User login
The Official Newspaper of the American Association for Thoracic Surgery
Targeted CT follow-up for incidental lung nodules?
CHICAGO – Limiting CT follow-up of incidental pulmonary nodules to a small area around the suspicious nodule may help resolve a common clinical dilemma and an Achilles heel of lung cancer screening, researchers suggest.
It could also reduce the radiation dose by more than 80%.
"Why should we radiate the entire thorax on follow-up?" Dr. Gregory D. Pearson asked rhetorically at the annual meeting of the Radiological Society of North America.
In the pivotal National Lung Cancer Screening Trial, annual low-dose CT reduced lung cancer deaths by 20% and all-cause mortality by 6.7% among heavy smokers, compared with traditional x-rays. Approximately 40% of the CT group, however, had findings of small, indeterminate pulmonary nodules considered suspicious for lung cancer on at least one scan, with 1.4% experiencing a complication as a result of additional testing (N. Engl. J. Med. 2011;365:395-409).
Several societies are working to devise the best protocol for further workup of detected nodules, but none have come up with the solution. The Fleischner Society, an international society for thoracic radiology, previously proposed serial follow-up imaging at intervals of less than 1 year for solid nodules smaller than 8 mm detected incidentally at nonscreening CT (Radiology 2005;237:395-400). For all semisolid nodules and ground-glass nodules at least 5 mm in size, researchers recommended a 3-month follow-up (Radiology 2005;237:395-400).
Follow-up CT scans, however, add costs and contribute to a patient’s cumulative radiation burden, said Dr. Pearson, a thoracic radiologist at New York–Presbyterian Hospital/Columbia University in New York City.
In an effort to develop a more practical solution, Dr. Pearson and his colleagues analyzed the variability in nodule location among 50 patients with subcentimeter nodules identified on CT screening for lung cancer and emphysema, and then devised a protocol for targeted CT follow-up that was validated in 50 additional patients.
Two experts and one novice reader, a medical student, independently measured the distances of the nodules from two anatomical landmarks, the lung apex and carina, on baseline and follow-up scans by cross-referencing the axial images with the CT scanogram on a PACS (picture archiving and communication system) workstation.
The interobserver variability was quite low, with mean differences of just 2-3 mm when the two experts were paired together or individually paired with the novice reader, Dr. Pearson said. Results were significantly better measuring from the apex than from the carina for two of the three reader pairings (P = .005 and .03), although the absolute difference was just 1 mm.
To allow for a greater margin of error, measurements in the validation phase of the study were only from the ipsilateral lung apex and covered a 60-mm range. At baseline, the expert identified the nodule and placed a cut line on the scan to measure the distance from the apex.
Medical students then measured the distance of the nodule from the apex on the follow-up scan, and reviewed a region of about 6 cm to determine whether the nodule would have been included in its entirety if the range of the CT scan had been narrowed to just 60 mm.
"The results here are pretty simple; 100% of the nodules in follow-up were scanned in their entirety," Dr. Pearson said.
The average craniocaudal coverage on follow-up CT was 363 mm.
By using a targeted 60-mm range, the average craniocaudal coverage and radiation dose would be reduced by 83%, although the actual dose reduction will depend on the location of the nodules, he added.
Still, the technique needs to be validated prospectively in larger groups, and would require buy-in from radiologists, medical societies, and Medicare and private insurers, Dr. Pearson said.
Session comoderator Dr. H. Page McAdams, division chief of cardiac and thoracic imaging at Duke University in Durham, N.C., said in an interview that the concept is intriguing, but raises a number of potential societal, reimbursement, and medical-legal issues.
Roughly 75% of the 100 consecutive patients in the study had a single nodule, Dr. Pearson told this publication.
Dr. McAdams reported grants from several imaging companies.
CHICAGO – Limiting CT follow-up of incidental pulmonary nodules to a small area around the suspicious nodule may help resolve a common clinical dilemma and an Achilles heel of lung cancer screening, researchers suggest.
It could also reduce the radiation dose by more than 80%.
"Why should we radiate the entire thorax on follow-up?" Dr. Gregory D. Pearson asked rhetorically at the annual meeting of the Radiological Society of North America.
In the pivotal National Lung Cancer Screening Trial, annual low-dose CT reduced lung cancer deaths by 20% and all-cause mortality by 6.7% among heavy smokers, compared with traditional x-rays. Approximately 40% of the CT group, however, had findings of small, indeterminate pulmonary nodules considered suspicious for lung cancer on at least one scan, with 1.4% experiencing a complication as a result of additional testing (N. Engl. J. Med. 2011;365:395-409).
Several societies are working to devise the best protocol for further workup of detected nodules, but none have come up with the solution. The Fleischner Society, an international society for thoracic radiology, previously proposed serial follow-up imaging at intervals of less than 1 year for solid nodules smaller than 8 mm detected incidentally at nonscreening CT (Radiology 2005;237:395-400). For all semisolid nodules and ground-glass nodules at least 5 mm in size, researchers recommended a 3-month follow-up (Radiology 2005;237:395-400).
Follow-up CT scans, however, add costs and contribute to a patient’s cumulative radiation burden, said Dr. Pearson, a thoracic radiologist at New York–Presbyterian Hospital/Columbia University in New York City.
In an effort to develop a more practical solution, Dr. Pearson and his colleagues analyzed the variability in nodule location among 50 patients with subcentimeter nodules identified on CT screening for lung cancer and emphysema, and then devised a protocol for targeted CT follow-up that was validated in 50 additional patients.
Two experts and one novice reader, a medical student, independently measured the distances of the nodules from two anatomical landmarks, the lung apex and carina, on baseline and follow-up scans by cross-referencing the axial images with the CT scanogram on a PACS (picture archiving and communication system) workstation.
The interobserver variability was quite low, with mean differences of just 2-3 mm when the two experts were paired together or individually paired with the novice reader, Dr. Pearson said. Results were significantly better measuring from the apex than from the carina for two of the three reader pairings (P = .005 and .03), although the absolute difference was just 1 mm.
To allow for a greater margin of error, measurements in the validation phase of the study were only from the ipsilateral lung apex and covered a 60-mm range. At baseline, the expert identified the nodule and placed a cut line on the scan to measure the distance from the apex.
Medical students then measured the distance of the nodule from the apex on the follow-up scan, and reviewed a region of about 6 cm to determine whether the nodule would have been included in its entirety if the range of the CT scan had been narrowed to just 60 mm.
"The results here are pretty simple; 100% of the nodules in follow-up were scanned in their entirety," Dr. Pearson said.
The average craniocaudal coverage on follow-up CT was 363 mm.
By using a targeted 60-mm range, the average craniocaudal coverage and radiation dose would be reduced by 83%, although the actual dose reduction will depend on the location of the nodules, he added.
Still, the technique needs to be validated prospectively in larger groups, and would require buy-in from radiologists, medical societies, and Medicare and private insurers, Dr. Pearson said.
Session comoderator Dr. H. Page McAdams, division chief of cardiac and thoracic imaging at Duke University in Durham, N.C., said in an interview that the concept is intriguing, but raises a number of potential societal, reimbursement, and medical-legal issues.
Roughly 75% of the 100 consecutive patients in the study had a single nodule, Dr. Pearson told this publication.
Dr. McAdams reported grants from several imaging companies.
CHICAGO – Limiting CT follow-up of incidental pulmonary nodules to a small area around the suspicious nodule may help resolve a common clinical dilemma and an Achilles heel of lung cancer screening, researchers suggest.
It could also reduce the radiation dose by more than 80%.
"Why should we radiate the entire thorax on follow-up?" Dr. Gregory D. Pearson asked rhetorically at the annual meeting of the Radiological Society of North America.
In the pivotal National Lung Cancer Screening Trial, annual low-dose CT reduced lung cancer deaths by 20% and all-cause mortality by 6.7% among heavy smokers, compared with traditional x-rays. Approximately 40% of the CT group, however, had findings of small, indeterminate pulmonary nodules considered suspicious for lung cancer on at least one scan, with 1.4% experiencing a complication as a result of additional testing (N. Engl. J. Med. 2011;365:395-409).
Several societies are working to devise the best protocol for further workup of detected nodules, but none have come up with the solution. The Fleischner Society, an international society for thoracic radiology, previously proposed serial follow-up imaging at intervals of less than 1 year for solid nodules smaller than 8 mm detected incidentally at nonscreening CT (Radiology 2005;237:395-400). For all semisolid nodules and ground-glass nodules at least 5 mm in size, researchers recommended a 3-month follow-up (Radiology 2005;237:395-400).
Follow-up CT scans, however, add costs and contribute to a patient’s cumulative radiation burden, said Dr. Pearson, a thoracic radiologist at New York–Presbyterian Hospital/Columbia University in New York City.
In an effort to develop a more practical solution, Dr. Pearson and his colleagues analyzed the variability in nodule location among 50 patients with subcentimeter nodules identified on CT screening for lung cancer and emphysema, and then devised a protocol for targeted CT follow-up that was validated in 50 additional patients.
Two experts and one novice reader, a medical student, independently measured the distances of the nodules from two anatomical landmarks, the lung apex and carina, on baseline and follow-up scans by cross-referencing the axial images with the CT scanogram on a PACS (picture archiving and communication system) workstation.
The interobserver variability was quite low, with mean differences of just 2-3 mm when the two experts were paired together or individually paired with the novice reader, Dr. Pearson said. Results were significantly better measuring from the apex than from the carina for two of the three reader pairings (P = .005 and .03), although the absolute difference was just 1 mm.
To allow for a greater margin of error, measurements in the validation phase of the study were only from the ipsilateral lung apex and covered a 60-mm range. At baseline, the expert identified the nodule and placed a cut line on the scan to measure the distance from the apex.
Medical students then measured the distance of the nodule from the apex on the follow-up scan, and reviewed a region of about 6 cm to determine whether the nodule would have been included in its entirety if the range of the CT scan had been narrowed to just 60 mm.
"The results here are pretty simple; 100% of the nodules in follow-up were scanned in their entirety," Dr. Pearson said.
The average craniocaudal coverage on follow-up CT was 363 mm.
By using a targeted 60-mm range, the average craniocaudal coverage and radiation dose would be reduced by 83%, although the actual dose reduction will depend on the location of the nodules, he added.
Still, the technique needs to be validated prospectively in larger groups, and would require buy-in from radiologists, medical societies, and Medicare and private insurers, Dr. Pearson said.
Session comoderator Dr. H. Page McAdams, division chief of cardiac and thoracic imaging at Duke University in Durham, N.C., said in an interview that the concept is intriguing, but raises a number of potential societal, reimbursement, and medical-legal issues.
Roughly 75% of the 100 consecutive patients in the study had a single nodule, Dr. Pearson told this publication.
Dr. McAdams reported grants from several imaging companies.
Major Finding: By using a targeted 60-mm range during CT follow-up of suspicious nodules, the average craniocaudal coverage and radiation dose would be reduced by 83%.
Data Source: Two-phase validation study in 100 consecutive patients with incidental subcentimeter lung nodules.
Disclosures: Dr. McAdams reported a research grant from General Electric, serving as a consultant for American College of Radiology Image Metrix, and working as an author for Reed Elsevier and UpToDate Inc.
COPD varies by state, peaks above 9%
The prevalence of chronic obstructive pulmonary disease is 6% nationwide, but varies from less than 4% in Washington and Minnesota to more than 9% in Alabama and Kentucky, according to data from the Centers for Disease Control and Prevention. The findings were published in the CDC’s Morbidity and Mortality Weekly Report.
A total of 13,306 adults who reported having chronic obstructive pulmonary disease (COPD) in the national survey also responded to the COPD module. Of these, 76% reported undergoing a diagnostic breathing test, 64% reported that COPD symptoms (specifically shortness of breath) had an adverse effect on their quality of life, and 51% reported taking at least one COPD medication (MMWR 2012;61:938-43).
In age-adjusted comparisons, women were more likely to report COPD compared with men (7% vs. 5%, respectively). COPD prevalence decreased from an average of 10% among individuals making less than $25,000 per year to 3% in those making more than $75,000 per year, and the prevalence was lower among employed individuals, homemakers, and students compared with those who were unemployed, retired, or otherwise unable to work. The prevalence of COPD was highest in current smokers (13%) compared with former smokers (7%) and never smokers (3%).
Data were taken from the 2011 Behavioral Risk Factor Surveillance System (BRFSS) survey. Additional COPD data were collected in an optional COPD module about COPD diagnosis and quality of life. This module was part of the BRFSS in 21 states, the District of Columbia, and Puerto Rico.
The 2011 BRFSS was conducted via telephone, either landline or mobile. The survey population included adults aged 18 years and older throughout the United States.
The findings were limited by several factors including the absence of data on individuals in institutions or nursing homes and by the use of self-reports for COPD diagnosis, the researchers said. However, the report is the first to analyze data on COPD prevalence in all 50 states, the District of Columbia, and Puerto Rico, they noted. State-level health officials should focus surveillance efforts, educational campaigns, and interventions on areas of highest COPD prevalence, they added.
The study was supported by the CDC and the National Heart, Lung, and Blood Institute of the National Institutes of Health.
The prevalence of chronic obstructive pulmonary disease is 6% nationwide, but varies from less than 4% in Washington and Minnesota to more than 9% in Alabama and Kentucky, according to data from the Centers for Disease Control and Prevention. The findings were published in the CDC’s Morbidity and Mortality Weekly Report.
A total of 13,306 adults who reported having chronic obstructive pulmonary disease (COPD) in the national survey also responded to the COPD module. Of these, 76% reported undergoing a diagnostic breathing test, 64% reported that COPD symptoms (specifically shortness of breath) had an adverse effect on their quality of life, and 51% reported taking at least one COPD medication (MMWR 2012;61:938-43).
