User login
For MD-IQ use only
European research team to study drug resistance in psychiatry
Having secured 11 million euros in funding from the European Union’s Horizon Health program, an international team of pharmacology, pharmacogenetics, and psychiatry experts has set to work in hopes of helping patients with severe mental illnesses.
On this team is a group of researchers from the University of Cagliari in Sardinia, Italy. They are part of a network of international experts from 26 universities, research centers, and European associations, all of whom have vast experience in the fields of psychiatry, pharmacology, genetics, and statistics. Coordinating the project is Bernhard T. Baune, MD, PhD, professor of psychiatry at the University of Münster, Germany.
The problem of drug resistance is of great relevance to psychiatrists. About one-third of patients do not respond to pharmacologic therapies; as a result, their illness becomes more and more severe. This development has a major impact on these patients’ quality of life. In addition, health care and social services face a rise in the costs associated with managing the illnesses.
The research team from the University of Cagliari has two members from the department of biomedical sciences – Alessio Squassina, PhD, head of the pharmacogenetics laboratory, and Claudia Pisanu, MD, PhD – and two translational clinical researchers from the department of medical sciences and public health – Bernardo Carpiniello, MD, head of the psychiatry division, and Mirko Manchia, MD, PhD. They will be in charge of recruiting and collecting biological material from one set of patients with mental illnesses, collecting DNA and performing genetic screenings for all of the patients recruited by the network’s members in the various European countries, and conducting and coordinating clinical trials in which the pharmacologic therapies will be guided based on the molecular results.
“The process of figuring out whether someone has drug resistance is complex,” explained Dr. Squassina. “It may require very long periods of treatment and observation which, in the end, severely impact the patient’s chances of seeing a significant improvement in their symptoms and of being able to reintegrate themselves into society in the shortest possible time frame.” The goal of the Psych-STRATA project is to come up with a predictive algorithm – consisting of molecular markers and clinical data – that, before a specific antidepressant is even given, will be able to identify the patients who have a greater probability of responding and those who have a greater probability of not responding. Psych-STRATA’s findings could have a meaningful positive effect on the lives of patients with mental illnesses, as they would provide psychiatrists with guidance for managing pharmacologic therapies more precisely and in a way that is based on patients’ biological characteristics. This, in turn, would increase the efficacy of drugs, lower the risks of adverse effects, and significantly contribute to achieving quick remission of symptoms.
A version of this article appeared on Medscape.com. This article was translated from Univadis Italy.
Having secured 11 million euros in funding from the European Union’s Horizon Health program, an international team of pharmacology, pharmacogenetics, and psychiatry experts has set to work in hopes of helping patients with severe mental illnesses.
On this team is a group of researchers from the University of Cagliari in Sardinia, Italy. They are part of a network of international experts from 26 universities, research centers, and European associations, all of whom have vast experience in the fields of psychiatry, pharmacology, genetics, and statistics. Coordinating the project is Bernhard T. Baune, MD, PhD, professor of psychiatry at the University of Münster, Germany.
The problem of drug resistance is of great relevance to psychiatrists. About one-third of patients do not respond to pharmacologic therapies; as a result, their illness becomes more and more severe. This development has a major impact on these patients’ quality of life. In addition, health care and social services face a rise in the costs associated with managing the illnesses.
The research team from the University of Cagliari has two members from the department of biomedical sciences – Alessio Squassina, PhD, head of the pharmacogenetics laboratory, and Claudia Pisanu, MD, PhD – and two translational clinical researchers from the department of medical sciences and public health – Bernardo Carpiniello, MD, head of the psychiatry division, and Mirko Manchia, MD, PhD. They will be in charge of recruiting and collecting biological material from one set of patients with mental illnesses, collecting DNA and performing genetic screenings for all of the patients recruited by the network’s members in the various European countries, and conducting and coordinating clinical trials in which the pharmacologic therapies will be guided based on the molecular results.
“The process of figuring out whether someone has drug resistance is complex,” explained Dr. Squassina. “It may require very long periods of treatment and observation which, in the end, severely impact the patient’s chances of seeing a significant improvement in their symptoms and of being able to reintegrate themselves into society in the shortest possible time frame.” The goal of the Psych-STRATA project is to come up with a predictive algorithm – consisting of molecular markers and clinical data – that, before a specific antidepressant is even given, will be able to identify the patients who have a greater probability of responding and those who have a greater probability of not responding. Psych-STRATA’s findings could have a meaningful positive effect on the lives of patients with mental illnesses, as they would provide psychiatrists with guidance for managing pharmacologic therapies more precisely and in a way that is based on patients’ biological characteristics. This, in turn, would increase the efficacy of drugs, lower the risks of adverse effects, and significantly contribute to achieving quick remission of symptoms.
A version of this article appeared on Medscape.com. This article was translated from Univadis Italy.
Having secured 11 million euros in funding from the European Union’s Horizon Health program, an international team of pharmacology, pharmacogenetics, and psychiatry experts has set to work in hopes of helping patients with severe mental illnesses.
On this team is a group of researchers from the University of Cagliari in Sardinia, Italy. They are part of a network of international experts from 26 universities, research centers, and European associations, all of whom have vast experience in the fields of psychiatry, pharmacology, genetics, and statistics. Coordinating the project is Bernhard T. Baune, MD, PhD, professor of psychiatry at the University of Münster, Germany.
The problem of drug resistance is of great relevance to psychiatrists. About one-third of patients do not respond to pharmacologic therapies; as a result, their illness becomes more and more severe. This development has a major impact on these patients’ quality of life. In addition, health care and social services face a rise in the costs associated with managing the illnesses.
The research team from the University of Cagliari has two members from the department of biomedical sciences – Alessio Squassina, PhD, head of the pharmacogenetics laboratory, and Claudia Pisanu, MD, PhD – and two translational clinical researchers from the department of medical sciences and public health – Bernardo Carpiniello, MD, head of the psychiatry division, and Mirko Manchia, MD, PhD. They will be in charge of recruiting and collecting biological material from one set of patients with mental illnesses, collecting DNA and performing genetic screenings for all of the patients recruited by the network’s members in the various European countries, and conducting and coordinating clinical trials in which the pharmacologic therapies will be guided based on the molecular results.
“The process of figuring out whether someone has drug resistance is complex,” explained Dr. Squassina. “It may require very long periods of treatment and observation which, in the end, severely impact the patient’s chances of seeing a significant improvement in their symptoms and of being able to reintegrate themselves into society in the shortest possible time frame.” The goal of the Psych-STRATA project is to come up with a predictive algorithm – consisting of molecular markers and clinical data – that, before a specific antidepressant is even given, will be able to identify the patients who have a greater probability of responding and those who have a greater probability of not responding. Psych-STRATA’s findings could have a meaningful positive effect on the lives of patients with mental illnesses, as they would provide psychiatrists with guidance for managing pharmacologic therapies more precisely and in a way that is based on patients’ biological characteristics. This, in turn, would increase the efficacy of drugs, lower the risks of adverse effects, and significantly contribute to achieving quick remission of symptoms.
A version of this article appeared on Medscape.com. This article was translated from Univadis Italy.
Don’t wait for patients to bring up their GI symptoms
Nearly three-quarters of Americans would wait before discussing GI symptoms with a health care provider if their bowel frequency or symptoms changed, with more than a quarter overall waiting for symptoms to become severe, according to a new survey from the American Gastroenterological Association.
Nearly 40% of people said GI symptoms had disrupted everyday activities such as exercising, running errands, and spending time with family or friends, but despite these disruptions, 30% of people said they would only discuss their bowel-related concerns if their doctor brought it up first. In response, the AGA launched “Trust Your Gut,” an awareness campaign aimed at shortening the time from the onset of bowel symptoms to discussions with health care providers.
“So many patients are either fearful or embarrassed about discussing their digestive symptoms such that they delay care unless the health care provider brings it up,” said Rajeev Jain, MD, a gastroenterologist with Texas Digestive Disease Consultants, AGA patient education adviser and a Trust Your Gut spokesperson.
“This potential delay could be detrimental in some cases, such as bleeding related to colon cancer,” he said. “If diagnosed sooner, an operation or chemotherapy could lead to treatment and a cure in those cases, versus advanced cancer that may be incurable.”
The AGA Trust Your Gut survey, conducted by Kelton Global during May 9-11, 2022, included 1,010 respondents from a nationally representative sample of U.S. adults.
Struggling with the issue
About 28% of respondents said they would see a clinician immediately if their bowel frequency or symptoms changed. However, 72% said they would wait, and on top of that, 27% said they would wait until the condition became severe or didn’t resolve over time. Women were more likely than men to say they would wait, at 72% versus 64%.
Overall, 39% of respondents said bowel issues have stopped them from doing some type of activity in the past year. Men were more likely than women to say that bowel issues have affected their ability to do an activity, at 44% versus 35%.
“Typically, when it comes to functional or motility disorders or bowel dysfunction, we tend to see a higher prevalence in women, so this was somewhat surprising to see,” said Andrea Shin, MD, a gastroenterology specialist and assistant professor of medicine at Indiana University, Indianapolis, and AGA patient education adviser designate.
“Part of this difference may be related to the communication barrier and how sex or gender affects that relationship between a clinician and a patient,” she said.
The reasons for patients’ reluctance varies, but themes of uncertainty and embarrassment are prevalent. About 33% said they’re not sure whether the symptoms are a problem, 31% said they hope the symptoms improve on their own, 23% said it’s embarrassing, and 12% don’t know what to tell the doctor. Men were more likely than women to say they don’t know what to say to a doctor about their symptoms, at 15% versus 9%.
Starting the conversation
From a young age, many respondents were raised to avoid the topic of bowel issues. About 23% said their parents encouraged them not to mention bathroom-related health issues, and 10% said they didn’t talk about bowel issues at all. Another 32% said they could talk about it but had to use code words, such as “go to the bathroom” or “potty.”
“What this highlights is that patients are culturally taught not to talk about their digestive tract, or they’re embarrassed or uncertain,” Dr. Jain said. “At the end of the day, we need to destigmatize discussions about digestive function and normalize it as part of overall health.”
The survey respondents said they’d feel most comfortable talking about bowel issues with doctors (63%) and nurses (41%), as well as a significant other (44%), parent (32%), or friend (27%). Women were more likely than men to feel comfortable turning to a nurse practitioner or physician’s assistant (47% versus 35%) or a friend (30% versus 24%).
To feel more comfortable with these conversations, 42% of survey participants said they would like their doctor or clinician to describe what’s normal. About 30% want to know the appropriate terms to describe their situation.
Health care providers should also consider the cultural and social factors that may affect a patient’s disease experience, as well as how they interact with the health care system, Shin said.
“Understanding these differences might help us to better engage with a community that is diverse,” she said. “In general, we also need to be more proactive about drawing these conversations out of patients, who may not mention it unless we ask because they find it so personal.”
The AGA Trust Your Gut campaign is supported by a sponsorship from Janssen. Dr. Jain and Dr. Shin reported to relevant disclosures.
Help your patients learn more by encouraging them to visit https://patient.gastro.org/trust-your-gut/.
Nearly three-quarters of Americans would wait before discussing GI symptoms with a health care provider if their bowel frequency or symptoms changed, with more than a quarter overall waiting for symptoms to become severe, according to a new survey from the American Gastroenterological Association.
Nearly 40% of people said GI symptoms had disrupted everyday activities such as exercising, running errands, and spending time with family or friends, but despite these disruptions, 30% of people said they would only discuss their bowel-related concerns if their doctor brought it up first. In response, the AGA launched “Trust Your Gut,” an awareness campaign aimed at shortening the time from the onset of bowel symptoms to discussions with health care providers.
“So many patients are either fearful or embarrassed about discussing their digestive symptoms such that they delay care unless the health care provider brings it up,” said Rajeev Jain, MD, a gastroenterologist with Texas Digestive Disease Consultants, AGA patient education adviser and a Trust Your Gut spokesperson.
“This potential delay could be detrimental in some cases, such as bleeding related to colon cancer,” he said. “If diagnosed sooner, an operation or chemotherapy could lead to treatment and a cure in those cases, versus advanced cancer that may be incurable.”
The AGA Trust Your Gut survey, conducted by Kelton Global during May 9-11, 2022, included 1,010 respondents from a nationally representative sample of U.S. adults.
Struggling with the issue
About 28% of respondents said they would see a clinician immediately if their bowel frequency or symptoms changed. However, 72% said they would wait, and on top of that, 27% said they would wait until the condition became severe or didn’t resolve over time. Women were more likely than men to say they would wait, at 72% versus 64%.
Overall, 39% of respondents said bowel issues have stopped them from doing some type of activity in the past year. Men were more likely than women to say that bowel issues have affected their ability to do an activity, at 44% versus 35%.
“Typically, when it comes to functional or motility disorders or bowel dysfunction, we tend to see a higher prevalence in women, so this was somewhat surprising to see,” said Andrea Shin, MD, a gastroenterology specialist and assistant professor of medicine at Indiana University, Indianapolis, and AGA patient education adviser designate.
“Part of this difference may be related to the communication barrier and how sex or gender affects that relationship between a clinician and a patient,” she said.
The reasons for patients’ reluctance varies, but themes of uncertainty and embarrassment are prevalent. About 33% said they’re not sure whether the symptoms are a problem, 31% said they hope the symptoms improve on their own, 23% said it’s embarrassing, and 12% don’t know what to tell the doctor. Men were more likely than women to say they don’t know what to say to a doctor about their symptoms, at 15% versus 9%.
Starting the conversation
From a young age, many respondents were raised to avoid the topic of bowel issues. About 23% said their parents encouraged them not to mention bathroom-related health issues, and 10% said they didn’t talk about bowel issues at all. Another 32% said they could talk about it but had to use code words, such as “go to the bathroom” or “potty.”
“What this highlights is that patients are culturally taught not to talk about their digestive tract, or they’re embarrassed or uncertain,” Dr. Jain said. “At the end of the day, we need to destigmatize discussions about digestive function and normalize it as part of overall health.”
The survey respondents said they’d feel most comfortable talking about bowel issues with doctors (63%) and nurses (41%), as well as a significant other (44%), parent (32%), or friend (27%). Women were more likely than men to feel comfortable turning to a nurse practitioner or physician’s assistant (47% versus 35%) or a friend (30% versus 24%).
To feel more comfortable with these conversations, 42% of survey participants said they would like their doctor or clinician to describe what’s normal. About 30% want to know the appropriate terms to describe their situation.
Health care providers should also consider the cultural and social factors that may affect a patient’s disease experience, as well as how they interact with the health care system, Shin said.
“Understanding these differences might help us to better engage with a community that is diverse,” she said. “In general, we also need to be more proactive about drawing these conversations out of patients, who may not mention it unless we ask because they find it so personal.”
The AGA Trust Your Gut campaign is supported by a sponsorship from Janssen. Dr. Jain and Dr. Shin reported to relevant disclosures.
Help your patients learn more by encouraging them to visit https://patient.gastro.org/trust-your-gut/.
Nearly three-quarters of Americans would wait before discussing GI symptoms with a health care provider if their bowel frequency or symptoms changed, with more than a quarter overall waiting for symptoms to become severe, according to a new survey from the American Gastroenterological Association.
Nearly 40% of people said GI symptoms had disrupted everyday activities such as exercising, running errands, and spending time with family or friends, but despite these disruptions, 30% of people said they would only discuss their bowel-related concerns if their doctor brought it up first. In response, the AGA launched “Trust Your Gut,” an awareness campaign aimed at shortening the time from the onset of bowel symptoms to discussions with health care providers.
“So many patients are either fearful or embarrassed about discussing their digestive symptoms such that they delay care unless the health care provider brings it up,” said Rajeev Jain, MD, a gastroenterologist with Texas Digestive Disease Consultants, AGA patient education adviser and a Trust Your Gut spokesperson.
“This potential delay could be detrimental in some cases, such as bleeding related to colon cancer,” he said. “If diagnosed sooner, an operation or chemotherapy could lead to treatment and a cure in those cases, versus advanced cancer that may be incurable.”
The AGA Trust Your Gut survey, conducted by Kelton Global during May 9-11, 2022, included 1,010 respondents from a nationally representative sample of U.S. adults.
Struggling with the issue
About 28% of respondents said they would see a clinician immediately if their bowel frequency or symptoms changed. However, 72% said they would wait, and on top of that, 27% said they would wait until the condition became severe or didn’t resolve over time. Women were more likely than men to say they would wait, at 72% versus 64%.
Overall, 39% of respondents said bowel issues have stopped them from doing some type of activity in the past year. Men were more likely than women to say that bowel issues have affected their ability to do an activity, at 44% versus 35%.
“Typically, when it comes to functional or motility disorders or bowel dysfunction, we tend to see a higher prevalence in women, so this was somewhat surprising to see,” said Andrea Shin, MD, a gastroenterology specialist and assistant professor of medicine at Indiana University, Indianapolis, and AGA patient education adviser designate.
“Part of this difference may be related to the communication barrier and how sex or gender affects that relationship between a clinician and a patient,” she said.
The reasons for patients’ reluctance varies, but themes of uncertainty and embarrassment are prevalent. About 33% said they’re not sure whether the symptoms are a problem, 31% said they hope the symptoms improve on their own, 23% said it’s embarrassing, and 12% don’t know what to tell the doctor. Men were more likely than women to say they don’t know what to say to a doctor about their symptoms, at 15% versus 9%.
Starting the conversation
From a young age, many respondents were raised to avoid the topic of bowel issues. About 23% said their parents encouraged them not to mention bathroom-related health issues, and 10% said they didn’t talk about bowel issues at all. Another 32% said they could talk about it but had to use code words, such as “go to the bathroom” or “potty.”
“What this highlights is that patients are culturally taught not to talk about their digestive tract, or they’re embarrassed or uncertain,” Dr. Jain said. “At the end of the day, we need to destigmatize discussions about digestive function and normalize it as part of overall health.”
The survey respondents said they’d feel most comfortable talking about bowel issues with doctors (63%) and nurses (41%), as well as a significant other (44%), parent (32%), or friend (27%). Women were more likely than men to feel comfortable turning to a nurse practitioner or physician’s assistant (47% versus 35%) or a friend (30% versus 24%).
To feel more comfortable with these conversations, 42% of survey participants said they would like their doctor or clinician to describe what’s normal. About 30% want to know the appropriate terms to describe their situation.
Health care providers should also consider the cultural and social factors that may affect a patient’s disease experience, as well as how they interact with the health care system, Shin said.
“Understanding these differences might help us to better engage with a community that is diverse,” she said. “In general, we also need to be more proactive about drawing these conversations out of patients, who may not mention it unless we ask because they find it so personal.”
The AGA Trust Your Gut campaign is supported by a sponsorship from Janssen. Dr. Jain and Dr. Shin reported to relevant disclosures.
Help your patients learn more by encouraging them to visit https://patient.gastro.org/trust-your-gut/.
VA Fast-Tracks Hiring to Address Critical Shortages
In an intensive push to fill acute workforce shortages, the US Department of Veterans Affairs (VA) is holding a “national onboarding surge event” the week of November 14. The goal is to get people who have already said yes to a job in the VA on that job more quickly. Every VA facility has been asked to submit a list of the highest-priority candidates, regardless of the position.
One of the most pressing reasons for getting more workers into the pipeline faster is that more and more veterans are entering VA care. As of October 1, tens of thousands of veterans will be eligible for VA health care, thanks to the Sergeant First Class Heath Robinson Honoring our Promise to Address Comprehensive Toxics Act of 2022 (PACT Act), passed in August, which expanded benefits for post-9/11 service members with illnesses due to toxic exposures.
Another reason is the need to fill the gaps left by attrition. In an October 19 press briefing, VA Undersecretary for Health Shereef Elnahal said the agency needs to hire about 52,000 employees per year just to keep up with the rate of health care professionals (HCPs) leaving the agency. At a September breakfast meeting with the Defense Writers Group, VA Secretary Denis McDonough said July 2022 marked the first month this year that the VA hired more nurses than it lost to retirement. He said the VA needs to hire 45,000 nurses over the next 3 years to keep up with attrition and growing demand for veteran care.
