User login
Cosmetics Safety
Ablative Lasers Effective, but Painful for Treating Acne Scars
Ablative fractional laser resurfacing is more effective than nonablative therapy for the treatment of acne scaring, albeit, with greater side effects and pain, according to a new review.
Ms. Michal Wen Sheue Ong and Dr. Saquib Bashir, of King’s College Hospital NHS Foundation Trust in London, conducted literature searches using the PubMed and Scopus databases for English-language articles published between 2003 and January 2011 that reported on "acne scars" and "fractional photothermolysis."
A total of 26 papers, published between 2008 and 2011, met the criteria – 13 papers on ablative fractional lasers and an equal number on nonablative fractional lasers (Br. J. Dermatol. 2012 Feb. 1 [doi: 10.1111/j.1365-2133.2012.10870.x]).
"Most ablative studies reported a percentage of improvement within the range of 26% to 75%," they wrote. In two cases, studies claimed 79.8% and 83% mean improvement, although the reviewers questioned the appropriateness of using mean values rather than medians, given that "the properties of the ordinal scales were unknown and points on the scale were not necessarily equidistant."
The nonablative studies reported an improvement range of 26% to 50%.
Only four studies were split-face randomized controlled trials, and most had follow-up criteria of just 1 to 6 months; only one study included a 2-year follow-up. Moreover, the methods and rating scales for measuring improvement varied widely.
Only five studies analyzed the histological degree of scar improvement, but in these, new collagen formation was noted with both ablative and nonablative fractional photothermolysis.
In one of the nonablative studies included in the review, an increase in elastic fibers framework in the papillary dermis, as well as the upper and mid dermis, was noted 12 weeks after final treatment (Photodermatol. Photoimmunol. Photomed. 2009;25:138-42).
Similarly, using 3D optical profiling, a study of ablative laser resurfacing showed a marked, statistically significant improvement in skin smoothness and scar volume 1 month after treatment. "However, there were no further improvements of skin smoothness or scar volume at 3- and 6-months follow-up," wrote the authors (J. Am. Acad. Dermatol. 2010;63:274-83).
Looking at side effects, "A higher proportion of patients (up to 92.3%) who undertake ablative FP [fractional photothermolysis] experience post inflammatory hyperpigmentation (PIH) than those who have nonablative FP (up to 13%)," wrote the reviewers, with a maximum duration of PIH of up to 6 months in ablative FP, vs. 1 week in nonablative treatment.
Pain ratings for nonablative procedures were also lower, compared with ablative procedures. "The mean pain score reported across ablative FP studies ranged from 5.9-8.1 (scale of 10)," reported the authors. In contrast, the mean pain scores for nonablative FP procedures were rated 3.9-5.7.
The authors pointed out that they found no evidence regarding the effects of FP lasers on patients’ psychological status and quality of life. "This information can be useful and should be obtained before and after treatment," they wrote.
Limitations of the review included the fact that none of the methods of assessing clinical outcome had had its validity or reliability investigated, wrote the reviewers. For the most part, however, the results were promising.
"Most studies had clinicians/dermatologists to assess overall scar improvement, and there were some studies which had patient assessment," they wrote. In many cases the evaluators were blinded, but at least three studies used evaluators who were not.
Fractional photothermolysis laser resurfacing improves facial acne scarring, despite dramatic methodological variability in efficacy studies. Nevertheless, more studies are needed, especially split-face, randomized controlled trials using objective assessment measures of improvement, like histological or 3D optical profiling, they concluded.
The review authors reported having no outside funding and stated that they had no conflicts of interest to declare.
Ablative fractional laser resurfacing is more effective than nonablative therapy for the treatment of acne scaring, albeit, with greater side effects and pain, according to a new review.
Ms. Michal Wen Sheue Ong and Dr. Saquib Bashir, of King’s College Hospital NHS Foundation Trust in London, conducted literature searches using the PubMed and Scopus databases for English-language articles published between 2003 and January 2011 that reported on "acne scars" and "fractional photothermolysis."
A total of 26 papers, published between 2008 and 2011, met the criteria – 13 papers on ablative fractional lasers and an equal number on nonablative fractional lasers (Br. J. Dermatol. 2012 Feb. 1 [doi: 10.1111/j.1365-2133.2012.10870.x]).
"Most ablative studies reported a percentage of improvement within the range of 26% to 75%," they wrote. In two cases, studies claimed 79.8% and 83% mean improvement, although the reviewers questioned the appropriateness of using mean values rather than medians, given that "the properties of the ordinal scales were unknown and points on the scale were not necessarily equidistant."
The nonablative studies reported an improvement range of 26% to 50%.
Only four studies were split-face randomized controlled trials, and most had follow-up criteria of just 1 to 6 months; only one study included a 2-year follow-up. Moreover, the methods and rating scales for measuring improvement varied widely.
Only five studies analyzed the histological degree of scar improvement, but in these, new collagen formation was noted with both ablative and nonablative fractional photothermolysis.
In one of the nonablative studies included in the review, an increase in elastic fibers framework in the papillary dermis, as well as the upper and mid dermis, was noted 12 weeks after final treatment (Photodermatol. Photoimmunol. Photomed. 2009;25:138-42).
Similarly, using 3D optical profiling, a study of ablative laser resurfacing showed a marked, statistically significant improvement in skin smoothness and scar volume 1 month after treatment. "However, there were no further improvements of skin smoothness or scar volume at 3- and 6-months follow-up," wrote the authors (J. Am. Acad. Dermatol. 2010;63:274-83).
Looking at side effects, "A higher proportion of patients (up to 92.3%) who undertake ablative FP [fractional photothermolysis] experience post inflammatory hyperpigmentation (PIH) than those who have nonablative FP (up to 13%)," wrote the reviewers, with a maximum duration of PIH of up to 6 months in ablative FP, vs. 1 week in nonablative treatment.
Pain ratings for nonablative procedures were also lower, compared with ablative procedures. "The mean pain score reported across ablative FP studies ranged from 5.9-8.1 (scale of 10)," reported the authors. In contrast, the mean pain scores for nonablative FP procedures were rated 3.9-5.7.
The authors pointed out that they found no evidence regarding the effects of FP lasers on patients’ psychological status and quality of life. "This information can be useful and should be obtained before and after treatment," they wrote.
Limitations of the review included the fact that none of the methods of assessing clinical outcome had had its validity or reliability investigated, wrote the reviewers. For the most part, however, the results were promising.
"Most studies had clinicians/dermatologists to assess overall scar improvement, and there were some studies which had patient assessment," they wrote. In many cases the evaluators were blinded, but at least three studies used evaluators who were not.
Fractional photothermolysis laser resurfacing improves facial acne scarring, despite dramatic methodological variability in efficacy studies. Nevertheless, more studies are needed, especially split-face, randomized controlled trials using objective assessment measures of improvement, like histological or 3D optical profiling, they concluded.
The review authors reported having no outside funding and stated that they had no conflicts of interest to declare.
Ablative fractional laser resurfacing is more effective than nonablative therapy for the treatment of acne scaring, albeit, with greater side effects and pain, according to a new review.
Ms. Michal Wen Sheue Ong and Dr. Saquib Bashir, of King’s College Hospital NHS Foundation Trust in London, conducted literature searches using the PubMed and Scopus databases for English-language articles published between 2003 and January 2011 that reported on "acne scars" and "fractional photothermolysis."
A total of 26 papers, published between 2008 and 2011, met the criteria – 13 papers on ablative fractional lasers and an equal number on nonablative fractional lasers (Br. J. Dermatol. 2012 Feb. 1 [doi: 10.1111/j.1365-2133.2012.10870.x]).
"Most ablative studies reported a percentage of improvement within the range of 26% to 75%," they wrote. In two cases, studies claimed 79.8% and 83% mean improvement, although the reviewers questioned the appropriateness of using mean values rather than medians, given that "the properties of the ordinal scales were unknown and points on the scale were not necessarily equidistant."
The nonablative studies reported an improvement range of 26% to 50%.
Only four studies were split-face randomized controlled trials, and most had follow-up criteria of just 1 to 6 months; only one study included a 2-year follow-up. Moreover, the methods and rating scales for measuring improvement varied widely.
Only five studies analyzed the histological degree of scar improvement, but in these, new collagen formation was noted with both ablative and nonablative fractional photothermolysis.
In one of the nonablative studies included in the review, an increase in elastic fibers framework in the papillary dermis, as well as the upper and mid dermis, was noted 12 weeks after final treatment (Photodermatol. Photoimmunol. Photomed. 2009;25:138-42).
Similarly, using 3D optical profiling, a study of ablative laser resurfacing showed a marked, statistically significant improvement in skin smoothness and scar volume 1 month after treatment. "However, there were no further improvements of skin smoothness or scar volume at 3- and 6-months follow-up," wrote the authors (J. Am. Acad. Dermatol. 2010;63:274-83).
Looking at side effects, "A higher proportion of patients (up to 92.3%) who undertake ablative FP [fractional photothermolysis] experience post inflammatory hyperpigmentation (PIH) than those who have nonablative FP (up to 13%)," wrote the reviewers, with a maximum duration of PIH of up to 6 months in ablative FP, vs. 1 week in nonablative treatment.
Pain ratings for nonablative procedures were also lower, compared with ablative procedures. "The mean pain score reported across ablative FP studies ranged from 5.9-8.1 (scale of 10)," reported the authors. In contrast, the mean pain scores for nonablative FP procedures were rated 3.9-5.7.
The authors pointed out that they found no evidence regarding the effects of FP lasers on patients’ psychological status and quality of life. "This information can be useful and should be obtained before and after treatment," they wrote.
Limitations of the review included the fact that none of the methods of assessing clinical outcome had had its validity or reliability investigated, wrote the reviewers. For the most part, however, the results were promising.
"Most studies had clinicians/dermatologists to assess overall scar improvement, and there were some studies which had patient assessment," they wrote. In many cases the evaluators were blinded, but at least three studies used evaluators who were not.
Fractional photothermolysis laser resurfacing improves facial acne scarring, despite dramatic methodological variability in efficacy studies. Nevertheless, more studies are needed, especially split-face, randomized controlled trials using objective assessment measures of improvement, like histological or 3D optical profiling, they concluded.
The review authors reported having no outside funding and stated that they had no conflicts of interest to declare.
FROM THE BRITISH JOURNAL OF DERMATOLOGY
Major Finding: Most ablative studies reported a percentage of improvement within the range of 26% to 75%, compared with a reported range of improvement of 26% to 50% for the nonablative studies.
Data Source: A review of 26 studies on ablative and nonablative fractional photothermolysis for facial acne scars.
Disclosures: The review authors reported having no outside funding and stated that they had no conflicts of interest to declare.
Skin of Color: Microskin Camouflages Imperfections
As a follow-up to our recent blog on using skin camouflage to cover skin disorders, a technology called Microskin is also available to mask skin imperfections.
Microskin, also known as simulated second skin, is a topical skin camouflage that is individually tailored to match a person's skin color and cover conditions such as birthmarks, vitiligo, burns, scars, striae, pigmentary disorders, rosacea, and photodamage.
