User login
The Official Newspaper of the American Association for Thoracic Surgery
Rigid Plating Speeds Sternal Healing
COLORADO SPRINGS – Rigid fixation with sternal plates resulted in superior sternal bone healing post sternotomy, compared with conventional wire cerclage in a randomized trial.
This was the first-ever randomized study to utilize CT scans to objectively assess sternal union. The results at 6 months of follow-up showed a striking advantage for rigid plate fixation using the proprietary SternaLock system, Dr. Jaishankar Raman said at the annual meeting of the Western Thoracic Surgical Association.
Most cardiac surgeons will be surprised, as was he, at how low the sternal union rates were 3 months poststernotomy. In fact, the sternal union rate then with conventional wire closure was zero, while for sternal plating it was 17%, added Dr. Raman of the University of Chicago.
He reported on 141 randomized cardiac surgery patients at six centers in the United States and Germany. All were at high risk for sternal wound complications, mostly due to multiple comorbid diseases. Their multilevel CT scans obtained at 3 or 6 months post surgery were independently scored in structured fashion by two independent radiologists at a core imaging center.
At 6 months, sternal union, or osteosynthesis – as defined by a CT score of 3 or more – was achieved in 70% of the rigid plate fixation group, compared with 20% of those with conventional wire cerclage.
There were no significant differences between the two study arms in rates of wound dehiscence or other adverse events.
Asked about the cost of SternaLock fixation, Dr. Raman replied, "That’s the biggest stumbling block in developing this technology."
The wire for conventional cerclage costs less than $50 per patient. In contrast, the SternaLock system costs about $1,000 per patient. It could be argued that if rigid plate fixation reduces the incidence of sternal wound complications in high-risk patients, the advanced technology would be cost effective. However, the randomized trial wasn’t powered to show a significant difference in such complications.
Dr. Raman observed that wire cerclage has been accepted as the time-honored and most widely employed means of sternal closure ever since the modern era of cardiac surgery began back in the 1950s, even though it is a crude method.
"Even though we may not like it, we in cardiac surgery do more bone approximation and bone fixation than most other bone-handling surgeons. Yet all other bone-handling surgeons have moved on to plate and screw fixation. Biomechanical studies show that plate fixation is significantly better than wire closure," according to the surgeon.
Discussant Dr. Matthew S. Slater, clinical director of adult cardiac surgery at Oregon Health & Sciences Center, Portland, said that based on the assumption that rigid plate fixation is a better method than conventional wire cerclage, what he’d really like to see next is a comparative study pitting the SternaLock system against other novel fixation technologies on the market, such as KLS Martin’s Sternal Talon and ACUTE Innovations’ AcuTie.
Dr. Raman agreed that would be a logical next step, adding that it’s his strong impression the industry is not interested in funding comparative trials.
He declared that he received a research grant from Biomet Microfixation, which markets the SternaLock and funded the randomized trial.
COLORADO SPRINGS – Rigid fixation with sternal plates resulted in superior sternal bone healing post sternotomy, compared with conventional wire cerclage in a randomized trial.
This was the first-ever randomized study to utilize CT scans to objectively assess sternal union. The results at 6 months of follow-up showed a striking advantage for rigid plate fixation using the proprietary SternaLock system, Dr. Jaishankar Raman said at the annual meeting of the Western Thoracic Surgical Association.
Most cardiac surgeons will be surprised, as was he, at how low the sternal union rates were 3 months poststernotomy. In fact, the sternal union rate then with conventional wire closure was zero, while for sternal plating it was 17%, added Dr. Raman of the University of Chicago.
He reported on 141 randomized cardiac surgery patients at six centers in the United States and Germany. All were at high risk for sternal wound complications, mostly due to multiple comorbid diseases. Their multilevel CT scans obtained at 3 or 6 months post surgery were independently scored in structured fashion by two independent radiologists at a core imaging center.
At 6 months, sternal union, or osteosynthesis – as defined by a CT score of 3 or more – was achieved in 70% of the rigid plate fixation group, compared with 20% of those with conventional wire cerclage.
There were no significant differences between the two study arms in rates of wound dehiscence or other adverse events.
Asked about the cost of SternaLock fixation, Dr. Raman replied, "That’s the biggest stumbling block in developing this technology."
The wire for conventional cerclage costs less than $50 per patient. In contrast, the SternaLock system costs about $1,000 per patient. It could be argued that if rigid plate fixation reduces the incidence of sternal wound complications in high-risk patients, the advanced technology would be cost effective. However, the randomized trial wasn’t powered to show a significant difference in such complications.
Dr. Raman observed that wire cerclage has been accepted as the time-honored and most widely employed means of sternal closure ever since the modern era of cardiac surgery began back in the 1950s, even though it is a crude method.
"Even though we may not like it, we in cardiac surgery do more bone approximation and bone fixation than most other bone-handling surgeons. Yet all other bone-handling surgeons have moved on to plate and screw fixation. Biomechanical studies show that plate fixation is significantly better than wire closure," according to the surgeon.
Discussant Dr. Matthew S. Slater, clinical director of adult cardiac surgery at Oregon Health & Sciences Center, Portland, said that based on the assumption that rigid plate fixation is a better method than conventional wire cerclage, what he’d really like to see next is a comparative study pitting the SternaLock system against other novel fixation technologies on the market, such as KLS Martin’s Sternal Talon and ACUTE Innovations’ AcuTie.
Dr. Raman agreed that would be a logical next step, adding that it’s his strong impression the industry is not interested in funding comparative trials.
He declared that he received a research grant from Biomet Microfixation, which markets the SternaLock and funded the randomized trial.
COLORADO SPRINGS – Rigid fixation with sternal plates resulted in superior sternal bone healing post sternotomy, compared with conventional wire cerclage in a randomized trial.
This was the first-ever randomized study to utilize CT scans to objectively assess sternal union. The results at 6 months of follow-up showed a striking advantage for rigid plate fixation using the proprietary SternaLock system, Dr. Jaishankar Raman said at the annual meeting of the Western Thoracic Surgical Association.
Most cardiac surgeons will be surprised, as was he, at how low the sternal union rates were 3 months poststernotomy. In fact, the sternal union rate then with conventional wire closure was zero, while for sternal plating it was 17%, added Dr. Raman of the University of Chicago.
He reported on 141 randomized cardiac surgery patients at six centers in the United States and Germany. All were at high risk for sternal wound complications, mostly due to multiple comorbid diseases. Their multilevel CT scans obtained at 3 or 6 months post surgery were independently scored in structured fashion by two independent radiologists at a core imaging center.
At 6 months, sternal union, or osteosynthesis – as defined by a CT score of 3 or more – was achieved in 70% of the rigid plate fixation group, compared with 20% of those with conventional wire cerclage.
There were no significant differences between the two study arms in rates of wound dehiscence or other adverse events.
Asked about the cost of SternaLock fixation, Dr. Raman replied, "That’s the biggest stumbling block in developing this technology."
The wire for conventional cerclage costs less than $50 per patient. In contrast, the SternaLock system costs about $1,000 per patient. It could be argued that if rigid plate fixation reduces the incidence of sternal wound complications in high-risk patients, the advanced technology would be cost effective. However, the randomized trial wasn’t powered to show a significant difference in such complications.
Dr. Raman observed that wire cerclage has been accepted as the time-honored and most widely employed means of sternal closure ever since the modern era of cardiac surgery began back in the 1950s, even though it is a crude method.
"Even though we may not like it, we in cardiac surgery do more bone approximation and bone fixation than most other bone-handling surgeons. Yet all other bone-handling surgeons have moved on to plate and screw fixation. Biomechanical studies show that plate fixation is significantly better than wire closure," according to the surgeon.
Discussant Dr. Matthew S. Slater, clinical director of adult cardiac surgery at Oregon Health & Sciences Center, Portland, said that based on the assumption that rigid plate fixation is a better method than conventional wire cerclage, what he’d really like to see next is a comparative study pitting the SternaLock system against other novel fixation technologies on the market, such as KLS Martin’s Sternal Talon and ACUTE Innovations’ AcuTie.
Dr. Raman agreed that would be a logical next step, adding that it’s his strong impression the industry is not interested in funding comparative trials.
He declared that he received a research grant from Biomet Microfixation, which markets the SternaLock and funded the randomized trial.
Major Finding: At 6 months, sternal union, or osteosynthesis – as defined by a CT score of 3 or more – was achieved in 70% of the rigid plate fixation group, compared with 20% who had conventional wire cerclage.
Data Source: A 141-patient multicenter randomized trial.
Disclosures: Dr. Raman received a research grant from Biomet Microfixation, which markets the SternaLock and funded the randomized trial.
In Coronary Artery Bypass, BIMA May Be Best
COLORADO SPRINGS ? Using bilateral internal mammary artery grafts provided a significant long-term survival advantage over single mammary artery grafts for coronary artery bypass surgery patients with normal or moderately impaired left ventricular function, according to a large retrospective study with lengthy follow-up. But when preoperative left ventricular ejection fraction (EF) was less than 30%, the procedure choice showed no difference in survival.
"BIMA grafting is the operation of choice in patients with a life expectancy beyond 1-2 decades," Dr. David Galbut said at the annual meeting of the Western Thoracic Surgical Association. He reported on 4,537 consecutive patients who had CABG with internal mammary artery grafting during 1972-1994 at three Florida hospitals. BIMA grafts were performed in 48% of the patients, an exceptionally high BIMA rate. In contrast, the Society of Thoracic Surgeons database shows that 4% of patients undergoing CABG nationally receive BIMA grafts. The reason for the 12-fold higher BIMA rate in the Florida study is that Dr. Galbut and colleagues had a decades-long conviction that BIMA has major clinical advantages.
In the Florida study, 233 patients had an EF below 30%, another 1,256 had an EF of 30%-50%, and 3,048 had a normal EF. In the low EF group, 87 BIMA patients were matched to an equal number of SIMA patients on the basis of 14 preoperative variables. In like manner, propensity scores were used to match 448 BIMA patients in the moderately impaired EF group and 1,137 BIMA patients with a normal EF to similar SIMA patients.
Many surgeons are reluctant to use BIMA grafting because of a concern that it will result in increased complications. This wasn?t the case in the Florida series. Indeed, operative morbidity ? including sternal wound infection rates ? were similar between BIMA and SIMA, according to Dr. Galbut of the Aventura (Fla.) Medical Center.
The 20-year survival rate in BIMA patients with moderately impaired EF was 33.1%, significantly better than the 19% survival in matched SIMA patients. In the normal EF group, the 20-year survival rate was 38.1% with BIMA and 35.8% with SIMA.
The general strategy the surgeons followed in BIMA grafting was to run the left internal mammary artery (LIMA) graft to the left anterior descending coronary artery. The LIMA is the dominant vessel in most patients and would therefore be the most durable conduit. The right internal mammary artery graft was placed wherever it fit best.
Discussant Dr. Anthony P. Furnary observed that retrospective studies can?t prove causality, not even when they?re large, painstakingly performed, and feature more than 2 decades of follow-up. Limitations in propensity score matching may account for much or all of the long-term survival advantage observed with BIMA grafting seen. Although patients were extensively matched in 14 preoperative variables, the year of surgery wasn?t among them.
The 22-year study period saw the introduction of many myocardial protection techniques. If more SIMA patients were operated on in earlier years, they might well have missed out on these therapies, said Dr. Furnary of the Providence Heart and Vascular Institute, Portland, Ore.
Dr. Galbut had no disclosures.
COLORADO SPRINGS ? Using bilateral internal mammary artery grafts provided a significant long-term survival advantage over single mammary artery grafts for coronary artery bypass surgery patients with normal or moderately impaired left ventricular function, according to a large retrospective study with lengthy follow-up. But when preoperative left ventricular ejection fraction (EF) was less than 30%, the procedure choice showed no difference in survival.
