User login
Scleroligation procedure proposed for gastroesophageal varices
In the treatment of gastroesophageal varices, scleroligation – a hybrid procedure that combines sclerotherapy and band ligation – performed as well as did band ligation, but required fewer sessions and had a shorter overall treatment duration. Sclerotherapy involves the injection of sclerosant to prompt occlusion of the varices, while ligation involves banding the varices to cut off blood flow.
The new approach combines them. The researchers ligated the varix 3-5 cm from the gastroesophageal junction and injected the sclerosant into the varix, below the ligated section. They reasoned that ligation should increase the contact time between the sclerosant and endothelial cells, and thus improve efficacy.
He noted that in the United States, band ligation is the standard of therapy, and the new study won’t change that. “These preliminary results from a single center are quite promising, and if they can be confirmed in a larger, multicenter trial, then this is something that can be added to our therapeutic armamentarium,” said Dr. Kwo.
Band ligation replaced sclerotherapy as the preferred treatment for gastroesophageal varices because it has equal efficacy but fewer severe side effects. However, it also suffers from a higher rate of recurrence because the bands cannot destroy deeper varices and perforating veins.
The combination technique, scleroligation, has been demonstrated in the treatment of esophageal varices, which prompted the authors’ investigation into gastroesophageal varices.
At a single center, the researchers recruited 120 patients with cirrhosis and acute gastroesophageal variceal bleeding above the gastroesophageal junction. They were randomized 1:1 to undergo endoscopic band ligation (EBL) or scleroligation (SL).
On average, 15.6 weeks were required to obliterate the varices in the EBL group versus 8.64 weeks in the SL group (P less than .001). The EBL group required an average of 3.43 sessions to reach that endpoint, compared with 2.22 sessions in the SL group (P less than .001). The EBL group required an average of 13.72 bands per patient, compared with 8.88 bands in the SL group (P less than .001). The EBL group also had a higher average number of units of blood transfused (2.30 vs 1.53; P less than .001).
No patients in either group experienced perforation, chest empyema, pericardial effusion, or strictures.
The good safety outcomes may be related to the small volume of sclerosant used, just 2 mL. “It’s probably because of their meticulous approach that they were able to reduce the complications that we have historically seen with sclerotherapy alone,” said Dr. Kwo.
There was no difference in the number of rebleeds or recurrences at follow-up, total cost, mortality due to rebleeding, or 12-month survival.
No funding source was disclosed. The authors reported no financial disclosures.
In the treatment of gastroesophageal varices, scleroligation – a hybrid procedure that combines sclerotherapy and band ligation – performed as well as did band ligation, but required fewer sessions and had a shorter overall treatment duration. Sclerotherapy involves the injection of sclerosant to prompt occlusion of the varices, while ligation involves banding the varices to cut off blood flow.
The new approach combines them. The researchers ligated the varix 3-5 cm from the gastroesophageal junction and injected the sclerosant into the varix, below the ligated section. They reasoned that ligation should increase the contact time between the sclerosant and endothelial cells, and thus improve efficacy.
He noted that in the United States, band ligation is the standard of therapy, and the new study won’t change that. “These preliminary results from a single center are quite promising, and if they can be confirmed in a larger, multicenter trial, then this is something that can be added to our therapeutic armamentarium,” said Dr. Kwo.
Band ligation replaced sclerotherapy as the preferred treatment for gastroesophageal varices because it has equal efficacy but fewer severe side effects. However, it also suffers from a higher rate of recurrence because the bands cannot destroy deeper varices and perforating veins.
The combination technique, scleroligation, has been demonstrated in the treatment of esophageal varices, which prompted the authors’ investigation into gastroesophageal varices.
At a single center, the researchers recruited 120 patients with cirrhosis and acute gastroesophageal variceal bleeding above the gastroesophageal junction. They were randomized 1:1 to undergo endoscopic band ligation (EBL) or scleroligation (SL).
On average, 15.6 weeks were required to obliterate the varices in the EBL group versus 8.64 weeks in the SL group (P less than .001). The EBL group required an average of 3.43 sessions to reach that endpoint, compared with 2.22 sessions in the SL group (P less than .001). The EBL group required an average of 13.72 bands per patient, compared with 8.88 bands in the SL group (P less than .001). The EBL group also had a higher average number of units of blood transfused (2.30 vs 1.53; P less than .001).
No patients in either group experienced perforation, chest empyema, pericardial effusion, or strictures.
The good safety outcomes may be related to the small volume of sclerosant used, just 2 mL. “It’s probably because of their meticulous approach that they were able to reduce the complications that we have historically seen with sclerotherapy alone,” said Dr. Kwo.
There was no difference in the number of rebleeds or recurrences at follow-up, total cost, mortality due to rebleeding, or 12-month survival.
No funding source was disclosed. The authors reported no financial disclosures.
In the treatment of gastroesophageal varices, scleroligation – a hybrid procedure that combines sclerotherapy and band ligation – performed as well as did band ligation, but required fewer sessions and had a shorter overall treatment duration. Sclerotherapy involves the injection of sclerosant to prompt occlusion of the varices, while ligation involves banding the varices to cut off blood flow.
The new approach combines them. The researchers ligated the varix 3-5 cm from the gastroesophageal junction and injected the sclerosant into the varix, below the ligated section. They reasoned that ligation should increase the contact time between the sclerosant and endothelial cells, and thus improve efficacy.
He noted that in the United States, band ligation is the standard of therapy, and the new study won’t change that. “These preliminary results from a single center are quite promising, and if they can be confirmed in a larger, multicenter trial, then this is something that can be added to our therapeutic armamentarium,” said Dr. Kwo.
Band ligation replaced sclerotherapy as the preferred treatment for gastroesophageal varices because it has equal efficacy but fewer severe side effects. However, it also suffers from a higher rate of recurrence because the bands cannot destroy deeper varices and perforating veins.
The combination technique, scleroligation, has been demonstrated in the treatment of esophageal varices, which prompted the authors’ investigation into gastroesophageal varices.
At a single center, the researchers recruited 120 patients with cirrhosis and acute gastroesophageal variceal bleeding above the gastroesophageal junction. They were randomized 1:1 to undergo endoscopic band ligation (EBL) or scleroligation (SL).
On average, 15.6 weeks were required to obliterate the varices in the EBL group versus 8.64 weeks in the SL group (P less than .001). The EBL group required an average of 3.43 sessions to reach that endpoint, compared with 2.22 sessions in the SL group (P less than .001). The EBL group required an average of 13.72 bands per patient, compared with 8.88 bands in the SL group (P less than .001). The EBL group also had a higher average number of units of blood transfused (2.30 vs 1.53; P less than .001).
No patients in either group experienced perforation, chest empyema, pericardial effusion, or strictures.
The good safety outcomes may be related to the small volume of sclerosant used, just 2 mL. “It’s probably because of their meticulous approach that they were able to reduce the complications that we have historically seen with sclerotherapy alone,” said Dr. Kwo.
There was no difference in the number of rebleeds or recurrences at follow-up, total cost, mortality due to rebleeding, or 12-month survival.
No funding source was disclosed. The authors reported no financial disclosures.
FROM GASTROINTESTINAL ENDOSCOPY
Key clinical point:
Major finding: Scleroligation required 2.22 sessions on average, compared with 3.43 for endoscopic band ligation.
Data source: Single-center randomized trial of 120 patients.
Disclosures: No funding source was disclosed. The authors reported no financial disclosures.
Addition of calcipotriene to 5-FU increases efficacy, tolerability as AK treatment
A combined formulation of calcipotriol and 5-fluorouracil (5-FU) outperformed 5-FU alone in reducing the number of actinic keratoses (AKs), with a shorter treatment course and less inflammation than typically seen with 5-FU alone, researchers reported in a study published online in November.
5-FU is effective, but it produces crusting and significant irritation, and is temporarily disfiguring, creating discomfort and inconvenience that often leads to poor patient compliance with treatment.
After demonstrating that the combined treatment reduces AKs in mice, they conducted the study of 131 patients with AKs, randomized to treatment with a cream containing 5% 5-FU and 0.005% calcipotriol, or Vaseline plus 5% 5-FU alone. Participants applied the treatments twice per day for 4 days.
Eight weeks after treatment, the combination group had a mean 87.8% reduction in the number of AKs on the face, compared with 26.3% of the 5-FU controls. The treatment group also had better responses on the scalp (a mean 76.4% reduction in AKs versus 5.7%), right upper extremity (68.8% versus 9.6%), and left upper extremity (79% versus 16.3%). All differences were statistically significant (P less than .0001 for all comparisons).
“The greater efficacy of calcipotriol plus 5-FU versus Vaseline plus 5-FU treatment in eliminating actinic keratoses remained highly significant after controlling for the baseline actinic keratosis count, age, and sex of the participants,” they wrote (J Clin Invest. 2016 Nov 21. pii: 89820. doi: 10.1172/JCI89820).
Significantly more of those in the combination group has skin redness during treatment, and 39% experienced a burning sensation on treated skin, compared with 13% of the 5-FU treated group. The rate of scaling and itching of treated skin during treatment was similar, and no patients had crusting or wounding of the treated skin.
“It was incredibly well tolerated. There wasn’t as much discomfort or crusting to where people had to stop. And patients who had used 5-FU in the past preferred this shorter treatment course as well as the type and amount of inflammation they had,” compared with their previous experience, Lynn Cornelius, MD, professor and chief of dermatology, Washington University, Saint Louis, said in an interview. “And it was more efficacious,” added Dr. Cornelius, who was one of the study authors.
The trial was investigator initiated. Two authors received grants from the American Skin Association, the Dermatology Foundation, the Burroughs Wellcome Fund, the American Philosophical Society, the La Roche-Posay Research Foundation, and the National Institutes of Health; three investigators were supported by an NIH grant. Dr. Cornelius reported having no financial disclosures.
A combined formulation of calcipotriol and 5-fluorouracil (5-FU) outperformed 5-FU alone in reducing the number of actinic keratoses (AKs), with a shorter treatment course and less inflammation than typically seen with 5-FU alone, researchers reported in a study published online in November.
5-FU is effective, but it produces crusting and significant irritation, and is temporarily disfiguring, creating discomfort and inconvenience that often leads to poor patient compliance with treatment.
After demonstrating that the combined treatment reduces AKs in mice, they conducted the study of 131 patients with AKs, randomized to treatment with a cream containing 5% 5-FU and 0.005% calcipotriol, or Vaseline plus 5% 5-FU alone. Participants applied the treatments twice per day for 4 days.
Eight weeks after treatment, the combination group had a mean 87.8% reduction in the number of AKs on the face, compared with 26.3% of the 5-FU controls. The treatment group also had better responses on the scalp (a mean 76.4% reduction in AKs versus 5.7%), right upper extremity (68.8% versus 9.6%), and left upper extremity (79% versus 16.3%). All differences were statistically significant (P less than .0001 for all comparisons).
“The greater efficacy of calcipotriol plus 5-FU versus Vaseline plus 5-FU treatment in eliminating actinic keratoses remained highly significant after controlling for the baseline actinic keratosis count, age, and sex of the participants,” they wrote (J Clin Invest. 2016 Nov 21. pii: 89820. doi: 10.1172/JCI89820).
Significantly more of those in the combination group has skin redness during treatment, and 39% experienced a burning sensation on treated skin, compared with 13% of the 5-FU treated group. The rate of scaling and itching of treated skin during treatment was similar, and no patients had crusting or wounding of the treated skin.
“It was incredibly well tolerated. There wasn’t as much discomfort or crusting to where people had to stop. And patients who had used 5-FU in the past preferred this shorter treatment course as well as the type and amount of inflammation they had,” compared with their previous experience, Lynn Cornelius, MD, professor and chief of dermatology, Washington University, Saint Louis, said in an interview. “And it was more efficacious,” added Dr. Cornelius, who was one of the study authors.
