User login
Sharon Worcester is an award-winning medical journalist for MDedge News. She has been with the company since 1996, first as the Southeast Bureau Chief (1996-2009) when the company was known as International Medical News Group, then as a freelance writer (2010-2015) before returning as a reporter in 2015. She previously worked as a daily newspaper reporter covering health and local government. Sharon currently reports primarily on oncology and hematology. She has a BA from Eckerd College and an MA in Mass Communication/Print Journalism from the University of Florida. Connect with her via LinkedIn and follow her on twitter @SW_MedReporter.
Many Children Still Not Receiving Appropriate Pneumococcal Vaccination
ATLANTA – A large proportion of children apparently are not receiving the 13-valent pneumococcal conjugate vaccine as recommended by the Advisory Committee on Immunization Practices, surveillance data from the Centers for Disease Control and Prevention suggest.
According to the data from an ongoing evaluation of PCV13 vaccine effectiveness, 86 (78%) vaccine-eligible children out of 110 diagnosed with invasive pneumococcal disease secondary to serotypes unique to PCV13 in the year after the vaccine was introduced had not received the dosing recommended by the Advisory Committee on Immunization Practices (ACIP), Dr. Chad M. Cox reported at the International Conference on Emerging Infectious Diseases.
The ACIP recommendations, published March 12, 2010, call for the same dosing schedule used for PCV7 (immunizations at ages 2, 4, and 6 months, with a booster dose at age 12-15 months). ACIP also called for a single supplemental dose of PCV13 in all children aged 14-59 months who previously received an age-appropriate series of PCV7, and for use of PCV13 for the fourth dose in those who had received only three of the four previously recommended doses of PCV7.
PCV13 includes six additional serotypes not included in PCV7, which was introduced in 2000 using the seven most commonly circulating serotypes.
After the introduction of PCV7, a sharp decrease occurred in disease caused by these seven serotypes, but in more recent years an increase was seen in disease caused by serotypes not covered by PC7. Because of the emergence of this "replacement disease," PCV13 was introduced, Dr. Cox explained.
"The [PCV13] vaccine was readily available soon after [the March 2010 ACIP recommendations], and quickly replaced PCV7 in most provider’s offices," said Dr. Cox of the CDC in Atlanta.
Nonetheless, in June 2011 the California Department of Health reported a fatal case of invasive pneumococcal disease in a 2-year-old, which was caused by a serotype in the PCV13 vaccine; 30 additional cases were identified in counties not included in the CDC surveillance area.
This led to a health advisory issued in August 2011 – reminding providers of the ACIP recommendations – and to this study of outcomes in 10 participating surveillance areas representing 3.8 million children under age 5 years.
The hospitalized children in this study included those from the surveillance areas for whom complete vaccination information was available. About two-thirds were aged 2-4 years, Dr. Cox said.
About two-thirds of patients in the study were noncompliant because they had not received a supplemental PCV13 dose after completion of the PCV7 series, and about one-fifth had not received the fourth dose in the series, which should have been a PCV13 dose, he noted.
The majority of the children (93%) had no underlying medical conditions, and 79% were hospitalized. No deaths occurred.
These findings demonstrate that invasive pneumococcal disease resulting from pneumococcal serotyopes unique to PCV13 continued to occur in those who did not receive the recommended dose of PCV13 in the year after it became available, Dr. Cox said.
Prevention of invasive pneumococcal disease requires that a single supplemental dose of PCV13 be given to all children aged 14-59 months who have received an age-appropriate series of PCV7, he said. Efforts have been made, using these and other CDC data, to better educate health care professionals about the ACIP recommendations.
"This is something we continue to watch," he said, noting that the vaccine effectiveness evaluation will continue for 2 more years.
Dr. Cox said that he had no relevant financial disclosures to report.
ATLANTA – A large proportion of children apparently are not receiving the 13-valent pneumococcal conjugate vaccine as recommended by the Advisory Committee on Immunization Practices, surveillance data from the Centers for Disease Control and Prevention suggest.
According to the data from an ongoing evaluation of PCV13 vaccine effectiveness, 86 (78%) vaccine-eligible children out of 110 diagnosed with invasive pneumococcal disease secondary to serotypes unique to PCV13 in the year after the vaccine was introduced had not received the dosing recommended by the Advisory Committee on Immunization Practices (ACIP), Dr. Chad M. Cox reported at the International Conference on Emerging Infectious Diseases.
The ACIP recommendations, published March 12, 2010, call for the same dosing schedule used for PCV7 (immunizations at ages 2, 4, and 6 months, with a booster dose at age 12-15 months). ACIP also called for a single supplemental dose of PCV13 in all children aged 14-59 months who previously received an age-appropriate series of PCV7, and for use of PCV13 for the fourth dose in those who had received only three of the four previously recommended doses of PCV7.
PCV13 includes six additional serotypes not included in PCV7, which was introduced in 2000 using the seven most commonly circulating serotypes.
After the introduction of PCV7, a sharp decrease occurred in disease caused by these seven serotypes, but in more recent years an increase was seen in disease caused by serotypes not covered by PC7. Because of the emergence of this "replacement disease," PCV13 was introduced, Dr. Cox explained.
"The [PCV13] vaccine was readily available soon after [the March 2010 ACIP recommendations], and quickly replaced PCV7 in most provider’s offices," said Dr. Cox of the CDC in Atlanta.
Nonetheless, in June 2011 the California Department of Health reported a fatal case of invasive pneumococcal disease in a 2-year-old, which was caused by a serotype in the PCV13 vaccine; 30 additional cases were identified in counties not included in the CDC surveillance area.
This led to a health advisory issued in August 2011 – reminding providers of the ACIP recommendations – and to this study of outcomes in 10 participating surveillance areas representing 3.8 million children under age 5 years.
The hospitalized children in this study included those from the surveillance areas for whom complete vaccination information was available. About two-thirds were aged 2-4 years, Dr. Cox said.
About two-thirds of patients in the study were noncompliant because they had not received a supplemental PCV13 dose after completion of the PCV7 series, and about one-fifth had not received the fourth dose in the series, which should have been a PCV13 dose, he noted.
The majority of the children (93%) had no underlying medical conditions, and 79% were hospitalized. No deaths occurred.
These findings demonstrate that invasive pneumococcal disease resulting from pneumococcal serotyopes unique to PCV13 continued to occur in those who did not receive the recommended dose of PCV13 in the year after it became available, Dr. Cox said.
Prevention of invasive pneumococcal disease requires that a single supplemental dose of PCV13 be given to all children aged 14-59 months who have received an age-appropriate series of PCV7, he said. Efforts have been made, using these and other CDC data, to better educate health care professionals about the ACIP recommendations.
"This is something we continue to watch," he said, noting that the vaccine effectiveness evaluation will continue for 2 more years.
Dr. Cox said that he had no relevant financial disclosures to report.
ATLANTA – A large proportion of children apparently are not receiving the 13-valent pneumococcal conjugate vaccine as recommended by the Advisory Committee on Immunization Practices, surveillance data from the Centers for Disease Control and Prevention suggest.
According to the data from an ongoing evaluation of PCV13 vaccine effectiveness, 86 (78%) vaccine-eligible children out of 110 diagnosed with invasive pneumococcal disease secondary to serotypes unique to PCV13 in the year after the vaccine was introduced had not received the dosing recommended by the Advisory Committee on Immunization Practices (ACIP), Dr. Chad M. Cox reported at the International Conference on Emerging Infectious Diseases.
The ACIP recommendations, published March 12, 2010, call for the same dosing schedule used for PCV7 (immunizations at ages 2, 4, and 6 months, with a booster dose at age 12-15 months). ACIP also called for a single supplemental dose of PCV13 in all children aged 14-59 months who previously received an age-appropriate series of PCV7, and for use of PCV13 for the fourth dose in those who had received only three of the four previously recommended doses of PCV7.
PCV13 includes six additional serotypes not included in PCV7, which was introduced in 2000 using the seven most commonly circulating serotypes.
After the introduction of PCV7, a sharp decrease occurred in disease caused by these seven serotypes, but in more recent years an increase was seen in disease caused by serotypes not covered by PC7. Because of the emergence of this "replacement disease," PCV13 was introduced, Dr. Cox explained.
"The [PCV13] vaccine was readily available soon after [the March 2010 ACIP recommendations], and quickly replaced PCV7 in most provider’s offices," said Dr. Cox of the CDC in Atlanta.
Nonetheless, in June 2011 the California Department of Health reported a fatal case of invasive pneumococcal disease in a 2-year-old, which was caused by a serotype in the PCV13 vaccine; 30 additional cases were identified in counties not included in the CDC surveillance area.
This led to a health advisory issued in August 2011 – reminding providers of the ACIP recommendations – and to this study of outcomes in 10 participating surveillance areas representing 3.8 million children under age 5 years.
The hospitalized children in this study included those from the surveillance areas for whom complete vaccination information was available. About two-thirds were aged 2-4 years, Dr. Cox said.
About two-thirds of patients in the study were noncompliant because they had not received a supplemental PCV13 dose after completion of the PCV7 series, and about one-fifth had not received the fourth dose in the series, which should have been a PCV13 dose, he noted.
The majority of the children (93%) had no underlying medical conditions, and 79% were hospitalized. No deaths occurred.
These findings demonstrate that invasive pneumococcal disease resulting from pneumococcal serotyopes unique to PCV13 continued to occur in those who did not receive the recommended dose of PCV13 in the year after it became available, Dr. Cox said.
Prevention of invasive pneumococcal disease requires that a single supplemental dose of PCV13 be given to all children aged 14-59 months who have received an age-appropriate series of PCV7, he said. Efforts have been made, using these and other CDC data, to better educate health care professionals about the ACIP recommendations.
"This is something we continue to watch," he said, noting that the vaccine effectiveness evaluation will continue for 2 more years.
Dr. Cox said that he had no relevant financial disclosures to report.
FROM THE INTERNATIONAL CONFERENCE ON EMERGING INFECTIOUS DISEASES
Major Finding: Of 110 patients diagnosed with invasive pneumococcal disease secondary to serotypes unique to PCV13 in the year after the vaccine was introduced, 86 (78%) vaccine-eligible children had not received the dosing recommended by ACIP.
Data Source: The data for the study were drawn from a 10-area CDC surveillance network across United States.
Disclosures: Dr. Cox said that he had no relevant financial disclosures to report.
Dengue Underreported in U.S. Travelers
ATLANTA – The risk of dengue remains a concern for residents of the United States who travel to the tropics, and the disease burden may be underestimated, surveillance data suggest.
Between 2005 and 2010, 1,697 laboratory-positive cases were reported to the Centers for Disease Control and Prevention’s arbovirus surveillance system (ArboNET) and/or to the CDC dengue branch, for an annual average of 285 cases. A substantial number of cases occurred in New York City and in Florida, and most travelers failed to take precautionary measures when traveling to endemic areas, according to data presented at the International Conference on Emerging Infectious Diseases.
Furthermore, when the estimated number of cases derived from laboratory testing data was compared with the number of laboratory-positive cases, there was a fourfold degree of underreporting, Dr. D. Fermin Arguello of the CDC, San Juan, Puerto Rico reported in a poster at the conference.
The CDC data indicated that half of the cases occurred in travelers to the Dominican Republic, Puerto Rico, India, Mexico, or Haiti.
Data from the New York City Department of Health and Mental Hygiene showed that between 2001 and 2009 the annual average was 36 cases, but that in 2010, when a global dengue epidemic occurred, 144 cases were identified, according to Brooke Bregman of the department.
This was more than any other single year, she pointed out.
Cases in New York also frequently occurred in travelers to the Dominican Republic and Puerto Rico. In fact, most cases there (68%) were associated with travel to the Caribbean. Others were associated with travel to Southeast Asia (13%), and South America (10%), Ms. Bregman said.
The New York data indicated that, although 81% of patients recalled being bitten by mosquitoes, only 29% reported using mosquito repellent and only 14% used a bed net.
Only 10% sought medical advice before traveling, Ms. Bregman said, noting that effective strategies are needed to encourage travelers to adopt protective measures.
Dr. Arguello agreed, noting also that travelers should seek pre-travel consultation, minimize mosquito exposure while traveling, and seek medical attention if they develop a fever either during travel or soon after return from travel.
He also noted a need for improvements in national surveillance reporting to determine the risk and impact of dengue in U.S. travelers.
In another poster presented at the conference, researchers noted that educational strategies do have a beneficial impact.
A 2011 population-based evaluation of knowledge, attitudes, and behaviors toward dengue prevention in Key West showed that of 526 households evaluated, more than 80% were able to identify infected mosquitoes as the transition mode for dengue, and standing water as an important source for the mosquito vector, according to Emily Zielinski-Gutiérrez, DrPH of the CDC, Fort Collins, Colo.
Respondents who reported being exposed to dengue educational messages were significantly more knowledgeable about the disease than were those with no recall of exposure to such messages, according to scores on a dengue knowledge scale, she said.
The Florida Keys Mosquito Control District and local newspaper articles were the most frequently cited sources of information about dengue.
This study highlighted areas where more effort is needed, however; less than half of the respondents were aware that some patients in Key West had been hospitalized for dengue, and a third could not name specific symptoms of dengue illness, Dr. Zielinski-Gutiérrez reported.