In age-adjusted comparisons, women were more likely to report COPD compared with men (7% vs. 5%, respectively). COPD prevalence decreased from an average of 10% among individuals making less than $25,000 per year to 3% in those making more than $75,000 per year, and the prevalence was lower among employed individuals, homemakers, and students compared with those who were unemployed, retired, or otherwise unable to work. The prevalence of COPD was highest in current smokers (13%) compared with former smokers (7%) and never smokers (3%).
Data were taken from the 2011 Behavioral Risk Factor Surveillance System (BRFSS) survey. Additional COPD data were collected in an optional COPD module about COPD diagnosis and quality of life. This module was part of the BRFSS in 21 states, the District of Columbia, and Puerto Rico.
The 2011 BRFSS was conducted via telephone, either landline or mobile. The survey population included adults aged 18 years and older throughout the United States.
The findings were limited by several factors including the absence of data on individuals in institutions or nursing homes and by the use of self-reports for COPD diagnosis, the researchers said. However, the report is the first to analyze data on COPD prevalence in all 50 states, the District of Columbia, and Puerto Rico, they noted. State-level health officials should focus surveillance efforts, educational campaigns, and interventions on areas of highest COPD prevalence, they added.
The study was supported by the CDC and the National Heart, Lung, and Blood Institute of the National Institutes of Health.
The prevalence of chronic obstructive pulmonary disease is 6% nationwide, but varies from less than 4% in Washington and Minnesota to more than 9% in Alabama and Kentucky, according to data from the Centers for Disease Control and Prevention. The findings were published in the CDC’s Morbidity and Mortality Weekly Report.
A total of 13,306 adults who reported having chronic obstructive pulmonary disease (COPD) in the national survey also responded to the COPD module. Of these, 76% reported undergoing a diagnostic breathing test, 64% reported that COPD symptoms (specifically shortness of breath) had an adverse effect on their quality of life, and 51% reported taking at least one COPD medication (MMWR 2012;61:938-43).
In age-adjusted comparisons, women were more likely to report COPD compared with men (7% vs. 5%, respectively). COPD prevalence decreased from an average of 10% among individuals making less than $25,000 per year to 3% in those making more than $75,000 per year, and the prevalence was lower among employed individuals, homemakers, and students compared with those who were unemployed, retired, or otherwise unable to work. The prevalence of COPD was highest in current smokers (13%) compared with former smokers (7%) and never smokers (3%).
Data were taken from the 2011 Behavioral Risk Factor Surveillance System (BRFSS) survey. Additional COPD data were collected in an optional COPD module about COPD diagnosis and quality of life. This module was part of the BRFSS in 21 states, the District of Columbia, and Puerto Rico.
The 2011 BRFSS was conducted via telephone, either landline or mobile. The survey population included adults aged 18 years and older throughout the United States.
The findings were limited by several factors including the absence of data on individuals in institutions or nursing homes and by the use of self-reports for COPD diagnosis, the researchers said. However, the report is the first to analyze data on COPD prevalence in all 50 states, the District of Columbia, and Puerto Rico, they noted. State-level health officials should focus surveillance efforts, educational campaigns, and interventions on areas of highest COPD prevalence, they added.
The study was supported by the CDC and the National Heart, Lung, and Blood Institute of the National Institutes of Health.
Major Finding: The overall prevalence of chronic obstructive pulmonary disease in the United States is approximately 6%.
Data Source: The data come from the 2011 Behavioral Risk Factor Surveillance System (BRFSS) survey.
Disclosures: The study was supported by the CDC and the National Heart, Lung, and Blood Institute of the National Institutes of Health.
Stereotactic body radiation boosts NSCLC survival
BOSTON – Delivering stereotactic body radiation for early-stage, inoperable non–small cell lung cancer doubled overall survival rates achieved in historical series with conventional radiation, investigators reported at the annual meeting of the American Society for Radiation Oncology.
The 3-year overall survival rate reached 59.9% for 100 patients whose stage IA non–small cell lung cancer (NSCLC) was treated with stereotactic body radiation therapy (SBRT), said Dr. Yasushi Nagata. He compared results of the nonrandomized phase II trial with 31%-39% in historical series with conventional radiation.
The 5-year overall survival rate was 40.8%, compared with 13%-22.2% historically, added Dr. Nagata from Hiroshima University, Japan.
He described SBRT as well tolerated with only mild toxicities, making it a suitable alternative to other therapies, particularly in older patients. "Patients with early inoperable lung cancer should consider this treatment," Dr. Nagata advised in a briefing.
The investigators concluded that the treatment should be the new standard, replacing conventional radiotherapy in this population.
Similar in concept to stereotactic radiosurgery with a cyberknife, SBRT is a technique for precise high-dose targeting of tissues from multiple angles and planes, allowing delivery of much larger doses by fraction than conformal 3-dimensional or intensity-modulated radiation therapy. With SBRT, radiation therapy sessions can often be compressed into as little as 4-6 fractions delivered over 2 to 2.5 weeks, compared with 8 to 9 weeks of daily fractions for other techniques.
The phase II Japanese Clinical Oncology Group trial, JCOG-0403, is said to be the first to evaluate SBRT in both operable and nonoperable NSCLC. At the 2010 ASTRO annual meeting, the investigators reported 3-year survival rates for 64 patients with surgically resectable NSCLC: overall survival was 76%; progression-free survival, 54.5%; local progression-free survival, 68.5%; and event-free survival, 51.4%.
In the current study, 77 men and 27 women with a median age of 78 years (range 59-90 years) were enrolled; four patients were later excluded from the study, three because they developed a second primary cancer.
The median tumor size was 21 mm (range 9-30 mm). Fifty patients had adenocarcinomas, 40 had squamous cell carcinomas, and 14 had other tumor histologies. All patients had histologically or cytologically proven NSCLC, clinical T1N0M0 disease, and were determined by thoracic surgeons to be inoperable.
All patients completed the treatment protocol, consisting of a dose of 48 Gy at the isocenter divided into 4 fractions over 4-8 days.
The progression-free survival rate at 3 years was 49.8%; the local progression-free survival rate was 52.8%, and event-free survival, 46.8%.
Dr. Nagata and Dr. Chang disclosed no relevant conflicts.
BOSTON – Delivering stereotactic body radiation for early-stage, inoperable non–small cell lung cancer doubled overall survival rates achieved in historical series with conventional radiation, investigators reported at the annual meeting of the American Society for Radiation Oncology.
The 3-year overall survival rate reached 59.9% for 100 patients whose stage IA non–small cell lung cancer (NSCLC) was treated with stereotactic body radiation therapy (SBRT), said Dr. Yasushi Nagata. He compared results of the nonrandomized phase II trial with 31%-39% in historical series with conventional radiation.
The 5-year overall survival rate was 40.8%, compared with 13%-22.2% historically, added Dr. Nagata from Hiroshima University, Japan.
He described SBRT as well tolerated with only mild toxicities, making it a suitable alternative to other therapies, particularly in older patients. "Patients with early inoperable lung cancer should consider this treatment," Dr. Nagata advised in a briefing.
The investigators concluded that the treatment should be the new standard, replacing conventional radiotherapy in this population.
Similar in concept to stereotactic radiosurgery with a cyberknife, SBRT is a technique for precise high-dose targeting of tissues from multiple angles and planes, allowing delivery of much larger doses by fraction than conformal 3-dimensional or intensity-modulated radiation therapy. With SBRT, radiation therapy sessions can often be compressed into as little as 4-6 fractions delivered over 2 to 2.5 weeks, compared with 8 to 9 weeks of daily fractions for other techniques.
The phase II Japanese Clinical Oncology Group trial, JCOG-0403, is said to be the first to evaluate SBRT in both operable and nonoperable NSCLC. At the 2010 ASTRO annual meeting, the investigators reported 3-year survival rates for 64 patients with surgically resectable NSCLC: overall survival was 76%; progression-free survival, 54.5%; local progression-free survival, 68.5%; and event-free survival, 51.4%.
In the current study, 77 men and 27 women with a median age of 78 years (range 59-90 years) were enrolled; four patients were later excluded from the study, three because they developed a second primary cancer.
The median tumor size was 21 mm (range 9-30 mm). Fifty patients had adenocarcinomas, 40 had squamous cell carcinomas, and 14 had other tumor histologies. All patients had histologically or cytologically proven NSCLC, clinical T1N0M0 disease, and were determined by thoracic surgeons to be inoperable.
All patients completed the treatment protocol, consisting of a dose of 48 Gy at the isocenter divided into 4 fractions over 4-8 days.
The progression-free survival rate at 3 years was 49.8%; the local progression-free survival rate was 52.8%, and event-free survival, 46.8%.
Dr. Nagata and Dr. Chang disclosed no relevant conflicts.
BOSTON – Delivering stereotactic body radiation for early-stage, inoperable non–small cell lung cancer doubled overall survival rates achieved in historical series with conventional radiation, investigators reported at the annual meeting of the American Society for Radiation Oncology.
The 3-year overall survival rate reached 59.9% for 100 patients whose stage IA non–small cell lung cancer (NSCLC) was treated with stereotactic body radiation therapy (SBRT), said Dr. Yasushi Nagata. He compared results of the nonrandomized phase II trial with 31%-39% in historical series with conventional radiation.
The 5-year overall survival rate was 40.8%, compared with 13%-22.2% historically, added Dr. Nagata from Hiroshima University, Japan.
He described SBRT as well tolerated with only mild toxicities, making it a suitable alternative to other therapies, particularly in older patients. "Patients with early inoperable lung cancer should consider this treatment," Dr. Nagata advised in a briefing.
The investigators concluded that the treatment should be the new standard, replacing conventional radiotherapy in this population.
Similar in concept to stereotactic radiosurgery with a cyberknife, SBRT is a technique for precise high-dose targeting of tissues from multiple angles and planes, allowing delivery of much larger doses by fraction than conformal 3-dimensional or intensity-modulated radiation therapy. With SBRT, radiation therapy sessions can often be compressed into as little as 4-6 fractions delivered over 2 to 2.5 weeks, compared with 8 to 9 weeks of daily fractions for other techniques.
The phase II Japanese Clinical Oncology Group trial, JCOG-0403, is said to be the first to evaluate SBRT in both operable and nonoperable NSCLC. At the 2010 ASTRO annual meeting, the investigators reported 3-year survival rates for 64 patients with surgically resectable NSCLC: overall survival was 76%; progression-free survival, 54.5%; local progression-free survival, 68.5%; and event-free survival, 51.4%.
In the current study, 77 men and 27 women with a median age of 78 years (range 59-90 years) were enrolled; four patients were later excluded from the study, three because they developed a second primary cancer.
The median tumor size was 21 mm (range 9-30 mm). Fifty patients had adenocarcinomas, 40 had squamous cell carcinomas, and 14 had other tumor histologies. All patients had histologically or cytologically proven NSCLC, clinical T1N0M0 disease, and were determined by thoracic surgeons to be inoperable.
All patients completed the treatment protocol, consisting of a dose of 48 Gy at the isocenter divided into 4 fractions over 4-8 days.
The progression-free survival rate at 3 years was 49.8%; the local progression-free survival rate was 52.8%, and event-free survival, 46.8%.
Dr. Nagata and Dr. Chang disclosed no relevant conflicts.
Major Finding: The 3-year overall survival rate for 100 patients with stage IA NSCLC treated with stereotactic body radiation therapy was 59.9%, compared with 31%-39% for conventional radiation.
Data Source: This was a nonrandomized phase II trial.
Disclosures: The study was supported by Japan’s Ministry of Health. Dr. Nagata and Dr. Chang disclosed no relevant conflicts of interest.
Crizotinib changes practice for ALK-positive NSCLC
VIENNA – Long-awaited data from the phase III PROFILE 1007 confirm that crizotinib provides superior progression-free survival and responses, compared with second-line chemo-therapy in advanced anaplastic lymphoma kinase–positive non–small cell lung cancer.
Median progression-free survival more than doubled from 3.0 months with single-agent chemotherapy to 7.7 months with crizotinib, according to an independent radiologic review (P value less than .0001; hazard ratio, 0.49). Crizotinib (Xalkori) remained superior regardless of whether chemotherapy contained docetaxel (Taxotere) (7.7 vs. 2.6 months; P less than .0001) or pemetrexed (Alimta) (7.7 vs. 4.2; P = .0004), an agent previously shown to be effective against ALK-positive NSCLC.
The overall response rate was 65.3% for crizotinib and 19.5% for chemotherapy in the intent to treat population of 347 patients (overall response rate ratio 3.4; P less than .0001).
Crizotinib was also associated with significantly greater improvement in lung cancer symptoms and quality of life, Dr. Alice Shaw said at the European Society for Medical Oncology Congress. "Taken together, these results establish crizotinib as the standard of care for patients with advanced, previously treated ALK-positive non–small cell lung cancer."
ALK rearrangements are present in about 5% of lung cancers, typically in younger, never smokers.
Overall survival in the study was 22.8 months for chemotherapy and 20.3 months for crizotinib (P = .5394; HR, 1.02). The interim survival analysis was immature with just 40% of expected deaths reported and likely confounded by the high number (87%) of chemotherapy patients who crossed over to crizotinib after progression, she noted. After adjusting for crossover, the hazard ratio suggests a survival advantage with crizotinib (HR, 0.83).
Discussant Jean-Charles Soria of Institut Gustave Roussy, Villejuif, France, agreed and said the survival times in either arm were impressive, observing that just 2 years ago survival in second-line ALK-positive NSCLC was just 9 months.