The trial was investigator initiated. Two authors received grants from the American Skin Association, the Dermatology Foundation, the Burroughs Wellcome Fund, the American Philosophical Society, the La Roche-Posay Research Foundation, and the National Institutes of Health; three investigators were supported by an NIH grant. Dr. Cornelius reported having no financial disclosures.
A combined formulation of calcipotriol and 5-fluorouracil (5-FU) outperformed 5-FU alone in reducing the number of actinic keratoses (AKs), with a shorter treatment course and less inflammation than typically seen with 5-FU alone, researchers reported in a study published online in November.
5-FU is effective, but it produces crusting and significant irritation, and is temporarily disfiguring, creating discomfort and inconvenience that often leads to poor patient compliance with treatment.
After demonstrating that the combined treatment reduces AKs in mice, they conducted the study of 131 patients with AKs, randomized to treatment with a cream containing 5% 5-FU and 0.005% calcipotriol, or Vaseline plus 5% 5-FU alone. Participants applied the treatments twice per day for 4 days.
Eight weeks after treatment, the combination group had a mean 87.8% reduction in the number of AKs on the face, compared with 26.3% of the 5-FU controls. The treatment group also had better responses on the scalp (a mean 76.4% reduction in AKs versus 5.7%), right upper extremity (68.8% versus 9.6%), and left upper extremity (79% versus 16.3%). All differences were statistically significant (P less than .0001 for all comparisons).
“The greater efficacy of calcipotriol plus 5-FU versus Vaseline plus 5-FU treatment in eliminating actinic keratoses remained highly significant after controlling for the baseline actinic keratosis count, age, and sex of the participants,” they wrote (J Clin Invest. 2016 Nov 21. pii: 89820. doi: 10.1172/JCI89820).
Significantly more of those in the combination group has skin redness during treatment, and 39% experienced a burning sensation on treated skin, compared with 13% of the 5-FU treated group. The rate of scaling and itching of treated skin during treatment was similar, and no patients had crusting or wounding of the treated skin.
“It was incredibly well tolerated. There wasn’t as much discomfort or crusting to where people had to stop. And patients who had used 5-FU in the past preferred this shorter treatment course as well as the type and amount of inflammation they had,” compared with their previous experience, Lynn Cornelius, MD, professor and chief of dermatology, Washington University, Saint Louis, said in an interview. “And it was more efficacious,” added Dr. Cornelius, who was one of the study authors.
The trial was investigator initiated. Two authors received grants from the American Skin Association, the Dermatology Foundation, the Burroughs Wellcome Fund, the American Philosophical Society, the La Roche-Posay Research Foundation, and the National Institutes of Health; three investigators were supported by an NIH grant. Dr. Cornelius reported having no financial disclosures.
FROM THE JOURNAL OF CLINICAL INVESTIGATION
Key clinical point:
Major finding: The combination cream reduced the number of AKs on the face by 87.8%, compared with 5-FU alone.
Data source: A randomized, placebo controlled trial of 131 subjects with AKs.
Disclosures: The trial was investigator initiated. Two authors received grants from the American Skin Association, the Dermatology Foundation, the Burroughs Wellcome Fund, the American Philosophical Society, the La Roche-Posay Research Foundation, and the National Institutes of Health; three investigators were supported by an NIH grant. Dr. Cornelius reported having no financial disclosures.
Blood pressure rise follows halting CPAP
Continuous positive airway pressure (CPAP) therapy for obstructive sleep apnea (OSA) has a significant beneficial effect on blood pressure, according to an analysis of participants in three randomized controlled trials.
Previous meta-analyses suggested that CPAP treatment led to an average of improvement of 2-3 mm Hg, but the estimates relied on heterogeneous trials that often had low levels of CPAP adherence, and those factors might have led to an underestimation of the treatment effect. The new analysis showed that halting CPAP increases blood pressure between 5.0 and 9.0 mm Hg, compared with patients who continued using CPAP (Chest. 2016;150[6]:1202-10).
To get around the problem of adherence, researchers led by Malcolm Kohler, MD, at University Hospital of Zürich analyzed the results of three previous studies looking at the effects of CPAP withdrawal. The analysis included 153 OSA patients on CPAP therapy, who had been randomized to continue therapy or to withdraw from therapy for 2 weeks. Eighty-seven of these patients discontinued CPAP, and the remaining 66 patients continued the therapy. Blood pressure was measured at home and in hospital.
On average, those who discontinued CPAP had an increase in office systolic blood pressure of 5.4 mm Hg (95% confidence interval, 1.8-8.9 mm Hg; P = .003) and an increase in home systolic blood pressure of 9.0 mm Hg (95% CI, 5.7-12.3 mm Hg; P less than .001), compared with patients who continued CPAP. The effects of stopping CPAP, instead of continuing the therapy, on office diastolic blood pressure and home diastolic pressure were increases of 5.0 mm Hg (95% CI, 2.7-7.3 mm Hg; P less than .001) and 7.8 mm Hg (95% CI, 5.6-10.0 mm Hg; P less than .001), respectively.
Patients who discontinued CPAP also experienced a significant increase in apnea-hypopnea index, from 2.8/h to 33.2/h, while those who continued using CPAP, on average, experienced only a 0.3/h increase in apnea-hypopnea index from baseline.
“One clinical implication is that if you do not need to stop CPAP for obstructive sleep apnea, do not stop it. This study also suggests the importance of monitoring your blood pressure in a home setting, under usual conditions,” summed up Robert Kloner, MD, PhD, director of the Huntington Medical Research Institutes Cardiovascular Research Lab, Pasadena, Calif., who was not involved in the study.
Previous studies of CPAP, such as the SAVE study published in the New England Journal of Medicine in September (N Engl J Med. 2016;375:919-31), often find little or no connection between CPAP therapy and cardiovascular outcomes. That is probably because of inadequate adherence to CPAP therapy. “That’s always been the bane of sleep apnea studies,” said Krishna M. Sundar, MD, FCCP, who also did not participate in the study.
The current work got around the problem by looking at patients who had already established use of CPAP. “This is a very good study,” said Dr. Sundar, who is the medical director of the Sleep-Wake Center at the University of Utah, Salt Lake City.
The study was funded by the Swiss National Science Foundation and the University of Zürich. The analysis’ authors and the outside experts quoted in this story reported no financial disclosures.
Continuous positive airway pressure (CPAP) therapy for obstructive sleep apnea (OSA) has a significant beneficial effect on blood pressure, according to an analysis of participants in three randomized controlled trials.
Previous meta-analyses suggested that CPAP treatment led to an average of improvement of 2-3 mm Hg, but the estimates relied on heterogeneous trials that often had low levels of CPAP adherence, and those factors might have led to an underestimation of the treatment effect. The new analysis showed that halting CPAP increases blood pressure between 5.0 and 9.0 mm Hg, compared with patients who continued using CPAP (Chest. 2016;150[6]:1202-10).
To get around the problem of adherence, researchers led by Malcolm Kohler, MD, at University Hospital of Zürich analyzed the results of three previous studies looking at the effects of CPAP withdrawal. The analysis included 153 OSA patients on CPAP therapy, who had been randomized to continue therapy or to withdraw from therapy for 2 weeks. Eighty-seven of these patients discontinued CPAP, and the remaining 66 patients continued the therapy. Blood pressure was measured at home and in hospital.
On average, those who discontinued CPAP had an increase in office systolic blood pressure of 5.4 mm Hg (95% confidence interval, 1.8-8.9 mm Hg; P = .003) and an increase in home systolic blood pressure of 9.0 mm Hg (95% CI, 5.7-12.3 mm Hg; P less than .001), compared with patients who continued CPAP. The effects of stopping CPAP, instead of continuing the therapy, on office diastolic blood pressure and home diastolic pressure were increases of 5.0 mm Hg (95% CI, 2.7-7.3 mm Hg; P less than .001) and 7.8 mm Hg (95% CI, 5.6-10.0 mm Hg; P less than .001), respectively.
Patients who discontinued CPAP also experienced a significant increase in apnea-hypopnea index, from 2.8/h to 33.2/h, while those who continued using CPAP, on average, experienced only a 0.3/h increase in apnea-hypopnea index from baseline.
“One clinical implication is that if you do not need to stop CPAP for obstructive sleep apnea, do not stop it. This study also suggests the importance of monitoring your blood pressure in a home setting, under usual conditions,” summed up Robert Kloner, MD, PhD, director of the Huntington Medical Research Institutes Cardiovascular Research Lab, Pasadena, Calif., who was not involved in the study.
Previous studies of CPAP, such as the SAVE study published in the New England Journal of Medicine in September (N Engl J Med. 2016;375:919-31), often find little or no connection between CPAP therapy and cardiovascular outcomes. That is probably because of inadequate adherence to CPAP therapy. “That’s always been the bane of sleep apnea studies,” said Krishna M. Sundar, MD, FCCP, who also did not participate in the study.
The current work got around the problem by looking at patients who had already established use of CPAP. “This is a very good study,” said Dr. Sundar, who is the medical director of the Sleep-Wake Center at the University of Utah, Salt Lake City.
The study was funded by the Swiss National Science Foundation and the University of Zürich. The analysis’ authors and the outside experts quoted in this story reported no financial disclosures.
Continuous positive airway pressure (CPAP) therapy for obstructive sleep apnea (OSA) has a significant beneficial effect on blood pressure, according to an analysis of participants in three randomized controlled trials.
Previous meta-analyses suggested that CPAP treatment led to an average of improvement of 2-3 mm Hg, but the estimates relied on heterogeneous trials that often had low levels of CPAP adherence, and those factors might have led to an underestimation of the treatment effect. The new analysis showed that halting CPAP increases blood pressure between 5.0 and 9.0 mm Hg, compared with patients who continued using CPAP (Chest. 2016;150[6]:1202-10).
To get around the problem of adherence, researchers led by Malcolm Kohler, MD, at University Hospital of Zürich analyzed the results of three previous studies looking at the effects of CPAP withdrawal. The analysis included 153 OSA patients on CPAP therapy, who had been randomized to continue therapy or to withdraw from therapy for 2 weeks. Eighty-seven of these patients discontinued CPAP, and the remaining 66 patients continued the therapy. Blood pressure was measured at home and in hospital.
On average, those who discontinued CPAP had an increase in office systolic blood pressure of 5.4 mm Hg (95% confidence interval, 1.8-8.9 mm Hg; P = .003) and an increase in home systolic blood pressure of 9.0 mm Hg (95% CI, 5.7-12.3 mm Hg; P less than .001), compared with patients who continued CPAP. The effects of stopping CPAP, instead of continuing the therapy, on office diastolic blood pressure and home diastolic pressure were increases of 5.0 mm Hg (95% CI, 2.7-7.3 mm Hg; P less than .001) and 7.8 mm Hg (95% CI, 5.6-10.0 mm Hg; P less than .001), respectively.
Patients who discontinued CPAP also experienced a significant increase in apnea-hypopnea index, from 2.8/h to 33.2/h, while those who continued using CPAP, on average, experienced only a 0.3/h increase in apnea-hypopnea index from baseline.
“One clinical implication is that if you do not need to stop CPAP for obstructive sleep apnea, do not stop it. This study also suggests the importance of monitoring your blood pressure in a home setting, under usual conditions,” summed up Robert Kloner, MD, PhD, director of the Huntington Medical Research Institutes Cardiovascular Research Lab, Pasadena, Calif., who was not involved in the study.
