User login
USPSTF affirms optional pelvic screening
Current evidence fails to support or reject routine screening pelvic exams for asymptomatic, low-risk, nonpregnant adult women, the U.S. Preventive Services Task Force concluded after reviewing the evidence on the accuracy, benefits, and potential harms.
The USPSTF issued an inconclusive “I” statement that was published online March 7 (JAMA. 2017;317[9]:947-53).
Researchers found no data comparing the impact of no screening versus screening pelvic examinations on patient health outcomes including reducing all-cause mortality, reducing cancer-specific and disease-specific morbidity and mortality, and improving quality of life.
“No direct evidence was identified for overall benefits and harms of the pelvic examination as a one-time or periodic screening test,” Janelle M. Guirguis-Blake, MD, of the University of Washington, Tacoma, and colleagues wrote in the accompanying evidence report (JAMA. 2017;317[9]:954-66). The review comprised nine studies: one addressing the harms of screening and eight addressing both harms and accuracy.
Although screening pelvic exams may identify serious conditions as well as benign ones, the potential remains for false-positive and false-negative results that might lead to invasive surgery and unnecessary testing and procedures, the researchers noted. However, the recommendations do not apply to certain conditions for which screening is already recommended, including cervical cancer (via Pap smear), gonorrhea, and chlamydia.
The recommendations are primarily a call for more research rather than a clear guide for clinicians, according to the USPSTF. The research gaps include studies on the physical and psychological harms of pelvic screening for asymptomatic women in primary care; the ability of screening to detect conditions beyond ovarian cancer, genital herpes, bacterial vaginosis, and trichomoniasis; and the impact of screening on a variety of health outcomes, including quality of life.
Given the inadequate evidence to recommend for or against screening, the USPSTF cited the recommendations of other organizations. Both the American College of Physicians and the American Academy of Family Physicians recommend against performing screening pelvic exams in asymptomatic, nonpregnant adult women. The American College of Obstetricians and Gynecologists recommends annual pelvic exams for women 21 years and older but acknowledges a lack of evidence and has said it should be a shared decision between the patient and clinician.
The USPSTF members reported having no relevant financial conflicts.
The USPSTF task force finding of insufficient evidence to support or refute screening pelvic exams conflicts with the views of other organizations, George F. Sawaya, MD, wrote in an editorial (JAMA 2017 Mar 7. doi: 10.1001/jamainternmed.2017.0271).
The American College of Physicians currently recommends against routine screening in asymptomatic, nonpregnant women, while the American College of Obstetricians and Gynecologists recommends in favor of an annual pelvic exam “based on expert opinion” despite the lack of evidence, he said.
“The USPSTF believes that in the setting of an ‘I’ statement, clinicians should be forthright with patients about the uncertainty concerning the balance of benefits and harms,” Dr. Sawaya wrote.
“But perhaps the conversation should focus on the uncertainty among the three professional groups,” he added. “Women should know the facts: that all three groups agree there is no scientific evidence that these examinations are beneficial; that there is evidence of harms including ‘false alarms,’ further testing, and even unnecessary surgery; and that one group strongly recommends against screening examinations, believing them to be more harmful than beneficial,” he said.
The USPSTF recommendation is not a surprise, Colleen McNicholas, DO, MSCI, and Jeffrey F. Peipert, MD, PhD, noted in a second editorial (JAMA 2017;317[9]:910-11). “Despite lack of rigorous research, many would argue that the periodic examination provides opportunity for counseling and trust building between the patient and physician and thus should be universally implemented,” they wrote. However, many women express fear and anxiety before the exam and discomfort, pain, or embarrassment during the exam. “To ignore this aspect when comparing individual parts of the examination seems insensitive and inappropriate,” they added.
“Women, as patients, should be involved in the decision regarding whether to perform a pelvic examination, and clinicians should not require that the patient undergo this procedure to obtain screening, counseling, and age-appropriate health services,” they concluded.
Dr. Sawaya is affiliated with the University of California, San Francisco. He reported having no financial conflicts. Dr. Peipert is affiliated with Indiana University School of Medicine, Indianapolis, and disclosed receiving grants from Teva Pharmaceuticals, Bayer Healthcare Pharmaceuticals, and Merck, as well as serving on the advisory boards of Perrigo and Teva. Dr. McNicholas is affiliated with Washington University, St. Louis, and reported having no financial conflicts.
The USPSTF task force finding of insufficient evidence to support or refute screening pelvic exams conflicts with the views of other organizations, George F. Sawaya, MD, wrote in an editorial (JAMA 2017 Mar 7. doi: 10.1001/jamainternmed.2017.0271).
The American College of Physicians currently recommends against routine screening in asymptomatic, nonpregnant women, while the American College of Obstetricians and Gynecologists recommends in favor of an annual pelvic exam “based on expert opinion” despite the lack of evidence, he said.
“The USPSTF believes that in the setting of an ‘I’ statement, clinicians should be forthright with patients about the uncertainty concerning the balance of benefits and harms,” Dr. Sawaya wrote.
“But perhaps the conversation should focus on the uncertainty among the three professional groups,” he added. “Women should know the facts: that all three groups agree there is no scientific evidence that these examinations are beneficial; that there is evidence of harms including ‘false alarms,’ further testing, and even unnecessary surgery; and that one group strongly recommends against screening examinations, believing them to be more harmful than beneficial,” he said.
The USPSTF recommendation is not a surprise, Colleen McNicholas, DO, MSCI, and Jeffrey F. Peipert, MD, PhD, noted in a second editorial (JAMA 2017;317[9]:910-11). “Despite lack of rigorous research, many would argue that the periodic examination provides opportunity for counseling and trust building between the patient and physician and thus should be universally implemented,” they wrote. However, many women express fear and anxiety before the exam and discomfort, pain, or embarrassment during the exam. “To ignore this aspect when comparing individual parts of the examination seems insensitive and inappropriate,” they added.
“Women, as patients, should be involved in the decision regarding whether to perform a pelvic examination, and clinicians should not require that the patient undergo this procedure to obtain screening, counseling, and age-appropriate health services,” they concluded.
Dr. Sawaya is affiliated with the University of California, San Francisco. He reported having no financial conflicts. Dr. Peipert is affiliated with Indiana University School of Medicine, Indianapolis, and disclosed receiving grants from Teva Pharmaceuticals, Bayer Healthcare Pharmaceuticals, and Merck, as well as serving on the advisory boards of Perrigo and Teva. Dr. McNicholas is affiliated with Washington University, St. Louis, and reported having no financial conflicts.
The USPSTF task force finding of insufficient evidence to support or refute screening pelvic exams conflicts with the views of other organizations, George F. Sawaya, MD, wrote in an editorial (JAMA 2017 Mar 7. doi: 10.1001/jamainternmed.2017.0271).
The American College of Physicians currently recommends against routine screening in asymptomatic, nonpregnant women, while the American College of Obstetricians and Gynecologists recommends in favor of an annual pelvic exam “based on expert opinion” despite the lack of evidence, he said.
“The USPSTF believes that in the setting of an ‘I’ statement, clinicians should be forthright with patients about the uncertainty concerning the balance of benefits and harms,” Dr. Sawaya wrote.
“But perhaps the conversation should focus on the uncertainty among the three professional groups,” he added. “Women should know the facts: that all three groups agree there is no scientific evidence that these examinations are beneficial; that there is evidence of harms including ‘false alarms,’ further testing, and even unnecessary surgery; and that one group strongly recommends against screening examinations, believing them to be more harmful than beneficial,” he said.
The USPSTF recommendation is not a surprise, Colleen McNicholas, DO, MSCI, and Jeffrey F. Peipert, MD, PhD, noted in a second editorial (JAMA 2017;317[9]:910-11). “Despite lack of rigorous research, many would argue that the periodic examination provides opportunity for counseling and trust building between the patient and physician and thus should be universally implemented,” they wrote. However, many women express fear and anxiety before the exam and discomfort, pain, or embarrassment during the exam. “To ignore this aspect when comparing individual parts of the examination seems insensitive and inappropriate,” they added.
“Women, as patients, should be involved in the decision regarding whether to perform a pelvic examination, and clinicians should not require that the patient undergo this procedure to obtain screening, counseling, and age-appropriate health services,” they concluded.
Dr. Sawaya is affiliated with the University of California, San Francisco. He reported having no financial conflicts. Dr. Peipert is affiliated with Indiana University School of Medicine, Indianapolis, and disclosed receiving grants from Teva Pharmaceuticals, Bayer Healthcare Pharmaceuticals, and Merck, as well as serving on the advisory boards of Perrigo and Teva. Dr. McNicholas is affiliated with Washington University, St. Louis, and reported having no financial conflicts.
Current evidence fails to support or reject routine screening pelvic exams for asymptomatic, low-risk, nonpregnant adult women, the U.S. Preventive Services Task Force concluded after reviewing the evidence on the accuracy, benefits, and potential harms.
The USPSTF issued an inconclusive “I” statement that was published online March 7 (JAMA. 2017;317[9]:947-53).
Researchers found no data comparing the impact of no screening versus screening pelvic examinations on patient health outcomes including reducing all-cause mortality, reducing cancer-specific and disease-specific morbidity and mortality, and improving quality of life.
“No direct evidence was identified for overall benefits and harms of the pelvic examination as a one-time or periodic screening test,” Janelle M. Guirguis-Blake, MD, of the University of Washington, Tacoma, and colleagues wrote in the accompanying evidence report (JAMA. 2017;317[9]:954-66). The review comprised nine studies: one addressing the harms of screening and eight addressing both harms and accuracy.
Although screening pelvic exams may identify serious conditions as well as benign ones, the potential remains for false-positive and false-negative results that might lead to invasive surgery and unnecessary testing and procedures, the researchers noted. However, the recommendations do not apply to certain conditions for which screening is already recommended, including cervical cancer (via Pap smear), gonorrhea, and chlamydia.