Crizotinib, an oral, first in class ALK inhibitor, was given accelerated approval in 2011 in the United States to treat advanced ALK-positive NSCLC but is not approved in Europe, where regulatory agencies have required data from the randomized trial.
Dr. Soria said that worldwide use of crizotinib will require that several financial and practical issues surrounding implementation of molecular testing in daily practice be addressed including the optimal technique, type of sample, and tissue availability.
Testing for epidermal growth factor receptor, another molecular alteration that directs targeted therapy in lung cancer, "should not compete with ALK," he said, adding that multiplexing test strategies "are key."
Investigators at 105 sites across 21 countries randomized 173 patients to crizotinib 250 mg twice-daily in a 21-day cycle and 174 patients to chemotherapy containing pemetrexed 500 mg/m2 or docetaxel 75 mg/m2 given intravenously on day 1 of a 21-day cycle.
Treatment duration varied significantly, with patients receiving a median of 11 cycles of crizotinib vs. 4 cycles of chemotherapy. This may have influenced the higher number of all-cause deaths among crizotinib patients (25 deaths vs. 7 deaths), said Dr. Shaw, a thoracic oncologist at Massachusetts General Hospital Cancer Center in Boston.
Crizotinib patients were more likely than chemotherapy patients to experience visual disturbances (any grade 60% vs. 9%), as well as diarrhea, nausea, elevated transaminases (16% grade 3/4 ), edema, upper respiratory infection, dysgeusia, and dizziness. In contrast, fatigue, alopecia, dyspnea, and rash were more common with chemotherapy.
Despite the fact that patients on crizotinib experienced more nausea and vomiting, antiemetic use was significantly higher in the chemotherapy arm (67% vs. 20%). Based on the EORTC Quality of Life Questionnaire (QLQ C-30) and QLQ-LC 13, crizotinib patients had greater improvement from baseline in cough, dyspnea, fatigue, alopecia, insomnia, and pain as well as global quality of life (both P less than .0001).
Dr. Soria reported financial relationshisps with several firms including Pfizer, the study sponsor.
VIENNA – Long-awaited data from the phase III PROFILE 1007 confirm that crizotinib provides superior progression-free survival and responses, compared with second-line chemo-therapy in advanced anaplastic lymphoma kinase–positive non–small cell lung cancer.
Median progression-free survival more than doubled from 3.0 months with single-agent chemotherapy to 7.7 months with crizotinib, according to an independent radiologic review (P value less than .0001; hazard ratio, 0.49). Crizotinib (Xalkori) remained superior regardless of whether chemotherapy contained docetaxel (Taxotere) (7.7 vs. 2.6 months; P less than .0001) or pemetrexed (Alimta) (7.7 vs. 4.2; P = .0004), an agent previously shown to be effective against ALK-positive NSCLC.
The overall response rate was 65.3% for crizotinib and 19.5% for chemotherapy in the intent to treat population of 347 patients (overall response rate ratio 3.4; P less than .0001).
Crizotinib was also associated with significantly greater improvement in lung cancer symptoms and quality of life, Dr. Alice Shaw said at the European Society for Medical Oncology Congress. "Taken together, these results establish crizotinib as the standard of care for patients with advanced, previously treated ALK-positive non–small cell lung cancer."
ALK rearrangements are present in about 5% of lung cancers, typically in younger, never smokers.
Overall survival in the study was 22.8 months for chemotherapy and 20.3 months for crizotinib (P = .5394; HR, 1.02). The interim survival analysis was immature with just 40% of expected deaths reported and likely confounded by the high number (87%) of chemotherapy patients who crossed over to crizotinib after progression, she noted. After adjusting for crossover, the hazard ratio suggests a survival advantage with crizotinib (HR, 0.83).
Discussant Jean-Charles Soria of Institut Gustave Roussy, Villejuif, France, agreed and said the survival times in either arm were impressive, observing that just 2 years ago survival in second-line ALK-positive NSCLC was just 9 months.
Crizotinib, an oral, first in class ALK inhibitor, was given accelerated approval in 2011 in the United States to treat advanced ALK-positive NSCLC but is not approved in Europe, where regulatory agencies have required data from the randomized trial.
Dr. Soria said that worldwide use of crizotinib will require that several financial and practical issues surrounding implementation of molecular testing in daily practice be addressed including the optimal technique, type of sample, and tissue availability.
Testing for epidermal growth factor receptor, another molecular alteration that directs targeted therapy in lung cancer, "should not compete with ALK," he said, adding that multiplexing test strategies "are key."
Investigators at 105 sites across 21 countries randomized 173 patients to crizotinib 250 mg twice-daily in a 21-day cycle and 174 patients to chemotherapy containing pemetrexed 500 mg/m2 or docetaxel 75 mg/m2 given intravenously on day 1 of a 21-day cycle.
Treatment duration varied significantly, with patients receiving a median of 11 cycles of crizotinib vs. 4 cycles of chemotherapy. This may have influenced the higher number of all-cause deaths among crizotinib patients (25 deaths vs. 7 deaths), said Dr. Shaw, a thoracic oncologist at Massachusetts General Hospital Cancer Center in Boston.
Crizotinib patients were more likely than chemotherapy patients to experience visual disturbances (any grade 60% vs. 9%), as well as diarrhea, nausea, elevated transaminases (16% grade 3/4 ), edema, upper respiratory infection, dysgeusia, and dizziness. In contrast, fatigue, alopecia, dyspnea, and rash were more common with chemotherapy.
Despite the fact that patients on crizotinib experienced more nausea and vomiting, antiemetic use was significantly higher in the chemotherapy arm (67% vs. 20%). Based on the EORTC Quality of Life Questionnaire (QLQ C-30) and QLQ-LC 13, crizotinib patients had greater improvement from baseline in cough, dyspnea, fatigue, alopecia, insomnia, and pain as well as global quality of life (both P less than .0001).
Dr. Soria reported financial relationshisps with several firms including Pfizer, the study sponsor.
VIENNA – Long-awaited data from the phase III PROFILE 1007 confirm that crizotinib provides superior progression-free survival and responses, compared with second-line chemo-therapy in advanced anaplastic lymphoma kinase–positive non–small cell lung cancer.
Median progression-free survival more than doubled from 3.0 months with single-agent chemotherapy to 7.7 months with crizotinib, according to an independent radiologic review (P value less than .0001; hazard ratio, 0.49). Crizotinib (Xalkori) remained superior regardless of whether chemotherapy contained docetaxel (Taxotere) (7.7 vs. 2.6 months; P less than .0001) or pemetrexed (Alimta) (7.7 vs. 4.2; P = .0004), an agent previously shown to be effective against ALK-positive NSCLC.
The overall response rate was 65.3% for crizotinib and 19.5% for chemotherapy in the intent to treat population of 347 patients (overall response rate ratio 3.4; P less than .0001).
Crizotinib was also associated with significantly greater improvement in lung cancer symptoms and quality of life, Dr. Alice Shaw said at the European Society for Medical Oncology Congress. "Taken together, these results establish crizotinib as the standard of care for patients with advanced, previously treated ALK-positive non–small cell lung cancer."
ALK rearrangements are present in about 5% of lung cancers, typically in younger, never smokers.
Overall survival in the study was 22.8 months for chemotherapy and 20.3 months for crizotinib (P = .5394; HR, 1.02). The interim survival analysis was immature with just 40% of expected deaths reported and likely confounded by the high number (87%) of chemotherapy patients who crossed over to crizotinib after progression, she noted. After adjusting for crossover, the hazard ratio suggests a survival advantage with crizotinib (HR, 0.83).
Discussant Jean-Charles Soria of Institut Gustave Roussy, Villejuif, France, agreed and said the survival times in either arm were impressive, observing that just 2 years ago survival in second-line ALK-positive NSCLC was just 9 months.
Crizotinib, an oral, first in class ALK inhibitor, was given accelerated approval in 2011 in the United States to treat advanced ALK-positive NSCLC but is not approved in Europe, where regulatory agencies have required data from the randomized trial.
Dr. Soria said that worldwide use of crizotinib will require that several financial and practical issues surrounding implementation of molecular testing in daily practice be addressed including the optimal technique, type of sample, and tissue availability.
Testing for epidermal growth factor receptor, another molecular alteration that directs targeted therapy in lung cancer, "should not compete with ALK," he said, adding that multiplexing test strategies "are key."
Investigators at 105 sites across 21 countries randomized 173 patients to crizotinib 250 mg twice-daily in a 21-day cycle and 174 patients to chemotherapy containing pemetrexed 500 mg/m2 or docetaxel 75 mg/m2 given intravenously on day 1 of a 21-day cycle.
Treatment duration varied significantly, with patients receiving a median of 11 cycles of crizotinib vs. 4 cycles of chemotherapy. This may have influenced the higher number of all-cause deaths among crizotinib patients (25 deaths vs. 7 deaths), said Dr. Shaw, a thoracic oncologist at Massachusetts General Hospital Cancer Center in Boston.
Crizotinib patients were more likely than chemotherapy patients to experience visual disturbances (any grade 60% vs. 9%), as well as diarrhea, nausea, elevated transaminases (16% grade 3/4 ), edema, upper respiratory infection, dysgeusia, and dizziness. In contrast, fatigue, alopecia, dyspnea, and rash were more common with chemotherapy.
Despite the fact that patients on crizotinib experienced more nausea and vomiting, antiemetic use was significantly higher in the chemotherapy arm (67% vs. 20%). Based on the EORTC Quality of Life Questionnaire (QLQ C-30) and QLQ-LC 13, crizotinib patients had greater improvement from baseline in cough, dyspnea, fatigue, alopecia, insomnia, and pain as well as global quality of life (both P less than .0001).
Dr. Soria reported financial relationshisps with several firms including Pfizer, the study sponsor.
Major Finding: Median progression-free survival was 3.0 months with chemotherapy and 7.7 months with crizotinib (P less than .0001; hazard ratio 0.49).
Data Source: Results came from a phase III study involving 318 patients with advanced ALK-positive non–small cell lung cancer.
Disclosures: Dr. Shaw reported an advisory relationship with Pfizer, Ariad, Chugai, Novartis, and Daiichi-Sankyo and research funding from AstraZeneca and Novartis.
Stem cell treatment post PCI didn’t improve outcomes
Intracoronary delivery of bone marrow mononuclear cells to the infarct zone of patients who have undergone percutaneous coronary intervention following an ST-segment elevation myocardial infarction did not improve left ventricular function at 6 months in the TIME trial.
The trial was designed to examine the difference in effect of infusing the bone marrow mononuclear cells (BMCs) into the infarct-related artery at 7 days after PCI and at 3 days, Dr. Jay H. Traverse said at the American Heart Association meeting.
Unfortunately, neither of these approaches were any better than placebo infusion at improving the recovery of left ventricular function, improving left ventricular volume, or reducing infarct size at 6 months’ follow-up in this double-blind Timing in Myocardial Infarction Evaluation (TIME) clinical trial, reported Dr. Traverse, of the Minneapolis Heart Institute at Abbott Northwestern Hospital.
"However, long-term follow-up of these patients and the development of new composite end points may still reveal a role for this cell type after AMI [acute myocardial infarction]," Dr. Traverse and his associates said in an article published online simultaneously with his presentation (JAMA 2012 Nov. 6 [doi: 10.1001/jama.2012.28726]).
Recent research indicates that the timing of BMC infusion after PCI due to ST-segment elevation myocardial infarction (STEMI) might be critical. In the days following STEMI, there are significant temporal changes in the release of cytokines and growth factors "that may support stem-cell homing and angiogenesis, leading to improved cell survival and engraftment," they noted.
In the TIME trial, a total of 132 high-risk patients were enrolled during a 3-year period after they had experienced STEMI, shown a left ventricular ejection fraction (LVEF) of 45% or less, and were slated for PCI with stenting. These subjects were randomly assigned to have stem cell therapy on either day 3 or day 7 after PCI. After some of these patients were excluded or withdrawn from the study, the remaining 120 patients underwent a second randomization to receive either the autologous BMCs (79 patients) or placebo infusions (41 patients).
The primary end points of TIME were changes in global and regional left ventricular function on MRI scanning at 6 months post PCI. There were no significant differences in these outcomes between subjects who received stem-cell therapy 3 days after PCI and those who received it 7 days after PCI, the investigators reported. There also were no significant differences among the study groups in secondary outcomes such as reduction in infarct volume or change in ventricular volumes.
However, there also were no significant differences in any outcomes between subjects who received active BMCs and those who received placebo infusions.
Dr. Traverse reported no conflicts.
The TIME trial, like two others in the series of studies from the Cardiovascular Cell Therapy Research Network, a consortium funded by the National Institutes of Health, is "well-intentioned, nicely designed, and impeccably executed, but difficult to interpret," said Dr. Eduardo Marban and Dr. Konstantinos Malliaras.
It may be that this treatment is ineffective in this patient population, "in which case the previous positive clinical studies were red herrings." Or it may be that, as Dr. Traverse suggests, the cell product used in TIME was somehow deficient, they said.
Dr. Marban and Dr. Malliaras are at Cedars-Sinai Heart Institute in Los Angeles. Dr. Marban reported being a founder of Capricor, a developer of cardiac stem-cell treatments; both he and Dr. Malliaras reported financial ties to Capricor. These remarks were taken from their editorial accompanying Dr. Traverse’s report (JAMA 2012 Nov. 6 [doi: 10.1001/jama.2012.64751]).
The TIME trial, like two others in the series of studies from the Cardiovascular Cell Therapy Research Network, a consortium funded by the National Institutes of Health, is "well-intentioned, nicely designed, and impeccably executed, but difficult to interpret," said Dr. Eduardo Marban and Dr. Konstantinos Malliaras.
