User login
Facial Contouring With Injectable Biphasic Filler Materials
The Skin Moisturizer Debate: Oil or Oil-Free?
Tretinoin for the Treatment of Photodamaged Skin
Controversy Rages Over Cosmetic Labial Surgery
Obstetrics and gynecology, under siege by diminishing reimbursement and escalating malpractice premiums, has broadly expanded its scope over recent years to include the cosmetic treatment of wrinkles, age spots, and love handles.
The trend has met with mild consternation voiced at medical meetings and in the commentary sections of professional journals, but little fervent pushback—with one notable exception: commercialization of cosmetic genital surgery.
Cosmetic labial surgery and vulvar fat transfers have been at the center of escalating controversy in the literature, pitting critics against proponents in a battle of words over medical ethics, evidence-based medicine, and philosophical questions of free choice and societal pressure.
An opinion about "procedures that are not medically indicated" issued in 2007 by the American College of Obstetricians and Gynecologists' Committee on Gynecologic Practice was considered too tepid by some in its recommendation that women be educated about the lack of evidence supporting the efficacy and safety of cosmetic vulvovaginal surgery.
Doing such procedures and advertising them with photographs of purportedly "attractive" versus "unattractive" genitalia constitutes a violation of the ethical relationship physicians have with their patients, maintains Dr. Paul Indman, an ob.gyn. in solo private practice in Los Gatos, Calif.
"What we do is destroy women's self-esteem [with such photographs] and then charge them a lot of money to fix what we have destroyed. I think our job … is to help women understand what the range of normal is, [to counteract] society-caused, society-influenced perceived differences," he said in an interview.
Dr. Robert D. Moore represents another point of view.
He and longtime partner Dr. John R. Miklos began incorporating cosmetic gynecologic procedures in their practice at the Atlanta Center for Laparoscopic Urogynecology and Reconstructive Pelvic Surgery 10 years ago to fill an unmet need, he said in an interview. "We were starting to see some of these procedures being done, and to be honest, the results were not very good at all. Clearly the surgeons who were doing it did not have experience or expertise in doing reconstructive surgery in this region, and patients were being harmed."
Whether women need the surgery is not a question Dr. Moore considers relevant, although he and the other physicians interviewed for this article all said they refuse to operate on women being pressured by a partner or those who have signs of psychiatric diagnoses such as body dysmorphic disorder.
To question whether patients know enough about normal genital variations to make an informed decision "is an insult to women's intelligence and confidence," he said.
In some cases, clinicians offering the procedures also cite functional indications, such as diminished sexual satisfaction or entrapment of hypertrophic labia with intercourse.
A review of 131 cases published by Dr. Miklos and Dr. Moore found that 37% of women undergoing labiaplasty cited purely aesthetic concerns (including their appearance in tight clothing), 32% cited functional impairment (such as discomfort while bicycling), and 31% had both concerns (J. Sex. Med. 2008;5:1492-5).
In his Los Angeles practice, though, only the "rare" woman cites functional discomfort, said Dr. David Matlock, who directs the Laser Vaginal Rejuvenation Institute of Los Angeles and has trademarked terms such as Laser Vaginal Rejuvenation, Designer Laser Vaginoplasty, and the G-Shot, or G-Spot Amplification.
In most cases, "it's aesthetic surgery. It's personal preference," driven in part by social trends, including Brazilian waxing.
"You don't need your breasts done, tummy tucked, or nose done. None of it is indicated. The patient wants to alter something. I listen to what the patient wants," he said in an interview.
As opposed to surgical innovations that enter the literature through clinical trials, results of which are presented at scientific meetings, "designer vaginoplasty" and aesthetic procedures are taught at profitable seminars and sponsored by surgeons such as Dr. Marco A. Pelosi II, director of the Pelosi Medical Center in Bayonne, N.J., and cofounder with his son, Dr. Marco A. Pelosi III, of the newly established International Society of Cosmetogynecology.
The elder Dr. Pelosi staunchly defended the profit motive for offering cosmetic training, saying that the objective is "totally different" from relatively inexpensive training obtained through professional medical societies. He and a small group of experts spent years developing these procedures and quite reasonably should be compensated for sharing their specialized knowledge with surgeons who stand to profit from what they learn, he said.
"We're not using this to cure cancer," he said in an interview. "This is something that is a service to enhance patients' self-concepts."
The idea that the seminars offer "industry secrets," as well as the general lack of solid data about indications and outcomes, is what concerns Dr. Erin Tracy, an ob.gyn. at Massachusetts General Hospital and a faculty member at Harvard Medical School, both in Boston.
"If they truly have procedures that are safe and beneficial for women, I would think they would want to share this data with the scientific community," she said. "Women need to be educated that at this point, these procedures are not proven to be safe or effective, and carry risks of bleeding, infection, pain with intercourse, and scar tissue."
She and other critics also questioned potential sexual and long-term complications of aesthetic gynecologic surgery, because the labia minora contain clitoral tissue, and the labia undergo physical changes over a woman's lifetime.
"Papers are coming," promised Dr. Matlock, who said a large, multicenter outcomes study of cosmetic genital procedures has been completed and accepted for publication.
Up to now, a handful of papers in scientific journals have been dwarfed by coverage of the procedures in women's magazines and the lay press, driving requests for the procedure.
"It's obviously interesting to the media," said Dr. Matlock. "Sex sells."
Papers decrying the lack of objective outcomes "miss the point," he said. "Is the patient happy or unhappy? That's what it's all about."
"Despite the fact that ob.gyns. are involved their whole lives in dealing with women, [they] have no idea how to meet the needs of female patients," said the elder Dr. Pelosi. "If they are treating anything objective—pain, infections—they are extremely competent, but anything beyond that, they don't want to hear about."
Frequently the argument is made that women have not seen hundreds of vulvas and labias to compare to their own genital appearance, and should be educated during about the wide range of normal anatomy, including labia minora widths at midline ranging from 7-50 mm (BJOG 2005;112:643-6).
The Web site for Dr. Miklos and Dr. Moore explains that labiaplasty can result in a "sleeker, thinner ... more youthful" appearance of the labia, and "inner lips [that] do not protrude past the labia majora at all, giving them a much more appealing shape and eliminating many of the symptoms of enlarged labia."
To question women's decision to obtain a different aesthetic appearance of their genitals is arrogant and demeaning, said Dr. Matlock.
Meanwhile, in the Netherlands, Dr. Karen Marieke Paarlberg reviews a booklet of 38 pictures of normal vulvas with patients requesting labiaplasty and discusses with them alternative means of addressing discomfort, if that is an issue.
"I think that more than 50% of women can be reassured by a doctor who can listen very well and who tries to reassure the woman that she is perfectly normal," she said in an interview.
Obstetrics and gynecology, under siege by diminishing reimbursement and escalating malpractice premiums, has broadly expanded its scope over recent years to include the cosmetic treatment of wrinkles, age spots, and love handles.
The trend has met with mild consternation voiced at medical meetings and in the commentary sections of professional journals, but little fervent pushback—with one notable exception: commercialization of cosmetic genital surgery.
Cosmetic labial surgery and vulvar fat transfers have been at the center of escalating controversy in the literature, pitting critics against proponents in a battle of words over medical ethics, evidence-based medicine, and philosophical questions of free choice and societal pressure.
An opinion about "procedures that are not medically indicated" issued in 2007 by the American College of Obstetricians and Gynecologists' Committee on Gynecologic Practice was considered too tepid by some in its recommendation that women be educated about the lack of evidence supporting the efficacy and safety of cosmetic vulvovaginal surgery.
Doing such procedures and advertising them with photographs of purportedly "attractive" versus "unattractive" genitalia constitutes a violation of the ethical relationship physicians have with their patients, maintains Dr. Paul Indman, an ob.gyn. in solo private practice in Los Gatos, Calif.
"What we do is destroy women's self-esteem [with such photographs] and then charge them a lot of money to fix what we have destroyed. I think our job … is to help women understand what the range of normal is, [to counteract] society-caused, society-influenced perceived differences," he said in an interview.
Dr. Robert D. Moore represents another point of view.
He and longtime partner Dr. John R. Miklos began incorporating cosmetic gynecologic procedures in their practice at the Atlanta Center for Laparoscopic Urogynecology and Reconstructive Pelvic Surgery 10 years ago to fill an unmet need, he said in an interview. "We were starting to see some of these procedures being done, and to be honest, the results were not very good at all. Clearly the surgeons who were doing it did not have experience or expertise in doing reconstructive surgery in this region, and patients were being harmed."
Whether women need the surgery is not a question Dr. Moore considers relevant, although he and the other physicians interviewed for this article all said they refuse to operate on women being pressured by a partner or those who have signs of psychiatric diagnoses such as body dysmorphic disorder.
To question whether patients know enough about normal genital variations to make an informed decision "is an insult to women's intelligence and confidence," he said.
In some cases, clinicians offering the procedures also cite functional indications, such as diminished sexual satisfaction or entrapment of hypertrophic labia with intercourse.
A review of 131 cases published by Dr. Miklos and Dr. Moore found that 37% of women undergoing labiaplasty cited purely aesthetic concerns (including their appearance in tight clothing), 32% cited functional impairment (such as discomfort while bicycling), and 31% had both concerns (J. Sex. Med. 2008;5:1492-5).
In his Los Angeles practice, though, only the "rare" woman cites functional discomfort, said Dr. David Matlock, who directs the Laser Vaginal Rejuvenation Institute of Los Angeles and has trademarked terms such as Laser Vaginal Rejuvenation, Designer Laser Vaginoplasty, and the G-Shot, or G-Spot Amplification.
In most cases, "it's aesthetic surgery. It's personal preference," driven in part by social trends, including Brazilian waxing.
"You don't need your breasts done, tummy tucked, or nose done. None of it is indicated. The patient wants to alter something. I listen to what the patient wants," he said in an interview.
As opposed to surgical innovations that enter the literature through clinical trials, results of which are presented at scientific meetings, "designer vaginoplasty" and aesthetic procedures are taught at profitable seminars and sponsored by surgeons such as Dr. Marco A. Pelosi II, director of the Pelosi Medical Center in Bayonne, N.J., and cofounder with his son, Dr. Marco A. Pelosi III, of the newly established International Society of Cosmetogynecology.
The elder Dr. Pelosi staunchly defended the profit motive for offering cosmetic training, saying that the objective is "totally different" from relatively inexpensive training obtained through professional medical societies. He and a small group of experts spent years developing these procedures and quite reasonably should be compensated for sharing their specialized knowledge with surgeons who stand to profit from what they learn, he said.
"We're not using this to cure cancer," he said in an interview. "This is something that is a service to enhance patients' self-concepts."
The idea that the seminars offer "industry secrets," as well as the general lack of solid data about indications and outcomes, is what concerns Dr. Erin Tracy, an ob.gyn. at Massachusetts General Hospital and a faculty member at Harvard Medical School, both in Boston.
