User login
Daily Recap: COVID-19 care delays mean excess cancer deaths; flu vaccine recommendations
Here are the stories our MDedge editors across specialties think you need to know about today:
COVID-related care delays mean excess cancer deaths
There could be 10,000 excess deaths from breast and colorectal cancer over the next 10 years as a result of missed screenings, delays in diagnosis, and reductions in oncology care caused by the COVID-19 pandemic, according to predictions generated by a National Cancer Institute model.
The number of excess deaths per year would peak in the next year or two, likely sooner for colorectal cancer than for breast cancer.
In an editorial published June 19 in Science, NCI Director Norman “Ned” Sharpless, MD, highlighted the modeling. In an interview, he pointed out that this analysis is conservative because the researchers evaluated only two types of cancer. They chose breast and colorectal cancer because these are common cancers – accounting for about one-sixth of all cancers – with relatively high screening rates.
“We didn’t model other cancer types, but we have no reason to think that we’re not going to see the same thing with other types of malignancies,” he said. “That is a significant amount of excess mortality.” Read more.
Diabetes control in U.S. youth has worsened over time
Glycemic control among youth with diabetes is no better today than it was in 2002 and in some subgroups it’s worse, according to data reported at the virtual American Diabetes Association scientific sessions. This finding comes despite the increased availability of diabetes technology, newer therapies, and more aggressive recommended blood glucose targets.
A particularly striking data point was seen among youth who had type 2 diabetes for 10 years or more: average A1c skyrocketed from 7.9% in 2008-2013 to 10.1% in 2014-2019. The numbers were small, 25 patients in the earlier cohort and 149 patients in the later, yet the difference was still statistically significant.
“Our finding that current youth and young adults with diabetes are not demonstrating improved glycemic control, compared to earlier cohorts in the SEARCH study, was surprising given how the landscape of diabetes management has changed dramatically over the past decade,” Faisal S. Malik, MD, of the University of Washington, Seattle, and Seattle Children’s Research Institute, said in an interview. Read more.
CDC advisors approve flu vaccine recommendations for 2020-2021
A pair of new vaccines for adults aged 65 years and older will be available for the 2020-2021 flu season – Fluzone high-dose quadrivalent, which replaces the trivalent Fluzone high-dose and Fluad quadrivalent (Seqirus), according to the Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices.
At a virtual meeting on June 24, the committee voted unanimously to approve the vaccine recommendations for annual influenza immunization of all individuals aged 6 months and older. They also voted to accept some guidance and language changes to the recommendations. Read more.
How can we better engage black men as patients?
In a new commentary, Kevin M. Simon, MD, seeks to answer a key question: “How do psychiatrists and other mental health clinicians better engage men of color?” Dr. Simon, a psychiatrist at Boston Children’s Hospital, recommends creating a comfortable environment, allowing for storytelling, assuring confidentiality, being aware of nonverbal language, and being respectful.
“Those on the front lines providing mental health services should understand black men’s mental health from an ecological perspective. Beyond the emotional burden that mental illness imposes on the individual, there are more considerable interpersonal and societal implications for the state of black men’s mental health. As such, in our full capacity like other men, black men play an essential role within families, churches, neighborhoods, and organizations,” Dr. Simon wrote. Read more.
For more on COVID-19, visit our Resource Center. All of our latest news is available on MDedge.com.
Here are the stories our MDedge editors across specialties think you need to know about today:
COVID-related care delays mean excess cancer deaths
There could be 10,000 excess deaths from breast and colorectal cancer over the next 10 years as a result of missed screenings, delays in diagnosis, and reductions in oncology care caused by the COVID-19 pandemic, according to predictions generated by a National Cancer Institute model.
The number of excess deaths per year would peak in the next year or two, likely sooner for colorectal cancer than for breast cancer.
In an editorial published June 19 in Science, NCI Director Norman “Ned” Sharpless, MD, highlighted the modeling. In an interview, he pointed out that this analysis is conservative because the researchers evaluated only two types of cancer. They chose breast and colorectal cancer because these are common cancers – accounting for about one-sixth of all cancers – with relatively high screening rates.
“We didn’t model other cancer types, but we have no reason to think that we’re not going to see the same thing with other types of malignancies,” he said. “That is a significant amount of excess mortality.” Read more.
Diabetes control in U.S. youth has worsened over time
Glycemic control among youth with diabetes is no better today than it was in 2002 and in some subgroups it’s worse, according to data reported at the virtual American Diabetes Association scientific sessions. This finding comes despite the increased availability of diabetes technology, newer therapies, and more aggressive recommended blood glucose targets.
A particularly striking data point was seen among youth who had type 2 diabetes for 10 years or more: average A1c skyrocketed from 7.9% in 2008-2013 to 10.1% in 2014-2019. The numbers were small, 25 patients in the earlier cohort and 149 patients in the later, yet the difference was still statistically significant.
“Our finding that current youth and young adults with diabetes are not demonstrating improved glycemic control, compared to earlier cohorts in the SEARCH study, was surprising given how the landscape of diabetes management has changed dramatically over the past decade,” Faisal S. Malik, MD, of the University of Washington, Seattle, and Seattle Children’s Research Institute, said in an interview. Read more.
CDC advisors approve flu vaccine recommendations for 2020-2021
A pair of new vaccines for adults aged 65 years and older will be available for the 2020-2021 flu season – Fluzone high-dose quadrivalent, which replaces the trivalent Fluzone high-dose and Fluad quadrivalent (Seqirus), according to the Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices.
At a virtual meeting on June 24, the committee voted unanimously to approve the vaccine recommendations for annual influenza immunization of all individuals aged 6 months and older. They also voted to accept some guidance and language changes to the recommendations. Read more.
How can we better engage black men as patients?
In a new commentary, Kevin M. Simon, MD, seeks to answer a key question: “How do psychiatrists and other mental health clinicians better engage men of color?” Dr. Simon, a psychiatrist at Boston Children’s Hospital, recommends creating a comfortable environment, allowing for storytelling, assuring confidentiality, being aware of nonverbal language, and being respectful.
“Those on the front lines providing mental health services should understand black men’s mental health from an ecological perspective. Beyond the emotional burden that mental illness imposes on the individual, there are more considerable interpersonal and societal implications for the state of black men’s mental health. As such, in our full capacity like other men, black men play an essential role within families, churches, neighborhoods, and organizations,” Dr. Simon wrote. Read more.
For more on COVID-19, visit our Resource Center. All of our latest news is available on MDedge.com.
Here are the stories our MDedge editors across specialties think you need to know about today:
COVID-related care delays mean excess cancer deaths
There could be 10,000 excess deaths from breast and colorectal cancer over the next 10 years as a result of missed screenings, delays in diagnosis, and reductions in oncology care caused by the COVID-19 pandemic, according to predictions generated by a National Cancer Institute model.
The number of excess deaths per year would peak in the next year or two, likely sooner for colorectal cancer than for breast cancer.
In an editorial published June 19 in Science, NCI Director Norman “Ned” Sharpless, MD, highlighted the modeling. In an interview, he pointed out that this analysis is conservative because the researchers evaluated only two types of cancer. They chose breast and colorectal cancer because these are common cancers – accounting for about one-sixth of all cancers – with relatively high screening rates.
“We didn’t model other cancer types, but we have no reason to think that we’re not going to see the same thing with other types of malignancies,” he said. “That is a significant amount of excess mortality.” Read more.
Diabetes control in U.S. youth has worsened over time
Glycemic control among youth with diabetes is no better today than it was in 2002 and in some subgroups it’s worse, according to data reported at the virtual American Diabetes Association scientific sessions. This finding comes despite the increased availability of diabetes technology, newer therapies, and more aggressive recommended blood glucose targets.
A particularly striking data point was seen among youth who had type 2 diabetes for 10 years or more: average A1c skyrocketed from 7.9% in 2008-2013 to 10.1% in 2014-2019. The numbers were small, 25 patients in the earlier cohort and 149 patients in the later, yet the difference was still statistically significant.
“Our finding that current youth and young adults with diabetes are not demonstrating improved glycemic control, compared to earlier cohorts in the SEARCH study, was surprising given how the landscape of diabetes management has changed dramatically over the past decade,” Faisal S. Malik, MD, of the University of Washington, Seattle, and Seattle Children’s Research Institute, said in an interview. Read more.
CDC advisors approve flu vaccine recommendations for 2020-2021
A pair of new vaccines for adults aged 65 years and older will be available for the 2020-2021 flu season – Fluzone high-dose quadrivalent, which replaces the trivalent Fluzone high-dose and Fluad quadrivalent (Seqirus), according to the Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices.
At a virtual meeting on June 24, the committee voted unanimously to approve the vaccine recommendations for annual influenza immunization of all individuals aged 6 months and older. They also voted to accept some guidance and language changes to the recommendations. Read more.
How can we better engage black men as patients?
In a new commentary, Kevin M. Simon, MD, seeks to answer a key question: “How do psychiatrists and other mental health clinicians better engage men of color?” Dr. Simon, a psychiatrist at Boston Children’s Hospital, recommends creating a comfortable environment, allowing for storytelling, assuring confidentiality, being aware of nonverbal language, and being respectful.
“Those on the front lines providing mental health services should understand black men’s mental health from an ecological perspective. Beyond the emotional burden that mental illness imposes on the individual, there are more considerable interpersonal and societal implications for the state of black men’s mental health. As such, in our full capacity like other men, black men play an essential role within families, churches, neighborhoods, and organizations,” Dr. Simon wrote. Read more.
For more on COVID-19, visit our Resource Center. All of our latest news is available on MDedge.com.
More than 10,000 excess cancer deaths because of COVID-19 delays
A model created by the National Cancer Institute predicts that tens of thousands of excess cancer deaths will occur over the next decade as a result of missed screenings, delays in diagnosis, and reductions in oncology care caused by the COVID-19 pandemic.
“As director of NCI, I am deeply concerned about the potential impacts of delayed diagnoses and deferred or modified treatment plans on cancer incidence and mortality,” said Norman “Ned” Sharpless, MD.
“In the past 3 decades, we have seen steady and strong progress against death and suffering from cancer, thanks to improvements in prevention, screening, diagnosis, and treatment. I worry that the SARS-CoV-2 pandemic has put those decades of steady progress at risk and may precipitate reversals of these trends.”
In an editorial published June 19 in Science, Dr. Sharpless highlighted modeling performed by the NCI that predicts an excess of 10,000 deaths from breast and colorectal cancer over the next 10 years.
The number of excess deaths per year would peak in the next year or 2, likely sooner for colorectal than for breast cancer, but “for both cancer types, we believe the pandemic will influence cancer deaths for at least a decade.”
In an interview, Dr. Sharpless pointed out that this analysis is conservative because the researchers only evaluated two types of cancer. They chose breast and colorectal cancer because these are common cancers (accounting for about one-sixth of all cancers) with relatively high screening rates.
“We didn’t model other cancer types, but we have no reason to think that we’re not going to see the same thing with other types of malignancies,” he said. “That is a significant amount of excess mortality.”
Delayed diagnosis, modified therapy
One of the effects of the pandemic has been to cause delays in cancer diagnosis. “Routine screening has plummeted and is running at less than 90% in some systems,” Dr. Sharpless said.
“Most cancers are diagnosed when people experience symptoms and go see their doctors, and those symptomatic screening events are also not happening,” he continued. “Fear of contracting the coronavirus in health care settings has dissuaded people from visits.”
In some cases, a delay in diagnosis will allow the cancer to progress to a more advanced stage. “The earlier the diagnosis, the better, and if the stages are more advanced, patients will not do as well for virtually every kind of cancer,” he said.
In addition to delays in diagnosis, treatments are being postponed or modified for patients recently diagnosed with cancer. Because of delays and reductions in curative therapies, patients may be receiving less than optimal care.
“We are seeing a lot of nonstandard care,” said Dr. Sharpless. “All of these things add up to increased cancer morbidity and mortality.”
He also pointed out that the term “elective” is confusing and problematic. “It doesn’t mean that it’s not needed, just that it’s not an emergency and doesn’t need to be done today,” said Dr. Sharpless. “But if we’re talking about chemotherapy and surgery, we don’t think they can be delayed for too long – maybe a week, but not for several months.”
Dr. Sharpless feels that overall it is time for cancer care to resume as much as possible, because “ignoring cancer for too long is an untenable choice and may turn one public health crisis into another.”
“If we act now, we can make up for lost time,” he wrote in the editorial. “Clearly, postponing procedures and deferring care due to the pandemic was prudent at one time, but now that we have made it through the initial shock of the pandemic, I believe it is time to resume robust cancer care.”
Through their network of cancer centers, researchers with the NCI can develop innovative solutions that allow screening and treatment to move forward while maintaining safety. “We need to make patients feel safe, and we have to answer important questions quickly,” he said.
Impact of COVID-19 on cancer care
The COVID-19 pandemic has overwhelmed health care systems worldwide and has created major challenges for clinicians who are caring for patients with cancer.
As previously reported, hospitals reprioritized resources for an impending onslaught of COVID-19 patients. Services and procedures deemed to be nonessential were canceled or delayed, including surgeries and imaging.
In a survey conducted by the American Cancer Society Cancer Action Network, half of the 1219 respondents reported changes, delays, or disruptions to the care they were receiving. The services most frequently affected included in-person provider visits (50%), supportive services (20%), and imaging procedures to monitor tumor growth (20%).
In addition, 8% reported that their treatment, including chemotherapy and immunotherapy, had been affected by the COVID-19 pandemic.
In the United Kingdom, Cancer Research UK estimated that because of the disruption to cancer services, 2.4 million people did not undergo cancer screening or further testing or did not receive cancer treatment and that tens of thousands of cases have gone undiagnosed.
Similarly, a survey by Macmillan Cancer Support showed that almost half (45%) of cancer patients have experienced delays or cancellations of cancer treatments, or their treatments have been altered as a result of coronavirus, leaving many living in fear. Calling cancer “the forgotten C” of the pandemic, it warned of a potential cancer “time bomb” when, as the number of deaths from COVID-19 falls, cancer returns as the leading cause of death in the United Kingdom.
Last month, a report also predicted that there will be an excess of cancer deaths in both the United States and United Kingdom because of patients not accessing health care services.
The authors calculated that there will be 6270 excess deaths among cancer patients 1 year from now in England and 33,890 excess deaths among cancer patients older than 40 years in the United States.
This article first appeared on Medscape.com.
A model created by the National Cancer Institute predicts that tens of thousands of excess cancer deaths will occur over the next decade as a result of missed screenings, delays in diagnosis, and reductions in oncology care caused by the COVID-19 pandemic.
“As director of NCI, I am deeply concerned about the potential impacts of delayed diagnoses and deferred or modified treatment plans on cancer incidence and mortality,” said Norman “Ned” Sharpless, MD.
“In the past 3 decades, we have seen steady and strong progress against death and suffering from cancer, thanks to improvements in prevention, screening, diagnosis, and treatment. I worry that the SARS-CoV-2 pandemic has put those decades of steady progress at risk and may precipitate reversals of these trends.”
In an editorial published June 19 in Science, Dr. Sharpless highlighted modeling performed by the NCI that predicts an excess of 10,000 deaths from breast and colorectal cancer over the next 10 years.
The number of excess deaths per year would peak in the next year or 2, likely sooner for colorectal than for breast cancer, but “for both cancer types, we believe the pandemic will influence cancer deaths for at least a decade.”
In an interview, Dr. Sharpless pointed out that this analysis is conservative because the researchers only evaluated two types of cancer. They chose breast and colorectal cancer because these are common cancers (accounting for about one-sixth of all cancers) with relatively high screening rates.