"BIMA grafting is the operation of choice in patients with a life expectancy beyond 1-2 decades," Dr. David Galbut said at the annual meeting of the Western Thoracic Surgical Association. He reported on 4,537 consecutive patients who had CABG with internal mammary artery grafting during 1972-1994 at three Florida hospitals. BIMA grafts were performed in 48% of the patients, an exceptionally high BIMA rate. In contrast, the Society of Thoracic Surgeons database shows that 4% of patients undergoing CABG nationally receive BIMA grafts. The reason for the 12-fold higher BIMA rate in the Florida study is that Dr. Galbut and colleagues had a decades-long conviction that BIMA has major clinical advantages.
In the Florida study, 233 patients had an EF below 30%, another 1,256 had an EF of 30%-50%, and 3,048 had a normal EF. In the low EF group, 87 BIMA patients were matched to an equal number of SIMA patients on the basis of 14 preoperative variables. In like manner, propensity scores were used to match 448 BIMA patients in the moderately impaired EF group and 1,137 BIMA patients with a normal EF to similar SIMA patients.
Many surgeons are reluctant to use BIMA grafting because of a concern that it will result in increased complications. This wasn?t the case in the Florida series. Indeed, operative morbidity ? including sternal wound infection rates ? were similar between BIMA and SIMA, according to Dr. Galbut of the Aventura (Fla.) Medical Center.
The 20-year survival rate in BIMA patients with moderately impaired EF was 33.1%, significantly better than the 19% survival in matched SIMA patients. In the normal EF group, the 20-year survival rate was 38.1% with BIMA and 35.8% with SIMA.
The general strategy the surgeons followed in BIMA grafting was to run the left internal mammary artery (LIMA) graft to the left anterior descending coronary artery. The LIMA is the dominant vessel in most patients and would therefore be the most durable conduit. The right internal mammary artery graft was placed wherever it fit best.
Discussant Dr. Anthony P. Furnary observed that retrospective studies can?t prove causality, not even when they?re large, painstakingly performed, and feature more than 2 decades of follow-up. Limitations in propensity score matching may account for much or all of the long-term survival advantage observed with BIMA grafting seen. Although patients were extensively matched in 14 preoperative variables, the year of surgery wasn?t among them.
The 22-year study period saw the introduction of many myocardial protection techniques. If more SIMA patients were operated on in earlier years, they might well have missed out on these therapies, said Dr. Furnary of the Providence Heart and Vascular Institute, Portland, Ore.
Dr. Galbut had no disclosures.
COLORADO SPRINGS ? Using bilateral internal mammary artery grafts provided a significant long-term survival advantage over single mammary artery grafts for coronary artery bypass surgery patients with normal or moderately impaired left ventricular function, according to a large retrospective study with lengthy follow-up. But when preoperative left ventricular ejection fraction (EF) was less than 30%, the procedure choice showed no difference in survival.
"BIMA grafting is the operation of choice in patients with a life expectancy beyond 1-2 decades," Dr. David Galbut said at the annual meeting of the Western Thoracic Surgical Association. He reported on 4,537 consecutive patients who had CABG with internal mammary artery grafting during 1972-1994 at three Florida hospitals. BIMA grafts were performed in 48% of the patients, an exceptionally high BIMA rate. In contrast, the Society of Thoracic Surgeons database shows that 4% of patients undergoing CABG nationally receive BIMA grafts. The reason for the 12-fold higher BIMA rate in the Florida study is that Dr. Galbut and colleagues had a decades-long conviction that BIMA has major clinical advantages.
In the Florida study, 233 patients had an EF below 30%, another 1,256 had an EF of 30%-50%, and 3,048 had a normal EF. In the low EF group, 87 BIMA patients were matched to an equal number of SIMA patients on the basis of 14 preoperative variables. In like manner, propensity scores were used to match 448 BIMA patients in the moderately impaired EF group and 1,137 BIMA patients with a normal EF to similar SIMA patients.
Many surgeons are reluctant to use BIMA grafting because of a concern that it will result in increased complications. This wasn?t the case in the Florida series. Indeed, operative morbidity ? including sternal wound infection rates ? were similar between BIMA and SIMA, according to Dr. Galbut of the Aventura (Fla.) Medical Center.
The 20-year survival rate in BIMA patients with moderately impaired EF was 33.1%, significantly better than the 19% survival in matched SIMA patients. In the normal EF group, the 20-year survival rate was 38.1% with BIMA and 35.8% with SIMA.
The general strategy the surgeons followed in BIMA grafting was to run the left internal mammary artery (LIMA) graft to the left anterior descending coronary artery. The LIMA is the dominant vessel in most patients and would therefore be the most durable conduit. The right internal mammary artery graft was placed wherever it fit best.
Discussant Dr. Anthony P. Furnary observed that retrospective studies can?t prove causality, not even when they?re large, painstakingly performed, and feature more than 2 decades of follow-up. Limitations in propensity score matching may account for much or all of the long-term survival advantage observed with BIMA grafting seen. Although patients were extensively matched in 14 preoperative variables, the year of surgery wasn?t among them.
The 22-year study period saw the introduction of many myocardial protection techniques. If more SIMA patients were operated on in earlier years, they might well have missed out on these therapies, said Dr. Furnary of the Providence Heart and Vascular Institute, Portland, Ore.
Dr. Galbut had no disclosures.
Major Finding: The 20-year survival rate in BIMA patients in the moderately impaired EF group was 33.1%, significantly better than the 19% in matched SIMA patients. In the normal EF group, the 20-year survival rate was 38.1% with BIMA and 35.8% with SIMA.
Data Source: A retrospective study of 4,537 consecutive patients who underwent CABG with internal mammary artery grafting during 1972-1994 at three Florida hospitals.
Disclosures: Dr. Galbut declared having no financial conflicts.
Training Residents And Their Mentors
In a world of rapidly changing technology and educational demands, innovative training methods are required to prepare the next generation of cardiothoracic surgeons. The Thoracic Surgery Directors Association and the Joint Council on Thoracic Surgery Education Inc. have developed programs to ensure that CT residents receive the best possible training.
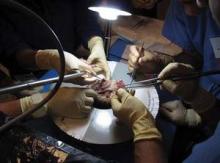
A prime example of these efforts is the annual TSDA Cardiothoracic Surgery Resident Boot Camp. The 2011 Boot Camp was held July 14-17 at the continuing education center of the University of North Carolina at Chapel Hill.
First-year residents from 24 thoracic surgery residency programs across the country joined faculty, led by Dr. James Fann of Stanford (Calif.) University, Dr. Rick Feins of UNC Chapel Hill, and Dr. George Hicks Jr. of the University of Rochester (N.Y.), with the goal of gaining valuable insights into surgical techniques and expanding their base of thoracic surgery knowledge.
The program was developed and hosted by the TSDA and was funded in part through a grant from the JTCSE.
|
|
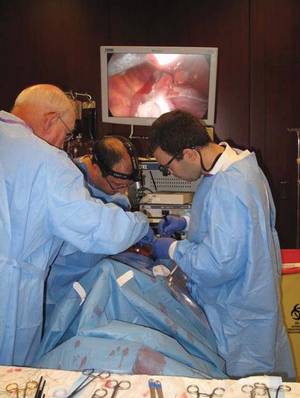
Photos courtesy of the Thoracic Surgery Directors Association
|
Now in its fourth year, the boot camp uses cardiothoracic simulator–based training to give residents some of the basic skill sets necessary to enhance their residency educational experience, especially in the operating room.
This year, procedures included cardiopulmonary bypass, aortic valve repair, anastomosis, lung ventilation, and lobectomy.
Seeking out multidisciplinary approaches to teaching, the TSDA boot camp faculty also brought in guest speakers from the world of 3-D gaming and aviation. Ron Maness, a former pilot with the U.S. Air Force Thunderbirds, offered insights into how pilots use simulation to avoid errors in the cockpit. Additionally, Richard Boyd from Lockheed Martin Virtual World Labs spoke about how 3-D simulation tools for health care could make analysis and training fast, safe, and measurable.
"Other professional fields have made great gains when it comes to quality by using simulations in teaching," said Dr. Feins. "Sharing multidisciplinary learning approaches with up-and-coming residents is a great way to expand and build on their current knowledge base."
Feedback from the residents that was reported at the TSDA website indicated that Boot Camp III was a success. "Boot Camp was perfectly [set up] to introduce career advancement in cardiac and thoracic surgery," noted one resident in an evaluation.
"The hand-picked faculty was a key element to the camp and collectively they shared the goal of introducing foreign concepts in the field and did it in a very [nonintimidating] fashion."
Director feedback also expressed strong support of the boot camp’s benefits, with 91% of program directors saying that their resident’s experience was very or extremely helpful. Resident boot camp participants displayed similar enthusiasm for the program, indicating that it was a "phenomenal experience," and a "fantastic opportunity," according to a TSDA summary.
This weekend-long course incorporated simulated emergency scenarios and surgery demonstrations, with residents able to spend extensive one-on-one time with the faculty, from whom they gained guidance along with the finer points of cardiothoracic surgery basics.
Faculty and resident assessments were integrated into the curriculum throughout the weekend, providing valuable data on surgical skills, teaching methods, and simulator-based competencies, according to the TSDA.
"We are pleased to have such a high level of participation this year," said Dr. Hicks, president of TSDA and the boot camp program director. "The faculty was enthusiastic and patient. Overall, it was a great experience, and TSDA is committed to providing continued simulation training for surgical residents."
Industry and institutional donations, including instruments, tissue, simulators, and supplies, were provided by the University of North Carolina, B-Line Medical, the Chamberlain Group, Covidien, CryoLife, Ethicon Endo-Surgery, Karl Storz Endoscopy, Maquet Cardiovascular, Medtronic, Olympus America, Pilling Division of Teleflex Medical, Scanlan International, Sorin Group, and St. Jude Medical.
Powerpoints of the educational session presentations, photos of the meeting, a faculty listing, and a list of supporting organizations are available at the TSDA website (www.tsda.org/sections/meetings/2011%20Boot%20Camp/index.html.)
Educating Mentors
For the second year, in conjunction with the residents’ boot camp, the JCTSE conducted its Educate the Educators (EtE) program. The EtE program was held July 14-17 in Chapel Hill and was developed based on the specific needs of cardiothoracic surgeons.
According to a statement by the JCTSE surgical director of education, Dr. Edward D. Verrier, "the combination of these two programs achieving their goals bodes well for the future of cardiothoracic surgery education. The TSDA’s [boot camp] provided incoming residents with an experiential foundation and hands-on practice in basic cardiothoracic operating skills and the JCTSE’s EtE program enhanced the teaching skills of cardiothoracic surgical faculty and promoted the concept of career advancement through education."
The objectives of the EtE course were derived from national surveys of U.S.-based cardiothoracic surgery faculty and residents. The findings from these surveys guided EtE course codirectors, Dr. Stephen C. Yang of Johns Hopkins University in Baltimore and Dr. Ara Vaporciyan of the University of Texas, Houston, according to the JCTSE.
The 2.5-day program focused on the effective delivery of skills-based education (simulation and intraoperative teaching) and methods to convert educational efforts into career advancement (grants and promotion); it included adult learning theory, how to teach in the operating room, curriculum development and implementation, how to improve assessment skills, and how to use the science of education as a faculty advancement tool.
The goal of the program, according to the JCTSE, is to better prepare attendees to enhance educational efforts at their home institution. This enhancement may come in the form of initiating a skills laboratory with a complete curriculum or developing a separate program to address a specific educational need.
Dr. Yang said in a JTCSE summary of the meeting, "I think EtE 2011 was even more successful than last year due in part to the return of stellar faculty from the 2010 program and additions to that faculty. Attendees arrived with a high level of enthusiasm, interest, and energy, most likely driven by the information they receive about the program they were about to attend but as well as feedback they received from last year’s attendees. This year’s attendees definitely left with an eagerness to encourage other colleagues to attend the course in the future."
According to the JCTSE, connections will be maintained with those who attended both the 2010 and 2011 EtE programs "to help guide them as they make inroads into improving cardiothoracic surgery education. The JCTSE remains committed to building an ‘army of educators’ who will lead the new wave of education for the next generation of CT surgeons."
