User login
ASDS/ASCDAS Meeting Highlights
International Dermatologic Surgery Exchange Fund Established
CHICAGO – Want to learn more about liposuction in Indonesia? Want to teach your cryosurgery technique to dermatologists in Greece? Want to help physicians in the Philippines perform fat transfer?
You can. Dermatologic surgeons in the United States now have more opportunities to travel, teach, and learn surgical techniques from colleagues in other countries, thanks to a unique collaboration that expands the International Mentorship Program and the International Preceptorship Program.
Earlier this year, Dr. Lawrence M. Field, traveling chair of the International Society for Dermatologic Surgery (ISDS) International Mentorship Program, donated $100,000 to the American Society for Dermatologic Surgeons (ASDS) to establish the Lawrence M. Field MD International Dermatologic Surgery Educational Exchange Fund.
"Dr. Field's donation will allow us to have two preceptorships, a fellowship here in the U.S. and [another] for what Dr. Field has been doing sending fellows to other countries," Dr. Jeffrey S. Dover, ASDS president, said at their annual meeting where the collaboration was announced.
Dr. Field is a "dermatologic surgeon, teacher, and benefactor. He has taught mostly hands-on in more than 60 countries," added ISDS president Dr. Gary J. Brauner.
The ISDS has run the mentorship program since 1986. Additional staffing and other resources provided by the ASDS will significantly expand its reach, said Dr. Field, who is in private practice in San Luis Obispo, Calif.
According to Dr. Field, the program has about 70 mentors from 19 nations.* The program continues to expand and is actively seeking host institutions around the world to work with the faculty. The ASDS/ISDS program is for established dermatologic surgeons and not residents.
Special language skills are a plus but not mandatory, Dr. Field said. In addition, there are no ethnic, cultural, religious or any other exclusions, only mutual acceptability is required.
The ASDS/ISDS program pays the airfare. All mentors, including Dr. Field, offer their expertise free of charge. "Pick me up at the airport; take me to a reasonably nice place; provide me with food, clothing, and shelter; licensure; and surgical scrubs," Dr. Field said, describing his requests to a host institution when he travels. In exchange, "I will give you everything I can ... from me to you, for nothing. Then take me back to the airport, I'll go home, and I'll remember these things forever."
A week commitment is the minimum, Dr. Field said. "You gain knowledge, experience, enjoyment, and the respect of your peers."
In his nearly 25 years as a traveling mentor, Dr. Field has taught and learned about scar revision in the Philippines, cryosurgery in Heraklion, Greece, and fat transfer in Saudi Arabia.** As a consultant to the DermaClinic, Dr. Field shared his expertise to transfer fat from a patient's abdomen to treat her facial atrophy.
Dr. Field praised the accomplishments of the many dermatologic surgeons who participated as ISDS international mentors. For example, Dr. John Strasswimmer, a dermatologic surgeon in Delray Beach, Fla. has treated albino patients in Africa. "Many great things will happen from that," Dr. Field said.
Another mentor, Dr. Rhoda Narins, worked with Dr. Indah Julianto to get permission from the Minister of Health in Indonesia to perform liposuction. "This program is just forming in Jakarta, Indonesia, so some of you might go there," Dr. Field said.
Dr. Field spent 31 years as a preceptor in his private office for dermatologic surgery fellows at University of California, San Francisco. During this time, he also
hosted international surgeons who, unlike the U.S. physicians, could not participate in hands-on training because of licensure requirements. This disparity led to the genesis of the international mentorship program.
The deadline for the first round of applications is Dec. 15, 2010. To apply or find out more, visit www.asds.net/InternationalEd/.
Dr. Field said that he has no relevant disclosures.
*CORRECTION 1/10/11: The article originally stated that the program had 29 U.S. dermatologic mentors and the program is active in 18 countries. The statement was corrected to: 70 mentors from 19 countries.
**CORRECTION 1/10/11: The article originally stated that Dr. Field has taught and learned about...fat transfer in Iran. That statement was revised to state: fat transfer in Saudi Arabia.
CHICAGO – Want to learn more about liposuction in Indonesia? Want to teach your cryosurgery technique to dermatologists in Greece? Want to help physicians in the Philippines perform fat transfer?
You can. Dermatologic surgeons in the United States now have more opportunities to travel, teach, and learn surgical techniques from colleagues in other countries, thanks to a unique collaboration that expands the International Mentorship Program and the International Preceptorship Program.
Earlier this year, Dr. Lawrence M. Field, traveling chair of the International Society for Dermatologic Surgery (ISDS) International Mentorship Program, donated $100,000 to the American Society for Dermatologic Surgeons (ASDS) to establish the Lawrence M. Field MD International Dermatologic Surgery Educational Exchange Fund.
"Dr. Field's donation will allow us to have two preceptorships, a fellowship here in the U.S. and [another] for what Dr. Field has been doing sending fellows to other countries," Dr. Jeffrey S. Dover, ASDS president, said at their annual meeting where the collaboration was announced.
Dr. Field is a "dermatologic surgeon, teacher, and benefactor. He has taught mostly hands-on in more than 60 countries," added ISDS president Dr. Gary J. Brauner.
The ISDS has run the mentorship program since 1986. Additional staffing and other resources provided by the ASDS will significantly expand its reach, said Dr. Field, who is in private practice in San Luis Obispo, Calif.
According to Dr. Field, the program has about 70 mentors from 19 nations.* The program continues to expand and is actively seeking host institutions around the world to work with the faculty. The ASDS/ISDS program is for established dermatologic surgeons and not residents.
Special language skills are a plus but not mandatory, Dr. Field said. In addition, there are no ethnic, cultural, religious or any other exclusions, only mutual acceptability is required.
The ASDS/ISDS program pays the airfare. All mentors, including Dr. Field, offer their expertise free of charge. "Pick me up at the airport; take me to a reasonably nice place; provide me with food, clothing, and shelter; licensure; and surgical scrubs," Dr. Field said, describing his requests to a host institution when he travels. In exchange, "I will give you everything I can ... from me to you, for nothing. Then take me back to the airport, I'll go home, and I'll remember these things forever."
A week commitment is the minimum, Dr. Field said. "You gain knowledge, experience, enjoyment, and the respect of your peers."
In his nearly 25 years as a traveling mentor, Dr. Field has taught and learned about scar revision in the Philippines, cryosurgery in Heraklion, Greece, and fat transfer in Saudi Arabia.** As a consultant to the DermaClinic, Dr. Field shared his expertise to transfer fat from a patient's abdomen to treat her facial atrophy.
