User login
Rebecca Gottesman, MD, PhD
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Redefine dysplastic nevi to stratify cancer risk
WAILEA, HAWAII – It is time for a new system of classifying nevi, according to Ashfaq Marghoob, MD, of Memorial Sloan Kettering Cancer Center, New York.
“It was known for the last 30 or 40 years that we do need to subclassify nevi into groups, so as to better stratify for melanoma risk,” identifying groups of individuals who would benefit most from targeted screening, Dr. Marghoob said in a video interview at the meeting, provided by Global Academy for Medical Education/Skin Disease Education Foundation. But it has been clear that there are many flaws in the current classification system, he added.
This is beginning to change as new data emerge about gene mutations and other science that can better stratify “or segregate” the nevi into subsets, and “the hope is we will be better able to predict which subsets are associated with melanoma risk either within the lesion itself or poses an increased risk to the patient,” he explained.
“As our understanding grows, we will start to come out with subsets of nevi that have a certain clinical and dermoscopic morphology,” to help predict which patients would benefit most from being monitored very closely, with the aim of detecting – and curing – melanomas early, said Dr. Marghoob, director of Memorial Sloan Kettering’s regional skin cancer clinic in Hauppauge, N.Y.
He had no financial conflicts to disclose.
SDEF and this news organization are owned by the same parent organization.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – It is time for a new system of classifying nevi, according to Ashfaq Marghoob, MD, of Memorial Sloan Kettering Cancer Center, New York.
“It was known for the last 30 or 40 years that we do need to subclassify nevi into groups, so as to better stratify for melanoma risk,” identifying groups of individuals who would benefit most from targeted screening, Dr. Marghoob said in a video interview at the meeting, provided by Global Academy for Medical Education/Skin Disease Education Foundation. But it has been clear that there are many flaws in the current classification system, he added.
This is beginning to change as new data emerge about gene mutations and other science that can better stratify “or segregate” the nevi into subsets, and “the hope is we will be better able to predict which subsets are associated with melanoma risk either within the lesion itself or poses an increased risk to the patient,” he explained.
“As our understanding grows, we will start to come out with subsets of nevi that have a certain clinical and dermoscopic morphology,” to help predict which patients would benefit most from being monitored very closely, with the aim of detecting – and curing – melanomas early, said Dr. Marghoob, director of Memorial Sloan Kettering’s regional skin cancer clinic in Hauppauge, N.Y.
He had no financial conflicts to disclose.
SDEF and this news organization are owned by the same parent organization.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – It is time for a new system of classifying nevi, according to Ashfaq Marghoob, MD, of Memorial Sloan Kettering Cancer Center, New York.
“It was known for the last 30 or 40 years that we do need to subclassify nevi into groups, so as to better stratify for melanoma risk,” identifying groups of individuals who would benefit most from targeted screening, Dr. Marghoob said in a video interview at the meeting, provided by Global Academy for Medical Education/Skin Disease Education Foundation. But it has been clear that there are many flaws in the current classification system, he added.
This is beginning to change as new data emerge about gene mutations and other science that can better stratify “or segregate” the nevi into subsets, and “the hope is we will be better able to predict which subsets are associated with melanoma risk either within the lesion itself or poses an increased risk to the patient,” he explained.
“As our understanding grows, we will start to come out with subsets of nevi that have a certain clinical and dermoscopic morphology,” to help predict which patients would benefit most from being monitored very closely, with the aim of detecting – and curing – melanomas early, said Dr. Marghoob, director of Memorial Sloan Kettering’s regional skin cancer clinic in Hauppauge, N.Y.
He had no financial conflicts to disclose.
SDEF and this news organization are owned by the same parent organization.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT SDEF HAWAII DERMATOLOGY SEMINAR
VIDEO: Molecular testing helps pinpoint ambiguous lesions
WAILEA, HAWAII – In a video interview, Pedram Gerami, MD, professor of dermatology, pathology, and pediatrics, Northwestern University, Chicago, discusses the use of molecular testing for melanoma and suspicious lesions.
Molecular tests are available for various components of diagnosis and prognosis of melanoma, and one of the most popular scenarios for their use is to confirm a diagnosis if a lesion is biopsied and the histopathologist “feels that the diagnosis is ambiguous by standard pathology methods,” Dr. Gerami said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
On average, between 1% and 5% of cases of suspicious lesions may need molecular testing to confirm the diagnosis, he noted. Of the available options for molecular testing, FISH (fluorescence in situ hybridization) testing is the most validated in the setting of ambiguous histology, he said.
