User login
DECAAF points way to improved AF ablation
DENVER – Preprocedural quantification of atrial fibrosis via delayed-enhancement MRI offers a potent means of boosting atrial fibrillation ablation success rates by weeding out likely nonresponders, a study has shown.
Results of the double-blind, multinational prospective DECAAF trial (Delayed-Enhancement MRI Determinant of Successful Catheter Ablation for Atrial Fibrillation) show that the extent of atrial fibrosis is a strong predictor of patient outcome. The more fibrosis present when measured preprocedurally by delayed-enhancement MRI (DE-MRI) with gadolinium contrast, the less likely a patient would remain in sinus rhythm at follow-up more than 1 year following ablation, Dr. Nassir Marrouche reported at the annual meeting of the Heart Rhythm Society.
"Hopefully this will help us better individualize the therapy. We have to accept at some point that we can’t cure everybody with atrial fibrillation. This modality helps us to better define which patients should be eligible," according to Dr. Marrouche, director of the comprehensive arrhythmia research and management center at the University of Utah, Salt Lake City.
One attractive feature of this management strategy is that patients who are candidates for AF ablation already routinely undergo a preprocedural 3-D scan with CT or MRI. It’s a straightforward matter to train an MRI technician to measure atrial fibrosis, as DECAAF showed.
This is a practice-changing development, he said: "We recommend that in every single ablation patient, before you touch their heart you really should know how extensive their disease is."
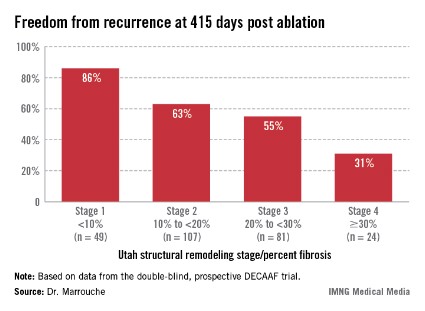
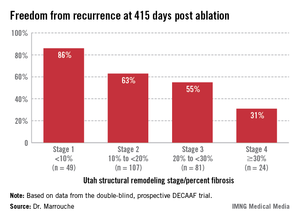
Patients undergoing a first ablation procedure for paroxysmal AF typically have about a 60% success rate, meaning they remain free of atrial arrhythmia at 1 year. In contrast, DECAAF participants with less than 10% fibrosis in their left atrium had a success rate of 86% at 415 days of follow-up.
Patients with less than 10% preprocedural atrial fibrosis are categorized as Utah stage 1 disease using a left atrial structural remodeling classification system previously described by Dr. Marrouche and his coworkers . At the other end of the spectrum, DECAAF subjects who were Utah stage 4, with at least 30% fibrosis, had a dismal 31% freedom of recurrence 415 days after the end of the standard 90-day postprocedural blanking period. Patients with stage 2 or 3 atrial fibrosis had intermediate long-term outcomes (see box).
"We sit down with a stage 4 patient and say, ‘Listen, your chance of being cured of this disease at long-term follow-up is not very high,’" the electrophysiologist explained. "We put our expectations on the table. We now have 5-year follow-up data showing a 5%-10% success in Utah 4 patients. We in Utah today are very reluctant to take such patients into the lab and ablate them. Instead, we try every option to rate-control them. But Utah stage 1 is straightforward. I make that decision for the patient: ‘You should be ablated early on.’ "
DECAAF included 261 patients with AF who underwent a first ablation procedure at 15 centers in the United States, Europe, and Australia. But first they all underwent DE-MRI, the results of which were sent to a core lab for blinded quantification of atrial fibrosis. The interventionalists remained blinded to the fibrosis findings.
Most DECAAF participants had paroxysmal AF. The ablation procedure consisted of pulmonary vein isolation alone in 68% of patients and pulmonary vein isolation plus other ablation maneuvers in the rest.
The only predictor of atrial fibrosis on DE-MRI was a history of hypertension. Duration of AF, patient age, AF type, and comorbid conditions were not associated with the extent of fibrosis.
In a multivariate analysis controlled for numerous potential confounders, the only significant predictor of AF recurrence was atrial fibrosis. For each 1% increase in fibrosis, the risk of recurrence climbed by 6.3%. Among the factors adjusted for in this multivariate analysis were age, sex, hypertension, heart failure, mitral valve disease, diabetes, AF type, left atrial volume, and procedure type.
Dr. Richard I. Fogel, chair of the scientific sessions program committee and HRS president-elect, commented that he found it surprising and counterintuitive that AF duration was not a predictor of the extent of atrial fibrosis in DECAAF.
"I thought that the theory was ‘atrial fibrillation begets atrial fibrillation,’ " said Dr. Fogel, a cardiologist and electrophysiologist in group practice in Indianapolis.
Dr. Marrouche replied that large gaps remain in understanding the pathophysiology of AF in humans.
"We’ve known for a long time from animal models that AF begets AF. With MRI, for the first time we’re opening the heart in humans with AF, and it doesn’t look like the animal models at all. The fibrosis in humans isn’t diffuse; it’s patchy, and it’s localized," according to Dr. Marrouche.
Every single participant in DECAAF had atrial fibrosis on the posterior left atrial wall; indeed, posterior wall fibrosis accounted for 57% of the total burden of fibrosis. But some patients with, say, a 15-year history of symptomatic AF, had minimal fibrosis, while some middle-aged marathon runners with recent-onset AF had 50% fibrosis indicative of advanced disease.
Why some patients with AF are relatively protected against tissue fibrosis while others aren’t is an important question for further study. Possible factors worthy of investigation include genetics and inflammation, he said.
Dr. Marrouche reported having no relevant financial conflicts.
DENVER – Preprocedural quantification of atrial fibrosis via delayed-enhancement MRI offers a potent means of boosting atrial fibrillation ablation success rates by weeding out likely nonresponders, a study has shown.
Results of the double-blind, multinational prospective DECAAF trial (Delayed-Enhancement MRI Determinant of Successful Catheter Ablation for Atrial Fibrillation) show that the extent of atrial fibrosis is a strong predictor of patient outcome. The more fibrosis present when measured preprocedurally by delayed-enhancement MRI (DE-MRI) with gadolinium contrast, the less likely a patient would remain in sinus rhythm at follow-up more than 1 year following ablation, Dr. Nassir Marrouche reported at the annual meeting of the Heart Rhythm Society.

"Hopefully this will help us better individualize the therapy. We have to accept at some point that we can’t cure everybody with atrial fibrillation. This modality helps us to better define which patients should be eligible," according to Dr. Marrouche, director of the comprehensive arrhythmia research and management center at the University of Utah, Salt Lake City.
One attractive feature of this management strategy is that patients who are candidates for AF ablation already routinely undergo a preprocedural 3-D scan with CT or MRI. It’s a straightforward matter to train an MRI technician to measure atrial fibrosis, as DECAAF showed.
This is a practice-changing development, he said: "We recommend that in every single ablation patient, before you touch their heart you really should know how extensive their disease is."
Patients undergoing a first ablation procedure for paroxysmal AF typically have about a 60% success rate, meaning they remain free of atrial arrhythmia at 1 year. In contrast, DECAAF participants with less than 10% fibrosis in their left atrium had a success rate of 86% at 415 days of follow-up.
Patients with less than 10% preprocedural atrial fibrosis are categorized as Utah stage 1 disease using a left atrial structural remodeling classification system previously described by Dr. Marrouche and his coworkers . At the other end of the spectrum, DECAAF subjects who were Utah stage 4, with at least 30% fibrosis, had a dismal 31% freedom of recurrence 415 days after the end of the standard 90-day postprocedural blanking period. Patients with stage 2 or 3 atrial fibrosis had intermediate long-term outcomes (see box).
"We sit down with a stage 4 patient and say, ‘Listen, your chance of being cured of this disease at long-term follow-up is not very high,’" the electrophysiologist explained. "We put our expectations on the table. We now have 5-year follow-up data showing a 5%-10% success in Utah 4 patients. We in Utah today are very reluctant to take such patients into the lab and ablate them. Instead, we try every option to rate-control them. But Utah stage 1 is straightforward. I make that decision for the patient: ‘You should be ablated early on.’ "
DECAAF included 261 patients with AF who underwent a first ablation procedure at 15 centers in the United States, Europe, and Australia. But first they all underwent DE-MRI, the results of which were sent to a core lab for blinded quantification of atrial fibrosis. The interventionalists remained blinded to the fibrosis findings.
Most DECAAF participants had paroxysmal AF. The ablation procedure consisted of pulmonary vein isolation alone in 68% of patients and pulmonary vein isolation plus other ablation maneuvers in the rest.
The only predictor of atrial fibrosis on DE-MRI was a history of hypertension. Duration of AF, patient age, AF type, and comorbid conditions were not associated with the extent of fibrosis.
In a multivariate analysis controlled for numerous potential confounders, the only significant predictor of AF recurrence was atrial fibrosis. For each 1% increase in fibrosis, the risk of recurrence climbed by 6.3%. Among the factors adjusted for in this multivariate analysis were age, sex, hypertension, heart failure, mitral valve disease, diabetes, AF type, left atrial volume, and procedure type.
Dr. Richard I. Fogel, chair of the scientific sessions program committee and HRS president-elect, commented that he found it surprising and counterintuitive that AF duration was not a predictor of the extent of atrial fibrosis in DECAAF.
"I thought that the theory was ‘atrial fibrillation begets atrial fibrillation,’ " said Dr. Fogel, a cardiologist and electrophysiologist in group practice in Indianapolis.
Dr. Marrouche replied that large gaps remain in understanding the pathophysiology of AF in humans.
"We’ve known for a long time from animal models that AF begets AF. With MRI, for the first time we’re opening the heart in humans with AF, and it doesn’t look like the animal models at all. The fibrosis in humans isn’t diffuse; it’s patchy, and it’s localized," according to Dr. Marrouche.
Every single participant in DECAAF had atrial fibrosis on the posterior left atrial wall; indeed, posterior wall fibrosis accounted for 57% of the total burden of fibrosis. But some patients with, say, a 15-year history of symptomatic AF, had minimal fibrosis, while some middle-aged marathon runners with recent-onset AF had 50% fibrosis indicative of advanced disease.
Why some patients with AF are relatively protected against tissue fibrosis while others aren’t is an important question for further study. Possible factors worthy of investigation include genetics and inflammation, he said.
Dr. Marrouche reported having no relevant financial conflicts.
DENVER – Preprocedural quantification of atrial fibrosis via delayed-enhancement MRI offers a potent means of boosting atrial fibrillation ablation success rates by weeding out likely nonresponders, a study has shown.
Results of the double-blind, multinational prospective DECAAF trial (Delayed-Enhancement MRI Determinant of Successful Catheter Ablation for Atrial Fibrillation) show that the extent of atrial fibrosis is a strong predictor of patient outcome. The more fibrosis present when measured preprocedurally by delayed-enhancement MRI (DE-MRI) with gadolinium contrast, the less likely a patient would remain in sinus rhythm at follow-up more than 1 year following ablation, Dr. Nassir Marrouche reported at the annual meeting of the Heart Rhythm Society.

"Hopefully this will help us better individualize the therapy. We have to accept at some point that we can’t cure everybody with atrial fibrillation. This modality helps us to better define which patients should be eligible," according to Dr. Marrouche, director of the comprehensive arrhythmia research and management center at the University of Utah, Salt Lake City.
One attractive feature of this management strategy is that patients who are candidates for AF ablation already routinely undergo a preprocedural 3-D scan with CT or MRI. It’s a straightforward matter to train an MRI technician to measure atrial fibrosis, as DECAAF showed.
This is a practice-changing development, he said: "We recommend that in every single ablation patient, before you touch their heart you really should know how extensive their disease is."
Patients undergoing a first ablation procedure for paroxysmal AF typically have about a 60% success rate, meaning they remain free of atrial arrhythmia at 1 year. In contrast, DECAAF participants with less than 10% fibrosis in their left atrium had a success rate of 86% at 415 days of follow-up.
Patients with less than 10% preprocedural atrial fibrosis are categorized as Utah stage 1 disease using a left atrial structural remodeling classification system previously described by Dr. Marrouche and his coworkers . At the other end of the spectrum, DECAAF subjects who were Utah stage 4, with at least 30% fibrosis, had a dismal 31% freedom of recurrence 415 days after the end of the standard 90-day postprocedural blanking period. Patients with stage 2 or 3 atrial fibrosis had intermediate long-term outcomes (see box).
"We sit down with a stage 4 patient and say, ‘Listen, your chance of being cured of this disease at long-term follow-up is not very high,’" the electrophysiologist explained. "We put our expectations on the table. We now have 5-year follow-up data showing a 5%-10% success in Utah 4 patients. We in Utah today are very reluctant to take such patients into the lab and ablate them. Instead, we try every option to rate-control them. But Utah stage 1 is straightforward. I make that decision for the patient: ‘You should be ablated early on.’ "
DECAAF included 261 patients with AF who underwent a first ablation procedure at 15 centers in the United States, Europe, and Australia. But first they all underwent DE-MRI, the results of which were sent to a core lab for blinded quantification of atrial fibrosis. The interventionalists remained blinded to the fibrosis findings.
Most DECAAF participants had paroxysmal AF. The ablation procedure consisted of pulmonary vein isolation alone in 68% of patients and pulmonary vein isolation plus other ablation maneuvers in the rest.
The only predictor of atrial fibrosis on DE-MRI was a history of hypertension. Duration of AF, patient age, AF type, and comorbid conditions were not associated with the extent of fibrosis.
In a multivariate analysis controlled for numerous potential confounders, the only significant predictor of AF recurrence was atrial fibrosis. For each 1% increase in fibrosis, the risk of recurrence climbed by 6.3%. Among the factors adjusted for in this multivariate analysis were age, sex, hypertension, heart failure, mitral valve disease, diabetes, AF type, left atrial volume, and procedure type.
Dr. Richard I. Fogel, chair of the scientific sessions program committee and HRS president-elect, commented that he found it surprising and counterintuitive that AF duration was not a predictor of the extent of atrial fibrosis in DECAAF.
"I thought that the theory was ‘atrial fibrillation begets atrial fibrillation,’ " said Dr. Fogel, a cardiologist and electrophysiologist in group practice in Indianapolis.
Dr. Marrouche replied that large gaps remain in understanding the pathophysiology of AF in humans.
"We’ve known for a long time from animal models that AF begets AF. With MRI, for the first time we’re opening the heart in humans with AF, and it doesn’t look like the animal models at all. The fibrosis in humans isn’t diffuse; it’s patchy, and it’s localized," according to Dr. Marrouche.
Every single participant in DECAAF had atrial fibrosis on the posterior left atrial wall; indeed, posterior wall fibrosis accounted for 57% of the total burden of fibrosis. But some patients with, say, a 15-year history of symptomatic AF, had minimal fibrosis, while some middle-aged marathon runners with recent-onset AF had 50% fibrosis indicative of advanced disease.
Why some patients with AF are relatively protected against tissue fibrosis while others aren’t is an important question for further study. Possible factors worthy of investigation include genetics and inflammation, he said.
Dr. Marrouche reported having no relevant financial conflicts.
AT HEART RHYTHM 2013
Major Finding: Patients undergoing a first ablation procedure for atrial fibrillation had an 86% long-term rate of maintenance of sinus rhythm if a preprocedural delayed-enhancement MRI showed minimal left atrial fibrosis. For every 1% of additional fibrosis present on MRI, the risk of atrial arrhythmia recurrence rose by 6.3%.
Data Source: A double-blind, prospective, multinational trial in 261 AF patients who underwent delayed enhancement MRI prior to catheter ablation with long-term follow-up.
Disclosures: The presenter reported having no relevant financial conflicts.
Upcoming guidelines on inherited arrhythmias contain surprises
DENVER – Major new guidelines on the diagnosis and management of patients with inherited primary arrhythmia syndromes have been jointly issued by the Heart Rhythm Society and its European and Asian counterparts.
The guidelines were sorely needed, according to Dr. Silvia G. Priori, cochair of the expert consensus panel writing group.
The field of inherited arrhythmias is rapidly evolving, with new pathogenic genetic mutations being found all the time. Much has changed in the 7 years since issuance of the last major guidelines: the American College of Cardiology/American Heart Association/European Society of Cardiology guidelines on prevention of sudden cardiac death (Circulation 2006;114:e385-484), noted Dr. Priori of the University of Pavia (Italy).
Her cochair, Dr. Arthur A. Wilde of the University of Amsterdam pointed out that the new 69-page report is the first major document to address some of the newer inherited arrhythmia syndromes, including catecholaminergic polymorphic ventricular tachycardia (CPVT), short QT syndrome, early repolarization, and progressive cardiac conduction disease (PCCD). In addition, the new report proposes major changes in the diagnostic criteria for the two most common primary arrhythmia syndromes: long QT syndrome (LQTS) and Brugada syndrome.
"Many of our colleagues in the field will be surprised," Dr. Priori predicted.
Here are the highlights:
• LQTS: With an estimated prevalence of roughly 1 per 2,000 live births worldwide, this is the most common of the inherited arrhythmia syndromes. What is likely to come as a surprise to many physicians is the expert consensus panel’s recommendation that the diagnosis of LQTS requires either the finding of an unequivocally causative mutation in one of the LQTS genes or, in the absence of such a defect, either a QTc interval of 480-499 ms in repeated 12-lead ECGs in a patient with unexplained syncope or a QTc of 500 ms in repeated ECGs in the absence of a secondary cause for QT prolongation in a nonsyncopal patient.
"A single ECG reading 10 ms above the upper limit of normal is not enough to establish the diagnosis. That’s quite different from what’s being done in common practice. Many of the patients who are referred to the centers of expertise on inherited arrhythmias are borderline patients in whom maybe one ECG was abnormal, and yet because of that they’ve been labeled as being affected by a genetic disease even if the genetic studies were negative. A single abnormal QTc measurement in a patient with negative genetic testing is not enough," Dr. Priori declared.
Dr. Wilde said the new guidelines loosen up the guidance on participation in competitive sports. The blanket prohibition of the past has been replaced by a case-by-case approach, with a Class I recommendation for routine referral to a clinical expert for evaluation of the risk posed by athletic activity. For example, although swimming is a very-high-risk activity for patients with the LQTS1 genotype, that’s not true for those who have LQTS2 or -3.
"It’s clear that if a patient with long QT syndrome has exercise-related syncopal events, that patient should not participate in competitive sports. But if the patient is asymptomatic and has minor QT prolongation, there’s probably not much reason for concern," he said.
"This is a sharp departure," Dr. Priori observed. "In several European countries, if you have the diagnosis of long QT syndrome, sports participation is not permitted, even if your physician clears you. So we hope with this document to slowly, carefully, begin to allow patients with this condition to do sports safely. We wanted to lift the ban so that a physician who feels a specific patient would have a low risk in the proper environment could make that recommendation."
• Brugada syndrome: Far more common in Asia than the western world, Brugada syndrome is 8- to 10-fold more frequent in males than females. The big change in the new guidelines is that the diagnosis no longer requires specific ECG changes plus clinical manifestations. Now, Brugada syndrome, like LQTS, is a pure ECG diagnosis. It is made definitively when a type 1 ST-segment elevation is noted either spontaneously or after administration of an intravenous sodium channel-blocking agent; the ST finding has to be observed in at least one right precordial lead placed in a standard or superior position up to the second intercostal space.
An implantable cardioverter-defibrillator is clearly indicated in a Brugada syndrome patient with a prior cardiac arrest or documented ventricular arrhythmias. The controversy lies in how to manage the asymptomatic patient. The guidelines give ICD implantation a weak Class IIb recommendation – meaning it "may be considered" – when such patients exhibit inducible ventricular arrhythmias during programmed electrical stimulation in the electrophysiology lab.