It may be that this treatment is ineffective in this patient population, "in which case the previous positive clinical studies were red herrings." Or it may be that, as Dr. Traverse suggests, the cell product used in TIME was somehow deficient, they said.
Dr. Marban and Dr. Malliaras are at Cedars-Sinai Heart Institute in Los Angeles. Dr. Marban reported being a founder of Capricor, a developer of cardiac stem-cell treatments; both he and Dr. Malliaras reported financial ties to Capricor. These remarks were taken from their editorial accompanying Dr. Traverse’s report (JAMA 2012 Nov. 6 [doi: 10.1001/jama.2012.64751]).
The TIME trial, like two others in the series of studies from the Cardiovascular Cell Therapy Research Network, a consortium funded by the National Institutes of Health, is "well-intentioned, nicely designed, and impeccably executed, but difficult to interpret," said Dr. Eduardo Marban and Dr. Konstantinos Malliaras.
It may be that this treatment is ineffective in this patient population, "in which case the previous positive clinical studies were red herrings." Or it may be that, as Dr. Traverse suggests, the cell product used in TIME was somehow deficient, they said.
Dr. Marban and Dr. Malliaras are at Cedars-Sinai Heart Institute in Los Angeles. Dr. Marban reported being a founder of Capricor, a developer of cardiac stem-cell treatments; both he and Dr. Malliaras reported financial ties to Capricor. These remarks were taken from their editorial accompanying Dr. Traverse’s report (JAMA 2012 Nov. 6 [doi: 10.1001/jama.2012.64751]).
Intracoronary delivery of bone marrow mononuclear cells to the infarct zone of patients who have undergone percutaneous coronary intervention following an ST-segment elevation myocardial infarction did not improve left ventricular function at 6 months in the TIME trial.
The trial was designed to examine the difference in effect of infusing the bone marrow mononuclear cells (BMCs) into the infarct-related artery at 7 days after PCI and at 3 days, Dr. Jay H. Traverse said at the American Heart Association meeting.
Unfortunately, neither of these approaches were any better than placebo infusion at improving the recovery of left ventricular function, improving left ventricular volume, or reducing infarct size at 6 months’ follow-up in this double-blind Timing in Myocardial Infarction Evaluation (TIME) clinical trial, reported Dr. Traverse, of the Minneapolis Heart Institute at Abbott Northwestern Hospital.
"However, long-term follow-up of these patients and the development of new composite end points may still reveal a role for this cell type after AMI [acute myocardial infarction]," Dr. Traverse and his associates said in an article published online simultaneously with his presentation (JAMA 2012 Nov. 6 [doi: 10.1001/jama.2012.28726]).
Recent research indicates that the timing of BMC infusion after PCI due to ST-segment elevation myocardial infarction (STEMI) might be critical. In the days following STEMI, there are significant temporal changes in the release of cytokines and growth factors "that may support stem-cell homing and angiogenesis, leading to improved cell survival and engraftment," they noted.
In the TIME trial, a total of 132 high-risk patients were enrolled during a 3-year period after they had experienced STEMI, shown a left ventricular ejection fraction (LVEF) of 45% or less, and were slated for PCI with stenting. These subjects were randomly assigned to have stem cell therapy on either day 3 or day 7 after PCI. After some of these patients were excluded or withdrawn from the study, the remaining 120 patients underwent a second randomization to receive either the autologous BMCs (79 patients) or placebo infusions (41 patients).
The primary end points of TIME were changes in global and regional left ventricular function on MRI scanning at 6 months post PCI. There were no significant differences in these outcomes between subjects who received stem-cell therapy 3 days after PCI and those who received it 7 days after PCI, the investigators reported. There also were no significant differences among the study groups in secondary outcomes such as reduction in infarct volume or change in ventricular volumes.
However, there also were no significant differences in any outcomes between subjects who received active BMCs and those who received placebo infusions.
Dr. Traverse reported no conflicts.
Intracoronary delivery of bone marrow mononuclear cells to the infarct zone of patients who have undergone percutaneous coronary intervention following an ST-segment elevation myocardial infarction did not improve left ventricular function at 6 months in the TIME trial.
The trial was designed to examine the difference in effect of infusing the bone marrow mononuclear cells (BMCs) into the infarct-related artery at 7 days after PCI and at 3 days, Dr. Jay H. Traverse said at the American Heart Association meeting.
Unfortunately, neither of these approaches were any better than placebo infusion at improving the recovery of left ventricular function, improving left ventricular volume, or reducing infarct size at 6 months’ follow-up in this double-blind Timing in Myocardial Infarction Evaluation (TIME) clinical trial, reported Dr. Traverse, of the Minneapolis Heart Institute at Abbott Northwestern Hospital.
"However, long-term follow-up of these patients and the development of new composite end points may still reveal a role for this cell type after AMI [acute myocardial infarction]," Dr. Traverse and his associates said in an article published online simultaneously with his presentation (JAMA 2012 Nov. 6 [doi: 10.1001/jama.2012.28726]).
Recent research indicates that the timing of BMC infusion after PCI due to ST-segment elevation myocardial infarction (STEMI) might be critical. In the days following STEMI, there are significant temporal changes in the release of cytokines and growth factors "that may support stem-cell homing and angiogenesis, leading to improved cell survival and engraftment," they noted.
In the TIME trial, a total of 132 high-risk patients were enrolled during a 3-year period after they had experienced STEMI, shown a left ventricular ejection fraction (LVEF) of 45% or less, and were slated for PCI with stenting. These subjects were randomly assigned to have stem cell therapy on either day 3 or day 7 after PCI. After some of these patients were excluded or withdrawn from the study, the remaining 120 patients underwent a second randomization to receive either the autologous BMCs (79 patients) or placebo infusions (41 patients).
The primary end points of TIME were changes in global and regional left ventricular function on MRI scanning at 6 months post PCI. There were no significant differences in these outcomes between subjects who received stem-cell therapy 3 days after PCI and those who received it 7 days after PCI, the investigators reported. There also were no significant differences among the study groups in secondary outcomes such as reduction in infarct volume or change in ventricular volumes.
However, there also were no significant differences in any outcomes between subjects who received active BMCs and those who received placebo infusions.
Dr. Traverse reported no conflicts.
Major Finding: The recovery of left ventricular function and volume did not differ between patients who received stem-cell (BMC) therapy in an infarcted artery 3 days after PCI and those who received it 7 days after PCI.
Data Source: This was a randomized, double-blind, placebo-controlled clinical trial involving 120 STEMI patients who underwent PCI with stent placement, received BMC or placebo infusions either 3 or 7 days later, and were followed for 6 months.
Disclosures: This study was funded by the National Heart, Lung, and Blood Institute. Dr. Traverse reported no financial conflicts of interest, but his associates reported numerous ties to industry sources.
Practice changes warrant residency reforms
Surgical residency programs have not kept up with radical changes in the practice of surgery over the past two decades, but innovations ranging from curriculum reform to increasing the length of residency could help to improve the overall performance of recent surgical residency graduates, according to an analysis in Annals of Surgery.
"The changes that have occurred have been disruptive to residency training, and to date there has been minimal compensation for these." The changes include not only the 80-hour workweek for surgical residents, but also clinical areas, according to Dr. Lewis, executive director of the American Board of Surgery, and Dr. Klingensmith, residency program director at Washington University in St. Louis ( Ann. Surg. 2012;256:553-9).
The effect of the 80-hour workweek has been a reduction by 6 months to a year of in-hospital experience during 5 years of residency. Most of that reduced time corresponds to night and weekends, when residents would be more likely to see urgent and emergent conditions, and to have a greater degree of independent functioning, autonomy, and indirect supervision, they said.
The effects of this and various technology changes "will undoubtedly continue, and the directions in which surgery will evolve in the future are not predictable," Dr. Lewis and Dr. Klingensmith wrote. They laid out potential ways in which residency programs can address the changes:
• There should be a continuous process to define and continually update the surgical residency curriculum, which needs to keep pace with the fast-changing surgical practice landscape, and to "prune" information related to diseases that no longer are seen frequently in practice.
"The starting point for making changes in residency is to recognize that much of what is being taught is obsolete, and addresses diseases that are no longer a significant problem, or those for which surgical treatment is rarely needed," they said.
• Residency programs should improve the efficacy of resident learning by reducing clerical functions for residents, using physician extenders where appropriate, and utilizing mobile computing technology to deliver "a more defined and comprehensive curriculum to residents at an individual level."
• Educators could make better use of simulators in certain areas..
• There should be earlier specialty focus in residency training for those residents who already know the specialty they would like to pursue.
• Residency should include expanded laparoscopic surgery training.
• Residency programs could increase in length to make up for the time lost to the 80-hour workweek rule. Four-fifths of surgical residents already elect to take a postresidency fellowship in a specialty or subspecialty area,
• Training should expand to include additional skills, such as the use of ultrasound and the use of interventional catheter techniques.
The authors reported no conflicts.
Surgical residency programs have not kept up with radical changes in the practice of surgery over the past two decades, but innovations ranging from curriculum reform to increasing the length of residency could help to improve the overall performance of recent surgical residency graduates, according to an analysis in Annals of Surgery.
"The changes that have occurred have been disruptive to residency training, and to date there has been minimal compensation for these." The changes include not only the 80-hour workweek for surgical residents, but also clinical areas, according to Dr. Lewis, executive director of the American Board of Surgery, and Dr. Klingensmith, residency program director at Washington University in St. Louis ( Ann. Surg. 2012;256:553-9).
The effect of the 80-hour workweek has been a reduction by 6 months to a year of in-hospital experience during 5 years of residency. Most of that reduced time corresponds to night and weekends, when residents would be more likely to see urgent and emergent conditions, and to have a greater degree of independent functioning, autonomy, and indirect supervision, they said.
The effects of this and various technology changes "will undoubtedly continue, and the directions in which surgery will evolve in the future are not predictable," Dr. Lewis and Dr. Klingensmith wrote. They laid out potential ways in which residency programs can address the changes:
• There should be a continuous process to define and continually update the surgical residency curriculum, which needs to keep pace with the fast-changing surgical practice landscape, and to "prune" information related to diseases that no longer are seen frequently in practice.
"The starting point for making changes in residency is to recognize that much of what is being taught is obsolete, and addresses diseases that are no longer a significant problem, or those for which surgical treatment is rarely needed," they said.
• Residency programs should improve the efficacy of resident learning by reducing clerical functions for residents, using physician extenders where appropriate, and utilizing mobile computing technology to deliver "a more defined and comprehensive curriculum to residents at an individual level."
• Educators could make better use of simulators in certain areas..
• There should be earlier specialty focus in residency training for those residents who already know the specialty they would like to pursue.
• Residency should include expanded laparoscopic surgery training.
• Residency programs could increase in length to make up for the time lost to the 80-hour workweek rule. Four-fifths of surgical residents already elect to take a postresidency fellowship in a specialty or subspecialty area,
• Training should expand to include additional skills, such as the use of ultrasound and the use of interventional catheter techniques.
The authors reported no conflicts.
Surgical residency programs have not kept up with radical changes in the practice of surgery over the past two decades, but innovations ranging from curriculum reform to increasing the length of residency could help to improve the overall performance of recent surgical residency graduates, according to an analysis in Annals of Surgery.
"The changes that have occurred have been disruptive to residency training, and to date there has been minimal compensation for these." The changes include not only the 80-hour workweek for surgical residents, but also clinical areas, according to Dr. Lewis, executive director of the American Board of Surgery, and Dr. Klingensmith, residency program director at Washington University in St. Louis ( Ann. Surg. 2012;256:553-9).
The effect of the 80-hour workweek has been a reduction by 6 months to a year of in-hospital experience during 5 years of residency. Most of that reduced time corresponds to night and weekends, when residents would be more likely to see urgent and emergent conditions, and to have a greater degree of independent functioning, autonomy, and indirect supervision, they said.
The effects of this and various technology changes "will undoubtedly continue, and the directions in which surgery will evolve in the future are not predictable," Dr. Lewis and Dr. Klingensmith wrote. They laid out potential ways in which residency programs can address the changes:
• There should be a continuous process to define and continually update the surgical residency curriculum, which needs to keep pace with the fast-changing surgical practice landscape, and to "prune" information related to diseases that no longer are seen frequently in practice.
"The starting point for making changes in residency is to recognize that much of what is being taught is obsolete, and addresses diseases that are no longer a significant problem, or those for which surgical treatment is rarely needed," they said.
• Residency programs should improve the efficacy of resident learning by reducing clerical functions for residents, using physician extenders where appropriate, and utilizing mobile computing technology to deliver "a more defined and comprehensive curriculum to residents at an individual level."
• Educators could make better use of simulators in certain areas..
• There should be earlier specialty focus in residency training for those residents who already know the specialty they would like to pursue.
• Residency should include expanded laparoscopic surgery training.
• Residency programs could increase in length to make up for the time lost to the 80-hour workweek rule. Four-fifths of surgical residents already elect to take a postresidency fellowship in a specialty or subspecialty area,
• Training should expand to include additional skills, such as the use of ultrasound and the use of interventional catheter techniques.
The authors reported no conflicts.
Apps proliferate amid concerns about medical use
DENVER – Do you need a stethoscope, a blood pressure monitor, or a tool to assess cardiac rhythms? There are apps for that. In fact, by recent count there are more than 200,000 applications of technology – or "apps" – available for smartphones or tablet devices, and they’re being used more and more for medical purposes.