None of the authors had disclosures to report.
ATLANTA – The risk of dengue remains a concern for residents of the United States who travel to the tropics, and the disease burden may be underestimated, surveillance data suggest.
Between 2005 and 2010, 1,697 laboratory-positive cases were reported to the Centers for Disease Control and Prevention’s arbovirus surveillance system (ArboNET) and/or to the CDC dengue branch, for an annual average of 285 cases. A substantial number of cases occurred in New York City and in Florida, and most travelers failed to take precautionary measures when traveling to endemic areas, according to data presented at the International Conference on Emerging Infectious Diseases.
Furthermore, when the estimated number of cases derived from laboratory testing data was compared with the number of laboratory-positive cases, there was a fourfold degree of underreporting, Dr. D. Fermin Arguello of the CDC, San Juan, Puerto Rico reported in a poster at the conference.
The CDC data indicated that half of the cases occurred in travelers to the Dominican Republic, Puerto Rico, India, Mexico, or Haiti.
Data from the New York City Department of Health and Mental Hygiene showed that between 2001 and 2009 the annual average was 36 cases, but that in 2010, when a global dengue epidemic occurred, 144 cases were identified, according to Brooke Bregman of the department.
This was more than any other single year, she pointed out.
Cases in New York also frequently occurred in travelers to the Dominican Republic and Puerto Rico. In fact, most cases there (68%) were associated with travel to the Caribbean. Others were associated with travel to Southeast Asia (13%), and South America (10%), Ms. Bregman said.
The New York data indicated that, although 81% of patients recalled being bitten by mosquitoes, only 29% reported using mosquito repellent and only 14% used a bed net.
Only 10% sought medical advice before traveling, Ms. Bregman said, noting that effective strategies are needed to encourage travelers to adopt protective measures.
Dr. Arguello agreed, noting also that travelers should seek pre-travel consultation, minimize mosquito exposure while traveling, and seek medical attention if they develop a fever either during travel or soon after return from travel.
He also noted a need for improvements in national surveillance reporting to determine the risk and impact of dengue in U.S. travelers.
In another poster presented at the conference, researchers noted that educational strategies do have a beneficial impact.
A 2011 population-based evaluation of knowledge, attitudes, and behaviors toward dengue prevention in Key West showed that of 526 households evaluated, more than 80% were able to identify infected mosquitoes as the transition mode for dengue, and standing water as an important source for the mosquito vector, according to Emily Zielinski-Gutiérrez, DrPH of the CDC, Fort Collins, Colo.
Respondents who reported being exposed to dengue educational messages were significantly more knowledgeable about the disease than were those with no recall of exposure to such messages, according to scores on a dengue knowledge scale, she said.
The Florida Keys Mosquito Control District and local newspaper articles were the most frequently cited sources of information about dengue.
This study highlighted areas where more effort is needed, however; less than half of the respondents were aware that some patients in Key West had been hospitalized for dengue, and a third could not name specific symptoms of dengue illness, Dr. Zielinski-Gutiérrez reported.
None of the authors had disclosures to report.
ATLANTA – The risk of dengue remains a concern for residents of the United States who travel to the tropics, and the disease burden may be underestimated, surveillance data suggest.
Between 2005 and 2010, 1,697 laboratory-positive cases were reported to the Centers for Disease Control and Prevention’s arbovirus surveillance system (ArboNET) and/or to the CDC dengue branch, for an annual average of 285 cases. A substantial number of cases occurred in New York City and in Florida, and most travelers failed to take precautionary measures when traveling to endemic areas, according to data presented at the International Conference on Emerging Infectious Diseases.
Furthermore, when the estimated number of cases derived from laboratory testing data was compared with the number of laboratory-positive cases, there was a fourfold degree of underreporting, Dr. D. Fermin Arguello of the CDC, San Juan, Puerto Rico reported in a poster at the conference.
The CDC data indicated that half of the cases occurred in travelers to the Dominican Republic, Puerto Rico, India, Mexico, or Haiti.
Data from the New York City Department of Health and Mental Hygiene showed that between 2001 and 2009 the annual average was 36 cases, but that in 2010, when a global dengue epidemic occurred, 144 cases were identified, according to Brooke Bregman of the department.
This was more than any other single year, she pointed out.
Cases in New York also frequently occurred in travelers to the Dominican Republic and Puerto Rico. In fact, most cases there (68%) were associated with travel to the Caribbean. Others were associated with travel to Southeast Asia (13%), and South America (10%), Ms. Bregman said.
The New York data indicated that, although 81% of patients recalled being bitten by mosquitoes, only 29% reported using mosquito repellent and only 14% used a bed net.
Only 10% sought medical advice before traveling, Ms. Bregman said, noting that effective strategies are needed to encourage travelers to adopt protective measures.
Dr. Arguello agreed, noting also that travelers should seek pre-travel consultation, minimize mosquito exposure while traveling, and seek medical attention if they develop a fever either during travel or soon after return from travel.
He also noted a need for improvements in national surveillance reporting to determine the risk and impact of dengue in U.S. travelers.
In another poster presented at the conference, researchers noted that educational strategies do have a beneficial impact.
A 2011 population-based evaluation of knowledge, attitudes, and behaviors toward dengue prevention in Key West showed that of 526 households evaluated, more than 80% were able to identify infected mosquitoes as the transition mode for dengue, and standing water as an important source for the mosquito vector, according to Emily Zielinski-Gutiérrez, DrPH of the CDC, Fort Collins, Colo.
Respondents who reported being exposed to dengue educational messages were significantly more knowledgeable about the disease than were those with no recall of exposure to such messages, according to scores on a dengue knowledge scale, she said.
The Florida Keys Mosquito Control District and local newspaper articles were the most frequently cited sources of information about dengue.
This study highlighted areas where more effort is needed, however; less than half of the respondents were aware that some patients in Key West had been hospitalized for dengue, and a third could not name specific symptoms of dengue illness, Dr. Zielinski-Gutiérrez reported.
None of the authors had disclosures to report.
FROM THE INTERNATIONAL CONFERENCE ON EMERGING INFECTIOUS DISEASES
Major Finding: Between 2005 and 2010, 1,697 laboratory-positive cases of dengue infection were reported to the Centers for Disease Control and Prevention’s arbovirus surveillance system (ArboNET) and/or to the CDC dengue branch, for an annual average of 285 cases. When the estimated number of cases derived from laboratory testing data was compared with the number of laboratory-positive cases, there was a fourfold degree of underreporting.
Data Source: Study findings are based on an analysis for surveillance data.
Disclosures: None of the authors had disclosures to report.
ACR Endorses Provisional Sjögren’s Classification Criteria
Provisional new classification criteria for Sjögren’s syndrome take into account the availability of new biologic treatment agents, rely solely on objective measures, and improve classification performance when compared with existing alternatives, according to the American College of Rheumatology.
The new criteria, which are the first to be endorsed by the ACR, target individuals with signs and symptoms suggestive of Sjögren’s syndrome and are based on expert opinion derived by analysis of data from the more than 1,300 patients in the SICCA (Sjögren’s International Collaborative Clinical Alliance) registry. They also differ from previous criteria in that only objective tests related to oral, ocular, and systemic manifestations of the syndrome are included.
This brings together three medical specialties – rheumatology, ophthalmology, and oral medicine – for the purpose of determining a patient’s disease status, and reinforces the importance of collaboration among these specialties when it comes to assessment and management of patients with Sjögren’s syndrome. It also protects patients by reducing the likelihood of misclassification, which could lead to unnecessary exposure to investigational drugs, according to Stephen C. Shiboski, Ph.D., of the University of California, San Francisco, and colleagues from the SICCA Research Groups, which authored the classification criteria.
Under the provisional guidelines, a classification as having Sjögren’s syndrome requires that a patient meet at least two of these three conditions:
• A blood test indicating the presence of anti–Sjögren’s syndrome antigen A and/or anti–Sjögren’s syndrome antigen B, or positive rheumatoid factor and antinuclear antibody titer of at least 1:320.
• An impaired ability to produce tears, as determined by an eye examination with an ocular staining score of 3 or greater.
• The presence of autoimmune impairment of salivary function, as determined by a focus score of 1 or more focus/4 mm2 in labial salivary gland biopsy samples, the investigators said (Arthritis Care Res. 2012;64:475-87).
A high level of consensus was reached by the 20 members of the expert panel with respect to the use of the these objective measures, with 86% agreeing or strongly agreeing that meeting two of these three criteria should be required to classify Sjögren’s syndrome.
Preliminary validation of the classification criteria was based on comparison with the American-European Consensus Group criteria, which are likely the most frequently used criteria, and with cases and controls from external sources to the population used for criteria development. These comparisons showed high levels of sensitivity (96.3%) and specificity (83%) for the new criteria, which exceeded those of the alternative criteria, the investigators noted.
The findings are important, given the availability and development of new biologic agents for the treatment of Sjögren’s syndrome.
"Until recently, since few therapeutic agents were being considered in the systemic management of [Sjögren’s syndrome], the development of classification criteria was mainly for the purpose of epidemiologic studies to estimate the prevalence of the disease. However, the development of new biologic immunomodulating agents that are being considered in the treatment of [Sjögren’s syndrome] increases the need and importance of developing stringent classification criteria that can be used in the context of clinical trials," the investigators wrote, explaining that the consequences of misclassifying someone as having Sjögren’s syndrome would be serious, given the potentially toxic side effects of the biologic agents.
The results of the validation analyses performed in the development of these criteria indicate that they constitute a set of criteria that are stringent enough to be used for allowing entry into clinical trials, they said.
These new classification criteria have been quantitatively validated using patient data, and have been approved by the ACR board of directors, but have not yet undergone validation based on an external data set.
This work was supported by the National Institutes of Health, including the National Institute for Dental and Craniofacial Research, the National Eye Institute, and the Office of Research on Women’s Health. Three authors made disclosures, including Dr. F. Vivino, who has received consultant fees and/or honoraria from Daiichi-Sankyo and Parion Sciences; Dr. A. Wu, who owns stock and/or stock options in Isis Pharmaceuticals and Schering-Plough; and Dr. J. S. Greenspan, who has received consultant fees from GlaxoSmithKline.
Provisional new classification criteria for Sjögren’s syndrome take into account the availability of new biologic treatment agents, rely solely on objective measures, and improve classification performance when compared with existing alternatives, according to the American College of Rheumatology.
The new criteria, which are the first to be endorsed by the ACR, target individuals with signs and symptoms suggestive of Sjögren’s syndrome and are based on expert opinion derived by analysis of data from the more than 1,300 patients in the SICCA (Sjögren’s International Collaborative Clinical Alliance) registry. They also differ from previous criteria in that only objective tests related to oral, ocular, and systemic manifestations of the syndrome are included.
This brings together three medical specialties – rheumatology, ophthalmology, and oral medicine – for the purpose of determining a patient’s disease status, and reinforces the importance of collaboration among these specialties when it comes to assessment and management of patients with Sjögren’s syndrome. It also protects patients by reducing the likelihood of misclassification, which could lead to unnecessary exposure to investigational drugs, according to Stephen C. Shiboski, Ph.D., of the University of California, San Francisco, and colleagues from the SICCA Research Groups, which authored the classification criteria.
Under the provisional guidelines, a classification as having Sjögren’s syndrome requires that a patient meet at least two of these three conditions:
• A blood test indicating the presence of anti–Sjögren’s syndrome antigen A and/or anti–Sjögren’s syndrome antigen B, or positive rheumatoid factor and antinuclear antibody titer of at least 1:320.
• An impaired ability to produce tears, as determined by an eye examination with an ocular staining score of 3 or greater.
• The presence of autoimmune impairment of salivary function, as determined by a focus score of 1 or more focus/4 mm2 in labial salivary gland biopsy samples, the investigators said (Arthritis Care Res. 2012;64:475-87).
A high level of consensus was reached by the 20 members of the expert panel with respect to the use of the these objective measures, with 86% agreeing or strongly agreeing that meeting two of these three criteria should be required to classify Sjögren’s syndrome.
Preliminary validation of the classification criteria was based on comparison with the American-European Consensus Group criteria, which are likely the most frequently used criteria, and with cases and controls from external sources to the population used for criteria development. These comparisons showed high levels of sensitivity (96.3%) and specificity (83%) for the new criteria, which exceeded those of the alternative criteria, the investigators noted.
The findings are important, given the availability and development of new biologic agents for the treatment of Sjögren’s syndrome.
"Until recently, since few therapeutic agents were being considered in the systemic management of [Sjögren’s syndrome], the development of classification criteria was mainly for the purpose of epidemiologic studies to estimate the prevalence of the disease. However, the development of new biologic immunomodulating agents that are being considered in the treatment of [Sjögren’s syndrome] increases the need and importance of developing stringent classification criteria that can be used in the context of clinical trials," the investigators wrote, explaining that the consequences of misclassifying someone as having Sjögren’s syndrome would be serious, given the potentially toxic side effects of the biologic agents.
The results of the validation analyses performed in the development of these criteria indicate that they constitute a set of criteria that are stringent enough to be used for allowing entry into clinical trials, they said.
