User login
Local Factors Play Major Role in Determining Compensation Rates for Pediatric Hospitalists
Although pediatricians make up less than 6% of the hospitalists surveyed by the Medical Group Management Association (MGMA), they represent a very different data profile from other specialties reported in SHM’s 2012 State of Hospital Medicine report.
The nonpediatric HM specialties (internal medicine, family medicine, and med/peds) have similar data profiles with regard to productivity and compensation statistics. They are all within 2% of the $233,855 “all adult hospitalists” median compensation. Although there is a bit more variability in the productivity data, all three groups are clustered within 10% of each other. The key to understanding their similarity is that they all serve mostly adult inpatients. While some of these physicians may also care for hospitalized children, I suspect this population is a small proportion of their daily workload.
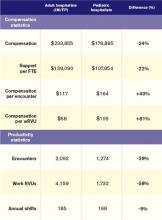
Pediatric hospitalists only treat pediatric patients and differ significantly from adult hospitalists, as summarized in Table 1.
Pediatricians remain among the lowest-earning specialties nationally, whether in the office or on children’s wards. The key to understanding the differences between adult and pediatric hospitalists is that they derive their compensation and productivity expectations from two separate and distinct physician marketplaces. Adult hospitalists benefit from more than a decade of rapidly growing demand for their services, as well as higher compensation for their office-based counterparts. Meanwhile, the market for pediatric hospitalists remains smaller and more segmented, allowing local factors to drive compensation more than a national demand for their services would.
Pediatric hospitalists appear to earn about a quarter less than their adult counterparts while receiving a similarly lower amount of hospital financial support per provider. Pediatric hospitalists also appear to work less than adult hospitalists, reflected in fewer shifts annually and fewer hours per shift; 75% of adult hospitalist groups report shift lengths of 12 hours or more, compared with 48% of pediatric hospitalist groups. This may stem from the frequent lulls in census common to a community hospital pediatrics service, in contrast to more consistent demand posed by geriatric populations. Although pediatric hospitalists receive more compensation per encounter or wRVU, they cannot generate those encounters or work RVUs at the same clip as adult hospitalists. Pediatricians must hold a family meeting for every single patient, and even something as seemingly simple as obtaining intravenous access might consume 45 minutes of a hospitalist’s time.
Thus, pediatric hospitalists find themselves caught in the same market as other pediatric specialists. These providers remain undervalued compared to virtually all other physicians. Those who seek to improve their financial prospects likely need to work more shifts or generate more workload relative to the expectations of their pediatrician peers.
Personally, I can’t help but wonder what attention pediatric care might enjoy if kids had a vote, a pension, an entitlement program, and a lobby on K Street like their grandparents do.
Dr. Ahlstrom is clinical director of Hospitalists of Northern Michigan and a member of SHM’s Practice Analysis Committee.
Although pediatricians make up less than 6% of the hospitalists surveyed by the Medical Group Management Association (MGMA), they represent a very different data profile from other specialties reported in SHM’s 2012 State of Hospital Medicine report.
The nonpediatric HM specialties (internal medicine, family medicine, and med/peds) have similar data profiles with regard to productivity and compensation statistics. They are all within 2% of the $233,855 “all adult hospitalists” median compensation. Although there is a bit more variability in the productivity data, all three groups are clustered within 10% of each other. The key to understanding their similarity is that they all serve mostly adult inpatients. While some of these physicians may also care for hospitalized children, I suspect this population is a small proportion of their daily workload.
Pediatric hospitalists only treat pediatric patients and differ significantly from adult hospitalists, as summarized in Table 1.
Pediatricians remain among the lowest-earning specialties nationally, whether in the office or on children’s wards. The key to understanding the differences between adult and pediatric hospitalists is that they derive their compensation and productivity expectations from two separate and distinct physician marketplaces. Adult hospitalists benefit from more than a decade of rapidly growing demand for their services, as well as higher compensation for their office-based counterparts. Meanwhile, the market for pediatric hospitalists remains smaller and more segmented, allowing local factors to drive compensation more than a national demand for their services would.
Pediatric hospitalists appear to earn about a quarter less than their adult counterparts while receiving a similarly lower amount of hospital financial support per provider. Pediatric hospitalists also appear to work less than adult hospitalists, reflected in fewer shifts annually and fewer hours per shift; 75% of adult hospitalist groups report shift lengths of 12 hours or more, compared with 48% of pediatric hospitalist groups. This may stem from the frequent lulls in census common to a community hospital pediatrics service, in contrast to more consistent demand posed by geriatric populations. Although pediatric hospitalists receive more compensation per encounter or wRVU, they cannot generate those encounters or work RVUs at the same clip as adult hospitalists. Pediatricians must hold a family meeting for every single patient, and even something as seemingly simple as obtaining intravenous access might consume 45 minutes of a hospitalist’s time.
