User login
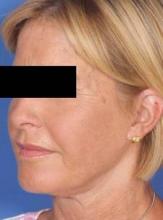
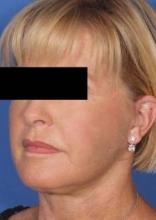
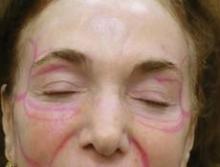
TCA Peel After Lift Improves Skin Texture
LAS VEGAS – In the early 1980s, combining facelift procedures with chemical skin peeling was considered a no-no because of skin necrosis concerns.
But Dr. David M. Morrow, founder and director of the Rancho Mirage, Calif.–based Morrow Institute, had a hunch that chemical peels that were made from phenols might be causing the necrosis, not those made from trichloroacetic acid (TCA). So in the late 1980s, he started combining TCA peels with lifting procedures of the upper face, midface, and neck – a practice that he has continued to this day.
At the annual meeting of the American Academy of Cosmetic Surgery, Dr. Sheila C. Barbarino presented results from 1,118 men and women aged 35-89 years who have undergone the combined procedures at the Morrow Institute since 1988, "all without a single case of skin necrosis," said Dr. Barbarino, an ophthalmic plastic surgeon at the institute.
Of the 1,118 procedures, 489 were performed using TCA 35%, 481 with TCA 18%, and 148 with TCA 15%. She noted that 483 of the procedures also involved the use of phenol 89%, which was applied to the lower eyelid and/or periorbital area. She said that the current practice at the institute is to use a moderately deep peel with TCA 18%.
The rationale for chemical skin peeling following lifting procedures is to improve skin color and texture "while creating new epidermis, dermal collagen, and elastic fibers," Dr. Barbarino said. "Combining these two procedures and performing them simultaneously is extremely efficient. It calls for only one operative setting for anesthesia [and] one window of healing time, and it saves the patient time and money."
In the upper face–, midface-, and neck-lifting procedures, undermining consisted of combined blunt and sharp dissection to create long, subcutaneous flaps of the neck and face. Suspension sutures were placed in a favorable vector via superficial musculoaponeurotic system (SMAS) plication and/or SMAS flaps. "The skin flaps were then trimmed and tailored and skin closure was performed, followed immediately by chemical skin peeling," Dr. Barbarino said.
Chemicals used were TCA 18%-35% and phenol 89% to nonundermined areas. "You can safely use phenol after transconjunctival lower lid blepharoplasty, but not after transcutaneous lower lid blepharoplasty, because the flap is a little too thin," she said.
Patients who underwent the combined procedures had Fitzpatrick skin types I-IV. Postoperatively, the skin was evaluated based on thickness, color, and condition. "Skin flap thickness and condition [were] also evaluated immediately after the surgery was performed," Dr. Barbarino said. "If significant swelling, ecchymosis, and/or hematoma were observed, we would defer the peel for another day."
Anesthesia used for the procedures consisted of IV or general sedation, supplemented with local infiltration of 0.5% lidocaine with epinephrine or a dilute local anesthetic solution.
"The benefit of combining these procedures is that you can address two problems with one healing period of approximately 2 weeks," Dr. Barbarino said. "We observed no clinical differences in outcomes from simultaneously performing these procedures versus performing each procedure at separate settings."
A key to preventing complications is to consider if the patient’s skin thickness will tolerate the combined procedures. Assessment for feasibility would involve analysis of the skin texture, turgor, and the presence or absence of ecchymoses under the skin after the face-lifting procedure. "If a patient’s skin was already very thin preoperatively, then the surgeon would be well advised not to proceed with the combined procedure," she said. "Ideally, you’d like to treat with topical vitamin C solution and tretinoin 0.1% cream for 1 month prior to any peel. Sun avoidance is mandatory during the healing process."
Infection with herpes simplex virus is a common complication of all chemical peels. If this occurs, Dr. Barbarino recommends treating with valacyclovir. "You can reassure your patients that these lesions will resolve without any scarring," she said.
No incidence of necrosis was noted in the patients, nor were there any objectionable permanent pigmentary changes. "Transient hyperpigmentation is responsive to bleaching agents or simply re-peeling the patient," she said.
Dr. Barbarino said that she had no relevant financial conflicts to disclose.
LAS VEGAS – In the early 1980s, combining facelift procedures with chemical skin peeling was considered a no-no because of skin necrosis concerns.
But Dr. David M. Morrow, founder and director of the Rancho Mirage, Calif.–based Morrow Institute, had a hunch that chemical peels that were made from phenols might be causing the necrosis, not those made from trichloroacetic acid (TCA). So in the late 1980s, he started combining TCA peels with lifting procedures of the upper face, midface, and neck – a practice that he has continued to this day.
At the annual meeting of the American Academy of Cosmetic Surgery, Dr. Sheila C. Barbarino presented results from 1,118 men and women aged 35-89 years who have undergone the combined procedures at the Morrow Institute since 1988, "all without a single case of skin necrosis," said Dr. Barbarino, an ophthalmic plastic surgeon at the institute.
Of the 1,118 procedures, 489 were performed using TCA 35%, 481 with TCA 18%, and 148 with TCA 15%. She noted that 483 of the procedures also involved the use of phenol 89%, which was applied to the lower eyelid and/or periorbital area. She said that the current practice at the institute is to use a moderately deep peel with TCA 18%.
The rationale for chemical skin peeling following lifting procedures is to improve skin color and texture "while creating new epidermis, dermal collagen, and elastic fibers," Dr. Barbarino said. "Combining these two procedures and performing them simultaneously is extremely efficient. It calls for only one operative setting for anesthesia [and] one window of healing time, and it saves the patient time and money."
In the upper face–, midface-, and neck-lifting procedures, undermining consisted of combined blunt and sharp dissection to create long, subcutaneous flaps of the neck and face. Suspension sutures were placed in a favorable vector via superficial musculoaponeurotic system (SMAS) plication and/or SMAS flaps. "The skin flaps were then trimmed and tailored and skin closure was performed, followed immediately by chemical skin peeling," Dr. Barbarino said.
Chemicals used were TCA 18%-35% and phenol 89% to nonundermined areas. "You can safely use phenol after transconjunctival lower lid blepharoplasty, but not after transcutaneous lower lid blepharoplasty, because the flap is a little too thin," she said.
Patients who underwent the combined procedures had Fitzpatrick skin types I-IV. Postoperatively, the skin was evaluated based on thickness, color, and condition. "Skin flap thickness and condition [were] also evaluated immediately after the surgery was performed," Dr. Barbarino said. "If significant swelling, ecchymosis, and/or hematoma were observed, we would defer the peel for another day."
Anesthesia used for the procedures consisted of IV or general sedation, supplemented with local infiltration of 0.5% lidocaine with epinephrine or a dilute local anesthetic solution.
"The benefit of combining these procedures is that you can address two problems with one healing period of approximately 2 weeks," Dr. Barbarino said. "We observed no clinical differences in outcomes from simultaneously performing these procedures versus performing each procedure at separate settings."
A key to preventing complications is to consider if the patient’s skin thickness will tolerate the combined procedures. Assessment for feasibility would involve analysis of the skin texture, turgor, and the presence or absence of ecchymoses under the skin after the face-lifting procedure. "If a patient’s skin was already very thin preoperatively, then the surgeon would be well advised not to proceed with the combined procedure," she said. "Ideally, you’d like to treat with topical vitamin C solution and tretinoin 0.1% cream for 1 month prior to any peel. Sun avoidance is mandatory during the healing process."