Dr. Field praised the accomplishments of the many dermatologic surgeons who participated as ISDS international mentors. For example, Dr. John Strasswimmer, a dermatologic surgeon in Delray Beach, Fla. has treated albino patients in Africa. "Many great things will happen from that," Dr. Field said.
Another mentor, Dr. Rhoda Narins, worked with Dr. Indah Julianto to get permission from the Minister of Health in Indonesia to perform liposuction. "This program is just forming in Jakarta, Indonesia, so some of you might go there," Dr. Field said.
Dr. Field spent 31 years as a preceptor in his private office for dermatologic surgery fellows at University of California, San Francisco. During this time, he also
hosted international surgeons who, unlike the U.S. physicians, could not participate in hands-on training because of licensure requirements. This disparity led to the genesis of the international mentorship program.
The deadline for the first round of applications is Dec. 15, 2010. To apply or find out more, visit www.asds.net/InternationalEd/.
Dr. Field said that he has no relevant disclosures.
*CORRECTION 1/10/11: The article originally stated that the program had 29 U.S. dermatologic mentors and the program is active in 18 countries. The statement was corrected to: 70 mentors from 19 countries.
**CORRECTION 1/10/11: The article originally stated that Dr. Field has taught and learned about...fat transfer in Iran. That statement was revised to state: fat transfer in Saudi Arabia.
CHICAGO – Want to learn more about liposuction in Indonesia? Want to teach your cryosurgery technique to dermatologists in Greece? Want to help physicians in the Philippines perform fat transfer?
You can. Dermatologic surgeons in the United States now have more opportunities to travel, teach, and learn surgical techniques from colleagues in other countries, thanks to a unique collaboration that expands the International Mentorship Program and the International Preceptorship Program.
Earlier this year, Dr. Lawrence M. Field, traveling chair of the International Society for Dermatologic Surgery (ISDS) International Mentorship Program, donated $100,000 to the American Society for Dermatologic Surgeons (ASDS) to establish the Lawrence M. Field MD International Dermatologic Surgery Educational Exchange Fund.
"Dr. Field's donation will allow us to have two preceptorships, a fellowship here in the U.S. and [another] for what Dr. Field has been doing sending fellows to other countries," Dr. Jeffrey S. Dover, ASDS president, said at their annual meeting where the collaboration was announced.
Dr. Field is a "dermatologic surgeon, teacher, and benefactor. He has taught mostly hands-on in more than 60 countries," added ISDS president Dr. Gary J. Brauner.
The ISDS has run the mentorship program since 1986. Additional staffing and other resources provided by the ASDS will significantly expand its reach, said Dr. Field, who is in private practice in San Luis Obispo, Calif.
According to Dr. Field, the program has about 70 mentors from 19 nations.* The program continues to expand and is actively seeking host institutions around the world to work with the faculty. The ASDS/ISDS program is for established dermatologic surgeons and not residents.
Special language skills are a plus but not mandatory, Dr. Field said. In addition, there are no ethnic, cultural, religious or any other exclusions, only mutual acceptability is required.
The ASDS/ISDS program pays the airfare. All mentors, including Dr. Field, offer their expertise free of charge. "Pick me up at the airport; take me to a reasonably nice place; provide me with food, clothing, and shelter; licensure; and surgical scrubs," Dr. Field said, describing his requests to a host institution when he travels. In exchange, "I will give you everything I can ... from me to you, for nothing. Then take me back to the airport, I'll go home, and I'll remember these things forever."
A week commitment is the minimum, Dr. Field said. "You gain knowledge, experience, enjoyment, and the respect of your peers."
In his nearly 25 years as a traveling mentor, Dr. Field has taught and learned about scar revision in the Philippines, cryosurgery in Heraklion, Greece, and fat transfer in Saudi Arabia.** As a consultant to the DermaClinic, Dr. Field shared his expertise to transfer fat from a patient's abdomen to treat her facial atrophy.
Dr. Field praised the accomplishments of the many dermatologic surgeons who participated as ISDS international mentors. For example, Dr. John Strasswimmer, a dermatologic surgeon in Delray Beach, Fla. has treated albino patients in Africa. "Many great things will happen from that," Dr. Field said.
Another mentor, Dr. Rhoda Narins, worked with Dr. Indah Julianto to get permission from the Minister of Health in Indonesia to perform liposuction. "This program is just forming in Jakarta, Indonesia, so some of you might go there," Dr. Field said.
Dr. Field spent 31 years as a preceptor in his private office for dermatologic surgery fellows at University of California, San Francisco. During this time, he also
hosted international surgeons who, unlike the U.S. physicians, could not participate in hands-on training because of licensure requirements. This disparity led to the genesis of the international mentorship program.
The deadline for the first round of applications is Dec. 15, 2010. To apply or find out more, visit www.asds.net/InternationalEd/.
Dr. Field said that he has no relevant disclosures.
*CORRECTION 1/10/11: The article originally stated that the program had 29 U.S. dermatologic mentors and the program is active in 18 countries. The statement was corrected to: 70 mentors from 19 countries.
**CORRECTION 1/10/11: The article originally stated that Dr. Field has taught and learned about...fat transfer in Iran. That statement was revised to state: fat transfer in Saudi Arabia.
FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY FOR DERMATOLOGIC SURGERY
Cryolipolysis: Realistic Expectations Key to Patient Satisfaction
CHICAGO - In contrast to claims made about some noninvasive body-contouring devices, cryolipolysis can and does work, Dr. Elizabeth Tanzi said.
However, careful patient selection and realistic expectations – on both the part of the patient and the physician – are essential to a successful outcome, said Dr. Tanzi, a private practice dermatologist in Washington, D.C.
"Noninvasive removal of fat to contour the body is a reality. However, as we've all been told: If something seems to be too good to be true, it probably is," Dr. Tanzi said. "There are limitations."
Educate patients that cryolipolysis is not a replacement for liposuction to remove large amounts of fat. The technique, instead, is best suited to flatten discreet bulges of fat – around the abdomen, the back, or the "love handles," for example, that are resistant to diet and exercise, Dr. Tanzi said at the annual meeting of the American Society for Dermatologic Surgery, which was held jointly with the American Society of Cosmetic Dermatology and Aesthetic Surgery.
You may need to counter some patient misperceptions about cryolipolysis as well. "This is not 'fat freezing,' no matter how many times you hear that in the media," she said.