Unlike traditional make-up, Microskin is an alcohol-based liquid that won't wipe off on clothing. It is waterproof and adheres to the epidermis forming a simulated second skin over the affected area.
One application typically lasts for 1-2 days on the face and several days longer on the body. Small areas are treated with a sponge, whereas larger areas may be airbrushed.
Microskin was developed in Australia, where it was studied at a pediatric burn center to assess the product's impact on burn patients. The U.S. headquarters are located in New York, but consultations are often set up at various cities around the country throughout the year.
Microskin is is not a treatment or medication for skin conditions, but it can be another acceptable option for helping patients achieve cosmetic improvement.
More information may be found at microskincenter.com.
- Naissan Wesley, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
As a follow-up to our recent blog on using skin camouflage to cover skin disorders, a technology called Microskin is also available to mask skin imperfections.
Microskin, also known as simulated second skin, is a topical skin camouflage that is individually tailored to match a person's skin color and cover conditions such as birthmarks, vitiligo, burns, scars, striae, pigmentary disorders, rosacea, and photodamage.
Unlike traditional make-up, Microskin is an alcohol-based liquid that won't wipe off on clothing. It is waterproof and adheres to the epidermis forming a simulated second skin over the affected area.
One application typically lasts for 1-2 days on the face and several days longer on the body. Small areas are treated with a sponge, whereas larger areas may be airbrushed.
Microskin was developed in Australia, where it was studied at a pediatric burn center to assess the product's impact on burn patients. The U.S. headquarters are located in New York, but consultations are often set up at various cities around the country throughout the year.
Microskin is is not a treatment or medication for skin conditions, but it can be another acceptable option for helping patients achieve cosmetic improvement.
More information may be found at microskincenter.com.
- Naissan Wesley, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
As a follow-up to our recent blog on using skin camouflage to cover skin disorders, a technology called Microskin is also available to mask skin imperfections.
Microskin, also known as simulated second skin, is a topical skin camouflage that is individually tailored to match a person's skin color and cover conditions such as birthmarks, vitiligo, burns, scars, striae, pigmentary disorders, rosacea, and photodamage.
Unlike traditional make-up, Microskin is an alcohol-based liquid that won't wipe off on clothing. It is waterproof and adheres to the epidermis forming a simulated second skin over the affected area.
One application typically lasts for 1-2 days on the face and several days longer on the body. Small areas are treated with a sponge, whereas larger areas may be airbrushed.
Microskin was developed in Australia, where it was studied at a pediatric burn center to assess the product's impact on burn patients. The U.S. headquarters are located in New York, but consultations are often set up at various cities around the country throughout the year.
Microskin is is not a treatment or medication for skin conditions, but it can be another acceptable option for helping patients achieve cosmetic improvement.
More information may be found at microskincenter.com.
- Naissan Wesley, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Skin of Color: Hair Practices and Scarring Alopecia
Scarring alopecia is a common and devastating disease in skin of color patients. Although many controversial studies have looked at the effects of styling techniques and chemical treatments on hair loss, no direct relationships have been found.
A recent study published in the Journal of Cosmetic Dermatology found that there was an increased baseline level of the profibrotic cytokine IL-1 alpha and the IL-1 receptor antagonist in the scalp sebum of afro-textured hair. The study also highlighted the increased susceptibility to scarring alopecia in black patients.
Interestingly, the levels of the profibrotic cytokines increased with chemical treatments and decreased with shampooing, which is also a feature unique to black patients.
When evaluating patients with scarring alopecia, I often inquire about shampooing frequency and chemical treatments. The frequency, type of treatment, chemical used, color used, and relaxing techniques are factors I document in order to evaluate hair loss for every patient.
This study sheds light on the increased risk of scarring alopecia in black patients; and it should alert dermatologists to elucidate hair practices in all patients with hair loss.
- Lily Talakoub, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Scarring alopecia is a common and devastating disease in skin of color patients. Although many controversial studies have looked at the effects of styling techniques and chemical treatments on hair loss, no direct relationships have been found.
A recent study published in the Journal of Cosmetic Dermatology found that there was an increased baseline level of the profibrotic cytokine IL-1 alpha and the IL-1 receptor antagonist in the scalp sebum of afro-textured hair. The study also highlighted the increased susceptibility to scarring alopecia in black patients.
Interestingly, the levels of the profibrotic cytokines increased with chemical treatments and decreased with shampooing, which is also a feature unique to black patients.
When evaluating patients with scarring alopecia, I often inquire about shampooing frequency and chemical treatments. The frequency, type of treatment, chemical used, color used, and relaxing techniques are factors I document in order to evaluate hair loss for every patient.
This study sheds light on the increased risk of scarring alopecia in black patients; and it should alert dermatologists to elucidate hair practices in all patients with hair loss.
- Lily Talakoub, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Scarring alopecia is a common and devastating disease in skin of color patients. Although many controversial studies have looked at the effects of styling techniques and chemical treatments on hair loss, no direct relationships have been found.
A recent study published in the Journal of Cosmetic Dermatology found that there was an increased baseline level of the profibrotic cytokine IL-1 alpha and the IL-1 receptor antagonist in the scalp sebum of afro-textured hair. The study also highlighted the increased susceptibility to scarring alopecia in black patients.
Interestingly, the levels of the profibrotic cytokines increased with chemical treatments and decreased with shampooing, which is also a feature unique to black patients.
When evaluating patients with scarring alopecia, I often inquire about shampooing frequency and chemical treatments. The frequency, type of treatment, chemical used, color used, and relaxing techniques are factors I document in order to evaluate hair loss for every patient.
This study sheds light on the increased risk of scarring alopecia in black patients; and it should alert dermatologists to elucidate hair practices in all patients with hair loss.
- Lily Talakoub, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
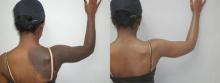
Blog: Ablative Fractional Resurfacing Improves Scar Mobility
When you think of ablative fractional resurfacing, you probably think of photo-damaged skin and acne scars, said Dr. Kenneth A. Arndt, a clinical professor of dermatology, emeritus, at Harvard.
So why would you use something that tightens skin to treat scars? When ablative fractional resurfacing is used on scars, it actually increases pliability, he said.
When you think of ablative fractional resurfacing, you probably think of photo-damaged skin and acne scars, said Dr. Kenneth A. Arndt, a clinical professor of dermatology, emeritus, at Harvard.
So why would you use something that tightens skin to treat scars? When ablative fractional resurfacing is used on scars, it actually increases pliability, he said.
When you think of ablative fractional resurfacing, you probably think of photo-damaged skin and acne scars, said Dr. Kenneth A. Arndt, a clinical professor of dermatology, emeritus, at Harvard.
So why would you use something that tightens skin to treat scars? When ablative fractional resurfacing is used on scars, it actually increases pliability, he said.
Setting Realistic Expectations Is Key to Happy Patients
To avoid unsatisfied patients, dermatologists should ensure patients have realistic expectations, according to Dr. Howard K. Steinman.
Dermatologists are often faced with patients with vague expectations, he said at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF). "They don’t know what they want improved, they’re just unhappy with the way they look, and they’re among the most difficult patients to deal with," said Dr. Steinman, director of dermatologic and skin cancer surgery at Scott and White Healthcare in Temple, Tex.
To successfully avoid leaving patients unsatisfied, he recommends the following strategies:
• Get the specifics. When meeting with a new patient, the first thing Dr. Steinman does is hand them a mirror and ask what they want changed. If there are several concerns, ask them to narrow it down to the top three.
• Burst their bubble. Make sure their expectations are realistic. Patients may be seeking a procedure that they saw in a magazine but it may not work for them. Patients with minor damage may request major treatments and vice versa. Be certain to clarify what each treatment will and will not accomplish.
• Rephrase. Summarize the patient’s concerns to ensure it was understood, he said.
• Assess lifestyle. To guarantee a successful experience, make sure patients will be able to tolerate the healing process and any possible complications. Ensure the patient has a supportive caregiver to assist in the process and that, after the procedure, the wound will be properly cared for.
• Overestimate. Depending on the procedure, make sure the patient understands how many treatments are required (include the cost for each treatment). When in doubt, overestimate. If the procedure requires between four and eight treatments, they’ll likely hear four, said Dr. Steinman. Make sure they are also aware of any necessary maintenance or touch-ups that may be needed.
• Base time frames on holidays. Patients are anxious to see results so they may hear 6 weeks when what was really said was 6 months. Therefore, pick a holiday closest to when patients are likely to see results; they’ll be more likely to remember it, and it’ll be easier for clinicians to keep track.
• Get on the same page. Make sure patient expectations match the likely results before they leave the office, he recommended. If the patient’s desires cannot fully be understood because of language or cultural barriers, refer the patient to another physician who can meet their needs.
Dr. Steinman did not have any relevant disclosures to report. SDEF and this news organization are owned by Elsevier.
To avoid unsatisfied patients, dermatologists should ensure patients have realistic expectations, according to Dr. Howard K. Steinman.
Dermatologists are often faced with patients with vague expectations, he said at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF). "They don’t know what they want improved, they’re just unhappy with the way they look, and they’re among the most difficult patients to deal with," said Dr. Steinman, director of dermatologic and skin cancer surgery at Scott and White Healthcare in Temple, Tex.
To successfully avoid leaving patients unsatisfied, he recommends the following strategies:
• Get the specifics. When meeting with a new patient, the first thing Dr. Steinman does is hand them a mirror and ask what they want changed. If there are several concerns, ask them to narrow it down to the top three.
• Burst their bubble. Make sure their expectations are realistic. Patients may be seeking a procedure that they saw in a magazine but it may not work for them. Patients with minor damage may request major treatments and vice versa. Be certain to clarify what each treatment will and will not accomplish.
• Rephrase. Summarize the patient’s concerns to ensure it was understood, he said.
• Assess lifestyle. To guarantee a successful experience, make sure patients will be able to tolerate the healing process and any possible complications. Ensure the patient has a supportive caregiver to assist in the process and that, after the procedure, the wound will be properly cared for.
• Overestimate. Depending on the procedure, make sure the patient understands how many treatments are required (include the cost for each treatment). When in doubt, overestimate. If the procedure requires between four and eight treatments, they’ll likely hear four, said Dr. Steinman. Make sure they are also aware of any necessary maintenance or touch-ups that may be needed.
• Base time frames on holidays. Patients are anxious to see results so they may hear 6 weeks when what was really said was 6 months. Therefore, pick a holiday closest to when patients are likely to see results; they’ll be more likely to remember it, and it’ll be easier for clinicians to keep track.
• Get on the same page. Make sure patient expectations match the likely results before they leave the office, he recommended. If the patient’s desires cannot fully be understood because of language or cultural barriers, refer the patient to another physician who can meet their needs.
Dr. Steinman did not have any relevant disclosures to report. SDEF and this news organization are owned by Elsevier.
To avoid unsatisfied patients, dermatologists should ensure patients have realistic expectations, according to Dr. Howard K. Steinman.
