User login
COVID-19: Social distancing with young children
Emma just celebrated her second birthday, and she has been working on the usual things that children start to master at this age: potty training, making friends, exerting her will through both actions and words, and generally enjoying life as the center of attention for both her parents and grandparents. Like everyone else in Maryland, Emma’s life changed suddenly with the coronavirus stay-at-home order that was issued on March 30. There is no more day care and her parents work from home while caring for her. Her grandparents visit, but only outside and only from a distance – there are no more hugs and there is no more sitting in her grandfather’s lap while he reads stories.
One afternoon a few weeks ago, Emma was looking out the window when she saw her friend, Max, walk by with his parents. Before her parents could stop her, Emma bolted out the door, and she and little Max wrapped each other in a tight embrace. Their parents snapped a photo of the smiling toddlers hugging before they separated the children. The photo is adorable, but as all struggle with social distancing, the poignance of two innocent toddlers in a forbidden embrace is a bit heartbreaking.
Everyone who has ever observed children knows that social distancing is not in their nature. Children play, they hug, they wrestle and tackle and poke, and sometimes even bite. And every student of social psychology has been taught about Harry Harlow’s experiments with rhesus macaques who were separated from their mothers and given access to an inanimate object to serve as a surrogate mother. The Harlow studies, while controversial, were revolutionary in demonstrating that early interactions with both a mother and with playmates were essential in the development of normal social relationships.
Regine Galanti, PhD, is a clinical psychologist at Long Island Behavioral Psychology, Cedarhurst, N.Y., who specializes in the treatment of anxiety and behavior problems. With young children she uses parent-child interaction therapy (PCIT) to help build relationships and discipline. Dr. Galanti said: “I don’t think we’re well prepared as a field to answer questions about the long-term effects of social distancing. If you need young children to socially distance, the responsibility has to fall on the adults. It’s important to explain to children what’s going on and to be honest in a developmentally appropriate way.”
Dr. Galanti has noticed that the issues that people had before COVID-19 are exacerbated by the stress of the current situation. What we do know is that young children thrive on structure.”
Tovah P. Klein, PhD, is the author of “How Toddlers Thrive” (Touchstone, 2015) and is the director of the Barnard College Center for Toddler Development in Manhattan. “When this started, we thought we would be closed for a few weeks,” Dr. Klein said. “We wanted to maintain a connection to the children, so we made videos for the parents to show to the kids, just to say ‘We’re still here.’ But as time went on and we realized it was going to be a while, we felt it was important to provide connection, so we launched a virtual program.”
Dr. Klein said that the teachers meet with their classes of 13 2-year-olds over Zoom, and when they first started, she asked the teachers to try to meet for 10 minutes. They are now meeting for 40 minutes twice a week. The children like seeing their teachers in their homes and they like seeing each other. In addition, the teachers make videos to send home and they are currently working on one to demystify masks. “We’re working on normalizing masks and showing children that when you put the mask on, you’re still there underneath.”
The center has existed for 48 years. There have been struggles for some of the children who attend; some of the parents have been hospitalized with the virus, and some work on the front line and so parents may be living away from a child.
“We’ve seen more challenging behaviors during this time, more tantrums, toileting issues, night awakenings, and more fragility. But as the new normal takes hold, things are settling in. Parents have been good about getting new routines and it helps if parents can handle their own stress,” Dr. Klein said. She also pointed out that for parents working at home while caring for their children, this can be particularly difficult on a young child. “The child knows the parent is home, but isn’t spending time with him, and he sees it as a rejection.”
Margaret Adams, MD, is a child psychiatrist in Maryland who works with very young children and their parents. She says that some of the children are thriving with the extra attention from their parents. “I often have seen difficulties with readjustment to the routine of separations to day care after a family vacation of a week, or sometimes even a weekend, even for those young ones who seem to love the social aspects of day care. I think it is likely a big impact will come upon return, depending on the developmental stage of the child,” Dr. Adams noted.
Despite the hardships of the moment, all three experts expressed hopefulness about the future for these children.
“Young children are super-resilient and that’s the blessing of this,” Dr. Galanti said. “I think they will be okay.”
Emma is home for now with her parents, who are expecting another child soon. Her mother notes: “The days are long and balancing work is an impossible challenge, but being with Emma has been a total blessing, and when would I ever have this much time to spend with my kid? She’s at such a fun age – so curious and adventurous – it’s amazing to watch her language and skills progress. I wish we weren’t in the midst of a pandemic, but Emma is definitely the bright spot.”
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore. Dr. Miller has no disclosures.
Emma just celebrated her second birthday, and she has been working on the usual things that children start to master at this age: potty training, making friends, exerting her will through both actions and words, and generally enjoying life as the center of attention for both her parents and grandparents. Like everyone else in Maryland, Emma’s life changed suddenly with the coronavirus stay-at-home order that was issued on March 30. There is no more day care and her parents work from home while caring for her. Her grandparents visit, but only outside and only from a distance – there are no more hugs and there is no more sitting in her grandfather’s lap while he reads stories.
One afternoon a few weeks ago, Emma was looking out the window when she saw her friend, Max, walk by with his parents. Before her parents could stop her, Emma bolted out the door, and she and little Max wrapped each other in a tight embrace. Their parents snapped a photo of the smiling toddlers hugging before they separated the children. The photo is adorable, but as all struggle with social distancing, the poignance of two innocent toddlers in a forbidden embrace is a bit heartbreaking.
Everyone who has ever observed children knows that social distancing is not in their nature. Children play, they hug, they wrestle and tackle and poke, and sometimes even bite. And every student of social psychology has been taught about Harry Harlow’s experiments with rhesus macaques who were separated from their mothers and given access to an inanimate object to serve as a surrogate mother. The Harlow studies, while controversial, were revolutionary in demonstrating that early interactions with both a mother and with playmates were essential in the development of normal social relationships.
Regine Galanti, PhD, is a clinical psychologist at Long Island Behavioral Psychology, Cedarhurst, N.Y., who specializes in the treatment of anxiety and behavior problems. With young children she uses parent-child interaction therapy (PCIT) to help build relationships and discipline. Dr. Galanti said: “I don’t think we’re well prepared as a field to answer questions about the long-term effects of social distancing. If you need young children to socially distance, the responsibility has to fall on the adults. It’s important to explain to children what’s going on and to be honest in a developmentally appropriate way.”
Dr. Galanti has noticed that the issues that people had before COVID-19 are exacerbated by the stress of the current situation. What we do know is that young children thrive on structure.”
Tovah P. Klein, PhD, is the author of “How Toddlers Thrive” (Touchstone, 2015) and is the director of the Barnard College Center for Toddler Development in Manhattan. “When this started, we thought we would be closed for a few weeks,” Dr. Klein said. “We wanted to maintain a connection to the children, so we made videos for the parents to show to the kids, just to say ‘We’re still here.’ But as time went on and we realized it was going to be a while, we felt it was important to provide connection, so we launched a virtual program.”
Dr. Klein said that the teachers meet with their classes of 13 2-year-olds over Zoom, and when they first started, she asked the teachers to try to meet for 10 minutes. They are now meeting for 40 minutes twice a week. The children like seeing their teachers in their homes and they like seeing each other. In addition, the teachers make videos to send home and they are currently working on one to demystify masks. “We’re working on normalizing masks and showing children that when you put the mask on, you’re still there underneath.”
The center has existed for 48 years. There have been struggles for some of the children who attend; some of the parents have been hospitalized with the virus, and some work on the front line and so parents may be living away from a child.
“We’ve seen more challenging behaviors during this time, more tantrums, toileting issues, night awakenings, and more fragility. But as the new normal takes hold, things are settling in. Parents have been good about getting new routines and it helps if parents can handle their own stress,” Dr. Klein said. She also pointed out that for parents working at home while caring for their children, this can be particularly difficult on a young child. “The child knows the parent is home, but isn’t spending time with him, and he sees it as a rejection.”
Margaret Adams, MD, is a child psychiatrist in Maryland who works with very young children and their parents. She says that some of the children are thriving with the extra attention from their parents. “I often have seen difficulties with readjustment to the routine of separations to day care after a family vacation of a week, or sometimes even a weekend, even for those young ones who seem to love the social aspects of day care. I think it is likely a big impact will come upon return, depending on the developmental stage of the child,” Dr. Adams noted.
Despite the hardships of the moment, all three experts expressed hopefulness about the future for these children.
“Young children are super-resilient and that’s the blessing of this,” Dr. Galanti said. “I think they will be okay.”
Emma is home for now with her parents, who are expecting another child soon. Her mother notes: “The days are long and balancing work is an impossible challenge, but being with Emma has been a total blessing, and when would I ever have this much time to spend with my kid? She’s at such a fun age – so curious and adventurous – it’s amazing to watch her language and skills progress. I wish we weren’t in the midst of a pandemic, but Emma is definitely the bright spot.”
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore. Dr. Miller has no disclosures.
Emma just celebrated her second birthday, and she has been working on the usual things that children start to master at this age: potty training, making friends, exerting her will through both actions and words, and generally enjoying life as the center of attention for both her parents and grandparents. Like everyone else in Maryland, Emma’s life changed suddenly with the coronavirus stay-at-home order that was issued on March 30. There is no more day care and her parents work from home while caring for her. Her grandparents visit, but only outside and only from a distance – there are no more hugs and there is no more sitting in her grandfather’s lap while he reads stories.
One afternoon a few weeks ago, Emma was looking out the window when she saw her friend, Max, walk by with his parents. Before her parents could stop her, Emma bolted out the door, and she and little Max wrapped each other in a tight embrace. Their parents snapped a photo of the smiling toddlers hugging before they separated the children. The photo is adorable, but as all struggle with social distancing, the poignance of two innocent toddlers in a forbidden embrace is a bit heartbreaking.
Everyone who has ever observed children knows that social distancing is not in their nature. Children play, they hug, they wrestle and tackle and poke, and sometimes even bite. And every student of social psychology has been taught about Harry Harlow’s experiments with rhesus macaques who were separated from their mothers and given access to an inanimate object to serve as a surrogate mother. The Harlow studies, while controversial, were revolutionary in demonstrating that early interactions with both a mother and with playmates were essential in the development of normal social relationships.
Regine Galanti, PhD, is a clinical psychologist at Long Island Behavioral Psychology, Cedarhurst, N.Y., who specializes in the treatment of anxiety and behavior problems. With young children she uses parent-child interaction therapy (PCIT) to help build relationships and discipline. Dr. Galanti said: “I don’t think we’re well prepared as a field to answer questions about the long-term effects of social distancing. If you need young children to socially distance, the responsibility has to fall on the adults. It’s important to explain to children what’s going on and to be honest in a developmentally appropriate way.”
Dr. Galanti has noticed that the issues that people had before COVID-19 are exacerbated by the stress of the current situation. What we do know is that young children thrive on structure.”
Tovah P. Klein, PhD, is the author of “How Toddlers Thrive” (Touchstone, 2015) and is the director of the Barnard College Center for Toddler Development in Manhattan. “When this started, we thought we would be closed for a few weeks,” Dr. Klein said. “We wanted to maintain a connection to the children, so we made videos for the parents to show to the kids, just to say ‘We’re still here.’ But as time went on and we realized it was going to be a while, we felt it was important to provide connection, so we launched a virtual program.”
Dr. Klein said that the teachers meet with their classes of 13 2-year-olds over Zoom, and when they first started, she asked the teachers to try to meet for 10 minutes. They are now meeting for 40 minutes twice a week. The children like seeing their teachers in their homes and they like seeing each other. In addition, the teachers make videos to send home and they are currently working on one to demystify masks. “We’re working on normalizing masks and showing children that when you put the mask on, you’re still there underneath.”
The center has existed for 48 years. There have been struggles for some of the children who attend; some of the parents have been hospitalized with the virus, and some work on the front line and so parents may be living away from a child.
“We’ve seen more challenging behaviors during this time, more tantrums, toileting issues, night awakenings, and more fragility. But as the new normal takes hold, things are settling in. Parents have been good about getting new routines and it helps if parents can handle their own stress,” Dr. Klein said. She also pointed out that for parents working at home while caring for their children, this can be particularly difficult on a young child. “The child knows the parent is home, but isn’t spending time with him, and he sees it as a rejection.”
Margaret Adams, MD, is a child psychiatrist in Maryland who works with very young children and their parents. She says that some of the children are thriving with the extra attention from their parents. “I often have seen difficulties with readjustment to the routine of separations to day care after a family vacation of a week, or sometimes even a weekend, even for those young ones who seem to love the social aspects of day care. I think it is likely a big impact will come upon return, depending on the developmental stage of the child,” Dr. Adams noted.
Despite the hardships of the moment, all three experts expressed hopefulness about the future for these children.
“Young children are super-resilient and that’s the blessing of this,” Dr. Galanti said. “I think they will be okay.”
Emma is home for now with her parents, who are expecting another child soon. Her mother notes: “The days are long and balancing work is an impossible challenge, but being with Emma has been a total blessing, and when would I ever have this much time to spend with my kid? She’s at such a fun age – so curious and adventurous – it’s amazing to watch her language and skills progress. I wish we weren’t in the midst of a pandemic, but Emma is definitely the bright spot.”
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore. Dr. Miller has no disclosures.
COVID 19: Confessions of an outpatient psychiatrist during the pandemic
It seems that some glitches would be inevitable. With a sudden shift to videoconferencing in private psychiatric practices, there were bound to be issues with both technology and privacy. One friend told me of such a glitch on the very first day she started telemental health: She was meeting with a patient who was sitting at her kitchen table. Unbeknownst to the patient, her husband walked into the kitchen behind her, fully naked, to get something from the refrigerator. “There was a full moon shot!” my friend said, initially quite shocked, and then eventually amused. As we all cope with a national tragedy and the total upheaval to our personal and professional lives, the stories just keep coming.
I left work on Friday, March 13, with plans to return on the following Monday to see patients. I had no idea that, by Sunday evening, I would be persuaded that for the safety of all I would need to shut down my real-life psychiatric practice and switch to a videoconferencing venue. I, along with many psychiatrists in Maryland, made this decision after Amy Huberman, MD, posted the following on the Maryland Psychiatric Society (MPS) listserv on Sunday, March 15:
“I want to make a case for starting video sessions with all your patients NOW. There is increasing evidence that the spread of coronavirus is driven primarily by asymptomatic or mildly ill people infected with the virus. Because of this, it’s not good enough to tell your patients not to come in if they have symptoms, or for you not to come into work if you have no symptoms. Even after I sent out a letter two weeks ago warning people not to come in if they had symptoms or had potentially come in contact with someone with COVID-19, several patients with coughs still came to my office, as well as several people who had just been on trips to New York City.
If we want to help slow the spread of this illness so that our health system has a better chance of being able to offer ventilators to the people who need them, we must limit all contacts as much as possible – even of asymptomatic people, given the emerging data.
I am planning to send out a message to all my patients today that they should do the same. Without the president or the media giving clear advice to people about what to do, it’s our job as physicians to do it.”
By that night, I had set up a home office with a blank wall behind me, windows in front of me, and books propping my computer at a height that would not have my patients looking up my nose. For the first time in over 20 years, I dusted my son’s Little League trophies, moved them and a 40,000 baseball card collection against the wall, carried a desk, chair, rug, houseplant, and a small Buddha into a room in which I would have some privacy, and my telepsychiatry practice found a home.
After some research, I registered for a free site called Doxy.me because it was HIPAA compliant and did not require patients to download an application; anyone with a camera on any Internet-enabled phone, computer, or tablet, could click on a link and enter my virtual waiting room. I soon discovered that images on the Doxy.me site are sometimes grainy and sometimes freeze up; in some sessions, we ended up switching to FaceTime, and as government mandates for HIPAA compliance relaxed, I offered to meet on any site that my patients might be comfortable with: if not Doxy.me (which remains my starting place for most sessions), Facetime, Skype, Zoom, or Whatsapp. I have not offered Bluejeans, Google Hangouts, or WebEx, and no one has requested those applications. I keep the phone next to the computer, and some sessions include a few minutes of tech support as I help patients (or they help me) navigate the various sites. In a few sessions, we could not get the audio to work and we used video on one venue while we talked on the phone. I haven’t figured out if the variations in the quality of the connection has to do with my Comcast connection, the fact that these websites are overloaded with users, or that my household now consists of three people, two large monitors, three laptops, two tablets, three cell phone lines (not to mention one dog and a transplanted cat), all going at the same time. The pets do not require any bandwidth, but all the people are talking to screens throughout the workday.
As my colleagues embarked on the same journey, the listserv questions and comments came quickly. What were the best platforms? Was it a good thing or a bad thing to suddenly be in people’s homes? Some felt the extraneous background to be helpful, others found it distracting and intrusive.
How do these sessions get coded for the purpose of billing? There was a tremendous amount of confusion over that, with the initial verdict being that Medicare wanted the place of service changed to “02” and that private insurers want one of two modifiers, and it was anyone’s guess which company wanted which modifier. Then there was the concern that Medicare was paying 25% less, until the MPS staff clarified that full fees would be paid, but the place of service should be filled in as “11” – not “02” – as with regular office visits, and the modifier “95” should be added on the Health Care Finance Administration claim form. We were left to wait and see what gets reimbursed and for what fees.
Could new patients be seen by videoconferencing? Could patients from other states be seen this way if the psychiatrist was not licensed in the state where the patient was calling from? One psychiatrist reported he had a patient in an adjacent state drive over the border into Maryland, but the patient brought her mother and the evaluation included unwanted input from the mom as the session consisted of the patient and her mother yelling at both each other in the car and at the psychiatrist on the screen!
Psychiatrists on the listserv began to comment that treatment sessions were intense and exhausting. I feel the literal face-to-face contact of another person’s head just inches from my own, with full eye contact, often gets to be a lot. No one asks why I’ve moved a trinket (ah, there are no trinkets) or gazes off around the room. I sometimes sit for long periods of time as I don’t even stand to see the patients to the door. Other patients move about or bounce their devices on their laps, and my stomach starts to feel queasy until I ask to have the device adjusted. In some sessions, I find I’m talking to partial heads, or that computer icons cover the patient’s mouth.
Being in people’s lives via screen has been interesting. Unlike my colleague, I have not had any streaking spouses, but I’ve greeted a few family members – often those serving as technical support – and I’ve toured part of a farm, met dogs, guinea pigs, and even a goat. I’ve made brief daily “visits” to a frightened patient in isolation on a COVID hospital unit and had the joy of celebrating the discharge to home. It’s odd to be in a bedroom with a patient, even virtually, and it is interesting to note where they choose to hold their sessions; I’ve had several patients hold sessions from their cars. Seeing my own image in the corner of the screen is also a bit distracting, and in one session, as I saw my own reaction, my patient said, “I knew you were going to make that face!”
The pandemic has usurped most of the activities of all of our lives, and without social interactions, travel, and work in the usual way, life does not hold its usual richness. In a few cases, I have ended the session after half the time as the patient insisted there was nothing to talk about. Many talk about the medical problems they can’t be seen for, what they are doing to keep safe (or not), how they are washing down their groceries, and who they are meeting with by Zoom. Of those who were terribly anxious before, some feel oddly calmer – the world has ramped up to meet their level of anxiety and they feel vindicated. No one thinks they are odd for worrying about germs on door knobs or elevator buttons. What were once neurotic fears are now our real-life reality. Others have been triggered by a paralyzing fear, often with panic attacks, and these sessions are certainly challenging as I figure out which medications will best help, while responding to requests for reassurance. And there is the troublesome aspect of trying to care for others who are fearful while living with the reality that these fears are not extraneous to our own lives: We, too, are scared for ourselves and our families.
For some people, stay-at-home mandates have been easier than for others. People who are naturally introverted, or those with social anxiety, have told me they find this time at home to be a relief. They no longer feel pressured to go out; there is permission to be alone, to read, or watch Netflix. No one is pressuring them to go to parties or look for a Tinder date. For others, the isolation and loneliness have been devastating, causing a range of emotions from being “stir crazy,” to triggering episodes of major depression and severe anxiety.
Health care workers in therapy talk about their fears of being contaminated with coronavirus, about the exposures they’ve had, their fears of bringing the virus home to family, and about the anger – sometimes rage – that their employers are not doing more to protect them.
Few people these past weeks are looking for insight into their patterns of behavior and emotion. Most of life has come to be about survival and not about personal striving. Students who are driven to excel are disappointed to have their scholastic worlds have switched to pass/fail. And for those struggling with milder forms of depression and anxiety, both the patients and I have all been a bit perplexed by losing the usual measures of what feelings are normal in a tragic world and we no longer use socializing as the hallmark that heralds a return to normalcy after a period of withdrawal.
In some aspects, it is not all been bad. I’ve enjoyed watching my neighbors walk by with their dogs through the window behind my computer screen and I’ve felt part of the daily evolution as the cherry tree outside that same window turns from dead brown wood to vibrant pink blossoms. I like the flexibility of my schedule and the sensation I always carry of being rushed has quelled. I take more walks and spend more time with the family members who are held captive with me. The dog, who no longer is left alone for hours each day, is certainly a winner.
Some of my colleagues tell me they are overwhelmed – patients they have not seen for years have returned, people are asking for more frequent sessions, and they are suddenly trying to work at home while homeschooling children. I have had only a few of those requests for crisis care, while new referrals are much quieter than normal. Some of my patients have even said that they simply aren’t comfortable meeting this way and they will see me at the other end of the pandemic. A few people I would have expected to hear from I have not, and I fear that those who have lost their jobs may avoiding the cost of treatment – this group I will reach out to in the coming weeks. A little extra time, however, has given me the opportunity to join the Johns Hopkins COVID-19 Mental Health team. And my first attempt at teaching a resident seminar by Zoom has gone well.
For some in the medical field, this has been a horrible and traumatic time; they are worked to exhaustion, and surrounded by distress, death, and personal fear with every shift. For others, life has come to a standstill as the elective procedures that fill their days have virtually stopped. For outpatient psychiatry, it’s been a bit of an in-between, we may feel an odd mix of relevant and useless all at the same time, as our services are appreciated by our patients, but as actual soldiers caring for the ill COVID patients, we are leaving that to our colleagues in the EDs, COVID units, and ICUs. As a physician who has not treated a patient in an ICU for decades, I wish I had something more concrete to contribute to the effort, and at the same time, I’m relieved that I don’t.
And what about the patients? How are they doing with remote psychiatry? Some are clearly flustered or frustrated by the technology issues. Other times sessions go smoothly, and the fact that we are talking through screens gets forgotten. Some like the convenience of not having to drive a far distance and no one misses my crowded parking lot.
Kristen, another doctor’s patient in Illinois, commented: “I appreciate the continuity in care, especially if the alternative is delaying appointments. I think that’s most important. The interaction helps manage added anxiety from isolating as well. I don’t think it diminishes the care I receive; it makes me feel that my doctor is still accessible. One other point, since I have had both telemedicine and in-person appointments with my current psychiatrist, is that during in-person meetings, he is usually on his computer and rarely looks at me or makes eye contact. In virtual meetings, I feel he is much more engaged with me.”
In normal times, I spend a good deal of time encouraging patients to work on building their relationships and community – these connections lead people to healthy and fulfilling lives – and now we talk about how to best be socially distant. We see each other as vectors of disease and to greet a friend with a handshake, much less a hug, would be unthinkable. Will our collective psyches ever recover? For those of us who will survive, that remains to be seen. In the meantime, perhaps we are all being forced to be more flexible and innovative.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
It seems that some glitches would be inevitable. With a sudden shift to videoconferencing in private psychiatric practices, there were bound to be issues with both technology and privacy. One friend told me of such a glitch on the very first day she started telemental health: She was meeting with a patient who was sitting at her kitchen table. Unbeknownst to the patient, her husband walked into the kitchen behind her, fully naked, to get something from the refrigerator. “There was a full moon shot!” my friend said, initially quite shocked, and then eventually amused. As we all cope with a national tragedy and the total upheaval to our personal and professional lives, the stories just keep coming.
I left work on Friday, March 13, with plans to return on the following Monday to see patients. I had no idea that, by Sunday evening, I would be persuaded that for the safety of all I would need to shut down my real-life psychiatric practice and switch to a videoconferencing venue. I, along with many psychiatrists in Maryland, made this decision after Amy Huberman, MD, posted the following on the Maryland Psychiatric Society (MPS) listserv on Sunday, March 15:
“I want to make a case for starting video sessions with all your patients NOW. There is increasing evidence that the spread of coronavirus is driven primarily by asymptomatic or mildly ill people infected with the virus. Because of this, it’s not good enough to tell your patients not to come in if they have symptoms, or for you not to come into work if you have no symptoms. Even after I sent out a letter two weeks ago warning people not to come in if they had symptoms or had potentially come in contact with someone with COVID-19, several patients with coughs still came to my office, as well as several people who had just been on trips to New York City.
