User login
Don't Disregard High-Dose Brachytherapy for Skin Cancer
ORLANDO – Although Mohs surgery remains a mainstay of skin cancer treatment, some patients benefit from targeted brachytherapy of their basal or squamous cell carcinoma lesions, according to Dr. Michael E. Kasper.
Patients who are elderly, infirm, or on blood thinners are good candidates for noninvasive brachytherapy using high-dose, small surface applicators, Dr. Kasper said. This therapeutic strategy also works well for treating lesions in anatomic locations at risk for delayed surgical healing.
"We are treating various small lesions with these surface applicators," Dr. Kasper said. For example, superficial squamous cell carcinoma (SCC) lesions up to 2 cm can be targeted "where we feel comfortable about the visible margins," he said at the annual meeting of the Florida Society of Dermatology and Dermatologic Surgery.
"We also see patients who are tired of [invasive resection] or who are poor candidates for surgery, and that is really the bulk of our patients," Dr. Kasper said. He assured meeting attendees that his goal as a radiation oncologist is not to take skin cancer patients away from dermatologists. "We’re not interested in treating 40- or 50-year-olds and really competing," said Dr. Kasper of Lynn Cancer Institute at Boca Raton (Fla.) Regional Hospital. "We are interested in working with dermatologists and really helping you with those patients who might be neglected or who are at high risk of developing a serious recurrence."
Neglected patients may include nursing home residents who do not get medical attention for their skin cancer in its earlier stages, he said.
Available data point to good local control and cosmesis for a majority of patients, Dr. Kasper said. A typical patient might experience acute effects such as crusting and some mild erythema about 10 days to 2 weeks after brachytherapy of a well differentiated SCC lesion of the lower extremity. More brisk erythema also occurs in about 10%-15% of patients, Dr. Kasper said.
Late hypopigmentation also develops in about 10% of patients, he said. "We are also seeing a few telangiectasias, but it’s fairly mild."
Interpret postradiation therapy biopsies with caution, Dr. Kasper warned. Of the 240 patients treated to date at his institution over about 6.5 years, there were three documented recurrences, including a couple at 3 and 4 months. "While we are counting those as recurrences, they probably aren’t. That’s way too early to biopsy these lesions." Use discretion and ideally wait until you see clear progression prior to performing a postradiation biopsy, he said. "There certainly are false positives that occur due to delayed tumor regression. The cancer cells die when they reproduce and many of these are slow growing tumors. So we would not expect them to all be completely resolved at 3 or 4 months although clinically, on the surface, they can appear that way."
Historically brachytherapy was delivered as a low-dose treatment over a long period of time at many sessions. Low-dose brachytherapy is typically in the 0.4 to 2.0 Gy/hr range, medium dose is greater than 2 and up to 12 Gy/hr, and the high dose exceeds 12 Gy/hr.
Availability of high-dose rate brachytherapy was a "major breakthrough" because patients no longer had to lie in the hospital all weekend to receive treatment. "It was a bit controversial at first, but now there are really good data to show there are radiobiologic reasons why the high dose rate may actually be advantageous in killing cancer cells compared to this low trickle effect that we were using with low-dose regimens."
Dr. Kasper determined that up to 30 sessions of low-dose rate brachytherapy can be a real impediment to patient compliance and worked to design a safe and effective regimen delivered in fewer sessions. "We wanted to be at six treatments and worked backwards." Striking a balance between the dose-response rate and the potential late side effects was another consideration.
A meeting attendee asked about the relative cost of brachytherapy, compared with other treatment modalities. Brachytherapy is generally more expensive than Mohs surgery, Dr. Kasper replied. The avoidance of cancer recurrences will hopefully justify the higher initial costs, he said. He added that brachytherapy costs are coming down, more so in outpatient centers, compared with hospital settings.
Dr. Kasper said he receives consulting fees from Nucletron/Elekta.
ORLANDO – Although Mohs surgery remains a mainstay of skin cancer treatment, some patients benefit from targeted brachytherapy of their basal or squamous cell carcinoma lesions, according to Dr. Michael E. Kasper.
Patients who are elderly, infirm, or on blood thinners are good candidates for noninvasive brachytherapy using high-dose, small surface applicators, Dr. Kasper said. This therapeutic strategy also works well for treating lesions in anatomic locations at risk for delayed surgical healing.
"We are treating various small lesions with these surface applicators," Dr. Kasper said. For example, superficial squamous cell carcinoma (SCC) lesions up to 2 cm can be targeted "where we feel comfortable about the visible margins," he said at the annual meeting of the Florida Society of Dermatology and Dermatologic Surgery.
"We also see patients who are tired of [invasive resection] or who are poor candidates for surgery, and that is really the bulk of our patients," Dr. Kasper said. He assured meeting attendees that his goal as a radiation oncologist is not to take skin cancer patients away from dermatologists. "We’re not interested in treating 40- or 50-year-olds and really competing," said Dr. Kasper of Lynn Cancer Institute at Boca Raton (Fla.) Regional Hospital. "We are interested in working with dermatologists and really helping you with those patients who might be neglected or who are at high risk of developing a serious recurrence."
Neglected patients may include nursing home residents who do not get medical attention for their skin cancer in its earlier stages, he said.
Available data point to good local control and cosmesis for a majority of patients, Dr. Kasper said. A typical patient might experience acute effects such as crusting and some mild erythema about 10 days to 2 weeks after brachytherapy of a well differentiated SCC lesion of the lower extremity. More brisk erythema also occurs in about 10%-15% of patients, Dr. Kasper said.
Late hypopigmentation also develops in about 10% of patients, he said. "We are also seeing a few telangiectasias, but it’s fairly mild."
Interpret postradiation therapy biopsies with caution, Dr. Kasper warned. Of the 240 patients treated to date at his institution over about 6.5 years, there were three documented recurrences, including a couple at 3 and 4 months. "While we are counting those as recurrences, they probably aren’t. That’s way too early to biopsy these lesions." Use discretion and ideally wait until you see clear progression prior to performing a postradiation biopsy, he said. "There certainly are false positives that occur due to delayed tumor regression. The cancer cells die when they reproduce and many of these are slow growing tumors. So we would not expect them to all be completely resolved at 3 or 4 months although clinically, on the surface, they can appear that way."
Historically brachytherapy was delivered as a low-dose treatment over a long period of time at many sessions. Low-dose brachytherapy is typically in the 0.4 to 2.0 Gy/hr range, medium dose is greater than 2 and up to 12 Gy/hr, and the high dose exceeds 12 Gy/hr.
Availability of high-dose rate brachytherapy was a "major breakthrough" because patients no longer had to lie in the hospital all weekend to receive treatment. "It was a bit controversial at first, but now there are really good data to show there are radiobiologic reasons why the high dose rate may actually be advantageous in killing cancer cells compared to this low trickle effect that we were using with low-dose regimens."
Dr. Kasper determined that up to 30 sessions of low-dose rate brachytherapy can be a real impediment to patient compliance and worked to design a safe and effective regimen delivered in fewer sessions. "We wanted to be at six treatments and worked backwards." Striking a balance between the dose-response rate and the potential late side effects was another consideration.
A meeting attendee asked about the relative cost of brachytherapy, compared with other treatment modalities. Brachytherapy is generally more expensive than Mohs surgery, Dr. Kasper replied. The avoidance of cancer recurrences will hopefully justify the higher initial costs, he said. He added that brachytherapy costs are coming down, more so in outpatient centers, compared with hospital settings.
Dr. Kasper said he receives consulting fees from Nucletron/Elekta.
ORLANDO – Although Mohs surgery remains a mainstay of skin cancer treatment, some patients benefit from targeted brachytherapy of their basal or squamous cell carcinoma lesions, according to Dr. Michael E. Kasper.
Patients who are elderly, infirm, or on blood thinners are good candidates for noninvasive brachytherapy using high-dose, small surface applicators, Dr. Kasper said. This therapeutic strategy also works well for treating lesions in anatomic locations at risk for delayed surgical healing.
"We are treating various small lesions with these surface applicators," Dr. Kasper said. For example, superficial squamous cell carcinoma (SCC) lesions up to 2 cm can be targeted "where we feel comfortable about the visible margins," he said at the annual meeting of the Florida Society of Dermatology and Dermatologic Surgery.
"We also see patients who are tired of [invasive resection] or who are poor candidates for surgery, and that is really the bulk of our patients," Dr. Kasper said. He assured meeting attendees that his goal as a radiation oncologist is not to take skin cancer patients away from dermatologists. "We’re not interested in treating 40- or 50-year-olds and really competing," said Dr. Kasper of Lynn Cancer Institute at Boca Raton (Fla.) Regional Hospital. "We are interested in working with dermatologists and really helping you with those patients who might be neglected or who are at high risk of developing a serious recurrence."
Neglected patients may include nursing home residents who do not get medical attention for their skin cancer in its earlier stages, he said.
Available data point to good local control and cosmesis for a majority of patients, Dr. Kasper said. A typical patient might experience acute effects such as crusting and some mild erythema about 10 days to 2 weeks after brachytherapy of a well differentiated SCC lesion of the lower extremity. More brisk erythema also occurs in about 10%-15% of patients, Dr. Kasper said.
Late hypopigmentation also develops in about 10% of patients, he said. "We are also seeing a few telangiectasias, but it’s fairly mild."
Interpret postradiation therapy biopsies with caution, Dr. Kasper warned. Of the 240 patients treated to date at his institution over about 6.5 years, there were three documented recurrences, including a couple at 3 and 4 months. "While we are counting those as recurrences, they probably aren’t. That’s way too early to biopsy these lesions." Use discretion and ideally wait until you see clear progression prior to performing a postradiation biopsy, he said. "There certainly are false positives that occur due to delayed tumor regression. The cancer cells die when they reproduce and many of these are slow growing tumors. So we would not expect them to all be completely resolved at 3 or 4 months although clinically, on the surface, they can appear that way."
Historically brachytherapy was delivered as a low-dose treatment over a long period of time at many sessions. Low-dose brachytherapy is typically in the 0.4 to 2.0 Gy/hr range, medium dose is greater than 2 and up to 12 Gy/hr, and the high dose exceeds 12 Gy/hr.
Availability of high-dose rate brachytherapy was a "major breakthrough" because patients no longer had to lie in the hospital all weekend to receive treatment. "It was a bit controversial at first, but now there are really good data to show there are radiobiologic reasons why the high dose rate may actually be advantageous in killing cancer cells compared to this low trickle effect that we were using with low-dose regimens."
Dr. Kasper determined that up to 30 sessions of low-dose rate brachytherapy can be a real impediment to patient compliance and worked to design a safe and effective regimen delivered in fewer sessions. "We wanted to be at six treatments and worked backwards." Striking a balance between the dose-response rate and the potential late side effects was another consideration.
A meeting attendee asked about the relative cost of brachytherapy, compared with other treatment modalities. Brachytherapy is generally more expensive than Mohs surgery, Dr. Kasper replied. The avoidance of cancer recurrences will hopefully justify the higher initial costs, he said. He added that brachytherapy costs are coming down, more so in outpatient centers, compared with hospital settings.
Dr. Kasper said he receives consulting fees from Nucletron/Elekta.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGY AND DERMATOLOGIC SURGERY
Most Cancers Not Elevated in Vasculitis
BERLIN – Nonmelanoma skin cancer was the only type of malignancy found to occur at an increased rate in new 5-year follow-up data on 535 patients treated for systemic small-vessel vasculitis in four major randomized trials sponsored by the European Vasculitis Society.
With 2,650 person-years of prospective observation of 281 clinical trial participants treated for granulomatosis with polyangiitis (formerly called Wegener’s granulomatosis) and 254 treated for microscopic polyangiitis, patients with circulating antineutrophil cytoplasmic antibody (ANCA)-associated vasculitis had a 2.78-fold greater incidence of nonmelanoma skin cancer than did the matched general population, based upon data from the European cancer registry. But no other type of cancer was significantly increased, Dr. Kerstin W.A. Westman reported at the annual European Congress of Rheumatology.
This finding came as a pleasant surprise. Earlier publications by other investigators have reported broadly elevated malignancy risks in the years following administration of the various toxic, largely cyclophosphamide-based therapeutic regimens for ANCA-associated vasculitis, noted Dr. Westman, a nephrologist at Lund (Sweden) University.
For example, Danish investigators reported significantly increased rates of bladder and prostate cancer and acute myeloid leukemia as well as nonmelanoma skin cancer in a study featuring 2,121 person-years of follow-up (J. Rheumatol.2008;35:100-5). However, the Danish patients were treated during 1973-1999, while participants in the four European Vasculitis Society randomized trials underwent treatment as recently as 2007, at which time, the research focus had shifted to trying to decrease the burden of immunosuppression while maintaining effectiveness, Dr. Westman observed. For this reason, she and her coworkers are cautiously optimistic about the limited cancer risk seen to date in their analysis.
"This may be caused by too short a period of time of follow-up or else, as we would like to think, maybe we have improved the treatment by lowering the cumulative dose of cyclophosphamide, making it less toxic. But that we don’t really know yet," she said.
Several audience members rose to relate that their own clinical experience has been that lymphoma, bladder cancer, and other malignancies crop up not within 5 years post treatment for ANCA-associated vasculitis, but 10-15 years later or even more.
"I completely agree," Dr. Westman replied. "It’s important for us to arrange longer-term follow-up to say anything conclusive about malignancy. We’re aiming for 10-year follow-up in these patients."
Still, she added, there is reason to be hopeful that some of the more recently evaluated treatment regimens are less oncogenic. For one thing, the earlier Danish study found increased rates of several types of cancer within 5 years.
Also, she cited a recent report on 445 patients with granulomatosis with polyangiitis treated during the past 4 decades at a single large German academic rheumatology center. The German investigators found no increase in malignancies. Moreover, the standardized mortality ratio – essentially, the risk of all-cause mortality compared to that of the matched general population – fell from 2.1 in patients treated during 1966-1993, to 1.41 in those treated in 1994-1998, to 1.03, meaning no increased risk, in patients treated in 1999-2002. Relapse rates during those three time periods dropped from 61% to 51% to 35% (Arthritis Rheum. 2011;63:257-66).
The four-study European Vasculitis Society cohort followed prospectively for 5 years had a median age of 61 years at the time of enrollment in the randomized trials. Of the 535 patients, 53% had antiproteinase-3 antibody positive ANCA (PR3-ANCA) and 38% had antimyeloperoxidase-positive ANCA.
Overall survival at 2 and 5 years was 85% and 78%, respectively. Mortality was 2.6-fold higher than in the age- and sex-matched general population. The mortality risk was greatest during the first year of follow up, with deaths mainly from infection or active vasculitis. After year 1, most deaths were caused by infection, cardiovascular events, or cancer.
Relapse, defined as new or worsened manifestations of ANCA-associated vasculitis requiring a change in therapy, occurred in 38% of patients. The two major risk factors for relapse were being PR3-ANCA positive or having cardiovascular involvement at enrollment.
The best 5-year overall survival was in patients younger than age 50 years at enrollment in their randomized trial. Survival was significantly worse in stepwise fashion in 50- to 60-year-olds, worse yet in 60- to 70-year-olds, and lowest of all in patients above age 70 years.
"Age matters," Dr. Westman declared.
One or more cardiovascular events occurred in 14% of the subjects during 5 years of follow-up. There were 32 cardiovascular deaths, 25 nonfatal strokes, and 42 nonfatal myocardial infarctions or revascularization procedures. Not surprisingly, older age was an independent risk factor for cardiovascular events. But PR3-ANCA–positive status proved to be an independent protector against cardiovascular events; it was associated with a 59% reduction in risk.
Also, in a new analysis of the CYCLOPS study, the most recent of the four European Vasculitis Society clinical trials, the risk of relapse was independently related to a participant’s PR3-ANCA status. The lowest relapse rate occurred in PR3-ANCA–negative patients randomized to daily oral cyclophosphamide for remission induction, while the worst relapse rate was in PR3-ANCA–positive patients assigned to pulse cyclophosphamide (Ann. Rheum. Dis. 2012;71:955-60). These findings may bring closer the day when individualized tailoring of immunosuppression might become possible.
