User login
Class I recall issued for Sapien 3 balloon
The Food and Drug Administration has issued a class I correction recall for Edward Lifescience’s Sapien 3 balloon system, which is used to deploy transcatheter aortic valve replacements, according to a release from the agency. A class I recall is the most serious the agency issues and indicates risk of severe injury or even death.
Rather than indicate removal of the device from market, this recall provides details on how to use the device cautiously and safely and instructs physicians on proper technique to safely retract the delivery system into the sheath in cases of a suspected balloon burst. Failure to observe these recommendations can result in vascular injury, bleeding, or surgical intervention.
These recommendations and instructions reiterate those issued in an Urgent Field Safety Notice that was provided by Edward Lifesciences on July 9, 2019. Edward Lifesciences could not be reached for comment.
The Food and Drug Administration has issued a class I correction recall for Edward Lifescience’s Sapien 3 balloon system, which is used to deploy transcatheter aortic valve replacements, according to a release from the agency. A class I recall is the most serious the agency issues and indicates risk of severe injury or even death.
Rather than indicate removal of the device from market, this recall provides details on how to use the device cautiously and safely and instructs physicians on proper technique to safely retract the delivery system into the sheath in cases of a suspected balloon burst. Failure to observe these recommendations can result in vascular injury, bleeding, or surgical intervention.
These recommendations and instructions reiterate those issued in an Urgent Field Safety Notice that was provided by Edward Lifesciences on July 9, 2019. Edward Lifesciences could not be reached for comment.
The Food and Drug Administration has issued a class I correction recall for Edward Lifescience’s Sapien 3 balloon system, which is used to deploy transcatheter aortic valve replacements, according to a release from the agency. A class I recall is the most serious the agency issues and indicates risk of severe injury or even death.
Rather than indicate removal of the device from market, this recall provides details on how to use the device cautiously and safely and instructs physicians on proper technique to safely retract the delivery system into the sheath in cases of a suspected balloon burst. Failure to observe these recommendations can result in vascular injury, bleeding, or surgical intervention.
These recommendations and instructions reiterate those issued in an Urgent Field Safety Notice that was provided by Edward Lifesciences on July 9, 2019. Edward Lifesciences could not be reached for comment.
Fifty-one percent of U.S. adolescents fully vaccinated against HPV
according to a report published in Morbidity and Mortality Weekly Report.
Researchers analyzed data from 18,700 adolescents aged 13-17 years – 48% of whom were female – in the 2018 National Immunization Survey–Teen to discover that 51% of adolescents were up to date with the human papillomavirus (HPV) vaccine, and 68% had received at least one dose of the vaccine.
There was an increase in HPV vaccination coverage from 2017 to 2018, but this was attributable to a 4.4 percentage point increase in males who were up to date, compared with a 0.6 percentage point increase in females.
“Although HPV vaccination coverage improved, increases among all adolescents were modest compared with increases in previous years and were observed only among males,” wrote Tanja Y. Walker of the National Center for Immunization and Respiratory Diseases at the Centers for Disease Control and Prevention, and coauthors.
The number of adolescents who had at least one dose of the quadrivalent meningococcal conjugate (4MenB) vaccine increased by 1.5 percentage points to 86.6%, while among individuals aged 17 years, coverage with two or more doses of 4MenB vaccine increased by 6.5 percentage points to 50.8%. Tdap coverage remained the same at 89% (MMWR 2019;68(33):718-23).
However, the study saw no significant increases in coverage with three or more hepatitis B vaccine doses, two or more MMR vaccine doses, or with one or more varicella vaccine doses in adolescents without a history of varicella disease.
Adolescents with Medicaid had higher HPV vaccination coverage than did adolescents with private health insurance. Uninsured adolescents had lower coverage overall, ranging from 4 percentage points lower for one or more varicella vaccine doses to 19 percentage points lower for two or more 4MenB vaccines, compared with adolescents with private health insurance.
Vaccination rates were lower among adolescents outside metropolitan areas, particularly when it came to being up to date with HPV vaccination, where there was a 15 percentage point difference, and with two or more doses of the quadrivalent meningococcal conjugate vaccine, where there was a 20 percentage point difference.
Provider recommendations to parents were associated with a higher rate of coverage with one or more doses of the HPV vaccine, but the prevalence of provider recommendations varied significantly from state to state. Overall, 78% of parents said they received a provider recommendation for the adolescent HPV vaccine, but that figure was as low as 60% in Mississippi and as high as 91% in Massachusetts.
Parents living in nonmetropolitan areas were less likely to report receiving a provider recommendation than were those in metropolitan principal cities.
“Equipping providers with the tools they need to give strong recommendations that emphasize the importance of HPV vaccination in preventing cancer and effectively address parental concerns is a priority, especially in states where provider recommendations were less commonly reported,” Ms. Walker and associates said.
No conflicts of interest were declared.
according to a report published in Morbidity and Mortality Weekly Report.
Researchers analyzed data from 18,700 adolescents aged 13-17 years – 48% of whom were female – in the 2018 National Immunization Survey–Teen to discover that 51% of adolescents were up to date with the human papillomavirus (HPV) vaccine, and 68% had received at least one dose of the vaccine.
There was an increase in HPV vaccination coverage from 2017 to 2018, but this was attributable to a 4.4 percentage point increase in males who were up to date, compared with a 0.6 percentage point increase in females.
“Although HPV vaccination coverage improved, increases among all adolescents were modest compared with increases in previous years and were observed only among males,” wrote Tanja Y. Walker of the National Center for Immunization and Respiratory Diseases at the Centers for Disease Control and Prevention, and coauthors.
The number of adolescents who had at least one dose of the quadrivalent meningococcal conjugate (4MenB) vaccine increased by 1.5 percentage points to 86.6%, while among individuals aged 17 years, coverage with two or more doses of 4MenB vaccine increased by 6.5 percentage points to 50.8%. Tdap coverage remained the same at 89% (MMWR 2019;68(33):718-23).
However, the study saw no significant increases in coverage with three or more hepatitis B vaccine doses, two or more MMR vaccine doses, or with one or more varicella vaccine doses in adolescents without a history of varicella disease.
Adolescents with Medicaid had higher HPV vaccination coverage than did adolescents with private health insurance. Uninsured adolescents had lower coverage overall, ranging from 4 percentage points lower for one or more varicella vaccine doses to 19 percentage points lower for two or more 4MenB vaccines, compared with adolescents with private health insurance.
Vaccination rates were lower among adolescents outside metropolitan areas, particularly when it came to being up to date with HPV vaccination, where there was a 15 percentage point difference, and with two or more doses of the quadrivalent meningococcal conjugate vaccine, where there was a 20 percentage point difference.
Provider recommendations to parents were associated with a higher rate of coverage with one or more doses of the HPV vaccine, but the prevalence of provider recommendations varied significantly from state to state. Overall, 78% of parents said they received a provider recommendation for the adolescent HPV vaccine, but that figure was as low as 60% in Mississippi and as high as 91% in Massachusetts.
Parents living in nonmetropolitan areas were less likely to report receiving a provider recommendation than were those in metropolitan principal cities.
“Equipping providers with the tools they need to give strong recommendations that emphasize the importance of HPV vaccination in preventing cancer and effectively address parental concerns is a priority, especially in states where provider recommendations were less commonly reported,” Ms. Walker and associates said.
No conflicts of interest were declared.
according to a report published in Morbidity and Mortality Weekly Report.
Researchers analyzed data from 18,700 adolescents aged 13-17 years – 48% of whom were female – in the 2018 National Immunization Survey–Teen to discover that 51% of adolescents were up to date with the human papillomavirus (HPV) vaccine, and 68% had received at least one dose of the vaccine.
There was an increase in HPV vaccination coverage from 2017 to 2018, but this was attributable to a 4.4 percentage point increase in males who were up to date, compared with a 0.6 percentage point increase in females.
“Although HPV vaccination coverage improved, increases among all adolescents were modest compared with increases in previous years and were observed only among males,” wrote Tanja Y. Walker of the National Center for Immunization and Respiratory Diseases at the Centers for Disease Control and Prevention, and coauthors.
The number of adolescents who had at least one dose of the quadrivalent meningococcal conjugate (4MenB) vaccine increased by 1.5 percentage points to 86.6%, while among individuals aged 17 years, coverage with two or more doses of 4MenB vaccine increased by 6.5 percentage points to 50.8%. Tdap coverage remained the same at 89% (MMWR 2019;68(33):718-23).
However, the study saw no significant increases in coverage with three or more hepatitis B vaccine doses, two or more MMR vaccine doses, or with one or more varicella vaccine doses in adolescents without a history of varicella disease.
Adolescents with Medicaid had higher HPV vaccination coverage than did adolescents with private health insurance. Uninsured adolescents had lower coverage overall, ranging from 4 percentage points lower for one or more varicella vaccine doses to 19 percentage points lower for two or more 4MenB vaccines, compared with adolescents with private health insurance.
Vaccination rates were lower among adolescents outside metropolitan areas, particularly when it came to being up to date with HPV vaccination, where there was a 15 percentage point difference, and with two or more doses of the quadrivalent meningococcal conjugate vaccine, where there was a 20 percentage point difference.
Provider recommendations to parents were associated with a higher rate of coverage with one or more doses of the HPV vaccine, but the prevalence of provider recommendations varied significantly from state to state. Overall, 78% of parents said they received a provider recommendation for the adolescent HPV vaccine, but that figure was as low as 60% in Mississippi and as high as 91% in Massachusetts.
