User login
Lidocaine-Delivery System, Emla 5% Comparable for Pain Control
PHOENIX — Patients reported less or a comparable amount of pain during needling roller treatment for upper lip rhytids when lidocaine was delivered with a jet-phoresis system, compared with an application of Emla 5% cream, results from a small study of 20 patients showed.
During a poster session at the annual meeting of the American Society for Laser Medicine and Surgery, researchers presented results from a study designed to compare administration of lidocaine with the jet-phoresis system, compared with the topical cream for pain control in patients scheduled for needling roller procedures for upper lip rhytids.
For the study, Dr. Michael Gold, a dermatologist who practices in Nashville, Tenn., and Dr. Ram Burvin, a plastic surgeon who practices in Tel-Aviv, had patients serve as their own control. The mean age of the patients was 56 years, and all were female.
The researchers treated half (left or right) of each patient's upper lip with Emla 5% cream for 45 minutes and the contralateral portion of the lip with lidocaine 3% jet phoresis for 5 minutes. They used a visual analog scale to measure pain elicited by application of a needling roller across the upper lip.
Each patient again served as her own control 12-16 weeks later when the treatments (lidocaine 3% with jet phoresis vs. Emla 5%) were repeated on the opposite lip sides for the same durations, so that in all, there were 40 full-lip applications of the two treatments. Different readings for the left and right sides were registered in some of the patients.
Of the total 40 treatments, pain control with lidocaine 3% with jet phoresis and Emla 5% was comparable in 19 applications, it was better with the lidocaine 3% with jet phoresis in 14 of the applications, and better with Emla 5% in 7 applications
The delivery device, the JetPeel 3, uses pressurized gas at supersonic velocities to deliver saline or other liquid nutrients through special handpieces into the superficial layers of the skin. It was cleared by the Food and Drug Administration in 2006 for delivery of saline into the skin.
The researchers received honoraria from TavTech Ltd., maker of the jet-phoresis system, to conduct the study.
PHOENIX — Patients reported less or a comparable amount of pain during needling roller treatment for upper lip rhytids when lidocaine was delivered with a jet-phoresis system, compared with an application of Emla 5% cream, results from a small study of 20 patients showed.
During a poster session at the annual meeting of the American Society for Laser Medicine and Surgery, researchers presented results from a study designed to compare administration of lidocaine with the jet-phoresis system, compared with the topical cream for pain control in patients scheduled for needling roller procedures for upper lip rhytids.
For the study, Dr. Michael Gold, a dermatologist who practices in Nashville, Tenn., and Dr. Ram Burvin, a plastic surgeon who practices in Tel-Aviv, had patients serve as their own control. The mean age of the patients was 56 years, and all were female.
The researchers treated half (left or right) of each patient's upper lip with Emla 5% cream for 45 minutes and the contralateral portion of the lip with lidocaine 3% jet phoresis for 5 minutes. They used a visual analog scale to measure pain elicited by application of a needling roller across the upper lip.
Each patient again served as her own control 12-16 weeks later when the treatments (lidocaine 3% with jet phoresis vs. Emla 5%) were repeated on the opposite lip sides for the same durations, so that in all, there were 40 full-lip applications of the two treatments. Different readings for the left and right sides were registered in some of the patients.
Of the total 40 treatments, pain control with lidocaine 3% with jet phoresis and Emla 5% was comparable in 19 applications, it was better with the lidocaine 3% with jet phoresis in 14 of the applications, and better with Emla 5% in 7 applications
The delivery device, the JetPeel 3, uses pressurized gas at supersonic velocities to deliver saline or other liquid nutrients through special handpieces into the superficial layers of the skin. It was cleared by the Food and Drug Administration in 2006 for delivery of saline into the skin.
The researchers received honoraria from TavTech Ltd., maker of the jet-phoresis system, to conduct the study.
PHOENIX — Patients reported less or a comparable amount of pain during needling roller treatment for upper lip rhytids when lidocaine was delivered with a jet-phoresis system, compared with an application of Emla 5% cream, results from a small study of 20 patients showed.
During a poster session at the annual meeting of the American Society for Laser Medicine and Surgery, researchers presented results from a study designed to compare administration of lidocaine with the jet-phoresis system, compared with the topical cream for pain control in patients scheduled for needling roller procedures for upper lip rhytids.
For the study, Dr. Michael Gold, a dermatologist who practices in Nashville, Tenn., and Dr. Ram Burvin, a plastic surgeon who practices in Tel-Aviv, had patients serve as their own control. The mean age of the patients was 56 years, and all were female.
The researchers treated half (left or right) of each patient's upper lip with Emla 5% cream for 45 minutes and the contralateral portion of the lip with lidocaine 3% jet phoresis for 5 minutes. They used a visual analog scale to measure pain elicited by application of a needling roller across the upper lip.
Each patient again served as her own control 12-16 weeks later when the treatments (lidocaine 3% with jet phoresis vs. Emla 5%) were repeated on the opposite lip sides for the same durations, so that in all, there were 40 full-lip applications of the two treatments. Different readings for the left and right sides were registered in some of the patients.
Of the total 40 treatments, pain control with lidocaine 3% with jet phoresis and Emla 5% was comparable in 19 applications, it was better with the lidocaine 3% with jet phoresis in 14 of the applications, and better with Emla 5% in 7 applications
The delivery device, the JetPeel 3, uses pressurized gas at supersonic velocities to deliver saline or other liquid nutrients through special handpieces into the superficial layers of the skin. It was cleared by the Food and Drug Administration in 2006 for delivery of saline into the skin.
The researchers received honoraria from TavTech Ltd., maker of the jet-phoresis system, to conduct the study.
Imiquimod Before Mohs Is No Help for Nodular, Nasal BCC
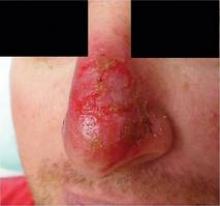
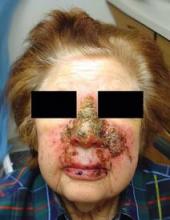
MONTEREY, Calif. — Using imiquimod on nodular basal cell carcinomas on the nose before Mohs surgery failed to simplify the surgery or reduce costs and significantly increased local adverse reactions, in a randomized, controlled study of 28 patients.
"Doctors across the country are using imiquimod 'off label' to treat BCCs on the nose, and they should know these findings before doing that," said Dr. David F. Butler.
The study was inspired by a patient who refused surgery or radiation for her nodular, nasal BCC and was treated with good results using imiquimod, he said at the annual meeting of the American Society for Mohs Surgery. Perhaps, he reasoned, adjunctive imiquimod might reduce similar tumors before treatment with Mohs surgery.
"I was surprised that imiquimod did not reduce the number of stages, reduce the cost of Mohs surgery, or reduce the cost of repair," said Dr. Butler, chair of dermatology at the Scott and White Clinic and professor of internal medicine at Texas A&M University, both in Temple, Tex.