“We didn’t model other cancer types, but we have no reason to think that we’re not going to see the same thing with other types of malignancies,” he said. “That is a significant amount of excess mortality.”
Delayed diagnosis, modified therapy
One of the effects of the pandemic has been to cause delays in cancer diagnosis. “Routine screening has plummeted and is running at less than 90% in some systems,” Dr. Sharpless said.
“Most cancers are diagnosed when people experience symptoms and go see their doctors, and those symptomatic screening events are also not happening,” he continued. “Fear of contracting the coronavirus in health care settings has dissuaded people from visits.”
In some cases, a delay in diagnosis will allow the cancer to progress to a more advanced stage. “The earlier the diagnosis, the better, and if the stages are more advanced, patients will not do as well for virtually every kind of cancer,” he said.
In addition to delays in diagnosis, treatments are being postponed or modified for patients recently diagnosed with cancer. Because of delays and reductions in curative therapies, patients may be receiving less than optimal care.
“We are seeing a lot of nonstandard care,” said Dr. Sharpless. “All of these things add up to increased cancer morbidity and mortality.”
He also pointed out that the term “elective” is confusing and problematic. “It doesn’t mean that it’s not needed, just that it’s not an emergency and doesn’t need to be done today,” said Dr. Sharpless. “But if we’re talking about chemotherapy and surgery, we don’t think they can be delayed for too long – maybe a week, but not for several months.”
Dr. Sharpless feels that overall it is time for cancer care to resume as much as possible, because “ignoring cancer for too long is an untenable choice and may turn one public health crisis into another.”
“If we act now, we can make up for lost time,” he wrote in the editorial. “Clearly, postponing procedures and deferring care due to the pandemic was prudent at one time, but now that we have made it through the initial shock of the pandemic, I believe it is time to resume robust cancer care.”
Through their network of cancer centers, researchers with the NCI can develop innovative solutions that allow screening and treatment to move forward while maintaining safety. “We need to make patients feel safe, and we have to answer important questions quickly,” he said.
Impact of COVID-19 on cancer care
The COVID-19 pandemic has overwhelmed health care systems worldwide and has created major challenges for clinicians who are caring for patients with cancer.
As previously reported, hospitals reprioritized resources for an impending onslaught of COVID-19 patients. Services and procedures deemed to be nonessential were canceled or delayed, including surgeries and imaging.
In a survey conducted by the American Cancer Society Cancer Action Network, half of the 1219 respondents reported changes, delays, or disruptions to the care they were receiving. The services most frequently affected included in-person provider visits (50%), supportive services (20%), and imaging procedures to monitor tumor growth (20%).
In addition, 8% reported that their treatment, including chemotherapy and immunotherapy, had been affected by the COVID-19 pandemic.
In the United Kingdom, Cancer Research UK estimated that because of the disruption to cancer services, 2.4 million people did not undergo cancer screening or further testing or did not receive cancer treatment and that tens of thousands of cases have gone undiagnosed.
Similarly, a survey by Macmillan Cancer Support showed that almost half (45%) of cancer patients have experienced delays or cancellations of cancer treatments, or their treatments have been altered as a result of coronavirus, leaving many living in fear. Calling cancer “the forgotten C” of the pandemic, it warned of a potential cancer “time bomb” when, as the number of deaths from COVID-19 falls, cancer returns as the leading cause of death in the United Kingdom.
Last month, a report also predicted that there will be an excess of cancer deaths in both the United States and United Kingdom because of patients not accessing health care services.
The authors calculated that there will be 6270 excess deaths among cancer patients 1 year from now in England and 33,890 excess deaths among cancer patients older than 40 years in the United States.
This article first appeared on Medscape.com.
A model created by the National Cancer Institute predicts that tens of thousands of excess cancer deaths will occur over the next decade as a result of missed screenings, delays in diagnosis, and reductions in oncology care caused by the COVID-19 pandemic.
“As director of NCI, I am deeply concerned about the potential impacts of delayed diagnoses and deferred or modified treatment plans on cancer incidence and mortality,” said Norman “Ned” Sharpless, MD.
“In the past 3 decades, we have seen steady and strong progress against death and suffering from cancer, thanks to improvements in prevention, screening, diagnosis, and treatment. I worry that the SARS-CoV-2 pandemic has put those decades of steady progress at risk and may precipitate reversals of these trends.”
In an editorial published June 19 in Science, Dr. Sharpless highlighted modeling performed by the NCI that predicts an excess of 10,000 deaths from breast and colorectal cancer over the next 10 years.
The number of excess deaths per year would peak in the next year or 2, likely sooner for colorectal than for breast cancer, but “for both cancer types, we believe the pandemic will influence cancer deaths for at least a decade.”
In an interview, Dr. Sharpless pointed out that this analysis is conservative because the researchers only evaluated two types of cancer. They chose breast and colorectal cancer because these are common cancers (accounting for about one-sixth of all cancers) with relatively high screening rates.
“We didn’t model other cancer types, but we have no reason to think that we’re not going to see the same thing with other types of malignancies,” he said. “That is a significant amount of excess mortality.”
Delayed diagnosis, modified therapy
One of the effects of the pandemic has been to cause delays in cancer diagnosis. “Routine screening has plummeted and is running at less than 90% in some systems,” Dr. Sharpless said.
“Most cancers are diagnosed when people experience symptoms and go see their doctors, and those symptomatic screening events are also not happening,” he continued. “Fear of contracting the coronavirus in health care settings has dissuaded people from visits.”
In some cases, a delay in diagnosis will allow the cancer to progress to a more advanced stage. “The earlier the diagnosis, the better, and if the stages are more advanced, patients will not do as well for virtually every kind of cancer,” he said.
In addition to delays in diagnosis, treatments are being postponed or modified for patients recently diagnosed with cancer. Because of delays and reductions in curative therapies, patients may be receiving less than optimal care.
“We are seeing a lot of nonstandard care,” said Dr. Sharpless. “All of these things add up to increased cancer morbidity and mortality.”
He also pointed out that the term “elective” is confusing and problematic. “It doesn’t mean that it’s not needed, just that it’s not an emergency and doesn’t need to be done today,” said Dr. Sharpless. “But if we’re talking about chemotherapy and surgery, we don’t think they can be delayed for too long – maybe a week, but not for several months.”
Dr. Sharpless feels that overall it is time for cancer care to resume as much as possible, because “ignoring cancer for too long is an untenable choice and may turn one public health crisis into another.”
“If we act now, we can make up for lost time,” he wrote in the editorial. “Clearly, postponing procedures and deferring care due to the pandemic was prudent at one time, but now that we have made it through the initial shock of the pandemic, I believe it is time to resume robust cancer care.”
Through their network of cancer centers, researchers with the NCI can develop innovative solutions that allow screening and treatment to move forward while maintaining safety. “We need to make patients feel safe, and we have to answer important questions quickly,” he said.
Impact of COVID-19 on cancer care
The COVID-19 pandemic has overwhelmed health care systems worldwide and has created major challenges for clinicians who are caring for patients with cancer.
As previously reported, hospitals reprioritized resources for an impending onslaught of COVID-19 patients. Services and procedures deemed to be nonessential were canceled or delayed, including surgeries and imaging.
In a survey conducted by the American Cancer Society Cancer Action Network, half of the 1219 respondents reported changes, delays, or disruptions to the care they were receiving. The services most frequently affected included in-person provider visits (50%), supportive services (20%), and imaging procedures to monitor tumor growth (20%).
In addition, 8% reported that their treatment, including chemotherapy and immunotherapy, had been affected by the COVID-19 pandemic.
In the United Kingdom, Cancer Research UK estimated that because of the disruption to cancer services, 2.4 million people did not undergo cancer screening or further testing or did not receive cancer treatment and that tens of thousands of cases have gone undiagnosed.
Similarly, a survey by Macmillan Cancer Support showed that almost half (45%) of cancer patients have experienced delays or cancellations of cancer treatments, or their treatments have been altered as a result of coronavirus, leaving many living in fear. Calling cancer “the forgotten C” of the pandemic, it warned of a potential cancer “time bomb” when, as the number of deaths from COVID-19 falls, cancer returns as the leading cause of death in the United Kingdom.
Last month, a report also predicted that there will be an excess of cancer deaths in both the United States and United Kingdom because of patients not accessing health care services.
The authors calculated that there will be 6270 excess deaths among cancer patients 1 year from now in England and 33,890 excess deaths among cancer patients older than 40 years in the United States.
This article first appeared on Medscape.com.
Daily Recap: Healthy lifestyle may stave off dementia; Tentative evidence on marijuana for migraine
Here are the stories our MDedge editors across specialties think you need to know about today:
First reported U.S. case of COVID-19 linked to Guillain-Barré syndrome
The first official U.S. case of Guillain-Barré syndrome (GBS) associated with COVID-19 has been reported by neurologists from Allegheny General Hospital in Pittsburgh, further supporting a link between the virus and neurologic complications, including GBS.
Physicians in China reported the first case that initially presented as acute GBS. Subsequently, physicians in Italy reported five cases of GBS in association with COVID-19.
“This onset is similar to a case report of acute Zika virus infection with concurrent GBS suggesting a parainfectious complication,” first author Sandeep Rana, MD, and colleagues noted. Read more.
Five healthy lifestyle choices tied to dramatic cut in dementia risk
Combining four of five healthy lifestyle choices has been linked to up to a 60% reduced risk for Alzheimer’s dementia in new research that strengthens ties between healthy behaviors and lower dementia risk. “I hope this study will motivate people to engage in a healthy lifestyle by not smoking, being physically and cognitively active, and having a high-quality diet,” lead investigator Klodian Dhana, MD, PhD, said in an interview.
They defined a healthy lifestyle score on the basis of the following factors: not smoking; engaging in 150 min/wk or more of physical exercise; light to moderate alcohol consumption; consuming a high-quality Mediterranean-DASH Diet Intervention for Neurodegenerative Delay diet (upper 40%); and engaging in late-life cognitive activities.
“What needs to be determined is how early should we start ‘behaving.’ We should all aim to score four to five factors across our entire lifespan, but this is not always feasible. So, when is the time to behave? Also, what is the relative weight of each of these factors?” said Luca Giliberto, MD, PhD. Read more.
Marijuana for migraine? Some tentative evidence
Medical marijuana may have promise for managing headache pain, according to results from a small study conducted at the Jefferson Headache Center at Thomas Jefferson University. The researchers found general satisfaction with medical marijuana, more frequent use as an abortive medication rather than a preventative, and more than two-thirds using the inhaled form rather than oral.
“A lot of patients are interested in medical marijuana but don’t know how to integrate it into the therapy plan they already have – whether it should be just to treat bad headaches when they happen, or is it meant to be a preventive medicine they use every day? We have some data out there that it can be helpful, but not a lot of specific information to guide your recommendations,” said Jefferson headache fellow Claire Ceriani, MD, in an interview. Read more.
Inside Mercy’s mission to care for non-COVID patients in Los Angeles
When the hospital ship USNS Mercy departed San Diego’s Naval Station North Island on March 23, 2020, to support the Department of Defense efforts in Los Angeles during the coronavirus outbreak, Commander Erin Blevins remembers the crew’s excitement was palpable. “We normally do partnerships abroad and respond to tsunamis and earthquakes,” said Cdr. Blevins, MD, a pediatric hematologist-oncologist who served as director of medical services for the mission.
Between March 29 and May 15, about 1,071 medical personnel aboard the Mercy cared for 77 patients with an average age of 53 years who were referred from 11 Los Angeles area hospitals.
Care aboard the ship ranged from basic medical and surgical care to critical care and trauma. The most common procedures were cholecystectomies and orthopedic procedures, and the average length of stay was 4-5 days, according to Cdr. Blevins. Over the course of the mission, the medical professionals conducted 36 surgeries, 77 x-ray exams, 26 CT scans, and administered hundreds of ancillary studies ranging from routine labs to high-end x-rays and blood transfusion support. Special Feature.
For more on COVID-19, visit our Resource Center. All of our latest news is available on MDedge.com.
Here are the stories our MDedge editors across specialties think you need to know about today:
First reported U.S. case of COVID-19 linked to Guillain-Barré syndrome
The first official U.S. case of Guillain-Barré syndrome (GBS) associated with COVID-19 has been reported by neurologists from Allegheny General Hospital in Pittsburgh, further supporting a link between the virus and neurologic complications, including GBS.
Physicians in China reported the first case that initially presented as acute GBS. Subsequently, physicians in Italy reported five cases of GBS in association with COVID-19.
“This onset is similar to a case report of acute Zika virus infection with concurrent GBS suggesting a parainfectious complication,” first author Sandeep Rana, MD, and colleagues noted. Read more.
Five healthy lifestyle choices tied to dramatic cut in dementia risk
Combining four of five healthy lifestyle choices has been linked to up to a 60% reduced risk for Alzheimer’s dementia in new research that strengthens ties between healthy behaviors and lower dementia risk. “I hope this study will motivate people to engage in a healthy lifestyle by not smoking, being physically and cognitively active, and having a high-quality diet,” lead investigator Klodian Dhana, MD, PhD, said in an interview.
They defined a healthy lifestyle score on the basis of the following factors: not smoking; engaging in 150 min/wk or more of physical exercise; light to moderate alcohol consumption; consuming a high-quality Mediterranean-DASH Diet Intervention for Neurodegenerative Delay diet (upper 40%); and engaging in late-life cognitive activities.
“What needs to be determined is how early should we start ‘behaving.’ We should all aim to score four to five factors across our entire lifespan, but this is not always feasible. So, when is the time to behave? Also, what is the relative weight of each of these factors?” said Luca Giliberto, MD, PhD. Read more.
Marijuana for migraine? Some tentative evidence
Medical marijuana may have promise for managing headache pain, according to results from a small study conducted at the Jefferson Headache Center at Thomas Jefferson University. The researchers found general satisfaction with medical marijuana, more frequent use as an abortive medication rather than a preventative, and more than two-thirds using the inhaled form rather than oral.
“A lot of patients are interested in medical marijuana but don’t know how to integrate it into the therapy plan they already have – whether it should be just to treat bad headaches when they happen, or is it meant to be a preventive medicine they use every day? We have some data out there that it can be helpful, but not a lot of specific information to guide your recommendations,” said Jefferson headache fellow Claire Ceriani, MD, in an interview. Read more.
Inside Mercy’s mission to care for non-COVID patients in Los Angeles
When the hospital ship USNS Mercy departed San Diego’s Naval Station North Island on March 23, 2020, to support the Department of Defense efforts in Los Angeles during the coronavirus outbreak, Commander Erin Blevins remembers the crew’s excitement was palpable. “We normally do partnerships abroad and respond to tsunamis and earthquakes,” said Cdr. Blevins, MD, a pediatric hematologist-oncologist who served as director of medical services for the mission.
Between March 29 and May 15, about 1,071 medical personnel aboard the Mercy cared for 77 patients with an average age of 53 years who were referred from 11 Los Angeles area hospitals.
Care aboard the ship ranged from basic medical and surgical care to critical care and trauma. The most common procedures were cholecystectomies and orthopedic procedures, and the average length of stay was 4-5 days, according to Cdr. Blevins. Over the course of the mission, the medical professionals conducted 36 surgeries, 77 x-ray exams, 26 CT scans, and administered hundreds of ancillary studies ranging from routine labs to high-end x-rays and blood transfusion support. Special Feature.
For more on COVID-19, visit our Resource Center. All of our latest news is available on MDedge.com.
Here are the stories our MDedge editors across specialties think you need to know about today:
First reported U.S. case of COVID-19 linked to Guillain-Barré syndrome
The first official U.S. case of Guillain-Barré syndrome (GBS) associated with COVID-19 has been reported by neurologists from Allegheny General Hospital in Pittsburgh, further supporting a link between the virus and neurologic complications, including GBS.