“We have to do a better job on hiring,” McDonough said. Streamlining the process is a major goal. Hiring rules loosened during the pandemic have since tightened back up. He pointed out that in many cases, the VA takes 90 to 100 days to onboard candidates and called the long-drawn-out process “being dragged through a bureaucratic morass.” During that time, he said, “They’re not being paid, they’re filling out paperwork… That’s disastrous.” In his press briefing, Elnahal said “we lose folks after we’ve made the selection” because the process is so long.
Moreover, the agency has a critical shortage not only of HCPs but the human resources professionals needed to fast-track the hirees’ progress. McDonough called it a “supply chain issue.” “We have the lowest ratio of human resource professionals per employee in the federal government by a long shot.” Partly, he said, because “a lot of our people end up hired away to other federal agencies.”
McDonough said the VA is also interested in transitioning more active-duty service members with in-demand skills, certifications, and talent into the VA workforce. “Cross-walking active duty into VA service much more aggressively,” he said, is another way to “grow that supply of ready, deployable, trained personnel.” The PACT Act gives the VA new incentives to entice workers, such as expanded recruitment, retention bonuses, and student loan repayment. The VA already provides training to about 1500 nurse and nurse residency programs across the VA, McDonough said but has plans for expanding to 5 times its current scope. He also addressed the question of a looming physician shortage: “Roughly 7 in 10 doctors in the United States will have had some portion of their training in a VA facility. We have to maintain that training function going forward.” The VA trains doctors, he added, “better than anybody else.”
The onboarding event will serve as a “national signal that we take this priority very seriously,” Elnahal said. “This will be not only a chance to have a step function improvement in the number of folks on board, which is an urgent priority, but to also set the groundwork for the more longitudinal work that we will need to do to improve the hiring process.”
Bulking up the workforce, he said, is “still far and away among our first priorities. Because if we don’t get our hospitals and facility staffed, it’s going to be a really hard effort to make process on the other priorities.”
In an intensive push to fill acute workforce shortages, the US Department of Veterans Affairs (VA) is holding a “national onboarding surge event” the week of November 14. The goal is to get people who have already said yes to a job in the VA on that job more quickly. Every VA facility has been asked to submit a list of the highest-priority candidates, regardless of the position.
One of the most pressing reasons for getting more workers into the pipeline faster is that more and more veterans are entering VA care. As of October 1, tens of thousands of veterans will be eligible for VA health care, thanks to the Sergeant First Class Heath Robinson Honoring our Promise to Address Comprehensive Toxics Act of 2022 (PACT Act), passed in August, which expanded benefits for post-9/11 service members with illnesses due to toxic exposures.
Another reason is the need to fill the gaps left by attrition. In an October 19 press briefing, VA Undersecretary for Health Shereef Elnahal said the agency needs to hire about 52,000 employees per year just to keep up with the rate of health care professionals (HCPs) leaving the agency. At a September breakfast meeting with the Defense Writers Group, VA Secretary Denis McDonough said July 2022 marked the first month this year that the VA hired more nurses than it lost to retirement. He said the VA needs to hire 45,000 nurses over the next 3 years to keep up with attrition and growing demand for veteran care.
“We have to do a better job on hiring,” McDonough said. Streamlining the process is a major goal. Hiring rules loosened during the pandemic have since tightened back up. He pointed out that in many cases, the VA takes 90 to 100 days to onboard candidates and called the long-drawn-out process “being dragged through a bureaucratic morass.” During that time, he said, “They’re not being paid, they’re filling out paperwork… That’s disastrous.” In his press briefing, Elnahal said “we lose folks after we’ve made the selection” because the process is so long.
Moreover, the agency has a critical shortage not only of HCPs but the human resources professionals needed to fast-track the hirees’ progress. McDonough called it a “supply chain issue.” “We have the lowest ratio of human resource professionals per employee in the federal government by a long shot.” Partly, he said, because “a lot of our people end up hired away to other federal agencies.”
McDonough said the VA is also interested in transitioning more active-duty service members with in-demand skills, certifications, and talent into the VA workforce. “Cross-walking active duty into VA service much more aggressively,” he said, is another way to “grow that supply of ready, deployable, trained personnel.” The PACT Act gives the VA new incentives to entice workers, such as expanded recruitment, retention bonuses, and student loan repayment. The VA already provides training to about 1500 nurse and nurse residency programs across the VA, McDonough said but has plans for expanding to 5 times its current scope. He also addressed the question of a looming physician shortage: “Roughly 7 in 10 doctors in the United States will have had some portion of their training in a VA facility. We have to maintain that training function going forward.” The VA trains doctors, he added, “better than anybody else.”
The onboarding event will serve as a “national signal that we take this priority very seriously,” Elnahal said. “This will be not only a chance to have a step function improvement in the number of folks on board, which is an urgent priority, but to also set the groundwork for the more longitudinal work that we will need to do to improve the hiring process.”
Bulking up the workforce, he said, is “still far and away among our first priorities. Because if we don’t get our hospitals and facility staffed, it’s going to be a really hard effort to make process on the other priorities.”
In an intensive push to fill acute workforce shortages, the US Department of Veterans Affairs (VA) is holding a “national onboarding surge event” the week of November 14. The goal is to get people who have already said yes to a job in the VA on that job more quickly. Every VA facility has been asked to submit a list of the highest-priority candidates, regardless of the position.
One of the most pressing reasons for getting more workers into the pipeline faster is that more and more veterans are entering VA care. As of October 1, tens of thousands of veterans will be eligible for VA health care, thanks to the Sergeant First Class Heath Robinson Honoring our Promise to Address Comprehensive Toxics Act of 2022 (PACT Act), passed in August, which expanded benefits for post-9/11 service members with illnesses due to toxic exposures.
Another reason is the need to fill the gaps left by attrition. In an October 19 press briefing, VA Undersecretary for Health Shereef Elnahal said the agency needs to hire about 52,000 employees per year just to keep up with the rate of health care professionals (HCPs) leaving the agency. At a September breakfast meeting with the Defense Writers Group, VA Secretary Denis McDonough said July 2022 marked the first month this year that the VA hired more nurses than it lost to retirement. He said the VA needs to hire 45,000 nurses over the next 3 years to keep up with attrition and growing demand for veteran care.
“We have to do a better job on hiring,” McDonough said. Streamlining the process is a major goal. Hiring rules loosened during the pandemic have since tightened back up. He pointed out that in many cases, the VA takes 90 to 100 days to onboard candidates and called the long-drawn-out process “being dragged through a bureaucratic morass.” During that time, he said, “They’re not being paid, they’re filling out paperwork… That’s disastrous.” In his press briefing, Elnahal said “we lose folks after we’ve made the selection” because the process is so long.
Moreover, the agency has a critical shortage not only of HCPs but the human resources professionals needed to fast-track the hirees’ progress. McDonough called it a “supply chain issue.” “We have the lowest ratio of human resource professionals per employee in the federal government by a long shot.” Partly, he said, because “a lot of our people end up hired away to other federal agencies.”
McDonough said the VA is also interested in transitioning more active-duty service members with in-demand skills, certifications, and talent into the VA workforce. “Cross-walking active duty into VA service much more aggressively,” he said, is another way to “grow that supply of ready, deployable, trained personnel.” The PACT Act gives the VA new incentives to entice workers, such as expanded recruitment, retention bonuses, and student loan repayment. The VA already provides training to about 1500 nurse and nurse residency programs across the VA, McDonough said but has plans for expanding to 5 times its current scope. He also addressed the question of a looming physician shortage: “Roughly 7 in 10 doctors in the United States will have had some portion of their training in a VA facility. We have to maintain that training function going forward.” The VA trains doctors, he added, “better than anybody else.”
The onboarding event will serve as a “national signal that we take this priority very seriously,” Elnahal said. “This will be not only a chance to have a step function improvement in the number of folks on board, which is an urgent priority, but to also set the groundwork for the more longitudinal work that we will need to do to improve the hiring process.”
Bulking up the workforce, he said, is “still far and away among our first priorities. Because if we don’t get our hospitals and facility staffed, it’s going to be a really hard effort to make process on the other priorities.”
Recurrent urinary tract infections: What’s good prophylaxis?
For those affected, recurrent urinary tract infections (UTIs) are sometimes stressful. However, even an informative discussion about risk factors and the imparting of behavioral recommendations can be very helpful for many women. Antibiotic prophylaxis should only be considered once all nonantibiotic therapy options have been exhausted.
One in seven women suffers at least once a year from cystitis. Around a third of those women develop a further urinary tract infection 6-12 months after the first infection. A urinary tract infection is classified as recurrent if two symptomatic episodes have occurred within the last 6 months or if three episodes have occurred within the last 12 months.
There are many different approaches to reducing the recurrence rate of urinary tract infections, Daniel Klussmann and Florian Wagenlehner, MD, of the department and outpatient clinic for urology at the University of Giessen (Germany) wrote in DMW Klinischer Fortschritt. Aside from general information and advice,
Fluids and D-mannose
An individual consultation discussion is the most important nonantibiotic strategy. Studies have shown that this strategy alone can lower the frequency of recurrent UTIs. According to the authors, special education programs on the causes and behavioral measures are especially helpful. Included in these programs is the recommendation to drink a sufficient, but not excessive, amount of fluids: approximately 1.5 liters per day. In one randomized study, this level of consumption halved UTI frequency. However, drinking an excessive amount of fluids should also be avoided, otherwise the antimicrobial peptides present in the urine become overly diluted.
The regular consumption of fruit juice, especially of that from berries, is also beneficial, according to the authors. However, study results on long-term prevention using cranberry products are inconsistent, and they are not recommended in the updated guideline. Like cranberries, D-mannose also inhibits the fimbriae of the Escherichia coli bacteria and therefore the bacteria’s ability to bind to the bladder epithelium. The authors cite a study in which, following the intake of 2 g of D-mannose dissolved in a glass of water every day, the rate of urinary tract infections dropped significantly, compared with consumption of placebo.
Additional recommendations in the S3 guideline include various phytotherapeutic products such as bearberry leaves, nasturtium herb, or horseradish root, although studies on the comparability of phytotherapeutic agents are very difficult to execute, the authors conceded.
It is already known that there is a positive correlation (by a factor of 60) between the recurrence rate of UTIs and the frequency of sexual intercourse. Even with contraceptive methods (such as vaginal suppositories, diaphragms or condoms coated with spermicide, and intrauterine devices), the risk of urinary tract infections increases by a factor of 2-14. Sexual abstinence, even if temporary, can be a remedy. Evidence for the recommendation to urinate immediately after coitus is contradictory in the literature, however. Excessive intimate hygiene clearly damages the local protective environment.
Estrogen substitution beneficial
For postmenopausal women, there is also the option of local estriol substitution (0.5 mg/day) as another nonantibiotic method of prophylaxis. This treatment serves as therapy for vaginal atrophy and reduces both vaginal colonization with uropathogens and the vaginal pH level. The authors cite Scandinavian studies that detected no increase in the risk of breast cancer from the local application of estriol.
Furthermore, the current guidelines recommend oral immunostimulation with bacterial cell wall components from uropathogenic strains of E. coli (OM-89, Uro-Vaxom). The authors reported on two meta-studies in which the average recurrence rate was reduced by 39%, compared with placebo. In addition, the treatment time for breakthrough infections decreased significantly, and prevention with OM-89 could even be started during acute therapy. Also recommended is parenteral immunostimulation with inactivated pathogens (StroVac). Acupuncture as cutaneous immunostimulation has also displayed a positive protective effect.
Only when nonantibiotic therapy fails and the patient is under a high amount of psychological strain should antibiotic prophylaxis be initiated, according to the authors. A period of 3-6 months should be the target here. When choosing an antibiotic and before starting therapy, the corresponding pathogen should be confirmed through a urine culture, and resistance testing should be performed. On the other hand, single-use, postcoital antibiotic prevention could be an alternative, particularly for women in whom a correlation between recurrent UTIs and sexual intercourse has been suspected, the authors wrote.
This article was translated from Univadis Germany. A version appeared on Medscape.com.
For those affected, recurrent urinary tract infections (UTIs) are sometimes stressful. However, even an informative discussion about risk factors and the imparting of behavioral recommendations can be very helpful for many women. Antibiotic prophylaxis should only be considered once all nonantibiotic therapy options have been exhausted.
One in seven women suffers at least once a year from cystitis. Around a third of those women develop a further urinary tract infection 6-12 months after the first infection. A urinary tract infection is classified as recurrent if two symptomatic episodes have occurred within the last 6 months or if three episodes have occurred within the last 12 months.
There are many different approaches to reducing the recurrence rate of urinary tract infections, Daniel Klussmann and Florian Wagenlehner, MD, of the department and outpatient clinic for urology at the University of Giessen (Germany) wrote in DMW Klinischer Fortschritt. Aside from general information and advice,
Fluids and D-mannose
An individual consultation discussion is the most important nonantibiotic strategy. Studies have shown that this strategy alone can lower the frequency of recurrent UTIs. According to the authors, special education programs on the causes and behavioral measures are especially helpful. Included in these programs is the recommendation to drink a sufficient, but not excessive, amount of fluids: approximately 1.5 liters per day. In one randomized study, this level of consumption halved UTI frequency. However, drinking an excessive amount of fluids should also be avoided, otherwise the antimicrobial peptides present in the urine become overly diluted.
The regular consumption of fruit juice, especially of that from berries, is also beneficial, according to the authors. However, study results on long-term prevention using cranberry products are inconsistent, and they are not recommended in the updated guideline. Like cranberries, D-mannose also inhibits the fimbriae of the Escherichia coli bacteria and therefore the bacteria’s ability to bind to the bladder epithelium. The authors cite a study in which, following the intake of 2 g of D-mannose dissolved in a glass of water every day, the rate of urinary tract infections dropped significantly, compared with consumption of placebo.
Additional recommendations in the S3 guideline include various phytotherapeutic products such as bearberry leaves, nasturtium herb, or horseradish root, although studies on the comparability of phytotherapeutic agents are very difficult to execute, the authors conceded.
It is already known that there is a positive correlation (by a factor of 60) between the recurrence rate of UTIs and the frequency of sexual intercourse. Even with contraceptive methods (such as vaginal suppositories, diaphragms or condoms coated with spermicide, and intrauterine devices), the risk of urinary tract infections increases by a factor of 2-14. Sexual abstinence, even if temporary, can be a remedy. Evidence for the recommendation to urinate immediately after coitus is contradictory in the literature, however. Excessive intimate hygiene clearly damages the local protective environment.
Estrogen substitution beneficial
For postmenopausal women, there is also the option of local estriol substitution (0.5 mg/day) as another nonantibiotic method of prophylaxis. This treatment serves as therapy for vaginal atrophy and reduces both vaginal colonization with uropathogens and the vaginal pH level. The authors cite Scandinavian studies that detected no increase in the risk of breast cancer from the local application of estriol.
Furthermore, the current guidelines recommend oral immunostimulation with bacterial cell wall components from uropathogenic strains of E. coli (OM-89, Uro-Vaxom). The authors reported on two meta-studies in which the average recurrence rate was reduced by 39%, compared with placebo. In addition, the treatment time for breakthrough infections decreased significantly, and prevention with OM-89 could even be started during acute therapy. Also recommended is parenteral immunostimulation with inactivated pathogens (StroVac). Acupuncture as cutaneous immunostimulation has also displayed a positive protective effect.
Only when nonantibiotic therapy fails and the patient is under a high amount of psychological strain should antibiotic prophylaxis be initiated, according to the authors. A period of 3-6 months should be the target here. When choosing an antibiotic and before starting therapy, the corresponding pathogen should be confirmed through a urine culture, and resistance testing should be performed. On the other hand, single-use, postcoital antibiotic prevention could be an alternative, particularly for women in whom a correlation between recurrent UTIs and sexual intercourse has been suspected, the authors wrote.
This article was translated from Univadis Germany. A version appeared on Medscape.com.
For those affected, recurrent urinary tract infections (UTIs) are sometimes stressful. However, even an informative discussion about risk factors and the imparting of behavioral recommendations can be very helpful for many women. Antibiotic prophylaxis should only be considered once all nonantibiotic therapy options have been exhausted.
One in seven women suffers at least once a year from cystitis. Around a third of those women develop a further urinary tract infection 6-12 months after the first infection. A urinary tract infection is classified as recurrent if two symptomatic episodes have occurred within the last 6 months or if three episodes have occurred within the last 12 months.
There are many different approaches to reducing the recurrence rate of urinary tract infections, Daniel Klussmann and Florian Wagenlehner, MD, of the department and outpatient clinic for urology at the University of Giessen (Germany) wrote in DMW Klinischer Fortschritt. Aside from general information and advice,
Fluids and D-mannose
An individual consultation discussion is the most important nonantibiotic strategy. Studies have shown that this strategy alone can lower the frequency of recurrent UTIs. According to the authors, special education programs on the causes and behavioral measures are especially helpful. Included in these programs is the recommendation to drink a sufficient, but not excessive, amount of fluids: approximately 1.5 liters per day. In one randomized study, this level of consumption halved UTI frequency. However, drinking an excessive amount of fluids should also be avoided, otherwise the antimicrobial peptides present in the urine become overly diluted.
The regular consumption of fruit juice, especially of that from berries, is also beneficial, according to the authors. However, study results on long-term prevention using cranberry products are inconsistent, and they are not recommended in the updated guideline. Like cranberries, D-mannose also inhibits the fimbriae of the Escherichia coli bacteria and therefore the bacteria’s ability to bind to the bladder epithelium. The authors cite a study in which, following the intake of 2 g of D-mannose dissolved in a glass of water every day, the rate of urinary tract infections dropped significantly, compared with consumption of placebo.
Additional recommendations in the S3 guideline include various phytotherapeutic products such as bearberry leaves, nasturtium herb, or horseradish root, although studies on the comparability of phytotherapeutic agents are very difficult to execute, the authors conceded.
It is already known that there is a positive correlation (by a factor of 60) between the recurrence rate of UTIs and the frequency of sexual intercourse. Even with contraceptive methods (such as vaginal suppositories, diaphragms or condoms coated with spermicide, and intrauterine devices), the risk of urinary tract infections increases by a factor of 2-14. Sexual abstinence, even if temporary, can be a remedy. Evidence for the recommendation to urinate immediately after coitus is contradictory in the literature, however. Excessive intimate hygiene clearly damages the local protective environment.
Estrogen substitution beneficial
For postmenopausal women, there is also the option of local estriol substitution (0.5 mg/day) as another nonantibiotic method of prophylaxis. This treatment serves as therapy for vaginal atrophy and reduces both vaginal colonization with uropathogens and the vaginal pH level. The authors cite Scandinavian studies that detected no increase in the risk of breast cancer from the local application of estriol.
Furthermore, the current guidelines recommend oral immunostimulation with bacterial cell wall components from uropathogenic strains of E. coli (OM-89, Uro-Vaxom). The authors reported on two meta-studies in which the average recurrence rate was reduced by 39%, compared with placebo. In addition, the treatment time for breakthrough infections decreased significantly, and prevention with OM-89 could even be started during acute therapy. Also recommended is parenteral immunostimulation with inactivated pathogens (StroVac). Acupuncture as cutaneous immunostimulation has also displayed a positive protective effect.
Only when nonantibiotic therapy fails and the patient is under a high amount of psychological strain should antibiotic prophylaxis be initiated, according to the authors. A period of 3-6 months should be the target here. When choosing an antibiotic and before starting therapy, the corresponding pathogen should be confirmed through a urine culture, and resistance testing should be performed. On the other hand, single-use, postcoital antibiotic prevention could be an alternative, particularly for women in whom a correlation between recurrent UTIs and sexual intercourse has been suspected, the authors wrote.
This article was translated from Univadis Germany. A version appeared on Medscape.com.
FROM DMW KLINISCHER FORTSCHRITT
Metabolites may distinguish severe subtypes of PAH
, based on data from approximately 1,500 individuals.
