User login
Sleep Deprivation Caused Insulin Resistance in Fat Cells
Sleep deprivation caused a 30% decline in the insulin sensitivity of fat cells of healthy, lean young adults, according to a study in the Oct. 6 issue of Annals of Internal Medicine.
Restricting sleep for 4 nights markedly impaired the phosphorylation of Akt within the adipocytes in subcutaneous fat, which is a crucial early step in the pathway that mediates most of insulin's metabolic action. "This finding identifies for the first time a molecular mechanism that may be involved in the reduction in total-body insulin sensitivity consistently observed in multiple laboratory studies of partial sleep deprivation in healthy adults," said Josiane L. Broussard, Ph.D., and her associates at the University of Chicago.
Moreover, "our finding of marked alterations in adipocyte function after experimental sleep restriction challenges the widely held belief that the primary function of sleep is the restoration of central nervous system function and suggests that sleep may play an equally important role in peripheral energy metabolism," they noted.
Insufficient sleep is known to raise the risk of metabolic disturbances, particularly insulin resistance, obesity, and type 2 diabetes. But "to our knowledge, no studies to date have linked sleep restriction to alterations in molecular metabolic pathways in any peripheral human tissue." Dr. Broussard and her colleagues examined whether experimental sleep restriction would reduce insulin sensitivity in subcutaneous fat, "a peripheral tissue that is a key site of insulin action and plays a pivotal role in energy metabolism as well as in the communication of energy balance to the brain."
Six men and one woman aged 18-30 years (mean age 23.7 years) who were healthy and lean were selected from the community as study subjects. All reported routine sleep times of 7.5-8.5 hours/night. All underwent overnight polysomnography to ensure they had no sleep disorders, standard glucose tolerance testing to rule out any occult disorders of insulin metabolism, and standard laboratory tests to rule out any other problem that could affect either sleep or metabolism.
These subjects were then assessed under two experimental sleep conditions in randomized order: after 4 consecutive nights of 8.5 hours of normal sleep and after 4 consecutive nights of 4.5 hours of restricted sleep. The subjects lived as sedentary inpatients during these experiments, with strictly controlled diets that were identical under the two sleep conditions.
At the conclusion of the sleep periods, abdominal subcutaneous fat tissue was sampled for in vitro measurement of phosphorylated Akt in response to increasing doses of insulin. Total body insulin sensitivity also was assessed using frequently sampled intravenous glucose tolerance tests.
The study subjects averaged 8.78 hours of sleep per night under the normal sleep condition and 4.35 hours under the restricted sleep condition. The amount of REM sleep was reduced by 56.8% in the latter condition.
After normal sleep, insulin provocation caused dose-dependent increases in phosphorylated Akt, as expected. In dramatic contrast, sleep restriction consistently induced an approximately 30% reduction in phosphorylated Akt in response to insulin provocation.
In addition, total-body insulin sensitivity was reduced by 16% after partial sleep deprivation, compared with normal sleep.
The 30% decline "lies within the range of the difference in insulin sensitivity in adipocytes from obese vs. lean participants and from diabetic patients vs. nondiabetic participants" in previous studies. "Thus, the impairment of insulin signalling in adipocytes from persons who are chronically sleep-deprived or have sleep disorders is likely to have important metabolic consequences," Dr. Broussard and her associates wrote (Ann. Intern. Med. 2012;157:549-57).
"From a clinical standpoint, our study provides additional evidence that insufficient sleep may contribute to the development of or exacerbate metabolic disorders." But the findings also "shed novel light on the still-elusive function of sleep, traditionally conceptualized as necessary only for the brain, because they suggest that sleep plays an important role for the functional integrity of multiple peripheral cell types, as well as for whole-body energy homeostasis," they said.
This study was limited in that it was performed at a single center, involved a very small sample size and involved only one woman. "The findings will therefore need to be replicated in a larger and more diverse population," the researchers added.
This study was funded by the National Institutes of Health. The researchers reported having no relevant conflicts of interest.
Dr. Broussard and her colleagues make a valuable contribution to our understanding of how sleep deprivation may directly contribute to diabetes and obesity, said Dr. Francesco P. Cappuccio and Dr. Michelle A. Miller.
Their findings also challenge "the traditional view that the primary purpose of sleep is confined to restorative effects on the CNS. [They] point to a much wider influence of sleep on bodily functions, including metabolism, adipose tissue, cardiovascular function, and possibly more," they said.
The results also highlight the need to address factors that limit sleep duration, as a strategy to improve the overall health of individuals as well as of society.
Francesco P. Cappuccio, M.D., and Michelle A. Miller, Ph.D., are at the University of Warwick, Coventry, England. They reported having no relevant conflicts of interest. These remarks were taken from their editorial accompanying Dr. Broussard’s report (Ann. Intern. Med. 2012;157:593-4).
Dr. Broussard and her colleagues make a valuable contribution to our understanding of how sleep deprivation may directly contribute to diabetes and obesity, said Dr. Francesco P. Cappuccio and Dr. Michelle A. Miller.
Their findings also challenge "the traditional view that the primary purpose of sleep is confined to restorative effects on the CNS. [They] point to a much wider influence of sleep on bodily functions, including metabolism, adipose tissue, cardiovascular function, and possibly more," they said.
The results also highlight the need to address factors that limit sleep duration, as a strategy to improve the overall health of individuals as well as of society.
Francesco P. Cappuccio, M.D., and Michelle A. Miller, Ph.D., are at the University of Warwick, Coventry, England. They reported having no relevant conflicts of interest. These remarks were taken from their editorial accompanying Dr. Broussard’s report (Ann. Intern. Med. 2012;157:593-4).
Dr. Broussard and her colleagues make a valuable contribution to our understanding of how sleep deprivation may directly contribute to diabetes and obesity, said Dr. Francesco P. Cappuccio and Dr. Michelle A. Miller.
Their findings also challenge "the traditional view that the primary purpose of sleep is confined to restorative effects on the CNS. [They] point to a much wider influence of sleep on bodily functions, including metabolism, adipose tissue, cardiovascular function, and possibly more," they said.
The results also highlight the need to address factors that limit sleep duration, as a strategy to improve the overall health of individuals as well as of society.
Francesco P. Cappuccio, M.D., and Michelle A. Miller, Ph.D., are at the University of Warwick, Coventry, England. They reported having no relevant conflicts of interest. These remarks were taken from their editorial accompanying Dr. Broussard’s report (Ann. Intern. Med. 2012;157:593-4).
Sleep deprivation caused a 30% decline in the insulin sensitivity of fat cells of healthy, lean young adults, according to a study in the Oct. 6 issue of Annals of Internal Medicine.
Restricting sleep for 4 nights markedly impaired the phosphorylation of Akt within the adipocytes in subcutaneous fat, which is a crucial early step in the pathway that mediates most of insulin's metabolic action. "This finding identifies for the first time a molecular mechanism that may be involved in the reduction in total-body insulin sensitivity consistently observed in multiple laboratory studies of partial sleep deprivation in healthy adults," said Josiane L. Broussard, Ph.D., and her associates at the University of Chicago.
Moreover, "our finding of marked alterations in adipocyte function after experimental sleep restriction challenges the widely held belief that the primary function of sleep is the restoration of central nervous system function and suggests that sleep may play an equally important role in peripheral energy metabolism," they noted.
Insufficient sleep is known to raise the risk of metabolic disturbances, particularly insulin resistance, obesity, and type 2 diabetes. But "to our knowledge, no studies to date have linked sleep restriction to alterations in molecular metabolic pathways in any peripheral human tissue." Dr. Broussard and her colleagues examined whether experimental sleep restriction would reduce insulin sensitivity in subcutaneous fat, "a peripheral tissue that is a key site of insulin action and plays a pivotal role in energy metabolism as well as in the communication of energy balance to the brain."
Six men and one woman aged 18-30 years (mean age 23.7 years) who were healthy and lean were selected from the community as study subjects. All reported routine sleep times of 7.5-8.5 hours/night. All underwent overnight polysomnography to ensure they had no sleep disorders, standard glucose tolerance testing to rule out any occult disorders of insulin metabolism, and standard laboratory tests to rule out any other problem that could affect either sleep or metabolism.
These subjects were then assessed under two experimental sleep conditions in randomized order: after 4 consecutive nights of 8.5 hours of normal sleep and after 4 consecutive nights of 4.5 hours of restricted sleep. The subjects lived as sedentary inpatients during these experiments, with strictly controlled diets that were identical under the two sleep conditions.
At the conclusion of the sleep periods, abdominal subcutaneous fat tissue was sampled for in vitro measurement of phosphorylated Akt in response to increasing doses of insulin. Total body insulin sensitivity also was assessed using frequently sampled intravenous glucose tolerance tests.
The study subjects averaged 8.78 hours of sleep per night under the normal sleep condition and 4.35 hours under the restricted sleep condition. The amount of REM sleep was reduced by 56.8% in the latter condition.
After normal sleep, insulin provocation caused dose-dependent increases in phosphorylated Akt, as expected. In dramatic contrast, sleep restriction consistently induced an approximately 30% reduction in phosphorylated Akt in response to insulin provocation.
In addition, total-body insulin sensitivity was reduced by 16% after partial sleep deprivation, compared with normal sleep.
The 30% decline "lies within the range of the difference in insulin sensitivity in adipocytes from obese vs. lean participants and from diabetic patients vs. nondiabetic participants" in previous studies. "Thus, the impairment of insulin signalling in adipocytes from persons who are chronically sleep-deprived or have sleep disorders is likely to have important metabolic consequences," Dr. Broussard and her associates wrote (Ann. Intern. Med. 2012;157:549-57).
"From a clinical standpoint, our study provides additional evidence that insufficient sleep may contribute to the development of or exacerbate metabolic disorders." But the findings also "shed novel light on the still-elusive function of sleep, traditionally conceptualized as necessary only for the brain, because they suggest that sleep plays an important role for the functional integrity of multiple peripheral cell types, as well as for whole-body energy homeostasis," they said.
This study was limited in that it was performed at a single center, involved a very small sample size and involved only one woman. "The findings will therefore need to be replicated in a larger and more diverse population," the researchers added.
This study was funded by the National Institutes of Health. The researchers reported having no relevant conflicts of interest.
Sleep deprivation caused a 30% decline in the insulin sensitivity of fat cells of healthy, lean young adults, according to a study in the Oct. 6 issue of Annals of Internal Medicine.
Restricting sleep for 4 nights markedly impaired the phosphorylation of Akt within the adipocytes in subcutaneous fat, which is a crucial early step in the pathway that mediates most of insulin's metabolic action. "This finding identifies for the first time a molecular mechanism that may be involved in the reduction in total-body insulin sensitivity consistently observed in multiple laboratory studies of partial sleep deprivation in healthy adults," said Josiane L. Broussard, Ph.D., and her associates at the University of Chicago.
Moreover, "our finding of marked alterations in adipocyte function after experimental sleep restriction challenges the widely held belief that the primary function of sleep is the restoration of central nervous system function and suggests that sleep may play an equally important role in peripheral energy metabolism," they noted.
Insufficient sleep is known to raise the risk of metabolic disturbances, particularly insulin resistance, obesity, and type 2 diabetes. But "to our knowledge, no studies to date have linked sleep restriction to alterations in molecular metabolic pathways in any peripheral human tissue." Dr. Broussard and her colleagues examined whether experimental sleep restriction would reduce insulin sensitivity in subcutaneous fat, "a peripheral tissue that is a key site of insulin action and plays a pivotal role in energy metabolism as well as in the communication of energy balance to the brain."
Six men and one woman aged 18-30 years (mean age 23.7 years) who were healthy and lean were selected from the community as study subjects. All reported routine sleep times of 7.5-8.5 hours/night. All underwent overnight polysomnography to ensure they had no sleep disorders, standard glucose tolerance testing to rule out any occult disorders of insulin metabolism, and standard laboratory tests to rule out any other problem that could affect either sleep or metabolism.
These subjects were then assessed under two experimental sleep conditions in randomized order: after 4 consecutive nights of 8.5 hours of normal sleep and after 4 consecutive nights of 4.5 hours of restricted sleep. The subjects lived as sedentary inpatients during these experiments, with strictly controlled diets that were identical under the two sleep conditions.
At the conclusion of the sleep periods, abdominal subcutaneous fat tissue was sampled for in vitro measurement of phosphorylated Akt in response to increasing doses of insulin. Total body insulin sensitivity also was assessed using frequently sampled intravenous glucose tolerance tests.
The study subjects averaged 8.78 hours of sleep per night under the normal sleep condition and 4.35 hours under the restricted sleep condition. The amount of REM sleep was reduced by 56.8% in the latter condition.
After normal sleep, insulin provocation caused dose-dependent increases in phosphorylated Akt, as expected. In dramatic contrast, sleep restriction consistently induced an approximately 30% reduction in phosphorylated Akt in response to insulin provocation.
In addition, total-body insulin sensitivity was reduced by 16% after partial sleep deprivation, compared with normal sleep.
The 30% decline "lies within the range of the difference in insulin sensitivity in adipocytes from obese vs. lean participants and from diabetic patients vs. nondiabetic participants" in previous studies. "Thus, the impairment of insulin signalling in adipocytes from persons who are chronically sleep-deprived or have sleep disorders is likely to have important metabolic consequences," Dr. Broussard and her associates wrote (Ann. Intern. Med. 2012;157:549-57).
"From a clinical standpoint, our study provides additional evidence that insufficient sleep may contribute to the development of or exacerbate metabolic disorders." But the findings also "shed novel light on the still-elusive function of sleep, traditionally conceptualized as necessary only for the brain, because they suggest that sleep plays an important role for the functional integrity of multiple peripheral cell types, as well as for whole-body energy homeostasis," they said.
This study was limited in that it was performed at a single center, involved a very small sample size and involved only one woman. "The findings will therefore need to be replicated in a larger and more diverse population," the researchers added.
This study was funded by the National Institutes of Health. The researchers reported having no relevant conflicts of interest.
FROM ANNALS OF INTERNAL MEDICINE
Major Finding: Partial sleep deprivation consistently caused a 30% reduction in fat cells’ response to insulin stimulation, as well as a 16% decline in total-body insulin sensitivity.
Data Source: Results were taken from a randomized crossover clinical study comparing the effects of sleep deprivation with those of normal sleep in 7 healthy, lean, young adults.
Disclosures: This study was funded by the National Institutes of Health. The researchers reported having no relevant conflicts of interest.
