User login
FDA effort focuses on approving more generic drugs
Pharmaceutical companies may be in for a more difficult time hiding behind a Risk Evaluation and Mitigation Strategy (REMS) as a way to prevent generic competition from entering the market.
The Food and Drug Administration issued two draft guidance documents on May 31 aimed at spurring on generic competition, items that are part of a broader White House strategy targeting the high price of prescription drugs.
“We have seen REMS requirements exploited in two ways,” FDA Commissioner Scott Gottlieb, MD, said in a statement. “One occurs at the front end of the drug development process, when generic drugs are being developed. The other occurs at the back end of the process, after necessary testing has been completed, when a generic drug seeks approval and market entry.”
On the front end, manufacturers use REMS to restrict the sale of drugs to keep them out of the hands of generic firms, which typically need about 5,000 doses to conduct bioequivalence and bioavailability studies, Dr. Gottlieb noted. The back-end obstacle, which happens after a generic manufacturer files application for generic approval, is what the two guidance documents address.
The first draft guidance document, “Development of a Shared System REMS,” outlines principles and recommendations for brand and generic manufacturers to develop a single REMS program that covers both products, which Dr. Gottlieb said will “enable timelier market entry for products that are part of these REMS.”
The second draft guidance document, “Waivers of the Single Shared System REMS Requirement,” describes the two circumstances under which the generic manufacturer can waive the single, shared REMS requirements:
- If the burden of forming a single, shared systems outweighs the benefits.
- If an aspect of the REMS is covered by a patent or is a trade secret and the generic company was unable to obtain a license for use.
“We believe that by making the process for developing a shared system REMS more efficient, we’ll discourage brand drug makers from using REMS as a way to block generic entry and help end some of the tactics that can delay access,” Dr. Gottlieb said. “Our safety programs shouldn’t be leveraged as a way to forestall generic entry after lawful IP has lapsed on a brand drug.”
“Today’s FDA guidance is a step in the right direction toward our common goal of lowering out-of-control drug prices,” the Campaign for Sustainable Rx Pricing said in a statement “When generic and biosimilar competition is thwarted by these abusive tactics, brand-name manufacturers, who alone control the price of their drugs, keep those prices artificially high. The problem is the price, and more competition is a proven solution.”
Comments on each of the draft guidance documents are due July 31 at www.regulations.gov.
Pharmaceutical companies may be in for a more difficult time hiding behind a Risk Evaluation and Mitigation Strategy (REMS) as a way to prevent generic competition from entering the market.
The Food and Drug Administration issued two draft guidance documents on May 31 aimed at spurring on generic competition, items that are part of a broader White House strategy targeting the high price of prescription drugs.
“We have seen REMS requirements exploited in two ways,” FDA Commissioner Scott Gottlieb, MD, said in a statement. “One occurs at the front end of the drug development process, when generic drugs are being developed. The other occurs at the back end of the process, after necessary testing has been completed, when a generic drug seeks approval and market entry.”
On the front end, manufacturers use REMS to restrict the sale of drugs to keep them out of the hands of generic firms, which typically need about 5,000 doses to conduct bioequivalence and bioavailability studies, Dr. Gottlieb noted. The back-end obstacle, which happens after a generic manufacturer files application for generic approval, is what the two guidance documents address.
The first draft guidance document, “Development of a Shared System REMS,” outlines principles and recommendations for brand and generic manufacturers to develop a single REMS program that covers both products, which Dr. Gottlieb said will “enable timelier market entry for products that are part of these REMS.”
The second draft guidance document, “Waivers of the Single Shared System REMS Requirement,” describes the two circumstances under which the generic manufacturer can waive the single, shared REMS requirements:
- If the burden of forming a single, shared systems outweighs the benefits.
- If an aspect of the REMS is covered by a patent or is a trade secret and the generic company was unable to obtain a license for use.
“We believe that by making the process for developing a shared system REMS more efficient, we’ll discourage brand drug makers from using REMS as a way to block generic entry and help end some of the tactics that can delay access,” Dr. Gottlieb said. “Our safety programs shouldn’t be leveraged as a way to forestall generic entry after lawful IP has lapsed on a brand drug.”
“Today’s FDA guidance is a step in the right direction toward our common goal of lowering out-of-control drug prices,” the Campaign for Sustainable Rx Pricing said in a statement “When generic and biosimilar competition is thwarted by these abusive tactics, brand-name manufacturers, who alone control the price of their drugs, keep those prices artificially high. The problem is the price, and more competition is a proven solution.”
Comments on each of the draft guidance documents are due July 31 at www.regulations.gov.
Pharmaceutical companies may be in for a more difficult time hiding behind a Risk Evaluation and Mitigation Strategy (REMS) as a way to prevent generic competition from entering the market.