Of patients with granulomatosis with polyangiitis, 49% experienced otolaryngologic involvement during 5 years of follow up, and in 65% of affected patients the otolaryngologic damage appeared to be permanent. An important study observation was that patients with frequent relapses were at increased risk of permanent otolaryngologic damage, Dr. Westman continued.
The four European Vasculitis Society randomized trials that tested various induction and maintenance-of-remission treatment regimens were known as NORAM, CYCAZAREM, MEPEX, and CYCLOPS.
The 5-year follow-up analysis of the four trials was funded by the European League Against Rheumatism. Dr. Westman reported having no financial conflicts.
BERLIN – Nonmelanoma skin cancer was the only type of malignancy found to occur at an increased rate in new 5-year follow-up data on 535 patients treated for systemic small-vessel vasculitis in four major randomized trials sponsored by the European Vasculitis Society.
With 2,650 person-years of prospective observation of 281 clinical trial participants treated for granulomatosis with polyangiitis (formerly called Wegener’s granulomatosis) and 254 treated for microscopic polyangiitis, patients with circulating antineutrophil cytoplasmic antibody (ANCA)-associated vasculitis had a 2.78-fold greater incidence of nonmelanoma skin cancer than did the matched general population, based upon data from the European cancer registry. But no other type of cancer was significantly increased, Dr. Kerstin W.A. Westman reported at the annual European Congress of Rheumatology.
This finding came as a pleasant surprise. Earlier publications by other investigators have reported broadly elevated malignancy risks in the years following administration of the various toxic, largely cyclophosphamide-based therapeutic regimens for ANCA-associated vasculitis, noted Dr. Westman, a nephrologist at Lund (Sweden) University.
For example, Danish investigators reported significantly increased rates of bladder and prostate cancer and acute myeloid leukemia as well as nonmelanoma skin cancer in a study featuring 2,121 person-years of follow-up (J. Rheumatol.2008;35:100-5). However, the Danish patients were treated during 1973-1999, while participants in the four European Vasculitis Society randomized trials underwent treatment as recently as 2007, at which time, the research focus had shifted to trying to decrease the burden of immunosuppression while maintaining effectiveness, Dr. Westman observed. For this reason, she and her coworkers are cautiously optimistic about the limited cancer risk seen to date in their analysis.
"This may be caused by too short a period of time of follow-up or else, as we would like to think, maybe we have improved the treatment by lowering the cumulative dose of cyclophosphamide, making it less toxic. But that we don’t really know yet," she said.
Several audience members rose to relate that their own clinical experience has been that lymphoma, bladder cancer, and other malignancies crop up not within 5 years post treatment for ANCA-associated vasculitis, but 10-15 years later or even more.
"I completely agree," Dr. Westman replied. "It’s important for us to arrange longer-term follow-up to say anything conclusive about malignancy. We’re aiming for 10-year follow-up in these patients."
Still, she added, there is reason to be hopeful that some of the more recently evaluated treatment regimens are less oncogenic. For one thing, the earlier Danish study found increased rates of several types of cancer within 5 years.
Also, she cited a recent report on 445 patients with granulomatosis with polyangiitis treated during the past 4 decades at a single large German academic rheumatology center. The German investigators found no increase in malignancies. Moreover, the standardized mortality ratio – essentially, the risk of all-cause mortality compared to that of the matched general population – fell from 2.1 in patients treated during 1966-1993, to 1.41 in those treated in 1994-1998, to 1.03, meaning no increased risk, in patients treated in 1999-2002. Relapse rates during those three time periods dropped from 61% to 51% to 35% (Arthritis Rheum. 2011;63:257-66).
The four-study European Vasculitis Society cohort followed prospectively for 5 years had a median age of 61 years at the time of enrollment in the randomized trials. Of the 535 patients, 53% had antiproteinase-3 antibody positive ANCA (PR3-ANCA) and 38% had antimyeloperoxidase-positive ANCA.
Overall survival at 2 and 5 years was 85% and 78%, respectively. Mortality was 2.6-fold higher than in the age- and sex-matched general population. The mortality risk was greatest during the first year of follow up, with deaths mainly from infection or active vasculitis. After year 1, most deaths were caused by infection, cardiovascular events, or cancer.
Relapse, defined as new or worsened manifestations of ANCA-associated vasculitis requiring a change in therapy, occurred in 38% of patients. The two major risk factors for relapse were being PR3-ANCA positive or having cardiovascular involvement at enrollment.
The best 5-year overall survival was in patients younger than age 50 years at enrollment in their randomized trial. Survival was significantly worse in stepwise fashion in 50- to 60-year-olds, worse yet in 60- to 70-year-olds, and lowest of all in patients above age 70 years.
"Age matters," Dr. Westman declared.
One or more cardiovascular events occurred in 14% of the subjects during 5 years of follow-up. There were 32 cardiovascular deaths, 25 nonfatal strokes, and 42 nonfatal myocardial infarctions or revascularization procedures. Not surprisingly, older age was an independent risk factor for cardiovascular events. But PR3-ANCA–positive status proved to be an independent protector against cardiovascular events; it was associated with a 59% reduction in risk.
Also, in a new analysis of the CYCLOPS study, the most recent of the four European Vasculitis Society clinical trials, the risk of relapse was independently related to a participant’s PR3-ANCA status. The lowest relapse rate occurred in PR3-ANCA–negative patients randomized to daily oral cyclophosphamide for remission induction, while the worst relapse rate was in PR3-ANCA–positive patients assigned to pulse cyclophosphamide (Ann. Rheum. Dis. 2012;71:955-60). These findings may bring closer the day when individualized tailoring of immunosuppression might become possible.
Of patients with granulomatosis with polyangiitis, 49% experienced otolaryngologic involvement during 5 years of follow up, and in 65% of affected patients the otolaryngologic damage appeared to be permanent. An important study observation was that patients with frequent relapses were at increased risk of permanent otolaryngologic damage, Dr. Westman continued.
The four European Vasculitis Society randomized trials that tested various induction and maintenance-of-remission treatment regimens were known as NORAM, CYCAZAREM, MEPEX, and CYCLOPS.
The 5-year follow-up analysis of the four trials was funded by the European League Against Rheumatism. Dr. Westman reported having no financial conflicts.
BERLIN – Nonmelanoma skin cancer was the only type of malignancy found to occur at an increased rate in new 5-year follow-up data on 535 patients treated for systemic small-vessel vasculitis in four major randomized trials sponsored by the European Vasculitis Society.
With 2,650 person-years of prospective observation of 281 clinical trial participants treated for granulomatosis with polyangiitis (formerly called Wegener’s granulomatosis) and 254 treated for microscopic polyangiitis, patients with circulating antineutrophil cytoplasmic antibody (ANCA)-associated vasculitis had a 2.78-fold greater incidence of nonmelanoma skin cancer than did the matched general population, based upon data from the European cancer registry. But no other type of cancer was significantly increased, Dr. Kerstin W.A. Westman reported at the annual European Congress of Rheumatology.
This finding came as a pleasant surprise. Earlier publications by other investigators have reported broadly elevated malignancy risks in the years following administration of the various toxic, largely cyclophosphamide-based therapeutic regimens for ANCA-associated vasculitis, noted Dr. Westman, a nephrologist at Lund (Sweden) University.
For example, Danish investigators reported significantly increased rates of bladder and prostate cancer and acute myeloid leukemia as well as nonmelanoma skin cancer in a study featuring 2,121 person-years of follow-up (J. Rheumatol.2008;35:100-5). However, the Danish patients were treated during 1973-1999, while participants in the four European Vasculitis Society randomized trials underwent treatment as recently as 2007, at which time, the research focus had shifted to trying to decrease the burden of immunosuppression while maintaining effectiveness, Dr. Westman observed. For this reason, she and her coworkers are cautiously optimistic about the limited cancer risk seen to date in their analysis.
"This may be caused by too short a period of time of follow-up or else, as we would like to think, maybe we have improved the treatment by lowering the cumulative dose of cyclophosphamide, making it less toxic. But that we don’t really know yet," she said.
Several audience members rose to relate that their own clinical experience has been that lymphoma, bladder cancer, and other malignancies crop up not within 5 years post treatment for ANCA-associated vasculitis, but 10-15 years later or even more.
"I completely agree," Dr. Westman replied. "It’s important for us to arrange longer-term follow-up to say anything conclusive about malignancy. We’re aiming for 10-year follow-up in these patients."
Still, she added, there is reason to be hopeful that some of the more recently evaluated treatment regimens are less oncogenic. For one thing, the earlier Danish study found increased rates of several types of cancer within 5 years.
Also, she cited a recent report on 445 patients with granulomatosis with polyangiitis treated during the past 4 decades at a single large German academic rheumatology center. The German investigators found no increase in malignancies. Moreover, the standardized mortality ratio – essentially, the risk of all-cause mortality compared to that of the matched general population – fell from 2.1 in patients treated during 1966-1993, to 1.41 in those treated in 1994-1998, to 1.03, meaning no increased risk, in patients treated in 1999-2002. Relapse rates during those three time periods dropped from 61% to 51% to 35% (Arthritis Rheum. 2011;63:257-66).
The four-study European Vasculitis Society cohort followed prospectively for 5 years had a median age of 61 years at the time of enrollment in the randomized trials. Of the 535 patients, 53% had antiproteinase-3 antibody positive ANCA (PR3-ANCA) and 38% had antimyeloperoxidase-positive ANCA.
Overall survival at 2 and 5 years was 85% and 78%, respectively. Mortality was 2.6-fold higher than in the age- and sex-matched general population. The mortality risk was greatest during the first year of follow up, with deaths mainly from infection or active vasculitis. After year 1, most deaths were caused by infection, cardiovascular events, or cancer.
Relapse, defined as new or worsened manifestations of ANCA-associated vasculitis requiring a change in therapy, occurred in 38% of patients. The two major risk factors for relapse were being PR3-ANCA positive or having cardiovascular involvement at enrollment.
The best 5-year overall survival was in patients younger than age 50 years at enrollment in their randomized trial. Survival was significantly worse in stepwise fashion in 50- to 60-year-olds, worse yet in 60- to 70-year-olds, and lowest of all in patients above age 70 years.
"Age matters," Dr. Westman declared.
One or more cardiovascular events occurred in 14% of the subjects during 5 years of follow-up. There were 32 cardiovascular deaths, 25 nonfatal strokes, and 42 nonfatal myocardial infarctions or revascularization procedures. Not surprisingly, older age was an independent risk factor for cardiovascular events. But PR3-ANCA–positive status proved to be an independent protector against cardiovascular events; it was associated with a 59% reduction in risk.
Also, in a new analysis of the CYCLOPS study, the most recent of the four European Vasculitis Society clinical trials, the risk of relapse was independently related to a participant’s PR3-ANCA status. The lowest relapse rate occurred in PR3-ANCA–negative patients randomized to daily oral cyclophosphamide for remission induction, while the worst relapse rate was in PR3-ANCA–positive patients assigned to pulse cyclophosphamide (Ann. Rheum. Dis. 2012;71:955-60). These findings may bring closer the day when individualized tailoring of immunosuppression might become possible.
Of patients with granulomatosis with polyangiitis, 49% experienced otolaryngologic involvement during 5 years of follow up, and in 65% of affected patients the otolaryngologic damage appeared to be permanent. An important study observation was that patients with frequent relapses were at increased risk of permanent otolaryngologic damage, Dr. Westman continued.
The four European Vasculitis Society randomized trials that tested various induction and maintenance-of-remission treatment regimens were known as NORAM, CYCAZAREM, MEPEX, and CYCLOPS.
The 5-year follow-up analysis of the four trials was funded by the European League Against Rheumatism. Dr. Westman reported having no financial conflicts.
AT THE ANNUAL EUROPEAN CONGRESS OF RHEUMATOLOGY
Major Finding: Patients with circulating antineutrophil cytoplasmic antibody (ANCA)-associated vasculitis had a 2.78-fold greater incidence of nonmelanoma skin cancer than did the matched general population, based upon European cancer registry data. But no other type of cancer was significantly increased in patients treated for ANCA-associated vasculitis. Patients in four European Vasculitis Society–sponsored randomized trials had an increased incidence of only one type of malignancy – nonmelanoma skin cancer – during 5 years of prospective follow-up.
Data Source: This finding is based on an analysis of data from a prospective follow-up of 281 patients with granulomatosis with polyangiitis and 254 with microscopic polyangiitis.
Disclosures: The long-term follow-up was funded by the European League Against Rheumatism. The investigators reported having no financial conflicts.
Baggy Eye Solutions: The Skinny Podcast
In this month's program, Miami dermatologist Dr. Jill Waibel shares her excitement about the effectiveness of fractional lasers to treat burn scars.
Then, Dr. Brett Coldiron, president of the American College of Mohs Surgery, explains why Mohs surgery rates are on the rise.
Health and Human Services Secretary Kathleen Sebelius asks for help and support in implementing the affordable care act.
And finally, Cosmetic Counter host Dr. Lily Talakoub offers tips for treating under-eye circles.
Don't miss another episode of The Skinny Podcast; subscribe on iTunes!
In this month's program, Miami dermatologist Dr. Jill Waibel shares her excitement about the effectiveness of fractional lasers to treat burn scars.
Then, Dr. Brett Coldiron, president of the American College of Mohs Surgery, explains why Mohs surgery rates are on the rise.
Health and Human Services Secretary Kathleen Sebelius asks for help and support in implementing the affordable care act.
And finally, Cosmetic Counter host Dr. Lily Talakoub offers tips for treating under-eye circles.
Don't miss another episode of The Skinny Podcast; subscribe on iTunes!
In this month's program, Miami dermatologist Dr. Jill Waibel shares her excitement about the effectiveness of fractional lasers to treat burn scars.
Then, Dr. Brett Coldiron, president of the American College of Mohs Surgery, explains why Mohs surgery rates are on the rise.
Health and Human Services Secretary Kathleen Sebelius asks for help and support in implementing the affordable care act.
And finally, Cosmetic Counter host Dr. Lily Talakoub offers tips for treating under-eye circles.
Don't miss another episode of The Skinny Podcast; subscribe on iTunes!
CTCL Proves Challenging in Skin of Color Patients
Over the past 4 decades, cutaneous T-cell lymphoma diagnoses have been on the rise, especially among black and other skin of color patients. Unfortunately, this form of skin cancer can be a diagnostic challenge.
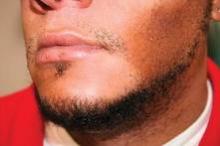
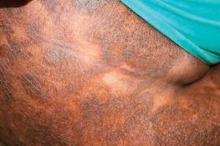
Regarding diagnosis, cutaneous T-cell lymphoma (CTCL) is the wild card of dermatology; it is a great mimicker of many skin disorders, and can look like almost anything. However, the most striking feature of the condition – and the key to diagnosis in ethnic skin – is its polymorphous pigmentation that is unique to skin of color.
CTCL lesions may be flat or raised, and may mimic other skin disorders associated with pigment change. These can include tinea versicolor, vitiligo, pityriasis rosea, and psoriasis. Lichen planus pigmentosus and progressive macular hypomelanosis are other important CTCL mimickers. Consider all of these conditions in the differential diagnosis.
An excellent resource for photos and descriptions of CTCL, as well as CTCL look-alikes, is an article by Dr. Ginette A. Hinds and Dr. Peter Heald (J. Am. Acad. Dermatol. 2009;60:359-75). The article also highlights the clinical variants within the mycosis fungoides subtype, the most common form of CTCL among blacks.
For example, look out for the "herald patch" of unilesional mycosis fungoides, which takes the form of a single large, dyspigmented patch. According to the authors, this variant has an excellent prognosis, possibly because of an active immune response that limits the initial spread of disease and contributes to preventing relapse.
Another variant is pigmented purpuric mycosis fungoides, which can often be confused with the benign pigmented purpura syndromes of Schamberg’s disease (progressive pigmented purpuric dermatitis), Gougerot-Blum syndrome (pigmented purpuric lichenoid dermatitis), Majocchi’s disease (purpura annularis telangiectodes), Doucas and Kapetanakis (lymphocytic capillaritis of unknown cause), and lichen aureus. The key to diagnosis in this case is recalling that "the lesions of the benign syndromes rarely assume the morphology and distribution found with mycosis fungoides," Dr. Hinds and Dr. Heald wrote.