The overall prognosis and therapeutic response for patients with pulmonary arterial hypertension associated with systemic sclerosis (SSc-PAH) tends to be worse than for patients with other types of PAH, such as idiopathic pulmonary arterial hypertension (IPAH), but the impact of different metabolite profiles among subtypes of disease has not been explored, wrote Mona Alotaibi, MD, of the University of California, San Diego, and colleagues.
“Recently, metabolic dysregulation has been proposed as a key mechanism by which IPAH and SSc-PAH differ and could control such disparities,” they noted. Clarifying the molecular mechanisms of SSc-PAH could inform management and treatment, they added.
In a study published in the journal Chest, the researchers sought to identify a bioactive lipid signature unique to SSc-PAH. They identified 400 patients with SSc-PAH and 1,082 with IPAH. An additional 100 patients with scleroderma but no PH and 44 patients with scleroderma who had PH were included for external validation. The mean ages of the patients with IPAH and SSc-PAH in the discovery and validation cohorts ranged from approximately 51 to 65 years; more than 75% of patients across the groups were women.
The researchers tested more than 700 bioactive lipid metabolites using liquid chromatography/mass spectrometry. They found five metabolites that distinguished SSc-PAH and IPAH that were significantly associated with markers of disease severity: 17-beta estradiol, novel Eic, nervonic acid, fatty acid esters of hydroxy fatty acids, and prostaglandin F2 alpha (PGF 2 alpha).
The biomarkers were increased in SSc-PAH patients compared to patients with SSC alone, which suggests that the biomarkers are related to PAH and not to scleroderma alone, the researchers noted.
In particular, nervonic acid was associated with worse functional capacity, in SSc-PAH patients, as were higher levels of 17-beta estradiol and prostaglandin F2 alpha. Also, 17-beta estradiol was associated with lower cardiac impairment (CI) and stroke volume index (SVI) in SSc-PAH patients, but higher SVI in IPAH patients. PGF 2 alpha was associated with lower CI and SVI and higher pulmonary vascular resistance in SSc-PAH and IPAH combined.
The study findings were limited by several factors including the inability to adjust for all potential confounders between IPAH and SSc-PAH, and the fact that a clear causal relationship could not be determined, the researchers noted. Inadequate statistical power to analyze SSc-PAH data was another limitation, and studies with detailed scleroderma phenotypes are needed to validate the results, they said.
However, the current study provides insight on the metabolic differences in SSc-PAH and the potential impact on disease pathology that may inform diagnosis, prognosis, and treatment strategies for SSc-PAH patients, they concluded.
The study was supported by the National Institutes of Health. Several individual investigators received support from organizations including the American Heart Association and the Chest Foundation, and from companies including Livanova, Equillium, Corvus, Bayer, and Actelion, but the authors had no relevant financial conflicts to disclose.
, based on data from approximately 1,500 individuals.
The overall prognosis and therapeutic response for patients with pulmonary arterial hypertension associated with systemic sclerosis (SSc-PAH) tends to be worse than for patients with other types of PAH, such as idiopathic pulmonary arterial hypertension (IPAH), but the impact of different metabolite profiles among subtypes of disease has not been explored, wrote Mona Alotaibi, MD, of the University of California, San Diego, and colleagues.
“Recently, metabolic dysregulation has been proposed as a key mechanism by which IPAH and SSc-PAH differ and could control such disparities,” they noted. Clarifying the molecular mechanisms of SSc-PAH could inform management and treatment, they added.
In a study published in the journal Chest, the researchers sought to identify a bioactive lipid signature unique to SSc-PAH. They identified 400 patients with SSc-PAH and 1,082 with IPAH. An additional 100 patients with scleroderma but no PH and 44 patients with scleroderma who had PH were included for external validation. The mean ages of the patients with IPAH and SSc-PAH in the discovery and validation cohorts ranged from approximately 51 to 65 years; more than 75% of patients across the groups were women.
The researchers tested more than 700 bioactive lipid metabolites using liquid chromatography/mass spectrometry. They found five metabolites that distinguished SSc-PAH and IPAH that were significantly associated with markers of disease severity: 17-beta estradiol, novel Eic, nervonic acid, fatty acid esters of hydroxy fatty acids, and prostaglandin F2 alpha (PGF 2 alpha).
The biomarkers were increased in SSc-PAH patients compared to patients with SSC alone, which suggests that the biomarkers are related to PAH and not to scleroderma alone, the researchers noted.
In particular, nervonic acid was associated with worse functional capacity, in SSc-PAH patients, as were higher levels of 17-beta estradiol and prostaglandin F2 alpha. Also, 17-beta estradiol was associated with lower cardiac impairment (CI) and stroke volume index (SVI) in SSc-PAH patients, but higher SVI in IPAH patients. PGF 2 alpha was associated with lower CI and SVI and higher pulmonary vascular resistance in SSc-PAH and IPAH combined.
The study findings were limited by several factors including the inability to adjust for all potential confounders between IPAH and SSc-PAH, and the fact that a clear causal relationship could not be determined, the researchers noted. Inadequate statistical power to analyze SSc-PAH data was another limitation, and studies with detailed scleroderma phenotypes are needed to validate the results, they said.
However, the current study provides insight on the metabolic differences in SSc-PAH and the potential impact on disease pathology that may inform diagnosis, prognosis, and treatment strategies for SSc-PAH patients, they concluded.
The study was supported by the National Institutes of Health. Several individual investigators received support from organizations including the American Heart Association and the Chest Foundation, and from companies including Livanova, Equillium, Corvus, Bayer, and Actelion, but the authors had no relevant financial conflicts to disclose.
, based on data from approximately 1,500 individuals.
The overall prognosis and therapeutic response for patients with pulmonary arterial hypertension associated with systemic sclerosis (SSc-PAH) tends to be worse than for patients with other types of PAH, such as idiopathic pulmonary arterial hypertension (IPAH), but the impact of different metabolite profiles among subtypes of disease has not been explored, wrote Mona Alotaibi, MD, of the University of California, San Diego, and colleagues.
“Recently, metabolic dysregulation has been proposed as a key mechanism by which IPAH and SSc-PAH differ and could control such disparities,” they noted. Clarifying the molecular mechanisms of SSc-PAH could inform management and treatment, they added.
In a study published in the journal Chest, the researchers sought to identify a bioactive lipid signature unique to SSc-PAH. They identified 400 patients with SSc-PAH and 1,082 with IPAH. An additional 100 patients with scleroderma but no PH and 44 patients with scleroderma who had PH were included for external validation. The mean ages of the patients with IPAH and SSc-PAH in the discovery and validation cohorts ranged from approximately 51 to 65 years; more than 75% of patients across the groups were women.
The researchers tested more than 700 bioactive lipid metabolites using liquid chromatography/mass spectrometry. They found five metabolites that distinguished SSc-PAH and IPAH that were significantly associated with markers of disease severity: 17-beta estradiol, novel Eic, nervonic acid, fatty acid esters of hydroxy fatty acids, and prostaglandin F2 alpha (PGF 2 alpha).
The biomarkers were increased in SSc-PAH patients compared to patients with SSC alone, which suggests that the biomarkers are related to PAH and not to scleroderma alone, the researchers noted.
In particular, nervonic acid was associated with worse functional capacity, in SSc-PAH patients, as were higher levels of 17-beta estradiol and prostaglandin F2 alpha. Also, 17-beta estradiol was associated with lower cardiac impairment (CI) and stroke volume index (SVI) in SSc-PAH patients, but higher SVI in IPAH patients. PGF 2 alpha was associated with lower CI and SVI and higher pulmonary vascular resistance in SSc-PAH and IPAH combined.
The study findings were limited by several factors including the inability to adjust for all potential confounders between IPAH and SSc-PAH, and the fact that a clear causal relationship could not be determined, the researchers noted. Inadequate statistical power to analyze SSc-PAH data was another limitation, and studies with detailed scleroderma phenotypes are needed to validate the results, they said.
However, the current study provides insight on the metabolic differences in SSc-PAH and the potential impact on disease pathology that may inform diagnosis, prognosis, and treatment strategies for SSc-PAH patients, they concluded.
The study was supported by the National Institutes of Health. Several individual investigators received support from organizations including the American Heart Association and the Chest Foundation, and from companies including Livanova, Equillium, Corvus, Bayer, and Actelion, but the authors had no relevant financial conflicts to disclose.
FROM CHEST
Sexual assault–related visits to the ED are on the rise
Data from the Federal Bureau of Investigation show an increase in reported rapes and sexual assaults (SAs) since 2006, and studies of victims show an increased risk of conditions such as suicidal ideation, PTSD, depression, substance use, and chronic conditions, write Emily L. Vogt of the University of Michigan, Ann Arbor, and colleagues.
However, trends and disparities in ED use by adults seeking care following SA have not been explored, they said.
For a study that was published in JAMA Network Open, researchers reviewed data from the Nationwide Emergency Department Sample (NEDS), a large, nationally representative database managed by the Agency for Healthcare Research and Quality. The dataset consisted of 120 million to 143 million weighted ED visits reported annually from 2006 through 2016. The study population included adults aged 18-65 years who had made an ED visit that was recorded in the NEDS and that was coded as an SA. SA was defined using ICD-9 codes until the fourth quarter of 2015, at which time ICD-10 codes came into use.
Overall, the number of SA-related ED visits increased by 1,533.0% during the study period, from 3,607 in 2006 to 55,296 in 2019. The average annual percentage change was 23.0% (P < .001). The greatest increase occurred from 2015 to 2016, when annual visits increased from 17,709 to 47,732. This increase likely reflected the updated ICD-10 codes, in which there are categories for suspected adult rape, confirmed adult rape, and adult forced sexual exploitation, the researchers note.
Patients presenting to the ED after an SA were mainly women (91.5%). Individuals aged 18-25 years accounted for nearly half of the presentations. Individuals in the lowest and second-lowest income quartiles also were overrepresented.
Despite the increased presentation to EDs, admission rates for SA decreased, from 12.6% to 4.3%, the researchers note. Patients who were older and were insured through Medicaid were more likely to be admitted than persons of other demographic groups.
The researchers also found that increases in ED presentations outpaced increases in SA reports to law enforcement. They compared the ED trends with FBI-reported rapes/SAs from 2015 to 2019 and found increases of 7% and 22% during the times of ICD-9 and ICD-10 codes, respectively. However, in 2019, the number of SA survivors who sought ED care remained below the number who reported to law enforcement (55,296 vs. 139,815, as determined on the basis of revised SA definitions).
“Although the association between increased coding specificity and documentation of SA is still unclear, ICD-10 likely contributed to increased ED documentation of SA,” but the data show steady increases that are independent of the coding change, the researchers write.
The study findings were limited by several factors, including the potential for multiple representations of patients, coding errors associated with the NEDS database, and the reliance on voluntary reports in the NEDS and FBI datasets, the researchers note. The results were strengthened by the large, diverse sample size and by the inclusion of hospital admissions and crime data for comparison, they say.
“As few as 21% of survivors seek medical care after SA, meaning that the survivors captured in this study represent a fraction of total SA-related care need,” the researchers write. “Our finding that most SA ED visits are by young, female, and low-income survivors can inform policy changes to better support these individuals,” which could include the development of outpatient and longitudinal care settings to better serve these populations, they conclude.
Better understanding not only of the trends underlying SA reporting but also of the demographics of survivors who seek treatment and evaluation after SA is vital, said Robert Glatter, MD, in an interview.
“Being able to better understand how social and societal movements affect a patient’s comfort in reporting an SA is vital in tracking the numbers of people who seek care in the ED,” said Dr. Glatter, an emergency medicine physician at Lenox Hill Hospital at Northwell Health, New York, and also of Hofstra University, Hempstead, N.Y.
Dr. Glatter said he was not surprised by the significant increase in sexual assault presentations, especially in light of increased awareness and the influence of the #MeToo movement and other social justice movements over the past decade.
“While I believe that victims of sexual violence may now feel more empowered to report an assault, the volume of SA that go unreported remains a serious public health issue and concern” in the United States and globally, he emphasized.
A key message from the current study is that there is a need for investment in “compassionate and comprehensive care for all survivors of SA,” Dr. Glatter said. “This includes recognition of the extensive mental health consequences of SA that can lead to not only depression, PTSD, and anxiety but also to suicidal ideation and suicide. The longer-term medical effects become life altering, permeating families and future generations,” he emphasized.
“As a society, we must also place a strong emphasis on caring for all SA survivors, but particularly those who come from economically or socially disadvantaged backgrounds who are uninsured or underinsured,” Dr. Glatter said. Issues of race, gender identity, and sexual identity among SA survivors also must be taken into consideration, he added.
“We need to better understand how our health care system can provide more nuanced follow-up care and reporting for survivors in outpatient settings. … Making access easier, while ensuring confidentiality, will allow more survivors of SA to seek treatment and care,” he said. “We also need to understand how using forensic nurses in this capacity, and beyond the ED, can better serve minority and racially diverse communities” and to increase the recruitment and training of such specialized nurses to care for SA victims, Dr. Glatter noted.
The study was supported by internal funding from the University of Michigan and the department of obstetrics and gynecology. Corresponding author Erica C. Marsh, MD, has received personal fees from Myovant Sciences and Pfizer unrelated to the current study. Dr. Glatter has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Data from the Federal Bureau of Investigation show an increase in reported rapes and sexual assaults (SAs) since 2006, and studies of victims show an increased risk of conditions such as suicidal ideation, PTSD, depression, substance use, and chronic conditions, write Emily L. Vogt of the University of Michigan, Ann Arbor, and colleagues.
However, trends and disparities in ED use by adults seeking care following SA have not been explored, they said.
For a study that was published in JAMA Network Open, researchers reviewed data from the Nationwide Emergency Department Sample (NEDS), a large, nationally representative database managed by the Agency for Healthcare Research and Quality. The dataset consisted of 120 million to 143 million weighted ED visits reported annually from 2006 through 2016. The study population included adults aged 18-65 years who had made an ED visit that was recorded in the NEDS and that was coded as an SA. SA was defined using ICD-9 codes until the fourth quarter of 2015, at which time ICD-10 codes came into use.
Overall, the number of SA-related ED visits increased by 1,533.0% during the study period, from 3,607 in 2006 to 55,296 in 2019. The average annual percentage change was 23.0% (P < .001). The greatest increase occurred from 2015 to 2016, when annual visits increased from 17,709 to 47,732. This increase likely reflected the updated ICD-10 codes, in which there are categories for suspected adult rape, confirmed adult rape, and adult forced sexual exploitation, the researchers note.
Patients presenting to the ED after an SA were mainly women (91.5%). Individuals aged 18-25 years accounted for nearly half of the presentations. Individuals in the lowest and second-lowest income quartiles also were overrepresented.
Despite the increased presentation to EDs, admission rates for SA decreased, from 12.6% to 4.3%, the researchers note. Patients who were older and were insured through Medicaid were more likely to be admitted than persons of other demographic groups.
The researchers also found that increases in ED presentations outpaced increases in SA reports to law enforcement. They compared the ED trends with FBI-reported rapes/SAs from 2015 to 2019 and found increases of 7% and 22% during the times of ICD-9 and ICD-10 codes, respectively. However, in 2019, the number of SA survivors who sought ED care remained below the number who reported to law enforcement (55,296 vs. 139,815, as determined on the basis of revised SA definitions).
“Although the association between increased coding specificity and documentation of SA is still unclear, ICD-10 likely contributed to increased ED documentation of SA,” but the data show steady increases that are independent of the coding change, the researchers write.
The study findings were limited by several factors, including the potential for multiple representations of patients, coding errors associated with the NEDS database, and the reliance on voluntary reports in the NEDS and FBI datasets, the researchers note. The results were strengthened by the large, diverse sample size and by the inclusion of hospital admissions and crime data for comparison, they say.
“As few as 21% of survivors seek medical care after SA, meaning that the survivors captured in this study represent a fraction of total SA-related care need,” the researchers write. “Our finding that most SA ED visits are by young, female, and low-income survivors can inform policy changes to better support these individuals,” which could include the development of outpatient and longitudinal care settings to better serve these populations, they conclude.
Better understanding not only of the trends underlying SA reporting but also of the demographics of survivors who seek treatment and evaluation after SA is vital, said Robert Glatter, MD, in an interview.
“Being able to better understand how social and societal movements affect a patient’s comfort in reporting an SA is vital in tracking the numbers of people who seek care in the ED,” said Dr. Glatter, an emergency medicine physician at Lenox Hill Hospital at Northwell Health, New York, and also of Hofstra University, Hempstead, N.Y.
Dr. Glatter said he was not surprised by the significant increase in sexual assault presentations, especially in light of increased awareness and the influence of the #MeToo movement and other social justice movements over the past decade.
“While I believe that victims of sexual violence may now feel more empowered to report an assault, the volume of SA that go unreported remains a serious public health issue and concern” in the United States and globally, he emphasized.
A key message from the current study is that there is a need for investment in “compassionate and comprehensive care for all survivors of SA,” Dr. Glatter said. “This includes recognition of the extensive mental health consequences of SA that can lead to not only depression, PTSD, and anxiety but also to suicidal ideation and suicide. The longer-term medical effects become life altering, permeating families and future generations,” he emphasized.
“As a society, we must also place a strong emphasis on caring for all SA survivors, but particularly those who come from economically or socially disadvantaged backgrounds who are uninsured or underinsured,” Dr. Glatter said. Issues of race, gender identity, and sexual identity among SA survivors also must be taken into consideration, he added.
“We need to better understand how our health care system can provide more nuanced follow-up care and reporting for survivors in outpatient settings. … Making access easier, while ensuring confidentiality, will allow more survivors of SA to seek treatment and care,” he said. “We also need to understand how using forensic nurses in this capacity, and beyond the ED, can better serve minority and racially diverse communities” and to increase the recruitment and training of such specialized nurses to care for SA victims, Dr. Glatter noted.
The study was supported by internal funding from the University of Michigan and the department of obstetrics and gynecology. Corresponding author Erica C. Marsh, MD, has received personal fees from Myovant Sciences and Pfizer unrelated to the current study. Dr. Glatter has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Data from the Federal Bureau of Investigation show an increase in reported rapes and sexual assaults (SAs) since 2006, and studies of victims show an increased risk of conditions such as suicidal ideation, PTSD, depression, substance use, and chronic conditions, write Emily L. Vogt of the University of Michigan, Ann Arbor, and colleagues.
However, trends and disparities in ED use by adults seeking care following SA have not been explored, they said.
For a study that was published in JAMA Network Open, researchers reviewed data from the Nationwide Emergency Department Sample (NEDS), a large, nationally representative database managed by the Agency for Healthcare Research and Quality. The dataset consisted of 120 million to 143 million weighted ED visits reported annually from 2006 through 2016. The study population included adults aged 18-65 years who had made an ED visit that was recorded in the NEDS and that was coded as an SA. SA was defined using ICD-9 codes until the fourth quarter of 2015, at which time ICD-10 codes came into use.
Overall, the number of SA-related ED visits increased by 1,533.0% during the study period, from 3,607 in 2006 to 55,296 in 2019. The average annual percentage change was 23.0% (P < .001). The greatest increase occurred from 2015 to 2016, when annual visits increased from 17,709 to 47,732. This increase likely reflected the updated ICD-10 codes, in which there are categories for suspected adult rape, confirmed adult rape, and adult forced sexual exploitation, the researchers note.
Patients presenting to the ED after an SA were mainly women (91.5%). Individuals aged 18-25 years accounted for nearly half of the presentations. Individuals in the lowest and second-lowest income quartiles also were overrepresented.
Despite the increased presentation to EDs, admission rates for SA decreased, from 12.6% to 4.3%, the researchers note. Patients who were older and were insured through Medicaid were more likely to be admitted than persons of other demographic groups.