If we want to help slow the spread of this illness so that our health system has a better chance of being able to offer ventilators to the people who need them, we must limit all contacts as much as possible – even of asymptomatic people, given the emerging data.
I am planning to send out a message to all my patients today that they should do the same. Without the president or the media giving clear advice to people about what to do, it’s our job as physicians to do it.”
By that night, I had set up a home office with a blank wall behind me, windows in front of me, and books propping my computer at a height that would not have my patients looking up my nose. For the first time in over 20 years, I dusted my son’s Little League trophies, moved them and a 40,000 baseball card collection against the wall, carried a desk, chair, rug, houseplant, and a small Buddha into a room in which I would have some privacy, and my telepsychiatry practice found a home.
After some research, I registered for a free site called Doxy.me because it was HIPAA compliant and did not require patients to download an application; anyone with a camera on any Internet-enabled phone, computer, or tablet, could click on a link and enter my virtual waiting room. I soon discovered that images on the Doxy.me site are sometimes grainy and sometimes freeze up; in some sessions, we ended up switching to FaceTime, and as government mandates for HIPAA compliance relaxed, I offered to meet on any site that my patients might be comfortable with: if not Doxy.me (which remains my starting place for most sessions), Facetime, Skype, Zoom, or Whatsapp. I have not offered Bluejeans, Google Hangouts, or WebEx, and no one has requested those applications. I keep the phone next to the computer, and some sessions include a few minutes of tech support as I help patients (or they help me) navigate the various sites. In a few sessions, we could not get the audio to work and we used video on one venue while we talked on the phone. I haven’t figured out if the variations in the quality of the connection has to do with my Comcast connection, the fact that these websites are overloaded with users, or that my household now consists of three people, two large monitors, three laptops, two tablets, three cell phone lines (not to mention one dog and a transplanted cat), all going at the same time. The pets do not require any bandwidth, but all the people are talking to screens throughout the workday.
As my colleagues embarked on the same journey, the listserv questions and comments came quickly. What were the best platforms? Was it a good thing or a bad thing to suddenly be in people’s homes? Some felt the extraneous background to be helpful, others found it distracting and intrusive.
How do these sessions get coded for the purpose of billing? There was a tremendous amount of confusion over that, with the initial verdict being that Medicare wanted the place of service changed to “02” and that private insurers want one of two modifiers, and it was anyone’s guess which company wanted which modifier. Then there was the concern that Medicare was paying 25% less, until the MPS staff clarified that full fees would be paid, but the place of service should be filled in as “11” – not “02” – as with regular office visits, and the modifier “95” should be added on the Health Care Finance Administration claim form. We were left to wait and see what gets reimbursed and for what fees.
Could new patients be seen by videoconferencing? Could patients from other states be seen this way if the psychiatrist was not licensed in the state where the patient was calling from? One psychiatrist reported he had a patient in an adjacent state drive over the border into Maryland, but the patient brought her mother and the evaluation included unwanted input from the mom as the session consisted of the patient and her mother yelling at both each other in the car and at the psychiatrist on the screen!
Psychiatrists on the listserv began to comment that treatment sessions were intense and exhausting. I feel the literal face-to-face contact of another person’s head just inches from my own, with full eye contact, often gets to be a lot. No one asks why I’ve moved a trinket (ah, there are no trinkets) or gazes off around the room. I sometimes sit for long periods of time as I don’t even stand to see the patients to the door. Other patients move about or bounce their devices on their laps, and my stomach starts to feel queasy until I ask to have the device adjusted. In some sessions, I find I’m talking to partial heads, or that computer icons cover the patient’s mouth.
Being in people’s lives via screen has been interesting. Unlike my colleague, I have not had any streaking spouses, but I’ve greeted a few family members – often those serving as technical support – and I’ve toured part of a farm, met dogs, guinea pigs, and even a goat. I’ve made brief daily “visits” to a frightened patient in isolation on a COVID hospital unit and had the joy of celebrating the discharge to home. It’s odd to be in a bedroom with a patient, even virtually, and it is interesting to note where they choose to hold their sessions; I’ve had several patients hold sessions from their cars. Seeing my own image in the corner of the screen is also a bit distracting, and in one session, as I saw my own reaction, my patient said, “I knew you were going to make that face!”
The pandemic has usurped most of the activities of all of our lives, and without social interactions, travel, and work in the usual way, life does not hold its usual richness. In a few cases, I have ended the session after half the time as the patient insisted there was nothing to talk about. Many talk about the medical problems they can’t be seen for, what they are doing to keep safe (or not), how they are washing down their groceries, and who they are meeting with by Zoom. Of those who were terribly anxious before, some feel oddly calmer – the world has ramped up to meet their level of anxiety and they feel vindicated. No one thinks they are odd for worrying about germs on door knobs or elevator buttons. What were once neurotic fears are now our real-life reality. Others have been triggered by a paralyzing fear, often with panic attacks, and these sessions are certainly challenging as I figure out which medications will best help, while responding to requests for reassurance. And there is the troublesome aspect of trying to care for others who are fearful while living with the reality that these fears are not extraneous to our own lives: We, too, are scared for ourselves and our families.
For some people, stay-at-home mandates have been easier than for others. People who are naturally introverted, or those with social anxiety, have told me they find this time at home to be a relief. They no longer feel pressured to go out; there is permission to be alone, to read, or watch Netflix. No one is pressuring them to go to parties or look for a Tinder date. For others, the isolation and loneliness have been devastating, causing a range of emotions from being “stir crazy,” to triggering episodes of major depression and severe anxiety.
Health care workers in therapy talk about their fears of being contaminated with coronavirus, about the exposures they’ve had, their fears of bringing the virus home to family, and about the anger – sometimes rage – that their employers are not doing more to protect them.
Few people these past weeks are looking for insight into their patterns of behavior and emotion. Most of life has come to be about survival and not about personal striving. Students who are driven to excel are disappointed to have their scholastic worlds have switched to pass/fail. And for those struggling with milder forms of depression and anxiety, both the patients and I have all been a bit perplexed by losing the usual measures of what feelings are normal in a tragic world and we no longer use socializing as the hallmark that heralds a return to normalcy after a period of withdrawal.
In some aspects, it is not all been bad. I’ve enjoyed watching my neighbors walk by with their dogs through the window behind my computer screen and I’ve felt part of the daily evolution as the cherry tree outside that same window turns from dead brown wood to vibrant pink blossoms. I like the flexibility of my schedule and the sensation I always carry of being rushed has quelled. I take more walks and spend more time with the family members who are held captive with me. The dog, who no longer is left alone for hours each day, is certainly a winner.
Some of my colleagues tell me they are overwhelmed – patients they have not seen for years have returned, people are asking for more frequent sessions, and they are suddenly trying to work at home while homeschooling children. I have had only a few of those requests for crisis care, while new referrals are much quieter than normal. Some of my patients have even said that they simply aren’t comfortable meeting this way and they will see me at the other end of the pandemic. A few people I would have expected to hear from I have not, and I fear that those who have lost their jobs may avoiding the cost of treatment – this group I will reach out to in the coming weeks. A little extra time, however, has given me the opportunity to join the Johns Hopkins COVID-19 Mental Health team. And my first attempt at teaching a resident seminar by Zoom has gone well.
For some in the medical field, this has been a horrible and traumatic time; they are worked to exhaustion, and surrounded by distress, death, and personal fear with every shift. For others, life has come to a standstill as the elective procedures that fill their days have virtually stopped. For outpatient psychiatry, it’s been a bit of an in-between, we may feel an odd mix of relevant and useless all at the same time, as our services are appreciated by our patients, but as actual soldiers caring for the ill COVID patients, we are leaving that to our colleagues in the EDs, COVID units, and ICUs. As a physician who has not treated a patient in an ICU for decades, I wish I had something more concrete to contribute to the effort, and at the same time, I’m relieved that I don’t.
And what about the patients? How are they doing with remote psychiatry? Some are clearly flustered or frustrated by the technology issues. Other times sessions go smoothly, and the fact that we are talking through screens gets forgotten. Some like the convenience of not having to drive a far distance and no one misses my crowded parking lot.
Kristen, another doctor’s patient in Illinois, commented: “I appreciate the continuity in care, especially if the alternative is delaying appointments. I think that’s most important. The interaction helps manage added anxiety from isolating as well. I don’t think it diminishes the care I receive; it makes me feel that my doctor is still accessible. One other point, since I have had both telemedicine and in-person appointments with my current psychiatrist, is that during in-person meetings, he is usually on his computer and rarely looks at me or makes eye contact. In virtual meetings, I feel he is much more engaged with me.”
In normal times, I spend a good deal of time encouraging patients to work on building their relationships and community – these connections lead people to healthy and fulfilling lives – and now we talk about how to best be socially distant. We see each other as vectors of disease and to greet a friend with a handshake, much less a hug, would be unthinkable. Will our collective psyches ever recover? For those of us who will survive, that remains to be seen. In the meantime, perhaps we are all being forced to be more flexible and innovative.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
It seems that some glitches would be inevitable. With a sudden shift to videoconferencing in private psychiatric practices, there were bound to be issues with both technology and privacy. One friend told me of such a glitch on the very first day she started telemental health: She was meeting with a patient who was sitting at her kitchen table. Unbeknownst to the patient, her husband walked into the kitchen behind her, fully naked, to get something from the refrigerator. “There was a full moon shot!” my friend said, initially quite shocked, and then eventually amused. As we all cope with a national tragedy and the total upheaval to our personal and professional lives, the stories just keep coming.
I left work on Friday, March 13, with plans to return on the following Monday to see patients. I had no idea that, by Sunday evening, I would be persuaded that for the safety of all I would need to shut down my real-life psychiatric practice and switch to a videoconferencing venue. I, along with many psychiatrists in Maryland, made this decision after Amy Huberman, MD, posted the following on the Maryland Psychiatric Society (MPS) listserv on Sunday, March 15:
“I want to make a case for starting video sessions with all your patients NOW. There is increasing evidence that the spread of coronavirus is driven primarily by asymptomatic or mildly ill people infected with the virus. Because of this, it’s not good enough to tell your patients not to come in if they have symptoms, or for you not to come into work if you have no symptoms. Even after I sent out a letter two weeks ago warning people not to come in if they had symptoms or had potentially come in contact with someone with COVID-19, several patients with coughs still came to my office, as well as several people who had just been on trips to New York City.
If we want to help slow the spread of this illness so that our health system has a better chance of being able to offer ventilators to the people who need them, we must limit all contacts as much as possible – even of asymptomatic people, given the emerging data.
I am planning to send out a message to all my patients today that they should do the same. Without the president or the media giving clear advice to people about what to do, it’s our job as physicians to do it.”
By that night, I had set up a home office with a blank wall behind me, windows in front of me, and books propping my computer at a height that would not have my patients looking up my nose. For the first time in over 20 years, I dusted my son’s Little League trophies, moved them and a 40,000 baseball card collection against the wall, carried a desk, chair, rug, houseplant, and a small Buddha into a room in which I would have some privacy, and my telepsychiatry practice found a home.
After some research, I registered for a free site called Doxy.me because it was HIPAA compliant and did not require patients to download an application; anyone with a camera on any Internet-enabled phone, computer, or tablet, could click on a link and enter my virtual waiting room. I soon discovered that images on the Doxy.me site are sometimes grainy and sometimes freeze up; in some sessions, we ended up switching to FaceTime, and as government mandates for HIPAA compliance relaxed, I offered to meet on any site that my patients might be comfortable with: if not Doxy.me (which remains my starting place for most sessions), Facetime, Skype, Zoom, or Whatsapp. I have not offered Bluejeans, Google Hangouts, or WebEx, and no one has requested those applications. I keep the phone next to the computer, and some sessions include a few minutes of tech support as I help patients (or they help me) navigate the various sites. In a few sessions, we could not get the audio to work and we used video on one venue while we talked on the phone. I haven’t figured out if the variations in the quality of the connection has to do with my Comcast connection, the fact that these websites are overloaded with users, or that my household now consists of three people, two large monitors, three laptops, two tablets, three cell phone lines (not to mention one dog and a transplanted cat), all going at the same time. The pets do not require any bandwidth, but all the people are talking to screens throughout the workday.
As my colleagues embarked on the same journey, the listserv questions and comments came quickly. What were the best platforms? Was it a good thing or a bad thing to suddenly be in people’s homes? Some felt the extraneous background to be helpful, others found it distracting and intrusive.
How do these sessions get coded for the purpose of billing? There was a tremendous amount of confusion over that, with the initial verdict being that Medicare wanted the place of service changed to “02” and that private insurers want one of two modifiers, and it was anyone’s guess which company wanted which modifier. Then there was the concern that Medicare was paying 25% less, until the MPS staff clarified that full fees would be paid, but the place of service should be filled in as “11” – not “02” – as with regular office visits, and the modifier “95” should be added on the Health Care Finance Administration claim form. We were left to wait and see what gets reimbursed and for what fees.
Could new patients be seen by videoconferencing? Could patients from other states be seen this way if the psychiatrist was not licensed in the state where the patient was calling from? One psychiatrist reported he had a patient in an adjacent state drive over the border into Maryland, but the patient brought her mother and the evaluation included unwanted input from the mom as the session consisted of the patient and her mother yelling at both each other in the car and at the psychiatrist on the screen!
Psychiatrists on the listserv began to comment that treatment sessions were intense and exhausting. I feel the literal face-to-face contact of another person’s head just inches from my own, with full eye contact, often gets to be a lot. No one asks why I’ve moved a trinket (ah, there are no trinkets) or gazes off around the room. I sometimes sit for long periods of time as I don’t even stand to see the patients to the door. Other patients move about or bounce their devices on their laps, and my stomach starts to feel queasy until I ask to have the device adjusted. In some sessions, I find I’m talking to partial heads, or that computer icons cover the patient’s mouth.
Being in people’s lives via screen has been interesting. Unlike my colleague, I have not had any streaking spouses, but I’ve greeted a few family members – often those serving as technical support – and I’ve toured part of a farm, met dogs, guinea pigs, and even a goat. I’ve made brief daily “visits” to a frightened patient in isolation on a COVID hospital unit and had the joy of celebrating the discharge to home. It’s odd to be in a bedroom with a patient, even virtually, and it is interesting to note where they choose to hold their sessions; I’ve had several patients hold sessions from their cars. Seeing my own image in the corner of the screen is also a bit distracting, and in one session, as I saw my own reaction, my patient said, “I knew you were going to make that face!”
The pandemic has usurped most of the activities of all of our lives, and without social interactions, travel, and work in the usual way, life does not hold its usual richness. In a few cases, I have ended the session after half the time as the patient insisted there was nothing to talk about. Many talk about the medical problems they can’t be seen for, what they are doing to keep safe (or not), how they are washing down their groceries, and who they are meeting with by Zoom. Of those who were terribly anxious before, some feel oddly calmer – the world has ramped up to meet their level of anxiety and they feel vindicated. No one thinks they are odd for worrying about germs on door knobs or elevator buttons. What were once neurotic fears are now our real-life reality. Others have been triggered by a paralyzing fear, often with panic attacks, and these sessions are certainly challenging as I figure out which medications will best help, while responding to requests for reassurance. And there is the troublesome aspect of trying to care for others who are fearful while living with the reality that these fears are not extraneous to our own lives: We, too, are scared for ourselves and our families.
For some people, stay-at-home mandates have been easier than for others. People who are naturally introverted, or those with social anxiety, have told me they find this time at home to be a relief. They no longer feel pressured to go out; there is permission to be alone, to read, or watch Netflix. No one is pressuring them to go to parties or look for a Tinder date. For others, the isolation and loneliness have been devastating, causing a range of emotions from being “stir crazy,” to triggering episodes of major depression and severe anxiety.
Health care workers in therapy talk about their fears of being contaminated with coronavirus, about the exposures they’ve had, their fears of bringing the virus home to family, and about the anger – sometimes rage – that their employers are not doing more to protect them.
Few people these past weeks are looking for insight into their patterns of behavior and emotion. Most of life has come to be about survival and not about personal striving. Students who are driven to excel are disappointed to have their scholastic worlds have switched to pass/fail. And for those struggling with milder forms of depression and anxiety, both the patients and I have all been a bit perplexed by losing the usual measures of what feelings are normal in a tragic world and we no longer use socializing as the hallmark that heralds a return to normalcy after a period of withdrawal.
In some aspects, it is not all been bad. I’ve enjoyed watching my neighbors walk by with their dogs through the window behind my computer screen and I’ve felt part of the daily evolution as the cherry tree outside that same window turns from dead brown wood to vibrant pink blossoms. I like the flexibility of my schedule and the sensation I always carry of being rushed has quelled. I take more walks and spend more time with the family members who are held captive with me. The dog, who no longer is left alone for hours each day, is certainly a winner.
Some of my colleagues tell me they are overwhelmed – patients they have not seen for years have returned, people are asking for more frequent sessions, and they are suddenly trying to work at home while homeschooling children. I have had only a few of those requests for crisis care, while new referrals are much quieter than normal. Some of my patients have even said that they simply aren’t comfortable meeting this way and they will see me at the other end of the pandemic. A few people I would have expected to hear from I have not, and I fear that those who have lost their jobs may avoiding the cost of treatment – this group I will reach out to in the coming weeks. A little extra time, however, has given me the opportunity to join the Johns Hopkins COVID-19 Mental Health team. And my first attempt at teaching a resident seminar by Zoom has gone well.
For some in the medical field, this has been a horrible and traumatic time; they are worked to exhaustion, and surrounded by distress, death, and personal fear with every shift. For others, life has come to a standstill as the elective procedures that fill their days have virtually stopped. For outpatient psychiatry, it’s been a bit of an in-between, we may feel an odd mix of relevant and useless all at the same time, as our services are appreciated by our patients, but as actual soldiers caring for the ill COVID patients, we are leaving that to our colleagues in the EDs, COVID units, and ICUs. As a physician who has not treated a patient in an ICU for decades, I wish I had something more concrete to contribute to the effort, and at the same time, I’m relieved that I don’t.
And what about the patients? How are they doing with remote psychiatry? Some are clearly flustered or frustrated by the technology issues. Other times sessions go smoothly, and the fact that we are talking through screens gets forgotten. Some like the convenience of not having to drive a far distance and no one misses my crowded parking lot.
Kristen, another doctor’s patient in Illinois, commented: “I appreciate the continuity in care, especially if the alternative is delaying appointments. I think that’s most important. The interaction helps manage added anxiety from isolating as well. I don’t think it diminishes the care I receive; it makes me feel that my doctor is still accessible. One other point, since I have had both telemedicine and in-person appointments with my current psychiatrist, is that during in-person meetings, he is usually on his computer and rarely looks at me or makes eye contact. In virtual meetings, I feel he is much more engaged with me.”
In normal times, I spend a good deal of time encouraging patients to work on building their relationships and community – these connections lead people to healthy and fulfilling lives – and now we talk about how to best be socially distant. We see each other as vectors of disease and to greet a friend with a handshake, much less a hug, would be unthinkable. Will our collective psyches ever recover? For those of us who will survive, that remains to be seen. In the meantime, perhaps we are all being forced to be more flexible and innovative.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
Coronavirus on the inpatient unit: A new challenge for psychiatry
For weeks now, the coronavirus epidemic has monopolized the media. As cases of COVID-19 have crossed borders and then oceans, the pandemic has caused fear and anxiety as Americans struggle with the uncertain nature of this highly contagious disease. Those exposed may be infectious before they are symptomatic, and the expression of the virus varies greatly: Some people have a mild illness and others quickly progress to severe pulmonary disease with a bilateral interstitial pneumonia that requires intubation and respiratory support. So far, the number of people infected and the absolute mortality is a fraction of what we have seen with this year’s seasonal flu, but in countries where the virus has spread quickly, medical systems have not been able to keep up with demand for high-intensity care and mortality rates have been many times higher than that of the flu. Italy, in particular, has not been able to halt the spread, even with the entire country on lockdown, and the medical system has been overwhelmed, resulting in rationing of care and many deaths.
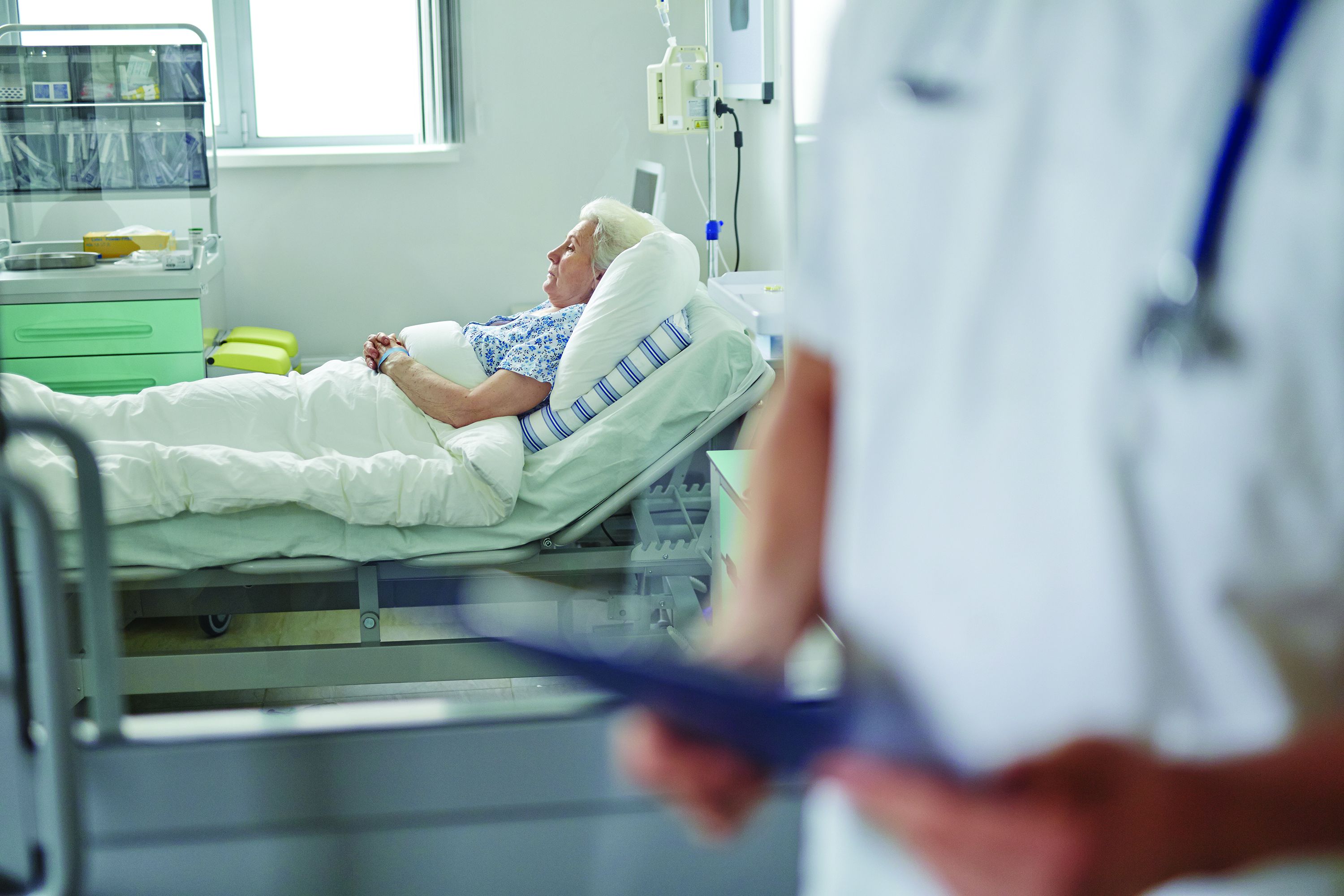
COVID-19 represents a new challenge for the inpatient psychiatry unit. Some patients on an acute psychiatric unit may be agitated, uncooperative, or even violent, and it’s not hard to imagine the distress of anyone who has a patient spit on them as we’re all trying to remember not to shake hands. Inevitably, there will be patients who present for psychiatric admission with no respiratory symptoms, who are admitted and then become ill and are diagnosed with COVID-19. In the meantime, the potential is there for contagion to other patients on the unit, the hospital staff, and visitors to the unit.