The Food and Drug Administration issued two draft guidance documents on May 31 aimed at spurring on generic competition, items that are part of a broader White House strategy targeting the high price of prescription drugs.
“We have seen REMS requirements exploited in two ways,” FDA Commissioner Scott Gottlieb, MD, said in a statement. “One occurs at the front end of the drug development process, when generic drugs are being developed. The other occurs at the back end of the process, after necessary testing has been completed, when a generic drug seeks approval and market entry.”
On the front end, manufacturers use REMS to restrict the sale of drugs to keep them out of the hands of generic firms, which typically need about 5,000 doses to conduct bioequivalence and bioavailability studies, Dr. Gottlieb noted. The back-end obstacle, which happens after a generic manufacturer files application for generic approval, is what the two guidance documents address.
The first draft guidance document, “Development of a Shared System REMS,” outlines principles and recommendations for brand and generic manufacturers to develop a single REMS program that covers both products, which Dr. Gottlieb said will “enable timelier market entry for products that are part of these REMS.”
The second draft guidance document, “Waivers of the Single Shared System REMS Requirement,” describes the two circumstances under which the generic manufacturer can waive the single, shared REMS requirements:
- If the burden of forming a single, shared systems outweighs the benefits.
- If an aspect of the REMS is covered by a patent or is a trade secret and the generic company was unable to obtain a license for use.
“We believe that by making the process for developing a shared system REMS more efficient, we’ll discourage brand drug makers from using REMS as a way to block generic entry and help end some of the tactics that can delay access,” Dr. Gottlieb said. “Our safety programs shouldn’t be leveraged as a way to forestall generic entry after lawful IP has lapsed on a brand drug.”
“Today’s FDA guidance is a step in the right direction toward our common goal of lowering out-of-control drug prices,” the Campaign for Sustainable Rx Pricing said in a statement “When generic and biosimilar competition is thwarted by these abusive tactics, brand-name manufacturers, who alone control the price of their drugs, keep those prices artificially high. The problem is the price, and more competition is a proven solution.”
Comments on each of the draft guidance documents are due July 31 at www.regulations.gov.
Emicizumab gets priority review for hemophilia A without inhibitors
The Food and Drug Administration has granted priority review to Roche’s emicizumab-kxwh (Hemlibra) for the treatment of adults and children with hemophilia A without factor VIII inhibitors.
The agency is scheduled to make a decision on approval in October 2018.
Among patients aged 12 years and older without factor VIII inhibitors, emicizumab-kxwh prophylaxis every week reduced treated bleeds by 96% (P less than .0001) and treated bleeds were reduced by 97% (P less than .0001) in patients who were treated every 2 weeks, according to Roche. The drug-treated group was compared with patients who received no prophylaxis. Another arm of the study examined patients who had previously received factor VIII prophylaxis and then switched to emicizumab-kxwh prophylaxis. In an intrapatient comparison, emicizumab-kxwh showed a 68% reduction in treated bleeds, which was statistically significant and demonstrated superior efficacy to factor VIII prophylaxis.
Emicizumab-kxwh was approved by FDA in November 2017 for routine prophylaxis for adults and children with hemophilia A with factor VIII inhibitors. That approval was based on results from the HAVEN 1 and HAVEN 2 studies.
The Food and Drug Administration has granted priority review to Roche’s emicizumab-kxwh (Hemlibra) for the treatment of adults and children with hemophilia A without factor VIII inhibitors.
The agency is scheduled to make a decision on approval in October 2018.
Among patients aged 12 years and older without factor VIII inhibitors, emicizumab-kxwh prophylaxis every week reduced treated bleeds by 96% (P less than .0001) and treated bleeds were reduced by 97% (P less than .0001) in patients who were treated every 2 weeks, according to Roche. The drug-treated group was compared with patients who received no prophylaxis. Another arm of the study examined patients who had previously received factor VIII prophylaxis and then switched to emicizumab-kxwh prophylaxis. In an intrapatient comparison, emicizumab-kxwh showed a 68% reduction in treated bleeds, which was statistically significant and demonstrated superior efficacy to factor VIII prophylaxis.
Emicizumab-kxwh was approved by FDA in November 2017 for routine prophylaxis for adults and children with hemophilia A with factor VIII inhibitors. That approval was based on results from the HAVEN 1 and HAVEN 2 studies.
The Food and Drug Administration has granted priority review to Roche’s emicizumab-kxwh (Hemlibra) for the treatment of adults and children with hemophilia A without factor VIII inhibitors.
The agency is scheduled to make a decision on approval in October 2018.