"If they truly have procedures that are safe and beneficial for women, I would think they would want to share this data with the scientific community," she said. "Women need to be educated that at this point, these procedures are not proven to be safe or effective, and carry risks of bleeding, infection, pain with intercourse, and scar tissue."
She and other critics also questioned potential sexual and long-term complications of aesthetic gynecologic surgery, because the labia minora contain clitoral tissue, and the labia undergo physical changes over a woman's lifetime.
"Papers are coming," promised Dr. Matlock, who said a large, multicenter outcomes study of cosmetic genital procedures has been completed and accepted for publication.
Up to now, a handful of papers in scientific journals have been dwarfed by coverage of the procedures in women's magazines and the lay press, driving requests for the procedure.
"It's obviously interesting to the media," said Dr. Matlock. "Sex sells."
Papers decrying the lack of objective outcomes "miss the point," he said. "Is the patient happy or unhappy? That's what it's all about."
"Despite the fact that ob.gyns. are involved their whole lives in dealing with women, [they] have no idea how to meet the needs of female patients," said the elder Dr. Pelosi. "If they are treating anything objective—pain, infections—they are extremely competent, but anything beyond that, they don't want to hear about."
Frequently the argument is made that women have not seen hundreds of vulvas and labias to compare to their own genital appearance, and should be educated during about the wide range of normal anatomy, including labia minora widths at midline ranging from 7-50 mm (BJOG 2005;112:643-6).
The Web site for Dr. Miklos and Dr. Moore explains that labiaplasty can result in a "sleeker, thinner ... more youthful" appearance of the labia, and "inner lips [that] do not protrude past the labia majora at all, giving them a much more appealing shape and eliminating many of the symptoms of enlarged labia."
To question women's decision to obtain a different aesthetic appearance of their genitals is arrogant and demeaning, said Dr. Matlock.
Meanwhile, in the Netherlands, Dr. Karen Marieke Paarlberg reviews a booklet of 38 pictures of normal vulvas with patients requesting labiaplasty and discusses with them alternative means of addressing discomfort, if that is an issue.
"I think that more than 50% of women can be reassured by a doctor who can listen very well and who tries to reassure the woman that she is perfectly normal," she said in an interview.
Obstetrics and gynecology, under siege by diminishing reimbursement and escalating malpractice premiums, has broadly expanded its scope over recent years to include the cosmetic treatment of wrinkles, age spots, and love handles.
The trend has met with mild consternation voiced at medical meetings and in the commentary sections of professional journals, but little fervent pushback—with one notable exception: commercialization of cosmetic genital surgery.
Cosmetic labial surgery and vulvar fat transfers have been at the center of escalating controversy in the literature, pitting critics against proponents in a battle of words over medical ethics, evidence-based medicine, and philosophical questions of free choice and societal pressure.
An opinion about "procedures that are not medically indicated" issued in 2007 by the American College of Obstetricians and Gynecologists' Committee on Gynecologic Practice was considered too tepid by some in its recommendation that women be educated about the lack of evidence supporting the efficacy and safety of cosmetic vulvovaginal surgery.
Doing such procedures and advertising them with photographs of purportedly "attractive" versus "unattractive" genitalia constitutes a violation of the ethical relationship physicians have with their patients, maintains Dr. Paul Indman, an ob.gyn. in solo private practice in Los Gatos, Calif.
"What we do is destroy women's self-esteem [with such photographs] and then charge them a lot of money to fix what we have destroyed. I think our job … is to help women understand what the range of normal is, [to counteract] society-caused, society-influenced perceived differences," he said in an interview.
Dr. Robert D. Moore represents another point of view.
He and longtime partner Dr. John R. Miklos began incorporating cosmetic gynecologic procedures in their practice at the Atlanta Center for Laparoscopic Urogynecology and Reconstructive Pelvic Surgery 10 years ago to fill an unmet need, he said in an interview. "We were starting to see some of these procedures being done, and to be honest, the results were not very good at all. Clearly the surgeons who were doing it did not have experience or expertise in doing reconstructive surgery in this region, and patients were being harmed."
Whether women need the surgery is not a question Dr. Moore considers relevant, although he and the other physicians interviewed for this article all said they refuse to operate on women being pressured by a partner or those who have signs of psychiatric diagnoses such as body dysmorphic disorder.
To question whether patients know enough about normal genital variations to make an informed decision "is an insult to women's intelligence and confidence," he said.
In some cases, clinicians offering the procedures also cite functional indications, such as diminished sexual satisfaction or entrapment of hypertrophic labia with intercourse.
A review of 131 cases published by Dr. Miklos and Dr. Moore found that 37% of women undergoing labiaplasty cited purely aesthetic concerns (including their appearance in tight clothing), 32% cited functional impairment (such as discomfort while bicycling), and 31% had both concerns (J. Sex. Med. 2008;5:1492-5).
In his Los Angeles practice, though, only the "rare" woman cites functional discomfort, said Dr. David Matlock, who directs the Laser Vaginal Rejuvenation Institute of Los Angeles and has trademarked terms such as Laser Vaginal Rejuvenation, Designer Laser Vaginoplasty, and the G-Shot, or G-Spot Amplification.
In most cases, "it's aesthetic surgery. It's personal preference," driven in part by social trends, including Brazilian waxing.
"You don't need your breasts done, tummy tucked, or nose done. None of it is indicated. The patient wants to alter something. I listen to what the patient wants," he said in an interview.
As opposed to surgical innovations that enter the literature through clinical trials, results of which are presented at scientific meetings, "designer vaginoplasty" and aesthetic procedures are taught at profitable seminars and sponsored by surgeons such as Dr. Marco A. Pelosi II, director of the Pelosi Medical Center in Bayonne, N.J., and cofounder with his son, Dr. Marco A. Pelosi III, of the newly established International Society of Cosmetogynecology.
The elder Dr. Pelosi staunchly defended the profit motive for offering cosmetic training, saying that the objective is "totally different" from relatively inexpensive training obtained through professional medical societies. He and a small group of experts spent years developing these procedures and quite reasonably should be compensated for sharing their specialized knowledge with surgeons who stand to profit from what they learn, he said.
"We're not using this to cure cancer," he said in an interview. "This is something that is a service to enhance patients' self-concepts."
The idea that the seminars offer "industry secrets," as well as the general lack of solid data about indications and outcomes, is what concerns Dr. Erin Tracy, an ob.gyn. at Massachusetts General Hospital and a faculty member at Harvard Medical School, both in Boston.
"If they truly have procedures that are safe and beneficial for women, I would think they would want to share this data with the scientific community," she said. "Women need to be educated that at this point, these procedures are not proven to be safe or effective, and carry risks of bleeding, infection, pain with intercourse, and scar tissue."
She and other critics also questioned potential sexual and long-term complications of aesthetic gynecologic surgery, because the labia minora contain clitoral tissue, and the labia undergo physical changes over a woman's lifetime.
"Papers are coming," promised Dr. Matlock, who said a large, multicenter outcomes study of cosmetic genital procedures has been completed and accepted for publication.
Up to now, a handful of papers in scientific journals have been dwarfed by coverage of the procedures in women's magazines and the lay press, driving requests for the procedure.
"It's obviously interesting to the media," said Dr. Matlock. "Sex sells."
Papers decrying the lack of objective outcomes "miss the point," he said. "Is the patient happy or unhappy? That's what it's all about."
"Despite the fact that ob.gyns. are involved their whole lives in dealing with women, [they] have no idea how to meet the needs of female patients," said the elder Dr. Pelosi. "If they are treating anything objective—pain, infections—they are extremely competent, but anything beyond that, they don't want to hear about."
Frequently the argument is made that women have not seen hundreds of vulvas and labias to compare to their own genital appearance, and should be educated during about the wide range of normal anatomy, including labia minora widths at midline ranging from 7-50 mm (BJOG 2005;112:643-6).
The Web site for Dr. Miklos and Dr. Moore explains that labiaplasty can result in a "sleeker, thinner ... more youthful" appearance of the labia, and "inner lips [that] do not protrude past the labia majora at all, giving them a much more appealing shape and eliminating many of the symptoms of enlarged labia."
To question women's decision to obtain a different aesthetic appearance of their genitals is arrogant and demeaning, said Dr. Matlock.
Meanwhile, in the Netherlands, Dr. Karen Marieke Paarlberg reviews a booklet of 38 pictures of normal vulvas with patients requesting labiaplasty and discusses with them alternative means of addressing discomfort, if that is an issue.
"I think that more than 50% of women can be reassured by a doctor who can listen very well and who tries to reassure the woman that she is perfectly normal," she said in an interview.
Evidence Backs Imiquimod Tx for Melanoma in Situ
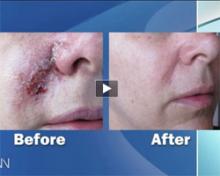
MIAMI — The topical immune response modulator imiquimod has a role in the treatment of melanoma in situ, particularly if patients refuse or fail surgery.
There are several concerns. The agent is only recommended for thinner lesions, and "failures do occur," said Dr. M. Shane Chapman of Darmouth-Hitchcock Medical Center in Lebanon, N.H. Also, "the 5-year follow-up data is not great—it's sparse. We are just not there yet."
Despite this, he said, imiquimod 5% cream (Aldara, Graceway) can have a role in the management of melanoma in situ, also known as lentigo maligna. Dr. Chapman acknowledged the controversial nature of his stance, and based his position on small case series, one "good prospective study" in the literature, and his own experience with more than 60 patients.
As an example, he discussed a 36-year-old man with metastatic melanoma. The patient had multiple surgeries and radiation therapy "and nothing seemed to work," he said. "I basically bathed him in imiquimod over several months." Six years later, the patient is doing well with no signs of nodal or metastatic disease. As with all melanoma patients, regardless of the therapy, they should be followed continuously for a lifetime, he said at the annual meeting of the American Academy of Dermatology.
In his regimen, imiquimod 5% cream is applied five times per week for 12 weeks, with a rest period on weekends. Inflammation can be intense with this aggressive protocol, so it is important to educate patients beforehand. Pretreatment with retinoids—such as tazarotene (Tazarac, Allergan) for 2 weeks—can increase the effectiveness of imiquimod in this setting, he added.
"The only good prospective study to date," Dr. Chapman said, is an open-label trial in which participants received daily treatment with topical 5% imiquimod for 3 months, followed by a biopsy 1 month post therapy (Br. J. Dermatol. 2003;149:66-70). The complete response rate was 93% in 28 patients with histologically confirmed lentigo maligna. Two patients were treatment failures.
Because of potential failures, "always go back and do a biopsy after clearance," he said.
For example, in a retrospective study of 40 patients pretreated with imiquimod (Dermatol. Surg. 2008;34:147-51), 30 appeared clinically clear after staged excision "but three of these had histologic evidence of disease—that is why I always do a follow-up biopsy."