Infection with herpes simplex virus is a common complication of all chemical peels. If this occurs, Dr. Barbarino recommends treating with valacyclovir. "You can reassure your patients that these lesions will resolve without any scarring," she said.
No incidence of necrosis was noted in the patients, nor were there any objectionable permanent pigmentary changes. "Transient hyperpigmentation is responsive to bleaching agents or simply re-peeling the patient," she said.
Dr. Barbarino said that she had no relevant financial conflicts to disclose.
LAS VEGAS – In the early 1980s, combining facelift procedures with chemical skin peeling was considered a no-no because of skin necrosis concerns.
But Dr. David M. Morrow, founder and director of the Rancho Mirage, Calif.–based Morrow Institute, had a hunch that chemical peels that were made from phenols might be causing the necrosis, not those made from trichloroacetic acid (TCA). So in the late 1980s, he started combining TCA peels with lifting procedures of the upper face, midface, and neck – a practice that he has continued to this day.
At the annual meeting of the American Academy of Cosmetic Surgery, Dr. Sheila C. Barbarino presented results from 1,118 men and women aged 35-89 years who have undergone the combined procedures at the Morrow Institute since 1988, "all without a single case of skin necrosis," said Dr. Barbarino, an ophthalmic plastic surgeon at the institute.
Of the 1,118 procedures, 489 were performed using TCA 35%, 481 with TCA 18%, and 148 with TCA 15%. She noted that 483 of the procedures also involved the use of phenol 89%, which was applied to the lower eyelid and/or periorbital area. She said that the current practice at the institute is to use a moderately deep peel with TCA 18%.
The rationale for chemical skin peeling following lifting procedures is to improve skin color and texture "while creating new epidermis, dermal collagen, and elastic fibers," Dr. Barbarino said. "Combining these two procedures and performing them simultaneously is extremely efficient. It calls for only one operative setting for anesthesia [and] one window of healing time, and it saves the patient time and money."
In the upper face–, midface-, and neck-lifting procedures, undermining consisted of combined blunt and sharp dissection to create long, subcutaneous flaps of the neck and face. Suspension sutures were placed in a favorable vector via superficial musculoaponeurotic system (SMAS) plication and/or SMAS flaps. "The skin flaps were then trimmed and tailored and skin closure was performed, followed immediately by chemical skin peeling," Dr. Barbarino said.
Chemicals used were TCA 18%-35% and phenol 89% to nonundermined areas. "You can safely use phenol after transconjunctival lower lid blepharoplasty, but not after transcutaneous lower lid blepharoplasty, because the flap is a little too thin," she said.
Patients who underwent the combined procedures had Fitzpatrick skin types I-IV. Postoperatively, the skin was evaluated based on thickness, color, and condition. "Skin flap thickness and condition [were] also evaluated immediately after the surgery was performed," Dr. Barbarino said. "If significant swelling, ecchymosis, and/or hematoma were observed, we would defer the peel for another day."
Anesthesia used for the procedures consisted of IV or general sedation, supplemented with local infiltration of 0.5% lidocaine with epinephrine or a dilute local anesthetic solution.
"The benefit of combining these procedures is that you can address two problems with one healing period of approximately 2 weeks," Dr. Barbarino said. "We observed no clinical differences in outcomes from simultaneously performing these procedures versus performing each procedure at separate settings."
A key to preventing complications is to consider if the patient’s skin thickness will tolerate the combined procedures. Assessment for feasibility would involve analysis of the skin texture, turgor, and the presence or absence of ecchymoses under the skin after the face-lifting procedure. "If a patient’s skin was already very thin preoperatively, then the surgeon would be well advised not to proceed with the combined procedure," she said. "Ideally, you’d like to treat with topical vitamin C solution and tretinoin 0.1% cream for 1 month prior to any peel. Sun avoidance is mandatory during the healing process."
Infection with herpes simplex virus is a common complication of all chemical peels. If this occurs, Dr. Barbarino recommends treating with valacyclovir. "You can reassure your patients that these lesions will resolve without any scarring," she said.
No incidence of necrosis was noted in the patients, nor were there any objectionable permanent pigmentary changes. "Transient hyperpigmentation is responsive to bleaching agents or simply re-peeling the patient," she said.
Dr. Barbarino said that she had no relevant financial conflicts to disclose.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF COSMETIC SURGERY
Attack Acne Early in Skin of Color Patients
MIAMI BEACH – Early and aggressive anti-inflammatory therapy – preferably combination – is the key to treating acne and postinflammatory hyperpigmentation in patients with skin of color.
Acne prevalence is about the same in black and white patients, said Dr. Valerie D. Callender. The same mechanisms cause acne and the same treatments, in general, are used regardless of skin type, she said. "What is important is ... there are sequelae of acne that make it a little different, and there are certain, special considerations we have to keep in mind when treating patients with darker skin types."
Prevention of keloids, hypertrophic scars, and postinflammatory hyperpigmentation are among the special considerations in this patient population, Dr. Callender said at the South Beach Symposium.
Keloids and hypertrophic scars usually result from inflammatory acne papules, nodules, and cysts, and can be challenging to treat. The keloids and scarring commonly arise along the jawline and on the chest, shoulder, and back. "It’s important to be very aggressive to resolve the inflammation, to treat them effectively. A lot of these patients do very well with isotretinoin and oral antibiotics," said Dr. Callender of the dermatology department at Howard University in Washington, D.C.
In patients with keloids, consider injection of 20 mg/cc intralesional triamcinolone every 4 weeks, sometimes every 2 weeks, to get these lesions to go down, she said. "Remember that is part of their acne regimen."
Postinflammatory hyperpigmentation (PIH) is a common presenting complaint among skin of color patients with acne or another inflammatory skin condition.
PIH is "psychologically devastating for these patients. We have to treat the PIH just as aggressively as we treat the acne," Dr. Callender said. In some cases, the disfigurement is severe and the hyperpigmented patches and macules can persist for months or even years.
In a study of 2,895 females aged 10-70, prevalence of PIH varied by ethnicity (J. Eur. Acad. Dermatol. Venereol. 2011;25:1054-60). The researchers at Massachusetts General Hospital in Boston found that PIH affected 65% of 384 black study patients and 48% of 258 Hispanic patients. "The other racial groups were less than 20% for PIH; this goes along with what we do in our practices," Dr. Callender said.
There are multiple options for prevention and treatment of PIH. Sunscreen, sun avoidance, and early diagnosis can prevent or minimize adverse effects. Hydroquinone, retinoids, azelaic acid, and/or kojic acid are recommended treatments.
"I love my hydroquinone, I use it a lot," Dr. Callender said. Hydroquinone lightens areas of hyperpigmentation through inhibition of tyrosine conversion to melanin, reduces the number of melanosomes, and inhibits DNA and RNA synthesis of melanocytes.
Topical retinoid agents are useful because they not only treat acne, but also address the hyperpigmentation, she said. Also, once the hyperpigmentation is under control, the topical retinoids help to exfoliate the skin and keep PIH from recurring. "We love to keep these patients on long-term topical retinoid therapy."
Tolerability is very important when prescribing topical retinoids and other agents. Carefully consider each patient’s potential risk for cutaneous irritation, including erythema, peeling, burning, and dryness. Be sure to inform nurses and office staff that when a patient calls about tolerability, "you have to inquire about any changes in pigmentation [as well], especially in skin of color patients," Dr. Callender said. Moisturizers, cleansers, and less irritating vehicles can improve tolerability.