• Catecholaminergic polymorphic ventricular tachycardia: The prevalence of CPVT is unclear, but it has been estimated at 1 per 5,000 live births, according to Dr. Wilde. This highly malignant condition is diagnosed in patients with a known pathogenic mutation, or in the presence of a structurally normal heart, a normal resting ECG, and unexplained exercise- or catecholamine-induced bidirectional VT of polymorphic ventricular premature beats or VT before age 40 years. First-line therapy is a long-acting beta-blocker such as nadolol, coupled with exercise restriction. ICD therapy is problematic because the inevitable inappropriate shocks increase sympathetic tone, triggering true shockable arrhythmias in a vicious cycle.
• Short QT syndrome: This is a rare channelopathy. It is diagnosed on the basis of a QTc of 330 ms or less, or a QTc of less than 360 ms in the presence of a pathogenic mutation, family history of sudden death before age 40 years, cardiac arrest in the absence of structural heart disease, or a family history of short QT syndrome.
• Progressive cardiac conduction disease: Still incompletely understood, PCCD is diagnosed in individuals under age 50 years who have unexplained progressive conduction abnormalities and a structurally normal heart with no skeletal myopathies. Pacemaker implantation is the most useful therapy.
• Early repolarization: The first report linking this extremely common ECG finding to sudden death came less than 5 years ago. Early repolarization, as characterized by J-point and ST-segment elevation in two or more contiguous leads, is present in up to 10% of normal individuals. In preparticipation athletic screening programs, it can be found in up to 15%-20% of subjects.
"There’s no reason for concern if that’s the only thing you find. It’s something you shouldn’t even communicate if there is no other issue. If a patient with early repolarization has no symptoms and no family history of premature sudden death, just leave it," Dr. Wilde advised.
On the other hand, if a patient with the early repolarization ECG pattern in two or more contiguous inferior and/or lateral leads experiences exercise-induced syncopal symptoms, further evaluation is warranted. Given how common and generally benign the early repolarization ECG pattern is, the expert panel recommended a conservative approach to diagnosis, urging that the formal diagnosis of early repolarization syndrome be restricted largely to those with the characteristic ECG findings who in addition have been resuscitated from unexplained ventricular fibrillation or polymorphic VT.
Dr. Priori emphasized that the guidelines have as a Class I recommendation that patients with a diagnosed or suspected inherited arrhythmia syndrome that can result in sudden cardiac death – and their first-degree relatives, as well – should be evaluated in a specialized multidisciplinary inherited arrhythmia clinic. Such clinics are more common in Europe than the United States; however, thought leaders in American electrophysiology now recognize that the increasing complexity of the field requires that more of these dedicated clinics be created in the United States, she said.
The expert consensus statement was a joint project of the Heart Rhythm Society, the European Heart Rhythm Association, and the Asia Pacific Heart Rhythm Society. The document is available at the HRS website and will be published this fall in Heart Rhythm, EP Europace, and the Journal of Arrhythmias.
Dr. Priori reported serving as a consultant to Medtronic, Boston Scientific, Biotronic, and Transgenomic. Dr. Wilde disclosed serving as a consultant to Sorin.
inherited primary arrhythmia, Dr. Silvia G. Priori, arrythmia guidelines, Arthur Wilde
DENVER – Major new guidelines on the diagnosis and management of patients with inherited primary arrhythmia syndromes have been jointly issued by the Heart Rhythm Society and its European and Asian counterparts.
The guidelines were sorely needed, according to Dr. Silvia G. Priori, cochair of the expert consensus panel writing group.
The field of inherited arrhythmias is rapidly evolving, with new pathogenic genetic mutations being found all the time. Much has changed in the 7 years since issuance of the last major guidelines: the American College of Cardiology/American Heart Association/European Society of Cardiology guidelines on prevention of sudden cardiac death (Circulation 2006;114:e385-484), noted Dr. Priori of the University of Pavia (Italy).
Her cochair, Dr. Arthur A. Wilde of the University of Amsterdam pointed out that the new 69-page report is the first major document to address some of the newer inherited arrhythmia syndromes, including catecholaminergic polymorphic ventricular tachycardia (CPVT), short QT syndrome, early repolarization, and progressive cardiac conduction disease (PCCD). In addition, the new report proposes major changes in the diagnostic criteria for the two most common primary arrhythmia syndromes: long QT syndrome (LQTS) and Brugada syndrome.
"Many of our colleagues in the field will be surprised," Dr. Priori predicted.
Here are the highlights:
• LQTS: With an estimated prevalence of roughly 1 per 2,000 live births worldwide, this is the most common of the inherited arrhythmia syndromes. What is likely to come as a surprise to many physicians is the expert consensus panel’s recommendation that the diagnosis of LQTS requires either the finding of an unequivocally causative mutation in one of the LQTS genes or, in the absence of such a defect, either a QTc interval of 480-499 ms in repeated 12-lead ECGs in a patient with unexplained syncope or a QTc of 500 ms in repeated ECGs in the absence of a secondary cause for QT prolongation in a nonsyncopal patient.
"A single ECG reading 10 ms above the upper limit of normal is not enough to establish the diagnosis. That’s quite different from what’s being done in common practice. Many of the patients who are referred to the centers of expertise on inherited arrhythmias are borderline patients in whom maybe one ECG was abnormal, and yet because of that they’ve been labeled as being affected by a genetic disease even if the genetic studies were negative. A single abnormal QTc measurement in a patient with negative genetic testing is not enough," Dr. Priori declared.
Dr. Wilde said the new guidelines loosen up the guidance on participation in competitive sports. The blanket prohibition of the past has been replaced by a case-by-case approach, with a Class I recommendation for routine referral to a clinical expert for evaluation of the risk posed by athletic activity. For example, although swimming is a very-high-risk activity for patients with the LQTS1 genotype, that’s not true for those who have LQTS2 or -3.
"It’s clear that if a patient with long QT syndrome has exercise-related syncopal events, that patient should not participate in competitive sports. But if the patient is asymptomatic and has minor QT prolongation, there’s probably not much reason for concern," he said.
"This is a sharp departure," Dr. Priori observed. "In several European countries, if you have the diagnosis of long QT syndrome, sports participation is not permitted, even if your physician clears you. So we hope with this document to slowly, carefully, begin to allow patients with this condition to do sports safely. We wanted to lift the ban so that a physician who feels a specific patient would have a low risk in the proper environment could make that recommendation."
• Brugada syndrome: Far more common in Asia than the western world, Brugada syndrome is 8- to 10-fold more frequent in males than females. The big change in the new guidelines is that the diagnosis no longer requires specific ECG changes plus clinical manifestations. Now, Brugada syndrome, like LQTS, is a pure ECG diagnosis. It is made definitively when a type 1 ST-segment elevation is noted either spontaneously or after administration of an intravenous sodium channel-blocking agent; the ST finding has to be observed in at least one right precordial lead placed in a standard or superior position up to the second intercostal space.
An implantable cardioverter-defibrillator is clearly indicated in a Brugada syndrome patient with a prior cardiac arrest or documented ventricular arrhythmias. The controversy lies in how to manage the asymptomatic patient. The guidelines give ICD implantation a weak Class IIb recommendation – meaning it "may be considered" – when such patients exhibit inducible ventricular arrhythmias during programmed electrical stimulation in the electrophysiology lab.
• Catecholaminergic polymorphic ventricular tachycardia: The prevalence of CPVT is unclear, but it has been estimated at 1 per 5,000 live births, according to Dr. Wilde. This highly malignant condition is diagnosed in patients with a known pathogenic mutation, or in the presence of a structurally normal heart, a normal resting ECG, and unexplained exercise- or catecholamine-induced bidirectional VT of polymorphic ventricular premature beats or VT before age 40 years. First-line therapy is a long-acting beta-blocker such as nadolol, coupled with exercise restriction. ICD therapy is problematic because the inevitable inappropriate shocks increase sympathetic tone, triggering true shockable arrhythmias in a vicious cycle.
• Short QT syndrome: This is a rare channelopathy. It is diagnosed on the basis of a QTc of 330 ms or less, or a QTc of less than 360 ms in the presence of a pathogenic mutation, family history of sudden death before age 40 years, cardiac arrest in the absence of structural heart disease, or a family history of short QT syndrome.
• Progressive cardiac conduction disease: Still incompletely understood, PCCD is diagnosed in individuals under age 50 years who have unexplained progressive conduction abnormalities and a structurally normal heart with no skeletal myopathies. Pacemaker implantation is the most useful therapy.
• Early repolarization: The first report linking this extremely common ECG finding to sudden death came less than 5 years ago. Early repolarization, as characterized by J-point and ST-segment elevation in two or more contiguous leads, is present in up to 10% of normal individuals. In preparticipation athletic screening programs, it can be found in up to 15%-20% of subjects.
"There’s no reason for concern if that’s the only thing you find. It’s something you shouldn’t even communicate if there is no other issue. If a patient with early repolarization has no symptoms and no family history of premature sudden death, just leave it," Dr. Wilde advised.
On the other hand, if a patient with the early repolarization ECG pattern in two or more contiguous inferior and/or lateral leads experiences exercise-induced syncopal symptoms, further evaluation is warranted. Given how common and generally benign the early repolarization ECG pattern is, the expert panel recommended a conservative approach to diagnosis, urging that the formal diagnosis of early repolarization syndrome be restricted largely to those with the characteristic ECG findings who in addition have been resuscitated from unexplained ventricular fibrillation or polymorphic VT.
Dr. Priori emphasized that the guidelines have as a Class I recommendation that patients with a diagnosed or suspected inherited arrhythmia syndrome that can result in sudden cardiac death – and their first-degree relatives, as well – should be evaluated in a specialized multidisciplinary inherited arrhythmia clinic. Such clinics are more common in Europe than the United States; however, thought leaders in American electrophysiology now recognize that the increasing complexity of the field requires that more of these dedicated clinics be created in the United States, she said.
The expert consensus statement was a joint project of the Heart Rhythm Society, the European Heart Rhythm Association, and the Asia Pacific Heart Rhythm Society. The document is available at the HRS website and will be published this fall in Heart Rhythm, EP Europace, and the Journal of Arrhythmias.
Dr. Priori reported serving as a consultant to Medtronic, Boston Scientific, Biotronic, and Transgenomic. Dr. Wilde disclosed serving as a consultant to Sorin.
DENVER – Major new guidelines on the diagnosis and management of patients with inherited primary arrhythmia syndromes have been jointly issued by the Heart Rhythm Society and its European and Asian counterparts.
The guidelines were sorely needed, according to Dr. Silvia G. Priori, cochair of the expert consensus panel writing group.
The field of inherited arrhythmias is rapidly evolving, with new pathogenic genetic mutations being found all the time. Much has changed in the 7 years since issuance of the last major guidelines: the American College of Cardiology/American Heart Association/European Society of Cardiology guidelines on prevention of sudden cardiac death (Circulation 2006;114:e385-484), noted Dr. Priori of the University of Pavia (Italy).
Her cochair, Dr. Arthur A. Wilde of the University of Amsterdam pointed out that the new 69-page report is the first major document to address some of the newer inherited arrhythmia syndromes, including catecholaminergic polymorphic ventricular tachycardia (CPVT), short QT syndrome, early repolarization, and progressive cardiac conduction disease (PCCD). In addition, the new report proposes major changes in the diagnostic criteria for the two most common primary arrhythmia syndromes: long QT syndrome (LQTS) and Brugada syndrome.
"Many of our colleagues in the field will be surprised," Dr. Priori predicted.
Here are the highlights:
• LQTS: With an estimated prevalence of roughly 1 per 2,000 live births worldwide, this is the most common of the inherited arrhythmia syndromes. What is likely to come as a surprise to many physicians is the expert consensus panel’s recommendation that the diagnosis of LQTS requires either the finding of an unequivocally causative mutation in one of the LQTS genes or, in the absence of such a defect, either a QTc interval of 480-499 ms in repeated 12-lead ECGs in a patient with unexplained syncope or a QTc of 500 ms in repeated ECGs in the absence of a secondary cause for QT prolongation in a nonsyncopal patient.
"A single ECG reading 10 ms above the upper limit of normal is not enough to establish the diagnosis. That’s quite different from what’s being done in common practice. Many of the patients who are referred to the centers of expertise on inherited arrhythmias are borderline patients in whom maybe one ECG was abnormal, and yet because of that they’ve been labeled as being affected by a genetic disease even if the genetic studies were negative. A single abnormal QTc measurement in a patient with negative genetic testing is not enough," Dr. Priori declared.
Dr. Wilde said the new guidelines loosen up the guidance on participation in competitive sports. The blanket prohibition of the past has been replaced by a case-by-case approach, with a Class I recommendation for routine referral to a clinical expert for evaluation of the risk posed by athletic activity. For example, although swimming is a very-high-risk activity for patients with the LQTS1 genotype, that’s not true for those who have LQTS2 or -3.
"It’s clear that if a patient with long QT syndrome has exercise-related syncopal events, that patient should not participate in competitive sports. But if the patient is asymptomatic and has minor QT prolongation, there’s probably not much reason for concern," he said.
"This is a sharp departure," Dr. Priori observed. "In several European countries, if you have the diagnosis of long QT syndrome, sports participation is not permitted, even if your physician clears you. So we hope with this document to slowly, carefully, begin to allow patients with this condition to do sports safely. We wanted to lift the ban so that a physician who feels a specific patient would have a low risk in the proper environment could make that recommendation."
• Brugada syndrome: Far more common in Asia than the western world, Brugada syndrome is 8- to 10-fold more frequent in males than females. The big change in the new guidelines is that the diagnosis no longer requires specific ECG changes plus clinical manifestations. Now, Brugada syndrome, like LQTS, is a pure ECG diagnosis. It is made definitively when a type 1 ST-segment elevation is noted either spontaneously or after administration of an intravenous sodium channel-blocking agent; the ST finding has to be observed in at least one right precordial lead placed in a standard or superior position up to the second intercostal space.
An implantable cardioverter-defibrillator is clearly indicated in a Brugada syndrome patient with a prior cardiac arrest or documented ventricular arrhythmias. The controversy lies in how to manage the asymptomatic patient. The guidelines give ICD implantation a weak Class IIb recommendation – meaning it "may be considered" – when such patients exhibit inducible ventricular arrhythmias during programmed electrical stimulation in the electrophysiology lab.
• Catecholaminergic polymorphic ventricular tachycardia: The prevalence of CPVT is unclear, but it has been estimated at 1 per 5,000 live births, according to Dr. Wilde. This highly malignant condition is diagnosed in patients with a known pathogenic mutation, or in the presence of a structurally normal heart, a normal resting ECG, and unexplained exercise- or catecholamine-induced bidirectional VT of polymorphic ventricular premature beats or VT before age 40 years. First-line therapy is a long-acting beta-blocker such as nadolol, coupled with exercise restriction. ICD therapy is problematic because the inevitable inappropriate shocks increase sympathetic tone, triggering true shockable arrhythmias in a vicious cycle.
• Short QT syndrome: This is a rare channelopathy. It is diagnosed on the basis of a QTc of 330 ms or less, or a QTc of less than 360 ms in the presence of a pathogenic mutation, family history of sudden death before age 40 years, cardiac arrest in the absence of structural heart disease, or a family history of short QT syndrome.
• Progressive cardiac conduction disease: Still incompletely understood, PCCD is diagnosed in individuals under age 50 years who have unexplained progressive conduction abnormalities and a structurally normal heart with no skeletal myopathies. Pacemaker implantation is the most useful therapy.
• Early repolarization: The first report linking this extremely common ECG finding to sudden death came less than 5 years ago. Early repolarization, as characterized by J-point and ST-segment elevation in two or more contiguous leads, is present in up to 10% of normal individuals. In preparticipation athletic screening programs, it can be found in up to 15%-20% of subjects.
"There’s no reason for concern if that’s the only thing you find. It’s something you shouldn’t even communicate if there is no other issue. If a patient with early repolarization has no symptoms and no family history of premature sudden death, just leave it," Dr. Wilde advised.
On the other hand, if a patient with the early repolarization ECG pattern in two or more contiguous inferior and/or lateral leads experiences exercise-induced syncopal symptoms, further evaluation is warranted. Given how common and generally benign the early repolarization ECG pattern is, the expert panel recommended a conservative approach to diagnosis, urging that the formal diagnosis of early repolarization syndrome be restricted largely to those with the characteristic ECG findings who in addition have been resuscitated from unexplained ventricular fibrillation or polymorphic VT.
Dr. Priori emphasized that the guidelines have as a Class I recommendation that patients with a diagnosed or suspected inherited arrhythmia syndrome that can result in sudden cardiac death – and their first-degree relatives, as well – should be evaluated in a specialized multidisciplinary inherited arrhythmia clinic. Such clinics are more common in Europe than the United States; however, thought leaders in American electrophysiology now recognize that the increasing complexity of the field requires that more of these dedicated clinics be created in the United States, she said.
The expert consensus statement was a joint project of the Heart Rhythm Society, the European Heart Rhythm Association, and the Asia Pacific Heart Rhythm Society. The document is available at the HRS website and will be published this fall in Heart Rhythm, EP Europace, and the Journal of Arrhythmias.
Dr. Priori reported serving as a consultant to Medtronic, Boston Scientific, Biotronic, and Transgenomic. Dr. Wilde disclosed serving as a consultant to Sorin.
inherited primary arrhythmia, Dr. Silvia G. Priori, arrythmia guidelines, Arthur Wilde
inherited primary arrhythmia, Dr. Silvia G. Priori, arrythmia guidelines, Arthur Wilde
AT HEART RHYTHM 2013
BRUISE CONTROL: Continue warfarin during cardiac device surgery
DENVER – Uninterrupted warfarin therapy during pacemaker or implantable cardioverter-defibrillator surgery in patients at high thromboembolic risk proved superior to the guideline-recommended practice of discontinuing warfarin and bridging with heparin, according to a large, multicenter, randomized clinical trial.
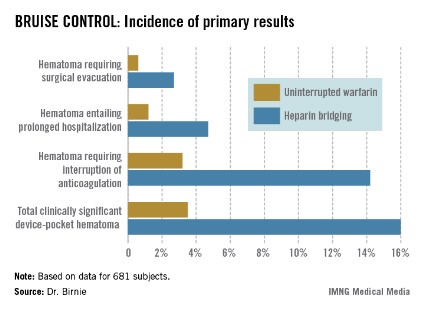
The primary outcome in the 17-center, 681-patient BRUISE CONTROL (Bridge or Continue Coumadin for Device Surgery Randomized Controlled Trial) trial was the incidence of clinically significant device-pocket hematoma. The rate was 16% in patients randomized to heparin bridging, compared with 3.5% with uninterrupted warfarin, Dr. David H. Birnie reported at the annual meeting of the Heart Rhythm Society.
These results are clearly practice changing. Heparin bridging has been the standard of care. It is recommended in this common clinical scenario in all of the major guidelines, but that’s bound to change as a result of BRUISE CONTROL, predicted Dr. Birnie of the University of Ottawa Heart Institute.
"This trial was a home run. It was unequivocally positive," he commented. "For sure, our clinical practice changed as soon as we saw those results."
Device-pocket hematoma is a "very nasty" complication of cardiac device surgery, Dr. Birnie noted. It is quite painful, can cause device infection, and is difficult to treat. Clinically significant device-pocket hematoma was defined in this trial as a hematoma resulting in prolonged hospitalization for an additional day or more, or interruption of oral anticoagulation for at least 24 hours, and/or requiring additional surgery. All three components of the primary endpoint were significantly less frequent in the uninterrupted warfarin group (see chart).
