User login
Underlying Mental Illness and Risk of Severe Outcomes Associated With COVID-19
The Centers for Disease Control and Prevention (CDC) has identified factors that put patients at a higher risk of severe COVID-19 infection, which include advanced age, obesity, cardiovascular disease, diabetes, chronic kidney disease, lung disease, and immunocompromising conditions. The CDC also acknowledges that mood disorders, including depression and schizophrenia, contribute to the progression to severe COVID-19.1 Antiviral therapies, such as nirmatrelvir and ritonavir combination, remdesivir, and molnupiravir, and monoclonal antibody (mAb) therapies, have been used to prevent hospitalization and mortality from COVID-19 infection for individuals with mild-to-moderate COVID-19 who are at high risk of progressing to severe infection.2 Although antiviral and mAb therapies likely have mitigated many infections, poor prognoses are prevalent. It is important to identify all patients at risk of progressing to severe COVID-19 infection.
Although the CDC considers depression and schizophrenia to be risk factors for severe COVID-19 infection, the Captain James A. Lovell Federal Health Care Center (FHCC) in North Chicago, Illinois, does not, making these patients ineligible for antiviral or mAb therapies unless they have another risk factor. As a result, these patients could be at risk of severe COVID-19 infection, but might not be treated appropriately. Psychiatric diagnoses are common among veterans, with 19.7% experiencing a mental illness in 2020.3 It is imperative to determine whether depression or schizophrenia play a role in the progression of COVID-19 to expand access to individuals who are eligible for antiviral or mAb therapies.
Because COVID-19 is a novel virus, there are few studies of psychiatric disorders and COVID-19 prognosis. A 2020 case control study determined that those with a recent mental illness diagnosis were at higher risk of COVID-19 infection with worse outcomes compared with those without psychiatric diagnoses. This effect was most prevalent among individuals with depression and schizophrenia.4 However, these individuals also were found to have additional comorbidities that could have contributed to poorer outcomes. A meta-analysis determined that psychiatric disorders were associated with increased COVID-19-related mortality.5 A 2022 cohort study that included vaccinated US Department of Veterans Affairs (VA) patients determined that having a psychiatric diagnosis was associated with increased incidence of breakthrough infections.6 Individuals with psychiatric conditions are thought to be at higher risk of severe COVID-19 outcomes because of poor access to care and higher incidence of untreated underlying health conditions.7 Lifestyle factors also could play a role. Because there is minimal data on COVID-19 prognosis and mental illness, further research is warranted to determine whether psychiatric diagnoses could contribute to more severe COVID-19 infections.
Methods
This was a retrospective cohort chart review study at FHCC that compared COVID-19 outcomes in individuals with depression or schizophrenia with those without these diagnoses. FHCC patients with the International Classification of Diseases code for COVID-19 (U07.1) from fiscal years 2020 to 2022 were included. We then selected patients with a depression or schizophrenia diagnosis noted in the electronic health record (EHR). These 2 patient lists were consolidated to identify every individual with a COVID-19 diagnosis and a diagnosis of depression or schizophrenia.
Patients were included if they were aged ≥ 18 years with a positive COVID-19 infection confirmed via polymerase chain reaction or blood test. Patients also had to have mild-to-moderate COVID-19 with ≥ 1 symptom such as fever, cough, sore throat, malaise, headache, muscle pain, loss of taste and smell, or shortness of breath. Patients were excluded if they had an asymptomatic infection, presented with severe COVID-19 infection, or were an FHCC employee. Severe COVID-19 was defined as having oxygen saturation < 94%, a respiratory rate > 30 breaths per minute, or supplemental oxygen requirement.
Patient EHRs were reviewed and analyzed using the VA Computerized Patient Record System and Joint Legacy Viewer. Collected data included age, medical history, use of antiviral or mAb therapy, and admission or death within 30 days of a positive COVID-19 test. The primary outcome of this study was severe COVID-19 outcomes defined as hospitalization, admission to the intensive care unit, intubation or mechanical ventilation, or death within 30 days of infection. The primary outcome was analyzed with a student t test; P < .05 was considered statistically significant.
Results
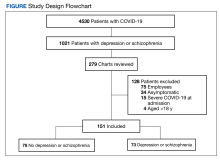
More than 5000 individuals had a COVID-19 diagnosis during the study period. Among these patients, 4530 had no depression or schizophrenia diagnosis; 1021 individuals had COVID-19 and a preexisting diagnosis of depression or schizophrenia. Among these 1021 patients, 279 charts were reviewed due to time constraints; 128 patients met exclusion criteria and 151 patients were included in the study. Of the 151 patients with COVID-19, 78 had no depression or schizophrenia and 73 patients with COVID-19 had a preexisting depression or schizophrenia diagnosis (Figure).
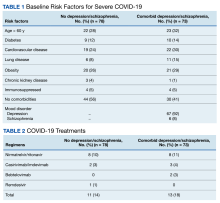
The 2 groups were similar at baseline. The most common risk factors for severe COVID-19 included age > 60 years, obesity, and cardiovascular disease. However, more than half of the individuals analyzed had no risk factors (Table 1). Some patients with risk factors received antiviral or mAb therapy to prevent severe COVID-19 infection; combination nirmatrelvir and ritonavir was the most common agent (Table 2). Of the 73 individuals with a psychiatric diagnosis, 67 had depression (91.8%), and 6 had schizophrenia (8.2%).
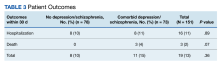
Hospitalization or death within 30 days of COVID-19 infection between patients with depression or schizophrenia and patients without these psychiatric diagnoses was not statistically significant (P = .36). Sixteen individuals were hospitalized, 8 in each group. Three individuals died within 30 days; death only occurred in patients who had depression or schizophrenia (Table 3).
Discussion
This study found that hospitalization or death within 30 days of COVID-19 infection occurred more frequently among individuals with depression or schizophrenia compared with those without these psychiatric comorbidities. However, this difference was not statistically significant.
This study had several limitations. It was a retrospective, chart review study, which relied on accurate documentation. In addition, we reviewed COVID-19 cases from fiscal years 2020 to 2022 and as a result, several viral variants were analyzed. This made it difficult to draw conclusions, especially because the omicron variant is thought to be less deadly, which may have skewed the data. Vaccinations and COVID-19 treatments became available in late 2020, which likely affected the progression to severe disease. Our study did not assess vaccination status, therefore it is unclear whether COVID-19 vaccination played a role in mitigating infection. When the pandemic began, many individuals were afraid to come to the hospital and did not receive care until they progressed to severe COVID-19, which would have excluded them from the study. Many individuals had additional comorbidities that likely impacted their COVID-19 outcomes. It is not possible to conclude if the depression or schizophrenia diagnoses were responsible for hospitalization or death within 30 days of infection or if it was because of other known risk factors. Future research is needed to address these limitations.
Conclusions
More COVID-19 hospitalizations and deaths occurred within 30 days of infection among those with depression and schizophrenia compared with individuals without these comorbidities. However, this effect was not statistically significant. Many limitations could have contributed to this finding, which should be addressed in future studies. Because the sample size was small, further research with a larger patient population is warranted to explore the association between psychiatric comorbidities such as depression and schizophrenia and COVID-19 disease progression. Future studies also could include assessment of vaccination status and exclude individuals with other high-risk comorbidities for severe COVID-19 outcomes. These studies could determine if depression and schizophrenia are correlated with worse COVID-19 outcomes and ensure that all high-risk patients are identified and treated appropriately to prevent morbidity and mortality.
Acknowledgements
Thank you to the research committee at the Captain James A. Lovell Federal Health Care Center who assisted in the completion of this project, including Shaiza Khan, PharmD, BCPS; Yinka Alaka, PharmD; and Hong-Yen Vi, PharmD, BCPS, BCCCP.
1. Centers for Disease Control and Prevention. Underlying medical conditions associated with higher risk for severe COVID-19: information for healthcare professionals. Updated February 9, 2023. Accessed February 27, 2024. https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-care/underlyingconditions.html
2. National Institutes of Health. Therapeutic management of nonhospitalized adults with COVID-19. Updated November 2, 2023. Accessed February 27, 2024. https://www.covid19treatmentguidelines.nih.gov/management/clinical-management-of-adults/nonhospitalized-adults-therapeutic-management
3. National Alliance on Mental Illness. Mental health by the numbers. Updated April 2023. Accessed February 27, 2024. https://www.nami.org/mhstats
4. Wang Q, Xu R, Volkow ND. Increased risk of COVID-19 infection and mortality in people with mental disorders: analysis from electronic health records in the United States. World Psychiatry . 2021;20(1):124-130. doi:10.1002/wps.20806
5. Fond G, Nemani K, Etchecopar-Etchart D, et al. Association Between Mental Health Disorders and Mortality Among Patients With COVID-19 in 7 Countries: A Systematic Review and Meta-analysis. JAMA Psychiatry . 2021;78(11):1208-1217. doi:10.1001/jamapsychiatry.2021.2274
6. Nishimi K, Neylan TC, Bertenthal D, Seal KH, O’Donovan A. Association of Psychiatric Disorders With Incidence of SARS-CoV-2 Breakthrough Infection Among Vaccinated Adults. JAMA Netw Open . 2022;5(4):e227287. Published 2022 Apr 1. doi:10.1001/jamanetworkopen.2022.7287
7. Koyama AK, Koumans EH, Sircar K, et al. Mental Health Conditions and Severe COVID-19 Outcomes after Hospitalization, United States. Emerg Infect Dis . 2022;28(7):1533-1536. doi:10.3201/eid2807.212208
The Centers for Disease Control and Prevention (CDC) has identified factors that put patients at a higher risk of severe COVID-19 infection, which include advanced age, obesity, cardiovascular disease, diabetes, chronic kidney disease, lung disease, and immunocompromising conditions. The CDC also acknowledges that mood disorders, including depression and schizophrenia, contribute to the progression to severe COVID-19.1 Antiviral therapies, such as nirmatrelvir and ritonavir combination, remdesivir, and molnupiravir, and monoclonal antibody (mAb) therapies, have been used to prevent hospitalization and mortality from COVID-19 infection for individuals with mild-to-moderate COVID-19 who are at high risk of progressing to severe infection.2 Although antiviral and mAb therapies likely have mitigated many infections, poor prognoses are prevalent. It is important to identify all patients at risk of progressing to severe COVID-19 infection.
Although the CDC considers depression and schizophrenia to be risk factors for severe COVID-19 infection, the Captain James A. Lovell Federal Health Care Center (FHCC) in North Chicago, Illinois, does not, making these patients ineligible for antiviral or mAb therapies unless they have another risk factor. As a result, these patients could be at risk of severe COVID-19 infection, but might not be treated appropriately. Psychiatric diagnoses are common among veterans, with 19.7% experiencing a mental illness in 2020.3 It is imperative to determine whether depression or schizophrenia play a role in the progression of COVID-19 to expand access to individuals who are eligible for antiviral or mAb therapies.
Because COVID-19 is a novel virus, there are few studies of psychiatric disorders and COVID-19 prognosis. A 2020 case control study determined that those with a recent mental illness diagnosis were at higher risk of COVID-19 infection with worse outcomes compared with those without psychiatric diagnoses. This effect was most prevalent among individuals with depression and schizophrenia.4 However, these individuals also were found to have additional comorbidities that could have contributed to poorer outcomes. A meta-analysis determined that psychiatric disorders were associated with increased COVID-19-related mortality.5 A 2022 cohort study that included vaccinated US Department of Veterans Affairs (VA) patients determined that having a psychiatric diagnosis was associated with increased incidence of breakthrough infections.6 Individuals with psychiatric conditions are thought to be at higher risk of severe COVID-19 outcomes because of poor access to care and higher incidence of untreated underlying health conditions.7 Lifestyle factors also could play a role. Because there is minimal data on COVID-19 prognosis and mental illness, further research is warranted to determine whether psychiatric diagnoses could contribute to more severe COVID-19 infections.
Methods
This was a retrospective cohort chart review study at FHCC that compared COVID-19 outcomes in individuals with depression or schizophrenia with those without these diagnoses. FHCC patients with the International Classification of Diseases code for COVID-19 (U07.1) from fiscal years 2020 to 2022 were included. We then selected patients with a depression or schizophrenia diagnosis noted in the electronic health record (EHR). These 2 patient lists were consolidated to identify every individual with a COVID-19 diagnosis and a diagnosis of depression or schizophrenia.
Patients were included if they were aged ≥ 18 years with a positive COVID-19 infection confirmed via polymerase chain reaction or blood test. Patients also had to have mild-to-moderate COVID-19 with ≥ 1 symptom such as fever, cough, sore throat, malaise, headache, muscle pain, loss of taste and smell, or shortness of breath. Patients were excluded if they had an asymptomatic infection, presented with severe COVID-19 infection, or were an FHCC employee. Severe COVID-19 was defined as having oxygen saturation < 94%, a respiratory rate > 30 breaths per minute, or supplemental oxygen requirement.
Patient EHRs were reviewed and analyzed using the VA Computerized Patient Record System and Joint Legacy Viewer. Collected data included age, medical history, use of antiviral or mAb therapy, and admission or death within 30 days of a positive COVID-19 test. The primary outcome of this study was severe COVID-19 outcomes defined as hospitalization, admission to the intensive care unit, intubation or mechanical ventilation, or death within 30 days of infection. The primary outcome was analyzed with a student t test; P < .05 was considered statistically significant.
Results
More than 5000 individuals had a COVID-19 diagnosis during the study period. Among these patients, 4530 had no depression or schizophrenia diagnosis; 1021 individuals had COVID-19 and a preexisting diagnosis of depression or schizophrenia. Among these 1021 patients, 279 charts were reviewed due to time constraints; 128 patients met exclusion criteria and 151 patients were included in the study. Of the 151 patients with COVID-19, 78 had no depression or schizophrenia and 73 patients with COVID-19 had a preexisting depression or schizophrenia diagnosis (Figure).
The 2 groups were similar at baseline. The most common risk factors for severe COVID-19 included age > 60 years, obesity, and cardiovascular disease. However, more than half of the individuals analyzed had no risk factors (Table 1). Some patients with risk factors received antiviral or mAb therapy to prevent severe COVID-19 infection; combination nirmatrelvir and ritonavir was the most common agent (Table 2). Of the 73 individuals with a psychiatric diagnosis, 67 had depression (91.8%), and 6 had schizophrenia (8.2%).
Hospitalization or death within 30 days of COVID-19 infection between patients with depression or schizophrenia and patients without these psychiatric diagnoses was not statistically significant (P = .36). Sixteen individuals were hospitalized, 8 in each group. Three individuals died within 30 days; death only occurred in patients who had depression or schizophrenia (Table 3).
Discussion
This study found that hospitalization or death within 30 days of COVID-19 infection occurred more frequently among individuals with depression or schizophrenia compared with those without these psychiatric comorbidities. However, this difference was not statistically significant.
This study had several limitations. It was a retrospective, chart review study, which relied on accurate documentation. In addition, we reviewed COVID-19 cases from fiscal years 2020 to 2022 and as a result, several viral variants were analyzed. This made it difficult to draw conclusions, especially because the omicron variant is thought to be less deadly, which may have skewed the data. Vaccinations and COVID-19 treatments became available in late 2020, which likely affected the progression to severe disease. Our study did not assess vaccination status, therefore it is unclear whether COVID-19 vaccination played a role in mitigating infection. When the pandemic began, many individuals were afraid to come to the hospital and did not receive care until they progressed to severe COVID-19, which would have excluded them from the study. Many individuals had additional comorbidities that likely impacted their COVID-19 outcomes. It is not possible to conclude if the depression or schizophrenia diagnoses were responsible for hospitalization or death within 30 days of infection or if it was because of other known risk factors. Future research is needed to address these limitations.
Conclusions
More COVID-19 hospitalizations and deaths occurred within 30 days of infection among those with depression and schizophrenia compared with individuals without these comorbidities. However, this effect was not statistically significant. Many limitations could have contributed to this finding, which should be addressed in future studies. Because the sample size was small, further research with a larger patient population is warranted to explore the association between psychiatric comorbidities such as depression and schizophrenia and COVID-19 disease progression. Future studies also could include assessment of vaccination status and exclude individuals with other high-risk comorbidities for severe COVID-19 outcomes. These studies could determine if depression and schizophrenia are correlated with worse COVID-19 outcomes and ensure that all high-risk patients are identified and treated appropriately to prevent morbidity and mortality.
Acknowledgements
Thank you to the research committee at the Captain James A. Lovell Federal Health Care Center who assisted in the completion of this project, including Shaiza Khan, PharmD, BCPS; Yinka Alaka, PharmD; and Hong-Yen Vi, PharmD, BCPS, BCCCP.
The Centers for Disease Control and Prevention (CDC) has identified factors that put patients at a higher risk of severe COVID-19 infection, which include advanced age, obesity, cardiovascular disease, diabetes, chronic kidney disease, lung disease, and immunocompromising conditions. The CDC also acknowledges that mood disorders, including depression and schizophrenia, contribute to the progression to severe COVID-19.1 Antiviral therapies, such as nirmatrelvir and ritonavir combination, remdesivir, and molnupiravir, and monoclonal antibody (mAb) therapies, have been used to prevent hospitalization and mortality from COVID-19 infection for individuals with mild-to-moderate COVID-19 who are at high risk of progressing to severe infection.2 Although antiviral and mAb therapies likely have mitigated many infections, poor prognoses are prevalent. It is important to identify all patients at risk of progressing to severe COVID-19 infection.
Although the CDC considers depression and schizophrenia to be risk factors for severe COVID-19 infection, the Captain James A. Lovell Federal Health Care Center (FHCC) in North Chicago, Illinois, does not, making these patients ineligible for antiviral or mAb therapies unless they have another risk factor. As a result, these patients could be at risk of severe COVID-19 infection, but might not be treated appropriately. Psychiatric diagnoses are common among veterans, with 19.7% experiencing a mental illness in 2020.3 It is imperative to determine whether depression or schizophrenia play a role in the progression of COVID-19 to expand access to individuals who are eligible for antiviral or mAb therapies.
Because COVID-19 is a novel virus, there are few studies of psychiatric disorders and COVID-19 prognosis. A 2020 case control study determined that those with a recent mental illness diagnosis were at higher risk of COVID-19 infection with worse outcomes compared with those without psychiatric diagnoses. This effect was most prevalent among individuals with depression and schizophrenia.4 However, these individuals also were found to have additional comorbidities that could have contributed to poorer outcomes. A meta-analysis determined that psychiatric disorders were associated with increased COVID-19-related mortality.5 A 2022 cohort study that included vaccinated US Department of Veterans Affairs (VA) patients determined that having a psychiatric diagnosis was associated with increased incidence of breakthrough infections.6 Individuals with psychiatric conditions are thought to be at higher risk of severe COVID-19 outcomes because of poor access to care and higher incidence of untreated underlying health conditions.7 Lifestyle factors also could play a role. Because there is minimal data on COVID-19 prognosis and mental illness, further research is warranted to determine whether psychiatric diagnoses could contribute to more severe COVID-19 infections.
Methods
This was a retrospective cohort chart review study at FHCC that compared COVID-19 outcomes in individuals with depression or schizophrenia with those without these diagnoses. FHCC patients with the International Classification of Diseases code for COVID-19 (U07.1) from fiscal years 2020 to 2022 were included. We then selected patients with a depression or schizophrenia diagnosis noted in the electronic health record (EHR). These 2 patient lists were consolidated to identify every individual with a COVID-19 diagnosis and a diagnosis of depression or schizophrenia.
Patients were included if they were aged ≥ 18 years with a positive COVID-19 infection confirmed via polymerase chain reaction or blood test. Patients also had to have mild-to-moderate COVID-19 with ≥ 1 symptom such as fever, cough, sore throat, malaise, headache, muscle pain, loss of taste and smell, or shortness of breath. Patients were excluded if they had an asymptomatic infection, presented with severe COVID-19 infection, or were an FHCC employee. Severe COVID-19 was defined as having oxygen saturation < 94%, a respiratory rate > 30 breaths per minute, or supplemental oxygen requirement.
Patient EHRs were reviewed and analyzed using the VA Computerized Patient Record System and Joint Legacy Viewer. Collected data included age, medical history, use of antiviral or mAb therapy, and admission or death within 30 days of a positive COVID-19 test. The primary outcome of this study was severe COVID-19 outcomes defined as hospitalization, admission to the intensive care unit, intubation or mechanical ventilation, or death within 30 days of infection. The primary outcome was analyzed with a student t test; P < .05 was considered statistically significant.
Results
More than 5000 individuals had a COVID-19 diagnosis during the study period. Among these patients, 4530 had no depression or schizophrenia diagnosis; 1021 individuals had COVID-19 and a preexisting diagnosis of depression or schizophrenia. Among these 1021 patients, 279 charts were reviewed due to time constraints; 128 patients met exclusion criteria and 151 patients were included in the study. Of the 151 patients with COVID-19, 78 had no depression or schizophrenia and 73 patients with COVID-19 had a preexisting depression or schizophrenia diagnosis (Figure).
The 2 groups were similar at baseline. The most common risk factors for severe COVID-19 included age > 60 years, obesity, and cardiovascular disease. However, more than half of the individuals analyzed had no risk factors (Table 1). Some patients with risk factors received antiviral or mAb therapy to prevent severe COVID-19 infection; combination nirmatrelvir and ritonavir was the most common agent (Table 2). Of the 73 individuals with a psychiatric diagnosis, 67 had depression (91.8%), and 6 had schizophrenia (8.2%).
