User login
Researchers link two genes to Raynaud’s disease
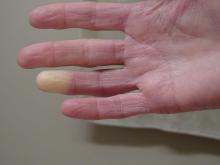
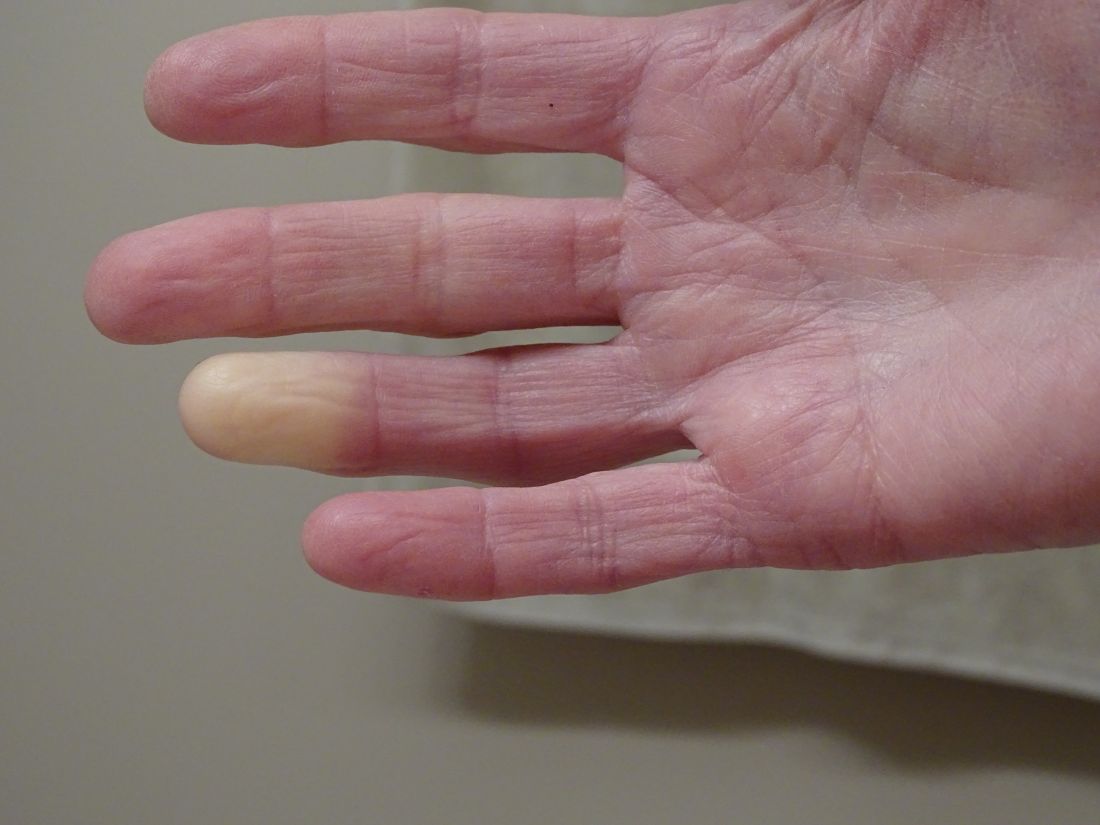
Researchers have identified two genes that may contribute to Raynaud’s phenomenon, a condition where blood vessels in the extremities constrict and limit blood flow.
Raynaud’s is a relatively common condition, affecting 2%-5% of the general population. Though Raynaud’s can be an annoyance for some, it can also cause severe pain and can require medication.
These newly identified genes will hopefully lead to new therapeutic options, said Maik Pietzner, PhD, chair in health data modeling at Queen Mary University of London’s Precision Healthcare University Research Institute (PHURI) and group leader in the Computational Medicine Group at the Berlin Institute of Health at Charité – Universitätsmedizin Berlin, Germany.
Dr. Pietzner led the research along with Claudia Langenberg, MD, PhD, director of PHURI.
The study was published in Nature Communications.
Largest genomic study of Raynaud’s to date
The researchers looked through electronic medical records from the UK Biobank, a large-scale database that contains genetic and health information on half a million participants. They identified more than 5,100 individuals with Raynaud’s, of which 68% had primary Raynaud’s. These participants were compared with more than 439,000 controls who did not have Raynaud’s.
In a secondary analysis, the team also used health records from the Queen Mary University of London Genes & Health Study, which contains health information on individuals of South Asian ancestry.
The researchers identified two genes that are likely involved with Raynaud’s. The first, ADRA2A, encodes for the alpha-2A adrenergic receptor that can cause vasoconstriction of small blood vessels in response to stress hormones. Researchers have long suspected that this type of receptor could be involved with Raynaud’s, but there was debate over which receptor subtype was responsible.
“Our finding of alpha-2A receptors is quite interesting because the focus has always been on alpha-2C receptors,” said Dr. Pietzner. “It’s only a letter, but it’s a massive difference in terms of biology and physiology,” he said, and could be why therapies targeting 2C receptors have been ineffective.
The second strongest association was for the transcription factor IRX1. Less is known about this gene, but the data we do have suggest that it is involved with regulating the dilation of blood vessels, Dr. Pietzner noted.
“There might be balance between the ADRA2A finding being responsible for constriction and the IRX1 finding indirectly linked to the dilation of those vessels following constrictions. Having both may explain why these prolonged episodes of vasoconstriction lead to a loss of oxygen to the tissues,” so they turn white and then blue, he said.
Because the Biobank cohort was European-centric, Dr. Pietzner and colleagues also identified 400 cases of Raynaud’s in British individuals of Bangladeshi and Pakistani ancestry and were able to replicate the association between IRX1 and Raynaud’s. Data on ADRA2A were unavailable.
The genes identified are associated with primary Raynaud’s. Secondary Raynaud’s is a rarer type of the condition that occurs along with autoimmune disorders, such as scleroderma, and is generally more severe.
It’s long been suspected that Raynaud’s had some genetic component, because half of patients with Raynaud’s have another family member with the same condition, said Laura Hummers, MD, who codirects the John Hopkins Scleroderma Center in Baltimore. She was not involved with the study.
This is “the largest study of this kind that’s been done,” she said, and the first to show a potential mechanism behind this genetic association.
The main gene finding, ADRA2A, “points to a receptor on the cells that regulate the tone of these blood vessels,” she continued. “It suggests maybe there’s too many of these receptors or they’re overly sensitive; something about them is different that makes patients more susceptible to these cold triggers. Knowing that is potentially really important, because it could give you a direct way to intervene, if true.”
New therapeutic avenues
The first-line treatment for primary Raynaud’s is behavioral interventions, such as maintaining body and extremity warmth and avoiding certain vasoconstricting drugs, said Kimberly Lakin, MD, a rheumatologist at the Hospital for Special Surgery in New York, who not involved in the research. These drugs could include over-the-counter decongestants and certain medications for attention-deficit/hyperactivity disorder.
If these behavioral interventions are not enough, clinicians most commonly prescribe calcium channel blockers. These medications are vasodilators but can be a concern for people with normal or already low blood pressure, Dr. Lakin said. They can also cause symptoms such as headache, leg swelling, constipation, and other gastrointestinal symptoms.
Other medications, such as fluoxetine, may also be considered as a later-line therapy, “but the effectiveness is fairly limited in Raynaud’s,” she said. “Certainly, other medication options that would be helpful and driven by the mechanisms of Raynaud’s would add to our ability to help patients.”
As it turns out, one of the genes identified in the study, ADRA2A, “is actually one of the most commonly targeted genes by drugs,” said Dr. Pietzner. Because the findings suggest that ADRA2A is overexpressed in Raynaud, a selective inhibitor like the antidepressant mirtazapine could be a promising candidate to repurpose for treating Raynaud’s, he said.
Limitations to electronic medical record analyses
Both Dr. Hummers and Dr. Lakin noted that research using diagnostic codes from medical records to identify cases has some limitations. The study may have included patients misdiagnosed with Raynaud’s when perhaps they had another condition. Patients with milder Raynaud’s who have not sought medical attention for the condition would not be represented in the study, Dr. Lakin said.
The UK Biobank includes individuals of mostly European descent, so an analysis confirming these findings in a more diverse population would be helpful, she said.
However, both Dr. Lakin and Dr. Hummers agreed that the study contributes to the understanding of the mechanisms behind Raynaud’s. Although the two identified genes were tied to primary Raynaud’s, the study’s findings could potentially apply to secondary Raynaud’s as well, Dr. Hummers said.
“Anything we learn about primary Raynaud’s may have implication for Raynaud’s more broadly,” she noted.
Dr. Hummers and Dr. Lakin disclosed no relevant financial relationships. Dr. Pietzner has received partnership funding for the MRC Clinical Pharmacology Training Scheme (cofunded by MRC and Roche, UCB, Eli Lilly, and Novartis) and a PhD studentship jointly funded by the UK Engineering and Physical Sciences Research Council and AstraZeneca. Dr. Pietzner also has unrestricted educational grant support for the UK Pharmacogenetics and Stratified Medicine Network from Bristol-Myers Squibb.
A version of this article appeared on Medscape.com.
Researchers have identified two genes that may contribute to Raynaud’s phenomenon, a condition where blood vessels in the extremities constrict and limit blood flow.
Raynaud’s is a relatively common condition, affecting 2%-5% of the general population. Though Raynaud’s can be an annoyance for some, it can also cause severe pain and can require medication.
These newly identified genes will hopefully lead to new therapeutic options, said Maik Pietzner, PhD, chair in health data modeling at Queen Mary University of London’s Precision Healthcare University Research Institute (PHURI) and group leader in the Computational Medicine Group at the Berlin Institute of Health at Charité – Universitätsmedizin Berlin, Germany.
Dr. Pietzner led the research along with Claudia Langenberg, MD, PhD, director of PHURI.
The study was published in Nature Communications.
Largest genomic study of Raynaud’s to date
The researchers looked through electronic medical records from the UK Biobank, a large-scale database that contains genetic and health information on half a million participants. They identified more than 5,100 individuals with Raynaud’s, of which 68% had primary Raynaud’s. These participants were compared with more than 439,000 controls who did not have Raynaud’s.
In a secondary analysis, the team also used health records from the Queen Mary University of London Genes & Health Study, which contains health information on individuals of South Asian ancestry.
The researchers identified two genes that are likely involved with Raynaud’s. The first, ADRA2A, encodes for the alpha-2A adrenergic receptor that can cause vasoconstriction of small blood vessels in response to stress hormones. Researchers have long suspected that this type of receptor could be involved with Raynaud’s, but there was debate over which receptor subtype was responsible.
“Our finding of alpha-2A receptors is quite interesting because the focus has always been on alpha-2C receptors,” said Dr. Pietzner. “It’s only a letter, but it’s a massive difference in terms of biology and physiology,” he said, and could be why therapies targeting 2C receptors have been ineffective.
The second strongest association was for the transcription factor IRX1. Less is known about this gene, but the data we do have suggest that it is involved with regulating the dilation of blood vessels, Dr. Pietzner noted.
“There might be balance between the ADRA2A finding being responsible for constriction and the IRX1 finding indirectly linked to the dilation of those vessels following constrictions. Having both may explain why these prolonged episodes of vasoconstriction lead to a loss of oxygen to the tissues,” so they turn white and then blue, he said.
Because the Biobank cohort was European-centric, Dr. Pietzner and colleagues also identified 400 cases of Raynaud’s in British individuals of Bangladeshi and Pakistani ancestry and were able to replicate the association between IRX1 and Raynaud’s. Data on ADRA2A were unavailable.
The genes identified are associated with primary Raynaud’s. Secondary Raynaud’s is a rarer type of the condition that occurs along with autoimmune disorders, such as scleroderma, and is generally more severe.
It’s long been suspected that Raynaud’s had some genetic component, because half of patients with Raynaud’s have another family member with the same condition, said Laura Hummers, MD, who codirects the John Hopkins Scleroderma Center in Baltimore. She was not involved with the study.
This is “the largest study of this kind that’s been done,” she said, and the first to show a potential mechanism behind this genetic association.
The main gene finding, ADRA2A, “points to a receptor on the cells that regulate the tone of these blood vessels,” she continued. “It suggests maybe there’s too many of these receptors or they’re overly sensitive; something about them is different that makes patients more susceptible to these cold triggers. Knowing that is potentially really important, because it could give you a direct way to intervene, if true.”
New therapeutic avenues
The first-line treatment for primary Raynaud’s is behavioral interventions, such as maintaining body and extremity warmth and avoiding certain vasoconstricting drugs, said Kimberly Lakin, MD, a rheumatologist at the Hospital for Special Surgery in New York, who not involved in the research. These drugs could include over-the-counter decongestants and certain medications for attention-deficit/hyperactivity disorder.
If these behavioral interventions are not enough, clinicians most commonly prescribe calcium channel blockers. These medications are vasodilators but can be a concern for people with normal or already low blood pressure, Dr. Lakin said. They can also cause symptoms such as headache, leg swelling, constipation, and other gastrointestinal symptoms.
Other medications, such as fluoxetine, may also be considered as a later-line therapy, “but the effectiveness is fairly limited in Raynaud’s,” she said. “Certainly, other medication options that would be helpful and driven by the mechanisms of Raynaud’s would add to our ability to help patients.”
As it turns out, one of the genes identified in the study, ADRA2A, “is actually one of the most commonly targeted genes by drugs,” said Dr. Pietzner. Because the findings suggest that ADRA2A is overexpressed in Raynaud, a selective inhibitor like the antidepressant mirtazapine could be a promising candidate to repurpose for treating Raynaud’s, he said.
Limitations to electronic medical record analyses
Both Dr. Hummers and Dr. Lakin noted that research using diagnostic codes from medical records to identify cases has some limitations. The study may have included patients misdiagnosed with Raynaud’s when perhaps they had another condition. Patients with milder Raynaud’s who have not sought medical attention for the condition would not be represented in the study, Dr. Lakin said.
The UK Biobank includes individuals of mostly European descent, so an analysis confirming these findings in a more diverse population would be helpful, she said.
However, both Dr. Lakin and Dr. Hummers agreed that the study contributes to the understanding of the mechanisms behind Raynaud’s. Although the two identified genes were tied to primary Raynaud’s, the study’s findings could potentially apply to secondary Raynaud’s as well, Dr. Hummers said.
“Anything we learn about primary Raynaud’s may have implication for Raynaud’s more broadly,” she noted.
Dr. Hummers and Dr. Lakin disclosed no relevant financial relationships. Dr. Pietzner has received partnership funding for the MRC Clinical Pharmacology Training Scheme (cofunded by MRC and Roche, UCB, Eli Lilly, and Novartis) and a PhD studentship jointly funded by the UK Engineering and Physical Sciences Research Council and AstraZeneca. Dr. Pietzner also has unrestricted educational grant support for the UK Pharmacogenetics and Stratified Medicine Network from Bristol-Myers Squibb.
A version of this article appeared on Medscape.com.