Of the 31 patients who enrolled in the study, 3 dropped out, 2 because of local adverse events and 1 because of other illness. Among the 28 patients who completed the study, 10 of 12 (83%) in the imiquimod arm and 4 of 16 (25%) in the control arm developed local adverse events after 3 weeks of treatment, including redness, blisters, erosions, and crusting. After 6 weeks, the same number in the imiquimod group and two patients in the control group (12%) had local adverse reactions. The differences between the groups were statistically significant.
The frequency of local adverse events limits the usefulness of imiquimod as adjunctive therapy in these cases, he said.
Only one stage of Mohs surgery was needed for 11 patients in each group. Two stages were needed for one patient in the imiquimod arm (8%) and five patients in the control arm (31%). Surgical defect sizes averaged 88 mm2 in the imiquimod arm and 100 mm2 in the control arm (Dermatol. Surg. 2009;35:24-9).
A larger study might show a difference, he acknowledged. The current study did not include the cost of imiquimod, so even if a larger study finds that adjunctive imiquimod therapy reduces the number of Mohs stages needed, the medication cost might negate any cost savings in the surgery.
Patients applied 5% imiquimod cream or vehicle to the tumor five nights a week for 6 weeks and covered it with a bandage supplied by investigators. One month after stopping the imiquimod, they underwent Mohs surgery.
Dr. Butler said in an interview that he was surprised by the "inordinately high" proportion of patients with tumor remaining at the time of Mohs surgery after imiquimod treatment.
Only 5 of 12 patients (42%) in the treatment group had complete clearance of the tumor after imiquimod therapy, with tumor absent (presumably destroyed) in the first stage block. "That's a relatively low number when you compare it to the 80% cure rate that you get when using imiquimod to treat superficial BCCs on the trunk or extremities," he said. "My concern is that nodular BCCs on the nose may be a different problem."
Imiquimod was approved in 2004 to treat superficial BCC on the trunk and extremities, with histologic cure rates of 79%-82% at those sites, previous studies have shown. Clearance rates have been lower, however, for nodular BCCs, with reports ranging from 65% to 76%, he noted. In addition, the most common site for BCCs is not the trunk or extremities but the nose, accounting for 25%-30%.
Dr. Butler advised against using imiquimod as a stand-alone therapy for nodular BCCs on the nose, but said it may be a reasonable option for patients who cannot or will not undergo other treatments.
"We do recommend, however, that if you're going to use imiquimod as a single therapy for nodular BCCs on the nose, that once you finish the treatment, that you go back and do a little biopsy of the area to document that the cancer is gone," he added.
Graceway Pharmaceuticals and 3M funded the study. Dr. Butler reported that he had no conflicts of interest.
MONTEREY, Calif. — Using imiquimod on nodular basal cell carcinomas on the nose before Mohs surgery failed to simplify the surgery or reduce costs and significantly increased local adverse reactions, in a randomized, controlled study of 28 patients.
"Doctors across the country are using imiquimod 'off label' to treat BCCs on the nose, and they should know these findings before doing that," said Dr. David F. Butler.
The study was inspired by a patient who refused surgery or radiation for her nodular, nasal BCC and was treated with good results using imiquimod, he said at the annual meeting of the American Society for Mohs Surgery. Perhaps, he reasoned, adjunctive imiquimod might reduce similar tumors before treatment with Mohs surgery.
"I was surprised that imiquimod did not reduce the number of stages, reduce the cost of Mohs surgery, or reduce the cost of repair," said Dr. Butler, chair of dermatology at the Scott and White Clinic and professor of internal medicine at Texas A&M University, both in Temple, Tex.
Of the 31 patients who enrolled in the study, 3 dropped out, 2 because of local adverse events and 1 because of other illness. Among the 28 patients who completed the study, 10 of 12 (83%) in the imiquimod arm and 4 of 16 (25%) in the control arm developed local adverse events after 3 weeks of treatment, including redness, blisters, erosions, and crusting. After 6 weeks, the same number in the imiquimod group and two patients in the control group (12%) had local adverse reactions. The differences between the groups were statistically significant.
The frequency of local adverse events limits the usefulness of imiquimod as adjunctive therapy in these cases, he said.
Only one stage of Mohs surgery was needed for 11 patients in each group. Two stages were needed for one patient in the imiquimod arm (8%) and five patients in the control arm (31%). Surgical defect sizes averaged 88 mm2 in the imiquimod arm and 100 mm2 in the control arm (Dermatol. Surg. 2009;35:24-9).
A larger study might show a difference, he acknowledged. The current study did not include the cost of imiquimod, so even if a larger study finds that adjunctive imiquimod therapy reduces the number of Mohs stages needed, the medication cost might negate any cost savings in the surgery.
Patients applied 5% imiquimod cream or vehicle to the tumor five nights a week for 6 weeks and covered it with a bandage supplied by investigators. One month after stopping the imiquimod, they underwent Mohs surgery.
Dr. Butler said in an interview that he was surprised by the "inordinately high" proportion of patients with tumor remaining at the time of Mohs surgery after imiquimod treatment.
Only 5 of 12 patients (42%) in the treatment group had complete clearance of the tumor after imiquimod therapy, with tumor absent (presumably destroyed) in the first stage block. "That's a relatively low number when you compare it to the 80% cure rate that you get when using imiquimod to treat superficial BCCs on the trunk or extremities," he said. "My concern is that nodular BCCs on the nose may be a different problem."
Imiquimod was approved in 2004 to treat superficial BCC on the trunk and extremities, with histologic cure rates of 79%-82% at those sites, previous studies have shown. Clearance rates have been lower, however, for nodular BCCs, with reports ranging from 65% to 76%, he noted. In addition, the most common site for BCCs is not the trunk or extremities but the nose, accounting for 25%-30%.
Dr. Butler advised against using imiquimod as a stand-alone therapy for nodular BCCs on the nose, but said it may be a reasonable option for patients who cannot or will not undergo other treatments.
"We do recommend, however, that if you're going to use imiquimod as a single therapy for nodular BCCs on the nose, that once you finish the treatment, that you go back and do a little biopsy of the area to document that the cancer is gone," he added.
Graceway Pharmaceuticals and 3M funded the study. Dr. Butler reported that he had no conflicts of interest.
MONTEREY, Calif. — Using imiquimod on nodular basal cell carcinomas on the nose before Mohs surgery failed to simplify the surgery or reduce costs and significantly increased local adverse reactions, in a randomized, controlled study of 28 patients.
"Doctors across the country are using imiquimod 'off label' to treat BCCs on the nose, and they should know these findings before doing that," said Dr. David F. Butler.
The study was inspired by a patient who refused surgery or radiation for her nodular, nasal BCC and was treated with good results using imiquimod, he said at the annual meeting of the American Society for Mohs Surgery. Perhaps, he reasoned, adjunctive imiquimod might reduce similar tumors before treatment with Mohs surgery.