Thus, pediatric hospitalists find themselves caught in the same market as other pediatric specialists. These providers remain undervalued compared to virtually all other physicians. Those who seek to improve their financial prospects likely need to work more shifts or generate more workload relative to the expectations of their pediatrician peers.
Personally, I can’t help but wonder what attention pediatric care might enjoy if kids had a vote, a pension, an entitlement program, and a lobby on K Street like their grandparents do.
Dr. Ahlstrom is clinical director of Hospitalists of Northern Michigan and a member of SHM’s Practice Analysis Committee.
Although pediatricians make up less than 6% of the hospitalists surveyed by the Medical Group Management Association (MGMA), they represent a very different data profile from other specialties reported in SHM’s 2012 State of Hospital Medicine report.
The nonpediatric HM specialties (internal medicine, family medicine, and med/peds) have similar data profiles with regard to productivity and compensation statistics. They are all within 2% of the $233,855 “all adult hospitalists” median compensation. Although there is a bit more variability in the productivity data, all three groups are clustered within 10% of each other. The key to understanding their similarity is that they all serve mostly adult inpatients. While some of these physicians may also care for hospitalized children, I suspect this population is a small proportion of their daily workload.
Pediatric hospitalists only treat pediatric patients and differ significantly from adult hospitalists, as summarized in Table 1.
Pediatricians remain among the lowest-earning specialties nationally, whether in the office or on children’s wards. The key to understanding the differences between adult and pediatric hospitalists is that they derive their compensation and productivity expectations from two separate and distinct physician marketplaces. Adult hospitalists benefit from more than a decade of rapidly growing demand for their services, as well as higher compensation for their office-based counterparts. Meanwhile, the market for pediatric hospitalists remains smaller and more segmented, allowing local factors to drive compensation more than a national demand for their services would.
Pediatric hospitalists appear to earn about a quarter less than their adult counterparts while receiving a similarly lower amount of hospital financial support per provider. Pediatric hospitalists also appear to work less than adult hospitalists, reflected in fewer shifts annually and fewer hours per shift; 75% of adult hospitalist groups report shift lengths of 12 hours or more, compared with 48% of pediatric hospitalist groups. This may stem from the frequent lulls in census common to a community hospital pediatrics service, in contrast to more consistent demand posed by geriatric populations. Although pediatric hospitalists receive more compensation per encounter or wRVU, they cannot generate those encounters or work RVUs at the same clip as adult hospitalists. Pediatricians must hold a family meeting for every single patient, and even something as seemingly simple as obtaining intravenous access might consume 45 minutes of a hospitalist’s time.
Thus, pediatric hospitalists find themselves caught in the same market as other pediatric specialists. These providers remain undervalued compared to virtually all other physicians. Those who seek to improve their financial prospects likely need to work more shifts or generate more workload relative to the expectations of their pediatrician peers.
Personally, I can’t help but wonder what attention pediatric care might enjoy if kids had a vote, a pension, an entitlement program, and a lobby on K Street like their grandparents do.
Dr. Ahlstrom is clinical director of Hospitalists of Northern Michigan and a member of SHM’s Practice Analysis Committee.
The Journal of Hospital Medicine Honors Top Reviewers for 2012
Journal of Hospital Medicine editors are recognizing 39 peer reviewers for the “collegial and insightful nature of their reviews.” The editors congratulate the reviewers for their contributions and thank them for the important role they play in making JHM an important and useful resource for its authors and readers.