The researchers also found that increases in ED presentations outpaced increases in SA reports to law enforcement. They compared the ED trends with FBI-reported rapes/SAs from 2015 to 2019 and found increases of 7% and 22% during the times of ICD-9 and ICD-10 codes, respectively. However, in 2019, the number of SA survivors who sought ED care remained below the number who reported to law enforcement (55,296 vs. 139,815, as determined on the basis of revised SA definitions).
“Although the association between increased coding specificity and documentation of SA is still unclear, ICD-10 likely contributed to increased ED documentation of SA,” but the data show steady increases that are independent of the coding change, the researchers write.
The study findings were limited by several factors, including the potential for multiple representations of patients, coding errors associated with the NEDS database, and the reliance on voluntary reports in the NEDS and FBI datasets, the researchers note. The results were strengthened by the large, diverse sample size and by the inclusion of hospital admissions and crime data for comparison, they say.
“As few as 21% of survivors seek medical care after SA, meaning that the survivors captured in this study represent a fraction of total SA-related care need,” the researchers write. “Our finding that most SA ED visits are by young, female, and low-income survivors can inform policy changes to better support these individuals,” which could include the development of outpatient and longitudinal care settings to better serve these populations, they conclude.
Better understanding not only of the trends underlying SA reporting but also of the demographics of survivors who seek treatment and evaluation after SA is vital, said Robert Glatter, MD, in an interview.
“Being able to better understand how social and societal movements affect a patient’s comfort in reporting an SA is vital in tracking the numbers of people who seek care in the ED,” said Dr. Glatter, an emergency medicine physician at Lenox Hill Hospital at Northwell Health, New York, and also of Hofstra University, Hempstead, N.Y.
Dr. Glatter said he was not surprised by the significant increase in sexual assault presentations, especially in light of increased awareness and the influence of the #MeToo movement and other social justice movements over the past decade.
“While I believe that victims of sexual violence may now feel more empowered to report an assault, the volume of SA that go unreported remains a serious public health issue and concern” in the United States and globally, he emphasized.
A key message from the current study is that there is a need for investment in “compassionate and comprehensive care for all survivors of SA,” Dr. Glatter said. “This includes recognition of the extensive mental health consequences of SA that can lead to not only depression, PTSD, and anxiety but also to suicidal ideation and suicide. The longer-term medical effects become life altering, permeating families and future generations,” he emphasized.
“As a society, we must also place a strong emphasis on caring for all SA survivors, but particularly those who come from economically or socially disadvantaged backgrounds who are uninsured or underinsured,” Dr. Glatter said. Issues of race, gender identity, and sexual identity among SA survivors also must be taken into consideration, he added.
“We need to better understand how our health care system can provide more nuanced follow-up care and reporting for survivors in outpatient settings. … Making access easier, while ensuring confidentiality, will allow more survivors of SA to seek treatment and care,” he said. “We also need to understand how using forensic nurses in this capacity, and beyond the ED, can better serve minority and racially diverse communities” and to increase the recruitment and training of such specialized nurses to care for SA victims, Dr. Glatter noted.
The study was supported by internal funding from the University of Michigan and the department of obstetrics and gynecology. Corresponding author Erica C. Marsh, MD, has received personal fees from Myovant Sciences and Pfizer unrelated to the current study. Dr. Glatter has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM JAMA NETWORK OPEN
Emergency contraception for psychiatric patients
Ms. A, age 22, is a college student who presents for an initial psychiatric evaluation. Her body mass index (BMI) is 20 (normal range: 18.5 to 24.9), and her medical history is positive only for childhood asthma. She has been treated for major depressive disorder with venlafaxine by her previous psychiatrist. While this antidepressant has been effective for some symptoms, she has experienced adverse effects and is interested in a different medication. During the evaluation, Ms. A remarks that she had a “scare” last night when the condom broke while having sex with her boyfriend. She says that she is interested in having children at some point, but not at present; she is concerned that getting pregnant now would cause her depression to “spiral out of control.”
Unwanted or mistimed pregnancies account for 45% of all pregnancies.1 While there are ramifications for any unintended pregnancy, the risks for patients with mental illness are greater and include potential adverse effects on the neonate from both psychiatric disease and psychiatric medication use, worse obstetrical outcomes for patients with untreated mental illness, and worsening of psychiatric symptoms and suicide risk in the peripartum period.2 These risks become even more pronounced when psychiatric medications are reflexively discontinued or reduced in pregnancy, which is commonly done contrary to best practice recommendations. In the United States, the recent Supreme Court decision in Dobbs v Jackson Women’s Health Organization has erased federal protections for abortion previously conferred by Roe v Wade. As a result, as of early October 2022, abortion had been made illegal in 11 states, and was likely to be banned in many others, most commonly in states where there is limited support for either parents or children. Thus, preventing unplanned pregnancies should be a treatment consideration for all medical disciplines.3
Psychiatrists may hesitate to prescribe emergency contraception (EC) due to fears it falls outside the scope of their practice. However, psychiatry has already moved towards prescribing nonpsychiatric medications when doing so clearly benefits the patient. One example is prescribing metformin to address metabolic syndrome related to the use of second-generation antipsychotics. Emergency contraceptives have strong safety profiles and are easy to prescribe. Unfortunately, there are many barriers to increasing access to emergency contraceptives for psychiatric patients.4 These include the erroneous belief that laboratory and physical exams are needed before starting EC, cost and/or limited stock of emergency contraceptives at pharmacies, and general confusion regarding what constitutes EC vs an oral abortive (Table 15-10). Psychiatrists are particularly well-positioned to support the reproductive autonomy and well-being of patients who struggle to engage with other clinicians. This article aims to help psychiatrists better understand EC so they can comfortably prescribe it before their patients need it.

What is emergency contraception?
EC is medications or devices that patients can use after sexual intercourse to prevent pregnancy. They do not impede the development of an established pregnancy and thus are not abortifacients. EC is not recommended as a primary means of contraception,9 but it can be extremely valuable to reduce pregnancy risk after unprotected intercourse or contraceptive failures such as broken condoms or missed doses of birth control pills. EC can prevent ≥95% of pregnancies when taken within 5 days of at-risk intercourse.11
Methods of EC fall into 2 categories: oral medications (sometimes referred to as “morning after pills”) and intrauterine devices (IUDs). IUDs are the most effective means of EC, especially for patients with higher BMIs or who may be taking medications such as cytochrome P450 (CYP)3A4 inducers that could interfere with the effectiveness of oral methods. IUDs also have the advantage of providing highly effective ongoing contraception.6 However, IUDs require in-office placement by a trained clinician, and patients may experience difficulty obtaining placement within 5 days of unprotected sex. Therefore, oral medication is the most common form of EC.
Oral EC is safe and effective, and professional societies (including the American College of Obstetricians and Gynecologists6 and the American Academy of Pediatrics7) recommend routinely prescribing oral EC for patients in advance of need. Advance prescribing eliminates barriers to accessing EC, increases the use of EC, and does not encourage risky sexual behaviors.10
Overview of oral emergency contraception
Two medications are FDA-approved for use as oral EC: ulipristal acetate and levonorgestrel. Both are available in generic and branded versions. While many common birth control pills can also be safely used off-label as emergency contraception (an approach known as the Yuzpe method), they are less effective, not as well-tolerated, and require knowledge of the specific type of pill the patient has available.9 Oral EC appears to work primarily through delay or inhibition of ovulation, and is unlikely to prevent implantation of a fertilized egg.9
Continue to: Ulipristal acetate
Ulipristal acetate (UPA) is an oral progesterone receptor agonist-antagonist taken as a single 30 mg dose up to 5 days after unprotected sex. Pregnancy rates from a single act of unprotected sex followed by UPA use range from 0% to 1.8%.4 Many pharmacies stock UPA, and others (especially chain pharmacies) report being able to order and fill it within 24 hours.12
Levonorgestrel (LNG) is an oral progestin that is available by prescription and has also been approved for over-the-counter sale to patients of all ages and sexes (without the need to show identification) since 2013.8 It is administered as a single 1.5 mg dose taken as soon as possible up to 3 days after unprotected sex, although it may continue to provide benefits when taken within 5 days. Pregnancy rates from a single act of unprotected sex followed by LNG use range from 0.3% to 2.6%, with much higher odds among women who are obese.4 LNG is available both by prescription or over-the-counter,13 although it is often kept in a locked cabinet or behind the counter, and staff are often misinformed regarding the lack of age restrictions for sale without a prescription.14
Safety and adverse effects. According to the CDC, there are no conditions for which the risks outweigh the advantages of use of either UPA or LNG,5 and patients for whom hormonal birth control is otherwise contraindicated can still use them safely. If a pregnancy has already occurred, taking EC will not harm the developing fetus; it is also safe to use when breastfeeding.5 Both medications are generally well-tolerated—neither has been causally linked to deaths or serious complications,5 and the most common adverse effects are headache (approximately 19%) and nausea (approximately 12%), in addition to irregular bleeding, fatigue, dizziness, and abdominal pain.15 Oral EC may be used more than once, even within the same menstrual cycle. Patients who use EC repeatedly should be encouraged to discuss more efficacious contraceptive options with their primary physician or gynecologist.
Will oral EC affect psychiatric treatment?
Oral EC is unlikely to have a meaningful effect on psychiatric symptoms or management, particularly when compared to the significant impacts of unintended pregnancies. Neither medication is known to have any clinically significant impacts on the pharmacokinetics or pharmacodynamics of psychotropic medications, although the effectiveness of both medications can be impaired by CYP3A4 inducers such as carbamazepine.5 In addition, while research has not specifically examined the impact of EC on psychiatric symptoms, the broader literature on hormonal contraception indicates that most patients with psychiatric disorders generally report similar or lower rates of mood symptoms associated with their use.16 Some women treated with hormonal contraceptives do develop dysphoric mood,16 but any such effects resulting from LNG would likely be transient. Mood disruptions or other psychiatric symptoms have not been associated with UPA use.
How to prescribe oral emergency contraception
Who and when. Women of reproductive age should be counseled about EC as part of anticipatory guidance, regardless of their current intentions for sexual behaviors. Patients do not need a physical examination or pregnancy test before being prescribed or using oral EC.9 Much like how intranasal naloxone is prescribed, prescriptions should be provided in advance of need, with multiple refills to facilitate ready access when needed.
Continue to: Which to prescribe
Which to prescribe. UPA is more effective in preventing pregnancy than LNG at all time points up to 120 hours after sex, including for women who are overweight or obese.15 As such, it is recommended as the first-line choice. However, because LNG is available without prescription and is more readily available (including via online order), it may be a good choice for patients who need rapid EC or who prefer a medication that does not require a prescription (Table 24,5,8,9,15).
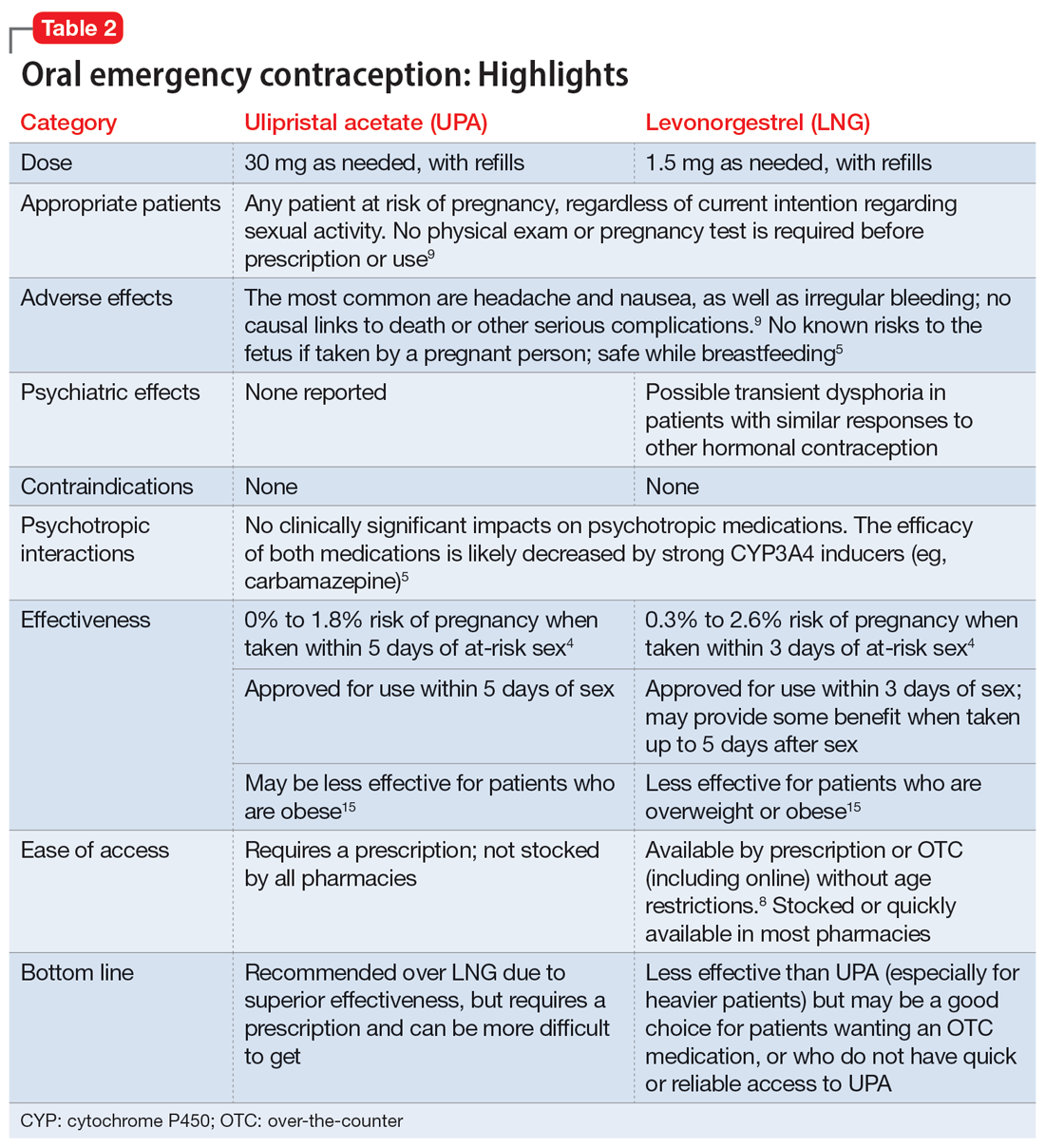
What to tell patients. Patients should be instructed to fill their prescription before they expect to use it, to ensure ready availability when desired (Table 35,9). Oral EC is shelf stable for at least 3 years when stored in a cool, dry environment. Patients should take the medication as soon as possible following at-risk sexual intercourse (Table 4). Tell them that if they vomit within 3 hours of taking the medication, they should take a second dose. Remind patients that EC does not protect against sexually transmitted infections, or from sex that occurs after the medication is taken (in fact, they can increase the possibility of pregnancy later in that menstrual cycle due to delayed ovulation).9 Counsel patients to abstain from sex or to use barrier contraception for 7 days after use. Those who take birth control pills can resume use immediately after using LNG; they should wait 5 days after taking UPA.

No routine follow-up is needed after taking UPA or LNG. However, patients should get a pregnancy test if their period does not start within 3 weeks, and should seek medical evaluation if they experience significant lower abdominal pain or persistent irregular bleeding in order to rule out pregnancy-related complications. Patients who use EC repeatedly should be recommended to pursue routine contraceptive care.

Billing. Counseling your patients about contraception can increase the reimbursement you receive by adding to the complexity of the encounter (regardless of whether you prescribe a medication) through use of the ICD-10 code Z30.0.
Emergency contraception for special populations
Some patients face additional challenges to effective EC that should be considered when counseling and prescribing. Table 54,5,7,15,17-21 discusses the use of EC in these special populations. Of particular importance for psychiatrists, LNG is less effective at preventing undesired pregnancy among patients who are overweight or obese,15,17,18 and strong CYP3A4-inducing agents may decrease the effectiveness of both LNG and UPA.5 Keep in mind, however, that the advantages of using either UPA or LNG outweigh the risks for all populations.5 Patients must be aware of appropriate information in order to make informed decisions, but should not be discouraged from using EC.

Continue to: Other groups of patients...
Other groups of patients may face barriers due to some clinicians’ hesitancy regarding their ability to consent to reproductive care. Most patients with psychiatric illnesses have decision-making capacity regarding reproductive issues.22 Although EC is supported by the American Academy of Pediatrics,7 patients age <18 have varying rights to consent across states,21 and merit special consideration.
CASE CONTINUED
Ms. A does not wish to get pregnant at this time, and expresses fears that her recent contraceptive failure could lead to an unintended pregnancy. In addition to her psychiatric treatment, her psychiatrist should discuss EC options with her. She has a healthy BMI and had inadequately protected sex <1 day ago, so her clinician may prescribe LNG (to ensure rapid access for immediate use) in addition to UPA for her to have available in case of future “scares.” The psychiatrist should consider pharmacologic treatment with an antidepressant with a relatively safe reproductive record (eg, sertraline).23 This is considered preventive ethics, since Ms. A is of reproductive age, even if she is not presently planning to get pregnant, due to the aforementioned high rate of unplanned pregnancy.23,24 It is also important for the psychiatrist to continue the dialogue in future sessions about preventing unintended pregnancy. Since Ms. A has benefited from a psychotropic medication when not pregnant, it will be important to discuss with her the risks and benefits of medication should she plan a pregnancy.
Bottom Line
Patients with mental illnesses are at increased risk of adverse outcomes resulting from unintended pregnancies. Clinicians should counsel patients about emergency contraception (EC) as a part of routine psychiatric care, and should prescribe oral EC in advance of patient need to facilitate effective use.
Related Resources
- American College of Obstetricians and Gynecologists Practice Bulletin on Emergency Contraception. https://www.acog.org/clinical/clinical-guidance/practice-bulletin/ articles/2015/09/emergency-contraception
- State policies on emergency contraception. https://www.guttmacher.org/state-policy/explore/emergency-contraception
- State policies on minors’ access to contraceptive services. https://www.guttmacher.org/state-policy/explore/minors-access-contraceptive-services
- Patient-oriented contraceptive education materials (in English and Spanish). https://shop.powertodecide.org/ptd-category/educational-materials
Drug Brand Names
Carbamazepine • Tegretol
Levonorgestrel • Plan B One-Step, Fallback
Metformin • Glucophage
Naloxone • Narcan
Norethindrone • Aygestin
Sertraline • Zoloft
Topiramate • Topamax
Ulipristal acetate • Ella
Venlafaxine • Effexor
1. Grossman D. Expanding access to short-acting hormonal contraceptive methods in the United States. JAMA Intern Med. 2019;179:1209-1210.
2. Gur TL, Kim DR, Epperson CN. Central nervous system effects of prenatal selective serotonin reuptake inhibitors: sensing the signal through the noise. Psychopharmacology (Berl). 2013;227:567-582.
3. Ross N, Landess J, Kaempf A, et al. Pregnancy termination: what psychiatrists need to know. Current Psychiatry. 2022;21:8-9.
4. Haeger KO, Lamme J, Cleland K. State of emergency contraception in the US, 2018. Contracept Reprod Med. 2018;3:20.
5. Curtis KM, Tepper NK, Jatlaoui TC, et al. US medical eligibility criteria for contraceptive use, 2016. MMWR Recomm Rep. 2016;65:1-3.
6. American College of Obstetricians and Gynecologists. Committee Opinion No 707: Access to emergency contraception. Obstet Gynecol. 2017;130:e48-e52.
7. Upadhya KK, Breuner CC, Alderman EM, et al. Emergency contraception. Pediatrics. 2019;144:e20193149.
8. Rowan A. Obama administration yields to the courts and the evidence, allows emergency contraception to be sold without restrictions. Guttmacher Institute. Published June 25, 2013. Accessed July 31, 2022. https://www.guttmacher.org/gpr/2013/06/obama-administration-yields-courts-and-evidence-allows-emergency-contraception-be-sold#
9. American College of Obstetricians and Gynecologists. Practice Bulletin No. 152: Emergency contraception. Obstet Gynecol. 2015;126:e1-e11.