"I was surprised that imiquimod did not reduce the number of stages, reduce the cost of Mohs surgery, or reduce the cost of repair," said Dr. Butler, chair of dermatology at the Scott and White Clinic and professor of internal medicine at Texas A&M University, both in Temple, Tex.
Of the 31 patients who enrolled in the study, 3 dropped out, 2 because of local adverse events and 1 because of other illness. Among the 28 patients who completed the study, 10 of 12 (83%) in the imiquimod arm and 4 of 16 (25%) in the control arm developed local adverse events after 3 weeks of treatment, including redness, blisters, erosions, and crusting. After 6 weeks, the same number in the imiquimod group and two patients in the control group (12%) had local adverse reactions. The differences between the groups were statistically significant.
The frequency of local adverse events limits the usefulness of imiquimod as adjunctive therapy in these cases, he said.
Only one stage of Mohs surgery was needed for 11 patients in each group. Two stages were needed for one patient in the imiquimod arm (8%) and five patients in the control arm (31%). Surgical defect sizes averaged 88 mm2 in the imiquimod arm and 100 mm2 in the control arm (Dermatol. Surg. 2009;35:24-9).
A larger study might show a difference, he acknowledged. The current study did not include the cost of imiquimod, so even if a larger study finds that adjunctive imiquimod therapy reduces the number of Mohs stages needed, the medication cost might negate any cost savings in the surgery.
Patients applied 5% imiquimod cream or vehicle to the tumor five nights a week for 6 weeks and covered it with a bandage supplied by investigators. One month after stopping the imiquimod, they underwent Mohs surgery.
Dr. Butler said in an interview that he was surprised by the "inordinately high" proportion of patients with tumor remaining at the time of Mohs surgery after imiquimod treatment.
Only 5 of 12 patients (42%) in the treatment group had complete clearance of the tumor after imiquimod therapy, with tumor absent (presumably destroyed) in the first stage block. "That's a relatively low number when you compare it to the 80% cure rate that you get when using imiquimod to treat superficial BCCs on the trunk or extremities," he said. "My concern is that nodular BCCs on the nose may be a different problem."
Imiquimod was approved in 2004 to treat superficial BCC on the trunk and extremities, with histologic cure rates of 79%-82% at those sites, previous studies have shown. Clearance rates have been lower, however, for nodular BCCs, with reports ranging from 65% to 76%, he noted. In addition, the most common site for BCCs is not the trunk or extremities but the nose, accounting for 25%-30%.
Dr. Butler advised against using imiquimod as a stand-alone therapy for nodular BCCs on the nose, but said it may be a reasonable option for patients who cannot or will not undergo other treatments.
"We do recommend, however, that if you're going to use imiquimod as a single therapy for nodular BCCs on the nose, that once you finish the treatment, that you go back and do a little biopsy of the area to document that the cancer is gone," he added.
Graceway Pharmaceuticals and 3M funded the study. Dr. Butler reported that he had no conflicts of interest.
Ultrasound-Assisted Lipoplasty Helps Recontour Jowls
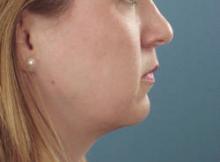
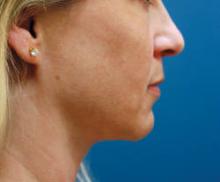
WASHINGTON — The removal of fat using ultrasound-assisted lipoplasty may be all it takes to recontour the jowls of younger patients and can complement techniques to recontour the jowls of older and more difficult-to-treat patients, said Dr. James C. Grotting.
Dr. Grotting has been using ultrasound-assisted liposuction (UAL) to recontour the jowls, "especially in the younger round-faced patient - who doesn't require a face lift - and the difficult, older, heavy-jowled patient."
"I think it's important to say that UAL is simply a tool that helps evenly and precisely remove the excess fat that contributes to the formation of the jowls," Dr. Grotting said at the annual meeting of the American Society for Aesthetic Plastic Surgery. "It's my opinion that UAL allows a little more control and may stimulate a modicum of skin retraction." This control helps to minimize the creation of visible lines, furrows, and other irregularities.
Dr. Grotting, a practicing plastic surgeon in Birmingham, Ala., grasps the fat to reposition and observe it to decide if he needs to reduce the amount of fat.
When performing UAL, he doubles the epinephrine injected, and hand-tunnels using the spatulated facial cannula to create the facial plane. Low power ultrasound helps provide additional control. An incision is then made right in front of the earlobe because "if you get behind the ear lobe, sometimes you get behind the platysma and you could potentially damage the mandibular branch," he said.
The area to be contoured is just the jowl area, extending down into the neck. "It's important to make sure that you're in the subcutaneous plane," he said.
"I've found this to be a very effective way to treat men - particularly men who are not interested in face lifts." He recommends being more aggressive when contouring the jowls in men because of the thickness of the skin. "I generally will come to the jowl from below."
Dr. Grotting did not have any relevant conflicts to disclose.
WASHINGTON — The removal of fat using ultrasound-assisted lipoplasty may be all it takes to recontour the jowls of younger patients and can complement techniques to recontour the jowls of older and more difficult-to-treat patients, said Dr. James C. Grotting.
Dr. Grotting has been using ultrasound-assisted liposuction (UAL) to recontour the jowls, "especially in the younger round-faced patient - who doesn't require a face lift - and the difficult, older, heavy-jowled patient."
"I think it's important to say that UAL is simply a tool that helps evenly and precisely remove the excess fat that contributes to the formation of the jowls," Dr. Grotting said at the annual meeting of the American Society for Aesthetic Plastic Surgery. "It's my opinion that UAL allows a little more control and may stimulate a modicum of skin retraction." This control helps to minimize the creation of visible lines, furrows, and other irregularities.
Dr. Grotting, a practicing plastic surgeon in Birmingham, Ala., grasps the fat to reposition and observe it to decide if he needs to reduce the amount of fat.
When performing UAL, he doubles the epinephrine injected, and hand-tunnels using the spatulated facial cannula to create the facial plane. Low power ultrasound helps provide additional control. An incision is then made right in front of the earlobe because "if you get behind the ear lobe, sometimes you get behind the platysma and you could potentially damage the mandibular branch," he said.
The area to be contoured is just the jowl area, extending down into the neck. "It's important to make sure that you're in the subcutaneous plane," he said.
"I've found this to be a very effective way to treat men - particularly men who are not interested in face lifts." He recommends being more aggressive when contouring the jowls in men because of the thickness of the skin. "I generally will come to the jowl from below."
Dr. Grotting did not have any relevant conflicts to disclose.
WASHINGTON — The removal of fat using ultrasound-assisted lipoplasty may be all it takes to recontour the jowls of younger patients and can complement techniques to recontour the jowls of older and more difficult-to-treat patients, said Dr. James C. Grotting.
Dr. Grotting has been using ultrasound-assisted liposuction (UAL) to recontour the jowls, "especially in the younger round-faced patient - who doesn't require a face lift - and the difficult, older, heavy-jowled patient."