One of his own patients failed after initial clearance of his lesion, Dr. Chapman said. The man had a large scalp lesion that cleared following use of topical imiquimod without retinoid treatment. "For 8 months, we thought he was cleared. He came back and had a node in middle of the lesion site—his third recurrence over 5 years." Dr. Chapman added, "He's doing well, but failures do occur."
It is important to realize that "we think we know when something is in situ, but we don't always know the entire lesion is in situ when we do this," Dr. Chapman said.
Even though surgical excision remains the first-line choice for most patients with melanoma in situ or thin melanoma lesions, surgery nonresponders or those who refuse resection can benefit from imiquimod. He cited three examples: a woman who did not want to have repeat surgery and whose lesion cleared with imiquimod; a man who did not want further surgery following two melanoma lesion excisions close together on his temple, who was treated well with imiquimod; and a patient with recurrent melanoma in situ at the forehead flap of the nose who is doing well 4 years out after imiquimod treatment.
In response to a question from the audience, Dr. Chapman said, "I don't think just any inflammatory response is going to make melanoma go away. Imiquimod is one of those serendipitous chemicals that is useful for a lot of skin tumors for some reason."
Dr. Chapman is a consultant for, and receives honoraria from, Graceway. He also receives honoraria from Abbott.
MIAMI — The topical immune response modulator imiquimod has a role in the treatment of melanoma in situ, particularly if patients refuse or fail surgery.
There are several concerns. The agent is only recommended for thinner lesions, and "failures do occur," said Dr. M. Shane Chapman of Darmouth-Hitchcock Medical Center in Lebanon, N.H. Also, "the 5-year follow-up data is not great—it's sparse. We are just not there yet."
Despite this, he said, imiquimod 5% cream (Aldara, Graceway) can have a role in the management of melanoma in situ, also known as lentigo maligna. Dr. Chapman acknowledged the controversial nature of his stance, and based his position on small case series, one "good prospective study" in the literature, and his own experience with more than 60 patients.
As an example, he discussed a 36-year-old man with metastatic melanoma. The patient had multiple surgeries and radiation therapy "and nothing seemed to work," he said. "I basically bathed him in imiquimod over several months." Six years later, the patient is doing well with no signs of nodal or metastatic disease. As with all melanoma patients, regardless of the therapy, they should be followed continuously for a lifetime, he said at the annual meeting of the American Academy of Dermatology.
In his regimen, imiquimod 5% cream is applied five times per week for 12 weeks, with a rest period on weekends. Inflammation can be intense with this aggressive protocol, so it is important to educate patients beforehand. Pretreatment with retinoids—such as tazarotene (Tazarac, Allergan) for 2 weeks—can increase the effectiveness of imiquimod in this setting, he added.
"The only good prospective study to date," Dr. Chapman said, is an open-label trial in which participants received daily treatment with topical 5% imiquimod for 3 months, followed by a biopsy 1 month post therapy (Br. J. Dermatol. 2003;149:66-70). The complete response rate was 93% in 28 patients with histologically confirmed lentigo maligna. Two patients were treatment failures.
Because of potential failures, "always go back and do a biopsy after clearance," he said.
For example, in a retrospective study of 40 patients pretreated with imiquimod (Dermatol. Surg. 2008;34:147-51), 30 appeared clinically clear after staged excision "but three of these had histologic evidence of disease—that is why I always do a follow-up biopsy."
One of his own patients failed after initial clearance of his lesion, Dr. Chapman said. The man had a large scalp lesion that cleared following use of topical imiquimod without retinoid treatment. "For 8 months, we thought he was cleared. He came back and had a node in middle of the lesion site—his third recurrence over 5 years." Dr. Chapman added, "He's doing well, but failures do occur."
It is important to realize that "we think we know when something is in situ, but we don't always know the entire lesion is in situ when we do this," Dr. Chapman said.
Even though surgical excision remains the first-line choice for most patients with melanoma in situ or thin melanoma lesions, surgery nonresponders or those who refuse resection can benefit from imiquimod. He cited three examples: a woman who did not want to have repeat surgery and whose lesion cleared with imiquimod; a man who did not want further surgery following two melanoma lesion excisions close together on his temple, who was treated well with imiquimod; and a patient with recurrent melanoma in situ at the forehead flap of the nose who is doing well 4 years out after imiquimod treatment.
In response to a question from the audience, Dr. Chapman said, "I don't think just any inflammatory response is going to make melanoma go away. Imiquimod is one of those serendipitous chemicals that is useful for a lot of skin tumors for some reason."
Dr. Chapman is a consultant for, and receives honoraria from, Graceway. He also receives honoraria from Abbott.
MIAMI — The topical immune response modulator imiquimod has a role in the treatment of melanoma in situ, particularly if patients refuse or fail surgery.
There are several concerns. The agent is only recommended for thinner lesions, and "failures do occur," said Dr. M. Shane Chapman of Darmouth-Hitchcock Medical Center in Lebanon, N.H. Also, "the 5-year follow-up data is not great—it's sparse. We are just not there yet."
Despite this, he said, imiquimod 5% cream (Aldara, Graceway) can have a role in the management of melanoma in situ, also known as lentigo maligna. Dr. Chapman acknowledged the controversial nature of his stance, and based his position on small case series, one "good prospective study" in the literature, and his own experience with more than 60 patients.
As an example, he discussed a 36-year-old man with metastatic melanoma. The patient had multiple surgeries and radiation therapy "and nothing seemed to work," he said. "I basically bathed him in imiquimod over several months." Six years later, the patient is doing well with no signs of nodal or metastatic disease. As with all melanoma patients, regardless of the therapy, they should be followed continuously for a lifetime, he said at the annual meeting of the American Academy of Dermatology.
In his regimen, imiquimod 5% cream is applied five times per week for 12 weeks, with a rest period on weekends. Inflammation can be intense with this aggressive protocol, so it is important to educate patients beforehand. Pretreatment with retinoids—such as tazarotene (Tazarac, Allergan) for 2 weeks—can increase the effectiveness of imiquimod in this setting, he added.
"The only good prospective study to date," Dr. Chapman said, is an open-label trial in which participants received daily treatment with topical 5% imiquimod for 3 months, followed by a biopsy 1 month post therapy (Br. J. Dermatol. 2003;149:66-70). The complete response rate was 93% in 28 patients with histologically confirmed lentigo maligna. Two patients were treatment failures.
Because of potential failures, "always go back and do a biopsy after clearance," he said.
For example, in a retrospective study of 40 patients pretreated with imiquimod (Dermatol. Surg. 2008;34:147-51), 30 appeared clinically clear after staged excision "but three of these had histologic evidence of disease—that is why I always do a follow-up biopsy."
One of his own patients failed after initial clearance of his lesion, Dr. Chapman said. The man had a large scalp lesion that cleared following use of topical imiquimod without retinoid treatment. "For 8 months, we thought he was cleared. He came back and had a node in middle of the lesion site—his third recurrence over 5 years." Dr. Chapman added, "He's doing well, but failures do occur."
It is important to realize that "we think we know when something is in situ, but we don't always know the entire lesion is in situ when we do this," Dr. Chapman said.
Even though surgical excision remains the first-line choice for most patients with melanoma in situ or thin melanoma lesions, surgery nonresponders or those who refuse resection can benefit from imiquimod. He cited three examples: a woman who did not want to have repeat surgery and whose lesion cleared with imiquimod; a man who did not want further surgery following two melanoma lesion excisions close together on his temple, who was treated well with imiquimod; and a patient with recurrent melanoma in situ at the forehead flap of the nose who is doing well 4 years out after imiquimod treatment.
In response to a question from the audience, Dr. Chapman said, "I don't think just any inflammatory response is going to make melanoma go away. Imiquimod is one of those serendipitous chemicals that is useful for a lot of skin tumors for some reason."
Dr. Chapman is a consultant for, and receives honoraria from, Graceway. He also receives honoraria from Abbott.
Oleuropein
Oleuropein is a phenolic compound derived from the leaves and oil of the olive tree Olea europaea as well as the leaves of the privet shrub. In the ancient world, olive oil was viewed as an essential substance and has been used for centuries in a wide variety of cutaneous treatments. Ancient Greeks bathed with olive oil (Phytother. Res. 2003;17:987-1,000), and ancient Egyptians and Romans used it in food, cosmetics, massage preparations for athletes, anointing substances, and salves for wounds.
Dietary Role of Olive Oil
The Mediterranean diet, reputed to be among the world's healthiest, features olive oil. Epidemiologic evidence now suggests that the Mediterranean diet, which also includes fruits, vegetables, and fish, is associated with reduced cancer and coronary heart disease risk. In addition, recent studies suggest that the olive oil-rich Mediterranean diet contributes to healthier aging and greater longevity (Eur. J. Clin. Invest. 2005;35:421-4).
The benefits of the Mediterranean diet have been partly attributed to the protective activity of the phenolic constituents caffeic acid and oleuropein present in extra-virgin olive oil (Med. Clin. (Barc) 2003;120:128-31). Oleuropein and hydroxytyrosol (a phenolic component of olive oil and a metabolite of oleuropein) have been found in vivo and in vitro to be potent antioxidants that confer significant biologic benefits, including cardioprotective effects (Med. Res. Rev. 2002;22:65-75; Curr. Atheroscler. Rep. 2001;3:64-7; Crit. Rev. Food Sci. Nutr. 2002;42:209-21).Visioli et al. have also shown that both compounds are strong scavengers of superoxide radicals and inhibitors of neutrophil respiratory burst (Biochem. Biophys. Res. Commun. 1998;247:60-4).
Benefits of Phenolic Compounds
Olive oils' phenolic compounds have demonstrated antimicrobial activity against several bacterial strains associated with intestinal and respiratory infections (Altern. Med. Rev. 2007;12:331-42; J. Nutr. Biochem. 2002;13:636-44). Bioavailable in humans, these compounds have also shown the ability to improve endothelial function as well as to modify hemostasis, exhibiting antithrombotic properties (Eur. J. Clin. Invest. 2005;35:421-4). Oleuropein is known to display numerous biologic properties, many of which have been ascribed to its antioxidant activities (Int. J. Cosmet. Sci. 2008;30:113-20). In addition to antioxidant and antibacterial properties, oleuropein is thought to possess antiviral and antifungal qualities.
The polyphenols oleuropein, tyrosol, hydroxytyrosol, and caffeic acid are the primary components of the polar fraction of virgin olive oil (Z. Naturforsch [C] 2000;55:814-9). A decade ago, de la Puerta et al. set out to ascertain the antieicosanoid and antioxidant effects in leukocytes of these olive oil constituents.
All four suppressed leukotriene B4 generation at the 5-lipoxygenase level in intact rat peritoneal leukocytes stimulated with calcium ionophore. None of the compounds was toxic to leukocytes at tested concentrations, and none significantly inhibited thromboxane generation through the cyclooxygenase pathway. The investigators concluded that oleuropein and the other phenolics present in virgin olive oil exhibit various antioxidant, lipoxygenase-inhibitory, and prostaglandin activities (Biochem. Pharmacol. 1999;57:445-9).