Researchers have identified two genes that may contribute to Raynaud’s phenomenon, a condition where blood vessels in the extremities constrict and limit blood flow.
Raynaud’s is a relatively common condition, affecting 2%-5% of the general population. Though Raynaud’s can be an annoyance for some, it can also cause severe pain and can require medication.
These newly identified genes will hopefully lead to new therapeutic options, said Maik Pietzner, PhD, chair in health data modeling at Queen Mary University of London’s Precision Healthcare University Research Institute (PHURI) and group leader in the Computational Medicine Group at the Berlin Institute of Health at Charité – Universitätsmedizin Berlin, Germany.
Dr. Pietzner led the research along with Claudia Langenberg, MD, PhD, director of PHURI.
The study was published in Nature Communications.
Largest genomic study of Raynaud’s to date
The researchers looked through electronic medical records from the UK Biobank, a large-scale database that contains genetic and health information on half a million participants. They identified more than 5,100 individuals with Raynaud’s, of which 68% had primary Raynaud’s. These participants were compared with more than 439,000 controls who did not have Raynaud’s.
In a secondary analysis, the team also used health records from the Queen Mary University of London Genes & Health Study, which contains health information on individuals of South Asian ancestry.
The researchers identified two genes that are likely involved with Raynaud’s. The first, ADRA2A, encodes for the alpha-2A adrenergic receptor that can cause vasoconstriction of small blood vessels in response to stress hormones. Researchers have long suspected that this type of receptor could be involved with Raynaud’s, but there was debate over which receptor subtype was responsible.
“Our finding of alpha-2A receptors is quite interesting because the focus has always been on alpha-2C receptors,” said Dr. Pietzner. “It’s only a letter, but it’s a massive difference in terms of biology and physiology,” he said, and could be why therapies targeting 2C receptors have been ineffective.
The second strongest association was for the transcription factor IRX1. Less is known about this gene, but the data we do have suggest that it is involved with regulating the dilation of blood vessels, Dr. Pietzner noted.
“There might be balance between the ADRA2A finding being responsible for constriction and the IRX1 finding indirectly linked to the dilation of those vessels following constrictions. Having both may explain why these prolonged episodes of vasoconstriction lead to a loss of oxygen to the tissues,” so they turn white and then blue, he said.
Because the Biobank cohort was European-centric, Dr. Pietzner and colleagues also identified 400 cases of Raynaud’s in British individuals of Bangladeshi and Pakistani ancestry and were able to replicate the association between IRX1 and Raynaud’s. Data on ADRA2A were unavailable.
The genes identified are associated with primary Raynaud’s. Secondary Raynaud’s is a rarer type of the condition that occurs along with autoimmune disorders, such as scleroderma, and is generally more severe.
It’s long been suspected that Raynaud’s had some genetic component, because half of patients with Raynaud’s have another family member with the same condition, said Laura Hummers, MD, who codirects the John Hopkins Scleroderma Center in Baltimore. She was not involved with the study.
This is “the largest study of this kind that’s been done,” she said, and the first to show a potential mechanism behind this genetic association.
The main gene finding, ADRA2A, “points to a receptor on the cells that regulate the tone of these blood vessels,” she continued. “It suggests maybe there’s too many of these receptors or they’re overly sensitive; something about them is different that makes patients more susceptible to these cold triggers. Knowing that is potentially really important, because it could give you a direct way to intervene, if true.”
New therapeutic avenues
The first-line treatment for primary Raynaud’s is behavioral interventions, such as maintaining body and extremity warmth and avoiding certain vasoconstricting drugs, said Kimberly Lakin, MD, a rheumatologist at the Hospital for Special Surgery in New York, who not involved in the research. These drugs could include over-the-counter decongestants and certain medications for attention-deficit/hyperactivity disorder.
If these behavioral interventions are not enough, clinicians most commonly prescribe calcium channel blockers. These medications are vasodilators but can be a concern for people with normal or already low blood pressure, Dr. Lakin said. They can also cause symptoms such as headache, leg swelling, constipation, and other gastrointestinal symptoms.
Other medications, such as fluoxetine, may also be considered as a later-line therapy, “but the effectiveness is fairly limited in Raynaud’s,” she said. “Certainly, other medication options that would be helpful and driven by the mechanisms of Raynaud’s would add to our ability to help patients.”
As it turns out, one of the genes identified in the study, ADRA2A, “is actually one of the most commonly targeted genes by drugs,” said Dr. Pietzner. Because the findings suggest that ADRA2A is overexpressed in Raynaud, a selective inhibitor like the antidepressant mirtazapine could be a promising candidate to repurpose for treating Raynaud’s, he said.
Limitations to electronic medical record analyses
Both Dr. Hummers and Dr. Lakin noted that research using diagnostic codes from medical records to identify cases has some limitations. The study may have included patients misdiagnosed with Raynaud’s when perhaps they had another condition. Patients with milder Raynaud’s who have not sought medical attention for the condition would not be represented in the study, Dr. Lakin said.
The UK Biobank includes individuals of mostly European descent, so an analysis confirming these findings in a more diverse population would be helpful, she said.
However, both Dr. Lakin and Dr. Hummers agreed that the study contributes to the understanding of the mechanisms behind Raynaud’s. Although the two identified genes were tied to primary Raynaud’s, the study’s findings could potentially apply to secondary Raynaud’s as well, Dr. Hummers said.
“Anything we learn about primary Raynaud’s may have implication for Raynaud’s more broadly,” she noted.
Dr. Hummers and Dr. Lakin disclosed no relevant financial relationships. Dr. Pietzner has received partnership funding for the MRC Clinical Pharmacology Training Scheme (cofunded by MRC and Roche, UCB, Eli Lilly, and Novartis) and a PhD studentship jointly funded by the UK Engineering and Physical Sciences Research Council and AstraZeneca. Dr. Pietzner also has unrestricted educational grant support for the UK Pharmacogenetics and Stratified Medicine Network from Bristol-Myers Squibb.
A version of this article appeared on Medscape.com.
FROM NATURE COMMUNICATIONS
Tool in development aims to steer telehealth visit appropriateness in rheumatology
Researchers have created a model to suggest which rheumatology visits can be effectively carried out via telehealth and which should remain in-person visits. The model not only could help to alleviate the decision burden on providers but also help to navigate how to incorporate telehealth into daily rheumatology practice as the COVID-19 pandemic subsides, experts say.
The beginning of the pandemic quickly drove rheumatology practices to adopt telehealth – which in the past has been studied only in selective groups of relatively stable patients. In Duke University’s department of rheumatology, nearly 90% of visits were conducted via telehealth for several weeks in April and May 2020, said David L. Leverenz, MD, an assistant professor of medicine at Duke University in Durham, N.C.
Since then, the practice has continued providing telehealth for a wider variety of patients: patients with high disease activity, those with low disease activity, people living 3 hours away or just 5 minutes from the medical center.
“Although the pandemic has really improved, and certainly we feel very safe providing in-person care, we’ve realized that it’s actually really possible to provide telehealth care to a lot of patients,” he said.
The model was then piloted with four Duke University rheumatologists for visits that took place from March through July 2022. A month prior to visits, researchers provided the rheumatologists a list of in-patient visits that the model suggested could be changed to telehealth visits. The list also included false changes, in which randomly selected visits were presented as being recommended for telehealth, although the model had not actually recommended the changes.
Dr. Leverenz and colleagues measured how frequently providers agreed with changes recommended by the model and the false changes. If a provider accepted a model-suggested change, the patient was contacted to either accept or reject the proposed switch. If a provider agreed with a false change, no additional action was taken.
Of the 201 patient encounters, there were 101 model-recommended changes and 100 artificial changes. Nearly all (99%) model-recommended changes suggested moving from in-person visits to telehealth visits. There was one recommendation to change a scheduled telehealth encounter to an in-person encounter. Of the false recommendations, 90 were for scheduled in-person visits, and 10 were for scheduled telehealth appointments.
Providers agreed with 71% of the model-recommended changes and with 21% of the false changes. Dr. Leverenz and colleagues reported “moderate agreement” between providers and model recommendations, reflected by a Cohen kappa coefficient of 0.45.
“This lined up pretty well with what providers thought was appropriate for the patient when presented with the information, and it also showed that, on top of current practice, that the model really does have the ability to expand appropriate telehealth care, which is really what we’re looking to do,” Dr. Leverenz said.
The article describing these results was published in Arthritis Care and Research.
Perhaps unsurprisingly, clinician preference for and experience with telemedicine were the biggest predictors of whether changes suggested by the model were accepted.
Focus model to specific diagnoses or many?
Currently, clinicians who are already juggling many other responsibilities throughout the day must use their own judgment to determine whether telemedicine may be appropriate. A model such as this could help alleviate that decision burden, said Kathleen Fear, PhD, the director of data and analytics at the University of Rochester Medical Center Health Lab, in New York.
“A model that can help with scheduling or prompt a provider or patient for when a visit is appropriate for telemedicine seems like a really effective way to make the most of telemedicine while reducing potential burden on providers,” she said.
Dr. Leverenz imagines that this model could be embedded into electronic health records as a “decision support tool” to aid discussions between patients and providers on whether telehealth might be appropriate for upcoming visits.
But developing a model that can generate predictions for the wide variety of conditions seen in daily rheumatology practice can be a challenge, said Christine Peoples, MD, a clinical associate professor of medicine and director of the tele-rheumatology program at the University of Pittsburgh.
“If you focus the model to certain diagnoses, at least in the beginning, that’s very helpful, because it’s too difficult to have one model for every single reason that folks see a rheumatologist,” she said.
Daniel A. Albert, MD, a professor of medicine and pediatrics at the Geisel School of Medicine at Dartmouth in Hanover, N,H., agreed. The model is “a good start,” he said, and highlights that tele-rheumatology continues to be underutilized in practice. But he argued that the moderate agreement found with the model was relatively low.
A more focused algorithm that targets a single or several more common conditions may be more accurate, he said. “You probably want to break it down,” Dr. Albert said.
But Dr. Leverenz argued that the novelty of this model is that it incorporates the many different conditions seen in daily rheumatology practice, whereas previous programs utilizing telehealth focused on specific conditions and patients with low disease activity.
In addition, the model is currently provider centric and does not take patient preference into account, Dr. Albert added. Dr. Leverenz said that that is the next step in further developing this model. He is currently conducting qualitative analyses with patients to better understand what patients think and how often their views on telehealth differ from that of their care providers.
“Hopefully, we can expand appropriate telehealth visits by teaching providers not just to do what they think is right for the patient but also meet the patient’s expectations and needs, based on what we learn,” he said.
The study was funded by a grant from Pfizer. Dr. Leverenz has received grants from Pfizer and has served as a consultant for Sanofi. None of the study’s other authors report relevant financial relationships. Dr. Peoples is an educational consultant on telehealth for Pfizer. Dr. Alberts has previously received grant funding from Pfizer. Dr. Fear has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Researchers have created a model to suggest which rheumatology visits can be effectively carried out via telehealth and which should remain in-person visits. The model not only could help to alleviate the decision burden on providers but also help to navigate how to incorporate telehealth into daily rheumatology practice as the COVID-19 pandemic subsides, experts say.
The beginning of the pandemic quickly drove rheumatology practices to adopt telehealth – which in the past has been studied only in selective groups of relatively stable patients. In Duke University’s department of rheumatology, nearly 90% of visits were conducted via telehealth for several weeks in April and May 2020, said David L. Leverenz, MD, an assistant professor of medicine at Duke University in Durham, N.C.
Since then, the practice has continued providing telehealth for a wider variety of patients: patients with high disease activity, those with low disease activity, people living 3 hours away or just 5 minutes from the medical center.
“Although the pandemic has really improved, and certainly we feel very safe providing in-person care, we’ve realized that it’s actually really possible to provide telehealth care to a lot of patients,” he said.
The model was then piloted with four Duke University rheumatologists for visits that took place from March through July 2022. A month prior to visits, researchers provided the rheumatologists a list of in-patient visits that the model suggested could be changed to telehealth visits. The list also included false changes, in which randomly selected visits were presented as being recommended for telehealth, although the model had not actually recommended the changes.
Dr. Leverenz and colleagues measured how frequently providers agreed with changes recommended by the model and the false changes. If a provider accepted a model-suggested change, the patient was contacted to either accept or reject the proposed switch. If a provider agreed with a false change, no additional action was taken.
Of the 201 patient encounters, there were 101 model-recommended changes and 100 artificial changes. Nearly all (99%) model-recommended changes suggested moving from in-person visits to telehealth visits. There was one recommendation to change a scheduled telehealth encounter to an in-person encounter. Of the false recommendations, 90 were for scheduled in-person visits, and 10 were for scheduled telehealth appointments.
Providers agreed with 71% of the model-recommended changes and with 21% of the false changes. Dr. Leverenz and colleagues reported “moderate agreement” between providers and model recommendations, reflected by a Cohen kappa coefficient of 0.45.
“This lined up pretty well with what providers thought was appropriate for the patient when presented with the information, and it also showed that, on top of current practice, that the model really does have the ability to expand appropriate telehealth care, which is really what we’re looking to do,” Dr. Leverenz said.
The article describing these results was published in Arthritis Care and Research.
Perhaps unsurprisingly, clinician preference for and experience with telemedicine were the biggest predictors of whether changes suggested by the model were accepted.
Focus model to specific diagnoses or many?
Currently, clinicians who are already juggling many other responsibilities throughout the day must use their own judgment to determine whether telemedicine may be appropriate. A model such as this could help alleviate that decision burden, said Kathleen Fear, PhD, the director of data and analytics at the University of Rochester Medical Center Health Lab, in New York.
“A model that can help with scheduling or prompt a provider or patient for when a visit is appropriate for telemedicine seems like a really effective way to make the most of telemedicine while reducing potential burden on providers,” she said.
Dr. Leverenz imagines that this model could be embedded into electronic health records as a “decision support tool” to aid discussions between patients and providers on whether telehealth might be appropriate for upcoming visits.
But developing a model that can generate predictions for the wide variety of conditions seen in daily rheumatology practice can be a challenge, said Christine Peoples, MD, a clinical associate professor of medicine and director of the tele-rheumatology program at the University of Pittsburgh.
“If you focus the model to certain diagnoses, at least in the beginning, that’s very helpful, because it’s too difficult to have one model for every single reason that folks see a rheumatologist,” she said.
Daniel A. Albert, MD, a professor of medicine and pediatrics at the Geisel School of Medicine at Dartmouth in Hanover, N,H., agreed. The model is “a good start,” he said, and highlights that tele-rheumatology continues to be underutilized in practice. But he argued that the moderate agreement found with the model was relatively low.
A more focused algorithm that targets a single or several more common conditions may be more accurate, he said. “You probably want to break it down,” Dr. Albert said.
But Dr. Leverenz argued that the novelty of this model is that it incorporates the many different conditions seen in daily rheumatology practice, whereas previous programs utilizing telehealth focused on specific conditions and patients with low disease activity.