- Brian Harte, MD, SFHM, South Pointe Hospital
- Michael DeVita, MD, St. Vincent’s Medical Center
- Gurpreet Dhaliwal, MD, University of California at San Francisco
- Evan Fieldston, MD, MBA, MSHP, Children’s Hospital of Philadelphia, University of Pennsylvania
- S. Ryan Greysen, MD, MHS, MA, University of California at San Francisco
- Luke Hansen, MD, Northwestern Memorial Hospital
- Luci Leykum, MD, FHM, University of Texas HSC
- Andrew Masica, MD, SFHM, Baylor Health Care System
- James C. Pile, MD, FACP, SFHM, Cleveland Clinic
- Steven Belknap, MD, Northwestern Memorial Hospital
- Vincent Liu, MD, Santa Clara (Calif.) Medical Center
- Basem Abdelmalak, MD, Cleveland Clinic
- Marisha Burden, MD, Denver Health Medical Center
- James Burke, MD, University of Michigan Health System, Ann Arbor
- Roy Carr-Hill, PhD, University of Liverpool
- Lawrence Haber, MD, University of California at San Francisco
- Keiki Hinami, MD,Northwestern Memorial Hospital
- Michael Hwa, MD, University of California at San Francisco
- Michael Jangigian, MD, New York University
- Mansoor Khalid, MD, Saint Francis Hospitalists
- Hilary Mosher, MD, University of Iowa Carver College of Medicine, Iowa City
- Andrew Odden, MD, Ann Arbor VA Medical Center, University of Michigan
- Maria Raven, MD, MPH, MSc, University of California at San Francisco
- Kristin Salottolo, MPH, St. Anthony Hospital
- Jonathan Sevransky, MD, MHS, Emory Healthcare
- Kittane Vishnupriya, MD, MBBS, Johns Hopkins Bayview Medical Center
- Robert S. Young, MD, Northwestern University
- Melissa Mattison, MD, SFHM, Beth Israel Deaconess Medical Center, Boston
- Jeff Rohde, MD, University of Michigan Health System, Ann Arbor
- Henry Michtalik, MD, Johns Hopkins
- Mark Shen, MD, Dell Children’s Medical Center of Central Texas, Austin
- Sumant Ranji, MD, University of California at San Francisco
- Greg Maynard, MD, SFHM, University of California at San Diego
- Anand Kartha, MD, MSc, Boston University
- Christopher Roy, MD, FHM, Brigham & Women’s Hospital, Boston
- Zachary Goldberger, MD, MS, University of Washington School of Medicine
- Chase Coffey, MD, Henry Ford Health System
- Quinn Czosnowski, PharmD, University of the Sciences
- Kenataro Iwata, MD, MSc, FACP, FIDSA, Kobe University Hospital
Journal of Hospital Medicine editors are recognizing 39 peer reviewers for the “collegial and insightful nature of their reviews.” The editors congratulate the reviewers for their contributions and thank them for the important role they play in making JHM an important and useful resource for its authors and readers.
- Brian Harte, MD, SFHM, South Pointe Hospital
- Michael DeVita, MD, St. Vincent’s Medical Center
- Gurpreet Dhaliwal, MD, University of California at San Francisco
- Evan Fieldston, MD, MBA, MSHP, Children’s Hospital of Philadelphia, University of Pennsylvania
- S. Ryan Greysen, MD, MHS, MA, University of California at San Francisco
- Luke Hansen, MD, Northwestern Memorial Hospital
- Luci Leykum, MD, FHM, University of Texas HSC
- Andrew Masica, MD, SFHM, Baylor Health Care System
- James C. Pile, MD, FACP, SFHM, Cleveland Clinic
- Steven Belknap, MD, Northwestern Memorial Hospital
- Vincent Liu, MD, Santa Clara (Calif.) Medical Center
- Basem Abdelmalak, MD, Cleveland Clinic
- Marisha Burden, MD, Denver Health Medical Center
- James Burke, MD, University of Michigan Health System, Ann Arbor
- Roy Carr-Hill, PhD, University of Liverpool
- Lawrence Haber, MD, University of California at San Francisco
- Keiki Hinami, MD,Northwestern Memorial Hospital
- Michael Hwa, MD, University of California at San Francisco
- Michael Jangigian, MD, New York University
- Mansoor Khalid, MD, Saint Francis Hospitalists
- Hilary Mosher, MD, University of Iowa Carver College of Medicine, Iowa City
- Andrew Odden, MD, Ann Arbor VA Medical Center, University of Michigan
- Maria Raven, MD, MPH, MSc, University of California at San Francisco
- Kristin Salottolo, MPH, St. Anthony Hospital
- Jonathan Sevransky, MD, MHS, Emory Healthcare
- Kittane Vishnupriya, MD, MBBS, Johns Hopkins Bayview Medical Center
- Robert S. Young, MD, Northwestern University
- Melissa Mattison, MD, SFHM, Beth Israel Deaconess Medical Center, Boston
- Jeff Rohde, MD, University of Michigan Health System, Ann Arbor
- Henry Michtalik, MD, Johns Hopkins
- Mark Shen, MD, Dell Children’s Medical Center of Central Texas, Austin
- Sumant Ranji, MD, University of California at San Francisco
- Greg Maynard, MD, SFHM, University of California at San Diego
- Anand Kartha, MD, MSc, Boston University
- Christopher Roy, MD, FHM, Brigham & Women’s Hospital, Boston
- Zachary Goldberger, MD, MS, University of Washington School of Medicine
- Chase Coffey, MD, Henry Ford Health System
- Quinn Czosnowski, PharmD, University of the Sciences
- Kenataro Iwata, MD, MSc, FACP, FIDSA, Kobe University Hospital
Journal of Hospital Medicine editors are recognizing 39 peer reviewers for the “collegial and insightful nature of their reviews.” The editors congratulate the reviewers for their contributions and thank them for the important role they play in making JHM an important and useful resource for its authors and readers.