Slightly less than a decade ago, researchers showed that all three different classes of phenolic constituents in olive oil, including simple phenols (hydroxytyrosol, tyrosol), secoiridoids (oleuropein, the aglycone of ligstroside, and their respective decarboxylated dialdehyde derivatives), and lignans [(+)-1-acetoxypinoresinol and pinoresinol], exhibit potent antioxidant activity. They stressed that consuming extra-virgin olive oil, which is laden with these phenolic antioxidants in addition to squalene and oleic acid, should hinder oxidative stress and thus yield significant protection against various cancers (such as colon, breast, and skin), coronary heart disease, and aging (Lancet Oncol. 2000;1:107-12).
In 2000, de la Puerta et al. investigated the anti-inflammatory effects of the unsaponifiable fraction of virgin olive oil and of the phenolic compounds of the polar fraction on edema in mice induced by arachidonic acid or 12-O-tetradecanoylphorbol-13- acetate (TPA). Of the phenolic constituents, oleuropein provoked the greatest inhibition of arachidonic acid-induced edema, similar to the reference drug dexamethasone. Varying degrees of anti-inflammatory activity were seen in both assays after the topical application of the olive oil compounds. The investigators concluded that both fractions may play a role in exerting the beneficial activity against various diseases that has been associated with olive oil (Z. Naturforsch [C] 2000;55:814-9).
In 2005, investigators studied the effects of several phenolic compounds (vanillic, p-coumaric, syringic, homovanillic and caffeic acids, kaempferol, oleuropein glycoside, and tyrosol) present in extra-virgin olive oil on inflammatory mediator production by human mononuclear cells. They stimulated diluted human blood cultures with lipopolysaccharide in the presence of the phenolics at various concentrations. Enzyme-linked immunosorbent assays were used to measure inflammatory cytokine concentration. Results showed that oleuropein glycoside and caffeic acid reduced the concentration of interleukin-1 beta by 80% and 40%, respectively. The investigators concluded that the effects seen from some phenolic compounds, including oleuropein, found in extra-virgin olive oil may play a role in the antiatherogenic activity attributed to the oil (Nutrition 2005;21:389-94).
Cosmetic Benefits
In 2008, researchers assessed the cosmetic activity of oleuropein against UVB-induced erythema by preparing an emulsion and emulgel that included the phenolic compound and then applying it on healthy volunteers exposed to UVB. Barrier function, skin color, and microcirculation were evaluated in the study, which considered protective effects delivered via preirradiation topical applications and mitigating effects after erythema induction. The investigators reported that the oleuropein preparations performed well, decreasing erythema, transepidermal water loss, and blood flow by 22%, 35%, and 30%, respectively. They concluded that oleuropein has the potential to be effective in combination with other active ingredients to mend the damage caused by UV radiation (Int. J. Cosmet. Sci. 2008;30:113-20).
In a study of olive oil and its disease-preventive capacity through the modulation of cell signaling, Wahle et al. suggested that the antioxidant effects of olive oil are likely multifactorial, resulting from a combination of its high oleic acid content (low oxidation potential in comparison to linoleic acid) and its high composition of various phenolic antioxidants, especially oleuropein, hydroxytyrosol, and tyrosol (Lipids 2004;39:1223-31).
Oleuropein is high on the long list of ingredients of Innovative Skincare's iS Clinical Moisturizing Treatment Sunscreen SPF 25, which, according to the manufacturer, incorporates innovative technology and several potent antioxidants to protect against sunburn and cutaneous aging. Innovative Skincare's Pro-Heal Serum also contains oleuropein--along with vitamins A, C, and E; kojic acid; and zinc sulfate--in a formulation intended to protect against UV damage and for the treatment of acne and rosacea. Oleuropein is also included among a cocktail of botanical ingredients, such as kaolin, glycolic acid, echinacea, peppermint, rosemary, and green tea extracts, in the Cellex-C Betaplex Clear Complexion Mask, which is designed to offer gentle exfoliation.
Conclusion
As is the case with numerous botanical ingredients, olive oil was used extensively in the ancient world, and its benefits are being relearned by the modern world.
Oleuropein is a key ingredient in olive oil, which is now known to be an integral part of the healthy Mediterranean diet and is used orally and topically to confer various health benefits. Indeed, oleuropein is one of the several key constituents in olive oil that have been demonstrated to impart antioxidant, antibacterial, anti-inflammatory, and anticarcinogenic effects.
Current data provide reasons for optimism, particularly if oleuropein, other olive oil components, and olive oil itself can be shown in topical form to consistently deliver such benefits. Nevertheless, much remains to be learned about oleuropein and the other constituents of olive oil in terms of mechanisms of action and the full range of health benefits they may confer.
Oleuropein is a phenolic compound derived from the leaves and oil of the olive tree Olea europaea as well as the leaves of the privet shrub. In the ancient world, olive oil was viewed as an essential substance and has been used for centuries in a wide variety of cutaneous treatments. Ancient Greeks bathed with olive oil (Phytother. Res. 2003;17:987-1,000), and ancient Egyptians and Romans used it in food, cosmetics, massage preparations for athletes, anointing substances, and salves for wounds.
Dietary Role of Olive Oil
The Mediterranean diet, reputed to be among the world's healthiest, features olive oil. Epidemiologic evidence now suggests that the Mediterranean diet, which also includes fruits, vegetables, and fish, is associated with reduced cancer and coronary heart disease risk. In addition, recent studies suggest that the olive oil-rich Mediterranean diet contributes to healthier aging and greater longevity (Eur. J. Clin. Invest. 2005;35:421-4).
The benefits of the Mediterranean diet have been partly attributed to the protective activity of the phenolic constituents caffeic acid and oleuropein present in extra-virgin olive oil (Med. Clin. (Barc) 2003;120:128-31). Oleuropein and hydroxytyrosol (a phenolic component of olive oil and a metabolite of oleuropein) have been found in vivo and in vitro to be potent antioxidants that confer significant biologic benefits, including cardioprotective effects (Med. Res. Rev. 2002;22:65-75; Curr. Atheroscler. Rep. 2001;3:64-7; Crit. Rev. Food Sci. Nutr. 2002;42:209-21).Visioli et al. have also shown that both compounds are strong scavengers of superoxide radicals and inhibitors of neutrophil respiratory burst (Biochem. Biophys. Res. Commun. 1998;247:60-4).
Benefits of Phenolic Compounds
Olive oils' phenolic compounds have demonstrated antimicrobial activity against several bacterial strains associated with intestinal and respiratory infections (Altern. Med. Rev. 2007;12:331-42; J. Nutr. Biochem. 2002;13:636-44). Bioavailable in humans, these compounds have also shown the ability to improve endothelial function as well as to modify hemostasis, exhibiting antithrombotic properties (Eur. J. Clin. Invest. 2005;35:421-4). Oleuropein is known to display numerous biologic properties, many of which have been ascribed to its antioxidant activities (Int. J. Cosmet. Sci. 2008;30:113-20). In addition to antioxidant and antibacterial properties, oleuropein is thought to possess antiviral and antifungal qualities.
The polyphenols oleuropein, tyrosol, hydroxytyrosol, and caffeic acid are the primary components of the polar fraction of virgin olive oil (Z. Naturforsch [C] 2000;55:814-9). A decade ago, de la Puerta et al. set out to ascertain the antieicosanoid and antioxidant effects in leukocytes of these olive oil constituents.
All four suppressed leukotriene B4 generation at the 5-lipoxygenase level in intact rat peritoneal leukocytes stimulated with calcium ionophore. None of the compounds was toxic to leukocytes at tested concentrations, and none significantly inhibited thromboxane generation through the cyclooxygenase pathway. The investigators concluded that oleuropein and the other phenolics present in virgin olive oil exhibit various antioxidant, lipoxygenase-inhibitory, and prostaglandin activities (Biochem. Pharmacol. 1999;57:445-9).
Slightly less than a decade ago, researchers showed that all three different classes of phenolic constituents in olive oil, including simple phenols (hydroxytyrosol, tyrosol), secoiridoids (oleuropein, the aglycone of ligstroside, and their respective decarboxylated dialdehyde derivatives), and lignans [(+)-1-acetoxypinoresinol and pinoresinol], exhibit potent antioxidant activity. They stressed that consuming extra-virgin olive oil, which is laden with these phenolic antioxidants in addition to squalene and oleic acid, should hinder oxidative stress and thus yield significant protection against various cancers (such as colon, breast, and skin), coronary heart disease, and aging (Lancet Oncol. 2000;1:107-12).
In 2000, de la Puerta et al. investigated the anti-inflammatory effects of the unsaponifiable fraction of virgin olive oil and of the phenolic compounds of the polar fraction on edema in mice induced by arachidonic acid or 12-O-tetradecanoylphorbol-13- acetate (TPA). Of the phenolic constituents, oleuropein provoked the greatest inhibition of arachidonic acid-induced edema, similar to the reference drug dexamethasone. Varying degrees of anti-inflammatory activity were seen in both assays after the topical application of the olive oil compounds. The investigators concluded that both fractions may play a role in exerting the beneficial activity against various diseases that has been associated with olive oil (Z. Naturforsch [C] 2000;55:814-9).
In 2005, investigators studied the effects of several phenolic compounds (vanillic, p-coumaric, syringic, homovanillic and caffeic acids, kaempferol, oleuropein glycoside, and tyrosol) present in extra-virgin olive oil on inflammatory mediator production by human mononuclear cells. They stimulated diluted human blood cultures with lipopolysaccharide in the presence of the phenolics at various concentrations. Enzyme-linked immunosorbent assays were used to measure inflammatory cytokine concentration. Results showed that oleuropein glycoside and caffeic acid reduced the concentration of interleukin-1 beta by 80% and 40%, respectively. The investigators concluded that the effects seen from some phenolic compounds, including oleuropein, found in extra-virgin olive oil may play a role in the antiatherogenic activity attributed to the oil (Nutrition 2005;21:389-94).
Cosmetic Benefits
In 2008, researchers assessed the cosmetic activity of oleuropein against UVB-induced erythema by preparing an emulsion and emulgel that included the phenolic compound and then applying it on healthy volunteers exposed to UVB. Barrier function, skin color, and microcirculation were evaluated in the study, which considered protective effects delivered via preirradiation topical applications and mitigating effects after erythema induction. The investigators reported that the oleuropein preparations performed well, decreasing erythema, transepidermal water loss, and blood flow by 22%, 35%, and 30%, respectively. They concluded that oleuropein has the potential to be effective in combination with other active ingredients to mend the damage caused by UV radiation (Int. J. Cosmet. Sci. 2008;30:113-20).
