User login
Stage 2 Sarcoidosis
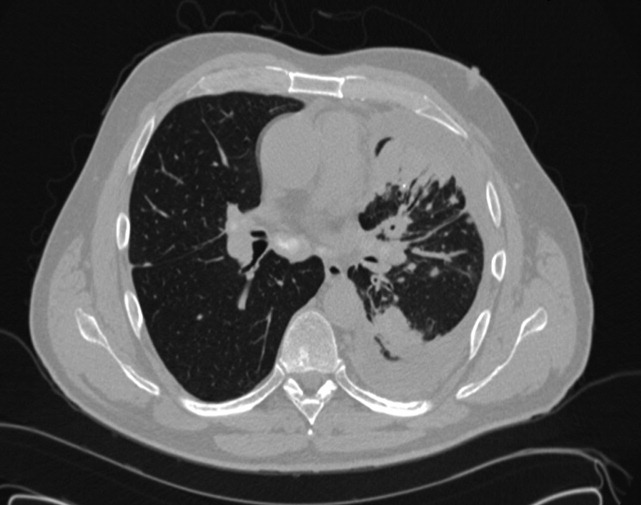
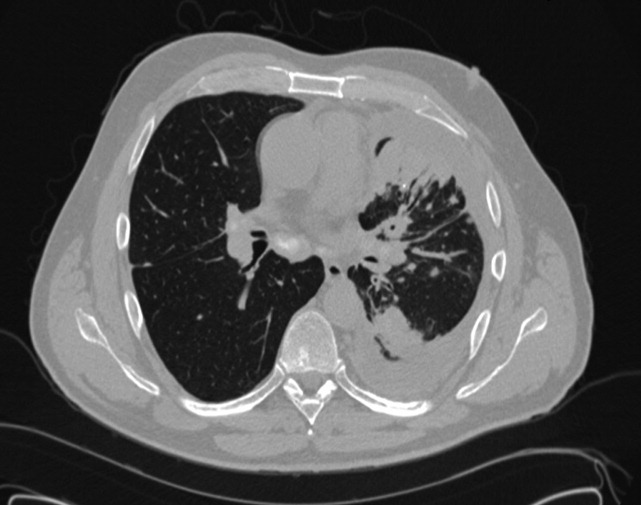
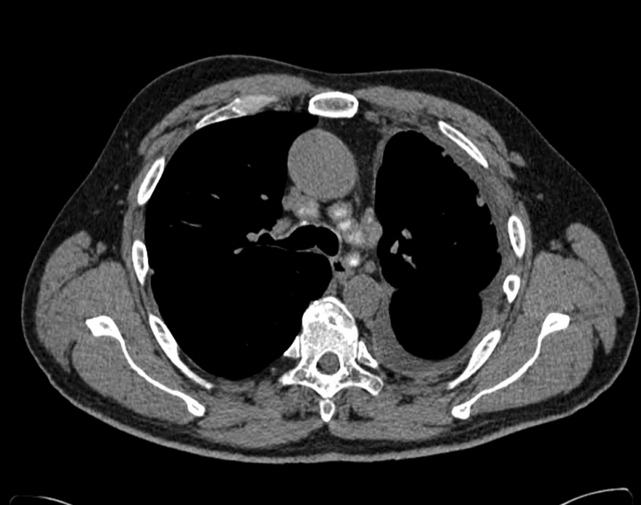
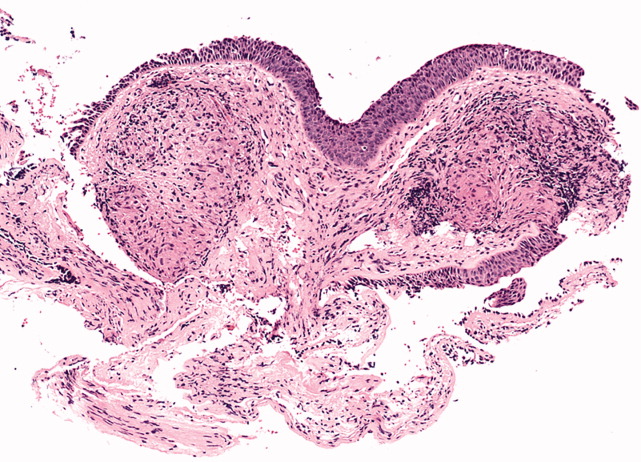
A 50‐year‐old man presented to the emergency department with progressive shortness of breath for 6 months. He described a dry cough, left‐sided chest pain, malaise, night sweats, and a 15‐pound weight loss. The patient had never smoked cigarettes, but he had been exposed to asbestos and wood dust when working at a sawmill. His physical examination was remarkable for decreased breath sounds at the left lung base. The admission blood tests were within normal limits. Chest radiography and a computed tomography (CT) scan of the chest were performed (the CT scan is shown in Figures 1 and 2). The CT scan showed a left pleural effusion with subpleural and peribronchovascular nodules. Also demonstrated on the CT scan were bilateral hilar and mediastinal lymphadenopathies with faint central calcification. As the left‐sided pleural effusion was initially suspected to be malignant, a thoracentesis was performed, and it revealed an exudative effusion. The total white cell count in fluid was 2100/L (lymphocytes, 76%), and cultures for aerobic and anaerobic bacteria, acid fasting bacilli, and fungi were negative. Cytology was negative for malignant cells. On the basis of the findings in the lung parenchyma and the presence of mediastinal lymphadenopathies, fiber‐optic bronchoscopy with bronchoalveolar lavage, protected specimen brushing, transbronchial needle aspiration, and transbronchial biopsies were performed. Mediastinal lymph node cytology was negative for malignant cells, whereas transbronchial biopsies showed noncaseating granulomas (Figure 3). At that time, our differential diagnoses of noncaseating granulomas included mycobacterium infection (although this usually presents caseating granulomas), berylliosis, histoplasmosis, and sarcoidosis. The tuberculin skin test (purified protein derivative) and serology for human immunodeficiency virus were negative. Bronchoalveolar lavage and cultures of lung tissue biopsies as well as needle aspiration from mediastinal lymph nodes were negative for mycobacterial, fungal, and bacterial organisms. The beryllium lymphocyte proliferation test was normal. Serologic antibodies for Aspergillus, Blastomyces, Coccidioides, and Histoplasma were negative. The urinary Histoplasma antigen was negative as well. The Department of Infectious Diseases was consulted, and an empirical treatment for histoplasmosis with itraconazole was started on the basis of the residence of the patient and the presence of noncaseating granulomas. After 1 month of antifungal treatment, there was no significant improvement. Video‐assisted thoracoscopic surgery with pleural biopsy was performed because of persistent pleural effusion and concern about an underlying infectious or malignant process. Pleural biopsies showed noncaseating granulomas (Figure 4). Pleural fluid was sent for adenosine deaminase (17 U/L) and flow cytometry (CD4/CD8 2.71). Cultures and cytology remained negative. A diagnosis of stage 2 sarcoidosis with pleural involvement was made, and treatment with prednisone was started.

Discussion
The overall prevalence of pleural involvement in sarcoidosis is about 3%. Patients with pleural sarcoidosis tend to be between 30 and 50 years of age, in contrast to the usual presentation of sarcoidosis between 20 and 30 years of age. The most common forms of pleural involvement are pleural effusions, pneumothorax, pleural thickening, and pleural nodules.1 Most effusions are usually small or modest in size, with few reports describing massive effusions.2 Recurrent pleural and pericardial effusions due to sarcoidosis have been reported as well.3 The fluid is typically a lymphocytic exudate, and almost all cases describe a CD4 predominant lymphocytic effusion with CD4/CD8 ratios ranging from 2.35 to 8.6.1 The presence of bloody pleural effusions in sarcoidosis most likely represents the rupture of small vessels that are compressed or infiltrated by granulomas.4
The majority of patients with reported sarcoid pleural effusions have stage 2 disease. With the progression of parenchymal disease, the prevalence of pleural effusions decreases, whereas pleural thickening and pneumothorax increase.5 It is important to emphasize that 40% of pleural effusions in sarcoidosis may be due to other causes, such as tuberculosis and mesothelioma. Our patient was initially treated with itraconazole as histoplasmosis is most prevalent in the Central and Eastern United States, especially in Ohio River valleys, where this patient lived.
The prevalence of a pneumothorax in sarcoidosis is up to 4%.1 Pleural thickening can be demonstrated in 11% to 71% of patients with pleural sarcoidosis, and 10% to 20% of these cases have thickening without effusion. Detection of subpleural nodules and cysts has been possible since the introduction of high‐resolution CT scans. Their prevalence in sarcoidosis ranges from 22% to 76%, and they are often described as masses that correspond to nodules seen in both parietal and visceral surfaces. Hilar or mediastinal lymphadenopathy is present on CT in 47% to 94% of patients with sarcoidosis. Lymph node enlargement is usually bilateral, most commonly with right‐sided predominance. The most involved stations are the right lower paratracheal, right hilar, subcarinal, aortopulmonary window, and right interlobar stations. Nodal calcification is noted in 53% with eggshell calcification present in 9%. The enlargement of internal mammary and pericardial lymph nodes requires the exclusion of lymphoma.6
The management of pleural sarcoidosis should be individualized because a majority of these effusions resolve spontaneously in 1 to 3 months.5 There have been reports of resolution in 2 weeks with steroid therapy. Incomplete resolution of the pleural effusions with progression to chronic pleural thickening or a trapped lung has been reported. There is agreement that oral corticosteroid treatment should be considered in patients with severe persistent or progressively worsening respiratory symptoms or declining lung function. Severe symptoms can be considered as those that interfere with essential aspects of the patient's daily life.7 The initial dosage of oral prednisone recommended by the American Thoracic Society, the European Respiratory Society, and the World Association of Sarcoidosis and Other Granulomatous Disorders guidelines is 20 to 40 mg/day.8 Further evaluation is recommended after 1 to 3 months. If the patient responds, the dose should be reduced gradually to a maintenance dose, such as 5 to 15 mg/day of prednisolone. American Thoracic Society/European Respiratory Society/World Association of Sarcoidosis and Other Granulomatous Disorders guidelines advise treatment for at least 1 year. Immunosuppressive, cytotoxic, and immunomodulatory agents have been used to treat patients failing or experiencing adverse effects of steroids. Favorable responses have been reported with methotrexate, leflunomide, azathioprine, cyclophosphamide, chlorambucil, cyclosporine A, antimalarials, tumor necrosis factor inhibitors, and thalidomide. Because of potential serious toxicities associated with cyclophosphamide and chlorambucil, these agents are not recommended.9
Our patient presented with pleural sarcoidosis with a pleural effusion and nodules. Treatment with 20 mg of prednisone daily was started initially. Four weeks after discharge, he was still dyspneic and had persistent left pleural effusion. He also had gained a significant amount of weight and developed bilateral lower extremity edema; these were thought to be secondary to prednisone treatment. Steroids were subsequently tapered, and leflunomide was started. His symptoms improved dramatically after 1 month of treatment with leflunomide and steroids, and 3 months later, his pleural effusion had completely resolved.
- ,.Pleural involvement in sarcoidosis.Curr Opin Pulm Med.2000;6(5):455–468.
- ,.Pleural sarcoidosis with massive effusion and lung entrapment.Kans Med.1990;91(4):103–105.
- ,,,,.Recurrent pleural and pericardial effusions due to sarcoidosis.PLoS Med.2005;2(3):e63.
- ,,,,.Pulmonary sarcoidosis with associated bloody pleurisy.Intern Med.2002;41(11):1021–1023.
- ,,,,.Pleural effusions in a series of 181 outpatients with sarcoidosis.Chest.2006;129(6):1599–1604.
- ,,,,.Imaging in sarcoidosis.Semin Respir Crit Care Med.2007;28(1):102–120.
- .Guidelines for the use of corticosteroids in the treatment of pulmonary sarcoidosis.Drugs.2007;67(8):1139–1147.
- ,,, et al.ATS/ERS/WASOG statement on sarcoidosis.Sarcoidosis Vasc Diffuse Lung Dis.1999;16(2):149–173.
- ,,,.Pulmonary sarcoidosis.Semin Respir Crit Care Med.2007;28(1):53–74.
A 50‐year‐old man presented to the emergency department with progressive shortness of breath for 6 months. He described a dry cough, left‐sided chest pain, malaise, night sweats, and a 15‐pound weight loss. The patient had never smoked cigarettes, but he had been exposed to asbestos and wood dust when working at a sawmill. His physical examination was remarkable for decreased breath sounds at the left lung base. The admission blood tests were within normal limits. Chest radiography and a computed tomography (CT) scan of the chest were performed (the CT scan is shown in Figures 1 and 2). The CT scan showed a left pleural effusion with subpleural and peribronchovascular nodules. Also demonstrated on the CT scan were bilateral hilar and mediastinal lymphadenopathies with faint central calcification. As the left‐sided pleural effusion was initially suspected to be malignant, a thoracentesis was performed, and it revealed an exudative effusion. The total white cell count in fluid was 2100/L (lymphocytes, 76%), and cultures for aerobic and anaerobic bacteria, acid fasting bacilli, and fungi were negative. Cytology was negative for malignant cells. On the basis of the findings in the lung parenchyma and the presence of mediastinal lymphadenopathies, fiber‐optic bronchoscopy with bronchoalveolar lavage, protected specimen brushing, transbronchial needle aspiration, and transbronchial biopsies were performed. Mediastinal lymph node cytology was negative for malignant cells, whereas transbronchial biopsies showed noncaseating granulomas (Figure 3). At that time, our differential diagnoses of noncaseating granulomas included mycobacterium infection (although this usually presents caseating granulomas), berylliosis, histoplasmosis, and sarcoidosis. The tuberculin skin test (purified protein derivative) and serology for human immunodeficiency virus were negative. Bronchoalveolar lavage and cultures of lung tissue biopsies as well as needle aspiration from mediastinal lymph nodes were negative for mycobacterial, fungal, and bacterial organisms. The beryllium lymphocyte proliferation test was normal. Serologic antibodies for Aspergillus, Blastomyces, Coccidioides, and Histoplasma were negative. The urinary Histoplasma antigen was negative as well. The Department of Infectious Diseases was consulted, and an empirical treatment for histoplasmosis with itraconazole was started on the basis of the residence of the patient and the presence of noncaseating granulomas. After 1 month of antifungal treatment, there was no significant improvement. Video‐assisted thoracoscopic surgery with pleural biopsy was performed because of persistent pleural effusion and concern about an underlying infectious or malignant process. Pleural biopsies showed noncaseating granulomas (Figure 4). Pleural fluid was sent for adenosine deaminase (17 U/L) and flow cytometry (CD4/CD8 2.71). Cultures and cytology remained negative. A diagnosis of stage 2 sarcoidosis with pleural involvement was made, and treatment with prednisone was started.




Discussion
The overall prevalence of pleural involvement in sarcoidosis is about 3%. Patients with pleural sarcoidosis tend to be between 30 and 50 years of age, in contrast to the usual presentation of sarcoidosis between 20 and 30 years of age. The most common forms of pleural involvement are pleural effusions, pneumothorax, pleural thickening, and pleural nodules.1 Most effusions are usually small or modest in size, with few reports describing massive effusions.2 Recurrent pleural and pericardial effusions due to sarcoidosis have been reported as well.3 The fluid is typically a lymphocytic exudate, and almost all cases describe a CD4 predominant lymphocytic effusion with CD4/CD8 ratios ranging from 2.35 to 8.6.1 The presence of bloody pleural effusions in sarcoidosis most likely represents the rupture of small vessels that are compressed or infiltrated by granulomas.4
The majority of patients with reported sarcoid pleural effusions have stage 2 disease. With the progression of parenchymal disease, the prevalence of pleural effusions decreases, whereas pleural thickening and pneumothorax increase.5 It is important to emphasize that 40% of pleural effusions in sarcoidosis may be due to other causes, such as tuberculosis and mesothelioma. Our patient was initially treated with itraconazole as histoplasmosis is most prevalent in the Central and Eastern United States, especially in Ohio River valleys, where this patient lived.
The prevalence of a pneumothorax in sarcoidosis is up to 4%.1 Pleural thickening can be demonstrated in 11% to 71% of patients with pleural sarcoidosis, and 10% to 20% of these cases have thickening without effusion. Detection of subpleural nodules and cysts has been possible since the introduction of high‐resolution CT scans. Their prevalence in sarcoidosis ranges from 22% to 76%, and they are often described as masses that correspond to nodules seen in both parietal and visceral surfaces. Hilar or mediastinal lymphadenopathy is present on CT in 47% to 94% of patients with sarcoidosis. Lymph node enlargement is usually bilateral, most commonly with right‐sided predominance. The most involved stations are the right lower paratracheal, right hilar, subcarinal, aortopulmonary window, and right interlobar stations. Nodal calcification is noted in 53% with eggshell calcification present in 9%. The enlargement of internal mammary and pericardial lymph nodes requires the exclusion of lymphoma.6
The management of pleural sarcoidosis should be individualized because a majority of these effusions resolve spontaneously in 1 to 3 months.5 There have been reports of resolution in 2 weeks with steroid therapy. Incomplete resolution of the pleural effusions with progression to chronic pleural thickening or a trapped lung has been reported. There is agreement that oral corticosteroid treatment should be considered in patients with severe persistent or progressively worsening respiratory symptoms or declining lung function. Severe symptoms can be considered as those that interfere with essential aspects of the patient's daily life.7 The initial dosage of oral prednisone recommended by the American Thoracic Society, the European Respiratory Society, and the World Association of Sarcoidosis and Other Granulomatous Disorders guidelines is 20 to 40 mg/day.8 Further evaluation is recommended after 1 to 3 months. If the patient responds, the dose should be reduced gradually to a maintenance dose, such as 5 to 15 mg/day of prednisolone. American Thoracic Society/European Respiratory Society/World Association of Sarcoidosis and Other Granulomatous Disorders guidelines advise treatment for at least 1 year. Immunosuppressive, cytotoxic, and immunomodulatory agents have been used to treat patients failing or experiencing adverse effects of steroids. Favorable responses have been reported with methotrexate, leflunomide, azathioprine, cyclophosphamide, chlorambucil, cyclosporine A, antimalarials, tumor necrosis factor inhibitors, and thalidomide. Because of potential serious toxicities associated with cyclophosphamide and chlorambucil, these agents are not recommended.9
Our patient presented with pleural sarcoidosis with a pleural effusion and nodules. Treatment with 20 mg of prednisone daily was started initially. Four weeks after discharge, he was still dyspneic and had persistent left pleural effusion. He also had gained a significant amount of weight and developed bilateral lower extremity edema; these were thought to be secondary to prednisone treatment. Steroids were subsequently tapered, and leflunomide was started. His symptoms improved dramatically after 1 month of treatment with leflunomide and steroids, and 3 months later, his pleural effusion had completely resolved.
A 50‐year‐old man presented to the emergency department with progressive shortness of breath for 6 months. He described a dry cough, left‐sided chest pain, malaise, night sweats, and a 15‐pound weight loss. The patient had never smoked cigarettes, but he had been exposed to asbestos and wood dust when working at a sawmill. His physical examination was remarkable for decreased breath sounds at the left lung base. The admission blood tests were within normal limits. Chest radiography and a computed tomography (CT) scan of the chest were performed (the CT scan is shown in Figures 1 and 2). The CT scan showed a left pleural effusion with subpleural and peribronchovascular nodules. Also demonstrated on the CT scan were bilateral hilar and mediastinal lymphadenopathies with faint central calcification. As the left‐sided pleural effusion was initially suspected to be malignant, a thoracentesis was performed, and it revealed an exudative effusion. The total white cell count in fluid was 2100/L (lymphocytes, 76%), and cultures for aerobic and anaerobic bacteria, acid fasting bacilli, and fungi were negative. Cytology was negative for malignant cells. On the basis of the findings in the lung parenchyma and the presence of mediastinal lymphadenopathies, fiber‐optic bronchoscopy with bronchoalveolar lavage, protected specimen brushing, transbronchial needle aspiration, and transbronchial biopsies were performed. Mediastinal lymph node cytology was negative for malignant cells, whereas transbronchial biopsies showed noncaseating granulomas (Figure 3). At that time, our differential diagnoses of noncaseating granulomas included mycobacterium infection (although this usually presents caseating granulomas), berylliosis, histoplasmosis, and sarcoidosis. The tuberculin skin test (purified protein derivative) and serology for human immunodeficiency virus were negative. Bronchoalveolar lavage and cultures of lung tissue biopsies as well as needle aspiration from mediastinal lymph nodes were negative for mycobacterial, fungal, and bacterial organisms. The beryllium lymphocyte proliferation test was normal. Serologic antibodies for Aspergillus, Blastomyces, Coccidioides, and Histoplasma were negative. The urinary Histoplasma antigen was negative as well. The Department of Infectious Diseases was consulted, and an empirical treatment for histoplasmosis with itraconazole was started on the basis of the residence of the patient and the presence of noncaseating granulomas. After 1 month of antifungal treatment, there was no significant improvement. Video‐assisted thoracoscopic surgery with pleural biopsy was performed because of persistent pleural effusion and concern about an underlying infectious or malignant process. Pleural biopsies showed noncaseating granulomas (Figure 4). Pleural fluid was sent for adenosine deaminase (17 U/L) and flow cytometry (CD4/CD8 2.71). Cultures and cytology remained negative. A diagnosis of stage 2 sarcoidosis with pleural involvement was made, and treatment with prednisone was started.




Discussion
The overall prevalence of pleural involvement in sarcoidosis is about 3%. Patients with pleural sarcoidosis tend to be between 30 and 50 years of age, in contrast to the usual presentation of sarcoidosis between 20 and 30 years of age. The most common forms of pleural involvement are pleural effusions, pneumothorax, pleural thickening, and pleural nodules.1 Most effusions are usually small or modest in size, with few reports describing massive effusions.2 Recurrent pleural and pericardial effusions due to sarcoidosis have been reported as well.3 The fluid is typically a lymphocytic exudate, and almost all cases describe a CD4 predominant lymphocytic effusion with CD4/CD8 ratios ranging from 2.35 to 8.6.1 The presence of bloody pleural effusions in sarcoidosis most likely represents the rupture of small vessels that are compressed or infiltrated by granulomas.4
The majority of patients with reported sarcoid pleural effusions have stage 2 disease. With the progression of parenchymal disease, the prevalence of pleural effusions decreases, whereas pleural thickening and pneumothorax increase.5 It is important to emphasize that 40% of pleural effusions in sarcoidosis may be due to other causes, such as tuberculosis and mesothelioma. Our patient was initially treated with itraconazole as histoplasmosis is most prevalent in the Central and Eastern United States, especially in Ohio River valleys, where this patient lived.
The prevalence of a pneumothorax in sarcoidosis is up to 4%.1 Pleural thickening can be demonstrated in 11% to 71% of patients with pleural sarcoidosis, and 10% to 20% of these cases have thickening without effusion. Detection of subpleural nodules and cysts has been possible since the introduction of high‐resolution CT scans. Their prevalence in sarcoidosis ranges from 22% to 76%, and they are often described as masses that correspond to nodules seen in both parietal and visceral surfaces. Hilar or mediastinal lymphadenopathy is present on CT in 47% to 94% of patients with sarcoidosis. Lymph node enlargement is usually bilateral, most commonly with right‐sided predominance. The most involved stations are the right lower paratracheal, right hilar, subcarinal, aortopulmonary window, and right interlobar stations. Nodal calcification is noted in 53% with eggshell calcification present in 9%. The enlargement of internal mammary and pericardial lymph nodes requires the exclusion of lymphoma.6
The management of pleural sarcoidosis should be individualized because a majority of these effusions resolve spontaneously in 1 to 3 months.5 There have been reports of resolution in 2 weeks with steroid therapy. Incomplete resolution of the pleural effusions with progression to chronic pleural thickening or a trapped lung has been reported. There is agreement that oral corticosteroid treatment should be considered in patients with severe persistent or progressively worsening respiratory symptoms or declining lung function. Severe symptoms can be considered as those that interfere with essential aspects of the patient's daily life.7 The initial dosage of oral prednisone recommended by the American Thoracic Society, the European Respiratory Society, and the World Association of Sarcoidosis and Other Granulomatous Disorders guidelines is 20 to 40 mg/day.8 Further evaluation is recommended after 1 to 3 months. If the patient responds, the dose should be reduced gradually to a maintenance dose, such as 5 to 15 mg/day of prednisolone. American Thoracic Society/European Respiratory Society/World Association of Sarcoidosis and Other Granulomatous Disorders guidelines advise treatment for at least 1 year. Immunosuppressive, cytotoxic, and immunomodulatory agents have been used to treat patients failing or experiencing adverse effects of steroids. Favorable responses have been reported with methotrexate, leflunomide, azathioprine, cyclophosphamide, chlorambucil, cyclosporine A, antimalarials, tumor necrosis factor inhibitors, and thalidomide. Because of potential serious toxicities associated with cyclophosphamide and chlorambucil, these agents are not recommended.9
Our patient presented with pleural sarcoidosis with a pleural effusion and nodules. Treatment with 20 mg of prednisone daily was started initially. Four weeks after discharge, he was still dyspneic and had persistent left pleural effusion. He also had gained a significant amount of weight and developed bilateral lower extremity edema; these were thought to be secondary to prednisone treatment. Steroids were subsequently tapered, and leflunomide was started. His symptoms improved dramatically after 1 month of treatment with leflunomide and steroids, and 3 months later, his pleural effusion had completely resolved.
- ,.Pleural involvement in sarcoidosis.Curr Opin Pulm Med.2000;6(5):455–468.
- ,.Pleural sarcoidosis with massive effusion and lung entrapment.Kans Med.1990;91(4):103–105.
- ,,,,.Recurrent pleural and pericardial effusions due to sarcoidosis.PLoS Med.2005;2(3):e63.
- ,,,,.Pulmonary sarcoidosis with associated bloody pleurisy.Intern Med.2002;41(11):1021–1023.
- ,,,,.Pleural effusions in a series of 181 outpatients with sarcoidosis.Chest.2006;129(6):1599–1604.
- ,,,,.Imaging in sarcoidosis.Semin Respir Crit Care Med.2007;28(1):102–120.
- .Guidelines for the use of corticosteroids in the treatment of pulmonary sarcoidosis.Drugs.2007;67(8):1139–1147.
- ,,, et al.ATS/ERS/WASOG statement on sarcoidosis.Sarcoidosis Vasc Diffuse Lung Dis.1999;16(2):149–173.
- ,,,.Pulmonary sarcoidosis.Semin Respir Crit Care Med.2007;28(1):53–74.
- ,.Pleural involvement in sarcoidosis.Curr Opin Pulm Med.2000;6(5):455–468.
- ,.Pleural sarcoidosis with massive effusion and lung entrapment.Kans Med.1990;91(4):103–105.
- ,,,,.Recurrent pleural and pericardial effusions due to sarcoidosis.PLoS Med.2005;2(3):e63.
- ,,,,.Pulmonary sarcoidosis with associated bloody pleurisy.Intern Med.2002;41(11):1021–1023.
- ,,,,.Pleural effusions in a series of 181 outpatients with sarcoidosis.Chest.2006;129(6):1599–1604.
- ,,,,.Imaging in sarcoidosis.Semin Respir Crit Care Med.2007;28(1):102–120.
- .Guidelines for the use of corticosteroids in the treatment of pulmonary sarcoidosis.Drugs.2007;67(8):1139–1147.
- ,,, et al.ATS/ERS/WASOG statement on sarcoidosis.Sarcoidosis Vasc Diffuse Lung Dis.1999;16(2):149–173.
- ,,,.Pulmonary sarcoidosis.Semin Respir Crit Care Med.2007;28(1):53–74.
Rube Goldberg Coordinated Care
I was 12 years old before I knew her actual name, Le Thi Canh, because we always called her Ba ngoai. She was my grandmother, and this is the story of how she died.
To see my grandmother for the warrior woman that she was to me, you have to know that her farmer father sent her to the city for schooling because he didn't know what else to do with a daughter who was so smart. In early 20th‐century Vietnam, this was an unusual thing to do with a girl. She met my grandfather there, when he was a campus activist, helping him hand out nationalist leaflets. He introduced her to his Communist friends. After the French jailed my grandfather, my grandmother courted him by sending him long letters and care packages while he was in prison. When he was finally released, they married and started a family while he struggled financially as a newspaper publisher and at other odd jobs. But in 1947 his own Communist comrades killed him as part of a party purge. He had been forewarned, and opted to go quietly rather than try to escape because he was promised that this would guarantee her safety. Before they killed him, somewhere in the mountains, my grandfather gave a soldier friend a poem he wrote for his wife. When she told me this story 8 years ago, more than half a century later, she recited his love missive from memory.
At the time of her husband's death, my grandmother had 6 children, the last born just a few weeks before. After a few years of scraping by (she ran her own one‐room school for a while), she decided to leave Hanoi, and migrated south to Saigon with her brood. She was a famously strict parent, to hear my aunts and uncles tell it. She watched them like a hawk, worked full‐time, put them all through school, and eventually rose to a leadership position in the Ministry of Social Work in South Vietnam. My memories of Saigon life are punctuated by scenes of siblings and cousins running around at her regal house, yellow stucco with porticos and black iron gates, at a corner turn in the road, past a cemetery.
On this side of the world, to see her, you would never have thought that my grandmother had led such an epic life. She never worked again after immigrating with us in 1975. She lived on Social Security checks, gardened, said Buddhist prayers, and was nanny to her grandchildren. She watched soap operas religiously, and could report their full plot lines while sitting and knitting. She bundled her many sadnesses in a contented, 4‐foot 9‐inch frame.
Having no home of her own, she would move from one child's house to another every few months so as not to wear out her welcome. But her children lived in Pennsylvania, New Jersey, Florida, Texas, and Maryland. And in most of these cities, she had a different primary care physician. She has 21 grandchildren; 8 of us are physicians. Yet the aunts and uncles told us very little about her medical care. She preferred older‐generation Vietnamese physicians and I'm not sure that they were all competent, but her children did not want to argue with an octogenarian war survivor, and we deferred to their judgment. So we would find out only incidentally, for example, that a doctor prescribed her tuberculosis drugs for a visit to Vietnam.
For many years, Ba ngoai had no major medical problems. She was hypothyroid and hypertensive but on medication and generally high functioning. She had a lumpectomy for early‐stage breast cancer. Then, a year or so after she told me the story of my grandfather's death, Alzheimer's set in. It became harder for her to report symptoms reliably, and she became mildly depressed. Her grandchildren were now birthing our own babies, and we offered these as a distraction, trying to surround her with celebrations of these new fruits of her life labors.
Ba ngoai's decline worsened 3 years ago. She became more easily fatigued, depressed, and confused. A few months before she died, she started to get dyspneic, and couldn't go for short walks any more. In retrospect, I think that her prescription for thyroid replacement somehow fell through the cracks, probably in the transfer of care from one city to another, although there remains a great deal of confusion in the family about exactly what happened. Her thyroxine levels dwindled. One evening in October of that year, at my uncle's house in Maryland, she became severely short of breath and nearly unconscious. They called her Maryland PCP, who sent her to an emergency room at a local hospital. She was admitted in severe congestive heart failure. When the hospitalist spoke with my mother and uncle, he explained that he could take some fluid off her lungs, but that she might need to be intubated and admitted to intensive care. Looking back, I guessed that she probably needed pressors and invasive monitoring. He asked them, Is this what you want? My uncle said, No, it's not. And the hospitalist and the huddle of relatives decided she should come home.
The question was, into whose care would she be discharged? My elders were wary of contacting her PCP, partly because some blamed him for not catching and addressing her symptoms sooner, partly because to even confront him with this perception would cause him, and hence them, to lose face. This seemed too excruciating a scenario to them.
So at last, my uncle called my brother, the oldest grandchild and a very talented clinician. My brother is a pulmonologist, the kind of physician who once did a history and physical on a patient complaining only of Really feeling bad, Doc, and confidently started a steroid infusion before returning the next day with test results confirming his suspicion of Wegener's granulomatosis. He took my grandmother's physical by phone, and told my uncle to increase her furosemide dose. Then he said, I'm on call, but I'll be down there tomorrow. Call everyone together. Most of my relatives were already in town; they had come at news of her decline. She became alert enough for a couple of days to see and recognize most of the faces around her, like so many markers on a long journey. And then she died, slipped away.
I find it hard to define good coordination of care. My instinct as a researcher is to list measurable elements, but the tools we currently have generate metrics that are either reductionistsuch as how rapidly a physician returns a patient's callor so global that they no longer seem actionablesuch as patient satisfaction. But if such metrics set the goal in the distance, it seems useful to also define its counterpartdiscoordinationas a marker of the reality we would like to leave behind us as far as possible. Discoordination includes elements of discontinuity (lost patient history), fragmentation (actions by multiple players), overuse and/or inappropriate use of services, and ultimately, ineffective care (that is, the patient's needs go unmet).
My experience of discoordination was that of a Rube Goldberg contraption. It's composed of innumerable subtasks, each cleverly designed as the easiest solution to a seemingly short‐term problem, as quick fixes, but that in aggregate generate such chaos that the ultimate purpose is lost. They include acts of denial, lies to avoid embarrassment or conflict, and choices of convenience. My mother and her siblings accommodated my grandmother's choice of physicians by (secretly) not always adhering to care recommendations they didn't agree with, instead of challenging her. They took her to different physicians in different cities rather than risk embarrassing (due to an exaggerated sense of the smallness of the Vietnamese community) any one physician by dropping him. Her grandchildren, despite our medical training, found it culturally easier to defer to our elders than to intervene in substandard care. And none of her physicians aggressively followed up to ensure that a frail Alzheimer's patient was getting the care she needed. This is not to suggest that coordination is a simple task because Rube Goldberg machines make simple tasks complicated. Rather, it is a depiction of how indirectly we tend to address the problem.
I imagine a different course of events for my grandmother in the absence of discoordination. What if her children and physicians had understood and acknowledged to one another that her care was fragmented and therefore suboptimal? What if we grandchildren had confronted both Ba Ngoai and our parents sooner about their choice of physicians and offered to take on more of the burden of helping with her care decisions? Would we, as physicians, have been better able to ensure that her providers made rational clinical decisions? And what if she and her family had consistently recognized a single physician as her medical home? Snowbirding is hardly a rare phenomenon among Medicare patients; we could have designated one physician as primarily responsible for coordinating her care even without limiting her travel.