Among patients aged 12 years and older without factor VIII inhibitors, emicizumab-kxwh prophylaxis every week reduced treated bleeds by 96% (P less than .0001) and treated bleeds were reduced by 97% (P less than .0001) in patients who were treated every 2 weeks, according to Roche. The drug-treated group was compared with patients who received no prophylaxis. Another arm of the study examined patients who had previously received factor VIII prophylaxis and then switched to emicizumab-kxwh prophylaxis. In an intrapatient comparison, emicizumab-kxwh showed a 68% reduction in treated bleeds, which was statistically significant and demonstrated superior efficacy to factor VIII prophylaxis.
Emicizumab-kxwh was approved by FDA in November 2017 for routine prophylaxis for adults and children with hemophilia A with factor VIII inhibitors. That approval was based on results from the HAVEN 1 and HAVEN 2 studies.
FDA approves first biosimilar to pegfilgrastim
to decrease the chance of infection in patients with nonmyeloid cancer who are receiving myelosuppressive chemotherapy and are at risk of febrile neutropenia.
The approval is based on structural and functional characterization, animal study data, human pharmacokinetic and pharmacodynamic data, clinical immunogenicity data, and other clinical safety and effectiveness data that demonstrates pegfilgrastim-jmdb is biosimilar to pegfilgrastim, the FDA said in a statement.
The FDA warns that “patients with a history of serious allergic reactions to human granulocyte colony–stimulating factors such as pegfilgrastim or filgrastim products should not take pegfilgrastim-jmdb.”
This approval is part of the FDA’s efforts to “help promote competition that can reduce drug costs and promote access,” FDA commissioner Scott Gottlieb, MD, said in the statement. “This summer, we’ll release a comprehensive new plan to advance new policy efforts that promote biosimilar product development. Biologics represent some of the most clinically important, but also costliest products that patients use to promote their health. We want to make sure that the pathway for developing biosimilar versions of approved biologics is efficient and effective, so that patients benefit from competition to existing biologics once lawful intellectual property has lapsed on these products.”
Pegfilgrastim-jmdb will be marketed as Fulphila by Mylan GmbH.
to decrease the chance of infection in patients with nonmyeloid cancer who are receiving myelosuppressive chemotherapy and are at risk of febrile neutropenia.
The approval is based on structural and functional characterization, animal study data, human pharmacokinetic and pharmacodynamic data, clinical immunogenicity data, and other clinical safety and effectiveness data that demonstrates pegfilgrastim-jmdb is biosimilar to pegfilgrastim, the FDA said in a statement.
The FDA warns that “patients with a history of serious allergic reactions to human granulocyte colony–stimulating factors such as pegfilgrastim or filgrastim products should not take pegfilgrastim-jmdb.”
This approval is part of the FDA’s efforts to “help promote competition that can reduce drug costs and promote access,” FDA commissioner Scott Gottlieb, MD, said in the statement. “This summer, we’ll release a comprehensive new plan to advance new policy efforts that promote biosimilar product development. Biologics represent some of the most clinically important, but also costliest products that patients use to promote their health. We want to make sure that the pathway for developing biosimilar versions of approved biologics is efficient and effective, so that patients benefit from competition to existing biologics once lawful intellectual property has lapsed on these products.”
Pegfilgrastim-jmdb will be marketed as Fulphila by Mylan GmbH.
to decrease the chance of infection in patients with nonmyeloid cancer who are receiving myelosuppressive chemotherapy and are at risk of febrile neutropenia.
The approval is based on structural and functional characterization, animal study data, human pharmacokinetic and pharmacodynamic data, clinical immunogenicity data, and other clinical safety and effectiveness data that demonstrates pegfilgrastim-jmdb is biosimilar to pegfilgrastim, the FDA said in a statement.
The FDA warns that “patients with a history of serious allergic reactions to human granulocyte colony–stimulating factors such as pegfilgrastim or filgrastim products should not take pegfilgrastim-jmdb.”
This approval is part of the FDA’s efforts to “help promote competition that can reduce drug costs and promote access,” FDA commissioner Scott Gottlieb, MD, said in the statement. “This summer, we’ll release a comprehensive new plan to advance new policy efforts that promote biosimilar product development. Biologics represent some of the most clinically important, but also costliest products that patients use to promote their health. We want to make sure that the pathway for developing biosimilar versions of approved biologics is efficient and effective, so that patients benefit from competition to existing biologics once lawful intellectual property has lapsed on these products.”
Pegfilgrastim-jmdb will be marketed as Fulphila by Mylan GmbH.
FDA alerts clinicians to gastric balloon deaths
according to an alert from the Food and Drug Administration issued on June 4.
Seven of these deaths occurred in patients in the United States; four involved the ORBERA Intragastric Balloon System, and three involved the ReShape Integrated Dual Balloon System.
The FDA has approved updated labeling for the ORBERA and ReShape balloon systems in the United States. The labels contain more information about possible death associated with the use of these devices in the United States. The manufacturers’ sites, Apollo Endosurgery and ReShape Lifesciences, provide more details about the new labeling.
