include loss-of-function mutations in mucA (mucoidy), lasR (quorum-sensing), mexS (regulates the antibiotic efflux pump), and other genes related to the production of the polysaccharides Psl and Pel (which contribute to biofilm formation).13 There may also be differences in low and high bacteria microbial networks that interact differently with host cytokines to create an unstable environment that predisposes to exacerbation.14
In an attempt to improve our eradication and suppression rates, investigators have begun to target specific aspects of Pseudomonas infection behavior. The GREAT-2 trial compares gremubamab (a bivalent, bispecific, monoclonal antibody targeting Psl exopolysaccharide and the type 3 secretion system component of PcrV) with placebo in patients with chronic Pseudomonas infection. A phase II trial with the phosphodiesterase inhibitor esifentrine, a phase III trial with a reversible DPP1 inhibitor called brensocatib (ASPEN), and a phase II trial with the CatC inhibitor BI 1291583 (Airleaf) are also being conducted. Each of these agents targets mediators of neutrophil inflammation.
In summary, NCFB with Pseudomonas infection is common and leads to an increase in costs, respiratory exacerbations, and hospitalizations. While eradication and suppression are recommended, they are difficult to achieve and require sustained durations of expensive medications that can be difficult to tolerate. Antibiotic therapies will continue to be studied (the ERASE randomized controlled trial to investigate the efficacy and safety of tobramycin to eradicate Pseudomonas infection is currently underway), but targeted therapies represent a promising new approach to combating this stubbornly resistant bacteria. The NCFB community will be watching closely to see whether medicines targeting molecular behavior and host interaction can achieve what antibiotic regimens thus far have not: consistent and sustainable eradication.
Dr. Green is Assistant Professor in Medicine, Medical Director, Bronchiectasis Program, UMass Chan/Baystate Health, Chest Infections Section, Member-at-Large
References
1. Weycker D, Hansen GL, Seifer FD. Prevalence and incidence of noncystic fibrosis bronchiectasis among US adults in 2013. Chron Respir Dis. 2017;14(4):377-384. doi: 10.1177/1479972317709649
2. Green O, Liautaud S, Knee A, Modahl L. Measuring accuracy of International Classification of Diseases codes in identification of patients with non-cystic fibrosis bronchiectasis. ERJ Open Res. 2024;10(2):00715-2023. doi: 10.1183/23120541.00715-2023
3. Franklin M, Minshall ME, Pontenani F, Devarajan S. Impact of Pseudomonas aeruginosa on resource utilization and costs in patients with exacerbated non-cystic fibrosis bronchiectasis. J Med Econ. 2024;27(1):671-677. doi: 10.1080/13696998.2024.2340382
4. Aksamit TR, Locantore N, Addrizzo-Harris D, et al. Five-year outcomes among U.S. bronchiectasis and NTM research registry patients. Am J Respir Crit Care Med. Accepted manuscript. Published online April 26, 2024.