In a world of rapidly changing technology and educational demands, innovative training methods are required to prepare the next generation of cardiothoracic surgeons. The Thoracic Surgery Directors Association and the Joint Council on Thoracic Surgery Education Inc. have developed programs to ensure that CT residents receive the best possible training.
A prime example of these efforts is the annual TSDA Cardiothoracic Surgery Resident Boot Camp. The 2011 Boot Camp was held July 14-17 at the continuing education center of the University of North Carolina at Chapel Hill.
First-year residents from 24 thoracic surgery residency programs across the country joined faculty, led by Dr. James Fann of Stanford (Calif.) University, Dr. Rick Feins of UNC Chapel Hill, and Dr. George Hicks Jr. of the University of Rochester (N.Y.), with the goal of gaining valuable insights into surgical techniques and expanding their base of thoracic surgery knowledge.
The program was developed and hosted by the TSDA and was funded in part through a grant from the JTCSE.

|
|
Photos courtesy of the Thoracic Surgery Directors Association
|
Now in its fourth year, the boot camp uses cardiothoracic simulator–based training to give residents some of the basic skill sets necessary to enhance their residency educational experience, especially in the operating room.
This year, procedures included cardiopulmonary bypass, aortic valve repair, anastomosis, lung ventilation, and lobectomy.
Seeking out multidisciplinary approaches to teaching, the TSDA boot camp faculty also brought in guest speakers from the world of 3-D gaming and aviation. Ron Maness, a former pilot with the U.S. Air Force Thunderbirds, offered insights into how pilots use simulation to avoid errors in the cockpit. Additionally, Richard Boyd from Lockheed Martin Virtual World Labs spoke about how 3-D simulation tools for health care could make analysis and training fast, safe, and measurable.
"Other professional fields have made great gains when it comes to quality by using simulations in teaching," said Dr. Feins. "Sharing multidisciplinary learning approaches with up-and-coming residents is a great way to expand and build on their current knowledge base."
Feedback from the residents that was reported at the TSDA website indicated that Boot Camp III was a success. "Boot Camp was perfectly [set up] to introduce career advancement in cardiac and thoracic surgery," noted one resident in an evaluation.
"The hand-picked faculty was a key element to the camp and collectively they shared the goal of introducing foreign concepts in the field and did it in a very [nonintimidating] fashion."
Director feedback also expressed strong support of the boot camp’s benefits, with 91% of program directors saying that their resident’s experience was very or extremely helpful. Resident boot camp participants displayed similar enthusiasm for the program, indicating that it was a "phenomenal experience," and a "fantastic opportunity," according to a TSDA summary.
This weekend-long course incorporated simulated emergency scenarios and surgery demonstrations, with residents able to spend extensive one-on-one time with the faculty, from whom they gained guidance along with the finer points of cardiothoracic surgery basics.
Faculty and resident assessments were integrated into the curriculum throughout the weekend, providing valuable data on surgical skills, teaching methods, and simulator-based competencies, according to the TSDA.
"We are pleased to have such a high level of participation this year," said Dr. Hicks, president of TSDA and the boot camp program director. "The faculty was enthusiastic and patient. Overall, it was a great experience, and TSDA is committed to providing continued simulation training for surgical residents."
Industry and institutional donations, including instruments, tissue, simulators, and supplies, were provided by the University of North Carolina, B-Line Medical, the Chamberlain Group, Covidien, CryoLife, Ethicon Endo-Surgery, Karl Storz Endoscopy, Maquet Cardiovascular, Medtronic, Olympus America, Pilling Division of Teleflex Medical, Scanlan International, Sorin Group, and St. Jude Medical.
Powerpoints of the educational session presentations, photos of the meeting, a faculty listing, and a list of supporting organizations are available at the TSDA website (www.tsda.org/sections/meetings/2011%20Boot%20Camp/index.html.)
Educating Mentors
For the second year, in conjunction with the residents’ boot camp, the JCTSE conducted its Educate the Educators (EtE) program. The EtE program was held July 14-17 in Chapel Hill and was developed based on the specific needs of cardiothoracic surgeons.
According to a statement by the JCTSE surgical director of education, Dr. Edward D. Verrier, "the combination of these two programs achieving their goals bodes well for the future of cardiothoracic surgery education. The TSDA’s [boot camp] provided incoming residents with an experiential foundation and hands-on practice in basic cardiothoracic operating skills and the JCTSE’s EtE program enhanced the teaching skills of cardiothoracic surgical faculty and promoted the concept of career advancement through education."
The objectives of the EtE course were derived from national surveys of U.S.-based cardiothoracic surgery faculty and residents. The findings from these surveys guided EtE course codirectors, Dr. Stephen C. Yang of Johns Hopkins University in Baltimore and Dr. Ara Vaporciyan of the University of Texas, Houston, according to the JCTSE.
The 2.5-day program focused on the effective delivery of skills-based education (simulation and intraoperative teaching) and methods to convert educational efforts into career advancement (grants and promotion); it included adult learning theory, how to teach in the operating room, curriculum development and implementation, how to improve assessment skills, and how to use the science of education as a faculty advancement tool.
The goal of the program, according to the JCTSE, is to better prepare attendees to enhance educational efforts at their home institution. This enhancement may come in the form of initiating a skills laboratory with a complete curriculum or developing a separate program to address a specific educational need.
Dr. Yang said in a JTCSE summary of the meeting, "I think EtE 2011 was even more successful than last year due in part to the return of stellar faculty from the 2010 program and additions to that faculty. Attendees arrived with a high level of enthusiasm, interest, and energy, most likely driven by the information they receive about the program they were about to attend but as well as feedback they received from last year’s attendees. This year’s attendees definitely left with an eagerness to encourage other colleagues to attend the course in the future."
According to the JCTSE, connections will be maintained with those who attended both the 2010 and 2011 EtE programs "to help guide them as they make inroads into improving cardiothoracic surgery education. The JCTSE remains committed to building an ‘army of educators’ who will lead the new wave of education for the next generation of CT surgeons."
In a world of rapidly changing technology and educational demands, innovative training methods are required to prepare the next generation of cardiothoracic surgeons. The Thoracic Surgery Directors Association and the Joint Council on Thoracic Surgery Education Inc. have developed programs to ensure that CT residents receive the best possible training.
A prime example of these efforts is the annual TSDA Cardiothoracic Surgery Resident Boot Camp. The 2011 Boot Camp was held July 14-17 at the continuing education center of the University of North Carolina at Chapel Hill.
First-year residents from 24 thoracic surgery residency programs across the country joined faculty, led by Dr. James Fann of Stanford (Calif.) University, Dr. Rick Feins of UNC Chapel Hill, and Dr. George Hicks Jr. of the University of Rochester (N.Y.), with the goal of gaining valuable insights into surgical techniques and expanding their base of thoracic surgery knowledge.
The program was developed and hosted by the TSDA and was funded in part through a grant from the JTCSE.

|
|
Photos courtesy of the Thoracic Surgery Directors Association
|
Now in its fourth year, the boot camp uses cardiothoracic simulator–based training to give residents some of the basic skill sets necessary to enhance their residency educational experience, especially in the operating room.
This year, procedures included cardiopulmonary bypass, aortic valve repair, anastomosis, lung ventilation, and lobectomy.
Seeking out multidisciplinary approaches to teaching, the TSDA boot camp faculty also brought in guest speakers from the world of 3-D gaming and aviation. Ron Maness, a former pilot with the U.S. Air Force Thunderbirds, offered insights into how pilots use simulation to avoid errors in the cockpit. Additionally, Richard Boyd from Lockheed Martin Virtual World Labs spoke about how 3-D simulation tools for health care could make analysis and training fast, safe, and measurable.
"Other professional fields have made great gains when it comes to quality by using simulations in teaching," said Dr. Feins. "Sharing multidisciplinary learning approaches with up-and-coming residents is a great way to expand and build on their current knowledge base."
Feedback from the residents that was reported at the TSDA website indicated that Boot Camp III was a success. "Boot Camp was perfectly [set up] to introduce career advancement in cardiac and thoracic surgery," noted one resident in an evaluation.
"The hand-picked faculty was a key element to the camp and collectively they shared the goal of introducing foreign concepts in the field and did it in a very [nonintimidating] fashion."
Director feedback also expressed strong support of the boot camp’s benefits, with 91% of program directors saying that their resident’s experience was very or extremely helpful. Resident boot camp participants displayed similar enthusiasm for the program, indicating that it was a "phenomenal experience," and a "fantastic opportunity," according to a TSDA summary.
This weekend-long course incorporated simulated emergency scenarios and surgery demonstrations, with residents able to spend extensive one-on-one time with the faculty, from whom they gained guidance along with the finer points of cardiothoracic surgery basics.
Faculty and resident assessments were integrated into the curriculum throughout the weekend, providing valuable data on surgical skills, teaching methods, and simulator-based competencies, according to the TSDA.
"We are pleased to have such a high level of participation this year," said Dr. Hicks, president of TSDA and the boot camp program director. "The faculty was enthusiastic and patient. Overall, it was a great experience, and TSDA is committed to providing continued simulation training for surgical residents."
Industry and institutional donations, including instruments, tissue, simulators, and supplies, were provided by the University of North Carolina, B-Line Medical, the Chamberlain Group, Covidien, CryoLife, Ethicon Endo-Surgery, Karl Storz Endoscopy, Maquet Cardiovascular, Medtronic, Olympus America, Pilling Division of Teleflex Medical, Scanlan International, Sorin Group, and St. Jude Medical.
Powerpoints of the educational session presentations, photos of the meeting, a faculty listing, and a list of supporting organizations are available at the TSDA website (www.tsda.org/sections/meetings/2011%20Boot%20Camp/index.html.)
Educating Mentors
For the second year, in conjunction with the residents’ boot camp, the JCTSE conducted its Educate the Educators (EtE) program. The EtE program was held July 14-17 in Chapel Hill and was developed based on the specific needs of cardiothoracic surgeons.
According to a statement by the JCTSE surgical director of education, Dr. Edward D. Verrier, "the combination of these two programs achieving their goals bodes well for the future of cardiothoracic surgery education. The TSDA’s [boot camp] provided incoming residents with an experiential foundation and hands-on practice in basic cardiothoracic operating skills and the JCTSE’s EtE program enhanced the teaching skills of cardiothoracic surgical faculty and promoted the concept of career advancement through education."
The objectives of the EtE course were derived from national surveys of U.S.-based cardiothoracic surgery faculty and residents. The findings from these surveys guided EtE course codirectors, Dr. Stephen C. Yang of Johns Hopkins University in Baltimore and Dr. Ara Vaporciyan of the University of Texas, Houston, according to the JCTSE.
The 2.5-day program focused on the effective delivery of skills-based education (simulation and intraoperative teaching) and methods to convert educational efforts into career advancement (grants and promotion); it included adult learning theory, how to teach in the operating room, curriculum development and implementation, how to improve assessment skills, and how to use the science of education as a faculty advancement tool.
The goal of the program, according to the JCTSE, is to better prepare attendees to enhance educational efforts at their home institution. This enhancement may come in the form of initiating a skills laboratory with a complete curriculum or developing a separate program to address a specific educational need.
Dr. Yang said in a JTCSE summary of the meeting, "I think EtE 2011 was even more successful than last year due in part to the return of stellar faculty from the 2010 program and additions to that faculty. Attendees arrived with a high level of enthusiasm, interest, and energy, most likely driven by the information they receive about the program they were about to attend but as well as feedback they received from last year’s attendees. This year’s attendees definitely left with an eagerness to encourage other colleagues to attend the course in the future."
According to the JCTSE, connections will be maintained with those who attended both the 2010 and 2011 EtE programs "to help guide them as they make inroads into improving cardiothoracic surgery education. The JCTSE remains committed to building an ‘army of educators’ who will lead the new wave of education for the next generation of CT surgeons."