Need a convenient way to look up drug interactions, pediatric dosing, or clinical decision rules from guidelines? Or how about a translator, a light to examine a finicky infant’s throat, or a "white board" to draw a picture for your patient? Yup – they’re all in apps, and chances are you already may be using some of these.
Dr. Joshua S. Broder expects an exponential increase in the use of apps in medicine as smartphones and tablets continue to proliferate, but their accuracy needs to be verified and potential problems need to be addressed, he said at the annual meeting of the American College of Emergency Physicians.
Apps will be used increasingly for bedside diagnosis and measurement of hemoglobin or other physiologic parameters. "Some of these tests may be taken over by smartphones in the near future," according to Dr. Broder of Duke University, Durham, N.C.
On the other hand, he cautioned, how do you sterilize a smartphone as you move from one hospital room or patient to another, so that you avoid transmitting infection? There are few independent studies so far testing the accuracy and reliability of medical apps, most of which were designed for lay consumers, not physicians.
The Food and Drug Administration is "very interested" in regulating any apps that might substitute for proven technologies such as stethoscopes or that physicians use as accessories to medical devices that already are regulated, he said. The FDA described its approach to deciding which mobile technology to regulate in a draft report in July 2012.
Even the basic functions of smartphones can be convenient in clinical practice, such as taking photos or videos and transmitting information by text or e-mail, but make sure you protect patient privacy and autonomy in ways that maintain trust and comply with HIPAA, Dr. Broder said.
The Duke University Health System has resolved any issues with HIPAA so that it’s safe for physicians to transmit images and video as long as they’re not sent outside the system. Talk to the HIPAA compliance officer at your medical center to establish the ground rules, he said. You can refresh your memory about which parts of data are considered by HIPAA to be protected information via a University of Miami site.
Dr. Broder reviewed some smartphone functions and apps that may be helpful and others that are not yet ready for medical prime time. Many are available for no cost or for as nominal fee. One study of health and fitness apps suggests that apps costing $0.99 or more tend to be higher quality and more trustworthy than less-expensive ones, he noted (J. Med. Internet Res. 2012;14:e72).
• Sleep: One of his residents swears by "smart alarm clock" apps that claim to use a smartphone’s accelerometer to assess where you are in your sleep cycle (based on your movements in bed) to wake you at a time that will leave you feeling less fatigued. You may set for 6 a.m., but the alarm may wake you at 5:45 a.m. Apps like Sleep Cycle ($0.99) and Sleep as Android have some underlying sleep science behind them, but no independent studies have verified their claims.
• CPR: The accelerometer also is used in the free app PocketCPR to give real-time feedback during CPR on the rate and depth of compression. Its has not been cleared by the FDA for use in humans, however, so the app warns that it’s meant for practice only. One prospective, randomized trial in 1,586 cardiac arrests that happened outside of hospitals found that use by emergency services personnel did not significantly change the likelihood of return of spontaneous circulation or other outcomes (BMJ 2011;342:d512).
• Chest: If you’re trying to teach students and residents about heart and lung sounds, or if you still get confused between mitral regurgitation and aortic stenosis, you might want to have a digital stethoscope app handy. These apps interpret heart and lung sounds heard typically through your smartphone’s microphone, which may not be good enough for clinical use. The Thinklabs Stethoscope app at $70 is pricey, compared with others, but it records sounds directly via the smartphone or through an attached electronic stethoscope.
A case that turns an iPhone into an ECG device has been submitted to the FDA for approval. The AliveCor iPhone ECG is expected to sell for between $100 and $200, compared with the usual price tag of thousands of dollars for conventional ECG machines, according to PC Magazine.
One small prospective study of experimental software that programs an iPhone to detect atrial fibrillation by placing a patient’s finger over the camera lens showed it was 98% sensitive and nearly 100% specific in detecting atrial fibrillation (IEEE Trans. Biomed. Eng. 2012 [doi:10.1109/TBME.2012.2208112]).
• Translation: When your hospital’s interpreter isn’t available, a free app like Google Translate can help. You can write or speak in one language and your device will write and say the message in a wide selection of language. You’ll need a wireless Internet connection for some translation apps.
• Eye chart: Your office has an eye chart, but you can’t find it. Pull up an app like the free EyeChart on your smartphone or tablet.
• Light: You want to inspect a patient’s sore throat, but the light in the exam room is broken. Use the flash on your smartphone camera, or use one of many free "flashlight" apps that turn the smartphone screen into a light source. Be sure to turn it off when you’re done, though, or your battery will run down quickly.
• Ultrasound: The miniaturization of ultrasound devices continues, with systems like the Mobisante MoblUS that attaches a probe to show images on your smartphone screen.
• Skin: For better evaluation of skin lesions, turn your iPhone into a dermatoscope by using the DermScope app ($4.99) and attaching the phone to the DermScope hardware (sold separately).
• Decision support: The PediStat app ($2.99 and up) makes it easy to determine the right pediatric drug dosing, among other features. The free Calculate (Medical Calculator) by QxMD app provides quick intuitive guides to common decision rules and can be customized by medical specialty.
• Drugs: Look up drug dosing, side effects, interactions and other information on free apps from Micromedex and others.
• Photos/videos: These apps are handy for documenting and sharing the appearance of a wound, a patients range of motion, or performance on a neurologic exam. Anyone who thinks they see uvula deviation in the throat of a struggling 3-year-old can snap a photo or video for review with other health care providers, medical students, or parents and avoid having to repeat the exam. Images of a wound problem after surgery can be sent to the surgeon when he or she is out of town.
Dr. Broder particularly finds the video useful for children having "pseudoseizures" whose parents demand a neurologic consult, even though the seizure event probably won’t be happening when the neurologist arrives. A video shows the neurologist exactly what Dr. Broder saw. (See the Dos and Don’ts for using photos and videos below.)
Once you’ve got an image or data you want to transmit, avoid texting as first-line means of communication because texts typically are not encrypted. Be careful when e-mailing to make sure it’s going to the correct address and only that address. Use e-mail options such as "confirm delivery" or "request read receipt," and add a sentence to the e-mail saying, "Please delete once no longer necessary for patient care," he advised.
Always document in the patient’s chart that you obtained patient consent and describe what was sent and who received it. Describe any images you send.
Don’t leave images on your portable devices. They’re easily lost, and most have inadequate encryption. Make images part of the medical record by uploading to the patient’s record, printing and scanning, or describing them clearly in the medical record. Then delete them from your device.
Store images and data in "cloud" computing sites with caution, Dr. Broder said. Services such as Google Drive or Dropbox allow sharing of very large files but provide no assurances about the quality of encryption or security. Cloud sites may be best used for giving patients access to instructions, instructional videos, reference papers, anatomic diagrams, etc.
The FDA approved the free Centricity Radiology Mobile Access app, which lets you view CT and MRI images on your iPhone if the images are stored in a GE Centricity PACS (picture archiving and communication system) platform – which may include 20% of U.S. radiology images, according to the company.
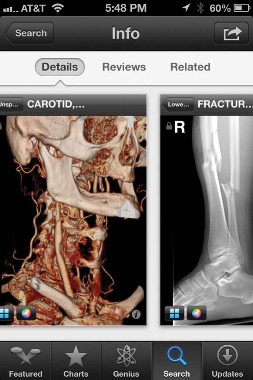
|
| Sherry Boschert/IMNG Medical Media A screen shot shows the Centricity Radiology Mobile Access app. |
The free CloudOn app lets you use MS Office software (including Word, Excel, and Powerpoint) on an iPad.
Various screen replicators that allow you to remotely access your computer desktop from your mobile device (such as ones by Citrix, or Splashtop Remote Desktop) all have the same problem, Dr. Broder said – they’re too clunky and not "touchscreen friendly."
And one final word on an underappreciated perk of medical apps on smartphones: When your medical director stops by, wanting to talk about your productivity, pull out your smartphone to show the data you’ve entered about patient encounters in your free iRVU app, which calculates total RVUs, charges, and average charge per encounter, among other features.
This list only begins to scratch the surface of app use in medicine. Other apps are available for immunization schedules, dictation, infectious disease guides, and teaching aids. Journals provide content to portable devices through apps, and some medical societies offer multifaceted apps such as ACEP Mobile.
Apps on smartphones and tablets will become part of daily medical practice, Dr. Broder predicted, but physicians need to be conscious about their limitations and potential problems as well as their assets.
Click here to view a video interview with Dr. Broder.
Dos and Don’ts for Medical Images on Smartphones
Do:
Obtain consent to acquire images or transmit them for the patient’s medical benefit.
Explain to the patient and get consent for any other intended use, such as education or publication.
Tell the patient what you will do with images when their use is completed – delete them or upload them to the medical record.
Confirm receipt if you send to other health care providers.
Specify in your message what that provider should do with the image.
Document in the patient’s chart that consent was obtained, what was sent, who received it, and content of the images.
Don’t:
Obtain images covertly.
Send to any unnecessary recipients.
Show images to anyone for fun.
Post to social media sites.
Blog about "funny" patient encounters.
Dr. Broder owns stock in Apple.
DENVER – Do you need a stethoscope, a blood pressure monitor, or a tool to assess cardiac rhythms? There are apps for that. In fact, by recent count there are more than 200,000 applications of technology – or "apps" – available for smartphones or tablet devices, and they’re being used more and more for medical purposes.
Need a convenient way to look up drug interactions, pediatric dosing, or clinical decision rules from guidelines? Or how about a translator, a light to examine a finicky infant’s throat, or a "white board" to draw a picture for your patient? Yup – they’re all in apps, and chances are you already may be using some of these.
Dr. Joshua S. Broder expects an exponential increase in the use of apps in medicine as smartphones and tablets continue to proliferate, but their accuracy needs to be verified and potential problems need to be addressed, he said at the annual meeting of the American College of Emergency Physicians.
Apps will be used increasingly for bedside diagnosis and measurement of hemoglobin or other physiologic parameters. "Some of these tests may be taken over by smartphones in the near future," according to Dr. Broder of Duke University, Durham, N.C.
On the other hand, he cautioned, how do you sterilize a smartphone as you move from one hospital room or patient to another, so that you avoid transmitting infection? There are few independent studies so far testing the accuracy and reliability of medical apps, most of which were designed for lay consumers, not physicians.
The Food and Drug Administration is "very interested" in regulating any apps that might substitute for proven technologies such as stethoscopes or that physicians use as accessories to medical devices that already are regulated, he said. The FDA described its approach to deciding which mobile technology to regulate in a draft report in July 2012.
Even the basic functions of smartphones can be convenient in clinical practice, such as taking photos or videos and transmitting information by text or e-mail, but make sure you protect patient privacy and autonomy in ways that maintain trust and comply with HIPAA, Dr. Broder said.
The Duke University Health System has resolved any issues with HIPAA so that it’s safe for physicians to transmit images and video as long as they’re not sent outside the system. Talk to the HIPAA compliance officer at your medical center to establish the ground rules, he said. You can refresh your memory about which parts of data are considered by HIPAA to be protected information via a University of Miami site.
Dr. Broder reviewed some smartphone functions and apps that may be helpful and others that are not yet ready for medical prime time. Many are available for no cost or for as nominal fee. One study of health and fitness apps suggests that apps costing $0.99 or more tend to be higher quality and more trustworthy than less-expensive ones, he noted (J. Med. Internet Res. 2012;14:e72).
• Sleep: One of his residents swears by "smart alarm clock" apps that claim to use a smartphone’s accelerometer to assess where you are in your sleep cycle (based on your movements in bed) to wake you at a time that will leave you feeling less fatigued. You may set for 6 a.m., but the alarm may wake you at 5:45 a.m. Apps like Sleep Cycle ($0.99) and Sleep as Android have some underlying sleep science behind them, but no independent studies have verified their claims.
• CPR: The accelerometer also is used in the free app PocketCPR to give real-time feedback during CPR on the rate and depth of compression. Its has not been cleared by the FDA for use in humans, however, so the app warns that it’s meant for practice only. One prospective, randomized trial in 1,586 cardiac arrests that happened outside of hospitals found that use by emergency services personnel did not significantly change the likelihood of return of spontaneous circulation or other outcomes (BMJ 2011;342:d512).
• Chest: If you’re trying to teach students and residents about heart and lung sounds, or if you still get confused between mitral regurgitation and aortic stenosis, you might want to have a digital stethoscope app handy. These apps interpret heart and lung sounds heard typically through your smartphone’s microphone, which may not be good enough for clinical use. The Thinklabs Stethoscope app at $70 is pricey, compared with others, but it records sounds directly via the smartphone or through an attached electronic stethoscope.
A case that turns an iPhone into an ECG device has been submitted to the FDA for approval. The AliveCor iPhone ECG is expected to sell for between $100 and $200, compared with the usual price tag of thousands of dollars for conventional ECG machines, according to PC Magazine.
One small prospective study of experimental software that programs an iPhone to detect atrial fibrillation by placing a patient’s finger over the camera lens showed it was 98% sensitive and nearly 100% specific in detecting atrial fibrillation (IEEE Trans. Biomed. Eng. 2012 [doi:10.1109/TBME.2012.2208112]).
• Translation: When your hospital’s interpreter isn’t available, a free app like Google Translate can help. You can write or speak in one language and your device will write and say the message in a wide selection of language. You’ll need a wireless Internet connection for some translation apps.
• Eye chart: Your office has an eye chart, but you can’t find it. Pull up an app like the free EyeChart on your smartphone or tablet.
• Light: You want to inspect a patient’s sore throat, but the light in the exam room is broken. Use the flash on your smartphone camera, or use one of many free "flashlight" apps that turn the smartphone screen into a light source. Be sure to turn it off when you’re done, though, or your battery will run down quickly.