Not only is mycosis fungoides difficult to diagnose, but it is especially prevalent among black patients. For instance, a 1988 study looking at Surveillance, Epidemiology, and End Results (SEER) data from 1973 through 1984 found that the incidence among black patients was twice that of white patients: 0.52/100,000 vs. 0.26 (JAMA 1988;260:42-46).
Similarly, in another study of 132 black patients with skin cancer, mycosis fungoides represented 12.1% of all skin neoplasms (Dermatol. Clin. 1988;6:397-405).
Mycosis fungoides is the fourth most common skin cancer among Japanese patients, representing approximately 5% of all skin malignancies in the population.
The incidence of CTCL and its subtypes is only increasing. A 2007 study that extended the SEER data mentioned above from 1973 to 2002 and included all CTCL cases found an incidence rate of 9.0 for black patients, per 1 million person-years, compared with 6.1 for white patients (Arch. Dermatol. 2007;143:854-9).
As in many skin cancers, early diagnosis can make the difference in successful outcomes. So add CTCL, and especially the mycosis fungoides subtype, to your differential when confronting pigmentation disorders in skin of color patients.
Dr. Roberts is past president of the Women’s Dermatologic Society (WDS) as well as past president of the California Society of Dermatology and Dermatologic Surgery (Calderm). She was a founding director of dermatopathology at the Loma Linda University Medical Center (Calif.). She currently runs a private practice in Rancho Mirage, Calif.
She disclosed financial relationships with Allergan, L’Oréal/La Roche Posay, Skin Medica, and Valeant Pharmaceuticals.
Over the past 4 decades, cutaneous T-cell lymphoma diagnoses have been on the rise, especially among black and other skin of color patients. Unfortunately, this form of skin cancer can be a diagnostic challenge.
Regarding diagnosis, cutaneous T-cell lymphoma (CTCL) is the wild card of dermatology; it is a great mimicker of many skin disorders, and can look like almost anything. However, the most striking feature of the condition – and the key to diagnosis in ethnic skin – is its polymorphous pigmentation that is unique to skin of color.
CTCL lesions may be flat or raised, and may mimic other skin disorders associated with pigment change. These can include tinea versicolor, vitiligo, pityriasis rosea, and psoriasis. Lichen planus pigmentosus and progressive macular hypomelanosis are other important CTCL mimickers. Consider all of these conditions in the differential diagnosis.
An excellent resource for photos and descriptions of CTCL, as well as CTCL look-alikes, is an article by Dr. Ginette A. Hinds and Dr. Peter Heald (J. Am. Acad. Dermatol. 2009;60:359-75). The article also highlights the clinical variants within the mycosis fungoides subtype, the most common form of CTCL among blacks.
For example, look out for the "herald patch" of unilesional mycosis fungoides, which takes the form of a single large, dyspigmented patch. According to the authors, this variant has an excellent prognosis, possibly because of an active immune response that limits the initial spread of disease and contributes to preventing relapse.
Another variant is pigmented purpuric mycosis fungoides, which can often be confused with the benign pigmented purpura syndromes of Schamberg’s disease (progressive pigmented purpuric dermatitis), Gougerot-Blum syndrome (pigmented purpuric lichenoid dermatitis), Majocchi’s disease (purpura annularis telangiectodes), Doucas and Kapetanakis (lymphocytic capillaritis of unknown cause), and lichen aureus. The key to diagnosis in this case is recalling that "the lesions of the benign syndromes rarely assume the morphology and distribution found with mycosis fungoides," Dr. Hinds and Dr. Heald wrote.
Not only is mycosis fungoides difficult to diagnose, but it is especially prevalent among black patients. For instance, a 1988 study looking at Surveillance, Epidemiology, and End Results (SEER) data from 1973 through 1984 found that the incidence among black patients was twice that of white patients: 0.52/100,000 vs. 0.26 (JAMA 1988;260:42-46).
Similarly, in another study of 132 black patients with skin cancer, mycosis fungoides represented 12.1% of all skin neoplasms (Dermatol. Clin. 1988;6:397-405).
Mycosis fungoides is the fourth most common skin cancer among Japanese patients, representing approximately 5% of all skin malignancies in the population.
The incidence of CTCL and its subtypes is only increasing. A 2007 study that extended the SEER data mentioned above from 1973 to 2002 and included all CTCL cases found an incidence rate of 9.0 for black patients, per 1 million person-years, compared with 6.1 for white patients (Arch. Dermatol. 2007;143:854-9).
As in many skin cancers, early diagnosis can make the difference in successful outcomes. So add CTCL, and especially the mycosis fungoides subtype, to your differential when confronting pigmentation disorders in skin of color patients.
Dr. Roberts is past president of the Women’s Dermatologic Society (WDS) as well as past president of the California Society of Dermatology and Dermatologic Surgery (Calderm). She was a founding director of dermatopathology at the Loma Linda University Medical Center (Calif.). She currently runs a private practice in Rancho Mirage, Calif.
She disclosed financial relationships with Allergan, L’Oréal/La Roche Posay, Skin Medica, and Valeant Pharmaceuticals.
Over the past 4 decades, cutaneous T-cell lymphoma diagnoses have been on the rise, especially among black and other skin of color patients. Unfortunately, this form of skin cancer can be a diagnostic challenge.
Regarding diagnosis, cutaneous T-cell lymphoma (CTCL) is the wild card of dermatology; it is a great mimicker of many skin disorders, and can look like almost anything. However, the most striking feature of the condition – and the key to diagnosis in ethnic skin – is its polymorphous pigmentation that is unique to skin of color.
CTCL lesions may be flat or raised, and may mimic other skin disorders associated with pigment change. These can include tinea versicolor, vitiligo, pityriasis rosea, and psoriasis. Lichen planus pigmentosus and progressive macular hypomelanosis are other important CTCL mimickers. Consider all of these conditions in the differential diagnosis.
An excellent resource for photos and descriptions of CTCL, as well as CTCL look-alikes, is an article by Dr. Ginette A. Hinds and Dr. Peter Heald (J. Am. Acad. Dermatol. 2009;60:359-75). The article also highlights the clinical variants within the mycosis fungoides subtype, the most common form of CTCL among blacks.
For example, look out for the "herald patch" of unilesional mycosis fungoides, which takes the form of a single large, dyspigmented patch. According to the authors, this variant has an excellent prognosis, possibly because of an active immune response that limits the initial spread of disease and contributes to preventing relapse.
Another variant is pigmented purpuric mycosis fungoides, which can often be confused with the benign pigmented purpura syndromes of Schamberg’s disease (progressive pigmented purpuric dermatitis), Gougerot-Blum syndrome (pigmented purpuric lichenoid dermatitis), Majocchi’s disease (purpura annularis telangiectodes), Doucas and Kapetanakis (lymphocytic capillaritis of unknown cause), and lichen aureus. The key to diagnosis in this case is recalling that "the lesions of the benign syndromes rarely assume the morphology and distribution found with mycosis fungoides," Dr. Hinds and Dr. Heald wrote.
Not only is mycosis fungoides difficult to diagnose, but it is especially prevalent among black patients. For instance, a 1988 study looking at Surveillance, Epidemiology, and End Results (SEER) data from 1973 through 1984 found that the incidence among black patients was twice that of white patients: 0.52/100,000 vs. 0.26 (JAMA 1988;260:42-46).
Similarly, in another study of 132 black patients with skin cancer, mycosis fungoides represented 12.1% of all skin neoplasms (Dermatol. Clin. 1988;6:397-405).
Mycosis fungoides is the fourth most common skin cancer among Japanese patients, representing approximately 5% of all skin malignancies in the population.
The incidence of CTCL and its subtypes is only increasing. A 2007 study that extended the SEER data mentioned above from 1973 to 2002 and included all CTCL cases found an incidence rate of 9.0 for black patients, per 1 million person-years, compared with 6.1 for white patients (Arch. Dermatol. 2007;143:854-9).
As in many skin cancers, early diagnosis can make the difference in successful outcomes. So add CTCL, and especially the mycosis fungoides subtype, to your differential when confronting pigmentation disorders in skin of color patients.
Dr. Roberts is past president of the Women’s Dermatologic Society (WDS) as well as past president of the California Society of Dermatology and Dermatologic Surgery (Calderm). She was a founding director of dermatopathology at the Loma Linda University Medical Center (Calif.). She currently runs a private practice in Rancho Mirage, Calif.
She disclosed financial relationships with Allergan, L’Oréal/La Roche Posay, Skin Medica, and Valeant Pharmaceuticals.
Aspirin Found to Protect Against Melanoma
RALEIGH, N.C. – Postmenopausal women who used aspirin regularly had a significantly reduced risk of developing melanoma during long-term prospective follow-up, according to a Women’s Health Initiative observational study analysis.
The magnitude of this risk reduction grew with greater duration of aspirin use, reported Christina A. Gamba, a medical student at Stanford (Calif.) University.
During 12 years of prospective follow-up, women who at the time of study enrollment reported they had been taking aspirin regularly for less than a year had roughly an 11% reduction in the likelihood of developing incident melanoma, compared with aspirin nonusers. Those who had been using aspirin regularly for 1-4 years at enrollment went on to have a 20% risk reduction. And women on aspirin for 5 years or longer at enrollment were 30% less likely to develop melanoma than nonusers.
These relative risk figures were fully adjusted for age, education, income, skin type, melanoma risk factors, physical activity, vitamin D intake, smoking status, body mass index, sunburn history, time spent outdoors, sunscreen use, and medical indications for aspirin use, such as cardiovascular disease, she noted.
The findings suggest a possible chemopreventive effect for aspirin against the development of melanoma. As such, these data are consistent with other studies that have linked NSAIDs with decreased risks of breast, colorectal, and gastric cancer. The specific mechanism of benefit is thought to involve inhibition of cyclo-oxygenase-2, which is proinflammatory.
Ms. Gamba explained that her Women’s Health Initiative observational study analysis included 59,806 postmenopausal white women for whom complete pertinent data were available. During nearly 12 years of follow-up, 548 incident melanomas occurred among the study population: 255 were invasive; the rest were in situ.
At enrollment, 25% of women reported using aspirin regularly; their melanoma incidence during follow-up was 0.76%. Fifteen percent of subjects used nonaspirin NSAIDs; their melanoma incidence was 0.97%, which was identical to the rate in the 60% of women who were nonusers of any NSAIDs. Regular users of acetaminophen, a drug that relieves pain but doesn’t inhibit cyclo-oxygenase-2, had the same melanoma incidence as nonusers of aspirin and other NSAIDs.
Three-quarters of the aspirin users were on regular- or extrastrength formulations. There were too few women on low-dose aspirin to be able to draw any conclusions as to whether it, too, protected against melanoma, she said at the annual meeting of the Society of Investigative Dermatology.
The study included one measure of consistency: At 3 years of follow-up, 60% of women who reported taking aspirin regularly at baseline were still doing so, as were 35% of those who had been on nonaspirin NSAIDs at enrollment.
Audience members posed this question: If aspirin’s presumed chemoprevention mechanism involves the inhibition of cyclooxygenase-2, why didn’t users of nonaspirin NSAIDs enjoy a similar benefit? Ms. Gamba offered two possible theories. One is that users of nonaspirin NSAIDs took the medication less frequently, in contrast to aspirin users who generally took the drug on a daily basis.
The other possibility, she continued, is that aspirin curbs tumorigenesis through cyclo-oxygenase-independent mechanisms – perhaps by promoting apoptotic genes and/or inhibiting tumor-promoting genes.
All cases of melanoma in the Women’s Health Initiative were pathologically confirmed. Ms. Gamba and her investigators are now going back and examining the pathology reports to learn what specific types of melanoma were involved. They are also reanalyzing their aspirin/NSAID usage data, this time restricting the analysis to cases of in situ melanoma.
The Women’s Health Initiative Observational Study was sponsored by the National Institutes of Health. Ms. Gamba reported having no relevant financial conflicts.
RALEIGH, N.C. – Postmenopausal women who used aspirin regularly had a significantly reduced risk of developing melanoma during long-term prospective follow-up, according to a Women’s Health Initiative observational study analysis.
The magnitude of this risk reduction grew with greater duration of aspirin use, reported Christina A. Gamba, a medical student at Stanford (Calif.) University.
During 12 years of prospective follow-up, women who at the time of study enrollment reported they had been taking aspirin regularly for less than a year had roughly an 11% reduction in the likelihood of developing incident melanoma, compared with aspirin nonusers. Those who had been using aspirin regularly for 1-4 years at enrollment went on to have a 20% risk reduction. And women on aspirin for 5 years or longer at enrollment were 30% less likely to develop melanoma than nonusers.
These relative risk figures were fully adjusted for age, education, income, skin type, melanoma risk factors, physical activity, vitamin D intake, smoking status, body mass index, sunburn history, time spent outdoors, sunscreen use, and medical indications for aspirin use, such as cardiovascular disease, she noted.
The findings suggest a possible chemopreventive effect for aspirin against the development of melanoma. As such, these data are consistent with other studies that have linked NSAIDs with decreased risks of breast, colorectal, and gastric cancer. The specific mechanism of benefit is thought to involve inhibition of cyclo-oxygenase-2, which is proinflammatory.
Ms. Gamba explained that her Women’s Health Initiative observational study analysis included 59,806 postmenopausal white women for whom complete pertinent data were available. During nearly 12 years of follow-up, 548 incident melanomas occurred among the study population: 255 were invasive; the rest were in situ.
At enrollment, 25% of women reported using aspirin regularly; their melanoma incidence during follow-up was 0.76%. Fifteen percent of subjects used nonaspirin NSAIDs; their melanoma incidence was 0.97%, which was identical to the rate in the 60% of women who were nonusers of any NSAIDs. Regular users of acetaminophen, a drug that relieves pain but doesn’t inhibit cyclo-oxygenase-2, had the same melanoma incidence as nonusers of aspirin and other NSAIDs.
Three-quarters of the aspirin users were on regular- or extrastrength formulations. There were too few women on low-dose aspirin to be able to draw any conclusions as to whether it, too, protected against melanoma, she said at the annual meeting of the Society of Investigative Dermatology.
The study included one measure of consistency: At 3 years of follow-up, 60% of women who reported taking aspirin regularly at baseline were still doing so, as were 35% of those who had been on nonaspirin NSAIDs at enrollment.
Audience members posed this question: If aspirin’s presumed chemoprevention mechanism involves the inhibition of cyclooxygenase-2, why didn’t users of nonaspirin NSAIDs enjoy a similar benefit? Ms. Gamba offered two possible theories. One is that users of nonaspirin NSAIDs took the medication less frequently, in contrast to aspirin users who generally took the drug on a daily basis.
The other possibility, she continued, is that aspirin curbs tumorigenesis through cyclo-oxygenase-independent mechanisms – perhaps by promoting apoptotic genes and/or inhibiting tumor-promoting genes.
All cases of melanoma in the Women’s Health Initiative were pathologically confirmed. Ms. Gamba and her investigators are now going back and examining the pathology reports to learn what specific types of melanoma were involved. They are also reanalyzing their aspirin/NSAID usage data, this time restricting the analysis to cases of in situ melanoma.
The Women’s Health Initiative Observational Study was sponsored by the National Institutes of Health. Ms. Gamba reported having no relevant financial conflicts.
RALEIGH, N.C. – Postmenopausal women who used aspirin regularly had a significantly reduced risk of developing melanoma during long-term prospective follow-up, according to a Women’s Health Initiative observational study analysis.
The magnitude of this risk reduction grew with greater duration of aspirin use, reported Christina A. Gamba, a medical student at Stanford (Calif.) University.
During 12 years of prospective follow-up, women who at the time of study enrollment reported they had been taking aspirin regularly for less than a year had roughly an 11% reduction in the likelihood of developing incident melanoma, compared with aspirin nonusers. Those who had been using aspirin regularly for 1-4 years at enrollment went on to have a 20% risk reduction. And women on aspirin for 5 years or longer at enrollment were 30% less likely to develop melanoma than nonusers.