This procedure, instead, relies on precise, controlled cooling of fat cells or adipocytes. This strategy exploits the natural vulnerability of adipocytes to prolonged cold exposure, Dr. Tanzi said, and causes the death of these cells without damage to surrounding tissues. The destroyed fat cells are cleared through the body's natural clearance mechanisms. The Food and Drug Administration approved a cryolipolysis device (CoolSculpting, Zeltiq) for marketing in September 2010.
You can tell inquisitive patients that a single cryolipolysis treatment reduced the fat layer an average of 22% for 32 patients in a prospective multicenter study, Dr. Tanzi said. Dr. Jeffrey Dover presented the results at the 2009 American Society for Laser Medicine and Surgery annual meeting.
Counsel patients that cryolipolysis results are not immediate, Dr. Tanzi said. Adipocytes appear intact immediately post treatment, followed by an inflammatory response seen at days 3, 5, and 7. It can take several months for fat cell clearance and full clinical results.
Patients also can expect temporary dulling of sensation in the treated area that typically resolves in 1-2 weeks, Dr. Tanzi said. Erythema can last minutes to hours post treatment but purpura is uncommon. In addition, patients might experience a "dull, deep soreness for several days. It is tolerable, and feels like they have just done a lot of sit-ups."
Patient and physician expectations have to be realistic, Dr. Tanzi said. "I get asked questions by patients over and over again. Does it really work? The answer is yes, but you have to define the terms." Cryolipolysis will improve the body’s contour, but it is not for skin tightening, for example, and it is not a weight loss strategy. "Yes, clothes fit better," she said. "Patients tell me about that, and now it’s part of my conversation in my consultation."
The noninvasive fat removal field – including cryolipolysis and the other body-contouring devices – is still in its infancy, Dr. Tanzi said in a follow-up interview.
Technology changes underway will expand the application of these technologies beyond the abdomen and love handle areas. "Soon we’ll be able to treat other areas, such as arms and thighs, to really get a nice contour improvement there as well," she said.
Dr. Tanzi disclosed that she is on the medical advisory board for Zeltiq.
CHICAGO - In contrast to claims made about some noninvasive body-contouring devices, cryolipolysis can and does work, Dr. Elizabeth Tanzi said.
However, careful patient selection and realistic expectations – on both the part of the patient and the physician – are essential to a successful outcome, said Dr. Tanzi, a private practice dermatologist in Washington, D.C.
"Noninvasive removal of fat to contour the body is a reality. However, as we've all been told: If something seems to be too good to be true, it probably is," Dr. Tanzi said. "There are limitations."
Educate patients that cryolipolysis is not a replacement for liposuction to remove large amounts of fat. The technique, instead, is best suited to flatten discreet bulges of fat – around the abdomen, the back, or the "love handles," for example, that are resistant to diet and exercise, Dr. Tanzi said at the annual meeting of the American Society for Dermatologic Surgery, which was held jointly with the American Society of Cosmetic Dermatology and Aesthetic Surgery.
You may need to counter some patient misperceptions about cryolipolysis as well. "This is not 'fat freezing,' no matter how many times you hear that in the media," she said.
This procedure, instead, relies on precise, controlled cooling of fat cells or adipocytes. This strategy exploits the natural vulnerability of adipocytes to prolonged cold exposure, Dr. Tanzi said, and causes the death of these cells without damage to surrounding tissues. The destroyed fat cells are cleared through the body's natural clearance mechanisms. The Food and Drug Administration approved a cryolipolysis device (CoolSculpting, Zeltiq) for marketing in September 2010.
You can tell inquisitive patients that a single cryolipolysis treatment reduced the fat layer an average of 22% for 32 patients in a prospective multicenter study, Dr. Tanzi said. Dr. Jeffrey Dover presented the results at the 2009 American Society for Laser Medicine and Surgery annual meeting.
Counsel patients that cryolipolysis results are not immediate, Dr. Tanzi said. Adipocytes appear intact immediately post treatment, followed by an inflammatory response seen at days 3, 5, and 7. It can take several months for fat cell clearance and full clinical results.
Patients also can expect temporary dulling of sensation in the treated area that typically resolves in 1-2 weeks, Dr. Tanzi said. Erythema can last minutes to hours post treatment but purpura is uncommon. In addition, patients might experience a "dull, deep soreness for several days. It is tolerable, and feels like they have just done a lot of sit-ups."
Patient and physician expectations have to be realistic, Dr. Tanzi said. "I get asked questions by patients over and over again. Does it really work? The answer is yes, but you have to define the terms." Cryolipolysis will improve the body’s contour, but it is not for skin tightening, for example, and it is not a weight loss strategy. "Yes, clothes fit better," she said. "Patients tell me about that, and now it’s part of my conversation in my consultation."
The noninvasive fat removal field – including cryolipolysis and the other body-contouring devices – is still in its infancy, Dr. Tanzi said in a follow-up interview.
Technology changes underway will expand the application of these technologies beyond the abdomen and love handle areas. "Soon we’ll be able to treat other areas, such as arms and thighs, to really get a nice contour improvement there as well," she said.
Dr. Tanzi disclosed that she is on the medical advisory board for Zeltiq.
CHICAGO - In contrast to claims made about some noninvasive body-contouring devices, cryolipolysis can and does work, Dr. Elizabeth Tanzi said.
However, careful patient selection and realistic expectations – on both the part of the patient and the physician – are essential to a successful outcome, said Dr. Tanzi, a private practice dermatologist in Washington, D.C.
"Noninvasive removal of fat to contour the body is a reality. However, as we've all been told: If something seems to be too good to be true, it probably is," Dr. Tanzi said. "There are limitations."
Educate patients that cryolipolysis is not a replacement for liposuction to remove large amounts of fat. The technique, instead, is best suited to flatten discreet bulges of fat – around the abdomen, the back, or the "love handles," for example, that are resistant to diet and exercise, Dr. Tanzi said at the annual meeting of the American Society for Dermatologic Surgery, which was held jointly with the American Society of Cosmetic Dermatology and Aesthetic Surgery.
You may need to counter some patient misperceptions about cryolipolysis as well. "This is not 'fat freezing,' no matter how many times you hear that in the media," she said.
This procedure, instead, relies on precise, controlled cooling of fat cells or adipocytes. This strategy exploits the natural vulnerability of adipocytes to prolonged cold exposure, Dr. Tanzi said, and causes the death of these cells without damage to surrounding tissues. The destroyed fat cells are cleared through the body's natural clearance mechanisms. The Food and Drug Administration approved a cryolipolysis device (CoolSculpting, Zeltiq) for marketing in September 2010.
You can tell inquisitive patients that a single cryolipolysis treatment reduced the fat layer an average of 22% for 32 patients in a prospective multicenter study, Dr. Tanzi said. Dr. Jeffrey Dover presented the results at the 2009 American Society for Laser Medicine and Surgery annual meeting.