5. Dean SG, Blakney RA, Ricotta EE, et al. Bronchiectasis-associated infections and outcomes in a large, geographically diverse electronic health record cohort in the United States. BMC Pulm Med. 2024;24(1):172. doi: 10.1186/s12890-024-02973-3
6. Chalmers JD, Polverino E, Crichton ML, et al. Bronchiectasis in Europe: data on disease characteristics from the European Bronchiectasis registry (EMBARC). Lancet Respir Med. 2023;11(7):637-649. doi: 10.1016/S2213-2600(23)00093-0
7. Polverino E, Goeminne PC, McDonnell MJ, et al. European Respiratory Society guidelines for the management of adult bronchiectasis. Eur Respir J. 2017;50(3):1700629. doi: 10.1183/13993003.00629-2017
8. Martínez-García MÁ, Máiz L, Olveira C, et al. Spanish guidelines on treatment of bronchiectasis in adults. Arch Bronconeumol. 2018;54(2):88-98. doi: 10.1016/j.arbres.2017.07.016
9. Hill AT, Sullivan AL, Chalmers JD, et al. British Thoracic Society guideline for bronchiectasis in adults. Thorax. 2019;74(Suppl 1):1-69. doi: 10.1136/thoraxjnl-2018-212463
10. Goolam Mahomed A, Maasdorp SD, Barnes R, et al. South African Thoracic Society position statement on the management of non-cystic fibrosis bronchiectasis in adults: 2023. Afr J Thorac Crit Care Med. 2023;29(2):10.7196/AJTCCM. 2023.v29i2.647. doi: 10.7196/AJTCCM.2023.v29i2.647
11. Brodt AM, Stovold E, Zhang L. Inhaled antibiotics for stable non-cystic fibrosis bronchiectasis: a systematic review. Eur Respir J. 2014;44(2):382-393. doi: 10.1183/09031936.00018414
12. Conceição M, Shteinberg M, Goeminne P, Altenburg J, Chalmers JD. Eradication treatment for Pseudomonas aeruginosa infection in adults with bronchiectasis: a systematic review and meta-analysis. Eur Respir Rev. 2024;33(171):230178. doi: 10.1183/16000617.0178-2023
13. Hilliam Y, Moore MP, Lamont IL, et al. Pseudomonas aeruginosa adaptation and diversification in the non-cystic fibrosis bronchiectasis lung. Eur Respir J. 2017;49(4):1602108. doi: 10.1183/13993003.02108-2016
14. Gramegna A, Kumar Narayana J, Amati F, et al. Microbial inflammatory networks in bronchiectasis exacerbators with Pseudomonas aeruginosa. Chest. 2023;164(1):65-68. doi: 10.1016/j.chest.2023.02.014
Pseudomonas aeruginosa is a clinically important organism that infects patients with noncystic fibrosis bronchiectasis (NCFB). In the United States, the estimated prevalence of NCFB is 213 per 100,000 across all age groups and 813 per 100,000 in the over 65 age group.1 A retrospective cohort study suggests the incidence of NCFB as ascertained from International Classification of Diseases codes may significantly underestimate its true prevalence.2
As the incidence of patients with NCFB continues to increase, the impact of the Pseudomonas infection is expected to grow. A recent retrospective cohort study of commercial claims from IQVIA’s PharMetrics Plus database for the period 2006 to 2020 showed that patients with NCFB and Pseudomonas infection had on average 2.58 hospital admissions per year, with a mean length of stay of 9.94 (± 11.06) days, compared with 1.18 admissions per year, with a mean length of stay of 6.5 (± 8.42) days, in patients with Pseudomonas-negative NCFB. The same trend applied to 30-day readmissions and ICU admissions, 1.32 (± 2.51 days) vs 0.47 (± 1.30 days) and 0.95 (± 1.62 days) vs 0.33 (± 0.76 days), respectively. The differential cost of care per patient per year between patients with NCFB with and without Pseudomonas infection ranged from $55,225 to $315,901.3
Recent data from the United States Bronchiectasis Registry showed the probability of acquiring Pseudomonas aeruginosa was 3% annually.4 The prevalence of Pseudomonas infection in a large, geographically diverse cohort in the United States was quoted at 15%.5 A retrospective analysis of the European Bronchiectasis Registry database showed Pseudomonas infection was the most commonly isolated pathogen (21.8%).6
Given the high incidence and prevalence of NCFB, the high prevalence of Pseudomonas infection in patients with NCFB, and the associated costs and morbidity from infection, identifying effective treatments has become a priority. The British, Spanish (SEPAR), South African, and European bronchiectasis guidelines outline several antibiotic regimens meant to achieve eradication. Generally, there is induction with a (1) quinolone, (2) β-lactam + aminoglycoside, or (3) quinolone with an inhaled antibiotic followed by three months of maintenance inhaled antibiotics.7-10 SEPAR allows for retreatment for recurrence at any time during the first year with any regimen.