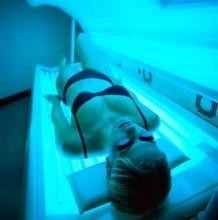
Tanning Bed Risks Not Communicated to 73% of Germans
Four out of 10 people in Germany reported ever using a tanning bed, according to the results of a recent population-based survey published online Oct. 15 in Archives of Dermatology.
The overall prevalence of tanning bed use was 39.2%, "and every seventh person ... had used a sunbed during the last 12 months," reported Sven Schneider, Ph.D., of the Mannheim Institute of Public Health, Heidelberg University (Germany), and his associates. "These findings emphasize the urgent need for standardized education of sunbed personnel by independent (not sunbed industry-associated) institutions."
Data on the prevalence of tanning bed use and on the behavior patterns associated with its use are "unavailable or limited," which is surprising because the prevalence and behavior patterns associated with exposure to other known carcinogens, such as tobacco and alcohol, "are studied and monitored extensively," reported Dr. Schneider and his colleagues. They sought "to obtain a more comprehensive overview of the current state of sunbed use in Germany."
They assessed 4,851 people aged 14-45 years using an anonymous telephone survey during both summer and winter months. The study population was equally divided between males and females, and the mean study patient age was 31 years. Of the participants, 32% reported having Fitzpatrick skin type I or II, 35% reported a Fitzpatrick skin type of III, and 28% reported having skin type IV. Skin types V and VI are rare in Germany, the researchers noted.
Tanning bed use was more common in people aged 18-25 years (mean prevalence, 21.4%) than in other age groups (mean prevalence, 12.6%). And women were more likely than were men to have ever used a tanning bed (49% vs 29.8%) or to be using tanning beds currently (17.7% vs 11.7%).
People used tanning beds predominantly in tanning salons (74.9%), fitness centers (10.1%), or at swimming pools/sauna facilities (7.9%). They were less likely to use tanning beds at home (3.8%), in hotels (1.5%), beauty salons (0.7%), or medical facilities (0.6%).
Among current users, 68.2% said that "advisory personnel" were present at their most recent visit. Only 41% of users reported use of protective goggles at their most recent visit, and 40% said they had never been advised to wear protective goggles.
Over 40% of current tanning bed users said they had never been given advice about skin type, and approximately 73% said they had never been informed about the potential health risks of tanning bed use. More than one-third of respondents who had Fitzpatrick type I or II skin had used a tanning bed at least once.
Seventy percent said they had not been asked by personnel about medications, skin care products, or skin disorders that may have contraindicated the use of a tanning bed. And nearly 78% of users said they had not received an individual tanning plan based on their skin type.
The most important reasons given for using tanning beds were for relaxation, to improve physical attractiveness, to "pretan" before vacation, and "the desire for a feeling of warmth." Other reasons given somewhat frequently were "for health care" and "vitamin D supplementation." Tanning bed personnel routinely failed to inform clients that these reasons "are not medically sound," Dr. Schneider and his associates reported (Arch. Dermatol. 2012 Oct. 15 [doi:10.1001/2013.jamadermatol.562]).
The study population may have been unusual in that a large proportion of the tanning bed users already had somewhat dark skin (Fitzgerald types III or higher). Also, results of the study showed that immigrants were more likely to use tanning beds. "This association might be explained by beauty ideals of users with a Turkish heritage: Turks represent the largest group of immigrants in Germany," wrote Dr. Schneider and colleagues.
The study was supported by the German Cancer Aid. No financial conflicts of interest were reported.
Four out of 10 people in Germany reported ever using a tanning bed, according to the results of a recent population-based survey published online Oct. 15 in Archives of Dermatology.
The overall prevalence of tanning bed use was 39.2%, "and every seventh person ... had used a sunbed during the last 12 months," reported Sven Schneider, Ph.D., of the Mannheim Institute of Public Health, Heidelberg University (Germany), and his associates. "These findings emphasize the urgent need for standardized education of sunbed personnel by independent (not sunbed industry-associated) institutions."
Data on the prevalence of tanning bed use and on the behavior patterns associated with its use are "unavailable or limited," which is surprising because the prevalence and behavior patterns associated with exposure to other known carcinogens, such as tobacco and alcohol, "are studied and monitored extensively," reported Dr. Schneider and his colleagues. They sought "to obtain a more comprehensive overview of the current state of sunbed use in Germany."
They assessed 4,851 people aged 14-45 years using an anonymous telephone survey during both summer and winter months. The study population was equally divided between males and females, and the mean study patient age was 31 years. Of the participants, 32% reported having Fitzpatrick skin type I or II, 35% reported a Fitzpatrick skin type of III, and 28% reported having skin type IV. Skin types V and VI are rare in Germany, the researchers noted.
Tanning bed use was more common in people aged 18-25 years (mean prevalence, 21.4%) than in other age groups (mean prevalence, 12.6%). And women were more likely than were men to have ever used a tanning bed (49% vs 29.8%) or to be using tanning beds currently (17.7% vs 11.7%).
People used tanning beds predominantly in tanning salons (74.9%), fitness centers (10.1%), or at swimming pools/sauna facilities (7.9%). They were less likely to use tanning beds at home (3.8%), in hotels (1.5%), beauty salons (0.7%), or medical facilities (0.6%).
Among current users, 68.2% said that "advisory personnel" were present at their most recent visit. Only 41% of users reported use of protective goggles at their most recent visit, and 40% said they had never been advised to wear protective goggles.
Over 40% of current tanning bed users said they had never been given advice about skin type, and approximately 73% said they had never been informed about the potential health risks of tanning bed use. More than one-third of respondents who had Fitzpatrick type I or II skin had used a tanning bed at least once.
Seventy percent said they had not been asked by personnel about medications, skin care products, or skin disorders that may have contraindicated the use of a tanning bed. And nearly 78% of users said they had not received an individual tanning plan based on their skin type.
The most important reasons given for using tanning beds were for relaxation, to improve physical attractiveness, to "pretan" before vacation, and "the desire for a feeling of warmth." Other reasons given somewhat frequently were "for health care" and "vitamin D supplementation." Tanning bed personnel routinely failed to inform clients that these reasons "are not medically sound," Dr. Schneider and his associates reported (Arch. Dermatol. 2012 Oct. 15 [doi:10.1001/2013.jamadermatol.562]).
The study population may have been unusual in that a large proportion of the tanning bed users already had somewhat dark skin (Fitzgerald types III or higher). Also, results of the study showed that immigrants were more likely to use tanning beds. "This association might be explained by beauty ideals of users with a Turkish heritage: Turks represent the largest group of immigrants in Germany," wrote Dr. Schneider and colleagues.
The study was supported by the German Cancer Aid. No financial conflicts of interest were reported.
Four out of 10 people in Germany reported ever using a tanning bed, according to the results of a recent population-based survey published online Oct. 15 in Archives of Dermatology.
The overall prevalence of tanning bed use was 39.2%, "and every seventh person ... had used a sunbed during the last 12 months," reported Sven Schneider, Ph.D., of the Mannheim Institute of Public Health, Heidelberg University (Germany), and his associates. "These findings emphasize the urgent need for standardized education of sunbed personnel by independent (not sunbed industry-associated) institutions."
Data on the prevalence of tanning bed use and on the behavior patterns associated with its use are "unavailable or limited," which is surprising because the prevalence and behavior patterns associated with exposure to other known carcinogens, such as tobacco and alcohol, "are studied and monitored extensively," reported Dr. Schneider and his colleagues. They sought "to obtain a more comprehensive overview of the current state of sunbed use in Germany."
They assessed 4,851 people aged 14-45 years using an anonymous telephone survey during both summer and winter months. The study population was equally divided between males and females, and the mean study patient age was 31 years. Of the participants, 32% reported having Fitzpatrick skin type I or II, 35% reported a Fitzpatrick skin type of III, and 28% reported having skin type IV. Skin types V and VI are rare in Germany, the researchers noted.
Tanning bed use was more common in people aged 18-25 years (mean prevalence, 21.4%) than in other age groups (mean prevalence, 12.6%). And women were more likely than were men to have ever used a tanning bed (49% vs 29.8%) or to be using tanning beds currently (17.7% vs 11.7%).
People used tanning beds predominantly in tanning salons (74.9%), fitness centers (10.1%), or at swimming pools/sauna facilities (7.9%). They were less likely to use tanning beds at home (3.8%), in hotels (1.5%), beauty salons (0.7%), or medical facilities (0.6%).
Among current users, 68.2% said that "advisory personnel" were present at their most recent visit. Only 41% of users reported use of protective goggles at their most recent visit, and 40% said they had never been advised to wear protective goggles.
Over 40% of current tanning bed users said they had never been given advice about skin type, and approximately 73% said they had never been informed about the potential health risks of tanning bed use. More than one-third of respondents who had Fitzpatrick type I or II skin had used a tanning bed at least once.
Seventy percent said they had not been asked by personnel about medications, skin care products, or skin disorders that may have contraindicated the use of a tanning bed. And nearly 78% of users said they had not received an individual tanning plan based on their skin type.
The most important reasons given for using tanning beds were for relaxation, to improve physical attractiveness, to "pretan" before vacation, and "the desire for a feeling of warmth." Other reasons given somewhat frequently were "for health care" and "vitamin D supplementation." Tanning bed personnel routinely failed to inform clients that these reasons "are not medically sound," Dr. Schneider and his associates reported (Arch. Dermatol. 2012 Oct. 15 [doi:10.1001/2013.jamadermatol.562]).
The study population may have been unusual in that a large proportion of the tanning bed users already had somewhat dark skin (Fitzgerald types III or higher). Also, results of the study showed that immigrants were more likely to use tanning beds. "This association might be explained by beauty ideals of users with a Turkish heritage: Turks represent the largest group of immigrants in Germany," wrote Dr. Schneider and colleagues.
The study was supported by the German Cancer Aid. No financial conflicts of interest were reported.
FROM ARCHIVES OF DERMATOLOGY
Major Finding: The overall prevalence of tanning bed use was nearly 40%, with most users being aged 18-25 years (mean prevalence, 21.4%).
Data Source: Investigators assessed 4,851 people aged 14-45 years using an anonymous telephone survey during both summer and winter months in Germany.
Disclosures: This study was supported by the German Cancer Aid. No financial conflicts of interest were reported.
More Evidence Links Tanning Beds to Skin Cancer
Indoor tanning is strongly associated with the development of both basal and squamous cell carcinoma, according to a recent meta-analysis.
Indoor tanning – the use of a sun bed, sun lamp, tanning booth, or solarium – was related to a 29% higher risk for basal cell carcinoma and a 67% higher risk for squamous cell carcinoma, compared with no such exposure, according to a meta-analysis of 12 studies that reported effect estimates.
This translates to nearly 171,000 cases of nonmelanoma skin cancer each year that are attributable to indoor tanning in the United States alone, reported Mackenzie R. Wehner, a medical student at Stanford (Calif.) University, and her associates.
Several studies have examined a potential link between indoor tanning and nonmelanoma skin cancers, but the study populations have been small and the results have not been consistent. Therefore, Ms. Wehner and her colleagues performed a systematic review and meta-analysis of 10 case-control studies, 1 nested case-control study, and 1 cohort study for a combined population of 80,661 patients, in which there were 9,328 cases of nonmelanoma skin cancer. The studies were conducted in six countries from 1985 to 2012.
The investigators found summary relative risks of 1.29 for basal cell carcinoma and 1.67 for squamous cell carcinoma. These findings did not change appreciably in sensitivity analyses (BMJ 2012;345:e5909 [doi:10.1136/bmj.e5909]).
To examine whether a dose-response effect was present, the researchers performed an additional analysis on the studies that included effect estimates for frequent or multiple exposures to indoor tanning. Such high-dose exposure was associated with an increased risk of basal cell carcinoma, but the increase was not statistically significant.
To examine whether exposure to indoor tanning at a young age was especially high risk, Ms. Wehner and her colleagues performed an additional analysis of studies that included effect estimates for exposure before age 25. They found that such exposure was associated with a relative risk of 1.40 for basal cell carcinoma and of 2.02 for squamous cell carcinoma. "This suggests a critical period for exposure during early life," they wrote.
"Applying our summary risk estimates to the prevalence of exposure to indoor tanning in the United States, we calculated the population attributable risk fraction at 3.7% for basal cell carcinoma and at 8.2% for squamous cell carcinoma. This corresponds to 98,408 cases of basal cell carcinoma and 72,244 cases of squamous cell carcinoma, making 170,652 cases of nonmelanoma skin cancer each year attributable to indoor tanning," the researchers noted.
The study results are consistent with those of a previous meta-analysis that pooled the results of five studies. "Our findings add to the growing body of evidence on the harms of indoor tanning," Ms. Wehner and her colleagues said. "We hope that these findings can support public health campaigns and motivate increased regulation to reduce exposure to this carcinogen, especially during early life."
The study was supported by the National Center for Research Resources and the National Institute of Arthritis and Musculoskeletal and Skin Diseases. One of the study investigators reported ties to Genentech. No other conflicts of interest were reported.
This study provides convincing evidence that exposure to artificial ultraviolet radiation is a cause of three main skin cancers, noted Catherine M. Olsen and Adèle C. Green.
Indoor tanning is already known to cause melanoma, and for that reason is classified as a group 1 carcinogen by the Word Health Organization, along with asbestos exposure and tobacco smoking. Now indoor tanning has been shown to have a strong positive association with basal and squamous cell cancers, with some evidence of a dose-response relationship, and confirmation that the risks are higher with earlier exposure.
The morbidity related to treatment of basal and squamous cell cancers, as well as the avoidable costs to the health care system, are substantial.
Ms. Olsen is a senior research officer and Ms. Green is head of cancer and population studies at the Queensland Institute of Medical Research, Australia. They reported no potential conflicts of interest. These remarks were taken from their editorial accompanying Ms. Wehner’s report (BMJ 2012;345:e6101 [doi:10.1136/bmj.e6101]).
This study provides convincing evidence that exposure to artificial ultraviolet radiation is a cause of three main skin cancers, noted Catherine M. Olsen and Adèle C. Green.
Indoor tanning is already known to cause melanoma, and for that reason is classified as a group 1 carcinogen by the Word Health Organization, along with asbestos exposure and tobacco smoking. Now indoor tanning has been shown to have a strong positive association with basal and squamous cell cancers, with some evidence of a dose-response relationship, and confirmation that the risks are higher with earlier exposure.
