User login
Healthy weight gain in pregnancy: What the USPSTF recommends
REFERENCES
- US Preventive Services Task Force. Behavioral counseling interventions for healthy weight and weight gain in pregnancy: US Preventive Services Task Force recommendation statement. JAMA. 2021;325:2087-2092. doi:10.1001/jama.2021.6949
- Rasmussen KM, Yaktine AL, eds. Weight Gain During Pregnancy: Reexamining the Guidelines. National Academies Press; 2009. doi: 10.17226/12584
REFERENCES
- US Preventive Services Task Force. Behavioral counseling interventions for healthy weight and weight gain in pregnancy: US Preventive Services Task Force recommendation statement. JAMA. 2021;325:2087-2092. doi:10.1001/jama.2021.6949
- Rasmussen KM, Yaktine AL, eds. Weight Gain During Pregnancy: Reexamining the Guidelines. National Academies Press; 2009. doi: 10.17226/12584
REFERENCES
- US Preventive Services Task Force. Behavioral counseling interventions for healthy weight and weight gain in pregnancy: US Preventive Services Task Force recommendation statement. JAMA. 2021;325:2087-2092. doi:10.1001/jama.2021.6949
- Rasmussen KM, Yaktine AL, eds. Weight Gain During Pregnancy: Reexamining the Guidelines. National Academies Press; 2009. doi: 10.17226/12584
AGA Clinical Practice Update: Early complications after bariatric/metabolic surgery
The American Gastroenterological Association recently published a clinical practice update concerning endoscopic evaluation and management of early complications after bariatric/metabolic surgery.
The seven best practice advice statements, based on available evidence and expert opinion, range from a general call for high familiarity with available interventions to specific approaches for managing postoperative leaks.
According to lead author Vivek Kumbhari, MD, PhD, director of advanced endoscopy, department of gastroenterology and hepatology, Mayo Clinic, Jacksonville, Fla., and colleagues, the update was written in consideration of increasing rates of bariatric/metabolic surgery.
“Bariatric/metabolic surgery is unmatched with respect to its weight loss and metabolic benefits,” the investigators wrote in Clinical Gastroenterology and Hepatology. “The selection criteria will continue to broaden, likely resulting in increasing numbers of less robust patients undergoing surgery (e.g., children, elderly, and those with significant cardiorespiratory comorbidities).”
Although the 90-day overall complication rate across all patients undergoing bariatric/metabolic surgery is only 4%, Dr. Kumbhari and colleagues noted that this rate is considerably higher, at 20.1%, among patients aged older than 65 years.
“As utilization escalates, so will the number of patients who suffer early complications,” they wrote.
The first three items of best practice advice describe who should be managing complications after bariatric/metabolic surgery, and how.
Foremost, Dr. Kumbhari and colleagues called for a multidisciplinary approach; they suggested that endoscopists should work closely with related specialists, such as bariatric/metabolic surgeons and interventional radiologists.
“Timely communication between the endoscopist, radiologist, surgeon, nutritionists, and inpatient medical team or primary care physician will result in efficient, effective care with prompt escalation and deescalation,” they wrote. “Daily communication is advised.”
The next two best practice advice statements encourage high familiarity with endoscopic treatments, postsurgical anatomy, interventional radiology, and surgical interventions, including risks and benefits of each approach.
“The endoscopist should ... have expertise in interventional endoscopy techniques, including but not limited to using concomitant fluoroscopy, stent deployment and retrieval, pneumatic balloon dilation, incisional therapies, endoscopic suturing, and managing percutaneous drains,” the investigators wrote. “Having the ability to perform a wide array of therapies will enhance the likelihood that the optimal endoscopic strategy will be employed, as opposed to simply performing a technique with which the endoscopist has experience.”
Following these best practices, Dr. Kumbhari and colleagues advised screening patients with postoperative complications for comorbidities, both medical in nature (such as infection) and psychological.
“Patients often have higher depression and anxiety scores, as well as a lower physical quality of life, and medical teams sometimes neglect the patient’s psychological state,” they wrote. “It is imperative that the multidisciplinary team recognize and acknowledge the patient’s psychological comorbidities and engage expertise to manage them.”
Next, the investigators advised that endoscopic intervention should be considered regardless of time interval since surgery, including the immediate postoperative period.
“Endoscopy is often indicated as the initial therapeutic modality, and it can safely be performed,” Dr. Kumbhari and colleagues wrote. “When endoscopy is performed, it is advised to use carbon dioxide for insufflation. Caution should be used when advancing the endoscope into the small bowel, as it is best to minimize pressure along the fresh staple lines. In cases in which the patient is critically ill or the interventional endoscopist does not have extensive experience with such a scenario, the endoscopy should be performed in the operating room with a surgeon present (preferably the surgeon who performed the operation).”
Dr. Kumbhari and colleagues discussed functional stenosis, which can precipitate and propagate leaks. They noted that “downstream stenosis is frequently seen at the level of the incisura angularis or in the proximal stomach when a sleeve gastrectomy is performed in a patient with a prior laparoscopic adjustable gastric band.”
To address stenosis, the update calls for “aggressive dilation” using a large pneumatic balloon, preferably with fluoroscopy to make sure the distal end of the balloon does not cross the pylorus. The investigators noted that endoscopic suturing may be needed if a tear involving the muscularis propria is encountered.
Lastly, the clinical practice update offers comprehensive guidance for managing staple-line leaks, which “most commonly occur along the staple line of the proximal stomach.”
As leaks are thought to stem from ischemia, “most leaks are not present upon completion of the operation, and they develop over the subsequent weeks, often in the setting of downstream stenosis,” the investigators wrote.
To guide management of staple-line leaks, the investigators presented a treatment algorithm that incorporates defect size, time since surgery, and presence or absence of stenosis.
For example, a defect smaller than 10 mm occurring within 6 weeks of surgery and lacking stenosis may be managed with a percutaneous drain and diversion. In contrast, a defect of similar size, also without stenosis, but occurring later than 6 weeks after the initial procedure, should be managed with endoscopic internal drainage or vacuum therapy.
“Clinicians should recognize that the goal for endoscopic management of staple-line leaks is often not necessarily initial closure of the leak site, but rather techniques to promote drainage of material from the perigastric collection into the gastric lumen such that the leak site closes by secondary intention,” wrote Dr. Kumbhari and colleagues.
The clinical practice update was commissioned and approved by the AGA Institute Clinical Practice Updates Committee and the AGA Governing Board. The investigators disclosed relationships with Boston Scientific, Medtronic, Apollo Endosurgery, and others.
The American Gastroenterological Association recently published a clinical practice update concerning endoscopic evaluation and management of early complications after bariatric/metabolic surgery.
The seven best practice advice statements, based on available evidence and expert opinion, range from a general call for high familiarity with available interventions to specific approaches for managing postoperative leaks.
According to lead author Vivek Kumbhari, MD, PhD, director of advanced endoscopy, department of gastroenterology and hepatology, Mayo Clinic, Jacksonville, Fla., and colleagues, the update was written in consideration of increasing rates of bariatric/metabolic surgery.
“Bariatric/metabolic surgery is unmatched with respect to its weight loss and metabolic benefits,” the investigators wrote in Clinical Gastroenterology and Hepatology. “The selection criteria will continue to broaden, likely resulting in increasing numbers of less robust patients undergoing surgery (e.g., children, elderly, and those with significant cardiorespiratory comorbidities).”
Although the 90-day overall complication rate across all patients undergoing bariatric/metabolic surgery is only 4%, Dr. Kumbhari and colleagues noted that this rate is considerably higher, at 20.1%, among patients aged older than 65 years.
“As utilization escalates, so will the number of patients who suffer early complications,” they wrote.
The first three items of best practice advice describe who should be managing complications after bariatric/metabolic surgery, and how.
Foremost, Dr. Kumbhari and colleagues called for a multidisciplinary approach; they suggested that endoscopists should work closely with related specialists, such as bariatric/metabolic surgeons and interventional radiologists.
“Timely communication between the endoscopist, radiologist, surgeon, nutritionists, and inpatient medical team or primary care physician will result in efficient, effective care with prompt escalation and deescalation,” they wrote. “Daily communication is advised.”
The next two best practice advice statements encourage high familiarity with endoscopic treatments, postsurgical anatomy, interventional radiology, and surgical interventions, including risks and benefits of each approach.
“The endoscopist should ... have expertise in interventional endoscopy techniques, including but not limited to using concomitant fluoroscopy, stent deployment and retrieval, pneumatic balloon dilation, incisional therapies, endoscopic suturing, and managing percutaneous drains,” the investigators wrote. “Having the ability to perform a wide array of therapies will enhance the likelihood that the optimal endoscopic strategy will be employed, as opposed to simply performing a technique with which the endoscopist has experience.”
Following these best practices, Dr. Kumbhari and colleagues advised screening patients with postoperative complications for comorbidities, both medical in nature (such as infection) and psychological.
“Patients often have higher depression and anxiety scores, as well as a lower physical quality of life, and medical teams sometimes neglect the patient’s psychological state,” they wrote. “It is imperative that the multidisciplinary team recognize and acknowledge the patient’s psychological comorbidities and engage expertise to manage them.”
Next, the investigators advised that endoscopic intervention should be considered regardless of time interval since surgery, including the immediate postoperative period.
“Endoscopy is often indicated as the initial therapeutic modality, and it can safely be performed,” Dr. Kumbhari and colleagues wrote. “When endoscopy is performed, it is advised to use carbon dioxide for insufflation. Caution should be used when advancing the endoscope into the small bowel, as it is best to minimize pressure along the fresh staple lines. In cases in which the patient is critically ill or the interventional endoscopist does not have extensive experience with such a scenario, the endoscopy should be performed in the operating room with a surgeon present (preferably the surgeon who performed the operation).”
Dr. Kumbhari and colleagues discussed functional stenosis, which can precipitate and propagate leaks. They noted that “downstream stenosis is frequently seen at the level of the incisura angularis or in the proximal stomach when a sleeve gastrectomy is performed in a patient with a prior laparoscopic adjustable gastric band.”
To address stenosis, the update calls for “aggressive dilation” using a large pneumatic balloon, preferably with fluoroscopy to make sure the distal end of the balloon does not cross the pylorus. The investigators noted that endoscopic suturing may be needed if a tear involving the muscularis propria is encountered.
Lastly, the clinical practice update offers comprehensive guidance for managing staple-line leaks, which “most commonly occur along the staple line of the proximal stomach.”
As leaks are thought to stem from ischemia, “most leaks are not present upon completion of the operation, and they develop over the subsequent weeks, often in the setting of downstream stenosis,” the investigators wrote.
To guide management of staple-line leaks, the investigators presented a treatment algorithm that incorporates defect size, time since surgery, and presence or absence of stenosis.
For example, a defect smaller than 10 mm occurring within 6 weeks of surgery and lacking stenosis may be managed with a percutaneous drain and diversion. In contrast, a defect of similar size, also without stenosis, but occurring later than 6 weeks after the initial procedure, should be managed with endoscopic internal drainage or vacuum therapy.
“Clinicians should recognize that the goal for endoscopic management of staple-line leaks is often not necessarily initial closure of the leak site, but rather techniques to promote drainage of material from the perigastric collection into the gastric lumen such that the leak site closes by secondary intention,” wrote Dr. Kumbhari and colleagues.
The clinical practice update was commissioned and approved by the AGA Institute Clinical Practice Updates Committee and the AGA Governing Board. The investigators disclosed relationships with Boston Scientific, Medtronic, Apollo Endosurgery, and others.
The American Gastroenterological Association recently published a clinical practice update concerning endoscopic evaluation and management of early complications after bariatric/metabolic surgery.
The seven best practice advice statements, based on available evidence and expert opinion, range from a general call for high familiarity with available interventions to specific approaches for managing postoperative leaks.
According to lead author Vivek Kumbhari, MD, PhD, director of advanced endoscopy, department of gastroenterology and hepatology, Mayo Clinic, Jacksonville, Fla., and colleagues, the update was written in consideration of increasing rates of bariatric/metabolic surgery.
“Bariatric/metabolic surgery is unmatched with respect to its weight loss and metabolic benefits,” the investigators wrote in Clinical Gastroenterology and Hepatology. “The selection criteria will continue to broaden, likely resulting in increasing numbers of less robust patients undergoing surgery (e.g., children, elderly, and those with significant cardiorespiratory comorbidities).”
Although the 90-day overall complication rate across all patients undergoing bariatric/metabolic surgery is only 4%, Dr. Kumbhari and colleagues noted that this rate is considerably higher, at 20.1%, among patients aged older than 65 years.
“As utilization escalates, so will the number of patients who suffer early complications,” they wrote.
The first three items of best practice advice describe who should be managing complications after bariatric/metabolic surgery, and how.
Foremost, Dr. Kumbhari and colleagues called for a multidisciplinary approach; they suggested that endoscopists should work closely with related specialists, such as bariatric/metabolic surgeons and interventional radiologists.
“Timely communication between the endoscopist, radiologist, surgeon, nutritionists, and inpatient medical team or primary care physician will result in efficient, effective care with prompt escalation and deescalation,” they wrote. “Daily communication is advised.”
The next two best practice advice statements encourage high familiarity with endoscopic treatments, postsurgical anatomy, interventional radiology, and surgical interventions, including risks and benefits of each approach.
“The endoscopist should ... have expertise in interventional endoscopy techniques, including but not limited to using concomitant fluoroscopy, stent deployment and retrieval, pneumatic balloon dilation, incisional therapies, endoscopic suturing, and managing percutaneous drains,” the investigators wrote. “Having the ability to perform a wide array of therapies will enhance the likelihood that the optimal endoscopic strategy will be employed, as opposed to simply performing a technique with which the endoscopist has experience.”
Following these best practices, Dr. Kumbhari and colleagues advised screening patients with postoperative complications for comorbidities, both medical in nature (such as infection) and psychological.
“Patients often have higher depression and anxiety scores, as well as a lower physical quality of life, and medical teams sometimes neglect the patient’s psychological state,” they wrote. “It is imperative that the multidisciplinary team recognize and acknowledge the patient’s psychological comorbidities and engage expertise to manage them.”
Next, the investigators advised that endoscopic intervention should be considered regardless of time interval since surgery, including the immediate postoperative period.
“Endoscopy is often indicated as the initial therapeutic modality, and it can safely be performed,” Dr. Kumbhari and colleagues wrote. “When endoscopy is performed, it is advised to use carbon dioxide for insufflation. Caution should be used when advancing the endoscope into the small bowel, as it is best to minimize pressure along the fresh staple lines. In cases in which the patient is critically ill or the interventional endoscopist does not have extensive experience with such a scenario, the endoscopy should be performed in the operating room with a surgeon present (preferably the surgeon who performed the operation).”
Dr. Kumbhari and colleagues discussed functional stenosis, which can precipitate and propagate leaks. They noted that “downstream stenosis is frequently seen at the level of the incisura angularis or in the proximal stomach when a sleeve gastrectomy is performed in a patient with a prior laparoscopic adjustable gastric band.”
To address stenosis, the update calls for “aggressive dilation” using a large pneumatic balloon, preferably with fluoroscopy to make sure the distal end of the balloon does not cross the pylorus. The investigators noted that endoscopic suturing may be needed if a tear involving the muscularis propria is encountered.
Lastly, the clinical practice update offers comprehensive guidance for managing staple-line leaks, which “most commonly occur along the staple line of the proximal stomach.”
As leaks are thought to stem from ischemia, “most leaks are not present upon completion of the operation, and they develop over the subsequent weeks, often in the setting of downstream stenosis,” the investigators wrote.
To guide management of staple-line leaks, the investigators presented a treatment algorithm that incorporates defect size, time since surgery, and presence or absence of stenosis.
For example, a defect smaller than 10 mm occurring within 6 weeks of surgery and lacking stenosis may be managed with a percutaneous drain and diversion. In contrast, a defect of similar size, also without stenosis, but occurring later than 6 weeks after the initial procedure, should be managed with endoscopic internal drainage or vacuum therapy.
“Clinicians should recognize that the goal for endoscopic management of staple-line leaks is often not necessarily initial closure of the leak site, but rather techniques to promote drainage of material from the perigastric collection into the gastric lumen such that the leak site closes by secondary intention,” wrote Dr. Kumbhari and colleagues.
The clinical practice update was commissioned and approved by the AGA Institute Clinical Practice Updates Committee and the AGA Governing Board. The investigators disclosed relationships with Boston Scientific, Medtronic, Apollo Endosurgery, and others.
FROM CLINICAL GASTROENTEROLOGY AND HEPATOLOGY
Obesity hypoventilation: Moving the needle on underrecognition
Obesity hypoventilation syndrome (OHS) is bound to be increasing because of the rising obesity epidemic but is underrecognized and “frequently underdiagnosed,” Saiprakash B. Venkateshiah, MD, said at the virtual annual meeting of the Associated Professional Sleep Societies.
The condition, which can cause significant morbidity and mortality, is defined by the combination of obesity and awake alveolar hypoventilation (PaCO2 ≥45 mm Hg), with the exclusion of alternate causes of hypoventilation. Sleep-disordered breathing (SDB) is almost universally present, with approximately 90% of individuals with OHS also having obstructive sleep apnea (OSA), most often severe, and approximately 10% having sleep-related hypoventilation, or a “pure hypoventilation subtype, if you will,” said Dr. Venkateshiah, assistant professor of medicine at Emory University, Atlanta.
The prevalence of OHS in the general population is unknown, but its prevalence in patients who present for the evaluation of SDB has ranged from 8%-20% across multiple studies, he said. Up to 40% of patients with OHS present for the first time with acute hypercapnic respiratory failure, which has an in-hospital mortality of 18%.
Postmenopausal women appear to have a higher prevalence, compared with premenopausal women and men, he noted, and women appear to be more likely than men to present with the clinical phenotype of OHS without associated OSA.
The arterial blood gas measurement needed to document alveolar hypoventilation and definitively diagnosis OHA is a “simple and economical test,” he said, “but it is logistically very difficult to obtain [these measurements] routinely in all patients in the clinic ... and is one of the reasons why OSH is underdiagnosed.”
Guideline advice
A practice guideline published in 2019 by the American Thoracic Society suggests that, for obese patients with SDB and a low to moderate probability of having OSH, a serum bicarbonate level be measured first. “In patients with serum bicarbonate less than 27 mmol/L, clinicians might forgo measuring PaCO2, as the diagnosis in them is very unlikely,” Dr. Venkateshiah said, referring to the guideline. “In patients with a serum bicarbonate greater than 27, you might need to measure PaCO2 to confirm or rule out the diagnosis of OHS.”
(Patients strongly suspected of having OHS, with more than a low to moderate probability – those in whom arterial blood gases should be measured – are “usually severely obese with typical signs and symptoms such as dyspnea, nocturia, lower-extremity edema, excessive daytime sleepiness, fatigue, loud disruptive snoring, witnessed apneas, as well as mild hypoxemia during wake and/or significant hypoxemia during sleep,” the ATS guideline says.)
The guideline panel considered the use of oxygen saturation measured with pulse oximetry during wakefulness to screen for OHS and decided to advise against it because of the paucity of evidence-based literature, Dr. Venkateshiah noted. (In making its five conditional recommendations, the guideline panel cited an overall very low quality of evidence.)
Symptoms of OHS overlap with those of OSA (for example, daytime hypersomnolence, witnessed apneas, loud snoring, and morning headaches), so “symptoms alone cannot be used to discriminate between the two disorders,” he advised. Signs of OHS commonly seen in clinical exams, however, are low resting daytime oxygen saturations and lower-extremity edema. A sleep study, he added, is needed to document and characterize SDB in patients with OHS.
Positive airway pressure therapy is the first-line treatment for OHS, and long-term outcomes of patients with OHS on PAP treatment are significantly better, compared with untreated individuals. There is no strong evidence to recommend one form of PAP therapy over another for patients with OHS and concomitant severe OSA, he said, but “the bottom line” from both short- and long-term randomized clinical trials comparing CPAP with noninvasive ventilation “is that CPAP is equivalent to noninvasive ventilation as far as outcomes are concerned.”
The ATS guideline panel recommends continuous positive airway pressure therapy for patients with OHS and severe OSA. And for OHS with nonsevere OSA, bilevel PAP is traditionally used – including pure hypoventilators, Dr. Venkateshiah said.
Weight-loss interventions are paramount, since “the primary driver of OHS is obesity,” he said at the meeting. There are only a few studies that have looked at bariatric surgery in patients with OHS, he said, “but they did note significant improvements in gas exchange, sleep apnea, lung volumes and pulmonary hypertension.”
The ATS guideline suggests weight-loss interventions that produce sustained weight loss of 25%-30% of the actual body weight. Such interventions are “most likely required to achieve resolution of hypoventilation,” Dr. Venkateshiah said.
OHS vs. COPD
In a separate presentation on OHS, Michelle Cao, DO, clinical associate professor at Stanford (Calif.) University, emphasized the importance of distinguishing the patient with OHS from the patient with hypercapnic chronic obstructive pulmonary disease (COPD). Spirometry and the flow volume curve can help rule out hypercapnic COPD and other conditions that cause daytime hypoventilation.
A study published in 2016 of 600 hospitalized patients determined to have unequivocal OHS found that 43% had been misdiagnosed as having COPD and none had been previously diagnosed with OHS, Dr. Cao noted. Patients in the study had a mean age of 58 and a mean body mass index of 48.2 kg/m2; 64% were women.
Dr. Venkateshiah and Dr. Cao had no relevant disclosures.
Obesity hypoventilation syndrome (OHS) is bound to be increasing because of the rising obesity epidemic but is underrecognized and “frequently underdiagnosed,” Saiprakash B. Venkateshiah, MD, said at the virtual annual meeting of the Associated Professional Sleep Societies.
