User login
Early cognitive impairment associated with later Parkinson’s disease
Adults with early cognitive impairment are at greater risk for developing parkinsonism than those without cognitive impairment, based on data from 7,386 adults participating in the ongoing Rotterdam Study. The findings were published online Sept. 25 in JAMA Neurology.
“Between 15% and 43% of patients with newly diagnosed Parkinson disease (PD) are cognitively impaired,” wrote Sirwan K. L. Darweesh, MD, of Erasmus MC University Medical Center, Rotterdam, the Netherlands, and his colleagues. However, data on the predictive value of cognitive impairment for parkinsonism has not been well studied, they wrote (JAMA Neurol. 2017. doi: 10.1001/jamaneurol.2017.2248).
Over approximately 8 years’ follow-up, 1% of the participants were diagnosed with incident parkinsonism.
“Poor global cognition at baseline was associated with a higher risk of incident parkinsonism” with a hazard ratio of 1.79, the researchers said.
“To enable translation of our findings to clinical practice, we present likelihood ratios (LRs) for the baseline presence of isolated or combined cognitive dysfunction and subtle motor features for incident parkinsonism during follow-up,” they noted.
Approximately half of participants diagnosed with incident parkinsonism during the study period had subtle motor features, cognitive dysfunction, or both, at baseline. Baseline cognitive impairment alone showed a likelihood ratio of 1.76 for development of parkinsonism, but the likelihood ratio was greater when both cognitive impairment and subtle motor findings were present (2.66).
“In individuals who received a diagnosis of both incident dementia and incident parkinsonism, baseline cognitive dysfunction was not associated with incident dementia,” the researchers noted.
The researchers determined that the most likely explanation for the association between cognitive decline and increased Parkinson’s risk was that “low baseline cognitive scores may indicate ongoing cognitive decline in prediagnostic patients who probably will develop parkinsonism, most of whom have prediagnostic PD,” they said.
The study findings were limited by several factors including the potential misclassification of parkinsonism diagnosis, the researchers noted. However, the association between poor cognitive function and the risk of parkinsonism and probably Parkinson’s disease remained for the executive, attention, cognitive speed, and memory domains of cognition, they said. “Our findings suggest that poor cognitive functioning can be considered a prodromal sign of PD,” they concluded.
This study was supported in part by Stichting ParkinsonFonds. The researchers had no financial conflicts to disclose.
The long-term nature of the Rotterdam Study makes it an excellent source for examining the association between poor cognition and parkinsonism, wrote Ethan G. Brown, MD, and Caroline M. Tanner, MD, in an accompanying editorial.
“This study reiterates the presence of cognitive impairment very early in PD, emphasizing the need for therapeutic trials to target this symptom as an outcome. Although only some patients with cognitive impairment progress to PD, the study provides some clues on how to distinguish those most at risk. Progression to parkinsonism was more likely with baseline impairment of several individual cognitive tests, but only changes in semantic fluency predicted probable PD. Semantic fluency has been previously found to be specific for progression of cognitive impairment in PD, and this study again suggests the importance of this cognitive test early on,” they wrote.
“Yet the presence of cognitive impairment so early also gives rise to questions about the underlying pathology of PD progression. A commonly cited mechanism for progression of PD involves prion-like spread of synuclein pathology up through the dorsal nucleus of the vagus and substantia nigra. This spread presumably causes the autonomic, sleep, and motor dysfunction common in PD and supposedly leads to cognitive impairment only once Lewy bodies enter the neocortex. The current evidence that cognitive impairment can be evident in the prodromal stage challenges the universality of the model of vagal spread,” they noted.
However, recognizing the role of cognitive impairment as an early sign of PD can help clinicians plan screening and care, they said.
“This recognition can allow physicians to screen for falls or other nonmotor aspects of PD in these cases and provide early treatment for these symptoms. Physicians may recommend interventions, such as physical activity, that are helpful for motor and cognitive changes in PD,” they added (JAMA Neurol. 2017. doi: 10.1001/jamaneurol.2017.1474).
Dr. Brown and Dr. Tanner are affiliated with the Movement Disorders and Neuromodulation Center in the department of neurology at the University of California, San Francisco. Dr. Brown disclosed compensation for serving on the Fellowship Advisory Board for AbbVie. Dr. Tanner disclosed grants from a variety of nonprofit sources, as well as compensation for serving on Data Monitoring Committees for Biotie Therapeutics, Voyager Therapeutics, and Intec Pharma. Dr. Tanner also disclosed personal consulting fees from Neurocrine Biosciences, Adamas Therapeutics, and PhotoPharmics.
The long-term nature of the Rotterdam Study makes it an excellent source for examining the association between poor cognition and parkinsonism, wrote Ethan G. Brown, MD, and Caroline M. Tanner, MD, in an accompanying editorial.
“This study reiterates the presence of cognitive impairment very early in PD, emphasizing the need for therapeutic trials to target this symptom as an outcome. Although only some patients with cognitive impairment progress to PD, the study provides some clues on how to distinguish those most at risk. Progression to parkinsonism was more likely with baseline impairment of several individual cognitive tests, but only changes in semantic fluency predicted probable PD. Semantic fluency has been previously found to be specific for progression of cognitive impairment in PD, and this study again suggests the importance of this cognitive test early on,” they wrote.
“Yet the presence of cognitive impairment so early also gives rise to questions about the underlying pathology of PD progression. A commonly cited mechanism for progression of PD involves prion-like spread of synuclein pathology up through the dorsal nucleus of the vagus and substantia nigra. This spread presumably causes the autonomic, sleep, and motor dysfunction common in PD and supposedly leads to cognitive impairment only once Lewy bodies enter the neocortex. The current evidence that cognitive impairment can be evident in the prodromal stage challenges the universality of the model of vagal spread,” they noted.
However, recognizing the role of cognitive impairment as an early sign of PD can help clinicians plan screening and care, they said.
“This recognition can allow physicians to screen for falls or other nonmotor aspects of PD in these cases and provide early treatment for these symptoms. Physicians may recommend interventions, such as physical activity, that are helpful for motor and cognitive changes in PD,” they added (JAMA Neurol. 2017. doi: 10.1001/jamaneurol.2017.1474).
Dr. Brown and Dr. Tanner are affiliated with the Movement Disorders and Neuromodulation Center in the department of neurology at the University of California, San Francisco. Dr. Brown disclosed compensation for serving on the Fellowship Advisory Board for AbbVie. Dr. Tanner disclosed grants from a variety of nonprofit sources, as well as compensation for serving on Data Monitoring Committees for Biotie Therapeutics, Voyager Therapeutics, and Intec Pharma. Dr. Tanner also disclosed personal consulting fees from Neurocrine Biosciences, Adamas Therapeutics, and PhotoPharmics.
The long-term nature of the Rotterdam Study makes it an excellent source for examining the association between poor cognition and parkinsonism, wrote Ethan G. Brown, MD, and Caroline M. Tanner, MD, in an accompanying editorial.
“This study reiterates the presence of cognitive impairment very early in PD, emphasizing the need for therapeutic trials to target this symptom as an outcome. Although only some patients with cognitive impairment progress to PD, the study provides some clues on how to distinguish those most at risk. Progression to parkinsonism was more likely with baseline impairment of several individual cognitive tests, but only changes in semantic fluency predicted probable PD. Semantic fluency has been previously found to be specific for progression of cognitive impairment in PD, and this study again suggests the importance of this cognitive test early on,” they wrote.
“Yet the presence of cognitive impairment so early also gives rise to questions about the underlying pathology of PD progression. A commonly cited mechanism for progression of PD involves prion-like spread of synuclein pathology up through the dorsal nucleus of the vagus and substantia nigra. This spread presumably causes the autonomic, sleep, and motor dysfunction common in PD and supposedly leads to cognitive impairment only once Lewy bodies enter the neocortex. The current evidence that cognitive impairment can be evident in the prodromal stage challenges the universality of the model of vagal spread,” they noted.
However, recognizing the role of cognitive impairment as an early sign of PD can help clinicians plan screening and care, they said.
“This recognition can allow physicians to screen for falls or other nonmotor aspects of PD in these cases and provide early treatment for these symptoms. Physicians may recommend interventions, such as physical activity, that are helpful for motor and cognitive changes in PD,” they added (JAMA Neurol. 2017. doi: 10.1001/jamaneurol.2017.1474).
Dr. Brown and Dr. Tanner are affiliated with the Movement Disorders and Neuromodulation Center in the department of neurology at the University of California, San Francisco. Dr. Brown disclosed compensation for serving on the Fellowship Advisory Board for AbbVie. Dr. Tanner disclosed grants from a variety of nonprofit sources, as well as compensation for serving on Data Monitoring Committees for Biotie Therapeutics, Voyager Therapeutics, and Intec Pharma. Dr. Tanner also disclosed personal consulting fees from Neurocrine Biosciences, Adamas Therapeutics, and PhotoPharmics.
Adults with early cognitive impairment are at greater risk for developing parkinsonism than those without cognitive impairment, based on data from 7,386 adults participating in the ongoing Rotterdam Study. The findings were published online Sept. 25 in JAMA Neurology.
“Between 15% and 43% of patients with newly diagnosed Parkinson disease (PD) are cognitively impaired,” wrote Sirwan K. L. Darweesh, MD, of Erasmus MC University Medical Center, Rotterdam, the Netherlands, and his colleagues. However, data on the predictive value of cognitive impairment for parkinsonism has not been well studied, they wrote (JAMA Neurol. 2017. doi: 10.1001/jamaneurol.2017.2248).
Over approximately 8 years’ follow-up, 1% of the participants were diagnosed with incident parkinsonism.
“Poor global cognition at baseline was associated with a higher risk of incident parkinsonism” with a hazard ratio of 1.79, the researchers said.
“To enable translation of our findings to clinical practice, we present likelihood ratios (LRs) for the baseline presence of isolated or combined cognitive dysfunction and subtle motor features for incident parkinsonism during follow-up,” they noted.
Approximately half of participants diagnosed with incident parkinsonism during the study period had subtle motor features, cognitive dysfunction, or both, at baseline. Baseline cognitive impairment alone showed a likelihood ratio of 1.76 for development of parkinsonism, but the likelihood ratio was greater when both cognitive impairment and subtle motor findings were present (2.66).
“In individuals who received a diagnosis of both incident dementia and incident parkinsonism, baseline cognitive dysfunction was not associated with incident dementia,” the researchers noted.
The researchers determined that the most likely explanation for the association between cognitive decline and increased Parkinson’s risk was that “low baseline cognitive scores may indicate ongoing cognitive decline in prediagnostic patients who probably will develop parkinsonism, most of whom have prediagnostic PD,” they said.
The study findings were limited by several factors including the potential misclassification of parkinsonism diagnosis, the researchers noted. However, the association between poor cognitive function and the risk of parkinsonism and probably Parkinson’s disease remained for the executive, attention, cognitive speed, and memory domains of cognition, they said. “Our findings suggest that poor cognitive functioning can be considered a prodromal sign of PD,” they concluded.
This study was supported in part by Stichting ParkinsonFonds. The researchers had no financial conflicts to disclose.
Adults with early cognitive impairment are at greater risk for developing parkinsonism than those without cognitive impairment, based on data from 7,386 adults participating in the ongoing Rotterdam Study. The findings were published online Sept. 25 in JAMA Neurology.