Hospitalization or death within 30 days of COVID-19 infection between patients with depression or schizophrenia and patients without these psychiatric diagnoses was not statistically significant (P = .36). Sixteen individuals were hospitalized, 8 in each group. Three individuals died within 30 days; death only occurred in patients who had depression or schizophrenia (Table 3).
Discussion
This study found that hospitalization or death within 30 days of COVID-19 infection occurred more frequently among individuals with depression or schizophrenia compared with those without these psychiatric comorbidities. However, this difference was not statistically significant.
This study had several limitations. It was a retrospective, chart review study, which relied on accurate documentation. In addition, we reviewed COVID-19 cases from fiscal years 2020 to 2022 and as a result, several viral variants were analyzed. This made it difficult to draw conclusions, especially because the omicron variant is thought to be less deadly, which may have skewed the data. Vaccinations and COVID-19 treatments became available in late 2020, which likely affected the progression to severe disease. Our study did not assess vaccination status, therefore it is unclear whether COVID-19 vaccination played a role in mitigating infection. When the pandemic began, many individuals were afraid to come to the hospital and did not receive care until they progressed to severe COVID-19, which would have excluded them from the study. Many individuals had additional comorbidities that likely impacted their COVID-19 outcomes. It is not possible to conclude if the depression or schizophrenia diagnoses were responsible for hospitalization or death within 30 days of infection or if it was because of other known risk factors. Future research is needed to address these limitations.
Conclusions
More COVID-19 hospitalizations and deaths occurred within 30 days of infection among those with depression and schizophrenia compared with individuals without these comorbidities. However, this effect was not statistically significant. Many limitations could have contributed to this finding, which should be addressed in future studies. Because the sample size was small, further research with a larger patient population is warranted to explore the association between psychiatric comorbidities such as depression and schizophrenia and COVID-19 disease progression. Future studies also could include assessment of vaccination status and exclude individuals with other high-risk comorbidities for severe COVID-19 outcomes. These studies could determine if depression and schizophrenia are correlated with worse COVID-19 outcomes and ensure that all high-risk patients are identified and treated appropriately to prevent morbidity and mortality.
Acknowledgements
Thank you to the research committee at the Captain James A. Lovell Federal Health Care Center who assisted in the completion of this project, including Shaiza Khan, PharmD, BCPS; Yinka Alaka, PharmD; and Hong-Yen Vi, PharmD, BCPS, BCCCP.
1. Centers for Disease Control and Prevention. Underlying medical conditions associated with higher risk for severe COVID-19: information for healthcare professionals. Updated February 9, 2023. Accessed February 27, 2024. https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-care/underlyingconditions.html
2. National Institutes of Health. Therapeutic management of nonhospitalized adults with COVID-19. Updated November 2, 2023. Accessed February 27, 2024. https://www.covid19treatmentguidelines.nih.gov/management/clinical-management-of-adults/nonhospitalized-adults-therapeutic-management
3. National Alliance on Mental Illness. Mental health by the numbers. Updated April 2023. Accessed February 27, 2024. https://www.nami.org/mhstats
4. Wang Q, Xu R, Volkow ND. Increased risk of COVID-19 infection and mortality in people with mental disorders: analysis from electronic health records in the United States. World Psychiatry . 2021;20(1):124-130. doi:10.1002/wps.20806
5. Fond G, Nemani K, Etchecopar-Etchart D, et al. Association Between Mental Health Disorders and Mortality Among Patients With COVID-19 in 7 Countries: A Systematic Review and Meta-analysis. JAMA Psychiatry . 2021;78(11):1208-1217. doi:10.1001/jamapsychiatry.2021.2274
6. Nishimi K, Neylan TC, Bertenthal D, Seal KH, O’Donovan A. Association of Psychiatric Disorders With Incidence of SARS-CoV-2 Breakthrough Infection Among Vaccinated Adults. JAMA Netw Open . 2022;5(4):e227287. Published 2022 Apr 1. doi:10.1001/jamanetworkopen.2022.7287
7. Koyama AK, Koumans EH, Sircar K, et al. Mental Health Conditions and Severe COVID-19 Outcomes after Hospitalization, United States. Emerg Infect Dis . 2022;28(7):1533-1536. doi:10.3201/eid2807.212208
1. Centers for Disease Control and Prevention. Underlying medical conditions associated with higher risk for severe COVID-19: information for healthcare professionals. Updated February 9, 2023. Accessed February 27, 2024. https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-care/underlyingconditions.html
2. National Institutes of Health. Therapeutic management of nonhospitalized adults with COVID-19. Updated November 2, 2023. Accessed February 27, 2024. https://www.covid19treatmentguidelines.nih.gov/management/clinical-management-of-adults/nonhospitalized-adults-therapeutic-management
3. National Alliance on Mental Illness. Mental health by the numbers. Updated April 2023. Accessed February 27, 2024. https://www.nami.org/mhstats
4. Wang Q, Xu R, Volkow ND. Increased risk of COVID-19 infection and mortality in people with mental disorders: analysis from electronic health records in the United States. World Psychiatry . 2021;20(1):124-130. doi:10.1002/wps.20806
5. Fond G, Nemani K, Etchecopar-Etchart D, et al. Association Between Mental Health Disorders and Mortality Among Patients With COVID-19 in 7 Countries: A Systematic Review and Meta-analysis. JAMA Psychiatry . 2021;78(11):1208-1217. doi:10.1001/jamapsychiatry.2021.2274
6. Nishimi K, Neylan TC, Bertenthal D, Seal KH, O’Donovan A. Association of Psychiatric Disorders With Incidence of SARS-CoV-2 Breakthrough Infection Among Vaccinated Adults. JAMA Netw Open . 2022;5(4):e227287. Published 2022 Apr 1. doi:10.1001/jamanetworkopen.2022.7287
7. Koyama AK, Koumans EH, Sircar K, et al. Mental Health Conditions and Severe COVID-19 Outcomes after Hospitalization, United States. Emerg Infect Dis . 2022;28(7):1533-1536. doi:10.3201/eid2807.212208
AI and Suicide Prevention in Primary Care: A Q&A
Primary care physicians play a critical role in identifying patients at risk for serious mental health issues, including suicidality. But the ever-increasing demands on their clinical time can hinder the ability to identify emotional distress in time to intervene. Can artificial intelligence (AI) help?
This news organization spoke with Tom Zaubler, MD, a psychiatrist and chief medical officer of NeuroFlow, about how AI can improve the ability of primary care physicians and other clinicians to screen their patients for suicidal ideation and boost rates of treatment for mental health issues in their patients. This interview has been edited for clarity and length.
Question: How can AI help in suicide prevention and mental health screening in primary care?
Answer: Recent studies have demonstrated the potential of AI in mental health screening and suicide prevention. One method is natural language processing (NLP), which can analyze patients› journal entries for signs of suicidal thoughts or behaviors. This technology has shown promise in detecting suicidal ideation in patients who may not report such thoughts on traditional screening tools like the Patient Health Questionnaire-9 (PHQ-9). AI can be part of an integrated approach to identify and provide support to individuals at risk for suicide or those without a psychiatric history but who may still be at risk.
Q: A recent study by [Maria] Oquendo and colleagues found that one fifth of patients who attempt suicide do not meet the criteria for a mental health disorder.
Improved screening is obviously important, but in some ways it’s not the most important part of the problem. The lack of accessibility to specialized mental health care is a critical obstacle to treating patients with acute psychiatric needs.
How can primary care doctors effectively connect patients with mental health support, given the scarcity of mental health professionals?
A: Primary care doctors can leverage technology to extend mental health support. This includes using platforms for safety screening and providing patients with immediate access to local and national resources and digital interventions. Alerts can be sent to professionals within the practice or employed by technology companies to offer immediate support, including suicide safety planning and counseling. Users can hit a button to “Find a Therapist.” Also, if they acknowledge feelings of self-harm, these keywords are detected within the app by NLP. “Urgent alerts” are then sent to clinicians who are overseeing patient care. If someone is flagged, a social worker or member of a response services team intervenes and calls the person at risk to tailor care. These interventions do not always require a psychiatrist or masters-prepared clinician but can be effectively managed by trained paraprofessionals. These staff members can provide suicide safety planning and lethal-means-restriction counseling, and can assess the need for escalation of care.
Q: How is technology likely to manifest in physician practices in the near future to support mental health care?
A: Automated screening platforms for depression and anxiety, alerts for physicians when patients screen positively, and integration with collaborative care models are a few of the ways technology will become part of clinical practice. Additionally, advanced data analytics and predictive modeling using electronic health records and claims data will help identify high-risk patients. Technologies like voice recognition and machine learning can analyze patient journals and possibly, in the future, social media feeds to detect mental health issues. These technologies aim to extend and augment the capabilities of healthcare practices, improving the identification and management of patients at risk for mental health issues.
Q: Are these technologies as effective in pediatric populations, and are there any specific challenges?
A: Technologies for mental health screening and support are effective in pediatric populations, with certain age-specific considerations and legal restrictions on technology use. For adolescents and older children comfortable with technology, digital tools can significantly impact mental health care. For younger children, technology must facilitate information-gathering from various sources, including parents and teachers. Despite challenges, technology is crucial for early identification and intervention in pediatric mental health, potentially shortening the time to diagnosis and improving outcomes.
The statistics are horrifying. One third of adolescent girls have seriously thought about suicide over the past year; 13% attempt suicide. So there’s a need in the adolescent population and in the preadolescent population, too, because there’s an 8- to 10-year lag between onset of symptoms and diagnosis of mental illness. If we can shorten that lag, you see improved performance in schools; you see decreased truancy; you see greater economic achievement and so on. It makes such a profound difference. Not to mention it saves lives. So, yes, technology is critical in a pediatric population. It exists and it’s happening right now. There are challenges, but the goal can be met.
Q: A 2014 study found that 45% of people who completed suicide visited a primary care physician in the preceding month. And only 23% of people who attempt suicide have not seen a primary care physician within the past year. What does that say about the importance of screening at the primary care level?
A: The fact that a significant percentage of individuals who die by suicide have visited a primary care physician within a month or year prior to their death underscores the critical role of primary care in suicide prevention. This highlights the potential for primary care settings to identify and intervene with individuals at risk for suicide, making the case for the importance of integrating effective mental health screenings and support technologies in primary care practices.
Q: In other words, we’re not talking about a marginal benefit.
A: No, the potential benefit is huge. The United States Preventive Services Task Force did not endorse universal screening for suicide in its 2023 recommendations; they felt — and I accept that conclusion — there wasn›t enough evidence [at the time] to really support that recommendation. I think when you talk to a lot of suicide researchers, what you will hear is that providing suicide assessments as far upstream as possible is critical, especially when you start seeing more and more research showing that 20% of the population who die by suicide are not likely to have any psychiatric pathology at all. I believe the evidence base will soon support a recommendation for universal screening for adults. I believe it is especially important to screen for suicidal ideation in kids, given the high rates of suicide in this population.
Dr. Zaubler has disclosed the following relevant financial relationships: chief medical officer, NeuroFlow.
A version of this article appeared on Medscape.com.
Primary care physicians play a critical role in identifying patients at risk for serious mental health issues, including suicidality. But the ever-increasing demands on their clinical time can hinder the ability to identify emotional distress in time to intervene. Can artificial intelligence (AI) help?
This news organization spoke with Tom Zaubler, MD, a psychiatrist and chief medical officer of NeuroFlow, about how AI can improve the ability of primary care physicians and other clinicians to screen their patients for suicidal ideation and boost rates of treatment for mental health issues in their patients. This interview has been edited for clarity and length.
Question: How can AI help in suicide prevention and mental health screening in primary care?
Answer: Recent studies have demonstrated the potential of AI in mental health screening and suicide prevention. One method is natural language processing (NLP), which can analyze patients› journal entries for signs of suicidal thoughts or behaviors. This technology has shown promise in detecting suicidal ideation in patients who may not report such thoughts on traditional screening tools like the Patient Health Questionnaire-9 (PHQ-9). AI can be part of an integrated approach to identify and provide support to individuals at risk for suicide or those without a psychiatric history but who may still be at risk.
Q: A recent study by [Maria] Oquendo and colleagues found that one fifth of patients who attempt suicide do not meet the criteria for a mental health disorder.
Improved screening is obviously important, but in some ways it’s not the most important part of the problem. The lack of accessibility to specialized mental health care is a critical obstacle to treating patients with acute psychiatric needs.
How can primary care doctors effectively connect patients with mental health support, given the scarcity of mental health professionals?
A: Primary care doctors can leverage technology to extend mental health support. This includes using platforms for safety screening and providing patients with immediate access to local and national resources and digital interventions. Alerts can be sent to professionals within the practice or employed by technology companies to offer immediate support, including suicide safety planning and counseling. Users can hit a button to “Find a Therapist.” Also, if they acknowledge feelings of self-harm, these keywords are detected within the app by NLP. “Urgent alerts” are then sent to clinicians who are overseeing patient care. If someone is flagged, a social worker or member of a response services team intervenes and calls the person at risk to tailor care. These interventions do not always require a psychiatrist or masters-prepared clinician but can be effectively managed by trained paraprofessionals. These staff members can provide suicide safety planning and lethal-means-restriction counseling, and can assess the need for escalation of care.
Q: How is technology likely to manifest in physician practices in the near future to support mental health care?
A: Automated screening platforms for depression and anxiety, alerts for physicians when patients screen positively, and integration with collaborative care models are a few of the ways technology will become part of clinical practice. Additionally, advanced data analytics and predictive modeling using electronic health records and claims data will help identify high-risk patients. Technologies like voice recognition and machine learning can analyze patient journals and possibly, in the future, social media feeds to detect mental health issues. These technologies aim to extend and augment the capabilities of healthcare practices, improving the identification and management of patients at risk for mental health issues.
Q: Are these technologies as effective in pediatric populations, and are there any specific challenges?
A: Technologies for mental health screening and support are effective in pediatric populations, with certain age-specific considerations and legal restrictions on technology use. For adolescents and older children comfortable with technology, digital tools can significantly impact mental health care. For younger children, technology must facilitate information-gathering from various sources, including parents and teachers. Despite challenges, technology is crucial for early identification and intervention in pediatric mental health, potentially shortening the time to diagnosis and improving outcomes.
The statistics are horrifying. One third of adolescent girls have seriously thought about suicide over the past year; 13% attempt suicide. So there’s a need in the adolescent population and in the preadolescent population, too, because there’s an 8- to 10-year lag between onset of symptoms and diagnosis of mental illness. If we can shorten that lag, you see improved performance in schools; you see decreased truancy; you see greater economic achievement and so on. It makes such a profound difference. Not to mention it saves lives. So, yes, technology is critical in a pediatric population. It exists and it’s happening right now. There are challenges, but the goal can be met.
Q: A 2014 study found that 45% of people who completed suicide visited a primary care physician in the preceding month. And only 23% of people who attempt suicide have not seen a primary care physician within the past year. What does that say about the importance of screening at the primary care level?
A: The fact that a significant percentage of individuals who die by suicide have visited a primary care physician within a month or year prior to their death underscores the critical role of primary care in suicide prevention. This highlights the potential for primary care settings to identify and intervene with individuals at risk for suicide, making the case for the importance of integrating effective mental health screenings and support technologies in primary care practices.
Q: In other words, we’re not talking about a marginal benefit.
A: No, the potential benefit is huge. The United States Preventive Services Task Force did not endorse universal screening for suicide in its 2023 recommendations; they felt — and I accept that conclusion — there wasn›t enough evidence [at the time] to really support that recommendation. I think when you talk to a lot of suicide researchers, what you will hear is that providing suicide assessments as far upstream as possible is critical, especially when you start seeing more and more research showing that 20% of the population who die by suicide are not likely to have any psychiatric pathology at all. I believe the evidence base will soon support a recommendation for universal screening for adults. I believe it is especially important to screen for suicidal ideation in kids, given the high rates of suicide in this population.
Dr. Zaubler has disclosed the following relevant financial relationships: chief medical officer, NeuroFlow.
A version of this article appeared on Medscape.com.
Primary care physicians play a critical role in identifying patients at risk for serious mental health issues, including suicidality. But the ever-increasing demands on their clinical time can hinder the ability to identify emotional distress in time to intervene. Can artificial intelligence (AI) help?
This news organization spoke with Tom Zaubler, MD, a psychiatrist and chief medical officer of NeuroFlow, about how AI can improve the ability of primary care physicians and other clinicians to screen their patients for suicidal ideation and boost rates of treatment for mental health issues in their patients. This interview has been edited for clarity and length.
Question: How can AI help in suicide prevention and mental health screening in primary care?
Answer: Recent studies have demonstrated the potential of AI in mental health screening and suicide prevention. One method is natural language processing (NLP), which can analyze patients› journal entries for signs of suicidal thoughts or behaviors. This technology has shown promise in detecting suicidal ideation in patients who may not report such thoughts on traditional screening tools like the Patient Health Questionnaire-9 (PHQ-9). AI can be part of an integrated approach to identify and provide support to individuals at risk for suicide or those without a psychiatric history but who may still be at risk.
Q: A recent study by [Maria] Oquendo and colleagues found that one fifth of patients who attempt suicide do not meet the criteria for a mental health disorder.
Improved screening is obviously important, but in some ways it’s not the most important part of the problem. The lack of accessibility to specialized mental health care is a critical obstacle to treating patients with acute psychiatric needs.
How can primary care doctors effectively connect patients with mental health support, given the scarcity of mental health professionals?
A: Primary care doctors can leverage technology to extend mental health support. This includes using platforms for safety screening and providing patients with immediate access to local and national resources and digital interventions. Alerts can be sent to professionals within the practice or employed by technology companies to offer immediate support, including suicide safety planning and counseling. Users can hit a button to “Find a Therapist.” Also, if they acknowledge feelings of self-harm, these keywords are detected within the app by NLP. “Urgent alerts” are then sent to clinicians who are overseeing patient care. If someone is flagged, a social worker or member of a response services team intervenes and calls the person at risk to tailor care. These interventions do not always require a psychiatrist or masters-prepared clinician but can be effectively managed by trained paraprofessionals. These staff members can provide suicide safety planning and lethal-means-restriction counseling, and can assess the need for escalation of care.
Q: How is technology likely to manifest in physician practices in the near future to support mental health care?
A: Automated screening platforms for depression and anxiety, alerts for physicians when patients screen positively, and integration with collaborative care models are a few of the ways technology will become part of clinical practice. Additionally, advanced data analytics and predictive modeling using electronic health records and claims data will help identify high-risk patients. Technologies like voice recognition and machine learning can analyze patient journals and possibly, in the future, social media feeds to detect mental health issues. These technologies aim to extend and augment the capabilities of healthcare practices, improving the identification and management of patients at risk for mental health issues.
Q: Are these technologies as effective in pediatric populations, and are there any specific challenges?
A: Technologies for mental health screening and support are effective in pediatric populations, with certain age-specific considerations and legal restrictions on technology use. For adolescents and older children comfortable with technology, digital tools can significantly impact mental health care. For younger children, technology must facilitate information-gathering from various sources, including parents and teachers. Despite challenges, technology is crucial for early identification and intervention in pediatric mental health, potentially shortening the time to diagnosis and improving outcomes.
The statistics are horrifying. One third of adolescent girls have seriously thought about suicide over the past year; 13% attempt suicide. So there’s a need in the adolescent population and in the preadolescent population, too, because there’s an 8- to 10-year lag between onset of symptoms and diagnosis of mental illness. If we can shorten that lag, you see improved performance in schools; you see decreased truancy; you see greater economic achievement and so on. It makes such a profound difference. Not to mention it saves lives. So, yes, technology is critical in a pediatric population. It exists and it’s happening right now. There are challenges, but the goal can be met.
Q: A 2014 study found that 45% of people who completed suicide visited a primary care physician in the preceding month. And only 23% of people who attempt suicide have not seen a primary care physician within the past year. What does that say about the importance of screening at the primary care level?
A: The fact that a significant percentage of individuals who die by suicide have visited a primary care physician within a month or year prior to their death underscores the critical role of primary care in suicide prevention. This highlights the potential for primary care settings to identify and intervene with individuals at risk for suicide, making the case for the importance of integrating effective mental health screenings and support technologies in primary care practices.
Q: In other words, we’re not talking about a marginal benefit.
A: No, the potential benefit is huge. The United States Preventive Services Task Force did not endorse universal screening for suicide in its 2023 recommendations; they felt — and I accept that conclusion — there wasn›t enough evidence [at the time] to really support that recommendation. I think when you talk to a lot of suicide researchers, what you will hear is that providing suicide assessments as far upstream as possible is critical, especially when you start seeing more and more research showing that 20% of the population who die by suicide are not likely to have any psychiatric pathology at all. I believe the evidence base will soon support a recommendation for universal screening for adults. I believe it is especially important to screen for suicidal ideation in kids, given the high rates of suicide in this population.
Dr. Zaubler has disclosed the following relevant financial relationships: chief medical officer, NeuroFlow.
A version of this article appeared on Medscape.com.
Perinatal Mood and Anxiety Disorder Increasing Rapidly
The number of women with perinatal mood and anxiety disorder (PMAD) has spiked sharply in the United States. A new study explores trends by state and time period.