The condition, which can cause significant morbidity and mortality, is defined by the combination of obesity and awake alveolar hypoventilation (PaCO2 ≥45 mm Hg), with the exclusion of alternate causes of hypoventilation. Sleep-disordered breathing (SDB) is almost universally present, with approximately 90% of individuals with OHS also having obstructive sleep apnea (OSA), most often severe, and approximately 10% having sleep-related hypoventilation, or a “pure hypoventilation subtype, if you will,” said Dr. Venkateshiah, assistant professor of medicine at Emory University, Atlanta.
The prevalence of OHS in the general population is unknown, but its prevalence in patients who present for the evaluation of SDB has ranged from 8%-20% across multiple studies, he said. Up to 40% of patients with OHS present for the first time with acute hypercapnic respiratory failure, which has an in-hospital mortality of 18%.
Postmenopausal women appear to have a higher prevalence, compared with premenopausal women and men, he noted, and women appear to be more likely than men to present with the clinical phenotype of OHS without associated OSA.
The arterial blood gas measurement needed to document alveolar hypoventilation and definitively diagnosis OHA is a “simple and economical test,” he said, “but it is logistically very difficult to obtain [these measurements] routinely in all patients in the clinic ... and is one of the reasons why OSH is underdiagnosed.”
Guideline advice
A practice guideline published in 2019 by the American Thoracic Society suggests that, for obese patients with SDB and a low to moderate probability of having OSH, a serum bicarbonate level be measured first. “In patients with serum bicarbonate less than 27 mmol/L, clinicians might forgo measuring PaCO2, as the diagnosis in them is very unlikely,” Dr. Venkateshiah said, referring to the guideline. “In patients with a serum bicarbonate greater than 27, you might need to measure PaCO2 to confirm or rule out the diagnosis of OHS.”
(Patients strongly suspected of having OHS, with more than a low to moderate probability – those in whom arterial blood gases should be measured – are “usually severely obese with typical signs and symptoms such as dyspnea, nocturia, lower-extremity edema, excessive daytime sleepiness, fatigue, loud disruptive snoring, witnessed apneas, as well as mild hypoxemia during wake and/or significant hypoxemia during sleep,” the ATS guideline says.)
The guideline panel considered the use of oxygen saturation measured with pulse oximetry during wakefulness to screen for OHS and decided to advise against it because of the paucity of evidence-based literature, Dr. Venkateshiah noted. (In making its five conditional recommendations, the guideline panel cited an overall very low quality of evidence.)
Symptoms of OHS overlap with those of OSA (for example, daytime hypersomnolence, witnessed apneas, loud snoring, and morning headaches), so “symptoms alone cannot be used to discriminate between the two disorders,” he advised. Signs of OHS commonly seen in clinical exams, however, are low resting daytime oxygen saturations and lower-extremity edema. A sleep study, he added, is needed to document and characterize SDB in patients with OHS.
Positive airway pressure therapy is the first-line treatment for OHS, and long-term outcomes of patients with OHS on PAP treatment are significantly better, compared with untreated individuals. There is no strong evidence to recommend one form of PAP therapy over another for patients with OHS and concomitant severe OSA, he said, but “the bottom line” from both short- and long-term randomized clinical trials comparing CPAP with noninvasive ventilation “is that CPAP is equivalent to noninvasive ventilation as far as outcomes are concerned.”
The ATS guideline panel recommends continuous positive airway pressure therapy for patients with OHS and severe OSA. And for OHS with nonsevere OSA, bilevel PAP is traditionally used – including pure hypoventilators, Dr. Venkateshiah said.
Weight-loss interventions are paramount, since “the primary driver of OHS is obesity,” he said at the meeting. There are only a few studies that have looked at bariatric surgery in patients with OHS, he said, “but they did note significant improvements in gas exchange, sleep apnea, lung volumes and pulmonary hypertension.”
The ATS guideline suggests weight-loss interventions that produce sustained weight loss of 25%-30% of the actual body weight. Such interventions are “most likely required to achieve resolution of hypoventilation,” Dr. Venkateshiah said.
OHS vs. COPD
In a separate presentation on OHS, Michelle Cao, DO, clinical associate professor at Stanford (Calif.) University, emphasized the importance of distinguishing the patient with OHS from the patient with hypercapnic chronic obstructive pulmonary disease (COPD). Spirometry and the flow volume curve can help rule out hypercapnic COPD and other conditions that cause daytime hypoventilation.
A study published in 2016 of 600 hospitalized patients determined to have unequivocal OHS found that 43% had been misdiagnosed as having COPD and none had been previously diagnosed with OHS, Dr. Cao noted. Patients in the study had a mean age of 58 and a mean body mass index of 48.2 kg/m2; 64% were women.
Dr. Venkateshiah and Dr. Cao had no relevant disclosures.
Obesity hypoventilation syndrome (OHS) is bound to be increasing because of the rising obesity epidemic but is underrecognized and “frequently underdiagnosed,” Saiprakash B. Venkateshiah, MD, said at the virtual annual meeting of the Associated Professional Sleep Societies.
The condition, which can cause significant morbidity and mortality, is defined by the combination of obesity and awake alveolar hypoventilation (PaCO2 ≥45 mm Hg), with the exclusion of alternate causes of hypoventilation. Sleep-disordered breathing (SDB) is almost universally present, with approximately 90% of individuals with OHS also having obstructive sleep apnea (OSA), most often severe, and approximately 10% having sleep-related hypoventilation, or a “pure hypoventilation subtype, if you will,” said Dr. Venkateshiah, assistant professor of medicine at Emory University, Atlanta.
The prevalence of OHS in the general population is unknown, but its prevalence in patients who present for the evaluation of SDB has ranged from 8%-20% across multiple studies, he said. Up to 40% of patients with OHS present for the first time with acute hypercapnic respiratory failure, which has an in-hospital mortality of 18%.
Postmenopausal women appear to have a higher prevalence, compared with premenopausal women and men, he noted, and women appear to be more likely than men to present with the clinical phenotype of OHS without associated OSA.
The arterial blood gas measurement needed to document alveolar hypoventilation and definitively diagnosis OHA is a “simple and economical test,” he said, “but it is logistically very difficult to obtain [these measurements] routinely in all patients in the clinic ... and is one of the reasons why OSH is underdiagnosed.”
Guideline advice
A practice guideline published in 2019 by the American Thoracic Society suggests that, for obese patients with SDB and a low to moderate probability of having OSH, a serum bicarbonate level be measured first. “In patients with serum bicarbonate less than 27 mmol/L, clinicians might forgo measuring PaCO2, as the diagnosis in them is very unlikely,” Dr. Venkateshiah said, referring to the guideline. “In patients with a serum bicarbonate greater than 27, you might need to measure PaCO2 to confirm or rule out the diagnosis of OHS.”
(Patients strongly suspected of having OHS, with more than a low to moderate probability – those in whom arterial blood gases should be measured – are “usually severely obese with typical signs and symptoms such as dyspnea, nocturia, lower-extremity edema, excessive daytime sleepiness, fatigue, loud disruptive snoring, witnessed apneas, as well as mild hypoxemia during wake and/or significant hypoxemia during sleep,” the ATS guideline says.)
The guideline panel considered the use of oxygen saturation measured with pulse oximetry during wakefulness to screen for OHS and decided to advise against it because of the paucity of evidence-based literature, Dr. Venkateshiah noted. (In making its five conditional recommendations, the guideline panel cited an overall very low quality of evidence.)
Symptoms of OHS overlap with those of OSA (for example, daytime hypersomnolence, witnessed apneas, loud snoring, and morning headaches), so “symptoms alone cannot be used to discriminate between the two disorders,” he advised. Signs of OHS commonly seen in clinical exams, however, are low resting daytime oxygen saturations and lower-extremity edema. A sleep study, he added, is needed to document and characterize SDB in patients with OHS.
Positive airway pressure therapy is the first-line treatment for OHS, and long-term outcomes of patients with OHS on PAP treatment are significantly better, compared with untreated individuals. There is no strong evidence to recommend one form of PAP therapy over another for patients with OHS and concomitant severe OSA, he said, but “the bottom line” from both short- and long-term randomized clinical trials comparing CPAP with noninvasive ventilation “is that CPAP is equivalent to noninvasive ventilation as far as outcomes are concerned.”
The ATS guideline panel recommends continuous positive airway pressure therapy for patients with OHS and severe OSA. And for OHS with nonsevere OSA, bilevel PAP is traditionally used – including pure hypoventilators, Dr. Venkateshiah said.
Weight-loss interventions are paramount, since “the primary driver of OHS is obesity,” he said at the meeting. There are only a few studies that have looked at bariatric surgery in patients with OHS, he said, “but they did note significant improvements in gas exchange, sleep apnea, lung volumes and pulmonary hypertension.”
The ATS guideline suggests weight-loss interventions that produce sustained weight loss of 25%-30% of the actual body weight. Such interventions are “most likely required to achieve resolution of hypoventilation,” Dr. Venkateshiah said.
OHS vs. COPD
In a separate presentation on OHS, Michelle Cao, DO, clinical associate professor at Stanford (Calif.) University, emphasized the importance of distinguishing the patient with OHS from the patient with hypercapnic chronic obstructive pulmonary disease (COPD). Spirometry and the flow volume curve can help rule out hypercapnic COPD and other conditions that cause daytime hypoventilation.
A study published in 2016 of 600 hospitalized patients determined to have unequivocal OHS found that 43% had been misdiagnosed as having COPD and none had been previously diagnosed with OHS, Dr. Cao noted. Patients in the study had a mean age of 58 and a mean body mass index of 48.2 kg/m2; 64% were women.
Dr. Venkateshiah and Dr. Cao had no relevant disclosures.
FROM SLEEP 2021
Semaglutide 2.4 mg ‘likely to usher in a new era’ in obesity treatment
The recently licensed weight-loss drug semaglutide 2.4 mg/week (Wegovy, Novo Nordisk) “is likely to usher in a new era in the medical treatment of obesity,” Lee M. Kaplan, MD, PhD, stated at the annual scientific sessions of the American Diabetes Association, held virtually.
Dr. Kaplan discussed the clinical implications of caring for patients with obesity now that the glucagon-like peptide-1 (GLP-1) receptor agonist is approved in the United States for weight loss.
Weight loss with semaglutide 2.4 mg was twice that achieved with liraglutide 3 mg (Saxenda, Novo Nordisk) – that is, roughly a 10%-15% weight loss at 68 weeks, said Dr. Kaplan, who was not involved in the pivotal STEP clinical trials of the agent.
“I think as we start to see more data come in over the next couple of years,” including from the cardiovascular outcome trial SELECT, he continued, “we’ll be able to use the data to create a nuanced [individualized patient treatment] approach, but we’ll also be able to use our clinical experience, which will grow rapidly over the next few years.”
In the future, semaglutide is likely to be combined with other drugs to provide even greater weight loss, predicts Dr. Kaplan, director of the Obesity, Metabolism, and Nutrition Institute at Massachusetts General Hospital in Boston.
In the meantime, “to be effective, semaglutide needs to be used,” he stressed, while noting that responses to the drug vary by individual, and so this will need to be taken into account.
“Obesity needs to be recognized as a disease in its own right, as well as a risk factor for numerous other diseases, [and] equitable access to obesity treatment needs to be broadened,” he emphasized.
Four pivotal phase 3 trials
As previously reported, four pivotal 68-week, phase 3 clinical trials in the Semaglutide Treatment Effect in People With Obesity (STEP) program tested the safety and efficacy of subcutaneous semaglutide 2.4 mg/week in more than 4,500 adults with overweight or obesity.
The trials have been published in high profile journals – the New England Journal of Medicine (STEP 1), The Lancet (STEP 2), and JAMA (STEP 3 and STEP 4) – said Robert F. Kushner, MD.
“I would encourage all of you to download and read each of these trials on your own,” Dr. Kushner, professor of medicine and medicine education at Northwestern University, Chicago, and coauthor of STEP 1, said before presenting a top-level review of key results.
STEP 1 examined weight management, STEP 3 added a background of intensive behavioral therapy, STEP 4 investigated sustained weight management, and STEP 2 (unlike the others) investigated weight management in patients with type 2 diabetes, he summarized.
In STEP 1, patients who received semaglutide had an average 15% weight loss, and those who stayed on the drug had a 17% weight loss, compared with the 2.4% weight loss in the placebo group.
“One-third of individuals in the trial achieved at least a 20% weight loss or more,” Dr. Kushner said, which is “really phenomenal.”
The results of STEP 3 “suggest that semaglutide with monthly brief lifestyle counseling alone is sufficient to produce a mean weight loss of 15%,” he noted, as adding a low-calorie diet and intensive behavior therapy sped up the initial weight loss but did not increase the final weight loss.
A post hoc analysis of STEP 2 showed “it’s clear that improvement in A1c” is greater with at least a 10% weight loss versus a smaller weight loss, Dr. Kushner said. A1c dropped by 2.2% versus 1.3%, with these two weight losses, respectively.
In STEP 4, after dose escalation to 2.4 mg at 20 weeks, patients had lost 10.6% of their initial weight. At 68 weeks, those who were switched to placebo at 20 weeks had lost 5.4% of their initial weight, whereas those who remained on semaglutide had lost 17.7% of their initial weight.
This shows that “if you remove the drug, the disease starts to come back,” Dr. Kushner pointed out.
Nausea, the most common side effect, occurred in 20% of patients, but was mostly mild or moderate, and gastrointestinal effects including constipation, vomiting, and diarrhea were transient and occurred early in the dose escalation phase.
Large individual variability, combination therapies on horizon
Dr. Kaplan pointed out, however, that “like [with] other antiobesity therapies ... there’s a large patient-to-patient variability.”
A third of patients exhibit more than 20% weight loss, and 10% exhibit more than 30% weight loss – approaching the efficacy of bariatric surgery.
However, nearly 10% of patients without diabetes and upwards of 30% of patients with diabetes will experience less than 5% weight loss, he said.
Therefore, “success or failure in one patient doesn’t predict response in another, and we should always remember that as we treat different patients with these medications,” Dr. Kaplan advised.
A recent phase 1b study suggests that combination therapy with semaglutide and the amylin agonist cagrilintide ups weight loss, as previously reported.
In this short trial with no lifestyle modification, it took 16 weeks for patients to reach full dosing, and at 20 weeks, patients on semaglutide had lost 8% of their initial weight, whereas those on combination therapy had lost 17% of their initial weight.
“There’s hope that, in combination with cagrilintide and probably with several other agents that are still in early development, we’ll be seeing average weight loss that is in the range of that seen with bariatric surgery,” Dr. Kushner said.
Doctors discuss two hypothetical cases
Session moderator Julio Rosenstock, MD, of the University of Texas, Dallas, a coinvestigator in several of the STEP trials, invited Dr. Kaplan and two other panelists to explain how they would manage two hypothetical patients.
Case 1
You have a patient with type 2 diabetes, a body mass index of 32, 33 kg/m2, and an A1c of 7.5% or 8% on metformin. Would you use semaglutide 1 mg (Ozempic, Novo Nordisk) that is indicated for type 2 diabetes, or would you use semaglutide 2.4 mg that is indicated for obesity and risk factors?
“We have the answer to that from STEP 2,” said Melanie J. Davies, MB ChB, MD, professor of diabetes medicine at the University of Leicester, England, who led the STEP 2 trial.
“For some patients, the 1-mg dose, which we use routinely in the clinic, may be reasonable to get good glycemic control for cardiovascular protection and will obviously achieve some weight loss. But if you really want to go for the weight-related comorbidities, then the 2.4-mg dose is what you need,” she said.
“A lot of [clinicians] might say: ‘I’ll see how [the patient goes] with the 1-mg dose, and then maybe if they’re not losing the weight and not getting to glycemic target, then maybe I’ll switch to 2.4 mg,’” said John Wilding, MD, who leads clinical research into obesity, diabetes, and endocrinology at the University of Liverpool, England, and led the STEP 1 trial.
“But the STEP 2 data show very clearly that you get almost the same A1c,” Dr. Rosenstock interjected. “I would go for 2.4 mg. The patient has a BMI of 32, 33 kg/m2. I would hit hard the BMI. We need to change that paradigm.”
“For other diseases we don’t always go to the maximum dose that’s available. We go to the dose that’s necessary to achieve the clinical endpoint that we want,” Dr. Kaplan noted. “I think one of the challenges is going to be to learn how to clinically nuance our therapy the way we do for other diseases.”
“That is the usual thinking,” Dr. Rosenstock agreed. But “with the 2.4-mg dose, one third get a 20% reduction of BMI, and 10% get almost a 30% reduction – and you [aren’t] going to see that with semaglutide 1 mg!”
“That’s true,” Dr. Kaplan conceded. However, a patient with a relatively low BMI of 32, 33 kg/m2 may not need the higher dose, unlike a patient who has a BMI of 45 kg/m2 and diabetes. But we’re going to find that out over the next couple of years, he expects.
Case 2
You have a patient with a BMI of 31 kg/m2 who is newly diagnosed with type 2 diabetes. Why should you start that patient with metformin? Why won’t you start with something that will directly tackle obesity and get the patient to lose 20 pounds and for sure the blood sugar is going to be better?
“I think if I have someone who is really keen to put their diabetes into remission,” Dr. Wilding said, “this would be a fantastic approach because they would have a really high chance of doing that.”
The prediabetes data from STEP showed that “we can put a lot of people from prediabetes back to normal glucose tolerance,” Dr. Wilding noted. “Maybe we can put people with early diabetes back to normal as well. I think that’s a trial that really does need to be done,” he said.
“We’re going to have to figure out the best pathway forward,” Dr. Kaplan observed, noting that multiple stakeholders, including payers, patients, and providers, play a role in the uptake of new obesity drugs.
“Do you think we will see less bariatric surgery with these drugs?” Dr. Rosenstock asked Dr. Kaplan.
“I think you have to remember that of the millions and millions of people with obesity, a very small portion are currently treated with antiobesity medication, and an even smaller portion are getting bariatric surgery,” Dr. Kaplan replied.
“In the United States, 90% of people who get bariatric surgery are self-referred,” he said, so, “I think initially we are not going to see much of a change” in rates of bariatric surgery.
Dr. Rosenstock, Dr. Kaplan, Dr. Wilding, and Dr. Davies disclosed ties with Novo Nordisk and numerous other companies.
A version of this article first appeared on Medscape.com.
The recently licensed weight-loss drug semaglutide 2.4 mg/week (Wegovy, Novo Nordisk) “is likely to usher in a new era in the medical treatment of obesity,” Lee M. Kaplan, MD, PhD, stated at the annual scientific sessions of the American Diabetes Association, held virtually.
Dr. Kaplan discussed the clinical implications of caring for patients with obesity now that the glucagon-like peptide-1 (GLP-1) receptor agonist is approved in the United States for weight loss.
Weight loss with semaglutide 2.4 mg was twice that achieved with liraglutide 3 mg (Saxenda, Novo Nordisk) – that is, roughly a 10%-15% weight loss at 68 weeks, said Dr. Kaplan, who was not involved in the pivotal STEP clinical trials of the agent.
“I think as we start to see more data come in over the next couple of years,” including from the cardiovascular outcome trial SELECT, he continued, “we’ll be able to use the data to create a nuanced [individualized patient treatment] approach, but we’ll also be able to use our clinical experience, which will grow rapidly over the next few years.”
In the future, semaglutide is likely to be combined with other drugs to provide even greater weight loss, predicts Dr. Kaplan, director of the Obesity, Metabolism, and Nutrition Institute at Massachusetts General Hospital in Boston.
In the meantime, “to be effective, semaglutide needs to be used,” he stressed, while noting that responses to the drug vary by individual, and so this will need to be taken into account.
“Obesity needs to be recognized as a disease in its own right, as well as a risk factor for numerous other diseases, [and] equitable access to obesity treatment needs to be broadened,” he emphasized.
Four pivotal phase 3 trials
As previously reported, four pivotal 68-week, phase 3 clinical trials in the Semaglutide Treatment Effect in People With Obesity (STEP) program tested the safety and efficacy of subcutaneous semaglutide 2.4 mg/week in more than 4,500 adults with overweight or obesity.
The trials have been published in high profile journals – the New England Journal of Medicine (STEP 1), The Lancet (STEP 2), and JAMA (STEP 3 and STEP 4) – said Robert F. Kushner, MD.
“I would encourage all of you to download and read each of these trials on your own,” Dr. Kushner, professor of medicine and medicine education at Northwestern University, Chicago, and coauthor of STEP 1, said before presenting a top-level review of key results.
STEP 1 examined weight management, STEP 3 added a background of intensive behavioral therapy, STEP 4 investigated sustained weight management, and STEP 2 (unlike the others) investigated weight management in patients with type 2 diabetes, he summarized.
In STEP 1, patients who received semaglutide had an average 15% weight loss, and those who stayed on the drug had a 17% weight loss, compared with the 2.4% weight loss in the placebo group.
“One-third of individuals in the trial achieved at least a 20% weight loss or more,” Dr. Kushner said, which is “really phenomenal.”
The results of STEP 3 “suggest that semaglutide with monthly brief lifestyle counseling alone is sufficient to produce a mean weight loss of 15%,” he noted, as adding a low-calorie diet and intensive behavior therapy sped up the initial weight loss but did not increase the final weight loss.
A post hoc analysis of STEP 2 showed “it’s clear that improvement in A1c” is greater with at least a 10% weight loss versus a smaller weight loss, Dr. Kushner said. A1c dropped by 2.2% versus 1.3%, with these two weight losses, respectively.
In STEP 4, after dose escalation to 2.4 mg at 20 weeks, patients had lost 10.6% of their initial weight. At 68 weeks, those who were switched to placebo at 20 weeks had lost 5.4% of their initial weight, whereas those who remained on semaglutide had lost 17.7% of their initial weight.