Parents living in nonmetropolitan areas were less likely to report receiving a provider recommendation than were those in metropolitan principal cities.
“Equipping providers with the tools they need to give strong recommendations that emphasize the importance of HPV vaccination in preventing cancer and effectively address parental concerns is a priority, especially in states where provider recommendations were less commonly reported,” Ms. Walker and associates said.
No conflicts of interest were declared.
FROM MMWR
Key clinical point: Slightly more than half of adolescents in the United States are fully vaccinated with the HPV vaccine.
Major finding: Rates of full HPV vaccination are 51% among adolescents aged 13-17 years.
Study details: Analysis of data from 18,700 adolescents aged 13-17 years in the 2018 National Immunization Survey–Teen.
Disclosures: No conflicts of interest were declared.
Source: Walker T et al. MMWR 2019 Aug 23;68(33):718-23.
EULAR updates vaccination recommendations for autoimmune inflammatory rheumatic disease patients
Vaccination status should be reviewed annually for patients with autoimmune inflammatory rheumatic diseases, according to updated recommendations from the European League Against Rheumatism.
Patients with autoimmune inflammatory rheumatic diseases (AIIRD) are at increased risk for infections, and vaccination has been shown to reduce risk by “potentially translating into a lower rate of hospital admissions due to infections, emergency room visits, and the rate of invasive infectious diseases,” wrote Victoria Furer, MD, of Tel Aviv Sourasky Medical Center, and members of the task force that updated the recommendations, which were published in Annals of the Rheumatic Diseases.
However, AIIRD patients often go unvaccinated because of a lack of awareness or concerns about vaccine safety and efficacy, they said (Ann Rheum Dis. 2019 Aug 14. doi: 10.1136/annrheumdis-2019-215882).
The task force consisted of 21 experts, including patients, rheumatologists, immunologists, an infectious disease specialist, and health professionals in rheumatology representing eight countries. They evaluated data from four systematic literature reviews and developed nine recommendations based on six key principles.
“For each recommendation, the level of evidence for the incidence/prevalence of vaccine preventable infection in AIIRD, and efficacy/immunogenicity/safety of vaccination were stated, when available, followed by the strength of recommendation and the level of agreement,” the task force wrote.
These overarching principles start with an annual assessment of vaccination status by the AIIRD patient’s rheumatology team. Other principles include explanation of an individualized vaccination program to the patient as a foundation for joint decision-making, vaccinating patients during quiescent disease periods, vaccinating in advance of planned immunosuppression when possible, considering non-live vaccines for AIIRD patients also treated with systemic glucocorticoids and DMARDs, and considering live-attenuated vaccines with caution.
Several of the nine recommendations developed by the task force are modified from the previous recommendations issued in 2011. The task force made its recommendations with an eye toward optimizing individual risk stratification and avoiding “unnecessary” vaccination in AIIRD patients with low risk of infection as part of the update process. A notable change from the 2011 guidelines is the recommendation of both influenza and pneumococcal vaccinations for the majority of patients with AIIRD as opposed to all patients to emphasize the importance of individualized risk assessment, the task force noted.
The recommendations state that influenza vaccination and pneumococcal vaccination should be “strongly considered” for patients with AIIRD, and patients also should receive tetanus toxoid vaccination according to recommendations for the general population. However, clinicians should consider passive immunization for patients treated with B-cell depleting therapy, the task force wrote.
AIIRD patients at risk for hepatitis A and B should receive vaccinations for those diseases, with boosters or passive immunization if indicated, and high-risk patients may consider herpes zoster vaccination, according to the recommendations.
In addition, AIIRD patients – especially patients with systemic lupus erythematosus – should receive human papilloma virus vaccination according to recommendations for the general population, but AIIRD patients should avoid yellow fever vaccination, the task force stated. However, for AIIRD patients traveling to areas of yellow fever risk, “withholding immunosuppressive therapy to allow a safe vaccination or measuring serology in previously exposed patients may be considered.”
Finally, mothers treated with biologics during the second half of pregnancy should avoid live-attenuated vaccines for their newborns, and immunocompetent household members of AIIRD patients should be encouraged to follow national guidelines for routine vaccination with the exception of the oral polio vaccine, the task force concluded.
Vaccination status should be reviewed annually for patients with autoimmune inflammatory rheumatic diseases, according to updated recommendations from the European League Against Rheumatism.
Patients with autoimmune inflammatory rheumatic diseases (AIIRD) are at increased risk for infections, and vaccination has been shown to reduce risk by “potentially translating into a lower rate of hospital admissions due to infections, emergency room visits, and the rate of invasive infectious diseases,” wrote Victoria Furer, MD, of Tel Aviv Sourasky Medical Center, and members of the task force that updated the recommendations, which were published in Annals of the Rheumatic Diseases.
However, AIIRD patients often go unvaccinated because of a lack of awareness or concerns about vaccine safety and efficacy, they said (Ann Rheum Dis. 2019 Aug 14. doi: 10.1136/annrheumdis-2019-215882).
The task force consisted of 21 experts, including patients, rheumatologists, immunologists, an infectious disease specialist, and health professionals in rheumatology representing eight countries. They evaluated data from four systematic literature reviews and developed nine recommendations based on six key principles.
“For each recommendation, the level of evidence for the incidence/prevalence of vaccine preventable infection in AIIRD, and efficacy/immunogenicity/safety of vaccination were stated, when available, followed by the strength of recommendation and the level of agreement,” the task force wrote.
These overarching principles start with an annual assessment of vaccination status by the AIIRD patient’s rheumatology team. Other principles include explanation of an individualized vaccination program to the patient as a foundation for joint decision-making, vaccinating patients during quiescent disease periods, vaccinating in advance of planned immunosuppression when possible, considering non-live vaccines for AIIRD patients also treated with systemic glucocorticoids and DMARDs, and considering live-attenuated vaccines with caution.
Several of the nine recommendations developed by the task force are modified from the previous recommendations issued in 2011. The task force made its recommendations with an eye toward optimizing individual risk stratification and avoiding “unnecessary” vaccination in AIIRD patients with low risk of infection as part of the update process. A notable change from the 2011 guidelines is the recommendation of both influenza and pneumococcal vaccinations for the majority of patients with AIIRD as opposed to all patients to emphasize the importance of individualized risk assessment, the task force noted.
The recommendations state that influenza vaccination and pneumococcal vaccination should be “strongly considered” for patients with AIIRD, and patients also should receive tetanus toxoid vaccination according to recommendations for the general population. However, clinicians should consider passive immunization for patients treated with B-cell depleting therapy, the task force wrote.
AIIRD patients at risk for hepatitis A and B should receive vaccinations for those diseases, with boosters or passive immunization if indicated, and high-risk patients may consider herpes zoster vaccination, according to the recommendations.
In addition, AIIRD patients – especially patients with systemic lupus erythematosus – should receive human papilloma virus vaccination according to recommendations for the general population, but AIIRD patients should avoid yellow fever vaccination, the task force stated. However, for AIIRD patients traveling to areas of yellow fever risk, “withholding immunosuppressive therapy to allow a safe vaccination or measuring serology in previously exposed patients may be considered.”
Finally, mothers treated with biologics during the second half of pregnancy should avoid live-attenuated vaccines for their newborns, and immunocompetent household members of AIIRD patients should be encouraged to follow national guidelines for routine vaccination with the exception of the oral polio vaccine, the task force concluded.
Vaccination status should be reviewed annually for patients with autoimmune inflammatory rheumatic diseases, according to updated recommendations from the European League Against Rheumatism.
Patients with autoimmune inflammatory rheumatic diseases (AIIRD) are at increased risk for infections, and vaccination has been shown to reduce risk by “potentially translating into a lower rate of hospital admissions due to infections, emergency room visits, and the rate of invasive infectious diseases,” wrote Victoria Furer, MD, of Tel Aviv Sourasky Medical Center, and members of the task force that updated the recommendations, which were published in Annals of the Rheumatic Diseases.
However, AIIRD patients often go unvaccinated because of a lack of awareness or concerns about vaccine safety and efficacy, they said (Ann Rheum Dis. 2019 Aug 14. doi: 10.1136/annrheumdis-2019-215882).
The task force consisted of 21 experts, including patients, rheumatologists, immunologists, an infectious disease specialist, and health professionals in rheumatology representing eight countries. They evaluated data from four systematic literature reviews and developed nine recommendations based on six key principles.
“For each recommendation, the level of evidence for the incidence/prevalence of vaccine preventable infection in AIIRD, and efficacy/immunogenicity/safety of vaccination were stated, when available, followed by the strength of recommendation and the level of agreement,” the task force wrote.
These overarching principles start with an annual assessment of vaccination status by the AIIRD patient’s rheumatology team. Other principles include explanation of an individualized vaccination program to the patient as a foundation for joint decision-making, vaccinating patients during quiescent disease periods, vaccinating in advance of planned immunosuppression when possible, considering non-live vaccines for AIIRD patients also treated with systemic glucocorticoids and DMARDs, and considering live-attenuated vaccines with caution.
Several of the nine recommendations developed by the task force are modified from the previous recommendations issued in 2011. The task force made its recommendations with an eye toward optimizing individual risk stratification and avoiding “unnecessary” vaccination in AIIRD patients with low risk of infection as part of the update process. A notable change from the 2011 guidelines is the recommendation of both influenza and pneumococcal vaccinations for the majority of patients with AIIRD as opposed to all patients to emphasize the importance of individualized risk assessment, the task force noted.