Performing device surgery in patients on uninterrupted warfarin with a median international normalized ratio (INR) of 2.3 was not associated with any increase in major perioperative bleeding or other surgical or thromboembolic complications. And patient satisfaction surveys indicated subjects greatly preferred having their procedure without stopping their warfarin.
BRUISE CONTROL was planned as a definitive 1,000-patient clinical trial. However, the Data and Safety Monitoring Board halted the study after an interim analysis involving the first 681 subjects.
Of note, this was a study restricted to patients at high stroke risk – greater than 5% annually – as defined by the presence of atrial fibrillation and a CHADS2 score of 3 or more or the presence of a mechanical heart valve.
Dr. Birnie said that although it seems counterintuitive to have less bleeding when cardiac device surgery is performed on a fully anticoagulated patient, as occurred in BRUISE CONTROL, he and his coinvestigators have an explanatory hypothesis: "When bleeding occurs in a fully anticoagulated patient, the operator can readily see it and address it. On the contrary, with bridging you get hemostasis at the time of surgery, but you may have missed a tiny little thing, and then 24 hours later when you start up your heparin bridging again, that’s when the bleeding occurs. It’s a physiologically plausible explanation," he said.
In a multivariate analysis, neither the use of pressure dressings, nor the use of sandbags, nor injection of antibleeding agents into the device pocket before closure had any significant impact on the incidence of clinically significant hematomas. Only three factors did: uninterrupted warfarin therapy, which reduced the risk by 84%; aspirin therapy, which doubled the risk; and the presence of diabetes mellitus, which was inexplicably associated with a 52% reduction in hematoma risk.
Each year roughly 1.6 million people worldwide undergo pacemaker or implantable cardioverter-defibrillator (ICD) implantation. Up to one-third of them are on long-term oral anticoagulation, most commonly with warfarin.
Dr. Birnie stressed that the BRUISE CONTROL findings have no relevance to patients on one of the new oral anticoagulants.
"The whole risk/benefit ratio of the new agents is completely different from warfarin. Their onset and offset of action is hours as opposed to the 5 days for warfarin," he noted.
With that point in mind, he and his coinvestigators have just started the BRUISE CONTROL-2 trial, which is examining whether it’s better to stop the new agents around the time of device surgery or continue the medication uninterrupted.
Simultaneous with Dr. Birnie’s presentation of the BRUISE CONTROL data in Denver, the study results were published online (N. Engl. J. Med. 2013 May 9 [doi: 10.1056/NEJMoa1302946]).
BRUISE CONTROL was funded by the Canadian Institutes of Health Research and the Ministry of Health and Long-Term Care of Ontario. Dr. Birnie reported having no conflicts of interest.
DENVER – Uninterrupted warfarin therapy during pacemaker or implantable cardioverter-defibrillator surgery in patients at high thromboembolic risk proved superior to the guideline-recommended practice of discontinuing warfarin and bridging with heparin, according to a large, multicenter, randomized clinical trial.
The primary outcome in the 17-center, 681-patient BRUISE CONTROL (Bridge or Continue Coumadin for Device Surgery Randomized Controlled Trial) trial was the incidence of clinically significant device-pocket hematoma. The rate was 16% in patients randomized to heparin bridging, compared with 3.5% with uninterrupted warfarin, Dr. David H. Birnie reported at the annual meeting of the Heart Rhythm Society.
These results are clearly practice changing. Heparin bridging has been the standard of care. It is recommended in this common clinical scenario in all of the major guidelines, but that’s bound to change as a result of BRUISE CONTROL, predicted Dr. Birnie of the University of Ottawa Heart Institute.
"This trial was a home run. It was unequivocally positive," he commented. "For sure, our clinical practice changed as soon as we saw those results."
Device-pocket hematoma is a "very nasty" complication of cardiac device surgery, Dr. Birnie noted. It is quite painful, can cause device infection, and is difficult to treat. Clinically significant device-pocket hematoma was defined in this trial as a hematoma resulting in prolonged hospitalization for an additional day or more, or interruption of oral anticoagulation for at least 24 hours, and/or requiring additional surgery. All three components of the primary endpoint were significantly less frequent in the uninterrupted warfarin group (see chart).
Performing device surgery in patients on uninterrupted warfarin with a median international normalized ratio (INR) of 2.3 was not associated with any increase in major perioperative bleeding or other surgical or thromboembolic complications. And patient satisfaction surveys indicated subjects greatly preferred having their procedure without stopping their warfarin.
BRUISE CONTROL was planned as a definitive 1,000-patient clinical trial. However, the Data and Safety Monitoring Board halted the study after an interim analysis involving the first 681 subjects.
Of note, this was a study restricted to patients at high stroke risk – greater than 5% annually – as defined by the presence of atrial fibrillation and a CHADS2 score of 3 or more or the presence of a mechanical heart valve.
Dr. Birnie said that although it seems counterintuitive to have less bleeding when cardiac device surgery is performed on a fully anticoagulated patient, as occurred in BRUISE CONTROL, he and his coinvestigators have an explanatory hypothesis: "When bleeding occurs in a fully anticoagulated patient, the operator can readily see it and address it. On the contrary, with bridging you get hemostasis at the time of surgery, but you may have missed a tiny little thing, and then 24 hours later when you start up your heparin bridging again, that’s when the bleeding occurs. It’s a physiologically plausible explanation," he said.
In a multivariate analysis, neither the use of pressure dressings, nor the use of sandbags, nor injection of antibleeding agents into the device pocket before closure had any significant impact on the incidence of clinically significant hematomas. Only three factors did: uninterrupted warfarin therapy, which reduced the risk by 84%; aspirin therapy, which doubled the risk; and the presence of diabetes mellitus, which was inexplicably associated with a 52% reduction in hematoma risk.
Each year roughly 1.6 million people worldwide undergo pacemaker or implantable cardioverter-defibrillator (ICD) implantation. Up to one-third of them are on long-term oral anticoagulation, most commonly with warfarin.
Dr. Birnie stressed that the BRUISE CONTROL findings have no relevance to patients on one of the new oral anticoagulants.
"The whole risk/benefit ratio of the new agents is completely different from warfarin. Their onset and offset of action is hours as opposed to the 5 days for warfarin," he noted.
With that point in mind, he and his coinvestigators have just started the BRUISE CONTROL-2 trial, which is examining whether it’s better to stop the new agents around the time of device surgery or continue the medication uninterrupted.
Simultaneous with Dr. Birnie’s presentation of the BRUISE CONTROL data in Denver, the study results were published online (N. Engl. J. Med. 2013 May 9 [doi: 10.1056/NEJMoa1302946]).
BRUISE CONTROL was funded by the Canadian Institutes of Health Research and the Ministry of Health and Long-Term Care of Ontario. Dr. Birnie reported having no conflicts of interest.
DENVER – Uninterrupted warfarin therapy during pacemaker or implantable cardioverter-defibrillator surgery in patients at high thromboembolic risk proved superior to the guideline-recommended practice of discontinuing warfarin and bridging with heparin, according to a large, multicenter, randomized clinical trial.
The primary outcome in the 17-center, 681-patient BRUISE CONTROL (Bridge or Continue Coumadin for Device Surgery Randomized Controlled Trial) trial was the incidence of clinically significant device-pocket hematoma. The rate was 16% in patients randomized to heparin bridging, compared with 3.5% with uninterrupted warfarin, Dr. David H. Birnie reported at the annual meeting of the Heart Rhythm Society.
These results are clearly practice changing. Heparin bridging has been the standard of care. It is recommended in this common clinical scenario in all of the major guidelines, but that’s bound to change as a result of BRUISE CONTROL, predicted Dr. Birnie of the University of Ottawa Heart Institute.
"This trial was a home run. It was unequivocally positive," he commented. "For sure, our clinical practice changed as soon as we saw those results."
Device-pocket hematoma is a "very nasty" complication of cardiac device surgery, Dr. Birnie noted. It is quite painful, can cause device infection, and is difficult to treat. Clinically significant device-pocket hematoma was defined in this trial as a hematoma resulting in prolonged hospitalization for an additional day or more, or interruption of oral anticoagulation for at least 24 hours, and/or requiring additional surgery. All three components of the primary endpoint were significantly less frequent in the uninterrupted warfarin group (see chart).
Performing device surgery in patients on uninterrupted warfarin with a median international normalized ratio (INR) of 2.3 was not associated with any increase in major perioperative bleeding or other surgical or thromboembolic complications. And patient satisfaction surveys indicated subjects greatly preferred having their procedure without stopping their warfarin.
BRUISE CONTROL was planned as a definitive 1,000-patient clinical trial. However, the Data and Safety Monitoring Board halted the study after an interim analysis involving the first 681 subjects.
Of note, this was a study restricted to patients at high stroke risk – greater than 5% annually – as defined by the presence of atrial fibrillation and a CHADS2 score of 3 or more or the presence of a mechanical heart valve.
Dr. Birnie said that although it seems counterintuitive to have less bleeding when cardiac device surgery is performed on a fully anticoagulated patient, as occurred in BRUISE CONTROL, he and his coinvestigators have an explanatory hypothesis: "When bleeding occurs in a fully anticoagulated patient, the operator can readily see it and address it. On the contrary, with bridging you get hemostasis at the time of surgery, but you may have missed a tiny little thing, and then 24 hours later when you start up your heparin bridging again, that’s when the bleeding occurs. It’s a physiologically plausible explanation," he said.
In a multivariate analysis, neither the use of pressure dressings, nor the use of sandbags, nor injection of antibleeding agents into the device pocket before closure had any significant impact on the incidence of clinically significant hematomas. Only three factors did: uninterrupted warfarin therapy, which reduced the risk by 84%; aspirin therapy, which doubled the risk; and the presence of diabetes mellitus, which was inexplicably associated with a 52% reduction in hematoma risk.
Each year roughly 1.6 million people worldwide undergo pacemaker or implantable cardioverter-defibrillator (ICD) implantation. Up to one-third of them are on long-term oral anticoagulation, most commonly with warfarin.
Dr. Birnie stressed that the BRUISE CONTROL findings have no relevance to patients on one of the new oral anticoagulants.
"The whole risk/benefit ratio of the new agents is completely different from warfarin. Their onset and offset of action is hours as opposed to the 5 days for warfarin," he noted.
With that point in mind, he and his coinvestigators have just started the BRUISE CONTROL-2 trial, which is examining whether it’s better to stop the new agents around the time of device surgery or continue the medication uninterrupted.
Simultaneous with Dr. Birnie’s presentation of the BRUISE CONTROL data in Denver, the study results were published online (N. Engl. J. Med. 2013 May 9 [doi: 10.1056/NEJMoa1302946]).
BRUISE CONTROL was funded by the Canadian Institutes of Health Research and the Ministry of Health and Long-Term Care of Ontario. Dr. Birnie reported having no conflicts of interest.
AT HEART RHYTHM 2013
Major finding: The incidence of clinically significant device-pocket hematoma in patients at high thromboembolic risk who underwent pacemaker or implantable cardioverter-defibrillator surgery was 3.5% if they remained on full-dose warfarin, compared with 16% with the guideline-recommended, standard-of-care practice of interrupting warfarin in favor of heparin bridging.
Data source: BRUISE CONTROL was a 681-patient, 17-center randomized clinical trial.
Disclosures: BRUISE CONTROL was funded by the Canadian Institutes of Health Research and the Ministry of Health and Long-Term Care of Ontario. Dr. Birnie reported having no conflicts of interest.
Biventricular pacing bests conventional tx in BLOCK HF trial
DENVER – Biventricular pacing rather than the right ventricular pacing recommended in current guidelines results in significantly better quality of life and symptom status, an analysis of secondary outcomes from the BLOCK HF trial have shown.
In a previous report of the trial’s primary outcome (N. Engl. J. Med. 2013;368:1585-93), the biventricular (BiV) pacing group showed a highly significant 26% reduction in risk of a composite of all-cause mortality, an urgent care visit for heart failure requiring intravenous therapy, or a 15% or greater increase in the left ventricular end-systolic volume index during an average of 37 months of follow-up, compared with patients who had right ventricular (RV) pacing.
The new report on prespecified secondary endpoints including quality of life and symptom status was undertaken because of researchers’ and regulatory agencies’ growing appreciation of the importance of such outcomes in patients with a chronic progressive disease such as heart failure, principal investigator Dr. Anne B. Curtis reported at the annual meeting of the Heart Rhythm Society.
BLOCK HF (Biventricular versus Right Ventricular Pacing in Patients with Left Ventricular Dysfunction and Atrioventricular Block) was a randomized, double-blind, prospective, 60-center clinical trial involving 691 patients in the United States and Canada. All had AV block warranting pacemaker therapy as well as New York Heart Association(NYHA) class I-III heart failure with a left ventricular ejection fraction of 50% or less. All participants got a cardiac resynchronization therapy device featuring BiV pacing. Patients were assigned in double-blind fashion for their device to run in BiV or conventional RV pacing mode, explained Dr. Curtis, professor and chair of the department of medicine at the University of Buffalo (N.Y.).
The new secondary analysis tabulated changes in the Packer clinical composite score, NYHA functional class, and quality of life, as measured by the Minnesota Living With Heart Failure Questionnaire, at 6, 12, 18, and 24 months.
The Packer clinical composite score classifies patients as improved, worsened, or unchanged based on patient global assessment, heart failure hospitalization, change in symptoms, and other factors. At all four time points through 24 months, significantly more patients in the BiV group were rated as improved and significantly fewer as worsened than in the RV group. For example, at 6 months 53% of the BiV group were categorized as improved and 23% as worsened, compared with 39% and 28% in the RV group, Dr. Curtis reported.
From a mean baseline quality of life score of 25, the BiV group improved by an average of 5 points at the 6-month assessment compared with a 0.3-point gain in the RV group. At 12 months, the BiV group still showed a 3.9-point improvement, significantly better than the average 0.9-point gain in the RV patients. At 18 and 24 months, however, there was no longer a significant difference between the two groups in terms of quality of life scores. Dr. Curtis attributed this drop-off to the fact that 86 patients in the RV arm crossed over to BiV pacing because of deteriorating heart failure, compared with 15 crossovers in the BiV group. In the intention-to-treat analysis employed in BLOCK HF, those crossovers to BiV pacing are still counted as being part of the RV group.
"If you could mandate that patients stayed in the same arm, I think you’d continue to see differences over time, but you can’t do that," she said.
An analysis of changes in NYHA functional class showed the BiV group had better outcomes at 12 months, but at not the other time points.
The BLOCK HF trial was undertaken in response to evidence suggesting that sustained RV apical pacing can degrade ventricular function, especially in patients with preexisting systolic dysfunction.
At present, cardiac resynchronization therapy devices aren’t approved by the Food and Drug Administration for patients with AV block with left ventricular dysfunction. Medtronic officials have indicated they plan to seek an expanded indication based on the BLOCK HF data.
One audience member, noting that the study outcomes were better with BiV pacing in patients across the full spectrum of depressed ejection fractions, asked Dr. Curtis if she expects an expansion of cardiac resynchronization therapy indications to include patients with heart block and a normal ejection fraction.
"I would anticipate that the guidelines will change for the type of patients studied here. But we didn’t study patients with a normal ejection fraction because the more normal the patient, the larger the sample size and longer the follow-up you’d need to show a difference. So I doubt that this study will change guidelines for patients with normal ejection fractions," she said.
Dr. Curtis reported that she serves as a consultant to Medtronic, which sponsored the BLOCK HF trial,
DENVER – Biventricular pacing rather than the right ventricular pacing recommended in current guidelines results in significantly better quality of life and symptom status, an analysis of secondary outcomes from the BLOCK HF trial have shown.
In a previous report of the trial’s primary outcome (N. Engl. J. Med. 2013;368:1585-93), the biventricular (BiV) pacing group showed a highly significant 26% reduction in risk of a composite of all-cause mortality, an urgent care visit for heart failure requiring intravenous therapy, or a 15% or greater increase in the left ventricular end-systolic volume index during an average of 37 months of follow-up, compared with patients who had right ventricular (RV) pacing.
The new report on prespecified secondary endpoints including quality of life and symptom status was undertaken because of researchers’ and regulatory agencies’ growing appreciation of the importance of such outcomes in patients with a chronic progressive disease such as heart failure, principal investigator Dr. Anne B. Curtis reported at the annual meeting of the Heart Rhythm Society.
BLOCK HF (Biventricular versus Right Ventricular Pacing in Patients with Left Ventricular Dysfunction and Atrioventricular Block) was a randomized, double-blind, prospective, 60-center clinical trial involving 691 patients in the United States and Canada. All had AV block warranting pacemaker therapy as well as New York Heart Association(NYHA) class I-III heart failure with a left ventricular ejection fraction of 50% or less. All participants got a cardiac resynchronization therapy device featuring BiV pacing. Patients were assigned in double-blind fashion for their device to run in BiV or conventional RV pacing mode, explained Dr. Curtis, professor and chair of the department of medicine at the University of Buffalo (N.Y.).
The new secondary analysis tabulated changes in the Packer clinical composite score, NYHA functional class, and quality of life, as measured by the Minnesota Living With Heart Failure Questionnaire, at 6, 12, 18, and 24 months.
The Packer clinical composite score classifies patients as improved, worsened, or unchanged based on patient global assessment, heart failure hospitalization, change in symptoms, and other factors. At all four time points through 24 months, significantly more patients in the BiV group were rated as improved and significantly fewer as worsened than in the RV group. For example, at 6 months 53% of the BiV group were categorized as improved and 23% as worsened, compared with 39% and 28% in the RV group, Dr. Curtis reported.
From a mean baseline quality of life score of 25, the BiV group improved by an average of 5 points at the 6-month assessment compared with a 0.3-point gain in the RV group. At 12 months, the BiV group still showed a 3.9-point improvement, significantly better than the average 0.9-point gain in the RV patients. At 18 and 24 months, however, there was no longer a significant difference between the two groups in terms of quality of life scores. Dr. Curtis attributed this drop-off to the fact that 86 patients in the RV arm crossed over to BiV pacing because of deteriorating heart failure, compared with 15 crossovers in the BiV group. In the intention-to-treat analysis employed in BLOCK HF, those crossovers to BiV pacing are still counted as being part of the RV group.
"If you could mandate that patients stayed in the same arm, I think you’d continue to see differences over time, but you can’t do that," she said.
An analysis of changes in NYHA functional class showed the BiV group had better outcomes at 12 months, but at not the other time points.
The BLOCK HF trial was undertaken in response to evidence suggesting that sustained RV apical pacing can degrade ventricular function, especially in patients with preexisting systolic dysfunction.
At present, cardiac resynchronization therapy devices aren’t approved by the Food and Drug Administration for patients with AV block with left ventricular dysfunction. Medtronic officials have indicated they plan to seek an expanded indication based on the BLOCK HF data.
One audience member, noting that the study outcomes were better with BiV pacing in patients across the full spectrum of depressed ejection fractions, asked Dr. Curtis if she expects an expansion of cardiac resynchronization therapy indications to include patients with heart block and a normal ejection fraction.
"I would anticipate that the guidelines will change for the type of patients studied here. But we didn’t study patients with a normal ejection fraction because the more normal the patient, the larger the sample size and longer the follow-up you’d need to show a difference. So I doubt that this study will change guidelines for patients with normal ejection fractions," she said.
Dr. Curtis reported that she serves as a consultant to Medtronic, which sponsored the BLOCK HF trial,
DENVER – Biventricular pacing rather than the right ventricular pacing recommended in current guidelines results in significantly better quality of life and symptom status, an analysis of secondary outcomes from the BLOCK HF trial have shown.