The morbidity related to treatment of basal and squamous cell cancers, as well as the avoidable costs to the health care system, are substantial.
Ms. Olsen is a senior research officer and Ms. Green is head of cancer and population studies at the Queensland Institute of Medical Research, Australia. They reported no potential conflicts of interest. These remarks were taken from their editorial accompanying Ms. Wehner’s report (BMJ 2012;345:e6101 [doi:10.1136/bmj.e6101]).
This study provides convincing evidence that exposure to artificial ultraviolet radiation is a cause of three main skin cancers, noted Catherine M. Olsen and Adèle C. Green.
Indoor tanning is already known to cause melanoma, and for that reason is classified as a group 1 carcinogen by the Word Health Organization, along with asbestos exposure and tobacco smoking. Now indoor tanning has been shown to have a strong positive association with basal and squamous cell cancers, with some evidence of a dose-response relationship, and confirmation that the risks are higher with earlier exposure.
The morbidity related to treatment of basal and squamous cell cancers, as well as the avoidable costs to the health care system, are substantial.
Ms. Olsen is a senior research officer and Ms. Green is head of cancer and population studies at the Queensland Institute of Medical Research, Australia. They reported no potential conflicts of interest. These remarks were taken from their editorial accompanying Ms. Wehner’s report (BMJ 2012;345:e6101 [doi:10.1136/bmj.e6101]).
Indoor tanning is strongly associated with the development of both basal and squamous cell carcinoma, according to a recent meta-analysis.
Indoor tanning – the use of a sun bed, sun lamp, tanning booth, or solarium – was related to a 29% higher risk for basal cell carcinoma and a 67% higher risk for squamous cell carcinoma, compared with no such exposure, according to a meta-analysis of 12 studies that reported effect estimates.
This translates to nearly 171,000 cases of nonmelanoma skin cancer each year that are attributable to indoor tanning in the United States alone, reported Mackenzie R. Wehner, a medical student at Stanford (Calif.) University, and her associates.
Several studies have examined a potential link between indoor tanning and nonmelanoma skin cancers, but the study populations have been small and the results have not been consistent. Therefore, Ms. Wehner and her colleagues performed a systematic review and meta-analysis of 10 case-control studies, 1 nested case-control study, and 1 cohort study for a combined population of 80,661 patients, in which there were 9,328 cases of nonmelanoma skin cancer. The studies were conducted in six countries from 1985 to 2012.
The investigators found summary relative risks of 1.29 for basal cell carcinoma and 1.67 for squamous cell carcinoma. These findings did not change appreciably in sensitivity analyses (BMJ 2012;345:e5909 [doi:10.1136/bmj.e5909]).
To examine whether a dose-response effect was present, the researchers performed an additional analysis on the studies that included effect estimates for frequent or multiple exposures to indoor tanning. Such high-dose exposure was associated with an increased risk of basal cell carcinoma, but the increase was not statistically significant.
To examine whether exposure to indoor tanning at a young age was especially high risk, Ms. Wehner and her colleagues performed an additional analysis of studies that included effect estimates for exposure before age 25. They found that such exposure was associated with a relative risk of 1.40 for basal cell carcinoma and of 2.02 for squamous cell carcinoma. "This suggests a critical period for exposure during early life," they wrote.
"Applying our summary risk estimates to the prevalence of exposure to indoor tanning in the United States, we calculated the population attributable risk fraction at 3.7% for basal cell carcinoma and at 8.2% for squamous cell carcinoma. This corresponds to 98,408 cases of basal cell carcinoma and 72,244 cases of squamous cell carcinoma, making 170,652 cases of nonmelanoma skin cancer each year attributable to indoor tanning," the researchers noted.
The study results are consistent with those of a previous meta-analysis that pooled the results of five studies. "Our findings add to the growing body of evidence on the harms of indoor tanning," Ms. Wehner and her colleagues said. "We hope that these findings can support public health campaigns and motivate increased regulation to reduce exposure to this carcinogen, especially during early life."
The study was supported by the National Center for Research Resources and the National Institute of Arthritis and Musculoskeletal and Skin Diseases. One of the study investigators reported ties to Genentech. No other conflicts of interest were reported.
Indoor tanning is strongly associated with the development of both basal and squamous cell carcinoma, according to a recent meta-analysis.
Indoor tanning – the use of a sun bed, sun lamp, tanning booth, or solarium – was related to a 29% higher risk for basal cell carcinoma and a 67% higher risk for squamous cell carcinoma, compared with no such exposure, according to a meta-analysis of 12 studies that reported effect estimates.
This translates to nearly 171,000 cases of nonmelanoma skin cancer each year that are attributable to indoor tanning in the United States alone, reported Mackenzie R. Wehner, a medical student at Stanford (Calif.) University, and her associates.
Several studies have examined a potential link between indoor tanning and nonmelanoma skin cancers, but the study populations have been small and the results have not been consistent. Therefore, Ms. Wehner and her colleagues performed a systematic review and meta-analysis of 10 case-control studies, 1 nested case-control study, and 1 cohort study for a combined population of 80,661 patients, in which there were 9,328 cases of nonmelanoma skin cancer. The studies were conducted in six countries from 1985 to 2012.
The investigators found summary relative risks of 1.29 for basal cell carcinoma and 1.67 for squamous cell carcinoma. These findings did not change appreciably in sensitivity analyses (BMJ 2012;345:e5909 [doi:10.1136/bmj.e5909]).
To examine whether a dose-response effect was present, the researchers performed an additional analysis on the studies that included effect estimates for frequent or multiple exposures to indoor tanning. Such high-dose exposure was associated with an increased risk of basal cell carcinoma, but the increase was not statistically significant.
To examine whether exposure to indoor tanning at a young age was especially high risk, Ms. Wehner and her colleagues performed an additional analysis of studies that included effect estimates for exposure before age 25. They found that such exposure was associated with a relative risk of 1.40 for basal cell carcinoma and of 2.02 for squamous cell carcinoma. "This suggests a critical period for exposure during early life," they wrote.
"Applying our summary risk estimates to the prevalence of exposure to indoor tanning in the United States, we calculated the population attributable risk fraction at 3.7% for basal cell carcinoma and at 8.2% for squamous cell carcinoma. This corresponds to 98,408 cases of basal cell carcinoma and 72,244 cases of squamous cell carcinoma, making 170,652 cases of nonmelanoma skin cancer each year attributable to indoor tanning," the researchers noted.
The study results are consistent with those of a previous meta-analysis that pooled the results of five studies. "Our findings add to the growing body of evidence on the harms of indoor tanning," Ms. Wehner and her colleagues said. "We hope that these findings can support public health campaigns and motivate increased regulation to reduce exposure to this carcinogen, especially during early life."
The study was supported by the National Center for Research Resources and the National Institute of Arthritis and Musculoskeletal and Skin Diseases. One of the study investigators reported ties to Genentech. No other conflicts of interest were reported.
FROM THE BRITISH MEDICAL JOURNAL
Major Finding: Exposure to indoor tanning was associated with a 29% higher risk for basal cell carcinoma and a 67% higher risk for squamous cell carcinoma.
Data Source: A systematic review and meta-analysis of 12 observational studies for a combined population of 80,661 patients that provided effect estimates for exposure to indoor tanning.
Disclosures: The study was supported by the National Center for Research Resources and the National Institute of Arthritis and Musculoskeletal and Skin Diseases. One of the study investigators reported ties to Genentech. No other conflicts of interest were reported.
Strikingly High Prevalence of Periodontal Disease Seen in New-Onset RA
Adults with new-onset rheumatoid arthritis showed a 75% prevalence of moderate to severe periodontal disease in a study profiling the oral microbiota in RA. The results were published in the October issue of Arthritis & Rheumatism.
The presence of periodontal disease was particularly striking because these study subjects were young, were mostly nonsmokers, and had never been treated with potentially immunosuppressive steroids or disease-modifying antirheumatic drugs (DMARDs), said Dr. Jose U. Scher, director of the arthritis clinic at New York University Hospital for Joint Diseases, and his associates.
The study finding is "consistent with the prevailing speculation" that Porphyromonas gingivalis and other species may be triggering factors for rheumatoid arthritis (RA) in susceptible people. But it also raises the intriguing alternative possibility that both the gums and the joints may be targets of the same autoimmune process and that periodontitis may be an extraarticular characteristic of RA, the investigators said.
RA has long been associated with both oral microbes and periodontal disease, but "data describing the subgingival microbiota in patients with RA are virtually nonexistent." Dr. Scher and his colleagues "aimed to determine the periodontal status of RA patients and healthy controls and to directly correlate, for the first time, the presence and abundance of subgingival microbiota with RA status."
They assessed 31 consecutive adults who presented to the university’s rheumatology clinics with new-onset RA; 34 adults who had chronic RA (mean duration, 5 years), most of whom were receiving oral and biologic DMARDs; and 18 healthy control subjects matched to the new-onset RA patients for age, sex, and ethnicity.
Oral samples were obtained from all study subjects using subgingival biofilm from the six sites with the greatest extent of periodontal disease. DNA was then extracted from the samples to identify the microorganisms that were present.
The prevalence of moderate to severe periodontal disease was 75% in patients with new-onset RA, equivalent to the 75% prevalence in patients with chronic RA and significantly higher than the 39% prevalence in the healthy controls. The rate in the control group was consistent with the 30%-40% rate found in the general population, the researchers said (Arthritis Rheum. 2012;64:3083-94).
This finding is consistent with the widely accepted idea that periodontal disease may be a risk factor for the development of RA. In fact, "it is reasonable to posit that a particular Porphyromonas species with defined virulent attributes (i.e., invasion properties, high PAD enzyme activity) might serve as a triggering factor for RA in susceptible individuals," they said.
Two species of bacteria, Prevotella and Leptotrichia, were found in many samples from patients with new-onset RA but in none of the samples from control subjects. The prevalence of Prevotella was 32.2% and that of Leptotrichia was 25.8% in new-onset RA. These organisms merit further study as possible periodontal triggers of RA, along with Porphyromonas gingivalis, Dr. Scher and his associates said.
Three of the most virulent periodontopathic bacteria – Tannerella, Treponema, and Porphyromonas – were more abundant in patients with new-onset RA than in those with chronic RA. It may be that these organisms diminish as patients begin therapeutic regimens, particularly those containing immunomodulatory agents that have antibacterial properties, such as methotrexate or hydroxychloroquine.
Dr. Scher and his colleagues noted that exposure to bacteria at other body sites, such as the lung or intestine, may also contribute to the development of RA. Their next project is to assess the role of the intestinal microbiota in the disease.
This study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. No financial conflicts of interest were reported.
Adults with new-onset rheumatoid arthritis showed a 75% prevalence of moderate to severe periodontal disease in a study profiling the oral microbiota in RA. The results were published in the October issue of Arthritis & Rheumatism.
The presence of periodontal disease was particularly striking because these study subjects were young, were mostly nonsmokers, and had never been treated with potentially immunosuppressive steroids or disease-modifying antirheumatic drugs (DMARDs), said Dr. Jose U. Scher, director of the arthritis clinic at New York University Hospital for Joint Diseases, and his associates.
The study finding is "consistent with the prevailing speculation" that Porphyromonas gingivalis and other species may be triggering factors for rheumatoid arthritis (RA) in susceptible people. But it also raises the intriguing alternative possibility that both the gums and the joints may be targets of the same autoimmune process and that periodontitis may be an extraarticular characteristic of RA, the investigators said.
RA has long been associated with both oral microbes and periodontal disease, but "data describing the subgingival microbiota in patients with RA are virtually nonexistent." Dr. Scher and his colleagues "aimed to determine the periodontal status of RA patients and healthy controls and to directly correlate, for the first time, the presence and abundance of subgingival microbiota with RA status."
They assessed 31 consecutive adults who presented to the university’s rheumatology clinics with new-onset RA; 34 adults who had chronic RA (mean duration, 5 years), most of whom were receiving oral and biologic DMARDs; and 18 healthy control subjects matched to the new-onset RA patients for age, sex, and ethnicity.
Oral samples were obtained from all study subjects using subgingival biofilm from the six sites with the greatest extent of periodontal disease. DNA was then extracted from the samples to identify the microorganisms that were present.
The prevalence of moderate to severe periodontal disease was 75% in patients with new-onset RA, equivalent to the 75% prevalence in patients with chronic RA and significantly higher than the 39% prevalence in the healthy controls. The rate in the control group was consistent with the 30%-40% rate found in the general population, the researchers said (Arthritis Rheum. 2012;64:3083-94).
This finding is consistent with the widely accepted idea that periodontal disease may be a risk factor for the development of RA. In fact, "it is reasonable to posit that a particular Porphyromonas species with defined virulent attributes (i.e., invasion properties, high PAD enzyme activity) might serve as a triggering factor for RA in susceptible individuals," they said.
Two species of bacteria, Prevotella and Leptotrichia, were found in many samples from patients with new-onset RA but in none of the samples from control subjects. The prevalence of Prevotella was 32.2% and that of Leptotrichia was 25.8% in new-onset RA. These organisms merit further study as possible periodontal triggers of RA, along with Porphyromonas gingivalis, Dr. Scher and his associates said.
Three of the most virulent periodontopathic bacteria – Tannerella, Treponema, and Porphyromonas – were more abundant in patients with new-onset RA than in those with chronic RA. It may be that these organisms diminish as patients begin therapeutic regimens, particularly those containing immunomodulatory agents that have antibacterial properties, such as methotrexate or hydroxychloroquine.
Dr. Scher and his colleagues noted that exposure to bacteria at other body sites, such as the lung or intestine, may also contribute to the development of RA. Their next project is to assess the role of the intestinal microbiota in the disease.
This study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. No financial conflicts of interest were reported.
Adults with new-onset rheumatoid arthritis showed a 75% prevalence of moderate to severe periodontal disease in a study profiling the oral microbiota in RA. The results were published in the October issue of Arthritis & Rheumatism.
The presence of periodontal disease was particularly striking because these study subjects were young, were mostly nonsmokers, and had never been treated with potentially immunosuppressive steroids or disease-modifying antirheumatic drugs (DMARDs), said Dr. Jose U. Scher, director of the arthritis clinic at New York University Hospital for Joint Diseases, and his associates.
