User login
Sharon Worcester is an award-winning medical journalist for MDedge News. She has been with the company since 1996, first as the Southeast Bureau Chief (1996-2009) when the company was known as International Medical News Group, then as a freelance writer (2010-2015) before returning as a reporter in 2015. She previously worked as a daily newspaper reporter covering health and local government. Sharon currently reports primarily on oncology and hematology. She has a BA from Eckerd College and an MA in Mass Communication/Print Journalism from the University of Florida. Connect with her via LinkedIn and follow her on twitter @SW_MedReporter.
VIDEO: DAWN2 shows need for patient-centered care in diabetes
ORLANDO – Nearly a decade after the results of the Diabetes Attitudes Wishes and Needs (DAWN) trial showed that the emotional health of patients with diabetes was not being adequately addressed, findings from the DAWN2 trial show that not much has changed in that regard.
Almost half of the more than 8,500 patients with diabetes who participated in the multinational DAWN2 trial reported experiencing emotional distress as a result of their diabetes, and 14% had likely clinical depression. The results also show that most patients with diabetes want to improve self-management, and that having a large social support network is associated with better psychosocial outcomes.
At the annual meeting of the American Association of Diabetes Educators, Martha Funnell, a certified diabetes educator, associate research scientist at the University of Michigan, Ann Arbor, and a member of the advisory committee for the Novo Nordisk–sponsored DAWN trials, discussed the findings and their clinical implications.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
ORLANDO – Nearly a decade after the results of the Diabetes Attitudes Wishes and Needs (DAWN) trial showed that the emotional health of patients with diabetes was not being adequately addressed, findings from the DAWN2 trial show that not much has changed in that regard.
Almost half of the more than 8,500 patients with diabetes who participated in the multinational DAWN2 trial reported experiencing emotional distress as a result of their diabetes, and 14% had likely clinical depression. The results also show that most patients with diabetes want to improve self-management, and that having a large social support network is associated with better psychosocial outcomes.
At the annual meeting of the American Association of Diabetes Educators, Martha Funnell, a certified diabetes educator, associate research scientist at the University of Michigan, Ann Arbor, and a member of the advisory committee for the Novo Nordisk–sponsored DAWN trials, discussed the findings and their clinical implications.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
ORLANDO – Nearly a decade after the results of the Diabetes Attitudes Wishes and Needs (DAWN) trial showed that the emotional health of patients with diabetes was not being adequately addressed, findings from the DAWN2 trial show that not much has changed in that regard.
Almost half of the more than 8,500 patients with diabetes who participated in the multinational DAWN2 trial reported experiencing emotional distress as a result of their diabetes, and 14% had likely clinical depression. The results also show that most patients with diabetes want to improve self-management, and that having a large social support network is associated with better psychosocial outcomes.
At the annual meeting of the American Association of Diabetes Educators, Martha Funnell, a certified diabetes educator, associate research scientist at the University of Michigan, Ann Arbor, and a member of the advisory committee for the Novo Nordisk–sponsored DAWN trials, discussed the findings and their clinical implications.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT AADE 14
DAWN2: Addressing emotional distress may improve diabetes self management
ORLANDO – Emotional distress associated with a diabetes diagnosis explains many patients’ difficulties with self-management, based on results from the DAWN2 study presented at the annual meeting of the American Association of Diabetes Educators.
The Novo Nordisk–sponsored DAWN2 (Diabetes Attitudes Wishes and Needs 2) study included 15,438 adults from 17 countries: 8,596 were people with diabetes (1,368 with type 1 and 7,228 with type 2), 2,057 were family members of people with diabetes, and 4,785 were health care providers. The researchers set out primarily to determine the factors that prevent and facilitate active and successful diabetes management.
"The ultimate goal for all of us and for this study is to enable all people with diabetes to live full, healthy, and productive lives, and to be engaged in their own care, preserving their health, and improving their quality of life," said Martha Funnell, a certified diabetes educator, associate research scientist at the University of Michigan, Ann Arbor, and a member of an advisory panel for the DAWN studies.
The first results from DAWN, published in 2005 and 2006, indicated that the psychosocial needs of patients with diabetes were not being met. The findings were based on the results of a survey that covered a broad range of topics, such as health and quality of life, attitudes and beliefs about diabetes, diabetes training, care and support, active self-management, and diabetes education and information. The first global benchmarking results were published in three articles in Diabetic Medicine (Diabet. Med. 2013;30:767-98).
Although a number of themes emerged from the DAWN findings, those with respect to emotional health stand out. In response to those results, emotional well-being has been incorporated into standards of care, Ms. Funnell said. In DAWN2, slightly more patients reported experiencing ongoing emotional distress as a result of diabetes (45% vs. 43%); 14% likely had clinical depression as a result of their diagnosis.
The findings are concerning as emotional distress – feelings of anger, fear, frustration, sadness, and guilt – are among the biggest influencers of self-management. Further, diabetes-related distress has an adverse impact on outcomes, including hemoglobin A1c levels, dietary and exercise behaviors, quality of life, and depression, Ms. Funnell said.
Diabetes also affects other aspects of life: 44% of people with diabetes in DAWN2 said their finances were affected, 38% said leisure activities were affected, 35% said that work and studies were affected, and 21% reported problems with family and peer relationships.
"We have to address diabetes-related distress if we want our patients to make changes and improve their outcomes," she said.
Notably, 52% of health care providers in DAWN2 reported asking patients how their life was affected by diabetes, yet only 24% of patients said their health care provider asked them that question.
"If I was going to do a one-question educational assessment, that would be the question [I would ask] because that tells pretty much all I need to know to work with that person," Ms. Funnell said.
Other findings from DAWN2 included the following:
• Family members of diabetes patients are burdened by the disease as well; 39% said they wanted to be more involved and 37% said they didn’t know how to be more involved.
• Most people with diabetes said that they want to be actively engaged and to participate in their care, but most aren’t.
• Half of the respondents with diabetes had never participated in a diabetes education program.
• Health care providers report a desire for more training in many aspects of diabetes care.
• Discrimination because of diabetes was reported by 19% of patients, implying a lack of awareness about diabetes.
An analysis of U.S.-only data from DAWN2 also shed light on important issues related to diabetes care and self-management.
The more than 500 U.S. respondents with diabetes in the DAWN2 study reported following a healthy eating plan for a mean of 4.7 days per week. They participated in at least 30 minutes of physical activity on a mean of 2.7 days per week and 65% expressed a desire to improve on this measure. Patients tested their blood sugar levels as recommended by their health care provider a mean of 4.5 days per week and took all medication as prescribed on a mean of 6.4 days per week. They checked their feet on a mean of 4.7 days per week (Curr. Med. Res. Opin. 2014 July 31:1-39).
Adherence varied considerably by ethnic group. For example, non-Hispanic white patients had the lowest scores for physical activity, Chinese Americans had the lowest scores for testing their blood sugar as recommended, and African Americans and Hispanics had the best scores for checking their feet.
Psychological outcomes also differed by ethnicity. African Americans had the best scores and non-Hispanic whites had the worst scores for well-being, quality of life, diabetes empowerment, and diabetes impact. Hispanics had the worst scores for quality of life and diabetes distress.
The DAWN2 data for U.S. survey respondents also indicated a substantial level of distress among people with diabetes and their family members. Having a large social support network for diabetes was related to better psychosocial outcomes, but few people with diabetes let others know how they can best provide support.
Also, U.S. respondents were pleased with the level of involvement of their family in diabetes care, and they feel that family members help a great deal by listening to them when they talk about difficulties associated with living with diabetes.
Diabetes is a burden from a management and psychological perspective. Patients need to be encouraged to ask for support when it is needed, and clinicians need to recognize that family members are untapped resources for patient support as well as a group in need of support as they deal with the burdens of caring for a family member with diabetes, Ms. Funnell added.
"Finally, we absolutely have to involve the person with diabetes and their family members as equal partners when developing care solutions," she said. Family members need to be taught how to help, and patients need to be asked how diabetes is affecting their life to identify problems and set appropriate goals for solving them.
"We need to truly focus on patient-centered care. ... We really need to surround the patient with their family and their friends, their health care, their communities, their workplaces, and the larger society if they are going to be successful in their self-management. It takes a village to manage diabetes, and every one of us has a role to play to make person-centered diabetes care and patient-centered diabetes education and ongoing support the reality that it needs to be," she said.
Ms. Funnell reported serving as a board or advisory panel member for Novo Nordisk, the sponsor of DAWN2, as well as several other drug companies involved in diabetes care, and receiving grant funding from BMS Foundation.
ORLANDO – Emotional distress associated with a diabetes diagnosis explains many patients’ difficulties with self-management, based on results from the DAWN2 study presented at the annual meeting of the American Association of Diabetes Educators.
The Novo Nordisk–sponsored DAWN2 (Diabetes Attitudes Wishes and Needs 2) study included 15,438 adults from 17 countries: 8,596 were people with diabetes (1,368 with type 1 and 7,228 with type 2), 2,057 were family members of people with diabetes, and 4,785 were health care providers. The researchers set out primarily to determine the factors that prevent and facilitate active and successful diabetes management.
"The ultimate goal for all of us and for this study is to enable all people with diabetes to live full, healthy, and productive lives, and to be engaged in their own care, preserving their health, and improving their quality of life," said Martha Funnell, a certified diabetes educator, associate research scientist at the University of Michigan, Ann Arbor, and a member of an advisory panel for the DAWN studies.
The first results from DAWN, published in 2005 and 2006, indicated that the psychosocial needs of patients with diabetes were not being met. The findings were based on the results of a survey that covered a broad range of topics, such as health and quality of life, attitudes and beliefs about diabetes, diabetes training, care and support, active self-management, and diabetes education and information. The first global benchmarking results were published in three articles in Diabetic Medicine (Diabet. Med. 2013;30:767-98).
Although a number of themes emerged from the DAWN findings, those with respect to emotional health stand out. In response to those results, emotional well-being has been incorporated into standards of care, Ms. Funnell said. In DAWN2, slightly more patients reported experiencing ongoing emotional distress as a result of diabetes (45% vs. 43%); 14% likely had clinical depression as a result of their diagnosis.
The findings are concerning as emotional distress – feelings of anger, fear, frustration, sadness, and guilt – are among the biggest influencers of self-management. Further, diabetes-related distress has an adverse impact on outcomes, including hemoglobin A1c levels, dietary and exercise behaviors, quality of life, and depression, Ms. Funnell said.
Diabetes also affects other aspects of life: 44% of people with diabetes in DAWN2 said their finances were affected, 38% said leisure activities were affected, 35% said that work and studies were affected, and 21% reported problems with family and peer relationships.
"We have to address diabetes-related distress if we want our patients to make changes and improve their outcomes," she said.
Notably, 52% of health care providers in DAWN2 reported asking patients how their life was affected by diabetes, yet only 24% of patients said their health care provider asked them that question.
"If I was going to do a one-question educational assessment, that would be the question [I would ask] because that tells pretty much all I need to know to work with that person," Ms. Funnell said.
Other findings from DAWN2 included the following:
• Family members of diabetes patients are burdened by the disease as well; 39% said they wanted to be more involved and 37% said they didn’t know how to be more involved.
• Most people with diabetes said that they want to be actively engaged and to participate in their care, but most aren’t.
• Half of the respondents with diabetes had never participated in a diabetes education program.
• Health care providers report a desire for more training in many aspects of diabetes care.
• Discrimination because of diabetes was reported by 19% of patients, implying a lack of awareness about diabetes.
An analysis of U.S.-only data from DAWN2 also shed light on important issues related to diabetes care and self-management.
The more than 500 U.S. respondents with diabetes in the DAWN2 study reported following a healthy eating plan for a mean of 4.7 days per week. They participated in at least 30 minutes of physical activity on a mean of 2.7 days per week and 65% expressed a desire to improve on this measure. Patients tested their blood sugar levels as recommended by their health care provider a mean of 4.5 days per week and took all medication as prescribed on a mean of 6.4 days per week. They checked their feet on a mean of 4.7 days per week (Curr. Med. Res. Opin. 2014 July 31:1-39).