Similar Survival in VLBW Infants with Delayed Surgery
PHILADELPHIA – When a very low birth weight (VLWBW) infant has congenital heart disease needing surgical repair, the two opposing strategies of immediate surgery or delaying surgery for several weeks until the newborn grows larger work equally well for survival. Survival rates after both approaches tracked nearly identically during 3 years of follow-up, in a single center review of 80 cases.
Because the review included a relatively small number of VLBW newborns, the analysis could not determine which benefited most from immediate surgery and which did better with a delayed operation. "But we were reassured that delay did not lead to excess risk," Dr. Edward J. Hickey said at the annual meeting of the American Association for Thoracic Surgery.
Results from a second, related analysis that he reported showed that birth weight surpassed gestational age as a predictor of survival in newborns with congenital heart disease. "Birth weight is a more reliable, independent risk factor for death," said Dr. Hickey, a cardiothoracic surgeon at the Hospital for Sick Children in Toronto. The analysis showed that the highest risk for survival occurred in newborns who weighed less than 2.0 kg at birth. As a result of this finding, Dr. Hickey’s comparison of immediate and delayed surgical repair focused on the 80 newborns in the series who weighed less than 2.0 kg and required prompt intervention.
Among these 80 infants, 34 had "immediate surgery," which meant they had their operation as soon as it could be scheduled and performed, generally within 3 weeks of birth. Surgery for the other 46 was an average of 8 weeks after birth. These differences reflected the way surgeons at Sick Children managed each case.
Among the delayed surgery cases, infants with truncus or coarctation had the slowest growth, with as little as 50 g gained per week. In contrast, infants with an atrial septal defect, tetralogy, or a total anomalous pulmonary venous connection had growth rates above average, often at a pace of more than 150 g/week.
"I was most struck by the infants with coarctation, who seemed to grow at very low rates. That suggests to us that these patients are the ones we should repair early," because it is less likely that a delay would lead to much weight gain and improved surgical prospects, Dr. Hickey said. Based on these findings, he and his associates now perform coarctation repairs in infants whose weight is as low as 1.4 kg, he said. But Dr. Hickey also stressed that the timing of surgical repair must be individualized for each patient.
The two analyses done by Dr. Hickey and his associates involved 1,557 children with congenital heart disease admitted to the Hospital for Sick Children at age 30 days or younger who underwent active management during a 10-year period. Overall survival in this group was 91% at 3 months after admission, 88% after 6 months, and 86% after 5 years.
They evaluated the impact of both gestational age and birth weight on survival among these children, and found that both parameters were linked to mortality. Infants born at 28 weeks’ gestational age had a roughly 40% survival rate after 1 year, those born at 32 weeks had about a 60% survival rate to 1 year, and those born at 36 weeks had about an 80% survival rate at 1 year.
When analyzed by birth weight, those born at 3.5 kg or larger had a greater than 90% 1-year survival rate, those born with a weight of 2.0 kg had about an 80% 1-year survival, and those born weighing 1.5 kg had about a 60% survival to 1 year. These data identified an inflection point where infants born weighing less than 2.0 kg had a substantially worse survival than those who weighed 2.0 kg or more. Additional analysis that compared the relative contributions of gestational age and birth weight also showed that birth weight was the much stronger factor influencing 1-year survival.
The series included 149 infants born at less than 2.0 kg, highlighting how uncommon it is for surgeons to face the question of how to manage VLBW infants with congenital heart disease. Eighty-five of these infants (57%) weighed 1.5-1.9 kg at birth, while the remainder weighed less than 1.5 kg. Thirty did not require immediate surgical intervention, 12 had other, noncardiovascular complications requiring initial intervention, and 27 received comfort care only, leaving 80 candidates that became part of the immediate – versus delayed – surgery analysis.
Among the 46 infants whose surgery was delayed for an average of 8 weeks, 18 (39%) had a total of 33 complications. Six of these 18 children died while awaiting surgery. "Despite this high complication rate, we see roughly equivalent survival" between the immediate and delayed surgery groups. That observation, coupled with the finding that many infants gained weight at an "acceptable" rate during the period of surgical delay, led to the conclusion that either strategy is reasonable and should depend on the specific features of each case, he said.
Dr. Hickey had no disclosures. ☐
PHILADELPHIA – When a very low birth weight (VLWBW) infant has congenital heart disease needing surgical repair, the two opposing strategies of immediate surgery or delaying surgery for several weeks until the newborn grows larger work equally well for survival. Survival rates after both approaches tracked nearly identically during 3 years of follow-up, in a single center review of 80 cases.
Because the review included a relatively small number of VLBW newborns, the analysis could not determine which benefited most from immediate surgery and which did better with a delayed operation. "But we were reassured that delay did not lead to excess risk," Dr. Edward J. Hickey said at the annual meeting of the American Association for Thoracic Surgery.
Results from a second, related analysis that he reported showed that birth weight surpassed gestational age as a predictor of survival in newborns with congenital heart disease. "Birth weight is a more reliable, independent risk factor for death," said Dr. Hickey, a cardiothoracic surgeon at the Hospital for Sick Children in Toronto. The analysis showed that the highest risk for survival occurred in newborns who weighed less than 2.0 kg at birth. As a result of this finding, Dr. Hickey’s comparison of immediate and delayed surgical repair focused on the 80 newborns in the series who weighed less than 2.0 kg and required prompt intervention.
Among these 80 infants, 34 had "immediate surgery," which meant they had their operation as soon as it could be scheduled and performed, generally within 3 weeks of birth. Surgery for the other 46 was an average of 8 weeks after birth. These differences reflected the way surgeons at Sick Children managed each case.
Among the delayed surgery cases, infants with truncus or coarctation had the slowest growth, with as little as 50 g gained per week. In contrast, infants with an atrial septal defect, tetralogy, or a total anomalous pulmonary venous connection had growth rates above average, often at a pace of more than 150 g/week.
"I was most struck by the infants with coarctation, who seemed to grow at very low rates. That suggests to us that these patients are the ones we should repair early," because it is less likely that a delay would lead to much weight gain and improved surgical prospects, Dr. Hickey said. Based on these findings, he and his associates now perform coarctation repairs in infants whose weight is as low as 1.4 kg, he said. But Dr. Hickey also stressed that the timing of surgical repair must be individualized for each patient.
The two analyses done by Dr. Hickey and his associates involved 1,557 children with congenital heart disease admitted to the Hospital for Sick Children at age 30 days or younger who underwent active management during a 10-year period. Overall survival in this group was 91% at 3 months after admission, 88% after 6 months, and 86% after 5 years.
They evaluated the impact of both gestational age and birth weight on survival among these children, and found that both parameters were linked to mortality. Infants born at 28 weeks’ gestational age had a roughly 40% survival rate after 1 year, those born at 32 weeks had about a 60% survival rate to 1 year, and those born at 36 weeks had about an 80% survival rate at 1 year.
When analyzed by birth weight, those born at 3.5 kg or larger had a greater than 90% 1-year survival rate, those born with a weight of 2.0 kg had about an 80% 1-year survival, and those born weighing 1.5 kg had about a 60% survival to 1 year. These data identified an inflection point where infants born weighing less than 2.0 kg had a substantially worse survival than those who weighed 2.0 kg or more. Additional analysis that compared the relative contributions of gestational age and birth weight also showed that birth weight was the much stronger factor influencing 1-year survival.
The series included 149 infants born at less than 2.0 kg, highlighting how uncommon it is for surgeons to face the question of how to manage VLBW infants with congenital heart disease. Eighty-five of these infants (57%) weighed 1.5-1.9 kg at birth, while the remainder weighed less than 1.5 kg. Thirty did not require immediate surgical intervention, 12 had other, noncardiovascular complications requiring initial intervention, and 27 received comfort care only, leaving 80 candidates that became part of the immediate – versus delayed – surgery analysis.
Among the 46 infants whose surgery was delayed for an average of 8 weeks, 18 (39%) had a total of 33 complications. Six of these 18 children died while awaiting surgery. "Despite this high complication rate, we see roughly equivalent survival" between the immediate and delayed surgery groups. That observation, coupled with the finding that many infants gained weight at an "acceptable" rate during the period of surgical delay, led to the conclusion that either strategy is reasonable and should depend on the specific features of each case, he said.
Dr. Hickey had no disclosures. ☐
PHILADELPHIA – When a very low birth weight (VLWBW) infant has congenital heart disease needing surgical repair, the two opposing strategies of immediate surgery or delaying surgery for several weeks until the newborn grows larger work equally well for survival. Survival rates after both approaches tracked nearly identically during 3 years of follow-up, in a single center review of 80 cases.
Because the review included a relatively small number of VLBW newborns, the analysis could not determine which benefited most from immediate surgery and which did better with a delayed operation. "But we were reassured that delay did not lead to excess risk," Dr. Edward J. Hickey said at the annual meeting of the American Association for Thoracic Surgery.
Results from a second, related analysis that he reported showed that birth weight surpassed gestational age as a predictor of survival in newborns with congenital heart disease. "Birth weight is a more reliable, independent risk factor for death," said Dr. Hickey, a cardiothoracic surgeon at the Hospital for Sick Children in Toronto. The analysis showed that the highest risk for survival occurred in newborns who weighed less than 2.0 kg at birth. As a result of this finding, Dr. Hickey’s comparison of immediate and delayed surgical repair focused on the 80 newborns in the series who weighed less than 2.0 kg and required prompt intervention.
Among these 80 infants, 34 had "immediate surgery," which meant they had their operation as soon as it could be scheduled and performed, generally within 3 weeks of birth. Surgery for the other 46 was an average of 8 weeks after birth. These differences reflected the way surgeons at Sick Children managed each case.
Among the delayed surgery cases, infants with truncus or coarctation had the slowest growth, with as little as 50 g gained per week. In contrast, infants with an atrial septal defect, tetralogy, or a total anomalous pulmonary venous connection had growth rates above average, often at a pace of more than 150 g/week.
"I was most struck by the infants with coarctation, who seemed to grow at very low rates. That suggests to us that these patients are the ones we should repair early," because it is less likely that a delay would lead to much weight gain and improved surgical prospects, Dr. Hickey said. Based on these findings, he and his associates now perform coarctation repairs in infants whose weight is as low as 1.4 kg, he said. But Dr. Hickey also stressed that the timing of surgical repair must be individualized for each patient.
The two analyses done by Dr. Hickey and his associates involved 1,557 children with congenital heart disease admitted to the Hospital for Sick Children at age 30 days or younger who underwent active management during a 10-year period. Overall survival in this group was 91% at 3 months after admission, 88% after 6 months, and 86% after 5 years.
They evaluated the impact of both gestational age and birth weight on survival among these children, and found that both parameters were linked to mortality. Infants born at 28 weeks’ gestational age had a roughly 40% survival rate after 1 year, those born at 32 weeks had about a 60% survival rate to 1 year, and those born at 36 weeks had about an 80% survival rate at 1 year.
When analyzed by birth weight, those born at 3.5 kg or larger had a greater than 90% 1-year survival rate, those born with a weight of 2.0 kg had about an 80% 1-year survival, and those born weighing 1.5 kg had about a 60% survival to 1 year. These data identified an inflection point where infants born weighing less than 2.0 kg had a substantially worse survival than those who weighed 2.0 kg or more. Additional analysis that compared the relative contributions of gestational age and birth weight also showed that birth weight was the much stronger factor influencing 1-year survival.
The series included 149 infants born at less than 2.0 kg, highlighting how uncommon it is for surgeons to face the question of how to manage VLBW infants with congenital heart disease. Eighty-five of these infants (57%) weighed 1.5-1.9 kg at birth, while the remainder weighed less than 1.5 kg. Thirty did not require immediate surgical intervention, 12 had other, noncardiovascular complications requiring initial intervention, and 27 received comfort care only, leaving 80 candidates that became part of the immediate – versus delayed – surgery analysis.
Among the 46 infants whose surgery was delayed for an average of 8 weeks, 18 (39%) had a total of 33 complications. Six of these 18 children died while awaiting surgery. "Despite this high complication rate, we see roughly equivalent survival" between the immediate and delayed surgery groups. That observation, coupled with the finding that many infants gained weight at an "acceptable" rate during the period of surgical delay, led to the conclusion that either strategy is reasonable and should depend on the specific features of each case, he said.
