User login
High-dose vitamin D fails against young children’s upper respiratory infections
A daily dose of 2,000 IU of vitamin D had no impact on reducing wintertime upper respiratory tract infections in young children, compared with a 400 IU dose, based on a study of 703 children aged 1-5 years. The report was published July 18 in JAMA.
“Vitamin D increases the synthesis of the antimicrobial peptide cathelicidin in respiratory epithelium, which has been shown to reduce disease severity and replication of the influenza virus in vitro,” but studies on the effect of vitamin D on upper respiratory infections have been limited, wrote Mary Aglipay of St. Michael’s Hospital, Toronto, and her colleagues.
The average number of laboratory-confirmed cases of upper respiratory tract infections per child was not significantly different between the high-dose and low-dose groups (1.05 vs. 1.03).
The median time to the first laboratory-confirmed infection was similar between the groups: 3.95 months in the high-dose group and 3.29 months in the low-dose group. In addition, the number of parent-reported upper respiratory tract infections was similar between the high-dose and low-dose groups (625 vs. 600).
Serum 25-hydroxyvitamin D levels also remained comparable between the high-dose and low-dose groups at the study’s end (48.7 ng/mL vs. 36.8 ng/mL).
The results were limited by several factors, including the lack of a placebo group and the high baseline vitamin D levels in the children at the end of the summer, the researchers noted.
However, “these findings do not support the routine use of high-dose vitamin D supplementation in children for the prevention of viral upper respiratory tract infection,” they said.
The study was supported by the Canadian Institutes of Health Research, Institute of Human Development, Child and Youth Health, and Institute of Nutrition, Metabolism and Diabetes, and the Thrasher Research Fund. The vitamin D formulations were donated by Ddrops. Ms. Aglipay had no financial conflicts to disclose. One coauthor, Muhammad Mamdani, MPH, had ties to a number of pharmaceutical companies.
A daily dose of 2,000 IU of vitamin D had no impact on reducing wintertime upper respiratory tract infections in young children, compared with a 400 IU dose, based on a study of 703 children aged 1-5 years. The report was published July 18 in JAMA.
“Vitamin D increases the synthesis of the antimicrobial peptide cathelicidin in respiratory epithelium, which has been shown to reduce disease severity and replication of the influenza virus in vitro,” but studies on the effect of vitamin D on upper respiratory infections have been limited, wrote Mary Aglipay of St. Michael’s Hospital, Toronto, and her colleagues.
The average number of laboratory-confirmed cases of upper respiratory tract infections per child was not significantly different between the high-dose and low-dose groups (1.05 vs. 1.03).
The median time to the first laboratory-confirmed infection was similar between the groups: 3.95 months in the high-dose group and 3.29 months in the low-dose group. In addition, the number of parent-reported upper respiratory tract infections was similar between the high-dose and low-dose groups (625 vs. 600).
Serum 25-hydroxyvitamin D levels also remained comparable between the high-dose and low-dose groups at the study’s end (48.7 ng/mL vs. 36.8 ng/mL).
The results were limited by several factors, including the lack of a placebo group and the high baseline vitamin D levels in the children at the end of the summer, the researchers noted.
However, “these findings do not support the routine use of high-dose vitamin D supplementation in children for the prevention of viral upper respiratory tract infection,” they said.
The study was supported by the Canadian Institutes of Health Research, Institute of Human Development, Child and Youth Health, and Institute of Nutrition, Metabolism and Diabetes, and the Thrasher Research Fund. The vitamin D formulations were donated by Ddrops. Ms. Aglipay had no financial conflicts to disclose. One coauthor, Muhammad Mamdani, MPH, had ties to a number of pharmaceutical companies.
A daily dose of 2,000 IU of vitamin D had no impact on reducing wintertime upper respiratory tract infections in young children, compared with a 400 IU dose, based on a study of 703 children aged 1-5 years. The report was published July 18 in JAMA.
“Vitamin D increases the synthesis of the antimicrobial peptide cathelicidin in respiratory epithelium, which has been shown to reduce disease severity and replication of the influenza virus in vitro,” but studies on the effect of vitamin D on upper respiratory infections have been limited, wrote Mary Aglipay of St. Michael’s Hospital, Toronto, and her colleagues.
The average number of laboratory-confirmed cases of upper respiratory tract infections per child was not significantly different between the high-dose and low-dose groups (1.05 vs. 1.03).
The median time to the first laboratory-confirmed infection was similar between the groups: 3.95 months in the high-dose group and 3.29 months in the low-dose group. In addition, the number of parent-reported upper respiratory tract infections was similar between the high-dose and low-dose groups (625 vs. 600).
Serum 25-hydroxyvitamin D levels also remained comparable between the high-dose and low-dose groups at the study’s end (48.7 ng/mL vs. 36.8 ng/mL).
The results were limited by several factors, including the lack of a placebo group and the high baseline vitamin D levels in the children at the end of the summer, the researchers noted.
However, “these findings do not support the routine use of high-dose vitamin D supplementation in children for the prevention of viral upper respiratory tract infection,” they said.
The study was supported by the Canadian Institutes of Health Research, Institute of Human Development, Child and Youth Health, and Institute of Nutrition, Metabolism and Diabetes, and the Thrasher Research Fund. The vitamin D formulations were donated by Ddrops. Ms. Aglipay had no financial conflicts to disclose. One coauthor, Muhammad Mamdani, MPH, had ties to a number of pharmaceutical companies.
FROM JAMA
Key clinical point:
Major finding: The average number of laboratory-confirmed upper respiratory tract infections per child was not significantly different between the high-dose and low-dose groups (1.05 vs. 1.03).
Data source: A study of 703 healthy children aged 1-5 years randomized to 2,000 IU or 400 IU of vitamin D.
Disclosures: The study was supported by the Canadian Institutes of Health Research, Institute of Human Development, Child and Youth Health, and Institute of Nutrition, Metabolism and Diabetes, and the Thrasher Research Fund. The vitamin D formulations were donated by Ddrops. Ms. Aglipay had no financial conflicts to disclose. One coauthor, Muhammad Mamdani, MPH, had ties to a number of pharmaceutical companies.
Counsel low-risk patients case by case on diet, exercise
Clinical judgment should drive referrals for diet and exercise behavioral counseling for adults with a low risk for cardiovascular disease (CVD), according to a new recommendation statement from the U.S. Preventive Services Task Force published online July 11 in JAMA.
“Persons who are interested and ready to make behavioral changes may be most likely to benefit from behavioral counseling,” according to the statement (JAMA 2017 Jul 11;318:167-74. doi: 10.1001/jama.2017.7171).
The recommendation is a C, which means that clinicians should consider patient preferences and clinical judgment, wrote David C. Grossman, MD, of Kaiser Permanente Washington Health Research Institute, Seattle, and his colleagues.
To assess the value of behavioral counseling in adults at low risk for cardiovascular disease, the USPSTF reviewed 88 trials including more than 120 interventions related to a healthful diet, physical activity, or both. None of the trials included in the review noted specific adverse events related to counseling.
Although the evidence was insufficient to support benefits from behavioral counseling for reducing death or CVD rates, the data showed that behavioral counseling was associated with improved systolic and diastolic blood pressure levels, cholesterol, body mass index, and waist circumference over 6-12 months.
In data from 34 trials, behavior counseling resulted in significant changes to several CVD risk factors, with average improvements of –1.26 mm Hg for systolic blood pressure, –0.49 mm Hg for diastolic blood pressure, –2.85 mg/dL for total cholesterol, –0.41 kg/m2 for body mass index, –1.04 kg for weight, and –0.19 cm for waist circumference.
The current recommendation updates the 2012 recommendations that primary care clinicians “selectively provide or refer patients who do not have hypertension, dyslipidemia, diabetes, or CVD to behavioral counseling to promote a healthful diet and physical activity rather than incorporating counseling into the routine care of adults.”
Separate USPSTF recommendations focus on behavioral counseling in adults with risk factors including obesity, abnormal blood glucose levels, diabetes, or CVD, therefore, the current recommendation “focuses on persons without these risk factors,” the researchers noted.
In the evidence report accompanying the recommendations, Carrie D. Patnode, PhD, of Kaiser Permanente in Portland, Ore., and her colleagues concluded that higher-intensity interventions may promote greater improvements in health outcomes, but that “there is very limited evidence on longer-term intermediate and health outcomes or on harmful effects of these interventions” (JAMA 2017;318:175-93. doi: 10.1001/jama.2017.3303).
The researchers had no financial conflicts to disclose.
“The evidence is strong, consistent, and persuasive that CVD risk factor prevention and treatment are associated with lower rates of CVD,” wrote Philip Greenland, MD, and Valentin Fuster, MD, PhD, in an accompanying editorial (JAMA 2017 Jul 11;318:130-1). “There are no universally effective solutions to accomplish this, but certain principles apply. Recommended dietary patterns focus on meals high in vegetables, fruit, whole grains, seafood, legumes, and nuts; moderate in low-fat and nonfat dairy products; lower in red and processed meat, foods and beverages containing added sugar, and refined grains,” they said. In addition, “physical activity must be encouraged in children and adults and emphasize a regular and consistent commitment to daily exercise habits. Research findings support the need to begin interventions in preschool children, [and should] involve the family, and continue lifelong,” they noted.
Although the guidelines address the challenges faced by clinicians in controlling CVD risk factors, “risk factor control in the clinical setting begins with risk assessment, aims at targeting all risk factors above ideal levels, and moves patients in measured steps toward more ideal cardiovascular health,” the editorialists said.
Dr. Greenland is affiliated with the department of preventive medicine at Northwestern University, Chicago. Dr. Fuster is director of the Zena and Michael A. Wiener Cardiovascular Institute, Icahn School of Medicine at Mount Sinai, N.Y. They had no financial conflicts to disclose.
“The evidence is strong, consistent, and persuasive that CVD risk factor prevention and treatment are associated with lower rates of CVD,” wrote Philip Greenland, MD, and Valentin Fuster, MD, PhD, in an accompanying editorial (JAMA 2017 Jul 11;318:130-1). “There are no universally effective solutions to accomplish this, but certain principles apply. Recommended dietary patterns focus on meals high in vegetables, fruit, whole grains, seafood, legumes, and nuts; moderate in low-fat and nonfat dairy products; lower in red and processed meat, foods and beverages containing added sugar, and refined grains,” they said. In addition, “physical activity must be encouraged in children and adults and emphasize a regular and consistent commitment to daily exercise habits. Research findings support the need to begin interventions in preschool children, [and should] involve the family, and continue lifelong,” they noted.