Physicians in China reported the first case that initially presented as acute GBS. Subsequently, physicians in Italy reported five cases of GBS in association with COVID-19.
“This onset is similar to a case report of acute Zika virus infection with concurrent GBS suggesting a parainfectious complication,” first author Sandeep Rana, MD, and colleagues noted. Read more.
Five healthy lifestyle choices tied to dramatic cut in dementia risk
Combining four of five healthy lifestyle choices has been linked to up to a 60% reduced risk for Alzheimer’s dementia in new research that strengthens ties between healthy behaviors and lower dementia risk. “I hope this study will motivate people to engage in a healthy lifestyle by not smoking, being physically and cognitively active, and having a high-quality diet,” lead investigator Klodian Dhana, MD, PhD, said in an interview.
They defined a healthy lifestyle score on the basis of the following factors: not smoking; engaging in 150 min/wk or more of physical exercise; light to moderate alcohol consumption; consuming a high-quality Mediterranean-DASH Diet Intervention for Neurodegenerative Delay diet (upper 40%); and engaging in late-life cognitive activities.
“What needs to be determined is how early should we start ‘behaving.’ We should all aim to score four to five factors across our entire lifespan, but this is not always feasible. So, when is the time to behave? Also, what is the relative weight of each of these factors?” said Luca Giliberto, MD, PhD. Read more.
Marijuana for migraine? Some tentative evidence
Medical marijuana may have promise for managing headache pain, according to results from a small study conducted at the Jefferson Headache Center at Thomas Jefferson University. The researchers found general satisfaction with medical marijuana, more frequent use as an abortive medication rather than a preventative, and more than two-thirds using the inhaled form rather than oral.
“A lot of patients are interested in medical marijuana but don’t know how to integrate it into the therapy plan they already have – whether it should be just to treat bad headaches when they happen, or is it meant to be a preventive medicine they use every day? We have some data out there that it can be helpful, but not a lot of specific information to guide your recommendations,” said Jefferson headache fellow Claire Ceriani, MD, in an interview. Read more.
Inside Mercy’s mission to care for non-COVID patients in Los Angeles
When the hospital ship USNS Mercy departed San Diego’s Naval Station North Island on March 23, 2020, to support the Department of Defense efforts in Los Angeles during the coronavirus outbreak, Commander Erin Blevins remembers the crew’s excitement was palpable. “We normally do partnerships abroad and respond to tsunamis and earthquakes,” said Cdr. Blevins, MD, a pediatric hematologist-oncologist who served as director of medical services for the mission.
Between March 29 and May 15, about 1,071 medical personnel aboard the Mercy cared for 77 patients with an average age of 53 years who were referred from 11 Los Angeles area hospitals.
Care aboard the ship ranged from basic medical and surgical care to critical care and trauma. The most common procedures were cholecystectomies and orthopedic procedures, and the average length of stay was 4-5 days, according to Cdr. Blevins. Over the course of the mission, the medical professionals conducted 36 surgeries, 77 x-ray exams, 26 CT scans, and administered hundreds of ancillary studies ranging from routine labs to high-end x-rays and blood transfusion support. Special Feature.
For more on COVID-19, visit our Resource Center. All of our latest news is available on MDedge.com.
COVID-associated pancreatitis may disproportionately affect young, overweight men
Patients with COVID-19 develop a distinct subset of pancreatitis hallmarked by duodenal and periduodenal inflammation, according to a recent case series.
Although all five patients presented with multiple predictive markers of severe pancreatitis, the subsequent clinical pathway “was much more benign than anticipated,” reported lead author Peter Szatmary, MB, BChir, PhD, of the University of Liverpool (England) and colleagues. Still, they noted prolonged hospital stays because of persistent inflammation and poor diabetic control.
“As the global pandemic of SARS-CoV-2 continues, nuances of the disease it precipitates in humans continue to emerge,” the investigators wrote in Gastroenterology. “[A] group from Wuhan reported a series of 9 patients with purported pancreatic injury in the context of SARS-CoV-2 infection, but did not provide robust evidence for pancreatitis relying on mild hyperamylasemia alone.”
For the present series, Dr. Szatmary and colleagues restricted diagnosis of pancreatitis to international consensus guidelines, which require “abdominal pain consistent with pancreatitis, serum amylase/lipase greater than three times the upper limit of normal, and characteristic findings on cross-sectional imaging.”
From middle of March to late April, the investigators identified 35 patients with acute pancreatitis at Royal Liverpool (England) University Hospital, 25 of whom tested negative for SARS-CoV-2, which resulted in study exclusion. An additional five patients were excluded from the series as another etiology for pancreatitis was clearly present, such as gallstones.
“The remaining 5 patients, all with SARS-CoV-2, presented atypically yet homogenously with a distinct metabolic-pancreatitis phenotype,” the investigators wrote.
All five patients were obese or overweight young men with a median body mass index of 30 kg/m2 and age of 42 years. On presentation, all patients had elevated, but nondiagnostic, levels of amylase (median, 149 U/L). Contrast-enhanced abdominal CT revealed moderate to severe hepatic steatosis (less than 104 HU), which rapidly regressed within a week among patients who underwent repeat imaging.
“The pattern of pancreatic inflammation was similarly unusual in these patients,” the investigators wrote, going on to describe “mild pancreatic edema without significant pancreatic or peripancreatic necrosis, with distinct duodenal/periduodenal inflammation involving the second and third part of the duodenum.”
According to Dr. Szatmary and colleagues, these findings were “accompanied by a profound systemic inflammatory response,” including 1-2 criteria for systemic inflammatory response syndrome that increased to 2-4 criteria within 48 hours. During hospitalization, patients also exhibited a “dramatic elevation” of C-reactive protein, from a median of 31 mg/L upon admission to 485 mg/L within 48 hours.
Although these markers predicted severe disease, all cases followed a clinical course similar to “a typical attack of moderate pancreatitis,” the investigators wrote.
All patients were treated with IV fluids, four out of five received broad-spectrum IV antibiotics for pneumonitis, three out of five received fibrate and/or insulin therapy, and two out of five received pancreatic enzyme replacement therapy. No patients required corticosteroids, organ support, or respiratory support beyond low-flow oxygen. Median hospital stay was 14 days.
“We ... propose the combination of male sex, abdominal pain, metabolic stress, and CT-findings of predominantly pancreatico-duodenal inflammation with steatosis represent a distinct subset of pancreatitis in patients infected with SARS-CoV-2,” the investigators wrote.
They suggested that the endocrine pancreas may be “particularly vulnerable to this infection,” citing prolonged hospital stays because of poor diabetic control.
“[T]ransient dyslipidemias and impaired glucose tolerance may be common in SARS-CoV-2 patients and warrant further investigation,” they concluded.
Oscar J. Hines, MD, chief of the division of general surgery at UCLA Medical Center and leader in the field of pancreatitis management, said that the case series has a limited impact.
“The findings are unlikely to change practice and only call attention for physicians to the possibility of pancreatitis in COVID-positive patients,” Dr. Hines said.
The investigators reported grants from NIHR, Wellcome Trust, Mylan, and others.
SOURCE: Szatmary P et al. Gastroenterology. 2020 Jun 1. doi: 10.1053/j.gastro.2020.05.069.
Patients with COVID-19 develop a distinct subset of pancreatitis hallmarked by duodenal and periduodenal inflammation, according to a recent case series.
Although all five patients presented with multiple predictive markers of severe pancreatitis, the subsequent clinical pathway “was much more benign than anticipated,” reported lead author Peter Szatmary, MB, BChir, PhD, of the University of Liverpool (England) and colleagues. Still, they noted prolonged hospital stays because of persistent inflammation and poor diabetic control.
“As the global pandemic of SARS-CoV-2 continues, nuances of the disease it precipitates in humans continue to emerge,” the investigators wrote in Gastroenterology. “[A] group from Wuhan reported a series of 9 patients with purported pancreatic injury in the context of SARS-CoV-2 infection, but did not provide robust evidence for pancreatitis relying on mild hyperamylasemia alone.”
For the present series, Dr. Szatmary and colleagues restricted diagnosis of pancreatitis to international consensus guidelines, which require “abdominal pain consistent with pancreatitis, serum amylase/lipase greater than three times the upper limit of normal, and characteristic findings on cross-sectional imaging.”
From middle of March to late April, the investigators identified 35 patients with acute pancreatitis at Royal Liverpool (England) University Hospital, 25 of whom tested negative for SARS-CoV-2, which resulted in study exclusion. An additional five patients were excluded from the series as another etiology for pancreatitis was clearly present, such as gallstones.
“The remaining 5 patients, all with SARS-CoV-2, presented atypically yet homogenously with a distinct metabolic-pancreatitis phenotype,” the investigators wrote.
All five patients were obese or overweight young men with a median body mass index of 30 kg/m2 and age of 42 years. On presentation, all patients had elevated, but nondiagnostic, levels of amylase (median, 149 U/L). Contrast-enhanced abdominal CT revealed moderate to severe hepatic steatosis (less than 104 HU), which rapidly regressed within a week among patients who underwent repeat imaging.
“The pattern of pancreatic inflammation was similarly unusual in these patients,” the investigators wrote, going on to describe “mild pancreatic edema without significant pancreatic or peripancreatic necrosis, with distinct duodenal/periduodenal inflammation involving the second and third part of the duodenum.”
According to Dr. Szatmary and colleagues, these findings were “accompanied by a profound systemic inflammatory response,” including 1-2 criteria for systemic inflammatory response syndrome that increased to 2-4 criteria within 48 hours. During hospitalization, patients also exhibited a “dramatic elevation” of C-reactive protein, from a median of 31 mg/L upon admission to 485 mg/L within 48 hours.
Although these markers predicted severe disease, all cases followed a clinical course similar to “a typical attack of moderate pancreatitis,” the investigators wrote.
All patients were treated with IV fluids, four out of five received broad-spectrum IV antibiotics for pneumonitis, three out of five received fibrate and/or insulin therapy, and two out of five received pancreatic enzyme replacement therapy. No patients required corticosteroids, organ support, or respiratory support beyond low-flow oxygen. Median hospital stay was 14 days.
“We ... propose the combination of male sex, abdominal pain, metabolic stress, and CT-findings of predominantly pancreatico-duodenal inflammation with steatosis represent a distinct subset of pancreatitis in patients infected with SARS-CoV-2,” the investigators wrote.
They suggested that the endocrine pancreas may be “particularly vulnerable to this infection,” citing prolonged hospital stays because of poor diabetic control.
“[T]ransient dyslipidemias and impaired glucose tolerance may be common in SARS-CoV-2 patients and warrant further investigation,” they concluded.
Oscar J. Hines, MD, chief of the division of general surgery at UCLA Medical Center and leader in the field of pancreatitis management, said that the case series has a limited impact.
“The findings are unlikely to change practice and only call attention for physicians to the possibility of pancreatitis in COVID-positive patients,” Dr. Hines said.
The investigators reported grants from NIHR, Wellcome Trust, Mylan, and others.
SOURCE: Szatmary P et al. Gastroenterology. 2020 Jun 1. doi: 10.1053/j.gastro.2020.05.069.
Patients with COVID-19 develop a distinct subset of pancreatitis hallmarked by duodenal and periduodenal inflammation, according to a recent case series.
Although all five patients presented with multiple predictive markers of severe pancreatitis, the subsequent clinical pathway “was much more benign than anticipated,” reported lead author Peter Szatmary, MB, BChir, PhD, of the University of Liverpool (England) and colleagues. Still, they noted prolonged hospital stays because of persistent inflammation and poor diabetic control.
“As the global pandemic of SARS-CoV-2 continues, nuances of the disease it precipitates in humans continue to emerge,” the investigators wrote in Gastroenterology. “[A] group from Wuhan reported a series of 9 patients with purported pancreatic injury in the context of SARS-CoV-2 infection, but did not provide robust evidence for pancreatitis relying on mild hyperamylasemia alone.”
For the present series, Dr. Szatmary and colleagues restricted diagnosis of pancreatitis to international consensus guidelines, which require “abdominal pain consistent with pancreatitis, serum amylase/lipase greater than three times the upper limit of normal, and characteristic findings on cross-sectional imaging.”
From middle of March to late April, the investigators identified 35 patients with acute pancreatitis at Royal Liverpool (England) University Hospital, 25 of whom tested negative for SARS-CoV-2, which resulted in study exclusion. An additional five patients were excluded from the series as another etiology for pancreatitis was clearly present, such as gallstones.
“The remaining 5 patients, all with SARS-CoV-2, presented atypically yet homogenously with a distinct metabolic-pancreatitis phenotype,” the investigators wrote.
All five patients were obese or overweight young men with a median body mass index of 30 kg/m2 and age of 42 years. On presentation, all patients had elevated, but nondiagnostic, levels of amylase (median, 149 U/L). Contrast-enhanced abdominal CT revealed moderate to severe hepatic steatosis (less than 104 HU), which rapidly regressed within a week among patients who underwent repeat imaging.
“The pattern of pancreatic inflammation was similarly unusual in these patients,” the investigators wrote, going on to describe “mild pancreatic edema without significant pancreatic or peripancreatic necrosis, with distinct duodenal/periduodenal inflammation involving the second and third part of the duodenum.”
According to Dr. Szatmary and colleagues, these findings were “accompanied by a profound systemic inflammatory response,” including 1-2 criteria for systemic inflammatory response syndrome that increased to 2-4 criteria within 48 hours. During hospitalization, patients also exhibited a “dramatic elevation” of C-reactive protein, from a median of 31 mg/L upon admission to 485 mg/L within 48 hours.
Although these markers predicted severe disease, all cases followed a clinical course similar to “a typical attack of moderate pancreatitis,” the investigators wrote.
All patients were treated with IV fluids, four out of five received broad-spectrum IV antibiotics for pneumonitis, three out of five received fibrate and/or insulin therapy, and two out of five received pancreatic enzyme replacement therapy. No patients required corticosteroids, organ support, or respiratory support beyond low-flow oxygen. Median hospital stay was 14 days.
“We ... propose the combination of male sex, abdominal pain, metabolic stress, and CT-findings of predominantly pancreatico-duodenal inflammation with steatosis represent a distinct subset of pancreatitis in patients infected with SARS-CoV-2,” the investigators wrote.
They suggested that the endocrine pancreas may be “particularly vulnerable to this infection,” citing prolonged hospital stays because of poor diabetic control.
“[T]ransient dyslipidemias and impaired glucose tolerance may be common in SARS-CoV-2 patients and warrant further investigation,” they concluded.
Oscar J. Hines, MD, chief of the division of general surgery at UCLA Medical Center and leader in the field of pancreatitis management, said that the case series has a limited impact.
“The findings are unlikely to change practice and only call attention for physicians to the possibility of pancreatitis in COVID-positive patients,” Dr. Hines said.
The investigators reported grants from NIHR, Wellcome Trust, Mylan, and others.
SOURCE: Szatmary P et al. Gastroenterology. 2020 Jun 1. doi: 10.1053/j.gastro.2020.05.069.
FROM GASTROENTEROLOGY
First reported U.S. case of COVID-19 linked to Guillain-Barré syndrome
further supporting a link between the virus and neurologic complications, including GBS.
Physicians in China reported the first case of COVID-19 that initially presented as acute GBS. The patient was a 61-year-old woman returning home from Wuhan during the pandemic.
Subsequently, physicians in Italy reported five cases of GBS in association with COVID-19.
The first U.S. case is described in the June issue of the Journal of Clinical Neuromuscular Disease.