While many hospital units treat infectious patients, the issues with psychiatry are different; psychiatry units are not set up to have aggressive infection control, staff and patients don’t typically wear protective gear, and people with psychiatric illnesses are ambulatory and interactive. The treatment of psychiatric illnesses involves more – not less – social interaction and patients attend groups and occupational therapy sessions; they dine in communal areas and watch television together in day rooms. Cell phones are typically not permitted for issues of privacy, and patients may use communal telephones. Patients who are very ill with psychiatric disorders may resist hygiene measures, and they may intrude on the personal space of others.
Patients with known COVID-19 can be isolated or transferred to another unit if more intensive medical care is necessary, but by that time, others have been exposed and potentially infected. How to contain this potential risk has been a topic of concern for psychiatric units everywhere. Following a potential or confirmed exposure, it’s not completely clear who should be sent home for self-quarantine: Do the staff who have had contact with the patient leave for 2 weeks, and if so, is there enough staff to replace them? Do they continue to work with protective equipment and leave only if they become symptomatic and test positive? Do staff remain at the hospital, or do they go home at night, potentially infecting those on public transportation and their family members? Presumably new patients would not be admitted to the unit, but our psychiatric system is taxed already with a lack of available beds.
In South Korea, patients and staff at the Daenam hospital reportedly faced this exact scenario. The hospital was locked down and 101 patients in the psychiatric facility developed COVID-19; 7 of those patients died, an outcome we hope to never see again. As of this writing, there are two patients on a 22-bed geropsychiatric unit at the UW Medical Center – Northwest in Seattle who developed COVID-19 after they were admitted to the unit. They have been isolated, and the rest of the patients on the unit have been quarantined. The staff are now wearing masks, gowns, and gloves.
“We started precautions for all 22 patients. ... We instituted our protocols for every room around, donning and doffing personal protective equipment (PPE). We had conversations with their family members,” said Santiago Neme, MD, MPH, an infectious disease physician at UW Medical Center – Northwest, in a press conference released by the university. “The patients were transferred and both remain stable. All patients on the unit were tested even though there were no concerning symptoms.”
These measures are necessary for infection control, but they are not helpful for the treatment of psychiatric disorders. Treatment consists, in part, of getting patients out of their rooms and involved in therapeutic activities in a milieu that removes them from the usual stresses of their daily lives. How insurance companies will respond to any need for extra days is one more concern to throw into the mix.
Paul Summergrad, MD, chairman of psychiatry at Tufts University in Boston, has been very interested in what facilities around the world have been doing. “In Washington state, after the nursing home infections, they sent home over a hundred staff members who had been exposed. In Hong Kong, the psychiatric hospitals have limited how patients circulate on the units even if no one is infected; this is not something that would go over well in the U.S.,” he said in an interview. Dr. Summergrad believes that higher death rates are seen in countries with higher smoking rates, and patients with psychiatric disorders are more likely to smoke than the general public, possibly placing them at higher risk for more severe morbidity and mortality.
Patrick Triplett, MD, clinical director of the department of psychiatry at Johns Hopkins University in Baltimore, communicated with me about their plans to manage a scenario in which a patient becomes ill on a psychiatry unit.
“If we think a patient might be infected, we will isolate them in a room with a closed door (We would need to account for their psychiatric needs as well during this period, say constant observation, for example.) and call the centralized command center, where the Hospital Epidemiology and Infection Control (HEIC) team gets involved. They will determine if the patient should be tested for COVID-19. If it’s determined that the patient is infected, they will likely be transferred to a floor with negative pressure rooms. We would coordinate psychiatric nursing needs with the receiving unit, based on the patient’s clinical needs.”
Dr. Triplett elaborated on the exposure of staff and visitors. “We take our lead on postexposure management from [HEIC] and Occupational Health. There are procedures in place for environmental cleaning, waste, linens, etc. The [Centers for Disease Control and Prevention] has guidelines on work restrictions for staff who have cared for patients with confirmed COVID-19, and HEIC helps determine the provider’s risk category. We would also involve them in determining risk levels and management for other patients on the floor and visitors. But prior to any known exposure, we are already limiting visitors for patients per the governor’s mandate of only one adult visitor per patient.”
The next couple of weeks will be telling, and as we readjust to a life of social distancing, it is certain to be a challenge to keep ourselves and our patients safe, healthy, and emotionally strong.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
For weeks now, the coronavirus epidemic has monopolized the media. As cases of COVID-19 have crossed borders and then oceans, the pandemic has caused fear and anxiety as Americans struggle with the uncertain nature of this highly contagious disease. Those exposed may be infectious before they are symptomatic, and the expression of the virus varies greatly: Some people have a mild illness and others quickly progress to severe pulmonary disease with a bilateral interstitial pneumonia that requires intubation and respiratory support. So far, the number of people infected and the absolute mortality is a fraction of what we have seen with this year’s seasonal flu, but in countries where the virus has spread quickly, medical systems have not been able to keep up with demand for high-intensity care and mortality rates have been many times higher than that of the flu. Italy, in particular, has not been able to halt the spread, even with the entire country on lockdown, and the medical system has been overwhelmed, resulting in rationing of care and many deaths.
COVID-19 represents a new challenge for the inpatient psychiatry unit. Some patients on an acute psychiatric unit may be agitated, uncooperative, or even violent, and it’s not hard to imagine the distress of anyone who has a patient spit on them as we’re all trying to remember not to shake hands. Inevitably, there will be patients who present for psychiatric admission with no respiratory symptoms, who are admitted and then become ill and are diagnosed with COVID-19. In the meantime, the potential is there for contagion to other patients on the unit, the hospital staff, and visitors to the unit.
While many hospital units treat infectious patients, the issues with psychiatry are different; psychiatry units are not set up to have aggressive infection control, staff and patients don’t typically wear protective gear, and people with psychiatric illnesses are ambulatory and interactive. The treatment of psychiatric illnesses involves more – not less – social interaction and patients attend groups and occupational therapy sessions; they dine in communal areas and watch television together in day rooms. Cell phones are typically not permitted for issues of privacy, and patients may use communal telephones. Patients who are very ill with psychiatric disorders may resist hygiene measures, and they may intrude on the personal space of others.
Patients with known COVID-19 can be isolated or transferred to another unit if more intensive medical care is necessary, but by that time, others have been exposed and potentially infected. How to contain this potential risk has been a topic of concern for psychiatric units everywhere. Following a potential or confirmed exposure, it’s not completely clear who should be sent home for self-quarantine: Do the staff who have had contact with the patient leave for 2 weeks, and if so, is there enough staff to replace them? Do they continue to work with protective equipment and leave only if they become symptomatic and test positive? Do staff remain at the hospital, or do they go home at night, potentially infecting those on public transportation and their family members? Presumably new patients would not be admitted to the unit, but our psychiatric system is taxed already with a lack of available beds.
In South Korea, patients and staff at the Daenam hospital reportedly faced this exact scenario. The hospital was locked down and 101 patients in the psychiatric facility developed COVID-19; 7 of those patients died, an outcome we hope to never see again. As of this writing, there are two patients on a 22-bed geropsychiatric unit at the UW Medical Center – Northwest in Seattle who developed COVID-19 after they were admitted to the unit. They have been isolated, and the rest of the patients on the unit have been quarantined. The staff are now wearing masks, gowns, and gloves.
“We started precautions for all 22 patients. ... We instituted our protocols for every room around, donning and doffing personal protective equipment (PPE). We had conversations with their family members,” said Santiago Neme, MD, MPH, an infectious disease physician at UW Medical Center – Northwest, in a press conference released by the university. “The patients were transferred and both remain stable. All patients on the unit were tested even though there were no concerning symptoms.”
These measures are necessary for infection control, but they are not helpful for the treatment of psychiatric disorders. Treatment consists, in part, of getting patients out of their rooms and involved in therapeutic activities in a milieu that removes them from the usual stresses of their daily lives. How insurance companies will respond to any need for extra days is one more concern to throw into the mix.
Paul Summergrad, MD, chairman of psychiatry at Tufts University in Boston, has been very interested in what facilities around the world have been doing. “In Washington state, after the nursing home infections, they sent home over a hundred staff members who had been exposed. In Hong Kong, the psychiatric hospitals have limited how patients circulate on the units even if no one is infected; this is not something that would go over well in the U.S.,” he said in an interview. Dr. Summergrad believes that higher death rates are seen in countries with higher smoking rates, and patients with psychiatric disorders are more likely to smoke than the general public, possibly placing them at higher risk for more severe morbidity and mortality.
Patrick Triplett, MD, clinical director of the department of psychiatry at Johns Hopkins University in Baltimore, communicated with me about their plans to manage a scenario in which a patient becomes ill on a psychiatry unit.
“If we think a patient might be infected, we will isolate them in a room with a closed door (We would need to account for their psychiatric needs as well during this period, say constant observation, for example.) and call the centralized command center, where the Hospital Epidemiology and Infection Control (HEIC) team gets involved. They will determine if the patient should be tested for COVID-19. If it’s determined that the patient is infected, they will likely be transferred to a floor with negative pressure rooms. We would coordinate psychiatric nursing needs with the receiving unit, based on the patient’s clinical needs.”
Dr. Triplett elaborated on the exposure of staff and visitors. “We take our lead on postexposure management from [HEIC] and Occupational Health. There are procedures in place for environmental cleaning, waste, linens, etc. The [Centers for Disease Control and Prevention] has guidelines on work restrictions for staff who have cared for patients with confirmed COVID-19, and HEIC helps determine the provider’s risk category. We would also involve them in determining risk levels and management for other patients on the floor and visitors. But prior to any known exposure, we are already limiting visitors for patients per the governor’s mandate of only one adult visitor per patient.”
The next couple of weeks will be telling, and as we readjust to a life of social distancing, it is certain to be a challenge to keep ourselves and our patients safe, healthy, and emotionally strong.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
For weeks now, the coronavirus epidemic has monopolized the media. As cases of COVID-19 have crossed borders and then oceans, the pandemic has caused fear and anxiety as Americans struggle with the uncertain nature of this highly contagious disease. Those exposed may be infectious before they are symptomatic, and the expression of the virus varies greatly: Some people have a mild illness and others quickly progress to severe pulmonary disease with a bilateral interstitial pneumonia that requires intubation and respiratory support. So far, the number of people infected and the absolute mortality is a fraction of what we have seen with this year’s seasonal flu, but in countries where the virus has spread quickly, medical systems have not been able to keep up with demand for high-intensity care and mortality rates have been many times higher than that of the flu. Italy, in particular, has not been able to halt the spread, even with the entire country on lockdown, and the medical system has been overwhelmed, resulting in rationing of care and many deaths.
COVID-19 represents a new challenge for the inpatient psychiatry unit. Some patients on an acute psychiatric unit may be agitated, uncooperative, or even violent, and it’s not hard to imagine the distress of anyone who has a patient spit on them as we’re all trying to remember not to shake hands. Inevitably, there will be patients who present for psychiatric admission with no respiratory symptoms, who are admitted and then become ill and are diagnosed with COVID-19. In the meantime, the potential is there for contagion to other patients on the unit, the hospital staff, and visitors to the unit.
While many hospital units treat infectious patients, the issues with psychiatry are different; psychiatry units are not set up to have aggressive infection control, staff and patients don’t typically wear protective gear, and people with psychiatric illnesses are ambulatory and interactive. The treatment of psychiatric illnesses involves more – not less – social interaction and patients attend groups and occupational therapy sessions; they dine in communal areas and watch television together in day rooms. Cell phones are typically not permitted for issues of privacy, and patients may use communal telephones. Patients who are very ill with psychiatric disorders may resist hygiene measures, and they may intrude on the personal space of others.
Patients with known COVID-19 can be isolated or transferred to another unit if more intensive medical care is necessary, but by that time, others have been exposed and potentially infected. How to contain this potential risk has been a topic of concern for psychiatric units everywhere. Following a potential or confirmed exposure, it’s not completely clear who should be sent home for self-quarantine: Do the staff who have had contact with the patient leave for 2 weeks, and if so, is there enough staff to replace them? Do they continue to work with protective equipment and leave only if they become symptomatic and test positive? Do staff remain at the hospital, or do they go home at night, potentially infecting those on public transportation and their family members? Presumably new patients would not be admitted to the unit, but our psychiatric system is taxed already with a lack of available beds.
In South Korea, patients and staff at the Daenam hospital reportedly faced this exact scenario. The hospital was locked down and 101 patients in the psychiatric facility developed COVID-19; 7 of those patients died, an outcome we hope to never see again. As of this writing, there are two patients on a 22-bed geropsychiatric unit at the UW Medical Center – Northwest in Seattle who developed COVID-19 after they were admitted to the unit. They have been isolated, and the rest of the patients on the unit have been quarantined. The staff are now wearing masks, gowns, and gloves.
“We started precautions for all 22 patients. ... We instituted our protocols for every room around, donning and doffing personal protective equipment (PPE). We had conversations with their family members,” said Santiago Neme, MD, MPH, an infectious disease physician at UW Medical Center – Northwest, in a press conference released by the university. “The patients were transferred and both remain stable. All patients on the unit were tested even though there were no concerning symptoms.”
These measures are necessary for infection control, but they are not helpful for the treatment of psychiatric disorders. Treatment consists, in part, of getting patients out of their rooms and involved in therapeutic activities in a milieu that removes them from the usual stresses of their daily lives. How insurance companies will respond to any need for extra days is one more concern to throw into the mix.
Paul Summergrad, MD, chairman of psychiatry at Tufts University in Boston, has been very interested in what facilities around the world have been doing. “In Washington state, after the nursing home infections, they sent home over a hundred staff members who had been exposed. In Hong Kong, the psychiatric hospitals have limited how patients circulate on the units even if no one is infected; this is not something that would go over well in the U.S.,” he said in an interview. Dr. Summergrad believes that higher death rates are seen in countries with higher smoking rates, and patients with psychiatric disorders are more likely to smoke than the general public, possibly placing them at higher risk for more severe morbidity and mortality.
Patrick Triplett, MD, clinical director of the department of psychiatry at Johns Hopkins University in Baltimore, communicated with me about their plans to manage a scenario in which a patient becomes ill on a psychiatry unit.
“If we think a patient might be infected, we will isolate them in a room with a closed door (We would need to account for their psychiatric needs as well during this period, say constant observation, for example.) and call the centralized command center, where the Hospital Epidemiology and Infection Control (HEIC) team gets involved. They will determine if the patient should be tested for COVID-19. If it’s determined that the patient is infected, they will likely be transferred to a floor with negative pressure rooms. We would coordinate psychiatric nursing needs with the receiving unit, based on the patient’s clinical needs.”
Dr. Triplett elaborated on the exposure of staff and visitors. “We take our lead on postexposure management from [HEIC] and Occupational Health. There are procedures in place for environmental cleaning, waste, linens, etc. The [Centers for Disease Control and Prevention] has guidelines on work restrictions for staff who have cared for patients with confirmed COVID-19, and HEIC helps determine the provider’s risk category. We would also involve them in determining risk levels and management for other patients on the floor and visitors. But prior to any known exposure, we are already limiting visitors for patients per the governor’s mandate of only one adult visitor per patient.”
The next couple of weeks will be telling, and as we readjust to a life of social distancing, it is certain to be a challenge to keep ourselves and our patients safe, healthy, and emotionally strong.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
Is anxiety about the coronavirus out of proportion?
A number of years ago, a patient I was treating mentioned that she was not eating tomatoes. There had been stories in the news about people contracting bacterial infections from tomatoes, but I paused for a moment, then asked her: “Have there been any contaminated tomatoes here in Maryland?” There had not been and I was still happily eating salsa, but my patient thought about this differently: If disease-causing tomatoes were to come to our state, someone would be the first person to become ill. She did not want to take any risks. My patient, however, was a heavy smoker and already grappling with health issues that were caused by smoking, so I found her choice of what she should worry about and how it influenced her behavior to be perplexing. I realize it’s not the same; nicotine is an addiction, while tomatoes remain a choice for most of us, and it’s common for people to worry about very unlikely events even when we are surrounded by very real and statistically more probable threats to our well-being.
Today’s news reports are filled with stories about 2019 Novel Coronavirus (2019-nCoV), an illness that started in Wuhan, China; as of Jan. 31, 2020, there were 9,776 confirmed cases and 213 deaths. There have been an additional 118 cases reported outside of mainland China, including 6 in the United States, and no one outside of China has died.
The response to the virus has been remarkable: Wuhan, a city of more than 11 million inhabitants, is on lockdown, as are 15 other cities in China; 46 million people have been affected, the largest quarantine in human history. Travel is restricted in parts of China, airports all over the world are screening those who fly in from Wuhan, foreign governments are bringing their citizens home from Wuhan, and even Starbucks has temporarily closed half its stores in China. The economics of containing this virus are astounding.
In the meantime, the Centers for Disease Control and Prevention reports that, as of the week of Jan. 25, there have been 19 million cases of the flu in the United States. Of those stricken, 180,000 people have been hospitalized and 10,000 have died, including 68 pediatric patients. No cities are on lockdown, public transportation runs as usual, airports don’t screen passengers for flu symptoms, and Starbucks continues to serve vanilla lattes to any willing customer. Anxiety about illness is not new; we’ve seen it with SARS, Ebola, measles, and even around Chipotle’s food poisoning cases – to name just a few recent scares. We have also seen a lot of media on vaping-related deaths, and as of early January 2020, vaping-related illnesses affected 2,602 people with 59 deaths. It has been a topic of discussion among legislators, with an emphasis on either outlawing the flavoring that might appeal to younger people or simply outlawing e-cigarettes. No one, however, is talking about outlawing regular cigarettes, despite the fact that many people have switched from cigarettes to vaping products as a way to quit smoking. So, while vaping has caused 59 deaths since 2018, cigarettes are responsible for 480,000 fatalities a year in the United States and smokers live, on average, 10 years less than nonsmokers.
So what fuels anxiety about the latest health scare, and why aren’t we more anxious about the more common causes of premature mortality? Certainly, the newness and the unknown are factors in the coronavirus scare. It’s not certain how this illness was introduced into the human population, although one theory is that it started with the consumption of bats who carry the virus. It’s spreading fast, and in some people, it has been lethal. The incubation period is not known, or whether it is contagious before symptoms appear. Coronavirus is getting a lot of public health attention and the World Health Organization just announced that the virus is a public health emergency of international concern. On the televised news on Jan. 29, 2020, coronavirus was the top story in the United States, even though an impeachment trial is in progress for our country’s president.
The public health response of locking down cities may help contain the outbreak and prevent a global epidemic, although millions of people had already left Wuhan, so the heavy-handed attempt to prevent spread of the virus may well be too late. In the case of the Ebola virus – a much more lethal disease that was also thought to be introduced by bats – public health measures certainly curtailed global spread, and the epidemic of 2014-2016 was limited to 28,600 cases and 11,325 deaths, nearly all of them in West Africa.
Most of the things that cause people to die are not new and are not topics the media chooses to sensationalize. Dissemination of news has changed over the decades, with so much more of it, instant reports on social media, and competition for viewers that leads journalists to pull at our emotions. And while we may, or may not, get flu shots and avoid those who have the flu, how and where we position both our anxiety and our resources does not always make sense. Certainly some people are predisposed to worry about both common and uncommon dangers, while others seem never to worry and engage in acts that many of us would consider dangerous. If we are looking for logic, it may be hard to find – there are those who would happily go bungee jumping but wouldn’t dream of leaving the house out without hand sanitizer.
The repercussions from this massive response to the Wuhan coronavirus are significant. For the millions of people on lockdown in China, each day gets emotionally harder; some may begin to have issues procuring food, and the financial losses for the economy will be significant. It’s not really possible to know yet if this response is warranted; we do know that infectious diseases can kill millions. The AIDS pandemic has taken the lives of 36 million people since 1981, and the influenza pandemic of 1918 resulted in an estimated 20 million to 50 million deaths after infecting 500 million people. Still, one might wonder if other, more mundane causes of morbidity and mortality – the ones that no longer garner our dread or make it to the front pages – might also be worthy of more hype and resources.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
A number of years ago, a patient I was treating mentioned that she was not eating tomatoes. There had been stories in the news about people contracting bacterial infections from tomatoes, but I paused for a moment, then asked her: “Have there been any contaminated tomatoes here in Maryland?” There had not been and I was still happily eating salsa, but my patient thought about this differently: If disease-causing tomatoes were to come to our state, someone would be the first person to become ill. She did not want to take any risks. My patient, however, was a heavy smoker and already grappling with health issues that were caused by smoking, so I found her choice of what she should worry about and how it influenced her behavior to be perplexing. I realize it’s not the same; nicotine is an addiction, while tomatoes remain a choice for most of us, and it’s common for people to worry about very unlikely events even when we are surrounded by very real and statistically more probable threats to our well-being.
Today’s news reports are filled with stories about 2019 Novel Coronavirus (2019-nCoV), an illness that started in Wuhan, China; as of Jan. 31, 2020, there were 9,776 confirmed cases and 213 deaths. There have been an additional 118 cases reported outside of mainland China, including 6 in the United States, and no one outside of China has died.
The response to the virus has been remarkable: Wuhan, a city of more than 11 million inhabitants, is on lockdown, as are 15 other cities in China; 46 million people have been affected, the largest quarantine in human history. Travel is restricted in parts of China, airports all over the world are screening those who fly in from Wuhan, foreign governments are bringing their citizens home from Wuhan, and even Starbucks has temporarily closed half its stores in China. The economics of containing this virus are astounding.
In the meantime, the Centers for Disease Control and Prevention reports that, as of the week of Jan. 25, there have been 19 million cases of the flu in the United States. Of those stricken, 180,000 people have been hospitalized and 10,000 have died, including 68 pediatric patients. No cities are on lockdown, public transportation runs as usual, airports don’t screen passengers for flu symptoms, and Starbucks continues to serve vanilla lattes to any willing customer. Anxiety about illness is not new; we’ve seen it with SARS, Ebola, measles, and even around Chipotle’s food poisoning cases – to name just a few recent scares. We have also seen a lot of media on vaping-related deaths, and as of early January 2020, vaping-related illnesses affected 2,602 people with 59 deaths. It has been a topic of discussion among legislators, with an emphasis on either outlawing the flavoring that might appeal to younger people or simply outlawing e-cigarettes. No one, however, is talking about outlawing regular cigarettes, despite the fact that many people have switched from cigarettes to vaping products as a way to quit smoking. So, while vaping has caused 59 deaths since 2018, cigarettes are responsible for 480,000 fatalities a year in the United States and smokers live, on average, 10 years less than nonsmokers.
So what fuels anxiety about the latest health scare, and why aren’t we more anxious about the more common causes of premature mortality? Certainly, the newness and the unknown are factors in the coronavirus scare. It’s not certain how this illness was introduced into the human population, although one theory is that it started with the consumption of bats who carry the virus. It’s spreading fast, and in some people, it has been lethal. The incubation period is not known, or whether it is contagious before symptoms appear. Coronavirus is getting a lot of public health attention and the World Health Organization just announced that the virus is a public health emergency of international concern. On the televised news on Jan. 29, 2020, coronavirus was the top story in the United States, even though an impeachment trial is in progress for our country’s president.
The public health response of locking down cities may help contain the outbreak and prevent a global epidemic, although millions of people had already left Wuhan, so the heavy-handed attempt to prevent spread of the virus may well be too late. In the case of the Ebola virus – a much more lethal disease that was also thought to be introduced by bats – public health measures certainly curtailed global spread, and the epidemic of 2014-2016 was limited to 28,600 cases and 11,325 deaths, nearly all of them in West Africa.
Most of the things that cause people to die are not new and are not topics the media chooses to sensationalize. Dissemination of news has changed over the decades, with so much more of it, instant reports on social media, and competition for viewers that leads journalists to pull at our emotions. And while we may, or may not, get flu shots and avoid those who have the flu, how and where we position both our anxiety and our resources does not always make sense. Certainly some people are predisposed to worry about both common and uncommon dangers, while others seem never to worry and engage in acts that many of us would consider dangerous. If we are looking for logic, it may be hard to find – there are those who would happily go bungee jumping but wouldn’t dream of leaving the house out without hand sanitizer.