"We also use adjunctive therapies and sunscreen protection [for PIH]. Remember combination therapy is the way to go," she said.
She and her associates conducted a meta-analysis looking at the tolerability of a fixed combination adapalene 0.1% and benzoyl peroxide 2.5% gel product (Epiduo) for acne in patients by Fitzpatrick skin type (J. Clin. Aesthet. Dermatol. 2010;3:15-9). They found erythema, scaling, and dryness scores higher for white patients in all three studies. Burning and stinging scores were not significantly different. "Tolerability is good for your skin of color patients. You don’t need to be overly concerned about a lot of irritation just because their skin is dark."
Chemical peels, lasers, and light-based therapies are additional treatment options for acne. Peels made with glycolic acid, salicylic acid, Jessner’s solution, or a combination is acceptable in skin of color patients. However, "be very, very careful with peels in skin of color patients. Make sure [to] use superficial peeling agents," Dr. Callender said.
More clinical studies of lasers and light-based therapies to treat acne are including the darker skin types, Dr. Callender said. Blue light, diode laser, intense pulse light, and photodynamic therapy are examples. "As we learn how to adjust the settings, they will be safer for skin of color patients," she said.
Dr. Callender disclosed that she is a consultant for Allergan and Galderma, which markets Epiduo; a researcher for Allergan, Galderma, and Intendis; and a member of the speakers’ bureau for Galderma.
MIAMI BEACH – Early and aggressive anti-inflammatory therapy – preferably combination – is the key to treating acne and postinflammatory hyperpigmentation in patients with skin of color.
Acne prevalence is about the same in black and white patients, said Dr. Valerie D. Callender. The same mechanisms cause acne and the same treatments, in general, are used regardless of skin type, she said. "What is important is ... there are sequelae of acne that make it a little different, and there are certain, special considerations we have to keep in mind when treating patients with darker skin types."
Prevention of keloids, hypertrophic scars, and postinflammatory hyperpigmentation are among the special considerations in this patient population, Dr. Callender said at the South Beach Symposium.
Keloids and hypertrophic scars usually result from inflammatory acne papules, nodules, and cysts, and can be challenging to treat. The keloids and scarring commonly arise along the jawline and on the chest, shoulder, and back. "It’s important to be very aggressive to resolve the inflammation, to treat them effectively. A lot of these patients do very well with isotretinoin and oral antibiotics," said Dr. Callender of the dermatology department at Howard University in Washington, D.C.
In patients with keloids, consider injection of 20 mg/cc intralesional triamcinolone every 4 weeks, sometimes every 2 weeks, to get these lesions to go down, she said. "Remember that is part of their acne regimen."
Postinflammatory hyperpigmentation (PIH) is a common presenting complaint among skin of color patients with acne or another inflammatory skin condition.
PIH is "psychologically devastating for these patients. We have to treat the PIH just as aggressively as we treat the acne," Dr. Callender said. In some cases, the disfigurement is severe and the hyperpigmented patches and macules can persist for months or even years.
In a study of 2,895 females aged 10-70, prevalence of PIH varied by ethnicity (J. Eur. Acad. Dermatol. Venereol. 2011;25:1054-60). The researchers at Massachusetts General Hospital in Boston found that PIH affected 65% of 384 black study patients and 48% of 258 Hispanic patients. "The other racial groups were less than 20% for PIH; this goes along with what we do in our practices," Dr. Callender said.
There are multiple options for prevention and treatment of PIH. Sunscreen, sun avoidance, and early diagnosis can prevent or minimize adverse effects. Hydroquinone, retinoids, azelaic acid, and/or kojic acid are recommended treatments.
"I love my hydroquinone, I use it a lot," Dr. Callender said. Hydroquinone lightens areas of hyperpigmentation through inhibition of tyrosine conversion to melanin, reduces the number of melanosomes, and inhibits DNA and RNA synthesis of melanocytes.
Topical retinoid agents are useful because they not only treat acne, but also address the hyperpigmentation, she said. Also, once the hyperpigmentation is under control, the topical retinoids help to exfoliate the skin and keep PIH from recurring. "We love to keep these patients on long-term topical retinoid therapy."
Tolerability is very important when prescribing topical retinoids and other agents. Carefully consider each patient’s potential risk for cutaneous irritation, including erythema, peeling, burning, and dryness. Be sure to inform nurses and office staff that when a patient calls about tolerability, "you have to inquire about any changes in pigmentation [as well], especially in skin of color patients," Dr. Callender said. Moisturizers, cleansers, and less irritating vehicles can improve tolerability.
"We also use adjunctive therapies and sunscreen protection [for PIH]. Remember combination therapy is the way to go," she said.
She and her associates conducted a meta-analysis looking at the tolerability of a fixed combination adapalene 0.1% and benzoyl peroxide 2.5% gel product (Epiduo) for acne in patients by Fitzpatrick skin type (J. Clin. Aesthet. Dermatol. 2010;3:15-9). They found erythema, scaling, and dryness scores higher for white patients in all three studies. Burning and stinging scores were not significantly different. "Tolerability is good for your skin of color patients. You don’t need to be overly concerned about a lot of irritation just because their skin is dark."
Chemical peels, lasers, and light-based therapies are additional treatment options for acne. Peels made with glycolic acid, salicylic acid, Jessner’s solution, or a combination is acceptable in skin of color patients. However, "be very, very careful with peels in skin of color patients. Make sure [to] use superficial peeling agents," Dr. Callender said.
More clinical studies of lasers and light-based therapies to treat acne are including the darker skin types, Dr. Callender said. Blue light, diode laser, intense pulse light, and photodynamic therapy are examples. "As we learn how to adjust the settings, they will be safer for skin of color patients," she said.
Dr. Callender disclosed that she is a consultant for Allergan and Galderma, which markets Epiduo; a researcher for Allergan, Galderma, and Intendis; and a member of the speakers’ bureau for Galderma.
MIAMI BEACH – Early and aggressive anti-inflammatory therapy – preferably combination – is the key to treating acne and postinflammatory hyperpigmentation in patients with skin of color.
Acne prevalence is about the same in black and white patients, said Dr. Valerie D. Callender. The same mechanisms cause acne and the same treatments, in general, are used regardless of skin type, she said. "What is important is ... there are sequelae of acne that make it a little different, and there are certain, special considerations we have to keep in mind when treating patients with darker skin types."
Prevention of keloids, hypertrophic scars, and postinflammatory hyperpigmentation are among the special considerations in this patient population, Dr. Callender said at the South Beach Symposium.
Keloids and hypertrophic scars usually result from inflammatory acne papules, nodules, and cysts, and can be challenging to treat. The keloids and scarring commonly arise along the jawline and on the chest, shoulder, and back. "It’s important to be very aggressive to resolve the inflammation, to treat them effectively. A lot of these patients do very well with isotretinoin and oral antibiotics," said Dr. Callender of the dermatology department at Howard University in Washington, D.C.
In patients with keloids, consider injection of 20 mg/cc intralesional triamcinolone every 4 weeks, sometimes every 2 weeks, to get these lesions to go down, she said. "Remember that is part of their acne regimen."
Postinflammatory hyperpigmentation (PIH) is a common presenting complaint among skin of color patients with acne or another inflammatory skin condition.
PIH is "psychologically devastating for these patients. We have to treat the PIH just as aggressively as we treat the acne," Dr. Callender said. In some cases, the disfigurement is severe and the hyperpigmented patches and macules can persist for months or even years.