These new classification criteria have been quantitatively validated using patient data, and have been approved by the ACR board of directors, but have not yet undergone validation based on an external data set.
This work was supported by the National Institutes of Health, including the National Institute for Dental and Craniofacial Research, the National Eye Institute, and the Office of Research on Women’s Health. Three authors made disclosures, including Dr. F. Vivino, who has received consultant fees and/or honoraria from Daiichi-Sankyo and Parion Sciences; Dr. A. Wu, who owns stock and/or stock options in Isis Pharmaceuticals and Schering-Plough; and Dr. J. S. Greenspan, who has received consultant fees from GlaxoSmithKline.
Provisional new classification criteria for Sjögren’s syndrome take into account the availability of new biologic treatment agents, rely solely on objective measures, and improve classification performance when compared with existing alternatives, according to the American College of Rheumatology.
The new criteria, which are the first to be endorsed by the ACR, target individuals with signs and symptoms suggestive of Sjögren’s syndrome and are based on expert opinion derived by analysis of data from the more than 1,300 patients in the SICCA (Sjögren’s International Collaborative Clinical Alliance) registry. They also differ from previous criteria in that only objective tests related to oral, ocular, and systemic manifestations of the syndrome are included.
This brings together three medical specialties – rheumatology, ophthalmology, and oral medicine – for the purpose of determining a patient’s disease status, and reinforces the importance of collaboration among these specialties when it comes to assessment and management of patients with Sjögren’s syndrome. It also protects patients by reducing the likelihood of misclassification, which could lead to unnecessary exposure to investigational drugs, according to Stephen C. Shiboski, Ph.D., of the University of California, San Francisco, and colleagues from the SICCA Research Groups, which authored the classification criteria.
Under the provisional guidelines, a classification as having Sjögren’s syndrome requires that a patient meet at least two of these three conditions:
• A blood test indicating the presence of anti–Sjögren’s syndrome antigen A and/or anti–Sjögren’s syndrome antigen B, or positive rheumatoid factor and antinuclear antibody titer of at least 1:320.
• An impaired ability to produce tears, as determined by an eye examination with an ocular staining score of 3 or greater.
• The presence of autoimmune impairment of salivary function, as determined by a focus score of 1 or more focus/4 mm2 in labial salivary gland biopsy samples, the investigators said (Arthritis Care Res. 2012;64:475-87).
A high level of consensus was reached by the 20 members of the expert panel with respect to the use of the these objective measures, with 86% agreeing or strongly agreeing that meeting two of these three criteria should be required to classify Sjögren’s syndrome.
Preliminary validation of the classification criteria was based on comparison with the American-European Consensus Group criteria, which are likely the most frequently used criteria, and with cases and controls from external sources to the population used for criteria development. These comparisons showed high levels of sensitivity (96.3%) and specificity (83%) for the new criteria, which exceeded those of the alternative criteria, the investigators noted.
The findings are important, given the availability and development of new biologic agents for the treatment of Sjögren’s syndrome.
"Until recently, since few therapeutic agents were being considered in the systemic management of [Sjögren’s syndrome], the development of classification criteria was mainly for the purpose of epidemiologic studies to estimate the prevalence of the disease. However, the development of new biologic immunomodulating agents that are being considered in the treatment of [Sjögren’s syndrome] increases the need and importance of developing stringent classification criteria that can be used in the context of clinical trials," the investigators wrote, explaining that the consequences of misclassifying someone as having Sjögren’s syndrome would be serious, given the potentially toxic side effects of the biologic agents.
The results of the validation analyses performed in the development of these criteria indicate that they constitute a set of criteria that are stringent enough to be used for allowing entry into clinical trials, they said.
These new classification criteria have been quantitatively validated using patient data, and have been approved by the ACR board of directors, but have not yet undergone validation based on an external data set.
This work was supported by the National Institutes of Health, including the National Institute for Dental and Craniofacial Research, the National Eye Institute, and the Office of Research on Women’s Health. Three authors made disclosures, including Dr. F. Vivino, who has received consultant fees and/or honoraria from Daiichi-Sankyo and Parion Sciences; Dr. A. Wu, who owns stock and/or stock options in Isis Pharmaceuticals and Schering-Plough; and Dr. J. S. Greenspan, who has received consultant fees from GlaxoSmithKline.
FROM ARTHRITIS CARE & RESEARCH
Major Finding: Preliminary validation of the classification criteria based on comparison with the AECG criteria and controls from external sources to the population used for criteria development show high levels of sensitivity (96.3%) and specificity (83%) for the new criteria, which exceeded those of the alternate criteria.
Data Source: The data came from the SICCA registry.
Disclosures: This work was supported by the National Institutes of Health, including the National Institute for Dental and Craniofacial Research, the National Eye Institute, and the Office of Research on Women’s Health. Three authors made disclosures, including Dr. F. Vivino, who has received consultant fees and/or honoraria from Daiichi-Sankyo and Parion Sciences; Dr. A. Wu, who owns stock and/or stock options in Isis Pharmaceuticals and Schering-Plough; and Dr. J. S. Greenspan, who has received consultant fees from GlaxoSmithKline.
Risk Factors for C. difficile Recurrence Identified
ATLANTA – People who take antacid therapy, the elderly, and individuals who reside in long-term care facilities are at increased risk of recurrent Clostridium difficile infections, according to data from the Connecticut Emerging Infections Program.
Of 826 children and adults with an initial incident episode of C. difficile infection, 130 (16%) had at least one recurrence. Those with vs. without recurrence were significantly older (75.1 vs. 69.9 years), and significantly more likely to reside in a long-term care facility (53% vs. 40%), Blanca Paccha reported in a poster at the International Conference on Emerging Infectious Diseases.
Individuals with recurrence were more likely than those without recurrence to be taking H2 blockers (10% vs. 3%), reported Ms. Paccha, a research assistant and student working on her master’s in Public Health at Yale University, New Haven, Conn.
When stratified based on whether the C. difficile infection was acquired in the health care setting or in the community, the only difference between the recurrence and nonrecurrence groups in those with health care–associated infection was the use of H2 blockers, which appeared to increase the risk for recurrence in this population. This finding contradicts those from previous studies that suggested a protective effect of antacid therapy, Ms. Paccha noted.
In those with community-associated infection, those with recurrence were older than those without recurrence (68.9 vs. 56.6 years). They also were significantly more likely to have used immunosuppressants (36% vs. 13%), and less likely to have used antimicrobials (73% vs. 43%), Ms. Paccha said in an interview.
C. difficile, which is often preceded by antibiotic use, has been a growing concern in the past decade because of the emergence of increasingly toxigenic strains. The Connecticut Emerging Infections Program has been conducting surveillance for the infection since 2009, she said.
Case patients were at least 1 year of age and were diagnosed on the basis of a positive C. difficile infection laboratory test. Those with health care–associated infection included patients with onset 3 days after hospital or long-term care facility admission (health care facility onset patients); patients with onset within 3 months of hospital discharge, outpatient surgery or long-term care facility residency (community-onset health care facility-associated patients); and patients with onset without prior health care exposure (community-associated infection patients). Information on the patients was obtained by chart review.
The study was limited by the use of a nonclinical definition of recurrence and by a lack of treatment data for the initial C. difficile infection.
Additional research to determine if those at risk for recurrence tend to harbor more toxigenic diseases is warranted, she said.
Ms. Paccha reported having no relevant conflicts of interest.
ATLANTA – People who take antacid therapy, the elderly, and individuals who reside in long-term care facilities are at increased risk of recurrent Clostridium difficile infections, according to data from the Connecticut Emerging Infections Program.
Of 826 children and adults with an initial incident episode of C. difficile infection, 130 (16%) had at least one recurrence. Those with vs. without recurrence were significantly older (75.1 vs. 69.9 years), and significantly more likely to reside in a long-term care facility (53% vs. 40%), Blanca Paccha reported in a poster at the International Conference on Emerging Infectious Diseases.
Individuals with recurrence were more likely than those without recurrence to be taking H2 blockers (10% vs. 3%), reported Ms. Paccha, a research assistant and student working on her master’s in Public Health at Yale University, New Haven, Conn.
When stratified based on whether the C. difficile infection was acquired in the health care setting or in the community, the only difference between the recurrence and nonrecurrence groups in those with health care–associated infection was the use of H2 blockers, which appeared to increase the risk for recurrence in this population. This finding contradicts those from previous studies that suggested a protective effect of antacid therapy, Ms. Paccha noted.
In those with community-associated infection, those with recurrence were older than those without recurrence (68.9 vs. 56.6 years). They also were significantly more likely to have used immunosuppressants (36% vs. 13%), and less likely to have used antimicrobials (73% vs. 43%), Ms. Paccha said in an interview.
C. difficile, which is often preceded by antibiotic use, has been a growing concern in the past decade because of the emergence of increasingly toxigenic strains. The Connecticut Emerging Infections Program has been conducting surveillance for the infection since 2009, she said.
Case patients were at least 1 year of age and were diagnosed on the basis of a positive C. difficile infection laboratory test. Those with health care–associated infection included patients with onset 3 days after hospital or long-term care facility admission (health care facility onset patients); patients with onset within 3 months of hospital discharge, outpatient surgery or long-term care facility residency (community-onset health care facility-associated patients); and patients with onset without prior health care exposure (community-associated infection patients). Information on the patients was obtained by chart review.
The study was limited by the use of a nonclinical definition of recurrence and by a lack of treatment data for the initial C. difficile infection.
Additional research to determine if those at risk for recurrence tend to harbor more toxigenic diseases is warranted, she said.
Ms. Paccha reported having no relevant conflicts of interest.
ATLANTA – People who take antacid therapy, the elderly, and individuals who reside in long-term care facilities are at increased risk of recurrent Clostridium difficile infections, according to data from the Connecticut Emerging Infections Program.
Of 826 children and adults with an initial incident episode of C. difficile infection, 130 (16%) had at least one recurrence. Those with vs. without recurrence were significantly older (75.1 vs. 69.9 years), and significantly more likely to reside in a long-term care facility (53% vs. 40%), Blanca Paccha reported in a poster at the International Conference on Emerging Infectious Diseases.
Individuals with recurrence were more likely than those without recurrence to be taking H2 blockers (10% vs. 3%), reported Ms. Paccha, a research assistant and student working on her master’s in Public Health at Yale University, New Haven, Conn.
When stratified based on whether the C. difficile infection was acquired in the health care setting or in the community, the only difference between the recurrence and nonrecurrence groups in those with health care–associated infection was the use of H2 blockers, which appeared to increase the risk for recurrence in this population. This finding contradicts those from previous studies that suggested a protective effect of antacid therapy, Ms. Paccha noted.
In those with community-associated infection, those with recurrence were older than those without recurrence (68.9 vs. 56.6 years). They also were significantly more likely to have used immunosuppressants (36% vs. 13%), and less likely to have used antimicrobials (73% vs. 43%), Ms. Paccha said in an interview.
C. difficile, which is often preceded by antibiotic use, has been a growing concern in the past decade because of the emergence of increasingly toxigenic strains. The Connecticut Emerging Infections Program has been conducting surveillance for the infection since 2009, she said.
Case patients were at least 1 year of age and were diagnosed on the basis of a positive C. difficile infection laboratory test. Those with health care–associated infection included patients with onset 3 days after hospital or long-term care facility admission (health care facility onset patients); patients with onset within 3 months of hospital discharge, outpatient surgery or long-term care facility residency (community-onset health care facility-associated patients); and patients with onset without prior health care exposure (community-associated infection patients). Information on the patients was obtained by chart review.
The study was limited by the use of a nonclinical definition of recurrence and by a lack of treatment data for the initial C. difficile infection.
Additional research to determine if those at risk for recurrence tend to harbor more toxigenic diseases is warranted, she said.
Ms. Paccha reported having no relevant conflicts of interest.
FROM THE INTERNATIONAL CONFERENCE ON EMERGING INFECTIOUS DISEASES
Major Finding: Of 826 children and adults with an initial incident episode of C. difficile infection, 130 (16%) had at least one recurrence. Those with vs. without recurrence were significantly older (75.1 vs. 69.9 years), more likely to reside in a long-term care facility (53% vs. 40%), and more likely be taking H2 blockers (10% vs. 3%).
Data Source: Surveillance data on C. difficile infection was gathered from the Connecticut Emerging Infections Program.
Disclosures: Ms. Paccha reported having no relevant conflicts of interest.
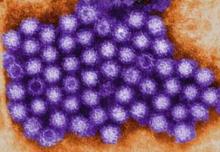
Gastroenteritis Deaths Soar, Largely Due to C. difficile, Norovirus
ATLANTA – The incidence of gastroenteritis-related deaths in the United States more than doubled from 1997 to 2007, largely because of Clostridium difficile and norovirus infections, mortality data from the National Center for Health Statistics show.
The apparent increase in C. difficile identified in this study is likely caused in part to increased recognition – and improved coding by physicians, but it also is likely because of a real increase resulting from the emergence of a hypervirulent and fluoroquinolone-resistant strain, Aron J. Hall, DVM, said at the International Conference on Emerging Infectious Diseases.