This shows that “if you remove the drug, the disease starts to come back,” Dr. Kushner pointed out.
Nausea, the most common side effect, occurred in 20% of patients, but was mostly mild or moderate, and gastrointestinal effects including constipation, vomiting, and diarrhea were transient and occurred early in the dose escalation phase.
Large individual variability, combination therapies on horizon
Dr. Kaplan pointed out, however, that “like [with] other antiobesity therapies ... there’s a large patient-to-patient variability.”
A third of patients exhibit more than 20% weight loss, and 10% exhibit more than 30% weight loss – approaching the efficacy of bariatric surgery.
However, nearly 10% of patients without diabetes and upwards of 30% of patients with diabetes will experience less than 5% weight loss, he said.
Therefore, “success or failure in one patient doesn’t predict response in another, and we should always remember that as we treat different patients with these medications,” Dr. Kaplan advised.
A recent phase 1b study suggests that combination therapy with semaglutide and the amylin agonist cagrilintide ups weight loss, as previously reported.
In this short trial with no lifestyle modification, it took 16 weeks for patients to reach full dosing, and at 20 weeks, patients on semaglutide had lost 8% of their initial weight, whereas those on combination therapy had lost 17% of their initial weight.
“There’s hope that, in combination with cagrilintide and probably with several other agents that are still in early development, we’ll be seeing average weight loss that is in the range of that seen with bariatric surgery,” Dr. Kushner said.
Doctors discuss two hypothetical cases
Session moderator Julio Rosenstock, MD, of the University of Texas, Dallas, a coinvestigator in several of the STEP trials, invited Dr. Kaplan and two other panelists to explain how they would manage two hypothetical patients.
Case 1
You have a patient with type 2 diabetes, a body mass index of 32, 33 kg/m2, and an A1c of 7.5% or 8% on metformin. Would you use semaglutide 1 mg (Ozempic, Novo Nordisk) that is indicated for type 2 diabetes, or would you use semaglutide 2.4 mg that is indicated for obesity and risk factors?
“We have the answer to that from STEP 2,” said Melanie J. Davies, MB ChB, MD, professor of diabetes medicine at the University of Leicester, England, who led the STEP 2 trial.
“For some patients, the 1-mg dose, which we use routinely in the clinic, may be reasonable to get good glycemic control for cardiovascular protection and will obviously achieve some weight loss. But if you really want to go for the weight-related comorbidities, then the 2.4-mg dose is what you need,” she said.
“A lot of [clinicians] might say: ‘I’ll see how [the patient goes] with the 1-mg dose, and then maybe if they’re not losing the weight and not getting to glycemic target, then maybe I’ll switch to 2.4 mg,’” said John Wilding, MD, who leads clinical research into obesity, diabetes, and endocrinology at the University of Liverpool, England, and led the STEP 1 trial.
“But the STEP 2 data show very clearly that you get almost the same A1c,” Dr. Rosenstock interjected. “I would go for 2.4 mg. The patient has a BMI of 32, 33 kg/m2. I would hit hard the BMI. We need to change that paradigm.”
“For other diseases we don’t always go to the maximum dose that’s available. We go to the dose that’s necessary to achieve the clinical endpoint that we want,” Dr. Kaplan noted. “I think one of the challenges is going to be to learn how to clinically nuance our therapy the way we do for other diseases.”
“That is the usual thinking,” Dr. Rosenstock agreed. But “with the 2.4-mg dose, one third get a 20% reduction of BMI, and 10% get almost a 30% reduction – and you [aren’t] going to see that with semaglutide 1 mg!”
“That’s true,” Dr. Kaplan conceded. However, a patient with a relatively low BMI of 32, 33 kg/m2 may not need the higher dose, unlike a patient who has a BMI of 45 kg/m2 and diabetes. But we’re going to find that out over the next couple of years, he expects.
Case 2
You have a patient with a BMI of 31 kg/m2 who is newly diagnosed with type 2 diabetes. Why should you start that patient with metformin? Why won’t you start with something that will directly tackle obesity and get the patient to lose 20 pounds and for sure the blood sugar is going to be better?
“I think if I have someone who is really keen to put their diabetes into remission,” Dr. Wilding said, “this would be a fantastic approach because they would have a really high chance of doing that.”
The prediabetes data from STEP showed that “we can put a lot of people from prediabetes back to normal glucose tolerance,” Dr. Wilding noted. “Maybe we can put people with early diabetes back to normal as well. I think that’s a trial that really does need to be done,” he said.
“We’re going to have to figure out the best pathway forward,” Dr. Kaplan observed, noting that multiple stakeholders, including payers, patients, and providers, play a role in the uptake of new obesity drugs.
“Do you think we will see less bariatric surgery with these drugs?” Dr. Rosenstock asked Dr. Kaplan.
“I think you have to remember that of the millions and millions of people with obesity, a very small portion are currently treated with antiobesity medication, and an even smaller portion are getting bariatric surgery,” Dr. Kaplan replied.
“In the United States, 90% of people who get bariatric surgery are self-referred,” he said, so, “I think initially we are not going to see much of a change” in rates of bariatric surgery.
Dr. Rosenstock, Dr. Kaplan, Dr. Wilding, and Dr. Davies disclosed ties with Novo Nordisk and numerous other companies.
A version of this article first appeared on Medscape.com.
The recently licensed weight-loss drug semaglutide 2.4 mg/week (Wegovy, Novo Nordisk) “is likely to usher in a new era in the medical treatment of obesity,” Lee M. Kaplan, MD, PhD, stated at the annual scientific sessions of the American Diabetes Association, held virtually.
Dr. Kaplan discussed the clinical implications of caring for patients with obesity now that the glucagon-like peptide-1 (GLP-1) receptor agonist is approved in the United States for weight loss.
Weight loss with semaglutide 2.4 mg was twice that achieved with liraglutide 3 mg (Saxenda, Novo Nordisk) – that is, roughly a 10%-15% weight loss at 68 weeks, said Dr. Kaplan, who was not involved in the pivotal STEP clinical trials of the agent.
“I think as we start to see more data come in over the next couple of years,” including from the cardiovascular outcome trial SELECT, he continued, “we’ll be able to use the data to create a nuanced [individualized patient treatment] approach, but we’ll also be able to use our clinical experience, which will grow rapidly over the next few years.”
In the future, semaglutide is likely to be combined with other drugs to provide even greater weight loss, predicts Dr. Kaplan, director of the Obesity, Metabolism, and Nutrition Institute at Massachusetts General Hospital in Boston.
In the meantime, “to be effective, semaglutide needs to be used,” he stressed, while noting that responses to the drug vary by individual, and so this will need to be taken into account.
“Obesity needs to be recognized as a disease in its own right, as well as a risk factor for numerous other diseases, [and] equitable access to obesity treatment needs to be broadened,” he emphasized.
Four pivotal phase 3 trials
As previously reported, four pivotal 68-week, phase 3 clinical trials in the Semaglutide Treatment Effect in People With Obesity (STEP) program tested the safety and efficacy of subcutaneous semaglutide 2.4 mg/week in more than 4,500 adults with overweight or obesity.
The trials have been published in high profile journals – the New England Journal of Medicine (STEP 1), The Lancet (STEP 2), and JAMA (STEP 3 and STEP 4) – said Robert F. Kushner, MD.
“I would encourage all of you to download and read each of these trials on your own,” Dr. Kushner, professor of medicine and medicine education at Northwestern University, Chicago, and coauthor of STEP 1, said before presenting a top-level review of key results.
STEP 1 examined weight management, STEP 3 added a background of intensive behavioral therapy, STEP 4 investigated sustained weight management, and STEP 2 (unlike the others) investigated weight management in patients with type 2 diabetes, he summarized.
In STEP 1, patients who received semaglutide had an average 15% weight loss, and those who stayed on the drug had a 17% weight loss, compared with the 2.4% weight loss in the placebo group.
“One-third of individuals in the trial achieved at least a 20% weight loss or more,” Dr. Kushner said, which is “really phenomenal.”
The results of STEP 3 “suggest that semaglutide with monthly brief lifestyle counseling alone is sufficient to produce a mean weight loss of 15%,” he noted, as adding a low-calorie diet and intensive behavior therapy sped up the initial weight loss but did not increase the final weight loss.
A post hoc analysis of STEP 2 showed “it’s clear that improvement in A1c” is greater with at least a 10% weight loss versus a smaller weight loss, Dr. Kushner said. A1c dropped by 2.2% versus 1.3%, with these two weight losses, respectively.
In STEP 4, after dose escalation to 2.4 mg at 20 weeks, patients had lost 10.6% of their initial weight. At 68 weeks, those who were switched to placebo at 20 weeks had lost 5.4% of their initial weight, whereas those who remained on semaglutide had lost 17.7% of their initial weight.
This shows that “if you remove the drug, the disease starts to come back,” Dr. Kushner pointed out.
Nausea, the most common side effect, occurred in 20% of patients, but was mostly mild or moderate, and gastrointestinal effects including constipation, vomiting, and diarrhea were transient and occurred early in the dose escalation phase.
Large individual variability, combination therapies on horizon
Dr. Kaplan pointed out, however, that “like [with] other antiobesity therapies ... there’s a large patient-to-patient variability.”
A third of patients exhibit more than 20% weight loss, and 10% exhibit more than 30% weight loss – approaching the efficacy of bariatric surgery.
However, nearly 10% of patients without diabetes and upwards of 30% of patients with diabetes will experience less than 5% weight loss, he said.
Therefore, “success or failure in one patient doesn’t predict response in another, and we should always remember that as we treat different patients with these medications,” Dr. Kaplan advised.
A recent phase 1b study suggests that combination therapy with semaglutide and the amylin agonist cagrilintide ups weight loss, as previously reported.
In this short trial with no lifestyle modification, it took 16 weeks for patients to reach full dosing, and at 20 weeks, patients on semaglutide had lost 8% of their initial weight, whereas those on combination therapy had lost 17% of their initial weight.
“There’s hope that, in combination with cagrilintide and probably with several other agents that are still in early development, we’ll be seeing average weight loss that is in the range of that seen with bariatric surgery,” Dr. Kushner said.
Doctors discuss two hypothetical cases
Session moderator Julio Rosenstock, MD, of the University of Texas, Dallas, a coinvestigator in several of the STEP trials, invited Dr. Kaplan and two other panelists to explain how they would manage two hypothetical patients.
Case 1
You have a patient with type 2 diabetes, a body mass index of 32, 33 kg/m2, and an A1c of 7.5% or 8% on metformin. Would you use semaglutide 1 mg (Ozempic, Novo Nordisk) that is indicated for type 2 diabetes, or would you use semaglutide 2.4 mg that is indicated for obesity and risk factors?
“We have the answer to that from STEP 2,” said Melanie J. Davies, MB ChB, MD, professor of diabetes medicine at the University of Leicester, England, who led the STEP 2 trial.
“For some patients, the 1-mg dose, which we use routinely in the clinic, may be reasonable to get good glycemic control for cardiovascular protection and will obviously achieve some weight loss. But if you really want to go for the weight-related comorbidities, then the 2.4-mg dose is what you need,” she said.
“A lot of [clinicians] might say: ‘I’ll see how [the patient goes] with the 1-mg dose, and then maybe if they’re not losing the weight and not getting to glycemic target, then maybe I’ll switch to 2.4 mg,’” said John Wilding, MD, who leads clinical research into obesity, diabetes, and endocrinology at the University of Liverpool, England, and led the STEP 1 trial.
“But the STEP 2 data show very clearly that you get almost the same A1c,” Dr. Rosenstock interjected. “I would go for 2.4 mg. The patient has a BMI of 32, 33 kg/m2. I would hit hard the BMI. We need to change that paradigm.”
“For other diseases we don’t always go to the maximum dose that’s available. We go to the dose that’s necessary to achieve the clinical endpoint that we want,” Dr. Kaplan noted. “I think one of the challenges is going to be to learn how to clinically nuance our therapy the way we do for other diseases.”
“That is the usual thinking,” Dr. Rosenstock agreed. But “with the 2.4-mg dose, one third get a 20% reduction of BMI, and 10% get almost a 30% reduction – and you [aren’t] going to see that with semaglutide 1 mg!”
“That’s true,” Dr. Kaplan conceded. However, a patient with a relatively low BMI of 32, 33 kg/m2 may not need the higher dose, unlike a patient who has a BMI of 45 kg/m2 and diabetes. But we’re going to find that out over the next couple of years, he expects.
Case 2
You have a patient with a BMI of 31 kg/m2 who is newly diagnosed with type 2 diabetes. Why should you start that patient with metformin? Why won’t you start with something that will directly tackle obesity and get the patient to lose 20 pounds and for sure the blood sugar is going to be better?
“I think if I have someone who is really keen to put their diabetes into remission,” Dr. Wilding said, “this would be a fantastic approach because they would have a really high chance of doing that.”
The prediabetes data from STEP showed that “we can put a lot of people from prediabetes back to normal glucose tolerance,” Dr. Wilding noted. “Maybe we can put people with early diabetes back to normal as well. I think that’s a trial that really does need to be done,” he said.
“We’re going to have to figure out the best pathway forward,” Dr. Kaplan observed, noting that multiple stakeholders, including payers, patients, and providers, play a role in the uptake of new obesity drugs.
“Do you think we will see less bariatric surgery with these drugs?” Dr. Rosenstock asked Dr. Kaplan.
“I think you have to remember that of the millions and millions of people with obesity, a very small portion are currently treated with antiobesity medication, and an even smaller portion are getting bariatric surgery,” Dr. Kaplan replied.
“In the United States, 90% of people who get bariatric surgery are self-referred,” he said, so, “I think initially we are not going to see much of a change” in rates of bariatric surgery.
Dr. Rosenstock, Dr. Kaplan, Dr. Wilding, and Dr. Davies disclosed ties with Novo Nordisk and numerous other companies.
A version of this article first appeared on Medscape.com.
SUSTAIN FORTE: Higher-dose semaglutide safely boosts glycemic control, weight loss
Accumulating evidence shows that
Just weeks after the Food and Drug Administration approved an increased, 2.4-mg/week dose of semaglutide (Wegovy) for the indication of weight loss, results from a new randomized study with 961 patients that directly compared the standard 1.0-mg weekly dose for glycemic control with a 2.0-mg weekly dose showed that, over 40 weeks, the higher dose produced modest incremental improvements in both A1c reduction and weight loss while maintaining safety.
“Once weekly 2.0-mg subcutaneous semaglutide [Ozempic] was superior to 1.0 mg in reducing A1c, with greater weight loss and a similar safety profile,” Juan P. Frias, MD, said at the annual scientific sessions of the American Diabetes Association while presenting results of the SUSTAIN FORTE trial.
Average impact of the increased efficacy was measured. In the study’s “treatment policy estimand” analysis (considered equivalent to an intention-to-treat analysis), the primary endpoint of the cut in average A1c fell by a further 0.18% among patients on the higher dose, compared with the lower-dose arm, a significant difference in patients who entered the study with an average A1c of 8.9%. The average incremental boost for weight loss on the higher dose was about 0.8 kg, a difference that just missed significance (P = .0535).
In the study’s “trial product estimand” analysis (which censors data when patients stop the study drug or add on rescue medications), the effects were slightly more robust. The 2-mg dose produced an average 0.23% incremental decrease in A1c, compared with 1 mg, and an average incremental 0.93-kg weight reduction, both significant, reported Dr. Frias, an endocrinologist and medical director of the National Research Institute in Los Angeles.
Dr. Frias highlighted that these modest average differences had a clinical impact for some patients. In the treatment product estimand analysis, the percentage of patients achieving an A1c level of less than 7.0% increased from 58% of those who received 1 mg semaglutide to 68% of those treated with 2 mg, and achievement of an A1c of less than 6.5% occurred in 39% of patients on 1 mg and in 52% of those on 2 mg.
A similar pattern existed for weight loss in the treatment product estimand. Weight loss of at least 5% happened in 51% of patients on the 1-mg dose and in 59% of those on the higher dose.
Gradual up-titration aids tolerance
“The GLP-1 receptor agonists have so many benefits, but we were concerned in the past about pushing the dose. We’ve learned more about how to do that so that patients can better tolerate it,” commented Robert A. Gabbay, MD, PhD, chief science and medicine officer of the ADA in Arlington, Va. “The challenge with the medications from this class has been tolerability.”
A key to minimizing adverse effects, especially gastrointestinal effects, from treatment with semaglutide and other GLP-1 receptor agonists has been more gradual up-titration to the target dose, Dr. Gabbay noted in an interview, and SUSTAIN FORTE took this approach. All patients started on a 0.25-mg injection of semaglutide once weekly for the first 4 weeks, followed by a 0.5-mg dose once weekly for 4 weeks, and then a 1.0 mg weekly dose. Patients in the arm randomized to receive 2.0 mg had one further dose escalation after receiving the 1.0-mg dose for 4 weeks.
The result was that gastrointestinal adverse effects occurred in 31% of patients maintained for 32 weeks on the 1-mg dose (with 40 total weeks of semaglutide treatment), and in 34% of patients who received the 2-mg dose for 28 weeks (and 40 total weeks of semaglutide treatment). Serious adverse events of all types occurred in 5% of patients in the 1-mg arm and in 4% of those on 2 mg. Total adverse events resulting in treatment discontinuation occurred in about 4.5% of patients in both arms, and discontinuations because of gastrointestinal effects occurred in about 3% of patients in both arms.
Severe hypoglycemia episodes occurred in 1 patient maintained on 1 mg weekly and in 2 patients in the 2-mg arm, while clinically significant episodes of hypoglycemia occurred in 18 patients on the 1-mg dose (4%) and in 12 of the patients on 2 mg (3%).
“It’s reassuring that the higher dose is tolerated,” commented Dr. Gabbay.
Several doses to choose from
SUSTAIN FORTE ran during 2019-2020 at about 125 centers in 10 countries, with roughly half the sites in the United States. It randomized adults with type 2 diabetes and an A1c of 8.0%-10.0% despite ongoing metformin treatment in all patients. Just over half the patients were also maintained on a sulfonylurea agent at entry. The enrolled patients had been diagnosed with diabetes for an average of about 10 years. They averaged 58 years of age, their body mass index averaged nearly 35 kg/m2, and about 58% were men.
The new evidence in support of a 2.0-mg weekly dose of semaglutide for patients with type 2 diabetes introduces a new wrinkle in a growing menu of dose options for this drug. On June 4, 2021, the FDA approved a weekly 2.4-mg dose of semaglutide for the indication of weight loss regardless of diabetes status in patients with a body mass index of 30 or higher (or in people at 27 or more with at least one weight-related comorbidity).
Dr. Gabbay suggested that, in practice, clinicians may focus more on treatment goals for individual patients rather than drug dose, especially with an agent that’s safer with slow dose titration.
In general, “clinicians establish a goal for each patient’s A1c; you use the drug dose that gets you there,” he observed.
SUSTAIN FORTE was sponsored by Novo Nordisk, the company that markets semaglutide. Dr. Frias has been a consultant to Novo Nordisk and numerous other companies, he has been a speaker on behalf of Lilly, Merck, and Sanofi, and he has received research funding from Novo Nordisk and numerous other companies. Dr. Gabbay had no relevant disclosures.
Accumulating evidence shows that
Just weeks after the Food and Drug Administration approved an increased, 2.4-mg/week dose of semaglutide (Wegovy) for the indication of weight loss, results from a new randomized study with 961 patients that directly compared the standard 1.0-mg weekly dose for glycemic control with a 2.0-mg weekly dose showed that, over 40 weeks, the higher dose produced modest incremental improvements in both A1c reduction and weight loss while maintaining safety.
“Once weekly 2.0-mg subcutaneous semaglutide [Ozempic] was superior to 1.0 mg in reducing A1c, with greater weight loss and a similar safety profile,” Juan P. Frias, MD, said at the annual scientific sessions of the American Diabetes Association while presenting results of the SUSTAIN FORTE trial.
Average impact of the increased efficacy was measured. In the study’s “treatment policy estimand” analysis (considered equivalent to an intention-to-treat analysis), the primary endpoint of the cut in average A1c fell by a further 0.18% among patients on the higher dose, compared with the lower-dose arm, a significant difference in patients who entered the study with an average A1c of 8.9%. The average incremental boost for weight loss on the higher dose was about 0.8 kg, a difference that just missed significance (P = .0535).
In the study’s “trial product estimand” analysis (which censors data when patients stop the study drug or add on rescue medications), the effects were slightly more robust. The 2-mg dose produced an average 0.23% incremental decrease in A1c, compared with 1 mg, and an average incremental 0.93-kg weight reduction, both significant, reported Dr. Frias, an endocrinologist and medical director of the National Research Institute in Los Angeles.
Dr. Frias highlighted that these modest average differences had a clinical impact for some patients. In the treatment product estimand analysis, the percentage of patients achieving an A1c level of less than 7.0% increased from 58% of those who received 1 mg semaglutide to 68% of those treated with 2 mg, and achievement of an A1c of less than 6.5% occurred in 39% of patients on 1 mg and in 52% of those on 2 mg.
A similar pattern existed for weight loss in the treatment product estimand. Weight loss of at least 5% happened in 51% of patients on the 1-mg dose and in 59% of those on the higher dose.
Gradual up-titration aids tolerance
“The GLP-1 receptor agonists have so many benefits, but we were concerned in the past about pushing the dose. We’ve learned more about how to do that so that patients can better tolerate it,” commented Robert A. Gabbay, MD, PhD, chief science and medicine officer of the ADA in Arlington, Va. “The challenge with the medications from this class has been tolerability.”