In a letter to health care providers, the FDA advised clinicians to educate bariatric surgery patients about the symptoms of complications from balloon procedures, including not only gastric perforation but also esophageal perforation, balloon deflation, gastrointestinal obstruction, and ulceration. In addition, the FDA reminded clinicians to monitor patients during the entire course of treatment for additional complications, including acute pancreatitis and spontaneous hyperinflation.
Any adverse events involving intragastric balloon systems should be reported to the FDA through MedWatch, the FDA Safety Information and Adverse Event Reporting program.
according to an alert from the Food and Drug Administration issued on June 4.
Seven of these deaths occurred in patients in the United States; four involved the ORBERA Intragastric Balloon System, and three involved the ReShape Integrated Dual Balloon System.
The FDA has approved updated labeling for the ORBERA and ReShape balloon systems in the United States. The labels contain more information about possible death associated with the use of these devices in the United States. The manufacturers’ sites, Apollo Endosurgery and ReShape Lifesciences, provide more details about the new labeling.
In a letter to health care providers, the FDA advised clinicians to educate bariatric surgery patients about the symptoms of complications from balloon procedures, including not only gastric perforation but also esophageal perforation, balloon deflation, gastrointestinal obstruction, and ulceration. In addition, the FDA reminded clinicians to monitor patients during the entire course of treatment for additional complications, including acute pancreatitis and spontaneous hyperinflation.
Any adverse events involving intragastric balloon systems should be reported to the FDA through MedWatch, the FDA Safety Information and Adverse Event Reporting program.
according to an alert from the Food and Drug Administration issued on June 4.
Seven of these deaths occurred in patients in the United States; four involved the ORBERA Intragastric Balloon System, and three involved the ReShape Integrated Dual Balloon System.
The FDA has approved updated labeling for the ORBERA and ReShape balloon systems in the United States. The labels contain more information about possible death associated with the use of these devices in the United States. The manufacturers’ sites, Apollo Endosurgery and ReShape Lifesciences, provide more details about the new labeling.
In a letter to health care providers, the FDA advised clinicians to educate bariatric surgery patients about the symptoms of complications from balloon procedures, including not only gastric perforation but also esophageal perforation, balloon deflation, gastrointestinal obstruction, and ulceration. In addition, the FDA reminded clinicians to monitor patients during the entire course of treatment for additional complications, including acute pancreatitis and spontaneous hyperinflation.
Any adverse events involving intragastric balloon systems should be reported to the FDA through MedWatch, the FDA Safety Information and Adverse Event Reporting program.
FDA grants priority review to first-line SAA treatment
The Food and Drug Administration has granted priority review to Novartis for their severe aplastic anemia drug.
in combination with standard immunosuppressive therapy (IST). The drug is already approved in the United States for treatment of refractory SAA patients. It is also approved for treatment of chronic immune thrombocytopenia in adults and children who are refractory to other treatments or patients with chronic hepatitis C virus. [[{"fid":"","view_mode":"","fields":{"format":"","field_file_image_alt_text[und][0][value]":"","field_file_image_credit[und][0][value]":"","field_file_image_caption[und][0][value]":"","field_file_image_caption[und][0][format]":"filtered_html"},"type":"media","attributes":{"class":"media-element file-"},"field_deltas":{"1":{"field_file_image_caption[und][0][format]":"filtered_html"}}}]]
The priority review status was granted based on preliminary findings showing that eltrombopag plus IST outperformed IST alone in treatment-naïve patients. The study showed that 52% of newly diagnosed patients achieved a complete response at 6 months with eltrombopag plus IST, which was 35% higher than patients treated with IST alone. The overall response rate was 85% at 6 months in the eltrombopag group, according to Novartis.
The drugmaker received a breakthrough therapy designation from the FDA for eltrombopag for first-line use in SAA in January 2018.
The Food and Drug Administration has granted priority review to Novartis for their severe aplastic anemia drug.
in combination with standard immunosuppressive therapy (IST). The drug is already approved in the United States for treatment of refractory SAA patients. It is also approved for treatment of chronic immune thrombocytopenia in adults and children who are refractory to other treatments or patients with chronic hepatitis C virus. [[{"fid":"","view_mode":"","fields":{"format":"","field_file_image_alt_text[und][0][value]":"","field_file_image_credit[und][0][value]":"","field_file_image_caption[und][0][value]":"","field_file_image_caption[und][0][format]":"filtered_html"},"type":"media","attributes":{"class":"media-element file-"},"field_deltas":{"1":{"field_file_image_caption[und][0][format]":"filtered_html"}}}]]
The priority review status was granted based on preliminary findings showing that eltrombopag plus IST outperformed IST alone in treatment-naïve patients. The study showed that 52% of newly diagnosed patients achieved a complete response at 6 months with eltrombopag plus IST, which was 35% higher than patients treated with IST alone. The overall response rate was 85% at 6 months in the eltrombopag group, according to Novartis.
