User login
Reactions to HPV Vaccine Found Brief, Minor
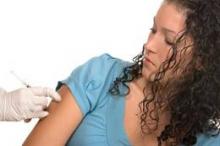
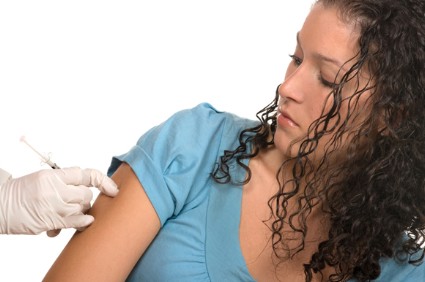
In a vaccine safety study, routine administration of the quadrivalent HPV vaccine was associated with only two minor short-term adverse events: syncope on the day of vaccination and skin infection during the 2 weeks thereafter, according to a report published online Oct. 1 in Archives of Pediatric and Adolescent Research.
"No other safety signals or potential signals following HPV4 were identified, including hospitalization/ED visits associated with autoimmune conditions" or any of the other categories of adverse outcomes they examined, said Dr. Nicola P. Klein of the Kaiser Permanente Vaccine Study Center, Oakland, Calif., and her associates.
"These findings support the general safety of routine vaccination with HPV4 to prevent cancer," they noted.
In the retrospective, observational study funded and largely designed by Merck, manufacturer of the Gardasil vaccine, Dr. Klein and her colleagues assessed the short-term safety of HPV4 administered to girls, adolescents, and young women during the course of routine clinical care at two large California HMOs from August 2006 through March 2008. This included all 189,629 females aged 9-26 years who received at least 1 dose of the vaccine during that time, with an additional detailed analysis of the 44,001 females who received all three doses.
All of the study subjects’ hospital and emergency department visits during the 60 days following vaccination were assessed, and the reasons for the visits were categorized according to the Healthcare Cost and Utilization Project’s (HCUP) list of 265 adverse health outcomes. The results for three risk intervals – the day of the vaccine, the 2 weeks following vaccination, and the 60 days following vaccination – were compared with those of a control interval remote from the vaccination date.
In an initial analysis of the data, 50 of these categories showed significantly elevated odds of an association with the vaccine during one or more of these risk intervals. But a detailed review of subjects’ medical records revealed that most of the diagnoses in these categories were present before the vaccine was administered; in other words, they were preexisting conditions. Only syncope and skin infections remained significantly associated with the vaccine after adjustment for these factors.
When the data were further analyzed by vaccine dose, only syncope on the day of vaccination and skin infection during the 2 weeks after vaccination remained significant.
"The association between HPV4 and syncope was not unexpected. Immunization and injections in general have a known association with syncope (particularly in this age group)," Dr. Klein and her associates said (Arch. Pediatr. Adolesc. Med. 2012 Oct. 1 [doi:10.1001/archpediatrics.2012.1451]).
Likewise, some illnesses categorized as "skin infections" may have been local injection-site reactions. But a more detailed review of the subjects’ medical records suggested that there was also a "real" increase in their seeking of medical care for skin conditions following vaccination. The reason for this association remains unknown, but it may be related to the fact that clinical visits in general tend to increase immediately following any injection, the researchers said.
Of note, there were no associations between vaccination and any serious adverse effects such as autoimmune disorders, venous embolism, thromboembolic events, clotting dysfunction, or anaphylaxis, they added.
This study did not address longer-term adverse responses to HPV4 vaccination. Even though the study population was quite large, the study also may have been underpowered to detect extremely rare reactions to the vaccine. "Ongoing monitoring of spontaneous reports and other sources such as the Vaccine Safety Datalink will further contribute to HPV4’s safety profile," Dr. Klein and her associates said.
This study was funded by Merck, which also "provided substantial input into the study design and analytic plan." Dr. Klein reported ties to Merck, GlaxoSmithKline, Pfizer, Novartis, and Sanofi-Pasteur, and a number of the other researchers reported ties to Merck.
In a vaccine safety study, routine administration of the quadrivalent HPV vaccine was associated with only two minor short-term adverse events: syncope on the day of vaccination and skin infection during the 2 weeks thereafter, according to a report published online Oct. 1 in Archives of Pediatric and Adolescent Research.
"No other safety signals or potential signals following HPV4 were identified, including hospitalization/ED visits associated with autoimmune conditions" or any of the other categories of adverse outcomes they examined, said Dr. Nicola P. Klein of the Kaiser Permanente Vaccine Study Center, Oakland, Calif., and her associates.
"These findings support the general safety of routine vaccination with HPV4 to prevent cancer," they noted.
In the retrospective, observational study funded and largely designed by Merck, manufacturer of the Gardasil vaccine, Dr. Klein and her colleagues assessed the short-term safety of HPV4 administered to girls, adolescents, and young women during the course of routine clinical care at two large California HMOs from August 2006 through March 2008. This included all 189,629 females aged 9-26 years who received at least 1 dose of the vaccine during that time, with an additional detailed analysis of the 44,001 females who received all three doses.
All of the study subjects’ hospital and emergency department visits during the 60 days following vaccination were assessed, and the reasons for the visits were categorized according to the Healthcare Cost and Utilization Project’s (HCUP) list of 265 adverse health outcomes. The results for three risk intervals – the day of the vaccine, the 2 weeks following vaccination, and the 60 days following vaccination – were compared with those of a control interval remote from the vaccination date.
In an initial analysis of the data, 50 of these categories showed significantly elevated odds of an association with the vaccine during one or more of these risk intervals. But a detailed review of subjects’ medical records revealed that most of the diagnoses in these categories were present before the vaccine was administered; in other words, they were preexisting conditions. Only syncope and skin infections remained significantly associated with the vaccine after adjustment for these factors.
When the data were further analyzed by vaccine dose, only syncope on the day of vaccination and skin infection during the 2 weeks after vaccination remained significant.
"The association between HPV4 and syncope was not unexpected. Immunization and injections in general have a known association with syncope (particularly in this age group)," Dr. Klein and her associates said (Arch. Pediatr. Adolesc. Med. 2012 Oct. 1 [doi:10.1001/archpediatrics.2012.1451]).
Likewise, some illnesses categorized as "skin infections" may have been local injection-site reactions. But a more detailed review of the subjects’ medical records suggested that there was also a "real" increase in their seeking of medical care for skin conditions following vaccination. The reason for this association remains unknown, but it may be related to the fact that clinical visits in general tend to increase immediately following any injection, the researchers said.
Of note, there were no associations between vaccination and any serious adverse effects such as autoimmune disorders, venous embolism, thromboembolic events, clotting dysfunction, or anaphylaxis, they added.
This study did not address longer-term adverse responses to HPV4 vaccination. Even though the study population was quite large, the study also may have been underpowered to detect extremely rare reactions to the vaccine. "Ongoing monitoring of spontaneous reports and other sources such as the Vaccine Safety Datalink will further contribute to HPV4’s safety profile," Dr. Klein and her associates said.
This study was funded by Merck, which also "provided substantial input into the study design and analytic plan." Dr. Klein reported ties to Merck, GlaxoSmithKline, Pfizer, Novartis, and Sanofi-Pasteur, and a number of the other researchers reported ties to Merck.
In a vaccine safety study, routine administration of the quadrivalent HPV vaccine was associated with only two minor short-term adverse events: syncope on the day of vaccination and skin infection during the 2 weeks thereafter, according to a report published online Oct. 1 in Archives of Pediatric and Adolescent Research.
"No other safety signals or potential signals following HPV4 were identified, including hospitalization/ED visits associated with autoimmune conditions" or any of the other categories of adverse outcomes they examined, said Dr. Nicola P. Klein of the Kaiser Permanente Vaccine Study Center, Oakland, Calif., and her associates.
"These findings support the general safety of routine vaccination with HPV4 to prevent cancer," they noted.
In the retrospective, observational study funded and largely designed by Merck, manufacturer of the Gardasil vaccine, Dr. Klein and her colleagues assessed the short-term safety of HPV4 administered to girls, adolescents, and young women during the course of routine clinical care at two large California HMOs from August 2006 through March 2008. This included all 189,629 females aged 9-26 years who received at least 1 dose of the vaccine during that time, with an additional detailed analysis of the 44,001 females who received all three doses.
All of the study subjects’ hospital and emergency department visits during the 60 days following vaccination were assessed, and the reasons for the visits were categorized according to the Healthcare Cost and Utilization Project’s (HCUP) list of 265 adverse health outcomes. The results for three risk intervals – the day of the vaccine, the 2 weeks following vaccination, and the 60 days following vaccination – were compared with those of a control interval remote from the vaccination date.
In an initial analysis of the data, 50 of these categories showed significantly elevated odds of an association with the vaccine during one or more of these risk intervals. But a detailed review of subjects’ medical records revealed that most of the diagnoses in these categories were present before the vaccine was administered; in other words, they were preexisting conditions. Only syncope and skin infections remained significantly associated with the vaccine after adjustment for these factors.
When the data were further analyzed by vaccine dose, only syncope on the day of vaccination and skin infection during the 2 weeks after vaccination remained significant.
"The association between HPV4 and syncope was not unexpected. Immunization and injections in general have a known association with syncope (particularly in this age group)," Dr. Klein and her associates said (Arch. Pediatr. Adolesc. Med. 2012 Oct. 1 [doi:10.1001/archpediatrics.2012.1451]).
Likewise, some illnesses categorized as "skin infections" may have been local injection-site reactions. But a more detailed review of the subjects’ medical records suggested that there was also a "real" increase in their seeking of medical care for skin conditions following vaccination. The reason for this association remains unknown, but it may be related to the fact that clinical visits in general tend to increase immediately following any injection, the researchers said.
Of note, there were no associations between vaccination and any serious adverse effects such as autoimmune disorders, venous embolism, thromboembolic events, clotting dysfunction, or anaphylaxis, they added.
This study did not address longer-term adverse responses to HPV4 vaccination. Even though the study population was quite large, the study also may have been underpowered to detect extremely rare reactions to the vaccine. "Ongoing monitoring of spontaneous reports and other sources such as the Vaccine Safety Datalink will further contribute to HPV4’s safety profile," Dr. Klein and her associates said.
This study was funded by Merck, which also "provided substantial input into the study design and analytic plan." Dr. Klein reported ties to Merck, GlaxoSmithKline, Pfizer, Novartis, and Sanofi-Pasteur, and a number of the other researchers reported ties to Merck.
FROM ARCHIVES OF PEDIATRIC AND ADOLESCENT MEDICINE
Major Finding: Only 2 of 265 possible categories of short-term adverse effects were found to be significantly associated with routine HPV4 vaccination: syncope and skin infections.
Data Source: A retrospective, observational cohort study involving 189,629 females aged 9-26 years who received at least 1 dose of the HPV4 vaccine in 2006-2008 at two large HMOs.
Disclosures: This study was funded by Merck, which also "provided substantial input into the study design and analytic plan." Dr. Klein reported ties to Merck, GlaxoSmithKline, Pfizer, Novartis, and Sanofi-Pasteur, and a number of the other researchers reported ties to Merck.
Doctors May Commonly Misdiagnose Creutzfeldt-Jakob Disease
Few patients with sporadic Creutzfeldt-Jakob disease appear to receive a correct diagnosis when first assessed by a physician, and many receive multiple misdiagnoses until finally being correctly diagnosed two-thirds of the way through the course of the fatal disease.
In a case series of 97 patients with the disease, only 17 (18%) were correctly diagnosed when first assessed by a physician. The average patient received four misdiagnoses and endured 8 months of evaluation before Creutzfeldt-Jakob disease (CJD) was finally identified, according to the report, published online Sept. 24 in Archives of Neurology.
CJD, which is almost always fatal within 1 year, can be difficult to diagnose because early symptoms and signs are so variable and are easily mistaken for those of other neurodegenerative conditions. But the "lack of recognition of this condition in the medical community" is also to blame, especially the fact that many physicians aren’t aware that diffusion-weighted MRI has a sensitivity of 91%-96% and a specificity of 91%-95% in differentiating CJD from other brain disorders, said Dr. Ross W. Paterson of the department of neurology, University of California, San Francisco, and his associates.
The investigators described their study as the first large-scale examination "of pathologically proven cases of spontaneous CJD that retrospectively determines what misdiagnoses are made in the work-up of [the disease], who makes these misdiagnoses, and how long it takes to reach the correct diagnosis."
A total of 76% of the patients in this study were first assessed by internists (40%) or neurologists (36%), comprising "the vast majority of the physicians making the misdiagnoses," the researchers noted. In 73% of the cases, a neurologist was the first specialist to perform an assessment.
Dr. Paterson and his colleagues studied the issue because they had observed that many families of patients referred to the UCSF Memory and Aging Center complained about the typical delay in diagnosis. Their loved ones had been subjected to extensive and costly evaluations for other conditions, and the families had failed to be protected from a transmissible prion disease. And the delay had deflected both patients and families from focusing on palliative care and end of life planning for this incurable disease.
The 40 female and 57 male subjects were treated at UCSF in 2001-2007. Their ages ranged from 26 to 83 years, with a mean age of 62 years.
Before being correctly diagnosed, the study subjects had received 373 misdiagnoses, with an average of approximately 4 per patient. Of 16 possible categories of disease under which they were misdiagnosed, the most frequent categories were neurodegenerative, autoimmune, infectious, toxic/metabolic, and "unknown dementia."
The most common individual misdiagnosis was viral encephalitis, most likely because of "the multifocality, acuity, and rapidity of symptoms seen in CJD," Dr. Paterson and his associates said (Arch. Neurol. 2012 Sept. 24 [doi:10.1001/2013.jamaneurol.79]).
In addition to internists and neurologists, a smattering of other physicians also misdiagnosed CJD when patients first presented with symptoms. These included six ophthalmologists, four psychiatrists, four cardiologists, two otolaryngologists, two orthopedists, and one neuro-oncologist.
The results of this study indicate that sporadic CJD should be considered "in any patient with a rapidly progressive dementia who has been given multiple potential diagnoses," such as those with neurodegenerative, autoimmune, infectious, or toxic/metabolic etiologies, the investigators wrote. And "if evidence to support a diagnosis of viral encephalitis, paraneoplastic disorder, depression, peripheral vertigo, Alzheimer’s disease, stroke, dementia (nonspecified), CNS vasculitis, peripheral neuropathy, or Hashimoto encephalopathy is lacking, then the clinician should think about requesting an MRI with diffusion-weighted imaging/apparent diffusion coefficient sequences to look for changes associated with sporadic CJD," they noted.
Moreover, since many radiology reports miss the pathognomonic MRI findings of CJD, "it is critical that physicians be aware of MRI findings in prion disease and read their patients’ MRIs [themselves]," Dr. Paterson and his associates added.
Although this study targeted patients with CJD, misdiagnosing CJD in a patient who has a different etiology for their rapidly progressive dementia is just as harmful, because many of these other dementias are treatable. A recent study demonstrated that 32% of patients referred to the National Prion Disease Pathology Surveillance Center for autopsy because of suspected CJD were actually found to have other diagnoses. A total of 7% had had a treatable etiology but went untreated because they were mistakenly diagnosed as having CJD, Dr. Paterson and his associates noted.
It is also incumbent on physicians to make the correct diagnosis so that transmission of this prion disease is avoided – particularly transmission via contaminated surgical equipment or medical procedures, they added.
This study was supported by the National Institute on Aging, the National Institute of Neurological Disorders and Stroke, the Michael J. Homer Family Fund, the National Center for Research Resources, and the John Douglas French Alzheimer’s Foundation. One of Dr. Paterson’s associates reported ties to TauRx Pharmaceuticals, Bristol-Myers Squibb, Siemens Molecular Imaging, and Allon Therapeutics.
Dr. Paterson and his associates at a major referral center for patients with suspected Creutzfeldt-Jakob disease should be commended for illustrating the diagnostic journey these patients and their families must travel "on their way to a final and very unfortunate diagnosis," said Dr. Richard J. Caselli.
|
|
|
Dr. Richard J. Caselli
|
Many of the most common alternative diagnoses can share many of the same features of CJD, including even MRI mimics, such as "anoxia/ischemia, viral encephalitis (acutely), and focal status epilepticus," which can usually be distinguished from CJD by the clinical context, he wrote.