The recommendations state that influenza vaccination and pneumococcal vaccination should be “strongly considered” for patients with AIIRD, and patients also should receive tetanus toxoid vaccination according to recommendations for the general population. However, clinicians should consider passive immunization for patients treated with B-cell depleting therapy, the task force wrote.
AIIRD patients at risk for hepatitis A and B should receive vaccinations for those diseases, with boosters or passive immunization if indicated, and high-risk patients may consider herpes zoster vaccination, according to the recommendations.
In addition, AIIRD patients – especially patients with systemic lupus erythematosus – should receive human papilloma virus vaccination according to recommendations for the general population, but AIIRD patients should avoid yellow fever vaccination, the task force stated. However, for AIIRD patients traveling to areas of yellow fever risk, “withholding immunosuppressive therapy to allow a safe vaccination or measuring serology in previously exposed patients may be considered.”
Finally, mothers treated with biologics during the second half of pregnancy should avoid live-attenuated vaccines for their newborns, and immunocompetent household members of AIIRD patients should be encouraged to follow national guidelines for routine vaccination with the exception of the oral polio vaccine, the task force concluded.
FROM ANNALS OF THE RHEUMATIC DISEASES
FUO, pneumonia often distinguishes influenza from RSV in hospitalized young children
LJUBLJANA, SLOVENIA – as the cause of hospitalization in infants and young children, Cihan Papan, MD, reported at the annual meeting of the European Society for Paediatric Infectious Diseases.
Dr. Papan, a pediatrician at University Children’s Hospital Mannheim (Germany) and Heidelberg (Germany) University, presented a retrospective single-center study of all 573 children aged under 2 years hospitalized over the course of several seasons for respiratory syncytial virus (RSV) or influenza as confirmed by rapid antigen testing. Even though these are two of the leading causes of hospitalization among young children, there is surprisingly sparse data comparing the two in terms of disease severity and hospital resource utilization, including antibiotic consumption. That information gap provided the basis for this study.
There were 476 children with confirmed RSV, 96 with influenza, and 1 RSV/influenza coinfection. Notably, even though the RSV group had lower temperatures and C-reactive protein levels, they were nevertheless more likely to be treated with antibiotics, by a margin of 29% to 23%.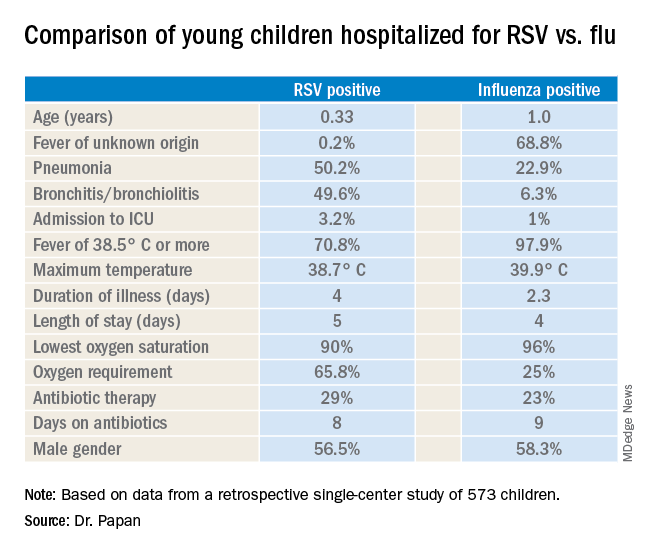
“These findings open new possibilities for antimicrobial stewardship in these groups of virally infected children,” observed Dr. Papan.
Fever of unknown origin was present in 68.8% of the influenza-positive patients, compared with just 0.2% of the RSV-positive children. In contrast, 50.2% of the RSV group had pneumonia and 49.6% had bronchitis or bronchiolitis, versus just 22.9% and 6.3% of the influenza patients, respectively. A larger proportion of the young children with RSV infection presented in a severely ill–looking condition. Children with RSV infection also were significantly younger.
Dr. Papan reported having no financial conflicts regarding his study.
LJUBLJANA, SLOVENIA – as the cause of hospitalization in infants and young children, Cihan Papan, MD, reported at the annual meeting of the European Society for Paediatric Infectious Diseases.
Dr. Papan, a pediatrician at University Children’s Hospital Mannheim (Germany) and Heidelberg (Germany) University, presented a retrospective single-center study of all 573 children aged under 2 years hospitalized over the course of several seasons for respiratory syncytial virus (RSV) or influenza as confirmed by rapid antigen testing. Even though these are two of the leading causes of hospitalization among young children, there is surprisingly sparse data comparing the two in terms of disease severity and hospital resource utilization, including antibiotic consumption. That information gap provided the basis for this study.
There were 476 children with confirmed RSV, 96 with influenza, and 1 RSV/influenza coinfection. Notably, even though the RSV group had lower temperatures and C-reactive protein levels, they were nevertheless more likely to be treated with antibiotics, by a margin of 29% to 23%.
“These findings open new possibilities for antimicrobial stewardship in these groups of virally infected children,” observed Dr. Papan.
Fever of unknown origin was present in 68.8% of the influenza-positive patients, compared with just 0.2% of the RSV-positive children. In contrast, 50.2% of the RSV group had pneumonia and 49.6% had bronchitis or bronchiolitis, versus just 22.9% and 6.3% of the influenza patients, respectively. A larger proportion of the young children with RSV infection presented in a severely ill–looking condition. Children with RSV infection also were significantly younger.
Dr. Papan reported having no financial conflicts regarding his study.
LJUBLJANA, SLOVENIA – as the cause of hospitalization in infants and young children, Cihan Papan, MD, reported at the annual meeting of the European Society for Paediatric Infectious Diseases.
Dr. Papan, a pediatrician at University Children’s Hospital Mannheim (Germany) and Heidelberg (Germany) University, presented a retrospective single-center study of all 573 children aged under 2 years hospitalized over the course of several seasons for respiratory syncytial virus (RSV) or influenza as confirmed by rapid antigen testing. Even though these are two of the leading causes of hospitalization among young children, there is surprisingly sparse data comparing the two in terms of disease severity and hospital resource utilization, including antibiotic consumption. That information gap provided the basis for this study.
There were 476 children with confirmed RSV, 96 with influenza, and 1 RSV/influenza coinfection. Notably, even though the RSV group had lower temperatures and C-reactive protein levels, they were nevertheless more likely to be treated with antibiotics, by a margin of 29% to 23%.
“These findings open new possibilities for antimicrobial stewardship in these groups of virally infected children,” observed Dr. Papan.
Fever of unknown origin was present in 68.8% of the influenza-positive patients, compared with just 0.2% of the RSV-positive children. In contrast, 50.2% of the RSV group had pneumonia and 49.6% had bronchitis or bronchiolitis, versus just 22.9% and 6.3% of the influenza patients, respectively. A larger proportion of the young children with RSV infection presented in a severely ill–looking condition. Children with RSV infection also were significantly younger.
Dr. Papan reported having no financial conflicts regarding his study.
REPORTING FROM ESPID 2019
Treating children with Kawasaki disease and coronary enlargement
IVIG plus steroids or infliximab, or IVIG alone?
Clinical question
Does use of corticosteroids or infliximab in addition to intravenous immunoglobulin improve cardiac outcomes in children with Kawasaki disease and enlarged coronary arteries?
Background
Kawasaki disease is a medium-vessel vasculitis primarily of young children. While the underlying cause remains unknown, treatment with intravenous immunoglobulin (IVIG) substantially lowers the risk of coronary artery aneurysms (CAA), the most serious sequelae of Kawasaki disease. Recent studies have suggested that – in cases of high-risk or treatment-resistant Kawasaki disease – using an immunomodulator, such as a corticosteroid or a TNF-alpha blocker, may improve outcomes, though these studies involved relatively small and homogeneous patient populations. It is unknown if these medications could prevent progression of CAA.
Study design
Retrospective multicenter study.
Setting
Two freestanding children’s hospitals and one mother-child hospital.
Synopsis
The study identified 121 children diagnosed with Kawasaki disease with CAA (z score 2.5-10) from 2008 through 2017 treated at the three study hospitals. Children with giant CAA at the time of diagnosis (z score greater than 10) or significant preexisting congenital heart disease were excluded.
All study hospitals had protocols for treatment of Kawasaki disease: Center 1 used IVIG and corticosteroids, Center 2 used IVIG and infliximab, and Center 3 used IVIG alone. Patients at all centers also received aspirin. Center 1 used methylprednisolone IV initially, changing to oral prednisolone after clinical improvement. The researchers reviewed the charts of each patient and classified them as having complete or incomplete Kawasaki disease. They assigned z scores for CAA size based on both initial and follow-up echocardiograms. The primary outcome was change in z score of CAA over the first year.
The population of patients treated at each center was significantly different. Center 1 reported older patients (median age 2.6 vs. 2.0 and 1.1), as well as a higher rate of male patients (83% vs. 77% and 58%). However, there was no difference in baseline z scores between centers. Patients who initially received IVIG and corticosteroids were less likely to require additional therapy because of persistent fever versus those receiving IVIG only, or IVIG and infliximab (0% vs. 21% vs. 14%, P = .03).
Patients receiving IVIG and corticosteroids, or IVIG and infliximab, were less likely to have progression of CAA size, with 23% and 24% having an increase in z score of more than 1 versus 58% of those who received IVIG alone. No group had significant differences in maximum z score, the rate of giant aneurysms, or the rate of regression of CAA.