In a study of 2,895 females aged 10-70, prevalence of PIH varied by ethnicity (J. Eur. Acad. Dermatol. Venereol. 2011;25:1054-60). The researchers at Massachusetts General Hospital in Boston found that PIH affected 65% of 384 black study patients and 48% of 258 Hispanic patients. "The other racial groups were less than 20% for PIH; this goes along with what we do in our practices," Dr. Callender said.
There are multiple options for prevention and treatment of PIH. Sunscreen, sun avoidance, and early diagnosis can prevent or minimize adverse effects. Hydroquinone, retinoids, azelaic acid, and/or kojic acid are recommended treatments.
"I love my hydroquinone, I use it a lot," Dr. Callender said. Hydroquinone lightens areas of hyperpigmentation through inhibition of tyrosine conversion to melanin, reduces the number of melanosomes, and inhibits DNA and RNA synthesis of melanocytes.
Topical retinoid agents are useful because they not only treat acne, but also address the hyperpigmentation, she said. Also, once the hyperpigmentation is under control, the topical retinoids help to exfoliate the skin and keep PIH from recurring. "We love to keep these patients on long-term topical retinoid therapy."
Tolerability is very important when prescribing topical retinoids and other agents. Carefully consider each patient’s potential risk for cutaneous irritation, including erythema, peeling, burning, and dryness. Be sure to inform nurses and office staff that when a patient calls about tolerability, "you have to inquire about any changes in pigmentation [as well], especially in skin of color patients," Dr. Callender said. Moisturizers, cleansers, and less irritating vehicles can improve tolerability.
"We also use adjunctive therapies and sunscreen protection [for PIH]. Remember combination therapy is the way to go," she said.
She and her associates conducted a meta-analysis looking at the tolerability of a fixed combination adapalene 0.1% and benzoyl peroxide 2.5% gel product (Epiduo) for acne in patients by Fitzpatrick skin type (J. Clin. Aesthet. Dermatol. 2010;3:15-9). They found erythema, scaling, and dryness scores higher for white patients in all three studies. Burning and stinging scores were not significantly different. "Tolerability is good for your skin of color patients. You don’t need to be overly concerned about a lot of irritation just because their skin is dark."
Chemical peels, lasers, and light-based therapies are additional treatment options for acne. Peels made with glycolic acid, salicylic acid, Jessner’s solution, or a combination is acceptable in skin of color patients. However, "be very, very careful with peels in skin of color patients. Make sure [to] use superficial peeling agents," Dr. Callender said.
More clinical studies of lasers and light-based therapies to treat acne are including the darker skin types, Dr. Callender said. Blue light, diode laser, intense pulse light, and photodynamic therapy are examples. "As we learn how to adjust the settings, they will be safer for skin of color patients," she said.
Dr. Callender disclosed that she is a consultant for Allergan and Galderma, which markets Epiduo; a researcher for Allergan, Galderma, and Intendis; and a member of the speakers’ bureau for Galderma.
EXPERT ANALYSIS FROM THE SOUTH BEACH SYMPOSIUM
Numbing Agents Cause More Pain in PDT
WAIKOLOA, HAWAII – Using EMLA or lidocaine cream in conjunction with topical 5-aminolevulinic acid photodynamic therapy may boost uptake of the photosensitizer, but the clinical outcomes can be unpredictable, according to Dr. E. Victor Ross.
"Our worst scenarios have been when we’ve used EMLA on the skin. We’ve stopped using EMLA or lidocaine cream on the skin in ALA-PDT because of the very pronounced, enhanced photodynamic effects. You get great long-term results, but such a bad short-term result that lots of people didn’t want to go through it," said Dr. Ross of Scripps Clinic Laser and Cosmetic Dermatology Center in Carmel Valley, Calif.
Using a topical numbing agent seemed to be an attractive option because patients often complain that photodynamic therapy (PDT) is painful. Plus, there seemed to be an added benefit: The anesthetic cream increased aminolevulanic acid (ALA) uptake by the skin, such that ALA incubation times before application of the light source could be greatly compressed. But clinical outcomes were too unpredictable, he said at the seminar sponsored by Skin Disease Education Foundation (SDEF). After several patients had unintended florid full photopeels involving 1½ weeks of downtime, it was time to abandon the practice.
When ALA-PDT first appeared about 10 years ago, the indication was for the treatment of actinic keratoses (AKs). Today this approved indication remains the No. 1 reason Dr. Ross utilizes the therapy, he said. But PDT’s role has expanded off label to include cosmetic procedures and the treatment of warts, nonmelanoma skin cancer, nevus sebaceous, as well as acne, which he considers "one of the great opportunities for PDT." In addition, in Asia, dermatologists are now refining the use of PDT with hematoporphyrin derivatives for the treatment of port wine stains and other vascular lesions.
Many U.S. dermatologists have incorporated PDT into their practices, with ALA being more widely used as a photosensitizer than methyl aminolevulinate (MAL). Yet PDT is a therapy that hasn’t been fully optimized; it is still fraught with side effects and suboptimal results, he said. Moreover, some fundamental issues regarding PDT remain unanswered: For example, the optimal duration of photosensitizer incubation time for various indications is still controversial.
Dr. Ross said he opts for what he considers a middle-of-the-road approach, with ALA application times of about 90-120 minutes, which he views as having an optimal balance between side effects and effectiveness. Even so, he noted that among the 8-10 patients per week he treats with ALA-PDT on average, 1 or 2 experience mild side effects.
"I don’t think we’re quite ‘there’ yet with PDT, although we’re getting closer. There are still so many tricks involved in making it work without side effects. We’ve still got some work to do," he said.
In addition to advising his colleagues to stay away from topical anesthetic creams, he offered additional tips for the use of ALA-PDT. Among them:
• Sending acne into long-term remission via PDT remains the Holy Grail, he said. The objective is to enhance the fluorescence of protoporphyrin 9 at the sebaceous gland while sparing the epidermis.
Some investigators are using low-intensity blue light at the skin surface while the photosensitizer is incubating in order to bleach it out of the epidermis, or, alternatively, warming and cooling the skin.
The best results Dr. Ross said he has seen have come through an arduous regimen involving three 3-hour-long ALA applications scheduled a month apart. There’s a delayed effect, with significant improvement coming at 3-6 months.
"It’s a tough, tough therapy to get through. There are lots of pustules and papules, and the acne invariably gets worse before it gets better. This doesn’t play into the hands of the typical teenager, who wants to get better right away," Dr. Ross said.
• A creamy solution of ALA will create more protoporphyrin 9 than an aqueous solution will.
• A red light source should be considered for deeper structures, such as basal cell carcinomas or sebaceous glands, and blue light for treating more superficial skin lesions. Although continuous blue light is 40 times more potent per photon than red light in exciting protoporphyrin 9, it doesn’t penetrate as deeply.
• Performing low-density fractional CO2 ablative laser therapy prior to application of the photosensitizing agent is "an exciting advance" in PDT, he said.
The innovation was developed by an international team led by investigators at the Wellman Center for Photomedicine at Massachusetts General Hospital, Boston, who published a split-face randomized study involving 15 patients with a total of 212 facial AKs. At the 3-month follow-up, the complete response rate of grade II-III lesions treated with MAL-PDT preceded by fractional ablative laser therapy was 87.5%, vs. 58.8% with conventional MAL-PDT. The complete response rate of grade I AKs was 100% with fractional laser/MAL-PDT, vs. 79% for MAL-PDT alone.
The fractional laser–pretreated areas also displayed significantly greater improvement in photoaging and fewer new AKs at follow-up: 3, compared with 11. But these superior outcomes came at a price: higher pain scores during illumination and significantly worse erythema and crusting post treatment (Br. J. Dermatol. 2012 Feb. 20 [doi:10.1111/j.1365-2133.2012.10893.x]).