Like cases from China and Italy, the U.S. patient’s symptoms of GBS reportedly occurred within days of being infected with SARS-CoV-2. “This onset is similar to a case report of acute Zika virus infection with concurrent GBS suggesting a parainfectious complication,” first author Sandeep Rana, MD, and colleagues noted.
The 54-year-old man was transferred to Allegheny General Hospital after developing ascending limb weakness and numbness that followed symptoms of a respiratory infection. Two weeks earlier, he initially developed rhinorrhea, odynophagia, fevers, chills, and night sweats. The man reported that his wife had tested positive for COVID-19 and that his symptoms started soon after her illness. The man also tested positive for COVID-19.
His deficits were characterized by quadriparesis and areflexia, burning dysesthesias, mild ophthalmoparesis, and dysautonomia. He did not have the loss of smell and taste documented in other COVID-19 patients. He briefly required mechanical ventilation and was successfully weaned after receiving a course of intravenous immunoglobulin.
Compared with other cases reported in the literature, the unique clinical features in the U.S. case are urinary retention secondary to dysautonomia and ocular symptoms of diplopia. These highlight the variability in the clinical presentation of GBS associated with COVID-19, the researchers noted.
They added that, with the Pittsburgh patient, electrophysiological findings were typical of demyelinating polyneuropathy seen in patients with GBS. The case series from Italy suggests that axonal variants could be as common in COVID-19–associated GBS.
“Although the number of documented cases internationally is notably small to date, it’s not completely surprising that a COVID-19 diagnosis may lead to a patient developing GBS. The increase of inflammation and inflammatory cells caused by the infection may trigger an irregular immune response that leads to the hallmark symptoms of this neurological disorder,” Dr. Rana said in a news release.
“Since GBS can significantly affect the respiratory system and other vital organs being pushed into overdrive during a COVID-19 immune response, it will be critically important to further investigate and understand this potential connection,” he added.
A version of this article originally appeared on Medscape.com.
further supporting a link between the virus and neurologic complications, including GBS.
Physicians in China reported the first case of COVID-19 that initially presented as acute GBS. The patient was a 61-year-old woman returning home from Wuhan during the pandemic.
Subsequently, physicians in Italy reported five cases of GBS in association with COVID-19.
The first U.S. case is described in the June issue of the Journal of Clinical Neuromuscular Disease.
Like cases from China and Italy, the U.S. patient’s symptoms of GBS reportedly occurred within days of being infected with SARS-CoV-2. “This onset is similar to a case report of acute Zika virus infection with concurrent GBS suggesting a parainfectious complication,” first author Sandeep Rana, MD, and colleagues noted.
The 54-year-old man was transferred to Allegheny General Hospital after developing ascending limb weakness and numbness that followed symptoms of a respiratory infection. Two weeks earlier, he initially developed rhinorrhea, odynophagia, fevers, chills, and night sweats. The man reported that his wife had tested positive for COVID-19 and that his symptoms started soon after her illness. The man also tested positive for COVID-19.
His deficits were characterized by quadriparesis and areflexia, burning dysesthesias, mild ophthalmoparesis, and dysautonomia. He did not have the loss of smell and taste documented in other COVID-19 patients. He briefly required mechanical ventilation and was successfully weaned after receiving a course of intravenous immunoglobulin.
Compared with other cases reported in the literature, the unique clinical features in the U.S. case are urinary retention secondary to dysautonomia and ocular symptoms of diplopia. These highlight the variability in the clinical presentation of GBS associated with COVID-19, the researchers noted.
They added that, with the Pittsburgh patient, electrophysiological findings were typical of demyelinating polyneuropathy seen in patients with GBS. The case series from Italy suggests that axonal variants could be as common in COVID-19–associated GBS.
“Although the number of documented cases internationally is notably small to date, it’s not completely surprising that a COVID-19 diagnosis may lead to a patient developing GBS. The increase of inflammation and inflammatory cells caused by the infection may trigger an irregular immune response that leads to the hallmark symptoms of this neurological disorder,” Dr. Rana said in a news release.
“Since GBS can significantly affect the respiratory system and other vital organs being pushed into overdrive during a COVID-19 immune response, it will be critically important to further investigate and understand this potential connection,” he added.
A version of this article originally appeared on Medscape.com.
further supporting a link between the virus and neurologic complications, including GBS.
Physicians in China reported the first case of COVID-19 that initially presented as acute GBS. The patient was a 61-year-old woman returning home from Wuhan during the pandemic.
Subsequently, physicians in Italy reported five cases of GBS in association with COVID-19.
The first U.S. case is described in the June issue of the Journal of Clinical Neuromuscular Disease.
Like cases from China and Italy, the U.S. patient’s symptoms of GBS reportedly occurred within days of being infected with SARS-CoV-2. “This onset is similar to a case report of acute Zika virus infection with concurrent GBS suggesting a parainfectious complication,” first author Sandeep Rana, MD, and colleagues noted.
The 54-year-old man was transferred to Allegheny General Hospital after developing ascending limb weakness and numbness that followed symptoms of a respiratory infection. Two weeks earlier, he initially developed rhinorrhea, odynophagia, fevers, chills, and night sweats. The man reported that his wife had tested positive for COVID-19 and that his symptoms started soon after her illness. The man also tested positive for COVID-19.
His deficits were characterized by quadriparesis and areflexia, burning dysesthesias, mild ophthalmoparesis, and dysautonomia. He did not have the loss of smell and taste documented in other COVID-19 patients. He briefly required mechanical ventilation and was successfully weaned after receiving a course of intravenous immunoglobulin.
Compared with other cases reported in the literature, the unique clinical features in the U.S. case are urinary retention secondary to dysautonomia and ocular symptoms of diplopia. These highlight the variability in the clinical presentation of GBS associated with COVID-19, the researchers noted.
They added that, with the Pittsburgh patient, electrophysiological findings were typical of demyelinating polyneuropathy seen in patients with GBS. The case series from Italy suggests that axonal variants could be as common in COVID-19–associated GBS.
“Although the number of documented cases internationally is notably small to date, it’s not completely surprising that a COVID-19 diagnosis may lead to a patient developing GBS. The increase of inflammation and inflammatory cells caused by the infection may trigger an irregular immune response that leads to the hallmark symptoms of this neurological disorder,” Dr. Rana said in a news release.
“Since GBS can significantly affect the respiratory system and other vital organs being pushed into overdrive during a COVID-19 immune response, it will be critically important to further investigate and understand this potential connection,” he added.
A version of this article originally appeared on Medscape.com.
The merger of personal and professional: A psychologist’s experience with the effects of COVID-19
The concepts of days, weeks, and months have all but lost their meaning during the times of coronavirus. This became all too clear when I found myself weeks into June before realizing that we were in the second half of 2020. The world has been in the grips of COVID-19 (the disease caused by SARS-CoV-2) for over half a year, and the end is still not in sight. Even more chilling is the fact that the virus’s effects will continue to be felt by humanity for years to come.
By now, most of us have been affected by COVID-19, whether directly or indirectly. Consequently, we’ve seen that the psychological toll the pandemic takes is as wide ranging as the disease caused by the novel coronavirus itself. Confusion, denial, fear, anxiety, depression/sadness, and emotional dysregulation have become all too common an experience. Many mental health experts have even likened our psychological response to COVID-19 to that of trauma survivors.
In early 2020, triggered by two separate but related threats. In addition to concerns regarding COVID-19, we also began to experience fear for our physical safety as anti-Chinese sentiment began to rise across the country and the world. Discrimination and acts of violence toward Chinese people worldwide began to spread almost as rapidly as the virus itself. Anxiety and fear became a common daily experience of countless people, myself included.
In late March, amid coping with existing stressors, my situation became significantly worse when my brother, a New York City firefighter, contracted COVID-19 while working on the front lines. Shortly thereafter, my parents, both aged 60 years and older, with whom my brother shares a home, contracted the virus as well. My anxiety triggers related to the spread of the virus and xenophobia suddenly became a distant memory. I now found myself grappling with the much greater fear of losing my entire family.
At the time, the availability of testing was very limited, even for those working on the front lines. Although not without a short delay, my brother was able to access testing through Fire Department of New York connections. After about 3 weeks in self-isolation at home and with the use of over the counter pain relievers, he made a full recovery and returned to work. My parents, on the other hand, were placed at the end of a weeks-long line for testing, during which time their conditions deteriorated. Nine days following the onset of my mother’s symptoms, her condition had gotten so bad, she required hospitalization. Six days later, my father followed suit.
Being in the epicenter of the COVID-19 outbreak, New York hospitals were severely overwhelmed. Upon admission, my mother was held in the ED and other temporary open spaces in the hospital for nearly 24 hours because there was a lack of available patient rooms. During this time, she was packed into small spaces with dozens of other patients afflicted with the same disease. Four days later, she was transferred to a different hospital 10 miles away to make room for new patients. Decisions needed to be made rapidly and often with limited communication, which made for a roller coaster of emotions that would not relent.
Confusion. One of the few things we know with certainty about coronavirus is how much we don’t know. The Centers for Disease Control and Prevention data indicate that older adults with underlying health conditions have worse outcomes. Yet my mother, who is younger and in better physical health than my father, became much sicker in a drastically shorter period of time. Furthermore, my parents’ symptoms were completely inconsistent with one another’s. Based on their symptoms alone, it appeared as though they were suffering with different conditions entirely. My mother experienced body aches and gastrointestinal symptoms, whereas my father developed the typical cough and fever associated with COVID-19. In addition to confusion regarding their symptoms and, therefore, in determining the best at-home supportive care prior to their hospitalizations, the lack of available testing made the very question of whether they even had COVID-19 an uncertainty.
Denial. When my family members first became symptomatic, I found myself in a state of denial not unlike that of individuals experiencing grief. I frequently engaged in both internal and external dialogues in which I would attempt to convince myself of the reasons why my family did not have COVID-19.
“My brother wears PPE while at work.”
“My father’s cough was mild.”
“My mother does not have a cough or a fever.”
Despite knowing better, I was initially unable to accept that everyone in my family had contracted a disease that had already claimed the lives of tens of thousands globally.
Fear. In order to prevent the spread of infection, many hospitals made changes to their visitor policies, placing greater restrictions on who can come and go. This has meant hospital patients who have died from COVID-19 complications have done so separated from their loved ones. After transporting my mother to the hospital ED, I was politely but firmly asked to leave per the new visitor policy. I felt as though there were cinder blocks attached to my feet as I reluctantly walked away, not knowing if it would be the last time I would see her. I experienced a fear and sadness so intense, it continues to elicit an emotional response today as I think back on that moment.
Anxiety. The difference between fear and anxiety is fear is an emotional response to a known threat or danger, and anxiety is a response to an unknown threat or danger. The days that followed my parents’ hospitalizations were riddled with anxiety that would come in waves. How were they doing? Could they breathe? Do the overwhelmed hospital staff have time to take care of them? What can I do to help? Is there anything I can do to help? The worrisome thoughts and unanswerable questions were incessant and seemed unresponsive to my efforts to quell them.
Sadness. To feel sadness is to be human. In my work as a psychologist, I emphasize the value in experiencing this emotion when therapeutically beneficial. This technique is used as part of acceptance and commitment therapy (ACT), which emphasizes the value of being present or in touch with one’s thoughts and emotions, instead of working to eliminate them. During these scary times, I leaned into this notion more than ever. I gave myself permission to not feel okay, to cry more than I had in a long time, and to be unapologetically sad. I flip-flopped between states of near-despair and hopeful, with the switch usually following a call from a member of the hospital care team with updates on my parents’ conditions.
My parents’ road to recovery extended far beyond their discharge from the hospital and was not without incident, but with support and appropriate follow-up care, they have since made full recoveries from COVID-19. Although the relief and happiness this brings me is immeasurable, the experience has left a lasting impression on me as both a person and a psychologist. Speaking as a person, I cannot overstate the value of relying on one’s social support network while coping with stressors related to COVID-19. Whether you are directly or indirectly affected by the disease, the emotional effects can feel equally intense. As in times of happiness and celebration, times of sadness can and should be shared by those who are equipped to provide support. This can be tricky in an era during which isolation is prescribed for our safety, but we have more options today for connecting virtually with others than ever before, including video conferencing, email, and that old friend, the telephone. Furthermore, identify and assert your boundaries. Sometimes, saying no to others is the best way to say yes to yourself. Certain work, chores, and social obligations that can wait, should wait.
As a psychologist, my experience has given me a renewed appreciation for the power of the therapeutic use of self in psychotherapy. The factor with the greatest effects on psychotherapy outcomes is the quality of the therapeutic alliance, a concept introduced by Sigmund Freud in 1912. I believe a therapist’s willingness to show that we, too, experience life’s ups and downs strengthens our ability to demonstrate empathy and further promote a sense of alliance. Therapists are not immune to the effects of COVID-19, and to acknowledge this fact allows us to relate to our patients on a basic human level, which is more important now than ever.
Dr. Tseng, a licensed clinical psychologist, is in private practice in New York. She disclosed no relevant financial relationships.
The concepts of days, weeks, and months have all but lost their meaning during the times of coronavirus. This became all too clear when I found myself weeks into June before realizing that we were in the second half of 2020. The world has been in the grips of COVID-19 (the disease caused by SARS-CoV-2) for over half a year, and the end is still not in sight. Even more chilling is the fact that the virus’s effects will continue to be felt by humanity for years to come.
By now, most of us have been affected by COVID-19, whether directly or indirectly. Consequently, we’ve seen that the psychological toll the pandemic takes is as wide ranging as the disease caused by the novel coronavirus itself. Confusion, denial, fear, anxiety, depression/sadness, and emotional dysregulation have become all too common an experience. Many mental health experts have even likened our psychological response to COVID-19 to that of trauma survivors.
In early 2020, triggered by two separate but related threats. In addition to concerns regarding COVID-19, we also began to experience fear for our physical safety as anti-Chinese sentiment began to rise across the country and the world. Discrimination and acts of violence toward Chinese people worldwide began to spread almost as rapidly as the virus itself. Anxiety and fear became a common daily experience of countless people, myself included.
In late March, amid coping with existing stressors, my situation became significantly worse when my brother, a New York City firefighter, contracted COVID-19 while working on the front lines. Shortly thereafter, my parents, both aged 60 years and older, with whom my brother shares a home, contracted the virus as well. My anxiety triggers related to the spread of the virus and xenophobia suddenly became a distant memory. I now found myself grappling with the much greater fear of losing my entire family.
At the time, the availability of testing was very limited, even for those working on the front lines. Although not without a short delay, my brother was able to access testing through Fire Department of New York connections. After about 3 weeks in self-isolation at home and with the use of over the counter pain relievers, he made a full recovery and returned to work. My parents, on the other hand, were placed at the end of a weeks-long line for testing, during which time their conditions deteriorated. Nine days following the onset of my mother’s symptoms, her condition had gotten so bad, she required hospitalization. Six days later, my father followed suit.
Being in the epicenter of the COVID-19 outbreak, New York hospitals were severely overwhelmed. Upon admission, my mother was held in the ED and other temporary open spaces in the hospital for nearly 24 hours because there was a lack of available patient rooms. During this time, she was packed into small spaces with dozens of other patients afflicted with the same disease. Four days later, she was transferred to a different hospital 10 miles away to make room for new patients. Decisions needed to be made rapidly and often with limited communication, which made for a roller coaster of emotions that would not relent.
Confusion. One of the few things we know with certainty about coronavirus is how much we don’t know. The Centers for Disease Control and Prevention data indicate that older adults with underlying health conditions have worse outcomes. Yet my mother, who is younger and in better physical health than my father, became much sicker in a drastically shorter period of time. Furthermore, my parents’ symptoms were completely inconsistent with one another’s. Based on their symptoms alone, it appeared as though they were suffering with different conditions entirely. My mother experienced body aches and gastrointestinal symptoms, whereas my father developed the typical cough and fever associated with COVID-19. In addition to confusion regarding their symptoms and, therefore, in determining the best at-home supportive care prior to their hospitalizations, the lack of available testing made the very question of whether they even had COVID-19 an uncertainty.