Although the guidelines address the challenges faced by clinicians in controlling CVD risk factors, “risk factor control in the clinical setting begins with risk assessment, aims at targeting all risk factors above ideal levels, and moves patients in measured steps toward more ideal cardiovascular health,” the editorialists said.
Dr. Greenland is affiliated with the department of preventive medicine at Northwestern University, Chicago. Dr. Fuster is director of the Zena and Michael A. Wiener Cardiovascular Institute, Icahn School of Medicine at Mount Sinai, N.Y. They had no financial conflicts to disclose.
“The evidence is strong, consistent, and persuasive that CVD risk factor prevention and treatment are associated with lower rates of CVD,” wrote Philip Greenland, MD, and Valentin Fuster, MD, PhD, in an accompanying editorial (JAMA 2017 Jul 11;318:130-1). “There are no universally effective solutions to accomplish this, but certain principles apply. Recommended dietary patterns focus on meals high in vegetables, fruit, whole grains, seafood, legumes, and nuts; moderate in low-fat and nonfat dairy products; lower in red and processed meat, foods and beverages containing added sugar, and refined grains,” they said. In addition, “physical activity must be encouraged in children and adults and emphasize a regular and consistent commitment to daily exercise habits. Research findings support the need to begin interventions in preschool children, [and should] involve the family, and continue lifelong,” they noted.
Although the guidelines address the challenges faced by clinicians in controlling CVD risk factors, “risk factor control in the clinical setting begins with risk assessment, aims at targeting all risk factors above ideal levels, and moves patients in measured steps toward more ideal cardiovascular health,” the editorialists said.
Dr. Greenland is affiliated with the department of preventive medicine at Northwestern University, Chicago. Dr. Fuster is director of the Zena and Michael A. Wiener Cardiovascular Institute, Icahn School of Medicine at Mount Sinai, N.Y. They had no financial conflicts to disclose.
Clinical judgment should drive referrals for diet and exercise behavioral counseling for adults with a low risk for cardiovascular disease (CVD), according to a new recommendation statement from the U.S. Preventive Services Task Force published online July 11 in JAMA.
“Persons who are interested and ready to make behavioral changes may be most likely to benefit from behavioral counseling,” according to the statement (JAMA 2017 Jul 11;318:167-74. doi: 10.1001/jama.2017.7171).
The recommendation is a C, which means that clinicians should consider patient preferences and clinical judgment, wrote David C. Grossman, MD, of Kaiser Permanente Washington Health Research Institute, Seattle, and his colleagues.
To assess the value of behavioral counseling in adults at low risk for cardiovascular disease, the USPSTF reviewed 88 trials including more than 120 interventions related to a healthful diet, physical activity, or both. None of the trials included in the review noted specific adverse events related to counseling.
Although the evidence was insufficient to support benefits from behavioral counseling for reducing death or CVD rates, the data showed that behavioral counseling was associated with improved systolic and diastolic blood pressure levels, cholesterol, body mass index, and waist circumference over 6-12 months.
In data from 34 trials, behavior counseling resulted in significant changes to several CVD risk factors, with average improvements of –1.26 mm Hg for systolic blood pressure, –0.49 mm Hg for diastolic blood pressure, –2.85 mg/dL for total cholesterol, –0.41 kg/m2 for body mass index, –1.04 kg for weight, and –0.19 cm for waist circumference.
The current recommendation updates the 2012 recommendations that primary care clinicians “selectively provide or refer patients who do not have hypertension, dyslipidemia, diabetes, or CVD to behavioral counseling to promote a healthful diet and physical activity rather than incorporating counseling into the routine care of adults.”
Separate USPSTF recommendations focus on behavioral counseling in adults with risk factors including obesity, abnormal blood glucose levels, diabetes, or CVD, therefore, the current recommendation “focuses on persons without these risk factors,” the researchers noted.
In the evidence report accompanying the recommendations, Carrie D. Patnode, PhD, of Kaiser Permanente in Portland, Ore., and her colleagues concluded that higher-intensity interventions may promote greater improvements in health outcomes, but that “there is very limited evidence on longer-term intermediate and health outcomes or on harmful effects of these interventions” (JAMA 2017;318:175-93. doi: 10.1001/jama.2017.3303).
The researchers had no financial conflicts to disclose.
Clinical judgment should drive referrals for diet and exercise behavioral counseling for adults with a low risk for cardiovascular disease (CVD), according to a new recommendation statement from the U.S. Preventive Services Task Force published online July 11 in JAMA.
“Persons who are interested and ready to make behavioral changes may be most likely to benefit from behavioral counseling,” according to the statement (JAMA 2017 Jul 11;318:167-74. doi: 10.1001/jama.2017.7171).
The recommendation is a C, which means that clinicians should consider patient preferences and clinical judgment, wrote David C. Grossman, MD, of Kaiser Permanente Washington Health Research Institute, Seattle, and his colleagues.
To assess the value of behavioral counseling in adults at low risk for cardiovascular disease, the USPSTF reviewed 88 trials including more than 120 interventions related to a healthful diet, physical activity, or both. None of the trials included in the review noted specific adverse events related to counseling.
Although the evidence was insufficient to support benefits from behavioral counseling for reducing death or CVD rates, the data showed that behavioral counseling was associated with improved systolic and diastolic blood pressure levels, cholesterol, body mass index, and waist circumference over 6-12 months.
In data from 34 trials, behavior counseling resulted in significant changes to several CVD risk factors, with average improvements of –1.26 mm Hg for systolic blood pressure, –0.49 mm Hg for diastolic blood pressure, –2.85 mg/dL for total cholesterol, –0.41 kg/m2 for body mass index, –1.04 kg for weight, and –0.19 cm for waist circumference.
The current recommendation updates the 2012 recommendations that primary care clinicians “selectively provide or refer patients who do not have hypertension, dyslipidemia, diabetes, or CVD to behavioral counseling to promote a healthful diet and physical activity rather than incorporating counseling into the routine care of adults.”
Separate USPSTF recommendations focus on behavioral counseling in adults with risk factors including obesity, abnormal blood glucose levels, diabetes, or CVD, therefore, the current recommendation “focuses on persons without these risk factors,” the researchers noted.
In the evidence report accompanying the recommendations, Carrie D. Patnode, PhD, of Kaiser Permanente in Portland, Ore., and her colleagues concluded that higher-intensity interventions may promote greater improvements in health outcomes, but that “there is very limited evidence on longer-term intermediate and health outcomes or on harmful effects of these interventions” (JAMA 2017;318:175-93. doi: 10.1001/jama.2017.3303).
The researchers had no financial conflicts to disclose.
FROM JAMA
Key clinical point: Even adults with no CVD risk factors benefit from behavioral counseling about diet and exercise, according to the USPSTF.
Major finding: In 34 trials involving intermediate outcomes, behavior counseling was associated with significant improvements in systolic blood pressure, diastolic blood pressure, total cholesterol, BMI, weight, and waist circumference.
Data source: The data come from a USPSTF review of 88 trials and more 120 interventions.
Disclosures: The researchers had no relevant financial conflicts to disclose.
Isotretinoin patients need not postpone skin surgery
Skin procedures including superficial chemical peels, laser hair removal, minor cutaneous surgery, manual dermabrasion, and fractional ablative and fractional nonablative laser procedures can be performed safely on patients who have recently been or are currently being treated with isotretinoin, according to new recommendations from a consensus panel.
The recommendations were published online in JAMA Dermatology.
Postponing surgical procedures in patients taking isotretinoin because of the potential for keloid formation and delayed wound healing “has persisted despite increasing reports to the contrary,” wrote Leah K. Spring, DO, of Naval Hospital Camp Lejeune, Camp Lejeune, N.C., and her colleagues (JAMA Dermatol. 2017. doi: 10.1001/jamadermatol.2017.2077).
This protocol is based on 11 patients with delayed healing and keloids, the researchers noted. “In our consensus-based assessment, these initial cases presented a hypothesis to be tested, rather than the foundation for medical dogma on which more than 30 years of clinical practice was built,” they wrote.
To establish the current level of evidence for delaying procedures in isotretinoin patients and to make recommendations, an expert panel reviewed data from 32 publications and more than 1,485 procedures. The literature was divided into five areas: dermabrasion, chemical peels, cutaneous surgery, laser hair removal, and ablative/nonablative laser treatments.
The researchers determined that evidence does not support the safety of mechanical dermabrasion or fully ablative laser surgeries for current or recent isotretinoin users. Manual dermabrasion and microdermabrasion were deemed safe for isotretinoin patients based on the latest evidence, however, as were fractional ablative and fractional nonablative procedures.
In addition, the evidence did not support refraining from chemical peels, laser hair removal, or cutaneous surgery for current and recent isotretinoin patients, although the panel recommended additional prospective, controlled clinical trials in these areas.
In the area of cutaneous surgery, the consensus panel also noted the need for “a rigorous evaluation of the aforementioned specific warning that muscle flap insertion should be delayed until the patient displays normal [creatine phosphokinase (CPK)] levels or, at least, CPK levels below twofold of normal.”
The recommendations can be a resource for discussions with patients about the risks of procedures concurrent with isotretinoin, Dr. Spring and her associates emphasized. “For some patients and some conditions, an informed decision may lead to earlier and potentially more effective interventions.”
Lead author Dr. Spring had no relevant financial conflicts to disclose. Several members of the consensus group disclosed relationships with multiple companies including Allergan, Merz, Leo, Promius, Lumenis, Cynosure, and Valeant.
Skin procedures including superficial chemical peels, laser hair removal, minor cutaneous surgery, manual dermabrasion, and fractional ablative and fractional nonablative laser procedures can be performed safely on patients who have recently been or are currently being treated with isotretinoin, according to new recommendations from a consensus panel.
The recommendations were published online in JAMA Dermatology.
Postponing surgical procedures in patients taking isotretinoin because of the potential for keloid formation and delayed wound healing “has persisted despite increasing reports to the contrary,” wrote Leah K. Spring, DO, of Naval Hospital Camp Lejeune, Camp Lejeune, N.C., and her colleagues (JAMA Dermatol. 2017. doi: 10.1001/jamadermatol.2017.2077).
This protocol is based on 11 patients with delayed healing and keloids, the researchers noted. “In our consensus-based assessment, these initial cases presented a hypothesis to be tested, rather than the foundation for medical dogma on which more than 30 years of clinical practice was built,” they wrote.