Counsel patients that cryolipolysis results are not immediate, Dr. Tanzi said. Adipocytes appear intact immediately post treatment, followed by an inflammatory response seen at days 3, 5, and 7. It can take several months for fat cell clearance and full clinical results.
Patients also can expect temporary dulling of sensation in the treated area that typically resolves in 1-2 weeks, Dr. Tanzi said. Erythema can last minutes to hours post treatment but purpura is uncommon. In addition, patients might experience a "dull, deep soreness for several days. It is tolerable, and feels like they have just done a lot of sit-ups."
Patient and physician expectations have to be realistic, Dr. Tanzi said. "I get asked questions by patients over and over again. Does it really work? The answer is yes, but you have to define the terms." Cryolipolysis will improve the body’s contour, but it is not for skin tightening, for example, and it is not a weight loss strategy. "Yes, clothes fit better," she said. "Patients tell me about that, and now it’s part of my conversation in my consultation."
The noninvasive fat removal field – including cryolipolysis and the other body-contouring devices – is still in its infancy, Dr. Tanzi said in a follow-up interview.
Technology changes underway will expand the application of these technologies beyond the abdomen and love handle areas. "Soon we’ll be able to treat other areas, such as arms and thighs, to really get a nice contour improvement there as well," she said.
Dr. Tanzi disclosed that she is on the medical advisory board for Zeltiq.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY FOR DERMATOLOGIC SURGERY
FDA: Tesamorelin Approved for Lipodystrophy in HIV
Tesamorelin, a growth hormone releasing factor drug, has been approved by the Food and Drug Administration to treat people with HIV who have lipodystrophy, a side effect of long-term antiretroviral drug therapy.
This is the first treatment approved for this indication, according to an FDA statement announcing the Nov. 10 approval.
Tesamorelin, which is administered in a subcutaneous injection once daily, was approved to "induce and maintain a reduction of excess visceral abdominal fat in HIV-infected patients with lipodystrophy," according to the FDA. Tesamorelin will be marketed as Egrifta by EMD Serono Inc. It was developed by Canadian-based Theratechnologies Inc.
At a meeting in May, the FDA’s Endocrinologic and Metabolic Drugs Advisory Committee unanimously agreed that tesamorelin had a favorable risk-benefit profile that supported approval in this population.
Lipodystrophy is characterized by the accumulation of excess fat in different parts of the body, mostly around the liver, stomach, and other abdominal organs.
Approval was based on two placebo-controlled studies of HIV-positive adults with lipodystrophy, who were on stable antiretroviral therapy. The studies showed that over a 26-week period, 534 patients who were treated with tesamorelin had greater reductions in abdominal fat as measured by CT scans, compared with 261 patients who received placebo injections. Some patients also reported improvements in self-image. "Whether Egrifta decreases the risk of cardiovascular disease or improves compliance with antiretroviral drugs has not been studied," the FDA statement noted.
Arthralgia, injection site reactions, stomach pain, and myalgia were among the most common side effects associated with treatment. Small increases in fasting blood sugar and increases in HbA1c levels were also reported among patients treated with tesamorelin, including cases that met the criteria for a diabetes diagnosis, according to data presented at the meeting.
Tesamorelin activates the growth hormone-releasing hormone receptor in the pituitary, stimulating the production of growth hormone.
Tesamorelin, a growth hormone releasing factor drug, has been approved by the Food and Drug Administration to treat people with HIV who have lipodystrophy, a side effect of long-term antiretroviral drug therapy.
This is the first treatment approved for this indication, according to an FDA statement announcing the Nov. 10 approval.
Tesamorelin, which is administered in a subcutaneous injection once daily, was approved to "induce and maintain a reduction of excess visceral abdominal fat in HIV-infected patients with lipodystrophy," according to the FDA. Tesamorelin will be marketed as Egrifta by EMD Serono Inc. It was developed by Canadian-based Theratechnologies Inc.
At a meeting in May, the FDA’s Endocrinologic and Metabolic Drugs Advisory Committee unanimously agreed that tesamorelin had a favorable risk-benefit profile that supported approval in this population.
Lipodystrophy is characterized by the accumulation of excess fat in different parts of the body, mostly around the liver, stomach, and other abdominal organs.
Approval was based on two placebo-controlled studies of HIV-positive adults with lipodystrophy, who were on stable antiretroviral therapy. The studies showed that over a 26-week period, 534 patients who were treated with tesamorelin had greater reductions in abdominal fat as measured by CT scans, compared with 261 patients who received placebo injections. Some patients also reported improvements in self-image. "Whether Egrifta decreases the risk of cardiovascular disease or improves compliance with antiretroviral drugs has not been studied," the FDA statement noted.
Arthralgia, injection site reactions, stomach pain, and myalgia were among the most common side effects associated with treatment. Small increases in fasting blood sugar and increases in HbA1c levels were also reported among patients treated with tesamorelin, including cases that met the criteria for a diabetes diagnosis, according to data presented at the meeting.
Tesamorelin activates the growth hormone-releasing hormone receptor in the pituitary, stimulating the production of growth hormone.
Tesamorelin, a growth hormone releasing factor drug, has been approved by the Food and Drug Administration to treat people with HIV who have lipodystrophy, a side effect of long-term antiretroviral drug therapy.
This is the first treatment approved for this indication, according to an FDA statement announcing the Nov. 10 approval.
Tesamorelin, which is administered in a subcutaneous injection once daily, was approved to "induce and maintain a reduction of excess visceral abdominal fat in HIV-infected patients with lipodystrophy," according to the FDA. Tesamorelin will be marketed as Egrifta by EMD Serono Inc. It was developed by Canadian-based Theratechnologies Inc.
At a meeting in May, the FDA’s Endocrinologic and Metabolic Drugs Advisory Committee unanimously agreed that tesamorelin had a favorable risk-benefit profile that supported approval in this population.
Lipodystrophy is characterized by the accumulation of excess fat in different parts of the body, mostly around the liver, stomach, and other abdominal organs.
Approval was based on two placebo-controlled studies of HIV-positive adults with lipodystrophy, who were on stable antiretroviral therapy. The studies showed that over a 26-week period, 534 patients who were treated with tesamorelin had greater reductions in abdominal fat as measured by CT scans, compared with 261 patients who received placebo injections. Some patients also reported improvements in self-image. "Whether Egrifta decreases the risk of cardiovascular disease or improves compliance with antiretroviral drugs has not been studied," the FDA statement noted.