Denial. When my family members first became symptomatic, I found myself in a state of denial not unlike that of individuals experiencing grief. I frequently engaged in both internal and external dialogues in which I would attempt to convince myself of the reasons why my family did not have COVID-19.
“My brother wears PPE while at work.”
“My father’s cough was mild.”
“My mother does not have a cough or a fever.”
Despite knowing better, I was initially unable to accept that everyone in my family had contracted a disease that had already claimed the lives of tens of thousands globally.
Fear. In order to prevent the spread of infection, many hospitals made changes to their visitor policies, placing greater restrictions on who can come and go. This has meant hospital patients who have died from COVID-19 complications have done so separated from their loved ones. After transporting my mother to the hospital ED, I was politely but firmly asked to leave per the new visitor policy. I felt as though there were cinder blocks attached to my feet as I reluctantly walked away, not knowing if it would be the last time I would see her. I experienced a fear and sadness so intense, it continues to elicit an emotional response today as I think back on that moment.
Anxiety. The difference between fear and anxiety is fear is an emotional response to a known threat or danger, and anxiety is a response to an unknown threat or danger. The days that followed my parents’ hospitalizations were riddled with anxiety that would come in waves. How were they doing? Could they breathe? Do the overwhelmed hospital staff have time to take care of them? What can I do to help? Is there anything I can do to help? The worrisome thoughts and unanswerable questions were incessant and seemed unresponsive to my efforts to quell them.
Sadness. To feel sadness is to be human. In my work as a psychologist, I emphasize the value in experiencing this emotion when therapeutically beneficial. This technique is used as part of acceptance and commitment therapy (ACT), which emphasizes the value of being present or in touch with one’s thoughts and emotions, instead of working to eliminate them. During these scary times, I leaned into this notion more than ever. I gave myself permission to not feel okay, to cry more than I had in a long time, and to be unapologetically sad. I flip-flopped between states of near-despair and hopeful, with the switch usually following a call from a member of the hospital care team with updates on my parents’ conditions.
My parents’ road to recovery extended far beyond their discharge from the hospital and was not without incident, but with support and appropriate follow-up care, they have since made full recoveries from COVID-19. Although the relief and happiness this brings me is immeasurable, the experience has left a lasting impression on me as both a person and a psychologist. Speaking as a person, I cannot overstate the value of relying on one’s social support network while coping with stressors related to COVID-19. Whether you are directly or indirectly affected by the disease, the emotional effects can feel equally intense. As in times of happiness and celebration, times of sadness can and should be shared by those who are equipped to provide support. This can be tricky in an era during which isolation is prescribed for our safety, but we have more options today for connecting virtually with others than ever before, including video conferencing, email, and that old friend, the telephone. Furthermore, identify and assert your boundaries. Sometimes, saying no to others is the best way to say yes to yourself. Certain work, chores, and social obligations that can wait, should wait.
As a psychologist, my experience has given me a renewed appreciation for the power of the therapeutic use of self in psychotherapy. The factor with the greatest effects on psychotherapy outcomes is the quality of the therapeutic alliance, a concept introduced by Sigmund Freud in 1912. I believe a therapist’s willingness to show that we, too, experience life’s ups and downs strengthens our ability to demonstrate empathy and further promote a sense of alliance. Therapists are not immune to the effects of COVID-19, and to acknowledge this fact allows us to relate to our patients on a basic human level, which is more important now than ever.
Dr. Tseng, a licensed clinical psychologist, is in private practice in New York. She disclosed no relevant financial relationships.
The concepts of days, weeks, and months have all but lost their meaning during the times of coronavirus. This became all too clear when I found myself weeks into June before realizing that we were in the second half of 2020. The world has been in the grips of COVID-19 (the disease caused by SARS-CoV-2) for over half a year, and the end is still not in sight. Even more chilling is the fact that the virus’s effects will continue to be felt by humanity for years to come.
By now, most of us have been affected by COVID-19, whether directly or indirectly. Consequently, we’ve seen that the psychological toll the pandemic takes is as wide ranging as the disease caused by the novel coronavirus itself. Confusion, denial, fear, anxiety, depression/sadness, and emotional dysregulation have become all too common an experience. Many mental health experts have even likened our psychological response to COVID-19 to that of trauma survivors.
In early 2020, triggered by two separate but related threats. In addition to concerns regarding COVID-19, we also began to experience fear for our physical safety as anti-Chinese sentiment began to rise across the country and the world. Discrimination and acts of violence toward Chinese people worldwide began to spread almost as rapidly as the virus itself. Anxiety and fear became a common daily experience of countless people, myself included.
In late March, amid coping with existing stressors, my situation became significantly worse when my brother, a New York City firefighter, contracted COVID-19 while working on the front lines. Shortly thereafter, my parents, both aged 60 years and older, with whom my brother shares a home, contracted the virus as well. My anxiety triggers related to the spread of the virus and xenophobia suddenly became a distant memory. I now found myself grappling with the much greater fear of losing my entire family.
At the time, the availability of testing was very limited, even for those working on the front lines. Although not without a short delay, my brother was able to access testing through Fire Department of New York connections. After about 3 weeks in self-isolation at home and with the use of over the counter pain relievers, he made a full recovery and returned to work. My parents, on the other hand, were placed at the end of a weeks-long line for testing, during which time their conditions deteriorated. Nine days following the onset of my mother’s symptoms, her condition had gotten so bad, she required hospitalization. Six days later, my father followed suit.
Being in the epicenter of the COVID-19 outbreak, New York hospitals were severely overwhelmed. Upon admission, my mother was held in the ED and other temporary open spaces in the hospital for nearly 24 hours because there was a lack of available patient rooms. During this time, she was packed into small spaces with dozens of other patients afflicted with the same disease. Four days later, she was transferred to a different hospital 10 miles away to make room for new patients. Decisions needed to be made rapidly and often with limited communication, which made for a roller coaster of emotions that would not relent.
Confusion. One of the few things we know with certainty about coronavirus is how much we don’t know. The Centers for Disease Control and Prevention data indicate that older adults with underlying health conditions have worse outcomes. Yet my mother, who is younger and in better physical health than my father, became much sicker in a drastically shorter period of time. Furthermore, my parents’ symptoms were completely inconsistent with one another’s. Based on their symptoms alone, it appeared as though they were suffering with different conditions entirely. My mother experienced body aches and gastrointestinal symptoms, whereas my father developed the typical cough and fever associated with COVID-19. In addition to confusion regarding their symptoms and, therefore, in determining the best at-home supportive care prior to their hospitalizations, the lack of available testing made the very question of whether they even had COVID-19 an uncertainty.
Denial. When my family members first became symptomatic, I found myself in a state of denial not unlike that of individuals experiencing grief. I frequently engaged in both internal and external dialogues in which I would attempt to convince myself of the reasons why my family did not have COVID-19.
“My brother wears PPE while at work.”
“My father’s cough was mild.”
“My mother does not have a cough or a fever.”
Despite knowing better, I was initially unable to accept that everyone in my family had contracted a disease that had already claimed the lives of tens of thousands globally.
Fear. In order to prevent the spread of infection, many hospitals made changes to their visitor policies, placing greater restrictions on who can come and go. This has meant hospital patients who have died from COVID-19 complications have done so separated from their loved ones. After transporting my mother to the hospital ED, I was politely but firmly asked to leave per the new visitor policy. I felt as though there were cinder blocks attached to my feet as I reluctantly walked away, not knowing if it would be the last time I would see her. I experienced a fear and sadness so intense, it continues to elicit an emotional response today as I think back on that moment.
Anxiety. The difference between fear and anxiety is fear is an emotional response to a known threat or danger, and anxiety is a response to an unknown threat or danger. The days that followed my parents’ hospitalizations were riddled with anxiety that would come in waves. How were they doing? Could they breathe? Do the overwhelmed hospital staff have time to take care of them? What can I do to help? Is there anything I can do to help? The worrisome thoughts and unanswerable questions were incessant and seemed unresponsive to my efforts to quell them.
Sadness. To feel sadness is to be human. In my work as a psychologist, I emphasize the value in experiencing this emotion when therapeutically beneficial. This technique is used as part of acceptance and commitment therapy (ACT), which emphasizes the value of being present or in touch with one’s thoughts and emotions, instead of working to eliminate them. During these scary times, I leaned into this notion more than ever. I gave myself permission to not feel okay, to cry more than I had in a long time, and to be unapologetically sad. I flip-flopped between states of near-despair and hopeful, with the switch usually following a call from a member of the hospital care team with updates on my parents’ conditions.
My parents’ road to recovery extended far beyond their discharge from the hospital and was not without incident, but with support and appropriate follow-up care, they have since made full recoveries from COVID-19. Although the relief and happiness this brings me is immeasurable, the experience has left a lasting impression on me as both a person and a psychologist. Speaking as a person, I cannot overstate the value of relying on one’s social support network while coping with stressors related to COVID-19. Whether you are directly or indirectly affected by the disease, the emotional effects can feel equally intense. As in times of happiness and celebration, times of sadness can and should be shared by those who are equipped to provide support. This can be tricky in an era during which isolation is prescribed for our safety, but we have more options today for connecting virtually with others than ever before, including video conferencing, email, and that old friend, the telephone. Furthermore, identify and assert your boundaries. Sometimes, saying no to others is the best way to say yes to yourself. Certain work, chores, and social obligations that can wait, should wait.
As a psychologist, my experience has given me a renewed appreciation for the power of the therapeutic use of self in psychotherapy. The factor with the greatest effects on psychotherapy outcomes is the quality of the therapeutic alliance, a concept introduced by Sigmund Freud in 1912. I believe a therapist’s willingness to show that we, too, experience life’s ups and downs strengthens our ability to demonstrate empathy and further promote a sense of alliance. Therapists are not immune to the effects of COVID-19, and to acknowledge this fact allows us to relate to our patients on a basic human level, which is more important now than ever.
Dr. Tseng, a licensed clinical psychologist, is in private practice in New York. She disclosed no relevant financial relationships.
What COVID-19 has taught us about senior care
Across the globe, there are marked differences in how countries responded to the COVID-19 outbreak, with varying degrees of success in limiting the spread of the virus. Some countries learned important lessons from previous outbreaks, including SARS and MERS, and put policies in place that contributed to lower infection and death rates from COVID-19 in these countries. Others struggled to respond appropriately to the outbreak.
The United States and most of the world was not affected significantly by SARS and MERS. Hence there is a need for different perspectives and observations on lessons that can be learned from this outbreak to help develop effective strategies and policies for the future. It also makes sense to focus intently on the demographic most affected by COVID-19 – the elderly.
Medical care, for the most part, is governed by protocols that clearly detail processes to be followed for the prevention and treatment of disease. Caring for older patients requires going above and beyond the protocols. That is one of the lessons learned from the COVID-19 pandemic – a wake-up call for a more proactive approach for at-risk patients, in this case everyone over the age of 60 years.
In this context, it is important for medical outreach to continue with the senior population long after the pandemic has run its course. Many seniors, particularly those susceptible to other illnesses or exhibiting ongoing issues, would benefit from a consistent and preplanned pattern of contacts by medical professionals and agencies that work with the aging population. These proactive follow-ups can facilitate prevention and treatment and, at the same time, reduce costs that would otherwise increase when health care is reactive.
Lessons in infectious disease containment
As COVID-19 spread globally, there were contrasting responses from individual countries in their efforts to contain the disease. Unfortunately, Italy suffered from its decision to lock down only specific regions of the country initially. The leadership in Italy may have ignored the advice of medical experts and been caught off guard by the intensity of the spread of COVID-19. In fact, they might not have taken strict actions right away because they did not want their responses to be viewed as an overreaction to the disease.
The government decided to shut down areas where the infection rates were high (“red zones”) rather than implement restrictions nationally. This may have inadvertently increased the spread as Italians vacated those “red zones” for other areas of the country not yet affected by COVID-19. Italy’s decentralized health care system also played a part in the effects of the disease, with some regions demonstrating more success in slowing the reach of the disease. According to an article in the Harvard Business Review, the neighboring regions of Lombardy and Veneto applied similar approaches to social distancing and retail closures. Veneto was more proactive, and its response to the outbreak was multipronged, including putting a “strong emphasis on home diagnosis and care” and “specific efforts to monitor and protect health care and other essential workers.” These measures most likely contributed to a slowdown of the spread of the disease in Veneto’s health care facilities, which lessened the load on medical providers.1
Conversely, Taiwan implemented proactive measures swiftly after learning about COVID-19. Taiwan was impacted adversely by the SARS outbreak in 2003 and, afterward, revised their medical policies and procedures to respond quickly to future infectious disease crises. In the beginning, little was known about COVID-19 or how it spread. However, Taiwan’s swift public health response to COVID-19 included early travel restrictions, patient screening, and quarantining of symptomatic patients. The government emphasized education and created real-time digital updates and alerts sent to their citizens, as well as partnering with media to broadcast crucial proactive health information and quickly disproving false information related to COVID-19. They coordinated with organizations throughout the country to increase supplies of personal protective equipment (PPE).2
Although countries and even cities within a country differ in terms of population demographics, health resources, government policies, and cultural practices, initial success stories have some similarities, including the following:
- Early travel restrictions from countries with positive cases, with some circumstances requiring compulsory quarantine periods and testing before entry.
- Extensive testing and proactive tracing of symptomatic cases early. Contacts of people testing positive were also tested, irrespective of being symptomatic or asymptomatic. If testing kits were unavailable, the contacts were self-quarantined.
- Emphasis on avoiding overburdening hospitals by having the public health infrastructure to divert people exhibiting symptoms, including using public health hotlines to send patients to dedicated testing sites and drive-through testing, rather than have patients presenting to emergency rooms and hospitals. This approach protected medical staff from exposure and allowed the focus to remain on treating severe symptomatic patients.
The vastly different response to the COVID-19 outbreak in these two countries illuminates the need for better preparation in the United States. At the onset of this outbreak, emergency room medical professionals, hospitalists, and outpatient primary care providers did not know how to screen for or treat this virus. Additionally, there was limited information on the most effective contact protocols for medical professionals, patients, and visitors. Finally, the lack of PPE and COVID-19 test kits hindered the U.S. response. Once the country is on the road to recovery from COVID-19, it is imperative to set the groundwork to prepare for future outbreaks and create mechanisms to quickly identify vulnerable populations when outbreaks occur.
Senior care in future infectious disease outbreaks
How can medical providers translate lessons learned from this outbreak into improving the quality of care for seniors? The National Institute on Aging (NIA) maintains a website with information about healthy aging. Seniors and their caregivers can use this website to learn more about chronic diseases, lifestyle modifications, disease prevention, and mental health.
In times of a pandemic, this website provides consistent and accurate information and education. One recommendation for reaching the elderly population during future outbreaks is for NIA to develop and implement strategies to increase the use of the website, including adding more audio and visual interfaces and developing a mobile app. Other recommendations for improving the quality of care for seniors include the following:
1. Identify which populations may be most affected when future outbreaks occur.
2. Consider nontraditional platforms, including social media, for communicating with the general population and for medical providers worldwide to learn from each other about new diseases, including the signs, symptoms, and treatment plans. Some medical professionals created specific WhatsApp groups to communicate, and the World Health Organization sent updated information about COVID-19 to anyone who texted them via WhatsApp.3
3. Create a checklist of signs and symptoms related to current infectious diseases and assess every vulnerable patient.
4. Share these guidelines with medical facilities that treat these populations, such as senior care, assisted living and rehabilitation facilities, hospitals, and outpatient treatment centers. Teach the staff at these medical facilities how to screen patients for signs and symptoms of the disease.