Dermatologists are often faced with patients with vague expectations, he said at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF). "They don’t know what they want improved, they’re just unhappy with the way they look, and they’re among the most difficult patients to deal with," said Dr. Steinman, director of dermatologic and skin cancer surgery at Scott and White Healthcare in Temple, Tex.
To successfully avoid leaving patients unsatisfied, he recommends the following strategies:
• Get the specifics. When meeting with a new patient, the first thing Dr. Steinman does is hand them a mirror and ask what they want changed. If there are several concerns, ask them to narrow it down to the top three.
• Burst their bubble. Make sure their expectations are realistic. Patients may be seeking a procedure that they saw in a magazine but it may not work for them. Patients with minor damage may request major treatments and vice versa. Be certain to clarify what each treatment will and will not accomplish.
• Rephrase. Summarize the patient’s concerns to ensure it was understood, he said.
• Assess lifestyle. To guarantee a successful experience, make sure patients will be able to tolerate the healing process and any possible complications. Ensure the patient has a supportive caregiver to assist in the process and that, after the procedure, the wound will be properly cared for.
• Overestimate. Depending on the procedure, make sure the patient understands how many treatments are required (include the cost for each treatment). When in doubt, overestimate. If the procedure requires between four and eight treatments, they’ll likely hear four, said Dr. Steinman. Make sure they are also aware of any necessary maintenance or touch-ups that may be needed.
• Base time frames on holidays. Patients are anxious to see results so they may hear 6 weeks when what was really said was 6 months. Therefore, pick a holiday closest to when patients are likely to see results; they’ll be more likely to remember it, and it’ll be easier for clinicians to keep track.
• Get on the same page. Make sure patient expectations match the likely results before they leave the office, he recommended. If the patient’s desires cannot fully be understood because of language or cultural barriers, refer the patient to another physician who can meet their needs.
Dr. Steinman did not have any relevant disclosures to report. SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM THE SDEF HAWAII DERMATOLOGY SEMINAR
Microwave Technology Outlasts Botulinum Toxin for Hyperhidrosis
Microwave technology is a new hyperhidrosis treatment that offers longer-term efficacy than botulinum toxin.
"With microwave thermolysis, we now have a reliable and safe method with long-term efficacy to treat our patients who suffer from hyperhidrosis," said Dr. Michael S. Kaminer, at the Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
A hyperhidrosis diagnosis is made in patients who have visible, excessive sweating for at least 6 months without apparent cause, and with at least two of the following characteristics (J. Am. Acad. Dermatol. 2004;51:274-86):
• Impairs daily activities.
• Frequency of at least one episode per week.
• Bilateral and symmetric.
• Age of onset before 25 years.
• Positive family history.
• Cessation during sleep.
In the United states, approximately 7.6 million people, or 4% of all U.S. adults, are estimated to have axillary hyperhidrosis with a level on the Hyperhidrosis Disease Severity Scale (HDSS) of either 3 ("My sweating is barely tolerable and frequently interferes with my daily activities.") or 4 ("My sweating is intolerable and always interferes with my daily activities."), according to Dr. Kaminer, managing partner, SkinCare Physicians, Chestnut Hill, Mass. Another 32.5 million are "sweat bothered," with an HDSS level of 2 ("My sweating is tolerable but sometimes interferes with my daily activities.") or 1 ("My sweating is never noticeable and never interferes with my daily activities.").
Axillary hyperhidrosis causes considerable distress among patients. In one survey of the Dermatology Life Quality Index, the condition scored just below atopic dermatitis, close to psoriasis, and above acne vulgaris in terms of quality of life impairment, with a mean baseline score of 10.45, compared with 11.20 for atopic dermatitis, 10.53 for psoriasis, and 7.45 for acne vulgaris (Br. J. Dermatol. 2008;159:997-1035).
Current treatment options include various topical over-the-counter products, iontophoresis, sympathectomy, botulinum toxin, ultrasound (in early trials), and now microwave thermolysis.
The proprietary microwave thermolysis system, MiraDry (Miramar Labs), focuses energy delivery to the dermal-fat interface. Microwave energy is absorbed by electric dipoles. The ion content of sweat is a perfect target for this, said Dr. Kaminer, who is also with the departments of dermatology at Yale University, New Haven, Conn.; Dartmouth College, Hanover, N.H.; and Brown University, Providence, R.I.
Energy becomes concentrated along this interface and creates a focal energy zone. Continuous hydroceramic cooling prevents thermal conduction of heat superficially, and creates a heat zone at the level of sweat glands resulting in thermolysis. The procedure involves injectable local anesthesia. Treatment time is about 30 minutes, with rapid recovery.
Long-term efficacy of the device was demonstrated in the DRIUP study (Dermatologic Reduction in Underarm Perspiration), in which 120 patients with HDSS scores of 3 or 4 were randomized in a 2:1 ratio to one to three active treatments (using a prior investigational version of the microwave device) or sham treatment at seven U.S. sites. Efficacy, defined as patients reporting a reduction to an HDSS score of 1 or 2, was 89% at 30 days, 74% at 3 months, 67% at 6 months, and 69% at the 9- and 12-month visits. In the sham group, efficacy was 54% at 30 days and 44% for the 3- and 6-month visits. At all time points, the differences between the treatment and sham groups were significant.
There were 45 treatment-related adverse events, with 28% of the treatment group and 13% of the sham group patients experiencing at least one adverse event. The most common of these was an area of transient altered sensation in the arm, occurring in 10% of patients in the active treatment group. All but one adverse event resolved over time; the patient withdrew from the study, reporting altered sweating on the face. In all, 71% of the events were rated as mild in severity and didn’t affect patients’ daily activities (Dermatol Surg. 2012;38:185-91). Swelling was common, self-limited, and proportional to the energy delivered, Dr. Kaminer noted.
When compared with botulinum toxin, both approaches are effective, noninvasive (injections only), and involve minimal to no downtime. However, the duration of effect is 6.7 months for botulinum toxin, compared with stable efficacy beginning at 3 months and lasting through 12 months follow-up for microwave thermolysis, he said.
Overall, the advantages of microwave thermolysis over other treatments are its long-term efficacy (greater than 12 months, and likely longer), and its efficacy in more than 90% of patients with the latest-generation device. Disadvantages include the need for two procedures and the less than 100% responder rate. Botulinum toxin, in contrast, is easier to perform, and nearly 100% effective. However, it has the downside of the need for repeat treatments approximately every 6 months, and its cost, along with problematic insurance coverage.
Dr. Kaminer said that his practice participated in a registry-type study in the summer and fall of 2011 and was one of the first clinics in the country to purchase a MiraDry System, in December 2011. "Our staff has found the procedure easy to incorporate into the flow of our practice, and patients have found it to be rather easy to have done. We have seen some modest swelling for up to 1 week after treatment, but that is expected. So far, our experience has been pretty much what we would have expected, and if anything, a little better."
He added that, "Interest in offering this new treatment option to patients with excessive underarm sweating has been extremely high. Between clinics in Japan and the U.S., there have been over 1,500 patients treated."
In all, safety results have been consistent with prior experiences. "As with any procedure that we do, it is important to clearly communicate with the patients what to expect from the procedure and the recovery. Our feedback allowed the company to fine-tune their training program so that clinics that purchase the system have tools they can use to make the experience a very positive one for their patients."
Miramar is in the early stages of commercialization for the MiraDry system. It is being placed in a controlled strategy and is expected to reach "a significant number of practices across the U.S. by the middle of this year," he said.
Dr. Kaminer is chairman of the Miramar Labs scientific advisory board. His institution served as a research study site for the phase II study. SDEF and this news organization are owned by Elsevier.
Microwave technology is a new hyperhidrosis treatment that offers longer-term efficacy than botulinum toxin.
"With microwave thermolysis, we now have a reliable and safe method with long-term efficacy to treat our patients who suffer from hyperhidrosis," said Dr. Michael S. Kaminer, at the Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
A hyperhidrosis diagnosis is made in patients who have visible, excessive sweating for at least 6 months without apparent cause, and with at least two of the following characteristics (J. Am. Acad. Dermatol. 2004;51:274-86):
• Impairs daily activities.
• Frequency of at least one episode per week.
• Bilateral and symmetric.
• Age of onset before 25 years.
• Positive family history.
• Cessation during sleep.
In the United states, approximately 7.6 million people, or 4% of all U.S. adults, are estimated to have axillary hyperhidrosis with a level on the Hyperhidrosis Disease Severity Scale (HDSS) of either 3 ("My sweating is barely tolerable and frequently interferes with my daily activities.") or 4 ("My sweating is intolerable and always interferes with my daily activities."), according to Dr. Kaminer, managing partner, SkinCare Physicians, Chestnut Hill, Mass. Another 32.5 million are "sweat bothered," with an HDSS level of 2 ("My sweating is tolerable but sometimes interferes with my daily activities.") or 1 ("My sweating is never noticeable and never interferes with my daily activities.").
Axillary hyperhidrosis causes considerable distress among patients. In one survey of the Dermatology Life Quality Index, the condition scored just below atopic dermatitis, close to psoriasis, and above acne vulgaris in terms of quality of life impairment, with a mean baseline score of 10.45, compared with 11.20 for atopic dermatitis, 10.53 for psoriasis, and 7.45 for acne vulgaris (Br. J. Dermatol. 2008;159:997-1035).
Current treatment options include various topical over-the-counter products, iontophoresis, sympathectomy, botulinum toxin, ultrasound (in early trials), and now microwave thermolysis.
The proprietary microwave thermolysis system, MiraDry (Miramar Labs), focuses energy delivery to the dermal-fat interface. Microwave energy is absorbed by electric dipoles. The ion content of sweat is a perfect target for this, said Dr. Kaminer, who is also with the departments of dermatology at Yale University, New Haven, Conn.; Dartmouth College, Hanover, N.H.; and Brown University, Providence, R.I.
Energy becomes concentrated along this interface and creates a focal energy zone. Continuous hydroceramic cooling prevents thermal conduction of heat superficially, and creates a heat zone at the level of sweat glands resulting in thermolysis. The procedure involves injectable local anesthesia. Treatment time is about 30 minutes, with rapid recovery.
Long-term efficacy of the device was demonstrated in the DRIUP study (Dermatologic Reduction in Underarm Perspiration), in which 120 patients with HDSS scores of 3 or 4 were randomized in a 2:1 ratio to one to three active treatments (using a prior investigational version of the microwave device) or sham treatment at seven U.S. sites. Efficacy, defined as patients reporting a reduction to an HDSS score of 1 or 2, was 89% at 30 days, 74% at 3 months, 67% at 6 months, and 69% at the 9- and 12-month visits. In the sham group, efficacy was 54% at 30 days and 44% for the 3- and 6-month visits. At all time points, the differences between the treatment and sham groups were significant.