Bottom line
Using IVIG + corticosteroids or IVIG + infliximab versus IVIG alone for children with Kawasaki disease with coronary artery aneurysms decreases the rate of aneurysm enlargement.
Citation
Dionne A et al. Treatment intensification in patients with Kawasaki disease and coronary aneurysm at diagnosis. Pediatrics. May 2019:e20183341. doi: 10.1542/peds.2018-3341.
Dr. Stubblefield is a pediatric hospitalist at Nemours/Alfred I. duPont Hospital for Children in Wilmington, Del., and clinical assistant professor of pediatrics at Sidney Kimmel Medical College at Thomas Jefferson University in Philadelphia.
IVIG plus steroids or infliximab, or IVIG alone?
IVIG plus steroids or infliximab, or IVIG alone?
Clinical question
Does use of corticosteroids or infliximab in addition to intravenous immunoglobulin improve cardiac outcomes in children with Kawasaki disease and enlarged coronary arteries?
Background
Kawasaki disease is a medium-vessel vasculitis primarily of young children. While the underlying cause remains unknown, treatment with intravenous immunoglobulin (IVIG) substantially lowers the risk of coronary artery aneurysms (CAA), the most serious sequelae of Kawasaki disease. Recent studies have suggested that – in cases of high-risk or treatment-resistant Kawasaki disease – using an immunomodulator, such as a corticosteroid or a TNF-alpha blocker, may improve outcomes, though these studies involved relatively small and homogeneous patient populations. It is unknown if these medications could prevent progression of CAA.
Study design
Retrospective multicenter study.
Setting
Two freestanding children’s hospitals and one mother-child hospital.
Synopsis
The study identified 121 children diagnosed with Kawasaki disease with CAA (z score 2.5-10) from 2008 through 2017 treated at the three study hospitals. Children with giant CAA at the time of diagnosis (z score greater than 10) or significant preexisting congenital heart disease were excluded.
All study hospitals had protocols for treatment of Kawasaki disease: Center 1 used IVIG and corticosteroids, Center 2 used IVIG and infliximab, and Center 3 used IVIG alone. Patients at all centers also received aspirin. Center 1 used methylprednisolone IV initially, changing to oral prednisolone after clinical improvement. The researchers reviewed the charts of each patient and classified them as having complete or incomplete Kawasaki disease. They assigned z scores for CAA size based on both initial and follow-up echocardiograms. The primary outcome was change in z score of CAA over the first year.
The population of patients treated at each center was significantly different. Center 1 reported older patients (median age 2.6 vs. 2.0 and 1.1), as well as a higher rate of male patients (83% vs. 77% and 58%). However, there was no difference in baseline z scores between centers. Patients who initially received IVIG and corticosteroids were less likely to require additional therapy because of persistent fever versus those receiving IVIG only, or IVIG and infliximab (0% vs. 21% vs. 14%, P = .03).
Patients receiving IVIG and corticosteroids, or IVIG and infliximab, were less likely to have progression of CAA size, with 23% and 24% having an increase in z score of more than 1 versus 58% of those who received IVIG alone. No group had significant differences in maximum z score, the rate of giant aneurysms, or the rate of regression of CAA.
Bottom line
Using IVIG + corticosteroids or IVIG + infliximab versus IVIG alone for children with Kawasaki disease with coronary artery aneurysms decreases the rate of aneurysm enlargement.
Citation
Dionne A et al. Treatment intensification in patients with Kawasaki disease and coronary aneurysm at diagnosis. Pediatrics. May 2019:e20183341. doi: 10.1542/peds.2018-3341.
Dr. Stubblefield is a pediatric hospitalist at Nemours/Alfred I. duPont Hospital for Children in Wilmington, Del., and clinical assistant professor of pediatrics at Sidney Kimmel Medical College at Thomas Jefferson University in Philadelphia.
Clinical question
Does use of corticosteroids or infliximab in addition to intravenous immunoglobulin improve cardiac outcomes in children with Kawasaki disease and enlarged coronary arteries?
Background
Kawasaki disease is a medium-vessel vasculitis primarily of young children. While the underlying cause remains unknown, treatment with intravenous immunoglobulin (IVIG) substantially lowers the risk of coronary artery aneurysms (CAA), the most serious sequelae of Kawasaki disease. Recent studies have suggested that – in cases of high-risk or treatment-resistant Kawasaki disease – using an immunomodulator, such as a corticosteroid or a TNF-alpha blocker, may improve outcomes, though these studies involved relatively small and homogeneous patient populations. It is unknown if these medications could prevent progression of CAA.
Study design
Retrospective multicenter study.
Setting
Two freestanding children’s hospitals and one mother-child hospital.
Synopsis
The study identified 121 children diagnosed with Kawasaki disease with CAA (z score 2.5-10) from 2008 through 2017 treated at the three study hospitals. Children with giant CAA at the time of diagnosis (z score greater than 10) or significant preexisting congenital heart disease were excluded.
All study hospitals had protocols for treatment of Kawasaki disease: Center 1 used IVIG and corticosteroids, Center 2 used IVIG and infliximab, and Center 3 used IVIG alone. Patients at all centers also received aspirin. Center 1 used methylprednisolone IV initially, changing to oral prednisolone after clinical improvement. The researchers reviewed the charts of each patient and classified them as having complete or incomplete Kawasaki disease. They assigned z scores for CAA size based on both initial and follow-up echocardiograms. The primary outcome was change in z score of CAA over the first year.
The population of patients treated at each center was significantly different. Center 1 reported older patients (median age 2.6 vs. 2.0 and 1.1), as well as a higher rate of male patients (83% vs. 77% and 58%). However, there was no difference in baseline z scores between centers. Patients who initially received IVIG and corticosteroids were less likely to require additional therapy because of persistent fever versus those receiving IVIG only, or IVIG and infliximab (0% vs. 21% vs. 14%, P = .03).
Patients receiving IVIG and corticosteroids, or IVIG and infliximab, were less likely to have progression of CAA size, with 23% and 24% having an increase in z score of more than 1 versus 58% of those who received IVIG alone. No group had significant differences in maximum z score, the rate of giant aneurysms, or the rate of regression of CAA.
Bottom line
Using IVIG + corticosteroids or IVIG + infliximab versus IVIG alone for children with Kawasaki disease with coronary artery aneurysms decreases the rate of aneurysm enlargement.
Citation
Dionne A et al. Treatment intensification in patients with Kawasaki disease and coronary aneurysm at diagnosis. Pediatrics. May 2019:e20183341. doi: 10.1542/peds.2018-3341.
Dr. Stubblefield is a pediatric hospitalist at Nemours/Alfred I. duPont Hospital for Children in Wilmington, Del., and clinical assistant professor of pediatrics at Sidney Kimmel Medical College at Thomas Jefferson University in Philadelphia.
Oncologists agree with AI treatment decisions about half the time
When it comes to treatment recommendations for high-risk breast cancer, oncologists agree with a leading artificial intelligence platform about half the time, according to investigators.
In the first study of its kind, involving 10 Chinese oncologists, recommendation concordance with the Watson for Oncology treatment advisory tool (WfO) was generally lower for hormone receptor–positive and metastatic cancers than hormone receptor–negative and nonmetastatic cases, reported Fengrui Xu, MD, of the Academy of Military Medical Sciences in Beijing, and colleagues. Refinement could enable broad use of Watson, not to dictate treatment decisions, but instead to propose alternate treatment approaches and offer point-of-care access to relevant evidence.
“[WfO] is an example of a quantitative oncology clinical decision support that leverages the clinical expertise of oncologists at Memorial Sloan Kettering Cancer Center [MSKCC],” the investigators wrote in JCO Clinical Cancer Informatics. The platform uses machine-learning software to interpret patient scenarios in light from MSKCC training cases, MSKCC treatment guidelines, and more than 300 medical textbooks and journals.
To compare WfO with real-world decision makers, the investigators recruited three chief physicians, four attending physicians, and three fellows to provide treatment recommendations for 1,977 patients with complex breast cancer who were treated at 10 hospitals in China. Participating physicians shared the workload; each evaluated an average of 198 different cases.
On average, oncologists and WfO made the same treatment recommendations 56% of the time. Out of the different types of physicians, fellows were most likely to agree with WfO, based on a 68% concordance rate, compared with 54% for chief physicians and 49% for attending physicians. Including all physicians, concordance was lowest for hormone receptor–positive/HER2-positive disease (48%) and highest for triple-negative cases (71%). Adjuvant and metastatic therapies were also evaluated, with high concordance for adjuvant endocrine (78%) and targeted therapy (100%), compared with moderate concordance for first- (52%) and second-line metastatic therapy (50%). The investigators described concordance results as generally “modest;” however, they noted that such levels are promising.
“This degree of concordance is encouraging because therapeutic decisions in these cases are often difficult as a result of the current limits of medical knowledge for treating complex breast cancers and the presence of local contextual factors that affect physician treatment choices,” the investigators wrote. “It is important to note that nonconcordance does not imply that one treatment is correct for a given patient and another is not, nor does it necessarily diminish the potential value of a decision support system that provides access to supporting evidence and insight into its reasoning process.”
The study was funded by Zefei Jiang. The investigators reported affiliations with IBM Watson Health, Pharmaceutical Manufacturer Institution, Merck, and others.
SOURCE: Xu F et al. JCO Clin Cancer Inform. 2019 Aug 16. doi: 10.1200/CCI.18.00159.