To establish the current level of evidence for delaying procedures in isotretinoin patients and to make recommendations, an expert panel reviewed data from 32 publications and more than 1,485 procedures. The literature was divided into five areas: dermabrasion, chemical peels, cutaneous surgery, laser hair removal, and ablative/nonablative laser treatments.
The researchers determined that evidence does not support the safety of mechanical dermabrasion or fully ablative laser surgeries for current or recent isotretinoin users. Manual dermabrasion and microdermabrasion were deemed safe for isotretinoin patients based on the latest evidence, however, as were fractional ablative and fractional nonablative procedures.
In addition, the evidence did not support refraining from chemical peels, laser hair removal, or cutaneous surgery for current and recent isotretinoin patients, although the panel recommended additional prospective, controlled clinical trials in these areas.
In the area of cutaneous surgery, the consensus panel also noted the need for “a rigorous evaluation of the aforementioned specific warning that muscle flap insertion should be delayed until the patient displays normal [creatine phosphokinase (CPK)] levels or, at least, CPK levels below twofold of normal.”
The recommendations can be a resource for discussions with patients about the risks of procedures concurrent with isotretinoin, Dr. Spring and her associates emphasized. “For some patients and some conditions, an informed decision may lead to earlier and potentially more effective interventions.”
Lead author Dr. Spring had no relevant financial conflicts to disclose. Several members of the consensus group disclosed relationships with multiple companies including Allergan, Merz, Leo, Promius, Lumenis, Cynosure, and Valeant.
Skin procedures including superficial chemical peels, laser hair removal, minor cutaneous surgery, manual dermabrasion, and fractional ablative and fractional nonablative laser procedures can be performed safely on patients who have recently been or are currently being treated with isotretinoin, according to new recommendations from a consensus panel.
The recommendations were published online in JAMA Dermatology.
Postponing surgical procedures in patients taking isotretinoin because of the potential for keloid formation and delayed wound healing “has persisted despite increasing reports to the contrary,” wrote Leah K. Spring, DO, of Naval Hospital Camp Lejeune, Camp Lejeune, N.C., and her colleagues (JAMA Dermatol. 2017. doi: 10.1001/jamadermatol.2017.2077).
This protocol is based on 11 patients with delayed healing and keloids, the researchers noted. “In our consensus-based assessment, these initial cases presented a hypothesis to be tested, rather than the foundation for medical dogma on which more than 30 years of clinical practice was built,” they wrote.
To establish the current level of evidence for delaying procedures in isotretinoin patients and to make recommendations, an expert panel reviewed data from 32 publications and more than 1,485 procedures. The literature was divided into five areas: dermabrasion, chemical peels, cutaneous surgery, laser hair removal, and ablative/nonablative laser treatments.
The researchers determined that evidence does not support the safety of mechanical dermabrasion or fully ablative laser surgeries for current or recent isotretinoin users. Manual dermabrasion and microdermabrasion were deemed safe for isotretinoin patients based on the latest evidence, however, as were fractional ablative and fractional nonablative procedures.
In addition, the evidence did not support refraining from chemical peels, laser hair removal, or cutaneous surgery for current and recent isotretinoin patients, although the panel recommended additional prospective, controlled clinical trials in these areas.
In the area of cutaneous surgery, the consensus panel also noted the need for “a rigorous evaluation of the aforementioned specific warning that muscle flap insertion should be delayed until the patient displays normal [creatine phosphokinase (CPK)] levels or, at least, CPK levels below twofold of normal.”
The recommendations can be a resource for discussions with patients about the risks of procedures concurrent with isotretinoin, Dr. Spring and her associates emphasized. “For some patients and some conditions, an informed decision may lead to earlier and potentially more effective interventions.”
Lead author Dr. Spring had no relevant financial conflicts to disclose. Several members of the consensus group disclosed relationships with multiple companies including Allergan, Merz, Leo, Promius, Lumenis, Cynosure, and Valeant.
FROM JAMA DERMATOLOGY
Key clinical point:
Major finding: Experts found insufficient evidence to postpone manual dermabrasion, superficial chemical peels, fractional ablative or nonablative laser resurfacing, laser hair removal, or cutaneous surgery in patients taking isotretinoin or those who have taken it within the past 6 to 12 months.
Data source: The data come from 32 clinical publications and a total of 1,485 procedures.
Disclosures: Lead author Dr. Spring had no relevant financial conflicts to disclose. Several members of the consensus group disclosed relationships with multiple companies, including Allergan, Merz, Leo, Promius, Lumenis, Cynosure, and Valeant.
Opioid prescribing drops nationally, remains high in some counties
Opioid prescribing in the United States declined overall between 2010 and 2015, but remained stable or increased in some counties, according to a report from the Centers for Disease Control and Prevention. The findings were published online in the CDC’s Morbidity and Mortality Weekly Report.
“The bottom line remains: We have too many people getting too many prescriptions at too high a dose,” Anne Schuchat, MD, acting director of the CDC, said in a July 6 teleconference.
CDC researchers calculated prescribing rates from 2006 to 2015 by dividing the number of opioid prescriptions by the population estimates from the U.S. census for each year and created quartiles using morphine milligram equivalent per capita to analyze opioid distribution. Annual opioid prescribing rates increased from 72 to 81 prescriptions per 100 persons from 2006 to 2010 and remained relatively constant from 2010 to 2012 before showing a 13% decrease to 71 prescriptions per 100 persons from 2012 to 2015 (MMWR. 2017 Jul 7;66[26]:697-704. doi: 10.15585/mmwr.mm6626a4).
But despite these overall declines, “We are now experiencing the highest overdose death rates ever recorded in the United States,” Dr. Schuchat said. Quartiles were created using MME per capita to characterize the distribution of opioids prescribed.
In the report, areas associated with higher opioid prescribing rates on a county level included small cities or towns, areas that had a higher proportion of white residents, areas with more doctors and dentists, and areas with more cases of arthritis, diabetes, or other disabilities, she said.
The findings suggest a need for more consistency among health care providers about prescription opioids, Dr. Schuchat said. “Clinical practice is all over the place, which is a sign that you need better standards; we hope the 2016 guidelines are a turning point for better prescribing,” she said.
The CDC’s guidelines on opioid prescribing were released in 2016. The guidelines recommend alternatives when possible. Clinicians should instead consider nonopioid therapy, other types of pain medication, and nondrug pain relief options, such as physical therapy and cognitive-behavioral therapy. Other concerns include the length and strength of opioid prescriptions. Even taking opioids for a few months increases the risk for addiction, Dr. Schuchat said.
“Physicians must continue to lead efforts to reverse the epidemic by using prescription drug–monitoring programs, eliminating stigma, prescribing the overdose reversal drug naloxone, and enhancing their education about safe opioid prescribing and effective pain management,” Patrice A. Harris, MD, chair of the American Medical Association Opioid Task Force, said in a statement in response to the report. “Our country must do more to provide evidence-based, comprehensive treatment for pain and for substance use disorders,” she said.
“We really encourage clinicians to look to the guidelines and the tools that are available,” Dr. Schuchat said. “We do know that internists and other primary care physicians prescribe most of the opioids, so it is important for them to be aware.” The CDC has developed a checklist and a mobile app that have been downloaded by thousands of clinicians so far, she noted. Changes in annual prescribing hold promise that practices can improve, she said.
The researchers reported no conflicts of interest.
Opioid prescribing in the United States declined overall between 2010 and 2015, but remained stable or increased in some counties, according to a report from the Centers for Disease Control and Prevention. The findings were published online in the CDC’s Morbidity and Mortality Weekly Report.
“The bottom line remains: We have too many people getting too many prescriptions at too high a dose,” Anne Schuchat, MD, acting director of the CDC, said in a July 6 teleconference.
CDC researchers calculated prescribing rates from 2006 to 2015 by dividing the number of opioid prescriptions by the population estimates from the U.S. census for each year and created quartiles using morphine milligram equivalent per capita to analyze opioid distribution. Annual opioid prescribing rates increased from 72 to 81 prescriptions per 100 persons from 2006 to 2010 and remained relatively constant from 2010 to 2012 before showing a 13% decrease to 71 prescriptions per 100 persons from 2012 to 2015 (MMWR. 2017 Jul 7;66[26]:697-704. doi: 10.15585/mmwr.mm6626a4).
But despite these overall declines, “We are now experiencing the highest overdose death rates ever recorded in the United States,” Dr. Schuchat said. Quartiles were created using MME per capita to characterize the distribution of opioids prescribed.
In the report, areas associated with higher opioid prescribing rates on a county level included small cities or towns, areas that had a higher proportion of white residents, areas with more doctors and dentists, and areas with more cases of arthritis, diabetes, or other disabilities, she said.
The findings suggest a need for more consistency among health care providers about prescription opioids, Dr. Schuchat said. “Clinical practice is all over the place, which is a sign that you need better standards; we hope the 2016 guidelines are a turning point for better prescribing,” she said.
The CDC’s guidelines on opioid prescribing were released in 2016. The guidelines recommend alternatives when possible. Clinicians should instead consider nonopioid therapy, other types of pain medication, and nondrug pain relief options, such as physical therapy and cognitive-behavioral therapy. Other concerns include the length and strength of opioid prescriptions. Even taking opioids for a few months increases the risk for addiction, Dr. Schuchat said.
“Physicians must continue to lead efforts to reverse the epidemic by using prescription drug–monitoring programs, eliminating stigma, prescribing the overdose reversal drug naloxone, and enhancing their education about safe opioid prescribing and effective pain management,” Patrice A. Harris, MD, chair of the American Medical Association Opioid Task Force, said in a statement in response to the report. “Our country must do more to provide evidence-based, comprehensive treatment for pain and for substance use disorders,” she said.
“We really encourage clinicians to look to the guidelines and the tools that are available,” Dr. Schuchat said. “We do know that internists and other primary care physicians prescribe most of the opioids, so it is important for them to be aware.” The CDC has developed a checklist and a mobile app that have been downloaded by thousands of clinicians so far, she noted. Changes in annual prescribing hold promise that practices can improve, she said.
The researchers reported no conflicts of interest.
Opioid prescribing in the United States declined overall between 2010 and 2015, but remained stable or increased in some counties, according to a report from the Centers for Disease Control and Prevention. The findings were published online in the CDC’s Morbidity and Mortality Weekly Report.
“The bottom line remains: We have too many people getting too many prescriptions at too high a dose,” Anne Schuchat, MD, acting director of the CDC, said in a July 6 teleconference.