The study finding is "consistent with the prevailing speculation" that Porphyromonas gingivalis and other species may be triggering factors for rheumatoid arthritis (RA) in susceptible people. But it also raises the intriguing alternative possibility that both the gums and the joints may be targets of the same autoimmune process and that periodontitis may be an extraarticular characteristic of RA, the investigators said.
RA has long been associated with both oral microbes and periodontal disease, but "data describing the subgingival microbiota in patients with RA are virtually nonexistent." Dr. Scher and his colleagues "aimed to determine the periodontal status of RA patients and healthy controls and to directly correlate, for the first time, the presence and abundance of subgingival microbiota with RA status."
They assessed 31 consecutive adults who presented to the university’s rheumatology clinics with new-onset RA; 34 adults who had chronic RA (mean duration, 5 years), most of whom were receiving oral and biologic DMARDs; and 18 healthy control subjects matched to the new-onset RA patients for age, sex, and ethnicity.
Oral samples were obtained from all study subjects using subgingival biofilm from the six sites with the greatest extent of periodontal disease. DNA was then extracted from the samples to identify the microorganisms that were present.
The prevalence of moderate to severe periodontal disease was 75% in patients with new-onset RA, equivalent to the 75% prevalence in patients with chronic RA and significantly higher than the 39% prevalence in the healthy controls. The rate in the control group was consistent with the 30%-40% rate found in the general population, the researchers said (Arthritis Rheum. 2012;64:3083-94).
This finding is consistent with the widely accepted idea that periodontal disease may be a risk factor for the development of RA. In fact, "it is reasonable to posit that a particular Porphyromonas species with defined virulent attributes (i.e., invasion properties, high PAD enzyme activity) might serve as a triggering factor for RA in susceptible individuals," they said.
Two species of bacteria, Prevotella and Leptotrichia, were found in many samples from patients with new-onset RA but in none of the samples from control subjects. The prevalence of Prevotella was 32.2% and that of Leptotrichia was 25.8% in new-onset RA. These organisms merit further study as possible periodontal triggers of RA, along with Porphyromonas gingivalis, Dr. Scher and his associates said.
Three of the most virulent periodontopathic bacteria – Tannerella, Treponema, and Porphyromonas – were more abundant in patients with new-onset RA than in those with chronic RA. It may be that these organisms diminish as patients begin therapeutic regimens, particularly those containing immunomodulatory agents that have antibacterial properties, such as methotrexate or hydroxychloroquine.
Dr. Scher and his colleagues noted that exposure to bacteria at other body sites, such as the lung or intestine, may also contribute to the development of RA. Their next project is to assess the role of the intestinal microbiota in the disease.
This study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. No financial conflicts of interest were reported.
FROM ARTHRITIS & RHEUMATISM
Major Finding: The prevalence of moderate to severe periodontal disease was 75% in patients with new-onset RA, which was just as high as the prevalence in longstanding RA and was markedly higher than the 39% prevalence in healthy controls.
Data Source: The data come from an analysis of subgingival bacteria and periodontal disease in 31 adults with new-onset RA, 34 with chronic RA, and 18 healthy control subjects.
Disclosures: This study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. No financial conflicts of interest were reported.
Nonpayment Fails to Improve Hospital Infection Rates
The 2008 Medicare policy to withhold payment for treating certain hospital-acquired infections failed to decrease infection rates in U.S. hospitals, according to a report published online Oct. 10 in the New England Journal of Medicine.
In a study involving 398 hospitals or medical systems across the country, implementing a Centers for Medicare and Medicaid Services policy of nonpayment for the treatment of preventable catheter-associated bloodstream infections and catheter-associated urinary tract infections appeared to have no impact at all on the acquisition of those infections, according to Dr. Ashish K. Jha of the department of health policy and management, Harvard School of Public Health, Boston, and his associates.
"As CMS continues to expand this policy to cover Medicaid through the Affordable Care Act, require public reporting of National Healthcare Safety Network [NHSN] data through the Hospital Compare website, and impose greater financial penalties on hospitals that perform poorly on these measures, careful evaluation is needed to determine when these programs work, when they have unintended consequences, and what might be done to improve patient outcomes," Dr. Jha noted.
Dr. Jha and his colleagues assessed data from the NHSN, a public health surveillance program for monitoring health care–associated infections across the country. A total of 1,166 nonfederal acute-care hospitals report their infection rates to this Centers for Disease Control and Prevention–sponsored network every month.
Dr. Jha and his colleagues assessed NHSN data on three types of infection at 398 of those hospitals in 41 states. They examined central catheter–associated bloodstream and catheter-associated urinary tract infections because these are the two hospital-acquired infections for which CMS currently does not pay. They also looked at ventilator-associated pneumonia, which is not targeted by the CMS policy, as a control.
Rates of central catheter–associated bloodstream infections were already decreasing at the time the CMS policy was implemented, likely because the federal government, national organizations, and accrediting agencies had already focused attention on preventing these nosocomial infections. The rate of these infections was 4.8% per quarter before the policy was implemented and 4.7% afterward, a nonsignificant difference, the investigators said (N. Engl. J. Med. 2012 [doi:10.1056/NEJMsa1202419]).
This pattern also was seen with catheter-associated UTIs, in which there was a small, nonsignificant increase in the infection rate after implementation of the CMS policy. For the control condition of ventilator-associated pneumonia, the infection rate was 7.3% before implementation and 8.2% after implementation of the policy, also showing no significant impact on infection rates.
These findings were consistent across all hospital types, regardless of size, regional location, type of ownership, or teaching status.
To assess whether any benefit of the nonpayment policy may have been offset by strategies to lower infection rates, such as mandatory reporting, the researchers performed a separate analysis involving only the hospital units located in states that didn’t have mandatory reporting. Again, no demonstrable effect on infection rates was seen.
To allow more time for hospitals to adapt to the policy change, the investigators performed a sensitivity analysis comparing infection rates 2 years after implementation with those before implementation. Again, they found no further decreases in the rates of any infections.
A possible explanation for these findings is that the amount of this financial disincentive was quite small. "Reductions in payment may have been equivalent to as little as 0.6% of Medicare revenue for the average hospital," Dr. Jha and his associates said. "Greater financial penalties might induce a greater change in hospital responsiveness to the CMS policy."
The study results are particularly important given the increasing use of financial disincentives to improve the quality of healthcare. There is very little evidence that this strategy, or other pay-for-performance strategies, actually improves patient outcomes, they said.
This study was supported by the Agency for Healthcare Research and Quality. No financial conflicts of interest were reported.
The 2008 Medicare policy to withhold payment for treating certain hospital-acquired infections failed to decrease infection rates in U.S. hospitals, according to a report published online Oct. 10 in the New England Journal of Medicine.
In a study involving 398 hospitals or medical systems across the country, implementing a Centers for Medicare and Medicaid Services policy of nonpayment for the treatment of preventable catheter-associated bloodstream infections and catheter-associated urinary tract infections appeared to have no impact at all on the acquisition of those infections, according to Dr. Ashish K. Jha of the department of health policy and management, Harvard School of Public Health, Boston, and his associates.
"As CMS continues to expand this policy to cover Medicaid through the Affordable Care Act, require public reporting of National Healthcare Safety Network [NHSN] data through the Hospital Compare website, and impose greater financial penalties on hospitals that perform poorly on these measures, careful evaluation is needed to determine when these programs work, when they have unintended consequences, and what might be done to improve patient outcomes," Dr. Jha noted.
Dr. Jha and his colleagues assessed data from the NHSN, a public health surveillance program for monitoring health care–associated infections across the country. A total of 1,166 nonfederal acute-care hospitals report their infection rates to this Centers for Disease Control and Prevention–sponsored network every month.
Dr. Jha and his colleagues assessed NHSN data on three types of infection at 398 of those hospitals in 41 states. They examined central catheter–associated bloodstream and catheter-associated urinary tract infections because these are the two hospital-acquired infections for which CMS currently does not pay. They also looked at ventilator-associated pneumonia, which is not targeted by the CMS policy, as a control.
Rates of central catheter–associated bloodstream infections were already decreasing at the time the CMS policy was implemented, likely because the federal government, national organizations, and accrediting agencies had already focused attention on preventing these nosocomial infections. The rate of these infections was 4.8% per quarter before the policy was implemented and 4.7% afterward, a nonsignificant difference, the investigators said (N. Engl. J. Med. 2012 [doi:10.1056/NEJMsa1202419]).
This pattern also was seen with catheter-associated UTIs, in which there was a small, nonsignificant increase in the infection rate after implementation of the CMS policy. For the control condition of ventilator-associated pneumonia, the infection rate was 7.3% before implementation and 8.2% after implementation of the policy, also showing no significant impact on infection rates.
These findings were consistent across all hospital types, regardless of size, regional location, type of ownership, or teaching status.
To assess whether any benefit of the nonpayment policy may have been offset by strategies to lower infection rates, such as mandatory reporting, the researchers performed a separate analysis involving only the hospital units located in states that didn’t have mandatory reporting. Again, no demonstrable effect on infection rates was seen.
To allow more time for hospitals to adapt to the policy change, the investigators performed a sensitivity analysis comparing infection rates 2 years after implementation with those before implementation. Again, they found no further decreases in the rates of any infections.
A possible explanation for these findings is that the amount of this financial disincentive was quite small. "Reductions in payment may have been equivalent to as little as 0.6% of Medicare revenue for the average hospital," Dr. Jha and his associates said. "Greater financial penalties might induce a greater change in hospital responsiveness to the CMS policy."
The study results are particularly important given the increasing use of financial disincentives to improve the quality of healthcare. There is very little evidence that this strategy, or other pay-for-performance strategies, actually improves patient outcomes, they said.
This study was supported by the Agency for Healthcare Research and Quality. No financial conflicts of interest were reported.
The 2008 Medicare policy to withhold payment for treating certain hospital-acquired infections failed to decrease infection rates in U.S. hospitals, according to a report published online Oct. 10 in the New England Journal of Medicine.
In a study involving 398 hospitals or medical systems across the country, implementing a Centers for Medicare and Medicaid Services policy of nonpayment for the treatment of preventable catheter-associated bloodstream infections and catheter-associated urinary tract infections appeared to have no impact at all on the acquisition of those infections, according to Dr. Ashish K. Jha of the department of health policy and management, Harvard School of Public Health, Boston, and his associates.
"As CMS continues to expand this policy to cover Medicaid through the Affordable Care Act, require public reporting of National Healthcare Safety Network [NHSN] data through the Hospital Compare website, and impose greater financial penalties on hospitals that perform poorly on these measures, careful evaluation is needed to determine when these programs work, when they have unintended consequences, and what might be done to improve patient outcomes," Dr. Jha noted.
Dr. Jha and his colleagues assessed data from the NHSN, a public health surveillance program for monitoring health care–associated infections across the country. A total of 1,166 nonfederal acute-care hospitals report their infection rates to this Centers for Disease Control and Prevention–sponsored network every month.
Dr. Jha and his colleagues assessed NHSN data on three types of infection at 398 of those hospitals in 41 states. They examined central catheter–associated bloodstream and catheter-associated urinary tract infections because these are the two hospital-acquired infections for which CMS currently does not pay. They also looked at ventilator-associated pneumonia, which is not targeted by the CMS policy, as a control.
Rates of central catheter–associated bloodstream infections were already decreasing at the time the CMS policy was implemented, likely because the federal government, national organizations, and accrediting agencies had already focused attention on preventing these nosocomial infections. The rate of these infections was 4.8% per quarter before the policy was implemented and 4.7% afterward, a nonsignificant difference, the investigators said (N. Engl. J. Med. 2012 [doi:10.1056/NEJMsa1202419]).
This pattern also was seen with catheter-associated UTIs, in which there was a small, nonsignificant increase in the infection rate after implementation of the CMS policy. For the control condition of ventilator-associated pneumonia, the infection rate was 7.3% before implementation and 8.2% after implementation of the policy, also showing no significant impact on infection rates.
These findings were consistent across all hospital types, regardless of size, regional location, type of ownership, or teaching status.
To assess whether any benefit of the nonpayment policy may have been offset by strategies to lower infection rates, such as mandatory reporting, the researchers performed a separate analysis involving only the hospital units located in states that didn’t have mandatory reporting. Again, no demonstrable effect on infection rates was seen.
To allow more time for hospitals to adapt to the policy change, the investigators performed a sensitivity analysis comparing infection rates 2 years after implementation with those before implementation. Again, they found no further decreases in the rates of any infections.
A possible explanation for these findings is that the amount of this financial disincentive was quite small. "Reductions in payment may have been equivalent to as little as 0.6% of Medicare revenue for the average hospital," Dr. Jha and his associates said. "Greater financial penalties might induce a greater change in hospital responsiveness to the CMS policy."
The study results are particularly important given the increasing use of financial disincentives to improve the quality of healthcare. There is very little evidence that this strategy, or other pay-for-performance strategies, actually improves patient outcomes, they said.
This study was supported by the Agency for Healthcare Research and Quality. No financial conflicts of interest were reported.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: The rate of central catheter–associated bloodstream infections was 4.8% before the nonpayment policy was implemented and 4.7% afterward, showing that the policy failed to decrease the infection rate.
Data Source: The data come from an analysis of trends in hospital-acquired infection rates before and after implementation of a federal policy to withhold payment for treating those infections, involving 398 hospitals in 41 states.
Disclosures: This study was supported by the Agency for Healthcare Research and Quality. No financial conflicts of interest were reported.
Use of PCI for MI Drops With Public Reporting of Patient Outcomes
The use of percutaneous coronary intervention for acute myocardial infarction was found to be lower in three states that implemented public reporting of PCI outcomes than in seven nearby states without public reporting, according to a study of nearly 98,000 cases in the October 10 issue of JAMA.
In addition, the use of PCI for acute MI declined in one state after public reporting of PCI outcomes was implemented there, said Dr. Karen E. Joynt of the departments of health policy and management at Harvard School of Public Health, Boston, and her associates.
Nevertheless, public reporting was not associated with any change in mortality for patients with acute MI in this study, they noted.
Collecting and publicly reporting patient outcomes is a tool intended to improve health care by motivating clinicians to improve their performance and allowing patients to choose the highest-quality hospitals. Critics of this strategy, however, say that it creates disincentives for physicians and hospitals to care for the sickest patients and may lead them to avoid offering lifesaving procedures such as PCI to the sickest or highest-risk patients.
To date, no national studies have examined whether public reporting of PCI outcomes has affected either the rates of PCI or the outcomes in patients with acute MI. Dr. Joynt and her colleagues did so using data from Medicare files.