Adherence varied considerably by ethnic group. For example, non-Hispanic white patients had the lowest scores for physical activity, Chinese Americans had the lowest scores for testing their blood sugar as recommended, and African Americans and Hispanics had the best scores for checking their feet.
Psychological outcomes also differed by ethnicity. African Americans had the best scores and non-Hispanic whites had the worst scores for well-being, quality of life, diabetes empowerment, and diabetes impact. Hispanics had the worst scores for quality of life and diabetes distress.
The DAWN2 data for U.S. survey respondents also indicated a substantial level of distress among people with diabetes and their family members. Having a large social support network for diabetes was related to better psychosocial outcomes, but few people with diabetes let others know how they can best provide support.
Also, U.S. respondents were pleased with the level of involvement of their family in diabetes care, and they feel that family members help a great deal by listening to them when they talk about difficulties associated with living with diabetes.
Diabetes is a burden from a management and psychological perspective. Patients need to be encouraged to ask for support when it is needed, and clinicians need to recognize that family members are untapped resources for patient support as well as a group in need of support as they deal with the burdens of caring for a family member with diabetes, Ms. Funnell added.
"Finally, we absolutely have to involve the person with diabetes and their family members as equal partners when developing care solutions," she said. Family members need to be taught how to help, and patients need to be asked how diabetes is affecting their life to identify problems and set appropriate goals for solving them.
"We need to truly focus on patient-centered care. ... We really need to surround the patient with their family and their friends, their health care, their communities, their workplaces, and the larger society if they are going to be successful in their self-management. It takes a village to manage diabetes, and every one of us has a role to play to make person-centered diabetes care and patient-centered diabetes education and ongoing support the reality that it needs to be," she said.
Ms. Funnell reported serving as a board or advisory panel member for Novo Nordisk, the sponsor of DAWN2, as well as several other drug companies involved in diabetes care, and receiving grant funding from BMS Foundation.
ORLANDO – Emotional distress associated with a diabetes diagnosis explains many patients’ difficulties with self-management, based on results from the DAWN2 study presented at the annual meeting of the American Association of Diabetes Educators.
The Novo Nordisk–sponsored DAWN2 (Diabetes Attitudes Wishes and Needs 2) study included 15,438 adults from 17 countries: 8,596 were people with diabetes (1,368 with type 1 and 7,228 with type 2), 2,057 were family members of people with diabetes, and 4,785 were health care providers. The researchers set out primarily to determine the factors that prevent and facilitate active and successful diabetes management.
"The ultimate goal for all of us and for this study is to enable all people with diabetes to live full, healthy, and productive lives, and to be engaged in their own care, preserving their health, and improving their quality of life," said Martha Funnell, a certified diabetes educator, associate research scientist at the University of Michigan, Ann Arbor, and a member of an advisory panel for the DAWN studies.
The first results from DAWN, published in 2005 and 2006, indicated that the psychosocial needs of patients with diabetes were not being met. The findings were based on the results of a survey that covered a broad range of topics, such as health and quality of life, attitudes and beliefs about diabetes, diabetes training, care and support, active self-management, and diabetes education and information. The first global benchmarking results were published in three articles in Diabetic Medicine (Diabet. Med. 2013;30:767-98).
Although a number of themes emerged from the DAWN findings, those with respect to emotional health stand out. In response to those results, emotional well-being has been incorporated into standards of care, Ms. Funnell said. In DAWN2, slightly more patients reported experiencing ongoing emotional distress as a result of diabetes (45% vs. 43%); 14% likely had clinical depression as a result of their diagnosis.
The findings are concerning as emotional distress – feelings of anger, fear, frustration, sadness, and guilt – are among the biggest influencers of self-management. Further, diabetes-related distress has an adverse impact on outcomes, including hemoglobin A1c levels, dietary and exercise behaviors, quality of life, and depression, Ms. Funnell said.
Diabetes also affects other aspects of life: 44% of people with diabetes in DAWN2 said their finances were affected, 38% said leisure activities were affected, 35% said that work and studies were affected, and 21% reported problems with family and peer relationships.
"We have to address diabetes-related distress if we want our patients to make changes and improve their outcomes," she said.
Notably, 52% of health care providers in DAWN2 reported asking patients how their life was affected by diabetes, yet only 24% of patients said their health care provider asked them that question.
"If I was going to do a one-question educational assessment, that would be the question [I would ask] because that tells pretty much all I need to know to work with that person," Ms. Funnell said.
Other findings from DAWN2 included the following:
• Family members of diabetes patients are burdened by the disease as well; 39% said they wanted to be more involved and 37% said they didn’t know how to be more involved.
• Most people with diabetes said that they want to be actively engaged and to participate in their care, but most aren’t.
• Half of the respondents with diabetes had never participated in a diabetes education program.
• Health care providers report a desire for more training in many aspects of diabetes care.
• Discrimination because of diabetes was reported by 19% of patients, implying a lack of awareness about diabetes.
An analysis of U.S.-only data from DAWN2 also shed light on important issues related to diabetes care and self-management.
The more than 500 U.S. respondents with diabetes in the DAWN2 study reported following a healthy eating plan for a mean of 4.7 days per week. They participated in at least 30 minutes of physical activity on a mean of 2.7 days per week and 65% expressed a desire to improve on this measure. Patients tested their blood sugar levels as recommended by their health care provider a mean of 4.5 days per week and took all medication as prescribed on a mean of 6.4 days per week. They checked their feet on a mean of 4.7 days per week (Curr. Med. Res. Opin. 2014 July 31:1-39).
Adherence varied considerably by ethnic group. For example, non-Hispanic white patients had the lowest scores for physical activity, Chinese Americans had the lowest scores for testing their blood sugar as recommended, and African Americans and Hispanics had the best scores for checking their feet.
Psychological outcomes also differed by ethnicity. African Americans had the best scores and non-Hispanic whites had the worst scores for well-being, quality of life, diabetes empowerment, and diabetes impact. Hispanics had the worst scores for quality of life and diabetes distress.
The DAWN2 data for U.S. survey respondents also indicated a substantial level of distress among people with diabetes and their family members. Having a large social support network for diabetes was related to better psychosocial outcomes, but few people with diabetes let others know how they can best provide support.
Also, U.S. respondents were pleased with the level of involvement of their family in diabetes care, and they feel that family members help a great deal by listening to them when they talk about difficulties associated with living with diabetes.
Diabetes is a burden from a management and psychological perspective. Patients need to be encouraged to ask for support when it is needed, and clinicians need to recognize that family members are untapped resources for patient support as well as a group in need of support as they deal with the burdens of caring for a family member with diabetes, Ms. Funnell added.
"Finally, we absolutely have to involve the person with diabetes and their family members as equal partners when developing care solutions," she said. Family members need to be taught how to help, and patients need to be asked how diabetes is affecting their life to identify problems and set appropriate goals for solving them.
"We need to truly focus on patient-centered care. ... We really need to surround the patient with their family and their friends, their health care, their communities, their workplaces, and the larger society if they are going to be successful in their self-management. It takes a village to manage diabetes, and every one of us has a role to play to make person-centered diabetes care and patient-centered diabetes education and ongoing support the reality that it needs to be," she said.
Ms. Funnell reported serving as a board or advisory panel member for Novo Nordisk, the sponsor of DAWN2, as well as several other drug companies involved in diabetes care, and receiving grant funding from BMS Foundation.
AT AADE 14
Key clinical point: Asking patients how their life is affected by diabetes may address emotional distress and improve self-management.
Major finding: Emotional distress was reported by 45% of diabetes patients surveyed.
Data source: The DAWN2 study, which analyzed survey responses of 15,438 adults.
Disclosures: Ms. Funnell reported serving as a board or advisory panel member for Novo Nordisk, the sponsor of DAWN2, as well as several other drug companies involved in diabetes care.
A low-fat vegan diet may lessen diabetic neuropathy pain
ORLANDO – A low-fat vegan diet reduced symptoms of peripheral neuropathy among patients with type 2 diabetes in the randomized, controlled Dietary Intervention for Chronic Diabetic Neuropathy Pain (DINE) study.
After 20 weeks, 17 patients who were assigned to the vegan diet group were more likely than were 18 control patients to have lost weight, to have reductions in pain scores, and to have neurologic improvements in their foot neuropathy.
The findings demonstrate "the potential of a low-fat vegan diet as a treatment for diabetic neuropathy pain," Anne E. Bunner, Ph.D., reported at the annual meeting of the American Association of Diabetes Educators. Other treatment options for diabetic neuropathy offer pain relief, but do not address the underlying nerve damage.
Support measures are needed to ensure the success of major dietary changes, said Dr. Bunner, associate director for clinical research at the Physicians Committee for Responsible Medicine, Washington, D.C.
The findings confirm those of a prior uncontrolled study (J. Nutr. Med. 1994;4:431-9) in which 81% of patients had pain relief with a low-fat, high-fiber vegan diet, Dr. Bunner said. A review of five studies involving more than 16,000 patients with type 2 diabetes showed that tight blood glucose control reduces the severity of diabetic neuropathy but does not eliminate the associated pain.
Dr. Bunner reported that the mean change scores in the diet group vs. the control group were –7.0 vs. –0.7 for body weight, –2.4 vs. –0.2 for body mass index, –9.1 vs. –0.9 for McGill Pain Questionnaire results, and 0.7 vs. –11.7 for foot conductance.
The diet group also experienced improvements in mean change scores for hemoglobin A1c (–0.8), Quality of Life score (–8.4), and Neuropathy Total Symptoms Score (–3.9), but the changes in these scores were not significantly better than those of the control group (–0.1, –4.7, –2.7, respectively).
The control group experienced greater improvements in pain as measured by a visual analogue scale (mean change scores of –1.2 and –2.1* for the diet and control groups, respectively). The change in the diet group was not statistically significant.
Patients in both groups used vitamin B12 supplements during the course of the study, which could explain the improvements in the control group, Dr. Bunner said. B12 deficiency is associated with diabetic neuropathy, but none of the patients had a B12 deficiency at baseline. It is possible that B12 may have been an active treatment or that the motivation associated with being a study participant was associated with the improvements.
Of note, 4 of 17 patients in the diet group were able to reduce the dosages of lipid-lowering medications; 1 increased the dosage. No one in the control group was able to reduce the dosages of lipid-lowering medications; 3 of 18 increased dosages. Ten of 17 diet group patients reduced the dosages of diabetes medications, and 2 of 18 controls reduced the dosages of diabetes medications.
Mean age of the study subjects was 57 years. Those assigned to the diet group were instructed to consume only plant foods, and to limit intake of oils, nuts, and fatty foods. Fat was limited to 3 g per serving or 20-30 g per day. Patients in the diet group also were advised to include 40 g/day of high-fiber foods, and to consume low–glycemic index foods. No limit was placed on portions.
The diet group participated in weekly classes involving nutrition education, social support, cooking demonstrations, and food product sampling.
Both groups used B12 supplements, and the control group was instructed to make no major dietary changes during the 20-week study.
Thirteen of 17 diet group patients were fully compliant with the vegan diet; 8 of the 13 were compliant with the low-fat instructions at both the 10- and 20-week assessment, and 3 of the 13 were compliant with the low-fat instructions at one of the two assessments. Two were fully compliant with the low-fat guidelines, but not the vegan guidelines, and two were noncompliant with both. One patient did not complete the study.
Dr. Bunner reported having no disclosures.
CORRECTED Aug 8: Improvement in pain in the control group, as measured by a visual analogue scale, was misstated in the original story. That value was –2.1.
ORLANDO – A low-fat vegan diet reduced symptoms of peripheral neuropathy among patients with type 2 diabetes in the randomized, controlled Dietary Intervention for Chronic Diabetic Neuropathy Pain (DINE) study.
After 20 weeks, 17 patients who were assigned to the vegan diet group were more likely than were 18 control patients to have lost weight, to have reductions in pain scores, and to have neurologic improvements in their foot neuropathy.
The findings demonstrate "the potential of a low-fat vegan diet as a treatment for diabetic neuropathy pain," Anne E. Bunner, Ph.D., reported at the annual meeting of the American Association of Diabetes Educators. Other treatment options for diabetic neuropathy offer pain relief, but do not address the underlying nerve damage.