Care coordination is an inherently human activity. Supportive elements such as efficient transfer of medical information, resources for patient education and self‐care, and adequate reimbursement can take us to the brink of, but not actually bridge, the chasm that we want to cross. Traversing that divide sometimes requires settling turf issues over undesirable responsibilities between different physicians and between physicians and other providers; clarifying who has primary responsibility for different types of decisions (I lead on cardiac issues and her son leads on health maintenance); and the violation of cultural norms of patients, families, and/or providers. These can be uncomfortable, unpleasant conversations that at times seem beside the point. But in aggregate, they are the work of coordination, because they force us to align our expectations of one another. No level of information technology could have dismantled the Rube Goldberg machine that trapped my grandmother. Her last of many lessons for me was that emotional courage, honesty, and perseverance offer a much more direct path through the muck.
I was 12 years old before I knew her actual name, Le Thi Canh, because we always called her Ba ngoai. She was my grandmother, and this is the story of how she died.
To see my grandmother for the warrior woman that she was to me, you have to know that her farmer father sent her to the city for schooling because he didn't know what else to do with a daughter who was so smart. In early 20th‐century Vietnam, this was an unusual thing to do with a girl. She met my grandfather there, when he was a campus activist, helping him hand out nationalist leaflets. He introduced her to his Communist friends. After the French jailed my grandfather, my grandmother courted him by sending him long letters and care packages while he was in prison. When he was finally released, they married and started a family while he struggled financially as a newspaper publisher and at other odd jobs. But in 1947 his own Communist comrades killed him as part of a party purge. He had been forewarned, and opted to go quietly rather than try to escape because he was promised that this would guarantee her safety. Before they killed him, somewhere in the mountains, my grandfather gave a soldier friend a poem he wrote for his wife. When she told me this story 8 years ago, more than half a century later, she recited his love missive from memory.
At the time of her husband's death, my grandmother had 6 children, the last born just a few weeks before. After a few years of scraping by (she ran her own one‐room school for a while), she decided to leave Hanoi, and migrated south to Saigon with her brood. She was a famously strict parent, to hear my aunts and uncles tell it. She watched them like a hawk, worked full‐time, put them all through school, and eventually rose to a leadership position in the Ministry of Social Work in South Vietnam. My memories of Saigon life are punctuated by scenes of siblings and cousins running around at her regal house, yellow stucco with porticos and black iron gates, at a corner turn in the road, past a cemetery.
On this side of the world, to see her, you would never have thought that my grandmother had led such an epic life. She never worked again after immigrating with us in 1975. She lived on Social Security checks, gardened, said Buddhist prayers, and was nanny to her grandchildren. She watched soap operas religiously, and could report their full plot lines while sitting and knitting. She bundled her many sadnesses in a contented, 4‐foot 9‐inch frame.
Having no home of her own, she would move from one child's house to another every few months so as not to wear out her welcome. But her children lived in Pennsylvania, New Jersey, Florida, Texas, and Maryland. And in most of these cities, she had a different primary care physician. She has 21 grandchildren; 8 of us are physicians. Yet the aunts and uncles told us very little about her medical care. She preferred older‐generation Vietnamese physicians and I'm not sure that they were all competent, but her children did not want to argue with an octogenarian war survivor, and we deferred to their judgment. So we would find out only incidentally, for example, that a doctor prescribed her tuberculosis drugs for a visit to Vietnam.
For many years, Ba ngoai had no major medical problems. She was hypothyroid and hypertensive but on medication and generally high functioning. She had a lumpectomy for early‐stage breast cancer. Then, a year or so after she told me the story of my grandfather's death, Alzheimer's set in. It became harder for her to report symptoms reliably, and she became mildly depressed. Her grandchildren were now birthing our own babies, and we offered these as a distraction, trying to surround her with celebrations of these new fruits of her life labors.
Ba ngoai's decline worsened 3 years ago. She became more easily fatigued, depressed, and confused. A few months before she died, she started to get dyspneic, and couldn't go for short walks any more. In retrospect, I think that her prescription for thyroid replacement somehow fell through the cracks, probably in the transfer of care from one city to another, although there remains a great deal of confusion in the family about exactly what happened. Her thyroxine levels dwindled. One evening in October of that year, at my uncle's house in Maryland, she became severely short of breath and nearly unconscious. They called her Maryland PCP, who sent her to an emergency room at a local hospital. She was admitted in severe congestive heart failure. When the hospitalist spoke with my mother and uncle, he explained that he could take some fluid off her lungs, but that she might need to be intubated and admitted to intensive care. Looking back, I guessed that she probably needed pressors and invasive monitoring. He asked them, Is this what you want? My uncle said, No, it's not. And the hospitalist and the huddle of relatives decided she should come home.
The question was, into whose care would she be discharged? My elders were wary of contacting her PCP, partly because some blamed him for not catching and addressing her symptoms sooner, partly because to even confront him with this perception would cause him, and hence them, to lose face. This seemed too excruciating a scenario to them.
So at last, my uncle called my brother, the oldest grandchild and a very talented clinician. My brother is a pulmonologist, the kind of physician who once did a history and physical on a patient complaining only of Really feeling bad, Doc, and confidently started a steroid infusion before returning the next day with test results confirming his suspicion of Wegener's granulomatosis. He took my grandmother's physical by phone, and told my uncle to increase her furosemide dose. Then he said, I'm on call, but I'll be down there tomorrow. Call everyone together. Most of my relatives were already in town; they had come at news of her decline. She became alert enough for a couple of days to see and recognize most of the faces around her, like so many markers on a long journey. And then she died, slipped away.
I find it hard to define good coordination of care. My instinct as a researcher is to list measurable elements, but the tools we currently have generate metrics that are either reductionistsuch as how rapidly a physician returns a patient's callor so global that they no longer seem actionablesuch as patient satisfaction. But if such metrics set the goal in the distance, it seems useful to also define its counterpartdiscoordinationas a marker of the reality we would like to leave behind us as far as possible. Discoordination includes elements of discontinuity (lost patient history), fragmentation (actions by multiple players), overuse and/or inappropriate use of services, and ultimately, ineffective care (that is, the patient's needs go unmet).
My experience of discoordination was that of a Rube Goldberg contraption. It's composed of innumerable subtasks, each cleverly designed as the easiest solution to a seemingly short‐term problem, as quick fixes, but that in aggregate generate such chaos that the ultimate purpose is lost. They include acts of denial, lies to avoid embarrassment or conflict, and choices of convenience. My mother and her siblings accommodated my grandmother's choice of physicians by (secretly) not always adhering to care recommendations they didn't agree with, instead of challenging her. They took her to different physicians in different cities rather than risk embarrassing (due to an exaggerated sense of the smallness of the Vietnamese community) any one physician by dropping him. Her grandchildren, despite our medical training, found it culturally easier to defer to our elders than to intervene in substandard care. And none of her physicians aggressively followed up to ensure that a frail Alzheimer's patient was getting the care she needed. This is not to suggest that coordination is a simple task because Rube Goldberg machines make simple tasks complicated. Rather, it is a depiction of how indirectly we tend to address the problem.
I imagine a different course of events for my grandmother in the absence of discoordination. What if her children and physicians had understood and acknowledged to one another that her care was fragmented and therefore suboptimal? What if we grandchildren had confronted both Ba Ngoai and our parents sooner about their choice of physicians and offered to take on more of the burden of helping with her care decisions? Would we, as physicians, have been better able to ensure that her providers made rational clinical decisions? And what if she and her family had consistently recognized a single physician as her medical home? Snowbirding is hardly a rare phenomenon among Medicare patients; we could have designated one physician as primarily responsible for coordinating her care even without limiting her travel.
Care coordination is an inherently human activity. Supportive elements such as efficient transfer of medical information, resources for patient education and self‐care, and adequate reimbursement can take us to the brink of, but not actually bridge, the chasm that we want to cross. Traversing that divide sometimes requires settling turf issues over undesirable responsibilities between different physicians and between physicians and other providers; clarifying who has primary responsibility for different types of decisions (I lead on cardiac issues and her son leads on health maintenance); and the violation of cultural norms of patients, families, and/or providers. These can be uncomfortable, unpleasant conversations that at times seem beside the point. But in aggregate, they are the work of coordination, because they force us to align our expectations of one another. No level of information technology could have dismantled the Rube Goldberg machine that trapped my grandmother. Her last of many lessons for me was that emotional courage, honesty, and perseverance offer a much more direct path through the muck.
I was 12 years old before I knew her actual name, Le Thi Canh, because we always called her Ba ngoai. She was my grandmother, and this is the story of how she died.
To see my grandmother for the warrior woman that she was to me, you have to know that her farmer father sent her to the city for schooling because he didn't know what else to do with a daughter who was so smart. In early 20th‐century Vietnam, this was an unusual thing to do with a girl. She met my grandfather there, when he was a campus activist, helping him hand out nationalist leaflets. He introduced her to his Communist friends. After the French jailed my grandfather, my grandmother courted him by sending him long letters and care packages while he was in prison. When he was finally released, they married and started a family while he struggled financially as a newspaper publisher and at other odd jobs. But in 1947 his own Communist comrades killed him as part of a party purge. He had been forewarned, and opted to go quietly rather than try to escape because he was promised that this would guarantee her safety. Before they killed him, somewhere in the mountains, my grandfather gave a soldier friend a poem he wrote for his wife. When she told me this story 8 years ago, more than half a century later, she recited his love missive from memory.
At the time of her husband's death, my grandmother had 6 children, the last born just a few weeks before. After a few years of scraping by (she ran her own one‐room school for a while), she decided to leave Hanoi, and migrated south to Saigon with her brood. She was a famously strict parent, to hear my aunts and uncles tell it. She watched them like a hawk, worked full‐time, put them all through school, and eventually rose to a leadership position in the Ministry of Social Work in South Vietnam. My memories of Saigon life are punctuated by scenes of siblings and cousins running around at her regal house, yellow stucco with porticos and black iron gates, at a corner turn in the road, past a cemetery.
On this side of the world, to see her, you would never have thought that my grandmother had led such an epic life. She never worked again after immigrating with us in 1975. She lived on Social Security checks, gardened, said Buddhist prayers, and was nanny to her grandchildren. She watched soap operas religiously, and could report their full plot lines while sitting and knitting. She bundled her many sadnesses in a contented, 4‐foot 9‐inch frame.
Having no home of her own, she would move from one child's house to another every few months so as not to wear out her welcome. But her children lived in Pennsylvania, New Jersey, Florida, Texas, and Maryland. And in most of these cities, she had a different primary care physician. She has 21 grandchildren; 8 of us are physicians. Yet the aunts and uncles told us very little about her medical care. She preferred older‐generation Vietnamese physicians and I'm not sure that they were all competent, but her children did not want to argue with an octogenarian war survivor, and we deferred to their judgment. So we would find out only incidentally, for example, that a doctor prescribed her tuberculosis drugs for a visit to Vietnam.
For many years, Ba ngoai had no major medical problems. She was hypothyroid and hypertensive but on medication and generally high functioning. She had a lumpectomy for early‐stage breast cancer. Then, a year or so after she told me the story of my grandfather's death, Alzheimer's set in. It became harder for her to report symptoms reliably, and she became mildly depressed. Her grandchildren were now birthing our own babies, and we offered these as a distraction, trying to surround her with celebrations of these new fruits of her life labors.
Ba ngoai's decline worsened 3 years ago. She became more easily fatigued, depressed, and confused. A few months before she died, she started to get dyspneic, and couldn't go for short walks any more. In retrospect, I think that her prescription for thyroid replacement somehow fell through the cracks, probably in the transfer of care from one city to another, although there remains a great deal of confusion in the family about exactly what happened. Her thyroxine levels dwindled. One evening in October of that year, at my uncle's house in Maryland, she became severely short of breath and nearly unconscious. They called her Maryland PCP, who sent her to an emergency room at a local hospital. She was admitted in severe congestive heart failure. When the hospitalist spoke with my mother and uncle, he explained that he could take some fluid off her lungs, but that she might need to be intubated and admitted to intensive care. Looking back, I guessed that she probably needed pressors and invasive monitoring. He asked them, Is this what you want? My uncle said, No, it's not. And the hospitalist and the huddle of relatives decided she should come home.
The question was, into whose care would she be discharged? My elders were wary of contacting her PCP, partly because some blamed him for not catching and addressing her symptoms sooner, partly because to even confront him with this perception would cause him, and hence them, to lose face. This seemed too excruciating a scenario to them.
So at last, my uncle called my brother, the oldest grandchild and a very talented clinician. My brother is a pulmonologist, the kind of physician who once did a history and physical on a patient complaining only of Really feeling bad, Doc, and confidently started a steroid infusion before returning the next day with test results confirming his suspicion of Wegener's granulomatosis. He took my grandmother's physical by phone, and told my uncle to increase her furosemide dose. Then he said, I'm on call, but I'll be down there tomorrow. Call everyone together. Most of my relatives were already in town; they had come at news of her decline. She became alert enough for a couple of days to see and recognize most of the faces around her, like so many markers on a long journey. And then she died, slipped away.
I find it hard to define good coordination of care. My instinct as a researcher is to list measurable elements, but the tools we currently have generate metrics that are either reductionistsuch as how rapidly a physician returns a patient's callor so global that they no longer seem actionablesuch as patient satisfaction. But if such metrics set the goal in the distance, it seems useful to also define its counterpartdiscoordinationas a marker of the reality we would like to leave behind us as far as possible. Discoordination includes elements of discontinuity (lost patient history), fragmentation (actions by multiple players), overuse and/or inappropriate use of services, and ultimately, ineffective care (that is, the patient's needs go unmet).
My experience of discoordination was that of a Rube Goldberg contraption. It's composed of innumerable subtasks, each cleverly designed as the easiest solution to a seemingly short‐term problem, as quick fixes, but that in aggregate generate such chaos that the ultimate purpose is lost. They include acts of denial, lies to avoid embarrassment or conflict, and choices of convenience. My mother and her siblings accommodated my grandmother's choice of physicians by (secretly) not always adhering to care recommendations they didn't agree with, instead of challenging her. They took her to different physicians in different cities rather than risk embarrassing (due to an exaggerated sense of the smallness of the Vietnamese community) any one physician by dropping him. Her grandchildren, despite our medical training, found it culturally easier to defer to our elders than to intervene in substandard care. And none of her physicians aggressively followed up to ensure that a frail Alzheimer's patient was getting the care she needed. This is not to suggest that coordination is a simple task because Rube Goldberg machines make simple tasks complicated. Rather, it is a depiction of how indirectly we tend to address the problem.
I imagine a different course of events for my grandmother in the absence of discoordination. What if her children and physicians had understood and acknowledged to one another that her care was fragmented and therefore suboptimal? What if we grandchildren had confronted both Ba Ngoai and our parents sooner about their choice of physicians and offered to take on more of the burden of helping with her care decisions? Would we, as physicians, have been better able to ensure that her providers made rational clinical decisions? And what if she and her family had consistently recognized a single physician as her medical home? Snowbirding is hardly a rare phenomenon among Medicare patients; we could have designated one physician as primarily responsible for coordinating her care even without limiting her travel.
Care coordination is an inherently human activity. Supportive elements such as efficient transfer of medical information, resources for patient education and self‐care, and adequate reimbursement can take us to the brink of, but not actually bridge, the chasm that we want to cross. Traversing that divide sometimes requires settling turf issues over undesirable responsibilities between different physicians and between physicians and other providers; clarifying who has primary responsibility for different types of decisions (I lead on cardiac issues and her son leads on health maintenance); and the violation of cultural norms of patients, families, and/or providers. These can be uncomfortable, unpleasant conversations that at times seem beside the point. But in aggregate, they are the work of coordination, because they force us to align our expectations of one another. No level of information technology could have dismantled the Rube Goldberg machine that trapped my grandmother. Her last of many lessons for me was that emotional courage, honesty, and perseverance offer a much more direct path through the muck.
BOOSTing the Hospital Discharge
Hospitalists recognize the importance of the care transition from the inpatient setting to the outpatient setting, despite being described as causing a divorce between inpatient and outpatient care.1 If you do not believe this, just glance at the table of contents for this issue of the Journal of Hospital Medicine, which has 5 reports on research about various aspects of the hospital discharge transition complemented by an eloquent story of how a hospitalist facilitated the care coordination of one family's matriarch.2 An accompanying editorial proposes that hospitalists embrace the need of patients and their caregivers for care coordination.3 Thankfully, a growing number of academic hospitalists are focusing their efforts on identifying problems in the process and evaluating potential interventions to optimize it.
The hospital discharge process commonly has been an afterthought, concluding a typically intense experience for patients, some of whom may have begun the episode of hospitalization near death. After diagnostic evaluations and treatments, a patient has achieved stable enough status to be discharged home, and the inpatient physician has signed off with a simple may go in the written orders. The physician may feel absolved of responsibility as he expects the nurses to take care of instructions and to find transportation home for the patient. Unfortunately, this experience often is consistent with Webster's definition of discharge: to relieve of a charge, load, or burden unload release from an obligation. Some patients may feel like a Nolan Ryan fastball flying out of the hospital, but with no one to catch them.
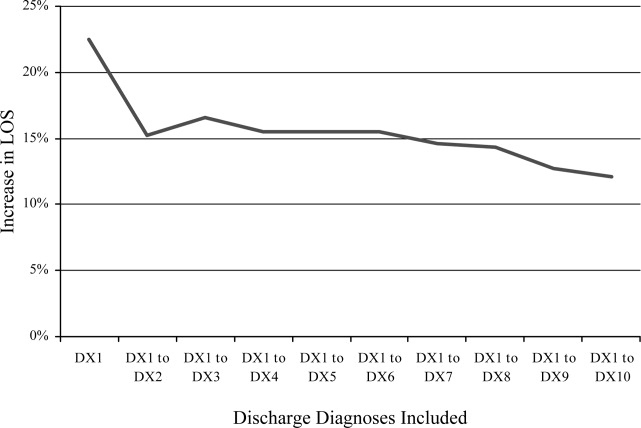
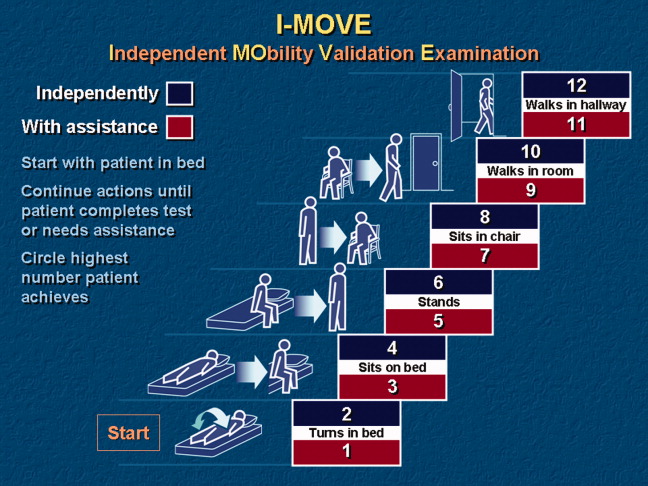
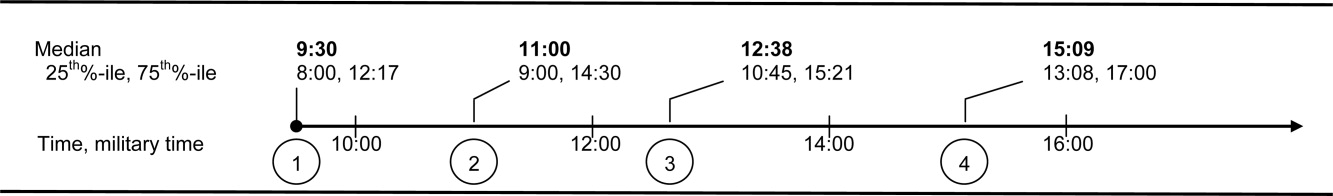
Recognizing how the hospital discharge transition to home can be a perilous process fraught with failure,4 we laid out a research agenda for transitions of care. We are gratified to see the robust response from researchers published in this issue of the Journal of Hospital Medicine. The studies range from the description of a new tool to assess patients' mobility before discharge5 to evidence that the length of stay is prolonged (ie, delayed discharge) when the discharge diagnosis differs from that made on admission.6 Chen and colleagues analyzed the timing of discharge during the day and found that the duration of the discharge process was influenced by the need for consultation or a procedure prior to discharge; this finding is not surprising to practicing hospitalists. We agree with their conclusion that broad institutional efforts will be needed to facilitate the process. Hospitalists are part of a system and must engage the entire team to improve efficiency.
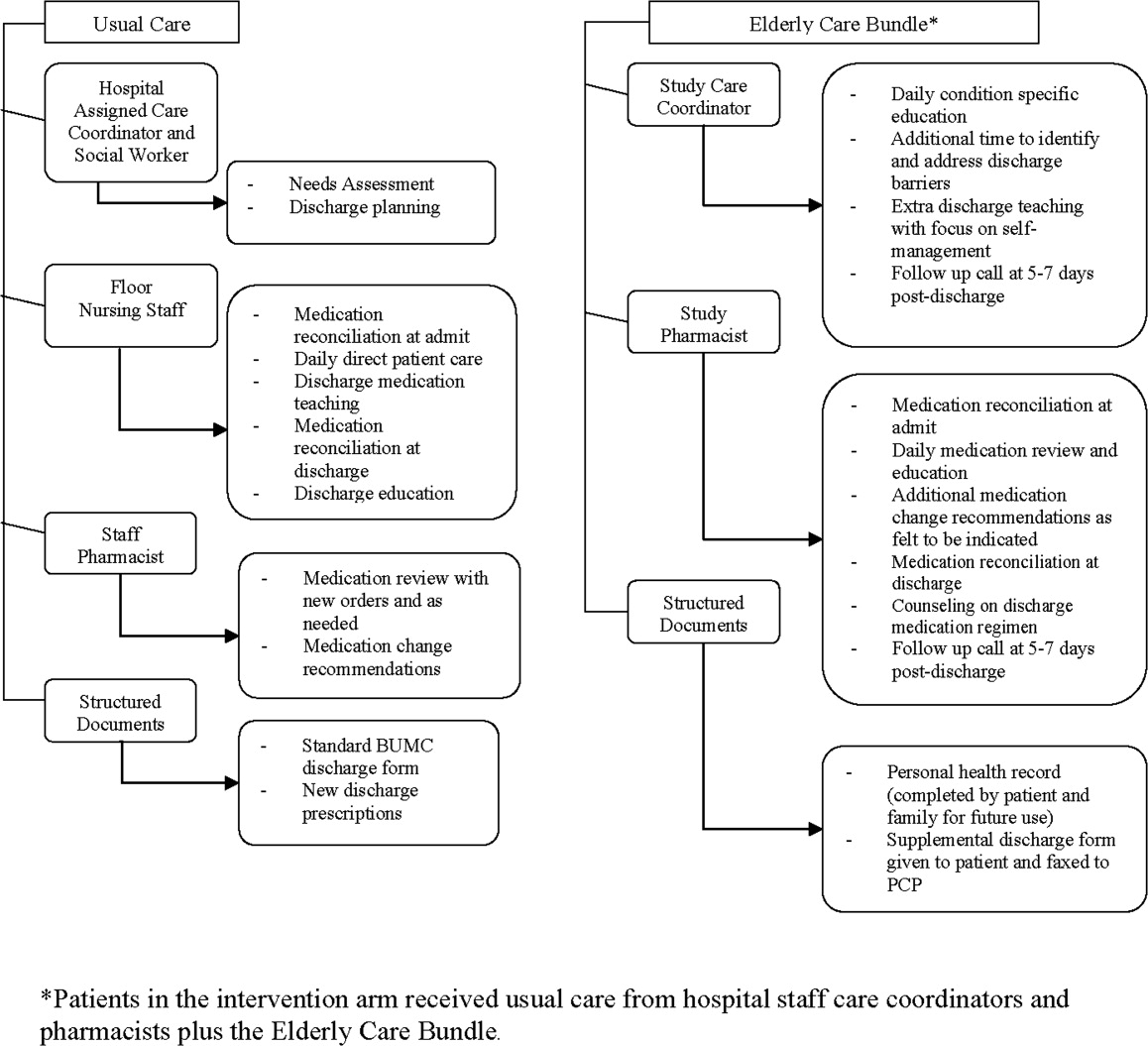
O'Leary and fellow hospitalists7 at Northwestern Memorial Hospital focused on creating a better discharge summary within their electronic health record with the aim of improved overall quality of the summaries and, just as important, timely completion. Despite some research indicating that absence of adequate communication between primary care providers and inpatient medical teams is not associated with adverse clinical outcomes,8 other research has demonstrated that it does affect outcomes and probably affects rehospitalization rates.9, 10 Moreover, another article in this issue describes a project undertaken at Baylor Health Care System (Dallas, TX) that demonstrated a reduction in emergency department visits and readmissions within 30 days post‐discharge among high‐risk elderly medical patients when a targeted care bundle was used.11 The results from this intervention, which consisted of medication counseling/reconciliation by a clinical pharmacist, condition‐specific enhanced discharge planning by a care coordinator, and phone follow‐up, confirm recent results from 2 similar studies.12, 13 These studies provide support for the idea that straightforward changes in the discharge process can improve patient outcomes.
Today in the United States, hospitalists likely care for the majority of hospitalized older patients.14 We strongly encourage them to use evidence‐based approaches to optimize the discharge process in their hospitals, and fortunately, clear guidance is available. Because of generous funding from the John A. Hartford Foundation, Project BOOST (Better Outcomes for Older Adults Through Safe Transitions) is mentoring 30 hospitals in an effort to implement the BOOST toolkit and improve their discharge transition processes.15 Another cost‐effective method involves the use of transition coaches to help the most vulnerable older patients with complex care needs.16 This approach is now being implemented by more than 100 healthcare organizations worldwide.17
Heartened by these exciting initiatives, we applaud the Society of Hospital Medicine's collaboration with the American College of Physicians, the Society of General Internal Medicine, the American Geriatrics Society, and the Society of Academic Emergency Medicine to produce a consensus policy statement on transitions of care that provides guiding principles for transitions both into and out of the hospital.18 Soon, all hospitalized patients and their caregivers may receive robust education prior to discharge, confirmation of their understanding with the teach‐back approach, medication reconciliation, and clear instructions for follow‐up, and the patient's primary care provider will be aware of all that has happened. Patients should expect nothing less than hospitalists ensuring their seamless transition from hospital to home.
- ,,,.Hospitalists and care transitions: the divorce of inpatient and outpatient care.Health Aff.2008;27:1315–1327.
- .Dismantling Rube Goldberg: cutting through chaos to achieve coordinated care.J Hosp Med.2009;4:259–260.
- ,,.A new narrative for hospitalists.J Hosp Med.2009;4:207–208.
- ,.Executing high‐quality care transitions: a call to do it right.J Hosp Med.2007;2:287–290.
- ,,.Home alone: mobility independence before discharge.J Hosp Med.2009;4:252–254.
- ,,,,.Discrepancy between admission and discharge diagnoses as a predictor of hospital length of stay.J Hosp Med.2009;4:234–239.
- ,,, et al.,Creating a better discharge summary: improvement in quality and timeliness using an electronic discharge summary.J Hosp Med.2009;4:219–225.
- ,,, et al.Association of communication between hospital‐based physicians and primary care providers with patient outcomes.J Gen Intern Med.2009;24:381–386.
- ,,,,,.Deficits in communication and information transfer between hospital‐based and primary care physicians: implications for patient safety and continuity of care.JAMA.2007;297:831–841.
- ,,.Rehospitalizations among patients in the Medicare fee‐for‐service program.N Engl J Med. In press.
- ,,, et al.Reduction of 30‐day post‐discharge hospital readmission or ED visit rates in high‐risk elderly medical patients through delivery of a targeted care bundle.J Hosp Med.2009;4:211–218.
- ,,, et al.A reengineered hospital discharge program to decrease rehospitalization: a randomized trial.Ann Intern Med.2009;150:178–187.
- ,,,.Redefining and redesigning hospital discharge to enhance patient care: a randomized controlled study.J Gen Intern Med.2008;23:1228–1233.
- ,,,.Growth in the care of older patients by hospitalists in the United States.N Engl J Med.2009;360:1102–1112.
- Society of Hospital Medicine. BOOSTing Care Transitions Resource Room. Available at: http://www.hospitalmedicine.org. Accessed March2009.
- ,,,.The care transitions intervention: results of a randomized controlled trial.Arch Intern Med.2006;166:1822–1828.
- Care Transitions Program. Available at: http://www.caretransitions.org. Accessed March2009.
- ,,, et al.Transitions of care consensus policy statement. American College of Physicians, Society of General Internal Medicine, Society of Hospital Medicine, American Geriatrics Society, American College of Emergency Physicians, and Society of Academic Emergency Medicine.J Hosp Med. In press.
Hospitalists recognize the importance of the care transition from the inpatient setting to the outpatient setting, despite being described as causing a divorce between inpatient and outpatient care.1 If you do not believe this, just glance at the table of contents for this issue of the Journal of Hospital Medicine, which has 5 reports on research about various aspects of the hospital discharge transition complemented by an eloquent story of how a hospitalist facilitated the care coordination of one family's matriarch.2 An accompanying editorial proposes that hospitalists embrace the need of patients and their caregivers for care coordination.3 Thankfully, a growing number of academic hospitalists are focusing their efforts on identifying problems in the process and evaluating potential interventions to optimize it.
The hospital discharge process commonly has been an afterthought, concluding a typically intense experience for patients, some of whom may have begun the episode of hospitalization near death. After diagnostic evaluations and treatments, a patient has achieved stable enough status to be discharged home, and the inpatient physician has signed off with a simple may go in the written orders. The physician may feel absolved of responsibility as he expects the nurses to take care of instructions and to find transportation home for the patient. Unfortunately, this experience often is consistent with Webster's definition of discharge: to relieve of a charge, load, or burden unload release from an obligation. Some patients may feel like a Nolan Ryan fastball flying out of the hospital, but with no one to catch them.
Recognizing how the hospital discharge transition to home can be a perilous process fraught with failure,4 we laid out a research agenda for transitions of care. We are gratified to see the robust response from researchers published in this issue of the Journal of Hospital Medicine. The studies range from the description of a new tool to assess patients' mobility before discharge5 to evidence that the length of stay is prolonged (ie, delayed discharge) when the discharge diagnosis differs from that made on admission.6 Chen and colleagues analyzed the timing of discharge during the day and found that the duration of the discharge process was influenced by the need for consultation or a procedure prior to discharge; this finding is not surprising to practicing hospitalists. We agree with their conclusion that broad institutional efforts will be needed to facilitate the process. Hospitalists are part of a system and must engage the entire team to improve efficiency.
O'Leary and fellow hospitalists7 at Northwestern Memorial Hospital focused on creating a better discharge summary within their electronic health record with the aim of improved overall quality of the summaries and, just as important, timely completion. Despite some research indicating that absence of adequate communication between primary care providers and inpatient medical teams is not associated with adverse clinical outcomes,8 other research has demonstrated that it does affect outcomes and probably affects rehospitalization rates.9, 10 Moreover, another article in this issue describes a project undertaken at Baylor Health Care System (Dallas, TX) that demonstrated a reduction in emergency department visits and readmissions within 30 days post‐discharge among high‐risk elderly medical patients when a targeted care bundle was used.11 The results from this intervention, which consisted of medication counseling/reconciliation by a clinical pharmacist, condition‐specific enhanced discharge planning by a care coordinator, and phone follow‐up, confirm recent results from 2 similar studies.12, 13 These studies provide support for the idea that straightforward changes in the discharge process can improve patient outcomes.
Today in the United States, hospitalists likely care for the majority of hospitalized older patients.14 We strongly encourage them to use evidence‐based approaches to optimize the discharge process in their hospitals, and fortunately, clear guidance is available. Because of generous funding from the John A. Hartford Foundation, Project BOOST (Better Outcomes for Older Adults Through Safe Transitions) is mentoring 30 hospitals in an effort to implement the BOOST toolkit and improve their discharge transition processes.15 Another cost‐effective method involves the use of transition coaches to help the most vulnerable older patients with complex care needs.16 This approach is now being implemented by more than 100 healthcare organizations worldwide.17
Heartened by these exciting initiatives, we applaud the Society of Hospital Medicine's collaboration with the American College of Physicians, the Society of General Internal Medicine, the American Geriatrics Society, and the Society of Academic Emergency Medicine to produce a consensus policy statement on transitions of care that provides guiding principles for transitions both into and out of the hospital.18 Soon, all hospitalized patients and their caregivers may receive robust education prior to discharge, confirmation of their understanding with the teach‐back approach, medication reconciliation, and clear instructions for follow‐up, and the patient's primary care provider will be aware of all that has happened. Patients should expect nothing less than hospitalists ensuring their seamless transition from hospital to home.
Hospitalists recognize the importance of the care transition from the inpatient setting to the outpatient setting, despite being described as causing a divorce between inpatient and outpatient care.1 If you do not believe this, just glance at the table of contents for this issue of the Journal of Hospital Medicine, which has 5 reports on research about various aspects of the hospital discharge transition complemented by an eloquent story of how a hospitalist facilitated the care coordination of one family's matriarch.2 An accompanying editorial proposes that hospitalists embrace the need of patients and their caregivers for care coordination.3 Thankfully, a growing number of academic hospitalists are focusing their efforts on identifying problems in the process and evaluating potential interventions to optimize it.
The hospital discharge process commonly has been an afterthought, concluding a typically intense experience for patients, some of whom may have begun the episode of hospitalization near death. After diagnostic evaluations and treatments, a patient has achieved stable enough status to be discharged home, and the inpatient physician has signed off with a simple may go in the written orders. The physician may feel absolved of responsibility as he expects the nurses to take care of instructions and to find transportation home for the patient. Unfortunately, this experience often is consistent with Webster's definition of discharge: to relieve of a charge, load, or burden unload release from an obligation. Some patients may feel like a Nolan Ryan fastball flying out of the hospital, but with no one to catch them.
Recognizing how the hospital discharge transition to home can be a perilous process fraught with failure,4 we laid out a research agenda for transitions of care. We are gratified to see the robust response from researchers published in this issue of the Journal of Hospital Medicine. The studies range from the description of a new tool to assess patients' mobility before discharge5 to evidence that the length of stay is prolonged (ie, delayed discharge) when the discharge diagnosis differs from that made on admission.6 Chen and colleagues analyzed the timing of discharge during the day and found that the duration of the discharge process was influenced by the need for consultation or a procedure prior to discharge; this finding is not surprising to practicing hospitalists. We agree with their conclusion that broad institutional efforts will be needed to facilitate the process. Hospitalists are part of a system and must engage the entire team to improve efficiency.