The recommendations are primarily a call for more research rather than a clear guide for clinicians, according to the USPSTF. The research gaps include studies on the physical and psychological harms of pelvic screening for asymptomatic women in primary care; the ability of screening to detect conditions beyond ovarian cancer, genital herpes, bacterial vaginosis, and trichomoniasis; and the impact of screening on a variety of health outcomes, including quality of life.
Given the inadequate evidence to recommend for or against screening, the USPSTF cited the recommendations of other organizations. Both the American College of Physicians and the American Academy of Family Physicians recommend against performing screening pelvic exams in asymptomatic, nonpregnant adult women. The American College of Obstetricians and Gynecologists recommends annual pelvic exams for women 21 years and older but acknowledges a lack of evidence and has said it should be a shared decision between the patient and clinician.
The USPSTF members reported having no relevant financial conflicts.
Current evidence fails to support or reject routine screening pelvic exams for asymptomatic, low-risk, nonpregnant adult women, the U.S. Preventive Services Task Force concluded after reviewing the evidence on the accuracy, benefits, and potential harms.
The USPSTF issued an inconclusive “I” statement that was published online March 7 (JAMA. 2017;317[9]:947-53).
Researchers found no data comparing the impact of no screening versus screening pelvic examinations on patient health outcomes including reducing all-cause mortality, reducing cancer-specific and disease-specific morbidity and mortality, and improving quality of life.
“No direct evidence was identified for overall benefits and harms of the pelvic examination as a one-time or periodic screening test,” Janelle M. Guirguis-Blake, MD, of the University of Washington, Tacoma, and colleagues wrote in the accompanying evidence report (JAMA. 2017;317[9]:954-66). The review comprised nine studies: one addressing the harms of screening and eight addressing both harms and accuracy.
Although screening pelvic exams may identify serious conditions as well as benign ones, the potential remains for false-positive and false-negative results that might lead to invasive surgery and unnecessary testing and procedures, the researchers noted. However, the recommendations do not apply to certain conditions for which screening is already recommended, including cervical cancer (via Pap smear), gonorrhea, and chlamydia.
The recommendations are primarily a call for more research rather than a clear guide for clinicians, according to the USPSTF. The research gaps include studies on the physical and psychological harms of pelvic screening for asymptomatic women in primary care; the ability of screening to detect conditions beyond ovarian cancer, genital herpes, bacterial vaginosis, and trichomoniasis; and the impact of screening on a variety of health outcomes, including quality of life.
Given the inadequate evidence to recommend for or against screening, the USPSTF cited the recommendations of other organizations. Both the American College of Physicians and the American Academy of Family Physicians recommend against performing screening pelvic exams in asymptomatic, nonpregnant adult women. The American College of Obstetricians and Gynecologists recommends annual pelvic exams for women 21 years and older but acknowledges a lack of evidence and has said it should be a shared decision between the patient and clinician.
The USPSTF members reported having no relevant financial conflicts.
FROM JAMA
Teen indoor tanning drops, but schools fall short on sun safety
Indoor tanning among adolescents in the United States has dropped significantly, but fewer than half of schools in the United States reported sun safety practices to help minimize students’ UV exposure in the school setting, based on data from two studies presented at the annual meeting of the American Academy of Dermatology and published simultaneously in JAMA Dermatology.
“Data suggest that intermittent, recreational exposure (vs. chronic exposure, as with outdoor workers) more often leads to sunburn,” wrote Sherry Everett Jones, PhD, MPH, and Gery P. Guy Jr, PhD, MPH, of the Centers for Disease Control and Prevention. “Although a small proportion of school districts and schools have adopted policies to address sun safety, most have not, even though it is common for students to be outside during the midday hours or after school when the sun is still at peak intensity.”
To characterize sun safety practices at schools, the researchers reviewed data from the 2014 School Health Policies and Practices Study Healthy and Safe School Environment questionnaire including 577 elementary, middle, and high schools (JAMA Dermatol. 2017. doi: 10.1001/jamadermatol.2016.6274).
Overall, 48% of schools reported that teachers allowed students time to apply sunscreen at school (the most frequent sun safety practice). However, only 13% made sunscreen available, 16% asked parents to ensure sunscreen application before school, and 15% made an effort to avoid scheduling outdoor activities during times of peak sun intensity. High schools were less likely than elementary or middle schools to follow sun safety practices.
“None of the sun safety policies or practices were statistically significantly associated with metropolitan status,” the researchers noted. However, the findings were limited by the cross-sectional nature of the study and lack of data about natural shade and man made shade structures in outdoor areas of the schools.
“Interventions driven by the public health and medical community educating school leadership and policy makers about the importance of sun safety are needed regardless of level, location, size, and poverty concentration of the school. These efforts could be instrumental in increasing the adoption of sun safety practices among schools,” Dr. Jones and Dr. Guy emphasized.
However, data from another study showed a significant reduction in the prevalence of indoor tanning among adolescents.
In particular, indoor tanning among non-Hispanic white females (the group at highest risk for skin cancer) dropped from 37% in 2009 to 15% in 2015. CDC researchers led by Dr. Guy pooled data from the 2009, 2011, 2013, and 2015 national Youth Risk Behavior Surveillance System Surveys (JAMA Dermatol. 2017. doi:10.1001/jamadermatol.2016.6273). Overall, the prevalence of indoor tanning among U.S. high school students decreased from 16% in 2009 to 7% in 2015.
“Despite declines in indoor tanning, continued efforts are needed,” the researchers wrote. “Public health efforts could help address the misconception that indoor tanning protects against sunburn. The medical community also can play a key role in counseling adolescents and young adults in accordance with the U.S. Preventive Services Task Force guidelines.”
The findings were limited by several factors including the use of self-reports and the inability to control for skin type, the researchers wrote. However, “Reducing the proportion of youth who engage in indoor tanning and experience sunburns presents an important cancer prevention opportunity.”
None of the researchers on either study had relevant financial conflicts to disclose.
Explore best practices for public education campaigns “For more than 10 years, much effort has been made to educate the public on sun-safety practices, including warnings about the harmful effects of indoor tanning on those at higher risk, such as young adults and children. In this issue of JAMA Dermatology, 2 important articles describe the progress made toward sun safety,” wrote Henry W. Lim, MD, and Samantha L. Schneider, MD, in the accompanying editorial.
Data from a study of indoor tanning showed a significant decrease in prevalence of indoor tanning among adolescents, from 16% in 2009 to 7% in 2015. Although these results are encouraging, public education is needed for further improvement, they said. “One myth is that UV radiation prevents vitamin D deficiency; however, oral vitamin D supplementation is known to be a safer alternative. Another myth is that obtaining a baseline tan before the summer or a vacation reduces the risk of sunburn. However, as Guy and colleagues observed, those who tanned indoors were more likely to develop sunburn than students who did not engage in indoor tanning.”
“Clearly, both the dermatology and medical communities need to continue public awareness campaigns regarding photoprotection, including sun-safety practices such as seeking shade when outdoors and wearing photoprotective clothing, wide-brimmed hats, and sunglasses,” they emphasized.
In addition, “A highly effective means of public education may be to identify a campaign, such as Portugal’s sugar packet initiative, that makes sun-safety awareness and practice a part of everyone’s daily routine,” they said (JAMA Dermatol. 2017. doi: 10.1001/jamadermatol.2016.6272).
Dr. Lim and Dr. Schneider are affiliated with the department of dermatology at Henry Ford Hospital in Detroit. Dr Lim disclosed serving as an investigator or coinvestigator on clinical research projects for Ferndale Pharma, Estée Lauder, and Allergan. Dr. Schneider had no relevant conflicts to disclose.
Explore best practices for public education campaigns “For more than 10 years, much effort has been made to educate the public on sun-safety practices, including warnings about the harmful effects of indoor tanning on those at higher risk, such as young adults and children. In this issue of JAMA Dermatology, 2 important articles describe the progress made toward sun safety,” wrote Henry W. Lim, MD, and Samantha L. Schneider, MD, in the accompanying editorial.
Data from a study of indoor tanning showed a significant decrease in prevalence of indoor tanning among adolescents, from 16% in 2009 to 7% in 2015. Although these results are encouraging, public education is needed for further improvement, they said. “One myth is that UV radiation prevents vitamin D deficiency; however, oral vitamin D supplementation is known to be a safer alternative. Another myth is that obtaining a baseline tan before the summer or a vacation reduces the risk of sunburn. However, as Guy and colleagues observed, those who tanned indoors were more likely to develop sunburn than students who did not engage in indoor tanning.”
“Clearly, both the dermatology and medical communities need to continue public awareness campaigns regarding photoprotection, including sun-safety practices such as seeking shade when outdoors and wearing photoprotective clothing, wide-brimmed hats, and sunglasses,” they emphasized.
In addition, “A highly effective means of public education may be to identify a campaign, such as Portugal’s sugar packet initiative, that makes sun-safety awareness and practice a part of everyone’s daily routine,” they said (JAMA Dermatol. 2017. doi: 10.1001/jamadermatol.2016.6272).
Dr. Lim and Dr. Schneider are affiliated with the department of dermatology at Henry Ford Hospital in Detroit. Dr Lim disclosed serving as an investigator or coinvestigator on clinical research projects for Ferndale Pharma, Estée Lauder, and Allergan. Dr. Schneider had no relevant conflicts to disclose.
Explore best practices for public education campaigns “For more than 10 years, much effort has been made to educate the public on sun-safety practices, including warnings about the harmful effects of indoor tanning on those at higher risk, such as young adults and children. In this issue of JAMA Dermatology, 2 important articles describe the progress made toward sun safety,” wrote Henry W. Lim, MD, and Samantha L. Schneider, MD, in the accompanying editorial.