A key to minimizing adverse effects, especially gastrointestinal effects, from treatment with semaglutide and other GLP-1 receptor agonists has been more gradual up-titration to the target dose, Dr. Gabbay noted in an interview, and SUSTAIN FORTE took this approach. All patients started on a 0.25-mg injection of semaglutide once weekly for the first 4 weeks, followed by a 0.5-mg dose once weekly for 4 weeks, and then a 1.0 mg weekly dose. Patients in the arm randomized to receive 2.0 mg had one further dose escalation after receiving the 1.0-mg dose for 4 weeks.
The result was that gastrointestinal adverse effects occurred in 31% of patients maintained for 32 weeks on the 1-mg dose (with 40 total weeks of semaglutide treatment), and in 34% of patients who received the 2-mg dose for 28 weeks (and 40 total weeks of semaglutide treatment). Serious adverse events of all types occurred in 5% of patients in the 1-mg arm and in 4% of those on 2 mg. Total adverse events resulting in treatment discontinuation occurred in about 4.5% of patients in both arms, and discontinuations because of gastrointestinal effects occurred in about 3% of patients in both arms.
Severe hypoglycemia episodes occurred in 1 patient maintained on 1 mg weekly and in 2 patients in the 2-mg arm, while clinically significant episodes of hypoglycemia occurred in 18 patients on the 1-mg dose (4%) and in 12 of the patients on 2 mg (3%).
“It’s reassuring that the higher dose is tolerated,” commented Dr. Gabbay.
Several doses to choose from
SUSTAIN FORTE ran during 2019-2020 at about 125 centers in 10 countries, with roughly half the sites in the United States. It randomized adults with type 2 diabetes and an A1c of 8.0%-10.0% despite ongoing metformin treatment in all patients. Just over half the patients were also maintained on a sulfonylurea agent at entry. The enrolled patients had been diagnosed with diabetes for an average of about 10 years. They averaged 58 years of age, their body mass index averaged nearly 35 kg/m2, and about 58% were men.
The new evidence in support of a 2.0-mg weekly dose of semaglutide for patients with type 2 diabetes introduces a new wrinkle in a growing menu of dose options for this drug. On June 4, 2021, the FDA approved a weekly 2.4-mg dose of semaglutide for the indication of weight loss regardless of diabetes status in patients with a body mass index of 30 or higher (or in people at 27 or more with at least one weight-related comorbidity).
Dr. Gabbay suggested that, in practice, clinicians may focus more on treatment goals for individual patients rather than drug dose, especially with an agent that’s safer with slow dose titration.
In general, “clinicians establish a goal for each patient’s A1c; you use the drug dose that gets you there,” he observed.
SUSTAIN FORTE was sponsored by Novo Nordisk, the company that markets semaglutide. Dr. Frias has been a consultant to Novo Nordisk and numerous other companies, he has been a speaker on behalf of Lilly, Merck, and Sanofi, and he has received research funding from Novo Nordisk and numerous other companies. Dr. Gabbay had no relevant disclosures.
Accumulating evidence shows that
Just weeks after the Food and Drug Administration approved an increased, 2.4-mg/week dose of semaglutide (Wegovy) for the indication of weight loss, results from a new randomized study with 961 patients that directly compared the standard 1.0-mg weekly dose for glycemic control with a 2.0-mg weekly dose showed that, over 40 weeks, the higher dose produced modest incremental improvements in both A1c reduction and weight loss while maintaining safety.
“Once weekly 2.0-mg subcutaneous semaglutide [Ozempic] was superior to 1.0 mg in reducing A1c, with greater weight loss and a similar safety profile,” Juan P. Frias, MD, said at the annual scientific sessions of the American Diabetes Association while presenting results of the SUSTAIN FORTE trial.
Average impact of the increased efficacy was measured. In the study’s “treatment policy estimand” analysis (considered equivalent to an intention-to-treat analysis), the primary endpoint of the cut in average A1c fell by a further 0.18% among patients on the higher dose, compared with the lower-dose arm, a significant difference in patients who entered the study with an average A1c of 8.9%. The average incremental boost for weight loss on the higher dose was about 0.8 kg, a difference that just missed significance (P = .0535).
In the study’s “trial product estimand” analysis (which censors data when patients stop the study drug or add on rescue medications), the effects were slightly more robust. The 2-mg dose produced an average 0.23% incremental decrease in A1c, compared with 1 mg, and an average incremental 0.93-kg weight reduction, both significant, reported Dr. Frias, an endocrinologist and medical director of the National Research Institute in Los Angeles.
Dr. Frias highlighted that these modest average differences had a clinical impact for some patients. In the treatment product estimand analysis, the percentage of patients achieving an A1c level of less than 7.0% increased from 58% of those who received 1 mg semaglutide to 68% of those treated with 2 mg, and achievement of an A1c of less than 6.5% occurred in 39% of patients on 1 mg and in 52% of those on 2 mg.
A similar pattern existed for weight loss in the treatment product estimand. Weight loss of at least 5% happened in 51% of patients on the 1-mg dose and in 59% of those on the higher dose.
Gradual up-titration aids tolerance
“The GLP-1 receptor agonists have so many benefits, but we were concerned in the past about pushing the dose. We’ve learned more about how to do that so that patients can better tolerate it,” commented Robert A. Gabbay, MD, PhD, chief science and medicine officer of the ADA in Arlington, Va. “The challenge with the medications from this class has been tolerability.”
A key to minimizing adverse effects, especially gastrointestinal effects, from treatment with semaglutide and other GLP-1 receptor agonists has been more gradual up-titration to the target dose, Dr. Gabbay noted in an interview, and SUSTAIN FORTE took this approach. All patients started on a 0.25-mg injection of semaglutide once weekly for the first 4 weeks, followed by a 0.5-mg dose once weekly for 4 weeks, and then a 1.0 mg weekly dose. Patients in the arm randomized to receive 2.0 mg had one further dose escalation after receiving the 1.0-mg dose for 4 weeks.
The result was that gastrointestinal adverse effects occurred in 31% of patients maintained for 32 weeks on the 1-mg dose (with 40 total weeks of semaglutide treatment), and in 34% of patients who received the 2-mg dose for 28 weeks (and 40 total weeks of semaglutide treatment). Serious adverse events of all types occurred in 5% of patients in the 1-mg arm and in 4% of those on 2 mg. Total adverse events resulting in treatment discontinuation occurred in about 4.5% of patients in both arms, and discontinuations because of gastrointestinal effects occurred in about 3% of patients in both arms.
Severe hypoglycemia episodes occurred in 1 patient maintained on 1 mg weekly and in 2 patients in the 2-mg arm, while clinically significant episodes of hypoglycemia occurred in 18 patients on the 1-mg dose (4%) and in 12 of the patients on 2 mg (3%).
“It’s reassuring that the higher dose is tolerated,” commented Dr. Gabbay.
Several doses to choose from
SUSTAIN FORTE ran during 2019-2020 at about 125 centers in 10 countries, with roughly half the sites in the United States. It randomized adults with type 2 diabetes and an A1c of 8.0%-10.0% despite ongoing metformin treatment in all patients. Just over half the patients were also maintained on a sulfonylurea agent at entry. The enrolled patients had been diagnosed with diabetes for an average of about 10 years. They averaged 58 years of age, their body mass index averaged nearly 35 kg/m2, and about 58% were men.
The new evidence in support of a 2.0-mg weekly dose of semaglutide for patients with type 2 diabetes introduces a new wrinkle in a growing menu of dose options for this drug. On June 4, 2021, the FDA approved a weekly 2.4-mg dose of semaglutide for the indication of weight loss regardless of diabetes status in patients with a body mass index of 30 or higher (or in people at 27 or more with at least one weight-related comorbidity).
Dr. Gabbay suggested that, in practice, clinicians may focus more on treatment goals for individual patients rather than drug dose, especially with an agent that’s safer with slow dose titration.
In general, “clinicians establish a goal for each patient’s A1c; you use the drug dose that gets you there,” he observed.
SUSTAIN FORTE was sponsored by Novo Nordisk, the company that markets semaglutide. Dr. Frias has been a consultant to Novo Nordisk and numerous other companies, he has been a speaker on behalf of Lilly, Merck, and Sanofi, and he has received research funding from Novo Nordisk and numerous other companies. Dr. Gabbay had no relevant disclosures.
FROM ADA 2021
‘Staggering’ doubling of type 2 diabetes in children during pandemic
The incidence of type 2 diabetes in children appears to have doubled during the COVID-19 pandemic, data from two new U.S. studies suggest, with the lead investigator of one saying she was “surprised by the staggering increase in cases of type 2 diabetes ... and the increase in severity of presentation.”
Findings from the two separate retrospective chart reviews – one conducted in Washington, D.C., and the other in Baton Rouge, La. – were presented June 25 at the annual scientific sessions of the American Diabetes Association.
Although the two studies differed somewhat in the clinical parameters examined, both revealed a similar doubling of the rates of hospitalizations for type 2 diabetes among youth during 2020, compared with the same time period in 2019, as well as greater severity of metabolic disturbance.
And, as has been previously described with type 2 diabetes in youth, African American ethnicity predominated in both cohorts.
“Although we could not assess the cause of the increases in type 2 diabetes from our data, these disparities suggest that indirect effects of social distancing measures, including school closure and unemployment, are placing undue burden on underserved communities. Decreases in well-child care and fears of seeking medical care during the pandemic may have also contributed,” lead investigator of one of the studies, pediatric endocrinologist Brynn E. Marks, MD, Children’s National Hospital, Washington, said in an interview.
More hospitalizations, racial disparities aggravated by COVID-19
Lead author of the other study, Daniel S. Hsia, MD, Pennington Biomedical Research Center, Baton Rouge, said in an interview: “Since the pandemic, our data suggest that more children may be diagnosed with type 2 diabetes and may require hospitalization when they are diagnosed. Looking at both datasets, there appears to be a racial disparity in type 2 diabetes diagnoses that has only been exacerbated by the COVID-19 pandemic.”
Of concern, Dr. Hsia said, “The incidence rate of type 2 diabetes in children was already on the rise before the pandemic. While there may be a brief leveling off now that children are getting regular health care and going back to school in person, I believe these rates will continue to rise especially in light of the childhood obesity rates not improving.”
Their dataset captured all youth who were newly diagnosed with type 2 diabetes during the first full year of the COVID-19 pandemic, from March 11, 2020, to March 10, 2021, and compared those data with the time period from March 11, 2019, to March 10, 2020.
During the pandemic, the number of cases of type 2 diabetes increased by 182%, from 50 in 2019 to 141 in 2020. The average age at diagnosis was about 14 years in both time periods.
In the prepandemic period, 18 (36%) diagnosed with type 2 diabetes required inpatient admission, compared with 85 (60.3%) during the pandemic. At Children’s National, youth with suspected new-onset type 2 diabetes aren’t typically hospitalized unless they have severe hyperglycemia, ketosis, or are unable to schedule urgent outpatient follow-up, Dr. Marks noted.
The proportions of youth with new-onset type 2 diabetes who presented in diabetic ketoacidosis (DKA) rose from 2 (4%) prepandemic to 33 (23.4%) during the pandemic. Presentation with hyperosmolar DKA rose from 0 to 13 (9.2%).
However, during the pandemic only five youth were actively infected with SARS-CoV-2 at the time of type 2 diabetes diagnosis among the 90 tested.
Dr. Marks said: “We believe the increase in inpatient admissions was due to more severe presentation during the pandemic. ...We were surprised by the staggering increase in cases of type 2 diabetes ... and the increase in severity of presentation.”
Shift in diagnoses to type 2 diabetes
The pandemic also appears to have shifted the proportion of youth diagnosed with type 2 diabetes, compared with type 1 diabetes. Whereas 24% of youth with new-onset diabetes prepandemic had type 2 diabetes and the rest had type 1 diabetes, during pandemic the proportion with type 2 diabetes rose to 44%.
“Rates of type 2 diabetes rose steadily at a rate of 1.45 cases per month throughout the course of the pandemic, suggesting a cumulative effect of the indirect effects of social distancing measures,” Dr. Marks said.
Furthermore, she added, whereas 60% of youth diagnosed with type 2 diabetes before the pandemic were female, the rate fell to 40% during the pandemic. This trend might be because of activity levels in that, while male adolescents are typically more active, rates of exercise fell in both sexes during the pandemic but declined more sharply in males such that activity levels between the sexes became equal.
Although type 2 diabetes in youth has always been more common in ethnic minorities, the pandemic appears to have exacerbated these disparities.
While 58% of youth diagnosed with type 2 diabetes prepandemic identified as non-Hispanic Black, that proportion rose to 76.7% during the pandemic. Among Black youth with new-onset type 2 diabetes, 31 of 33 presented in DKA, and 12 of the 13 who presented in hyperosmolar DKA during the pandemic were Black.
“Strategies to promote health equity and address the undue burden of the COVID-19 pandemic on underserved communities must be developed to avoid worsening disparities and long-term health outcomes,” Dr. Marks said.
‘A microcosm’: Similar findings in a smaller population
Dr. Hsia and colleagues looked at a smaller number of patients in a shorter time period. In March–December 2019, the hospitalization rate for new-onset type 2 diabetes was 0.27% (8 out of 2,964 hospitalizations), compared with 0.62% (17 out of 2,729 hospitalizations) during the same period in 2020 (P < .048) – also more than a doubling. Age at admission, sex, and body mass index didn’t differ between the two groups.
Criteria for DKA were met by three children in 2019 versus eight in 2020, and hyperosmolar hyperglycemic syndrome in zero versus two, respectively. Mean hemoglobin A1c on admission was 12.4% in 2019 versus 13.1% in 2020 (P = .59), and mean serum glucose was 441 mg/dL versus 669 mg/dL (P = .14), respectively. Serum osmolality on admission was 314 mmol/kg in 2019 versus 335 mmol/kg in 2020 (P = .19).
“Clinically speaking the differences in the lab values were significant, but we did not have enough numbers ... to see a statistically significant difference. I think by looking at more centers, our site likely represents a microcosm of what is happening across the country,” Dr. Hsia said.
In 2019, 7 of the 8 children were African American, as were 16 of the 17 children in 2020. The other single child in each group was White.
Dr. Hsia said: “Larger studies that include more patients are needed to confirm our initial findings. More research is needed to understand why this increasing trend of type 2 diabetes diagnoses in children may be occurring [and] to better understand how stay-at-home orders and other restrictions due to COVID-19 have worsened risk factors for type 2 diabetes.”
“These include decreased physical activity, more screen time, disturbed sleep, and increased intake of processed foods, which can all lead to weight gain,” he concluded.
Dr. Marks reported receiving research support from Tandem, Dexcom, and the Cystic Fibrosis Foundation. Dr. Hsia reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The incidence of type 2 diabetes in children appears to have doubled during the COVID-19 pandemic, data from two new U.S. studies suggest, with the lead investigator of one saying she was “surprised by the staggering increase in cases of type 2 diabetes ... and the increase in severity of presentation.”
Findings from the two separate retrospective chart reviews – one conducted in Washington, D.C., and the other in Baton Rouge, La. – were presented June 25 at the annual scientific sessions of the American Diabetes Association.
Although the two studies differed somewhat in the clinical parameters examined, both revealed a similar doubling of the rates of hospitalizations for type 2 diabetes among youth during 2020, compared with the same time period in 2019, as well as greater severity of metabolic disturbance.
And, as has been previously described with type 2 diabetes in youth, African American ethnicity predominated in both cohorts.
“Although we could not assess the cause of the increases in type 2 diabetes from our data, these disparities suggest that indirect effects of social distancing measures, including school closure and unemployment, are placing undue burden on underserved communities. Decreases in well-child care and fears of seeking medical care during the pandemic may have also contributed,” lead investigator of one of the studies, pediatric endocrinologist Brynn E. Marks, MD, Children’s National Hospital, Washington, said in an interview.
More hospitalizations, racial disparities aggravated by COVID-19
Lead author of the other study, Daniel S. Hsia, MD, Pennington Biomedical Research Center, Baton Rouge, said in an interview: “Since the pandemic, our data suggest that more children may be diagnosed with type 2 diabetes and may require hospitalization when they are diagnosed. Looking at both datasets, there appears to be a racial disparity in type 2 diabetes diagnoses that has only been exacerbated by the COVID-19 pandemic.”
Of concern, Dr. Hsia said, “The incidence rate of type 2 diabetes in children was already on the rise before the pandemic. While there may be a brief leveling off now that children are getting regular health care and going back to school in person, I believe these rates will continue to rise especially in light of the childhood obesity rates not improving.”
Their dataset captured all youth who were newly diagnosed with type 2 diabetes during the first full year of the COVID-19 pandemic, from March 11, 2020, to March 10, 2021, and compared those data with the time period from March 11, 2019, to March 10, 2020.
During the pandemic, the number of cases of type 2 diabetes increased by 182%, from 50 in 2019 to 141 in 2020. The average age at diagnosis was about 14 years in both time periods.
In the prepandemic period, 18 (36%) diagnosed with type 2 diabetes required inpatient admission, compared with 85 (60.3%) during the pandemic. At Children’s National, youth with suspected new-onset type 2 diabetes aren’t typically hospitalized unless they have severe hyperglycemia, ketosis, or are unable to schedule urgent outpatient follow-up, Dr. Marks noted.
The proportions of youth with new-onset type 2 diabetes who presented in diabetic ketoacidosis (DKA) rose from 2 (4%) prepandemic to 33 (23.4%) during the pandemic. Presentation with hyperosmolar DKA rose from 0 to 13 (9.2%).
However, during the pandemic only five youth were actively infected with SARS-CoV-2 at the time of type 2 diabetes diagnosis among the 90 tested.
Dr. Marks said: “We believe the increase in inpatient admissions was due to more severe presentation during the pandemic. ...We were surprised by the staggering increase in cases of type 2 diabetes ... and the increase in severity of presentation.”
Shift in diagnoses to type 2 diabetes
The pandemic also appears to have shifted the proportion of youth diagnosed with type 2 diabetes, compared with type 1 diabetes. Whereas 24% of youth with new-onset diabetes prepandemic had type 2 diabetes and the rest had type 1 diabetes, during pandemic the proportion with type 2 diabetes rose to 44%.
“Rates of type 2 diabetes rose steadily at a rate of 1.45 cases per month throughout the course of the pandemic, suggesting a cumulative effect of the indirect effects of social distancing measures,” Dr. Marks said.
Furthermore, she added, whereas 60% of youth diagnosed with type 2 diabetes before the pandemic were female, the rate fell to 40% during the pandemic. This trend might be because of activity levels in that, while male adolescents are typically more active, rates of exercise fell in both sexes during the pandemic but declined more sharply in males such that activity levels between the sexes became equal.
Although type 2 diabetes in youth has always been more common in ethnic minorities, the pandemic appears to have exacerbated these disparities.
While 58% of youth diagnosed with type 2 diabetes prepandemic identified as non-Hispanic Black, that proportion rose to 76.7% during the pandemic. Among Black youth with new-onset type 2 diabetes, 31 of 33 presented in DKA, and 12 of the 13 who presented in hyperosmolar DKA during the pandemic were Black.
“Strategies to promote health equity and address the undue burden of the COVID-19 pandemic on underserved communities must be developed to avoid worsening disparities and long-term health outcomes,” Dr. Marks said.
‘A microcosm’: Similar findings in a smaller population
Dr. Hsia and colleagues looked at a smaller number of patients in a shorter time period. In March–December 2019, the hospitalization rate for new-onset type 2 diabetes was 0.27% (8 out of 2,964 hospitalizations), compared with 0.62% (17 out of 2,729 hospitalizations) during the same period in 2020 (P < .048) – also more than a doubling. Age at admission, sex, and body mass index didn’t differ between the two groups.
Criteria for DKA were met by three children in 2019 versus eight in 2020, and hyperosmolar hyperglycemic syndrome in zero versus two, respectively. Mean hemoglobin A1c on admission was 12.4% in 2019 versus 13.1% in 2020 (P = .59), and mean serum glucose was 441 mg/dL versus 669 mg/dL (P = .14), respectively. Serum osmolality on admission was 314 mmol/kg in 2019 versus 335 mmol/kg in 2020 (P = .19).
“Clinically speaking the differences in the lab values were significant, but we did not have enough numbers ... to see a statistically significant difference. I think by looking at more centers, our site likely represents a microcosm of what is happening across the country,” Dr. Hsia said.
In 2019, 7 of the 8 children were African American, as were 16 of the 17 children in 2020. The other single child in each group was White.
Dr. Hsia said: “Larger studies that include more patients are needed to confirm our initial findings. More research is needed to understand why this increasing trend of type 2 diabetes diagnoses in children may be occurring [and] to better understand how stay-at-home orders and other restrictions due to COVID-19 have worsened risk factors for type 2 diabetes.”
“These include decreased physical activity, more screen time, disturbed sleep, and increased intake of processed foods, which can all lead to weight gain,” he concluded.
Dr. Marks reported receiving research support from Tandem, Dexcom, and the Cystic Fibrosis Foundation. Dr. Hsia reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The incidence of type 2 diabetes in children appears to have doubled during the COVID-19 pandemic, data from two new U.S. studies suggest, with the lead investigator of one saying she was “surprised by the staggering increase in cases of type 2 diabetes ... and the increase in severity of presentation.”
Findings from the two separate retrospective chart reviews – one conducted in Washington, D.C., and the other in Baton Rouge, La. – were presented June 25 at the annual scientific sessions of the American Diabetes Association.
Although the two studies differed somewhat in the clinical parameters examined, both revealed a similar doubling of the rates of hospitalizations for type 2 diabetes among youth during 2020, compared with the same time period in 2019, as well as greater severity of metabolic disturbance.
And, as has been previously described with type 2 diabetes in youth, African American ethnicity predominated in both cohorts.
“Although we could not assess the cause of the increases in type 2 diabetes from our data, these disparities suggest that indirect effects of social distancing measures, including school closure and unemployment, are placing undue burden on underserved communities. Decreases in well-child care and fears of seeking medical care during the pandemic may have also contributed,” lead investigator of one of the studies, pediatric endocrinologist Brynn E. Marks, MD, Children’s National Hospital, Washington, said in an interview.