In a study of olive oil and its disease-preventive capacity through the modulation of cell signaling, Wahle et al. suggested that the antioxidant effects of olive oil are likely multifactorial, resulting from a combination of its high oleic acid content (low oxidation potential in comparison to linoleic acid) and its high composition of various phenolic antioxidants, especially oleuropein, hydroxytyrosol, and tyrosol (Lipids 2004;39:1223-31).
Oleuropein is high on the long list of ingredients of Innovative Skincare's iS Clinical Moisturizing Treatment Sunscreen SPF 25, which, according to the manufacturer, incorporates innovative technology and several potent antioxidants to protect against sunburn and cutaneous aging. Innovative Skincare's Pro-Heal Serum also contains oleuropein--along with vitamins A, C, and E; kojic acid; and zinc sulfate--in a formulation intended to protect against UV damage and for the treatment of acne and rosacea. Oleuropein is also included among a cocktail of botanical ingredients, such as kaolin, glycolic acid, echinacea, peppermint, rosemary, and green tea extracts, in the Cellex-C Betaplex Clear Complexion Mask, which is designed to offer gentle exfoliation.
Conclusion
As is the case with numerous botanical ingredients, olive oil was used extensively in the ancient world, and its benefits are being relearned by the modern world.
Oleuropein is a key ingredient in olive oil, which is now known to be an integral part of the healthy Mediterranean diet and is used orally and topically to confer various health benefits. Indeed, oleuropein is one of the several key constituents in olive oil that have been demonstrated to impart antioxidant, antibacterial, anti-inflammatory, and anticarcinogenic effects.
Current data provide reasons for optimism, particularly if oleuropein, other olive oil components, and olive oil itself can be shown in topical form to consistently deliver such benefits. Nevertheless, much remains to be learned about oleuropein and the other constituents of olive oil in terms of mechanisms of action and the full range of health benefits they may confer.
Oleuropein is a phenolic compound derived from the leaves and oil of the olive tree Olea europaea as well as the leaves of the privet shrub. In the ancient world, olive oil was viewed as an essential substance and has been used for centuries in a wide variety of cutaneous treatments. Ancient Greeks bathed with olive oil (Phytother. Res. 2003;17:987-1,000), and ancient Egyptians and Romans used it in food, cosmetics, massage preparations for athletes, anointing substances, and salves for wounds.
Dietary Role of Olive Oil
The Mediterranean diet, reputed to be among the world's healthiest, features olive oil. Epidemiologic evidence now suggests that the Mediterranean diet, which also includes fruits, vegetables, and fish, is associated with reduced cancer and coronary heart disease risk. In addition, recent studies suggest that the olive oil-rich Mediterranean diet contributes to healthier aging and greater longevity (Eur. J. Clin. Invest. 2005;35:421-4).
The benefits of the Mediterranean diet have been partly attributed to the protective activity of the phenolic constituents caffeic acid and oleuropein present in extra-virgin olive oil (Med. Clin. (Barc) 2003;120:128-31). Oleuropein and hydroxytyrosol (a phenolic component of olive oil and a metabolite of oleuropein) have been found in vivo and in vitro to be potent antioxidants that confer significant biologic benefits, including cardioprotective effects (Med. Res. Rev. 2002;22:65-75; Curr. Atheroscler. Rep. 2001;3:64-7; Crit. Rev. Food Sci. Nutr. 2002;42:209-21).Visioli et al. have also shown that both compounds are strong scavengers of superoxide radicals and inhibitors of neutrophil respiratory burst (Biochem. Biophys. Res. Commun. 1998;247:60-4).
Benefits of Phenolic Compounds
Olive oils' phenolic compounds have demonstrated antimicrobial activity against several bacterial strains associated with intestinal and respiratory infections (Altern. Med. Rev. 2007;12:331-42; J. Nutr. Biochem. 2002;13:636-44). Bioavailable in humans, these compounds have also shown the ability to improve endothelial function as well as to modify hemostasis, exhibiting antithrombotic properties (Eur. J. Clin. Invest. 2005;35:421-4). Oleuropein is known to display numerous biologic properties, many of which have been ascribed to its antioxidant activities (Int. J. Cosmet. Sci. 2008;30:113-20). In addition to antioxidant and antibacterial properties, oleuropein is thought to possess antiviral and antifungal qualities.
The polyphenols oleuropein, tyrosol, hydroxytyrosol, and caffeic acid are the primary components of the polar fraction of virgin olive oil (Z. Naturforsch [C] 2000;55:814-9). A decade ago, de la Puerta et al. set out to ascertain the antieicosanoid and antioxidant effects in leukocytes of these olive oil constituents.
All four suppressed leukotriene B4 generation at the 5-lipoxygenase level in intact rat peritoneal leukocytes stimulated with calcium ionophore. None of the compounds was toxic to leukocytes at tested concentrations, and none significantly inhibited thromboxane generation through the cyclooxygenase pathway. The investigators concluded that oleuropein and the other phenolics present in virgin olive oil exhibit various antioxidant, lipoxygenase-inhibitory, and prostaglandin activities (Biochem. Pharmacol. 1999;57:445-9).
Slightly less than a decade ago, researchers showed that all three different classes of phenolic constituents in olive oil, including simple phenols (hydroxytyrosol, tyrosol), secoiridoids (oleuropein, the aglycone of ligstroside, and their respective decarboxylated dialdehyde derivatives), and lignans [(+)-1-acetoxypinoresinol and pinoresinol], exhibit potent antioxidant activity. They stressed that consuming extra-virgin olive oil, which is laden with these phenolic antioxidants in addition to squalene and oleic acid, should hinder oxidative stress and thus yield significant protection against various cancers (such as colon, breast, and skin), coronary heart disease, and aging (Lancet Oncol. 2000;1:107-12).
In 2000, de la Puerta et al. investigated the anti-inflammatory effects of the unsaponifiable fraction of virgin olive oil and of the phenolic compounds of the polar fraction on edema in mice induced by arachidonic acid or 12-O-tetradecanoylphorbol-13- acetate (TPA). Of the phenolic constituents, oleuropein provoked the greatest inhibition of arachidonic acid-induced edema, similar to the reference drug dexamethasone. Varying degrees of anti-inflammatory activity were seen in both assays after the topical application of the olive oil compounds. The investigators concluded that both fractions may play a role in exerting the beneficial activity against various diseases that has been associated with olive oil (Z. Naturforsch [C] 2000;55:814-9).
In 2005, investigators studied the effects of several phenolic compounds (vanillic, p-coumaric, syringic, homovanillic and caffeic acids, kaempferol, oleuropein glycoside, and tyrosol) present in extra-virgin olive oil on inflammatory mediator production by human mononuclear cells. They stimulated diluted human blood cultures with lipopolysaccharide in the presence of the phenolics at various concentrations. Enzyme-linked immunosorbent assays were used to measure inflammatory cytokine concentration. Results showed that oleuropein glycoside and caffeic acid reduced the concentration of interleukin-1 beta by 80% and 40%, respectively. The investigators concluded that the effects seen from some phenolic compounds, including oleuropein, found in extra-virgin olive oil may play a role in the antiatherogenic activity attributed to the oil (Nutrition 2005;21:389-94).
Cosmetic Benefits
In 2008, researchers assessed the cosmetic activity of oleuropein against UVB-induced erythema by preparing an emulsion and emulgel that included the phenolic compound and then applying it on healthy volunteers exposed to UVB. Barrier function, skin color, and microcirculation were evaluated in the study, which considered protective effects delivered via preirradiation topical applications and mitigating effects after erythema induction. The investigators reported that the oleuropein preparations performed well, decreasing erythema, transepidermal water loss, and blood flow by 22%, 35%, and 30%, respectively. They concluded that oleuropein has the potential to be effective in combination with other active ingredients to mend the damage caused by UV radiation (Int. J. Cosmet. Sci. 2008;30:113-20).
In a study of olive oil and its disease-preventive capacity through the modulation of cell signaling, Wahle et al. suggested that the antioxidant effects of olive oil are likely multifactorial, resulting from a combination of its high oleic acid content (low oxidation potential in comparison to linoleic acid) and its high composition of various phenolic antioxidants, especially oleuropein, hydroxytyrosol, and tyrosol (Lipids 2004;39:1223-31).
Oleuropein is high on the long list of ingredients of Innovative Skincare's iS Clinical Moisturizing Treatment Sunscreen SPF 25, which, according to the manufacturer, incorporates innovative technology and several potent antioxidants to protect against sunburn and cutaneous aging. Innovative Skincare's Pro-Heal Serum also contains oleuropein--along with vitamins A, C, and E; kojic acid; and zinc sulfate--in a formulation intended to protect against UV damage and for the treatment of acne and rosacea. Oleuropein is also included among a cocktail of botanical ingredients, such as kaolin, glycolic acid, echinacea, peppermint, rosemary, and green tea extracts, in the Cellex-C Betaplex Clear Complexion Mask, which is designed to offer gentle exfoliation.
Conclusion
As is the case with numerous botanical ingredients, olive oil was used extensively in the ancient world, and its benefits are being relearned by the modern world.
Oleuropein is a key ingredient in olive oil, which is now known to be an integral part of the healthy Mediterranean diet and is used orally and topically to confer various health benefits. Indeed, oleuropein is one of the several key constituents in olive oil that have been demonstrated to impart antioxidant, antibacterial, anti-inflammatory, and anticarcinogenic effects.
Current data provide reasons for optimism, particularly if oleuropein, other olive oil components, and olive oil itself can be shown in topical form to consistently deliver such benefits. Nevertheless, much remains to be learned about oleuropein and the other constituents of olive oil in terms of mechanisms of action and the full range of health benefits they may confer.
Intra-Arterial Embolization With Fillers Is Rare, But Severe
WASHINGTON — Intra-arterial embolization during filler injection is rare, but it can happen to even the most experienced physician, said Dr. Claudio DeLorenzi.
Intra-arterial embolization occurs when a filler needle enters an artery. During injection, the filler flows retrograde in the vessel. Once the pressure from injection is stopped, the product is carried through the vasculature and the results can be disastrous, Dr. DeLorenzi said at the annual meeting of the American Society for Aesthetic Plastic Surgery.
Local and distal necrosis can occur following intra-arterial embolization. Typically the whole angiosome--the vascular territory of skin and underlying muscles, tendons, nerves, and bones--is affected, resulting in full-thickness necrosis.
The first sign of trouble is severe pain, followed typically by a bluish livedo pattern.
This can progress to hemorrhagic blisters, necrotic eschar, and late scarring. "The severity of some of these complications is extreme by any measure," said Dr. DeLorenzi, who is a plastic surgeon in Kitchener, Ont.
"So if you see this reticular bluish pattern, it means that you need to take action," he said. A crash cart for this complication allows for an immediate response. The cart should contain hyaluronidase--which can reverse the effects of hyaluronic acid fillers--aspirin, nitroglycerine paste, and heat compresses.