The repercussions from this massive response to the Wuhan coronavirus are significant. For the millions of people on lockdown in China, each day gets emotionally harder; some may begin to have issues procuring food, and the financial losses for the economy will be significant. It’s not really possible to know yet if this response is warranted; we do know that infectious diseases can kill millions. The AIDS pandemic has taken the lives of 36 million people since 1981, and the influenza pandemic of 1918 resulted in an estimated 20 million to 50 million deaths after infecting 500 million people. Still, one might wonder if other, more mundane causes of morbidity and mortality – the ones that no longer garner our dread or make it to the front pages – might also be worthy of more hype and resources.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
A number of years ago, a patient I was treating mentioned that she was not eating tomatoes. There had been stories in the news about people contracting bacterial infections from tomatoes, but I paused for a moment, then asked her: “Have there been any contaminated tomatoes here in Maryland?” There had not been and I was still happily eating salsa, but my patient thought about this differently: If disease-causing tomatoes were to come to our state, someone would be the first person to become ill. She did not want to take any risks. My patient, however, was a heavy smoker and already grappling with health issues that were caused by smoking, so I found her choice of what she should worry about and how it influenced her behavior to be perplexing. I realize it’s not the same; nicotine is an addiction, while tomatoes remain a choice for most of us, and it’s common for people to worry about very unlikely events even when we are surrounded by very real and statistically more probable threats to our well-being.
Today’s news reports are filled with stories about 2019 Novel Coronavirus (2019-nCoV), an illness that started in Wuhan, China; as of Jan. 31, 2020, there were 9,776 confirmed cases and 213 deaths. There have been an additional 118 cases reported outside of mainland China, including 6 in the United States, and no one outside of China has died.
The response to the virus has been remarkable: Wuhan, a city of more than 11 million inhabitants, is on lockdown, as are 15 other cities in China; 46 million people have been affected, the largest quarantine in human history. Travel is restricted in parts of China, airports all over the world are screening those who fly in from Wuhan, foreign governments are bringing their citizens home from Wuhan, and even Starbucks has temporarily closed half its stores in China. The economics of containing this virus are astounding.
In the meantime, the Centers for Disease Control and Prevention reports that, as of the week of Jan. 25, there have been 19 million cases of the flu in the United States. Of those stricken, 180,000 people have been hospitalized and 10,000 have died, including 68 pediatric patients. No cities are on lockdown, public transportation runs as usual, airports don’t screen passengers for flu symptoms, and Starbucks continues to serve vanilla lattes to any willing customer. Anxiety about illness is not new; we’ve seen it with SARS, Ebola, measles, and even around Chipotle’s food poisoning cases – to name just a few recent scares. We have also seen a lot of media on vaping-related deaths, and as of early January 2020, vaping-related illnesses affected 2,602 people with 59 deaths. It has been a topic of discussion among legislators, with an emphasis on either outlawing the flavoring that might appeal to younger people or simply outlawing e-cigarettes. No one, however, is talking about outlawing regular cigarettes, despite the fact that many people have switched from cigarettes to vaping products as a way to quit smoking. So, while vaping has caused 59 deaths since 2018, cigarettes are responsible for 480,000 fatalities a year in the United States and smokers live, on average, 10 years less than nonsmokers.
So what fuels anxiety about the latest health scare, and why aren’t we more anxious about the more common causes of premature mortality? Certainly, the newness and the unknown are factors in the coronavirus scare. It’s not certain how this illness was introduced into the human population, although one theory is that it started with the consumption of bats who carry the virus. It’s spreading fast, and in some people, it has been lethal. The incubation period is not known, or whether it is contagious before symptoms appear. Coronavirus is getting a lot of public health attention and the World Health Organization just announced that the virus is a public health emergency of international concern. On the televised news on Jan. 29, 2020, coronavirus was the top story in the United States, even though an impeachment trial is in progress for our country’s president.
The public health response of locking down cities may help contain the outbreak and prevent a global epidemic, although millions of people had already left Wuhan, so the heavy-handed attempt to prevent spread of the virus may well be too late. In the case of the Ebola virus – a much more lethal disease that was also thought to be introduced by bats – public health measures certainly curtailed global spread, and the epidemic of 2014-2016 was limited to 28,600 cases and 11,325 deaths, nearly all of them in West Africa.
Most of the things that cause people to die are not new and are not topics the media chooses to sensationalize. Dissemination of news has changed over the decades, with so much more of it, instant reports on social media, and competition for viewers that leads journalists to pull at our emotions. And while we may, or may not, get flu shots and avoid those who have the flu, how and where we position both our anxiety and our resources does not always make sense. Certainly some people are predisposed to worry about both common and uncommon dangers, while others seem never to worry and engage in acts that many of us would consider dangerous. If we are looking for logic, it may be hard to find – there are those who would happily go bungee jumping but wouldn’t dream of leaving the house out without hand sanitizer.
The repercussions from this massive response to the Wuhan coronavirus are significant. For the millions of people on lockdown in China, each day gets emotionally harder; some may begin to have issues procuring food, and the financial losses for the economy will be significant. It’s not really possible to know yet if this response is warranted; we do know that infectious diseases can kill millions. The AIDS pandemic has taken the lives of 36 million people since 1981, and the influenza pandemic of 1918 resulted in an estimated 20 million to 50 million deaths after infecting 500 million people. Still, one might wonder if other, more mundane causes of morbidity and mortality – the ones that no longer garner our dread or make it to the front pages – might also be worthy of more hype and resources.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
The suicide wars
Topic of suicide prevention causing divisions within psychiatry
At every swipe through my social media feeds, I’m greeted with another topic that has advocates clustered at the extremes. People align, and they align quickly in our strangely polarized world in which anyone who might sit in the middle lies low.
It seems we’re divided: On the left you are a CNN fan or you’re one of those soulless monsters who tunes in to Fox News. You’re pro-life or you’re a baby killer, advocating for late-term abortions or even the execution of live infants. When it comes to firearm regulation, one side says you’re a threat to the Constitution, while the other says that those opposed are responsible for the death of every person who was ever the victim of a discharged firearm. And those who feel strongly about a given topic often justify their attacks on those who disagree. Psychiatry is no stranger to this thinking, and we are the only medical specialty with organized “antipsychiatry” groups who oppose our work. I have been a bit surprised, however, that the topic of suicide prevention is one that has us divided within our own specialty.
Amy Barnhorst, MD, is a psychiatrist at the University of California, Davis, and the author of “The empty promise of suicide prevention: Many of the problems that lead people to kill themselves cannot be fixed with a little serotonin,” an op-ed piece that appeared in the New York Times on April 26, 2019. Dr. Barnhorst began her essay with the story of a patient who was hospitalized after a relative realized she was planning her suicide. That story had an ending that psychiatrists relish: A person with previously unrecognized and untreated bipolar disorder received care, including medication, and got better. This suicide was preventable, a life was saved, and this story followed a model we all hope is being replicated over and over.
Dr. Barnhorst went on to say that this was an outlier in her career, that most of the suicidal patients she sees are impoverished, homeless, addicted, and she wrote about how little the treatment setting has to offer: The idea that a pill would fix these problems is almost laughable. She suggests that there is more to suicide prevention than identifying prospective patients and getting them acute psychiatric care.
The decision to stop living is one that people arrive at by different paths, some over months, but many in a matter of minutes. Those people won’t be intercepted by the mental health system. We certainly need more psychiatric services and more research into better, faster-acting treatments for severe depression and suicidal thoughts, but that will never be enough.
We need to address the root causes of our nation’s suicide problem – poverty, homelessness, and the accompanying exposure to trauma, crime, and drugs. That means better alcohol and drug treatment, family counseling, low-income housing resources, job training, and individual therapy. And for those at risk who still slip past all the checkpoints, we need to make sure they don’t have access to guns and lethal medications.
Psychological autopsies done after suicides have indicated that more than 90% of people who die from suicide suffered from a mental illness, yet 54% of those who ended their own lives had never received a psychiatric diagnosis. There is a hopefulness that, if only we had more – more services, more therapy, more medication – then we could prevent suicide. Unfortunately, this line of thinking, with a “Zero Suicide” initiative, points a finger at those who survive: Suicide is preventable, so someone is to blame, if not a family member for missing the warning signs then the clinician who offered treatment that wasn’t good enough.
Along this line, the New York Times printed another opinion piece on Jan. 6 by Richard A. Friedman, MD, titled, “Why are young Americans killing themselves?” Dr. Friedman’s conclusion was more along the psychiatrist party line: “The good news is that we don’t have to wait for all the answers to know what to do. We know that various psychotherapies and medication are highly effective in treating depression. We just need to do a better job of identifying, reaching out to and providing resources for at-risk youths.”
Dr. Friedman goes on to propose universal screening at school, among other measures to identify those at risk. It is no surprise that Dr. Friedman’s article had more than 1,700 comments before commenting was closed by the Times. I have written about the pros and cons of screening adolescents for depression in a primary care setting, so putting the responsibility of identifying suicidal teenagers on school teachers seems like an ominous responsibility to add to a teacher’s obligations.
I did not read Dr. Barnhorst’s earlier op-ed piece as a condemnation of psychiatric care, but rather as a call to action and a reality check on the idea that psychiatry is the only answer to our suicide epidemic. More people than ever get treatment – from psychiatrists, from primary care doctors, from nonphysician prescribing clinicians, and from so many varieties of psychotherapists, and yet our suicide rates continue to rise.
In a post on the Psychology Today website, Sara Gorman, PhD, and Jack M. Gorman, MD, discussed Dr. Barnhorst’s article. “In the process of making her point, Barnhorst also manages to seriously trivialize the role of antidepressant medication in the treatment of depression and to imply that, given societal woes, there isn’t much we can do to try to prevent suicides – aside from limiting access to lethal means,” they wrote.
The Gormans were not alone in their objections; the day after the op-ed appeared in the New York Times, a well-respected psychiatry department chairman took on not just the content of the op-ed, but also the author, in his Twitter feed. He wrote, “@amybarnhorst doesn’t read scientific literature or skipped training. this article is wrong. #suicide is largely preventable, if proper measures taken n Rx provided. @nytimes please vet authors better @APAPsychiatric.” Dr. Barnhorst, also a voice on Twitter, added the wry response, “I skipped training.” When Twitter users responded that initial Twitter comment conveyed a lack of civility toward a colleague, the original Tweeter – I’m withholding his name with the hope that even writing about these interactions won’t put me on anyone’s enemy list – like many others sitting on the poles of these contentious topics, responded with the following, “All for civility except in the case of misinformation that puts lives at risk, especially when purveyed by a professional who wears the patina of credibility.”
If it’s not yet obvious, I don’t believe there is a simple answer to our suicide problem, nor do I think it puts lives at risk to point out that, so far, our treatments have not lowered suicide rates. The issue is complex and we have no perfect explanation as to why countries differ so greatly with regard to suicide. There are impoverished, war-torn countries with remarkably lower suicide rates, and nations with much stricter gun laws that have higher statistics. Honduras, deemed “the murder capital of the world,” has an enviable suicide rate of only 2.9 per 100,000.
If the solution were as simple as making medications more accessible, the answer might be an easy one (or at least worth trying) – make antidepressants available over-the-counter, a move that would both increase access and decrease stigma.
Some people are determined to end their own lives. They aren’t looking to see psychiatrists or to call hotlines, and they may well resort to an alternate method if any given one is not readily available. For these individuals, suicide may not be preventable, and we may be left to say that this tragic phenomena with its diverse causes should also lead us to explore the root causes of human misery and our cultural features that lead some people to end their own lives while others endure.
Clearly, there are those who have untreated psychiatric illnesses and who make impulsive and lethal decisions – access to care and means restrictions certainly save some lives. And while it is obvious to us as psychiatrists that anyone who is depressed or is having suicidal thoughts is deserving of a psychiatric evaluation and intervention, the truth remains that access to treatment in this country is limited by finances, by the availability of mental health professionals, and by stigma and shame. In the end, The one thing I am certain of is that our efforts to prevent suicide should unite, and not fracture, our profession.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
Topic of suicide prevention causing divisions within psychiatry
Topic of suicide prevention causing divisions within psychiatry
At every swipe through my social media feeds, I’m greeted with another topic that has advocates clustered at the extremes. People align, and they align quickly in our strangely polarized world in which anyone who might sit in the middle lies low.
It seems we’re divided: On the left you are a CNN fan or you’re one of those soulless monsters who tunes in to Fox News. You’re pro-life or you’re a baby killer, advocating for late-term abortions or even the execution of live infants. When it comes to firearm regulation, one side says you’re a threat to the Constitution, while the other says that those opposed are responsible for the death of every person who was ever the victim of a discharged firearm. And those who feel strongly about a given topic often justify their attacks on those who disagree. Psychiatry is no stranger to this thinking, and we are the only medical specialty with organized “antipsychiatry” groups who oppose our work. I have been a bit surprised, however, that the topic of suicide prevention is one that has us divided within our own specialty.
Amy Barnhorst, MD, is a psychiatrist at the University of California, Davis, and the author of “The empty promise of suicide prevention: Many of the problems that lead people to kill themselves cannot be fixed with a little serotonin,” an op-ed piece that appeared in the New York Times on April 26, 2019. Dr. Barnhorst began her essay with the story of a patient who was hospitalized after a relative realized she was planning her suicide. That story had an ending that psychiatrists relish: A person with previously unrecognized and untreated bipolar disorder received care, including medication, and got better. This suicide was preventable, a life was saved, and this story followed a model we all hope is being replicated over and over.
Dr. Barnhorst went on to say that this was an outlier in her career, that most of the suicidal patients she sees are impoverished, homeless, addicted, and she wrote about how little the treatment setting has to offer: The idea that a pill would fix these problems is almost laughable. She suggests that there is more to suicide prevention than identifying prospective patients and getting them acute psychiatric care.
The decision to stop living is one that people arrive at by different paths, some over months, but many in a matter of minutes. Those people won’t be intercepted by the mental health system. We certainly need more psychiatric services and more research into better, faster-acting treatments for severe depression and suicidal thoughts, but that will never be enough.
We need to address the root causes of our nation’s suicide problem – poverty, homelessness, and the accompanying exposure to trauma, crime, and drugs. That means better alcohol and drug treatment, family counseling, low-income housing resources, job training, and individual therapy. And for those at risk who still slip past all the checkpoints, we need to make sure they don’t have access to guns and lethal medications.
Psychological autopsies done after suicides have indicated that more than 90% of people who die from suicide suffered from a mental illness, yet 54% of those who ended their own lives had never received a psychiatric diagnosis. There is a hopefulness that, if only we had more – more services, more therapy, more medication – then we could prevent suicide. Unfortunately, this line of thinking, with a “Zero Suicide” initiative, points a finger at those who survive: Suicide is preventable, so someone is to blame, if not a family member for missing the warning signs then the clinician who offered treatment that wasn’t good enough.
Along this line, the New York Times printed another opinion piece on Jan. 6 by Richard A. Friedman, MD, titled, “Why are young Americans killing themselves?” Dr. Friedman’s conclusion was more along the psychiatrist party line: “The good news is that we don’t have to wait for all the answers to know what to do. We know that various psychotherapies and medication are highly effective in treating depression. We just need to do a better job of identifying, reaching out to and providing resources for at-risk youths.”
Dr. Friedman goes on to propose universal screening at school, among other measures to identify those at risk. It is no surprise that Dr. Friedman’s article had more than 1,700 comments before commenting was closed by the Times. I have written about the pros and cons of screening adolescents for depression in a primary care setting, so putting the responsibility of identifying suicidal teenagers on school teachers seems like an ominous responsibility to add to a teacher’s obligations.
I did not read Dr. Barnhorst’s earlier op-ed piece as a condemnation of psychiatric care, but rather as a call to action and a reality check on the idea that psychiatry is the only answer to our suicide epidemic. More people than ever get treatment – from psychiatrists, from primary care doctors, from nonphysician prescribing clinicians, and from so many varieties of psychotherapists, and yet our suicide rates continue to rise.
In a post on the Psychology Today website, Sara Gorman, PhD, and Jack M. Gorman, MD, discussed Dr. Barnhorst’s article. “In the process of making her point, Barnhorst also manages to seriously trivialize the role of antidepressant medication in the treatment of depression and to imply that, given societal woes, there isn’t much we can do to try to prevent suicides – aside from limiting access to lethal means,” they wrote.
The Gormans were not alone in their objections; the day after the op-ed appeared in the New York Times, a well-respected psychiatry department chairman took on not just the content of the op-ed, but also the author, in his Twitter feed. He wrote, “@amybarnhorst doesn’t read scientific literature or skipped training. this article is wrong. #suicide is largely preventable, if proper measures taken n Rx provided. @nytimes please vet authors better @APAPsychiatric.” Dr. Barnhorst, also a voice on Twitter, added the wry response, “I skipped training.” When Twitter users responded that initial Twitter comment conveyed a lack of civility toward a colleague, the original Tweeter – I’m withholding his name with the hope that even writing about these interactions won’t put me on anyone’s enemy list – like many others sitting on the poles of these contentious topics, responded with the following, “All for civility except in the case of misinformation that puts lives at risk, especially when purveyed by a professional who wears the patina of credibility.”
If it’s not yet obvious, I don’t believe there is a simple answer to our suicide problem, nor do I think it puts lives at risk to point out that, so far, our treatments have not lowered suicide rates. The issue is complex and we have no perfect explanation as to why countries differ so greatly with regard to suicide. There are impoverished, war-torn countries with remarkably lower suicide rates, and nations with much stricter gun laws that have higher statistics. Honduras, deemed “the murder capital of the world,” has an enviable suicide rate of only 2.9 per 100,000.
If the solution were as simple as making medications more accessible, the answer might be an easy one (or at least worth trying) – make antidepressants available over-the-counter, a move that would both increase access and decrease stigma.
Some people are determined to end their own lives. They aren’t looking to see psychiatrists or to call hotlines, and they may well resort to an alternate method if any given one is not readily available. For these individuals, suicide may not be preventable, and we may be left to say that this tragic phenomena with its diverse causes should also lead us to explore the root causes of human misery and our cultural features that lead some people to end their own lives while others endure.
Clearly, there are those who have untreated psychiatric illnesses and who make impulsive and lethal decisions – access to care and means restrictions certainly save some lives. And while it is obvious to us as psychiatrists that anyone who is depressed or is having suicidal thoughts is deserving of a psychiatric evaluation and intervention, the truth remains that access to treatment in this country is limited by finances, by the availability of mental health professionals, and by stigma and shame. In the end, The one thing I am certain of is that our efforts to prevent suicide should unite, and not fracture, our profession.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
At every swipe through my social media feeds, I’m greeted with another topic that has advocates clustered at the extremes. People align, and they align quickly in our strangely polarized world in which anyone who might sit in the middle lies low.
It seems we’re divided: On the left you are a CNN fan or you’re one of those soulless monsters who tunes in to Fox News. You’re pro-life or you’re a baby killer, advocating for late-term abortions or even the execution of live infants. When it comes to firearm regulation, one side says you’re a threat to the Constitution, while the other says that those opposed are responsible for the death of every person who was ever the victim of a discharged firearm. And those who feel strongly about a given topic often justify their attacks on those who disagree. Psychiatry is no stranger to this thinking, and we are the only medical specialty with organized “antipsychiatry” groups who oppose our work. I have been a bit surprised, however, that the topic of suicide prevention is one that has us divided within our own specialty.
Amy Barnhorst, MD, is a psychiatrist at the University of California, Davis, and the author of “The empty promise of suicide prevention: Many of the problems that lead people to kill themselves cannot be fixed with a little serotonin,” an op-ed piece that appeared in the New York Times on April 26, 2019. Dr. Barnhorst began her essay with the story of a patient who was hospitalized after a relative realized she was planning her suicide. That story had an ending that psychiatrists relish: A person with previously unrecognized and untreated bipolar disorder received care, including medication, and got better. This suicide was preventable, a life was saved, and this story followed a model we all hope is being replicated over and over.
Dr. Barnhorst went on to say that this was an outlier in her career, that most of the suicidal patients she sees are impoverished, homeless, addicted, and she wrote about how little the treatment setting has to offer: The idea that a pill would fix these problems is almost laughable. She suggests that there is more to suicide prevention than identifying prospective patients and getting them acute psychiatric care.
The decision to stop living is one that people arrive at by different paths, some over months, but many in a matter of minutes. Those people won’t be intercepted by the mental health system. We certainly need more psychiatric services and more research into better, faster-acting treatments for severe depression and suicidal thoughts, but that will never be enough.
We need to address the root causes of our nation’s suicide problem – poverty, homelessness, and the accompanying exposure to trauma, crime, and drugs. That means better alcohol and drug treatment, family counseling, low-income housing resources, job training, and individual therapy. And for those at risk who still slip past all the checkpoints, we need to make sure they don’t have access to guns and lethal medications.
Psychological autopsies done after suicides have indicated that more than 90% of people who die from suicide suffered from a mental illness, yet 54% of those who ended their own lives had never received a psychiatric diagnosis. There is a hopefulness that, if only we had more – more services, more therapy, more medication – then we could prevent suicide. Unfortunately, this line of thinking, with a “Zero Suicide” initiative, points a finger at those who survive: Suicide is preventable, so someone is to blame, if not a family member for missing the warning signs then the clinician who offered treatment that wasn’t good enough.
Along this line, the New York Times printed another opinion piece on Jan. 6 by Richard A. Friedman, MD, titled, “Why are young Americans killing themselves?” Dr. Friedman’s conclusion was more along the psychiatrist party line: “The good news is that we don’t have to wait for all the answers to know what to do. We know that various psychotherapies and medication are highly effective in treating depression. We just need to do a better job of identifying, reaching out to and providing resources for at-risk youths.”
Dr. Friedman goes on to propose universal screening at school, among other measures to identify those at risk. It is no surprise that Dr. Friedman’s article had more than 1,700 comments before commenting was closed by the Times. I have written about the pros and cons of screening adolescents for depression in a primary care setting, so putting the responsibility of identifying suicidal teenagers on school teachers seems like an ominous responsibility to add to a teacher’s obligations.
I did not read Dr. Barnhorst’s earlier op-ed piece as a condemnation of psychiatric care, but rather as a call to action and a reality check on the idea that psychiatry is the only answer to our suicide epidemic. More people than ever get treatment – from psychiatrists, from primary care doctors, from nonphysician prescribing clinicians, and from so many varieties of psychotherapists, and yet our suicide rates continue to rise.
In a post on the Psychology Today website, Sara Gorman, PhD, and Jack M. Gorman, MD, discussed Dr. Barnhorst’s article. “In the process of making her point, Barnhorst also manages to seriously trivialize the role of antidepressant medication in the treatment of depression and to imply that, given societal woes, there isn’t much we can do to try to prevent suicides – aside from limiting access to lethal means,” they wrote.
The Gormans were not alone in their objections; the day after the op-ed appeared in the New York Times, a well-respected psychiatry department chairman took on not just the content of the op-ed, but also the author, in his Twitter feed. He wrote, “@amybarnhorst doesn’t read scientific literature or skipped training. this article is wrong. #suicide is largely preventable, if proper measures taken n Rx provided. @nytimes please vet authors better @APAPsychiatric.” Dr. Barnhorst, also a voice on Twitter, added the wry response, “I skipped training.” When Twitter users responded that initial Twitter comment conveyed a lack of civility toward a colleague, the original Tweeter – I’m withholding his name with the hope that even writing about these interactions won’t put me on anyone’s enemy list – like many others sitting on the poles of these contentious topics, responded with the following, “All for civility except in the case of misinformation that puts lives at risk, especially when purveyed by a professional who wears the patina of credibility.”
If it’s not yet obvious, I don’t believe there is a simple answer to our suicide problem, nor do I think it puts lives at risk to point out that, so far, our treatments have not lowered suicide rates. The issue is complex and we have no perfect explanation as to why countries differ so greatly with regard to suicide. There are impoverished, war-torn countries with remarkably lower suicide rates, and nations with much stricter gun laws that have higher statistics. Honduras, deemed “the murder capital of the world,” has an enviable suicide rate of only 2.9 per 100,000.
If the solution were as simple as making medications more accessible, the answer might be an easy one (or at least worth trying) – make antidepressants available over-the-counter, a move that would both increase access and decrease stigma.
Some people are determined to end their own lives. They aren’t looking to see psychiatrists or to call hotlines, and they may well resort to an alternate method if any given one is not readily available. For these individuals, suicide may not be preventable, and we may be left to say that this tragic phenomena with its diverse causes should also lead us to explore the root causes of human misery and our cultural features that lead some people to end their own lives while others endure.