CDC researchers calculated prescribing rates from 2006 to 2015 by dividing the number of opioid prescriptions by the population estimates from the U.S. census for each year and created quartiles using morphine milligram equivalent per capita to analyze opioid distribution. Annual opioid prescribing rates increased from 72 to 81 prescriptions per 100 persons from 2006 to 2010 and remained relatively constant from 2010 to 2012 before showing a 13% decrease to 71 prescriptions per 100 persons from 2012 to 2015 (MMWR. 2017 Jul 7;66[26]:697-704. doi: 10.15585/mmwr.mm6626a4).
But despite these overall declines, “We are now experiencing the highest overdose death rates ever recorded in the United States,” Dr. Schuchat said. Quartiles were created using MME per capita to characterize the distribution of opioids prescribed.
In the report, areas associated with higher opioid prescribing rates on a county level included small cities or towns, areas that had a higher proportion of white residents, areas with more doctors and dentists, and areas with more cases of arthritis, diabetes, or other disabilities, she said.
The findings suggest a need for more consistency among health care providers about prescription opioids, Dr. Schuchat said. “Clinical practice is all over the place, which is a sign that you need better standards; we hope the 2016 guidelines are a turning point for better prescribing,” she said.
The CDC’s guidelines on opioid prescribing were released in 2016. The guidelines recommend alternatives when possible. Clinicians should instead consider nonopioid therapy, other types of pain medication, and nondrug pain relief options, such as physical therapy and cognitive-behavioral therapy. Other concerns include the length and strength of opioid prescriptions. Even taking opioids for a few months increases the risk for addiction, Dr. Schuchat said.
“Physicians must continue to lead efforts to reverse the epidemic by using prescription drug–monitoring programs, eliminating stigma, prescribing the overdose reversal drug naloxone, and enhancing their education about safe opioid prescribing and effective pain management,” Patrice A. Harris, MD, chair of the American Medical Association Opioid Task Force, said in a statement in response to the report. “Our country must do more to provide evidence-based, comprehensive treatment for pain and for substance use disorders,” she said.
“We really encourage clinicians to look to the guidelines and the tools that are available,” Dr. Schuchat said. “We do know that internists and other primary care physicians prescribe most of the opioids, so it is important for them to be aware.” The CDC has developed a checklist and a mobile app that have been downloaded by thousands of clinicians so far, she noted. Changes in annual prescribing hold promise that practices can improve, she said.
The researchers reported no conflicts of interest.
FROM MMWR
Imaging after bariatric surgery appears overdone
Nearly 70% of bariatric surgery patients received postoperative imaging, with more than one-third receiving CT imaging. This high level of screening resulted in symptom-related findings in only 23% of cases, and may be excessive, according to researchers who studied nearly 600 adults who underwent bariatric surgery.
As the volume of bariatric surgery has increased, so has the role of postoperative imaging, wrote Dana Haddad, MD, and her colleagues at Harlem Hospital Center, New York.
“However, there is a lack of well-defined postoperative imaging guidelines,” they said. “Detrimental aspects of postoperative imaging include the potential for false-positive findings leading to further and often unnecessary investigations, radiation exposure, and additional cost,” they added.
The primary outcomes were the numbers of initial postimaging studies and whether the findings supported subsequent studies.
The study population included 399 adults who underwent laparoscopic bypass and 144 who underwent sleeve gastrectomy. The average age of the patients was 41 years and 90% were women.
The researchers identified 907 imaging studies performed in 400 patients (69% of the study population). Of these, 38% were ultrasound, 36% were CT, 15% were x-ray, 6.6% were fluoroscopy, 3.3% were MRI, and .6% were nuclear medicine.
On review of the imaging findings, the researchers found that half (50%) were unremarkable, while 13% were either surgery related or symptom related, 6.8% were not related to surgery but might have explained patients’ symptoms, 4.3% were surgery-related but not likely to explain symptoms, and 26% were incidental. “Interestingly, no incidental findings were found to be of major clinical importance; all were benign,” according to the researchers.
However, incidental findings led to a total of 71 additional studies, and to 5 laparoscopic cholecystectomies.
A univariate analysis showed that the factors with a significant impact a patient’s odds of undergoing postoperative abdominal imaging included having a bypass procedure vs. a sleeve procedure, older age, and lower baseline body mass index. In addition, patients with a history of abdominal surgery or dyspepsia or those who had a routine postoperative upper gastrointestinal series were significantly more likely to undergo CT scans. Patients with history of ulcer or reflux were significantly less likely to undergo CT scans.
Although the study was limited by the retrospective design and lack of information about possible imaging of patients at other centers, “results suggest that nonroutine postoperative abdominal imaging in the bariatric population is common and requires streamlined protocols, with almost 70% of patients undergoing imaging and greater than 70% of findings being unrelated to symptoms or negative,” the researchers said.
A clinical algorithm for imaging of bariatric patients should be based on clinical parameters collected during a physical exam. “Once an algorithm is in place, further studies will be needed to validate its accuracy and efficiency,” the researchers stated.
Dr. Haddad and her colleagues had no financial conflicts to disclose.
Nearly 70% of bariatric surgery patients received postoperative imaging, with more than one-third receiving CT imaging. This high level of screening resulted in symptom-related findings in only 23% of cases, and may be excessive, according to researchers who studied nearly 600 adults who underwent bariatric surgery.
As the volume of bariatric surgery has increased, so has the role of postoperative imaging, wrote Dana Haddad, MD, and her colleagues at Harlem Hospital Center, New York.
“However, there is a lack of well-defined postoperative imaging guidelines,” they said. “Detrimental aspects of postoperative imaging include the potential for false-positive findings leading to further and often unnecessary investigations, radiation exposure, and additional cost,” they added.
The primary outcomes were the numbers of initial postimaging studies and whether the findings supported subsequent studies.
The study population included 399 adults who underwent laparoscopic bypass and 144 who underwent sleeve gastrectomy. The average age of the patients was 41 years and 90% were women.
The researchers identified 907 imaging studies performed in 400 patients (69% of the study population). Of these, 38% were ultrasound, 36% were CT, 15% were x-ray, 6.6% were fluoroscopy, 3.3% were MRI, and .6% were nuclear medicine.
On review of the imaging findings, the researchers found that half (50%) were unremarkable, while 13% were either surgery related or symptom related, 6.8% were not related to surgery but might have explained patients’ symptoms, 4.3% were surgery-related but not likely to explain symptoms, and 26% were incidental. “Interestingly, no incidental findings were found to be of major clinical importance; all were benign,” according to the researchers.
However, incidental findings led to a total of 71 additional studies, and to 5 laparoscopic cholecystectomies.
A univariate analysis showed that the factors with a significant impact a patient’s odds of undergoing postoperative abdominal imaging included having a bypass procedure vs. a sleeve procedure, older age, and lower baseline body mass index. In addition, patients with a history of abdominal surgery or dyspepsia or those who had a routine postoperative upper gastrointestinal series were significantly more likely to undergo CT scans. Patients with history of ulcer or reflux were significantly less likely to undergo CT scans.
Although the study was limited by the retrospective design and lack of information about possible imaging of patients at other centers, “results suggest that nonroutine postoperative abdominal imaging in the bariatric population is common and requires streamlined protocols, with almost 70% of patients undergoing imaging and greater than 70% of findings being unrelated to symptoms or negative,” the researchers said.
A clinical algorithm for imaging of bariatric patients should be based on clinical parameters collected during a physical exam. “Once an algorithm is in place, further studies will be needed to validate its accuracy and efficiency,” the researchers stated.
Dr. Haddad and her colleagues had no financial conflicts to disclose.
Nearly 70% of bariatric surgery patients received postoperative imaging, with more than one-third receiving CT imaging. This high level of screening resulted in symptom-related findings in only 23% of cases, and may be excessive, according to researchers who studied nearly 600 adults who underwent bariatric surgery.
As the volume of bariatric surgery has increased, so has the role of postoperative imaging, wrote Dana Haddad, MD, and her colleagues at Harlem Hospital Center, New York.
“However, there is a lack of well-defined postoperative imaging guidelines,” they said. “Detrimental aspects of postoperative imaging include the potential for false-positive findings leading to further and often unnecessary investigations, radiation exposure, and additional cost,” they added.
The primary outcomes were the numbers of initial postimaging studies and whether the findings supported subsequent studies.
The study population included 399 adults who underwent laparoscopic bypass and 144 who underwent sleeve gastrectomy. The average age of the patients was 41 years and 90% were women.
The researchers identified 907 imaging studies performed in 400 patients (69% of the study population). Of these, 38% were ultrasound, 36% were CT, 15% were x-ray, 6.6% were fluoroscopy, 3.3% were MRI, and .6% were nuclear medicine.
On review of the imaging findings, the researchers found that half (50%) were unremarkable, while 13% were either surgery related or symptom related, 6.8% were not related to surgery but might have explained patients’ symptoms, 4.3% were surgery-related but not likely to explain symptoms, and 26% were incidental. “Interestingly, no incidental findings were found to be of major clinical importance; all were benign,” according to the researchers.
However, incidental findings led to a total of 71 additional studies, and to 5 laparoscopic cholecystectomies.
A univariate analysis showed that the factors with a significant impact a patient’s odds of undergoing postoperative abdominal imaging included having a bypass procedure vs. a sleeve procedure, older age, and lower baseline body mass index. In addition, patients with a history of abdominal surgery or dyspepsia or those who had a routine postoperative upper gastrointestinal series were significantly more likely to undergo CT scans. Patients with history of ulcer or reflux were significantly less likely to undergo CT scans.
Although the study was limited by the retrospective design and lack of information about possible imaging of patients at other centers, “results suggest that nonroutine postoperative abdominal imaging in the bariatric population is common and requires streamlined protocols, with almost 70% of patients undergoing imaging and greater than 70% of findings being unrelated to symptoms or negative,” the researchers said.
A clinical algorithm for imaging of bariatric patients should be based on clinical parameters collected during a physical exam. “Once an algorithm is in place, further studies will be needed to validate its accuracy and efficiency,” the researchers stated.
Dr. Haddad and her colleagues had no financial conflicts to disclose.
FROM SURGERY FOR OBESITY AND RELATED DISEASES
Key clinical point: No well-defined guidelines exist for when to use postoperative imaging in bariatric surgery patients.
Major finding: Approximately 70% of postoperative imaging findings were not symptom related, and incidental findings led to 71 additional studies.
Data source: A review of 578 patients who underwent gastric bypass or sleeve gastrectomy.