Previous studies of CPAP, such as the SAVE study published in the New England Journal of Medicine in September (N Engl J Med. 2016;375:919-31), often find little or no connection between CPAP therapy and cardiovascular outcomes. That is probably because of inadequate adherence to CPAP therapy. “That’s always been the bane of sleep apnea studies,” said Krishna M. Sundar, MD, FCCP, who also did not participate in the study.
The current work got around the problem by looking at patients who had already established use of CPAP. “This is a very good study,” said Dr. Sundar, who is the medical director of the Sleep-Wake Center at the University of Utah, Salt Lake City.
The study was funded by the Swiss National Science Foundation and the University of Zürich. The analysis’ authors and the outside experts quoted in this story reported no financial disclosures.
FROM CHEST
Key clinical point: Interrupting CPAP therapy leads to a rise in blood pressure.
Major finding: Stopping CPAP was associated with 5.0-9.0 mm Hg blood pressure increase.
Data source: Analysis of 153 patients with moderate to severe OSA, who had participated in three randomized controlled trials.
Disclosures: The study was funded by the Swiss National Science Foundation and the University of Zürich. The authors of the analysis and the outside experts quoted in this story reported no financial disclosures.
Dr. Sundar and Dr. Kloner reported having no financial disclosures.
In lung cancer screening, patient education works
A counseling and shared decision-making visit improved patient knowledge of the eligibility criteria, benefits, and potential risks of lung cancer screening via a low-radiation chest CT scan.
The Center for Medicare & Medicaid Services has added the type of visit addressed in this study to Medicare’s preventive services benefits for individuals meeting certain criteria, but no previous study had looked at how the implementation of such a visit impacted a patient’s knowledge and understanding.
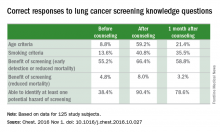
The researchers noted significant improvement in all questions before and after a counseling session (P = .03 to P less than .0001). Those improvements lessened at 1 month, but were still higher than precounseling scores.
The percentages of participants who knew the age criteria for lung cancer screening before counseling, immediately after counseling, and 1 month after counseling, for example, were 8.8% (11 patients), 59.2% (74 patients), and 21.4% (24 patients), respectively. The percentage of participants able to identify at least one of the potential hazards of screening increased by a similar amount immediately after receiving counseling, as did the percentage of participants able to identify the age criteria for lung cancer screening immediately after receiving counseling. The percentages of patients able to identify at least one of the potential hazards of screening were 38.4% before counseling and 90.4% immediately after receiving counseling. One month following counseling, the percentage of patients with such knowledge remained fairly high, dropping to 78.6%.
“Showing the value of these visits is very important to encourage policymakers and payers to continue to support the counseling and shared decision-making visit,” Peter J. Mazzone, MD, MPH, who led the study, said in an interview.
These types of conversations are important because of the uncertainties surrounding lung cancer screening, which leads to about a 20% reduction in mortality risk. That translates to the need to screen about 250 people to save 1 life. “I think the public sometimes doesn’t realize that the effectiveness of some of these preventive screenings may not be as large as they think they are,” said David Grossman, vice chair of the US Preventive Services Task Force and a senior investigator at the Group Health Research Institute, Seattle, who was not involved in the study.
The researchers developed a centralized counseling and shared decision-making visit that included a narrated slide show and individualized risk assessment. They approached 423 consecutive patients who had been identified by their primary care provider or a specialist as potential candidates for screening. Of those 423 patients, 125 agreed to participate in the study (Chest. 2016 Nov 1. doi: 10.1016/j.chest.2016.10.027).
The session delivered expected improvements in patient knowledge, but there were some surprises. “The starting point of knowledge was perhaps less than we would have anticipated, and the gains, though very substantial, weren’t perfect,” said Dr. Mazzone, who is also director of the lung cancer screening program at the Cleveland Clinic.
The drop in knowledge at 1 month suggests that the information needs to be reinforced, possibly each time patients come in for an annual screening visit, Dr. Mazzone added.
Counseling sessions can also help convince patients to quit smoking, if tobacco use is a concern. “It’s not appropriate to screen for lung cancer without making a commitment to try to quit,” said Dr. Grossman.
No funding source was disclosed. Dr. Mazzone and Dr. Grossman reported having no financial disclosures.
A counseling and shared decision-making visit improved patient knowledge of the eligibility criteria, benefits, and potential risks of lung cancer screening via a low-radiation chest CT scan.
The Center for Medicare & Medicaid Services has added the type of visit addressed in this study to Medicare’s preventive services benefits for individuals meeting certain criteria, but no previous study had looked at how the implementation of such a visit impacted a patient’s knowledge and understanding.
The researchers noted significant improvement in all questions before and after a counseling session (P = .03 to P less than .0001). Those improvements lessened at 1 month, but were still higher than precounseling scores.
The percentages of participants who knew the age criteria for lung cancer screening before counseling, immediately after counseling, and 1 month after counseling, for example, were 8.8% (11 patients), 59.2% (74 patients), and 21.4% (24 patients), respectively. The percentage of participants able to identify at least one of the potential hazards of screening increased by a similar amount immediately after receiving counseling, as did the percentage of participants able to identify the age criteria for lung cancer screening immediately after receiving counseling. The percentages of patients able to identify at least one of the potential hazards of screening were 38.4% before counseling and 90.4% immediately after receiving counseling. One month following counseling, the percentage of patients with such knowledge remained fairly high, dropping to 78.6%.
“Showing the value of these visits is very important to encourage policymakers and payers to continue to support the counseling and shared decision-making visit,” Peter J. Mazzone, MD, MPH, who led the study, said in an interview.
These types of conversations are important because of the uncertainties surrounding lung cancer screening, which leads to about a 20% reduction in mortality risk. That translates to the need to screen about 250 people to save 1 life. “I think the public sometimes doesn’t realize that the effectiveness of some of these preventive screenings may not be as large as they think they are,” said David Grossman, vice chair of the US Preventive Services Task Force and a senior investigator at the Group Health Research Institute, Seattle, who was not involved in the study.
The researchers developed a centralized counseling and shared decision-making visit that included a narrated slide show and individualized risk assessment. They approached 423 consecutive patients who had been identified by their primary care provider or a specialist as potential candidates for screening. Of those 423 patients, 125 agreed to participate in the study (Chest. 2016 Nov 1. doi: 10.1016/j.chest.2016.10.027).
The session delivered expected improvements in patient knowledge, but there were some surprises. “The starting point of knowledge was perhaps less than we would have anticipated, and the gains, though very substantial, weren’t perfect,” said Dr. Mazzone, who is also director of the lung cancer screening program at the Cleveland Clinic.
The drop in knowledge at 1 month suggests that the information needs to be reinforced, possibly each time patients come in for an annual screening visit, Dr. Mazzone added.
Counseling sessions can also help convince patients to quit smoking, if tobacco use is a concern. “It’s not appropriate to screen for lung cancer without making a commitment to try to quit,” said Dr. Grossman.
No funding source was disclosed. Dr. Mazzone and Dr. Grossman reported having no financial disclosures.
A counseling and shared decision-making visit improved patient knowledge of the eligibility criteria, benefits, and potential risks of lung cancer screening via a low-radiation chest CT scan.
The Center for Medicare & Medicaid Services has added the type of visit addressed in this study to Medicare’s preventive services benefits for individuals meeting certain criteria, but no previous study had looked at how the implementation of such a visit impacted a patient’s knowledge and understanding.
The researchers noted significant improvement in all questions before and after a counseling session (P = .03 to P less than .0001). Those improvements lessened at 1 month, but were still higher than precounseling scores.
The percentages of participants who knew the age criteria for lung cancer screening before counseling, immediately after counseling, and 1 month after counseling, for example, were 8.8% (11 patients), 59.2% (74 patients), and 21.4% (24 patients), respectively. The percentage of participants able to identify at least one of the potential hazards of screening increased by a similar amount immediately after receiving counseling, as did the percentage of participants able to identify the age criteria for lung cancer screening immediately after receiving counseling. The percentages of patients able to identify at least one of the potential hazards of screening were 38.4% before counseling and 90.4% immediately after receiving counseling. One month following counseling, the percentage of patients with such knowledge remained fairly high, dropping to 78.6%.
“Showing the value of these visits is very important to encourage policymakers and payers to continue to support the counseling and shared decision-making visit,” Peter J. Mazzone, MD, MPH, who led the study, said in an interview.
These types of conversations are important because of the uncertainties surrounding lung cancer screening, which leads to about a 20% reduction in mortality risk. That translates to the need to screen about 250 people to save 1 life. “I think the public sometimes doesn’t realize that the effectiveness of some of these preventive screenings may not be as large as they think they are,” said David Grossman, vice chair of the US Preventive Services Task Force and a senior investigator at the Group Health Research Institute, Seattle, who was not involved in the study.
The researchers developed a centralized counseling and shared decision-making visit that included a narrated slide show and individualized risk assessment. They approached 423 consecutive patients who had been identified by their primary care provider or a specialist as potential candidates for screening. Of those 423 patients, 125 agreed to participate in the study (Chest. 2016 Nov 1. doi: 10.1016/j.chest.2016.10.027).
The session delivered expected improvements in patient knowledge, but there were some surprises. “The starting point of knowledge was perhaps less than we would have anticipated, and the gains, though very substantial, weren’t perfect,” said Dr. Mazzone, who is also director of the lung cancer screening program at the Cleveland Clinic.
The drop in knowledge at 1 month suggests that the information needs to be reinforced, possibly each time patients come in for an annual screening visit, Dr. Mazzone added.
Counseling sessions can also help convince patients to quit smoking, if tobacco use is a concern. “It’s not appropriate to screen for lung cancer without making a commitment to try to quit,” said Dr. Grossman.
No funding source was disclosed. Dr. Mazzone and Dr. Grossman reported having no financial disclosures.
FROM CHEST
Key clinical point:
Major finding: Failure to identify potential harm dropped from 61.6% to 21.4%.
Data source: Prospective study of 125 patients.
Disclosures: No funding source was disclosed. Dr. Mazzone and Dr. Grossman reported having no financial disclosures.
Early paternal emotional involvement tied to children’s preadolescent behavior
Children whose fathers have a positive emotional response to parenting and provide a sense of security early on are less likely to exhibit behavioral problems at age 9, a cohort study of more than 13,000 children shows. However, the researchers found no association between behavioral problems and paternal involvement with child care and household tasks.
The researchers used data from the Avon Longitudinal Study of Parents and Children, a birth cohort study of children in southwest England that is also known as Children of the 90s. In this study, the children’s fathers completed questionnaires at 8 weeks (37 questions) and 8 months (21 questions) after the birth. They were asked to rate their level of agreement with 58 statements related to several issues, including direct care, household tasks, attitudes about parenting, and relationships with the child. The mothers were interviewed at child age 9 (N = 6,898) and 11 (N = 6,328) to determine the presence or absence of behavioral problems, which were measured via the total difficulties score of the Strengths and Difficulties Questionnaire.
Previous studies have tended toward the assumption that paternal involvement with the child is unidimensional, which might explain why other studies have not found a clear association with behavioral problems. This study is the first to look at paternal involvement as multidimensional, reported Charles Opondo, PhD, of the University of Oxford (England), and his colleagues (BMJ Open. 2016;6:e012034. doi: 10.1136/bmjopen-2016-012034).
The questions for fathers related to emotional response to the childhood, how often fathers participated in domestic and child care activity, and feelings of security about their paternal role.
Children of fathers who scored high on questions about emotional response were less likely to have behavioral problems at age 9 (odds ratio, 0.86; 95% confidence interval, 0.79-0.94; P = .001), as were children of fathers who scored high on their sense of security (OR, 0.87; 95% CI, 0.79-0.96; P = .006). The same patterns were true at age 11.