Fractional CO2 laser pretreatment enhances conversion of the photosensitizing agent to protoporphyrin 9, Dr. Ross explained. He compared the tiny holes in the skin created by the fractional laser to the process of aerating a lawn. The holes create conduits for the photosensitizer to bypass the stratum corneum, which is the major obstacle to uptake of ALA or MAL. Once the photosensitizer skips past the stratum corneum, it quickly spreads laterally throughout the epidermis.
However, Dr. Ross offered a note of caution regarding this novel approach. He said that he performed the therapy recently and found that 30 minutes of ALA incubation was too much.
"If you do these procedures, I would say go very light and just leave the ALA for less than 30 minutes to start, because the response you’re going to get when using a fractional laser beforehand is profound. It’s a huge difference," he said.
Dr. Ross reported that he serves as a consultant to and receives research support from Palomar. He also disclosed receiving research support from Candela, Cutera, Lumenis, Sciton, and Ulthera.
SDEF and this news organization are owned by Elsevier.
WAIKOLOA, HAWAII – Using EMLA or lidocaine cream in conjunction with topical 5-aminolevulinic acid photodynamic therapy may boost uptake of the photosensitizer, but the clinical outcomes can be unpredictable, according to Dr. E. Victor Ross.
"Our worst scenarios have been when we’ve used EMLA on the skin. We’ve stopped using EMLA or lidocaine cream on the skin in ALA-PDT because of the very pronounced, enhanced photodynamic effects. You get great long-term results, but such a bad short-term result that lots of people didn’t want to go through it," said Dr. Ross of Scripps Clinic Laser and Cosmetic Dermatology Center in Carmel Valley, Calif.
Using a topical numbing agent seemed to be an attractive option because patients often complain that photodynamic therapy (PDT) is painful. Plus, there seemed to be an added benefit: The anesthetic cream increased aminolevulanic acid (ALA) uptake by the skin, such that ALA incubation times before application of the light source could be greatly compressed. But clinical outcomes were too unpredictable, he said at the seminar sponsored by Skin Disease Education Foundation (SDEF). After several patients had unintended florid full photopeels involving 1½ weeks of downtime, it was time to abandon the practice.
When ALA-PDT first appeared about 10 years ago, the indication was for the treatment of actinic keratoses (AKs). Today this approved indication remains the No. 1 reason Dr. Ross utilizes the therapy, he said. But PDT’s role has expanded off label to include cosmetic procedures and the treatment of warts, nonmelanoma skin cancer, nevus sebaceous, as well as acne, which he considers "one of the great opportunities for PDT." In addition, in Asia, dermatologists are now refining the use of PDT with hematoporphyrin derivatives for the treatment of port wine stains and other vascular lesions.
Many U.S. dermatologists have incorporated PDT into their practices, with ALA being more widely used as a photosensitizer than methyl aminolevulinate (MAL). Yet PDT is a therapy that hasn’t been fully optimized; it is still fraught with side effects and suboptimal results, he said. Moreover, some fundamental issues regarding PDT remain unanswered: For example, the optimal duration of photosensitizer incubation time for various indications is still controversial.
Dr. Ross said he opts for what he considers a middle-of-the-road approach, with ALA application times of about 90-120 minutes, which he views as having an optimal balance between side effects and effectiveness. Even so, he noted that among the 8-10 patients per week he treats with ALA-PDT on average, 1 or 2 experience mild side effects.
"I don’t think we’re quite ‘there’ yet with PDT, although we’re getting closer. There are still so many tricks involved in making it work without side effects. We’ve still got some work to do," he said.
In addition to advising his colleagues to stay away from topical anesthetic creams, he offered additional tips for the use of ALA-PDT. Among them:
• Sending acne into long-term remission via PDT remains the Holy Grail, he said. The objective is to enhance the fluorescence of protoporphyrin 9 at the sebaceous gland while sparing the epidermis.
Some investigators are using low-intensity blue light at the skin surface while the photosensitizer is incubating in order to bleach it out of the epidermis, or, alternatively, warming and cooling the skin.
The best results Dr. Ross said he has seen have come through an arduous regimen involving three 3-hour-long ALA applications scheduled a month apart. There’s a delayed effect, with significant improvement coming at 3-6 months.
"It’s a tough, tough therapy to get through. There are lots of pustules and papules, and the acne invariably gets worse before it gets better. This doesn’t play into the hands of the typical teenager, who wants to get better right away," Dr. Ross said.
• A creamy solution of ALA will create more protoporphyrin 9 than an aqueous solution will.
• A red light source should be considered for deeper structures, such as basal cell carcinomas or sebaceous glands, and blue light for treating more superficial skin lesions. Although continuous blue light is 40 times more potent per photon than red light in exciting protoporphyrin 9, it doesn’t penetrate as deeply.
• Performing low-density fractional CO2 ablative laser therapy prior to application of the photosensitizing agent is "an exciting advance" in PDT, he said.
The innovation was developed by an international team led by investigators at the Wellman Center for Photomedicine at Massachusetts General Hospital, Boston, who published a split-face randomized study involving 15 patients with a total of 212 facial AKs. At the 3-month follow-up, the complete response rate of grade II-III lesions treated with MAL-PDT preceded by fractional ablative laser therapy was 87.5%, vs. 58.8% with conventional MAL-PDT. The complete response rate of grade I AKs was 100% with fractional laser/MAL-PDT, vs. 79% for MAL-PDT alone.
The fractional laser–pretreated areas also displayed significantly greater improvement in photoaging and fewer new AKs at follow-up: 3, compared with 11. But these superior outcomes came at a price: higher pain scores during illumination and significantly worse erythema and crusting post treatment (Br. J. Dermatol. 2012 Feb. 20 [doi:10.1111/j.1365-2133.2012.10893.x]).
Fractional CO2 laser pretreatment enhances conversion of the photosensitizing agent to protoporphyrin 9, Dr. Ross explained. He compared the tiny holes in the skin created by the fractional laser to the process of aerating a lawn. The holes create conduits for the photosensitizer to bypass the stratum corneum, which is the major obstacle to uptake of ALA or MAL. Once the photosensitizer skips past the stratum corneum, it quickly spreads laterally throughout the epidermis.
However, Dr. Ross offered a note of caution regarding this novel approach. He said that he performed the therapy recently and found that 30 minutes of ALA incubation was too much.
"If you do these procedures, I would say go very light and just leave the ALA for less than 30 minutes to start, because the response you’re going to get when using a fractional laser beforehand is profound. It’s a huge difference," he said.
Dr. Ross reported that he serves as a consultant to and receives research support from Palomar. He also disclosed receiving research support from Candela, Cutera, Lumenis, Sciton, and Ulthera.
SDEF and this news organization are owned by Elsevier.
WAIKOLOA, HAWAII – Using EMLA or lidocaine cream in conjunction with topical 5-aminolevulinic acid photodynamic therapy may boost uptake of the photosensitizer, but the clinical outcomes can be unpredictable, according to Dr. E. Victor Ross.
"Our worst scenarios have been when we’ve used EMLA on the skin. We’ve stopped using EMLA or lidocaine cream on the skin in ALA-PDT because of the very pronounced, enhanced photodynamic effects. You get great long-term results, but such a bad short-term result that lots of people didn’t want to go through it," said Dr. Ross of Scripps Clinic Laser and Cosmetic Dermatology Center in Carmel Valley, Calif.