More hospitalizations, racial disparities aggravated by COVID-19
Lead author of the other study, Daniel S. Hsia, MD, Pennington Biomedical Research Center, Baton Rouge, said in an interview: “Since the pandemic, our data suggest that more children may be diagnosed with type 2 diabetes and may require hospitalization when they are diagnosed. Looking at both datasets, there appears to be a racial disparity in type 2 diabetes diagnoses that has only been exacerbated by the COVID-19 pandemic.”
Of concern, Dr. Hsia said, “The incidence rate of type 2 diabetes in children was already on the rise before the pandemic. While there may be a brief leveling off now that children are getting regular health care and going back to school in person, I believe these rates will continue to rise especially in light of the childhood obesity rates not improving.”
Their dataset captured all youth who were newly diagnosed with type 2 diabetes during the first full year of the COVID-19 pandemic, from March 11, 2020, to March 10, 2021, and compared those data with the time period from March 11, 2019, to March 10, 2020.
During the pandemic, the number of cases of type 2 diabetes increased by 182%, from 50 in 2019 to 141 in 2020. The average age at diagnosis was about 14 years in both time periods.
In the prepandemic period, 18 (36%) diagnosed with type 2 diabetes required inpatient admission, compared with 85 (60.3%) during the pandemic. At Children’s National, youth with suspected new-onset type 2 diabetes aren’t typically hospitalized unless they have severe hyperglycemia, ketosis, or are unable to schedule urgent outpatient follow-up, Dr. Marks noted.
The proportions of youth with new-onset type 2 diabetes who presented in diabetic ketoacidosis (DKA) rose from 2 (4%) prepandemic to 33 (23.4%) during the pandemic. Presentation with hyperosmolar DKA rose from 0 to 13 (9.2%).
However, during the pandemic only five youth were actively infected with SARS-CoV-2 at the time of type 2 diabetes diagnosis among the 90 tested.
Dr. Marks said: “We believe the increase in inpatient admissions was due to more severe presentation during the pandemic. ...We were surprised by the staggering increase in cases of type 2 diabetes ... and the increase in severity of presentation.”
Shift in diagnoses to type 2 diabetes
The pandemic also appears to have shifted the proportion of youth diagnosed with type 2 diabetes, compared with type 1 diabetes. Whereas 24% of youth with new-onset diabetes prepandemic had type 2 diabetes and the rest had type 1 diabetes, during pandemic the proportion with type 2 diabetes rose to 44%.
“Rates of type 2 diabetes rose steadily at a rate of 1.45 cases per month throughout the course of the pandemic, suggesting a cumulative effect of the indirect effects of social distancing measures,” Dr. Marks said.
Furthermore, she added, whereas 60% of youth diagnosed with type 2 diabetes before the pandemic were female, the rate fell to 40% during the pandemic. This trend might be because of activity levels in that, while male adolescents are typically more active, rates of exercise fell in both sexes during the pandemic but declined more sharply in males such that activity levels between the sexes became equal.
Although type 2 diabetes in youth has always been more common in ethnic minorities, the pandemic appears to have exacerbated these disparities.
While 58% of youth diagnosed with type 2 diabetes prepandemic identified as non-Hispanic Black, that proportion rose to 76.7% during the pandemic. Among Black youth with new-onset type 2 diabetes, 31 of 33 presented in DKA, and 12 of the 13 who presented in hyperosmolar DKA during the pandemic were Black.
“Strategies to promote health equity and address the undue burden of the COVID-19 pandemic on underserved communities must be developed to avoid worsening disparities and long-term health outcomes,” Dr. Marks said.
‘A microcosm’: Similar findings in a smaller population
Dr. Hsia and colleagues looked at a smaller number of patients in a shorter time period. In March–December 2019, the hospitalization rate for new-onset type 2 diabetes was 0.27% (8 out of 2,964 hospitalizations), compared with 0.62% (17 out of 2,729 hospitalizations) during the same period in 2020 (P < .048) – also more than a doubling. Age at admission, sex, and body mass index didn’t differ between the two groups.
Criteria for DKA were met by three children in 2019 versus eight in 2020, and hyperosmolar hyperglycemic syndrome in zero versus two, respectively. Mean hemoglobin A1c on admission was 12.4% in 2019 versus 13.1% in 2020 (P = .59), and mean serum glucose was 441 mg/dL versus 669 mg/dL (P = .14), respectively. Serum osmolality on admission was 314 mmol/kg in 2019 versus 335 mmol/kg in 2020 (P = .19).
“Clinically speaking the differences in the lab values were significant, but we did not have enough numbers ... to see a statistically significant difference. I think by looking at more centers, our site likely represents a microcosm of what is happening across the country,” Dr. Hsia said.
In 2019, 7 of the 8 children were African American, as were 16 of the 17 children in 2020. The other single child in each group was White.
Dr. Hsia said: “Larger studies that include more patients are needed to confirm our initial findings. More research is needed to understand why this increasing trend of type 2 diabetes diagnoses in children may be occurring [and] to better understand how stay-at-home orders and other restrictions due to COVID-19 have worsened risk factors for type 2 diabetes.”
“These include decreased physical activity, more screen time, disturbed sleep, and increased intake of processed foods, which can all lead to weight gain,” he concluded.
Dr. Marks reported receiving research support from Tandem, Dexcom, and the Cystic Fibrosis Foundation. Dr. Hsia reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
‘Stunning’ twincretin beats semaglutide for A1c, weight reduction in T2D
Tirzepatide, a novel “twincretin” agent, was superior to 1-mg semaglutide treatments for reducing both hemoglobin A1c levels and body weight in patients with type 2 diabetes in a pivotal, 40-week, head-to-head trial with nearly 1,900 randomized patients, one of four positive pivotal trial results reported for tirzepatide at the annual scientific sessions of the American Diabetes Association.
“Across all four studies we see a significant and clinically meaningful decrease in A1c, and robust weight loss. The results exceeded our expectations” for both these outcomes, said Laura Fernández Landó, MD, senior medical director for tirzepatide at Lilly, the company developing the agent, and a coauthor on the semaglutide comparison study as well as on other tirzepatide reports at the meeting.
“This opens up a new avenue for results in diabetes therapy,” Jens Juul Holst, MD, remarked in a press conference.
SURPASS-2 compared three different tirzepatide doses delivered once weekly by subcutaneous injection against a 1-mg weekly, subcutaneous dose of semaglutide (Ozempic) in 1,879 adults who had been diagnosed with type 2 diabetes for an average of almost 9 years. All patients were already on metformin treatment that had proved inadequate for controlling their hyperglycemia; enrolled patients had an average A1c of 8.28%. The trial’s primary endpoint was change from baseline in A1c levels after 40 weeks.
Significant differences at each dose level
Patients on each of the three tirzepatide doses – 5 mg, 10 mg, or 15 mg once weekly – showed dose-dependent reductions in A1c that, for each dose, were significantly better than the reduction achieved with semaglutide. The highest tirzepatide dose reduced A1c levels by an average of 0.45% more than what semaglutide achieved, reported first author Juan P. Frias, MD; Dr. Landó; and their coauthors.
One key secondary endpoint was weight reduction, and each of the three tirzepatide doses again produced significant incremental loss beyond what semaglutide produced. The 5-mg weekly dose of tirzepatide produced an average 1.9-kg additional weight loss, compared with semaglutide, while the 15-mg dose resulted in an average 5.5-kg loss beyond what semaglutide achieved and a total average weight loss of 11.2 kg from baseline.
The study’s additional key secondary endpoints, the percentages of patients reaching an A1c of less than 7%, and less than 5.7%, also showed significantly better numbers with tirzepatide. The highest tirzepatide dose pushed 86% of patients below the 7% mark, compared with 79% on semaglutide, and the top tirzepatide dose resulted in 46% of patients getting their A1c below 5.7%, compared with 19% of patients on semaglutide.
The findings are “stunning, I must stay, and those results included that up to half of the patients treated with high doses of tirzepatide may reach A1c levels of less than 5.7%, which is really, really unheard of,” said Dr. Holst, professor of endocrinology and metabolism at the University of Copenhagen. Along with the “weight losses at the same time of up to 12% in that patient group, we are seeing some completely unexpected and really shocking and wonderful new advances in the therapy,” added Dr. Holst.
The safety profile of tirzepatide was roughly similar to semaglutide’s and to that other agents in the glucagonlike peptide-1 receptor agonist (GLP-1 RA) class. Concurrently with the report at the meeting, the results also appeared in an article published online in the New England Journal of Medicine.
An ‘impressive’ weight loss effect
Weight loss on tirzepatide was “impressive,” commented Katherine R. Tuttle, MD, a nephrologist affiliated with the University of Washington and executive director for research at Providence Health Care in Spokane, Wash. Another striking feature of tirzepatide’s weight-loss effect was that it did not plateau during the 40 weeks of the study, Dr. Tuttle noted in an accompanying editorial that accompanied the published report, a finding that suggests the potential for additional weight loss from continued treatment .
“The weight loss is remarkable,” commented Rodolfo J. Galindo, MD, an endocrinologist at Emory University, Atlanta. While incremental reduction of A1c on the order of less than 0.5% is helpful, incremental weight loss of more than 10 lbs on tirzepatide, compared with semaglutide “will likely be a tie-breaker” for many clinicians and patients to favor tirzepatide over semaglutide or another GLP-1 RA agent, he said in an interview. Dr. Galindo also cited other important factors that he predicted will drive decisions on using tirzepatide or a GLP-1 RA once tirzepatide reaches the U.S. market: relative cost, access, and tolerability.
The important issue of dose
But the edge that tirzepatide showed over semaglutide for weight loss did not occur on a completely level playing field. The 1 mg/week dose of semaglutide used as the comparator in SURPASS-2 was the maximum dose available at the time the study began, but in June 2021 the Food and Drug Administration approved a 2.4 mg/week dose (Wegovy) labeled specifically for weight loss. Dr. Tuttle cited the limitation this introduces in her editorial.
“The dose issue is important,” she wrote. The doses of tirzepatide and semaglutide compared in SURPASS-2 “were not comparable in terms of weight outcomes” given that prior evidence showed that the 2.4 mg/week semaglutide dose is more appropriate for weight loss.
Dr. Tuttle also cited other factors to consider when assessing tirzepatide compared with agents in the GLP-1 RA class.
Several GLP-1 RA agents, including semaglutide, have proven efficacy for reducing rates of atherosclerotic cardiovascular events and albuminuria, and they also slow decline in kidney function and progression of diabetic kidney disease. No details on the renal effects of tirzepatide appeared in the SURPASS-2 report. A press release from Lilly in May 2021 briefly mentioned results from a meta-analysis of several clinical studies of tirzepatide that showed a nonsignificant effect from tirzepatide on the incidence of major cardiovascular adverse events (death from cardiovascular or undetermined causes, MI, stroke, and hospitalization for unstable angina) relative to comparator groups. Results from a dedicated cardiovascular outcomes trial in high-risk patients treated with tirzepatide, SURPASS-CVOT, are not expected until 2024.
A further limitation of SURPASS-2 was the demographics of the enrolled population, which had a low (0.4%) enrollment rate of Black patients, and a high proportion (70%) of Hispanic patients, Dr. Tuttle observed.
Low rates of hypoglycemia
Another notable finding from SURPASS-2 was the low incidence of clinically significant hypoglycemic events (blood glucose levels less than 54 mg/dL), which occurred in 0.2%-1.7% of patients on tirzepatide, depending on their dose, and in 0.4% of patients on semaglutide. Two patients in the tirzepatide cohort had severe hypoglycemia.
These numbers are reassuring, said Dr. Galindo, and reflect the safety of tirzepatide’s dual, incretin-like mechanisms of action that make it a “twincretin.” The molecule acts as both a GLP-1 RA, and as glucose-dependent insulinotropic polypeptide, an incretin that stimulates insulin release when blood sugar is high but also increases glucagon levels when blood sugar levels are normal or low. This dual action may help explain the apparent increased potency tirzepatide showed for both A1c reduction and weight loss, compared with semaglutide, which acts only as a GLP-1 RA.
Some experts have cited the uncertainty introduced by the open-label design of SURPASS-2, a decision necessitated by the distinctly different delivery devices used for tirzepatide and semaglutide, explained Dr. Landó. But she highlighted that double blinding applied to the three different tirzepatide dosages tested in the trial. Dr. Landó said that Lilly plans to seek FDA approval for all three tested tirzepatide doses to give clinicians and patients flexibility in applying the treatment.
SURPASS-2 used a prolonged dose-escalation protocol designed to minimize gastrointestinal adverse effects that started patients on a 2.5 mg weekly dose that then increased by 2.5 mg increments every 4 weeks until patients reached their assigned target dose. This meant that patients did not begin receiving the 15-mg/week dose until halfway through the trial.
Several more tirzepatide trials
Reports from two other pivotal trials for tirzepatide also appeared as posters at the meeting. SURPASS-5 compared tirzepatide with placebo in 475 patients inadequately controlled with titrated insulin glargine (Lantus). SURPASS-3 randomized 1,444 patients to tirzepatide or titrated insulin degludec (Tresiba). In both studies treatment with tirzepatide led to significantly better reductions in A1c and in weight loss than the comparator treatments. Results from a third pivotal trial, SURPASS-1 which compared tirzepatide against placebo in 478 treatment-naive patients, will come in a report scheduled for the second day of the meeting.
The results from all the recent tirzepatide trials show a consistent benefit across the continuum of patients with type 2 diabetes regardless of whether it’s recent onset or well-established disease, said Dr. Landó.
The SURPASS studies were sponsored by Lilly, the company developing tirzepatide, and the reports include several authors who are Lilly employees. Dr. Landó is a Lilly employee and stockholder. Dr. Tuttle has been a consultant to Lilly and to Novo Nordisk, the company that markets semaglutide, as well as to AstraZeneca, Bayer, Boehringer Ingelheim, Gilead, and Janssen. She has also received travel expenses from Kyokawa Hakko Kirin, and research funding from Bayer, Goldfinch Bio, and Lilly. Dr. Galindo has been a consultant to Lilly and to Novo Nordisk, as well as to Abbott Diabetes Care, Sanofi, Valeritas, and Weight Watchers, and his institution has received grant support on his behalf from Lilly, Novo Nordisk and Dexcom. Dr. Holst had no disclosures.
Tirzepatide, a novel “twincretin” agent, was superior to 1-mg semaglutide treatments for reducing both hemoglobin A1c levels and body weight in patients with type 2 diabetes in a pivotal, 40-week, head-to-head trial with nearly 1,900 randomized patients, one of four positive pivotal trial results reported for tirzepatide at the annual scientific sessions of the American Diabetes Association.
“Across all four studies we see a significant and clinically meaningful decrease in A1c, and robust weight loss. The results exceeded our expectations” for both these outcomes, said Laura Fernández Landó, MD, senior medical director for tirzepatide at Lilly, the company developing the agent, and a coauthor on the semaglutide comparison study as well as on other tirzepatide reports at the meeting.
“This opens up a new avenue for results in diabetes therapy,” Jens Juul Holst, MD, remarked in a press conference.
SURPASS-2 compared three different tirzepatide doses delivered once weekly by subcutaneous injection against a 1-mg weekly, subcutaneous dose of semaglutide (Ozempic) in 1,879 adults who had been diagnosed with type 2 diabetes for an average of almost 9 years. All patients were already on metformin treatment that had proved inadequate for controlling their hyperglycemia; enrolled patients had an average A1c of 8.28%. The trial’s primary endpoint was change from baseline in A1c levels after 40 weeks.
Significant differences at each dose level
Patients on each of the three tirzepatide doses – 5 mg, 10 mg, or 15 mg once weekly – showed dose-dependent reductions in A1c that, for each dose, were significantly better than the reduction achieved with semaglutide. The highest tirzepatide dose reduced A1c levels by an average of 0.45% more than what semaglutide achieved, reported first author Juan P. Frias, MD; Dr. Landó; and their coauthors.
One key secondary endpoint was weight reduction, and each of the three tirzepatide doses again produced significant incremental loss beyond what semaglutide produced. The 5-mg weekly dose of tirzepatide produced an average 1.9-kg additional weight loss, compared with semaglutide, while the 15-mg dose resulted in an average 5.5-kg loss beyond what semaglutide achieved and a total average weight loss of 11.2 kg from baseline.
The study’s additional key secondary endpoints, the percentages of patients reaching an A1c of less than 7%, and less than 5.7%, also showed significantly better numbers with tirzepatide. The highest tirzepatide dose pushed 86% of patients below the 7% mark, compared with 79% on semaglutide, and the top tirzepatide dose resulted in 46% of patients getting their A1c below 5.7%, compared with 19% of patients on semaglutide.
The findings are “stunning, I must stay, and those results included that up to half of the patients treated with high doses of tirzepatide may reach A1c levels of less than 5.7%, which is really, really unheard of,” said Dr. Holst, professor of endocrinology and metabolism at the University of Copenhagen. Along with the “weight losses at the same time of up to 12% in that patient group, we are seeing some completely unexpected and really shocking and wonderful new advances in the therapy,” added Dr. Holst.
The safety profile of tirzepatide was roughly similar to semaglutide’s and to that other agents in the glucagonlike peptide-1 receptor agonist (GLP-1 RA) class. Concurrently with the report at the meeting, the results also appeared in an article published online in the New England Journal of Medicine.
An ‘impressive’ weight loss effect
Weight loss on tirzepatide was “impressive,” commented Katherine R. Tuttle, MD, a nephrologist affiliated with the University of Washington and executive director for research at Providence Health Care in Spokane, Wash. Another striking feature of tirzepatide’s weight-loss effect was that it did not plateau during the 40 weeks of the study, Dr. Tuttle noted in an accompanying editorial that accompanied the published report, a finding that suggests the potential for additional weight loss from continued treatment .
“The weight loss is remarkable,” commented Rodolfo J. Galindo, MD, an endocrinologist at Emory University, Atlanta. While incremental reduction of A1c on the order of less than 0.5% is helpful, incremental weight loss of more than 10 lbs on tirzepatide, compared with semaglutide “will likely be a tie-breaker” for many clinicians and patients to favor tirzepatide over semaglutide or another GLP-1 RA agent, he said in an interview. Dr. Galindo also cited other important factors that he predicted will drive decisions on using tirzepatide or a GLP-1 RA once tirzepatide reaches the U.S. market: relative cost, access, and tolerability.
The important issue of dose
But the edge that tirzepatide showed over semaglutide for weight loss did not occur on a completely level playing field. The 1 mg/week dose of semaglutide used as the comparator in SURPASS-2 was the maximum dose available at the time the study began, but in June 2021 the Food and Drug Administration approved a 2.4 mg/week dose (Wegovy) labeled specifically for weight loss. Dr. Tuttle cited the limitation this introduces in her editorial.
“The dose issue is important,” she wrote. The doses of tirzepatide and semaglutide compared in SURPASS-2 “were not comparable in terms of weight outcomes” given that prior evidence showed that the 2.4 mg/week semaglutide dose is more appropriate for weight loss.
Dr. Tuttle also cited other factors to consider when assessing tirzepatide compared with agents in the GLP-1 RA class.
Several GLP-1 RA agents, including semaglutide, have proven efficacy for reducing rates of atherosclerotic cardiovascular events and albuminuria, and they also slow decline in kidney function and progression of diabetic kidney disease. No details on the renal effects of tirzepatide appeared in the SURPASS-2 report. A press release from Lilly in May 2021 briefly mentioned results from a meta-analysis of several clinical studies of tirzepatide that showed a nonsignificant effect from tirzepatide on the incidence of major cardiovascular adverse events (death from cardiovascular or undetermined causes, MI, stroke, and hospitalization for unstable angina) relative to comparator groups. Results from a dedicated cardiovascular outcomes trial in high-risk patients treated with tirzepatide, SURPASS-CVOT, are not expected until 2024.
A further limitation of SURPASS-2 was the demographics of the enrolled population, which had a low (0.4%) enrollment rate of Black patients, and a high proportion (70%) of Hispanic patients, Dr. Tuttle observed.
Low rates of hypoglycemia
Another notable finding from SURPASS-2 was the low incidence of clinically significant hypoglycemic events (blood glucose levels less than 54 mg/dL), which occurred in 0.2%-1.7% of patients on tirzepatide, depending on their dose, and in 0.4% of patients on semaglutide. Two patients in the tirzepatide cohort had severe hypoglycemia.
These numbers are reassuring, said Dr. Galindo, and reflect the safety of tirzepatide’s dual, incretin-like mechanisms of action that make it a “twincretin.” The molecule acts as both a GLP-1 RA, and as glucose-dependent insulinotropic polypeptide, an incretin that stimulates insulin release when blood sugar is high but also increases glucagon levels when blood sugar levels are normal or low. This dual action may help explain the apparent increased potency tirzepatide showed for both A1c reduction and weight loss, compared with semaglutide, which acts only as a GLP-1 RA.
Some experts have cited the uncertainty introduced by the open-label design of SURPASS-2, a decision necessitated by the distinctly different delivery devices used for tirzepatide and semaglutide, explained Dr. Landó. But she highlighted that double blinding applied to the three different tirzepatide dosages tested in the trial. Dr. Landó said that Lilly plans to seek FDA approval for all three tested tirzepatide doses to give clinicians and patients flexibility in applying the treatment.
SURPASS-2 used a prolonged dose-escalation protocol designed to minimize gastrointestinal adverse effects that started patients on a 2.5 mg weekly dose that then increased by 2.5 mg increments every 4 weeks until patients reached their assigned target dose. This meant that patients did not begin receiving the 15-mg/week dose until halfway through the trial.