Disclosures: The researchers had no financial conflicts to disclose.
Obeticholic acid fails to prevent liver damage in an animal model of short-bowel syndrome
Obeticholic acid failed to prevent the development of short-bowel syndrome–associated liver disease in a preliminary study using piglet models. The findings were published in the July issue of Cellular and Molecular Gastroenterology and Hepatology (doi: 10.1016/j.jcmgh.2017.02.008).
Current treatment options for short-bowel syndrome-associated liver disease are limited, wrote Prue M. Pereira-Fantini, PhD, of Murdoch Childrens Research Institute, Victoria, Australia, and colleagues. However, the farnesoid X receptor, which regulates genes involved in bile acid synthesis, absorption, and transport in the intestine and liver, has shown promise as a pharmaceutical target.
“Recently, we described SBS-ALD-associated alterations in bile acid composition associated with disrupted farnesoid X receptor (FXR) signaling mechanisms,” the researchers said. Obeticholic acid (OCA) has been shown to prevent liver disease in mouse models and human disease, and the researchers explored whether it would be effective in the context of short-bowel syndrome associated liver disease (SBS-ALD).
The researchers randomized piglets into four groups to receive small-bowel resection or sham surgery, and either a daily dose of 2.4 mg/kg per day of OCA or no treatment. The pigs were euthanized 2 weeks after their surgeries, and the researchers collected portal plasma samples, bile samples, and liver samples.
OCA treatment in piglets in the SBS surgery group was associated with decreased stool fat that suggested improved fat absorption, but impacted liver morphology, the researchers noted. “Untreated, sham-operated piglets showed normal liver histology when compared with SBS piglets who showed decreased hepatic lobule area and small clusters of inflammatory cells together with mild-to-moderate vesicular zone 2 lipidosis,” they wrote.
Overall, OCA treatment prevented the depletion of taurine; taurine concentration was approximately 8 ng/mL for piglets with SBS treated with OCA compared with 8 ng/mL in the sham group, 9 ng/mL in the sham plus OCA group, and 3 ng/mL in the SBS-only group. However, bile acid dysmetabolism occurred as shown by HDCA levels, which increased with OCA treatment compared to sham controls but were significantly reduced in SBS piglets treated with OCA vs. untreated SBS piglets.
In addition, the researchers found that small-bowel resection did not impact gene expression levels of FXR targets in the intestine or liver. However, “intestinal FXR gene expression was 11-fold higher in untreated SBS piglets when compared with untreated sham piglets,” they wrote. OCA treatment had no significant impact on FXR gene expression in the OCA-treated group vs. the untreated group and in the OCA-treated SBS group.
Although the findings were limited by use of an animal model, the results suggest that OCA treatment may have clinical benefits for SBS patients by reducing fat malabsorption, which remains a challenge, the researchers wrote. However, OCA “did not prevent the development of SBS-ALD, thereby limiting the potential therapeutic benefit in patients with SBS,” they concluded.
The researchers had no financial conflicts to disclose. The study was supported in part by the National Health and Medical Research Council of Australia and by a research grant from the Science Foundation Ireland.
Obeticholic acid failed to prevent the development of short-bowel syndrome–associated liver disease in a preliminary study using piglet models. The findings were published in the July issue of Cellular and Molecular Gastroenterology and Hepatology (doi: 10.1016/j.jcmgh.2017.02.008).
Current treatment options for short-bowel syndrome-associated liver disease are limited, wrote Prue M. Pereira-Fantini, PhD, of Murdoch Childrens Research Institute, Victoria, Australia, and colleagues. However, the farnesoid X receptor, which regulates genes involved in bile acid synthesis, absorption, and transport in the intestine and liver, has shown promise as a pharmaceutical target.
“Recently, we described SBS-ALD-associated alterations in bile acid composition associated with disrupted farnesoid X receptor (FXR) signaling mechanisms,” the researchers said. Obeticholic acid (OCA) has been shown to prevent liver disease in mouse models and human disease, and the researchers explored whether it would be effective in the context of short-bowel syndrome associated liver disease (SBS-ALD).
The researchers randomized piglets into four groups to receive small-bowel resection or sham surgery, and either a daily dose of 2.4 mg/kg per day of OCA or no treatment. The pigs were euthanized 2 weeks after their surgeries, and the researchers collected portal plasma samples, bile samples, and liver samples.
OCA treatment in piglets in the SBS surgery group was associated with decreased stool fat that suggested improved fat absorption, but impacted liver morphology, the researchers noted. “Untreated, sham-operated piglets showed normal liver histology when compared with SBS piglets who showed decreased hepatic lobule area and small clusters of inflammatory cells together with mild-to-moderate vesicular zone 2 lipidosis,” they wrote.
Overall, OCA treatment prevented the depletion of taurine; taurine concentration was approximately 8 ng/mL for piglets with SBS treated with OCA compared with 8 ng/mL in the sham group, 9 ng/mL in the sham plus OCA group, and 3 ng/mL in the SBS-only group. However, bile acid dysmetabolism occurred as shown by HDCA levels, which increased with OCA treatment compared to sham controls but were significantly reduced in SBS piglets treated with OCA vs. untreated SBS piglets.
In addition, the researchers found that small-bowel resection did not impact gene expression levels of FXR targets in the intestine or liver. However, “intestinal FXR gene expression was 11-fold higher in untreated SBS piglets when compared with untreated sham piglets,” they wrote. OCA treatment had no significant impact on FXR gene expression in the OCA-treated group vs. the untreated group and in the OCA-treated SBS group.
Although the findings were limited by use of an animal model, the results suggest that OCA treatment may have clinical benefits for SBS patients by reducing fat malabsorption, which remains a challenge, the researchers wrote. However, OCA “did not prevent the development of SBS-ALD, thereby limiting the potential therapeutic benefit in patients with SBS,” they concluded.
The researchers had no financial conflicts to disclose. The study was supported in part by the National Health and Medical Research Council of Australia and by a research grant from the Science Foundation Ireland.
Obeticholic acid failed to prevent the development of short-bowel syndrome–associated liver disease in a preliminary study using piglet models. The findings were published in the July issue of Cellular and Molecular Gastroenterology and Hepatology (doi: 10.1016/j.jcmgh.2017.02.008).
Current treatment options for short-bowel syndrome-associated liver disease are limited, wrote Prue M. Pereira-Fantini, PhD, of Murdoch Childrens Research Institute, Victoria, Australia, and colleagues. However, the farnesoid X receptor, which regulates genes involved in bile acid synthesis, absorption, and transport in the intestine and liver, has shown promise as a pharmaceutical target.
“Recently, we described SBS-ALD-associated alterations in bile acid composition associated with disrupted farnesoid X receptor (FXR) signaling mechanisms,” the researchers said. Obeticholic acid (OCA) has been shown to prevent liver disease in mouse models and human disease, and the researchers explored whether it would be effective in the context of short-bowel syndrome associated liver disease (SBS-ALD).
The researchers randomized piglets into four groups to receive small-bowel resection or sham surgery, and either a daily dose of 2.4 mg/kg per day of OCA or no treatment. The pigs were euthanized 2 weeks after their surgeries, and the researchers collected portal plasma samples, bile samples, and liver samples.
OCA treatment in piglets in the SBS surgery group was associated with decreased stool fat that suggested improved fat absorption, but impacted liver morphology, the researchers noted. “Untreated, sham-operated piglets showed normal liver histology when compared with SBS piglets who showed decreased hepatic lobule area and small clusters of inflammatory cells together with mild-to-moderate vesicular zone 2 lipidosis,” they wrote.
Overall, OCA treatment prevented the depletion of taurine; taurine concentration was approximately 8 ng/mL for piglets with SBS treated with OCA compared with 8 ng/mL in the sham group, 9 ng/mL in the sham plus OCA group, and 3 ng/mL in the SBS-only group. However, bile acid dysmetabolism occurred as shown by HDCA levels, which increased with OCA treatment compared to sham controls but were significantly reduced in SBS piglets treated with OCA vs. untreated SBS piglets.
In addition, the researchers found that small-bowel resection did not impact gene expression levels of FXR targets in the intestine or liver. However, “intestinal FXR gene expression was 11-fold higher in untreated SBS piglets when compared with untreated sham piglets,” they wrote. OCA treatment had no significant impact on FXR gene expression in the OCA-treated group vs. the untreated group and in the OCA-treated SBS group.
Although the findings were limited by use of an animal model, the results suggest that OCA treatment may have clinical benefits for SBS patients by reducing fat malabsorption, which remains a challenge, the researchers wrote. However, OCA “did not prevent the development of SBS-ALD, thereby limiting the potential therapeutic benefit in patients with SBS,” they concluded.
The researchers had no financial conflicts to disclose. The study was supported in part by the National Health and Medical Research Council of Australia and by a research grant from the Science Foundation Ireland.
FROM CMGH
Key clinical point: Treatment with obeticholic acid improved absorption and altered bile acid, but did not prevent liver damage in a piglet model of short-bowel syndrome.
Major finding: Overall, taurine concentration was approximately 8 ng/mL for piglets with SBS treated with OCA compared with 8 ng/mL in the sham surgery group, 9 ng/mL in the sham treated with OCA group, and 3 ng/mL in the SBS-only group.
Data source: The data come from piglets treated with obeticholic acid or untreated, and randomized to a small-bowel resection or a sham surgery.
Disclosures: The researchers had no financial conflicts to disclose,
Proper catheter removal promotes colorectal surgery recovery
Adherence to guidelines for urinary catheter removal significantly reduced rates of urinary tract infection and length of hospital stay, based on data from almost 3,000 patients.
UTIs occurred in 0.8% of colonic surgery patients who were guideline compliant, compared with 4.1% of noncompliant patients. Similarly, UTIs were significantly less likely in rectal surgery patients who complied with guidelines, compared with those who did not (3.5% vs. 9.6%).
The Implementation of the Enhanced Recovery After Surgery (iERAS) program involved 15 academic hospitals in Ontario, Canada. The guidelines include prompt removal of catheters from colonic and rectal surgery patients. Recommended removal times ranged from 24 hours to 72 hours, depending on the procedure.