Between 2008 and 2020, in a national cohort of 750,004 commercially insured women with a live birth, nearly 1 in 5 (144,037 [19.2%]) were diagnosed with PMAD, according to a paper published in Health Affairs. PMAD diagnoses among privately insured women increased by 93.3% over those years, wrote lead author Kara Zivin, PhD, of the University of Michigan, Veterans Affairs Ann Arbor Healthcare System, and colleagues.
PMAD describes a spectrum of emotional complications with mild to severe symptoms that can affect women while pregnant and through the first year after giving birth.
The total number of perinatal women decreased from a high of 64,842 in 2008 to a low of 52,479 in 2020, a 19.1% decrease, but over the same time, women with diagnosed PMAD increased 56.4% from 9,520 in 2008 to 14,890 in 2020. Prevalence of PMAD doubled from 1,468 per 10,000 deliveries to 2,837 per 10,000 deliveries in 2020, according to the analysis.
Differences by State
Increases differed substantially by state. Though average annual changes across all states reached 109 additional PMAD diagnoses per 10,000 deliveries, Iowa had the greatest increase with an additional 163 PMAD diagnoses per 10,000 deliveries annually. New Mexico had the smallest annual growth, at an additional 49 per 10,000 deliveries.
The increases were accompanied by maternal health improvement efforts. The Affordable Care Act (ACA) required insurance companies to cover maternity and preventive services, which likely increased PMAD screening and detection, the researchers noted.
“Diagnosis of PMAD is rising due to increased awareness and in all likelihood, decrease in stigma, but availability of providers is so challenging,” said Lee S. Cohen, MD, who was not part of the study. Dr. Cohen is director of the Ammon-Pinizzotto Center for Women’s Mental Health and Perinatal and Reproductive Psychiatry at Massachusetts General Hospital in Boston. “The navigation to providers by women who are suffering is beyond challenging,” he said.
The authors reported that all states except Vermont saw increasing rates of PMAD diagnoses post-ACA vs. pre-ACA. The researchers also found that relative to the period from 2008 to 2014, psychotherapy rates continued rising from 2015 to 2020 and suicidality (suicidal ideation or self-harm diagnoses) rates declined.
States’ Suicidality Rates Vary Widely
“Overall, access to psychotherapy may have stemmed suicidality despite increasing PMAD diagnoses. But although more PMAD diagnoses may have led to increased psychotherapy, therapy access depends on provider availability, which varies by geographic region and insurance coverage network,” the authors wrote.
Suicidality rates differed greatly by state. Louisiana’s annual rate of increase was greatest, at 22 per 10,000 while Maryland had the greatest negative annual rate of change, at −15 per 10,000 deliveries, the authors explained.
“Observed trends in PMAD diagnoses among privately insured people during 2008-2020 and in associated suicidality and psychotherapy use suggest an increasingly rapid worsening of US maternal mental health,” the authors wrote.
The authors noted that this study did not include those on public insurance, a group that may experience disproportionate maternal morbidity and mortality burden, and urged that future studies include them.
Strengths of Study
Kimberly McKee, PhD, MPH, assistant professor in the department of family medicine at University of Michigan in Ann Arbor, who was not part of this research, said this paper gives a broader look than prior work because it includes the year before and after birth, rather than delivery and hospitalization.
“It’s really important to look out at least 12 months postpartum,” she noted.
Another strength is that the study was able to look at use of services such as psychotherapy before and post ACA. She noted the increased use of psychotherapy and the decrease in suicidal ideation was an association, but said, “I think it’s reasonable to assume that there was a benefit.”
She noted that these data go through 2020 and the COVID-19 pandemic has even further stressed the healthcare system, which could affect these numbers.
Primary Care’s Role
“The opportunity for primary care to really be the medical home for reproductive-age women is key here,” Dr. McKee said, adding that primary care can provide the continuity if women go off and on insurance around pregnancy and make sure the women get follow-up care and referrals to specialty care.
Models that integrate behavioral health and primary care are particularly promising, she said. Inclusion of social workers at the point of care can also help meet needs regarding social determinants of health.
Telehealth is another avenue for expansion extending the reach for following perinatal women, she said. “Using every tool we have to reach individuals where they are can allow for more frequent check-ins, which is really important here.”
Dr. McKee said the paper highlights an important reality: Mental health is a leading cause and contributor to maternal mortality, which “is 100% preventable.” Yet, current literature continues to show increases.
“This is a fairly common problem that affects not just women, but the fetus, their children, their families,” she noted.
The authors and Dr. Cohen and Dr. McKee reported no relevant financial relationships.
The number of women with perinatal mood and anxiety disorder (PMAD) has spiked sharply in the United States. A new study explores trends by state and time period.
Between 2008 and 2020, in a national cohort of 750,004 commercially insured women with a live birth, nearly 1 in 5 (144,037 [19.2%]) were diagnosed with PMAD, according to a paper published in Health Affairs. PMAD diagnoses among privately insured women increased by 93.3% over those years, wrote lead author Kara Zivin, PhD, of the University of Michigan, Veterans Affairs Ann Arbor Healthcare System, and colleagues.
PMAD describes a spectrum of emotional complications with mild to severe symptoms that can affect women while pregnant and through the first year after giving birth.
The total number of perinatal women decreased from a high of 64,842 in 2008 to a low of 52,479 in 2020, a 19.1% decrease, but over the same time, women with diagnosed PMAD increased 56.4% from 9,520 in 2008 to 14,890 in 2020. Prevalence of PMAD doubled from 1,468 per 10,000 deliveries to 2,837 per 10,000 deliveries in 2020, according to the analysis.
Differences by State
Increases differed substantially by state. Though average annual changes across all states reached 109 additional PMAD diagnoses per 10,000 deliveries, Iowa had the greatest increase with an additional 163 PMAD diagnoses per 10,000 deliveries annually. New Mexico had the smallest annual growth, at an additional 49 per 10,000 deliveries.
The increases were accompanied by maternal health improvement efforts. The Affordable Care Act (ACA) required insurance companies to cover maternity and preventive services, which likely increased PMAD screening and detection, the researchers noted.
“Diagnosis of PMAD is rising due to increased awareness and in all likelihood, decrease in stigma, but availability of providers is so challenging,” said Lee S. Cohen, MD, who was not part of the study. Dr. Cohen is director of the Ammon-Pinizzotto Center for Women’s Mental Health and Perinatal and Reproductive Psychiatry at Massachusetts General Hospital in Boston. “The navigation to providers by women who are suffering is beyond challenging,” he said.
The authors reported that all states except Vermont saw increasing rates of PMAD diagnoses post-ACA vs. pre-ACA. The researchers also found that relative to the period from 2008 to 2014, psychotherapy rates continued rising from 2015 to 2020 and suicidality (suicidal ideation or self-harm diagnoses) rates declined.
States’ Suicidality Rates Vary Widely
“Overall, access to psychotherapy may have stemmed suicidality despite increasing PMAD diagnoses. But although more PMAD diagnoses may have led to increased psychotherapy, therapy access depends on provider availability, which varies by geographic region and insurance coverage network,” the authors wrote.
Suicidality rates differed greatly by state. Louisiana’s annual rate of increase was greatest, at 22 per 10,000 while Maryland had the greatest negative annual rate of change, at −15 per 10,000 deliveries, the authors explained.
“Observed trends in PMAD diagnoses among privately insured people during 2008-2020 and in associated suicidality and psychotherapy use suggest an increasingly rapid worsening of US maternal mental health,” the authors wrote.
The authors noted that this study did not include those on public insurance, a group that may experience disproportionate maternal morbidity and mortality burden, and urged that future studies include them.
Strengths of Study
Kimberly McKee, PhD, MPH, assistant professor in the department of family medicine at University of Michigan in Ann Arbor, who was not part of this research, said this paper gives a broader look than prior work because it includes the year before and after birth, rather than delivery and hospitalization.
“It’s really important to look out at least 12 months postpartum,” she noted.
Another strength is that the study was able to look at use of services such as psychotherapy before and post ACA. She noted the increased use of psychotherapy and the decrease in suicidal ideation was an association, but said, “I think it’s reasonable to assume that there was a benefit.”
She noted that these data go through 2020 and the COVID-19 pandemic has even further stressed the healthcare system, which could affect these numbers.
Primary Care’s Role
“The opportunity for primary care to really be the medical home for reproductive-age women is key here,” Dr. McKee said, adding that primary care can provide the continuity if women go off and on insurance around pregnancy and make sure the women get follow-up care and referrals to specialty care.
Models that integrate behavioral health and primary care are particularly promising, she said. Inclusion of social workers at the point of care can also help meet needs regarding social determinants of health.
Telehealth is another avenue for expansion extending the reach for following perinatal women, she said. “Using every tool we have to reach individuals where they are can allow for more frequent check-ins, which is really important here.”
Dr. McKee said the paper highlights an important reality: Mental health is a leading cause and contributor to maternal mortality, which “is 100% preventable.” Yet, current literature continues to show increases.
“This is a fairly common problem that affects not just women, but the fetus, their children, their families,” she noted.
The authors and Dr. Cohen and Dr. McKee reported no relevant financial relationships.
The number of women with perinatal mood and anxiety disorder (PMAD) has spiked sharply in the United States. A new study explores trends by state and time period.
Between 2008 and 2020, in a national cohort of 750,004 commercially insured women with a live birth, nearly 1 in 5 (144,037 [19.2%]) were diagnosed with PMAD, according to a paper published in Health Affairs. PMAD diagnoses among privately insured women increased by 93.3% over those years, wrote lead author Kara Zivin, PhD, of the University of Michigan, Veterans Affairs Ann Arbor Healthcare System, and colleagues.
PMAD describes a spectrum of emotional complications with mild to severe symptoms that can affect women while pregnant and through the first year after giving birth.
The total number of perinatal women decreased from a high of 64,842 in 2008 to a low of 52,479 in 2020, a 19.1% decrease, but over the same time, women with diagnosed PMAD increased 56.4% from 9,520 in 2008 to 14,890 in 2020. Prevalence of PMAD doubled from 1,468 per 10,000 deliveries to 2,837 per 10,000 deliveries in 2020, according to the analysis.
Differences by State
Increases differed substantially by state. Though average annual changes across all states reached 109 additional PMAD diagnoses per 10,000 deliveries, Iowa had the greatest increase with an additional 163 PMAD diagnoses per 10,000 deliveries annually. New Mexico had the smallest annual growth, at an additional 49 per 10,000 deliveries.
The increases were accompanied by maternal health improvement efforts. The Affordable Care Act (ACA) required insurance companies to cover maternity and preventive services, which likely increased PMAD screening and detection, the researchers noted.
“Diagnosis of PMAD is rising due to increased awareness and in all likelihood, decrease in stigma, but availability of providers is so challenging,” said Lee S. Cohen, MD, who was not part of the study. Dr. Cohen is director of the Ammon-Pinizzotto Center for Women’s Mental Health and Perinatal and Reproductive Psychiatry at Massachusetts General Hospital in Boston. “The navigation to providers by women who are suffering is beyond challenging,” he said.
The authors reported that all states except Vermont saw increasing rates of PMAD diagnoses post-ACA vs. pre-ACA. The researchers also found that relative to the period from 2008 to 2014, psychotherapy rates continued rising from 2015 to 2020 and suicidality (suicidal ideation or self-harm diagnoses) rates declined.
States’ Suicidality Rates Vary Widely
“Overall, access to psychotherapy may have stemmed suicidality despite increasing PMAD diagnoses. But although more PMAD diagnoses may have led to increased psychotherapy, therapy access depends on provider availability, which varies by geographic region and insurance coverage network,” the authors wrote.
Suicidality rates differed greatly by state. Louisiana’s annual rate of increase was greatest, at 22 per 10,000 while Maryland had the greatest negative annual rate of change, at −15 per 10,000 deliveries, the authors explained.
“Observed trends in PMAD diagnoses among privately insured people during 2008-2020 and in associated suicidality and psychotherapy use suggest an increasingly rapid worsening of US maternal mental health,” the authors wrote.
The authors noted that this study did not include those on public insurance, a group that may experience disproportionate maternal morbidity and mortality burden, and urged that future studies include them.
Strengths of Study
Kimberly McKee, PhD, MPH, assistant professor in the department of family medicine at University of Michigan in Ann Arbor, who was not part of this research, said this paper gives a broader look than prior work because it includes the year before and after birth, rather than delivery and hospitalization.
“It’s really important to look out at least 12 months postpartum,” she noted.
Another strength is that the study was able to look at use of services such as psychotherapy before and post ACA. She noted the increased use of psychotherapy and the decrease in suicidal ideation was an association, but said, “I think it’s reasonable to assume that there was a benefit.”
She noted that these data go through 2020 and the COVID-19 pandemic has even further stressed the healthcare system, which could affect these numbers.
Primary Care’s Role
“The opportunity for primary care to really be the medical home for reproductive-age women is key here,” Dr. McKee said, adding that primary care can provide the continuity if women go off and on insurance around pregnancy and make sure the women get follow-up care and referrals to specialty care.
Models that integrate behavioral health and primary care are particularly promising, she said. Inclusion of social workers at the point of care can also help meet needs regarding social determinants of health.
Telehealth is another avenue for expansion extending the reach for following perinatal women, she said. “Using every tool we have to reach individuals where they are can allow for more frequent check-ins, which is really important here.”
Dr. McKee said the paper highlights an important reality: Mental health is a leading cause and contributor to maternal mortality, which “is 100% preventable.” Yet, current literature continues to show increases.
“This is a fairly common problem that affects not just women, but the fetus, their children, their families,” she noted.
The authors and Dr. Cohen and Dr. McKee reported no relevant financial relationships.
FROM HEALTH AFFAIRS
Childhood Adversity Robustly Linked to Adult Mental Illness
Adverse childhood experiences (ACEs) are associated with a significantly increased risk for adult depressive, anxiety, and stress-related disorders, new data from a large registry study of twins showed.
Researchers found that each additional adverse event placed children at a 52% greater risk for a psychiatric disorder as an adult, with sexual abuse associated with the greatest risk.
The findings showed that the association held even after controlling for shared genetic and environmental factors.
The results suggested that “interventions targeting ACEs, including primary prevention and enhanced access to evidence-based trauma therapies to individuals who experienced ACEs, may be associated with reduced risk of future psychopathology,” the investigators, with first author Hilda Björk Daníelsdóttir, MSc, of the University of Iceland, Reykjavik, Iceland, wrote.
The findings were published online on March 6 in JAMA Psychiatry.
Dose-Dependent Effect
Previous research has shown a robust link between childhood abuse and an increased risk for psychiatric disorders in adulthood, but evidence of this association in studies that adjust for familial confounding is “completely lacking,” the investigators wrote.
To learn more about how genetic factors may affect the relationship between ACEs and later psychiatric diagnoses, the investigators used data from the nationwide Swedish Twin Registry, which includes data on more than 25,000 identical and nonidentical twins.
The twin registry is linked to the Swedish National Patient Registry, which includes information on inpatient or outpatient psychiatric diagnoses after age 19.
The twins responded to a large web-based questionnaire about past-week depressive symptoms as a measure of current mental health and distinct types of ACEs including family violence, emotional abuse or neglect, physical neglect, physical abuse, sexual abuse, rape, and hate crime.
Three birth cohorts from the twin registry were surveyed between 2005 and 2016 and followed up in the national registry from age 19 until the end of 2016.
Among the sample of 25,000 twin pairs (15,000 female; mean age at assessment, 29 years), 9750 (39%) participants reported exposure to at least one ACE, while 2000 (8%) reported exposure to three or more ACEs. Most respondents — 61% — reported no ACE exposure.
More than 2300 participants received a psychiatric diagnosis as an adult. The incidence of any psychiatric disorder increased from 503 individuals (6.4%) among participants without any ACEs to 993 individuals (24.6%) among those reporting three or more.
At the cohort level, a greater number of ACEs was associated with increased odds of any psychiatric disorder in a dose-dependent manner, the investigators noted (odds ratio [OR], 1.52; 95% CI, 1.48-1.57).
Untangling Genes and Environment
To determine how much of the increased risk for adult mental illness is due to ACEs and how much can be attributed to genetics and environment, the researchers focused on twin pairs where one had exposure to one type of ACEs and the other did not. This analysis revealed that the association remained but was attenuated. In identical twins, the effect of each ACE raised the odds of having a psychiatric condition by 20% (1.20; 95% CI, 1.02-1.40), and for nonidentical twins, the odds increased by 29% (1.29; 95% CI, 1.14-1.47).
The weakening of the risk “suggests that familial confounding contributed to the association between ACEs and adult mental health outcomes,” the authors wrote.
Of all the ACEs, sexual abuse carried the highest risk for adult psychiatric disorders. Children who were exposed to sexual abuse, compared with those who were not, had up to a 200% higher risk for any psychiatric disorder in the following comparisons: Full cohort (OR, 3.09; 95% CI, 2.68-3.56), dizygotic twin pairs (OR, 2.10; 95% CI, 1.33-3.32), and monozygotic twin pairs (1.80; 95% CI, 1.04-3.11).
“Our results demonstrated that familial factors contributed to a lesser extent to the association between sexual abuse and adult psychiatric disorders,” the authors wrote.
One major limitation of the study was that ACEs were based on retrospective report and thus may be subject to recall bias. Also, the findings cannot be generalized to other countries or cultures.
The study was funded by the European Research Council, the Icelandic Center for Research, and the European Union Horizon 2020. Disclosures are noted in the original article.
A version of this article appeared on Medscape.com.
Adverse childhood experiences (ACEs) are associated with a significantly increased risk for adult depressive, anxiety, and stress-related disorders, new data from a large registry study of twins showed.
Researchers found that each additional adverse event placed children at a 52% greater risk for a psychiatric disorder as an adult, with sexual abuse associated with the greatest risk.
The findings showed that the association held even after controlling for shared genetic and environmental factors.
The results suggested that “interventions targeting ACEs, including primary prevention and enhanced access to evidence-based trauma therapies to individuals who experienced ACEs, may be associated with reduced risk of future psychopathology,” the investigators, with first author Hilda Björk Daníelsdóttir, MSc, of the University of Iceland, Reykjavik, Iceland, wrote.
The findings were published online on March 6 in JAMA Psychiatry.
Dose-Dependent Effect
Previous research has shown a robust link between childhood abuse and an increased risk for psychiatric disorders in adulthood, but evidence of this association in studies that adjust for familial confounding is “completely lacking,” the investigators wrote.
To learn more about how genetic factors may affect the relationship between ACEs and later psychiatric diagnoses, the investigators used data from the nationwide Swedish Twin Registry, which includes data on more than 25,000 identical and nonidentical twins.
The twin registry is linked to the Swedish National Patient Registry, which includes information on inpatient or outpatient psychiatric diagnoses after age 19.
The twins responded to a large web-based questionnaire about past-week depressive symptoms as a measure of current mental health and distinct types of ACEs including family violence, emotional abuse or neglect, physical neglect, physical abuse, sexual abuse, rape, and hate crime.
Three birth cohorts from the twin registry were surveyed between 2005 and 2016 and followed up in the national registry from age 19 until the end of 2016.
Among the sample of 25,000 twin pairs (15,000 female; mean age at assessment, 29 years), 9750 (39%) participants reported exposure to at least one ACE, while 2000 (8%) reported exposure to three or more ACEs. Most respondents — 61% — reported no ACE exposure.
More than 2300 participants received a psychiatric diagnosis as an adult. The incidence of any psychiatric disorder increased from 503 individuals (6.4%) among participants without any ACEs to 993 individuals (24.6%) among those reporting three or more.
At the cohort level, a greater number of ACEs was associated with increased odds of any psychiatric disorder in a dose-dependent manner, the investigators noted (odds ratio [OR], 1.52; 95% CI, 1.48-1.57).
Untangling Genes and Environment
To determine how much of the increased risk for adult mental illness is due to ACEs and how much can be attributed to genetics and environment, the researchers focused on twin pairs where one had exposure to one type of ACEs and the other did not. This analysis revealed that the association remained but was attenuated. In identical twins, the effect of each ACE raised the odds of having a psychiatric condition by 20% (1.20; 95% CI, 1.02-1.40), and for nonidentical twins, the odds increased by 29% (1.29; 95% CI, 1.14-1.47).
The weakening of the risk “suggests that familial confounding contributed to the association between ACEs and adult mental health outcomes,” the authors wrote.
Of all the ACEs, sexual abuse carried the highest risk for adult psychiatric disorders. Children who were exposed to sexual abuse, compared with those who were not, had up to a 200% higher risk for any psychiatric disorder in the following comparisons: Full cohort (OR, 3.09; 95% CI, 2.68-3.56), dizygotic twin pairs (OR, 2.10; 95% CI, 1.33-3.32), and monozygotic twin pairs (1.80; 95% CI, 1.04-3.11).
“Our results demonstrated that familial factors contributed to a lesser extent to the association between sexual abuse and adult psychiatric disorders,” the authors wrote.
One major limitation of the study was that ACEs were based on retrospective report and thus may be subject to recall bias. Also, the findings cannot be generalized to other countries or cultures.
The study was funded by the European Research Council, the Icelandic Center for Research, and the European Union Horizon 2020. Disclosures are noted in the original article.
A version of this article appeared on Medscape.com.
Adverse childhood experiences (ACEs) are associated with a significantly increased risk for adult depressive, anxiety, and stress-related disorders, new data from a large registry study of twins showed.