Using a topical numbing agent seemed to be an attractive option because patients often complain that photodynamic therapy (PDT) is painful. Plus, there seemed to be an added benefit: The anesthetic cream increased aminolevulanic acid (ALA) uptake by the skin, such that ALA incubation times before application of the light source could be greatly compressed. But clinical outcomes were too unpredictable, he said at the seminar sponsored by Skin Disease Education Foundation (SDEF). After several patients had unintended florid full photopeels involving 1½ weeks of downtime, it was time to abandon the practice.
When ALA-PDT first appeared about 10 years ago, the indication was for the treatment of actinic keratoses (AKs). Today this approved indication remains the No. 1 reason Dr. Ross utilizes the therapy, he said. But PDT’s role has expanded off label to include cosmetic procedures and the treatment of warts, nonmelanoma skin cancer, nevus sebaceous, as well as acne, which he considers "one of the great opportunities for PDT." In addition, in Asia, dermatologists are now refining the use of PDT with hematoporphyrin derivatives for the treatment of port wine stains and other vascular lesions.
Many U.S. dermatologists have incorporated PDT into their practices, with ALA being more widely used as a photosensitizer than methyl aminolevulinate (MAL). Yet PDT is a therapy that hasn’t been fully optimized; it is still fraught with side effects and suboptimal results, he said. Moreover, some fundamental issues regarding PDT remain unanswered: For example, the optimal duration of photosensitizer incubation time for various indications is still controversial.
Dr. Ross said he opts for what he considers a middle-of-the-road approach, with ALA application times of about 90-120 minutes, which he views as having an optimal balance between side effects and effectiveness. Even so, he noted that among the 8-10 patients per week he treats with ALA-PDT on average, 1 or 2 experience mild side effects.
"I don’t think we’re quite ‘there’ yet with PDT, although we’re getting closer. There are still so many tricks involved in making it work without side effects. We’ve still got some work to do," he said.
In addition to advising his colleagues to stay away from topical anesthetic creams, he offered additional tips for the use of ALA-PDT. Among them:
• Sending acne into long-term remission via PDT remains the Holy Grail, he said. The objective is to enhance the fluorescence of protoporphyrin 9 at the sebaceous gland while sparing the epidermis.
Some investigators are using low-intensity blue light at the skin surface while the photosensitizer is incubating in order to bleach it out of the epidermis, or, alternatively, warming and cooling the skin.
The best results Dr. Ross said he has seen have come through an arduous regimen involving three 3-hour-long ALA applications scheduled a month apart. There’s a delayed effect, with significant improvement coming at 3-6 months.
"It’s a tough, tough therapy to get through. There are lots of pustules and papules, and the acne invariably gets worse before it gets better. This doesn’t play into the hands of the typical teenager, who wants to get better right away," Dr. Ross said.
• A creamy solution of ALA will create more protoporphyrin 9 than an aqueous solution will.
• A red light source should be considered for deeper structures, such as basal cell carcinomas or sebaceous glands, and blue light for treating more superficial skin lesions. Although continuous blue light is 40 times more potent per photon than red light in exciting protoporphyrin 9, it doesn’t penetrate as deeply.
• Performing low-density fractional CO2 ablative laser therapy prior to application of the photosensitizing agent is "an exciting advance" in PDT, he said.
The innovation was developed by an international team led by investigators at the Wellman Center for Photomedicine at Massachusetts General Hospital, Boston, who published a split-face randomized study involving 15 patients with a total of 212 facial AKs. At the 3-month follow-up, the complete response rate of grade II-III lesions treated with MAL-PDT preceded by fractional ablative laser therapy was 87.5%, vs. 58.8% with conventional MAL-PDT. The complete response rate of grade I AKs was 100% with fractional laser/MAL-PDT, vs. 79% for MAL-PDT alone.
The fractional laser–pretreated areas also displayed significantly greater improvement in photoaging and fewer new AKs at follow-up: 3, compared with 11. But these superior outcomes came at a price: higher pain scores during illumination and significantly worse erythema and crusting post treatment (Br. J. Dermatol. 2012 Feb. 20 [doi:10.1111/j.1365-2133.2012.10893.x]).
Fractional CO2 laser pretreatment enhances conversion of the photosensitizing agent to protoporphyrin 9, Dr. Ross explained. He compared the tiny holes in the skin created by the fractional laser to the process of aerating a lawn. The holes create conduits for the photosensitizer to bypass the stratum corneum, which is the major obstacle to uptake of ALA or MAL. Once the photosensitizer skips past the stratum corneum, it quickly spreads laterally throughout the epidermis.
However, Dr. Ross offered a note of caution regarding this novel approach. He said that he performed the therapy recently and found that 30 minutes of ALA incubation was too much.
"If you do these procedures, I would say go very light and just leave the ALA for less than 30 minutes to start, because the response you’re going to get when using a fractional laser beforehand is profound. It’s a huge difference," he said.
Dr. Ross reported that he serves as a consultant to and receives research support from Palomar. He also disclosed receiving research support from Candela, Cutera, Lumenis, Sciton, and Ulthera.
SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM THE SDEF HAWAII DERMATOLOGY SEMINAR
Don't Delay Psoriasis Treatment: The Skinny Podcast
In this month's program, Dr. Alexa B. Kimball discusses why psoriasis treatment shouldn't be delayed.
Dr. James M. Spencer offers his insights on the pros and cons of bringing radiation treatment back to the dermatologist's office.
Then, a marketing guru offers tips on how to keep cosmetic patients coming back.
Cosmetic counter host Dr. Lily Talakoub explains what it really means when a product claims to be all "natural."
And finally, Dr. Alan Rockoff shares one of the more humorous places people have gone to read his new book.
In this month's program, Dr. Alexa B. Kimball discusses why psoriasis treatment shouldn't be delayed.
Dr. James M. Spencer offers his insights on the pros and cons of bringing radiation treatment back to the dermatologist's office.
Then, a marketing guru offers tips on how to keep cosmetic patients coming back.
Cosmetic counter host Dr. Lily Talakoub explains what it really means when a product claims to be all "natural."
And finally, Dr. Alan Rockoff shares one of the more humorous places people have gone to read his new book.
In this month's program, Dr. Alexa B. Kimball discusses why psoriasis treatment shouldn't be delayed.
Dr. James M. Spencer offers his insights on the pros and cons of bringing radiation treatment back to the dermatologist's office.
Then, a marketing guru offers tips on how to keep cosmetic patients coming back.
Cosmetic counter host Dr. Lily Talakoub explains what it really means when a product claims to be all "natural."
And finally, Dr. Alan Rockoff shares one of the more humorous places people have gone to read his new book.
Mineral Makeup Is a Dermatologist's 'Fire Extinguisher'
WAIKOLOA, HAWAII – Mineral makeup has been game changing for everything from covering acne blemishes to masking postprocedure discoloration, noted Dr. Howard K. Steinman.
"Mineral makeup has done to medical makeup what fillers and Botox have done to the field of facial cosmetic surgery. You now have little excuse for not using makeup in your office," said Steinman, director of dermatologic and skin cancer surgery at Scott and White Medical Center, Temple, Texas.
Mineral makeup is easy for patients to learn how to apply effectively; anyone on the office staff can be trained to teach patients how, he said. The products take up a trivial amount of office space, cost very little, pose negligible risk, and generate considerable patient satisfaction.
"Mineral makeup achieves really spectacular results," said Dr. Steinman at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Patients go to a dermatologist because they want cure or control of a medical condition, symptomatic relief, and an improved appearance. But while successful treatment of melasma, for example, may take months, the patient’s appearance can be improved immediately in the interim – on day 1 of therapy –through the use of mineral makeup.