O'Leary and fellow hospitalists7 at Northwestern Memorial Hospital focused on creating a better discharge summary within their electronic health record with the aim of improved overall quality of the summaries and, just as important, timely completion. Despite some research indicating that absence of adequate communication between primary care providers and inpatient medical teams is not associated with adverse clinical outcomes,8 other research has demonstrated that it does affect outcomes and probably affects rehospitalization rates.9, 10 Moreover, another article in this issue describes a project undertaken at Baylor Health Care System (Dallas, TX) that demonstrated a reduction in emergency department visits and readmissions within 30 days post‐discharge among high‐risk elderly medical patients when a targeted care bundle was used.11 The results from this intervention, which consisted of medication counseling/reconciliation by a clinical pharmacist, condition‐specific enhanced discharge planning by a care coordinator, and phone follow‐up, confirm recent results from 2 similar studies.12, 13 These studies provide support for the idea that straightforward changes in the discharge process can improve patient outcomes.
Today in the United States, hospitalists likely care for the majority of hospitalized older patients.14 We strongly encourage them to use evidence‐based approaches to optimize the discharge process in their hospitals, and fortunately, clear guidance is available. Because of generous funding from the John A. Hartford Foundation, Project BOOST (Better Outcomes for Older Adults Through Safe Transitions) is mentoring 30 hospitals in an effort to implement the BOOST toolkit and improve their discharge transition processes.15 Another cost‐effective method involves the use of transition coaches to help the most vulnerable older patients with complex care needs.16 This approach is now being implemented by more than 100 healthcare organizations worldwide.17
Heartened by these exciting initiatives, we applaud the Society of Hospital Medicine's collaboration with the American College of Physicians, the Society of General Internal Medicine, the American Geriatrics Society, and the Society of Academic Emergency Medicine to produce a consensus policy statement on transitions of care that provides guiding principles for transitions both into and out of the hospital.18 Soon, all hospitalized patients and their caregivers may receive robust education prior to discharge, confirmation of their understanding with the teach‐back approach, medication reconciliation, and clear instructions for follow‐up, and the patient's primary care provider will be aware of all that has happened. Patients should expect nothing less than hospitalists ensuring their seamless transition from hospital to home.
- ,,,.Hospitalists and care transitions: the divorce of inpatient and outpatient care.Health Aff.2008;27:1315–1327.
- .Dismantling Rube Goldberg: cutting through chaos to achieve coordinated care.J Hosp Med.2009;4:259–260.
- ,,.A new narrative for hospitalists.J Hosp Med.2009;4:207–208.
- ,.Executing high‐quality care transitions: a call to do it right.J Hosp Med.2007;2:287–290.
- ,,.Home alone: mobility independence before discharge.J Hosp Med.2009;4:252–254.
- ,,,,.Discrepancy between admission and discharge diagnoses as a predictor of hospital length of stay.J Hosp Med.2009;4:234–239.
- ,,, et al.,Creating a better discharge summary: improvement in quality and timeliness using an electronic discharge summary.J Hosp Med.2009;4:219–225.
- ,,, et al.Association of communication between hospital‐based physicians and primary care providers with patient outcomes.J Gen Intern Med.2009;24:381–386.
- ,,,,,.Deficits in communication and information transfer between hospital‐based and primary care physicians: implications for patient safety and continuity of care.JAMA.2007;297:831–841.
- ,,.Rehospitalizations among patients in the Medicare fee‐for‐service program.N Engl J Med. In press.
- ,,, et al.Reduction of 30‐day post‐discharge hospital readmission or ED visit rates in high‐risk elderly medical patients through delivery of a targeted care bundle.J Hosp Med.2009;4:211–218.
- ,,, et al.A reengineered hospital discharge program to decrease rehospitalization: a randomized trial.Ann Intern Med.2009;150:178–187.
- ,,,.Redefining and redesigning hospital discharge to enhance patient care: a randomized controlled study.J Gen Intern Med.2008;23:1228–1233.
- ,,,.Growth in the care of older patients by hospitalists in the United States.N Engl J Med.2009;360:1102–1112.
- Society of Hospital Medicine. BOOSTing Care Transitions Resource Room. Available at: http://www.hospitalmedicine.org. Accessed March2009.
- ,,,.The care transitions intervention: results of a randomized controlled trial.Arch Intern Med.2006;166:1822–1828.
- Care Transitions Program. Available at: http://www.caretransitions.org. Accessed March2009.
- ,,, et al.Transitions of care consensus policy statement. American College of Physicians, Society of General Internal Medicine, Society of Hospital Medicine, American Geriatrics Society, American College of Emergency Physicians, and Society of Academic Emergency Medicine.J Hosp Med. In press.
- ,,,.Hospitalists and care transitions: the divorce of inpatient and outpatient care.Health Aff.2008;27:1315–1327.
- .Dismantling Rube Goldberg: cutting through chaos to achieve coordinated care.J Hosp Med.2009;4:259–260.
- ,,.A new narrative for hospitalists.J Hosp Med.2009;4:207–208.
- ,.Executing high‐quality care transitions: a call to do it right.J Hosp Med.2007;2:287–290.
- ,,.Home alone: mobility independence before discharge.J Hosp Med.2009;4:252–254.
- ,,,,.Discrepancy between admission and discharge diagnoses as a predictor of hospital length of stay.J Hosp Med.2009;4:234–239.
- ,,, et al.,Creating a better discharge summary: improvement in quality and timeliness using an electronic discharge summary.J Hosp Med.2009;4:219–225.
- ,,, et al.Association of communication between hospital‐based physicians and primary care providers with patient outcomes.J Gen Intern Med.2009;24:381–386.
- ,,,,,.Deficits in communication and information transfer between hospital‐based and primary care physicians: implications for patient safety and continuity of care.JAMA.2007;297:831–841.
- ,,.Rehospitalizations among patients in the Medicare fee‐for‐service program.N Engl J Med. In press.
- ,,, et al.Reduction of 30‐day post‐discharge hospital readmission or ED visit rates in high‐risk elderly medical patients through delivery of a targeted care bundle.J Hosp Med.2009;4:211–218.
- ,,, et al.A reengineered hospital discharge program to decrease rehospitalization: a randomized trial.Ann Intern Med.2009;150:178–187.
- ,,,.Redefining and redesigning hospital discharge to enhance patient care: a randomized controlled study.J Gen Intern Med.2008;23:1228–1233.
- ,,,.Growth in the care of older patients by hospitalists in the United States.N Engl J Med.2009;360:1102–1112.
- Society of Hospital Medicine. BOOSTing Care Transitions Resource Room. Available at: http://www.hospitalmedicine.org. Accessed March2009.
- ,,,.The care transitions intervention: results of a randomized controlled trial.Arch Intern Med.2006;166:1822–1828.
- Care Transitions Program. Available at: http://www.caretransitions.org. Accessed March2009.
- ,,, et al.Transitions of care consensus policy statement. American College of Physicians, Society of General Internal Medicine, Society of Hospital Medicine, American Geriatrics Society, American College of Emergency Physicians, and Society of Academic Emergency Medicine.J Hosp Med. In press.
Risk Stratification Tools for TIA
Transient ischemic attacks (TIAs) are common and represent a clarion call to action to prevent disabling stroke. Incidence estimates for TIA range from 37 to 107 per 100,000 persons each year.1 Extrapolating from these data, there are likely greater than 100,000 to 300,000 TIAs in the US annually. Within 3 months, approximately 10% of these patients will suffer a stroke, with approximately one‐half of these events occurring within the first 48 hours after the sentinel TIA.26 Nearly two‐thirds of secondary strokes result in disability and 21% are fatal.3 Hospitalists are frequently called to provide care for patients with TIA and, as such, in order to establish an appropriate care plan, they require tools to better predict the likelihood and timing of a disabling stroke.7 In this review we examine the rationale for early aggressive TIA evaluation and treatment in the hospital, overview risk stratification models to identify the patients at highest risk for early recurrent ischemia, and explore application of these tools to admission policy and individualized patient care planning.
Definition
TIA is defined as a brief episode of neurological dysfunction caused by focal brain or retinal ischemia with clinical symptoms typically lasting less than 1 hour and without evidence of brain infarction.8, 9 Prior arbitrary time limits are being abandoned as advanced imaging techniques demonstrate that clinical examination lacks the sensitivity to detect small cerebral infarctions leading to misclassification of as many as 30% to 40% of strokes as TIAs.811 For cases in which imaging is not available, the diagnosis of clinically probable TIA is suggested. Patients with imaging consistent with stroke appear to be at 4‐fold to 10‐fold higher risk for subsequent ischemic events, thus the presence of subclinical infarcts may have clinical importance.2, 12 The majority of TIAs resolve within 1 hour of onset and neurologic deficit continuance beyond this time frame is more consistent with a stroke.13 Continuing symptoms after 1 hour mandates aggressive therapy in lieu of withholding intervention in the hopes of a spontaneous recovery.
Rationale for Hospitalization
Urgent evaluation and treatment within 24 to 48 hours of a TIA is recommended by the National Stroke Association (Table 1).14 These guidelines also recommend hospital admission for high‐risk patients. There are a number of compelling arguments for the hospitalization of a patient at high risk for subsequent stroke.
| Test | Rationale | Therapy |
|---|---|---|
| ||
| Electrocardiogram and rhythm strip | To detect atrial fibrillation. | Long‐term warfarin indicated for suspected cardioembolic etiology. |
| Echocardiogram | To detect intracardiac thrombus or vegetations. Bubble study to detect patent foramen ovale in young patients. | Warfarin indicated for suspected cardioembolic etiology. Patent foramen ovale closure is an option for selected patients. |
| Carotid ultrasound | To detect large vessel atherosclerotic disease. | Antiplatelet therapy* indicated for atherosclerotic etiologies. Early carotid endarterectomy following TIA considered for 50% symptomatic ipsilateral stenosis. |
| Fasting lipid profile, complete blood count, serum electrolytes and creatinine | Secondary prevention of stroke by treating hyperlipidemia. Signs and symptoms associated with severe laboratory abnormalities may mimic TIA. | LDL >100 mg/dL (optional goal >70 mg/dL) is indication for cholesterol lowering therapy. |
| Neuroimaging‐MRI with diffusion images MRA or CT CTA | To detect clinically inapparent lesions of stroke. Useful in ruling out some mimics of TIA. | Patients with abnormal MRI diffusion images represent a population at increased risk for recurrent stroke. |
First, hospitalization offers potential for reduced time to thrombolysis for those patients who have a second ischemic event in the early period following TIA. Outpatients with new ischemic stroke may see hours pass between symptom onset and presentation to the emergency department (ED). This delay frequently places them outside of the thrombolytic window.1517 Hospitalization, assuming a well‐designed inpatient stroke care system, has great potential to reduce this delay. Approximately 50% of the stroke risk following a TIA is evident within 48 hours and rapid thrombolysis, available in an inpatient setting, is associated with improved outcome after stroke.3, 18 A cost‐utility analysis found that a 24‐hour admission for TIA patients to allow tissue plasminogen activator (t‐PA) for recurrent ischemia has a cost‐effectiveness ratio of $55,044 per quality‐adjusted life year with increasing cost effectiveness for the highest risk patients, such as those with a 24‐hour stroke risk of >5%.19
Second, hospital admission often facilitates the reliable and efficient evaluation for etiology and early initiation of secondary prevention. Neuroimaging, carotid ultrasound, echocardiography, and telemetry can be expedited with rapid initiation of proven secondary preventive therapies such as statin treatment, blood pressure control, and antithrombotic therapy. When indicated, carotid revascularization is recommended as soon as possible following TIA, with retrospective reviews suggesting improved outcomes when performed within 2 weeks of the event.1420 In one analysis, a negative association between hospitalization for TIA and subsequent stroke was discovered by review of Canadian population‐based administrative databases.5 While the mechanism for the negative association could not be established, the literature provides some support for hospitalization being associated with decreased risk for second strokes (hazard ratio [HR], 0.73; 95% confidence interval [CI], 0.570.95).5
Theoretically, much of this evaluation and treatment could occur in the outpatient setting but delays commonly seen in outpatient evaluation and the high potential for early second strokes for some patients may make this a risky care plan. Despite the high likelihood for serious outcomes following TIA and clear guidelines for early evaluation and management, current care often lacks a sense of urgency. A 2004 Canadian study revealed that three‐quarters of patients with a TIA were discharged directly from the ED with a resultant delay in diagnostic investigation.4 Over one‐third of patients were discharged without a prescription for antithrombotic therapy. American primary care practice patterns reveal even more significant delays in therapy, with only 2% of patients admitted to a hospital on the day of presentation for TIA, despite 80% of patients presenting for evaluation on the day of symptom onset.21 In this study less than one‐half of patients with atrial fibrillation were started on immediate anticoagulation.21 Further, as many as one‐third of patients did not have any evaluation in the month after the index event.21 Hospitalization for high‐risk patients has the potential to avoid these delays in outpatient evaluation and initiation of therapy.
Still, not all patients will require admission to a hospital setting. American EDs admit approximately one‐half of all TIAs, with regional variability not explained exclusively by clinical characteristics.22 Focusing on identifying the cohort of patients who would most benefit from hospitalization is paramount. In general, hospitalization should be reserved for patients with higher risk of an early secondary stroke. Specifically, admission is generally recommended for patients with crescendo symptoms, TIA on antithrombotic therapy, or symptoms lasting >1 hour.14 Additionally, patients with symptomatic carotid stenosis of 50% and presumed cardioembolic or hypercoagulable etiology merit hospital admission.14 In many cases these etiologies may not be known at time of presentation. Evaluation, such as carotid ultrasound, may not be readily available in the ED to inform the admission decision. Several new scoring systems that utilize routine clinical features available within an hour of presentation have been developed to more objectively assess the risk of secondary stroke following a TIA. The use of these prognostic scoring systems is recommended by the National Stroke Association to aid in triaging this cohort of patients.14
Prognostic Scoring Systems
California Score
The 2000 California Score (Tables 2 and 3) is a 5‐point tool retrospectively developed from a database of 1,707 TIA patients seen in the ED of a California hospital system to predict the likelihood of stroke within 90 days of an initial presentation with transient neurologic deficits.3 Multivariate logistic regression models were used to test the clinical factors associated with stroke risk, resulting in a tool using clinical features of age, diabetes, symptom duration, and the type of deficit to provide quantitative estimates of intermediate term risk. Within 90 days, none of the patients with a score of zero had a stroke whereas the highest score had a 34% risk of stroke (Table 3). While it is possible that some patients with lower scores had a nonischemic etiology for their transient neurological symptoms, clinical practice contains similar ambiguity, and such patients would be correctly predicted to have a low risk for subsequent strokes. Additionally, the derivation and validation of this tool did not include a neurologist confirmation of TIA diagnosis; however, this likely mirrors the practice in most EDs. The California Score has subsequently been validated and expanded upon during the development of the ABCD2 score.23 The California Score's utility is limited in the acute decision‐making process, especially regarding the decision to admit, as it focuses on 90‐day outcomes. For that, shorter‐term risk assessments are more useful.
| Clinical Feature | California Score (points) | ABCD (points) | ABCD2 (points) | |
|---|---|---|---|---|
| ||||
| Age | 60 years | 1 | 1 | 1 |
| Blood pressure | Systolic blood pressure 140 or diastolic blood pressure 90 mmHg | N/A | 1 | 1 |
| Clinical deficits* | Unilateral weakness (focal motor weakness of 1 or more of face, arm, hand, or leg) | 1 | 2 | 2 |
| Speech impairment (dysarthria, dysphasia, or both) | 1 | 1 | 1 | |
| Duration | 60 minutes | 1 | 2 | 2 |
| 10‐59 minutes | 1 | 1 | 1 | |
| Diabetes | Present | 1 | N/A | 1 |
| Maximum score | 5 | 6 | 7 | |
| California Score | 0 | 1 | 2 | 3 | 4 | 5 |
|---|---|---|---|---|---|---|
| ||||||
| 90‐day stroke risk (%) | 0 | 3 | 7 | 11 | 15 | 34 |
ABCD Score
The 2005 ABCD (Tables 2 and 4) is a 6‐point tool designed to predict 7‐day risk of stroke following TIA from the Oxfordshire Community Stroke Project, a UK prospective population‐based cohort of 209 patients with diagnosis of TIA made by a neurologist.24 It evaluated factors previously found to be independent predictors of stroke after TIA, and determined that risk factors of age, blood pressure, type of clinical deficit, and symptom duration predicted 7‐day risk of stroke following TIA. Unlike the California score, the ABCD authors found presenting blood pressure, but not diabetes, to be independent predictors of future events. The authors validated the score with a second population of TIA patients in the Oxford Vascular Study and in a hospital‐based TIA clinic cohort.24 In the validation cohorts the score was highly predictive of stroke at 7 days (P 0.001). Patients with the lowest scores of 0 to 3 had no strokes in the week following the index TIA, whereas patients with the highest score of 6 carried a 35.5% risk of early second stroke. The primary limitation of the ABCD score lies in the small sample size, with only 18 recurrent strokes in the week after TIA in the derivation cohort.
| ABCD Score | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
|---|---|---|---|---|---|---|---|
| |||||||
| 7‐Day stroke risk (%) | 0 | 0 | 0 | 0 | 2.2 | 16.3 | 35.5 |
The ABCD score has subsequently been tested in other settings with mixed results. Two studies found limited utility.25, 26 Other trials found high scores to be overly inclusive but highly predictive and thus the majority of evidence appears to support the validity of the ABCD score in predicting risk of early recurrent ischemic events.2729 The ABCD score has been used to triage patients with high scores to inpatient management although the benefit of this strategy on outcomes has not been proven.30
ABCD2 Score
The 2007 ABCD2 (Tables 2 and 5) is a 7‐point tool that uses the original ABCD criteria along with an additional point for diabetes.23 The ABCD2 derived a unified prognostic score for optimal prediction of the 2‐day stroke risk from multivariate analysis of the original data sets used to create the California and ABCD scores. This score was then validated by the authors in 4 independent cohorts from the United States and the United Kingdom.23 In sum, 4809 patients with TIA were included in the ABCD2 analysis. Similar to prior studies, stroke occurred in 9.2% of patients by 90 days of which 20% were fatal. The authors created low (03 points), intermediate (45 points), and high (67 points) risk categories. In the validation cohorts the prediction rule for the ABCD2 functioned better than the California or ABCD scores with c statistics of 0.62 to 0.83 (ideal prediction produces a c statistic of 1 and prediction no better than chance would have a c statistic of 0.5). They found a 2‐day risk of stroke of 1% for low, 4.1% for intermediate, and 8.1% for the high risk group. Data from the study suggest 34% of TIA patients will be in low‐risk, 45% in intermediate‐risk, and 21% in high‐risk categories. While the ABCD2 score overcomes some of the problems with the 2 prior systems it shares many of the limitations as it was derived from the combined data sets. All scoring systems lack the ability to provide guidance on the management of TIAs associated with rare conditions, such as vasculitis, that are underrepresented in the derivation data sets. The ABCD2 also does not incorporate imaging data and this will likely require further exploration.
| ABCD2 Score | 0‐3 | 4‐5 | 6‐7 |
|---|---|---|---|
| |||
| Risk stratification | Low | Intermediate | High |
| 2‐Day stroke risk (%) | 1 | 4.1 | 8.1 |
| 7‐Day stroke risk (%) | 1.2 | 5.9 | 11.7 |
| 90‐Day stroke risk (%) | 3.1 | 9.8 | 17.8 |
The ABCD2 score can be used to predict risk for a variety of time intervals, has now been validated in independent Greek and British populations, and appears to be the best performing tool at predicting early risk of stroke regardless of underlying etiology.23, 31, 32 The authors suggest that admission for patients in the high‐risk group is prudent whereas outpatient evaluation is reasonable for patients in the low‐risk group.23 Admission for patients in the intermediate‐risk group will depend on individualized decision making, local practice standards, and available community resources.
New Models of Care: An Opportunity for Hospitalists
The key to improving TIA outcomes appears to be more contingent on the speed of evaluation and initiation of appropriate therapy than on the location of the care. The EXPRESS trial studied the effect of an immediate access neurovascular clinic providing urgent evaluation and immediate treatment of nonhospitalized TIA patients versus usual care. Statistically significant reductions were seen in time to evaluation, first treatment prescription, and in 90‐day risk of recurrent stroke (10.3% versus 2.1%, P 0.0001) after the clinic was changed to the rapid evaluation and treatment model.33
The SOS‐TIA study used a 24‐hour access hospital‐based TIA clinic to evaluate the effects of rapid assessment and interventions on hospital length of stay and clinical outcomes.34 The 90‐day stroke rate was 1.24% (95% CI, 0.712.12), which represents a 79% reduction compared to the predicted stroke rate from the ABCD2 scores. With expedited evaluation and treatment, 74% of patients were able to be sent home on the same day.
The results of these 2 new studies provide compelling evidence that rapid evaluation and treatment in the first 48 hours after TIA has the potential to alter outcomes. Unfortunately not all communities have access to same day TIA clinics. Still, these findings should embolden hospitalists to advocate for urgent evaluation, such as neurology and cardiac imaging and carotid evaluation, with immediate initiation of secondary preventive therapy and early surgical intervention when appropriate. In most cases these changes will require process transformations that present prime opportunities for hospitalists to reengineer systems of care.
Incorporating Prognostic Scores into Clinical Practice
Applying the evidence to practice requires calculation of the early risk but also awareness of the community resources available. High‐risk patients with an ABCD2 score of 6 or 7 have a very high 8.1% risk of stroke within the next 48 hours. Given the catastrophic outcomes frequently seen after second strokes, these patients warrant inpatient admission to facilitate the immediate initiation of appropriate secondary prevention and potentially shorten time to thrombolysis if an early stroke occurs. Intermediate‐risk patients with ABCD2 scores of 4 and 5 have a 4.1% 2‐day risk of stroke and may be considered for admission, hospital observation, or expedited clinic evaluation contingent on local availability. As many as one‐third of TIA patients will be categorized as low risk with a score of 0 to 3. These patients have a 2‐day risk of stroke of only 1% and are likely safe for prompt outpatient evaluation and management. The new, validated, ABCD2 score is not a substitute for individualized judgment, but is helpful in developing admission guidelines in cooperation between neurologists, emergency room physicians, and hospitalists, and in using evidence‐based medicine to provide optimal care for the patient presenting with a TIA.
Stroke and TIA arise from identical etiologies, respond to the same secondary preventive measures, and should be considered part of the spectrum of an ischemic cerebral syndrome. Recognizing TIA as a medical emergency with high rates of secondary stroke and subsequent disability allows institution of therapies with appropriate urgency. Hospitalization offers the ability to rapidly coordinate the testing and secondary prevention measures but also, for high‐risk patients, offers the opportunity to reduce the time to thrombolysis for early recurrent strokes. New, validated scoring systems such as the ABCD2 score help the hospitalist to decide which patients are appropriate for admission and which can be managed in progressive and traditional outpatient settings.
- ,,.Epidemiological impact in the United States of a tissue‐based definition of transient ischemic attack.Stroke.2003;34:919–924.
- ,,, et al.Head computed tomography findings predict short‐term stroke risk after transient ischemic attack.Stroke.2003;34:2894–2899.
- ,,, et al.Short‐term prognosis after emergency department diagnosis of TIA.JAMA.2000;284:2901–2906.
- ,,, et al.Management and outcomes of transient ischemic attacks in Ontario.CMAJ.2004;170:1099–1104.
- ,,, et al.The high risk of stroke immediately after transient ischemic attack: a population based study.Neurology.2004;62:2015–2020.
- ,,, et al.Early risk of stroke after transient ischemic attack: a systematic review and meta‐analysis.Arch Intern Med.2007;167:2417–2422.
- ,,, et al.The spectrum of community‐based hospitalist practice: a call to tailor internal medicine residency training.Arch Intern Med.2007;167:727–729.
- .Transient ischemic attack with abnormal diffusion‐weighted imaging results: what's in a name?Arch Neurol.2007;64:1080–1082.
- ,.A reappraisal of the definition and pathophysiology of the transient ischemic attack.Med Sci Monit.2007;13:RA50–53.
- ,,, et al.Diffusion‐weighted imaging‐negative patients with transient ischemic attack are at risk of recurrent transient events.Stroke.2007;38:2367–2369.
- ,,, et al.Transient ischemic attack—proposal for a new definition.N Engl J Med.2002;347:1713–1716.
- ,,, et al.Management and outcome of patients with transient ischemic attack admitted to a stroke unit.Cerebrovasc Dis.2007;24:80–85.
- .How transient are transient ischemic attacks.Neurology.1988;38:674–677.
- ,,, et al.National Stroke Association guidelines for the management of transient ischemic attacks.Ann Neurol.2006;60:301–313.
- ,,, et al.Out‐of‐hospital delays in patients with acute stroke.Ann Emerg Med.2004;44:476–483.
- ,,, et al.Factors associated with delayed admission to hospital and in‐hospital delays in acute stroke and TIA: a prospective multicenter study.Stroke.1999;30:40–48.
- ,,, et al.Prehospital and emergency department delays after acute stroke: the Genentech Stroke Presentation Survey.Stroke.2000;31:2585–2590.
- Tissue plasminogen activator for acute ischemic stroke.The National Institute of Neurological Disorders and Stroke rt‐PA Stroke Study Group.N Engl J Med.1995;333:1581–1587.
- ,.Is hospitalization after TIA cost effective on the basis of treatment with tPA?Neurology.2005;65:1799–1801.
- ,,, et al.Endarterectomy for symptomatic carotid stenosis in relation to clinical subgroups and timing of surgery.Lancet.2004;363:915–924.
- ,,, et al.New transient ischemic attack and stroke: outpatient management by primary care physicians.Arch Intern Med.2000;160:2941–2946.
- ,,, et al.Hospital and demographic influences on the disposition of transient ischemic attack.Acad Emerg Med.2008;15:171–176.
- ,,, et al.Validation and refinement of scores to predict very early stroke risk after transient ischaemic attack.Lancet.2007;369:283–292.
- ,,, et al.A simple score (ABCD) to identify individuals at high early risk of stroke after transient ischaemic attack.Lancet.2005;366:29–36.
- ,,, et al.Is the ABCD score useful for risk stratification of patients with acute transient ischemic attack?Stroke.2006;37:1710–1714.
- ,,, et al.Absence of usefulness of ABCD score in the early risk of recurrent stroke in transient ischemic attack patients.Stroke.2007;38:855–856.
- ,,, et al.Validation of the ABCD score in identifying individuals at high early risk of stroke after a transient ischemic attack: a hospital‐based case series study.Stroke.2006;37:2892–2897.
- ,.Rapid identification of high‐risk transient ischemic attacks: prospective validation of the ABCD score.Stroke.2008;39:297–302.
- ,,.Can the ABCD score be dichotomized to identify high‐risk patients with transient ischaemic attack in the emergency department?Emerg Med J.2007;24:92–95.
- ,,, et al.Can risk stratification of transient ischaemic attacks improve patient care in the emergency department?Emerg Med J.2007;24:637–640.
- ,,, et al.Prognosis in patients with transient ischaemic attack (TIA) and minor stroke attending TIA services in the north west of England: The NORTHSTAR Study.J Neurol Neurosurg Psychiatry.2007:1–6.
- ,,.Potential applicability of the ABCD2 in triaging TIA patients.Lancet.2007;369:1082.
- ,,, et al.Effect of urgent treatment of transient ischemic attack and minor stroke on early recurrent stroke (EXPRESS Study): a prospective population‐based sequential comparison.Lancet.2007;370;1432–1442.
- ,,, et al.A transient ischemic attack clinic with round‐the‐clock access (SOS‐TIA): feasibility and effects.Lancet Neurol.2007;6:953–960.
Transient ischemic attacks (TIAs) are common and represent a clarion call to action to prevent disabling stroke. Incidence estimates for TIA range from 37 to 107 per 100,000 persons each year.1 Extrapolating from these data, there are likely greater than 100,000 to 300,000 TIAs in the US annually. Within 3 months, approximately 10% of these patients will suffer a stroke, with approximately one‐half of these events occurring within the first 48 hours after the sentinel TIA.26 Nearly two‐thirds of secondary strokes result in disability and 21% are fatal.3 Hospitalists are frequently called to provide care for patients with TIA and, as such, in order to establish an appropriate care plan, they require tools to better predict the likelihood and timing of a disabling stroke.7 In this review we examine the rationale for early aggressive TIA evaluation and treatment in the hospital, overview risk stratification models to identify the patients at highest risk for early recurrent ischemia, and explore application of these tools to admission policy and individualized patient care planning.
Definition
TIA is defined as a brief episode of neurological dysfunction caused by focal brain or retinal ischemia with clinical symptoms typically lasting less than 1 hour and without evidence of brain infarction.8, 9 Prior arbitrary time limits are being abandoned as advanced imaging techniques demonstrate that clinical examination lacks the sensitivity to detect small cerebral infarctions leading to misclassification of as many as 30% to 40% of strokes as TIAs.811 For cases in which imaging is not available, the diagnosis of clinically probable TIA is suggested. Patients with imaging consistent with stroke appear to be at 4‐fold to 10‐fold higher risk for subsequent ischemic events, thus the presence of subclinical infarcts may have clinical importance.2, 12 The majority of TIAs resolve within 1 hour of onset and neurologic deficit continuance beyond this time frame is more consistent with a stroke.13 Continuing symptoms after 1 hour mandates aggressive therapy in lieu of withholding intervention in the hopes of a spontaneous recovery.
Rationale for Hospitalization
Urgent evaluation and treatment within 24 to 48 hours of a TIA is recommended by the National Stroke Association (Table 1).14 These guidelines also recommend hospital admission for high‐risk patients. There are a number of compelling arguments for the hospitalization of a patient at high risk for subsequent stroke.
| Test | Rationale | Therapy |
|---|---|---|
| ||
| Electrocardiogram and rhythm strip | To detect atrial fibrillation. | Long‐term warfarin indicated for suspected cardioembolic etiology. |
| Echocardiogram | To detect intracardiac thrombus or vegetations. Bubble study to detect patent foramen ovale in young patients. | Warfarin indicated for suspected cardioembolic etiology. Patent foramen ovale closure is an option for selected patients. |
| Carotid ultrasound | To detect large vessel atherosclerotic disease. | Antiplatelet therapy* indicated for atherosclerotic etiologies. Early carotid endarterectomy following TIA considered for 50% symptomatic ipsilateral stenosis. |
| Fasting lipid profile, complete blood count, serum electrolytes and creatinine | Secondary prevention of stroke by treating hyperlipidemia. Signs and symptoms associated with severe laboratory abnormalities may mimic TIA. | LDL >100 mg/dL (optional goal >70 mg/dL) is indication for cholesterol lowering therapy. |
| Neuroimaging‐MRI with diffusion images MRA or CT CTA | To detect clinically inapparent lesions of stroke. Useful in ruling out some mimics of TIA. | Patients with abnormal MRI diffusion images represent a population at increased risk for recurrent stroke. |
First, hospitalization offers potential for reduced time to thrombolysis for those patients who have a second ischemic event in the early period following TIA. Outpatients with new ischemic stroke may see hours pass between symptom onset and presentation to the emergency department (ED). This delay frequently places them outside of the thrombolytic window.1517 Hospitalization, assuming a well‐designed inpatient stroke care system, has great potential to reduce this delay. Approximately 50% of the stroke risk following a TIA is evident within 48 hours and rapid thrombolysis, available in an inpatient setting, is associated with improved outcome after stroke.3, 18 A cost‐utility analysis found that a 24‐hour admission for TIA patients to allow tissue plasminogen activator (t‐PA) for recurrent ischemia has a cost‐effectiveness ratio of $55,044 per quality‐adjusted life year with increasing cost effectiveness for the highest risk patients, such as those with a 24‐hour stroke risk of >5%.19
Second, hospital admission often facilitates the reliable and efficient evaluation for etiology and early initiation of secondary prevention. Neuroimaging, carotid ultrasound, echocardiography, and telemetry can be expedited with rapid initiation of proven secondary preventive therapies such as statin treatment, blood pressure control, and antithrombotic therapy. When indicated, carotid revascularization is recommended as soon as possible following TIA, with retrospective reviews suggesting improved outcomes when performed within 2 weeks of the event.1420 In one analysis, a negative association between hospitalization for TIA and subsequent stroke was discovered by review of Canadian population‐based administrative databases.5 While the mechanism for the negative association could not be established, the literature provides some support for hospitalization being associated with decreased risk for second strokes (hazard ratio [HR], 0.73; 95% confidence interval [CI], 0.570.95).5
Theoretically, much of this evaluation and treatment could occur in the outpatient setting but delays commonly seen in outpatient evaluation and the high potential for early second strokes for some patients may make this a risky care plan. Despite the high likelihood for serious outcomes following TIA and clear guidelines for early evaluation and management, current care often lacks a sense of urgency. A 2004 Canadian study revealed that three‐quarters of patients with a TIA were discharged directly from the ED with a resultant delay in diagnostic investigation.4 Over one‐third of patients were discharged without a prescription for antithrombotic therapy. American primary care practice patterns reveal even more significant delays in therapy, with only 2% of patients admitted to a hospital on the day of presentation for TIA, despite 80% of patients presenting for evaluation on the day of symptom onset.21 In this study less than one‐half of patients with atrial fibrillation were started on immediate anticoagulation.21 Further, as many as one‐third of patients did not have any evaluation in the month after the index event.21 Hospitalization for high‐risk patients has the potential to avoid these delays in outpatient evaluation and initiation of therapy.