Researchers found that each additional adverse event placed children at a 52% greater risk for a psychiatric disorder as an adult, with sexual abuse associated with the greatest risk.
The findings showed that the association held even after controlling for shared genetic and environmental factors.
The results suggested that “interventions targeting ACEs, including primary prevention and enhanced access to evidence-based trauma therapies to individuals who experienced ACEs, may be associated with reduced risk of future psychopathology,” the investigators, with first author Hilda Björk Daníelsdóttir, MSc, of the University of Iceland, Reykjavik, Iceland, wrote.
The findings were published online on March 6 in JAMA Psychiatry.
Dose-Dependent Effect
Previous research has shown a robust link between childhood abuse and an increased risk for psychiatric disorders in adulthood, but evidence of this association in studies that adjust for familial confounding is “completely lacking,” the investigators wrote.
To learn more about how genetic factors may affect the relationship between ACEs and later psychiatric diagnoses, the investigators used data from the nationwide Swedish Twin Registry, which includes data on more than 25,000 identical and nonidentical twins.
The twin registry is linked to the Swedish National Patient Registry, which includes information on inpatient or outpatient psychiatric diagnoses after age 19.
The twins responded to a large web-based questionnaire about past-week depressive symptoms as a measure of current mental health and distinct types of ACEs including family violence, emotional abuse or neglect, physical neglect, physical abuse, sexual abuse, rape, and hate crime.
Three birth cohorts from the twin registry were surveyed between 2005 and 2016 and followed up in the national registry from age 19 until the end of 2016.
Among the sample of 25,000 twin pairs (15,000 female; mean age at assessment, 29 years), 9750 (39%) participants reported exposure to at least one ACE, while 2000 (8%) reported exposure to three or more ACEs. Most respondents — 61% — reported no ACE exposure.
More than 2300 participants received a psychiatric diagnosis as an adult. The incidence of any psychiatric disorder increased from 503 individuals (6.4%) among participants without any ACEs to 993 individuals (24.6%) among those reporting three or more.
At the cohort level, a greater number of ACEs was associated with increased odds of any psychiatric disorder in a dose-dependent manner, the investigators noted (odds ratio [OR], 1.52; 95% CI, 1.48-1.57).
Untangling Genes and Environment
To determine how much of the increased risk for adult mental illness is due to ACEs and how much can be attributed to genetics and environment, the researchers focused on twin pairs where one had exposure to one type of ACEs and the other did not. This analysis revealed that the association remained but was attenuated. In identical twins, the effect of each ACE raised the odds of having a psychiatric condition by 20% (1.20; 95% CI, 1.02-1.40), and for nonidentical twins, the odds increased by 29% (1.29; 95% CI, 1.14-1.47).
The weakening of the risk “suggests that familial confounding contributed to the association between ACEs and adult mental health outcomes,” the authors wrote.
Of all the ACEs, sexual abuse carried the highest risk for adult psychiatric disorders. Children who were exposed to sexual abuse, compared with those who were not, had up to a 200% higher risk for any psychiatric disorder in the following comparisons: Full cohort (OR, 3.09; 95% CI, 2.68-3.56), dizygotic twin pairs (OR, 2.10; 95% CI, 1.33-3.32), and monozygotic twin pairs (1.80; 95% CI, 1.04-3.11).
“Our results demonstrated that familial factors contributed to a lesser extent to the association between sexual abuse and adult psychiatric disorders,” the authors wrote.
One major limitation of the study was that ACEs were based on retrospective report and thus may be subject to recall bias. Also, the findings cannot be generalized to other countries or cultures.
The study was funded by the European Research Council, the Icelandic Center for Research, and the European Union Horizon 2020. Disclosures are noted in the original article.
A version of this article appeared on Medscape.com.
Mental Health and Slow Concussion Recovery
Those of you who are regular readers of Letters from Maine have probably noticed that concussion is one of my favorite topics. The explanation for this perseveration is personal and may lie in the fact that I played two contact sports in college. In high school we still wore leather helmets and in college the lacrosse helmets were constructed of plastic-coated cardboard. I can recall just a few of what might be now labeled as sports-related concussions. Ironically, my only loss of consciousness came on the first dinner date with the woman who would eventually become my wife. A hypotensive episode resulting from the combination of sweat loss (2 hours of basketball) and blood loss from selling some platelets earlier in the day (to pay for the dinner) led to the unfortunate meeting of my head and the beautifully tiled floor at the restaurant.
Postconcussion Recovery
The phenomenon of delayed symptomatic recovery has been a particular interest of mine. Within the last 12 months I have written about an excellent companion commentary in Pediatricsby Talin Babikian PhD, a psychologist at University of California, Los Angeles, in which he urges us to “Consider the comorbidities or premorbidities,” including, among others, anxiety and/or depression, post-traumatic stress, and poor sleep when we are faced with a patient who is slow in shedding his postconcussion symptoms. A short 6 months after reading Dr. Babikian’s prescient commentary, I have encountered some evidence supporting his advice.
Investigators at the Sports Medicine and Performance Center at the Children’s Hospital of Philadelphia have recently published a study in which they have found “Preexisting mental health diagnoses are associated with greater postinjury emotional symptom burden and longer concussion recovery in a dose-response fashion.” In their prospective study of over 3000 children and adolescents, they found that, although patients with more mental health diagnoses were at greater risk of increased emotional symptoms after concussion, “Children and adolescents with any preexisting mental health diagnosis took longer to recover.”
Female patients and those with abnormal visio-vestibular test results at the initial postinjury evaluation took longer to recover, although boys with prolonged recovery had more emotional symptoms. In general, patients with preexisting mental health diagnoses returned to exercise later, a known factor in delayed concussion recovery.
Making Sense of It All
There are a couple of ways to look at this paper’s findings. The first is through the lens that focuses on the population of children and adolescents who have known mental health conditions. If our patient has a mental health diagnosis, we shouldn’t be surprised that he/she is taking longer to recover from his/her concussion and is experiencing an increase in symptoms. Most of us probably suspected this already. However, we should be particularly aware of this phenomenon if the patient is male.
The other perspective is probably more valuable to us as primary care physicians. Even one diagnosis so subtle that we may have overlooked it is likely to slow his/her progress toward recovery. And, of course, it may be that injury has triggered an underlying condition that none — not even the most astute diagnostician — would have found without a focused investigation.
I can’t leave this subject without wondering whether the findings in this paper should be extrapolated to other conditions of delayed recovery, including Lyme disease and COVID 19. Patients with these conditions are understandably resistant to the suggestion that their mental health may be contributing to the situation. Too many have been told too often it is “all in their head.” However, I think we as clinicians should keep open minds when symptoms are resolving more slowly than we would expect.
Finally, in their conclusion the authors of this paper reinforce a principle that has unfortunately taken some of us a while to accept. Early introduction of symptom-limited exercise should be a standard of postconcussion management, especially for patients with a mental health diagnosis.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at pdnews@mdedge.com.
Those of you who are regular readers of Letters from Maine have probably noticed that concussion is one of my favorite topics. The explanation for this perseveration is personal and may lie in the fact that I played two contact sports in college. In high school we still wore leather helmets and in college the lacrosse helmets were constructed of plastic-coated cardboard. I can recall just a few of what might be now labeled as sports-related concussions. Ironically, my only loss of consciousness came on the first dinner date with the woman who would eventually become my wife. A hypotensive episode resulting from the combination of sweat loss (2 hours of basketball) and blood loss from selling some platelets earlier in the day (to pay for the dinner) led to the unfortunate meeting of my head and the beautifully tiled floor at the restaurant.
Postconcussion Recovery
The phenomenon of delayed symptomatic recovery has been a particular interest of mine. Within the last 12 months I have written about an excellent companion commentary in Pediatricsby Talin Babikian PhD, a psychologist at University of California, Los Angeles, in which he urges us to “Consider the comorbidities or premorbidities,” including, among others, anxiety and/or depression, post-traumatic stress, and poor sleep when we are faced with a patient who is slow in shedding his postconcussion symptoms. A short 6 months after reading Dr. Babikian’s prescient commentary, I have encountered some evidence supporting his advice.
Investigators at the Sports Medicine and Performance Center at the Children’s Hospital of Philadelphia have recently published a study in which they have found “Preexisting mental health diagnoses are associated with greater postinjury emotional symptom burden and longer concussion recovery in a dose-response fashion.” In their prospective study of over 3000 children and adolescents, they found that, although patients with more mental health diagnoses were at greater risk of increased emotional symptoms after concussion, “Children and adolescents with any preexisting mental health diagnosis took longer to recover.”
Female patients and those with abnormal visio-vestibular test results at the initial postinjury evaluation took longer to recover, although boys with prolonged recovery had more emotional symptoms. In general, patients with preexisting mental health diagnoses returned to exercise later, a known factor in delayed concussion recovery.
Making Sense of It All
There are a couple of ways to look at this paper’s findings. The first is through the lens that focuses on the population of children and adolescents who have known mental health conditions. If our patient has a mental health diagnosis, we shouldn’t be surprised that he/she is taking longer to recover from his/her concussion and is experiencing an increase in symptoms. Most of us probably suspected this already. However, we should be particularly aware of this phenomenon if the patient is male.
The other perspective is probably more valuable to us as primary care physicians. Even one diagnosis so subtle that we may have overlooked it is likely to slow his/her progress toward recovery. And, of course, it may be that injury has triggered an underlying condition that none — not even the most astute diagnostician — would have found without a focused investigation.
I can’t leave this subject without wondering whether the findings in this paper should be extrapolated to other conditions of delayed recovery, including Lyme disease and COVID 19. Patients with these conditions are understandably resistant to the suggestion that their mental health may be contributing to the situation. Too many have been told too often it is “all in their head.” However, I think we as clinicians should keep open minds when symptoms are resolving more slowly than we would expect.
Finally, in their conclusion the authors of this paper reinforce a principle that has unfortunately taken some of us a while to accept. Early introduction of symptom-limited exercise should be a standard of postconcussion management, especially for patients with a mental health diagnosis.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at pdnews@mdedge.com.
Those of you who are regular readers of Letters from Maine have probably noticed that concussion is one of my favorite topics. The explanation for this perseveration is personal and may lie in the fact that I played two contact sports in college. In high school we still wore leather helmets and in college the lacrosse helmets were constructed of plastic-coated cardboard. I can recall just a few of what might be now labeled as sports-related concussions. Ironically, my only loss of consciousness came on the first dinner date with the woman who would eventually become my wife. A hypotensive episode resulting from the combination of sweat loss (2 hours of basketball) and blood loss from selling some platelets earlier in the day (to pay for the dinner) led to the unfortunate meeting of my head and the beautifully tiled floor at the restaurant.
Postconcussion Recovery
The phenomenon of delayed symptomatic recovery has been a particular interest of mine. Within the last 12 months I have written about an excellent companion commentary in Pediatricsby Talin Babikian PhD, a psychologist at University of California, Los Angeles, in which he urges us to “Consider the comorbidities or premorbidities,” including, among others, anxiety and/or depression, post-traumatic stress, and poor sleep when we are faced with a patient who is slow in shedding his postconcussion symptoms. A short 6 months after reading Dr. Babikian’s prescient commentary, I have encountered some evidence supporting his advice.
Investigators at the Sports Medicine and Performance Center at the Children’s Hospital of Philadelphia have recently published a study in which they have found “Preexisting mental health diagnoses are associated with greater postinjury emotional symptom burden and longer concussion recovery in a dose-response fashion.” In their prospective study of over 3000 children and adolescents, they found that, although patients with more mental health diagnoses were at greater risk of increased emotional symptoms after concussion, “Children and adolescents with any preexisting mental health diagnosis took longer to recover.”
Female patients and those with abnormal visio-vestibular test results at the initial postinjury evaluation took longer to recover, although boys with prolonged recovery had more emotional symptoms. In general, patients with preexisting mental health diagnoses returned to exercise later, a known factor in delayed concussion recovery.
Making Sense of It All
There are a couple of ways to look at this paper’s findings. The first is through the lens that focuses on the population of children and adolescents who have known mental health conditions. If our patient has a mental health diagnosis, we shouldn’t be surprised that he/she is taking longer to recover from his/her concussion and is experiencing an increase in symptoms. Most of us probably suspected this already. However, we should be particularly aware of this phenomenon if the patient is male.
The other perspective is probably more valuable to us as primary care physicians. Even one diagnosis so subtle that we may have overlooked it is likely to slow his/her progress toward recovery. And, of course, it may be that injury has triggered an underlying condition that none — not even the most astute diagnostician — would have found without a focused investigation.
I can’t leave this subject without wondering whether the findings in this paper should be extrapolated to other conditions of delayed recovery, including Lyme disease and COVID 19. Patients with these conditions are understandably resistant to the suggestion that their mental health may be contributing to the situation. Too many have been told too often it is “all in their head.” However, I think we as clinicians should keep open minds when symptoms are resolving more slowly than we would expect.
Finally, in their conclusion the authors of this paper reinforce a principle that has unfortunately taken some of us a while to accept. Early introduction of symptom-limited exercise should be a standard of postconcussion management, especially for patients with a mental health diagnosis.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at pdnews@mdedge.com.
Methylphenidate Linked to Small Increase in CV Event Risk
TOPLINE:
Methylphenidate was associated with a small increased risk for cardiovascular events in individuals taking the drug for more than 6 months in a new cohort study.
METHODOLOGY:
- The retrospective, population-based cohort study was based on national Swedish registry data and included 26,710 patients with attention-deficit/hyperactivity disorder (ADHD) aged 12-60 years (median age 20) who had been prescribed methylphenidate between 2007 and 2012. They were each matched on birth date, sex, and county with up to 10 nonusers without ADHD (a total of 225,672 controls).
- Rates of cardiovascular events, including ischemic heart disease, venous thromboembolism, heart failure, or tachyarrhythmias 1 year before methylphenidate treatment and 6 months after treatment initiation were compared between individuals receiving methylphenidate and matched controls using a Bayesian within-individual design.
TAKEAWAY:
- The overall incidence of cardiovascular events was 1.51 per 10,000 person-weeks for individuals receiving methylphenidate and 0.77 for the matched controls.
- Individuals taking methylphenidate had a 70% posterior probability for a greater than 10% increased risk for cardiovascular events than controls and a 49% posterior probability for an increased risk larger than 20%.
- No difference was found in this risk between individuals with and without a history of cardiovascular disease.
IN PRACTICE:
The researchers concluded that these results support a small (10%) increased risk for cardiovascular events in individuals receiving methylphenidate compared with matched controls after 6 months of treatment. The probability of finding a difference in risk between users and nonusers decreased when considering risk for 20% or larger, with no evidence of differences between those with and without a history of cardiovascular disease. They said the findings suggest the decision to initiate methylphenidate should incorporate considerations of potential adverse cardiovascular effects among the broader benefits and risks for treatment for individual patients.
SOURCE:
The study, led by Miguel Garcia-Argibay, PhD, Örebro University, Örebro, Sweden, was published online in JAMA Network Open on March 6.
LIMITATIONS:
The data were observational, and thus, causality could not be inferred. Lack of information on methylphenidate dose meant that it was not possible to assess a dose effect. Compliance with the medication was also not known, and the association may therefore have been underestimated. The findings of this study were based on data collected from a Swedish population, which may not be representative of other populations.
DISCLOSURES:
The study received funding from the European Union’s Horizon 2020 research and innovation program and the Swedish Research Council for Health, Working Life, and Welfare.
A version of this article appeared on Medscape.com.
TOPLINE:
Methylphenidate was associated with a small increased risk for cardiovascular events in individuals taking the drug for more than 6 months in a new cohort study.
METHODOLOGY:
- The retrospective, population-based cohort study was based on national Swedish registry data and included 26,710 patients with attention-deficit/hyperactivity disorder (ADHD) aged 12-60 years (median age 20) who had been prescribed methylphenidate between 2007 and 2012. They were each matched on birth date, sex, and county with up to 10 nonusers without ADHD (a total of 225,672 controls).
- Rates of cardiovascular events, including ischemic heart disease, venous thromboembolism, heart failure, or tachyarrhythmias 1 year before methylphenidate treatment and 6 months after treatment initiation were compared between individuals receiving methylphenidate and matched controls using a Bayesian within-individual design.
TAKEAWAY:
- The overall incidence of cardiovascular events was 1.51 per 10,000 person-weeks for individuals receiving methylphenidate and 0.77 for the matched controls.
- Individuals taking methylphenidate had a 70% posterior probability for a greater than 10% increased risk for cardiovascular events than controls and a 49% posterior probability for an increased risk larger than 20%.
- No difference was found in this risk between individuals with and without a history of cardiovascular disease.
IN PRACTICE:
The researchers concluded that these results support a small (10%) increased risk for cardiovascular events in individuals receiving methylphenidate compared with matched controls after 6 months of treatment. The probability of finding a difference in risk between users and nonusers decreased when considering risk for 20% or larger, with no evidence of differences between those with and without a history of cardiovascular disease. They said the findings suggest the decision to initiate methylphenidate should incorporate considerations of potential adverse cardiovascular effects among the broader benefits and risks for treatment for individual patients.
SOURCE:
The study, led by Miguel Garcia-Argibay, PhD, Örebro University, Örebro, Sweden, was published online in JAMA Network Open on March 6.
LIMITATIONS:
The data were observational, and thus, causality could not be inferred. Lack of information on methylphenidate dose meant that it was not possible to assess a dose effect. Compliance with the medication was also not known, and the association may therefore have been underestimated. The findings of this study were based on data collected from a Swedish population, which may not be representative of other populations.
DISCLOSURES:
The study received funding from the European Union’s Horizon 2020 research and innovation program and the Swedish Research Council for Health, Working Life, and Welfare.
A version of this article appeared on Medscape.com.
TOPLINE:
Methylphenidate was associated with a small increased risk for cardiovascular events in individuals taking the drug for more than 6 months in a new cohort study.
METHODOLOGY:
- The retrospective, population-based cohort study was based on national Swedish registry data and included 26,710 patients with attention-deficit/hyperactivity disorder (ADHD) aged 12-60 years (median age 20) who had been prescribed methylphenidate between 2007 and 2012. They were each matched on birth date, sex, and county with up to 10 nonusers without ADHD (a total of 225,672 controls).
- Rates of cardiovascular events, including ischemic heart disease, venous thromboembolism, heart failure, or tachyarrhythmias 1 year before methylphenidate treatment and 6 months after treatment initiation were compared between individuals receiving methylphenidate and matched controls using a Bayesian within-individual design.
TAKEAWAY:
- The overall incidence of cardiovascular events was 1.51 per 10,000 person-weeks for individuals receiving methylphenidate and 0.77 for the matched controls.
- Individuals taking methylphenidate had a 70% posterior probability for a greater than 10% increased risk for cardiovascular events than controls and a 49% posterior probability for an increased risk larger than 20%.
- No difference was found in this risk between individuals with and without a history of cardiovascular disease.
IN PRACTICE:
The researchers concluded that these results support a small (10%) increased risk for cardiovascular events in individuals receiving methylphenidate compared with matched controls after 6 months of treatment. The probability of finding a difference in risk between users and nonusers decreased when considering risk for 20% or larger, with no evidence of differences between those with and without a history of cardiovascular disease. They said the findings suggest the decision to initiate methylphenidate should incorporate considerations of potential adverse cardiovascular effects among the broader benefits and risks for treatment for individual patients.
SOURCE:
The study, led by Miguel Garcia-Argibay, PhD, Örebro University, Örebro, Sweden, was published online in JAMA Network Open on March 6.
LIMITATIONS:
The data were observational, and thus, causality could not be inferred. Lack of information on methylphenidate dose meant that it was not possible to assess a dose effect. Compliance with the medication was also not known, and the association may therefore have been underestimated. The findings of this study were based on data collected from a Swedish population, which may not be representative of other populations.
DISCLOSURES:
The study received funding from the European Union’s Horizon 2020 research and innovation program and the Swedish Research Council for Health, Working Life, and Welfare.
A version of this article appeared on Medscape.com.
Paid Parental Leave: Impact on Maternal Mental Health and Child Wellbeing
Maternal mental health has a profound impact on the health and wellbeing of the child. Since the onset of the pandemic, rates of postpartum depression have increased, affecting an estimated 1 in 5 women.1 Numerous studies show the impact of postpartum depression on the newborn child across multiple domains, from bonding to healthy weight gain to meeting developmental milestones.
While new medications are being studied and approved to specifically target postpartum depression, these treatments are inaccessible to many because of high costs and long wait lists. Beyond medication, structural changes such as paid parental leave have been shown to have a substantial impact on maternal mental health, thus impacting the health of children as well.
Implications for Mothers and Children
Psychiatric diagnoses such as postpartum depression are on the rise.1,2 This is likely attributable to a combination of factors, including increased isolation since the start of the pandemic, worsening health inequities across race and socioeconomic status, and difficulty accessing mental health care.3-5 The effect that postpartum depression has on the family is significant for the newborn as well as other children in the home.
Data suggest that postpartum depression impacts both the physical and mental health of the child. Infants of mothers with postpartum depression may experience challenges with weight gain, decreased breastfeeding, sleep disruptions, and delays in achieving developmental milestones.6-9 They may also show decreased maternal infant bonding, challenges with cognitive development including language and IQ, and increased risk of behavioral disturbances.10,11 These effects are likely attributable to a combination of factors, including decreased maternal responsiveness to infant cues.7,12 Many of these effects are mediated by the chronicity and severity of depressive symptoms, suggesting the importance of screening and treatment of postpartum depression.10,11 However, treatment for postpartum depression can be difficult to access, particularly given the increased level of need.