"Most health care expenditures occur during the final year of life, and CJD is no exception to this general rule. As we attempt to rein in health care costs while sacrificing no degree of medical accuracy or compassion, we owe it to our patients and to society to have the necessary knowledge to consider the diagnosis, establish the diagnosis as efficiently as possible, and then work with patients, families, and palliative care providers to maximize the quality of life for our dying patients," he said.
Richard J. Caselli, M.D., is a professor of neurology at the Mayo Clinic in Scottsdale, Ariz. He reported no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Paterson’s report (Arch. Neurol. 2012 [doi:10.1001/2013.jamaneurol.1]).
Dr. Paterson and his associates at a major referral center for patients with suspected Creutzfeldt-Jakob disease should be commended for illustrating the diagnostic journey these patients and their families must travel "on their way to a final and very unfortunate diagnosis," said Dr. Richard J. Caselli.
|
|
|
Dr. Richard J. Caselli
|
Many of the most common alternative diagnoses can share many of the same features of CJD, including even MRI mimics, such as "anoxia/ischemia, viral encephalitis (acutely), and focal status epilepticus," which can usually be distinguished from CJD by the clinical context, he wrote.
"Most health care expenditures occur during the final year of life, and CJD is no exception to this general rule. As we attempt to rein in health care costs while sacrificing no degree of medical accuracy or compassion, we owe it to our patients and to society to have the necessary knowledge to consider the diagnosis, establish the diagnosis as efficiently as possible, and then work with patients, families, and palliative care providers to maximize the quality of life for our dying patients," he said.
Richard J. Caselli, M.D., is a professor of neurology at the Mayo Clinic in Scottsdale, Ariz. He reported no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Paterson’s report (Arch. Neurol. 2012 [doi:10.1001/2013.jamaneurol.1]).
Dr. Paterson and his associates at a major referral center for patients with suspected Creutzfeldt-Jakob disease should be commended for illustrating the diagnostic journey these patients and their families must travel "on their way to a final and very unfortunate diagnosis," said Dr. Richard J. Caselli.
|
|
|
Dr. Richard J. Caselli
|
Many of the most common alternative diagnoses can share many of the same features of CJD, including even MRI mimics, such as "anoxia/ischemia, viral encephalitis (acutely), and focal status epilepticus," which can usually be distinguished from CJD by the clinical context, he wrote.
"Most health care expenditures occur during the final year of life, and CJD is no exception to this general rule. As we attempt to rein in health care costs while sacrificing no degree of medical accuracy or compassion, we owe it to our patients and to society to have the necessary knowledge to consider the diagnosis, establish the diagnosis as efficiently as possible, and then work with patients, families, and palliative care providers to maximize the quality of life for our dying patients," he said.
Richard J. Caselli, M.D., is a professor of neurology at the Mayo Clinic in Scottsdale, Ariz. He reported no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Paterson’s report (Arch. Neurol. 2012 [doi:10.1001/2013.jamaneurol.1]).
Few patients with sporadic Creutzfeldt-Jakob disease appear to receive a correct diagnosis when first assessed by a physician, and many receive multiple misdiagnoses until finally being correctly diagnosed two-thirds of the way through the course of the fatal disease.
In a case series of 97 patients with the disease, only 17 (18%) were correctly diagnosed when first assessed by a physician. The average patient received four misdiagnoses and endured 8 months of evaluation before Creutzfeldt-Jakob disease (CJD) was finally identified, according to the report, published online Sept. 24 in Archives of Neurology.
CJD, which is almost always fatal within 1 year, can be difficult to diagnose because early symptoms and signs are so variable and are easily mistaken for those of other neurodegenerative conditions. But the "lack of recognition of this condition in the medical community" is also to blame, especially the fact that many physicians aren’t aware that diffusion-weighted MRI has a sensitivity of 91%-96% and a specificity of 91%-95% in differentiating CJD from other brain disorders, said Dr. Ross W. Paterson of the department of neurology, University of California, San Francisco, and his associates.
The investigators described their study as the first large-scale examination "of pathologically proven cases of spontaneous CJD that retrospectively determines what misdiagnoses are made in the work-up of [the disease], who makes these misdiagnoses, and how long it takes to reach the correct diagnosis."
A total of 76% of the patients in this study were first assessed by internists (40%) or neurologists (36%), comprising "the vast majority of the physicians making the misdiagnoses," the researchers noted. In 73% of the cases, a neurologist was the first specialist to perform an assessment.
Dr. Paterson and his colleagues studied the issue because they had observed that many families of patients referred to the UCSF Memory and Aging Center complained about the typical delay in diagnosis. Their loved ones had been subjected to extensive and costly evaluations for other conditions, and the families had failed to be protected from a transmissible prion disease. And the delay had deflected both patients and families from focusing on palliative care and end of life planning for this incurable disease.
The 40 female and 57 male subjects were treated at UCSF in 2001-2007. Their ages ranged from 26 to 83 years, with a mean age of 62 years.
Before being correctly diagnosed, the study subjects had received 373 misdiagnoses, with an average of approximately 4 per patient. Of 16 possible categories of disease under which they were misdiagnosed, the most frequent categories were neurodegenerative, autoimmune, infectious, toxic/metabolic, and "unknown dementia."
The most common individual misdiagnosis was viral encephalitis, most likely because of "the multifocality, acuity, and rapidity of symptoms seen in CJD," Dr. Paterson and his associates said (Arch. Neurol. 2012 Sept. 24 [doi:10.1001/2013.jamaneurol.79]).
In addition to internists and neurologists, a smattering of other physicians also misdiagnosed CJD when patients first presented with symptoms. These included six ophthalmologists, four psychiatrists, four cardiologists, two otolaryngologists, two orthopedists, and one neuro-oncologist.
The results of this study indicate that sporadic CJD should be considered "in any patient with a rapidly progressive dementia who has been given multiple potential diagnoses," such as those with neurodegenerative, autoimmune, infectious, or toxic/metabolic etiologies, the investigators wrote. And "if evidence to support a diagnosis of viral encephalitis, paraneoplastic disorder, depression, peripheral vertigo, Alzheimer’s disease, stroke, dementia (nonspecified), CNS vasculitis, peripheral neuropathy, or Hashimoto encephalopathy is lacking, then the clinician should think about requesting an MRI with diffusion-weighted imaging/apparent diffusion coefficient sequences to look for changes associated with sporadic CJD," they noted.
Moreover, since many radiology reports miss the pathognomonic MRI findings of CJD, "it is critical that physicians be aware of MRI findings in prion disease and read their patients’ MRIs [themselves]," Dr. Paterson and his associates added.
Although this study targeted patients with CJD, misdiagnosing CJD in a patient who has a different etiology for their rapidly progressive dementia is just as harmful, because many of these other dementias are treatable. A recent study demonstrated that 32% of patients referred to the National Prion Disease Pathology Surveillance Center for autopsy because of suspected CJD were actually found to have other diagnoses. A total of 7% had had a treatable etiology but went untreated because they were mistakenly diagnosed as having CJD, Dr. Paterson and his associates noted.
It is also incumbent on physicians to make the correct diagnosis so that transmission of this prion disease is avoided – particularly transmission via contaminated surgical equipment or medical procedures, they added.
This study was supported by the National Institute on Aging, the National Institute of Neurological Disorders and Stroke, the Michael J. Homer Family Fund, the National Center for Research Resources, and the John Douglas French Alzheimer’s Foundation. One of Dr. Paterson’s associates reported ties to TauRx Pharmaceuticals, Bristol-Myers Squibb, Siemens Molecular Imaging, and Allon Therapeutics.
Few patients with sporadic Creutzfeldt-Jakob disease appear to receive a correct diagnosis when first assessed by a physician, and many receive multiple misdiagnoses until finally being correctly diagnosed two-thirds of the way through the course of the fatal disease.
In a case series of 97 patients with the disease, only 17 (18%) were correctly diagnosed when first assessed by a physician. The average patient received four misdiagnoses and endured 8 months of evaluation before Creutzfeldt-Jakob disease (CJD) was finally identified, according to the report, published online Sept. 24 in Archives of Neurology.
CJD, which is almost always fatal within 1 year, can be difficult to diagnose because early symptoms and signs are so variable and are easily mistaken for those of other neurodegenerative conditions. But the "lack of recognition of this condition in the medical community" is also to blame, especially the fact that many physicians aren’t aware that diffusion-weighted MRI has a sensitivity of 91%-96% and a specificity of 91%-95% in differentiating CJD from other brain disorders, said Dr. Ross W. Paterson of the department of neurology, University of California, San Francisco, and his associates.
The investigators described their study as the first large-scale examination "of pathologically proven cases of spontaneous CJD that retrospectively determines what misdiagnoses are made in the work-up of [the disease], who makes these misdiagnoses, and how long it takes to reach the correct diagnosis."
A total of 76% of the patients in this study were first assessed by internists (40%) or neurologists (36%), comprising "the vast majority of the physicians making the misdiagnoses," the researchers noted. In 73% of the cases, a neurologist was the first specialist to perform an assessment.
Dr. Paterson and his colleagues studied the issue because they had observed that many families of patients referred to the UCSF Memory and Aging Center complained about the typical delay in diagnosis. Their loved ones had been subjected to extensive and costly evaluations for other conditions, and the families had failed to be protected from a transmissible prion disease. And the delay had deflected both patients and families from focusing on palliative care and end of life planning for this incurable disease.
The 40 female and 57 male subjects were treated at UCSF in 2001-2007. Their ages ranged from 26 to 83 years, with a mean age of 62 years.
Before being correctly diagnosed, the study subjects had received 373 misdiagnoses, with an average of approximately 4 per patient. Of 16 possible categories of disease under which they were misdiagnosed, the most frequent categories were neurodegenerative, autoimmune, infectious, toxic/metabolic, and "unknown dementia."
The most common individual misdiagnosis was viral encephalitis, most likely because of "the multifocality, acuity, and rapidity of symptoms seen in CJD," Dr. Paterson and his associates said (Arch. Neurol. 2012 Sept. 24 [doi:10.1001/2013.jamaneurol.79]).
In addition to internists and neurologists, a smattering of other physicians also misdiagnosed CJD when patients first presented with symptoms. These included six ophthalmologists, four psychiatrists, four cardiologists, two otolaryngologists, two orthopedists, and one neuro-oncologist.
The results of this study indicate that sporadic CJD should be considered "in any patient with a rapidly progressive dementia who has been given multiple potential diagnoses," such as those with neurodegenerative, autoimmune, infectious, or toxic/metabolic etiologies, the investigators wrote. And "if evidence to support a diagnosis of viral encephalitis, paraneoplastic disorder, depression, peripheral vertigo, Alzheimer’s disease, stroke, dementia (nonspecified), CNS vasculitis, peripheral neuropathy, or Hashimoto encephalopathy is lacking, then the clinician should think about requesting an MRI with diffusion-weighted imaging/apparent diffusion coefficient sequences to look for changes associated with sporadic CJD," they noted.
Moreover, since many radiology reports miss the pathognomonic MRI findings of CJD, "it is critical that physicians be aware of MRI findings in prion disease and read their patients’ MRIs [themselves]," Dr. Paterson and his associates added.
Although this study targeted patients with CJD, misdiagnosing CJD in a patient who has a different etiology for their rapidly progressive dementia is just as harmful, because many of these other dementias are treatable. A recent study demonstrated that 32% of patients referred to the National Prion Disease Pathology Surveillance Center for autopsy because of suspected CJD were actually found to have other diagnoses. A total of 7% had had a treatable etiology but went untreated because they were mistakenly diagnosed as having CJD, Dr. Paterson and his associates noted.
It is also incumbent on physicians to make the correct diagnosis so that transmission of this prion disease is avoided – particularly transmission via contaminated surgical equipment or medical procedures, they added.
This study was supported by the National Institute on Aging, the National Institute of Neurological Disorders and Stroke, the Michael J. Homer Family Fund, the National Center for Research Resources, and the John Douglas French Alzheimer’s Foundation. One of Dr. Paterson’s associates reported ties to TauRx Pharmaceuticals, Bristol-Myers Squibb, Siemens Molecular Imaging, and Allon Therapeutics.
FROM THE ARCHIVES OF NEUROLOGY
Major Finding: There were 373 misdiagnoses in this series of 97 patients with spontaneous CJD, and only 17 patients were correctly diagnosed when first evaluated by a physician, who was an internist in 40% of cases and a neurologist in 36%.
Data Source: Results were taken from a retrospective analysis of the medical records of 97 adults with CJD who were seen over a 5-year period at a major referral center for diseases of memory and aging.
Disclosures: This study was supported by the National Institute on Aging, the National Institute of Neurological Disorders and Stroke, the Michael J. Homer Family Fund, the National Center for Research Resources, and the John Douglas French Alzheimer's Foundation. One of Dr. Paterson’s associates reported ties to TauRx Pharmaceuticals, Bristol-Myers Squibb, Siemens Molecular Imaging, and Allon Therapeutics.
Active Surveillance Favored for Low-Risk Prostate Cancer
Compared with immediate radical prostatectomy, active surveillance for men with low-risk prostate cancer produces only a "very modest" 1.8-month decrease in cancer-specific survival, according to a report published online Sept. 24 in Clinical Cancer Research.
However, men on active surveillance enjoyed 6 more years of life free from treatment and its adverse effects than men who had immediate surgery, said Dr. Ruth Etzioni of the division of public health services, Fred Hutchinson Cancer Research Center, Seattle, and her associates.
These are the findings of a new simulation model they developed to predict prostate cancer mortality in a virtual population of 1 million contemporary U.S. cases, using the best available data from contemporary studies of the issue.
The investigators first incorporated into their simulation model the findings from an active surveillance program in which men with low-risk prostate cancer are biopsied every year and referred for further treatment if any adverse changes are found. This program also allows patients to self-refer for further treatment for several other reasons, including if their prostate-specific antigen level rises or if they become too anxious over "watchful waiting."
The researchers then incorporated into the model information from a large longitudinal database on the interval between radical prostatectomy and recurrence. The Cancer of the Prostate Strategic Urologic Research Endeavor (CaPSURE) database enrolled nearly 14,000 men treated at 40 urology practices, and included 1,000 clinical and patient variables.
Lastly, Dr. Etzioni and her colleagues used data from another cohort study of 3,470 men to model the time from prostate cancer recurrence until death. They then computed the cumulative cancer-specific mortality in their virtual cohort for men under active surveillance compared with men who underwent immediate radical prostatectomy.
The model projected that the 20-year cumulative rate of prostate cancer–specific mortality would be 2.78% with active surveillance and 1.64% with immediate radical prostatectomy. This corresponded with an average of 1.8 months of life saved per case, which was considered a "very modest" advantage, the investigators said (Clin. Cancer Res. 2012 Sept. 24 [doi:10.1158/1078-0432.CCR-12-1502]).
However, the model also showed that men on active surveillance "had on average 6.4 more years of life free from treatment and its side effects," which could be a substantial advantage.
Three separate sensitivity analyses demonstrated that the model’s projections were robust even when multiple variables were altered. "All sensitivity analyses produced only modest differences in cumulative prostate cancer mortality under active surveillance, and supported our projection that active surveillance would have a minimal impact on life expectancy for low-risk cancer cases," Dr. Etzioni and her associates said.
"Ultimately, the model predicts that approximately 64% of men on active surveillance would be treated [for prostate cancer] within their lifetimes. ... Thus, under active surveillance, 36% of men could avoid being treated," they said.
These findings are consistent with those of at least one other modeling study and with those of the longitudinal PIVOT (Prostate Cancer Intervention versus Observation Trial) study that tracked disease-free survival for 12 years.
"Although this is not a new result, it is confirmation of what we expected, and it substantiates data from previous studies looking at watchful waiting. Very few men with low-risk disease die from prostate cancer regardless, and the difference between treatments appears to be very modest," Dr. Etzioni said in a press statement accompanying this report.
This study was supported by the National Cancer Institute and the Centers for Disease Control and Prevention. No financial conflicts of interest were reported.
Compared with immediate radical prostatectomy, active surveillance for men with low-risk prostate cancer produces only a "very modest" 1.8-month decrease in cancer-specific survival, according to a report published online Sept. 24 in Clinical Cancer Research.
However, men on active surveillance enjoyed 6 more years of life free from treatment and its adverse effects than men who had immediate surgery, said Dr. Ruth Etzioni of the division of public health services, Fred Hutchinson Cancer Research Center, Seattle, and her associates.