"I think it's important to say that UAL is simply a tool that helps evenly and precisely remove the excess fat that contributes to the formation of the jowls," Dr. Grotting said at the annual meeting of the American Society for Aesthetic Plastic Surgery. "It's my opinion that UAL allows a little more control and may stimulate a modicum of skin retraction." This control helps to minimize the creation of visible lines, furrows, and other irregularities.
Dr. Grotting, a practicing plastic surgeon in Birmingham, Ala., grasps the fat to reposition and observe it to decide if he needs to reduce the amount of fat.
When performing UAL, he doubles the epinephrine injected, and hand-tunnels using the spatulated facial cannula to create the facial plane. Low power ultrasound helps provide additional control. An incision is then made right in front of the earlobe because "if you get behind the ear lobe, sometimes you get behind the platysma and you could potentially damage the mandibular branch," he said.
The area to be contoured is just the jowl area, extending down into the neck. "It's important to make sure that you're in the subcutaneous plane," he said.
"I've found this to be a very effective way to treat men - particularly men who are not interested in face lifts." He recommends being more aggressive when contouring the jowls in men because of the thickness of the skin. "I generally will come to the jowl from below."
Dr. Grotting did not have any relevant conflicts to disclose.
Tips for Treating Acne Scarring in Darker Skinned Patients
PHOENIX — Educate darker skinned patients who seek treatment for acne scars that there is no remedy to make the scars completely disappear.
"Depending on the patient's skin type, the sensitivity of their skin, and how aggressively you treat them, the risk of hyperpigmentation can be relatively modest, or well over 50%. The expected degree of improvement, on the other hand, even with multiple modalities and multiple treatments, is 40%-50%. I think it's very important to explain that," said Dr. Murad Alam at the annual meeting of the American Society for Laser Medicine and Surgery.
Dr. Alam, chief of cutaneous and aesthetic surgery at Northwestern University, Chicago, said that clinicians face certain challenges in treating acne scars in patients of color, including the risk of exacerbation of active acne, risk of focal or diffuse hyperpigmentation or hypopigmentation, risk of nodularity or surface texture change, and risk of minimal effect.
To mitigate risks, Dr. Alam considers oral antibiotics in patients who have any degree of active acne, "even if they get one or two acne pimples once in a blue moon," he said. "If the acne is more than very mild, you may wish to target that as the primary goal and defer treatment of the acne scarring until the acne is under good control."
If the acne is mild, "you can start oral antibiotics at least 1 month before the acne scarring intervention, so they do have something on board to reduce the risk of an acne flare," he said. "You may also consider pretreatment with bleaching agents. I'm personally not that convinced that pre-treatment is that helpful, but post-treatment with bleaching agents is of definite efficacy in mitigating postinflammatory hyperpigmentation."
As for treatment, nonablative resurfacing with mid-infrared lasers, including 1320-nm, 1450-nm, and 1540-nm devices, has been shown to be effective in patients with lighter skin. "This heating process causes collagen remodeling, and can have a modest effect on so-called rolling scars, which can be quite disfiguring," he said.
Another option is ablative resurfacing with non-CO2 fractional lasers such as the 1550-nm laser. "This is one of the most gentle devices in this category, but even so you have risks of postinflammatory hyperpigmentation," Dr. Alam said. "I like to err on the side of being very modest with regard to fluences. It's much better to do more treatments than to push each individual treatment at the risk of having pigmentary abnormalities."
A more aggressive approach is ablative resurfacing with CO2 fractional lasers, which "should be restricted to patients who are of lighter skin type. If they do choose this [modality], they need to understand the significant risk of postinflammatory hyperpigmentation. I would say that virtually every patient of skin of color who undergoes this treatment will have some degree of postinflammatory hyperpigmentation. In some cases they might consider that worth it if it makes their scarring better and if it can be managed after treatment so it eventually goes away."
Perhaps the most beneficial treatment for acne scars in patients of color, Dr. Alam said, is subdermal manipulation.
In one procedure, known as subcision, clinicians insert a needle with a sphere-like tip, often an 18-guage Nokor needle, underneath the skin. "By debriding the underside of the skin, you can cause some of the acne scars to float upward," he explained. "You want to ensure very good hemostasis before doing this—lidocaine with epinephrine—because you want to avoid bruising during the procedure. If done properly, this can result in modest improvement of rolling scars, and it can be done repeatedly."
Dermal fillers can be used as an adjunct. About a month after subcision procedures Dr. Alam considers collagen for fine defects, hyaluronic acid for medium defects, and calcium hydroxylapatite for deeper defects.
The best way to develop a treatment plan for acne scarring, he said, is to assess the patient's commitment to improvement and their tolerance for adverse events.
"How much annoyance and disfigurement are they willing to tolerate?" Dr. Alam asked. "If both of these are low, you might wish to restrict yourself to subcision with or without fillers, because if done properly, that almost eliminates the risk of adverse events like hyperpigmentation, and it does provide some modest improvement with relatively little cost."
If the patient is highly committed to achieving improvement but is wary of adverse events, "then you might consider subcision and fillers, followed by nonablative laser or repeated low energy non-CO2 fractional laser treatments."
In those rare patients with a high tolerance for adverse events, he said, consider CO2 fractional laser treatments "at very modest settings."
Dr. Alam said that he had no relevant financial conflicts.
PHOENIX — Educate darker skinned patients who seek treatment for acne scars that there is no remedy to make the scars completely disappear.
"Depending on the patient's skin type, the sensitivity of their skin, and how aggressively you treat them, the risk of hyperpigmentation can be relatively modest, or well over 50%. The expected degree of improvement, on the other hand, even with multiple modalities and multiple treatments, is 40%-50%. I think it's very important to explain that," said Dr. Murad Alam at the annual meeting of the American Society for Laser Medicine and Surgery.
Dr. Alam, chief of cutaneous and aesthetic surgery at Northwestern University, Chicago, said that clinicians face certain challenges in treating acne scars in patients of color, including the risk of exacerbation of active acne, risk of focal or diffuse hyperpigmentation or hypopigmentation, risk of nodularity or surface texture change, and risk of minimal effect.
To mitigate risks, Dr. Alam considers oral antibiotics in patients who have any degree of active acne, "even if they get one or two acne pimples once in a blue moon," he said. "If the acne is more than very mild, you may wish to target that as the primary goal and defer treatment of the acne scarring until the acne is under good control."
If the acne is mild, "you can start oral antibiotics at least 1 month before the acne scarring intervention, so they do have something on board to reduce the risk of an acne flare," he said. "You may also consider pretreatment with bleaching agents. I'm personally not that convinced that pre-treatment is that helpful, but post-treatment with bleaching agents is of definite efficacy in mitigating postinflammatory hyperpigmentation."