It is therefore critical to consider what structural interventions and policy changes can decrease the risk of developing postpartum depression. Data consistently show that access to paid parental leave improves maternal mental health outcomes. Among patients with access to parental leave, research shows that paid leave of longer duration, at least 2-3 months, is the most protective.13 Studies have identified decreased depressive symptoms, decreased stress, decreased use of mental health services, and decreased hospital admissions among women with longer parental leave.13 The positive effects of paid parental leave on maternal mental health can extend beyond the postpartum period, solidifying its impact on the long-term health outcomes of both mother and child.13
Advocacy Is Imperative
In 2024, the United States is the only high-income country, and one of only seven countries in the world, that does not guarantee access to paid parental leave. The Family Medical Leave Act is a 31-year-old federal law that requires some employers to provide unpaid leave to eligible employees. It is narrow in scope, and it excludes many low-wage workers and LGBTQ+ families. Thirteen states — California, Colorado, Connecticut, Delaware, Maine, Massachusetts, Maryland, Minnesota, New Jersey, New York, Oregon, Rhode Island, and Washington — as well as the District of Columbia, have enacted their own paid leave policies. However, there are no federal laws requiring access to paid parental leave. As of 2023, fewer than 30% of workers in the United States have access to paid parental leave, and only 16% of employees in the service industry have access to paid parental leave.14 This disproportionately affects families from lower income backgrounds, and further exacerbates socioeconomic, racial, and gender inequities. From a health systems lens, this increases risk of adverse maternal mental health outcomes among those who already have decreased access to mental health services, worsening health disparities.
Paid parental leave has strong public support across party lines, with polls showing the majority of Americans support comprehensive paid family and medical leave.15 Despite this, the United States has failed to enact legislation on this issue since 1993. Multiple attempts at expanding leave have not come to fruition. In the past year, both the house and the senate have announced bipartisan efforts to expand access to paid parental leave. However, legislative frameworks are still in early stages.
As physicians, it is crucial that we advocate for expanded access to paid parental leave. We must use our expertise to speak to the impact that paid parental leave can have on the mental and physical health of parents, children, and families. By advocating for paid parental leave, we can help create a more just and equitable healthcare system.
Dr. Shannon is a second-year psychiatry resident at University of California, Los Angeles. She attended Stanford University for her undergraduate degree and Dartmouth Geisel School of Medicine for medical school. Her interests include perinatal psychiatry, health systems research, and mental health policy advocacy. Dr. Richards is assistant clinical professor in the department of psychiatry and biobehavioral sciences; program director of the child and adolescent psychiatry fellowship; and associate medical director of the perinatal program at the UCLA Semel Institute for Neuroscience and Human Behavior, Los Angeles.
References
1. Wang Z et al. Mapping Global Prevalence of Depression Among Postpartum Women. Transl Psychiatry. 2021 Oct 20. doi: 10.1038/s41398-021-01663-6.
2. Iyengar U et al. One Year Into the Pandemic: A Systematic Review of Perinatal Mental Health Outcomes During COVID-19. Front Psychiatry. 2021 Jun 24. doi: 10.3389/fpsyt.2021.674194.
3. World Health Organization. Mental Health and COVID-19: Early Evidence of the Pandemic’s Impact: Scientific Brief. 2022 Mar 2. www.who.int/publications/i/item/WHO-2019-nCoV-Sci_Brief-Mental_health-2022.1.
4. Masters GA et al. Impact of the COVID-19 Pandemic on Mental Health, Access to Care, and Health Disparities in the Perinatal Period. J Psychiatr Res. 2021 May. doi: 10.1016/j.jpsychires.2021.02.056.
5. Shuffrey LC et al. Improving Perinatal Maternal Mental Health Starts With Addressing Structural Inequities. JAMA Psychiatry. 2022 May 1. doi: 10.1001/jamapsychiatry.2022.0097.
6. Lubotzky-Gete S et al. Postpartum Depression and Infant Development Up to 24 months: A Nationwide Population-Based Study. J Affect Disord. 2021 Apr 15. doi: 10.1016/j.jad.2021.02.042.
7. Saharoy R et al. Postpartum Depression and Maternal Care: Exploring the Complex Effects on Mothers and Infants. Cureus. 2023 Jul 4. doi: 10.7759/cureus.41381..
8. Gress-Smith JL et al. Postpartum Depression Prevalence and Impact on Infant Health, Weight, and Sleep in Low-Income and Ethnic Minority Women and Infants. Matern Child Health J. 2012 May. doi: 10.1007/s10995-011-0812-y.
9. Kim S et al. The Impact of Antepartum Depression and Postpartum Depression on Exclusive Breastfeeding: A Systematic Review and Meta-Analysis. Clin Nurs Res. 2022 Jun. doi: 10.1177/10547738211053507.
10. Mirhosseini H et al. Cognitive Behavioral Development in Children Following Maternal Postpartum Depression: A Review Article. Electron Physician. 2015 Dec 20. doi: 10.19082/1673.
11. Grace SL et al. The Effect of Postpartum Depression on Child Cognitive Development and Behavior: A Review and Critical Analysis of the Literature. Arch Womens Ment Health. 2003 Nov. doi: 10.1007/s00737-003-0024-6.
12. Milgrom J et al. The Mediating Role of Maternal Responsiveness in Some Longer Term Effects of Postnatal Depression on Infant Development. Infant Behavior and Development. 2004 Sep 11. doi.org/10.1016/j.infbeh.2004.03.003.
13. Heshmati A et al. The Effect of Parental Leave on Parents’ Mental Health: A Systematic Review. Lancet Public Health. 2023 Jan. doi: 10.1016/S2468-2667(22)00311-5.
14. U.S. Bureau of Labor Statistics, What Data Does the BLS Publish on Family Leave? 2023 Sept 21. www.bls.gov/ebs/factsheets/family-leave-benefits-fact-sheet.htm.
15. Horowitz JM et al. Americans Widely Support Paid Family and Medical Leave, But Differ Over Specific Policies. Pew Research Center’s Social & Demographic Trends Project, Pew Research Center. 2017 Mar 23. www.pewresearch.org/social-trends/2017/03/23/americans-widely-support-paid-family-and-medical-leave-but-differ-over-specific-policies/.
Maternal mental health has a profound impact on the health and wellbeing of the child. Since the onset of the pandemic, rates of postpartum depression have increased, affecting an estimated 1 in 5 women.1 Numerous studies show the impact of postpartum depression on the newborn child across multiple domains, from bonding to healthy weight gain to meeting developmental milestones.
While new medications are being studied and approved to specifically target postpartum depression, these treatments are inaccessible to many because of high costs and long wait lists. Beyond medication, structural changes such as paid parental leave have been shown to have a substantial impact on maternal mental health, thus impacting the health of children as well.
Implications for Mothers and Children
Psychiatric diagnoses such as postpartum depression are on the rise.1,2 This is likely attributable to a combination of factors, including increased isolation since the start of the pandemic, worsening health inequities across race and socioeconomic status, and difficulty accessing mental health care.3-5 The effect that postpartum depression has on the family is significant for the newborn as well as other children in the home.
Data suggest that postpartum depression impacts both the physical and mental health of the child. Infants of mothers with postpartum depression may experience challenges with weight gain, decreased breastfeeding, sleep disruptions, and delays in achieving developmental milestones.6-9 They may also show decreased maternal infant bonding, challenges with cognitive development including language and IQ, and increased risk of behavioral disturbances.10,11 These effects are likely attributable to a combination of factors, including decreased maternal responsiveness to infant cues.7,12 Many of these effects are mediated by the chronicity and severity of depressive symptoms, suggesting the importance of screening and treatment of postpartum depression.10,11 However, treatment for postpartum depression can be difficult to access, particularly given the increased level of need.
It is therefore critical to consider what structural interventions and policy changes can decrease the risk of developing postpartum depression. Data consistently show that access to paid parental leave improves maternal mental health outcomes. Among patients with access to parental leave, research shows that paid leave of longer duration, at least 2-3 months, is the most protective.13 Studies have identified decreased depressive symptoms, decreased stress, decreased use of mental health services, and decreased hospital admissions among women with longer parental leave.13 The positive effects of paid parental leave on maternal mental health can extend beyond the postpartum period, solidifying its impact on the long-term health outcomes of both mother and child.13
Advocacy Is Imperative
In 2024, the United States is the only high-income country, and one of only seven countries in the world, that does not guarantee access to paid parental leave. The Family Medical Leave Act is a 31-year-old federal law that requires some employers to provide unpaid leave to eligible employees. It is narrow in scope, and it excludes many low-wage workers and LGBTQ+ families. Thirteen states — California, Colorado, Connecticut, Delaware, Maine, Massachusetts, Maryland, Minnesota, New Jersey, New York, Oregon, Rhode Island, and Washington — as well as the District of Columbia, have enacted their own paid leave policies. However, there are no federal laws requiring access to paid parental leave. As of 2023, fewer than 30% of workers in the United States have access to paid parental leave, and only 16% of employees in the service industry have access to paid parental leave.14 This disproportionately affects families from lower income backgrounds, and further exacerbates socioeconomic, racial, and gender inequities. From a health systems lens, this increases risk of adverse maternal mental health outcomes among those who already have decreased access to mental health services, worsening health disparities.
Paid parental leave has strong public support across party lines, with polls showing the majority of Americans support comprehensive paid family and medical leave.15 Despite this, the United States has failed to enact legislation on this issue since 1993. Multiple attempts at expanding leave have not come to fruition. In the past year, both the house and the senate have announced bipartisan efforts to expand access to paid parental leave. However, legislative frameworks are still in early stages.
As physicians, it is crucial that we advocate for expanded access to paid parental leave. We must use our expertise to speak to the impact that paid parental leave can have on the mental and physical health of parents, children, and families. By advocating for paid parental leave, we can help create a more just and equitable healthcare system.
Dr. Shannon is a second-year psychiatry resident at University of California, Los Angeles. She attended Stanford University for her undergraduate degree and Dartmouth Geisel School of Medicine for medical school. Her interests include perinatal psychiatry, health systems research, and mental health policy advocacy. Dr. Richards is assistant clinical professor in the department of psychiatry and biobehavioral sciences; program director of the child and adolescent psychiatry fellowship; and associate medical director of the perinatal program at the UCLA Semel Institute for Neuroscience and Human Behavior, Los Angeles.
References
1. Wang Z et al. Mapping Global Prevalence of Depression Among Postpartum Women. Transl Psychiatry. 2021 Oct 20. doi: 10.1038/s41398-021-01663-6.
2. Iyengar U et al. One Year Into the Pandemic: A Systematic Review of Perinatal Mental Health Outcomes During COVID-19. Front Psychiatry. 2021 Jun 24. doi: 10.3389/fpsyt.2021.674194.
3. World Health Organization. Mental Health and COVID-19: Early Evidence of the Pandemic’s Impact: Scientific Brief. 2022 Mar 2. www.who.int/publications/i/item/WHO-2019-nCoV-Sci_Brief-Mental_health-2022.1.
4. Masters GA et al. Impact of the COVID-19 Pandemic on Mental Health, Access to Care, and Health Disparities in the Perinatal Period. J Psychiatr Res. 2021 May. doi: 10.1016/j.jpsychires.2021.02.056.
5. Shuffrey LC et al. Improving Perinatal Maternal Mental Health Starts With Addressing Structural Inequities. JAMA Psychiatry. 2022 May 1. doi: 10.1001/jamapsychiatry.2022.0097.
6. Lubotzky-Gete S et al. Postpartum Depression and Infant Development Up to 24 months: A Nationwide Population-Based Study. J Affect Disord. 2021 Apr 15. doi: 10.1016/j.jad.2021.02.042.
7. Saharoy R et al. Postpartum Depression and Maternal Care: Exploring the Complex Effects on Mothers and Infants. Cureus. 2023 Jul 4. doi: 10.7759/cureus.41381..
8. Gress-Smith JL et al. Postpartum Depression Prevalence and Impact on Infant Health, Weight, and Sleep in Low-Income and Ethnic Minority Women and Infants. Matern Child Health J. 2012 May. doi: 10.1007/s10995-011-0812-y.
9. Kim S et al. The Impact of Antepartum Depression and Postpartum Depression on Exclusive Breastfeeding: A Systematic Review and Meta-Analysis. Clin Nurs Res. 2022 Jun. doi: 10.1177/10547738211053507.
10. Mirhosseini H et al. Cognitive Behavioral Development in Children Following Maternal Postpartum Depression: A Review Article. Electron Physician. 2015 Dec 20. doi: 10.19082/1673.
11. Grace SL et al. The Effect of Postpartum Depression on Child Cognitive Development and Behavior: A Review and Critical Analysis of the Literature. Arch Womens Ment Health. 2003 Nov. doi: 10.1007/s00737-003-0024-6.
12. Milgrom J et al. The Mediating Role of Maternal Responsiveness in Some Longer Term Effects of Postnatal Depression on Infant Development. Infant Behavior and Development. 2004 Sep 11. doi.org/10.1016/j.infbeh.2004.03.003.
13. Heshmati A et al. The Effect of Parental Leave on Parents’ Mental Health: A Systematic Review. Lancet Public Health. 2023 Jan. doi: 10.1016/S2468-2667(22)00311-5.
14. U.S. Bureau of Labor Statistics, What Data Does the BLS Publish on Family Leave? 2023 Sept 21. www.bls.gov/ebs/factsheets/family-leave-benefits-fact-sheet.htm.
15. Horowitz JM et al. Americans Widely Support Paid Family and Medical Leave, But Differ Over Specific Policies. Pew Research Center’s Social & Demographic Trends Project, Pew Research Center. 2017 Mar 23. www.pewresearch.org/social-trends/2017/03/23/americans-widely-support-paid-family-and-medical-leave-but-differ-over-specific-policies/.
Maternal mental health has a profound impact on the health and wellbeing of the child. Since the onset of the pandemic, rates of postpartum depression have increased, affecting an estimated 1 in 5 women.1 Numerous studies show the impact of postpartum depression on the newborn child across multiple domains, from bonding to healthy weight gain to meeting developmental milestones.
While new medications are being studied and approved to specifically target postpartum depression, these treatments are inaccessible to many because of high costs and long wait lists. Beyond medication, structural changes such as paid parental leave have been shown to have a substantial impact on maternal mental health, thus impacting the health of children as well.
Implications for Mothers and Children
Psychiatric diagnoses such as postpartum depression are on the rise.1,2 This is likely attributable to a combination of factors, including increased isolation since the start of the pandemic, worsening health inequities across race and socioeconomic status, and difficulty accessing mental health care.3-5 The effect that postpartum depression has on the family is significant for the newborn as well as other children in the home.
Data suggest that postpartum depression impacts both the physical and mental health of the child. Infants of mothers with postpartum depression may experience challenges with weight gain, decreased breastfeeding, sleep disruptions, and delays in achieving developmental milestones.6-9 They may also show decreased maternal infant bonding, challenges with cognitive development including language and IQ, and increased risk of behavioral disturbances.10,11 These effects are likely attributable to a combination of factors, including decreased maternal responsiveness to infant cues.7,12 Many of these effects are mediated by the chronicity and severity of depressive symptoms, suggesting the importance of screening and treatment of postpartum depression.10,11 However, treatment for postpartum depression can be difficult to access, particularly given the increased level of need.
It is therefore critical to consider what structural interventions and policy changes can decrease the risk of developing postpartum depression. Data consistently show that access to paid parental leave improves maternal mental health outcomes. Among patients with access to parental leave, research shows that paid leave of longer duration, at least 2-3 months, is the most protective.13 Studies have identified decreased depressive symptoms, decreased stress, decreased use of mental health services, and decreased hospital admissions among women with longer parental leave.13 The positive effects of paid parental leave on maternal mental health can extend beyond the postpartum period, solidifying its impact on the long-term health outcomes of both mother and child.13
Advocacy Is Imperative
In 2024, the United States is the only high-income country, and one of only seven countries in the world, that does not guarantee access to paid parental leave. The Family Medical Leave Act is a 31-year-old federal law that requires some employers to provide unpaid leave to eligible employees. It is narrow in scope, and it excludes many low-wage workers and LGBTQ+ families. Thirteen states — California, Colorado, Connecticut, Delaware, Maine, Massachusetts, Maryland, Minnesota, New Jersey, New York, Oregon, Rhode Island, and Washington — as well as the District of Columbia, have enacted their own paid leave policies. However, there are no federal laws requiring access to paid parental leave. As of 2023, fewer than 30% of workers in the United States have access to paid parental leave, and only 16% of employees in the service industry have access to paid parental leave.14 This disproportionately affects families from lower income backgrounds, and further exacerbates socioeconomic, racial, and gender inequities. From a health systems lens, this increases risk of adverse maternal mental health outcomes among those who already have decreased access to mental health services, worsening health disparities.
Paid parental leave has strong public support across party lines, with polls showing the majority of Americans support comprehensive paid family and medical leave.15 Despite this, the United States has failed to enact legislation on this issue since 1993. Multiple attempts at expanding leave have not come to fruition. In the past year, both the house and the senate have announced bipartisan efforts to expand access to paid parental leave. However, legislative frameworks are still in early stages.
As physicians, it is crucial that we advocate for expanded access to paid parental leave. We must use our expertise to speak to the impact that paid parental leave can have on the mental and physical health of parents, children, and families. By advocating for paid parental leave, we can help create a more just and equitable healthcare system.
Dr. Shannon is a second-year psychiatry resident at University of California, Los Angeles. She attended Stanford University for her undergraduate degree and Dartmouth Geisel School of Medicine for medical school. Her interests include perinatal psychiatry, health systems research, and mental health policy advocacy. Dr. Richards is assistant clinical professor in the department of psychiatry and biobehavioral sciences; program director of the child and adolescent psychiatry fellowship; and associate medical director of the perinatal program at the UCLA Semel Institute for Neuroscience and Human Behavior, Los Angeles.
References
1. Wang Z et al. Mapping Global Prevalence of Depression Among Postpartum Women. Transl Psychiatry. 2021 Oct 20. doi: 10.1038/s41398-021-01663-6.
2. Iyengar U et al. One Year Into the Pandemic: A Systematic Review of Perinatal Mental Health Outcomes During COVID-19. Front Psychiatry. 2021 Jun 24. doi: 10.3389/fpsyt.2021.674194.
3. World Health Organization. Mental Health and COVID-19: Early Evidence of the Pandemic’s Impact: Scientific Brief. 2022 Mar 2. www.who.int/publications/i/item/WHO-2019-nCoV-Sci_Brief-Mental_health-2022.1.
4. Masters GA et al. Impact of the COVID-19 Pandemic on Mental Health, Access to Care, and Health Disparities in the Perinatal Period. J Psychiatr Res. 2021 May. doi: 10.1016/j.jpsychires.2021.02.056.
5. Shuffrey LC et al. Improving Perinatal Maternal Mental Health Starts With Addressing Structural Inequities. JAMA Psychiatry. 2022 May 1. doi: 10.1001/jamapsychiatry.2022.0097.
6. Lubotzky-Gete S et al. Postpartum Depression and Infant Development Up to 24 months: A Nationwide Population-Based Study. J Affect Disord. 2021 Apr 15. doi: 10.1016/j.jad.2021.02.042.
7. Saharoy R et al. Postpartum Depression and Maternal Care: Exploring the Complex Effects on Mothers and Infants. Cureus. 2023 Jul 4. doi: 10.7759/cureus.41381..
8. Gress-Smith JL et al. Postpartum Depression Prevalence and Impact on Infant Health, Weight, and Sleep in Low-Income and Ethnic Minority Women and Infants. Matern Child Health J. 2012 May. doi: 10.1007/s10995-011-0812-y.
9. Kim S et al. The Impact of Antepartum Depression and Postpartum Depression on Exclusive Breastfeeding: A Systematic Review and Meta-Analysis. Clin Nurs Res. 2022 Jun. doi: 10.1177/10547738211053507.
10. Mirhosseini H et al. Cognitive Behavioral Development in Children Following Maternal Postpartum Depression: A Review Article. Electron Physician. 2015 Dec 20. doi: 10.19082/1673.
11. Grace SL et al. The Effect of Postpartum Depression on Child Cognitive Development and Behavior: A Review and Critical Analysis of the Literature. Arch Womens Ment Health. 2003 Nov. doi: 10.1007/s00737-003-0024-6.
12. Milgrom J et al. The Mediating Role of Maternal Responsiveness in Some Longer Term Effects of Postnatal Depression on Infant Development. Infant Behavior and Development. 2004 Sep 11. doi.org/10.1016/j.infbeh.2004.03.003.
13. Heshmati A et al. The Effect of Parental Leave on Parents’ Mental Health: A Systematic Review. Lancet Public Health. 2023 Jan. doi: 10.1016/S2468-2667(22)00311-5.
14. U.S. Bureau of Labor Statistics, What Data Does the BLS Publish on Family Leave? 2023 Sept 21. www.bls.gov/ebs/factsheets/family-leave-benefits-fact-sheet.htm.
15. Horowitz JM et al. Americans Widely Support Paid Family and Medical Leave, But Differ Over Specific Policies. Pew Research Center’s Social & Demographic Trends Project, Pew Research Center. 2017 Mar 23. www.pewresearch.org/social-trends/2017/03/23/americans-widely-support-paid-family-and-medical-leave-but-differ-over-specific-policies/.