Mineral makeup provides complete coverage for macular medical conditions including acne erythema, rosacea, vitiligo, sarcoidosis, port wine stains, and spider vessels. These products are also the answer to postprocedure discoloration following chemical peels, laser resurfacing, and fillers.
"It’s your fire extinguisher for procedural misadventures. The nice thing about having mineral makeups in your office is you don’t have to worry about these things as much because the problem is going to leave the office fixed," Dr. Steinman explained.
Green-tinted concealer is a popular but ineffective solution for red discoloration of skin. The results tend to be muddy looking and unconvincing. Mineral makeup, he said, is far superior.
Dr. Steinman singled out four companies as the major players in the mineral makeup market: Youngblood, Bare Minerals, Color Science, and Jane Iredale. All have been in business a long time, offer products of excellent quality, and provide reasonably good service to physicians, he said.
He prefers Youngblood in his own office because his wife, a paramedical camouflage therapist trained to cover burn scars and disfiguring surgical wounds, prefers the quality.
"My suggestion is to have your esthetician, or whoever will be doing your makeup, try them all and decide which one they prefer," said Dr. Steinman.
He also recommends Dermacolor (Kryolan), a specialized camouflage foundation system made in Germany that is formulated for postoperative skin and contains an opaque sunscreen. Unlike mineral makeup, Dermacolor is waterproof even with swimming. The company offers more than 70 premixed colors, although a selection of about 20 is sufficient to cover virtually any clinical situation, he said.
Dr. Steinman suggested that the makeup artist match the patient’s skin tones before surgery so Dermacolor is ready to be applied at the first postoperative visit.
Dr. Steinman said a relatively new comprehensive line of makeup products he recommends is Cover FX. The product texture and coverage are outstanding, it’s easy for patients to apply, and the company caters to physicians, he said.
Camouflage makeup does have limitations. It won’t effectively cover three-dimensional lesions, such as acne scars or keloids. And it can’t do much for burn scars with absent hair and skin pores, he noted.
That being said, Dr. Steinman considers makeup in the office an indispensable part of his practice. "Makeup is just essential, I think, if you’re going to do cosmetic surgery or you want to treat patients with medical macular problems," he said.
Dr. Steinman reported having no financial relationships with any of the companies he discussed.
SDEF and this news organization are owned by Elsevier.
*This post was updated on 3/7/12.
WAIKOLOA, HAWAII – Mineral makeup has been game changing for everything from covering acne blemishes to masking postprocedure discoloration, noted Dr. Howard K. Steinman.
"Mineral makeup has done to medical makeup what fillers and Botox have done to the field of facial cosmetic surgery. You now have little excuse for not using makeup in your office," said Steinman, director of dermatologic and skin cancer surgery at Scott and White Medical Center, Temple, Texas.
Mineral makeup is easy for patients to learn how to apply effectively; anyone on the office staff can be trained to teach patients how, he said. The products take up a trivial amount of office space, cost very little, pose negligible risk, and generate considerable patient satisfaction.
"Mineral makeup achieves really spectacular results," said Dr. Steinman at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Patients go to a dermatologist because they want cure or control of a medical condition, symptomatic relief, and an improved appearance. But while successful treatment of melasma, for example, may take months, the patient’s appearance can be improved immediately in the interim – on day 1 of therapy –through the use of mineral makeup.
Mineral makeup provides complete coverage for macular medical conditions including acne erythema, rosacea, vitiligo, sarcoidosis, port wine stains, and spider vessels. These products are also the answer to postprocedure discoloration following chemical peels, laser resurfacing, and fillers.
"It’s your fire extinguisher for procedural misadventures. The nice thing about having mineral makeups in your office is you don’t have to worry about these things as much because the problem is going to leave the office fixed," Dr. Steinman explained.
Green-tinted concealer is a popular but ineffective solution for red discoloration of skin. The results tend to be muddy looking and unconvincing. Mineral makeup, he said, is far superior.
Dr. Steinman singled out four companies as the major players in the mineral makeup market: Youngblood, Bare Minerals, Color Science, and Jane Iredale. All have been in business a long time, offer products of excellent quality, and provide reasonably good service to physicians, he said.
He prefers Youngblood in his own office because his wife, a paramedical camouflage therapist trained to cover burn scars and disfiguring surgical wounds, prefers the quality.
"My suggestion is to have your esthetician, or whoever will be doing your makeup, try them all and decide which one they prefer," said Dr. Steinman.
He also recommends Dermacolor (Kryolan), a specialized camouflage foundation system made in Germany that is formulated for postoperative skin and contains an opaque sunscreen. Unlike mineral makeup, Dermacolor is waterproof even with swimming. The company offers more than 70 premixed colors, although a selection of about 20 is sufficient to cover virtually any clinical situation, he said.
Dr. Steinman suggested that the makeup artist match the patient’s skin tones before surgery so Dermacolor is ready to be applied at the first postoperative visit.
Dr. Steinman said a relatively new comprehensive line of makeup products he recommends is Cover FX. The product texture and coverage are outstanding, it’s easy for patients to apply, and the company caters to physicians, he said.
Camouflage makeup does have limitations. It won’t effectively cover three-dimensional lesions, such as acne scars or keloids. And it can’t do much for burn scars with absent hair and skin pores, he noted.
That being said, Dr. Steinman considers makeup in the office an indispensable part of his practice. "Makeup is just essential, I think, if you’re going to do cosmetic surgery or you want to treat patients with medical macular problems," he said.
Dr. Steinman reported having no financial relationships with any of the companies he discussed.
SDEF and this news organization are owned by Elsevier.
*This post was updated on 3/7/12.
WAIKOLOA, HAWAII – Mineral makeup has been game changing for everything from covering acne blemishes to masking postprocedure discoloration, noted Dr. Howard K. Steinman.
"Mineral makeup has done to medical makeup what fillers and Botox have done to the field of facial cosmetic surgery. You now have little excuse for not using makeup in your office," said Steinman, director of dermatologic and skin cancer surgery at Scott and White Medical Center, Temple, Texas.
Mineral makeup is easy for patients to learn how to apply effectively; anyone on the office staff can be trained to teach patients how, he said. The products take up a trivial amount of office space, cost very little, pose negligible risk, and generate considerable patient satisfaction.
"Mineral makeup achieves really spectacular results," said Dr. Steinman at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Patients go to a dermatologist because they want cure or control of a medical condition, symptomatic relief, and an improved appearance. But while successful treatment of melasma, for example, may take months, the patient’s appearance can be improved immediately in the interim – on day 1 of therapy –through the use of mineral makeup.
Mineral makeup provides complete coverage for macular medical conditions including acne erythema, rosacea, vitiligo, sarcoidosis, port wine stains, and spider vessels. These products are also the answer to postprocedure discoloration following chemical peels, laser resurfacing, and fillers.
"It’s your fire extinguisher for procedural misadventures. The nice thing about having mineral makeups in your office is you don’t have to worry about these things as much because the problem is going to leave the office fixed," Dr. Steinman explained.
Green-tinted concealer is a popular but ineffective solution for red discoloration of skin. The results tend to be muddy looking and unconvincing. Mineral makeup, he said, is far superior.
Dr. Steinman singled out four companies as the major players in the mineral makeup market: Youngblood, Bare Minerals, Color Science, and Jane Iredale. All have been in business a long time, offer products of excellent quality, and provide reasonably good service to physicians, he said.