These are the findings of a new simulation model they developed to predict prostate cancer mortality in a virtual population of 1 million contemporary U.S. cases, using the best available data from contemporary studies of the issue.
The investigators first incorporated into their simulation model the findings from an active surveillance program in which men with low-risk prostate cancer are biopsied every year and referred for further treatment if any adverse changes are found. This program also allows patients to self-refer for further treatment for several other reasons, including if their prostate-specific antigen level rises or if they become too anxious over "watchful waiting."
The researchers then incorporated into the model information from a large longitudinal database on the interval between radical prostatectomy and recurrence. The Cancer of the Prostate Strategic Urologic Research Endeavor (CaPSURE) database enrolled nearly 14,000 men treated at 40 urology practices, and included 1,000 clinical and patient variables.
Lastly, Dr. Etzioni and her colleagues used data from another cohort study of 3,470 men to model the time from prostate cancer recurrence until death. They then computed the cumulative cancer-specific mortality in their virtual cohort for men under active surveillance compared with men who underwent immediate radical prostatectomy.
The model projected that the 20-year cumulative rate of prostate cancer–specific mortality would be 2.78% with active surveillance and 1.64% with immediate radical prostatectomy. This corresponded with an average of 1.8 months of life saved per case, which was considered a "very modest" advantage, the investigators said (Clin. Cancer Res. 2012 Sept. 24 [doi:10.1158/1078-0432.CCR-12-1502]).
However, the model also showed that men on active surveillance "had on average 6.4 more years of life free from treatment and its side effects," which could be a substantial advantage.
Three separate sensitivity analyses demonstrated that the model’s projections were robust even when multiple variables were altered. "All sensitivity analyses produced only modest differences in cumulative prostate cancer mortality under active surveillance, and supported our projection that active surveillance would have a minimal impact on life expectancy for low-risk cancer cases," Dr. Etzioni and her associates said.
"Ultimately, the model predicts that approximately 64% of men on active surveillance would be treated [for prostate cancer] within their lifetimes. ... Thus, under active surveillance, 36% of men could avoid being treated," they said.
These findings are consistent with those of at least one other modeling study and with those of the longitudinal PIVOT (Prostate Cancer Intervention versus Observation Trial) study that tracked disease-free survival for 12 years.
"Although this is not a new result, it is confirmation of what we expected, and it substantiates data from previous studies looking at watchful waiting. Very few men with low-risk disease die from prostate cancer regardless, and the difference between treatments appears to be very modest," Dr. Etzioni said in a press statement accompanying this report.
This study was supported by the National Cancer Institute and the Centers for Disease Control and Prevention. No financial conflicts of interest were reported.
Compared with immediate radical prostatectomy, active surveillance for men with low-risk prostate cancer produces only a "very modest" 1.8-month decrease in cancer-specific survival, according to a report published online Sept. 24 in Clinical Cancer Research.
However, men on active surveillance enjoyed 6 more years of life free from treatment and its adverse effects than men who had immediate surgery, said Dr. Ruth Etzioni of the division of public health services, Fred Hutchinson Cancer Research Center, Seattle, and her associates.
These are the findings of a new simulation model they developed to predict prostate cancer mortality in a virtual population of 1 million contemporary U.S. cases, using the best available data from contemporary studies of the issue.
The investigators first incorporated into their simulation model the findings from an active surveillance program in which men with low-risk prostate cancer are biopsied every year and referred for further treatment if any adverse changes are found. This program also allows patients to self-refer for further treatment for several other reasons, including if their prostate-specific antigen level rises or if they become too anxious over "watchful waiting."
The researchers then incorporated into the model information from a large longitudinal database on the interval between radical prostatectomy and recurrence. The Cancer of the Prostate Strategic Urologic Research Endeavor (CaPSURE) database enrolled nearly 14,000 men treated at 40 urology practices, and included 1,000 clinical and patient variables.
Lastly, Dr. Etzioni and her colleagues used data from another cohort study of 3,470 men to model the time from prostate cancer recurrence until death. They then computed the cumulative cancer-specific mortality in their virtual cohort for men under active surveillance compared with men who underwent immediate radical prostatectomy.
The model projected that the 20-year cumulative rate of prostate cancer–specific mortality would be 2.78% with active surveillance and 1.64% with immediate radical prostatectomy. This corresponded with an average of 1.8 months of life saved per case, which was considered a "very modest" advantage, the investigators said (Clin. Cancer Res. 2012 Sept. 24 [doi:10.1158/1078-0432.CCR-12-1502]).
However, the model also showed that men on active surveillance "had on average 6.4 more years of life free from treatment and its side effects," which could be a substantial advantage.
Three separate sensitivity analyses demonstrated that the model’s projections were robust even when multiple variables were altered. "All sensitivity analyses produced only modest differences in cumulative prostate cancer mortality under active surveillance, and supported our projection that active surveillance would have a minimal impact on life expectancy for low-risk cancer cases," Dr. Etzioni and her associates said.
"Ultimately, the model predicts that approximately 64% of men on active surveillance would be treated [for prostate cancer] within their lifetimes. ... Thus, under active surveillance, 36% of men could avoid being treated," they said.
These findings are consistent with those of at least one other modeling study and with those of the longitudinal PIVOT (Prostate Cancer Intervention versus Observation Trial) study that tracked disease-free survival for 12 years.
"Although this is not a new result, it is confirmation of what we expected, and it substantiates data from previous studies looking at watchful waiting. Very few men with low-risk disease die from prostate cancer regardless, and the difference between treatments appears to be very modest," Dr. Etzioni said in a press statement accompanying this report.
This study was supported by the National Cancer Institute and the Centers for Disease Control and Prevention. No financial conflicts of interest were reported.
FROM CLINICAL CANCER RESEARCH
Major Finding: The predicted 20-year cumulative rate of prostate cancer–specific mortality showed 1.8 months of life saved per patient who chose surgery over watchful waiting, but the watchful waiting group benefited from 6.4 more years of freedom from treatment and treatment-related side effects.
Data Source: Investigators ran a simulation model that predicted prostate cancer–specific mortality in a virtual population of 1,000 U.S. men with low-risk disease.
Disclosures: This study was supported by the National Cancer Institute and the Centers for Disease Control and Prevention. No financial conflicts of interest were reported.
Hypoglycemia in ICU Patients Strongly Linked to Death
Hypoglycemia in patients in the intensive care unit is strongly associated with increased mortality, according to a subanalysis of the NICE-SUGAR trial published online Sept. 19 in the New England Journal of Medicine.
Researchers performed a more detailed, post hoc analysis of data collected in the previously published NICE-SUGAR (Normoglycemia in Intensive Care Evaluation–Survival Using Glucose Algorithm Regulation) trial, in which ICU patients assigned to intensive glucose control had a significant, 14% increased risk of death, compared with those assigned to conventional treatment (N. Engl. J. Med. 2009;360:1283-97).
In this analysis, the investigators confirmed that both moderate and severe hypoglycemia were significantly more common in ICU patients randomly assigned to receive intensive glucose control than in those assigned to receive conventional glucose control, and that hypoglycemia – in either group – was significantly linked to mortality.
Moreover, the findings show that there is a dose-response relationship between the intensity of glucose control and the rates of hypoglycemia and of death, that the association is consistent across several subgroups of patients, and that the link is strongest for death caused by distributive (vasodilative) shock. All of these findings point to a causal relationship between hypoglycemia and adverse outcomes, but causality cannot be proved because of the design of this study, said Dr. Simon Finfer, of the NICE-SUGAR writing committee and Royal North Shore Hospital and the George Institute for Global Health, University of Sydney, and his associates.
Nevertheless, "it would seem rather prudent to ensure that strategies for managing blood glucose concentration in critically ill patients focus not only on the control of hyperglycemia but also on avoidance of both moderate and severe hypoglycemia," they noted.
Hyperglycemia occurs frequently in ICU patients and is associated with increased morbidity and mortality. A study published in 2001 suggested that intensive glucose control, using insulin if necessary, reduced that morbidity and mortality (N. Engl. J. Med. 2001;345:1359-67), and the practice became widespread.
From that point until the publication of the NICE-SUGAR study in 2009, glucose control in hospital patients was primarily aimed at avoiding hyperglycemia. But NICE-SUGAR and other studies prompted a revision of guidelines for inpatient glycemic control with an increased focus on avoiding hypoglycemia (Diabetes Care 2009;32:1119-31).
For the current analysis, the NICE-SUGAR investigators looked at the associations between moderate hypoglycemia (blood glucose 41-70 mg/dL) and severe hypoglycemia (40 mg/dL or below) and death in 6,026 of the study subjects, who had been randomized to receive either intensive blood glucose control, with a target blood glucose range of 81-108 mg/dL, or conventional control, with a target of 180 mg/dL.
Moderate hypoglycemia developed 45% of patients, and severe hypoglycemia occurred in 3.7% of patients. Broken down by treatment group, moderate hypoglycemia occurred in 74% of the intensive-control group and 16% of the conventional-control group; severe hypoglycemia developed in 6.9% and 0.5%, respectively.
Overall mortality was 26.2%. Mortality in the 3,089 patients with no hypoglycemia was 23.5%. That rate was 28.5% in the 2,714 patients who developed moderate hypoglycemia and 35.4% in the 223 who developed severe hypoglycemia, for highly significant adjusted hazard ratios of 1.41 and 2.10, respectively. The association was stronger in patients whose hypoglycemia lasted more than 1 day than in those with shorter durations of hypoglycemia.
"Even after adjustment for events occurring after the first episode of hypoglycemia, moderate hypoglycemia was associated with an increase in the risk of death of 40%, and severe hypoglycemia with a doubling of the risk," Dr. Finfer and his colleagues said (N. Engl. J. Med. 2012;367:1108-18 [doi: 10.1056/NEJMoa1204942]).
The link between hypoglycemia and death also was robust across subgroups of patients, including patients who had underlying diabetes and those who did not have underlying diabetes.
In a minority of patients, hypoglycemia appears to be a marker, rather than a cause, of an increased risk of death. In these cases it probably signals very severe underlying disease processes and impending death, the investigators said.
This study was supported by the Australian National Health and Medical Research Council, the Health Research Council of New Zealand, and the Canadian Institutes of Health Research. Dr. Finfer reported ties to Edwards, and his associates reported ties to Fresenius Kabi, AstraZeneca, and Eisai.
Intensive glucose control aimed at achieving very low blood glucose levels in ICU patients should now be considered unacceptable, "and older, nonchalant attitudes need to be abandoned," said Dr. Irl B. Hirsch.
Instead, "maintaining blood glucose at levels similar to those in the conventional-control group of the NICE-SUGAR population is safe," and is consistent with existing guidelines recommending 140-180 mg/dL (Diabetes Care 2009;32:1119-31). "Continued assessment of the quality of care and the appropriate use of insulin protocol should be the standard for every ICU," he said.
Dr. Hirsch is professor of medicine at the University of Washington, Seattle. He reported ties to Johnson & Johnson, Roche, Abbott, CellNovo, Sanofi, and Halozyme. These remarks were taken from his editorial comment accompanying Dr. Finfer’s report (N. Engl. J. Med. 2012 Sept. 19 [doi: 10.1056/NEJMe1208208]).
Intensive glucose control aimed at achieving very low blood glucose levels in ICU patients should now be considered unacceptable, "and older, nonchalant attitudes need to be abandoned," said Dr. Irl B. Hirsch.
Instead, "maintaining blood glucose at levels similar to those in the conventional-control group of the NICE-SUGAR population is safe," and is consistent with existing guidelines recommending 140-180 mg/dL (Diabetes Care 2009;32:1119-31). "Continued assessment of the quality of care and the appropriate use of insulin protocol should be the standard for every ICU," he said.
Dr. Hirsch is professor of medicine at the University of Washington, Seattle. He reported ties to Johnson & Johnson, Roche, Abbott, CellNovo, Sanofi, and Halozyme. These remarks were taken from his editorial comment accompanying Dr. Finfer’s report (N. Engl. J. Med. 2012 Sept. 19 [doi: 10.1056/NEJMe1208208]).
Intensive glucose control aimed at achieving very low blood glucose levels in ICU patients should now be considered unacceptable, "and older, nonchalant attitudes need to be abandoned," said Dr. Irl B. Hirsch.
Instead, "maintaining blood glucose at levels similar to those in the conventional-control group of the NICE-SUGAR population is safe," and is consistent with existing guidelines recommending 140-180 mg/dL (Diabetes Care 2009;32:1119-31). "Continued assessment of the quality of care and the appropriate use of insulin protocol should be the standard for every ICU," he said.
Dr. Hirsch is professor of medicine at the University of Washington, Seattle. He reported ties to Johnson & Johnson, Roche, Abbott, CellNovo, Sanofi, and Halozyme. These remarks were taken from his editorial comment accompanying Dr. Finfer’s report (N. Engl. J. Med. 2012 Sept. 19 [doi: 10.1056/NEJMe1208208]).
Hypoglycemia in patients in the intensive care unit is strongly associated with increased mortality, according to a subanalysis of the NICE-SUGAR trial published online Sept. 19 in the New England Journal of Medicine.
Researchers performed a more detailed, post hoc analysis of data collected in the previously published NICE-SUGAR (Normoglycemia in Intensive Care Evaluation–Survival Using Glucose Algorithm Regulation) trial, in which ICU patients assigned to intensive glucose control had a significant, 14% increased risk of death, compared with those assigned to conventional treatment (N. Engl. J. Med. 2009;360:1283-97).
In this analysis, the investigators confirmed that both moderate and severe hypoglycemia were significantly more common in ICU patients randomly assigned to receive intensive glucose control than in those assigned to receive conventional glucose control, and that hypoglycemia – in either group – was significantly linked to mortality.
Moreover, the findings show that there is a dose-response relationship between the intensity of glucose control and the rates of hypoglycemia and of death, that the association is consistent across several subgroups of patients, and that the link is strongest for death caused by distributive (vasodilative) shock. All of these findings point to a causal relationship between hypoglycemia and adverse outcomes, but causality cannot be proved because of the design of this study, said Dr. Simon Finfer, of the NICE-SUGAR writing committee and Royal North Shore Hospital and the George Institute for Global Health, University of Sydney, and his associates.
Nevertheless, "it would seem rather prudent to ensure that strategies for managing blood glucose concentration in critically ill patients focus not only on the control of hyperglycemia but also on avoidance of both moderate and severe hypoglycemia," they noted.
Hyperglycemia occurs frequently in ICU patients and is associated with increased morbidity and mortality. A study published in 2001 suggested that intensive glucose control, using insulin if necessary, reduced that morbidity and mortality (N. Engl. J. Med. 2001;345:1359-67), and the practice became widespread.
From that point until the publication of the NICE-SUGAR study in 2009, glucose control in hospital patients was primarily aimed at avoiding hyperglycemia. But NICE-SUGAR and other studies prompted a revision of guidelines for inpatient glycemic control with an increased focus on avoiding hypoglycemia (Diabetes Care 2009;32:1119-31).
For the current analysis, the NICE-SUGAR investigators looked at the associations between moderate hypoglycemia (blood glucose 41-70 mg/dL) and severe hypoglycemia (40 mg/dL or below) and death in 6,026 of the study subjects, who had been randomized to receive either intensive blood glucose control, with a target blood glucose range of 81-108 mg/dL, or conventional control, with a target of 180 mg/dL.
Moderate hypoglycemia developed 45% of patients, and severe hypoglycemia occurred in 3.7% of patients. Broken down by treatment group, moderate hypoglycemia occurred in 74% of the intensive-control group and 16% of the conventional-control group; severe hypoglycemia developed in 6.9% and 0.5%, respectively.
Overall mortality was 26.2%. Mortality in the 3,089 patients with no hypoglycemia was 23.5%. That rate was 28.5% in the 2,714 patients who developed moderate hypoglycemia and 35.4% in the 223 who developed severe hypoglycemia, for highly significant adjusted hazard ratios of 1.41 and 2.10, respectively. The association was stronger in patients whose hypoglycemia lasted more than 1 day than in those with shorter durations of hypoglycemia.
"Even after adjustment for events occurring after the first episode of hypoglycemia, moderate hypoglycemia was associated with an increase in the risk of death of 40%, and severe hypoglycemia with a doubling of the risk," Dr. Finfer and his colleagues said (N. Engl. J. Med. 2012;367:1108-18 [doi: 10.1056/NEJMoa1204942]).