Data from a study of indoor tanning showed a significant decrease in prevalence of indoor tanning among adolescents, from 16% in 2009 to 7% in 2015. Although these results are encouraging, public education is needed for further improvement, they said. “One myth is that UV radiation prevents vitamin D deficiency; however, oral vitamin D supplementation is known to be a safer alternative. Another myth is that obtaining a baseline tan before the summer or a vacation reduces the risk of sunburn. However, as Guy and colleagues observed, those who tanned indoors were more likely to develop sunburn than students who did not engage in indoor tanning.”
“Clearly, both the dermatology and medical communities need to continue public awareness campaigns regarding photoprotection, including sun-safety practices such as seeking shade when outdoors and wearing photoprotective clothing, wide-brimmed hats, and sunglasses,” they emphasized.
In addition, “A highly effective means of public education may be to identify a campaign, such as Portugal’s sugar packet initiative, that makes sun-safety awareness and practice a part of everyone’s daily routine,” they said (JAMA Dermatol. 2017. doi: 10.1001/jamadermatol.2016.6272).
Dr. Lim and Dr. Schneider are affiliated with the department of dermatology at Henry Ford Hospital in Detroit. Dr Lim disclosed serving as an investigator or coinvestigator on clinical research projects for Ferndale Pharma, Estée Lauder, and Allergan. Dr. Schneider had no relevant conflicts to disclose.
Indoor tanning among adolescents in the United States has dropped significantly, but fewer than half of schools in the United States reported sun safety practices to help minimize students’ UV exposure in the school setting, based on data from two studies presented at the annual meeting of the American Academy of Dermatology and published simultaneously in JAMA Dermatology.
“Data suggest that intermittent, recreational exposure (vs. chronic exposure, as with outdoor workers) more often leads to sunburn,” wrote Sherry Everett Jones, PhD, MPH, and Gery P. Guy Jr, PhD, MPH, of the Centers for Disease Control and Prevention. “Although a small proportion of school districts and schools have adopted policies to address sun safety, most have not, even though it is common for students to be outside during the midday hours or after school when the sun is still at peak intensity.”
To characterize sun safety practices at schools, the researchers reviewed data from the 2014 School Health Policies and Practices Study Healthy and Safe School Environment questionnaire including 577 elementary, middle, and high schools (JAMA Dermatol. 2017. doi: 10.1001/jamadermatol.2016.6274).
Overall, 48% of schools reported that teachers allowed students time to apply sunscreen at school (the most frequent sun safety practice). However, only 13% made sunscreen available, 16% asked parents to ensure sunscreen application before school, and 15% made an effort to avoid scheduling outdoor activities during times of peak sun intensity. High schools were less likely than elementary or middle schools to follow sun safety practices.
“None of the sun safety policies or practices were statistically significantly associated with metropolitan status,” the researchers noted. However, the findings were limited by the cross-sectional nature of the study and lack of data about natural shade and man made shade structures in outdoor areas of the schools.
“Interventions driven by the public health and medical community educating school leadership and policy makers about the importance of sun safety are needed regardless of level, location, size, and poverty concentration of the school. These efforts could be instrumental in increasing the adoption of sun safety practices among schools,” Dr. Jones and Dr. Guy emphasized.
However, data from another study showed a significant reduction in the prevalence of indoor tanning among adolescents.
In particular, indoor tanning among non-Hispanic white females (the group at highest risk for skin cancer) dropped from 37% in 2009 to 15% in 2015. CDC researchers led by Dr. Guy pooled data from the 2009, 2011, 2013, and 2015 national Youth Risk Behavior Surveillance System Surveys (JAMA Dermatol. 2017. doi:10.1001/jamadermatol.2016.6273). Overall, the prevalence of indoor tanning among U.S. high school students decreased from 16% in 2009 to 7% in 2015.
“Despite declines in indoor tanning, continued efforts are needed,” the researchers wrote. “Public health efforts could help address the misconception that indoor tanning protects against sunburn. The medical community also can play a key role in counseling adolescents and young adults in accordance with the U.S. Preventive Services Task Force guidelines.”
The findings were limited by several factors including the use of self-reports and the inability to control for skin type, the researchers wrote. However, “Reducing the proportion of youth who engage in indoor tanning and experience sunburns presents an important cancer prevention opportunity.”
None of the researchers on either study had relevant financial conflicts to disclose.
Indoor tanning among adolescents in the United States has dropped significantly, but fewer than half of schools in the United States reported sun safety practices to help minimize students’ UV exposure in the school setting, based on data from two studies presented at the annual meeting of the American Academy of Dermatology and published simultaneously in JAMA Dermatology.
“Data suggest that intermittent, recreational exposure (vs. chronic exposure, as with outdoor workers) more often leads to sunburn,” wrote Sherry Everett Jones, PhD, MPH, and Gery P. Guy Jr, PhD, MPH, of the Centers for Disease Control and Prevention. “Although a small proportion of school districts and schools have adopted policies to address sun safety, most have not, even though it is common for students to be outside during the midday hours or after school when the sun is still at peak intensity.”
To characterize sun safety practices at schools, the researchers reviewed data from the 2014 School Health Policies and Practices Study Healthy and Safe School Environment questionnaire including 577 elementary, middle, and high schools (JAMA Dermatol. 2017. doi: 10.1001/jamadermatol.2016.6274).
Overall, 48% of schools reported that teachers allowed students time to apply sunscreen at school (the most frequent sun safety practice). However, only 13% made sunscreen available, 16% asked parents to ensure sunscreen application before school, and 15% made an effort to avoid scheduling outdoor activities during times of peak sun intensity. High schools were less likely than elementary or middle schools to follow sun safety practices.
“None of the sun safety policies or practices were statistically significantly associated with metropolitan status,” the researchers noted. However, the findings were limited by the cross-sectional nature of the study and lack of data about natural shade and man made shade structures in outdoor areas of the schools.
“Interventions driven by the public health and medical community educating school leadership and policy makers about the importance of sun safety are needed regardless of level, location, size, and poverty concentration of the school. These efforts could be instrumental in increasing the adoption of sun safety practices among schools,” Dr. Jones and Dr. Guy emphasized.
However, data from another study showed a significant reduction in the prevalence of indoor tanning among adolescents.
In particular, indoor tanning among non-Hispanic white females (the group at highest risk for skin cancer) dropped from 37% in 2009 to 15% in 2015. CDC researchers led by Dr. Guy pooled data from the 2009, 2011, 2013, and 2015 national Youth Risk Behavior Surveillance System Surveys (JAMA Dermatol. 2017. doi:10.1001/jamadermatol.2016.6273). Overall, the prevalence of indoor tanning among U.S. high school students decreased from 16% in 2009 to 7% in 2015.
“Despite declines in indoor tanning, continued efforts are needed,” the researchers wrote. “Public health efforts could help address the misconception that indoor tanning protects against sunburn. The medical community also can play a key role in counseling adolescents and young adults in accordance with the U.S. Preventive Services Task Force guidelines.”
The findings were limited by several factors including the use of self-reports and the inability to control for skin type, the researchers wrote. However, “Reducing the proportion of youth who engage in indoor tanning and experience sunburns presents an important cancer prevention opportunity.”
None of the researchers on either study had relevant financial conflicts to disclose.
FROM AAD 2017
Key clinical point:
Major finding: Fewer than half (48%) of schools in the United States allowed time for sunscreen application, and fewer than 15% provided sunscreen. However, overall prevalence of indoor tanning among U.S. adolescents dropped from 16% in 2009 to 7% in 2015.
Data source: Data were taken from the 2014 School Health Policies and Practices Study in the first study and from the 2009, 2011, 2013, and 2015 national Youth Risk Behavior Surveys in the second.
Disclosures: The researchers had no financial conflicts to disclose.
Chikungunya implicated in long-term joint disease
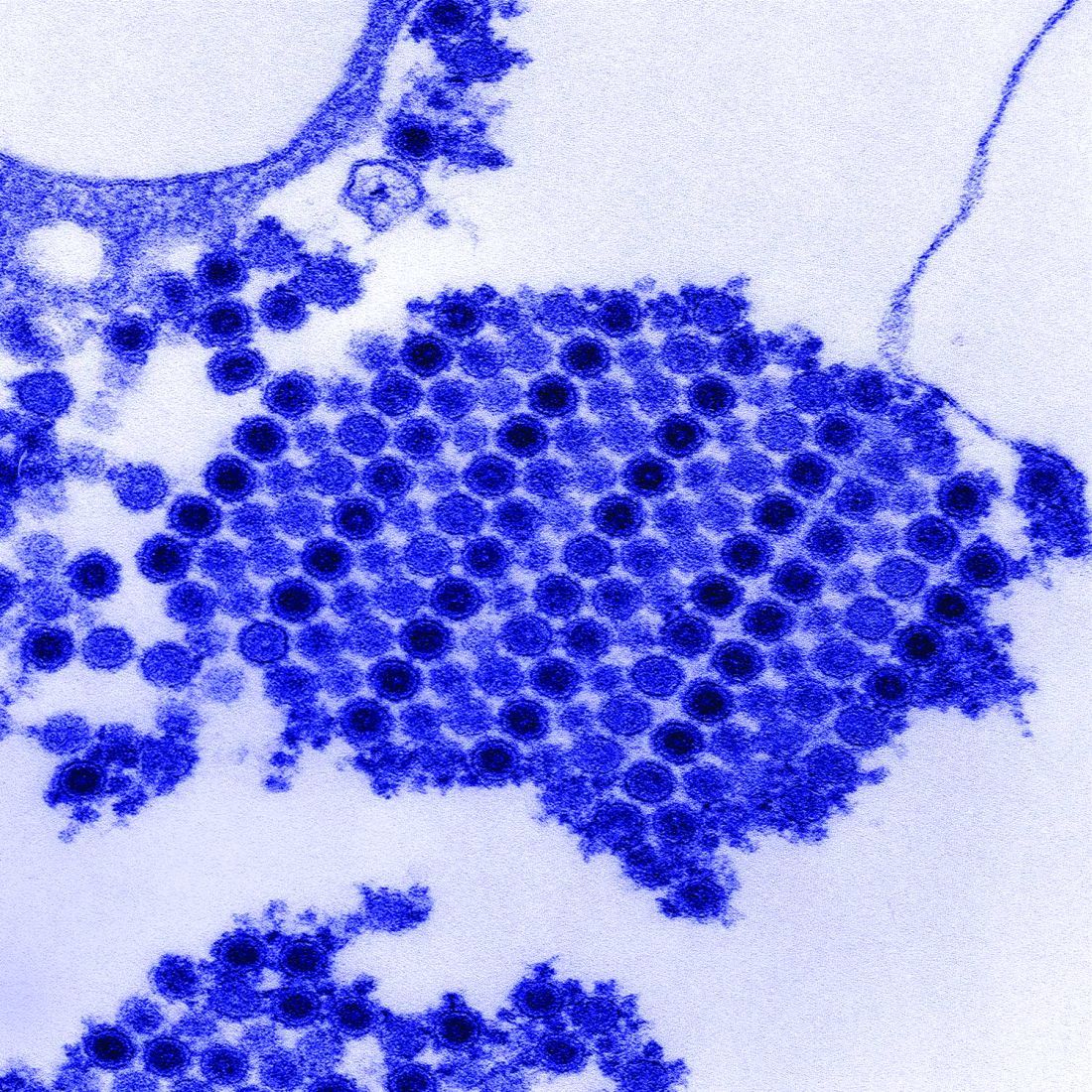
A majority of Chikungunya infections can cause arthritis and arthralgia months or years after the initial infection, based on data from a prospective study of 307 patients.