Clearly, there are those who have untreated psychiatric illnesses and who make impulsive and lethal decisions – access to care and means restrictions certainly save some lives. And while it is obvious to us as psychiatrists that anyone who is depressed or is having suicidal thoughts is deserving of a psychiatric evaluation and intervention, the truth remains that access to treatment in this country is limited by finances, by the availability of mental health professionals, and by stigma and shame. In the end, The one thing I am certain of is that our efforts to prevent suicide should unite, and not fracture, our profession.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
The Great Pretender
Susannah Cahalan’s new book challenges an experiment that changed psychiatry
As an undergraduate psychology major, I was taught about the Rosenhan study in several of my courses. My professors lectured about the shocking findings psychologist David Rosenhan, PhD, documented in a 1973 Science article, “On Being Sane in Insane Places” and these findings lent themselves to lecture hall drama. Eight people presented to hospitals and said they heard voices saying: “empty, hollow, thud.” These “pseudopatients” exhibited no other psychiatric symptoms but were admitted, diagnosed with schizophrenia, and observations of their behavior were made. The charts included notes such as, “Patient exhibits writing behavior,” my professors said. The pseudopatients were kept for an average of 19 days, and one for as long as 51 days. The decades have passed, and there are many things I learned in college that I have since forgotten, but I remember “empty, hollow, thud,” and the famous Rosenhan experiment.
I was eager to read Susannah Cahalan’s book, “The Great Pretender” (Grand Central Publishing, 2019), which puts both Dr. Rosenhan and his pseudopatient study under a microscope. Ms. Cahalan is the author of the page-turner, Brain on Fire: My Month of Madness (Free Press, 2012), where she recounted her own struggle with a psychotic episode. Ms. Cahalan, a young reporter in New York City, became psychotic and then catatonic; her condition perplexed the neurologists who were treating her on an inpatient unit, and they were on the verge of transferring her to psychiatry when a diagnosis of anti-NMDA receptor encephalitis was suspected and then confirmed with a brain biopsy. Ms. Cahalan made a full recovery after treatment with steroids, intravenous immunoglobulin, and plasmapheresis. While Ms. Cahalan’s symptoms were classic for a severe psychotic disorder, there was reason to believe that this was not a primary psychiatric disorder: She was having grand mal seizures. Her book was a bestseller, and she has spoken widely to make others aware of this rare illness that masquerades as psychosis. I heard her speak at the opening session of the American Psychiatric Association’s annual meeting in May of 2017.“My family, like many families before them, fought against the tyranny of the mental illness label,” Ms. Cahalan writes at the very beginning of “The Great Pretender.” She goes on to talk about how psychiatry differs from other medical fields: It’s the only specialty where people can be treated against their will; psychiatry casts judgments on the person; mental illness is poorly defined – perhaps there is no clear divide between normal and mad; and psychiatric disorders are less “real” than other illnesses. Throughout the book she refers to psychiatrists as smug and arrogant.
Ms. Cahalan takes on the task of documenting the horrors of psychiatry’s often sordid history, starting with journalist Nellie Bly’s 1887 journey into to a psychiatric facility to expose the abuses there. Certainly, psychiatry’s history is sordid. Ms. Cahalan talks about inhumane conditions in overcrowded psychiatric hospitals, about our sad chapter of lobotomies, about the influence of psychoanalysis on diagnosis and treatment, and about how homosexuality was once an illness and now is not. She includes “One Flew Over the Cuckoo’s Nest,” “The Myth of Mental Illness,” big pharma, and the Goldwater fiasco. In her recounting of the history, it’s all bad. She mentions Benjamin Rush, MD, only once, as the creator of “ ‘... the tranquilizing chair’ (a case of the worst false advertising ever), a terrifying sensory-deprivation apparatus in which patients were strapped down to a chair with a wooden box placed over their heads to block stimulation, restrict movement, and reduce blood to the brain.” Dr. Rush’s role as the father of American psychiatry who challenged the belief that mental illness was the result of demonic possession, gets no mention. Nor does Ms. Cahalan note that he founded Pennsylvania Hospital, where moral and occupational therapy revolutionized the treatment of those with mental illness.
So there’s her story, her rendition of the history of American psychiatry, and through this she weaves in the story of the Rosenhan experiment.
“ ‘It all started out as a dare,’ Dr. Rosenhan told a local newspaper, ‘I was teaching psychology at Swarthmore, and my students were saying that the course was too conceptual and abstract. So I said, ‘Okay, if you really want to know what mental patients are like, become mental patients.’ ”
Really? I read this and wondered how a psychologist could talk about people who had been hospitalized with psychiatric disorders as though they were aliens. Certainly, some of these students, their family members, or their friends must have been hospitalized at some point. Yet all through, there is this sense that the patients are other, and the discovery of the undercover operation is that the patients are actually human beings! Dr. Rosenhan, who was one of the pseudopatients, goes on to conclude that the label is everything, that once labeled they are treated differently by the nurses in “cages” and the doctors who walk by and avert their gaze. A second man Ms. Cahalan named, also one of the pseudopatients, had a similar experience. A third subject she located was not included in the study: His experience was counter to the findings of the study, his time in the hospital was a positive, he found it comforting, and the experiences he had there had a lasting positive influence on his life.
Ms. Cahalan talks about the publication of “On Being Sane in Insane Places” as a study that was finally scientific, one that changed all of psychiatry, and was the driving force for the creation of the DSM-III and the closure of state hospitals. I wondered if it was as influential as Ms. Cahalan claims, and I asked some psychiatrists who were practicing in 1973 when the article was published. I wanted to know if this study rocked their world.
“At first, with the great amount of publicity the study generated, it was added fodder for the antipsychiatrists, including the Scientologists and Szaszians,” Steven Sharfstein, MD, a former president of the American Psychiatric Association, told me. “But as young psychiatrists in the trenches, business continued to boom, and we continued to do the best job we could with diagnosis, assessment of risk, involuntary commitment, and treatment. And from what I recall, morale was high in the 1970s. We had some new medications and psychotherapies, and there was community activism. Faking symptoms to gain admission seemed to be a no-brainer, but keeping people for long stays was more problematic.”
E. Fuller Torrey, MD, the founder of the Treatment Advocacy Center who worked for many years treating patients at St. Elizabeth’s Hospital, replied: “It is important to remember that this study was published at the height of the deinstitutionalization movement and quite likely accelerated it. As I recall, at the time it seemed odd that all eight patients claimed to have had similar experiences while hospitalized. I think the main effect of the study was to provide ammunition for the antipsychiatrists.”
Ms. Cahalan has bought into the antipsychiatry movement full force. It’s not until the very end that there is any acknowledgment that psychiatry ever helped anyone, and even then, it’s a bit begrudging. Worse, she neglects to mention that people with psychiatric disorders suffer because of their psychic pain; one could get through this book and believe that people with mental illness struggle only because they are labeled and then mistreated, and for someone who has suffered herself, she misses the essence of how awful it is to be ill, and that people are often helped by psychiatric treatments. When she finally adds a paragraph talking about the usefulness of psychotropics, it’s with a caveat. “But I’m not here to rail against the drugs. There are plenty of places you can get that perspective. I see that these drugs help many people lead full and meaningful lives. It would be folly to discount their worth. We also can’t deny that the situation is complicated.”
There are moments in the manuscript where I found it difficult to know what were Dr. Rosenhan’s interpretations and what were Ms. Callahan’s interpretations of Dr. Rosenhan’s experiences. A lot of assumptions are made – particularly about the motivations of the hospital staff – and I wasn’t always sure they were correct. For example, on his second day in the hospital, Dr. Rosenhan asked a nurse for the newspaper. When she tells him it hasn’t come yet, he concludes that the staff is keeping the newspapers from the patients. And when a staff member is initially chatty then later shuns Dr. Rosenhan, he concludes that the man initially mistook him for a psychiatrist because he looks professorial. Both Ms. Cahalan and Dr. Rosenhan approach psychiatry with biases, and they don’t always question their assumptions.
, a professor who didn’t treat patients. This intermixing of the two fields felt contrived to me, and gave too much credence to the idea that no one really knows sane from disordered, and everyone was embracing the antipsychiatry dogma. Surely, someone during the those years must have liked their psychiatrist.
That said, Ms. Cahalan does a phenomenal job of infiltrating the world of the late Dr. Rosenhan. She starts out enamored by him and by his finding that psychiatrists can’t tell real illness from faked disorder. She meets with his friends, his son, his colleagues, his students, and she flies all over the country to meet with those who can help her understand him. She gains access to his personal files and to the book he started to write about the experiment, then abandoned, which eventually resulted in a lawsuit by Doubleday to have the book’s advance returned. At one point, she even hires a private detective.
What is Ms. Cahalan looking for so desperately? She’s looking for these anonymous pseudopatients, the people who were admitted to these unnamed state hospitals, who made observations and took notes, who were diagnosed with schizophrenia and then finally released. She’s looking for the truth, and while she identifies Dr. Rosenhan and two other pseudopatients as people who faked their way into the hospital, she finds a mass of contradictions. The one pseudopatient was excluded from the study – he is the one who felt comforted by his time in the hospital. The other six pseudopatients could not be found, despite Ms. Cahalan’s heroic attempts. Furthermore, she found many inconsistencies in what Dr. Rosenhan reported, and his hospital notes revealed more than a presentation for voices saying “empty, hollow, thud.” He reported it had been going on for months, that he had put copper over his ears to block the sound, and that he felt suicidal.
Ultimately, Ms. Cahalan was left to conclude that the Rosenhan experiment was a lie, that the pseudopatients likely never existed and the article was a fabrication. She brings up other studies that have been proven to be fraudulent, and by this point, our faith in all of science is pretty shaken.
Ms. Cahalan took a long journey to get us to this place, one that spent a lot of effort in bashing psychiatry, finally concluding that, as a result of this fraudulent experiment, too many hospitals have been shuttered – leaving our sickest patients to the streets and to the jails – and that there are not enough mental health professionals. As a psychiatrist – one who is often willing to question our practices – I was distracted by the flagrant antipsychiatry sentiments. Reading past that, Ms. Cahalan’s remarkable detective work and creative intermingling of the Rosenhan experiment layered on the history of psychiatry, further layered on her own experience with psychosis, makes for an amazing story. The Rosenhan study may have rocked the world of psychiatry; the fact that it was fabricated should rock us even more.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
Susannah Cahalan’s new book challenges an experiment that changed psychiatry
Susannah Cahalan’s new book challenges an experiment that changed psychiatry
As an undergraduate psychology major, I was taught about the Rosenhan study in several of my courses. My professors lectured about the shocking findings psychologist David Rosenhan, PhD, documented in a 1973 Science article, “On Being Sane in Insane Places” and these findings lent themselves to lecture hall drama. Eight people presented to hospitals and said they heard voices saying: “empty, hollow, thud.” These “pseudopatients” exhibited no other psychiatric symptoms but were admitted, diagnosed with schizophrenia, and observations of their behavior were made. The charts included notes such as, “Patient exhibits writing behavior,” my professors said. The pseudopatients were kept for an average of 19 days, and one for as long as 51 days. The decades have passed, and there are many things I learned in college that I have since forgotten, but I remember “empty, hollow, thud,” and the famous Rosenhan experiment.
I was eager to read Susannah Cahalan’s book, “The Great Pretender” (Grand Central Publishing, 2019), which puts both Dr. Rosenhan and his pseudopatient study under a microscope. Ms. Cahalan is the author of the page-turner, Brain on Fire: My Month of Madness (Free Press, 2012), where she recounted her own struggle with a psychotic episode. Ms. Cahalan, a young reporter in New York City, became psychotic and then catatonic; her condition perplexed the neurologists who were treating her on an inpatient unit, and they were on the verge of transferring her to psychiatry when a diagnosis of anti-NMDA receptor encephalitis was suspected and then confirmed with a brain biopsy. Ms. Cahalan made a full recovery after treatment with steroids, intravenous immunoglobulin, and plasmapheresis. While Ms. Cahalan’s symptoms were classic for a severe psychotic disorder, there was reason to believe that this was not a primary psychiatric disorder: She was having grand mal seizures. Her book was a bestseller, and she has spoken widely to make others aware of this rare illness that masquerades as psychosis. I heard her speak at the opening session of the American Psychiatric Association’s annual meeting in May of 2017.“My family, like many families before them, fought against the tyranny of the mental illness label,” Ms. Cahalan writes at the very beginning of “The Great Pretender.” She goes on to talk about how psychiatry differs from other medical fields: It’s the only specialty where people can be treated against their will; psychiatry casts judgments on the person; mental illness is poorly defined – perhaps there is no clear divide between normal and mad; and psychiatric disorders are less “real” than other illnesses. Throughout the book she refers to psychiatrists as smug and arrogant.
Ms. Cahalan takes on the task of documenting the horrors of psychiatry’s often sordid history, starting with journalist Nellie Bly’s 1887 journey into to a psychiatric facility to expose the abuses there. Certainly, psychiatry’s history is sordid. Ms. Cahalan talks about inhumane conditions in overcrowded psychiatric hospitals, about our sad chapter of lobotomies, about the influence of psychoanalysis on diagnosis and treatment, and about how homosexuality was once an illness and now is not. She includes “One Flew Over the Cuckoo’s Nest,” “The Myth of Mental Illness,” big pharma, and the Goldwater fiasco. In her recounting of the history, it’s all bad. She mentions Benjamin Rush, MD, only once, as the creator of “ ‘... the tranquilizing chair’ (a case of the worst false advertising ever), a terrifying sensory-deprivation apparatus in which patients were strapped down to a chair with a wooden box placed over their heads to block stimulation, restrict movement, and reduce blood to the brain.” Dr. Rush’s role as the father of American psychiatry who challenged the belief that mental illness was the result of demonic possession, gets no mention. Nor does Ms. Cahalan note that he founded Pennsylvania Hospital, where moral and occupational therapy revolutionized the treatment of those with mental illness.
So there’s her story, her rendition of the history of American psychiatry, and through this she weaves in the story of the Rosenhan experiment.
“ ‘It all started out as a dare,’ Dr. Rosenhan told a local newspaper, ‘I was teaching psychology at Swarthmore, and my students were saying that the course was too conceptual and abstract. So I said, ‘Okay, if you really want to know what mental patients are like, become mental patients.’ ”
Really? I read this and wondered how a psychologist could talk about people who had been hospitalized with psychiatric disorders as though they were aliens. Certainly, some of these students, their family members, or their friends must have been hospitalized at some point. Yet all through, there is this sense that the patients are other, and the discovery of the undercover operation is that the patients are actually human beings! Dr. Rosenhan, who was one of the pseudopatients, goes on to conclude that the label is everything, that once labeled they are treated differently by the nurses in “cages” and the doctors who walk by and avert their gaze. A second man Ms. Cahalan named, also one of the pseudopatients, had a similar experience. A third subject she located was not included in the study: His experience was counter to the findings of the study, his time in the hospital was a positive, he found it comforting, and the experiences he had there had a lasting positive influence on his life.
Ms. Cahalan talks about the publication of “On Being Sane in Insane Places” as a study that was finally scientific, one that changed all of psychiatry, and was the driving force for the creation of the DSM-III and the closure of state hospitals. I wondered if it was as influential as Ms. Cahalan claims, and I asked some psychiatrists who were practicing in 1973 when the article was published. I wanted to know if this study rocked their world.
“At first, with the great amount of publicity the study generated, it was added fodder for the antipsychiatrists, including the Scientologists and Szaszians,” Steven Sharfstein, MD, a former president of the American Psychiatric Association, told me. “But as young psychiatrists in the trenches, business continued to boom, and we continued to do the best job we could with diagnosis, assessment of risk, involuntary commitment, and treatment. And from what I recall, morale was high in the 1970s. We had some new medications and psychotherapies, and there was community activism. Faking symptoms to gain admission seemed to be a no-brainer, but keeping people for long stays was more problematic.”
E. Fuller Torrey, MD, the founder of the Treatment Advocacy Center who worked for many years treating patients at St. Elizabeth’s Hospital, replied: “It is important to remember that this study was published at the height of the deinstitutionalization movement and quite likely accelerated it. As I recall, at the time it seemed odd that all eight patients claimed to have had similar experiences while hospitalized. I think the main effect of the study was to provide ammunition for the antipsychiatrists.”
Ms. Cahalan has bought into the antipsychiatry movement full force. It’s not until the very end that there is any acknowledgment that psychiatry ever helped anyone, and even then, it’s a bit begrudging. Worse, she neglects to mention that people with psychiatric disorders suffer because of their psychic pain; one could get through this book and believe that people with mental illness struggle only because they are labeled and then mistreated, and for someone who has suffered herself, she misses the essence of how awful it is to be ill, and that people are often helped by psychiatric treatments. When she finally adds a paragraph talking about the usefulness of psychotropics, it’s with a caveat. “But I’m not here to rail against the drugs. There are plenty of places you can get that perspective. I see that these drugs help many people lead full and meaningful lives. It would be folly to discount their worth. We also can’t deny that the situation is complicated.”
There are moments in the manuscript where I found it difficult to know what were Dr. Rosenhan’s interpretations and what were Ms. Callahan’s interpretations of Dr. Rosenhan’s experiences. A lot of assumptions are made – particularly about the motivations of the hospital staff – and I wasn’t always sure they were correct. For example, on his second day in the hospital, Dr. Rosenhan asked a nurse for the newspaper. When she tells him it hasn’t come yet, he concludes that the staff is keeping the newspapers from the patients. And when a staff member is initially chatty then later shuns Dr. Rosenhan, he concludes that the man initially mistook him for a psychiatrist because he looks professorial. Both Ms. Cahalan and Dr. Rosenhan approach psychiatry with biases, and they don’t always question their assumptions.
, a professor who didn’t treat patients. This intermixing of the two fields felt contrived to me, and gave too much credence to the idea that no one really knows sane from disordered, and everyone was embracing the antipsychiatry dogma. Surely, someone during the those years must have liked their psychiatrist.
That said, Ms. Cahalan does a phenomenal job of infiltrating the world of the late Dr. Rosenhan. She starts out enamored by him and by his finding that psychiatrists can’t tell real illness from faked disorder. She meets with his friends, his son, his colleagues, his students, and she flies all over the country to meet with those who can help her understand him. She gains access to his personal files and to the book he started to write about the experiment, then abandoned, which eventually resulted in a lawsuit by Doubleday to have the book’s advance returned. At one point, she even hires a private detective.
What is Ms. Cahalan looking for so desperately? She’s looking for these anonymous pseudopatients, the people who were admitted to these unnamed state hospitals, who made observations and took notes, who were diagnosed with schizophrenia and then finally released. She’s looking for the truth, and while she identifies Dr. Rosenhan and two other pseudopatients as people who faked their way into the hospital, she finds a mass of contradictions. The one pseudopatient was excluded from the study – he is the one who felt comforted by his time in the hospital. The other six pseudopatients could not be found, despite Ms. Cahalan’s heroic attempts. Furthermore, she found many inconsistencies in what Dr. Rosenhan reported, and his hospital notes revealed more than a presentation for voices saying “empty, hollow, thud.” He reported it had been going on for months, that he had put copper over his ears to block the sound, and that he felt suicidal.
Ultimately, Ms. Cahalan was left to conclude that the Rosenhan experiment was a lie, that the pseudopatients likely never existed and the article was a fabrication. She brings up other studies that have been proven to be fraudulent, and by this point, our faith in all of science is pretty shaken.
Ms. Cahalan took a long journey to get us to this place, one that spent a lot of effort in bashing psychiatry, finally concluding that, as a result of this fraudulent experiment, too many hospitals have been shuttered – leaving our sickest patients to the streets and to the jails – and that there are not enough mental health professionals. As a psychiatrist – one who is often willing to question our practices – I was distracted by the flagrant antipsychiatry sentiments. Reading past that, Ms. Cahalan’s remarkable detective work and creative intermingling of the Rosenhan experiment layered on the history of psychiatry, further layered on her own experience with psychosis, makes for an amazing story. The Rosenhan study may have rocked the world of psychiatry; the fact that it was fabricated should rock us even more.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
As an undergraduate psychology major, I was taught about the Rosenhan study in several of my courses. My professors lectured about the shocking findings psychologist David Rosenhan, PhD, documented in a 1973 Science article, “On Being Sane in Insane Places” and these findings lent themselves to lecture hall drama. Eight people presented to hospitals and said they heard voices saying: “empty, hollow, thud.” These “pseudopatients” exhibited no other psychiatric symptoms but were admitted, diagnosed with schizophrenia, and observations of their behavior were made. The charts included notes such as, “Patient exhibits writing behavior,” my professors said. The pseudopatients were kept for an average of 19 days, and one for as long as 51 days. The decades have passed, and there are many things I learned in college that I have since forgotten, but I remember “empty, hollow, thud,” and the famous Rosenhan experiment.
I was eager to read Susannah Cahalan’s book, “The Great Pretender” (Grand Central Publishing, 2019), which puts both Dr. Rosenhan and his pseudopatient study under a microscope. Ms. Cahalan is the author of the page-turner, Brain on Fire: My Month of Madness (Free Press, 2012), where she recounted her own struggle with a psychotic episode. Ms. Cahalan, a young reporter in New York City, became psychotic and then catatonic; her condition perplexed the neurologists who were treating her on an inpatient unit, and they were on the verge of transferring her to psychiatry when a diagnosis of anti-NMDA receptor encephalitis was suspected and then confirmed with a brain biopsy. Ms. Cahalan made a full recovery after treatment with steroids, intravenous immunoglobulin, and plasmapheresis. While Ms. Cahalan’s symptoms were classic for a severe psychotic disorder, there was reason to believe that this was not a primary psychiatric disorder: She was having grand mal seizures. Her book was a bestseller, and she has spoken widely to make others aware of this rare illness that masquerades as psychosis. I heard her speak at the opening session of the American Psychiatric Association’s annual meeting in May of 2017.“My family, like many families before them, fought against the tyranny of the mental illness label,” Ms. Cahalan writes at the very beginning of “The Great Pretender.” She goes on to talk about how psychiatry differs from other medical fields: It’s the only specialty where people can be treated against their will; psychiatry casts judgments on the person; mental illness is poorly defined – perhaps there is no clear divide between normal and mad; and psychiatric disorders are less “real” than other illnesses. Throughout the book she refers to psychiatrists as smug and arrogant.
Ms. Cahalan takes on the task of documenting the horrors of psychiatry’s often sordid history, starting with journalist Nellie Bly’s 1887 journey into to a psychiatric facility to expose the abuses there. Certainly, psychiatry’s history is sordid. Ms. Cahalan talks about inhumane conditions in overcrowded psychiatric hospitals, about our sad chapter of lobotomies, about the influence of psychoanalysis on diagnosis and treatment, and about how homosexuality was once an illness and now is not. She includes “One Flew Over the Cuckoo’s Nest,” “The Myth of Mental Illness,” big pharma, and the Goldwater fiasco. In her recounting of the history, it’s all bad. She mentions Benjamin Rush, MD, only once, as the creator of “ ‘... the tranquilizing chair’ (a case of the worst false advertising ever), a terrifying sensory-deprivation apparatus in which patients were strapped down to a chair with a wooden box placed over their heads to block stimulation, restrict movement, and reduce blood to the brain.” Dr. Rush’s role as the father of American psychiatry who challenged the belief that mental illness was the result of demonic possession, gets no mention. Nor does Ms. Cahalan note that he founded Pennsylvania Hospital, where moral and occupational therapy revolutionized the treatment of those with mental illness.
So there’s her story, her rendition of the history of American psychiatry, and through this she weaves in the story of the Rosenhan experiment.
“ ‘It all started out as a dare,’ Dr. Rosenhan told a local newspaper, ‘I was teaching psychology at Swarthmore, and my students were saying that the course was too conceptual and abstract. So I said, ‘Okay, if you really want to know what mental patients are like, become mental patients.’ ”
Really? I read this and wondered how a psychologist could talk about people who had been hospitalized with psychiatric disorders as though they were aliens. Certainly, some of these students, their family members, or their friends must have been hospitalized at some point. Yet all through, there is this sense that the patients are other, and the discovery of the undercover operation is that the patients are actually human beings! Dr. Rosenhan, who was one of the pseudopatients, goes on to conclude that the label is everything, that once labeled they are treated differently by the nurses in “cages” and the doctors who walk by and avert their gaze. A second man Ms. Cahalan named, also one of the pseudopatients, had a similar experience. A third subject she located was not included in the study: His experience was counter to the findings of the study, his time in the hospital was a positive, he found it comforting, and the experiences he had there had a lasting positive influence on his life.
Ms. Cahalan talks about the publication of “On Being Sane in Insane Places” as a study that was finally scientific, one that changed all of psychiatry, and was the driving force for the creation of the DSM-III and the closure of state hospitals. I wondered if it was as influential as Ms. Cahalan claims, and I asked some psychiatrists who were practicing in 1973 when the article was published. I wanted to know if this study rocked their world.