For chronic Pseudomonas infection, SEPAR recommends treatment with inhaled antibiotics for patients with more than two exacerbations or one hospitalization, while the threshold in the British and European guidelines is more than three exacerbations. Azithromycin may be used for those who are intolerant or allergic to the nebulized antibiotics. It is worth noting that in the United States, the antibiotics colistin, ciprofloxacin, aztreonam, gentamicin, and tobramycin are administered off label for this indication. A systematic review found a 10% rate of bronchospasm in the treated group compared with 2.3% in the control group, and premedication with albuterol is often needed.11
Unfortunately, the data supporting the listed eradication and suppressive regimens are weak. A systematic review and meta-analysis of six observational studies including 289 patients showed a 12-month eradication rate of only 40% (95% CI, 34-45; P < 0.00001; I2 = 0).12 These results are disappointing and identify a need for further research into the manner in which Pseudomonas infection interacts with the host lung.
We currently know Pseudomonas infection evades antibiotics and host defenses by accumulating mutations and deletions. These include loss-of-function mutations in mucA (mucoidy), lasR (quorum-sensing), mexS (regulates the antibiotic efflux pump), and other genes related to the production of the polysaccharides Psl and Pel (which contribute to biofilm formation).13 There may also be differences in low and high bacteria microbial networks that interact differently with host cytokines to create an unstable environment that predisposes to exacerbation.14
In an attempt to improve our eradication and suppression rates, investigators have begun to target specific aspects of Pseudomonas infection behavior. The GREAT-2 trial compares gremubamab (a bivalent, bispecific, monoclonal antibody targeting Psl exopolysaccharide and the type 3 secretion system component of PcrV) with placebo in patients with chronic Pseudomonas infection. A phase II trial with the phosphodiesterase inhibitor esifentrine, a phase III trial with a reversible DPP1 inhibitor called brensocatib (ASPEN), and a phase II trial with the CatC inhibitor BI 1291583 (Airleaf) are also being conducted. Each of these agents targets mediators of neutrophil inflammation.
In summary, NCFB with Pseudomonas infection is common and leads to an increase in costs, respiratory exacerbations, and hospitalizations. While eradication and suppression are recommended, they are difficult to achieve and require sustained durations of expensive medications that can be difficult to tolerate. Antibiotic therapies will continue to be studied (the ERASE randomized controlled trial to investigate the efficacy and safety of tobramycin to eradicate Pseudomonas infection is currently underway), but targeted therapies represent a promising new approach to combating this stubbornly resistant bacteria. The NCFB community will be watching closely to see whether medicines targeting molecular behavior and host interaction can achieve what antibiotic regimens thus far have not: consistent and sustainable eradication.
Dr. Green is Assistant Professor in Medicine, Medical Director, Bronchiectasis Program, UMass Chan/Baystate Health, Chest Infections Section, Member-at-Large
References
1. Weycker D, Hansen GL, Seifer FD. Prevalence and incidence of noncystic fibrosis bronchiectasis among US adults in 2013. Chron Respir Dis. 2017;14(4):377-384. doi: 10.1177/1479972317709649
2. Green O, Liautaud S, Knee A, Modahl L. Measuring accuracy of International Classification of Diseases codes in identification of patients with non-cystic fibrosis bronchiectasis. ERJ Open Res. 2024;10(2):00715-2023. doi: 10.1183/23120541.00715-2023
3. Franklin M, Minshall ME, Pontenani F, Devarajan S. Impact of Pseudomonas aeruginosa on resource utilization and costs in patients with exacerbated non-cystic fibrosis bronchiectasis. J Med Econ. 2024;27(1):671-677. doi: 10.1080/13696998.2024.2340382
4. Aksamit TR, Locantore N, Addrizzo-Harris D, et al. Five-year outcomes among U.S. bronchiectasis and NTM research registry patients. Am J Respir Crit Care Med. Accepted manuscript. Published online April 26, 2024.