“The most common symptoms of Chikungunya virus infection are fever associated with rheumatic manifestations,” wrote rheumatologist Eric Bouquillard, MD, of Saint-Pierre, Reunion, France, and his colleagues.
Overall, 83% of the patients showed persistent joint pain after an average of 32 months. In addition, synovitis occurred in 64% of the patients who experienced chronic joint pain, mainly in the wrists, fingers, and ankles.
At baseline, the average number of painful joints was 6.5. At follow-up, the average number of painful joints was 3.3, and 43% of patients reported persistence of one or more swollen joints.
However, the patients reported little functional impairment; the average Health Assessment Questionnaire score was 0.44.
“RT-PCR [reverse transcription–polymerase chain reaction] was used in an attempt to detect the viral genome in synovial fluid samples from 10 patients, including 2 patients in the viremic phase, but the results were always negative,” the researchers noted.
Dr. Bouquillard and his colleagues enrolled the patients during April 2005-December 2006. Rheumatologic exams were conducted at baseline, and follow-up data were collected by phone surveys at 1 and 2 years after the onset of Chikungunya infection. Phone surveys were conducted by the Reunion Island Clinical Investigation Centre for Clinical Epidemiology, and interviewers also assessed patients for signs of anxiety, depression, and weakness.
The study was not designed to address treatment, but data from previous studies suggest that combination disease-modifying antirheumatic drug therapy may be more effective than hydroxychloroquine monotherapy for chronic joint pain post Chikungunya, the researchers noted.
The researchers had no financial conflicts to disclose. The study was supported in part by the Union Régionale des Médecins Libéraux de La Réunion.
A majority of Chikungunya infections can cause arthritis and arthralgia months or years after the initial infection, based on data from a prospective study of 307 patients.
“The most common symptoms of Chikungunya virus infection are fever associated with rheumatic manifestations,” wrote rheumatologist Eric Bouquillard, MD, of Saint-Pierre, Reunion, France, and his colleagues.
Overall, 83% of the patients showed persistent joint pain after an average of 32 months. In addition, synovitis occurred in 64% of the patients who experienced chronic joint pain, mainly in the wrists, fingers, and ankles.
At baseline, the average number of painful joints was 6.5. At follow-up, the average number of painful joints was 3.3, and 43% of patients reported persistence of one or more swollen joints.
However, the patients reported little functional impairment; the average Health Assessment Questionnaire score was 0.44.
“RT-PCR [reverse transcription–polymerase chain reaction] was used in an attempt to detect the viral genome in synovial fluid samples from 10 patients, including 2 patients in the viremic phase, but the results were always negative,” the researchers noted.
Dr. Bouquillard and his colleagues enrolled the patients during April 2005-December 2006. Rheumatologic exams were conducted at baseline, and follow-up data were collected by phone surveys at 1 and 2 years after the onset of Chikungunya infection. Phone surveys were conducted by the Reunion Island Clinical Investigation Centre for Clinical Epidemiology, and interviewers also assessed patients for signs of anxiety, depression, and weakness.
The study was not designed to address treatment, but data from previous studies suggest that combination disease-modifying antirheumatic drug therapy may be more effective than hydroxychloroquine monotherapy for chronic joint pain post Chikungunya, the researchers noted.
The researchers had no financial conflicts to disclose. The study was supported in part by the Union Régionale des Médecins Libéraux de La Réunion.
A majority of Chikungunya infections can cause arthritis and arthralgia months or years after the initial infection, based on data from a prospective study of 307 patients.
“The most common symptoms of Chikungunya virus infection are fever associated with rheumatic manifestations,” wrote rheumatologist Eric Bouquillard, MD, of Saint-Pierre, Reunion, France, and his colleagues.
Overall, 83% of the patients showed persistent joint pain after an average of 32 months. In addition, synovitis occurred in 64% of the patients who experienced chronic joint pain, mainly in the wrists, fingers, and ankles.
At baseline, the average number of painful joints was 6.5. At follow-up, the average number of painful joints was 3.3, and 43% of patients reported persistence of one or more swollen joints.
However, the patients reported little functional impairment; the average Health Assessment Questionnaire score was 0.44.
“RT-PCR [reverse transcription–polymerase chain reaction] was used in an attempt to detect the viral genome in synovial fluid samples from 10 patients, including 2 patients in the viremic phase, but the results were always negative,” the researchers noted.
Dr. Bouquillard and his colleagues enrolled the patients during April 2005-December 2006. Rheumatologic exams were conducted at baseline, and follow-up data were collected by phone surveys at 1 and 2 years after the onset of Chikungunya infection. Phone surveys were conducted by the Reunion Island Clinical Investigation Centre for Clinical Epidemiology, and interviewers also assessed patients for signs of anxiety, depression, and weakness.
The study was not designed to address treatment, but data from previous studies suggest that combination disease-modifying antirheumatic drug therapy may be more effective than hydroxychloroquine monotherapy for chronic joint pain post Chikungunya, the researchers noted.
The researchers had no financial conflicts to disclose. The study was supported in part by the Union Régionale des Médecins Libéraux de La Réunion.
FROM JOINT BONE SPINE
Key clinical point:
Major finding: Approximately 83% of adults with Chikungunya virus infections reported persistent joint pain after an average of 32 months.
Data source: A prospective, multicenter study of 307 adults with a history of Chikungunya virus infections.
Disclosures: The researchers had no financial conflicts to disclose. The study was supported in part by the Union Régionale des Médecins Libéraux de La Réunion.
Electrical stimulation skin patch shows promise in easing migraine pain
A wireless skin patch using electrical stimulation at an intensity lower than pain threshold reduced migraine pain when compared against sham stimulation in a trial of 71 adults with episodic migraine. The findings were published online March 1 in Neurology.
“Our rationale is activation of pain inhibitory centers, via the conditioned pain modulation effect; remote noxious stimuli can exert a generalized analgesic effect,” wrote David Yarnitsky, MD, of the Rambam Healthcare Campus and Technion Faculty of Medicine, Haifa, Israel, and his colleagues.
The devices were randomized to give a nonpainful sham stimulation at a very low frequency (controls) or a nonpainful active stimulation at one of four levels (active treatment). Patients were asked to place the wireless patch on the arm of their choice, regardless of the location of migraine pain, and activate the device for 20 minutes as soon as possible after a migraine attack began. They were instructed to use their smartphones to adjust the stimulation as appropriate during the treatment time. The stimulations were active programs at 80-120 Hz with pulse widths of 200, 150, 100, and 50 microseconds. The sham stimulation was a 0.1-Hz frequency with 45-microsecond pulses.
Overall, 64% of patients at the top three stimuli levels reduced their pain level by at least half 2 hours after the treatment, compared with 26% of patients using the sham stimulation. Average reductions were 46% for the 200-microsecond stimulus, 48% for 150, and 39% for 100.
In addition, 58% of the patients in the 200-microsecond group with moderate to severe pain at baseline reported reductions to mild or no pain, compared with 24% of sham patients.
Treatment with stimulation within 20 minutes of migraine onset was the most helpful, resulting in a 47% pain reduction, compared with a 25% reduction with delayed treatment, the researchers noted.
No patients reported side effects or adverse events related to the device.
The investigators said that complete 20-minute treatments were obtained for 70% of each of the top three stimuli levels, for 58% of treatments at 50-microsecond pulse widths, and for just 28% of placebo treatments. This low rate of completion of placebo stimuli may be the result of a loss of blinding for some of the sham activations, the investigators acknowledged, but they argued that “it is likely that this fact did not lead to falsely improved results; on the contrary, had those incomplete stimuli periods been completed, it is most likely that sham effectiveness results would have been lower than currently reported, making the results even more distinct.”
The study was funded by Theranica, and Dr. Yarnitsky disclosed serving on the company’s medical advisory board.
A wireless skin patch using electrical stimulation at an intensity lower than pain threshold reduced migraine pain when compared against sham stimulation in a trial of 71 adults with episodic migraine. The findings were published online March 1 in Neurology.