“Between 15% and 43% of patients with newly diagnosed Parkinson disease (PD) are cognitively impaired,” wrote Sirwan K. L. Darweesh, MD, of Erasmus MC University Medical Center, Rotterdam, the Netherlands, and his colleagues. However, data on the predictive value of cognitive impairment for parkinsonism has not been well studied, they wrote (JAMA Neurol. 2017. doi: 10.1001/jamaneurol.2017.2248).
Over approximately 8 years’ follow-up, 1% of the participants were diagnosed with incident parkinsonism.
“Poor global cognition at baseline was associated with a higher risk of incident parkinsonism” with a hazard ratio of 1.79, the researchers said.
“To enable translation of our findings to clinical practice, we present likelihood ratios (LRs) for the baseline presence of isolated or combined cognitive dysfunction and subtle motor features for incident parkinsonism during follow-up,” they noted.
Approximately half of participants diagnosed with incident parkinsonism during the study period had subtle motor features, cognitive dysfunction, or both, at baseline. Baseline cognitive impairment alone showed a likelihood ratio of 1.76 for development of parkinsonism, but the likelihood ratio was greater when both cognitive impairment and subtle motor findings were present (2.66).
“In individuals who received a diagnosis of both incident dementia and incident parkinsonism, baseline cognitive dysfunction was not associated with incident dementia,” the researchers noted.
The researchers determined that the most likely explanation for the association between cognitive decline and increased Parkinson’s risk was that “low baseline cognitive scores may indicate ongoing cognitive decline in prediagnostic patients who probably will develop parkinsonism, most of whom have prediagnostic PD,” they said.
The study findings were limited by several factors including the potential misclassification of parkinsonism diagnosis, the researchers noted. However, the association between poor cognitive function and the risk of parkinsonism and probably Parkinson’s disease remained for the executive, attention, cognitive speed, and memory domains of cognition, they said. “Our findings suggest that poor cognitive functioning can be considered a prodromal sign of PD,” they concluded.
This study was supported in part by Stichting ParkinsonFonds. The researchers had no financial conflicts to disclose.
FROM JAMA NEUROLOGY
Key clinical point: Mild cognitive impairment may appear early in adults who go on to develop Parkinson’s disease.
Major finding: Poor global cognition at baseline was associated with a greater risk of incident parkinsonism (hazard ratio, 1.79) over approximately 8 years.
Data source: The data come from 7,386 adults in the population-based Rotterdam Study.
Disclosures: This study was supported in part by Stichting ParkinsonFonds. The researchers had no financial conflicts to disclose.
Alopecia patients share their struggles
SILVER SPRING, MD. – Alopecia areata patients struggle as much, if not more so, with the social and emotional challenges of the disease as with the physical challenges, according to patients and others who spoke at a public meeting on alopecia areata patient-focused drug development.
Alopecia areata affects as many as 6.8 million individuals in the United States, according to the National Alopecia Areata Foundation (NAAF). However, the particulars of alopecia can vary widely from one person to another; some patients experience total hair loss (alopecia universalis), while others retain eyebrows, eyelashes, or some body hair.
The FDA meeting, held on Sept. 11, is part of the agency’s patient-focused drug development initiative. “We wanted to hear the broader patient’s voice,” Theresa M. Mullin, PhD, director of the FDA’s Office of Strategic Programs, said in her opening remarks. Gary Sherwood, communications director for NAAF, said that the meeting was the culmination of a 5-year effort, begun in 2012 when alopecia areata was named as one of 39 disease categories under consideration for such a meeting. “It is too early to know what the exact results will be … but if the past is any indication, they may be significant. The meeting held with psoriasis yielded FDA approval of a treatment previously denied,” he added in an interview.
Two panel presentations featured patients who discussed their experiences with alopecia; each was followed by a discussion period where patients and family members in the audience were invited to share their experiences.
The “Health Effects and Daily Impacts” panel allowed several patients and their family members the opportunity to identify specific issues that may surprise clinicians.
“One thing I learned was how much the patients are bothered by sweating of the scalp; this can affect what type of head covering, hair piece, or hat/helmet they are able to wear, and thus limits activities,” Dr. Marathe continued. “This is not something I had focused on previously. I will be more inclined to ask about sweating and offer treatments, such as scalp botulinum toxin or aluminum chloride now that I have been alerted to this concern. Also, the challenges of facial makeup such as pencil for eyebrows was another thing that the FDA session brought home for me; I’m more inclined to suggest things such as microblading for eyebrows, or to try treatments like latanoprost for eyebrows/lashes.”
The second panel, “Current Approaches to Treatment,” included a different group of patients who shared stories of treatments that had been successful and those that had not. “The patients at the FDA meeting expressed very eloquently what our patients feel – different treatments may work temporarily and then stop working, which leads to a roller coaster of emotions of hope and disappointment,” A. Yasmine Kirkorian, MD, also a dermatologist at Children’s National Health System, said in an interview. “Patients and physicians would be interested in a treatment option with a track record for predictable efficacy with durable and sustained hair regrowth and minimal side effects.”
Dr. Marathe noted that in her experience, those who develop alopecia totalis or universalis at a younger age tend to have more recalcitrant disease. “It is still very hard for me to predict which children will regrow their hair spontaneously, or with topical therapies, versus those with more resistant disease. I hope that continued study will allow us to offer a more realistic prognosis for these patients,” she said.
Discussion after the treatment panel included testimonials from patients who reported successful treatment with tofacitinib (Xeljanz), a Janus kinase inhibitor approved for rheumatoid arthritis, which is not approved for treatment of alopecia.
“I absolutely agree with the focus on JAK inhibitors and increasing our understanding of how they work, as well as what some of the long-term effects are,” said Dr. Marathe. “The better we are able to target the pathogenesis of this condition, the more easily we can treat in a more focused fashion and reduce side effects,” but more clinical trials are needed to determine safety and efficacy for children and teens, she noted.
One of her hesitations in prescribing tofacitinib to her patients is that she cannot provide them with a sense of how long they will need to be on the treatment. “Current data show that the hair growth on the medication is usually lost upon stopping it; the question I still struggle with is whether it is realistic to put a 4- or 5-year-old on a medication that has no estimated or anticipated stop date,” she said.
As for what she offers patients in terms of resources for emotional support, Dr. Kirkorian said the psychosocial aspects of alopecia areata are always discussed at patient visits. “Psychosocial needs vary based on age, personality, and personal philosophy. We offer the gamut of outside resources from local support groups, the National Alopecia Areata Foundation, referral to psychology/psychiatry and, very importantly, referral to Camp Discovery. Children have told us across the board how important and meaningful it was to them to be able to just be themselves around other children who look like them.”
Dr. Marathe and Dr. Kirkorian were attendees at the meeting; they had no relevant disclosures. They are members of the Dermatology News Editorial Advisory Board.
SILVER SPRING, MD. – Alopecia areata patients struggle as much, if not more so, with the social and emotional challenges of the disease as with the physical challenges, according to patients and others who spoke at a public meeting on alopecia areata patient-focused drug development.
Alopecia areata affects as many as 6.8 million individuals in the United States, according to the National Alopecia Areata Foundation (NAAF). However, the particulars of alopecia can vary widely from one person to another; some patients experience total hair loss (alopecia universalis), while others retain eyebrows, eyelashes, or some body hair.
The FDA meeting, held on Sept. 11, is part of the agency’s patient-focused drug development initiative. “We wanted to hear the broader patient’s voice,” Theresa M. Mullin, PhD, director of the FDA’s Office of Strategic Programs, said in her opening remarks. Gary Sherwood, communications director for NAAF, said that the meeting was the culmination of a 5-year effort, begun in 2012 when alopecia areata was named as one of 39 disease categories under consideration for such a meeting. “It is too early to know what the exact results will be … but if the past is any indication, they may be significant. The meeting held with psoriasis yielded FDA approval of a treatment previously denied,” he added in an interview.
Two panel presentations featured patients who discussed their experiences with alopecia; each was followed by a discussion period where patients and family members in the audience were invited to share their experiences.
The “Health Effects and Daily Impacts” panel allowed several patients and their family members the opportunity to identify specific issues that may surprise clinicians.
“One thing I learned was how much the patients are bothered by sweating of the scalp; this can affect what type of head covering, hair piece, or hat/helmet they are able to wear, and thus limits activities,” Dr. Marathe continued. “This is not something I had focused on previously. I will be more inclined to ask about sweating and offer treatments, such as scalp botulinum toxin or aluminum chloride now that I have been alerted to this concern. Also, the challenges of facial makeup such as pencil for eyebrows was another thing that the FDA session brought home for me; I’m more inclined to suggest things such as microblading for eyebrows, or to try treatments like latanoprost for eyebrows/lashes.”
The second panel, “Current Approaches to Treatment,” included a different group of patients who shared stories of treatments that had been successful and those that had not. “The patients at the FDA meeting expressed very eloquently what our patients feel – different treatments may work temporarily and then stop working, which leads to a roller coaster of emotions of hope and disappointment,” A. Yasmine Kirkorian, MD, also a dermatologist at Children’s National Health System, said in an interview. “Patients and physicians would be interested in a treatment option with a track record for predictable efficacy with durable and sustained hair regrowth and minimal side effects.”
Dr. Marathe noted that in her experience, those who develop alopecia totalis or universalis at a younger age tend to have more recalcitrant disease. “It is still very hard for me to predict which children will regrow their hair spontaneously, or with topical therapies, versus those with more resistant disease. I hope that continued study will allow us to offer a more realistic prognosis for these patients,” she said.
Discussion after the treatment panel included testimonials from patients who reported successful treatment with tofacitinib (Xeljanz), a Janus kinase inhibitor approved for rheumatoid arthritis, which is not approved for treatment of alopecia.
“I absolutely agree with the focus on JAK inhibitors and increasing our understanding of how they work, as well as what some of the long-term effects are,” said Dr. Marathe. “The better we are able to target the pathogenesis of this condition, the more easily we can treat in a more focused fashion and reduce side effects,” but more clinical trials are needed to determine safety and efficacy for children and teens, she noted.
One of her hesitations in prescribing tofacitinib to her patients is that she cannot provide them with a sense of how long they will need to be on the treatment. “Current data show that the hair growth on the medication is usually lost upon stopping it; the question I still struggle with is whether it is realistic to put a 4- or 5-year-old on a medication that has no estimated or anticipated stop date,” she said.
As for what she offers patients in terms of resources for emotional support, Dr. Kirkorian said the psychosocial aspects of alopecia areata are always discussed at patient visits. “Psychosocial needs vary based on age, personality, and personal philosophy. We offer the gamut of outside resources from local support groups, the National Alopecia Areata Foundation, referral to psychology/psychiatry and, very importantly, referral to Camp Discovery. Children have told us across the board how important and meaningful it was to them to be able to just be themselves around other children who look like them.”
Dr. Marathe and Dr. Kirkorian were attendees at the meeting; they had no relevant disclosures. They are members of the Dermatology News Editorial Advisory Board.
SILVER SPRING, MD. – Alopecia areata patients struggle as much, if not more so, with the social and emotional challenges of the disease as with the physical challenges, according to patients and others who spoke at a public meeting on alopecia areata patient-focused drug development.