“At first, with the great amount of publicity the study generated, it was added fodder for the antipsychiatrists, including the Scientologists and Szaszians,” Steven Sharfstein, MD, a former president of the American Psychiatric Association, told me. “But as young psychiatrists in the trenches, business continued to boom, and we continued to do the best job we could with diagnosis, assessment of risk, involuntary commitment, and treatment. And from what I recall, morale was high in the 1970s. We had some new medications and psychotherapies, and there was community activism. Faking symptoms to gain admission seemed to be a no-brainer, but keeping people for long stays was more problematic.”
E. Fuller Torrey, MD, the founder of the Treatment Advocacy Center who worked for many years treating patients at St. Elizabeth’s Hospital, replied: “It is important to remember that this study was published at the height of the deinstitutionalization movement and quite likely accelerated it. As I recall, at the time it seemed odd that all eight patients claimed to have had similar experiences while hospitalized. I think the main effect of the study was to provide ammunition for the antipsychiatrists.”
Ms. Cahalan has bought into the antipsychiatry movement full force. It’s not until the very end that there is any acknowledgment that psychiatry ever helped anyone, and even then, it’s a bit begrudging. Worse, she neglects to mention that people with psychiatric disorders suffer because of their psychic pain; one could get through this book and believe that people with mental illness struggle only because they are labeled and then mistreated, and for someone who has suffered herself, she misses the essence of how awful it is to be ill, and that people are often helped by psychiatric treatments. When she finally adds a paragraph talking about the usefulness of psychotropics, it’s with a caveat. “But I’m not here to rail against the drugs. There are plenty of places you can get that perspective. I see that these drugs help many people lead full and meaningful lives. It would be folly to discount their worth. We also can’t deny that the situation is complicated.”
There are moments in the manuscript where I found it difficult to know what were Dr. Rosenhan’s interpretations and what were Ms. Callahan’s interpretations of Dr. Rosenhan’s experiences. A lot of assumptions are made – particularly about the motivations of the hospital staff – and I wasn’t always sure they were correct. For example, on his second day in the hospital, Dr. Rosenhan asked a nurse for the newspaper. When she tells him it hasn’t come yet, he concludes that the staff is keeping the newspapers from the patients. And when a staff member is initially chatty then later shuns Dr. Rosenhan, he concludes that the man initially mistook him for a psychiatrist because he looks professorial. Both Ms. Cahalan and Dr. Rosenhan approach psychiatry with biases, and they don’t always question their assumptions.
, a professor who didn’t treat patients. This intermixing of the two fields felt contrived to me, and gave too much credence to the idea that no one really knows sane from disordered, and everyone was embracing the antipsychiatry dogma. Surely, someone during the those years must have liked their psychiatrist.
That said, Ms. Cahalan does a phenomenal job of infiltrating the world of the late Dr. Rosenhan. She starts out enamored by him and by his finding that psychiatrists can’t tell real illness from faked disorder. She meets with his friends, his son, his colleagues, his students, and she flies all over the country to meet with those who can help her understand him. She gains access to his personal files and to the book he started to write about the experiment, then abandoned, which eventually resulted in a lawsuit by Doubleday to have the book’s advance returned. At one point, she even hires a private detective.
What is Ms. Cahalan looking for so desperately? She’s looking for these anonymous pseudopatients, the people who were admitted to these unnamed state hospitals, who made observations and took notes, who were diagnosed with schizophrenia and then finally released. She’s looking for the truth, and while she identifies Dr. Rosenhan and two other pseudopatients as people who faked their way into the hospital, she finds a mass of contradictions. The one pseudopatient was excluded from the study – he is the one who felt comforted by his time in the hospital. The other six pseudopatients could not be found, despite Ms. Cahalan’s heroic attempts. Furthermore, she found many inconsistencies in what Dr. Rosenhan reported, and his hospital notes revealed more than a presentation for voices saying “empty, hollow, thud.” He reported it had been going on for months, that he had put copper over his ears to block the sound, and that he felt suicidal.
Ultimately, Ms. Cahalan was left to conclude that the Rosenhan experiment was a lie, that the pseudopatients likely never existed and the article was a fabrication. She brings up other studies that have been proven to be fraudulent, and by this point, our faith in all of science is pretty shaken.
Ms. Cahalan took a long journey to get us to this place, one that spent a lot of effort in bashing psychiatry, finally concluding that, as a result of this fraudulent experiment, too many hospitals have been shuttered – leaving our sickest patients to the streets and to the jails – and that there are not enough mental health professionals. As a psychiatrist – one who is often willing to question our practices – I was distracted by the flagrant antipsychiatry sentiments. Reading past that, Ms. Cahalan’s remarkable detective work and creative intermingling of the Rosenhan experiment layered on the history of psychiatry, further layered on her own experience with psychosis, makes for an amazing story. The Rosenhan study may have rocked the world of psychiatry; the fact that it was fabricated should rock us even more.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
Proposed RESPONSE Act targets potential shooters
As I’m writing, my Twitter feed announces yet another public shooting, this one at a Walmart in Oklahoma. It’s a problem that gets worse as it gets more attention and the argument over how to approach the issue of mass shootings still continues down two separate and distinct pathways: Is this the result of too-easy access to firearms or is it one of untreated mental illness?
Sen. John Cornyn (R-Tex.) spoke on the Senate floor on Oct. 23, 2019, about new legislation he is cosponsoring in the aftermath of two mass shootings in Texas this past August. The Restoring, Enhancing, Strengthening, and Promoting Our Nation’s Safety Efforts Act of 2019 (S. 2690), or the RESPONSE Act, is designed to “reduce mass violence, strengthen mental health collaboration in communities, improve school safety, and for other purposes.” Sen. Cornyn notes that in the aftermath of those shootings he met with his constituents and he heard a common refrain: Please do something.
“Unfortunately, there is no quick fix, no simple answer, instead we are left to look at the factors that led to these attacks and to try to do something to prevent the sequence of events from playing out again in the future,” Sen. Cornyn said.
“While mental illness is not the prevailing cause of mass violence, enhanced mental health resources are critical to saving lives,” he said, adding that most gun deaths are from suicide. In his speech, he outlined the issues it would address – and despite his statement that mental illness is not the cause of mass violence – he went on to elaborate on the issues that the bill would address.
“First, this legislation takes aim at unlicensed firearms dealers who are breaking the law,” he said. This legislation would create a task force to prosecute those who buy and sell firearms through unlicensed dealers, and he notes that one of the Texas shooters was denied a gun by a licensed firearms dealer before purchasing one from an unlicensed dealer. That Sen. Cornyn’s proposed legislation would not create any new gun legislation is not a surprise: he has an A+ rating from the National Rifle Association and his website’s fun facts include the statement: “Sen. Cornyn owns several firearms and hunts as often as he can.”
The rest of the RESPONSE Act takes aim at those who have or might have psychiatric disorders or a tendency toward violence. Sen. Cornyn noted that the act would expand assisted outpatient treatment (AOT, or outpatient civil commitment). He referenced this as a way for families to get care for their loved ones in the community rather than in a hospital and did not allude to the involuntary nature of the treatment.
Marvin Swartz, MD, is professor of psychiatry at Duke University, Durham, N.C., and lead investigator on outcome studies following the implementation of outpatient civil commitment legislation.
“AOT may be justified in improving treatment adherence and service provision,” Dr. Swartz noted, “but there is no direct line to serious violence. The violence we documented as reduced were mainly minor acts of interpersonal violence – pushing and shoving – what we call minor acts of violence. There is no evidence that AOT is a remedy to serious acts of violence – mass shootings included.”
In addition, Sen. Cornyn noted there would be expanded crisis intervention teams and increased coordination between mental health providers and law enforcement. Furthermore, the bill would make schools safer by identifying students whose behavior indicated a threat of violence and providing those students with the services they need. This would be done “by promoting best practices within our schools and promoting Internet safety.”
Finally, Sen. Cornyn talked about using social media as a means to identify those who might be a danger. “Because so often these shooters advertise on social media ... this legislation includes provisions to [ensure] that law enforcement can receive timely information about threats made online.”
The bill already has garnered both support and opposition. It has been supported by the National Council for Behavioral Health, the National Alliance on Mental Illness (NAMI), and the Treatment Advocacy Center. Those opposed to the legislation include the National Disability Rights Network, the American Association of People with Disabilities, the National Council on Independent Living, the Disability Rights Education & Defense Fund, the Bazelon Center for Mental Health Law, and the Autistic Self Advocacy Network. The American Psychiatric Association has not made a statement on the proposed legislation as of this writing.
The National Council for Behavioral Health posted an endorsement on its website. It notes: “The RESPONSE Act authorizes up to $10 million of existing funds in the Department of Justice for partnership between law enforcement and mental health providers to increase access to long-acting medically assisted treatment. Additionally, it requires the Department of Health and Human Services (HHS) to develop and disseminate guidance for states to fund mental health programs and crisis intervention teams through Medicaid as well as to issue a report to Congress on best practices to expand the mental health workforce. These provisions aim to divert more individuals from incarceration and will create more opportunities for community-based treatment and recovery.”
There is no question that psychiatric treatment for those with mental illness is underfunded and often inaccessible. But while it is true that some individuals become violent when they are ill, most do not, and targeting those one in five Americans who suffer from a psychiatric disorder each year in an effort to identify, then thwart, the rare mass murderer among us makes no sense.
Acts of mass violence remain rare. In 2018, the year we had a record-breaking number of mass shootings, there were 12 mass murders in the United States, according to the criteria used by Mother Jones, and 27 active shooter incidents using the FBI’s criteria. Approximately half of all mass shooters showed signs of mental illness prior to the shooting and of those, some had never come to the attention of mental health professionals in a way that would have predicted violence. While linking mass violence to mental illness may seem reasonable, the numbers just don’t make sense and targeting this presumed link between mental illness and mass violence is stigmatizing.
The text of the RESPONSE Act reveals proposed legislation that is perhaps more thoughtful than Sen. Cornyn’s speech suggested; the bill starts with funding services for those with psychiatric disorders who are being released from the correctional system, a population that may be at higher risk for acts of violence. The funding for outpatient civil commitment is worded in such a way that it is hard to know exactly what is required. The bill starts by mandating that each state must use 10% of the funding it gets from this bill for court-ordered treatment (AOT), but then lists alternative ways states may use that 10%, including “otherwise support evidence-based programs that address the needs of eligible patients.” In all, the proposed legislation is long and complex and attempts to address issues related to terrorism, the Internet, mental health, and the educational system. It’s an ambitious use of $10 million a year for our entire country.
At a time when mental health care is desperately underfunded and many are unable to access treatment, it is tempting to endorse any legislation that improves funding. But does it serve society to endorse legislation that suggests psychiatrists can prevent mass shootings? Does that ultimately serve our patients?
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle of Inpatient Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016), and has a private practice in Baltimore.
As I’m writing, my Twitter feed announces yet another public shooting, this one at a Walmart in Oklahoma. It’s a problem that gets worse as it gets more attention and the argument over how to approach the issue of mass shootings still continues down two separate and distinct pathways: Is this the result of too-easy access to firearms or is it one of untreated mental illness?
Sen. John Cornyn (R-Tex.) spoke on the Senate floor on Oct. 23, 2019, about new legislation he is cosponsoring in the aftermath of two mass shootings in Texas this past August. The Restoring, Enhancing, Strengthening, and Promoting Our Nation’s Safety Efforts Act of 2019 (S. 2690), or the RESPONSE Act, is designed to “reduce mass violence, strengthen mental health collaboration in communities, improve school safety, and for other purposes.” Sen. Cornyn notes that in the aftermath of those shootings he met with his constituents and he heard a common refrain: Please do something.
“Unfortunately, there is no quick fix, no simple answer, instead we are left to look at the factors that led to these attacks and to try to do something to prevent the sequence of events from playing out again in the future,” Sen. Cornyn said.
“While mental illness is not the prevailing cause of mass violence, enhanced mental health resources are critical to saving lives,” he said, adding that most gun deaths are from suicide. In his speech, he outlined the issues it would address – and despite his statement that mental illness is not the cause of mass violence – he went on to elaborate on the issues that the bill would address.
“First, this legislation takes aim at unlicensed firearms dealers who are breaking the law,” he said. This legislation would create a task force to prosecute those who buy and sell firearms through unlicensed dealers, and he notes that one of the Texas shooters was denied a gun by a licensed firearms dealer before purchasing one from an unlicensed dealer. That Sen. Cornyn’s proposed legislation would not create any new gun legislation is not a surprise: he has an A+ rating from the National Rifle Association and his website’s fun facts include the statement: “Sen. Cornyn owns several firearms and hunts as often as he can.”
The rest of the RESPONSE Act takes aim at those who have or might have psychiatric disorders or a tendency toward violence. Sen. Cornyn noted that the act would expand assisted outpatient treatment (AOT, or outpatient civil commitment). He referenced this as a way for families to get care for their loved ones in the community rather than in a hospital and did not allude to the involuntary nature of the treatment.
Marvin Swartz, MD, is professor of psychiatry at Duke University, Durham, N.C., and lead investigator on outcome studies following the implementation of outpatient civil commitment legislation.
“AOT may be justified in improving treatment adherence and service provision,” Dr. Swartz noted, “but there is no direct line to serious violence. The violence we documented as reduced were mainly minor acts of interpersonal violence – pushing and shoving – what we call minor acts of violence. There is no evidence that AOT is a remedy to serious acts of violence – mass shootings included.”
In addition, Sen. Cornyn noted there would be expanded crisis intervention teams and increased coordination between mental health providers and law enforcement. Furthermore, the bill would make schools safer by identifying students whose behavior indicated a threat of violence and providing those students with the services they need. This would be done “by promoting best practices within our schools and promoting Internet safety.”
Finally, Sen. Cornyn talked about using social media as a means to identify those who might be a danger. “Because so often these shooters advertise on social media ... this legislation includes provisions to [ensure] that law enforcement can receive timely information about threats made online.”
The bill already has garnered both support and opposition. It has been supported by the National Council for Behavioral Health, the National Alliance on Mental Illness (NAMI), and the Treatment Advocacy Center. Those opposed to the legislation include the National Disability Rights Network, the American Association of People with Disabilities, the National Council on Independent Living, the Disability Rights Education & Defense Fund, the Bazelon Center for Mental Health Law, and the Autistic Self Advocacy Network. The American Psychiatric Association has not made a statement on the proposed legislation as of this writing.
The National Council for Behavioral Health posted an endorsement on its website. It notes: “The RESPONSE Act authorizes up to $10 million of existing funds in the Department of Justice for partnership between law enforcement and mental health providers to increase access to long-acting medically assisted treatment. Additionally, it requires the Department of Health and Human Services (HHS) to develop and disseminate guidance for states to fund mental health programs and crisis intervention teams through Medicaid as well as to issue a report to Congress on best practices to expand the mental health workforce. These provisions aim to divert more individuals from incarceration and will create more opportunities for community-based treatment and recovery.”
There is no question that psychiatric treatment for those with mental illness is underfunded and often inaccessible. But while it is true that some individuals become violent when they are ill, most do not, and targeting those one in five Americans who suffer from a psychiatric disorder each year in an effort to identify, then thwart, the rare mass murderer among us makes no sense.
Acts of mass violence remain rare. In 2018, the year we had a record-breaking number of mass shootings, there were 12 mass murders in the United States, according to the criteria used by Mother Jones, and 27 active shooter incidents using the FBI’s criteria. Approximately half of all mass shooters showed signs of mental illness prior to the shooting and of those, some had never come to the attention of mental health professionals in a way that would have predicted violence. While linking mass violence to mental illness may seem reasonable, the numbers just don’t make sense and targeting this presumed link between mental illness and mass violence is stigmatizing.
The text of the RESPONSE Act reveals proposed legislation that is perhaps more thoughtful than Sen. Cornyn’s speech suggested; the bill starts with funding services for those with psychiatric disorders who are being released from the correctional system, a population that may be at higher risk for acts of violence. The funding for outpatient civil commitment is worded in such a way that it is hard to know exactly what is required. The bill starts by mandating that each state must use 10% of the funding it gets from this bill for court-ordered treatment (AOT), but then lists alternative ways states may use that 10%, including “otherwise support evidence-based programs that address the needs of eligible patients.” In all, the proposed legislation is long and complex and attempts to address issues related to terrorism, the Internet, mental health, and the educational system. It’s an ambitious use of $10 million a year for our entire country.
At a time when mental health care is desperately underfunded and many are unable to access treatment, it is tempting to endorse any legislation that improves funding. But does it serve society to endorse legislation that suggests psychiatrists can prevent mass shootings? Does that ultimately serve our patients?
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle of Inpatient Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016), and has a private practice in Baltimore.
As I’m writing, my Twitter feed announces yet another public shooting, this one at a Walmart in Oklahoma. It’s a problem that gets worse as it gets more attention and the argument over how to approach the issue of mass shootings still continues down two separate and distinct pathways: Is this the result of too-easy access to firearms or is it one of untreated mental illness?
Sen. John Cornyn (R-Tex.) spoke on the Senate floor on Oct. 23, 2019, about new legislation he is cosponsoring in the aftermath of two mass shootings in Texas this past August. The Restoring, Enhancing, Strengthening, and Promoting Our Nation’s Safety Efforts Act of 2019 (S. 2690), or the RESPONSE Act, is designed to “reduce mass violence, strengthen mental health collaboration in communities, improve school safety, and for other purposes.” Sen. Cornyn notes that in the aftermath of those shootings he met with his constituents and he heard a common refrain: Please do something.
“Unfortunately, there is no quick fix, no simple answer, instead we are left to look at the factors that led to these attacks and to try to do something to prevent the sequence of events from playing out again in the future,” Sen. Cornyn said.
“While mental illness is not the prevailing cause of mass violence, enhanced mental health resources are critical to saving lives,” he said, adding that most gun deaths are from suicide. In his speech, he outlined the issues it would address – and despite his statement that mental illness is not the cause of mass violence – he went on to elaborate on the issues that the bill would address.
“First, this legislation takes aim at unlicensed firearms dealers who are breaking the law,” he said. This legislation would create a task force to prosecute those who buy and sell firearms through unlicensed dealers, and he notes that one of the Texas shooters was denied a gun by a licensed firearms dealer before purchasing one from an unlicensed dealer. That Sen. Cornyn’s proposed legislation would not create any new gun legislation is not a surprise: he has an A+ rating from the National Rifle Association and his website’s fun facts include the statement: “Sen. Cornyn owns several firearms and hunts as often as he can.”
The rest of the RESPONSE Act takes aim at those who have or might have psychiatric disorders or a tendency toward violence. Sen. Cornyn noted that the act would expand assisted outpatient treatment (AOT, or outpatient civil commitment). He referenced this as a way for families to get care for their loved ones in the community rather than in a hospital and did not allude to the involuntary nature of the treatment.
Marvin Swartz, MD, is professor of psychiatry at Duke University, Durham, N.C., and lead investigator on outcome studies following the implementation of outpatient civil commitment legislation.
“AOT may be justified in improving treatment adherence and service provision,” Dr. Swartz noted, “but there is no direct line to serious violence. The violence we documented as reduced were mainly minor acts of interpersonal violence – pushing and shoving – what we call minor acts of violence. There is no evidence that AOT is a remedy to serious acts of violence – mass shootings included.”
In addition, Sen. Cornyn noted there would be expanded crisis intervention teams and increased coordination between mental health providers and law enforcement. Furthermore, the bill would make schools safer by identifying students whose behavior indicated a threat of violence and providing those students with the services they need. This would be done “by promoting best practices within our schools and promoting Internet safety.”
Finally, Sen. Cornyn talked about using social media as a means to identify those who might be a danger. “Because so often these shooters advertise on social media ... this legislation includes provisions to [ensure] that law enforcement can receive timely information about threats made online.”
The bill already has garnered both support and opposition. It has been supported by the National Council for Behavioral Health, the National Alliance on Mental Illness (NAMI), and the Treatment Advocacy Center. Those opposed to the legislation include the National Disability Rights Network, the American Association of People with Disabilities, the National Council on Independent Living, the Disability Rights Education & Defense Fund, the Bazelon Center for Mental Health Law, and the Autistic Self Advocacy Network. The American Psychiatric Association has not made a statement on the proposed legislation as of this writing.
The National Council for Behavioral Health posted an endorsement on its website. It notes: “The RESPONSE Act authorizes up to $10 million of existing funds in the Department of Justice for partnership between law enforcement and mental health providers to increase access to long-acting medically assisted treatment. Additionally, it requires the Department of Health and Human Services (HHS) to develop and disseminate guidance for states to fund mental health programs and crisis intervention teams through Medicaid as well as to issue a report to Congress on best practices to expand the mental health workforce. These provisions aim to divert more individuals from incarceration and will create more opportunities for community-based treatment and recovery.”
There is no question that psychiatric treatment for those with mental illness is underfunded and often inaccessible. But while it is true that some individuals become violent when they are ill, most do not, and targeting those one in five Americans who suffer from a psychiatric disorder each year in an effort to identify, then thwart, the rare mass murderer among us makes no sense.
Acts of mass violence remain rare. In 2018, the year we had a record-breaking number of mass shootings, there were 12 mass murders in the United States, according to the criteria used by Mother Jones, and 27 active shooter incidents using the FBI’s criteria. Approximately half of all mass shooters showed signs of mental illness prior to the shooting and of those, some had never come to the attention of mental health professionals in a way that would have predicted violence. While linking mass violence to mental illness may seem reasonable, the numbers just don’t make sense and targeting this presumed link between mental illness and mass violence is stigmatizing.
The text of the RESPONSE Act reveals proposed legislation that is perhaps more thoughtful than Sen. Cornyn’s speech suggested; the bill starts with funding services for those with psychiatric disorders who are being released from the correctional system, a population that may be at higher risk for acts of violence. The funding for outpatient civil commitment is worded in such a way that it is hard to know exactly what is required. The bill starts by mandating that each state must use 10% of the funding it gets from this bill for court-ordered treatment (AOT), but then lists alternative ways states may use that 10%, including “otherwise support evidence-based programs that address the needs of eligible patients.” In all, the proposed legislation is long and complex and attempts to address issues related to terrorism, the Internet, mental health, and the educational system. It’s an ambitious use of $10 million a year for our entire country.
At a time when mental health care is desperately underfunded and many are unable to access treatment, it is tempting to endorse any legislation that improves funding. But does it serve society to endorse legislation that suggests psychiatrists can prevent mass shootings? Does that ultimately serve our patients?
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle of Inpatient Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016), and has a private practice in Baltimore.
Psilocybin research at Johns Hopkins
A new center opens to study novel treatment uses for psychedelics
Psychiatry Grand Rounds started on Monday, Oct. 7, 2019, as they do every Monday at Johns Hopkins, with the department chair interviewing a patient.
The patient told James Potash, MD, that he had suffered with depression for many years and that medications were only a partial fix. His participation in a psilocybin trial at Johns Hopkins in Baltimore was different, and 3 months after the second, and final, treatment, he felt remarkably better. The treatment had quieted the self-deprecating script that had looped through his thoughts for years. “It was nothing like what I was expecting,” the patient said. “I didn’t feel out of control. And now I’m not fighting with myself all day.”
Grand Rounds at Hopkins are different from those at other institutions in that the rounds are given by departments’ full-time faculty members; psychiatrists from other institutions are invited to come speak at other times during the week. But Grand Rounds are reserved for the faculty to present their own research. The patient interview was followed by a lecture by Roland Griffiths, PhD, on “Psilocybin: A potentially promising treatment for depression.” Dr. Griffiths has been studying the effects of psychedelic drugs for the past 40 years; he’s been at Hopkins since 1972. The Grand Rounds presentation came just weeks after it was announced that Dr. Griffiths would be heading the Johns Hopkins Center for Psychedelic & Consciousness Research, funded with $17 million in private donations.
Dr. Griffiths began by talking about the history of psychedelic drug research and the fact that research had been dormant for several decades. “There was – and still is – concern about potential adverse reactions, including panic reactions and the possibility of precipitating psychosis,” he said.
Originally, he conducted several studies in healthy volunteers with no history of psychedelic use. Participants had one or more day-long sessions with staff members who would then serve as monitors when psilocybin was administered; these preliminary meetings were designed to build trust and rapport with the team and to decrease the risk of adverse reactions. On session days when psilocybin was administered, participants were told to eat a low-fat breakfast and then were given a high dose of psilocybin in a capsule. The next 6 hours were spent with the volunteer lying on a couch with an eye mask, headphones with soft music, and two monitors in the room. “The room is decorated like a living room. We created a container for people to explore their inner experience.”
Dr. Griffiths talked about the experiences people reported.
“There were large increases in personally meaningful and insight-type experiences. People reported a sense of unity and interconnectedness of all things, accompanied by a sense of preciousness or reverence, and by the sense that ... the experience was more real or true than everyday waking consciousness. Although the acute effects of psilocybin resolved by the end of the session day, the memories remain and people reported enduring changes in mood, attitude, and behavior.”