Dr. Gerami disclosed serving as a consultant and researcher for Castle Biosciences, Myriad Genetics, and DermTech.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – In a video interview, Pedram Gerami, MD, professor of dermatology, pathology, and pediatrics, Northwestern University, Chicago, discusses the use of molecular testing for melanoma and suspicious lesions.
Molecular tests are available for various components of diagnosis and prognosis of melanoma, and one of the most popular scenarios for their use is to confirm a diagnosis if a lesion is biopsied and the histopathologist “feels that the diagnosis is ambiguous by standard pathology methods,” Dr. Gerami said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
On average, between 1% and 5% of cases of suspicious lesions may need molecular testing to confirm the diagnosis, he noted. Of the available options for molecular testing, FISH (fluorescence in situ hybridization) testing is the most validated in the setting of ambiguous histology, he said.
Dr. Gerami disclosed serving as a consultant and researcher for Castle Biosciences, Myriad Genetics, and DermTech.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – In a video interview, Pedram Gerami, MD, professor of dermatology, pathology, and pediatrics, Northwestern University, Chicago, discusses the use of molecular testing for melanoma and suspicious lesions.
Molecular tests are available for various components of diagnosis and prognosis of melanoma, and one of the most popular scenarios for their use is to confirm a diagnosis if a lesion is biopsied and the histopathologist “feels that the diagnosis is ambiguous by standard pathology methods,” Dr. Gerami said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
On average, between 1% and 5% of cases of suspicious lesions may need molecular testing to confirm the diagnosis, he noted. Of the available options for molecular testing, FISH (fluorescence in situ hybridization) testing is the most validated in the setting of ambiguous histology, he said.
Dr. Gerami disclosed serving as a consultant and researcher for Castle Biosciences, Myriad Genetics, and DermTech.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT SDEF HAWAII DERMATOLOGY SEMINAR
Adrenal “incidentalomas”
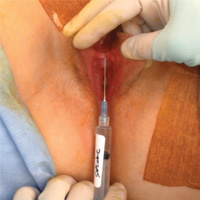
Novel classification of labial anatomy and evaluation in the treatment of labial agglutination

References
Pardo J, Sola V, Ricci P, Guillof E. Laser labioplasty of labia minora. Int J Gynaecol Obstet. 2006;93(1):38–43.
Chang P, Salisbury MA, Narsete T, Buckspan R, Derrick D, Ersek RA. Vaginal labiaplasty: defense of the simple "clip and snip" and a new classification system. Aesthetic Plast Surg. 2013;37(5): p. 887–891.
Malone DG, Clark TB, Wei N. Ultrasound-guided percutaneous injection, hydrodissection, and fenestration for carpel tunnel syndrome description of a new technique. J Appl Res. 2010;10(3):116–123.
Visit the Society of Gynecologic Surgeons online: sgsonline.org
More videos from SGS:
- Strategies for prophylactic oophoropexy
- Tips and tricks for open laparoscopy
- Complete colpectomy & colpocleisis: Model for simulation
- Natural orifice sacral colpopexy
- Alternative options for visualizing ureteral patency during intraoperative cystoscopy
- Use of suprapubic Carter-Thomason needle to assist in cystoscopic excision of an intravesical foreign object
- Uterine artery ligation: Advanced techniques and considerations for the difficult laparoscopic hysterectomy
- Cervical injection of methylene blue for identification of sentinel lymph nodes in cervical cancer
- Misplaced hysteroscopic sterilization micro-insert in the peritoneal cavity: A corpus alienum
- Laparoscopic cystectomy for large, bilateral ovarian dermoids
- Small bowel surgery for the benign gynecologist

References
Pardo J, Sola V, Ricci P, Guillof E. Laser labioplasty of labia minora. Int J Gynaecol Obstet. 2006;93(1):38–43.
Chang P, Salisbury MA, Narsete T, Buckspan R, Derrick D, Ersek RA. Vaginal labiaplasty: defense of the simple "clip and snip" and a new classification system. Aesthetic Plast Surg. 2013;37(5): p. 887–891.
Malone DG, Clark TB, Wei N. Ultrasound-guided percutaneous injection, hydrodissection, and fenestration for carpel tunnel syndrome description of a new technique. J Appl Res. 2010;10(3):116–123.