Alopecia areata affects as many as 6.8 million individuals in the United States, according to the National Alopecia Areata Foundation (NAAF). However, the particulars of alopecia can vary widely from one person to another; some patients experience total hair loss (alopecia universalis), while others retain eyebrows, eyelashes, or some body hair.
The FDA meeting, held on Sept. 11, is part of the agency’s patient-focused drug development initiative. “We wanted to hear the broader patient’s voice,” Theresa M. Mullin, PhD, director of the FDA’s Office of Strategic Programs, said in her opening remarks. Gary Sherwood, communications director for NAAF, said that the meeting was the culmination of a 5-year effort, begun in 2012 when alopecia areata was named as one of 39 disease categories under consideration for such a meeting. “It is too early to know what the exact results will be … but if the past is any indication, they may be significant. The meeting held with psoriasis yielded FDA approval of a treatment previously denied,” he added in an interview.
Two panel presentations featured patients who discussed their experiences with alopecia; each was followed by a discussion period where patients and family members in the audience were invited to share their experiences.
The “Health Effects and Daily Impacts” panel allowed several patients and their family members the opportunity to identify specific issues that may surprise clinicians.
“One thing I learned was how much the patients are bothered by sweating of the scalp; this can affect what type of head covering, hair piece, or hat/helmet they are able to wear, and thus limits activities,” Dr. Marathe continued. “This is not something I had focused on previously. I will be more inclined to ask about sweating and offer treatments, such as scalp botulinum toxin or aluminum chloride now that I have been alerted to this concern. Also, the challenges of facial makeup such as pencil for eyebrows was another thing that the FDA session brought home for me; I’m more inclined to suggest things such as microblading for eyebrows, or to try treatments like latanoprost for eyebrows/lashes.”
The second panel, “Current Approaches to Treatment,” included a different group of patients who shared stories of treatments that had been successful and those that had not. “The patients at the FDA meeting expressed very eloquently what our patients feel – different treatments may work temporarily and then stop working, which leads to a roller coaster of emotions of hope and disappointment,” A. Yasmine Kirkorian, MD, also a dermatologist at Children’s National Health System, said in an interview. “Patients and physicians would be interested in a treatment option with a track record for predictable efficacy with durable and sustained hair regrowth and minimal side effects.”
Dr. Marathe noted that in her experience, those who develop alopecia totalis or universalis at a younger age tend to have more recalcitrant disease. “It is still very hard for me to predict which children will regrow their hair spontaneously, or with topical therapies, versus those with more resistant disease. I hope that continued study will allow us to offer a more realistic prognosis for these patients,” she said.
Discussion after the treatment panel included testimonials from patients who reported successful treatment with tofacitinib (Xeljanz), a Janus kinase inhibitor approved for rheumatoid arthritis, which is not approved for treatment of alopecia.
“I absolutely agree with the focus on JAK inhibitors and increasing our understanding of how they work, as well as what some of the long-term effects are,” said Dr. Marathe. “The better we are able to target the pathogenesis of this condition, the more easily we can treat in a more focused fashion and reduce side effects,” but more clinical trials are needed to determine safety and efficacy for children and teens, she noted.
One of her hesitations in prescribing tofacitinib to her patients is that she cannot provide them with a sense of how long they will need to be on the treatment. “Current data show that the hair growth on the medication is usually lost upon stopping it; the question I still struggle with is whether it is realistic to put a 4- or 5-year-old on a medication that has no estimated or anticipated stop date,” she said.
As for what she offers patients in terms of resources for emotional support, Dr. Kirkorian said the psychosocial aspects of alopecia areata are always discussed at patient visits. “Psychosocial needs vary based on age, personality, and personal philosophy. We offer the gamut of outside resources from local support groups, the National Alopecia Areata Foundation, referral to psychology/psychiatry and, very importantly, referral to Camp Discovery. Children have told us across the board how important and meaningful it was to them to be able to just be themselves around other children who look like them.”
Dr. Marathe and Dr. Kirkorian were attendees at the meeting; they had no relevant disclosures. They are members of the Dermatology News Editorial Advisory Board.
AT AN FDA PUBLIC MEETING
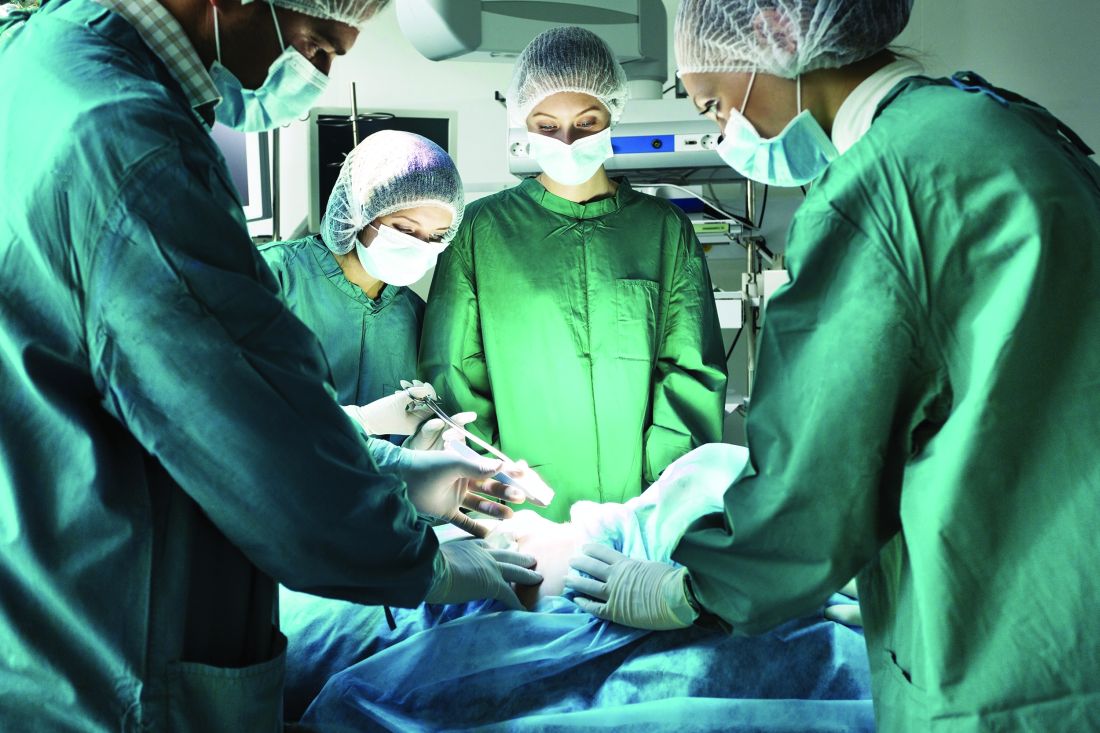
GERD postop relapse rates highest in women, older adults
Healthy men younger than 45 years have the lowest risk of relapse after reflux surgery compared with other demographic subgroups, according to data from a population-based study of 2,655 adults in Sweden. The findings were published online in JAMA.
“Cohort studies have shown a high risk of recurrent symptoms of GERD after surgery, which may have contributed to the decline in the use of antireflux surgery,” but long-term reflux recurrence rates and potential risk factors have not been well studied, wrote John Maret-Ouda, MD, and colleagues at the Karolinska Institutet in Stockholm, Sweden.
Overall, 18% of the patients suffered a reflux relapse; 84% of these were prescribed long-term medication, and 16% underwent additional surgery.
The highest relapse rates occurred among women, older patients, and those with comorbid conditions. Reflux occurred in 22% of women vs. 14% of men (hazard ratio 1.57), and the hazard ratio was 1.41 for patients aged 61 years and older compared with those aged 45 years and younger. Patients with one or more comorbidities were approximately one-third more likely to have a recurrence of reflux, compared with those who had no comorbidities (hazard ratio 1.36).
Approximately 4% of patients reported complications; the most common complication was infection (1.1%), followed by bleeding (0.9%), and esophageal perforation (0.9%).
The recurrence rate of 18% is low compared with other studies, the researchers noted. Possible reasons for the difference include the population-based design of the current study, which meant that no patients were lost to follow-up, as well as the recent time period, “in which laparoscopic antireflux surgery has become more centralized to expert centers where selection of patients might be stricter and the quality of surgery might be higher,” they wrote.
The study findings were limited by several factors including clinical variations on coding, lack of data on certain confounding variables including body mass index and smoking, and a lack of control GERD patients who did not undergo antireflux surgery, the researchers said. The results suggest that the benefits of laparoscopic antireflux surgery may be diminished by the potential for recurrent GERD, they added.
The Swedish Research Council funded the study. The researchers had no financial conflicts to disclose.
“The operation can be performed with a relatively low rate of morbidity and a very low mortality rate,” Stuart J. Spechler, MD, wrote in an editorial. “Although findings regarding GERD symptom relief and patient satisfaction based on medication usage data should be interpreted with caution, the observation that more than 80% of patients did not restart antireflux medications after laparoscopic antireflux surgery suggests that the operation provided long-lasting relief of GERD symptoms for most patients,” he said. Although surgery is not a permanent cure for all patients with GERD, “the ever-increasing number of proposed [proton pump inhibitor] risks has caused the greatest concern among clinicians and their patients,” said Dr. Spechler. “Whether the greater than 80% possibility of long-term freedom from PPIs and their associated risks warrants the 4% risk of acute surgical complications and the 17.7% risk of GERD recurrence is a decision that individual patients should make after a detailed discussion of these risks and benefits with their physicians,” he said. However, the study findings suggest “that laparoscopic antireflux surgery might be an especially appealing option for young and otherwise healthy men, who seem to have the lowest rate of GERD recurrence after antireflux surgery and who otherwise would likely require decades of PPI treatment without the operation,” he wrote (JAMA 2017;318:913-5).
Dr. Spechler is affiliated with Baylor University in Dallas. He disclosed serving as a consultant for Ironwood Pharmaceuticals and Takeda Pharmaceuticals, and funding support from the National Institutes of Health.
“The operation can be performed with a relatively low rate of morbidity and a very low mortality rate,” Stuart J. Spechler, MD, wrote in an editorial. “Although findings regarding GERD symptom relief and patient satisfaction based on medication usage data should be interpreted with caution, the observation that more than 80% of patients did not restart antireflux medications after laparoscopic antireflux surgery suggests that the operation provided long-lasting relief of GERD symptoms for most patients,” he said. Although surgery is not a permanent cure for all patients with GERD, “the ever-increasing number of proposed [proton pump inhibitor] risks has caused the greatest concern among clinicians and their patients,” said Dr. Spechler. “Whether the greater than 80% possibility of long-term freedom from PPIs and their associated risks warrants the 4% risk of acute surgical complications and the 17.7% risk of GERD recurrence is a decision that individual patients should make after a detailed discussion of these risks and benefits with their physicians,” he said. However, the study findings suggest “that laparoscopic antireflux surgery might be an especially appealing option for young and otherwise healthy men, who seem to have the lowest rate of GERD recurrence after antireflux surgery and who otherwise would likely require decades of PPI treatment without the operation,” he wrote (JAMA 2017;318:913-5).
Dr. Spechler is affiliated with Baylor University in Dallas. He disclosed serving as a consultant for Ironwood Pharmaceuticals and Takeda Pharmaceuticals, and funding support from the National Institutes of Health.