In a previous report of the trial’s primary outcome (N. Engl. J. Med. 2013;368:1585-93), the biventricular (BiV) pacing group showed a highly significant 26% reduction in risk of a composite of all-cause mortality, an urgent care visit for heart failure requiring intravenous therapy, or a 15% or greater increase in the left ventricular end-systolic volume index during an average of 37 months of follow-up, compared with patients who had right ventricular (RV) pacing.
The new report on prespecified secondary endpoints including quality of life and symptom status was undertaken because of researchers’ and regulatory agencies’ growing appreciation of the importance of such outcomes in patients with a chronic progressive disease such as heart failure, principal investigator Dr. Anne B. Curtis reported at the annual meeting of the Heart Rhythm Society.
BLOCK HF (Biventricular versus Right Ventricular Pacing in Patients with Left Ventricular Dysfunction and Atrioventricular Block) was a randomized, double-blind, prospective, 60-center clinical trial involving 691 patients in the United States and Canada. All had AV block warranting pacemaker therapy as well as New York Heart Association(NYHA) class I-III heart failure with a left ventricular ejection fraction of 50% or less. All participants got a cardiac resynchronization therapy device featuring BiV pacing. Patients were assigned in double-blind fashion for their device to run in BiV or conventional RV pacing mode, explained Dr. Curtis, professor and chair of the department of medicine at the University of Buffalo (N.Y.).
The new secondary analysis tabulated changes in the Packer clinical composite score, NYHA functional class, and quality of life, as measured by the Minnesota Living With Heart Failure Questionnaire, at 6, 12, 18, and 24 months.
The Packer clinical composite score classifies patients as improved, worsened, or unchanged based on patient global assessment, heart failure hospitalization, change in symptoms, and other factors. At all four time points through 24 months, significantly more patients in the BiV group were rated as improved and significantly fewer as worsened than in the RV group. For example, at 6 months 53% of the BiV group were categorized as improved and 23% as worsened, compared with 39% and 28% in the RV group, Dr. Curtis reported.
From a mean baseline quality of life score of 25, the BiV group improved by an average of 5 points at the 6-month assessment compared with a 0.3-point gain in the RV group. At 12 months, the BiV group still showed a 3.9-point improvement, significantly better than the average 0.9-point gain in the RV patients. At 18 and 24 months, however, there was no longer a significant difference between the two groups in terms of quality of life scores. Dr. Curtis attributed this drop-off to the fact that 86 patients in the RV arm crossed over to BiV pacing because of deteriorating heart failure, compared with 15 crossovers in the BiV group. In the intention-to-treat analysis employed in BLOCK HF, those crossovers to BiV pacing are still counted as being part of the RV group.
"If you could mandate that patients stayed in the same arm, I think you’d continue to see differences over time, but you can’t do that," she said.
An analysis of changes in NYHA functional class showed the BiV group had better outcomes at 12 months, but at not the other time points.
The BLOCK HF trial was undertaken in response to evidence suggesting that sustained RV apical pacing can degrade ventricular function, especially in patients with preexisting systolic dysfunction.
At present, cardiac resynchronization therapy devices aren’t approved by the Food and Drug Administration for patients with AV block with left ventricular dysfunction. Medtronic officials have indicated they plan to seek an expanded indication based on the BLOCK HF data.
One audience member, noting that the study outcomes were better with BiV pacing in patients across the full spectrum of depressed ejection fractions, asked Dr. Curtis if she expects an expansion of cardiac resynchronization therapy indications to include patients with heart block and a normal ejection fraction.
"I would anticipate that the guidelines will change for the type of patients studied here. But we didn’t study patients with a normal ejection fraction because the more normal the patient, the larger the sample size and longer the follow-up you’d need to show a difference. So I doubt that this study will change guidelines for patients with normal ejection fractions," she said.
Dr. Curtis reported that she serves as a consultant to Medtronic, which sponsored the BLOCK HF trial,
AT HEART RHYTHM 2013
Major finding: Fifty-three percent of patients with atrioventricular block and systolic dysfunction were rated as "improved" after 6 months of biventricular pacing, compared with just 39% of patients on conventional right ventricular pacing.
Data source: A prespecified secondary analysis of the BLOCK HF trial, a randomized, double-blind, prospective multicenter study involving 691 patients.
Disclosures: The BLOCK HF trial was sponsored by Medtronic. The presenter disclosed that she serves as a paid consultant to the device company.
Antitachycardia pacing in ICDs linked to higher mortality
DENVER – The use of antitachycardia pacing was associated with increased mortality in a proprietary registry of patients with an implantable cardioverter defibrillator or cardiac resynchronization therapy defibrillator.
The finding from the ALTITUDE study of Boston Scientific’s Latitude remote electronic monitoring system is an early warning signal of a potentially serious issue in cardiac device programming, Dr. Leslie A. Saxon said at the annual meeting of the Heart Rhythm Society. The database encompasses 225,000 device recipients who have received 195,000 shocks recorded during 21 million device transmissions.
Antitachycardia pacing (ATP) is an essentially painless means of terminating ventricular tachycardia (VT) without resorting to an unpleasant "full-on" shock. Moreover, major randomized trials including MADIT-II and SCD-HeFT as well as ALTITUDE data have consistently shown that mortality risk following first use of shock therapy is two- to threefold higher in implantable cardioverter defibrillator (ICD) or cardiac resynchronization therapy defibrillator (CRT-D) recipients.
ATP detection programming has burgeoned since 2008, when devices with two-zone ATP detection became available. In 2006, roughly 60% of patients in the Latitude registry had ATP programming switched on. By 2011, virtually all patients had "ATP on," which has become the device industry’s out-of-the-box device setting.
ALTITUDE shows that nearly one-quarter of device recipients now receive ATP therapy during the first year after device implantation. Unexpectedly, however, shock rates have remained essentially stable during this period of first-year ATP therapy. Thus, ATP has not resulted in the anticipated meaningful reduction in shock rates, said Dr. Saxon, professor of medicine and chief of the division of cardiovascular medicine at the University of Southern California, Los Angeles.
Moreover, mortality risk during an average 3.5 years of follow-up was lowest in device recipients who received no therapy, greater in those with shock-only or ATP-only therapy, and worst in those who received ATP that accelerated VT; indeed, the mortality risk in that subgroup was threefold higher than in patients who received no device therapy, she said.
Further, device VT detection programming set to a rate of greater than 170 bpm was independently associated with a significant 8% improvement in survival compared with a setting of 170 bpm or less. Programming the VT detection to more than 170 bpm resulted in a significantly lower incidence of shock (7.6% vs.10.4%) and ATP therapy (13.9% vs. 22.4%).
ALTITUDE is not a randomized study, she noted. The decisions for particular programming settings aren’t known. Only limited information on clinical comorbidities is available. Thus, the study findings should be considered hypothesis generating and nondefinitive, although they are concerning.
"It’s unclear if the need for ATP or the ATP itself is a marker of increased risk. However – given the frequency of ATP and the mortality association found in this study – strategies to explore reducing ATP therapies seem justified," Dr. Saxon said. "We’ve put so much emphasis on device shocks, and here we are with a fourfold greater number of patients getting ATP, which is associated with a mortality risk similar to shock. There’s no reason not to explore withholding ATP treatment to try to further improve device outcomes."
Audience member Dr. James G. Porterfield of the University of Tennessee, Memphis, asked: "Do you have enough confidence in this data to start programming ATP off yet?"
"I do," she replied. "But I think it’s very important that we individualize therapy because I also have scores of patients who have symptomatic VT terminated with two-zone therapy."
The current practice in her cardiology group is to turn on ATP only in those patients who have documented VT, and to test the ATP to make sure it’s effective, added Dr. Saxon, who chairs the ALTITUDE study physician panel.
She reported receiving consultant fees from Boston Scientific, which operates the Latitude registry.
DENVER – The use of antitachycardia pacing was associated with increased mortality in a proprietary registry of patients with an implantable cardioverter defibrillator or cardiac resynchronization therapy defibrillator.
The finding from the ALTITUDE study of Boston Scientific’s Latitude remote electronic monitoring system is an early warning signal of a potentially serious issue in cardiac device programming, Dr. Leslie A. Saxon said at the annual meeting of the Heart Rhythm Society. The database encompasses 225,000 device recipients who have received 195,000 shocks recorded during 21 million device transmissions.
Antitachycardia pacing (ATP) is an essentially painless means of terminating ventricular tachycardia (VT) without resorting to an unpleasant "full-on" shock. Moreover, major randomized trials including MADIT-II and SCD-HeFT as well as ALTITUDE data have consistently shown that mortality risk following first use of shock therapy is two- to threefold higher in implantable cardioverter defibrillator (ICD) or cardiac resynchronization therapy defibrillator (CRT-D) recipients.
ATP detection programming has burgeoned since 2008, when devices with two-zone ATP detection became available. In 2006, roughly 60% of patients in the Latitude registry had ATP programming switched on. By 2011, virtually all patients had "ATP on," which has become the device industry’s out-of-the-box device setting.
ALTITUDE shows that nearly one-quarter of device recipients now receive ATP therapy during the first year after device implantation. Unexpectedly, however, shock rates have remained essentially stable during this period of first-year ATP therapy. Thus, ATP has not resulted in the anticipated meaningful reduction in shock rates, said Dr. Saxon, professor of medicine and chief of the division of cardiovascular medicine at the University of Southern California, Los Angeles.
Moreover, mortality risk during an average 3.5 years of follow-up was lowest in device recipients who received no therapy, greater in those with shock-only or ATP-only therapy, and worst in those who received ATP that accelerated VT; indeed, the mortality risk in that subgroup was threefold higher than in patients who received no device therapy, she said.
Further, device VT detection programming set to a rate of greater than 170 bpm was independently associated with a significant 8% improvement in survival compared with a setting of 170 bpm or less. Programming the VT detection to more than 170 bpm resulted in a significantly lower incidence of shock (7.6% vs.10.4%) and ATP therapy (13.9% vs. 22.4%).
ALTITUDE is not a randomized study, she noted. The decisions for particular programming settings aren’t known. Only limited information on clinical comorbidities is available. Thus, the study findings should be considered hypothesis generating and nondefinitive, although they are concerning.
"It’s unclear if the need for ATP or the ATP itself is a marker of increased risk. However – given the frequency of ATP and the mortality association found in this study – strategies to explore reducing ATP therapies seem justified," Dr. Saxon said. "We’ve put so much emphasis on device shocks, and here we are with a fourfold greater number of patients getting ATP, which is associated with a mortality risk similar to shock. There’s no reason not to explore withholding ATP treatment to try to further improve device outcomes."
Audience member Dr. James G. Porterfield of the University of Tennessee, Memphis, asked: "Do you have enough confidence in this data to start programming ATP off yet?"
"I do," she replied. "But I think it’s very important that we individualize therapy because I also have scores of patients who have symptomatic VT terminated with two-zone therapy."
The current practice in her cardiology group is to turn on ATP only in those patients who have documented VT, and to test the ATP to make sure it’s effective, added Dr. Saxon, who chairs the ALTITUDE study physician panel.
She reported receiving consultant fees from Boston Scientific, which operates the Latitude registry.
DENVER – The use of antitachycardia pacing was associated with increased mortality in a proprietary registry of patients with an implantable cardioverter defibrillator or cardiac resynchronization therapy defibrillator.
The finding from the ALTITUDE study of Boston Scientific’s Latitude remote electronic monitoring system is an early warning signal of a potentially serious issue in cardiac device programming, Dr. Leslie A. Saxon said at the annual meeting of the Heart Rhythm Society. The database encompasses 225,000 device recipients who have received 195,000 shocks recorded during 21 million device transmissions.
Antitachycardia pacing (ATP) is an essentially painless means of terminating ventricular tachycardia (VT) without resorting to an unpleasant "full-on" shock. Moreover, major randomized trials including MADIT-II and SCD-HeFT as well as ALTITUDE data have consistently shown that mortality risk following first use of shock therapy is two- to threefold higher in implantable cardioverter defibrillator (ICD) or cardiac resynchronization therapy defibrillator (CRT-D) recipients.
ATP detection programming has burgeoned since 2008, when devices with two-zone ATP detection became available. In 2006, roughly 60% of patients in the Latitude registry had ATP programming switched on. By 2011, virtually all patients had "ATP on," which has become the device industry’s out-of-the-box device setting.
ALTITUDE shows that nearly one-quarter of device recipients now receive ATP therapy during the first year after device implantation. Unexpectedly, however, shock rates have remained essentially stable during this period of first-year ATP therapy. Thus, ATP has not resulted in the anticipated meaningful reduction in shock rates, said Dr. Saxon, professor of medicine and chief of the division of cardiovascular medicine at the University of Southern California, Los Angeles.
Moreover, mortality risk during an average 3.5 years of follow-up was lowest in device recipients who received no therapy, greater in those with shock-only or ATP-only therapy, and worst in those who received ATP that accelerated VT; indeed, the mortality risk in that subgroup was threefold higher than in patients who received no device therapy, she said.
Further, device VT detection programming set to a rate of greater than 170 bpm was independently associated with a significant 8% improvement in survival compared with a setting of 170 bpm or less. Programming the VT detection to more than 170 bpm resulted in a significantly lower incidence of shock (7.6% vs.10.4%) and ATP therapy (13.9% vs. 22.4%).
ALTITUDE is not a randomized study, she noted. The decisions for particular programming settings aren’t known. Only limited information on clinical comorbidities is available. Thus, the study findings should be considered hypothesis generating and nondefinitive, although they are concerning.
"It’s unclear if the need for ATP or the ATP itself is a marker of increased risk. However – given the frequency of ATP and the mortality association found in this study – strategies to explore reducing ATP therapies seem justified," Dr. Saxon said. "We’ve put so much emphasis on device shocks, and here we are with a fourfold greater number of patients getting ATP, which is associated with a mortality risk similar to shock. There’s no reason not to explore withholding ATP treatment to try to further improve device outcomes."
Audience member Dr. James G. Porterfield of the University of Tennessee, Memphis, asked: "Do you have enough confidence in this data to start programming ATP off yet?"
"I do," she replied. "But I think it’s very important that we individualize therapy because I also have scores of patients who have symptomatic VT terminated with two-zone therapy."
The current practice in her cardiology group is to turn on ATP only in those patients who have documented VT, and to test the ATP to make sure it’s effective, added Dr. Saxon, who chairs the ALTITUDE study physician panel.
She reported receiving consultant fees from Boston Scientific, which operates the Latitude registry.
AT HEART RHYTHM 2013
Major finding: Programming the device’s VT detection to more than 170 bpm resulted in a significantly lower incidence of shock (7.6% vs. 10.4%) and ATP therapy (13.9% vs. 22.4%).
Data source: The ALTITUDE study of data obtained from 225,000 cardiac device recipients in the proprietary Latitude network device remote monitoring system.
Disclosures: Boston Scientific sponsors the Latitude network and the ongoing ALTITUDE study. Dr. Saxon disclosed that she is a consultant to the company.
Better endografts mean fewer reinterventions for endovascular AAA
INDIANAPOLIS – Reintervention rates following endovascular repair of abdominal aortic aneurysms have fallen steadily with the introduction of each successive generation of endografts, while reintervention rates after open surgical repair remained stable during a recent 15-year period.
This was among the key findings from the first in-depth analysis of reinterventions occurring in contemporaneous cohorts of abdominal aortic aneurysm (AAA) patients undergoing endovascular aneurysm repair (EVAR) or open repair. The large single-center retrospective study demonstrated major differences between the two treatment strategies in terms of the incidence, nature, timing, and mortality associated with complications requiring reintervention, Dr. Mustafa Al-Jubouri said at the annual meeting of the American Surgical Association.
Dr. Al-Jubouri of Jobst Vascular Institute, Toledo, Ohio, reported on the 1,144 patients who underwent AAA repair there during 1996-2011. Forty-nine percent had EVAR, 51% open surgical repair. Beginning in 2003, more EVARs than open repairs were done annually at the Toledo institute, consistent with the experience at many major centers in the United States and elsewhere, where EVAR has become the first-line treatment based upon evidence that it offers lower operative mortality, less blood loss, and shorter ICU and hospital lengths of stay.
These advantages come at a cost, however: namely, a greater rate of secondary interventions, mainly due to device migration, failure, or endoleaks. The purpose of Dr. Al-Jubouri’s study was to evaluate the rates and reasons for reintervention over time in the two cohorts, as well as the impact of reintervention on long-term survival.
Reintervention was required in 13.6% of the EVAR group during a mean follow-up of 4.58 years, and in 5.1% of the open surgery group during 6.58 years. A single reintervention occurred in 7.9% of EVAR patients and 3.6% of the open repair group. More than one reintervention was required in 5.8% of EVAR patients compared to just 1.6% of the open repair group.
The types and timing of complications leading to reintervention were very different in the two groups. Sixty-eight percent of reinterventions in the EVAR group were for treatment of endoleaks. Another 11.5% were to address device migration, and an equal number were for occlusion.
In contrast, the three most frequent causes of reintervention in the open repair group were colonic ischemia, accounting for 30.4% of reintervention procedures; severe bleeding, 21.7%; and incisional hernia, which triggered another 21.7% of reinterventions.
Notably, 60% of all reinterventions in the open repair group occurred during the initial hospitalization, while less than 7% of reinterventions in the EVAR patients happened within 1 month of the index procedure and only one-third within the first year, the surgeon continued.
Thirty-day mortality in EVAR patients who underwent reintervention within the first month was zero, compared to a 23.3% mortality rate in open repair patients requiring reintervention within 1 month. However, when patients did not require early reintervention, 30-day mortality rates in the two groups did not differ significantly: 1.9% in EVAR group and in the open repair group. That means when patients in the open surgery group required early reintervention, their mortality rate shot up sevenfold.
After the first 30 days post-index procedure, long-term survival rates in the two groups were similar.
Need for reintervention in the open repair group was strongly related to larger aneurysm size. In contrast, reintervention rates were similar in the EVAR group regardless of aneurysm size.
A first reintervention after EVAR occurred in 23.7% of patients who received a first-generation endograft, such as the Ancure or Talent; in 16.2% of those who got the second-generation AneuRx endograft; and in 9.1% with a third-generation endograft, such as the Excluder, Endurant, Powerlink, or Zenith. The annualized rate of reintervention during the first 3 years of follow-up was 6.8% per year with first-generation devices, 7.2% per year with second-generation endografts, and significantly lower at 3.4% per year with the third-generation.
One major reason reintervention rates in EVAR patients have declined over time is that each newer generation of endograft is lower-profile, easier to deploy, and more durable. Also, many of the surgeons now putting in third-generation endografts were performing EVAR 15 years ago; they’re very experienced operators, Dr. Al-Jubouri noted.
Discussant Dr. James R. Debord proposed another explanation for the decrease in EVAR reinterventions over time.
"Isn’t it much more likely that it’s due to recognition of the fact that many of these type 2 endoleaks that we used to intervene on early on don’t require reintervention unless there’s sac enlargement?" commented Dr. Debord, professor of clinical surgery and chief of vascular surgery at the University of Illinois at Peoria.
Dr. Al-Jubouri concurred that this is an important factor in the declining rate of EVAR reinterventions.
"We saw a significant decrease in reinterventions for type 2 endoleaks between the first, second, and third generations," he said.
Asked how his study findings have changed the follow-up protocols at Jobst Vascular Institute, the surgeon replied that in the early years of the series EVAR patients got a CT scan at 6 weeks, 6 months, 1 year, and annually thereafter. This evaluation has evolved over time. Now EVAR patients get a CT scan at 6-12 weeks, and duplex ultrasounds at 6 months, 1 year, and annually thereafter.