- Brian Harte, MD, SFHM, South Pointe Hospital
- Michael DeVita, MD, St. Vincent’s Medical Center
- Gurpreet Dhaliwal, MD, University of California at San Francisco
- Evan Fieldston, MD, MBA, MSHP, Children’s Hospital of Philadelphia, University of Pennsylvania
- S. Ryan Greysen, MD, MHS, MA, University of California at San Francisco
- Luke Hansen, MD, Northwestern Memorial Hospital
- Luci Leykum, MD, FHM, University of Texas HSC
- Andrew Masica, MD, SFHM, Baylor Health Care System
- James C. Pile, MD, FACP, SFHM, Cleveland Clinic
- Steven Belknap, MD, Northwestern Memorial Hospital
- Vincent Liu, MD, Santa Clara (Calif.) Medical Center
- Basem Abdelmalak, MD, Cleveland Clinic
- Marisha Burden, MD, Denver Health Medical Center
- James Burke, MD, University of Michigan Health System, Ann Arbor
- Roy Carr-Hill, PhD, University of Liverpool
- Lawrence Haber, MD, University of California at San Francisco
- Keiki Hinami, MD,Northwestern Memorial Hospital
- Michael Hwa, MD, University of California at San Francisco
- Michael Jangigian, MD, New York University
- Mansoor Khalid, MD, Saint Francis Hospitalists
- Hilary Mosher, MD, University of Iowa Carver College of Medicine, Iowa City
- Andrew Odden, MD, Ann Arbor VA Medical Center, University of Michigan
- Maria Raven, MD, MPH, MSc, University of California at San Francisco
- Kristin Salottolo, MPH, St. Anthony Hospital
- Jonathan Sevransky, MD, MHS, Emory Healthcare
- Kittane Vishnupriya, MD, MBBS, Johns Hopkins Bayview Medical Center
- Robert S. Young, MD, Northwestern University
- Melissa Mattison, MD, SFHM, Beth Israel Deaconess Medical Center, Boston
- Jeff Rohde, MD, University of Michigan Health System, Ann Arbor
- Henry Michtalik, MD, Johns Hopkins
- Mark Shen, MD, Dell Children’s Medical Center of Central Texas, Austin
- Sumant Ranji, MD, University of California at San Francisco
- Greg Maynard, MD, SFHM, University of California at San Diego
- Anand Kartha, MD, MSc, Boston University
- Christopher Roy, MD, FHM, Brigham & Women’s Hospital, Boston
- Zachary Goldberger, MD, MS, University of Washington School of Medicine
- Chase Coffey, MD, Henry Ford Health System
- Quinn Czosnowski, PharmD, University of the Sciences
- Kenataro Iwata, MD, MSc, FACP, FIDSA, Kobe University Hospital
Fellow in Hospital Medicine Spotlight: Danielle Smith, MD, SFHM
Dr. Smith is president of the Southeastern Wisconsin chapter of SHM, and is a member of SHM’s Physician in Training Committee, for which she promotes hospital medicine as a career.
Undergraduate education: University of Wisconsin at La Crosse.
Medical school: Medical College of Wisconsin, Milwaukee.
Notable: Dr. Smith has increased her hospital’s patient satisfaction levels to the 90th percentile from the 60th percentile by creating a program that keeps patients’ family members informed daily about their condition. She says the hardest part of keeping patients happy is bonding with them and building a rapport in a short amount of time; only after bonding with patients will they be aware of hospitalists as physicians. Dr. Smith also is a Six Sigma black belt.
FYI: When she was growing up, she wanted to be a Dallas Cowboys cheerleader. Today, she enjoys dance and gymnastics with her children. Dr. Smith is looking forward to receiving her MBA, which she plans to use to help fix parts of the healthcare system in a time of change.
Quotable: “To me, being an SHM fellow means a validation of the years of commitment I have to quality patient care, not only of the individual patient, but of the way we deliver healthcare as a society. I am honored to be an SHM Senior Fellow and privileged to be part of a group of hospitalists truly committed to providing quality patient care, lifelong learning, and improving the ways we deliver care.”
Dr. Smith is president of the Southeastern Wisconsin chapter of SHM, and is a member of SHM’s Physician in Training Committee, for which she promotes hospital medicine as a career.
Undergraduate education: University of Wisconsin at La Crosse.
Medical school: Medical College of Wisconsin, Milwaukee.
Notable: Dr. Smith has increased her hospital’s patient satisfaction levels to the 90th percentile from the 60th percentile by creating a program that keeps patients’ family members informed daily about their condition. She says the hardest part of keeping patients happy is bonding with them and building a rapport in a short amount of time; only after bonding with patients will they be aware of hospitalists as physicians. Dr. Smith also is a Six Sigma black belt.