There were 45 treatment-related adverse events, with 28% of the treatment group and 13% of the sham group patients experiencing at least one adverse event. The most common of these was an area of transient altered sensation in the arm, occurring in 10% of patients in the active treatment group. All but one adverse event resolved over time; the patient withdrew from the study, reporting altered sweating on the face. In all, 71% of the events were rated as mild in severity and didn’t affect patients’ daily activities (Dermatol Surg. 2012;38:185-91). Swelling was common, self-limited, and proportional to the energy delivered, Dr. Kaminer noted.
When compared with botulinum toxin, both approaches are effective, noninvasive (injections only), and involve minimal to no downtime. However, the duration of effect is 6.7 months for botulinum toxin, compared with stable efficacy beginning at 3 months and lasting through 12 months follow-up for microwave thermolysis, he said.
Overall, the advantages of microwave thermolysis over other treatments are its long-term efficacy (greater than 12 months, and likely longer), and its efficacy in more than 90% of patients with the latest-generation device. Disadvantages include the need for two procedures and the less than 100% responder rate. Botulinum toxin, in contrast, is easier to perform, and nearly 100% effective. However, it has the downside of the need for repeat treatments approximately every 6 months, and its cost, along with problematic insurance coverage.
Dr. Kaminer said that his practice participated in a registry-type study in the summer and fall of 2011 and was one of the first clinics in the country to purchase a MiraDry System, in December 2011. "Our staff has found the procedure easy to incorporate into the flow of our practice, and patients have found it to be rather easy to have done. We have seen some modest swelling for up to 1 week after treatment, but that is expected. So far, our experience has been pretty much what we would have expected, and if anything, a little better."
He added that, "Interest in offering this new treatment option to patients with excessive underarm sweating has been extremely high. Between clinics in Japan and the U.S., there have been over 1,500 patients treated."
In all, safety results have been consistent with prior experiences. "As with any procedure that we do, it is important to clearly communicate with the patients what to expect from the procedure and the recovery. Our feedback allowed the company to fine-tune their training program so that clinics that purchase the system have tools they can use to make the experience a very positive one for their patients."
Miramar is in the early stages of commercialization for the MiraDry system. It is being placed in a controlled strategy and is expected to reach "a significant number of practices across the U.S. by the middle of this year," he said.
Dr. Kaminer is chairman of the Miramar Labs scientific advisory board. His institution served as a research study site for the phase II study. SDEF and this news organization are owned by Elsevier.
Microwave technology is a new hyperhidrosis treatment that offers longer-term efficacy than botulinum toxin.
"With microwave thermolysis, we now have a reliable and safe method with long-term efficacy to treat our patients who suffer from hyperhidrosis," said Dr. Michael S. Kaminer, at the Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
A hyperhidrosis diagnosis is made in patients who have visible, excessive sweating for at least 6 months without apparent cause, and with at least two of the following characteristics (J. Am. Acad. Dermatol. 2004;51:274-86):
• Impairs daily activities.
• Frequency of at least one episode per week.
• Bilateral and symmetric.
• Age of onset before 25 years.
• Positive family history.
• Cessation during sleep.
In the United states, approximately 7.6 million people, or 4% of all U.S. adults, are estimated to have axillary hyperhidrosis with a level on the Hyperhidrosis Disease Severity Scale (HDSS) of either 3 ("My sweating is barely tolerable and frequently interferes with my daily activities.") or 4 ("My sweating is intolerable and always interferes with my daily activities."), according to Dr. Kaminer, managing partner, SkinCare Physicians, Chestnut Hill, Mass. Another 32.5 million are "sweat bothered," with an HDSS level of 2 ("My sweating is tolerable but sometimes interferes with my daily activities.") or 1 ("My sweating is never noticeable and never interferes with my daily activities.").
Axillary hyperhidrosis causes considerable distress among patients. In one survey of the Dermatology Life Quality Index, the condition scored just below atopic dermatitis, close to psoriasis, and above acne vulgaris in terms of quality of life impairment, with a mean baseline score of 10.45, compared with 11.20 for atopic dermatitis, 10.53 for psoriasis, and 7.45 for acne vulgaris (Br. J. Dermatol. 2008;159:997-1035).
Current treatment options include various topical over-the-counter products, iontophoresis, sympathectomy, botulinum toxin, ultrasound (in early trials), and now microwave thermolysis.
The proprietary microwave thermolysis system, MiraDry (Miramar Labs), focuses energy delivery to the dermal-fat interface. Microwave energy is absorbed by electric dipoles. The ion content of sweat is a perfect target for this, said Dr. Kaminer, who is also with the departments of dermatology at Yale University, New Haven, Conn.; Dartmouth College, Hanover, N.H.; and Brown University, Providence, R.I.
Energy becomes concentrated along this interface and creates a focal energy zone. Continuous hydroceramic cooling prevents thermal conduction of heat superficially, and creates a heat zone at the level of sweat glands resulting in thermolysis. The procedure involves injectable local anesthesia. Treatment time is about 30 minutes, with rapid recovery.
Long-term efficacy of the device was demonstrated in the DRIUP study (Dermatologic Reduction in Underarm Perspiration), in which 120 patients with HDSS scores of 3 or 4 were randomized in a 2:1 ratio to one to three active treatments (using a prior investigational version of the microwave device) or sham treatment at seven U.S. sites. Efficacy, defined as patients reporting a reduction to an HDSS score of 1 or 2, was 89% at 30 days, 74% at 3 months, 67% at 6 months, and 69% at the 9- and 12-month visits. In the sham group, efficacy was 54% at 30 days and 44% for the 3- and 6-month visits. At all time points, the differences between the treatment and sham groups were significant.
There were 45 treatment-related adverse events, with 28% of the treatment group and 13% of the sham group patients experiencing at least one adverse event. The most common of these was an area of transient altered sensation in the arm, occurring in 10% of patients in the active treatment group. All but one adverse event resolved over time; the patient withdrew from the study, reporting altered sweating on the face. In all, 71% of the events were rated as mild in severity and didn’t affect patients’ daily activities (Dermatol Surg. 2012;38:185-91). Swelling was common, self-limited, and proportional to the energy delivered, Dr. Kaminer noted.
When compared with botulinum toxin, both approaches are effective, noninvasive (injections only), and involve minimal to no downtime. However, the duration of effect is 6.7 months for botulinum toxin, compared with stable efficacy beginning at 3 months and lasting through 12 months follow-up for microwave thermolysis, he said.
Overall, the advantages of microwave thermolysis over other treatments are its long-term efficacy (greater than 12 months, and likely longer), and its efficacy in more than 90% of patients with the latest-generation device. Disadvantages include the need for two procedures and the less than 100% responder rate. Botulinum toxin, in contrast, is easier to perform, and nearly 100% effective. However, it has the downside of the need for repeat treatments approximately every 6 months, and its cost, along with problematic insurance coverage.
Dr. Kaminer said that his practice participated in a registry-type study in the summer and fall of 2011 and was one of the first clinics in the country to purchase a MiraDry System, in December 2011. "Our staff has found the procedure easy to incorporate into the flow of our practice, and patients have found it to be rather easy to have done. We have seen some modest swelling for up to 1 week after treatment, but that is expected. So far, our experience has been pretty much what we would have expected, and if anything, a little better."
He added that, "Interest in offering this new treatment option to patients with excessive underarm sweating has been extremely high. Between clinics in Japan and the U.S., there have been over 1,500 patients treated."
In all, safety results have been consistent with prior experiences. "As with any procedure that we do, it is important to clearly communicate with the patients what to expect from the procedure and the recovery. Our feedback allowed the company to fine-tune their training program so that clinics that purchase the system have tools they can use to make the experience a very positive one for their patients."
Miramar is in the early stages of commercialization for the MiraDry system. It is being placed in a controlled strategy and is expected to reach "a significant number of practices across the U.S. by the middle of this year," he said.
Dr. Kaminer is chairman of the Miramar Labs scientific advisory board. His institution served as a research study site for the phase II study. SDEF and this news organization are owned by Elsevier.
FROM THE SDEF HAWAII DERMATOLOGY SEMINAR
Major Finding: Efficacy was 89% at 30 days, 74% at 3 months, 67% at 6 months, and 69% at the 9- and 12-month visits.
Data Source: Patients (120) with HDSS scores of 3 or 4 were randomized in a 2:1 ratio to one to three active treatments (using a prior investigational version of the microwave device) or sham treatment at seven U.S. sites.
Disclosures: Dr. Kaminer is chairman of the Miramar Labs scientific advisory board. His institution served as a research study site for the phase II study. SDEF and this news organization are owned by Elsevier.
Let Balance, Aesthetics Guide Volume Replacement
Volume replacement can give an aging face some lift, but it’s not for everyone, according to Dr. Mark G. Rubin.
In a woman with a round face, for example, adding volume to the lower half of the face can create a fuller, heavier appearance rather than a more youthful appearance, he said at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
"We all agree that volume loss is a significant part of aging, but without attention to facial balance and aesthetics, the results of volume replacement can be less than satisfactory," he added, noting that when it comes to facial contouring, an understanding of balance and aesthetics becomes more important than technique.
One important concept to keep in mind is the "triangle of youth," said Dr. Rubin who practices dermatology in Beverly Hills, Calif. He explained that a triangular face is more youthful, which is why volume that promotes roundness can have the opposite effect, even if the volume tends to smooth wrinkles.
Creating a triangular shape by providing fullness and prominence of the cheekbone – as long as it isn’t overdone – can create a youthful, attractive look, he said.
The aging lower half of the face has volume loss in several areas, including the medial cheek/nasojugal groove, the central cheek, the nasolabial folds, the marionette lines, and the prejowl area.
Volume replacement in the marionette lines and at the jaw line can be particularly effective.
In the marionette fold, one technique that can be useful is building a layer of support to push up on the descending cheek, thereby camouflaging its leading edge.
"Sometime you need to add a little support into the lateral lower lip, as well as the horseshoe of the modiolus," he said. "Remember, as you push up on the corner of the lip, that you can accidentally create or aggravate fullness laterally."
Adding filler to the upper vermilion border can also support this approach by tightening the lip and providing some lift to the corner, thereby helping reduce the puffiness created by treating the upper marionette area.
Volume at the jawline can also provide a more youthful look, but keep in mind that the two areas of apparent volume loss – the pre- and postjowl – are actually normal areas, whereas the skin in between has descended, Dr. Rubin explained. Filling these pre- and postjowl pseudodepressions will provide something of an optical illusion, making the jowl look less prominent. Similarly, adding volume at the prejowl sulcus can reduce the sagging appearance of the jowl.
However, a patient with a round face may not be a good candidate for this approach. "Too much volume at the prejowl sulcus in a patient with a round face will make the face look fat," he explained.
Also, in some patients the smoothing of the jaw line may look good on profile, but it can have a masculinizing effect by widening the lateral face when viewed head on.
As for the cheeks, not all "deflate" in the same way, and thus not all will benefit from volume replacement. In those with central cheek hollowing, volume can be very effective in creating a more youthful appearance, as well as in tightening loose skin.
A number of filler options can be considered, including hyaluronic acid (HA) fillers, poly-L-lactic acid, calcium hydroxylapatite, and polymethyl methacrylate (PMMA).
