User login
Sharon Worcester is an award-winning medical journalist for MDedge News. She has been with the company since 1996, first as the Southeast Bureau Chief (1996-2009) when the company was known as International Medical News Group, then as a freelance writer (2010-2015) before returning as a reporter in 2015. She previously worked as a daily newspaper reporter covering health and local government. Sharon currently reports primarily on oncology and hematology. She has a BA from Eckerd College and an MA in Mass Communication/Print Journalism from the University of Florida. Connect with her via LinkedIn and follow her on twitter @SW_MedReporter.
Analysis: Push for expanded hepatitis C screening appears premature
The recent advent of new treatments for hepatitis C prompted organizations including the Centers for Disease Control and Prevention, the U.S. Preventive Services Task Force, and the World Health Organization to recommend expanded hepatitis C screening, but such screening may be premature, according to a subject analysis.
Too much uncertainty exists regarding the validity of surrogate markers for treatment efficacy that were used in trials, and evidence regarding clinical outcomes and screening strategies is lacking, according to Dr. Ronald L. Koretz of the University of California, Los Angeles, and his colleagues, who evaluated the current understanding of the incidence and natural course of hepatitis C infection, treatment efficacy, and potential harms of treatment for their analysis.
The best available data suggest that 80%-85% of patients with chronic hepatitis C will die of nonhepatic causes; thus screening could lead to unnecessary treatment. This is important, as safety data for newer drugs are limited, and the existing data suggest a small but concerning rate of serious adverse events associated with the use of some treatments and treatment regimens; the risk-benefit profile of treatment cannot be adequately evaluated because of the lack of data regarding treatment benefits, the investigators reported online Jan. 13 in the British Medical Journal ([doi:10.10036/bmj.g7809]).
Clinical trials to determine the outcomes of treatment in screen-detected patients, as well as the long-term hazards of treatment, are needed, they said, noting that currently available trials included small numbers of patients and/or only short-term follow-up. Until data from such trials are available, physicians should not be pressured to enforce recommended screening strategies “out of enthusiasm for new treatments that have not yet been shown to cause long-term clinical improvement,” they concluded.
Dr. Koretz is a member of the editorial board of the Cochrane Hepato-Biliary Group. The authors reported having no other financial conflicts.
The authors question the merits of hepatitis C (HCV) screening despite the endorsement of the Centers for Disease Control and Prevention, U.S. Preventive Services Task Force, and World Health Organization. They suggest HCV does not lead to sufficient mortality, treatment may cause harm, sustained virologic response (SVR) does not represent a ‘cure’ and question if treating HCV truly reduces long term morbidity/mortality. While it is true the majority of patients with HCV will not develop cirrhosis or death attributable to their liver disease, the authors downplayed the morbidity and mortality related to HCV and the significant cost to the health care system as well (Ann. Intern. Med. 2012;156:271; Hepatology 2013;57:2164]. The authors also downplayed the importance of sustained viral response (SVR), suggesting that it does not represent a cure, yet neglect to mention several studies demonstrating late recurrence in only 1%-3% of patients who have achieved SVR. Furthermore, the authors describe the “harms of treatment,” yet they largely reference therapies that are no longer used and make minimal comment on the clear safety and efficacy of the current interferon-free regimens. Additionally, they report that while clearing HCV may reduce the risk of decompensated cirrhosis and hepatocellular carcinoma, it does not completely eliminate these risks and therefore treatment may not be of value. This brings us back to the motivation of the CDC, USPSTF, and WHO to recommend screening for HCV – identifying asymptomatic infection to allow for administration of safe, effective antiviral therapies before the development of cirrhosis and all of its complications.
Dr. Sean Koppe is director of hepatology, University of Illinois Hospital & Health Sciences System. He has no conflicts of interest.
The authors question the merits of hepatitis C (HCV) screening despite the endorsement of the Centers for Disease Control and Prevention, U.S. Preventive Services Task Force, and World Health Organization. They suggest HCV does not lead to sufficient mortality, treatment may cause harm, sustained virologic response (SVR) does not represent a ‘cure’ and question if treating HCV truly reduces long term morbidity/mortality. While it is true the majority of patients with HCV will not develop cirrhosis or death attributable to their liver disease, the authors downplayed the morbidity and mortality related to HCV and the significant cost to the health care system as well (Ann. Intern. Med. 2012;156:271; Hepatology 2013;57:2164]. The authors also downplayed the importance of sustained viral response (SVR), suggesting that it does not represent a cure, yet neglect to mention several studies demonstrating late recurrence in only 1%-3% of patients who have achieved SVR. Furthermore, the authors describe the “harms of treatment,” yet they largely reference therapies that are no longer used and make minimal comment on the clear safety and efficacy of the current interferon-free regimens. Additionally, they report that while clearing HCV may reduce the risk of decompensated cirrhosis and hepatocellular carcinoma, it does not completely eliminate these risks and therefore treatment may not be of value. This brings us back to the motivation of the CDC, USPSTF, and WHO to recommend screening for HCV – identifying asymptomatic infection to allow for administration of safe, effective antiviral therapies before the development of cirrhosis and all of its complications.
Dr. Sean Koppe is director of hepatology, University of Illinois Hospital & Health Sciences System. He has no conflicts of interest.
The authors question the merits of hepatitis C (HCV) screening despite the endorsement of the Centers for Disease Control and Prevention, U.S. Preventive Services Task Force, and World Health Organization. They suggest HCV does not lead to sufficient mortality, treatment may cause harm, sustained virologic response (SVR) does not represent a ‘cure’ and question if treating HCV truly reduces long term morbidity/mortality. While it is true the majority of patients with HCV will not develop cirrhosis or death attributable to their liver disease, the authors downplayed the morbidity and mortality related to HCV and the significant cost to the health care system as well (Ann. Intern. Med. 2012;156:271; Hepatology 2013;57:2164]. The authors also downplayed the importance of sustained viral response (SVR), suggesting that it does not represent a cure, yet neglect to mention several studies demonstrating late recurrence in only 1%-3% of patients who have achieved SVR. Furthermore, the authors describe the “harms of treatment,” yet they largely reference therapies that are no longer used and make minimal comment on the clear safety and efficacy of the current interferon-free regimens. Additionally, they report that while clearing HCV may reduce the risk of decompensated cirrhosis and hepatocellular carcinoma, it does not completely eliminate these risks and therefore treatment may not be of value. This brings us back to the motivation of the CDC, USPSTF, and WHO to recommend screening for HCV – identifying asymptomatic infection to allow for administration of safe, effective antiviral therapies before the development of cirrhosis and all of its complications.
Dr. Sean Koppe is director of hepatology, University of Illinois Hospital & Health Sciences System. He has no conflicts of interest.
The recent advent of new treatments for hepatitis C prompted organizations including the Centers for Disease Control and Prevention, the U.S. Preventive Services Task Force, and the World Health Organization to recommend expanded hepatitis C screening, but such screening may be premature, according to a subject analysis.
Too much uncertainty exists regarding the validity of surrogate markers for treatment efficacy that were used in trials, and evidence regarding clinical outcomes and screening strategies is lacking, according to Dr. Ronald L. Koretz of the University of California, Los Angeles, and his colleagues, who evaluated the current understanding of the incidence and natural course of hepatitis C infection, treatment efficacy, and potential harms of treatment for their analysis.
The best available data suggest that 80%-85% of patients with chronic hepatitis C will die of nonhepatic causes; thus screening could lead to unnecessary treatment. This is important, as safety data for newer drugs are limited, and the existing data suggest a small but concerning rate of serious adverse events associated with the use of some treatments and treatment regimens; the risk-benefit profile of treatment cannot be adequately evaluated because of the lack of data regarding treatment benefits, the investigators reported online Jan. 13 in the British Medical Journal ([doi:10.10036/bmj.g7809]).
Clinical trials to determine the outcomes of treatment in screen-detected patients, as well as the long-term hazards of treatment, are needed, they said, noting that currently available trials included small numbers of patients and/or only short-term follow-up. Until data from such trials are available, physicians should not be pressured to enforce recommended screening strategies “out of enthusiasm for new treatments that have not yet been shown to cause long-term clinical improvement,” they concluded.
Dr. Koretz is a member of the editorial board of the Cochrane Hepato-Biliary Group. The authors reported having no other financial conflicts.
The recent advent of new treatments for hepatitis C prompted organizations including the Centers for Disease Control and Prevention, the U.S. Preventive Services Task Force, and the World Health Organization to recommend expanded hepatitis C screening, but such screening may be premature, according to a subject analysis.
Too much uncertainty exists regarding the validity of surrogate markers for treatment efficacy that were used in trials, and evidence regarding clinical outcomes and screening strategies is lacking, according to Dr. Ronald L. Koretz of the University of California, Los Angeles, and his colleagues, who evaluated the current understanding of the incidence and natural course of hepatitis C infection, treatment efficacy, and potential harms of treatment for their analysis.
The best available data suggest that 80%-85% of patients with chronic hepatitis C will die of nonhepatic causes; thus screening could lead to unnecessary treatment. This is important, as safety data for newer drugs are limited, and the existing data suggest a small but concerning rate of serious adverse events associated with the use of some treatments and treatment regimens; the risk-benefit profile of treatment cannot be adequately evaluated because of the lack of data regarding treatment benefits, the investigators reported online Jan. 13 in the British Medical Journal ([doi:10.10036/bmj.g7809]).
Clinical trials to determine the outcomes of treatment in screen-detected patients, as well as the long-term hazards of treatment, are needed, they said, noting that currently available trials included small numbers of patients and/or only short-term follow-up. Until data from such trials are available, physicians should not be pressured to enforce recommended screening strategies “out of enthusiasm for new treatments that have not yet been shown to cause long-term clinical improvement,” they concluded.
Dr. Koretz is a member of the editorial board of the Cochrane Hepato-Biliary Group. The authors reported having no other financial conflicts.
Key clinical point: Evidence to support expanded hepatitis C screening is lacking.
Major finding: An estimated 80%-85% of patients with chronic hepatitis C will die from nonhepatic causes.
Data source: An analysis of existing evidence.
Disclosures: Dr. Koretz is a member of the editorial board of the Cochrane Hepato-Biliary Group. The authors reported having no other relevant financial disclosures.
CDC: Flu remains widespread; antivirals underutilized
The approximate midpoint of the 2014-2015 flu season has been reached, disease remains widespread, and antiviral flu medications remain underutilized, according to the Centers for Disease Control and Prevention.
As predicted, this season is proving particularly severe due to the predominance of antigenically drifted H3N2 virus strains, and the CDC is urging clinicians to maintain a high index of suspicion for flu and to prescribe antivirals earlier and more aggressively for patients presenting with flulike illness – especially young children, those over age 65 years, and those with underlying conditions, even if their symptoms are mild, CDC Director Thomas R. Frieden said during a press briefing.
A health advisory on the topic was issued Jan. 9, he noted.
“The CDC has recommended the use of antiviral drugs as an adjunct to vaccination. They are the only medicines that can specifically treat influenza illness, and in the context of an H3N2 predominant season with a less effective vaccine, treatment with antiflu drugs is even more important than usual,” he said, referring to the two neuraminidase inhibitors currently approved for treating influenza: oseltamivir and zanamivir.
About two-thirds of the H3N2 viruses analyzed this season are different from the H3N2 virus included in this year’s vaccine, which is why the vaccine is expected to have reduced effectiveness, he explained.
This makes early antiviral treatment all the more important, he added, noting that treatment within 2 days of symptom onset is optimal, but later treatment can also offer benefit.