Adolescent Risk and Resilience
Bullying, heavy social media use, experimentation with drugs and alcohol: These are the well-described hazards of adolescence. We have growing knowledge of the risks associated with these experiences and which youth are more vulnerable to these risks. Developmentally, adolescence is a time of critical brain development marked by heightened sensitivity to social approval and limited impulse control. Adolescents also have growing autonomy from parents alongside a stronger need for time with friends (the new peer home away from the parental home). These factors alone make adolescence a period of heightened sensitivity to these experiences, but some youth have greater vulnerability to develop psychopathology such as anxiety, depression, eating disorders, or addiction after exposure to these common experiences. Pediatricians can assess these broader vulnerabilities during well child visits of pre- and early teens and offer patients and their parents strategies for minimizing risk and cultivating resilience.
Bullying
Bullying, both verbal and physical, has long been an unwelcome part of youth. Cellphones and social media have brought bullying into the 21st century. Cyberbullying has meant that targeted youth are no longer safe after school and it carries higher risk of self-harm and suicidality than the analog version. No child benefits from bullying, but some children are more vulnerable to develop an anxiety or mood disorder, self-injury, or suicidality, whereas others experience stress and distress, but are able to adaptively seek support from friends and adults and stay on track developmentally, even to flourish. There is evidence that girls and LGBTQ youth are more commonly bullied and at higher risk for depression, self-harm, and suicidality as a consequence of cyberbullying. Youth already suffering from a psychiatric illness or substance abuse who are bullied are at higher risk for self-harm and suicidality than that of their bullied peers. Youth whose parents score high on measures of distress and family dysfunction also face higher risk of self-harm and suicidality after bullying.1
Social Media
Unlike bullying, social media has been a force only in 21st century life, with Facebook starting in 2004 and cellphones in common use by adolescents in the past 2 decades. While there are potential benefits of social media use, such as stronger connections to supportive peers for isolated LGBTQ youth or youth who live in rural areas, there are also risks. Of course, social media carries the risk of cyberbullying. It also carries the risk for very heavy patterns of use that can interfere with physical activity, adequate sleep, academic performance, and healthy in-person social activities. There is robust emerging evidence that heavy users have higher rates of mood disorders and anxiety symptoms, although it is unclear whether social media exacerbates, or more social media use is the result of depression and/or anxiety. Adolescents’ desire for social acceptance makes them especially sensitive to the social rewards of “likes” and they are thus vulnerable to becoming heavy users. Adolescent girls who are heavy users are vulnerable to developing a disordered body image and eating disorders. Those youth with especially low levels of impulse control, such as those with ADHD, have greater risk of developing problematic use.2-4
Substance Use and Abuse
Exploration of alcohol and drug use has been a common experience, and hazard, of adolescence for many generations. As a result, we have richer knowledge of those factors that are associated with risk of and protection against that use progressing to a use disorder. Earlier age at first experimentation appears to be independently correlated with increased risk of developing a substance use disorder. Every pediatrician should be aware of a family history of substance use disorders, especially alcohol, as they are strongly associated with higher risk. Youth with temperaments that are sensation seeking, externalizing and impulsive are at higher risk. Youth with anxiety and mood disorders and untreated attention deficit disorders are at higher risk. Youth whose parents have high levels of conflict or “permissive” parenting styles are at higher risk as are those who as children experienced abuse or neglect.5-7
Minimizing Risk and Cultivating Resilience
Protective factors balance these risks: adequate sleep; positive relationships with friends and parents; and confidence in their academic, athletic, or social abilities all are correlated with good outcomes after bullying, drug and alcohol use, and social media use. These teenagers are meaningfully connected to caring adults and peers, have a future orientation, and typically have higher self-esteem. Youth whose parents balance attunement with rules and expectations (“authoritative” parenting) appear to be at lower risk of poor mental health outcomes associated with heavy social media use as well as other risk behaviors. These parents have clear rules and expectations, including about drugs and alcohol, and enforce rules reasonably calmly and consistently. Youth whose families eat dinner together at least three times weekly, who attend schools that offer a wide range of after-school activities, and who learn to use problem-focused coping skills rather than emotion-focused coping skills are protected against poor mental health outcomes in the face of these challenges.
While bullying is a stressor, social media and substances may seem like ways of managing stress and connecting with peers. There are youth with clear vulnerabilities to the risks associated with each of them. Shared factors include vulnerable temperaments, high conflict or permissive parenting, family history of substance use disorders or preexisting psychiatric illness. Pediatricians are in a unique position to raise teenagers’ awareness of their specific vulnerabilities. Talk about the heightened risk of experimentation with alcohol or drugs in your patients who are in treatment for an anxiety or mood disorder. Help them cultivate critical thinking — an adolescent specialty — around marketing and peer pressure. Remind them that social media companies make money from keeping them online longer. Then help them identify what strategies are in their control, such as limiting their time online. What else could they be doing with their time that they actually enjoy? Remind them about the value of protecting time for adequate sleep, regular exercise, and sitting down for dinner with their family. Ask about their nourishing relationships with peers and adults and talk about the value of protecting time for them. Ask your patients and their parents about how they face stress, emphasizing their ability to locate what is within their control. While awareness of feelings is important, learning to manage intense emotions is more connected to healthy habits of sleep and exercise and strategies to get support or pivot to engaging activities. Discussing this openly models for parents how to bear difficulty alongside their children without becoming distressed or punitive themselves. Talk with worried parents about the value of regular meals together, shared physical activities, and supporting time for their children’s emerging interests and hobbies. Equipping your patients and their parents with knowledge about their particular vulnerabilities, reminders about what is known about these risks, and all that is in their power to build resilience, may be as meaningful a public health intervention as asking them about biking with helmets and using seat belts.
Dr. Swick is physician in chief at Ohana, Center for Child and Adolescent Behavioral Health, Community Hospital of the Monterey (Calif.) Peninsula. Dr. Jellinek is professor emeritus of psychiatry and pediatrics, Harvard Medical School, Boston. Email them at pdnews@mdedge.com.
References
1. Zych I et al. Protective Factors Against Bullying and Cyberbullying: A Systematic Review of Meta-Analyses. Aggress Violent Behav. 2019;45:4-19. doi: 10.1016/j.avb.2018.06.008.
2. Office of the Surgeon General. Social Media and Youth Mental Health: The U.S. Surgeon General’s Advisory. 2023. https://www.ncbi.nlm.nih.gov/books/NBK594761/.
3. Uhls Y et al. Benefits and Costs of Social Media in Adolescence. Pediatrics. 2017 Nov;140(Suppl 2):S67-S70. doi: 10.1542/peds.2016-1758E.
4. Health Advisory on Social Media Use in Adolescence. American Psychological Association (2023).
5. Sloboda Z et al. Revisiting the Concepts of Risk and Protective Factors for Understanding the Etiology and Development of Substance Use and Substance Use Disorders: Implications for Prevention, Substance Use and Misuse, Subst Use Misuse. 2012 Jun-Jul;47(8-9):944-62. doi: 10.3109/10826084.2012.663280.
6. O’Connell M et al. Preventing Mental, Emotional, and Behavioral Disorders Among Young People: Progress and Possibilities. Washington, DC: The National Academies Press and US Department of Health and Human Services, Substance Abuse and Mental Health Administration. 2009 (https://nap.nationalacademies.org/catalog/12480/preventing-mental-emotional-and-behavioral-disorders-among-young-people-progress).
7. Staiger P et al. Can Emotion-Focused Coping Help Explain the Link Between Posttraumatic Stress Disorder Severity and Triggers for Substance Use in Young Adults? J Subst Abuse Treat. 2009 Mar;36(2):220-6. doi: 10.1016/j.jsat.2008.05.008.
Bullying, heavy social media use, experimentation with drugs and alcohol: These are the well-described hazards of adolescence. We have growing knowledge of the risks associated with these experiences and which youth are more vulnerable to these risks. Developmentally, adolescence is a time of critical brain development marked by heightened sensitivity to social approval and limited impulse control. Adolescents also have growing autonomy from parents alongside a stronger need for time with friends (the new peer home away from the parental home). These factors alone make adolescence a period of heightened sensitivity to these experiences, but some youth have greater vulnerability to develop psychopathology such as anxiety, depression, eating disorders, or addiction after exposure to these common experiences. Pediatricians can assess these broader vulnerabilities during well child visits of pre- and early teens and offer patients and their parents strategies for minimizing risk and cultivating resilience.
Bullying
Bullying, both verbal and physical, has long been an unwelcome part of youth. Cellphones and social media have brought bullying into the 21st century. Cyberbullying has meant that targeted youth are no longer safe after school and it carries higher risk of self-harm and suicidality than the analog version. No child benefits from bullying, but some children are more vulnerable to develop an anxiety or mood disorder, self-injury, or suicidality, whereas others experience stress and distress, but are able to adaptively seek support from friends and adults and stay on track developmentally, even to flourish. There is evidence that girls and LGBTQ youth are more commonly bullied and at higher risk for depression, self-harm, and suicidality as a consequence of cyberbullying. Youth already suffering from a psychiatric illness or substance abuse who are bullied are at higher risk for self-harm and suicidality than that of their bullied peers. Youth whose parents score high on measures of distress and family dysfunction also face higher risk of self-harm and suicidality after bullying.1
Social Media
Unlike bullying, social media has been a force only in 21st century life, with Facebook starting in 2004 and cellphones in common use by adolescents in the past 2 decades. While there are potential benefits of social media use, such as stronger connections to supportive peers for isolated LGBTQ youth or youth who live in rural areas, there are also risks. Of course, social media carries the risk of cyberbullying. It also carries the risk for very heavy patterns of use that can interfere with physical activity, adequate sleep, academic performance, and healthy in-person social activities. There is robust emerging evidence that heavy users have higher rates of mood disorders and anxiety symptoms, although it is unclear whether social media exacerbates, or more social media use is the result of depression and/or anxiety. Adolescents’ desire for social acceptance makes them especially sensitive to the social rewards of “likes” and they are thus vulnerable to becoming heavy users. Adolescent girls who are heavy users are vulnerable to developing a disordered body image and eating disorders. Those youth with especially low levels of impulse control, such as those with ADHD, have greater risk of developing problematic use.2-4
Substance Use and Abuse
Exploration of alcohol and drug use has been a common experience, and hazard, of adolescence for many generations. As a result, we have richer knowledge of those factors that are associated with risk of and protection against that use progressing to a use disorder. Earlier age at first experimentation appears to be independently correlated with increased risk of developing a substance use disorder. Every pediatrician should be aware of a family history of substance use disorders, especially alcohol, as they are strongly associated with higher risk. Youth with temperaments that are sensation seeking, externalizing and impulsive are at higher risk. Youth with anxiety and mood disorders and untreated attention deficit disorders are at higher risk. Youth whose parents have high levels of conflict or “permissive” parenting styles are at higher risk as are those who as children experienced abuse or neglect.5-7
Minimizing Risk and Cultivating Resilience
Protective factors balance these risks: adequate sleep; positive relationships with friends and parents; and confidence in their academic, athletic, or social abilities all are correlated with good outcomes after bullying, drug and alcohol use, and social media use. These teenagers are meaningfully connected to caring adults and peers, have a future orientation, and typically have higher self-esteem. Youth whose parents balance attunement with rules and expectations (“authoritative” parenting) appear to be at lower risk of poor mental health outcomes associated with heavy social media use as well as other risk behaviors. These parents have clear rules and expectations, including about drugs and alcohol, and enforce rules reasonably calmly and consistently. Youth whose families eat dinner together at least three times weekly, who attend schools that offer a wide range of after-school activities, and who learn to use problem-focused coping skills rather than emotion-focused coping skills are protected against poor mental health outcomes in the face of these challenges.
While bullying is a stressor, social media and substances may seem like ways of managing stress and connecting with peers. There are youth with clear vulnerabilities to the risks associated with each of them. Shared factors include vulnerable temperaments, high conflict or permissive parenting, family history of substance use disorders or preexisting psychiatric illness. Pediatricians are in a unique position to raise teenagers’ awareness of their specific vulnerabilities. Talk about the heightened risk of experimentation with alcohol or drugs in your patients who are in treatment for an anxiety or mood disorder. Help them cultivate critical thinking — an adolescent specialty — around marketing and peer pressure. Remind them that social media companies make money from keeping them online longer. Then help them identify what strategies are in their control, such as limiting their time online. What else could they be doing with their time that they actually enjoy? Remind them about the value of protecting time for adequate sleep, regular exercise, and sitting down for dinner with their family. Ask about their nourishing relationships with peers and adults and talk about the value of protecting time for them. Ask your patients and their parents about how they face stress, emphasizing their ability to locate what is within their control. While awareness of feelings is important, learning to manage intense emotions is more connected to healthy habits of sleep and exercise and strategies to get support or pivot to engaging activities. Discussing this openly models for parents how to bear difficulty alongside their children without becoming distressed or punitive themselves. Talk with worried parents about the value of regular meals together, shared physical activities, and supporting time for their children’s emerging interests and hobbies. Equipping your patients and their parents with knowledge about their particular vulnerabilities, reminders about what is known about these risks, and all that is in their power to build resilience, may be as meaningful a public health intervention as asking them about biking with helmets and using seat belts.
Dr. Swick is physician in chief at Ohana, Center for Child and Adolescent Behavioral Health, Community Hospital of the Monterey (Calif.) Peninsula. Dr. Jellinek is professor emeritus of psychiatry and pediatrics, Harvard Medical School, Boston. Email them at pdnews@mdedge.com.
References
1. Zych I et al. Protective Factors Against Bullying and Cyberbullying: A Systematic Review of Meta-Analyses. Aggress Violent Behav. 2019;45:4-19. doi: 10.1016/j.avb.2018.06.008.
2. Office of the Surgeon General. Social Media and Youth Mental Health: The U.S. Surgeon General’s Advisory. 2023. https://www.ncbi.nlm.nih.gov/books/NBK594761/.
3. Uhls Y et al. Benefits and Costs of Social Media in Adolescence. Pediatrics. 2017 Nov;140(Suppl 2):S67-S70. doi: 10.1542/peds.2016-1758E.
4. Health Advisory on Social Media Use in Adolescence. American Psychological Association (2023).
5. Sloboda Z et al. Revisiting the Concepts of Risk and Protective Factors for Understanding the Etiology and Development of Substance Use and Substance Use Disorders: Implications for Prevention, Substance Use and Misuse, Subst Use Misuse. 2012 Jun-Jul;47(8-9):944-62. doi: 10.3109/10826084.2012.663280.
6. O’Connell M et al. Preventing Mental, Emotional, and Behavioral Disorders Among Young People: Progress and Possibilities. Washington, DC: The National Academies Press and US Department of Health and Human Services, Substance Abuse and Mental Health Administration. 2009 (https://nap.nationalacademies.org/catalog/12480/preventing-mental-emotional-and-behavioral-disorders-among-young-people-progress).
7. Staiger P et al. Can Emotion-Focused Coping Help Explain the Link Between Posttraumatic Stress Disorder Severity and Triggers for Substance Use in Young Adults? J Subst Abuse Treat. 2009 Mar;36(2):220-6. doi: 10.1016/j.jsat.2008.05.008.
Bullying, heavy social media use, experimentation with drugs and alcohol: These are the well-described hazards of adolescence. We have growing knowledge of the risks associated with these experiences and which youth are more vulnerable to these risks. Developmentally, adolescence is a time of critical brain development marked by heightened sensitivity to social approval and limited impulse control. Adolescents also have growing autonomy from parents alongside a stronger need for time with friends (the new peer home away from the parental home). These factors alone make adolescence a period of heightened sensitivity to these experiences, but some youth have greater vulnerability to develop psychopathology such as anxiety, depression, eating disorders, or addiction after exposure to these common experiences. Pediatricians can assess these broader vulnerabilities during well child visits of pre- and early teens and offer patients and their parents strategies for minimizing risk and cultivating resilience.
Bullying
Bullying, both verbal and physical, has long been an unwelcome part of youth. Cellphones and social media have brought bullying into the 21st century. Cyberbullying has meant that targeted youth are no longer safe after school and it carries higher risk of self-harm and suicidality than the analog version. No child benefits from bullying, but some children are more vulnerable to develop an anxiety or mood disorder, self-injury, or suicidality, whereas others experience stress and distress, but are able to adaptively seek support from friends and adults and stay on track developmentally, even to flourish. There is evidence that girls and LGBTQ youth are more commonly bullied and at higher risk for depression, self-harm, and suicidality as a consequence of cyberbullying. Youth already suffering from a psychiatric illness or substance abuse who are bullied are at higher risk for self-harm and suicidality than that of their bullied peers. Youth whose parents score high on measures of distress and family dysfunction also face higher risk of self-harm and suicidality after bullying.1
Social Media
Unlike bullying, social media has been a force only in 21st century life, with Facebook starting in 2004 and cellphones in common use by adolescents in the past 2 decades. While there are potential benefits of social media use, such as stronger connections to supportive peers for isolated LGBTQ youth or youth who live in rural areas, there are also risks. Of course, social media carries the risk of cyberbullying. It also carries the risk for very heavy patterns of use that can interfere with physical activity, adequate sleep, academic performance, and healthy in-person social activities. There is robust emerging evidence that heavy users have higher rates of mood disorders and anxiety symptoms, although it is unclear whether social media exacerbates, or more social media use is the result of depression and/or anxiety. Adolescents’ desire for social acceptance makes them especially sensitive to the social rewards of “likes” and they are thus vulnerable to becoming heavy users. Adolescent girls who are heavy users are vulnerable to developing a disordered body image and eating disorders. Those youth with especially low levels of impulse control, such as those with ADHD, have greater risk of developing problematic use.2-4
Substance Use and Abuse
Exploration of alcohol and drug use has been a common experience, and hazard, of adolescence for many generations. As a result, we have richer knowledge of those factors that are associated with risk of and protection against that use progressing to a use disorder. Earlier age at first experimentation appears to be independently correlated with increased risk of developing a substance use disorder. Every pediatrician should be aware of a family history of substance use disorders, especially alcohol, as they are strongly associated with higher risk. Youth with temperaments that are sensation seeking, externalizing and impulsive are at higher risk. Youth with anxiety and mood disorders and untreated attention deficit disorders are at higher risk. Youth whose parents have high levels of conflict or “permissive” parenting styles are at higher risk as are those who as children experienced abuse or neglect.5-7
Minimizing Risk and Cultivating Resilience
Protective factors balance these risks: adequate sleep; positive relationships with friends and parents; and confidence in their academic, athletic, or social abilities all are correlated with good outcomes after bullying, drug and alcohol use, and social media use. These teenagers are meaningfully connected to caring adults and peers, have a future orientation, and typically have higher self-esteem. Youth whose parents balance attunement with rules and expectations (“authoritative” parenting) appear to be at lower risk of poor mental health outcomes associated with heavy social media use as well as other risk behaviors. These parents have clear rules and expectations, including about drugs and alcohol, and enforce rules reasonably calmly and consistently. Youth whose families eat dinner together at least three times weekly, who attend schools that offer a wide range of after-school activities, and who learn to use problem-focused coping skills rather than emotion-focused coping skills are protected against poor mental health outcomes in the face of these challenges.
While bullying is a stressor, social media and substances may seem like ways of managing stress and connecting with peers. There are youth with clear vulnerabilities to the risks associated with each of them. Shared factors include vulnerable temperaments, high conflict or permissive parenting, family history of substance use disorders or preexisting psychiatric illness. Pediatricians are in a unique position to raise teenagers’ awareness of their specific vulnerabilities. Talk about the heightened risk of experimentation with alcohol or drugs in your patients who are in treatment for an anxiety or mood disorder. Help them cultivate critical thinking — an adolescent specialty — around marketing and peer pressure. Remind them that social media companies make money from keeping them online longer. Then help them identify what strategies are in their control, such as limiting their time online. What else could they be doing with their time that they actually enjoy? Remind them about the value of protecting time for adequate sleep, regular exercise, and sitting down for dinner with their family. Ask about their nourishing relationships with peers and adults and talk about the value of protecting time for them. Ask your patients and their parents about how they face stress, emphasizing their ability to locate what is within their control. While awareness of feelings is important, learning to manage intense emotions is more connected to healthy habits of sleep and exercise and strategies to get support or pivot to engaging activities. Discussing this openly models for parents how to bear difficulty alongside their children without becoming distressed or punitive themselves. Talk with worried parents about the value of regular meals together, shared physical activities, and supporting time for their children’s emerging interests and hobbies. Equipping your patients and their parents with knowledge about their particular vulnerabilities, reminders about what is known about these risks, and all that is in their power to build resilience, may be as meaningful a public health intervention as asking them about biking with helmets and using seat belts.
Dr. Swick is physician in chief at Ohana, Center for Child and Adolescent Behavioral Health, Community Hospital of the Monterey (Calif.) Peninsula. Dr. Jellinek is professor emeritus of psychiatry and pediatrics, Harvard Medical School, Boston. Email them at pdnews@mdedge.com.
References
1. Zych I et al. Protective Factors Against Bullying and Cyberbullying: A Systematic Review of Meta-Analyses. Aggress Violent Behav. 2019;45:4-19. doi: 10.1016/j.avb.2018.06.008.
2. Office of the Surgeon General. Social Media and Youth Mental Health: The U.S. Surgeon General’s Advisory. 2023. https://www.ncbi.nlm.nih.gov/books/NBK594761/.