“The operation can be performed with a relatively low rate of morbidity and a very low mortality rate,” Stuart J. Spechler, MD, wrote in an editorial. “Although findings regarding GERD symptom relief and patient satisfaction based on medication usage data should be interpreted with caution, the observation that more than 80% of patients did not restart antireflux medications after laparoscopic antireflux surgery suggests that the operation provided long-lasting relief of GERD symptoms for most patients,” he said. Although surgery is not a permanent cure for all patients with GERD, “the ever-increasing number of proposed [proton pump inhibitor] risks has caused the greatest concern among clinicians and their patients,” said Dr. Spechler. “Whether the greater than 80% possibility of long-term freedom from PPIs and their associated risks warrants the 4% risk of acute surgical complications and the 17.7% risk of GERD recurrence is a decision that individual patients should make after a detailed discussion of these risks and benefits with their physicians,” he said. However, the study findings suggest “that laparoscopic antireflux surgery might be an especially appealing option for young and otherwise healthy men, who seem to have the lowest rate of GERD recurrence after antireflux surgery and who otherwise would likely require decades of PPI treatment without the operation,” he wrote (JAMA 2017;318:913-5).
Dr. Spechler is affiliated with Baylor University in Dallas. He disclosed serving as a consultant for Ironwood Pharmaceuticals and Takeda Pharmaceuticals, and funding support from the National Institutes of Health.
Healthy men younger than 45 years have the lowest risk of relapse after reflux surgery compared with other demographic subgroups, according to data from a population-based study of 2,655 adults in Sweden. The findings were published online in JAMA.
“Cohort studies have shown a high risk of recurrent symptoms of GERD after surgery, which may have contributed to the decline in the use of antireflux surgery,” but long-term reflux recurrence rates and potential risk factors have not been well studied, wrote John Maret-Ouda, MD, and colleagues at the Karolinska Institutet in Stockholm, Sweden.
Overall, 18% of the patients suffered a reflux relapse; 84% of these were prescribed long-term medication, and 16% underwent additional surgery.
The highest relapse rates occurred among women, older patients, and those with comorbid conditions. Reflux occurred in 22% of women vs. 14% of men (hazard ratio 1.57), and the hazard ratio was 1.41 for patients aged 61 years and older compared with those aged 45 years and younger. Patients with one or more comorbidities were approximately one-third more likely to have a recurrence of reflux, compared with those who had no comorbidities (hazard ratio 1.36).
Approximately 4% of patients reported complications; the most common complication was infection (1.1%), followed by bleeding (0.9%), and esophageal perforation (0.9%).
The recurrence rate of 18% is low compared with other studies, the researchers noted. Possible reasons for the difference include the population-based design of the current study, which meant that no patients were lost to follow-up, as well as the recent time period, “in which laparoscopic antireflux surgery has become more centralized to expert centers where selection of patients might be stricter and the quality of surgery might be higher,” they wrote.
The study findings were limited by several factors including clinical variations on coding, lack of data on certain confounding variables including body mass index and smoking, and a lack of control GERD patients who did not undergo antireflux surgery, the researchers said. The results suggest that the benefits of laparoscopic antireflux surgery may be diminished by the potential for recurrent GERD, they added.
The Swedish Research Council funded the study. The researchers had no financial conflicts to disclose.
Healthy men younger than 45 years have the lowest risk of relapse after reflux surgery compared with other demographic subgroups, according to data from a population-based study of 2,655 adults in Sweden. The findings were published online in JAMA.
“Cohort studies have shown a high risk of recurrent symptoms of GERD after surgery, which may have contributed to the decline in the use of antireflux surgery,” but long-term reflux recurrence rates and potential risk factors have not been well studied, wrote John Maret-Ouda, MD, and colleagues at the Karolinska Institutet in Stockholm, Sweden.
Overall, 18% of the patients suffered a reflux relapse; 84% of these were prescribed long-term medication, and 16% underwent additional surgery.
The highest relapse rates occurred among women, older patients, and those with comorbid conditions. Reflux occurred in 22% of women vs. 14% of men (hazard ratio 1.57), and the hazard ratio was 1.41 for patients aged 61 years and older compared with those aged 45 years and younger. Patients with one or more comorbidities were approximately one-third more likely to have a recurrence of reflux, compared with those who had no comorbidities (hazard ratio 1.36).
Approximately 4% of patients reported complications; the most common complication was infection (1.1%), followed by bleeding (0.9%), and esophageal perforation (0.9%).
The recurrence rate of 18% is low compared with other studies, the researchers noted. Possible reasons for the difference include the population-based design of the current study, which meant that no patients were lost to follow-up, as well as the recent time period, “in which laparoscopic antireflux surgery has become more centralized to expert centers where selection of patients might be stricter and the quality of surgery might be higher,” they wrote.
The study findings were limited by several factors including clinical variations on coding, lack of data on certain confounding variables including body mass index and smoking, and a lack of control GERD patients who did not undergo antireflux surgery, the researchers said. The results suggest that the benefits of laparoscopic antireflux surgery may be diminished by the potential for recurrent GERD, they added.
The Swedish Research Council funded the study. The researchers had no financial conflicts to disclose.
FROM JAMA
Key clinical point: Young men were less likely than were other demographic groups to experience recurrence of gastroesophageal reflux after surgery.
Major finding: Overall, 18% of 2,655 adults who underwent reflux surgery experienced recurrent reflux requiring long-term medication or additional surgery.
Data source: A population-based, retrospective cohort study of reflux surgery patients in Sweden.
Disclosures: The Swedish Research Council supported the study.
VIDEO: Alopecia areata patients seek emotional support
SILVER SPRING, MD. – The emotional challenges facing alopecia areata patients are as tough, or tougher, than the physical challenges, according to many patients participating in a public meeting on alopecia areata patient-focused drug development.
A panel of patients shared their experiences of living with alopecia areata, including Elizabeth DeCarlo of Wilmington, Delaware. In a video interview at the meeting, held at FDA headquarters on Sept. 11, Ms. DeCarlo elaborated on what she would like clinicians to understand about alopecia patients that might surprise them, and what matters to her as a patient.
“I would tell them to be more compassionate,” Ms. DeCarlo said. “It’s very emotional.” She also emphasized the value of giving alopecia patients information about local support groups, as well as national organizations such as the National Alopecia Areata Foundation.
Ms. DeCarlo had no financial conflicts to disclose.
SILVER SPRING, MD. – The emotional challenges facing alopecia areata patients are as tough, or tougher, than the physical challenges, according to many patients participating in a public meeting on alopecia areata patient-focused drug development.
A panel of patients shared their experiences of living with alopecia areata, including Elizabeth DeCarlo of Wilmington, Delaware. In a video interview at the meeting, held at FDA headquarters on Sept. 11, Ms. DeCarlo elaborated on what she would like clinicians to understand about alopecia patients that might surprise them, and what matters to her as a patient.
“I would tell them to be more compassionate,” Ms. DeCarlo said. “It’s very emotional.” She also emphasized the value of giving alopecia patients information about local support groups, as well as national organizations such as the National Alopecia Areata Foundation.
Ms. DeCarlo had no financial conflicts to disclose.
SILVER SPRING, MD. – The emotional challenges facing alopecia areata patients are as tough, or tougher, than the physical challenges, according to many patients participating in a public meeting on alopecia areata patient-focused drug development.
A panel of patients shared their experiences of living with alopecia areata, including Elizabeth DeCarlo of Wilmington, Delaware. In a video interview at the meeting, held at FDA headquarters on Sept. 11, Ms. DeCarlo elaborated on what she would like clinicians to understand about alopecia patients that might surprise them, and what matters to her as a patient.
“I would tell them to be more compassionate,” Ms. DeCarlo said. “It’s very emotional.” She also emphasized the value of giving alopecia patients information about local support groups, as well as national organizations such as the National Alopecia Areata Foundation.
Ms. DeCarlo had no financial conflicts to disclose.
AT AN FDA PUBLIC MEETING
USPSTF backs away from cotesting in cervical cancer screening
Women aged 30-65 years should be offered a choice between two cervical cancer screening methods, according to draft recommendations from the U.S. Preventive Services Task Force. The recommendations were released on Sept. 12.
The Task Force continues to recommend that women in their 20s be screened every 3 years via cervical cytology, but in a change from the 2012 recommendations, the researchers now advise clinicians to offer women aged 30-65 years a choice of either cytology every 3 years or the high-risk human papillomavirus (hrHPV) test every 5 years as a method of screening for cervical cancer. Cotesting is no longer recommended.
Offering women aged 30-65 years a screening choice received an A recommendation. The draft retains the previous Task Force position and D recommendation against cervical cancer screening for certain groups, including women younger than 21 years, women aged 65 and older with a history of screening and a low risk of cervical cancer, and women who have had a hysterectomy.
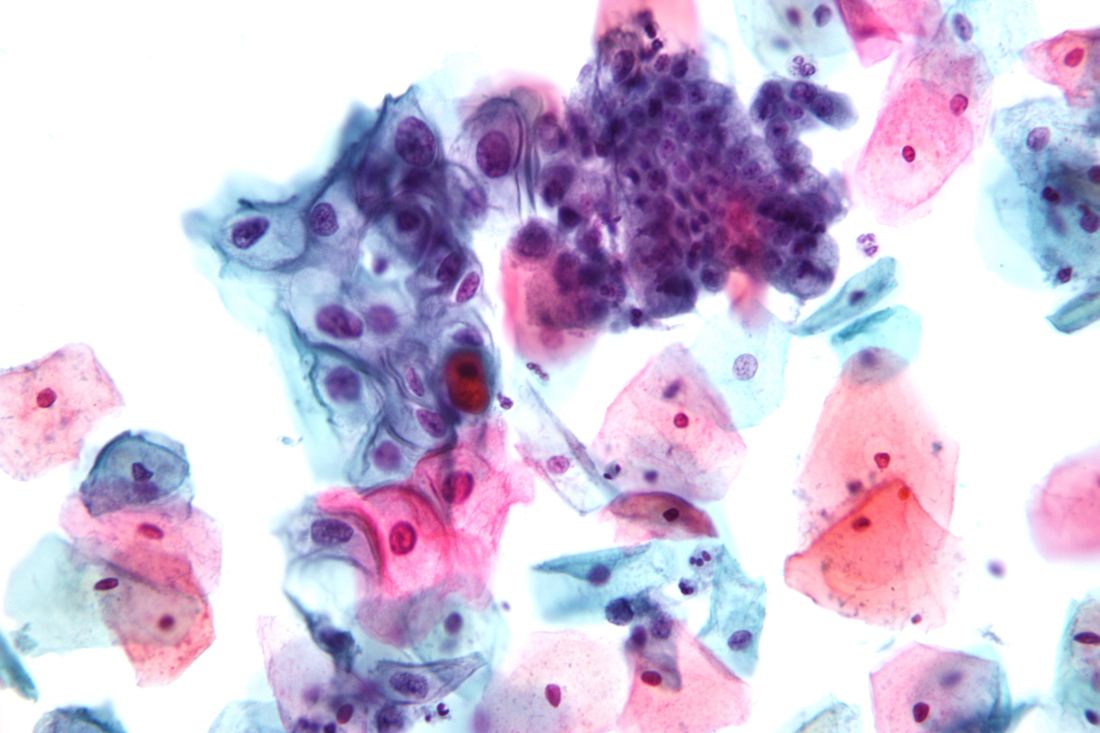
The USPSTF based the draft recommendations in part on a review of four randomized, controlled trials of cotesting hrHPV and cytology that included more than 130,000 women.