The impact of paternal involvement on mothers could be an important factor. “There is evidence that fathers’ involvement can also alleviate the impact of factors such as maternal depression, which are known to increase children’s risk of behavioral problems,” the researchers wrote.
Meanwhile, Dr. Opondo and his colleagues found no significant relationship between behavioral problems, and time spent in domestic and child care activity at either age.
“The findings of this research study suggest that it is psychological and emotional aspects of paternal involvement in a child’s infancy that are most powerful in influencing later child behavior and not the amount of time that fathers are engaged in child care or domestic tasks in the household,” Dr. Opondo and his colleagues said.
The researchers cited several limitations. The study was observational, for example, and could be subject to unobserved confounders. In addition, the study relied on self-reporting, which can produce bias.
The Policy Research Program in the Department of Health, England, funded the study. The authors reported having no financial disclosures.
Children whose fathers have a positive emotional response to parenting and provide a sense of security early on are less likely to exhibit behavioral problems at age 9, a cohort study of more than 13,000 children shows. However, the researchers found no association between behavioral problems and paternal involvement with child care and household tasks.
The researchers used data from the Avon Longitudinal Study of Parents and Children, a birth cohort study of children in southwest England that is also known as Children of the 90s. In this study, the children’s fathers completed questionnaires at 8 weeks (37 questions) and 8 months (21 questions) after the birth. They were asked to rate their level of agreement with 58 statements related to several issues, including direct care, household tasks, attitudes about parenting, and relationships with the child. The mothers were interviewed at child age 9 (N = 6,898) and 11 (N = 6,328) to determine the presence or absence of behavioral problems, which were measured via the total difficulties score of the Strengths and Difficulties Questionnaire.
Previous studies have tended toward the assumption that paternal involvement with the child is unidimensional, which might explain why other studies have not found a clear association with behavioral problems. This study is the first to look at paternal involvement as multidimensional, reported Charles Opondo, PhD, of the University of Oxford (England), and his colleagues (BMJ Open. 2016;6:e012034. doi: 10.1136/bmjopen-2016-012034).
The questions for fathers related to emotional response to the childhood, how often fathers participated in domestic and child care activity, and feelings of security about their paternal role.
Children of fathers who scored high on questions about emotional response were less likely to have behavioral problems at age 9 (odds ratio, 0.86; 95% confidence interval, 0.79-0.94; P = .001), as were children of fathers who scored high on their sense of security (OR, 0.87; 95% CI, 0.79-0.96; P = .006). The same patterns were true at age 11.
The impact of paternal involvement on mothers could be an important factor. “There is evidence that fathers’ involvement can also alleviate the impact of factors such as maternal depression, which are known to increase children’s risk of behavioral problems,” the researchers wrote.
Meanwhile, Dr. Opondo and his colleagues found no significant relationship between behavioral problems, and time spent in domestic and child care activity at either age.
“The findings of this research study suggest that it is psychological and emotional aspects of paternal involvement in a child’s infancy that are most powerful in influencing later child behavior and not the amount of time that fathers are engaged in child care or domestic tasks in the household,” Dr. Opondo and his colleagues said.
The researchers cited several limitations. The study was observational, for example, and could be subject to unobserved confounders. In addition, the study relied on self-reporting, which can produce bias.
The Policy Research Program in the Department of Health, England, funded the study. The authors reported having no financial disclosures.
Children whose fathers have a positive emotional response to parenting and provide a sense of security early on are less likely to exhibit behavioral problems at age 9, a cohort study of more than 13,000 children shows. However, the researchers found no association between behavioral problems and paternal involvement with child care and household tasks.
The researchers used data from the Avon Longitudinal Study of Parents and Children, a birth cohort study of children in southwest England that is also known as Children of the 90s. In this study, the children’s fathers completed questionnaires at 8 weeks (37 questions) and 8 months (21 questions) after the birth. They were asked to rate their level of agreement with 58 statements related to several issues, including direct care, household tasks, attitudes about parenting, and relationships with the child. The mothers were interviewed at child age 9 (N = 6,898) and 11 (N = 6,328) to determine the presence or absence of behavioral problems, which were measured via the total difficulties score of the Strengths and Difficulties Questionnaire.
Previous studies have tended toward the assumption that paternal involvement with the child is unidimensional, which might explain why other studies have not found a clear association with behavioral problems. This study is the first to look at paternal involvement as multidimensional, reported Charles Opondo, PhD, of the University of Oxford (England), and his colleagues (BMJ Open. 2016;6:e012034. doi: 10.1136/bmjopen-2016-012034).
The questions for fathers related to emotional response to the childhood, how often fathers participated in domestic and child care activity, and feelings of security about their paternal role.
Children of fathers who scored high on questions about emotional response were less likely to have behavioral problems at age 9 (odds ratio, 0.86; 95% confidence interval, 0.79-0.94; P = .001), as were children of fathers who scored high on their sense of security (OR, 0.87; 95% CI, 0.79-0.96; P = .006). The same patterns were true at age 11.
The impact of paternal involvement on mothers could be an important factor. “There is evidence that fathers’ involvement can also alleviate the impact of factors such as maternal depression, which are known to increase children’s risk of behavioral problems,” the researchers wrote.
Meanwhile, Dr. Opondo and his colleagues found no significant relationship between behavioral problems, and time spent in domestic and child care activity at either age.
“The findings of this research study suggest that it is psychological and emotional aspects of paternal involvement in a child’s infancy that are most powerful in influencing later child behavior and not the amount of time that fathers are engaged in child care or domestic tasks in the household,” Dr. Opondo and his colleagues said.
The researchers cited several limitations. The study was observational, for example, and could be subject to unobserved confounders. In addition, the study relied on self-reporting, which can produce bias.
The Policy Research Program in the Department of Health, England, funded the study. The authors reported having no financial disclosures.
Key clinical point:
Major finding: The children of fathers who reported strong emotional attachment and security as a parent had a lower risk of behavioral problems.
Data source: Cohort study of 14,440 children in southwest England.
Disclosures: The Policy Research Program in the Department of Health, England, funded the study. The authors reported having no financial disclosures.
Two doses of HPV vaccine may be noninferior to three
A two-dose schedule of the 9-valent human papillomavirus (HPV) vaccine in children aged 9-14 years is noninferior to a three-dose schedule in adolescent girls and women (aged 16-26 years), based on immunogenicity measurements.
Many countries have poor HPV vaccination rates, in part because the current regimen requires three doses over a 6-month span, and it can be challenging in some areas for children to make three health care visits in the required time span. “Using an effective two-dose regimen entailing fewer visits could improve adherence to HPV vaccination programs. Coadministration of the 9-valent HPV vaccine with diphtheria, tetanus, pertussis, polio, and meningococcal vaccines could also be completed at the same visit,” reported Ole-Erik Iversen, MD, PhD, of the University of Bergen (Norway) and his colleagues (JAMA. 2016 Nov 21. doi: 10.1001/jama.2016.17615).
The researchers measured serum anti-HPV antibodies 1 month after the final dose. At least 98% of the participants in each group seroconverted to a response against all 9 HPV subtypes, and analysis of the antibody geometric mean titers revealed that the groups who received two doses had noninferior responses to the control group of adolescent girls and young women who received three doses.
Antibody geometric mean titers against all 9 HPV types were higher in subgroups of boys and girls (aged 9-10 years, aged 11-12 years, and aged 13-14 years) who received two doses, compared with girls and young women who received three doses. “These observations suggest that the overall results of the primary immunogenicity analyses may be applicable across the entire studied age range of girls and boys,” Dr. Iversen and his associates wrote.
The study cannot prove that the two-dose regimen has equal efficacy to the three-dose regimen in preventing HPV infection, only that the immunogenicity is noninferior, they said.
The study was sponsored by Merck, which manufactures the vaccine. Study authors have financial ties to Merck and a number of other pharmaceutical companies.
Evidence now supports a two-dose schedule in adolescents (aged 9-14 years) for all three licensed HPV vaccines. When the vaccination series is initiated before the age of 15 years, two doses administered at a 0- and 6-month interval or at a 0- and 12-month interval were found to be just as immunogenic as (or even better than) three doses.
The coverage of HPV vaccination in the United States is lower than that for other vaccines recommended for adolescents, such as quadrivalent meningococcal conjugate vaccine and tetanus, diphtheria, and acellular pertussis vaccine. In 2015, three-dose HPV vaccination coverage among 13- to 17-year-olds was only 41.9% for girls and 28.1% for boys; at least one-dose coverage was 62.8% for girls and 49.8% for boys.
Going forward, a two-dose schedule should make it easier to complete the recommended vaccination series. A two-dose schedule (at 0 and 6-12 months) will decrease health care appointments needed for HPV vaccination and facilitate clinicians’ ability to deliver vaccine at preventive health visits. Nevertheless, efforts will be needed to increase vaccine initiation and ensure delivery of the second dose.
Lauri E. Markowitz, MD, is at the division of viral diseases, National Center for Immunization and Respiratory Diseases at the Centers for Disease Control and Prevention, Atlanta. Elizabeth R. Unger, MD, MPH, is at the division of high-consequence pathogens and pathology, National Center for Emerging and Zoonotic Infectious Diseases at the CDC. Elissa Meites, PhD, MD, is at the division of viral diseases, National Center for Immunization and Respiratory Diseases at the CDC. Their comments were excerpted from an editorial accompanying the article by Iversen et al. (JAMA. 2016 Nov 21. doi: 10.1001/jama.2016.16393). The authors declared no financial conflicts of interest.
Evidence now supports a two-dose schedule in adolescents (aged 9-14 years) for all three licensed HPV vaccines. When the vaccination series is initiated before the age of 15 years, two doses administered at a 0- and 6-month interval or at a 0- and 12-month interval were found to be just as immunogenic as (or even better than) three doses.
The coverage of HPV vaccination in the United States is lower than that for other vaccines recommended for adolescents, such as quadrivalent meningococcal conjugate vaccine and tetanus, diphtheria, and acellular pertussis vaccine. In 2015, three-dose HPV vaccination coverage among 13- to 17-year-olds was only 41.9% for girls and 28.1% for boys; at least one-dose coverage was 62.8% for girls and 49.8% for boys.
Going forward, a two-dose schedule should make it easier to complete the recommended vaccination series. A two-dose schedule (at 0 and 6-12 months) will decrease health care appointments needed for HPV vaccination and facilitate clinicians’ ability to deliver vaccine at preventive health visits. Nevertheless, efforts will be needed to increase vaccine initiation and ensure delivery of the second dose.
Lauri E. Markowitz, MD, is at the division of viral diseases, National Center for Immunization and Respiratory Diseases at the Centers for Disease Control and Prevention, Atlanta. Elizabeth R. Unger, MD, MPH, is at the division of high-consequence pathogens and pathology, National Center for Emerging and Zoonotic Infectious Diseases at the CDC. Elissa Meites, PhD, MD, is at the division of viral diseases, National Center for Immunization and Respiratory Diseases at the CDC. Their comments were excerpted from an editorial accompanying the article by Iversen et al. (JAMA. 2016 Nov 21. doi: 10.1001/jama.2016.16393). The authors declared no financial conflicts of interest.
Evidence now supports a two-dose schedule in adolescents (aged 9-14 years) for all three licensed HPV vaccines. When the vaccination series is initiated before the age of 15 years, two doses administered at a 0- and 6-month interval or at a 0- and 12-month interval were found to be just as immunogenic as (or even better than) three doses.
The coverage of HPV vaccination in the United States is lower than that for other vaccines recommended for adolescents, such as quadrivalent meningococcal conjugate vaccine and tetanus, diphtheria, and acellular pertussis vaccine. In 2015, three-dose HPV vaccination coverage among 13- to 17-year-olds was only 41.9% for girls and 28.1% for boys; at least one-dose coverage was 62.8% for girls and 49.8% for boys.