10. Rodriguez MI, Curtis KM, Gaffield ML, et al. Advance supply of emergency contraception: a systematic review. Contraception. 2013;87:590-601.
11. World Health Organization. Emergency contraception. Published November 9, 2021. Accessed August 4, 2022. https://www.who.int/news-room/fact-sheets/detail/emergency-contraception
12. Shigesato M, Elia J, Tschann M, et al. Pharmacy access to ulipristal acetate in major cities throughout the United States. Contraception. 2018;97:264-269.
13. Wilkinson TA, Clark P, Rafie S, et al. Access to emergency contraception after removal of age restrictions. Pediatrics. 2017;140:e20164262.
14. Cleland K, Bass J, Doci F, et al. Access to emergency contraception in the over-the-counter era. Women’s Health Issues. 2016;26:622-627.
15. Glasier AF, Cameron ST, Fine PM, et al. Ulipristal acetate versus levonorgestrel for emergency contraception: a randomised non-inferiority trial and meta-analysis. Lancet. 2010;375:555-562.
16. McCloskey LR, Wisner KL, Cattan MK, et al. Contraception for women with psychiatric disorders. Am J Psychiatry. 2021;178:247-255.
17. Kapp N, Abitbol JL, Mathé H, et al. Effect of body weight and BMI on the efficacy of levonorgestrel emergency contraception. Contraception. 2015;91:97-104.
18. Festin MP, Peregoudov A, Seuc A, et al. Effect of BMI and body weight on pregnancy rates with LNG as emergency contraception: analysis of four WHO HRP studies. Contraception. 2017;95:50-54.
19. Edelman AB, Hennebold JD, Bond K, et al. Double dosing levonorgestrel-based emergency contraception for individuals with obesity: a randomized controlled trial. Obstet Gynecol. 2022;140(1):48-54.
20. FSRH Clinical Effectiveness Unit. FSRH clinical guideline: Emergency contraception. Published March 2017. Amended December 2020. Faculty of Sexual & Reproductive Healthcare. Accessed August 4, 2022. https://www.fsrh.org/documents/ceu-clinical-guidance-emergency-contraception-march-2017/
21. Guttmacher Institute. Minors’ access to contraceptive services. Guttmacher Institute. Accessed August 4, 2022. https://www.guttmacher.org/state-policy/explore/minors-access-contraceptive-services
22. Ross NE, Webster TG, Tastenhoye CA, et al. Reproductive decision-making capacity in women with psychiatric illness: a systematic review. J Acad Consult Liaison Psychiatry. 2022;63:61-70.
23. Friedman SH, Hall RCW. Avoiding malpractice while treating depression in pregnant women. Current Psychiatry. 2021;20:30-36.
24. Friedman SH. The ethics of treating depression in pregnancy. J Primary Healthcare. 2015;7:81-83.
Ms. A, age 22, is a college student who presents for an initial psychiatric evaluation. Her body mass index (BMI) is 20 (normal range: 18.5 to 24.9), and her medical history is positive only for childhood asthma. She has been treated for major depressive disorder with venlafaxine by her previous psychiatrist. While this antidepressant has been effective for some symptoms, she has experienced adverse effects and is interested in a different medication. During the evaluation, Ms. A remarks that she had a “scare” last night when the condom broke while having sex with her boyfriend. She says that she is interested in having children at some point, but not at present; she is concerned that getting pregnant now would cause her depression to “spiral out of control.”
Unwanted or mistimed pregnancies account for 45% of all pregnancies.1 While there are ramifications for any unintended pregnancy, the risks for patients with mental illness are greater and include potential adverse effects on the neonate from both psychiatric disease and psychiatric medication use, worse obstetrical outcomes for patients with untreated mental illness, and worsening of psychiatric symptoms and suicide risk in the peripartum period.2 These risks become even more pronounced when psychiatric medications are reflexively discontinued or reduced in pregnancy, which is commonly done contrary to best practice recommendations. In the United States, the recent Supreme Court decision in Dobbs v Jackson Women’s Health Organization has erased federal protections for abortion previously conferred by Roe v Wade. As a result, as of early October 2022, abortion had been made illegal in 11 states, and was likely to be banned in many others, most commonly in states where there is limited support for either parents or children. Thus, preventing unplanned pregnancies should be a treatment consideration for all medical disciplines.3
Psychiatrists may hesitate to prescribe emergency contraception (EC) due to fears it falls outside the scope of their practice. However, psychiatry has already moved towards prescribing nonpsychiatric medications when doing so clearly benefits the patient. One example is prescribing metformin to address metabolic syndrome related to the use of second-generation antipsychotics. Emergency contraceptives have strong safety profiles and are easy to prescribe. Unfortunately, there are many barriers to increasing access to emergency contraceptives for psychiatric patients.4 These include the erroneous belief that laboratory and physical exams are needed before starting EC, cost and/or limited stock of emergency contraceptives at pharmacies, and general confusion regarding what constitutes EC vs an oral abortive (Table 15-10). Psychiatrists are particularly well-positioned to support the reproductive autonomy and well-being of patients who struggle to engage with other clinicians. This article aims to help psychiatrists better understand EC so they can comfortably prescribe it before their patients need it.

What is emergency contraception?
EC is medications or devices that patients can use after sexual intercourse to prevent pregnancy. They do not impede the development of an established pregnancy and thus are not abortifacients. EC is not recommended as a primary means of contraception,9 but it can be extremely valuable to reduce pregnancy risk after unprotected intercourse or contraceptive failures such as broken condoms or missed doses of birth control pills. EC can prevent ≥95% of pregnancies when taken within 5 days of at-risk intercourse.11
Methods of EC fall into 2 categories: oral medications (sometimes referred to as “morning after pills”) and intrauterine devices (IUDs). IUDs are the most effective means of EC, especially for patients with higher BMIs or who may be taking medications such as cytochrome P450 (CYP)3A4 inducers that could interfere with the effectiveness of oral methods. IUDs also have the advantage of providing highly effective ongoing contraception.6 However, IUDs require in-office placement by a trained clinician, and patients may experience difficulty obtaining placement within 5 days of unprotected sex. Therefore, oral medication is the most common form of EC.
Oral EC is safe and effective, and professional societies (including the American College of Obstetricians and Gynecologists6 and the American Academy of Pediatrics7) recommend routinely prescribing oral EC for patients in advance of need. Advance prescribing eliminates barriers to accessing EC, increases the use of EC, and does not encourage risky sexual behaviors.10
Overview of oral emergency contraception
Two medications are FDA-approved for use as oral EC: ulipristal acetate and levonorgestrel. Both are available in generic and branded versions. While many common birth control pills can also be safely used off-label as emergency contraception (an approach known as the Yuzpe method), they are less effective, not as well-tolerated, and require knowledge of the specific type of pill the patient has available.9 Oral EC appears to work primarily through delay or inhibition of ovulation, and is unlikely to prevent implantation of a fertilized egg.9
Continue to: Ulipristal acetate
Ulipristal acetate (UPA) is an oral progesterone receptor agonist-antagonist taken as a single 30 mg dose up to 5 days after unprotected sex. Pregnancy rates from a single act of unprotected sex followed by UPA use range from 0% to 1.8%.4 Many pharmacies stock UPA, and others (especially chain pharmacies) report being able to order and fill it within 24 hours.12
Levonorgestrel (LNG) is an oral progestin that is available by prescription and has also been approved for over-the-counter sale to patients of all ages and sexes (without the need to show identification) since 2013.8 It is administered as a single 1.5 mg dose taken as soon as possible up to 3 days after unprotected sex, although it may continue to provide benefits when taken within 5 days. Pregnancy rates from a single act of unprotected sex followed by LNG use range from 0.3% to 2.6%, with much higher odds among women who are obese.4 LNG is available both by prescription or over-the-counter,13 although it is often kept in a locked cabinet or behind the counter, and staff are often misinformed regarding the lack of age restrictions for sale without a prescription.14
Safety and adverse effects. According to the CDC, there are no conditions for which the risks outweigh the advantages of use of either UPA or LNG,5 and patients for whom hormonal birth control is otherwise contraindicated can still use them safely. If a pregnancy has already occurred, taking EC will not harm the developing fetus; it is also safe to use when breastfeeding.5 Both medications are generally well-tolerated—neither has been causally linked to deaths or serious complications,5 and the most common adverse effects are headache (approximately 19%) and nausea (approximately 12%), in addition to irregular bleeding, fatigue, dizziness, and abdominal pain.15 Oral EC may be used more than once, even within the same menstrual cycle. Patients who use EC repeatedly should be encouraged to discuss more efficacious contraceptive options with their primary physician or gynecologist.
Will oral EC affect psychiatric treatment?
Oral EC is unlikely to have a meaningful effect on psychiatric symptoms or management, particularly when compared to the significant impacts of unintended pregnancies. Neither medication is known to have any clinically significant impacts on the pharmacokinetics or pharmacodynamics of psychotropic medications, although the effectiveness of both medications can be impaired by CYP3A4 inducers such as carbamazepine.5 In addition, while research has not specifically examined the impact of EC on psychiatric symptoms, the broader literature on hormonal contraception indicates that most patients with psychiatric disorders generally report similar or lower rates of mood symptoms associated with their use.16 Some women treated with hormonal contraceptives do develop dysphoric mood,16 but any such effects resulting from LNG would likely be transient. Mood disruptions or other psychiatric symptoms have not been associated with UPA use.
How to prescribe oral emergency contraception
Who and when. Women of reproductive age should be counseled about EC as part of anticipatory guidance, regardless of their current intentions for sexual behaviors. Patients do not need a physical examination or pregnancy test before being prescribed or using oral EC.9 Much like how intranasal naloxone is prescribed, prescriptions should be provided in advance of need, with multiple refills to facilitate ready access when needed.
Continue to: Which to prescribe
Which to prescribe. UPA is more effective in preventing pregnancy than LNG at all time points up to 120 hours after sex, including for women who are overweight or obese.15 As such, it is recommended as the first-line choice. However, because LNG is available without prescription and is more readily available (including via online order), it may be a good choice for patients who need rapid EC or who prefer a medication that does not require a prescription (Table 24,5,8,9,15).

What to tell patients. Patients should be instructed to fill their prescription before they expect to use it, to ensure ready availability when desired (Table 35,9). Oral EC is shelf stable for at least 3 years when stored in a cool, dry environment. Patients should take the medication as soon as possible following at-risk sexual intercourse (Table 4). Tell them that if they vomit within 3 hours of taking the medication, they should take a second dose. Remind patients that EC does not protect against sexually transmitted infections, or from sex that occurs after the medication is taken (in fact, they can increase the possibility of pregnancy later in that menstrual cycle due to delayed ovulation).9 Counsel patients to abstain from sex or to use barrier contraception for 7 days after use. Those who take birth control pills can resume use immediately after using LNG; they should wait 5 days after taking UPA.

No routine follow-up is needed after taking UPA or LNG. However, patients should get a pregnancy test if their period does not start within 3 weeks, and should seek medical evaluation if they experience significant lower abdominal pain or persistent irregular bleeding in order to rule out pregnancy-related complications. Patients who use EC repeatedly should be recommended to pursue routine contraceptive care.

Billing. Counseling your patients about contraception can increase the reimbursement you receive by adding to the complexity of the encounter (regardless of whether you prescribe a medication) through use of the ICD-10 code Z30.0.
Emergency contraception for special populations
Some patients face additional challenges to effective EC that should be considered when counseling and prescribing. Table 54,5,7,15,17-21 discusses the use of EC in these special populations. Of particular importance for psychiatrists, LNG is less effective at preventing undesired pregnancy among patients who are overweight or obese,15,17,18 and strong CYP3A4-inducing agents may decrease the effectiveness of both LNG and UPA.5 Keep in mind, however, that the advantages of using either UPA or LNG outweigh the risks for all populations.5 Patients must be aware of appropriate information in order to make informed decisions, but should not be discouraged from using EC.

Continue to: Other groups of patients...
Other groups of patients may face barriers due to some clinicians’ hesitancy regarding their ability to consent to reproductive care. Most patients with psychiatric illnesses have decision-making capacity regarding reproductive issues.22 Although EC is supported by the American Academy of Pediatrics,7 patients age <18 have varying rights to consent across states,21 and merit special consideration.
CASE CONTINUED
Ms. A does not wish to get pregnant at this time, and expresses fears that her recent contraceptive failure could lead to an unintended pregnancy. In addition to her psychiatric treatment, her psychiatrist should discuss EC options with her. She has a healthy BMI and had inadequately protected sex <1 day ago, so her clinician may prescribe LNG (to ensure rapid access for immediate use) in addition to UPA for her to have available in case of future “scares.” The psychiatrist should consider pharmacologic treatment with an antidepressant with a relatively safe reproductive record (eg, sertraline).23 This is considered preventive ethics, since Ms. A is of reproductive age, even if she is not presently planning to get pregnant, due to the aforementioned high rate of unplanned pregnancy.23,24 It is also important for the psychiatrist to continue the dialogue in future sessions about preventing unintended pregnancy. Since Ms. A has benefited from a psychotropic medication when not pregnant, it will be important to discuss with her the risks and benefits of medication should she plan a pregnancy.
Bottom Line
Patients with mental illnesses are at increased risk of adverse outcomes resulting from unintended pregnancies. Clinicians should counsel patients about emergency contraception (EC) as a part of routine psychiatric care, and should prescribe oral EC in advance of patient need to facilitate effective use.
Related Resources
- American College of Obstetricians and Gynecologists Practice Bulletin on Emergency Contraception. https://www.acog.org/clinical/clinical-guidance/practice-bulletin/ articles/2015/09/emergency-contraception
- State policies on emergency contraception. https://www.guttmacher.org/state-policy/explore/emergency-contraception
- State policies on minors’ access to contraceptive services. https://www.guttmacher.org/state-policy/explore/minors-access-contraceptive-services
- Patient-oriented contraceptive education materials (in English and Spanish). https://shop.powertodecide.org/ptd-category/educational-materials
Drug Brand Names
Carbamazepine • Tegretol
Levonorgestrel • Plan B One-Step, Fallback
Metformin • Glucophage
Naloxone • Narcan
Norethindrone • Aygestin
Sertraline • Zoloft
Topiramate • Topamax
Ulipristal acetate • Ella
Venlafaxine • Effexor
Ms. A, age 22, is a college student who presents for an initial psychiatric evaluation. Her body mass index (BMI) is 20 (normal range: 18.5 to 24.9), and her medical history is positive only for childhood asthma. She has been treated for major depressive disorder with venlafaxine by her previous psychiatrist. While this antidepressant has been effective for some symptoms, she has experienced adverse effects and is interested in a different medication. During the evaluation, Ms. A remarks that she had a “scare” last night when the condom broke while having sex with her boyfriend. She says that she is interested in having children at some point, but not at present; she is concerned that getting pregnant now would cause her depression to “spiral out of control.”
Unwanted or mistimed pregnancies account for 45% of all pregnancies.1 While there are ramifications for any unintended pregnancy, the risks for patients with mental illness are greater and include potential adverse effects on the neonate from both psychiatric disease and psychiatric medication use, worse obstetrical outcomes for patients with untreated mental illness, and worsening of psychiatric symptoms and suicide risk in the peripartum period.2 These risks become even more pronounced when psychiatric medications are reflexively discontinued or reduced in pregnancy, which is commonly done contrary to best practice recommendations. In the United States, the recent Supreme Court decision in Dobbs v Jackson Women’s Health Organization has erased federal protections for abortion previously conferred by Roe v Wade. As a result, as of early October 2022, abortion had been made illegal in 11 states, and was likely to be banned in many others, most commonly in states where there is limited support for either parents or children. Thus, preventing unplanned pregnancies should be a treatment consideration for all medical disciplines.3
Psychiatrists may hesitate to prescribe emergency contraception (EC) due to fears it falls outside the scope of their practice. However, psychiatry has already moved towards prescribing nonpsychiatric medications when doing so clearly benefits the patient. One example is prescribing metformin to address metabolic syndrome related to the use of second-generation antipsychotics. Emergency contraceptives have strong safety profiles and are easy to prescribe. Unfortunately, there are many barriers to increasing access to emergency contraceptives for psychiatric patients.4 These include the erroneous belief that laboratory and physical exams are needed before starting EC, cost and/or limited stock of emergency contraceptives at pharmacies, and general confusion regarding what constitutes EC vs an oral abortive (Table 15-10). Psychiatrists are particularly well-positioned to support the reproductive autonomy and well-being of patients who struggle to engage with other clinicians. This article aims to help psychiatrists better understand EC so they can comfortably prescribe it before their patients need it.

What is emergency contraception?
EC is medications or devices that patients can use after sexual intercourse to prevent pregnancy. They do not impede the development of an established pregnancy and thus are not abortifacients. EC is not recommended as a primary means of contraception,9 but it can be extremely valuable to reduce pregnancy risk after unprotected intercourse or contraceptive failures such as broken condoms or missed doses of birth control pills. EC can prevent ≥95% of pregnancies when taken within 5 days of at-risk intercourse.11
Methods of EC fall into 2 categories: oral medications (sometimes referred to as “morning after pills”) and intrauterine devices (IUDs). IUDs are the most effective means of EC, especially for patients with higher BMIs or who may be taking medications such as cytochrome P450 (CYP)3A4 inducers that could interfere with the effectiveness of oral methods. IUDs also have the advantage of providing highly effective ongoing contraception.6 However, IUDs require in-office placement by a trained clinician, and patients may experience difficulty obtaining placement within 5 days of unprotected sex. Therefore, oral medication is the most common form of EC.
Oral EC is safe and effective, and professional societies (including the American College of Obstetricians and Gynecologists6 and the American Academy of Pediatrics7) recommend routinely prescribing oral EC for patients in advance of need. Advance prescribing eliminates barriers to accessing EC, increases the use of EC, and does not encourage risky sexual behaviors.10
Overview of oral emergency contraception
Two medications are FDA-approved for use as oral EC: ulipristal acetate and levonorgestrel. Both are available in generic and branded versions. While many common birth control pills can also be safely used off-label as emergency contraception (an approach known as the Yuzpe method), they are less effective, not as well-tolerated, and require knowledge of the specific type of pill the patient has available.9 Oral EC appears to work primarily through delay or inhibition of ovulation, and is unlikely to prevent implantation of a fertilized egg.9
Continue to: Ulipristal acetate
Ulipristal acetate (UPA) is an oral progesterone receptor agonist-antagonist taken as a single 30 mg dose up to 5 days after unprotected sex. Pregnancy rates from a single act of unprotected sex followed by UPA use range from 0% to 1.8%.4 Many pharmacies stock UPA, and others (especially chain pharmacies) report being able to order and fill it within 24 hours.12
Levonorgestrel (LNG) is an oral progestin that is available by prescription and has also been approved for over-the-counter sale to patients of all ages and sexes (without the need to show identification) since 2013.8 It is administered as a single 1.5 mg dose taken as soon as possible up to 3 days after unprotected sex, although it may continue to provide benefits when taken within 5 days. Pregnancy rates from a single act of unprotected sex followed by LNG use range from 0.3% to 2.6%, with much higher odds among women who are obese.4 LNG is available both by prescription or over-the-counter,13 although it is often kept in a locked cabinet or behind the counter, and staff are often misinformed regarding the lack of age restrictions for sale without a prescription.14
Safety and adverse effects. According to the CDC, there are no conditions for which the risks outweigh the advantages of use of either UPA or LNG,5 and patients for whom hormonal birth control is otherwise contraindicated can still use them safely. If a pregnancy has already occurred, taking EC will not harm the developing fetus; it is also safe to use when breastfeeding.5 Both medications are generally well-tolerated—neither has been causally linked to deaths or serious complications,5 and the most common adverse effects are headache (approximately 19%) and nausea (approximately 12%), in addition to irregular bleeding, fatigue, dizziness, and abdominal pain.15 Oral EC may be used more than once, even within the same menstrual cycle. Patients who use EC repeatedly should be encouraged to discuss more efficacious contraceptive options with their primary physician or gynecologist.