Support measures are needed to ensure the success of major dietary changes, said Dr. Bunner, associate director for clinical research at the Physicians Committee for Responsible Medicine, Washington, D.C.
The findings confirm those of a prior uncontrolled study (J. Nutr. Med. 1994;4:431-9) in which 81% of patients had pain relief with a low-fat, high-fiber vegan diet, Dr. Bunner said. A review of five studies involving more than 16,000 patients with type 2 diabetes showed that tight blood glucose control reduces the severity of diabetic neuropathy but does not eliminate the associated pain.
Dr. Bunner reported that the mean change scores in the diet group vs. the control group were –7.0 vs. –0.7 for body weight, –2.4 vs. –0.2 for body mass index, –9.1 vs. –0.9 for McGill Pain Questionnaire results, and 0.7 vs. –11.7 for foot conductance.
The diet group also experienced improvements in mean change scores for hemoglobin A1c (–0.8), Quality of Life score (–8.4), and Neuropathy Total Symptoms Score (–3.9), but the changes in these scores were not significantly better than those of the control group (–0.1, –4.7, –2.7, respectively).
The control group experienced greater improvements in pain as measured by a visual analogue scale (mean change scores of –1.2 and –2.1* for the diet and control groups, respectively). The change in the diet group was not statistically significant.
Patients in both groups used vitamin B12 supplements during the course of the study, which could explain the improvements in the control group, Dr. Bunner said. B12 deficiency is associated with diabetic neuropathy, but none of the patients had a B12 deficiency at baseline. It is possible that B12 may have been an active treatment or that the motivation associated with being a study participant was associated with the improvements.
Of note, 4 of 17 patients in the diet group were able to reduce the dosages of lipid-lowering medications; 1 increased the dosage. No one in the control group was able to reduce the dosages of lipid-lowering medications; 3 of 18 increased dosages. Ten of 17 diet group patients reduced the dosages of diabetes medications, and 2 of 18 controls reduced the dosages of diabetes medications.
Mean age of the study subjects was 57 years. Those assigned to the diet group were instructed to consume only plant foods, and to limit intake of oils, nuts, and fatty foods. Fat was limited to 3 g per serving or 20-30 g per day. Patients in the diet group also were advised to include 40 g/day of high-fiber foods, and to consume low–glycemic index foods. No limit was placed on portions.
The diet group participated in weekly classes involving nutrition education, social support, cooking demonstrations, and food product sampling.
Both groups used B12 supplements, and the control group was instructed to make no major dietary changes during the 20-week study.
Thirteen of 17 diet group patients were fully compliant with the vegan diet; 8 of the 13 were compliant with the low-fat instructions at both the 10- and 20-week assessment, and 3 of the 13 were compliant with the low-fat instructions at one of the two assessments. Two were fully compliant with the low-fat guidelines, but not the vegan guidelines, and two were noncompliant with both. One patient did not complete the study.
Dr. Bunner reported having no disclosures.
CORRECTED Aug 8: Improvement in pain in the control group, as measured by a visual analogue scale, was misstated in the original story. That value was –2.1.
ORLANDO – A low-fat vegan diet reduced symptoms of peripheral neuropathy among patients with type 2 diabetes in the randomized, controlled Dietary Intervention for Chronic Diabetic Neuropathy Pain (DINE) study.
After 20 weeks, 17 patients who were assigned to the vegan diet group were more likely than were 18 control patients to have lost weight, to have reductions in pain scores, and to have neurologic improvements in their foot neuropathy.
The findings demonstrate "the potential of a low-fat vegan diet as a treatment for diabetic neuropathy pain," Anne E. Bunner, Ph.D., reported at the annual meeting of the American Association of Diabetes Educators. Other treatment options for diabetic neuropathy offer pain relief, but do not address the underlying nerve damage.
Support measures are needed to ensure the success of major dietary changes, said Dr. Bunner, associate director for clinical research at the Physicians Committee for Responsible Medicine, Washington, D.C.
The findings confirm those of a prior uncontrolled study (J. Nutr. Med. 1994;4:431-9) in which 81% of patients had pain relief with a low-fat, high-fiber vegan diet, Dr. Bunner said. A review of five studies involving more than 16,000 patients with type 2 diabetes showed that tight blood glucose control reduces the severity of diabetic neuropathy but does not eliminate the associated pain.
Dr. Bunner reported that the mean change scores in the diet group vs. the control group were –7.0 vs. –0.7 for body weight, –2.4 vs. –0.2 for body mass index, –9.1 vs. –0.9 for McGill Pain Questionnaire results, and 0.7 vs. –11.7 for foot conductance.
The diet group also experienced improvements in mean change scores for hemoglobin A1c (–0.8), Quality of Life score (–8.4), and Neuropathy Total Symptoms Score (–3.9), but the changes in these scores were not significantly better than those of the control group (–0.1, –4.7, –2.7, respectively).
The control group experienced greater improvements in pain as measured by a visual analogue scale (mean change scores of –1.2 and –2.1* for the diet and control groups, respectively). The change in the diet group was not statistically significant.
Patients in both groups used vitamin B12 supplements during the course of the study, which could explain the improvements in the control group, Dr. Bunner said. B12 deficiency is associated with diabetic neuropathy, but none of the patients had a B12 deficiency at baseline. It is possible that B12 may have been an active treatment or that the motivation associated with being a study participant was associated with the improvements.
Of note, 4 of 17 patients in the diet group were able to reduce the dosages of lipid-lowering medications; 1 increased the dosage. No one in the control group was able to reduce the dosages of lipid-lowering medications; 3 of 18 increased dosages. Ten of 17 diet group patients reduced the dosages of diabetes medications, and 2 of 18 controls reduced the dosages of diabetes medications.
Mean age of the study subjects was 57 years. Those assigned to the diet group were instructed to consume only plant foods, and to limit intake of oils, nuts, and fatty foods. Fat was limited to 3 g per serving or 20-30 g per day. Patients in the diet group also were advised to include 40 g/day of high-fiber foods, and to consume low–glycemic index foods. No limit was placed on portions.
The diet group participated in weekly classes involving nutrition education, social support, cooking demonstrations, and food product sampling.
Both groups used B12 supplements, and the control group was instructed to make no major dietary changes during the 20-week study.
Thirteen of 17 diet group patients were fully compliant with the vegan diet; 8 of the 13 were compliant with the low-fat instructions at both the 10- and 20-week assessment, and 3 of the 13 were compliant with the low-fat instructions at one of the two assessments. Two were fully compliant with the low-fat guidelines, but not the vegan guidelines, and two were noncompliant with both. One patient did not complete the study.
Dr. Bunner reported having no disclosures.
CORRECTED Aug 8: Improvement in pain in the control group, as measured by a visual analogue scale, was misstated in the original story. That value was –2.1.
AT AADE 14
Key clinical point: Following a vegan diet might relieve neuropathy pain in patients with type 2 diabetes.
Major finding: After 20 weeks, mean change scores on the McGill Pain Questionnaire were –9.1 for the vegan diet group vs. –0.9 for the control group.
Data source: The randomized, controlled DINE study of 35 patients.
Disclosures: Dr. Bunner reported having no disclosures.
Findings support endovascular-first approach for ruptured VAAs
BOSTON – Endovascular interventions for ruptured visceral artery aneurysms are associated with reduced morbidity and mortality, compared with open interventions, according to findings from a retrospective chart review.
Both endovascular and open repairs are safe and durable for intact visceral artery aneurysms, Dr. Ankur J. Shukla reported at a the 2014 Vascular Annual Meeting.
Of 261 patients who presented with visceral artery aneurysms (VAAs), 174 underwent repair: 74 who presented with ruptured VAA and 100 who presented with intact VAA. The majority – 73% of ruptured VAA and 62% of intact VAA – were repaired with an endovascular approach.
Among those with ruptured VAA, 30-day mortality was 7.4% following endovascular repair, compared with 28.6% following open repair, a significant difference, said Dr. Shukla of the University of Pittsburgh Medical Center.
Survival at 3 years of ruptured VAA was about 70% vs. 46.4% in the endovascular and open repair groups, respectively, he said.
About 65% of patients with ruptured VAA presented with pain, and about 30% presented in hemodynamic shock. The most commonly identified etiology was "inflammatory/pancreatitis inflammatory," and 80% of the aneurysms were pseudoaneurysmal in nature.
A large proportion of the aneurysms were in the splenic and arterial beds, but 26% were located in the pancreaticoduodenal arcade, and those had a mean size of 12.7 mm. Most (95%) were pseudoaneurysms.
The outcomes with ruptured VAA were quite good, Dr. Shukla said, noting that the technical success rate was 98.7%.
Although the 30-day reintervention rate with endovascular repair was higher, the difference between the groups was not statistically significant, and there was a trend toward a lower rate of major complications with endovascular repair.
Factors found to be predictors of mortality risk were older age and steroid use, while endovascular repair was found to be protective.
As for the patients with intact VAA, most presented without symptoms, and the most common etiology was atherosclerosis.
"When we looked at the distribution, this was very consistent with what has been reported in the literature, with the splenic and arterial beds really making up the lion’s share of this group. Notable is the fact that 6.7% of our patients had intact aneurysms in the pancreaticoduodenal arcade," he said.
Outcomes in those with intact aneurysms were good. A slightly higher 30-day reintervention rate in those who underwent endovascular repair did not reach statistical significance, and both the endovascular and open repair groups had low rates of major complications.
Survival at 3 years for intact aneurysms did not differ in the endovascular and open repair groups. This was partly due to a 0% 30-day mortality, and – despite the fact that the overall mortality in those with intact aneurysms was 10% – there was zero overall aneurysm-related mortality, he said.
Patients in the study were treated at a single institution between 2003 and 2013. Most were in their mid to late 50s, and there were more men and more individuals on immunosuppressive therapy in the ruptured VAA group. However, comorbidities were similar in the ruptured and intact VAA groups.
Visceral artery aneurysms occur only rarely, affecting 0.1% to 2% of the general population, but because of the increasing use of noninvasive imaging, more of these aneurysms are being detected incidentally.
When they are not found incidentally, they often go undetected and present when they rupture, Dr. Shukla said.
"Because of the increasing utilization and improvement of endovascular technology, we now have a lot of options to fix these aneurysms. But the outcomes are not well defined. Even less well defined is the outcome of ruptured visceral artery aneurysms," he said, noting that most studies have a small sample size or look only at endovascular or open repairs.
Overall, the current study showed that there is "an acute and sharp drop-off in survival with open repair," related, most likely, to operative mortality, he said.
"Based on the findings, we recommend aggressive treatment of pseudoaneurysms and true aneurysms in the pancreaticoduodenal arcade, and advocate for an endovascular-first approach to treating ruptured visceral artery aneurysms, acknowledging that success in this is really predicated on good planning based on advanced imaging and endovascular set-up," he concluded.
Dr. Shukla reported having no disclosures
Visceral Artery Aneurysms (VAA) can be challenging to treat from an open approach especially when the aneurysm is adherent to the surrounding pancreatic, visceral or retroperitoneal tissue. In most areas of vascular disease endovascular therapy is easier. But, endovascular therapy for VAA can be as challenging as the open surgical repair because of vessel tortuosity and access, imaging challenges, and the few options available for durable aneurysm treatment. Dr. Shukla and colleagues reviewed their outcomes in treating VAA over a 10-year period and report high rates of technical success, low morbidity and mortality using endovascular means for both intact and ruptured VAA. The results for endovascular therapy for ruptured VAA were particularly promising. These results indicate that coils and other ablative maneuvers may suffice in the setting of hemorrhage and be preferable to open surgical repair or ligation. This study provides important information on a rare problem and reassures us that the mid-term durability of ablative techniques for VAA is acceptable.
Dr. Vikram Kashyap is professor of surgery, Case Western Reserve University and chief, Division of Vascular Surgery and Endovascular Therapy, and co-director, Harrington Heart & Vascular Institute, University Hospitals Case Medical Center,Cleveland.