They first performed a cross-sectional analysis of PCI rates in 30,745 patients who had a discharge diagnosis of acute MI in a single year, 2010. They compared the rates in three states that mandated public reporting – Massachusetts, Pennsylvania, and New York – against rates in seven nearby states that did not (Maine, Vermont, New Hampshire, Connecticut, Rhode Island, Maryland, and Delaware).
Patients in the public-reporting states were significantly less likely to receive PCI (37.7%) than were those in nonreporting states (42.7%). This trend was most pronounced in MI patients who had ST-elevation MI, cardiogenic shock, or cardiac arrest and was not seen in patients with non–ST-elevation MI, the investigators said (JAMA 2012:308;1460-8).
When the patients were categorized by age – 65-74 years vs. 75 years and older – the results were the same: Regardless of their age, patients in publicly reporting states were less likely to receive PCI than were those in nonreporting states.
The researchers then performed a longitudinal analysis of trends in PCI rates for 49,660 acute MI patients in reporting states and 48,142 in nonreporting states who were treated in 2002-2010. They focused on the experience in Massachusetts, tracking the rates before public reporting of PCI was implemented there (2002-2004) with the rates after it was implemented (2006-2010).
Before public reporting of PCI was implemented, the PCI rate in Massachusetts (40.6%) was comparable with that in nonreporting states (41.8%), but PCI rates in Massachusetts began to decline when reporting was implemented and by 2010 patients in Massachusetts were significantly less likely to receive PCI than were those in nonreporting states.
As in the cross-sectional study, PCI rates in Massachusetts declined the most among MI patients who had cardiogenic shock or cardiac arrest, and these findings did not change when patients were categorized by younger vs. older age.
Despite these declines in PCI rates, there was no significant difference in 30-day mortality between acute MI patients in reporting states (12.8%) and those in nonreporting states (12.1%). Some may find it reassuring that mandating public reporting did not increase patient mortality, but, conversely, it also did not reduce mortality, the researchers said.
Although the study was not designed to find out why mortality was not affected by reductions in PCI rates, Dr. Joynt and her associates proposed two explanations.
First, it may be that public reporting had its intended effect of focusing clinicians on performing PCI in only the most appropriate patients, and that they correctly avoided doing it in cases in which it would have been futile or unnecessary.
Alternatively, it’s possible that public reporting had an unintended effect of pressuring physicians to avoid PCI in eligible but high-risk patients because of concern that poor outcomes would color their performance rating.
"Our data cannot definitively differentiate between these two potential mechanisms," the investigators said.
This study was supported by the National Heart, Lung, and Blood Institute. No financial conflicts of interest were reported.
There are three explanations for the observed lack of difference in mortality between reporting and nonreporting states, said Dr. Mauro Moscucci.
First, "futility assessments" in reporting states may have led to avoidance of PCI in patients who were less likely to benefit. Second, public reporting might have resulted in a drive toward improved quality of care and improved outcomes in patients receiving PCI, offsetting the adverse effect of not performing PCI in high-risk patients. Third, the optimal coding of comorbid condition required in risk adjustment may have been gamed through upcoding, thus leading to observed outcomes that are better than predicted. Better coding in public reporting states might have mitigated the adverse effect of denial of care after risk adjustment, he suggested.
This study highlights the possible unintended consequences of public reporting. The findings "may help spearhead a new focus on procedures that, while perceived [to be] appropriate based on current use criteria, might not result in added benefit in selected patients," he added.
Mauro Moscucci, M.D., is chief of the cardiovascular division at the University of Miami. He reported no relevant conflicts of interest. These remarks were taken from his editorial accompanying Dr. Joynt’s report (JAMA 2012;308:148-9).
There are three explanations for the observed lack of difference in mortality between reporting and nonreporting states, said Dr. Mauro Moscucci.
First, "futility assessments" in reporting states may have led to avoidance of PCI in patients who were less likely to benefit. Second, public reporting might have resulted in a drive toward improved quality of care and improved outcomes in patients receiving PCI, offsetting the adverse effect of not performing PCI in high-risk patients. Third, the optimal coding of comorbid condition required in risk adjustment may have been gamed through upcoding, thus leading to observed outcomes that are better than predicted. Better coding in public reporting states might have mitigated the adverse effect of denial of care after risk adjustment, he suggested.
This study highlights the possible unintended consequences of public reporting. The findings "may help spearhead a new focus on procedures that, while perceived [to be] appropriate based on current use criteria, might not result in added benefit in selected patients," he added.
Mauro Moscucci, M.D., is chief of the cardiovascular division at the University of Miami. He reported no relevant conflicts of interest. These remarks were taken from his editorial accompanying Dr. Joynt’s report (JAMA 2012;308:148-9).
There are three explanations for the observed lack of difference in mortality between reporting and nonreporting states, said Dr. Mauro Moscucci.
First, "futility assessments" in reporting states may have led to avoidance of PCI in patients who were less likely to benefit. Second, public reporting might have resulted in a drive toward improved quality of care and improved outcomes in patients receiving PCI, offsetting the adverse effect of not performing PCI in high-risk patients. Third, the optimal coding of comorbid condition required in risk adjustment may have been gamed through upcoding, thus leading to observed outcomes that are better than predicted. Better coding in public reporting states might have mitigated the adverse effect of denial of care after risk adjustment, he suggested.
This study highlights the possible unintended consequences of public reporting. The findings "may help spearhead a new focus on procedures that, while perceived [to be] appropriate based on current use criteria, might not result in added benefit in selected patients," he added.
Mauro Moscucci, M.D., is chief of the cardiovascular division at the University of Miami. He reported no relevant conflicts of interest. These remarks were taken from his editorial accompanying Dr. Joynt’s report (JAMA 2012;308:148-9).
The use of percutaneous coronary intervention for acute myocardial infarction was found to be lower in three states that implemented public reporting of PCI outcomes than in seven nearby states without public reporting, according to a study of nearly 98,000 cases in the October 10 issue of JAMA.
In addition, the use of PCI for acute MI declined in one state after public reporting of PCI outcomes was implemented there, said Dr. Karen E. Joynt of the departments of health policy and management at Harvard School of Public Health, Boston, and her associates.
Nevertheless, public reporting was not associated with any change in mortality for patients with acute MI in this study, they noted.
Collecting and publicly reporting patient outcomes is a tool intended to improve health care by motivating clinicians to improve their performance and allowing patients to choose the highest-quality hospitals. Critics of this strategy, however, say that it creates disincentives for physicians and hospitals to care for the sickest patients and may lead them to avoid offering lifesaving procedures such as PCI to the sickest or highest-risk patients.
To date, no national studies have examined whether public reporting of PCI outcomes has affected either the rates of PCI or the outcomes in patients with acute MI. Dr. Joynt and her colleagues did so using data from Medicare files.
They first performed a cross-sectional analysis of PCI rates in 30,745 patients who had a discharge diagnosis of acute MI in a single year, 2010. They compared the rates in three states that mandated public reporting – Massachusetts, Pennsylvania, and New York – against rates in seven nearby states that did not (Maine, Vermont, New Hampshire, Connecticut, Rhode Island, Maryland, and Delaware).
Patients in the public-reporting states were significantly less likely to receive PCI (37.7%) than were those in nonreporting states (42.7%). This trend was most pronounced in MI patients who had ST-elevation MI, cardiogenic shock, or cardiac arrest and was not seen in patients with non–ST-elevation MI, the investigators said (JAMA 2012:308;1460-8).
When the patients were categorized by age – 65-74 years vs. 75 years and older – the results were the same: Regardless of their age, patients in publicly reporting states were less likely to receive PCI than were those in nonreporting states.
The researchers then performed a longitudinal analysis of trends in PCI rates for 49,660 acute MI patients in reporting states and 48,142 in nonreporting states who were treated in 2002-2010. They focused on the experience in Massachusetts, tracking the rates before public reporting of PCI was implemented there (2002-2004) with the rates after it was implemented (2006-2010).
Before public reporting of PCI was implemented, the PCI rate in Massachusetts (40.6%) was comparable with that in nonreporting states (41.8%), but PCI rates in Massachusetts began to decline when reporting was implemented and by 2010 patients in Massachusetts were significantly less likely to receive PCI than were those in nonreporting states.
As in the cross-sectional study, PCI rates in Massachusetts declined the most among MI patients who had cardiogenic shock or cardiac arrest, and these findings did not change when patients were categorized by younger vs. older age.
Despite these declines in PCI rates, there was no significant difference in 30-day mortality between acute MI patients in reporting states (12.8%) and those in nonreporting states (12.1%). Some may find it reassuring that mandating public reporting did not increase patient mortality, but, conversely, it also did not reduce mortality, the researchers said.
Although the study was not designed to find out why mortality was not affected by reductions in PCI rates, Dr. Joynt and her associates proposed two explanations.
First, it may be that public reporting had its intended effect of focusing clinicians on performing PCI in only the most appropriate patients, and that they correctly avoided doing it in cases in which it would have been futile or unnecessary.
Alternatively, it’s possible that public reporting had an unintended effect of pressuring physicians to avoid PCI in eligible but high-risk patients because of concern that poor outcomes would color their performance rating.
"Our data cannot definitively differentiate between these two potential mechanisms," the investigators said.
This study was supported by the National Heart, Lung, and Blood Institute. No financial conflicts of interest were reported.
The use of percutaneous coronary intervention for acute myocardial infarction was found to be lower in three states that implemented public reporting of PCI outcomes than in seven nearby states without public reporting, according to a study of nearly 98,000 cases in the October 10 issue of JAMA.
In addition, the use of PCI for acute MI declined in one state after public reporting of PCI outcomes was implemented there, said Dr. Karen E. Joynt of the departments of health policy and management at Harvard School of Public Health, Boston, and her associates.
Nevertheless, public reporting was not associated with any change in mortality for patients with acute MI in this study, they noted.
Collecting and publicly reporting patient outcomes is a tool intended to improve health care by motivating clinicians to improve their performance and allowing patients to choose the highest-quality hospitals. Critics of this strategy, however, say that it creates disincentives for physicians and hospitals to care for the sickest patients and may lead them to avoid offering lifesaving procedures such as PCI to the sickest or highest-risk patients.
To date, no national studies have examined whether public reporting of PCI outcomes has affected either the rates of PCI or the outcomes in patients with acute MI. Dr. Joynt and her colleagues did so using data from Medicare files.
They first performed a cross-sectional analysis of PCI rates in 30,745 patients who had a discharge diagnosis of acute MI in a single year, 2010. They compared the rates in three states that mandated public reporting – Massachusetts, Pennsylvania, and New York – against rates in seven nearby states that did not (Maine, Vermont, New Hampshire, Connecticut, Rhode Island, Maryland, and Delaware).
Patients in the public-reporting states were significantly less likely to receive PCI (37.7%) than were those in nonreporting states (42.7%). This trend was most pronounced in MI patients who had ST-elevation MI, cardiogenic shock, or cardiac arrest and was not seen in patients with non–ST-elevation MI, the investigators said (JAMA 2012:308;1460-8).
When the patients were categorized by age – 65-74 years vs. 75 years and older – the results were the same: Regardless of their age, patients in publicly reporting states were less likely to receive PCI than were those in nonreporting states.
The researchers then performed a longitudinal analysis of trends in PCI rates for 49,660 acute MI patients in reporting states and 48,142 in nonreporting states who were treated in 2002-2010. They focused on the experience in Massachusetts, tracking the rates before public reporting of PCI was implemented there (2002-2004) with the rates after it was implemented (2006-2010).
Before public reporting of PCI was implemented, the PCI rate in Massachusetts (40.6%) was comparable with that in nonreporting states (41.8%), but PCI rates in Massachusetts began to decline when reporting was implemented and by 2010 patients in Massachusetts were significantly less likely to receive PCI than were those in nonreporting states.
As in the cross-sectional study, PCI rates in Massachusetts declined the most among MI patients who had cardiogenic shock or cardiac arrest, and these findings did not change when patients were categorized by younger vs. older age.
Despite these declines in PCI rates, there was no significant difference in 30-day mortality between acute MI patients in reporting states (12.8%) and those in nonreporting states (12.1%). Some may find it reassuring that mandating public reporting did not increase patient mortality, but, conversely, it also did not reduce mortality, the researchers said.
Although the study was not designed to find out why mortality was not affected by reductions in PCI rates, Dr. Joynt and her associates proposed two explanations.
First, it may be that public reporting had its intended effect of focusing clinicians on performing PCI in only the most appropriate patients, and that they correctly avoided doing it in cases in which it would have been futile or unnecessary.
Alternatively, it’s possible that public reporting had an unintended effect of pressuring physicians to avoid PCI in eligible but high-risk patients because of concern that poor outcomes would color their performance rating.
"Our data cannot definitively differentiate between these two potential mechanisms," the investigators said.
This study was supported by the National Heart, Lung, and Blood Institute. No financial conflicts of interest were reported.
FROM JAMA
Major Finding: Patients with acute MI were less likely to receive PCI in states with mandatory public reporting of PCI outcomes (37.7%) than in those without public reporting (42.7%).
Data Source: A longitudinal analysis included PCI rates and outcomes for 49,660 acute MI patients treated in reporting states and 48,142 treated in nonreporting states in 2002-2010; there also was a cross-sectional analysis of 30,745 patients treated in 2010 only.
Disclosures: This study was supported by the National Heart, Lung, and Blood Institute. No financial conflicts of interest were reported.
Disparity in HIV Mortality Widens Between Whites, Nonwhites
HIV-related mortality decreased markedly since the mid-1990s across all demographic groups except among non-Hispanic blacks with low levels of educational attainment, according to a report published online Oct. 8 in Archives of Internal Medicine.
The inevitable result of these temporal trends is a widening gap between whites and nonwhites in deaths from HIV.
"These findings suggest the need for focused interventions and resources to facilitate the identification of high-risk individuals, as well as entry and retention into care for these most vulnerable groups affected by the HIV epidemic in the United States," said Edgar P. Simard, Ph.D., of the American Cancer Society’s Surveillance Research Program, and his associates.
HIV has become a more predominant cause of death among blacks at the same time that its prominence as a cause of death among whites has been on the decline. It was the ninth-leading cause of death among blacks in the most recent year for which data are available, but only the 24th-leading cause of death among whites, the authors noted.