The drugmaker received a breakthrough therapy designation from the FDA for eltrombopag for first-line use in SAA in January 2018.
The Food and Drug Administration has granted priority review to Novartis for their severe aplastic anemia drug.
in combination with standard immunosuppressive therapy (IST). The drug is already approved in the United States for treatment of refractory SAA patients. It is also approved for treatment of chronic immune thrombocytopenia in adults and children who are refractory to other treatments or patients with chronic hepatitis C virus. [[{"fid":"","view_mode":"","fields":{"format":"","field_file_image_alt_text[und][0][value]":"","field_file_image_credit[und][0][value]":"","field_file_image_caption[und][0][value]":"","field_file_image_caption[und][0][format]":"filtered_html"},"type":"media","attributes":{"class":"media-element file-"},"field_deltas":{"1":{"field_file_image_caption[und][0][format]":"filtered_html"}}}]]
The priority review status was granted based on preliminary findings showing that eltrombopag plus IST outperformed IST alone in treatment-naïve patients. The study showed that 52% of newly diagnosed patients achieved a complete response at 6 months with eltrombopag plus IST, which was 35% higher than patients treated with IST alone. The overall response rate was 85% at 6 months in the eltrombopag group, according to Novartis.
The drugmaker received a breakthrough therapy designation from the FDA for eltrombopag for first-line use in SAA in January 2018.
FDA approves Olumiant for treatment of rheumatoid arthritis
, an orally administered Janus kinase (JAK) inhibitor, to treat adults with moderate to severe rheumatoid arthritis (RA) who have responded inadequately or poorly to methotrexate, its manufacturer, Eli Lilly, announced June 1. The regulators voted against approval of the 4-mg dose because of concerns about the safety profile.
Olumiant is accompanied by a boxed warning about the risk of serious infections, malignancies, and thrombosis. Patients taking Olumiant also have experienced tuberculosis and opportunistic viral, fungal, and bacterial infections. These infections have led to hospitalization or death.
As part of the approval, Lilly and the original developer of baricitinib, Incyte, have agreed to conduct further randomized and controlled clinical trials to evaluate the long-term safety of Olumiant.
Lilly said in its announcement that it expects to launch Olumiant in the United States by the end of the second quarter of 2018 at a targeted price that is 60% less than “the leading TNF inhibitor.” Additionally, Lilly will offer patient support in the form of a patient support program called Olumiant Together. More information for the program can be obtained by calling 844-OLUMIANT.
, an orally administered Janus kinase (JAK) inhibitor, to treat adults with moderate to severe rheumatoid arthritis (RA) who have responded inadequately or poorly to methotrexate, its manufacturer, Eli Lilly, announced June 1. The regulators voted against approval of the 4-mg dose because of concerns about the safety profile.
Olumiant is accompanied by a boxed warning about the risk of serious infections, malignancies, and thrombosis. Patients taking Olumiant also have experienced tuberculosis and opportunistic viral, fungal, and bacterial infections. These infections have led to hospitalization or death.
As part of the approval, Lilly and the original developer of baricitinib, Incyte, have agreed to conduct further randomized and controlled clinical trials to evaluate the long-term safety of Olumiant.
Lilly said in its announcement that it expects to launch Olumiant in the United States by the end of the second quarter of 2018 at a targeted price that is 60% less than “the leading TNF inhibitor.” Additionally, Lilly will offer patient support in the form of a patient support program called Olumiant Together. More information for the program can be obtained by calling 844-OLUMIANT.
, an orally administered Janus kinase (JAK) inhibitor, to treat adults with moderate to severe rheumatoid arthritis (RA) who have responded inadequately or poorly to methotrexate, its manufacturer, Eli Lilly, announced June 1. The regulators voted against approval of the 4-mg dose because of concerns about the safety profile.
Olumiant is accompanied by a boxed warning about the risk of serious infections, malignancies, and thrombosis. Patients taking Olumiant also have experienced tuberculosis and opportunistic viral, fungal, and bacterial infections. These infections have led to hospitalization or death.
As part of the approval, Lilly and the original developer of baricitinib, Incyte, have agreed to conduct further randomized and controlled clinical trials to evaluate the long-term safety of Olumiant.
Lilly said in its announcement that it expects to launch Olumiant in the United States by the end of the second quarter of 2018 at a targeted price that is 60% less than “the leading TNF inhibitor.” Additionally, Lilly will offer patient support in the form of a patient support program called Olumiant Together. More information for the program can be obtained by calling 844-OLUMIANT.