“CDC scientists have looked very carefully at the use of influenza drugs in the clinical setting, and the conclusion is clear: They work, but they aren’t being used nearly enough. They can reduce symptoms, shorten duration of illness, and prevent serious complications,” he said.
Early treatment may help patients avoid hospitalization and could be life saving, he added.
Many patients are unaware that effective prescription treatments exist, and many doctors are not using the treatments as recommended. In one study, fewer than one in five eligible high-risk patients received treatment.
“So we’re expanding our efforts to reach clinicians about reminders about the importance of these drugs,” he said, noting that if high-risk patients with underlying conditions such as asthma, sickle cell disease, renal disease, or diabetes were treated, “tens of thousands of hospitalizations, and thousands of deaths could potentially be prevented.”
Dr. Frieden suggested that clinicians consider phone triage lines for high-risk patients to discuss symptoms over the phone and to “facilitate early initiation of treatment.”
An antiviral prescription can be provided without testing and before an office visit, he added.
The typical flu season lasts about 13 weeks on average, and the season began about 7 weeks ago. The continued high rate of H3N2 disease has had the greatest impact on older adults; that is typical of such seasons, which often involve a higher rate of hospitalizations and deaths.
In fact, hospitalization rates in the over 65 age group are rising sharply, Dr. Frieden said.
Last week the rate was 52 per 100,000 population, and this week the rate was 92 per 100,000 population. The cumulative rate 2 years ago when H3N2 viruses last predominated was 183 per 100,000, he noted.
“We wouldn’t be surprised to see something very similar this year,” he said.
Young children are also severely affected; thus far in the season there have been 26 reported pediatric flu-related deaths.
However, there are early signs that infection rates are declining in areas where the season started earlier, such as the Southeast, and the number of patients presenting to a doctor with flulike symptoms has also declined slightly, but it is too soon to tell whether disease activity has peaked, he said, stressing that “we still have several weeks of flu activity ahead.”
It’s not too late to get vaccinated, and despite the reduced efficacy of this year’s vaccine against the circulating H3N2 strains, vaccination may still offer some benefit.
“There are other strains out there as well,” he said, noting that a proportion of cases from other strains, such as influenza B, tend to occur late in the season, and this year’s vaccine offers a good match for influenza B viruses.
Pneumococcal vaccination is also important, particularly for older adults and those at high risk , he said.
Last September the CDC announced a new recommendation that all adults over age 65 years should get two different pneumococcal vaccines. Such vaccination may help prevent flu-related pneumonia.
Patients with the flu or flulike illness should be advised to cover their cough and to stay home from work or school to protect those who are most vulnerable to the flu, he said.
The approximate midpoint of the 2014-2015 flu season has been reached, disease remains widespread, and antiviral flu medications remain underutilized, according to the Centers for Disease Control and Prevention.
As predicted, this season is proving particularly severe due to the predominance of antigenically drifted H3N2 virus strains, and the CDC is urging clinicians to maintain a high index of suspicion for flu and to prescribe antivirals earlier and more aggressively for patients presenting with flulike illness – especially young children, those over age 65 years, and those with underlying conditions, even if their symptoms are mild, CDC Director Thomas R. Frieden said during a press briefing.
A health advisory on the topic was issued Jan. 9, he noted.
“The CDC has recommended the use of antiviral drugs as an adjunct to vaccination. They are the only medicines that can specifically treat influenza illness, and in the context of an H3N2 predominant season with a less effective vaccine, treatment with antiflu drugs is even more important than usual,” he said, referring to the two neuraminidase inhibitors currently approved for treating influenza: oseltamivir and zanamivir.
About two-thirds of the H3N2 viruses analyzed this season are different from the H3N2 virus included in this year’s vaccine, which is why the vaccine is expected to have reduced effectiveness, he explained.
This makes early antiviral treatment all the more important, he added, noting that treatment within 2 days of symptom onset is optimal, but later treatment can also offer benefit.
“CDC scientists have looked very carefully at the use of influenza drugs in the clinical setting, and the conclusion is clear: They work, but they aren’t being used nearly enough. They can reduce symptoms, shorten duration of illness, and prevent serious complications,” he said.
Early treatment may help patients avoid hospitalization and could be life saving, he added.
Many patients are unaware that effective prescription treatments exist, and many doctors are not using the treatments as recommended. In one study, fewer than one in five eligible high-risk patients received treatment.
“So we’re expanding our efforts to reach clinicians about reminders about the importance of these drugs,” he said, noting that if high-risk patients with underlying conditions such as asthma, sickle cell disease, renal disease, or diabetes were treated, “tens of thousands of hospitalizations, and thousands of deaths could potentially be prevented.”
Dr. Frieden suggested that clinicians consider phone triage lines for high-risk patients to discuss symptoms over the phone and to “facilitate early initiation of treatment.”
An antiviral prescription can be provided without testing and before an office visit, he added.
The typical flu season lasts about 13 weeks on average, and the season began about 7 weeks ago. The continued high rate of H3N2 disease has had the greatest impact on older adults; that is typical of such seasons, which often involve a higher rate of hospitalizations and deaths.
In fact, hospitalization rates in the over 65 age group are rising sharply, Dr. Frieden said.
Last week the rate was 52 per 100,000 population, and this week the rate was 92 per 100,000 population. The cumulative rate 2 years ago when H3N2 viruses last predominated was 183 per 100,000, he noted.
“We wouldn’t be surprised to see something very similar this year,” he said.
Young children are also severely affected; thus far in the season there have been 26 reported pediatric flu-related deaths.
However, there are early signs that infection rates are declining in areas where the season started earlier, such as the Southeast, and the number of patients presenting to a doctor with flulike symptoms has also declined slightly, but it is too soon to tell whether disease activity has peaked, he said, stressing that “we still have several weeks of flu activity ahead.”
It’s not too late to get vaccinated, and despite the reduced efficacy of this year’s vaccine against the circulating H3N2 strains, vaccination may still offer some benefit.
“There are other strains out there as well,” he said, noting that a proportion of cases from other strains, such as influenza B, tend to occur late in the season, and this year’s vaccine offers a good match for influenza B viruses.
Pneumococcal vaccination is also important, particularly for older adults and those at high risk , he said.
Last September the CDC announced a new recommendation that all adults over age 65 years should get two different pneumococcal vaccines. Such vaccination may help prevent flu-related pneumonia.
Patients with the flu or flulike illness should be advised to cover their cough and to stay home from work or school to protect those who are most vulnerable to the flu, he said.
The approximate midpoint of the 2014-2015 flu season has been reached, disease remains widespread, and antiviral flu medications remain underutilized, according to the Centers for Disease Control and Prevention.
As predicted, this season is proving particularly severe due to the predominance of antigenically drifted H3N2 virus strains, and the CDC is urging clinicians to maintain a high index of suspicion for flu and to prescribe antivirals earlier and more aggressively for patients presenting with flulike illness – especially young children, those over age 65 years, and those with underlying conditions, even if their symptoms are mild, CDC Director Thomas R. Frieden said during a press briefing.
A health advisory on the topic was issued Jan. 9, he noted.
“The CDC has recommended the use of antiviral drugs as an adjunct to vaccination. They are the only medicines that can specifically treat influenza illness, and in the context of an H3N2 predominant season with a less effective vaccine, treatment with antiflu drugs is even more important than usual,” he said, referring to the two neuraminidase inhibitors currently approved for treating influenza: oseltamivir and zanamivir.
About two-thirds of the H3N2 viruses analyzed this season are different from the H3N2 virus included in this year’s vaccine, which is why the vaccine is expected to have reduced effectiveness, he explained.
This makes early antiviral treatment all the more important, he added, noting that treatment within 2 days of symptom onset is optimal, but later treatment can also offer benefit.
“CDC scientists have looked very carefully at the use of influenza drugs in the clinical setting, and the conclusion is clear: They work, but they aren’t being used nearly enough. They can reduce symptoms, shorten duration of illness, and prevent serious complications,” he said.
Early treatment may help patients avoid hospitalization and could be life saving, he added.
Many patients are unaware that effective prescription treatments exist, and many doctors are not using the treatments as recommended. In one study, fewer than one in five eligible high-risk patients received treatment.
“So we’re expanding our efforts to reach clinicians about reminders about the importance of these drugs,” he said, noting that if high-risk patients with underlying conditions such as asthma, sickle cell disease, renal disease, or diabetes were treated, “tens of thousands of hospitalizations, and thousands of deaths could potentially be prevented.”
Dr. Frieden suggested that clinicians consider phone triage lines for high-risk patients to discuss symptoms over the phone and to “facilitate early initiation of treatment.”
An antiviral prescription can be provided without testing and before an office visit, he added.
The typical flu season lasts about 13 weeks on average, and the season began about 7 weeks ago. The continued high rate of H3N2 disease has had the greatest impact on older adults; that is typical of such seasons, which often involve a higher rate of hospitalizations and deaths.
In fact, hospitalization rates in the over 65 age group are rising sharply, Dr. Frieden said.
Last week the rate was 52 per 100,000 population, and this week the rate was 92 per 100,000 population. The cumulative rate 2 years ago when H3N2 viruses last predominated was 183 per 100,000, he noted.
“We wouldn’t be surprised to see something very similar this year,” he said.
Young children are also severely affected; thus far in the season there have been 26 reported pediatric flu-related deaths.
However, there are early signs that infection rates are declining in areas where the season started earlier, such as the Southeast, and the number of patients presenting to a doctor with flulike symptoms has also declined slightly, but it is too soon to tell whether disease activity has peaked, he said, stressing that “we still have several weeks of flu activity ahead.”
It’s not too late to get vaccinated, and despite the reduced efficacy of this year’s vaccine against the circulating H3N2 strains, vaccination may still offer some benefit.
“There are other strains out there as well,” he said, noting that a proportion of cases from other strains, such as influenza B, tend to occur late in the season, and this year’s vaccine offers a good match for influenza B viruses.
Pneumococcal vaccination is also important, particularly for older adults and those at high risk , he said.
Last September the CDC announced a new recommendation that all adults over age 65 years should get two different pneumococcal vaccines. Such vaccination may help prevent flu-related pneumonia.
Patients with the flu or flulike illness should be advised to cover their cough and to stay home from work or school to protect those who are most vulnerable to the flu, he said.
HIM Study: Prevalent HVP-16 infections tend to persist
Prevalent oral human papillomavirus 16 infections in men persist longer than newly acquired infections, and the rate of persistence for incident infections increases with age, according to findings from the HPV Infection in Men (HIM) study.
Of 23 oral HPV-16–positive men aged 18 to 64 years who provided an oral gargle sample during at least two visits during the course of the ongoing multinational cohort study and who were followed for a median of 44.4 months, 13 acquired a new incident infection and 10 entered the study with a prevalent infection. Of the incident infections, 38.5% persisted for at least 1 month, and 10% persisted for at least 24 months; none persisted for more than 36 months (median duration, 7 months), but the rate of persistence for 12 months or longer increased significantly with age (100% of men aged 45 years or older had persistent infection vs. 50% of those aged 31-44 years, and 0% of those aged 18-30 years), Dr. Christine M. Pierce Campbell of the Moffitt Cancer Center and Research Institute, Tampa, Fla., and her colleagues reported online Jan. 9 in Cancer Prevention Research.