"There is no standardized follow-up for open repair patients. However, most [patients] get an annual duplex ultrasound for their follow-up. A CT scan is not part of the follow-up of patients with open repair. But most if not all of the complications that developed in the open repair group were symptomatic," he explained.
He reported having no financial conflicts.
Dr. Mustafa Al-Jubouri and his colleagues assessed reinterventions and outcomes after EVAR and open AAA repair over a long time period, and found decreasing rates of reintervention after EVAR, which they attribute to improvements in technology from first to third and later-generation devices. I would concur with the one discussant, that some of the decrease may also be due to the understanding that not all type II endoleaks require repair. Further, much of the decrease may be due to physician experience – both with appropriate patient and device selection, and technical expertise, including with deployment. However, regardless of the underlying reason for the improvement in the reintervention rate, it is heartening that reintervention is decreasing as physicians become more facile, and industry provides technological improvements to the devices.
Dr. Linda Harris, FACS, is division chief and program director of vascular surgery at State University of New York, Buffalo. Dr. Harris has no disclosures
Dr. Mustafa Al-Jubouri and his colleagues assessed reinterventions and outcomes after EVAR and open AAA repair over a long time period, and found decreasing rates of reintervention after EVAR, which they attribute to improvements in technology from first to third and later-generation devices. I would concur with the one discussant, that some of the decrease may also be due to the understanding that not all type II endoleaks require repair. Further, much of the decrease may be due to physician experience – both with appropriate patient and device selection, and technical expertise, including with deployment. However, regardless of the underlying reason for the improvement in the reintervention rate, it is heartening that reintervention is decreasing as physicians become more facile, and industry provides technological improvements to the devices.
Dr. Linda Harris, FACS, is division chief and program director of vascular surgery at State University of New York, Buffalo. Dr. Harris has no disclosures
Dr. Mustafa Al-Jubouri and his colleagues assessed reinterventions and outcomes after EVAR and open AAA repair over a long time period, and found decreasing rates of reintervention after EVAR, which they attribute to improvements in technology from first to third and later-generation devices. I would concur with the one discussant, that some of the decrease may also be due to the understanding that not all type II endoleaks require repair. Further, much of the decrease may be due to physician experience – both with appropriate patient and device selection, and technical expertise, including with deployment. However, regardless of the underlying reason for the improvement in the reintervention rate, it is heartening that reintervention is decreasing as physicians become more facile, and industry provides technological improvements to the devices.
Dr. Linda Harris, FACS, is division chief and program director of vascular surgery at State University of New York, Buffalo. Dr. Harris has no disclosures
INDIANAPOLIS – Reintervention rates following endovascular repair of abdominal aortic aneurysms have fallen steadily with the introduction of each successive generation of endografts, while reintervention rates after open surgical repair remained stable during a recent 15-year period.
This was among the key findings from the first in-depth analysis of reinterventions occurring in contemporaneous cohorts of abdominal aortic aneurysm (AAA) patients undergoing endovascular aneurysm repair (EVAR) or open repair. The large single-center retrospective study demonstrated major differences between the two treatment strategies in terms of the incidence, nature, timing, and mortality associated with complications requiring reintervention, Dr. Mustafa Al-Jubouri said at the annual meeting of the American Surgical Association.
Dr. Al-Jubouri of Jobst Vascular Institute, Toledo, Ohio, reported on the 1,144 patients who underwent AAA repair there during 1996-2011. Forty-nine percent had EVAR, 51% open surgical repair. Beginning in 2003, more EVARs than open repairs were done annually at the Toledo institute, consistent with the experience at many major centers in the United States and elsewhere, where EVAR has become the first-line treatment based upon evidence that it offers lower operative mortality, less blood loss, and shorter ICU and hospital lengths of stay.
These advantages come at a cost, however: namely, a greater rate of secondary interventions, mainly due to device migration, failure, or endoleaks. The purpose of Dr. Al-Jubouri’s study was to evaluate the rates and reasons for reintervention over time in the two cohorts, as well as the impact of reintervention on long-term survival.
Reintervention was required in 13.6% of the EVAR group during a mean follow-up of 4.58 years, and in 5.1% of the open surgery group during 6.58 years. A single reintervention occurred in 7.9% of EVAR patients and 3.6% of the open repair group. More than one reintervention was required in 5.8% of EVAR patients compared to just 1.6% of the open repair group.
The types and timing of complications leading to reintervention were very different in the two groups. Sixty-eight percent of reinterventions in the EVAR group were for treatment of endoleaks. Another 11.5% were to address device migration, and an equal number were for occlusion.
In contrast, the three most frequent causes of reintervention in the open repair group were colonic ischemia, accounting for 30.4% of reintervention procedures; severe bleeding, 21.7%; and incisional hernia, which triggered another 21.7% of reinterventions.
Notably, 60% of all reinterventions in the open repair group occurred during the initial hospitalization, while less than 7% of reinterventions in the EVAR patients happened within 1 month of the index procedure and only one-third within the first year, the surgeon continued.
Thirty-day mortality in EVAR patients who underwent reintervention within the first month was zero, compared to a 23.3% mortality rate in open repair patients requiring reintervention within 1 month. However, when patients did not require early reintervention, 30-day mortality rates in the two groups did not differ significantly: 1.9% in EVAR group and in the open repair group. That means when patients in the open surgery group required early reintervention, their mortality rate shot up sevenfold.
After the first 30 days post-index procedure, long-term survival rates in the two groups were similar.
Need for reintervention in the open repair group was strongly related to larger aneurysm size. In contrast, reintervention rates were similar in the EVAR group regardless of aneurysm size.
A first reintervention after EVAR occurred in 23.7% of patients who received a first-generation endograft, such as the Ancure or Talent; in 16.2% of those who got the second-generation AneuRx endograft; and in 9.1% with a third-generation endograft, such as the Excluder, Endurant, Powerlink, or Zenith. The annualized rate of reintervention during the first 3 years of follow-up was 6.8% per year with first-generation devices, 7.2% per year with second-generation endografts, and significantly lower at 3.4% per year with the third-generation.
One major reason reintervention rates in EVAR patients have declined over time is that each newer generation of endograft is lower-profile, easier to deploy, and more durable. Also, many of the surgeons now putting in third-generation endografts were performing EVAR 15 years ago; they’re very experienced operators, Dr. Al-Jubouri noted.
Discussant Dr. James R. Debord proposed another explanation for the decrease in EVAR reinterventions over time.
"Isn’t it much more likely that it’s due to recognition of the fact that many of these type 2 endoleaks that we used to intervene on early on don’t require reintervention unless there’s sac enlargement?" commented Dr. Debord, professor of clinical surgery and chief of vascular surgery at the University of Illinois at Peoria.
Dr. Al-Jubouri concurred that this is an important factor in the declining rate of EVAR reinterventions.
"We saw a significant decrease in reinterventions for type 2 endoleaks between the first, second, and third generations," he said.
Asked how his study findings have changed the follow-up protocols at Jobst Vascular Institute, the surgeon replied that in the early years of the series EVAR patients got a CT scan at 6 weeks, 6 months, 1 year, and annually thereafter. This evaluation has evolved over time. Now EVAR patients get a CT scan at 6-12 weeks, and duplex ultrasounds at 6 months, 1 year, and annually thereafter.
"There is no standardized follow-up for open repair patients. However, most [patients] get an annual duplex ultrasound for their follow-up. A CT scan is not part of the follow-up of patients with open repair. But most if not all of the complications that developed in the open repair group were symptomatic," he explained.
He reported having no financial conflicts.
INDIANAPOLIS – Reintervention rates following endovascular repair of abdominal aortic aneurysms have fallen steadily with the introduction of each successive generation of endografts, while reintervention rates after open surgical repair remained stable during a recent 15-year period.
This was among the key findings from the first in-depth analysis of reinterventions occurring in contemporaneous cohorts of abdominal aortic aneurysm (AAA) patients undergoing endovascular aneurysm repair (EVAR) or open repair. The large single-center retrospective study demonstrated major differences between the two treatment strategies in terms of the incidence, nature, timing, and mortality associated with complications requiring reintervention, Dr. Mustafa Al-Jubouri said at the annual meeting of the American Surgical Association.
Dr. Al-Jubouri of Jobst Vascular Institute, Toledo, Ohio, reported on the 1,144 patients who underwent AAA repair there during 1996-2011. Forty-nine percent had EVAR, 51% open surgical repair. Beginning in 2003, more EVARs than open repairs were done annually at the Toledo institute, consistent with the experience at many major centers in the United States and elsewhere, where EVAR has become the first-line treatment based upon evidence that it offers lower operative mortality, less blood loss, and shorter ICU and hospital lengths of stay.
These advantages come at a cost, however: namely, a greater rate of secondary interventions, mainly due to device migration, failure, or endoleaks. The purpose of Dr. Al-Jubouri’s study was to evaluate the rates and reasons for reintervention over time in the two cohorts, as well as the impact of reintervention on long-term survival.
Reintervention was required in 13.6% of the EVAR group during a mean follow-up of 4.58 years, and in 5.1% of the open surgery group during 6.58 years. A single reintervention occurred in 7.9% of EVAR patients and 3.6% of the open repair group. More than one reintervention was required in 5.8% of EVAR patients compared to just 1.6% of the open repair group.
The types and timing of complications leading to reintervention were very different in the two groups. Sixty-eight percent of reinterventions in the EVAR group were for treatment of endoleaks. Another 11.5% were to address device migration, and an equal number were for occlusion.
In contrast, the three most frequent causes of reintervention in the open repair group were colonic ischemia, accounting for 30.4% of reintervention procedures; severe bleeding, 21.7%; and incisional hernia, which triggered another 21.7% of reinterventions.
Notably, 60% of all reinterventions in the open repair group occurred during the initial hospitalization, while less than 7% of reinterventions in the EVAR patients happened within 1 month of the index procedure and only one-third within the first year, the surgeon continued.
Thirty-day mortality in EVAR patients who underwent reintervention within the first month was zero, compared to a 23.3% mortality rate in open repair patients requiring reintervention within 1 month. However, when patients did not require early reintervention, 30-day mortality rates in the two groups did not differ significantly: 1.9% in EVAR group and in the open repair group. That means when patients in the open surgery group required early reintervention, their mortality rate shot up sevenfold.
After the first 30 days post-index procedure, long-term survival rates in the two groups were similar.
Need for reintervention in the open repair group was strongly related to larger aneurysm size. In contrast, reintervention rates were similar in the EVAR group regardless of aneurysm size.
A first reintervention after EVAR occurred in 23.7% of patients who received a first-generation endograft, such as the Ancure or Talent; in 16.2% of those who got the second-generation AneuRx endograft; and in 9.1% with a third-generation endograft, such as the Excluder, Endurant, Powerlink, or Zenith. The annualized rate of reintervention during the first 3 years of follow-up was 6.8% per year with first-generation devices, 7.2% per year with second-generation endografts, and significantly lower at 3.4% per year with the third-generation.
One major reason reintervention rates in EVAR patients have declined over time is that each newer generation of endograft is lower-profile, easier to deploy, and more durable. Also, many of the surgeons now putting in third-generation endografts were performing EVAR 15 years ago; they’re very experienced operators, Dr. Al-Jubouri noted.
Discussant Dr. James R. Debord proposed another explanation for the decrease in EVAR reinterventions over time.
"Isn’t it much more likely that it’s due to recognition of the fact that many of these type 2 endoleaks that we used to intervene on early on don’t require reintervention unless there’s sac enlargement?" commented Dr. Debord, professor of clinical surgery and chief of vascular surgery at the University of Illinois at Peoria.
Dr. Al-Jubouri concurred that this is an important factor in the declining rate of EVAR reinterventions.
"We saw a significant decrease in reinterventions for type 2 endoleaks between the first, second, and third generations," he said.
Asked how his study findings have changed the follow-up protocols at Jobst Vascular Institute, the surgeon replied that in the early years of the series EVAR patients got a CT scan at 6 weeks, 6 months, 1 year, and annually thereafter. This evaluation has evolved over time. Now EVAR patients get a CT scan at 6-12 weeks, and duplex ultrasounds at 6 months, 1 year, and annually thereafter.
"There is no standardized follow-up for open repair patients. However, most [patients] get an annual duplex ultrasound for their follow-up. A CT scan is not part of the follow-up of patients with open repair. But most if not all of the complications that developed in the open repair group were symptomatic," he explained.
He reported having no financial conflicts.
AT THE ASA ANNUAL MEETING
Major Finding: Reintervention rates were markedly higher following endovascular repair compared with open surgical repair of abdominal aortic aneurysms, but the adverse effects associated with reintervention after open repair were far more serious.
Data Source: A retrospective study of the 15-year experience at a large-volume vascular surgery. It encompassed 1,144 patients who underwent abdominal aortic aneurysm repair and their subsequent reintervention rates.
Disclosures: The presenter reported having no conflicts of interest.
Robotic pancreatic resection safe in 250-patient series
INDIANAPOLIS – Robotic-assisted major pancreatic resection is safe, feasible, reliable, and versatile, according to the findings of the largest reported single-center series of such procedures.
That being said, the next and absolutely critical step needs to be comparative effectiveness studies pitting robotic versus laparoscopic or open pancreatic resections, Dr. Herbert J. Zeh III reported at the annual meeting of the American Surgical Association.
He noted that there was a considerable learning curve with the procedure in this single-center series of 250 consecutive robotic-assisted major pancreatic resections. "If we had compared our first 30, 40, or even 60 cases, we would have been comparing an innovative procedure to one that’s been refined continuously since 1937," noted Dr. Zeh of the University of Pittsburgh.
Discussants praised Dr. Zeh and his coinvestigators as innovators who are taking a rigorously scientific and cautious approach in investigating the applicability of robotic techniques to major pancreatic surgery. But some discussants were concerned that the growing dissemination of robotic surgery is based largely upon what they consider to be marketing hype and competitive pressure.
Dr. Zeh explained that he and his coworkers have undertaken the study of robotic-assisted major pancreatic resections because they believe that a minimally invasive approach will reduce the substantial morbidity traditionally associated with open procedures, and that laparoscopic techniques aren’t the answer in these complex resections, which often require resuturing the pancreas to the GI tract.
"It was our perception as a group of dedicated pancreatic surgeons that we could not utilize the laparoscopic technology to adhere to the standard principles of open surgery that we thought were important for safe performance of pancreatic resections. These include meticulous dissection, safe control of major vascular structures, and precise suturing," he said.
The 250 consecutive robotic-assisted major pancreatic resections in this series included the full range of complex pancreatic operations. The two most common procedures were pancreaticoduodenectomy, also known as the Whipple procedure, in 132 patients and distal pancreatectomy in 83.
Overall 30- and 90-day mortality rates were 0.8% and 2.0%, respectively. All deaths were in pancreaticoduodenectomy patients, with 30- and 90-day mortality rates of 1.5% and 3.8%.
Clinically significant complications occurred in 21% of patients. The most common was intra-abdominal fluid collection requiring drainage via interventional radiology. Morbidity rates were similar to those reported in large series of open and laparoscopic pancreatic resections.
Estimated blood loss in pancreaticoduodenectomy averaged 499 mL in the first one-third of patients who had the robotic procedure; thereafter, the blood loss improved to 401 mL.
Rates of conversion from robotic to open surgery also improved over time, from 18.2% in the first third of the patient series to 3.4% in the latter two-thirds.
Mean operative time was 529 minutes for pancreaticoduodenectomy and 256 minutes for distal pancreatectomy. These times have dropped steadily with experience such that mean operative time in the last 50 pancreaticoduodenectomies was 444 minutes, while in the last 50 distal pancreatectomies it was 222 minutes, which approaches reported times for laparoscopic and open operations, Dr. Zeh noted.
The median length of stay was 10 days for pancreaticoduodenectomy patients and 6 days for those undergoing distal pancreatectomy. As a precautionary measure, surgeons kept patients treated early in the series in the hospital longer than was probably necessary. Length of stay has come down over time, although this trend hasn’t yet reached statistical significance.
The readmission rate was 24% in pancreaticoduodenectomy patients and 28% in distal pancreatectomy patients; 2% of patients required a reoperation.
As experience has grown, the group’s criteria for selecting patients for the robotic approach have loosened considerably. Many recent patients have been obese or superobese.
"Currently the only absolute contraindication is some sort of vascular involvement that would entail resecting a vein and reanastomosing it using a minimally invasive approach. That’s really the only frontier we haven’t crossed," said Dr. Zeh.
The potential advantages of the robotic platform that drew the researchers’ interest include greater range of motion for the robotic needle driver and other tools, compared with what is achievable laparoscopically; enhanced visualization with magnification; computerized smoothing of a surgeon’s tremor; and the ability to see structures in three dimensions, unlike in laparoscopy.
"I think the real advantage is the computer," he added. "Robotic surgery is probably misnamed; it’s really computer-assisted surgery. What this is going to allow us to do is to take the skill sets that we have to the next level. Pilots couldn’t control fighter jets without a computer between them and the plane. In the end, I think the addition of the computer between us and the patient is going to allow us to do things that we haven’t even thought about."
He reported having received an honorarium from Medtronic on a single occasion for participation in a symposium on minimally invasive pancreatic surgery.
When it comes to robotic surgery, the emperor is not wearing any clothes. I don’t believe there has ever been a series that has conclusively shown that the robot has made any difference in patient outcomes or quality of the procedure. I believe that it is a technology that enables surgeons who cannot otherwise perform the procedure to perform the procedure. That’s been shown in the urology literature, particularly.
What’s going on in my community and others throughout the country is a terrible abuse of this technology, where we have doctors in our local hospitals taking out ovaries with this technology, taking out a uterus, and who are doing single-site robotic cholecystectomies in 4 hours at $4,000 in cost. They’re using robotic technology to do simple procedures that could otherwise be done better and faster without this technology.
We need to be outspoken and realistic about the use of robotic surgery. We need to advance this technology, but carefully and with a caveat.
Dr. Jeffrey L. Ponsky is professor and chairman of the department of surgery at Case Western Reserve University, Cleveland. He made his remarks as a discussant at the meeting.
When it comes to robotic surgery, the emperor is not wearing any clothes. I don’t believe there has ever been a series that has conclusively shown that the robot has made any difference in patient outcomes or quality of the procedure. I believe that it is a technology that enables surgeons who cannot otherwise perform the procedure to perform the procedure. That’s been shown in the urology literature, particularly.
What’s going on in my community and others throughout the country is a terrible abuse of this technology, where we have doctors in our local hospitals taking out ovaries with this technology, taking out a uterus, and who are doing single-site robotic cholecystectomies in 4 hours at $4,000 in cost. They’re using robotic technology to do simple procedures that could otherwise be done better and faster without this technology.
We need to be outspoken and realistic about the use of robotic surgery. We need to advance this technology, but carefully and with a caveat.
Dr. Jeffrey L. Ponsky is professor and chairman of the department of surgery at Case Western Reserve University, Cleveland. He made his remarks as a discussant at the meeting.
When it comes to robotic surgery, the emperor is not wearing any clothes. I don’t believe there has ever been a series that has conclusively shown that the robot has made any difference in patient outcomes or quality of the procedure. I believe that it is a technology that enables surgeons who cannot otherwise perform the procedure to perform the procedure. That’s been shown in the urology literature, particularly.
What’s going on in my community and others throughout the country is a terrible abuse of this technology, where we have doctors in our local hospitals taking out ovaries with this technology, taking out a uterus, and who are doing single-site robotic cholecystectomies in 4 hours at $4,000 in cost. They’re using robotic technology to do simple procedures that could otherwise be done better and faster without this technology.
We need to be outspoken and realistic about the use of robotic surgery. We need to advance this technology, but carefully and with a caveat.