Still, not all patients will require admission to a hospital setting. American EDs admit approximately one‐half of all TIAs, with regional variability not explained exclusively by clinical characteristics.22 Focusing on identifying the cohort of patients who would most benefit from hospitalization is paramount. In general, hospitalization should be reserved for patients with higher risk of an early secondary stroke. Specifically, admission is generally recommended for patients with crescendo symptoms, TIA on antithrombotic therapy, or symptoms lasting >1 hour.14 Additionally, patients with symptomatic carotid stenosis of 50% and presumed cardioembolic or hypercoagulable etiology merit hospital admission.14 In many cases these etiologies may not be known at time of presentation. Evaluation, such as carotid ultrasound, may not be readily available in the ED to inform the admission decision. Several new scoring systems that utilize routine clinical features available within an hour of presentation have been developed to more objectively assess the risk of secondary stroke following a TIA. The use of these prognostic scoring systems is recommended by the National Stroke Association to aid in triaging this cohort of patients.14
Prognostic Scoring Systems
California Score
The 2000 California Score (Tables 2 and 3) is a 5‐point tool retrospectively developed from a database of 1,707 TIA patients seen in the ED of a California hospital system to predict the likelihood of stroke within 90 days of an initial presentation with transient neurologic deficits.3 Multivariate logistic regression models were used to test the clinical factors associated with stroke risk, resulting in a tool using clinical features of age, diabetes, symptom duration, and the type of deficit to provide quantitative estimates of intermediate term risk. Within 90 days, none of the patients with a score of zero had a stroke whereas the highest score had a 34% risk of stroke (Table 3). While it is possible that some patients with lower scores had a nonischemic etiology for their transient neurological symptoms, clinical practice contains similar ambiguity, and such patients would be correctly predicted to have a low risk for subsequent strokes. Additionally, the derivation and validation of this tool did not include a neurologist confirmation of TIA diagnosis; however, this likely mirrors the practice in most EDs. The California Score has subsequently been validated and expanded upon during the development of the ABCD2 score.23 The California Score's utility is limited in the acute decision‐making process, especially regarding the decision to admit, as it focuses on 90‐day outcomes. For that, shorter‐term risk assessments are more useful.
| Clinical Feature | California Score (points) | ABCD (points) | ABCD2 (points) | |
|---|---|---|---|---|
| ||||
| Age | 60 years | 1 | 1 | 1 |
| Blood pressure | Systolic blood pressure 140 or diastolic blood pressure 90 mmHg | N/A | 1 | 1 |
| Clinical deficits* | Unilateral weakness (focal motor weakness of 1 or more of face, arm, hand, or leg) | 1 | 2 | 2 |
| Speech impairment (dysarthria, dysphasia, or both) | 1 | 1 | 1 | |
| Duration | 60 minutes | 1 | 2 | 2 |
| 10‐59 minutes | 1 | 1 | 1 | |
| Diabetes | Present | 1 | N/A | 1 |
| Maximum score | 5 | 6 | 7 | |
| California Score | 0 | 1 | 2 | 3 | 4 | 5 |
|---|---|---|---|---|---|---|
| ||||||
| 90‐day stroke risk (%) | 0 | 3 | 7 | 11 | 15 | 34 |
ABCD Score
The 2005 ABCD (Tables 2 and 4) is a 6‐point tool designed to predict 7‐day risk of stroke following TIA from the Oxfordshire Community Stroke Project, a UK prospective population‐based cohort of 209 patients with diagnosis of TIA made by a neurologist.24 It evaluated factors previously found to be independent predictors of stroke after TIA, and determined that risk factors of age, blood pressure, type of clinical deficit, and symptom duration predicted 7‐day risk of stroke following TIA. Unlike the California score, the ABCD authors found presenting blood pressure, but not diabetes, to be independent predictors of future events. The authors validated the score with a second population of TIA patients in the Oxford Vascular Study and in a hospital‐based TIA clinic cohort.24 In the validation cohorts the score was highly predictive of stroke at 7 days (P 0.001). Patients with the lowest scores of 0 to 3 had no strokes in the week following the index TIA, whereas patients with the highest score of 6 carried a 35.5% risk of early second stroke. The primary limitation of the ABCD score lies in the small sample size, with only 18 recurrent strokes in the week after TIA in the derivation cohort.
| ABCD Score | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
|---|---|---|---|---|---|---|---|
| |||||||
| 7‐Day stroke risk (%) | 0 | 0 | 0 | 0 | 2.2 | 16.3 | 35.5 |
The ABCD score has subsequently been tested in other settings with mixed results. Two studies found limited utility.25, 26 Other trials found high scores to be overly inclusive but highly predictive and thus the majority of evidence appears to support the validity of the ABCD score in predicting risk of early recurrent ischemic events.2729 The ABCD score has been used to triage patients with high scores to inpatient management although the benefit of this strategy on outcomes has not been proven.30
ABCD2 Score
The 2007 ABCD2 (Tables 2 and 5) is a 7‐point tool that uses the original ABCD criteria along with an additional point for diabetes.23 The ABCD2 derived a unified prognostic score for optimal prediction of the 2‐day stroke risk from multivariate analysis of the original data sets used to create the California and ABCD scores. This score was then validated by the authors in 4 independent cohorts from the United States and the United Kingdom.23 In sum, 4809 patients with TIA were included in the ABCD2 analysis. Similar to prior studies, stroke occurred in 9.2% of patients by 90 days of which 20% were fatal. The authors created low (03 points), intermediate (45 points), and high (67 points) risk categories. In the validation cohorts the prediction rule for the ABCD2 functioned better than the California or ABCD scores with c statistics of 0.62 to 0.83 (ideal prediction produces a c statistic of 1 and prediction no better than chance would have a c statistic of 0.5). They found a 2‐day risk of stroke of 1% for low, 4.1% for intermediate, and 8.1% for the high risk group. Data from the study suggest 34% of TIA patients will be in low‐risk, 45% in intermediate‐risk, and 21% in high‐risk categories. While the ABCD2 score overcomes some of the problems with the 2 prior systems it shares many of the limitations as it was derived from the combined data sets. All scoring systems lack the ability to provide guidance on the management of TIAs associated with rare conditions, such as vasculitis, that are underrepresented in the derivation data sets. The ABCD2 also does not incorporate imaging data and this will likely require further exploration.
| ABCD2 Score | 0‐3 | 4‐5 | 6‐7 |
|---|---|---|---|
| |||
| Risk stratification | Low | Intermediate | High |
| 2‐Day stroke risk (%) | 1 | 4.1 | 8.1 |
| 7‐Day stroke risk (%) | 1.2 | 5.9 | 11.7 |
| 90‐Day stroke risk (%) | 3.1 | 9.8 | 17.8 |
The ABCD2 score can be used to predict risk for a variety of time intervals, has now been validated in independent Greek and British populations, and appears to be the best performing tool at predicting early risk of stroke regardless of underlying etiology.23, 31, 32 The authors suggest that admission for patients in the high‐risk group is prudent whereas outpatient evaluation is reasonable for patients in the low‐risk group.23 Admission for patients in the intermediate‐risk group will depend on individualized decision making, local practice standards, and available community resources.
New Models of Care: An Opportunity for Hospitalists
The key to improving TIA outcomes appears to be more contingent on the speed of evaluation and initiation of appropriate therapy than on the location of the care. The EXPRESS trial studied the effect of an immediate access neurovascular clinic providing urgent evaluation and immediate treatment of nonhospitalized TIA patients versus usual care. Statistically significant reductions were seen in time to evaluation, first treatment prescription, and in 90‐day risk of recurrent stroke (10.3% versus 2.1%, P 0.0001) after the clinic was changed to the rapid evaluation and treatment model.33
The SOS‐TIA study used a 24‐hour access hospital‐based TIA clinic to evaluate the effects of rapid assessment and interventions on hospital length of stay and clinical outcomes.34 The 90‐day stroke rate was 1.24% (95% CI, 0.712.12), which represents a 79% reduction compared to the predicted stroke rate from the ABCD2 scores. With expedited evaluation and treatment, 74% of patients were able to be sent home on the same day.
The results of these 2 new studies provide compelling evidence that rapid evaluation and treatment in the first 48 hours after TIA has the potential to alter outcomes. Unfortunately not all communities have access to same day TIA clinics. Still, these findings should embolden hospitalists to advocate for urgent evaluation, such as neurology and cardiac imaging and carotid evaluation, with immediate initiation of secondary preventive therapy and early surgical intervention when appropriate. In most cases these changes will require process transformations that present prime opportunities for hospitalists to reengineer systems of care.
Incorporating Prognostic Scores into Clinical Practice
Applying the evidence to practice requires calculation of the early risk but also awareness of the community resources available. High‐risk patients with an ABCD2 score of 6 or 7 have a very high 8.1% risk of stroke within the next 48 hours. Given the catastrophic outcomes frequently seen after second strokes, these patients warrant inpatient admission to facilitate the immediate initiation of appropriate secondary prevention and potentially shorten time to thrombolysis if an early stroke occurs. Intermediate‐risk patients with ABCD2 scores of 4 and 5 have a 4.1% 2‐day risk of stroke and may be considered for admission, hospital observation, or expedited clinic evaluation contingent on local availability. As many as one‐third of TIA patients will be categorized as low risk with a score of 0 to 3. These patients have a 2‐day risk of stroke of only 1% and are likely safe for prompt outpatient evaluation and management. The new, validated, ABCD2 score is not a substitute for individualized judgment, but is helpful in developing admission guidelines in cooperation between neurologists, emergency room physicians, and hospitalists, and in using evidence‐based medicine to provide optimal care for the patient presenting with a TIA.
Stroke and TIA arise from identical etiologies, respond to the same secondary preventive measures, and should be considered part of the spectrum of an ischemic cerebral syndrome. Recognizing TIA as a medical emergency with high rates of secondary stroke and subsequent disability allows institution of therapies with appropriate urgency. Hospitalization offers the ability to rapidly coordinate the testing and secondary prevention measures but also, for high‐risk patients, offers the opportunity to reduce the time to thrombolysis for early recurrent strokes. New, validated scoring systems such as the ABCD2 score help the hospitalist to decide which patients are appropriate for admission and which can be managed in progressive and traditional outpatient settings.
Transient ischemic attacks (TIAs) are common and represent a clarion call to action to prevent disabling stroke. Incidence estimates for TIA range from 37 to 107 per 100,000 persons each year.1 Extrapolating from these data, there are likely greater than 100,000 to 300,000 TIAs in the US annually. Within 3 months, approximately 10% of these patients will suffer a stroke, with approximately one‐half of these events occurring within the first 48 hours after the sentinel TIA.26 Nearly two‐thirds of secondary strokes result in disability and 21% are fatal.3 Hospitalists are frequently called to provide care for patients with TIA and, as such, in order to establish an appropriate care plan, they require tools to better predict the likelihood and timing of a disabling stroke.7 In this review we examine the rationale for early aggressive TIA evaluation and treatment in the hospital, overview risk stratification models to identify the patients at highest risk for early recurrent ischemia, and explore application of these tools to admission policy and individualized patient care planning.
Definition
TIA is defined as a brief episode of neurological dysfunction caused by focal brain or retinal ischemia with clinical symptoms typically lasting less than 1 hour and without evidence of brain infarction.8, 9 Prior arbitrary time limits are being abandoned as advanced imaging techniques demonstrate that clinical examination lacks the sensitivity to detect small cerebral infarctions leading to misclassification of as many as 30% to 40% of strokes as TIAs.811 For cases in which imaging is not available, the diagnosis of clinically probable TIA is suggested. Patients with imaging consistent with stroke appear to be at 4‐fold to 10‐fold higher risk for subsequent ischemic events, thus the presence of subclinical infarcts may have clinical importance.2, 12 The majority of TIAs resolve within 1 hour of onset and neurologic deficit continuance beyond this time frame is more consistent with a stroke.13 Continuing symptoms after 1 hour mandates aggressive therapy in lieu of withholding intervention in the hopes of a spontaneous recovery.
Rationale for Hospitalization
Urgent evaluation and treatment within 24 to 48 hours of a TIA is recommended by the National Stroke Association (Table 1).14 These guidelines also recommend hospital admission for high‐risk patients. There are a number of compelling arguments for the hospitalization of a patient at high risk for subsequent stroke.
| Test | Rationale | Therapy |
|---|---|---|
| ||
| Electrocardiogram and rhythm strip | To detect atrial fibrillation. | Long‐term warfarin indicated for suspected cardioembolic etiology. |
| Echocardiogram | To detect intracardiac thrombus or vegetations. Bubble study to detect patent foramen ovale in young patients. | Warfarin indicated for suspected cardioembolic etiology. Patent foramen ovale closure is an option for selected patients. |
| Carotid ultrasound | To detect large vessel atherosclerotic disease. | Antiplatelet therapy* indicated for atherosclerotic etiologies. Early carotid endarterectomy following TIA considered for 50% symptomatic ipsilateral stenosis. |
| Fasting lipid profile, complete blood count, serum electrolytes and creatinine | Secondary prevention of stroke by treating hyperlipidemia. Signs and symptoms associated with severe laboratory abnormalities may mimic TIA. | LDL >100 mg/dL (optional goal >70 mg/dL) is indication for cholesterol lowering therapy. |
| Neuroimaging‐MRI with diffusion images MRA or CT CTA | To detect clinically inapparent lesions of stroke. Useful in ruling out some mimics of TIA. | Patients with abnormal MRI diffusion images represent a population at increased risk for recurrent stroke. |
First, hospitalization offers potential for reduced time to thrombolysis for those patients who have a second ischemic event in the early period following TIA. Outpatients with new ischemic stroke may see hours pass between symptom onset and presentation to the emergency department (ED). This delay frequently places them outside of the thrombolytic window.1517 Hospitalization, assuming a well‐designed inpatient stroke care system, has great potential to reduce this delay. Approximately 50% of the stroke risk following a TIA is evident within 48 hours and rapid thrombolysis, available in an inpatient setting, is associated with improved outcome after stroke.3, 18 A cost‐utility analysis found that a 24‐hour admission for TIA patients to allow tissue plasminogen activator (t‐PA) for recurrent ischemia has a cost‐effectiveness ratio of $55,044 per quality‐adjusted life year with increasing cost effectiveness for the highest risk patients, such as those with a 24‐hour stroke risk of >5%.19
Second, hospital admission often facilitates the reliable and efficient evaluation for etiology and early initiation of secondary prevention. Neuroimaging, carotid ultrasound, echocardiography, and telemetry can be expedited with rapid initiation of proven secondary preventive therapies such as statin treatment, blood pressure control, and antithrombotic therapy. When indicated, carotid revascularization is recommended as soon as possible following TIA, with retrospective reviews suggesting improved outcomes when performed within 2 weeks of the event.1420 In one analysis, a negative association between hospitalization for TIA and subsequent stroke was discovered by review of Canadian population‐based administrative databases.5 While the mechanism for the negative association could not be established, the literature provides some support for hospitalization being associated with decreased risk for second strokes (hazard ratio [HR], 0.73; 95% confidence interval [CI], 0.570.95).5
Theoretically, much of this evaluation and treatment could occur in the outpatient setting but delays commonly seen in outpatient evaluation and the high potential for early second strokes for some patients may make this a risky care plan. Despite the high likelihood for serious outcomes following TIA and clear guidelines for early evaluation and management, current care often lacks a sense of urgency. A 2004 Canadian study revealed that three‐quarters of patients with a TIA were discharged directly from the ED with a resultant delay in diagnostic investigation.4 Over one‐third of patients were discharged without a prescription for antithrombotic therapy. American primary care practice patterns reveal even more significant delays in therapy, with only 2% of patients admitted to a hospital on the day of presentation for TIA, despite 80% of patients presenting for evaluation on the day of symptom onset.21 In this study less than one‐half of patients with atrial fibrillation were started on immediate anticoagulation.21 Further, as many as one‐third of patients did not have any evaluation in the month after the index event.21 Hospitalization for high‐risk patients has the potential to avoid these delays in outpatient evaluation and initiation of therapy.
Still, not all patients will require admission to a hospital setting. American EDs admit approximately one‐half of all TIAs, with regional variability not explained exclusively by clinical characteristics.22 Focusing on identifying the cohort of patients who would most benefit from hospitalization is paramount. In general, hospitalization should be reserved for patients with higher risk of an early secondary stroke. Specifically, admission is generally recommended for patients with crescendo symptoms, TIA on antithrombotic therapy, or symptoms lasting >1 hour.14 Additionally, patients with symptomatic carotid stenosis of 50% and presumed cardioembolic or hypercoagulable etiology merit hospital admission.14 In many cases these etiologies may not be known at time of presentation. Evaluation, such as carotid ultrasound, may not be readily available in the ED to inform the admission decision. Several new scoring systems that utilize routine clinical features available within an hour of presentation have been developed to more objectively assess the risk of secondary stroke following a TIA. The use of these prognostic scoring systems is recommended by the National Stroke Association to aid in triaging this cohort of patients.14
Prognostic Scoring Systems
California Score
The 2000 California Score (Tables 2 and 3) is a 5‐point tool retrospectively developed from a database of 1,707 TIA patients seen in the ED of a California hospital system to predict the likelihood of stroke within 90 days of an initial presentation with transient neurologic deficits.3 Multivariate logistic regression models were used to test the clinical factors associated with stroke risk, resulting in a tool using clinical features of age, diabetes, symptom duration, and the type of deficit to provide quantitative estimates of intermediate term risk. Within 90 days, none of the patients with a score of zero had a stroke whereas the highest score had a 34% risk of stroke (Table 3). While it is possible that some patients with lower scores had a nonischemic etiology for their transient neurological symptoms, clinical practice contains similar ambiguity, and such patients would be correctly predicted to have a low risk for subsequent strokes. Additionally, the derivation and validation of this tool did not include a neurologist confirmation of TIA diagnosis; however, this likely mirrors the practice in most EDs. The California Score has subsequently been validated and expanded upon during the development of the ABCD2 score.23 The California Score's utility is limited in the acute decision‐making process, especially regarding the decision to admit, as it focuses on 90‐day outcomes. For that, shorter‐term risk assessments are more useful.
| Clinical Feature | California Score (points) | ABCD (points) | ABCD2 (points) | |
|---|---|---|---|---|
| ||||
| Age | 60 years | 1 | 1 | 1 |
| Blood pressure | Systolic blood pressure 140 or diastolic blood pressure 90 mmHg | N/A | 1 | 1 |
| Clinical deficits* | Unilateral weakness (focal motor weakness of 1 or more of face, arm, hand, or leg) | 1 | 2 | 2 |
| Speech impairment (dysarthria, dysphasia, or both) | 1 | 1 | 1 | |
| Duration | 60 minutes | 1 | 2 | 2 |
| 10‐59 minutes | 1 | 1 | 1 | |
| Diabetes | Present | 1 | N/A | 1 |
| Maximum score | 5 | 6 | 7 | |
| California Score | 0 | 1 | 2 | 3 | 4 | 5 |
|---|---|---|---|---|---|---|
| ||||||
| 90‐day stroke risk (%) | 0 | 3 | 7 | 11 | 15 | 34 |
ABCD Score
The 2005 ABCD (Tables 2 and 4) is a 6‐point tool designed to predict 7‐day risk of stroke following TIA from the Oxfordshire Community Stroke Project, a UK prospective population‐based cohort of 209 patients with diagnosis of TIA made by a neurologist.24 It evaluated factors previously found to be independent predictors of stroke after TIA, and determined that risk factors of age, blood pressure, type of clinical deficit, and symptom duration predicted 7‐day risk of stroke following TIA. Unlike the California score, the ABCD authors found presenting blood pressure, but not diabetes, to be independent predictors of future events. The authors validated the score with a second population of TIA patients in the Oxford Vascular Study and in a hospital‐based TIA clinic cohort.24 In the validation cohorts the score was highly predictive of stroke at 7 days (P 0.001). Patients with the lowest scores of 0 to 3 had no strokes in the week following the index TIA, whereas patients with the highest score of 6 carried a 35.5% risk of early second stroke. The primary limitation of the ABCD score lies in the small sample size, with only 18 recurrent strokes in the week after TIA in the derivation cohort.
| ABCD Score | 0 | 1 | 2 | 3 | 4 | 5 | 6 |
|---|---|---|---|---|---|---|---|
| |||||||
| 7‐Day stroke risk (%) | 0 | 0 | 0 | 0 | 2.2 | 16.3 | 35.5 |
The ABCD score has subsequently been tested in other settings with mixed results. Two studies found limited utility.25, 26 Other trials found high scores to be overly inclusive but highly predictive and thus the majority of evidence appears to support the validity of the ABCD score in predicting risk of early recurrent ischemic events.2729 The ABCD score has been used to triage patients with high scores to inpatient management although the benefit of this strategy on outcomes has not been proven.30
ABCD2 Score
The 2007 ABCD2 (Tables 2 and 5) is a 7‐point tool that uses the original ABCD criteria along with an additional point for diabetes.23 The ABCD2 derived a unified prognostic score for optimal prediction of the 2‐day stroke risk from multivariate analysis of the original data sets used to create the California and ABCD scores. This score was then validated by the authors in 4 independent cohorts from the United States and the United Kingdom.23 In sum, 4809 patients with TIA were included in the ABCD2 analysis. Similar to prior studies, stroke occurred in 9.2% of patients by 90 days of which 20% were fatal. The authors created low (03 points), intermediate (45 points), and high (67 points) risk categories. In the validation cohorts the prediction rule for the ABCD2 functioned better than the California or ABCD scores with c statistics of 0.62 to 0.83 (ideal prediction produces a c statistic of 1 and prediction no better than chance would have a c statistic of 0.5). They found a 2‐day risk of stroke of 1% for low, 4.1% for intermediate, and 8.1% for the high risk group. Data from the study suggest 34% of TIA patients will be in low‐risk, 45% in intermediate‐risk, and 21% in high‐risk categories. While the ABCD2 score overcomes some of the problems with the 2 prior systems it shares many of the limitations as it was derived from the combined data sets. All scoring systems lack the ability to provide guidance on the management of TIAs associated with rare conditions, such as vasculitis, that are underrepresented in the derivation data sets. The ABCD2 also does not incorporate imaging data and this will likely require further exploration.
| ABCD2 Score | 0‐3 | 4‐5 | 6‐7 |
|---|---|---|---|
| |||
| Risk stratification | Low | Intermediate | High |
| 2‐Day stroke risk (%) | 1 | 4.1 | 8.1 |
| 7‐Day stroke risk (%) | 1.2 | 5.9 | 11.7 |
| 90‐Day stroke risk (%) | 3.1 | 9.8 | 17.8 |
The ABCD2 score can be used to predict risk for a variety of time intervals, has now been validated in independent Greek and British populations, and appears to be the best performing tool at predicting early risk of stroke regardless of underlying etiology.23, 31, 32 The authors suggest that admission for patients in the high‐risk group is prudent whereas outpatient evaluation is reasonable for patients in the low‐risk group.23 Admission for patients in the intermediate‐risk group will depend on individualized decision making, local practice standards, and available community resources.
New Models of Care: An Opportunity for Hospitalists
The key to improving TIA outcomes appears to be more contingent on the speed of evaluation and initiation of appropriate therapy than on the location of the care. The EXPRESS trial studied the effect of an immediate access neurovascular clinic providing urgent evaluation and immediate treatment of nonhospitalized TIA patients versus usual care. Statistically significant reductions were seen in time to evaluation, first treatment prescription, and in 90‐day risk of recurrent stroke (10.3% versus 2.1%, P 0.0001) after the clinic was changed to the rapid evaluation and treatment model.33
The SOS‐TIA study used a 24‐hour access hospital‐based TIA clinic to evaluate the effects of rapid assessment and interventions on hospital length of stay and clinical outcomes.34 The 90‐day stroke rate was 1.24% (95% CI, 0.712.12), which represents a 79% reduction compared to the predicted stroke rate from the ABCD2 scores. With expedited evaluation and treatment, 74% of patients were able to be sent home on the same day.
The results of these 2 new studies provide compelling evidence that rapid evaluation and treatment in the first 48 hours after TIA has the potential to alter outcomes. Unfortunately not all communities have access to same day TIA clinics. Still, these findings should embolden hospitalists to advocate for urgent evaluation, such as neurology and cardiac imaging and carotid evaluation, with immediate initiation of secondary preventive therapy and early surgical intervention when appropriate. In most cases these changes will require process transformations that present prime opportunities for hospitalists to reengineer systems of care.
Incorporating Prognostic Scores into Clinical Practice
Applying the evidence to practice requires calculation of the early risk but also awareness of the community resources available. High‐risk patients with an ABCD2 score of 6 or 7 have a very high 8.1% risk of stroke within the next 48 hours. Given the catastrophic outcomes frequently seen after second strokes, these patients warrant inpatient admission to facilitate the immediate initiation of appropriate secondary prevention and potentially shorten time to thrombolysis if an early stroke occurs. Intermediate‐risk patients with ABCD2 scores of 4 and 5 have a 4.1% 2‐day risk of stroke and may be considered for admission, hospital observation, or expedited clinic evaluation contingent on local availability. As many as one‐third of TIA patients will be categorized as low risk with a score of 0 to 3. These patients have a 2‐day risk of stroke of only 1% and are likely safe for prompt outpatient evaluation and management. The new, validated, ABCD2 score is not a substitute for individualized judgment, but is helpful in developing admission guidelines in cooperation between neurologists, emergency room physicians, and hospitalists, and in using evidence‐based medicine to provide optimal care for the patient presenting with a TIA.
Stroke and TIA arise from identical etiologies, respond to the same secondary preventive measures, and should be considered part of the spectrum of an ischemic cerebral syndrome. Recognizing TIA as a medical emergency with high rates of secondary stroke and subsequent disability allows institution of therapies with appropriate urgency. Hospitalization offers the ability to rapidly coordinate the testing and secondary prevention measures but also, for high‐risk patients, offers the opportunity to reduce the time to thrombolysis for early recurrent strokes. New, validated scoring systems such as the ABCD2 score help the hospitalist to decide which patients are appropriate for admission and which can be managed in progressive and traditional outpatient settings.
- ,,.Epidemiological impact in the United States of a tissue‐based definition of transient ischemic attack.Stroke.2003;34:919–924.
- ,,, et al.Head computed tomography findings predict short‐term stroke risk after transient ischemic attack.Stroke.2003;34:2894–2899.
- ,,, et al.Short‐term prognosis after emergency department diagnosis of TIA.JAMA.2000;284:2901–2906.
- ,,, et al.Management and outcomes of transient ischemic attacks in Ontario.CMAJ.2004;170:1099–1104.
- ,,, et al.The high risk of stroke immediately after transient ischemic attack: a population based study.Neurology.2004;62:2015–2020.
- ,,, et al.Early risk of stroke after transient ischemic attack: a systematic review and meta‐analysis.Arch Intern Med.2007;167:2417–2422.
- ,,, et al.The spectrum of community‐based hospitalist practice: a call to tailor internal medicine residency training.Arch Intern Med.2007;167:727–729.
- .Transient ischemic attack with abnormal diffusion‐weighted imaging results: what's in a name?Arch Neurol.2007;64:1080–1082.
- ,.A reappraisal of the definition and pathophysiology of the transient ischemic attack.Med Sci Monit.2007;13:RA50–53.
- ,,, et al.Diffusion‐weighted imaging‐negative patients with transient ischemic attack are at risk of recurrent transient events.Stroke.2007;38:2367–2369.
- ,,, et al.Transient ischemic attack—proposal for a new definition.N Engl J Med.2002;347:1713–1716.
- ,,, et al.Management and outcome of patients with transient ischemic attack admitted to a stroke unit.Cerebrovasc Dis.2007;24:80–85.
- .How transient are transient ischemic attacks.Neurology.1988;38:674–677.
- ,,, et al.National Stroke Association guidelines for the management of transient ischemic attacks.Ann Neurol.2006;60:301–313.
- ,,, et al.Out‐of‐hospital delays in patients with acute stroke.Ann Emerg Med.2004;44:476–483.
- ,,, et al.Factors associated with delayed admission to hospital and in‐hospital delays in acute stroke and TIA: a prospective multicenter study.Stroke.1999;30:40–48.
- ,,, et al.Prehospital and emergency department delays after acute stroke: the Genentech Stroke Presentation Survey.Stroke.2000;31:2585–2590.
- Tissue plasminogen activator for acute ischemic stroke.The National Institute of Neurological Disorders and Stroke rt‐PA Stroke Study Group.N Engl J Med.1995;333:1581–1587.
- ,.Is hospitalization after TIA cost effective on the basis of treatment with tPA?Neurology.2005;65:1799–1801.
- ,,, et al.Endarterectomy for symptomatic carotid stenosis in relation to clinical subgroups and timing of surgery.Lancet.2004;363:915–924.
- ,,, et al.New transient ischemic attack and stroke: outpatient management by primary care physicians.Arch Intern Med.2000;160:2941–2946.
- ,,, et al.Hospital and demographic influences on the disposition of transient ischemic attack.Acad Emerg Med.2008;15:171–176.
- ,,, et al.Validation and refinement of scores to predict very early stroke risk after transient ischaemic attack.Lancet.2007;369:283–292.
- ,,, et al.A simple score (ABCD) to identify individuals at high early risk of stroke after transient ischaemic attack.Lancet.2005;366:29–36.
- ,,, et al.Is the ABCD score useful for risk stratification of patients with acute transient ischemic attack?Stroke.2006;37:1710–1714.
- ,,, et al.Absence of usefulness of ABCD score in the early risk of recurrent stroke in transient ischemic attack patients.Stroke.2007;38:855–856.
- ,,, et al.Validation of the ABCD score in identifying individuals at high early risk of stroke after a transient ischemic attack: a hospital‐based case series study.Stroke.2006;37:2892–2897.
- ,.Rapid identification of high‐risk transient ischemic attacks: prospective validation of the ABCD score.Stroke.2008;39:297–302.
- ,,.Can the ABCD score be dichotomized to identify high‐risk patients with transient ischaemic attack in the emergency department?Emerg Med J.2007;24:92–95.
- ,,, et al.Can risk stratification of transient ischaemic attacks improve patient care in the emergency department?Emerg Med J.2007;24:637–640.
- ,,, et al.Prognosis in patients with transient ischaemic attack (TIA) and minor stroke attending TIA services in the north west of England: The NORTHSTAR Study.J Neurol Neurosurg Psychiatry.2007:1–6.
- ,,.Potential applicability of the ABCD2 in triaging TIA patients.Lancet.2007;369:1082.
- ,,, et al.Effect of urgent treatment of transient ischemic attack and minor stroke on early recurrent stroke (EXPRESS Study): a prospective population‐based sequential comparison.Lancet.2007;370;1432–1442.
- ,,, et al.A transient ischemic attack clinic with round‐the‐clock access (SOS‐TIA): feasibility and effects.Lancet Neurol.2007;6:953–960.
- ,,.Epidemiological impact in the United States of a tissue‐based definition of transient ischemic attack.Stroke.2003;34:919–924.
- ,,, et al.Head computed tomography findings predict short‐term stroke risk after transient ischemic attack.Stroke.2003;34:2894–2899.
- ,,, et al.Short‐term prognosis after emergency department diagnosis of TIA.JAMA.2000;284:2901–2906.
- ,,, et al.Management and outcomes of transient ischemic attacks in Ontario.CMAJ.2004;170:1099–1104.
- ,,, et al.The high risk of stroke immediately after transient ischemic attack: a population based study.Neurology.2004;62:2015–2020.
- ,,, et al.Early risk of stroke after transient ischemic attack: a systematic review and meta‐analysis.Arch Intern Med.2007;167:2417–2422.
- ,,, et al.The spectrum of community‐based hospitalist practice: a call to tailor internal medicine residency training.Arch Intern Med.2007;167:727–729.
- .Transient ischemic attack with abnormal diffusion‐weighted imaging results: what's in a name?Arch Neurol.2007;64:1080–1082.
- ,.A reappraisal of the definition and pathophysiology of the transient ischemic attack.Med Sci Monit.2007;13:RA50–53.
- ,,, et al.Diffusion‐weighted imaging‐negative patients with transient ischemic attack are at risk of recurrent transient events.Stroke.2007;38:2367–2369.
- ,,, et al.Transient ischemic attack—proposal for a new definition.N Engl J Med.2002;347:1713–1716.
- ,,, et al.Management and outcome of patients with transient ischemic attack admitted to a stroke unit.Cerebrovasc Dis.2007;24:80–85.
- .How transient are transient ischemic attacks.Neurology.1988;38:674–677.
- ,,, et al.National Stroke Association guidelines for the management of transient ischemic attacks.Ann Neurol.2006;60:301–313.
- ,,, et al.Out‐of‐hospital delays in patients with acute stroke.Ann Emerg Med.2004;44:476–483.
- ,,, et al.Factors associated with delayed admission to hospital and in‐hospital delays in acute stroke and TIA: a prospective multicenter study.Stroke.1999;30:40–48.
- ,,, et al.Prehospital and emergency department delays after acute stroke: the Genentech Stroke Presentation Survey.Stroke.2000;31:2585–2590.
- Tissue plasminogen activator for acute ischemic stroke.The National Institute of Neurological Disorders and Stroke rt‐PA Stroke Study Group.N Engl J Med.1995;333:1581–1587.
- ,.Is hospitalization after TIA cost effective on the basis of treatment with tPA?Neurology.2005;65:1799–1801.
- ,,, et al.Endarterectomy for symptomatic carotid stenosis in relation to clinical subgroups and timing of surgery.Lancet.2004;363:915–924.
- ,,, et al.New transient ischemic attack and stroke: outpatient management by primary care physicians.Arch Intern Med.2000;160:2941–2946.
- ,,, et al.Hospital and demographic influences on the disposition of transient ischemic attack.Acad Emerg Med.2008;15:171–176.
- ,,, et al.Validation and refinement of scores to predict very early stroke risk after transient ischaemic attack.Lancet.2007;369:283–292.
- ,,, et al.A simple score (ABCD) to identify individuals at high early risk of stroke after transient ischaemic attack.Lancet.2005;366:29–36.
- ,,, et al.Is the ABCD score useful for risk stratification of patients with acute transient ischemic attack?Stroke.2006;37:1710–1714.
- ,,, et al.Absence of usefulness of ABCD score in the early risk of recurrent stroke in transient ischemic attack patients.Stroke.2007;38:855–856.
- ,,, et al.Validation of the ABCD score in identifying individuals at high early risk of stroke after a transient ischemic attack: a hospital‐based case series study.Stroke.2006;37:2892–2897.
- ,.Rapid identification of high‐risk transient ischemic attacks: prospective validation of the ABCD score.Stroke.2008;39:297–302.
- ,,.Can the ABCD score be dichotomized to identify high‐risk patients with transient ischaemic attack in the emergency department?Emerg Med J.2007;24:92–95.
- ,,, et al.Can risk stratification of transient ischaemic attacks improve patient care in the emergency department?Emerg Med J.2007;24:637–640.
- ,,, et al.Prognosis in patients with transient ischaemic attack (TIA) and minor stroke attending TIA services in the north west of England: The NORTHSTAR Study.J Neurol Neurosurg Psychiatry.2007:1–6.
- ,,.Potential applicability of the ABCD2 in triaging TIA patients.Lancet.2007;369:1082.
- ,,, et al.Effect of urgent treatment of transient ischemic attack and minor stroke on early recurrent stroke (EXPRESS Study): a prospective population‐based sequential comparison.Lancet.2007;370;1432–1442.
- ,,, et al.A transient ischemic attack clinic with round‐the‐clock access (SOS‐TIA): feasibility and effects.Lancet Neurol.2007;6:953–960.
Diagnosis Discrepancies and LOS
Recent research has found that the addition of clinical data to administrative data strengthens the accuracy of predicting inpatient mortality.1, 2 Pine et al.1 showed that including present on admission (POA) codes and numerical laboratory data resulted in substantially better fitting risk adjustment models than those based on administrative data alone. Risk adjustment models, despite improvement with the use of POA codes, are still imperfect and severity adjustment alone does not explain differences in mortality as well as we would hope.2
The addition of POA codes improves prediction of mortality, since they distinguish between conditions that were present at the time of admission and conditions that were acquired during the hospitalization, but it is not known if the addition of these codes is related to other measures of hospital performancesuch as differences in length of stay (LOS). Which of the factors related to the patient's clinical condition at the time of hospital admission drive differences in outcomes?