These relative risk figures were fully adjusted for age, education, income, skin type, melanoma risk factors, physical activity, vitamin D intake, smoking status, body mass index, sunburn history, time spent outdoors, sunscreen use, and medical indications for aspirin use, such as cardiovascular disease, she noted.
The findings suggest a possible chemopreventive effect for aspirin against the development of melanoma. As such, these data are consistent with other studies that have linked NSAIDs with decreased risks of breast, colorectal, and gastric cancer. The specific mechanism of benefit is thought to involve inhibition of cyclo-oxygenase-2, which is proinflammatory.
Ms. Gamba explained that her Women’s Health Initiative observational study analysis included 59,806 postmenopausal white women for whom complete pertinent data were available. During nearly 12 years of follow-up, 548 incident melanomas occurred among the study population: 255 were invasive; the rest were in situ.
At enrollment, 25% of women reported using aspirin regularly; their melanoma incidence during follow-up was 0.76%. Fifteen percent of subjects used nonaspirin NSAIDs; their melanoma incidence was 0.97%, which was identical to the rate in the 60% of women who were nonusers of any NSAIDs. Regular users of acetaminophen, a drug that relieves pain but doesn’t inhibit cyclo-oxygenase-2, had the same melanoma incidence as nonusers of aspirin and other NSAIDs.
Three-quarters of the aspirin users were on regular- or extrastrength formulations. There were too few women on low-dose aspirin to be able to draw any conclusions as to whether it, too, protected against melanoma, she said at the annual meeting of the Society of Investigative Dermatology.
The study included one measure of consistency: At 3 years of follow-up, 60% of women who reported taking aspirin regularly at baseline were still doing so, as were 35% of those who had been on nonaspirin NSAIDs at enrollment.
Audience members posed this question: If aspirin’s presumed chemoprevention mechanism involves the inhibition of cyclooxygenase-2, why didn’t users of nonaspirin NSAIDs enjoy a similar benefit? Ms. Gamba offered two possible theories. One is that users of nonaspirin NSAIDs took the medication less frequently, in contrast to aspirin users who generally took the drug on a daily basis.
The other possibility, she continued, is that aspirin curbs tumorigenesis through cyclo-oxygenase-independent mechanisms – perhaps by promoting apoptotic genes and/or inhibiting tumor-promoting genes.
All cases of melanoma in the Women’s Health Initiative were pathologically confirmed. Ms. Gamba and her investigators are now going back and examining the pathology reports to learn what specific types of melanoma were involved. They are also reanalyzing their aspirin/NSAID usage data, this time restricting the analysis to cases of in situ melanoma.
The Women’s Health Initiative Observational Study was sponsored by the National Institutes of Health. Ms. Gamba reported having no relevant financial conflicts.
FROM THE ANNUAL MEETING OF THE SOCIETY FOR INVESTIGATIVE DERMATOLOGY
Major Finding: Postmenopausal women who reported using aspirin regularly at baseline went on to have an 11%-30% reduction in the risk for developing melanoma, compared with aspirin nonusers.
Data Source: Data were from an analysis of nearly 60,000 postmenopausal white participants in the Women’s Health Initiative observational study.
Disclosures: The Women’s Health Initiative study was funded by the National Institutes of Health. Ms. Gamba reported having no relevant financial conflicts.
Vismodegib Continues to Prove BCC Effectiveness
Two small, early-phase studies found that vismodegib is effective for the treatment of basal cell nevus syndrome and advanced basal cell carcinoma, according to results published June 6 in the New England Journal of Medicine.
Basal cell malignancies are among the most common nonmelanoma skin cancers in the United States, accounting for at least 80% of the 2.1 million cases. It is a highly disfiguring cancer but is only sometimes life threatening. Almost all basal cell carcinomas (BCCs) are caused by alterations in the hedgehog signaling pathway.
Vismodegib (Erivedge) was approved by the Food and Drug Administration in January for treating locally advanced and metastatic BCC. Vismodegib (manufactured by Genentech) is a small molecule inhibitor that steps in to repair the hedgehog pathway.
Study 1: Locally Advanced and Metastatic BCC
In the first study, conducted before vismodegib received FDA approval for locally advanced and metastatic BCC, Dr. Aleksandar Sekulic and colleagues conducted a phase II, nonrandomized, two-cohort trial at multiple sites around the United States and overseas. Vismodegib was given to 33 patients with metastatic BCC and 63 patients with locally advanced disease. Both cohorts had inoperable disease or were not eligible for surgery.
All the patients were treated with 150 mg of oral vismodegib daily. The median age of patients was 62 years and all were white, noted Dr. Sekulic of the Mayo Clinic in Scottsdale, Ariz.
The patients were treated with vismodegib until disease progression, until side effects became intolerable, or until end of study. Patients could stop the drug for up to a month if side effects were intolerable.
There was no standard end point for measuring response in locally advanced BCC when the study was designed. The definition used was a decrease of 30% or more of the externally visible or radiographic dimension or complete resolution of ulceration. Progressive disease was an increase of 20% or more in the externally visible or radiographic dimension, new ulceration, or a new lesion.
The response rate for the metastatic group treated with vismodegib was 30%. All of the responses were partial, defined as an absence of residual BCC in a biopsy specimen. In locally advanced disease, the response rate was 43%. Thirteen of the 63 patients had a complete response. The median duration of response was 7.6 months for metastatic and locally advanced BCC patients (N. Engl. J. Med. 2012;366:2171-9).
Half of the patients stopped the drug early, with 18% of metastatic patients discontinuing because of disease progression. Twenty-five percent of locally advanced patients decided on their own to stop therapy, for unknown reasons, according to the investigators. Adverse events – primarily muscle spasms, weight loss, fatigue, and loss of appetite – took a toll on patients. A quarter reported serious adverse events.
Seven patients died, but the relation to vismodegib is not clear at this point. "The deaths were considered by the site investigator to be unrelated to vismodegib," the investigators wrote.
The locally advanced and metastatic BCC trial was funded by Genentech and was jointly designed by Genetech and Dr. Sekulic. A majority of his colleagues reported being employees and/or receiving grants or financial support from the company.
In an interview, Dr. Ali Hendi, assistant clinical professor of dermatology at Georgetown University Medical Center, Washington, said that he felt the investigators in the study were overly subjective in defining locally advanced tumors. "These are tumors that are aggressive, but that does not make them inoperable in the right hands," said Dr. Hendi, who is also a Mohs surgeon.
He also noted the slim complete response rate, which, when coupled with the toxicity and the high cost of the therapy – which might run as much as $70,000 per treatment course – make it a less desirable therapy for many patients.
"For locally advanced [disease] I think the utility is limited if there is good surgical care available," he said. Vismodegib may be more useful for BCC nevus syndrome and for metastatic disease, where it may be the only therapy available, he added.
Dr. Hendi reported no conflicts.
Study 2: Basal Cell Nevus Syndrome
In a second randomized, double-blind, placebo-controlled trial of 41 patients with basal cell nevus syndrome, Dr. Jean Y. Tang and colleagues found that vismodegib reduced BCC tumors and blocked the development of new BCCs.
Basal cell nevus syndrome is rare, but it causes hundreds or thousands of carcinomas in each patient. There is no therapy, and often patients have to undergo multiple surgeries to remove the tumors.
Patients with the condition have one defective copy of the tumor suppressor gene (PTCH1), which inhibits the hedgehog signaling pathway, noted Dr. Tang of Stanford University (Calif.), and her colleagues.
The study enrolled patients from Sept. 2009 through Jan. 2011, but in Dec. 2010 the data safety and monitoring board decided to end the placebo treatment because the results so highly favored vismodegib. Patients were randomized to placebo or 150 mg daily of the drug for a planned 18 months.
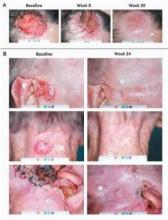
The primary end point was the comparative rate of appearance of new BCCs that were eligible for surgery. Patients were followed for a mean of 8 months. Those who took vismodegib had a much lower rate of surgically eligible disease: 2 vs. 29 cases for placebo. Existing carcinomas shrunk by 65% in vismodegib-treated patients, compared with only 11% for placebo patients. Vismodegib patients also had fewer surgeries than patients receiving placebo: 0.31 per patient compared with 4.4 per patient, respectively.
At 1 month, there was a 90% reduction in hedgehog target-gene expression. There was no residual carcinoma in 83% of the biopsy samples taken from sites where the disease had been judged to be clinically regressed (N. Engl. J. Med. 2012;366:2180-8).
Fifty-four percent of study patients discontinued treatment because of adverse events. Patients treated with vismodegib were more likely to have grade 1 or 2 dysgeusia, muscle cramps, hair loss, and weight loss. They also had more grade 3 or 4 adverse events. The authors said that these side effects were similar to those reported in phase 1 and 2 trials of vismodegib, and also in other studies of therapies that inhibit the hedgehog pathway.
The authors concluded that vismodegib reduces tumor burden and blocks new tumor growth, but whether some of the clinically regressed tumors still harbor residual tumor cells cannot be ruled out – which could explain why there is tumor regrowth after therapy is stopped.
However, the "findings confirm the essential role of the hedgehog pathway in basal cell carcinomas," they wrote.
The trial was funded by Genentech and by grants from the National Institutes of Health, the National Institute of Arthritis and Musculoskeletal and Skin Diseases, the National Cancer Institute, the Swim Across America Foundation, and the Michael J. Rainen Family Foundation. Dr. Tang reported receiving consulting fees from Genentech. Several coauthors of the study reported receiving grants or fees from Genentech.
The two studies show that vismodegib is highly effective. "It is a landmark day for patients with basal cell carcinoma and all those involved in their care – the greatest advance in therapy yet seen for this disease," Dr. John T. Lear wrote in an accompanying editorial.
The response rates were impressive, especially in patients with basal cell nevus syndrome.
"However, the side effects are considerable and frequent, resulting in high rates of drug discontinuation, and these rates will probably be even higher in clinical practice," he said.
Another question raised is whether hedgehog pathway inhibition truly clears the BCC or whether it leaves residual resistant cells that could give rise to a recurrence. Follow-up studies are needed to address this question, Dr. Lear said (N. Engl. J. Med. 2012;366:2225-6).
Intermittent dosing might allow more patients to benefit by preventing new lesions. This would be especially important for BCC nevus syndrome. And for patients with large, symptomatic lesions, "the usefulness of local control in improving quality of life should not be underestimated," he noted.
Dr. Lear is affiliated with the Manchester Academic Health Science Centre at Manchester (England) University and the departments of dermatology at Salford Royal Hospital and Central Manchester National Health Service Foundation Trusts. He has received consulting fees from Novartis for an ongoing BCC study.
The two studies show that vismodegib is highly effective. "It is a landmark day for patients with basal cell carcinoma and all those involved in their care – the greatest advance in therapy yet seen for this disease," Dr. John T. Lear wrote in an accompanying editorial.
The response rates were impressive, especially in patients with basal cell nevus syndrome.
"However, the side effects are considerable and frequent, resulting in high rates of drug discontinuation, and these rates will probably be even higher in clinical practice," he said.
Another question raised is whether hedgehog pathway inhibition truly clears the BCC or whether it leaves residual resistant cells that could give rise to a recurrence. Follow-up studies are needed to address this question, Dr. Lear said (N. Engl. J. Med. 2012;366:2225-6).
Intermittent dosing might allow more patients to benefit by preventing new lesions. This would be especially important for BCC nevus syndrome. And for patients with large, symptomatic lesions, "the usefulness of local control in improving quality of life should not be underestimated," he noted.
Dr. Lear is affiliated with the Manchester Academic Health Science Centre at Manchester (England) University and the departments of dermatology at Salford Royal Hospital and Central Manchester National Health Service Foundation Trusts. He has received consulting fees from Novartis for an ongoing BCC study.
The two studies show that vismodegib is highly effective. "It is a landmark day for patients with basal cell carcinoma and all those involved in their care – the greatest advance in therapy yet seen for this disease," Dr. John T. Lear wrote in an accompanying editorial.
The response rates were impressive, especially in patients with basal cell nevus syndrome.
"However, the side effects are considerable and frequent, resulting in high rates of drug discontinuation, and these rates will probably be even higher in clinical practice," he said.
Another question raised is whether hedgehog pathway inhibition truly clears the BCC or whether it leaves residual resistant cells that could give rise to a recurrence. Follow-up studies are needed to address this question, Dr. Lear said (N. Engl. J. Med. 2012;366:2225-6).
Intermittent dosing might allow more patients to benefit by preventing new lesions. This would be especially important for BCC nevus syndrome. And for patients with large, symptomatic lesions, "the usefulness of local control in improving quality of life should not be underestimated," he noted.
Dr. Lear is affiliated with the Manchester Academic Health Science Centre at Manchester (England) University and the departments of dermatology at Salford Royal Hospital and Central Manchester National Health Service Foundation Trusts. He has received consulting fees from Novartis for an ongoing BCC study.
Two small, early-phase studies found that vismodegib is effective for the treatment of basal cell nevus syndrome and advanced basal cell carcinoma, according to results published June 6 in the New England Journal of Medicine.
Basal cell malignancies are among the most common nonmelanoma skin cancers in the United States, accounting for at least 80% of the 2.1 million cases. It is a highly disfiguring cancer but is only sometimes life threatening. Almost all basal cell carcinomas (BCCs) are caused by alterations in the hedgehog signaling pathway.
Vismodegib (Erivedge) was approved by the Food and Drug Administration in January for treating locally advanced and metastatic BCC. Vismodegib (manufactured by Genentech) is a small molecule inhibitor that steps in to repair the hedgehog pathway.
Study 1: Locally Advanced and Metastatic BCC
In the first study, conducted before vismodegib received FDA approval for locally advanced and metastatic BCC, Dr. Aleksandar Sekulic and colleagues conducted a phase II, nonrandomized, two-cohort trial at multiple sites around the United States and overseas. Vismodegib was given to 33 patients with metastatic BCC and 63 patients with locally advanced disease. Both cohorts had inoperable disease or were not eligible for surgery.
All the patients were treated with 150 mg of oral vismodegib daily. The median age of patients was 62 years and all were white, noted Dr. Sekulic of the Mayo Clinic in Scottsdale, Ariz.
The patients were treated with vismodegib until disease progression, until side effects became intolerable, or until end of study. Patients could stop the drug for up to a month if side effects were intolerable.
There was no standard end point for measuring response in locally advanced BCC when the study was designed. The definition used was a decrease of 30% or more of the externally visible or radiographic dimension or complete resolution of ulceration. Progressive disease was an increase of 20% or more in the externally visible or radiographic dimension, new ulceration, or a new lesion.
The response rate for the metastatic group treated with vismodegib was 30%. All of the responses were partial, defined as an absence of residual BCC in a biopsy specimen. In locally advanced disease, the response rate was 43%. Thirteen of the 63 patients had a complete response. The median duration of response was 7.6 months for metastatic and locally advanced BCC patients (N. Engl. J. Med. 2012;366:2171-9).
Half of the patients stopped the drug early, with 18% of metastatic patients discontinuing because of disease progression. Twenty-five percent of locally advanced patients decided on their own to stop therapy, for unknown reasons, according to the investigators. Adverse events – primarily muscle spasms, weight loss, fatigue, and loss of appetite – took a toll on patients. A quarter reported serious adverse events.
Seven patients died, but the relation to vismodegib is not clear at this point. "The deaths were considered by the site investigator to be unrelated to vismodegib," the investigators wrote.
The locally advanced and metastatic BCC trial was funded by Genentech and was jointly designed by Genetech and Dr. Sekulic. A majority of his colleagues reported being employees and/or receiving grants or financial support from the company.
In an interview, Dr. Ali Hendi, assistant clinical professor of dermatology at Georgetown University Medical Center, Washington, said that he felt the investigators in the study were overly subjective in defining locally advanced tumors. "These are tumors that are aggressive, but that does not make them inoperable in the right hands," said Dr. Hendi, who is also a Mohs surgeon.
He also noted the slim complete response rate, which, when coupled with the toxicity and the high cost of the therapy – which might run as much as $70,000 per treatment course – make it a less desirable therapy for many patients.