Dr. DeLorenzi recommended having a low threshold for using hyaluronidase. Recommendations in the literature on the amount to use vary from 25 to 150 units.
Hyaluronidase should be injected diffusely in the affected area, which should then be massaged to distribute the filler. "Even if you've selected a non-hyaluronic acid filler, there may be some role for using hyaluronidase. You may get some improvement in circulation," he said.
Increased risk for intra-arterial embolization appears to be associated with large volumes of filler, small sharp needles, high pressure, deeper injections, and compound type.
"Prevention, of course, is best," said Dr. DeLorenzi. To avoid intra-arterial embolization, he recommends using a small bolus (less than 0.1 cc), a blunt cannula, low pressure, slow injection; knowing the relevant anatomy; being prepared; and using epinephrine prior to the filler procedure (this may reduce the vessel size and the risk of hitting a vessel).
Dr. Delorenzi reported that he is a speaker for Allergan Inc.
WASHINGTON — Intra-arterial embolization during filler injection is rare, but it can happen to even the most experienced physician, said Dr. Claudio DeLorenzi.
Intra-arterial embolization occurs when a filler needle enters an artery. During injection, the filler flows retrograde in the vessel. Once the pressure from injection is stopped, the product is carried through the vasculature and the results can be disastrous, Dr. DeLorenzi said at the annual meeting of the American Society for Aesthetic Plastic Surgery.
Local and distal necrosis can occur following intra-arterial embolization. Typically the whole angiosome--the vascular territory of skin and underlying muscles, tendons, nerves, and bones--is affected, resulting in full-thickness necrosis.
The first sign of trouble is severe pain, followed typically by a bluish livedo pattern.
This can progress to hemorrhagic blisters, necrotic eschar, and late scarring. "The severity of some of these complications is extreme by any measure," said Dr. DeLorenzi, who is a plastic surgeon in Kitchener, Ont.
"So if you see this reticular bluish pattern, it means that you need to take action," he said. A crash cart for this complication allows for an immediate response. The cart should contain hyaluronidase--which can reverse the effects of hyaluronic acid fillers--aspirin, nitroglycerine paste, and heat compresses.
Dr. DeLorenzi recommended having a low threshold for using hyaluronidase. Recommendations in the literature on the amount to use vary from 25 to 150 units.
Hyaluronidase should be injected diffusely in the affected area, which should then be massaged to distribute the filler. "Even if you've selected a non-hyaluronic acid filler, there may be some role for using hyaluronidase. You may get some improvement in circulation," he said.
Increased risk for intra-arterial embolization appears to be associated with large volumes of filler, small sharp needles, high pressure, deeper injections, and compound type.
"Prevention, of course, is best," said Dr. DeLorenzi. To avoid intra-arterial embolization, he recommends using a small bolus (less than 0.1 cc), a blunt cannula, low pressure, slow injection; knowing the relevant anatomy; being prepared; and using epinephrine prior to the filler procedure (this may reduce the vessel size and the risk of hitting a vessel).
Dr. Delorenzi reported that he is a speaker for Allergan Inc.
WASHINGTON — Intra-arterial embolization during filler injection is rare, but it can happen to even the most experienced physician, said Dr. Claudio DeLorenzi.
Intra-arterial embolization occurs when a filler needle enters an artery. During injection, the filler flows retrograde in the vessel. Once the pressure from injection is stopped, the product is carried through the vasculature and the results can be disastrous, Dr. DeLorenzi said at the annual meeting of the American Society for Aesthetic Plastic Surgery.
Local and distal necrosis can occur following intra-arterial embolization. Typically the whole angiosome--the vascular territory of skin and underlying muscles, tendons, nerves, and bones--is affected, resulting in full-thickness necrosis.
The first sign of trouble is severe pain, followed typically by a bluish livedo pattern.
This can progress to hemorrhagic blisters, necrotic eschar, and late scarring. "The severity of some of these complications is extreme by any measure," said Dr. DeLorenzi, who is a plastic surgeon in Kitchener, Ont.
"So if you see this reticular bluish pattern, it means that you need to take action," he said. A crash cart for this complication allows for an immediate response. The cart should contain hyaluronidase--which can reverse the effects of hyaluronic acid fillers--aspirin, nitroglycerine paste, and heat compresses.
Dr. DeLorenzi recommended having a low threshold for using hyaluronidase. Recommendations in the literature on the amount to use vary from 25 to 150 units.
Hyaluronidase should be injected diffusely in the affected area, which should then be massaged to distribute the filler. "Even if you've selected a non-hyaluronic acid filler, there may be some role for using hyaluronidase. You may get some improvement in circulation," he said.
Increased risk for intra-arterial embolization appears to be associated with large volumes of filler, small sharp needles, high pressure, deeper injections, and compound type.
"Prevention, of course, is best," said Dr. DeLorenzi. To avoid intra-arterial embolization, he recommends using a small bolus (less than 0.1 cc), a blunt cannula, low pressure, slow injection; knowing the relevant anatomy; being prepared; and using epinephrine prior to the filler procedure (this may reduce the vessel size and the risk of hitting a vessel).
Dr. Delorenzi reported that he is a speaker for Allergan Inc.
After Mohs, Cancer Recurrence Less Than 2% in New Study
MADRID — Mohs surgery for lentigo maligna and lentigo maligna melanoma yields a substantially lower recurrence rate and smaller surgical deficit than does conventional surgery, according to Dr. Leonard H. Goldberg.
"It's especially useful on cosmetically sensitive areas of the body like the eyelids, where a 5-mm or 1-cm or 2-cm margin is virtually impossible because you'd destroy the patient's cosmetic appearance," Dr. Goldberg said at the 13th World Congress on Cancers of the Skin.
Of 708 cases of lentigo maligna and lentigo maligna melanoma that he treated using Mohs surgery from 1997 through 2007, the recurrence rate was 1.3%.
In contrast, conventional surgery is associated with recurrence rates of 8%-20%, he said. That's because the clinical margins of lentigo maligna are often indistinct, being masked by actinic keratoses or other sun-induced dysplastic changes.
The lentigines are "often much larger than what you'd expect," he said. "There's always the problem of where does the lentigo maligna end? Are those single cells in the periphery also lentigo maligna?"
Dr. Goldberg utilizes Dr. Helmut Breuninger's "Tübingen torte" technique of surgical specimen cutting using 90-degree sectioning, along with immunostaining. En-face (parallel) control of the entire surgical margin is considerably more reliable than bread-loafed cross-sectioning of the excised melanoma specimen.
"Bread-loafing doesn't always find the tumor. We don't bread-loaf tumors anymore," he said.
The change in practice came as a result of a study that Dr. Goldberg and his colleagues conducted in 36 patients with melanoma in situ treated with Mohs surgery with positive margins after initial excision with 5-mm margins (Dermatol. Surg. 2007;33:1434-9).
Because the average linear extent of melanoma at the surgical margin was 1.4 mm, they calculated that bread-loafing at 1-, 4-, and 10-mm intervals would have a 58%, 19%, and 7% chance, respectively, of detecting positive margins. To detect positive margins with 100% certainty, the bread-loafing would have to be done at 0.1-mm intervals, which is impractical, he said.
Dr. Goldberg noted that his personal 1.3% recurrence rate is in the same ballpark as outcomes reported by other Mohs surgeons. For example, researchers reported a 0.3% recurrence rate in 331 patients with melanoma in situ or lentigo maligna, compared with a 20% rate in 81 historical controls who underwent conventional surgery (J. Am. Acad. Dermatol. 2005;52:92-100).
In a separate review of four other published studies totaling 546 patients with lentigo maligna and lentigo maligna melanoma with margin control by various modifications of Mohs surgery, recurrence rates were 0.5%-2.8% (J. Am. Acad. Dermatol. 2007;57:659-64).
Dr. Goldberg reported no financial conflicts.
MADRID — Mohs surgery for lentigo maligna and lentigo maligna melanoma yields a substantially lower recurrence rate and smaller surgical deficit than does conventional surgery, according to Dr. Leonard H. Goldberg.
"It's especially useful on cosmetically sensitive areas of the body like the eyelids, where a 5-mm or 1-cm or 2-cm margin is virtually impossible because you'd destroy the patient's cosmetic appearance," Dr. Goldberg said at the 13th World Congress on Cancers of the Skin.
Of 708 cases of lentigo maligna and lentigo maligna melanoma that he treated using Mohs surgery from 1997 through 2007, the recurrence rate was 1.3%.
In contrast, conventional surgery is associated with recurrence rates of 8%-20%, he said. That's because the clinical margins of lentigo maligna are often indistinct, being masked by actinic keratoses or other sun-induced dysplastic changes.
The lentigines are "often much larger than what you'd expect," he said. "There's always the problem of where does the lentigo maligna end? Are those single cells in the periphery also lentigo maligna?"
Dr. Goldberg utilizes Dr. Helmut Breuninger's "Tübingen torte" technique of surgical specimen cutting using 90-degree sectioning, along with immunostaining. En-face (parallel) control of the entire surgical margin is considerably more reliable than bread-loafed cross-sectioning of the excised melanoma specimen.
"Bread-loafing doesn't always find the tumor. We don't bread-loaf tumors anymore," he said.
The change in practice came as a result of a study that Dr. Goldberg and his colleagues conducted in 36 patients with melanoma in situ treated with Mohs surgery with positive margins after initial excision with 5-mm margins (Dermatol. Surg. 2007;33:1434-9).
Because the average linear extent of melanoma at the surgical margin was 1.4 mm, they calculated that bread-loafing at 1-, 4-, and 10-mm intervals would have a 58%, 19%, and 7% chance, respectively, of detecting positive margins. To detect positive margins with 100% certainty, the bread-loafing would have to be done at 0.1-mm intervals, which is impractical, he said.
Dr. Goldberg noted that his personal 1.3% recurrence rate is in the same ballpark as outcomes reported by other Mohs surgeons. For example, researchers reported a 0.3% recurrence rate in 331 patients with melanoma in situ or lentigo maligna, compared with a 20% rate in 81 historical controls who underwent conventional surgery (J. Am. Acad. Dermatol. 2005;52:92-100).
In a separate review of four other published studies totaling 546 patients with lentigo maligna and lentigo maligna melanoma with margin control by various modifications of Mohs surgery, recurrence rates were 0.5%-2.8% (J. Am. Acad. Dermatol. 2007;57:659-64).
Dr. Goldberg reported no financial conflicts.
MADRID — Mohs surgery for lentigo maligna and lentigo maligna melanoma yields a substantially lower recurrence rate and smaller surgical deficit than does conventional surgery, according to Dr. Leonard H. Goldberg.
"It's especially useful on cosmetically sensitive areas of the body like the eyelids, where a 5-mm or 1-cm or 2-cm margin is virtually impossible because you'd destroy the patient's cosmetic appearance," Dr. Goldberg said at the 13th World Congress on Cancers of the Skin.