FDA issues Ebola preparedness statement
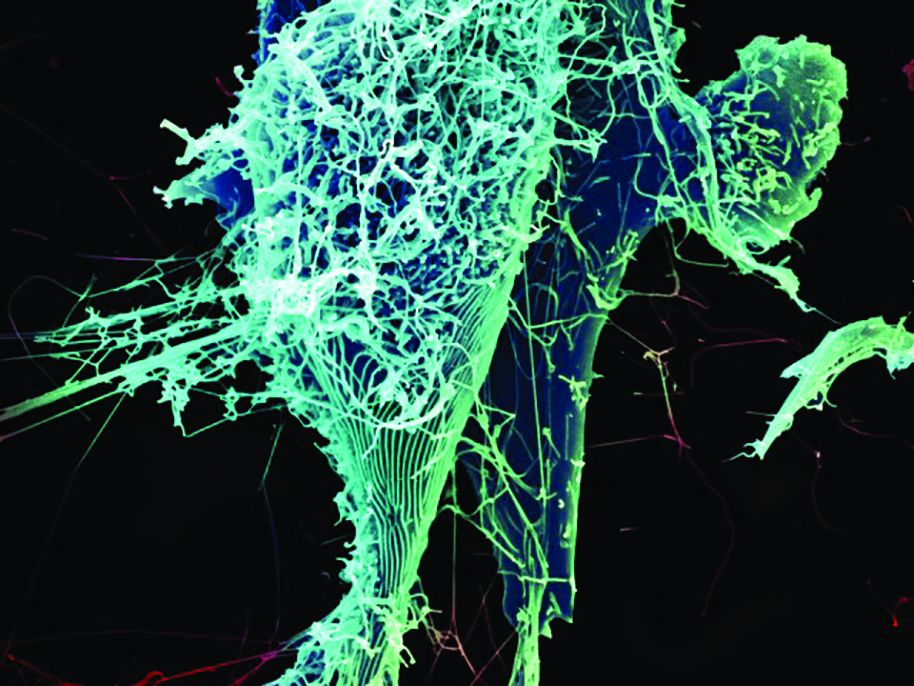
In response to the Ebola outbreak in the Democratic Republic of Congo (DRC), the Food and Drug Administration has announced steps the agency is taking to make diagnostic and medical products available as part of critical response efforts.
In addition to providing scientific and regulatory advice to medical product developers, the FDA is using its authorities to ensure Merck’s investigational Ebola Zaire vaccine is made available appropriately to vaccinate high-risk populations in the DRC. Additionally, the FDA also is committed to facilitating the development of investigational drugs for the treatment of Ebola virus and supporting access to these products under appropriate regulatory pathways, FDA Commissioner Scott Gottlieb, MD, said in a statement.
Clinical trials that are adaptive to the circumstances of an outbreak are essential, he added. “During the 2014-2015 Ebola outbreak, the FDA recognized that some of the medical products that initially appeared to show great promise sometimes, when subjected to objective testing, were not effective or may have done more harm than good.”
Further, as there are no approved treatments or vaccines for Ebola, the agency will be monitoring for false product claims to protect consumers from fraudulent products claiming to prevent, treat, or cure the disease.
“The FDA knows that it takes a sustained, robust, and globally coordinated effort to best protect our nation from various infectious disease threats,” Dr. Gottlieb wrote. “We’re committed to supporting the people of the DRC and preventing a worsening circumstance during the current outbreak. And we remain highly engaged in the international response efforts.”
In response to the Ebola outbreak in the Democratic Republic of Congo (DRC), the Food and Drug Administration has announced steps the agency is taking to make diagnostic and medical products available as part of critical response efforts.
In addition to providing scientific and regulatory advice to medical product developers, the FDA is using its authorities to ensure Merck’s investigational Ebola Zaire vaccine is made available appropriately to vaccinate high-risk populations in the DRC. Additionally, the FDA also is committed to facilitating the development of investigational drugs for the treatment of Ebola virus and supporting access to these products under appropriate regulatory pathways, FDA Commissioner Scott Gottlieb, MD, said in a statement.
Clinical trials that are adaptive to the circumstances of an outbreak are essential, he added. “During the 2014-2015 Ebola outbreak, the FDA recognized that some of the medical products that initially appeared to show great promise sometimes, when subjected to objective testing, were not effective or may have done more harm than good.”
Further, as there are no approved treatments or vaccines for Ebola, the agency will be monitoring for false product claims to protect consumers from fraudulent products claiming to prevent, treat, or cure the disease.
“The FDA knows that it takes a sustained, robust, and globally coordinated effort to best protect our nation from various infectious disease threats,” Dr. Gottlieb wrote. “We’re committed to supporting the people of the DRC and preventing a worsening circumstance during the current outbreak. And we remain highly engaged in the international response efforts.”
In response to the Ebola outbreak in the Democratic Republic of Congo (DRC), the Food and Drug Administration has announced steps the agency is taking to make diagnostic and medical products available as part of critical response efforts.