“Although numerous reports have documented the overall effectiveness of bundled ERAS interventions improving outcome, the contribution of individual components of the pathway in the context of an ERAS implementation program is uncertain,” wrote Allan Okrainec, MD, of the University of Toronto, and his colleagues.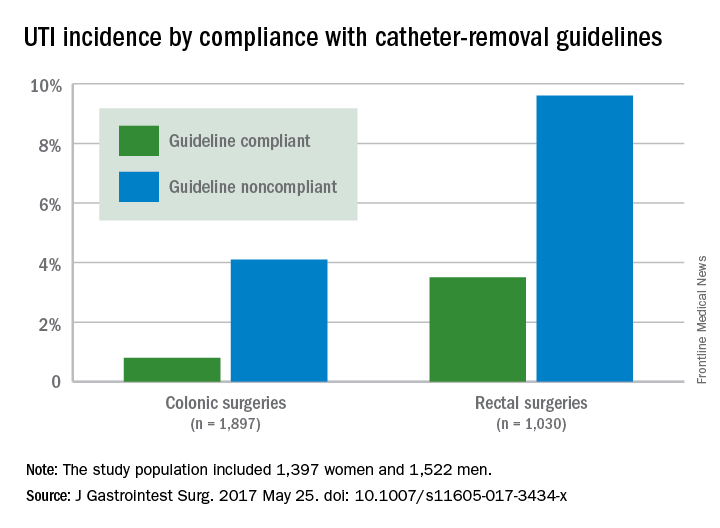
Overall, 53% of patients had catheters removed in compliance with the guidelines, including 47.2% of those with colonic resections and 69.5% of those with rectal resections.
The average length of hospital stay for colonic surgery patients who complied with the urinary catheter guideline was 4 days, compared with 5 days for noncompliant patients, a statistically significant difference. Similarly, the average length of stay was significantly shorter for compliant rectal surgery patients, compared with noncompliant patients (5 days vs. 8 days, respectively).
Reinsertion of the urinary catheter was needed for 6% of the patients, including 122 patients with suspected or confirmed urinary retention and 36 patients who had other indications for reinsertion.
“One of the concerns about early removal of catheters is that it might lead to an increased need for reinsertion,” the researchers noted. “In our study, guideline compliance was associated with an increased rate of catheter reinsertion, but [it] only increased the risk by 2%-3% in patients having rectal or colonic procedures,” the investigators said.
The study results were limited by a lack of information about reasons for noncompliance with the guidelines, the researchers added. However, the data support the value of early catheter removal for surgical patients. “It is noteworthy that, in our study, as well as others, urinary retention rates are relatively low,” they said.
The Council of Academic Hospitals of Ontario funded the study. The researchers had no financial conflicts to disclose.
Adherence to guidelines for urinary catheter removal significantly reduced rates of urinary tract infection and length of hospital stay, based on data from almost 3,000 patients.
UTIs occurred in 0.8% of colonic surgery patients who were guideline compliant, compared with 4.1% of noncompliant patients. Similarly, UTIs were significantly less likely in rectal surgery patients who complied with guidelines, compared with those who did not (3.5% vs. 9.6%).
The Implementation of the Enhanced Recovery After Surgery (iERAS) program involved 15 academic hospitals in Ontario, Canada. The guidelines include prompt removal of catheters from colonic and rectal surgery patients. Recommended removal times ranged from 24 hours to 72 hours, depending on the procedure.
“Although numerous reports have documented the overall effectiveness of bundled ERAS interventions improving outcome, the contribution of individual components of the pathway in the context of an ERAS implementation program is uncertain,” wrote Allan Okrainec, MD, of the University of Toronto, and his colleagues.
Overall, 53% of patients had catheters removed in compliance with the guidelines, including 47.2% of those with colonic resections and 69.5% of those with rectal resections.
The average length of hospital stay for colonic surgery patients who complied with the urinary catheter guideline was 4 days, compared with 5 days for noncompliant patients, a statistically significant difference. Similarly, the average length of stay was significantly shorter for compliant rectal surgery patients, compared with noncompliant patients (5 days vs. 8 days, respectively).
Reinsertion of the urinary catheter was needed for 6% of the patients, including 122 patients with suspected or confirmed urinary retention and 36 patients who had other indications for reinsertion.
“One of the concerns about early removal of catheters is that it might lead to an increased need for reinsertion,” the researchers noted. “In our study, guideline compliance was associated with an increased rate of catheter reinsertion, but [it] only increased the risk by 2%-3% in patients having rectal or colonic procedures,” the investigators said.
The study results were limited by a lack of information about reasons for noncompliance with the guidelines, the researchers added. However, the data support the value of early catheter removal for surgical patients. “It is noteworthy that, in our study, as well as others, urinary retention rates are relatively low,” they said.
The Council of Academic Hospitals of Ontario funded the study. The researchers had no financial conflicts to disclose.
Adherence to guidelines for urinary catheter removal significantly reduced rates of urinary tract infection and length of hospital stay, based on data from almost 3,000 patients.
UTIs occurred in 0.8% of colonic surgery patients who were guideline compliant, compared with 4.1% of noncompliant patients. Similarly, UTIs were significantly less likely in rectal surgery patients who complied with guidelines, compared with those who did not (3.5% vs. 9.6%).
The Implementation of the Enhanced Recovery After Surgery (iERAS) program involved 15 academic hospitals in Ontario, Canada. The guidelines include prompt removal of catheters from colonic and rectal surgery patients. Recommended removal times ranged from 24 hours to 72 hours, depending on the procedure.
“Although numerous reports have documented the overall effectiveness of bundled ERAS interventions improving outcome, the contribution of individual components of the pathway in the context of an ERAS implementation program is uncertain,” wrote Allan Okrainec, MD, of the University of Toronto, and his colleagues.
Overall, 53% of patients had catheters removed in compliance with the guidelines, including 47.2% of those with colonic resections and 69.5% of those with rectal resections.
The average length of hospital stay for colonic surgery patients who complied with the urinary catheter guideline was 4 days, compared with 5 days for noncompliant patients, a statistically significant difference. Similarly, the average length of stay was significantly shorter for compliant rectal surgery patients, compared with noncompliant patients (5 days vs. 8 days, respectively).
Reinsertion of the urinary catheter was needed for 6% of the patients, including 122 patients with suspected or confirmed urinary retention and 36 patients who had other indications for reinsertion.
“One of the concerns about early removal of catheters is that it might lead to an increased need for reinsertion,” the researchers noted. “In our study, guideline compliance was associated with an increased rate of catheter reinsertion, but [it] only increased the risk by 2%-3% in patients having rectal or colonic procedures,” the investigators said.
The study results were limited by a lack of information about reasons for noncompliance with the guidelines, the researchers added. However, the data support the value of early catheter removal for surgical patients. “It is noteworthy that, in our study, as well as others, urinary retention rates are relatively low,” they said.
The Council of Academic Hospitals of Ontario funded the study. The researchers had no financial conflicts to disclose.
FROM THE JOURNAL OF GASTROINTESTINAL SURGERY
Key clinical point: Compliance with guidelines for urinary catheter removal significantly reduced hospital stay and UTI rates in colon and rectal surgery patients.
Major finding: UTI rates in colonic surgery patients were 0.8% and 4.1%, respectively, for those who were compliant and noncompliant with the guidelines. Rates were 3.5% and 9.6%, respectively, for compliant and noncompliant rectal surgery patients.
Data source: A prospective study of 2,927 adults who underwent colonic or rectal surgery between September 2012 and April 2015.
Disclosures: The Council of Academic Hospitals of Ontario funded the study. The researchers had no financial conflicts to disclose.
Breastfeeding may reduce moms’ stroke risk
Breastfeeding not only benefits babies; it also may lower the risk for a heart attack or stroke later in life for mothers who breastfeed more than for women who don’t.
The findings, which were published online June 21 in the Journal of the American Heart Association, are based on data from a prospective study of nearly 300,000 women in China.
To assess the impact of breastfeeding on maternal cardiovascular health, the researchers reviewed data from 289,573 women who were participating in the China Kadoorie Biobank study to assess their reproductive history and lifestyle. At the time of study enrollment, none of the women had a history of cardiovascular disease and 99% reported at least one live birth. The average age of the women at baseline was 51 years.
Of the women who had given birth, 97% reported ever breastfeeding, and 91% reported breastfeeding each child for at least 6 months. The median duration of breastfeeding was 12 months per child (J Am Heart Assoc. 2017 Jun 21. doi: JAHA/2017/006081-T2).
During an 8-year follow-up period, participants experienced 16,671 cases of coronary heart disease and 23,983 strokes.
Overall, women who breastfed babies had a 9% reduction in risk of coronary heart disease and an 8% reduction in risk of stroke, compared with women who never breastfed. The longer the duration of breastfeeding, the greater the risk reduction; for every additional 6 months of breastfeeding, researchers found a 4% reduction in heart disease risk and a 3% reduction in stroke risk. Mothers who breastfed for 2 years or more had the most protection – an 18% reduced risk of heart disease and a 17% reduced risk of stroke, compared with mothers who never breastfed.
The study was limited by several factors, including its observational nature, which cannot confirm a causal relationship between breastfeeding and CVD. However, the results suggest that, if causal, “interventions to increase the likelihood and duration of breastfeeding could have persistent benefits to maternal cardiovascular health,” they wrote.
The baseline study was funded by the Kadoorie Charitable Foundation in Hong Kong; long-term support came from the UK Wellcome Trust, Chinese Ministry of Science and Technology, and the Chinese National Natural Science Foundation. Other support came from the British Heart Foundation, UK Medical Research Council and Cancer Research UK, and the National Natural Science Foundation of China. Dr. Peters has received support from the British Heart Foundation.
Breastfeeding not only benefits babies; it also may lower the risk for a heart attack or stroke later in life for mothers who breastfeed more than for women who don’t.
The findings, which were published online June 21 in the Journal of the American Heart Association, are based on data from a prospective study of nearly 300,000 women in China.
To assess the impact of breastfeeding on maternal cardiovascular health, the researchers reviewed data from 289,573 women who were participating in the China Kadoorie Biobank study to assess their reproductive history and lifestyle. At the time of study enrollment, none of the women had a history of cardiovascular disease and 99% reported at least one live birth. The average age of the women at baseline was 51 years.
Of the women who had given birth, 97% reported ever breastfeeding, and 91% reported breastfeeding each child for at least 6 months. The median duration of breastfeeding was 12 months per child (J Am Heart Assoc. 2017 Jun 21. doi: JAHA/2017/006081-T2).
During an 8-year follow-up period, participants experienced 16,671 cases of coronary heart disease and 23,983 strokes.