Of 708 cases of lentigo maligna and lentigo maligna melanoma that he treated using Mohs surgery from 1997 through 2007, the recurrence rate was 1.3%.
In contrast, conventional surgery is associated with recurrence rates of 8%-20%, he said. That's because the clinical margins of lentigo maligna are often indistinct, being masked by actinic keratoses or other sun-induced dysplastic changes.
The lentigines are "often much larger than what you'd expect," he said. "There's always the problem of where does the lentigo maligna end? Are those single cells in the periphery also lentigo maligna?"
Dr. Goldberg utilizes Dr. Helmut Breuninger's "Tübingen torte" technique of surgical specimen cutting using 90-degree sectioning, along with immunostaining. En-face (parallel) control of the entire surgical margin is considerably more reliable than bread-loafed cross-sectioning of the excised melanoma specimen.
"Bread-loafing doesn't always find the tumor. We don't bread-loaf tumors anymore," he said.
The change in practice came as a result of a study that Dr. Goldberg and his colleagues conducted in 36 patients with melanoma in situ treated with Mohs surgery with positive margins after initial excision with 5-mm margins (Dermatol. Surg. 2007;33:1434-9).
Because the average linear extent of melanoma at the surgical margin was 1.4 mm, they calculated that bread-loafing at 1-, 4-, and 10-mm intervals would have a 58%, 19%, and 7% chance, respectively, of detecting positive margins. To detect positive margins with 100% certainty, the bread-loafing would have to be done at 0.1-mm intervals, which is impractical, he said.
Dr. Goldberg noted that his personal 1.3% recurrence rate is in the same ballpark as outcomes reported by other Mohs surgeons. For example, researchers reported a 0.3% recurrence rate in 331 patients with melanoma in situ or lentigo maligna, compared with a 20% rate in 81 historical controls who underwent conventional surgery (J. Am. Acad. Dermatol. 2005;52:92-100).
In a separate review of four other published studies totaling 546 patients with lentigo maligna and lentigo maligna melanoma with margin control by various modifications of Mohs surgery, recurrence rates were 0.5%-2.8% (J. Am. Acad. Dermatol. 2007;57:659-64).
Dr. Goldberg reported no financial conflicts.
Expertise Is Essential for Effective Laser Tattoo Removal
NAPLES, Fla. — Patients present with different reasons for tattoo removal—such as regret following a crazy night or a change in relationship status. The number of options for laser tattoo removal, however, is more limited, Dr. Albert J. Nemeth said.
Specific Q-switched Nd:YAG laser wavelengths are good at shattering tattoo ink but must be applied specific to the ink color. Also, do not use non-Q-switched Nd:YAG lasers or other lasers designed for different dermatologic indications, Dr. Nemeth said at the annual meeting of the Florida Society of Dermatology and Dermatologic Surgery.
In general, 95% of amateur tattoos take one to three laser treatment sessions for removal. In contrast, six or more sessions are often required to remove most professional tattoos. Variables include the depth at which pigment was placed and type of ink. "Tattoo depth can vary. That is important to conceptualize when treating these tattoos," Dr. Nemeth said.
Tattoos applied by a friend or family member and those inked professionally share a common challenge for dermatologists—a lack of regulation on what can be used for pigment. "It's really quite interesting in terms of the secret concoctions that I've heard … cigarette ash; for some reason Crest toothpaste seems to be a magic ingredient; and—I don't understand why—but urine seems to be important in there also," Dr. Nemeth said in an interview.
|
An important caveat: If the patient reports or displays any symptoms of allergic dermatitis to the ink (constant oozing or crusting), lasers can worsen those symptoms. Physical removal of the tattoo is the only option for these patients, said Dr. Nemeth, a private-practice dermatologist in Clearwater, Fla., and FSDDS president. Dermabrasion, for example, is an option "if you are extraordinarily proficient at that."
An estimated 14% of all adults in the United States have at least one tattoo, according to a Harris Poll by Harris Interactive in 2008. A predominance of tattooing among a younger segment of the population means dermatologists are likely to see more and more patients with tattoos.
Removal of tattoos via laser can be life changing and/or life saving for some patients. For example, former gang members might feel safer after removal of an identifying tattoo, said Dr. Nemeth, also of the department of dermatology and cutaneous surgery at the University of South Florida, Tampa.
For removal of green tattoo inks, Dr. Nemeth uses a 694-nm Q-switched ruby or 755-nm Q-switched alexandrite laser. To shatter black, blue, sky blue, or darker inks, he employs a 1064-nm Q switched Nd:YAG laser. If a patient's tattoo features red, orange, or purple inks, these can be effectively treated with a 532-nm Q-switched Nd:YAG laser, he said. Also be aware that laser therapy can darken tattoo inks if they contain iron oxide or titanium oxide.
Avoid the temptation to use lasers for other indications. "An EpiTouch ruby laser made for hair removal should not be used for tattoo removal," Dr. Nemeth said. "This is an important take-home message: Just because the wavelength is close, it does not mean the indications are the same."
Also, intense pulsed light systems are not appropriate for this indication, Dr. Nemeth said. "If your salesperson told you IPL can be used to remove tattoos, [he] lied to you. IPL cannot be used to remove a tattoo, in my humble opinion."
The Q-switched lasers have afforded patients a much better aesthetic outcome following tattoo removal. "It used to be every patient knew they were switching their tattoo for a scar, "Dr. Nemeth said. "Now you can get some very, very nice results."
Dr. Nemeth had no relevant financial disclosures.
NAPLES, Fla. — Patients present with different reasons for tattoo removal—such as regret following a crazy night or a change in relationship status. The number of options for laser tattoo removal, however, is more limited, Dr. Albert J. Nemeth said.
Specific Q-switched Nd:YAG laser wavelengths are good at shattering tattoo ink but must be applied specific to the ink color. Also, do not use non-Q-switched Nd:YAG lasers or other lasers designed for different dermatologic indications, Dr. Nemeth said at the annual meeting of the Florida Society of Dermatology and Dermatologic Surgery.
In general, 95% of amateur tattoos take one to three laser treatment sessions for removal. In contrast, six or more sessions are often required to remove most professional tattoos. Variables include the depth at which pigment was placed and type of ink. "Tattoo depth can vary. That is important to conceptualize when treating these tattoos," Dr. Nemeth said.
Tattoos applied by a friend or family member and those inked professionally share a common challenge for dermatologists—a lack of regulation on what can be used for pigment. "It's really quite interesting in terms of the secret concoctions that I've heard … cigarette ash; for some reason Crest toothpaste seems to be a magic ingredient; and—I don't understand why—but urine seems to be important in there also," Dr. Nemeth said in an interview.
|
An important caveat: If the patient reports or displays any symptoms of allergic dermatitis to the ink (constant oozing or crusting), lasers can worsen those symptoms. Physical removal of the tattoo is the only option for these patients, said Dr. Nemeth, a private-practice dermatologist in Clearwater, Fla., and FSDDS president. Dermabrasion, for example, is an option "if you are extraordinarily proficient at that."
An estimated 14% of all adults in the United States have at least one tattoo, according to a Harris Poll by Harris Interactive in 2008. A predominance of tattooing among a younger segment of the population means dermatologists are likely to see more and more patients with tattoos.
Removal of tattoos via laser can be life changing and/or life saving for some patients. For example, former gang members might feel safer after removal of an identifying tattoo, said Dr. Nemeth, also of the department of dermatology and cutaneous surgery at the University of South Florida, Tampa.
For removal of green tattoo inks, Dr. Nemeth uses a 694-nm Q-switched ruby or 755-nm Q-switched alexandrite laser. To shatter black, blue, sky blue, or darker inks, he employs a 1064-nm Q switched Nd:YAG laser. If a patient's tattoo features red, orange, or purple inks, these can be effectively treated with a 532-nm Q-switched Nd:YAG laser, he said. Also be aware that laser therapy can darken tattoo inks if they contain iron oxide or titanium oxide.
Avoid the temptation to use lasers for other indications. "An EpiTouch ruby laser made for hair removal should not be used for tattoo removal," Dr. Nemeth said. "This is an important take-home message: Just because the wavelength is close, it does not mean the indications are the same."
Also, intense pulsed light systems are not appropriate for this indication, Dr. Nemeth said. "If your salesperson told you IPL can be used to remove tattoos, [he] lied to you. IPL cannot be used to remove a tattoo, in my humble opinion."
The Q-switched lasers have afforded patients a much better aesthetic outcome following tattoo removal. "It used to be every patient knew they were switching their tattoo for a scar, "Dr. Nemeth said. "Now you can get some very, very nice results."
Dr. Nemeth had no relevant financial disclosures.
NAPLES, Fla. — Patients present with different reasons for tattoo removal—such as regret following a crazy night or a change in relationship status. The number of options for laser tattoo removal, however, is more limited, Dr. Albert J. Nemeth said.
Specific Q-switched Nd:YAG laser wavelengths are good at shattering tattoo ink but must be applied specific to the ink color. Also, do not use non-Q-switched Nd:YAG lasers or other lasers designed for different dermatologic indications, Dr. Nemeth said at the annual meeting of the Florida Society of Dermatology and Dermatologic Surgery.
In general, 95% of amateur tattoos take one to three laser treatment sessions for removal. In contrast, six or more sessions are often required to remove most professional tattoos. Variables include the depth at which pigment was placed and type of ink. "Tattoo depth can vary. That is important to conceptualize when treating these tattoos," Dr. Nemeth said.
Tattoos applied by a friend or family member and those inked professionally share a common challenge for dermatologists—a lack of regulation on what can be used for pigment. "It's really quite interesting in terms of the secret concoctions that I've heard … cigarette ash; for some reason Crest toothpaste seems to be a magic ingredient; and—I don't understand why—but urine seems to be important in there also," Dr. Nemeth said in an interview.
|
An important caveat: If the patient reports or displays any symptoms of allergic dermatitis to the ink (constant oozing or crusting), lasers can worsen those symptoms. Physical removal of the tattoo is the only option for these patients, said Dr. Nemeth, a private-practice dermatologist in Clearwater, Fla., and FSDDS president. Dermabrasion, for example, is an option "if you are extraordinarily proficient at that."
An estimated 14% of all adults in the United States have at least one tattoo, according to a Harris Poll by Harris Interactive in 2008. A predominance of tattooing among a younger segment of the population means dermatologists are likely to see more and more patients with tattoos.
Removal of tattoos via laser can be life changing and/or life saving for some patients. For example, former gang members might feel safer after removal of an identifying tattoo, said Dr. Nemeth, also of the department of dermatology and cutaneous surgery at the University of South Florida, Tampa.
For removal of green tattoo inks, Dr. Nemeth uses a 694-nm Q-switched ruby or 755-nm Q-switched alexandrite laser. To shatter black, blue, sky blue, or darker inks, he employs a 1064-nm Q switched Nd:YAG laser. If a patient's tattoo features red, orange, or purple inks, these can be effectively treated with a 532-nm Q-switched Nd:YAG laser, he said. Also be aware that laser therapy can darken tattoo inks if they contain iron oxide or titanium oxide.