The elderly are disproportionately affected by these deadly infections, with those aged 65 years and older accounting for 83% of the gastroenteritis deaths during the study period, said Dr. Hall of the Centers for Disease Control and Prevention’s Viral Gastroenteritis Team.
"The mortality rate increases with increasing age, even within this older age group." These findings could help guide clinical management and development of candidate vaccines.
Between 1997 and 2007, all-cause gastroenteritis mortality increased from 25/1,000,000 person-years, to 57/1,000,000, which equates to an increase from about 7,000 to about 17,000 gastroenteritis-related deaths per year. The rate among those aged 65 years and older in 2007 was 259/1,000,000 person-years, Dr. Hall noted.
C. difficile was the leading cause of gastroenteritis-related death, and the incidence of C. difficile infection increased fivefold, from 10/1,000,000 in 1999-2000 to 48/1,000,000 in 2006-2007 – or from about 2,700 to 14,500 deaths per year.
Further, this study is the first to demonstrate that norovirus is likely the second leading infectious cause, Dr. Hall said.
On average, norovirus contributed to nearly 800 deaths per year during the study period (3/1,000,000 person-years), but mortality rates surged about every 3 years by up to 50%; these surges coincided with outbreaks associated with emergent viral strains, he explained.
As with C. difficile–related gastroenteritis deaths, most of these were in the elderly. However, a "small, but perhaps important" fraction of deaths occurred among children younger than age 5 years, Dr. Hall noted.
Seasonal variations also were apparent in this study, with C. difficile–associated deaths occurring most often during the spring months of March through May, and with norovirus-related deaths peaking in the winter months of December through February.
C. difficile and norovirus have emerged in recent years and are recognized as important contributors to gastroenteritis, but there have been limited data on deaths, Dr. Hall explained, adding that this is due in part to limited availability and/or sensitivity of clinical diagnostic assays, and also because deaths have historically not been coded specifically as being associated with a particular pathogen.
In fact, half of the gastroenteritis deaths included in the National Center for Health Statistics multiple cause of death mortality data are uncoded.
For this study, deaths with gastroenteritis listed as an underlying or contributing cause were included in the analysis, and an indirect attribution model was used to estimate the proportion of cause-unspecified gastroenteritis deaths that likely were due to specific causes. C. difficile, using this model, accounted for nearly 70% of gastroenteritis deaths.
The estimates of norovirus-associated gastroenteritis deaths in this study represent a 40% higher incidence than previously estimated based on extrapolation from community studies and studies from other industrialized countries, he added.
Gastroenteritis has long been recognized as an important contributor to mortality among children in developing countries, but less has been known about gastroenteritis-related mortality among adults and about the contributions of specific pathogens. These findings provide the first comprehensive analysis of data in more than 2 decades to characterize gastroenteritis deaths across all aged, he said.
The disease burden and seasonal patterns identified in this study could be helpful for the development of clinical management strategies, he said, adding that the mortality burden of these pathogens – particularly in the elderly – underscores the need for judicious use of antibiotics and proper infection control, as well as the need for effective interventions.
Dr. Hall noted that candidate vaccines are currently in development for both C. difficile and norovirus.
He reported having no relevant conflicts of interest.
ATLANTA – The incidence of gastroenteritis-related deaths in the United States more than doubled from 1997 to 2007, largely because of Clostridium difficile and norovirus infections, mortality data from the National Center for Health Statistics show.
The apparent increase in C. difficile identified in this study is likely caused in part to increased recognition – and improved coding by physicians, but it also is likely because of a real increase resulting from the emergence of a hypervirulent and fluoroquinolone-resistant strain, Aron J. Hall, DVM, said at the International Conference on Emerging Infectious Diseases.
The elderly are disproportionately affected by these deadly infections, with those aged 65 years and older accounting for 83% of the gastroenteritis deaths during the study period, said Dr. Hall of the Centers for Disease Control and Prevention’s Viral Gastroenteritis Team.
"The mortality rate increases with increasing age, even within this older age group." These findings could help guide clinical management and development of candidate vaccines.
Between 1997 and 2007, all-cause gastroenteritis mortality increased from 25/1,000,000 person-years, to 57/1,000,000, which equates to an increase from about 7,000 to about 17,000 gastroenteritis-related deaths per year. The rate among those aged 65 years and older in 2007 was 259/1,000,000 person-years, Dr. Hall noted.
C. difficile was the leading cause of gastroenteritis-related death, and the incidence of C. difficile infection increased fivefold, from 10/1,000,000 in 1999-2000 to 48/1,000,000 in 2006-2007 – or from about 2,700 to 14,500 deaths per year.
Further, this study is the first to demonstrate that norovirus is likely the second leading infectious cause, Dr. Hall said.
On average, norovirus contributed to nearly 800 deaths per year during the study period (3/1,000,000 person-years), but mortality rates surged about every 3 years by up to 50%; these surges coincided with outbreaks associated with emergent viral strains, he explained.
As with C. difficile–related gastroenteritis deaths, most of these were in the elderly. However, a "small, but perhaps important" fraction of deaths occurred among children younger than age 5 years, Dr. Hall noted.
Seasonal variations also were apparent in this study, with C. difficile–associated deaths occurring most often during the spring months of March through May, and with norovirus-related deaths peaking in the winter months of December through February.
C. difficile and norovirus have emerged in recent years and are recognized as important contributors to gastroenteritis, but there have been limited data on deaths, Dr. Hall explained, adding that this is due in part to limited availability and/or sensitivity of clinical diagnostic assays, and also because deaths have historically not been coded specifically as being associated with a particular pathogen.
In fact, half of the gastroenteritis deaths included in the National Center for Health Statistics multiple cause of death mortality data are uncoded.
For this study, deaths with gastroenteritis listed as an underlying or contributing cause were included in the analysis, and an indirect attribution model was used to estimate the proportion of cause-unspecified gastroenteritis deaths that likely were due to specific causes. C. difficile, using this model, accounted for nearly 70% of gastroenteritis deaths.
The estimates of norovirus-associated gastroenteritis deaths in this study represent a 40% higher incidence than previously estimated based on extrapolation from community studies and studies from other industrialized countries, he added.
Gastroenteritis has long been recognized as an important contributor to mortality among children in developing countries, but less has been known about gastroenteritis-related mortality among adults and about the contributions of specific pathogens. These findings provide the first comprehensive analysis of data in more than 2 decades to characterize gastroenteritis deaths across all aged, he said.
The disease burden and seasonal patterns identified in this study could be helpful for the development of clinical management strategies, he said, adding that the mortality burden of these pathogens – particularly in the elderly – underscores the need for judicious use of antibiotics and proper infection control, as well as the need for effective interventions.
Dr. Hall noted that candidate vaccines are currently in development for both C. difficile and norovirus.
He reported having no relevant conflicts of interest.
ATLANTA – The incidence of gastroenteritis-related deaths in the United States more than doubled from 1997 to 2007, largely because of Clostridium difficile and norovirus infections, mortality data from the National Center for Health Statistics show.
The apparent increase in C. difficile identified in this study is likely caused in part to increased recognition – and improved coding by physicians, but it also is likely because of a real increase resulting from the emergence of a hypervirulent and fluoroquinolone-resistant strain, Aron J. Hall, DVM, said at the International Conference on Emerging Infectious Diseases.
The elderly are disproportionately affected by these deadly infections, with those aged 65 years and older accounting for 83% of the gastroenteritis deaths during the study period, said Dr. Hall of the Centers for Disease Control and Prevention’s Viral Gastroenteritis Team.
"The mortality rate increases with increasing age, even within this older age group." These findings could help guide clinical management and development of candidate vaccines.
Between 1997 and 2007, all-cause gastroenteritis mortality increased from 25/1,000,000 person-years, to 57/1,000,000, which equates to an increase from about 7,000 to about 17,000 gastroenteritis-related deaths per year. The rate among those aged 65 years and older in 2007 was 259/1,000,000 person-years, Dr. Hall noted.
C. difficile was the leading cause of gastroenteritis-related death, and the incidence of C. difficile infection increased fivefold, from 10/1,000,000 in 1999-2000 to 48/1,000,000 in 2006-2007 – or from about 2,700 to 14,500 deaths per year.
Further, this study is the first to demonstrate that norovirus is likely the second leading infectious cause, Dr. Hall said.
On average, norovirus contributed to nearly 800 deaths per year during the study period (3/1,000,000 person-years), but mortality rates surged about every 3 years by up to 50%; these surges coincided with outbreaks associated with emergent viral strains, he explained.
As with C. difficile–related gastroenteritis deaths, most of these were in the elderly. However, a "small, but perhaps important" fraction of deaths occurred among children younger than age 5 years, Dr. Hall noted.
Seasonal variations also were apparent in this study, with C. difficile–associated deaths occurring most often during the spring months of March through May, and with norovirus-related deaths peaking in the winter months of December through February.
C. difficile and norovirus have emerged in recent years and are recognized as important contributors to gastroenteritis, but there have been limited data on deaths, Dr. Hall explained, adding that this is due in part to limited availability and/or sensitivity of clinical diagnostic assays, and also because deaths have historically not been coded specifically as being associated with a particular pathogen.
In fact, half of the gastroenteritis deaths included in the National Center for Health Statistics multiple cause of death mortality data are uncoded.
For this study, deaths with gastroenteritis listed as an underlying or contributing cause were included in the analysis, and an indirect attribution model was used to estimate the proportion of cause-unspecified gastroenteritis deaths that likely were due to specific causes. C. difficile, using this model, accounted for nearly 70% of gastroenteritis deaths.
The estimates of norovirus-associated gastroenteritis deaths in this study represent a 40% higher incidence than previously estimated based on extrapolation from community studies and studies from other industrialized countries, he added.
Gastroenteritis has long been recognized as an important contributor to mortality among children in developing countries, but less has been known about gastroenteritis-related mortality among adults and about the contributions of specific pathogens. These findings provide the first comprehensive analysis of data in more than 2 decades to characterize gastroenteritis deaths across all aged, he said.
The disease burden and seasonal patterns identified in this study could be helpful for the development of clinical management strategies, he said, adding that the mortality burden of these pathogens – particularly in the elderly – underscores the need for judicious use of antibiotics and proper infection control, as well as the need for effective interventions.
Dr. Hall noted that candidate vaccines are currently in development for both C. difficile and norovirus.
He reported having no relevant conflicts of interest.
FROM THE INTERNATIONAL CONFERENCE ON EMERGING INFECTIOUS DISEASES
Major Finding: Between 1997 and 2007, all-cause gastroenteritis mortality increased from 25/1,000,000 person-years, to 57/1,000,000, which equates to an increase from about 7,000 to about 17,000 gastroenteritis-related deaths per year. The rate among those aged 65 years and older in 2007 was 259/1,000,000 person-years.
Data Source: An analysis of data from the National Center for Health Statistics. An indirect attribution model was used to estimate the proportion of cause-unspecified gastroenteritis deaths that likely were from specific causes.
Disclosures: Dr. Hall had no disclosures to report.
Lyme Disease Presents Differently in Men and Women
ATLANTA – Women with Lyme disease display more clinical symptoms than do men with the disease and also are less likely to seroconvert following treatment, according to findings from a prospective cohort study involving 77 patients.
Numerous symptoms were reported more often by the 37 women in the study than by the 40 men. For example, significantly more women than men reported joint pain, muscle pain, headache, back pain, heart palpitations, nausea, vomiting, anxiety, numbness and tingling, and changes in vision during at least one of six preplanned study visits with a physician, Lauren A. Crowder, M.P.H. reported in a poster at the International Conference on Emerging Infectious Diseases.
Joint pain, heart palpitations, nausea, vomiting, and changes in vision were reported significantly more often by women at two of the six visits, and headache was reported significantly more often by women at four of the six visits.
"The second preliminary finding we observed in our cohort of patients was that women were less likely to seroconvert on the antibody tests for serodiagnosis of Lyme disease," Ms. Crowder of the Lyme Disease Research Foundation, Lutherville, Md., said in an interview.
At the initial study visit, a similar proportion of men and women (about 60% of each) tested negative for Lyme disease using the Centers for Disease Control and Prevention’s recommended two-tier testing criteria for serodiagnosis. However, at the second visit, which was performed immediately post treatment, 70% of women who tested negative at the first visit remained negative, compared with only 35% of the men who initially tested negative.
Additionally, polychromatic flow cytometry performed on patient samples indicated that women had significantly higher frequency of CD4+CCR5+ T-cells prior to treatment than did men (mean of 9.82% vs. 5.96%).
"These findings suggest to us that there may be a difference between how men and women respond to infection with Lyme disease. One hypothesis for these differences is that there may be an immunological variation in response to Borrelia burgdorferi, the bacterial infection that causes Lyme disease, between men and women," Ms. Crowder said.
Study participants had early, untreated erythema migrans and clinically confirmed Lyme disease. At the first of the six study visits, they were tested using the CDC criteria by a commercial laboratory. All were treated with 3-week course of doxycycline and were then followed for up to 2 years. At each study visit, participants underwent a physical examination and interval history, reported clinical symptoms and completed self-administered surveys, and underwent repeat laboratory evaluations.