“Modeling found that cotesting does not offer any benefit in terms of cancer reduction or life-years gained over hrHPV testing alone but increases the number of tests and procedures per each cancer case averted,” the Task Force members noted in the draft recommendation statement. “Therefore, the USPSTF concluded that there is convincing evidence that screening with either cytology alone or hrHPV testing alone provides substantial benefit and is preferable to cotesting” in otherwise healthy women aged 30-65 years.
The American College of Obstetricians and Gynecologists currently recommends cotesting with cytology and HPV testing every 5 years or cytology alone every 3 years in women aged 30-65 years (Obstet Gynecol. 2016;128[4]:e111-30).
The USPSTF draft recommendations do not apply to women at increased risk for cervical cancer, including those with compromised immune systems or those who have cervical intraepithelial neoplasia grade 2 or 3.
The draft recommendations are available online for public comment from Sept. 12 through Oct. 9, 2017, at the USPSTF website, www.uspreventiveservicestaskforce.org.
Women aged 30-65 years should be offered a choice between two cervical cancer screening methods, according to draft recommendations from the U.S. Preventive Services Task Force. The recommendations were released on Sept. 12.
The Task Force continues to recommend that women in their 20s be screened every 3 years via cervical cytology, but in a change from the 2012 recommendations, the researchers now advise clinicians to offer women aged 30-65 years a choice of either cytology every 3 years or the high-risk human papillomavirus (hrHPV) test every 5 years as a method of screening for cervical cancer. Cotesting is no longer recommended.
Offering women aged 30-65 years a screening choice received an A recommendation. The draft retains the previous Task Force position and D recommendation against cervical cancer screening for certain groups, including women younger than 21 years, women aged 65 and older with a history of screening and a low risk of cervical cancer, and women who have had a hysterectomy.

The USPSTF based the draft recommendations in part on a review of four randomized, controlled trials of cotesting hrHPV and cytology that included more than 130,000 women.
“Modeling found that cotesting does not offer any benefit in terms of cancer reduction or life-years gained over hrHPV testing alone but increases the number of tests and procedures per each cancer case averted,” the Task Force members noted in the draft recommendation statement. “Therefore, the USPSTF concluded that there is convincing evidence that screening with either cytology alone or hrHPV testing alone provides substantial benefit and is preferable to cotesting” in otherwise healthy women aged 30-65 years.
The American College of Obstetricians and Gynecologists currently recommends cotesting with cytology and HPV testing every 5 years or cytology alone every 3 years in women aged 30-65 years (Obstet Gynecol. 2016;128[4]:e111-30).
The USPSTF draft recommendations do not apply to women at increased risk for cervical cancer, including those with compromised immune systems or those who have cervical intraepithelial neoplasia grade 2 or 3.
The draft recommendations are available online for public comment from Sept. 12 through Oct. 9, 2017, at the USPSTF website, www.uspreventiveservicestaskforce.org.
Women aged 30-65 years should be offered a choice between two cervical cancer screening methods, according to draft recommendations from the U.S. Preventive Services Task Force. The recommendations were released on Sept. 12.
The Task Force continues to recommend that women in their 20s be screened every 3 years via cervical cytology, but in a change from the 2012 recommendations, the researchers now advise clinicians to offer women aged 30-65 years a choice of either cytology every 3 years or the high-risk human papillomavirus (hrHPV) test every 5 years as a method of screening for cervical cancer. Cotesting is no longer recommended.
Offering women aged 30-65 years a screening choice received an A recommendation. The draft retains the previous Task Force position and D recommendation against cervical cancer screening for certain groups, including women younger than 21 years, women aged 65 and older with a history of screening and a low risk of cervical cancer, and women who have had a hysterectomy.

The USPSTF based the draft recommendations in part on a review of four randomized, controlled trials of cotesting hrHPV and cytology that included more than 130,000 women.
“Modeling found that cotesting does not offer any benefit in terms of cancer reduction or life-years gained over hrHPV testing alone but increases the number of tests and procedures per each cancer case averted,” the Task Force members noted in the draft recommendation statement. “Therefore, the USPSTF concluded that there is convincing evidence that screening with either cytology alone or hrHPV testing alone provides substantial benefit and is preferable to cotesting” in otherwise healthy women aged 30-65 years.
The American College of Obstetricians and Gynecologists currently recommends cotesting with cytology and HPV testing every 5 years or cytology alone every 3 years in women aged 30-65 years (Obstet Gynecol. 2016;128[4]:e111-30).
The USPSTF draft recommendations do not apply to women at increased risk for cervical cancer, including those with compromised immune systems or those who have cervical intraepithelial neoplasia grade 2 or 3.
The draft recommendations are available online for public comment from Sept. 12 through Oct. 9, 2017, at the USPSTF website, www.uspreventiveservicestaskforce.org.
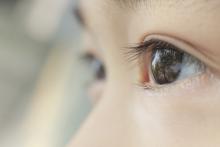
Check children’s eyes early for best corrections
or its risk factors with the goal of improving visual acuity, publishing its final recommendation statement and evidence summary online Sept. 5 in JAMA.
A review of the latest evidence supports a B recommendation for vision screening at least once in children aged 3-5 years, but the evidence is insufficient to determine the balance of risks and benefits for vision screening in children younger than 3 years (meriting an I statement from the USPSTF). The recommendation updates the 2011 USPSTF recommendation, which also recommended vision screening for children aged 3-5 years with a B recommendation.
“The prevalence of amblyopia, strabismus, and anisometropia ranges from 1% to 6% among children younger than 6 years in the United States,” which can lead to permanent vision loss if left untreated, chair and corresponding author David C. Grossman, MD, of Kaiser Permanente Washington Health Research Institute, Seattle, and colleagues noted in the recommendation statement (JAMA. 2017;318:836-44).
The USPSTF found “inadequate evidence that treatment reduced the incidence of long-term amblyopia or improved school performance, functioning, or quality of life.” However, the USPSTF concluded that the harms of screening and treating preschool children for amblyopia and its risk factors were small, and that treatment improved visual acuity, “which is likely to result in permanent improvements throughout life.”
The benefits of early treatment were characterized as moderate because of the risk of permanent, uncorrectable vision loss associated with untreated amblyopia, “and the benefits of screening and treatment can be experienced over a child’s lifetime,” the researchers said.
The evidence report accompanying the recommendations contained data from 40 studies with 34,709 participants, and addressed issues including the benefits of screening, accuracy of vision screening tests, and the potential harms and benefits of treatments including eye patches and glasses (JAMA. 2017;318:845-58).
“Studies directly evaluating the effectiveness of screening were limited and do not establish whether vision screening in preschool children is better than no screening,” Daniel E. Jonas, MD, of RTI International–University of North Carolina at Chapel Hill Evidence-based Practice Center and his colleagues wrote in the evidence report.
Therefore, the Task Force called for additional research while recommending at least one screening.
The study was funded by the Agency for Healthcare Research and Quality. The researchers had no financial conflicts to disclose.
Read the complete recommendations online at http://www.uspreventiveservicestaskforce.org.
or its risk factors with the goal of improving visual acuity, publishing its final recommendation statement and evidence summary online Sept. 5 in JAMA.
A review of the latest evidence supports a B recommendation for vision screening at least once in children aged 3-5 years, but the evidence is insufficient to determine the balance of risks and benefits for vision screening in children younger than 3 years (meriting an I statement from the USPSTF). The recommendation updates the 2011 USPSTF recommendation, which also recommended vision screening for children aged 3-5 years with a B recommendation.
“The prevalence of amblyopia, strabismus, and anisometropia ranges from 1% to 6% among children younger than 6 years in the United States,” which can lead to permanent vision loss if left untreated, chair and corresponding author David C. Grossman, MD, of Kaiser Permanente Washington Health Research Institute, Seattle, and colleagues noted in the recommendation statement (JAMA. 2017;318:836-44).
The USPSTF found “inadequate evidence that treatment reduced the incidence of long-term amblyopia or improved school performance, functioning, or quality of life.” However, the USPSTF concluded that the harms of screening and treating preschool children for amblyopia and its risk factors were small, and that treatment improved visual acuity, “which is likely to result in permanent improvements throughout life.”
The benefits of early treatment were characterized as moderate because of the risk of permanent, uncorrectable vision loss associated with untreated amblyopia, “and the benefits of screening and treatment can be experienced over a child’s lifetime,” the researchers said.
The evidence report accompanying the recommendations contained data from 40 studies with 34,709 participants, and addressed issues including the benefits of screening, accuracy of vision screening tests, and the potential harms and benefits of treatments including eye patches and glasses (JAMA. 2017;318:845-58).
“Studies directly evaluating the effectiveness of screening were limited and do not establish whether vision screening in preschool children is better than no screening,” Daniel E. Jonas, MD, of RTI International–University of North Carolina at Chapel Hill Evidence-based Practice Center and his colleagues wrote in the evidence report.
Therefore, the Task Force called for additional research while recommending at least one screening.
The study was funded by the Agency for Healthcare Research and Quality. The researchers had no financial conflicts to disclose.
Read the complete recommendations online at http://www.uspreventiveservicestaskforce.org.
or its risk factors with the goal of improving visual acuity, publishing its final recommendation statement and evidence summary online Sept. 5 in JAMA.
A review of the latest evidence supports a B recommendation for vision screening at least once in children aged 3-5 years, but the evidence is insufficient to determine the balance of risks and benefits for vision screening in children younger than 3 years (meriting an I statement from the USPSTF). The recommendation updates the 2011 USPSTF recommendation, which also recommended vision screening for children aged 3-5 years with a B recommendation.
“The prevalence of amblyopia, strabismus, and anisometropia ranges from 1% to 6% among children younger than 6 years in the United States,” which can lead to permanent vision loss if left untreated, chair and corresponding author David C. Grossman, MD, of Kaiser Permanente Washington Health Research Institute, Seattle, and colleagues noted in the recommendation statement (JAMA. 2017;318:836-44).
The USPSTF found “inadequate evidence that treatment reduced the incidence of long-term amblyopia or improved school performance, functioning, or quality of life.” However, the USPSTF concluded that the harms of screening and treating preschool children for amblyopia and its risk factors were small, and that treatment improved visual acuity, “which is likely to result in permanent improvements throughout life.”
The benefits of early treatment were characterized as moderate because of the risk of permanent, uncorrectable vision loss associated with untreated amblyopia, “and the benefits of screening and treatment can be experienced over a child’s lifetime,” the researchers said.
The evidence report accompanying the recommendations contained data from 40 studies with 34,709 participants, and addressed issues including the benefits of screening, accuracy of vision screening tests, and the potential harms and benefits of treatments including eye patches and glasses (JAMA. 2017;318:845-58).
“Studies directly evaluating the effectiveness of screening were limited and do not establish whether vision screening in preschool children is better than no screening,” Daniel E. Jonas, MD, of RTI International–University of North Carolina at Chapel Hill Evidence-based Practice Center and his colleagues wrote in the evidence report.
Therefore, the Task Force called for additional research while recommending at least one screening.
The study was funded by the Agency for Healthcare Research and Quality. The researchers had no financial conflicts to disclose.
Read the complete recommendations online at http://www.uspreventiveservicestaskforce.org.