Arthralgia, injection site reactions, stomach pain, and myalgia were among the most common side effects associated with treatment. Small increases in fasting blood sugar and increases in HbA1c levels were also reported among patients treated with tesamorelin, including cases that met the criteria for a diabetes diagnosis, according to data presented at the meeting.
Tesamorelin activates the growth hormone-releasing hormone receptor in the pituitary, stimulating the production of growth hormone.
FROM THE FDA
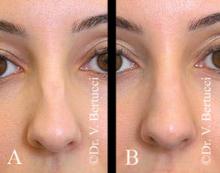
Nonsurgical Rhinoplasty Made Possible With Injectables
CHICAGO - Some patients are ideal candidates for nonsurgical rhinoplasty to reshape the nose, according to experts.
Patients unready or unwilling to undergo surgery, for example, could opt for more temporary aesthetic changes through injectable products, two presenters noted at the annual meeting of the American Society for Dermatologic Surgery.
Unlike more familiar facial cosmetic procedures, patients might need to be educated that injectables in the nose are a valid option, said Dr. Jean-François Tremblay, chief of the dermatologic surgery unit at the University of Montreal’s hospital center. Some will also need guidance as to what constitutes an ideal nose.
"We are not going to replace rhinoplasty, but there is a lot we can do with fillers in an in-and-out procedure," said Dr. Vince Bertucci, Immediate Past President of the Canadian Society for Dermatologic Surgery and the Medical Director of Bertucci MedSpa in Woodbridge, just outside Toronto.
Fillers can increase nasal tip projection and give the nose a longer, more refined appearance. Botulinum toxin can reduce dynamic changes that occur for some during facial expression, such as tip movement, "bunny lines," or alar flare. "Some patients with bunny lines really pull up their ali when they smile, but post botulinum toxin injection, they do not raise up as high," Dr. Bertucci said.
In some cases, fillers and botulinum toxin can be used in combination. Nasal tip droop is a common concern, Dr. Bertucci said. Botulinum toxin injected into the depressor septi nasi at the base of the columella can reverse this common effect of aging. He cautioned, however, the upper lip can be widened or elongated with this technique, and the upper lip tends to be already elongated in some elderly patients.
Dr. Bertucci emphasized the importance of knowing the nasal anatomy and danger zones. For example, inject botulinum toxin approximately half way between the nasal-facial junction and dorsum of the nose to avoid hitting the muscle that lifts the mouth. If the levator labii superioris alaeque nasi is inadvertently treated, the patient may end up with an unusual or asymmetric smile. "The message here is do not inject too far down the side of the nose."
The best candidates for nonsurgical rhinoplasty have minor deformities, not major deviations or bony anomalies, Dr. Tremblay said. Lower cost, little to no downtime, and the reversible or modifiable nature of the filler correction are among the appeals, he said. A temporary duration of effect can be a disadvantage. In addition, "we can only add volume and not remove anything," said Dr. Tremblay during the joint presentation.
An important caveat is patients who seek correction with injectables after a rhinoplasty require additional caution and expertise. "I would not recommend starting out on post-rhinoplasty patients," Dr. Bertucci said. Vascular changes and modification of bone and tissue from surgery can increase the risk of necrosis.
Regardless of history, begin by asking all patients what bothers them, Dr. Tremblay advised. "I want to understand their expectations, what their notion of an ideal nose is, and do a quick psychoanalysis 101." He added, "The rate of people having body dysmorphic disorder is higher when people complain about their noses versus other concerns. So it could be a sign someone does not have balanced psychological health."
Ensure you view the nose from all angles (frontal, lateral, and basal) and consider any aesthetic changes in the context of the entire face. "The basal view can show underlying anomalies that might explain superficial features we are trying to correct," Dr. Tremblay said.
An ideal nose "cannot be defined for any given individual without taking into consideration the rest of the facial features," Dr. Tremblay said. For example, he increased the chin projection of a woman who initially wanted the size of her nose reduced. She was happy with her nose after the chin augmentation.
Skin thickness varies in different parts of the nose. In general, the mid-nose skin tends to be thinner and more delicate than the proximal and distal areas. "So when you inject the mid-nose, keep in mind the need to [massage] material around so you don’t get a prominence," Dr. Bertucci said. Also avoid superficial placement and overcorrection with fillers (consider a staged correction). He added, "Injecting slowly is really important. It seems like a simple thing, but look at the skin as you inject is it blanching?"
A tip with filler enhancement on the dorsum of the nose is to pinch the skin and pull it gently up before injecting. Dr. Bertucci said, "I am still underneath the level of the skin, and I am off the vessels that may be lying on the bone or muscle."
"I also find that useful and that is what I do," Dr. Tremblay said. I try to generate with pinching the correction I am trying to achieve, and inject until I reach the volume I want."
A long-lasting but nonpermanent filler product is more ideal than a permanent one in the nose, Dr. Bertucci said. "This leaves you a way out, and the anatomy changes with age." Hyaluronic acid or calcium hydroxylapatite products are examples. In contrast, use of silicone can be riskier in terms of overcorrection and granulomatous effects.
A meeting attendee countered that he prefers silicone because hyaluronic acid corrections only last 2-3 months in his patients. Dr. Bertucci replied that, because of its permanent nature, "I would not use silicone unless you are very skilled in its use."
Injection-related pain, redness, bleeding, ecchymosis, and hematoma are possible complications regardless of the product type injected, Dr. Bertucci said.
Dr. Bertucci disclosed that he is a consultant for Allergan, Medicis Pharmaceutical Corp., and Merz Pharmaceutical, and an investigator for Allergen and Merz. Dr. Tromblay disclosed that he is a medical consultant for Allergan, Medicis, Canderm Pharma Inc., La Roche-Posay, Procter & Gamble, and Johnson & Johnson.
CHICAGO - Some patients are ideal candidates for nonsurgical rhinoplasty to reshape the nose, according to experts.
Patients unready or unwilling to undergo surgery, for example, could opt for more temporary aesthetic changes through injectable products, two presenters noted at the annual meeting of the American Society for Dermatologic Surgery.
Unlike more familiar facial cosmetic procedures, patients might need to be educated that injectables in the nose are a valid option, said Dr. Jean-François Tremblay, chief of the dermatologic surgery unit at the University of Montreal’s hospital center. Some will also need guidance as to what constitutes an ideal nose.
"We are not going to replace rhinoplasty, but there is a lot we can do with fillers in an in-and-out procedure," said Dr. Vince Bertucci, Immediate Past President of the Canadian Society for Dermatologic Surgery and the Medical Director of Bertucci MedSpa in Woodbridge, just outside Toronto.