5. Implement social isolation strategies, travel and visitor restrictions, and testing and screening as soon as possible at these medical facilities.
6. Recognize that these strategies may affect the psychological and emotional well-being of seniors, increasing their risk for depression and anxiety and negatively affecting their immunity and mental health. Additionally, the use of PPE, either by the medical providers or the patient, may cause anxiety in seniors and those with mild cognitive impairment.
7. Encourage these medical facilities to improve coping strategies with older patients, such as incorporating communication technology that helps seniors stay connected with their families, and participating in physical and mental exercise, as well as religious activities.
8. Ask these medical facilities to create isolation or quarantine rooms for infected seniors.
9. Work with family members to proactively report to medical professionals any symptoms noticed in their senior relatives. Educate seniors to report symptoms earlier.
10. Offer incentives for medical professionals to conduct on-site testing in primary care offices or senior care facilities instead of sending patients to hospital emergency rooms for evaluation. This will only be effective if there are enough test kits available.
11. Urge insurance companies and Medicare to allow additional medical visits for screening vulnerable populations. Encourage the use of telemedicine in place of in-office visits (preferably billed at the same rate as an in-office visit) where appropriate, especially with nonambulatory patients or those with transportation issues. Many insurance companies, including Medicare, approved COVID-19–related coverage of telemedicine in place of office visits to limit the spread of the disease.
12. Provide community health care and integration and better coordination of local, state, and national health care.
13. Hold regular epidemic and pandemic preparedness exercises in every hospital, nursing home, and assisted living facility.
Proactive health care outreach
It is easier to identify the signs and symptoms of already identified infectious diseases as opposed to a novel one like COVID-19. The United States faced a steep learning curve with COVID-19. Hospitalists and other medical professionals were not able to learn about COVID-19 in a journal. At first, they did not know how to screen patients coming into the ER, how to protect staff, or what the treatment plan was for this new disease. As a result, the medical system experienced disorder and confusion. Investing in community health care and better coordination of local, state, and national health care resources is a priority.
The senior citizen population appears to be most vulnerable to this virus and may be just as vulnerable in future outbreaks. Yet the insights gained from this pandemic can lead to a more comprehensive outreach to senior patients and increased screenings for comorbidities and future contagious diseases. An emphasis on proactive health care and outreach for seniors, with a focus on identifying and treating comorbid conditions, improves the medical care system overall and may prevent or slow future community outbreaks.
Dr. Kasarla is a hospitalist with APOGEE Physicians at Wise Surgical at Parkway in Fort Worth, Tex. He did his internal medicine residency at Mercy Hospital & Medical Center, Chicago. Readers can contact him at madhukarreddy.kasarla@apogeephysicians.com. Dr. Devireddy is a family physician at Positive Health Medical Center, Kingston, Jamaica. Contact him at drjaisheel@gmail.com.
References
1. Pisano GP et al. Lessons from Italy’s response to coronavirus. Harvard Business Review. 2020 Mar 27. https://hbr.org/2020/03/lessons-from-italys-response-to-coronavirus.
2. Tu C. Lessons from Taiwan’s experience with COVID-19. New Atlanticist. 2020 Apr 7. https://atlanticcouncil.org/blogs/new-atlanticist/lessons-from-taiwans-experience-with-covid-19/.
3. Newman LH. WhatsApp is at the center of coronavirus response. WIRED. 2020 Mar 20. https://www.wired.com/story/whatsapp-coronavirus-who-information-app/.
Across the globe, there are marked differences in how countries responded to the COVID-19 outbreak, with varying degrees of success in limiting the spread of the virus. Some countries learned important lessons from previous outbreaks, including SARS and MERS, and put policies in place that contributed to lower infection and death rates from COVID-19 in these countries. Others struggled to respond appropriately to the outbreak.
The United States and most of the world was not affected significantly by SARS and MERS. Hence there is a need for different perspectives and observations on lessons that can be learned from this outbreak to help develop effective strategies and policies for the future. It also makes sense to focus intently on the demographic most affected by COVID-19 – the elderly.
Medical care, for the most part, is governed by protocols that clearly detail processes to be followed for the prevention and treatment of disease. Caring for older patients requires going above and beyond the protocols. That is one of the lessons learned from the COVID-19 pandemic – a wake-up call for a more proactive approach for at-risk patients, in this case everyone over the age of 60 years.
In this context, it is important for medical outreach to continue with the senior population long after the pandemic has run its course. Many seniors, particularly those susceptible to other illnesses or exhibiting ongoing issues, would benefit from a consistent and preplanned pattern of contacts by medical professionals and agencies that work with the aging population. These proactive follow-ups can facilitate prevention and treatment and, at the same time, reduce costs that would otherwise increase when health care is reactive.
Lessons in infectious disease containment
As COVID-19 spread globally, there were contrasting responses from individual countries in their efforts to contain the disease. Unfortunately, Italy suffered from its decision to lock down only specific regions of the country initially. The leadership in Italy may have ignored the advice of medical experts and been caught off guard by the intensity of the spread of COVID-19. In fact, they might not have taken strict actions right away because they did not want their responses to be viewed as an overreaction to the disease.
The government decided to shut down areas where the infection rates were high (“red zones”) rather than implement restrictions nationally. This may have inadvertently increased the spread as Italians vacated those “red zones” for other areas of the country not yet affected by COVID-19. Italy’s decentralized health care system also played a part in the effects of the disease, with some regions demonstrating more success in slowing the reach of the disease. According to an article in the Harvard Business Review, the neighboring regions of Lombardy and Veneto applied similar approaches to social distancing and retail closures. Veneto was more proactive, and its response to the outbreak was multipronged, including putting a “strong emphasis on home diagnosis and care” and “specific efforts to monitor and protect health care and other essential workers.” These measures most likely contributed to a slowdown of the spread of the disease in Veneto’s health care facilities, which lessened the load on medical providers.1
Conversely, Taiwan implemented proactive measures swiftly after learning about COVID-19. Taiwan was impacted adversely by the SARS outbreak in 2003 and, afterward, revised their medical policies and procedures to respond quickly to future infectious disease crises. In the beginning, little was known about COVID-19 or how it spread. However, Taiwan’s swift public health response to COVID-19 included early travel restrictions, patient screening, and quarantining of symptomatic patients. The government emphasized education and created real-time digital updates and alerts sent to their citizens, as well as partnering with media to broadcast crucial proactive health information and quickly disproving false information related to COVID-19. They coordinated with organizations throughout the country to increase supplies of personal protective equipment (PPE).2
Although countries and even cities within a country differ in terms of population demographics, health resources, government policies, and cultural practices, initial success stories have some similarities, including the following:
- Early travel restrictions from countries with positive cases, with some circumstances requiring compulsory quarantine periods and testing before entry.
- Extensive testing and proactive tracing of symptomatic cases early. Contacts of people testing positive were also tested, irrespective of being symptomatic or asymptomatic. If testing kits were unavailable, the contacts were self-quarantined.
- Emphasis on avoiding overburdening hospitals by having the public health infrastructure to divert people exhibiting symptoms, including using public health hotlines to send patients to dedicated testing sites and drive-through testing, rather than have patients presenting to emergency rooms and hospitals. This approach protected medical staff from exposure and allowed the focus to remain on treating severe symptomatic patients.
The vastly different response to the COVID-19 outbreak in these two countries illuminates the need for better preparation in the United States. At the onset of this outbreak, emergency room medical professionals, hospitalists, and outpatient primary care providers did not know how to screen for or treat this virus. Additionally, there was limited information on the most effective contact protocols for medical professionals, patients, and visitors. Finally, the lack of PPE and COVID-19 test kits hindered the U.S. response. Once the country is on the road to recovery from COVID-19, it is imperative to set the groundwork to prepare for future outbreaks and create mechanisms to quickly identify vulnerable populations when outbreaks occur.
Senior care in future infectious disease outbreaks
How can medical providers translate lessons learned from this outbreak into improving the quality of care for seniors? The National Institute on Aging (NIA) maintains a website with information about healthy aging. Seniors and their caregivers can use this website to learn more about chronic diseases, lifestyle modifications, disease prevention, and mental health.
In times of a pandemic, this website provides consistent and accurate information and education. One recommendation for reaching the elderly population during future outbreaks is for NIA to develop and implement strategies to increase the use of the website, including adding more audio and visual interfaces and developing a mobile app. Other recommendations for improving the quality of care for seniors include the following:
1. Identify which populations may be most affected when future outbreaks occur.
2. Consider nontraditional platforms, including social media, for communicating with the general population and for medical providers worldwide to learn from each other about new diseases, including the signs, symptoms, and treatment plans. Some medical professionals created specific WhatsApp groups to communicate, and the World Health Organization sent updated information about COVID-19 to anyone who texted them via WhatsApp.3
3. Create a checklist of signs and symptoms related to current infectious diseases and assess every vulnerable patient.
4. Share these guidelines with medical facilities that treat these populations, such as senior care, assisted living and rehabilitation facilities, hospitals, and outpatient treatment centers. Teach the staff at these medical facilities how to screen patients for signs and symptoms of the disease.
5. Implement social isolation strategies, travel and visitor restrictions, and testing and screening as soon as possible at these medical facilities.
6. Recognize that these strategies may affect the psychological and emotional well-being of seniors, increasing their risk for depression and anxiety and negatively affecting their immunity and mental health. Additionally, the use of PPE, either by the medical providers or the patient, may cause anxiety in seniors and those with mild cognitive impairment.
7. Encourage these medical facilities to improve coping strategies with older patients, such as incorporating communication technology that helps seniors stay connected with their families, and participating in physical and mental exercise, as well as religious activities.
8. Ask these medical facilities to create isolation or quarantine rooms for infected seniors.
9. Work with family members to proactively report to medical professionals any symptoms noticed in their senior relatives. Educate seniors to report symptoms earlier.
10. Offer incentives for medical professionals to conduct on-site testing in primary care offices or senior care facilities instead of sending patients to hospital emergency rooms for evaluation. This will only be effective if there are enough test kits available.
11. Urge insurance companies and Medicare to allow additional medical visits for screening vulnerable populations. Encourage the use of telemedicine in place of in-office visits (preferably billed at the same rate as an in-office visit) where appropriate, especially with nonambulatory patients or those with transportation issues. Many insurance companies, including Medicare, approved COVID-19–related coverage of telemedicine in place of office visits to limit the spread of the disease.
12. Provide community health care and integration and better coordination of local, state, and national health care.
13. Hold regular epidemic and pandemic preparedness exercises in every hospital, nursing home, and assisted living facility.
Proactive health care outreach
It is easier to identify the signs and symptoms of already identified infectious diseases as opposed to a novel one like COVID-19. The United States faced a steep learning curve with COVID-19. Hospitalists and other medical professionals were not able to learn about COVID-19 in a journal. At first, they did not know how to screen patients coming into the ER, how to protect staff, or what the treatment plan was for this new disease. As a result, the medical system experienced disorder and confusion. Investing in community health care and better coordination of local, state, and national health care resources is a priority.
The senior citizen population appears to be most vulnerable to this virus and may be just as vulnerable in future outbreaks. Yet the insights gained from this pandemic can lead to a more comprehensive outreach to senior patients and increased screenings for comorbidities and future contagious diseases. An emphasis on proactive health care and outreach for seniors, with a focus on identifying and treating comorbid conditions, improves the medical care system overall and may prevent or slow future community outbreaks.
Dr. Kasarla is a hospitalist with APOGEE Physicians at Wise Surgical at Parkway in Fort Worth, Tex. He did his internal medicine residency at Mercy Hospital & Medical Center, Chicago. Readers can contact him at madhukarreddy.kasarla@apogeephysicians.com. Dr. Devireddy is a family physician at Positive Health Medical Center, Kingston, Jamaica. Contact him at drjaisheel@gmail.com.
References
1. Pisano GP et al. Lessons from Italy’s response to coronavirus. Harvard Business Review. 2020 Mar 27. https://hbr.org/2020/03/lessons-from-italys-response-to-coronavirus.
2. Tu C. Lessons from Taiwan’s experience with COVID-19. New Atlanticist. 2020 Apr 7. https://atlanticcouncil.org/blogs/new-atlanticist/lessons-from-taiwans-experience-with-covid-19/.
3. Newman LH. WhatsApp is at the center of coronavirus response. WIRED. 2020 Mar 20. https://www.wired.com/story/whatsapp-coronavirus-who-information-app/.
Across the globe, there are marked differences in how countries responded to the COVID-19 outbreak, with varying degrees of success in limiting the spread of the virus. Some countries learned important lessons from previous outbreaks, including SARS and MERS, and put policies in place that contributed to lower infection and death rates from COVID-19 in these countries. Others struggled to respond appropriately to the outbreak.
The United States and most of the world was not affected significantly by SARS and MERS. Hence there is a need for different perspectives and observations on lessons that can be learned from this outbreak to help develop effective strategies and policies for the future. It also makes sense to focus intently on the demographic most affected by COVID-19 – the elderly.
Medical care, for the most part, is governed by protocols that clearly detail processes to be followed for the prevention and treatment of disease. Caring for older patients requires going above and beyond the protocols. That is one of the lessons learned from the COVID-19 pandemic – a wake-up call for a more proactive approach for at-risk patients, in this case everyone over the age of 60 years.
In this context, it is important for medical outreach to continue with the senior population long after the pandemic has run its course. Many seniors, particularly those susceptible to other illnesses or exhibiting ongoing issues, would benefit from a consistent and preplanned pattern of contacts by medical professionals and agencies that work with the aging population. These proactive follow-ups can facilitate prevention and treatment and, at the same time, reduce costs that would otherwise increase when health care is reactive.
Lessons in infectious disease containment
As COVID-19 spread globally, there were contrasting responses from individual countries in their efforts to contain the disease. Unfortunately, Italy suffered from its decision to lock down only specific regions of the country initially. The leadership in Italy may have ignored the advice of medical experts and been caught off guard by the intensity of the spread of COVID-19. In fact, they might not have taken strict actions right away because they did not want their responses to be viewed as an overreaction to the disease.
The government decided to shut down areas where the infection rates were high (“red zones”) rather than implement restrictions nationally. This may have inadvertently increased the spread as Italians vacated those “red zones” for other areas of the country not yet affected by COVID-19. Italy’s decentralized health care system also played a part in the effects of the disease, with some regions demonstrating more success in slowing the reach of the disease. According to an article in the Harvard Business Review, the neighboring regions of Lombardy and Veneto applied similar approaches to social distancing and retail closures. Veneto was more proactive, and its response to the outbreak was multipronged, including putting a “strong emphasis on home diagnosis and care” and “specific efforts to monitor and protect health care and other essential workers.” These measures most likely contributed to a slowdown of the spread of the disease in Veneto’s health care facilities, which lessened the load on medical providers.1
Conversely, Taiwan implemented proactive measures swiftly after learning about COVID-19. Taiwan was impacted adversely by the SARS outbreak in 2003 and, afterward, revised their medical policies and procedures to respond quickly to future infectious disease crises. In the beginning, little was known about COVID-19 or how it spread. However, Taiwan’s swift public health response to COVID-19 included early travel restrictions, patient screening, and quarantining of symptomatic patients. The government emphasized education and created real-time digital updates and alerts sent to their citizens, as well as partnering with media to broadcast crucial proactive health information and quickly disproving false information related to COVID-19. They coordinated with organizations throughout the country to increase supplies of personal protective equipment (PPE).2
Although countries and even cities within a country differ in terms of population demographics, health resources, government policies, and cultural practices, initial success stories have some similarities, including the following:
- Early travel restrictions from countries with positive cases, with some circumstances requiring compulsory quarantine periods and testing before entry.