In addition, the model is currently provider centric and does not take patient preference into account, Dr. Albert added. Dr. Leverenz said that that is the next step in further developing this model. He is currently conducting qualitative analyses with patients to better understand what patients think and how often their views on telehealth differ from that of their care providers.
“Hopefully, we can expand appropriate telehealth visits by teaching providers not just to do what they think is right for the patient but also meet the patient’s expectations and needs, based on what we learn,” he said.
The study was funded by a grant from Pfizer. Dr. Leverenz has received grants from Pfizer and has served as a consultant for Sanofi. None of the study’s other authors report relevant financial relationships. Dr. Peoples is an educational consultant on telehealth for Pfizer. Dr. Alberts has previously received grant funding from Pfizer. Dr. Fear has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Researchers have created a model to suggest which rheumatology visits can be effectively carried out via telehealth and which should remain in-person visits. The model not only could help to alleviate the decision burden on providers but also help to navigate how to incorporate telehealth into daily rheumatology practice as the COVID-19 pandemic subsides, experts say.
The beginning of the pandemic quickly drove rheumatology practices to adopt telehealth – which in the past has been studied only in selective groups of relatively stable patients. In Duke University’s department of rheumatology, nearly 90% of visits were conducted via telehealth for several weeks in April and May 2020, said David L. Leverenz, MD, an assistant professor of medicine at Duke University in Durham, N.C.
Since then, the practice has continued providing telehealth for a wider variety of patients: patients with high disease activity, those with low disease activity, people living 3 hours away or just 5 minutes from the medical center.
“Although the pandemic has really improved, and certainly we feel very safe providing in-person care, we’ve realized that it’s actually really possible to provide telehealth care to a lot of patients,” he said.
The model was then piloted with four Duke University rheumatologists for visits that took place from March through July 2022. A month prior to visits, researchers provided the rheumatologists a list of in-patient visits that the model suggested could be changed to telehealth visits. The list also included false changes, in which randomly selected visits were presented as being recommended for telehealth, although the model had not actually recommended the changes.
Dr. Leverenz and colleagues measured how frequently providers agreed with changes recommended by the model and the false changes. If a provider accepted a model-suggested change, the patient was contacted to either accept or reject the proposed switch. If a provider agreed with a false change, no additional action was taken.
Of the 201 patient encounters, there were 101 model-recommended changes and 100 artificial changes. Nearly all (99%) model-recommended changes suggested moving from in-person visits to telehealth visits. There was one recommendation to change a scheduled telehealth encounter to an in-person encounter. Of the false recommendations, 90 were for scheduled in-person visits, and 10 were for scheduled telehealth appointments.
Providers agreed with 71% of the model-recommended changes and with 21% of the false changes. Dr. Leverenz and colleagues reported “moderate agreement” between providers and model recommendations, reflected by a Cohen kappa coefficient of 0.45.
“This lined up pretty well with what providers thought was appropriate for the patient when presented with the information, and it also showed that, on top of current practice, that the model really does have the ability to expand appropriate telehealth care, which is really what we’re looking to do,” Dr. Leverenz said.
The article describing these results was published in Arthritis Care and Research.
Perhaps unsurprisingly, clinician preference for and experience with telemedicine were the biggest predictors of whether changes suggested by the model were accepted.
Focus model to specific diagnoses or many?
Currently, clinicians who are already juggling many other responsibilities throughout the day must use their own judgment to determine whether telemedicine may be appropriate. A model such as this could help alleviate that decision burden, said Kathleen Fear, PhD, the director of data and analytics at the University of Rochester Medical Center Health Lab, in New York.
“A model that can help with scheduling or prompt a provider or patient for when a visit is appropriate for telemedicine seems like a really effective way to make the most of telemedicine while reducing potential burden on providers,” she said.
Dr. Leverenz imagines that this model could be embedded into electronic health records as a “decision support tool” to aid discussions between patients and providers on whether telehealth might be appropriate for upcoming visits.
But developing a model that can generate predictions for the wide variety of conditions seen in daily rheumatology practice can be a challenge, said Christine Peoples, MD, a clinical associate professor of medicine and director of the tele-rheumatology program at the University of Pittsburgh.
“If you focus the model to certain diagnoses, at least in the beginning, that’s very helpful, because it’s too difficult to have one model for every single reason that folks see a rheumatologist,” she said.
Daniel A. Albert, MD, a professor of medicine and pediatrics at the Geisel School of Medicine at Dartmouth in Hanover, N,H., agreed. The model is “a good start,” he said, and highlights that tele-rheumatology continues to be underutilized in practice. But he argued that the moderate agreement found with the model was relatively low.
A more focused algorithm that targets a single or several more common conditions may be more accurate, he said. “You probably want to break it down,” Dr. Albert said.
But Dr. Leverenz argued that the novelty of this model is that it incorporates the many different conditions seen in daily rheumatology practice, whereas previous programs utilizing telehealth focused on specific conditions and patients with low disease activity.
In addition, the model is currently provider centric and does not take patient preference into account, Dr. Albert added. Dr. Leverenz said that that is the next step in further developing this model. He is currently conducting qualitative analyses with patients to better understand what patients think and how often their views on telehealth differ from that of their care providers.
“Hopefully, we can expand appropriate telehealth visits by teaching providers not just to do what they think is right for the patient but also meet the patient’s expectations and needs, based on what we learn,” he said.
The study was funded by a grant from Pfizer. Dr. Leverenz has received grants from Pfizer and has served as a consultant for Sanofi. None of the study’s other authors report relevant financial relationships. Dr. Peoples is an educational consultant on telehealth for Pfizer. Dr. Alberts has previously received grant funding from Pfizer. Dr. Fear has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM ARTHRITIS CARE AND RESEARCH
Intravenous formulation of secukinumab gets FDA approval
The Food and Drug Administration has approved an intravenous (IV) formulation of secukinumab (Cosentyx) for the treatment of adults with psoriatic arthritis (PsA), ankylosing spondylitis (AS), and nonradiographic axial spondyloarthritis (nr-axSpA).
Secukinumab is the only treatment approved in an IV formulation that specifically targets and blocks interleukin-17A and the only non–tumor necrosis factor alpha IV option available to treat the three indications of PsA, AS, and nr-axSpA, according to a press release from the drug’s manufacturer, Novartis.
The approval marks the first new IV treatment in 6 years for these three conditions. The drug was first approved in 2015 and up to now has been available only as a subcutaneous injection.
The new formulation is also approved for secukinumab’s other indications of plaque psoriasis in people aged 6 years or older, children aged 2 years or older with PsA, and enthesitis-related arthritis in patients aged 4 years or older.
“A significant portion of the millions of PsA, AS, and nr-axSpA patients in the United States require treatment through IV infusions for a variety of reasons, including not being comfortable with self-injections or simply preferring to have treatments administered in their health care provider’s office,” Philip J. Mease, MD, clinical professor at the University of Washington, Seattle, and director of rheumatology research at the Swedish Medical Center, Seattle, said in the press release. “The approval of Cosentyx as an IV formulation is an important milestone for patients because it expands the treatment options available to them with a different mechanism of action than existing biologic IV therapies, along with the comfort and familiarity of an established treatment.”
This IV formulation is administered monthly in a 30-minute, weight-based dosing regimen. This new option will become available before the end of the year, Novartis said.
“With this approval of Cosentyx as an IV formulation, along with the subcutaneous formulation, we can broaden the use of Cosentyx to help more patients manage their condition with a medicine backed by more than a decade of clinical research and 8 years of real-world experience,” said Christy Siegel, vice president and head of immunology, Novartis U.S.
A version of this article first appeared on Medscape.com.
The Food and Drug Administration has approved an intravenous (IV) formulation of secukinumab (Cosentyx) for the treatment of adults with psoriatic arthritis (PsA), ankylosing spondylitis (AS), and nonradiographic axial spondyloarthritis (nr-axSpA).
Secukinumab is the only treatment approved in an IV formulation that specifically targets and blocks interleukin-17A and the only non–tumor necrosis factor alpha IV option available to treat the three indications of PsA, AS, and nr-axSpA, according to a press release from the drug’s manufacturer, Novartis.
The approval marks the first new IV treatment in 6 years for these three conditions. The drug was first approved in 2015 and up to now has been available only as a subcutaneous injection.
The new formulation is also approved for secukinumab’s other indications of plaque psoriasis in people aged 6 years or older, children aged 2 years or older with PsA, and enthesitis-related arthritis in patients aged 4 years or older.
“A significant portion of the millions of PsA, AS, and nr-axSpA patients in the United States require treatment through IV infusions for a variety of reasons, including not being comfortable with self-injections or simply preferring to have treatments administered in their health care provider’s office,” Philip J. Mease, MD, clinical professor at the University of Washington, Seattle, and director of rheumatology research at the Swedish Medical Center, Seattle, said in the press release. “The approval of Cosentyx as an IV formulation is an important milestone for patients because it expands the treatment options available to them with a different mechanism of action than existing biologic IV therapies, along with the comfort and familiarity of an established treatment.”
This IV formulation is administered monthly in a 30-minute, weight-based dosing regimen. This new option will become available before the end of the year, Novartis said.
“With this approval of Cosentyx as an IV formulation, along with the subcutaneous formulation, we can broaden the use of Cosentyx to help more patients manage their condition with a medicine backed by more than a decade of clinical research and 8 years of real-world experience,” said Christy Siegel, vice president and head of immunology, Novartis U.S.
A version of this article first appeared on Medscape.com.
The Food and Drug Administration has approved an intravenous (IV) formulation of secukinumab (Cosentyx) for the treatment of adults with psoriatic arthritis (PsA), ankylosing spondylitis (AS), and nonradiographic axial spondyloarthritis (nr-axSpA).
Secukinumab is the only treatment approved in an IV formulation that specifically targets and blocks interleukin-17A and the only non–tumor necrosis factor alpha IV option available to treat the three indications of PsA, AS, and nr-axSpA, according to a press release from the drug’s manufacturer, Novartis.
The approval marks the first new IV treatment in 6 years for these three conditions. The drug was first approved in 2015 and up to now has been available only as a subcutaneous injection.
The new formulation is also approved for secukinumab’s other indications of plaque psoriasis in people aged 6 years or older, children aged 2 years or older with PsA, and enthesitis-related arthritis in patients aged 4 years or older.
“A significant portion of the millions of PsA, AS, and nr-axSpA patients in the United States require treatment through IV infusions for a variety of reasons, including not being comfortable with self-injections or simply preferring to have treatments administered in their health care provider’s office,” Philip J. Mease, MD, clinical professor at the University of Washington, Seattle, and director of rheumatology research at the Swedish Medical Center, Seattle, said in the press release. “The approval of Cosentyx as an IV formulation is an important milestone for patients because it expands the treatment options available to them with a different mechanism of action than existing biologic IV therapies, along with the comfort and familiarity of an established treatment.”
This IV formulation is administered monthly in a 30-minute, weight-based dosing regimen. This new option will become available before the end of the year, Novartis said.
“With this approval of Cosentyx as an IV formulation, along with the subcutaneous formulation, we can broaden the use of Cosentyx to help more patients manage their condition with a medicine backed by more than a decade of clinical research and 8 years of real-world experience,” said Christy Siegel, vice president and head of immunology, Novartis U.S.
A version of this article first appeared on Medscape.com.
More evidence shows COVID-19’s link to risk for autoimmune disease
TOPLINE:
Research from South Korea provides additional evidence for the connection between COVID-19 and an increased risk for autoimmune conditions post infection.
METHODOLOGY:
- In this retrospective study, researchers identified 354,527 individuals diagnosed with COVID-19 via polymerase chain reaction (PCR) testing from Oct. 8, 2020, to Dec. 31, 2021.
- Researchers compared the COVID-19 group with 6,134,940 healthy individuals who had no evidence of COVID-19 to quantify the risk for autoimmune and autoinflammatory connective tissue disorders.
- Patients were followed until diagnosis, death, or end of study period (Dec. 31, 2021).
TAKEAWAY:
- Risks for alopecia areata, alopecia totalis, antineutrophil cytoplasmic antibody–associated vasculitis, Crohn’s disease, and sarcoidosis were higher in the COVID-19 group.
- Patients with more severe COVID-19 (admitted to the ICU) were at greater risk for many autoimmune conditions, including alopecia totalis, psoriasis, vitiligo, and vasculitis.
IN PRACTICE:
“Our results emphasize the need to focus on managing not only the acute stages of COVID-19 itself but also autoimmune diseases as complications of COVID-19,” the authors wrote.
SOURCE:
Sung Ha Lim, MD, of Yonsei University, Wonju, South Korea, was the first author of the study, published in JAMA Network Open.
LIMITATIONS:
The study was retrospective and was composed almost exclusively of individuals from a single ethnicity. The study could have included individuals with COVID-19 in the control group who did not undergo PCR testing. The analysis did not include detailed information on each patient, including genetic information, that could have contributed to autoimmune disease risk.
DISCLOSURES:
The study was supported by a fund from the research program of the Korea Medical Institute and by grants from the Korea Health Industry Development Institute, the Korean Ministry of Health & Welfare, and the National Research Foundation of Korea. The authors disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
TOPLINE:
Research from South Korea provides additional evidence for the connection between COVID-19 and an increased risk for autoimmune conditions post infection.
METHODOLOGY:
- In this retrospective study, researchers identified 354,527 individuals diagnosed with COVID-19 via polymerase chain reaction (PCR) testing from Oct. 8, 2020, to Dec. 31, 2021.
- Researchers compared the COVID-19 group with 6,134,940 healthy individuals who had no evidence of COVID-19 to quantify the risk for autoimmune and autoinflammatory connective tissue disorders.
- Patients were followed until diagnosis, death, or end of study period (Dec. 31, 2021).
TAKEAWAY:
- Risks for alopecia areata, alopecia totalis, antineutrophil cytoplasmic antibody–associated vasculitis, Crohn’s disease, and sarcoidosis were higher in the COVID-19 group.
- Patients with more severe COVID-19 (admitted to the ICU) were at greater risk for many autoimmune conditions, including alopecia totalis, psoriasis, vitiligo, and vasculitis.
IN PRACTICE:
“Our results emphasize the need to focus on managing not only the acute stages of COVID-19 itself but also autoimmune diseases as complications of COVID-19,” the authors wrote.
SOURCE:
Sung Ha Lim, MD, of Yonsei University, Wonju, South Korea, was the first author of the study, published in JAMA Network Open.
LIMITATIONS:
The study was retrospective and was composed almost exclusively of individuals from a single ethnicity. The study could have included individuals with COVID-19 in the control group who did not undergo PCR testing. The analysis did not include detailed information on each patient, including genetic information, that could have contributed to autoimmune disease risk.
DISCLOSURES:
The study was supported by a fund from the research program of the Korea Medical Institute and by grants from the Korea Health Industry Development Institute, the Korean Ministry of Health & Welfare, and the National Research Foundation of Korea. The authors disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
TOPLINE:
Research from South Korea provides additional evidence for the connection between COVID-19 and an increased risk for autoimmune conditions post infection.