Visceral Artery Aneurysms (VAA) can be challenging to treat from an open approach especially when the aneurysm is adherent to the surrounding pancreatic, visceral or retroperitoneal tissue. In most areas of vascular disease endovascular therapy is easier. But, endovascular therapy for VAA can be as challenging as the open surgical repair because of vessel tortuosity and access, imaging challenges, and the few options available for durable aneurysm treatment. Dr. Shukla and colleagues reviewed their outcomes in treating VAA over a 10-year period and report high rates of technical success, low morbidity and mortality using endovascular means for both intact and ruptured VAA. The results for endovascular therapy for ruptured VAA were particularly promising. These results indicate that coils and other ablative maneuvers may suffice in the setting of hemorrhage and be preferable to open surgical repair or ligation. This study provides important information on a rare problem and reassures us that the mid-term durability of ablative techniques for VAA is acceptable.
Dr. Vikram Kashyap is professor of surgery, Case Western Reserve University and chief, Division of Vascular Surgery and Endovascular Therapy, and co-director, Harrington Heart & Vascular Institute, University Hospitals Case Medical Center,Cleveland.
Visceral Artery Aneurysms (VAA) can be challenging to treat from an open approach especially when the aneurysm is adherent to the surrounding pancreatic, visceral or retroperitoneal tissue. In most areas of vascular disease endovascular therapy is easier. But, endovascular therapy for VAA can be as challenging as the open surgical repair because of vessel tortuosity and access, imaging challenges, and the few options available for durable aneurysm treatment. Dr. Shukla and colleagues reviewed their outcomes in treating VAA over a 10-year period and report high rates of technical success, low morbidity and mortality using endovascular means for both intact and ruptured VAA. The results for endovascular therapy for ruptured VAA were particularly promising. These results indicate that coils and other ablative maneuvers may suffice in the setting of hemorrhage and be preferable to open surgical repair or ligation. This study provides important information on a rare problem and reassures us that the mid-term durability of ablative techniques for VAA is acceptable.
Dr. Vikram Kashyap is professor of surgery, Case Western Reserve University and chief, Division of Vascular Surgery and Endovascular Therapy, and co-director, Harrington Heart & Vascular Institute, University Hospitals Case Medical Center,Cleveland.
BOSTON – Endovascular interventions for ruptured visceral artery aneurysms are associated with reduced morbidity and mortality, compared with open interventions, according to findings from a retrospective chart review.
Both endovascular and open repairs are safe and durable for intact visceral artery aneurysms, Dr. Ankur J. Shukla reported at a the 2014 Vascular Annual Meeting.
Of 261 patients who presented with visceral artery aneurysms (VAAs), 174 underwent repair: 74 who presented with ruptured VAA and 100 who presented with intact VAA. The majority – 73% of ruptured VAA and 62% of intact VAA – were repaired with an endovascular approach.
Among those with ruptured VAA, 30-day mortality was 7.4% following endovascular repair, compared with 28.6% following open repair, a significant difference, said Dr. Shukla of the University of Pittsburgh Medical Center.
Survival at 3 years of ruptured VAA was about 70% vs. 46.4% in the endovascular and open repair groups, respectively, he said.
About 65% of patients with ruptured VAA presented with pain, and about 30% presented in hemodynamic shock. The most commonly identified etiology was "inflammatory/pancreatitis inflammatory," and 80% of the aneurysms were pseudoaneurysmal in nature.
A large proportion of the aneurysms were in the splenic and arterial beds, but 26% were located in the pancreaticoduodenal arcade, and those had a mean size of 12.7 mm. Most (95%) were pseudoaneurysms.
The outcomes with ruptured VAA were quite good, Dr. Shukla said, noting that the technical success rate was 98.7%.
Although the 30-day reintervention rate with endovascular repair was higher, the difference between the groups was not statistically significant, and there was a trend toward a lower rate of major complications with endovascular repair.
Factors found to be predictors of mortality risk were older age and steroid use, while endovascular repair was found to be protective.
As for the patients with intact VAA, most presented without symptoms, and the most common etiology was atherosclerosis.
"When we looked at the distribution, this was very consistent with what has been reported in the literature, with the splenic and arterial beds really making up the lion’s share of this group. Notable is the fact that 6.7% of our patients had intact aneurysms in the pancreaticoduodenal arcade," he said.
Outcomes in those with intact aneurysms were good. A slightly higher 30-day reintervention rate in those who underwent endovascular repair did not reach statistical significance, and both the endovascular and open repair groups had low rates of major complications.
Survival at 3 years for intact aneurysms did not differ in the endovascular and open repair groups. This was partly due to a 0% 30-day mortality, and – despite the fact that the overall mortality in those with intact aneurysms was 10% – there was zero overall aneurysm-related mortality, he said.
Patients in the study were treated at a single institution between 2003 and 2013. Most were in their mid to late 50s, and there were more men and more individuals on immunosuppressive therapy in the ruptured VAA group. However, comorbidities were similar in the ruptured and intact VAA groups.
Visceral artery aneurysms occur only rarely, affecting 0.1% to 2% of the general population, but because of the increasing use of noninvasive imaging, more of these aneurysms are being detected incidentally.
When they are not found incidentally, they often go undetected and present when they rupture, Dr. Shukla said.
"Because of the increasing utilization and improvement of endovascular technology, we now have a lot of options to fix these aneurysms. But the outcomes are not well defined. Even less well defined is the outcome of ruptured visceral artery aneurysms," he said, noting that most studies have a small sample size or look only at endovascular or open repairs.
Overall, the current study showed that there is "an acute and sharp drop-off in survival with open repair," related, most likely, to operative mortality, he said.
"Based on the findings, we recommend aggressive treatment of pseudoaneurysms and true aneurysms in the pancreaticoduodenal arcade, and advocate for an endovascular-first approach to treating ruptured visceral artery aneurysms, acknowledging that success in this is really predicated on good planning based on advanced imaging and endovascular set-up," he concluded.
Dr. Shukla reported having no disclosures
BOSTON – Endovascular interventions for ruptured visceral artery aneurysms are associated with reduced morbidity and mortality, compared with open interventions, according to findings from a retrospective chart review.
Both endovascular and open repairs are safe and durable for intact visceral artery aneurysms, Dr. Ankur J. Shukla reported at a the 2014 Vascular Annual Meeting.
Of 261 patients who presented with visceral artery aneurysms (VAAs), 174 underwent repair: 74 who presented with ruptured VAA and 100 who presented with intact VAA. The majority – 73% of ruptured VAA and 62% of intact VAA – were repaired with an endovascular approach.
Among those with ruptured VAA, 30-day mortality was 7.4% following endovascular repair, compared with 28.6% following open repair, a significant difference, said Dr. Shukla of the University of Pittsburgh Medical Center.
Survival at 3 years of ruptured VAA was about 70% vs. 46.4% in the endovascular and open repair groups, respectively, he said.
About 65% of patients with ruptured VAA presented with pain, and about 30% presented in hemodynamic shock. The most commonly identified etiology was "inflammatory/pancreatitis inflammatory," and 80% of the aneurysms were pseudoaneurysmal in nature.
A large proportion of the aneurysms were in the splenic and arterial beds, but 26% were located in the pancreaticoduodenal arcade, and those had a mean size of 12.7 mm. Most (95%) were pseudoaneurysms.
The outcomes with ruptured VAA were quite good, Dr. Shukla said, noting that the technical success rate was 98.7%.
Although the 30-day reintervention rate with endovascular repair was higher, the difference between the groups was not statistically significant, and there was a trend toward a lower rate of major complications with endovascular repair.
Factors found to be predictors of mortality risk were older age and steroid use, while endovascular repair was found to be protective.
As for the patients with intact VAA, most presented without symptoms, and the most common etiology was atherosclerosis.
"When we looked at the distribution, this was very consistent with what has been reported in the literature, with the splenic and arterial beds really making up the lion’s share of this group. Notable is the fact that 6.7% of our patients had intact aneurysms in the pancreaticoduodenal arcade," he said.
Outcomes in those with intact aneurysms were good. A slightly higher 30-day reintervention rate in those who underwent endovascular repair did not reach statistical significance, and both the endovascular and open repair groups had low rates of major complications.
Survival at 3 years for intact aneurysms did not differ in the endovascular and open repair groups. This was partly due to a 0% 30-day mortality, and – despite the fact that the overall mortality in those with intact aneurysms was 10% – there was zero overall aneurysm-related mortality, he said.
Patients in the study were treated at a single institution between 2003 and 2013. Most were in their mid to late 50s, and there were more men and more individuals on immunosuppressive therapy in the ruptured VAA group. However, comorbidities were similar in the ruptured and intact VAA groups.
Visceral artery aneurysms occur only rarely, affecting 0.1% to 2% of the general population, but because of the increasing use of noninvasive imaging, more of these aneurysms are being detected incidentally.
When they are not found incidentally, they often go undetected and present when they rupture, Dr. Shukla said.
"Because of the increasing utilization and improvement of endovascular technology, we now have a lot of options to fix these aneurysms. But the outcomes are not well defined. Even less well defined is the outcome of ruptured visceral artery aneurysms," he said, noting that most studies have a small sample size or look only at endovascular or open repairs.
Overall, the current study showed that there is "an acute and sharp drop-off in survival with open repair," related, most likely, to operative mortality, he said.
"Based on the findings, we recommend aggressive treatment of pseudoaneurysms and true aneurysms in the pancreaticoduodenal arcade, and advocate for an endovascular-first approach to treating ruptured visceral artery aneurysms, acknowledging that success in this is really predicated on good planning based on advanced imaging and endovascular set-up," he concluded.
Dr. Shukla reported having no disclosures
AT THE 2014 VASCULAR ANNUAL MEETING
Key clinical point: The researchers recommend aggressive treatment of visceral artery pseudoaneurysms and true aneurysms, with an endovascular-first approach to treating ruptured aneurysms.
Major finding: Thirty-day mortality was 7.4% vs. 26% with endovascular vs. open repair of ruptured VAAs.
Data source: A retrospective chart review involving 174 cases.
Disclosures: Dr. Shukla reported having no disclosures.
Data increasingly support plant-based diet for diabetes prevention, care
ORLANDO – Evidence increasingly supports plant-based nutrition for preventing diabetes or improving outcomes in those with diabetes.
The Adventist Health Study-2 (AHS-2), for example, demonstrated that a plant-based eating pattern – defined as ad libitum whole grains, legumes, fruits, and vegetables, and avoidance of all animal products, added oils, and high-fat foods – reduced the incidence of type 2 diabetes. The prospective cohort study involving more than 96,000 adults demonstrated that body mass index and the incidence of diabetes increased in tandem with the amount of animal products in the diet, according to Meghan Jardine, who reviewed the recent literature on plant-based nutrition in a poster presented at the annual meeting of the American Association of Diabetes Educators.
The prevalence of type 2 diabetes among nonvegetarians, semivegetarians, pescovegetarians, lacto-ovovegetarians, and vegans in that study was 7.6%, 6.1%, 4.9%, 3.2%, and 2.9%, respectively, and BMI for each of those groups was 28.8, 27.3, 26.3, 25.7, and 23.6 kg/m2, respectively, said Ms. Jardine, a registered and licensed dietician, certified diabetes educator, and diabetes education coordinator at Parkland Health and Hospital System, Dallas.
AHS-2 also demonstrated increased longevity in those who followed a plant-based eating pattern, with men living 9.5 years longer and women living 6.1 years longer than their meat-eating counterparts (JAMA 2013;173:1230-8).
In addition, a National Institutes of Health study demonstrated that a low-fat vegan diet led to significantly greater improvements in glycemic and lipid control than did a conventional diabetes diet in patients with type 2 diabetes.
Hemoglobin A1c levels in 49 patients on the low-fat vegan diet improved from 8.06 to 7.65 at 74 weeks, but while the levels in 50 patients on the conventional diabetes diet initially improved from 7.93 to about 7.7 at 11 weeks, at 74 weeks they had increased to 7.94 (Diabetes Care 2006;29:1777-83).
Among the other findings that Ms. Jardine mentioned were those from "a remarkable study" in which 17 of 21 patients with sharp, burning pain characteristic of distal polyneuropathy experienced complete pain relief after initiating a low-fat, high-fiber, vegan diet along with a daily 30-minute walk, and findings from several studies that have suggested that plant-based eating preserved renal function.