A patient's admission diagnosis may be an important piece of information that accounts for differences in hospital care. A patient's diagnosis at the time of hospital admission leads to the initial course of treatment. If the admitting diagnosis is inaccurate, a physician may spend critical time following a course of unneeded treatment until the correct diagnosis is made (reflected by a discrepancy between the admitting and discharge diagnosis codes). This discrepancy may be a marker of the fact that, while some patients are admitted to the hospital for treatment of a previously diagnosed condition, other patients require a diagnostic workup to determine the clinical problem.
A discrepancy may also reflect poor systems of documenting critical information and result in delays in care, with potentially serious health consequences.3, 4 If diagnosis discrepancy is a marker of difficult‐to‐diagnose cases, leading to delays in care, we may be able to improve our understanding of perceived differences in the production of high‐quality medical care and proactively identify cases which need more attention at admission to ensure that necessary care is provided as quickly as possible.
Almost universally, comparisons of hospital performance are risk‐adjusted to account for differences in case mix and severity across institutions. These risk‐adjustment models rely on discharge diagnoses to adjust for clinical differences among patients, even though recent research has shown that models using discharge diagnoses alone are inadequate predictors of variation in mortality among hospitals. While the findings of Pine et al.1 suggest the need to add certain clinical information, such as laboratory values, to improve these models, this information may be costly for some institutions to collect and report. We aimed to explore whether other simple to measure factors that are independent of the quality of care provided and routinely collected by hospitals' electronic information systems can be used to improve risk‐adjustment models. To assess the potential of other routinely collected diagnostic information in explaining differences in health outcomes, this study examined whether a discrepancy between the admission and discharge diagnoses was associated with hospital LOS.
Patients and Methods
Patient Population
The sample included all patients age 18 years and older who were admitted to and discharged from the general medicine units at Rush University Medical Center between July 2005 and June 2006. We further limited the sample to patients who were admitted via the emergency department (ED) or directly by their physician, excluding patients with scheduled admissions for which LOS may vary little and patients transferred from other hospitals. We also excluded patients admitted directly to the intensive care units. However, some patients were transferred to the intensive care units during their stay and we retained these patients. Only a small percent of cases fit this designation (1.2%). We did not explore the effects of this clinical situation due to small numbers of patients. Our attempt was to constitute a sample that would include patients for whom admission is more likely for an episodic and diagnostically complex set of symptoms and signs.
Diagnosis Discrepancy
Admission and discharge diagnosis codes were classified using the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD‐9‐CM). An admission diagnosis is routinely documented and coded by hospitals but is not used by most private and public payers for reimbursement purposes, unlike the discharge diagnosis codes. The admission diagnosis code summarizes information known at the time the patient is admitted to the hospital and corresponds to the chief complaint in the history and physical report. Its specificity may depend on a variety of patient and physician‐related factors, and neither the quality of the information collected at admission nor the specificity of the coded information is externally regulated. Only one admission diagnosis code is captured and, like the discharge diagnosis codes, coded at the time of discharge. The admission diagnosis code reflects the amount of information known at the time of admission but is retrospectively coded.
A patient may have multiple discharge diagnosis codes. These codes summarize information collected throughout a hospitalization. The discharge diagnosis codes are used to bill third‐party payers and patients. In addition, governmental agencies, benchmarking institutions, and researchers use the discharge diagnosis codes to classify a patient's condition, identify comorbidities, and measure severity of illness.
We measured discrepancy between admission and discharge diagnoses in two ways. We first compared the admitting diagnosis code with the principal discharge diagnosis code. A match was defined as a patient record in which the two codes were exactly the same at the terminal digit. If the two codes did not match exactly at the terminal digit, we classified the patient as having a discrepancy or mismatch between diagnosis codes. For example, if the admitting diagnosis code was 786.05 (shortness of breath) and the principal discharge diagnosis code was 428 (congestive heart failure, unspecified), the diagnosis codes were classified as discrepant. To test the robustness of our definition of discrepancy between admitting and discharge diagnoses, we created a second variable that compared the admitting diagnosis code with the first five discharge diagnosis codes. If the admitting diagnosis code did not match any of the first five discharge diagnosis codes, the diagnosis codes were classified as discrepant.
We use the term diagnosis discrepancy to refer to records that have a mismatch between admitting and discharge diagnosis codes.
Models and Data Collection
The outcome of interest was inpatient LOS. The primary independent variable was whether the patient record had a discrepancy between the admitting and discharge diagnosis codes.
Our models controlled for the following variables: age; sex; admission source (ED or primary care provider); primary source of insurance (Medicare, Medicaid, or commercial coverage); and severity of illness, measured by the number of comorbid conditions.5, 6 We also controlled for the general type of clinical condition, which was classified by the principal discharge diagnosis code using the Healthcare Cost and Utilization Project's Clinical Classifications Software 2007.7 Data were collected from the institution's clinical data warehouse.
Statistical Analysis
A generalized linear regression model fit with a negative binomial distribution was used to test for an association between inpatient LOS and a discrepancy between admitting and discharge diagnosis codes, adjusting for the variables described above. We reestimated our models without the respective diagnosis discrepancy variable and calculated a likelihood ratio test statistic for the two models to determine whether the addition of diagnosis discrepancy significantly improved our models.
We used two sensitivity tests to assess the specification of our models. First, we included two interaction terms: one for diagnosis discrepancy and ED admissions, to assess whether the association between diagnosis discrepancy and LOS differed by admission source; and another for diagnosis discrepancy and the number of comorbidities, to assess whether the association between diagnosis discrepancy and LOS differed by level of patient complexity. Second, we incrementally broadened our definition of a match in admitting and discharge diagnoses by comparing the admitting diagnosis with the first two discharge diagnoses, then the first three discharge diagnoses, through the 10th discharge diagnosis, and reestimated the regression models using the successively broader definition of match (principal, first two, first three, first four, through the first 10 discharge diagnoses) to further assess the robustness of our measurement of diagnosis discrepancy as a predictor of LOS.
Results
Of the 5,375 patients discharged between July 2005 and June 2006, 75.6% had a discrepancy between their admitting and principal discharge diagnosis. Patients with a discrepancy between their admitting and principal discharge diagnosis codes had significantly longer LOS, were older, had more comorbid conditions, and were more likely to be male, admitted through the ED, and have Medicare (Table 1). Results were similar for the more encompassing definition of a discrepancy between admitting and the top 5 discharge diagnoses (results not shown).
| Variables | n | No Discrepancy (n = 1,313) | Discrepancy (n = 4,062) | P* |
|---|---|---|---|---|
| ||||
| LOS (days), mean (SE) | 3.4 (3.6) | 4.2 (4.1) | <0.001 | |
| Age (years), mean (SE) | 56.3 (18.8) | 59.7 (18.6) | <0.001 | |
| Comorbid conditions (number), mean (SE) | 1.2 (1.2) | 1.4 (1.3) | <0.001 | |
| Gender (%) | 0.019 | |||
| Male | 2,201 | 29.8 | 70.3 | |
| Female | 3,174 | 26.1 | 73.9 | |
| Admission source (%) | ||||
| Direct | 4,202 | 29.8 | 70.3 | <0.001 |
| ED | 1,173 | 22.9 | 77.1 | |
| Insurance coverage | ||||
| Medicare | 2,677 | 21.6 | 78.4 | <0.001 |
| Medicaid | 908 | 26.3 | 73.7 | |
| Commercial | 1,790 | 27.7 | 72.3 | |
| Clinical domain (%) | <0.001 | |||
| Endocrine | 370 | 22.7 | 77.3 | |
| Nervous system | 230 | 35.7 | 64.4 | |
| Circulatory | 1,008 | 19.0 | 81.1 | |
| Respiratory | 483 | 16.4 | 83.6 | |
| Digestive | 852 | 14.2 | 85.8 | |
| Genitourinary | 372 | 19.6 | 80.4 | |
| Skin | 249 | 53.0 | 47.0 | |
| Musculoskeletal | 276 | 20.3 | 79.7 | |
| Injury/poisoning | 549 | 27.9 | 72.1 | |
| Other | 986 | 34.7 | 65.3 | |
Table 2 reports the 10 most common admitting diagnoses that did not match the principal discharge diagnosis code and the 10 most common principal discharge diagnoses that did not match the admitting diagnosis code. The top 10 discrepant admitting diagnosis codes represented nearly one‐half of all cases with a discrepancy between the admitting and discharge diagnoses. The top 10 principal discharge diagnosis codes represented 23% of all discrepant diagnoses. Table 3 lists the 10 most common pairs of mismatched admitting and principal discharge diagnosis codes. The most common mismatched pair was a principal admitting diagnosis code of 786.05 (shortness of breath) and discharge diagnosis code of 428.0 (congestive heart failure, unspecified).
| Rank | Admission Diagnosis Code Not Matching Primary Discharge Diagnosis | Rank | Principal Discharge Diagnosis Code Not Matching Admission Diagnosis Code | ||||
|---|---|---|---|---|---|---|---|
| Code | Description | % | Code | Description | % | ||
| 1 | 786.05 | Shortness of breath | 11.1 | 1 | 428.0 | Congestive heart failure, unspecified | 6.0 |
| 2 | 789.00 | Abdominal pain, unspecified site | 8.5 | 2 | 486 | Pneumonia, organism unspecified | 3.3 |
| 3 | 780.6 | Fever | 6.7 | 3 | 584.9 | Acute renal failure, unspecified | 2.2 |
| 4 | 786.50 | Chest pain, unspecified | 5.6 | 4 | 786.59 | Chest pain, other | 2.1 |
| 5 | 787.01 | Nausea without vomiting | 3.9 | 5 | 599.0 | Urinary tract infection, site not specified | 2.1 |
| 6 | 780.99 | Other general symptoms | 3.4 | 6 | 996.81 | Complications of kidney transplant | 1.8 |
| 7 | 780.79 | Other malaise and fatigue | 3.0 | 7 | 577.0 | Acute pancreatitis | 1.7 |
| 8 | 780.2 | Syncope and collapse | 2.6 | 8 | 996.62 | Infection and inflammatory reaction due to other vascular device, implant or graft | 1.4 |
| 9 | 729.5 | Pain in limb | 2.1 | 9 | 434.91 | Cerebral artery occlusion with cerebral infarction, unspecified | 1.3 |
| 10 | 729.81 | Swelling of limb | 2.0 | 10 | 008.8 | Intestinal infection, not elsewhere classified | 1.0 |
| Admission Diagnosis | Principal Discharge Diagnosis | ||
|---|---|---|---|
| Code | Description | Code | Description |
| 786.05 | Shortness of breath | 428.0 | Congestive heart failure, unspecified |
| 786.50 | Chest pain, unspecified | 786.59 | Chest pain, other |
| 786.05 | Shortness of breath | 486 | Pneumonia, organism unspecified |
| 780.6 | Fever | 486 | Pneumonia, organism unspecified |
| 780.6 | Fever | 996.62 | Infection and inflammatory reaction due to other vascular device, implant or graft |
| 789.00 | Abdominal pain, unspecified site | 577.0 | Acute pancreatitis |
| 780.6 | Fever | 599.0 | Urinary tract infection, site not specified |
| 786.05 | Shortness of breath | 491.21 | Obstructive chronic bronchitis with acute exacerbation |
| 786.05 | Shortness of breath | 415.19 | Pulmonary embolism and infarction, other |
| 786.05 | Shortness of breath | 493.22 | Chronic obstructive asthma, with acute exacerbation |
Table 4 reports the results of the generalized linear model predicting LOS. Discrepancy between the admitting and principal discharge diagnoses was associated with a 22.5% longer LOS (P < 0.01), translating into a 0.76‐day increase at the mean for those with discrepant diagnoses. Our results are robust to our definition of discrepancy between admitting and discharge diagnoses. Using the discrepancy definition based on the top five discharge diagnosis codes, a discrepancy between admitting and discharge diagnoses was associated with a 15.4% longer LOS (P < 0.01), translating into a 0.52‐day increase. Results of the likelihood ratio test showed that the addition of diagnosis discrepancy significantly improved the fit of the regression models using both the principal and top five discharge diagnosis codes.
| Variable | Coefficient | ||
|---|---|---|---|
| Model 1 | Model 2 | Model 3 | |
| |||
| Intercept | 0.98* (0.06) | 0.84* (0.06) | 0.89* (0.06) |
| Diagnosis discrepancy with principal discharge diagnosis | 0.20* (0.03) | ||
| Diagnosis discrepancy with top 5 discharge diagnoses | 0.14* (0.02) | ||
| Age | 0.001 (0.001) | 0.001 (0.001) | 0.001 (0.001) |
| Female | 0.03 (0.02) | 0.03 (0.02) | 0.03 (0.02) |
| Emergency department admission | 0.02 (0.03) | 0.03 (0.03) | 0.03 (0.03) |
| Medicare | 0.15* (0.03) | 0.15* (0.03) | 0.15* (0.03) |
| Medicaid | 0.04 (0.03) | 0.04 (0.03) | 0.05 (0.03) |
| Number of comorbid conditions | 0.13* (0.01) | 0.13* (0.01) | 0.13* (0.01) |
| Log likelihood for model | 11737.23 | 11797.54 | 11771.76 |
| Likelihood ratio test statistic | 120.62* | 69.06* | |
Broadening our definition of a match between admitting and discharge diagnosis codes from matching only on the principal discharge diagnosis code to the first 10 discharge diagnosis codes showed that even when using the first 10 discharge diagnoses, a diagnosis discrepancy still significantly increased LOS. The magnitude weakened, however, as the definition of a match in diagnosis codes was broadened, ranging from 22.5% when including the principal discharge diagnosis code only to 12.1% when including the first 10 discharge diagnosis codes (Figure 1).
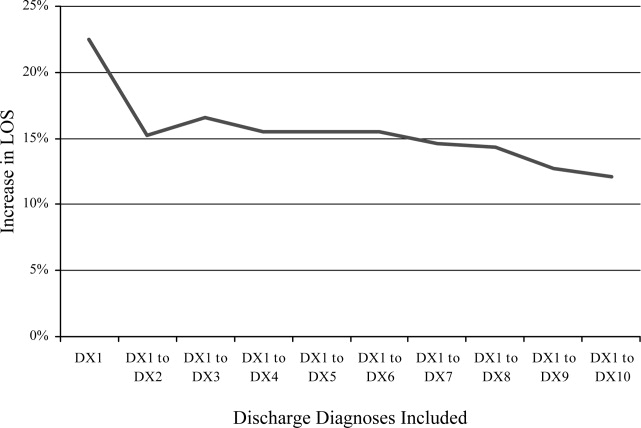
Discussion
Discrepancy between admitting and discharge diagnosis codes was associated with a large increase in LOS, even after controlling for age, sex, admission source, insurance, number of comorbid conditions, and clinical domain. This discrepancy translated into an increase of 0.76 days in LOS per general medicine patient, nearly two‐thirds larger than the increase in LOS of 0.47 days associated with having one comorbid condition, and equated to 4,102 additional patient days for the 5,375 general internal medicine patients admitted.
The relative and absolute increase in LOS associated with a diagnosis discrepancy is considerably larger than that associated with measures of comorbid illness found in other studies. In a study examining the predictive power of comorbidity measures based on diagnosis codes and outpatient pharmacy records, Parker et al.8 found that the inclusion of comorbid conditions based on only discharge diagnosis codes was associated with up to a 0.28‐day increase in LOS, and the further inclusion of comorbidity markers based on pharmacy data was associated with up to an additional 0.09‐day LOS. In a study comparing different measures of disease severity and comorbidities in predicting LOS for total knee replacement patients, Melfi et al.9 found that the addition of one diagnosis code was associated with a 3.3% increase in LOS. Similarly, Kieszak et al.10 found that the likelihood of having an LOS greater than 10 days increased two‐fold for patients with carotid endartectomy and at least one comorbidity.
While a discrepancy between the admitting and discharge diagnosis codes was consistently associated with an increased LOS, the underlying reasons are not yet understood. We can only speculate about the reasons for this association, and further work is needed to test these hypotheses. There are several possible explanations for discrepant cases: (1) poorer documentation at the time of admission, (2) more complexity in terms of the diagnostic task, and (3) less thorough diagnostic workup at the time of admission.
First, we do not think that poor documentation at the time of admission is the most likely explanation. Our ED uses documentation templates for all admitted patients, hence equalizing the amount of documentation for many patients. However, the main reason we do not think this is the reason for discrepancy is that diagnosis codes at the time of admission via the ED are assigned by physicians and not those who code based on documented information.
We do think that the most likely reason is that patients with discrepant diagnoses are truly harder to diagnose cases. For example, we assume that the time to provide care to patients once admitted is the same regardless of the ED or preadmission triage. For example, assume all patients are seen nearly as soon as admitted and the workup promptly ensues. Hence, under these conditions, variation in LOS may be due to more care needed for the most severely ill. If this assertion is true, our finding is a new one and adds a new candidate variable to explain variation in care due to patient severity (beyond comorbid illness, which we controlled for). We think we are showing that diagnostic uncertainty is a common, previously unexamined component of the complexity of clinical presentations (we propose that diagnosis discrepancy is a complexity variable rather than a comorbid, severity of illness variable). For example, discrepancy between admitting and discharge diagnosis codes could be due to other patient characteristics such as a patient's inability to communicate his or her symptoms to the physician due to language or cultural barriers.
However, regarding the third possible reason, if the ED or the preadmission setting fails to provide diagnostic services prior to admission for those patients with discrepant diagnoses regardless of diagnostic complexity, then our finding is a hospital or system performance variable. Those patients with discrepant diagnoses may have had a less thorough workup prior to admission leading to more workup being needed during the admission.
Regardless of the reason (perhaps all three reasons are involved at some level), our study points to a new component of patient care variations. We hope our finding spurs future research efforts. We are about to embark on a comparison of patients with identical discharge diagnoses but discrepant or not discrepant admission diagnoses to explore variations in the amount/type of diagnostic and treatment plans provided both before and during hospitalization.
In further support of diagnosis complexity as the reason for discrepancy is that the codes on admission for discrepantly coded patients are nonspecific, symptom or sign diagnoses (ie, shortness of breath, abdominal pain) while discharge diagnoses are more specific (ie, congestive heart failure, pancreatitis) (Tables 2 and 3). The nonspecific nature of the preliminary codes likely signifies more clinically complex situations and when noted, over and above previously described risk adjustment models, the discrepancy portends more healthcare needs. For patients admitted without a clear diagnosis of a clinical problem, diagnostic workups may be more complex and require longer hospitalization. For these patients, a longer LOS may not be a marker of poor quality of care, but instead the lack of critical information present at the time of admission.
Our comparison of the association between LOS and a discrepancy in diagnosis codes when the admitting diagnosis code was successively matched to a larger number of discharge diagnosis codes suggests that LOS increases not only when the admitting diagnosis is incorrect or not sufficiently specific, but also when the admitting diagnosis is correct, but not the principal discharge diagnosis. Taken together, these findings suggest that delays in care may result from lack of clear patient diagnostic information at the time of admission.
Our findings may advance the understanding of variations in hospital care from two standpoints. First, noting the discrepant diagnoses may significantly improve prediction in health services research studies examining variations in hospital performance, even beyond the addition of POA coding. Second, and perhaps more importantly, prospectively identifying patients at the time of admission with the nonspecific, preliminary codes identified in our study may allow physicians to target earlier in care patients with more demanding care needs. We realize, however, that before we could use this information to prospectively attempt to improve care, coding would have to be done at admission rather than discharge. At our site, this is true in the ED setting. Patients are assigned an admission diagnosis code as they leave the ED and this code is carried through to discharge without alteration. A nonspecific admission code could, for example, alert those taking care of the patient in the hospital that this is perhaps a more complex clinical situation requiring earlier consultation. Concurrent coding could also jumpstart studies to better understand whether what we have found in this preliminary study is due to poor assessment or difficult patient situations. However, this contingency may not be possible for those admitted directly from physician offices, as both the admission and discharge codes are determined at the time of discharge and based on documentation. Yet, on admission, a chief complaint is provided that may serve the same purpose as an admission diagnosis code if they are sufficiently in agreement.
Our study has limitations. It is from a single medical center and uses administrative data alone. We did not have access to clinical records for more detailed information about the content and completeness of medical records at the time of admission. Our observations should be tested in other hospital systems. Another limitation may be that we focus on discrepancy and not on those patients without a discrepancy. However, the aim of testing for discrepancy is to focus on improvement. Conducting a more in‐depth chart review of patients with similar final diagnoses, some with discrepant codes and others with nondiscrepant codes, may be a way to assess the reasons why LOS varied in the two groups. The next step, should our observations be confirmed, is to systematically assess whether other characteristics exist that differentiate cases in which a discrepancy between diagnosis codes is due to diagnostic uncertainty from those in which it is due to diagnostic oversight or error. A method to systematically identify conditions at admission that are likely to be misdiagnosed or have a delay in diagnosis may substantially improve the overall quality of care provided in the hospital.
- ,,, et al.Enhancement of claims data to improve risk adjustment of hospital mortality.JAMA.2007;297:71–76.
- .The risks of risk adjustment.JAMA.1997;278:1600–1607.
- ,,.Change in the quality of care delivered to Medicare beneficiaries, 1998–1999 to 2000–2001.JAMA.2003;289:305–312.
- ,,, et al.Delay in the diagnosis of acute myocardial infarction: Effect on quality of care and its assessment.Acad Emerg Med.2006;13:931–938.
- ,,, et al.Comorbid illness is associated with survival and length of hospital stay in patients with chronic disability. A prospective comparison of three comorbidity indices.Med Care.1996;34:1093–1101.
- ,,,,,.Comorbidities, complications and coding bias: does the number of diagnosis codes matter in predicting in‐hospital mortality?JAMA.1992;267:2197–2203.
- ,,. Clinical classifications software (CCS), 2007. Available at: http://www.hcup‐us.ahrq.gov/toolssoftware/ccs/ccs.jsp. Accessed December2008.
- ,,.Can pharmacy data improve prediction of hospital outcomes? Comparison with a diagnosis‐based comorbidity measure.Med Care.2003;41:407–419.
- ,,,.Selecting a patient characteristics index for the prediction of medical outcomes using administrative data.J Clin Epidemiol.1995;48:917–926.
- ,,,,.A comparison of the Charlson Comorbidity Index derived from medical record data and administrative billing data.J Clin Epidemiol.1999;52:137–142.
Recent research has found that the addition of clinical data to administrative data strengthens the accuracy of predicting inpatient mortality.1, 2 Pine et al.1 showed that including present on admission (POA) codes and numerical laboratory data resulted in substantially better fitting risk adjustment models than those based on administrative data alone. Risk adjustment models, despite improvement with the use of POA codes, are still imperfect and severity adjustment alone does not explain differences in mortality as well as we would hope.2
The addition of POA codes improves prediction of mortality, since they distinguish between conditions that were present at the time of admission and conditions that were acquired during the hospitalization, but it is not known if the addition of these codes is related to other measures of hospital performancesuch as differences in length of stay (LOS). Which of the factors related to the patient's clinical condition at the time of hospital admission drive differences in outcomes?
A patient's admission diagnosis may be an important piece of information that accounts for differences in hospital care. A patient's diagnosis at the time of hospital admission leads to the initial course of treatment. If the admitting diagnosis is inaccurate, a physician may spend critical time following a course of unneeded treatment until the correct diagnosis is made (reflected by a discrepancy between the admitting and discharge diagnosis codes). This discrepancy may be a marker of the fact that, while some patients are admitted to the hospital for treatment of a previously diagnosed condition, other patients require a diagnostic workup to determine the clinical problem.
A discrepancy may also reflect poor systems of documenting critical information and result in delays in care, with potentially serious health consequences.3, 4 If diagnosis discrepancy is a marker of difficult‐to‐diagnose cases, leading to delays in care, we may be able to improve our understanding of perceived differences in the production of high‐quality medical care and proactively identify cases which need more attention at admission to ensure that necessary care is provided as quickly as possible.
Almost universally, comparisons of hospital performance are risk‐adjusted to account for differences in case mix and severity across institutions. These risk‐adjustment models rely on discharge diagnoses to adjust for clinical differences among patients, even though recent research has shown that models using discharge diagnoses alone are inadequate predictors of variation in mortality among hospitals. While the findings of Pine et al.1 suggest the need to add certain clinical information, such as laboratory values, to improve these models, this information may be costly for some institutions to collect and report. We aimed to explore whether other simple to measure factors that are independent of the quality of care provided and routinely collected by hospitals' electronic information systems can be used to improve risk‐adjustment models. To assess the potential of other routinely collected diagnostic information in explaining differences in health outcomes, this study examined whether a discrepancy between the admission and discharge diagnoses was associated with hospital LOS.
Patients and Methods
Patient Population
The sample included all patients age 18 years and older who were admitted to and discharged from the general medicine units at Rush University Medical Center between July 2005 and June 2006. We further limited the sample to patients who were admitted via the emergency department (ED) or directly by their physician, excluding patients with scheduled admissions for which LOS may vary little and patients transferred from other hospitals. We also excluded patients admitted directly to the intensive care units. However, some patients were transferred to the intensive care units during their stay and we retained these patients. Only a small percent of cases fit this designation (1.2%). We did not explore the effects of this clinical situation due to small numbers of patients. Our attempt was to constitute a sample that would include patients for whom admission is more likely for an episodic and diagnostically complex set of symptoms and signs.
Diagnosis Discrepancy
Admission and discharge diagnosis codes were classified using the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD‐9‐CM). An admission diagnosis is routinely documented and coded by hospitals but is not used by most private and public payers for reimbursement purposes, unlike the discharge diagnosis codes. The admission diagnosis code summarizes information known at the time the patient is admitted to the hospital and corresponds to the chief complaint in the history and physical report. Its specificity may depend on a variety of patient and physician‐related factors, and neither the quality of the information collected at admission nor the specificity of the coded information is externally regulated. Only one admission diagnosis code is captured and, like the discharge diagnosis codes, coded at the time of discharge. The admission diagnosis code reflects the amount of information known at the time of admission but is retrospectively coded.
A patient may have multiple discharge diagnosis codes. These codes summarize information collected throughout a hospitalization. The discharge diagnosis codes are used to bill third‐party payers and patients. In addition, governmental agencies, benchmarking institutions, and researchers use the discharge diagnosis codes to classify a patient's condition, identify comorbidities, and measure severity of illness.
We measured discrepancy between admission and discharge diagnoses in two ways. We first compared the admitting diagnosis code with the principal discharge diagnosis code. A match was defined as a patient record in which the two codes were exactly the same at the terminal digit. If the two codes did not match exactly at the terminal digit, we classified the patient as having a discrepancy or mismatch between diagnosis codes. For example, if the admitting diagnosis code was 786.05 (shortness of breath) and the principal discharge diagnosis code was 428 (congestive heart failure, unspecified), the diagnosis codes were classified as discrepant. To test the robustness of our definition of discrepancy between admitting and discharge diagnoses, we created a second variable that compared the admitting diagnosis code with the first five discharge diagnosis codes. If the admitting diagnosis code did not match any of the first five discharge diagnosis codes, the diagnosis codes were classified as discrepant.
We use the term diagnosis discrepancy to refer to records that have a mismatch between admitting and discharge diagnosis codes.
Models and Data Collection
The outcome of interest was inpatient LOS. The primary independent variable was whether the patient record had a discrepancy between the admitting and discharge diagnosis codes.
Our models controlled for the following variables: age; sex; admission source (ED or primary care provider); primary source of insurance (Medicare, Medicaid, or commercial coverage); and severity of illness, measured by the number of comorbid conditions.5, 6 We also controlled for the general type of clinical condition, which was classified by the principal discharge diagnosis code using the Healthcare Cost and Utilization Project's Clinical Classifications Software 2007.7 Data were collected from the institution's clinical data warehouse.
Statistical Analysis
A generalized linear regression model fit with a negative binomial distribution was used to test for an association between inpatient LOS and a discrepancy between admitting and discharge diagnosis codes, adjusting for the variables described above. We reestimated our models without the respective diagnosis discrepancy variable and calculated a likelihood ratio test statistic for the two models to determine whether the addition of diagnosis discrepancy significantly improved our models.
We used two sensitivity tests to assess the specification of our models. First, we included two interaction terms: one for diagnosis discrepancy and ED admissions, to assess whether the association between diagnosis discrepancy and LOS differed by admission source; and another for diagnosis discrepancy and the number of comorbidities, to assess whether the association between diagnosis discrepancy and LOS differed by level of patient complexity. Second, we incrementally broadened our definition of a match in admitting and discharge diagnoses by comparing the admitting diagnosis with the first two discharge diagnoses, then the first three discharge diagnoses, through the 10th discharge diagnosis, and reestimated the regression models using the successively broader definition of match (principal, first two, first three, first four, through the first 10 discharge diagnoses) to further assess the robustness of our measurement of diagnosis discrepancy as a predictor of LOS.
Results
Of the 5,375 patients discharged between July 2005 and June 2006, 75.6% had a discrepancy between their admitting and principal discharge diagnosis. Patients with a discrepancy between their admitting and principal discharge diagnosis codes had significantly longer LOS, were older, had more comorbid conditions, and were more likely to be male, admitted through the ED, and have Medicare (Table 1). Results were similar for the more encompassing definition of a discrepancy between admitting and the top 5 discharge diagnoses (results not shown).
| Variables | n | No Discrepancy (n = 1,313) | Discrepancy (n = 4,062) | P* |
|---|---|---|---|---|
| ||||
| LOS (days), mean (SE) | 3.4 (3.6) | 4.2 (4.1) | <0.001 | |
| Age (years), mean (SE) | 56.3 (18.8) | 59.7 (18.6) | <0.001 | |
| Comorbid conditions (number), mean (SE) | 1.2 (1.2) | 1.4 (1.3) | <0.001 | |
| Gender (%) | 0.019 | |||
| Male | 2,201 | 29.8 | 70.3 | |
| Female | 3,174 | 26.1 | 73.9 | |
| Admission source (%) | ||||
| Direct | 4,202 | 29.8 | 70.3 | <0.001 |
| ED | 1,173 | 22.9 | 77.1 | |
| Insurance coverage | ||||
| Medicare | 2,677 | 21.6 | 78.4 | <0.001 |
| Medicaid | 908 | 26.3 | 73.7 | |
| Commercial | 1,790 | 27.7 | 72.3 | |
| Clinical domain (%) | <0.001 | |||
| Endocrine | 370 | 22.7 | 77.3 | |
| Nervous system | 230 | 35.7 | 64.4 | |
| Circulatory | 1,008 | 19.0 | 81.1 | |
| Respiratory | 483 | 16.4 | 83.6 | |
| Digestive | 852 | 14.2 | 85.8 | |
| Genitourinary | 372 | 19.6 | 80.4 | |
| Skin | 249 | 53.0 | 47.0 | |
| Musculoskeletal | 276 | 20.3 | 79.7 | |
| Injury/poisoning | 549 | 27.9 | 72.1 | |
| Other | 986 | 34.7 | 65.3 | |
Table 2 reports the 10 most common admitting diagnoses that did not match the principal discharge diagnosis code and the 10 most common principal discharge diagnoses that did not match the admitting diagnosis code. The top 10 discrepant admitting diagnosis codes represented nearly one‐half of all cases with a discrepancy between the admitting and discharge diagnoses. The top 10 principal discharge diagnosis codes represented 23% of all discrepant diagnoses. Table 3 lists the 10 most common pairs of mismatched admitting and principal discharge diagnosis codes. The most common mismatched pair was a principal admitting diagnosis code of 786.05 (shortness of breath) and discharge diagnosis code of 428.0 (congestive heart failure, unspecified).
| Rank | Admission Diagnosis Code Not Matching Primary Discharge Diagnosis | Rank | Principal Discharge Diagnosis Code Not Matching Admission Diagnosis Code | ||||
|---|---|---|---|---|---|---|---|
| Code | Description | % | Code | Description | % | ||
| 1 | 786.05 | Shortness of breath | 11.1 | 1 | 428.0 | Congestive heart failure, unspecified | 6.0 |
| 2 | 789.00 | Abdominal pain, unspecified site | 8.5 | 2 | 486 | Pneumonia, organism unspecified | 3.3 |
| 3 | 780.6 | Fever | 6.7 | 3 | 584.9 | Acute renal failure, unspecified | 2.2 |
| 4 | 786.50 | Chest pain, unspecified | 5.6 | 4 | 786.59 | Chest pain, other | 2.1 |
| 5 | 787.01 | Nausea without vomiting | 3.9 | 5 | 599.0 | Urinary tract infection, site not specified | 2.1 |
| 6 | 780.99 | Other general symptoms | 3.4 | 6 | 996.81 | Complications of kidney transplant | 1.8 |
| 7 | 780.79 | Other malaise and fatigue | 3.0 | 7 | 577.0 | Acute pancreatitis | 1.7 |
| 8 | 780.2 | Syncope and collapse | 2.6 | 8 | 996.62 | Infection and inflammatory reaction due to other vascular device, implant or graft | 1.4 |
| 9 | 729.5 | Pain in limb | 2.1 | 9 | 434.91 | Cerebral artery occlusion with cerebral infarction, unspecified | 1.3 |
| 10 | 729.81 | Swelling of limb | 2.0 | 10 | 008.8 | Intestinal infection, not elsewhere classified | 1.0 |
| Admission Diagnosis | Principal Discharge Diagnosis | ||
|---|---|---|---|
| Code | Description | Code | Description |
| 786.05 | Shortness of breath | 428.0 | Congestive heart failure, unspecified |
| 786.50 | Chest pain, unspecified | 786.59 | Chest pain, other |
| 786.05 | Shortness of breath | 486 | Pneumonia, organism unspecified |
| 780.6 | Fever | 486 | Pneumonia, organism unspecified |
| 780.6 | Fever | 996.62 | Infection and inflammatory reaction due to other vascular device, implant or graft |
| 789.00 | Abdominal pain, unspecified site | 577.0 | Acute pancreatitis |
| 780.6 | Fever | 599.0 | Urinary tract infection, site not specified |
| 786.05 | Shortness of breath | 491.21 | Obstructive chronic bronchitis with acute exacerbation |
| 786.05 | Shortness of breath | 415.19 | Pulmonary embolism and infarction, other |
| 786.05 | Shortness of breath | 493.22 | Chronic obstructive asthma, with acute exacerbation |
Table 4 reports the results of the generalized linear model predicting LOS. Discrepancy between the admitting and principal discharge diagnoses was associated with a 22.5% longer LOS (P < 0.01), translating into a 0.76‐day increase at the mean for those with discrepant diagnoses. Our results are robust to our definition of discrepancy between admitting and discharge diagnoses. Using the discrepancy definition based on the top five discharge diagnosis codes, a discrepancy between admitting and discharge diagnoses was associated with a 15.4% longer LOS (P < 0.01), translating into a 0.52‐day increase. Results of the likelihood ratio test showed that the addition of diagnosis discrepancy significantly improved the fit of the regression models using both the principal and top five discharge diagnosis codes.
| Variable | Coefficient | ||
|---|---|---|---|
| Model 1 | Model 2 | Model 3 | |
| |||
| Intercept | 0.98* (0.06) | 0.84* (0.06) | 0.89* (0.06) |
| Diagnosis discrepancy with principal discharge diagnosis | 0.20* (0.03) | ||
| Diagnosis discrepancy with top 5 discharge diagnoses | 0.14* (0.02) | ||
| Age | 0.001 (0.001) | 0.001 (0.001) | 0.001 (0.001) |
| Female | 0.03 (0.02) | 0.03 (0.02) | 0.03 (0.02) |
| Emergency department admission | 0.02 (0.03) | 0.03 (0.03) | 0.03 (0.03) |
| Medicare | 0.15* (0.03) | 0.15* (0.03) | 0.15* (0.03) |
| Medicaid | 0.04 (0.03) | 0.04 (0.03) | 0.05 (0.03) |
| Number of comorbid conditions | 0.13* (0.01) | 0.13* (0.01) | 0.13* (0.01) |
| Log likelihood for model | 11737.23 | 11797.54 | 11771.76 |
| Likelihood ratio test statistic | 120.62* | 69.06* | |
Broadening our definition of a match between admitting and discharge diagnosis codes from matching only on the principal discharge diagnosis code to the first 10 discharge diagnosis codes showed that even when using the first 10 discharge diagnoses, a diagnosis discrepancy still significantly increased LOS. The magnitude weakened, however, as the definition of a match in diagnosis codes was broadened, ranging from 22.5% when including the principal discharge diagnosis code only to 12.1% when including the first 10 discharge diagnosis codes (Figure 1).