METHODOLOGY:
- In this retrospective study, researchers identified 354,527 individuals diagnosed with COVID-19 via polymerase chain reaction (PCR) testing from Oct. 8, 2020, to Dec. 31, 2021.
- Researchers compared the COVID-19 group with 6,134,940 healthy individuals who had no evidence of COVID-19 to quantify the risk for autoimmune and autoinflammatory connective tissue disorders.
- Patients were followed until diagnosis, death, or end of study period (Dec. 31, 2021).
TAKEAWAY:
- Risks for alopecia areata, alopecia totalis, antineutrophil cytoplasmic antibody–associated vasculitis, Crohn’s disease, and sarcoidosis were higher in the COVID-19 group.
- Patients with more severe COVID-19 (admitted to the ICU) were at greater risk for many autoimmune conditions, including alopecia totalis, psoriasis, vitiligo, and vasculitis.
IN PRACTICE:
“Our results emphasize the need to focus on managing not only the acute stages of COVID-19 itself but also autoimmune diseases as complications of COVID-19,” the authors wrote.
SOURCE:
Sung Ha Lim, MD, of Yonsei University, Wonju, South Korea, was the first author of the study, published in JAMA Network Open.
LIMITATIONS:
The study was retrospective and was composed almost exclusively of individuals from a single ethnicity. The study could have included individuals with COVID-19 in the control group who did not undergo PCR testing. The analysis did not include detailed information on each patient, including genetic information, that could have contributed to autoimmune disease risk.
DISCLOSURES:
The study was supported by a fund from the research program of the Korea Medical Institute and by grants from the Korea Health Industry Development Institute, the Korean Ministry of Health & Welfare, and the National Research Foundation of Korea. The authors disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM JAMA NETWORK OPEN
FDA approves ninth Humira biosimilar, with interchangeability
The Food and Drug Administration has granted an interchangeability designation to adalimumab-afzb (Abrilada), according to an announcement from Pfizer.
This is the second adalimumab biosimilar granted interchangeability. The first, adalimumab-adbm (Cyltezo), became available in July.
Biosimilars introduce market competition that can help lower drug prices. Adalimumab-afzb is one of nine approved biosimilars for Humira, and the last to launch in 2023.
Adalimumab-afzb is indicated for:
- Adults with rheumatoid arthritis.
- Polyarticular juvenile idiopathic arthritis in patients 2 years of age and older.
- Adults with psoriatic arthritis.
- Adults with ankylosing spondylitis.
- Crohn’s disease in adults and children 6 years of age and older.
- Adults with ulcerative colitis.
- Adults with plaque psoriasis.
- Adults with hidradenitis suppurativa.
- Adults with noninfectious intermediate and posterior uveitis and panuveitis.
“With this designation, Abrilada is now both biosimilar to and interchangeable with Humira, reinforcing confidence among physicians and pharmacists that there is no decrease in effectiveness or increase in safety risk associated with switching between Abrilada and the reference product,” Roy Fleischmann, MD, clinical professor of medicine, University of Texas Southwestern Medical Center, Dallas, said in Pfizer’s statement.
An interchangeability designation allows pharmacists to substitute the biosimilar for the reference product without involving the prescribing clinician (according to state law). To achieve this designation, Pfizer submitted data from a phase 3 study led by Dr. Fleischmann that evaluated adalimumab-afzb in patients with RA. Patients who were switched three times between the biosimilar and the reference product had outcomes similar to those of patients continuously treated with the reference product.
Adalimumab-afzb will be available later in October at a 5% discount from Humira’s price. Later this year, the drug will launch at a second price, a 60% discount from Humira.
Full prescribing information for adalimumab-afzb is available here.
A version of this article first appeared on Medscape.com.
The Food and Drug Administration has granted an interchangeability designation to adalimumab-afzb (Abrilada), according to an announcement from Pfizer.
This is the second adalimumab biosimilar granted interchangeability. The first, adalimumab-adbm (Cyltezo), became available in July.
Biosimilars introduce market competition that can help lower drug prices. Adalimumab-afzb is one of nine approved biosimilars for Humira, and the last to launch in 2023.
Adalimumab-afzb is indicated for:
- Adults with rheumatoid arthritis.
- Polyarticular juvenile idiopathic arthritis in patients 2 years of age and older.
- Adults with psoriatic arthritis.
- Adults with ankylosing spondylitis.
- Crohn’s disease in adults and children 6 years of age and older.
- Adults with ulcerative colitis.
- Adults with plaque psoriasis.
- Adults with hidradenitis suppurativa.
- Adults with noninfectious intermediate and posterior uveitis and panuveitis.
“With this designation, Abrilada is now both biosimilar to and interchangeable with Humira, reinforcing confidence among physicians and pharmacists that there is no decrease in effectiveness or increase in safety risk associated with switching between Abrilada and the reference product,” Roy Fleischmann, MD, clinical professor of medicine, University of Texas Southwestern Medical Center, Dallas, said in Pfizer’s statement.
An interchangeability designation allows pharmacists to substitute the biosimilar for the reference product without involving the prescribing clinician (according to state law). To achieve this designation, Pfizer submitted data from a phase 3 study led by Dr. Fleischmann that evaluated adalimumab-afzb in patients with RA. Patients who were switched three times between the biosimilar and the reference product had outcomes similar to those of patients continuously treated with the reference product.
Adalimumab-afzb will be available later in October at a 5% discount from Humira’s price. Later this year, the drug will launch at a second price, a 60% discount from Humira.
Full prescribing information for adalimumab-afzb is available here.
A version of this article first appeared on Medscape.com.
The Food and Drug Administration has granted an interchangeability designation to adalimumab-afzb (Abrilada), according to an announcement from Pfizer.
This is the second adalimumab biosimilar granted interchangeability. The first, adalimumab-adbm (Cyltezo), became available in July.
Biosimilars introduce market competition that can help lower drug prices. Adalimumab-afzb is one of nine approved biosimilars for Humira, and the last to launch in 2023.
Adalimumab-afzb is indicated for:
- Adults with rheumatoid arthritis.
- Polyarticular juvenile idiopathic arthritis in patients 2 years of age and older.
- Adults with psoriatic arthritis.
- Adults with ankylosing spondylitis.
- Crohn’s disease in adults and children 6 years of age and older.
- Adults with ulcerative colitis.
- Adults with plaque psoriasis.
- Adults with hidradenitis suppurativa.
- Adults with noninfectious intermediate and posterior uveitis and panuveitis.
“With this designation, Abrilada is now both biosimilar to and interchangeable with Humira, reinforcing confidence among physicians and pharmacists that there is no decrease in effectiveness or increase in safety risk associated with switching between Abrilada and the reference product,” Roy Fleischmann, MD, clinical professor of medicine, University of Texas Southwestern Medical Center, Dallas, said in Pfizer’s statement.
An interchangeability designation allows pharmacists to substitute the biosimilar for the reference product without involving the prescribing clinician (according to state law). To achieve this designation, Pfizer submitted data from a phase 3 study led by Dr. Fleischmann that evaluated adalimumab-afzb in patients with RA. Patients who were switched three times between the biosimilar and the reference product had outcomes similar to those of patients continuously treated with the reference product.
Adalimumab-afzb will be available later in October at a 5% discount from Humira’s price. Later this year, the drug will launch at a second price, a 60% discount from Humira.
Full prescribing information for adalimumab-afzb is available here.
A version of this article first appeared on Medscape.com.
PET scan at diagnosis may help to predict aneurysm risk in patients with giant cell arteritis
PET scans may serve as both a diagnostic and prognostic tool in giant cell arteritis (GCA), according to a new study.
In over 100 patients with GCA who underwent 18F-fluorodeoxyglucose PET imaging, those with elevated FDG uptake at diagnosis were more likely to develop thoracic aortic aneurysms.
“PET-CT has an excellent diagnostic accuracy for the diagnosis of GCA, certainly if both extracranial and intracranial vessels were assessed. This study shows that performing PET imaging at diagnosis in patients with GCA may also help estimate the future risk for aortic aneurysm formation,” lead author Lien Moreel, MD, of the department of internal medicine at University Hospitals Leuven (Belgium), wrote in an email. “PET imaging at diagnosis can provide both diagnostic and prognostic information in one imaging tool in patients with GCA.”
Previous retrospective studies have found an association between FDG uptake at diagnosis and risk for aortic complications, but “prospective studies confirming these findings are lacking,” the investigators wrote. The study was published online in Annals of Internal Medicine.
In the study, Dr. Moreel and colleagues prospectively followed 106 individuals diagnosed with GCA who received FDG-PET within 3 days after starting glucocorticoids. Patients also had CT imaging at diagnosis and then CT imaging annually for up to 10 years.
A PET scan was considered positive with an FDG uptake of grade 2 or higher in any of seven vascular regions (thoracic and abdominal aorta, subclavian, axillary, carotid, iliac, and femoral arteries). Researchers also used the results to quantify a total vascular score (TVS). Out of the entire cohort, 75 patients had a positive PET scan result.
These patients had a larger increase in the diameter of the ascending aorta and the descending aorta, as well the volume of thoracic aorta after 5 years, compared with those who had a negative PET scan result. These changes were also associated with higher TVS at diagnosis. Of the 23 patients who developed an aortic aneurysm, 18 had a positive PET scan at diagnosis.
The risk of incident thoracic aortic aneurysms was calculated to be 10 times higher in patients with positive PET scans. Fourteen of the 15 patients (93%) with an incident thoracic aortic aneurysm had positive PET results.
Up to now, “we’ve had no way of predicting which patients might be at risk of this potentially serious complication,” Kenneth Warrington, MD, chair of the department of rheumatology and director of the Vasculitis Clinic at the Mayo Clinic in Rochester, Minn., said in an interview. He was not involved with the research.
He hopes that the findings will help inform clinicians on how patients with GCA should be evaluated and monitored. Although the American College of Rheumatology conditionally recommends noninvasive imaging in patients newly diagnosed with GCA, guidance for follow-up on these patients is less clear.
“There are no clear guidelines, but most clinicians who take care of patients with GCA do obtain imaging periodically,” he said. “There is a lot of variability in the practice in terms of which type of scan is used and how often it’s done.”
Although this study did not specifically look at the benefit of screening patients, “we think that follow-up of aortic dimensions seems to be warranted in GCA patients with a positive PET scan result, especially in those with high intensity and broad extent of vascular inflammation,” Dr. Moreel said. “However, the added value of screening and the interval required should be addressed in future studies.”
Applying this study’s protocol in practice in the United States might be difficult, Dr. Warrington noted, as it can be challenging logistically to get imaging done within 3 days of starting steroids. However, Dr. Moreel said it is possible to delay the start of glucocorticoids until the PET scan is performed in patients without visual symptoms or jaw claudication.
PET scans are also expensive, and it can be difficult to get insurance coverage in the United States. However, other imaging modalities could potentially be used in similar ways, Dr. Warrington said. “One could potentially extrapolate to say that if there is difficulty with accessing PET scan, we could use other modalities like CT or MRI basically to see whether the aorta is inflamed or not.”
Dr. Moreel disclosed no relevant financial relationships. Dr. Warrington has received compensation for consulting activities with Sanofi. Eli Lilly, Kiniksa, and Bristol-Myers Squibb have provided support to the Mayo Clinic for clinical trials related to GCA, of which Dr. Warrington served as subinvestigator.
A version of this article appeared on Medscape.com.
PET scans may serve as both a diagnostic and prognostic tool in giant cell arteritis (GCA), according to a new study.
In over 100 patients with GCA who underwent 18F-fluorodeoxyglucose PET imaging, those with elevated FDG uptake at diagnosis were more likely to develop thoracic aortic aneurysms.
“PET-CT has an excellent diagnostic accuracy for the diagnosis of GCA, certainly if both extracranial and intracranial vessels were assessed. This study shows that performing PET imaging at diagnosis in patients with GCA may also help estimate the future risk for aortic aneurysm formation,” lead author Lien Moreel, MD, of the department of internal medicine at University Hospitals Leuven (Belgium), wrote in an email. “PET imaging at diagnosis can provide both diagnostic and prognostic information in one imaging tool in patients with GCA.”
Previous retrospective studies have found an association between FDG uptake at diagnosis and risk for aortic complications, but “prospective studies confirming these findings are lacking,” the investigators wrote. The study was published online in Annals of Internal Medicine.
In the study, Dr. Moreel and colleagues prospectively followed 106 individuals diagnosed with GCA who received FDG-PET within 3 days after starting glucocorticoids. Patients also had CT imaging at diagnosis and then CT imaging annually for up to 10 years.
A PET scan was considered positive with an FDG uptake of grade 2 or higher in any of seven vascular regions (thoracic and abdominal aorta, subclavian, axillary, carotid, iliac, and femoral arteries). Researchers also used the results to quantify a total vascular score (TVS). Out of the entire cohort, 75 patients had a positive PET scan result.
These patients had a larger increase in the diameter of the ascending aorta and the descending aorta, as well the volume of thoracic aorta after 5 years, compared with those who had a negative PET scan result. These changes were also associated with higher TVS at diagnosis. Of the 23 patients who developed an aortic aneurysm, 18 had a positive PET scan at diagnosis.
The risk of incident thoracic aortic aneurysms was calculated to be 10 times higher in patients with positive PET scans. Fourteen of the 15 patients (93%) with an incident thoracic aortic aneurysm had positive PET results.
Up to now, “we’ve had no way of predicting which patients might be at risk of this potentially serious complication,” Kenneth Warrington, MD, chair of the department of rheumatology and director of the Vasculitis Clinic at the Mayo Clinic in Rochester, Minn., said in an interview. He was not involved with the research.
He hopes that the findings will help inform clinicians on how patients with GCA should be evaluated and monitored. Although the American College of Rheumatology conditionally recommends noninvasive imaging in patients newly diagnosed with GCA, guidance for follow-up on these patients is less clear.
“There are no clear guidelines, but most clinicians who take care of patients with GCA do obtain imaging periodically,” he said. “There is a lot of variability in the practice in terms of which type of scan is used and how often it’s done.”
Although this study did not specifically look at the benefit of screening patients, “we think that follow-up of aortic dimensions seems to be warranted in GCA patients with a positive PET scan result, especially in those with high intensity and broad extent of vascular inflammation,” Dr. Moreel said. “However, the added value of screening and the interval required should be addressed in future studies.”
Applying this study’s protocol in practice in the United States might be difficult, Dr. Warrington noted, as it can be challenging logistically to get imaging done within 3 days of starting steroids. However, Dr. Moreel said it is possible to delay the start of glucocorticoids until the PET scan is performed in patients without visual symptoms or jaw claudication.
PET scans are also expensive, and it can be difficult to get insurance coverage in the United States. However, other imaging modalities could potentially be used in similar ways, Dr. Warrington said. “One could potentially extrapolate to say that if there is difficulty with accessing PET scan, we could use other modalities like CT or MRI basically to see whether the aorta is inflamed or not.”