"But for first-time patients, or if you are learning your way, don’t underestimate the value of a reversible filler," he said.
As with the use of neurotoxins, the approach to using fillers can vary without necessarily affecting the outcome. Various physicians have their own preferences for products and injection techniques, yet almost everyone seems to be able to achieve the intended aesthetic goal, he explained.
"So I don’t think the ‘what’ is that important. It’s knowing the ‘where’ and the mastering of an injection technique that means more," he said.
In fact, Food and Drug Administration trial data for most fillers suggest that they are more similar than dissimilar in terms of efficacy, longevity, and adverse effects. Still, although conventional wisdom suggests that particle size, concentration, or lift should affect the final result, and thus in theory there should be one product that is best for each location, there is a lack of agreement.
In Dr. Rubin’s experience, however, HA, PMMA, and calcium hydroxylapatite fillers can have a slight rippling effect when they are injected in areas of soft tissue, such as the central cheek.
"It’s hard to make a smooth contour across 6-8 cm when you are injecting droplets or linear filaments of a filler," he said, noting that poly-L-lactic acid seems to create a smoother contour in that area.
When injecting over bony areas, HA products and calcium hydroxylapatite are acceptable, because the defects are generally smaller and there is less surface area on which to see ripples.
Dr. Rubin is a consultant for Medicis. He also has been involved in FDA clinical trials for Restylane, Perlane, and Artefill. SDEF and this news organization are owned by Elsevier.
Volume replacement can give an aging face some lift, but it’s not for everyone, according to Dr. Mark G. Rubin.
In a woman with a round face, for example, adding volume to the lower half of the face can create a fuller, heavier appearance rather than a more youthful appearance, he said at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
"We all agree that volume loss is a significant part of aging, but without attention to facial balance and aesthetics, the results of volume replacement can be less than satisfactory," he added, noting that when it comes to facial contouring, an understanding of balance and aesthetics becomes more important than technique.
One important concept to keep in mind is the "triangle of youth," said Dr. Rubin who practices dermatology in Beverly Hills, Calif. He explained that a triangular face is more youthful, which is why volume that promotes roundness can have the opposite effect, even if the volume tends to smooth wrinkles.
Creating a triangular shape by providing fullness and prominence of the cheekbone – as long as it isn’t overdone – can create a youthful, attractive look, he said.
The aging lower half of the face has volume loss in several areas, including the medial cheek/nasojugal groove, the central cheek, the nasolabial folds, the marionette lines, and the prejowl area.
Volume replacement in the marionette lines and at the jaw line can be particularly effective.
In the marionette fold, one technique that can be useful is building a layer of support to push up on the descending cheek, thereby camouflaging its leading edge.
"Sometime you need to add a little support into the lateral lower lip, as well as the horseshoe of the modiolus," he said. "Remember, as you push up on the corner of the lip, that you can accidentally create or aggravate fullness laterally."
Adding filler to the upper vermilion border can also support this approach by tightening the lip and providing some lift to the corner, thereby helping reduce the puffiness created by treating the upper marionette area.
Volume at the jawline can also provide a more youthful look, but keep in mind that the two areas of apparent volume loss – the pre- and postjowl – are actually normal areas, whereas the skin in between has descended, Dr. Rubin explained. Filling these pre- and postjowl pseudodepressions will provide something of an optical illusion, making the jowl look less prominent. Similarly, adding volume at the prejowl sulcus can reduce the sagging appearance of the jowl.
However, a patient with a round face may not be a good candidate for this approach. "Too much volume at the prejowl sulcus in a patient with a round face will make the face look fat," he explained.
Also, in some patients the smoothing of the jaw line may look good on profile, but it can have a masculinizing effect by widening the lateral face when viewed head on.
As for the cheeks, not all "deflate" in the same way, and thus not all will benefit from volume replacement. In those with central cheek hollowing, volume can be very effective in creating a more youthful appearance, as well as in tightening loose skin.
A number of filler options can be considered, including hyaluronic acid (HA) fillers, poly-L-lactic acid, calcium hydroxylapatite, and polymethyl methacrylate (PMMA).
"But for first-time patients, or if you are learning your way, don’t underestimate the value of a reversible filler," he said.
As with the use of neurotoxins, the approach to using fillers can vary without necessarily affecting the outcome. Various physicians have their own preferences for products and injection techniques, yet almost everyone seems to be able to achieve the intended aesthetic goal, he explained.
"So I don’t think the ‘what’ is that important. It’s knowing the ‘where’ and the mastering of an injection technique that means more," he said.
In fact, Food and Drug Administration trial data for most fillers suggest that they are more similar than dissimilar in terms of efficacy, longevity, and adverse effects. Still, although conventional wisdom suggests that particle size, concentration, or lift should affect the final result, and thus in theory there should be one product that is best for each location, there is a lack of agreement.
In Dr. Rubin’s experience, however, HA, PMMA, and calcium hydroxylapatite fillers can have a slight rippling effect when they are injected in areas of soft tissue, such as the central cheek.
"It’s hard to make a smooth contour across 6-8 cm when you are injecting droplets or linear filaments of a filler," he said, noting that poly-L-lactic acid seems to create a smoother contour in that area.
When injecting over bony areas, HA products and calcium hydroxylapatite are acceptable, because the defects are generally smaller and there is less surface area on which to see ripples.
Dr. Rubin is a consultant for Medicis. He also has been involved in FDA clinical trials for Restylane, Perlane, and Artefill. SDEF and this news organization are owned by Elsevier.
Volume replacement can give an aging face some lift, but it’s not for everyone, according to Dr. Mark G. Rubin.
In a woman with a round face, for example, adding volume to the lower half of the face can create a fuller, heavier appearance rather than a more youthful appearance, he said at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
"We all agree that volume loss is a significant part of aging, but without attention to facial balance and aesthetics, the results of volume replacement can be less than satisfactory," he added, noting that when it comes to facial contouring, an understanding of balance and aesthetics becomes more important than technique.
One important concept to keep in mind is the "triangle of youth," said Dr. Rubin who practices dermatology in Beverly Hills, Calif. He explained that a triangular face is more youthful, which is why volume that promotes roundness can have the opposite effect, even if the volume tends to smooth wrinkles.
Creating a triangular shape by providing fullness and prominence of the cheekbone – as long as it isn’t overdone – can create a youthful, attractive look, he said.
The aging lower half of the face has volume loss in several areas, including the medial cheek/nasojugal groove, the central cheek, the nasolabial folds, the marionette lines, and the prejowl area.
Volume replacement in the marionette lines and at the jaw line can be particularly effective.
In the marionette fold, one technique that can be useful is building a layer of support to push up on the descending cheek, thereby camouflaging its leading edge.
"Sometime you need to add a little support into the lateral lower lip, as well as the horseshoe of the modiolus," he said. "Remember, as you push up on the corner of the lip, that you can accidentally create or aggravate fullness laterally."
Adding filler to the upper vermilion border can also support this approach by tightening the lip and providing some lift to the corner, thereby helping reduce the puffiness created by treating the upper marionette area.
Volume at the jawline can also provide a more youthful look, but keep in mind that the two areas of apparent volume loss – the pre- and postjowl – are actually normal areas, whereas the skin in between has descended, Dr. Rubin explained. Filling these pre- and postjowl pseudodepressions will provide something of an optical illusion, making the jowl look less prominent. Similarly, adding volume at the prejowl sulcus can reduce the sagging appearance of the jowl.
However, a patient with a round face may not be a good candidate for this approach. "Too much volume at the prejowl sulcus in a patient with a round face will make the face look fat," he explained.
Also, in some patients the smoothing of the jaw line may look good on profile, but it can have a masculinizing effect by widening the lateral face when viewed head on.
As for the cheeks, not all "deflate" in the same way, and thus not all will benefit from volume replacement. In those with central cheek hollowing, volume can be very effective in creating a more youthful appearance, as well as in tightening loose skin.
A number of filler options can be considered, including hyaluronic acid (HA) fillers, poly-L-lactic acid, calcium hydroxylapatite, and polymethyl methacrylate (PMMA).
"But for first-time patients, or if you are learning your way, don’t underestimate the value of a reversible filler," he said.
As with the use of neurotoxins, the approach to using fillers can vary without necessarily affecting the outcome. Various physicians have their own preferences for products and injection techniques, yet almost everyone seems to be able to achieve the intended aesthetic goal, he explained.
"So I don’t think the ‘what’ is that important. It’s knowing the ‘where’ and the mastering of an injection technique that means more," he said.
In fact, Food and Drug Administration trial data for most fillers suggest that they are more similar than dissimilar in terms of efficacy, longevity, and adverse effects. Still, although conventional wisdom suggests that particle size, concentration, or lift should affect the final result, and thus in theory there should be one product that is best for each location, there is a lack of agreement.
In Dr. Rubin’s experience, however, HA, PMMA, and calcium hydroxylapatite fillers can have a slight rippling effect when they are injected in areas of soft tissue, such as the central cheek.
"It’s hard to make a smooth contour across 6-8 cm when you are injecting droplets or linear filaments of a filler," he said, noting that poly-L-lactic acid seems to create a smoother contour in that area.
When injecting over bony areas, HA products and calcium hydroxylapatite are acceptable, because the defects are generally smaller and there is less surface area on which to see ripples.
Dr. Rubin is a consultant for Medicis. He also has been involved in FDA clinical trials for Restylane, Perlane, and Artefill. SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM THE SDEF HAWAII DERMATOLOGY SEMINAR
Astaxanthin
Certain plant constituents have been established as exerting photoprotective effects, such as antioxidants, which include carotenoids, tocopherols, vitamin C, and flavonoids and other polyphenols. Researchers have shown that carotenoids are superior scavengers of singlet oxygen and sufficient scavengers of other reactive oxygen species (Nutrition 2001;17:818-22). As dietary antioxidants, carotenoids have been shown to confer photoprotective benefits to human skin, efficiently scavenging peroxyl radicals and hampering lipid peroxidation (Photochem. Photobiol. 2002;75:503-6).
Carotenoid pigments, which consist of more than 600 compounds, are secondary metabolic plant products that confer yellow, green, red, or orange color to fruits and vegetables. They are precursors of vitamin A (retinol). Astaxanthin, a member of the xanthophyll class of carotenoids and closely related to beta-carotene, lutein, and zeaxanthin (J. Nat. Prod. 2006;69:443-9), is a red-orange carotenoid present in plants and algae that is also known to contribute to the color of seafood such as salmon, shrimp, and lobster. It is synthesized by only a few bacteria, including Brevibacterium, Mycobacterium lacticola, Agrobacterium auratim, and Haematococcus pluvialis, and the yeast Phaffia rhodozyma (Bioresour. Technol. 2004;92:209-14). Astaxanthin is also found in bird species, such as flamingos and quails, but cannot be synthesized by them (J. Nat. Prod. 2006;69:443-9).