The data were remarkable. One month after these high-dose psilocybin sessions, 78% of the volunteers rated the experience as among the top five most personally meaningful experiences of their lives, 94% said they had an increased sense of well-being with improved life satisfaction, and nearly 90% endorsed positive behavior change. Six months after the last session, participants still endorsed having more positive relationships, feeling more love, tolerance, empathy and compassion, friends, family members, and others. Family members and work colleagues who were interviewed noted these positive changes as well.
At this point in Grand Rounds, I was ready to volunteer. My best estimate (tongue in cheek, with no corroboration) is that about half of the audience was waiting on free psilocybin samples, while the other half was remembering Timothy Leary, PhD, bad trips, and psychosis. “We’ve been down this road before,” the gentleman next to me commented.
Dr. Griffiths went on to talk about trials of psilocybin in clinical populations. In one study, the effects of psilocybin were examined in cancer patients with depression and anxiety. Of the 51 cancer patients, half previously had been treated with psychotropic medications before coming to the study. This randomized, double-blind crossover study compared high-dose psilocybin with an extremely low dose of psilocybin used as the placebo.
Another study looked at patients with major depression who, like the patient interviewed, had not had full resolution of symptoms with conventional antidepressants. Of the 24 participants in that group, 69% reported clinically significant improvement 12 weeks after the treatment. Just over half of participants reported a full remission to normal.
Dr. Griffiths ended by concluding that the positive experiences people have with psilocybin are associated with “enduring positive trait changes in attitudes, mood and behavior, spirituality, and altruism ... and that such experiences are now amenable to systematic prospective scientific study.”
J. Raymond DePaulo, MD, chair of the National Network of Depression Centers and former chair of psychiatry at Johns Hopkins, noted that he used to be skeptical. He has been impressed that Dr. Griffiths has listened to criticism and addressed concerns others have raised. “When it was suggested that this was the result of delirium, he started giving people cognitive tests while they were using psilocybin and he showed it wasn’t the case.”
“I have always objected to words like ‘psychedelic’ and ‘hallucinogen,’ ” said Dr. DePaulo. “They are confusing and inaccurate. No one takes these medications because they want to hallucinate. They take them to change their mood. That said, I am thrilled that we are on the precipice of being able to use this to treat depression.”
Since 1999, the Johns Hopkins Psilocybin Research Project has conducted more than 700 sessions with 369 participants. When might psilocybin be available to patients outside of a research protocol? Two companies have obtained approval from the Food and Drug Administration to initiate registration in trials for treatment of depression. Dr. Griffiths estimates that it could be another 5 years before psilocybin will be available for medical use.
The new center with its generous funding will allow for more studies with more patient populations. The center’s projects will look at using psilocybin as a treatment for opioid use disorder, comorbid depression and alcohol use disorder, anorexia nervosa, depression in Alzheimer’s disease, posttreatment Lyme disease syndrome, and PTSD.
Scott Aaronson, MD, is a mood disorder expert and director of clinical research at the Sheppard Pratt Health System in Towson/Baltimore. Dr. Aaronson, who also studies psilocybin as a treatment for depression, noted: “The problem with the development of psychedelics is that we are not really prepared to capture the improvement we see with their use, as the main changes are not in the classic markers of depression like the Montgomery-Åsberg or the Hamilton Depression rating scales, but [rather] in the patient’s perception of who they are, how they fit in with the world, and what is most important. We need to develop ways to capture those critical changes and work with the FDA to develop an entirely new vision of what constitutes improvement in psychiatric illness. My overall take is that it is a terrific time to specialize in treatment-resistant mood disorders!”
Dr. Miller is coauthor of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
A new center opens to study novel treatment uses for psychedelics
A new center opens to study novel treatment uses for psychedelics
Psychiatry Grand Rounds started on Monday, Oct. 7, 2019, as they do every Monday at Johns Hopkins, with the department chair interviewing a patient.
The patient told James Potash, MD, that he had suffered with depression for many years and that medications were only a partial fix. His participation in a psilocybin trial at Johns Hopkins in Baltimore was different, and 3 months after the second, and final, treatment, he felt remarkably better. The treatment had quieted the self-deprecating script that had looped through his thoughts for years. “It was nothing like what I was expecting,” the patient said. “I didn’t feel out of control. And now I’m not fighting with myself all day.”
Grand Rounds at Hopkins are different from those at other institutions in that the rounds are given by departments’ full-time faculty members; psychiatrists from other institutions are invited to come speak at other times during the week. But Grand Rounds are reserved for the faculty to present their own research. The patient interview was followed by a lecture by Roland Griffiths, PhD, on “Psilocybin: A potentially promising treatment for depression.” Dr. Griffiths has been studying the effects of psychedelic drugs for the past 40 years; he’s been at Hopkins since 1972. The Grand Rounds presentation came just weeks after it was announced that Dr. Griffiths would be heading the Johns Hopkins Center for Psychedelic & Consciousness Research, funded with $17 million in private donations.
Dr. Griffiths began by talking about the history of psychedelic drug research and the fact that research had been dormant for several decades. “There was – and still is – concern about potential adverse reactions, including panic reactions and the possibility of precipitating psychosis,” he said.
Originally, he conducted several studies in healthy volunteers with no history of psychedelic use. Participants had one or more day-long sessions with staff members who would then serve as monitors when psilocybin was administered; these preliminary meetings were designed to build trust and rapport with the team and to decrease the risk of adverse reactions. On session days when psilocybin was administered, participants were told to eat a low-fat breakfast and then were given a high dose of psilocybin in a capsule. The next 6 hours were spent with the volunteer lying on a couch with an eye mask, headphones with soft music, and two monitors in the room. “The room is decorated like a living room. We created a container for people to explore their inner experience.”
Dr. Griffiths talked about the experiences people reported.
“There were large increases in personally meaningful and insight-type experiences. People reported a sense of unity and interconnectedness of all things, accompanied by a sense of preciousness or reverence, and by the sense that ... the experience was more real or true than everyday waking consciousness. Although the acute effects of psilocybin resolved by the end of the session day, the memories remain and people reported enduring changes in mood, attitude, and behavior.”
The data were remarkable. One month after these high-dose psilocybin sessions, 78% of the volunteers rated the experience as among the top five most personally meaningful experiences of their lives, 94% said they had an increased sense of well-being with improved life satisfaction, and nearly 90% endorsed positive behavior change. Six months after the last session, participants still endorsed having more positive relationships, feeling more love, tolerance, empathy and compassion, friends, family members, and others. Family members and work colleagues who were interviewed noted these positive changes as well.
At this point in Grand Rounds, I was ready to volunteer. My best estimate (tongue in cheek, with no corroboration) is that about half of the audience was waiting on free psilocybin samples, while the other half was remembering Timothy Leary, PhD, bad trips, and psychosis. “We’ve been down this road before,” the gentleman next to me commented.
Dr. Griffiths went on to talk about trials of psilocybin in clinical populations. In one study, the effects of psilocybin were examined in cancer patients with depression and anxiety. Of the 51 cancer patients, half previously had been treated with psychotropic medications before coming to the study. This randomized, double-blind crossover study compared high-dose psilocybin with an extremely low dose of psilocybin used as the placebo.
Another study looked at patients with major depression who, like the patient interviewed, had not had full resolution of symptoms with conventional antidepressants. Of the 24 participants in that group, 69% reported clinically significant improvement 12 weeks after the treatment. Just over half of participants reported a full remission to normal.
Dr. Griffiths ended by concluding that the positive experiences people have with psilocybin are associated with “enduring positive trait changes in attitudes, mood and behavior, spirituality, and altruism ... and that such experiences are now amenable to systematic prospective scientific study.”
J. Raymond DePaulo, MD, chair of the National Network of Depression Centers and former chair of psychiatry at Johns Hopkins, noted that he used to be skeptical. He has been impressed that Dr. Griffiths has listened to criticism and addressed concerns others have raised. “When it was suggested that this was the result of delirium, he started giving people cognitive tests while they were using psilocybin and he showed it wasn’t the case.”
“I have always objected to words like ‘psychedelic’ and ‘hallucinogen,’ ” said Dr. DePaulo. “They are confusing and inaccurate. No one takes these medications because they want to hallucinate. They take them to change their mood. That said, I am thrilled that we are on the precipice of being able to use this to treat depression.”
Since 1999, the Johns Hopkins Psilocybin Research Project has conducted more than 700 sessions with 369 participants. When might psilocybin be available to patients outside of a research protocol? Two companies have obtained approval from the Food and Drug Administration to initiate registration in trials for treatment of depression. Dr. Griffiths estimates that it could be another 5 years before psilocybin will be available for medical use.
The new center with its generous funding will allow for more studies with more patient populations. The center’s projects will look at using psilocybin as a treatment for opioid use disorder, comorbid depression and alcohol use disorder, anorexia nervosa, depression in Alzheimer’s disease, posttreatment Lyme disease syndrome, and PTSD.
Scott Aaronson, MD, is a mood disorder expert and director of clinical research at the Sheppard Pratt Health System in Towson/Baltimore. Dr. Aaronson, who also studies psilocybin as a treatment for depression, noted: “The problem with the development of psychedelics is that we are not really prepared to capture the improvement we see with their use, as the main changes are not in the classic markers of depression like the Montgomery-Åsberg or the Hamilton Depression rating scales, but [rather] in the patient’s perception of who they are, how they fit in with the world, and what is most important. We need to develop ways to capture those critical changes and work with the FDA to develop an entirely new vision of what constitutes improvement in psychiatric illness. My overall take is that it is a terrific time to specialize in treatment-resistant mood disorders!”
Dr. Miller is coauthor of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
Psychiatry Grand Rounds started on Monday, Oct. 7, 2019, as they do every Monday at Johns Hopkins, with the department chair interviewing a patient.
The patient told James Potash, MD, that he had suffered with depression for many years and that medications were only a partial fix. His participation in a psilocybin trial at Johns Hopkins in Baltimore was different, and 3 months after the second, and final, treatment, he felt remarkably better. The treatment had quieted the self-deprecating script that had looped through his thoughts for years. “It was nothing like what I was expecting,” the patient said. “I didn’t feel out of control. And now I’m not fighting with myself all day.”
Grand Rounds at Hopkins are different from those at other institutions in that the rounds are given by departments’ full-time faculty members; psychiatrists from other institutions are invited to come speak at other times during the week. But Grand Rounds are reserved for the faculty to present their own research. The patient interview was followed by a lecture by Roland Griffiths, PhD, on “Psilocybin: A potentially promising treatment for depression.” Dr. Griffiths has been studying the effects of psychedelic drugs for the past 40 years; he’s been at Hopkins since 1972. The Grand Rounds presentation came just weeks after it was announced that Dr. Griffiths would be heading the Johns Hopkins Center for Psychedelic & Consciousness Research, funded with $17 million in private donations.
Dr. Griffiths began by talking about the history of psychedelic drug research and the fact that research had been dormant for several decades. “There was – and still is – concern about potential adverse reactions, including panic reactions and the possibility of precipitating psychosis,” he said.
Originally, he conducted several studies in healthy volunteers with no history of psychedelic use. Participants had one or more day-long sessions with staff members who would then serve as monitors when psilocybin was administered; these preliminary meetings were designed to build trust and rapport with the team and to decrease the risk of adverse reactions. On session days when psilocybin was administered, participants were told to eat a low-fat breakfast and then were given a high dose of psilocybin in a capsule. The next 6 hours were spent with the volunteer lying on a couch with an eye mask, headphones with soft music, and two monitors in the room. “The room is decorated like a living room. We created a container for people to explore their inner experience.”
Dr. Griffiths talked about the experiences people reported.
“There were large increases in personally meaningful and insight-type experiences. People reported a sense of unity and interconnectedness of all things, accompanied by a sense of preciousness or reverence, and by the sense that ... the experience was more real or true than everyday waking consciousness. Although the acute effects of psilocybin resolved by the end of the session day, the memories remain and people reported enduring changes in mood, attitude, and behavior.”
The data were remarkable. One month after these high-dose psilocybin sessions, 78% of the volunteers rated the experience as among the top five most personally meaningful experiences of their lives, 94% said they had an increased sense of well-being with improved life satisfaction, and nearly 90% endorsed positive behavior change. Six months after the last session, participants still endorsed having more positive relationships, feeling more love, tolerance, empathy and compassion, friends, family members, and others. Family members and work colleagues who were interviewed noted these positive changes as well.
At this point in Grand Rounds, I was ready to volunteer. My best estimate (tongue in cheek, with no corroboration) is that about half of the audience was waiting on free psilocybin samples, while the other half was remembering Timothy Leary, PhD, bad trips, and psychosis. “We’ve been down this road before,” the gentleman next to me commented.
Dr. Griffiths went on to talk about trials of psilocybin in clinical populations. In one study, the effects of psilocybin were examined in cancer patients with depression and anxiety. Of the 51 cancer patients, half previously had been treated with psychotropic medications before coming to the study. This randomized, double-blind crossover study compared high-dose psilocybin with an extremely low dose of psilocybin used as the placebo.
Another study looked at patients with major depression who, like the patient interviewed, had not had full resolution of symptoms with conventional antidepressants. Of the 24 participants in that group, 69% reported clinically significant improvement 12 weeks after the treatment. Just over half of participants reported a full remission to normal.
Dr. Griffiths ended by concluding that the positive experiences people have with psilocybin are associated with “enduring positive trait changes in attitudes, mood and behavior, spirituality, and altruism ... and that such experiences are now amenable to systematic prospective scientific study.”
J. Raymond DePaulo, MD, chair of the National Network of Depression Centers and former chair of psychiatry at Johns Hopkins, noted that he used to be skeptical. He has been impressed that Dr. Griffiths has listened to criticism and addressed concerns others have raised. “When it was suggested that this was the result of delirium, he started giving people cognitive tests while they were using psilocybin and he showed it wasn’t the case.”
“I have always objected to words like ‘psychedelic’ and ‘hallucinogen,’ ” said Dr. DePaulo. “They are confusing and inaccurate. No one takes these medications because they want to hallucinate. They take them to change their mood. That said, I am thrilled that we are on the precipice of being able to use this to treat depression.”
Since 1999, the Johns Hopkins Psilocybin Research Project has conducted more than 700 sessions with 369 participants. When might psilocybin be available to patients outside of a research protocol? Two companies have obtained approval from the Food and Drug Administration to initiate registration in trials for treatment of depression. Dr. Griffiths estimates that it could be another 5 years before psilocybin will be available for medical use.
The new center with its generous funding will allow for more studies with more patient populations. The center’s projects will look at using psilocybin as a treatment for opioid use disorder, comorbid depression and alcohol use disorder, anorexia nervosa, depression in Alzheimer’s disease, posttreatment Lyme disease syndrome, and PTSD.
Scott Aaronson, MD, is a mood disorder expert and director of clinical research at the Sheppard Pratt Health System in Towson/Baltimore. Dr. Aaronson, who also studies psilocybin as a treatment for depression, noted: “The problem with the development of psychedelics is that we are not really prepared to capture the improvement we see with their use, as the main changes are not in the classic markers of depression like the Montgomery-Åsberg or the Hamilton Depression rating scales, but [rather] in the patient’s perception of who they are, how they fit in with the world, and what is most important. We need to develop ways to capture those critical changes and work with the FDA to develop an entirely new vision of what constitutes improvement in psychiatric illness. My overall take is that it is a terrific time to specialize in treatment-resistant mood disorders!”
Dr. Miller is coauthor of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
Baltimore’s pilot project in outpatient civil commitment
Novel program has gotten off to a rough start
No topic is quite so controversial in psychiatry as outpatient civil commitment.
We all value the right to make our own medical decisions, perhaps even more so when it comes to issues of mental health. The concern, however, is that some patients lack the ability to see that they are ill, and their refusal to participate in treatment leads them to repeated involuntary hospitalizations or to behaviors that result in their incarceration. Mandated care for forensic patients – those who have ended up in the criminal justice system – is not as controversial, but for those who have committed no crime, the legislative struggles can get very heated. Add to that the cost of implementing outpatient civil commitment (OCC), the difficulties in enforcing the orders, the call to include an array of services for participants, the difficulties in ascertaining if these mandates are successful in helping patients live better lives, and the fact that treatment doesn’t always work, then what seems like a simple solution to the problem of noncompliance is actually quite complex.
Maryland is one of four states that does not have OCC. In 2017, it was announced that the city of Baltimore would begin an OCC pilot program. The program, administered by Behavioral Health System Baltimore (BHSB) in partnership with numerous other mental health organizations, has had several fits and starts. The program initially was funded by the Substance Abuse and Mental Health Services Administration (SAMHSA), and the grant required the program to serve a minimum of 75 patients. However, it was soon discovered that there were no written regulations, and that began a 1-year delay while regulations were written, including two periods for open public comment. Once set, BHSB needed to let local hospitals know the program existed and solicit referrals.
When it became clear that they would not be able to serve 75 individuals, BHSB elected to give its funding back to SAMHSA, and a second 3-month delay ensued until the state of Maryland picked up the cost. The Baltimore pilot project in OCC is different from other civil commitment programs. The criteria for inclusion are brief: The patient must be aged over 18 years, be a resident of Baltimore, and must have been retained by a judge at a hospital inpatient civil commitment hearing at least two times in the past year because of noncompliance with outpatient treatment. The referral needs to come from the inpatient unit before the patient is discharged, and entails a “settlement agreement” with a judge, typically the same administrative law judge that visits the hospital weekly for the inpatient commitment hearings. A connection is made with the patient prior to discharge from the inpatient facility.
The Baltimore project also differs in many ways from traditional outpatient commitment programs in other states. In this program, the patient is not mandated to treatment. Instead, the patient is required to meet with the program’s peer-recovery specialist. The recovery specialist provides support for the patient after discharge, facilitates engagement in both psychiatric and somatic medical care, and helps with transportation to appointments. Services for each participant continue for 6 months; the initial SAMHSA grant was for $2.8 million for 4 years.
Nicole McGill, the program’s monitor notes: “When people are repeatedly hospitalized, it signals to us that maybe the system hasn’t been doing what it needs to do. For those people, the OCC pilot aims to be the connection to existing services in the community.”
Of the 19 people who have been referred to the program since October 2017, 9 have been accepted. Six of those patients enrolled voluntarily; three were ordered into the program against their will. Of those three, one patient has refused to meet with the peer-recovery specialist. That patient, however, is enrolled with an Assertive Community Treatment and is not someone who is refusing psychiatric treatment. That patient was enlisted with the hope that more engagement might prevent future hospitalizations.
“We didn’t want to create a program that forced people into treatment,” said Adrienne Breidenstine, vice president for policy and communications for BHSB. “Those programs don’t work. If a program participant chooses not to engage in services, the OCC peers will step up their engagement. There are no punitive or legal consequences; they aren’t brought back to the hospital or taken to jail.”
So far, the program has been well received by its clients. Feedback is solicited through the Mental Health Association of Maryland. One client provided a testimonial saying: “I didn’t know there were so many resources out there. They took me to the food co-op and gave me free sheets. I got a fan. They didn’t waste time getting me that. It helped a lot with the heat. They get me to appointments. They helped so much.”
This fall, BHSB is expanding its services; as of Sept. 9, 2019, any Baltimore resident who is currently hospitalized and has been hospitalized at least one other time in the past 12 months will be eligible for the outpatient “commitment” program; there will no longer be a requirement that these inpatient stays involved retention at a civil commitment hearing or that the patient ever had an involuntary status. Patients who have not been committed to the hospital, however, will only be able to enter the program on a voluntary track.
This model of OCC is a bit of a misnomer: Most of the patients are in the program voluntarily, and they are not being required to go to treatment or take medications. It is a way to get a higher level of service to the sickest of patients who have needed repeated hospitalizations without the objections that get raised when patients are mandated to care. Given the distress that involuntary hospitalization causes, it may well be helpful to expand a voluntary offer of services to all patients who are retained at a hearing, even if only once; perhaps the added support could prevent future decompensations.
For now, the program has had a rough beginning, and the expense is hard to justify for so few patients. For advocates who support outpatient commitment, this program does not go far enough, as there is no requirement to take medications and no consequence for refusal to participate. As the criteria for inclusion are loosened to include those who are repeatedly hospitalized on a voluntary basis, it will be interesting to see if hospitalizations can be prevented and if the quality of life can be improved for these patients.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice, and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
Novel program has gotten off to a rough start
Novel program has gotten off to a rough start
No topic is quite so controversial in psychiatry as outpatient civil commitment.
We all value the right to make our own medical decisions, perhaps even more so when it comes to issues of mental health. The concern, however, is that some patients lack the ability to see that they are ill, and their refusal to participate in treatment leads them to repeated involuntary hospitalizations or to behaviors that result in their incarceration. Mandated care for forensic patients – those who have ended up in the criminal justice system – is not as controversial, but for those who have committed no crime, the legislative struggles can get very heated. Add to that the cost of implementing outpatient civil commitment (OCC), the difficulties in enforcing the orders, the call to include an array of services for participants, the difficulties in ascertaining if these mandates are successful in helping patients live better lives, and the fact that treatment doesn’t always work, then what seems like a simple solution to the problem of noncompliance is actually quite complex.
Maryland is one of four states that does not have OCC. In 2017, it was announced that the city of Baltimore would begin an OCC pilot program. The program, administered by Behavioral Health System Baltimore (BHSB) in partnership with numerous other mental health organizations, has had several fits and starts. The program initially was funded by the Substance Abuse and Mental Health Services Administration (SAMHSA), and the grant required the program to serve a minimum of 75 patients. However, it was soon discovered that there were no written regulations, and that began a 1-year delay while regulations were written, including two periods for open public comment. Once set, BHSB needed to let local hospitals know the program existed and solicit referrals.
When it became clear that they would not be able to serve 75 individuals, BHSB elected to give its funding back to SAMHSA, and a second 3-month delay ensued until the state of Maryland picked up the cost. The Baltimore pilot project in OCC is different from other civil commitment programs. The criteria for inclusion are brief: The patient must be aged over 18 years, be a resident of Baltimore, and must have been retained by a judge at a hospital inpatient civil commitment hearing at least two times in the past year because of noncompliance with outpatient treatment. The referral needs to come from the inpatient unit before the patient is discharged, and entails a “settlement agreement” with a judge, typically the same administrative law judge that visits the hospital weekly for the inpatient commitment hearings. A connection is made with the patient prior to discharge from the inpatient facility.
The Baltimore project also differs in many ways from traditional outpatient commitment programs in other states. In this program, the patient is not mandated to treatment. Instead, the patient is required to meet with the program’s peer-recovery specialist. The recovery specialist provides support for the patient after discharge, facilitates engagement in both psychiatric and somatic medical care, and helps with transportation to appointments. Services for each participant continue for 6 months; the initial SAMHSA grant was for $2.8 million for 4 years.
Nicole McGill, the program’s monitor notes: “When people are repeatedly hospitalized, it signals to us that maybe the system hasn’t been doing what it needs to do. For those people, the OCC pilot aims to be the connection to existing services in the community.”
Of the 19 people who have been referred to the program since October 2017, 9 have been accepted. Six of those patients enrolled voluntarily; three were ordered into the program against their will. Of those three, one patient has refused to meet with the peer-recovery specialist. That patient, however, is enrolled with an Assertive Community Treatment and is not someone who is refusing psychiatric treatment. That patient was enlisted with the hope that more engagement might prevent future hospitalizations.
“We didn’t want to create a program that forced people into treatment,” said Adrienne Breidenstine, vice president for policy and communications for BHSB. “Those programs don’t work. If a program participant chooses not to engage in services, the OCC peers will step up their engagement. There are no punitive or legal consequences; they aren’t brought back to the hospital or taken to jail.”
So far, the program has been well received by its clients. Feedback is solicited through the Mental Health Association of Maryland. One client provided a testimonial saying: “I didn’t know there were so many resources out there. They took me to the food co-op and gave me free sheets. I got a fan. They didn’t waste time getting me that. It helped a lot with the heat. They get me to appointments. They helped so much.”
This fall, BHSB is expanding its services; as of Sept. 9, 2019, any Baltimore resident who is currently hospitalized and has been hospitalized at least one other time in the past 12 months will be eligible for the outpatient “commitment” program; there will no longer be a requirement that these inpatient stays involved retention at a civil commitment hearing or that the patient ever had an involuntary status. Patients who have not been committed to the hospital, however, will only be able to enter the program on a voluntary track.