Dr. Moreel disclosed no relevant financial relationships. Dr. Warrington has received compensation for consulting activities with Sanofi. Eli Lilly, Kiniksa, and Bristol-Myers Squibb have provided support to the Mayo Clinic for clinical trials related to GCA, of which Dr. Warrington served as subinvestigator.
A version of this article appeared on Medscape.com.
PET scans may serve as both a diagnostic and prognostic tool in giant cell arteritis (GCA), according to a new study.
In over 100 patients with GCA who underwent 18F-fluorodeoxyglucose PET imaging, those with elevated FDG uptake at diagnosis were more likely to develop thoracic aortic aneurysms.
“PET-CT has an excellent diagnostic accuracy for the diagnosis of GCA, certainly if both extracranial and intracranial vessels were assessed. This study shows that performing PET imaging at diagnosis in patients with GCA may also help estimate the future risk for aortic aneurysm formation,” lead author Lien Moreel, MD, of the department of internal medicine at University Hospitals Leuven (Belgium), wrote in an email. “PET imaging at diagnosis can provide both diagnostic and prognostic information in one imaging tool in patients with GCA.”
Previous retrospective studies have found an association between FDG uptake at diagnosis and risk for aortic complications, but “prospective studies confirming these findings are lacking,” the investigators wrote. The study was published online in Annals of Internal Medicine.
In the study, Dr. Moreel and colleagues prospectively followed 106 individuals diagnosed with GCA who received FDG-PET within 3 days after starting glucocorticoids. Patients also had CT imaging at diagnosis and then CT imaging annually for up to 10 years.
A PET scan was considered positive with an FDG uptake of grade 2 or higher in any of seven vascular regions (thoracic and abdominal aorta, subclavian, axillary, carotid, iliac, and femoral arteries). Researchers also used the results to quantify a total vascular score (TVS). Out of the entire cohort, 75 patients had a positive PET scan result.
These patients had a larger increase in the diameter of the ascending aorta and the descending aorta, as well the volume of thoracic aorta after 5 years, compared with those who had a negative PET scan result. These changes were also associated with higher TVS at diagnosis. Of the 23 patients who developed an aortic aneurysm, 18 had a positive PET scan at diagnosis.
The risk of incident thoracic aortic aneurysms was calculated to be 10 times higher in patients with positive PET scans. Fourteen of the 15 patients (93%) with an incident thoracic aortic aneurysm had positive PET results.
Up to now, “we’ve had no way of predicting which patients might be at risk of this potentially serious complication,” Kenneth Warrington, MD, chair of the department of rheumatology and director of the Vasculitis Clinic at the Mayo Clinic in Rochester, Minn., said in an interview. He was not involved with the research.
He hopes that the findings will help inform clinicians on how patients with GCA should be evaluated and monitored. Although the American College of Rheumatology conditionally recommends noninvasive imaging in patients newly diagnosed with GCA, guidance for follow-up on these patients is less clear.
“There are no clear guidelines, but most clinicians who take care of patients with GCA do obtain imaging periodically,” he said. “There is a lot of variability in the practice in terms of which type of scan is used and how often it’s done.”
Although this study did not specifically look at the benefit of screening patients, “we think that follow-up of aortic dimensions seems to be warranted in GCA patients with a positive PET scan result, especially in those with high intensity and broad extent of vascular inflammation,” Dr. Moreel said. “However, the added value of screening and the interval required should be addressed in future studies.”
Applying this study’s protocol in practice in the United States might be difficult, Dr. Warrington noted, as it can be challenging logistically to get imaging done within 3 days of starting steroids. However, Dr. Moreel said it is possible to delay the start of glucocorticoids until the PET scan is performed in patients without visual symptoms or jaw claudication.
PET scans are also expensive, and it can be difficult to get insurance coverage in the United States. However, other imaging modalities could potentially be used in similar ways, Dr. Warrington said. “One could potentially extrapolate to say that if there is difficulty with accessing PET scan, we could use other modalities like CT or MRI basically to see whether the aorta is inflamed or not.”
Dr. Moreel disclosed no relevant financial relationships. Dr. Warrington has received compensation for consulting activities with Sanofi. Eli Lilly, Kiniksa, and Bristol-Myers Squibb have provided support to the Mayo Clinic for clinical trials related to GCA, of which Dr. Warrington served as subinvestigator.
A version of this article appeared on Medscape.com.
FROM ANNALS OF INTERNAL MEDICINE
FDA approves first tocilizumab biosimilar
The Food and Drug Administration has approved the biosimilar tocilizumab-bavi (Tofidence), Biogen, the drug’s manufacturer, announced on Sept. 29.
It is the first tocilizumab biosimilar approved by the FDA. The reference product, Actemra (Genentech), was first approved by the agency in 2010.
“The approval of Tofidence in the U.S. marks another positive step toward helping more people with chronic autoimmune conditions gain access to leading therapies,” Ian Henshaw, global head of biosimilars at Biogen, said in a statement. “With the increasing numbers of approved biosimilars, we expect increased savings and sustainability for health care systems and an increase in physician choice and patient access to biologics.”
Biogen’s pricing for tocilizumab-bavi will be available closer to the product’s launch date, which has yet to be determined, a company spokesman said. The U.S. average monthly cost of Actemra for rheumatoid arthritis, administered intravenously, is $2,134-$4,268 depending on dosage, according to a Genentech spokesperson.
Tocilizumab-bavi is an intravenous formulation (20 mg/mL) indicated for treatment of moderately to severely active RA, polyarticular juvenile idiopathic arthritis (PJIA), and systemic juvenile idiopathic arthritis (SJIA). The medication is administered every 4 weeks in RA and PJIA and every 8 weeks in SJIA as a single intravenous drip infusion over 1 hour.
The European Commission approved its first tocilizumab biosimilar, Tyenne (Fresenius Kabi), earlier in 2023 in both subcutaneous and intravenous formulations. Biogen did not comment on whether the company is working on a subcutaneous formulation for tocilizumab-bavi.
A version of this article appeared on Medscape.com.
The Food and Drug Administration has approved the biosimilar tocilizumab-bavi (Tofidence), Biogen, the drug’s manufacturer, announced on Sept. 29.
It is the first tocilizumab biosimilar approved by the FDA. The reference product, Actemra (Genentech), was first approved by the agency in 2010.
“The approval of Tofidence in the U.S. marks another positive step toward helping more people with chronic autoimmune conditions gain access to leading therapies,” Ian Henshaw, global head of biosimilars at Biogen, said in a statement. “With the increasing numbers of approved biosimilars, we expect increased savings and sustainability for health care systems and an increase in physician choice and patient access to biologics.”
Biogen’s pricing for tocilizumab-bavi will be available closer to the product’s launch date, which has yet to be determined, a company spokesman said. The U.S. average monthly cost of Actemra for rheumatoid arthritis, administered intravenously, is $2,134-$4,268 depending on dosage, according to a Genentech spokesperson.
Tocilizumab-bavi is an intravenous formulation (20 mg/mL) indicated for treatment of moderately to severely active RA, polyarticular juvenile idiopathic arthritis (PJIA), and systemic juvenile idiopathic arthritis (SJIA). The medication is administered every 4 weeks in RA and PJIA and every 8 weeks in SJIA as a single intravenous drip infusion over 1 hour.
The European Commission approved its first tocilizumab biosimilar, Tyenne (Fresenius Kabi), earlier in 2023 in both subcutaneous and intravenous formulations. Biogen did not comment on whether the company is working on a subcutaneous formulation for tocilizumab-bavi.
A version of this article appeared on Medscape.com.
The Food and Drug Administration has approved the biosimilar tocilizumab-bavi (Tofidence), Biogen, the drug’s manufacturer, announced on Sept. 29.
It is the first tocilizumab biosimilar approved by the FDA. The reference product, Actemra (Genentech), was first approved by the agency in 2010.
“The approval of Tofidence in the U.S. marks another positive step toward helping more people with chronic autoimmune conditions gain access to leading therapies,” Ian Henshaw, global head of biosimilars at Biogen, said in a statement. “With the increasing numbers of approved biosimilars, we expect increased savings and sustainability for health care systems and an increase in physician choice and patient access to biologics.”
Biogen’s pricing for tocilizumab-bavi will be available closer to the product’s launch date, which has yet to be determined, a company spokesman said. The U.S. average monthly cost of Actemra for rheumatoid arthritis, administered intravenously, is $2,134-$4,268 depending on dosage, according to a Genentech spokesperson.
Tocilizumab-bavi is an intravenous formulation (20 mg/mL) indicated for treatment of moderately to severely active RA, polyarticular juvenile idiopathic arthritis (PJIA), and systemic juvenile idiopathic arthritis (SJIA). The medication is administered every 4 weeks in RA and PJIA and every 8 weeks in SJIA as a single intravenous drip infusion over 1 hour.
The European Commission approved its first tocilizumab biosimilar, Tyenne (Fresenius Kabi), earlier in 2023 in both subcutaneous and intravenous formulations. Biogen did not comment on whether the company is working on a subcutaneous formulation for tocilizumab-bavi.
A version of this article appeared on Medscape.com.
Are cellular therapies the future of autoimmune disease?
A revolutionary treatment for cancers may also be able to treat and reset the immune system to provide long-term remission or possibly even cure certain autoimmune diseases.
Chimeric antigen receptor (CAR) T-cell therapy has offered a novel approach to treating hematologic cancers since 2017, but there are early signs that these cellular immunotherapies could be repurposed for B-cell mediated autoimmune diseases.
In September of last year, researchers in Germany reported that five patients with refractory systemic lupus erythematosus (SLE) treated with CAR T-cell therapy all achieved drug-free remission. At the time of publication, no patients had relapsed for up to 17 months after treatment. The authors described seroconversion of antinuclear antibodies in two patients with the longest follow-up, “indicating that abrogation of autoimmune B-cell clones may lead to a more widespread correction of autoimmunity,” the researchers write.
In another case study published in June, researchers used CD-19 targeted CAR-T cells to treat a 41-year-old man with refractory antisynthetase syndrome with progressive myositis and interstitial lung disease. Six months after treatment, there were no signs of myositis on MRI and a chest CT scan showed full regression of alveolitis.
Since then, two biotechnology companies – Cabaletta Bio in Philadelphia and Kyverna Therapeutics in Emeryville, Calif. – have already been granted fast-track designations from the U.S. Food and Drug Administration for CAR T-cell therapy for SLE and lupus nephritis. Bristol-Myers Squibb is also conducting a phase 1 trial in patients with severe, refractory SLE. Several biotechnology companies and hospitals in China are also conducting clinical trials for SLE. But this is only the tip of the iceberg regarding cellular therapies for autoimmune disease, said Max Konig, MD, PhD, an assistant professor of medicine in the division of rheumatology at Johns Hopkins University, Baltimore.
“It’s an incredibly exciting time. It’s unprecedented in the history of autoimmunity,” he noted.
A ‘reboot’ for the immune system
B-cell targeted therapies have been around since the early 2000s with drugs like rituximab, a monoclonal antibody medication that targets CD20, an antigen expressed on the surface of B cells. The CAR T cells currently available target another surface antigen, CD19, and are a much more potent therapy. Both are effective at depleting B cells in blood, but these engineered CD19-targeted T cells can reach B cells sitting in tissues in a way that antibody therapies cannot, Dr. Konig explained.
“If you have a patient with myositis, for example, where autoreactive B cells are sitting in the inflamed muscle, or a patient with rheumatoid arthritis, where you have disease-relevant B cells in hard-to-reach tissues like the synovium, those cells are much harder to deplete with an antibody, compared to a T cell that evolved to surveil and effectively kill in all tissues,” he explained.
In this process, T cells are collected from patients via leukapheresis and then re-engineered to express chimeric antigen receptors. A few days before these modified T cells are infused back into the patient, the patients are given a low-dose chemotherapy (lymphodepletion) regimen to help increase the effectiveness of the therapy. The one-time infusion is generally given on an inpatient basis, and patients are then monitored in hospital for side effects.
Once B cells are depleted, disease symptoms improve. But in the case studies published to date, once B cells re-emerge, they are naïve and no longer producing autoreactive B cells.
“Maybe it’s like a tabula rasa: You wipe [the B cells] out and start with a clean slate. Then, the immune system reboots, and now it’s working, whereas before it was messed up,” said Carl June, MD, who directs the Center for Cellular Immunotherapies at the at the University of Pennsylvania, Philadelphia. Dr. June and his research team led the development of CAR T-cell therapies for blood cancers.
The findings suggest that autoantibodies “might not be hardwired into the immune system,” he said.
But Dr. Konig stressed that we are still in the early days of clinical trials, and more research is necessary to understand the safety and efficacy of these therapies.
“There’s an incredible buzz around CAR T cells at the moment in rheumatology, which is great because I think that’s where the future is,” he said. “But we still need to learn how to appropriately apply these therapies in randomized, controlled trials.”
So far, the evidence behind CD19 CAR T-cell therapies in autoimmune disease is from case studies and phase 1 trials in a very small number of selected patients. (The upcoming Cabaletta and Kyverna trials in lupus will also be small, consisting of 12 patients each.)
Risks of intensive therapy
But while these therapies show promise, the process is very intensive. The lymphodepleting regimen increases the risk for infection and patients are commonly hospitalized for a week or more following infusion for toxicity monitoring. Serious adverse events such as cytokine release syndrome (CRS) can occur days to weeks after CAR T-cell infusion. In the five-patient case series reported in 2022, patients were hospitalized for 10 days following treatment.
The patient with antisynthetase syndrome, as well as three of five patients in the SLE case series study experienced mild CRS following infusion. Patients are also at a high risk for infection, as the engineered T cells target all B cells, not just the autoreactive immune cells.
The inability to differentiate between disease-causing and protective immune cells is an issue for all currently available drugs treating autoimmune disease, Dr. Konig said. But scientists are already working on how to make these potent cellular therapies safer and more precise.
Alternatives to standard CAR T-cell therapies
Engineering T cells with RNA is a new approach to limit the side effects and toxicity of CAR T-cell therapy, said Chris Jewell, PhD, the chief scientific officer at Cartesian Therapeutics, a biotechnology company based in Gaithersburg, Md. The company’s RNA CAR T-cell (rCAR-T) therapy – called DESCARTES-08 – is in phase 2 clinical trials for treatment of myasthenia gravis. Once these rCAR-T cells are infused in patients, as they divide, the RNAnaturally decays, he explained, meaning that after a certain point, the CAR is no longer expressed.
DESCARTES-08 targets B-cell maturation antigen (BCMA), which is primarily expressed on plasma cells, rather than all B cells, Dr. Jewell said.
“Targeting BCMA, we actually have a more selective profile,” he explained. “We are targeting the cells primarily responsible for the pathogenicity; many plasma cells – such as long-lived plasma cells – also take a long time to repopulate.”
This therapy also does not require lymphodepletion prior to infusion and can be done in an outpatient setting. The therapy is given in multiple infusions, once per week.