“Our rationale is activation of pain inhibitory centers, via the conditioned pain modulation effect; remote noxious stimuli can exert a generalized analgesic effect,” wrote David Yarnitsky, MD, of the Rambam Healthcare Campus and Technion Faculty of Medicine, Haifa, Israel, and his colleagues.
The devices were randomized to give a nonpainful sham stimulation at a very low frequency (controls) or a nonpainful active stimulation at one of four levels (active treatment). Patients were asked to place the wireless patch on the arm of their choice, regardless of the location of migraine pain, and activate the device for 20 minutes as soon as possible after a migraine attack began. They were instructed to use their smartphones to adjust the stimulation as appropriate during the treatment time. The stimulations were active programs at 80-120 Hz with pulse widths of 200, 150, 100, and 50 microseconds. The sham stimulation was a 0.1-Hz frequency with 45-microsecond pulses.
Overall, 64% of patients at the top three stimuli levels reduced their pain level by at least half 2 hours after the treatment, compared with 26% of patients using the sham stimulation. Average reductions were 46% for the 200-microsecond stimulus, 48% for 150, and 39% for 100.
In addition, 58% of the patients in the 200-microsecond group with moderate to severe pain at baseline reported reductions to mild or no pain, compared with 24% of sham patients.
Treatment with stimulation within 20 minutes of migraine onset was the most helpful, resulting in a 47% pain reduction, compared with a 25% reduction with delayed treatment, the researchers noted.
No patients reported side effects or adverse events related to the device.
The investigators said that complete 20-minute treatments were obtained for 70% of each of the top three stimuli levels, for 58% of treatments at 50-microsecond pulse widths, and for just 28% of placebo treatments. This low rate of completion of placebo stimuli may be the result of a loss of blinding for some of the sham activations, the investigators acknowledged, but they argued that “it is likely that this fact did not lead to falsely improved results; on the contrary, had those incomplete stimuli periods been completed, it is most likely that sham effectiveness results would have been lower than currently reported, making the results even more distinct.”
The study was funded by Theranica, and Dr. Yarnitsky disclosed serving on the company’s medical advisory board.
A wireless skin patch using electrical stimulation at an intensity lower than pain threshold reduced migraine pain when compared against sham stimulation in a trial of 71 adults with episodic migraine. The findings were published online March 1 in Neurology.
“Our rationale is activation of pain inhibitory centers, via the conditioned pain modulation effect; remote noxious stimuli can exert a generalized analgesic effect,” wrote David Yarnitsky, MD, of the Rambam Healthcare Campus and Technion Faculty of Medicine, Haifa, Israel, and his colleagues.
The devices were randomized to give a nonpainful sham stimulation at a very low frequency (controls) or a nonpainful active stimulation at one of four levels (active treatment). Patients were asked to place the wireless patch on the arm of their choice, regardless of the location of migraine pain, and activate the device for 20 minutes as soon as possible after a migraine attack began. They were instructed to use their smartphones to adjust the stimulation as appropriate during the treatment time. The stimulations were active programs at 80-120 Hz with pulse widths of 200, 150, 100, and 50 microseconds. The sham stimulation was a 0.1-Hz frequency with 45-microsecond pulses.
Overall, 64% of patients at the top three stimuli levels reduced their pain level by at least half 2 hours after the treatment, compared with 26% of patients using the sham stimulation. Average reductions were 46% for the 200-microsecond stimulus, 48% for 150, and 39% for 100.
In addition, 58% of the patients in the 200-microsecond group with moderate to severe pain at baseline reported reductions to mild or no pain, compared with 24% of sham patients.
Treatment with stimulation within 20 minutes of migraine onset was the most helpful, resulting in a 47% pain reduction, compared with a 25% reduction with delayed treatment, the researchers noted.
No patients reported side effects or adverse events related to the device.
The investigators said that complete 20-minute treatments were obtained for 70% of each of the top three stimuli levels, for 58% of treatments at 50-microsecond pulse widths, and for just 28% of placebo treatments. This low rate of completion of placebo stimuli may be the result of a loss of blinding for some of the sham activations, the investigators acknowledged, but they argued that “it is likely that this fact did not lead to falsely improved results; on the contrary, had those incomplete stimuli periods been completed, it is most likely that sham effectiveness results would have been lower than currently reported, making the results even more distinct.”
The study was funded by Theranica, and Dr. Yarnitsky disclosed serving on the company’s medical advisory board.
FROM NEUROLOGY
Key clinical point:
Major finding: A total of 64% of migraine patients experienced a 50% pain reduction when treated with a skin patch that delivered wireless, painless electrical stimulation, compared with 26% of patients who received sham treatment.
Data source: A prospective, double-blind, randomized, crossover, sham-controlled study including 71 adults and 299 episodes of migraine.
Disclosures: The study was funded by Theranica, and lead author Dr. Yarnitsky disclosed serving on the company’s medical advisory board.
Updated SSI prevention guidance highlights glucose control, MRSA
The guidelines for controlling surgical site infections have been updated to reflect evidence-based findings of a collaboration between surgeons and infection control experts from the American College of Surgeons, the ACS National Surgical Quality Improvement Program, and the Surgical Infection Society.
Updated strategies to reduce the risk of surgical site infections (SSIs) include perioperative glucose control in all patients and the use of oral antibiotics as an element of colon procedures, according to guidelines published in Journal of the American College of Surgeons (J Am Coll Surg. 2017;224:59-74).
Surgical site infections now account for 20% of all hospital-acquired infections, wrote lead author Kristen A. Ban, MD, a surgical resident at Loyola University Medical Center, Maywood, Ill., and her colleagues.
The most recent guidelines for preventing surgical site infections came from the Centers for Disease Control and Prevention in 1999; “the CDC has been working on an update since 2011, but this has been incredibly slow,” E. Patchen Dellinger, MD, of the University of Washington, Seattle, one of the guidelines’ authors, said in an interview. “A publication should be coming out sometime this year, but in the meantime, it was useful to have something for clinicians to refer to,” he said.
The researchers used PubMed to review specific topics in the SSI literature and address knowledge gaps.
Based on their findings, the new guidelines add recommendations to previous versions that address SSI prevention in the prehospital setting, at the hospital, and after discharge. The level of evidence to support each guideline varies; the researchers strongly recommend certain points, such as perioperative glucose control for all patients, not only those with diabetes; other recommendations such as postoperative showering 12 hours after surgery vs. delayed showering are left to the surgeon’s discretion.
“The changes/new recommendations since the 1999 guideline include the recommendation for the use of oral antibiotics with mechanical bowel prep for colon operations (in combination with intravenous prophylactic antibiotics), the control of perioperative glucose levels in ALL patients (not just diabetics), the maintenance of normothermia in the OR, the use of wound protectors for clean-contaminated cases, the use of antimicrobial sutures, and the use of increased FiO2 levels for intubated patients,” Dr. Dellinger said. These new elements also will be recommended when the updated CDC guidelines are released, and already have been recommended in recent guidelines from the World Health Organization, he added.
Guidelines for prehospital interventions include smoking cessation 4-6 weeks before surgery, preoperative bathing with chlorhexidine, glucose control for diabetes patients, MRSA screening, and bowel preparation (combining mechanical and antibiotic) for all elective colectomies.
Recommended hospital interventions include the following:
• Intraoperative normothermia.
• Use of wound protectors in open abdominal surgery.
• Use of triclosan antibiotic sutures.
• Supplemental oxygen.
• Antibiotic prophylaxis when indicated.
• Glucose control for all patients perioperatively.
• Hair removal only when necessary, avoiding a razor if possible.
• Alcohol-based skin preparation when possible.
• Surgical hand scrub.
• Facility scrub laundering and use of a skull cap if minimal hair is exposed.
• Use of double gloves and changing gloves before incision closure in colorectal cases.
• Use of new instruments for closure in colorectal cases.
• Purse string closure of stoma sites.
• Use of topical antibiotics as part of wound care.
• Using wound vacuum therapy over stapled skin.
Data on interventions after hospital discharge that may reduce SSI incidence are limited, the researchers said. No specific wound care protocols or surveillance methods have been identified. However, “promising new methods of surveillance are being explored, many of which use smartphone technology to help patients send their surgeon daily photos or updates,” they noted.
“Strategies to decrease SSI are multimodal and occur across a range of settings under the supervision of numerous providers,” the researchers wrote. “Ensuring high compliance with these risk-reduction strategies is crucial to the success of SSI reduction efforts,” they added.
However, changes to surgical practice don’t happen overnight, Dr. Dellinger said. “If all of these are actually adapted it should decrease SSI rates in all areas,” he noted. “Oral antibiotics for colorectal cases and glucose control for all patients will probably make the biggest benefit if actually adopted,” he said.
“We could use some better studies on the precise timing of parenteral prophylactic antibiotics,” said Dr. Dellinger. “One such study has been submitted from Switzerland and should be published sometime this year. Hard evidence on the best timing is missing although observational data allows some of us to come to conclusions on that,” he said. “Additional studies on perioperative oxygenation where fluid management and temperature management are better controlled would be helpful, and more and better studies are need for antimicrobial sutures,” he added.
The authors had nothing to disclose relevant to the scope of the guidelines. Outside the scope of this work, Dr. Dellinger disclosed serving on the advisory boards for 3M, Melinta, and Theravance, as well as receiving a grant from Motif for a clinical trial of iclaprim vs. vancomycin for the treatment of skin and soft tissue infections.
The guidelines for controlling surgical site infections have been updated to reflect evidence-based findings of a collaboration between surgeons and infection control experts from the American College of Surgeons, the ACS National Surgical Quality Improvement Program, and the Surgical Infection Society.
Updated strategies to reduce the risk of surgical site infections (SSIs) include perioperative glucose control in all patients and the use of oral antibiotics as an element of colon procedures, according to guidelines published in Journal of the American College of Surgeons (J Am Coll Surg. 2017;224:59-74).