Of the prevalent infections, 90% persisted for at least 12 months, 80% persisted for at least 24 months, 57% persisted for at least 36 months, and 40% persisted for 48 months or longer, the investigators said, noting that persistence of prevalent infections also increased with age, but this finding was not statistically significant (Cancer Prev. Res. 2015 Jan. 9 [doi:10.1158/1940-6207.CAPR-14-0296]).
The findings may explain the high prevalence of oral HPV among older patients and could have implications for identifying men at high risk for developing HPV-related oropharyngeal cancer, they said, noting that evidence increasingly suggests that most oropharyngeal cancers among men are caused by HPV infection, and that most cases are diagnosed at an advanced clinical stage.
“Given that the overwhelming majority of prevalent oral HPV-16 infections detected here persisted beyond 1 year, and 40% persisted beyond 4 years, there is a clear need to evaluate whether long-term persistent oral HPV-16 infection can predict future oropharyngeal cancer risk. … mid-adult and older men appear to be at the highest risk of oral HPV infection and should be the focus of prevention interventions, they concluded.
The HIM study cohort was supported by grants from the National Cancer Institute and Merck Sharp & Dohme to individual authors. Dr. Campbell was supported, in part, by a postdoctoral fellowship and reported having no other disclosures.
Prevalent oral human papillomavirus 16 infections in men persist longer than newly acquired infections, and the rate of persistence for incident infections increases with age, according to findings from the HPV Infection in Men (HIM) study.
Of 23 oral HPV-16–positive men aged 18 to 64 years who provided an oral gargle sample during at least two visits during the course of the ongoing multinational cohort study and who were followed for a median of 44.4 months, 13 acquired a new incident infection and 10 entered the study with a prevalent infection. Of the incident infections, 38.5% persisted for at least 1 month, and 10% persisted for at least 24 months; none persisted for more than 36 months (median duration, 7 months), but the rate of persistence for 12 months or longer increased significantly with age (100% of men aged 45 years or older had persistent infection vs. 50% of those aged 31-44 years, and 0% of those aged 18-30 years), Dr. Christine M. Pierce Campbell of the Moffitt Cancer Center and Research Institute, Tampa, Fla., and her colleagues reported online Jan. 9 in Cancer Prevention Research.
Of the prevalent infections, 90% persisted for at least 12 months, 80% persisted for at least 24 months, 57% persisted for at least 36 months, and 40% persisted for 48 months or longer, the investigators said, noting that persistence of prevalent infections also increased with age, but this finding was not statistically significant (Cancer Prev. Res. 2015 Jan. 9 [doi:10.1158/1940-6207.CAPR-14-0296]).
The findings may explain the high prevalence of oral HPV among older patients and could have implications for identifying men at high risk for developing HPV-related oropharyngeal cancer, they said, noting that evidence increasingly suggests that most oropharyngeal cancers among men are caused by HPV infection, and that most cases are diagnosed at an advanced clinical stage.
“Given that the overwhelming majority of prevalent oral HPV-16 infections detected here persisted beyond 1 year, and 40% persisted beyond 4 years, there is a clear need to evaluate whether long-term persistent oral HPV-16 infection can predict future oropharyngeal cancer risk. … mid-adult and older men appear to be at the highest risk of oral HPV infection and should be the focus of prevention interventions, they concluded.
The HIM study cohort was supported by grants from the National Cancer Institute and Merck Sharp & Dohme to individual authors. Dr. Campbell was supported, in part, by a postdoctoral fellowship and reported having no other disclosures.
Prevalent oral human papillomavirus 16 infections in men persist longer than newly acquired infections, and the rate of persistence for incident infections increases with age, according to findings from the HPV Infection in Men (HIM) study.
Of 23 oral HPV-16–positive men aged 18 to 64 years who provided an oral gargle sample during at least two visits during the course of the ongoing multinational cohort study and who were followed for a median of 44.4 months, 13 acquired a new incident infection and 10 entered the study with a prevalent infection. Of the incident infections, 38.5% persisted for at least 1 month, and 10% persisted for at least 24 months; none persisted for more than 36 months (median duration, 7 months), but the rate of persistence for 12 months or longer increased significantly with age (100% of men aged 45 years or older had persistent infection vs. 50% of those aged 31-44 years, and 0% of those aged 18-30 years), Dr. Christine M. Pierce Campbell of the Moffitt Cancer Center and Research Institute, Tampa, Fla., and her colleagues reported online Jan. 9 in Cancer Prevention Research.
Of the prevalent infections, 90% persisted for at least 12 months, 80% persisted for at least 24 months, 57% persisted for at least 36 months, and 40% persisted for 48 months or longer, the investigators said, noting that persistence of prevalent infections also increased with age, but this finding was not statistically significant (Cancer Prev. Res. 2015 Jan. 9 [doi:10.1158/1940-6207.CAPR-14-0296]).
The findings may explain the high prevalence of oral HPV among older patients and could have implications for identifying men at high risk for developing HPV-related oropharyngeal cancer, they said, noting that evidence increasingly suggests that most oropharyngeal cancers among men are caused by HPV infection, and that most cases are diagnosed at an advanced clinical stage.
“Given that the overwhelming majority of prevalent oral HPV-16 infections detected here persisted beyond 1 year, and 40% persisted beyond 4 years, there is a clear need to evaluate whether long-term persistent oral HPV-16 infection can predict future oropharyngeal cancer risk. … mid-adult and older men appear to be at the highest risk of oral HPV infection and should be the focus of prevention interventions, they concluded.
The HIM study cohort was supported by grants from the National Cancer Institute and Merck Sharp & Dohme to individual authors. Dr. Campbell was supported, in part, by a postdoctoral fellowship and reported having no other disclosures.
Key clinical point: Prevalent oral HPV-16 infections tend to be persistent, and infection risk is highest for middle-aged and older men.
Major finding: 90% of prevalent infections persisted for at least 12 months; 40% persisted for at least 48 months.
Data source: An analysis of data from 23 patients in a multinational cohort study (HIM study).
Disclosures: The HIM study cohort was supported by grants from the National Cancer Institute and Merck Sharp & Dohme to individual authors. Dr. Campbell was supported, in part, by a postdoctoral fellowship and reported having no other disclosures.
Patients cured of gestational trophoblastic tumors rarely develop subsequent malignancy
Patients cured of gestational trophoblastic tumors using modern chemotherapy regimens have no overall increased risk of subsequent malignancy, according to findings from a review of nearly 2,000 patients treated at a single institution.
There is evidence, however, of an increased risk of leukemia in patients treated with etoposide, methotrexate, and dactinomycin followed by cyclophosphamide and vincristine (EMA-CO) on alternating weeks, of other site-specific malignancies in small numbers of patients, and of early menopause with most regimens, Dr. Philip Savage of Charing Cross Hospital, London, and his colleagues reported online Dec. 29 in the Journal of Clinical Oncology.
Of 1,903 patients treated between 1958 and 2000 with a mean follow-up of 16.9 years, 86 developed a subsequent malignancy, compared with the expected number of 79, based on a national age-matched population (standardized incidence ratio, 1.1). The risk was low among those treated with EMA-CO (standardized incidence ratio, 0.9), as well as among those treated with methotrexate and folinic acid (MTX-FA; standardized incidence ratio, 0.7), but was slightly higher when these two regimens were used with other nonalkylating agents and with other combination regimens including alkylating agents or cisplatin (standardized incidence ratios ranged from 1.4 to 1.9). The risk also increased with increasing numbers of chemotherapy cycles (standardized incidence ratio for 7-12 cycles, 1.4, and for 13 or more cycles, 2.5), the investigators said (J. Clin. Oncol. 2014 Dec. 29 [doi:10.1200/JCO.2014.57.5332]).
Leukemia occurred in six patients, including four who developed acute myeloid leukemia, and all cases developed within 10 years following chemotherapy. All four patients with acute myeloid leukemia had been treated with prolonged therapy involving “complex multidrug historical regimens,” and had etoposide exposure. Other risks included oral cancers – primarily in those treated with MTX-FA plus other nonalkylating agents, and melanoma and meningioma, which were nonsignificantly increased in several treatment categories, they noted.
Patients treated with MTX-FA had a low risk of early menopause, but the risk was 13% by age 40, and 36% by age 45 years among those treated with EMA-CO, they said.
Dr Savage reported having no disclosures.
Patients cured of gestational trophoblastic tumors using modern chemotherapy regimens have no overall increased risk of subsequent malignancy, according to findings from a review of nearly 2,000 patients treated at a single institution.
There is evidence, however, of an increased risk of leukemia in patients treated with etoposide, methotrexate, and dactinomycin followed by cyclophosphamide and vincristine (EMA-CO) on alternating weeks, of other site-specific malignancies in small numbers of patients, and of early menopause with most regimens, Dr. Philip Savage of Charing Cross Hospital, London, and his colleagues reported online Dec. 29 in the Journal of Clinical Oncology.
Of 1,903 patients treated between 1958 and 2000 with a mean follow-up of 16.9 years, 86 developed a subsequent malignancy, compared with the expected number of 79, based on a national age-matched population (standardized incidence ratio, 1.1). The risk was low among those treated with EMA-CO (standardized incidence ratio, 0.9), as well as among those treated with methotrexate and folinic acid (MTX-FA; standardized incidence ratio, 0.7), but was slightly higher when these two regimens were used with other nonalkylating agents and with other combination regimens including alkylating agents or cisplatin (standardized incidence ratios ranged from 1.4 to 1.9). The risk also increased with increasing numbers of chemotherapy cycles (standardized incidence ratio for 7-12 cycles, 1.4, and for 13 or more cycles, 2.5), the investigators said (J. Clin. Oncol. 2014 Dec. 29 [doi:10.1200/JCO.2014.57.5332]).
Leukemia occurred in six patients, including four who developed acute myeloid leukemia, and all cases developed within 10 years following chemotherapy. All four patients with acute myeloid leukemia had been treated with prolonged therapy involving “complex multidrug historical regimens,” and had etoposide exposure. Other risks included oral cancers – primarily in those treated with MTX-FA plus other nonalkylating agents, and melanoma and meningioma, which were nonsignificantly increased in several treatment categories, they noted.
Patients treated with MTX-FA had a low risk of early menopause, but the risk was 13% by age 40, and 36% by age 45 years among those treated with EMA-CO, they said.
Dr Savage reported having no disclosures.
Patients cured of gestational trophoblastic tumors using modern chemotherapy regimens have no overall increased risk of subsequent malignancy, according to findings from a review of nearly 2,000 patients treated at a single institution.
There is evidence, however, of an increased risk of leukemia in patients treated with etoposide, methotrexate, and dactinomycin followed by cyclophosphamide and vincristine (EMA-CO) on alternating weeks, of other site-specific malignancies in small numbers of patients, and of early menopause with most regimens, Dr. Philip Savage of Charing Cross Hospital, London, and his colleagues reported online Dec. 29 in the Journal of Clinical Oncology.
Of 1,903 patients treated between 1958 and 2000 with a mean follow-up of 16.9 years, 86 developed a subsequent malignancy, compared with the expected number of 79, based on a national age-matched population (standardized incidence ratio, 1.1). The risk was low among those treated with EMA-CO (standardized incidence ratio, 0.9), as well as among those treated with methotrexate and folinic acid (MTX-FA; standardized incidence ratio, 0.7), but was slightly higher when these two regimens were used with other nonalkylating agents and with other combination regimens including alkylating agents or cisplatin (standardized incidence ratios ranged from 1.4 to 1.9). The risk also increased with increasing numbers of chemotherapy cycles (standardized incidence ratio for 7-12 cycles, 1.4, and for 13 or more cycles, 2.5), the investigators said (J. Clin. Oncol. 2014 Dec. 29 [doi:10.1200/JCO.2014.57.5332]).