Sources. The richest source of astaxanthin is the green microalga H. pluvialis (J. Nat. Prod. 2006;69:443-9), which contains more than 80% astaxanthin in its cells (Bioresour. Technol. 2004;92:209-14). Because of its rapid growth and high astaxanthin content, H. pluvialis is now produced at industrial scale, and its commercial production has grown significantly worldwide during the last decade (Trends Biotechnol. 2003;21:210-6). Astaxanthin also can be derived from the fermentation of the pink yeast Xanthophyllomyces dendrorhous, extracted from crustacea (e.g., Antarctic krill, Euphausia superba), which have a limited ability to synthesize astaxanthin from dietary carotenoids, and produced synthetically. Mammals can neither produce astaxanthin nor convert dietary astaxanthin into vitamin A (Trends Biotechnol. 2003;21:210-6).
Although this potent carotenoid is expensive to produce, isolate, and purify, investigators recently demonstrated a method of fermenting P. rhodozyma (X. dendrorhous) yeast cells with brewer malt waste, yielding a significant amount of astaxanthin with demonstrated antiproliferative effectiveness in two tested breast cancer cell lines (Int. J. Mol. Med. 2005;16:931-6). Indeed, astaxanthin is known to exhibit antiproliferative properties against skin and breast cancer (Int. J. Mol. Med. 2005;16:931-6).
Research Findings. In in vitro studies performed during the last two decades, astaxanthin has been shown to exhibit significantly greater antioxidant capacity than beta-carotene (Nutr. Res. 1995;15:1695-1704; Arch. Biochem. Biophys. 1992;297:291-5; Lipids 1989;24:659-61). In fact, this xanthophyllic carotenoid has demonstrated up to several-fold stronger antioxidant activity than vitamin E and beta-carotene (Trends Biotechnol. 2003;21:210-6; Physiol. Chem. Phys. Med. NMR 1990;22:27-38), as well as other carotenoids (J. Nat. Prod. 2006;69:443-9; Trends Biotechnol. 2003;21:210-6; Crit. Rev. Food Sci. Nutr. 2006;46:185-96).
Astaxanthin also appears to have the potential to be significantly more effective than beta-carotene and lutein at preventing UV-induced lipid photo-oxidation (J. Dermatol. Sci. 1998;16:226-30; Trends Biotechnol. 2003;21:210-6).
In a study conducted in 1998, investigators found that beta-carotene, lutein, and astaxanthin exhibited protective activity against UVA-induced oxidative stress in cultured rat kidney fibroblasts. Of the three carotenoids, astaxanthin demonstrated the most potent protective capacity (J. Dermatol. Sci. 1998;16:226-30).
Ten years ago, investigators tested a proprietary algal extract containing a significant amount of astaxanthin to determine its protective capacity against UVA-induced DNA damage in human skin fibroblasts, human melanocytes, and human intestinal CaCo-2 cells. They also compared the effects with those of a synthetic astaxanthin. The results showed that the synthetic astaxanthin prevented UVA-induced damage in all cell types at all tested concentrations (10 nmol, 100 nmol, and 10 micromol), whereas the algal extract conferred protection in all cell types only at the highest concentration. In addition, 2-hour exposure to UVA led to significant cellular superoxide dismutase activity in fibroblast cells, along with a substantial decrease in cellular glutathione content. Eighteen-hour preincubation with 10 micromol of either form of astaxanthin, however, prevented both of these UVA-induced changes in fibroblast cells. Simultaneous incubation with either form of astaxanthin also prevented UVA-induced depletion of glutathione content in CaCo-2 cells, but did not affect superoxide dismutase activity. Overall, the researchers concluded that the algal extract containing astaxanthin performed comparably to synthetic astaxanthin, and warrants attention as an antioxidant that may deliver health benefits (J. Dermatol. Sci. 2002;30:73-84).
Recently, investigators studied in vitro the effects of the carotenoids astaxanthin and canthaxanthin on gap junctional intercellular communication, which is integral in homeostasis, growth control, and cell development, and is known to be impaired in cancer cells. They exposed primary human skin fibroblasts to 0.001 to 10 micromol/L of the carotenoids, and used a dye transfer assay to measure gap junctional communication. Intercellular communication increased after 24 and 72 hours of incubation with canthaxanthin, but decreased significantly with astaxanthin, with a reverse seen upon withdrawal of astaxanthin. Using Western blot analysis, the investigators found that astaxanthin influences channel function by altering the phosphorylation pattern of the protein connexin, lowering the phosphorylation state (J. Nutr. 2005;135:2507-11).
Products. Derived primarily from algae or yeasts, a wide variety of astaxanthin products are available as nutritional supplements in health food stores (Crit. Rev. Food Sci. Nutr. 2006;46:185-96). Increasingly, astaxanthin is finding inclusion as an active ingredient in topical formulations.
Philosophy’s when hope is not enough SPF age-defense sunscreen is a broad-spectrum UVA/UVB SPF 20 sun protection formulation that contains astaxanthin, tocotrienol, vitamin C, peptides, and beta-glucan. It is designed to moisturize and protect the skin from sun damage.
In addition, astaxanthin, termed "the most potent antioxidant yet discovered" by Derma E, is a staple in products from by manufacturer, including Age-Defying Night Crème with Astaxanthin and Pycnogenol, Age-Defying Day Crème with Astaxanthin and Pycnogenol, Age-Defying Eye Crème with Astaxanthin and Pycnogenol, Anti-Aging Moisturizing Complex with SPF 15, Orange Blossom Age-Defying Hand and Body Lotion, and Lavender Age-Defying Hand and Body Lotion.
ShenDea also includes astaxanthin as a main ingredient in its line of facial creams, gels and lotions, combining the carotenoid with pearl and grape seed extract.
Derma MD features astaxanthin in AstaXanthin Micro Peel; AstaXanthin Concentrate Tri-Complex, intended for postprocedural application; and "D" Puff Eye Repair Gel.
Conclusion. Along with pigmentary and other functions, carotenoids exhibit significant antioxidant activity. Much more research has been conducted on carotenoids such as beta-carotene, lutein, and lycopene than on astaxanthin, but the evidence for this latter carotenoid is compelling. The effects of astaxanthin on crustaceans and seafood are well established, but recent research suggests that this potent antioxidant has the capacity to impart significant health benefits to human beings. More research, in the form of randomized controlled trials, is warranted to determine the efficacy and safety of this carotenoid in formulations intended to benefit the skin.
Certain plant constituents have been established as exerting photoprotective effects, such as antioxidants, which include carotenoids, tocopherols, vitamin C, and flavonoids and other polyphenols. Researchers have shown that carotenoids are superior scavengers of singlet oxygen and sufficient scavengers of other reactive oxygen species (Nutrition 2001;17:818-22). As dietary antioxidants, carotenoids have been shown to confer photoprotective benefits to human skin, efficiently scavenging peroxyl radicals and hampering lipid peroxidation (Photochem. Photobiol. 2002;75:503-6).
Carotenoid pigments, which consist of more than 600 compounds, are secondary metabolic plant products that confer yellow, green, red, or orange color to fruits and vegetables. They are precursors of vitamin A (retinol). Astaxanthin, a member of the xanthophyll class of carotenoids and closely related to beta-carotene, lutein, and zeaxanthin (J. Nat. Prod. 2006;69:443-9), is a red-orange carotenoid present in plants and algae that is also known to contribute to the color of seafood such as salmon, shrimp, and lobster. It is synthesized by only a few bacteria, including Brevibacterium, Mycobacterium lacticola, Agrobacterium auratim, and Haematococcus pluvialis, and the yeast Phaffia rhodozyma (Bioresour. Technol. 2004;92:209-14). Astaxanthin is also found in bird species, such as flamingos and quails, but cannot be synthesized by them (J. Nat. Prod. 2006;69:443-9).
Sources. The richest source of astaxanthin is the green microalga H. pluvialis (J. Nat. Prod. 2006;69:443-9), which contains more than 80% astaxanthin in its cells (Bioresour. Technol. 2004;92:209-14). Because of its rapid growth and high astaxanthin content, H. pluvialis is now produced at industrial scale, and its commercial production has grown significantly worldwide during the last decade (Trends Biotechnol. 2003;21:210-6). Astaxanthin also can be derived from the fermentation of the pink yeast Xanthophyllomyces dendrorhous, extracted from crustacea (e.g., Antarctic krill, Euphausia superba), which have a limited ability to synthesize astaxanthin from dietary carotenoids, and produced synthetically. Mammals can neither produce astaxanthin nor convert dietary astaxanthin into vitamin A (Trends Biotechnol. 2003;21:210-6).
Although this potent carotenoid is expensive to produce, isolate, and purify, investigators recently demonstrated a method of fermenting P. rhodozyma (X. dendrorhous) yeast cells with brewer malt waste, yielding a significant amount of astaxanthin with demonstrated antiproliferative effectiveness in two tested breast cancer cell lines (Int. J. Mol. Med. 2005;16:931-6). Indeed, astaxanthin is known to exhibit antiproliferative properties against skin and breast cancer (Int. J. Mol. Med. 2005;16:931-6).
Research Findings. In in vitro studies performed during the last two decades, astaxanthin has been shown to exhibit significantly greater antioxidant capacity than beta-carotene (Nutr. Res. 1995;15:1695-1704; Arch. Biochem. Biophys. 1992;297:291-5; Lipids 1989;24:659-61). In fact, this xanthophyllic carotenoid has demonstrated up to several-fold stronger antioxidant activity than vitamin E and beta-carotene (Trends Biotechnol. 2003;21:210-6; Physiol. Chem. Phys. Med. NMR 1990;22:27-38), as well as other carotenoids (J. Nat. Prod. 2006;69:443-9; Trends Biotechnol. 2003;21:210-6; Crit. Rev. Food Sci. Nutr. 2006;46:185-96).
Astaxanthin also appears to have the potential to be significantly more effective than beta-carotene and lutein at preventing UV-induced lipid photo-oxidation (J. Dermatol. Sci. 1998;16:226-30; Trends Biotechnol. 2003;21:210-6).
In a study conducted in 1998, investigators found that beta-carotene, lutein, and astaxanthin exhibited protective activity against UVA-induced oxidative stress in cultured rat kidney fibroblasts. Of the three carotenoids, astaxanthin demonstrated the most potent protective capacity (J. Dermatol. Sci. 1998;16:226-30).
Ten years ago, investigators tested a proprietary algal extract containing a significant amount of astaxanthin to determine its protective capacity against UVA-induced DNA damage in human skin fibroblasts, human melanocytes, and human intestinal CaCo-2 cells. They also compared the effects with those of a synthetic astaxanthin. The results showed that the synthetic astaxanthin prevented UVA-induced damage in all cell types at all tested concentrations (10 nmol, 100 nmol, and 10 micromol), whereas the algal extract conferred protection in all cell types only at the highest concentration. In addition, 2-hour exposure to UVA led to significant cellular superoxide dismutase activity in fibroblast cells, along with a substantial decrease in cellular glutathione content. Eighteen-hour preincubation with 10 micromol of either form of astaxanthin, however, prevented both of these UVA-induced changes in fibroblast cells. Simultaneous incubation with either form of astaxanthin also prevented UVA-induced depletion of glutathione content in CaCo-2 cells, but did not affect superoxide dismutase activity. Overall, the researchers concluded that the algal extract containing astaxanthin performed comparably to synthetic astaxanthin, and warrants attention as an antioxidant that may deliver health benefits (J. Dermatol. Sci. 2002;30:73-84).