As for treatment, nonablative resurfacing with mid-infrared lasers, including 1320-nm, 1450-nm, and 1540-nm devices, has been shown to be effective in patients with lighter skin. "This heating process causes collagen remodeling, and can have a modest effect on so-called rolling scars, which can be quite disfiguring," he said.
Another option is ablative resurfacing with non-CO2 fractional lasers such as the 1550-nm laser. "This is one of the most gentle devices in this category, but even so you have risks of postinflammatory hyperpigmentation," Dr. Alam said. "I like to err on the side of being very modest with regard to fluences. It's much better to do more treatments than to push each individual treatment at the risk of having pigmentary abnormalities."
A more aggressive approach is ablative resurfacing with CO2 fractional lasers, which "should be restricted to patients who are of lighter skin type. If they do choose this [modality], they need to understand the significant risk of postinflammatory hyperpigmentation. I would say that virtually every patient of skin of color who undergoes this treatment will have some degree of postinflammatory hyperpigmentation. In some cases they might consider that worth it if it makes their scarring better and if it can be managed after treatment so it eventually goes away."
Perhaps the most beneficial treatment for acne scars in patients of color, Dr. Alam said, is subdermal manipulation.
In one procedure, known as subcision, clinicians insert a needle with a sphere-like tip, often an 18-guage Nokor needle, underneath the skin. "By debriding the underside of the skin, you can cause some of the acne scars to float upward," he explained. "You want to ensure very good hemostasis before doing this—lidocaine with epinephrine—because you want to avoid bruising during the procedure. If done properly, this can result in modest improvement of rolling scars, and it can be done repeatedly."
Dermal fillers can be used as an adjunct. About a month after subcision procedures Dr. Alam considers collagen for fine defects, hyaluronic acid for medium defects, and calcium hydroxylapatite for deeper defects.
The best way to develop a treatment plan for acne scarring, he said, is to assess the patient's commitment to improvement and their tolerance for adverse events.
"How much annoyance and disfigurement are they willing to tolerate?" Dr. Alam asked. "If both of these are low, you might wish to restrict yourself to subcision with or without fillers, because if done properly, that almost eliminates the risk of adverse events like hyperpigmentation, and it does provide some modest improvement with relatively little cost."
If the patient is highly committed to achieving improvement but is wary of adverse events, "then you might consider subcision and fillers, followed by nonablative laser or repeated low energy non-CO2 fractional laser treatments."
In those rare patients with a high tolerance for adverse events, he said, consider CO2 fractional laser treatments "at very modest settings."
Dr. Alam said that he had no relevant financial conflicts.
PHOENIX — Educate darker skinned patients who seek treatment for acne scars that there is no remedy to make the scars completely disappear.
"Depending on the patient's skin type, the sensitivity of their skin, and how aggressively you treat them, the risk of hyperpigmentation can be relatively modest, or well over 50%. The expected degree of improvement, on the other hand, even with multiple modalities and multiple treatments, is 40%-50%. I think it's very important to explain that," said Dr. Murad Alam at the annual meeting of the American Society for Laser Medicine and Surgery.
Dr. Alam, chief of cutaneous and aesthetic surgery at Northwestern University, Chicago, said that clinicians face certain challenges in treating acne scars in patients of color, including the risk of exacerbation of active acne, risk of focal or diffuse hyperpigmentation or hypopigmentation, risk of nodularity or surface texture change, and risk of minimal effect.
To mitigate risks, Dr. Alam considers oral antibiotics in patients who have any degree of active acne, "even if they get one or two acne pimples once in a blue moon," he said. "If the acne is more than very mild, you may wish to target that as the primary goal and defer treatment of the acne scarring until the acne is under good control."
If the acne is mild, "you can start oral antibiotics at least 1 month before the acne scarring intervention, so they do have something on board to reduce the risk of an acne flare," he said. "You may also consider pretreatment with bleaching agents. I'm personally not that convinced that pre-treatment is that helpful, but post-treatment with bleaching agents is of definite efficacy in mitigating postinflammatory hyperpigmentation."
As for treatment, nonablative resurfacing with mid-infrared lasers, including 1320-nm, 1450-nm, and 1540-nm devices, has been shown to be effective in patients with lighter skin. "This heating process causes collagen remodeling, and can have a modest effect on so-called rolling scars, which can be quite disfiguring," he said.
Another option is ablative resurfacing with non-CO2 fractional lasers such as the 1550-nm laser. "This is one of the most gentle devices in this category, but even so you have risks of postinflammatory hyperpigmentation," Dr. Alam said. "I like to err on the side of being very modest with regard to fluences. It's much better to do more treatments than to push each individual treatment at the risk of having pigmentary abnormalities."
A more aggressive approach is ablative resurfacing with CO2 fractional lasers, which "should be restricted to patients who are of lighter skin type. If they do choose this [modality], they need to understand the significant risk of postinflammatory hyperpigmentation. I would say that virtually every patient of skin of color who undergoes this treatment will have some degree of postinflammatory hyperpigmentation. In some cases they might consider that worth it if it makes their scarring better and if it can be managed after treatment so it eventually goes away."
Perhaps the most beneficial treatment for acne scars in patients of color, Dr. Alam said, is subdermal manipulation.
In one procedure, known as subcision, clinicians insert a needle with a sphere-like tip, often an 18-guage Nokor needle, underneath the skin. "By debriding the underside of the skin, you can cause some of the acne scars to float upward," he explained. "You want to ensure very good hemostasis before doing this—lidocaine with epinephrine—because you want to avoid bruising during the procedure. If done properly, this can result in modest improvement of rolling scars, and it can be done repeatedly."
Dermal fillers can be used as an adjunct. About a month after subcision procedures Dr. Alam considers collagen for fine defects, hyaluronic acid for medium defects, and calcium hydroxylapatite for deeper defects.
The best way to develop a treatment plan for acne scarring, he said, is to assess the patient's commitment to improvement and their tolerance for adverse events.
"How much annoyance and disfigurement are they willing to tolerate?" Dr. Alam asked. "If both of these are low, you might wish to restrict yourself to subcision with or without fillers, because if done properly, that almost eliminates the risk of adverse events like hyperpigmentation, and it does provide some modest improvement with relatively little cost."
If the patient is highly committed to achieving improvement but is wary of adverse events, "then you might consider subcision and fillers, followed by nonablative laser or repeated low energy non-CO2 fractional laser treatments."
In those rare patients with a high tolerance for adverse events, he said, consider CO2 fractional laser treatments "at very modest settings."
Dr. Alam said that he had no relevant financial conflicts.
Cosmeceuticals Enhance Cosmetic Procedures for Melasma
SANTA MONICA, Calif. - Melasma is notoriously difficult to eliminate, but adding cosmeceuticals to the treatment can improve chemical peel results, according to Dr. Cherie M. Ditre.
"I use a combination of retinols, combinations of antioxidants such as green tea, along with hydroquinones," Dr. Ditre said in an interview at a cosmetic dermatology seminar sponsored by Skin Disease Education Foundation (SDEF).