FROM JAMA
Intraoperative ketamine makes no dent in postop delirium or pain
Postoperative delirium remains a problem without an effective solution, wrote Michael S. Avidan, MBBCh, FCASA, of Washington University, Saint Louis, and his colleagues (Lancet 2017;390[10091]:267-75).
Recent guidelines published by the American Pain Society, the American Society of Regional Anesthesia and Pain Medicine, and the American Society of Anesthesiologists’ Committee on Regional Anesthesia, Executive Committee, and Administrative Council include ketamine as a recommended component of multimodal pain therapy for several commonly performed surgeries. “Before recommending widespread administration of an intraoperative bolus of subanaesthetic ketamine, demonstrating that ketamine decreases either delirium or pain, or both, without incurring adverse effects in a large, pragmatic trial was warranted,” the researchers said.
In the PODCAST (Prevention of Delirium and Complications Associated With Surgical Treatments) trial, the researchers randomized 672 patients over the age of 60 undergoing major open surgery under general anesthesia (such as open cardiac or noncardiac surgery, urological surgery, gynecologic surgery, or intra-abdominal surgery) to 0.5 mg/kg ketamine (227), 1.0 mg/kg ketamine (223), or placebo (222). The ketamine or placebo was given after anesthesia and before surgical incision.
Overall, no difference in the incidence of delirium occurred between patients in the combined ketamine groups (19.5%) and the placebo group (19.8%), and there was no significant difference in delirium across all three treatment groups.
No differences in pain based on visual analog scale scores were observed across the three groups, and overall adverse event rates were similar as well: approximately 40.8% in the 1.0-mg ketamine group, 39.6% in the 0.5-mg ketamine group, and 36.9% in the placebo group.
The study findings were limited by several factors, including a study population potentially too small to show an effect of ketamine on delirium, and a lack of data on other variables that might contribute to delirium and pain, the researchers noted. However, the results suggest that “despite present evidence and guidelines, the administration of a subanaesthetic ketamine dose during surgery is not useful for preventing postoperative delirium (primary outcome) or reducing postoperative pain and minimising opioid consumption (related secondary outcomes),” and appears to increase postoperative hallucinations and nightmares to an extent that might be prohibitive, they said.
The National Institutes of Health and Cancer Center Support funded the study. The researchers had no financial conflicts to disclose.
Postoperative delirium remains a problem without an effective solution, wrote Michael S. Avidan, MBBCh, FCASA, of Washington University, Saint Louis, and his colleagues (Lancet 2017;390[10091]:267-75).
Recent guidelines published by the American Pain Society, the American Society of Regional Anesthesia and Pain Medicine, and the American Society of Anesthesiologists’ Committee on Regional Anesthesia, Executive Committee, and Administrative Council include ketamine as a recommended component of multimodal pain therapy for several commonly performed surgeries. “Before recommending widespread administration of an intraoperative bolus of subanaesthetic ketamine, demonstrating that ketamine decreases either delirium or pain, or both, without incurring adverse effects in a large, pragmatic trial was warranted,” the researchers said.
In the PODCAST (Prevention of Delirium and Complications Associated With Surgical Treatments) trial, the researchers randomized 672 patients over the age of 60 undergoing major open surgery under general anesthesia (such as open cardiac or noncardiac surgery, urological surgery, gynecologic surgery, or intra-abdominal surgery) to 0.5 mg/kg ketamine (227), 1.0 mg/kg ketamine (223), or placebo (222). The ketamine or placebo was given after anesthesia and before surgical incision.
Overall, no difference in the incidence of delirium occurred between patients in the combined ketamine groups (19.5%) and the placebo group (19.8%), and there was no significant difference in delirium across all three treatment groups.
No differences in pain based on visual analog scale scores were observed across the three groups, and overall adverse event rates were similar as well: approximately 40.8% in the 1.0-mg ketamine group, 39.6% in the 0.5-mg ketamine group, and 36.9% in the placebo group.
The study findings were limited by several factors, including a study population potentially too small to show an effect of ketamine on delirium, and a lack of data on other variables that might contribute to delirium and pain, the researchers noted. However, the results suggest that “despite present evidence and guidelines, the administration of a subanaesthetic ketamine dose during surgery is not useful for preventing postoperative delirium (primary outcome) or reducing postoperative pain and minimising opioid consumption (related secondary outcomes),” and appears to increase postoperative hallucinations and nightmares to an extent that might be prohibitive, they said.
The National Institutes of Health and Cancer Center Support funded the study. The researchers had no financial conflicts to disclose.
Postoperative delirium remains a problem without an effective solution, wrote Michael S. Avidan, MBBCh, FCASA, of Washington University, Saint Louis, and his colleagues (Lancet 2017;390[10091]:267-75).
Recent guidelines published by the American Pain Society, the American Society of Regional Anesthesia and Pain Medicine, and the American Society of Anesthesiologists’ Committee on Regional Anesthesia, Executive Committee, and Administrative Council include ketamine as a recommended component of multimodal pain therapy for several commonly performed surgeries. “Before recommending widespread administration of an intraoperative bolus of subanaesthetic ketamine, demonstrating that ketamine decreases either delirium or pain, or both, without incurring adverse effects in a large, pragmatic trial was warranted,” the researchers said.
In the PODCAST (Prevention of Delirium and Complications Associated With Surgical Treatments) trial, the researchers randomized 672 patients over the age of 60 undergoing major open surgery under general anesthesia (such as open cardiac or noncardiac surgery, urological surgery, gynecologic surgery, or intra-abdominal surgery) to 0.5 mg/kg ketamine (227), 1.0 mg/kg ketamine (223), or placebo (222). The ketamine or placebo was given after anesthesia and before surgical incision.
Overall, no difference in the incidence of delirium occurred between patients in the combined ketamine groups (19.5%) and the placebo group (19.8%), and there was no significant difference in delirium across all three treatment groups.
No differences in pain based on visual analog scale scores were observed across the three groups, and overall adverse event rates were similar as well: approximately 40.8% in the 1.0-mg ketamine group, 39.6% in the 0.5-mg ketamine group, and 36.9% in the placebo group.
The study findings were limited by several factors, including a study population potentially too small to show an effect of ketamine on delirium, and a lack of data on other variables that might contribute to delirium and pain, the researchers noted. However, the results suggest that “despite present evidence and guidelines, the administration of a subanaesthetic ketamine dose during surgery is not useful for preventing postoperative delirium (primary outcome) or reducing postoperative pain and minimising opioid consumption (related secondary outcomes),” and appears to increase postoperative hallucinations and nightmares to an extent that might be prohibitive, they said.
The National Institutes of Health and Cancer Center Support funded the study. The researchers had no financial conflicts to disclose.
FROM THE LANCET
Key clinical point: Ketamine failed to reduce postoperative delirium in older adults.
Major finding: No difference was observed in the incidence of postoperative delirium between patients given ketamine before surgical incision and patients on placebo.
Data source: The Prevention of Delirium and Complications Associated With Surgical Treatments study, a randomized, multicenter trial of 672 adults older than 60 years.
Disclosures: The National Institutes of Health and Cancer Center Support funded the study. The researchers had no financial conflicts to disclose.
BMI z scores fall short for tracking severe obesity
, based on data from nearly 7,000 children in the Bogalusa Heart Study.
The current parameters used in the Centers for Disease Control and Prevention growth charts for children with high body mass index (BMI) “can result in estimates that differ substantially from those that are observed and constrains the maximum BMI z that is attainable at a given sex and age,” wrote David S. Freedman, PhD, of the Centers for Disease Control and Prevention in Atlanta, and Gerald S. Berenson, MD, of Louisiana State University Health Sciences Center, New Orleans, (Pediatrics. 2017;140:e20171072).
The BMI adjusted z score (BMIaz) or the BMI expressed as a percentage of the 95th percentile (%BMIp95) “will provide more accurate information on body size over time among children with very high BMIs,” they said.
In children with severe obesity, BMI z was a weaker measure (r = 0.46) than were measures of %BMIp95 (r = 0.61) or BMIaz scores with no upper boundary (r = 0.65).
BMI z scores were weakest when applied to children younger than 10 years, with correlations of r = 0.36 for BMI z vs. correlations of 0.60 and 0.57 for BMIaz and %BMIp95, respectively.
The results were limited by several factors including the age of the data (40 years ago, when the prevalence of severe obesity was lower, 2% compared with approximately 6% now) and long intervals between exams in some cases (5 years or more), the researchers noted. However, the results suggest that BMI z values “can differ substantially from empirical estimates, have an effective upper limit, and are strongly influenced by sex and age,” they said. As an alternative, the researchers recommended that “very high BMIs should be should expressed as z scores on the basis of linear extrapolations of a fixed SD or as percentage of the CDC 95th percentile,” or using multilevel models that adjust for age and sex.
The researchers had no financial conflicts to disclose. The National Institute on Aging, the National Heart, Lung, and Blood Institute, and the National Institutes of Health funded the study.
The use of BMI z scores to assess and track severe obesity in children should be abandoned.
In the study by Freedman et al., BMI z scores, which are extrapolations of BMI measurements, did not correlate well with other measures of adiposity. Their use to assess severe obesity is problematic because large changes in weight and BMI are linked to small changes in BMI z or BMI percentiles.
William H. Dietz, MD, PhD, is at the Sumner M. Redstone Global Center for Prevention and Wellness, Milken Institute School of Public Health at George Washington University in Washington. He had no relevant financial disclosures, but disclosed that he serves on the scientific advisory board for Weight Watchers and is on the board of directors for the Partnership for a Healthier America. He discussed the article by Freedman et al. in an editorial (Pediatrics. 2017;140:e20172148).
The use of BMI z scores to assess and track severe obesity in children should be abandoned.
In the study by Freedman et al., BMI z scores, which are extrapolations of BMI measurements, did not correlate well with other measures of adiposity. Their use to assess severe obesity is problematic because large changes in weight and BMI are linked to small changes in BMI z or BMI percentiles.
William H. Dietz, MD, PhD, is at the Sumner M. Redstone Global Center for Prevention and Wellness, Milken Institute School of Public Health at George Washington University in Washington. He had no relevant financial disclosures, but disclosed that he serves on the scientific advisory board for Weight Watchers and is on the board of directors for the Partnership for a Healthier America. He discussed the article by Freedman et al. in an editorial (Pediatrics. 2017;140:e20172148).
The use of BMI z scores to assess and track severe obesity in children should be abandoned.
In the study by Freedman et al., BMI z scores, which are extrapolations of BMI measurements, did not correlate well with other measures of adiposity. Their use to assess severe obesity is problematic because large changes in weight and BMI are linked to small changes in BMI z or BMI percentiles.
William H. Dietz, MD, PhD, is at the Sumner M. Redstone Global Center for Prevention and Wellness, Milken Institute School of Public Health at George Washington University in Washington. He had no relevant financial disclosures, but disclosed that he serves on the scientific advisory board for Weight Watchers and is on the board of directors for the Partnership for a Healthier America. He discussed the article by Freedman et al. in an editorial (Pediatrics. 2017;140:e20172148).
, based on data from nearly 7,000 children in the Bogalusa Heart Study.
The current parameters used in the Centers for Disease Control and Prevention growth charts for children with high body mass index (BMI) “can result in estimates that differ substantially from those that are observed and constrains the maximum BMI z that is attainable at a given sex and age,” wrote David S. Freedman, PhD, of the Centers for Disease Control and Prevention in Atlanta, and Gerald S. Berenson, MD, of Louisiana State University Health Sciences Center, New Orleans, (Pediatrics. 2017;140:e20171072).