Going forward, a two-dose schedule should make it easier to complete the recommended vaccination series. A two-dose schedule (at 0 and 6-12 months) will decrease health care appointments needed for HPV vaccination and facilitate clinicians’ ability to deliver vaccine at preventive health visits. Nevertheless, efforts will be needed to increase vaccine initiation and ensure delivery of the second dose.
Lauri E. Markowitz, MD, is at the division of viral diseases, National Center for Immunization and Respiratory Diseases at the Centers for Disease Control and Prevention, Atlanta. Elizabeth R. Unger, MD, MPH, is at the division of high-consequence pathogens and pathology, National Center for Emerging and Zoonotic Infectious Diseases at the CDC. Elissa Meites, PhD, MD, is at the division of viral diseases, National Center for Immunization and Respiratory Diseases at the CDC. Their comments were excerpted from an editorial accompanying the article by Iversen et al. (JAMA. 2016 Nov 21. doi: 10.1001/jama.2016.16393). The authors declared no financial conflicts of interest.
A two-dose schedule of the 9-valent human papillomavirus (HPV) vaccine in children aged 9-14 years is noninferior to a three-dose schedule in adolescent girls and women (aged 16-26 years), based on immunogenicity measurements.
Many countries have poor HPV vaccination rates, in part because the current regimen requires three doses over a 6-month span, and it can be challenging in some areas for children to make three health care visits in the required time span. “Using an effective two-dose regimen entailing fewer visits could improve adherence to HPV vaccination programs. Coadministration of the 9-valent HPV vaccine with diphtheria, tetanus, pertussis, polio, and meningococcal vaccines could also be completed at the same visit,” reported Ole-Erik Iversen, MD, PhD, of the University of Bergen (Norway) and his colleagues (JAMA. 2016 Nov 21. doi: 10.1001/jama.2016.17615).
The researchers measured serum anti-HPV antibodies 1 month after the final dose. At least 98% of the participants in each group seroconverted to a response against all 9 HPV subtypes, and analysis of the antibody geometric mean titers revealed that the groups who received two doses had noninferior responses to the control group of adolescent girls and young women who received three doses.
Antibody geometric mean titers against all 9 HPV types were higher in subgroups of boys and girls (aged 9-10 years, aged 11-12 years, and aged 13-14 years) who received two doses, compared with girls and young women who received three doses. “These observations suggest that the overall results of the primary immunogenicity analyses may be applicable across the entire studied age range of girls and boys,” Dr. Iversen and his associates wrote.
The study cannot prove that the two-dose regimen has equal efficacy to the three-dose regimen in preventing HPV infection, only that the immunogenicity is noninferior, they said.
The study was sponsored by Merck, which manufactures the vaccine. Study authors have financial ties to Merck and a number of other pharmaceutical companies.
A two-dose schedule of the 9-valent human papillomavirus (HPV) vaccine in children aged 9-14 years is noninferior to a three-dose schedule in adolescent girls and women (aged 16-26 years), based on immunogenicity measurements.
Many countries have poor HPV vaccination rates, in part because the current regimen requires three doses over a 6-month span, and it can be challenging in some areas for children to make three health care visits in the required time span. “Using an effective two-dose regimen entailing fewer visits could improve adherence to HPV vaccination programs. Coadministration of the 9-valent HPV vaccine with diphtheria, tetanus, pertussis, polio, and meningococcal vaccines could also be completed at the same visit,” reported Ole-Erik Iversen, MD, PhD, of the University of Bergen (Norway) and his colleagues (JAMA. 2016 Nov 21. doi: 10.1001/jama.2016.17615).
The researchers measured serum anti-HPV antibodies 1 month after the final dose. At least 98% of the participants in each group seroconverted to a response against all 9 HPV subtypes, and analysis of the antibody geometric mean titers revealed that the groups who received two doses had noninferior responses to the control group of adolescent girls and young women who received three doses.
Antibody geometric mean titers against all 9 HPV types were higher in subgroups of boys and girls (aged 9-10 years, aged 11-12 years, and aged 13-14 years) who received two doses, compared with girls and young women who received three doses. “These observations suggest that the overall results of the primary immunogenicity analyses may be applicable across the entire studied age range of girls and boys,” Dr. Iversen and his associates wrote.
The study cannot prove that the two-dose regimen has equal efficacy to the three-dose regimen in preventing HPV infection, only that the immunogenicity is noninferior, they said.
The study was sponsored by Merck, which manufactures the vaccine. Study authors have financial ties to Merck and a number of other pharmaceutical companies.
FROM JAMA
Key clinical point:
Major finding: Antibody geometric mean titers against all 9 HPV types were higher in subgroups of boys and girls (aged 9-10 years, aged 11-12 years, and aged 13-14 years) who received two doses, compared with girls and young women who received three doses.
Data source: Prospective, randomized trial of 1,377 children and young adults.
Disclosures: The study was sponsored by Merck, which manufactures the vaccine. Study authors have financial ties to Merck and a number of other pharmaceutical companies.
Higher sRAGE found in nonfocal ARDS
A biomarker may show whether acute respiratory distress syndrome (ARDS) is focal or nonfocal, a study showed.
This is an important distinction because some research suggests nonfocal ARDS, characterized by diffuse lung aeration loss, may have a worse prognosis and the two subtypes may respond differently to interventions such as positive end-expiratory pressure and recruitment maneuvers.
At present, the only way to identify focal versus nonfocal ARDS is a computed tomography scan, but that is often impractical because of the risks of moving the patient.
The current research, published in the November issue of CHEST (2016;150:998-1007), revealed that patients with nonfocal ARDS have higher plasma levels of the soluble form of the receptor for advanced glycation end product (sRAGE). At a cutoff of 1,188 pg/ml, the blood test differentiated between focal and nonfocal ARDS with a 94% sensitivity and an 84% specificity.
“Elevated baseline plasma sRAGE is a strong marker of nonfocal CT-based lung-imaging pattern in patients with early ARDS,” reported Jean-Michel Constantin of University Hospital of Clermont-Ferrand (France) and colleagues in the Azurea network.
The researchers recruited 119 consecutive ARDS patients from 10 intensive care units in France. They measured plasma levels of sRAGE, plasminogen activator inhibitor–1 (PAI-1), soluble intercellular adhesion molecule–1, and surfactant protein–D within 24 hours of ARDS onset. Each patient underwent a lung CT scan within 48 hours to assess focal versus nonfocal lung morphology.
Twenty-seven percent of patients had focal ARDS, while 73% were categorized as nonfocal. Mean plasma levels of sRAGE were much higher in nonfocal patients (3,074 pg/ml vs. 877 pg/ml, P less than .001). A cutoff value of 1,188 ng/ml distinguished focal and nonfocal ARDS with a sensitivity of 93% (95% confidence interval, 85%-97%) and a specificity of 84% (95% CI, 66%-95%). The test’s positive predictive value was 94% (95% CI, 87%-98%), and its negative predictive value was 81% (95% CI, 64%-93%).
The research is still in its early stage, but has a couple possible applications, according to Daniel R. Ouellette, MD, of Henry Ford Hospital, Detroit. “We might conceive of using this as a marker for nonfocal ARDS, and potentially use it to identify patients with worse outcomes. The other thing is, it may be a clue to help us learn about the underlying physiology of the disease,” he said in an interview.
If physicians can confidently categorize a patient, it could inform treatment. “We know that patients who have diffuse disease may be more likely to be treated successfully with advanced ventilator techniques. These techniques would be more useful and likely to lead to recovery in patients that don’t have focal disease,” said Dr. Ouellette.
However, he added that more research is needed. “These results are exciting, but they are very preliminary,” Dr Ouellette said.
The study was funded by the Auvergne Regional Council, the French Agence Nationale de la Recherche, and the Direction Generale de l’Offre de Soins, and the University Hospital of Clermont-Ferrand. The authors reported receiving funds from various pharmaceutical companies.
“Mechanical stress is concentrated at the border zones between well-[aerated] and poorly aerated lung units, which is thought to predispose to mechanical lung injury in these regions during tidal ventilation. … The results of the current study support this possibility that mechanical lung injury persists in regions of stress concentration during low tidal volume ventilation, contributing to higher mortality in nonfocal ARDS.
“The current study also provides additional evidence that a plasma biomarker, such as sRAGE, could improve our ability to endotype patients with [acute respiratory distress syndrome], forecast prognosis, and identify subgroups for targeting of specific therapies early in the course of [acute respiratory distress syndrome].”
Michael A. Matthay , MD, is a professor of medicine and anesthesia at the University of California, San Francisco, and is with the Cardiovascular Research Institute. Jeremy R. Beitler, MD, is with the department of medicine at the University of California, San Diego. Dr. Matthay consults for Cerus Therapeutics, GlaxoSmithKline, Boerhinger-Ingleheim, Bayer, Biogen, Quark Pharmaceuticals, and Incardia. Dr. Beitler has received research support from Amgen and GlaxoSmithKline.
“Mechanical stress is concentrated at the border zones between well-[aerated] and poorly aerated lung units, which is thought to predispose to mechanical lung injury in these regions during tidal ventilation. … The results of the current study support this possibility that mechanical lung injury persists in regions of stress concentration during low tidal volume ventilation, contributing to higher mortality in nonfocal ARDS.
“The current study also provides additional evidence that a plasma biomarker, such as sRAGE, could improve our ability to endotype patients with [acute respiratory distress syndrome], forecast prognosis, and identify subgroups for targeting of specific therapies early in the course of [acute respiratory distress syndrome].”
Michael A. Matthay , MD, is a professor of medicine and anesthesia at the University of California, San Francisco, and is with the Cardiovascular Research Institute. Jeremy R. Beitler, MD, is with the department of medicine at the University of California, San Diego. Dr. Matthay consults for Cerus Therapeutics, GlaxoSmithKline, Boerhinger-Ingleheim, Bayer, Biogen, Quark Pharmaceuticals, and Incardia. Dr. Beitler has received research support from Amgen and GlaxoSmithKline.
“Mechanical stress is concentrated at the border zones between well-[aerated] and poorly aerated lung units, which is thought to predispose to mechanical lung injury in these regions during tidal ventilation. … The results of the current study support this possibility that mechanical lung injury persists in regions of stress concentration during low tidal volume ventilation, contributing to higher mortality in nonfocal ARDS.
“The current study also provides additional evidence that a plasma biomarker, such as sRAGE, could improve our ability to endotype patients with [acute respiratory distress syndrome], forecast prognosis, and identify subgroups for targeting of specific therapies early in the course of [acute respiratory distress syndrome].”
Michael A. Matthay , MD, is a professor of medicine and anesthesia at the University of California, San Francisco, and is with the Cardiovascular Research Institute. Jeremy R. Beitler, MD, is with the department of medicine at the University of California, San Diego. Dr. Matthay consults for Cerus Therapeutics, GlaxoSmithKline, Boerhinger-Ingleheim, Bayer, Biogen, Quark Pharmaceuticals, and Incardia. Dr. Beitler has received research support from Amgen and GlaxoSmithKline.
A biomarker may show whether acute respiratory distress syndrome (ARDS) is focal or nonfocal, a study showed.
This is an important distinction because some research suggests nonfocal ARDS, characterized by diffuse lung aeration loss, may have a worse prognosis and the two subtypes may respond differently to interventions such as positive end-expiratory pressure and recruitment maneuvers.
At present, the only way to identify focal versus nonfocal ARDS is a computed tomography scan, but that is often impractical because of the risks of moving the patient.
The current research, published in the November issue of CHEST (2016;150:998-1007), revealed that patients with nonfocal ARDS have higher plasma levels of the soluble form of the receptor for advanced glycation end product (sRAGE). At a cutoff of 1,188 pg/ml, the blood test differentiated between focal and nonfocal ARDS with a 94% sensitivity and an 84% specificity.