Fillers can increase nasal tip projection and give the nose a longer, more refined appearance. Botulinum toxin can reduce dynamic changes that occur for some during facial expression, such as tip movement, "bunny lines," or alar flare. "Some patients with bunny lines really pull up their ali when they smile, but post botulinum toxin injection, they do not raise up as high," Dr. Bertucci said.
In some cases, fillers and botulinum toxin can be used in combination. Nasal tip droop is a common concern, Dr. Bertucci said. Botulinum toxin injected into the depressor septi nasi at the base of the columella can reverse this common effect of aging. He cautioned, however, the upper lip can be widened or elongated with this technique, and the upper lip tends to be already elongated in some elderly patients.
Dr. Bertucci emphasized the importance of knowing the nasal anatomy and danger zones. For example, inject botulinum toxin approximately half way between the nasal-facial junction and dorsum of the nose to avoid hitting the muscle that lifts the mouth. If the levator labii superioris alaeque nasi is inadvertently treated, the patient may end up with an unusual or asymmetric smile. "The message here is do not inject too far down the side of the nose."
The best candidates for nonsurgical rhinoplasty have minor deformities, not major deviations or bony anomalies, Dr. Tremblay said. Lower cost, little to no downtime, and the reversible or modifiable nature of the filler correction are among the appeals, he said. A temporary duration of effect can be a disadvantage. In addition, "we can only add volume and not remove anything," said Dr. Tremblay during the joint presentation.
An important caveat is patients who seek correction with injectables after a rhinoplasty require additional caution and expertise. "I would not recommend starting out on post-rhinoplasty patients," Dr. Bertucci said. Vascular changes and modification of bone and tissue from surgery can increase the risk of necrosis.
Regardless of history, begin by asking all patients what bothers them, Dr. Tremblay advised. "I want to understand their expectations, what their notion of an ideal nose is, and do a quick psychoanalysis 101." He added, "The rate of people having body dysmorphic disorder is higher when people complain about their noses versus other concerns. So it could be a sign someone does not have balanced psychological health."
Ensure you view the nose from all angles (frontal, lateral, and basal) and consider any aesthetic changes in the context of the entire face. "The basal view can show underlying anomalies that might explain superficial features we are trying to correct," Dr. Tremblay said.
An ideal nose "cannot be defined for any given individual without taking into consideration the rest of the facial features," Dr. Tremblay said. For example, he increased the chin projection of a woman who initially wanted the size of her nose reduced. She was happy with her nose after the chin augmentation.
Skin thickness varies in different parts of the nose. In general, the mid-nose skin tends to be thinner and more delicate than the proximal and distal areas. "So when you inject the mid-nose, keep in mind the need to [massage] material around so you don’t get a prominence," Dr. Bertucci said. Also avoid superficial placement and overcorrection with fillers (consider a staged correction). He added, "Injecting slowly is really important. It seems like a simple thing, but look at the skin as you inject is it blanching?"
A tip with filler enhancement on the dorsum of the nose is to pinch the skin and pull it gently up before injecting. Dr. Bertucci said, "I am still underneath the level of the skin, and I am off the vessels that may be lying on the bone or muscle."
"I also find that useful and that is what I do," Dr. Tremblay said. I try to generate with pinching the correction I am trying to achieve, and inject until I reach the volume I want."
A long-lasting but nonpermanent filler product is more ideal than a permanent one in the nose, Dr. Bertucci said. "This leaves you a way out, and the anatomy changes with age." Hyaluronic acid or calcium hydroxylapatite products are examples. In contrast, use of silicone can be riskier in terms of overcorrection and granulomatous effects.
A meeting attendee countered that he prefers silicone because hyaluronic acid corrections only last 2-3 months in his patients. Dr. Bertucci replied that, because of its permanent nature, "I would not use silicone unless you are very skilled in its use."
Injection-related pain, redness, bleeding, ecchymosis, and hematoma are possible complications regardless of the product type injected, Dr. Bertucci said.
Dr. Bertucci disclosed that he is a consultant for Allergan, Medicis Pharmaceutical Corp., and Merz Pharmaceutical, and an investigator for Allergen and Merz. Dr. Tromblay disclosed that he is a medical consultant for Allergan, Medicis, Canderm Pharma Inc., La Roche-Posay, Procter & Gamble, and Johnson & Johnson.
CHICAGO - Some patients are ideal candidates for nonsurgical rhinoplasty to reshape the nose, according to experts.
Patients unready or unwilling to undergo surgery, for example, could opt for more temporary aesthetic changes through injectable products, two presenters noted at the annual meeting of the American Society for Dermatologic Surgery.
Unlike more familiar facial cosmetic procedures, patients might need to be educated that injectables in the nose are a valid option, said Dr. Jean-François Tremblay, chief of the dermatologic surgery unit at the University of Montreal’s hospital center. Some will also need guidance as to what constitutes an ideal nose.
"We are not going to replace rhinoplasty, but there is a lot we can do with fillers in an in-and-out procedure," said Dr. Vince Bertucci, Immediate Past President of the Canadian Society for Dermatologic Surgery and the Medical Director of Bertucci MedSpa in Woodbridge, just outside Toronto.
Fillers can increase nasal tip projection and give the nose a longer, more refined appearance. Botulinum toxin can reduce dynamic changes that occur for some during facial expression, such as tip movement, "bunny lines," or alar flare. "Some patients with bunny lines really pull up their ali when they smile, but post botulinum toxin injection, they do not raise up as high," Dr. Bertucci said.
In some cases, fillers and botulinum toxin can be used in combination. Nasal tip droop is a common concern, Dr. Bertucci said. Botulinum toxin injected into the depressor septi nasi at the base of the columella can reverse this common effect of aging. He cautioned, however, the upper lip can be widened or elongated with this technique, and the upper lip tends to be already elongated in some elderly patients.
Dr. Bertucci emphasized the importance of knowing the nasal anatomy and danger zones. For example, inject botulinum toxin approximately half way between the nasal-facial junction and dorsum of the nose to avoid hitting the muscle that lifts the mouth. If the levator labii superioris alaeque nasi is inadvertently treated, the patient may end up with an unusual or asymmetric smile. "The message here is do not inject too far down the side of the nose."
The best candidates for nonsurgical rhinoplasty have minor deformities, not major deviations or bony anomalies, Dr. Tremblay said. Lower cost, little to no downtime, and the reversible or modifiable nature of the filler correction are among the appeals, he said. A temporary duration of effect can be a disadvantage. In addition, "we can only add volume and not remove anything," said Dr. Tremblay during the joint presentation.