Overall, women who breastfed babies had a 9% reduction in risk of coronary heart disease and an 8% reduction in risk of stroke, compared with women who never breastfed. The longer the duration of breastfeeding, the greater the risk reduction; for every additional 6 months of breastfeeding, researchers found a 4% reduction in heart disease risk and a 3% reduction in stroke risk. Mothers who breastfed for 2 years or more had the most protection – an 18% reduced risk of heart disease and a 17% reduced risk of stroke, compared with mothers who never breastfed.
The study was limited by several factors, including its observational nature, which cannot confirm a causal relationship between breastfeeding and CVD. However, the results suggest that, if causal, “interventions to increase the likelihood and duration of breastfeeding could have persistent benefits to maternal cardiovascular health,” they wrote.
The baseline study was funded by the Kadoorie Charitable Foundation in Hong Kong; long-term support came from the UK Wellcome Trust, Chinese Ministry of Science and Technology, and the Chinese National Natural Science Foundation. Other support came from the British Heart Foundation, UK Medical Research Council and Cancer Research UK, and the National Natural Science Foundation of China. Dr. Peters has received support from the British Heart Foundation.
Breastfeeding not only benefits babies; it also may lower the risk for a heart attack or stroke later in life for mothers who breastfeed more than for women who don’t.
The findings, which were published online June 21 in the Journal of the American Heart Association, are based on data from a prospective study of nearly 300,000 women in China.
To assess the impact of breastfeeding on maternal cardiovascular health, the researchers reviewed data from 289,573 women who were participating in the China Kadoorie Biobank study to assess their reproductive history and lifestyle. At the time of study enrollment, none of the women had a history of cardiovascular disease and 99% reported at least one live birth. The average age of the women at baseline was 51 years.
Of the women who had given birth, 97% reported ever breastfeeding, and 91% reported breastfeeding each child for at least 6 months. The median duration of breastfeeding was 12 months per child (J Am Heart Assoc. 2017 Jun 21. doi: JAHA/2017/006081-T2).
During an 8-year follow-up period, participants experienced 16,671 cases of coronary heart disease and 23,983 strokes.
Overall, women who breastfed babies had a 9% reduction in risk of coronary heart disease and an 8% reduction in risk of stroke, compared with women who never breastfed. The longer the duration of breastfeeding, the greater the risk reduction; for every additional 6 months of breastfeeding, researchers found a 4% reduction in heart disease risk and a 3% reduction in stroke risk. Mothers who breastfed for 2 years or more had the most protection – an 18% reduced risk of heart disease and a 17% reduced risk of stroke, compared with mothers who never breastfed.
The study was limited by several factors, including its observational nature, which cannot confirm a causal relationship between breastfeeding and CVD. However, the results suggest that, if causal, “interventions to increase the likelihood and duration of breastfeeding could have persistent benefits to maternal cardiovascular health,” they wrote.
The baseline study was funded by the Kadoorie Charitable Foundation in Hong Kong; long-term support came from the UK Wellcome Trust, Chinese Ministry of Science and Technology, and the Chinese National Natural Science Foundation. Other support came from the British Heart Foundation, UK Medical Research Council and Cancer Research UK, and the National Natural Science Foundation of China. Dr. Peters has received support from the British Heart Foundation.
FROM THE JOURNAL OF THE AMERICAN HEART ASSOCIATION
Key clinical point: Interventions to encourage breastfeeding may benefit mothers’ cardiovascular health later in life.
Major finding: Women who breastfed their babies had a 10% reduction in risk of cardiovascular disease later in life.
Data source: A prospective study of approximately 300,000 women in China.
Disclosures: The baseline study was funded by the Kadoorie Charitable Foundation in Hong Kong; long-term support came from the UK Wellcome Trust, Chinese Ministry of Science and Technology, and the Chinese National Natural Science Foundation. Dr. Peters has received support from the British Heart Foundation.
Knee OA structural defects predict pain trajectories
The presence of bone marrow lesions and cartilage defects on baseline MRI scans of knee osteoarthritis (OA) patients may help to predict moderate to severe pain trajectories, based on data from a population-based study presented here at the European Congress of Rheumatology.
Three pain trajectories were identified: 52% of the patients reported stable mild pain over time, 33% reported moderate pain over time, and 15% reported fluctuating or severe pain over time.
“Knee pain is the most prominent symptom of knee osteoarthritis,” Dr. Pan said in an interview. “It is also a main reason for people to seek joint replacement. Despite this, the causes of knee pain are poorly understood. Therapy will only improve if we understand this better.”
Dr. Pan and his colleagues studied 1,099 adults with knee OA who participated in a population-based study. The mean age was 63 years (ranging from 51 to 81 years). A total of 875 participants were assessed using the knee pain components of the Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) at 2.6 years’ follow-up, 768 at 5.1 years’ follow-up, and 563 at 10.7 years’ follow-up.
Knee OA was assessed at baseline by x-ray, and T1-weighted or T2-weighted MRI scans of the right knee were used to assess knee structural pathology. The researchers applied group-based trajectory modeling to identify pain trajectories.
“We identified three distinct trajectories over time,” Dr. Pan said. “Remarkably, structural, environmental, sociodemographic, and psychological factors are associated with a more ‘severe pain’ trajectory, suggesting that pain course is determined by an integrated mix of all these factors.”
Dr. Pan added: “We already know that structural damage is a major driver in the development and maintenance of pain severity, but less is known about the other factors.”
The researchers found a significant dose-response relationship between the number of knee structural abnormalities, including cartilage defects and bone marrow lesions, and the ‘moderate pain’ and ‘severe pain’ trajectories (P less than .001 comparing both categories to the ‘mild pain’ trajectory).
Other factors that were significantly associated with both moderate and severe pain, compared with mild pain, included higher body mass index (overweight but not obese), emotional problems, and musculoskeletal diseases.
The findings provide support to the concept that “pain experience is both complex and individual in nature, suggesting the clinician should target treatments according to which of these factors predominate in the individual,” Dr. Pan said.
Future research may aim to develop “a predictive model that could be utilized in clinical practice and target therapies based on these trajectories.”
Dr. Pan had no financial conflicts to disclose.
The presence of bone marrow lesions and cartilage defects on baseline MRI scans of knee osteoarthritis (OA) patients may help to predict moderate to severe pain trajectories, based on data from a population-based study presented here at the European Congress of Rheumatology.
Three pain trajectories were identified: 52% of the patients reported stable mild pain over time, 33% reported moderate pain over time, and 15% reported fluctuating or severe pain over time.
“Knee pain is the most prominent symptom of knee osteoarthritis,” Dr. Pan said in an interview. “It is also a main reason for people to seek joint replacement. Despite this, the causes of knee pain are poorly understood. Therapy will only improve if we understand this better.”
Dr. Pan and his colleagues studied 1,099 adults with knee OA who participated in a population-based study. The mean age was 63 years (ranging from 51 to 81 years). A total of 875 participants were assessed using the knee pain components of the Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) at 2.6 years’ follow-up, 768 at 5.1 years’ follow-up, and 563 at 10.7 years’ follow-up.
Knee OA was assessed at baseline by x-ray, and T1-weighted or T2-weighted MRI scans of the right knee were used to assess knee structural pathology. The researchers applied group-based trajectory modeling to identify pain trajectories.
“We identified three distinct trajectories over time,” Dr. Pan said. “Remarkably, structural, environmental, sociodemographic, and psychological factors are associated with a more ‘severe pain’ trajectory, suggesting that pain course is determined by an integrated mix of all these factors.”
Dr. Pan added: “We already know that structural damage is a major driver in the development and maintenance of pain severity, but less is known about the other factors.”
The researchers found a significant dose-response relationship between the number of knee structural abnormalities, including cartilage defects and bone marrow lesions, and the ‘moderate pain’ and ‘severe pain’ trajectories (P less than .001 comparing both categories to the ‘mild pain’ trajectory).
Other factors that were significantly associated with both moderate and severe pain, compared with mild pain, included higher body mass index (overweight but not obese), emotional problems, and musculoskeletal diseases.
The findings provide support to the concept that “pain experience is both complex and individual in nature, suggesting the clinician should target treatments according to which of these factors predominate in the individual,” Dr. Pan said.
Future research may aim to develop “a predictive model that could be utilized in clinical practice and target therapies based on these trajectories.”
Dr. Pan had no financial conflicts to disclose.
The presence of bone marrow lesions and cartilage defects on baseline MRI scans of knee osteoarthritis (OA) patients may help to predict moderate to severe pain trajectories, based on data from a population-based study presented here at the European Congress of Rheumatology.
Three pain trajectories were identified: 52% of the patients reported stable mild pain over time, 33% reported moderate pain over time, and 15% reported fluctuating or severe pain over time.
“Knee pain is the most prominent symptom of knee osteoarthritis,” Dr. Pan said in an interview. “It is also a main reason for people to seek joint replacement. Despite this, the causes of knee pain are poorly understood. Therapy will only improve if we understand this better.”
Dr. Pan and his colleagues studied 1,099 adults with knee OA who participated in a population-based study. The mean age was 63 years (ranging from 51 to 81 years). A total of 875 participants were assessed using the knee pain components of the Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) at 2.6 years’ follow-up, 768 at 5.1 years’ follow-up, and 563 at 10.7 years’ follow-up.
Knee OA was assessed at baseline by x-ray, and T1-weighted or T2-weighted MRI scans of the right knee were used to assess knee structural pathology. The researchers applied group-based trajectory modeling to identify pain trajectories.
“We identified three distinct trajectories over time,” Dr. Pan said. “Remarkably, structural, environmental, sociodemographic, and psychological factors are associated with a more ‘severe pain’ trajectory, suggesting that pain course is determined by an integrated mix of all these factors.”
Dr. Pan added: “We already know that structural damage is a major driver in the development and maintenance of pain severity, but less is known about the other factors.”
The researchers found a significant dose-response relationship between the number of knee structural abnormalities, including cartilage defects and bone marrow lesions, and the ‘moderate pain’ and ‘severe pain’ trajectories (P less than .001 comparing both categories to the ‘mild pain’ trajectory).
Other factors that were significantly associated with both moderate and severe pain, compared with mild pain, included higher body mass index (overweight but not obese), emotional problems, and musculoskeletal diseases.
The findings provide support to the concept that “pain experience is both complex and individual in nature, suggesting the clinician should target treatments according to which of these factors predominate in the individual,” Dr. Pan said.
Future research may aim to develop “a predictive model that could be utilized in clinical practice and target therapies based on these trajectories.”
Dr. Pan had no financial conflicts to disclose.
FROM THE EULAR 2017 CONGRESS
Key clinical point:
Major finding: Three pain trajectories were identified: stable mild pain (52% of patients), moderate pain (33%), and fluctuating or severe pain (15%).