Avoid the temptation to use lasers for other indications. "An EpiTouch ruby laser made for hair removal should not be used for tattoo removal," Dr. Nemeth said. "This is an important take-home message: Just because the wavelength is close, it does not mean the indications are the same."
Also, intense pulsed light systems are not appropriate for this indication, Dr. Nemeth said. "If your salesperson told you IPL can be used to remove tattoos, [he] lied to you. IPL cannot be used to remove a tattoo, in my humble opinion."
The Q-switched lasers have afforded patients a much better aesthetic outcome following tattoo removal. "It used to be every patient knew they were switching their tattoo for a scar, "Dr. Nemeth said. "Now you can get some very, very nice results."
Dr. Nemeth had no relevant financial disclosures.
Repeat Suction Enhances Subcision Efficacy for Depressed Facial Scars
A novel technique that combines subcision and suction proved safe and effective for promoting significant and lasting improvement of mild to severe depressed facial scars in a study of 58 patients.
In 46 patients who strictly followed the study protocol of subcision followed by frequent suctioning at the time of postsubcision depression recurrence, the depth and size of scars decreased significantly by a mean of nearly 72% at 6-month follow-up, according to assessment by two investigators, and by 75% according to patient assessment.
An improvement of at least 80% occurred in about 28% of patients, according to investigator assessment, and in 42%, according to patient assessment, Dr. S. Aalami Harandi of the Parsian Laser Clinic, Bandar Abbas, Iran, and colleagues reported online in the June 9 issue of the Journal of the European Academy of Dermatology and Venereology.
Mean improvement at 6 months in 12 patients who started suction late or had long intervals between suction sessions was 44% by investigator assessment and 49% by patient assessment, the investigators reported (J. Eur. Acad. Dermatol. Venereol. 2010 June 9 [doi:10.1111/ j.1468-3083.2010.03711.x]).
The study participants - 34 women and 24 men aged 16-44 years - had depressed acne scars of various types, including rolling, superficial boxcar, deep boxcar, and pitted, as well as scars from chicken pox, trauma, and surgery. Superficial dermal undermining was performed on 1-70 scars per patient using mainly 23-gauge needles. Suctioning was initiated on the third day following subcision, and was performed at least every other day for 2 weeks, per protocol.
The best results (80% or better improvement) were seen in 24 of the 46 patients on protocol who had the most frequent suctioning (almost daily versus every other day interval in the first week of suction period), the investigators noted.
Although subcision is a safe, valuable, and practical method in itself, it has only mild to moderate efficacy because of the frequency of depression recurrence. In the investigators' experience, recurrence with subcision alone generally starts 2-5 days after subcision, with rapid progression of re-depression for up to 10 days, and gradual progression of re-depression for about 1 week more; therefore, the protocol for this study involved repeated suctioning at the recurrence period.
The addition of suctioning, which prevents redepression by "induction of repeated haemorrhage in dermal pocket, delay in healing, and more new connective tissue formation at the scar area," appears to improve the efficacy of subcision alone.
The combined subcision and suction treatment in this study was associated with "significant" (greater than 60% improvement) and "excellent" (80% improvement or greater) efficacy, the investigators said.
Bruising occurred in all cases, but resolved within 12 days, and any discoloration that occurred resolved within 2 months; hypertrophic scarring occurred in 1.7% of treated scars (22 scars in six patients), which was mostly due to sub-epidermal like undermining( technical error), and was managed successfully in all cases; and hemorrhagic papules and pustules occurred in 5.6% of subcised scars, and were treated successfully with drainage and topical antibiotics or steroids.
Advantages of the subcision-suction method include ease of application, low cost, short down-time, applicability for various skin types (most had type III in this study), applicability for various scar types, lack of significant complications, and "remarkable and persistent improvement in short time without injury to the skin surface," the investigators reported.
"It seems that this method has the potential to be used as the first step for acne and other depressed scars management," they wrote, adding that since multistep treatment is necessary for optimal correction of acne scars, treatment may involve the use of other techniques or repeat subcision-suction after several months.
Further study of this technique is warranted, particularly given the prevalence of the problem of depressed scars of the face, they noted.
The investigators had no conflicts of interest to declare.
A novel technique that combines subcision and suction proved safe and effective for promoting significant and lasting improvement of mild to severe depressed facial scars in a study of 58 patients.
In 46 patients who strictly followed the study protocol of subcision followed by frequent suctioning at the time of postsubcision depression recurrence, the depth and size of scars decreased significantly by a mean of nearly 72% at 6-month follow-up, according to assessment by two investigators, and by 75% according to patient assessment.
An improvement of at least 80% occurred in about 28% of patients, according to investigator assessment, and in 42%, according to patient assessment, Dr. S. Aalami Harandi of the Parsian Laser Clinic, Bandar Abbas, Iran, and colleagues reported online in the June 9 issue of the Journal of the European Academy of Dermatology and Venereology.
Mean improvement at 6 months in 12 patients who started suction late or had long intervals between suction sessions was 44% by investigator assessment and 49% by patient assessment, the investigators reported (J. Eur. Acad. Dermatol. Venereol. 2010 June 9 [doi:10.1111/ j.1468-3083.2010.03711.x]).
The study participants - 34 women and 24 men aged 16-44 years - had depressed acne scars of various types, including rolling, superficial boxcar, deep boxcar, and pitted, as well as scars from chicken pox, trauma, and surgery. Superficial dermal undermining was performed on 1-70 scars per patient using mainly 23-gauge needles. Suctioning was initiated on the third day following subcision, and was performed at least every other day for 2 weeks, per protocol.
The best results (80% or better improvement) were seen in 24 of the 46 patients on protocol who had the most frequent suctioning (almost daily versus every other day interval in the first week of suction period), the investigators noted.
Although subcision is a safe, valuable, and practical method in itself, it has only mild to moderate efficacy because of the frequency of depression recurrence. In the investigators' experience, recurrence with subcision alone generally starts 2-5 days after subcision, with rapid progression of re-depression for up to 10 days, and gradual progression of re-depression for about 1 week more; therefore, the protocol for this study involved repeated suctioning at the recurrence period.
The addition of suctioning, which prevents redepression by "induction of repeated haemorrhage in dermal pocket, delay in healing, and more new connective tissue formation at the scar area," appears to improve the efficacy of subcision alone.
The combined subcision and suction treatment in this study was associated with "significant" (greater than 60% improvement) and "excellent" (80% improvement or greater) efficacy, the investigators said.
Bruising occurred in all cases, but resolved within 12 days, and any discoloration that occurred resolved within 2 months; hypertrophic scarring occurred in 1.7% of treated scars (22 scars in six patients), which was mostly due to sub-epidermal like undermining( technical error), and was managed successfully in all cases; and hemorrhagic papules and pustules occurred in 5.6% of subcised scars, and were treated successfully with drainage and topical antibiotics or steroids.
Advantages of the subcision-suction method include ease of application, low cost, short down-time, applicability for various skin types (most had type III in this study), applicability for various scar types, lack of significant complications, and "remarkable and persistent improvement in short time without injury to the skin surface," the investigators reported.
"It seems that this method has the potential to be used as the first step for acne and other depressed scars management," they wrote, adding that since multistep treatment is necessary for optimal correction of acne scars, treatment may involve the use of other techniques or repeat subcision-suction after several months.
Further study of this technique is warranted, particularly given the prevalence of the problem of depressed scars of the face, they noted.
The investigators had no conflicts of interest to declare.
A novel technique that combines subcision and suction proved safe and effective for promoting significant and lasting improvement of mild to severe depressed facial scars in a study of 58 patients.
In 46 patients who strictly followed the study protocol of subcision followed by frequent suctioning at the time of postsubcision depression recurrence, the depth and size of scars decreased significantly by a mean of nearly 72% at 6-month follow-up, according to assessment by two investigators, and by 75% according to patient assessment.
An improvement of at least 80% occurred in about 28% of patients, according to investigator assessment, and in 42%, according to patient assessment, Dr. S. Aalami Harandi of the Parsian Laser Clinic, Bandar Abbas, Iran, and colleagues reported online in the June 9 issue of the Journal of the European Academy of Dermatology and Venereology.
Mean improvement at 6 months in 12 patients who started suction late or had long intervals between suction sessions was 44% by investigator assessment and 49% by patient assessment, the investigators reported (J. Eur. Acad. Dermatol. Venereol. 2010 June 9 [doi:10.1111/ j.1468-3083.2010.03711.x]).
The study participants - 34 women and 24 men aged 16-44 years - had depressed acne scars of various types, including rolling, superficial boxcar, deep boxcar, and pitted, as well as scars from chicken pox, trauma, and surgery. Superficial dermal undermining was performed on 1-70 scars per patient using mainly 23-gauge needles. Suctioning was initiated on the third day following subcision, and was performed at least every other day for 2 weeks, per protocol.
The best results (80% or better improvement) were seen in 24 of the 46 patients on protocol who had the most frequent suctioning (almost daily versus every other day interval in the first week of suction period), the investigators noted.
Although subcision is a safe, valuable, and practical method in itself, it has only mild to moderate efficacy because of the frequency of depression recurrence. In the investigators' experience, recurrence with subcision alone generally starts 2-5 days after subcision, with rapid progression of re-depression for up to 10 days, and gradual progression of re-depression for about 1 week more; therefore, the protocol for this study involved repeated suctioning at the recurrence period.
The addition of suctioning, which prevents redepression by "induction of repeated haemorrhage in dermal pocket, delay in healing, and more new connective tissue formation at the scar area," appears to improve the efficacy of subcision alone.
The combined subcision and suction treatment in this study was associated with "significant" (greater than 60% improvement) and "excellent" (80% improvement or greater) efficacy, the investigators said.
Bruising occurred in all cases, but resolved within 12 days, and any discoloration that occurred resolved within 2 months; hypertrophic scarring occurred in 1.7% of treated scars (22 scars in six patients), which was mostly due to sub-epidermal like undermining( technical error), and was managed successfully in all cases; and hemorrhagic papules and pustules occurred in 5.6% of subcised scars, and were treated successfully with drainage and topical antibiotics or steroids.
Advantages of the subcision-suction method include ease of application, low cost, short down-time, applicability for various skin types (most had type III in this study), applicability for various scar types, lack of significant complications, and "remarkable and persistent improvement in short time without injury to the skin surface," the investigators reported.
"It seems that this method has the potential to be used as the first step for acne and other depressed scars management," they wrote, adding that since multistep treatment is necessary for optimal correction of acne scars, treatment may involve the use of other techniques or repeat subcision-suction after several months.
Further study of this technique is warranted, particularly given the prevalence of the problem of depressed scars of the face, they noted.
The investigators had no conflicts of interest to declare.