Several more tirzepatide trials
Reports from two other pivotal trials for tirzepatide also appeared as posters at the meeting. SURPASS-5 compared tirzepatide with placebo in 475 patients inadequately controlled with titrated insulin glargine (Lantus). SURPASS-3 randomized 1,444 patients to tirzepatide or titrated insulin degludec (Tresiba). In both studies treatment with tirzepatide led to significantly better reductions in A1c and in weight loss than the comparator treatments. Results from a third pivotal trial, SURPASS-1 which compared tirzepatide against placebo in 478 treatment-naive patients, will come in a report scheduled for the second day of the meeting.
The results from all the recent tirzepatide trials show a consistent benefit across the continuum of patients with type 2 diabetes regardless of whether it’s recent onset or well-established disease, said Dr. Landó.
The SURPASS studies were sponsored by Lilly, the company developing tirzepatide, and the reports include several authors who are Lilly employees. Dr. Landó is a Lilly employee and stockholder. Dr. Tuttle has been a consultant to Lilly and to Novo Nordisk, the company that markets semaglutide, as well as to AstraZeneca, Bayer, Boehringer Ingelheim, Gilead, and Janssen. She has also received travel expenses from Kyokawa Hakko Kirin, and research funding from Bayer, Goldfinch Bio, and Lilly. Dr. Galindo has been a consultant to Lilly and to Novo Nordisk, as well as to Abbott Diabetes Care, Sanofi, Valeritas, and Weight Watchers, and his institution has received grant support on his behalf from Lilly, Novo Nordisk and Dexcom. Dr. Holst had no disclosures.
Tirzepatide, a novel “twincretin” agent, was superior to 1-mg semaglutide treatments for reducing both hemoglobin A1c levels and body weight in patients with type 2 diabetes in a pivotal, 40-week, head-to-head trial with nearly 1,900 randomized patients, one of four positive pivotal trial results reported for tirzepatide at the annual scientific sessions of the American Diabetes Association.
“Across all four studies we see a significant and clinically meaningful decrease in A1c, and robust weight loss. The results exceeded our expectations” for both these outcomes, said Laura Fernández Landó, MD, senior medical director for tirzepatide at Lilly, the company developing the agent, and a coauthor on the semaglutide comparison study as well as on other tirzepatide reports at the meeting.
“This opens up a new avenue for results in diabetes therapy,” Jens Juul Holst, MD, remarked in a press conference.
SURPASS-2 compared three different tirzepatide doses delivered once weekly by subcutaneous injection against a 1-mg weekly, subcutaneous dose of semaglutide (Ozempic) in 1,879 adults who had been diagnosed with type 2 diabetes for an average of almost 9 years. All patients were already on metformin treatment that had proved inadequate for controlling their hyperglycemia; enrolled patients had an average A1c of 8.28%. The trial’s primary endpoint was change from baseline in A1c levels after 40 weeks.
Significant differences at each dose level
Patients on each of the three tirzepatide doses – 5 mg, 10 mg, or 15 mg once weekly – showed dose-dependent reductions in A1c that, for each dose, were significantly better than the reduction achieved with semaglutide. The highest tirzepatide dose reduced A1c levels by an average of 0.45% more than what semaglutide achieved, reported first author Juan P. Frias, MD; Dr. Landó; and their coauthors.
One key secondary endpoint was weight reduction, and each of the three tirzepatide doses again produced significant incremental loss beyond what semaglutide produced. The 5-mg weekly dose of tirzepatide produced an average 1.9-kg additional weight loss, compared with semaglutide, while the 15-mg dose resulted in an average 5.5-kg loss beyond what semaglutide achieved and a total average weight loss of 11.2 kg from baseline.
The study’s additional key secondary endpoints, the percentages of patients reaching an A1c of less than 7%, and less than 5.7%, also showed significantly better numbers with tirzepatide. The highest tirzepatide dose pushed 86% of patients below the 7% mark, compared with 79% on semaglutide, and the top tirzepatide dose resulted in 46% of patients getting their A1c below 5.7%, compared with 19% of patients on semaglutide.
The findings are “stunning, I must stay, and those results included that up to half of the patients treated with high doses of tirzepatide may reach A1c levels of less than 5.7%, which is really, really unheard of,” said Dr. Holst, professor of endocrinology and metabolism at the University of Copenhagen. Along with the “weight losses at the same time of up to 12% in that patient group, we are seeing some completely unexpected and really shocking and wonderful new advances in the therapy,” added Dr. Holst.
The safety profile of tirzepatide was roughly similar to semaglutide’s and to that other agents in the glucagonlike peptide-1 receptor agonist (GLP-1 RA) class. Concurrently with the report at the meeting, the results also appeared in an article published online in the New England Journal of Medicine.
An ‘impressive’ weight loss effect
Weight loss on tirzepatide was “impressive,” commented Katherine R. Tuttle, MD, a nephrologist affiliated with the University of Washington and executive director for research at Providence Health Care in Spokane, Wash. Another striking feature of tirzepatide’s weight-loss effect was that it did not plateau during the 40 weeks of the study, Dr. Tuttle noted in an accompanying editorial that accompanied the published report, a finding that suggests the potential for additional weight loss from continued treatment .
“The weight loss is remarkable,” commented Rodolfo J. Galindo, MD, an endocrinologist at Emory University, Atlanta. While incremental reduction of A1c on the order of less than 0.5% is helpful, incremental weight loss of more than 10 lbs on tirzepatide, compared with semaglutide “will likely be a tie-breaker” for many clinicians and patients to favor tirzepatide over semaglutide or another GLP-1 RA agent, he said in an interview. Dr. Galindo also cited other important factors that he predicted will drive decisions on using tirzepatide or a GLP-1 RA once tirzepatide reaches the U.S. market: relative cost, access, and tolerability.
The important issue of dose
But the edge that tirzepatide showed over semaglutide for weight loss did not occur on a completely level playing field. The 1 mg/week dose of semaglutide used as the comparator in SURPASS-2 was the maximum dose available at the time the study began, but in June 2021 the Food and Drug Administration approved a 2.4 mg/week dose (Wegovy) labeled specifically for weight loss. Dr. Tuttle cited the limitation this introduces in her editorial.
“The dose issue is important,” she wrote. The doses of tirzepatide and semaglutide compared in SURPASS-2 “were not comparable in terms of weight outcomes” given that prior evidence showed that the 2.4 mg/week semaglutide dose is more appropriate for weight loss.
Dr. Tuttle also cited other factors to consider when assessing tirzepatide compared with agents in the GLP-1 RA class.
Several GLP-1 RA agents, including semaglutide, have proven efficacy for reducing rates of atherosclerotic cardiovascular events and albuminuria, and they also slow decline in kidney function and progression of diabetic kidney disease. No details on the renal effects of tirzepatide appeared in the SURPASS-2 report. A press release from Lilly in May 2021 briefly mentioned results from a meta-analysis of several clinical studies of tirzepatide that showed a nonsignificant effect from tirzepatide on the incidence of major cardiovascular adverse events (death from cardiovascular or undetermined causes, MI, stroke, and hospitalization for unstable angina) relative to comparator groups. Results from a dedicated cardiovascular outcomes trial in high-risk patients treated with tirzepatide, SURPASS-CVOT, are not expected until 2024.
A further limitation of SURPASS-2 was the demographics of the enrolled population, which had a low (0.4%) enrollment rate of Black patients, and a high proportion (70%) of Hispanic patients, Dr. Tuttle observed.
Low rates of hypoglycemia
Another notable finding from SURPASS-2 was the low incidence of clinically significant hypoglycemic events (blood glucose levels less than 54 mg/dL), which occurred in 0.2%-1.7% of patients on tirzepatide, depending on their dose, and in 0.4% of patients on semaglutide. Two patients in the tirzepatide cohort had severe hypoglycemia.
These numbers are reassuring, said Dr. Galindo, and reflect the safety of tirzepatide’s dual, incretin-like mechanisms of action that make it a “twincretin.” The molecule acts as both a GLP-1 RA, and as glucose-dependent insulinotropic polypeptide, an incretin that stimulates insulin release when blood sugar is high but also increases glucagon levels when blood sugar levels are normal or low. This dual action may help explain the apparent increased potency tirzepatide showed for both A1c reduction and weight loss, compared with semaglutide, which acts only as a GLP-1 RA.
Some experts have cited the uncertainty introduced by the open-label design of SURPASS-2, a decision necessitated by the distinctly different delivery devices used for tirzepatide and semaglutide, explained Dr. Landó. But she highlighted that double blinding applied to the three different tirzepatide dosages tested in the trial. Dr. Landó said that Lilly plans to seek FDA approval for all three tested tirzepatide doses to give clinicians and patients flexibility in applying the treatment.
SURPASS-2 used a prolonged dose-escalation protocol designed to minimize gastrointestinal adverse effects that started patients on a 2.5 mg weekly dose that then increased by 2.5 mg increments every 4 weeks until patients reached their assigned target dose. This meant that patients did not begin receiving the 15-mg/week dose until halfway through the trial.
Several more tirzepatide trials
Reports from two other pivotal trials for tirzepatide also appeared as posters at the meeting. SURPASS-5 compared tirzepatide with placebo in 475 patients inadequately controlled with titrated insulin glargine (Lantus). SURPASS-3 randomized 1,444 patients to tirzepatide or titrated insulin degludec (Tresiba). In both studies treatment with tirzepatide led to significantly better reductions in A1c and in weight loss than the comparator treatments. Results from a third pivotal trial, SURPASS-1 which compared tirzepatide against placebo in 478 treatment-naive patients, will come in a report scheduled for the second day of the meeting.
The results from all the recent tirzepatide trials show a consistent benefit across the continuum of patients with type 2 diabetes regardless of whether it’s recent onset or well-established disease, said Dr. Landó.
The SURPASS studies were sponsored by Lilly, the company developing tirzepatide, and the reports include several authors who are Lilly employees. Dr. Landó is a Lilly employee and stockholder. Dr. Tuttle has been a consultant to Lilly and to Novo Nordisk, the company that markets semaglutide, as well as to AstraZeneca, Bayer, Boehringer Ingelheim, Gilead, and Janssen. She has also received travel expenses from Kyokawa Hakko Kirin, and research funding from Bayer, Goldfinch Bio, and Lilly. Dr. Galindo has been a consultant to Lilly and to Novo Nordisk, as well as to Abbott Diabetes Care, Sanofi, Valeritas, and Weight Watchers, and his institution has received grant support on his behalf from Lilly, Novo Nordisk and Dexcom. Dr. Holst had no disclosures.
FROM ADA 2021
Time-restricted eating ‘promising, but more data are needed’
Time-restricted eating – that is, reducing the number of hours a person is allowed to eat during the day – may produce a modest 1%-4% weight loss, even without cutting calories, early studies in humans suggest. But more research is needed to provide definitive evidence.
This type of intermittent fasting also appears to improve blood glucose, blood pressure, and oxidative stress, said Courtney M. Peterson, PhD, a researcher at the University of Alabama at Birmingham, summarizing what is known about the potential weight-loss strategy at the annual scientific sessions of the American Diabetes Association.
The best results were seen with early time-restricted eating (that is, ending the nighttime fasting early in the day) and allowing a person to eat 8-10 hours each day (for example, 8 a.m. to 4 p.m. or 8 a.m. to 6 p.m.), with fasting and only water allowed the remaining hours, she reported.
However, the 3 dozen or so studies in humans to date are mainly small, pilot, or single-arm studies lasting up to 3 months, and there are only three main randomized, controlled trials with 25 or more participants in each group.
Large trials with around 260 participants are needed, Dr. Peterson said, “before drawing definitive conclusions” about the weight-loss and cardiometabolic benefits of time-restricted eating.
Invited to comment, session chair Lisa S. Chow, MD, an associate professor of medicine in the endocrine and diabetes division at the University of Minnesota, Minneapolis, similarly said: “I think time-restricted eating is promising because of its simple message and noted weight-loss benefit, yet more data are needed.”
“Many uncertainties remain,” she added, “including the potential concern that time-restricted eating may be associated with lean [muscle] mass loss and identifying the populations most likely to benefit from time-restricted eating,” she said.
36 small studies, a review, a meta-analysis, 3 RCTs
There have been about three dozen small studies of time-restricted eating in humans, which examined 4- to 11-hour eating windows, Dr. Peterson explained.
A systematic review of 23 trials of time-restricted eating reported that, on average, participants lost 3% of their initial weight. And a meta-analysis of 19 trials in 475 participants found a –0.9 kg mean difference effect for weight loss.
However, those two analyses did not compare time-restricted eating with a control treatment, she stressed.
The largest randomized, controlled trial is a 12-week study in 271 adults with nonalcoholic fatty liver disease in China, Dr. Peterson said.
The researchers compared three groups:
- Alternate-day modified fasting: healthy meal provided.
- Time-restricted eating: 8-hour window, healthy meal provided.
- Control: 20% calorie reduction, no meal provided.
At 4 and 12 weeks, adults in the two treatment groups lost more weight than those in the control group, but “this was not a fair comparison” because of the lack of a provided meal in the control group, Dr. Peterson pointed out.
The next largest randomized, controlled study is the 12-week TREAT trial, published online in JAMA Internal Medicine in October 2020.
The researchers, from the University of California, San Francisco, randomized 116 adults into two groups:
- 8-hour time-restricted eating from noon to 8 p.m..
- Control: three meals/day.
Time-restricted eating did not lead to greater weight loss, compared with three structured meals a day, which was not surprising, Dr. Chow said, as “participants just reported whether they were engaged in time-restricted eating in a yes/no answer.”
Moreover, “there was no objective measure of their eating window. From our study, we showed that the extent of eating window restriction matters, not just time-restricted eating participation.”
Also, in TREAT, the eating window was noon to 8 p.m. (considered late for time-restricted eating), and the trial also allowed noncaloric beverages outside the window, whereas most studies only allow water and medications.
Lastly, TREAT showed that time-restricted eating reduced weight, compared with baseline, but the weight loss was not significant, compared with the control group, and there was a wide spread of effects (that is, some lost a lot of weight, others didn’t lose much weight).
“That being said, the JAMA Internal Medicine paper is the largest paper to date of time-restricted eating randomized versus control, so its findings need to be acknowledged and recognized,” Dr. Chow said.
Peterson reported that her group recently completed a 14-week intervention in 90 adults with obesity divided into two groups:
- Control: Continuous energy restriction, self-selected ≥ 12-hour window.
- Early time-restricted eating: 8-hour window from 7 a.m. to 3 p.m.
The findings will provide further insight into the benefits of time-restricted eating.
How might time-restricted eating lead to weight loss?
Dr. Peterson concluded by presenting data suggesting how time-restricted eating may induce weight loss.
In a 4-day crossover study in 11 overweight adults, time-restricted eating did not affect energy expenditure, but it lessened swings in subjective hunger, improved appetite hormones including ghrelin, and increased fat oxidation.
Most trials have reported that time-restricted eating improves one or more cardiometabolic endpoints, she noted.
Early time-restricted eating was associated with improved insulin sensitivity and secretion, blood pressure, and oxidative stress, but not better lipid levels.
In contrast, compared with eating 3 meals/day (control), late time-restricted eating (eating 1 meal/day from 5 p.m. to 9 p.m.) was associated with worsened cardiometabolic health (glucose, insulin, blood pressure, and lipid levels) in an 8-week crossover study in 15 participants.
Dr. Peterson and Dr. Chow reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Time-restricted eating – that is, reducing the number of hours a person is allowed to eat during the day – may produce a modest 1%-4% weight loss, even without cutting calories, early studies in humans suggest. But more research is needed to provide definitive evidence.
This type of intermittent fasting also appears to improve blood glucose, blood pressure, and oxidative stress, said Courtney M. Peterson, PhD, a researcher at the University of Alabama at Birmingham, summarizing what is known about the potential weight-loss strategy at the annual scientific sessions of the American Diabetes Association.
The best results were seen with early time-restricted eating (that is, ending the nighttime fasting early in the day) and allowing a person to eat 8-10 hours each day (for example, 8 a.m. to 4 p.m. or 8 a.m. to 6 p.m.), with fasting and only water allowed the remaining hours, she reported.
However, the 3 dozen or so studies in humans to date are mainly small, pilot, or single-arm studies lasting up to 3 months, and there are only three main randomized, controlled trials with 25 or more participants in each group.
Large trials with around 260 participants are needed, Dr. Peterson said, “before drawing definitive conclusions” about the weight-loss and cardiometabolic benefits of time-restricted eating.
Invited to comment, session chair Lisa S. Chow, MD, an associate professor of medicine in the endocrine and diabetes division at the University of Minnesota, Minneapolis, similarly said: “I think time-restricted eating is promising because of its simple message and noted weight-loss benefit, yet more data are needed.”
“Many uncertainties remain,” she added, “including the potential concern that time-restricted eating may be associated with lean [muscle] mass loss and identifying the populations most likely to benefit from time-restricted eating,” she said.
36 small studies, a review, a meta-analysis, 3 RCTs
There have been about three dozen small studies of time-restricted eating in humans, which examined 4- to 11-hour eating windows, Dr. Peterson explained.
A systematic review of 23 trials of time-restricted eating reported that, on average, participants lost 3% of their initial weight. And a meta-analysis of 19 trials in 475 participants found a –0.9 kg mean difference effect for weight loss.
However, those two analyses did not compare time-restricted eating with a control treatment, she stressed.
The largest randomized, controlled trial is a 12-week study in 271 adults with nonalcoholic fatty liver disease in China, Dr. Peterson said.
The researchers compared three groups:
- Alternate-day modified fasting: healthy meal provided.
- Time-restricted eating: 8-hour window, healthy meal provided.
- Control: 20% calorie reduction, no meal provided.
At 4 and 12 weeks, adults in the two treatment groups lost more weight than those in the control group, but “this was not a fair comparison” because of the lack of a provided meal in the control group, Dr. Peterson pointed out.
The next largest randomized, controlled study is the 12-week TREAT trial, published online in JAMA Internal Medicine in October 2020.
The researchers, from the University of California, San Francisco, randomized 116 adults into two groups:
- 8-hour time-restricted eating from noon to 8 p.m..
- Control: three meals/day.
Time-restricted eating did not lead to greater weight loss, compared with three structured meals a day, which was not surprising, Dr. Chow said, as “participants just reported whether they were engaged in time-restricted eating in a yes/no answer.”
Moreover, “there was no objective measure of their eating window. From our study, we showed that the extent of eating window restriction matters, not just time-restricted eating participation.”
Also, in TREAT, the eating window was noon to 8 p.m. (considered late for time-restricted eating), and the trial also allowed noncaloric beverages outside the window, whereas most studies only allow water and medications.
Lastly, TREAT showed that time-restricted eating reduced weight, compared with baseline, but the weight loss was not significant, compared with the control group, and there was a wide spread of effects (that is, some lost a lot of weight, others didn’t lose much weight).
“That being said, the JAMA Internal Medicine paper is the largest paper to date of time-restricted eating randomized versus control, so its findings need to be acknowledged and recognized,” Dr. Chow said.
Peterson reported that her group recently completed a 14-week intervention in 90 adults with obesity divided into two groups:
- Control: Continuous energy restriction, self-selected ≥ 12-hour window.
- Early time-restricted eating: 8-hour window from 7 a.m. to 3 p.m.
The findings will provide further insight into the benefits of time-restricted eating.
How might time-restricted eating lead to weight loss?
Dr. Peterson concluded by presenting data suggesting how time-restricted eating may induce weight loss.
In a 4-day crossover study in 11 overweight adults, time-restricted eating did not affect energy expenditure, but it lessened swings in subjective hunger, improved appetite hormones including ghrelin, and increased fat oxidation.
Most trials have reported that time-restricted eating improves one or more cardiometabolic endpoints, she noted.
Early time-restricted eating was associated with improved insulin sensitivity and secretion, blood pressure, and oxidative stress, but not better lipid levels.
In contrast, compared with eating 3 meals/day (control), late time-restricted eating (eating 1 meal/day from 5 p.m. to 9 p.m.) was associated with worsened cardiometabolic health (glucose, insulin, blood pressure, and lipid levels) in an 8-week crossover study in 15 participants.
Dr. Peterson and Dr. Chow reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Time-restricted eating – that is, reducing the number of hours a person is allowed to eat during the day – may produce a modest 1%-4% weight loss, even without cutting calories, early studies in humans suggest. But more research is needed to provide definitive evidence.
This type of intermittent fasting also appears to improve blood glucose, blood pressure, and oxidative stress, said Courtney M. Peterson, PhD, a researcher at the University of Alabama at Birmingham, summarizing what is known about the potential weight-loss strategy at the annual scientific sessions of the American Diabetes Association.
The best results were seen with early time-restricted eating (that is, ending the nighttime fasting early in the day) and allowing a person to eat 8-10 hours each day (for example, 8 a.m. to 4 p.m. or 8 a.m. to 6 p.m.), with fasting and only water allowed the remaining hours, she reported.
However, the 3 dozen or so studies in humans to date are mainly small, pilot, or single-arm studies lasting up to 3 months, and there are only three main randomized, controlled trials with 25 or more participants in each group.
Large trials with around 260 participants are needed, Dr. Peterson said, “before drawing definitive conclusions” about the weight-loss and cardiometabolic benefits of time-restricted eating.
Invited to comment, session chair Lisa S. Chow, MD, an associate professor of medicine in the endocrine and diabetes division at the University of Minnesota, Minneapolis, similarly said: “I think time-restricted eating is promising because of its simple message and noted weight-loss benefit, yet more data are needed.”
“Many uncertainties remain,” she added, “including the potential concern that time-restricted eating may be associated with lean [muscle] mass loss and identifying the populations most likely to benefit from time-restricted eating,” she said.
36 small studies, a review, a meta-analysis, 3 RCTs
There have been about three dozen small studies of time-restricted eating in humans, which examined 4- to 11-hour eating windows, Dr. Peterson explained.