FYI: When she was growing up, she wanted to be a Dallas Cowboys cheerleader. Today, she enjoys dance and gymnastics with her children. Dr. Smith is looking forward to receiving her MBA, which she plans to use to help fix parts of the healthcare system in a time of change.
Quotable: “To me, being an SHM fellow means a validation of the years of commitment I have to quality patient care, not only of the individual patient, but of the way we deliver healthcare as a society. I am honored to be an SHM Senior Fellow and privileged to be part of a group of hospitalists truly committed to providing quality patient care, lifelong learning, and improving the ways we deliver care.”
Dr. Smith is president of the Southeastern Wisconsin chapter of SHM, and is a member of SHM’s Physician in Training Committee, for which she promotes hospital medicine as a career.
Undergraduate education: University of Wisconsin at La Crosse.
Medical school: Medical College of Wisconsin, Milwaukee.
Notable: Dr. Smith has increased her hospital’s patient satisfaction levels to the 90th percentile from the 60th percentile by creating a program that keeps patients’ family members informed daily about their condition. She says the hardest part of keeping patients happy is bonding with them and building a rapport in a short amount of time; only after bonding with patients will they be aware of hospitalists as physicians. Dr. Smith also is a Six Sigma black belt.
FYI: When she was growing up, she wanted to be a Dallas Cowboys cheerleader. Today, she enjoys dance and gymnastics with her children. Dr. Smith is looking forward to receiving her MBA, which she plans to use to help fix parts of the healthcare system in a time of change.
Quotable: “To me, being an SHM fellow means a validation of the years of commitment I have to quality patient care, not only of the individual patient, but of the way we deliver healthcare as a society. I am honored to be an SHM Senior Fellow and privileged to be part of a group of hospitalists truly committed to providing quality patient care, lifelong learning, and improving the ways we deliver care.”
HMX Term of the Month: CMS 1500
Medical claim form established by CMS to submit paper claims to Medicare and Medicaid. Most commercial insurance carriers also require paper claims be submitted on CMS 1500s. The form is distinguished by its red ink.
Medical claim form established by CMS to submit paper claims to Medicare and Medicaid. Most commercial insurance carriers also require paper claims be submitted on CMS 1500s. The form is distinguished by its red ink.
Medical claim form established by CMS to submit paper claims to Medicare and Medicaid. Most commercial insurance carriers also require paper claims be submitted on CMS 1500s. The form is distinguished by its red ink.
Hospitalists Get Peek at Hospital Medicine 2013 Annual Meeting Schedule Online
After the welcomes and plenary sessions by leaders in healthcare, will you go to a breakout session called “More Non-Evidence-Based Medicine: Things We Do for No Reason” or the workshop on point-of-care evidence?
Now is the time to start deciding with the new HM13 “Day at a Glance” schedules, available at www.hospitalmedicine2013.org. With more than 100 events, sessions, and work groups, the schedule is a roadmap for hospitalists planning their annual meeting experience in advance.
This year, hospitalists will have extra help in planning their HM13 strategy digitally. For the first time, hospitalists will be able to use their smartphones and tablet devices to review the HM13 agenda and plan their own personal schedules before they arrive at the conference.
To download a printable PDF of the HM13 “Day at a Glance,” visit www.hospitalmedicine2013.org/pdf/At-A-Glance.pdf.
After the welcomes and plenary sessions by leaders in healthcare, will you go to a breakout session called “More Non-Evidence-Based Medicine: Things We Do for No Reason” or the workshop on point-of-care evidence?
Now is the time to start deciding with the new HM13 “Day at a Glance” schedules, available at www.hospitalmedicine2013.org. With more than 100 events, sessions, and work groups, the schedule is a roadmap for hospitalists planning their annual meeting experience in advance.
This year, hospitalists will have extra help in planning their HM13 strategy digitally. For the first time, hospitalists will be able to use their smartphones and tablet devices to review the HM13 agenda and plan their own personal schedules before they arrive at the conference.
To download a printable PDF of the HM13 “Day at a Glance,” visit www.hospitalmedicine2013.org/pdf/At-A-Glance.pdf.
After the welcomes and plenary sessions by leaders in healthcare, will you go to a breakout session called “More Non-Evidence-Based Medicine: Things We Do for No Reason” or the workshop on point-of-care evidence?
Now is the time to start deciding with the new HM13 “Day at a Glance” schedules, available at www.hospitalmedicine2013.org. With more than 100 events, sessions, and work groups, the schedule is a roadmap for hospitalists planning their annual meeting experience in advance.
This year, hospitalists will have extra help in planning their HM13 strategy digitally. For the first time, hospitalists will be able to use their smartphones and tablet devices to review the HM13 agenda and plan their own personal schedules before they arrive at the conference.