“Elevated baseline plasma sRAGE is a strong marker of nonfocal CT-based lung-imaging pattern in patients with early ARDS,” reported Jean-Michel Constantin of University Hospital of Clermont-Ferrand (France) and colleagues in the Azurea network.
The researchers recruited 119 consecutive ARDS patients from 10 intensive care units in France. They measured plasma levels of sRAGE, plasminogen activator inhibitor–1 (PAI-1), soluble intercellular adhesion molecule–1, and surfactant protein–D within 24 hours of ARDS onset. Each patient underwent a lung CT scan within 48 hours to assess focal versus nonfocal lung morphology.
Twenty-seven percent of patients had focal ARDS, while 73% were categorized as nonfocal. Mean plasma levels of sRAGE were much higher in nonfocal patients (3,074 pg/ml vs. 877 pg/ml, P less than .001). A cutoff value of 1,188 ng/ml distinguished focal and nonfocal ARDS with a sensitivity of 93% (95% confidence interval, 85%-97%) and a specificity of 84% (95% CI, 66%-95%). The test’s positive predictive value was 94% (95% CI, 87%-98%), and its negative predictive value was 81% (95% CI, 64%-93%).
The research is still in its early stage, but has a couple possible applications, according to Daniel R. Ouellette, MD, of Henry Ford Hospital, Detroit. “We might conceive of using this as a marker for nonfocal ARDS, and potentially use it to identify patients with worse outcomes. The other thing is, it may be a clue to help us learn about the underlying physiology of the disease,” he said in an interview.
If physicians can confidently categorize a patient, it could inform treatment. “We know that patients who have diffuse disease may be more likely to be treated successfully with advanced ventilator techniques. These techniques would be more useful and likely to lead to recovery in patients that don’t have focal disease,” said Dr. Ouellette.
However, he added that more research is needed. “These results are exciting, but they are very preliminary,” Dr Ouellette said.
The study was funded by the Auvergne Regional Council, the French Agence Nationale de la Recherche, and the Direction Generale de l’Offre de Soins, and the University Hospital of Clermont-Ferrand. The authors reported receiving funds from various pharmaceutical companies.
A biomarker may show whether acute respiratory distress syndrome (ARDS) is focal or nonfocal, a study showed.
This is an important distinction because some research suggests nonfocal ARDS, characterized by diffuse lung aeration loss, may have a worse prognosis and the two subtypes may respond differently to interventions such as positive end-expiratory pressure and recruitment maneuvers.
At present, the only way to identify focal versus nonfocal ARDS is a computed tomography scan, but that is often impractical because of the risks of moving the patient.
The current research, published in the November issue of CHEST (2016;150:998-1007), revealed that patients with nonfocal ARDS have higher plasma levels of the soluble form of the receptor for advanced glycation end product (sRAGE). At a cutoff of 1,188 pg/ml, the blood test differentiated between focal and nonfocal ARDS with a 94% sensitivity and an 84% specificity.
“Elevated baseline plasma sRAGE is a strong marker of nonfocal CT-based lung-imaging pattern in patients with early ARDS,” reported Jean-Michel Constantin of University Hospital of Clermont-Ferrand (France) and colleagues in the Azurea network.
The researchers recruited 119 consecutive ARDS patients from 10 intensive care units in France. They measured plasma levels of sRAGE, plasminogen activator inhibitor–1 (PAI-1), soluble intercellular adhesion molecule–1, and surfactant protein–D within 24 hours of ARDS onset. Each patient underwent a lung CT scan within 48 hours to assess focal versus nonfocal lung morphology.
Twenty-seven percent of patients had focal ARDS, while 73% were categorized as nonfocal. Mean plasma levels of sRAGE were much higher in nonfocal patients (3,074 pg/ml vs. 877 pg/ml, P less than .001). A cutoff value of 1,188 ng/ml distinguished focal and nonfocal ARDS with a sensitivity of 93% (95% confidence interval, 85%-97%) and a specificity of 84% (95% CI, 66%-95%). The test’s positive predictive value was 94% (95% CI, 87%-98%), and its negative predictive value was 81% (95% CI, 64%-93%).
The research is still in its early stage, but has a couple possible applications, according to Daniel R. Ouellette, MD, of Henry Ford Hospital, Detroit. “We might conceive of using this as a marker for nonfocal ARDS, and potentially use it to identify patients with worse outcomes. The other thing is, it may be a clue to help us learn about the underlying physiology of the disease,” he said in an interview.
If physicians can confidently categorize a patient, it could inform treatment. “We know that patients who have diffuse disease may be more likely to be treated successfully with advanced ventilator techniques. These techniques would be more useful and likely to lead to recovery in patients that don’t have focal disease,” said Dr. Ouellette.
However, he added that more research is needed. “These results are exciting, but they are very preliminary,” Dr Ouellette said.
The study was funded by the Auvergne Regional Council, the French Agence Nationale de la Recherche, and the Direction Generale de l’Offre de Soins, and the University Hospital of Clermont-Ferrand. The authors reported receiving funds from various pharmaceutical companies.
FROM CHEST
Key clinical point:
Major finding: At a cutoff of 1,188 pg/ml, the sRAGE blood test differentiated between focal and nonfocal ARDS with a 94% sensitivity and an 84% specificity.
Data source: A prospective multicenter cohort study.
Disclosures: The study was funded by the Auvergne Regional Council, the French Agence Nationale de la Recherche, and the Direction Generale de l’Offre de Soins, and the University Hospital of Clermont-Ferrand. The authors reported receiving funds from various pharmaceutical companies.
Flu susceptibility driven by birth year
Differences in susceptibility to an influenza A virus (IAV) strain may be traceable to the first lifetime influenza infection, according to a new statistical model, which could have implications for epidemiology and future flu vaccines.
In the Nov. 11 issue of Science, researchers described infection models of the H5N1 and H7N9 strains of influenza A. The former occurs more commonly in younger people, and the latter in older individuals, but the reasons for those associations have puzzled scientists.
The researchers, led by James Lloyd-Smith, PhD, of the department of ecology and evolutionary biology at the University of California, Los Angeles, looked at susceptibility to IAV strains by birth year, and found that this was the best predictor of vulnerability. For example, an analysis of H5N1 cases in Egypt, where had many H5N1 cases spread over the past decade, showed that individuals born in the same year had the same average risk of severe H5N1 infection, even after they had aged by 10 years. That suggests that it is the birth year, not advancing age, which influences susceptibility (Science. 2016 Nov 11;354[6313]:721-5. doi:10.1126/science.aag1322).
The researchers suggest that the immune system “imprints” on the hemagglutinin (HA) subtype during an individual’s first infection, which confers protection against severe disease caused by other, related viruses, though it may not reduce infection rates overall.
The year 1968 may have marked an important inflection point. That year marked a shift in the identify of circulating viruses, from group 1 HA (which includes H5N1) to group 2 HA (which includes H7N9). Individuals born before 1968 were likely first infected with a group 1 virus, while those born later were most likely initially exposed to a group 2 virus. If the imprint theory is correct, younger people would have imprinted on group 2 viruses similar to H7N9, which would explain their greater vulnerability to group 1 viruses like H5N1.
“Imprinting was the dominant explanatory factor for observed incidence and mortality patterns for both H5N1 and H7N9. It was the only tested factor included in all plausible models for both viruses,” the researchers wrote.
According to the model, imprinting explains 75% of protection against severe infection and 80% of the protection against mortality for H5N1 and H7N9.
That information adds a previously unrecognized layer to influenza epidemiology, which should be accounted for in public health measures. “The methods shown here can provide rolling estimates of which age groups would be at highest risk for severe disease should particular novel HA subtypes emerge,” the researchers wrote.
The researchers received funding from the National Institutes of Health, the National Science Foundation, the David and Lucile Packard Foundation, and the Department of Homeland Security. They reported having no financial disclosures.
A growing body of epidemiological evidence points to the prolonged effects of cross-immunity, including competition between strains during seasonal and pandemic outbreaks, reduced risk of pandemic infection in those with previous seasonal exposure, and – as reported by Gostic et al. – lifelong protection against viruses of different subtypes but in the same hemagglutinin (HA) homology group. Basic science efforts are now needed to fully validate the HA imprinting hypothesis. More broadly, further experimental and theoretical work should map the relationship between early childhood exposure to influenza and immune protection and the implications of lifelong immunity for vaccination strategies and pandemic risk.
Cécile Viboud, PhD, is the acting director of the division of international epidemiology and population studies at the Fogarty International Center at the National Institutes of Health. Suzanne L. Epstein, PhD, is the associate director for research at the office of tissues and advanced therapies at the Food and Drug Administration Center for Biologics Evaluation and Research. They had no relevant financial disclosures and made these remarks in an editorial that accompanied the published study (Science. 2016 Nov 11;354[6313]:706-7. doi:10.1126/science.aak9816).
A growing body of epidemiological evidence points to the prolonged effects of cross-immunity, including competition between strains during seasonal and pandemic outbreaks, reduced risk of pandemic infection in those with previous seasonal exposure, and – as reported by Gostic et al. – lifelong protection against viruses of different subtypes but in the same hemagglutinin (HA) homology group. Basic science efforts are now needed to fully validate the HA imprinting hypothesis. More broadly, further experimental and theoretical work should map the relationship between early childhood exposure to influenza and immune protection and the implications of lifelong immunity for vaccination strategies and pandemic risk.
Cécile Viboud, PhD, is the acting director of the division of international epidemiology and population studies at the Fogarty International Center at the National Institutes of Health. Suzanne L. Epstein, PhD, is the associate director for research at the office of tissues and advanced therapies at the Food and Drug Administration Center for Biologics Evaluation and Research. They had no relevant financial disclosures and made these remarks in an editorial that accompanied the published study (Science. 2016 Nov 11;354[6313]:706-7. doi:10.1126/science.aak9816).
A growing body of epidemiological evidence points to the prolonged effects of cross-immunity, including competition between strains during seasonal and pandemic outbreaks, reduced risk of pandemic infection in those with previous seasonal exposure, and – as reported by Gostic et al. – lifelong protection against viruses of different subtypes but in the same hemagglutinin (HA) homology group. Basic science efforts are now needed to fully validate the HA imprinting hypothesis. More broadly, further experimental and theoretical work should map the relationship between early childhood exposure to influenza and immune protection and the implications of lifelong immunity for vaccination strategies and pandemic risk.
Cécile Viboud, PhD, is the acting director of the division of international epidemiology and population studies at the Fogarty International Center at the National Institutes of Health. Suzanne L. Epstein, PhD, is the associate director for research at the office of tissues and advanced therapies at the Food and Drug Administration Center for Biologics Evaluation and Research. They had no relevant financial disclosures and made these remarks in an editorial that accompanied the published study (Science. 2016 Nov 11;354[6313]:706-7. doi:10.1126/science.aak9816).
Differences in susceptibility to an influenza A virus (IAV) strain may be traceable to the first lifetime influenza infection, according to a new statistical model, which could have implications for epidemiology and future flu vaccines.
In the Nov. 11 issue of Science, researchers described infection models of the H5N1 and H7N9 strains of influenza A. The former occurs more commonly in younger people, and the latter in older individuals, but the reasons for those associations have puzzled scientists.
The researchers, led by James Lloyd-Smith, PhD, of the department of ecology and evolutionary biology at the University of California, Los Angeles, looked at susceptibility to IAV strains by birth year, and found that this was the best predictor of vulnerability. For example, an analysis of H5N1 cases in Egypt, where had many H5N1 cases spread over the past decade, showed that individuals born in the same year had the same average risk of severe H5N1 infection, even after they had aged by 10 years. That suggests that it is the birth year, not advancing age, which influences susceptibility (Science. 2016 Nov 11;354[6313]:721-5. doi:10.1126/science.aag1322).