In the most recent clinical trial, patients with myasthenia gravis received six infusions over 6 weeks and experienced notable decreases in myasthenia gravis severity scale at up to 9 months of follow-up.
While standard CAR T-cell therapies under clinical investigational up to now all use effector T cells, regulatory T cells (Tregs) can also be engineered to target autoimmune disease. Abata Therapeutics, based in Boston, is using this approach for therapies for progressive multiple sclerosis and type 1 diabetes. These engineered Tregs express a T-cell receptor (TCR) that recognizes tissue-specific antigens and suppress inflammation at the site of the disease. “Treg-based cell therapies are really harnessing the natural power of regulatory cells to reset immune tolerance and recalibrate the immune system,” said their chief medical officer, Leonard Dragone, MD, PhD.
These therapies are derived from terminally differentiated cells that have limited capacity to produce pro-inflammatory cytokines including interleukin-2 or interferon gamma, Dr. Dragone explained. “CRS is difficult to envision from engineered Treg products and hasn’t been observed in any clinical experience with polyclonal Tregs,” he said.
This approach also does not require lymphodepletion prior to treatment. The company’s Treg cellular therapy for progressive MS is currently in investigational new drug-enabling studies, and they aim to dose their first patients in 2024.
Precision immunotherapy
For B-cell driven autoimmune diseases where the autoantibody is known, researchers have begun to re-engineer T cells to recognize only autoreactive B cells. While CD19 CAR T cells act more like a sledgehammer, these precision cellular immunotherapies are “like a razor’s strike,” Dr. June said.
“The chimeric autoantibody receptor (CAAR) approach targets autoantibodies that are expressed only on the surface of autoimmune B cells and are not expressed on normal B cells, which ideally should lead to precision targeting of just the cells that cause autoimmune disease,” explained Aimee Payne, MD, PhD, professor of dermatology and director of the Penn Clinical Autoimmunity Center of Excellence at the University of Pennsylvania, Philadelphia.
She and her research team used this approach to develop a treatment for mucosal pemphigus vulgaris, an autoimmune blistering disease of mucous membranes driven by autoantibodies against desmoglein 3.
“The current standard of care for pemphigus is to treat with steroids and rituximab, an infusion therapy that results in global, but temporary, B-cell depletion,” she said. “By expressing desmoglein 3 (DSG3) on the surface of the CAAR T-cell therapy, we target just the anti-DSG3 B cells that cause disease in mucosal pemphigus vulgaris and spare the healthy B cells.”
The therapy – called DSG3-CAART – is being developed by Cabaletta Bio and is now in phase 1 clinical trials. The approach is also being investigated to treat certain types of myasthenia gravis and membranous nephropathy.
Dr. Konig’s lab at Johns Hopkins developed and is now exploring a new precision cellular immunotherapy approach, chimeric autoantigen-T cell receptor (CATCR) T-cell therapy, to treat antiphospholipid syndrome, which is in preclinical stages. In this approach, Dr. Konig and his team are “re-engineering the natural T-cell receptor to selectively kill disease-causing B cells that drive antiphospholipid syndrome,” he explained.
He anticipates the CD19 CAR T-cell therapies currently in clinical trials will help to pave the way for this new generation of precision cellular therapies. The ultimate goal of these therapies, he said, is to uncouple therapeutic potency from infection risk.
“That’s really the holy grail in the treatment of autoimmune diseases. It’s tantalizingly close, but we’re not there yet.”
Dr. June is an inventor on patents and/or patent applications licensed to Novartis Institutes of Biomedical Research and receives license revenue from such licenses. Dr. June is a scientific founder of Tmunity Therapeutics and Capstan Therapeutics and is a member of the scientific advisory boards of AC Immune SA, Alaunos, BlueSphere Bio, Cabaletta, Carisma, Cartography Biosciences, Cellares, Celldex, Decheng Capital, Poseida, Verismo, and WIRB-Copernicus Group. Dr. Konig is a consultant for argenx and Revel and is listed as inventor for patent applications filed by John Hopkins University. Dr. Payne holds equity, grants, payments, and patent licensing from Cabaletta Bio and consults for Janssen.
A version of this article first appeared on Medscape.com.
A revolutionary treatment for cancers may also be able to treat and reset the immune system to provide long-term remission or possibly even cure certain autoimmune diseases.
Chimeric antigen receptor (CAR) T-cell therapy has offered a novel approach to treating hematologic cancers since 2017, but there are early signs that these cellular immunotherapies could be repurposed for B-cell mediated autoimmune diseases.
In September of last year, researchers in Germany reported that five patients with refractory systemic lupus erythematosus (SLE) treated with CAR T-cell therapy all achieved drug-free remission. At the time of publication, no patients had relapsed for up to 17 months after treatment. The authors described seroconversion of antinuclear antibodies in two patients with the longest follow-up, “indicating that abrogation of autoimmune B-cell clones may lead to a more widespread correction of autoimmunity,” the researchers write.
In another case study published in June, researchers used CD-19 targeted CAR-T cells to treat a 41-year-old man with refractory antisynthetase syndrome with progressive myositis and interstitial lung disease. Six months after treatment, there were no signs of myositis on MRI and a chest CT scan showed full regression of alveolitis.
Since then, two biotechnology companies – Cabaletta Bio in Philadelphia and Kyverna Therapeutics in Emeryville, Calif. – have already been granted fast-track designations from the U.S. Food and Drug Administration for CAR T-cell therapy for SLE and lupus nephritis. Bristol-Myers Squibb is also conducting a phase 1 trial in patients with severe, refractory SLE. Several biotechnology companies and hospitals in China are also conducting clinical trials for SLE. But this is only the tip of the iceberg regarding cellular therapies for autoimmune disease, said Max Konig, MD, PhD, an assistant professor of medicine in the division of rheumatology at Johns Hopkins University, Baltimore.
“It’s an incredibly exciting time. It’s unprecedented in the history of autoimmunity,” he noted.
A ‘reboot’ for the immune system
B-cell targeted therapies have been around since the early 2000s with drugs like rituximab, a monoclonal antibody medication that targets CD20, an antigen expressed on the surface of B cells. The CAR T cells currently available target another surface antigen, CD19, and are a much more potent therapy. Both are effective at depleting B cells in blood, but these engineered CD19-targeted T cells can reach B cells sitting in tissues in a way that antibody therapies cannot, Dr. Konig explained.
“If you have a patient with myositis, for example, where autoreactive B cells are sitting in the inflamed muscle, or a patient with rheumatoid arthritis, where you have disease-relevant B cells in hard-to-reach tissues like the synovium, those cells are much harder to deplete with an antibody, compared to a T cell that evolved to surveil and effectively kill in all tissues,” he explained.
In this process, T cells are collected from patients via leukapheresis and then re-engineered to express chimeric antigen receptors. A few days before these modified T cells are infused back into the patient, the patients are given a low-dose chemotherapy (lymphodepletion) regimen to help increase the effectiveness of the therapy. The one-time infusion is generally given on an inpatient basis, and patients are then monitored in hospital for side effects.
Once B cells are depleted, disease symptoms improve. But in the case studies published to date, once B cells re-emerge, they are naïve and no longer producing autoreactive B cells.
“Maybe it’s like a tabula rasa: You wipe [the B cells] out and start with a clean slate. Then, the immune system reboots, and now it’s working, whereas before it was messed up,” said Carl June, MD, who directs the Center for Cellular Immunotherapies at the at the University of Pennsylvania, Philadelphia. Dr. June and his research team led the development of CAR T-cell therapies for blood cancers.
The findings suggest that autoantibodies “might not be hardwired into the immune system,” he said.
But Dr. Konig stressed that we are still in the early days of clinical trials, and more research is necessary to understand the safety and efficacy of these therapies.
“There’s an incredible buzz around CAR T cells at the moment in rheumatology, which is great because I think that’s where the future is,” he said. “But we still need to learn how to appropriately apply these therapies in randomized, controlled trials.”
So far, the evidence behind CD19 CAR T-cell therapies in autoimmune disease is from case studies and phase 1 trials in a very small number of selected patients. (The upcoming Cabaletta and Kyverna trials in lupus will also be small, consisting of 12 patients each.)
Risks of intensive therapy
But while these therapies show promise, the process is very intensive. The lymphodepleting regimen increases the risk for infection and patients are commonly hospitalized for a week or more following infusion for toxicity monitoring. Serious adverse events such as cytokine release syndrome (CRS) can occur days to weeks after CAR T-cell infusion. In the five-patient case series reported in 2022, patients were hospitalized for 10 days following treatment.
The patient with antisynthetase syndrome, as well as three of five patients in the SLE case series study experienced mild CRS following infusion. Patients are also at a high risk for infection, as the engineered T cells target all B cells, not just the autoreactive immune cells.
The inability to differentiate between disease-causing and protective immune cells is an issue for all currently available drugs treating autoimmune disease, Dr. Konig said. But scientists are already working on how to make these potent cellular therapies safer and more precise.
Alternatives to standard CAR T-cell therapies
Engineering T cells with RNA is a new approach to limit the side effects and toxicity of CAR T-cell therapy, said Chris Jewell, PhD, the chief scientific officer at Cartesian Therapeutics, a biotechnology company based in Gaithersburg, Md. The company’s RNA CAR T-cell (rCAR-T) therapy – called DESCARTES-08 – is in phase 2 clinical trials for treatment of myasthenia gravis. Once these rCAR-T cells are infused in patients, as they divide, the RNAnaturally decays, he explained, meaning that after a certain point, the CAR is no longer expressed.
DESCARTES-08 targets B-cell maturation antigen (BCMA), which is primarily expressed on plasma cells, rather than all B cells, Dr. Jewell said.
“Targeting BCMA, we actually have a more selective profile,” he explained. “We are targeting the cells primarily responsible for the pathogenicity; many plasma cells – such as long-lived plasma cells – also take a long time to repopulate.”
This therapy also does not require lymphodepletion prior to infusion and can be done in an outpatient setting. The therapy is given in multiple infusions, once per week.
In the most recent clinical trial, patients with myasthenia gravis received six infusions over 6 weeks and experienced notable decreases in myasthenia gravis severity scale at up to 9 months of follow-up.
While standard CAR T-cell therapies under clinical investigational up to now all use effector T cells, regulatory T cells (Tregs) can also be engineered to target autoimmune disease. Abata Therapeutics, based in Boston, is using this approach for therapies for progressive multiple sclerosis and type 1 diabetes. These engineered Tregs express a T-cell receptor (TCR) that recognizes tissue-specific antigens and suppress inflammation at the site of the disease. “Treg-based cell therapies are really harnessing the natural power of regulatory cells to reset immune tolerance and recalibrate the immune system,” said their chief medical officer, Leonard Dragone, MD, PhD.
These therapies are derived from terminally differentiated cells that have limited capacity to produce pro-inflammatory cytokines including interleukin-2 or interferon gamma, Dr. Dragone explained. “CRS is difficult to envision from engineered Treg products and hasn’t been observed in any clinical experience with polyclonal Tregs,” he said.
This approach also does not require lymphodepletion prior to treatment. The company’s Treg cellular therapy for progressive MS is currently in investigational new drug-enabling studies, and they aim to dose their first patients in 2024.
Precision immunotherapy
For B-cell driven autoimmune diseases where the autoantibody is known, researchers have begun to re-engineer T cells to recognize only autoreactive B cells. While CD19 CAR T cells act more like a sledgehammer, these precision cellular immunotherapies are “like a razor’s strike,” Dr. June said.
“The chimeric autoantibody receptor (CAAR) approach targets autoantibodies that are expressed only on the surface of autoimmune B cells and are not expressed on normal B cells, which ideally should lead to precision targeting of just the cells that cause autoimmune disease,” explained Aimee Payne, MD, PhD, professor of dermatology and director of the Penn Clinical Autoimmunity Center of Excellence at the University of Pennsylvania, Philadelphia.
She and her research team used this approach to develop a treatment for mucosal pemphigus vulgaris, an autoimmune blistering disease of mucous membranes driven by autoantibodies against desmoglein 3.
“The current standard of care for pemphigus is to treat with steroids and rituximab, an infusion therapy that results in global, but temporary, B-cell depletion,” she said. “By expressing desmoglein 3 (DSG3) on the surface of the CAAR T-cell therapy, we target just the anti-DSG3 B cells that cause disease in mucosal pemphigus vulgaris and spare the healthy B cells.”
The therapy – called DSG3-CAART – is being developed by Cabaletta Bio and is now in phase 1 clinical trials. The approach is also being investigated to treat certain types of myasthenia gravis and membranous nephropathy.
Dr. Konig’s lab at Johns Hopkins developed and is now exploring a new precision cellular immunotherapy approach, chimeric autoantigen-T cell receptor (CATCR) T-cell therapy, to treat antiphospholipid syndrome, which is in preclinical stages. In this approach, Dr. Konig and his team are “re-engineering the natural T-cell receptor to selectively kill disease-causing B cells that drive antiphospholipid syndrome,” he explained.
He anticipates the CD19 CAR T-cell therapies currently in clinical trials will help to pave the way for this new generation of precision cellular therapies. The ultimate goal of these therapies, he said, is to uncouple therapeutic potency from infection risk.
“That’s really the holy grail in the treatment of autoimmune diseases. It’s tantalizingly close, but we’re not there yet.”
Dr. June is an inventor on patents and/or patent applications licensed to Novartis Institutes of Biomedical Research and receives license revenue from such licenses. Dr. June is a scientific founder of Tmunity Therapeutics and Capstan Therapeutics and is a member of the scientific advisory boards of AC Immune SA, Alaunos, BlueSphere Bio, Cabaletta, Carisma, Cartography Biosciences, Cellares, Celldex, Decheng Capital, Poseida, Verismo, and WIRB-Copernicus Group. Dr. Konig is a consultant for argenx and Revel and is listed as inventor for patent applications filed by John Hopkins University. Dr. Payne holds equity, grants, payments, and patent licensing from Cabaletta Bio and consults for Janssen.
A version of this article first appeared on Medscape.com.
A revolutionary treatment for cancers may also be able to treat and reset the immune system to provide long-term remission or possibly even cure certain autoimmune diseases.
Chimeric antigen receptor (CAR) T-cell therapy has offered a novel approach to treating hematologic cancers since 2017, but there are early signs that these cellular immunotherapies could be repurposed for B-cell mediated autoimmune diseases.
In September of last year, researchers in Germany reported that five patients with refractory systemic lupus erythematosus (SLE) treated with CAR T-cell therapy all achieved drug-free remission. At the time of publication, no patients had relapsed for up to 17 months after treatment. The authors described seroconversion of antinuclear antibodies in two patients with the longest follow-up, “indicating that abrogation of autoimmune B-cell clones may lead to a more widespread correction of autoimmunity,” the researchers write.
In another case study published in June, researchers used CD-19 targeted CAR-T cells to treat a 41-year-old man with refractory antisynthetase syndrome with progressive myositis and interstitial lung disease. Six months after treatment, there were no signs of myositis on MRI and a chest CT scan showed full regression of alveolitis.