Moreover, a plant-based eating pattern has been shown to reverse coronary artery disease and improve magnesium intake (which reduces insulin resistance), and the high fiber intake associated with plant-based eating improves glucose control and decreases mortality from circulatory, digestive, and inflammatory disease, she said.
Two recent studies demonstrated that meat consumption substantially increases the risk of type 2 diabetes. Even just a half serving per day increase was associated with a 48% increase over 4 years in one study (JAMA Intern. Med. 2013;173:1328-35).
Ms. Jardine noted that the Academy of Nutrition and Dietetics position is that "appropriately planned vegetarian diets, including total vegetarian or vegan diets, are healthful, nutritionally adequate and may provide health benefits in the prevention and treatment of certain disease," and that such diets have been found to be "highly acceptable in diverse populations with various disease states" (Diabetes Educ. 2010:36:33-48).
She warned that patients with diabetes who are on medications and who begin to follow a plant-based eating pattern should be instructed about how to recognize and treat hypoglycemia, as adjustments to medications that lower glucose, blood pressure, and cholesterol may be needed.
ORLANDO – Evidence increasingly supports plant-based nutrition for preventing diabetes or improving outcomes in those with diabetes.
The Adventist Health Study-2 (AHS-2), for example, demonstrated that a plant-based eating pattern – defined as ad libitum whole grains, legumes, fruits, and vegetables, and avoidance of all animal products, added oils, and high-fat foods – reduced the incidence of type 2 diabetes. The prospective cohort study involving more than 96,000 adults demonstrated that body mass index and the incidence of diabetes increased in tandem with the amount of animal products in the diet, according to Meghan Jardine, who reviewed the recent literature on plant-based nutrition in a poster presented at the annual meeting of the American Association of Diabetes Educators.
The prevalence of type 2 diabetes among nonvegetarians, semivegetarians, pescovegetarians, lacto-ovovegetarians, and vegans in that study was 7.6%, 6.1%, 4.9%, 3.2%, and 2.9%, respectively, and BMI for each of those groups was 28.8, 27.3, 26.3, 25.7, and 23.6 kg/m2, respectively, said Ms. Jardine, a registered and licensed dietician, certified diabetes educator, and diabetes education coordinator at Parkland Health and Hospital System, Dallas.
AHS-2 also demonstrated increased longevity in those who followed a plant-based eating pattern, with men living 9.5 years longer and women living 6.1 years longer than their meat-eating counterparts (JAMA 2013;173:1230-8).
In addition, a National Institutes of Health study demonstrated that a low-fat vegan diet led to significantly greater improvements in glycemic and lipid control than did a conventional diabetes diet in patients with type 2 diabetes.
Hemoglobin A1c levels in 49 patients on the low-fat vegan diet improved from 8.06 to 7.65 at 74 weeks, but while the levels in 50 patients on the conventional diabetes diet initially improved from 7.93 to about 7.7 at 11 weeks, at 74 weeks they had increased to 7.94 (Diabetes Care 2006;29:1777-83).
Among the other findings that Ms. Jardine mentioned were those from "a remarkable study" in which 17 of 21 patients with sharp, burning pain characteristic of distal polyneuropathy experienced complete pain relief after initiating a low-fat, high-fiber, vegan diet along with a daily 30-minute walk, and findings from several studies that have suggested that plant-based eating preserved renal function.
Moreover, a plant-based eating pattern has been shown to reverse coronary artery disease and improve magnesium intake (which reduces insulin resistance), and the high fiber intake associated with plant-based eating improves glucose control and decreases mortality from circulatory, digestive, and inflammatory disease, she said.
Two recent studies demonstrated that meat consumption substantially increases the risk of type 2 diabetes. Even just a half serving per day increase was associated with a 48% increase over 4 years in one study (JAMA Intern. Med. 2013;173:1328-35).
Ms. Jardine noted that the Academy of Nutrition and Dietetics position is that "appropriately planned vegetarian diets, including total vegetarian or vegan diets, are healthful, nutritionally adequate and may provide health benefits in the prevention and treatment of certain disease," and that such diets have been found to be "highly acceptable in diverse populations with various disease states" (Diabetes Educ. 2010:36:33-48).
She warned that patients with diabetes who are on medications and who begin to follow a plant-based eating pattern should be instructed about how to recognize and treat hypoglycemia, as adjustments to medications that lower glucose, blood pressure, and cholesterol may be needed.
ORLANDO – Evidence increasingly supports plant-based nutrition for preventing diabetes or improving outcomes in those with diabetes.
The Adventist Health Study-2 (AHS-2), for example, demonstrated that a plant-based eating pattern – defined as ad libitum whole grains, legumes, fruits, and vegetables, and avoidance of all animal products, added oils, and high-fat foods – reduced the incidence of type 2 diabetes. The prospective cohort study involving more than 96,000 adults demonstrated that body mass index and the incidence of diabetes increased in tandem with the amount of animal products in the diet, according to Meghan Jardine, who reviewed the recent literature on plant-based nutrition in a poster presented at the annual meeting of the American Association of Diabetes Educators.
The prevalence of type 2 diabetes among nonvegetarians, semivegetarians, pescovegetarians, lacto-ovovegetarians, and vegans in that study was 7.6%, 6.1%, 4.9%, 3.2%, and 2.9%, respectively, and BMI for each of those groups was 28.8, 27.3, 26.3, 25.7, and 23.6 kg/m2, respectively, said Ms. Jardine, a registered and licensed dietician, certified diabetes educator, and diabetes education coordinator at Parkland Health and Hospital System, Dallas.
AHS-2 also demonstrated increased longevity in those who followed a plant-based eating pattern, with men living 9.5 years longer and women living 6.1 years longer than their meat-eating counterparts (JAMA 2013;173:1230-8).
In addition, a National Institutes of Health study demonstrated that a low-fat vegan diet led to significantly greater improvements in glycemic and lipid control than did a conventional diabetes diet in patients with type 2 diabetes.
Hemoglobin A1c levels in 49 patients on the low-fat vegan diet improved from 8.06 to 7.65 at 74 weeks, but while the levels in 50 patients on the conventional diabetes diet initially improved from 7.93 to about 7.7 at 11 weeks, at 74 weeks they had increased to 7.94 (Diabetes Care 2006;29:1777-83).
Among the other findings that Ms. Jardine mentioned were those from "a remarkable study" in which 17 of 21 patients with sharp, burning pain characteristic of distal polyneuropathy experienced complete pain relief after initiating a low-fat, high-fiber, vegan diet along with a daily 30-minute walk, and findings from several studies that have suggested that plant-based eating preserved renal function.
Moreover, a plant-based eating pattern has been shown to reverse coronary artery disease and improve magnesium intake (which reduces insulin resistance), and the high fiber intake associated with plant-based eating improves glucose control and decreases mortality from circulatory, digestive, and inflammatory disease, she said.
Two recent studies demonstrated that meat consumption substantially increases the risk of type 2 diabetes. Even just a half serving per day increase was associated with a 48% increase over 4 years in one study (JAMA Intern. Med. 2013;173:1328-35).
Ms. Jardine noted that the Academy of Nutrition and Dietetics position is that "appropriately planned vegetarian diets, including total vegetarian or vegan diets, are healthful, nutritionally adequate and may provide health benefits in the prevention and treatment of certain disease," and that such diets have been found to be "highly acceptable in diverse populations with various disease states" (Diabetes Educ. 2010:36:33-48).
She warned that patients with diabetes who are on medications and who begin to follow a plant-based eating pattern should be instructed about how to recognize and treat hypoglycemia, as adjustments to medications that lower glucose, blood pressure, and cholesterol may be needed.
AT AADE 14
Key clinical point: Vegan diets help.
Major finding: Longevity was increased in men (by 9.5 years) and women (by 6.1 years) with a plant- vs. meat-based diet in one study.
Data source: A review of the literature on plant-based nutrition.
Disclosures: Ms. Jardine reported having no disclosures.
Patient decision aid eases diabetes treatment choices
ORLANDO – A new online tool designed to guide patients who had inadequately controlled type 2 diabetes in making decisions about their self-care got high marks from users during pilot clinical testing.
The patient decision aid (PDA), which was developed with input from patients, clinicians, and an expert panel using a process guided by the International Patient Decision Aid Standards (IPDAS) Collaboration, received an average survey score of 73.31 out of 100 for preparing users for decision making, based on post-test responses from 10 patients. Decision self-efficacy survey scores improved from 84.32 at baseline to 94.32 post test, knowledge (about diabetes and treatment) scores improved from 56.41 to 74.00, and decisional conflict scores improved from 47.32 to 29.11, Alicia C. Shillington, Ph.D., R.N., reported in a poster at the annual meeting of the American Association of Diabetes Educators.
Two-week post-test scores for knowledge and decisional conflict showed sustained benefit, with slight improvement to 74.90 and 26.79, respectively, according to Dr. Shillington of EPI-Q Inc., Oak Brook, Ill.
The final PDA was first tested in two patient focus groups, then in the 10 patients in the pilot study. The patients had type 2 diabetes and were taking metformin. They were evaluated prior to receiving the PDA, immediately after, and again at a 2-week follow-up.
All clinicians who tested the PDA endorsed it, and the vast majority (90%-100% on all measures) said the PDA could help facilitate key aspects of shared decision making (SDM). For example, they said the PDA could help patients understand the risks and benefits of adding a second diabetic medication, identify the importance patients place on those risks and benefits, prepare for the follow-up consultation visit, be involved in decision making as much as they desire, and make more informed decisions.
In addition, the PDA could help clinicians understand the issues that are most important to the patient, tailor counseling to patient preferences for decision participation, positively facilitate the follow-up consultation, positively affect the patient-physician relationship, improve the way time is spent during the follow-up consultation visit, and improve the quality of the follow-up consultation visit.
PDAs are SDM tools that can help patients make treatment choices that are consistent with their values and preferences, Dr. Shillington said, noting that the American Diabetes Association "embraces SDM in selecting antihyperglycemic treatment."
The new PDA, which achieved the highest quality rating from the IPDAS, includes an introduction that covers the reason patients have reached a particular decision point (for example, they are not achieving adequate glycemic control with metformin and lifestyle changes). Next, patients are presented with their options, including various benefits and side effects for different medications.
Patients can then provide feedback via questionnaires that allow them to communicate long-term goals and the relative importance of factors such as the degree of blood sugar reduction, avoiding blood glucose lability, maintaining or losing weight, achieving a convenient dosing schedule, and avoiding injections. Responses on this section are available to clinicians.
Finally, a summary is provided, including a fact sheet that reiterates the risks and benefits of each class of medication in a balanced and unbiased manner; and an option is given for the patient to print the information.
The PDA is currently being evaluated in a randomized controlled validation study involving 220 patients. A Spanish version has also been developed and is in testing to expand access, Dr. Shillington said.
"PDAs for type 2 diabetes mellitus can potentially promote patient-centered care and improve self-management behaviors. Access to high-quality, well-developed SDM tools is needed and may improve the quality of care and better align care with individual patient values," she concluded.
Dr. Shillington reported having no disclosures.
ORLANDO – A new online tool designed to guide patients who had inadequately controlled type 2 diabetes in making decisions about their self-care got high marks from users during pilot clinical testing.
The patient decision aid (PDA), which was developed with input from patients, clinicians, and an expert panel using a process guided by the International Patient Decision Aid Standards (IPDAS) Collaboration, received an average survey score of 73.31 out of 100 for preparing users for decision making, based on post-test responses from 10 patients. Decision self-efficacy survey scores improved from 84.32 at baseline to 94.32 post test, knowledge (about diabetes and treatment) scores improved from 56.41 to 74.00, and decisional conflict scores improved from 47.32 to 29.11, Alicia C. Shillington, Ph.D., R.N., reported in a poster at the annual meeting of the American Association of Diabetes Educators.
Two-week post-test scores for knowledge and decisional conflict showed sustained benefit, with slight improvement to 74.90 and 26.79, respectively, according to Dr. Shillington of EPI-Q Inc., Oak Brook, Ill.