Discussion
Discrepancy between admitting and discharge diagnosis codes was associated with a large increase in LOS, even after controlling for age, sex, admission source, insurance, number of comorbid conditions, and clinical domain. This discrepancy translated into an increase of 0.76 days in LOS per general medicine patient, nearly two‐thirds larger than the increase in LOS of 0.47 days associated with having one comorbid condition, and equated to 4,102 additional patient days for the 5,375 general internal medicine patients admitted.
The relative and absolute increase in LOS associated with a diagnosis discrepancy is considerably larger than that associated with measures of comorbid illness found in other studies. In a study examining the predictive power of comorbidity measures based on diagnosis codes and outpatient pharmacy records, Parker et al.8 found that the inclusion of comorbid conditions based on only discharge diagnosis codes was associated with up to a 0.28‐day increase in LOS, and the further inclusion of comorbidity markers based on pharmacy data was associated with up to an additional 0.09‐day LOS. In a study comparing different measures of disease severity and comorbidities in predicting LOS for total knee replacement patients, Melfi et al.9 found that the addition of one diagnosis code was associated with a 3.3% increase in LOS. Similarly, Kieszak et al.10 found that the likelihood of having an LOS greater than 10 days increased two‐fold for patients with carotid endartectomy and at least one comorbidity.
While a discrepancy between the admitting and discharge diagnosis codes was consistently associated with an increased LOS, the underlying reasons are not yet understood. We can only speculate about the reasons for this association, and further work is needed to test these hypotheses. There are several possible explanations for discrepant cases: (1) poorer documentation at the time of admission, (2) more complexity in terms of the diagnostic task, and (3) less thorough diagnostic workup at the time of admission.
First, we do not think that poor documentation at the time of admission is the most likely explanation. Our ED uses documentation templates for all admitted patients, hence equalizing the amount of documentation for many patients. However, the main reason we do not think this is the reason for discrepancy is that diagnosis codes at the time of admission via the ED are assigned by physicians and not those who code based on documented information.
We do think that the most likely reason is that patients with discrepant diagnoses are truly harder to diagnose cases. For example, we assume that the time to provide care to patients once admitted is the same regardless of the ED or preadmission triage. For example, assume all patients are seen nearly as soon as admitted and the workup promptly ensues. Hence, under these conditions, variation in LOS may be due to more care needed for the most severely ill. If this assertion is true, our finding is a new one and adds a new candidate variable to explain variation in care due to patient severity (beyond comorbid illness, which we controlled for). We think we are showing that diagnostic uncertainty is a common, previously unexamined component of the complexity of clinical presentations (we propose that diagnosis discrepancy is a complexity variable rather than a comorbid, severity of illness variable). For example, discrepancy between admitting and discharge diagnosis codes could be due to other patient characteristics such as a patient's inability to communicate his or her symptoms to the physician due to language or cultural barriers.
However, regarding the third possible reason, if the ED or the preadmission setting fails to provide diagnostic services prior to admission for those patients with discrepant diagnoses regardless of diagnostic complexity, then our finding is a hospital or system performance variable. Those patients with discrepant diagnoses may have had a less thorough workup prior to admission leading to more workup being needed during the admission.
Regardless of the reason (perhaps all three reasons are involved at some level), our study points to a new component of patient care variations. We hope our finding spurs future research efforts. We are about to embark on a comparison of patients with identical discharge diagnoses but discrepant or not discrepant admission diagnoses to explore variations in the amount/type of diagnostic and treatment plans provided both before and during hospitalization.
In further support of diagnosis complexity as the reason for discrepancy is that the codes on admission for discrepantly coded patients are nonspecific, symptom or sign diagnoses (ie, shortness of breath, abdominal pain) while discharge diagnoses are more specific (ie, congestive heart failure, pancreatitis) (Tables 2 and 3). The nonspecific nature of the preliminary codes likely signifies more clinically complex situations and when noted, over and above previously described risk adjustment models, the discrepancy portends more healthcare needs. For patients admitted without a clear diagnosis of a clinical problem, diagnostic workups may be more complex and require longer hospitalization. For these patients, a longer LOS may not be a marker of poor quality of care, but instead the lack of critical information present at the time of admission.
Our comparison of the association between LOS and a discrepancy in diagnosis codes when the admitting diagnosis code was successively matched to a larger number of discharge diagnosis codes suggests that LOS increases not only when the admitting diagnosis is incorrect or not sufficiently specific, but also when the admitting diagnosis is correct, but not the principal discharge diagnosis. Taken together, these findings suggest that delays in care may result from lack of clear patient diagnostic information at the time of admission.
Our findings may advance the understanding of variations in hospital care from two standpoints. First, noting the discrepant diagnoses may significantly improve prediction in health services research studies examining variations in hospital performance, even beyond the addition of POA coding. Second, and perhaps more importantly, prospectively identifying patients at the time of admission with the nonspecific, preliminary codes identified in our study may allow physicians to target earlier in care patients with more demanding care needs. We realize, however, that before we could use this information to prospectively attempt to improve care, coding would have to be done at admission rather than discharge. At our site, this is true in the ED setting. Patients are assigned an admission diagnosis code as they leave the ED and this code is carried through to discharge without alteration. A nonspecific admission code could, for example, alert those taking care of the patient in the hospital that this is perhaps a more complex clinical situation requiring earlier consultation. Concurrent coding could also jumpstart studies to better understand whether what we have found in this preliminary study is due to poor assessment or difficult patient situations. However, this contingency may not be possible for those admitted directly from physician offices, as both the admission and discharge codes are determined at the time of discharge and based on documentation. Yet, on admission, a chief complaint is provided that may serve the same purpose as an admission diagnosis code if they are sufficiently in agreement.
Our study has limitations. It is from a single medical center and uses administrative data alone. We did not have access to clinical records for more detailed information about the content and completeness of medical records at the time of admission. Our observations should be tested in other hospital systems. Another limitation may be that we focus on discrepancy and not on those patients without a discrepancy. However, the aim of testing for discrepancy is to focus on improvement. Conducting a more in‐depth chart review of patients with similar final diagnoses, some with discrepant codes and others with nondiscrepant codes, may be a way to assess the reasons why LOS varied in the two groups. The next step, should our observations be confirmed, is to systematically assess whether other characteristics exist that differentiate cases in which a discrepancy between diagnosis codes is due to diagnostic uncertainty from those in which it is due to diagnostic oversight or error. A method to systematically identify conditions at admission that are likely to be misdiagnosed or have a delay in diagnosis may substantially improve the overall quality of care provided in the hospital.
Recent research has found that the addition of clinical data to administrative data strengthens the accuracy of predicting inpatient mortality.1, 2 Pine et al.1 showed that including present on admission (POA) codes and numerical laboratory data resulted in substantially better fitting risk adjustment models than those based on administrative data alone. Risk adjustment models, despite improvement with the use of POA codes, are still imperfect and severity adjustment alone does not explain differences in mortality as well as we would hope.2
The addition of POA codes improves prediction of mortality, since they distinguish between conditions that were present at the time of admission and conditions that were acquired during the hospitalization, but it is not known if the addition of these codes is related to other measures of hospital performancesuch as differences in length of stay (LOS). Which of the factors related to the patient's clinical condition at the time of hospital admission drive differences in outcomes?
A patient's admission diagnosis may be an important piece of information that accounts for differences in hospital care. A patient's diagnosis at the time of hospital admission leads to the initial course of treatment. If the admitting diagnosis is inaccurate, a physician may spend critical time following a course of unneeded treatment until the correct diagnosis is made (reflected by a discrepancy between the admitting and discharge diagnosis codes). This discrepancy may be a marker of the fact that, while some patients are admitted to the hospital for treatment of a previously diagnosed condition, other patients require a diagnostic workup to determine the clinical problem.
A discrepancy may also reflect poor systems of documenting critical information and result in delays in care, with potentially serious health consequences.3, 4 If diagnosis discrepancy is a marker of difficult‐to‐diagnose cases, leading to delays in care, we may be able to improve our understanding of perceived differences in the production of high‐quality medical care and proactively identify cases which need more attention at admission to ensure that necessary care is provided as quickly as possible.
Almost universally, comparisons of hospital performance are risk‐adjusted to account for differences in case mix and severity across institutions. These risk‐adjustment models rely on discharge diagnoses to adjust for clinical differences among patients, even though recent research has shown that models using discharge diagnoses alone are inadequate predictors of variation in mortality among hospitals. While the findings of Pine et al.1 suggest the need to add certain clinical information, such as laboratory values, to improve these models, this information may be costly for some institutions to collect and report. We aimed to explore whether other simple to measure factors that are independent of the quality of care provided and routinely collected by hospitals' electronic information systems can be used to improve risk‐adjustment models. To assess the potential of other routinely collected diagnostic information in explaining differences in health outcomes, this study examined whether a discrepancy between the admission and discharge diagnoses was associated with hospital LOS.
Patients and Methods
Patient Population
The sample included all patients age 18 years and older who were admitted to and discharged from the general medicine units at Rush University Medical Center between July 2005 and June 2006. We further limited the sample to patients who were admitted via the emergency department (ED) or directly by their physician, excluding patients with scheduled admissions for which LOS may vary little and patients transferred from other hospitals. We also excluded patients admitted directly to the intensive care units. However, some patients were transferred to the intensive care units during their stay and we retained these patients. Only a small percent of cases fit this designation (1.2%). We did not explore the effects of this clinical situation due to small numbers of patients. Our attempt was to constitute a sample that would include patients for whom admission is more likely for an episodic and diagnostically complex set of symptoms and signs.
Diagnosis Discrepancy
Admission and discharge diagnosis codes were classified using the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD‐9‐CM). An admission diagnosis is routinely documented and coded by hospitals but is not used by most private and public payers for reimbursement purposes, unlike the discharge diagnosis codes. The admission diagnosis code summarizes information known at the time the patient is admitted to the hospital and corresponds to the chief complaint in the history and physical report. Its specificity may depend on a variety of patient and physician‐related factors, and neither the quality of the information collected at admission nor the specificity of the coded information is externally regulated. Only one admission diagnosis code is captured and, like the discharge diagnosis codes, coded at the time of discharge. The admission diagnosis code reflects the amount of information known at the time of admission but is retrospectively coded.
A patient may have multiple discharge diagnosis codes. These codes summarize information collected throughout a hospitalization. The discharge diagnosis codes are used to bill third‐party payers and patients. In addition, governmental agencies, benchmarking institutions, and researchers use the discharge diagnosis codes to classify a patient's condition, identify comorbidities, and measure severity of illness.
We measured discrepancy between admission and discharge diagnoses in two ways. We first compared the admitting diagnosis code with the principal discharge diagnosis code. A match was defined as a patient record in which the two codes were exactly the same at the terminal digit. If the two codes did not match exactly at the terminal digit, we classified the patient as having a discrepancy or mismatch between diagnosis codes. For example, if the admitting diagnosis code was 786.05 (shortness of breath) and the principal discharge diagnosis code was 428 (congestive heart failure, unspecified), the diagnosis codes were classified as discrepant. To test the robustness of our definition of discrepancy between admitting and discharge diagnoses, we created a second variable that compared the admitting diagnosis code with the first five discharge diagnosis codes. If the admitting diagnosis code did not match any of the first five discharge diagnosis codes, the diagnosis codes were classified as discrepant.
We use the term diagnosis discrepancy to refer to records that have a mismatch between admitting and discharge diagnosis codes.
Models and Data Collection
The outcome of interest was inpatient LOS. The primary independent variable was whether the patient record had a discrepancy between the admitting and discharge diagnosis codes.
Our models controlled for the following variables: age; sex; admission source (ED or primary care provider); primary source of insurance (Medicare, Medicaid, or commercial coverage); and severity of illness, measured by the number of comorbid conditions.5, 6 We also controlled for the general type of clinical condition, which was classified by the principal discharge diagnosis code using the Healthcare Cost and Utilization Project's Clinical Classifications Software 2007.7 Data were collected from the institution's clinical data warehouse.
Statistical Analysis
A generalized linear regression model fit with a negative binomial distribution was used to test for an association between inpatient LOS and a discrepancy between admitting and discharge diagnosis codes, adjusting for the variables described above. We reestimated our models without the respective diagnosis discrepancy variable and calculated a likelihood ratio test statistic for the two models to determine whether the addition of diagnosis discrepancy significantly improved our models.
We used two sensitivity tests to assess the specification of our models. First, we included two interaction terms: one for diagnosis discrepancy and ED admissions, to assess whether the association between diagnosis discrepancy and LOS differed by admission source; and another for diagnosis discrepancy and the number of comorbidities, to assess whether the association between diagnosis discrepancy and LOS differed by level of patient complexity. Second, we incrementally broadened our definition of a match in admitting and discharge diagnoses by comparing the admitting diagnosis with the first two discharge diagnoses, then the first three discharge diagnoses, through the 10th discharge diagnosis, and reestimated the regression models using the successively broader definition of match (principal, first two, first three, first four, through the first 10 discharge diagnoses) to further assess the robustness of our measurement of diagnosis discrepancy as a predictor of LOS.
Results
Of the 5,375 patients discharged between July 2005 and June 2006, 75.6% had a discrepancy between their admitting and principal discharge diagnosis. Patients with a discrepancy between their admitting and principal discharge diagnosis codes had significantly longer LOS, were older, had more comorbid conditions, and were more likely to be male, admitted through the ED, and have Medicare (Table 1). Results were similar for the more encompassing definition of a discrepancy between admitting and the top 5 discharge diagnoses (results not shown).
| Variables | n | No Discrepancy (n = 1,313) | Discrepancy (n = 4,062) | P* |
|---|---|---|---|---|
| ||||
| LOS (days), mean (SE) | 3.4 (3.6) | 4.2 (4.1) | <0.001 | |
| Age (years), mean (SE) | 56.3 (18.8) | 59.7 (18.6) | <0.001 | |
| Comorbid conditions (number), mean (SE) | 1.2 (1.2) | 1.4 (1.3) | <0.001 | |
| Gender (%) | 0.019 | |||
| Male | 2,201 | 29.8 | 70.3 | |
| Female | 3,174 | 26.1 | 73.9 | |
| Admission source (%) | ||||
| Direct | 4,202 | 29.8 | 70.3 | <0.001 |
| ED | 1,173 | 22.9 | 77.1 | |
| Insurance coverage | ||||
| Medicare | 2,677 | 21.6 | 78.4 | <0.001 |
| Medicaid | 908 | 26.3 | 73.7 | |
| Commercial | 1,790 | 27.7 | 72.3 | |
| Clinical domain (%) | <0.001 | |||
| Endocrine | 370 | 22.7 | 77.3 | |
| Nervous system | 230 | 35.7 | 64.4 | |
| Circulatory | 1,008 | 19.0 | 81.1 | |
| Respiratory | 483 | 16.4 | 83.6 | |
| Digestive | 852 | 14.2 | 85.8 | |
| Genitourinary | 372 | 19.6 | 80.4 | |
| Skin | 249 | 53.0 | 47.0 | |
| Musculoskeletal | 276 | 20.3 | 79.7 | |
| Injury/poisoning | 549 | 27.9 | 72.1 | |
| Other | 986 | 34.7 | 65.3 | |
Table 2 reports the 10 most common admitting diagnoses that did not match the principal discharge diagnosis code and the 10 most common principal discharge diagnoses that did not match the admitting diagnosis code. The top 10 discrepant admitting diagnosis codes represented nearly one‐half of all cases with a discrepancy between the admitting and discharge diagnoses. The top 10 principal discharge diagnosis codes represented 23% of all discrepant diagnoses. Table 3 lists the 10 most common pairs of mismatched admitting and principal discharge diagnosis codes. The most common mismatched pair was a principal admitting diagnosis code of 786.05 (shortness of breath) and discharge diagnosis code of 428.0 (congestive heart failure, unspecified).
| Rank | Admission Diagnosis Code Not Matching Primary Discharge Diagnosis | Rank | Principal Discharge Diagnosis Code Not Matching Admission Diagnosis Code | ||||
|---|---|---|---|---|---|---|---|
| Code | Description | % | Code | Description | % | ||
| 1 | 786.05 | Shortness of breath | 11.1 | 1 | 428.0 | Congestive heart failure, unspecified | 6.0 |
| 2 | 789.00 | Abdominal pain, unspecified site | 8.5 | 2 | 486 | Pneumonia, organism unspecified | 3.3 |
| 3 | 780.6 | Fever | 6.7 | 3 | 584.9 | Acute renal failure, unspecified | 2.2 |
| 4 | 786.50 | Chest pain, unspecified | 5.6 | 4 | 786.59 | Chest pain, other | 2.1 |
| 5 | 787.01 | Nausea without vomiting | 3.9 | 5 | 599.0 | Urinary tract infection, site not specified | 2.1 |
| 6 | 780.99 | Other general symptoms | 3.4 | 6 | 996.81 | Complications of kidney transplant | 1.8 |
| 7 | 780.79 | Other malaise and fatigue | 3.0 | 7 | 577.0 | Acute pancreatitis | 1.7 |
| 8 | 780.2 | Syncope and collapse | 2.6 | 8 | 996.62 | Infection and inflammatory reaction due to other vascular device, implant or graft | 1.4 |
| 9 | 729.5 | Pain in limb | 2.1 | 9 | 434.91 | Cerebral artery occlusion with cerebral infarction, unspecified | 1.3 |
| 10 | 729.81 | Swelling of limb | 2.0 | 10 | 008.8 | Intestinal infection, not elsewhere classified | 1.0 |
| Admission Diagnosis | Principal Discharge Diagnosis | ||
|---|---|---|---|
| Code | Description | Code | Description |
| 786.05 | Shortness of breath | 428.0 | Congestive heart failure, unspecified |
| 786.50 | Chest pain, unspecified | 786.59 | Chest pain, other |
| 786.05 | Shortness of breath | 486 | Pneumonia, organism unspecified |
| 780.6 | Fever | 486 | Pneumonia, organism unspecified |
| 780.6 | Fever | 996.62 | Infection and inflammatory reaction due to other vascular device, implant or graft |
| 789.00 | Abdominal pain, unspecified site | 577.0 | Acute pancreatitis |
| 780.6 | Fever | 599.0 | Urinary tract infection, site not specified |
| 786.05 | Shortness of breath | 491.21 | Obstructive chronic bronchitis with acute exacerbation |
| 786.05 | Shortness of breath | 415.19 | Pulmonary embolism and infarction, other |
| 786.05 | Shortness of breath | 493.22 | Chronic obstructive asthma, with acute exacerbation |
Table 4 reports the results of the generalized linear model predicting LOS. Discrepancy between the admitting and principal discharge diagnoses was associated with a 22.5% longer LOS (P < 0.01), translating into a 0.76‐day increase at the mean for those with discrepant diagnoses. Our results are robust to our definition of discrepancy between admitting and discharge diagnoses. Using the discrepancy definition based on the top five discharge diagnosis codes, a discrepancy between admitting and discharge diagnoses was associated with a 15.4% longer LOS (P < 0.01), translating into a 0.52‐day increase. Results of the likelihood ratio test showed that the addition of diagnosis discrepancy significantly improved the fit of the regression models using both the principal and top five discharge diagnosis codes.
| Variable | Coefficient | ||
|---|---|---|---|
| Model 1 | Model 2 | Model 3 | |
| |||
| Intercept | 0.98* (0.06) | 0.84* (0.06) | 0.89* (0.06) |
| Diagnosis discrepancy with principal discharge diagnosis | 0.20* (0.03) | ||
| Diagnosis discrepancy with top 5 discharge diagnoses | 0.14* (0.02) | ||
| Age | 0.001 (0.001) | 0.001 (0.001) | 0.001 (0.001) |
| Female | 0.03 (0.02) | 0.03 (0.02) | 0.03 (0.02) |
| Emergency department admission | 0.02 (0.03) | 0.03 (0.03) | 0.03 (0.03) |
| Medicare | 0.15* (0.03) | 0.15* (0.03) | 0.15* (0.03) |
| Medicaid | 0.04 (0.03) | 0.04 (0.03) | 0.05 (0.03) |
| Number of comorbid conditions | 0.13* (0.01) | 0.13* (0.01) | 0.13* (0.01) |
| Log likelihood for model | 11737.23 | 11797.54 | 11771.76 |
| Likelihood ratio test statistic | 120.62* | 69.06* | |
Broadening our definition of a match between admitting and discharge diagnosis codes from matching only on the principal discharge diagnosis code to the first 10 discharge diagnosis codes showed that even when using the first 10 discharge diagnoses, a diagnosis discrepancy still significantly increased LOS. The magnitude weakened, however, as the definition of a match in diagnosis codes was broadened, ranging from 22.5% when including the principal discharge diagnosis code only to 12.1% when including the first 10 discharge diagnosis codes (Figure 1).

Discussion
Discrepancy between admitting and discharge diagnosis codes was associated with a large increase in LOS, even after controlling for age, sex, admission source, insurance, number of comorbid conditions, and clinical domain. This discrepancy translated into an increase of 0.76 days in LOS per general medicine patient, nearly two‐thirds larger than the increase in LOS of 0.47 days associated with having one comorbid condition, and equated to 4,102 additional patient days for the 5,375 general internal medicine patients admitted.
The relative and absolute increase in LOS associated with a diagnosis discrepancy is considerably larger than that associated with measures of comorbid illness found in other studies. In a study examining the predictive power of comorbidity measures based on diagnosis codes and outpatient pharmacy records, Parker et al.8 found that the inclusion of comorbid conditions based on only discharge diagnosis codes was associated with up to a 0.28‐day increase in LOS, and the further inclusion of comorbidity markers based on pharmacy data was associated with up to an additional 0.09‐day LOS. In a study comparing different measures of disease severity and comorbidities in predicting LOS for total knee replacement patients, Melfi et al.9 found that the addition of one diagnosis code was associated with a 3.3% increase in LOS. Similarly, Kieszak et al.10 found that the likelihood of having an LOS greater than 10 days increased two‐fold for patients with carotid endartectomy and at least one comorbidity.
While a discrepancy between the admitting and discharge diagnosis codes was consistently associated with an increased LOS, the underlying reasons are not yet understood. We can only speculate about the reasons for this association, and further work is needed to test these hypotheses. There are several possible explanations for discrepant cases: (1) poorer documentation at the time of admission, (2) more complexity in terms of the diagnostic task, and (3) less thorough diagnostic workup at the time of admission.
First, we do not think that poor documentation at the time of admission is the most likely explanation. Our ED uses documentation templates for all admitted patients, hence equalizing the amount of documentation for many patients. However, the main reason we do not think this is the reason for discrepancy is that diagnosis codes at the time of admission via the ED are assigned by physicians and not those who code based on documented information.
We do think that the most likely reason is that patients with discrepant diagnoses are truly harder to diagnose cases. For example, we assume that the time to provide care to patients once admitted is the same regardless of the ED or preadmission triage. For example, assume all patients are seen nearly as soon as admitted and the workup promptly ensues. Hence, under these conditions, variation in LOS may be due to more care needed for the most severely ill. If this assertion is true, our finding is a new one and adds a new candidate variable to explain variation in care due to patient severity (beyond comorbid illness, which we controlled for). We think we are showing that diagnostic uncertainty is a common, previously unexamined component of the complexity of clinical presentations (we propose that diagnosis discrepancy is a complexity variable rather than a comorbid, severity of illness variable). For example, discrepancy between admitting and discharge diagnosis codes could be due to other patient characteristics such as a patient's inability to communicate his or her symptoms to the physician due to language or cultural barriers.
However, regarding the third possible reason, if the ED or the preadmission setting fails to provide diagnostic services prior to admission for those patients with discrepant diagnoses regardless of diagnostic complexity, then our finding is a hospital or system performance variable. Those patients with discrepant diagnoses may have had a less thorough workup prior to admission leading to more workup being needed during the admission.
Regardless of the reason (perhaps all three reasons are involved at some level), our study points to a new component of patient care variations. We hope our finding spurs future research efforts. We are about to embark on a comparison of patients with identical discharge diagnoses but discrepant or not discrepant admission diagnoses to explore variations in the amount/type of diagnostic and treatment plans provided both before and during hospitalization.
In further support of diagnosis complexity as the reason for discrepancy is that the codes on admission for discrepantly coded patients are nonspecific, symptom or sign diagnoses (ie, shortness of breath, abdominal pain) while discharge diagnoses are more specific (ie, congestive heart failure, pancreatitis) (Tables 2 and 3). The nonspecific nature of the preliminary codes likely signifies more clinically complex situations and when noted, over and above previously described risk adjustment models, the discrepancy portends more healthcare needs. For patients admitted without a clear diagnosis of a clinical problem, diagnostic workups may be more complex and require longer hospitalization. For these patients, a longer LOS may not be a marker of poor quality of care, but instead the lack of critical information present at the time of admission.
Our comparison of the association between LOS and a discrepancy in diagnosis codes when the admitting diagnosis code was successively matched to a larger number of discharge diagnosis codes suggests that LOS increases not only when the admitting diagnosis is incorrect or not sufficiently specific, but also when the admitting diagnosis is correct, but not the principal discharge diagnosis. Taken together, these findings suggest that delays in care may result from lack of clear patient diagnostic information at the time of admission.
Our findings may advance the understanding of variations in hospital care from two standpoints. First, noting the discrepant diagnoses may significantly improve prediction in health services research studies examining variations in hospital performance, even beyond the addition of POA coding. Second, and perhaps more importantly, prospectively identifying patients at the time of admission with the nonspecific, preliminary codes identified in our study may allow physicians to target earlier in care patients with more demanding care needs. We realize, however, that before we could use this information to prospectively attempt to improve care, coding would have to be done at admission rather than discharge. At our site, this is true in the ED setting. Patients are assigned an admission diagnosis code as they leave the ED and this code is carried through to discharge without alteration. A nonspecific admission code could, for example, alert those taking care of the patient in the hospital that this is perhaps a more complex clinical situation requiring earlier consultation. Concurrent coding could also jumpstart studies to better understand whether what we have found in this preliminary study is due to poor assessment or difficult patient situations. However, this contingency may not be possible for those admitted directly from physician offices, as both the admission and discharge codes are determined at the time of discharge and based on documentation. Yet, on admission, a chief complaint is provided that may serve the same purpose as an admission diagnosis code if they are sufficiently in agreement.
Our study has limitations. It is from a single medical center and uses administrative data alone. We did not have access to clinical records for more detailed information about the content and completeness of medical records at the time of admission. Our observations should be tested in other hospital systems. Another limitation may be that we focus on discrepancy and not on those patients without a discrepancy. However, the aim of testing for discrepancy is to focus on improvement. Conducting a more in‐depth chart review of patients with similar final diagnoses, some with discrepant codes and others with nondiscrepant codes, may be a way to assess the reasons why LOS varied in the two groups. The next step, should our observations be confirmed, is to systematically assess whether other characteristics exist that differentiate cases in which a discrepancy between diagnosis codes is due to diagnostic uncertainty from those in which it is due to diagnostic oversight or error. A method to systematically identify conditions at admission that are likely to be misdiagnosed or have a delay in diagnosis may substantially improve the overall quality of care provided in the hospital.
- ,,, et al.Enhancement of claims data to improve risk adjustment of hospital mortality.JAMA.2007;297:71–76.
- .The risks of risk adjustment.JAMA.1997;278:1600–1607.
- ,,.Change in the quality of care delivered to Medicare beneficiaries, 1998–1999 to 2000–2001.JAMA.2003;289:305–312.
- ,,, et al.Delay in the diagnosis of acute myocardial infarction: Effect on quality of care and its assessment.Acad Emerg Med.2006;13:931–938.
- ,,, et al.Comorbid illness is associated with survival and length of hospital stay in patients with chronic disability. A prospective comparison of three comorbidity indices.Med Care.1996;34:1093–1101.
- ,,,,,.Comorbidities, complications and coding bias: does the number of diagnosis codes matter in predicting in‐hospital mortality?JAMA.1992;267:2197–2203.
- ,,. Clinical classifications software (CCS), 2007. Available at: http://www.hcup‐us.ahrq.gov/toolssoftware/ccs/ccs.jsp. Accessed December2008.
- ,,.Can pharmacy data improve prediction of hospital outcomes? Comparison with a diagnosis‐based comorbidity measure.Med Care.2003;41:407–419.
- ,,,.Selecting a patient characteristics index for the prediction of medical outcomes using administrative data.J Clin Epidemiol.1995;48:917–926.
- ,,,,.A comparison of the Charlson Comorbidity Index derived from medical record data and administrative billing data.J Clin Epidemiol.1999;52:137–142.
- ,,, et al.Enhancement of claims data to improve risk adjustment of hospital mortality.JAMA.2007;297:71–76.
- .The risks of risk adjustment.JAMA.1997;278:1600–1607.
- ,,.Change in the quality of care delivered to Medicare beneficiaries, 1998–1999 to 2000–2001.JAMA.2003;289:305–312.
- ,,, et al.Delay in the diagnosis of acute myocardial infarction: Effect on quality of care and its assessment.Acad Emerg Med.2006;13:931–938.
- ,,, et al.Comorbid illness is associated with survival and length of hospital stay in patients with chronic disability. A prospective comparison of three comorbidity indices.Med Care.1996;34:1093–1101.
- ,,,,,.Comorbidities, complications and coding bias: does the number of diagnosis codes matter in predicting in‐hospital mortality?JAMA.1992;267:2197–2203.
- ,,. Clinical classifications software (CCS), 2007. Available at: http://www.hcup‐us.ahrq.gov/toolssoftware/ccs/ccs.jsp. Accessed December2008.
- ,,.Can pharmacy data improve prediction of hospital outcomes? Comparison with a diagnosis‐based comorbidity measure.Med Care.2003;41:407–419.
- ,,,.Selecting a patient characteristics index for the prediction of medical outcomes using administrative data.J Clin Epidemiol.1995;48:917–926.
- ,,,,.A comparison of the Charlson Comorbidity Index derived from medical record data and administrative billing data.J Clin Epidemiol.1999;52:137–142.
Copyright © 2009 Society of Hospital Medicine
Discharge Planning
Hospitalized patients are often debilitated, either from their admitting illness or from the deconditioning that occurs with inactivity. Functional decline, which appears to progress in a hierarchical pattern,1 occurs in 24% to 50% of geriatric patients during hospitalization and is poorly documented.2 Such a decline is associated not only with longer hospital stays and increased health care costs but also with higher mortality.3 The American College of Physicians, through its Assessing Care of Vulnerable Elders project, expressly endorsed gait and mobility evaluation as a quality indicator, and examination insufficiency is well documented.4
Of the several existing mobility assessment tools, few are used routinely in hospital. Some require complex scoring; others require timing and/or a trained occupational therapist.5 We created a simplified tool named Independent Mobility Validation Examination (I‐MOVE) for use by bedside caregivers. We evaluated the tool's face validity and interobserver agreement.
I‐MOVE
I‐MOVE, represented schematically in Figure 1, is a performance test that assesses the patient's ability to perform a sequence of 6 basic tasks: rolling over in bed, sitting up, standing, transferring to a chair, walking in the room, and walking in the hallway. Most motor functions can be assumed to be hierarchical in nature; any patient who can perform at the highest level, such as walking safely, also would be expected to perform at the lowest level.
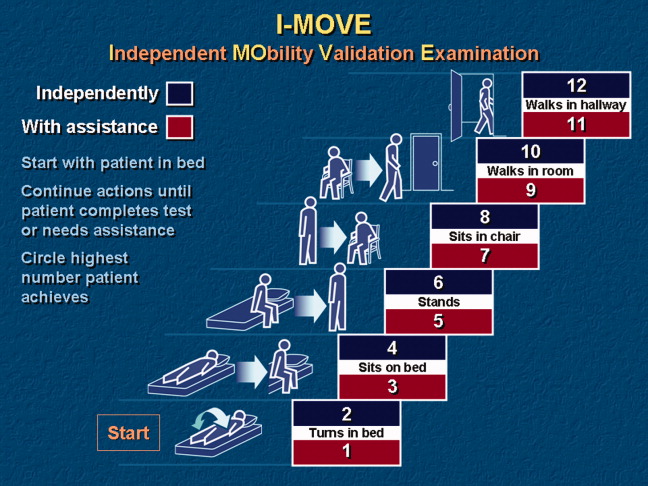
Instructions for administering I‐MOVE are as follows:
-
Review current orders. Exclude patients ordered on bed rest or non‐weight‐bearing or other orders precluding any of the 6 requested actions.
-
Prepare environment.
-
Chair at bedside.
-
Lower side bed rail closest to chair.
-
Clear path for patient to ambulate.
-
Ensure patient dons slippers.
-
Flatten bed.