Recently, investigators studied in vitro the effects of the carotenoids astaxanthin and canthaxanthin on gap junctional intercellular communication, which is integral in homeostasis, growth control, and cell development, and is known to be impaired in cancer cells. They exposed primary human skin fibroblasts to 0.001 to 10 micromol/L of the carotenoids, and used a dye transfer assay to measure gap junctional communication. Intercellular communication increased after 24 and 72 hours of incubation with canthaxanthin, but decreased significantly with astaxanthin, with a reverse seen upon withdrawal of astaxanthin. Using Western blot analysis, the investigators found that astaxanthin influences channel function by altering the phosphorylation pattern of the protein connexin, lowering the phosphorylation state (J. Nutr. 2005;135:2507-11).
Products. Derived primarily from algae or yeasts, a wide variety of astaxanthin products are available as nutritional supplements in health food stores (Crit. Rev. Food Sci. Nutr. 2006;46:185-96). Increasingly, astaxanthin is finding inclusion as an active ingredient in topical formulations.
Philosophy’s when hope is not enough SPF age-defense sunscreen is a broad-spectrum UVA/UVB SPF 20 sun protection formulation that contains astaxanthin, tocotrienol, vitamin C, peptides, and beta-glucan. It is designed to moisturize and protect the skin from sun damage.
In addition, astaxanthin, termed "the most potent antioxidant yet discovered" by Derma E, is a staple in products from by manufacturer, including Age-Defying Night Crème with Astaxanthin and Pycnogenol, Age-Defying Day Crème with Astaxanthin and Pycnogenol, Age-Defying Eye Crème with Astaxanthin and Pycnogenol, Anti-Aging Moisturizing Complex with SPF 15, Orange Blossom Age-Defying Hand and Body Lotion, and Lavender Age-Defying Hand and Body Lotion.
ShenDea also includes astaxanthin as a main ingredient in its line of facial creams, gels and lotions, combining the carotenoid with pearl and grape seed extract.
Derma MD features astaxanthin in AstaXanthin Micro Peel; AstaXanthin Concentrate Tri-Complex, intended for postprocedural application; and "D" Puff Eye Repair Gel.
Conclusion. Along with pigmentary and other functions, carotenoids exhibit significant antioxidant activity. Much more research has been conducted on carotenoids such as beta-carotene, lutein, and lycopene than on astaxanthin, but the evidence for this latter carotenoid is compelling. The effects of astaxanthin on crustaceans and seafood are well established, but recent research suggests that this potent antioxidant has the capacity to impart significant health benefits to human beings. More research, in the form of randomized controlled trials, is warranted to determine the efficacy and safety of this carotenoid in formulations intended to benefit the skin.
Certain plant constituents have been established as exerting photoprotective effects, such as antioxidants, which include carotenoids, tocopherols, vitamin C, and flavonoids and other polyphenols. Researchers have shown that carotenoids are superior scavengers of singlet oxygen and sufficient scavengers of other reactive oxygen species (Nutrition 2001;17:818-22). As dietary antioxidants, carotenoids have been shown to confer photoprotective benefits to human skin, efficiently scavenging peroxyl radicals and hampering lipid peroxidation (Photochem. Photobiol. 2002;75:503-6).
Carotenoid pigments, which consist of more than 600 compounds, are secondary metabolic plant products that confer yellow, green, red, or orange color to fruits and vegetables. They are precursors of vitamin A (retinol). Astaxanthin, a member of the xanthophyll class of carotenoids and closely related to beta-carotene, lutein, and zeaxanthin (J. Nat. Prod. 2006;69:443-9), is a red-orange carotenoid present in plants and algae that is also known to contribute to the color of seafood such as salmon, shrimp, and lobster. It is synthesized by only a few bacteria, including Brevibacterium, Mycobacterium lacticola, Agrobacterium auratim, and Haematococcus pluvialis, and the yeast Phaffia rhodozyma (Bioresour. Technol. 2004;92:209-14). Astaxanthin is also found in bird species, such as flamingos and quails, but cannot be synthesized by them (J. Nat. Prod. 2006;69:443-9).
Sources. The richest source of astaxanthin is the green microalga H. pluvialis (J. Nat. Prod. 2006;69:443-9), which contains more than 80% astaxanthin in its cells (Bioresour. Technol. 2004;92:209-14). Because of its rapid growth and high astaxanthin content, H. pluvialis is now produced at industrial scale, and its commercial production has grown significantly worldwide during the last decade (Trends Biotechnol. 2003;21:210-6). Astaxanthin also can be derived from the fermentation of the pink yeast Xanthophyllomyces dendrorhous, extracted from crustacea (e.g., Antarctic krill, Euphausia superba), which have a limited ability to synthesize astaxanthin from dietary carotenoids, and produced synthetically. Mammals can neither produce astaxanthin nor convert dietary astaxanthin into vitamin A (Trends Biotechnol. 2003;21:210-6).
Although this potent carotenoid is expensive to produce, isolate, and purify, investigators recently demonstrated a method of fermenting P. rhodozyma (X. dendrorhous) yeast cells with brewer malt waste, yielding a significant amount of astaxanthin with demonstrated antiproliferative effectiveness in two tested breast cancer cell lines (Int. J. Mol. Med. 2005;16:931-6). Indeed, astaxanthin is known to exhibit antiproliferative properties against skin and breast cancer (Int. J. Mol. Med. 2005;16:931-6).
Research Findings. In in vitro studies performed during the last two decades, astaxanthin has been shown to exhibit significantly greater antioxidant capacity than beta-carotene (Nutr. Res. 1995;15:1695-1704; Arch. Biochem. Biophys. 1992;297:291-5; Lipids 1989;24:659-61). In fact, this xanthophyllic carotenoid has demonstrated up to several-fold stronger antioxidant activity than vitamin E and beta-carotene (Trends Biotechnol. 2003;21:210-6; Physiol. Chem. Phys. Med. NMR 1990;22:27-38), as well as other carotenoids (J. Nat. Prod. 2006;69:443-9; Trends Biotechnol. 2003;21:210-6; Crit. Rev. Food Sci. Nutr. 2006;46:185-96).
Astaxanthin also appears to have the potential to be significantly more effective than beta-carotene and lutein at preventing UV-induced lipid photo-oxidation (J. Dermatol. Sci. 1998;16:226-30; Trends Biotechnol. 2003;21:210-6).
In a study conducted in 1998, investigators found that beta-carotene, lutein, and astaxanthin exhibited protective activity against UVA-induced oxidative stress in cultured rat kidney fibroblasts. Of the three carotenoids, astaxanthin demonstrated the most potent protective capacity (J. Dermatol. Sci. 1998;16:226-30).
Ten years ago, investigators tested a proprietary algal extract containing a significant amount of astaxanthin to determine its protective capacity against UVA-induced DNA damage in human skin fibroblasts, human melanocytes, and human intestinal CaCo-2 cells. They also compared the effects with those of a synthetic astaxanthin. The results showed that the synthetic astaxanthin prevented UVA-induced damage in all cell types at all tested concentrations (10 nmol, 100 nmol, and 10 micromol), whereas the algal extract conferred protection in all cell types only at the highest concentration. In addition, 2-hour exposure to UVA led to significant cellular superoxide dismutase activity in fibroblast cells, along with a substantial decrease in cellular glutathione content. Eighteen-hour preincubation with 10 micromol of either form of astaxanthin, however, prevented both of these UVA-induced changes in fibroblast cells. Simultaneous incubation with either form of astaxanthin also prevented UVA-induced depletion of glutathione content in CaCo-2 cells, but did not affect superoxide dismutase activity. Overall, the researchers concluded that the algal extract containing astaxanthin performed comparably to synthetic astaxanthin, and warrants attention as an antioxidant that may deliver health benefits (J. Dermatol. Sci. 2002;30:73-84).
Recently, investigators studied in vitro the effects of the carotenoids astaxanthin and canthaxanthin on gap junctional intercellular communication, which is integral in homeostasis, growth control, and cell development, and is known to be impaired in cancer cells. They exposed primary human skin fibroblasts to 0.001 to 10 micromol/L of the carotenoids, and used a dye transfer assay to measure gap junctional communication. Intercellular communication increased after 24 and 72 hours of incubation with canthaxanthin, but decreased significantly with astaxanthin, with a reverse seen upon withdrawal of astaxanthin. Using Western blot analysis, the investigators found that astaxanthin influences channel function by altering the phosphorylation pattern of the protein connexin, lowering the phosphorylation state (J. Nutr. 2005;135:2507-11).
Products. Derived primarily from algae or yeasts, a wide variety of astaxanthin products are available as nutritional supplements in health food stores (Crit. Rev. Food Sci. Nutr. 2006;46:185-96). Increasingly, astaxanthin is finding inclusion as an active ingredient in topical formulations.
Philosophy’s when hope is not enough SPF age-defense sunscreen is a broad-spectrum UVA/UVB SPF 20 sun protection formulation that contains astaxanthin, tocotrienol, vitamin C, peptides, and beta-glucan. It is designed to moisturize and protect the skin from sun damage.
In addition, astaxanthin, termed "the most potent antioxidant yet discovered" by Derma E, is a staple in products from by manufacturer, including Age-Defying Night Crème with Astaxanthin and Pycnogenol, Age-Defying Day Crème with Astaxanthin and Pycnogenol, Age-Defying Eye Crème with Astaxanthin and Pycnogenol, Anti-Aging Moisturizing Complex with SPF 15, Orange Blossom Age-Defying Hand and Body Lotion, and Lavender Age-Defying Hand and Body Lotion.
ShenDea also includes astaxanthin as a main ingredient in its line of facial creams, gels and lotions, combining the carotenoid with pearl and grape seed extract.
Derma MD features astaxanthin in AstaXanthin Micro Peel; AstaXanthin Concentrate Tri-Complex, intended for postprocedural application; and "D" Puff Eye Repair Gel.
Conclusion. Along with pigmentary and other functions, carotenoids exhibit significant antioxidant activity. Much more research has been conducted on carotenoids such as beta-carotene, lutein, and lycopene than on astaxanthin, but the evidence for this latter carotenoid is compelling. The effects of astaxanthin on crustaceans and seafood are well established, but recent research suggests that this potent antioxidant has the capacity to impart significant health benefits to human beings. More research, in the form of randomized controlled trials, is warranted to determine the efficacy and safety of this carotenoid in formulations intended to benefit the skin.
Observation Okayed as Option for Some Skin Cancers
MIAMI BEACH – Observation or a "watchful waiting" approach is an acceptable option vs. re-excision for patients with positive margins remaining after removal of head and neck skin cancers, according to a retrospective study.