Leukemia occurred in six patients, including four who developed acute myeloid leukemia, and all cases developed within 10 years following chemotherapy. All four patients with acute myeloid leukemia had been treated with prolonged therapy involving “complex multidrug historical regimens,” and had etoposide exposure. Other risks included oral cancers – primarily in those treated with MTX-FA plus other nonalkylating agents, and melanoma and meningioma, which were nonsignificantly increased in several treatment categories, they noted.
Patients treated with MTX-FA had a low risk of early menopause, but the risk was 13% by age 40, and 36% by age 45 years among those treated with EMA-CO, they said.
Dr Savage reported having no disclosures.
FROM THE JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: The findings should reassure those using MTX-FA therapy that risk of second malignancy and early menopause is low.
Major finding: No overall increased incidence of subsequent malignancies after chemotherapy for gestational trophoblastic tumors (standardized incidence ratio, 1.1).
Data source: A review of 1,903 patients at a single institution.
Disclosures: Dr Savage reported having no disclosures.
Bundled intervention tackles S. aureus SSIs
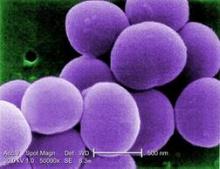
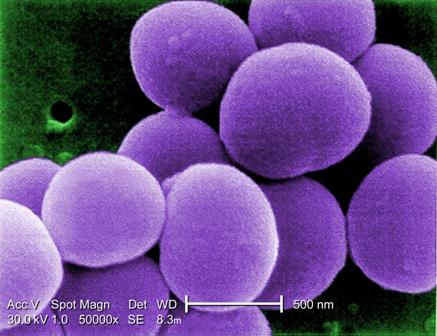
PHILADELPHIA – A bundled intervention including Staphylococcus aureus screening, decolonization, and targeted perioperative prophylaxis significantly decreased the rate of complex S. aureus surgical site infections in a multicenter quasi-experimental effectiveness study of patients undergoing cardiac operations or total joint arthroplasty.
The pooled rate of complex S. aureus surgical site infections (SSIs) decreased from 0.36% following 28,218 procedures performed during the preintervention period to 0.20% after 14,316 procedures performed during the intervention period (rate ratio, 0.58), Dr. Loreen A. Herwaldt of the University of Iowa, Iowa City, reported at an annual scientific meeting on infectious diseases.
Further, the number of months with no complex S. aureus SSIs increased from 2 of 39 months (5.1%) to 8 of 22 months (36.4%) Dr. Herwaldt said, noting that the median rate and range of complex SSIs became zero by intervention month 4.
The decrease in SSIs was greatest for joint arthroplasties, she said at the combined annual meetings of the Infectious Diseases Society of America, the Society for Healthcare Epidemiology of America, the HIV Medicine Association, and the Pediatric Infectious Diseases Society.
Subgroup analyses also demonstrated significantly lower rates of complex SSIs for scheduled vs. nonscheduled or emergent operations (rate ratio, 0.55), fully adherent vs. partially or nonadherent operations (rate ratio, 0.26), and for operations in which the surgeon (in accordance with hospital participation) implemented at least some bundle elements vs. no bundle elements (rate ratio, 0.54), she said, explaining that surgeons could opt out of the study even if a hospital was participating.
The rate of complex SSIs caused by any pathogen also was reduced (rate ratio, 0.67).
“We were very pleased to note that gram negative SSIs did not increase. The rate ratio was 0.86, and the confidence interval did cross 1 and the P value was 0.67,” she said.
The study, known as STOP SSI, was conducted at 20 Hospital Corporation of America (HCA) hospitals in nine states from March 1, 2009, to March 31, 2014. Patients who tested positive for methicillin-resistant or methicillin-susceptible S. aureus on a preoperative nares screen within 30 days before surgery were asked to apply mupirocin intranasally twice daily for 5 days and to bathe with chlorhexidine gluconate once daily for 5 days prior to their operation, including on the night before and the morning of surgery. Those who tested negative for MRSA and MSSA bathed with chlorhexidine gluconate only on the night before surgery and the morning of surgery.
Those with MRSA were treated with vancomycin and cefazolin perioperatively, and those without MRSA received only cefazolin.
If the patient’s status was unknown at the time of the operation, the goal was to have the patient bathe in chlorhexidine and to give as many intranasal doses of mupirocin as possible before surgery. The patient was treated perioperatively with vancomycin and cefazolin, and if it was later determined that the patient was positive for MRSA, the mupirocin was continued after surgery until the patient had been treated for 5 days.
After a 3-month phase-in period, 48% of the hospitals were fully compliant with this protocol, and 20% were partially compliant.
The use of a bundled intervention similar to the one used in this study was shown in a recent meta-analysis (BMJ 2013;346:f2743) to be likely to reduce the rate of S. aureus SSIs, but the approach had not been studied in a multicenter trial, Dr. Herwaldt said.
“Implementation of this SSI bundle was associated with significantly lower rates of complex S. aureus SSIs in the total cohort and in the hip and knee arthroplasty group. It was not associated with an increase in gram-negative SSIs, and thus we feel that if people actually did implement this bundle, it could substantially reduce patient morbidity and the cost of care,” she concluded, noting that the effect was seen only with implementation of the full bundle.
The Agency for Healthcare Research and Quality funded the study. Dr. Herwaldt reported having no disclosures.
PHILADELPHIA – A bundled intervention including Staphylococcus aureus screening, decolonization, and targeted perioperative prophylaxis significantly decreased the rate of complex S. aureus surgical site infections in a multicenter quasi-experimental effectiveness study of patients undergoing cardiac operations or total joint arthroplasty.
The pooled rate of complex S. aureus surgical site infections (SSIs) decreased from 0.36% following 28,218 procedures performed during the preintervention period to 0.20% after 14,316 procedures performed during the intervention period (rate ratio, 0.58), Dr. Loreen A. Herwaldt of the University of Iowa, Iowa City, reported at an annual scientific meeting on infectious diseases.
Further, the number of months with no complex S. aureus SSIs increased from 2 of 39 months (5.1%) to 8 of 22 months (36.4%) Dr. Herwaldt said, noting that the median rate and range of complex SSIs became zero by intervention month 4.
The decrease in SSIs was greatest for joint arthroplasties, she said at the combined annual meetings of the Infectious Diseases Society of America, the Society for Healthcare Epidemiology of America, the HIV Medicine Association, and the Pediatric Infectious Diseases Society.
Subgroup analyses also demonstrated significantly lower rates of complex SSIs for scheduled vs. nonscheduled or emergent operations (rate ratio, 0.55), fully adherent vs. partially or nonadherent operations (rate ratio, 0.26), and for operations in which the surgeon (in accordance with hospital participation) implemented at least some bundle elements vs. no bundle elements (rate ratio, 0.54), she said, explaining that surgeons could opt out of the study even if a hospital was participating.
The rate of complex SSIs caused by any pathogen also was reduced (rate ratio, 0.67).
“We were very pleased to note that gram negative SSIs did not increase. The rate ratio was 0.86, and the confidence interval did cross 1 and the P value was 0.67,” she said.
The study, known as STOP SSI, was conducted at 20 Hospital Corporation of America (HCA) hospitals in nine states from March 1, 2009, to March 31, 2014. Patients who tested positive for methicillin-resistant or methicillin-susceptible S. aureus on a preoperative nares screen within 30 days before surgery were asked to apply mupirocin intranasally twice daily for 5 days and to bathe with chlorhexidine gluconate once daily for 5 days prior to their operation, including on the night before and the morning of surgery. Those who tested negative for MRSA and MSSA bathed with chlorhexidine gluconate only on the night before surgery and the morning of surgery.
Those with MRSA were treated with vancomycin and cefazolin perioperatively, and those without MRSA received only cefazolin.
If the patient’s status was unknown at the time of the operation, the goal was to have the patient bathe in chlorhexidine and to give as many intranasal doses of mupirocin as possible before surgery. The patient was treated perioperatively with vancomycin and cefazolin, and if it was later determined that the patient was positive for MRSA, the mupirocin was continued after surgery until the patient had been treated for 5 days.
After a 3-month phase-in period, 48% of the hospitals were fully compliant with this protocol, and 20% were partially compliant.
The use of a bundled intervention similar to the one used in this study was shown in a recent meta-analysis (BMJ 2013;346:f2743) to be likely to reduce the rate of S. aureus SSIs, but the approach had not been studied in a multicenter trial, Dr. Herwaldt said.
“Implementation of this SSI bundle was associated with significantly lower rates of complex S. aureus SSIs in the total cohort and in the hip and knee arthroplasty group. It was not associated with an increase in gram-negative SSIs, and thus we feel that if people actually did implement this bundle, it could substantially reduce patient morbidity and the cost of care,” she concluded, noting that the effect was seen only with implementation of the full bundle.
The Agency for Healthcare Research and Quality funded the study. Dr. Herwaldt reported having no disclosures.
PHILADELPHIA – A bundled intervention including Staphylococcus aureus screening, decolonization, and targeted perioperative prophylaxis significantly decreased the rate of complex S. aureus surgical site infections in a multicenter quasi-experimental effectiveness study of patients undergoing cardiac operations or total joint arthroplasty.
The pooled rate of complex S. aureus surgical site infections (SSIs) decreased from 0.36% following 28,218 procedures performed during the preintervention period to 0.20% after 14,316 procedures performed during the intervention period (rate ratio, 0.58), Dr. Loreen A. Herwaldt of the University of Iowa, Iowa City, reported at an annual scientific meeting on infectious diseases.
Further, the number of months with no complex S. aureus SSIs increased from 2 of 39 months (5.1%) to 8 of 22 months (36.4%) Dr. Herwaldt said, noting that the median rate and range of complex SSIs became zero by intervention month 4.
The decrease in SSIs was greatest for joint arthroplasties, she said at the combined annual meetings of the Infectious Diseases Society of America, the Society for Healthcare Epidemiology of America, the HIV Medicine Association, and the Pediatric Infectious Diseases Society.
Subgroup analyses also demonstrated significantly lower rates of complex SSIs for scheduled vs. nonscheduled or emergent operations (rate ratio, 0.55), fully adherent vs. partially or nonadherent operations (rate ratio, 0.26), and for operations in which the surgeon (in accordance with hospital participation) implemented at least some bundle elements vs. no bundle elements (rate ratio, 0.54), she said, explaining that surgeons could opt out of the study even if a hospital was participating.
The rate of complex SSIs caused by any pathogen also was reduced (rate ratio, 0.67).
“We were very pleased to note that gram negative SSIs did not increase. The rate ratio was 0.86, and the confidence interval did cross 1 and the P value was 0.67,” she said.
The study, known as STOP SSI, was conducted at 20 Hospital Corporation of America (HCA) hospitals in nine states from March 1, 2009, to March 31, 2014. Patients who tested positive for methicillin-resistant or methicillin-susceptible S. aureus on a preoperative nares screen within 30 days before surgery were asked to apply mupirocin intranasally twice daily for 5 days and to bathe with chlorhexidine gluconate once daily for 5 days prior to their operation, including on the night before and the morning of surgery. Those who tested negative for MRSA and MSSA bathed with chlorhexidine gluconate only on the night before surgery and the morning of surgery.
Those with MRSA were treated with vancomycin and cefazolin perioperatively, and those without MRSA received only cefazolin.