"Those three together are a powerhouse. And, occasionally, I'll add in alpha-hydroxy acids to actually help increase permeation through the skin."
The exact combinations depend on the procedure planned, said Dr. Ditre director of the University of Pennsylvania Health System's Skin Enhancement Center in Radnor.
If she is planning a chemical peel, for example, she has the patients "prepped first in the morning with an alpha-hydroxy acid cleanser starting at 10% and moving up. And then I also have them use hydroquinone at 4%. I can also titrate that in office to 6% or 8% depending on what they need. And then I go with an antioxidant such as green tea and a sunscreen."
She prefers sunscreens containing titanium dioxide and zinc oxide, and recommends Anthelios, which contains Mexoryl, and is a Food and Drug Administration-approved sun filter.
For the evening, Dr. Ditre instructs her chemical peel patients to use an alpha-hydroxy acid cleanser with a retinol that she titrates based on skin type and condition. She mixes that with an antioxidant such as green tea.
"I do that for a period of about 2 weeks prior to the chemical peel," she said. "The chemical peel that I'm presently using is a combination of a 1% retinol with 14% hydroquinone, and we leave it on as a masque for about 5-8 hours to wash off at home. And then, for the following 2 weeks, they use a regimen of a retinol and hydroquinone along with their sunscreen and a calming lotion," after which patients will return for follow-up.
Dr. Ditre said she has never seen an adverse reaction to green tea, which she described as "very gentle." Retinols are another story, however.
"Some of the retinols can approximate retinoic acid, so you have to be careful in very sensitive skin patients," she said. "I think that starting with the 2X [concentration] is better for sensitive skin patients. And that's why you do it as a prep prior to actually doing procedures, to make sure it's agreeable with them prior to doing a more invasive procedure."
Dr. Ditre reported having no disclosures. SDEF and this news organization are owned by Elsevier.
SANTA MONICA, Calif. - Melasma is notoriously difficult to eliminate, but adding cosmeceuticals to the treatment can improve chemical peel results, according to Dr. Cherie M. Ditre.
"I use a combination of retinols, combinations of antioxidants such as green tea, along with hydroquinones," Dr. Ditre said in an interview at a cosmetic dermatology seminar sponsored by Skin Disease Education Foundation (SDEF).
"Those three together are a powerhouse. And, occasionally, I'll add in alpha-hydroxy acids to actually help increase permeation through the skin."
The exact combinations depend on the procedure planned, said Dr. Ditre director of the University of Pennsylvania Health System's Skin Enhancement Center in Radnor.
If she is planning a chemical peel, for example, she has the patients "prepped first in the morning with an alpha-hydroxy acid cleanser starting at 10% and moving up. And then I also have them use hydroquinone at 4%. I can also titrate that in office to 6% or 8% depending on what they need. And then I go with an antioxidant such as green tea and a sunscreen."
She prefers sunscreens containing titanium dioxide and zinc oxide, and recommends Anthelios, which contains Mexoryl, and is a Food and Drug Administration-approved sun filter.
For the evening, Dr. Ditre instructs her chemical peel patients to use an alpha-hydroxy acid cleanser with a retinol that she titrates based on skin type and condition. She mixes that with an antioxidant such as green tea.
"I do that for a period of about 2 weeks prior to the chemical peel," she said. "The chemical peel that I'm presently using is a combination of a 1% retinol with 14% hydroquinone, and we leave it on as a masque for about 5-8 hours to wash off at home. And then, for the following 2 weeks, they use a regimen of a retinol and hydroquinone along with their sunscreen and a calming lotion," after which patients will return for follow-up.
Dr. Ditre said she has never seen an adverse reaction to green tea, which she described as "very gentle." Retinols are another story, however.
"Some of the retinols can approximate retinoic acid, so you have to be careful in very sensitive skin patients," she said. "I think that starting with the 2X [concentration] is better for sensitive skin patients. And that's why you do it as a prep prior to actually doing procedures, to make sure it's agreeable with them prior to doing a more invasive procedure."
Dr. Ditre reported having no disclosures. SDEF and this news organization are owned by Elsevier.
SANTA MONICA, Calif. - Melasma is notoriously difficult to eliminate, but adding cosmeceuticals to the treatment can improve chemical peel results, according to Dr. Cherie M. Ditre.
"I use a combination of retinols, combinations of antioxidants such as green tea, along with hydroquinones," Dr. Ditre said in an interview at a cosmetic dermatology seminar sponsored by Skin Disease Education Foundation (SDEF).
"Those three together are a powerhouse. And, occasionally, I'll add in alpha-hydroxy acids to actually help increase permeation through the skin."
The exact combinations depend on the procedure planned, said Dr. Ditre director of the University of Pennsylvania Health System's Skin Enhancement Center in Radnor.
If she is planning a chemical peel, for example, she has the patients "prepped first in the morning with an alpha-hydroxy acid cleanser starting at 10% and moving up. And then I also have them use hydroquinone at 4%. I can also titrate that in office to 6% or 8% depending on what they need. And then I go with an antioxidant such as green tea and a sunscreen."
She prefers sunscreens containing titanium dioxide and zinc oxide, and recommends Anthelios, which contains Mexoryl, and is a Food and Drug Administration-approved sun filter.
For the evening, Dr. Ditre instructs her chemical peel patients to use an alpha-hydroxy acid cleanser with a retinol that she titrates based on skin type and condition. She mixes that with an antioxidant such as green tea.
"I do that for a period of about 2 weeks prior to the chemical peel," she said. "The chemical peel that I'm presently using is a combination of a 1% retinol with 14% hydroquinone, and we leave it on as a masque for about 5-8 hours to wash off at home. And then, for the following 2 weeks, they use a regimen of a retinol and hydroquinone along with their sunscreen and a calming lotion," after which patients will return for follow-up.
Dr. Ditre said she has never seen an adverse reaction to green tea, which she described as "very gentle." Retinols are another story, however.
"Some of the retinols can approximate retinoic acid, so you have to be careful in very sensitive skin patients," she said. "I think that starting with the 2X [concentration] is better for sensitive skin patients. And that's why you do it as a prep prior to actually doing procedures, to make sure it's agreeable with them prior to doing a more invasive procedure."
Dr. Ditre reported having no disclosures. SDEF and this news organization are owned by Elsevier.
A Market Overview of Nutricosmetics
Shedding Light at the Tanning Parlor: A Review of the Recent Research on Teenage Tanning Behavior
Burn Scar Treatment Called ‘Work in Progress’
PHOENIX — Burn scars rank as one of the most difficult dermatologic conditions to treat, Dr. Jill S. Waibel said at the annual meeting of the American Society for Laser Medicine and Surgery.
"Burn scars are the worst we see in clinical medicine," said Dr. Waibel, a dermatologist with a laser practice in Miami. "I believe that if we can treat a burn scar, we can treat any scar."