Dr. Jeffrey L. Ponsky is professor and chairman of the department of surgery at Case Western Reserve University, Cleveland. He made his remarks as a discussant at the meeting.
INDIANAPOLIS – Robotic-assisted major pancreatic resection is safe, feasible, reliable, and versatile, according to the findings of the largest reported single-center series of such procedures.
That being said, the next and absolutely critical step needs to be comparative effectiveness studies pitting robotic versus laparoscopic or open pancreatic resections, Dr. Herbert J. Zeh III reported at the annual meeting of the American Surgical Association.
He noted that there was a considerable learning curve with the procedure in this single-center series of 250 consecutive robotic-assisted major pancreatic resections. "If we had compared our first 30, 40, or even 60 cases, we would have been comparing an innovative procedure to one that’s been refined continuously since 1937," noted Dr. Zeh of the University of Pittsburgh.
Discussants praised Dr. Zeh and his coinvestigators as innovators who are taking a rigorously scientific and cautious approach in investigating the applicability of robotic techniques to major pancreatic surgery. But some discussants were concerned that the growing dissemination of robotic surgery is based largely upon what they consider to be marketing hype and competitive pressure.
Dr. Zeh explained that he and his coworkers have undertaken the study of robotic-assisted major pancreatic resections because they believe that a minimally invasive approach will reduce the substantial morbidity traditionally associated with open procedures, and that laparoscopic techniques aren’t the answer in these complex resections, which often require resuturing the pancreas to the GI tract.
"It was our perception as a group of dedicated pancreatic surgeons that we could not utilize the laparoscopic technology to adhere to the standard principles of open surgery that we thought were important for safe performance of pancreatic resections. These include meticulous dissection, safe control of major vascular structures, and precise suturing," he said.
The 250 consecutive robotic-assisted major pancreatic resections in this series included the full range of complex pancreatic operations. The two most common procedures were pancreaticoduodenectomy, also known as the Whipple procedure, in 132 patients and distal pancreatectomy in 83.
Overall 30- and 90-day mortality rates were 0.8% and 2.0%, respectively. All deaths were in pancreaticoduodenectomy patients, with 30- and 90-day mortality rates of 1.5% and 3.8%.
Clinically significant complications occurred in 21% of patients. The most common was intra-abdominal fluid collection requiring drainage via interventional radiology. Morbidity rates were similar to those reported in large series of open and laparoscopic pancreatic resections.
Estimated blood loss in pancreaticoduodenectomy averaged 499 mL in the first one-third of patients who had the robotic procedure; thereafter, the blood loss improved to 401 mL.
Rates of conversion from robotic to open surgery also improved over time, from 18.2% in the first third of the patient series to 3.4% in the latter two-thirds.
Mean operative time was 529 minutes for pancreaticoduodenectomy and 256 minutes for distal pancreatectomy. These times have dropped steadily with experience such that mean operative time in the last 50 pancreaticoduodenectomies was 444 minutes, while in the last 50 distal pancreatectomies it was 222 minutes, which approaches reported times for laparoscopic and open operations, Dr. Zeh noted.
The median length of stay was 10 days for pancreaticoduodenectomy patients and 6 days for those undergoing distal pancreatectomy. As a precautionary measure, surgeons kept patients treated early in the series in the hospital longer than was probably necessary. Length of stay has come down over time, although this trend hasn’t yet reached statistical significance.
The readmission rate was 24% in pancreaticoduodenectomy patients and 28% in distal pancreatectomy patients; 2% of patients required a reoperation.
As experience has grown, the group’s criteria for selecting patients for the robotic approach have loosened considerably. Many recent patients have been obese or superobese.
"Currently the only absolute contraindication is some sort of vascular involvement that would entail resecting a vein and reanastomosing it using a minimally invasive approach. That’s really the only frontier we haven’t crossed," said Dr. Zeh.
The potential advantages of the robotic platform that drew the researchers’ interest include greater range of motion for the robotic needle driver and other tools, compared with what is achievable laparoscopically; enhanced visualization with magnification; computerized smoothing of a surgeon’s tremor; and the ability to see structures in three dimensions, unlike in laparoscopy.
"I think the real advantage is the computer," he added. "Robotic surgery is probably misnamed; it’s really computer-assisted surgery. What this is going to allow us to do is to take the skill sets that we have to the next level. Pilots couldn’t control fighter jets without a computer between them and the plane. In the end, I think the addition of the computer between us and the patient is going to allow us to do things that we haven’t even thought about."
He reported having received an honorarium from Medtronic on a single occasion for participation in a symposium on minimally invasive pancreatic surgery.
INDIANAPOLIS – Robotic-assisted major pancreatic resection is safe, feasible, reliable, and versatile, according to the findings of the largest reported single-center series of such procedures.
That being said, the next and absolutely critical step needs to be comparative effectiveness studies pitting robotic versus laparoscopic or open pancreatic resections, Dr. Herbert J. Zeh III reported at the annual meeting of the American Surgical Association.
He noted that there was a considerable learning curve with the procedure in this single-center series of 250 consecutive robotic-assisted major pancreatic resections. "If we had compared our first 30, 40, or even 60 cases, we would have been comparing an innovative procedure to one that’s been refined continuously since 1937," noted Dr. Zeh of the University of Pittsburgh.
Discussants praised Dr. Zeh and his coinvestigators as innovators who are taking a rigorously scientific and cautious approach in investigating the applicability of robotic techniques to major pancreatic surgery. But some discussants were concerned that the growing dissemination of robotic surgery is based largely upon what they consider to be marketing hype and competitive pressure.
Dr. Zeh explained that he and his coworkers have undertaken the study of robotic-assisted major pancreatic resections because they believe that a minimally invasive approach will reduce the substantial morbidity traditionally associated with open procedures, and that laparoscopic techniques aren’t the answer in these complex resections, which often require resuturing the pancreas to the GI tract.
"It was our perception as a group of dedicated pancreatic surgeons that we could not utilize the laparoscopic technology to adhere to the standard principles of open surgery that we thought were important for safe performance of pancreatic resections. These include meticulous dissection, safe control of major vascular structures, and precise suturing," he said.
The 250 consecutive robotic-assisted major pancreatic resections in this series included the full range of complex pancreatic operations. The two most common procedures were pancreaticoduodenectomy, also known as the Whipple procedure, in 132 patients and distal pancreatectomy in 83.
Overall 30- and 90-day mortality rates were 0.8% and 2.0%, respectively. All deaths were in pancreaticoduodenectomy patients, with 30- and 90-day mortality rates of 1.5% and 3.8%.
Clinically significant complications occurred in 21% of patients. The most common was intra-abdominal fluid collection requiring drainage via interventional radiology. Morbidity rates were similar to those reported in large series of open and laparoscopic pancreatic resections.
Estimated blood loss in pancreaticoduodenectomy averaged 499 mL in the first one-third of patients who had the robotic procedure; thereafter, the blood loss improved to 401 mL.
Rates of conversion from robotic to open surgery also improved over time, from 18.2% in the first third of the patient series to 3.4% in the latter two-thirds.
Mean operative time was 529 minutes for pancreaticoduodenectomy and 256 minutes for distal pancreatectomy. These times have dropped steadily with experience such that mean operative time in the last 50 pancreaticoduodenectomies was 444 minutes, while in the last 50 distal pancreatectomies it was 222 minutes, which approaches reported times for laparoscopic and open operations, Dr. Zeh noted.
The median length of stay was 10 days for pancreaticoduodenectomy patients and 6 days for those undergoing distal pancreatectomy. As a precautionary measure, surgeons kept patients treated early in the series in the hospital longer than was probably necessary. Length of stay has come down over time, although this trend hasn’t yet reached statistical significance.
The readmission rate was 24% in pancreaticoduodenectomy patients and 28% in distal pancreatectomy patients; 2% of patients required a reoperation.
As experience has grown, the group’s criteria for selecting patients for the robotic approach have loosened considerably. Many recent patients have been obese or superobese.
"Currently the only absolute contraindication is some sort of vascular involvement that would entail resecting a vein and reanastomosing it using a minimally invasive approach. That’s really the only frontier we haven’t crossed," said Dr. Zeh.
The potential advantages of the robotic platform that drew the researchers’ interest include greater range of motion for the robotic needle driver and other tools, compared with what is achievable laparoscopically; enhanced visualization with magnification; computerized smoothing of a surgeon’s tremor; and the ability to see structures in three dimensions, unlike in laparoscopy.
"I think the real advantage is the computer," he added. "Robotic surgery is probably misnamed; it’s really computer-assisted surgery. What this is going to allow us to do is to take the skill sets that we have to the next level. Pilots couldn’t control fighter jets without a computer between them and the plane. In the end, I think the addition of the computer between us and the patient is going to allow us to do things that we haven’t even thought about."
He reported having received an honorarium from Medtronic on a single occasion for participation in a symposium on minimally invasive pancreatic surgery.
AT THE ASA ANNUAL MEETING
Major finding: Overall 30- and 90-day mortality rates were 0.8% and 2.0%, respectively, following various types of robotic-assisted major pancreatic resection, with deaths occurring only in the subset of patients undergoing pancreaticoduodenectomy.
Data source: A retrospective review of a prospectively maintained single-center database of 250 consecutive patients undergoing robotic-assisted major pancreatic resections.
Disclosures: The presenter reported having received an honorarium from Medtronic on a single occasion.
Big trials show no advantage to using off-pump CABG
SAN FRANCISCO - Off-pump coronary artery bypass graft surgery offered no advantages over on-pump CABG in any major end points at 1 year of follow-up in two major prospective randomized trials totaling more than 7,000 patients.
Among the key 1-year outcomes - which didn't differ between off- and on-pump CABG patients in the GOPCABE and CORONARY trials - were death, MI, stroke, neurocognitive function, quality of life, renal failure, and repeat revascularization, investigators reported at the annual meeting of the American College of Cardiology.
A third randomized trial presented at the same session of the ACC meeting did find a significant outcome advantage favoring off-pump CABG in high-operative-risk patients at 1 year. However, experts discounted this Czech study because it was small, single center, reported only 30-day results, and the advantage found for off-pump surgery hinged on an outdated and inadequate definition of MI.
The new study findings signal a striking fall from grace for off-pump CABG. Not long ago, this technique, while controversial, was viewed by many as a progressive development within heart surgery, one that would revitalize a mature operation whose annual case numbers were declining in the face of stiff competition from percutaneous coronary intervention by cardiologists. Off-pump CABG was an innovation designed to avoid the perioperative complications related to aortic cross-clamping and the heart-lung machine, including the lingering neurocognitive dysfunction known informally in surgical circles as "pump head."
However, the resounding lack of any demonstrable advantages for off-pump CABG in the two large trials presented in San Francisco left analysts scratching their heads as to the role remaining for this beating heart surgical technique, which is more difficult to learn and perform skillfully than on-pump bypass.
Discussant Dr. Michael J. Mack, a cardiac surgeon, voiced a similar sentiment. "I was an early advocate of off-pump surgery. But as a card-carrying off-pump bypass surgeon, it's getting harder and harder for me to maintain enthusiasm for a potential benefit from this," declared Dr. Mack, medical director of cardiovascular surgery for the Baylor Health Care System and director of cardiovascular research at the Heart Hospital in Plano, Tex. He noted that the CORONARY and GOPCABE trials follow upon the earlier ROOBY (Randomized On/Off Bypass) trial, which actually showed worse outcomes in the off-pump group. ROOBY enrolled 2,203 Veterans Affairs patients, with the off-pump CABG group having a significantly higher 1-year rate of the primary composite endpoint comprising death, nonfatal MI, or repeat revascularization, along with worse graft patency (N. Engl. J. Med. 2009;361:1827-37).
GOPCABE and CORONARY were designed in part to answer critics of ROOBY, who have argued that the VA trial used insufficiently experienced off-pump CABG surgeons and featured a patient population at too low an operative risk to detect a signal of benefit favoring off-pump surgery. The GOPCABE (German Off-Pump Coronary Artery Bypass Grafting in Elderly Patients) study involved 2,539 patients aged 75 years or older randomized at 12 German centers. A total of 60% of patients had triple-vessel disease, and no one was excluded from the trial because of left ventricular function or coronary artery anatomy. Participating surgeons were highly experienced. Those who performed off-pump CABG in the study had previously done an average of 514 of them, while the on-pump surgeons had done an average of 1,378 of those operations.
"We wanted to have the best off-pump vs. the best on-pump surgeons, like in a competition," explained Dr. Anno Diegeler, a surgeon at the Bad Neustadt (Germany) Heart Center.
He and his coinvestigators conducted GOPCABE because they believed it would be easier to show advantages for off-pump CABG in a population at high operative risk, such as elderly patients with many comorbidities. Indeed, the study hypothesis was that the off-pump group would show a robust 30% reduction in the primary endpoint, a composite of death, stroke, myocardial infarction, repeat revascularization, or new renal-replacement therapy at 1 year.
That didn't happen. The 30-day rate of the primary endpoint was 7.8% in the off-pump group and 8.2% with on-pump CABG, while the 1-year rates were 13.1% and 14.0%, respectively. None of the individual components of the composite endpoint differed significantly between the groups, either.
Neurocognitive function wasn't measured in GOPCABE, but it was in CORONARY (the CABG Off or On Pump Revascularization Study), which involved 4,752 randomized patients in 19 countries.
Dr. Andre Lamy presented the 1-year results. The primary endpoint was a composite of death, MI, stroke, or new renal failure requiring dialysis. The rate was 12.1% in patients in the off-pump group and similar at 13.3% in the on-pump group. As in GOPCABE, the surgeons participating in CORONARY were highly proficient. They had to have at least 2 years' experience as a staff cardiac surgeon and at least 100 prior cases of whichever operation they were assigned to. The vast majority met that standard for both procedures.
Quality of life and neurocognitive tests showed significant difference between the two groups.
However, neurocognitive testing was declared optional because it's so time consuming, and many patients opted out. For example, only 1,273 of the original 4,752 patients returned to take the Montreal Cognitive Assessment at 1 year, noted Dr. Lamy, a heart surgeon at the Population Health Research Institute at McMaster University in Hamilton, Ont.
Discussant Dr. Bernard Gersh zeroed in on the incomplete neurocognitive testing. "I think this is really a significant limitation. There's a huge bias. If there's any advantage to off-pump CABG, it may be in neurocognitive dysfunction," commented Dr. Gersh, professor of medicine at the Mayo Clinic, Rochester, Minn.
In response to questioning as to where off-pump CABG fits into clinical practice in light of the disappointing CORONARY and GOPCABE findings, Dr. Diegeler said he remains convinced that some high-operative-risk patients - those with aortic calcification or other evidence of generalized vascular disease - do benefit preferentially from off-pump surgery when performed by expert surgeons.
Dr. Lamy said a post hoc analysis of the CORONARY data showed that low-operative-risk patients as defined by a EuroScore of 0-2 tended to do better with on- than off-pump CABG, while the converse was true in those with moderate- or high-risk scores.
"In my personal practice now, my low-risk patients go on-pump and my moderate- and high-risk patients go off-pump," he added.
Dr. Jan Hlavicka presented the results of the PRAGUE-6 trial, in which 206 patients at high operative risk - a EuroScore of 6 or greater - were randomized to off- or on-pump CABG at Charles University, Prague. The operations were performed by five surgeons proficient in both procedures. The 30-day primary composite endpoint comprising death, MI, stroke, or new renal failure requiring dialysis occurred in 20.6% of the on-pump group, compared with 9.2% of off-pump patients.
The off-pump group required significantly fewer RBC transfusions. There were no significant differences between the two groups in terms of average hospital length of stay, wound infection rates, or total hospital costs.
Dr. Gersh noted that the only significant difference between the two groups in the individual components of the primary endpoint was in acute MI rates: 12.1% in the on- vs. 4.1% in the off-pump CABG group. He took issue with the Czech investigators? use of the 2004 Society of Thoracic Surgeons definition of acute MI. That's not sufficiently stringent. It surely captures many patients who don't really have an acute MI. The data should be reanalyzed using a contemporary definition which requires new Q waves, he added.
Dr. Hlavicka, Dr. Lamy, and Dr. Diegeler declared no conflicts.
SAN FRANCISCO - Off-pump coronary artery bypass graft surgery offered no advantages over on-pump CABG in any major end points at 1 year of follow-up in two major prospective randomized trials totaling more than 7,000 patients.
Among the key 1-year outcomes - which didn't differ between off- and on-pump CABG patients in the GOPCABE and CORONARY trials - were death, MI, stroke, neurocognitive function, quality of life, renal failure, and repeat revascularization, investigators reported at the annual meeting of the American College of Cardiology.
A third randomized trial presented at the same session of the ACC meeting did find a significant outcome advantage favoring off-pump CABG in high-operative-risk patients at 1 year. However, experts discounted this Czech study because it was small, single center, reported only 30-day results, and the advantage found for off-pump surgery hinged on an outdated and inadequate definition of MI.
The new study findings signal a striking fall from grace for off-pump CABG. Not long ago, this technique, while controversial, was viewed by many as a progressive development within heart surgery, one that would revitalize a mature operation whose annual case numbers were declining in the face of stiff competition from percutaneous coronary intervention by cardiologists. Off-pump CABG was an innovation designed to avoid the perioperative complications related to aortic cross-clamping and the heart-lung machine, including the lingering neurocognitive dysfunction known informally in surgical circles as "pump head."
However, the resounding lack of any demonstrable advantages for off-pump CABG in the two large trials presented in San Francisco left analysts scratching their heads as to the role remaining for this beating heart surgical technique, which is more difficult to learn and perform skillfully than on-pump bypass.
Discussant Dr. Michael J. Mack, a cardiac surgeon, voiced a similar sentiment. "I was an early advocate of off-pump surgery. But as a card-carrying off-pump bypass surgeon, it's getting harder and harder for me to maintain enthusiasm for a potential benefit from this," declared Dr. Mack, medical director of cardiovascular surgery for the Baylor Health Care System and director of cardiovascular research at the Heart Hospital in Plano, Tex. He noted that the CORONARY and GOPCABE trials follow upon the earlier ROOBY (Randomized On/Off Bypass) trial, which actually showed worse outcomes in the off-pump group. ROOBY enrolled 2,203 Veterans Affairs patients, with the off-pump CABG group having a significantly higher 1-year rate of the primary composite endpoint comprising death, nonfatal MI, or repeat revascularization, along with worse graft patency (N. Engl. J. Med. 2009;361:1827-37).
GOPCABE and CORONARY were designed in part to answer critics of ROOBY, who have argued that the VA trial used insufficiently experienced off-pump CABG surgeons and featured a patient population at too low an operative risk to detect a signal of benefit favoring off-pump surgery. The GOPCABE (German Off-Pump Coronary Artery Bypass Grafting in Elderly Patients) study involved 2,539 patients aged 75 years or older randomized at 12 German centers. A total of 60% of patients had triple-vessel disease, and no one was excluded from the trial because of left ventricular function or coronary artery anatomy. Participating surgeons were highly experienced. Those who performed off-pump CABG in the study had previously done an average of 514 of them, while the on-pump surgeons had done an average of 1,378 of those operations.
"We wanted to have the best off-pump vs. the best on-pump surgeons, like in a competition," explained Dr. Anno Diegeler, a surgeon at the Bad Neustadt (Germany) Heart Center.
He and his coinvestigators conducted GOPCABE because they believed it would be easier to show advantages for off-pump CABG in a population at high operative risk, such as elderly patients with many comorbidities. Indeed, the study hypothesis was that the off-pump group would show a robust 30% reduction in the primary endpoint, a composite of death, stroke, myocardial infarction, repeat revascularization, or new renal-replacement therapy at 1 year.