The findings highlight a need for additional research on sex-based differences in the effects of early Lyme disease. Such differences have been seen in other infectious disease, but have not been thoroughly explored in early Lyme disease, Ms. Crowder noted.
Such study is important given that Lyme disease is the most common vector-borne infectious disease in the United States. Although most patients recover from acute infection with proper antibiotic treatment, a subset of patients develop Post-Treatment Lyme Disease Syndrome. The CDC defines this syndrome as involving lingering symptoms of fatigue, pain, or joint and muscle aches. In some cases, these can last for more than 6 months.
"We will continue to explore these suggested differences both in this cohort and in future research studies," she said.
Ms. Crowder also stressed the importance of encouraging patients to look for ticks if they live in Lyme endemic areas.
This study was supported by the Lyme Disease Research Foundation. Ms. Crowder had no disclosures to report.
ATLANTA – Women with Lyme disease display more clinical symptoms than do men with the disease and also are less likely to seroconvert following treatment, according to findings from a prospective cohort study involving 77 patients.
Numerous symptoms were reported more often by the 37 women in the study than by the 40 men. For example, significantly more women than men reported joint pain, muscle pain, headache, back pain, heart palpitations, nausea, vomiting, anxiety, numbness and tingling, and changes in vision during at least one of six preplanned study visits with a physician, Lauren A. Crowder, M.P.H. reported in a poster at the International Conference on Emerging Infectious Diseases.
Joint pain, heart palpitations, nausea, vomiting, and changes in vision were reported significantly more often by women at two of the six visits, and headache was reported significantly more often by women at four of the six visits.
"The second preliminary finding we observed in our cohort of patients was that women were less likely to seroconvert on the antibody tests for serodiagnosis of Lyme disease," Ms. Crowder of the Lyme Disease Research Foundation, Lutherville, Md., said in an interview.
At the initial study visit, a similar proportion of men and women (about 60% of each) tested negative for Lyme disease using the Centers for Disease Control and Prevention’s recommended two-tier testing criteria for serodiagnosis. However, at the second visit, which was performed immediately post treatment, 70% of women who tested negative at the first visit remained negative, compared with only 35% of the men who initially tested negative.
Additionally, polychromatic flow cytometry performed on patient samples indicated that women had significantly higher frequency of CD4+CCR5+ T-cells prior to treatment than did men (mean of 9.82% vs. 5.96%).
"These findings suggest to us that there may be a difference between how men and women respond to infection with Lyme disease. One hypothesis for these differences is that there may be an immunological variation in response to Borrelia burgdorferi, the bacterial infection that causes Lyme disease, between men and women," Ms. Crowder said.
Study participants had early, untreated erythema migrans and clinically confirmed Lyme disease. At the first of the six study visits, they were tested using the CDC criteria by a commercial laboratory. All were treated with 3-week course of doxycycline and were then followed for up to 2 years. At each study visit, participants underwent a physical examination and interval history, reported clinical symptoms and completed self-administered surveys, and underwent repeat laboratory evaluations.
The findings highlight a need for additional research on sex-based differences in the effects of early Lyme disease. Such differences have been seen in other infectious disease, but have not been thoroughly explored in early Lyme disease, Ms. Crowder noted.
Such study is important given that Lyme disease is the most common vector-borne infectious disease in the United States. Although most patients recover from acute infection with proper antibiotic treatment, a subset of patients develop Post-Treatment Lyme Disease Syndrome. The CDC defines this syndrome as involving lingering symptoms of fatigue, pain, or joint and muscle aches. In some cases, these can last for more than 6 months.
"We will continue to explore these suggested differences both in this cohort and in future research studies," she said.
Ms. Crowder also stressed the importance of encouraging patients to look for ticks if they live in Lyme endemic areas.
This study was supported by the Lyme Disease Research Foundation. Ms. Crowder had no disclosures to report.
ATLANTA – Women with Lyme disease display more clinical symptoms than do men with the disease and also are less likely to seroconvert following treatment, according to findings from a prospective cohort study involving 77 patients.
Numerous symptoms were reported more often by the 37 women in the study than by the 40 men. For example, significantly more women than men reported joint pain, muscle pain, headache, back pain, heart palpitations, nausea, vomiting, anxiety, numbness and tingling, and changes in vision during at least one of six preplanned study visits with a physician, Lauren A. Crowder, M.P.H. reported in a poster at the International Conference on Emerging Infectious Diseases.
Joint pain, heart palpitations, nausea, vomiting, and changes in vision were reported significantly more often by women at two of the six visits, and headache was reported significantly more often by women at four of the six visits.
"The second preliminary finding we observed in our cohort of patients was that women were less likely to seroconvert on the antibody tests for serodiagnosis of Lyme disease," Ms. Crowder of the Lyme Disease Research Foundation, Lutherville, Md., said in an interview.
At the initial study visit, a similar proportion of men and women (about 60% of each) tested negative for Lyme disease using the Centers for Disease Control and Prevention’s recommended two-tier testing criteria for serodiagnosis. However, at the second visit, which was performed immediately post treatment, 70% of women who tested negative at the first visit remained negative, compared with only 35% of the men who initially tested negative.
Additionally, polychromatic flow cytometry performed on patient samples indicated that women had significantly higher frequency of CD4+CCR5+ T-cells prior to treatment than did men (mean of 9.82% vs. 5.96%).
"These findings suggest to us that there may be a difference between how men and women respond to infection with Lyme disease. One hypothesis for these differences is that there may be an immunological variation in response to Borrelia burgdorferi, the bacterial infection that causes Lyme disease, between men and women," Ms. Crowder said.
Study participants had early, untreated erythema migrans and clinically confirmed Lyme disease. At the first of the six study visits, they were tested using the CDC criteria by a commercial laboratory. All were treated with 3-week course of doxycycline and were then followed for up to 2 years. At each study visit, participants underwent a physical examination and interval history, reported clinical symptoms and completed self-administered surveys, and underwent repeat laboratory evaluations.
The findings highlight a need for additional research on sex-based differences in the effects of early Lyme disease. Such differences have been seen in other infectious disease, but have not been thoroughly explored in early Lyme disease, Ms. Crowder noted.
Such study is important given that Lyme disease is the most common vector-borne infectious disease in the United States. Although most patients recover from acute infection with proper antibiotic treatment, a subset of patients develop Post-Treatment Lyme Disease Syndrome. The CDC defines this syndrome as involving lingering symptoms of fatigue, pain, or joint and muscle aches. In some cases, these can last for more than 6 months.
"We will continue to explore these suggested differences both in this cohort and in future research studies," she said.
Ms. Crowder also stressed the importance of encouraging patients to look for ticks if they live in Lyme endemic areas.
This study was supported by the Lyme Disease Research Foundation. Ms. Crowder had no disclosures to report.
FROM THE INTERNATIONAL CONFERENCE ON EMERGING INFECTIOUS DISEASES
Lyme Disease Presents Differently in Men and Women
ATLANTA – Women with Lyme disease display more clinical symptoms than do men with the disease and also are less likely to seroconvert following treatment, according to findings from a prospective cohort study involving 77 patients.
Numerous symptoms were reported more often by the 37 women in the study than by the 40 men. For example, significantly more women than men reported joint pain, muscle pain, headache, back pain, heart palpitations, nausea, vomiting, anxiety, numbness and tingling, and changes in vision during at least one of six preplanned study visits with a physician, Lauren A. Crowder, M.P.H. reported in a poster at the International Conference on Emerging Infectious Diseases.
Joint pain, heart palpitations, nausea, vomiting, and changes in vision were reported significantly more often by women at two of the six visits, and headache was reported significantly more often by women at four of the six visits.
"The second preliminary finding we observed in our cohort of patients was that women were less likely to seroconvert on the antibody tests for serodiagnosis of Lyme disease," Ms. Crowder of the Lyme Disease Research Foundation, Lutherville, Md., said in an interview.
At the initial study visit, a similar proportion of men and women (about 60% of each) tested negative for Lyme disease using the Centers for Disease Control and Prevention’s recommended two-tier testing criteria for serodiagnosis. However, at the second visit, which was performed immediately post treatment, 70% of women who tested negative at the first visit remained negative, compared with only 35% of the men who initially tested negative.
Additionally, polychromatic flow cytometry performed on patient samples indicated that women had significantly higher frequency of CD4+CCR5+ T-cells prior to treatment than did men (mean of 9.82% vs. 5.96%).
"These findings suggest to us that there may be a difference between how men and women respond to infection with Lyme disease. One hypothesis for these differences is that there may be an immunological variation in response to Borrelia burgdorferi, the bacterial infection that causes Lyme disease, between men and women," Ms. Crowder said.
Study participants had early, untreated erythema migrans and clinically confirmed Lyme disease. At the first of the six study visits, they were tested using the CDC criteria by a commercial laboratory. All were treated with 3-week course of doxycycline and were then followed for up to 2 years. At each study visit, participants underwent a physical examination and interval history, reported clinical symptoms and completed self-administered surveys, and underwent repeat laboratory evaluations.
The findings highlight a need for additional research on sex-based differences in the effects of early Lyme disease. Such differences have been seen in other infectious disease, but have not been thoroughly explored in early Lyme disease, Ms. Crowder noted.
Such study is important given that Lyme disease is the most common vector-borne infectious disease in the United States. Although most patients recover from acute infection with proper antibiotic treatment, a subset of patients develop Post-Treatment Lyme Disease Syndrome. The CDC defines this syndrome as involving lingering symptoms of fatigue, pain, or joint and muscle aches. In some cases, these can last for more than 6 months.
"We will continue to explore these suggested differences both in this cohort and in future research studies," she said.
Ms. Crowder also stressed the importance of encouraging patients to look for ticks if they live in Lyme endemic areas.
This study was supported by the Lyme Disease Research Foundation. Ms. Crowder had no disclosures to report.
ATLANTA – Women with Lyme disease display more clinical symptoms than do men with the disease and also are less likely to seroconvert following treatment, according to findings from a prospective cohort study involving 77 patients.
Numerous symptoms were reported more often by the 37 women in the study than by the 40 men. For example, significantly more women than men reported joint pain, muscle pain, headache, back pain, heart palpitations, nausea, vomiting, anxiety, numbness and tingling, and changes in vision during at least one of six preplanned study visits with a physician, Lauren A. Crowder, M.P.H. reported in a poster at the International Conference on Emerging Infectious Diseases.
Joint pain, heart palpitations, nausea, vomiting, and changes in vision were reported significantly more often by women at two of the six visits, and headache was reported significantly more often by women at four of the six visits.
"The second preliminary finding we observed in our cohort of patients was that women were less likely to seroconvert on the antibody tests for serodiagnosis of Lyme disease," Ms. Crowder of the Lyme Disease Research Foundation, Lutherville, Md., said in an interview.
At the initial study visit, a similar proportion of men and women (about 60% of each) tested negative for Lyme disease using the Centers for Disease Control and Prevention’s recommended two-tier testing criteria for serodiagnosis. However, at the second visit, which was performed immediately post treatment, 70% of women who tested negative at the first visit remained negative, compared with only 35% of the men who initially tested negative.
Additionally, polychromatic flow cytometry performed on patient samples indicated that women had significantly higher frequency of CD4+CCR5+ T-cells prior to treatment than did men (mean of 9.82% vs. 5.96%).
"These findings suggest to us that there may be a difference between how men and women respond to infection with Lyme disease. One hypothesis for these differences is that there may be an immunological variation in response to Borrelia burgdorferi, the bacterial infection that causes Lyme disease, between men and women," Ms. Crowder said.
Study participants had early, untreated erythema migrans and clinically confirmed Lyme disease. At the first of the six study visits, they were tested using the CDC criteria by a commercial laboratory. All were treated with 3-week course of doxycycline and were then followed for up to 2 years. At each study visit, participants underwent a physical examination and interval history, reported clinical symptoms and completed self-administered surveys, and underwent repeat laboratory evaluations.
The findings highlight a need for additional research on sex-based differences in the effects of early Lyme disease. Such differences have been seen in other infectious disease, but have not been thoroughly explored in early Lyme disease, Ms. Crowder noted.
Such study is important given that Lyme disease is the most common vector-borne infectious disease in the United States. Although most patients recover from acute infection with proper antibiotic treatment, a subset of patients develop Post-Treatment Lyme Disease Syndrome. The CDC defines this syndrome as involving lingering symptoms of fatigue, pain, or joint and muscle aches. In some cases, these can last for more than 6 months.
"We will continue to explore these suggested differences both in this cohort and in future research studies," she said.
Ms. Crowder also stressed the importance of encouraging patients to look for ticks if they live in Lyme endemic areas.
This study was supported by the Lyme Disease Research Foundation. Ms. Crowder had no disclosures to report.
ATLANTA – Women with Lyme disease display more clinical symptoms than do men with the disease and also are less likely to seroconvert following treatment, according to findings from a prospective cohort study involving 77 patients.
Numerous symptoms were reported more often by the 37 women in the study than by the 40 men. For example, significantly more women than men reported joint pain, muscle pain, headache, back pain, heart palpitations, nausea, vomiting, anxiety, numbness and tingling, and changes in vision during at least one of six preplanned study visits with a physician, Lauren A. Crowder, M.P.H. reported in a poster at the International Conference on Emerging Infectious Diseases.