"For locally advanced [disease] I think the utility is limited if there is good surgical care available," he said. Vismodegib may be more useful for BCC nevus syndrome and for metastatic disease, where it may be the only therapy available, he added.
Dr. Hendi reported no conflicts.
Study 2: Basal Cell Nevus Syndrome
In a second randomized, double-blind, placebo-controlled trial of 41 patients with basal cell nevus syndrome, Dr. Jean Y. Tang and colleagues found that vismodegib reduced BCC tumors and blocked the development of new BCCs.
Basal cell nevus syndrome is rare, but it causes hundreds or thousands of carcinomas in each patient. There is no therapy, and often patients have to undergo multiple surgeries to remove the tumors.
Patients with the condition have one defective copy of the tumor suppressor gene (PTCH1), which inhibits the hedgehog signaling pathway, noted Dr. Tang of Stanford University (Calif.), and her colleagues.
The study enrolled patients from Sept. 2009 through Jan. 2011, but in Dec. 2010 the data safety and monitoring board decided to end the placebo treatment because the results so highly favored vismodegib. Patients were randomized to placebo or 150 mg daily of the drug for a planned 18 months.
The primary end point was the comparative rate of appearance of new BCCs that were eligible for surgery. Patients were followed for a mean of 8 months. Those who took vismodegib had a much lower rate of surgically eligible disease: 2 vs. 29 cases for placebo. Existing carcinomas shrunk by 65% in vismodegib-treated patients, compared with only 11% for placebo patients. Vismodegib patients also had fewer surgeries than patients receiving placebo: 0.31 per patient compared with 4.4 per patient, respectively.
At 1 month, there was a 90% reduction in hedgehog target-gene expression. There was no residual carcinoma in 83% of the biopsy samples taken from sites where the disease had been judged to be clinically regressed (N. Engl. J. Med. 2012;366:2180-8).
Fifty-four percent of study patients discontinued treatment because of adverse events. Patients treated with vismodegib were more likely to have grade 1 or 2 dysgeusia, muscle cramps, hair loss, and weight loss. They also had more grade 3 or 4 adverse events. The authors said that these side effects were similar to those reported in phase 1 and 2 trials of vismodegib, and also in other studies of therapies that inhibit the hedgehog pathway.
The authors concluded that vismodegib reduces tumor burden and blocks new tumor growth, but whether some of the clinically regressed tumors still harbor residual tumor cells cannot be ruled out – which could explain why there is tumor regrowth after therapy is stopped.
However, the "findings confirm the essential role of the hedgehog pathway in basal cell carcinomas," they wrote.
The trial was funded by Genentech and by grants from the National Institutes of Health, the National Institute of Arthritis and Musculoskeletal and Skin Diseases, the National Cancer Institute, the Swim Across America Foundation, and the Michael J. Rainen Family Foundation. Dr. Tang reported receiving consulting fees from Genentech. Several coauthors of the study reported receiving grants or fees from Genentech.
Two small, early-phase studies found that vismodegib is effective for the treatment of basal cell nevus syndrome and advanced basal cell carcinoma, according to results published June 6 in the New England Journal of Medicine.
Basal cell malignancies are among the most common nonmelanoma skin cancers in the United States, accounting for at least 80% of the 2.1 million cases. It is a highly disfiguring cancer but is only sometimes life threatening. Almost all basal cell carcinomas (BCCs) are caused by alterations in the hedgehog signaling pathway.
Vismodegib (Erivedge) was approved by the Food and Drug Administration in January for treating locally advanced and metastatic BCC. Vismodegib (manufactured by Genentech) is a small molecule inhibitor that steps in to repair the hedgehog pathway.
Study 1: Locally Advanced and Metastatic BCC
In the first study, conducted before vismodegib received FDA approval for locally advanced and metastatic BCC, Dr. Aleksandar Sekulic and colleagues conducted a phase II, nonrandomized, two-cohort trial at multiple sites around the United States and overseas. Vismodegib was given to 33 patients with metastatic BCC and 63 patients with locally advanced disease. Both cohorts had inoperable disease or were not eligible for surgery.
All the patients were treated with 150 mg of oral vismodegib daily. The median age of patients was 62 years and all were white, noted Dr. Sekulic of the Mayo Clinic in Scottsdale, Ariz.
The patients were treated with vismodegib until disease progression, until side effects became intolerable, or until end of study. Patients could stop the drug for up to a month if side effects were intolerable.
There was no standard end point for measuring response in locally advanced BCC when the study was designed. The definition used was a decrease of 30% or more of the externally visible or radiographic dimension or complete resolution of ulceration. Progressive disease was an increase of 20% or more in the externally visible or radiographic dimension, new ulceration, or a new lesion.
The response rate for the metastatic group treated with vismodegib was 30%. All of the responses were partial, defined as an absence of residual BCC in a biopsy specimen. In locally advanced disease, the response rate was 43%. Thirteen of the 63 patients had a complete response. The median duration of response was 7.6 months for metastatic and locally advanced BCC patients (N. Engl. J. Med. 2012;366:2171-9).
Half of the patients stopped the drug early, with 18% of metastatic patients discontinuing because of disease progression. Twenty-five percent of locally advanced patients decided on their own to stop therapy, for unknown reasons, according to the investigators. Adverse events – primarily muscle spasms, weight loss, fatigue, and loss of appetite – took a toll on patients. A quarter reported serious adverse events.
Seven patients died, but the relation to vismodegib is not clear at this point. "The deaths were considered by the site investigator to be unrelated to vismodegib," the investigators wrote.
The locally advanced and metastatic BCC trial was funded by Genentech and was jointly designed by Genetech and Dr. Sekulic. A majority of his colleagues reported being employees and/or receiving grants or financial support from the company.
In an interview, Dr. Ali Hendi, assistant clinical professor of dermatology at Georgetown University Medical Center, Washington, said that he felt the investigators in the study were overly subjective in defining locally advanced tumors. "These are tumors that are aggressive, but that does not make them inoperable in the right hands," said Dr. Hendi, who is also a Mohs surgeon.
He also noted the slim complete response rate, which, when coupled with the toxicity and the high cost of the therapy – which might run as much as $70,000 per treatment course – make it a less desirable therapy for many patients.
"For locally advanced [disease] I think the utility is limited if there is good surgical care available," he said. Vismodegib may be more useful for BCC nevus syndrome and for metastatic disease, where it may be the only therapy available, he added.
Dr. Hendi reported no conflicts.
Study 2: Basal Cell Nevus Syndrome
In a second randomized, double-blind, placebo-controlled trial of 41 patients with basal cell nevus syndrome, Dr. Jean Y. Tang and colleagues found that vismodegib reduced BCC tumors and blocked the development of new BCCs.
Basal cell nevus syndrome is rare, but it causes hundreds or thousands of carcinomas in each patient. There is no therapy, and often patients have to undergo multiple surgeries to remove the tumors.
Patients with the condition have one defective copy of the tumor suppressor gene (PTCH1), which inhibits the hedgehog signaling pathway, noted Dr. Tang of Stanford University (Calif.), and her colleagues.
The study enrolled patients from Sept. 2009 through Jan. 2011, but in Dec. 2010 the data safety and monitoring board decided to end the placebo treatment because the results so highly favored vismodegib. Patients were randomized to placebo or 150 mg daily of the drug for a planned 18 months.
The primary end point was the comparative rate of appearance of new BCCs that were eligible for surgery. Patients were followed for a mean of 8 months. Those who took vismodegib had a much lower rate of surgically eligible disease: 2 vs. 29 cases for placebo. Existing carcinomas shrunk by 65% in vismodegib-treated patients, compared with only 11% for placebo patients. Vismodegib patients also had fewer surgeries than patients receiving placebo: 0.31 per patient compared with 4.4 per patient, respectively.
At 1 month, there was a 90% reduction in hedgehog target-gene expression. There was no residual carcinoma in 83% of the biopsy samples taken from sites where the disease had been judged to be clinically regressed (N. Engl. J. Med. 2012;366:2180-8).
Fifty-four percent of study patients discontinued treatment because of adverse events. Patients treated with vismodegib were more likely to have grade 1 or 2 dysgeusia, muscle cramps, hair loss, and weight loss. They also had more grade 3 or 4 adverse events. The authors said that these side effects were similar to those reported in phase 1 and 2 trials of vismodegib, and also in other studies of therapies that inhibit the hedgehog pathway.
The authors concluded that vismodegib reduces tumor burden and blocks new tumor growth, but whether some of the clinically regressed tumors still harbor residual tumor cells cannot be ruled out – which could explain why there is tumor regrowth after therapy is stopped.
However, the "findings confirm the essential role of the hedgehog pathway in basal cell carcinomas," they wrote.
The trial was funded by Genentech and by grants from the National Institutes of Health, the National Institute of Arthritis and Musculoskeletal and Skin Diseases, the National Cancer Institute, the Swim Across America Foundation, and the Michael J. Rainen Family Foundation. Dr. Tang reported receiving consulting fees from Genentech. Several coauthors of the study reported receiving grants or fees from Genentech.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: In the first trial, the response rate for vismodegib-treated patients was 30% for the metastatic group and 43% for the locally advanced BCC group. In the basal cell nevus syndrome trial, vismodegib-treated patients had a lower rate of surgically eligible disease: 2 cases vs. 29 cases for placebo.
Data Source: In the first trial, the data came from a nonrandomized, dual-cohort, multicenter, phase II trial of 96 patients. The data for the second trial came from a randomized, placebo-controlled study of 41 patients.
Disclosures: The locally advanced and metastatic BCC trial was funded by Genentech and was jointly designed by Genentech and Dr. Sekulic. A majority of his colleagues reported being employees and/or receiving grants or financial support from the company. The basal cell nevus syndrome trial was funded by Genentech and by grants from the National Institutes of Health, the National Institute of Arthritis and Musculoskeletal and Skin Diseases, the National Cancer Institute, the Swim Across America Foundation, and the Michael J. Rainen Family Foundation. Dr. Tang reported receiving consulting fees from Genentech. Several coauthors of the study reported receiving grants or fees from Genentech.
Stanford Experience Shows Long Metastatic BCC Survival
RALEIGH, N.C. – The prognosis for patients with metastatic basal cell carcinoma may be better than previous reports have suggested, according to Christina Danial.
A single-center case series found a median overall survival of 7.8 years from diagnosis of BCC metastasis to all-cause mortality, which was significantly better than the 10- to 14-month overall survival described in meta-analyses of roughly 300 case reports of metastatic BCC published since the 1890s, noted Ms. Danial, a medical student at Stanford (Calif.) University.
The Stanford series involved 17 patients with metastatic BCC treated there from 1998 to 2011. Although 17 patients may not sound like a lot, it is in fact the largest single-center experience ever reported – a fact that’s testimony to the rarity of metastatic BCC. The BCC metastasis rate has been estimated at 0.003%-0.55%, Ms. Danial said.
The mean overall survival from the date of diagnosis of the primary tumor to death from any cause was 15.96 years. The mean progression-free survival from diagnosis of the metastasis to disease progression based on physician assessment or radiologic findings was 2.4 years.
The most important predictor of metastasis identified by Ms. Danial and her coinvestigators was having a primary tumor of the basosquamous histologic subtype. This was associated with a 6.5-fold increased risk of metastasis.
Eleven patients experienced metastasis to the lung. The second most common site was bone, in eight patients. All metastases were pathologically confirmed by tissue diagnosis.
The explanation for the markedly better overall survival in the Stanford series than in earlier reports is unclear. Improvements in treatment are one possibility. Another is that reporting bias may have been a factor in previous reports, with more aggressive cases of metastatic BCC having a greater likelihood of being published. Yet another possibility is that patients who are referred to Stanford for treatment are in better overall health than those featured in prior case reports, since they are able to travel to the academic medical center, Ms. Danial noted.
None of the various forms of chemotherapy, surgery, and radiation treatment utilized in Stanford patients with metastatic BCC was associated with a significant increase in overall survival. That being said, it’s too soon to know whether the Stanford patients involved in a clinical trial of vismodegib (Erivedge), the novel Hedgehog signaling pathway inhibitor, will experience a significant survival advantage over those who didn’t receive the drug.
The Stanford series presented by Ms. Danial also included 32 patients with locally advanced BCC. Their mean overall survival from the time of diagnosis of the primary tumor was 10.1 years. The primary tumor was located on the head or neck in 22 of the 32 patients, as was the case in 8 of 17 patients with metastatic BCC.
Ms. Danial reported having no relevant financial conflicts.
RALEIGH, N.C. – The prognosis for patients with metastatic basal cell carcinoma may be better than previous reports have suggested, according to Christina Danial.
A single-center case series found a median overall survival of 7.8 years from diagnosis of BCC metastasis to all-cause mortality, which was significantly better than the 10- to 14-month overall survival described in meta-analyses of roughly 300 case reports of metastatic BCC published since the 1890s, noted Ms. Danial, a medical student at Stanford (Calif.) University.
The Stanford series involved 17 patients with metastatic BCC treated there from 1998 to 2011. Although 17 patients may not sound like a lot, it is in fact the largest single-center experience ever reported – a fact that’s testimony to the rarity of metastatic BCC. The BCC metastasis rate has been estimated at 0.003%-0.55%, Ms. Danial said.
The mean overall survival from the date of diagnosis of the primary tumor to death from any cause was 15.96 years. The mean progression-free survival from diagnosis of the metastasis to disease progression based on physician assessment or radiologic findings was 2.4 years.
The most important predictor of metastasis identified by Ms. Danial and her coinvestigators was having a primary tumor of the basosquamous histologic subtype. This was associated with a 6.5-fold increased risk of metastasis.
Eleven patients experienced metastasis to the lung. The second most common site was bone, in eight patients. All metastases were pathologically confirmed by tissue diagnosis.
The explanation for the markedly better overall survival in the Stanford series than in earlier reports is unclear. Improvements in treatment are one possibility. Another is that reporting bias may have been a factor in previous reports, with more aggressive cases of metastatic BCC having a greater likelihood of being published. Yet another possibility is that patients who are referred to Stanford for treatment are in better overall health than those featured in prior case reports, since they are able to travel to the academic medical center, Ms. Danial noted.
None of the various forms of chemotherapy, surgery, and radiation treatment utilized in Stanford patients with metastatic BCC was associated with a significant increase in overall survival. That being said, it’s too soon to know whether the Stanford patients involved in a clinical trial of vismodegib (Erivedge), the novel Hedgehog signaling pathway inhibitor, will experience a significant survival advantage over those who didn’t receive the drug.
The Stanford series presented by Ms. Danial also included 32 patients with locally advanced BCC. Their mean overall survival from the time of diagnosis of the primary tumor was 10.1 years. The primary tumor was located on the head or neck in 22 of the 32 patients, as was the case in 8 of 17 patients with metastatic BCC.
Ms. Danial reported having no relevant financial conflicts.
RALEIGH, N.C. – The prognosis for patients with metastatic basal cell carcinoma may be better than previous reports have suggested, according to Christina Danial.
A single-center case series found a median overall survival of 7.8 years from diagnosis of BCC metastasis to all-cause mortality, which was significantly better than the 10- to 14-month overall survival described in meta-analyses of roughly 300 case reports of metastatic BCC published since the 1890s, noted Ms. Danial, a medical student at Stanford (Calif.) University.
The Stanford series involved 17 patients with metastatic BCC treated there from 1998 to 2011. Although 17 patients may not sound like a lot, it is in fact the largest single-center experience ever reported – a fact that’s testimony to the rarity of metastatic BCC. The BCC metastasis rate has been estimated at 0.003%-0.55%, Ms. Danial said.
The mean overall survival from the date of diagnosis of the primary tumor to death from any cause was 15.96 years. The mean progression-free survival from diagnosis of the metastasis to disease progression based on physician assessment or radiologic findings was 2.4 years.
The most important predictor of metastasis identified by Ms. Danial and her coinvestigators was having a primary tumor of the basosquamous histologic subtype. This was associated with a 6.5-fold increased risk of metastasis.
Eleven patients experienced metastasis to the lung. The second most common site was bone, in eight patients. All metastases were pathologically confirmed by tissue diagnosis.