An important caveat is patients who seek correction with injectables after a rhinoplasty require additional caution and expertise. "I would not recommend starting out on post-rhinoplasty patients," Dr. Bertucci said. Vascular changes and modification of bone and tissue from surgery can increase the risk of necrosis.
Regardless of history, begin by asking all patients what bothers them, Dr. Tremblay advised. "I want to understand their expectations, what their notion of an ideal nose is, and do a quick psychoanalysis 101." He added, "The rate of people having body dysmorphic disorder is higher when people complain about their noses versus other concerns. So it could be a sign someone does not have balanced psychological health."
Ensure you view the nose from all angles (frontal, lateral, and basal) and consider any aesthetic changes in the context of the entire face. "The basal view can show underlying anomalies that might explain superficial features we are trying to correct," Dr. Tremblay said.
An ideal nose "cannot be defined for any given individual without taking into consideration the rest of the facial features," Dr. Tremblay said. For example, he increased the chin projection of a woman who initially wanted the size of her nose reduced. She was happy with her nose after the chin augmentation.
Skin thickness varies in different parts of the nose. In general, the mid-nose skin tends to be thinner and more delicate than the proximal and distal areas. "So when you inject the mid-nose, keep in mind the need to [massage] material around so you don’t get a prominence," Dr. Bertucci said. Also avoid superficial placement and overcorrection with fillers (consider a staged correction). He added, "Injecting slowly is really important. It seems like a simple thing, but look at the skin as you inject is it blanching?"
A tip with filler enhancement on the dorsum of the nose is to pinch the skin and pull it gently up before injecting. Dr. Bertucci said, "I am still underneath the level of the skin, and I am off the vessels that may be lying on the bone or muscle."
"I also find that useful and that is what I do," Dr. Tremblay said. I try to generate with pinching the correction I am trying to achieve, and inject until I reach the volume I want."
A long-lasting but nonpermanent filler product is more ideal than a permanent one in the nose, Dr. Bertucci said. "This leaves you a way out, and the anatomy changes with age." Hyaluronic acid or calcium hydroxylapatite products are examples. In contrast, use of silicone can be riskier in terms of overcorrection and granulomatous effects.
A meeting attendee countered that he prefers silicone because hyaluronic acid corrections only last 2-3 months in his patients. Dr. Bertucci replied that, because of its permanent nature, "I would not use silicone unless you are very skilled in its use."
Injection-related pain, redness, bleeding, ecchymosis, and hematoma are possible complications regardless of the product type injected, Dr. Bertucci said.
Dr. Bertucci disclosed that he is a consultant for Allergan, Medicis Pharmaceutical Corp., and Merz Pharmaceutical, and an investigator for Allergen and Merz. Dr. Tromblay disclosed that he is a medical consultant for Allergan, Medicis, Canderm Pharma Inc., La Roche-Posay, Procter & Gamble, and Johnson & Johnson.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE AMERICAN SOCIETY FOR DERMATOLOGIC SURGERY
Make Effort to Create Calm Environment During Pediatric Surgery
Many factors contribute to a child's perception of pain, including their age, past experiences, and cognitive development, according to Dr. Brandie J. Metz.
Dr. Metz shared tips and techniques to improve the pediatric dermatologic surgery experience for the doctor, patient, and parent at the Las Vegas Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Create a calm environment. When talking with a pediatric patient, get down on their level – sit at or below the child's height, and talk directly to him or her. Explain the procedure in a nonthreatening way, but do not leave anything out, and be honest about what is going to happen, noted Dr. Metz, the director of pediatric dermatology at the University of California, Irvine. "There should be no surprises."
Allow the child to have some control over the situation by allowing him or her to choose a radio station to play in the background or a DVD to watch if possible. Engage children in conversation, and let them choose the color for a surgical dressing, said Dr. Metz.
During the procedure, position the parent at the head of the table and strategically drape the surgical field so the parent and child cannot see the actual procedure. Take extra time to cover surgical trays or blood-soaked gauze that could increase the anxiety of the parent or child, she said.
When performing injections, slow infiltration is best; also, consider using a topical anesthetic and 30-gauge needles, she recommended. Dr. Metz prefers buffered, warmed lidocaine, with 1 cc 8.4% sodium bicarbonate/10 cc of 1% lidocaine.
The issue of anesthesia is an important one for pediatric surgery patients. There are no set rules or guidelines about the age at which surgical procedures can be performed with local vs. general anesthesia, Dr. Metz said. She recommended local anesthesia as an option for girls aged 8-9 years and older, and boys aged 9-10 years and older, but it ultimately depends on the maturity of the child. "Consider general anesthesia for larger procedures and in younger children," she said.
Remember that some elective dermatologic surgeries can be postponed until the preadolescent or adolescent years, she noted. Few data exist on the risks of general anesthesia for young children, but the risk appears highest during the first month of life, and complications are more common in emergency procedures, compared with elective procedures, she said. According to the American Society of Anesthesiologists, the risk of a complication from anesthesia in a healthy child ranges from 1:20,000 to 1:80,000 or less.
When performing excisions in children, 2-octyl cyanoacrylate (Dermabond) is an option, Dr. Metz reported. Several studies have shown the advantage of this skin glue over sutures or staples. However, studies of Dermabond have not controlled for confounding factors including excision location, patient ethnicity, and previous keloids.
Advantages of 2-octyl cyanoacrylate include speed of use, avoidance of a follow-up visit to remove sutures, and ability to withstand getting wet. Also, the antibacterial properties of the product might reduce the risk of post-surgery infections, Dr. Metz noted.
Disadvantages of 2-octyl cyanoacrylate include cost ($30/vial), the inability to place the product in the wound, and the lack of strength for use in high-tension areas, she reported.
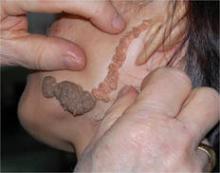
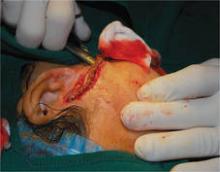
Dr. Metz also shared tips for the staged excision of congenital nevi in children, which is an option when tissue expansion is not advisable and primary closure is not possible. Her recommendations for a successful excision include:
- Take as much of the lesion as possible during the first stage.
- Don't wait too long between stages. The timing should be about 6 to 8 weeks; long enough for the tension on the skin to relax, but not long enough for the scar to spread.
- Consider absorbable sutures to avoid the need for a suture removal visit.
Dr. Metz disclosed having no conflicts of interest. SDEF and this news organization are owned by Elsevier.