Surgical site infections now account for 20% of all hospital-acquired infections, wrote lead author Kristen A. Ban, MD, a surgical resident at Loyola University Medical Center, Maywood, Ill., and her colleagues.
The most recent guidelines for preventing surgical site infections came from the Centers for Disease Control and Prevention in 1999; “the CDC has been working on an update since 2011, but this has been incredibly slow,” E. Patchen Dellinger, MD, of the University of Washington, Seattle, one of the guidelines’ authors, said in an interview. “A publication should be coming out sometime this year, but in the meantime, it was useful to have something for clinicians to refer to,” he said.
The researchers used PubMed to review specific topics in the SSI literature and address knowledge gaps.
Based on their findings, the new guidelines add recommendations to previous versions that address SSI prevention in the prehospital setting, at the hospital, and after discharge. The level of evidence to support each guideline varies; the researchers strongly recommend certain points, such as perioperative glucose control for all patients, not only those with diabetes; other recommendations such as postoperative showering 12 hours after surgery vs. delayed showering are left to the surgeon’s discretion.
“The changes/new recommendations since the 1999 guideline include the recommendation for the use of oral antibiotics with mechanical bowel prep for colon operations (in combination with intravenous prophylactic antibiotics), the control of perioperative glucose levels in ALL patients (not just diabetics), the maintenance of normothermia in the OR, the use of wound protectors for clean-contaminated cases, the use of antimicrobial sutures, and the use of increased FiO2 levels for intubated patients,” Dr. Dellinger said. These new elements also will be recommended when the updated CDC guidelines are released, and already have been recommended in recent guidelines from the World Health Organization, he added.
Guidelines for prehospital interventions include smoking cessation 4-6 weeks before surgery, preoperative bathing with chlorhexidine, glucose control for diabetes patients, MRSA screening, and bowel preparation (combining mechanical and antibiotic) for all elective colectomies.
Recommended hospital interventions include the following:
• Intraoperative normothermia.
• Use of wound protectors in open abdominal surgery.
• Use of triclosan antibiotic sutures.
• Supplemental oxygen.
• Antibiotic prophylaxis when indicated.
• Glucose control for all patients perioperatively.
• Hair removal only when necessary, avoiding a razor if possible.
• Alcohol-based skin preparation when possible.
• Surgical hand scrub.
• Facility scrub laundering and use of a skull cap if minimal hair is exposed.
• Use of double gloves and changing gloves before incision closure in colorectal cases.
• Use of new instruments for closure in colorectal cases.
• Purse string closure of stoma sites.
• Use of topical antibiotics as part of wound care.
• Using wound vacuum therapy over stapled skin.
Data on interventions after hospital discharge that may reduce SSI incidence are limited, the researchers said. No specific wound care protocols or surveillance methods have been identified. However, “promising new methods of surveillance are being explored, many of which use smartphone technology to help patients send their surgeon daily photos or updates,” they noted.
“Strategies to decrease SSI are multimodal and occur across a range of settings under the supervision of numerous providers,” the researchers wrote. “Ensuring high compliance with these risk-reduction strategies is crucial to the success of SSI reduction efforts,” they added.
However, changes to surgical practice don’t happen overnight, Dr. Dellinger said. “If all of these are actually adapted it should decrease SSI rates in all areas,” he noted. “Oral antibiotics for colorectal cases and glucose control for all patients will probably make the biggest benefit if actually adopted,” he said.
“We could use some better studies on the precise timing of parenteral prophylactic antibiotics,” said Dr. Dellinger. “One such study has been submitted from Switzerland and should be published sometime this year. Hard evidence on the best timing is missing although observational data allows some of us to come to conclusions on that,” he said. “Additional studies on perioperative oxygenation where fluid management and temperature management are better controlled would be helpful, and more and better studies are need for antimicrobial sutures,” he added.
The authors had nothing to disclose relevant to the scope of the guidelines. Outside the scope of this work, Dr. Dellinger disclosed serving on the advisory boards for 3M, Melinta, and Theravance, as well as receiving a grant from Motif for a clinical trial of iclaprim vs. vancomycin for the treatment of skin and soft tissue infections.
The guidelines for controlling surgical site infections have been updated to reflect evidence-based findings of a collaboration between surgeons and infection control experts from the American College of Surgeons, the ACS National Surgical Quality Improvement Program, and the Surgical Infection Society.
Updated strategies to reduce the risk of surgical site infections (SSIs) include perioperative glucose control in all patients and the use of oral antibiotics as an element of colon procedures, according to guidelines published in Journal of the American College of Surgeons (J Am Coll Surg. 2017;224:59-74).
Surgical site infections now account for 20% of all hospital-acquired infections, wrote lead author Kristen A. Ban, MD, a surgical resident at Loyola University Medical Center, Maywood, Ill., and her colleagues.
The most recent guidelines for preventing surgical site infections came from the Centers for Disease Control and Prevention in 1999; “the CDC has been working on an update since 2011, but this has been incredibly slow,” E. Patchen Dellinger, MD, of the University of Washington, Seattle, one of the guidelines’ authors, said in an interview. “A publication should be coming out sometime this year, but in the meantime, it was useful to have something for clinicians to refer to,” he said.
The researchers used PubMed to review specific topics in the SSI literature and address knowledge gaps.
Based on their findings, the new guidelines add recommendations to previous versions that address SSI prevention in the prehospital setting, at the hospital, and after discharge. The level of evidence to support each guideline varies; the researchers strongly recommend certain points, such as perioperative glucose control for all patients, not only those with diabetes; other recommendations such as postoperative showering 12 hours after surgery vs. delayed showering are left to the surgeon’s discretion.
“The changes/new recommendations since the 1999 guideline include the recommendation for the use of oral antibiotics with mechanical bowel prep for colon operations (in combination with intravenous prophylactic antibiotics), the control of perioperative glucose levels in ALL patients (not just diabetics), the maintenance of normothermia in the OR, the use of wound protectors for clean-contaminated cases, the use of antimicrobial sutures, and the use of increased FiO2 levels for intubated patients,” Dr. Dellinger said. These new elements also will be recommended when the updated CDC guidelines are released, and already have been recommended in recent guidelines from the World Health Organization, he added.
Guidelines for prehospital interventions include smoking cessation 4-6 weeks before surgery, preoperative bathing with chlorhexidine, glucose control for diabetes patients, MRSA screening, and bowel preparation (combining mechanical and antibiotic) for all elective colectomies.
Recommended hospital interventions include the following:
• Intraoperative normothermia.
• Use of wound protectors in open abdominal surgery.
• Use of triclosan antibiotic sutures.
• Supplemental oxygen.
• Antibiotic prophylaxis when indicated.
• Glucose control for all patients perioperatively.
• Hair removal only when necessary, avoiding a razor if possible.
• Alcohol-based skin preparation when possible.
• Surgical hand scrub.
• Facility scrub laundering and use of a skull cap if minimal hair is exposed.
• Use of double gloves and changing gloves before incision closure in colorectal cases.
• Use of new instruments for closure in colorectal cases.
• Purse string closure of stoma sites.
• Use of topical antibiotics as part of wound care.
• Using wound vacuum therapy over stapled skin.
Data on interventions after hospital discharge that may reduce SSI incidence are limited, the researchers said. No specific wound care protocols or surveillance methods have been identified. However, “promising new methods of surveillance are being explored, many of which use smartphone technology to help patients send their surgeon daily photos or updates,” they noted.
“Strategies to decrease SSI are multimodal and occur across a range of settings under the supervision of numerous providers,” the researchers wrote. “Ensuring high compliance with these risk-reduction strategies is crucial to the success of SSI reduction efforts,” they added.
However, changes to surgical practice don’t happen overnight, Dr. Dellinger said. “If all of these are actually adapted it should decrease SSI rates in all areas,” he noted. “Oral antibiotics for colorectal cases and glucose control for all patients will probably make the biggest benefit if actually adopted,” he said.
“We could use some better studies on the precise timing of parenteral prophylactic antibiotics,” said Dr. Dellinger. “One such study has been submitted from Switzerland and should be published sometime this year. Hard evidence on the best timing is missing although observational data allows some of us to come to conclusions on that,” he said. “Additional studies on perioperative oxygenation where fluid management and temperature management are better controlled would be helpful, and more and better studies are need for antimicrobial sutures,” he added.
The authors had nothing to disclose relevant to the scope of the guidelines. Outside the scope of this work, Dr. Dellinger disclosed serving on the advisory boards for 3M, Melinta, and Theravance, as well as receiving a grant from Motif for a clinical trial of iclaprim vs. vancomycin for the treatment of skin and soft tissue infections.
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF SURGEONS
Redefine dysplastic nevi to stratify cancer risk
WAILEA, HAWAII – It is time for a new system of classifying nevi, according to Ashfaq Marghoob, MD, of Memorial Sloan Kettering Cancer Center, New York.
“It was known for the last 30 or 40 years that we do need to subclassify nevi into groups, so as to better stratify for melanoma risk,” identifying groups of individuals who would benefit most from targeted screening, Dr. Marghoob said in a video interview at the meeting, provided by Global Academy for Medical Education/Skin Disease Education Foundation. But it has been clear that there are many flaws in the current classification system, he added.
This is beginning to change as new data emerge about gene mutations and other science that can better stratify “or segregate” the nevi into subsets, and “the hope is we will be better able to predict which subsets are associated with melanoma risk either within the lesion itself or poses an increased risk to the patient,” he explained.
“As our understanding grows, we will start to come out with subsets of nevi that have a certain clinical and dermoscopic morphology,” to help predict which patients would benefit most from being monitored very closely, with the aim of detecting – and curing – melanomas early, said Dr. Marghoob, director of Memorial Sloan Kettering’s regional skin cancer clinic in Hauppauge, N.Y.