The explanation for the markedly better overall survival in the Stanford series than in earlier reports is unclear. Improvements in treatment are one possibility. Another is that reporting bias may have been a factor in previous reports, with more aggressive cases of metastatic BCC having a greater likelihood of being published. Yet another possibility is that patients who are referred to Stanford for treatment are in better overall health than those featured in prior case reports, since they are able to travel to the academic medical center, Ms. Danial noted.
None of the various forms of chemotherapy, surgery, and radiation treatment utilized in Stanford patients with metastatic BCC was associated with a significant increase in overall survival. That being said, it’s too soon to know whether the Stanford patients involved in a clinical trial of vismodegib (Erivedge), the novel Hedgehog signaling pathway inhibitor, will experience a significant survival advantage over those who didn’t receive the drug.
The Stanford series presented by Ms. Danial also included 32 patients with locally advanced BCC. Their mean overall survival from the time of diagnosis of the primary tumor was 10.1 years. The primary tumor was located on the head or neck in 22 of the 32 patients, as was the case in 8 of 17 patients with metastatic BCC.
Ms. Danial reported having no relevant financial conflicts.
FROM THE ANNUAL MEETING OF THE SOCIETY FOR INVESTIGATIVE DERMATOLOGY
Major Finding: The median overall survival from the time of diagnosis of metastatic basal cell carcinoma was 7.8 years in a single-center series, compared with 10-14 months reported in prior studies.
Data Source: Data came from a series of 17 cases of metastatic basal cell carcinoma managed at Stanford University from1998 to 2011.
Disclosures: Ms. Danial reported having no relevant financial conflicts.
60 Years and Counting: A Celebration of Dermatologic Surgery
It was questionable whether in 1952, when Dr. Norman Orentreich performed the first hair transplant and Dr. George Mackee reported on his 50-year experience with phenol chemical peels, anyone envisioned how far the field of dermatologic surgery would advance, but there’s no question now: The specialty has come a long way.
"Dermatologic surgery has blossomed into a full and diverse specialty with many elements," Dr. C. William Hanke noted in the June issue of Seminars in Cutaneous Medicine and Surgery (2012;31:52-9). He highlighted key events that shaped the burgeoning specialty.
Historical Highlights
From the first report on phenol peels by Dr. Mackee (Br. J. Dermatol. 1952;64:456-9), to the coining of the term "tumescent local anesthesia" by Dr. Hanke and his colleagues in 1998 – and publication of a comprehensive text on the tumescent technique 2 years later by Dr. Jeffery A. Klein ("Tumescent Technique: Tumescent Anesthesia and Microcannular Liposuction," St. Louis, Mosby, 2000) – Dr. Hanke chronicled the specialty’s evolution.
For example, he noted that in 1961, Dr. Leon Goldman became the first physician to treat patients with lasers. "He is acknowledged as the father of lasers in medicine and surgery," Dr. Hanke, a dermatologist in private practice in Carmel, Indiana, wrote. He added that the pioneer's first medicinal use of a laser launched 3 decades of related leadership, practice, and research.
Among other events that stand out in the history of the specialty, according to Dr. Hanke, are the first reports on cryosurgery with liquid nitrogen in 1966 by Dr. Setrag Zacarian ("Cryosurgery of Skin Cancer and Cutaneous Disorders," Mosby, St. Louis, 1985), and on ambulatory phlebectomy by Dr. Robert Muller the same year (Phlebologie 1966;19:227-9).
And, in 1967, Dr. Frederic E. Mohs founded the American College of Chemosurgery, which is today known as the American College of Mohs Surgery. "Mohs surgery continues to be an important part of the dermatologic surgery curriculum," Dr. Hanke said.
Advancements in vein ablation took pace in 1982 when the first report on hypertonic saline injections for treating leg veins, by Bruce Chrisman, was published (Hawaii Med. J. 1982;41:406-8).
In 1986, Dr. Saul Asken published the "Manual of Liposuction Surgery and Autologous Fat Transplantation Under Local Anesthesia" (Terry and Associates, Irvine, Calif.), and the following year, Dr. Jeffery A. Klein published the first report on the tumescent technique for liposuction (Am. J. Cosm. Surg. 1987;4:263-7).
Dr. Alastair Carruthers and Dr. Jean Carruthers revolutionized the field in 1987 when they began using botulinum toxin for cosmetic purposes. "Their joint observation that botulinum toxin can affect the muscles of facial expression began a revolution in cosmetic dermatology," wrote Dr. Hanke.
He also highlighted the launch of numerous societies and publications that helped to advance the specialty, including the founding of the American Society for Dermatologic Surgery in 1970, the launch of the Journal of Dermatologic Surgery in 1975, and the founding of the American Society for Lasers in Medicine and Surgery in 1981. And the specialty has continued to evolve at a rapid pace since that time, he noted.
Work by Dr. R. Rox Anderson and Dr. John A. Parrish on selective photothermolysis, for example, launched research leading to the fractionated laser technology in use today; and ongoing work by the Carruthers on botulinum toxin launched a new era in noninvasive facial rejuvenation, he said.
"Facelift bypass" procedures have satisfied many patients without subjecting them to the expense or morbidity of extensive facial surgery, Dr. Hanke noted, adding that new filler materials can be placed in the subcutaneous or supraperiosteal planes of the face with good results and minimal complications.
"A newly approved hyaluronic acid from Germany will allow treatment of very superficial wrinkles without the risk of the 'Tyndall effect,' " he added.
Also in the last decade, dermatologic surgery-related educational initiatives have been advanced. In 2004, 1-year fellowship training programs were approved by the Accreditation Council for Graduate Medical Education for training in dermatologic surgery; and last year, there were 47 ACGME-accredited procedural dermatology fellowship training programs in place, he said.
"Dermatologic surgery is an important component of nearly all dermatology postgraduate courses," added Dr. Hanke.
The history of fractional laser technology and fillers were addressed in separate articles in the same issue of Seminars in Cutaneous Medicine and Surgery, underscoring the importance of the two recent developments.
Fillers
The next phase of development in injectable fillers has begun, according to Dr. Richard G. Glogau.
"The concept of augmentation has moved from simple lines, scars, and wrinkles to revolumizing the aging face," noted Dr. Glogau, a clinical professor of dermatology at the University of California, San Francisco. "While seeking extended duration of effect balanced against the safety profile of the injectable, our focus is now directed to extending the lifting or volumizing effect that one can achieve with these fillers."
The initial movement into 3-dimensional correction with injectable fillers began with the dramatic improvement seen in lip volume championed in the 1980s, and each of a litany of fillers that followed, including fat, collagen, silicone, hyaluronic acids, poly-l-lactic acids, calcium hydroxylapatite, and polymethylmethacrylate (Sem. Cut. Med. Surg. 2012;31:78-87).
New fillers, some which represent refinements of existing technologies, continue to undergo review. Aquamid a biocompatible, nonabsorbable, permanent injectable hydrogel implant is currently under review by the Food and Drug Administration and is approved for use in Europe.
It is also possible that fillers will move beyond the traditional concept of inert medical devices and into the realm of true biologics – "materials that will improve the texture, elasticity, radiance, and possibly color, of the skin itself," he added.
"Just as the last 40 years has seen the movement from 2 to 3 dimensions, the next 2 decades will see movement form the macro to the micro level, and fillers will become systems for active metabolic manipulation and protection of the aging skin," he concluded.
Fractionation
The development of fractional photothermolysis was "a milestone in the history of laser technology and cutaneous resurfacing," according to Dr. Nazanin Saedi, a dermatologist in private practice in Chestnut Hill, Mass., and her colleagues.
The technology, noted the study authors, builds on the knowledge gained from early CO2 and Er:YAG laser treatment experiences, achieving greater optimization of parameters to induce the types of benefits seen with CO2 resurfacing, but without the significant postoperative morbidity, complications, and discomfort associated with the earlier technologies.
Furthermore, the older therapies destroyed the barrier protection, which "significantly increased the risk of infection throughout the recovery period and required extensive home care. The risk of scarring, delayed-onset permanent hypopigmentation, and demarcation lines was significant even in the hands of an experienced operator," they wrote (Sem. Cut. Med. Surg. 2012;31:105-9).
In an en effort to overcome these problems, what followed was nonablative dermal remodeling (with less than impressive results), and ultimately, the "idea of fractionated laser technology," they continued.
First used in hair transplant surgery, the technology led to development of the 1,550-nm nonablative "Fraxel" laser (now called the Fraxel Re:Store by Solta Medical), which debuted in the literature in 2004. This and other fractional laser technologies are now used to treat photoaging, superficial and deep rhytids, scars (including in patients with darker skin types), and pigmentation.
Both nonablative and ablative fractional resurfacing have proved to be safer than have traditional ablative lasers, Dr. Saedi and her colleagues noted. However, complications can still occur, such as infections (with herpes simplex virus being the most common), acneiform eruptions, prolonged erythema, pigmentary alteration, and scarring (rare, but can also result from infection associated with treatment).
"Counterintuitively, nonablative or ablative fractionated devices at low energies and densities can be useful in the treatment of scarring, including hypertrophic scars" as previously mentioned, they noted.
"While [fractional lasers are] inherently safer due to the pixelated manner of the treatment, complications can be further prevented with attentive surgical technique and judicious use of prophylaxis," they wrote.
The future of fractional laser technology promises to hold exciting developments. For example, since ablative fractional resurfacing creates microscopic vertical holes in tissue, the delivery of topical drugs through these holes is possible. In animal models, the photosensitizer methylaminolevulinic acid has been delivered using this approach, and tests suggest that low density treatment would be sufficient for deep dermal drug delivery.
"Treatment of skin in a porcine model showed enhanced depth of photodynamic therapy following porphyrin application after pretreatment with fractional resurfacing. An in vitro study utilizing low fluence fractionated Erbium:YAG demonstrated upwards of a 125-fold increase in imiquimod delivery," they noted.
Trials in humans are underway to assess the feasibility and safety of enhanced drug delivery using this approach, and there is speculation that ultimately, it could be used for delivery of biologic peptides and vaccines.
Tattoo removal is another promising use for fractional lasers, with early studies demonstrating good results, noted Dr. Saedi and her colleagues, explaining that ablative fractional lasers, when used in conjunction with a Q-switched laser, appear to provide enhanced tattoo removal capabilities.
"With new devices and wavelengths, the applications of this technology continue to grow," they wrote, concluding that "the future remains bright for fractionated laser devices."
Likewise, the future of dermatologic surgery in general remains promising, Dr. Hanke said. "Many new procedures and advances lie ahead."
Neither Dr. Hanke nor Dr. Saedi had disclosures to report. Another author on the article by Dr. Saedi (Dr. Christopher Zachary) reported receiving an honorarium from Solta Medical.
It was questionable whether in 1952, when Dr. Norman Orentreich performed the first hair transplant and Dr. George Mackee reported on his 50-year experience with phenol chemical peels, anyone envisioned how far the field of dermatologic surgery would advance, but there’s no question now: The specialty has come a long way.
"Dermatologic surgery has blossomed into a full and diverse specialty with many elements," Dr. C. William Hanke noted in the June issue of Seminars in Cutaneous Medicine and Surgery (2012;31:52-9). He highlighted key events that shaped the burgeoning specialty.
Historical Highlights
From the first report on phenol peels by Dr. Mackee (Br. J. Dermatol. 1952;64:456-9), to the coining of the term "tumescent local anesthesia" by Dr. Hanke and his colleagues in 1998 – and publication of a comprehensive text on the tumescent technique 2 years later by Dr. Jeffery A. Klein ("Tumescent Technique: Tumescent Anesthesia and Microcannular Liposuction," St. Louis, Mosby, 2000) – Dr. Hanke chronicled the specialty’s evolution.
For example, he noted that in 1961, Dr. Leon Goldman became the first physician to treat patients with lasers. "He is acknowledged as the father of lasers in medicine and surgery," Dr. Hanke, a dermatologist in private practice in Carmel, Indiana, wrote. He added that the pioneer's first medicinal use of a laser launched 3 decades of related leadership, practice, and research.
Among other events that stand out in the history of the specialty, according to Dr. Hanke, are the first reports on cryosurgery with liquid nitrogen in 1966 by Dr. Setrag Zacarian ("Cryosurgery of Skin Cancer and Cutaneous Disorders," Mosby, St. Louis, 1985), and on ambulatory phlebectomy by Dr. Robert Muller the same year (Phlebologie 1966;19:227-9).
And, in 1967, Dr. Frederic E. Mohs founded the American College of Chemosurgery, which is today known as the American College of Mohs Surgery. "Mohs surgery continues to be an important part of the dermatologic surgery curriculum," Dr. Hanke said.
Advancements in vein ablation took pace in 1982 when the first report on hypertonic saline injections for treating leg veins, by Bruce Chrisman, was published (Hawaii Med. J. 1982;41:406-8).
In 1986, Dr. Saul Asken published the "Manual of Liposuction Surgery and Autologous Fat Transplantation Under Local Anesthesia" (Terry and Associates, Irvine, Calif.), and the following year, Dr. Jeffery A. Klein published the first report on the tumescent technique for liposuction (Am. J. Cosm. Surg. 1987;4:263-7).
Dr. Alastair Carruthers and Dr. Jean Carruthers revolutionized the field in 1987 when they began using botulinum toxin for cosmetic purposes. "Their joint observation that botulinum toxin can affect the muscles of facial expression began a revolution in cosmetic dermatology," wrote Dr. Hanke.
He also highlighted the launch of numerous societies and publications that helped to advance the specialty, including the founding of the American Society for Dermatologic Surgery in 1970, the launch of the Journal of Dermatologic Surgery in 1975, and the founding of the American Society for Lasers in Medicine and Surgery in 1981. And the specialty has continued to evolve at a rapid pace since that time, he noted.
Work by Dr. R. Rox Anderson and Dr. John A. Parrish on selective photothermolysis, for example, launched research leading to the fractionated laser technology in use today; and ongoing work by the Carruthers on botulinum toxin launched a new era in noninvasive facial rejuvenation, he said.
"Facelift bypass" procedures have satisfied many patients without subjecting them to the expense or morbidity of extensive facial surgery, Dr. Hanke noted, adding that new filler materials can be placed in the subcutaneous or supraperiosteal planes of the face with good results and minimal complications.
"A newly approved hyaluronic acid from Germany will allow treatment of very superficial wrinkles without the risk of the 'Tyndall effect,' " he added.
Also in the last decade, dermatologic surgery-related educational initiatives have been advanced. In 2004, 1-year fellowship training programs were approved by the Accreditation Council for Graduate Medical Education for training in dermatologic surgery; and last year, there were 47 ACGME-accredited procedural dermatology fellowship training programs in place, he said.
"Dermatologic surgery is an important component of nearly all dermatology postgraduate courses," added Dr. Hanke.
The history of fractional laser technology and fillers were addressed in separate articles in the same issue of Seminars in Cutaneous Medicine and Surgery, underscoring the importance of the two recent developments.
Fillers
The next phase of development in injectable fillers has begun, according to Dr. Richard G. Glogau.
"The concept of augmentation has moved from simple lines, scars, and wrinkles to revolumizing the aging face," noted Dr. Glogau, a clinical professor of dermatology at the University of California, San Francisco. "While seeking extended duration of effect balanced against the safety profile of the injectable, our focus is now directed to extending the lifting or volumizing effect that one can achieve with these fillers."
The initial movement into 3-dimensional correction with injectable fillers began with the dramatic improvement seen in lip volume championed in the 1980s, and each of a litany of fillers that followed, including fat, collagen, silicone, hyaluronic acids, poly-l-lactic acids, calcium hydroxylapatite, and polymethylmethacrylate (Sem. Cut. Med. Surg. 2012;31:78-87).
New fillers, some which represent refinements of existing technologies, continue to undergo review. Aquamid a biocompatible, nonabsorbable, permanent injectable hydrogel implant is currently under review by the Food and Drug Administration and is approved for use in Europe.
It is also possible that fillers will move beyond the traditional concept of inert medical devices and into the realm of true biologics – "materials that will improve the texture, elasticity, radiance, and possibly color, of the skin itself," he added.
"Just as the last 40 years has seen the movement from 2 to 3 dimensions, the next 2 decades will see movement form the macro to the micro level, and fillers will become systems for active metabolic manipulation and protection of the aging skin," he concluded.