The link between hypoglycemia and death also was robust across subgroups of patients, including patients who had underlying diabetes and those who did not have underlying diabetes.
In a minority of patients, hypoglycemia appears to be a marker, rather than a cause, of an increased risk of death. In these cases it probably signals very severe underlying disease processes and impending death, the investigators said.
This study was supported by the Australian National Health and Medical Research Council, the Health Research Council of New Zealand, and the Canadian Institutes of Health Research. Dr. Finfer reported ties to Edwards, and his associates reported ties to Fresenius Kabi, AstraZeneca, and Eisai.
Hypoglycemia in patients in the intensive care unit is strongly associated with increased mortality, according to a subanalysis of the NICE-SUGAR trial published online Sept. 19 in the New England Journal of Medicine.
Researchers performed a more detailed, post hoc analysis of data collected in the previously published NICE-SUGAR (Normoglycemia in Intensive Care Evaluation–Survival Using Glucose Algorithm Regulation) trial, in which ICU patients assigned to intensive glucose control had a significant, 14% increased risk of death, compared with those assigned to conventional treatment (N. Engl. J. Med. 2009;360:1283-97).
In this analysis, the investigators confirmed that both moderate and severe hypoglycemia were significantly more common in ICU patients randomly assigned to receive intensive glucose control than in those assigned to receive conventional glucose control, and that hypoglycemia – in either group – was significantly linked to mortality.
Moreover, the findings show that there is a dose-response relationship between the intensity of glucose control and the rates of hypoglycemia and of death, that the association is consistent across several subgroups of patients, and that the link is strongest for death caused by distributive (vasodilative) shock. All of these findings point to a causal relationship between hypoglycemia and adverse outcomes, but causality cannot be proved because of the design of this study, said Dr. Simon Finfer, of the NICE-SUGAR writing committee and Royal North Shore Hospital and the George Institute for Global Health, University of Sydney, and his associates.
Nevertheless, "it would seem rather prudent to ensure that strategies for managing blood glucose concentration in critically ill patients focus not only on the control of hyperglycemia but also on avoidance of both moderate and severe hypoglycemia," they noted.
Hyperglycemia occurs frequently in ICU patients and is associated with increased morbidity and mortality. A study published in 2001 suggested that intensive glucose control, using insulin if necessary, reduced that morbidity and mortality (N. Engl. J. Med. 2001;345:1359-67), and the practice became widespread.
From that point until the publication of the NICE-SUGAR study in 2009, glucose control in hospital patients was primarily aimed at avoiding hyperglycemia. But NICE-SUGAR and other studies prompted a revision of guidelines for inpatient glycemic control with an increased focus on avoiding hypoglycemia (Diabetes Care 2009;32:1119-31).
For the current analysis, the NICE-SUGAR investigators looked at the associations between moderate hypoglycemia (blood glucose 41-70 mg/dL) and severe hypoglycemia (40 mg/dL or below) and death in 6,026 of the study subjects, who had been randomized to receive either intensive blood glucose control, with a target blood glucose range of 81-108 mg/dL, or conventional control, with a target of 180 mg/dL.
Moderate hypoglycemia developed 45% of patients, and severe hypoglycemia occurred in 3.7% of patients. Broken down by treatment group, moderate hypoglycemia occurred in 74% of the intensive-control group and 16% of the conventional-control group; severe hypoglycemia developed in 6.9% and 0.5%, respectively.
Overall mortality was 26.2%. Mortality in the 3,089 patients with no hypoglycemia was 23.5%. That rate was 28.5% in the 2,714 patients who developed moderate hypoglycemia and 35.4% in the 223 who developed severe hypoglycemia, for highly significant adjusted hazard ratios of 1.41 and 2.10, respectively. The association was stronger in patients whose hypoglycemia lasted more than 1 day than in those with shorter durations of hypoglycemia.
"Even after adjustment for events occurring after the first episode of hypoglycemia, moderate hypoglycemia was associated with an increase in the risk of death of 40%, and severe hypoglycemia with a doubling of the risk," Dr. Finfer and his colleagues said (N. Engl. J. Med. 2012;367:1108-18 [doi: 10.1056/NEJMoa1204942]).
The link between hypoglycemia and death also was robust across subgroups of patients, including patients who had underlying diabetes and those who did not have underlying diabetes.
In a minority of patients, hypoglycemia appears to be a marker, rather than a cause, of an increased risk of death. In these cases it probably signals very severe underlying disease processes and impending death, the investigators said.
This study was supported by the Australian National Health and Medical Research Council, the Health Research Council of New Zealand, and the Canadian Institutes of Health Research. Dr. Finfer reported ties to Edwards, and his associates reported ties to Fresenius Kabi, AstraZeneca, and Eisai.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: Mortality was 28.5% in 2,714 ICU patients who developed moderate hypoglycemia and 35.4% in the 223 who developed severe hypoglycemia, for highly significant adjusted hazard ratios of 1.41 and 2.10, respectively.
Data Source: This was a post hoc analysis of 3,013 ICU patients in the NICE-SUGAR trial who received intensive glucose control and 3,013 who received conventional glucose control during treatment at 42 hospitals.
Disclosures: This study was supported by the Australian National Health and Medical Research Council, the Health Research Council of New Zealand, and the Canadian Institutes of Health Research. Dr. Finfer reported ties to Edwards, and his associates reported ties to Fresenius Kabi, AstraZeneca, and Eisai.
DNA Alone Inadequate to Identify HPV-Related Cancers
Testing for the presence of human papillomavirus DNA alone, especially using polymerase chain reaction methods, is not adequate to identify which head and neck squamous cell carcinomas are caused by the virus, according to two studies published online Sept. 18 in Cancer Research.
Identifying HPV-driven malignancies is important because they respond better to treatment and have better outcomes than those unrelated to HPV infection. Indeed, treatment of head and neck squamous cell carcinoma (HNSCC) may soon be guided by the tumor’s HPV status, since trials are now underway to determine whether de-escalation of chemo- and radiotherapy is safe and effective in such patients.
At present, however, the biomarkers that are best suited to making this identification are unclear.
Case Series Assesses Biomarkers
In the first study, researchers assessed the usefulness of four biomarkers in determining which HNSCCs in a case series were driven by HPV. They began by examining fresh-frozen tumor biopsy samples from 199 German adults diagnosed as having oropharyngeal squamous cell cancer between 1990 and 2008.
The four biomarkers were HPV-16 viral load, viral oncogene RNA (E6 and E7), p16INK4a, and RNA patterns similar to those characteristic of cervical carcinomas (CxCa RNA), said Dr. Dana Holzinger of the German Cancer Research Center at Heidelberg (Germany) University and her associates.
The simple presence of HPV DNA in a tumor sample was found to be a poor indicator of prognosis, likely because it often signaled past HPV infections or recent oral exposure, rather than active HPV infection that progressed to malignancy, the investigators said (Cancer Res. 2012 Sept. 18 [doi: 10.1158/0008-5472.CAN-11-3934]).
Instead, "we showed that high viral load and a cancer-specific pattern of viral gene expression are most suited to identify patients with HPV-driven tumors among patients with oropharyngeal cancer. Viral expression pattern is a completely new marker in this field, and viral load has hardly been analyzed before," Dr. Holzinger said in a press statement accompanying the publication of these findings.
"Once standardized assays for these markers, applicable in routine clinical laboratories, are established, they will allow precise identification" of cancers that are or are not HPV-driven, which will in turn influence prognosis and treatment, she added.
Results Back Combination Approach
In the second study, Dr. Caihua Liang of Brown University, Providence, R.I., and her associates examined 488 HNSCC samples as well as serum samples collected in a population-based study in the Boston area during 1999-2003.
As in the first study, these investigators found that the mere presence of HPV-16 DNA in these tumors, particularly when detected by PCR analysis, did not accurately predict overall survival or progression-free survival.
Instead, "our study strongly suggests that the combination of detection of HPV-16 DNA in HNSCC tumors [plus] p16 immunostaining with E6/E7 antibodies represents the most clinically valuable surrogate marker for the identification of patients . . . who have a better prognosis," they said (Cancer Res. 2012 Sept. 28 [doi: 10.1158/0008-5472.CAN-11-3277]).
"Assessment of HPV DNA using polymerase chain reaction methods as a biomarker in individual head and neck cancers is a poor predictor of outcome, and is also poorly associated with antibody response indicative of exposure and/or infection by HPV," senior author Dr. Karl T. Kelsey added in the press statement.
"We may not be diagnosing these tumors as accurately and precisely as we need to for adjusting treatments," said Dr. Kelsey, a professor in the department of epidemiology and the department of pathology and laboratory medicine at Brown University.
Dr. Holzinger’s study was funded in part by the European Commission, BMBG/HGAF-Canceropole Grand-Est, and the German Research Foundation. Her associates reported ties to Qiagen and Roche. Dr. Liang’s study was supported by the National Institutes of Health and the Flight Attendant Medical Research Institute, and one associate reported ties to Bristol-Myers Squibb.
Both of these studies demonstrate that the HPV DNA status of head and neck squamous cell carcinomas should be interpreted with caution, said Dr. Eduardo Mendez.
"Further testing to confirm HPV active infection may be warranted, particularly in consideration of de-escalation regimens," he said. In addition, other prognostic factors should be taken into account, such as tumor classification and lymph node status.
Dr. Mendez is at the University of Washington/Fred Hutchinson Cancer Research Center, Seattle. He reported ties to Intuitive Surgical. These remarks were taken from his commentary accompanying Dr. Holzinger’s and Dr. Liang’s reports (Cancer Res. 2012 Sept. 18 [doi: 10.1158/0008-5472.CAN-12-3285]).
Both of these studies demonstrate that the HPV DNA status of head and neck squamous cell carcinomas should be interpreted with caution, said Dr. Eduardo Mendez.
"Further testing to confirm HPV active infection may be warranted, particularly in consideration of de-escalation regimens," he said. In addition, other prognostic factors should be taken into account, such as tumor classification and lymph node status.
Dr. Mendez is at the University of Washington/Fred Hutchinson Cancer Research Center, Seattle. He reported ties to Intuitive Surgical. These remarks were taken from his commentary accompanying Dr. Holzinger’s and Dr. Liang’s reports (Cancer Res. 2012 Sept. 18 [doi: 10.1158/0008-5472.CAN-12-3285]).
Both of these studies demonstrate that the HPV DNA status of head and neck squamous cell carcinomas should be interpreted with caution, said Dr. Eduardo Mendez.
"Further testing to confirm HPV active infection may be warranted, particularly in consideration of de-escalation regimens," he said. In addition, other prognostic factors should be taken into account, such as tumor classification and lymph node status.
Dr. Mendez is at the University of Washington/Fred Hutchinson Cancer Research Center, Seattle. He reported ties to Intuitive Surgical. These remarks were taken from his commentary accompanying Dr. Holzinger’s and Dr. Liang’s reports (Cancer Res. 2012 Sept. 18 [doi: 10.1158/0008-5472.CAN-12-3285]).
Testing for the presence of human papillomavirus DNA alone, especially using polymerase chain reaction methods, is not adequate to identify which head and neck squamous cell carcinomas are caused by the virus, according to two studies published online Sept. 18 in Cancer Research.
Identifying HPV-driven malignancies is important because they respond better to treatment and have better outcomes than those unrelated to HPV infection. Indeed, treatment of head and neck squamous cell carcinoma (HNSCC) may soon be guided by the tumor’s HPV status, since trials are now underway to determine whether de-escalation of chemo- and radiotherapy is safe and effective in such patients.
At present, however, the biomarkers that are best suited to making this identification are unclear.
Case Series Assesses Biomarkers
In the first study, researchers assessed the usefulness of four biomarkers in determining which HNSCCs in a case series were driven by HPV. They began by examining fresh-frozen tumor biopsy samples from 199 German adults diagnosed as having oropharyngeal squamous cell cancer between 1990 and 2008.
The four biomarkers were HPV-16 viral load, viral oncogene RNA (E6 and E7), p16INK4a, and RNA patterns similar to those characteristic of cervical carcinomas (CxCa RNA), said Dr. Dana Holzinger of the German Cancer Research Center at Heidelberg (Germany) University and her associates.
The simple presence of HPV DNA in a tumor sample was found to be a poor indicator of prognosis, likely because it often signaled past HPV infections or recent oral exposure, rather than active HPV infection that progressed to malignancy, the investigators said (Cancer Res. 2012 Sept. 18 [doi: 10.1158/0008-5472.CAN-11-3934]).
Instead, "we showed that high viral load and a cancer-specific pattern of viral gene expression are most suited to identify patients with HPV-driven tumors among patients with oropharyngeal cancer. Viral expression pattern is a completely new marker in this field, and viral load has hardly been analyzed before," Dr. Holzinger said in a press statement accompanying the publication of these findings.
"Once standardized assays for these markers, applicable in routine clinical laboratories, are established, they will allow precise identification" of cancers that are or are not HPV-driven, which will in turn influence prognosis and treatment, she added.
Results Back Combination Approach
In the second study, Dr. Caihua Liang of Brown University, Providence, R.I., and her associates examined 488 HNSCC samples as well as serum samples collected in a population-based study in the Boston area during 1999-2003.
As in the first study, these investigators found that the mere presence of HPV-16 DNA in these tumors, particularly when detected by PCR analysis, did not accurately predict overall survival or progression-free survival.
Instead, "our study strongly suggests that the combination of detection of HPV-16 DNA in HNSCC tumors [plus] p16 immunostaining with E6/E7 antibodies represents the most clinically valuable surrogate marker for the identification of patients . . . who have a better prognosis," they said (Cancer Res. 2012 Sept. 28 [doi: 10.1158/0008-5472.CAN-11-3277]).
"Assessment of HPV DNA using polymerase chain reaction methods as a biomarker in individual head and neck cancers is a poor predictor of outcome, and is also poorly associated with antibody response indicative of exposure and/or infection by HPV," senior author Dr. Karl T. Kelsey added in the press statement.
"We may not be diagnosing these tumors as accurately and precisely as we need to for adjusting treatments," said Dr. Kelsey, a professor in the department of epidemiology and the department of pathology and laboratory medicine at Brown University.
Dr. Holzinger’s study was funded in part by the European Commission, BMBG/HGAF-Canceropole Grand-Est, and the German Research Foundation. Her associates reported ties to Qiagen and Roche. Dr. Liang’s study was supported by the National Institutes of Health and the Flight Attendant Medical Research Institute, and one associate reported ties to Bristol-Myers Squibb.
Testing for the presence of human papillomavirus DNA alone, especially using polymerase chain reaction methods, is not adequate to identify which head and neck squamous cell carcinomas are caused by the virus, according to two studies published online Sept. 18 in Cancer Research.
Identifying HPV-driven malignancies is important because they respond better to treatment and have better outcomes than those unrelated to HPV infection. Indeed, treatment of head and neck squamous cell carcinoma (HNSCC) may soon be guided by the tumor’s HPV status, since trials are now underway to determine whether de-escalation of chemo- and radiotherapy is safe and effective in such patients.
At present, however, the biomarkers that are best suited to making this identification are unclear.
Case Series Assesses Biomarkers
In the first study, researchers assessed the usefulness of four biomarkers in determining which HNSCCs in a case series were driven by HPV. They began by examining fresh-frozen tumor biopsy samples from 199 German adults diagnosed as having oropharyngeal squamous cell cancer between 1990 and 2008.
The four biomarkers were HPV-16 viral load, viral oncogene RNA (E6 and E7), p16INK4a, and RNA patterns similar to those characteristic of cervical carcinomas (CxCa RNA), said Dr. Dana Holzinger of the German Cancer Research Center at Heidelberg (Germany) University and her associates.
The simple presence of HPV DNA in a tumor sample was found to be a poor indicator of prognosis, likely because it often signaled past HPV infections or recent oral exposure, rather than active HPV infection that progressed to malignancy, the investigators said (Cancer Res. 2012 Sept. 18 [doi: 10.1158/0008-5472.CAN-11-3934]).
Instead, "we showed that high viral load and a cancer-specific pattern of viral gene expression are most suited to identify patients with HPV-driven tumors among patients with oropharyngeal cancer. Viral expression pattern is a completely new marker in this field, and viral load has hardly been analyzed before," Dr. Holzinger said in a press statement accompanying the publication of these findings.