"We posit that black men and minority women, in particular those with low socioeconomic status, may be exceptionally vulnerable to HIV deaths owing to a combined lack of knowledge of HIV prevention, lack of knowledge of their own HIV status, lack of access to the health care system, social stigma, and marginalization." --Dr. Simard and associates.
Dr. Simard and his colleagues examined trends in HIV mortality using data recorded on death certificates and filed in the National Vital Statistics System, which is administered by the National Center for Health Statistics. In recent years, death certificates have included patients’ educational attainment, which these investigators used as a proxy for the subjects’ socioeconomic status. The lowest level of educational attainment was defined as less than or equal to 12 years of education as reported by next of kin.
The researchers also categorized the data according to the subjects’ sex and race/ethnicity. They assessed 91,307 HIV-related deaths among adults aged 25-64 years across 26 states, focusing on comparing the data from 1993-1995 against that from 2005-2007.
Overall, HIV mortality declined over time for most men and women of all ethnicities and educational levels. The main exceptions to the across-the-board sharp decline in HIV-related mortality were found among non-Hispanic black women of low educational attainment, in whom HIV mortality remained markedly high, and Hispanic women with 13 to 15 years of education.
In addition, the reductions in mortality were much greater among whites than among nonwhites. Declines in mortality also generally were much greater among people with high educational attainment than among those with lower educational attainment. Both trends caused a widening in the already large gap between these groups.
For example, among non-Hispanic black men with the highest educational attainment, HIV mortality decreased from 117.89 to 15.35 per 100,000, a dramatic reduction. But this rate of 15.35 is still more than three times higher than the 5.04 per 100,000 rate in non-Hispanic white men with the highest educational attainment.
Although this study was not designed to find the reasons underlying these disparities, "We posit that black men and minority women, in particular those with low socioeconomic status, may be exceptionally vulnerable to HIV deaths owing to a combined lack of knowledge of HIV prevention, lack of knowledge of their own HIV status, lack of access to the health care system, social stigma, and marginalization," Dr. Simard and his associates said (Arch. Intern. Med. 2012 Oct. 8 [doi:10.1001/archinternmed.2012.4508]).
"Our findings suggest the importance of considering individuals not only on the basis of race/ethnicity but also by socioeconomic status for the purposes of allocating resources for HIV prevention and treatment," they added.
This study was funded by the American Cancer Society. No financial conflicts of interest were reported.
The findings of Edgar P. Simard, Ph.D., and his colleagues demonstrate that it is high time for "a major commitment of resources to address these shameful disparities in HIV outcomes," said Dr. William Cunningham.
Currently most funding is funneled to research on antiretroviral therapy and vaccines to prevent primary infection, while funding for research specifically targeting low-income persons of color "is frankly relatively small." Agencies such as the Centers for Disease Control and Prevention, the Agency for Health Research and Quality, and the Health Resources and Services Administration "have been heroically attempting to address such issues, but with relatively miniscule budgets that are constantly under threat of further cuts," he said.
Dr. Cunningham is affiliated with the department of internal medicine at the University of California, Los Angeles. He reported no financial conflicts of interest. These remarks were taken from his invited commentary accompanying Dr. Simard’s report (Arch. Intern. Med. 2012 Oct. 8 [doi:10.1001/2013.jamainternmed.613]).
The findings of Edgar P. Simard, Ph.D., and his colleagues demonstrate that it is high time for "a major commitment of resources to address these shameful disparities in HIV outcomes," said Dr. William Cunningham.
Currently most funding is funneled to research on antiretroviral therapy and vaccines to prevent primary infection, while funding for research specifically targeting low-income persons of color "is frankly relatively small." Agencies such as the Centers for Disease Control and Prevention, the Agency for Health Research and Quality, and the Health Resources and Services Administration "have been heroically attempting to address such issues, but with relatively miniscule budgets that are constantly under threat of further cuts," he said.
Dr. Cunningham is affiliated with the department of internal medicine at the University of California, Los Angeles. He reported no financial conflicts of interest. These remarks were taken from his invited commentary accompanying Dr. Simard’s report (Arch. Intern. Med. 2012 Oct. 8 [doi:10.1001/2013.jamainternmed.613]).
The findings of Edgar P. Simard, Ph.D., and his colleagues demonstrate that it is high time for "a major commitment of resources to address these shameful disparities in HIV outcomes," said Dr. William Cunningham.
Currently most funding is funneled to research on antiretroviral therapy and vaccines to prevent primary infection, while funding for research specifically targeting low-income persons of color "is frankly relatively small." Agencies such as the Centers for Disease Control and Prevention, the Agency for Health Research and Quality, and the Health Resources and Services Administration "have been heroically attempting to address such issues, but with relatively miniscule budgets that are constantly under threat of further cuts," he said.
Dr. Cunningham is affiliated with the department of internal medicine at the University of California, Los Angeles. He reported no financial conflicts of interest. These remarks were taken from his invited commentary accompanying Dr. Simard’s report (Arch. Intern. Med. 2012 Oct. 8 [doi:10.1001/2013.jamainternmed.613]).
HIV-related mortality decreased markedly since the mid-1990s across all demographic groups except among non-Hispanic blacks with low levels of educational attainment, according to a report published online Oct. 8 in Archives of Internal Medicine.
The inevitable result of these temporal trends is a widening gap between whites and nonwhites in deaths from HIV.
"These findings suggest the need for focused interventions and resources to facilitate the identification of high-risk individuals, as well as entry and retention into care for these most vulnerable groups affected by the HIV epidemic in the United States," said Edgar P. Simard, Ph.D., of the American Cancer Society’s Surveillance Research Program, and his associates.
HIV has become a more predominant cause of death among blacks at the same time that its prominence as a cause of death among whites has been on the decline. It was the ninth-leading cause of death among blacks in the most recent year for which data are available, but only the 24th-leading cause of death among whites, the authors noted.
"We posit that black men and minority women, in particular those with low socioeconomic status, may be exceptionally vulnerable to HIV deaths owing to a combined lack of knowledge of HIV prevention, lack of knowledge of their own HIV status, lack of access to the health care system, social stigma, and marginalization." --Dr. Simard and associates.
Dr. Simard and his colleagues examined trends in HIV mortality using data recorded on death certificates and filed in the National Vital Statistics System, which is administered by the National Center for Health Statistics. In recent years, death certificates have included patients’ educational attainment, which these investigators used as a proxy for the subjects’ socioeconomic status. The lowest level of educational attainment was defined as less than or equal to 12 years of education as reported by next of kin.
The researchers also categorized the data according to the subjects’ sex and race/ethnicity. They assessed 91,307 HIV-related deaths among adults aged 25-64 years across 26 states, focusing on comparing the data from 1993-1995 against that from 2005-2007.
Overall, HIV mortality declined over time for most men and women of all ethnicities and educational levels. The main exceptions to the across-the-board sharp decline in HIV-related mortality were found among non-Hispanic black women of low educational attainment, in whom HIV mortality remained markedly high, and Hispanic women with 13 to 15 years of education.
In addition, the reductions in mortality were much greater among whites than among nonwhites. Declines in mortality also generally were much greater among people with high educational attainment than among those with lower educational attainment. Both trends caused a widening in the already large gap between these groups.
For example, among non-Hispanic black men with the highest educational attainment, HIV mortality decreased from 117.89 to 15.35 per 100,000, a dramatic reduction. But this rate of 15.35 is still more than three times higher than the 5.04 per 100,000 rate in non-Hispanic white men with the highest educational attainment.
Although this study was not designed to find the reasons underlying these disparities, "We posit that black men and minority women, in particular those with low socioeconomic status, may be exceptionally vulnerable to HIV deaths owing to a combined lack of knowledge of HIV prevention, lack of knowledge of their own HIV status, lack of access to the health care system, social stigma, and marginalization," Dr. Simard and his associates said (Arch. Intern. Med. 2012 Oct. 8 [doi:10.1001/archinternmed.2012.4508]).
"Our findings suggest the importance of considering individuals not only on the basis of race/ethnicity but also by socioeconomic status for the purposes of allocating resources for HIV prevention and treatment," they added.
This study was funded by the American Cancer Society. No financial conflicts of interest were reported.
HIV-related mortality decreased markedly since the mid-1990s across all demographic groups except among non-Hispanic blacks with low levels of educational attainment, according to a report published online Oct. 8 in Archives of Internal Medicine.
The inevitable result of these temporal trends is a widening gap between whites and nonwhites in deaths from HIV.
"These findings suggest the need for focused interventions and resources to facilitate the identification of high-risk individuals, as well as entry and retention into care for these most vulnerable groups affected by the HIV epidemic in the United States," said Edgar P. Simard, Ph.D., of the American Cancer Society’s Surveillance Research Program, and his associates.
HIV has become a more predominant cause of death among blacks at the same time that its prominence as a cause of death among whites has been on the decline. It was the ninth-leading cause of death among blacks in the most recent year for which data are available, but only the 24th-leading cause of death among whites, the authors noted.
"We posit that black men and minority women, in particular those with low socioeconomic status, may be exceptionally vulnerable to HIV deaths owing to a combined lack of knowledge of HIV prevention, lack of knowledge of their own HIV status, lack of access to the health care system, social stigma, and marginalization." --Dr. Simard and associates.
Dr. Simard and his colleagues examined trends in HIV mortality using data recorded on death certificates and filed in the National Vital Statistics System, which is administered by the National Center for Health Statistics. In recent years, death certificates have included patients’ educational attainment, which these investigators used as a proxy for the subjects’ socioeconomic status. The lowest level of educational attainment was defined as less than or equal to 12 years of education as reported by next of kin.
The researchers also categorized the data according to the subjects’ sex and race/ethnicity. They assessed 91,307 HIV-related deaths among adults aged 25-64 years across 26 states, focusing on comparing the data from 1993-1995 against that from 2005-2007.
Overall, HIV mortality declined over time for most men and women of all ethnicities and educational levels. The main exceptions to the across-the-board sharp decline in HIV-related mortality were found among non-Hispanic black women of low educational attainment, in whom HIV mortality remained markedly high, and Hispanic women with 13 to 15 years of education.
In addition, the reductions in mortality were much greater among whites than among nonwhites. Declines in mortality also generally were much greater among people with high educational attainment than among those with lower educational attainment. Both trends caused a widening in the already large gap between these groups.
For example, among non-Hispanic black men with the highest educational attainment, HIV mortality decreased from 117.89 to 15.35 per 100,000, a dramatic reduction. But this rate of 15.35 is still more than three times higher than the 5.04 per 100,000 rate in non-Hispanic white men with the highest educational attainment.
Although this study was not designed to find the reasons underlying these disparities, "We posit that black men and minority women, in particular those with low socioeconomic status, may be exceptionally vulnerable to HIV deaths owing to a combined lack of knowledge of HIV prevention, lack of knowledge of their own HIV status, lack of access to the health care system, social stigma, and marginalization," Dr. Simard and his associates said (Arch. Intern. Med. 2012 Oct. 8 [doi:10.1001/archinternmed.2012.4508]).
"Our findings suggest the importance of considering individuals not only on the basis of race/ethnicity but also by socioeconomic status for the purposes of allocating resources for HIV prevention and treatment," they added.
This study was funded by the American Cancer Society. No financial conflicts of interest were reported.
FROM ARCHIVES OF INTERNAL MEDICINE
Major Finding: Among non-Hispanic black men with the highest educational attainment, HIV mortality decreased from 117.89 to 15.35 per 100,000. But the rate of 15.35 is still more than three times higher than the 5.04 per 100,000 rate among non-Hispanic white men with the highest educational attainment.
Data Source: An analysis of death certificate data for 91,307 American adults who died from HIV-related causes, focusing on comparing deaths in 1993-95 against deaths in 2005-07.
Disclosures: This study was funded by the American Cancer Society. No financial conflicts of interest were reported.
MRI Identifies Candidates for Prostate Cancer Surveillance
Adding an MRI exam to the initial clinical evaluation of men thought to have low-risk prostate cancer can help identify which of them are the best candidates for active surveillance, according to study findings published online Oct. 3 in the Journal of Urology.
In a retrospective study of 388 men believed to have low-risk prostate cancer, tumors that were clearly visualized on an initial MRI were significantly more likely to be upgraded or upstaged on later confirmatory biopsy, and to prompt prostatectomy at that time. In contrast, tumors that could not be clearly visualized on MRI at the initial evaluation were significantly more likely to remain low grade on later confirmatory biopsy, and lent themselves to active surveillance rather than surgery, said Dr. Hebert Alberto Vargas of the department of radiology, Memorial Sloan-Kettering Cancer Center, New York, and his associates.
"These results suggest that MRI of the prostate, if read by radiologists with appropriate training and experience, could help determine active surveillance eligibility and obviate the need for confirmatory biopsy in substantial numbers of patients," they noted.
Initial biopsy samples of prostate cancers can miss areas of high-grade cancer, and "even the most stringent criteria misclassify 16%-42% of cases, which, despite low-risk features on initial biopsy, [are found to have] unfavorable pathological features at radical prostatectomy." Accordingly, some treatment centers recommend a second, confirmatory biopsy before pursuing active surveillance, the investigators said.
In one study of the issue, 27% of men with very low-risk features on initial biopsy proved to have upgraded or upstaged tumors at confirmatory biopsy.
Dr. Vargas and his colleagues decided to examine retrospectively whether standard transrectal T2-weighted MRI of the prostate would be useful in predicting which tumors were likely to be upgraded or upstaged on confirmatory biopsy.
The investigators identified 388 cases in their institution’s database in which men had an initial Gleason score of 6 or less on initial prostate biopsy performed in 1999-2010, had a prostate-specific antigen level less than 10 ng/mL, and had a confirmatory biopsy performed within 6 months of the initial biopsy.
Three radiologists independently interpreted the archived MRI scans and assigned each one a score indicating that tumor tissue was definitely evident, probably evident, definitely absent, probably absent, or indeterminate.
For all three radiologist readers, MRI scores indicating the probable or definite absence of tumor were highly predictive that confirmatory biopsy would show only very low-risk features and that active surveillance would be sufficient for those patients. In contrast, in a multivariate analysis, MRI scores showing the probable or definite presence of tumor were highly predictive that confirmatory biopsy would find upgraded or upstaged cancer (odds ratio, 2.16-3.97), and that radical prostatectomy would be recommended, the investigators said (J. Urol. 2012 Oct. 3 [doi:10.1016/j.juro.2012.07.024]).