Fractionation
The development of fractional photothermolysis was "a milestone in the history of laser technology and cutaneous resurfacing," according to Dr. Nazanin Saedi, a dermatologist in private practice in Chestnut Hill, Mass., and her colleagues.
The technology, noted the study authors, builds on the knowledge gained from early CO2 and Er:YAG laser treatment experiences, achieving greater optimization of parameters to induce the types of benefits seen with CO2 resurfacing, but without the significant postoperative morbidity, complications, and discomfort associated with the earlier technologies.
Furthermore, the older therapies destroyed the barrier protection, which "significantly increased the risk of infection throughout the recovery period and required extensive home care. The risk of scarring, delayed-onset permanent hypopigmentation, and demarcation lines was significant even in the hands of an experienced operator," they wrote (Sem. Cut. Med. Surg. 2012;31:105-9).
In an en effort to overcome these problems, what followed was nonablative dermal remodeling (with less than impressive results), and ultimately, the "idea of fractionated laser technology," they continued.
First used in hair transplant surgery, the technology led to development of the 1,550-nm nonablative "Fraxel" laser (now called the Fraxel Re:Store by Solta Medical), which debuted in the literature in 2004. This and other fractional laser technologies are now used to treat photoaging, superficial and deep rhytids, scars (including in patients with darker skin types), and pigmentation.
Both nonablative and ablative fractional resurfacing have proved to be safer than have traditional ablative lasers, Dr. Saedi and her colleagues noted. However, complications can still occur, such as infections (with herpes simplex virus being the most common), acneiform eruptions, prolonged erythema, pigmentary alteration, and scarring (rare, but can also result from infection associated with treatment).
"Counterintuitively, nonablative or ablative fractionated devices at low energies and densities can be useful in the treatment of scarring, including hypertrophic scars" as previously mentioned, they noted.
"While [fractional lasers are] inherently safer due to the pixelated manner of the treatment, complications can be further prevented with attentive surgical technique and judicious use of prophylaxis," they wrote.
The future of fractional laser technology promises to hold exciting developments. For example, since ablative fractional resurfacing creates microscopic vertical holes in tissue, the delivery of topical drugs through these holes is possible. In animal models, the photosensitizer methylaminolevulinic acid has been delivered using this approach, and tests suggest that low density treatment would be sufficient for deep dermal drug delivery.
"Treatment of skin in a porcine model showed enhanced depth of photodynamic therapy following porphyrin application after pretreatment with fractional resurfacing. An in vitro study utilizing low fluence fractionated Erbium:YAG demonstrated upwards of a 125-fold increase in imiquimod delivery," they noted.
Trials in humans are underway to assess the feasibility and safety of enhanced drug delivery using this approach, and there is speculation that ultimately, it could be used for delivery of biologic peptides and vaccines.
Tattoo removal is another promising use for fractional lasers, with early studies demonstrating good results, noted Dr. Saedi and her colleagues, explaining that ablative fractional lasers, when used in conjunction with a Q-switched laser, appear to provide enhanced tattoo removal capabilities.
"With new devices and wavelengths, the applications of this technology continue to grow," they wrote, concluding that "the future remains bright for fractionated laser devices."
Likewise, the future of dermatologic surgery in general remains promising, Dr. Hanke said. "Many new procedures and advances lie ahead."
Neither Dr. Hanke nor Dr. Saedi had disclosures to report. Another author on the article by Dr. Saedi (Dr. Christopher Zachary) reported receiving an honorarium from Solta Medical.
It was questionable whether in 1952, when Dr. Norman Orentreich performed the first hair transplant and Dr. George Mackee reported on his 50-year experience with phenol chemical peels, anyone envisioned how far the field of dermatologic surgery would advance, but there’s no question now: The specialty has come a long way.
"Dermatologic surgery has blossomed into a full and diverse specialty with many elements," Dr. C. William Hanke noted in the June issue of Seminars in Cutaneous Medicine and Surgery (2012;31:52-9). He highlighted key events that shaped the burgeoning specialty.
Historical Highlights
From the first report on phenol peels by Dr. Mackee (Br. J. Dermatol. 1952;64:456-9), to the coining of the term "tumescent local anesthesia" by Dr. Hanke and his colleagues in 1998 – and publication of a comprehensive text on the tumescent technique 2 years later by Dr. Jeffery A. Klein ("Tumescent Technique: Tumescent Anesthesia and Microcannular Liposuction," St. Louis, Mosby, 2000) – Dr. Hanke chronicled the specialty’s evolution.
For example, he noted that in 1961, Dr. Leon Goldman became the first physician to treat patients with lasers. "He is acknowledged as the father of lasers in medicine and surgery," Dr. Hanke, a dermatologist in private practice in Carmel, Indiana, wrote. He added that the pioneer's first medicinal use of a laser launched 3 decades of related leadership, practice, and research.
Among other events that stand out in the history of the specialty, according to Dr. Hanke, are the first reports on cryosurgery with liquid nitrogen in 1966 by Dr. Setrag Zacarian ("Cryosurgery of Skin Cancer and Cutaneous Disorders," Mosby, St. Louis, 1985), and on ambulatory phlebectomy by Dr. Robert Muller the same year (Phlebologie 1966;19:227-9).
And, in 1967, Dr. Frederic E. Mohs founded the American College of Chemosurgery, which is today known as the American College of Mohs Surgery. "Mohs surgery continues to be an important part of the dermatologic surgery curriculum," Dr. Hanke said.
Advancements in vein ablation took pace in 1982 when the first report on hypertonic saline injections for treating leg veins, by Bruce Chrisman, was published (Hawaii Med. J. 1982;41:406-8).
In 1986, Dr. Saul Asken published the "Manual of Liposuction Surgery and Autologous Fat Transplantation Under Local Anesthesia" (Terry and Associates, Irvine, Calif.), and the following year, Dr. Jeffery A. Klein published the first report on the tumescent technique for liposuction (Am. J. Cosm. Surg. 1987;4:263-7).
Dr. Alastair Carruthers and Dr. Jean Carruthers revolutionized the field in 1987 when they began using botulinum toxin for cosmetic purposes. "Their joint observation that botulinum toxin can affect the muscles of facial expression began a revolution in cosmetic dermatology," wrote Dr. Hanke.
He also highlighted the launch of numerous societies and publications that helped to advance the specialty, including the founding of the American Society for Dermatologic Surgery in 1970, the launch of the Journal of Dermatologic Surgery in 1975, and the founding of the American Society for Lasers in Medicine and Surgery in 1981. And the specialty has continued to evolve at a rapid pace since that time, he noted.
Work by Dr. R. Rox Anderson and Dr. John A. Parrish on selective photothermolysis, for example, launched research leading to the fractionated laser technology in use today; and ongoing work by the Carruthers on botulinum toxin launched a new era in noninvasive facial rejuvenation, he said.
"Facelift bypass" procedures have satisfied many patients without subjecting them to the expense or morbidity of extensive facial surgery, Dr. Hanke noted, adding that new filler materials can be placed in the subcutaneous or supraperiosteal planes of the face with good results and minimal complications.
"A newly approved hyaluronic acid from Germany will allow treatment of very superficial wrinkles without the risk of the 'Tyndall effect,' " he added.
Also in the last decade, dermatologic surgery-related educational initiatives have been advanced. In 2004, 1-year fellowship training programs were approved by the Accreditation Council for Graduate Medical Education for training in dermatologic surgery; and last year, there were 47 ACGME-accredited procedural dermatology fellowship training programs in place, he said.
"Dermatologic surgery is an important component of nearly all dermatology postgraduate courses," added Dr. Hanke.
The history of fractional laser technology and fillers were addressed in separate articles in the same issue of Seminars in Cutaneous Medicine and Surgery, underscoring the importance of the two recent developments.
Fillers
The next phase of development in injectable fillers has begun, according to Dr. Richard G. Glogau.
"The concept of augmentation has moved from simple lines, scars, and wrinkles to revolumizing the aging face," noted Dr. Glogau, a clinical professor of dermatology at the University of California, San Francisco. "While seeking extended duration of effect balanced against the safety profile of the injectable, our focus is now directed to extending the lifting or volumizing effect that one can achieve with these fillers."
The initial movement into 3-dimensional correction with injectable fillers began with the dramatic improvement seen in lip volume championed in the 1980s, and each of a litany of fillers that followed, including fat, collagen, silicone, hyaluronic acids, poly-l-lactic acids, calcium hydroxylapatite, and polymethylmethacrylate (Sem. Cut. Med. Surg. 2012;31:78-87).
New fillers, some which represent refinements of existing technologies, continue to undergo review. Aquamid a biocompatible, nonabsorbable, permanent injectable hydrogel implant is currently under review by the Food and Drug Administration and is approved for use in Europe.
It is also possible that fillers will move beyond the traditional concept of inert medical devices and into the realm of true biologics – "materials that will improve the texture, elasticity, radiance, and possibly color, of the skin itself," he added.
"Just as the last 40 years has seen the movement from 2 to 3 dimensions, the next 2 decades will see movement form the macro to the micro level, and fillers will become systems for active metabolic manipulation and protection of the aging skin," he concluded.
Fractionation
The development of fractional photothermolysis was "a milestone in the history of laser technology and cutaneous resurfacing," according to Dr. Nazanin Saedi, a dermatologist in private practice in Chestnut Hill, Mass., and her colleagues.
The technology, noted the study authors, builds on the knowledge gained from early CO2 and Er:YAG laser treatment experiences, achieving greater optimization of parameters to induce the types of benefits seen with CO2 resurfacing, but without the significant postoperative morbidity, complications, and discomfort associated with the earlier technologies.
Furthermore, the older therapies destroyed the barrier protection, which "significantly increased the risk of infection throughout the recovery period and required extensive home care. The risk of scarring, delayed-onset permanent hypopigmentation, and demarcation lines was significant even in the hands of an experienced operator," they wrote (Sem. Cut. Med. Surg. 2012;31:105-9).
In an en effort to overcome these problems, what followed was nonablative dermal remodeling (with less than impressive results), and ultimately, the "idea of fractionated laser technology," they continued.
First used in hair transplant surgery, the technology led to development of the 1,550-nm nonablative "Fraxel" laser (now called the Fraxel Re:Store by Solta Medical), which debuted in the literature in 2004. This and other fractional laser technologies are now used to treat photoaging, superficial and deep rhytids, scars (including in patients with darker skin types), and pigmentation.
Both nonablative and ablative fractional resurfacing have proved to be safer than have traditional ablative lasers, Dr. Saedi and her colleagues noted. However, complications can still occur, such as infections (with herpes simplex virus being the most common), acneiform eruptions, prolonged erythema, pigmentary alteration, and scarring (rare, but can also result from infection associated with treatment).
"Counterintuitively, nonablative or ablative fractionated devices at low energies and densities can be useful in the treatment of scarring, including hypertrophic scars" as previously mentioned, they noted.
"While [fractional lasers are] inherently safer due to the pixelated manner of the treatment, complications can be further prevented with attentive surgical technique and judicious use of prophylaxis," they wrote.
The future of fractional laser technology promises to hold exciting developments. For example, since ablative fractional resurfacing creates microscopic vertical holes in tissue, the delivery of topical drugs through these holes is possible. In animal models, the photosensitizer methylaminolevulinic acid has been delivered using this approach, and tests suggest that low density treatment would be sufficient for deep dermal drug delivery.
"Treatment of skin in a porcine model showed enhanced depth of photodynamic therapy following porphyrin application after pretreatment with fractional resurfacing. An in vitro study utilizing low fluence fractionated Erbium:YAG demonstrated upwards of a 125-fold increase in imiquimod delivery," they noted.
Trials in humans are underway to assess the feasibility and safety of enhanced drug delivery using this approach, and there is speculation that ultimately, it could be used for delivery of biologic peptides and vaccines.
Tattoo removal is another promising use for fractional lasers, with early studies demonstrating good results, noted Dr. Saedi and her colleagues, explaining that ablative fractional lasers, when used in conjunction with a Q-switched laser, appear to provide enhanced tattoo removal capabilities.
"With new devices and wavelengths, the applications of this technology continue to grow," they wrote, concluding that "the future remains bright for fractionated laser devices."
Likewise, the future of dermatologic surgery in general remains promising, Dr. Hanke said. "Many new procedures and advances lie ahead."
Neither Dr. Hanke nor Dr. Saedi had disclosures to report. Another author on the article by Dr. Saedi (Dr. Christopher Zachary) reported receiving an honorarium from Solta Medical.
FROM SEMINARS IN CUTANEOUS MEDICINE AND SURGERY
Dermatologic Surgery Milestones
Dermatologic surgery has come a long way since the 1950s. This look at some of the highlights – from phenol peels and hair transplants to tumescent liposuction and botulinum toxin injections – covers the subspecialty's evolution and influence.
Dermatologic surgery has come a long way since the 1950s. This look at some of the highlights – from phenol peels and hair transplants to tumescent liposuction and botulinum toxin injections – covers the subspecialty's evolution and influence.
Dermatologic surgery has come a long way since the 1950s. This look at some of the highlights – from phenol peels and hair transplants to tumescent liposuction and botulinum toxin injections – covers the subspecialty's evolution and influence.
Two Targeted Agents Best Chemotherapy in BRAF-Mutant Melanoma
CHICAGO – Two new oral targeted agents that have yielded positive results in phase III clinical trials are likely to change the treatment landscape for the half of patients with melanoma whose tumors have a mutation of BRAF driving their behavior.
The drugs – trametinib and dabrafenib – both interfere with signaling in the BRAF pathway and respectively reduced the risk of progression or death by 55% and 70% relative to chemotherapy in patients with advanced melanoma harboring common BRAF mutations, according to data presented at the annual meeting of the American Society of Clinical Oncology. These drugs also had good safety profiles.
Thus, trametinib and dabrafenib are likely to join vemurafenib (Zelboraf), the only targeted agent currently approved specifically for the treatment of BRAF-mutant melanoma.
The trials’ findings "show the promise of personalized medicine or precision medicine, using a patient-focused approach that targets treatment to the genetic abnormalities that drive cancer growth and metastatic behavior," Dr. Sylvia Adams of New York University Langone Medical Center commented in a press briefing that she moderated, where the findings were initially reported.
In the first trial, known as METRIC, investigators led by Dr. Caroline Robert, head of the department of dermatology at the Institut Gustave Roussy in Villejuif, France, compared trametinib – an oral selective inhibitor of MEK, which lies downstream of BRAF – with chemotherapy (dacarbazine or paclitaxel) in 322 patients with V600E or V600K BRAF-mutant locally advanced or metastatic melanoma.
Patients in the trametinib group had a higher rate of grade 3 or worse hypertension (12% vs. 3%) and rash (8% vs. 0%). Cases of decreased ejection fraction or ventricular dysfunction (7%) and chorioretinopathy (less than 1%) with the drug were reversible. Of note – in contrast to what has been seen with vemurafenib – none of the patients developed cutaneous squamous cell carcinomas.
Median progression-free survival was longer with trametinib than with chemotherapy (4.8 vs. 1.5 months; hazard ratio, 0.45; P less than .0001), according to data reported at the meeting. (Full results are also being simultaneously published in the New England Journal of Medicine.)
Trametinib reduced the risk of death as well (HR, 0.54; P = .01). "Crossover was allowed," Dr. Robert noted. "That of course can blend the results of overall survival, but even in spite of this crossover in 47% of the patients [in the chemotherapy group], we still have a difference in overall survival.
"Trametinib is the first-in-class MEK inhibitor to show a statistically significant activity in progression-free survival, response rate, and overall survival benefit in a randomized trial and here in this population of BRAF-mutant melanoma patients. The safety profile is very manageable," she commented. "Thus, this phase III trial provides a really positive risk-benefit ratio of trametinib in patients with BRAF-mutant melanoma and delivers an alternate treatment option for these patients."
Dr. Robert said that she didn’t view it as problematic that oncologists may soon have to select among multiple drugs for this patient population. "Let me remind you, for 50 years, we had nothing. And very recently, we have one drug on the market, a BRAF inhibitor; now, hopefully we will have others. So we are very happy to have more than one drug. The future will tell us how to use these drugs, and we are looking forward to try[ing] the combination of BRAF and MEK inhibitors."