• Ultrasound: The miniaturization of ultrasound devices continues, with systems like the Mobisante MoblUS that attaches a probe to show images on your smartphone screen.
• Skin: For better evaluation of skin lesions, turn your iPhone into a dermatoscope by using the DermScope app ($4.99) and attaching the phone to the DermScope hardware (sold separately).
• Decision support: The PediStat app ($2.99 and up) makes it easy to determine the right pediatric drug dosing, among other features. The free Calculate (Medical Calculator) by QxMD app provides quick intuitive guides to common decision rules and can be customized by medical specialty.
• Drugs: Look up drug dosing, side effects, interactions and other information on free apps from Micromedex and others.
• Photos/videos: These apps are handy for documenting and sharing the appearance of a wound, a patients range of motion, or performance on a neurologic exam. Anyone who thinks they see uvula deviation in the throat of a struggling 3-year-old can snap a photo or video for review with other health care providers, medical students, or parents and avoid having to repeat the exam. Images of a wound problem after surgery can be sent to the surgeon when he or she is out of town.
Dr. Broder particularly finds the video useful for children having "pseudoseizures" whose parents demand a neurologic consult, even though the seizure event probably won’t be happening when the neurologist arrives. A video shows the neurologist exactly what Dr. Broder saw. (See the Dos and Don’ts for using photos and videos below.)
Once you’ve got an image or data you want to transmit, avoid texting as first-line means of communication because texts typically are not encrypted. Be careful when e-mailing to make sure it’s going to the correct address and only that address. Use e-mail options such as "confirm delivery" or "request read receipt," and add a sentence to the e-mail saying, "Please delete once no longer necessary for patient care," he advised.
Always document in the patient’s chart that you obtained patient consent and describe what was sent and who received it. Describe any images you send.
Don’t leave images on your portable devices. They’re easily lost, and most have inadequate encryption. Make images part of the medical record by uploading to the patient’s record, printing and scanning, or describing them clearly in the medical record. Then delete them from your device.
Store images and data in "cloud" computing sites with caution, Dr. Broder said. Services such as Google Drive or Dropbox allow sharing of very large files but provide no assurances about the quality of encryption or security. Cloud sites may be best used for giving patients access to instructions, instructional videos, reference papers, anatomic diagrams, etc.
The FDA approved the free Centricity Radiology Mobile Access app, which lets you view CT and MRI images on your iPhone if the images are stored in a GE Centricity PACS (picture archiving and communication system) platform – which may include 20% of U.S. radiology images, according to the company.

|
| Sherry Boschert/IMNG Medical Media A screen shot shows the Centricity Radiology Mobile Access app. |
The free CloudOn app lets you use MS Office software (including Word, Excel, and Powerpoint) on an iPad.
Various screen replicators that allow you to remotely access your computer desktop from your mobile device (such as ones by Citrix, or Splashtop Remote Desktop) all have the same problem, Dr. Broder said – they’re too clunky and not "touchscreen friendly."
And one final word on an underappreciated perk of medical apps on smartphones: When your medical director stops by, wanting to talk about your productivity, pull out your smartphone to show the data you’ve entered about patient encounters in your free iRVU app, which calculates total RVUs, charges, and average charge per encounter, among other features.
This list only begins to scratch the surface of app use in medicine. Other apps are available for immunization schedules, dictation, infectious disease guides, and teaching aids. Journals provide content to portable devices through apps, and some medical societies offer multifaceted apps such as ACEP Mobile.
Apps on smartphones and tablets will become part of daily medical practice, Dr. Broder predicted, but physicians need to be conscious about their limitations and potential problems as well as their assets.
Click here to view a video interview with Dr. Broder.
Dos and Don’ts for Medical Images on Smartphones
Do:
Obtain consent to acquire images or transmit them for the patient’s medical benefit.
Explain to the patient and get consent for any other intended use, such as education or publication.
Tell the patient what you will do with images when their use is completed – delete them or upload them to the medical record.
Confirm receipt if you send to other health care providers.
Specify in your message what that provider should do with the image.
Document in the patient’s chart that consent was obtained, what was sent, who received it, and content of the images.
Don’t:
Obtain images covertly.
Send to any unnecessary recipients.
Show images to anyone for fun.
Post to social media sites.
Blog about "funny" patient encounters.
Dr. Broder owns stock in Apple.
DENVER – Do you need a stethoscope, a blood pressure monitor, or a tool to assess cardiac rhythms? There are apps for that. In fact, by recent count there are more than 200,000 applications of technology – or "apps" – available for smartphones or tablet devices, and they’re being used more and more for medical purposes.
Need a convenient way to look up drug interactions, pediatric dosing, or clinical decision rules from guidelines? Or how about a translator, a light to examine a finicky infant’s throat, or a "white board" to draw a picture for your patient? Yup – they’re all in apps, and chances are you already may be using some of these.
Dr. Joshua S. Broder expects an exponential increase in the use of apps in medicine as smartphones and tablets continue to proliferate, but their accuracy needs to be verified and potential problems need to be addressed, he said at the annual meeting of the American College of Emergency Physicians.
Apps will be used increasingly for bedside diagnosis and measurement of hemoglobin or other physiologic parameters. "Some of these tests may be taken over by smartphones in the near future," according to Dr. Broder of Duke University, Durham, N.C.
On the other hand, he cautioned, how do you sterilize a smartphone as you move from one hospital room or patient to another, so that you avoid transmitting infection? There are few independent studies so far testing the accuracy and reliability of medical apps, most of which were designed for lay consumers, not physicians.
The Food and Drug Administration is "very interested" in regulating any apps that might substitute for proven technologies such as stethoscopes or that physicians use as accessories to medical devices that already are regulated, he said. The FDA described its approach to deciding which mobile technology to regulate in a draft report in July 2012.
Even the basic functions of smartphones can be convenient in clinical practice, such as taking photos or videos and transmitting information by text or e-mail, but make sure you protect patient privacy and autonomy in ways that maintain trust and comply with HIPAA, Dr. Broder said.
The Duke University Health System has resolved any issues with HIPAA so that it’s safe for physicians to transmit images and video as long as they’re not sent outside the system. Talk to the HIPAA compliance officer at your medical center to establish the ground rules, he said. You can refresh your memory about which parts of data are considered by HIPAA to be protected information via a University of Miami site.
Dr. Broder reviewed some smartphone functions and apps that may be helpful and others that are not yet ready for medical prime time. Many are available for no cost or for as nominal fee. One study of health and fitness apps suggests that apps costing $0.99 or more tend to be higher quality and more trustworthy than less-expensive ones, he noted (J. Med. Internet Res. 2012;14:e72).
• Sleep: One of his residents swears by "smart alarm clock" apps that claim to use a smartphone’s accelerometer to assess where you are in your sleep cycle (based on your movements in bed) to wake you at a time that will leave you feeling less fatigued. You may set for 6 a.m., but the alarm may wake you at 5:45 a.m. Apps like Sleep Cycle ($0.99) and Sleep as Android have some underlying sleep science behind them, but no independent studies have verified their claims.
• CPR: The accelerometer also is used in the free app PocketCPR to give real-time feedback during CPR on the rate and depth of compression. Its has not been cleared by the FDA for use in humans, however, so the app warns that it’s meant for practice only. One prospective, randomized trial in 1,586 cardiac arrests that happened outside of hospitals found that use by emergency services personnel did not significantly change the likelihood of return of spontaneous circulation or other outcomes (BMJ 2011;342:d512).
• Chest: If you’re trying to teach students and residents about heart and lung sounds, or if you still get confused between mitral regurgitation and aortic stenosis, you might want to have a digital stethoscope app handy. These apps interpret heart and lung sounds heard typically through your smartphone’s microphone, which may not be good enough for clinical use. The Thinklabs Stethoscope app at $70 is pricey, compared with others, but it records sounds directly via the smartphone or through an attached electronic stethoscope.
A case that turns an iPhone into an ECG device has been submitted to the FDA for approval. The AliveCor iPhone ECG is expected to sell for between $100 and $200, compared with the usual price tag of thousands of dollars for conventional ECG machines, according to PC Magazine.
One small prospective study of experimental software that programs an iPhone to detect atrial fibrillation by placing a patient’s finger over the camera lens showed it was 98% sensitive and nearly 100% specific in detecting atrial fibrillation (IEEE Trans. Biomed. Eng. 2012 [doi:10.1109/TBME.2012.2208112]).
• Translation: When your hospital’s interpreter isn’t available, a free app like Google Translate can help. You can write or speak in one language and your device will write and say the message in a wide selection of language. You’ll need a wireless Internet connection for some translation apps.
• Eye chart: Your office has an eye chart, but you can’t find it. Pull up an app like the free EyeChart on your smartphone or tablet.
• Light: You want to inspect a patient’s sore throat, but the light in the exam room is broken. Use the flash on your smartphone camera, or use one of many free "flashlight" apps that turn the smartphone screen into a light source. Be sure to turn it off when you’re done, though, or your battery will run down quickly.
• Ultrasound: The miniaturization of ultrasound devices continues, with systems like the Mobisante MoblUS that attaches a probe to show images on your smartphone screen.
• Skin: For better evaluation of skin lesions, turn your iPhone into a dermatoscope by using the DermScope app ($4.99) and attaching the phone to the DermScope hardware (sold separately).
• Decision support: The PediStat app ($2.99 and up) makes it easy to determine the right pediatric drug dosing, among other features. The free Calculate (Medical Calculator) by QxMD app provides quick intuitive guides to common decision rules and can be customized by medical specialty.
• Drugs: Look up drug dosing, side effects, interactions and other information on free apps from Micromedex and others.
• Photos/videos: These apps are handy for documenting and sharing the appearance of a wound, a patients range of motion, or performance on a neurologic exam. Anyone who thinks they see uvula deviation in the throat of a struggling 3-year-old can snap a photo or video for review with other health care providers, medical students, or parents and avoid having to repeat the exam. Images of a wound problem after surgery can be sent to the surgeon when he or she is out of town.
Dr. Broder particularly finds the video useful for children having "pseudoseizures" whose parents demand a neurologic consult, even though the seizure event probably won’t be happening when the neurologist arrives. A video shows the neurologist exactly what Dr. Broder saw. (See the Dos and Don’ts for using photos and videos below.)
Once you’ve got an image or data you want to transmit, avoid texting as first-line means of communication because texts typically are not encrypted. Be careful when e-mailing to make sure it’s going to the correct address and only that address. Use e-mail options such as "confirm delivery" or "request read receipt," and add a sentence to the e-mail saying, "Please delete once no longer necessary for patient care," he advised.
Always document in the patient’s chart that you obtained patient consent and describe what was sent and who received it. Describe any images you send.
Don’t leave images on your portable devices. They’re easily lost, and most have inadequate encryption. Make images part of the medical record by uploading to the patient’s record, printing and scanning, or describing them clearly in the medical record. Then delete them from your device.
Store images and data in "cloud" computing sites with caution, Dr. Broder said. Services such as Google Drive or Dropbox allow sharing of very large files but provide no assurances about the quality of encryption or security. Cloud sites may be best used for giving patients access to instructions, instructional videos, reference papers, anatomic diagrams, etc.
The FDA approved the free Centricity Radiology Mobile Access app, which lets you view CT and MRI images on your iPhone if the images are stored in a GE Centricity PACS (picture archiving and communication system) platform – which may include 20% of U.S. radiology images, according to the company.

|
| Sherry Boschert/IMNG Medical Media A screen shot shows the Centricity Radiology Mobile Access app. |
The free CloudOn app lets you use MS Office software (including Word, Excel, and Powerpoint) on an iPad.
Various screen replicators that allow you to remotely access your computer desktop from your mobile device (such as ones by Citrix, or Splashtop Remote Desktop) all have the same problem, Dr. Broder said – they’re too clunky and not "touchscreen friendly."
And one final word on an underappreciated perk of medical apps on smartphones: When your medical director stops by, wanting to talk about your productivity, pull out your smartphone to show the data you’ve entered about patient encounters in your free iRVU app, which calculates total RVUs, charges, and average charge per encounter, among other features.
This list only begins to scratch the surface of app use in medicine. Other apps are available for immunization schedules, dictation, infectious disease guides, and teaching aids. Journals provide content to portable devices through apps, and some medical societies offer multifaceted apps such as ACEP Mobile.
Apps on smartphones and tablets will become part of daily medical practice, Dr. Broder predicted, but physicians need to be conscious about their limitations and potential problems as well as their assets.
Click here to view a video interview with Dr. Broder.
Dos and Don’ts for Medical Images on Smartphones
Do:
Obtain consent to acquire images or transmit them for the patient’s medical benefit.
Explain to the patient and get consent for any other intended use, such as education or publication.
Tell the patient what you will do with images when their use is completed – delete them or upload them to the medical record.
Confirm receipt if you send to other health care providers.
Specify in your message what that provider should do with the image.
Document in the patient’s chart that consent was obtained, what was sent, who received it, and content of the images.
Don’t:
Obtain images covertly.
Send to any unnecessary recipients.
Show images to anyone for fun.
Post to social media sites.
Blog about "funny" patient encounters.
Dr. Broder owns stock in Apple.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE AMERICAN COLLEGE OF EMERGENCY PHYSICIANS
PCI without surgery backup shows no economic benefit
LOS ANGELES – There are perfectly good reasons for hospitals to offer elective percutaneous coronary intervention without on-site cardiac surgery backup, but saving institutional dollars isn’t among them.
That’s the bottom line from CPORT-E (Cardiovascular Patient Outcomes Research Team/Non-Primary Percutaneous Coronary Intervention Economic Study), the prespecified economic analysis conducted as part of the landmark CPORT trial.