When it comes to treatment recommendations for high-risk breast cancer, oncologists agree with a leading artificial intelligence platform about half the time, according to investigators.
In the first study of its kind, involving 10 Chinese oncologists, recommendation concordance with the Watson for Oncology treatment advisory tool (WfO) was generally lower for hormone receptor–positive and metastatic cancers than hormone receptor–negative and nonmetastatic cases, reported Fengrui Xu, MD, of the Academy of Military Medical Sciences in Beijing, and colleagues. Refinement could enable broad use of Watson, not to dictate treatment decisions, but instead to propose alternate treatment approaches and offer point-of-care access to relevant evidence.
“[WfO] is an example of a quantitative oncology clinical decision support that leverages the clinical expertise of oncologists at Memorial Sloan Kettering Cancer Center [MSKCC],” the investigators wrote in JCO Clinical Cancer Informatics. The platform uses machine-learning software to interpret patient scenarios in light from MSKCC training cases, MSKCC treatment guidelines, and more than 300 medical textbooks and journals.
To compare WfO with real-world decision makers, the investigators recruited three chief physicians, four attending physicians, and three fellows to provide treatment recommendations for 1,977 patients with complex breast cancer who were treated at 10 hospitals in China. Participating physicians shared the workload; each evaluated an average of 198 different cases.
On average, oncologists and WfO made the same treatment recommendations 56% of the time. Out of the different types of physicians, fellows were most likely to agree with WfO, based on a 68% concordance rate, compared with 54% for chief physicians and 49% for attending physicians. Including all physicians, concordance was lowest for hormone receptor–positive/HER2-positive disease (48%) and highest for triple-negative cases (71%). Adjuvant and metastatic therapies were also evaluated, with high concordance for adjuvant endocrine (78%) and targeted therapy (100%), compared with moderate concordance for first- (52%) and second-line metastatic therapy (50%). The investigators described concordance results as generally “modest;” however, they noted that such levels are promising.
“This degree of concordance is encouraging because therapeutic decisions in these cases are often difficult as a result of the current limits of medical knowledge for treating complex breast cancers and the presence of local contextual factors that affect physician treatment choices,” the investigators wrote. “It is important to note that nonconcordance does not imply that one treatment is correct for a given patient and another is not, nor does it necessarily diminish the potential value of a decision support system that provides access to supporting evidence and insight into its reasoning process.”
The study was funded by Zefei Jiang. The investigators reported affiliations with IBM Watson Health, Pharmaceutical Manufacturer Institution, Merck, and others.
SOURCE: Xu F et al. JCO Clin Cancer Inform. 2019 Aug 16. doi: 10.1200/CCI.18.00159.
When it comes to treatment recommendations for high-risk breast cancer, oncologists agree with a leading artificial intelligence platform about half the time, according to investigators.
In the first study of its kind, involving 10 Chinese oncologists, recommendation concordance with the Watson for Oncology treatment advisory tool (WfO) was generally lower for hormone receptor–positive and metastatic cancers than hormone receptor–negative and nonmetastatic cases, reported Fengrui Xu, MD, of the Academy of Military Medical Sciences in Beijing, and colleagues. Refinement could enable broad use of Watson, not to dictate treatment decisions, but instead to propose alternate treatment approaches and offer point-of-care access to relevant evidence.
“[WfO] is an example of a quantitative oncology clinical decision support that leverages the clinical expertise of oncologists at Memorial Sloan Kettering Cancer Center [MSKCC],” the investigators wrote in JCO Clinical Cancer Informatics. The platform uses machine-learning software to interpret patient scenarios in light from MSKCC training cases, MSKCC treatment guidelines, and more than 300 medical textbooks and journals.
To compare WfO with real-world decision makers, the investigators recruited three chief physicians, four attending physicians, and three fellows to provide treatment recommendations for 1,977 patients with complex breast cancer who were treated at 10 hospitals in China. Participating physicians shared the workload; each evaluated an average of 198 different cases.
On average, oncologists and WfO made the same treatment recommendations 56% of the time. Out of the different types of physicians, fellows were most likely to agree with WfO, based on a 68% concordance rate, compared with 54% for chief physicians and 49% for attending physicians. Including all physicians, concordance was lowest for hormone receptor–positive/HER2-positive disease (48%) and highest for triple-negative cases (71%). Adjuvant and metastatic therapies were also evaluated, with high concordance for adjuvant endocrine (78%) and targeted therapy (100%), compared with moderate concordance for first- (52%) and second-line metastatic therapy (50%). The investigators described concordance results as generally “modest;” however, they noted that such levels are promising.
“This degree of concordance is encouraging because therapeutic decisions in these cases are often difficult as a result of the current limits of medical knowledge for treating complex breast cancers and the presence of local contextual factors that affect physician treatment choices,” the investigators wrote. “It is important to note that nonconcordance does not imply that one treatment is correct for a given patient and another is not, nor does it necessarily diminish the potential value of a decision support system that provides access to supporting evidence and insight into its reasoning process.”
The study was funded by Zefei Jiang. The investigators reported affiliations with IBM Watson Health, Pharmaceutical Manufacturer Institution, Merck, and others.
SOURCE: Xu F et al. JCO Clin Cancer Inform. 2019 Aug 16. doi: 10.1200/CCI.18.00159.
FROM JCO CLINICAL CANCER INFORMATICS
Galcanezumab benefits patients with migraine and medication overuse
PHILADELPHIA –
“When you have targeted preventive treatment and you reduce the burden of illness, medication overuse seems to be reduced as well,” said Sheena Aurora, MD, adjunct clinical associate professor of anesthesiology and perioperative and pain medicine at Stanford (Calif.) Health Care. Dr. Aurora also is a medical fellow and global launch leader for galcanezumab at Eli Lilly, which has developed the treatment.
Galcanezumab is a humanized monoclonal antibody that selectively binds to the calcitonin gene-related peptide. The phase 3 EVOLVE-1, EVOLVE-2, and REGAIN studies indicated galcanezumab’s superiority to placebo in preventing episodic and chronic migraine.
A post hoc analysis of phase 3 data
Dr. Aurora and colleagues conducted a post hoc analysis of data from the three phase 3 studies to examine galcanezumab’s effect in patients with medication overuse. EVOLVE-1 and EVOLVE-2 included patients with episodic migraine, and REGAIN included patients with chronic migraine. All participants were randomized to monthly subcutaneous injections of placebo or galcanezumab (120 mg/month or 240 mg/month) for 3-6 months. Based on information obtained through electronic patient-reported outcome diaries, investigators determined headache medication overuse using criteria adapted from the International Classification of Headache Disorders, third edition. They estimated mean changes in monthly headache days and the proportion of patients with medication overuse after randomization using mixed modeling.
The demographic characteristics of the three study populations were similar to those reported in epidemiologic studies of migraine, said Dr. Aurora. Most participants were women, and most patients were between ages 40 and 49 years. At baseline, the mean number of monthly migraine headache days was 20 among patients with chronic migraine and 9 among patients with episodic migraine.
The rate of medication overuse was higher in the combined study population than in the literature. Patients with medication overuse had greater disability and greater health care resource utilization, compared with patients without medication overuse. Among patients with chronic migraine, participants who overused medication were not significantly different from those who did not. But among patients with episodic migraine, participants who overused medication had higher headache frequency than those who did not.
In the EVOLVE trials, the proportion of patients with baseline medication overuse was 19.3% in the placebo arm, 17.0% in the galcanezumab 120-mg arm, and 19.2% in the galcanezumab 240-mg arm. In REGAIN, the proportion of patients with baseline medication overuse was 63.4% in the placebo arm, 64.3% in the galcanezumab 120-mg arm, and 64.1% in the galcanezumab 240-mg arm.
Galcanezumab reduced medication overuse
Compared with placebo, both doses of galcanezumab significantly decreased mean monthly migraine headache days in patients with baseline medication overuse. In the EVOLVE studies, this endpoint decreased by 2.71 in the placebo group, 6.26 in the galcanezumab 120-mg group, and 5.77 in the galcanezumab 240-mg group. In REGAIN, the reductions were 2.25 in the placebo group, 4.78 in the galcanezumab 120-mg group, and 4.51 in the galcanezumab 240-mg group. The effect size was higher in patients who were overusing medications, compared with those who were not, said Dr. Aurora. “This is clinically relevant, because most of us ... had this belief that patients who were overusing medications may be more treatment-resistant to prevention.”
In addition, galcanezumab was associated with significantly lower rates of average monthly medication overuse, compared with placebo. In the EVOLVE studies, the average rate of monthly medication overuse was 15.9% for the placebo group, 6.2% for the galcanezumab 120-mg group, and 7.9% for the galcanezumab 240-mg group. In REGAIN, the average rate of monthly medication overuse was 40.6% in the placebo group, 24.3% in the galcanezumab 120-mg group, and 23.1% in the galcanezumab 240-mg group. About 85% of patients with episodic migraine and medication overuse had a reduction in medication overuse, and approximately 50% of patients with chronic migraine and medication overuse had a reduction in medication overuse, said Dr. Aurora.
Dr. Aurora and coinvestigators are employees of Eli Lilly, which developed galcanezumab and funded the EVOLVE and REGAIN studies.
SOURCE: Aurora S et al. AHS 2019. Abstract IOR07.