"Once standardized assays for these markers, applicable in routine clinical laboratories, are established, they will allow precise identification" of cancers that are or are not HPV-driven, which will in turn influence prognosis and treatment, she added.
Results Back Combination Approach
In the second study, Dr. Caihua Liang of Brown University, Providence, R.I., and her associates examined 488 HNSCC samples as well as serum samples collected in a population-based study in the Boston area during 1999-2003.
As in the first study, these investigators found that the mere presence of HPV-16 DNA in these tumors, particularly when detected by PCR analysis, did not accurately predict overall survival or progression-free survival.
Instead, "our study strongly suggests that the combination of detection of HPV-16 DNA in HNSCC tumors [plus] p16 immunostaining with E6/E7 antibodies represents the most clinically valuable surrogate marker for the identification of patients . . . who have a better prognosis," they said (Cancer Res. 2012 Sept. 28 [doi: 10.1158/0008-5472.CAN-11-3277]).
"Assessment of HPV DNA using polymerase chain reaction methods as a biomarker in individual head and neck cancers is a poor predictor of outcome, and is also poorly associated with antibody response indicative of exposure and/or infection by HPV," senior author Dr. Karl T. Kelsey added in the press statement.
"We may not be diagnosing these tumors as accurately and precisely as we need to for adjusting treatments," said Dr. Kelsey, a professor in the department of epidemiology and the department of pathology and laboratory medicine at Brown University.
Dr. Holzinger’s study was funded in part by the European Commission, BMBG/HGAF-Canceropole Grand-Est, and the German Research Foundation. Her associates reported ties to Qiagen and Roche. Dr. Liang’s study was supported by the National Institutes of Health and the Flight Attendant Medical Research Institute, and one associate reported ties to Bristol-Myers Squibb.
FROM CANCER RESEARCH
Major Finding: The simple presence of HPV DNA in tumor samples did not accurately identify which cancers were driven by active HPV infection, and thus did not predict which would show the greatest response to treatment.
Data Source: Two analyses were used to assess the prognostic accuracy of various biomarkers in tumor samples from adults with head and neck squamous cell carcinoma.
Disclosures: Dr. Holzinger’s study was funded in part by the European Commission, BMBG/HGAF-Canceropole Grand-Est, and the German Research Foundation. Her associates reported ties to Qiagen and Roche. Dr. Liang’s study was supported by the National Institutes of Health and the Flight Attendant Medical Research Institute, and one associate reported ties to Bristol-Myers Squibb.
Gastric Bypass Benefits Persist at 6 Years' Follow-Up
Both weight loss and its associated improvements in cardiovascular and metabolic risk factors persisted for 6 years in most of the 418 severely obese adults who underwent Roux-en-Y gastric bypass surgery in a prospective study published in the Sept. 19 JAMA.
Despite some weight regain over time, surgery patients showed a mean weight loss of 28% at 6-year follow-up, as well as higher remission rates for diabetes, dyslipidemia, and hypertension, compared with the two control groups, said Ted D. Adams, Ph.D., of the department of internal medicine, University of Utah, Salt Lake City, and his associates.
"Considering the 5%-9% weight loss at 1 year with only 2%-6% weight loss after 4 years of intensive lifestyle-based and medication-based therapy, the weight-loss maintenance of 28% ... in our Utah study is quite significant," they noted.
The study involved severely obese adults with a body mass index of 35 kg/m2 or higher (mean BMI 45.9 kg/m2), of whom 82% were women and 96% were white. In addition to the patients who underwent either open or laparoscopic gastric bypass, there were 417 obese subjects in the first control group who were assessed for the surgery at the same time as the intervention group but did not have the surgery, and 321 obese subjects in the second control group who were randomly selected from a population-based sample of Utah residents.
Subjects in the control groups did not receive any weight-loss intervention as part of the study but were free to pursue it on their own. Over time, 101 of the subjects from both control groups chose to have bariatric surgery.
In the surgical group, mean weight loss was 35% at 2 years and 28% at 6 years, representing a 7% regain over time. By comparison, neither control group showed any significant weight loss or regain.
Diabetes remitted in 75% of the bypass group at 2 years, decreasing to 62% at 6 years. Despite the recurrence of diabetes in some patients, this long-term remission rate was dramatically better than the remission rates in the control groups (8% and 6%, respectively).
Similarly, the proportion of bypass patients who developed index diabetes during follow-up was markedly lower in the bypass group (2%) than in either control group (17% and 15%, respectively).
Remission of hypertension also was greater 6 years after bypass surgery (42%) than in the control groups (18% and 9%, respectively). Rates of high LDL cholesterol and triglycerides followed the same pattern, Dr. Adams and his colleagues wrote (JAMA 2012;308:1122-31).
Importantly, the weight loss and the concurrent improvement in cardiovascular and metabolic risk factors did not improve mortality. There were 29 deaths: 12 in the bypass group (3%); 14 in the first control group (3%); and 3 in the second control group (1%).
Notably, suicide was significantly more common in the bypass patients than in the control subjects. There were four suicides and three poisonings "of undetermined intention" overall, and six of these seven events occurred in bypass patients. The reason for this excess in the surgery group is unknown, but it is consistent with the finding that the mental component of the SF-36 fails to improve during follow-up, even though the physical component improves markedly among gastric bypass patients.
Other investigators have postulated that bariatric surgery precipitates profound changes "that may generate tension and pose special social, psychological, and lifestyle challenges. Preoperative and postoperative psychological assessment of social and emotional status related to post–bariatric surgical expectations and the potential risk of self-destructive behavior might be warranted," Dr. Adams and his associates said.
The rate of perioperative complications was 3% in the surgery group, and there were 38 hospitalizations for bypass-related indications.
This study was supported by the National Institutes of Health, the National Institute of Diabetes and Digestive and Kidney Diseases, and the National Center for Research Resources. Dr. Adams’s associates reported ties to Vivus, Orexigen, GlaxoSmithKline, Health Outcome Solutions, and Ethicon Endo-Surgery.
Dr. Adams and his associates show that, despite some weight regain and some recurrence of diabetes, "the control of comorbid conditions remained very good" several years after severely obese patients underwent gastric bypass surgery, said Dr. Anita P. Courcoulas.
Most weight-loss studies are limited by very high dropout rates, so it was remarkable that follow-up was 96% in the intervention group in this study. "These findings are important because they show in a Roux-en-Y cohort and control group with nearly complete follow-up at 6 years that weight loss and associated health benefits ... are durable," she noted.
Anita P. Courcoulas, M.D., is in the department of minimally invasive bariatric and general surgery at the University of Pittsburgh Medical Center. She reported ties to Ethicon, Endogastric Solutions, Pfizer, Allergan, Stryker Endoscopy, Covidien, and Nutrisystem. These remarks were taken from her editorial comment accompanying the report (JAMA 2012;308:1160-1).
Dr. Adams and his associates show that, despite some weight regain and some recurrence of diabetes, "the control of comorbid conditions remained very good" several years after severely obese patients underwent gastric bypass surgery, said Dr. Anita P. Courcoulas.
Most weight-loss studies are limited by very high dropout rates, so it was remarkable that follow-up was 96% in the intervention group in this study. "These findings are important because they show in a Roux-en-Y cohort and control group with nearly complete follow-up at 6 years that weight loss and associated health benefits ... are durable," she noted.
Anita P. Courcoulas, M.D., is in the department of minimally invasive bariatric and general surgery at the University of Pittsburgh Medical Center. She reported ties to Ethicon, Endogastric Solutions, Pfizer, Allergan, Stryker Endoscopy, Covidien, and Nutrisystem. These remarks were taken from her editorial comment accompanying the report (JAMA 2012;308:1160-1).
Dr. Adams and his associates show that, despite some weight regain and some recurrence of diabetes, "the control of comorbid conditions remained very good" several years after severely obese patients underwent gastric bypass surgery, said Dr. Anita P. Courcoulas.
Most weight-loss studies are limited by very high dropout rates, so it was remarkable that follow-up was 96% in the intervention group in this study. "These findings are important because they show in a Roux-en-Y cohort and control group with nearly complete follow-up at 6 years that weight loss and associated health benefits ... are durable," she noted.
Anita P. Courcoulas, M.D., is in the department of minimally invasive bariatric and general surgery at the University of Pittsburgh Medical Center. She reported ties to Ethicon, Endogastric Solutions, Pfizer, Allergan, Stryker Endoscopy, Covidien, and Nutrisystem. These remarks were taken from her editorial comment accompanying the report (JAMA 2012;308:1160-1).
Both weight loss and its associated improvements in cardiovascular and metabolic risk factors persisted for 6 years in most of the 418 severely obese adults who underwent Roux-en-Y gastric bypass surgery in a prospective study published in the Sept. 19 JAMA.
Despite some weight regain over time, surgery patients showed a mean weight loss of 28% at 6-year follow-up, as well as higher remission rates for diabetes, dyslipidemia, and hypertension, compared with the two control groups, said Ted D. Adams, Ph.D., of the department of internal medicine, University of Utah, Salt Lake City, and his associates.
"Considering the 5%-9% weight loss at 1 year with only 2%-6% weight loss after 4 years of intensive lifestyle-based and medication-based therapy, the weight-loss maintenance of 28% ... in our Utah study is quite significant," they noted.
The study involved severely obese adults with a body mass index of 35 kg/m2 or higher (mean BMI 45.9 kg/m2), of whom 82% were women and 96% were white. In addition to the patients who underwent either open or laparoscopic gastric bypass, there were 417 obese subjects in the first control group who were assessed for the surgery at the same time as the intervention group but did not have the surgery, and 321 obese subjects in the second control group who were randomly selected from a population-based sample of Utah residents.
Subjects in the control groups did not receive any weight-loss intervention as part of the study but were free to pursue it on their own. Over time, 101 of the subjects from both control groups chose to have bariatric surgery.
In the surgical group, mean weight loss was 35% at 2 years and 28% at 6 years, representing a 7% regain over time. By comparison, neither control group showed any significant weight loss or regain.
Diabetes remitted in 75% of the bypass group at 2 years, decreasing to 62% at 6 years. Despite the recurrence of diabetes in some patients, this long-term remission rate was dramatically better than the remission rates in the control groups (8% and 6%, respectively).
Similarly, the proportion of bypass patients who developed index diabetes during follow-up was markedly lower in the bypass group (2%) than in either control group (17% and 15%, respectively).
Remission of hypertension also was greater 6 years after bypass surgery (42%) than in the control groups (18% and 9%, respectively). Rates of high LDL cholesterol and triglycerides followed the same pattern, Dr. Adams and his colleagues wrote (JAMA 2012;308:1122-31).
Importantly, the weight loss and the concurrent improvement in cardiovascular and metabolic risk factors did not improve mortality. There were 29 deaths: 12 in the bypass group (3%); 14 in the first control group (3%); and 3 in the second control group (1%).
Notably, suicide was significantly more common in the bypass patients than in the control subjects. There were four suicides and three poisonings "of undetermined intention" overall, and six of these seven events occurred in bypass patients. The reason for this excess in the surgery group is unknown, but it is consistent with the finding that the mental component of the SF-36 fails to improve during follow-up, even though the physical component improves markedly among gastric bypass patients.
Other investigators have postulated that bariatric surgery precipitates profound changes "that may generate tension and pose special social, psychological, and lifestyle challenges. Preoperative and postoperative psychological assessment of social and emotional status related to post–bariatric surgical expectations and the potential risk of self-destructive behavior might be warranted," Dr. Adams and his associates said.
The rate of perioperative complications was 3% in the surgery group, and there were 38 hospitalizations for bypass-related indications.
This study was supported by the National Institutes of Health, the National Institute of Diabetes and Digestive and Kidney Diseases, and the National Center for Research Resources. Dr. Adams’s associates reported ties to Vivus, Orexigen, GlaxoSmithKline, Health Outcome Solutions, and Ethicon Endo-Surgery.
Both weight loss and its associated improvements in cardiovascular and metabolic risk factors persisted for 6 years in most of the 418 severely obese adults who underwent Roux-en-Y gastric bypass surgery in a prospective study published in the Sept. 19 JAMA.
Despite some weight regain over time, surgery patients showed a mean weight loss of 28% at 6-year follow-up, as well as higher remission rates for diabetes, dyslipidemia, and hypertension, compared with the two control groups, said Ted D. Adams, Ph.D., of the department of internal medicine, University of Utah, Salt Lake City, and his associates.
"Considering the 5%-9% weight loss at 1 year with only 2%-6% weight loss after 4 years of intensive lifestyle-based and medication-based therapy, the weight-loss maintenance of 28% ... in our Utah study is quite significant," they noted.
The study involved severely obese adults with a body mass index of 35 kg/m2 or higher (mean BMI 45.9 kg/m2), of whom 82% were women and 96% were white. In addition to the patients who underwent either open or laparoscopic gastric bypass, there were 417 obese subjects in the first control group who were assessed for the surgery at the same time as the intervention group but did not have the surgery, and 321 obese subjects in the second control group who were randomly selected from a population-based sample of Utah residents.
Subjects in the control groups did not receive any weight-loss intervention as part of the study but were free to pursue it on their own. Over time, 101 of the subjects from both control groups chose to have bariatric surgery.
In the surgical group, mean weight loss was 35% at 2 years and 28% at 6 years, representing a 7% regain over time. By comparison, neither control group showed any significant weight loss or regain.
Diabetes remitted in 75% of the bypass group at 2 years, decreasing to 62% at 6 years. Despite the recurrence of diabetes in some patients, this long-term remission rate was dramatically better than the remission rates in the control groups (8% and 6%, respectively).
Similarly, the proportion of bypass patients who developed index diabetes during follow-up was markedly lower in the bypass group (2%) than in either control group (17% and 15%, respectively).
Remission of hypertension also was greater 6 years after bypass surgery (42%) than in the control groups (18% and 9%, respectively). Rates of high LDL cholesterol and triglycerides followed the same pattern, Dr. Adams and his colleagues wrote (JAMA 2012;308:1122-31).
Importantly, the weight loss and the concurrent improvement in cardiovascular and metabolic risk factors did not improve mortality. There were 29 deaths: 12 in the bypass group (3%); 14 in the first control group (3%); and 3 in the second control group (1%).
Notably, suicide was significantly more common in the bypass patients than in the control subjects. There were four suicides and three poisonings "of undetermined intention" overall, and six of these seven events occurred in bypass patients. The reason for this excess in the surgery group is unknown, but it is consistent with the finding that the mental component of the SF-36 fails to improve during follow-up, even though the physical component improves markedly among gastric bypass patients.
Other investigators have postulated that bariatric surgery precipitates profound changes "that may generate tension and pose special social, psychological, and lifestyle challenges. Preoperative and postoperative psychological assessment of social and emotional status related to post–bariatric surgical expectations and the potential risk of self-destructive behavior might be warranted," Dr. Adams and his associates said.
The rate of perioperative complications was 3% in the surgery group, and there were 38 hospitalizations for bypass-related indications.
This study was supported by the National Institutes of Health, the National Institute of Diabetes and Digestive and Kidney Diseases, and the National Center for Research Resources. Dr. Adams’s associates reported ties to Vivus, Orexigen, GlaxoSmithKline, Health Outcome Solutions, and Ethicon Endo-Surgery.
FROM JAMA
Major Finding: Six years after undergoing gastric bypass, patients showed a mean weight loss of 28%, a diabetes remission rate of 62%, a hypertension remission rate of 42%, and improved lipid profiles.
Data Source: A prospective case-control study involving 1,156 severely obese adults, comparing outcomes at long-term follow-up between 418 who had undergone Roux-en-Y gastric bypass and 738 who had not.
Disclosures: This study was supported by the National Institutes of Health, the National Institute of Diabetes and Digestive and Kidney Diseases, and the National Center for Research Resources. Dr. Adams’s associates reported ties to Vivus, Orexigen, GlaxoSmithKline, Health Outcome Solutions, and Ethicon Endo-Surgery.
Variability Hampers True Comparison of Handoff Interventions
Most interventions have a positive effect on patient handoffs from hospital discharge back into primary care, but trials examining them are of such mixed sizes and types that it is extremely difficult to compare them, researchers say.
A review of randomized trials of transition-of-care interventions found great variability in methodologies, patient populations, outcome measures, and the interventions themselves. It is impossible, at least at present, to identify which approaches are the most effective, wrote Gijs Hesselink of the Scientific Institute for Quality of Healthcare, Radboud University, Nijmegen, the Netherlands, and his associates. They reported their findings in the Sept.17 issue of Annals of Internal Medicine.