The researchers suggest that the immune system “imprints” on the hemagglutinin (HA) subtype during an individual’s first infection, which confers protection against severe disease caused by other, related viruses, though it may not reduce infection rates overall.
The year 1968 may have marked an important inflection point. That year marked a shift in the identify of circulating viruses, from group 1 HA (which includes H5N1) to group 2 HA (which includes H7N9). Individuals born before 1968 were likely first infected with a group 1 virus, while those born later were most likely initially exposed to a group 2 virus. If the imprint theory is correct, younger people would have imprinted on group 2 viruses similar to H7N9, which would explain their greater vulnerability to group 1 viruses like H5N1.
“Imprinting was the dominant explanatory factor for observed incidence and mortality patterns for both H5N1 and H7N9. It was the only tested factor included in all plausible models for both viruses,” the researchers wrote.
According to the model, imprinting explains 75% of protection against severe infection and 80% of the protection against mortality for H5N1 and H7N9.
That information adds a previously unrecognized layer to influenza epidemiology, which should be accounted for in public health measures. “The methods shown here can provide rolling estimates of which age groups would be at highest risk for severe disease should particular novel HA subtypes emerge,” the researchers wrote.
The researchers received funding from the National Institutes of Health, the National Science Foundation, the David and Lucile Packard Foundation, and the Department of Homeland Security. They reported having no financial disclosures.
Differences in susceptibility to an influenza A virus (IAV) strain may be traceable to the first lifetime influenza infection, according to a new statistical model, which could have implications for epidemiology and future flu vaccines.
In the Nov. 11 issue of Science, researchers described infection models of the H5N1 and H7N9 strains of influenza A. The former occurs more commonly in younger people, and the latter in older individuals, but the reasons for those associations have puzzled scientists.
The researchers, led by James Lloyd-Smith, PhD, of the department of ecology and evolutionary biology at the University of California, Los Angeles, looked at susceptibility to IAV strains by birth year, and found that this was the best predictor of vulnerability. For example, an analysis of H5N1 cases in Egypt, where had many H5N1 cases spread over the past decade, showed that individuals born in the same year had the same average risk of severe H5N1 infection, even after they had aged by 10 years. That suggests that it is the birth year, not advancing age, which influences susceptibility (Science. 2016 Nov 11;354[6313]:721-5. doi:10.1126/science.aag1322).
The researchers suggest that the immune system “imprints” on the hemagglutinin (HA) subtype during an individual’s first infection, which confers protection against severe disease caused by other, related viruses, though it may not reduce infection rates overall.
The year 1968 may have marked an important inflection point. That year marked a shift in the identify of circulating viruses, from group 1 HA (which includes H5N1) to group 2 HA (which includes H7N9). Individuals born before 1968 were likely first infected with a group 1 virus, while those born later were most likely initially exposed to a group 2 virus. If the imprint theory is correct, younger people would have imprinted on group 2 viruses similar to H7N9, which would explain their greater vulnerability to group 1 viruses like H5N1.
“Imprinting was the dominant explanatory factor for observed incidence and mortality patterns for both H5N1 and H7N9. It was the only tested factor included in all plausible models for both viruses,” the researchers wrote.
According to the model, imprinting explains 75% of protection against severe infection and 80% of the protection against mortality for H5N1 and H7N9.
That information adds a previously unrecognized layer to influenza epidemiology, which should be accounted for in public health measures. “The methods shown here can provide rolling estimates of which age groups would be at highest risk for severe disease should particular novel HA subtypes emerge,” the researchers wrote.
The researchers received funding from the National Institutes of Health, the National Science Foundation, the David and Lucile Packard Foundation, and the Department of Homeland Security. They reported having no financial disclosures.
Key clinical point:
Major finding: Early exposure to virus subtype explains 75% of protection against severe disease in later life.
Data source: Statistical model of retrospective data.
Disclosures: The researchers received funding from the National Institutes of Health, the National Science Foundation, the David and Lucile Packard Foundation, and the Department of Homeland Security. They reported having no financial disclosures.
Diabetes, stroke linked to recurrent C. difficile
LAS VEGAS – Diabetes and stroke are risk factors for recurrent Clostridium difficile infection (CDI), with stroke patients at about 10 times the risk of recurrence.
The underlying cause for the association is a mystery, but one-sided paralysis is one possibility. “A lot of stroke patients may be hemiplegic, and they may be bedridden, so that may be a risk factor by itself. It’s something that may need to be studied in the future,” Alan Putrus, MD, a gastroenterology fellow at St. John Providence Hospital, Detroit, said in an interview.
CDI recurrence rates range from 5% to 47%, depending on the institution. Although risk factors of initial CDI have been well defined, few studies have looked at risk factors associated with recurrence.
In order to get at the question, the researchers conducted a study of 108 initial CDIs and 113 recurrences at two urban and one suburban hospital. Patients who experienced recurrence were matched 1:1 to age- and gender-matched controls with no recurrent CDI.
CDI recurrence rates were 16.5% and 15.9% in the two urban hospitals, and 14.9% in the suburban hospital.
Logistic regression revealed risk factors associated with CDI recurrence, including diabetes (odds ratio, 1.91; 95% confidence interval, 1.05-3.47; P = .04), stroke (OR, 9.73; 95% CI, 1.15-82.35; P = .04), exposure to proton pump inhibitors in the past 3 months (OR, 1.82; 95% CI, 1.03-3.23; P = .04), and admission to an intensive care unit in the past 3 months (OR, 1.95; 95% CI, 1.0-3.83; P = .04).
The results suggest that diabetes and especially stroke may be important risk factors for CDI recurrence, and their presence should prompt physicians to alter patient care accordingly, according to Dr. Putrus.
He stressed the importance of antibiotic stewardship. “Once you find a certain bug or pathogen, try to deescalate the antibiotics as soon as you can. If a patient is diabetic, controlling their blood sugar may also help,” Dr. Putrus said.
Finally, physicians should consider whether proton pump inhibitors are really necessary. Some patients start on PPIs but remain on the drugs long after symptoms have abated. “A lot of patients just have some discomfort in their abdomen, and they never stop taking it. They keep refilling it. So that’s a problem,” said Dr. Putrus.
Dr. Putrus has declared no conflicts of interest.
AGA Resource
AGA offers information to educate your patients about C. difficile and fecal microbiota transplant. Learn more at http://www.gastro.org/patient-care/conditions-diseases/clostridium-difficile-infection.
LAS VEGAS – Diabetes and stroke are risk factors for recurrent Clostridium difficile infection (CDI), with stroke patients at about 10 times the risk of recurrence.
The underlying cause for the association is a mystery, but one-sided paralysis is one possibility. “A lot of stroke patients may be hemiplegic, and they may be bedridden, so that may be a risk factor by itself. It’s something that may need to be studied in the future,” Alan Putrus, MD, a gastroenterology fellow at St. John Providence Hospital, Detroit, said in an interview.
CDI recurrence rates range from 5% to 47%, depending on the institution. Although risk factors of initial CDI have been well defined, few studies have looked at risk factors associated with recurrence.
In order to get at the question, the researchers conducted a study of 108 initial CDIs and 113 recurrences at two urban and one suburban hospital. Patients who experienced recurrence were matched 1:1 to age- and gender-matched controls with no recurrent CDI.
CDI recurrence rates were 16.5% and 15.9% in the two urban hospitals, and 14.9% in the suburban hospital.
Logistic regression revealed risk factors associated with CDI recurrence, including diabetes (odds ratio, 1.91; 95% confidence interval, 1.05-3.47; P = .04), stroke (OR, 9.73; 95% CI, 1.15-82.35; P = .04), exposure to proton pump inhibitors in the past 3 months (OR, 1.82; 95% CI, 1.03-3.23; P = .04), and admission to an intensive care unit in the past 3 months (OR, 1.95; 95% CI, 1.0-3.83; P = .04).
The results suggest that diabetes and especially stroke may be important risk factors for CDI recurrence, and their presence should prompt physicians to alter patient care accordingly, according to Dr. Putrus.
He stressed the importance of antibiotic stewardship. “Once you find a certain bug or pathogen, try to deescalate the antibiotics as soon as you can. If a patient is diabetic, controlling their blood sugar may also help,” Dr. Putrus said.
Finally, physicians should consider whether proton pump inhibitors are really necessary. Some patients start on PPIs but remain on the drugs long after symptoms have abated. “A lot of patients just have some discomfort in their abdomen, and they never stop taking it. They keep refilling it. So that’s a problem,” said Dr. Putrus.
Dr. Putrus has declared no conflicts of interest.
AGA Resource
AGA offers information to educate your patients about C. difficile and fecal microbiota transplant. Learn more at http://www.gastro.org/patient-care/conditions-diseases/clostridium-difficile-infection.
LAS VEGAS – Diabetes and stroke are risk factors for recurrent Clostridium difficile infection (CDI), with stroke patients at about 10 times the risk of recurrence.
The underlying cause for the association is a mystery, but one-sided paralysis is one possibility. “A lot of stroke patients may be hemiplegic, and they may be bedridden, so that may be a risk factor by itself. It’s something that may need to be studied in the future,” Alan Putrus, MD, a gastroenterology fellow at St. John Providence Hospital, Detroit, said in an interview.
CDI recurrence rates range from 5% to 47%, depending on the institution. Although risk factors of initial CDI have been well defined, few studies have looked at risk factors associated with recurrence.
In order to get at the question, the researchers conducted a study of 108 initial CDIs and 113 recurrences at two urban and one suburban hospital. Patients who experienced recurrence were matched 1:1 to age- and gender-matched controls with no recurrent CDI.
CDI recurrence rates were 16.5% and 15.9% in the two urban hospitals, and 14.9% in the suburban hospital.
Logistic regression revealed risk factors associated with CDI recurrence, including diabetes (odds ratio, 1.91; 95% confidence interval, 1.05-3.47; P = .04), stroke (OR, 9.73; 95% CI, 1.15-82.35; P = .04), exposure to proton pump inhibitors in the past 3 months (OR, 1.82; 95% CI, 1.03-3.23; P = .04), and admission to an intensive care unit in the past 3 months (OR, 1.95; 95% CI, 1.0-3.83; P = .04).
The results suggest that diabetes and especially stroke may be important risk factors for CDI recurrence, and their presence should prompt physicians to alter patient care accordingly, according to Dr. Putrus.
He stressed the importance of antibiotic stewardship. “Once you find a certain bug or pathogen, try to deescalate the antibiotics as soon as you can. If a patient is diabetic, controlling their blood sugar may also help,” Dr. Putrus said.
Finally, physicians should consider whether proton pump inhibitors are really necessary. Some patients start on PPIs but remain on the drugs long after symptoms have abated. “A lot of patients just have some discomfort in their abdomen, and they never stop taking it. They keep refilling it. So that’s a problem,” said Dr. Putrus.
Dr. Putrus has declared no conflicts of interest.
AGA Resource
AGA offers information to educate your patients about C. difficile and fecal microbiota transplant. Learn more at http://www.gastro.org/patient-care/conditions-diseases/clostridium-difficile-infection.
AT ACG 2016
Key clinical point:
Major finding: Diabetes, stroke, and a history of PPI use were all associated with higher risks of recurrence.
Data source: Case-control, retrospective study.
Disclosures: Dr. Putrus has declared no conflicts of interest.
Ozanimod has lasting effect on ulcerative colitis
LAS VEGAS – Ozanimod, an oral agent that selectively modulates the sphingosine 1-phosphate (S1P) 1 and 5 receptor, has a lasting effect on symptoms of ulcerative colitis, according to results from an open-label extension study.