Will oral EC affect psychiatric treatment?
Oral EC is unlikely to have a meaningful effect on psychiatric symptoms or management, particularly when compared to the significant impacts of unintended pregnancies. Neither medication is known to have any clinically significant impacts on the pharmacokinetics or pharmacodynamics of psychotropic medications, although the effectiveness of both medications can be impaired by CYP3A4 inducers such as carbamazepine.5 In addition, while research has not specifically examined the impact of EC on psychiatric symptoms, the broader literature on hormonal contraception indicates that most patients with psychiatric disorders generally report similar or lower rates of mood symptoms associated with their use.16 Some women treated with hormonal contraceptives do develop dysphoric mood,16 but any such effects resulting from LNG would likely be transient. Mood disruptions or other psychiatric symptoms have not been associated with UPA use.
How to prescribe oral emergency contraception
Who and when. Women of reproductive age should be counseled about EC as part of anticipatory guidance, regardless of their current intentions for sexual behaviors. Patients do not need a physical examination or pregnancy test before being prescribed or using oral EC.9 Much like how intranasal naloxone is prescribed, prescriptions should be provided in advance of need, with multiple refills to facilitate ready access when needed.
Continue to: Which to prescribe
Which to prescribe. UPA is more effective in preventing pregnancy than LNG at all time points up to 120 hours after sex, including for women who are overweight or obese.15 As such, it is recommended as the first-line choice. However, because LNG is available without prescription and is more readily available (including via online order), it may be a good choice for patients who need rapid EC or who prefer a medication that does not require a prescription (Table 24,5,8,9,15).

What to tell patients. Patients should be instructed to fill their prescription before they expect to use it, to ensure ready availability when desired (Table 35,9). Oral EC is shelf stable for at least 3 years when stored in a cool, dry environment. Patients should take the medication as soon as possible following at-risk sexual intercourse (Table 4). Tell them that if they vomit within 3 hours of taking the medication, they should take a second dose. Remind patients that EC does not protect against sexually transmitted infections, or from sex that occurs after the medication is taken (in fact, they can increase the possibility of pregnancy later in that menstrual cycle due to delayed ovulation).9 Counsel patients to abstain from sex or to use barrier contraception for 7 days after use. Those who take birth control pills can resume use immediately after using LNG; they should wait 5 days after taking UPA.

No routine follow-up is needed after taking UPA or LNG. However, patients should get a pregnancy test if their period does not start within 3 weeks, and should seek medical evaluation if they experience significant lower abdominal pain or persistent irregular bleeding in order to rule out pregnancy-related complications. Patients who use EC repeatedly should be recommended to pursue routine contraceptive care.

Billing. Counseling your patients about contraception can increase the reimbursement you receive by adding to the complexity of the encounter (regardless of whether you prescribe a medication) through use of the ICD-10 code Z30.0.
Emergency contraception for special populations
Some patients face additional challenges to effective EC that should be considered when counseling and prescribing. Table 54,5,7,15,17-21 discusses the use of EC in these special populations. Of particular importance for psychiatrists, LNG is less effective at preventing undesired pregnancy among patients who are overweight or obese,15,17,18 and strong CYP3A4-inducing agents may decrease the effectiveness of both LNG and UPA.5 Keep in mind, however, that the advantages of using either UPA or LNG outweigh the risks for all populations.5 Patients must be aware of appropriate information in order to make informed decisions, but should not be discouraged from using EC.

Continue to: Other groups of patients...
Other groups of patients may face barriers due to some clinicians’ hesitancy regarding their ability to consent to reproductive care. Most patients with psychiatric illnesses have decision-making capacity regarding reproductive issues.22 Although EC is supported by the American Academy of Pediatrics,7 patients age <18 have varying rights to consent across states,21 and merit special consideration.
CASE CONTINUED
Ms. A does not wish to get pregnant at this time, and expresses fears that her recent contraceptive failure could lead to an unintended pregnancy. In addition to her psychiatric treatment, her psychiatrist should discuss EC options with her. She has a healthy BMI and had inadequately protected sex <1 day ago, so her clinician may prescribe LNG (to ensure rapid access for immediate use) in addition to UPA for her to have available in case of future “scares.” The psychiatrist should consider pharmacologic treatment with an antidepressant with a relatively safe reproductive record (eg, sertraline).23 This is considered preventive ethics, since Ms. A is of reproductive age, even if she is not presently planning to get pregnant, due to the aforementioned high rate of unplanned pregnancy.23,24 It is also important for the psychiatrist to continue the dialogue in future sessions about preventing unintended pregnancy. Since Ms. A has benefited from a psychotropic medication when not pregnant, it will be important to discuss with her the risks and benefits of medication should she plan a pregnancy.
Bottom Line
Patients with mental illnesses are at increased risk of adverse outcomes resulting from unintended pregnancies. Clinicians should counsel patients about emergency contraception (EC) as a part of routine psychiatric care, and should prescribe oral EC in advance of patient need to facilitate effective use.
Related Resources
- American College of Obstetricians and Gynecologists Practice Bulletin on Emergency Contraception. https://www.acog.org/clinical/clinical-guidance/practice-bulletin/ articles/2015/09/emergency-contraception
- State policies on emergency contraception. https://www.guttmacher.org/state-policy/explore/emergency-contraception
- State policies on minors’ access to contraceptive services. https://www.guttmacher.org/state-policy/explore/minors-access-contraceptive-services
- Patient-oriented contraceptive education materials (in English and Spanish). https://shop.powertodecide.org/ptd-category/educational-materials
Drug Brand Names
Carbamazepine • Tegretol
Levonorgestrel • Plan B One-Step, Fallback
Metformin • Glucophage
Naloxone • Narcan
Norethindrone • Aygestin
Sertraline • Zoloft
Topiramate • Topamax
Ulipristal acetate • Ella
Venlafaxine • Effexor
1. Grossman D. Expanding access to short-acting hormonal contraceptive methods in the United States. JAMA Intern Med. 2019;179:1209-1210.
2. Gur TL, Kim DR, Epperson CN. Central nervous system effects of prenatal selective serotonin reuptake inhibitors: sensing the signal through the noise. Psychopharmacology (Berl). 2013;227:567-582.
3. Ross N, Landess J, Kaempf A, et al. Pregnancy termination: what psychiatrists need to know. Current Psychiatry. 2022;21:8-9.
4. Haeger KO, Lamme J, Cleland K. State of emergency contraception in the US, 2018. Contracept Reprod Med. 2018;3:20.
5. Curtis KM, Tepper NK, Jatlaoui TC, et al. US medical eligibility criteria for contraceptive use, 2016. MMWR Recomm Rep. 2016;65:1-3.
6. American College of Obstetricians and Gynecologists. Committee Opinion No 707: Access to emergency contraception. Obstet Gynecol. 2017;130:e48-e52.
7. Upadhya KK, Breuner CC, Alderman EM, et al. Emergency contraception. Pediatrics. 2019;144:e20193149.
8. Rowan A. Obama administration yields to the courts and the evidence, allows emergency contraception to be sold without restrictions. Guttmacher Institute. Published June 25, 2013. Accessed July 31, 2022. https://www.guttmacher.org/gpr/2013/06/obama-administration-yields-courts-and-evidence-allows-emergency-contraception-be-sold#
9. American College of Obstetricians and Gynecologists. Practice Bulletin No. 152: Emergency contraception. Obstet Gynecol. 2015;126:e1-e11.
10. Rodriguez MI, Curtis KM, Gaffield ML, et al. Advance supply of emergency contraception: a systematic review. Contraception. 2013;87:590-601.
11. World Health Organization. Emergency contraception. Published November 9, 2021. Accessed August 4, 2022. https://www.who.int/news-room/fact-sheets/detail/emergency-contraception
12. Shigesato M, Elia J, Tschann M, et al. Pharmacy access to ulipristal acetate in major cities throughout the United States. Contraception. 2018;97:264-269.
13. Wilkinson TA, Clark P, Rafie S, et al. Access to emergency contraception after removal of age restrictions. Pediatrics. 2017;140:e20164262.
14. Cleland K, Bass J, Doci F, et al. Access to emergency contraception in the over-the-counter era. Women’s Health Issues. 2016;26:622-627.
15. Glasier AF, Cameron ST, Fine PM, et al. Ulipristal acetate versus levonorgestrel for emergency contraception: a randomised non-inferiority trial and meta-analysis. Lancet. 2010;375:555-562.
16. McCloskey LR, Wisner KL, Cattan MK, et al. Contraception for women with psychiatric disorders. Am J Psychiatry. 2021;178:247-255.
17. Kapp N, Abitbol JL, Mathé H, et al. Effect of body weight and BMI on the efficacy of levonorgestrel emergency contraception. Contraception. 2015;91:97-104.
18. Festin MP, Peregoudov A, Seuc A, et al. Effect of BMI and body weight on pregnancy rates with LNG as emergency contraception: analysis of four WHO HRP studies. Contraception. 2017;95:50-54.
19. Edelman AB, Hennebold JD, Bond K, et al. Double dosing levonorgestrel-based emergency contraception for individuals with obesity: a randomized controlled trial. Obstet Gynecol. 2022;140(1):48-54.
20. FSRH Clinical Effectiveness Unit. FSRH clinical guideline: Emergency contraception. Published March 2017. Amended December 2020. Faculty of Sexual & Reproductive Healthcare. Accessed August 4, 2022. https://www.fsrh.org/documents/ceu-clinical-guidance-emergency-contraception-march-2017/
21. Guttmacher Institute. Minors’ access to contraceptive services. Guttmacher Institute. Accessed August 4, 2022. https://www.guttmacher.org/state-policy/explore/minors-access-contraceptive-services
22. Ross NE, Webster TG, Tastenhoye CA, et al. Reproductive decision-making capacity in women with psychiatric illness: a systematic review. J Acad Consult Liaison Psychiatry. 2022;63:61-70.
23. Friedman SH, Hall RCW. Avoiding malpractice while treating depression in pregnant women. Current Psychiatry. 2021;20:30-36.
24. Friedman SH. The ethics of treating depression in pregnancy. J Primary Healthcare. 2015;7:81-83.
1. Grossman D. Expanding access to short-acting hormonal contraceptive methods in the United States. JAMA Intern Med. 2019;179:1209-1210.
2. Gur TL, Kim DR, Epperson CN. Central nervous system effects of prenatal selective serotonin reuptake inhibitors: sensing the signal through the noise. Psychopharmacology (Berl). 2013;227:567-582.
3. Ross N, Landess J, Kaempf A, et al. Pregnancy termination: what psychiatrists need to know. Current Psychiatry. 2022;21:8-9.
4. Haeger KO, Lamme J, Cleland K. State of emergency contraception in the US, 2018. Contracept Reprod Med. 2018;3:20.
5. Curtis KM, Tepper NK, Jatlaoui TC, et al. US medical eligibility criteria for contraceptive use, 2016. MMWR Recomm Rep. 2016;65:1-3.
6. American College of Obstetricians and Gynecologists. Committee Opinion No 707: Access to emergency contraception. Obstet Gynecol. 2017;130:e48-e52.
7. Upadhya KK, Breuner CC, Alderman EM, et al. Emergency contraception. Pediatrics. 2019;144:e20193149.
8. Rowan A. Obama administration yields to the courts and the evidence, allows emergency contraception to be sold without restrictions. Guttmacher Institute. Published June 25, 2013. Accessed July 31, 2022. https://www.guttmacher.org/gpr/2013/06/obama-administration-yields-courts-and-evidence-allows-emergency-contraception-be-sold#
9. American College of Obstetricians and Gynecologists. Practice Bulletin No. 152: Emergency contraception. Obstet Gynecol. 2015;126:e1-e11.
10. Rodriguez MI, Curtis KM, Gaffield ML, et al. Advance supply of emergency contraception: a systematic review. Contraception. 2013;87:590-601.
11. World Health Organization. Emergency contraception. Published November 9, 2021. Accessed August 4, 2022. https://www.who.int/news-room/fact-sheets/detail/emergency-contraception
12. Shigesato M, Elia J, Tschann M, et al. Pharmacy access to ulipristal acetate in major cities throughout the United States. Contraception. 2018;97:264-269.
13. Wilkinson TA, Clark P, Rafie S, et al. Access to emergency contraception after removal of age restrictions. Pediatrics. 2017;140:e20164262.
14. Cleland K, Bass J, Doci F, et al. Access to emergency contraception in the over-the-counter era. Women’s Health Issues. 2016;26:622-627.
15. Glasier AF, Cameron ST, Fine PM, et al. Ulipristal acetate versus levonorgestrel for emergency contraception: a randomised non-inferiority trial and meta-analysis. Lancet. 2010;375:555-562.
16. McCloskey LR, Wisner KL, Cattan MK, et al. Contraception for women with psychiatric disorders. Am J Psychiatry. 2021;178:247-255.
17. Kapp N, Abitbol JL, Mathé H, et al. Effect of body weight and BMI on the efficacy of levonorgestrel emergency contraception. Contraception. 2015;91:97-104.
18. Festin MP, Peregoudov A, Seuc A, et al. Effect of BMI and body weight on pregnancy rates with LNG as emergency contraception: analysis of four WHO HRP studies. Contraception. 2017;95:50-54.
19. Edelman AB, Hennebold JD, Bond K, et al. Double dosing levonorgestrel-based emergency contraception for individuals with obesity: a randomized controlled trial. Obstet Gynecol. 2022;140(1):48-54.
20. FSRH Clinical Effectiveness Unit. FSRH clinical guideline: Emergency contraception. Published March 2017. Amended December 2020. Faculty of Sexual & Reproductive Healthcare. Accessed August 4, 2022. https://www.fsrh.org/documents/ceu-clinical-guidance-emergency-contraception-march-2017/
21. Guttmacher Institute. Minors’ access to contraceptive services. Guttmacher Institute. Accessed August 4, 2022. https://www.guttmacher.org/state-policy/explore/minors-access-contraceptive-services
22. Ross NE, Webster TG, Tastenhoye CA, et al. Reproductive decision-making capacity in women with psychiatric illness: a systematic review. J Acad Consult Liaison Psychiatry. 2022;63:61-70.
23. Friedman SH, Hall RCW. Avoiding malpractice while treating depression in pregnant women. Current Psychiatry. 2021;20:30-36.
24. Friedman SH. The ethics of treating depression in pregnancy. J Primary Healthcare. 2015;7:81-83.
A heartwarming welcome
Dear colleagues,
This November issue of The New Gastroenterologist marks my official transition as the new Editor in Chief! I am humbled with this opportunity to be a part of such a unique publication and have received immense support from Dr. Vijaya Rao, the TNG staff, as well as my mentors and colleagues. With its foundation built by Dr. Bryson Katona and then taken to the next level by Dr. Rao, TNG has grown over the years, and I hope that I can continue to extend its reach to more trainees and early faculty.
In this issue’s In Focus, Dr. Wenfei Wang and Dr. Neil Sengupta (both from University of Chicago) review the management of antithrombotic medications in elective endoscopic procedures and emphasize individualizing the approach while providing guideline recommendations on how to navigate the gastrointestinal bleeding risk and cardiovascular disease in this day and age.
With endoscopic bariatric therapy and antiobesity medications burgeoning within gastroenterology, Dr. Singrid Young (New York University), Dr. Cameron Zenger (New York University), Dr. Erik Holzwanger (Harvard Medical School in Boston), and Dr. Violeta Popov (New York University) review how their multidisciplinary approach has made their endoscopic bariatric program successful in treating patients struggling with obesity. In our Ethics section, Dr. David Ney (Thomas Jefferson University Hospital, Philadelphia) and Dr. Jason Karlawish (University of Pennsylvania, Philadelphia) delve into patient capacity, particularly when consenting for procedures.
Being involved with national society committees may seem daunting to a lot of trainees and early faculty, but Dr. Peter S. Liang (New York University Langone Health) and Dr. Stephanie D. Pointer (Tristar Hendersonville Medical Center in Tennessee) describe their journeys to becoming AGA committee chairs as early-career physicians. While you ponder whether to join a committee, it may be a good time to learn new ways to increase your financial portfolio through passive income, detailed by Dr. Latifat Alli-Akintade (Kaiser Permanente South Sacramento Medical Center in California).
Last but not least, I am excited to introduce a personal favorite in this newsletter – a piece on females supporting female gastroenterologists in career development and more. Dr. Tonya Adams outlines action items on how to create a culture that fosters professional and leadership development among females, using the Gastro Health Women’s Network as an example of how this network has succeeded in cultivating such an environment.
If you are interested in contributing or have ideas for future TNG topics, please contact me (jtrieu23@gmail.com), or Jillian Schweitzer (jschweitzer@gastro.org), managing editor of TNG.
Until next time, I leave you with an interesting historical fact: William Beaumont, the father of Gastroenterology, published the first findings on the digestive system after performing experiments on Alexis St. Martin when he developed a large gastrocutaneous fistula from an abdominal gunshot wound.
Yours truly,
Judy A. Trieu, MD, MPH
Editor in Chief
Advanced Endoscopy Fellow, University of North Carolina at Chapel Hill, Division of Gastroenterology & Hepatology
Dear colleagues,
This November issue of The New Gastroenterologist marks my official transition as the new Editor in Chief! I am humbled with this opportunity to be a part of such a unique publication and have received immense support from Dr. Vijaya Rao, the TNG staff, as well as my mentors and colleagues. With its foundation built by Dr. Bryson Katona and then taken to the next level by Dr. Rao, TNG has grown over the years, and I hope that I can continue to extend its reach to more trainees and early faculty.
In this issue’s In Focus, Dr. Wenfei Wang and Dr. Neil Sengupta (both from University of Chicago) review the management of antithrombotic medications in elective endoscopic procedures and emphasize individualizing the approach while providing guideline recommendations on how to navigate the gastrointestinal bleeding risk and cardiovascular disease in this day and age.
With endoscopic bariatric therapy and antiobesity medications burgeoning within gastroenterology, Dr. Singrid Young (New York University), Dr. Cameron Zenger (New York University), Dr. Erik Holzwanger (Harvard Medical School in Boston), and Dr. Violeta Popov (New York University) review how their multidisciplinary approach has made their endoscopic bariatric program successful in treating patients struggling with obesity. In our Ethics section, Dr. David Ney (Thomas Jefferson University Hospital, Philadelphia) and Dr. Jason Karlawish (University of Pennsylvania, Philadelphia) delve into patient capacity, particularly when consenting for procedures.
Being involved with national society committees may seem daunting to a lot of trainees and early faculty, but Dr. Peter S. Liang (New York University Langone Health) and Dr. Stephanie D. Pointer (Tristar Hendersonville Medical Center in Tennessee) describe their journeys to becoming AGA committee chairs as early-career physicians. While you ponder whether to join a committee, it may be a good time to learn new ways to increase your financial portfolio through passive income, detailed by Dr. Latifat Alli-Akintade (Kaiser Permanente South Sacramento Medical Center in California).
Last but not least, I am excited to introduce a personal favorite in this newsletter – a piece on females supporting female gastroenterologists in career development and more. Dr. Tonya Adams outlines action items on how to create a culture that fosters professional and leadership development among females, using the Gastro Health Women’s Network as an example of how this network has succeeded in cultivating such an environment.
If you are interested in contributing or have ideas for future TNG topics, please contact me (jtrieu23@gmail.com), or Jillian Schweitzer (jschweitzer@gastro.org), managing editor of TNG.
Until next time, I leave you with an interesting historical fact: William Beaumont, the father of Gastroenterology, published the first findings on the digestive system after performing experiments on Alexis St. Martin when he developed a large gastrocutaneous fistula from an abdominal gunshot wound.