The final PDA was first tested in two patient focus groups, then in the 10 patients in the pilot study. The patients had type 2 diabetes and were taking metformin. They were evaluated prior to receiving the PDA, immediately after, and again at a 2-week follow-up.
All clinicians who tested the PDA endorsed it, and the vast majority (90%-100% on all measures) said the PDA could help facilitate key aspects of shared decision making (SDM). For example, they said the PDA could help patients understand the risks and benefits of adding a second diabetic medication, identify the importance patients place on those risks and benefits, prepare for the follow-up consultation visit, be involved in decision making as much as they desire, and make more informed decisions.
In addition, the PDA could help clinicians understand the issues that are most important to the patient, tailor counseling to patient preferences for decision participation, positively facilitate the follow-up consultation, positively affect the patient-physician relationship, improve the way time is spent during the follow-up consultation visit, and improve the quality of the follow-up consultation visit.
PDAs are SDM tools that can help patients make treatment choices that are consistent with their values and preferences, Dr. Shillington said, noting that the American Diabetes Association "embraces SDM in selecting antihyperglycemic treatment."
The new PDA, which achieved the highest quality rating from the IPDAS, includes an introduction that covers the reason patients have reached a particular decision point (for example, they are not achieving adequate glycemic control with metformin and lifestyle changes). Next, patients are presented with their options, including various benefits and side effects for different medications.
Patients can then provide feedback via questionnaires that allow them to communicate long-term goals and the relative importance of factors such as the degree of blood sugar reduction, avoiding blood glucose lability, maintaining or losing weight, achieving a convenient dosing schedule, and avoiding injections. Responses on this section are available to clinicians.
Finally, a summary is provided, including a fact sheet that reiterates the risks and benefits of each class of medication in a balanced and unbiased manner; and an option is given for the patient to print the information.
The PDA is currently being evaluated in a randomized controlled validation study involving 220 patients. A Spanish version has also been developed and is in testing to expand access, Dr. Shillington said.
"PDAs for type 2 diabetes mellitus can potentially promote patient-centered care and improve self-management behaviors. Access to high-quality, well-developed SDM tools is needed and may improve the quality of care and better align care with individual patient values," she concluded.
Dr. Shillington reported having no disclosures.
ORLANDO – A new online tool designed to guide patients who had inadequately controlled type 2 diabetes in making decisions about their self-care got high marks from users during pilot clinical testing.
The patient decision aid (PDA), which was developed with input from patients, clinicians, and an expert panel using a process guided by the International Patient Decision Aid Standards (IPDAS) Collaboration, received an average survey score of 73.31 out of 100 for preparing users for decision making, based on post-test responses from 10 patients. Decision self-efficacy survey scores improved from 84.32 at baseline to 94.32 post test, knowledge (about diabetes and treatment) scores improved from 56.41 to 74.00, and decisional conflict scores improved from 47.32 to 29.11, Alicia C. Shillington, Ph.D., R.N., reported in a poster at the annual meeting of the American Association of Diabetes Educators.
Two-week post-test scores for knowledge and decisional conflict showed sustained benefit, with slight improvement to 74.90 and 26.79, respectively, according to Dr. Shillington of EPI-Q Inc., Oak Brook, Ill.
The final PDA was first tested in two patient focus groups, then in the 10 patients in the pilot study. The patients had type 2 diabetes and were taking metformin. They were evaluated prior to receiving the PDA, immediately after, and again at a 2-week follow-up.
All clinicians who tested the PDA endorsed it, and the vast majority (90%-100% on all measures) said the PDA could help facilitate key aspects of shared decision making (SDM). For example, they said the PDA could help patients understand the risks and benefits of adding a second diabetic medication, identify the importance patients place on those risks and benefits, prepare for the follow-up consultation visit, be involved in decision making as much as they desire, and make more informed decisions.
In addition, the PDA could help clinicians understand the issues that are most important to the patient, tailor counseling to patient preferences for decision participation, positively facilitate the follow-up consultation, positively affect the patient-physician relationship, improve the way time is spent during the follow-up consultation visit, and improve the quality of the follow-up consultation visit.
PDAs are SDM tools that can help patients make treatment choices that are consistent with their values and preferences, Dr. Shillington said, noting that the American Diabetes Association "embraces SDM in selecting antihyperglycemic treatment."
The new PDA, which achieved the highest quality rating from the IPDAS, includes an introduction that covers the reason patients have reached a particular decision point (for example, they are not achieving adequate glycemic control with metformin and lifestyle changes). Next, patients are presented with their options, including various benefits and side effects for different medications.
Patients can then provide feedback via questionnaires that allow them to communicate long-term goals and the relative importance of factors such as the degree of blood sugar reduction, avoiding blood glucose lability, maintaining or losing weight, achieving a convenient dosing schedule, and avoiding injections. Responses on this section are available to clinicians.
Finally, a summary is provided, including a fact sheet that reiterates the risks and benefits of each class of medication in a balanced and unbiased manner; and an option is given for the patient to print the information.
The PDA is currently being evaluated in a randomized controlled validation study involving 220 patients. A Spanish version has also been developed and is in testing to expand access, Dr. Shillington said.
"PDAs for type 2 diabetes mellitus can potentially promote patient-centered care and improve self-management behaviors. Access to high-quality, well-developed SDM tools is needed and may improve the quality of care and better align care with individual patient values," she concluded.
Dr. Shillington reported having no disclosures.
AT AADE 14
Attention to risk factors could reduce CAP-related emergency revisits
LAKE BUENA VISTA, FLA. – Fever or lack of an antibiotic prescription are two factors that increase the risk of a return visit to the emergency department and subsequent hospital admission in children with community-acquired pneumonia, according to a review of ED medical records.
Of 1,857 children aged 3 months to 18 years with a diagnosis of pneumonia who were discharged to home after the index ED visit between November 2009 and April 2013, 131 (7.1%) returned to the ED within 7 days, 90 of those (4.8%) were discharged to home, and 41 (2.2%) were admitted, Dr. Emily Fain of Cincinnati Children’s Hospital reported in a poster at the Pediatric Hospital Medicine 2014 meeting.
Factors shown on multivariable analyses to be significantly associated with a return visit were tachycardia at discharge (odds ratio, 1.48), fever at discharge (OR, 1.89 for a temperature of 99.5-101.2° F, and 2.35 for a temperature greater than 101.3° F, compared with a temperature less than 99.5° F), and lack of an antibiotic prescription (OR, 0.44 among those who received a prescription).
Factors associated with admission at the time of the ED revisit were tachypnea in the ED (OR, 2.01), fever at discharge (OR, 3.48 for a temperature of 99.5-101.2° F, and 4.51 for a temperature greater than 101.3° F, compared with a temperature less than 99.5° F), history of community-acquired pneumonia (CAP) (OR, 3.98), lack of an antibiotic prescription (OR, 0.32 for those who received a prescription), time of visit (OR, 0.43 for those who arrived between 4 p.m. and 12 a.m., compared with arrival between 8 a.m. and 4 p.m.), and race (OR, 0.44 for African Americans vs. whites).
Revisits to the ED are an indicator of quality of care and disease progression, and CAP is among the most common reasons for ED visits, the investigators noted at the meeting sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
"Attention to these risk factors, particularly potentially modifiable factors such as vital signs, could influence decision making when treating patients for CAP. Further investigation is warranted to better understand the association between lack of antibiotic prescription and revisit to the ED with and without subsequent hospitalization," they concluded.
This study was supported by the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health. Dr. Fain and her colleagues reported having no disclosures.
LAKE BUENA VISTA, FLA. – Fever or lack of an antibiotic prescription are two factors that increase the risk of a return visit to the emergency department and subsequent hospital admission in children with community-acquired pneumonia, according to a review of ED medical records.
Of 1,857 children aged 3 months to 18 years with a diagnosis of pneumonia who were discharged to home after the index ED visit between November 2009 and April 2013, 131 (7.1%) returned to the ED within 7 days, 90 of those (4.8%) were discharged to home, and 41 (2.2%) were admitted, Dr. Emily Fain of Cincinnati Children’s Hospital reported in a poster at the Pediatric Hospital Medicine 2014 meeting.
Factors shown on multivariable analyses to be significantly associated with a return visit were tachycardia at discharge (odds ratio, 1.48), fever at discharge (OR, 1.89 for a temperature of 99.5-101.2° F, and 2.35 for a temperature greater than 101.3° F, compared with a temperature less than 99.5° F), and lack of an antibiotic prescription (OR, 0.44 among those who received a prescription).
Factors associated with admission at the time of the ED revisit were tachypnea in the ED (OR, 2.01), fever at discharge (OR, 3.48 for a temperature of 99.5-101.2° F, and 4.51 for a temperature greater than 101.3° F, compared with a temperature less than 99.5° F), history of community-acquired pneumonia (CAP) (OR, 3.98), lack of an antibiotic prescription (OR, 0.32 for those who received a prescription), time of visit (OR, 0.43 for those who arrived between 4 p.m. and 12 a.m., compared with arrival between 8 a.m. and 4 p.m.), and race (OR, 0.44 for African Americans vs. whites).
Revisits to the ED are an indicator of quality of care and disease progression, and CAP is among the most common reasons for ED visits, the investigators noted at the meeting sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
"Attention to these risk factors, particularly potentially modifiable factors such as vital signs, could influence decision making when treating patients for CAP. Further investigation is warranted to better understand the association between lack of antibiotic prescription and revisit to the ED with and without subsequent hospitalization," they concluded.
This study was supported by the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health. Dr. Fain and her colleagues reported having no disclosures.
LAKE BUENA VISTA, FLA. – Fever or lack of an antibiotic prescription are two factors that increase the risk of a return visit to the emergency department and subsequent hospital admission in children with community-acquired pneumonia, according to a review of ED medical records.
Of 1,857 children aged 3 months to 18 years with a diagnosis of pneumonia who were discharged to home after the index ED visit between November 2009 and April 2013, 131 (7.1%) returned to the ED within 7 days, 90 of those (4.8%) were discharged to home, and 41 (2.2%) were admitted, Dr. Emily Fain of Cincinnati Children’s Hospital reported in a poster at the Pediatric Hospital Medicine 2014 meeting.
Factors shown on multivariable analyses to be significantly associated with a return visit were tachycardia at discharge (odds ratio, 1.48), fever at discharge (OR, 1.89 for a temperature of 99.5-101.2° F, and 2.35 for a temperature greater than 101.3° F, compared with a temperature less than 99.5° F), and lack of an antibiotic prescription (OR, 0.44 among those who received a prescription).
Factors associated with admission at the time of the ED revisit were tachypnea in the ED (OR, 2.01), fever at discharge (OR, 3.48 for a temperature of 99.5-101.2° F, and 4.51 for a temperature greater than 101.3° F, compared with a temperature less than 99.5° F), history of community-acquired pneumonia (CAP) (OR, 3.98), lack of an antibiotic prescription (OR, 0.32 for those who received a prescription), time of visit (OR, 0.43 for those who arrived between 4 p.m. and 12 a.m., compared with arrival between 8 a.m. and 4 p.m.), and race (OR, 0.44 for African Americans vs. whites).
Revisits to the ED are an indicator of quality of care and disease progression, and CAP is among the most common reasons for ED visits, the investigators noted at the meeting sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
"Attention to these risk factors, particularly potentially modifiable factors such as vital signs, could influence decision making when treating patients for CAP. Further investigation is warranted to better understand the association between lack of antibiotic prescription and revisit to the ED with and without subsequent hospitalization," they concluded.
This study was supported by the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health. Dr. Fain and her colleagues reported having no disclosures.
AT PEDIATRIC HOSPITAL MEDICINE 2014
Key clinical point: In children with community-acquired pneumonia, fever or lack of an antibiotic prescription are two factors that increase the risk of a return visit to the ED.
Major finding: A total of 7.1% of children seen in the ED for CAP had a return visit within 7 days.
Data source: A retrospective cohort study involving 1,857 children.
Disclosures: This study was supported by the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health. Dr. Fain and her colleagues reported having no disclosures.