Many factors contribute to a child's perception of pain, including their age, past experiences, and cognitive development, according to Dr. Brandie J. Metz.
Dr. Metz shared tips and techniques to improve the pediatric dermatologic surgery experience for the doctor, patient, and parent at the Las Vegas Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Create a calm environment. When talking with a pediatric patient, get down on their level – sit at or below the child's height, and talk directly to him or her. Explain the procedure in a nonthreatening way, but do not leave anything out, and be honest about what is going to happen, noted Dr. Metz, the director of pediatric dermatology at the University of California, Irvine. "There should be no surprises."
Allow the child to have some control over the situation by allowing him or her to choose a radio station to play in the background or a DVD to watch if possible. Engage children in conversation, and let them choose the color for a surgical dressing, said Dr. Metz.
During the procedure, position the parent at the head of the table and strategically drape the surgical field so the parent and child cannot see the actual procedure. Take extra time to cover surgical trays or blood-soaked gauze that could increase the anxiety of the parent or child, she said.
When performing injections, slow infiltration is best; also, consider using a topical anesthetic and 30-gauge needles, she recommended. Dr. Metz prefers buffered, warmed lidocaine, with 1 cc 8.4% sodium bicarbonate/10 cc of 1% lidocaine.
The issue of anesthesia is an important one for pediatric surgery patients. There are no set rules or guidelines about the age at which surgical procedures can be performed with local vs. general anesthesia, Dr. Metz said. She recommended local anesthesia as an option for girls aged 8-9 years and older, and boys aged 9-10 years and older, but it ultimately depends on the maturity of the child. "Consider general anesthesia for larger procedures and in younger children," she said.
Remember that some elective dermatologic surgeries can be postponed until the preadolescent or adolescent years, she noted. Few data exist on the risks of general anesthesia for young children, but the risk appears highest during the first month of life, and complications are more common in emergency procedures, compared with elective procedures, she said. According to the American Society of Anesthesiologists, the risk of a complication from anesthesia in a healthy child ranges from 1:20,000 to 1:80,000 or less.
When performing excisions in children, 2-octyl cyanoacrylate (Dermabond) is an option, Dr. Metz reported. Several studies have shown the advantage of this skin glue over sutures or staples. However, studies of Dermabond have not controlled for confounding factors including excision location, patient ethnicity, and previous keloids.
Advantages of 2-octyl cyanoacrylate include speed of use, avoidance of a follow-up visit to remove sutures, and ability to withstand getting wet. Also, the antibacterial properties of the product might reduce the risk of post-surgery infections, Dr. Metz noted.
Disadvantages of 2-octyl cyanoacrylate include cost ($30/vial), the inability to place the product in the wound, and the lack of strength for use in high-tension areas, she reported.
Dr. Metz also shared tips for the staged excision of congenital nevi in children, which is an option when tissue expansion is not advisable and primary closure is not possible. Her recommendations for a successful excision include:
- Take as much of the lesion as possible during the first stage.
- Don't wait too long between stages. The timing should be about 6 to 8 weeks; long enough for the tension on the skin to relax, but not long enough for the scar to spread.
- Consider absorbable sutures to avoid the need for a suture removal visit.
Dr. Metz disclosed having no conflicts of interest. SDEF and this news organization are owned by Elsevier.
Many factors contribute to a child's perception of pain, including their age, past experiences, and cognitive development, according to Dr. Brandie J. Metz.
Dr. Metz shared tips and techniques to improve the pediatric dermatologic surgery experience for the doctor, patient, and parent at the Las Vegas Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Create a calm environment. When talking with a pediatric patient, get down on their level – sit at or below the child's height, and talk directly to him or her. Explain the procedure in a nonthreatening way, but do not leave anything out, and be honest about what is going to happen, noted Dr. Metz, the director of pediatric dermatology at the University of California, Irvine. "There should be no surprises."
Allow the child to have some control over the situation by allowing him or her to choose a radio station to play in the background or a DVD to watch if possible. Engage children in conversation, and let them choose the color for a surgical dressing, said Dr. Metz.
During the procedure, position the parent at the head of the table and strategically drape the surgical field so the parent and child cannot see the actual procedure. Take extra time to cover surgical trays or blood-soaked gauze that could increase the anxiety of the parent or child, she said.
When performing injections, slow infiltration is best; also, consider using a topical anesthetic and 30-gauge needles, she recommended. Dr. Metz prefers buffered, warmed lidocaine, with 1 cc 8.4% sodium bicarbonate/10 cc of 1% lidocaine.
The issue of anesthesia is an important one for pediatric surgery patients. There are no set rules or guidelines about the age at which surgical procedures can be performed with local vs. general anesthesia, Dr. Metz said. She recommended local anesthesia as an option for girls aged 8-9 years and older, and boys aged 9-10 years and older, but it ultimately depends on the maturity of the child. "Consider general anesthesia for larger procedures and in younger children," she said.
Remember that some elective dermatologic surgeries can be postponed until the preadolescent or adolescent years, she noted. Few data exist on the risks of general anesthesia for young children, but the risk appears highest during the first month of life, and complications are more common in emergency procedures, compared with elective procedures, she said. According to the American Society of Anesthesiologists, the risk of a complication from anesthesia in a healthy child ranges from 1:20,000 to 1:80,000 or less.
When performing excisions in children, 2-octyl cyanoacrylate (Dermabond) is an option, Dr. Metz reported. Several studies have shown the advantage of this skin glue over sutures or staples. However, studies of Dermabond have not controlled for confounding factors including excision location, patient ethnicity, and previous keloids.
Advantages of 2-octyl cyanoacrylate include speed of use, avoidance of a follow-up visit to remove sutures, and ability to withstand getting wet. Also, the antibacterial properties of the product might reduce the risk of post-surgery infections, Dr. Metz noted.
Disadvantages of 2-octyl cyanoacrylate include cost ($30/vial), the inability to place the product in the wound, and the lack of strength for use in high-tension areas, she reported.
Dr. Metz also shared tips for the staged excision of congenital nevi in children, which is an option when tissue expansion is not advisable and primary closure is not possible. Her recommendations for a successful excision include:
- Take as much of the lesion as possible during the first stage.
- Don't wait too long between stages. The timing should be about 6 to 8 weeks; long enough for the tension on the skin to relax, but not long enough for the scar to spread.
- Consider absorbable sutures to avoid the need for a suture removal visit.
Dr. Metz disclosed having no conflicts of interest. SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM THE SDEF LAS VEGAS DERMATOLOGY SEMINAR