If the patient’s status was unknown at the time of the operation, the goal was to have the patient bathe in chlorhexidine and to give as many intranasal doses of mupirocin as possible before surgery. The patient was treated perioperatively with vancomycin and cefazolin, and if it was later determined that the patient was positive for MRSA, the mupirocin was continued after surgery until the patient had been treated for 5 days.
After a 3-month phase-in period, 48% of the hospitals were fully compliant with this protocol, and 20% were partially compliant.
The use of a bundled intervention similar to the one used in this study was shown in a recent meta-analysis (BMJ 2013;346:f2743) to be likely to reduce the rate of S. aureus SSIs, but the approach had not been studied in a multicenter trial, Dr. Herwaldt said.
“Implementation of this SSI bundle was associated with significantly lower rates of complex S. aureus SSIs in the total cohort and in the hip and knee arthroplasty group. It was not associated with an increase in gram-negative SSIs, and thus we feel that if people actually did implement this bundle, it could substantially reduce patient morbidity and the cost of care,” she concluded, noting that the effect was seen only with implementation of the full bundle.
The Agency for Healthcare Research and Quality funded the study. Dr. Herwaldt reported having no disclosures.
AT IDWEEK 2014
Key clinical point: Implementing a bundled intervention reduced S. aureus SSIs and could reduce patient morbidity and costs.
Major finding: The pooled S. aureus SSI rate decreased from 0.36% to 0.20% (rate ratio, 0.58).
Data source: A multicenter quasi-experimental effectiveness study of 42,534 procedures.
Disclosures: The Agency for Healthcare Research and Quality funded the study. Dr. Herwaldt reported having no disclosures.
Number, not level, of positive antibodies predicts mortality in early RA
Seropositivity for both rheumatoid factor and anti-citrullinated protein antibody was associated with increased mortality, compared with single positivity or seronegativity in patients with early inflammatory arthritis in two large, independent observational cohorts.
However, higher levels of the antibodies did not appear to be associated with early deaths as the influence of increasing antibody level was not consistent in the two cohorts, Dr. Jennifer H. Humphreys of the University of Manchester (England) and her colleagues reported (Arthritis Res. Ther. 2014 Dec. 4 [doi:10.1186/s13075-014-0483-3]).
Among 3,053 patients in the Norfolk Arthritis Register (NOAR) cohort and 1,909 in the Leiden Early Arthritis Clinic (EAC) cohort, double antibody positivity – which occurred in 35% and 42% of patients in the cohorts, respectively – was associated with excess mortality (adjusted hazard ratios, 1.35 and 1.57). However, when antibody status was negative, low-positive, or high-positive, findings in one cohort were not replicated in the other. For example, there was a marked difference in rheumatoid factor high and low positivity in the NOAR cohort (adjusted HRs of 0.80 and 1.49, respectively), but not in the EAC cohort (adjusted HRs of 1.62 and 1.63, respectively), the investigators said.
Median patient age at symptom onset was 56 years in NOAR and 54 years in EAC, and 65% and 63% of subjects in the cohorts, respectively, were women. They were followed for a mean of 11.8 years and 8.5 years, until death or censor date, and analyses were adjusted for age, sex, smoking status, inflammatory markers, and year of enrollment.
The findings suggest that in patients presenting with early rheumatoid arthritis, mortality risk may be better assessed by the number of positive antibodies than by the antibody levels, the investigators concluded.
NOAR is funded by Arthritis Research UK grants, as is Dr. Humphreys. The current study was also funded by the European Community Seventh Framework Program FP7 and a Vidi grant of the Netherlands Organization for Scientific Research. The authors reported having no other disclosures.
Seropositivity for both rheumatoid factor and anti-citrullinated protein antibody was associated with increased mortality, compared with single positivity or seronegativity in patients with early inflammatory arthritis in two large, independent observational cohorts.
However, higher levels of the antibodies did not appear to be associated with early deaths as the influence of increasing antibody level was not consistent in the two cohorts, Dr. Jennifer H. Humphreys of the University of Manchester (England) and her colleagues reported (Arthritis Res. Ther. 2014 Dec. 4 [doi:10.1186/s13075-014-0483-3]).
Among 3,053 patients in the Norfolk Arthritis Register (NOAR) cohort and 1,909 in the Leiden Early Arthritis Clinic (EAC) cohort, double antibody positivity – which occurred in 35% and 42% of patients in the cohorts, respectively – was associated with excess mortality (adjusted hazard ratios, 1.35 and 1.57). However, when antibody status was negative, low-positive, or high-positive, findings in one cohort were not replicated in the other. For example, there was a marked difference in rheumatoid factor high and low positivity in the NOAR cohort (adjusted HRs of 0.80 and 1.49, respectively), but not in the EAC cohort (adjusted HRs of 1.62 and 1.63, respectively), the investigators said.
Median patient age at symptom onset was 56 years in NOAR and 54 years in EAC, and 65% and 63% of subjects in the cohorts, respectively, were women. They were followed for a mean of 11.8 years and 8.5 years, until death or censor date, and analyses were adjusted for age, sex, smoking status, inflammatory markers, and year of enrollment.
The findings suggest that in patients presenting with early rheumatoid arthritis, mortality risk may be better assessed by the number of positive antibodies than by the antibody levels, the investigators concluded.
NOAR is funded by Arthritis Research UK grants, as is Dr. Humphreys. The current study was also funded by the European Community Seventh Framework Program FP7 and a Vidi grant of the Netherlands Organization for Scientific Research. The authors reported having no other disclosures.
Seropositivity for both rheumatoid factor and anti-citrullinated protein antibody was associated with increased mortality, compared with single positivity or seronegativity in patients with early inflammatory arthritis in two large, independent observational cohorts.
However, higher levels of the antibodies did not appear to be associated with early deaths as the influence of increasing antibody level was not consistent in the two cohorts, Dr. Jennifer H. Humphreys of the University of Manchester (England) and her colleagues reported (Arthritis Res. Ther. 2014 Dec. 4 [doi:10.1186/s13075-014-0483-3]).
Among 3,053 patients in the Norfolk Arthritis Register (NOAR) cohort and 1,909 in the Leiden Early Arthritis Clinic (EAC) cohort, double antibody positivity – which occurred in 35% and 42% of patients in the cohorts, respectively – was associated with excess mortality (adjusted hazard ratios, 1.35 and 1.57). However, when antibody status was negative, low-positive, or high-positive, findings in one cohort were not replicated in the other. For example, there was a marked difference in rheumatoid factor high and low positivity in the NOAR cohort (adjusted HRs of 0.80 and 1.49, respectively), but not in the EAC cohort (adjusted HRs of 1.62 and 1.63, respectively), the investigators said.
Median patient age at symptom onset was 56 years in NOAR and 54 years in EAC, and 65% and 63% of subjects in the cohorts, respectively, were women. They were followed for a mean of 11.8 years and 8.5 years, until death or censor date, and analyses were adjusted for age, sex, smoking status, inflammatory markers, and year of enrollment.
The findings suggest that in patients presenting with early rheumatoid arthritis, mortality risk may be better assessed by the number of positive antibodies than by the antibody levels, the investigators concluded.
NOAR is funded by Arthritis Research UK grants, as is Dr. Humphreys. The current study was also funded by the European Community Seventh Framework Program FP7 and a Vidi grant of the Netherlands Organization for Scientific Research. The authors reported having no other disclosures.
FROM ARTHRITIS RESEARCH & THERAPY
Key clinical point: Dual rheumatoid factor and anti-citrullinated protein antibody positivity may be better than antibody levels for predicting mortality risk in patients with early inflammatory arthritis.
Major finding: Double antibody positivity was associated with excess mortality in the NOAR and EAC cohorts (adjusted hazard ratios, 1.35 and 1.57).
Data source: Two observational cohorts totaling 4,962 patients.
Disclosures: NOAR is funded by Arthritis Research UK grants, as is Dr. Humphreys. The current study was also funded by the European Community Seventh Framework Program FP7 and a Vidi grant of the Netherlands Organization for Scientific Research. The authors reported having no other disclosures.
Bisphosphonates May Protect Against Endometrial Cancer
The use of nitrogenous bisphosphonates was associated with a nearly 50% reduction in the incidence of endometrial cancer among women in the PLCO, or Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial.
The endometrial cancer incidence rate among women in the study who reported ever using nitrogenous bisphosphonates was 8.7/10,000 person-years, compared with 17.7/10,000 person-years among those who reported never being exposed to nitrogenous bisphosphonates (rate ratio, 0.49), Sharon Hensley Alford, Ph.D., of the Henry Ford Health System, Detroit, and her colleagues reported online Dec. 22 in Cancer.
The effect was similar after adjustment for age, race, body mass index, smoking status, and use of hormone therapy (hazard ratio, 0.56). The effect was also similar for both type I and type II disease, although there were only nine cases of type II disease, so the finding did not reach statistical significance, the investigators reported (Cancer 2014 Dec. 22 [doi:10.1002/cncr.28952]).
PLCO study subjects included in the current analysis were 23,485 women aged 55-74 years at study entry between 1993 and 2001, who had no cancer diagnosed prior to year 5 of the study when they completed a supplemental questionnaire to assess bone medication use. The women were followed until last known contact, death, or endometrial cancer diagnosis.
The findings support those of preclinical studies demonstrating antitumor effects of bisphosphonates, and suggest that their use may protect against endometrial cancer, the investigators said.
“However, additional studies are needed that include other potential confounders and a larger sample so that type II endometrial cancer could be assessed more confidently,” they concluded, adding that a trial assessing for endometrial, breast, and colorectal cancer in postmenopausal women would be ideal.
The PLCO trial was funded by the National Institutes of Health. The authors reported having no relevant financial disclosures.
The use of nitrogenous bisphosphonates was associated with a nearly 50% reduction in the incidence of endometrial cancer among women in the PLCO, or Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial.
The endometrial cancer incidence rate among women in the study who reported ever using nitrogenous bisphosphonates was 8.7/10,000 person-years, compared with 17.7/10,000 person-years among those who reported never being exposed to nitrogenous bisphosphonates (rate ratio, 0.49), Sharon Hensley Alford, Ph.D., of the Henry Ford Health System, Detroit, and her colleagues reported online Dec. 22 in Cancer.
The effect was similar after adjustment for age, race, body mass index, smoking status, and use of hormone therapy (hazard ratio, 0.56). The effect was also similar for both type I and type II disease, although there were only nine cases of type II disease, so the finding did not reach statistical significance, the investigators reported (Cancer 2014 Dec. 22 [doi:10.1002/cncr.28952]).
PLCO study subjects included in the current analysis were 23,485 women aged 55-74 years at study entry between 1993 and 2001, who had no cancer diagnosed prior to year 5 of the study when they completed a supplemental questionnaire to assess bone medication use. The women were followed until last known contact, death, or endometrial cancer diagnosis.
The findings support those of preclinical studies demonstrating antitumor effects of bisphosphonates, and suggest that their use may protect against endometrial cancer, the investigators said.
“However, additional studies are needed that include other potential confounders and a larger sample so that type II endometrial cancer could be assessed more confidently,” they concluded, adding that a trial assessing for endometrial, breast, and colorectal cancer in postmenopausal women would be ideal.
The PLCO trial was funded by the National Institutes of Health. The authors reported having no relevant financial disclosures.
The use of nitrogenous bisphosphonates was associated with a nearly 50% reduction in the incidence of endometrial cancer among women in the PLCO, or Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial.