Dr. Hickey had no disclosures. ☐
Major Finding: In infants with congenital heart disease with a birth weight below 2.0 kg who required surgical intervention, immediate surgery or surgery delayed for an average of 8 weeks led to similar survival rates during the following 3 years.
Data Source: Review of 80 VLBW infants who required surgery for congenital heart disease at one center during a 10-year period.
Disclosures: Dr. Hickey said that he had no disclosures.
Cardiothoracic Clinical Trails Move Forward
The Cardiothoracic Surgical Trials Network is a major collaborative effort focusing on surgical approaches for cardiac disease. Two of their trials recently reached enrollment milestones, according to the CTSN.
In August the University of Pennsylvania randomized the 200th patient in the severe ischemic mitral regurgitation (SMR) trial. As of the end of the month, the Network randomized 205 patients in the trial designed to evaluate the efficacy and safety of mitral valve repair and replacement for severe MR patients.
There is a companion trial, the moderate MR (MMR) trial, to evaluate the safety and efficacy of mitral valve repair and coronary artery bypass grafting (CABG) vs. CABG alone.
The goal of these trials is to determine the optimal approach to treatment of patients with ischemic MR, a controversial subject involving significant variations in surgical practice. Investigators expect to complete enrollment in the SMR trial (n=250) in the fall of 2011, and in the MMR trial (n=300) by summer of 202.
Also in August, the University of Virginia randomized the 100th patient in the atrial fibrillation (AF) trial. The Network designed a comparative effectiveness randomized trial of surgical ablation with left atrial appendage (LAA) closure versus LAA closure alone in patients with (longstanding) persistent AF undergoing MVS. According to CTSN, nested within this trial, is a further randomized comparison of 2 different lesions sets (pulmonary vein isolation only and Maze lesion set).
The FDA recently approved expansion from 13 to 23 clinical centers and these new sites are now being launched to enable completion of enrollment in 2012.
Two new CTSN-sponsored cell therapy trials are also in the works.
Left ventricular assist device (LVAD) therapy has become widely used and outcomes have improved over time. However, adverse events are still noted and could be minimized. In addition, quality of life could be improved if the duration of support could be limited. One potential way to do this is by inducing myocardial recovery through cell therapy, according to the CTSN.
In collaboration with the Cardiovascular Cell Therapy Research Network, CTSN has developed a translational trial that is intended to evaluate the safety, and explore the efficacy, of direct myocardial injection of off-the-shelf mesenchymal precursor cells in LVAD recipients. The FDA recently approved the protocol, and start-up activities are underway. The ttraining of site coordinators is scheduled to begin in mid-fall 2011.
The second cell therapy trial planned involves the use of intracoronary injections of autologous cardiac stem cells to be performed following cardiac transplantation. According to the CSTN, this trial will be designed to provide "important exploratory information regarding safety and the ability of stem cells to engraft and differentiate within the scaffold of the transplanted heart."
The rationale for this research is to modulate tolerance of the transplanted heart in order to reduce the incidence of allograft rejection. A pre-IND meeting to discuss the protocol was initiated with the FDA.
In the important area of drug support for cardiac surgery patients, CTSN is collaborating with the VA Cooperative Clinical Studies Program, to design what is intended to be a large, simple trial evaluating the effect of adding ticagrelor to aspirin after coronary artery bypass grafting.
The primary efficacy endpoint in the trial will be MACCE and the primary safety endpoint will be severe bleeding. The sample size will be close to 5,000 patients, and the trial is designed to detect a 20% reduction in the primary efficacy endpoint.
Further information on these and other upcoming and ongoing trials can be found on the CSTN website: www.ctsurgerynet.org along with access to their monthly newsletter.n
The Cardiothoracic Surgical Trials Network is a major collaborative effort focusing on surgical approaches for cardiac disease. Two of their trials recently reached enrollment milestones, according to the CTSN.
In August the University of Pennsylvania randomized the 200th patient in the severe ischemic mitral regurgitation (SMR) trial. As of the end of the month, the Network randomized 205 patients in the trial designed to evaluate the efficacy and safety of mitral valve repair and replacement for severe MR patients.
There is a companion trial, the moderate MR (MMR) trial, to evaluate the safety and efficacy of mitral valve repair and coronary artery bypass grafting (CABG) vs. CABG alone.
The goal of these trials is to determine the optimal approach to treatment of patients with ischemic MR, a controversial subject involving significant variations in surgical practice. Investigators expect to complete enrollment in the SMR trial (n=250) in the fall of 2011, and in the MMR trial (n=300) by summer of 202.
Also in August, the University of Virginia randomized the 100th patient in the atrial fibrillation (AF) trial. The Network designed a comparative effectiveness randomized trial of surgical ablation with left atrial appendage (LAA) closure versus LAA closure alone in patients with (longstanding) persistent AF undergoing MVS. According to CTSN, nested within this trial, is a further randomized comparison of 2 different lesions sets (pulmonary vein isolation only and Maze lesion set).
The FDA recently approved expansion from 13 to 23 clinical centers and these new sites are now being launched to enable completion of enrollment in 2012.
Two new CTSN-sponsored cell therapy trials are also in the works.
Left ventricular assist device (LVAD) therapy has become widely used and outcomes have improved over time. However, adverse events are still noted and could be minimized. In addition, quality of life could be improved if the duration of support could be limited. One potential way to do this is by inducing myocardial recovery through cell therapy, according to the CTSN.
In collaboration with the Cardiovascular Cell Therapy Research Network, CTSN has developed a translational trial that is intended to evaluate the safety, and explore the efficacy, of direct myocardial injection of off-the-shelf mesenchymal precursor cells in LVAD recipients. The FDA recently approved the protocol, and start-up activities are underway. The ttraining of site coordinators is scheduled to begin in mid-fall 2011.
The second cell therapy trial planned involves the use of intracoronary injections of autologous cardiac stem cells to be performed following cardiac transplantation. According to the CSTN, this trial will be designed to provide "important exploratory information regarding safety and the ability of stem cells to engraft and differentiate within the scaffold of the transplanted heart."
The rationale for this research is to modulate tolerance of the transplanted heart in order to reduce the incidence of allograft rejection. A pre-IND meeting to discuss the protocol was initiated with the FDA.
In the important area of drug support for cardiac surgery patients, CTSN is collaborating with the VA Cooperative Clinical Studies Program, to design what is intended to be a large, simple trial evaluating the effect of adding ticagrelor to aspirin after coronary artery bypass grafting.
The primary efficacy endpoint in the trial will be MACCE and the primary safety endpoint will be severe bleeding. The sample size will be close to 5,000 patients, and the trial is designed to detect a 20% reduction in the primary efficacy endpoint.
Further information on these and other upcoming and ongoing trials can be found on the CSTN website: www.ctsurgerynet.org along with access to their monthly newsletter.n
The Cardiothoracic Surgical Trials Network is a major collaborative effort focusing on surgical approaches for cardiac disease. Two of their trials recently reached enrollment milestones, according to the CTSN.
In August the University of Pennsylvania randomized the 200th patient in the severe ischemic mitral regurgitation (SMR) trial. As of the end of the month, the Network randomized 205 patients in the trial designed to evaluate the efficacy and safety of mitral valve repair and replacement for severe MR patients.
There is a companion trial, the moderate MR (MMR) trial, to evaluate the safety and efficacy of mitral valve repair and coronary artery bypass grafting (CABG) vs. CABG alone.
The goal of these trials is to determine the optimal approach to treatment of patients with ischemic MR, a controversial subject involving significant variations in surgical practice. Investigators expect to complete enrollment in the SMR trial (n=250) in the fall of 2011, and in the MMR trial (n=300) by summer of 202.
Also in August, the University of Virginia randomized the 100th patient in the atrial fibrillation (AF) trial. The Network designed a comparative effectiveness randomized trial of surgical ablation with left atrial appendage (LAA) closure versus LAA closure alone in patients with (longstanding) persistent AF undergoing MVS. According to CTSN, nested within this trial, is a further randomized comparison of 2 different lesions sets (pulmonary vein isolation only and Maze lesion set).
The FDA recently approved expansion from 13 to 23 clinical centers and these new sites are now being launched to enable completion of enrollment in 2012.
Two new CTSN-sponsored cell therapy trials are also in the works.
Left ventricular assist device (LVAD) therapy has become widely used and outcomes have improved over time. However, adverse events are still noted and could be minimized. In addition, quality of life could be improved if the duration of support could be limited. One potential way to do this is by inducing myocardial recovery through cell therapy, according to the CTSN.
In collaboration with the Cardiovascular Cell Therapy Research Network, CTSN has developed a translational trial that is intended to evaluate the safety, and explore the efficacy, of direct myocardial injection of off-the-shelf mesenchymal precursor cells in LVAD recipients. The FDA recently approved the protocol, and start-up activities are underway. The ttraining of site coordinators is scheduled to begin in mid-fall 2011.
The second cell therapy trial planned involves the use of intracoronary injections of autologous cardiac stem cells to be performed following cardiac transplantation. According to the CSTN, this trial will be designed to provide "important exploratory information regarding safety and the ability of stem cells to engraft and differentiate within the scaffold of the transplanted heart."
The rationale for this research is to modulate tolerance of the transplanted heart in order to reduce the incidence of allograft rejection. A pre-IND meeting to discuss the protocol was initiated with the FDA.
In the important area of drug support for cardiac surgery patients, CTSN is collaborating with the VA Cooperative Clinical Studies Program, to design what is intended to be a large, simple trial evaluating the effect of adding ticagrelor to aspirin after coronary artery bypass grafting.
The primary efficacy endpoint in the trial will be MACCE and the primary safety endpoint will be severe bleeding. The sample size will be close to 5,000 patients, and the trial is designed to detect a 20% reduction in the primary efficacy endpoint.
Further information on these and other upcoming and ongoing trials can be found on the CSTN website: www.ctsurgerynet.org along with access to their monthly newsletter.n
Medicare to Begin Testing Bundling
Physicians and hospitals now have the chance to test out bundled payments on a range of conditions under a new Medicare initiative.
Officials at the Centers for Medicare and Medicaid Services have invited physicians, hospitals, and other health care providers to participate in the Bundled Payments for Care Improvement initiative. The program, which was mandated under the Affordable Care Act, offers a variety of options for bundling payments for a hospital stay, for post-discharge services, or for both the hospital stay and the post-discharge care.
The move toward bundled payments is a major shift in how the government pays for medical care. Instead of paying hospitals, physicians, and other providers separately, this initiative would combine the payment over an episode of care for a specific condition. The aim of the program is to incentivize clinicians to work together and provide better continuity of care, resulting in better quality and lower costs.
"Today, Medicare pays for care the wrong way," Health and Human Services Secretary Kathleen Sebelius said during a teleconference to announce the bundling program. "Payments are based on the quantity of care, the amount of services delivered, not the quality of that care. And that leaves us too often with a system that actually can punish the providers that are most successful at getting and keeping their patients healthy."
The new bundling program offers four ways that health care providers can receive a bundled payment, three of which provide payment retrospectively, and one that offers a prospective payment. For example, under some of the retrospective payment models, CMS and the providers would agree on a target payment amount for the episode of care and providers would be paid under the original Medicare fee-for-service system, but at a negotiated discount of 2% to 3% or greater. At the end of the care episode, the total payment would be compared with the target price and providers would be able to share in the savings, according to CMS.
The prospective payment model would work differently. Under that option, CMS would make a single bundled payment to the hospital to cover all services provided during the inpatient stay by the hospital, physicians, and other providers. That payment would offer at least a 3% discount to Medicare. Under this option, physicians and other providers would submit "no pay" claims to Medicare and the hospital would pay them out of the single bundled payment.
In addition to the options of prospective or retrospective payment, providers could choose how long the episode of care will be and what conditions they want to bundle payment for, and what services would be included in the payment. CMS officials said they wanted to make the program flexible so that a range of hospitals, physicians, and other providers could participate.