Under normal circumstances, wounded skin re-epithelizes from hair follicles and dermal glands, but because burn scars are often partially or completely deprived of their epidermal appendages, "healing is severely affected," she noted.
Thanks to surgical advances in the past decade, survival of burn patients has risen from about 30% to 95%. The types of scars they present with include hypertrophic, keloid, contracture, and atrophic.
Current efforts to treat burn scars fall into one of two camps: prevention of scar formation and late reconstruction of mature scars.
"We do have a model for a scarless wound," Dr. Waibel said. "A fetus in utero does not scar. We don't understand that process. There are also a number of topical applications to prevent scars at the time of the wound. Over 200 cytokines are involved in wound healing."
Research efforts are also under way on laser-assisted skin healing with a diode laser, she said, which alters the wound-healing process by thermal stress.
Current treatment for late reconstruction of mature scars includes surgery, followed by laser combination therapy. "I think fractional therapy is the … standard, but I really don't think we understand the mechanism of action in laser and scar reduction," Dr. Waibel commented. "I think we break it down into two areas: either fractional versus thermal, or probably it's fractional and thermal. The thermal effects are the most interesting. How much heat is required for the most constructive healing versus too much thermal injury? We need to look more at what that [ideal] temperature is."
She tells her burn scar patients to consider their treatment as a "work in progress" and asks them to give her a year before they start to assess efficacy. In 2005, her first burn patient underwent five treatments with a 1550-nm, nonablative, erbium-fiber fractional laser; intralesional Kenalog (triamcinolone); and a shave biopsy.
"We see functional improvement as well as cosmetic, especially with contracture scars, and we're working on some range-of-motion studies right now," Dr. Waibel said.
In a study presented at the society's 2009 meeting, Dr. Waibel and her associates presented results from a proof-of-concept study of 10 patients who had burn scars that were treated with a 1550-nm, nonablative, erbium-fiber fractional laser.
Objective scoring by blinded investigators of photos taken pretreatment and at 3 months posttreatment indicated that 78% of patients had excellent to moderate results.
Dr. Waibel acknowledged certain limitations in current efforts to improve treatment for patients with burn scars, including the need for surgery for anatomical fixes and the lack of understanding of the processes of scar formation and the laser effects on scars. "We need better technology, and we need to maximize treatment modalities," she said. "We really need to develop a scar laser. All of the lasers that we use for scars right now were invented for wrinkles."
Dr. Waibel has conducted research for Solta Medical and Sciton, and she has received honoraria from Lumenis for lectures.
PHOENIX — Burn scars rank as one of the most difficult dermatologic conditions to treat, Dr. Jill S. Waibel said at the annual meeting of the American Society for Laser Medicine and Surgery.
"Burn scars are the worst we see in clinical medicine," said Dr. Waibel, a dermatologist with a laser practice in Miami. "I believe that if we can treat a burn scar, we can treat any scar."
Under normal circumstances, wounded skin re-epithelizes from hair follicles and dermal glands, but because burn scars are often partially or completely deprived of their epidermal appendages, "healing is severely affected," she noted.
Thanks to surgical advances in the past decade, survival of burn patients has risen from about 30% to 95%. The types of scars they present with include hypertrophic, keloid, contracture, and atrophic.
Current efforts to treat burn scars fall into one of two camps: prevention of scar formation and late reconstruction of mature scars.
"We do have a model for a scarless wound," Dr. Waibel said. "A fetus in utero does not scar. We don't understand that process. There are also a number of topical applications to prevent scars at the time of the wound. Over 200 cytokines are involved in wound healing."
Research efforts are also under way on laser-assisted skin healing with a diode laser, she said, which alters the wound-healing process by thermal stress.
Current treatment for late reconstruction of mature scars includes surgery, followed by laser combination therapy. "I think fractional therapy is the … standard, but I really don't think we understand the mechanism of action in laser and scar reduction," Dr. Waibel commented. "I think we break it down into two areas: either fractional versus thermal, or probably it's fractional and thermal. The thermal effects are the most interesting. How much heat is required for the most constructive healing versus too much thermal injury? We need to look more at what that [ideal] temperature is."
She tells her burn scar patients to consider their treatment as a "work in progress" and asks them to give her a year before they start to assess efficacy. In 2005, her first burn patient underwent five treatments with a 1550-nm, nonablative, erbium-fiber fractional laser; intralesional Kenalog (triamcinolone); and a shave biopsy.
"We see functional improvement as well as cosmetic, especially with contracture scars, and we're working on some range-of-motion studies right now," Dr. Waibel said.
In a study presented at the society's 2009 meeting, Dr. Waibel and her associates presented results from a proof-of-concept study of 10 patients who had burn scars that were treated with a 1550-nm, nonablative, erbium-fiber fractional laser.
Objective scoring by blinded investigators of photos taken pretreatment and at 3 months posttreatment indicated that 78% of patients had excellent to moderate results.
Dr. Waibel acknowledged certain limitations in current efforts to improve treatment for patients with burn scars, including the need for surgery for anatomical fixes and the lack of understanding of the processes of scar formation and the laser effects on scars. "We need better technology, and we need to maximize treatment modalities," she said. "We really need to develop a scar laser. All of the lasers that we use for scars right now were invented for wrinkles."
Dr. Waibel has conducted research for Solta Medical and Sciton, and she has received honoraria from Lumenis for lectures.
PHOENIX — Burn scars rank as one of the most difficult dermatologic conditions to treat, Dr. Jill S. Waibel said at the annual meeting of the American Society for Laser Medicine and Surgery.
"Burn scars are the worst we see in clinical medicine," said Dr. Waibel, a dermatologist with a laser practice in Miami. "I believe that if we can treat a burn scar, we can treat any scar."
Under normal circumstances, wounded skin re-epithelizes from hair follicles and dermal glands, but because burn scars are often partially or completely deprived of their epidermal appendages, "healing is severely affected," she noted.
Thanks to surgical advances in the past decade, survival of burn patients has risen from about 30% to 95%. The types of scars they present with include hypertrophic, keloid, contracture, and atrophic.
Current efforts to treat burn scars fall into one of two camps: prevention of scar formation and late reconstruction of mature scars.
"We do have a model for a scarless wound," Dr. Waibel said. "A fetus in utero does not scar. We don't understand that process. There are also a number of topical applications to prevent scars at the time of the wound. Over 200 cytokines are involved in wound healing."
Research efforts are also under way on laser-assisted skin healing with a diode laser, she said, which alters the wound-healing process by thermal stress.
Current treatment for late reconstruction of mature scars includes surgery, followed by laser combination therapy. "I think fractional therapy is the … standard, but I really don't think we understand the mechanism of action in laser and scar reduction," Dr. Waibel commented. "I think we break it down into two areas: either fractional versus thermal, or probably it's fractional and thermal. The thermal effects are the most interesting. How much heat is required for the most constructive healing versus too much thermal injury? We need to look more at what that [ideal] temperature is."