Yours truly,
Judy A. Trieu, MD, MPH
Editor in Chief
Advanced Endoscopy Fellow, University of North Carolina at Chapel Hill, Division of Gastroenterology & Hepatology
Dear colleagues,
This November issue of The New Gastroenterologist marks my official transition as the new Editor in Chief! I am humbled with this opportunity to be a part of such a unique publication and have received immense support from Dr. Vijaya Rao, the TNG staff, as well as my mentors and colleagues. With its foundation built by Dr. Bryson Katona and then taken to the next level by Dr. Rao, TNG has grown over the years, and I hope that I can continue to extend its reach to more trainees and early faculty.
In this issue’s In Focus, Dr. Wenfei Wang and Dr. Neil Sengupta (both from University of Chicago) review the management of antithrombotic medications in elective endoscopic procedures and emphasize individualizing the approach while providing guideline recommendations on how to navigate the gastrointestinal bleeding risk and cardiovascular disease in this day and age.
With endoscopic bariatric therapy and antiobesity medications burgeoning within gastroenterology, Dr. Singrid Young (New York University), Dr. Cameron Zenger (New York University), Dr. Erik Holzwanger (Harvard Medical School in Boston), and Dr. Violeta Popov (New York University) review how their multidisciplinary approach has made their endoscopic bariatric program successful in treating patients struggling with obesity. In our Ethics section, Dr. David Ney (Thomas Jefferson University Hospital, Philadelphia) and Dr. Jason Karlawish (University of Pennsylvania, Philadelphia) delve into patient capacity, particularly when consenting for procedures.
Being involved with national society committees may seem daunting to a lot of trainees and early faculty, but Dr. Peter S. Liang (New York University Langone Health) and Dr. Stephanie D. Pointer (Tristar Hendersonville Medical Center in Tennessee) describe their journeys to becoming AGA committee chairs as early-career physicians. While you ponder whether to join a committee, it may be a good time to learn new ways to increase your financial portfolio through passive income, detailed by Dr. Latifat Alli-Akintade (Kaiser Permanente South Sacramento Medical Center in California).
Last but not least, I am excited to introduce a personal favorite in this newsletter – a piece on females supporting female gastroenterologists in career development and more. Dr. Tonya Adams outlines action items on how to create a culture that fosters professional and leadership development among females, using the Gastro Health Women’s Network as an example of how this network has succeeded in cultivating such an environment.
If you are interested in contributing or have ideas for future TNG topics, please contact me (jtrieu23@gmail.com), or Jillian Schweitzer (jschweitzer@gastro.org), managing editor of TNG.
Until next time, I leave you with an interesting historical fact: William Beaumont, the father of Gastroenterology, published the first findings on the digestive system after performing experiments on Alexis St. Martin when he developed a large gastrocutaneous fistula from an abdominal gunshot wound.
Yours truly,
Judy A. Trieu, MD, MPH
Editor in Chief
Advanced Endoscopy Fellow, University of North Carolina at Chapel Hill, Division of Gastroenterology & Hepatology
Innovation in GI: What’s the next big thing?
Dear colleagues,
Innovation is the livelihood of our field, driving major advances in endoscopy and attracting many of us to Gastroenterology. From the development of endoscopic retrograde cholangiopancreatography to the wide-spread adoption of third space endoscopy, we continue to push the boundaries of our practice. But what is the next big disruption in GI, and how will it impact us? Dr. Jeremy Glissen Brown discusses the application of artificial intelligence in GI highlighting its promise but also raising important questions. Dr. Raman Muthusamy elaborates on single-use endoscopes – are they the wave of the future in preventing infection and meeting patient preference? Or will their long-term cost and environmental impact limit their use? I welcome your own thoughts on disruptive innovation in Gastroenterology – share with us on Twitter @AGA_GIHN and by email at ginews@gastro.org.
Gyanprakash A. Ketwaroo, MD, MSc, is an associate professor of medicine, Yale University, New Haven, Conn., and chief of endoscopy at West Haven (Conn.) VA Medical Center. He is an associate editor for GI & Hepatology News.
The AI revolution, with some important caveats
BY JEREMY R. GLISSEN BROWN, MD, MSC
In 2018, Japan’s Pharmaceutical and Medical Device Agency approved the first artificial intelligence (AI)–based tool, a computer-aided diagnosis system (CADx) for use in clinical practice.1 Since that time, we have seen regulatory approval for a variety of deep learning and AI-based tools in endoscopy and beyond. In addition, there has been an enormous amount of commercial and research interest in AI-based tools in clinical medicine and gastroenterology, and it is almost impossible to open a major gastroenterology journal or go to an academic conference without encountering a slew of AI-based projects.
Many thought and industry leaders say that we are in the midst of an AI revolution in gastroenterology. Indeed, we are at a period of unprecedented growth for deep learning and AI for several reasons, including a recent shift toward data-driven approaches, advancement of machine-learning techniques, and increased computing power. There is, however, also an unprecedented amount of scrutiny and thoughtful conversation about the role AI might play in clinical practice and how we use and regulate these tools in the clinical setting. We are thus in a unique position to ask ourselves the essential question: “Are we on the cusp of an AI revolution in gastroenterology, or are we seeing the release of medical software that is perhaps at best useful in a niche environment and at worse a hype-driven novelty without much clinical benefit?” We will use the most popular use-case, computer aided detection (CADe) of polyps in the colon, to explore this question. In the end, I believe that deep-learning technology will fundamentally change the way we practice gastroenterology. However, this is the perfect time to explore what this means now, and what we can do to shape what it will mean for the future.
CADe: Promise and questions
CADe is a computer vision task that involves localization, such as finding a polyp during colonoscopy and highlighting it with a hollow box. CADe in colonoscopy is perhaps the most well-studied application of deep learning in GI endoscopy to date and is furthest along in the development-implementation pipeline. Because of this, it is an ideal use-case for examining both the evidence that currently supports its use as well as the questions that have come up as we are starting to see CADe algorithms deployed in clinical practice. It is honestly astounding to think that, just 5 years ago, we were talking about CADe as a research concept. While early efforts applying traditional machine learning date back at least to the 1990s, we started to see prospective studies of CADe systems with undetectable or nearly undetectable latency in 2019.2 Since that time we have seen the publication of at least 10 randomized clinical trials involving CADe.
CADe clearly has an impact on some of the conventional quality metrics we use for colonoscopy. While there is considerable heterogeneity in region and design among these trials, most show a significant increase in adenoma detection rate (ADR) and adenomas per colonoscopy. Tandem studies show decreases in adenoma miss rate, and at least one study showed a decrease in sessile serrated lesion miss rate as well. In one of the first randomized, controlled trials across multiple endoscopy centers in Italy, Repici and colleagues showed an increase in ADR from 40.4% in the control group to 54.8% in the CADe group (RR, 1.30; 95% confidence interval, 1.14-1.45).3 Because of pioneering trials such as this one, there are currently several CADe systems that have received regulatory approval in Europe, Asia, and the United States and are being deployed commercially.
It is also clear that the technology is there. In clinical practice, the Food and Drug Administration–approved systems work smoothly, with little to no detectable latency and generally low false-positive and false-negative rates. With clinical deployment, however, we have seen the emergence of healthy debate surrounding every aspect of this task-specific AI. On the development side, important questions include transparency of development data, ensuring that algorithm development is ethical and equitable (as deep learning is susceptible to exacerbating human biases) and methods of data labeling. On the deployment level, important concerns include proper regulation of locked versus “open” algorithms and downstream effects on cost.
In addition, with CADe we have seen a variety of clinical questions crop up because of the novelty of the technology. These include the concern that the increase in ADR we have seen thus far is driven in large part by diminutive and small adenomas (with healthy debate in turn as to these entities’ influence on interval colorectal cancer rates), the effect CADe might have on fellowship training to detect polyps with the human eye, and whether the technology affects sessile serrated lesion detection rates or not. The great thing about such questions is that they have inspired novel research related to CADe in the clinical setting, including how CADe affects trainee ADR, how CADe affects gaze patterns, and how CADe affects recommended surveillance intervals.
CADx, novel applications, and the future
Though there is not space to expand in this particular forum, it is safe to say that with the advancement of CADx in endoscopy and colonoscopy, we have seen similar and novel questions come up. The beautiful thing about all of this is that we are just scratching the surface of what is achievable with deep learning. We have started to see novel projects utilizing deep-learning algorithms, from detecting cirrhosis on ECG to automatically classifying stool consistency on the Bristol Stool Scale from pictures of stool. I ultimately do think that the deployment of AI tools will fundamentally change the way we practice and think about gastroenterology. We are at an incredibly exciting time where we as physicians have the power to shape what that looks like, how we think about AI deployment and regulation and where we go from here.
Dr. Glissen Brown is with the division of gastroenterology and hepatology at Duke University Medical Center, Durham, N.C. He has served as a consultant for Medtronic.
References
1. Aisu N et al. PLOS Digital Health. 2021 Jan 18. doi: 10.1371/journal.pdig.0000001.
2. Wang P et al. Gut. 2019 Oct;68(10):1813-9.
3. Repici A et al. Gastroenterology. 2020 Aug;159(2):512-20.e7.
What’s the future of single-use endoscopes?
BY V. RAMAN MUTHUSAMY, MD, MAS
Single-use endoscopes have been proposed as a definitive solution to the risk of endoscope-transmitted infections. While these infections have been reported for several decades, they have traditionally been associated with identified breaches in the reprocessing protocol. In 2015, numerous cases of duodenoscope-transmitted infections were reported after endoscopic retrograde cholangiopancreatography (ERCP) procedures. Many, if not most, of these cases were not associated with identified deviations from standard high-level disinfection protocols and occurred at high-volume experienced facilities. A subsequent FDA postmarket surveillance study found contamination rates were linked with potentially pathogenic bacteria in approximately 5% of duodenoscopes. Thus, amid growing concerns about the ability to adequately clean these complex devices, these events prompted the development of single-use duodenoscopes. Given the multifactorial causes leading to contaminated duodenoscopes, the advantages of such single-use devices are their ability to ensure the elimination of the potential of infection transmission as these devices are never reused. In addition to this primary benefit, the ability to create single-use devices could lead to more easily available specialty scopes and allow variations in endoscope design that could improve ergonomics. Single-use devices may also expand the ability to provide endoscopic services by eliminating the need for device reprocessing equipment at low-volume sites. However, several concerns have been raised regarding their use, especially if it were to become widespread. These include issues of device quality and performance (potentially leading to more failed cases or adverse events), cost, their environmental impact and current uncertainty regarding their indications for use. Furthermore, new alternatives such as reusable devices with partially disposable components or future low-temperature sterilization options may minimize the need for such devices. We will briefly discuss these issues in more detail below.
Given that nearly all cases of GI device–transmitted infections where standard reprocessing protocols were followed have occurred in duodenoscopes, I will focus on single-use duodenoscopes in this article. It is important that we reassure our patients and colleagues that standard reprocessing appears to be extremely effective with all other types of devices, including elevator containing linear echoendoscopes. Studies investigating the causes of why duodenoscopes have primarily been associated with device-transmitted outbreaks have focused on the complexity of the elevator including its recesses, fixed end-cap and wire channels. However, culturing has shown that up to one-third of contamination may occur in the instrument channels or in the region of the biopsy cap, leading to some potential residual sites of infection even when newly developed reusable devices with disposable elevators/end-caps are utilized.1 Another challenge with reprocessing is the ability to prove residual contamination does not exist. While culturing the devices after reprocessing is most used, it should be noted many sites with outbreaks failed to culture the culprit bacteria from the devices as accessing the sites of contamination can be challenging. The use of other markers of residual contamination such as ATP and tests for residual blood/protein have yielded variable results. Specifically, ATP testing has not correlated well with culture results but may be helpful in assessing the quality of manual cleaning.2
These challenges have made the concept of single-use devices more appealing given the lack of a need reprocess devices or validate cleaning efficacy. Currently, there are two FDA-approved devices on the market, but the published literature to date has largely involved one of these devices. To date, in four published studies that have assessed the clinical performance of single-use duodenoscopes in over 400 patients, procedural success rates have ranged from 91% to 97% with adverse event rates and endoscopist satisfaction scores comparable to reusable devices. Most of these users were expert biliary endoscopists and more data are needed regarding the performance of the device in lower-volume and nonexpert users. While indications for use in these studies have varied, I feel that there are four potential scenarios to utilize these devices: in patients with known multidrug-resistant organisms undergoing ERCP; to facilitate logistics/operations when a reusable device is not available; in critically ill patients who would not tolerate a scope-acquired infection; and in procedures associated with a risk of bacteremia.
While preliminary data suggest single-use duodenoscopes are safe and effective in expert hands, concerns exist regarding their implementation more broadly into clinical practice. First, the devices cost between $1,500-3,000, making them impractical for many health systems. One study estimated the break-even cost of the device to be $800-1,300 based on variation in site volume and device contamination rates.3 However, it should be noted that current enhanced reprocessing protocols for reusable devices may add an additional $75,000-$400,000 per year based on center volume.4 In the United States, there is currently payment by federal and some commercial payors that cover part or all of the device cost, but whether this will continue long-term is unclear. In addition, there is significant concern regarding the environmental impact of a broader mover to single-use devices. Reprocessing programs do exist for these devices, but detailed analyses regarding the environmental effects of a strategy using single-use versus reusable devices and the waste generated from each are needed.
Finally, while primarily created to avoid device-related infection transmission, other benefits can be realized with single-use devices. The potential for ergonomic enhancements (variable handle sizes or shaft stiffness, R- and L-handed scopes) as well as the creation of specialty devices (extra-long or thin devices, devices with special optical or rotational capabilities) may become more feasible with a single-use platform. Finally, the pace of endoscopic innovation and refinement is likely to quicken with a single use platform, and new advancements can be incorporated in a timelier manner.
Conclusion
In summary, I believe single-use devices offer the potential to improve the safety of endoscopic procedures as well as improve procedural access, enhance ergonomics, and foster and expedite device innovation. However, reductions in cost, refining their indications, and developing recycling programs to minimize their environmental impact will be essential before more widespread adoption is achieved.
Dr. Muthusamy is a professor of clinical medicine at the University of California, Los Angeles, and the medical director of endoscopy at the UCLA Health System. He reported relationships with Medtronic, Boston Scientific, Motus GI, Endogastric Solutions, and Capsovision.
References
1. Bartles RL et al. Gastrointest Endosc. 2018 Aug;88(2):306-13.e2.
2. Day LW et al. Gastrointest Endosc. 2021 Jan;93(1):11-33.e6.
3. Bang JY et al. Gut. 2019 Nov;68(11):1915-7.
4. Bomman S et al. Endosc Int Open. 2021 Aug 23;9(9):E1404-12.
Dear colleagues,
Innovation is the livelihood of our field, driving major advances in endoscopy and attracting many of us to Gastroenterology. From the development of endoscopic retrograde cholangiopancreatography to the wide-spread adoption of third space endoscopy, we continue to push the boundaries of our practice. But what is the next big disruption in GI, and how will it impact us? Dr. Jeremy Glissen Brown discusses the application of artificial intelligence in GI highlighting its promise but also raising important questions. Dr. Raman Muthusamy elaborates on single-use endoscopes – are they the wave of the future in preventing infection and meeting patient preference? Or will their long-term cost and environmental impact limit their use? I welcome your own thoughts on disruptive innovation in Gastroenterology – share with us on Twitter @AGA_GIHN and by email at ginews@gastro.org.
Gyanprakash A. Ketwaroo, MD, MSc, is an associate professor of medicine, Yale University, New Haven, Conn., and chief of endoscopy at West Haven (Conn.) VA Medical Center. He is an associate editor for GI & Hepatology News.
The AI revolution, with some important caveats
BY JEREMY R. GLISSEN BROWN, MD, MSC
In 2018, Japan’s Pharmaceutical and Medical Device Agency approved the first artificial intelligence (AI)–based tool, a computer-aided diagnosis system (CADx) for use in clinical practice.1 Since that time, we have seen regulatory approval for a variety of deep learning and AI-based tools in endoscopy and beyond. In addition, there has been an enormous amount of commercial and research interest in AI-based tools in clinical medicine and gastroenterology, and it is almost impossible to open a major gastroenterology journal or go to an academic conference without encountering a slew of AI-based projects.
Many thought and industry leaders say that we are in the midst of an AI revolution in gastroenterology. Indeed, we are at a period of unprecedented growth for deep learning and AI for several reasons, including a recent shift toward data-driven approaches, advancement of machine-learning techniques, and increased computing power. There is, however, also an unprecedented amount of scrutiny and thoughtful conversation about the role AI might play in clinical practice and how we use and regulate these tools in the clinical setting. We are thus in a unique position to ask ourselves the essential question: “Are we on the cusp of an AI revolution in gastroenterology, or are we seeing the release of medical software that is perhaps at best useful in a niche environment and at worse a hype-driven novelty without much clinical benefit?” We will use the most popular use-case, computer aided detection (CADe) of polyps in the colon, to explore this question. In the end, I believe that deep-learning technology will fundamentally change the way we practice gastroenterology. However, this is the perfect time to explore what this means now, and what we can do to shape what it will mean for the future.
CADe: Promise and questions
CADe is a computer vision task that involves localization, such as finding a polyp during colonoscopy and highlighting it with a hollow box. CADe in colonoscopy is perhaps the most well-studied application of deep learning in GI endoscopy to date and is furthest along in the development-implementation pipeline. Because of this, it is an ideal use-case for examining both the evidence that currently supports its use as well as the questions that have come up as we are starting to see CADe algorithms deployed in clinical practice. It is honestly astounding to think that, just 5 years ago, we were talking about CADe as a research concept. While early efforts applying traditional machine learning date back at least to the 1990s, we started to see prospective studies of CADe systems with undetectable or nearly undetectable latency in 2019.2 Since that time we have seen the publication of at least 10 randomized clinical trials involving CADe.
CADe clearly has an impact on some of the conventional quality metrics we use for colonoscopy. While there is considerable heterogeneity in region and design among these trials, most show a significant increase in adenoma detection rate (ADR) and adenomas per colonoscopy. Tandem studies show decreases in adenoma miss rate, and at least one study showed a decrease in sessile serrated lesion miss rate as well. In one of the first randomized, controlled trials across multiple endoscopy centers in Italy, Repici and colleagues showed an increase in ADR from 40.4% in the control group to 54.8% in the CADe group (RR, 1.30; 95% confidence interval, 1.14-1.45).3 Because of pioneering trials such as this one, there are currently several CADe systems that have received regulatory approval in Europe, Asia, and the United States and are being deployed commercially.
It is also clear that the technology is there. In clinical practice, the Food and Drug Administration–approved systems work smoothly, with little to no detectable latency and generally low false-positive and false-negative rates. With clinical deployment, however, we have seen the emergence of healthy debate surrounding every aspect of this task-specific AI. On the development side, important questions include transparency of development data, ensuring that algorithm development is ethical and equitable (as deep learning is susceptible to exacerbating human biases) and methods of data labeling. On the deployment level, important concerns include proper regulation of locked versus “open” algorithms and downstream effects on cost.
In addition, with CADe we have seen a variety of clinical questions crop up because of the novelty of the technology. These include the concern that the increase in ADR we have seen thus far is driven in large part by diminutive and small adenomas (with healthy debate in turn as to these entities’ influence on interval colorectal cancer rates), the effect CADe might have on fellowship training to detect polyps with the human eye, and whether the technology affects sessile serrated lesion detection rates or not. The great thing about such questions is that they have inspired novel research related to CADe in the clinical setting, including how CADe affects trainee ADR, how CADe affects gaze patterns, and how CADe affects recommended surveillance intervals.
CADx, novel applications, and the future
Though there is not space to expand in this particular forum, it is safe to say that with the advancement of CADx in endoscopy and colonoscopy, we have seen similar and novel questions come up. The beautiful thing about all of this is that we are just scratching the surface of what is achievable with deep learning. We have started to see novel projects utilizing deep-learning algorithms, from detecting cirrhosis on ECG to automatically classifying stool consistency on the Bristol Stool Scale from pictures of stool. I ultimately do think that the deployment of AI tools will fundamentally change the way we practice and think about gastroenterology. We are at an incredibly exciting time where we as physicians have the power to shape what that looks like, how we think about AI deployment and regulation and where we go from here.