To download a printable PDF of the HM13 “Day at a Glance,” visit www.hospitalmedicine2013.org/pdf/At-A-Glance.pdf.
Neurotoxin Techniques for Men
Hospitalists to Unveil Patient Care Recommendations As Part of Choosing Wisely Campaign
This month, hospitalists will be a vital part of Choosing Wisely, an important public initiative from the American Board of Internal Medicine (ABIM) Foundation that identifies treatments and procedures that might be overused by caregivers.
On Feb. 21 in Washington, D.C., the ABIM Foundation, SHM, and more than a dozen other medical specialties will announce recommendations that, in the ABIM Foundation’s words, “represent specific, evidence-based recommendations physicians and patients should discuss to help make wise decisions about the most appropriate care based on their individual situation.” Hospitalists who helped SHM develop its recommendations will be in attendance to help field questions about SHM’s work with Choosing Wisely and its lists.
SHM has developed two lists of recommendations: one for adult HM and another for pediatric HM. SHM will make a special announcement Feb. 21 in The Hospitalist eWire with both lists and commentary for how hospitalists can have informed conversations with their patients about the lists. The Hospitalist will follow up with a feature story and other information about Choosing Wisely in its March issue.
As part of the campaign, the ABIM Foundation, SHM, and consumer magazine Consumer Reports have teamed up to develop material specifically designed to educate patients about the Choosing Wisely recommendations. Materials will be available on the ABIM Foundation and SHM websites.
SHM will continue the conversation about high-value care and working with patients to make wise decisions well beyond February and March. At HM13, SHM’s annual meeting in Washington, D.C., SHM will offer a pre-course on Choosing Wisely and its philosophy. The pre-course is May 16, the day before the official start of HM13.
For more information about Choosing Wisely, visit www.choosingwisely.org. To register for the Choosing Wisely pre-course at HM13, visit www.hospitalmedicine2013.org.
This month, hospitalists will be a vital part of Choosing Wisely, an important public initiative from the American Board of Internal Medicine (ABIM) Foundation that identifies treatments and procedures that might be overused by caregivers.
On Feb. 21 in Washington, D.C., the ABIM Foundation, SHM, and more than a dozen other medical specialties will announce recommendations that, in the ABIM Foundation’s words, “represent specific, evidence-based recommendations physicians and patients should discuss to help make wise decisions about the most appropriate care based on their individual situation.” Hospitalists who helped SHM develop its recommendations will be in attendance to help field questions about SHM’s work with Choosing Wisely and its lists.
SHM has developed two lists of recommendations: one for adult HM and another for pediatric HM. SHM will make a special announcement Feb. 21 in The Hospitalist eWire with both lists and commentary for how hospitalists can have informed conversations with their patients about the lists. The Hospitalist will follow up with a feature story and other information about Choosing Wisely in its March issue.
As part of the campaign, the ABIM Foundation, SHM, and consumer magazine Consumer Reports have teamed up to develop material specifically designed to educate patients about the Choosing Wisely recommendations. Materials will be available on the ABIM Foundation and SHM websites.
SHM will continue the conversation about high-value care and working with patients to make wise decisions well beyond February and March. At HM13, SHM’s annual meeting in Washington, D.C., SHM will offer a pre-course on Choosing Wisely and its philosophy. The pre-course is May 16, the day before the official start of HM13.
For more information about Choosing Wisely, visit www.choosingwisely.org. To register for the Choosing Wisely pre-course at HM13, visit www.hospitalmedicine2013.org.
This month, hospitalists will be a vital part of Choosing Wisely, an important public initiative from the American Board of Internal Medicine (ABIM) Foundation that identifies treatments and procedures that might be overused by caregivers.
On Feb. 21 in Washington, D.C., the ABIM Foundation, SHM, and more than a dozen other medical specialties will announce recommendations that, in the ABIM Foundation’s words, “represent specific, evidence-based recommendations physicians and patients should discuss to help make wise decisions about the most appropriate care based on their individual situation.” Hospitalists who helped SHM develop its recommendations will be in attendance to help field questions about SHM’s work with Choosing Wisely and its lists.
SHM has developed two lists of recommendations: one for adult HM and another for pediatric HM. SHM will make a special announcement Feb. 21 in The Hospitalist eWire with both lists and commentary for how hospitalists can have informed conversations with their patients about the lists. The Hospitalist will follow up with a feature story and other information about Choosing Wisely in its March issue.
As part of the campaign, the ABIM Foundation, SHM, and consumer magazine Consumer Reports have teamed up to develop material specifically designed to educate patients about the Choosing Wisely recommendations. Materials will be available on the ABIM Foundation and SHM websites.
SHM will continue the conversation about high-value care and working with patients to make wise decisions well beyond February and March. At HM13, SHM’s annual meeting in Washington, D.C., SHM will offer a pre-course on Choosing Wisely and its philosophy. The pre-course is May 16, the day before the official start of HM13.