"There is no strong evidence that a single intervention is regularly associated with positive effects on a specific outcome measure," they noted.
Mr. Hesselink and his colleagues performed a systematic review of 36 randomized clinical trials performed between 1990 and 2011 that assessed interventions aimed at improving adult patients’ transitions from the hospital to primary care. They excluded studies of psychiatric patients and pregnant women and included studies of patients with general medical, surgical, heart failure, geriatric, stroke, or breast cancer diagnoses.
The studies included patients who had stayed in urban, secondary, tertiary, teaching, and university-affiliated hospitals. The sample sizes ranged from 20 subjects to 1,098 subjects.
The following factors were assessed in these clinical trials: the quality of the information exchanged between the hospital and primary care providers, including the completeness, accuracy, and clarity of that information; the quality of the coordination of health care, including patient assessment, care planning, and organization of follow-up services; and the quality of communication, including personal contact, accessibility, and time lines.
"Because of heterogeneity of the study designs, participants, and outcome measures, meta-analysis was not possible," the researchers said.
Overall, the quality of the 36 trials was judged to be "relatively high." However, 12 of the studies were not blinded, and the blinding status was unclear in another 10. And, in 10 studies, the intervention group was not similar to the control group at baseline.
The interventions were found to be significantly more effective than usual care for at least 1 outcome in 25 of the 36 trials, Mr. Hesselink and his associates said (Ann. Intern. Med. 2012;157;417-28).
In particular, discharge interventions that focused on structuring and reconciling discharge information, coordinating follow-up care, and direct, timely communication between hospital and primary providers were effective at reducing rehospitalization and emergency department visits and at improving patient satisfaction and quality of life.
A total of 22 trials examined interventions aimed at improving the quality of information exchanged at hospital discharge, and 14 of them showed a statistically significant improvement in quality of care, errors, and adverse events. Similarly, 27 trials examined interventions aimed at improving coordination of care, and 20 of them showed a significant improvement in continuity of care, early assessment of patient needs and resources, and postdischarge contact with the patient.
A total of 31 trials examined interventions aimed at improving communication, such as use of liaison nurses, liaison pharmacists, faxes, or e-mail to quickly transmit discharge summaries, plans, and other information. And 22 of them showed a significant improvement in patient status, rehospitalization, and appropriate use of postdischarge primary care.
"More attention should be directed to developing standardized measures of continuity of care for a better evaluation of, and comparison between, discharge interventions," the investigators said.
This study was supported by the European Union. No industry-related conflicts of interest were reported.
This systematic review of the highest-quality clinical trials examining interventions to improve patients’ transition from the hospital into primary care could not identify the most effective interventions but did lay the groundwork for the next important steps, said Dr. Susan T. Bray-Hall.
Researchers now need to identify the most pertinent outcomes, define simple and reproducible interventions, assess costs, and eventually design multicenter studies "to translate the most effective programs into wider practice," she said.
Susan T. Bray-Hall, M.D., is at the University of Colorado, Denver. These remarks were taken from her editorial accompanying Dr. Hesselink’s report (Ann. Intern. Med. 2012;157:448-9).
This systematic review of the highest-quality clinical trials examining interventions to improve patients’ transition from the hospital into primary care could not identify the most effective interventions but did lay the groundwork for the next important steps, said Dr. Susan T. Bray-Hall.
Researchers now need to identify the most pertinent outcomes, define simple and reproducible interventions, assess costs, and eventually design multicenter studies "to translate the most effective programs into wider practice," she said.
Susan T. Bray-Hall, M.D., is at the University of Colorado, Denver. These remarks were taken from her editorial accompanying Dr. Hesselink’s report (Ann. Intern. Med. 2012;157:448-9).
This systematic review of the highest-quality clinical trials examining interventions to improve patients’ transition from the hospital into primary care could not identify the most effective interventions but did lay the groundwork for the next important steps, said Dr. Susan T. Bray-Hall.
Researchers now need to identify the most pertinent outcomes, define simple and reproducible interventions, assess costs, and eventually design multicenter studies "to translate the most effective programs into wider practice," she said.
Susan T. Bray-Hall, M.D., is at the University of Colorado, Denver. These remarks were taken from her editorial accompanying Dr. Hesselink’s report (Ann. Intern. Med. 2012;157:448-9).
Most interventions have a positive effect on patient handoffs from hospital discharge back into primary care, but trials examining them are of such mixed sizes and types that it is extremely difficult to compare them, researchers say.
A review of randomized trials of transition-of-care interventions found great variability in methodologies, patient populations, outcome measures, and the interventions themselves. It is impossible, at least at present, to identify which approaches are the most effective, wrote Gijs Hesselink of the Scientific Institute for Quality of Healthcare, Radboud University, Nijmegen, the Netherlands, and his associates. They reported their findings in the Sept.17 issue of Annals of Internal Medicine.
"There is no strong evidence that a single intervention is regularly associated with positive effects on a specific outcome measure," they noted.
Mr. Hesselink and his colleagues performed a systematic review of 36 randomized clinical trials performed between 1990 and 2011 that assessed interventions aimed at improving adult patients’ transitions from the hospital to primary care. They excluded studies of psychiatric patients and pregnant women and included studies of patients with general medical, surgical, heart failure, geriatric, stroke, or breast cancer diagnoses.
The studies included patients who had stayed in urban, secondary, tertiary, teaching, and university-affiliated hospitals. The sample sizes ranged from 20 subjects to 1,098 subjects.
The following factors were assessed in these clinical trials: the quality of the information exchanged between the hospital and primary care providers, including the completeness, accuracy, and clarity of that information; the quality of the coordination of health care, including patient assessment, care planning, and organization of follow-up services; and the quality of communication, including personal contact, accessibility, and time lines.
"Because of heterogeneity of the study designs, participants, and outcome measures, meta-analysis was not possible," the researchers said.
Overall, the quality of the 36 trials was judged to be "relatively high." However, 12 of the studies were not blinded, and the blinding status was unclear in another 10. And, in 10 studies, the intervention group was not similar to the control group at baseline.
The interventions were found to be significantly more effective than usual care for at least 1 outcome in 25 of the 36 trials, Mr. Hesselink and his associates said (Ann. Intern. Med. 2012;157;417-28).
In particular, discharge interventions that focused on structuring and reconciling discharge information, coordinating follow-up care, and direct, timely communication between hospital and primary providers were effective at reducing rehospitalization and emergency department visits and at improving patient satisfaction and quality of life.
A total of 22 trials examined interventions aimed at improving the quality of information exchanged at hospital discharge, and 14 of them showed a statistically significant improvement in quality of care, errors, and adverse events. Similarly, 27 trials examined interventions aimed at improving coordination of care, and 20 of them showed a significant improvement in continuity of care, early assessment of patient needs and resources, and postdischarge contact with the patient.
A total of 31 trials examined interventions aimed at improving communication, such as use of liaison nurses, liaison pharmacists, faxes, or e-mail to quickly transmit discharge summaries, plans, and other information. And 22 of them showed a significant improvement in patient status, rehospitalization, and appropriate use of postdischarge primary care.
"More attention should be directed to developing standardized measures of continuity of care for a better evaluation of, and comparison between, discharge interventions," the investigators said.
This study was supported by the European Union. No industry-related conflicts of interest were reported.
Most interventions have a positive effect on patient handoffs from hospital discharge back into primary care, but trials examining them are of such mixed sizes and types that it is extremely difficult to compare them, researchers say.
A review of randomized trials of transition-of-care interventions found great variability in methodologies, patient populations, outcome measures, and the interventions themselves. It is impossible, at least at present, to identify which approaches are the most effective, wrote Gijs Hesselink of the Scientific Institute for Quality of Healthcare, Radboud University, Nijmegen, the Netherlands, and his associates. They reported their findings in the Sept.17 issue of Annals of Internal Medicine.
"There is no strong evidence that a single intervention is regularly associated with positive effects on a specific outcome measure," they noted.
Mr. Hesselink and his colleagues performed a systematic review of 36 randomized clinical trials performed between 1990 and 2011 that assessed interventions aimed at improving adult patients’ transitions from the hospital to primary care. They excluded studies of psychiatric patients and pregnant women and included studies of patients with general medical, surgical, heart failure, geriatric, stroke, or breast cancer diagnoses.
The studies included patients who had stayed in urban, secondary, tertiary, teaching, and university-affiliated hospitals. The sample sizes ranged from 20 subjects to 1,098 subjects.
The following factors were assessed in these clinical trials: the quality of the information exchanged between the hospital and primary care providers, including the completeness, accuracy, and clarity of that information; the quality of the coordination of health care, including patient assessment, care planning, and organization of follow-up services; and the quality of communication, including personal contact, accessibility, and time lines.
"Because of heterogeneity of the study designs, participants, and outcome measures, meta-analysis was not possible," the researchers said.
Overall, the quality of the 36 trials was judged to be "relatively high." However, 12 of the studies were not blinded, and the blinding status was unclear in another 10. And, in 10 studies, the intervention group was not similar to the control group at baseline.
The interventions were found to be significantly more effective than usual care for at least 1 outcome in 25 of the 36 trials, Mr. Hesselink and his associates said (Ann. Intern. Med. 2012;157;417-28).
In particular, discharge interventions that focused on structuring and reconciling discharge information, coordinating follow-up care, and direct, timely communication between hospital and primary providers were effective at reducing rehospitalization and emergency department visits and at improving patient satisfaction and quality of life.
A total of 22 trials examined interventions aimed at improving the quality of information exchanged at hospital discharge, and 14 of them showed a statistically significant improvement in quality of care, errors, and adverse events. Similarly, 27 trials examined interventions aimed at improving coordination of care, and 20 of them showed a significant improvement in continuity of care, early assessment of patient needs and resources, and postdischarge contact with the patient.
A total of 31 trials examined interventions aimed at improving communication, such as use of liaison nurses, liaison pharmacists, faxes, or e-mail to quickly transmit discharge summaries, plans, and other information. And 22 of them showed a significant improvement in patient status, rehospitalization, and appropriate use of postdischarge primary care.
"More attention should be directed to developing standardized measures of continuity of care for a better evaluation of, and comparison between, discharge interventions," the investigators said.
This study was supported by the European Union. No industry-related conflicts of interest were reported.
FROM ANNALS OF INTERNAL MEDICINE
Major Finding: Interventions aimed at improving patients’ transition from the hospital back into primary care significantly more effective than usual care for at least 1 outcome in trials reviewed.
Data Source: Results were taken from a systematic review of 36 randomized clinical trials performed in 1990-2011 that assessed interventions to improve patients’ transition from the hospital back into primary care.
Disclosures: This study was supported by the European Union. No industry-related conflicts of interest were reported.
Withholding Warfarin After GI Bleed Raises Risk of Thrombosis, Death
Deciding not to resume warfarin therapy after an episode of gastrointestinal bleeding raises the risk of thrombosis by a factor of 10 and the risk of death threefold, according to a retrospective cohort study published online September 17 in Archives of Internal Medicine.
"For many patients who have experienced gastrointestinal bleeding, the benefits of resuming warfarin therapy will outweigh the risks," said Daniel M. Witt, Pharm.D., of the clinical pharmacy anticoagulation service at Kaiser Permanente of Colorado, Aurora, and his associates.
"Surprisingly little is known about warfarin therapy and resumption" following a GI bleed, and there is no consensus as to the optimal timing or the risks of restarting anticoagulation. Dr. Witt and his colleagues used Kaiser’s administrative and clinical databases to study the incidence of thrombosis, recurrent bleeding episodes, and death from any cause in 442 adults who presented to a hospital or emergency department with warfarin-associated GI bleeding in 2005-2009 and who were followed for 90 days.
The mean patient age was 74 years, and the study population was equally comprised of men and women. Half of the study subjects were taking warfarin to prevent atrial fibrillation–related stroke or systemic embolization. One-quarter of patients used it to treat or prevent a second venous thrombosis, 10% were on it to prevent thromboembolic complications from prosthetic heart valves, and the remainder took it for other indications.
After an index GI bleed, 260 patients (59%) resumed warfarin therapy, usually within a week. The median time to resumption of warfarin was 4 days. In 41 of these patients, warfarin therapy was never suspended. It was suspended and never resumed in the remaining 182 patients.
During the 90-day follow-up, 11 patients (2.5%) had a thrombotic event. There were six arterial events, including five strokes and one systemic embolus, and five venous events, including three pulmonary embolisms and two deep vein thromboses (DVTs).
The rate of thrombotic events was 0.4% among the patients who resumed warfarin therapy (one DVT), compared with 5.5% among those who did not resume warfarin (five strokes, one systemic embolus, three pulmonary embolisms, and one DVT), a significant difference, the investigators said (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2012.5261]).
"Patients who either never interrupted warfarin therapy or resumed therapy within 14 days of the index GI bleed experienced no thromboses," they added.
GI bleeding recurred in 36 patients (8.4%) overall. A numerically higher proportion of patients who resumed warfarin therapy had recurrent GI bleeding (10%) than those who did not resume warfarin (5.5%), but this difference was not statistically significant.
In addition, a multivariable analysis that accounted for numerous possible confounders – including patient age, sex, propensity for complications; the INR at admission; acute treatment for the GI bleed; and location of GI bleed – also showed that the risk for rebleeding was not significantly greater in patients who resumed warfarin therapy than in those who did not.
Moreover, recurrent GI bleeding was never fatal. Fatal strokes did occur, however, in three patients with atrial fibrillation whose warfarin therapy was withdrawn and never resumed, Dr. Witt and his associates said.
A total of 52 patients (12%) died during follow-up. The most common cause of death was related to malignancy (29% of deaths), infection (19% of deaths), or cardiac disease (17%).
Resumption of warfarin therapy was strongly associated with a threefold decrease in the risk of death from any cause.
The investigators also performed a post hoc analysis excluding all patients who died within 1 week of the index GI bleed to rule out those who may not have had an opportunity to resume warfarin therapy. In this analysis, the strong association between resumption of warfarin and decreased mortality persisted.
Mortality was lowest among patients who resumed warfarin therapy within 15-90 days of the index GI bleed, the researchers said.
"Our results provide some guidance regarding the optimal timing of warfarin therapy resumption following GI bleeding, but clinical judgment remains a critical factor in this difficult decision," they noted.
This study was funded by CSL Behring. Dr. Witt’s associates, but not Dr. Witt, reported ties to numerous industry sources.
This study provides high-quality, real-world data showing that the risk of recurrent bleeding was acceptably low (10%), none of the episodes of recurrence were fatal, and most physicians and patients were willing to resume anticoagulation soon after GI bleeding, said Dr. Daniel J. Brotman and Dr. Amir K. Jaffer.
Dr. Amir K. Jaffer |
"We would hesitate to continue concurrent antiplatelet therapy in these patients without a compelling indication to do so (such as a recent coronary stent), and also would caution against extrapolating these findings to newer anticoagulants, such as dabigatran and rivaroxaban, that may be associated with more GI bleeding than warfarin when used long term and whose effects are not easily reversed," they said.
Dr. Brotman is with the hospitalist program at Johns Hopkins Hospital, Baltimore. Dr. Jaffer is with the division of hospital medicine at the University of Miami. Dr. Brotman reported ties to Gerson Lehrman Group, the Dunn Group, Quantia Communications, Siemens Healthcare Diagnostics, and Amerigroup Corporation. Dr. Jaffer reported ties to Sanofi-Aventis, Boehringer Ingelheim, Bristol Myers Squibb, Janssen Pharmaceuticals, Canyon Pharmaceuticals, and CSL. These remarks were taken from their invited commentary accompanying Dr. Witt’s report (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2012.4309]).
This study provides high-quality, real-world data showing that the risk of recurrent bleeding was acceptably low (10%), none of the episodes of recurrence were fatal, and most physicians and patients were willing to resume anticoagulation soon after GI bleeding, said Dr. Daniel J. Brotman and Dr. Amir K. Jaffer.
Dr. Amir K. Jaffer |
"We would hesitate to continue concurrent antiplatelet therapy in these patients without a compelling indication to do so (such as a recent coronary stent), and also would caution against extrapolating these findings to newer anticoagulants, such as dabigatran and rivaroxaban, that may be associated with more GI bleeding than warfarin when used long term and whose effects are not easily reversed," they said.