The estimated medical costs per CPORT participant, including the index revascularization and hospitalization as well as costs incurred during 9 months of follow-up, averaged $29,136 in hospitals without on-site coronary artery bypass surgery backup and $25,412 in centers with backup. This 15% difference did not reach statistical significance, Eric L. Eisenstein, DBA, reported at the annual scientific sessions of the American Heart Association.
Patients assigned to PCI at hospitals without on-site cardiac surgery actually had a shorter average length of stay; however, their total hospitalization costs ran higher because the study protocol dictated that their post-PCI care take place in the intensive care unit. Patients in centers with no on-site CABG backup also had a significantly higher rate of repeat target vessel revascularization during 9 months of follow-up: 6.5% compared with 5.4% when PCI was performed in hospitals with surgical backup, explained Dr. Eisenstein of Duke Clinical Research Institute, Durham, N.C.
CPORT was a randomized, prospective trial in which elective PCI performed at hospitals with or without on-site cardiac surgery backup was compared for nearly 19,000 participants. As previously reported (N. Engl. J. Med. 2012;366:1792-802), there were no significant differences between the two patient populations in terms of the coprimary end points of 6-week mortality (0.9% at hospitals without on-site surgery and 1.0% at those with backup) and 9-month major adverse cardiac events (12.1% without versus 11.2% with on-site surgical backup).
Discussant Dr. Mark A. Hlatky noted that 9-month total costs in CPORT-E were 22% higher at low-PCI-volume sites without surgery but only 7% higher at high-volume sites without surgery than at hospitals having on-site CABG backup.
"That’s a very interesting issue: The crucial factor driving costs may not be whether surgery is present on site or not, but the PCI volume at the site. If we have a low-volume site there may be higher costs and more adverse events. Whenever you do something in higher volumes you’re more efficient economically and you may actually do a little bit better job," said Dr. Hlatky of Stanford (Calif.) University.
As a matter of health policy, introducing elective PCI at hospitals without on-site cardiac surgery is attractive because it improves access, particularly for patients in rural areas. Another consideration is that these centers without on-site surgery may be available for emergency PCI, thereby avoiding the delays inherent in patient transfer to a distant center, he observed.
Discussant Dr. David O. Williams called CPORT "an extremely well-organized and well-conducted trial. It was a large study and the findings, I believe, are quite valid. To be applicable, however, hospitals will need to replicate all the necessary operational and training activities inherent in the trial, which were really quite extensive." That means no money-saving shortcuts, such as eliminating a post-PCI stay in the ICU.
"I believe this trial is significant and will likely impact the manner in which PCI is performed in the U.S. The performance of PCI in hospitals without on-site CABG surgery, I believe, will be adopted and become the standard of care," predicted Dr. Williams, an interventional cardiologist at Brigham and Women’s Hospital, Boston.
Dr. Eisenstein had research grants from Medtronic and Eli Lilly. Dr. Williams reported grants from medical device companies. Dr. Hlatky had no conflicts.
LOS ANGELES – There are perfectly good reasons for hospitals to offer elective percutaneous coronary intervention without on-site cardiac surgery backup, but saving institutional dollars isn’t among them.
That’s the bottom line from CPORT-E (Cardiovascular Patient Outcomes Research Team/Non-Primary Percutaneous Coronary Intervention Economic Study), the prespecified economic analysis conducted as part of the landmark CPORT trial.
The estimated medical costs per CPORT participant, including the index revascularization and hospitalization as well as costs incurred during 9 months of follow-up, averaged $29,136 in hospitals without on-site coronary artery bypass surgery backup and $25,412 in centers with backup. This 15% difference did not reach statistical significance, Eric L. Eisenstein, DBA, reported at the annual scientific sessions of the American Heart Association.
Patients assigned to PCI at hospitals without on-site cardiac surgery actually had a shorter average length of stay; however, their total hospitalization costs ran higher because the study protocol dictated that their post-PCI care take place in the intensive care unit. Patients in centers with no on-site CABG backup also had a significantly higher rate of repeat target vessel revascularization during 9 months of follow-up: 6.5% compared with 5.4% when PCI was performed in hospitals with surgical backup, explained Dr. Eisenstein of Duke Clinical Research Institute, Durham, N.C.
CPORT was a randomized, prospective trial in which elective PCI performed at hospitals with or without on-site cardiac surgery backup was compared for nearly 19,000 participants. As previously reported (N. Engl. J. Med. 2012;366:1792-802), there were no significant differences between the two patient populations in terms of the coprimary end points of 6-week mortality (0.9% at hospitals without on-site surgery and 1.0% at those with backup) and 9-month major adverse cardiac events (12.1% without versus 11.2% with on-site surgical backup).
Discussant Dr. Mark A. Hlatky noted that 9-month total costs in CPORT-E were 22% higher at low-PCI-volume sites without surgery but only 7% higher at high-volume sites without surgery than at hospitals having on-site CABG backup.
"That’s a very interesting issue: The crucial factor driving costs may not be whether surgery is present on site or not, but the PCI volume at the site. If we have a low-volume site there may be higher costs and more adverse events. Whenever you do something in higher volumes you’re more efficient economically and you may actually do a little bit better job," said Dr. Hlatky of Stanford (Calif.) University.
As a matter of health policy, introducing elective PCI at hospitals without on-site cardiac surgery is attractive because it improves access, particularly for patients in rural areas. Another consideration is that these centers without on-site surgery may be available for emergency PCI, thereby avoiding the delays inherent in patient transfer to a distant center, he observed.
Discussant Dr. David O. Williams called CPORT "an extremely well-organized and well-conducted trial. It was a large study and the findings, I believe, are quite valid. To be applicable, however, hospitals will need to replicate all the necessary operational and training activities inherent in the trial, which were really quite extensive." That means no money-saving shortcuts, such as eliminating a post-PCI stay in the ICU.
"I believe this trial is significant and will likely impact the manner in which PCI is performed in the U.S. The performance of PCI in hospitals without on-site CABG surgery, I believe, will be adopted and become the standard of care," predicted Dr. Williams, an interventional cardiologist at Brigham and Women’s Hospital, Boston.
Dr. Eisenstein had research grants from Medtronic and Eli Lilly. Dr. Williams reported grants from medical device companies. Dr. Hlatky had no conflicts.
LOS ANGELES – There are perfectly good reasons for hospitals to offer elective percutaneous coronary intervention without on-site cardiac surgery backup, but saving institutional dollars isn’t among them.
That’s the bottom line from CPORT-E (Cardiovascular Patient Outcomes Research Team/Non-Primary Percutaneous Coronary Intervention Economic Study), the prespecified economic analysis conducted as part of the landmark CPORT trial.
The estimated medical costs per CPORT participant, including the index revascularization and hospitalization as well as costs incurred during 9 months of follow-up, averaged $29,136 in hospitals without on-site coronary artery bypass surgery backup and $25,412 in centers with backup. This 15% difference did not reach statistical significance, Eric L. Eisenstein, DBA, reported at the annual scientific sessions of the American Heart Association.
Patients assigned to PCI at hospitals without on-site cardiac surgery actually had a shorter average length of stay; however, their total hospitalization costs ran higher because the study protocol dictated that their post-PCI care take place in the intensive care unit. Patients in centers with no on-site CABG backup also had a significantly higher rate of repeat target vessel revascularization during 9 months of follow-up: 6.5% compared with 5.4% when PCI was performed in hospitals with surgical backup, explained Dr. Eisenstein of Duke Clinical Research Institute, Durham, N.C.
CPORT was a randomized, prospective trial in which elective PCI performed at hospitals with or without on-site cardiac surgery backup was compared for nearly 19,000 participants. As previously reported (N. Engl. J. Med. 2012;366:1792-802), there were no significant differences between the two patient populations in terms of the coprimary end points of 6-week mortality (0.9% at hospitals without on-site surgery and 1.0% at those with backup) and 9-month major adverse cardiac events (12.1% without versus 11.2% with on-site surgical backup).
Discussant Dr. Mark A. Hlatky noted that 9-month total costs in CPORT-E were 22% higher at low-PCI-volume sites without surgery but only 7% higher at high-volume sites without surgery than at hospitals having on-site CABG backup.
"That’s a very interesting issue: The crucial factor driving costs may not be whether surgery is present on site or not, but the PCI volume at the site. If we have a low-volume site there may be higher costs and more adverse events. Whenever you do something in higher volumes you’re more efficient economically and you may actually do a little bit better job," said Dr. Hlatky of Stanford (Calif.) University.
As a matter of health policy, introducing elective PCI at hospitals without on-site cardiac surgery is attractive because it improves access, particularly for patients in rural areas. Another consideration is that these centers without on-site surgery may be available for emergency PCI, thereby avoiding the delays inherent in patient transfer to a distant center, he observed.
Discussant Dr. David O. Williams called CPORT "an extremely well-organized and well-conducted trial. It was a large study and the findings, I believe, are quite valid. To be applicable, however, hospitals will need to replicate all the necessary operational and training activities inherent in the trial, which were really quite extensive." That means no money-saving shortcuts, such as eliminating a post-PCI stay in the ICU.
"I believe this trial is significant and will likely impact the manner in which PCI is performed in the U.S. The performance of PCI in hospitals without on-site CABG surgery, I believe, will be adopted and become the standard of care," predicted Dr. Williams, an interventional cardiologist at Brigham and Women’s Hospital, Boston.
Dr. Eisenstein had research grants from Medtronic and Eli Lilly. Dr. Williams reported grants from medical device companies. Dr. Hlatky had no conflicts.
Major Finding: The mean total cost of elective percutaneous intervention and subsequent cardiovascular hospital care during 9 months of follow-up was 22% higher in patients at low-volume PCI centers without on-site cardiac surgery backup, but only 7% higher at high-volume centers without surgical backup, than when PCI was performed at centers with cardiac surgery backup.
Data Source: The CPORT trial included almost 19,000 patients who were randomized to elective percutaneous coronary intervention at hospitals with or without on-site cardiac surgery backup.
Disclosures: The CPORT Economic Study was funded by Johns Hopkins University. Dr. Eisenstein reported receiving research grants from Medtronic and Eli Lilly.
Medicare Spending Increased When Consult Pay Was Eliminated
A change in Medicare policy regarding payments for consultations vs. office visits had the unintended consequence of raising overall costs the first year it was implemented, according to a report published online in Archives of Internal Medicine.
Prior to 2010, the Medicare Physician Fee Schedule provided higher payments for consultations than for office visits at every level of complexity. For example, in 2009 Medicare paid $124.79 on average for a consultation of medium complexity, compared with $91.97 for a new patient office visit and $61.31 for an established patient office visit of similar complexity.
Since primary care physicians billed primarily for office visits and specialists billed primarily for consultations, this resulted in a large discrepancy in reimbursement between primary and specialist physicians for doing similarly complex work, according to Zirui Song, Ph.D., of the department of health care policy, Harvard Medical School, Boston, and his associates.
With the fee schedule for calendar 2010, the Centers for Medicare and Medicaid Services eliminated payments for consultations altogether, so that all outpatient physician encounters would be billed as office visits, and simultaneously raised the fees for office visits. The change was designed specifically to be budget-neutral for the Medicare program.
Dr. Song and his colleagues assessed the effects of this policy change on Medicare payments in 2010. They used data from a sample of 2.2 million Medicare beneficiaries who had a diagnosis related to diabetes or cardiovascular conditions, or prescriptions for any cardiovascular or cholesterol-reducing drugs, and who were seen as outpatients in 2007 through the end of 2010.
During 2010, payments for consultations decreased an average of $18.52 per beneficiary per quarter.
However, payments for new patient office visits rose by $13.64 per beneficiary per quarter and payments for established patient office visits rose by $15.08 per beneficiary per quarter. This represents an increase of 131% in the number of new patient office visits billed to Medicare and an increase of 12% in the number of established patient office visits billed to Medicare, compared with the preceding year.
"On net, spending on all physician encounters was higher by $10.20 per beneficiary per quarter after the policy" for an increase of 6.5%, Dr. Song and his associates said (Arch. Intern. Med. 2012 [doi:10.1001/jamainternmend.2013.1125]).
The volume of patient encounters did not increase during this period, the researchers found. Rather, it appears that "an increase in the intensity of coding" was responsible for approximately one-third of the 6.5% rise, while the fee increase for office visits was responsible for the other two-thirds.
The income gap between specialists and primary care physicians did narrow somewhat after this policy change was implemented. Primary care physicians accounted for a slightly greater proportion (58%) of the rise in spending than did specialists (42%), the researchers noted.
They added that this study pertained only to Medicare payments for outpatient encounters, and did not address all other physician services. "The overall discrepancy in Medicare payments" between primary care and specialist physicians "derives largely from procedural services, which this policy does not address," Dr. Song and his colleagues said.
Similarly, this study examined only the policy’s effect on the first year after implementation, and these results may not be generalizable to longer term effects, they said.
This study was supported by The Commonwealth Fund, the National Institute on Aging, and the National Bureau of Economic Research. The investigators reported no relevant financial conflicts of interest.
A change in Medicare policy regarding payments for consultations vs. office visits had the unintended consequence of raising overall costs the first year it was implemented, according to a report published online in Archives of Internal Medicine.
Prior to 2010, the Medicare Physician Fee Schedule provided higher payments for consultations than for office visits at every level of complexity. For example, in 2009 Medicare paid $124.79 on average for a consultation of medium complexity, compared with $91.97 for a new patient office visit and $61.31 for an established patient office visit of similar complexity.
Since primary care physicians billed primarily for office visits and specialists billed primarily for consultations, this resulted in a large discrepancy in reimbursement between primary and specialist physicians for doing similarly complex work, according to Zirui Song, Ph.D., of the department of health care policy, Harvard Medical School, Boston, and his associates.