5. Dean SG, Blakney RA, Ricotta EE, et al. Bronchiectasis-associated infections and outcomes in a large, geographically diverse electronic health record cohort in the United States. BMC Pulm Med. 2024;24(1):172. doi: 10.1186/s12890-024-02973-3
6. Chalmers JD, Polverino E, Crichton ML, et al. Bronchiectasis in Europe: data on disease characteristics from the European Bronchiectasis registry (EMBARC). Lancet Respir Med. 2023;11(7):637-649. doi: 10.1016/S2213-2600(23)00093-0
7. Polverino E, Goeminne PC, McDonnell MJ, et al. European Respiratory Society guidelines for the management of adult bronchiectasis. Eur Respir J. 2017;50(3):1700629. doi: 10.1183/13993003.00629-2017
8. Martínez-García MÁ, Máiz L, Olveira C, et al. Spanish guidelines on treatment of bronchiectasis in adults. Arch Bronconeumol. 2018;54(2):88-98. doi: 10.1016/j.arbres.2017.07.016
9. Hill AT, Sullivan AL, Chalmers JD, et al. British Thoracic Society guideline for bronchiectasis in adults. Thorax. 2019;74(Suppl 1):1-69. doi: 10.1136/thoraxjnl-2018-212463
10. Goolam Mahomed A, Maasdorp SD, Barnes R, et al. South African Thoracic Society position statement on the management of non-cystic fibrosis bronchiectasis in adults: 2023. Afr J Thorac Crit Care Med. 2023;29(2):10.7196/AJTCCM. 2023.v29i2.647. doi: 10.7196/AJTCCM.2023.v29i2.647
11. Brodt AM, Stovold E, Zhang L. Inhaled antibiotics for stable non-cystic fibrosis bronchiectasis: a systematic review. Eur Respir J. 2014;44(2):382-393. doi: 10.1183/09031936.00018414
12. Conceição M, Shteinberg M, Goeminne P, Altenburg J, Chalmers JD. Eradication treatment for Pseudomonas aeruginosa infection in adults with bronchiectasis: a systematic review and meta-analysis. Eur Respir Rev. 2024;33(171):230178. doi: 10.1183/16000617.0178-2023
13. Hilliam Y, Moore MP, Lamont IL, et al. Pseudomonas aeruginosa adaptation and diversification in the non-cystic fibrosis bronchiectasis lung. Eur Respir J. 2017;49(4):1602108. doi: 10.1183/13993003.02108-2016
14. Gramegna A, Kumar Narayana J, Amati F, et al. Microbial inflammatory networks in bronchiectasis exacerbators with Pseudomonas aeruginosa. Chest. 2023;164(1):65-68. doi: 10.1016/j.chest.2023.02.014
Pseudomonas aeruginosa is a clinically important organism that infects patients with noncystic fibrosis bronchiectasis (NCFB). In the United States, the estimated prevalence of NCFB is 213 per 100,000 across all age groups and 813 per 100,000 in the over 65 age group.1 A retrospective cohort study suggests the incidence of NCFB as ascertained from International Classification of Diseases codes may significantly underestimate its true prevalence.2
As the incidence of patients with NCFB continues to increase, the impact of the Pseudomonas infection is expected to grow. A recent retrospective cohort study of commercial claims from IQVIA’s PharMetrics Plus database for the period 2006 to 2020 showed that patients with NCFB and Pseudomonas infection had on average 2.58 hospital admissions per year, with a mean length of stay of 9.94 (± 11.06) days, compared with 1.18 admissions per year, with a mean length of stay of 6.5 (± 8.42) days, in patients with Pseudomonas-negative NCFB. The same trend applied to 30-day readmissions and ICU admissions, 1.32 (± 2.51 days) vs 0.47 (± 1.30 days) and 0.95 (± 1.62 days) vs 0.33 (± 0.76 days), respectively. The differential cost of care per patient per year between patients with NCFB with and without Pseudomonas infection ranged from $55,225 to $315,901.3
Recent data from the United States Bronchiectasis Registry showed the probability of acquiring Pseudomonas aeruginosa was 3% annually.4 The prevalence of Pseudomonas infection in a large, geographically diverse cohort in the United States was quoted at 15%.5 A retrospective analysis of the European Bronchiectasis Registry database showed Pseudomonas infection was the most commonly isolated pathogen (21.8%).6
Given the high incidence and prevalence of NCFB, the high prevalence of Pseudomonas infection in patients with NCFB, and the associated costs and morbidity from infection, identifying effective treatments has become a priority. The British, Spanish (SEPAR), South African, and European bronchiectasis guidelines outline several antibiotic regimens meant to achieve eradication. Generally, there is induction with a (1) quinolone, (2) β-lactam + aminoglycoside, or (3) quinolone with an inhaled antibiotic followed by three months of maintenance inhaled antibiotics.7-10 SEPAR allows for retreatment for recurrence at any time during the first year with any regimen.