She tells her burn scar patients to consider their treatment as a "work in progress" and asks them to give her a year before they start to assess efficacy. In 2005, her first burn patient underwent five treatments with a 1550-nm, nonablative, erbium-fiber fractional laser; intralesional Kenalog (triamcinolone); and a shave biopsy.
"We see functional improvement as well as cosmetic, especially with contracture scars, and we're working on some range-of-motion studies right now," Dr. Waibel said.
In a study presented at the society's 2009 meeting, Dr. Waibel and her associates presented results from a proof-of-concept study of 10 patients who had burn scars that were treated with a 1550-nm, nonablative, erbium-fiber fractional laser.
Objective scoring by blinded investigators of photos taken pretreatment and at 3 months posttreatment indicated that 78% of patients had excellent to moderate results.
Dr. Waibel acknowledged certain limitations in current efforts to improve treatment for patients with burn scars, including the need for surgery for anatomical fixes and the lack of understanding of the processes of scar formation and the laser effects on scars. "We need better technology, and we need to maximize treatment modalities," she said. "We really need to develop a scar laser. All of the lasers that we use for scars right now were invented for wrinkles."
Dr. Waibel has conducted research for Solta Medical and Sciton, and she has received honoraria from Lumenis for lectures.
Video: Advances in Treating the Aging Face
Dr. Rebecca Fitzgerald talks about advances made in treating the aging face. Instead of fixing specific folds and lines, she recommends considering the entire face.
Markette Smith interviewed Dr. Fitzgerald, a dermatologist in private practice in Los Angeles, at the annual meeting of The American Society for Aesthetic Plastic Surgery.
Dr. Rebecca Fitzgerald talks about advances made in treating the aging face. Instead of fixing specific folds and lines, she recommends considering the entire face.
Markette Smith interviewed Dr. Fitzgerald, a dermatologist in private practice in Los Angeles, at the annual meeting of The American Society for Aesthetic Plastic Surgery.
Dr. Rebecca Fitzgerald talks about advances made in treating the aging face. Instead of fixing specific folds and lines, she recommends considering the entire face.
Markette Smith interviewed Dr. Fitzgerald, a dermatologist in private practice in Los Angeles, at the annual meeting of The American Society for Aesthetic Plastic Surgery.
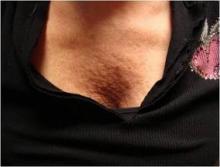
"Peach Pit" Décolleté Defect Can Be Repaired With Fillers
SANTA MONICA, CALIF. — The volume loss and wrinkled skin that appears in the décolleté area of some older women can be significantly softened with filler followed by fractionated laser treatments, Dr. Joel L. Cohen said at a cosmetic dermatology seminar sponsored by Skin Disease Education Foundation.
This cosmetic defect, which Dr. Cohen has dubbed "the peach pit," responds well to injections of hyaluronic acid fillers along with fractionated laser sessions.
"Over the course of many years, I've noticed that many patients become concerned about their décolleté area," said Dr. Cohen, director of AboutSkin Dermatology and DermSurgery, Englewood, Colo., in an interview. "I've tried botulinum toxin [type A]. And despite some reports of efficacy, I haven't been able to actually see this type of efficacy myself. People have topically treated it with retinoids and although that can be helpful, there are patients who have more severe crumpling of the skin."
Instead, he uses Juvéderm (Allergan) or Restylane (Medicis). With such hyaluronic acid fillers, "If you do get lumps or bumps, or the patients aren't happy with it, you could inject the enzyme hyaluronidase and make it go away," he said. "It's easier to mold out little contour irregularities with these types of agents as well."
Using only topical anesthesia, Dr. Cohen injects two or sometimes three syringes of the hyaluronic acid product, after which he asks a female assistant to massage it in. He follows up a few weeks later with two or more treatments with a fractionated laser, often combined with a light erbium laser peel for more texture improvement.
Pharmaceuticals Inc. Skin Disease Education Foundation (SDEF) and this news organization are owned by Elsevier.
SANTA MONICA, CALIF. — The volume loss and wrinkled skin that appears in the décolleté area of some older women can be significantly softened with filler followed by fractionated laser treatments, Dr. Joel L. Cohen said at a cosmetic dermatology seminar sponsored by Skin Disease Education Foundation.
This cosmetic defect, which Dr. Cohen has dubbed "the peach pit," responds well to injections of hyaluronic acid fillers along with fractionated laser sessions.
"Over the course of many years, I've noticed that many patients become concerned about their décolleté area," said Dr. Cohen, director of AboutSkin Dermatology and DermSurgery, Englewood, Colo., in an interview. "I've tried botulinum toxin [type A]. And despite some reports of efficacy, I haven't been able to actually see this type of efficacy myself. People have topically treated it with retinoids and although that can be helpful, there are patients who have more severe crumpling of the skin."
Instead, he uses Juvéderm (Allergan) or Restylane (Medicis). With such hyaluronic acid fillers, "If you do get lumps or bumps, or the patients aren't happy with it, you could inject the enzyme hyaluronidase and make it go away," he said. "It's easier to mold out little contour irregularities with these types of agents as well."
Using only topical anesthesia, Dr. Cohen injects two or sometimes three syringes of the hyaluronic acid product, after which he asks a female assistant to massage it in. He follows up a few weeks later with two or more treatments with a fractionated laser, often combined with a light erbium laser peel for more texture improvement.
Pharmaceuticals Inc. Skin Disease Education Foundation (SDEF) and this news organization are owned by Elsevier.
SANTA MONICA, CALIF. — The volume loss and wrinkled skin that appears in the décolleté area of some older women can be significantly softened with filler followed by fractionated laser treatments, Dr. Joel L. Cohen said at a cosmetic dermatology seminar sponsored by Skin Disease Education Foundation.
This cosmetic defect, which Dr. Cohen has dubbed "the peach pit," responds well to injections of hyaluronic acid fillers along with fractionated laser sessions.
"Over the course of many years, I've noticed that many patients become concerned about their décolleté area," said Dr. Cohen, director of AboutSkin Dermatology and DermSurgery, Englewood, Colo., in an interview. "I've tried botulinum toxin [type A]. And despite some reports of efficacy, I haven't been able to actually see this type of efficacy myself. People have topically treated it with retinoids and although that can be helpful, there are patients who have more severe crumpling of the skin."
Instead, he uses Juvéderm (Allergan) or Restylane (Medicis). With such hyaluronic acid fillers, "If you do get lumps or bumps, or the patients aren't happy with it, you could inject the enzyme hyaluronidase and make it go away," he said. "It's easier to mold out little contour irregularities with these types of agents as well."
Using only topical anesthesia, Dr. Cohen injects two or sometimes three syringes of the hyaluronic acid product, after which he asks a female assistant to massage it in. He follows up a few weeks later with two or more treatments with a fractionated laser, often combined with a light erbium laser peel for more texture improvement.
Pharmaceuticals Inc. Skin Disease Education Foundation (SDEF) and this news organization are owned by Elsevier.