3. Uhls Y et al. Benefits and Costs of Social Media in Adolescence. Pediatrics. 2017 Nov;140(Suppl 2):S67-S70. doi: 10.1542/peds.2016-1758E.
4. Health Advisory on Social Media Use in Adolescence. American Psychological Association (2023).
5. Sloboda Z et al. Revisiting the Concepts of Risk and Protective Factors for Understanding the Etiology and Development of Substance Use and Substance Use Disorders: Implications for Prevention, Substance Use and Misuse, Subst Use Misuse. 2012 Jun-Jul;47(8-9):944-62. doi: 10.3109/10826084.2012.663280.
6. O’Connell M et al. Preventing Mental, Emotional, and Behavioral Disorders Among Young People: Progress and Possibilities. Washington, DC: The National Academies Press and US Department of Health and Human Services, Substance Abuse and Mental Health Administration. 2009 (https://nap.nationalacademies.org/catalog/12480/preventing-mental-emotional-and-behavioral-disorders-among-young-people-progress).
7. Staiger P et al. Can Emotion-Focused Coping Help Explain the Link Between Posttraumatic Stress Disorder Severity and Triggers for Substance Use in Young Adults? J Subst Abuse Treat. 2009 Mar;36(2):220-6. doi: 10.1016/j.jsat.2008.05.008.
RA Outcomes Worsened by Depression and Anxiety, Signaling Need for Multidisciplinary Action
Patients diagnosed with rheumatoid arthritis (RA) and co-occurring anxiety or depression are less likely to achieve low disease activity (LDA) and better symptom control after 3 months of treatment, according to new research presented at the at the annual meeting of the Canadian Rheumatology Association.
The findings emphasized the importance of taking a multidisciplinary approach to RA treatment, said presenter Susan Bartlett, PhD, a professor in the Divisions of Clinical Epidemiology, Rheumatology, and Respiratory Epidemiology at McGill University in Montreal, Quebec, Canada.
“In the absence of directly addressing anxiety and depression, people are not going to improve to the same extent we hope that they will,” she told this news organization.
Symptom Clusters in RA
In her research, presented on February 29, Dr. Bartlett explored how certain symptom clusters in RA predicted prognosis.
Symptom clusters are related symptoms that occur together and can be associated with worse outcomes than one symptom alone. Symptom science has been a growing interest in precision medicine, particularly for cancer, Dr. Bartlett noted, and this same approach could help pinpoint RA subtypes, disease trajectories, and personalized treatment.
In the study, Dr. Bartlett and colleagues used data from the Canadian Early Arthritis Cohort (CATCH), a multisite prospective research study following individuals with new-onset RA. They identified patients starting methotrexate (MTX) therapy who also had clinical and patient-reported outcome measures available. Individuals included in the analysis may have also been taking additional disease-modifying antirheumatic drugs beyond MTX.
Across the 310 selected individuals, researchers identified four key symptoms: Pain, fatigue, anxiety, and depression. Pain and fatigue were defined as physical symptoms, while anxiety and depression were classified as emotional symptoms. Results showed that the patients could be sorted into four distinct symptom clusters: Minimal symptoms (12%), mild physical and emotional symptoms (11%), moderate to severe pain and fatigue (40%), and moderate to severe physical and emotional symptoms (37%).
Researchers then followed patients during the first 6 months of treatment to evaluate if patients’ symptoms improved.
Symptom improvement mostly occurred during the first 3 months of treatment and remained consistent at 6 months. Overall, patients with moderate to severe emotional symptoms had a worse prognosis and were less likely to achieve milder symptoms than those who had only pain and fatigue or mild emotional symptoms. While 64% of patients in the moderate to severe physical symptoms group achieved minimal symptoms after 3 months of treatment, only 13% of patients with moderate to severe physical and emotional systems reported minimal symptoms during this same time frame.
The study builds on previous work that “suggests that there are different factors that we can identify around the time of diagnosis that point to how well a person is likely to respond,” Dr. Bartlett added. “What our work is showing pretty clearly [is that] the presence of anxiety and depression is one of those important markers.”
Patients With Depression Report Worse Disease Activity
In a related study, researchers from the University of Ottawa explored how depression in RA affected subjective and objective disease measures.
The study included patients from the Ottawa Rheumatology Comprehensive Treatment and Assessment (ORCHESTRA) clinic at The Ottawa Hospital, Ottawa, Ontario, Canada, which sees patients with inflammatory arthritis who are starting biologic therapy or switching to another biologic. The clinic is designed to take a more comprehensive approach to managing inflammatory arthritis, including addressing comorbidities such as cardiac disease, depression, and cancer. Patients seen at the clinic can opt to be included in the ORCHESTRA cohort to be a part of ongoing research.
From this cohort, researchers identified 98 patients with RA. At enrollment, patients were screened for depression using patient health questionnaire scores and asked about duration of morning stiffness and tender joint counts. Swollen joint counts, ultrasound, and clinical scores were used to evaluate disease activity.
In the study group, 47 patients had no depression, 21 patients had mild depression, and 30 patients had moderate to severe depression. Researchers found that subjective disease measures, including visual analog pain scale, health assessment questionnaire, and disease activity score in 28 joints were all higher in patients with depression; however, depression did not appear to affect objective disease measures, such as the Global OMERACT-EULAR Synovitis Score or Doppler scores.
While there is a known link between inflammation and depression, these findings suggest that depression is “a concomitant comorbidity just like cardiovascular disease, just like fibromyalgia, just like some other comorbidity that also needs to be addressed in its own right to improve the outcomes,” noted Elliot Hepworth, MD, a rheumatologist and ORCHESTRA clinic lead at The Ottawa Hospital, in an interview.
Dr. Hepworth presented the findings on March 1.
The data also suggested that patients with depression had poorer outcomes. For the 79 patients who had 3-month follow-up visit data, 43.9% of patients with no or mild depression achieved LDA and remission compared with 21.7% of patients with moderate to severe depression, though this difference was not statistically significant (P = .064). There was a similar trend for the 39 patients with 6-month follow-up data: Only 20% of patients with moderate to severe depression had reached LDA and remission compared with 37.9% of patients with no or mild depression (P = .445). The researchers noted this could be an issue with a smaller sample size.
“Every time more patients get added we approach closer to significance,” Dr. Hepworth added.
Some Disagreement, Same Takeaway
Commenting on the Ottawa study, Dr. Bartlett was skeptical of the conclusion that depression may not directly influence disease activity. “There’s just too much good evidence these days that [depression] very much coexists with worse disease activity,” she said. “It is not in the person’s head.”
Dr. Hepworth added that patient-reported outcomes are important for clinicians to address during treatment.
“There’s the tender joints, there’s the pain, there’s the fatigue, there’s the patient global assessment, which are subjective,” he said, “but that does not mean that they are not important. Those are important to the patient: That is how they’re living their life, and that is how they’re experiencing their disease.”
This is why efforts to treat depression in patients with RA such as cognitive behavioral therapy are so important, he said, to which Dr. Bartlett agreed.
“A comprehensive approach is required, which includes addressing depression,” she said. Otherwise, data show “that people just never make it to remission.”
The studies looked at different patient populations but ultimately complement each other, added Sibel Aydin, MD, a professor of medicine in the Division of Rheumatology at the University of Ottawa, Ottawa, Ontario, Canada, and senior author of the Ottawa study.
“Two different cohorts with different patient populations still reached the same result,” she said. “If you don’t address the emotional aspect, you are not going to achieve the good outcomes.”
“It’s remarkable when you have two independent researchers coming to the same conclusion without ever talking to each other,” added Dr. Hepworth. “That really shows that this is something that’s pervasive, and it’s not just within our patient population.”
CATCH is funded by unrestricted research grants from programs with Pfizer, AbbVie, Roche, Sandoz, Fresenius Kabi, Organon, Viatris, JAMP, and Celltrion. Dr. Bartlett is president of the PROMIS Health Organization. She is a member of speakers bureaus or has consulted for Pfizer, Sandoz, Merck, Janssen, and Organon. Dr. Hepworth and Dr. Aydin declared no conflicts of interest.
A version of this article appeared on Medscape.com .
Patients diagnosed with rheumatoid arthritis (RA) and co-occurring anxiety or depression are less likely to achieve low disease activity (LDA) and better symptom control after 3 months of treatment, according to new research presented at the at the annual meeting of the Canadian Rheumatology Association.
The findings emphasized the importance of taking a multidisciplinary approach to RA treatment, said presenter Susan Bartlett, PhD, a professor in the Divisions of Clinical Epidemiology, Rheumatology, and Respiratory Epidemiology at McGill University in Montreal, Quebec, Canada.
“In the absence of directly addressing anxiety and depression, people are not going to improve to the same extent we hope that they will,” she told this news organization.
Symptom Clusters in RA
In her research, presented on February 29, Dr. Bartlett explored how certain symptom clusters in RA predicted prognosis.
Symptom clusters are related symptoms that occur together and can be associated with worse outcomes than one symptom alone. Symptom science has been a growing interest in precision medicine, particularly for cancer, Dr. Bartlett noted, and this same approach could help pinpoint RA subtypes, disease trajectories, and personalized treatment.
In the study, Dr. Bartlett and colleagues used data from the Canadian Early Arthritis Cohort (CATCH), a multisite prospective research study following individuals with new-onset RA. They identified patients starting methotrexate (MTX) therapy who also had clinical and patient-reported outcome measures available. Individuals included in the analysis may have also been taking additional disease-modifying antirheumatic drugs beyond MTX.
Across the 310 selected individuals, researchers identified four key symptoms: Pain, fatigue, anxiety, and depression. Pain and fatigue were defined as physical symptoms, while anxiety and depression were classified as emotional symptoms. Results showed that the patients could be sorted into four distinct symptom clusters: Minimal symptoms (12%), mild physical and emotional symptoms (11%), moderate to severe pain and fatigue (40%), and moderate to severe physical and emotional symptoms (37%).
Researchers then followed patients during the first 6 months of treatment to evaluate if patients’ symptoms improved.
Symptom improvement mostly occurred during the first 3 months of treatment and remained consistent at 6 months. Overall, patients with moderate to severe emotional symptoms had a worse prognosis and were less likely to achieve milder symptoms than those who had only pain and fatigue or mild emotional symptoms. While 64% of patients in the moderate to severe physical symptoms group achieved minimal symptoms after 3 months of treatment, only 13% of patients with moderate to severe physical and emotional systems reported minimal symptoms during this same time frame.
The study builds on previous work that “suggests that there are different factors that we can identify around the time of diagnosis that point to how well a person is likely to respond,” Dr. Bartlett added. “What our work is showing pretty clearly [is that] the presence of anxiety and depression is one of those important markers.”
Patients With Depression Report Worse Disease Activity
In a related study, researchers from the University of Ottawa explored how depression in RA affected subjective and objective disease measures.
The study included patients from the Ottawa Rheumatology Comprehensive Treatment and Assessment (ORCHESTRA) clinic at The Ottawa Hospital, Ottawa, Ontario, Canada, which sees patients with inflammatory arthritis who are starting biologic therapy or switching to another biologic. The clinic is designed to take a more comprehensive approach to managing inflammatory arthritis, including addressing comorbidities such as cardiac disease, depression, and cancer. Patients seen at the clinic can opt to be included in the ORCHESTRA cohort to be a part of ongoing research.
From this cohort, researchers identified 98 patients with RA. At enrollment, patients were screened for depression using patient health questionnaire scores and asked about duration of morning stiffness and tender joint counts. Swollen joint counts, ultrasound, and clinical scores were used to evaluate disease activity.
In the study group, 47 patients had no depression, 21 patients had mild depression, and 30 patients had moderate to severe depression. Researchers found that subjective disease measures, including visual analog pain scale, health assessment questionnaire, and disease activity score in 28 joints were all higher in patients with depression; however, depression did not appear to affect objective disease measures, such as the Global OMERACT-EULAR Synovitis Score or Doppler scores.
While there is a known link between inflammation and depression, these findings suggest that depression is “a concomitant comorbidity just like cardiovascular disease, just like fibromyalgia, just like some other comorbidity that also needs to be addressed in its own right to improve the outcomes,” noted Elliot Hepworth, MD, a rheumatologist and ORCHESTRA clinic lead at The Ottawa Hospital, in an interview.
Dr. Hepworth presented the findings on March 1.
The data also suggested that patients with depression had poorer outcomes. For the 79 patients who had 3-month follow-up visit data, 43.9% of patients with no or mild depression achieved LDA and remission compared with 21.7% of patients with moderate to severe depression, though this difference was not statistically significant (P = .064). There was a similar trend for the 39 patients with 6-month follow-up data: Only 20% of patients with moderate to severe depression had reached LDA and remission compared with 37.9% of patients with no or mild depression (P = .445). The researchers noted this could be an issue with a smaller sample size.
“Every time more patients get added we approach closer to significance,” Dr. Hepworth added.
Some Disagreement, Same Takeaway
Commenting on the Ottawa study, Dr. Bartlett was skeptical of the conclusion that depression may not directly influence disease activity. “There’s just too much good evidence these days that [depression] very much coexists with worse disease activity,” she said. “It is not in the person’s head.”
Dr. Hepworth added that patient-reported outcomes are important for clinicians to address during treatment.
“There’s the tender joints, there’s the pain, there’s the fatigue, there’s the patient global assessment, which are subjective,” he said, “but that does not mean that they are not important. Those are important to the patient: That is how they’re living their life, and that is how they’re experiencing their disease.”
This is why efforts to treat depression in patients with RA such as cognitive behavioral therapy are so important, he said, to which Dr. Bartlett agreed.
“A comprehensive approach is required, which includes addressing depression,” she said. Otherwise, data show “that people just never make it to remission.”
The studies looked at different patient populations but ultimately complement each other, added Sibel Aydin, MD, a professor of medicine in the Division of Rheumatology at the University of Ottawa, Ottawa, Ontario, Canada, and senior author of the Ottawa study.
“Two different cohorts with different patient populations still reached the same result,” she said. “If you don’t address the emotional aspect, you are not going to achieve the good outcomes.”
“It’s remarkable when you have two independent researchers coming to the same conclusion without ever talking to each other,” added Dr. Hepworth. “That really shows that this is something that’s pervasive, and it’s not just within our patient population.”
CATCH is funded by unrestricted research grants from programs with Pfizer, AbbVie, Roche, Sandoz, Fresenius Kabi, Organon, Viatris, JAMP, and Celltrion. Dr. Bartlett is president of the PROMIS Health Organization. She is a member of speakers bureaus or has consulted for Pfizer, Sandoz, Merck, Janssen, and Organon. Dr. Hepworth and Dr. Aydin declared no conflicts of interest.
A version of this article appeared on Medscape.com .
Patients diagnosed with rheumatoid arthritis (RA) and co-occurring anxiety or depression are less likely to achieve low disease activity (LDA) and better symptom control after 3 months of treatment, according to new research presented at the at the annual meeting of the Canadian Rheumatology Association.
The findings emphasized the importance of taking a multidisciplinary approach to RA treatment, said presenter Susan Bartlett, PhD, a professor in the Divisions of Clinical Epidemiology, Rheumatology, and Respiratory Epidemiology at McGill University in Montreal, Quebec, Canada.
“In the absence of directly addressing anxiety and depression, people are not going to improve to the same extent we hope that they will,” she told this news organization.
Symptom Clusters in RA
In her research, presented on February 29, Dr. Bartlett explored how certain symptom clusters in RA predicted prognosis.
Symptom clusters are related symptoms that occur together and can be associated with worse outcomes than one symptom alone. Symptom science has been a growing interest in precision medicine, particularly for cancer, Dr. Bartlett noted, and this same approach could help pinpoint RA subtypes, disease trajectories, and personalized treatment.
In the study, Dr. Bartlett and colleagues used data from the Canadian Early Arthritis Cohort (CATCH), a multisite prospective research study following individuals with new-onset RA. They identified patients starting methotrexate (MTX) therapy who also had clinical and patient-reported outcome measures available. Individuals included in the analysis may have also been taking additional disease-modifying antirheumatic drugs beyond MTX.
Across the 310 selected individuals, researchers identified four key symptoms: Pain, fatigue, anxiety, and depression. Pain and fatigue were defined as physical symptoms, while anxiety and depression were classified as emotional symptoms. Results showed that the patients could be sorted into four distinct symptom clusters: Minimal symptoms (12%), mild physical and emotional symptoms (11%), moderate to severe pain and fatigue (40%), and moderate to severe physical and emotional symptoms (37%).
Researchers then followed patients during the first 6 months of treatment to evaluate if patients’ symptoms improved.
Symptom improvement mostly occurred during the first 3 months of treatment and remained consistent at 6 months. Overall, patients with moderate to severe emotional symptoms had a worse prognosis and were less likely to achieve milder symptoms than those who had only pain and fatigue or mild emotional symptoms. While 64% of patients in the moderate to severe physical symptoms group achieved minimal symptoms after 3 months of treatment, only 13% of patients with moderate to severe physical and emotional systems reported minimal symptoms during this same time frame.
The study builds on previous work that “suggests that there are different factors that we can identify around the time of diagnosis that point to how well a person is likely to respond,” Dr. Bartlett added. “What our work is showing pretty clearly [is that] the presence of anxiety and depression is one of those important markers.”
Patients With Depression Report Worse Disease Activity
In a related study, researchers from the University of Ottawa explored how depression in RA affected subjective and objective disease measures.
The study included patients from the Ottawa Rheumatology Comprehensive Treatment and Assessment (ORCHESTRA) clinic at The Ottawa Hospital, Ottawa, Ontario, Canada, which sees patients with inflammatory arthritis who are starting biologic therapy or switching to another biologic. The clinic is designed to take a more comprehensive approach to managing inflammatory arthritis, including addressing comorbidities such as cardiac disease, depression, and cancer. Patients seen at the clinic can opt to be included in the ORCHESTRA cohort to be a part of ongoing research.
From this cohort, researchers identified 98 patients with RA. At enrollment, patients were screened for depression using patient health questionnaire scores and asked about duration of morning stiffness and tender joint counts. Swollen joint counts, ultrasound, and clinical scores were used to evaluate disease activity.
In the study group, 47 patients had no depression, 21 patients had mild depression, and 30 patients had moderate to severe depression. Researchers found that subjective disease measures, including visual analog pain scale, health assessment questionnaire, and disease activity score in 28 joints were all higher in patients with depression; however, depression did not appear to affect objective disease measures, such as the Global OMERACT-EULAR Synovitis Score or Doppler scores.
While there is a known link between inflammation and depression, these findings suggest that depression is “a concomitant comorbidity just like cardiovascular disease, just like fibromyalgia, just like some other comorbidity that also needs to be addressed in its own right to improve the outcomes,” noted Elliot Hepworth, MD, a rheumatologist and ORCHESTRA clinic lead at The Ottawa Hospital, in an interview.
Dr. Hepworth presented the findings on March 1.
The data also suggested that patients with depression had poorer outcomes. For the 79 patients who had 3-month follow-up visit data, 43.9% of patients with no or mild depression achieved LDA and remission compared with 21.7% of patients with moderate to severe depression, though this difference was not statistically significant (P = .064). There was a similar trend for the 39 patients with 6-month follow-up data: Only 20% of patients with moderate to severe depression had reached LDA and remission compared with 37.9% of patients with no or mild depression (P = .445). The researchers noted this could be an issue with a smaller sample size.
“Every time more patients get added we approach closer to significance,” Dr. Hepworth added.
Some Disagreement, Same Takeaway
Commenting on the Ottawa study, Dr. Bartlett was skeptical of the conclusion that depression may not directly influence disease activity. “There’s just too much good evidence these days that [depression] very much coexists with worse disease activity,” she said. “It is not in the person’s head.”
Dr. Hepworth added that patient-reported outcomes are important for clinicians to address during treatment.
“There’s the tender joints, there’s the pain, there’s the fatigue, there’s the patient global assessment, which are subjective,” he said, “but that does not mean that they are not important. Those are important to the patient: That is how they’re living their life, and that is how they’re experiencing their disease.”
This is why efforts to treat depression in patients with RA such as cognitive behavioral therapy are so important, he said, to which Dr. Bartlett agreed.
“A comprehensive approach is required, which includes addressing depression,” she said. Otherwise, data show “that people just never make it to remission.”
The studies looked at different patient populations but ultimately complement each other, added Sibel Aydin, MD, a professor of medicine in the Division of Rheumatology at the University of Ottawa, Ottawa, Ontario, Canada, and senior author of the Ottawa study.
“Two different cohorts with different patient populations still reached the same result,” she said. “If you don’t address the emotional aspect, you are not going to achieve the good outcomes.”
“It’s remarkable when you have two independent researchers coming to the same conclusion without ever talking to each other,” added Dr. Hepworth. “That really shows that this is something that’s pervasive, and it’s not just within our patient population.”
CATCH is funded by unrestricted research grants from programs with Pfizer, AbbVie, Roche, Sandoz, Fresenius Kabi, Organon, Viatris, JAMP, and Celltrion. Dr. Bartlett is president of the PROMIS Health Organization. She is a member of speakers bureaus or has consulted for Pfizer, Sandoz, Merck, Janssen, and Organon. Dr. Hepworth and Dr. Aydin declared no conflicts of interest.
A version of this article appeared on Medscape.com .