The endometrial cancer incidence rate among women in the study who reported ever using nitrogenous bisphosphonates was 8.7/10,000 person-years, compared with 17.7/10,000 person-years among those who reported never being exposed to nitrogenous bisphosphonates (rate ratio, 0.49), Sharon Hensley Alford, Ph.D., of the Henry Ford Health System, Detroit, and her colleagues reported online Dec. 22 in Cancer.
The effect was similar after adjustment for age, race, body mass index, smoking status, and use of hormone therapy (hazard ratio, 0.56). The effect was also similar for both type I and type II disease, although there were only nine cases of type II disease, so the finding did not reach statistical significance, the investigators reported (Cancer 2014 Dec. 22 [doi:10.1002/cncr.28952]).
PLCO study subjects included in the current analysis were 23,485 women aged 55-74 years at study entry between 1993 and 2001, who had no cancer diagnosed prior to year 5 of the study when they completed a supplemental questionnaire to assess bone medication use. The women were followed until last known contact, death, or endometrial cancer diagnosis.
The findings support those of preclinical studies demonstrating antitumor effects of bisphosphonates, and suggest that their use may protect against endometrial cancer, the investigators said.
“However, additional studies are needed that include other potential confounders and a larger sample so that type II endometrial cancer could be assessed more confidently,” they concluded, adding that a trial assessing for endometrial, breast, and colorectal cancer in postmenopausal women would be ideal.
The PLCO trial was funded by the National Institutes of Health. The authors reported having no relevant financial disclosures.
FROM CANCER
Bisphosphonates may protect against endometrial cancer
The use of nitrogenous bisphosphonates was associated with a nearly 50% reduction in the incidence of endometrial cancer among women in the PLCO, or Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial.
The endometrial cancer incidence rate among women in the study who reported ever using nitrogenous bisphosphonates was 8.7/10,000 person-years, compared with 17.7/10,000 person-years among those who reported never being exposed to nitrogenous bisphosphonates (rate ratio, 0.49), Sharon Hensley Alford, Ph.D., of the Henry Ford Health System, Detroit, and her colleagues reported online Dec. 22 in Cancer.
The effect was similar after adjustment for age, race, body mass index, smoking status, and use of hormone therapy (hazard ratio, 0.56). The effect was also similar for both type I and type II disease, although there were only nine cases of type II disease, so the finding did not reach statistical significance, the investigators reported (Cancer 2014 Dec. 22 [doi:10.1002/cncr.28952]).
PLCO study subjects included in the current analysis were 23,485 women aged 55-74 years at study entry between 1993 and 2001, who had no cancer diagnosed prior to year 5 of the study when they completed a supplemental questionnaire to assess bone medication use. The women were followed until last known contact, death, or endometrial cancer diagnosis.
The findings support those of preclinical studies demonstrating antitumor effects of bisphosphonates, and suggest that their use may protect against endometrial cancer, the investigators said.
“However, additional studies are needed that include other potential confounders and a larger sample so that type II endometrial cancer could be assessed more confidently,” they concluded, adding that a trial assessing for endometrial, breast, and colorectal cancer in postmenopausal women would be ideal.
The PLCO trial was funded by the National Institutes of Health. The authors reported having no relevant financial disclosures.
The use of nitrogenous bisphosphonates was associated with a nearly 50% reduction in the incidence of endometrial cancer among women in the PLCO, or Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial.
The endometrial cancer incidence rate among women in the study who reported ever using nitrogenous bisphosphonates was 8.7/10,000 person-years, compared with 17.7/10,000 person-years among those who reported never being exposed to nitrogenous bisphosphonates (rate ratio, 0.49), Sharon Hensley Alford, Ph.D., of the Henry Ford Health System, Detroit, and her colleagues reported online Dec. 22 in Cancer.
The effect was similar after adjustment for age, race, body mass index, smoking status, and use of hormone therapy (hazard ratio, 0.56). The effect was also similar for both type I and type II disease, although there were only nine cases of type II disease, so the finding did not reach statistical significance, the investigators reported (Cancer 2014 Dec. 22 [doi:10.1002/cncr.28952]).
PLCO study subjects included in the current analysis were 23,485 women aged 55-74 years at study entry between 1993 and 2001, who had no cancer diagnosed prior to year 5 of the study when they completed a supplemental questionnaire to assess bone medication use. The women were followed until last known contact, death, or endometrial cancer diagnosis.
The findings support those of preclinical studies demonstrating antitumor effects of bisphosphonates, and suggest that their use may protect against endometrial cancer, the investigators said.
“However, additional studies are needed that include other potential confounders and a larger sample so that type II endometrial cancer could be assessed more confidently,” they concluded, adding that a trial assessing for endometrial, breast, and colorectal cancer in postmenopausal women would be ideal.
The PLCO trial was funded by the National Institutes of Health. The authors reported having no relevant financial disclosures.
The use of nitrogenous bisphosphonates was associated with a nearly 50% reduction in the incidence of endometrial cancer among women in the PLCO, or Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial.
The endometrial cancer incidence rate among women in the study who reported ever using nitrogenous bisphosphonates was 8.7/10,000 person-years, compared with 17.7/10,000 person-years among those who reported never being exposed to nitrogenous bisphosphonates (rate ratio, 0.49), Sharon Hensley Alford, Ph.D., of the Henry Ford Health System, Detroit, and her colleagues reported online Dec. 22 in Cancer.
The effect was similar after adjustment for age, race, body mass index, smoking status, and use of hormone therapy (hazard ratio, 0.56). The effect was also similar for both type I and type II disease, although there were only nine cases of type II disease, so the finding did not reach statistical significance, the investigators reported (Cancer 2014 Dec. 22 [doi:10.1002/cncr.28952]).
PLCO study subjects included in the current analysis were 23,485 women aged 55-74 years at study entry between 1993 and 2001, who had no cancer diagnosed prior to year 5 of the study when they completed a supplemental questionnaire to assess bone medication use. The women were followed until last known contact, death, or endometrial cancer diagnosis.
The findings support those of preclinical studies demonstrating antitumor effects of bisphosphonates, and suggest that their use may protect against endometrial cancer, the investigators said.
“However, additional studies are needed that include other potential confounders and a larger sample so that type II endometrial cancer could be assessed more confidently,” they concluded, adding that a trial assessing for endometrial, breast, and colorectal cancer in postmenopausal women would be ideal.
The PLCO trial was funded by the National Institutes of Health. The authors reported having no relevant financial disclosures.
FROM CANCER
Key clinical point: Women with a history of bisphosphonate use had a reduced risk of developing endometrial cancer.
Major finding: The endometrial cancer incidence rate was 8.7 vs. 17.7/10,000 person-years for ever vs. never users of nitrogenous bisphosphonates (rate ratio, 0.49).
Data source: An analysis of data from 23,485 women from a randomized population-based trial.
Disclosures: The PLCO trial was funded by the National Institutes of Health. The authors reported having no financial disclosures.
Anti-TGF-beta 1 therapy for diabetic nephropathy disappoints
PHILADELPHIA– Anti-TGF-beta 1 therapy was safe and well-tolerated, but failed to slow disease progression in patients with advanced diabetic nephropathy in a randomized, double-masked, phase 2 dose-ranging study.
In fact, the trial was terminated 4 months early for efficacy futility, Dr. James R. Voelker reported at Kidney Week 2014.
In 416 patients with type 1 or type 2 diabetes and a likelihood of rapid disease progression who were randomized to receive subcutaneous treatment with either placebo or various doses of a beta-1-specific humanized monoclonal neutralizing antibody known as LY2382770 (LY).
Treatment at any dose was not significantly more effective than placebo with respect to the primary outcome measure of mean change in serum creatinine. Mean serum creatinine increased from 2.22 to 2.48 mg/dl in the placebo group, and in the treatment groups it increased from 2.15 to 2.49 mg/dl (2 mg/month group), from 2.13 to 2.49 mg/dl (10 mg/month group), and from 2.15 to 2.50 mg/dl (50 mg/month group), Dr. Voelker of Eli Lilly and Co., Indianapolis, said at the meeting, which was sponsored by the American Society of Nephrology.
Patients in the study were adults aged 25 years or older (mean 62.2 years ) with serum creatinine of 1.3 to 3.3 mg/dl for women, and 1.5 to 3.5 mg/dl for men, or estimated glomerular filtration rate of 20 to 60 ml/min/1.73 m2, and they had a 24-hour urine protein/creatinine ratio of at least 800 mg/g. The groups were similar with respect to demographics and baseline characteristic, and most (75%) were men with type 2 diabetes (90%). All patient were receiving stable renin-angiotensin-system inhibition (RASi) therapy.
The intent was to select a population with a likelihood of fairly rapid disease progression during the course of the study to enable detection of a treatment effect, Dr. Voelker explained.
“Diabetic nephropathy is a disease of significant unmet medical need, as it is the leading cause of end-stage renal disease in much of the world. Thus. it is incumbent upon the nephrology community to identify new and more effective treatments than are currently available,” Dr. Voelker said.
TGF-beta over-activity has been implicated as a key pathogenic factor in diabetic neuropathy, and it was previously demonstrated that a TGF-beta 1-specific humanized monoclonal antibody was as effective as an antibody against all three TGF-beta isoforms, he said.
“We also had demonstrated that beta 1-specific inhibition in preclinical animal toxicology testing was far more tolerated than when you inhibit all 3 TGF-beta isoforms, which I should mention are all differentially expressed and regulated, but all signal through the same receptor complex,” he added, noting that based on these and other data, it was hypothesized that modulating excessive beta 1 activity with LY would safely slow renal progression in patients with diabetes on background RASi therapy.
The study was overseen by an independent data safety monitoring committee that reviewed unblinded safety data at periodic intervals. No safety issues emerged, but in the later stages of the study the committee did recommend that an unscheduled utility analysis be performed. Based on the results of that analysis, the decision was made to prematurely terminate the study about 4 months before its scheduled completion.
“Unfortunately there was no evidence in any of the study arms of a slowing of the rate of (serum creatinine increase),” Dr. Voelker said, adding that there also was no evidence of a benefit in numerous subgroup analyses, including analyses based on diabetes type.
Dr. Voelker is an employee of Eli Lilly and Co, which sponsored this study.
PHILADELPHIA– Anti-TGF-beta 1 therapy was safe and well-tolerated, but failed to slow disease progression in patients with advanced diabetic nephropathy in a randomized, double-masked, phase 2 dose-ranging study.
In fact, the trial was terminated 4 months early for efficacy futility, Dr. James R. Voelker reported at Kidney Week 2014.
In 416 patients with type 1 or type 2 diabetes and a likelihood of rapid disease progression who were randomized to receive subcutaneous treatment with either placebo or various doses of a beta-1-specific humanized monoclonal neutralizing antibody known as LY2382770 (LY).
Treatment at any dose was not significantly more effective than placebo with respect to the primary outcome measure of mean change in serum creatinine. Mean serum creatinine increased from 2.22 to 2.48 mg/dl in the placebo group, and in the treatment groups it increased from 2.15 to 2.49 mg/dl (2 mg/month group), from 2.13 to 2.49 mg/dl (10 mg/month group), and from 2.15 to 2.50 mg/dl (50 mg/month group), Dr. Voelker of Eli Lilly and Co., Indianapolis, said at the meeting, which was sponsored by the American Society of Nephrology.