For chronic Pseudomonas infection, SEPAR recommends treatment with inhaled antibiotics for patients with more than two exacerbations or one hospitalization, while the threshold in the British and European guidelines is more than three exacerbations. Azithromycin may be used for those who are intolerant or allergic to the nebulized antibiotics. It is worth noting that in the United States, the antibiotics colistin, ciprofloxacin, aztreonam, gentamicin, and tobramycin are administered off label for this indication. A systematic review found a 10% rate of bronchospasm in the treated group compared with 2.3% in the control group, and premedication with albuterol is often needed.11
Unfortunately, the data supporting the listed eradication and suppressive regimens are weak. A systematic review and meta-analysis of six observational studies including 289 patients showed a 12-month eradication rate of only 40% (95% CI, 34-45; P < 0.00001; I2 = 0).12 These results are disappointing and identify a need for further research into the manner in which Pseudomonas infection interacts with the host lung.
We currently know Pseudomonas infection evades antibiotics and host defenses by accumulating mutations and deletions. These include loss-of-function mutations in mucA (mucoidy), lasR (quorum-sensing), mexS (regulates the antibiotic efflux pump), and other genes related to the production of the polysaccharides Psl and Pel (which contribute to biofilm formation).13 There may also be differences in low and high bacteria microbial networks that interact differently with host cytokines to create an unstable environment that predisposes to exacerbation.14
In an attempt to improve our eradication and suppression rates, investigators have begun to target specific aspects of Pseudomonas infection behavior. The GREAT-2 trial compares gremubamab (a bivalent, bispecific, monoclonal antibody targeting Psl exopolysaccharide and the type 3 secretion system component of PcrV) with placebo in patients with chronic Pseudomonas infection. A phase II trial with the phosphodiesterase inhibitor esifentrine, a phase III trial with a reversible DPP1 inhibitor called brensocatib (ASPEN), and a phase II trial with the CatC inhibitor BI 1291583 (Airleaf) are also being conducted. Each of these agents targets mediators of neutrophil inflammation.
In summary, NCFB with Pseudomonas infection is common and leads to an increase in costs, respiratory exacerbations, and hospitalizations. While eradication and suppression are recommended, they are difficult to achieve and require sustained durations of expensive medications that can be difficult to tolerate. Antibiotic therapies will continue to be studied (the ERASE randomized controlled trial to investigate the efficacy and safety of tobramycin to eradicate Pseudomonas infection is currently underway), but targeted therapies represent a promising new approach to combating this stubbornly resistant bacteria. The NCFB community will be watching closely to see whether medicines targeting molecular behavior and host interaction can achieve what antibiotic regimens thus far have not: consistent and sustainable eradication.