A systematic review of 23 trials of time-restricted eating reported that, on average, participants lost 3% of their initial weight. And a meta-analysis of 19 trials in 475 participants found a –0.9 kg mean difference effect for weight loss.
However, those two analyses did not compare time-restricted eating with a control treatment, she stressed.
The largest randomized, controlled trial is a 12-week study in 271 adults with nonalcoholic fatty liver disease in China, Dr. Peterson said.
The researchers compared three groups:
- Alternate-day modified fasting: healthy meal provided.
- Time-restricted eating: 8-hour window, healthy meal provided.
- Control: 20% calorie reduction, no meal provided.
At 4 and 12 weeks, adults in the two treatment groups lost more weight than those in the control group, but “this was not a fair comparison” because of the lack of a provided meal in the control group, Dr. Peterson pointed out.
The next largest randomized, controlled study is the 12-week TREAT trial, published online in JAMA Internal Medicine in October 2020.
The researchers, from the University of California, San Francisco, randomized 116 adults into two groups:
- 8-hour time-restricted eating from noon to 8 p.m..
- Control: three meals/day.
Time-restricted eating did not lead to greater weight loss, compared with three structured meals a day, which was not surprising, Dr. Chow said, as “participants just reported whether they were engaged in time-restricted eating in a yes/no answer.”
Moreover, “there was no objective measure of their eating window. From our study, we showed that the extent of eating window restriction matters, not just time-restricted eating participation.”
Also, in TREAT, the eating window was noon to 8 p.m. (considered late for time-restricted eating), and the trial also allowed noncaloric beverages outside the window, whereas most studies only allow water and medications.
Lastly, TREAT showed that time-restricted eating reduced weight, compared with baseline, but the weight loss was not significant, compared with the control group, and there was a wide spread of effects (that is, some lost a lot of weight, others didn’t lose much weight).
“That being said, the JAMA Internal Medicine paper is the largest paper to date of time-restricted eating randomized versus control, so its findings need to be acknowledged and recognized,” Dr. Chow said.
Peterson reported that her group recently completed a 14-week intervention in 90 adults with obesity divided into two groups:
- Control: Continuous energy restriction, self-selected ≥ 12-hour window.
- Early time-restricted eating: 8-hour window from 7 a.m. to 3 p.m.
The findings will provide further insight into the benefits of time-restricted eating.
How might time-restricted eating lead to weight loss?
Dr. Peterson concluded by presenting data suggesting how time-restricted eating may induce weight loss.
In a 4-day crossover study in 11 overweight adults, time-restricted eating did not affect energy expenditure, but it lessened swings in subjective hunger, improved appetite hormones including ghrelin, and increased fat oxidation.
Most trials have reported that time-restricted eating improves one or more cardiometabolic endpoints, she noted.
Early time-restricted eating was associated with improved insulin sensitivity and secretion, blood pressure, and oxidative stress, but not better lipid levels.
In contrast, compared with eating 3 meals/day (control), late time-restricted eating (eating 1 meal/day from 5 p.m. to 9 p.m.) was associated with worsened cardiometabolic health (glucose, insulin, blood pressure, and lipid levels) in an 8-week crossover study in 15 participants.
Dr. Peterson and Dr. Chow reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Bariatric surgery leads to better cardiovascular function in pregnancy
Pregnant women with a history of bariatric surgery have better cardiovascular adaptation to pregnancy compared with women who have similar early-pregnancy body mass index (BMI) but no history of weight loss surgery, new data suggest.
“Pregnant women who have had bariatric surgery demonstrate better cardiovascular adaptation through lower blood pressure, heart rate, and cardiac output, more favorable diastolic indices, and better systolic function,” reported Deesha Patel, MBBS MRCOG, specialist registrar, Chelsea and Westminster Hospital, London.
“Because the groups were matched for early pregnancy BMI, it’s unlikely that the results are due to weight loss alone but indicate that the metabolic alterations as a result of the surgery, via the enterocardiac axis, play an important role,” Dr. Patel continued.
The findings were presented at the Royal College of Obstetricians and Gynecologists 2021 Virtual World Congress.
Although obesity is known for its inflammatory and toxic effects on the cardiovascular system, it is not clear to what extent the various treatment options for obesity modify these risks in the long term, said Hutan Ashrafian, MD, clinical lecturer in surgery, Imperial College London.
“It is even less clear how anti-obesity interventions affect the cardiovascular system in pregnancy,” Dr. Ashrafian told this news organization.
“This very novel study in pregnant mothers having undergone the most successful and consistent intervention for severe obesity – bariatric or metabolic surgery – gives new clues as to the extent that bariatric procedures can alter cardiovascular risk in pregnant mothers,” continued Dr. Ashrafian, who was not involved in the study.
The results show how bariatric surgery has favorable effects on cardiac adaptation in pregnancy and in turn “might offer protection from pregnancy-related cardiovascular pathology such as preeclampsia,” explained Dr. Ashrafian. “This adds to the known effects of cardiovascular protection of bariatric surgery through the enterocardiac axis, which may explain a wider range of effects that can be translated within pregnancy and possibly following pregnancy in the postpartum era and beyond.”
A history of bariatric surgery versus no surgery
The prospective, longitudinal study compared 41 women who had a history of bariatric surgery with 41 women who had not undergone surgery. Patients’ characteristics were closely matched for age, BMI (34.5 kg/m2 and 34.3 kg/m2 in the surgery and bariatric surgery groups, respectively) and race. Hypertensive disorders in the post-surgery group were significantly less common compared with the no-surgery group (0% vs. 9.8%).
During the study, participants underwent cardiovascular assessment at 12-14 weeks, 20-24 weeks, and 30-32 weeks of gestation. The assessment included measurement of blood pressure and heart rate, transthoracic echocardiography, and 2D speckle tracking, performed offline to assess global longitudinal and circumferential strain.
Blood pressure readings across the three trimesters were consistently lower in the women who had undergone bariatric surgery compared with those in the no-surgery group, and all differences were statistically significant. Likewise, heart rate and cardiac output across the three trimesters were lower in the post-surgery cohort. However, there was no difference in stroke volume between the two groups.
As for diastolic function, there were more favorable indices in the post-surgery group with a higher E/A ratio, a marker of left ventricle filling (P < .001), and lower left atrial volume (P < .05), Dr. Patel reported.
With respect to systolic function, there was no difference in ejection fraction, but there was lower global longitudinal strain (P < .01) and global circumferential strain in the post-bariatric group (P = .02), suggesting better systolic function.
“Strain is a measure of differences in motion and velocity between regions of the myocardium through the cardiac cycle and can detect subclinical changes when ejection fraction is normal,” she added.
“This is a fascinating piece of work. The author should be congratulated on gathering so many [pregnant] women who had had bariatric surgery. The work gives a unique glimpse into metabolic syndrome,” said Philip Toozs-Hobson, MD, who moderated the session.
“We are increasingly recognizing the impact [of bariatric surgery] on metabolic syndrome, and the fact that this study demonstrates that there is more to it than just weight is important,” continued Dr. Toosz-Hobson, who is a consultant gynecologist at Birmingham Women’s Hospital NHS Foundation Trust, United Kingdom.
Cardiovascular benefits of bariatric surgery
Bariatric surgery has been associated with loss of excess body weight of up to 55% and with approximately 40% reduction in all-cause mortality in the general population. The procedure also reduces the risk for heart disease, diabetes, and cancer.
The cardiovascular benefits of bariatric surgery include reduced hypertension, remodeling of the heart with a reduction in left ventricular mass, and an improvement in diastolic and systolic function.
“Traditionally, the cardiac changes were thought to be due to weight loss and blood pressure reduction, but it is now conceivable that the metabolic components contribute to the reverse modeling via changes to the enterocardiac axis involving changes to gut hormones,” said Dr. Patel. These hormones include secretin, glucagon, and vasoactive intestinal peptide, which are known to have inotropic effects, as well as adiponectin and leptin, which are known to have cardiac effects, she added.
“Pregnancy following bariatric surgery is associated with a reduced risk of hypertensive disorders, as well as a reduced risk of gestational diabetes, large-for-gestational-age neonates, and a small increased risk of small-for-gestational-age neonates,” said Dr. Patel.
Dr. Patel and Dr. Toosz-Hobson have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Pregnant women with a history of bariatric surgery have better cardiovascular adaptation to pregnancy compared with women who have similar early-pregnancy body mass index (BMI) but no history of weight loss surgery, new data suggest.
“Pregnant women who have had bariatric surgery demonstrate better cardiovascular adaptation through lower blood pressure, heart rate, and cardiac output, more favorable diastolic indices, and better systolic function,” reported Deesha Patel, MBBS MRCOG, specialist registrar, Chelsea and Westminster Hospital, London.
“Because the groups were matched for early pregnancy BMI, it’s unlikely that the results are due to weight loss alone but indicate that the metabolic alterations as a result of the surgery, via the enterocardiac axis, play an important role,” Dr. Patel continued.
The findings were presented at the Royal College of Obstetricians and Gynecologists 2021 Virtual World Congress.
Although obesity is known for its inflammatory and toxic effects on the cardiovascular system, it is not clear to what extent the various treatment options for obesity modify these risks in the long term, said Hutan Ashrafian, MD, clinical lecturer in surgery, Imperial College London.
“It is even less clear how anti-obesity interventions affect the cardiovascular system in pregnancy,” Dr. Ashrafian told this news organization.
“This very novel study in pregnant mothers having undergone the most successful and consistent intervention for severe obesity – bariatric or metabolic surgery – gives new clues as to the extent that bariatric procedures can alter cardiovascular risk in pregnant mothers,” continued Dr. Ashrafian, who was not involved in the study.
The results show how bariatric surgery has favorable effects on cardiac adaptation in pregnancy and in turn “might offer protection from pregnancy-related cardiovascular pathology such as preeclampsia,” explained Dr. Ashrafian. “This adds to the known effects of cardiovascular protection of bariatric surgery through the enterocardiac axis, which may explain a wider range of effects that can be translated within pregnancy and possibly following pregnancy in the postpartum era and beyond.”
A history of bariatric surgery versus no surgery
The prospective, longitudinal study compared 41 women who had a history of bariatric surgery with 41 women who had not undergone surgery. Patients’ characteristics were closely matched for age, BMI (34.5 kg/m2 and 34.3 kg/m2 in the surgery and bariatric surgery groups, respectively) and race. Hypertensive disorders in the post-surgery group were significantly less common compared with the no-surgery group (0% vs. 9.8%).
During the study, participants underwent cardiovascular assessment at 12-14 weeks, 20-24 weeks, and 30-32 weeks of gestation. The assessment included measurement of blood pressure and heart rate, transthoracic echocardiography, and 2D speckle tracking, performed offline to assess global longitudinal and circumferential strain.
Blood pressure readings across the three trimesters were consistently lower in the women who had undergone bariatric surgery compared with those in the no-surgery group, and all differences were statistically significant. Likewise, heart rate and cardiac output across the three trimesters were lower in the post-surgery cohort. However, there was no difference in stroke volume between the two groups.
As for diastolic function, there were more favorable indices in the post-surgery group with a higher E/A ratio, a marker of left ventricle filling (P < .001), and lower left atrial volume (P < .05), Dr. Patel reported.
With respect to systolic function, there was no difference in ejection fraction, but there was lower global longitudinal strain (P < .01) and global circumferential strain in the post-bariatric group (P = .02), suggesting better systolic function.
“Strain is a measure of differences in motion and velocity between regions of the myocardium through the cardiac cycle and can detect subclinical changes when ejection fraction is normal,” she added.
“This is a fascinating piece of work. The author should be congratulated on gathering so many [pregnant] women who had had bariatric surgery. The work gives a unique glimpse into metabolic syndrome,” said Philip Toozs-Hobson, MD, who moderated the session.
“We are increasingly recognizing the impact [of bariatric surgery] on metabolic syndrome, and the fact that this study demonstrates that there is more to it than just weight is important,” continued Dr. Toosz-Hobson, who is a consultant gynecologist at Birmingham Women’s Hospital NHS Foundation Trust, United Kingdom.
Cardiovascular benefits of bariatric surgery
Bariatric surgery has been associated with loss of excess body weight of up to 55% and with approximately 40% reduction in all-cause mortality in the general population. The procedure also reduces the risk for heart disease, diabetes, and cancer.
The cardiovascular benefits of bariatric surgery include reduced hypertension, remodeling of the heart with a reduction in left ventricular mass, and an improvement in diastolic and systolic function.
“Traditionally, the cardiac changes were thought to be due to weight loss and blood pressure reduction, but it is now conceivable that the metabolic components contribute to the reverse modeling via changes to the enterocardiac axis involving changes to gut hormones,” said Dr. Patel. These hormones include secretin, glucagon, and vasoactive intestinal peptide, which are known to have inotropic effects, as well as adiponectin and leptin, which are known to have cardiac effects, she added.
“Pregnancy following bariatric surgery is associated with a reduced risk of hypertensive disorders, as well as a reduced risk of gestational diabetes, large-for-gestational-age neonates, and a small increased risk of small-for-gestational-age neonates,” said Dr. Patel.
Dr. Patel and Dr. Toosz-Hobson have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Pregnant women with a history of bariatric surgery have better cardiovascular adaptation to pregnancy compared with women who have similar early-pregnancy body mass index (BMI) but no history of weight loss surgery, new data suggest.
“Pregnant women who have had bariatric surgery demonstrate better cardiovascular adaptation through lower blood pressure, heart rate, and cardiac output, more favorable diastolic indices, and better systolic function,” reported Deesha Patel, MBBS MRCOG, specialist registrar, Chelsea and Westminster Hospital, London.
“Because the groups were matched for early pregnancy BMI, it’s unlikely that the results are due to weight loss alone but indicate that the metabolic alterations as a result of the surgery, via the enterocardiac axis, play an important role,” Dr. Patel continued.
The findings were presented at the Royal College of Obstetricians and Gynecologists 2021 Virtual World Congress.
Although obesity is known for its inflammatory and toxic effects on the cardiovascular system, it is not clear to what extent the various treatment options for obesity modify these risks in the long term, said Hutan Ashrafian, MD, clinical lecturer in surgery, Imperial College London.
“It is even less clear how anti-obesity interventions affect the cardiovascular system in pregnancy,” Dr. Ashrafian told this news organization.
“This very novel study in pregnant mothers having undergone the most successful and consistent intervention for severe obesity – bariatric or metabolic surgery – gives new clues as to the extent that bariatric procedures can alter cardiovascular risk in pregnant mothers,” continued Dr. Ashrafian, who was not involved in the study.
The results show how bariatric surgery has favorable effects on cardiac adaptation in pregnancy and in turn “might offer protection from pregnancy-related cardiovascular pathology such as preeclampsia,” explained Dr. Ashrafian. “This adds to the known effects of cardiovascular protection of bariatric surgery through the enterocardiac axis, which may explain a wider range of effects that can be translated within pregnancy and possibly following pregnancy in the postpartum era and beyond.”
A history of bariatric surgery versus no surgery
The prospective, longitudinal study compared 41 women who had a history of bariatric surgery with 41 women who had not undergone surgery. Patients’ characteristics were closely matched for age, BMI (34.5 kg/m2 and 34.3 kg/m2 in the surgery and bariatric surgery groups, respectively) and race. Hypertensive disorders in the post-surgery group were significantly less common compared with the no-surgery group (0% vs. 9.8%).
During the study, participants underwent cardiovascular assessment at 12-14 weeks, 20-24 weeks, and 30-32 weeks of gestation. The assessment included measurement of blood pressure and heart rate, transthoracic echocardiography, and 2D speckle tracking, performed offline to assess global longitudinal and circumferential strain.
Blood pressure readings across the three trimesters were consistently lower in the women who had undergone bariatric surgery compared with those in the no-surgery group, and all differences were statistically significant. Likewise, heart rate and cardiac output across the three trimesters were lower in the post-surgery cohort. However, there was no difference in stroke volume between the two groups.
As for diastolic function, there were more favorable indices in the post-surgery group with a higher E/A ratio, a marker of left ventricle filling (P < .001), and lower left atrial volume (P < .05), Dr. Patel reported.
With respect to systolic function, there was no difference in ejection fraction, but there was lower global longitudinal strain (P < .01) and global circumferential strain in the post-bariatric group (P = .02), suggesting better systolic function.
“Strain is a measure of differences in motion and velocity between regions of the myocardium through the cardiac cycle and can detect subclinical changes when ejection fraction is normal,” she added.
“This is a fascinating piece of work. The author should be congratulated on gathering so many [pregnant] women who had had bariatric surgery. The work gives a unique glimpse into metabolic syndrome,” said Philip Toozs-Hobson, MD, who moderated the session.
“We are increasingly recognizing the impact [of bariatric surgery] on metabolic syndrome, and the fact that this study demonstrates that there is more to it than just weight is important,” continued Dr. Toosz-Hobson, who is a consultant gynecologist at Birmingham Women’s Hospital NHS Foundation Trust, United Kingdom.
Cardiovascular benefits of bariatric surgery
Bariatric surgery has been associated with loss of excess body weight of up to 55% and with approximately 40% reduction in all-cause mortality in the general population. The procedure also reduces the risk for heart disease, diabetes, and cancer.
The cardiovascular benefits of bariatric surgery include reduced hypertension, remodeling of the heart with a reduction in left ventricular mass, and an improvement in diastolic and systolic function.
“Traditionally, the cardiac changes were thought to be due to weight loss and blood pressure reduction, but it is now conceivable that the metabolic components contribute to the reverse modeling via changes to the enterocardiac axis involving changes to gut hormones,” said Dr. Patel. These hormones include secretin, glucagon, and vasoactive intestinal peptide, which are known to have inotropic effects, as well as adiponectin and leptin, which are known to have cardiac effects, she added.
“Pregnancy following bariatric surgery is associated with a reduced risk of hypertensive disorders, as well as a reduced risk of gestational diabetes, large-for-gestational-age neonates, and a small increased risk of small-for-gestational-age neonates,” said Dr. Patel.
Dr. Patel and Dr. Toosz-Hobson have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
No overall statin effect seen on dementia, cognition in ASPREE analysis
Statin therapy likely didn’t lead to dementia or even mild cognitive impairment (MCI) in older patients taking the drugs for cardiovascular (CV) primary prevention in a post hoc analysis of a trial that required normal cognitive ability for entry.
Nor did statins, whether lipophilic or hydrophilic, appear to influence changes in cognition or affect separate domains of mental performance, such as memory, language ability, or executive function, over the trial’s follow-up, which averaged almost 5 years.
Although such findings aren’t novel – they are consistent with observations from a number of earlier studies – the new analysis included a possible signal for a statin association with new-onset dementia in a subgroup of more than 18,000 patients. Researchers attribute the retrospective finding, from a trial not designed to explore the issue, to confounding or chance.
Still, the adjusted risk for dementia seemed to go up by a third among statin users who at baseline placed in the lowest quartile for cognitive function, based on a composite test score, in the ASPREE trial, a test of primary-prevention low-dose aspirin in patients 65 or older. The better the baseline cognitive score by quartile, the lower the risk for dementia ( interaction P < .001).
The bottom-quartile association of statins with dementia was driven by new diagnoses of Alzheimer’s disease, as opposed to the study’s other “mixed presentation” dementia subtype, wrote the authors of analysis, published June 21, 2021, in the Journal of the American College of Cardiology), led by Zhen Zhou, PhD, Menzies Institute for Medical Research, University of Tasmania, Hobart, Australia.
“I wouldn’t overinterpret that,” said senior author Mark R. Nelson, MBBS, PhD, of the same institution. Indeed, it should be “reassuring” for physicians prescribing statins to older patients that there was no overall statin effect on cognition or new-onset dementia, he said in an interview.
“This is a post hoc analysis within a dataset, although a very-high-quality dataset, it must be said.” The patients were prospectively followed for a range of cognition domains, and the results were adjudicated, Dr. Nelson observed. Although the question of statins and dementia risk is thought to be largely settled, the analysis “was just too tempting not to do.”
On the basis of the current analysis and the bulk of preceding evidence, “lipid lowering in the short term does not appear to result in improvement or deterioration of cognition irrespective of baseline LDL cholesterol levels and medication used,” Christie M. Ballantyne, MD, and Vijay Nambi, MD, PhD, both from Baylor College of Medicine, Houston, wrote in an accompanying editorial.
The current study “provides additional information that the lipo- or hydrophilicity of the statin does not affect changes in cognition. However, the potential increased risk for Alzheimer’s disease, especially among patients with baseline cognitive impairment, requires further investigation.”
The current analysis is reassuring that the likelihood of such statin effects on cognition “is vanishingly small,” Neil J. Stone MD, Northwestern University, Chicago, said in an interview. In fact, its primary finding of no such association “best summarizes what we know in 2021 about statin therapy” after exploration of the issue in a number of prospective trials and systematic reviews, said Dr. Stone, who was not a coauthor on the report.
The observed interaction between statin use and baseline neurocognitive ability “is hypothesis raising at best. It should be explored in randomized, controlled trials that can look at this question in an unbiased manner,” he agreed.
If patients believe or suspect that a statin is causing symptoms that suggest cognitive dysfunction, “what they really need to do is to stop it for 3 weeks and check out other causes. And in rechallenging, the guidelines say, if they think that it’s causing a memory problem that occurs anecdotally, then they can be given another statin, usually, which doesn’t cause it.”
ASPREE compared daily low-dose aspirin with placebo in a community-based older population numbering about 19,000 in Australia and the United States. Patients were initially without known CV disease, dementia, or physical disabilities. It did not randomize patients by statin therapy.
Of note, entry to the trial required a score of at least 78 on the Modified Mini-Mental State Examination (3MS), corresponding to normal cognition.