Joint pain, heart palpitations, nausea, vomiting, and changes in vision were reported significantly more often by women at two of the six visits, and headache was reported significantly more often by women at four of the six visits.
"The second preliminary finding we observed in our cohort of patients was that women were less likely to seroconvert on the antibody tests for serodiagnosis of Lyme disease," Ms. Crowder of the Lyme Disease Research Foundation, Lutherville, Md., said in an interview.
At the initial study visit, a similar proportion of men and women (about 60% of each) tested negative for Lyme disease using the Centers for Disease Control and Prevention’s recommended two-tier testing criteria for serodiagnosis. However, at the second visit, which was performed immediately post treatment, 70% of women who tested negative at the first visit remained negative, compared with only 35% of the men who initially tested negative.
Additionally, polychromatic flow cytometry performed on patient samples indicated that women had significantly higher frequency of CD4+CCR5+ T-cells prior to treatment than did men (mean of 9.82% vs. 5.96%).
"These findings suggest to us that there may be a difference between how men and women respond to infection with Lyme disease. One hypothesis for these differences is that there may be an immunological variation in response to Borrelia burgdorferi, the bacterial infection that causes Lyme disease, between men and women," Ms. Crowder said.
Study participants had early, untreated erythema migrans and clinically confirmed Lyme disease. At the first of the six study visits, they were tested using the CDC criteria by a commercial laboratory. All were treated with 3-week course of doxycycline and were then followed for up to 2 years. At each study visit, participants underwent a physical examination and interval history, reported clinical symptoms and completed self-administered surveys, and underwent repeat laboratory evaluations.
The findings highlight a need for additional research on sex-based differences in the effects of early Lyme disease. Such differences have been seen in other infectious disease, but have not been thoroughly explored in early Lyme disease, Ms. Crowder noted.
Such study is important given that Lyme disease is the most common vector-borne infectious disease in the United States. Although most patients recover from acute infection with proper antibiotic treatment, a subset of patients develop Post-Treatment Lyme Disease Syndrome. The CDC defines this syndrome as involving lingering symptoms of fatigue, pain, or joint and muscle aches. In some cases, these can last for more than 6 months.
"We will continue to explore these suggested differences both in this cohort and in future research studies," she said.
Ms. Crowder also stressed the importance of encouraging patients to look for ticks if they live in Lyme endemic areas.
This study was supported by the Lyme Disease Research Foundation. Ms. Crowder had no disclosures to report.
FROM THE INTERNATIONAL CONFERENCE ON EMERGING INFECTIOUS DISEASES
Major Finding: Significantly more women than men with Lyme disease reported joint pain, muscle pain, headache, back pain, heart palpitations, nausea, vomiting, anxiety, numbness and tingling, and changes in vision during at least one of six preplanned study visits with a physician.
Data Source: Findings were from a prospective cohort study.
Disclosures: This study was supported by the Lyme Disease Research Foundation. Ms. Crowder had no disclosures to report.
WBCs Help Identify More Severe Pertussis in Infants
ATLANTA – Infants with more-severe pertussis infections are more likely to have higher white blood cell counts and more-rapid increases in those counts than are infants with less-severe infections, according to findings from a California study of 31 infants.
These 31 infants, aged 90 days or younger, were admitted to the pediatric ICU at one of five participating centers in California following a 2010 Bordetella pertussis epidemic in the state, during which 10 infants died from the infection. The findings have implications for identifying infants with potentially severe infections early in the course of their illness, to allow for more rapid implementation of interventions such as exchange transfusion that may improve outcomes, Dr. James D. Cherry reported at the International Conference on Emerging Infectious Diseases.
Of the 31 infants who were admitted between September 1, 2009, and June 30, 2011, at a median age of 36 days, 8 had more-severe infections (defined by the presence of pulmonary hypertension or by infection-related mortality). Seven had pulmonary hypertension, and four of the eight infants died.
Compared with the 23 infants who had less-severe infections, the 8 with more-severe infections had significantly higher peak WBC counts (72.8 vs. 26.3 x 103/mcL), their WBC count exceeded 30.0 more rapidly following onset of illness (5.1 vs. 14.6 days), and they were more likely to have a 50% increase in their WBC count within 24 hours of illness onset (50% vs. 0%), said Dr. Cherry, a pediatric infectious disease specialist with Mattel Children’s Hospital at the University of California, Los Angeles.
Those with more severe infection also were significantly more likely to receive an exchange transfusion (75% vs. 0%), to be diagnosed with pneumonia (100% vs. 43%), and to be intubated (75% vs. 9%), he noted.
The more-severe and less-severe patient groups were similar with respect to sex, ethnicity, and median age at onset. Overall, 54% were girls and 94% were Hispanic.
This study is unique in that all patients in the pediatric ICU were younger than 3 months of age, Dr. Cherry said, noting that based on earlier data, it was assumed that this differences in outcomes among infants with pertussis was associated with delays in getting appropriate care.
"But after seeing [these new] data, I think it’s a lot more complicated than that," he said, explaining that no differences were seen between the groups in demographic factors that are health care indicators.
The findings suggest that it is imperative in these very young babies to assess WBC immediately so the trajectory can be tracked. Those at risk for a more-severe course should be considered for exchange transfusion, he concluded.
Dr. Cherry said he had no relevant financial disclosures.
ATLANTA – Infants with more-severe pertussis infections are more likely to have higher white blood cell counts and more-rapid increases in those counts than are infants with less-severe infections, according to findings from a California study of 31 infants.
These 31 infants, aged 90 days or younger, were admitted to the pediatric ICU at one of five participating centers in California following a 2010 Bordetella pertussis epidemic in the state, during which 10 infants died from the infection. The findings have implications for identifying infants with potentially severe infections early in the course of their illness, to allow for more rapid implementation of interventions such as exchange transfusion that may improve outcomes, Dr. James D. Cherry reported at the International Conference on Emerging Infectious Diseases.
Of the 31 infants who were admitted between September 1, 2009, and June 30, 2011, at a median age of 36 days, 8 had more-severe infections (defined by the presence of pulmonary hypertension or by infection-related mortality). Seven had pulmonary hypertension, and four of the eight infants died.
Compared with the 23 infants who had less-severe infections, the 8 with more-severe infections had significantly higher peak WBC counts (72.8 vs. 26.3 x 103/mcL), their WBC count exceeded 30.0 more rapidly following onset of illness (5.1 vs. 14.6 days), and they were more likely to have a 50% increase in their WBC count within 24 hours of illness onset (50% vs. 0%), said Dr. Cherry, a pediatric infectious disease specialist with Mattel Children’s Hospital at the University of California, Los Angeles.
Those with more severe infection also were significantly more likely to receive an exchange transfusion (75% vs. 0%), to be diagnosed with pneumonia (100% vs. 43%), and to be intubated (75% vs. 9%), he noted.
The more-severe and less-severe patient groups were similar with respect to sex, ethnicity, and median age at onset. Overall, 54% were girls and 94% were Hispanic.
This study is unique in that all patients in the pediatric ICU were younger than 3 months of age, Dr. Cherry said, noting that based on earlier data, it was assumed that this differences in outcomes among infants with pertussis was associated with delays in getting appropriate care.
"But after seeing [these new] data, I think it’s a lot more complicated than that," he said, explaining that no differences were seen between the groups in demographic factors that are health care indicators.
The findings suggest that it is imperative in these very young babies to assess WBC immediately so the trajectory can be tracked. Those at risk for a more-severe course should be considered for exchange transfusion, he concluded.
Dr. Cherry said he had no relevant financial disclosures.
ATLANTA – Infants with more-severe pertussis infections are more likely to have higher white blood cell counts and more-rapid increases in those counts than are infants with less-severe infections, according to findings from a California study of 31 infants.
These 31 infants, aged 90 days or younger, were admitted to the pediatric ICU at one of five participating centers in California following a 2010 Bordetella pertussis epidemic in the state, during which 10 infants died from the infection. The findings have implications for identifying infants with potentially severe infections early in the course of their illness, to allow for more rapid implementation of interventions such as exchange transfusion that may improve outcomes, Dr. James D. Cherry reported at the International Conference on Emerging Infectious Diseases.
Of the 31 infants who were admitted between September 1, 2009, and June 30, 2011, at a median age of 36 days, 8 had more-severe infections (defined by the presence of pulmonary hypertension or by infection-related mortality). Seven had pulmonary hypertension, and four of the eight infants died.
Compared with the 23 infants who had less-severe infections, the 8 with more-severe infections had significantly higher peak WBC counts (72.8 vs. 26.3 x 103/mcL), their WBC count exceeded 30.0 more rapidly following onset of illness (5.1 vs. 14.6 days), and they were more likely to have a 50% increase in their WBC count within 24 hours of illness onset (50% vs. 0%), said Dr. Cherry, a pediatric infectious disease specialist with Mattel Children’s Hospital at the University of California, Los Angeles.
Those with more severe infection also were significantly more likely to receive an exchange transfusion (75% vs. 0%), to be diagnosed with pneumonia (100% vs. 43%), and to be intubated (75% vs. 9%), he noted.
The more-severe and less-severe patient groups were similar with respect to sex, ethnicity, and median age at onset. Overall, 54% were girls and 94% were Hispanic.
This study is unique in that all patients in the pediatric ICU were younger than 3 months of age, Dr. Cherry said, noting that based on earlier data, it was assumed that this differences in outcomes among infants with pertussis was associated with delays in getting appropriate care.
"But after seeing [these new] data, I think it’s a lot more complicated than that," he said, explaining that no differences were seen between the groups in demographic factors that are health care indicators.
The findings suggest that it is imperative in these very young babies to assess WBC immediately so the trajectory can be tracked. Those at risk for a more-severe course should be considered for exchange transfusion, he concluded.
Dr. Cherry said he had no relevant financial disclosures.
FROM THE INTERNATIONAL CONFERENCE ON EMERGING INFECTIOUS DISEASES
Major Finding: Compared with 23 infants with less-severe infections, the 8 with more-severe infections had significantly higher peak WBC counts (72.8 vs. 26.3 x 103/mcL), their WBC count exceeded 30.0 more rapidly following onset of illness (5.1 vs. 14.6 days), and they were more likely to have a 50% increase in their WBC count within 24 hours of illness onset (50% vs. 0%).
Data Source: Data are from an observational study of 31 infants looking at characteristics of infants with severe pertussis infection.
Disclosures: Dr. Cherry said he had no relevant financial disclosures.
Connecticut Sees Overall Decline in MRSA Infections
ATLANTA – The overall incidence of methicillin-resistant Staphylococcus aureus infection has been declining in Connecticut since 2007, due entirely to decreases in infections caused by health care–related strains, according to laboratory reports on invasive MRSA isolates from across the state.
From 2001 to 2010, the overall incidence of MRSA infections declined significantly from 26.0 to 22.1 per 100,000 population. The incidence of health care–related MRSA infections declined significantly from 14.4 to 13.8 per 100,000 population, and the incidence of hospital-onset MRSA infections declined significantly from 10.0 to 5.2 per 100,000 population, which together were enough to offset a significant increase in the incidence of community-acquired MRSA infection during the same time period from 1.4 to 3.1 per 100,000 population, Dr. James Hadler reported during a poster session at the International Conference on Emerging Infectious Diseases.
The improvements in the health care–related strains of MRSA coincided with increased public, public health, and hospital attention to the problem of MRSA infections, said Dr. Hadler of the Connecticut and Yale Emerging Infections Program, Yale School of Public Health, New Haven, Conn.
MRSA has posed two distinct problems over the years, including hospital-onset bloodstream infections associated with highly-resistant strains, and community-onset infections, which mostly involve skin and soft-tissue infections caused by less resistant community MRSA strains. These started to increase in the 1980s and 1990s, respectively. Now hospital strains are causing infection in the community, and community strains are causing infections in the hospital, Dr. Hadler said.
Laboratory reporting for invasive MRSA became mandatory in Connecticut in 2001, and legislative initiatives in Connecticut in 2006 resulted in laws requiring reporting of hospital-related infection. In 2007, national attention was called to MRSA in a publication by the Emerging Infections Program that highlighted the magnitude of the problem, and the passing of legislation in Connecticut and other states mandating reporting of hospital infections.
From 2001 to 2007, the incidence of MRSA in Connecticut was either increasing or stable, but after 2007 the incidence began to decline, he explained.
Furthermore, an examination of incidence trends in three time periods (2001-2003, 2004-2006, and 2007-2010) showed that the trends for decline did indeed occur only from 2007 to 2010 for the overall, health care–associated, and hospital-onset cases. The increase in community-acquired disease occurred from 2004 to 2006.
Between 2007 and 2010, the overall incidence decreased 18.8%, the hospital-onset incidence decreased by 33.2%, and health care–associated infections decreased by 12.8%. After the initial increase from 2004 to 2006, the incidence of community-acquired cases decreased by 12.7%.
MRSA cases in this study were defined as those with MRSA isolated from normally sterile body sites. Cases were classified, based on a medical record review, as being a hospital-onset case (with MRSA isolated greater than 2 days after admission), a community-onset case, or a health care–associated case (with MRSA acquired during hospitalization, surgery, dialysis, or a stay in a long-term care facility in the past year, or central line at diagnosis).