Visit the Society of Gynecologic Surgeons online: sgsonline.org
More videos from SGS:
- Strategies for prophylactic oophoropexy
- Tips and tricks for open laparoscopy
- Complete colpectomy & colpocleisis: Model for simulation
- Natural orifice sacral colpopexy
- Alternative options for visualizing ureteral patency during intraoperative cystoscopy
- Use of suprapubic Carter-Thomason needle to assist in cystoscopic excision of an intravesical foreign object
- Uterine artery ligation: Advanced techniques and considerations for the difficult laparoscopic hysterectomy
- Cervical injection of methylene blue for identification of sentinel lymph nodes in cervical cancer
- Misplaced hysteroscopic sterilization micro-insert in the peritoneal cavity: A corpus alienum
- Laparoscopic cystectomy for large, bilateral ovarian dermoids
- Small bowel surgery for the benign gynecologist

References
Pardo J, Sola V, Ricci P, Guillof E. Laser labioplasty of labia minora. Int J Gynaecol Obstet. 2006;93(1):38–43.
Chang P, Salisbury MA, Narsete T, Buckspan R, Derrick D, Ersek RA. Vaginal labiaplasty: defense of the simple "clip and snip" and a new classification system. Aesthetic Plast Surg. 2013;37(5): p. 887–891.
Malone DG, Clark TB, Wei N. Ultrasound-guided percutaneous injection, hydrodissection, and fenestration for carpel tunnel syndrome description of a new technique. J Appl Res. 2010;10(3):116–123.
Visit the Society of Gynecologic Surgeons online: sgsonline.org
More videos from SGS:
- Strategies for prophylactic oophoropexy
- Tips and tricks for open laparoscopy
- Complete colpectomy & colpocleisis: Model for simulation
- Natural orifice sacral colpopexy
- Alternative options for visualizing ureteral patency during intraoperative cystoscopy
- Use of suprapubic Carter-Thomason needle to assist in cystoscopic excision of an intravesical foreign object
- Uterine artery ligation: Advanced techniques and considerations for the difficult laparoscopic hysterectomy
- Cervical injection of methylene blue for identification of sentinel lymph nodes in cervical cancer
- Misplaced hysteroscopic sterilization micro-insert in the peritoneal cavity: A corpus alienum
- Laparoscopic cystectomy for large, bilateral ovarian dermoids
- Small bowel surgery for the benign gynecologist
This video is brought to you by
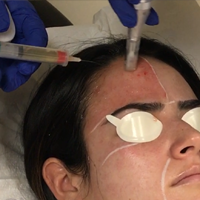
Microneedling With Platelet-Rich Plasma



A Surgeon's Intuition: Listen Before You Operate (An interview with associate editor, Brian J. Cole, MD)
In this DocThoughts interview, The American Journal of Orthopedics' associate editor, Dr. Cole, delves into the mind of a surgeon and gives insight into the surgical decision making process for his athletes.
In this DocThoughts interview, The American Journal of Orthopedics' associate editor, Dr. Cole, delves into the mind of a surgeon and gives insight into the surgical decision making process for his athletes.
In this DocThoughts interview, The American Journal of Orthopedics' associate editor, Dr. Cole, delves into the mind of a surgeon and gives insight into the surgical decision making process for his athletes.
VIDEO: Distinctive features define pediatric psoriasis
WAILEA, HAWAII – Plaque type psoriasis continues to be the most common type of psoriasis in children, but there are other presentations that should be considered, said Wynnis Tom, MD, a pediatric dermatologist at the University of California, San Diego, and Rady Children’s Hospital, San Diego.
“We certainly see a form of what some people would call napkin dermatitis,” or “diaper psoriasis,” affecting the diaper area in young infants, Dr. Tom said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
So when a child has a more refractory diaper rash, “look around to see if there are other lesions in the surrounding area that might be more typical for psoriasis,” she noted.
“We also see a lot more guttate disease” in children with psoriasis, which is more likely to be related to infections and triggers, Dr. Tom said. The face and scalp are often affected in children, and it is important to attend to these areas early to help avoid social stigma, she added.
Dr. Tom disclosed financial relationships with companies including Celgene, Janssen, and Promius. SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – Plaque type psoriasis continues to be the most common type of psoriasis in children, but there are other presentations that should be considered, said Wynnis Tom, MD, a pediatric dermatologist at the University of California, San Diego, and Rady Children’s Hospital, San Diego.