Aspirin showed no significant benefit for disability-free survival, an endpoint that included death and dementia, or CV events over a median of 4.7 years. It was associated with slightly more cases of major hemorrhage, as previously reported.
A subsequent ASPREE analysis suggested that the aspirin had no effect on risks of mild cognitive impairment, cognitive decline, or dementia.
Of the 18,846 patients in the current post hoc analysis, the average age of the patients was 74 years, and 56.4% were women; 31.3% were taking statins at baseline. The incidence of dementia per 1,000 person-years for those taking statins in comparison with those not taking statins was 6.91 and 6.48, respectively. Any cognitive changes were tracked by the 3MS and three other validated tests in different domains of cognition, with results contributing to the composite score.
The corresponding incidence of dementia considered probable Alzheimer’s disease was 2.97 and 2.65 for those receiving versus not receiving statins, respectively. The incidence of dementia with mixed presentation was 3.94 and 3.84, respectively.
There were no significant differences in risk for dementia overall or for either dementia subtype in multivariate analyses. Adjustments included demographics, CV lifestyle risk factors, family medical history, including dementia, ASPREE randomization group, and individual scores on the four tests of cognition.
Results for development of MCI mirrored those for dementia, as did results stratified for baseline lipids and for use of lipophilic statins, such as atorvastatin or simvastatin versus hydrophilic statins, including pravastatin and rosuvastatin.
Significant interactions were observed between composite cognitive scores and statin therapy at baseline; as scores increased, indicating better cognitive performance, the risks for dementia and its subtypes went down. Statins were associated with incident dementia at the lowest cognitive performance quartile.
That association is probably a function of the cohort’s advanced age, Dr. Nelson said. “If you get into old age, and you’ve got high cognitive scores, you’ve probably got protective factors. That’s how I would interpret that.”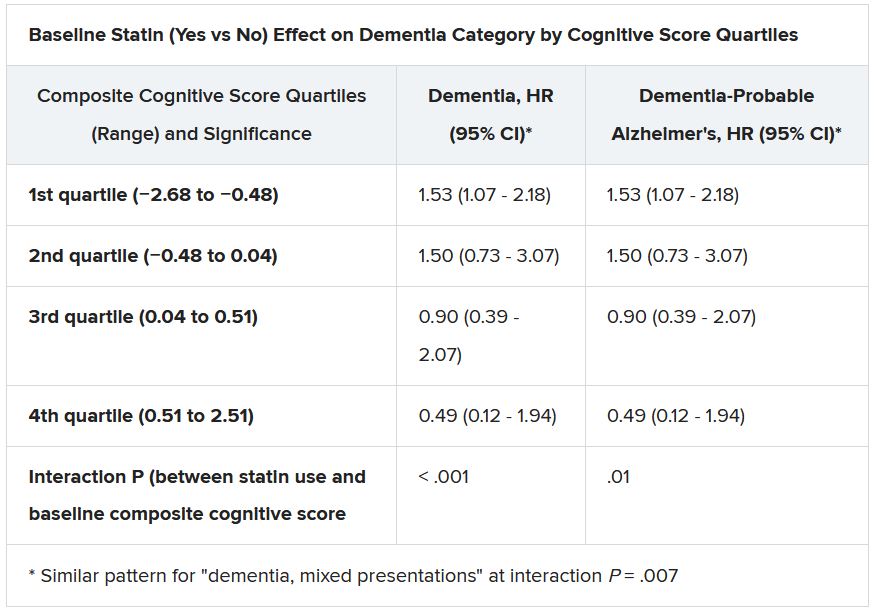
Dr. Ballantyne and Dr. Nambi also emphasized the difficulties of controlling for potential biases even with extensive covariate adjustments. The statin dosages at which patients were treated were not part of the analysis, “and achieved LDL [cholesterol levels over the study period were not known,” they wrote.
“Furthermore, patients who were treated with statins were more likely to have diabetes, hypertension, chronic kidney disease, and obesity, all of which are known to increase risk for cognitive decline, and, as might have been predicted, statin users therefore had significantly lower scores for global cognition and episodic memory.”
Dr. Nelson pointed to an ongoing prospective atorvastatin trial that includes dementia in its primary endpoint and should be “the definitive study.” STAREE (Statin Therapy for Reducing Events in the Elderly) is running throughout Australia with a projected enrollment of 18,000 and primary completion by the end of 2022. “We’ve already enrolled 8,000 patients.”
Less far along is the PREVENTABLE (Pragmatic Evaluation of Events and Benefits of Lipid-Lowering in Older Adults) trial, based in the United States and also randomizing to atorvastatin or placebo, that will have an estimated 20,000 older patients and completion in 5 years. The primary endpoint is new dementia or persistent disability.
Both trials “are powered to enable firm conclusions concerning any statin effects,” said Dr. Ballantyne and Dr. Nambi. “In the meantime, practicing clinicians can have confidence and share with their patients that short-term lipid-lowering therapy in older patients, including with statins, is unlikely to have a major impact on cognition.”
ASPREE was supported by grants from the U.S. National Institute on Aging and the National Cancer Institute and the National Health and Medical Research Council of Australia, by Monash University, and by the Victorian Cancer Agency. Dr. Nelson reported receiving honoraria from Sanofi and Amgen; support from Bayer for ASPREE; and grant support for STAREE. Disclosures for the other authors are in the report. Dr. Ballantyne disclosed grant and research support from Abbott Diagnostic, Akcea, Amgen, Esperion, Ionis, Novartis, Regeneron, and Roche Diagnostics; and consulting for Abbott Diagnostics, Althera, Amarin, Amgen, Arrowhead, AstraZeneca, Corvidia, Denka Seiken, Esperion, Genentech, Gilead, Matinas BioPharma, New Amsterdam, Novartis, Novo Nordisk, Pfizer, Regeneron, Roche Diagnostics, and Sanofi-Synthelabo. Dr. Nambi is a coinvestigator on a provisional patent along with Baylor College of Medicine and Roche on the use of biomarkers to predict heart failure, and a site principal investigator for studies sponsored by Amgen and Merck. Dr. Stone had no disclosures.
A version of this article first appeared on Medscape.com.
Statin therapy likely didn’t lead to dementia or even mild cognitive impairment (MCI) in older patients taking the drugs for cardiovascular (CV) primary prevention in a post hoc analysis of a trial that required normal cognitive ability for entry.
Nor did statins, whether lipophilic or hydrophilic, appear to influence changes in cognition or affect separate domains of mental performance, such as memory, language ability, or executive function, over the trial’s follow-up, which averaged almost 5 years.
Although such findings aren’t novel – they are consistent with observations from a number of earlier studies – the new analysis included a possible signal for a statin association with new-onset dementia in a subgroup of more than 18,000 patients. Researchers attribute the retrospective finding, from a trial not designed to explore the issue, to confounding or chance.
Still, the adjusted risk for dementia seemed to go up by a third among statin users who at baseline placed in the lowest quartile for cognitive function, based on a composite test score, in the ASPREE trial, a test of primary-prevention low-dose aspirin in patients 65 or older. The better the baseline cognitive score by quartile, the lower the risk for dementia ( interaction P < .001).
The bottom-quartile association of statins with dementia was driven by new diagnoses of Alzheimer’s disease, as opposed to the study’s other “mixed presentation” dementia subtype, wrote the authors of analysis, published June 21, 2021, in the Journal of the American College of Cardiology), led by Zhen Zhou, PhD, Menzies Institute for Medical Research, University of Tasmania, Hobart, Australia.
“I wouldn’t overinterpret that,” said senior author Mark R. Nelson, MBBS, PhD, of the same institution. Indeed, it should be “reassuring” for physicians prescribing statins to older patients that there was no overall statin effect on cognition or new-onset dementia, he said in an interview.
“This is a post hoc analysis within a dataset, although a very-high-quality dataset, it must be said.” The patients were prospectively followed for a range of cognition domains, and the results were adjudicated, Dr. Nelson observed. Although the question of statins and dementia risk is thought to be largely settled, the analysis “was just too tempting not to do.”
On the basis of the current analysis and the bulk of preceding evidence, “lipid lowering in the short term does not appear to result in improvement or deterioration of cognition irrespective of baseline LDL cholesterol levels and medication used,” Christie M. Ballantyne, MD, and Vijay Nambi, MD, PhD, both from Baylor College of Medicine, Houston, wrote in an accompanying editorial.
The current study “provides additional information that the lipo- or hydrophilicity of the statin does not affect changes in cognition. However, the potential increased risk for Alzheimer’s disease, especially among patients with baseline cognitive impairment, requires further investigation.”
The current analysis is reassuring that the likelihood of such statin effects on cognition “is vanishingly small,” Neil J. Stone MD, Northwestern University, Chicago, said in an interview. In fact, its primary finding of no such association “best summarizes what we know in 2021 about statin therapy” after exploration of the issue in a number of prospective trials and systematic reviews, said Dr. Stone, who was not a coauthor on the report.
The observed interaction between statin use and baseline neurocognitive ability “is hypothesis raising at best. It should be explored in randomized, controlled trials that can look at this question in an unbiased manner,” he agreed.
If patients believe or suspect that a statin is causing symptoms that suggest cognitive dysfunction, “what they really need to do is to stop it for 3 weeks and check out other causes. And in rechallenging, the guidelines say, if they think that it’s causing a memory problem that occurs anecdotally, then they can be given another statin, usually, which doesn’t cause it.”
ASPREE compared daily low-dose aspirin with placebo in a community-based older population numbering about 19,000 in Australia and the United States. Patients were initially without known CV disease, dementia, or physical disabilities. It did not randomize patients by statin therapy.
Of note, entry to the trial required a score of at least 78 on the Modified Mini-Mental State Examination (3MS), corresponding to normal cognition.
Aspirin showed no significant benefit for disability-free survival, an endpoint that included death and dementia, or CV events over a median of 4.7 years. It was associated with slightly more cases of major hemorrhage, as previously reported.
A subsequent ASPREE analysis suggested that the aspirin had no effect on risks of mild cognitive impairment, cognitive decline, or dementia.
Of the 18,846 patients in the current post hoc analysis, the average age of the patients was 74 years, and 56.4% were women; 31.3% were taking statins at baseline. The incidence of dementia per 1,000 person-years for those taking statins in comparison with those not taking statins was 6.91 and 6.48, respectively. Any cognitive changes were tracked by the 3MS and three other validated tests in different domains of cognition, with results contributing to the composite score.
The corresponding incidence of dementia considered probable Alzheimer’s disease was 2.97 and 2.65 for those receiving versus not receiving statins, respectively. The incidence of dementia with mixed presentation was 3.94 and 3.84, respectively.
There were no significant differences in risk for dementia overall or for either dementia subtype in multivariate analyses. Adjustments included demographics, CV lifestyle risk factors, family medical history, including dementia, ASPREE randomization group, and individual scores on the four tests of cognition.
Results for development of MCI mirrored those for dementia, as did results stratified for baseline lipids and for use of lipophilic statins, such as atorvastatin or simvastatin versus hydrophilic statins, including pravastatin and rosuvastatin.
Significant interactions were observed between composite cognitive scores and statin therapy at baseline; as scores increased, indicating better cognitive performance, the risks for dementia and its subtypes went down. Statins were associated with incident dementia at the lowest cognitive performance quartile.
That association is probably a function of the cohort’s advanced age, Dr. Nelson said. “If you get into old age, and you’ve got high cognitive scores, you’ve probably got protective factors. That’s how I would interpret that.”
Dr. Ballantyne and Dr. Nambi also emphasized the difficulties of controlling for potential biases even with extensive covariate adjustments. The statin dosages at which patients were treated were not part of the analysis, “and achieved LDL [cholesterol levels over the study period were not known,” they wrote.
“Furthermore, patients who were treated with statins were more likely to have diabetes, hypertension, chronic kidney disease, and obesity, all of which are known to increase risk for cognitive decline, and, as might have been predicted, statin users therefore had significantly lower scores for global cognition and episodic memory.”
Dr. Nelson pointed to an ongoing prospective atorvastatin trial that includes dementia in its primary endpoint and should be “the definitive study.” STAREE (Statin Therapy for Reducing Events in the Elderly) is running throughout Australia with a projected enrollment of 18,000 and primary completion by the end of 2022. “We’ve already enrolled 8,000 patients.”
Less far along is the PREVENTABLE (Pragmatic Evaluation of Events and Benefits of Lipid-Lowering in Older Adults) trial, based in the United States and also randomizing to atorvastatin or placebo, that will have an estimated 20,000 older patients and completion in 5 years. The primary endpoint is new dementia or persistent disability.
Both trials “are powered to enable firm conclusions concerning any statin effects,” said Dr. Ballantyne and Dr. Nambi. “In the meantime, practicing clinicians can have confidence and share with their patients that short-term lipid-lowering therapy in older patients, including with statins, is unlikely to have a major impact on cognition.”
ASPREE was supported by grants from the U.S. National Institute on Aging and the National Cancer Institute and the National Health and Medical Research Council of Australia, by Monash University, and by the Victorian Cancer Agency. Dr. Nelson reported receiving honoraria from Sanofi and Amgen; support from Bayer for ASPREE; and grant support for STAREE. Disclosures for the other authors are in the report. Dr. Ballantyne disclosed grant and research support from Abbott Diagnostic, Akcea, Amgen, Esperion, Ionis, Novartis, Regeneron, and Roche Diagnostics; and consulting for Abbott Diagnostics, Althera, Amarin, Amgen, Arrowhead, AstraZeneca, Corvidia, Denka Seiken, Esperion, Genentech, Gilead, Matinas BioPharma, New Amsterdam, Novartis, Novo Nordisk, Pfizer, Regeneron, Roche Diagnostics, and Sanofi-Synthelabo. Dr. Nambi is a coinvestigator on a provisional patent along with Baylor College of Medicine and Roche on the use of biomarkers to predict heart failure, and a site principal investigator for studies sponsored by Amgen and Merck. Dr. Stone had no disclosures.
A version of this article first appeared on Medscape.com.
Statin therapy likely didn’t lead to dementia or even mild cognitive impairment (MCI) in older patients taking the drugs for cardiovascular (CV) primary prevention in a post hoc analysis of a trial that required normal cognitive ability for entry.
Nor did statins, whether lipophilic or hydrophilic, appear to influence changes in cognition or affect separate domains of mental performance, such as memory, language ability, or executive function, over the trial’s follow-up, which averaged almost 5 years.
Although such findings aren’t novel – they are consistent with observations from a number of earlier studies – the new analysis included a possible signal for a statin association with new-onset dementia in a subgroup of more than 18,000 patients. Researchers attribute the retrospective finding, from a trial not designed to explore the issue, to confounding or chance.
Still, the adjusted risk for dementia seemed to go up by a third among statin users who at baseline placed in the lowest quartile for cognitive function, based on a composite test score, in the ASPREE trial, a test of primary-prevention low-dose aspirin in patients 65 or older. The better the baseline cognitive score by quartile, the lower the risk for dementia ( interaction P < .001).
The bottom-quartile association of statins with dementia was driven by new diagnoses of Alzheimer’s disease, as opposed to the study’s other “mixed presentation” dementia subtype, wrote the authors of analysis, published June 21, 2021, in the Journal of the American College of Cardiology), led by Zhen Zhou, PhD, Menzies Institute for Medical Research, University of Tasmania, Hobart, Australia.
“I wouldn’t overinterpret that,” said senior author Mark R. Nelson, MBBS, PhD, of the same institution. Indeed, it should be “reassuring” for physicians prescribing statins to older patients that there was no overall statin effect on cognition or new-onset dementia, he said in an interview.
“This is a post hoc analysis within a dataset, although a very-high-quality dataset, it must be said.” The patients were prospectively followed for a range of cognition domains, and the results were adjudicated, Dr. Nelson observed. Although the question of statins and dementia risk is thought to be largely settled, the analysis “was just too tempting not to do.”
On the basis of the current analysis and the bulk of preceding evidence, “lipid lowering in the short term does not appear to result in improvement or deterioration of cognition irrespective of baseline LDL cholesterol levels and medication used,” Christie M. Ballantyne, MD, and Vijay Nambi, MD, PhD, both from Baylor College of Medicine, Houston, wrote in an accompanying editorial.
The current study “provides additional information that the lipo- or hydrophilicity of the statin does not affect changes in cognition. However, the potential increased risk for Alzheimer’s disease, especially among patients with baseline cognitive impairment, requires further investigation.”
The current analysis is reassuring that the likelihood of such statin effects on cognition “is vanishingly small,” Neil J. Stone MD, Northwestern University, Chicago, said in an interview. In fact, its primary finding of no such association “best summarizes what we know in 2021 about statin therapy” after exploration of the issue in a number of prospective trials and systematic reviews, said Dr. Stone, who was not a coauthor on the report.
The observed interaction between statin use and baseline neurocognitive ability “is hypothesis raising at best. It should be explored in randomized, controlled trials that can look at this question in an unbiased manner,” he agreed.
If patients believe or suspect that a statin is causing symptoms that suggest cognitive dysfunction, “what they really need to do is to stop it for 3 weeks and check out other causes. And in rechallenging, the guidelines say, if they think that it’s causing a memory problem that occurs anecdotally, then they can be given another statin, usually, which doesn’t cause it.”
ASPREE compared daily low-dose aspirin with placebo in a community-based older population numbering about 19,000 in Australia and the United States. Patients were initially without known CV disease, dementia, or physical disabilities. It did not randomize patients by statin therapy.
Of note, entry to the trial required a score of at least 78 on the Modified Mini-Mental State Examination (3MS), corresponding to normal cognition.
Aspirin showed no significant benefit for disability-free survival, an endpoint that included death and dementia, or CV events over a median of 4.7 years. It was associated with slightly more cases of major hemorrhage, as previously reported.
A subsequent ASPREE analysis suggested that the aspirin had no effect on risks of mild cognitive impairment, cognitive decline, or dementia.
Of the 18,846 patients in the current post hoc analysis, the average age of the patients was 74 years, and 56.4% were women; 31.3% were taking statins at baseline. The incidence of dementia per 1,000 person-years for those taking statins in comparison with those not taking statins was 6.91 and 6.48, respectively. Any cognitive changes were tracked by the 3MS and three other validated tests in different domains of cognition, with results contributing to the composite score.
The corresponding incidence of dementia considered probable Alzheimer’s disease was 2.97 and 2.65 for those receiving versus not receiving statins, respectively. The incidence of dementia with mixed presentation was 3.94 and 3.84, respectively.
There were no significant differences in risk for dementia overall or for either dementia subtype in multivariate analyses. Adjustments included demographics, CV lifestyle risk factors, family medical history, including dementia, ASPREE randomization group, and individual scores on the four tests of cognition.
Results for development of MCI mirrored those for dementia, as did results stratified for baseline lipids and for use of lipophilic statins, such as atorvastatin or simvastatin versus hydrophilic statins, including pravastatin and rosuvastatin.
Significant interactions were observed between composite cognitive scores and statin therapy at baseline; as scores increased, indicating better cognitive performance, the risks for dementia and its subtypes went down. Statins were associated with incident dementia at the lowest cognitive performance quartile.
That association is probably a function of the cohort’s advanced age, Dr. Nelson said. “If you get into old age, and you’ve got high cognitive scores, you’ve probably got protective factors. That’s how I would interpret that.”
Dr. Ballantyne and Dr. Nambi also emphasized the difficulties of controlling for potential biases even with extensive covariate adjustments. The statin dosages at which patients were treated were not part of the analysis, “and achieved LDL [cholesterol levels over the study period were not known,” they wrote.
“Furthermore, patients who were treated with statins were more likely to have diabetes, hypertension, chronic kidney disease, and obesity, all of which are known to increase risk for cognitive decline, and, as might have been predicted, statin users therefore had significantly lower scores for global cognition and episodic memory.”
Dr. Nelson pointed to an ongoing prospective atorvastatin trial that includes dementia in its primary endpoint and should be “the definitive study.” STAREE (Statin Therapy for Reducing Events in the Elderly) is running throughout Australia with a projected enrollment of 18,000 and primary completion by the end of 2022. “We’ve already enrolled 8,000 patients.”
Less far along is the PREVENTABLE (Pragmatic Evaluation of Events and Benefits of Lipid-Lowering in Older Adults) trial, based in the United States and also randomizing to atorvastatin or placebo, that will have an estimated 20,000 older patients and completion in 5 years. The primary endpoint is new dementia or persistent disability.
Both trials “are powered to enable firm conclusions concerning any statin effects,” said Dr. Ballantyne and Dr. Nambi. “In the meantime, practicing clinicians can have confidence and share with their patients that short-term lipid-lowering therapy in older patients, including with statins, is unlikely to have a major impact on cognition.”
ASPREE was supported by grants from the U.S. National Institute on Aging and the National Cancer Institute and the National Health and Medical Research Council of Australia, by Monash University, and by the Victorian Cancer Agency. Dr. Nelson reported receiving honoraria from Sanofi and Amgen; support from Bayer for ASPREE; and grant support for STAREE. Disclosures for the other authors are in the report. Dr. Ballantyne disclosed grant and research support from Abbott Diagnostic, Akcea, Amgen, Esperion, Ionis, Novartis, Regeneron, and Roche Diagnostics; and consulting for Abbott Diagnostics, Althera, Amarin, Amgen, Arrowhead, AstraZeneca, Corvidia, Denka Seiken, Esperion, Genentech, Gilead, Matinas BioPharma, New Amsterdam, Novartis, Novo Nordisk, Pfizer, Regeneron, Roche Diagnostics, and Sanofi-Synthelabo. Dr. Nambi is a coinvestigator on a provisional patent along with Baylor College of Medicine and Roche on the use of biomarkers to predict heart failure, and a site principal investigator for studies sponsored by Amgen and Merck. Dr. Stone had no disclosures.
A version of this article first appeared on Medscape.com.