The findings are encouraging, although continued monitoring to assess the sustainability of these apparent improvements in MRSA prevention is needed, according to Dr. Hadler.
"It looks like we’re making real progress with MRSA-related hospital- and health care–associated infections, but bigger improvements have been dampened by the community MRSA strains," he said in an interview.
The findings in Connecticut may reflect those of other areas in the United States, because Connecticut, which serves as one of seven MRSA surveillance areas that are part of the Centers for Disease Control and Prevention’s Emerging Infections Programs, is demographically diverse and representative of the larger U.S. population, he added.
Dr. Hadler said he had no relevant financial disclosures.
ATLANTA – The overall incidence of methicillin-resistant Staphylococcus aureus infection has been declining in Connecticut since 2007, due entirely to decreases in infections caused by health care–related strains, according to laboratory reports on invasive MRSA isolates from across the state.
From 2001 to 2010, the overall incidence of MRSA infections declined significantly from 26.0 to 22.1 per 100,000 population. The incidence of health care–related MRSA infections declined significantly from 14.4 to 13.8 per 100,000 population, and the incidence of hospital-onset MRSA infections declined significantly from 10.0 to 5.2 per 100,000 population, which together were enough to offset a significant increase in the incidence of community-acquired MRSA infection during the same time period from 1.4 to 3.1 per 100,000 population, Dr. James Hadler reported during a poster session at the International Conference on Emerging Infectious Diseases.
The improvements in the health care–related strains of MRSA coincided with increased public, public health, and hospital attention to the problem of MRSA infections, said Dr. Hadler of the Connecticut and Yale Emerging Infections Program, Yale School of Public Health, New Haven, Conn.
MRSA has posed two distinct problems over the years, including hospital-onset bloodstream infections associated with highly-resistant strains, and community-onset infections, which mostly involve skin and soft-tissue infections caused by less resistant community MRSA strains. These started to increase in the 1980s and 1990s, respectively. Now hospital strains are causing infection in the community, and community strains are causing infections in the hospital, Dr. Hadler said.
Laboratory reporting for invasive MRSA became mandatory in Connecticut in 2001, and legislative initiatives in Connecticut in 2006 resulted in laws requiring reporting of hospital-related infection. In 2007, national attention was called to MRSA in a publication by the Emerging Infections Program that highlighted the magnitude of the problem, and the passing of legislation in Connecticut and other states mandating reporting of hospital infections.
From 2001 to 2007, the incidence of MRSA in Connecticut was either increasing or stable, but after 2007 the incidence began to decline, he explained.
Furthermore, an examination of incidence trends in three time periods (2001-2003, 2004-2006, and 2007-2010) showed that the trends for decline did indeed occur only from 2007 to 2010 for the overall, health care–associated, and hospital-onset cases. The increase in community-acquired disease occurred from 2004 to 2006.
Between 2007 and 2010, the overall incidence decreased 18.8%, the hospital-onset incidence decreased by 33.2%, and health care–associated infections decreased by 12.8%. After the initial increase from 2004 to 2006, the incidence of community-acquired cases decreased by 12.7%.
MRSA cases in this study were defined as those with MRSA isolated from normally sterile body sites. Cases were classified, based on a medical record review, as being a hospital-onset case (with MRSA isolated greater than 2 days after admission), a community-onset case, or a health care–associated case (with MRSA acquired during hospitalization, surgery, dialysis, or a stay in a long-term care facility in the past year, or central line at diagnosis).
The findings are encouraging, although continued monitoring to assess the sustainability of these apparent improvements in MRSA prevention is needed, according to Dr. Hadler.
"It looks like we’re making real progress with MRSA-related hospital- and health care–associated infections, but bigger improvements have been dampened by the community MRSA strains," he said in an interview.
The findings in Connecticut may reflect those of other areas in the United States, because Connecticut, which serves as one of seven MRSA surveillance areas that are part of the Centers for Disease Control and Prevention’s Emerging Infections Programs, is demographically diverse and representative of the larger U.S. population, he added.
Dr. Hadler said he had no relevant financial disclosures.
ATLANTA – The overall incidence of methicillin-resistant Staphylococcus aureus infection has been declining in Connecticut since 2007, due entirely to decreases in infections caused by health care–related strains, according to laboratory reports on invasive MRSA isolates from across the state.
From 2001 to 2010, the overall incidence of MRSA infections declined significantly from 26.0 to 22.1 per 100,000 population. The incidence of health care–related MRSA infections declined significantly from 14.4 to 13.8 per 100,000 population, and the incidence of hospital-onset MRSA infections declined significantly from 10.0 to 5.2 per 100,000 population, which together were enough to offset a significant increase in the incidence of community-acquired MRSA infection during the same time period from 1.4 to 3.1 per 100,000 population, Dr. James Hadler reported during a poster session at the International Conference on Emerging Infectious Diseases.
The improvements in the health care–related strains of MRSA coincided with increased public, public health, and hospital attention to the problem of MRSA infections, said Dr. Hadler of the Connecticut and Yale Emerging Infections Program, Yale School of Public Health, New Haven, Conn.
MRSA has posed two distinct problems over the years, including hospital-onset bloodstream infections associated with highly-resistant strains, and community-onset infections, which mostly involve skin and soft-tissue infections caused by less resistant community MRSA strains. These started to increase in the 1980s and 1990s, respectively. Now hospital strains are causing infection in the community, and community strains are causing infections in the hospital, Dr. Hadler said.
Laboratory reporting for invasive MRSA became mandatory in Connecticut in 2001, and legislative initiatives in Connecticut in 2006 resulted in laws requiring reporting of hospital-related infection. In 2007, national attention was called to MRSA in a publication by the Emerging Infections Program that highlighted the magnitude of the problem, and the passing of legislation in Connecticut and other states mandating reporting of hospital infections.
From 2001 to 2007, the incidence of MRSA in Connecticut was either increasing or stable, but after 2007 the incidence began to decline, he explained.
Furthermore, an examination of incidence trends in three time periods (2001-2003, 2004-2006, and 2007-2010) showed that the trends for decline did indeed occur only from 2007 to 2010 for the overall, health care–associated, and hospital-onset cases. The increase in community-acquired disease occurred from 2004 to 2006.
Between 2007 and 2010, the overall incidence decreased 18.8%, the hospital-onset incidence decreased by 33.2%, and health care–associated infections decreased by 12.8%. After the initial increase from 2004 to 2006, the incidence of community-acquired cases decreased by 12.7%.
MRSA cases in this study were defined as those with MRSA isolated from normally sterile body sites. Cases were classified, based on a medical record review, as being a hospital-onset case (with MRSA isolated greater than 2 days after admission), a community-onset case, or a health care–associated case (with MRSA acquired during hospitalization, surgery, dialysis, or a stay in a long-term care facility in the past year, or central line at diagnosis).
The findings are encouraging, although continued monitoring to assess the sustainability of these apparent improvements in MRSA prevention is needed, according to Dr. Hadler.
"It looks like we’re making real progress with MRSA-related hospital- and health care–associated infections, but bigger improvements have been dampened by the community MRSA strains," he said in an interview.
The findings in Connecticut may reflect those of other areas in the United States, because Connecticut, which serves as one of seven MRSA surveillance areas that are part of the Centers for Disease Control and Prevention’s Emerging Infections Programs, is demographically diverse and representative of the larger U.S. population, he added.
Dr. Hadler said he had no relevant financial disclosures.
FROM THE INTERNATIONAL CONFERENCE ON EMERGING INFECTIOUS DISEASES
Major Finding: The incidence of health care–related MRSA infections declined significantly from 14.4 to 13.8 per 100,000 population, and the incidence of hospital-onset MRSA infections declined significantly from 10.0 to 5.2 per 100,000 population, which together were enough to offset a significant increase in the incidence of community-acquired MRSA infection during the same time period from 1.4 to 3.1 per 100,000 population.
Data Source: Surveillance data/statewide lab reports from 2001 to 2010 were studied.
Disclosures: Dr. Hadler said he had no relevant financial disclosures.
Exposure to Diesel Exhaust Tied to More Lung Cancer Deaths
Exposure to diesel exhaust increases the risk of developing and dying from lung cancer, according to the results of a large cohort mortality study in more than 12,000 exposed workers and a related nested case-control study.
The Diesel Exhaust in Miners Study confirms prior studies demonstrating a possible causal relationship between diesel exhaust exposure and lung cancer, and suggests that this association represents an important public health burden in urban areas worldwide.
Both studies were published online March 5 in the Journal of the National Cancer Institute.
In the main cohort mortality study, the standardized mortality ratio (SMR) of 1.26 for lung cancer among 12,315 exposed workers was significantly greater than were state-based mortality rates, wrote Michael D. Attfield. Ph.D., formerly with the National Institute for Occupational Safety and Health in Morgantown, W.Va., and his colleagues.
Esophageal cancer and pneumoconiosis mortality also were significantly elevated in the exposed workers (SMRs, 1.83 and 12.20, respectively), the researchers found (J. Natl. Cancer Inst. 2012 [doi:10.1093/jnci/djs035]).
Outcomes were evaluated in workers exposed to diesel exhaust at eight nonmetal mining facilities in the United States using retrospective quantitative estimates of respirable elemental carbon (REC) exposures as a surrogate for diesel exhaust exposure. The data covered the periods from the introduction (between 1947 and 1967) of diesel-powered equipment to 1997.
A dose-response relationship between exposure and lung cancer mortality was not apparent in the overall cohort, but clear evidence of such a relationship emerged after the investigators divided the population, comparing those who had worked underground at some point (ever-underground) with surface workers.
"In contrast to the complete cohort, hazard ratios that increased with level of exposure were seen for ever-underground workers using quartiles of REC exposure. Using the expanded exposure categories, hazard ratios for 15-year lagged cumulative REC exposure rose with increasing exposure, the trend being more pronounced when workers with shorter tenures were excluded," the investigators said.
As for the surface-only workers, no clear exposure-response trend was seen in the quartile analysis, but there was evidence of an increasing trend in risk with increasing exposure, they said.
The overall findings were "essentially unchanged" after the researchers controlled for cumulative exposures to silica, asbestos, nondiesel exhaust polycyclic aromatic hydrocarbons, and respirable dust.
Though limited by factors typical of cohort mortality studies, such as uncertainty in exposure assessments and lack of information on lifestyle factors, this study had strong statistical power and the findings suggest that despite ongoing efforts to reduce diesel engine emissions, diesel exhaust exposure remains a problem.
"Certainly, many workers around the world, in mining and in other industries and jobs, continue to be exposed to REC at levels similar to those observed in this study; in addition, environmental exposures have been shown to reach the levels seen for average REC intensity in surface workers in this study," the investigators concluded.
The findings are bolstered by those from the companion nested case-control study, which also evaluated the relationship between diesel exhaust exposure and lung cancer mortality, but which included adjustment for smoking and other established and hypothesized potential confounders.
For this companion study, Debra T. Silverman, Sc.D., of the National Cancer Institute, Bethesda, Md., and her colleagues compared 198 lung cancer death cases and 562 incidence density–sampled control subjects.
After adjustment for smoking, history of employment in high-risk occupations for lung cancer, and a history of respiratory disease, they also found statistically significant increasing trends in lung cancer risk with increasing exposure (J. Natl. Cancer Inst. 2012;104:1-14 [doi:10.1093/jnci/djs034]).
"Our findings are important not only for miners but also for the 1.4 million American workers and the 3 million European workers exposed to diesel exhaust and for urban populations worldwide," the investigators said.
Citing Los Angeles; the Bronx borough of New York City; Mexico City; Estarreja, Portugal; and nine urban centers in China, they noted that some of the higher-average elemental carbon levels reported in major cities represent potential lifetime exposures that approximate the cumulative exposures experienced by underground miners with low exposures in this study.
"Because such workers had at least a 50% increased lung cancer risk, our results suggest that the high air concentrations of elemental carbon reported in some urban areas may confer increased risk of lung cancer. Thus, if the diesel exhaust/lung cancer relation is causal, the public health burden of the carcinogenicity of inhaled diesel exhaust in workers and in populations of urban areas with high levels of diesel exposure may be substantial," they concluded.
The Diesel Exhaust in Miners Study was funded by the Intramural Research Program of the National Institutes of Health, National Cancer Institute, Division of Cancer Epidemiology and Genetics, and the National Institute for Occupational Safety and Health, Division of Respiratory Disease Studies. The authors had no disclosures to report.
In an accompanying editorial, Lesley Rushton, Ph.D., said that the Diesel Exhaust in Miners Study represents an important contribution to the body of evidence about diesel exhaust, and is particularly timely given that the current categorization of diesel exhaust exposure as a "probable human carcinogen" by the International Agency for Research on Cancer will be reconsidered at a meeting of that agency later this year.
"The issue of causality is fundamental when estimating and ranking burden of disease attributable to various exposures," she said, noting that the data in this study indicate a "sharp rise in risk at lower levels and show that background levels of 1-2 mcg/m3 are still likely to carry a small excess risk; substantial proportions of the population exposed at these low levels of exposure would thus continue to contribute to the burden of cancer from diesel exhaust exposure" (J. Natl. Cancer Inst. 2012 March 5 [doi: 10.1093/jnci/djs137]).