Dr. Adams, the press briefing moderator, characterized the findings as "exciting" for two reasons. "Number one, it shows that in metastatic melanoma, MEK pathway–targeted therapy, as seen here for MEK inhibition, is very effective. So there is tumor shrinkage; there is survival benefit for those patients. And second, it also opens the landscape of treatments for BRAF-mutant melanomas and provides patients with additional options."
In the second trial, known as BREAK-3, a team led by Dr. Axel Hauschild, professor of dermatology at the University Hospital in Kiel, Germany, compared dabrafenib, an oral inhibitor of BRAF, with chemotherapy (dacarbazine) in 250 patients with locally advanced or metastatic V600E BRAF-mutant melanoma. In this trial, 68% of patients in the chemotherapy group ultimately crossed over to the other group.
Compared with chemotherapy, dabrafenib improved median progression-free survival (5.1 vs. 2.7 months; HR, 0.30; P less than .0001). The rate of complete or partial response was more than double with the targeted therapy (53% vs. 19%).
"The data for overall survival are very immature; only 12% of the patients have died so far, and therefore the data are not presented here," Dr. Hauschild explained.
Dabrafenib was associated with higher rates of grade 3 or worse hyperkeratosis (2% vs. 0%) and squamous cell carcinoma (5% vs. 0%), whereas chemotherapy was associated with higher rates of grade 3 or worse hematologic adverse events.
"The next step is the combination of dabrafenib and the drug trametinib, not only for stage IV but also for the adjuvant setting," Dr. Hauschild commented. In fact, updated results of a phase I/II trial testing the combination are also being reported at the meeting.
Given the availability of BRAF-targeted therapy today, all melanomas should have mutational testing at minimum for BRAF status, he said. Additionally, clinical trials will be essential to sorting out the various new treatment options.
"It’s not the end of the story for me: It’s the beginning of a completely new era of treatment of metastatic melanoma, and I strongly believe in combinations. Therefore, it’s very much appreciated if patients are brought to clinical trials," he said. "But they need to receive in these clinical trials standard of care. And for BRAF-mutated patients, standard of care is no longer [dacarbazine]; it’s no longer placebo. It needs to be a BRAF inhibitor."
Dr. Adams, the moderator, commented, "This phase III study of dabrafenib confirms that BRAF targeting in mutant melanoma is highly effective as seen by tumor shrinkage in about half of the patients, similar to the [Food and Drug Administration]–approved drug vemurafenib and potentially with less severe skin side effects. We are eagerly awaiting results of combinatorial therapy to see if combinations can actually push out the onset of resistance."
Dr. Robert disclosed that she is a consultant to Bristol-Myers Squibb, GlaxoSmithKline, and Roche. Dr. Hauschild disclosed that he is a consultant to and receives honoraria and research funding from GlaxoSmithKline. Both trials were funded by GlaxoSmithKline. Dr. Adams disclosed that she is a consultant to GlaxoSmithKline.
trametinib, dabrafenib, the American Society of Clinical Oncology, vemurafenib, Zelboraf, Dr. Sylvia Adams, METRIC, Dr. Caroline Robert, oral selective inhibitor of MEK, metastatic melanoma, melanoma drugs
CHICAGO – Two new oral targeted agents that have yielded positive results in phase III clinical trials are likely to change the treatment landscape for the half of patients with melanoma whose tumors have a mutation of BRAF driving their behavior.
The drugs – trametinib and dabrafenib – both interfere with signaling in the BRAF pathway and respectively reduced the risk of progression or death by 55% and 70% relative to chemotherapy in patients with advanced melanoma harboring common BRAF mutations, according to data presented at the annual meeting of the American Society of Clinical Oncology. These drugs also had good safety profiles.
Thus, trametinib and dabrafenib are likely to join vemurafenib (Zelboraf), the only targeted agent currently approved specifically for the treatment of BRAF-mutant melanoma.
The trials’ findings "show the promise of personalized medicine or precision medicine, using a patient-focused approach that targets treatment to the genetic abnormalities that drive cancer growth and metastatic behavior," Dr. Sylvia Adams of New York University Langone Medical Center commented in a press briefing that she moderated, where the findings were initially reported.
In the first trial, known as METRIC, investigators led by Dr. Caroline Robert, head of the department of dermatology at the Institut Gustave Roussy in Villejuif, France, compared trametinib – an oral selective inhibitor of MEK, which lies downstream of BRAF – with chemotherapy (dacarbazine or paclitaxel) in 322 patients with V600E or V600K BRAF-mutant locally advanced or metastatic melanoma.
Patients in the trametinib group had a higher rate of grade 3 or worse hypertension (12% vs. 3%) and rash (8% vs. 0%). Cases of decreased ejection fraction or ventricular dysfunction (7%) and chorioretinopathy (less than 1%) with the drug were reversible. Of note – in contrast to what has been seen with vemurafenib – none of the patients developed cutaneous squamous cell carcinomas.
Median progression-free survival was longer with trametinib than with chemotherapy (4.8 vs. 1.5 months; hazard ratio, 0.45; P less than .0001), according to data reported at the meeting. (Full results are also being simultaneously published in the New England Journal of Medicine.)
Trametinib reduced the risk of death as well (HR, 0.54; P = .01). "Crossover was allowed," Dr. Robert noted. "That of course can blend the results of overall survival, but even in spite of this crossover in 47% of the patients [in the chemotherapy group], we still have a difference in overall survival.
"Trametinib is the first-in-class MEK inhibitor to show a statistically significant activity in progression-free survival, response rate, and overall survival benefit in a randomized trial and here in this population of BRAF-mutant melanoma patients. The safety profile is very manageable," she commented. "Thus, this phase III trial provides a really positive risk-benefit ratio of trametinib in patients with BRAF-mutant melanoma and delivers an alternate treatment option for these patients."
Dr. Robert said that she didn’t view it as problematic that oncologists may soon have to select among multiple drugs for this patient population. "Let me remind you, for 50 years, we had nothing. And very recently, we have one drug on the market, a BRAF inhibitor; now, hopefully we will have others. So we are very happy to have more than one drug. The future will tell us how to use these drugs, and we are looking forward to try[ing] the combination of BRAF and MEK inhibitors."
Dr. Adams, the press briefing moderator, characterized the findings as "exciting" for two reasons. "Number one, it shows that in metastatic melanoma, MEK pathway–targeted therapy, as seen here for MEK inhibition, is very effective. So there is tumor shrinkage; there is survival benefit for those patients. And second, it also opens the landscape of treatments for BRAF-mutant melanomas and provides patients with additional options."
In the second trial, known as BREAK-3, a team led by Dr. Axel Hauschild, professor of dermatology at the University Hospital in Kiel, Germany, compared dabrafenib, an oral inhibitor of BRAF, with chemotherapy (dacarbazine) in 250 patients with locally advanced or metastatic V600E BRAF-mutant melanoma. In this trial, 68% of patients in the chemotherapy group ultimately crossed over to the other group.
Compared with chemotherapy, dabrafenib improved median progression-free survival (5.1 vs. 2.7 months; HR, 0.30; P less than .0001). The rate of complete or partial response was more than double with the targeted therapy (53% vs. 19%).
"The data for overall survival are very immature; only 12% of the patients have died so far, and therefore the data are not presented here," Dr. Hauschild explained.
Dabrafenib was associated with higher rates of grade 3 or worse hyperkeratosis (2% vs. 0%) and squamous cell carcinoma (5% vs. 0%), whereas chemotherapy was associated with higher rates of grade 3 or worse hematologic adverse events.
"The next step is the combination of dabrafenib and the drug trametinib, not only for stage IV but also for the adjuvant setting," Dr. Hauschild commented. In fact, updated results of a phase I/II trial testing the combination are also being reported at the meeting.
Given the availability of BRAF-targeted therapy today, all melanomas should have mutational testing at minimum for BRAF status, he said. Additionally, clinical trials will be essential to sorting out the various new treatment options.
"It’s not the end of the story for me: It’s the beginning of a completely new era of treatment of metastatic melanoma, and I strongly believe in combinations. Therefore, it’s very much appreciated if patients are brought to clinical trials," he said. "But they need to receive in these clinical trials standard of care. And for BRAF-mutated patients, standard of care is no longer [dacarbazine]; it’s no longer placebo. It needs to be a BRAF inhibitor."
Dr. Adams, the moderator, commented, "This phase III study of dabrafenib confirms that BRAF targeting in mutant melanoma is highly effective as seen by tumor shrinkage in about half of the patients, similar to the [Food and Drug Administration]–approved drug vemurafenib and potentially with less severe skin side effects. We are eagerly awaiting results of combinatorial therapy to see if combinations can actually push out the onset of resistance."
Dr. Robert disclosed that she is a consultant to Bristol-Myers Squibb, GlaxoSmithKline, and Roche. Dr. Hauschild disclosed that he is a consultant to and receives honoraria and research funding from GlaxoSmithKline. Both trials were funded by GlaxoSmithKline. Dr. Adams disclosed that she is a consultant to GlaxoSmithKline.
CHICAGO – Two new oral targeted agents that have yielded positive results in phase III clinical trials are likely to change the treatment landscape for the half of patients with melanoma whose tumors have a mutation of BRAF driving their behavior.
The drugs – trametinib and dabrafenib – both interfere with signaling in the BRAF pathway and respectively reduced the risk of progression or death by 55% and 70% relative to chemotherapy in patients with advanced melanoma harboring common BRAF mutations, according to data presented at the annual meeting of the American Society of Clinical Oncology. These drugs also had good safety profiles.
Thus, trametinib and dabrafenib are likely to join vemurafenib (Zelboraf), the only targeted agent currently approved specifically for the treatment of BRAF-mutant melanoma.
The trials’ findings "show the promise of personalized medicine or precision medicine, using a patient-focused approach that targets treatment to the genetic abnormalities that drive cancer growth and metastatic behavior," Dr. Sylvia Adams of New York University Langone Medical Center commented in a press briefing that she moderated, where the findings were initially reported.
In the first trial, known as METRIC, investigators led by Dr. Caroline Robert, head of the department of dermatology at the Institut Gustave Roussy in Villejuif, France, compared trametinib – an oral selective inhibitor of MEK, which lies downstream of BRAF – with chemotherapy (dacarbazine or paclitaxel) in 322 patients with V600E or V600K BRAF-mutant locally advanced or metastatic melanoma.
Patients in the trametinib group had a higher rate of grade 3 or worse hypertension (12% vs. 3%) and rash (8% vs. 0%). Cases of decreased ejection fraction or ventricular dysfunction (7%) and chorioretinopathy (less than 1%) with the drug were reversible. Of note – in contrast to what has been seen with vemurafenib – none of the patients developed cutaneous squamous cell carcinomas.
Median progression-free survival was longer with trametinib than with chemotherapy (4.8 vs. 1.5 months; hazard ratio, 0.45; P less than .0001), according to data reported at the meeting. (Full results are also being simultaneously published in the New England Journal of Medicine.)
Trametinib reduced the risk of death as well (HR, 0.54; P = .01). "Crossover was allowed," Dr. Robert noted. "That of course can blend the results of overall survival, but even in spite of this crossover in 47% of the patients [in the chemotherapy group], we still have a difference in overall survival.
"Trametinib is the first-in-class MEK inhibitor to show a statistically significant activity in progression-free survival, response rate, and overall survival benefit in a randomized trial and here in this population of BRAF-mutant melanoma patients. The safety profile is very manageable," she commented. "Thus, this phase III trial provides a really positive risk-benefit ratio of trametinib in patients with BRAF-mutant melanoma and delivers an alternate treatment option for these patients."
Dr. Robert said that she didn’t view it as problematic that oncologists may soon have to select among multiple drugs for this patient population. "Let me remind you, for 50 years, we had nothing. And very recently, we have one drug on the market, a BRAF inhibitor; now, hopefully we will have others. So we are very happy to have more than one drug. The future will tell us how to use these drugs, and we are looking forward to try[ing] the combination of BRAF and MEK inhibitors."
Dr. Adams, the press briefing moderator, characterized the findings as "exciting" for two reasons. "Number one, it shows that in metastatic melanoma, MEK pathway–targeted therapy, as seen here for MEK inhibition, is very effective. So there is tumor shrinkage; there is survival benefit for those patients. And second, it also opens the landscape of treatments for BRAF-mutant melanomas and provides patients with additional options."
In the second trial, known as BREAK-3, a team led by Dr. Axel Hauschild, professor of dermatology at the University Hospital in Kiel, Germany, compared dabrafenib, an oral inhibitor of BRAF, with chemotherapy (dacarbazine) in 250 patients with locally advanced or metastatic V600E BRAF-mutant melanoma. In this trial, 68% of patients in the chemotherapy group ultimately crossed over to the other group.
Compared with chemotherapy, dabrafenib improved median progression-free survival (5.1 vs. 2.7 months; HR, 0.30; P less than .0001). The rate of complete or partial response was more than double with the targeted therapy (53% vs. 19%).
"The data for overall survival are very immature; only 12% of the patients have died so far, and therefore the data are not presented here," Dr. Hauschild explained.
Dabrafenib was associated with higher rates of grade 3 or worse hyperkeratosis (2% vs. 0%) and squamous cell carcinoma (5% vs. 0%), whereas chemotherapy was associated with higher rates of grade 3 or worse hematologic adverse events.
"The next step is the combination of dabrafenib and the drug trametinib, not only for stage IV but also for the adjuvant setting," Dr. Hauschild commented. In fact, updated results of a phase I/II trial testing the combination are also being reported at the meeting.
Given the availability of BRAF-targeted therapy today, all melanomas should have mutational testing at minimum for BRAF status, he said. Additionally, clinical trials will be essential to sorting out the various new treatment options.
"It’s not the end of the story for me: It’s the beginning of a completely new era of treatment of metastatic melanoma, and I strongly believe in combinations. Therefore, it’s very much appreciated if patients are brought to clinical trials," he said. "But they need to receive in these clinical trials standard of care. And for BRAF-mutated patients, standard of care is no longer [dacarbazine]; it’s no longer placebo. It needs to be a BRAF inhibitor."
Dr. Adams, the moderator, commented, "This phase III study of dabrafenib confirms that BRAF targeting in mutant melanoma is highly effective as seen by tumor shrinkage in about half of the patients, similar to the [Food and Drug Administration]–approved drug vemurafenib and potentially with less severe skin side effects. We are eagerly awaiting results of combinatorial therapy to see if combinations can actually push out the onset of resistance."
Dr. Robert disclosed that she is a consultant to Bristol-Myers Squibb, GlaxoSmithKline, and Roche. Dr. Hauschild disclosed that he is a consultant to and receives honoraria and research funding from GlaxoSmithKline. Both trials were funded by GlaxoSmithKline. Dr. Adams disclosed that she is a consultant to GlaxoSmithKline.
trametinib, dabrafenib, the American Society of Clinical Oncology, vemurafenib, Zelboraf, Dr. Sylvia Adams, METRIC, Dr. Caroline Robert, oral selective inhibitor of MEK, metastatic melanoma, melanoma drugs
trametinib, dabrafenib, the American Society of Clinical Oncology, vemurafenib, Zelboraf, Dr. Sylvia Adams, METRIC, Dr. Caroline Robert, oral selective inhibitor of MEK, metastatic melanoma, melanoma drugs
FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY OF CLINICAL ONCOLOGY
Major Finding: Relative to chemotherapy, trametinib improved progression-free survival (hazard ratio, 0.45) and overall survival (HR, 0.54), and dabrafenib improved progression-free survival (HR, 0.30).
Data Source: A pair of randomized phase III trials among 322 patients with V600E/K BRAF-mutant advanced melanoma (the METRIC trial) and 250 patients with V600E BRAF-mutant advanced melanoma (the BREAK-3 trial)
Disclosures: Dr. Robert disclosed that she is a consultant to Bristol-Myers Squibb, GlaxoSmithKline, and Roche. Dr. Hauschild disclosed that he is a consultant to and receives honoraria and research funding from GlaxoSmithKline. Both trials were funded by GlaxoSmithKline. Dr. Adams disclosed that she is a consultant to GlaxoSmithKline.