In addition to providing scientific and regulatory advice to medical product developers, the FDA is using its authorities to ensure Merck’s investigational Ebola Zaire vaccine is made available appropriately to vaccinate high-risk populations in the DRC. Additionally, the FDA also is committed to facilitating the development of investigational drugs for the treatment of Ebola virus and supporting access to these products under appropriate regulatory pathways, FDA Commissioner Scott Gottlieb, MD, said in a statement.
Clinical trials that are adaptive to the circumstances of an outbreak are essential, he added. “During the 2014-2015 Ebola outbreak, the FDA recognized that some of the medical products that initially appeared to show great promise sometimes, when subjected to objective testing, were not effective or may have done more harm than good.”
Further, as there are no approved treatments or vaccines for Ebola, the agency will be monitoring for false product claims to protect consumers from fraudulent products claiming to prevent, treat, or cure the disease.
“The FDA knows that it takes a sustained, robust, and globally coordinated effort to best protect our nation from various infectious disease threats,” Dr. Gottlieb wrote. “We’re committed to supporting the people of the DRC and preventing a worsening circumstance during the current outbreak. And we remain highly engaged in the international response efforts.”
FDA expands Xeljanz approval to certain adults with ulcerative colitis
In two 8-week placebo-controlled trials, 10 mg of Xeljanz given twice daily induced remissions in 17%-18% of patients. In a placebo-controlled trial among the patients who responded by week 8, Xeljanz, at a 5-mg or 10-mg dose given twice daily, was effective in inducing remission by week 52 in 34% and 41% of patients, respectively. Additionally, 35% and 47% of those patients sustained corticosteroid-free remissions when treated with 5-mg and 10-mg doses, respectively.
“New treatments are needed for patients with moderately to severely active ulcerative colitis,” said Julie Beitz, MD, director of the Office of Drug Evaluation III in FDA’s Center for Drug Evaluation and Research in a press release. “Today’s approval provides an alternative therapy for a debilitating disease with limited treatment options.”
Xeljanz is the first oral medication approved for chronic use in moderately to severely active UC. The FDA states that other FDA-approved treatments for the chronic treatment of moderately to severely active ulcerative colitis must be administered through an intravenous infusion or subcutaneous injection.
Xeljanz, made by Pfizer Labs, was previously approved in 2012 for rheumatoid arthritis and in 2017 for psoriatic arthritis.
Find the full press release on the FDA’s website.
In two 8-week placebo-controlled trials, 10 mg of Xeljanz given twice daily induced remissions in 17%-18% of patients. In a placebo-controlled trial among the patients who responded by week 8, Xeljanz, at a 5-mg or 10-mg dose given twice daily, was effective in inducing remission by week 52 in 34% and 41% of patients, respectively. Additionally, 35% and 47% of those patients sustained corticosteroid-free remissions when treated with 5-mg and 10-mg doses, respectively.
“New treatments are needed for patients with moderately to severely active ulcerative colitis,” said Julie Beitz, MD, director of the Office of Drug Evaluation III in FDA’s Center for Drug Evaluation and Research in a press release. “Today’s approval provides an alternative therapy for a debilitating disease with limited treatment options.”
Xeljanz is the first oral medication approved for chronic use in moderately to severely active UC. The FDA states that other FDA-approved treatments for the chronic treatment of moderately to severely active ulcerative colitis must be administered through an intravenous infusion or subcutaneous injection.
Xeljanz, made by Pfizer Labs, was previously approved in 2012 for rheumatoid arthritis and in 2017 for psoriatic arthritis.
Find the full press release on the FDA’s website.
In two 8-week placebo-controlled trials, 10 mg of Xeljanz given twice daily induced remissions in 17%-18% of patients. In a placebo-controlled trial among the patients who responded by week 8, Xeljanz, at a 5-mg or 10-mg dose given twice daily, was effective in inducing remission by week 52 in 34% and 41% of patients, respectively. Additionally, 35% and 47% of those patients sustained corticosteroid-free remissions when treated with 5-mg and 10-mg doses, respectively.
“New treatments are needed for patients with moderately to severely active ulcerative colitis,” said Julie Beitz, MD, director of the Office of Drug Evaluation III in FDA’s Center for Drug Evaluation and Research in a press release. “Today’s approval provides an alternative therapy for a debilitating disease with limited treatment options.”
Xeljanz is the first oral medication approved for chronic use in moderately to severely active UC. The FDA states that other FDA-approved treatments for the chronic treatment of moderately to severely active ulcerative colitis must be administered through an intravenous infusion or subcutaneous injection.
Xeljanz, made by Pfizer Labs, was previously approved in 2012 for rheumatoid arthritis and in 2017 for psoriatic arthritis.
Find the full press release on the FDA’s website.
FDA approves estradiol vaginal inserts for dyspareunia*
, in a 4-mcg and 10-mcg dose. The 4-mcg dose is a lower dose than any currently available.