Dr. Brotman is with the hospitalist program at Johns Hopkins Hospital, Baltimore. Dr. Jaffer is with the division of hospital medicine at the University of Miami. Dr. Brotman reported ties to Gerson Lehrman Group, the Dunn Group, Quantia Communications, Siemens Healthcare Diagnostics, and Amerigroup Corporation. Dr. Jaffer reported ties to Sanofi-Aventis, Boehringer Ingelheim, Bristol Myers Squibb, Janssen Pharmaceuticals, Canyon Pharmaceuticals, and CSL. These remarks were taken from their invited commentary accompanying Dr. Witt’s report (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2012.4309]).
This study provides high-quality, real-world data showing that the risk of recurrent bleeding was acceptably low (10%), none of the episodes of recurrence were fatal, and most physicians and patients were willing to resume anticoagulation soon after GI bleeding, said Dr. Daniel J. Brotman and Dr. Amir K. Jaffer.
Dr. Amir K. Jaffer |
"We would hesitate to continue concurrent antiplatelet therapy in these patients without a compelling indication to do so (such as a recent coronary stent), and also would caution against extrapolating these findings to newer anticoagulants, such as dabigatran and rivaroxaban, that may be associated with more GI bleeding than warfarin when used long term and whose effects are not easily reversed," they said.
Dr. Brotman is with the hospitalist program at Johns Hopkins Hospital, Baltimore. Dr. Jaffer is with the division of hospital medicine at the University of Miami. Dr. Brotman reported ties to Gerson Lehrman Group, the Dunn Group, Quantia Communications, Siemens Healthcare Diagnostics, and Amerigroup Corporation. Dr. Jaffer reported ties to Sanofi-Aventis, Boehringer Ingelheim, Bristol Myers Squibb, Janssen Pharmaceuticals, Canyon Pharmaceuticals, and CSL. These remarks were taken from their invited commentary accompanying Dr. Witt’s report (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2012.4309]).
Deciding not to resume warfarin therapy after an episode of gastrointestinal bleeding raises the risk of thrombosis by a factor of 10 and the risk of death threefold, according to a retrospective cohort study published online September 17 in Archives of Internal Medicine.
"For many patients who have experienced gastrointestinal bleeding, the benefits of resuming warfarin therapy will outweigh the risks," said Daniel M. Witt, Pharm.D., of the clinical pharmacy anticoagulation service at Kaiser Permanente of Colorado, Aurora, and his associates.
"Surprisingly little is known about warfarin therapy and resumption" following a GI bleed, and there is no consensus as to the optimal timing or the risks of restarting anticoagulation. Dr. Witt and his colleagues used Kaiser’s administrative and clinical databases to study the incidence of thrombosis, recurrent bleeding episodes, and death from any cause in 442 adults who presented to a hospital or emergency department with warfarin-associated GI bleeding in 2005-2009 and who were followed for 90 days.
The mean patient age was 74 years, and the study population was equally comprised of men and women. Half of the study subjects were taking warfarin to prevent atrial fibrillation–related stroke or systemic embolization. One-quarter of patients used it to treat or prevent a second venous thrombosis, 10% were on it to prevent thromboembolic complications from prosthetic heart valves, and the remainder took it for other indications.
After an index GI bleed, 260 patients (59%) resumed warfarin therapy, usually within a week. The median time to resumption of warfarin was 4 days. In 41 of these patients, warfarin therapy was never suspended. It was suspended and never resumed in the remaining 182 patients.
During the 90-day follow-up, 11 patients (2.5%) had a thrombotic event. There were six arterial events, including five strokes and one systemic embolus, and five venous events, including three pulmonary embolisms and two deep vein thromboses (DVTs).
The rate of thrombotic events was 0.4% among the patients who resumed warfarin therapy (one DVT), compared with 5.5% among those who did not resume warfarin (five strokes, one systemic embolus, three pulmonary embolisms, and one DVT), a significant difference, the investigators said (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2012.5261]).
"Patients who either never interrupted warfarin therapy or resumed therapy within 14 days of the index GI bleed experienced no thromboses," they added.
GI bleeding recurred in 36 patients (8.4%) overall. A numerically higher proportion of patients who resumed warfarin therapy had recurrent GI bleeding (10%) than those who did not resume warfarin (5.5%), but this difference was not statistically significant.
In addition, a multivariable analysis that accounted for numerous possible confounders – including patient age, sex, propensity for complications; the INR at admission; acute treatment for the GI bleed; and location of GI bleed – also showed that the risk for rebleeding was not significantly greater in patients who resumed warfarin therapy than in those who did not.
Moreover, recurrent GI bleeding was never fatal. Fatal strokes did occur, however, in three patients with atrial fibrillation whose warfarin therapy was withdrawn and never resumed, Dr. Witt and his associates said.
A total of 52 patients (12%) died during follow-up. The most common cause of death was related to malignancy (29% of deaths), infection (19% of deaths), or cardiac disease (17%).
Resumption of warfarin therapy was strongly associated with a threefold decrease in the risk of death from any cause.
The investigators also performed a post hoc analysis excluding all patients who died within 1 week of the index GI bleed to rule out those who may not have had an opportunity to resume warfarin therapy. In this analysis, the strong association between resumption of warfarin and decreased mortality persisted.
Mortality was lowest among patients who resumed warfarin therapy within 15-90 days of the index GI bleed, the researchers said.
"Our results provide some guidance regarding the optimal timing of warfarin therapy resumption following GI bleeding, but clinical judgment remains a critical factor in this difficult decision," they noted.
This study was funded by CSL Behring. Dr. Witt’s associates, but not Dr. Witt, reported ties to numerous industry sources.
Deciding not to resume warfarin therapy after an episode of gastrointestinal bleeding raises the risk of thrombosis by a factor of 10 and the risk of death threefold, according to a retrospective cohort study published online September 17 in Archives of Internal Medicine.
"For many patients who have experienced gastrointestinal bleeding, the benefits of resuming warfarin therapy will outweigh the risks," said Daniel M. Witt, Pharm.D., of the clinical pharmacy anticoagulation service at Kaiser Permanente of Colorado, Aurora, and his associates.
"Surprisingly little is known about warfarin therapy and resumption" following a GI bleed, and there is no consensus as to the optimal timing or the risks of restarting anticoagulation. Dr. Witt and his colleagues used Kaiser’s administrative and clinical databases to study the incidence of thrombosis, recurrent bleeding episodes, and death from any cause in 442 adults who presented to a hospital or emergency department with warfarin-associated GI bleeding in 2005-2009 and who were followed for 90 days.
The mean patient age was 74 years, and the study population was equally comprised of men and women. Half of the study subjects were taking warfarin to prevent atrial fibrillation–related stroke or systemic embolization. One-quarter of patients used it to treat or prevent a second venous thrombosis, 10% were on it to prevent thromboembolic complications from prosthetic heart valves, and the remainder took it for other indications.
After an index GI bleed, 260 patients (59%) resumed warfarin therapy, usually within a week. The median time to resumption of warfarin was 4 days. In 41 of these patients, warfarin therapy was never suspended. It was suspended and never resumed in the remaining 182 patients.
During the 90-day follow-up, 11 patients (2.5%) had a thrombotic event. There were six arterial events, including five strokes and one systemic embolus, and five venous events, including three pulmonary embolisms and two deep vein thromboses (DVTs).
The rate of thrombotic events was 0.4% among the patients who resumed warfarin therapy (one DVT), compared with 5.5% among those who did not resume warfarin (five strokes, one systemic embolus, three pulmonary embolisms, and one DVT), a significant difference, the investigators said (Arch. Intern. Med. 2012 [doi:10.1001/archinternmed.2012.5261]).
"Patients who either never interrupted warfarin therapy or resumed therapy within 14 days of the index GI bleed experienced no thromboses," they added.
GI bleeding recurred in 36 patients (8.4%) overall. A numerically higher proportion of patients who resumed warfarin therapy had recurrent GI bleeding (10%) than those who did not resume warfarin (5.5%), but this difference was not statistically significant.
In addition, a multivariable analysis that accounted for numerous possible confounders – including patient age, sex, propensity for complications; the INR at admission; acute treatment for the GI bleed; and location of GI bleed – also showed that the risk for rebleeding was not significantly greater in patients who resumed warfarin therapy than in those who did not.
Moreover, recurrent GI bleeding was never fatal. Fatal strokes did occur, however, in three patients with atrial fibrillation whose warfarin therapy was withdrawn and never resumed, Dr. Witt and his associates said.
A total of 52 patients (12%) died during follow-up. The most common cause of death was related to malignancy (29% of deaths), infection (19% of deaths), or cardiac disease (17%).
Resumption of warfarin therapy was strongly associated with a threefold decrease in the risk of death from any cause.
The investigators also performed a post hoc analysis excluding all patients who died within 1 week of the index GI bleed to rule out those who may not have had an opportunity to resume warfarin therapy. In this analysis, the strong association between resumption of warfarin and decreased mortality persisted.
Mortality was lowest among patients who resumed warfarin therapy within 15-90 days of the index GI bleed, the researchers said.
"Our results provide some guidance regarding the optimal timing of warfarin therapy resumption following GI bleeding, but clinical judgment remains a critical factor in this difficult decision," they noted.
This study was funded by CSL Behring. Dr. Witt’s associates, but not Dr. Witt, reported ties to numerous industry sources.
FROM ARCHIVES OF INTERNAL MEDICINE
Major Finding: The rate of thrombotic events was 0.4% in patients who resumed warfarin therapy after an episode of GI bleeding, compared with 5.5% in those who did not resume warfarin.
Data Source: A retrospective cohort study compared outcomes between 260 patients who resumed warfarin therapy and 182 who did not, who were followed for 90 days.
Disclosures: This study was funded by CSL Behring. Dr. Witt’s associates, but not Dr. Witt, reported ties to numerous industry sources.
DTaP's Pertussis Protection Waned After 5 Years
Protection against pertussis "wanes substantially" 5 years after completion of the series of acellular pertussis vaccines, according to a report published online Sept. 12 in the New England Journal of Medicine.
In a study prompted by the 2010 pertussis outbreak in California, researchers found that the risk of pertussis rose by 42% each year after the fifth dose of DTaP was received.
They could not determine the vaccine’s initial effectiveness, however, because California’s near-100% vaccine coverage meant there was no control group of unvaccinated children. Nonetheless, the investigators extrapolated that if the initial effectiveness was 95% – making the risk of pertussis in vaccinated children only 5% – that risk would increase to 29% after 5 years.
"The corresponding decrease in DTaP effectiveness would be from 95% to 71%," said Dr. Nicola P. Klein, director of the Kaiser Permanente Vaccine Study Center, Oakland, Calif., and her associates.
"Our findings highlight the need to develop new pertussis-containing vaccines that will provide long-lasting immunity," they noted (N. Engl. J. Med. 2012;367:1012-9 [doi:10.1056/NEJMoa1200850]).
During the 2010 outbreak, the incidence of pertussis was the highest California has seen since 1958.
Dr. Klein and her colleagues performed a case-control study using information in the Kaiser Permanente database on 277 patients aged 4-12 years who had received the full series of the DTaP vaccine but had nevertheless tested positive for pertussis between 2006 and 2011. There were two control groups: 3,318 patients who had tested negative for pertussis during the same period, and 6,086 patients matched for age, sex, race/ethnicity, and residence.
"The large population in the health plan allowed controls to be matched to PCR-positive children on many potential confounders," the investigators said.
The overall incidence of pertussis in the study population as a whole during this period was 5.4%.
Both older age and increasing time since receiving the fifth dose of DTaP were associated with a higher rate of pertussis. The incidence was 4.5% among 6-year-olds, 12.2% among 8-year-olds, and 18.5% among 10-year-olds.
"The incidence of pertussis was highest among the population of children who were 8-11 years of age and who had received the full five-dose series of DTaP in childhood, suggesting that the waning efficacy of the fifth dose among school-age children played a key role in both allowing and sustaining the recent pertussis outbreak," the researchers said.
The researchers were surprised by the fact that pertussis incidence was higher in these preteens than in teenagers, who had likely received the whole-cell pertussis vaccine rather than the acellular DTaP. Teenagers traditionally have higher rates of pertussis and are considered a major reservoir of the infection.
"The odds ratio for pertussis was 1.42 per year, indicating that each year after the fifth dose of DTaP was associated with a 42% increased odds of acquiring pertussis," Dr. Klein and her associates said.
The findings are consistent with the results of clinical trials that assessed the duration of the vaccine’s protection, as well as other observational studies. "Taken together, these studies indicate that protection is less enduring with DTaP than with whole-cell pertussis vaccines," they said.
The Centers for Disease Control and Prevention recommends routine administration of the Tdap vaccine, a vaccine with reduced pertussis-antigen content, beginning at 11 years of age. But the limited duration of protection from the acellular vaccine found in these studies "raises the question of whether routine administration of Tdap in younger children is warranted," the investigators added.
"Prevention of future outbreaks will be best achieved by developing new pertussis-containing vaccines that provide long-lasting immunity," they noted.
This study was supported by Kaiser Permanente. Dr. Klein and an associate reported grants to their institution by GlaxoSmithKline, Merck, Novartis, Pfizer, and Sanofi Pasteur.
Protection against pertussis "wanes substantially" 5 years after completion of the series of acellular pertussis vaccines, according to a report published online Sept. 12 in the New England Journal of Medicine.
In a study prompted by the 2010 pertussis outbreak in California, researchers found that the risk of pertussis rose by 42% each year after the fifth dose of DTaP was received.
They could not determine the vaccine’s initial effectiveness, however, because California’s near-100% vaccine coverage meant there was no control group of unvaccinated children. Nonetheless, the investigators extrapolated that if the initial effectiveness was 95% – making the risk of pertussis in vaccinated children only 5% – that risk would increase to 29% after 5 years.
"The corresponding decrease in DTaP effectiveness would be from 95% to 71%," said Dr. Nicola P. Klein, director of the Kaiser Permanente Vaccine Study Center, Oakland, Calif., and her associates.
"Our findings highlight the need to develop new pertussis-containing vaccines that will provide long-lasting immunity," they noted (N. Engl. J. Med. 2012;367:1012-9 [doi:10.1056/NEJMoa1200850]).
During the 2010 outbreak, the incidence of pertussis was the highest California has seen since 1958.
Dr. Klein and her colleagues performed a case-control study using information in the Kaiser Permanente database on 277 patients aged 4-12 years who had received the full series of the DTaP vaccine but had nevertheless tested positive for pertussis between 2006 and 2011. There were two control groups: 3,318 patients who had tested negative for pertussis during the same period, and 6,086 patients matched for age, sex, race/ethnicity, and residence.
"The large population in the health plan allowed controls to be matched to PCR-positive children on many potential confounders," the investigators said.
The overall incidence of pertussis in the study population as a whole during this period was 5.4%.
Both older age and increasing time since receiving the fifth dose of DTaP were associated with a higher rate of pertussis. The incidence was 4.5% among 6-year-olds, 12.2% among 8-year-olds, and 18.5% among 10-year-olds.
"The incidence of pertussis was highest among the population of children who were 8-11 years of age and who had received the full five-dose series of DTaP in childhood, suggesting that the waning efficacy of the fifth dose among school-age children played a key role in both allowing and sustaining the recent pertussis outbreak," the researchers said.
The researchers were surprised by the fact that pertussis incidence was higher in these preteens than in teenagers, who had likely received the whole-cell pertussis vaccine rather than the acellular DTaP. Teenagers traditionally have higher rates of pertussis and are considered a major reservoir of the infection.
"The odds ratio for pertussis was 1.42 per year, indicating that each year after the fifth dose of DTaP was associated with a 42% increased odds of acquiring pertussis," Dr. Klein and her associates said.
The findings are consistent with the results of clinical trials that assessed the duration of the vaccine’s protection, as well as other observational studies. "Taken together, these studies indicate that protection is less enduring with DTaP than with whole-cell pertussis vaccines," they said.
The Centers for Disease Control and Prevention recommends routine administration of the Tdap vaccine, a vaccine with reduced pertussis-antigen content, beginning at 11 years of age. But the limited duration of protection from the acellular vaccine found in these studies "raises the question of whether routine administration of Tdap in younger children is warranted," the investigators added.
"Prevention of future outbreaks will be best achieved by developing new pertussis-containing vaccines that provide long-lasting immunity," they noted.