Notably, one of the three radiologists, who had read only about 50 prostate MRI scans at the time of this study, had consistently less accurate readings than either of the other radiologists. The second radiologist had a fellowship in body imaging plus specialized training in prostate imaging, and had interpreted approximately 500 prostate MRIs. The third radiologist had completed a fellowship in genitourinary radiology and had read more than 5,000 prostate MRI scans.
The study findings thus confirm the importance of training and experience for the accurate interpretation of MRI scans of the prostate, Dr. Vargas and his associates noted.
This study was supported by the National Institutes of Health. No financial conflicts were reported.
Adding an MRI exam to the initial clinical evaluation of men thought to have low-risk prostate cancer can help identify which of them are the best candidates for active surveillance, according to study findings published online Oct. 3 in the Journal of Urology.
In a retrospective study of 388 men believed to have low-risk prostate cancer, tumors that were clearly visualized on an initial MRI were significantly more likely to be upgraded or upstaged on later confirmatory biopsy, and to prompt prostatectomy at that time. In contrast, tumors that could not be clearly visualized on MRI at the initial evaluation were significantly more likely to remain low grade on later confirmatory biopsy, and lent themselves to active surveillance rather than surgery, said Dr. Hebert Alberto Vargas of the department of radiology, Memorial Sloan-Kettering Cancer Center, New York, and his associates.
"These results suggest that MRI of the prostate, if read by radiologists with appropriate training and experience, could help determine active surveillance eligibility and obviate the need for confirmatory biopsy in substantial numbers of patients," they noted.
Initial biopsy samples of prostate cancers can miss areas of high-grade cancer, and "even the most stringent criteria misclassify 16%-42% of cases, which, despite low-risk features on initial biopsy, [are found to have] unfavorable pathological features at radical prostatectomy." Accordingly, some treatment centers recommend a second, confirmatory biopsy before pursuing active surveillance, the investigators said.
In one study of the issue, 27% of men with very low-risk features on initial biopsy proved to have upgraded or upstaged tumors at confirmatory biopsy.
Dr. Vargas and his colleagues decided to examine retrospectively whether standard transrectal T2-weighted MRI of the prostate would be useful in predicting which tumors were likely to be upgraded or upstaged on confirmatory biopsy.
The investigators identified 388 cases in their institution’s database in which men had an initial Gleason score of 6 or less on initial prostate biopsy performed in 1999-2010, had a prostate-specific antigen level less than 10 ng/mL, and had a confirmatory biopsy performed within 6 months of the initial biopsy.
Three radiologists independently interpreted the archived MRI scans and assigned each one a score indicating that tumor tissue was definitely evident, probably evident, definitely absent, probably absent, or indeterminate.
For all three radiologist readers, MRI scores indicating the probable or definite absence of tumor were highly predictive that confirmatory biopsy would show only very low-risk features and that active surveillance would be sufficient for those patients. In contrast, in a multivariate analysis, MRI scores showing the probable or definite presence of tumor were highly predictive that confirmatory biopsy would find upgraded or upstaged cancer (odds ratio, 2.16-3.97), and that radical prostatectomy would be recommended, the investigators said (J. Urol. 2012 Oct. 3 [doi:10.1016/j.juro.2012.07.024]).
Notably, one of the three radiologists, who had read only about 50 prostate MRI scans at the time of this study, had consistently less accurate readings than either of the other radiologists. The second radiologist had a fellowship in body imaging plus specialized training in prostate imaging, and had interpreted approximately 500 prostate MRIs. The third radiologist had completed a fellowship in genitourinary radiology and had read more than 5,000 prostate MRI scans.
The study findings thus confirm the importance of training and experience for the accurate interpretation of MRI scans of the prostate, Dr. Vargas and his associates noted.
This study was supported by the National Institutes of Health. No financial conflicts were reported.
Adding an MRI exam to the initial clinical evaluation of men thought to have low-risk prostate cancer can help identify which of them are the best candidates for active surveillance, according to study findings published online Oct. 3 in the Journal of Urology.
In a retrospective study of 388 men believed to have low-risk prostate cancer, tumors that were clearly visualized on an initial MRI were significantly more likely to be upgraded or upstaged on later confirmatory biopsy, and to prompt prostatectomy at that time. In contrast, tumors that could not be clearly visualized on MRI at the initial evaluation were significantly more likely to remain low grade on later confirmatory biopsy, and lent themselves to active surveillance rather than surgery, said Dr. Hebert Alberto Vargas of the department of radiology, Memorial Sloan-Kettering Cancer Center, New York, and his associates.
"These results suggest that MRI of the prostate, if read by radiologists with appropriate training and experience, could help determine active surveillance eligibility and obviate the need for confirmatory biopsy in substantial numbers of patients," they noted.
Initial biopsy samples of prostate cancers can miss areas of high-grade cancer, and "even the most stringent criteria misclassify 16%-42% of cases, which, despite low-risk features on initial biopsy, [are found to have] unfavorable pathological features at radical prostatectomy." Accordingly, some treatment centers recommend a second, confirmatory biopsy before pursuing active surveillance, the investigators said.
In one study of the issue, 27% of men with very low-risk features on initial biopsy proved to have upgraded or upstaged tumors at confirmatory biopsy.
Dr. Vargas and his colleagues decided to examine retrospectively whether standard transrectal T2-weighted MRI of the prostate would be useful in predicting which tumors were likely to be upgraded or upstaged on confirmatory biopsy.
The investigators identified 388 cases in their institution’s database in which men had an initial Gleason score of 6 or less on initial prostate biopsy performed in 1999-2010, had a prostate-specific antigen level less than 10 ng/mL, and had a confirmatory biopsy performed within 6 months of the initial biopsy.
Three radiologists independently interpreted the archived MRI scans and assigned each one a score indicating that tumor tissue was definitely evident, probably evident, definitely absent, probably absent, or indeterminate.
For all three radiologist readers, MRI scores indicating the probable or definite absence of tumor were highly predictive that confirmatory biopsy would show only very low-risk features and that active surveillance would be sufficient for those patients. In contrast, in a multivariate analysis, MRI scores showing the probable or definite presence of tumor were highly predictive that confirmatory biopsy would find upgraded or upstaged cancer (odds ratio, 2.16-3.97), and that radical prostatectomy would be recommended, the investigators said (J. Urol. 2012 Oct. 3 [doi:10.1016/j.juro.2012.07.024]).
Notably, one of the three radiologists, who had read only about 50 prostate MRI scans at the time of this study, had consistently less accurate readings than either of the other radiologists. The second radiologist had a fellowship in body imaging plus specialized training in prostate imaging, and had interpreted approximately 500 prostate MRIs. The third radiologist had completed a fellowship in genitourinary radiology and had read more than 5,000 prostate MRI scans.
The study findings thus confirm the importance of training and experience for the accurate interpretation of MRI scans of the prostate, Dr. Vargas and his associates noted.
This study was supported by the National Institutes of Health. No financial conflicts were reported.
FROM THE JOURNAL OF UROLOGY
Major Finding: In a multivariate analysis, MRI scores showing the probable or definite presence of tumor were highly predictive that confirmatory biopsy would find upgraded or upstaged cancer (odds ratio, 2.16-3.97), and that radical prostatectomy would be recommended.
Data Source: A retrospective study of MRI scans of the prostate in 388 men treated for low-risk prostate cancer at a single medical center during a 10-year period was conducted.
Disclosures: This study was supported by the National Institutes of Health. No financial conflicts were reported.
High-Dose Vitamin D Did Not Curb URTIs
Monthly high-dose vitamin D supplementation failed to reduce the number of upper respiratory tract infections in healthy adults of European extraction who already had adequate serum 25-hydroxyvitamin D levels, according to a report in the Oct. 3 issue of JAMA.
The treatment also failed to reduce the severity or duration of URTIs, or the number of days patients missed work, said Dr. David R. Murdoch of the department of pathology, University of Otago, Christchurch, New Zealand, and his associates (JAMA 2012;308:1333-9).
However, it is still possible that monthly high-dose vitamin-D supplementation may prevent or ameliorate URTIs in other populations, the authors noted, particularly those with a high prevalence of vitamin D deficiency. And different regimens with smaller, steadier dosing might prove effective, they added.
Epidemiologic and observational studies have reported an association between low vitamin D levels and a high rate of a variety of respiratory tract infections. But the few clinical trials to examine the issue have been hampered by small study populations, short durations, and low doses of vitamin D.
This large, randomized, double-blind, placebo-controlled clinical trial was designed to overcome those drawbacks, the investigators said.
Dr. Murdoch and his colleagues assessed 322 healthy adults with a mean age of 47 years, of whom 75% were women. The patients were randomly assigned to receive either oral vitamin D3 or matching placebo tablets every month for 18 months, and were followed closely for signs and symptoms of URTIs. Nasopharyngeal swabs were collected and analyzed for the presence of 20 viruses whenever a patient developed a runny nose, nasal stuffiness, sore throat, or cough that was not attributed to allergy.
The active-treatment group received a loading dose of 200,000 IU of vitamin D3 for months 1 and 2, then a maintenance dose of 100,000 IU for the remainder of the study. A total of 91% of the patients completed the study, and there were only three missed appointments throughout.
Serum levels of 25-hydroxyvitamin D rose dramatically in the patients who received active treatment but not in those who received placebo.
The main outcome measure of this study was the number of URTIs that developed during follow-up.
There were 593 URTIs in the vitamin D group, with a mean of 3.7 infections per person, and 611 URTIs in the placebo group, with a mean of 3.8 infections per person. This was not a statistically significant difference, the investigators said.
The results didn’t change when the data were categorized according to patients’ scores on the Wisconsin Upper Respiratory Symptom Survey 24, which measures the severity and functional impact of URTIs. Nor were outcomes altered by an analysis based on patients’ serum vitamin D levels at baseline.
The lack of a treatment effect also persisted across one summer and two winter seasons, even though the number of URTIs nearly doubled during the winter. The mean number of URTIs was 1.3 for both study groups in summer, and 2.5 and 2.3 in winter for the placebo and treatment groups, respectively.
There also was no difference in URTI severity between patients who received vitamin D and those who received placebo. The number of URTIs associated with positive nasopharyngeal swabs also was not significantly different between the two groups.
Another measure of URTI severity – the percentage of patients who missed at least 1 day of work when sick with a cold – also was exactly the same, at 41% in both groups.
There were no cases of asymptomatic hypercalcemia and no other adverse events attributed to vitamin D supplementation. The number of serious adverse events was not significantly different between the active-treatment and placebo groups.
"Further research is required to clarify whether there is benefit from supplementation in other populations and with other dosing regimens," Dr. Murdoch and his associates concluded.
The study was supported by the Health Research Council of New Zealand. The researchers reported no conflicts of interest.
This randomized, controlled trial rigorously addressed the question of whether vitamin D therapy can cut the number of respiratory infections, said Dr. Jeffrey A. Linder.
The trial was well powered to detect meaningful differences between the two study groups, boasted very good adherence to treatment assignments and a low dropout rate, and used a well-validated outcome tool to assess patients’ signs and symptoms. Not only did the treatment fail to decrease the rate of URTIs, but it also failed to show any impact on the severity, duration, or microbiologic characteristics of infections between the two study groups. Vitamin D should be added to the list of ineffective therapies for the common cold, he said.
Dr. Linder is in the division of general medicine and primary care at Brigham and Women’s Hospital and Harvard Medical School, Boston. He reported no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Murdoch’s report (JAMA 2012;308:1375-6).
This randomized, controlled trial rigorously addressed the question of whether vitamin D therapy can cut the number of respiratory infections, said Dr. Jeffrey A. Linder.
The trial was well powered to detect meaningful differences between the two study groups, boasted very good adherence to treatment assignments and a low dropout rate, and used a well-validated outcome tool to assess patients’ signs and symptoms. Not only did the treatment fail to decrease the rate of URTIs, but it also failed to show any impact on the severity, duration, or microbiologic characteristics of infections between the two study groups. Vitamin D should be added to the list of ineffective therapies for the common cold, he said.
Dr. Linder is in the division of general medicine and primary care at Brigham and Women’s Hospital and Harvard Medical School, Boston. He reported no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Murdoch’s report (JAMA 2012;308:1375-6).
This randomized, controlled trial rigorously addressed the question of whether vitamin D therapy can cut the number of respiratory infections, said Dr. Jeffrey A. Linder.
The trial was well powered to detect meaningful differences between the two study groups, boasted very good adherence to treatment assignments and a low dropout rate, and used a well-validated outcome tool to assess patients’ signs and symptoms. Not only did the treatment fail to decrease the rate of URTIs, but it also failed to show any impact on the severity, duration, or microbiologic characteristics of infections between the two study groups. Vitamin D should be added to the list of ineffective therapies for the common cold, he said.
Dr. Linder is in the division of general medicine and primary care at Brigham and Women’s Hospital and Harvard Medical School, Boston. He reported no financial conflicts of interest. These remarks were taken from his editorial accompanying Dr. Murdoch’s report (JAMA 2012;308:1375-6).
Monthly high-dose vitamin D supplementation failed to reduce the number of upper respiratory tract infections in healthy adults of European extraction who already had adequate serum 25-hydroxyvitamin D levels, according to a report in the Oct. 3 issue of JAMA.
The treatment also failed to reduce the severity or duration of URTIs, or the number of days patients missed work, said Dr. David R. Murdoch of the department of pathology, University of Otago, Christchurch, New Zealand, and his associates (JAMA 2012;308:1333-9).
However, it is still possible that monthly high-dose vitamin-D supplementation may prevent or ameliorate URTIs in other populations, the authors noted, particularly those with a high prevalence of vitamin D deficiency. And different regimens with smaller, steadier dosing might prove effective, they added.
Epidemiologic and observational studies have reported an association between low vitamin D levels and a high rate of a variety of respiratory tract infections. But the few clinical trials to examine the issue have been hampered by small study populations, short durations, and low doses of vitamin D.
This large, randomized, double-blind, placebo-controlled clinical trial was designed to overcome those drawbacks, the investigators said.
Dr. Murdoch and his colleagues assessed 322 healthy adults with a mean age of 47 years, of whom 75% were women. The patients were randomly assigned to receive either oral vitamin D3 or matching placebo tablets every month for 18 months, and were followed closely for signs and symptoms of URTIs. Nasopharyngeal swabs were collected and analyzed for the presence of 20 viruses whenever a patient developed a runny nose, nasal stuffiness, sore throat, or cough that was not attributed to allergy.