Dr. Glissen Brown is with the division of gastroenterology and hepatology at Duke University Medical Center, Durham, N.C. He has served as a consultant for Medtronic.
References
1. Aisu N et al. PLOS Digital Health. 2021 Jan 18. doi: 10.1371/journal.pdig.0000001.
2. Wang P et al. Gut. 2019 Oct;68(10):1813-9.
3. Repici A et al. Gastroenterology. 2020 Aug;159(2):512-20.e7.
What’s the future of single-use endoscopes?
BY V. RAMAN MUTHUSAMY, MD, MAS
Single-use endoscopes have been proposed as a definitive solution to the risk of endoscope-transmitted infections. While these infections have been reported for several decades, they have traditionally been associated with identified breaches in the reprocessing protocol. In 2015, numerous cases of duodenoscope-transmitted infections were reported after endoscopic retrograde cholangiopancreatography (ERCP) procedures. Many, if not most, of these cases were not associated with identified deviations from standard high-level disinfection protocols and occurred at high-volume experienced facilities. A subsequent FDA postmarket surveillance study found contamination rates were linked with potentially pathogenic bacteria in approximately 5% of duodenoscopes. Thus, amid growing concerns about the ability to adequately clean these complex devices, these events prompted the development of single-use duodenoscopes. Given the multifactorial causes leading to contaminated duodenoscopes, the advantages of such single-use devices are their ability to ensure the elimination of the potential of infection transmission as these devices are never reused. In addition to this primary benefit, the ability to create single-use devices could lead to more easily available specialty scopes and allow variations in endoscope design that could improve ergonomics. Single-use devices may also expand the ability to provide endoscopic services by eliminating the need for device reprocessing equipment at low-volume sites. However, several concerns have been raised regarding their use, especially if it were to become widespread. These include issues of device quality and performance (potentially leading to more failed cases or adverse events), cost, their environmental impact and current uncertainty regarding their indications for use. Furthermore, new alternatives such as reusable devices with partially disposable components or future low-temperature sterilization options may minimize the need for such devices. We will briefly discuss these issues in more detail below.
Given that nearly all cases of GI device–transmitted infections where standard reprocessing protocols were followed have occurred in duodenoscopes, I will focus on single-use duodenoscopes in this article. It is important that we reassure our patients and colleagues that standard reprocessing appears to be extremely effective with all other types of devices, including elevator containing linear echoendoscopes. Studies investigating the causes of why duodenoscopes have primarily been associated with device-transmitted outbreaks have focused on the complexity of the elevator including its recesses, fixed end-cap and wire channels. However, culturing has shown that up to one-third of contamination may occur in the instrument channels or in the region of the biopsy cap, leading to some potential residual sites of infection even when newly developed reusable devices with disposable elevators/end-caps are utilized.1 Another challenge with reprocessing is the ability to prove residual contamination does not exist. While culturing the devices after reprocessing is most used, it should be noted many sites with outbreaks failed to culture the culprit bacteria from the devices as accessing the sites of contamination can be challenging. The use of other markers of residual contamination such as ATP and tests for residual blood/protein have yielded variable results. Specifically, ATP testing has not correlated well with culture results but may be helpful in assessing the quality of manual cleaning.2
These challenges have made the concept of single-use devices more appealing given the lack of a need reprocess devices or validate cleaning efficacy. Currently, there are two FDA-approved devices on the market, but the published literature to date has largely involved one of these devices. To date, in four published studies that have assessed the clinical performance of single-use duodenoscopes in over 400 patients, procedural success rates have ranged from 91% to 97% with adverse event rates and endoscopist satisfaction scores comparable to reusable devices. Most of these users were expert biliary endoscopists and more data are needed regarding the performance of the device in lower-volume and nonexpert users. While indications for use in these studies have varied, I feel that there are four potential scenarios to utilize these devices: in patients with known multidrug-resistant organisms undergoing ERCP; to facilitate logistics/operations when a reusable device is not available; in critically ill patients who would not tolerate a scope-acquired infection; and in procedures associated with a risk of bacteremia.
While preliminary data suggest single-use duodenoscopes are safe and effective in expert hands, concerns exist regarding their implementation more broadly into clinical practice. First, the devices cost between $1,500-3,000, making them impractical for many health systems. One study estimated the break-even cost of the device to be $800-1,300 based on variation in site volume and device contamination rates.3 However, it should be noted that current enhanced reprocessing protocols for reusable devices may add an additional $75,000-$400,000 per year based on center volume.4 In the United States, there is currently payment by federal and some commercial payors that cover part or all of the device cost, but whether this will continue long-term is unclear. In addition, there is significant concern regarding the environmental impact of a broader mover to single-use devices. Reprocessing programs do exist for these devices, but detailed analyses regarding the environmental effects of a strategy using single-use versus reusable devices and the waste generated from each are needed.
Finally, while primarily created to avoid device-related infection transmission, other benefits can be realized with single-use devices. The potential for ergonomic enhancements (variable handle sizes or shaft stiffness, R- and L-handed scopes) as well as the creation of specialty devices (extra-long or thin devices, devices with special optical or rotational capabilities) may become more feasible with a single-use platform. Finally, the pace of endoscopic innovation and refinement is likely to quicken with a single use platform, and new advancements can be incorporated in a timelier manner.
Conclusion
In summary, I believe single-use devices offer the potential to improve the safety of endoscopic procedures as well as improve procedural access, enhance ergonomics, and foster and expedite device innovation. However, reductions in cost, refining their indications, and developing recycling programs to minimize their environmental impact will be essential before more widespread adoption is achieved.
Dr. Muthusamy is a professor of clinical medicine at the University of California, Los Angeles, and the medical director of endoscopy at the UCLA Health System. He reported relationships with Medtronic, Boston Scientific, Motus GI, Endogastric Solutions, and Capsovision.
References
1. Bartles RL et al. Gastrointest Endosc. 2018 Aug;88(2):306-13.e2.
2. Day LW et al. Gastrointest Endosc. 2021 Jan;93(1):11-33.e6.
3. Bang JY et al. Gut. 2019 Nov;68(11):1915-7.
4. Bomman S et al. Endosc Int Open. 2021 Aug 23;9(9):E1404-12.
Dear colleagues,
Innovation is the livelihood of our field, driving major advances in endoscopy and attracting many of us to Gastroenterology. From the development of endoscopic retrograde cholangiopancreatography to the wide-spread adoption of third space endoscopy, we continue to push the boundaries of our practice. But what is the next big disruption in GI, and how will it impact us? Dr. Jeremy Glissen Brown discusses the application of artificial intelligence in GI highlighting its promise but also raising important questions. Dr. Raman Muthusamy elaborates on single-use endoscopes – are they the wave of the future in preventing infection and meeting patient preference? Or will their long-term cost and environmental impact limit their use? I welcome your own thoughts on disruptive innovation in Gastroenterology – share with us on Twitter @AGA_GIHN and by email at ginews@gastro.org.
Gyanprakash A. Ketwaroo, MD, MSc, is an associate professor of medicine, Yale University, New Haven, Conn., and chief of endoscopy at West Haven (Conn.) VA Medical Center. He is an associate editor for GI & Hepatology News.
The AI revolution, with some important caveats
BY JEREMY R. GLISSEN BROWN, MD, MSC
In 2018, Japan’s Pharmaceutical and Medical Device Agency approved the first artificial intelligence (AI)–based tool, a computer-aided diagnosis system (CADx) for use in clinical practice.1 Since that time, we have seen regulatory approval for a variety of deep learning and AI-based tools in endoscopy and beyond. In addition, there has been an enormous amount of commercial and research interest in AI-based tools in clinical medicine and gastroenterology, and it is almost impossible to open a major gastroenterology journal or go to an academic conference without encountering a slew of AI-based projects.
Many thought and industry leaders say that we are in the midst of an AI revolution in gastroenterology. Indeed, we are at a period of unprecedented growth for deep learning and AI for several reasons, including a recent shift toward data-driven approaches, advancement of machine-learning techniques, and increased computing power. There is, however, also an unprecedented amount of scrutiny and thoughtful conversation about the role AI might play in clinical practice and how we use and regulate these tools in the clinical setting. We are thus in a unique position to ask ourselves the essential question: “Are we on the cusp of an AI revolution in gastroenterology, or are we seeing the release of medical software that is perhaps at best useful in a niche environment and at worse a hype-driven novelty without much clinical benefit?” We will use the most popular use-case, computer aided detection (CADe) of polyps in the colon, to explore this question. In the end, I believe that deep-learning technology will fundamentally change the way we practice gastroenterology. However, this is the perfect time to explore what this means now, and what we can do to shape what it will mean for the future.
CADe: Promise and questions
CADe is a computer vision task that involves localization, such as finding a polyp during colonoscopy and highlighting it with a hollow box. CADe in colonoscopy is perhaps the most well-studied application of deep learning in GI endoscopy to date and is furthest along in the development-implementation pipeline. Because of this, it is an ideal use-case for examining both the evidence that currently supports its use as well as the questions that have come up as we are starting to see CADe algorithms deployed in clinical practice. It is honestly astounding to think that, just 5 years ago, we were talking about CADe as a research concept. While early efforts applying traditional machine learning date back at least to the 1990s, we started to see prospective studies of CADe systems with undetectable or nearly undetectable latency in 2019.2 Since that time we have seen the publication of at least 10 randomized clinical trials involving CADe.
CADe clearly has an impact on some of the conventional quality metrics we use for colonoscopy. While there is considerable heterogeneity in region and design among these trials, most show a significant increase in adenoma detection rate (ADR) and adenomas per colonoscopy. Tandem studies show decreases in adenoma miss rate, and at least one study showed a decrease in sessile serrated lesion miss rate as well. In one of the first randomized, controlled trials across multiple endoscopy centers in Italy, Repici and colleagues showed an increase in ADR from 40.4% in the control group to 54.8% in the CADe group (RR, 1.30; 95% confidence interval, 1.14-1.45).3 Because of pioneering trials such as this one, there are currently several CADe systems that have received regulatory approval in Europe, Asia, and the United States and are being deployed commercially.
It is also clear that the technology is there. In clinical practice, the Food and Drug Administration–approved systems work smoothly, with little to no detectable latency and generally low false-positive and false-negative rates. With clinical deployment, however, we have seen the emergence of healthy debate surrounding every aspect of this task-specific AI. On the development side, important questions include transparency of development data, ensuring that algorithm development is ethical and equitable (as deep learning is susceptible to exacerbating human biases) and methods of data labeling. On the deployment level, important concerns include proper regulation of locked versus “open” algorithms and downstream effects on cost.
In addition, with CADe we have seen a variety of clinical questions crop up because of the novelty of the technology. These include the concern that the increase in ADR we have seen thus far is driven in large part by diminutive and small adenomas (with healthy debate in turn as to these entities’ influence on interval colorectal cancer rates), the effect CADe might have on fellowship training to detect polyps with the human eye, and whether the technology affects sessile serrated lesion detection rates or not. The great thing about such questions is that they have inspired novel research related to CADe in the clinical setting, including how CADe affects trainee ADR, how CADe affects gaze patterns, and how CADe affects recommended surveillance intervals.
CADx, novel applications, and the future
Though there is not space to expand in this particular forum, it is safe to say that with the advancement of CADx in endoscopy and colonoscopy, we have seen similar and novel questions come up. The beautiful thing about all of this is that we are just scratching the surface of what is achievable with deep learning. We have started to see novel projects utilizing deep-learning algorithms, from detecting cirrhosis on ECG to automatically classifying stool consistency on the Bristol Stool Scale from pictures of stool. I ultimately do think that the deployment of AI tools will fundamentally change the way we practice and think about gastroenterology. We are at an incredibly exciting time where we as physicians have the power to shape what that looks like, how we think about AI deployment and regulation and where we go from here.
Dr. Glissen Brown is with the division of gastroenterology and hepatology at Duke University Medical Center, Durham, N.C. He has served as a consultant for Medtronic.
References
1. Aisu N et al. PLOS Digital Health. 2021 Jan 18. doi: 10.1371/journal.pdig.0000001.
2. Wang P et al. Gut. 2019 Oct;68(10):1813-9.
3. Repici A et al. Gastroenterology. 2020 Aug;159(2):512-20.e7.
What’s the future of single-use endoscopes?
BY V. RAMAN MUTHUSAMY, MD, MAS
Single-use endoscopes have been proposed as a definitive solution to the risk of endoscope-transmitted infections. While these infections have been reported for several decades, they have traditionally been associated with identified breaches in the reprocessing protocol. In 2015, numerous cases of duodenoscope-transmitted infections were reported after endoscopic retrograde cholangiopancreatography (ERCP) procedures. Many, if not most, of these cases were not associated with identified deviations from standard high-level disinfection protocols and occurred at high-volume experienced facilities. A subsequent FDA postmarket surveillance study found contamination rates were linked with potentially pathogenic bacteria in approximately 5% of duodenoscopes. Thus, amid growing concerns about the ability to adequately clean these complex devices, these events prompted the development of single-use duodenoscopes. Given the multifactorial causes leading to contaminated duodenoscopes, the advantages of such single-use devices are their ability to ensure the elimination of the potential of infection transmission as these devices are never reused. In addition to this primary benefit, the ability to create single-use devices could lead to more easily available specialty scopes and allow variations in endoscope design that could improve ergonomics. Single-use devices may also expand the ability to provide endoscopic services by eliminating the need for device reprocessing equipment at low-volume sites. However, several concerns have been raised regarding their use, especially if it were to become widespread. These include issues of device quality and performance (potentially leading to more failed cases or adverse events), cost, their environmental impact and current uncertainty regarding their indications for use. Furthermore, new alternatives such as reusable devices with partially disposable components or future low-temperature sterilization options may minimize the need for such devices. We will briefly discuss these issues in more detail below.
Given that nearly all cases of GI device–transmitted infections where standard reprocessing protocols were followed have occurred in duodenoscopes, I will focus on single-use duodenoscopes in this article. It is important that we reassure our patients and colleagues that standard reprocessing appears to be extremely effective with all other types of devices, including elevator containing linear echoendoscopes. Studies investigating the causes of why duodenoscopes have primarily been associated with device-transmitted outbreaks have focused on the complexity of the elevator including its recesses, fixed end-cap and wire channels. However, culturing has shown that up to one-third of contamination may occur in the instrument channels or in the region of the biopsy cap, leading to some potential residual sites of infection even when newly developed reusable devices with disposable elevators/end-caps are utilized.1 Another challenge with reprocessing is the ability to prove residual contamination does not exist. While culturing the devices after reprocessing is most used, it should be noted many sites with outbreaks failed to culture the culprit bacteria from the devices as accessing the sites of contamination can be challenging. The use of other markers of residual contamination such as ATP and tests for residual blood/protein have yielded variable results. Specifically, ATP testing has not correlated well with culture results but may be helpful in assessing the quality of manual cleaning.2
These challenges have made the concept of single-use devices more appealing given the lack of a need reprocess devices or validate cleaning efficacy. Currently, there are two FDA-approved devices on the market, but the published literature to date has largely involved one of these devices. To date, in four published studies that have assessed the clinical performance of single-use duodenoscopes in over 400 patients, procedural success rates have ranged from 91% to 97% with adverse event rates and endoscopist satisfaction scores comparable to reusable devices. Most of these users were expert biliary endoscopists and more data are needed regarding the performance of the device in lower-volume and nonexpert users. While indications for use in these studies have varied, I feel that there are four potential scenarios to utilize these devices: in patients with known multidrug-resistant organisms undergoing ERCP; to facilitate logistics/operations when a reusable device is not available; in critically ill patients who would not tolerate a scope-acquired infection; and in procedures associated with a risk of bacteremia.
While preliminary data suggest single-use duodenoscopes are safe and effective in expert hands, concerns exist regarding their implementation more broadly into clinical practice. First, the devices cost between $1,500-3,000, making them impractical for many health systems. One study estimated the break-even cost of the device to be $800-1,300 based on variation in site volume and device contamination rates.3 However, it should be noted that current enhanced reprocessing protocols for reusable devices may add an additional $75,000-$400,000 per year based on center volume.4 In the United States, there is currently payment by federal and some commercial payors that cover part or all of the device cost, but whether this will continue long-term is unclear. In addition, there is significant concern regarding the environmental impact of a broader mover to single-use devices. Reprocessing programs do exist for these devices, but detailed analyses regarding the environmental effects of a strategy using single-use versus reusable devices and the waste generated from each are needed.
Finally, while primarily created to avoid device-related infection transmission, other benefits can be realized with single-use devices. The potential for ergonomic enhancements (variable handle sizes or shaft stiffness, R- and L-handed scopes) as well as the creation of specialty devices (extra-long or thin devices, devices with special optical or rotational capabilities) may become more feasible with a single-use platform. Finally, the pace of endoscopic innovation and refinement is likely to quicken with a single use platform, and new advancements can be incorporated in a timelier manner.
Conclusion
In summary, I believe single-use devices offer the potential to improve the safety of endoscopic procedures as well as improve procedural access, enhance ergonomics, and foster and expedite device innovation. However, reductions in cost, refining their indications, and developing recycling programs to minimize their environmental impact will be essential before more widespread adoption is achieved.
Dr. Muthusamy is a professor of clinical medicine at the University of California, Los Angeles, and the medical director of endoscopy at the UCLA Health System. He reported relationships with Medtronic, Boston Scientific, Motus GI, Endogastric Solutions, and Capsovision.
References
1. Bartles RL et al. Gastrointest Endosc. 2018 Aug;88(2):306-13.e2.
2. Day LW et al. Gastrointest Endosc. 2021 Jan;93(1):11-33.e6.
3. Bang JY et al. Gut. 2019 Nov;68(11):1915-7.
4. Bomman S et al. Endosc Int Open. 2021 Aug 23;9(9):E1404-12.
Question 2
Correct answer: B. Selenium exposure.
Rationale
Helicobacter pylori infection is by far the most important risk factor for gastric cancer worldwide. Less common risk factors for gastric cancer include Lynch syndrome, Peutz-Jeghers syndrome, Menetrier's disease, and germline mutations in the CDH gene (encoding E-cadherin). However, there is some evidence that selenium, as well as high consumption of fruits and vegetables, may have protective effects against gastric cancer.
References
de Martel C et al. Gastroenterol Clin North Am. 2013 Jun;42(2):219-40.
Giardiello FM et al. N Engl J Med. 1987 Jun 11;316(24):1511-4.
Qiao YL et al. J Natl Cancer Inst. 2009 Apr 1;101(7):507-18.
Correct answer: B. Selenium exposure.
Rationale
Helicobacter pylori infection is by far the most important risk factor for gastric cancer worldwide. Less common risk factors for gastric cancer include Lynch syndrome, Peutz-Jeghers syndrome, Menetrier's disease, and germline mutations in the CDH gene (encoding E-cadherin). However, there is some evidence that selenium, as well as high consumption of fruits and vegetables, may have protective effects against gastric cancer.
References
de Martel C et al. Gastroenterol Clin North Am. 2013 Jun;42(2):219-40.
Giardiello FM et al. N Engl J Med. 1987 Jun 11;316(24):1511-4.
Qiao YL et al. J Natl Cancer Inst. 2009 Apr 1;101(7):507-18.
Correct answer: B. Selenium exposure.
Rationale
Helicobacter pylori infection is by far the most important risk factor for gastric cancer worldwide. Less common risk factors for gastric cancer include Lynch syndrome, Peutz-Jeghers syndrome, Menetrier's disease, and germline mutations in the CDH gene (encoding E-cadherin). However, there is some evidence that selenium, as well as high consumption of fruits and vegetables, may have protective effects against gastric cancer.
References
de Martel C et al. Gastroenterol Clin North Am. 2013 Jun;42(2):219-40.
Giardiello FM et al. N Engl J Med. 1987 Jun 11;316(24):1511-4.
Qiao YL et al. J Natl Cancer Inst. 2009 Apr 1;101(7):507-18.
.