This study was supported by Kaiser Permanente. Dr. Klein and an associate reported grants to their institution by GlaxoSmithKline, Merck, Novartis, Pfizer, and Sanofi Pasteur.
Protection against pertussis "wanes substantially" 5 years after completion of the series of acellular pertussis vaccines, according to a report published online Sept. 12 in the New England Journal of Medicine.
In a study prompted by the 2010 pertussis outbreak in California, researchers found that the risk of pertussis rose by 42% each year after the fifth dose of DTaP was received.
They could not determine the vaccine’s initial effectiveness, however, because California’s near-100% vaccine coverage meant there was no control group of unvaccinated children. Nonetheless, the investigators extrapolated that if the initial effectiveness was 95% – making the risk of pertussis in vaccinated children only 5% – that risk would increase to 29% after 5 years.
"The corresponding decrease in DTaP effectiveness would be from 95% to 71%," said Dr. Nicola P. Klein, director of the Kaiser Permanente Vaccine Study Center, Oakland, Calif., and her associates.
"Our findings highlight the need to develop new pertussis-containing vaccines that will provide long-lasting immunity," they noted (N. Engl. J. Med. 2012;367:1012-9 [doi:10.1056/NEJMoa1200850]).
During the 2010 outbreak, the incidence of pertussis was the highest California has seen since 1958.
Dr. Klein and her colleagues performed a case-control study using information in the Kaiser Permanente database on 277 patients aged 4-12 years who had received the full series of the DTaP vaccine but had nevertheless tested positive for pertussis between 2006 and 2011. There were two control groups: 3,318 patients who had tested negative for pertussis during the same period, and 6,086 patients matched for age, sex, race/ethnicity, and residence.
"The large population in the health plan allowed controls to be matched to PCR-positive children on many potential confounders," the investigators said.
The overall incidence of pertussis in the study population as a whole during this period was 5.4%.
Both older age and increasing time since receiving the fifth dose of DTaP were associated with a higher rate of pertussis. The incidence was 4.5% among 6-year-olds, 12.2% among 8-year-olds, and 18.5% among 10-year-olds.
"The incidence of pertussis was highest among the population of children who were 8-11 years of age and who had received the full five-dose series of DTaP in childhood, suggesting that the waning efficacy of the fifth dose among school-age children played a key role in both allowing and sustaining the recent pertussis outbreak," the researchers said.
The researchers were surprised by the fact that pertussis incidence was higher in these preteens than in teenagers, who had likely received the whole-cell pertussis vaccine rather than the acellular DTaP. Teenagers traditionally have higher rates of pertussis and are considered a major reservoir of the infection.
"The odds ratio for pertussis was 1.42 per year, indicating that each year after the fifth dose of DTaP was associated with a 42% increased odds of acquiring pertussis," Dr. Klein and her associates said.
The findings are consistent with the results of clinical trials that assessed the duration of the vaccine’s protection, as well as other observational studies. "Taken together, these studies indicate that protection is less enduring with DTaP than with whole-cell pertussis vaccines," they said.
The Centers for Disease Control and Prevention recommends routine administration of the Tdap vaccine, a vaccine with reduced pertussis-antigen content, beginning at 11 years of age. But the limited duration of protection from the acellular vaccine found in these studies "raises the question of whether routine administration of Tdap in younger children is warranted," the investigators added.
"Prevention of future outbreaks will be best achieved by developing new pertussis-containing vaccines that provide long-lasting immunity," they noted.
This study was supported by Kaiser Permanente. Dr. Klein and an associate reported grants to their institution by GlaxoSmithKline, Merck, Novartis, Pfizer, and Sanofi Pasteur.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: The risk of pertussis rose 42% per year each year following completion of the DTaP vaccine series, suggesting that the protection it confers drops from approximately 95% to approximately 71% after 5 years.
Data Source: A case-control study involving 277 children aged 4-12 years in 2006-2011 who developed pertussis after receiving the full series of the DTaP vaccine, 3,318 controls who tested negative for pertussis during the same time, and 6,086 controls matched for several potential confounders.
Disclosures: This study was supported by Kaiser Permanente. Dr. Klein and an associate reported grants to their institution by GlaxoSmithKline, Merck, Novartis, Pfizer, and Sanofi Pasteur.
Two Common Genetic Variants Linked to Barrett's Esophagus
Two common genetic variants on chromosomes 6p21 and 16q24 were found to be associated with Barrett’s esophagus in the first genome-wide association study of susceptibility to the disorder, according to a letter to the editor published online Sept. 9 in Nature Genetics.
Genetic factors have long been suspected to play a role in the development of Barrett’s esophagus since relative risks for the disorder, as well as for gastroesophageal reflux disease and esophageal adenocarcinoma, are increased two- to fourfold in first-degree relatives of affected patients.
However, "extensive candidate gene and linkage searches have to date been unsuccessful in identifying genetic variants that are associated with risk of Barrett’s esophagus," wrote Dr. Zhan Su of the Wellcome Trust Centre for Human Genetics in Oxford, England, and his associates.
Their findings provide the first direct evidence that the etiology of Barrett’s esophagus has a genetic component, the researchers noted.
Dr. Su and his colleagues performed the genome-wide association study as part of a Wellcome Trust consortium study of the genetic components of 15 common disorders and traits. They identified the two genetic variants in a discovery analysis and confirmed the findings in another five replication cohorts.
The discovery analysis involved genotyping of 1,852 adults with histologically confirmed Barrett’s esophagus who were recruited from sites across the United Kingdom. A representative sample of 5,172 control subjects also was analyzed. A total of 521,744 single-nucleotide polymorphisms (SNPs) were typed.
The 100 SNPs that were associated to some degree with Barrett’s esophagus were then analyzed in a separate cohort of 1,105 cases from two clinical trials, 4,421 controls from another U.K. sample, and 2,578 controls from yet another U.K .sample.
The top 16 SNPs from these analyses were then analyzed in a second replication cohort of 473 cases and 1,780 controls from a Dutch genotyping database. Two of the SNPs were found to be significantly associated with Barrett\'’s esophagus: rs9257809 on chromosome 6p21 and rs9936833 on chromosome 16q24.
It is notable that the closest coding gene to the rs9936833 SNP on chromosome 16q24 is a gene that encodes a protein involved in the development of the gastrointestinal tract. It has been reported that, when this gene is inactivated, structural alterations in the esophagus, especially atresia, occur. The rs9257809 SNP on 6p21 is near the telomeric edge of the major histocompatibility complex region.
The two SNPs were then examined further in an Irish cohort of 245 cases and 473 controls, a U.K. cohort of 1,765 cases and 1,586 controls, and a cohort of 2,398 cases and 2,167 controls from Europe, Australia, and the United States.
Overall, the two SNPs "showed compelling evidence for association," with Barrett’s esophagus, reflected in the significance of the combined P values for rs9257809 (odds ratio, 1.21) and rs9936833 (odds ratio, 1.14), the investigators reported (Nat. Genet. 2012 Sept. 9 [doi:10.1038/ng.2408]).
In a subgroup analysis involving only patients who had histologic evidence of intestinal metaplasia, the same two SNPs were again strongly associated with Barrett’s esophagus. Neither SNP, however, was associated with either the circumferential extent or the maximal length of the affected segment of esophagus.
Given that men are known to be more susceptible than women to Barrett’s esophagus, the investigators also performed a sex-stratified analysis of the data and found that the association between both SNPs and the disorder was stronger in men than in women. "This finding warrants further investigation," they noted.
Similarly, given the known association between obesity and Barrett’s esophagus, the researchers analyzed the 40 SNPs that previously have been linked with either body mass index or waist-to-hip ratio. These latter SNPs were "more likely than expected by chance to show effects in the same direction in association with Barrett’s esophagus, suggesting that genetic effects may in part underpin the epidemiologic observation that BMI is a risk factor for Barrett’s esophagus," Dr. Su and his associates said.
"Given that Barrett’s esophagus has an accepted status as a precursor lesion, the SNPs that we have identified could also essentially be risk factors for esophageal adenocarcinoma and may give clues as to the biology of both of these important phenotypes," they added.
The financial disclosures of Dr. Su and his 143 coauthors are listed in the online version of this article.
Two common genetic variants on chromosomes 6p21 and 16q24 were found to be associated with Barrett’s esophagus in the first genome-wide association study of susceptibility to the disorder, according to a letter to the editor published online Sept. 9 in Nature Genetics.
Genetic factors have long been suspected to play a role in the development of Barrett’s esophagus since relative risks for the disorder, as well as for gastroesophageal reflux disease and esophageal adenocarcinoma, are increased two- to fourfold in first-degree relatives of affected patients.
However, "extensive candidate gene and linkage searches have to date been unsuccessful in identifying genetic variants that are associated with risk of Barrett’s esophagus," wrote Dr. Zhan Su of the Wellcome Trust Centre for Human Genetics in Oxford, England, and his associates.
Their findings provide the first direct evidence that the etiology of Barrett’s esophagus has a genetic component, the researchers noted.
Dr. Su and his colleagues performed the genome-wide association study as part of a Wellcome Trust consortium study of the genetic components of 15 common disorders and traits. They identified the two genetic variants in a discovery analysis and confirmed the findings in another five replication cohorts.
The discovery analysis involved genotyping of 1,852 adults with histologically confirmed Barrett’s esophagus who were recruited from sites across the United Kingdom. A representative sample of 5,172 control subjects also was analyzed. A total of 521,744 single-nucleotide polymorphisms (SNPs) were typed.
The 100 SNPs that were associated to some degree with Barrett’s esophagus were then analyzed in a separate cohort of 1,105 cases from two clinical trials, 4,421 controls from another U.K. sample, and 2,578 controls from yet another U.K .sample.
The top 16 SNPs from these analyses were then analyzed in a second replication cohort of 473 cases and 1,780 controls from a Dutch genotyping database. Two of the SNPs were found to be significantly associated with Barrett\'’s esophagus: rs9257809 on chromosome 6p21 and rs9936833 on chromosome 16q24.
It is notable that the closest coding gene to the rs9936833 SNP on chromosome 16q24 is a gene that encodes a protein involved in the development of the gastrointestinal tract. It has been reported that, when this gene is inactivated, structural alterations in the esophagus, especially atresia, occur. The rs9257809 SNP on 6p21 is near the telomeric edge of the major histocompatibility complex region.
The two SNPs were then examined further in an Irish cohort of 245 cases and 473 controls, a U.K. cohort of 1,765 cases and 1,586 controls, and a cohort of 2,398 cases and 2,167 controls from Europe, Australia, and the United States.
Overall, the two SNPs "showed compelling evidence for association," with Barrett’s esophagus, reflected in the significance of the combined P values for rs9257809 (odds ratio, 1.21) and rs9936833 (odds ratio, 1.14), the investigators reported (Nat. Genet. 2012 Sept. 9 [doi:10.1038/ng.2408]).
In a subgroup analysis involving only patients who had histologic evidence of intestinal metaplasia, the same two SNPs were again strongly associated with Barrett’s esophagus. Neither SNP, however, was associated with either the circumferential extent or the maximal length of the affected segment of esophagus.
Given that men are known to be more susceptible than women to Barrett’s esophagus, the investigators also performed a sex-stratified analysis of the data and found that the association between both SNPs and the disorder was stronger in men than in women. "This finding warrants further investigation," they noted.
Similarly, given the known association between obesity and Barrett’s esophagus, the researchers analyzed the 40 SNPs that previously have been linked with either body mass index or waist-to-hip ratio. These latter SNPs were "more likely than expected by chance to show effects in the same direction in association with Barrett’s esophagus, suggesting that genetic effects may in part underpin the epidemiologic observation that BMI is a risk factor for Barrett’s esophagus," Dr. Su and his associates said.
"Given that Barrett’s esophagus has an accepted status as a precursor lesion, the SNPs that we have identified could also essentially be risk factors for esophageal adenocarcinoma and may give clues as to the biology of both of these important phenotypes," they added.
The financial disclosures of Dr. Su and his 143 coauthors are listed in the online version of this article.
Two common genetic variants on chromosomes 6p21 and 16q24 were found to be associated with Barrett’s esophagus in the first genome-wide association study of susceptibility to the disorder, according to a letter to the editor published online Sept. 9 in Nature Genetics.
Genetic factors have long been suspected to play a role in the development of Barrett’s esophagus since relative risks for the disorder, as well as for gastroesophageal reflux disease and esophageal adenocarcinoma, are increased two- to fourfold in first-degree relatives of affected patients.
However, "extensive candidate gene and linkage searches have to date been unsuccessful in identifying genetic variants that are associated with risk of Barrett’s esophagus," wrote Dr. Zhan Su of the Wellcome Trust Centre for Human Genetics in Oxford, England, and his associates.
Their findings provide the first direct evidence that the etiology of Barrett’s esophagus has a genetic component, the researchers noted.
Dr. Su and his colleagues performed the genome-wide association study as part of a Wellcome Trust consortium study of the genetic components of 15 common disorders and traits. They identified the two genetic variants in a discovery analysis and confirmed the findings in another five replication cohorts.
The discovery analysis involved genotyping of 1,852 adults with histologically confirmed Barrett’s esophagus who were recruited from sites across the United Kingdom. A representative sample of 5,172 control subjects also was analyzed. A total of 521,744 single-nucleotide polymorphisms (SNPs) were typed.
The 100 SNPs that were associated to some degree with Barrett’s esophagus were then analyzed in a separate cohort of 1,105 cases from two clinical trials, 4,421 controls from another U.K. sample, and 2,578 controls from yet another U.K .sample.
The top 16 SNPs from these analyses were then analyzed in a second replication cohort of 473 cases and 1,780 controls from a Dutch genotyping database. Two of the SNPs were found to be significantly associated with Barrett\'’s esophagus: rs9257809 on chromosome 6p21 and rs9936833 on chromosome 16q24.
It is notable that the closest coding gene to the rs9936833 SNP on chromosome 16q24 is a gene that encodes a protein involved in the development of the gastrointestinal tract. It has been reported that, when this gene is inactivated, structural alterations in the esophagus, especially atresia, occur. The rs9257809 SNP on 6p21 is near the telomeric edge of the major histocompatibility complex region.
The two SNPs were then examined further in an Irish cohort of 245 cases and 473 controls, a U.K. cohort of 1,765 cases and 1,586 controls, and a cohort of 2,398 cases and 2,167 controls from Europe, Australia, and the United States.
Overall, the two SNPs "showed compelling evidence for association," with Barrett’s esophagus, reflected in the significance of the combined P values for rs9257809 (odds ratio, 1.21) and rs9936833 (odds ratio, 1.14), the investigators reported (Nat. Genet. 2012 Sept. 9 [doi:10.1038/ng.2408]).
In a subgroup analysis involving only patients who had histologic evidence of intestinal metaplasia, the same two SNPs were again strongly associated with Barrett’s esophagus. Neither SNP, however, was associated with either the circumferential extent or the maximal length of the affected segment of esophagus.
Given that men are known to be more susceptible than women to Barrett’s esophagus, the investigators also performed a sex-stratified analysis of the data and found that the association between both SNPs and the disorder was stronger in men than in women. "This finding warrants further investigation," they noted.
Similarly, given the known association between obesity and Barrett’s esophagus, the researchers analyzed the 40 SNPs that previously have been linked with either body mass index or waist-to-hip ratio. These latter SNPs were "more likely than expected by chance to show effects in the same direction in association with Barrett’s esophagus, suggesting that genetic effects may in part underpin the epidemiologic observation that BMI is a risk factor for Barrett’s esophagus," Dr. Su and his associates said.
"Given that Barrett’s esophagus has an accepted status as a precursor lesion, the SNPs that we have identified could also essentially be risk factors for esophageal adenocarcinoma and may give clues as to the biology of both of these important phenotypes," they added.
The financial disclosures of Dr. Su and his 143 coauthors are listed in the online version of this article.
FROM NATURE GENETICS
Major Finding: The rs9257809 SNP on chromosome 6p21 and the rs9936833 SNP on chromosome 16q24 both were strongly associated with an increased risk of developing Barrett's esophagus.
Data Source: The investigators conducted a genome-wide association study of susceptibility to Barrett’s esophagus, analyzing the genotypes of 7,838 patients and 15,599 control subjects in several countries.
Disclosures: The financial disclosures of Dr. Su and his 143 coauthors are listed in the online version of this article.