With the fee schedule for calendar 2010, the Centers for Medicare and Medicaid Services eliminated payments for consultations altogether, so that all outpatient physician encounters would be billed as office visits, and simultaneously raised the fees for office visits. The change was designed specifically to be budget-neutral for the Medicare program.
Dr. Song and his colleagues assessed the effects of this policy change on Medicare payments in 2010. They used data from a sample of 2.2 million Medicare beneficiaries who had a diagnosis related to diabetes or cardiovascular conditions, or prescriptions for any cardiovascular or cholesterol-reducing drugs, and who were seen as outpatients in 2007 through the end of 2010.
During 2010, payments for consultations decreased an average of $18.52 per beneficiary per quarter.
However, payments for new patient office visits rose by $13.64 per beneficiary per quarter and payments for established patient office visits rose by $15.08 per beneficiary per quarter. This represents an increase of 131% in the number of new patient office visits billed to Medicare and an increase of 12% in the number of established patient office visits billed to Medicare, compared with the preceding year.
"On net, spending on all physician encounters was higher by $10.20 per beneficiary per quarter after the policy" for an increase of 6.5%, Dr. Song and his associates said (Arch. Intern. Med. 2012 [doi:10.1001/jamainternmend.2013.1125]).
The volume of patient encounters did not increase during this period, the researchers found. Rather, it appears that "an increase in the intensity of coding" was responsible for approximately one-third of the 6.5% rise, while the fee increase for office visits was responsible for the other two-thirds.
The income gap between specialists and primary care physicians did narrow somewhat after this policy change was implemented. Primary care physicians accounted for a slightly greater proportion (58%) of the rise in spending than did specialists (42%), the researchers noted.
They added that this study pertained only to Medicare payments for outpatient encounters, and did not address all other physician services. "The overall discrepancy in Medicare payments" between primary care and specialist physicians "derives largely from procedural services, which this policy does not address," Dr. Song and his colleagues said.
Similarly, this study examined only the policy’s effect on the first year after implementation, and these results may not be generalizable to longer term effects, they said.
This study was supported by The Commonwealth Fund, the National Institute on Aging, and the National Bureau of Economic Research. The investigators reported no relevant financial conflicts of interest.
A change in Medicare policy regarding payments for consultations vs. office visits had the unintended consequence of raising overall costs the first year it was implemented, according to a report published online in Archives of Internal Medicine.
Prior to 2010, the Medicare Physician Fee Schedule provided higher payments for consultations than for office visits at every level of complexity. For example, in 2009 Medicare paid $124.79 on average for a consultation of medium complexity, compared with $91.97 for a new patient office visit and $61.31 for an established patient office visit of similar complexity.
Since primary care physicians billed primarily for office visits and specialists billed primarily for consultations, this resulted in a large discrepancy in reimbursement between primary and specialist physicians for doing similarly complex work, according to Zirui Song, Ph.D., of the department of health care policy, Harvard Medical School, Boston, and his associates.
With the fee schedule for calendar 2010, the Centers for Medicare and Medicaid Services eliminated payments for consultations altogether, so that all outpatient physician encounters would be billed as office visits, and simultaneously raised the fees for office visits. The change was designed specifically to be budget-neutral for the Medicare program.
Dr. Song and his colleagues assessed the effects of this policy change on Medicare payments in 2010. They used data from a sample of 2.2 million Medicare beneficiaries who had a diagnosis related to diabetes or cardiovascular conditions, or prescriptions for any cardiovascular or cholesterol-reducing drugs, and who were seen as outpatients in 2007 through the end of 2010.
During 2010, payments for consultations decreased an average of $18.52 per beneficiary per quarter.
However, payments for new patient office visits rose by $13.64 per beneficiary per quarter and payments for established patient office visits rose by $15.08 per beneficiary per quarter. This represents an increase of 131% in the number of new patient office visits billed to Medicare and an increase of 12% in the number of established patient office visits billed to Medicare, compared with the preceding year.
"On net, spending on all physician encounters was higher by $10.20 per beneficiary per quarter after the policy" for an increase of 6.5%, Dr. Song and his associates said (Arch. Intern. Med. 2012 [doi:10.1001/jamainternmend.2013.1125]).
The volume of patient encounters did not increase during this period, the researchers found. Rather, it appears that "an increase in the intensity of coding" was responsible for approximately one-third of the 6.5% rise, while the fee increase for office visits was responsible for the other two-thirds.
The income gap between specialists and primary care physicians did narrow somewhat after this policy change was implemented. Primary care physicians accounted for a slightly greater proportion (58%) of the rise in spending than did specialists (42%), the researchers noted.
They added that this study pertained only to Medicare payments for outpatient encounters, and did not address all other physician services. "The overall discrepancy in Medicare payments" between primary care and specialist physicians "derives largely from procedural services, which this policy does not address," Dr. Song and his colleagues said.
Similarly, this study examined only the policy’s effect on the first year after implementation, and these results may not be generalizable to longer term effects, they said.
This study was supported by The Commonwealth Fund, the National Institute on Aging, and the National Bureau of Economic Research. The investigators reported no relevant financial conflicts of interest.
FROM ARCHIVES OF INTERNAL MEDICINE
Major Finding: Medicare payments for outpatient visits rose 6.5%, or $10.20 per beneficiary per quarter, during the first year after consultations were eliminated from the Physician Fee Schedule in an effort to redistribute payments more fairly between specialists and primary care physicians.
Data Source: An analysis of Medicare data on 2.2 million patients with diagnoses related to diabetes or cardiovascular disease who were seen as outpatients by primary care physicians and specialists in 2007-2010.
Disclosures: This study was supported by The Commonwealth Fund, the National Institute on Aging, and the National Bureau of Economic Research. The investigators reported no relevant financial conflicts of interest.
ADVANCE: TAVI survival remains high with CoreValve
At 1 year, overall survival after implantation with the transcatheter aortic CoreValve in the postmarket ADVANCE study was 82.1% and cardiovascular survival 88.2%. This compares with survival rates of 87.4% and 91.7% at 6 months and 95.5% and 96.6% at 30 days, principal investigator Dr. Axel Linke said at Transcatheter Cardiovascular Therapeutics 2012.
"If you put it into the perspective of the PARTNER A and B cohorts [in the pivotal trial in the Sapien transcatheter valve system], our mortality rate is, in absolute values, 8% to 13% lower," he said in an interview.
One explanation is that the 1,015-patient, postmarket ADVANCE study sought out centers experienced with transcatheter aortic valve implantation (TAVI). The 44 centers in Western Europe, Asia, and South America had to have performed at least 40 TAVI procedures, with some German centers having done as many as 500, to be certified by a TAVI proctor and to have a heart team in place. In comparison, some centers in the PARTNER trial of the Edwards Lifesciences Sapien valve contributed just six or seven patients and were selected based on their experience with general cardiologic intervention, he observed.
The 1-year survival rates in ADVANCE also surpass those from early registries, notably the French Aortic National CoreValve and Edwards Registry, where the initial experience with TAVI was associated with interventional mistakes, which were linked to early mortality, Dr. Linke said. The CoreValve System has been implanted in more than 30,000 patients since approval in the European Union in 2007, but is limited to investigational use in the United States.
No details were presented regarding mortality in various subgroups or complications such as stroke, paravalvular leaks or left bundle branch block (LBBB). A recent analysis raised concerns about LBBB, showing that one-third of 202 consecutive patients with no prior conduction disturbances developed new-onset LBBB after TAVI with a balloon-expandable valve (Sapien or Sapien XT). Although it resolved in 37.7% by hospital discharge and 57.3% at 6- to 12-month follow-up, patients with persistent LBBB had a significantly higher incidence of syncope and complete atrioventricular block requiring a permanent pacemaker (J. Am. Coll. Cardiol. 2012;60:1743-52 [doi:10.1016/j.jacc.2012.035].
The researchers will look at LBBB in detailed analyses expected from ADVANCE, but there’s been no evidence of a problem with LBBB in earlier follow-up in ADVANCE or from other CoreValve users.
Quality of life data from ADVANCE, reported in a separate poster session at the meeting, showed significant benefits with CoreValve, even in higher-risk patients. The access route used during TAVI had no impact on quality of life improvement at 6 months.
Dr. Linke has served as a consultant for Medtronic, the study sponsor.
At 1 year, overall survival after implantation with the transcatheter aortic CoreValve in the postmarket ADVANCE study was 82.1% and cardiovascular survival 88.2%. This compares with survival rates of 87.4% and 91.7% at 6 months and 95.5% and 96.6% at 30 days, principal investigator Dr. Axel Linke said at Transcatheter Cardiovascular Therapeutics 2012.
"If you put it into the perspective of the PARTNER A and B cohorts [in the pivotal trial in the Sapien transcatheter valve system], our mortality rate is, in absolute values, 8% to 13% lower," he said in an interview.
One explanation is that the 1,015-patient, postmarket ADVANCE study sought out centers experienced with transcatheter aortic valve implantation (TAVI). The 44 centers in Western Europe, Asia, and South America had to have performed at least 40 TAVI procedures, with some German centers having done as many as 500, to be certified by a TAVI proctor and to have a heart team in place. In comparison, some centers in the PARTNER trial of the Edwards Lifesciences Sapien valve contributed just six or seven patients and were selected based on their experience with general cardiologic intervention, he observed.
The 1-year survival rates in ADVANCE also surpass those from early registries, notably the French Aortic National CoreValve and Edwards Registry, where the initial experience with TAVI was associated with interventional mistakes, which were linked to early mortality, Dr. Linke said. The CoreValve System has been implanted in more than 30,000 patients since approval in the European Union in 2007, but is limited to investigational use in the United States.
No details were presented regarding mortality in various subgroups or complications such as stroke, paravalvular leaks or left bundle branch block (LBBB). A recent analysis raised concerns about LBBB, showing that one-third of 202 consecutive patients with no prior conduction disturbances developed new-onset LBBB after TAVI with a balloon-expandable valve (Sapien or Sapien XT). Although it resolved in 37.7% by hospital discharge and 57.3% at 6- to 12-month follow-up, patients with persistent LBBB had a significantly higher incidence of syncope and complete atrioventricular block requiring a permanent pacemaker (J. Am. Coll. Cardiol. 2012;60:1743-52 [doi:10.1016/j.jacc.2012.035].
The researchers will look at LBBB in detailed analyses expected from ADVANCE, but there’s been no evidence of a problem with LBBB in earlier follow-up in ADVANCE or from other CoreValve users.
Quality of life data from ADVANCE, reported in a separate poster session at the meeting, showed significant benefits with CoreValve, even in higher-risk patients. The access route used during TAVI had no impact on quality of life improvement at 6 months.
Dr. Linke has served as a consultant for Medtronic, the study sponsor.
At 1 year, overall survival after implantation with the transcatheter aortic CoreValve in the postmarket ADVANCE study was 82.1% and cardiovascular survival 88.2%. This compares with survival rates of 87.4% and 91.7% at 6 months and 95.5% and 96.6% at 30 days, principal investigator Dr. Axel Linke said at Transcatheter Cardiovascular Therapeutics 2012.
"If you put it into the perspective of the PARTNER A and B cohorts [in the pivotal trial in the Sapien transcatheter valve system], our mortality rate is, in absolute values, 8% to 13% lower," he said in an interview.
One explanation is that the 1,015-patient, postmarket ADVANCE study sought out centers experienced with transcatheter aortic valve implantation (TAVI). The 44 centers in Western Europe, Asia, and South America had to have performed at least 40 TAVI procedures, with some German centers having done as many as 500, to be certified by a TAVI proctor and to have a heart team in place. In comparison, some centers in the PARTNER trial of the Edwards Lifesciences Sapien valve contributed just six or seven patients and were selected based on their experience with general cardiologic intervention, he observed.
The 1-year survival rates in ADVANCE also surpass those from early registries, notably the French Aortic National CoreValve and Edwards Registry, where the initial experience with TAVI was associated with interventional mistakes, which were linked to early mortality, Dr. Linke said. The CoreValve System has been implanted in more than 30,000 patients since approval in the European Union in 2007, but is limited to investigational use in the United States.
No details were presented regarding mortality in various subgroups or complications such as stroke, paravalvular leaks or left bundle branch block (LBBB). A recent analysis raised concerns about LBBB, showing that one-third of 202 consecutive patients with no prior conduction disturbances developed new-onset LBBB after TAVI with a balloon-expandable valve (Sapien or Sapien XT). Although it resolved in 37.7% by hospital discharge and 57.3% at 6- to 12-month follow-up, patients with persistent LBBB had a significantly higher incidence of syncope and complete atrioventricular block requiring a permanent pacemaker (J. Am. Coll. Cardiol. 2012;60:1743-52 [doi:10.1016/j.jacc.2012.035].
The researchers will look at LBBB in detailed analyses expected from ADVANCE, but there’s been no evidence of a problem with LBBB in earlier follow-up in ADVANCE or from other CoreValve users.
Quality of life data from ADVANCE, reported in a separate poster session at the meeting, showed significant benefits with CoreValve, even in higher-risk patients. The access route used during TAVI had no impact on quality of life improvement at 6 months.
Dr. Linke has served as a consultant for Medtronic, the study sponsor.
Major Finding: At 1 year, overall survival was 82.1% and cardiovascular survival 88.2%.
Data Source: International, postmarket phase IV study of 1,015 patients with severe aortic stenosis implanted with the transcatheter CoreValve.
Disclosures: Dr. Linke reported serving as an advisor or consultant for Medtronic, which sponsored the study.