PHILADELPHIA –
“When you have targeted preventive treatment and you reduce the burden of illness, medication overuse seems to be reduced as well,” said Sheena Aurora, MD, adjunct clinical associate professor of anesthesiology and perioperative and pain medicine at Stanford (Calif.) Health Care. Dr. Aurora also is a medical fellow and global launch leader for galcanezumab at Eli Lilly, which has developed the treatment.
Galcanezumab is a humanized monoclonal antibody that selectively binds to the calcitonin gene-related peptide. The phase 3 EVOLVE-1, EVOLVE-2, and REGAIN studies indicated galcanezumab’s superiority to placebo in preventing episodic and chronic migraine.
A post hoc analysis of phase 3 data
Dr. Aurora and colleagues conducted a post hoc analysis of data from the three phase 3 studies to examine galcanezumab’s effect in patients with medication overuse. EVOLVE-1 and EVOLVE-2 included patients with episodic migraine, and REGAIN included patients with chronic migraine. All participants were randomized to monthly subcutaneous injections of placebo or galcanezumab (120 mg/month or 240 mg/month) for 3-6 months. Based on information obtained through electronic patient-reported outcome diaries, investigators determined headache medication overuse using criteria adapted from the International Classification of Headache Disorders, third edition. They estimated mean changes in monthly headache days and the proportion of patients with medication overuse after randomization using mixed modeling.
The demographic characteristics of the three study populations were similar to those reported in epidemiologic studies of migraine, said Dr. Aurora. Most participants were women, and most patients were between ages 40 and 49 years. At baseline, the mean number of monthly migraine headache days was 20 among patients with chronic migraine and 9 among patients with episodic migraine.
The rate of medication overuse was higher in the combined study population than in the literature. Patients with medication overuse had greater disability and greater health care resource utilization, compared with patients without medication overuse. Among patients with chronic migraine, participants who overused medication were not significantly different from those who did not. But among patients with episodic migraine, participants who overused medication had higher headache frequency than those who did not.
In the EVOLVE trials, the proportion of patients with baseline medication overuse was 19.3% in the placebo arm, 17.0% in the galcanezumab 120-mg arm, and 19.2% in the galcanezumab 240-mg arm. In REGAIN, the proportion of patients with baseline medication overuse was 63.4% in the placebo arm, 64.3% in the galcanezumab 120-mg arm, and 64.1% in the galcanezumab 240-mg arm.
Galcanezumab reduced medication overuse
Compared with placebo, both doses of galcanezumab significantly decreased mean monthly migraine headache days in patients with baseline medication overuse. In the EVOLVE studies, this endpoint decreased by 2.71 in the placebo group, 6.26 in the galcanezumab 120-mg group, and 5.77 in the galcanezumab 240-mg group. In REGAIN, the reductions were 2.25 in the placebo group, 4.78 in the galcanezumab 120-mg group, and 4.51 in the galcanezumab 240-mg group. The effect size was higher in patients who were overusing medications, compared with those who were not, said Dr. Aurora. “This is clinically relevant, because most of us ... had this belief that patients who were overusing medications may be more treatment-resistant to prevention.”
In addition, galcanezumab was associated with significantly lower rates of average monthly medication overuse, compared with placebo. In the EVOLVE studies, the average rate of monthly medication overuse was 15.9% for the placebo group, 6.2% for the galcanezumab 120-mg group, and 7.9% for the galcanezumab 240-mg group. In REGAIN, the average rate of monthly medication overuse was 40.6% in the placebo group, 24.3% in the galcanezumab 120-mg group, and 23.1% in the galcanezumab 240-mg group. About 85% of patients with episodic migraine and medication overuse had a reduction in medication overuse, and approximately 50% of patients with chronic migraine and medication overuse had a reduction in medication overuse, said Dr. Aurora.
Dr. Aurora and coinvestigators are employees of Eli Lilly, which developed galcanezumab and funded the EVOLVE and REGAIN studies.
SOURCE: Aurora S et al. AHS 2019. Abstract IOR07.
PHILADELPHIA –
“When you have targeted preventive treatment and you reduce the burden of illness, medication overuse seems to be reduced as well,” said Sheena Aurora, MD, adjunct clinical associate professor of anesthesiology and perioperative and pain medicine at Stanford (Calif.) Health Care. Dr. Aurora also is a medical fellow and global launch leader for galcanezumab at Eli Lilly, which has developed the treatment.
Galcanezumab is a humanized monoclonal antibody that selectively binds to the calcitonin gene-related peptide. The phase 3 EVOLVE-1, EVOLVE-2, and REGAIN studies indicated galcanezumab’s superiority to placebo in preventing episodic and chronic migraine.
A post hoc analysis of phase 3 data
Dr. Aurora and colleagues conducted a post hoc analysis of data from the three phase 3 studies to examine galcanezumab’s effect in patients with medication overuse. EVOLVE-1 and EVOLVE-2 included patients with episodic migraine, and REGAIN included patients with chronic migraine. All participants were randomized to monthly subcutaneous injections of placebo or galcanezumab (120 mg/month or 240 mg/month) for 3-6 months. Based on information obtained through electronic patient-reported outcome diaries, investigators determined headache medication overuse using criteria adapted from the International Classification of Headache Disorders, third edition. They estimated mean changes in monthly headache days and the proportion of patients with medication overuse after randomization using mixed modeling.
The demographic characteristics of the three study populations were similar to those reported in epidemiologic studies of migraine, said Dr. Aurora. Most participants were women, and most patients were between ages 40 and 49 years. At baseline, the mean number of monthly migraine headache days was 20 among patients with chronic migraine and 9 among patients with episodic migraine.
The rate of medication overuse was higher in the combined study population than in the literature. Patients with medication overuse had greater disability and greater health care resource utilization, compared with patients without medication overuse. Among patients with chronic migraine, participants who overused medication were not significantly different from those who did not. But among patients with episodic migraine, participants who overused medication had higher headache frequency than those who did not.
In the EVOLVE trials, the proportion of patients with baseline medication overuse was 19.3% in the placebo arm, 17.0% in the galcanezumab 120-mg arm, and 19.2% in the galcanezumab 240-mg arm. In REGAIN, the proportion of patients with baseline medication overuse was 63.4% in the placebo arm, 64.3% in the galcanezumab 120-mg arm, and 64.1% in the galcanezumab 240-mg arm.
Galcanezumab reduced medication overuse
Compared with placebo, both doses of galcanezumab significantly decreased mean monthly migraine headache days in patients with baseline medication overuse. In the EVOLVE studies, this endpoint decreased by 2.71 in the placebo group, 6.26 in the galcanezumab 120-mg group, and 5.77 in the galcanezumab 240-mg group. In REGAIN, the reductions were 2.25 in the placebo group, 4.78 in the galcanezumab 120-mg group, and 4.51 in the galcanezumab 240-mg group. The effect size was higher in patients who were overusing medications, compared with those who were not, said Dr. Aurora. “This is clinically relevant, because most of us ... had this belief that patients who were overusing medications may be more treatment-resistant to prevention.”
In addition, galcanezumab was associated with significantly lower rates of average monthly medication overuse, compared with placebo. In the EVOLVE studies, the average rate of monthly medication overuse was 15.9% for the placebo group, 6.2% for the galcanezumab 120-mg group, and 7.9% for the galcanezumab 240-mg group. In REGAIN, the average rate of monthly medication overuse was 40.6% in the placebo group, 24.3% in the galcanezumab 120-mg group, and 23.1% in the galcanezumab 240-mg group. About 85% of patients with episodic migraine and medication overuse had a reduction in medication overuse, and approximately 50% of patients with chronic migraine and medication overuse had a reduction in medication overuse, said Dr. Aurora.
Dr. Aurora and coinvestigators are employees of Eli Lilly, which developed galcanezumab and funded the EVOLVE and REGAIN studies.
SOURCE: Aurora S et al. AHS 2019. Abstract IOR07.
REPORTING FROM AHS 2019
Green thumbnail
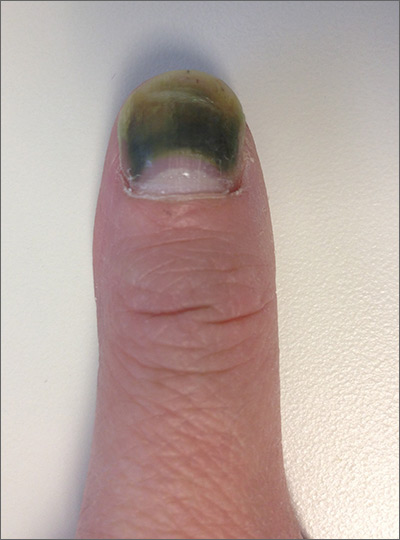
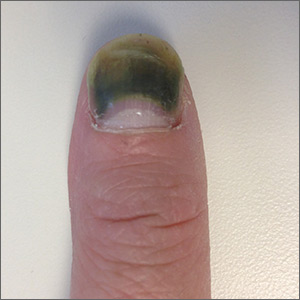
The patient was given a diagnosis of green nail syndrome (GNS), an infection of the nail bed caused by Pseudomonas aeruginosa. These bacteria produce pyocyanin, a blue-green pigment that discolors the nail. GNS often occurs in patients with prior nail problems, such as onychomycosis, onycholysis, trauma, chronic paronychia, or psoriasis.
Nail disease disrupts the integumentary barrier and allows a portal of entry for bacteria. Scanning electron microscopy of patients with GNS has shown that fungal infections create tunnel-like structures in the nail keratin, and P aeruginosa can grow in these spaces. Nails with prior nail disease that are chronically exposed to moisture are at greatest risk of developing GNS, and it is typical for only one nail to be involved.