Patients in the study were adults aged 25 years or older (mean 62.2 years ) with serum creatinine of 1.3 to 3.3 mg/dl for women, and 1.5 to 3.5 mg/dl for men, or estimated glomerular filtration rate of 20 to 60 ml/min/1.73 m2, and they had a 24-hour urine protein/creatinine ratio of at least 800 mg/g. The groups were similar with respect to demographics and baseline characteristic, and most (75%) were men with type 2 diabetes (90%). All patient were receiving stable renin-angiotensin-system inhibition (RASi) therapy.
The intent was to select a population with a likelihood of fairly rapid disease progression during the course of the study to enable detection of a treatment effect, Dr. Voelker explained.
“Diabetic nephropathy is a disease of significant unmet medical need, as it is the leading cause of end-stage renal disease in much of the world. Thus. it is incumbent upon the nephrology community to identify new and more effective treatments than are currently available,” Dr. Voelker said.
TGF-beta over-activity has been implicated as a key pathogenic factor in diabetic neuropathy, and it was previously demonstrated that a TGF-beta 1-specific humanized monoclonal antibody was as effective as an antibody against all three TGF-beta isoforms, he said.
“We also had demonstrated that beta 1-specific inhibition in preclinical animal toxicology testing was far more tolerated than when you inhibit all 3 TGF-beta isoforms, which I should mention are all differentially expressed and regulated, but all signal through the same receptor complex,” he added, noting that based on these and other data, it was hypothesized that modulating excessive beta 1 activity with LY would safely slow renal progression in patients with diabetes on background RASi therapy.
The study was overseen by an independent data safety monitoring committee that reviewed unblinded safety data at periodic intervals. No safety issues emerged, but in the later stages of the study the committee did recommend that an unscheduled utility analysis be performed. Based on the results of that analysis, the decision was made to prematurely terminate the study about 4 months before its scheduled completion.
“Unfortunately there was no evidence in any of the study arms of a slowing of the rate of (serum creatinine increase),” Dr. Voelker said, adding that there also was no evidence of a benefit in numerous subgroup analyses, including analyses based on diabetes type.
Dr. Voelker is an employee of Eli Lilly and Co, which sponsored this study.
PHILADELPHIA– Anti-TGF-beta 1 therapy was safe and well-tolerated, but failed to slow disease progression in patients with advanced diabetic nephropathy in a randomized, double-masked, phase 2 dose-ranging study.
In fact, the trial was terminated 4 months early for efficacy futility, Dr. James R. Voelker reported at Kidney Week 2014.
In 416 patients with type 1 or type 2 diabetes and a likelihood of rapid disease progression who were randomized to receive subcutaneous treatment with either placebo or various doses of a beta-1-specific humanized monoclonal neutralizing antibody known as LY2382770 (LY).
Treatment at any dose was not significantly more effective than placebo with respect to the primary outcome measure of mean change in serum creatinine. Mean serum creatinine increased from 2.22 to 2.48 mg/dl in the placebo group, and in the treatment groups it increased from 2.15 to 2.49 mg/dl (2 mg/month group), from 2.13 to 2.49 mg/dl (10 mg/month group), and from 2.15 to 2.50 mg/dl (50 mg/month group), Dr. Voelker of Eli Lilly and Co., Indianapolis, said at the meeting, which was sponsored by the American Society of Nephrology.
Patients in the study were adults aged 25 years or older (mean 62.2 years ) with serum creatinine of 1.3 to 3.3 mg/dl for women, and 1.5 to 3.5 mg/dl for men, or estimated glomerular filtration rate of 20 to 60 ml/min/1.73 m2, and they had a 24-hour urine protein/creatinine ratio of at least 800 mg/g. The groups were similar with respect to demographics and baseline characteristic, and most (75%) were men with type 2 diabetes (90%). All patient were receiving stable renin-angiotensin-system inhibition (RASi) therapy.
The intent was to select a population with a likelihood of fairly rapid disease progression during the course of the study to enable detection of a treatment effect, Dr. Voelker explained.
“Diabetic nephropathy is a disease of significant unmet medical need, as it is the leading cause of end-stage renal disease in much of the world. Thus. it is incumbent upon the nephrology community to identify new and more effective treatments than are currently available,” Dr. Voelker said.
TGF-beta over-activity has been implicated as a key pathogenic factor in diabetic neuropathy, and it was previously demonstrated that a TGF-beta 1-specific humanized monoclonal antibody was as effective as an antibody against all three TGF-beta isoforms, he said.
“We also had demonstrated that beta 1-specific inhibition in preclinical animal toxicology testing was far more tolerated than when you inhibit all 3 TGF-beta isoforms, which I should mention are all differentially expressed and regulated, but all signal through the same receptor complex,” he added, noting that based on these and other data, it was hypothesized that modulating excessive beta 1 activity with LY would safely slow renal progression in patients with diabetes on background RASi therapy.
The study was overseen by an independent data safety monitoring committee that reviewed unblinded safety data at periodic intervals. No safety issues emerged, but in the later stages of the study the committee did recommend that an unscheduled utility analysis be performed. Based on the results of that analysis, the decision was made to prematurely terminate the study about 4 months before its scheduled completion.
“Unfortunately there was no evidence in any of the study arms of a slowing of the rate of (serum creatinine increase),” Dr. Voelker said, adding that there also was no evidence of a benefit in numerous subgroup analyses, including analyses based on diabetes type.
Dr. Voelker is an employee of Eli Lilly and Co, which sponsored this study.
Key clinical point: Anti-TGF-beta 1 therapy failed to slow the progression of diabetic kidney disease.
Major finding: Mean serum creatinine increased from 2.22 to 2.48 mg/dl in the placebo group and in the treatment arms; 2.15 to 2.49 mg/dl (2 mg/month), 2.13 to 2.49 mg/dl (10 mg/month), and 2.15 to 2.50 mg/dl (50 mg/month).
Data source: A randomized, double-masked, phase-2 dose-ranging study involving 416 patients.
Disclosures: Dr. Voelker is an employee of Eli Lilly and Co, which sponsored this study.
Lower BP slows disease process in early PKD
PHILADELPHIA – Dual blockade of the renin-angiotensin-aldosterone system with combined angiotensin-converting enzyme inhibitor and angiotensin receptor blocker therapy was no more effective than ACE inhibitor therapy alone for slowing the rate of increase in total kidney volume in patients with early autosomal dominant polycystic kidney disease, investigators have reported.
Notably, though, aggressive blood pressure control, as compared with standard control, was associated with a slower rate of increase in total kidney volume in study A of the Halt Progression of Polycystic Kidney Disease (HALT-PKD) trial, Dr. Arlene B. Chapman reported at Kidney Week 2014.
Participants in the randomized, placebo-controlled 2x2 factorial trial were 423 hypertensive patients aged 15 to 49 years who had an estimated glomerular filtration rate (eGFR) of greater than 60 ml/min/1.73 m2 of body surface area. They were enrolled at 7 sites from February 2000 through June 2009, underwent a 2-4 week washout period during which antihypertensive therapy was discontinued and clonidine and labetalol therapy was maintained, and were randomized to receive either lisinopril plus telmisartan, or lisinopril plus placebo. They were also randomized to a standard blood pressure target of 120/70 to 130/80 mm Hg, or to a low blood pressure target of 95/60 to 110/75 mm Hg. Treatment doses were adjusted to achieve the target blood pressure, said Dr. Chapman of Emory University, Atlanta.
With respect to dual blockade of the renin-angiotensin-aldosterone system (RAAS) and the primary outcome of percentage change in total kidney volume over time, the rate of total kidney volume increase was similar at 6.0% and 6.2% per year in the lisinopril plus telmisartan group and the lisinopril plus placebo group, respectively, according to findings simultaneously published online Nov. 15 in the New England Journal of Medicine, which showed that total kidney volume increased by 40.5% and 42.2% at 60 months in the groups, respectively (N Engl J Med 2014 Nov. 15[doi:10.1056/NEJMoa1402685])
With respect to the standard vs. low blood pressure target, which was the focus of Dr. Chapman’s talk, significant differences were seen in systolic and diastolic blood pressure, with a difference of 13.4 mm Hg and 9.3 mm Hg, respectively, between the groups at the end of the trial, she said.
“Urinary aldosterone levels decreased significantly in both groups. However, there were no differences in the levels of change between the low and standard blood pressure groups,” she said.
The low target group had a 14.2% slower annual increase in total kidney volume at the end of the study as compared with those in the standard blood pressure target group (annualized change of 5.57% in the low target group vs. 6.57% in the standard target group), she said.
Overall, the change in eGFR did not differ between the groups. Urinary albumin excretion and left ventricular mass declined significantly more in the low vs. standard blood pressure control group, and renal vascular resistance remained the same in the low blood pressure control group, but increased in the standard blood pressure control group.
During a mean follow-up of 5 years, no differences were seen between the groups in the rate of hyperkalemia, acute kidney injury, hospitalizations, cardiac-related hospitalizations or mortality, and the event rates were low, she noted.
“Polycystic kidney disease is the fourth leading cause of renal failure in the United States. It is characterized by renal cyst growth with increased total kidney volume, resulting in activation of the renin-angiotensin system, the development of hypertension early, and progression to renal failure. To date there is no evidence that blood pressure control or blockade of the renin-angiotensin-system slows the progression of renal disease,” she said.
This portion of the HALT-PKD trial showed that both dual blockade of the RAAS and rigorous blood pressure control were safe, but that dual blockade provides no benefit as compared with lisinopril monotherapy with regard to change in total kidney volume and eGFR.
Aggressive blood pressure control, however, was of benefit.
“Low blood pressure treatment in young, healthy, hypertensive polycystic kidney disease patients with blockade of the renin-angiotensin-system was well-tolerated and safe and resulted in a 14.2% slower rate of total kidney volume growth over 5 years, reduced left ventricular mass index, urinary albumin secretion, and renal vascular resistance. This is without impact overall on the change in kidney function,” she concluded.
The HALT-PKD trial was funded by grants from the National Institute of Diabetes and Digestive and Kidney Diseases (including a grant to Dr. Chapman), the National Center for Research Resources General Clinical Research Centers, the National Center for Advancing Translational Sciences Clinical and Translational Science Awards, the Zell Family Foundation, and the PKD Foundation. Detailed author disclosures are available with the full text of the HALT-PKD study at NEJM.org.
Studies A and B of the HALT-PKD trial add to the growing number of studies showing no benefit with dual RAAS blockade over single blockade in patients with kidney disease, therefore, the observation in both studies that an ACE inhibitor used alone is effective for blood pressure control is encouraging, according to Dr. David H. Ellison and Dr. Julie Ingelfinger.
“These two studies provide important guidance for the care of patients with [autosomal dominant polycystic kidney disease}. They show that blood pressure can be controlled with ACE inhibitors, drugs that have an acceptable safety profile. They suggest that rigorous blood-pressure control, early in the disease process, may slow cyst growth and reduce the left-ventricular-mass index, but this approach is complicated by increased dizziness” they wrote in an editorial (N Engl J Med 2014, Nov. 15[doi:10.1056/NEJMe1412586]).
Also, the studies dissociate kidney-volume growth from a decline in renal function, which emphasizes the importance of hard outcomes in clinical trials involving patients with ADPKD, they said.
“Despite these limitations, the studies indicate that, with careful medical care, including meticulous attention to blood pressure, the prognosis for patients with ADPKD remains good,” they concluded.
Dr. Ellison is with Oregon Health and Science University, Portland. Dr. Ingelfinger is with Massachusetts General Hospital, Boston.
Studies A and B of the HALT-PKD trial add to the growing number of studies showing no benefit with dual RAAS blockade over single blockade in patients with kidney disease, therefore, the observation in both studies that an ACE inhibitor used alone is effective for blood pressure control is encouraging, according to Dr. David H. Ellison and Dr. Julie Ingelfinger.