That didn't happen. The 30-day rate of the primary endpoint was 7.8% in the off-pump group and 8.2% with on-pump CABG, while the 1-year rates were 13.1% and 14.0%, respectively. None of the individual components of the composite endpoint differed significantly between the groups, either.
Neurocognitive function wasn't measured in GOPCABE, but it was in CORONARY (the CABG Off or On Pump Revascularization Study), which involved 4,752 randomized patients in 19 countries.
Dr. Andre Lamy presented the 1-year results. The primary endpoint was a composite of death, MI, stroke, or new renal failure requiring dialysis. The rate was 12.1% in patients in the off-pump group and similar at 13.3% in the on-pump group. As in GOPCABE, the surgeons participating in CORONARY were highly proficient. They had to have at least 2 years' experience as a staff cardiac surgeon and at least 100 prior cases of whichever operation they were assigned to. The vast majority met that standard for both procedures.
Quality of life and neurocognitive tests showed significant difference between the two groups.
However, neurocognitive testing was declared optional because it's so time consuming, and many patients opted out. For example, only 1,273 of the original 4,752 patients returned to take the Montreal Cognitive Assessment at 1 year, noted Dr. Lamy, a heart surgeon at the Population Health Research Institute at McMaster University in Hamilton, Ont.
Discussant Dr. Bernard Gersh zeroed in on the incomplete neurocognitive testing. "I think this is really a significant limitation. There's a huge bias. If there's any advantage to off-pump CABG, it may be in neurocognitive dysfunction," commented Dr. Gersh, professor of medicine at the Mayo Clinic, Rochester, Minn.
In response to questioning as to where off-pump CABG fits into clinical practice in light of the disappointing CORONARY and GOPCABE findings, Dr. Diegeler said he remains convinced that some high-operative-risk patients - those with aortic calcification or other evidence of generalized vascular disease - do benefit preferentially from off-pump surgery when performed by expert surgeons.
Dr. Lamy said a post hoc analysis of the CORONARY data showed that low-operative-risk patients as defined by a EuroScore of 0-2 tended to do better with on- than off-pump CABG, while the converse was true in those with moderate- or high-risk scores.
"In my personal practice now, my low-risk patients go on-pump and my moderate- and high-risk patients go off-pump," he added.
Dr. Jan Hlavicka presented the results of the PRAGUE-6 trial, in which 206 patients at high operative risk - a EuroScore of 6 or greater - were randomized to off- or on-pump CABG at Charles University, Prague. The operations were performed by five surgeons proficient in both procedures. The 30-day primary composite endpoint comprising death, MI, stroke, or new renal failure requiring dialysis occurred in 20.6% of the on-pump group, compared with 9.2% of off-pump patients.
The off-pump group required significantly fewer RBC transfusions. There were no significant differences between the two groups in terms of average hospital length of stay, wound infection rates, or total hospital costs.
Dr. Gersh noted that the only significant difference between the two groups in the individual components of the primary endpoint was in acute MI rates: 12.1% in the on- vs. 4.1% in the off-pump CABG group. He took issue with the Czech investigators? use of the 2004 Society of Thoracic Surgeons definition of acute MI. That's not sufficiently stringent. It surely captures many patients who don't really have an acute MI. The data should be reanalyzed using a contemporary definition which requires new Q waves, he added.
Dr. Hlavicka, Dr. Lamy, and Dr. Diegeler declared no conflicts.
SAN FRANCISCO - Off-pump coronary artery bypass graft surgery offered no advantages over on-pump CABG in any major end points at 1 year of follow-up in two major prospective randomized trials totaling more than 7,000 patients.
Among the key 1-year outcomes - which didn't differ between off- and on-pump CABG patients in the GOPCABE and CORONARY trials - were death, MI, stroke, neurocognitive function, quality of life, renal failure, and repeat revascularization, investigators reported at the annual meeting of the American College of Cardiology.
A third randomized trial presented at the same session of the ACC meeting did find a significant outcome advantage favoring off-pump CABG in high-operative-risk patients at 1 year. However, experts discounted this Czech study because it was small, single center, reported only 30-day results, and the advantage found for off-pump surgery hinged on an outdated and inadequate definition of MI.
The new study findings signal a striking fall from grace for off-pump CABG. Not long ago, this technique, while controversial, was viewed by many as a progressive development within heart surgery, one that would revitalize a mature operation whose annual case numbers were declining in the face of stiff competition from percutaneous coronary intervention by cardiologists. Off-pump CABG was an innovation designed to avoid the perioperative complications related to aortic cross-clamping and the heart-lung machine, including the lingering neurocognitive dysfunction known informally in surgical circles as "pump head."
However, the resounding lack of any demonstrable advantages for off-pump CABG in the two large trials presented in San Francisco left analysts scratching their heads as to the role remaining for this beating heart surgical technique, which is more difficult to learn and perform skillfully than on-pump bypass.
Discussant Dr. Michael J. Mack, a cardiac surgeon, voiced a similar sentiment. "I was an early advocate of off-pump surgery. But as a card-carrying off-pump bypass surgeon, it's getting harder and harder for me to maintain enthusiasm for a potential benefit from this," declared Dr. Mack, medical director of cardiovascular surgery for the Baylor Health Care System and director of cardiovascular research at the Heart Hospital in Plano, Tex. He noted that the CORONARY and GOPCABE trials follow upon the earlier ROOBY (Randomized On/Off Bypass) trial, which actually showed worse outcomes in the off-pump group. ROOBY enrolled 2,203 Veterans Affairs patients, with the off-pump CABG group having a significantly higher 1-year rate of the primary composite endpoint comprising death, nonfatal MI, or repeat revascularization, along with worse graft patency (N. Engl. J. Med. 2009;361:1827-37).
GOPCABE and CORONARY were designed in part to answer critics of ROOBY, who have argued that the VA trial used insufficiently experienced off-pump CABG surgeons and featured a patient population at too low an operative risk to detect a signal of benefit favoring off-pump surgery. The GOPCABE (German Off-Pump Coronary Artery Bypass Grafting in Elderly Patients) study involved 2,539 patients aged 75 years or older randomized at 12 German centers. A total of 60% of patients had triple-vessel disease, and no one was excluded from the trial because of left ventricular function or coronary artery anatomy. Participating surgeons were highly experienced. Those who performed off-pump CABG in the study had previously done an average of 514 of them, while the on-pump surgeons had done an average of 1,378 of those operations.
"We wanted to have the best off-pump vs. the best on-pump surgeons, like in a competition," explained Dr. Anno Diegeler, a surgeon at the Bad Neustadt (Germany) Heart Center.
He and his coinvestigators conducted GOPCABE because they believed it would be easier to show advantages for off-pump CABG in a population at high operative risk, such as elderly patients with many comorbidities. Indeed, the study hypothesis was that the off-pump group would show a robust 30% reduction in the primary endpoint, a composite of death, stroke, myocardial infarction, repeat revascularization, or new renal-replacement therapy at 1 year.
That didn't happen. The 30-day rate of the primary endpoint was 7.8% in the off-pump group and 8.2% with on-pump CABG, while the 1-year rates were 13.1% and 14.0%, respectively. None of the individual components of the composite endpoint differed significantly between the groups, either.
Neurocognitive function wasn't measured in GOPCABE, but it was in CORONARY (the CABG Off or On Pump Revascularization Study), which involved 4,752 randomized patients in 19 countries.
Dr. Andre Lamy presented the 1-year results. The primary endpoint was a composite of death, MI, stroke, or new renal failure requiring dialysis. The rate was 12.1% in patients in the off-pump group and similar at 13.3% in the on-pump group. As in GOPCABE, the surgeons participating in CORONARY were highly proficient. They had to have at least 2 years' experience as a staff cardiac surgeon and at least 100 prior cases of whichever operation they were assigned to. The vast majority met that standard for both procedures.
Quality of life and neurocognitive tests showed significant difference between the two groups.
However, neurocognitive testing was declared optional because it's so time consuming, and many patients opted out. For example, only 1,273 of the original 4,752 patients returned to take the Montreal Cognitive Assessment at 1 year, noted Dr. Lamy, a heart surgeon at the Population Health Research Institute at McMaster University in Hamilton, Ont.
Discussant Dr. Bernard Gersh zeroed in on the incomplete neurocognitive testing. "I think this is really a significant limitation. There's a huge bias. If there's any advantage to off-pump CABG, it may be in neurocognitive dysfunction," commented Dr. Gersh, professor of medicine at the Mayo Clinic, Rochester, Minn.
In response to questioning as to where off-pump CABG fits into clinical practice in light of the disappointing CORONARY and GOPCABE findings, Dr. Diegeler said he remains convinced that some high-operative-risk patients - those with aortic calcification or other evidence of generalized vascular disease - do benefit preferentially from off-pump surgery when performed by expert surgeons.
Dr. Lamy said a post hoc analysis of the CORONARY data showed that low-operative-risk patients as defined by a EuroScore of 0-2 tended to do better with on- than off-pump CABG, while the converse was true in those with moderate- or high-risk scores.
"In my personal practice now, my low-risk patients go on-pump and my moderate- and high-risk patients go off-pump," he added.
Dr. Jan Hlavicka presented the results of the PRAGUE-6 trial, in which 206 patients at high operative risk - a EuroScore of 6 or greater - were randomized to off- or on-pump CABG at Charles University, Prague. The operations were performed by five surgeons proficient in both procedures. The 30-day primary composite endpoint comprising death, MI, stroke, or new renal failure requiring dialysis occurred in 20.6% of the on-pump group, compared with 9.2% of off-pump patients.
The off-pump group required significantly fewer RBC transfusions. There were no significant differences between the two groups in terms of average hospital length of stay, wound infection rates, or total hospital costs.
Dr. Gersh noted that the only significant difference between the two groups in the individual components of the primary endpoint was in acute MI rates: 12.1% in the on- vs. 4.1% in the off-pump CABG group. He took issue with the Czech investigators? use of the 2004 Society of Thoracic Surgeons definition of acute MI. That's not sufficiently stringent. It surely captures many patients who don't really have an acute MI. The data should be reanalyzed using a contemporary definition which requires new Q waves, he added.
Dr. Hlavicka, Dr. Lamy, and Dr. Diegeler declared no conflicts.
Endovascular AAA repair superior for kidney disease patients
INDIANAPOLIS – Contrary to conventional wisdom, endovascular aneurysm repair (EVAR) provides outcomes superior to those achieved with open surgical repair of abdominal aortic aneurysm in patients with chronic renal insufficiency, a large study indicates.
"EVAR should be the first-line therapy in the patient with chronic renal insufficiency when the patient has the appropriate anatomy. However, in patients with severe renal impairment, a higher threshold should be applied for repair because the risks of both open repair and EVAR are significantly higher," Dr. Bao-Ngoc H. Nguyen declared at the annual meeting of the American Surgical Association.
"Chronic renal failure is quite prevalent in patients with abdominal aortic aneurysm: up to 30%. It is quite worrisome because any further decline in renal function in these patients could push them toward dialysis. More than that, postoperative renal failure is a predictor for early and late mortality," noted Dr. Nguyen of George Washington University, Washington.
She presented a retrospective study in patients with abdominal aortic aneurysm and chronic kidney disease. The aim, she explained, was to answer a key question: "Which one of these two treatment modalities is the lesser of two evils?"
For answers, Dr. Nguyen and coinvestigators turned to the American College of Surgeons National Quality Improvement Program (NSQIP) database for 2005-2010. They identified 3,523 patients with moderate chronic renal insufficiency, defined as an estimated glomerular filtration rate (eGFR) of 30-60 mL/minute, who underwent EVAR for abdominal aortic aneurysm and 1,117 treated via open surgical repair. Another 363 EVAR patients had severe chronic renal insufficiency, with an eGFR of less than 30 mL/minute, as did 139 patients who underwent open repair. Vascular surgeons performed all procedures in this study.
Patients with moderate renal insufficiency who underwent EVAR had markedly lower 30-day rates of mortality, pulmonary complications, cardiovascular events, and postoperative renal dysfunction, including acute kidney injury, than did those who had open surgical repair. One or more adverse events occurred in 6% of the EVAR group, compared with 24.1% of open repair patients. In a multivariate analysis controlled for preoperative differences in the patient groups, those undergoing open repair had an adjusted 4.1-fold greater risk of mortality as well as a 2.2-fold increased risk of cardiovascular events, a 4.2-fold increased risk of renal deterioration including a 5.2-fold greater risk of dialysis, and additional hazards.
In contrast, among the much smaller population of patients with baseline severe chronic renal insufficiency, there was no significant difference between the two treatment groups in terms of 30-day mortality, postoperative renal deterioration, or cardiovascular complications, although pulmonary complications were an adjusted fivefold more likely in the open surgery than among EVAR patients. Of note, rates of all adverse outcomes were markedly higher in both groups than in those with moderate chronic renal insufficiency, such that one or more adverse events occurred in 16.9% of EVAR patients and 42.5% of the open repair patients with severe chronic renal insufficiency.
Discussant Dr. Michael Watkins commented that this study has one glaring shortcoming resulting from a limitation of the NSQIP database.
While NSQIP contains only validated data entered by unbiased, well-trained professionals and NSQIP is "far superior" to the various administrative databases commonly used in evaluating outcomes, it doesn’t include key details about patients’ presenting anatomy, observed Dr. Watkins, director of the vascular research laboratory at Massachusetts General Hospital, Boston.
"Was the anatomy really similar in the two groups, or were patients who underwent open repair not candidates for EVAR?" he asked.
Dr. Nguyen conceded that this constitutes a major study limitation, adding that she agrees with Dr. Watkins that anatomy should be the first and foremost factor considered in deciding upon the surgical approach in abdominal aortic aneurysm repair.
She reported having no financial conflicts.
INDIANAPOLIS – Contrary to conventional wisdom, endovascular aneurysm repair (EVAR) provides outcomes superior to those achieved with open surgical repair of abdominal aortic aneurysm in patients with chronic renal insufficiency, a large study indicates.
"EVAR should be the first-line therapy in the patient with chronic renal insufficiency when the patient has the appropriate anatomy. However, in patients with severe renal impairment, a higher threshold should be applied for repair because the risks of both open repair and EVAR are significantly higher," Dr. Bao-Ngoc H. Nguyen declared at the annual meeting of the American Surgical Association.
"Chronic renal failure is quite prevalent in patients with abdominal aortic aneurysm: up to 30%. It is quite worrisome because any further decline in renal function in these patients could push them toward dialysis. More than that, postoperative renal failure is a predictor for early and late mortality," noted Dr. Nguyen of George Washington University, Washington.
She presented a retrospective study in patients with abdominal aortic aneurysm and chronic kidney disease. The aim, she explained, was to answer a key question: "Which one of these two treatment modalities is the lesser of two evils?"
For answers, Dr. Nguyen and coinvestigators turned to the American College of Surgeons National Quality Improvement Program (NSQIP) database for 2005-2010. They identified 3,523 patients with moderate chronic renal insufficiency, defined as an estimated glomerular filtration rate (eGFR) of 30-60 mL/minute, who underwent EVAR for abdominal aortic aneurysm and 1,117 treated via open surgical repair. Another 363 EVAR patients had severe chronic renal insufficiency, with an eGFR of less than 30 mL/minute, as did 139 patients who underwent open repair. Vascular surgeons performed all procedures in this study.
Patients with moderate renal insufficiency who underwent EVAR had markedly lower 30-day rates of mortality, pulmonary complications, cardiovascular events, and postoperative renal dysfunction, including acute kidney injury, than did those who had open surgical repair. One or more adverse events occurred in 6% of the EVAR group, compared with 24.1% of open repair patients. In a multivariate analysis controlled for preoperative differences in the patient groups, those undergoing open repair had an adjusted 4.1-fold greater risk of mortality as well as a 2.2-fold increased risk of cardiovascular events, a 4.2-fold increased risk of renal deterioration including a 5.2-fold greater risk of dialysis, and additional hazards.
In contrast, among the much smaller population of patients with baseline severe chronic renal insufficiency, there was no significant difference between the two treatment groups in terms of 30-day mortality, postoperative renal deterioration, or cardiovascular complications, although pulmonary complications were an adjusted fivefold more likely in the open surgery than among EVAR patients. Of note, rates of all adverse outcomes were markedly higher in both groups than in those with moderate chronic renal insufficiency, such that one or more adverse events occurred in 16.9% of EVAR patients and 42.5% of the open repair patients with severe chronic renal insufficiency.
Discussant Dr. Michael Watkins commented that this study has one glaring shortcoming resulting from a limitation of the NSQIP database.
While NSQIP contains only validated data entered by unbiased, well-trained professionals and NSQIP is "far superior" to the various administrative databases commonly used in evaluating outcomes, it doesn’t include key details about patients’ presenting anatomy, observed Dr. Watkins, director of the vascular research laboratory at Massachusetts General Hospital, Boston.
"Was the anatomy really similar in the two groups, or were patients who underwent open repair not candidates for EVAR?" he asked.
Dr. Nguyen conceded that this constitutes a major study limitation, adding that she agrees with Dr. Watkins that anatomy should be the first and foremost factor considered in deciding upon the surgical approach in abdominal aortic aneurysm repair.
She reported having no financial conflicts.
INDIANAPOLIS – Contrary to conventional wisdom, endovascular aneurysm repair (EVAR) provides outcomes superior to those achieved with open surgical repair of abdominal aortic aneurysm in patients with chronic renal insufficiency, a large study indicates.
"EVAR should be the first-line therapy in the patient with chronic renal insufficiency when the patient has the appropriate anatomy. However, in patients with severe renal impairment, a higher threshold should be applied for repair because the risks of both open repair and EVAR are significantly higher," Dr. Bao-Ngoc H. Nguyen declared at the annual meeting of the American Surgical Association.
"Chronic renal failure is quite prevalent in patients with abdominal aortic aneurysm: up to 30%. It is quite worrisome because any further decline in renal function in these patients could push them toward dialysis. More than that, postoperative renal failure is a predictor for early and late mortality," noted Dr. Nguyen of George Washington University, Washington.
She presented a retrospective study in patients with abdominal aortic aneurysm and chronic kidney disease. The aim, she explained, was to answer a key question: "Which one of these two treatment modalities is the lesser of two evils?"
For answers, Dr. Nguyen and coinvestigators turned to the American College of Surgeons National Quality Improvement Program (NSQIP) database for 2005-2010. They identified 3,523 patients with moderate chronic renal insufficiency, defined as an estimated glomerular filtration rate (eGFR) of 30-60 mL/minute, who underwent EVAR for abdominal aortic aneurysm and 1,117 treated via open surgical repair. Another 363 EVAR patients had severe chronic renal insufficiency, with an eGFR of less than 30 mL/minute, as did 139 patients who underwent open repair. Vascular surgeons performed all procedures in this study.
Patients with moderate renal insufficiency who underwent EVAR had markedly lower 30-day rates of mortality, pulmonary complications, cardiovascular events, and postoperative renal dysfunction, including acute kidney injury, than did those who had open surgical repair. One or more adverse events occurred in 6% of the EVAR group, compared with 24.1% of open repair patients. In a multivariate analysis controlled for preoperative differences in the patient groups, those undergoing open repair had an adjusted 4.1-fold greater risk of mortality as well as a 2.2-fold increased risk of cardiovascular events, a 4.2-fold increased risk of renal deterioration including a 5.2-fold greater risk of dialysis, and additional hazards.
In contrast, among the much smaller population of patients with baseline severe chronic renal insufficiency, there was no significant difference between the two treatment groups in terms of 30-day mortality, postoperative renal deterioration, or cardiovascular complications, although pulmonary complications were an adjusted fivefold more likely in the open surgery than among EVAR patients. Of note, rates of all adverse outcomes were markedly higher in both groups than in those with moderate chronic renal insufficiency, such that one or more adverse events occurred in 16.9% of EVAR patients and 42.5% of the open repair patients with severe chronic renal insufficiency.