“We certainly see a form of what some people would call napkin dermatitis,” or “diaper psoriasis,” affecting the diaper area in young infants, Dr. Tom said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
So when a child has a more refractory diaper rash, “look around to see if there are other lesions in the surrounding area that might be more typical for psoriasis,” she noted.
“We also see a lot more guttate disease” in children with psoriasis, which is more likely to be related to infections and triggers, Dr. Tom said. The face and scalp are often affected in children, and it is important to attend to these areas early to help avoid social stigma, she added.
Dr. Tom disclosed financial relationships with companies including Celgene, Janssen, and Promius. SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – Plaque type psoriasis continues to be the most common type of psoriasis in children, but there are other presentations that should be considered, said Wynnis Tom, MD, a pediatric dermatologist at the University of California, San Diego, and Rady Children’s Hospital, San Diego.
“We certainly see a form of what some people would call napkin dermatitis,” or “diaper psoriasis,” affecting the diaper area in young infants, Dr. Tom said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
So when a child has a more refractory diaper rash, “look around to see if there are other lesions in the surrounding area that might be more typical for psoriasis,” she noted.
“We also see a lot more guttate disease” in children with psoriasis, which is more likely to be related to infections and triggers, Dr. Tom said. The face and scalp are often affected in children, and it is important to attend to these areas early to help avoid social stigma, she added.
Dr. Tom disclosed financial relationships with companies including Celgene, Janssen, and Promius. SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT SDEF HAWAII DERMATOLOGY SEMINAR
VIDEO: Dosing an important consideration when using neuromodulators in men
WAILEA, HAWAII – Using larger doses and avoiding overarching of the brows are among the considerations to keep in mind when using neuromodulators in men, advised Canadian dermatologist Katie Beleznay, MD.
In general, men have a very different anatomy with a different brow position, and have needs different from those of women, said Dr. Beleznay of the University of British Columbia, Vancouver.
One secret for successful injections of toxins in male patients: Dose matters. Men have stronger muscles in the face and need larger doses to overcome their muscular strength, Dr. Beleznay said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
On average, “if you use 20-30 units in a female glabella, maybe you’d use 40-50, maybe even 60 units in a male patient,” she said. However, the volume depends on the strength of the muscles in the area, and some men may need less to avoid a frozen look. “You can always treat less and bring them back in a couple of weeks and add more,” especially with patients who are new to treatment, Dr. Beleznay noted.
She disclosed financial relationships with Allergan, Revance, Evolus, Galderma, and Zeltiq.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – Using larger doses and avoiding overarching of the brows are among the considerations to keep in mind when using neuromodulators in men, advised Canadian dermatologist Katie Beleznay, MD.
In general, men have a very different anatomy with a different brow position, and have needs different from those of women, said Dr. Beleznay of the University of British Columbia, Vancouver.
One secret for successful injections of toxins in male patients: Dose matters. Men have stronger muscles in the face and need larger doses to overcome their muscular strength, Dr. Beleznay said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
On average, “if you use 20-30 units in a female glabella, maybe you’d use 40-50, maybe even 60 units in a male patient,” she said. However, the volume depends on the strength of the muscles in the area, and some men may need less to avoid a frozen look. “You can always treat less and bring them back in a couple of weeks and add more,” especially with patients who are new to treatment, Dr. Beleznay noted.
She disclosed financial relationships with Allergan, Revance, Evolus, Galderma, and Zeltiq.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – Using larger doses and avoiding overarching of the brows are among the considerations to keep in mind when using neuromodulators in men, advised Canadian dermatologist Katie Beleznay, MD.
In general, men have a very different anatomy with a different brow position, and have needs different from those of women, said Dr. Beleznay of the University of British Columbia, Vancouver.
One secret for successful injections of toxins in male patients: Dose matters. Men have stronger muscles in the face and need larger doses to overcome their muscular strength, Dr. Beleznay said in a video interview at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
On average, “if you use 20-30 units in a female glabella, maybe you’d use 40-50, maybe even 60 units in a male patient,” she said. However, the volume depends on the strength of the muscles in the area, and some men may need less to avoid a frozen look. “You can always treat less and bring them back in a couple of weeks and add more,” especially with patients who are new to treatment, Dr. Beleznay noted.