-
Ensure any gait assistive device, if generally used by the patient, is within reach from the bedside.
-
Requests for patient action (for steps c through f, make available and within reach any appropriate gait‐assistance device such as walker or cane, if such is customarily used at home or newly prescribed):
-
With patient lying supine in bed, with close supervision, ask patient to turn from side to side in bed (request when both bed rails are up).
-
Lower side rail closer to chair and ask the patient to rise up to a sitting position and turn to sit up with legs dangling off the bed.
-
Ask the patient to stand.
-
Ask the patient to take a seat in the chair next to the bed.
-
Ask the patient to ambulate in the room.
-
Ask the patient to ambulate in the hallway.
-
At any point if the patient seems incapable, unsteady, or unsafe to accomplish the requested task, render hands‐on assistance and immediately end the test.
-
Document, by number (1‐12), the activity level successfully accomplished independently by the patient (even number levels) or accomplished with assistance (odd number levels).
-
Patient may be considered independent if able to perform the activity with a normal assistive device (cane, walker, brace, or crutches) but not using furniture.
-
Assistance is defined as any physical contact with the patient.
Findings
Face Validity
We sent surveys to 6 experienced practicing clinicians at our hospital: a geriatrician, a physiatrist, an exercise physiologist, an occupational therapist, a physical therapist, and a registered nurse. We asked each clinician to rate the 6 I‐MOVE elements (requested actions) for clinical relevance to mobility independence. Relevance of each element was measured on an ordinal scale with scores ranging from 1 to 4, with: 1 not relevant; 2 somewhat relevant; 3 quite relevant; and 4 very relevant. From the 5 responses we received, 4 evaluators ranked all 6 I‐MOVE requested actions as very relevant. The fifth evaluator ranked 5 of the 6 actions as very relevant and 1 action (walking in the room) as quite relevant. These results demonstrate general agreement that I‐MOVE is, at face value, a reasonable measure of independent mobility.
Interrater Reliability
The protocol was approved by the hospital's institutional review board. On a general medical unita non‐electrocardiographic telemetry, nonsurgical unit of an acute care hospital, where patients are assigned the primary service of an internal medicine physicianwe instructed 2 registered nurse (RN) volunteers (RN1 and RN2) in the I‐MOVE protocol. Each RN administered I‐MOVE independently to 41 consecutive, cognitively intact patients in a blinded fashion (ie, neither nurse was aware of the other's scoring of each patient) and within 1 hour of each other's assessment.
After administering I‐MOVE to each patient, the nurse judged and scored the patient's performance using the 12‐level I‐MOVE ordinal scale, ranging from a low value of 1, complete dependence, to the highest value of 12, complete independence. The patients' I‐MOVE score pairs recorded by RN1 and RN2 were statistically compared. Interrater reliability, a comparison of the 41 patients' score pairs, is graphically represented in Figure 2. The calculated intraclass correlation coefficient (r) was 0.90, indicating excellent agreement (r > 0.75).
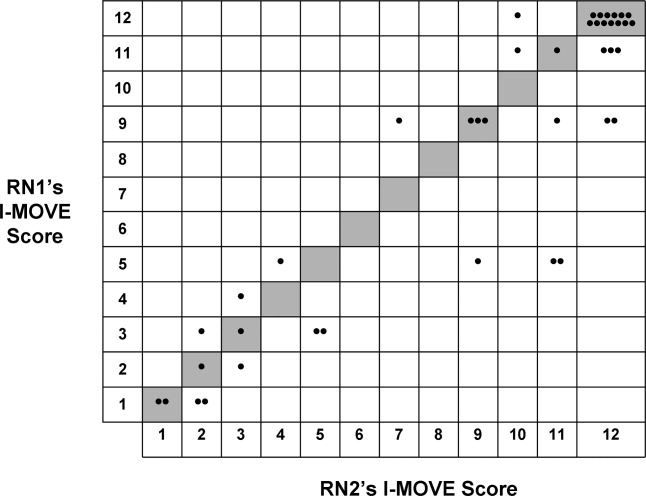
Discussion
Traditional physical examinations by physicians and assessments by nurses do not routinely extend to standardized mobility testing and may fail to recognize disability. Of the existing mobility assessment tools, we believe that most are not suited to patients hospitalized on general medical units. I‐MOVE has been designed to address this need, with an emphasis on practicality and brevity to allow repetition at appropriate intervals (tracking), as is done for vital signs. In this initial study, I‐MOVE was found to have face‐valid content and excellent interrater agreement.
Our study had several limitations. Only 1 pair of test administrators was involved; the sample population was chosen by convenience; clustering of outcomes occurred at level 12, which may have augmented the agreement; and the study was limited to cognitively intact patients. Note that we chose to use the intraclass correlation coefficient rather than the statistic because the weighting between the ordinal I‐MOVE scores has not yet been studied and defined. Also, the weighted is asymptotically equivalent to the intraclass correlation coefficient.
I‐MOVE is intended to aid caregivers in the recognition of debility so that appropriate interventions such as physical therapy may be prescribed. It was designed to complement, not replace, specialized evaluations such as those performed by physical therapists, occupational therapists, or comprehensive geriatric assessments. This practical assessment of basic functioning may enhance communication among caregivers, patients, and patients' family members, especially with regard to discharge planning. Further study is needed to validate I‐MOVE against existing tools, evaluate I‐MOVE's utility as a vital sign, and discern whether a sharp or unexpected decline portends a medical complication.
- .Health status and physical capacity. In:Osterweil D,Brummel‐Smith K,Beck JC, eds.Comprehensive Geriatric Assessment.New York:McGraw‐Hill;2000:41–66.
- ,,, et al.A predictive index for functional decline in hospitalized elderly medical patients.J Gen Intern Med.1993;8(12):645–652.
- ,,.Prevalence and outcomes of low mobility in hospitalized older patients.J Am Geriatr Soc.2004;52(8):1263–1270.
- ,,, et al.Detection and management of falls and instability in vulnerable elders by community physicians.J Am Geriatr Soc.2004;52(9):1527–1531.
- ,,.Exercising body and mind: an integrated approach to functional independence in hospitalized older people.J Am Geriatr Soc.2008;56(4):630–635.
Hospitalized patients are often debilitated, either from their admitting illness or from the deconditioning that occurs with inactivity. Functional decline, which appears to progress in a hierarchical pattern,1 occurs in 24% to 50% of geriatric patients during hospitalization and is poorly documented.2 Such a decline is associated not only with longer hospital stays and increased health care costs but also with higher mortality.3 The American College of Physicians, through its Assessing Care of Vulnerable Elders project, expressly endorsed gait and mobility evaluation as a quality indicator, and examination insufficiency is well documented.4
Of the several existing mobility assessment tools, few are used routinely in hospital. Some require complex scoring; others require timing and/or a trained occupational therapist.5 We created a simplified tool named Independent Mobility Validation Examination (I‐MOVE) for use by bedside caregivers. We evaluated the tool's face validity and interobserver agreement.
I‐MOVE
I‐MOVE, represented schematically in Figure 1, is a performance test that assesses the patient's ability to perform a sequence of 6 basic tasks: rolling over in bed, sitting up, standing, transferring to a chair, walking in the room, and walking in the hallway. Most motor functions can be assumed to be hierarchical in nature; any patient who can perform at the highest level, such as walking safely, also would be expected to perform at the lowest level.

Instructions for administering I‐MOVE are as follows:
-
Review current orders. Exclude patients ordered on bed rest or non‐weight‐bearing or other orders precluding any of the 6 requested actions.
-
Prepare environment.
-
Chair at bedside.
-
Lower side bed rail closest to chair.
-
Clear path for patient to ambulate.
-
Ensure patient dons slippers.
-
Flatten bed.
-
Ensure any gait assistive device, if generally used by the patient, is within reach from the bedside.
-
Requests for patient action (for steps c through f, make available and within reach any appropriate gait‐assistance device such as walker or cane, if such is customarily used at home or newly prescribed):
-
With patient lying supine in bed, with close supervision, ask patient to turn from side to side in bed (request when both bed rails are up).
-
Lower side rail closer to chair and ask the patient to rise up to a sitting position and turn to sit up with legs dangling off the bed.
-
Ask the patient to stand.
-
Ask the patient to take a seat in the chair next to the bed.
-
Ask the patient to ambulate in the room.
-
Ask the patient to ambulate in the hallway.
-
At any point if the patient seems incapable, unsteady, or unsafe to accomplish the requested task, render hands‐on assistance and immediately end the test.
-
Document, by number (1‐12), the activity level successfully accomplished independently by the patient (even number levels) or accomplished with assistance (odd number levels).
-
Patient may be considered independent if able to perform the activity with a normal assistive device (cane, walker, brace, or crutches) but not using furniture.
-
Assistance is defined as any physical contact with the patient.
Findings
Face Validity
We sent surveys to 6 experienced practicing clinicians at our hospital: a geriatrician, a physiatrist, an exercise physiologist, an occupational therapist, a physical therapist, and a registered nurse. We asked each clinician to rate the 6 I‐MOVE elements (requested actions) for clinical relevance to mobility independence. Relevance of each element was measured on an ordinal scale with scores ranging from 1 to 4, with: 1 not relevant; 2 somewhat relevant; 3 quite relevant; and 4 very relevant. From the 5 responses we received, 4 evaluators ranked all 6 I‐MOVE requested actions as very relevant. The fifth evaluator ranked 5 of the 6 actions as very relevant and 1 action (walking in the room) as quite relevant. These results demonstrate general agreement that I‐MOVE is, at face value, a reasonable measure of independent mobility.
Interrater Reliability
The protocol was approved by the hospital's institutional review board. On a general medical unita non‐electrocardiographic telemetry, nonsurgical unit of an acute care hospital, where patients are assigned the primary service of an internal medicine physicianwe instructed 2 registered nurse (RN) volunteers (RN1 and RN2) in the I‐MOVE protocol. Each RN administered I‐MOVE independently to 41 consecutive, cognitively intact patients in a blinded fashion (ie, neither nurse was aware of the other's scoring of each patient) and within 1 hour of each other's assessment.
After administering I‐MOVE to each patient, the nurse judged and scored the patient's performance using the 12‐level I‐MOVE ordinal scale, ranging from a low value of 1, complete dependence, to the highest value of 12, complete independence. The patients' I‐MOVE score pairs recorded by RN1 and RN2 were statistically compared. Interrater reliability, a comparison of the 41 patients' score pairs, is graphically represented in Figure 2. The calculated intraclass correlation coefficient (r) was 0.90, indicating excellent agreement (r > 0.75).

Discussion
Traditional physical examinations by physicians and assessments by nurses do not routinely extend to standardized mobility testing and may fail to recognize disability. Of the existing mobility assessment tools, we believe that most are not suited to patients hospitalized on general medical units. I‐MOVE has been designed to address this need, with an emphasis on practicality and brevity to allow repetition at appropriate intervals (tracking), as is done for vital signs. In this initial study, I‐MOVE was found to have face‐valid content and excellent interrater agreement.
Our study had several limitations. Only 1 pair of test administrators was involved; the sample population was chosen by convenience; clustering of outcomes occurred at level 12, which may have augmented the agreement; and the study was limited to cognitively intact patients. Note that we chose to use the intraclass correlation coefficient rather than the statistic because the weighting between the ordinal I‐MOVE scores has not yet been studied and defined. Also, the weighted is asymptotically equivalent to the intraclass correlation coefficient.
I‐MOVE is intended to aid caregivers in the recognition of debility so that appropriate interventions such as physical therapy may be prescribed. It was designed to complement, not replace, specialized evaluations such as those performed by physical therapists, occupational therapists, or comprehensive geriatric assessments. This practical assessment of basic functioning may enhance communication among caregivers, patients, and patients' family members, especially with regard to discharge planning. Further study is needed to validate I‐MOVE against existing tools, evaluate I‐MOVE's utility as a vital sign, and discern whether a sharp or unexpected decline portends a medical complication.
Hospitalized patients are often debilitated, either from their admitting illness or from the deconditioning that occurs with inactivity. Functional decline, which appears to progress in a hierarchical pattern,1 occurs in 24% to 50% of geriatric patients during hospitalization and is poorly documented.2 Such a decline is associated not only with longer hospital stays and increased health care costs but also with higher mortality.3 The American College of Physicians, through its Assessing Care of Vulnerable Elders project, expressly endorsed gait and mobility evaluation as a quality indicator, and examination insufficiency is well documented.4
Of the several existing mobility assessment tools, few are used routinely in hospital. Some require complex scoring; others require timing and/or a trained occupational therapist.5 We created a simplified tool named Independent Mobility Validation Examination (I‐MOVE) for use by bedside caregivers. We evaluated the tool's face validity and interobserver agreement.
I‐MOVE
I‐MOVE, represented schematically in Figure 1, is a performance test that assesses the patient's ability to perform a sequence of 6 basic tasks: rolling over in bed, sitting up, standing, transferring to a chair, walking in the room, and walking in the hallway. Most motor functions can be assumed to be hierarchical in nature; any patient who can perform at the highest level, such as walking safely, also would be expected to perform at the lowest level.

Instructions for administering I‐MOVE are as follows:
-
Review current orders. Exclude patients ordered on bed rest or non‐weight‐bearing or other orders precluding any of the 6 requested actions.
-
Prepare environment.
-
Chair at bedside.
-
Lower side bed rail closest to chair.
-
Clear path for patient to ambulate.
-
Ensure patient dons slippers.
-
Flatten bed.
-
Ensure any gait assistive device, if generally used by the patient, is within reach from the bedside.
-
Requests for patient action (for steps c through f, make available and within reach any appropriate gait‐assistance device such as walker or cane, if such is customarily used at home or newly prescribed):
-
With patient lying supine in bed, with close supervision, ask patient to turn from side to side in bed (request when both bed rails are up).
-
Lower side rail closer to chair and ask the patient to rise up to a sitting position and turn to sit up with legs dangling off the bed.
-
Ask the patient to stand.
-
Ask the patient to take a seat in the chair next to the bed.
-
Ask the patient to ambulate in the room.
-
Ask the patient to ambulate in the hallway.
-
At any point if the patient seems incapable, unsteady, or unsafe to accomplish the requested task, render hands‐on assistance and immediately end the test.
-
Document, by number (1‐12), the activity level successfully accomplished independently by the patient (even number levels) or accomplished with assistance (odd number levels).
-
Patient may be considered independent if able to perform the activity with a normal assistive device (cane, walker, brace, or crutches) but not using furniture.
-
Assistance is defined as any physical contact with the patient.
Findings
Face Validity
We sent surveys to 6 experienced practicing clinicians at our hospital: a geriatrician, a physiatrist, an exercise physiologist, an occupational therapist, a physical therapist, and a registered nurse. We asked each clinician to rate the 6 I‐MOVE elements (requested actions) for clinical relevance to mobility independence. Relevance of each element was measured on an ordinal scale with scores ranging from 1 to 4, with: 1 not relevant; 2 somewhat relevant; 3 quite relevant; and 4 very relevant. From the 5 responses we received, 4 evaluators ranked all 6 I‐MOVE requested actions as very relevant. The fifth evaluator ranked 5 of the 6 actions as very relevant and 1 action (walking in the room) as quite relevant. These results demonstrate general agreement that I‐MOVE is, at face value, a reasonable measure of independent mobility.
Interrater Reliability
The protocol was approved by the hospital's institutional review board. On a general medical unita non‐electrocardiographic telemetry, nonsurgical unit of an acute care hospital, where patients are assigned the primary service of an internal medicine physicianwe instructed 2 registered nurse (RN) volunteers (RN1 and RN2) in the I‐MOVE protocol. Each RN administered I‐MOVE independently to 41 consecutive, cognitively intact patients in a blinded fashion (ie, neither nurse was aware of the other's scoring of each patient) and within 1 hour of each other's assessment.
After administering I‐MOVE to each patient, the nurse judged and scored the patient's performance using the 12‐level I‐MOVE ordinal scale, ranging from a low value of 1, complete dependence, to the highest value of 12, complete independence. The patients' I‐MOVE score pairs recorded by RN1 and RN2 were statistically compared. Interrater reliability, a comparison of the 41 patients' score pairs, is graphically represented in Figure 2. The calculated intraclass correlation coefficient (r) was 0.90, indicating excellent agreement (r > 0.75).

Discussion
Traditional physical examinations by physicians and assessments by nurses do not routinely extend to standardized mobility testing and may fail to recognize disability. Of the existing mobility assessment tools, we believe that most are not suited to patients hospitalized on general medical units. I‐MOVE has been designed to address this need, with an emphasis on practicality and brevity to allow repetition at appropriate intervals (tracking), as is done for vital signs. In this initial study, I‐MOVE was found to have face‐valid content and excellent interrater agreement.
Our study had several limitations. Only 1 pair of test administrators was involved; the sample population was chosen by convenience; clustering of outcomes occurred at level 12, which may have augmented the agreement; and the study was limited to cognitively intact patients. Note that we chose to use the intraclass correlation coefficient rather than the statistic because the weighting between the ordinal I‐MOVE scores has not yet been studied and defined. Also, the weighted is asymptotically equivalent to the intraclass correlation coefficient.
I‐MOVE is intended to aid caregivers in the recognition of debility so that appropriate interventions such as physical therapy may be prescribed. It was designed to complement, not replace, specialized evaluations such as those performed by physical therapists, occupational therapists, or comprehensive geriatric assessments. This practical assessment of basic functioning may enhance communication among caregivers, patients, and patients' family members, especially with regard to discharge planning. Further study is needed to validate I‐MOVE against existing tools, evaluate I‐MOVE's utility as a vital sign, and discern whether a sharp or unexpected decline portends a medical complication.
- .Health status and physical capacity. In:Osterweil D,Brummel‐Smith K,Beck JC, eds.Comprehensive Geriatric Assessment.New York:McGraw‐Hill;2000:41–66.
- ,,, et al.A predictive index for functional decline in hospitalized elderly medical patients.J Gen Intern Med.1993;8(12):645–652.
- ,,.Prevalence and outcomes of low mobility in hospitalized older patients.J Am Geriatr Soc.2004;52(8):1263–1270.
- ,,, et al.Detection and management of falls and instability in vulnerable elders by community physicians.J Am Geriatr Soc.2004;52(9):1527–1531.
- ,,.Exercising body and mind: an integrated approach to functional independence in hospitalized older people.J Am Geriatr Soc.2008;56(4):630–635.
- .Health status and physical capacity. In:Osterweil D,Brummel‐Smith K,Beck JC, eds.Comprehensive Geriatric Assessment.New York:McGraw‐Hill;2000:41–66.
- ,,, et al.A predictive index for functional decline in hospitalized elderly medical patients.J Gen Intern Med.1993;8(12):645–652.
- ,,.Prevalence and outcomes of low mobility in hospitalized older patients.J Am Geriatr Soc.2004;52(8):1263–1270.
- ,,, et al.Detection and management of falls and instability in vulnerable elders by community physicians.J Am Geriatr Soc.2004;52(9):1527–1531.
- ,,.Exercising body and mind: an integrated approach to functional independence in hospitalized older people.J Am Geriatr Soc.2008;56(4):630–635.
A New Narrative for Hospitalists
The hospitalist is not typically the hero in contemporary narratives about medical practice. More often, the hospitalist is portrayed as an interloper, a doctor who works for the hospital and not the patient, an employee focused on efficiency and rapid discharge rather than continuous medical care. Elsewhere in this issue, Mai Pham1 offers an updated story in which a hospitalist organizes the loose ends of a patient's medical history and contributes significantly to healthcare coordination.
Hospitalists acknowledge that an admission to the hospital disrupts established outpatient continuity and that discharge can be a perilous event, with potential for medical errors. The Society of Hospital Medicine has recognized discontinuity as enough of a concern that care transitions are considered a core competency for hospital physicians.2 This competency requires hospitalists to be able to move a patient safely from the outpatient setting through the hospital wards and back home again.
As our specialty approaches two decades of practice experience, the work that we do in coordinating medical care and ensuring continuity has evolved and deepened. Initial efforts to coordinate care from the inpatient setting focused on how key hospital events could be best communicated to the patient's primary physician.3, 4 Communication at admission and at critical junctures was encouraged, and research demonstrated that a timely discharge summary sent to the primary care office could decrease hospital readmission.5
Experienced hospitalists recognize, however, that not every inpatient can identify a primary care doctor; sometimes, it is this very lack of established outpatient care that triggers a patient's admission. Reasons for discontinuous prehospital care include disrupted outpatient relationships, particularly as provider networks and insurance status are re‐evaluated, as well as cultural and social barriers. Complex, overcrowded outpatient health systems can be challenging to navigate even for the savviest of patients.
These concerns have helped us to focus on the hospital as a critical setting for delivering continuity of care. The mechanisms for ensuring continuity include, harnessing the inpatient capability for real‐time diagnosis and treatment synthesis, which, in Mai Pham's case,1 enabled decision‐making and timely care coordination for her dying grandmother. Hospitals typically offer an array of tools needed to assist physicians in coordinating a patient's care, including rapid diagnostic testing and simultaneous multidisciplinary evaluation with consulting physicians; nurses; case managers; physical, occupational, and speech therapists; pharmacists; nutritionists; social workers; and palliative care teams. The patient's family members and friends are frequently present in the inpatient setting and can provide additional data points that are not always available in a timely manner in the ambulatory setting. Each of these inpatient interactions can help patients to develop routes of access to healthcare after they are discharged from the hospital.
Despite the advantages of the hospital setting, however, the knock on hospitalists is that we are just on the clock. Frequent handoffs, both when physician shifts change and when a fresh hospitalist rotates on service, present a significant concern to seamless care.6 Increasing fragmentation in hospital staffing may correlate with lengthened hospital stay and increased difficulty in receiving follow‐up outpatient care.7 A new narrative for hospitalists, one focused on enhancing continuity, requires mindfulness toward schedule fragmentation and balances personal desires with the need to maintain a continued presence and availability for patients.
Enhancing continuity and care coordination in the hospital also means continually working to improve provider‐to‐provider communications. Solutions may include well‐executed chart documentation, with active concerns flagged for the oncoming physician, and an electronic medical record that is easy to access from various locations. Computerized templates may enable more thorough handoffs in certain settings.8 As the use of systems and checklists gains traction for their ability to reduce iatrogenic complications and save money,9 hospitalists may come to rely more widely on systems that improve continuity, especially for aspects of inpatient care such as medication reconciliation.10
We believe that the most critical way in which hospitalists can ensure continuous care involves increasing physician efforts to engage with patients during their hospitalization. Hospitalists meet patients at particularly intense and vulnerable times of life, and we have all observed how patients can lose autonomy simply by being hospitalized. In the hospital, things happen to patients, sometimes because of the sheer size and force of the inpatient team and the momentum of a hospital stay.
Yet hospitalists can quickly develop a rapport with their patients through the number and intensity of their patient interactions. The free‐form structure of the inpatient schedule means a flexibility to be present with patients on short notice, to respond to acute events in real time, and to be available to talk with family members and other caregivers at their convenience. Hospitalists can take part in multiple bedside interactions in a single day and on consecutive days. Because of this flexibility, hospitalists can bond with their patients in a short time frame11 as they access critical social and clinical contexts, often more efficiently than possible elsewhere. As one primary care physician wrote when she gave up caring for her hospitalized patients, I know what happened to my patient, but I didn't really experience it with my patient.12 Hospitalists do get to share in this drama.
The medical community has been slow to recognize that hospitalists, as much as any generalist physician, can and do engage patients actively in their medical care. The hospital can be an ideal setting to ensure continuity through real‐time diagnostics and therapeutics and even more so through the intense bonding that can happen between physicians and patients on the wards. The old story of an outpatient provider single‐handedly managing a patient's care is rapidly disappearing in many locales. However, the story of the hospitalist is more than that of the hero in waiting. The story is a cautionary tale, one in which the relationship between the hospitalist and his or her patients is still under development, a tale for which much work remains. As hospitalists, we must continue to refine our skills and systems to deliver continuous care for patients in transition. We must also continue to focus on experiences with our patients and their families and, when called upon, to engage in those challenging conversations that Mai Pham1 says force us to align our expectations of one another. Forging this human connection will always be part of seamless healthcare for every physician, not least for the hospitalist.
Acknowledgements
The authors acknowledge Andrew Auerbach, MD, and John Choe, MD, MPH, for their comments on this article.
- .Dismantling Rube Goldberg: Cutting through chaos to achieve coordinated care.J Hosp Med.2009;4(4):259–260.
- Transitions of care.J Hosp Med.2006;1(suppl 1):95.
- ,,,,,.Deficits in communication and information transfer between hospital‐based and primary care physicians: implications for patient safety and continuity of care.JAMA.2007;297(8):831–841.
- ,,,.Promoting effective transitions of care at hospital discharge: a review of key issues for hospitalists.J Hosp Med.2007;2(5):314–323.
- ,,,.Effect of discharge summary availability during post‐discharge visits on hospital readmission.J Gen Intern Med.2002;17(3):186–192.
- ,.Care transitions for hospitalized patients.Med Clin North Am.2008;92(2):315–324, viii.
- ,,,,.Impact of fragmentation of hospitalist care on length of stay and postdischarge issues. Abstract presented at: Society of Hospital Medicine 2008 Annual Meeting; April 2008; San Diego, CA.
- ,,,,.A randomized, controlled trial evaluating the impact of a computerized rounding and sign‐out system on continuity of care and resident work hours.J Am Coll Surg.2005;200(4):538–545.
- .The checklist.New Yorker. December 10, 2007.
- ,,, et al.Transition of care for hospitalized elderly patients—development of a discharge checklist for hospitalists.J Hosp Med.2006;1(6):354–360.
- ,.The hospitalist's story.JAMA.2006;296(17):2067–2068.
- .Satisfaction?JAMA.2005;293(18):2193.
The hospitalist is not typically the hero in contemporary narratives about medical practice. More often, the hospitalist is portrayed as an interloper, a doctor who works for the hospital and not the patient, an employee focused on efficiency and rapid discharge rather than continuous medical care. Elsewhere in this issue, Mai Pham1 offers an updated story in which a hospitalist organizes the loose ends of a patient's medical history and contributes significantly to healthcare coordination.
Hospitalists acknowledge that an admission to the hospital disrupts established outpatient continuity and that discharge can be a perilous event, with potential for medical errors. The Society of Hospital Medicine has recognized discontinuity as enough of a concern that care transitions are considered a core competency for hospital physicians.2 This competency requires hospitalists to be able to move a patient safely from the outpatient setting through the hospital wards and back home again.
As our specialty approaches two decades of practice experience, the work that we do in coordinating medical care and ensuring continuity has evolved and deepened. Initial efforts to coordinate care from the inpatient setting focused on how key hospital events could be best communicated to the patient's primary physician.3, 4 Communication at admission and at critical junctures was encouraged, and research demonstrated that a timely discharge summary sent to the primary care office could decrease hospital readmission.5
Experienced hospitalists recognize, however, that not every inpatient can identify a primary care doctor; sometimes, it is this very lack of established outpatient care that triggers a patient's admission. Reasons for discontinuous prehospital care include disrupted outpatient relationships, particularly as provider networks and insurance status are re‐evaluated, as well as cultural and social barriers. Complex, overcrowded outpatient health systems can be challenging to navigate even for the savviest of patients.
These concerns have helped us to focus on the hospital as a critical setting for delivering continuity of care. The mechanisms for ensuring continuity include, harnessing the inpatient capability for real‐time diagnosis and treatment synthesis, which, in Mai Pham's case,1 enabled decision‐making and timely care coordination for her dying grandmother. Hospitals typically offer an array of tools needed to assist physicians in coordinating a patient's care, including rapid diagnostic testing and simultaneous multidisciplinary evaluation with consulting physicians; nurses; case managers; physical, occupational, and speech therapists; pharmacists; nutritionists; social workers; and palliative care teams. The patient's family members and friends are frequently present in the inpatient setting and can provide additional data points that are not always available in a timely manner in the ambulatory setting. Each of these inpatient interactions can help patients to develop routes of access to healthcare after they are discharged from the hospital.
Despite the advantages of the hospital setting, however, the knock on hospitalists is that we are just on the clock. Frequent handoffs, both when physician shifts change and when a fresh hospitalist rotates on service, present a significant concern to seamless care.6 Increasing fragmentation in hospital staffing may correlate with lengthened hospital stay and increased difficulty in receiving follow‐up outpatient care.7 A new narrative for hospitalists, one focused on enhancing continuity, requires mindfulness toward schedule fragmentation and balances personal desires with the need to maintain a continued presence and availability for patients.
Enhancing continuity and care coordination in the hospital also means continually working to improve provider‐to‐provider communications. Solutions may include well‐executed chart documentation, with active concerns flagged for the oncoming physician, and an electronic medical record that is easy to access from various locations. Computerized templates may enable more thorough handoffs in certain settings.8 As the use of systems and checklists gains traction for their ability to reduce iatrogenic complications and save money,9 hospitalists may come to rely more widely on systems that improve continuity, especially for aspects of inpatient care such as medication reconciliation.10
We believe that the most critical way in which hospitalists can ensure continuous care involves increasing physician efforts to engage with patients during their hospitalization. Hospitalists meet patients at particularly intense and vulnerable times of life, and we have all observed how patients can lose autonomy simply by being hospitalized. In the hospital, things happen to patients, sometimes because of the sheer size and force of the inpatient team and the momentum of a hospital stay.
Yet hospitalists can quickly develop a rapport with their patients through the number and intensity of their patient interactions. The free‐form structure of the inpatient schedule means a flexibility to be present with patients on short notice, to respond to acute events in real time, and to be available to talk with family members and other caregivers at their convenience. Hospitalists can take part in multiple bedside interactions in a single day and on consecutive days. Because of this flexibility, hospitalists can bond with their patients in a short time frame11 as they access critical social and clinical contexts, often more efficiently than possible elsewhere. As one primary care physician wrote when she gave up caring for her hospitalized patients, I know what happened to my patient, but I didn't really experience it with my patient.12 Hospitalists do get to share in this drama.
The medical community has been slow to recognize that hospitalists, as much as any generalist physician, can and do engage patients actively in their medical care. The hospital can be an ideal setting to ensure continuity through real‐time diagnostics and therapeutics and even more so through the intense bonding that can happen between physicians and patients on the wards. The old story of an outpatient provider single‐handedly managing a patient's care is rapidly disappearing in many locales. However, the story of the hospitalist is more than that of the hero in waiting. The story is a cautionary tale, one in which the relationship between the hospitalist and his or her patients is still under development, a tale for which much work remains. As hospitalists, we must continue to refine our skills and systems to deliver continuous care for patients in transition. We must also continue to focus on experiences with our patients and their families and, when called upon, to engage in those challenging conversations that Mai Pham1 says force us to align our expectations of one another. Forging this human connection will always be part of seamless healthcare for every physician, not least for the hospitalist.
Acknowledgements
The authors acknowledge Andrew Auerbach, MD, and John Choe, MD, MPH, for their comments on this article.
The hospitalist is not typically the hero in contemporary narratives about medical practice. More often, the hospitalist is portrayed as an interloper, a doctor who works for the hospital and not the patient, an employee focused on efficiency and rapid discharge rather than continuous medical care. Elsewhere in this issue, Mai Pham1 offers an updated story in which a hospitalist organizes the loose ends of a patient's medical history and contributes significantly to healthcare coordination.
Hospitalists acknowledge that an admission to the hospital disrupts established outpatient continuity and that discharge can be a perilous event, with potential for medical errors. The Society of Hospital Medicine has recognized discontinuity as enough of a concern that care transitions are considered a core competency for hospital physicians.2 This competency requires hospitalists to be able to move a patient safely from the outpatient setting through the hospital wards and back home again.
As our specialty approaches two decades of practice experience, the work that we do in coordinating medical care and ensuring continuity has evolved and deepened. Initial efforts to coordinate care from the inpatient setting focused on how key hospital events could be best communicated to the patient's primary physician.3, 4 Communication at admission and at critical junctures was encouraged, and research demonstrated that a timely discharge summary sent to the primary care office could decrease hospital readmission.5
Experienced hospitalists recognize, however, that not every inpatient can identify a primary care doctor; sometimes, it is this very lack of established outpatient care that triggers a patient's admission. Reasons for discontinuous prehospital care include disrupted outpatient relationships, particularly as provider networks and insurance status are re‐evaluated, as well as cultural and social barriers. Complex, overcrowded outpatient health systems can be challenging to navigate even for the savviest of patients.
These concerns have helped us to focus on the hospital as a critical setting for delivering continuity of care. The mechanisms for ensuring continuity include, harnessing the inpatient capability for real‐time diagnosis and treatment synthesis, which, in Mai Pham's case,1 enabled decision‐making and timely care coordination for her dying grandmother. Hospitals typically offer an array of tools needed to assist physicians in coordinating a patient's care, including rapid diagnostic testing and simultaneous multidisciplinary evaluation with consulting physicians; nurses; case managers; physical, occupational, and speech therapists; pharmacists; nutritionists; social workers; and palliative care teams. The patient's family members and friends are frequently present in the inpatient setting and can provide additional data points that are not always available in a timely manner in the ambulatory setting. Each of these inpatient interactions can help patients to develop routes of access to healthcare after they are discharged from the hospital.
Despite the advantages of the hospital setting, however, the knock on hospitalists is that we are just on the clock. Frequent handoffs, both when physician shifts change and when a fresh hospitalist rotates on service, present a significant concern to seamless care.6 Increasing fragmentation in hospital staffing may correlate with lengthened hospital stay and increased difficulty in receiving follow‐up outpatient care.7 A new narrative for hospitalists, one focused on enhancing continuity, requires mindfulness toward schedule fragmentation and balances personal desires with the need to maintain a continued presence and availability for patients.
Enhancing continuity and care coordination in the hospital also means continually working to improve provider‐to‐provider communications. Solutions may include well‐executed chart documentation, with active concerns flagged for the oncoming physician, and an electronic medical record that is easy to access from various locations. Computerized templates may enable more thorough handoffs in certain settings.8 As the use of systems and checklists gains traction for their ability to reduce iatrogenic complications and save money,9 hospitalists may come to rely more widely on systems that improve continuity, especially for aspects of inpatient care such as medication reconciliation.10
We believe that the most critical way in which hospitalists can ensure continuous care involves increasing physician efforts to engage with patients during their hospitalization. Hospitalists meet patients at particularly intense and vulnerable times of life, and we have all observed how patients can lose autonomy simply by being hospitalized. In the hospital, things happen to patients, sometimes because of the sheer size and force of the inpatient team and the momentum of a hospital stay.