The hormone treatment is intended for dyspareunia resulting from menopausal vulvar and vaginal atrophy. The patient places a soft gel capsule in the lower part of the vagina, daily for 2 weeks, then at a reduced rate of twice per week. The capsule dissolves and reintroduces estrogen to the tissue.
The manufacturer of the product, TherapeuticsMD, has committed to conduct a postapproval observational study, as a condition of approval.
Estradiol comes with a boxed warning of risks of endometrial cancer, stroke, deep vein thrombosis, pulmonary embolism, myocardial infarction, breast cancer, and “probable dementia.” The most common adverse reaction to the estradiol vaginal inserts was headache.
Editor's Note: This article has been corrected to state that the 4-mcg dose showed significant improvement in severity of dyspareunia.
dwatson@mdedge.com
, in a 4-mcg and 10-mcg dose. The 4-mcg dose is a lower dose than any currently available.
The hormone treatment is intended for dyspareunia resulting from menopausal vulvar and vaginal atrophy. The patient places a soft gel capsule in the lower part of the vagina, daily for 2 weeks, then at a reduced rate of twice per week. The capsule dissolves and reintroduces estrogen to the tissue.
The manufacturer of the product, TherapeuticsMD, has committed to conduct a postapproval observational study, as a condition of approval.
Estradiol comes with a boxed warning of risks of endometrial cancer, stroke, deep vein thrombosis, pulmonary embolism, myocardial infarction, breast cancer, and “probable dementia.” The most common adverse reaction to the estradiol vaginal inserts was headache.
Editor's Note: This article has been corrected to state that the 4-mcg dose showed significant improvement in severity of dyspareunia.
dwatson@mdedge.com
, in a 4-mcg and 10-mcg dose. The 4-mcg dose is a lower dose than any currently available.
The hormone treatment is intended for dyspareunia resulting from menopausal vulvar and vaginal atrophy. The patient places a soft gel capsule in the lower part of the vagina, daily for 2 weeks, then at a reduced rate of twice per week. The capsule dissolves and reintroduces estrogen to the tissue.
The manufacturer of the product, TherapeuticsMD, has committed to conduct a postapproval observational study, as a condition of approval.
Estradiol comes with a boxed warning of risks of endometrial cancer, stroke, deep vein thrombosis, pulmonary embolism, myocardial infarction, breast cancer, and “probable dementia.” The most common adverse reaction to the estradiol vaginal inserts was headache.
Editor's Note: This article has been corrected to state that the 4-mcg dose showed significant improvement in severity of dyspareunia.
dwatson@mdedge.com
FDA to review FLT3 agent for refractory AML
The Food and Drug Administration has granted priority review to an FMS-like tyrosine kinase 3 (FLT3)–targeting agent for the treatment of adults with relapsed or refractory acute myeloid leukemia (AML).
If approved, it would be the first FLT3 inhibitor available for this indication.
The application is based on the ongoing ADMIRAL trial, a phase 3, open-label, randomized study of gilteritinib versus salvage chemotherapy. The trial is designed to enroll 369 patients with FLT3 mutations present in bone marrow or whole blood who are refractory or have relapsed on first-line therapy. The primary endpoints are overall survival and rates of complete remission and complete remission with partial hematologic recovery.
The FDA has set Nov. 29 as a target date for reaching a decision on approval of the drug.
The Food and Drug Administration has granted priority review to an FMS-like tyrosine kinase 3 (FLT3)–targeting agent for the treatment of adults with relapsed or refractory acute myeloid leukemia (AML).
If approved, it would be the first FLT3 inhibitor available for this indication.
The application is based on the ongoing ADMIRAL trial, a phase 3, open-label, randomized study of gilteritinib versus salvage chemotherapy. The trial is designed to enroll 369 patients with FLT3 mutations present in bone marrow or whole blood who are refractory or have relapsed on first-line therapy. The primary endpoints are overall survival and rates of complete remission and complete remission with partial hematologic recovery.
The FDA has set Nov. 29 as a target date for reaching a decision on approval of the drug.
The Food and Drug Administration has granted priority review to an FMS-like tyrosine kinase 3 (FLT3)–targeting agent for the treatment of adults with relapsed or refractory acute myeloid leukemia (AML).
If approved, it would be the first FLT3 inhibitor available for this indication.
The application is based on the ongoing ADMIRAL trial, a phase 3, open-label, randomized study of gilteritinib versus salvage chemotherapy. The trial is designed to enroll 369 patients with FLT3 mutations present in bone marrow or whole blood who are refractory or have relapsed on first-line therapy. The primary endpoints are overall survival and rates of complete remission and complete remission with partial hematologic recovery.
The FDA has set Nov. 29 as a target date for reaching a decision on approval of the drug.