Organizations interested in applying must submit a letter of intent by Sept. 22 for Model 1 and by Nov. 4 for Models 2, 3, and 4. More information on the program and how to apply is seen at www.innovations.cms.gov/areas-of-focus/patient-care-models/bundled-payments-for-care-improvement.html.
Dr. Richard Gilfillan, the acting director of the CMS Innovation Center, which is overseeing the bundling initiative, said he expects that hundreds of organizations will apply. CMS will consider a number of factors in choosing participants for the program including the best proposals for care improvement, the number of patients involved, and the conditions addressed, and the price discounts offered, he said.
The program is a unique opportunity for hospitals to redesign their systems to promote better care coordination, Dr. Gilfillan said, and have that effort supported through Medicare payments.
The idea is to eliminate the traditional barriers between physicians and other providers – both inpatient and outpatient – all of whom may be involved in the care of a single condition, said Dr. Nancy Nielson, senior advisor to the CMS Innovation Center and past president of the American Medical Association. "I do believe that both physicians and hospitals will find this [to be] an opportunity that’s flexible enough to give them the opportunity to begin to learn how to get paid for care differently," she said.
Dr. Cecil B. Wilson, AMA immediate past president, said the organization will urge federal officials to encourage applications for physician-led bundling projects.
"For this to be successful, and for physicians to participate actively, then they need to be a part of that process rather than just some larger corporation or larger hospital system or health plan that’s organizing these," he said. "We think those are important as well, but we also think it’s important that physicians be a part of that leadership."
While there are physicians working in large group practices that have had some experience with bundled payments, most doctors aren’t prepared for these types of payment changes, Dr. Wilson said. So the AMA is also recommending that CMS provide technical assistance and data to interested physicians.
Health care consultant Robert Minkin urged physicians to apply for the bundling program. "The implications of bundled payments and other clinical integration models are that we come to a common, best-evidence practice approach to care that manages on a fixed budget," said Mr. Minkin, of the Camden Group. "Physicians who can survive in an environment like that will thrive. For those who have difficulty in those situations, it’s going to be very tough."
Physicians and hospitals now have the chance to test out bundled payments on a range of conditions under a new Medicare initiative.
Officials at the Centers for Medicare and Medicaid Services have invited physicians, hospitals, and other health care providers to participate in the Bundled Payments for Care Improvement initiative. The program, which was mandated under the Affordable Care Act, offers a variety of options for bundling payments for a hospital stay, for post-discharge services, or for both the hospital stay and the post-discharge care.
The move toward bundled payments is a major shift in how the government pays for medical care. Instead of paying hospitals, physicians, and other providers separately, this initiative would combine the payment over an episode of care for a specific condition. The aim of the program is to incentivize clinicians to work together and provide better continuity of care, resulting in better quality and lower costs.
"Today, Medicare pays for care the wrong way," Health and Human Services Secretary Kathleen Sebelius said during a teleconference to announce the bundling program. "Payments are based on the quantity of care, the amount of services delivered, not the quality of that care. And that leaves us too often with a system that actually can punish the providers that are most successful at getting and keeping their patients healthy."
The new bundling program offers four ways that health care providers can receive a bundled payment, three of which provide payment retrospectively, and one that offers a prospective payment. For example, under some of the retrospective payment models, CMS and the providers would agree on a target payment amount for the episode of care and providers would be paid under the original Medicare fee-for-service system, but at a negotiated discount of 2% to 3% or greater. At the end of the care episode, the total payment would be compared with the target price and providers would be able to share in the savings, according to CMS.
The prospective payment model would work differently. Under that option, CMS would make a single bundled payment to the hospital to cover all services provided during the inpatient stay by the hospital, physicians, and other providers. That payment would offer at least a 3% discount to Medicare. Under this option, physicians and other providers would submit "no pay" claims to Medicare and the hospital would pay them out of the single bundled payment.
In addition to the options of prospective or retrospective payment, providers could choose how long the episode of care will be and what conditions they want to bundle payment for, and what services would be included in the payment. CMS officials said they wanted to make the program flexible so that a range of hospitals, physicians, and other providers could participate.
Organizations interested in applying must submit a letter of intent by Sept. 22 for Model 1 and by Nov. 4 for Models 2, 3, and 4. More information on the program and how to apply is seen at www.innovations.cms.gov/areas-of-focus/patient-care-models/bundled-payments-for-care-improvement.html.
Dr. Richard Gilfillan, the acting director of the CMS Innovation Center, which is overseeing the bundling initiative, said he expects that hundreds of organizations will apply. CMS will consider a number of factors in choosing participants for the program including the best proposals for care improvement, the number of patients involved, and the conditions addressed, and the price discounts offered, he said.
The program is a unique opportunity for hospitals to redesign their systems to promote better care coordination, Dr. Gilfillan said, and have that effort supported through Medicare payments.
The idea is to eliminate the traditional barriers between physicians and other providers – both inpatient and outpatient – all of whom may be involved in the care of a single condition, said Dr. Nancy Nielson, senior advisor to the CMS Innovation Center and past president of the American Medical Association. "I do believe that both physicians and hospitals will find this [to be] an opportunity that’s flexible enough to give them the opportunity to begin to learn how to get paid for care differently," she said.
Dr. Cecil B. Wilson, AMA immediate past president, said the organization will urge federal officials to encourage applications for physician-led bundling projects.
"For this to be successful, and for physicians to participate actively, then they need to be a part of that process rather than just some larger corporation or larger hospital system or health plan that’s organizing these," he said. "We think those are important as well, but we also think it’s important that physicians be a part of that leadership."
While there are physicians working in large group practices that have had some experience with bundled payments, most doctors aren’t prepared for these types of payment changes, Dr. Wilson said. So the AMA is also recommending that CMS provide technical assistance and data to interested physicians.
Health care consultant Robert Minkin urged physicians to apply for the bundling program. "The implications of bundled payments and other clinical integration models are that we come to a common, best-evidence practice approach to care that manages on a fixed budget," said Mr. Minkin, of the Camden Group. "Physicians who can survive in an environment like that will thrive. For those who have difficulty in those situations, it’s going to be very tough."
Physicians and hospitals now have the chance to test out bundled payments on a range of conditions under a new Medicare initiative.
Officials at the Centers for Medicare and Medicaid Services have invited physicians, hospitals, and other health care providers to participate in the Bundled Payments for Care Improvement initiative. The program, which was mandated under the Affordable Care Act, offers a variety of options for bundling payments for a hospital stay, for post-discharge services, or for both the hospital stay and the post-discharge care.
The move toward bundled payments is a major shift in how the government pays for medical care. Instead of paying hospitals, physicians, and other providers separately, this initiative would combine the payment over an episode of care for a specific condition. The aim of the program is to incentivize clinicians to work together and provide better continuity of care, resulting in better quality and lower costs.
"Today, Medicare pays for care the wrong way," Health and Human Services Secretary Kathleen Sebelius said during a teleconference to announce the bundling program. "Payments are based on the quantity of care, the amount of services delivered, not the quality of that care. And that leaves us too often with a system that actually can punish the providers that are most successful at getting and keeping their patients healthy."
The new bundling program offers four ways that health care providers can receive a bundled payment, three of which provide payment retrospectively, and one that offers a prospective payment. For example, under some of the retrospective payment models, CMS and the providers would agree on a target payment amount for the episode of care and providers would be paid under the original Medicare fee-for-service system, but at a negotiated discount of 2% to 3% or greater. At the end of the care episode, the total payment would be compared with the target price and providers would be able to share in the savings, according to CMS.
The prospective payment model would work differently. Under that option, CMS would make a single bundled payment to the hospital to cover all services provided during the inpatient stay by the hospital, physicians, and other providers. That payment would offer at least a 3% discount to Medicare. Under this option, physicians and other providers would submit "no pay" claims to Medicare and the hospital would pay them out of the single bundled payment.
In addition to the options of prospective or retrospective payment, providers could choose how long the episode of care will be and what conditions they want to bundle payment for, and what services would be included in the payment. CMS officials said they wanted to make the program flexible so that a range of hospitals, physicians, and other providers could participate.
Organizations interested in applying must submit a letter of intent by Sept. 22 for Model 1 and by Nov. 4 for Models 2, 3, and 4. More information on the program and how to apply is seen at www.innovations.cms.gov/areas-of-focus/patient-care-models/bundled-payments-for-care-improvement.html.
Dr. Richard Gilfillan, the acting director of the CMS Innovation Center, which is overseeing the bundling initiative, said he expects that hundreds of organizations will apply. CMS will consider a number of factors in choosing participants for the program including the best proposals for care improvement, the number of patients involved, and the conditions addressed, and the price discounts offered, he said.
The program is a unique opportunity for hospitals to redesign their systems to promote better care coordination, Dr. Gilfillan said, and have that effort supported through Medicare payments.
The idea is to eliminate the traditional barriers between physicians and other providers – both inpatient and outpatient – all of whom may be involved in the care of a single condition, said Dr. Nancy Nielson, senior advisor to the CMS Innovation Center and past president of the American Medical Association. "I do believe that both physicians and hospitals will find this [to be] an opportunity that’s flexible enough to give them the opportunity to begin to learn how to get paid for care differently," she said.
Dr. Cecil B. Wilson, AMA immediate past president, said the organization will urge federal officials to encourage applications for physician-led bundling projects.
"For this to be successful, and for physicians to participate actively, then they need to be a part of that process rather than just some larger corporation or larger hospital system or health plan that’s organizing these," he said. "We think those are important as well, but we also think it’s important that physicians be a part of that leadership."
While there are physicians working in large group practices that have had some experience with bundled payments, most doctors aren’t prepared for these types of payment changes, Dr. Wilson said. So the AMA is also recommending that CMS provide technical assistance and data to interested physicians.
Health care consultant Robert Minkin urged physicians to apply for the bundling program. "The implications of bundled payments and other clinical integration models are that we come to a common, best-evidence practice approach to care that manages on a fixed budget," said Mr. Minkin, of the Camden Group. "Physicians who can survive in an environment like that will thrive. For those who have difficulty in those situations, it’s going to be very tough."
Welcome Our New Resident Editors
Our sincerest thanks go to outgoing resident editors, Dr. Stephanie Mick and Dr. Christian Peyre for helping to establish the "Residents’ Corner" and creating excellent content for the section. To replace them, we have been fortunate to recruit two talented cardiothoracic residents representing a broad range of cardiothoracic educational interests.
In alphabetical order, Dr. Robroy MacIver grew up in Minnesota and attended the University of Minnesota medical school. He took a work-study job in the cardiothoracic research lab with Dr. Sara Shumway and Dick Bianco where he
"got hooked on surgery." From there he moved to Chicago to work with Dr. Constantine Mavroudis and Dr. Carl Backer at the Children’s Memorial Hospital, where he decided to focus on congenital heart surgery. He spent 2 years in the lab with Dr. Mavroudis and Dr. Backer working on tissue engineering in a heart block model. He was given the opportunity to travel to Melbourne for a year as an "add on" to his current pediatric fellowship at Seattle Children’s Hospital.
Dr. Bryan A. Whitson is a third-year Cardiovascular and Thoracic Surgery Fellow at the University of Minnesota. A native Hoosier, he completed his undergraduate degree in mechanical engineering at Purdue University, his medical doctorate at Indiana University, and his PhD at the University of Minnesota in Surgery investigating the immunobiology of minimally invasive surgery and cancer. His general surgery training was at the University of Minnesota where he also completed a Clinical Fellowship in Surgical Infectious Diseases.
He is currently the cardiovascular and thoracic surgery senior fellow at the University of Minnesota. He has 30 United States and international patents, received several grants, and over 60 publications.
Dr. Whitson’s research interests include lung transplantation, minimally invasive cardiothoracic surgery, medical device design, nanomedicine, and pulmonary assist devices.