Dr. Green is Assistant Professor in Medicine, Medical Director, Bronchiectasis Program, UMass Chan/Baystate Health, Chest Infections Section, Member-at-Large
References
1. Weycker D, Hansen GL, Seifer FD. Prevalence and incidence of noncystic fibrosis bronchiectasis among US adults in 2013. Chron Respir Dis. 2017;14(4):377-384. doi: 10.1177/1479972317709649
2. Green O, Liautaud S, Knee A, Modahl L. Measuring accuracy of International Classification of Diseases codes in identification of patients with non-cystic fibrosis bronchiectasis. ERJ Open Res. 2024;10(2):00715-2023. doi: 10.1183/23120541.00715-2023
3. Franklin M, Minshall ME, Pontenani F, Devarajan S. Impact of Pseudomonas aeruginosa on resource utilization and costs in patients with exacerbated non-cystic fibrosis bronchiectasis. J Med Econ. 2024;27(1):671-677. doi: 10.1080/13696998.2024.2340382
4. Aksamit TR, Locantore N, Addrizzo-Harris D, et al. Five-year outcomes among U.S. bronchiectasis and NTM research registry patients. Am J Respir Crit Care Med. Accepted manuscript. Published online April 26, 2024.
5. Dean SG, Blakney RA, Ricotta EE, et al. Bronchiectasis-associated infections and outcomes in a large, geographically diverse electronic health record cohort in the United States. BMC Pulm Med. 2024;24(1):172. doi: 10.1186/s12890-024-02973-3
6. Chalmers JD, Polverino E, Crichton ML, et al. Bronchiectasis in Europe: data on disease characteristics from the European Bronchiectasis registry (EMBARC). Lancet Respir Med. 2023;11(7):637-649. doi: 10.1016/S2213-2600(23)00093-0
7. Polverino E, Goeminne PC, McDonnell MJ, et al. European Respiratory Society guidelines for the management of adult bronchiectasis. Eur Respir J. 2017;50(3):1700629. doi: 10.1183/13993003.00629-2017
8. Martínez-García MÁ, Máiz L, Olveira C, et al. Spanish guidelines on treatment of bronchiectasis in adults. Arch Bronconeumol. 2018;54(2):88-98. doi: 10.1016/j.arbres.2017.07.016
9. Hill AT, Sullivan AL, Chalmers JD, et al. British Thoracic Society guideline for bronchiectasis in adults. Thorax. 2019;74(Suppl 1):1-69. doi: 10.1136/thoraxjnl-2018-212463
10. Goolam Mahomed A, Maasdorp SD, Barnes R, et al. South African Thoracic Society position statement on the management of non-cystic fibrosis bronchiectasis in adults: 2023. Afr J Thorac Crit Care Med. 2023;29(2):10.7196/AJTCCM. 2023.v29i2.647. doi: 10.7196/AJTCCM.2023.v29i2.647
11. Brodt AM, Stovold E, Zhang L. Inhaled antibiotics for stable non-cystic fibrosis bronchiectasis: a systematic review. Eur Respir J. 2014;44(2):382-393. doi: 10.1183/09031936.00018414
12. Conceição M, Shteinberg M, Goeminne P, Altenburg J, Chalmers JD. Eradication treatment for Pseudomonas aeruginosa infection in adults with bronchiectasis: a systematic review and meta-analysis. Eur Respir Rev. 2024;33(171):230178. doi: 10.1183/16000617.0178-2023
13. Hilliam Y, Moore MP, Lamont IL, et al. Pseudomonas aeruginosa adaptation and diversification in the non-cystic fibrosis bronchiectasis lung. Eur Respir J. 2017;49(4):1602108. doi: 10.1183/13993003.02108-2016
14. Gramegna A, Kumar Narayana J, Amati F, et al. Microbial inflammatory networks in bronchiectasis exacerbators with Pseudomonas aeruginosa. Chest. 2023;164(1):65-68. doi: 10.1016/j.chest.2023.02.014