"A lot of times we take these lesions off and they appear to be benign, not really knowing what the preoperative histologic diagnosis is. [Then we] find out the diagnosis is cancer, and not only that, but they have a positive margin." Dr. Justin Douglas said at the Triological Society Combined Sections meeting.
The question is, he said, "Do you have to rush them back in [and re-excise] or can you sit on them for a while?"
"Dr. Douglas addresses an interesting question," said session moderator Dr. Jeffrey H. Spiegel, chief of the division of facial plastic and reconstructive surgery at Boston University Medical Center and otolaryngology faculty member at Boston University. "I see a lot of people who had squamous cells and basal cells excised sent back for re-excision ... and he’ll help us understand if I even need to be doing that."
Dr. Douglas and his colleagues studied 492 patients at the Clarksburg Veterans Affairs Hospital in Morgantown, W.Va. All had skin cancers removed from their head or neck, including 387 basal cell carcinomas and 105 squamous cell carcinomas, over 5 years.
"Do you have to rush them back in [and re-excise] or can you sit on them for a while?"
About 40% or 197 lesions had a negative margin after wide local excision. The remaining 295 lesions featured a positive margin on permanent section analysis. The positive lesions included 232 basal cell carcinomas (BCCs) and 63 squamous cell carcinomas (SCCs).
"In the group of 232 positive basal cell lesions, everybody was offered re-excision. A total 105 chose re-excision and 127 decided to just watch it, despite our best judgment," said Dr. Douglas, an otolaryngologist at the Morgantown V.A.
"Even of the squamous cell patients, 26 still said they wanted to watch it," Dr. Douglas said at the meeting, which was cosponsored by the Triological Society and the American College of Surgeons.
Of the positive margin group, none of the BCC and four (3.8%) of the SCC lesions recurred within a median follow-up of 3.7 years. This finding suggests a role for clinical observation of low-risk, nonmelanomatous cancers, Dr. Douglas said.
The four SCC lesions that recurred included one lesion in the observation-only group and three in the re-excision group. Some of these patients likely had a more aggressive form of cancer, Dr. Douglas said.
"Essentially, we feel what we learned from this study is that ... given the fact that you can handle any recurrence of these lesions if they occur, you can watch the basal cells, even with positive margins," Dr. Douglas said. "We still feel all squamous cell lesions should be taken out until you get a clear margin."
Why the majority of positive margin patients who chose observation did not experience recurrence is poorly understood, Dr. Douglas said. However, it could be the patient’s immune system, secondary to the wound healing process, comes in and cleans up any residual cells. Another possibility is that patients die from other causes before recurrence can occur. "The truth of the matter is: We don’t know. We need more studies to figure this out."
The nose was the most common site for the T1, nonmelanoma lesions. The average size was 1.2 cm. Mean patient age was 61 years and 484 (98%) were men. Patients were excluded from the study if their lesion was previously treated or they chose an option other than re-excision or observation.
Although initial excision by a Mohs surgeon would be ideal, Dr. Douglas said, in his study dermatologists and otolaryngologists removed the lesions at one of the hospital ambulatory clinics. This strategy reflects some real-world limitations. "The problem is, at least in West Virginia, Mohs surgeons are very sparse. There are probably only a handful in the state." Operating room time and scheduling (particularly for patients with many lesions), availability of a pathologist to read frozen sections, and costs are additional challenges.
Dr. Douglas and Dr. Spiegel said that they had no relevant financial disclosures.
MIAMI BEACH – Observation or a "watchful waiting" approach is an acceptable option vs. re-excision for patients with positive margins remaining after removal of head and neck skin cancers, according to a retrospective study.
"A lot of times we take these lesions off and they appear to be benign, not really knowing what the preoperative histologic diagnosis is. [Then we] find out the diagnosis is cancer, and not only that, but they have a positive margin." Dr. Justin Douglas said at the Triological Society Combined Sections meeting.
The question is, he said, "Do you have to rush them back in [and re-excise] or can you sit on them for a while?"
"Dr. Douglas addresses an interesting question," said session moderator Dr. Jeffrey H. Spiegel, chief of the division of facial plastic and reconstructive surgery at Boston University Medical Center and otolaryngology faculty member at Boston University. "I see a lot of people who had squamous cells and basal cells excised sent back for re-excision ... and he’ll help us understand if I even need to be doing that."
Dr. Douglas and his colleagues studied 492 patients at the Clarksburg Veterans Affairs Hospital in Morgantown, W.Va. All had skin cancers removed from their head or neck, including 387 basal cell carcinomas and 105 squamous cell carcinomas, over 5 years.
"Do you have to rush them back in [and re-excise] or can you sit on them for a while?"
About 40% or 197 lesions had a negative margin after wide local excision. The remaining 295 lesions featured a positive margin on permanent section analysis. The positive lesions included 232 basal cell carcinomas (BCCs) and 63 squamous cell carcinomas (SCCs).
"In the group of 232 positive basal cell lesions, everybody was offered re-excision. A total 105 chose re-excision and 127 decided to just watch it, despite our best judgment," said Dr. Douglas, an otolaryngologist at the Morgantown V.A.
"Even of the squamous cell patients, 26 still said they wanted to watch it," Dr. Douglas said at the meeting, which was cosponsored by the Triological Society and the American College of Surgeons.
Of the positive margin group, none of the BCC and four (3.8%) of the SCC lesions recurred within a median follow-up of 3.7 years. This finding suggests a role for clinical observation of low-risk, nonmelanomatous cancers, Dr. Douglas said.
The four SCC lesions that recurred included one lesion in the observation-only group and three in the re-excision group. Some of these patients likely had a more aggressive form of cancer, Dr. Douglas said.
"Essentially, we feel what we learned from this study is that ... given the fact that you can handle any recurrence of these lesions if they occur, you can watch the basal cells, even with positive margins," Dr. Douglas said. "We still feel all squamous cell lesions should be taken out until you get a clear margin."
Why the majority of positive margin patients who chose observation did not experience recurrence is poorly understood, Dr. Douglas said. However, it could be the patient’s immune system, secondary to the wound healing process, comes in and cleans up any residual cells. Another possibility is that patients die from other causes before recurrence can occur. "The truth of the matter is: We don’t know. We need more studies to figure this out."
The nose was the most common site for the T1, nonmelanoma lesions. The average size was 1.2 cm. Mean patient age was 61 years and 484 (98%) were men. Patients were excluded from the study if their lesion was previously treated or they chose an option other than re-excision or observation.
Although initial excision by a Mohs surgeon would be ideal, Dr. Douglas said, in his study dermatologists and otolaryngologists removed the lesions at one of the hospital ambulatory clinics. This strategy reflects some real-world limitations. "The problem is, at least in West Virginia, Mohs surgeons are very sparse. There are probably only a handful in the state." Operating room time and scheduling (particularly for patients with many lesions), availability of a pathologist to read frozen sections, and costs are additional challenges.
Dr. Douglas and Dr. Spiegel said that they had no relevant financial disclosures.
MIAMI BEACH – Observation or a "watchful waiting" approach is an acceptable option vs. re-excision for patients with positive margins remaining after removal of head and neck skin cancers, according to a retrospective study.
"A lot of times we take these lesions off and they appear to be benign, not really knowing what the preoperative histologic diagnosis is. [Then we] find out the diagnosis is cancer, and not only that, but they have a positive margin." Dr. Justin Douglas said at the Triological Society Combined Sections meeting.
The question is, he said, "Do you have to rush them back in [and re-excise] or can you sit on them for a while?"
"Dr. Douglas addresses an interesting question," said session moderator Dr. Jeffrey H. Spiegel, chief of the division of facial plastic and reconstructive surgery at Boston University Medical Center and otolaryngology faculty member at Boston University. "I see a lot of people who had squamous cells and basal cells excised sent back for re-excision ... and he’ll help us understand if I even need to be doing that."
Dr. Douglas and his colleagues studied 492 patients at the Clarksburg Veterans Affairs Hospital in Morgantown, W.Va. All had skin cancers removed from their head or neck, including 387 basal cell carcinomas and 105 squamous cell carcinomas, over 5 years.
"Do you have to rush them back in [and re-excise] or can you sit on them for a while?"
About 40% or 197 lesions had a negative margin after wide local excision. The remaining 295 lesions featured a positive margin on permanent section analysis. The positive lesions included 232 basal cell carcinomas (BCCs) and 63 squamous cell carcinomas (SCCs).
"In the group of 232 positive basal cell lesions, everybody was offered re-excision. A total 105 chose re-excision and 127 decided to just watch it, despite our best judgment," said Dr. Douglas, an otolaryngologist at the Morgantown V.A.
"Even of the squamous cell patients, 26 still said they wanted to watch it," Dr. Douglas said at the meeting, which was cosponsored by the Triological Society and the American College of Surgeons.
Of the positive margin group, none of the BCC and four (3.8%) of the SCC lesions recurred within a median follow-up of 3.7 years. This finding suggests a role for clinical observation of low-risk, nonmelanomatous cancers, Dr. Douglas said.
The four SCC lesions that recurred included one lesion in the observation-only group and three in the re-excision group. Some of these patients likely had a more aggressive form of cancer, Dr. Douglas said.
"Essentially, we feel what we learned from this study is that ... given the fact that you can handle any recurrence of these lesions if they occur, you can watch the basal cells, even with positive margins," Dr. Douglas said. "We still feel all squamous cell lesions should be taken out until you get a clear margin."
Why the majority of positive margin patients who chose observation did not experience recurrence is poorly understood, Dr. Douglas said. However, it could be the patient’s immune system, secondary to the wound healing process, comes in and cleans up any residual cells. Another possibility is that patients die from other causes before recurrence can occur. "The truth of the matter is: We don’t know. We need more studies to figure this out."
The nose was the most common site for the T1, nonmelanoma lesions. The average size was 1.2 cm. Mean patient age was 61 years and 484 (98%) were men. Patients were excluded from the study if their lesion was previously treated or they chose an option other than re-excision or observation.
Although initial excision by a Mohs surgeon would be ideal, Dr. Douglas said, in his study dermatologists and otolaryngologists removed the lesions at one of the hospital ambulatory clinics. This strategy reflects some real-world limitations. "The problem is, at least in West Virginia, Mohs surgeons are very sparse. There are probably only a handful in the state." Operating room time and scheduling (particularly for patients with many lesions), availability of a pathologist to read frozen sections, and costs are additional challenges.
Dr. Douglas and Dr. Spiegel said that they had no relevant financial disclosures.
FROM THE TRIOLOGICAL SOCIETY COMBINED SECTIONS MEETING
Major Finding: None of 232 basal cell carcinoma lesions and 4 (3.8%) of 63 positive squamous cell carcinoma lesions with an initial positive margin recurred over a median follow-up of 3.7 years.
Data Source: Retrospective, single-center study of 492 patients diagnosed with head and neck skin cancers over 5 years.
Disclosures: Dr. Douglas reported having no financial disclosures.