Data source: Population-based cohort study of 1,099 patients with knee OA.
Disclosures: The presenter had no financial conflicts to disclose.
Aspirin triples major bleeding risk after age 75 years
Older adults who take aspirin daily are at greater risk for serious bleeding than previously thought, based on data from roughly 3,000 patients.
“The risk of upper gastrointestinal bleeding on antiplatelet treatment increases with age, but it is uncertain whether older age alone is a sufficient indicator of high risk to justify routine coprescription of PPIs [proton pump inhibitors],” wrote Linxin Li, DPhil, of the University of Oxford (England) and her colleagues.
To assess the rate of bleeding among older adults on long-term aspirin therapy, Dr. Li and her colleagues reviewed data from the Oxford Vascular Study, a prospective population-based study of 3,166 patients. Of those, 1,584 were younger than 75 years, with an average age of 61 years, and 1,582 were at least 75 years old, with average age of 83 years. Patients were followed at 30 days, 6 months, and 1, 5, and 10 years to determine bleeding, recurrent ischemic events, and disability (Lancet. 2017. doi: 10.1016/S0140-6736[17]30770-5).
In addition, more than twice the major upper GI bleeds were disabling or fatal in adults aged 75 years and older than in the younger patients (62% vs. 25%).
Only a third of the patients in the study were taking proton pump inhibitors (PPIs), partly because current clinical guidelines don’t specifically recommend their use and partly in the absence of an accepted definition of which patients are at high risk for upper GI bleeding, the researchers said. They estimated that the number needed to treat with PPIs to prevent a major GI bleed after 5 years decreased with age: “80 for patients younger than 65 years, 75 for patients aged 65-74 years, 23 for patients aged 75-84 years, and 21 for patients aged 85 years or older.” In addition, the number needed to treat with PPIs to prevent a disabling or fatal upper GI bleed after 5 years was 338 for patients younger than 65 years but dropped to 25 for patients aged 85 years and older.
The findings were limited by the observational nature of the study and inability to show that increased risk of bleeding was caused by aspirin alone, the researchers said. However, based on the data, “age 75 years would be an appropriate threshold to start a PPI both in patients newly initiated on antiplatelet drugs and in patients on established treatment,” they wrote.
The study data were taken from the Oxford Vascular Study, which was funded by the National Institute of Health Research and several other research institutions. Corresponding author Peter Rothwell, MD, disclosed financial relationships with Bayer.
In patients with stroke with a cardiac source of embolism who qualify for oral anticoagulation, we obsess about the association between benefit and bleeding risk. Specific risk scores were developed to assess the bleeding risk for patients with atrial fibrillation who qualified for anticoagulation. However, similar risk scores are not applied for patients who undergo long-term prevention with antiplatelet therapy.
On the basis of this study’s results, the benefit-risk association in long-term antiplatelet therapy should be evaluated every 3-5 years in patients older than 75 years, and PPIs should be used in patients on antiplatelet therapy who are at least 75 years old or in patients with a history of gastrointestinal bleeds.
Hans-Christoph Diener, MD, of the department of neurology at the University Duisburg-Essen in Essen, Germany, made these remarks in an accompanying editorial (Lancet. 2017 Jun 13. doi: 10.1016/S0140-6736[17]31507-6). He disclosed relationships with multiple companies, including AstraZeneca, Bristol-Myers Squibb, GlaxoSmithKline, Merck, and Novartis.
In patients with stroke with a cardiac source of embolism who qualify for oral anticoagulation, we obsess about the association between benefit and bleeding risk. Specific risk scores were developed to assess the bleeding risk for patients with atrial fibrillation who qualified for anticoagulation. However, similar risk scores are not applied for patients who undergo long-term prevention with antiplatelet therapy.
On the basis of this study’s results, the benefit-risk association in long-term antiplatelet therapy should be evaluated every 3-5 years in patients older than 75 years, and PPIs should be used in patients on antiplatelet therapy who are at least 75 years old or in patients with a history of gastrointestinal bleeds.
Hans-Christoph Diener, MD, of the department of neurology at the University Duisburg-Essen in Essen, Germany, made these remarks in an accompanying editorial (Lancet. 2017 Jun 13. doi: 10.1016/S0140-6736[17]31507-6). He disclosed relationships with multiple companies, including AstraZeneca, Bristol-Myers Squibb, GlaxoSmithKline, Merck, and Novartis.
In patients with stroke with a cardiac source of embolism who qualify for oral anticoagulation, we obsess about the association between benefit and bleeding risk. Specific risk scores were developed to assess the bleeding risk for patients with atrial fibrillation who qualified for anticoagulation. However, similar risk scores are not applied for patients who undergo long-term prevention with antiplatelet therapy.
On the basis of this study’s results, the benefit-risk association in long-term antiplatelet therapy should be evaluated every 3-5 years in patients older than 75 years, and PPIs should be used in patients on antiplatelet therapy who are at least 75 years old or in patients with a history of gastrointestinal bleeds.
Hans-Christoph Diener, MD, of the department of neurology at the University Duisburg-Essen in Essen, Germany, made these remarks in an accompanying editorial (Lancet. 2017 Jun 13. doi: 10.1016/S0140-6736[17]31507-6). He disclosed relationships with multiple companies, including AstraZeneca, Bristol-Myers Squibb, GlaxoSmithKline, Merck, and Novartis.
Older adults who take aspirin daily are at greater risk for serious bleeding than previously thought, based on data from roughly 3,000 patients.
“The risk of upper gastrointestinal bleeding on antiplatelet treatment increases with age, but it is uncertain whether older age alone is a sufficient indicator of high risk to justify routine coprescription of PPIs [proton pump inhibitors],” wrote Linxin Li, DPhil, of the University of Oxford (England) and her colleagues.
To assess the rate of bleeding among older adults on long-term aspirin therapy, Dr. Li and her colleagues reviewed data from the Oxford Vascular Study, a prospective population-based study of 3,166 patients. Of those, 1,584 were younger than 75 years, with an average age of 61 years, and 1,582 were at least 75 years old, with average age of 83 years. Patients were followed at 30 days, 6 months, and 1, 5, and 10 years to determine bleeding, recurrent ischemic events, and disability (Lancet. 2017. doi: 10.1016/S0140-6736[17]30770-5).
In addition, more than twice the major upper GI bleeds were disabling or fatal in adults aged 75 years and older than in the younger patients (62% vs. 25%).
Only a third of the patients in the study were taking proton pump inhibitors (PPIs), partly because current clinical guidelines don’t specifically recommend their use and partly in the absence of an accepted definition of which patients are at high risk for upper GI bleeding, the researchers said. They estimated that the number needed to treat with PPIs to prevent a major GI bleed after 5 years decreased with age: “80 for patients younger than 65 years, 75 for patients aged 65-74 years, 23 for patients aged 75-84 years, and 21 for patients aged 85 years or older.” In addition, the number needed to treat with PPIs to prevent a disabling or fatal upper GI bleed after 5 years was 338 for patients younger than 65 years but dropped to 25 for patients aged 85 years and older.
The findings were limited by the observational nature of the study and inability to show that increased risk of bleeding was caused by aspirin alone, the researchers said. However, based on the data, “age 75 years would be an appropriate threshold to start a PPI both in patients newly initiated on antiplatelet drugs and in patients on established treatment,” they wrote.
The study data were taken from the Oxford Vascular Study, which was funded by the National Institute of Health Research and several other research institutions. Corresponding author Peter Rothwell, MD, disclosed financial relationships with Bayer.
Older adults who take aspirin daily are at greater risk for serious bleeding than previously thought, based on data from roughly 3,000 patients.
“The risk of upper gastrointestinal bleeding on antiplatelet treatment increases with age, but it is uncertain whether older age alone is a sufficient indicator of high risk to justify routine coprescription of PPIs [proton pump inhibitors],” wrote Linxin Li, DPhil, of the University of Oxford (England) and her colleagues.
To assess the rate of bleeding among older adults on long-term aspirin therapy, Dr. Li and her colleagues reviewed data from the Oxford Vascular Study, a prospective population-based study of 3,166 patients. Of those, 1,584 were younger than 75 years, with an average age of 61 years, and 1,582 were at least 75 years old, with average age of 83 years. Patients were followed at 30 days, 6 months, and 1, 5, and 10 years to determine bleeding, recurrent ischemic events, and disability (Lancet. 2017. doi: 10.1016/S0140-6736[17]30770-5).
In addition, more than twice the major upper GI bleeds were disabling or fatal in adults aged 75 years and older than in the younger patients (62% vs. 25%).
Only a third of the patients in the study were taking proton pump inhibitors (PPIs), partly because current clinical guidelines don’t specifically recommend their use and partly in the absence of an accepted definition of which patients are at high risk for upper GI bleeding, the researchers said. They estimated that the number needed to treat with PPIs to prevent a major GI bleed after 5 years decreased with age: “80 for patients younger than 65 years, 75 for patients aged 65-74 years, 23 for patients aged 75-84 years, and 21 for patients aged 85 years or older.” In addition, the number needed to treat with PPIs to prevent a disabling or fatal upper GI bleed after 5 years was 338 for patients younger than 65 years but dropped to 25 for patients aged 85 years and older.
The findings were limited by the observational nature of the study and inability to show that increased risk of bleeding was caused by aspirin alone, the researchers said. However, based on the data, “age 75 years would be an appropriate threshold to start a PPI both in patients newly initiated on antiplatelet drugs and in patients on established treatment,” they wrote.
The study data were taken from the Oxford Vascular Study, which was funded by the National Institute of Health Research and several other research institutions. Corresponding author Peter Rothwell, MD, disclosed financial relationships with Bayer.
FROM THE LANCET
Key clinical point:
Major finding: The annual rate of life-threatening or fatal bleeding episodes was less than 0.5% for patients younger than 65 years but rose to 1.5% in those aged 75-84 years and 2.5% in those aged 85 years and older.
Data source: A prospective, population-based cohort study of 3,166 adults who had one transient ischemic attack, ischemic stroke, or MI and who were treated with antiplatelet drugs.
Disclosures: The study data were taken from the Oxford Vascular Study, which was funded by the Wellcome Trust, Wolfson Foundation, British Heart Foundation, Dunhill Medical Trust, the National Institute of Health Research (NIHR), and the NIHR Oxford Biomedical Research Centre. Corresponding author Peter Rothwell, MD, disclosed financial relationships with Bayer.