Thus, stringent occupational and environmental standards for such exposure should be set, and compliance should be ensured, she argued.
In addition to lower emissions and more efficient engines, she suggested a number of strategies for reducing exposure in occupational settings, including engineering controls such as improved ventilation and regular vehicle maintenance, limiting the number of vehicles – particularly in closed spaces – turning off engines when not in use, and use of appropriate respiratory protective equipment.
Although reductions in the general environment pose more of a challenge, some of these occupational measures are nonetheless relevant in that setting. "The necessity for such reduction is becoming increasingly apparent and is essential if the health of large numbers of people is not to be compromised," she said.
Dr. Rushton is with Imperial College London. She had no disclosures to report.
In an accompanying editorial, Lesley Rushton, Ph.D., said that the Diesel Exhaust in Miners Study represents an important contribution to the body of evidence about diesel exhaust, and is particularly timely given that the current categorization of diesel exhaust exposure as a "probable human carcinogen" by the International Agency for Research on Cancer will be reconsidered at a meeting of that agency later this year.
"The issue of causality is fundamental when estimating and ranking burden of disease attributable to various exposures," she said, noting that the data in this study indicate a "sharp rise in risk at lower levels and show that background levels of 1-2 mcg/m3 are still likely to carry a small excess risk; substantial proportions of the population exposed at these low levels of exposure would thus continue to contribute to the burden of cancer from diesel exhaust exposure" (J. Natl. Cancer Inst. 2012 March 5 [doi: 10.1093/jnci/djs137]).
Thus, stringent occupational and environmental standards for such exposure should be set, and compliance should be ensured, she argued.
In addition to lower emissions and more efficient engines, she suggested a number of strategies for reducing exposure in occupational settings, including engineering controls such as improved ventilation and regular vehicle maintenance, limiting the number of vehicles – particularly in closed spaces – turning off engines when not in use, and use of appropriate respiratory protective equipment.
Although reductions in the general environment pose more of a challenge, some of these occupational measures are nonetheless relevant in that setting. "The necessity for such reduction is becoming increasingly apparent and is essential if the health of large numbers of people is not to be compromised," she said.
Dr. Rushton is with Imperial College London. She had no disclosures to report.
In an accompanying editorial, Lesley Rushton, Ph.D., said that the Diesel Exhaust in Miners Study represents an important contribution to the body of evidence about diesel exhaust, and is particularly timely given that the current categorization of diesel exhaust exposure as a "probable human carcinogen" by the International Agency for Research on Cancer will be reconsidered at a meeting of that agency later this year.
"The issue of causality is fundamental when estimating and ranking burden of disease attributable to various exposures," she said, noting that the data in this study indicate a "sharp rise in risk at lower levels and show that background levels of 1-2 mcg/m3 are still likely to carry a small excess risk; substantial proportions of the population exposed at these low levels of exposure would thus continue to contribute to the burden of cancer from diesel exhaust exposure" (J. Natl. Cancer Inst. 2012 March 5 [doi: 10.1093/jnci/djs137]).
Thus, stringent occupational and environmental standards for such exposure should be set, and compliance should be ensured, she argued.
In addition to lower emissions and more efficient engines, she suggested a number of strategies for reducing exposure in occupational settings, including engineering controls such as improved ventilation and regular vehicle maintenance, limiting the number of vehicles – particularly in closed spaces – turning off engines when not in use, and use of appropriate respiratory protective equipment.
Although reductions in the general environment pose more of a challenge, some of these occupational measures are nonetheless relevant in that setting. "The necessity for such reduction is becoming increasingly apparent and is essential if the health of large numbers of people is not to be compromised," she said.
Dr. Rushton is with Imperial College London. She had no disclosures to report.
Exposure to diesel exhaust increases the risk of developing and dying from lung cancer, according to the results of a large cohort mortality study in more than 12,000 exposed workers and a related nested case-control study.
The Diesel Exhaust in Miners Study confirms prior studies demonstrating a possible causal relationship between diesel exhaust exposure and lung cancer, and suggests that this association represents an important public health burden in urban areas worldwide.
Both studies were published online March 5 in the Journal of the National Cancer Institute.
In the main cohort mortality study, the standardized mortality ratio (SMR) of 1.26 for lung cancer among 12,315 exposed workers was significantly greater than were state-based mortality rates, wrote Michael D. Attfield. Ph.D., formerly with the National Institute for Occupational Safety and Health in Morgantown, W.Va., and his colleagues.
Esophageal cancer and pneumoconiosis mortality also were significantly elevated in the exposed workers (SMRs, 1.83 and 12.20, respectively), the researchers found (J. Natl. Cancer Inst. 2012 [doi:10.1093/jnci/djs035]).
Outcomes were evaluated in workers exposed to diesel exhaust at eight nonmetal mining facilities in the United States using retrospective quantitative estimates of respirable elemental carbon (REC) exposures as a surrogate for diesel exhaust exposure. The data covered the periods from the introduction (between 1947 and 1967) of diesel-powered equipment to 1997.
A dose-response relationship between exposure and lung cancer mortality was not apparent in the overall cohort, but clear evidence of such a relationship emerged after the investigators divided the population, comparing those who had worked underground at some point (ever-underground) with surface workers.
"In contrast to the complete cohort, hazard ratios that increased with level of exposure were seen for ever-underground workers using quartiles of REC exposure. Using the expanded exposure categories, hazard ratios for 15-year lagged cumulative REC exposure rose with increasing exposure, the trend being more pronounced when workers with shorter tenures were excluded," the investigators said.
As for the surface-only workers, no clear exposure-response trend was seen in the quartile analysis, but there was evidence of an increasing trend in risk with increasing exposure, they said.
The overall findings were "essentially unchanged" after the researchers controlled for cumulative exposures to silica, asbestos, nondiesel exhaust polycyclic aromatic hydrocarbons, and respirable dust.
Though limited by factors typical of cohort mortality studies, such as uncertainty in exposure assessments and lack of information on lifestyle factors, this study had strong statistical power and the findings suggest that despite ongoing efforts to reduce diesel engine emissions, diesel exhaust exposure remains a problem.
"Certainly, many workers around the world, in mining and in other industries and jobs, continue to be exposed to REC at levels similar to those observed in this study; in addition, environmental exposures have been shown to reach the levels seen for average REC intensity in surface workers in this study," the investigators concluded.
The findings are bolstered by those from the companion nested case-control study, which also evaluated the relationship between diesel exhaust exposure and lung cancer mortality, but which included adjustment for smoking and other established and hypothesized potential confounders.
For this companion study, Debra T. Silverman, Sc.D., of the National Cancer Institute, Bethesda, Md., and her colleagues compared 198 lung cancer death cases and 562 incidence density–sampled control subjects.
After adjustment for smoking, history of employment in high-risk occupations for lung cancer, and a history of respiratory disease, they also found statistically significant increasing trends in lung cancer risk with increasing exposure (J. Natl. Cancer Inst. 2012;104:1-14 [doi:10.1093/jnci/djs034]).
"Our findings are important not only for miners but also for the 1.4 million American workers and the 3 million European workers exposed to diesel exhaust and for urban populations worldwide," the investigators said.
Citing Los Angeles; the Bronx borough of New York City; Mexico City; Estarreja, Portugal; and nine urban centers in China, they noted that some of the higher-average elemental carbon levels reported in major cities represent potential lifetime exposures that approximate the cumulative exposures experienced by underground miners with low exposures in this study.
"Because such workers had at least a 50% increased lung cancer risk, our results suggest that the high air concentrations of elemental carbon reported in some urban areas may confer increased risk of lung cancer. Thus, if the diesel exhaust/lung cancer relation is causal, the public health burden of the carcinogenicity of inhaled diesel exhaust in workers and in populations of urban areas with high levels of diesel exposure may be substantial," they concluded.
The Diesel Exhaust in Miners Study was funded by the Intramural Research Program of the National Institutes of Health, National Cancer Institute, Division of Cancer Epidemiology and Genetics, and the National Institute for Occupational Safety and Health, Division of Respiratory Disease Studies. The authors had no disclosures to report.
Exposure to diesel exhaust increases the risk of developing and dying from lung cancer, according to the results of a large cohort mortality study in more than 12,000 exposed workers and a related nested case-control study.
The Diesel Exhaust in Miners Study confirms prior studies demonstrating a possible causal relationship between diesel exhaust exposure and lung cancer, and suggests that this association represents an important public health burden in urban areas worldwide.
Both studies were published online March 5 in the Journal of the National Cancer Institute.
In the main cohort mortality study, the standardized mortality ratio (SMR) of 1.26 for lung cancer among 12,315 exposed workers was significantly greater than were state-based mortality rates, wrote Michael D. Attfield. Ph.D., formerly with the National Institute for Occupational Safety and Health in Morgantown, W.Va., and his colleagues.
Esophageal cancer and pneumoconiosis mortality also were significantly elevated in the exposed workers (SMRs, 1.83 and 12.20, respectively), the researchers found (J. Natl. Cancer Inst. 2012 [doi:10.1093/jnci/djs035]).
Outcomes were evaluated in workers exposed to diesel exhaust at eight nonmetal mining facilities in the United States using retrospective quantitative estimates of respirable elemental carbon (REC) exposures as a surrogate for diesel exhaust exposure. The data covered the periods from the introduction (between 1947 and 1967) of diesel-powered equipment to 1997.
A dose-response relationship between exposure and lung cancer mortality was not apparent in the overall cohort, but clear evidence of such a relationship emerged after the investigators divided the population, comparing those who had worked underground at some point (ever-underground) with surface workers.
"In contrast to the complete cohort, hazard ratios that increased with level of exposure were seen for ever-underground workers using quartiles of REC exposure. Using the expanded exposure categories, hazard ratios for 15-year lagged cumulative REC exposure rose with increasing exposure, the trend being more pronounced when workers with shorter tenures were excluded," the investigators said.
As for the surface-only workers, no clear exposure-response trend was seen in the quartile analysis, but there was evidence of an increasing trend in risk with increasing exposure, they said.
The overall findings were "essentially unchanged" after the researchers controlled for cumulative exposures to silica, asbestos, nondiesel exhaust polycyclic aromatic hydrocarbons, and respirable dust.
Though limited by factors typical of cohort mortality studies, such as uncertainty in exposure assessments and lack of information on lifestyle factors, this study had strong statistical power and the findings suggest that despite ongoing efforts to reduce diesel engine emissions, diesel exhaust exposure remains a problem.
"Certainly, many workers around the world, in mining and in other industries and jobs, continue to be exposed to REC at levels similar to those observed in this study; in addition, environmental exposures have been shown to reach the levels seen for average REC intensity in surface workers in this study," the investigators concluded.
The findings are bolstered by those from the companion nested case-control study, which also evaluated the relationship between diesel exhaust exposure and lung cancer mortality, but which included adjustment for smoking and other established and hypothesized potential confounders.
For this companion study, Debra T. Silverman, Sc.D., of the National Cancer Institute, Bethesda, Md., and her colleagues compared 198 lung cancer death cases and 562 incidence density–sampled control subjects.
After adjustment for smoking, history of employment in high-risk occupations for lung cancer, and a history of respiratory disease, they also found statistically significant increasing trends in lung cancer risk with increasing exposure (J. Natl. Cancer Inst. 2012;104:1-14 [doi:10.1093/jnci/djs034]).
"Our findings are important not only for miners but also for the 1.4 million American workers and the 3 million European workers exposed to diesel exhaust and for urban populations worldwide," the investigators said.
Citing Los Angeles; the Bronx borough of New York City; Mexico City; Estarreja, Portugal; and nine urban centers in China, they noted that some of the higher-average elemental carbon levels reported in major cities represent potential lifetime exposures that approximate the cumulative exposures experienced by underground miners with low exposures in this study.
"Because such workers had at least a 50% increased lung cancer risk, our results suggest that the high air concentrations of elemental carbon reported in some urban areas may confer increased risk of lung cancer. Thus, if the diesel exhaust/lung cancer relation is causal, the public health burden of the carcinogenicity of inhaled diesel exhaust in workers and in populations of urban areas with high levels of diesel exposure may be substantial," they concluded.
The Diesel Exhaust in Miners Study was funded by the Intramural Research Program of the National Institutes of Health, National Cancer Institute, Division of Cancer Epidemiology and Genetics, and the National Institute for Occupational Safety and Health, Division of Respiratory Disease Studies. The authors had no disclosures to report.
FROM THE JOURNAL OF THE NATIONAL CANCER INSTITUTE
Major Finding: The standardized mortality ratio (SMR) of 1.26 for lung cancer among 12,315 exposed workers was significantly greater than were state-based mortality rates .
Data Source: Data came from a large cohort mortality study and a companion nested case-control study.
Disclosures: The Diesel Exhaust in Miners Study was funded by the Intramural Research Program of the National Institutes of Health, National Cancer Institute, Division of Cancer Epidemiology and Genetics and the National Institute for Occupational Safety and Health, Division of Respiratory Disease Studies. The authors had no disclosures to report.