- Extensive testing and proactive tracing of symptomatic cases early. Contacts of people testing positive were also tested, irrespective of being symptomatic or asymptomatic. If testing kits were unavailable, the contacts were self-quarantined.
- Emphasis on avoiding overburdening hospitals by having the public health infrastructure to divert people exhibiting symptoms, including using public health hotlines to send patients to dedicated testing sites and drive-through testing, rather than have patients presenting to emergency rooms and hospitals. This approach protected medical staff from exposure and allowed the focus to remain on treating severe symptomatic patients.
The vastly different response to the COVID-19 outbreak in these two countries illuminates the need for better preparation in the United States. At the onset of this outbreak, emergency room medical professionals, hospitalists, and outpatient primary care providers did not know how to screen for or treat this virus. Additionally, there was limited information on the most effective contact protocols for medical professionals, patients, and visitors. Finally, the lack of PPE and COVID-19 test kits hindered the U.S. response. Once the country is on the road to recovery from COVID-19, it is imperative to set the groundwork to prepare for future outbreaks and create mechanisms to quickly identify vulnerable populations when outbreaks occur.
Senior care in future infectious disease outbreaks
How can medical providers translate lessons learned from this outbreak into improving the quality of care for seniors? The National Institute on Aging (NIA) maintains a website with information about healthy aging. Seniors and their caregivers can use this website to learn more about chronic diseases, lifestyle modifications, disease prevention, and mental health.
In times of a pandemic, this website provides consistent and accurate information and education. One recommendation for reaching the elderly population during future outbreaks is for NIA to develop and implement strategies to increase the use of the website, including adding more audio and visual interfaces and developing a mobile app. Other recommendations for improving the quality of care for seniors include the following:
1. Identify which populations may be most affected when future outbreaks occur.
2. Consider nontraditional platforms, including social media, for communicating with the general population and for medical providers worldwide to learn from each other about new diseases, including the signs, symptoms, and treatment plans. Some medical professionals created specific WhatsApp groups to communicate, and the World Health Organization sent updated information about COVID-19 to anyone who texted them via WhatsApp.3
3. Create a checklist of signs and symptoms related to current infectious diseases and assess every vulnerable patient.
4. Share these guidelines with medical facilities that treat these populations, such as senior care, assisted living and rehabilitation facilities, hospitals, and outpatient treatment centers. Teach the staff at these medical facilities how to screen patients for signs and symptoms of the disease.
5. Implement social isolation strategies, travel and visitor restrictions, and testing and screening as soon as possible at these medical facilities.
6. Recognize that these strategies may affect the psychological and emotional well-being of seniors, increasing their risk for depression and anxiety and negatively affecting their immunity and mental health. Additionally, the use of PPE, either by the medical providers or the patient, may cause anxiety in seniors and those with mild cognitive impairment.
7. Encourage these medical facilities to improve coping strategies with older patients, such as incorporating communication technology that helps seniors stay connected with their families, and participating in physical and mental exercise, as well as religious activities.
8. Ask these medical facilities to create isolation or quarantine rooms for infected seniors.
9. Work with family members to proactively report to medical professionals any symptoms noticed in their senior relatives. Educate seniors to report symptoms earlier.
10. Offer incentives for medical professionals to conduct on-site testing in primary care offices or senior care facilities instead of sending patients to hospital emergency rooms for evaluation. This will only be effective if there are enough test kits available.
11. Urge insurance companies and Medicare to allow additional medical visits for screening vulnerable populations. Encourage the use of telemedicine in place of in-office visits (preferably billed at the same rate as an in-office visit) where appropriate, especially with nonambulatory patients or those with transportation issues. Many insurance companies, including Medicare, approved COVID-19–related coverage of telemedicine in place of office visits to limit the spread of the disease.
12. Provide community health care and integration and better coordination of local, state, and national health care.
13. Hold regular epidemic and pandemic preparedness exercises in every hospital, nursing home, and assisted living facility.
Proactive health care outreach
It is easier to identify the signs and symptoms of already identified infectious diseases as opposed to a novel one like COVID-19. The United States faced a steep learning curve with COVID-19. Hospitalists and other medical professionals were not able to learn about COVID-19 in a journal. At first, they did not know how to screen patients coming into the ER, how to protect staff, or what the treatment plan was for this new disease. As a result, the medical system experienced disorder and confusion. Investing in community health care and better coordination of local, state, and national health care resources is a priority.
The senior citizen population appears to be most vulnerable to this virus and may be just as vulnerable in future outbreaks. Yet the insights gained from this pandemic can lead to a more comprehensive outreach to senior patients and increased screenings for comorbidities and future contagious diseases. An emphasis on proactive health care and outreach for seniors, with a focus on identifying and treating comorbid conditions, improves the medical care system overall and may prevent or slow future community outbreaks.
Dr. Kasarla is a hospitalist with APOGEE Physicians at Wise Surgical at Parkway in Fort Worth, Tex. He did his internal medicine residency at Mercy Hospital & Medical Center, Chicago. Readers can contact him at madhukarreddy.kasarla@apogeephysicians.com. Dr. Devireddy is a family physician at Positive Health Medical Center, Kingston, Jamaica. Contact him at drjaisheel@gmail.com.
References
1. Pisano GP et al. Lessons from Italy’s response to coronavirus. Harvard Business Review. 2020 Mar 27. https://hbr.org/2020/03/lessons-from-italys-response-to-coronavirus.
2. Tu C. Lessons from Taiwan’s experience with COVID-19. New Atlanticist. 2020 Apr 7. https://atlanticcouncil.org/blogs/new-atlanticist/lessons-from-taiwans-experience-with-covid-19/.
3. Newman LH. WhatsApp is at the center of coronavirus response. WIRED. 2020 Mar 20. https://www.wired.com/story/whatsapp-coronavirus-who-information-app/.
A tribute to Edward Ross Ritvo, MD, 1930-2020
Reflections on loss amid COVID-19
I sit here on Father’s Day during a global pandemic and can’t help but think of Mark Twain’s quote, “Truth is stranger than fiction.” Isn’t that what calls us to our profession? When friends ask if I have watched a particular movie or TV show, I almost always say no. Why would I? Day after day at “work” I am hearing the most remarkable stories – many unfolding right before my eyes.
My Dad’s story is no less remarkable. As he was a pioneer in our field, I hope you will allow me to share a few recollections.
June 10, just 10 days after turning 90, Dad died peacefully in his home. His obituary, written by James McCracken, MD, says: “He was an internationally known child psychiatrist who, with colleagues, formed the vanguard of UCLA researchers establishing the biomedical basis of autism in the 1960s despite the prevailing psychological theories of the day ... who would later break new ground in identifying the role of genetics, sleep, and neurophysiological differences, perinatal risk factors, and biomarkers relating to autism and autism risk.”
Dad had extensive training in psychoanalysis and worked hard to maintain expertise in both the psychological and biological arenas. While he helped established autism as a neurologic disease and advocated for DSM criteria changes, he continued teaching Psychodynamic Theory of Personality to the UCLA medical students and maintained a clinical practice based in psychotherapeutic techniques. He was practicing biopsychosocial medicine long before the concept was articulated.
He conducted the first epidemiologic survey of autism in the state of Utah. He chose Utah because the Mormons keep perfect genealogical records. He identified multiple families with more than one child affected as well as examining, pre-, peri-, and postnatal factors affecting these families. Being a maverick has its challenges. One paper about parents with mild autism was rejected from publication seven times before a watered-down version of clinical vignettes finally got accepted. In collaboration with his wife, Riva Ariella Ritvo, he developed the Ritvo Autism Asperger Diagnostic Scale–Revised, (RAADS-R) still in use today.
Dad’s career was complicated by medical issues beginning in his 40s when he had a near-fatal heart attack at the top of Mammoth Mountain while skiing. After struggling for 20 years, he ultimately had a heart transplant at Cedars-Sinai Medical Center at 69 years old. Months after the transplant, he was back at work. He was unstoppable and maintained his optimism and great sense of humor throughout this complicated ordeal. He always remembered his commitment to his donor and his new heart, and worked out every day. Living to 90 was against all the odds.
Dad also persevered throughout his youngest son’s 10-year battle with Ewing’s sarcoma. Despite losing Max in 2016, Dad was active in research and clinical practice until the very end. He was doing telepsychiatry with patients in prisons and rehabilitation hospitals the last few years because he was too weak to travel to an office. He continued his research, and his last paper on eye movement responses as a possible biological marker of autism was published in February 2020.
Although Dad did not have COVID-19, the social isolation and stress of the last few months hastened his decline. The last week in the hospital with no visitors was too much for such a social man, and he died days after he was discharged. Always a trailblazer, Dad’s Zoom funeral was watched across the country by his children, grandchildren, extended family, and friends. Choosing to honor his wish to be cautious in this pandemic, we remained sheltering in place.
As Dad was the ultimate professor, I know he would want us to learn from his life and his passing. We are in an accelerated growth phase now as our lives and the lives of our patients are radically altered.
I hope, like Dad, we can choose to feel nourished by our meaningful work as we travel through life’s ups and downs. We must learn new ways to care for ourselves, our families, and our patients during these challenging times. We must find ways to mourn and celebrate those lost during the pandemic.
I know Dad would love synchronicity that I spent Father’s Day writing about him for Clinical Psychiatry News! Thank you for giving me this gift of reflection on this special day.
Dr. Ritvo, a psychiatrist with more than 25 years’ experience, practices in Miami Beach. She is the author of “Bekindr – The Transformative Power of Kindness” (Hellertown, Pa.: Momosa Publishing, 2018) and is the founder of the Bekindr Global Initiative, a movement aimed at cultivating kindness in the world. Dr. Ritvo also is the cofounder of the Bold Beauty Project, a nonprofit group that pairs women with disabilities with photographers who create art exhibitions to raise awareness.
Reflections on loss amid COVID-19
Reflections on loss amid COVID-19
I sit here on Father’s Day during a global pandemic and can’t help but think of Mark Twain’s quote, “Truth is stranger than fiction.” Isn’t that what calls us to our profession? When friends ask if I have watched a particular movie or TV show, I almost always say no. Why would I? Day after day at “work” I am hearing the most remarkable stories – many unfolding right before my eyes.
My Dad’s story is no less remarkable. As he was a pioneer in our field, I hope you will allow me to share a few recollections.
June 10, just 10 days after turning 90, Dad died peacefully in his home. His obituary, written by James McCracken, MD, says: “He was an internationally known child psychiatrist who, with colleagues, formed the vanguard of UCLA researchers establishing the biomedical basis of autism in the 1960s despite the prevailing psychological theories of the day ... who would later break new ground in identifying the role of genetics, sleep, and neurophysiological differences, perinatal risk factors, and biomarkers relating to autism and autism risk.”
Dad had extensive training in psychoanalysis and worked hard to maintain expertise in both the psychological and biological arenas. While he helped established autism as a neurologic disease and advocated for DSM criteria changes, he continued teaching Psychodynamic Theory of Personality to the UCLA medical students and maintained a clinical practice based in psychotherapeutic techniques. He was practicing biopsychosocial medicine long before the concept was articulated.
He conducted the first epidemiologic survey of autism in the state of Utah. He chose Utah because the Mormons keep perfect genealogical records. He identified multiple families with more than one child affected as well as examining, pre-, peri-, and postnatal factors affecting these families. Being a maverick has its challenges. One paper about parents with mild autism was rejected from publication seven times before a watered-down version of clinical vignettes finally got accepted. In collaboration with his wife, Riva Ariella Ritvo, he developed the Ritvo Autism Asperger Diagnostic Scale–Revised, (RAADS-R) still in use today.
Dad’s career was complicated by medical issues beginning in his 40s when he had a near-fatal heart attack at the top of Mammoth Mountain while skiing. After struggling for 20 years, he ultimately had a heart transplant at Cedars-Sinai Medical Center at 69 years old. Months after the transplant, he was back at work. He was unstoppable and maintained his optimism and great sense of humor throughout this complicated ordeal. He always remembered his commitment to his donor and his new heart, and worked out every day. Living to 90 was against all the odds.
Dad also persevered throughout his youngest son’s 10-year battle with Ewing’s sarcoma. Despite losing Max in 2016, Dad was active in research and clinical practice until the very end. He was doing telepsychiatry with patients in prisons and rehabilitation hospitals the last few years because he was too weak to travel to an office. He continued his research, and his last paper on eye movement responses as a possible biological marker of autism was published in February 2020.
Although Dad did not have COVID-19, the social isolation and stress of the last few months hastened his decline. The last week in the hospital with no visitors was too much for such a social man, and he died days after he was discharged. Always a trailblazer, Dad’s Zoom funeral was watched across the country by his children, grandchildren, extended family, and friends. Choosing to honor his wish to be cautious in this pandemic, we remained sheltering in place.
As Dad was the ultimate professor, I know he would want us to learn from his life and his passing. We are in an accelerated growth phase now as our lives and the lives of our patients are radically altered.
I hope, like Dad, we can choose to feel nourished by our meaningful work as we travel through life’s ups and downs. We must learn new ways to care for ourselves, our families, and our patients during these challenging times. We must find ways to mourn and celebrate those lost during the pandemic.
I know Dad would love synchronicity that I spent Father’s Day writing about him for Clinical Psychiatry News! Thank you for giving me this gift of reflection on this special day.
Dr. Ritvo, a psychiatrist with more than 25 years’ experience, practices in Miami Beach. She is the author of “Bekindr – The Transformative Power of Kindness” (Hellertown, Pa.: Momosa Publishing, 2018) and is the founder of the Bekindr Global Initiative, a movement aimed at cultivating kindness in the world. Dr. Ritvo also is the cofounder of the Bold Beauty Project, a nonprofit group that pairs women with disabilities with photographers who create art exhibitions to raise awareness.
I sit here on Father’s Day during a global pandemic and can’t help but think of Mark Twain’s quote, “Truth is stranger than fiction.” Isn’t that what calls us to our profession? When friends ask if I have watched a particular movie or TV show, I almost always say no. Why would I? Day after day at “work” I am hearing the most remarkable stories – many unfolding right before my eyes.
My Dad’s story is no less remarkable. As he was a pioneer in our field, I hope you will allow me to share a few recollections.
June 10, just 10 days after turning 90, Dad died peacefully in his home. His obituary, written by James McCracken, MD, says: “He was an internationally known child psychiatrist who, with colleagues, formed the vanguard of UCLA researchers establishing the biomedical basis of autism in the 1960s despite the prevailing psychological theories of the day ... who would later break new ground in identifying the role of genetics, sleep, and neurophysiological differences, perinatal risk factors, and biomarkers relating to autism and autism risk.”
Dad had extensive training in psychoanalysis and worked hard to maintain expertise in both the psychological and biological arenas. While he helped established autism as a neurologic disease and advocated for DSM criteria changes, he continued teaching Psychodynamic Theory of Personality to the UCLA medical students and maintained a clinical practice based in psychotherapeutic techniques. He was practicing biopsychosocial medicine long before the concept was articulated.
He conducted the first epidemiologic survey of autism in the state of Utah. He chose Utah because the Mormons keep perfect genealogical records. He identified multiple families with more than one child affected as well as examining, pre-, peri-, and postnatal factors affecting these families. Being a maverick has its challenges. One paper about parents with mild autism was rejected from publication seven times before a watered-down version of clinical vignettes finally got accepted. In collaboration with his wife, Riva Ariella Ritvo, he developed the Ritvo Autism Asperger Diagnostic Scale–Revised, (RAADS-R) still in use today.