He had no financial conflicts to disclose.
SDEF and this news organization are owned by the same parent organization.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – It is time for a new system of classifying nevi, according to Ashfaq Marghoob, MD, of Memorial Sloan Kettering Cancer Center, New York.
“It was known for the last 30 or 40 years that we do need to subclassify nevi into groups, so as to better stratify for melanoma risk,” identifying groups of individuals who would benefit most from targeted screening, Dr. Marghoob said in a video interview at the meeting, provided by Global Academy for Medical Education/Skin Disease Education Foundation. But it has been clear that there are many flaws in the current classification system, he added.
This is beginning to change as new data emerge about gene mutations and other science that can better stratify “or segregate” the nevi into subsets, and “the hope is we will be better able to predict which subsets are associated with melanoma risk either within the lesion itself or poses an increased risk to the patient,” he explained.
“As our understanding grows, we will start to come out with subsets of nevi that have a certain clinical and dermoscopic morphology,” to help predict which patients would benefit most from being monitored very closely, with the aim of detecting – and curing – melanomas early, said Dr. Marghoob, director of Memorial Sloan Kettering’s regional skin cancer clinic in Hauppauge, N.Y.
He had no financial conflicts to disclose.
SDEF and this news organization are owned by the same parent organization.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – It is time for a new system of classifying nevi, according to Ashfaq Marghoob, MD, of Memorial Sloan Kettering Cancer Center, New York.
“It was known for the last 30 or 40 years that we do need to subclassify nevi into groups, so as to better stratify for melanoma risk,” identifying groups of individuals who would benefit most from targeted screening, Dr. Marghoob said in a video interview at the meeting, provided by Global Academy for Medical Education/Skin Disease Education Foundation. But it has been clear that there are many flaws in the current classification system, he added.
This is beginning to change as new data emerge about gene mutations and other science that can better stratify “or segregate” the nevi into subsets, and “the hope is we will be better able to predict which subsets are associated with melanoma risk either within the lesion itself or poses an increased risk to the patient,” he explained.
“As our understanding grows, we will start to come out with subsets of nevi that have a certain clinical and dermoscopic morphology,” to help predict which patients would benefit most from being monitored very closely, with the aim of detecting – and curing – melanomas early, said Dr. Marghoob, director of Memorial Sloan Kettering’s regional skin cancer clinic in Hauppauge, N.Y.
He had no financial conflicts to disclose.
SDEF and this news organization are owned by the same parent organization.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT SDEF HAWAII DERMATOLOGY SEMINAR
VIDEO: Molecular testing helps pinpoint ambiguous lesions
WAILEA, HAWAII – In a video interview, Pedram Gerami, MD, professor of dermatology, pathology, and pediatrics, Northwestern University, Chicago, discusses the use of molecular testing for melanoma and suspicious lesions.
Molecular tests are available for various components of diagnosis and prognosis of melanoma, and one of the most popular scenarios for their use is to confirm a diagnosis if a lesion is biopsied and the histopathologist “feels that the diagnosis is ambiguous by standard pathology methods,” Dr. Gerami said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
On average, between 1% and 5% of cases of suspicious lesions may need molecular testing to confirm the diagnosis, he noted. Of the available options for molecular testing, FISH (fluorescence in situ hybridization) testing is the most validated in the setting of ambiguous histology, he said.
Dr. Gerami disclosed serving as a consultant and researcher for Castle Biosciences, Myriad Genetics, and DermTech.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – In a video interview, Pedram Gerami, MD, professor of dermatology, pathology, and pediatrics, Northwestern University, Chicago, discusses the use of molecular testing for melanoma and suspicious lesions.
Molecular tests are available for various components of diagnosis and prognosis of melanoma, and one of the most popular scenarios for their use is to confirm a diagnosis if a lesion is biopsied and the histopathologist “feels that the diagnosis is ambiguous by standard pathology methods,” Dr. Gerami said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
On average, between 1% and 5% of cases of suspicious lesions may need molecular testing to confirm the diagnosis, he noted. Of the available options for molecular testing, FISH (fluorescence in situ hybridization) testing is the most validated in the setting of ambiguous histology, he said.
Dr. Gerami disclosed serving as a consultant and researcher for Castle Biosciences, Myriad Genetics, and DermTech.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – In a video interview, Pedram Gerami, MD, professor of dermatology, pathology, and pediatrics, Northwestern University, Chicago, discusses the use of molecular testing for melanoma and suspicious lesions.
Molecular tests are available for various components of diagnosis and prognosis of melanoma, and one of the most popular scenarios for their use is to confirm a diagnosis if a lesion is biopsied and the histopathologist “feels that the diagnosis is ambiguous by standard pathology methods,” Dr. Gerami said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
On average, between 1% and 5% of cases of suspicious lesions may need molecular testing to confirm the diagnosis, he noted. Of the available options for molecular testing, FISH (fluorescence in situ hybridization) testing is the most validated in the setting of ambiguous histology, he said.
Dr. Gerami disclosed serving as a consultant and researcher for Castle Biosciences, Myriad Genetics, and DermTech.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT SDEF HAWAII DERMATOLOGY SEMINAR
FDA confirms complications from intragastric balloons
Complications from overinflation and acute pancreatitis can create problems for obesity patients treated with intragastric balloons, according to a statement from the Food and Drug Administration. In a letter to health care providers published on February 9, 2017, the FDA warned of the two specific issues that have been the subject of multiple adverse event reports.
“We recommend that you closely monitor patients with these devices for these adverse events, and to submit reports to help us better understand any complications from the use of these obesity treatment devices,” the letter said.
Most of the overinflation reports involved the Orbera Intragastric Balloon System (Apollo Endosurgery) that uses a single balloon, although some reports involved the ReShape Integrated Dual Balloon System (ReShape Medical) that uses two balloons. Neither product mentions overinflation risk in its labeling. “At this moment there is not enough information to determine what is causing the balloon to overinflate,” according to the FDA letter.
A separate set of adverse event reports noted the development of acute pancreatitis caused when the balloons compressed other gastrointestinal structures. Both the Orbera and ReShape products were associated with pancreatitis, although neither lists pancreatitis as a potential complication on their labels. Pancreatitis was reported as early as 3 days after implantation, and symptoms included severe back and abdominal pain.
The FDA letter recommends that health care providers consider overinflation and pancreatitis in their differential diagnoses of obesity patients with intragastric balloons who present with the symptoms described, and to report any type of serious adverse events associated with intragastric balloons to the FDA through the MedWatch program. For more information about reporting adverse events to the FDA, visit the MedWatch site.
Complications from overinflation and acute pancreatitis can create problems for obesity patients treated with intragastric balloons, according to a statement from the Food and Drug Administration. In a letter to health care providers published on February 9, 2017, the FDA warned of the two specific issues that have been the subject of multiple adverse event reports.
“We recommend that you closely monitor patients with these devices for these adverse events, and to submit reports to help us better understand any complications from the use of these obesity treatment devices,” the letter said.
Most of the overinflation reports involved the Orbera Intragastric Balloon System (Apollo Endosurgery) that uses a single balloon, although some reports involved the ReShape Integrated Dual Balloon System (ReShape Medical) that uses two balloons. Neither product mentions overinflation risk in its labeling. “At this moment there is not enough information to determine what is causing the balloon to overinflate,” according to the FDA letter.
A separate set of adverse event reports noted the development of acute pancreatitis caused when the balloons compressed other gastrointestinal structures. Both the Orbera and ReShape products were associated with pancreatitis, although neither lists pancreatitis as a potential complication on their labels. Pancreatitis was reported as early as 3 days after implantation, and symptoms included severe back and abdominal pain.
The FDA letter recommends that health care providers consider overinflation and pancreatitis in their differential diagnoses of obesity patients with intragastric balloons who present with the symptoms described, and to report any type of serious adverse events associated with intragastric balloons to the FDA through the MedWatch program. For more information about reporting adverse events to the FDA, visit the MedWatch site.
Complications from overinflation and acute pancreatitis can create problems for obesity patients treated with intragastric balloons, according to a statement from the Food and Drug Administration. In a letter to health care providers published on February 9, 2017, the FDA warned of the two specific issues that have been the subject of multiple adverse event reports.
“We recommend that you closely monitor patients with these devices for these adverse events, and to submit reports to help us better understand any complications from the use of these obesity treatment devices,” the letter said.
Most of the overinflation reports involved the Orbera Intragastric Balloon System (Apollo Endosurgery) that uses a single balloon, although some reports involved the ReShape Integrated Dual Balloon System (ReShape Medical) that uses two balloons. Neither product mentions overinflation risk in its labeling. “At this moment there is not enough information to determine what is causing the balloon to overinflate,” according to the FDA letter.
A separate set of adverse event reports noted the development of acute pancreatitis caused when the balloons compressed other gastrointestinal structures. Both the Orbera and ReShape products were associated with pancreatitis, although neither lists pancreatitis as a potential complication on their labels. Pancreatitis was reported as early as 3 days after implantation, and symptoms included severe back and abdominal pain.
The FDA letter recommends that health care providers consider overinflation and pancreatitis in their differential diagnoses of obesity patients with intragastric balloons who present with the symptoms described, and to report any type of serious adverse events associated with intragastric balloons to the FDA through the MedWatch program. For more information about reporting adverse events to the FDA, visit the MedWatch site.
Collaborative care aids seniors’ mild depression
A collaborative care model significantly mitigated mild depression in adults aged 65 and older, compared with usual care in the short term, based on data from 705 patients. The findings were published online Feb. 21.
“There is limited research about older people with mild depressive disorders who have insufficient levels of depressive symptoms to meet diagnostic criteria (called subclinical, subthreshold, or subsyndromal depression) but also reduced quality of life and function,” wrote Simon Gilbody, PhD, of the University of York (England) and colleagues. However, subthreshold depression increases the risk of a severe depressive illness, the researchers added.