It’s likely that this patient’s earlier nail problem had been a case of onycholysis, based on her description of a “spongy” nail bed and loose nail. This created a favorable environment for an infection by allowing moisture and bacteria to infiltrate the space. The patient also acknowledged that she washed dishes by hand and bathed her young children. This frequent soaking of her hands likely helped to provide a moist environment in which P aeruginosa could thrive. In addition, onycholysis is associated with hypothyroidism, which the patient also had.
GNS can be diagnosed by clinical observation and characteristic pigmentation along with an appropriate patient history. Nail discoloration, or chromonychia, can present in a variety of colors. Nail findings may represent an isolated disease or provide an important clinical clue to other systemic diseases. The specific shade of discoloration helps to differentiate the underlying pathology. Culture of the nail bed may be helpful if bacterial resistance or co-infection with fungal organisms is suspected. GNS is often painless, but may be accompanied by mild tenderness of the nail.
The patient was prescribed ciprofloxacin 500 mg twice a day for 10 days, plus bleach soaks (1 part bleach to 4 parts water) twice a day. She also was advised to wear gloves for household tasks that involved immersing her hands in water, and to dry her finger with a hair dryer after bathing.
This case was adapted from: Gish D, Romero BJ. Green fingernail. J Fam Pract. 2017;66:E7-E9.

The patient was given a diagnosis of green nail syndrome (GNS), an infection of the nail bed caused by Pseudomonas aeruginosa. These bacteria produce pyocyanin, a blue-green pigment that discolors the nail. GNS often occurs in patients with prior nail problems, such as onychomycosis, onycholysis, trauma, chronic paronychia, or psoriasis.
Nail disease disrupts the integumentary barrier and allows a portal of entry for bacteria. Scanning electron microscopy of patients with GNS has shown that fungal infections create tunnel-like structures in the nail keratin, and P aeruginosa can grow in these spaces. Nails with prior nail disease that are chronically exposed to moisture are at greatest risk of developing GNS, and it is typical for only one nail to be involved.
It’s likely that this patient’s earlier nail problem had been a case of onycholysis, based on her description of a “spongy” nail bed and loose nail. This created a favorable environment for an infection by allowing moisture and bacteria to infiltrate the space. The patient also acknowledged that she washed dishes by hand and bathed her young children. This frequent soaking of her hands likely helped to provide a moist environment in which P aeruginosa could thrive. In addition, onycholysis is associated with hypothyroidism, which the patient also had.
GNS can be diagnosed by clinical observation and characteristic pigmentation along with an appropriate patient history. Nail discoloration, or chromonychia, can present in a variety of colors. Nail findings may represent an isolated disease or provide an important clinical clue to other systemic diseases. The specific shade of discoloration helps to differentiate the underlying pathology. Culture of the nail bed may be helpful if bacterial resistance or co-infection with fungal organisms is suspected. GNS is often painless, but may be accompanied by mild tenderness of the nail.
The patient was prescribed ciprofloxacin 500 mg twice a day for 10 days, plus bleach soaks (1 part bleach to 4 parts water) twice a day. She also was advised to wear gloves for household tasks that involved immersing her hands in water, and to dry her finger with a hair dryer after bathing.
This case was adapted from: Gish D, Romero BJ. Green fingernail. J Fam Pract. 2017;66:E7-E9.

The patient was given a diagnosis of green nail syndrome (GNS), an infection of the nail bed caused by Pseudomonas aeruginosa. These bacteria produce pyocyanin, a blue-green pigment that discolors the nail. GNS often occurs in patients with prior nail problems, such as onychomycosis, onycholysis, trauma, chronic paronychia, or psoriasis.
Nail disease disrupts the integumentary barrier and allows a portal of entry for bacteria. Scanning electron microscopy of patients with GNS has shown that fungal infections create tunnel-like structures in the nail keratin, and P aeruginosa can grow in these spaces. Nails with prior nail disease that are chronically exposed to moisture are at greatest risk of developing GNS, and it is typical for only one nail to be involved.
It’s likely that this patient’s earlier nail problem had been a case of onycholysis, based on her description of a “spongy” nail bed and loose nail. This created a favorable environment for an infection by allowing moisture and bacteria to infiltrate the space. The patient also acknowledged that she washed dishes by hand and bathed her young children. This frequent soaking of her hands likely helped to provide a moist environment in which P aeruginosa could thrive. In addition, onycholysis is associated with hypothyroidism, which the patient also had.
GNS can be diagnosed by clinical observation and characteristic pigmentation along with an appropriate patient history. Nail discoloration, or chromonychia, can present in a variety of colors. Nail findings may represent an isolated disease or provide an important clinical clue to other systemic diseases. The specific shade of discoloration helps to differentiate the underlying pathology. Culture of the nail bed may be helpful if bacterial resistance or co-infection with fungal organisms is suspected. GNS is often painless, but may be accompanied by mild tenderness of the nail.
The patient was prescribed ciprofloxacin 500 mg twice a day for 10 days, plus bleach soaks (1 part bleach to 4 parts water) twice a day. She also was advised to wear gloves for household tasks that involved immersing her hands in water, and to dry her finger with a hair dryer after bathing.
This case was adapted from: Gish D, Romero BJ. Green fingernail. J Fam Pract. 2017;66:E7-E9.
PTSD symptom reduction tied to lower risk of type 2 diabetes
Veterans with a clinically meaningful reduction in symptoms of PTSD are less likely to develop type 2 diabetes, research from a retrospective study shows.
“We cautiously speculate that normalization of hypothalamic-pituitary-adrenal axis and cortisol levels could be one mechanism behind our results,” wrote Jeffrey F. Scherrer, PhD, and colleagues. “PTSD is associated with inflammation, which may in turn be associated with increased risk for [type 2 diabetes].” The study was published in JAMA Psychiatry.
Using medical record data from the Veterans Health Administration, Dr. Scherrer and colleagues identified 5,916 patients with PTSD who visited a VHA medical center between 2008 and 2012, and scored at least 50 points or higher on the PTSD Checklist (PCL) followed by another PCL score at least 8 months after the previous score. The mean age of patients in the study was 42.1 years, the cohort consisted of 84.3% men, and 66.3% patients were white. PCL score reduction was deemed clinically meaningful if there was a decrease of 20 points or more in the score, reported Dr. Scherrer of the department of family and community medicine at Saint Louis University and colleagues.
Patients who were older (mean 43.6 years vs. mean 41.7 years; P = .02) and those who underwent minimally adequate duration of PTSD psychotherapy (P less than .001) were significantly more likely to have a clinically meaningful decrease in PCL scores. Patients who received antidepressants (P = .004) or antipsychotics (P less than .001) were significantly more likely to have less than clinically meaningful decreases in PCL scores. Factors that put patients at significantly higher risk of developing type 2 diabetes included older age (hazard ratio, 1.05; 95% confidence interval, 1.04-1.07; P less than .001), black race/ethnicity (HR, 1.86; 95% CI, 1.23-2.83; P = .004), hypertension (HR, 3.46; 95% CI, 2.33-5.16), hyperlipidemia (HR, 2.82; 95% CI, 1.91-4.16), and obesity (HR, 3.32; 95% CI, 2.12-5.21) (all P less than .001).
Minimally adequate duration of PTSD psychotherapy and high use of primary care health services also were associated with developing type 2 diabetes.
In a Cox proportional hazards regression model, patients with clinically meaningful decreases in PCL scores had significantly lower risk of developing type 2 diabetes, and those results remained consistent after adjusting for age, calculating the results using weighted data, and factoring in hypertension, obesity, and hyperlipidemia.
“This result was independent of numerous demographics and psychiatric and physical comorbidities,” said Dr. Scherrer and colleagues. “The association was also independent of the number of PTSD psychotherapy sessions used, suggesting that a healthy adherer effect, or a general orientation to improve health, is unlikely to explain our observations.”
Dr. Scherrer and colleagues cited several limitations, such as unmeasured confounding and the difficulty of generalizing the results beyond PTSD patients in a VHA setting. In addition, the researchers were unable to calculate the lifetime effect of reduced PTSD symptoms and incidence of type 2 diabetes.
This study was funded in part by a grant from the National Heart, Lung, and Blood Institute. Four authors reported receiving one or more grants from the National Heart, Lung, and Blood Institute during the study period. Some authors reported receiving other support from Noblis Therapeutics and Saint Louis University both during and outside the study period. The other authors reported no relevant conflicts of interest.
SOURCE: Scherrer JF et al. JAMA Psychiatry. 2019 Aug 21. doi: 10.1001/jamapsychiatry.2019.2096.
Veterans with a clinically meaningful reduction in symptoms of PTSD are less likely to develop type 2 diabetes, research from a retrospective study shows.
“We cautiously speculate that normalization of hypothalamic-pituitary-adrenal axis and cortisol levels could be one mechanism behind our results,” wrote Jeffrey F. Scherrer, PhD, and colleagues. “PTSD is associated with inflammation, which may in turn be associated with increased risk for [type 2 diabetes].” The study was published in JAMA Psychiatry.
Using medical record data from the Veterans Health Administration, Dr. Scherrer and colleagues identified 5,916 patients with PTSD who visited a VHA medical center between 2008 and 2012, and scored at least 50 points or higher on the PTSD Checklist (PCL) followed by another PCL score at least 8 months after the previous score. The mean age of patients in the study was 42.1 years, the cohort consisted of 84.3% men, and 66.3% patients were white. PCL score reduction was deemed clinically meaningful if there was a decrease of 20 points or more in the score, reported Dr. Scherrer of the department of family and community medicine at Saint Louis University and colleagues.