Renal ultrasound in neonates with febrile UTI can rule out high-grade vesicoureteral reflux
LAKE BUENA VISTA, FLA. – Renal ultrasound in infants under 2 months of age with febrile urinary tract infection can be used to rule out high-grade vesicoureteral reflux, according to findings from a retrospective cross-sectional study.
This is because renal ultrasound has a high negative predictive value for detecting high-grade vesicoureteral reflux (VUR) in neonates, and although it has poor sensitivity for detecting low-grade VUR, its sensitivity for detecting high-grade VUR is quite good in this population.
The findings could have important implications for the management of neonates with febrile urinary tract infection (UTI), who are not included in American Academy of Pediatrics guidelines for febrile UTI. A 2011 update to those guidelines calls for the use of screening renal and bladder ultrasound, but recommends against routine voiding cystourethrogram (VCUG) after an initial febrile UTI in young children unless indicated by sonographic findings; however, these guidelines apply to children aged 2 months to 2 years only.
Younger infants who present with febrile UTI differ from those over 2 months of age in that they are more likely to be male – a high percentage of whom are uncircumcised and prone to UTI because of colonization, they have a more immature immune system that can also contribute to greater likelihood of UTI, and they can have higher rates of reflux and anatomical anomalies, Dr. Sowdhamini S. Wallace, director of pediatric hospital medicine research at Texas Children’s Hospital, Houston, reported at the Pediatric Hospital Medicine 2014 meeting.
Although many studies have included older children, they have limited applicability to younger infants because of these differences, and those studies that have included infants less than 2 months of age have been of small size or questionable quality, Dr. Wallace noted.
"So the objective of our study was to determine the test properties of renal ultrasound for detecting VUR and high-grade VUR and obstructive uropathies in this [younger] age group," she said at the meeting, which was sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
Of 200 eligible neonates with a mean age of 33 days, 30% had an abnormal renal ultrasound after presenting with febrile UTI. The most common reason for an abnormal finding was hydronephrosis.
Twenty-six percent of the neonates had reflux and 8% had high-grade reflux; 8% had obstructive uropathies or nonobstructive lower tract anomalies, Dr. Wallace said.
The sensitivity of renal ultrasound for all grades of VUR was 31% overall, but was 87% for high-grade VUR.
"For high-grade VUR, the negative predictive value was 99%, with a 95%-100% confidence interval. There were no obstructive uropathies that were diagnosed by VCUG in patients with a normal renal ultrasound," she said.
The number of patients with a normal ultrasound who would need to undergo VCUG to detect one case of high-grade VUR was 70; the number needed to test to detect one case of low-grade VUR was 4, she said.
The number needed to test "should be very helpful for physicians when they are deciding whether to get a VCUG on a neonate under 2 months if they have a normal renal ultrasound, Dr. Wallace said.
"Overall, I think you can see, with the number needed to test of 70, that you would have to test many babies with normal renal ultrasound to detect one case of high-grade VUR, so you may be able to spare many infants from VCUG," she concluded.
The infants presented to the emergency department during 2008-2011 with culture-proven UTI and fever of at least 100.4° F. They were identified through a microbiology database; those included in the study had urine collected through a catheterization or suprapubic aspiration, and those with a history of abnormal prenatal ultrasound, a previous diagnosis of genitourinary tract anomalies, or greater than 30 days between ultrasound and VCUG were excluded.
Imaging studies were reviewed independently by two radiologists who were blinded to the VCUG findings. Any discrepancies were resolved by a third radiologist.
Renal ultrasound was categorized as abnormal if it showed hydronephrosis and/or caliectasis, or if there was renal size discrepancy greater than 10%, findings of a duplicated collecting system, or urethral thickening, urethral dilatation, or bladder abnormalities.
VUR severity was determined by the standard classification system.
The study is limited by the fact that most renal ultrasounds were performed at the time of UTI diagnosis when inflammation is likely present. Inflammation may also be present in patients with VUR, thus the sensitivity of renal ultrasound in this study may have been higher than with renal ultrasound performed after a UTI has resolved. Also, in the absence of a standard definition for hydronephrosis in infants less than 2 months of age the prenatal parameter of 4 mL was used.
Dr. Wallace reported having no disclosures.
LAKE BUENA VISTA, FLA. – Renal ultrasound in infants under 2 months of age with febrile urinary tract infection can be used to rule out high-grade vesicoureteral reflux, according to findings from a retrospective cross-sectional study.
This is because renal ultrasound has a high negative predictive value for detecting high-grade vesicoureteral reflux (VUR) in neonates, and although it has poor sensitivity for detecting low-grade VUR, its sensitivity for detecting high-grade VUR is quite good in this population.
The findings could have important implications for the management of neonates with febrile urinary tract infection (UTI), who are not included in American Academy of Pediatrics guidelines for febrile UTI. A 2011 update to those guidelines calls for the use of screening renal and bladder ultrasound, but recommends against routine voiding cystourethrogram (VCUG) after an initial febrile UTI in young children unless indicated by sonographic findings; however, these guidelines apply to children aged 2 months to 2 years only.
Younger infants who present with febrile UTI differ from those over 2 months of age in that they are more likely to be male – a high percentage of whom are uncircumcised and prone to UTI because of colonization, they have a more immature immune system that can also contribute to greater likelihood of UTI, and they can have higher rates of reflux and anatomical anomalies, Dr. Sowdhamini S. Wallace, director of pediatric hospital medicine research at Texas Children’s Hospital, Houston, reported at the Pediatric Hospital Medicine 2014 meeting.
Although many studies have included older children, they have limited applicability to younger infants because of these differences, and those studies that have included infants less than 2 months of age have been of small size or questionable quality, Dr. Wallace noted.
"So the objective of our study was to determine the test properties of renal ultrasound for detecting VUR and high-grade VUR and obstructive uropathies in this [younger] age group," she said at the meeting, which was sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
Of 200 eligible neonates with a mean age of 33 days, 30% had an abnormal renal ultrasound after presenting with febrile UTI. The most common reason for an abnormal finding was hydronephrosis.
Twenty-six percent of the neonates had reflux and 8% had high-grade reflux; 8% had obstructive uropathies or nonobstructive lower tract anomalies, Dr. Wallace said.
The sensitivity of renal ultrasound for all grades of VUR was 31% overall, but was 87% for high-grade VUR.
"For high-grade VUR, the negative predictive value was 99%, with a 95%-100% confidence interval. There were no obstructive uropathies that were diagnosed by VCUG in patients with a normal renal ultrasound," she said.
The number of patients with a normal ultrasound who would need to undergo VCUG to detect one case of high-grade VUR was 70; the number needed to test to detect one case of low-grade VUR was 4, she said.
The number needed to test "should be very helpful for physicians when they are deciding whether to get a VCUG on a neonate under 2 months if they have a normal renal ultrasound, Dr. Wallace said.
"Overall, I think you can see, with the number needed to test of 70, that you would have to test many babies with normal renal ultrasound to detect one case of high-grade VUR, so you may be able to spare many infants from VCUG," she concluded.
The infants presented to the emergency department during 2008-2011 with culture-proven UTI and fever of at least 100.4° F. They were identified through a microbiology database; those included in the study had urine collected through a catheterization or suprapubic aspiration, and those with a history of abnormal prenatal ultrasound, a previous diagnosis of genitourinary tract anomalies, or greater than 30 days between ultrasound and VCUG were excluded.
Imaging studies were reviewed independently by two radiologists who were blinded to the VCUG findings. Any discrepancies were resolved by a third radiologist.
Renal ultrasound was categorized as abnormal if it showed hydronephrosis and/or caliectasis, or if there was renal size discrepancy greater than 10%, findings of a duplicated collecting system, or urethral thickening, urethral dilatation, or bladder abnormalities.
VUR severity was determined by the standard classification system.
The study is limited by the fact that most renal ultrasounds were performed at the time of UTI diagnosis when inflammation is likely present. Inflammation may also be present in patients with VUR, thus the sensitivity of renal ultrasound in this study may have been higher than with renal ultrasound performed after a UTI has resolved. Also, in the absence of a standard definition for hydronephrosis in infants less than 2 months of age the prenatal parameter of 4 mL was used.
Dr. Wallace reported having no disclosures.
LAKE BUENA VISTA, FLA. – Renal ultrasound in infants under 2 months of age with febrile urinary tract infection can be used to rule out high-grade vesicoureteral reflux, according to findings from a retrospective cross-sectional study.
This is because renal ultrasound has a high negative predictive value for detecting high-grade vesicoureteral reflux (VUR) in neonates, and although it has poor sensitivity for detecting low-grade VUR, its sensitivity for detecting high-grade VUR is quite good in this population.
The findings could have important implications for the management of neonates with febrile urinary tract infection (UTI), who are not included in American Academy of Pediatrics guidelines for febrile UTI. A 2011 update to those guidelines calls for the use of screening renal and bladder ultrasound, but recommends against routine voiding cystourethrogram (VCUG) after an initial febrile UTI in young children unless indicated by sonographic findings; however, these guidelines apply to children aged 2 months to 2 years only.
Younger infants who present with febrile UTI differ from those over 2 months of age in that they are more likely to be male – a high percentage of whom are uncircumcised and prone to UTI because of colonization, they have a more immature immune system that can also contribute to greater likelihood of UTI, and they can have higher rates of reflux and anatomical anomalies, Dr. Sowdhamini S. Wallace, director of pediatric hospital medicine research at Texas Children’s Hospital, Houston, reported at the Pediatric Hospital Medicine 2014 meeting.
Although many studies have included older children, they have limited applicability to younger infants because of these differences, and those studies that have included infants less than 2 months of age have been of small size or questionable quality, Dr. Wallace noted.
"So the objective of our study was to determine the test properties of renal ultrasound for detecting VUR and high-grade VUR and obstructive uropathies in this [younger] age group," she said at the meeting, which was sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
Of 200 eligible neonates with a mean age of 33 days, 30% had an abnormal renal ultrasound after presenting with febrile UTI. The most common reason for an abnormal finding was hydronephrosis.
Twenty-six percent of the neonates had reflux and 8% had high-grade reflux; 8% had obstructive uropathies or nonobstructive lower tract anomalies, Dr. Wallace said.
The sensitivity of renal ultrasound for all grades of VUR was 31% overall, but was 87% for high-grade VUR.
"For high-grade VUR, the negative predictive value was 99%, with a 95%-100% confidence interval. There were no obstructive uropathies that were diagnosed by VCUG in patients with a normal renal ultrasound," she said.
The number of patients with a normal ultrasound who would need to undergo VCUG to detect one case of high-grade VUR was 70; the number needed to test to detect one case of low-grade VUR was 4, she said.
The number needed to test "should be very helpful for physicians when they are deciding whether to get a VCUG on a neonate under 2 months if they have a normal renal ultrasound, Dr. Wallace said.
"Overall, I think you can see, with the number needed to test of 70, that you would have to test many babies with normal renal ultrasound to detect one case of high-grade VUR, so you may be able to spare many infants from VCUG," she concluded.
The infants presented to the emergency department during 2008-2011 with culture-proven UTI and fever of at least 100.4° F. They were identified through a microbiology database; those included in the study had urine collected through a catheterization or suprapubic aspiration, and those with a history of abnormal prenatal ultrasound, a previous diagnosis of genitourinary tract anomalies, or greater than 30 days between ultrasound and VCUG were excluded.
Imaging studies were reviewed independently by two radiologists who were blinded to the VCUG findings. Any discrepancies were resolved by a third radiologist.
Renal ultrasound was categorized as abnormal if it showed hydronephrosis and/or caliectasis, or if there was renal size discrepancy greater than 10%, findings of a duplicated collecting system, or urethral thickening, urethral dilatation, or bladder abnormalities.
VUR severity was determined by the standard classification system.
The study is limited by the fact that most renal ultrasounds were performed at the time of UTI diagnosis when inflammation is likely present. Inflammation may also be present in patients with VUR, thus the sensitivity of renal ultrasound in this study may have been higher than with renal ultrasound performed after a UTI has resolved. Also, in the absence of a standard definition for hydronephrosis in infants less than 2 months of age the prenatal parameter of 4 mL was used.
Dr. Wallace reported having no disclosures.