He prefers Youngblood in his own office because his wife, a paramedical camouflage therapist trained to cover burn scars and disfiguring surgical wounds, prefers the quality.
"My suggestion is to have your esthetician, or whoever will be doing your makeup, try them all and decide which one they prefer," said Dr. Steinman.
He also recommends Dermacolor (Kryolan), a specialized camouflage foundation system made in Germany that is formulated for postoperative skin and contains an opaque sunscreen. Unlike mineral makeup, Dermacolor is waterproof even with swimming. The company offers more than 70 premixed colors, although a selection of about 20 is sufficient to cover virtually any clinical situation, he said.
Dr. Steinman suggested that the makeup artist match the patient’s skin tones before surgery so Dermacolor is ready to be applied at the first postoperative visit.
Dr. Steinman said a relatively new comprehensive line of makeup products he recommends is Cover FX. The product texture and coverage are outstanding, it’s easy for patients to apply, and the company caters to physicians, he said.
Camouflage makeup does have limitations. It won’t effectively cover three-dimensional lesions, such as acne scars or keloids. And it can’t do much for burn scars with absent hair and skin pores, he noted.
That being said, Dr. Steinman considers makeup in the office an indispensable part of his practice. "Makeup is just essential, I think, if you’re going to do cosmetic surgery or you want to treat patients with medical macular problems," he said.
Dr. Steinman reported having no financial relationships with any of the companies he discussed.
SDEF and this news organization are owned by Elsevier.
*This post was updated on 3/7/12.
EXPERT ANALYSIS FROM THE SDEF HAWAII DERMATOLOGY SEMINAR
Dial 'Derm' for Murder
Skin & Allergy News editor Amy Pfeiffer and Terry Rudd review hot news in dermatology with the experts in this month's Skinny Vodcast.
Skin & Allergy News editor Amy Pfeiffer and Terry Rudd review hot news in dermatology with the experts in this month's Skinny Vodcast.
Skin & Allergy News editor Amy Pfeiffer and Terry Rudd review hot news in dermatology with the experts in this month's Skinny Vodcast.
Several Sharp Needles Needed for Tear Trough Deformities
LAS VEGAS – When treating tear trough deformities with hyaluronic acid fillers, Dr. Suzan Obagi makes it a point to have a set of sharp 30-gauge needles handy.
"There’s nothing worse than trying to do a treatment in the periorbital region, and then have your needles dull," she said during a demonstration on dermal fillers at the annual meeting of the American Academy of Cosmetic Surgery. "This can cause discomfort for the patient and probably more bruising. In a single session I may go through four or five needles. You’re better off having a sharp needle handy."
Dr. Obagi, who directs the University of Pittsburgh Medical Center's Cosmetic Surgery and Skin Health Center, likes to have an assistant on hand during periorbital injections of hyaluronic acid fillers, "so if you need to finish one side, the assistant can hold very gentle pressure on the treated area to minimize swelling and bruising," she said. "What you don’t want to do is push too hard. You’re in an area where you can easily move this filler to different regions. It should always be very light pressure on the area. I always tell patients not to rub or massage for 24 hours after the injection."
Some clinicians will treat the tear trough deformity without treating the rest of the orbital rim, she continued. "If patients have volume loss, it’s not just going to be the tear trough; it’s going to continue out to the sides of the orbit rim, especially in older patients," she said. "So it’s important to build up that area as well."
Dr. Obagi, who is also the immediate past vice president of the American Board of Cosmetic Surgery, prefers to use hyaluronic acid fillers that are smaller in particle size such as Medicis’ Restylane for tear trough deformities, adding lidocaine plus epinephrine prior to injection. "I use 0.3 mL 1% lidocaine with epinephrine and 0.2 mL sodium bicarbonate, and I use a Luer lock adapter to mix them together," she said. "I’m going to be working in an area where I want no bruising; in order to do that I need the epinephrine in there."
Dr. Obagi said that she had no relevant financial conflicts to disclose.
LAS VEGAS – When treating tear trough deformities with hyaluronic acid fillers, Dr. Suzan Obagi makes it a point to have a set of sharp 30-gauge needles handy.
"There’s nothing worse than trying to do a treatment in the periorbital region, and then have your needles dull," she said during a demonstration on dermal fillers at the annual meeting of the American Academy of Cosmetic Surgery. "This can cause discomfort for the patient and probably more bruising. In a single session I may go through four or five needles. You’re better off having a sharp needle handy."
Dr. Obagi, who directs the University of Pittsburgh Medical Center's Cosmetic Surgery and Skin Health Center, likes to have an assistant on hand during periorbital injections of hyaluronic acid fillers, "so if you need to finish one side, the assistant can hold very gentle pressure on the treated area to minimize swelling and bruising," she said. "What you don’t want to do is push too hard. You’re in an area where you can easily move this filler to different regions. It should always be very light pressure on the area. I always tell patients not to rub or massage for 24 hours after the injection."
Some clinicians will treat the tear trough deformity without treating the rest of the orbital rim, she continued. "If patients have volume loss, it’s not just going to be the tear trough; it’s going to continue out to the sides of the orbit rim, especially in older patients," she said. "So it’s important to build up that area as well."
Dr. Obagi, who is also the immediate past vice president of the American Board of Cosmetic Surgery, prefers to use hyaluronic acid fillers that are smaller in particle size such as Medicis’ Restylane for tear trough deformities, adding lidocaine plus epinephrine prior to injection. "I use 0.3 mL 1% lidocaine with epinephrine and 0.2 mL sodium bicarbonate, and I use a Luer lock adapter to mix them together," she said. "I’m going to be working in an area where I want no bruising; in order to do that I need the epinephrine in there."
Dr. Obagi said that she had no relevant financial conflicts to disclose.
LAS VEGAS – When treating tear trough deformities with hyaluronic acid fillers, Dr. Suzan Obagi makes it a point to have a set of sharp 30-gauge needles handy.
"There’s nothing worse than trying to do a treatment in the periorbital region, and then have your needles dull," she said during a demonstration on dermal fillers at the annual meeting of the American Academy of Cosmetic Surgery. "This can cause discomfort for the patient and probably more bruising. In a single session I may go through four or five needles. You’re better off having a sharp needle handy."
Dr. Obagi, who directs the University of Pittsburgh Medical Center's Cosmetic Surgery and Skin Health Center, likes to have an assistant on hand during periorbital injections of hyaluronic acid fillers, "so if you need to finish one side, the assistant can hold very gentle pressure on the treated area to minimize swelling and bruising," she said. "What you don’t want to do is push too hard. You’re in an area where you can easily move this filler to different regions. It should always be very light pressure on the area. I always tell patients not to rub or massage for 24 hours after the injection."
Some clinicians will treat the tear trough deformity without treating the rest of the orbital rim, she continued. "If patients have volume loss, it’s not just going to be the tear trough; it’s going to continue out to the sides of the orbit rim, especially in older patients," she said. "So it’s important to build up that area as well."
Dr. Obagi, who is also the immediate past vice president of the American Board of Cosmetic Surgery, prefers to use hyaluronic acid fillers that are smaller in particle size such as Medicis’ Restylane for tear trough deformities, adding lidocaine plus epinephrine prior to injection. "I use 0.3 mL 1% lidocaine with epinephrine and 0.2 mL sodium bicarbonate, and I use a Luer lock adapter to mix them together," she said. "I’m going to be working in an area where I want no bruising; in order to do that I need the epinephrine in there."
Dr. Obagi said that she had no relevant financial conflicts to disclose.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF COSMETIC SURGERY