“These two studies provide important guidance for the care of patients with [autosomal dominant polycystic kidney disease}. They show that blood pressure can be controlled with ACE inhibitors, drugs that have an acceptable safety profile. They suggest that rigorous blood-pressure control, early in the disease process, may slow cyst growth and reduce the left-ventricular-mass index, but this approach is complicated by increased dizziness” they wrote in an editorial (N Engl J Med 2014, Nov. 15[doi:10.1056/NEJMe1412586]).
Also, the studies dissociate kidney-volume growth from a decline in renal function, which emphasizes the importance of hard outcomes in clinical trials involving patients with ADPKD, they said.
“Despite these limitations, the studies indicate that, with careful medical care, including meticulous attention to blood pressure, the prognosis for patients with ADPKD remains good,” they concluded.
Dr. Ellison is with Oregon Health and Science University, Portland. Dr. Ingelfinger is with Massachusetts General Hospital, Boston.
Studies A and B of the HALT-PKD trial add to the growing number of studies showing no benefit with dual RAAS blockade over single blockade in patients with kidney disease, therefore, the observation in both studies that an ACE inhibitor used alone is effective for blood pressure control is encouraging, according to Dr. David H. Ellison and Dr. Julie Ingelfinger.
“These two studies provide important guidance for the care of patients with [autosomal dominant polycystic kidney disease}. They show that blood pressure can be controlled with ACE inhibitors, drugs that have an acceptable safety profile. They suggest that rigorous blood-pressure control, early in the disease process, may slow cyst growth and reduce the left-ventricular-mass index, but this approach is complicated by increased dizziness” they wrote in an editorial (N Engl J Med 2014, Nov. 15[doi:10.1056/NEJMe1412586]).
Also, the studies dissociate kidney-volume growth from a decline in renal function, which emphasizes the importance of hard outcomes in clinical trials involving patients with ADPKD, they said.
“Despite these limitations, the studies indicate that, with careful medical care, including meticulous attention to blood pressure, the prognosis for patients with ADPKD remains good,” they concluded.
Dr. Ellison is with Oregon Health and Science University, Portland. Dr. Ingelfinger is with Massachusetts General Hospital, Boston.
PHILADELPHIA – Dual blockade of the renin-angiotensin-aldosterone system with combined angiotensin-converting enzyme inhibitor and angiotensin receptor blocker therapy was no more effective than ACE inhibitor therapy alone for slowing the rate of increase in total kidney volume in patients with early autosomal dominant polycystic kidney disease, investigators have reported.
Notably, though, aggressive blood pressure control, as compared with standard control, was associated with a slower rate of increase in total kidney volume in study A of the Halt Progression of Polycystic Kidney Disease (HALT-PKD) trial, Dr. Arlene B. Chapman reported at Kidney Week 2014.
Participants in the randomized, placebo-controlled 2x2 factorial trial were 423 hypertensive patients aged 15 to 49 years who had an estimated glomerular filtration rate (eGFR) of greater than 60 ml/min/1.73 m2 of body surface area. They were enrolled at 7 sites from February 2000 through June 2009, underwent a 2-4 week washout period during which antihypertensive therapy was discontinued and clonidine and labetalol therapy was maintained, and were randomized to receive either lisinopril plus telmisartan, or lisinopril plus placebo. They were also randomized to a standard blood pressure target of 120/70 to 130/80 mm Hg, or to a low blood pressure target of 95/60 to 110/75 mm Hg. Treatment doses were adjusted to achieve the target blood pressure, said Dr. Chapman of Emory University, Atlanta.
With respect to dual blockade of the renin-angiotensin-aldosterone system (RAAS) and the primary outcome of percentage change in total kidney volume over time, the rate of total kidney volume increase was similar at 6.0% and 6.2% per year in the lisinopril plus telmisartan group and the lisinopril plus placebo group, respectively, according to findings simultaneously published online Nov. 15 in the New England Journal of Medicine, which showed that total kidney volume increased by 40.5% and 42.2% at 60 months in the groups, respectively (N Engl J Med 2014 Nov. 15[doi:10.1056/NEJMoa1402685])
With respect to the standard vs. low blood pressure target, which was the focus of Dr. Chapman’s talk, significant differences were seen in systolic and diastolic blood pressure, with a difference of 13.4 mm Hg and 9.3 mm Hg, respectively, between the groups at the end of the trial, she said.
“Urinary aldosterone levels decreased significantly in both groups. However, there were no differences in the levels of change between the low and standard blood pressure groups,” she said.
The low target group had a 14.2% slower annual increase in total kidney volume at the end of the study as compared with those in the standard blood pressure target group (annualized change of 5.57% in the low target group vs. 6.57% in the standard target group), she said.
Overall, the change in eGFR did not differ between the groups. Urinary albumin excretion and left ventricular mass declined significantly more in the low vs. standard blood pressure control group, and renal vascular resistance remained the same in the low blood pressure control group, but increased in the standard blood pressure control group.
During a mean follow-up of 5 years, no differences were seen between the groups in the rate of hyperkalemia, acute kidney injury, hospitalizations, cardiac-related hospitalizations or mortality, and the event rates were low, she noted.
“Polycystic kidney disease is the fourth leading cause of renal failure in the United States. It is characterized by renal cyst growth with increased total kidney volume, resulting in activation of the renin-angiotensin system, the development of hypertension early, and progression to renal failure. To date there is no evidence that blood pressure control or blockade of the renin-angiotensin-system slows the progression of renal disease,” she said.
This portion of the HALT-PKD trial showed that both dual blockade of the RAAS and rigorous blood pressure control were safe, but that dual blockade provides no benefit as compared with lisinopril monotherapy with regard to change in total kidney volume and eGFR.
Aggressive blood pressure control, however, was of benefit.
“Low blood pressure treatment in young, healthy, hypertensive polycystic kidney disease patients with blockade of the renin-angiotensin-system was well-tolerated and safe and resulted in a 14.2% slower rate of total kidney volume growth over 5 years, reduced left ventricular mass index, urinary albumin secretion, and renal vascular resistance. This is without impact overall on the change in kidney function,” she concluded.
The HALT-PKD trial was funded by grants from the National Institute of Diabetes and Digestive and Kidney Diseases (including a grant to Dr. Chapman), the National Center for Research Resources General Clinical Research Centers, the National Center for Advancing Translational Sciences Clinical and Translational Science Awards, the Zell Family Foundation, and the PKD Foundation. Detailed author disclosures are available with the full text of the HALT-PKD study at NEJM.org.
PHILADELPHIA – Dual blockade of the renin-angiotensin-aldosterone system with combined angiotensin-converting enzyme inhibitor and angiotensin receptor blocker therapy was no more effective than ACE inhibitor therapy alone for slowing the rate of increase in total kidney volume in patients with early autosomal dominant polycystic kidney disease, investigators have reported.
Notably, though, aggressive blood pressure control, as compared with standard control, was associated with a slower rate of increase in total kidney volume in study A of the Halt Progression of Polycystic Kidney Disease (HALT-PKD) trial, Dr. Arlene B. Chapman reported at Kidney Week 2014.
Participants in the randomized, placebo-controlled 2x2 factorial trial were 423 hypertensive patients aged 15 to 49 years who had an estimated glomerular filtration rate (eGFR) of greater than 60 ml/min/1.73 m2 of body surface area. They were enrolled at 7 sites from February 2000 through June 2009, underwent a 2-4 week washout period during which antihypertensive therapy was discontinued and clonidine and labetalol therapy was maintained, and were randomized to receive either lisinopril plus telmisartan, or lisinopril plus placebo. They were also randomized to a standard blood pressure target of 120/70 to 130/80 mm Hg, or to a low blood pressure target of 95/60 to 110/75 mm Hg. Treatment doses were adjusted to achieve the target blood pressure, said Dr. Chapman of Emory University, Atlanta.
With respect to dual blockade of the renin-angiotensin-aldosterone system (RAAS) and the primary outcome of percentage change in total kidney volume over time, the rate of total kidney volume increase was similar at 6.0% and 6.2% per year in the lisinopril plus telmisartan group and the lisinopril plus placebo group, respectively, according to findings simultaneously published online Nov. 15 in the New England Journal of Medicine, which showed that total kidney volume increased by 40.5% and 42.2% at 60 months in the groups, respectively (N Engl J Med 2014 Nov. 15[doi:10.1056/NEJMoa1402685])
With respect to the standard vs. low blood pressure target, which was the focus of Dr. Chapman’s talk, significant differences were seen in systolic and diastolic blood pressure, with a difference of 13.4 mm Hg and 9.3 mm Hg, respectively, between the groups at the end of the trial, she said.
“Urinary aldosterone levels decreased significantly in both groups. However, there were no differences in the levels of change between the low and standard blood pressure groups,” she said.
The low target group had a 14.2% slower annual increase in total kidney volume at the end of the study as compared with those in the standard blood pressure target group (annualized change of 5.57% in the low target group vs. 6.57% in the standard target group), she said.
Overall, the change in eGFR did not differ between the groups. Urinary albumin excretion and left ventricular mass declined significantly more in the low vs. standard blood pressure control group, and renal vascular resistance remained the same in the low blood pressure control group, but increased in the standard blood pressure control group.
During a mean follow-up of 5 years, no differences were seen between the groups in the rate of hyperkalemia, acute kidney injury, hospitalizations, cardiac-related hospitalizations or mortality, and the event rates were low, she noted.
“Polycystic kidney disease is the fourth leading cause of renal failure in the United States. It is characterized by renal cyst growth with increased total kidney volume, resulting in activation of the renin-angiotensin system, the development of hypertension early, and progression to renal failure. To date there is no evidence that blood pressure control or blockade of the renin-angiotensin-system slows the progression of renal disease,” she said.
This portion of the HALT-PKD trial showed that both dual blockade of the RAAS and rigorous blood pressure control were safe, but that dual blockade provides no benefit as compared with lisinopril monotherapy with regard to change in total kidney volume and eGFR.
Aggressive blood pressure control, however, was of benefit.
“Low blood pressure treatment in young, healthy, hypertensive polycystic kidney disease patients with blockade of the renin-angiotensin-system was well-tolerated and safe and resulted in a 14.2% slower rate of total kidney volume growth over 5 years, reduced left ventricular mass index, urinary albumin secretion, and renal vascular resistance. This is without impact overall on the change in kidney function,” she concluded.
The HALT-PKD trial was funded by grants from the National Institute of Diabetes and Digestive and Kidney Diseases (including a grant to Dr. Chapman), the National Center for Research Resources General Clinical Research Centers, the National Center for Advancing Translational Sciences Clinical and Translational Science Awards, the Zell Family Foundation, and the PKD Foundation. Detailed author disclosures are available with the full text of the HALT-PKD study at NEJM.org.
Key clinical point: Aggressive blood pressure control may be of benefit in patients with early PKD.
Major finding: Low vs. standard blood pressure control resulted in a 14.2% slower rate of total kidney volume increase.
Data source: The randomized, placebo-controlled HALT-PKD trial (Study A).
Disclosures: The HALT-PKD trial was funded by grants from the National Institute of Diabetes and Digestive and Kidney Diseases (including a grant to Dr. Chapman), The National Center for Research Resources General Clinical Research Centers, the National Center for Advancing Translational Sciences Clinical and Translational Science Awards, the Zell Family Foundation, and the PKD Foundation.