Discussant Dr. Michael Watkins commented that this study has one glaring shortcoming resulting from a limitation of the NSQIP database.
While NSQIP contains only validated data entered by unbiased, well-trained professionals and NSQIP is "far superior" to the various administrative databases commonly used in evaluating outcomes, it doesn’t include key details about patients’ presenting anatomy, observed Dr. Watkins, director of the vascular research laboratory at Massachusetts General Hospital, Boston.
"Was the anatomy really similar in the two groups, or were patients who underwent open repair not candidates for EVAR?" he asked.
Dr. Nguyen conceded that this constitutes a major study limitation, adding that she agrees with Dr. Watkins that anatomy should be the first and foremost factor considered in deciding upon the surgical approach in abdominal aortic aneurysm repair.
She reported having no financial conflicts.
AT THE ASA ANNUAL MEETING
Major Finding: Patients with moderate chronic renal insufficiency who underwent open surgical repair of abdominal aortic aneurysm had a 4.2-fold greater risk of postoperative renal deterioration than did those who had an endovascular aneurysm repair.
Data Source: A retrospective study of a large national surgical database.
Disclosures: The presenter reported having no conflicts of interest.
Surgical educators flag training gaps
INDIANAPOLIS – The nation’s elite surgical educators are up in arms over reported widespread deficiencies in the skill set and judgment of recent graduates of 5-year general surgery residencies.
The source of their ire is a detailed new survey of the nation’s subspecialty fellowship program directors. Today 80% of graduating general surgery residents seek these year-long fellowships to obtain advanced training in bariatric, colorectal, thoracic, hepatobiliary, or other surgical areas. The surveyed program directors indicated many trainees arrive unprepared in essential areas.
"Many new fellows must gain basic and fundamental skills at the beginning of their fellowship before they can commence to benefit from the advanced skills that they originally came to obtain. The current high demand for fellowship training and the lack of readiness upon completion of general surgery residencies should be a call to action for all stakeholders in surgical training," Dr. Samer Mattar declared in presenting the survey results at the annual meeting of the American Surgical Association.
The survey was conducted by the Fellowship Council, an umbrella organization in charge of standardizing curricula, accrediting programs, and matching residents to fellowships. The group distributed the surveys to all 145 subspecialty fellowship program directors and drew a 63% response rate. That’s considered high for such a lengthy survey and is an indication of the importance educators place on the subject matter, said Dr. Mattar of Indiana University, Indianapolis.
The survey assessed five key educational domains: professionalism, independent practice, psychomotor skills, expertise in their chosen disease state, and scholarly focus.
"Incoming fellows exhibited high levels of professionalism, but there were deficiencies in autonomy and independence, psychomotor abilities, and – most profoundly – academics and scholarship," Dr. Mattar noted in summarizing the survey results.
The underlying theme of the responses is that many fellows are pursuing fellowship positions to make up for inadequacies in their residency rather than to push their skills to the next level. Among the key survey findings:
• Forty-three percent of program directors felt incoming fellows were unable to independently perform half an hour of a major procedure.
• Thirty percent of incoming fellows couldn’t independently perform basic operations such as laparoscopic cholecystectomy.
• Fifty-six percent were unable to laparoscopically suture and tie knots properly, and 26% couldn’t recognize anatomic planes through the laparoscope.
• One-quarter were deemed unable to recognize early signs of complications.
• Nearly 40% of program directors said new fellows display a lack of "patient ownership." "We promote patient ownership in our programs. We are somewhat disappointed and dismayed that the fellows feel that the patient is part of a service and not their own," Dr. Mattar commented.
• Only 51% of program directors indicated their incoming fellows demonstrated independence in the operating room and on call, although fellows did show marked improvement in these areas as the year went on.
• A large majority of program directors thought their fellows were disinterested in research and advancing the field, even though, as Dr. Mattar noted, "This is a mandate in our curriculum."
Discussant Dr. Michael G. Sarr was blunt: "This is a scary situation."
"There’s a clear message here from this study: We have a problem. I maintain that we have to stop being bullied by naive, public, politically driven agendas and by some of our own graybeard pundits – and I think we all know who those groups are – and once again take over the control of educating our successors," said Dr. Sarr, professor of surgery at the Mayo Medical School, Rochester, Minn.
He attributed the decline in graduating general surgery residents’ technical skills, patient ownership, and ability to function as trustworthy independent surgeons in large part to the mandated 80-hour maximum work week.
"We all admit and acknowledge that prior to the duty hours reduction of 2003, the expected duty hours most of us trained in were barbaric and often dangerous, and they involved too much scut work. But in the past the final product was superb," Dr. Sarr recalled.
He argued that while it would be folly to return to those days, some flexibility regarding the work hours limit would be beneficial.
"Should our politically driven ACGME [Accreditation Council for Graduate Medical Education] and our own RRC [Residency Review Committee] – yes, our own elected overseeing organization – liberalize its rigid, unbending, stringent rules to allow our residents to make more liberal decisions and to develop professionalism by exceeding their 80-hour work restriction when clinical situations demand their presence?" he asked.
Discussant Dr. Frank R. Lewis, executive director of the American Board of Surgery, said that even though the 80-hour work limit has effectively subtracted 6-12 months from the general surgery residency, he doesn’t believe this emotional and contentious issue is the main problem. He noted that at present the average number of operations done by a first-year resident is less than two per week, while second-year residents average only two to three per week.
"Our residents are spending 80 hours a week while doing two or three operations per week, which arguably could be done in half a day. It would be hard to imagine a less efficient educational process," Dr. Lewis complained.
He added that nobody should be surprised by the Fellowship Council survey results. During the past decade the failure rate on the American Board of Surgery’s oral exam has climbed steadily from 16% to 28%. At present the percentage of examinees who fail either the oral or written ABS exam the first time around is in the mid-30s.
"That’s arguably an absurd failure rate for a 5-year training program in a group of people who should have mastered the subject," the surgeon added.
He asserted that most of the factors responsible for the decline in the competence of graduating general surgery residents are beyond the control of academic surgeons. These factors include the gutting of surgical clerkship opportunities in the fourth year of medical school, along with changes in the surgical landscape that have caused once-popular operations to essentially go away due to technical advances or improved drug therapy.
Discussant Dr. Mark A. Malangoni, associate executive director of the ABS, noted that the more complex open surgery operations previously done by general surgery residents have in many cases been converted to complex laparoscopic procedures that have become the purview of the subspecialty fellowships. Why not abolish the fellowships and drive all those interesting cases and that dedicated training effort back into the residency years? he asked.
That’s not going to happen, Dr. Mattar replied, citing the huge market demand and need for these fellowships.
"They’re very rewarding to all stakeholders," he added.
But constructive changes are afoot, according to Dr. Mattar. Plans are well underway to change the fourth year of medical school so that students interested in a career in surgery can begin to prepare for it then. And there are also efforts to custom-tailor the final year of general surgery residency so that residents can prepare for their fellowship year. Toward that end the Fellowship Council has moved the fellowship match date up to June so residents who know they are fellowship bound can put their fifth year to the best use.
The survey was conducted by the Fellowship Council, an umbrella organization with oversight over surgical subspecialty fellowships. Dr. Mattar reported having no financial conflicts.
INDIANAPOLIS – The nation’s elite surgical educators are up in arms over reported widespread deficiencies in the skill set and judgment of recent graduates of 5-year general surgery residencies.
The source of their ire is a detailed new survey of the nation’s subspecialty fellowship program directors. Today 80% of graduating general surgery residents seek these year-long fellowships to obtain advanced training in bariatric, colorectal, thoracic, hepatobiliary, or other surgical areas. The surveyed program directors indicated many trainees arrive unprepared in essential areas.
"Many new fellows must gain basic and fundamental skills at the beginning of their fellowship before they can commence to benefit from the advanced skills that they originally came to obtain. The current high demand for fellowship training and the lack of readiness upon completion of general surgery residencies should be a call to action for all stakeholders in surgical training," Dr. Samer Mattar declared in presenting the survey results at the annual meeting of the American Surgical Association.
The survey was conducted by the Fellowship Council, an umbrella organization in charge of standardizing curricula, accrediting programs, and matching residents to fellowships. The group distributed the surveys to all 145 subspecialty fellowship program directors and drew a 63% response rate. That’s considered high for such a lengthy survey and is an indication of the importance educators place on the subject matter, said Dr. Mattar of Indiana University, Indianapolis.
The survey assessed five key educational domains: professionalism, independent practice, psychomotor skills, expertise in their chosen disease state, and scholarly focus.
"Incoming fellows exhibited high levels of professionalism, but there were deficiencies in autonomy and independence, psychomotor abilities, and – most profoundly – academics and scholarship," Dr. Mattar noted in summarizing the survey results.
The underlying theme of the responses is that many fellows are pursuing fellowship positions to make up for inadequacies in their residency rather than to push their skills to the next level. Among the key survey findings:
• Forty-three percent of program directors felt incoming fellows were unable to independently perform half an hour of a major procedure.
• Thirty percent of incoming fellows couldn’t independently perform basic operations such as laparoscopic cholecystectomy.
• Fifty-six percent were unable to laparoscopically suture and tie knots properly, and 26% couldn’t recognize anatomic planes through the laparoscope.
• One-quarter were deemed unable to recognize early signs of complications.
• Nearly 40% of program directors said new fellows display a lack of "patient ownership." "We promote patient ownership in our programs. We are somewhat disappointed and dismayed that the fellows feel that the patient is part of a service and not their own," Dr. Mattar commented.
• Only 51% of program directors indicated their incoming fellows demonstrated independence in the operating room and on call, although fellows did show marked improvement in these areas as the year went on.
• A large majority of program directors thought their fellows were disinterested in research and advancing the field, even though, as Dr. Mattar noted, "This is a mandate in our curriculum."
Discussant Dr. Michael G. Sarr was blunt: "This is a scary situation."
"There’s a clear message here from this study: We have a problem. I maintain that we have to stop being bullied by naive, public, politically driven agendas and by some of our own graybeard pundits – and I think we all know who those groups are – and once again take over the control of educating our successors," said Dr. Sarr, professor of surgery at the Mayo Medical School, Rochester, Minn.
He attributed the decline in graduating general surgery residents’ technical skills, patient ownership, and ability to function as trustworthy independent surgeons in large part to the mandated 80-hour maximum work week.
"We all admit and acknowledge that prior to the duty hours reduction of 2003, the expected duty hours most of us trained in were barbaric and often dangerous, and they involved too much scut work. But in the past the final product was superb," Dr. Sarr recalled.
He argued that while it would be folly to return to those days, some flexibility regarding the work hours limit would be beneficial.
"Should our politically driven ACGME [Accreditation Council for Graduate Medical Education] and our own RRC [Residency Review Committee] – yes, our own elected overseeing organization – liberalize its rigid, unbending, stringent rules to allow our residents to make more liberal decisions and to develop professionalism by exceeding their 80-hour work restriction when clinical situations demand their presence?" he asked.
Discussant Dr. Frank R. Lewis, executive director of the American Board of Surgery, said that even though the 80-hour work limit has effectively subtracted 6-12 months from the general surgery residency, he doesn’t believe this emotional and contentious issue is the main problem. He noted that at present the average number of operations done by a first-year resident is less than two per week, while second-year residents average only two to three per week.
"Our residents are spending 80 hours a week while doing two or three operations per week, which arguably could be done in half a day. It would be hard to imagine a less efficient educational process," Dr. Lewis complained.
He added that nobody should be surprised by the Fellowship Council survey results. During the past decade the failure rate on the American Board of Surgery’s oral exam has climbed steadily from 16% to 28%. At present the percentage of examinees who fail either the oral or written ABS exam the first time around is in the mid-30s.
"That’s arguably an absurd failure rate for a 5-year training program in a group of people who should have mastered the subject," the surgeon added.
He asserted that most of the factors responsible for the decline in the competence of graduating general surgery residents are beyond the control of academic surgeons. These factors include the gutting of surgical clerkship opportunities in the fourth year of medical school, along with changes in the surgical landscape that have caused once-popular operations to essentially go away due to technical advances or improved drug therapy.
Discussant Dr. Mark A. Malangoni, associate executive director of the ABS, noted that the more complex open surgery operations previously done by general surgery residents have in many cases been converted to complex laparoscopic procedures that have become the purview of the subspecialty fellowships. Why not abolish the fellowships and drive all those interesting cases and that dedicated training effort back into the residency years? he asked.
That’s not going to happen, Dr. Mattar replied, citing the huge market demand and need for these fellowships.
"They’re very rewarding to all stakeholders," he added.
But constructive changes are afoot, according to Dr. Mattar. Plans are well underway to change the fourth year of medical school so that students interested in a career in surgery can begin to prepare for it then. And there are also efforts to custom-tailor the final year of general surgery residency so that residents can prepare for their fellowship year. Toward that end the Fellowship Council has moved the fellowship match date up to June so residents who know they are fellowship bound can put their fifth year to the best use.
The survey was conducted by the Fellowship Council, an umbrella organization with oversight over surgical subspecialty fellowships. Dr. Mattar reported having no financial conflicts.
INDIANAPOLIS – The nation’s elite surgical educators are up in arms over reported widespread deficiencies in the skill set and judgment of recent graduates of 5-year general surgery residencies.
The source of their ire is a detailed new survey of the nation’s subspecialty fellowship program directors. Today 80% of graduating general surgery residents seek these year-long fellowships to obtain advanced training in bariatric, colorectal, thoracic, hepatobiliary, or other surgical areas. The surveyed program directors indicated many trainees arrive unprepared in essential areas.
"Many new fellows must gain basic and fundamental skills at the beginning of their fellowship before they can commence to benefit from the advanced skills that they originally came to obtain. The current high demand for fellowship training and the lack of readiness upon completion of general surgery residencies should be a call to action for all stakeholders in surgical training," Dr. Samer Mattar declared in presenting the survey results at the annual meeting of the American Surgical Association.
The survey was conducted by the Fellowship Council, an umbrella organization in charge of standardizing curricula, accrediting programs, and matching residents to fellowships. The group distributed the surveys to all 145 subspecialty fellowship program directors and drew a 63% response rate. That’s considered high for such a lengthy survey and is an indication of the importance educators place on the subject matter, said Dr. Mattar of Indiana University, Indianapolis.
The survey assessed five key educational domains: professionalism, independent practice, psychomotor skills, expertise in their chosen disease state, and scholarly focus.
"Incoming fellows exhibited high levels of professionalism, but there were deficiencies in autonomy and independence, psychomotor abilities, and – most profoundly – academics and scholarship," Dr. Mattar noted in summarizing the survey results.
The underlying theme of the responses is that many fellows are pursuing fellowship positions to make up for inadequacies in their residency rather than to push their skills to the next level. Among the key survey findings:
• Forty-three percent of program directors felt incoming fellows were unable to independently perform half an hour of a major procedure.
• Thirty percent of incoming fellows couldn’t independently perform basic operations such as laparoscopic cholecystectomy.
• Fifty-six percent were unable to laparoscopically suture and tie knots properly, and 26% couldn’t recognize anatomic planes through the laparoscope.
• One-quarter were deemed unable to recognize early signs of complications.
• Nearly 40% of program directors said new fellows display a lack of "patient ownership." "We promote patient ownership in our programs. We are somewhat disappointed and dismayed that the fellows feel that the patient is part of a service and not their own," Dr. Mattar commented.
• Only 51% of program directors indicated their incoming fellows demonstrated independence in the operating room and on call, although fellows did show marked improvement in these areas as the year went on.
• A large majority of program directors thought their fellows were disinterested in research and advancing the field, even though, as Dr. Mattar noted, "This is a mandate in our curriculum."
Discussant Dr. Michael G. Sarr was blunt: "This is a scary situation."
"There’s a clear message here from this study: We have a problem. I maintain that we have to stop being bullied by naive, public, politically driven agendas and by some of our own graybeard pundits – and I think we all know who those groups are – and once again take over the control of educating our successors," said Dr. Sarr, professor of surgery at the Mayo Medical School, Rochester, Minn.
He attributed the decline in graduating general surgery residents’ technical skills, patient ownership, and ability to function as trustworthy independent surgeons in large part to the mandated 80-hour maximum work week.
"We all admit and acknowledge that prior to the duty hours reduction of 2003, the expected duty hours most of us trained in were barbaric and often dangerous, and they involved too much scut work. But in the past the final product was superb," Dr. Sarr recalled.
He argued that while it would be folly to return to those days, some flexibility regarding the work hours limit would be beneficial.
"Should our politically driven ACGME [Accreditation Council for Graduate Medical Education] and our own RRC [Residency Review Committee] – yes, our own elected overseeing organization – liberalize its rigid, unbending, stringent rules to allow our residents to make more liberal decisions and to develop professionalism by exceeding their 80-hour work restriction when clinical situations demand their presence?" he asked.
Discussant Dr. Frank R. Lewis, executive director of the American Board of Surgery, said that even though the 80-hour work limit has effectively subtracted 6-12 months from the general surgery residency, he doesn’t believe this emotional and contentious issue is the main problem. He noted that at present the average number of operations done by a first-year resident is less than two per week, while second-year residents average only two to three per week.
"Our residents are spending 80 hours a week while doing two or three operations per week, which arguably could be done in half a day. It would be hard to imagine a less efficient educational process," Dr. Lewis complained.
He added that nobody should be surprised by the Fellowship Council survey results. During the past decade the failure rate on the American Board of Surgery’s oral exam has climbed steadily from 16% to 28%. At present the percentage of examinees who fail either the oral or written ABS exam the first time around is in the mid-30s.
"That’s arguably an absurd failure rate for a 5-year training program in a group of people who should have mastered the subject," the surgeon added.
He asserted that most of the factors responsible for the decline in the competence of graduating general surgery residents are beyond the control of academic surgeons. These factors include the gutting of surgical clerkship opportunities in the fourth year of medical school, along with changes in the surgical landscape that have caused once-popular operations to essentially go away due to technical advances or improved drug therapy.
Discussant Dr. Mark A. Malangoni, associate executive director of the ABS, noted that the more complex open surgery operations previously done by general surgery residents have in many cases been converted to complex laparoscopic procedures that have become the purview of the subspecialty fellowships. Why not abolish the fellowships and drive all those interesting cases and that dedicated training effort back into the residency years? he asked.
That’s not going to happen, Dr. Mattar replied, citing the huge market demand and need for these fellowships.
"They’re very rewarding to all stakeholders," he added.
But constructive changes are afoot, according to Dr. Mattar. Plans are well underway to change the fourth year of medical school so that students interested in a career in surgery can begin to prepare for it then. And there are also efforts to custom-tailor the final year of general surgery residency so that residents can prepare for their fellowship year. Toward that end the Fellowship Council has moved the fellowship match date up to June so residents who know they are fellowship bound can put their fifth year to the best use.
The survey was conducted by the Fellowship Council, an umbrella organization with oversight over surgical subspecialty fellowships. Dr. Mattar reported having no financial conflicts.
AT THE ASA ANNUAL MEETING
Major finding: Forty-three percent of incoming fellows in the nation’s surgical subspecialty programs were deemed by their program directors to be unable to independently perform half an hour of a major procedure.
Data source: A survey of the nation’s 145 surgical subspecialty program directors. It drew responses from 91 (63%).
Disclosures: The survey was conducted by the Fellowship Council, an umbrella organization with oversight over surgical subspecialty fellowships. Dr. Mattar reported having no financial conflicts.