AT PEDIATRIC HOSPITAL MEDICINE 2014
Key clinical finding: With the number needed to test of 70, you would have to test many babies with normal renal ultrasound to detect one case of high-grade VUR, so you may be able to spare many infants from VCUG.
Major finding: Number needed to test to detect one case of high-grade VUR: 70.
Data source: A retrospective cross-sectional study of 200 neonates.
Disclosures: Dr. Wallace reported having no disclosures.
Subspecialty outpatient clinics, EDs miss many flu vaccination opportunities
LAKE BUENA VISTA, FLA. – Nearly 44% of incompletely vaccinated inpatients with influenza had a missed opportunity for vaccination, according to retrospective chart review at Children’s Hospital Colorado.
Among 197 such children admitted with confirmed influenza in 2010-2014, 86 (44%) had a total of 507 medical visits during which influenza vaccine was available, Dr. Suchitra Rao of the University of Colorado, Denver, reported in a poster at the Pediatric Hospital Medicine 2014 meeting.
The majority of patients with missed opportunity visits were considered high risk for severe complications from influenza from factors such as age younger than 2 years, immunosuppression, pregnancy, or an underlying chronic pulmonary, cardiovascular, renal, hepatic, neurological, hematologic, or metabolic disorder, although this finding was not statistically significant, Dr. Rao reported.
The bulk of missed opportunity visits occurred during September, October, and November (20%-23% each month) prior to onset of the influenza season, with declining percentages taking place between December and April. Most of the visits (45%) occurred at specialty clinics, followed by the emergency department or urgent care setting (22%).
"Subspecialty outpatient visits provide an excellent opportunity for influenza vaccination because they target high-risk patients and they represent the highest proportion of missed opportunities for vaccination," Dr. Rao and her colleagues wrote.
Future analyses will explore independent risk factors for missed opportunities, and identify differences in visit characteristic for high vs. low risk groups, they noted.
The Pediatric Hospital Medicine 2014 meeting was sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
The authors reported having no relevant financial disclosures.
LAKE BUENA VISTA, FLA. – Nearly 44% of incompletely vaccinated inpatients with influenza had a missed opportunity for vaccination, according to retrospective chart review at Children’s Hospital Colorado.
Among 197 such children admitted with confirmed influenza in 2010-2014, 86 (44%) had a total of 507 medical visits during which influenza vaccine was available, Dr. Suchitra Rao of the University of Colorado, Denver, reported in a poster at the Pediatric Hospital Medicine 2014 meeting.
The majority of patients with missed opportunity visits were considered high risk for severe complications from influenza from factors such as age younger than 2 years, immunosuppression, pregnancy, or an underlying chronic pulmonary, cardiovascular, renal, hepatic, neurological, hematologic, or metabolic disorder, although this finding was not statistically significant, Dr. Rao reported.
The bulk of missed opportunity visits occurred during September, October, and November (20%-23% each month) prior to onset of the influenza season, with declining percentages taking place between December and April. Most of the visits (45%) occurred at specialty clinics, followed by the emergency department or urgent care setting (22%).
"Subspecialty outpatient visits provide an excellent opportunity for influenza vaccination because they target high-risk patients and they represent the highest proportion of missed opportunities for vaccination," Dr. Rao and her colleagues wrote.
Future analyses will explore independent risk factors for missed opportunities, and identify differences in visit characteristic for high vs. low risk groups, they noted.
The Pediatric Hospital Medicine 2014 meeting was sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
The authors reported having no relevant financial disclosures.
LAKE BUENA VISTA, FLA. – Nearly 44% of incompletely vaccinated inpatients with influenza had a missed opportunity for vaccination, according to retrospective chart review at Children’s Hospital Colorado.
Among 197 such children admitted with confirmed influenza in 2010-2014, 86 (44%) had a total of 507 medical visits during which influenza vaccine was available, Dr. Suchitra Rao of the University of Colorado, Denver, reported in a poster at the Pediatric Hospital Medicine 2014 meeting.
The majority of patients with missed opportunity visits were considered high risk for severe complications from influenza from factors such as age younger than 2 years, immunosuppression, pregnancy, or an underlying chronic pulmonary, cardiovascular, renal, hepatic, neurological, hematologic, or metabolic disorder, although this finding was not statistically significant, Dr. Rao reported.
The bulk of missed opportunity visits occurred during September, October, and November (20%-23% each month) prior to onset of the influenza season, with declining percentages taking place between December and April. Most of the visits (45%) occurred at specialty clinics, followed by the emergency department or urgent care setting (22%).
"Subspecialty outpatient visits provide an excellent opportunity for influenza vaccination because they target high-risk patients and they represent the highest proportion of missed opportunities for vaccination," Dr. Rao and her colleagues wrote.
Future analyses will explore independent risk factors for missed opportunities, and identify differences in visit characteristic for high vs. low risk groups, they noted.
The Pediatric Hospital Medicine 2014 meeting was sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
The authors reported having no relevant financial disclosures.
AT PEDIATRIC HOSPITAL MEDICINE 2014
Key clinical point: Specialty outpatient visits offer an important opportunity for influenza vaccinations.
Major finding: A total of 44% of 197 patients had a total of 507 missed opportunities for vaccination.
Data source: A retrospective review of the charts of 197 incompletely vaccinated children with the flu.
Disclosures: The authors reported having no relevant financial disclosures.
High-flow nasal cannulas support children outside the ICU
LAKE BUENA VISTA, FLA. – The use of high-flow nasal cannulas for respiratory support in young children with acute bronchiolitis is safe outside the intensive care unit setting, according to a retrospective cohort study.
However, initiating the use of high-flow nasal cannulas (HFNCs) on the pediatric floor increases length of stay and direct cost, Dr. Jaime Pittenger of the University of Kentucky, Lexington, reported in a poster at the Pediatric Hospital Medicine 2014 meeting.
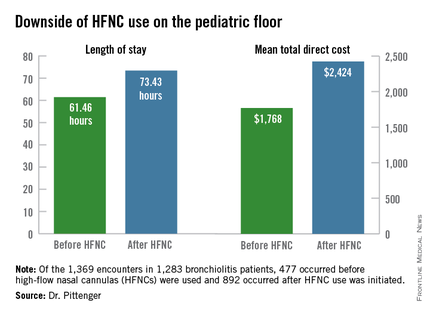
Of 1,369 encounters in 1,283 non-ICU bronchiolitis patients under age 2 who were seen between October 2008 and May 2013, 477 occurred before HFNC use on the floor was initiated in 2010, and 892 occurred after such use was initiated. Of these, 139 involved receipt of HFNCs outside the ICU, Dr. Pittenger reported at the meeting, which was sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
Of those who received HFNCs outside the ICU, 66% who would have previously gone to the ICU remained on the floor, she noted.
Furthermore, a reduction was seen in noninvasive and invasive ventilation in the ICU after HFNC use outside the ICU was initiated, although this did not reach significance (P = .19).
Use of HFNCs on the floor was associated with a relatively low frequency of complications, but mean length of stay was 61.46 hours before HFNC was used outside the ICU, compared with 73.43 hours. Mean total direct cost was $1,768 before HFNC was used outside the ICU, vs. $2,424 after it began to be used outside the ICU after non-ICU HFNC initiation.
HFNC use outside the ICU for respiratory support in pediatric patients with bronchiolitis has increased in recent years, but there has been little evidence to support the safety and effectiveness of this paradigm shift. Though limited by lack of standardization, patient and treatment selection biases, and a small cohort size for ascertaining the frequency of complications, these findings suggest that the practice is feasible.
However, future studies should evaluate the cost-effectiveness of using HFNC on the floor, Dr. Pittenger concluded, noting that standardization of initiation, escalation, and de-escalation of HFNC are also needed.
Dr. Pittenger reported having no disclosures.
LAKE BUENA VISTA, FLA. – The use of high-flow nasal cannulas for respiratory support in young children with acute bronchiolitis is safe outside the intensive care unit setting, according to a retrospective cohort study.
However, initiating the use of high-flow nasal cannulas (HFNCs) on the pediatric floor increases length of stay and direct cost, Dr. Jaime Pittenger of the University of Kentucky, Lexington, reported in a poster at the Pediatric Hospital Medicine 2014 meeting.

Of 1,369 encounters in 1,283 non-ICU bronchiolitis patients under age 2 who were seen between October 2008 and May 2013, 477 occurred before HFNC use on the floor was initiated in 2010, and 892 occurred after such use was initiated. Of these, 139 involved receipt of HFNCs outside the ICU, Dr. Pittenger reported at the meeting, which was sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
Of those who received HFNCs outside the ICU, 66% who would have previously gone to the ICU remained on the floor, she noted.
Furthermore, a reduction was seen in noninvasive and invasive ventilation in the ICU after HFNC use outside the ICU was initiated, although this did not reach significance (P = .19).
Use of HFNCs on the floor was associated with a relatively low frequency of complications, but mean length of stay was 61.46 hours before HFNC was used outside the ICU, compared with 73.43 hours. Mean total direct cost was $1,768 before HFNC was used outside the ICU, vs. $2,424 after it began to be used outside the ICU after non-ICU HFNC initiation.
HFNC use outside the ICU for respiratory support in pediatric patients with bronchiolitis has increased in recent years, but there has been little evidence to support the safety and effectiveness of this paradigm shift. Though limited by lack of standardization, patient and treatment selection biases, and a small cohort size for ascertaining the frequency of complications, these findings suggest that the practice is feasible.
However, future studies should evaluate the cost-effectiveness of using HFNC on the floor, Dr. Pittenger concluded, noting that standardization of initiation, escalation, and de-escalation of HFNC are also needed.
Dr. Pittenger reported having no disclosures.
LAKE BUENA VISTA, FLA. – The use of high-flow nasal cannulas for respiratory support in young children with acute bronchiolitis is safe outside the intensive care unit setting, according to a retrospective cohort study.
However, initiating the use of high-flow nasal cannulas (HFNCs) on the pediatric floor increases length of stay and direct cost, Dr. Jaime Pittenger of the University of Kentucky, Lexington, reported in a poster at the Pediatric Hospital Medicine 2014 meeting.

Of 1,369 encounters in 1,283 non-ICU bronchiolitis patients under age 2 who were seen between October 2008 and May 2013, 477 occurred before HFNC use on the floor was initiated in 2010, and 892 occurred after such use was initiated. Of these, 139 involved receipt of HFNCs outside the ICU, Dr. Pittenger reported at the meeting, which was sponsored by the Society of Hospital Medicine, the American Academy of Pediatrics, the AAP Section on Hospital Medicine, and the Academic Pediatric Association.
Of those who received HFNCs outside the ICU, 66% who would have previously gone to the ICU remained on the floor, she noted.
Furthermore, a reduction was seen in noninvasive and invasive ventilation in the ICU after HFNC use outside the ICU was initiated, although this did not reach significance (P = .19).
Use of HFNCs on the floor was associated with a relatively low frequency of complications, but mean length of stay was 61.46 hours before HFNC was used outside the ICU, compared with 73.43 hours. Mean total direct cost was $1,768 before HFNC was used outside the ICU, vs. $2,424 after it began to be used outside the ICU after non-ICU HFNC initiation.
HFNC use outside the ICU for respiratory support in pediatric patients with bronchiolitis has increased in recent years, but there has been little evidence to support the safety and effectiveness of this paradigm shift. Though limited by lack of standardization, patient and treatment selection biases, and a small cohort size for ascertaining the frequency of complications, these findings suggest that the practice is feasible.
However, future studies should evaluate the cost-effectiveness of using HFNC on the floor, Dr. Pittenger concluded, noting that standardization of initiation, escalation, and de-escalation of HFNC are also needed.
Dr. Pittenger reported having no disclosures.
AT PEDIATRIC HOSPITAL MEDICINE 2014
Key clinical point: HFNC use outside the ICU is feasible for respiratory support in young children with bronchiolitis.
Major finding: A total of 66% of HFNC patients who would have been sent to the ICU remained on the pediatric floor.
Data source: A retrospective cohort study of 1,369 encounters in 1,283 non-ICU bronchiolitis patients under age 2.
Disclosures: Dr. Pittenger reported having no disclosures.