Overall, patients in the collaborative care group improved from an average score of 7.8 at baseline to 5.4 after 4 months; the usual care group improved from an average of 7.8 at baseline to 6.7 at 4 months. The difference in scores persisted at 12 months in the secondary analysis (JAMA. 2017;317:728-37. doi: 10.1001/jama.2017.0130). “For populations with case-level depression, a successful treatment outcome has been defined as 5 points on the PHQ-9,” the researchers noted. “This magnitude of benefit was not observed in either group of the trial when comparing scores before and after treatment, although this result would be anticipated given the lower baseline PHQ-9 scores in populations with subthreshold depression.’
The study participants came from 32 primary care practices in northern England; the average age was 77 years, and 58% were women.
The results were limited by several factors, including the absence of a standardized interview to diagnose depression, differences in retention and attrition between groups, and the absence of long-term follow-up, “and further research is needed to assess longer-term efficacy,” the researchers said.
Neither Dr. Gilbody nor his colleagues had financial conflicts to disclose.
The CASPER trial “provides the first evidence that collaborative care may benefit patients with subthreshold depression,” Kurt Kroenke, MD, wrote in an accompanying editorial. In addition to the improvements on the Patient Health Questionnaire and the reduction in risk of progression to threshold level depression, the findings further support the use of behavioral activation, which was the core treatment in the study, he said. “Strong evidence for the effectiveness of behavioral activation was provided by the recent COBRA trial. … and behavioral activation was found to be noninferior to cognitive-behavioral therapy for the outcome of depression,” he wrote. However, more research is needed before clinicians routinely expand treatment beyond major depression to include subthreshold depression, Dr. Kroenke noted. Key factors include the variable rate of progression from subthreshold depression to major depression, the duration and context of subthreshold depression, patient preferences, and the possible role of antidepressants, he noted. However, the CASPER findings show “new evidence that collaborative care improves outcomes for at least some patients with subthreshold depression,” Dr. Kroenke said. “Patients with persistent symptoms, functional impairment, and a desire for treatment may particularly benefit,” he added (JAMA. 2017;317:702-4).
Kurt Kroenke, MD, is affiliated with the VA Health Services Research and Development Service Center for Health Communication and Information, Regenstrief Institute and Indiana University, both in Indianapolis. He had no financial conflicts to disclose.
The CASPER trial “provides the first evidence that collaborative care may benefit patients with subthreshold depression,” Kurt Kroenke, MD, wrote in an accompanying editorial. In addition to the improvements on the Patient Health Questionnaire and the reduction in risk of progression to threshold level depression, the findings further support the use of behavioral activation, which was the core treatment in the study, he said. “Strong evidence for the effectiveness of behavioral activation was provided by the recent COBRA trial. … and behavioral activation was found to be noninferior to cognitive-behavioral therapy for the outcome of depression,” he wrote. However, more research is needed before clinicians routinely expand treatment beyond major depression to include subthreshold depression, Dr. Kroenke noted. Key factors include the variable rate of progression from subthreshold depression to major depression, the duration and context of subthreshold depression, patient preferences, and the possible role of antidepressants, he noted. However, the CASPER findings show “new evidence that collaborative care improves outcomes for at least some patients with subthreshold depression,” Dr. Kroenke said. “Patients with persistent symptoms, functional impairment, and a desire for treatment may particularly benefit,” he added (JAMA. 2017;317:702-4).
Kurt Kroenke, MD, is affiliated with the VA Health Services Research and Development Service Center for Health Communication and Information, Regenstrief Institute and Indiana University, both in Indianapolis. He had no financial conflicts to disclose.
The CASPER trial “provides the first evidence that collaborative care may benefit patients with subthreshold depression,” Kurt Kroenke, MD, wrote in an accompanying editorial. In addition to the improvements on the Patient Health Questionnaire and the reduction in risk of progression to threshold level depression, the findings further support the use of behavioral activation, which was the core treatment in the study, he said. “Strong evidence for the effectiveness of behavioral activation was provided by the recent COBRA trial. … and behavioral activation was found to be noninferior to cognitive-behavioral therapy for the outcome of depression,” he wrote. However, more research is needed before clinicians routinely expand treatment beyond major depression to include subthreshold depression, Dr. Kroenke noted. Key factors include the variable rate of progression from subthreshold depression to major depression, the duration and context of subthreshold depression, patient preferences, and the possible role of antidepressants, he noted. However, the CASPER findings show “new evidence that collaborative care improves outcomes for at least some patients with subthreshold depression,” Dr. Kroenke said. “Patients with persistent symptoms, functional impairment, and a desire for treatment may particularly benefit,” he added (JAMA. 2017;317:702-4).
Kurt Kroenke, MD, is affiliated with the VA Health Services Research and Development Service Center for Health Communication and Information, Regenstrief Institute and Indiana University, both in Indianapolis. He had no financial conflicts to disclose.
A collaborative care model significantly mitigated mild depression in adults aged 65 and older, compared with usual care in the short term, based on data from 705 patients. The findings were published online Feb. 21.
“There is limited research about older people with mild depressive disorders who have insufficient levels of depressive symptoms to meet diagnostic criteria (called subclinical, subthreshold, or subsyndromal depression) but also reduced quality of life and function,” wrote Simon Gilbody, PhD, of the University of York (England) and colleagues. However, subthreshold depression increases the risk of a severe depressive illness, the researchers added.
Overall, patients in the collaborative care group improved from an average score of 7.8 at baseline to 5.4 after 4 months; the usual care group improved from an average of 7.8 at baseline to 6.7 at 4 months. The difference in scores persisted at 12 months in the secondary analysis (JAMA. 2017;317:728-37. doi: 10.1001/jama.2017.0130). “For populations with case-level depression, a successful treatment outcome has been defined as 5 points on the PHQ-9,” the researchers noted. “This magnitude of benefit was not observed in either group of the trial when comparing scores before and after treatment, although this result would be anticipated given the lower baseline PHQ-9 scores in populations with subthreshold depression.’
The study participants came from 32 primary care practices in northern England; the average age was 77 years, and 58% were women.
The results were limited by several factors, including the absence of a standardized interview to diagnose depression, differences in retention and attrition between groups, and the absence of long-term follow-up, “and further research is needed to assess longer-term efficacy,” the researchers said.
Neither Dr. Gilbody nor his colleagues had financial conflicts to disclose.
A collaborative care model significantly mitigated mild depression in adults aged 65 and older, compared with usual care in the short term, based on data from 705 patients. The findings were published online Feb. 21.
“There is limited research about older people with mild depressive disorders who have insufficient levels of depressive symptoms to meet diagnostic criteria (called subclinical, subthreshold, or subsyndromal depression) but also reduced quality of life and function,” wrote Simon Gilbody, PhD, of the University of York (England) and colleagues. However, subthreshold depression increases the risk of a severe depressive illness, the researchers added.
Overall, patients in the collaborative care group improved from an average score of 7.8 at baseline to 5.4 after 4 months; the usual care group improved from an average of 7.8 at baseline to 6.7 at 4 months. The difference in scores persisted at 12 months in the secondary analysis (JAMA. 2017;317:728-37. doi: 10.1001/jama.2017.0130). “For populations with case-level depression, a successful treatment outcome has been defined as 5 points on the PHQ-9,” the researchers noted. “This magnitude of benefit was not observed in either group of the trial when comparing scores before and after treatment, although this result would be anticipated given the lower baseline PHQ-9 scores in populations with subthreshold depression.’
The study participants came from 32 primary care practices in northern England; the average age was 77 years, and 58% were women.
The results were limited by several factors, including the absence of a standardized interview to diagnose depression, differences in retention and attrition between groups, and the absence of long-term follow-up, “and further research is needed to assess longer-term efficacy,” the researchers said.
Neither Dr. Gilbody nor his colleagues had financial conflicts to disclose.
FROM JAMA
Key clinical point: Collaborative care reduced subthreshold depression in older adults, compared with usual care after 4 months.
Major finding: Older adults with subthreshold depression who received collaborative care had lower depression scores on the Patient Health Questionnaire than those who received usual care after 4 months (average scores 5.4 and 6.7, respectively).
Data source: A randomized trial of 705 adults aged 65 years and older with subthreshold depression.
Disclosures: The researchers had no financial conflicts to disclose.
VIDEO: Coffee break at the Hawaii Dermatology Seminar
WAILEA, HAWAII – A few attendees at the Hawaii Dermatology Seminar discussed some of the highlights of the presentations during a coffee break at the meeting.
New treatment protocols for psoriasis, details about skin disease in children, managing medication side effects, and promising data about biologics are discussed in this video, as are updates on the latest tips for treating atopic dermatitis.
The interviewees had no conflicts to disclose.
The meeting is provided by Global Academy for Medical Education/Skin Disease Education Foundation. SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – A few attendees at the Hawaii Dermatology Seminar discussed some of the highlights of the presentations during a coffee break at the meeting.
New treatment protocols for psoriasis, details about skin disease in children, managing medication side effects, and promising data about biologics are discussed in this video, as are updates on the latest tips for treating atopic dermatitis.
The interviewees had no conflicts to disclose.
The meeting is provided by Global Academy for Medical Education/Skin Disease Education Foundation. SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – A few attendees at the Hawaii Dermatology Seminar discussed some of the highlights of the presentations during a coffee break at the meeting.
New treatment protocols for psoriasis, details about skin disease in children, managing medication side effects, and promising data about biologics are discussed in this video, as are updates on the latest tips for treating atopic dermatitis.
The interviewees had no conflicts to disclose.
The meeting is provided by Global Academy for Medical Education/Skin Disease Education Foundation. SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT SDEF HAWAII DERMATOLOGY SEMINAR