She disclosed financial relationships with Allergan, Revance, Evolus, Galderma, and Zeltiq.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT SDEF HAWAII DERMATOLOGY SEMINAR
VIDEO: Patient survey data yield useful information on acne and different contraceptives
WAILEA, HAWAII – A study that used patient-reported outcomes to assess the impact of different contraceptive methods on acne provided “fascinating results,” Lawrence F. Eichenfield, MD, said at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
“Progestins are present in birth control for the birth control, but they’re not usually good for the acne,” Dr. Eichenfield said in a video interview at the meeting.
Dr. Eichenfield, professor of dermatology and pediatrics at the University of California, San Diego, and his colleagues reviewed patient reports from an Internet-based survey of more than 2,000 adolescent and young adult acne patients asking whether they were on any contraceptive, and if so, how they thought the contraceptive method affected their acne.
Overall, hormonal progestin-only IUDs and some progestin-only implants correlated with worse acne. Of the combined oral contraceptives, those on the OCs containing drospirenone performed best, he said. Also of interest, the triphasic OCs, with the progestin in three phases, had a better impact on the acne than did the dual ones, he added.
The review of patient-reported outcomes can not only inform clinicians on how they should prescribe hormonal therapy, but also raises awareness of the impact of contraceptives on acne in general, Dr. Eichenfield said.
The results were published last year (J Drugs Dermatol. 2016 Jun 1;15[6]:670-4).
Dr. Eichenfield disclosed relationships with Anacor/Pfizer, Genentech, Lilly, Regeneron/Sanofi, Medimetriks, and Otsuka.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – A study that used patient-reported outcomes to assess the impact of different contraceptive methods on acne provided “fascinating results,” Lawrence F. Eichenfield, MD, said at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
“Progestins are present in birth control for the birth control, but they’re not usually good for the acne,” Dr. Eichenfield said in a video interview at the meeting.
Dr. Eichenfield, professor of dermatology and pediatrics at the University of California, San Diego, and his colleagues reviewed patient reports from an Internet-based survey of more than 2,000 adolescent and young adult acne patients asking whether they were on any contraceptive, and if so, how they thought the contraceptive method affected their acne.
Overall, hormonal progestin-only IUDs and some progestin-only implants correlated with worse acne. Of the combined oral contraceptives, those on the OCs containing drospirenone performed best, he said. Also of interest, the triphasic OCs, with the progestin in three phases, had a better impact on the acne than did the dual ones, he added.
The review of patient-reported outcomes can not only inform clinicians on how they should prescribe hormonal therapy, but also raises awareness of the impact of contraceptives on acne in general, Dr. Eichenfield said.
The results were published last year (J Drugs Dermatol. 2016 Jun 1;15[6]:670-4).
Dr. Eichenfield disclosed relationships with Anacor/Pfizer, Genentech, Lilly, Regeneron/Sanofi, Medimetriks, and Otsuka.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WAILEA, HAWAII – A study that used patient-reported outcomes to assess the impact of different contraceptive methods on acne provided “fascinating results,” Lawrence F. Eichenfield, MD, said at the Hawaii Dermatology Seminar provided by Global Academy for Medical Education/Skin Disease Education Foundation.
“Progestins are present in birth control for the birth control, but they’re not usually good for the acne,” Dr. Eichenfield said in a video interview at the meeting.
Dr. Eichenfield, professor of dermatology and pediatrics at the University of California, San Diego, and his colleagues reviewed patient reports from an Internet-based survey of more than 2,000 adolescent and young adult acne patients asking whether they were on any contraceptive, and if so, how they thought the contraceptive method affected their acne.
Overall, hormonal progestin-only IUDs and some progestin-only implants correlated with worse acne. Of the combined oral contraceptives, those on the OCs containing drospirenone performed best, he said. Also of interest, the triphasic OCs, with the progestin in three phases, had a better impact on the acne than did the dual ones, he added.
The review of patient-reported outcomes can not only inform clinicians on how they should prescribe hormonal therapy, but also raises awareness of the impact of contraceptives on acne in general, Dr. Eichenfield said.
The results were published last year (J Drugs Dermatol. 2016 Jun 1;15[6]:670-4).
Dr. Eichenfield disclosed relationships with Anacor/Pfizer, Genentech, Lilly, Regeneron/Sanofi, Medimetriks, and Otsuka.
SDEF and this news organization are owned by the same parent company.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
EXPERT ANALYSIS FROM SDEF HAWAII DERMATOLOGY SEMINAR