FROM CRA 2024
No End in Sight for National ADHD Drug Shortage
Nearly 18 months after the US Food and Drug Administration (FDA) first acknowledged a national shortage of Adderall, the most common drug used to treat attention-deficit/hyperactivity disorder (ADHD),
The first shortage of immediate release formulations of amphetamine mixed salts (Adderall, Adderall IR) was reported by the FDA in October 2022. Now, the list includes Focalin, Ritalin, and Vyvanse, among others.
Adding to the ongoing crisis, the FDA announced in early February that Azurity Pharmaceuticals was voluntarily withdrawing one lot of its Zenzedi (dextroamphetamine sulfate) 30 mg tablets because of contamination with the antihistamine, carbinoxamine.
For the roughly 10 million adults and 6 million children in the United States grappling with ADHD, getting a prescription filled with the exact medication ordered by a physician is dictated by geographic location, insurance formularies, and pharmacy supply chains. It’s particularly challenging for those who live in rural or underserved areas with limited access to nearby pharmacies.
“Not a day goes by when I don’t hear from a number of unfortunately struggling patients about this shortage,” said Aditya Pawar, MD, a child and adolescent psychiatrist with the Kennedy Krieger Institute and an assistant professor of psychiatry and behavioral sciences at Johns Hopkins School of Medicine, Baltimore, Maryland.
The ADHD drug shortage is now well into its second year, and clinicians and advocates alike say there is no apparent end in sight.
How Did We Get Here?
Manufacturers and federal agencies blame the shortage on rising demand and each other, while clinicians say that insurers, drug distributors, and middlemen are also playing a role in keeping medications out of patients’ hands.
In August 2023, the Drug Enforcement Administration (DEA), which sets quotas for the production of controlled substances, and the FDA publicly blamed manufacturers for the shortages, claiming they were not using up their allocations.
At the time, the DEA said manufacturers made and sold only 70% of their quota, nearly 1 billion doses short of what they were allowed to produce and ship that year.
The agencies also noted a record-high number of prescriptions for stimulants from 2012 to 2021. Driven in part by telehealth, the demand intensified during the pandemic. One recent study reported a 14% increase in ADHD stimulant prescriptions between 2020 and 2022.
Insurers also play a role in the shortage, David Goodman, MD, an assistant professor of psychiatry and behavioral sciences also at Johns Hopkins University, told this news organization.
Stepped therapy — in which patients must try one, two, or three medications before they are authorized to receive a more expensive or newer drug — contributes to the problem, Dr. Goodman said. Demand for such medications is high and supply low. In addition, some insurers only provide coverage for in-network pharmacies, regardless of the ability of other providers outside such networks to fill prescriptions.
“If the insurance dictates where you get your pills, and that pharmacy doesn’t have the pills or that pharmacy chain in your area doesn’t have those pills, you’re out of luck,” Dr. Goodman said.
Patients as Detectives
To get prescriptions filled, patients must “turn into detectives,” Laurie Kulikosky, CEO of Children and Adults with Attention-Deficit/Hyperactivity Disorder, told this news organization. “It’s a huge stressor.”
Tracking which ADHD medications are available, on back order, or discontinued requires frequent checking of the FDA’s drug shortages website.
Some manufacturers of generic versions of mixed amphetamine salts are only fulfilling orders for existing contracts, while others say new product won’t be available until at least April or as late as September. All blame the delay on the shortage of active ingredients.
Teva, which makes both the brand and generic of Adderall, reported on the FDA’s site that its manufacturing and distribution is at record-high levels, but demand continues to rise.
The branded Concerta is available, but some makers of generic methylphenidate reported supplies won’t be available until July.
Lisdexamfetamine dimesylate in almost all dosages is either unavailable, available in restricted quantities, or on extended back order. However, the branded product Vyvanse is available.
Industry, Government Respond
In a November 2023 statement, the DEA reported that 17 of 18 drug manufacturers the agency contacted planned to use their full DEA quota and increase production for that year. The agency said it had made it easier for manufacturers to request changes in allocations and that periodically updating quotas was a possibility.
This news organization asked the DEA whether any manufacturers had not met their 2023 quotas, but an agency spokesperson said it would not comment.
An FDA spokesperson said it could help manufacturers ask for bigger quotas and to increase production, noting that in 2023, the DEA increased the quota for methylphenidate following an FDA request.
“The FDA is in frequent communication with the manufacturers of ADHD stimulant medications and the DEA, and we will continue to monitor supply,” the spokesperson said.
For 2024, the FDA told the DEA that it predicted a 3.1% increase in use of amphetamine, methylphenidate (including dexmethylphenidate), and lisdexamfetamine. The DEA took that into account when it issued its final quotas for 2024. Whether those amounts will be enough remains to be seen.
With many drugs — not just those for ADHD — in short supply, in February, the US Department of Health and Human Services (HHS) and the Federal Trade Commission opened an inquiry of sorts, seeking comments on how middlemen and others were influencing pricing and supply of generic drugs.
“When you’re prescribed an important medication by your doctor and you learn the drug is out of stock, your heart sinks,” HHS Secretary Xavier Becerra said in a statement. “This devastating reality is the case for too many Americans who need generic drugs for ADHD, cancer, and other conditions.”
On the comments site, which is open until April 15, many of the 4000-plus complaints filed to-date are from individuals with ADHD.
Dr. Pawar said clinicians can’t know what’s going on between the FDA, the DEA, and manufacturers, adding that, “they need to sit together and figure something out.”
Even Members of Congress have had trouble getting answers. In October, Rep. Abigail Spanberger (D-Virginia) and a dozen colleagues wrote to the FDA and DEA seeking information on how the agencies were responding to stimulant shortages. The DEA has still not replied.
Workarounds the Only Option?
In the past, physicians would prescribe the optimal medication for individual patients based on clinical factors. Now, one of the major factors in determining drug choice is the agent that has “the highest likelihood of benefit and the lowest likelihood of administrative demand or burden,” Dr. Goodman said.
With so many medications in short supply, clinicians have figured out workarounds to get prescriptions filled, but they don’t often pan out.
If a patient needs a 60-mg daily dose of a medication and the pharmacy doesn’t have any 60-mg pills, Dr. Goodman said he might write a prescription for a 30-mg pill to be taken twice a day. However, insurers often will cover only 30 pills for a month, which can thwart this strategy.
Dr. Pawar said he sometimes prescribes Journay PM in lieu of Concerta because it is often available. But insurers may deny coverage of Journay PM because it is a newer medication, he said. When prescribing ADHD medications, he also provides his patients with a list of potential substitutes so they can ask the pharmacist if any are in stock.
With no end to the shortage in sight, clinicians must often prescribe multiple medications until their patients are able to find one that’s available. In addition, patients are burdened with making calls and visits to multiple pharmacies until they find one that can fill their prescription.
Meanwhile, the ripple effects to the ADHD drug shortage continue to spread. Extended periods without treatment can lead to declining job performance or job loss, fractured relationships, and even financial distress, Dr. Goodman said.
“If you go without your pills for a month and you’re not performing, your work declines and you lose your job as a result, that’s not on you — that’s on the fact that you can’t get your treatment,” he noted. “The shortage is no longer an inconvenience.”
Dr. Goodman, Dr. Pawar, and Ms. Kulikosky reported no relevant financial relationships.
A version of this article appeared on Medscape.com.
Nearly 18 months after the US Food and Drug Administration (FDA) first acknowledged a national shortage of Adderall, the most common drug used to treat attention-deficit/hyperactivity disorder (ADHD),
The first shortage of immediate release formulations of amphetamine mixed salts (Adderall, Adderall IR) was reported by the FDA in October 2022. Now, the list includes Focalin, Ritalin, and Vyvanse, among others.
Adding to the ongoing crisis, the FDA announced in early February that Azurity Pharmaceuticals was voluntarily withdrawing one lot of its Zenzedi (dextroamphetamine sulfate) 30 mg tablets because of contamination with the antihistamine, carbinoxamine.
For the roughly 10 million adults and 6 million children in the United States grappling with ADHD, getting a prescription filled with the exact medication ordered by a physician is dictated by geographic location, insurance formularies, and pharmacy supply chains. It’s particularly challenging for those who live in rural or underserved areas with limited access to nearby pharmacies.
“Not a day goes by when I don’t hear from a number of unfortunately struggling patients about this shortage,” said Aditya Pawar, MD, a child and adolescent psychiatrist with the Kennedy Krieger Institute and an assistant professor of psychiatry and behavioral sciences at Johns Hopkins School of Medicine, Baltimore, Maryland.
The ADHD drug shortage is now well into its second year, and clinicians and advocates alike say there is no apparent end in sight.
How Did We Get Here?
Manufacturers and federal agencies blame the shortage on rising demand and each other, while clinicians say that insurers, drug distributors, and middlemen are also playing a role in keeping medications out of patients’ hands.
In August 2023, the Drug Enforcement Administration (DEA), which sets quotas for the production of controlled substances, and the FDA publicly blamed manufacturers for the shortages, claiming they were not using up their allocations.
At the time, the DEA said manufacturers made and sold only 70% of their quota, nearly 1 billion doses short of what they were allowed to produce and ship that year.
The agencies also noted a record-high number of prescriptions for stimulants from 2012 to 2021. Driven in part by telehealth, the demand intensified during the pandemic. One recent study reported a 14% increase in ADHD stimulant prescriptions between 2020 and 2022.
Insurers also play a role in the shortage, David Goodman, MD, an assistant professor of psychiatry and behavioral sciences also at Johns Hopkins University, told this news organization.
Stepped therapy — in which patients must try one, two, or three medications before they are authorized to receive a more expensive or newer drug — contributes to the problem, Dr. Goodman said. Demand for such medications is high and supply low. In addition, some insurers only provide coverage for in-network pharmacies, regardless of the ability of other providers outside such networks to fill prescriptions.
“If the insurance dictates where you get your pills, and that pharmacy doesn’t have the pills or that pharmacy chain in your area doesn’t have those pills, you’re out of luck,” Dr. Goodman said.
Patients as Detectives
To get prescriptions filled, patients must “turn into detectives,” Laurie Kulikosky, CEO of Children and Adults with Attention-Deficit/Hyperactivity Disorder, told this news organization. “It’s a huge stressor.”
Tracking which ADHD medications are available, on back order, or discontinued requires frequent checking of the FDA’s drug shortages website.
Some manufacturers of generic versions of mixed amphetamine salts are only fulfilling orders for existing contracts, while others say new product won’t be available until at least April or as late as September. All blame the delay on the shortage of active ingredients.
Teva, which makes both the brand and generic of Adderall, reported on the FDA’s site that its manufacturing and distribution is at record-high levels, but demand continues to rise.
The branded Concerta is available, but some makers of generic methylphenidate reported supplies won’t be available until July.
Lisdexamfetamine dimesylate in almost all dosages is either unavailable, available in restricted quantities, or on extended back order. However, the branded product Vyvanse is available.
Industry, Government Respond
In a November 2023 statement, the DEA reported that 17 of 18 drug manufacturers the agency contacted planned to use their full DEA quota and increase production for that year. The agency said it had made it easier for manufacturers to request changes in allocations and that periodically updating quotas was a possibility.
This news organization asked the DEA whether any manufacturers had not met their 2023 quotas, but an agency spokesperson said it would not comment.
An FDA spokesperson said it could help manufacturers ask for bigger quotas and to increase production, noting that in 2023, the DEA increased the quota for methylphenidate following an FDA request.
“The FDA is in frequent communication with the manufacturers of ADHD stimulant medications and the DEA, and we will continue to monitor supply,” the spokesperson said.
For 2024, the FDA told the DEA that it predicted a 3.1% increase in use of amphetamine, methylphenidate (including dexmethylphenidate), and lisdexamfetamine. The DEA took that into account when it issued its final quotas for 2024. Whether those amounts will be enough remains to be seen.
With many drugs — not just those for ADHD — in short supply, in February, the US Department of Health and Human Services (HHS) and the Federal Trade Commission opened an inquiry of sorts, seeking comments on how middlemen and others were influencing pricing and supply of generic drugs.
“When you’re prescribed an important medication by your doctor and you learn the drug is out of stock, your heart sinks,” HHS Secretary Xavier Becerra said in a statement. “This devastating reality is the case for too many Americans who need generic drugs for ADHD, cancer, and other conditions.”
On the comments site, which is open until April 15, many of the 4000-plus complaints filed to-date are from individuals with ADHD.
Dr. Pawar said clinicians can’t know what’s going on between the FDA, the DEA, and manufacturers, adding that, “they need to sit together and figure something out.”
Even Members of Congress have had trouble getting answers. In October, Rep. Abigail Spanberger (D-Virginia) and a dozen colleagues wrote to the FDA and DEA seeking information on how the agencies were responding to stimulant shortages. The DEA has still not replied.
Workarounds the Only Option?
In the past, physicians would prescribe the optimal medication for individual patients based on clinical factors. Now, one of the major factors in determining drug choice is the agent that has “the highest likelihood of benefit and the lowest likelihood of administrative demand or burden,” Dr. Goodman said.
With so many medications in short supply, clinicians have figured out workarounds to get prescriptions filled, but they don’t often pan out.
If a patient needs a 60-mg daily dose of a medication and the pharmacy doesn’t have any 60-mg pills, Dr. Goodman said he might write a prescription for a 30-mg pill to be taken twice a day. However, insurers often will cover only 30 pills for a month, which can thwart this strategy.
Dr. Pawar said he sometimes prescribes Journay PM in lieu of Concerta because it is often available. But insurers may deny coverage of Journay PM because it is a newer medication, he said. When prescribing ADHD medications, he also provides his patients with a list of potential substitutes so they can ask the pharmacist if any are in stock.
With no end to the shortage in sight, clinicians must often prescribe multiple medications until their patients are able to find one that’s available. In addition, patients are burdened with making calls and visits to multiple pharmacies until they find one that can fill their prescription.
Meanwhile, the ripple effects to the ADHD drug shortage continue to spread. Extended periods without treatment can lead to declining job performance or job loss, fractured relationships, and even financial distress, Dr. Goodman said.
“If you go without your pills for a month and you’re not performing, your work declines and you lose your job as a result, that’s not on you — that’s on the fact that you can’t get your treatment,” he noted. “The shortage is no longer an inconvenience.”
Dr. Goodman, Dr. Pawar, and Ms. Kulikosky reported no relevant financial relationships.
A version of this article appeared on Medscape.com.
Nearly 18 months after the US Food and Drug Administration (FDA) first acknowledged a national shortage of Adderall, the most common drug used to treat attention-deficit/hyperactivity disorder (ADHD),
The first shortage of immediate release formulations of amphetamine mixed salts (Adderall, Adderall IR) was reported by the FDA in October 2022. Now, the list includes Focalin, Ritalin, and Vyvanse, among others.
Adding to the ongoing crisis, the FDA announced in early February that Azurity Pharmaceuticals was voluntarily withdrawing one lot of its Zenzedi (dextroamphetamine sulfate) 30 mg tablets because of contamination with the antihistamine, carbinoxamine.
For the roughly 10 million adults and 6 million children in the United States grappling with ADHD, getting a prescription filled with the exact medication ordered by a physician is dictated by geographic location, insurance formularies, and pharmacy supply chains. It’s particularly challenging for those who live in rural or underserved areas with limited access to nearby pharmacies.
“Not a day goes by when I don’t hear from a number of unfortunately struggling patients about this shortage,” said Aditya Pawar, MD, a child and adolescent psychiatrist with the Kennedy Krieger Institute and an assistant professor of psychiatry and behavioral sciences at Johns Hopkins School of Medicine, Baltimore, Maryland.
The ADHD drug shortage is now well into its second year, and clinicians and advocates alike say there is no apparent end in sight.
How Did We Get Here?
Manufacturers and federal agencies blame the shortage on rising demand and each other, while clinicians say that insurers, drug distributors, and middlemen are also playing a role in keeping medications out of patients’ hands.
In August 2023, the Drug Enforcement Administration (DEA), which sets quotas for the production of controlled substances, and the FDA publicly blamed manufacturers for the shortages, claiming they were not using up their allocations.
At the time, the DEA said manufacturers made and sold only 70% of their quota, nearly 1 billion doses short of what they were allowed to produce and ship that year.
The agencies also noted a record-high number of prescriptions for stimulants from 2012 to 2021. Driven in part by telehealth, the demand intensified during the pandemic. One recent study reported a 14% increase in ADHD stimulant prescriptions between 2020 and 2022.
Insurers also play a role in the shortage, David Goodman, MD, an assistant professor of psychiatry and behavioral sciences also at Johns Hopkins University, told this news organization.
Stepped therapy — in which patients must try one, two, or three medications before they are authorized to receive a more expensive or newer drug — contributes to the problem, Dr. Goodman said. Demand for such medications is high and supply low. In addition, some insurers only provide coverage for in-network pharmacies, regardless of the ability of other providers outside such networks to fill prescriptions.
“If the insurance dictates where you get your pills, and that pharmacy doesn’t have the pills or that pharmacy chain in your area doesn’t have those pills, you’re out of luck,” Dr. Goodman said.
Patients as Detectives
To get prescriptions filled, patients must “turn into detectives,” Laurie Kulikosky, CEO of Children and Adults with Attention-Deficit/Hyperactivity Disorder, told this news organization. “It’s a huge stressor.”
Tracking which ADHD medications are available, on back order, or discontinued requires frequent checking of the FDA’s drug shortages website.
Some manufacturers of generic versions of mixed amphetamine salts are only fulfilling orders for existing contracts, while others say new product won’t be available until at least April or as late as September. All blame the delay on the shortage of active ingredients.
Teva, which makes both the brand and generic of Adderall, reported on the FDA’s site that its manufacturing and distribution is at record-high levels, but demand continues to rise.
The branded Concerta is available, but some makers of generic methylphenidate reported supplies won’t be available until July.
Lisdexamfetamine dimesylate in almost all dosages is either unavailable, available in restricted quantities, or on extended back order. However, the branded product Vyvanse is available.
Industry, Government Respond
In a November 2023 statement, the DEA reported that 17 of 18 drug manufacturers the agency contacted planned to use their full DEA quota and increase production for that year. The agency said it had made it easier for manufacturers to request changes in allocations and that periodically updating quotas was a possibility.
This news organization asked the DEA whether any manufacturers had not met their 2023 quotas, but an agency spokesperson said it would not comment.
An FDA spokesperson said it could help manufacturers ask for bigger quotas and to increase production, noting that in 2023, the DEA increased the quota for methylphenidate following an FDA request.
“The FDA is in frequent communication with the manufacturers of ADHD stimulant medications and the DEA, and we will continue to monitor supply,” the spokesperson said.
For 2024, the FDA told the DEA that it predicted a 3.1% increase in use of amphetamine, methylphenidate (including dexmethylphenidate), and lisdexamfetamine. The DEA took that into account when it issued its final quotas for 2024. Whether those amounts will be enough remains to be seen.
With many drugs — not just those for ADHD — in short supply, in February, the US Department of Health and Human Services (HHS) and the Federal Trade Commission opened an inquiry of sorts, seeking comments on how middlemen and others were influencing pricing and supply of generic drugs.
“When you’re prescribed an important medication by your doctor and you learn the drug is out of stock, your heart sinks,” HHS Secretary Xavier Becerra said in a statement. “This devastating reality is the case for too many Americans who need generic drugs for ADHD, cancer, and other conditions.”
On the comments site, which is open until April 15, many of the 4000-plus complaints filed to-date are from individuals with ADHD.
Dr. Pawar said clinicians can’t know what’s going on between the FDA, the DEA, and manufacturers, adding that, “they need to sit together and figure something out.”
Even Members of Congress have had trouble getting answers. In October, Rep. Abigail Spanberger (D-Virginia) and a dozen colleagues wrote to the FDA and DEA seeking information on how the agencies were responding to stimulant shortages. The DEA has still not replied.
Workarounds the Only Option?
In the past, physicians would prescribe the optimal medication for individual patients based on clinical factors. Now, one of the major factors in determining drug choice is the agent that has “the highest likelihood of benefit and the lowest likelihood of administrative demand or burden,” Dr. Goodman said.
With so many medications in short supply, clinicians have figured out workarounds to get prescriptions filled, but they don’t often pan out.
If a patient needs a 60-mg daily dose of a medication and the pharmacy doesn’t have any 60-mg pills, Dr. Goodman said he might write a prescription for a 30-mg pill to be taken twice a day. However, insurers often will cover only 30 pills for a month, which can thwart this strategy.
Dr. Pawar said he sometimes prescribes Journay PM in lieu of Concerta because it is often available. But insurers may deny coverage of Journay PM because it is a newer medication, he said. When prescribing ADHD medications, he also provides his patients with a list of potential substitutes so they can ask the pharmacist if any are in stock.
With no end to the shortage in sight, clinicians must often prescribe multiple medications until their patients are able to find one that’s available. In addition, patients are burdened with making calls and visits to multiple pharmacies until they find one that can fill their prescription.
Meanwhile, the ripple effects to the ADHD drug shortage continue to spread. Extended periods without treatment can lead to declining job performance or job loss, fractured relationships, and even financial distress, Dr. Goodman said.
“If you go without your pills for a month and you’re not performing, your work declines and you lose your job as a result, that’s not on you — that’s on the fact that you can’t get your treatment,” he noted. “The shortage is no longer an inconvenience.”
Dr. Goodman, Dr. Pawar, and Ms. Kulikosky reported no relevant financial relationships.
A version of this article appeared on Medscape.com.