Together, Dr. MacIver and Dr. Whitson will work with the rest of the TSN staff to develop and improve our Residents’ Corner in print and online.☐
Our sincerest thanks go to outgoing resident editors, Dr. Stephanie Mick and Dr. Christian Peyre for helping to establish the "Residents’ Corner" and creating excellent content for the section. To replace them, we have been fortunate to recruit two talented cardiothoracic residents representing a broad range of cardiothoracic educational interests.
In alphabetical order, Dr. Robroy MacIver grew up in Minnesota and attended the University of Minnesota medical school. He took a work-study job in the cardiothoracic research lab with Dr. Sara Shumway and Dick Bianco where he
"got hooked on surgery." From there he moved to Chicago to work with Dr. Constantine Mavroudis and Dr. Carl Backer at the Children’s Memorial Hospital, where he decided to focus on congenital heart surgery. He spent 2 years in the lab with Dr. Mavroudis and Dr. Backer working on tissue engineering in a heart block model. He was given the opportunity to travel to Melbourne for a year as an "add on" to his current pediatric fellowship at Seattle Children’s Hospital.
Dr. Bryan A. Whitson is a third-year Cardiovascular and Thoracic Surgery Fellow at the University of Minnesota. A native Hoosier, he completed his undergraduate degree in mechanical engineering at Purdue University, his medical doctorate at Indiana University, and his PhD at the University of Minnesota in Surgery investigating the immunobiology of minimally invasive surgery and cancer. His general surgery training was at the University of Minnesota where he also completed a Clinical Fellowship in Surgical Infectious Diseases.
He is currently the cardiovascular and thoracic surgery senior fellow at the University of Minnesota. He has 30 United States and international patents, received several grants, and over 60 publications.
Dr. Whitson’s research interests include lung transplantation, minimally invasive cardiothoracic surgery, medical device design, nanomedicine, and pulmonary assist devices.
Together, Dr. MacIver and Dr. Whitson will work with the rest of the TSN staff to develop and improve our Residents’ Corner in print and online.☐
Our sincerest thanks go to outgoing resident editors, Dr. Stephanie Mick and Dr. Christian Peyre for helping to establish the "Residents’ Corner" and creating excellent content for the section. To replace them, we have been fortunate to recruit two talented cardiothoracic residents representing a broad range of cardiothoracic educational interests.
In alphabetical order, Dr. Robroy MacIver grew up in Minnesota and attended the University of Minnesota medical school. He took a work-study job in the cardiothoracic research lab with Dr. Sara Shumway and Dick Bianco where he
"got hooked on surgery." From there he moved to Chicago to work with Dr. Constantine Mavroudis and Dr. Carl Backer at the Children’s Memorial Hospital, where he decided to focus on congenital heart surgery. He spent 2 years in the lab with Dr. Mavroudis and Dr. Backer working on tissue engineering in a heart block model. He was given the opportunity to travel to Melbourne for a year as an "add on" to his current pediatric fellowship at Seattle Children’s Hospital.
Dr. Bryan A. Whitson is a third-year Cardiovascular and Thoracic Surgery Fellow at the University of Minnesota. A native Hoosier, he completed his undergraduate degree in mechanical engineering at Purdue University, his medical doctorate at Indiana University, and his PhD at the University of Minnesota in Surgery investigating the immunobiology of minimally invasive surgery and cancer. His general surgery training was at the University of Minnesota where he also completed a Clinical Fellowship in Surgical Infectious Diseases.
He is currently the cardiovascular and thoracic surgery senior fellow at the University of Minnesota. He has 30 United States and international patents, received several grants, and over 60 publications.
Dr. Whitson’s research interests include lung transplantation, minimally invasive cardiothoracic surgery, medical device design, nanomedicine, and pulmonary assist devices.
Together, Dr. MacIver and Dr. Whitson will work with the rest of the TSN staff to develop and improve our Residents’ Corner in print and online.☐
TSRA Review of Cardiothoracic Surgery Available
Some of the most useful review materials in General Surgery are those written by residents, for residents. Until now, nothing like this has existed in Cardiothoracic Surgery. The Thoracic Surgery Residents Association (TSRA) is proud to announce the recent creation of just such a resource, the TSRA Review of Cardiothoracic Surgery. More than 50 cardiothoracic surgery residents from around the country contributed to the book, which covers General Thoracic, Adult Cardiac and Congenital Cardiac Surgery as well as Cardiothoracic Trauma and Critical Care. Details on obtaining the book (including free-of-charge formats) can be found at the TSRA website: (http://www.tsranet.org/sections/review_of_cardiothor/index.html).
Some of the most useful review materials in General Surgery are those written by residents, for residents. Until now, nothing like this has existed in Cardiothoracic Surgery. The Thoracic Surgery Residents Association (TSRA) is proud to announce the recent creation of just such a resource, the TSRA Review of Cardiothoracic Surgery. More than 50 cardiothoracic surgery residents from around the country contributed to the book, which covers General Thoracic, Adult Cardiac and Congenital Cardiac Surgery as well as Cardiothoracic Trauma and Critical Care. Details on obtaining the book (including free-of-charge formats) can be found at the TSRA website: (http://www.tsranet.org/sections/review_of_cardiothor/index.html).
Some of the most useful review materials in General Surgery are those written by residents, for residents. Until now, nothing like this has existed in Cardiothoracic Surgery. The Thoracic Surgery Residents Association (TSRA) is proud to announce the recent creation of just such a resource, the TSRA Review of Cardiothoracic Surgery. More than 50 cardiothoracic surgery residents from around the country contributed to the book, which covers General Thoracic, Adult Cardiac and Congenital Cardiac Surgery as well as Cardiothoracic Trauma and Critical Care. Details on obtaining the book (including free-of-charge formats) can be found at the TSRA website: (http://www.tsranet.org/sections/review_of_cardiothor/index.html).
Resection Works Well for High-Risk NSCLC Patients
COLORADO SPRINGS – Patients with stage 1a non–small cell lung cancer deemed medically inoperable or high risk can undergo surgical resection safely and with excellent results, judging by results of a single-center retrospective study.
Indeed, their perioperative morbidity and mortality and 5-year recurrence-free survival rates were similar to those of low-risk patients undergoing tumor resection, Dr. Andrea S. Wolf said at the annual meeting of the Western Thoracic Surgical Association.
"These outcomes in high-risk patients provide the standard to which nonoperative therapies should be compared," said Dr. Wolf of Brigham and Women’s Hospital, Boston.
Of the 170,000 new cases of non–small cell lung cancer (NSCLC) diagnosed annually in the United States, 80% are deemed inoperable because of extensive malignancy or severe comorbidities, including chronic obstructive pulmonary disease, which affects roughly half of patients with NSCLC. Stereotactic body radiation therapy (SBRT), which uses advanced imaging techniques to deliver a targeted radiation dose to a tumor, is making substantial inroads in these inoperable patients. But Dr. Wolf’s study suggests that surgery is feasible for many patients considered high risk for pulmonary resection.
She reviewed the records of 66 patients with stage 1a disease considered high risk and 158 low-risk controls, all of whom underwent surgical resection at Brigham and Women’s Hospital during 1997-2006. None had pure bronchoalveolar carcinoma. Patients were deemed high risk if they were aged 80 years or older, or if their forced expiratory volume in 1 second (FEV1) was 50% or less of the predicted amount. Forty percent of the high-risk patients met the age criterion, 60% met the diminished pulmonary function standard, and 5% fulfilled both. Pathologic findings were similar in the high- and low-risk groups, with a median tumor size of 1.5 cm.
With a median 6 years of follow-up, the local recurrence rate was 18% in the high-risk population and 16% in the low-risk cohort. The distant recurrence rate was 15% in both groups.
The 5-year overall survival rate was 54% in the high-risk group and significantly better at 68% in the low-risk group (P = .04). However, there was no significant difference in 5-year recurrence-free survival: 73% and 77% in the high- and low-risk groups, respectively.
Perioperative mortality occurred in 2% of low-risk patients and none of the high-risk patients. The perioperative major morbidity rate was 14% in the high-risk group and 8% in the low-risk group. Similarly, there were no significant between-group differences in the rates of any individual major complications, which included MI, pulmonary embolus, and reoperation for bleeding.
"Your rationale is right on target," discussant Dr. Joseph B. Shrager told Dr. Wolf. "It’s highly important in this era of SBRT to document the excellent results we can get with surgery in very-high-risk patients. And zero deaths, which is what you showed here and was equivalent to the experience with low-risk patients, is certainly admirable."
That being said, he added that he was disappointed with the Boston surgeons’ low use of anatomic resection in the high-risk group. Only 18% underwent lobectomy and another 6% received segmentectomy, while 76% had a wedge resection.
"There were less than one-tenth as many segmentectomies as wedges in the high-risk patients. So, really, what you’ve shown is that a lesser operation – or you might even say our least-good operation – can safely be done in high-risk patients. The question now is, is that lesser operation better than SBRT? Because if it’s not, then SBRT will probably win that argument. I have to say, I think we have a better chance of winning out over SBRT with surgery if we’re comparing it to segmentectomy than if we’re comparing it to wedge," said Dr. Shrager, professor and chief of the division of thoracic surgery at Stanford (Calif.) University.
Dr. Wolf replied that, like Dr. Shrager, she and her coinvestigators were "surprised" at the high rate of wedge resection because thoracic surgeons at Brigham and Women’s Hospital tend to promote anatomic resection whenever possible. She suspects some of the wedges were performed in an effort to spare parenchyma when a tumor bordered segmental boundaries.
Dr. Shrager also took the Boston surgeons to task for the fact that only 38% of high-risk patients in the series underwent lymph node sampling.
"Short of a proven survival advantage for surgery over SBRT, which we don’t have yet, all we can say is at least we’re providing better lymph node staging. So why not more lymph node sampling?" Dr. Shrager asked.
Dr. Wolf said this, too, came as a surprise to her and her colleagues. The most likely explanation is that in many instances patients and surgeons sought smaller, quicker operations in an effort to spare the patient. But given the compelling evidence showing that lymph node sampling is critical for accurate staging and for determining the need for adjunctive therapy, that’s not an adequate excuse.
"Going forward, we’re very interested in making sure nodes are sampled, even with wedge resections," she said.
Dr. Wolf declared no conflicts.☐
COLORADO SPRINGS – Patients with stage 1a non–small cell lung cancer deemed medically inoperable or high risk can undergo surgical resection safely and with excellent results, judging by results of a single-center retrospective study.
Indeed, their perioperative morbidity and mortality and 5-year recurrence-free survival rates were similar to those of low-risk patients undergoing tumor resection, Dr. Andrea S. Wolf said at the annual meeting of the Western Thoracic Surgical Association.
"These outcomes in high-risk patients provide the standard to which nonoperative therapies should be compared," said Dr. Wolf of Brigham and Women’s Hospital, Boston.
Of the 170,000 new cases of non–small cell lung cancer (NSCLC) diagnosed annually in the United States, 80% are deemed inoperable because of extensive malignancy or severe comorbidities, including chronic obstructive pulmonary disease, which affects roughly half of patients with NSCLC. Stereotactic body radiation therapy (SBRT), which uses advanced imaging techniques to deliver a targeted radiation dose to a tumor, is making substantial inroads in these inoperable patients. But Dr. Wolf’s study suggests that surgery is feasible for many patients considered high risk for pulmonary resection.
She reviewed the records of 66 patients with stage 1a disease considered high risk and 158 low-risk controls, all of whom underwent surgical resection at Brigham and Women’s Hospital during 1997-2006. None had pure bronchoalveolar carcinoma. Patients were deemed high risk if they were aged 80 years or older, or if their forced expiratory volume in 1 second (FEV1) was 50% or less of the predicted amount. Forty percent of the high-risk patients met the age criterion, 60% met the diminished pulmonary function standard, and 5% fulfilled both. Pathologic findings were similar in the high- and low-risk groups, with a median tumor size of 1.5 cm.
With a median 6 years of follow-up, the local recurrence rate was 18% in the high-risk population and 16% in the low-risk cohort. The distant recurrence rate was 15% in both groups.