Since then, two biotechnology companies – Cabaletta Bio in Philadelphia and Kyverna Therapeutics in Emeryville, Calif. – have already been granted fast-track designations from the U.S. Food and Drug Administration for CAR T-cell therapy for SLE and lupus nephritis. Bristol-Myers Squibb is also conducting a phase 1 trial in patients with severe, refractory SLE. Several biotechnology companies and hospitals in China are also conducting clinical trials for SLE. But this is only the tip of the iceberg regarding cellular therapies for autoimmune disease, said Max Konig, MD, PhD, an assistant professor of medicine in the division of rheumatology at Johns Hopkins University, Baltimore.
“It’s an incredibly exciting time. It’s unprecedented in the history of autoimmunity,” he noted.
A ‘reboot’ for the immune system
B-cell targeted therapies have been around since the early 2000s with drugs like rituximab, a monoclonal antibody medication that targets CD20, an antigen expressed on the surface of B cells. The CAR T cells currently available target another surface antigen, CD19, and are a much more potent therapy. Both are effective at depleting B cells in blood, but these engineered CD19-targeted T cells can reach B cells sitting in tissues in a way that antibody therapies cannot, Dr. Konig explained.
“If you have a patient with myositis, for example, where autoreactive B cells are sitting in the inflamed muscle, or a patient with rheumatoid arthritis, where you have disease-relevant B cells in hard-to-reach tissues like the synovium, those cells are much harder to deplete with an antibody, compared to a T cell that evolved to surveil and effectively kill in all tissues,” he explained.
In this process, T cells are collected from patients via leukapheresis and then re-engineered to express chimeric antigen receptors. A few days before these modified T cells are infused back into the patient, the patients are given a low-dose chemotherapy (lymphodepletion) regimen to help increase the effectiveness of the therapy. The one-time infusion is generally given on an inpatient basis, and patients are then monitored in hospital for side effects.
Once B cells are depleted, disease symptoms improve. But in the case studies published to date, once B cells re-emerge, they are naïve and no longer producing autoreactive B cells.
“Maybe it’s like a tabula rasa: You wipe [the B cells] out and start with a clean slate. Then, the immune system reboots, and now it’s working, whereas before it was messed up,” said Carl June, MD, who directs the Center for Cellular Immunotherapies at the at the University of Pennsylvania, Philadelphia. Dr. June and his research team led the development of CAR T-cell therapies for blood cancers.
The findings suggest that autoantibodies “might not be hardwired into the immune system,” he said.
But Dr. Konig stressed that we are still in the early days of clinical trials, and more research is necessary to understand the safety and efficacy of these therapies.
“There’s an incredible buzz around CAR T cells at the moment in rheumatology, which is great because I think that’s where the future is,” he said. “But we still need to learn how to appropriately apply these therapies in randomized, controlled trials.”
So far, the evidence behind CD19 CAR T-cell therapies in autoimmune disease is from case studies and phase 1 trials in a very small number of selected patients. (The upcoming Cabaletta and Kyverna trials in lupus will also be small, consisting of 12 patients each.)
Risks of intensive therapy
But while these therapies show promise, the process is very intensive. The lymphodepleting regimen increases the risk for infection and patients are commonly hospitalized for a week or more following infusion for toxicity monitoring. Serious adverse events such as cytokine release syndrome (CRS) can occur days to weeks after CAR T-cell infusion. In the five-patient case series reported in 2022, patients were hospitalized for 10 days following treatment.
The patient with antisynthetase syndrome, as well as three of five patients in the SLE case series study experienced mild CRS following infusion. Patients are also at a high risk for infection, as the engineered T cells target all B cells, not just the autoreactive immune cells.
The inability to differentiate between disease-causing and protective immune cells is an issue for all currently available drugs treating autoimmune disease, Dr. Konig said. But scientists are already working on how to make these potent cellular therapies safer and more precise.
Alternatives to standard CAR T-cell therapies
Engineering T cells with RNA is a new approach to limit the side effects and toxicity of CAR T-cell therapy, said Chris Jewell, PhD, the chief scientific officer at Cartesian Therapeutics, a biotechnology company based in Gaithersburg, Md. The company’s RNA CAR T-cell (rCAR-T) therapy – called DESCARTES-08 – is in phase 2 clinical trials for treatment of myasthenia gravis. Once these rCAR-T cells are infused in patients, as they divide, the RNAnaturally decays, he explained, meaning that after a certain point, the CAR is no longer expressed.
DESCARTES-08 targets B-cell maturation antigen (BCMA), which is primarily expressed on plasma cells, rather than all B cells, Dr. Jewell said.
“Targeting BCMA, we actually have a more selective profile,” he explained. “We are targeting the cells primarily responsible for the pathogenicity; many plasma cells – such as long-lived plasma cells – also take a long time to repopulate.”
This therapy also does not require lymphodepletion prior to infusion and can be done in an outpatient setting. The therapy is given in multiple infusions, once per week.
In the most recent clinical trial, patients with myasthenia gravis received six infusions over 6 weeks and experienced notable decreases in myasthenia gravis severity scale at up to 9 months of follow-up.
While standard CAR T-cell therapies under clinical investigational up to now all use effector T cells, regulatory T cells (Tregs) can also be engineered to target autoimmune disease. Abata Therapeutics, based in Boston, is using this approach for therapies for progressive multiple sclerosis and type 1 diabetes. These engineered Tregs express a T-cell receptor (TCR) that recognizes tissue-specific antigens and suppress inflammation at the site of the disease. “Treg-based cell therapies are really harnessing the natural power of regulatory cells to reset immune tolerance and recalibrate the immune system,” said their chief medical officer, Leonard Dragone, MD, PhD.
These therapies are derived from terminally differentiated cells that have limited capacity to produce pro-inflammatory cytokines including interleukin-2 or interferon gamma, Dr. Dragone explained. “CRS is difficult to envision from engineered Treg products and hasn’t been observed in any clinical experience with polyclonal Tregs,” he said.
This approach also does not require lymphodepletion prior to treatment. The company’s Treg cellular therapy for progressive MS is currently in investigational new drug-enabling studies, and they aim to dose their first patients in 2024.
Precision immunotherapy
For B-cell driven autoimmune diseases where the autoantibody is known, researchers have begun to re-engineer T cells to recognize only autoreactive B cells. While CD19 CAR T cells act more like a sledgehammer, these precision cellular immunotherapies are “like a razor’s strike,” Dr. June said.
“The chimeric autoantibody receptor (CAAR) approach targets autoantibodies that are expressed only on the surface of autoimmune B cells and are not expressed on normal B cells, which ideally should lead to precision targeting of just the cells that cause autoimmune disease,” explained Aimee Payne, MD, PhD, professor of dermatology and director of the Penn Clinical Autoimmunity Center of Excellence at the University of Pennsylvania, Philadelphia.
She and her research team used this approach to develop a treatment for mucosal pemphigus vulgaris, an autoimmune blistering disease of mucous membranes driven by autoantibodies against desmoglein 3.
“The current standard of care for pemphigus is to treat with steroids and rituximab, an infusion therapy that results in global, but temporary, B-cell depletion,” she said. “By expressing desmoglein 3 (DSG3) on the surface of the CAAR T-cell therapy, we target just the anti-DSG3 B cells that cause disease in mucosal pemphigus vulgaris and spare the healthy B cells.”
The therapy – called DSG3-CAART – is being developed by Cabaletta Bio and is now in phase 1 clinical trials. The approach is also being investigated to treat certain types of myasthenia gravis and membranous nephropathy.
Dr. Konig’s lab at Johns Hopkins developed and is now exploring a new precision cellular immunotherapy approach, chimeric autoantigen-T cell receptor (CATCR) T-cell therapy, to treat antiphospholipid syndrome, which is in preclinical stages. In this approach, Dr. Konig and his team are “re-engineering the natural T-cell receptor to selectively kill disease-causing B cells that drive antiphospholipid syndrome,” he explained.
He anticipates the CD19 CAR T-cell therapies currently in clinical trials will help to pave the way for this new generation of precision cellular therapies. The ultimate goal of these therapies, he said, is to uncouple therapeutic potency from infection risk.
“That’s really the holy grail in the treatment of autoimmune diseases. It’s tantalizingly close, but we’re not there yet.”
Dr. June is an inventor on patents and/or patent applications licensed to Novartis Institutes of Biomedical Research and receives license revenue from such licenses. Dr. June is a scientific founder of Tmunity Therapeutics and Capstan Therapeutics and is a member of the scientific advisory boards of AC Immune SA, Alaunos, BlueSphere Bio, Cabaletta, Carisma, Cartography Biosciences, Cellares, Celldex, Decheng Capital, Poseida, Verismo, and WIRB-Copernicus Group. Dr. Konig is a consultant for argenx and Revel and is listed as inventor for patent applications filed by John Hopkins University. Dr. Payne holds equity, grants, payments, and patent licensing from Cabaletta Bio and consults for Janssen.
A version of this article first appeared on Medscape.com.
Colchicine still needed to prevent gout flares in allopurinol ‘start-low, go-slow’ strategy
The use of colchicine prophylaxis during the process of up-titrating allopurinol slowly to reach target serum urate levels for patients with gout proved necessary to reduce the risk of flares in a randomized, double-blind, placebo-controlled noninferiority trial conducted by researchers in New Zealand.
Use of colchicine led to fewer flares during the first 6 months after initiating treatment with allopurinol, but when colchicine and placebo were stopped at 6 months, the number of flares rose, and there was no overall difference in the average number of flares between the placebo and colchicine groups over 12 months.
“Gout flares are common when starting urate-lowering therapy, although may be less frequent using the newer allopurinol ‘start-low, go-slow’ dose escalation strategy,” Lisa Stamp, MBChB, PhD, of the University of Otago, Christchurch, New Zealand, and colleagues write in Annals of the Rheumatic Diseases. “This study was undertaken to determine whether colchicine prophylaxis is required with the more gradual dose escalation of allopurinol to achieve target serum urate.”
The study was published online in the BMJ.
The researchers randomly assigned 200 participants to receive colchicine 0.5 mg daily or placebo. At the same time, allopurinol 50 mg daily was initially given to those with an estimated glomerular filtration rate (eGFR) less than 60 mL/min/1.73 m2, and 100 mg daily was given to those with eGFR greater than or equal to 60 mL/min/1.73 m2; doses were increased monthly by 50 mg daily for those with eGFR less than 60 and by 100 mg daily for those with eGFR greater than or equal to 60 until the target urate level of less than 0.36 mmol/L (about < 6 mg/dL) was achieved. In total, 93% of patients were male, and 69% were White. Patients were enrolled from February 2019 through December 2021. The final study visit was in January 2023. Researchers tracked the mean number of patient-reported gout flares per month with a prespecified noninferiority margin of 0.12 gout flares/month. After the first 6 months, colchicine and placebo were stopped, and researchers continued to track outcomes up to month 12.
From baseline to 6 months, there were more gout flares per month in the placebo group (0.61) than in the colchicine group (0.35). From 6 to 12 months, there were more gout flares among patients who previously received colchicine, compared with those who received placebo. While 22.8% of patients in the colchicine group experienced flares at month 6, the following month – after stopping the drug – 41.2% experienced flares. For comparison, 30.8% of the placebo group experienced flares at month 6, and in month 7, 23.5% experienced flares. The spike in flares in the colchicine group began to decline after month 9.
Among the colchicine and placebo groups, reductions in serum urate at 6 and 12 months were similar, and mean serum urate levels declined below 0.36 mmol/L at 4 months and thereafter. Both groups reached a mean allopurinol dose of 280 mg/d at 6 months.
It is not clear what caused this rise in flares in the colchicine group, Stamp noted in an email to this news organization. Overall, there was no difference in the average number of gout flares between either group over the entire 12-month study period.
The study findings make a case for continuing colchicine prophylaxis considerably beyond the point at which the target urate serum level is reached, said Robert Terkeltaub, MD, professor emeritus of medicine in the division of rheumatology, allergy, and immunology at the University of California, San Diego. He was not involved with the research.
“The flare burden with this really conservative allopurinol dosing regimen is really stunning,” he said in an interview. Despite this “start low and go slow” strategy, flares remained a problem, he noted. “It argues that you need at least a year to get out of the woods and have a lower flare burden, even if colchicine prophylaxis is used for the first 6 months.”
The current standard of care in rheumatology for gout treatment includes flare prophylaxis when starting urate-lowering therapy. In daily practice, “this can (and often does) mean continuing flare prophylaxis for longer than the recommended minimum duration from [established] gout treatment guidelines for an individual patient,” explained Elizabeth R. Graef, DO, assistant professor of medicine at Boston University and a rheumatologist at Boston Medical Center.
There are many different factors to consider when determining a patient’s flare risk beyond serum urate levels and date of last flare, she noted. Flare severity, concurrent diuretic use, dose changes, tophus count, and additional health conditions such as diabetes can all contribute to individual patient outcomes.
“Gout is an erosive arthritis, and every time someone flares, there’s a risk of permanent erosive damage, so I tend to be more aggressive with prophylaxis,” she said.
The study was funded by the Health Research Council of New Zealand. Dr. Graef disclosed no relevant financial relationships. Dr. Terkeltaub consults for LG Chem, Fortress/Urica, Selecta Biosciences, Horizon Therapeutics, Atom Biosciences, Acquist Therapeutics, Generate Biomedicines, AstraZeneca, and Synlogic. Dr. Terkeltaub serves as the nonsalaried president of the Gout, Hyperuricemia, and Crystal-Associated Disease Network, which annually receives unrestricted arms-length grant support from pharma donors.
A version of this article first appeared on Medscape.com.
The use of colchicine prophylaxis during the process of up-titrating allopurinol slowly to reach target serum urate levels for patients with gout proved necessary to reduce the risk of flares in a randomized, double-blind, placebo-controlled noninferiority trial conducted by researchers in New Zealand.
Use of colchicine led to fewer flares during the first 6 months after initiating treatment with allopurinol, but when colchicine and placebo were stopped at 6 months, the number of flares rose, and there was no overall difference in the average number of flares between the placebo and colchicine groups over 12 months.
“Gout flares are common when starting urate-lowering therapy, although may be less frequent using the newer allopurinol ‘start-low, go-slow’ dose escalation strategy,” Lisa Stamp, MBChB, PhD, of the University of Otago, Christchurch, New Zealand, and colleagues write in Annals of the Rheumatic Diseases. “This study was undertaken to determine whether colchicine prophylaxis is required with the more gradual dose escalation of allopurinol to achieve target serum urate.”
The study was published online in the BMJ.