The BMI adjusted z score (BMIaz) or the BMI expressed as a percentage of the 95th percentile (%BMIp95) “will provide more accurate information on body size over time among children with very high BMIs,” they said.
In children with severe obesity, BMI z was a weaker measure (r = 0.46) than were measures of %BMIp95 (r = 0.61) or BMIaz scores with no upper boundary (r = 0.65).
BMI z scores were weakest when applied to children younger than 10 years, with correlations of r = 0.36 for BMI z vs. correlations of 0.60 and 0.57 for BMIaz and %BMIp95, respectively.
The results were limited by several factors including the age of the data (40 years ago, when the prevalence of severe obesity was lower, 2% compared with approximately 6% now) and long intervals between exams in some cases (5 years or more), the researchers noted. However, the results suggest that BMI z values “can differ substantially from empirical estimates, have an effective upper limit, and are strongly influenced by sex and age,” they said. As an alternative, the researchers recommended that “very high BMIs should be should expressed as z scores on the basis of linear extrapolations of a fixed SD or as percentage of the CDC 95th percentile,” or using multilevel models that adjust for age and sex.
The researchers had no financial conflicts to disclose. The National Institute on Aging, the National Heart, Lung, and Blood Institute, and the National Institutes of Health funded the study.
, based on data from nearly 7,000 children in the Bogalusa Heart Study.
The current parameters used in the Centers for Disease Control and Prevention growth charts for children with high body mass index (BMI) “can result in estimates that differ substantially from those that are observed and constrains the maximum BMI z that is attainable at a given sex and age,” wrote David S. Freedman, PhD, of the Centers for Disease Control and Prevention in Atlanta, and Gerald S. Berenson, MD, of Louisiana State University Health Sciences Center, New Orleans, (Pediatrics. 2017;140:e20171072).
The BMI adjusted z score (BMIaz) or the BMI expressed as a percentage of the 95th percentile (%BMIp95) “will provide more accurate information on body size over time among children with very high BMIs,” they said.
In children with severe obesity, BMI z was a weaker measure (r = 0.46) than were measures of %BMIp95 (r = 0.61) or BMIaz scores with no upper boundary (r = 0.65).
BMI z scores were weakest when applied to children younger than 10 years, with correlations of r = 0.36 for BMI z vs. correlations of 0.60 and 0.57 for BMIaz and %BMIp95, respectively.
The results were limited by several factors including the age of the data (40 years ago, when the prevalence of severe obesity was lower, 2% compared with approximately 6% now) and long intervals between exams in some cases (5 years or more), the researchers noted. However, the results suggest that BMI z values “can differ substantially from empirical estimates, have an effective upper limit, and are strongly influenced by sex and age,” they said. As an alternative, the researchers recommended that “very high BMIs should be should expressed as z scores on the basis of linear extrapolations of a fixed SD or as percentage of the CDC 95th percentile,” or using multilevel models that adjust for age and sex.
The researchers had no financial conflicts to disclose. The National Institute on Aging, the National Heart, Lung, and Blood Institute, and the National Institutes of Health funded the study.
FROM PEDIATRICS
Key clinical point: BMI z scores are weak trackers of severe obesity in children.
Major finding: Correlations were weaker for BMI z scores (r = 0.46) than for metrics of BMI using the 95th percentile or z scores with no upper bound (r = approximately 0.6) over 2.8 years.
Data source: The study is based on longitudinal data from 6,994 children participating in the Bogalusa Heart study, including 247 children with severe obesity.
Disclosures: The researchers had no relevant financial conflicts to disclose. The National Institute on Aging, the National Heart, Lung, and Blood Institute, and the National Institutes of Health funded the study.
Brain scan study suggests serotonin drives early cognitive decline
Serotonin levels may play an early role in cognitive decline, according to imaging data from a group of study participants with mild cognitive impairment.
Previous studies have shown a link between a loss of serotonin neurons as part of normal aging and as part of the development of Alzheimer’s disease, wrote Gwenn S. Smith, PhD, of Johns Hopkins University in Baltimore, and her colleagues. However, “it is not known whether serotonin degeneration occurs in the preclinical stages or later in the course of AD,” the researchers said. The researchers used MRI and PET imaging to measure serotonin transporters (SERT) in the brains of 28 adults with mild cognitive impairment (MCI) and 28 healthy controls.
Overall, MCI participants showed significantly lower SERT, compared with the healthy controls; the loss of SERT in the MCI group ranged from 10% to 38%. No significant regions of higher SERT were noted in the MCI group, compared with the controls, and no significant differences were noted in gray matter volume.
The participants were recruited from the community or from the Johns Hopkins University Alzheimer’s Disease Research Center. All of the subjects underwent several evaluations, including the Clinical Dementia Rating Scale and the Mini-Mental State Examination, and mild cognitive impairment was defined as a cognitive decline mainly in the ability to remember sequences or organization, as well as having lower scores on tests such as the California Verbal Learning Test (Neurobiol Dis. 2017 Sep;105:33-41). The average age of the participants was 66 years, and about 45% were women.
The study results were limited by several factors, including lack of arterial blood for quantification purposes and the absence of partial-volume correction in assessing the brain images, reported Dr. Smith, a professor of psychiatry and behavioral sciences at the university, and her colleagues.
However, the findings suggest that “the loss of SERT in MCI may have a substantial impact on brain function and behavior given the widespread distribution of SERT in the brain and the evidence that serotonin modulates other neurotransmitters (glutamate, norepinephrine, dopamine, and acetylcholine) implicated in AD and potentially MCI,” they emphasized.
Based on the findings, next steps for research could include targeting receptors that detect serotonin on message-receiving cells. “The substantially lower SERT in MCI observed in the present study suggests that the serotonin system may represent an important target for prevention and treatment,” the researchers noted.
Dr. Smith has received research funding from the National Institutes of Health and Functional Neuromodulation. This study was supported by the NIH.
Serotonin levels may play an early role in cognitive decline, according to imaging data from a group of study participants with mild cognitive impairment.
Previous studies have shown a link between a loss of serotonin neurons as part of normal aging and as part of the development of Alzheimer’s disease, wrote Gwenn S. Smith, PhD, of Johns Hopkins University in Baltimore, and her colleagues. However, “it is not known whether serotonin degeneration occurs in the preclinical stages or later in the course of AD,” the researchers said. The researchers used MRI and PET imaging to measure serotonin transporters (SERT) in the brains of 28 adults with mild cognitive impairment (MCI) and 28 healthy controls.
Overall, MCI participants showed significantly lower SERT, compared with the healthy controls; the loss of SERT in the MCI group ranged from 10% to 38%. No significant regions of higher SERT were noted in the MCI group, compared with the controls, and no significant differences were noted in gray matter volume.
The participants were recruited from the community or from the Johns Hopkins University Alzheimer’s Disease Research Center. All of the subjects underwent several evaluations, including the Clinical Dementia Rating Scale and the Mini-Mental State Examination, and mild cognitive impairment was defined as a cognitive decline mainly in the ability to remember sequences or organization, as well as having lower scores on tests such as the California Verbal Learning Test (Neurobiol Dis. 2017 Sep;105:33-41). The average age of the participants was 66 years, and about 45% were women.
The study results were limited by several factors, including lack of arterial blood for quantification purposes and the absence of partial-volume correction in assessing the brain images, reported Dr. Smith, a professor of psychiatry and behavioral sciences at the university, and her colleagues.
However, the findings suggest that “the loss of SERT in MCI may have a substantial impact on brain function and behavior given the widespread distribution of SERT in the brain and the evidence that serotonin modulates other neurotransmitters (glutamate, norepinephrine, dopamine, and acetylcholine) implicated in AD and potentially MCI,” they emphasized.
Based on the findings, next steps for research could include targeting receptors that detect serotonin on message-receiving cells. “The substantially lower SERT in MCI observed in the present study suggests that the serotonin system may represent an important target for prevention and treatment,” the researchers noted.
Dr. Smith has received research funding from the National Institutes of Health and Functional Neuromodulation. This study was supported by the NIH.
Serotonin levels may play an early role in cognitive decline, according to imaging data from a group of study participants with mild cognitive impairment.
Previous studies have shown a link between a loss of serotonin neurons as part of normal aging and as part of the development of Alzheimer’s disease, wrote Gwenn S. Smith, PhD, of Johns Hopkins University in Baltimore, and her colleagues. However, “it is not known whether serotonin degeneration occurs in the preclinical stages or later in the course of AD,” the researchers said. The researchers used MRI and PET imaging to measure serotonin transporters (SERT) in the brains of 28 adults with mild cognitive impairment (MCI) and 28 healthy controls.
Overall, MCI participants showed significantly lower SERT, compared with the healthy controls; the loss of SERT in the MCI group ranged from 10% to 38%. No significant regions of higher SERT were noted in the MCI group, compared with the controls, and no significant differences were noted in gray matter volume.
The participants were recruited from the community or from the Johns Hopkins University Alzheimer’s Disease Research Center. All of the subjects underwent several evaluations, including the Clinical Dementia Rating Scale and the Mini-Mental State Examination, and mild cognitive impairment was defined as a cognitive decline mainly in the ability to remember sequences or organization, as well as having lower scores on tests such as the California Verbal Learning Test (Neurobiol Dis. 2017 Sep;105:33-41). The average age of the participants was 66 years, and about 45% were women.
The study results were limited by several factors, including lack of arterial blood for quantification purposes and the absence of partial-volume correction in assessing the brain images, reported Dr. Smith, a professor of psychiatry and behavioral sciences at the university, and her colleagues.
However, the findings suggest that “the loss of SERT in MCI may have a substantial impact on brain function and behavior given the widespread distribution of SERT in the brain and the evidence that serotonin modulates other neurotransmitters (glutamate, norepinephrine, dopamine, and acetylcholine) implicated in AD and potentially MCI,” they emphasized.
Based on the findings, next steps for research could include targeting receptors that detect serotonin on message-receiving cells. “The substantially lower SERT in MCI observed in the present study suggests that the serotonin system may represent an important target for prevention and treatment,” the researchers noted.
Dr. Smith has received research funding from the National Institutes of Health and Functional Neuromodulation. This study was supported by the NIH.
FROM NEUROBIOLOGY OF DISEASE
Key clinical point: Levels of serotonin transporters were significantly lower in the cortical, striatal, thalamic, and limbic regions of the brain of adults with mild cognitive impairment, compared with healthy controls.
Major finding: The decrease in serotonin transporters (SERT) ranged from 10% to 38% in MCI adults, compared with healthy controls.
Data source: The data come from a comparison study of 28 adults with MCI and 28 healthy controls.
Disclosures: Dr. Smith has received research funding from the National Institutes of Health and Functional Neuromodulation. The study was supported by the NIH.
Cannabis shows inconsistent benefits for pain, PTSD
Chronic pain and posttraumatic stress disorder are among the top reasons given by patients seeking medical marijuana in states where it is legal, but there is little scientific evidence to support its value for treating either condition, based on the results of a pair of systemic evidence reviews conducted by the U.S. Department of Veterans Affairs.
The findings were published online Aug. 14 in the Annals of Internal Medicine.