For more information about Choosing Wisely, visit www.choosingwisely.org. To register for the Choosing Wisely pre-course at HM13, visit www.hospitalmedicine2013.org.
Assessment of safety of a rapid desensitization regimen for patients with hypersensitivity reactions to chemotherapy infusions
Background Hypersensitivity reactions to chemotherapy agents occur with relatively high frequency with some of the most widely used chemotherapeutic drug classes. Desensitization using a standard 12-step protocol has been successful, but takes about 6.5 hours. Limited studies have shown that a faster protocol may also be safe.
Objective To determine when desensitization could be safely speeded up.
Methods Patients with documented HSRs (24 patients) were desensitized initially with the standard 12-step protocol for 1 or 2 treatments, for a total of 180 desensitizations. Those patients who had negative skin testing and who tolerated the desensitizations were switched to the more rapid desensitization protocol (16 patients).
Results All 16 patients were successfully desensitized, having received the full dose of their chemotherapy. Eight patients were not advanced to the rapid protocol because they had reactions during initial desensitizations or they had a positive skin test; all of them were successfully desensitized using the 12-step protocol at the slower rate of infusion. These data present criteria for defining which patients may be safely transitioned to a rapid desensitization protocol.
Limitation Most of the patients in the study (21 of 24) were women.
Conclusions Patients with HSRs to chemotherapy agents, who tolerate an initial 12-step desensitization and have a negative skin test, can be advanced to a more rapid protocol. It is likely that patients with HSRs to the taxanes can be started on the more rapid protocol without starting on the 12-step protocol.
*Click on the PDF icon at the top of this introduction to read the full article.
Background Hypersensitivity reactions to chemotherapy agents occur with relatively high frequency with some of the most widely used chemotherapeutic drug classes. Desensitization using a standard 12-step protocol has been successful, but takes about 6.5 hours. Limited studies have shown that a faster protocol may also be safe.
Objective To determine when desensitization could be safely speeded up.
Methods Patients with documented HSRs (24 patients) were desensitized initially with the standard 12-step protocol for 1 or 2 treatments, for a total of 180 desensitizations. Those patients who had negative skin testing and who tolerated the desensitizations were switched to the more rapid desensitization protocol (16 patients).
Results All 16 patients were successfully desensitized, having received the full dose of their chemotherapy. Eight patients were not advanced to the rapid protocol because they had reactions during initial desensitizations or they had a positive skin test; all of them were successfully desensitized using the 12-step protocol at the slower rate of infusion. These data present criteria for defining which patients may be safely transitioned to a rapid desensitization protocol.
Limitation Most of the patients in the study (21 of 24) were women.
Conclusions Patients with HSRs to chemotherapy agents, who tolerate an initial 12-step desensitization and have a negative skin test, can be advanced to a more rapid protocol. It is likely that patients with HSRs to the taxanes can be started on the more rapid protocol without starting on the 12-step protocol.
*Click on the PDF icon at the top of this introduction to read the full article.
Background Hypersensitivity reactions to chemotherapy agents occur with relatively high frequency with some of the most widely used chemotherapeutic drug classes. Desensitization using a standard 12-step protocol has been successful, but takes about 6.5 hours. Limited studies have shown that a faster protocol may also be safe.
Objective To determine when desensitization could be safely speeded up.
Methods Patients with documented HSRs (24 patients) were desensitized initially with the standard 12-step protocol for 1 or 2 treatments, for a total of 180 desensitizations. Those patients who had negative skin testing and who tolerated the desensitizations were switched to the more rapid desensitization protocol (16 patients).
Results All 16 patients were successfully desensitized, having received the full dose of their chemotherapy. Eight patients were not advanced to the rapid protocol because they had reactions during initial desensitizations or they had a positive skin test; all of them were successfully desensitized using the 12-step protocol at the slower rate of infusion. These data present criteria for defining which patients may be safely transitioned to a rapid desensitization protocol.
Limitation Most of the patients in the study (21 of 24) were women.
Conclusions Patients with HSRs to chemotherapy agents, who tolerate an initial 12-step desensitization and have a negative skin test, can be advanced to a more rapid protocol. It is likely that patients with HSRs to the taxanes can be started on the more rapid protocol without starting on the 12-step protocol.
*Click on the PDF icon at the top of this introduction to read the full article.
Cost-benefit analysis of decision support methods for patients with breast cancer in a rural community
Background Decision support interventions help patients who are facing difficult treatment decisions and improve shared decision making. There is little evidence of the economic impact of these interventions.
Objective To determine the costs of providing a decision support intervention in the form of consultation planning (CP) and consultation planning with recording and summary (CPRS) to women with breast cancer and to compare the cost benefit of CP and CPRS by telephone versus in person.