Patients who were older (mean 43.6 years vs. mean 41.7 years; P = .02) and those who underwent minimally adequate duration of PTSD psychotherapy (P less than .001) were significantly more likely to have a clinically meaningful decrease in PCL scores. Patients who received antidepressants (P = .004) or antipsychotics (P less than .001) were significantly more likely to have less than clinically meaningful decreases in PCL scores. Factors that put patients at significantly higher risk of developing type 2 diabetes included older age (hazard ratio, 1.05; 95% confidence interval, 1.04-1.07; P less than .001), black race/ethnicity (HR, 1.86; 95% CI, 1.23-2.83; P = .004), hypertension (HR, 3.46; 95% CI, 2.33-5.16), hyperlipidemia (HR, 2.82; 95% CI, 1.91-4.16), and obesity (HR, 3.32; 95% CI, 2.12-5.21) (all P less than .001).
Minimally adequate duration of PTSD psychotherapy and high use of primary care health services also were associated with developing type 2 diabetes.
In a Cox proportional hazards regression model, patients with clinically meaningful decreases in PCL scores had significantly lower risk of developing type 2 diabetes, and those results remained consistent after adjusting for age, calculating the results using weighted data, and factoring in hypertension, obesity, and hyperlipidemia.
“This result was independent of numerous demographics and psychiatric and physical comorbidities,” said Dr. Scherrer and colleagues. “The association was also independent of the number of PTSD psychotherapy sessions used, suggesting that a healthy adherer effect, or a general orientation to improve health, is unlikely to explain our observations.”
Dr. Scherrer and colleagues cited several limitations, such as unmeasured confounding and the difficulty of generalizing the results beyond PTSD patients in a VHA setting. In addition, the researchers were unable to calculate the lifetime effect of reduced PTSD symptoms and incidence of type 2 diabetes.
This study was funded in part by a grant from the National Heart, Lung, and Blood Institute. Four authors reported receiving one or more grants from the National Heart, Lung, and Blood Institute during the study period. Some authors reported receiving other support from Noblis Therapeutics and Saint Louis University both during and outside the study period. The other authors reported no relevant conflicts of interest.
SOURCE: Scherrer JF et al. JAMA Psychiatry. 2019 Aug 21. doi: 10.1001/jamapsychiatry.2019.2096.
Veterans with a clinically meaningful reduction in symptoms of PTSD are less likely to develop type 2 diabetes, research from a retrospective study shows.
“We cautiously speculate that normalization of hypothalamic-pituitary-adrenal axis and cortisol levels could be one mechanism behind our results,” wrote Jeffrey F. Scherrer, PhD, and colleagues. “PTSD is associated with inflammation, which may in turn be associated with increased risk for [type 2 diabetes].” The study was published in JAMA Psychiatry.
Using medical record data from the Veterans Health Administration, Dr. Scherrer and colleagues identified 5,916 patients with PTSD who visited a VHA medical center between 2008 and 2012, and scored at least 50 points or higher on the PTSD Checklist (PCL) followed by another PCL score at least 8 months after the previous score. The mean age of patients in the study was 42.1 years, the cohort consisted of 84.3% men, and 66.3% patients were white. PCL score reduction was deemed clinically meaningful if there was a decrease of 20 points or more in the score, reported Dr. Scherrer of the department of family and community medicine at Saint Louis University and colleagues.
Patients who were older (mean 43.6 years vs. mean 41.7 years; P = .02) and those who underwent minimally adequate duration of PTSD psychotherapy (P less than .001) were significantly more likely to have a clinically meaningful decrease in PCL scores. Patients who received antidepressants (P = .004) or antipsychotics (P less than .001) were significantly more likely to have less than clinically meaningful decreases in PCL scores. Factors that put patients at significantly higher risk of developing type 2 diabetes included older age (hazard ratio, 1.05; 95% confidence interval, 1.04-1.07; P less than .001), black race/ethnicity (HR, 1.86; 95% CI, 1.23-2.83; P = .004), hypertension (HR, 3.46; 95% CI, 2.33-5.16), hyperlipidemia (HR, 2.82; 95% CI, 1.91-4.16), and obesity (HR, 3.32; 95% CI, 2.12-5.21) (all P less than .001).
Minimally adequate duration of PTSD psychotherapy and high use of primary care health services also were associated with developing type 2 diabetes.
In a Cox proportional hazards regression model, patients with clinically meaningful decreases in PCL scores had significantly lower risk of developing type 2 diabetes, and those results remained consistent after adjusting for age, calculating the results using weighted data, and factoring in hypertension, obesity, and hyperlipidemia.
“This result was independent of numerous demographics and psychiatric and physical comorbidities,” said Dr. Scherrer and colleagues. “The association was also independent of the number of PTSD psychotherapy sessions used, suggesting that a healthy adherer effect, or a general orientation to improve health, is unlikely to explain our observations.”
Dr. Scherrer and colleagues cited several limitations, such as unmeasured confounding and the difficulty of generalizing the results beyond PTSD patients in a VHA setting. In addition, the researchers were unable to calculate the lifetime effect of reduced PTSD symptoms and incidence of type 2 diabetes.
This study was funded in part by a grant from the National Heart, Lung, and Blood Institute. Four authors reported receiving one or more grants from the National Heart, Lung, and Blood Institute during the study period. Some authors reported receiving other support from Noblis Therapeutics and Saint Louis University both during and outside the study period. The other authors reported no relevant conflicts of interest.
SOURCE: Scherrer JF et al. JAMA Psychiatry. 2019 Aug 21. doi: 10.1001/jamapsychiatry.2019.2096.
FROM JAMA PSYCHIATRY
Vaping illness cases now over 150, CDC says
Officials from the CDC and the Food and Drug Administration are working with state health officials to gather information on the cases as well as any products or substances that might be involved.
A total of 153 potential cases were reported between June 28 and Aug. 20 in 16 states – California, Connecticut, Florida, Illinois, Indiana, Iowa, Michigan, Minnesota, New Jersey, New Mexico, New York, North Carolina, Pennsylvania, Texas, Utah, and Wisconsin.
Health officials have yet to find a cause for these illnesses; however, all patients have reported e-cigarette use or vaping, according to a CDC statement. Evidence to date does not seem to indicate that an infectious agent is the cause.
In general, patients have reported a gradual onset of symptoms including shortness of breath and/or chest pain that increased over days or weeks before hospital admission. Gastrointestinal symptoms including vomiting, diarrhea, and fatigue have been reported by some.
Many patients reported using products containing tetrahydrocannabinol, though no specific or consistent product has been linked definitively.
While cases reported across the country seem to be similar, there is no evidence currently indicating they have a common cause, according to the CDC statement.
The CDC is urging health care professionals to report possible cases to their state or local health department and the FDA is urging the public to provide detailed reports of any unusual or unexpected health concerns related to tobacco use or e-cigarette use through its Safety Reporting Portal.
Officials from the CDC and the Food and Drug Administration are working with state health officials to gather information on the cases as well as any products or substances that might be involved.
A total of 153 potential cases were reported between June 28 and Aug. 20 in 16 states – California, Connecticut, Florida, Illinois, Indiana, Iowa, Michigan, Minnesota, New Jersey, New Mexico, New York, North Carolina, Pennsylvania, Texas, Utah, and Wisconsin.
Health officials have yet to find a cause for these illnesses; however, all patients have reported e-cigarette use or vaping, according to a CDC statement. Evidence to date does not seem to indicate that an infectious agent is the cause.
In general, patients have reported a gradual onset of symptoms including shortness of breath and/or chest pain that increased over days or weeks before hospital admission. Gastrointestinal symptoms including vomiting, diarrhea, and fatigue have been reported by some.
Many patients reported using products containing tetrahydrocannabinol, though no specific or consistent product has been linked definitively.
While cases reported across the country seem to be similar, there is no evidence currently indicating they have a common cause, according to the CDC statement.
The CDC is urging health care professionals to report possible cases to their state or local health department and the FDA is urging the public to provide detailed reports of any unusual or unexpected health concerns related to tobacco use or e-cigarette use through its Safety Reporting Portal.
Officials from the CDC and the Food and Drug Administration are working with state health officials to gather information on the cases as well as any products or substances that might be involved.
A total of 153 potential cases were reported between June 28 and Aug. 20 in 16 states – California, Connecticut, Florida, Illinois, Indiana, Iowa, Michigan, Minnesota, New Jersey, New Mexico, New York, North Carolina, Pennsylvania, Texas, Utah, and Wisconsin.
Health officials have yet to find a cause for these illnesses; however, all patients have reported e-cigarette use or vaping, according to a CDC statement. Evidence to date does not seem to indicate that an infectious agent is the cause.
In general, patients have reported a gradual onset of symptoms including shortness of breath and/or chest pain that increased over days or weeks before hospital admission. Gastrointestinal symptoms including vomiting, diarrhea, and fatigue have been reported by some.
Many patients reported using products containing tetrahydrocannabinol, though no specific or consistent product has been linked definitively.
While cases reported across the country seem to be similar, there is no evidence currently indicating they have a common cause, according to the CDC statement.
The CDC is urging health care professionals to report possible cases to their state or local health department and the FDA is urging the public to provide detailed reports of any unusual or unexpected health concerns related to tobacco use or e-cigarette use through its Safety Reporting Portal.