The active-treatment group received a loading dose of 200,000 IU of vitamin D3 for months 1 and 2, then a maintenance dose of 100,000 IU for the remainder of the study. A total of 91% of the patients completed the study, and there were only three missed appointments throughout.
Serum levels of 25-hydroxyvitamin D rose dramatically in the patients who received active treatment but not in those who received placebo.
The main outcome measure of this study was the number of URTIs that developed during follow-up.
There were 593 URTIs in the vitamin D group, with a mean of 3.7 infections per person, and 611 URTIs in the placebo group, with a mean of 3.8 infections per person. This was not a statistically significant difference, the investigators said.
The results didn’t change when the data were categorized according to patients’ scores on the Wisconsin Upper Respiratory Symptom Survey 24, which measures the severity and functional impact of URTIs. Nor were outcomes altered by an analysis based on patients’ serum vitamin D levels at baseline.
The lack of a treatment effect also persisted across one summer and two winter seasons, even though the number of URTIs nearly doubled during the winter. The mean number of URTIs was 1.3 for both study groups in summer, and 2.5 and 2.3 in winter for the placebo and treatment groups, respectively.
There also was no difference in URTI severity between patients who received vitamin D and those who received placebo. The number of URTIs associated with positive nasopharyngeal swabs also was not significantly different between the two groups.
Another measure of URTI severity – the percentage of patients who missed at least 1 day of work when sick with a cold – also was exactly the same, at 41% in both groups.
There were no cases of asymptomatic hypercalcemia and no other adverse events attributed to vitamin D supplementation. The number of serious adverse events was not significantly different between the active-treatment and placebo groups.
"Further research is required to clarify whether there is benefit from supplementation in other populations and with other dosing regimens," Dr. Murdoch and his associates concluded.
The study was supported by the Health Research Council of New Zealand. The researchers reported no conflicts of interest.
Monthly high-dose vitamin D supplementation failed to reduce the number of upper respiratory tract infections in healthy adults of European extraction who already had adequate serum 25-hydroxyvitamin D levels, according to a report in the Oct. 3 issue of JAMA.
The treatment also failed to reduce the severity or duration of URTIs, or the number of days patients missed work, said Dr. David R. Murdoch of the department of pathology, University of Otago, Christchurch, New Zealand, and his associates (JAMA 2012;308:1333-9).
However, it is still possible that monthly high-dose vitamin-D supplementation may prevent or ameliorate URTIs in other populations, the authors noted, particularly those with a high prevalence of vitamin D deficiency. And different regimens with smaller, steadier dosing might prove effective, they added.
Epidemiologic and observational studies have reported an association between low vitamin D levels and a high rate of a variety of respiratory tract infections. But the few clinical trials to examine the issue have been hampered by small study populations, short durations, and low doses of vitamin D.
This large, randomized, double-blind, placebo-controlled clinical trial was designed to overcome those drawbacks, the investigators said.
Dr. Murdoch and his colleagues assessed 322 healthy adults with a mean age of 47 years, of whom 75% were women. The patients were randomly assigned to receive either oral vitamin D3 or matching placebo tablets every month for 18 months, and were followed closely for signs and symptoms of URTIs. Nasopharyngeal swabs were collected and analyzed for the presence of 20 viruses whenever a patient developed a runny nose, nasal stuffiness, sore throat, or cough that was not attributed to allergy.
The active-treatment group received a loading dose of 200,000 IU of vitamin D3 for months 1 and 2, then a maintenance dose of 100,000 IU for the remainder of the study. A total of 91% of the patients completed the study, and there were only three missed appointments throughout.
Serum levels of 25-hydroxyvitamin D rose dramatically in the patients who received active treatment but not in those who received placebo.
The main outcome measure of this study was the number of URTIs that developed during follow-up.
There were 593 URTIs in the vitamin D group, with a mean of 3.7 infections per person, and 611 URTIs in the placebo group, with a mean of 3.8 infections per person. This was not a statistically significant difference, the investigators said.
The results didn’t change when the data were categorized according to patients’ scores on the Wisconsin Upper Respiratory Symptom Survey 24, which measures the severity and functional impact of URTIs. Nor were outcomes altered by an analysis based on patients’ serum vitamin D levels at baseline.
The lack of a treatment effect also persisted across one summer and two winter seasons, even though the number of URTIs nearly doubled during the winter. The mean number of URTIs was 1.3 for both study groups in summer, and 2.5 and 2.3 in winter for the placebo and treatment groups, respectively.
There also was no difference in URTI severity between patients who received vitamin D and those who received placebo. The number of URTIs associated with positive nasopharyngeal swabs also was not significantly different between the two groups.
Another measure of URTI severity – the percentage of patients who missed at least 1 day of work when sick with a cold – also was exactly the same, at 41% in both groups.
There were no cases of asymptomatic hypercalcemia and no other adverse events attributed to vitamin D supplementation. The number of serious adverse events was not significantly different between the active-treatment and placebo groups.
"Further research is required to clarify whether there is benefit from supplementation in other populations and with other dosing regimens," Dr. Murdoch and his associates concluded.
The study was supported by the Health Research Council of New Zealand. The researchers reported no conflicts of interest.
FROM JAMA
Major Finding: The mean number of upper respiratory tract infections was 3.7 per person in healthy adult patients who received vitamin D supplements, which was not significantly different from the 3.8 rate in the control group.
Data Source: A randomized, double-blind, placebo-controlled clinical trial involving 322 healthy adults who were followed for 18 months for the incidence and severity of URTIs.
Disclosures: This study was supported by the Health Research Council of New Zealand. No financial conflicts of interest were reported.
Use of EHR Helps Improve Diabetes Control
Use of a certified electronic health record system improved drug therapy and follow-up monitoring of patients with type 2 diabetes, as well as improving their glycemic and lipid control, according to a report published online Oct. 1 in Annals of Internal Medicine.
The greatest improvements were seen in patients who had the poorest disease control at baseline, as measured by hemoglobin A1c and LDL-cholesterol levels. Electronic health record (EHR) use also reduced inappropriate medication changes and retesting of patients who already met glycemic and lipid control targets, said Mary Reed, Dr.P.H., of Kaiser Permanente Northern California, Oakland, and her associates.
"[An] EHR may be a powerful tool to help clinicians deliver well-targeted, high-quality chronic disease care and improve patient outcomes," they noted.
Implementation of EHR systems is being driven by federal stimulus legislation that provides incentive payments of up to $44,000 per physician for the "meaningful use" of such a system; penalties for not doing so begin in 2015.
Dr. Reed and her colleagues were able to compare patient outcomes before and after EHR adoption because of the staggered roll-out of the technology across the 17 medical centers of their HMO over 3 years.
The investigators examined testing intervals, glycemic control, and LDL-cholesterol control in the 169,711 patients in their plan’s diabetes registry during the 5 years before, during, and after EHR implementation. There were more than 1.3 million HbA1c tests and 1.2 million LDL cholesterol tests during that time.
After EHR implementation, patients with an HbA1c levels of 7% or greater were significantly more likely to receive treatment intensification than they had been before the EHR was used. In contrast, patients with HbA1c values under 7% did not experience unnecessary intensification.
Similarly, after implementation, patients with high HbA1c levels were significantly more likely to undergo retesting within 90 days than they had been before, while those with normal HbA1c levels were not subjected to unnecessary retesting.
The findings were the same with regard to high LDL-cholesterol levels. Diabetic patients with high LDL were more likely to receive treatment intensification and to be retested within 90 days than they had been before the EHR program was implemented.
Correspondingly, both glycemic control and cholesterol control improved with use of the EHR and the improvement in these clinical outcomes was greatest among patients whose HbA1c and LDL-cholesterol levels had been the highest at baseline, Dr. Reed and her associates said (Ann. Intern. Med. 2012;157:482-9).
Improvements were characterized as "modest," but the investigators noted that could be due in part to the fact that this patient population was already participating in "a sophisticated and systematic [diabetes] management program" and therefore had good control at baseline.
"It is likely that EHR implementation could bring more dramatic improvements in other settings, where baseline rates of control are lower or disease management capabilities are more limited," they said.
They added that as an observational study, their study could not establish cause and effect. But the findings do suggest that using an EHR improves the clinical care of patients with diabetes, they said.
"The lack of any measurable unintended harm in the outcomes for this study" is also an important finding, because it refutes the results of previous studies that suggested an EHR could have no effect on, or could even worsen, patient care.
The study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases.
Use of a certified electronic health record system improved drug therapy and follow-up monitoring of patients with type 2 diabetes, as well as improving their glycemic and lipid control, according to a report published online Oct. 1 in Annals of Internal Medicine.
The greatest improvements were seen in patients who had the poorest disease control at baseline, as measured by hemoglobin A1c and LDL-cholesterol levels. Electronic health record (EHR) use also reduced inappropriate medication changes and retesting of patients who already met glycemic and lipid control targets, said Mary Reed, Dr.P.H., of Kaiser Permanente Northern California, Oakland, and her associates.
"[An] EHR may be a powerful tool to help clinicians deliver well-targeted, high-quality chronic disease care and improve patient outcomes," they noted.
Implementation of EHR systems is being driven by federal stimulus legislation that provides incentive payments of up to $44,000 per physician for the "meaningful use" of such a system; penalties for not doing so begin in 2015.
Dr. Reed and her colleagues were able to compare patient outcomes before and after EHR adoption because of the staggered roll-out of the technology across the 17 medical centers of their HMO over 3 years.
The investigators examined testing intervals, glycemic control, and LDL-cholesterol control in the 169,711 patients in their plan’s diabetes registry during the 5 years before, during, and after EHR implementation. There were more than 1.3 million HbA1c tests and 1.2 million LDL cholesterol tests during that time.
After EHR implementation, patients with an HbA1c levels of 7% or greater were significantly more likely to receive treatment intensification than they had been before the EHR was used. In contrast, patients with HbA1c values under 7% did not experience unnecessary intensification.
Similarly, after implementation, patients with high HbA1c levels were significantly more likely to undergo retesting within 90 days than they had been before, while those with normal HbA1c levels were not subjected to unnecessary retesting.
The findings were the same with regard to high LDL-cholesterol levels. Diabetic patients with high LDL were more likely to receive treatment intensification and to be retested within 90 days than they had been before the EHR program was implemented.
Correspondingly, both glycemic control and cholesterol control improved with use of the EHR and the improvement in these clinical outcomes was greatest among patients whose HbA1c and LDL-cholesterol levels had been the highest at baseline, Dr. Reed and her associates said (Ann. Intern. Med. 2012;157:482-9).
Improvements were characterized as "modest," but the investigators noted that could be due in part to the fact that this patient population was already participating in "a sophisticated and systematic [diabetes] management program" and therefore had good control at baseline.
"It is likely that EHR implementation could bring more dramatic improvements in other settings, where baseline rates of control are lower or disease management capabilities are more limited," they said.
They added that as an observational study, their study could not establish cause and effect. But the findings do suggest that using an EHR improves the clinical care of patients with diabetes, they said.
"The lack of any measurable unintended harm in the outcomes for this study" is also an important finding, because it refutes the results of previous studies that suggested an EHR could have no effect on, or could even worsen, patient care.
The study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases.
Use of a certified electronic health record system improved drug therapy and follow-up monitoring of patients with type 2 diabetes, as well as improving their glycemic and lipid control, according to a report published online Oct. 1 in Annals of Internal Medicine.
The greatest improvements were seen in patients who had the poorest disease control at baseline, as measured by hemoglobin A1c and LDL-cholesterol levels. Electronic health record (EHR) use also reduced inappropriate medication changes and retesting of patients who already met glycemic and lipid control targets, said Mary Reed, Dr.P.H., of Kaiser Permanente Northern California, Oakland, and her associates.
"[An] EHR may be a powerful tool to help clinicians deliver well-targeted, high-quality chronic disease care and improve patient outcomes," they noted.
Implementation of EHR systems is being driven by federal stimulus legislation that provides incentive payments of up to $44,000 per physician for the "meaningful use" of such a system; penalties for not doing so begin in 2015.
Dr. Reed and her colleagues were able to compare patient outcomes before and after EHR adoption because of the staggered roll-out of the technology across the 17 medical centers of their HMO over 3 years.
The investigators examined testing intervals, glycemic control, and LDL-cholesterol control in the 169,711 patients in their plan’s diabetes registry during the 5 years before, during, and after EHR implementation. There were more than 1.3 million HbA1c tests and 1.2 million LDL cholesterol tests during that time.
After EHR implementation, patients with an HbA1c levels of 7% or greater were significantly more likely to receive treatment intensification than they had been before the EHR was used. In contrast, patients with HbA1c values under 7% did not experience unnecessary intensification.
Similarly, after implementation, patients with high HbA1c levels were significantly more likely to undergo retesting within 90 days than they had been before, while those with normal HbA1c levels were not subjected to unnecessary retesting.
The findings were the same with regard to high LDL-cholesterol levels. Diabetic patients with high LDL were more likely to receive treatment intensification and to be retested within 90 days than they had been before the EHR program was implemented.
Correspondingly, both glycemic control and cholesterol control improved with use of the EHR and the improvement in these clinical outcomes was greatest among patients whose HbA1c and LDL-cholesterol levels had been the highest at baseline, Dr. Reed and her associates said (Ann. Intern. Med. 2012;157:482-9).
Improvements were characterized as "modest," but the investigators noted that could be due in part to the fact that this patient population was already participating in "a sophisticated and systematic [diabetes] management program" and therefore had good control at baseline.
"It is likely that EHR implementation could bring more dramatic improvements in other settings, where baseline rates of control are lower or disease management capabilities are more limited," they said.
They added that as an observational study, their study could not establish cause and effect. But the findings do suggest that using an EHR improves the clinical care of patients with diabetes, they said.
"The lack of any measurable unintended harm in the outcomes for this study" is also an important finding, because it refutes the results of previous studies that suggested an EHR could have no effect on, or could even worsen, patient care.
The study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases.
FROM ANNALS OF INTERNAL MEDICINE
Major Finding: After a certified EHR system was introduced, intensification of drug therapy, follow-up monitoring of response to treatment, and both glycemic and lipid control all improved.
Data Source: The findings come from an observational study of outcomes in 169,711 diabetes patients treated at 17 medical centers during the staggered implementation of an EHR system.
Disclosures: This study was supported by the National Institute of Diabetes and Digestive and Kidney Diseases. The investigators' reported conflicts of interest were not available.