The study extends the phase II TOUCHSTONE trial, in which patients with ulcerative colitis showed significant clinical improvement out to 32 weeks. The current study showed those improvements lasting out to at least 1 year, with about 80% of patients staying on the drug at the end of the study.
With other drug regimens, “the loss rates are at least 50% of the patients, so this is a remarkable level of durability over time,” William Sandborn, MD, chief of gastroenterology at the University of California at San Diego, said at the annual meeting of the American College of Gastroenterology. “With biologics, if you follow patients out for a year or 2, you see a fair amount of loss of response and some of that probably has to do with the formation of antidrug antibodies and immunogenicity,” Dr. Sandborn added.
In the original TOUCHSTONE study, 197 patients were randomized to placebo, ozanimod 0.5 mg, or ozanimod 1.0 mg, and followed out to week 32. Twenty-one percent of those in the 1.0-mg group achieved clinical remission, compared with 26% in the 0.5-mg group and 6% of those receiving placebo. Clinical response rates were 51%, 35%, and 20%, respectively.
In the open-label study, patients from all arms who did not respond to treatment after the induction phase, or relapsed during the maintenance phase, or completed the maintenance phase (170 patients in total) entered the open-label study with a dose of 1.0 mg ozanimod. At the time of the cut-off, patients in the extension study had been taking ozanimod for at least 1 year.
At the start of the extension study, the partial Mayo Score (pMS) for patients on placebo, ozanimod 0.5 mg, and 1.0 mg were 4.6, 4.5, and 3.3, respectively. All groups showed improvement in pMS by week 44 (1.7, 1.7, and 1.9, respectively)
At week 44, 90.9% of patients had little or no active disease (physician global assessment 0 or 1), 98.4% had little or no blood in their stools, and 84.7% had no blood in their stools.
Adverse events with a frequency higher than 2% included ulcerative colitis flare (5.9%), anemia (3.5%), upper respiratory tract infection (4.1%), nasal pharyngitis (3.5%), back pain (2.9%), arthralgia (2.4%), and headache (2.4%). The researchers noted some transient elevation of alanine aminotransferase or aspartate aminotransferase, but these elevations were temporary and reversed during ongoing treatment; 2.4% of patients experienced ALT and AST levels higher than three times the upper limit of normal, and all were asymptomatic.
Serious adverse events that occurred in two or more patients included anemia (1.2%) and ulcerative colitis flare (2.4%).
“This is a promising oral product with a similar mechanism of action to other lymphocyte trafficking agents,” said Stephen Hanauer, MD, medical director of the digestive health center at the Northwestern University, Chicago, who attended the session.
Ozanimod and other lymphocyte trafficking agents may offer a slightly different profile than some of the other drug classes, such as the anti–tumor necrosis factor agents, according to Dr. Hanauer, because the agents don’t affect lymphocytes already in the tissues. On the other hand, once the drug has acted, its effect may linger. “The time to effect may be a little slower, but the long-term effect seems to be as good or better as other mechanisms of action.”
The drug’s real place could be in early disease, Dr. Hanauer said. “If this is truly an effective and safe agent, the real positioning should be earlier in the disease, before patients are exposed to steroids and other immune suppressants, or biologics that have an infection risk.”
Celgene funded the study. Dr. Sandborn has received funding from Receptos and Celgene and consulted for both companies. Dr. Hanauer has consulted with Receptos, Celgene, Pfizer, Jansen, and AbbVie.
AGA Resource
AGA offers an IBD Clinical Service Line that provides tools to help you become more efficient, understand quality standards, and improve the process of care for patients. Learn more at http://www.gastro.org/patient-care/conditions-diseases/ibd
LAS VEGAS – Ozanimod, an oral agent that selectively modulates the sphingosine 1-phosphate (S1P) 1 and 5 receptor, has a lasting effect on symptoms of ulcerative colitis, according to results from an open-label extension study.
The study extends the phase II TOUCHSTONE trial, in which patients with ulcerative colitis showed significant clinical improvement out to 32 weeks. The current study showed those improvements lasting out to at least 1 year, with about 80% of patients staying on the drug at the end of the study.
With other drug regimens, “the loss rates are at least 50% of the patients, so this is a remarkable level of durability over time,” William Sandborn, MD, chief of gastroenterology at the University of California at San Diego, said at the annual meeting of the American College of Gastroenterology. “With biologics, if you follow patients out for a year or 2, you see a fair amount of loss of response and some of that probably has to do with the formation of antidrug antibodies and immunogenicity,” Dr. Sandborn added.
In the original TOUCHSTONE study, 197 patients were randomized to placebo, ozanimod 0.5 mg, or ozanimod 1.0 mg, and followed out to week 32. Twenty-one percent of those in the 1.0-mg group achieved clinical remission, compared with 26% in the 0.5-mg group and 6% of those receiving placebo. Clinical response rates were 51%, 35%, and 20%, respectively.
In the open-label study, patients from all arms who did not respond to treatment after the induction phase, or relapsed during the maintenance phase, or completed the maintenance phase (170 patients in total) entered the open-label study with a dose of 1.0 mg ozanimod. At the time of the cut-off, patients in the extension study had been taking ozanimod for at least 1 year.
At the start of the extension study, the partial Mayo Score (pMS) for patients on placebo, ozanimod 0.5 mg, and 1.0 mg were 4.6, 4.5, and 3.3, respectively. All groups showed improvement in pMS by week 44 (1.7, 1.7, and 1.9, respectively)
At week 44, 90.9% of patients had little or no active disease (physician global assessment 0 or 1), 98.4% had little or no blood in their stools, and 84.7% had no blood in their stools.
Adverse events with a frequency higher than 2% included ulcerative colitis flare (5.9%), anemia (3.5%), upper respiratory tract infection (4.1%), nasal pharyngitis (3.5%), back pain (2.9%), arthralgia (2.4%), and headache (2.4%). The researchers noted some transient elevation of alanine aminotransferase or aspartate aminotransferase, but these elevations were temporary and reversed during ongoing treatment; 2.4% of patients experienced ALT and AST levels higher than three times the upper limit of normal, and all were asymptomatic.
Serious adverse events that occurred in two or more patients included anemia (1.2%) and ulcerative colitis flare (2.4%).
“This is a promising oral product with a similar mechanism of action to other lymphocyte trafficking agents,” said Stephen Hanauer, MD, medical director of the digestive health center at the Northwestern University, Chicago, who attended the session.
Ozanimod and other lymphocyte trafficking agents may offer a slightly different profile than some of the other drug classes, such as the anti–tumor necrosis factor agents, according to Dr. Hanauer, because the agents don’t affect lymphocytes already in the tissues. On the other hand, once the drug has acted, its effect may linger. “The time to effect may be a little slower, but the long-term effect seems to be as good or better as other mechanisms of action.”
The drug’s real place could be in early disease, Dr. Hanauer said. “If this is truly an effective and safe agent, the real positioning should be earlier in the disease, before patients are exposed to steroids and other immune suppressants, or biologics that have an infection risk.”
Celgene funded the study. Dr. Sandborn has received funding from Receptos and Celgene and consulted for both companies. Dr. Hanauer has consulted with Receptos, Celgene, Pfizer, Jansen, and AbbVie.
AGA Resource
AGA offers an IBD Clinical Service Line that provides tools to help you become more efficient, understand quality standards, and improve the process of care for patients. Learn more at http://www.gastro.org/patient-care/conditions-diseases/ibd
LAS VEGAS – Ozanimod, an oral agent that selectively modulates the sphingosine 1-phosphate (S1P) 1 and 5 receptor, has a lasting effect on symptoms of ulcerative colitis, according to results from an open-label extension study.
The study extends the phase II TOUCHSTONE trial, in which patients with ulcerative colitis showed significant clinical improvement out to 32 weeks. The current study showed those improvements lasting out to at least 1 year, with about 80% of patients staying on the drug at the end of the study.
With other drug regimens, “the loss rates are at least 50% of the patients, so this is a remarkable level of durability over time,” William Sandborn, MD, chief of gastroenterology at the University of California at San Diego, said at the annual meeting of the American College of Gastroenterology. “With biologics, if you follow patients out for a year or 2, you see a fair amount of loss of response and some of that probably has to do with the formation of antidrug antibodies and immunogenicity,” Dr. Sandborn added.
In the original TOUCHSTONE study, 197 patients were randomized to placebo, ozanimod 0.5 mg, or ozanimod 1.0 mg, and followed out to week 32. Twenty-one percent of those in the 1.0-mg group achieved clinical remission, compared with 26% in the 0.5-mg group and 6% of those receiving placebo. Clinical response rates were 51%, 35%, and 20%, respectively.
In the open-label study, patients from all arms who did not respond to treatment after the induction phase, or relapsed during the maintenance phase, or completed the maintenance phase (170 patients in total) entered the open-label study with a dose of 1.0 mg ozanimod. At the time of the cut-off, patients in the extension study had been taking ozanimod for at least 1 year.
At the start of the extension study, the partial Mayo Score (pMS) for patients on placebo, ozanimod 0.5 mg, and 1.0 mg were 4.6, 4.5, and 3.3, respectively. All groups showed improvement in pMS by week 44 (1.7, 1.7, and 1.9, respectively)
At week 44, 90.9% of patients had little or no active disease (physician global assessment 0 or 1), 98.4% had little or no blood in their stools, and 84.7% had no blood in their stools.
Adverse events with a frequency higher than 2% included ulcerative colitis flare (5.9%), anemia (3.5%), upper respiratory tract infection (4.1%), nasal pharyngitis (3.5%), back pain (2.9%), arthralgia (2.4%), and headache (2.4%). The researchers noted some transient elevation of alanine aminotransferase or aspartate aminotransferase, but these elevations were temporary and reversed during ongoing treatment; 2.4% of patients experienced ALT and AST levels higher than three times the upper limit of normal, and all were asymptomatic.
Serious adverse events that occurred in two or more patients included anemia (1.2%) and ulcerative colitis flare (2.4%).
“This is a promising oral product with a similar mechanism of action to other lymphocyte trafficking agents,” said Stephen Hanauer, MD, medical director of the digestive health center at the Northwestern University, Chicago, who attended the session.
Ozanimod and other lymphocyte trafficking agents may offer a slightly different profile than some of the other drug classes, such as the anti–tumor necrosis factor agents, according to Dr. Hanauer, because the agents don’t affect lymphocytes already in the tissues. On the other hand, once the drug has acted, its effect may linger. “The time to effect may be a little slower, but the long-term effect seems to be as good or better as other mechanisms of action.”
The drug’s real place could be in early disease, Dr. Hanauer said. “If this is truly an effective and safe agent, the real positioning should be earlier in the disease, before patients are exposed to steroids and other immune suppressants, or biologics that have an infection risk.”
Celgene funded the study. Dr. Sandborn has received funding from Receptos and Celgene and consulted for both companies. Dr. Hanauer has consulted with Receptos, Celgene, Pfizer, Jansen, and AbbVie.
AGA Resource
AGA offers an IBD Clinical Service Line that provides tools to help you become more efficient, understand quality standards, and improve the process of care for patients. Learn more at http://www.gastro.org/patient-care/conditions-diseases/ibd
AT ACG 2016
Key clinical point:
Major finding: Ozanimod maintains efficacy in ulcerative colitis out to 1 year, with 90% of patients having little or no evidence of active disease.
Data source: Open-label extension study following a phase II clinical trial.
Disclosures: Celgene funded the study. Dr. Sandborn has received funding from Receptos and Celgene and consulted for both companies. Dr. Hanauer has consulted with Receptos, Celgene, Pfizer, Jansen, and AbbVie.