Methods Sixty-eight women with breast cancer who were being treated at a rural cancer resource center were randomized to CP in person or by telephone. All participants were then provided with an audio-recording of the physician consultation along with a typed summary for the full intervention (CPRS). Surveys completed by the participants and center staff provided data for measuring costs and willingness-to-pay (WTP) benefits. Societal perspective costs and incremental net benefit (INB) across delivery methods was determined.
Results Total CP costs were $208.72 for telephone and $264.00 for in-person delivery. Significantly lower telephone-group costs (P ˂ .001) were a result of lower participant travel expenses. Participants were willing to pay $154.12 for telephone and $144.03 for in-person CP (P = .85). WTP did not exceed costs of either delivery method compared with no intervention. INB of providing CP for telephone versus in person was $65.37, favoring telephone delivery. Sensitivity analysis revealed that with more efficient CP training, WTP became greater than the costs of delivering CP by telephone versus no intervention.
Limitations There may be some income distribution effects in the measurement of WTP.
Conclusions Providing CP by telephone was significantly less costly with no significant difference in benefit. Participants’ WTP only exceeded the full cost of CP with more efficient training or higher participant volume. A positive INB showed telephone delivery is efficient and may increase accessibility to decision support services, particularly in rural communities.
Click on the PDF icon at the top of this introduction to read the full article.
Background Decision support interventions help patients who are facing difficult treatment decisions and improve shared decision making. There is little evidence of the economic impact of these interventions.
Objective To determine the costs of providing a decision support intervention in the form of consultation planning (CP) and consultation planning with recording and summary (CPRS) to women with breast cancer and to compare the cost benefit of CP and CPRS by telephone versus in person.
Methods Sixty-eight women with breast cancer who were being treated at a rural cancer resource center were randomized to CP in person or by telephone. All participants were then provided with an audio-recording of the physician consultation along with a typed summary for the full intervention (CPRS). Surveys completed by the participants and center staff provided data for measuring costs and willingness-to-pay (WTP) benefits. Societal perspective costs and incremental net benefit (INB) across delivery methods was determined.
Results Total CP costs were $208.72 for telephone and $264.00 for in-person delivery. Significantly lower telephone-group costs (P ˂ .001) were a result of lower participant travel expenses. Participants were willing to pay $154.12 for telephone and $144.03 for in-person CP (P = .85). WTP did not exceed costs of either delivery method compared with no intervention. INB of providing CP for telephone versus in person was $65.37, favoring telephone delivery. Sensitivity analysis revealed that with more efficient CP training, WTP became greater than the costs of delivering CP by telephone versus no intervention.
Limitations There may be some income distribution effects in the measurement of WTP.
Conclusions Providing CP by telephone was significantly less costly with no significant difference in benefit. Participants’ WTP only exceeded the full cost of CP with more efficient training or higher participant volume. A positive INB showed telephone delivery is efficient and may increase accessibility to decision support services, particularly in rural communities.
Click on the PDF icon at the top of this introduction to read the full article.
Background Decision support interventions help patients who are facing difficult treatment decisions and improve shared decision making. There is little evidence of the economic impact of these interventions.
Objective To determine the costs of providing a decision support intervention in the form of consultation planning (CP) and consultation planning with recording and summary (CPRS) to women with breast cancer and to compare the cost benefit of CP and CPRS by telephone versus in person.
Methods Sixty-eight women with breast cancer who were being treated at a rural cancer resource center were randomized to CP in person or by telephone. All participants were then provided with an audio-recording of the physician consultation along with a typed summary for the full intervention (CPRS). Surveys completed by the participants and center staff provided data for measuring costs and willingness-to-pay (WTP) benefits. Societal perspective costs and incremental net benefit (INB) across delivery methods was determined.
Results Total CP costs were $208.72 for telephone and $264.00 for in-person delivery. Significantly lower telephone-group costs (P ˂ .001) were a result of lower participant travel expenses. Participants were willing to pay $154.12 for telephone and $144.03 for in-person CP (P = .85). WTP did not exceed costs of either delivery method compared with no intervention. INB of providing CP for telephone versus in person was $65.37, favoring telephone delivery. Sensitivity analysis revealed that with more efficient CP training, WTP became greater than the costs of delivering CP by telephone versus no intervention.
Limitations There may be some income distribution effects in the measurement of WTP.
Conclusions Providing CP by telephone was significantly less costly with no significant difference in benefit. Participants’ WTP only exceeded the full cost of CP with more efficient training or higher participant volume. A positive INB showed telephone delivery is efficient and may increase accessibility to decision support services, particularly in rural communities.
Click on the PDF icon at the top of this introduction to read the full article.