Dad’s career was complicated by medical issues beginning in his 40s when he had a near-fatal heart attack at the top of Mammoth Mountain while skiing. After struggling for 20 years, he ultimately had a heart transplant at Cedars-Sinai Medical Center at 69 years old. Months after the transplant, he was back at work. He was unstoppable and maintained his optimism and great sense of humor throughout this complicated ordeal. He always remembered his commitment to his donor and his new heart, and worked out every day. Living to 90 was against all the odds.
Dad also persevered throughout his youngest son’s 10-year battle with Ewing’s sarcoma. Despite losing Max in 2016, Dad was active in research and clinical practice until the very end. He was doing telepsychiatry with patients in prisons and rehabilitation hospitals the last few years because he was too weak to travel to an office. He continued his research, and his last paper on eye movement responses as a possible biological marker of autism was published in February 2020.
Although Dad did not have COVID-19, the social isolation and stress of the last few months hastened his decline. The last week in the hospital with no visitors was too much for such a social man, and he died days after he was discharged. Always a trailblazer, Dad’s Zoom funeral was watched across the country by his children, grandchildren, extended family, and friends. Choosing to honor his wish to be cautious in this pandemic, we remained sheltering in place.
As Dad was the ultimate professor, I know he would want us to learn from his life and his passing. We are in an accelerated growth phase now as our lives and the lives of our patients are radically altered.
I hope, like Dad, we can choose to feel nourished by our meaningful work as we travel through life’s ups and downs. We must learn new ways to care for ourselves, our families, and our patients during these challenging times. We must find ways to mourn and celebrate those lost during the pandemic.
I know Dad would love synchronicity that I spent Father’s Day writing about him for Clinical Psychiatry News! Thank you for giving me this gift of reflection on this special day.
Dr. Ritvo, a psychiatrist with more than 25 years’ experience, practices in Miami Beach. She is the author of “Bekindr – The Transformative Power of Kindness” (Hellertown, Pa.: Momosa Publishing, 2018) and is the founder of the Bekindr Global Initiative, a movement aimed at cultivating kindness in the world. Dr. Ritvo also is the cofounder of the Bold Beauty Project, a nonprofit group that pairs women with disabilities with photographers who create art exhibitions to raise awareness.
School daze
A few weeks ago I was asked by the head of our local parks and recreation department for my opinion on whether the town should open its summer recreation camps program. He had been receiving multiple inquiries from parents who in the past had relied on the day camps for day care. The director already had surveyed health care administrators and other providers in the town and his team had crafted a plan based on what guidelines they could glean from state and federal advisory groups. The feedback he had received from town officials and health care representatives was that they felt opening would be a bad decision. One physician observed that there is just “so much we don’t know about the virus at this point.”
I certainly agreed that we still have much to learn about COVID-19, but I told the director that we know enough that I would feel comfortable with opening the day camps, which have traditionally been held outdoors under open-sided tents. If group sizes were kept small, staff personnel were dedicated to just one group, and temperatures were taken at the beginning and at the midpoint of each daily session, I felt that the risk of triggering an outbreak was small. I told him that in my mind the Achilles heel of the plan was whether the camp staff, who are generally high school and college-age young people, could be trusted to follow rigorous social distancing in their off-work hours.
Eventually the decision was made by the traditionally risk-averse town officials to open the camps. I hope that this step forward will spur the process of reopening the schools in the fall by demonstrating that, at least in an open-air environment, some simple common sense measures could create a safe environment for children to congregate in. Unfortunately, the long delay in formulating the plan and a basic hesitancy on the part of some parents has resulted in disappointing enrollment figures so far.
I suspect that many of you have been asked to participate in the planning and decision-making processes for opening the school systems in your community or at least have some thoughts of your own about how best to begin the reopening process.
I suspect you agree that, if the number of new cases detected each day in your state is still rising and/or your state’s ability to test, track, case find, and quarantine is inadequate, reopening schools is probably just asking for trouble. However, a recent study has found that children and young adults under the age of 20 years were almost half as likely to become infected as those over the age of 20 (Nat Med. 2020 Jun 16. doi: 10.1038/s41591-020-0962-9). We already know that, in general, children are presenting with less severe illness. Although the authors observe that we still need to learn more about the transmissibility of subclinical infections, particularly in children, they suggest that “interventions aimed at children might have relatively little impact on reducing SARS-CoV-2 transmission.” It is sounding like reopening schools will place the children at relatively low risk. However, until we know more about transmissibility we have to assume reopening schools may place the community at an increased risk.
If this new information is confirmed by other studies, how would this change the recommendations you would make to the community about reopening its schools? What about masks? We are learning that they make a difference for adults, but is this true for very young children as well? Masks should probably remain part of the hygiene education program as well for at least the foreseeable future.
Do you think your school system can broaden its focus beyond surface cleaning to air handling and ventilation? Here in Maine, keeping the windows open for more than a few weeks a year is going to present problems that may be expensive to remedy.
There are always more questions than answers, but my hope is that here in Maine our apparent success on a state level will allow us to reopen the schools as long as we remain vigilant for the first signs that we need to return to lock down. How do you feel about your community’s situation?
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at pdnews@mdedge.com.
A few weeks ago I was asked by the head of our local parks and recreation department for my opinion on whether the town should open its summer recreation camps program. He had been receiving multiple inquiries from parents who in the past had relied on the day camps for day care. The director already had surveyed health care administrators and other providers in the town and his team had crafted a plan based on what guidelines they could glean from state and federal advisory groups. The feedback he had received from town officials and health care representatives was that they felt opening would be a bad decision. One physician observed that there is just “so much we don’t know about the virus at this point.”
I certainly agreed that we still have much to learn about COVID-19, but I told the director that we know enough that I would feel comfortable with opening the day camps, which have traditionally been held outdoors under open-sided tents. If group sizes were kept small, staff personnel were dedicated to just one group, and temperatures were taken at the beginning and at the midpoint of each daily session, I felt that the risk of triggering an outbreak was small. I told him that in my mind the Achilles heel of the plan was whether the camp staff, who are generally high school and college-age young people, could be trusted to follow rigorous social distancing in their off-work hours.
Eventually the decision was made by the traditionally risk-averse town officials to open the camps. I hope that this step forward will spur the process of reopening the schools in the fall by demonstrating that, at least in an open-air environment, some simple common sense measures could create a safe environment for children to congregate in. Unfortunately, the long delay in formulating the plan and a basic hesitancy on the part of some parents has resulted in disappointing enrollment figures so far.
I suspect that many of you have been asked to participate in the planning and decision-making processes for opening the school systems in your community or at least have some thoughts of your own about how best to begin the reopening process.
I suspect you agree that, if the number of new cases detected each day in your state is still rising and/or your state’s ability to test, track, case find, and quarantine is inadequate, reopening schools is probably just asking for trouble. However, a recent study has found that children and young adults under the age of 20 years were almost half as likely to become infected as those over the age of 20 (Nat Med. 2020 Jun 16. doi: 10.1038/s41591-020-0962-9). We already know that, in general, children are presenting with less severe illness. Although the authors observe that we still need to learn more about the transmissibility of subclinical infections, particularly in children, they suggest that “interventions aimed at children might have relatively little impact on reducing SARS-CoV-2 transmission.” It is sounding like reopening schools will place the children at relatively low risk. However, until we know more about transmissibility we have to assume reopening schools may place the community at an increased risk.
If this new information is confirmed by other studies, how would this change the recommendations you would make to the community about reopening its schools? What about masks? We are learning that they make a difference for adults, but is this true for very young children as well? Masks should probably remain part of the hygiene education program as well for at least the foreseeable future.
Do you think your school system can broaden its focus beyond surface cleaning to air handling and ventilation? Here in Maine, keeping the windows open for more than a few weeks a year is going to present problems that may be expensive to remedy.
There are always more questions than answers, but my hope is that here in Maine our apparent success on a state level will allow us to reopen the schools as long as we remain vigilant for the first signs that we need to return to lock down. How do you feel about your community’s situation?
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at pdnews@mdedge.com.
A few weeks ago I was asked by the head of our local parks and recreation department for my opinion on whether the town should open its summer recreation camps program. He had been receiving multiple inquiries from parents who in the past had relied on the day camps for day care. The director already had surveyed health care administrators and other providers in the town and his team had crafted a plan based on what guidelines they could glean from state and federal advisory groups. The feedback he had received from town officials and health care representatives was that they felt opening would be a bad decision. One physician observed that there is just “so much we don’t know about the virus at this point.”
I certainly agreed that we still have much to learn about COVID-19, but I told the director that we know enough that I would feel comfortable with opening the day camps, which have traditionally been held outdoors under open-sided tents. If group sizes were kept small, staff personnel were dedicated to just one group, and temperatures were taken at the beginning and at the midpoint of each daily session, I felt that the risk of triggering an outbreak was small. I told him that in my mind the Achilles heel of the plan was whether the camp staff, who are generally high school and college-age young people, could be trusted to follow rigorous social distancing in their off-work hours.
Eventually the decision was made by the traditionally risk-averse town officials to open the camps. I hope that this step forward will spur the process of reopening the schools in the fall by demonstrating that, at least in an open-air environment, some simple common sense measures could create a safe environment for children to congregate in. Unfortunately, the long delay in formulating the plan and a basic hesitancy on the part of some parents has resulted in disappointing enrollment figures so far.
I suspect that many of you have been asked to participate in the planning and decision-making processes for opening the school systems in your community or at least have some thoughts of your own about how best to begin the reopening process.
I suspect you agree that, if the number of new cases detected each day in your state is still rising and/or your state’s ability to test, track, case find, and quarantine is inadequate, reopening schools is probably just asking for trouble. However, a recent study has found that children and young adults under the age of 20 years were almost half as likely to become infected as those over the age of 20 (Nat Med. 2020 Jun 16. doi: 10.1038/s41591-020-0962-9). We already know that, in general, children are presenting with less severe illness. Although the authors observe that we still need to learn more about the transmissibility of subclinical infections, particularly in children, they suggest that “interventions aimed at children might have relatively little impact on reducing SARS-CoV-2 transmission.” It is sounding like reopening schools will place the children at relatively low risk. However, until we know more about transmissibility we have to assume reopening schools may place the community at an increased risk.
If this new information is confirmed by other studies, how would this change the recommendations you would make to the community about reopening its schools? What about masks? We are learning that they make a difference for adults, but is this true for very young children as well? Masks should probably remain part of the hygiene education program as well for at least the foreseeable future.
Do you think your school system can broaden its focus beyond surface cleaning to air handling and ventilation? Here in Maine, keeping the windows open for more than a few weeks a year is going to present problems that may be expensive to remedy.
There are always more questions than answers, but my hope is that here in Maine our apparent success on a state level will allow us to reopen the schools as long as we remain vigilant for the first signs that we need to return to lock down. How do you feel about your community’s situation?
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at pdnews@mdedge.com.
COVID-19: Medicare data show long hospital stays, disparities
according to a new analysis by the Centers for Medicare & Medicaid Services.
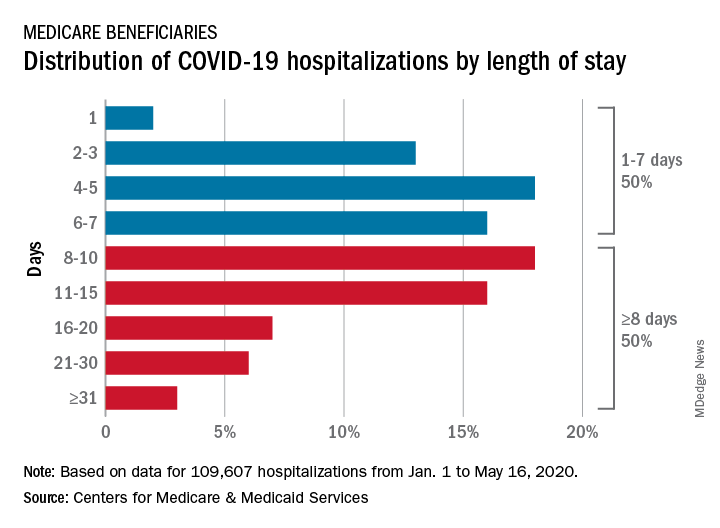
CMS encounter and claims data show almost 110,000 hospital stays for COVID-19 from Jan. 1 to May 16, 2020. Of the longer admissions, 18% were 8-10 days, 16% were 11-15 days, and another 16% were 16 days or longer, the CMS reported in a preliminary data snapshot released June 22.
The hospitalization rate for the Medicare population was 175 per 100,000 as of May 16, but the CMS data show a number of disparities involving race/ethnicity and other demographic characteristics were uncovered, such as the following:
- Black patients were hospitalized for COVID-19 at a much higher rate, at 465 per 100,000 beneficiaries, than were Hispanics (258), Asians (187), and whites (123).
- Residents of urban/suburban areas had a much higher hospitalization rate than did those living in rural areas: 205 versus 57 per 100,000.
- Beneficiaries enrolled in both Medicare and Medicaid had 473 hospitalizations per 100,000, but the rate for those with Medicare only was 112.
“The disparities in the data reflect longstanding challenges facing minority communities and low-income older adults, many of whom face structural challenges to their health that go far beyond what is traditionally considered ‘medical,’ ” CMS Administrator Seema Verma said in a separate statement.
according to a new analysis by the Centers for Medicare & Medicaid Services.

CMS encounter and claims data show almost 110,000 hospital stays for COVID-19 from Jan. 1 to May 16, 2020. Of the longer admissions, 18% were 8-10 days, 16% were 11-15 days, and another 16% were 16 days or longer, the CMS reported in a preliminary data snapshot released June 22.
The hospitalization rate for the Medicare population was 175 per 100,000 as of May 16, but the CMS data show a number of disparities involving race/ethnicity and other demographic characteristics were uncovered, such as the following:
- Black patients were hospitalized for COVID-19 at a much higher rate, at 465 per 100,000 beneficiaries, than were Hispanics (258), Asians (187), and whites (123).
- Residents of urban/suburban areas had a much higher hospitalization rate than did those living in rural areas: 205 versus 57 per 100,000.
- Beneficiaries enrolled in both Medicare and Medicaid had 473 hospitalizations per 100,000, but the rate for those with Medicare only was 112.
“The disparities in the data reflect longstanding challenges facing minority communities and low-income older adults, many of whom face structural challenges to their health that go far beyond what is traditionally considered ‘medical,’ ” CMS Administrator Seema Verma said in a separate statement.
according to a new analysis by the Centers for Medicare & Medicaid Services.

CMS encounter and claims data show almost 110,000 hospital stays for COVID-19 from Jan. 1 to May 16, 2020. Of the longer admissions, 18% were 8-10 days, 16% were 11-15 days, and another 16% were 16 days or longer, the CMS reported in a preliminary data snapshot released June 22.
The hospitalization rate for the Medicare population was 175 per 100,000 as of May 16, but the CMS data show a number of disparities involving race/ethnicity and other demographic characteristics were uncovered, such as the following:
- Black patients were hospitalized for COVID-19 at a much higher rate, at 465 per 100,000 beneficiaries, than were Hispanics (258), Asians (187), and whites (123).
- Residents of urban/suburban areas had a much higher hospitalization rate than did those living in rural areas: 205 versus 57 per 100,000.
- Beneficiaries enrolled in both Medicare and Medicaid had 473 hospitalizations per 100,000, but the rate for those with Medicare only was 112.
“The disparities in the data reflect longstanding challenges facing minority communities and low-income older adults, many of whom face structural challenges to their health that go far beyond what is traditionally considered ‘medical,’ ” CMS Administrator Seema Verma said in a separate statement.