In the PTSD study, Maya E. O’Neil, PhD, of the VA Portland (Ore.) Health Care System, and colleagues found no significant evidence to support the effectiveness of cannabis for relieving symptoms (Ann Intern Med. 2017 Aug 14. doi: 10.7326/M17-0477). The researchers reviewed data from two systematic reviews and three primary studies.
One of the larger studies (included in one of the systematic reviews) included 47,000 veterans in VA intensive PTSD programs during 1992-2011. In fact, after controlling for demographic factors and other confounding variables, individuals who continued to use cannabis or started using cannabis showed worse PTSD symptoms than did nonusers after 4 months.
“Findings from [randomized, controlled trials] are needed to help determine whether and to what extent cannabis may improve PTSD symptoms, and further studies also are needed to clarify harms in patients with PTSD,” the researchers noted.
In the review of chronic pain literature, Shannon M. Nugent, PhD, also of the VA Portland (Ore.) Health Care System, and her colleagues examined 27 trials, 11 reviews, and 32 primary studies (Ann Intern Med. 2017 Aug 14. doi: 10.7326/M17-0155).
“Across nine studies, intervention patients were more likely to report at least 30% improvement in pain,” the investigators said. But this finding was specific to tetrahydrocannabinol (THC), the researchers said, and evidence of the ability of cannabis to relieve other types of pain, such as cancer pain and multiple sclerosis pain, was insufficient.
In addition, the researchers found a low strength of evidence association between cannabis use and the development of psychotic symptoms, and a moderate strength of evidence association between cannabis use and impaired cognitive function in the general population. “However, our confidence in the findings is limited by inconsistent findings among included studies, inadequate assessment of exposure, and inadequate adjustment for confounding among the studies” they said.
Although no significant differences were noted in rates of adverse events between cannabis users and nonusers, some data suggested users had an increased risk for short-term adverse events that ranged from dizziness to paranoia and suicide attempts.
Other potential harms associated with cannabis use included decreased lung function, increased risk of complications from infectious diseases, cannabis hyperemesis syndrome, and increased risk of violent behavior.
“Even though we did not find strong, consistent evidence of benefit, clinicians will still need to engage in evidence-based discussions with patients managing chronic pain who are using or requesting to use cannabis,” the researchers wrote.
The researchers had no financial conflicts to disclose. The study was commissioned by the Veterans Health Administration.
“The systematic reviews highlight an alarming lack of high-quality data from which to draw firm conclusions about the efficacy of cannabis for these conditions, for which cannabis is both sanctioned and commonly used,” wrote Sachin Patel, MD, PhD, in an accompanying editorial (Ann Intern Med. 2017 Aug 14. doi: 10.7326/M17-1713).
“Even if future studies reveal a clear lack of substantial benefit of cannabis for pain or PTSD, legislation is unlikely to remove these conditions from the lists of indications for medical cannabis,” he cautioned. “It will be up to front-line practicing physicians to learn about the harms and benefits of cannabis, educate their patients on these topics, and make evidence-based recommendations about using cannabis and related products for various health conditions.
“In parallel, the research community must pursue high-quality studies and disseminate the results to clinicians and the public. In this context, these reviews are must-reads for all physicians, especially those practicing in states where medical cannabis is legal,” Dr. Patel added.
Dr. Patel is affiliated with Vanderbilt Psychiatric Hospital in Nashville, Tenn. He had no relevant financial conflicts to disclose, but reported receiving grants from Lundbeck.
“The systematic reviews highlight an alarming lack of high-quality data from which to draw firm conclusions about the efficacy of cannabis for these conditions, for which cannabis is both sanctioned and commonly used,” wrote Sachin Patel, MD, PhD, in an accompanying editorial (Ann Intern Med. 2017 Aug 14. doi: 10.7326/M17-1713).
“Even if future studies reveal a clear lack of substantial benefit of cannabis for pain or PTSD, legislation is unlikely to remove these conditions from the lists of indications for medical cannabis,” he cautioned. “It will be up to front-line practicing physicians to learn about the harms and benefits of cannabis, educate their patients on these topics, and make evidence-based recommendations about using cannabis and related products for various health conditions.
“In parallel, the research community must pursue high-quality studies and disseminate the results to clinicians and the public. In this context, these reviews are must-reads for all physicians, especially those practicing in states where medical cannabis is legal,” Dr. Patel added.
Dr. Patel is affiliated with Vanderbilt Psychiatric Hospital in Nashville, Tenn. He had no relevant financial conflicts to disclose, but reported receiving grants from Lundbeck.
“The systematic reviews highlight an alarming lack of high-quality data from which to draw firm conclusions about the efficacy of cannabis for these conditions, for which cannabis is both sanctioned and commonly used,” wrote Sachin Patel, MD, PhD, in an accompanying editorial (Ann Intern Med. 2017 Aug 14. doi: 10.7326/M17-1713).
“Even if future studies reveal a clear lack of substantial benefit of cannabis for pain or PTSD, legislation is unlikely to remove these conditions from the lists of indications for medical cannabis,” he cautioned. “It will be up to front-line practicing physicians to learn about the harms and benefits of cannabis, educate their patients on these topics, and make evidence-based recommendations about using cannabis and related products for various health conditions.
“In parallel, the research community must pursue high-quality studies and disseminate the results to clinicians and the public. In this context, these reviews are must-reads for all physicians, especially those practicing in states where medical cannabis is legal,” Dr. Patel added.
Dr. Patel is affiliated with Vanderbilt Psychiatric Hospital in Nashville, Tenn. He had no relevant financial conflicts to disclose, but reported receiving grants from Lundbeck.
Chronic pain and posttraumatic stress disorder are among the top reasons given by patients seeking medical marijuana in states where it is legal, but there is little scientific evidence to support its value for treating either condition, based on the results of a pair of systemic evidence reviews conducted by the U.S. Department of Veterans Affairs.
The findings were published online Aug. 14 in the Annals of Internal Medicine.
In the PTSD study, Maya E. O’Neil, PhD, of the VA Portland (Ore.) Health Care System, and colleagues found no significant evidence to support the effectiveness of cannabis for relieving symptoms (Ann Intern Med. 2017 Aug 14. doi: 10.7326/M17-0477). The researchers reviewed data from two systematic reviews and three primary studies.
One of the larger studies (included in one of the systematic reviews) included 47,000 veterans in VA intensive PTSD programs during 1992-2011. In fact, after controlling for demographic factors and other confounding variables, individuals who continued to use cannabis or started using cannabis showed worse PTSD symptoms than did nonusers after 4 months.
“Findings from [randomized, controlled trials] are needed to help determine whether and to what extent cannabis may improve PTSD symptoms, and further studies also are needed to clarify harms in patients with PTSD,” the researchers noted.
In the review of chronic pain literature, Shannon M. Nugent, PhD, also of the VA Portland (Ore.) Health Care System, and her colleagues examined 27 trials, 11 reviews, and 32 primary studies (Ann Intern Med. 2017 Aug 14. doi: 10.7326/M17-0155).
“Across nine studies, intervention patients were more likely to report at least 30% improvement in pain,” the investigators said. But this finding was specific to tetrahydrocannabinol (THC), the researchers said, and evidence of the ability of cannabis to relieve other types of pain, such as cancer pain and multiple sclerosis pain, was insufficient.
In addition, the researchers found a low strength of evidence association between cannabis use and the development of psychotic symptoms, and a moderate strength of evidence association between cannabis use and impaired cognitive function in the general population. “However, our confidence in the findings is limited by inconsistent findings among included studies, inadequate assessment of exposure, and inadequate adjustment for confounding among the studies” they said.
Although no significant differences were noted in rates of adverse events between cannabis users and nonusers, some data suggested users had an increased risk for short-term adverse events that ranged from dizziness to paranoia and suicide attempts.
Other potential harms associated with cannabis use included decreased lung function, increased risk of complications from infectious diseases, cannabis hyperemesis syndrome, and increased risk of violent behavior.
“Even though we did not find strong, consistent evidence of benefit, clinicians will still need to engage in evidence-based discussions with patients managing chronic pain who are using or requesting to use cannabis,” the researchers wrote.
The researchers had no financial conflicts to disclose. The study was commissioned by the Veterans Health Administration.
Chronic pain and posttraumatic stress disorder are among the top reasons given by patients seeking medical marijuana in states where it is legal, but there is little scientific evidence to support its value for treating either condition, based on the results of a pair of systemic evidence reviews conducted by the U.S. Department of Veterans Affairs.
The findings were published online Aug. 14 in the Annals of Internal Medicine.
In the PTSD study, Maya E. O’Neil, PhD, of the VA Portland (Ore.) Health Care System, and colleagues found no significant evidence to support the effectiveness of cannabis for relieving symptoms (Ann Intern Med. 2017 Aug 14. doi: 10.7326/M17-0477). The researchers reviewed data from two systematic reviews and three primary studies.
One of the larger studies (included in one of the systematic reviews) included 47,000 veterans in VA intensive PTSD programs during 1992-2011. In fact, after controlling for demographic factors and other confounding variables, individuals who continued to use cannabis or started using cannabis showed worse PTSD symptoms than did nonusers after 4 months.
“Findings from [randomized, controlled trials] are needed to help determine whether and to what extent cannabis may improve PTSD symptoms, and further studies also are needed to clarify harms in patients with PTSD,” the researchers noted.
In the review of chronic pain literature, Shannon M. Nugent, PhD, also of the VA Portland (Ore.) Health Care System, and her colleagues examined 27 trials, 11 reviews, and 32 primary studies (Ann Intern Med. 2017 Aug 14. doi: 10.7326/M17-0155).
“Across nine studies, intervention patients were more likely to report at least 30% improvement in pain,” the investigators said. But this finding was specific to tetrahydrocannabinol (THC), the researchers said, and evidence of the ability of cannabis to relieve other types of pain, such as cancer pain and multiple sclerosis pain, was insufficient.
In addition, the researchers found a low strength of evidence association between cannabis use and the development of psychotic symptoms, and a moderate strength of evidence association between cannabis use and impaired cognitive function in the general population. “However, our confidence in the findings is limited by inconsistent findings among included studies, inadequate assessment of exposure, and inadequate adjustment for confounding among the studies” they said.
Although no significant differences were noted in rates of adverse events between cannabis users and nonusers, some data suggested users had an increased risk for short-term adverse events that ranged from dizziness to paranoia and suicide attempts.
Other potential harms associated with cannabis use included decreased lung function, increased risk of complications from infectious diseases, cannabis hyperemesis syndrome, and increased risk of violent behavior.
“Even though we did not find strong, consistent evidence of benefit, clinicians will still need to engage in evidence-based discussions with patients managing chronic pain who are using or requesting to use cannabis,” the researchers wrote.
The researchers had no financial conflicts to disclose. The study was commissioned by the Veterans Health Administration.
FROM ANNALS OF INTERNAL MEDICINE
Key clinical point:
Major finding: One study of cannabis use for neuropathic pain showed an approximately 30% improvement in pain, but researchers found no significant impact on relieving other types of chronic pain or PTSD symptoms.
Data source: The data come from a chronic pain review that included 27 trials, 11 systematic reviews, and 32 primary studies; and a PTSD review that included 2 systematic reviews and 3 primary studies.
Disclosures: The researchers had no financial conflicts to disclose. The study was commissioned by the Veterans Health Administration.