This model of OCC is a bit of a misnomer: Most of the patients are in the program voluntarily, and they are not being required to go to treatment or take medications. It is a way to get a higher level of service to the sickest of patients who have needed repeated hospitalizations without the objections that get raised when patients are mandated to care. Given the distress that involuntary hospitalization causes, it may well be helpful to expand a voluntary offer of services to all patients who are retained at a hearing, even if only once; perhaps the added support could prevent future decompensations.
For now, the program has had a rough beginning, and the expense is hard to justify for so few patients. For advocates who support outpatient commitment, this program does not go far enough, as there is no requirement to take medications and no consequence for refusal to participate. As the criteria for inclusion are loosened to include those who are repeatedly hospitalized on a voluntary basis, it will be interesting to see if hospitalizations can be prevented and if the quality of life can be improved for these patients.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice, and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
No topic is quite so controversial in psychiatry as outpatient civil commitment.
We all value the right to make our own medical decisions, perhaps even more so when it comes to issues of mental health. The concern, however, is that some patients lack the ability to see that they are ill, and their refusal to participate in treatment leads them to repeated involuntary hospitalizations or to behaviors that result in their incarceration. Mandated care for forensic patients – those who have ended up in the criminal justice system – is not as controversial, but for those who have committed no crime, the legislative struggles can get very heated. Add to that the cost of implementing outpatient civil commitment (OCC), the difficulties in enforcing the orders, the call to include an array of services for participants, the difficulties in ascertaining if these mandates are successful in helping patients live better lives, and the fact that treatment doesn’t always work, then what seems like a simple solution to the problem of noncompliance is actually quite complex.
Maryland is one of four states that does not have OCC. In 2017, it was announced that the city of Baltimore would begin an OCC pilot program. The program, administered by Behavioral Health System Baltimore (BHSB) in partnership with numerous other mental health organizations, has had several fits and starts. The program initially was funded by the Substance Abuse and Mental Health Services Administration (SAMHSA), and the grant required the program to serve a minimum of 75 patients. However, it was soon discovered that there were no written regulations, and that began a 1-year delay while regulations were written, including two periods for open public comment. Once set, BHSB needed to let local hospitals know the program existed and solicit referrals.
When it became clear that they would not be able to serve 75 individuals, BHSB elected to give its funding back to SAMHSA, and a second 3-month delay ensued until the state of Maryland picked up the cost. The Baltimore pilot project in OCC is different from other civil commitment programs. The criteria for inclusion are brief: The patient must be aged over 18 years, be a resident of Baltimore, and must have been retained by a judge at a hospital inpatient civil commitment hearing at least two times in the past year because of noncompliance with outpatient treatment. The referral needs to come from the inpatient unit before the patient is discharged, and entails a “settlement agreement” with a judge, typically the same administrative law judge that visits the hospital weekly for the inpatient commitment hearings. A connection is made with the patient prior to discharge from the inpatient facility.
The Baltimore project also differs in many ways from traditional outpatient commitment programs in other states. In this program, the patient is not mandated to treatment. Instead, the patient is required to meet with the program’s peer-recovery specialist. The recovery specialist provides support for the patient after discharge, facilitates engagement in both psychiatric and somatic medical care, and helps with transportation to appointments. Services for each participant continue for 6 months; the initial SAMHSA grant was for $2.8 million for 4 years.
Nicole McGill, the program’s monitor notes: “When people are repeatedly hospitalized, it signals to us that maybe the system hasn’t been doing what it needs to do. For those people, the OCC pilot aims to be the connection to existing services in the community.”
Of the 19 people who have been referred to the program since October 2017, 9 have been accepted. Six of those patients enrolled voluntarily; three were ordered into the program against their will. Of those three, one patient has refused to meet with the peer-recovery specialist. That patient, however, is enrolled with an Assertive Community Treatment and is not someone who is refusing psychiatric treatment. That patient was enlisted with the hope that more engagement might prevent future hospitalizations.
“We didn’t want to create a program that forced people into treatment,” said Adrienne Breidenstine, vice president for policy and communications for BHSB. “Those programs don’t work. If a program participant chooses not to engage in services, the OCC peers will step up their engagement. There are no punitive or legal consequences; they aren’t brought back to the hospital or taken to jail.”
So far, the program has been well received by its clients. Feedback is solicited through the Mental Health Association of Maryland. One client provided a testimonial saying: “I didn’t know there were so many resources out there. They took me to the food co-op and gave me free sheets. I got a fan. They didn’t waste time getting me that. It helped a lot with the heat. They get me to appointments. They helped so much.”
This fall, BHSB is expanding its services; as of Sept. 9, 2019, any Baltimore resident who is currently hospitalized and has been hospitalized at least one other time in the past 12 months will be eligible for the outpatient “commitment” program; there will no longer be a requirement that these inpatient stays involved retention at a civil commitment hearing or that the patient ever had an involuntary status. Patients who have not been committed to the hospital, however, will only be able to enter the program on a voluntary track.
This model of OCC is a bit of a misnomer: Most of the patients are in the program voluntarily, and they are not being required to go to treatment or take medications. It is a way to get a higher level of service to the sickest of patients who have needed repeated hospitalizations without the objections that get raised when patients are mandated to care. Given the distress that involuntary hospitalization causes, it may well be helpful to expand a voluntary offer of services to all patients who are retained at a hearing, even if only once; perhaps the added support could prevent future decompensations.
For now, the program has had a rough beginning, and the expense is hard to justify for so few patients. For advocates who support outpatient commitment, this program does not go far enough, as there is no requirement to take medications and no consequence for refusal to participate. As the criteria for inclusion are loosened to include those who are repeatedly hospitalized on a voluntary basis, it will be interesting to see if hospitalizations can be prevented and if the quality of life can be improved for these patients.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle Over Involuntary Psychiatric Care” (Baltimore: Johns Hopkins University, 2016). She has a private practice, and is assistant professor of psychiatry and behavioral sciences at Johns Hopkins, both in Baltimore.
Insurance networks: Is it time to abandon them?
Bob has been coming to therapy for a few months now. Initially, we met every week, but as his depression lifted, he asked to space the sessions out to twice a month, even as he continues to struggle with many challenges in his life. The cost, he says, is prohibitive, and while Bob believed he had good commercial insurance coverage, he’s learned a few things about insurance and mental health care.
Bob was referred to me by his internist. He knew I did not participate in his insurance network, but his policy covers out-of-network care. He’d had a number of imaging studies and then knee surgery earlier in the year, so he believed he’d met his deductible. He learned that, while he’d met his in-network deductible, he’d had no out-of-network expenses and there was a separate, much higher deductible – one he was not likely to meet with outpatient psychiatric care. In fact, the full cost of his treatment was not being subtracted from the deductible he needed to meet, but rather he was getting credit for lower usual and customary evaluation and management and psychotherapy fees for each session. It became clear that it would be many months – if ever – before Bob could expect any reimbursement for his out-of-network visits.
What Bob didn’t know was that, had he decided to switch to an in-network psychiatrist, he might well have trouble finding one, since half of psychiatrists don’t participate with any health insurance plans. And if he did see an in-network psychiatrist, he would likely need to find a separate in-network social worker or psychologist for psychotherapy, because most in-network psychiatrists see patients for short medication-management appointments. While the insurance companies would give Bob a list of providers, those lists are not kept up to date and include psychiatrists who have died, moved, aren’t taking new patients, or who have retired. The insurance company clearly states on its voicemail that verification of services does not guarantee payment, and Bob was told that the only way he could be certain of the reimbursement would be to submit the claims and wait. He went into treatment fully understanding that he might get no help with the cost from his health insurance.
When I first started in private practice in the 1990s, I joined only one panel. An older colleague told me I was foolish to hesitate, and that soon the panels would fill and it would be too late; psychiatrists wouldn’t be able to get on to the panels and would be unable to attract patients. A few years later, that same psychiatrist withdrew from all the insurance panels he was on; working on their terms was not rewarding. This division of in-network and out-of-network care is crucial to managed care: They must attract panels of doctors who will work for lower rates or with stipulations on how the doctor practices in order to save money.
But managed care came with a price: An entire administration was created to oversee the regulation of treatment. With time, some aspects of care management have vanished; it has been years since I have been asked to fill out a treatment plan to justify a need for outpatient psychotherapy. In Bob’s case, it’s clear how they save money; since he will not reach his high deductible, he will bear the full cost of his psychotherapy. Other patients who cannot afford to go out of network may give up searching and decide to go without treatment – this is not always an easy service to negotiate when one is distressed and compromised. Half of people with serious psychiatric disorders are not in treatment, and barriers to getting care are certainly one reason why.
Many psychiatrists have discovered that they can maintain a practice without being on insurance panels, as managed care only works if there are enough players willing to toss the ball. As psychiatrists have shied away from these panels, insurers have raised their reimbursement rates, and in Maryland, Medicaid also has had to raise their rates. The struggle has become one of how to get enough mental health professionals, and psychiatrists in particular, to join insurance panels in what is a shortage field.
Perhaps there are better ways to spend health care dollars than on the administration and management that come with limiting which doctors patients can see. The logistics of in-network versus out-of-network care are an expensive one, and create unconscionable scenarios in other fields. For example, such scenarios include ones in which a patient is brought in for emergency care to a facility where the doctors are not in network, or a patient has a procedure with an in-network surgeon but is unaware that the anesthesiologist or other members of the care team are not on the panel.
What if insurers controlled costs by setting a reasonable fee they would pay for services and paid any licensed physician for these services? Would market forces sort this out? Would fees then set to one which insurers would be willing to pay and physicians would be willing to accept? Or would those who are ill and impoverished be blocked from getting any care? What if we tried a whole new paradigm for psychiatric care?
Richard G. Frank, PhD, is a professor of health economics at Harvard. He specializes in mental health economics and is coauthor of the book “Better But Not Well: Mental Health Policy in the United States Since 1950” (Baltimore: Johns Hopkins University Press, 2006). Dr. Frank is a proponent of insurance panels.
“In the world we live in, we need to have panels; they are essential to controlling cost. They create a balance in terms of cost and utilization control in ways that protect patients, and they create a way for the insurance companies to bargain,” he said.
Dr. Frank noted that the concept that insurers should pay a set reasonable fee to any physician a patient wants to see has been tried. “It’s called ‘reference pricing,’ and when they did that with hip replacement surgery in California, it just hasn’t worked out. Patients ended up getting larger bills than they anticipated.
“The issues with psychiatry are different,” he continued. “There is a lot of bad behavior on the part of insurers and it’s an issue of parity. We shouldn’t let insurers differentially pay psychiatrists less. They have had an incentive to reduce the availability of mental health care and it’s bad for patients. It’s about lower payments to psychiatrists and the way those payments are currently structured drives patients out of care and defeats the purpose of insurance.”
Steven Sharfstein, MD, is the former CEO of Sheppard Pratt Health Systems, a past president of the American Psychiatric Association, and coauthor of several books on the economics of psychiatry. He refers to the current practice of credentialing network psychiatrists as a means of “rationing by supply.”
“The networks create a barrier to accessing care. I don’t think it’s an efficient way to take on the high cost of care, and it creates a tiered system.” Like Dr. Frank, Dr. Sharfstein believes parity is a large part of the problem. When asked about the idea of ending networks and establishing uniform deductibles and reimbursement rates, Dr. Sharfstein replied: “It really depends. We would need fees to hit a sweet spot that supports care while controlling costs.”
One thing is clear: With the current paradigm, it is often difficult to access treatment, and the well-insured patients may bear a significant and disproportionate cost (if not the entire cost) for getting care. Many who need care do not get it, regardless of their insurance status. Our status quo for psychiatric care falls short and I don’t predict that psychiatrists will rush to join networks so long as the demand for psychiatrists is greater than the supply.
Might another financial model work better? We know the system is lacking and one option, as Dr. Frank suggests, is to find solutions within the current model. But perhaps the question should not be one of how to get more psychiatrists to join networks, but of how to rework the system without the assumption that networks are the only way. While Bob is pleased that his symptoms are getting better and he’s managed a way to tackle his own bills, it’s certainly time to explore new ways of delivering and reimbursing psychiatric care.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle of Inpatient Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016), and has a private practice in Baltimore.
Bob has been coming to therapy for a few months now. Initially, we met every week, but as his depression lifted, he asked to space the sessions out to twice a month, even as he continues to struggle with many challenges in his life. The cost, he says, is prohibitive, and while Bob believed he had good commercial insurance coverage, he’s learned a few things about insurance and mental health care.
Bob was referred to me by his internist. He knew I did not participate in his insurance network, but his policy covers out-of-network care. He’d had a number of imaging studies and then knee surgery earlier in the year, so he believed he’d met his deductible. He learned that, while he’d met his in-network deductible, he’d had no out-of-network expenses and there was a separate, much higher deductible – one he was not likely to meet with outpatient psychiatric care. In fact, the full cost of his treatment was not being subtracted from the deductible he needed to meet, but rather he was getting credit for lower usual and customary evaluation and management and psychotherapy fees for each session. It became clear that it would be many months – if ever – before Bob could expect any reimbursement for his out-of-network visits.
What Bob didn’t know was that, had he decided to switch to an in-network psychiatrist, he might well have trouble finding one, since half of psychiatrists don’t participate with any health insurance plans. And if he did see an in-network psychiatrist, he would likely need to find a separate in-network social worker or psychologist for psychotherapy, because most in-network psychiatrists see patients for short medication-management appointments. While the insurance companies would give Bob a list of providers, those lists are not kept up to date and include psychiatrists who have died, moved, aren’t taking new patients, or who have retired. The insurance company clearly states on its voicemail that verification of services does not guarantee payment, and Bob was told that the only way he could be certain of the reimbursement would be to submit the claims and wait. He went into treatment fully understanding that he might get no help with the cost from his health insurance.
When I first started in private practice in the 1990s, I joined only one panel. An older colleague told me I was foolish to hesitate, and that soon the panels would fill and it would be too late; psychiatrists wouldn’t be able to get on to the panels and would be unable to attract patients. A few years later, that same psychiatrist withdrew from all the insurance panels he was on; working on their terms was not rewarding. This division of in-network and out-of-network care is crucial to managed care: They must attract panels of doctors who will work for lower rates or with stipulations on how the doctor practices in order to save money.
But managed care came with a price: An entire administration was created to oversee the regulation of treatment. With time, some aspects of care management have vanished; it has been years since I have been asked to fill out a treatment plan to justify a need for outpatient psychotherapy. In Bob’s case, it’s clear how they save money; since he will not reach his high deductible, he will bear the full cost of his psychotherapy. Other patients who cannot afford to go out of network may give up searching and decide to go without treatment – this is not always an easy service to negotiate when one is distressed and compromised. Half of people with serious psychiatric disorders are not in treatment, and barriers to getting care are certainly one reason why.
Many psychiatrists have discovered that they can maintain a practice without being on insurance panels, as managed care only works if there are enough players willing to toss the ball. As psychiatrists have shied away from these panels, insurers have raised their reimbursement rates, and in Maryland, Medicaid also has had to raise their rates. The struggle has become one of how to get enough mental health professionals, and psychiatrists in particular, to join insurance panels in what is a shortage field.
Perhaps there are better ways to spend health care dollars than on the administration and management that come with limiting which doctors patients can see. The logistics of in-network versus out-of-network care are an expensive one, and create unconscionable scenarios in other fields. For example, such scenarios include ones in which a patient is brought in for emergency care to a facility where the doctors are not in network, or a patient has a procedure with an in-network surgeon but is unaware that the anesthesiologist or other members of the care team are not on the panel.
What if insurers controlled costs by setting a reasonable fee they would pay for services and paid any licensed physician for these services? Would market forces sort this out? Would fees then set to one which insurers would be willing to pay and physicians would be willing to accept? Or would those who are ill and impoverished be blocked from getting any care? What if we tried a whole new paradigm for psychiatric care?
Richard G. Frank, PhD, is a professor of health economics at Harvard. He specializes in mental health economics and is coauthor of the book “Better But Not Well: Mental Health Policy in the United States Since 1950” (Baltimore: Johns Hopkins University Press, 2006). Dr. Frank is a proponent of insurance panels.
“In the world we live in, we need to have panels; they are essential to controlling cost. They create a balance in terms of cost and utilization control in ways that protect patients, and they create a way for the insurance companies to bargain,” he said.
Dr. Frank noted that the concept that insurers should pay a set reasonable fee to any physician a patient wants to see has been tried. “It’s called ‘reference pricing,’ and when they did that with hip replacement surgery in California, it just hasn’t worked out. Patients ended up getting larger bills than they anticipated.
“The issues with psychiatry are different,” he continued. “There is a lot of bad behavior on the part of insurers and it’s an issue of parity. We shouldn’t let insurers differentially pay psychiatrists less. They have had an incentive to reduce the availability of mental health care and it’s bad for patients. It’s about lower payments to psychiatrists and the way those payments are currently structured drives patients out of care and defeats the purpose of insurance.”
Steven Sharfstein, MD, is the former CEO of Sheppard Pratt Health Systems, a past president of the American Psychiatric Association, and coauthor of several books on the economics of psychiatry. He refers to the current practice of credentialing network psychiatrists as a means of “rationing by supply.”
“The networks create a barrier to accessing care. I don’t think it’s an efficient way to take on the high cost of care, and it creates a tiered system.” Like Dr. Frank, Dr. Sharfstein believes parity is a large part of the problem. When asked about the idea of ending networks and establishing uniform deductibles and reimbursement rates, Dr. Sharfstein replied: “It really depends. We would need fees to hit a sweet spot that supports care while controlling costs.”
One thing is clear: With the current paradigm, it is often difficult to access treatment, and the well-insured patients may bear a significant and disproportionate cost (if not the entire cost) for getting care. Many who need care do not get it, regardless of their insurance status. Our status quo for psychiatric care falls short and I don’t predict that psychiatrists will rush to join networks so long as the demand for psychiatrists is greater than the supply.
Might another financial model work better? We know the system is lacking and one option, as Dr. Frank suggests, is to find solutions within the current model. But perhaps the question should not be one of how to get more psychiatrists to join networks, but of how to rework the system without the assumption that networks are the only way. While Bob is pleased that his symptoms are getting better and he’s managed a way to tackle his own bills, it’s certainly time to explore new ways of delivering and reimbursing psychiatric care.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle of Inpatient Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016), and has a private practice in Baltimore.
Bob has been coming to therapy for a few months now. Initially, we met every week, but as his depression lifted, he asked to space the sessions out to twice a month, even as he continues to struggle with many challenges in his life. The cost, he says, is prohibitive, and while Bob believed he had good commercial insurance coverage, he’s learned a few things about insurance and mental health care.
Bob was referred to me by his internist. He knew I did not participate in his insurance network, but his policy covers out-of-network care. He’d had a number of imaging studies and then knee surgery earlier in the year, so he believed he’d met his deductible. He learned that, while he’d met his in-network deductible, he’d had no out-of-network expenses and there was a separate, much higher deductible – one he was not likely to meet with outpatient psychiatric care. In fact, the full cost of his treatment was not being subtracted from the deductible he needed to meet, but rather he was getting credit for lower usual and customary evaluation and management and psychotherapy fees for each session. It became clear that it would be many months – if ever – before Bob could expect any reimbursement for his out-of-network visits.
What Bob didn’t know was that, had he decided to switch to an in-network psychiatrist, he might well have trouble finding one, since half of psychiatrists don’t participate with any health insurance plans. And if he did see an in-network psychiatrist, he would likely need to find a separate in-network social worker or psychologist for psychotherapy, because most in-network psychiatrists see patients for short medication-management appointments. While the insurance companies would give Bob a list of providers, those lists are not kept up to date and include psychiatrists who have died, moved, aren’t taking new patients, or who have retired. The insurance company clearly states on its voicemail that verification of services does not guarantee payment, and Bob was told that the only way he could be certain of the reimbursement would be to submit the claims and wait. He went into treatment fully understanding that he might get no help with the cost from his health insurance.
When I first started in private practice in the 1990s, I joined only one panel. An older colleague told me I was foolish to hesitate, and that soon the panels would fill and it would be too late; psychiatrists wouldn’t be able to get on to the panels and would be unable to attract patients. A few years later, that same psychiatrist withdrew from all the insurance panels he was on; working on their terms was not rewarding. This division of in-network and out-of-network care is crucial to managed care: They must attract panels of doctors who will work for lower rates or with stipulations on how the doctor practices in order to save money.
But managed care came with a price: An entire administration was created to oversee the regulation of treatment. With time, some aspects of care management have vanished; it has been years since I have been asked to fill out a treatment plan to justify a need for outpatient psychotherapy. In Bob’s case, it’s clear how they save money; since he will not reach his high deductible, he will bear the full cost of his psychotherapy. Other patients who cannot afford to go out of network may give up searching and decide to go without treatment – this is not always an easy service to negotiate when one is distressed and compromised. Half of people with serious psychiatric disorders are not in treatment, and barriers to getting care are certainly one reason why.
Many psychiatrists have discovered that they can maintain a practice without being on insurance panels, as managed care only works if there are enough players willing to toss the ball. As psychiatrists have shied away from these panels, insurers have raised their reimbursement rates, and in Maryland, Medicaid also has had to raise their rates. The struggle has become one of how to get enough mental health professionals, and psychiatrists in particular, to join insurance panels in what is a shortage field.
Perhaps there are better ways to spend health care dollars than on the administration and management that come with limiting which doctors patients can see. The logistics of in-network versus out-of-network care are an expensive one, and create unconscionable scenarios in other fields. For example, such scenarios include ones in which a patient is brought in for emergency care to a facility where the doctors are not in network, or a patient has a procedure with an in-network surgeon but is unaware that the anesthesiologist or other members of the care team are not on the panel.
What if insurers controlled costs by setting a reasonable fee they would pay for services and paid any licensed physician for these services? Would market forces sort this out? Would fees then set to one which insurers would be willing to pay and physicians would be willing to accept? Or would those who are ill and impoverished be blocked from getting any care? What if we tried a whole new paradigm for psychiatric care?
Richard G. Frank, PhD, is a professor of health economics at Harvard. He specializes in mental health economics and is coauthor of the book “Better But Not Well: Mental Health Policy in the United States Since 1950” (Baltimore: Johns Hopkins University Press, 2006). Dr. Frank is a proponent of insurance panels.
“In the world we live in, we need to have panels; they are essential to controlling cost. They create a balance in terms of cost and utilization control in ways that protect patients, and they create a way for the insurance companies to bargain,” he said.
Dr. Frank noted that the concept that insurers should pay a set reasonable fee to any physician a patient wants to see has been tried. “It’s called ‘reference pricing,’ and when they did that with hip replacement surgery in California, it just hasn’t worked out. Patients ended up getting larger bills than they anticipated.
“The issues with psychiatry are different,” he continued. “There is a lot of bad behavior on the part of insurers and it’s an issue of parity. We shouldn’t let insurers differentially pay psychiatrists less. They have had an incentive to reduce the availability of mental health care and it’s bad for patients. It’s about lower payments to psychiatrists and the way those payments are currently structured drives patients out of care and defeats the purpose of insurance.”
Steven Sharfstein, MD, is the former CEO of Sheppard Pratt Health Systems, a past president of the American Psychiatric Association, and coauthor of several books on the economics of psychiatry. He refers to the current practice of credentialing network psychiatrists as a means of “rationing by supply.”
“The networks create a barrier to accessing care. I don’t think it’s an efficient way to take on the high cost of care, and it creates a tiered system.” Like Dr. Frank, Dr. Sharfstein believes parity is a large part of the problem. When asked about the idea of ending networks and establishing uniform deductibles and reimbursement rates, Dr. Sharfstein replied: “It really depends. We would need fees to hit a sweet spot that supports care while controlling costs.”
One thing is clear: With the current paradigm, it is often difficult to access treatment, and the well-insured patients may bear a significant and disproportionate cost (if not the entire cost) for getting care. Many who need care do not get it, regardless of their insurance status. Our status quo for psychiatric care falls short and I don’t predict that psychiatrists will rush to join networks so long as the demand for psychiatrists is greater than the supply.
Might another financial model work better? We know the system is lacking and one option, as Dr. Frank suggests, is to find solutions within the current model. But perhaps the question should not be one of how to get more psychiatrists to join networks, but of how to rework the system without the assumption that networks are the only way. While Bob is pleased that his symptoms are getting better and he’s managed a way to tackle his own bills, it’s certainly time to explore new ways of delivering and reimbursing psychiatric care.
Dr. Miller is coauthor with Annette Hanson, MD, of “Committed: The Battle of Inpatient Psychiatric Care” (Baltimore: Johns Hopkins University Press, 2016), and has a private practice in Baltimore.