The 5-year overall survival rate was 54% in the high-risk group and significantly better at 68% in the low-risk group (P = .04). However, there was no significant difference in 5-year recurrence-free survival: 73% and 77% in the high- and low-risk groups, respectively.
Perioperative mortality occurred in 2% of low-risk patients and none of the high-risk patients. The perioperative major morbidity rate was 14% in the high-risk group and 8% in the low-risk group. Similarly, there were no significant between-group differences in the rates of any individual major complications, which included MI, pulmonary embolus, and reoperation for bleeding.
"Your rationale is right on target," discussant Dr. Joseph B. Shrager told Dr. Wolf. "It’s highly important in this era of SBRT to document the excellent results we can get with surgery in very-high-risk patients. And zero deaths, which is what you showed here and was equivalent to the experience with low-risk patients, is certainly admirable."
That being said, he added that he was disappointed with the Boston surgeons’ low use of anatomic resection in the high-risk group. Only 18% underwent lobectomy and another 6% received segmentectomy, while 76% had a wedge resection.
"There were less than one-tenth as many segmentectomies as wedges in the high-risk patients. So, really, what you’ve shown is that a lesser operation – or you might even say our least-good operation – can safely be done in high-risk patients. The question now is, is that lesser operation better than SBRT? Because if it’s not, then SBRT will probably win that argument. I have to say, I think we have a better chance of winning out over SBRT with surgery if we’re comparing it to segmentectomy than if we’re comparing it to wedge," said Dr. Shrager, professor and chief of the division of thoracic surgery at Stanford (Calif.) University.
Dr. Wolf replied that, like Dr. Shrager, she and her coinvestigators were "surprised" at the high rate of wedge resection because thoracic surgeons at Brigham and Women’s Hospital tend to promote anatomic resection whenever possible. She suspects some of the wedges were performed in an effort to spare parenchyma when a tumor bordered segmental boundaries.
Dr. Shrager also took the Boston surgeons to task for the fact that only 38% of high-risk patients in the series underwent lymph node sampling.
"Short of a proven survival advantage for surgery over SBRT, which we don’t have yet, all we can say is at least we’re providing better lymph node staging. So why not more lymph node sampling?" Dr. Shrager asked.
Dr. Wolf said this, too, came as a surprise to her and her colleagues. The most likely explanation is that in many instances patients and surgeons sought smaller, quicker operations in an effort to spare the patient. But given the compelling evidence showing that lymph node sampling is critical for accurate staging and for determining the need for adjunctive therapy, that’s not an adequate excuse.
"Going forward, we’re very interested in making sure nodes are sampled, even with wedge resections," she said.
Dr. Wolf declared no conflicts.☐
COLORADO SPRINGS – Patients with stage 1a non–small cell lung cancer deemed medically inoperable or high risk can undergo surgical resection safely and with excellent results, judging by results of a single-center retrospective study.
Indeed, their perioperative morbidity and mortality and 5-year recurrence-free survival rates were similar to those of low-risk patients undergoing tumor resection, Dr. Andrea S. Wolf said at the annual meeting of the Western Thoracic Surgical Association.
"These outcomes in high-risk patients provide the standard to which nonoperative therapies should be compared," said Dr. Wolf of Brigham and Women’s Hospital, Boston.
Of the 170,000 new cases of non–small cell lung cancer (NSCLC) diagnosed annually in the United States, 80% are deemed inoperable because of extensive malignancy or severe comorbidities, including chronic obstructive pulmonary disease, which affects roughly half of patients with NSCLC. Stereotactic body radiation therapy (SBRT), which uses advanced imaging techniques to deliver a targeted radiation dose to a tumor, is making substantial inroads in these inoperable patients. But Dr. Wolf’s study suggests that surgery is feasible for many patients considered high risk for pulmonary resection.
She reviewed the records of 66 patients with stage 1a disease considered high risk and 158 low-risk controls, all of whom underwent surgical resection at Brigham and Women’s Hospital during 1997-2006. None had pure bronchoalveolar carcinoma. Patients were deemed high risk if they were aged 80 years or older, or if their forced expiratory volume in 1 second (FEV1) was 50% or less of the predicted amount. Forty percent of the high-risk patients met the age criterion, 60% met the diminished pulmonary function standard, and 5% fulfilled both. Pathologic findings were similar in the high- and low-risk groups, with a median tumor size of 1.5 cm.
With a median 6 years of follow-up, the local recurrence rate was 18% in the high-risk population and 16% in the low-risk cohort. The distant recurrence rate was 15% in both groups.
The 5-year overall survival rate was 54% in the high-risk group and significantly better at 68% in the low-risk group (P = .04). However, there was no significant difference in 5-year recurrence-free survival: 73% and 77% in the high- and low-risk groups, respectively.
Perioperative mortality occurred in 2% of low-risk patients and none of the high-risk patients. The perioperative major morbidity rate was 14% in the high-risk group and 8% in the low-risk group. Similarly, there were no significant between-group differences in the rates of any individual major complications, which included MI, pulmonary embolus, and reoperation for bleeding.
"Your rationale is right on target," discussant Dr. Joseph B. Shrager told Dr. Wolf. "It’s highly important in this era of SBRT to document the excellent results we can get with surgery in very-high-risk patients. And zero deaths, which is what you showed here and was equivalent to the experience with low-risk patients, is certainly admirable."
That being said, he added that he was disappointed with the Boston surgeons’ low use of anatomic resection in the high-risk group. Only 18% underwent lobectomy and another 6% received segmentectomy, while 76% had a wedge resection.
"There were less than one-tenth as many segmentectomies as wedges in the high-risk patients. So, really, what you’ve shown is that a lesser operation – or you might even say our least-good operation – can safely be done in high-risk patients. The question now is, is that lesser operation better than SBRT? Because if it’s not, then SBRT will probably win that argument. I have to say, I think we have a better chance of winning out over SBRT with surgery if we’re comparing it to segmentectomy than if we’re comparing it to wedge," said Dr. Shrager, professor and chief of the division of thoracic surgery at Stanford (Calif.) University.
Dr. Wolf replied that, like Dr. Shrager, she and her coinvestigators were "surprised" at the high rate of wedge resection because thoracic surgeons at Brigham and Women’s Hospital tend to promote anatomic resection whenever possible. She suspects some of the wedges were performed in an effort to spare parenchyma when a tumor bordered segmental boundaries.
Dr. Shrager also took the Boston surgeons to task for the fact that only 38% of high-risk patients in the series underwent lymph node sampling.
"Short of a proven survival advantage for surgery over SBRT, which we don’t have yet, all we can say is at least we’re providing better lymph node staging. So why not more lymph node sampling?" Dr. Shrager asked.
Dr. Wolf said this, too, came as a surprise to her and her colleagues. The most likely explanation is that in many instances patients and surgeons sought smaller, quicker operations in an effort to spare the patient. But given the compelling evidence showing that lymph node sampling is critical for accurate staging and for determining the need for adjunctive therapy, that’s not an adequate excuse.
"Going forward, we’re very interested in making sure nodes are sampled, even with wedge resections," she said.
Dr. Wolf declared no conflicts.☐
Major Finding: High-risk surgical candidates with stage 1a non–small-cell lung cancer underwent pulmonary resection with zero perioperative mortality, little major morbidity, and a 5-year recurrence-free survival rate similar to that of low-risk patients.
Data Source: Retrospective analysis of the Brigham and Women’s Hospital experience.
Disclosures: Dr. Wolf declared having no financial conflicts.
Trend of Hospital-Employed Docs Could Raise Costs
Hospital employment of physicians continues to rise rapidly around the country, but the trend could drive up costs at least in the short term, according to a report from the Center for Studying Health System Change.
Physicians employed by hospitals are often paid based on their productivity, which offers an incentive to increase the volume of services. And in some cases, physicians are under pressure from their hospitals to order more expensive tests, according to the report.
The researchers from the Center for Studying Health System Change based their analysis on interviews with nearly 550 physicians, hospital executives, health plan officials, and others, in 12 nationally representative metropolitan communities: Boston; Cleveland; Greenville, S.C.; Indianapolis; Lansing, Mich.; Little Rock, Ark.; Miami; northern New Jersey, Orange County, Calif.; Phoenix; Seattle; and Syracuse, N.Y.
"The acceleration in hospital employment of physicians risks raising costs and not improving quality of care unless payment reforms shift provider incentives away from volume toward higher quality and efficiency," said Dr. Ann S. O’Malley of the Center for Studying Health System Change and a coauthor of the study.
The trend toward hospitals’ employing more physicians can also drive up costs because hospitals are able to charge hospital facility fees for office visits and procedures, even when those services are administered in a physician’s office. That means that Medicare – and in some cases private insurers – are paying significantly more for the same services simply because the physician is employed by the hospital.
Hospital employment of physicians does have the potential to improve quality through better integration of care and communication between physicians. The problem, the researchers noted, is that integration and communication can be slow to improve just because physicians get their paychecks from the hospital.
The research was funded by the Robert Wood Johnson Foundation and the National Institute for Health Care Reform.
Hospital employment of physicians continues to rise rapidly around the country, but the trend could drive up costs at least in the short term, according to a report from the Center for Studying Health System Change.
Physicians employed by hospitals are often paid based on their productivity, which offers an incentive to increase the volume of services. And in some cases, physicians are under pressure from their hospitals to order more expensive tests, according to the report.
The researchers from the Center for Studying Health System Change based their analysis on interviews with nearly 550 physicians, hospital executives, health plan officials, and others, in 12 nationally representative metropolitan communities: Boston; Cleveland; Greenville, S.C.; Indianapolis; Lansing, Mich.; Little Rock, Ark.; Miami; northern New Jersey, Orange County, Calif.; Phoenix; Seattle; and Syracuse, N.Y.
"The acceleration in hospital employment of physicians risks raising costs and not improving quality of care unless payment reforms shift provider incentives away from volume toward higher quality and efficiency," said Dr. Ann S. O’Malley of the Center for Studying Health System Change and a coauthor of the study.
The trend toward hospitals’ employing more physicians can also drive up costs because hospitals are able to charge hospital facility fees for office visits and procedures, even when those services are administered in a physician’s office. That means that Medicare – and in some cases private insurers – are paying significantly more for the same services simply because the physician is employed by the hospital.
Hospital employment of physicians does have the potential to improve quality through better integration of care and communication between physicians. The problem, the researchers noted, is that integration and communication can be slow to improve just because physicians get their paychecks from the hospital.
The research was funded by the Robert Wood Johnson Foundation and the National Institute for Health Care Reform.
Hospital employment of physicians continues to rise rapidly around the country, but the trend could drive up costs at least in the short term, according to a report from the Center for Studying Health System Change.
Physicians employed by hospitals are often paid based on their productivity, which offers an incentive to increase the volume of services. And in some cases, physicians are under pressure from their hospitals to order more expensive tests, according to the report.
The researchers from the Center for Studying Health System Change based their analysis on interviews with nearly 550 physicians, hospital executives, health plan officials, and others, in 12 nationally representative metropolitan communities: Boston; Cleveland; Greenville, S.C.; Indianapolis; Lansing, Mich.; Little Rock, Ark.; Miami; northern New Jersey, Orange County, Calif.; Phoenix; Seattle; and Syracuse, N.Y.
"The acceleration in hospital employment of physicians risks raising costs and not improving quality of care unless payment reforms shift provider incentives away from volume toward higher quality and efficiency," said Dr. Ann S. O’Malley of the Center for Studying Health System Change and a coauthor of the study.
The trend toward hospitals’ employing more physicians can also drive up costs because hospitals are able to charge hospital facility fees for office visits and procedures, even when those services are administered in a physician’s office. That means that Medicare – and in some cases private insurers – are paying significantly more for the same services simply because the physician is employed by the hospital.
Hospital employment of physicians does have the potential to improve quality through better integration of care and communication between physicians. The problem, the researchers noted, is that integration and communication can be slow to improve just because physicians get their paychecks from the hospital.
The research was funded by the Robert Wood Johnson Foundation and the National Institute for Health Care Reform.