The researchers randomly assigned 200 participants to receive colchicine 0.5 mg daily or placebo. At the same time, allopurinol 50 mg daily was initially given to those with an estimated glomerular filtration rate (eGFR) less than 60 mL/min/1.73 m2, and 100 mg daily was given to those with eGFR greater than or equal to 60 mL/min/1.73 m2; doses were increased monthly by 50 mg daily for those with eGFR less than 60 and by 100 mg daily for those with eGFR greater than or equal to 60 until the target urate level of less than 0.36 mmol/L (about < 6 mg/dL) was achieved. In total, 93% of patients were male, and 69% were White. Patients were enrolled from February 2019 through December 2021. The final study visit was in January 2023. Researchers tracked the mean number of patient-reported gout flares per month with a prespecified noninferiority margin of 0.12 gout flares/month. After the first 6 months, colchicine and placebo were stopped, and researchers continued to track outcomes up to month 12.
From baseline to 6 months, there were more gout flares per month in the placebo group (0.61) than in the colchicine group (0.35). From 6 to 12 months, there were more gout flares among patients who previously received colchicine, compared with those who received placebo. While 22.8% of patients in the colchicine group experienced flares at month 6, the following month – after stopping the drug – 41.2% experienced flares. For comparison, 30.8% of the placebo group experienced flares at month 6, and in month 7, 23.5% experienced flares. The spike in flares in the colchicine group began to decline after month 9.
Among the colchicine and placebo groups, reductions in serum urate at 6 and 12 months were similar, and mean serum urate levels declined below 0.36 mmol/L at 4 months and thereafter. Both groups reached a mean allopurinol dose of 280 mg/d at 6 months.
It is not clear what caused this rise in flares in the colchicine group, Stamp noted in an email to this news organization. Overall, there was no difference in the average number of gout flares between either group over the entire 12-month study period.
The study findings make a case for continuing colchicine prophylaxis considerably beyond the point at which the target urate serum level is reached, said Robert Terkeltaub, MD, professor emeritus of medicine in the division of rheumatology, allergy, and immunology at the University of California, San Diego. He was not involved with the research.
“The flare burden with this really conservative allopurinol dosing regimen is really stunning,” he said in an interview. Despite this “start low and go slow” strategy, flares remained a problem, he noted. “It argues that you need at least a year to get out of the woods and have a lower flare burden, even if colchicine prophylaxis is used for the first 6 months.”
The current standard of care in rheumatology for gout treatment includes flare prophylaxis when starting urate-lowering therapy. In daily practice, “this can (and often does) mean continuing flare prophylaxis for longer than the recommended minimum duration from [established] gout treatment guidelines for an individual patient,” explained Elizabeth R. Graef, DO, assistant professor of medicine at Boston University and a rheumatologist at Boston Medical Center.
There are many different factors to consider when determining a patient’s flare risk beyond serum urate levels and date of last flare, she noted. Flare severity, concurrent diuretic use, dose changes, tophus count, and additional health conditions such as diabetes can all contribute to individual patient outcomes.
“Gout is an erosive arthritis, and every time someone flares, there’s a risk of permanent erosive damage, so I tend to be more aggressive with prophylaxis,” she said.
The study was funded by the Health Research Council of New Zealand. Dr. Graef disclosed no relevant financial relationships. Dr. Terkeltaub consults for LG Chem, Fortress/Urica, Selecta Biosciences, Horizon Therapeutics, Atom Biosciences, Acquist Therapeutics, Generate Biomedicines, AstraZeneca, and Synlogic. Dr. Terkeltaub serves as the nonsalaried president of the Gout, Hyperuricemia, and Crystal-Associated Disease Network, which annually receives unrestricted arms-length grant support from pharma donors.
A version of this article first appeared on Medscape.com.
The use of colchicine prophylaxis during the process of up-titrating allopurinol slowly to reach target serum urate levels for patients with gout proved necessary to reduce the risk of flares in a randomized, double-blind, placebo-controlled noninferiority trial conducted by researchers in New Zealand.
Use of colchicine led to fewer flares during the first 6 months after initiating treatment with allopurinol, but when colchicine and placebo were stopped at 6 months, the number of flares rose, and there was no overall difference in the average number of flares between the placebo and colchicine groups over 12 months.
“Gout flares are common when starting urate-lowering therapy, although may be less frequent using the newer allopurinol ‘start-low, go-slow’ dose escalation strategy,” Lisa Stamp, MBChB, PhD, of the University of Otago, Christchurch, New Zealand, and colleagues write in Annals of the Rheumatic Diseases. “This study was undertaken to determine whether colchicine prophylaxis is required with the more gradual dose escalation of allopurinol to achieve target serum urate.”
The study was published online in the BMJ.
The researchers randomly assigned 200 participants to receive colchicine 0.5 mg daily or placebo. At the same time, allopurinol 50 mg daily was initially given to those with an estimated glomerular filtration rate (eGFR) less than 60 mL/min/1.73 m2, and 100 mg daily was given to those with eGFR greater than or equal to 60 mL/min/1.73 m2; doses were increased monthly by 50 mg daily for those with eGFR less than 60 and by 100 mg daily for those with eGFR greater than or equal to 60 until the target urate level of less than 0.36 mmol/L (about < 6 mg/dL) was achieved. In total, 93% of patients were male, and 69% were White. Patients were enrolled from February 2019 through December 2021. The final study visit was in January 2023. Researchers tracked the mean number of patient-reported gout flares per month with a prespecified noninferiority margin of 0.12 gout flares/month. After the first 6 months, colchicine and placebo were stopped, and researchers continued to track outcomes up to month 12.
From baseline to 6 months, there were more gout flares per month in the placebo group (0.61) than in the colchicine group (0.35). From 6 to 12 months, there were more gout flares among patients who previously received colchicine, compared with those who received placebo. While 22.8% of patients in the colchicine group experienced flares at month 6, the following month – after stopping the drug – 41.2% experienced flares. For comparison, 30.8% of the placebo group experienced flares at month 6, and in month 7, 23.5% experienced flares. The spike in flares in the colchicine group began to decline after month 9.
Among the colchicine and placebo groups, reductions in serum urate at 6 and 12 months were similar, and mean serum urate levels declined below 0.36 mmol/L at 4 months and thereafter. Both groups reached a mean allopurinol dose of 280 mg/d at 6 months.
It is not clear what caused this rise in flares in the colchicine group, Stamp noted in an email to this news organization. Overall, there was no difference in the average number of gout flares between either group over the entire 12-month study period.
The study findings make a case for continuing colchicine prophylaxis considerably beyond the point at which the target urate serum level is reached, said Robert Terkeltaub, MD, professor emeritus of medicine in the division of rheumatology, allergy, and immunology at the University of California, San Diego. He was not involved with the research.
“The flare burden with this really conservative allopurinol dosing regimen is really stunning,” he said in an interview. Despite this “start low and go slow” strategy, flares remained a problem, he noted. “It argues that you need at least a year to get out of the woods and have a lower flare burden, even if colchicine prophylaxis is used for the first 6 months.”
The current standard of care in rheumatology for gout treatment includes flare prophylaxis when starting urate-lowering therapy. In daily practice, “this can (and often does) mean continuing flare prophylaxis for longer than the recommended minimum duration from [established] gout treatment guidelines for an individual patient,” explained Elizabeth R. Graef, DO, assistant professor of medicine at Boston University and a rheumatologist at Boston Medical Center.
There are many different factors to consider when determining a patient’s flare risk beyond serum urate levels and date of last flare, she noted. Flare severity, concurrent diuretic use, dose changes, tophus count, and additional health conditions such as diabetes can all contribute to individual patient outcomes.
“Gout is an erosive arthritis, and every time someone flares, there’s a risk of permanent erosive damage, so I tend to be more aggressive with prophylaxis,” she said.
The study was funded by the Health Research Council of New Zealand. Dr. Graef disclosed no relevant financial relationships. Dr. Terkeltaub consults for LG Chem, Fortress/Urica, Selecta Biosciences, Horizon Therapeutics, Atom Biosciences, Acquist Therapeutics, Generate Biomedicines, AstraZeneca, and Synlogic. Dr. Terkeltaub serves as the nonsalaried president of the Gout, Hyperuricemia, and Crystal-Associated Disease Network, which annually receives unrestricted arms-length grant support from pharma donors.
A version of this article first appeared on Medscape.com.
Precision blood test for rheumatoid arthritis receives Medicare coverage
Medicare will now cover a molecular diagnostic test to predict treatment response for certain patients with rheumatoid arthritis.
The blood test, PrismRA, is the first and only commercially available test that can help predict which patients with RA are unlikely to respond to tumor necrosis factor inhibitor therapy, according to the test manufacturer, Scipher Medicine.
“Precision medicine will now be accessible to many patients suffering from RA, a potentially debilitating disease if not treated with the right therapy,” Alif Saleh, the company’s chief executive officer, said in a press release on Sept. 7. “This coverage decision not only represents a significant benefit for patients today but also ushers in a new era of precision medicine in autoimmune diseases.”
PrismRA was first made available in December 2021 for commercial billing. The test costs about $5,000, but most patients with insurance coverage pay less than $75 out-of-pocket after insurance, according to Scipher.
On Sept. 1, 2022, the Medicare administrative contractor Palmetto GBA published a draft recommendation that the test should not be covered by the national health insurance program, stating that biomarker tests “have not yet demonstrated definitive value above the combination of available clinical, laboratory, and demographic data.”
During the comment period, clinicians urged the contractor to reconsider.
“I do not have a test or clinical assessment to inform me of the right biologic for my patients. I utilize the PrismRA test to inform me which biologic is the best start. Without this valuable tool, I am left with prescribing based on what is dictated by the patient’s insurance,” wrote one commenter.
These responses and additional data published during the comment period resulted in Palmetto GBA revising their decision.
“We agree that despite the many limitations of predictive biomarker tests, a review of the evidence supports their limited use given their demonstrated validity and utility,” the company wrote in response. “Specifically, when a nonresponse signature is obtained by the molecular signature response classifier, nearly 90% of those patients will prove to not clinically respond to TNFi therapies using multiple validated disease response criteria including the ACR50 and CDAI. For these patients, a change in management would ultimately serve to avoid time on an unnecessary therapy and shorten the time to an appropriate therapy.”
The local coverage determination provides Medicare coverage nationally for patients who have a confirmed diagnosis of moderate to severely active RA, have failed first-line therapy for RA treatment, and have not started biologic or targeted synthetic therapy for RA or who are being considered for an alternative class of targeted therapy due to failure of an initially targeted therapy despite adequate dosing.
The LCD becomes effective for tests performed on or after Oct. 15, 2023.
A version of this article first appeared on Medscape.com.
Medicare will now cover a molecular diagnostic test to predict treatment response for certain patients with rheumatoid arthritis.
The blood test, PrismRA, is the first and only commercially available test that can help predict which patients with RA are unlikely to respond to tumor necrosis factor inhibitor therapy, according to the test manufacturer, Scipher Medicine.
“Precision medicine will now be accessible to many patients suffering from RA, a potentially debilitating disease if not treated with the right therapy,” Alif Saleh, the company’s chief executive officer, said in a press release on Sept. 7. “This coverage decision not only represents a significant benefit for patients today but also ushers in a new era of precision medicine in autoimmune diseases.”
PrismRA was first made available in December 2021 for commercial billing. The test costs about $5,000, but most patients with insurance coverage pay less than $75 out-of-pocket after insurance, according to Scipher.
On Sept. 1, 2022, the Medicare administrative contractor Palmetto GBA published a draft recommendation that the test should not be covered by the national health insurance program, stating that biomarker tests “have not yet demonstrated definitive value above the combination of available clinical, laboratory, and demographic data.”
During the comment period, clinicians urged the contractor to reconsider.
“I do not have a test or clinical assessment to inform me of the right biologic for my patients. I utilize the PrismRA test to inform me which biologic is the best start. Without this valuable tool, I am left with prescribing based on what is dictated by the patient’s insurance,” wrote one commenter.
These responses and additional data published during the comment period resulted in Palmetto GBA revising their decision.
“We agree that despite the many limitations of predictive biomarker tests, a review of the evidence supports their limited use given their demonstrated validity and utility,” the company wrote in response. “Specifically, when a nonresponse signature is obtained by the molecular signature response classifier, nearly 90% of those patients will prove to not clinically respond to TNFi therapies using multiple validated disease response criteria including the ACR50 and CDAI. For these patients, a change in management would ultimately serve to avoid time on an unnecessary therapy and shorten the time to an appropriate therapy.”
The local coverage determination provides Medicare coverage nationally for patients who have a confirmed diagnosis of moderate to severely active RA, have failed first-line therapy for RA treatment, and have not started biologic or targeted synthetic therapy for RA or who are being considered for an alternative class of targeted therapy due to failure of an initially targeted therapy despite adequate dosing.
The LCD becomes effective for tests performed on or after Oct. 15, 2023.
A version of this article first appeared on Medscape.com.
Medicare will now cover a molecular diagnostic test to predict treatment response for certain patients with rheumatoid arthritis.
The blood test, PrismRA, is the first and only commercially available test that can help predict which patients with RA are unlikely to respond to tumor necrosis factor inhibitor therapy, according to the test manufacturer, Scipher Medicine.
“Precision medicine will now be accessible to many patients suffering from RA, a potentially debilitating disease if not treated with the right therapy,” Alif Saleh, the company’s chief executive officer, said in a press release on Sept. 7. “This coverage decision not only represents a significant benefit for patients today but also ushers in a new era of precision medicine in autoimmune diseases.”
PrismRA was first made available in December 2021 for commercial billing. The test costs about $5,000, but most patients with insurance coverage pay less than $75 out-of-pocket after insurance, according to Scipher.
On Sept. 1, 2022, the Medicare administrative contractor Palmetto GBA published a draft recommendation that the test should not be covered by the national health insurance program, stating that biomarker tests “have not yet demonstrated definitive value above the combination of available clinical, laboratory, and demographic data.”
During the comment period, clinicians urged the contractor to reconsider.
“I do not have a test or clinical assessment to inform me of the right biologic for my patients. I utilize the PrismRA test to inform me which biologic is the best start. Without this valuable tool, I am left with prescribing based on what is dictated by the patient’s insurance,” wrote one commenter.
These responses and additional data published during the comment period resulted in Palmetto GBA revising their decision.
“We agree that despite the many limitations of predictive biomarker tests, a review of the evidence supports their limited use given their demonstrated validity and utility,” the company wrote in response. “Specifically, when a nonresponse signature is obtained by the molecular signature response classifier, nearly 90% of those patients will prove to not clinically respond to TNFi therapies using multiple validated disease response criteria including the ACR50 and CDAI. For these patients, a change in management would ultimately serve to avoid time on an unnecessary therapy and shorten the time to an appropriate therapy.”
The local coverage determination provides Medicare coverage nationally for patients who have a confirmed diagnosis of moderate to severely active RA, have failed first-line therapy for RA treatment, and have not started biologic or targeted synthetic therapy for RA or who are being considered for an alternative class of targeted therapy due to failure of an initially targeted therapy despite adequate dosing.
The LCD becomes effective for tests performed on or after Oct. 15, 2023.
A version of this article first appeared on Medscape.com.