Yet hospitalists can quickly develop a rapport with their patients through the number and intensity of their patient interactions. The free‐form structure of the inpatient schedule means a flexibility to be present with patients on short notice, to respond to acute events in real time, and to be available to talk with family members and other caregivers at their convenience. Hospitalists can take part in multiple bedside interactions in a single day and on consecutive days. Because of this flexibility, hospitalists can bond with their patients in a short time frame11 as they access critical social and clinical contexts, often more efficiently than possible elsewhere. As one primary care physician wrote when she gave up caring for her hospitalized patients, I know what happened to my patient, but I didn't really experience it with my patient.12 Hospitalists do get to share in this drama.
The medical community has been slow to recognize that hospitalists, as much as any generalist physician, can and do engage patients actively in their medical care. The hospital can be an ideal setting to ensure continuity through real‐time diagnostics and therapeutics and even more so through the intense bonding that can happen between physicians and patients on the wards. The old story of an outpatient provider single‐handedly managing a patient's care is rapidly disappearing in many locales. However, the story of the hospitalist is more than that of the hero in waiting. The story is a cautionary tale, one in which the relationship between the hospitalist and his or her patients is still under development, a tale for which much work remains. As hospitalists, we must continue to refine our skills and systems to deliver continuous care for patients in transition. We must also continue to focus on experiences with our patients and their families and, when called upon, to engage in those challenging conversations that Mai Pham1 says force us to align our expectations of one another. Forging this human connection will always be part of seamless healthcare for every physician, not least for the hospitalist.
Acknowledgements
The authors acknowledge Andrew Auerbach, MD, and John Choe, MD, MPH, for their comments on this article.
- .Dismantling Rube Goldberg: Cutting through chaos to achieve coordinated care.J Hosp Med.2009;4(4):259–260.
- Transitions of care.J Hosp Med.2006;1(suppl 1):95.
- ,,,,,.Deficits in communication and information transfer between hospital‐based and primary care physicians: implications for patient safety and continuity of care.JAMA.2007;297(8):831–841.
- ,,,.Promoting effective transitions of care at hospital discharge: a review of key issues for hospitalists.J Hosp Med.2007;2(5):314–323.
- ,,,.Effect of discharge summary availability during post‐discharge visits on hospital readmission.J Gen Intern Med.2002;17(3):186–192.
- ,.Care transitions for hospitalized patients.Med Clin North Am.2008;92(2):315–324, viii.
- ,,,,.Impact of fragmentation of hospitalist care on length of stay and postdischarge issues. Abstract presented at: Society of Hospital Medicine 2008 Annual Meeting; April 2008; San Diego, CA.
- ,,,,.A randomized, controlled trial evaluating the impact of a computerized rounding and sign‐out system on continuity of care and resident work hours.J Am Coll Surg.2005;200(4):538–545.
- .The checklist.New Yorker. December 10, 2007.
- ,,, et al.Transition of care for hospitalized elderly patients—development of a discharge checklist for hospitalists.J Hosp Med.2006;1(6):354–360.
- ,.The hospitalist's story.JAMA.2006;296(17):2067–2068.
- .Satisfaction?JAMA.2005;293(18):2193.
- .Dismantling Rube Goldberg: Cutting through chaos to achieve coordinated care.J Hosp Med.2009;4(4):259–260.
- Transitions of care.J Hosp Med.2006;1(suppl 1):95.
- ,,,,,.Deficits in communication and information transfer between hospital‐based and primary care physicians: implications for patient safety and continuity of care.JAMA.2007;297(8):831–841.
- ,,,.Promoting effective transitions of care at hospital discharge: a review of key issues for hospitalists.J Hosp Med.2007;2(5):314–323.
- ,,,.Effect of discharge summary availability during post‐discharge visits on hospital readmission.J Gen Intern Med.2002;17(3):186–192.
- ,.Care transitions for hospitalized patients.Med Clin North Am.2008;92(2):315–324, viii.
- ,,,,.Impact of fragmentation of hospitalist care on length of stay and postdischarge issues. Abstract presented at: Society of Hospital Medicine 2008 Annual Meeting; April 2008; San Diego, CA.
- ,,,,.A randomized, controlled trial evaluating the impact of a computerized rounding and sign‐out system on continuity of care and resident work hours.J Am Coll Surg.2005;200(4):538–545.
- .The checklist.New Yorker. December 10, 2007.
- ,,, et al.Transition of care for hospitalized elderly patients—development of a discharge checklist for hospitalists.J Hosp Med.2006;1(6):354–360.
- ,.The hospitalist's story.JAMA.2006;296(17):2067–2068.
- .Satisfaction?JAMA.2005;293(18):2193.
Impact of Elderly Inpatient Care Bundle
Elderly patients (aged 65 years and older) consume a disproportionate amount of acute health care resources, composing up to 20% of emergency department (ED) visits,1, 2 having a 2‐fold to 5‐fold increase in likelihood of hospital admission,1 and frequently incurring lengths of hospital stay (LOS) approximately 15% higher than the national averages.3 In addition, they are at increased risk for hospital readmission in the 90‐day interval following hospital discharge.1, 4, 5 Specific risk factors for readmission include age above 80 years, discharge within the previous 30 days, the presence of 3 or more comorbid diagnoses, use of 5 or more prescription medications, difficulty with at least 1 activity of daily living (ADL), and lack of discharge education.6 These risk factors can translate into adverse drug events,79 exacerbations of chronic diseases,10 or functional decline4, 5 that can trigger ED visits or hospital readmission.
Hospital‐based care coordinationdefined as a multidisciplinary interaction between inpatients and providers that focuses on education, communication, and discharge planning with the primary aim of improving outcomeshas demonstrated inconsistent results as a mechanism to reduce LOS, postdischarge ED visits, or hospital readmission rates. While disease‐specific care coordination programs for congestive heart failure and chronic obstructive pulmonary disease have been effective in reducing rehospitalization rates,1015 the benefits of comprehensive care coordination for elderly general medical inpatients with a broader range of diagnoses are less clear. In a group of 750 elderly patients with 1 of 11 common inpatient diagnoses (such as stroke or hip fracture) likely to ultimately require a high level of home support, Coleman et al.16 found that a structured transitional care program centered on a personal coach decreased rehospitalization rates at 30 and 90 days. Preen et al.17 found improved patient involvement and perceived quality of life with care coordination focused on discharge planning, but no impact on LOS. Likewise, a recent meta‐analysis18 failed to demonstrate statistically significant differences in mortality, LOS, or readmission rates in hospitalized patients who received intensive care coordination versus usual care; however, variation in the components of the care coordination intervention and reported outcomes restricted the ability to pool data in this study.
Care coordination programs demonstrating efficacy in reducing health care utilization in elderly medical patients have generally included an outpatient transitional component with out‐of‐hospital postacute care visits by health care personnel such as a nurse, pharmacist, or physician.1923 These offsite interventions generate additional expenses and resource demands that may not be practical for smaller hospitals to implement.24, 25 In contrast, hospital‐based care coordination programs have clear ownership and thus may be more practical to disseminate. Individual elements of hospital‐based care coordination such as pharmacist counseling, discharge education, and telephone follow‐up have been shown to reduce ED visitation and readmission rates in high‐risk elderly patients. Less information is available regarding the impact of these interventions delivered in an aggregate bundle by hospital staff in the absence of bridging transitional visits.2629
The objective of this pilot study was to determine whether a supplemental elderly care bundle, targeted to high‐risk inpatients by hospital staff as an enhancement to existing care coordination, would affect postdischarge readmission and ED visit rates. The intervention was designed to capitalize on existing resources, and focused specifically on elderly inpatients who were hospitalized with diagnoses commonly encountered in a general medical unit and predisposed to recidivism.
Patients and Methods
Patient Selection and Enrollment
The screening population consisted of elderly patients admitted to 1 of 2 hospital‐medicine groups (MedProvider Inpatient Care Unit or Texas Primary Care) at the 900‐bed Baylor University Medical Center (BUMC, Dallas, TX) between March and June 2007 with a diagnosis likely to fall within 1 of 20 frequent Medicare medical diagnosis reimbursement groups (DRGs) at BUMC, as listed in Table 1. Study personnel performed daily chart review to establish eligibility criteria, which included age 70 years, use of 5 medications regularly, 3 chronic comorbid conditions, requirement for assistance with 1 ADL, and preadmission residence at home or assisted living with a reasonable expectation of disposition back to that domicile. These criteria were based on factors found in the literature to be associated with extended LOS and postdischarge readmission/ED visit events.5, 6, 3032 Potential enrollees needed to be conversant in English (a multilingual staff was not feasible due to limited resources for this pilot project) and have reliable phone contact, or have a proxy caregiver who could speak English and be reached by phone. Predefined exclusion criteria were admission primarily for a surgical procedure, terminal diagnosis with life expectancy 6 months, residence in a long‐term care facility (long‐term acute care [LTAC], skilled nursing facility [SNF], or nursing home) prior to hospitalization with anticipated discharge back to that facility, and patient/family refusal to participate. Additionally, with an average LOS between 5 and 6 days in BUMC's Medicare population for the DRGs of interest, it was felt that the effects of the care bundle intervention would be obscured unless initiated early in the hospitalization. Thus, patients who could not be enrolled within 72 hours following admission were subsequently excluded. The Baylor Health Care System (BHCS) Institutional Review Board (IRB) approved this study, and written informed consent was obtained from all patients or their surrogates.
| DRG | DRG Name |
|---|---|
| |
| 127 | Heart failure and shock |
| 14 | Intracranial hemorrhage or cerebral infarction |
| 89 | Simple pneumonia/pleurisy |
| 416 | Septicemia |
| 316 | Renal failure |
| 182 | Esophagitis/gastroenterological/miscellaneous digestive disorders with complications |
| 174 | Gastrointestinal hemorrhage with complications |
| 88 | Chronic obstructive pulmonary disease |
| 320 | Kidney/urinary tract infection with complications |
| 144 | Other circulatory diagnoses with complications |
| 138 | Arrhythmia/conduction disorders with complications |
| 277 | Cellulitis with complications |
| 124 | Circulatory disorders except acute myocardial infarction with cardiac catheterization and complex diagnosis |
| 430 | Psychoses |
| 188 | Other digestive diagnoses with complications |
| 395 | Red blood cell disorders |
| 79 | Respiratory infections and inflammations with complications |
| 524 | Transient ischemia |
| 143 | Chest pain |
| 141 | Syncope and collapse with complications |
Patients meeting eligibility criteria were approached within 72 hours of admission for study participation. After consent and enrollment, patients were randomized to intervention or usual care arms in permuted blocks of 8 via a random number generator and sealed opaque envelopes. Nursing and care coordination staff providing usual care to patients (independent of the research team) were blinded to the treatment group status of enrollees; trial design precluded blinding of study personnel and patients.
Delivery of the Supplemental Care Bundle
Starting no later than 24 hours after enrollment and continuing up to 1 week following hospital discharge, intervention group patients received a targeted care bundle provided by 1 of 3 care coordinators (CCs) and 1 of 4 clinical pharmacists (CPs) working with the study team. The care bundle was designed as an intensive patient‐centered educational program that would augment BUMC's existing care coordination processes (delivered to all patients regardless of study participation); specific elements are displayed in Figure 1. Study CCs saw patients daily throughout their hospital stay, and instructed patients on specific health conditions, with an emphasis on optimizing home self‐care and contingency plans if problems arose. CP visits focused on medication reconciliation and education regarding any new agents started during the hospitalization. The personal health record (PHR) provided a tool to engage patients in self‐care, and as discussed by Coleman et al.,7, 16, 33 promoted information transfer from the hospital to outpatient settings. During the postdischarge phone call, CCs followed a basic script to confirm receipt of medical equipment, medications, home health arrangements, and scheduling of follow‐up appointments. They also used this contact as an opportunity to reinforce patient education on managing their conditions. CPs reviewed medication use (type, schedule, dose), and spoke with patients about any symptoms they may have experienced as medication side effects. If indicated based on their phone discussions, both CCs and CPs could recommend an action plan to the patient.
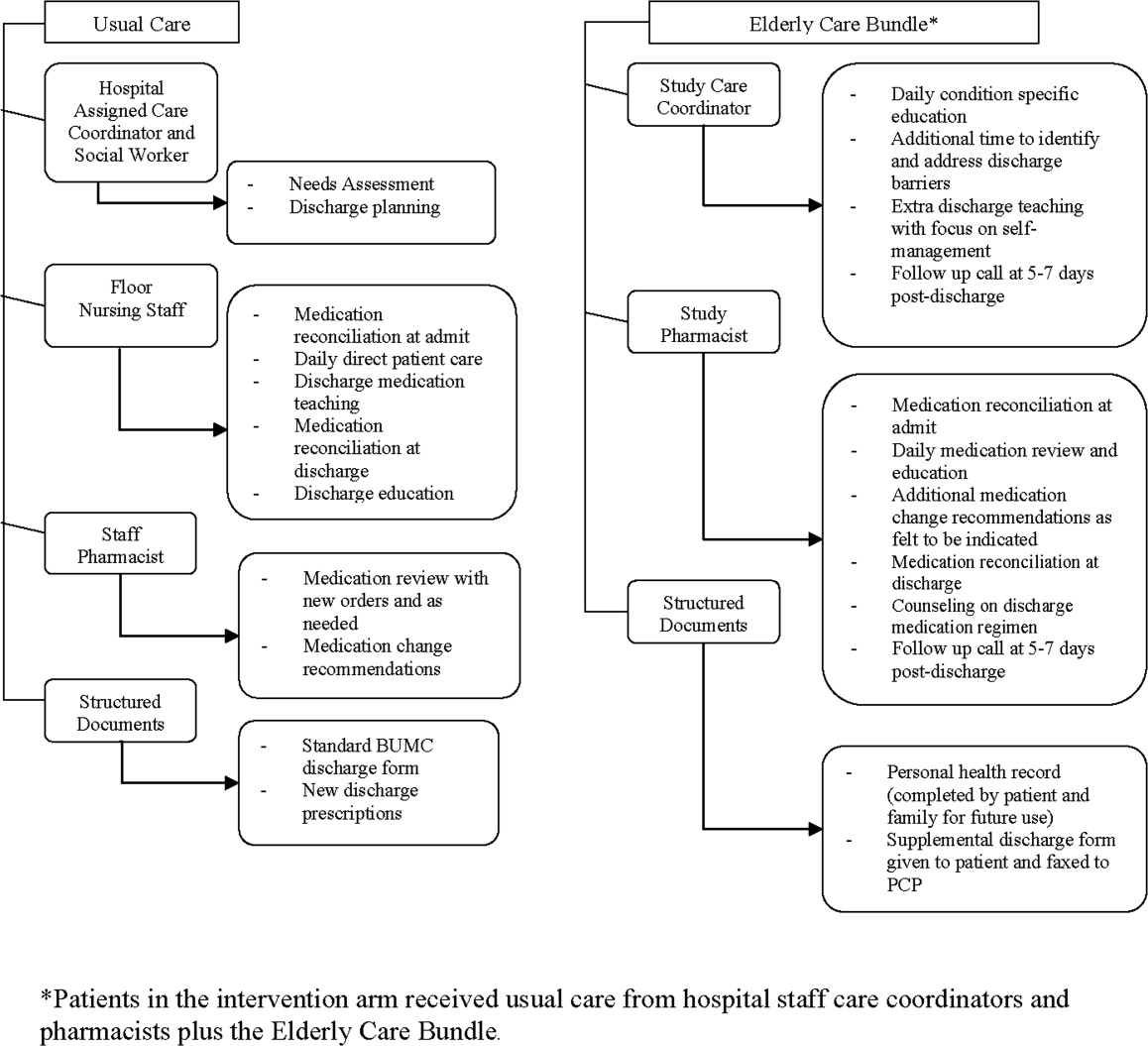
The study CCs and CPs were existing hospital staff and performed their research activities in addition to their usual duties. Study CCs were highly experienced (averaging 8 years of inpatient floor nursing plus 10 years as CCs) and all had advanced nursing certifications (ACM, BSN, or MSN). The CPs were upper‐level pharmacy residents completing their inpatient clinical rotations. Additional training for both study CCs and CPs was limited to a series of 3 meetings (each 45 minutes in duration) regarding the intent and delivery of the supplemental care bundle, including use of study forms.
At the time of the trial, the particular CCs and CPs chosen to deliver the supplemental care bundle had work assignments ensuring that crossover between intervention and usual care groups would not occur. For example, 1 of the study CCs normally covered a surgical floor such that her normal scope of responsibilities would not influence the medical patients in the study (their baseline care coordination was provided by nonstudy personnel). Medication reconciliation and medication education is generally performed by floor nursing staff rather than CPs at BUMC.
Data Collection and Outcomes Measurement
Following enrollment, demographic information and a basic medical history were documented by research staff. Inaccuracies in medication lists discovered by pharmacists during the medication reconciliation process were entered directly into the universal medication list on the hospital chart. CPs also kept a log of the medication education given to patients (and recommendations for changes to patients' regimens given to physicians) throughout their hospital stay. Study CCs recorded their assessments of patient needs and associated responses. Furthermore, the research team CC prepared an enhanced discharge form that was given to intervention patients in addition to BUMC's standard form. Data on LOS, illness severity (APR‐DRGs), and unplanned hospital readmission or ED visitation at 30 and 60 days postdischarge were collected via BUMC's electronic reporting systems. All patient follow‐up was completed as of September 1, 2007.
Statistical Analyses
Resource and time constraints necessitated a sample size that would allow implementation of the intervention despite a limited number of study CCs and pharmacists. To accommodate these conditions while still generating pilot data, an a priori decision was made to enroll up to 80 patients. Continuous data variables were normally distributed. Differences between groups for continuous variables were assessed with the Student t‐test; differences in proportions between groups were compared with Fisher's exact tests. Time to readmission events between the groups were evaluated in a post hoc manner using the log‐rank test. Data were analyzed using Prism version 5 for Windows (GraphPad Software, Inc., San Diego, CA) and SPSS version 15 for Windows (SPSS Inc., Chicago, IL). P values < 0.05 were considered statistically significant.
Results
The final sample size for this pilot was small, with 41 total patients (21 controls, 20 interventions). The main reason for enrollment failure of patients meeting study criteria was an inability to obtain informed consent. Sixty patients declined participation after being approached, and another 56 patients were unable to give their informed consent due to impairments (poor cognition, medication induced sedation, severity of illness) with lack of an available proxy to give written consent during the 72‐hour postadmission recruitment window. There were no statistically significant differences in the baseline characteristics of the intervention and control groups (Table 2). A similar proportion of patients (23% in the intervention, 15% in controls; P = 0.70) had preexisting diagnoses of dementia or depression. However, on APR‐DRG measures relating to acuity of illness and mortality risk, patients in the intervention group trended toward higher severity (Table 2). Likewise, although it was not a statistically significant difference, 13 of 20 patients in the intervention group were taking medications from 2 drug classes commonly implicated in adverse drug events (warfarin, insulin, diuretics, sedating agents) as part of their discharge medication regimen compared to 10 of 21 patients in the control group.
| Control (n = 21) | Intervention (n = 20) | P Value | |
|---|---|---|---|
| Age in years (mean SD) | 79.8 5.6 | 77.2 5.3 | 0.14 |
| Males, n (%) | 8 (38) | 3 (15) | 0.10 |
| Females, n (%) | 13 (62) | 17 (85) | 0.10 |
| Race, n (%) | |||
| African‐American | 3 (14) | 5 (25) | 0.45 |
| Asian | 0 (0) | 1 (5) | 0.49 |
| Caucasian | 17 (81) | 14 (70) | 0.48 |
| Hispanic | 1 (5) | 0 | 1.0 |
| Preadmission living status, n (%) | |||
| Alone | 6 (29) | 4 (20) | 0.72 |
| With spouse or other family | 11 (52) | 15 (75) | 0.20 |
| Assisted living | 4 (19) | 1 (5) | 0.34 |
| Inpatient medications (mean SD) | 11 3 | 12 5 | 0.18 |
| Charlson score (mean, SD) | 3.2 1.3 | 3.7 1.1 | 0.21 |
| % with APR DRG severity rating 3 | 57.5 | 83.3 | 0.12 |
| % with APR DRG mortality rating 3 | 20.0 | 55.6 | 0.07 |
| Primary admission diagnoses (n cases, in order of frequency) | 3 pneumonia | 3 pneumonia | |
| 3 CHF | 3 syncope | ||
| 2 syncope | 2 CHF | ||
| 2 COPD | 2 COPD | ||
| 2 cellulitis | 2 cellulitis | ||
| 2 GI disorder (nonbleed) | 2 GI disorder (nonbleed) | ||
| 2 GI bleed | 1 GI bleed | ||
| 2 UTI | 1 atrial fibrillation | ||
| 1 atrial fibrillation | 1 encephalopathy | ||
| 1 stroke | 1 TIA | ||
| 1 renal failure | 1 renal failure | ||
| 1 volume depletion |
Study outcomes are displayed in Table 3. Mean LOS is reported as a descriptive finding; there was insufficient power to compare this outcome statistically between groups. The majority of patients were discharged to home. A similar proportion of patients in the intervention (20%) and control groups (22%) who had lived at home immediately prior to admission were discharged from the hospital to skilled care facilities (P = 0.87). The number of readmissions/ED visits (taken as a composite measure of unplanned healthcare utilization) within 30 days of discharge was lower in the intervention group; by 60 days, there was no longer a statistically significant difference in readmission/ED visit rates between groups. For those patients who had a readmission or ED visit following hospital discharge, the intervention group had a longer time interval to first event compared to controls (36.2 versus 15.7 days, P = 0.05). Of the patients discharged to skilled care, 1 in the intervention group (at 53 days) and 1 in the control group (at 16 days) had a readmission/ED visit event. Figure 2 shows time‐to‐first readmission or ED visit event curves at 30 and 60 days for both intervention and control groups. For patients who had a readmission/ED visit event, LOS for this episode was 2.2 2.1 days in controls and 3.7 2.1 days in the intervention group (insufficient power for statistical comparison). The study's small sample size prevented development of a meaningful regression model.
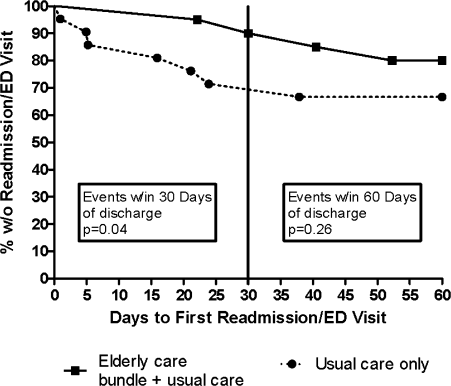
| Outcome Measure | Control (n = 21) | Intervention (n = 20) | P Value |
|---|---|---|---|
| |||
| Length of stay for index hospitalization (days)* | 4.7 3.7 | 6.2 4.1 | |
| 0‐30 day postdischarge readmissions/ED visits | 8 (38%) | 2 (10%) | 0.03 |
| 31‐60 day postdischarge readmissions/ED visits | 1 (5%) | 4 (20%) | 0.18 |
| Total postdischarge readmissions/ED visits at 60 days | 9 | 6 | 0.52 |
Resource utilization and the specifics of patient‐study personnel interaction associated with the intervention were tracked. Research assistants spent an average of 50 minutes daily screening charts for potential candidates. For the 20 patients who received the supplemental elderly care bundle, study CCs averaged 20 to 25 minutes per patient daily of additional time counseling patients and families, identifying and attending to discharge barriers, filling out documentation, and faxing the supplemental study discharge form to the patient's primary care physician. Any residual home care needs or issues unresolved at discharge were addressed with the patient in the 5 to 7 day follow‐up phone call. Similarly, study CPs expended approximately 20 minutes daily per patient providing medication education, reconciliation, and optimization of drug therapy. Study pharmacists recommended a change to the medication regimens of 10 patients in the intervention group; physicians acted upon these recommendations for 7 of the patients. The changes included dosage adjustment, discontinuation of medications due to possible drug interaction or duplication of drugs with the same pharmacologic effect, and addition of medications as indicated by patient condition or to reconcile with patients' at‐home medication regimens. Patients contacted via phone by the study pharmacist within 1 week after discharge were able to describe proper use of new medications started in the hospital and confirm that they obtained or had the means to obtain the prescribed drugs.
Discussion
This pilot study examined the effects of a supplemental care bundle involving patient education and discharge planning delivered by hospital‐based CCs and CPs on the rate of readmission/ED visitation in 41 elderly (70 years of age) patients. The study was not adequately powered to detect an impact of the intervention on index LOS. The care bundle did lead to significantly fewer readmissions or ED visits 30 days postdischarge and appeared to increase the time interval to first unplanned readmission or ED visit compared to usual care. This effect was no longer present at 60 days postdischarge. Resource allocations and scope of duties for CCs and CPs (an average of 20 minutes per patient per day) related to delivering the intervention were realistic for broader implementation in the hospitalized elderly population at high risk for readmission or ED visitation following discharge.
Length of stay for the initial hospitalization associated with the care bundle was an original outcome of interest to the study team. However, with the final enrollment of 41 patients and a power of 0.8, the between group difference would have needed to be 2.6 days to be statistically significant. It is likely that any change in LOS related to the care bundle would be much smaller, particularly since 2 key determinants of LOS, severity of illness and physician behavior, were beyond this patient education‐oriented intervention's scope of influence.3437 Furthermore, the diverse range of eligible diagnoses limited the study CCs' ability to reduce variability through use of clinical care pathways. One approach in leveraging an elderly care bundle to reduce LOS may be to focus on a specific disease that has well‐established inpatient benchmarks and treatment algorithms. For example, in patients with community‐acquired pneumonia, the use of care coordination in combination with standardized order sets decreased LOS without compromising safety, mainly by shortening the time from clinical stability to discharge.38
On separation of the readmission/ED visit outcome into 30 and 60 day postdischarge time frames, the intervention group had a lower rate of unplanned acute health care use within 30 days postdischarge; the difference between groups had dissipated by 60 days postdischarge. This convergence suggests that a hospital‐based intervention's influence is strongest closer to the time of the initial hospital stay, and wanes as more time has elapsed. Indeed, interventions that have successfully maintained lower readmission rates beyond 60 and 90 days postdischarge in a high‐risk elderly population (such as the program advocated by Coleman et al.16) have included a transitional care provider engaging patients during the hospitalization and performing subsequent visits to the home or nursing facility.33 An optimal intervention would capitalize on the hospital‐based staff's ability to improve short‐term readmission/ED visit rates while linking patients to longer‐term transitional care to extend these outcomes. Electronic health records could potentially facilitate these care transitions, beginning with an automated screening process for identification of high‐risk inpatients and continuing through postdischarge follow‐up. How to develop these resources in settings where outpatient practices are independent or only loosely affiliated with hospitals is an area for continued investigation.
In a group of elderly patients with multiple comorbidities and complex pharmacotherapy regimens, the study bundle component targeting medication management appears to be a high‐yield intervention to reduce unplanned health care utilization following hospital discharge. These patients are more susceptible to nonadherence and drug‐related adverse events, which may contribute to hospital readmission or ED visitation.7, 9, 39 Consistent with findings at other sites,28, 40 a heightened level of CP involvement in the care of high‐risk elderly patients may have helped reduce these undesirable outcomes. Of the 9 readmission/ED visit events in the control group, 3 were attributable to medication related complications (2 from sedatives, 1 from a diuretic). None of the readmission/ED visit events in intervention group patients stemmed from medication effects.
Correspondingly, the research CCs' provision of daily condition‐specific education, additional time to more thoroughly investigate discharge needs, engagement of patients' families as active partners in self‐care, and the use of a structured discharge form along with follow‐up phone calls may have better prepared patients to manage their health problems once released from the hospital.26, 28, 29 For example, 1 patient in the control group was readmitted less than 24 hours after initial discharge due to inability to perform self‐care at home. Given the study power issues described previously, data on LOS for the second hospitalization for patients who had a readmission event are difficult to interpret, but could suggest the occurrence of some shorter, preventable readmissions in the control group. Conversely, the readmission/ED visit events in intervention patients appeared to be associated with a specific medical condition (eg, failure of diabetic cellulitis to respond to appropriate outpatient treatment) rather than problems that would have been corrected with an educational/self‐management program such as this targeted care bundle.
This pilot study had several limitations. The main issue was a small patient sample size that was primarily due to an inability to obtain informed consent. Design of the study as a randomized controlled trial and plans to disseminate study findings beyond BHCS necessitated IRB approval rather than delivery of the supplemental care bundle as a quality improvement (QI) project. Placing QI initiatives under research regulations can lead to project delays, higher costs, and patient frustrations with the process.41, 42 This tension was evident during study screening and enrollment, as many patients who otherwise met criteria and would potentially benefit from the intervention were hesitant to participate in a research study or refused to sign a multipage consent document. The difficulties of enrolling elderly patients in clinical trials have been well‐described.43, 44 Further research involving a minimal‐risk, educational intervention such as this elderly care‐bundle would likely better fit under the category of expedited IRB review with waiver or modification of the informed consent process.45
Incomplete blinding could have potentially affected our results. At the study site, the team members delivering the care bundle were a regular part of the hospital staff (as opposed to external researchers), and it is not unusual for a CC or a pharmacist to enter a patient's room (eg, to confirm a drug allergy history). In view of this, the impact of imperfect blinding on 30‐day outcomes would likely be minimal. Furthermore, a floor staff perception that a specific patient was being taken care of by the study team resulting in a lower than usual level of care, would tend to bias the result of the intervention toward the null effect.
vThe study cohort did not have enough subjects to perform analyses (ie, modeling or examination of subgroups) beyond basic comparative findings. Issues such as preadmission living situation and the presence of depression or cognitive impairment (Mini‐Mental Status Exams were not performed on these patients) may potentially influence postdischarge recidivism; their effects can not be reliably ascertained from these data. Additionally, to prevent study personnel from engaging patients who would soon be going home, it was felt that the benefits from the care bundle would be recognized only if the intervention could be initiated within 72 hours of admission and delivered in full, a requirement that further reduced the enrollment pool. The intent of this pilot work was to guide future investigations surrounding hospital‐to‐home transitional care. The next phase of research in this area will need an enhanced sample size with more extensive baseline data collection so that potential confounding factors or outcomes in specific populations can be explored.
Another problem restricting applicability of study findings was the use of only 3 different CCs and 3 pharmacists on the research team to deliver the components of patient education, discharge planning, and medication counseling in the elderly care bundle. Personnel for the trial were chosen for their experience and interest in the area of care transitions. To distinguish the benefit of the elderly care bundle in general versus the expertise of these particular CCs and study pharmacists, a larger‐scale, multisite trial would be necessary. Lastly, due to resource constraints, patients who resided in long‐term care (either LTAC, SNFs, or nursing homes) prior to admission with anticipated return to those sites were not eligible for the study. Similar to the patients whose comorbidities or acute severity of illness prevented informed consent, this segment of the elderly population may have derived even more benefit from receipt of the elderly care bundle.10, 15, 46 Despite exclusion of this group (which would be expected to lessen the impact of the intervention), a difference in readmission/ED visits rates at 30 days following discharge was observed.
Conclusions
This pilot randomized clinical trial (RCT) evaluated the effects of a supplemental, aggregate care bundle centered on patient education, discharge planning, and medication counseling and reconciliation compared to usual care in a group of elderly patients at high risk of readmission or ED visitation following an index hospitalization. The intervention was designed to be reproducible and make use of existing hospital resources. Probably through facilitation of patient self‐care and home management, the elderly care bundle reduced the composite outcome of readmission/ED visits at 30 days postdischarge. By 60 days, this effect had waned, demonstrating the short‐term benefit of a hospital‐based educational intervention and stressing the need to incorporate additional outpatient transitional care support to sustain favorable outcomes. The study was not powered to detect small differences (which would be more likely than a change of multiple days) in length of index hospital stay related to the care bundle. There were important study limitations (primarily associated with small sample size), and this work should be viewed as hypothesis‐generating. Future trials should assess the impact of a standardized targeted care bundle delivered across multiple healthcare systems on a larger cohort of high‐risk elderly patients, including analysis of financial and personnel allocations relative to the benefits of the intervention.
Acknowledgements
The authors thank study pharmacists Kristen Hesch (PharmD), Renee Danysh (PharmD), Rema Thyagarajan (PharmD), and Betina Thomas (PharmD) for providing patients with medication education and conducting medication reconciliation. They also thank Jeanne Bradbury (RN, ACM), Diana Davis (RN, BSN), and Gail McVea (RN, MSN) for their involvement as care coordinators; Veronica Odom (RN) for her contributions as a research nurse; and Marilyn Callies (RN, MBA) for her role as project advisor.
- ,.Older adults in the emergency department: a systematic review of patterns of use, adverse outcomes, and effectiveness of interventions.Ann Emerg Med.2002;39(3):238–247.
- ,,,,,.Emergency department utilization by the elderly: analysis of the National Hospital Ambulatory Medical Care Survey.Acad Emerg Med.1996;3(7):694–699.
- ,.2005 National Hospital Discharge Survey.Adv Data.2007(385):1–19.
- ,,,,.Short‐term outcomes of elderly patients discharged from an emergency department.J Am Geriatr Soc.1989;37(10):937–943.
- ,,,,.The discharge of elderly patients from an accident and emergency department: functional changes and risk of readmission.Age Ageing.1990;19(6):415–418.
- ,,,,,.Factors associated with unplanned hospital readmission among patients 65 years of age and older in a Medicare managed care plan.Am J Med.1999;107(1):13–17.
- ,,,.Posthospital medication discrepancies: prevalence and contributing factors.Arch Intern Med.2005;165(16):1842–1847.
- ,.From the emergency department to home.J Clin Nurs.2005;14(6):776–785.
- ,,.Adverse drug events in elderly patients receiving home health services following hospital discharge.Ann Pharmacother.1999;33(11):1147–1153.
- ,,, et al.A randomized trial of the efficacy of multidisciplinary care in heart failure outpatients at high risk of hospital readmission.J Am Coll Cardiol.2002;39(3):471–480.
- ,,,.A systematic review of randomized trials of disease management programs in heart failure.Am J Med.2001;110(5):378–384.
- ,,,,,.Comprehensive discharge planning with postdischarge support for older patients with congestive heart failure: a meta‐analysis.JAMA.2004;291(11):1358–1367.
- ,,,.Case management may reduce length of hospital stay in patients with recurrent admissions for chronic obstructive pulmonary disease.Respirology.2001;6(1):37–42.
- ,,,,,.A chronic disease management programme can reduce days in hospital for patients with chronic obstructive pulmonary disease.Intern Med J.2004;34(11):608–614.
- ,,.Disease management programmes for older people with heart failure: crucial characteristics which improve post‐discharge outcomes.Eur Heart J.2006;27(5):596–612.
- ,,,.The care transitions intervention: results of a randomized controlled trial.Arch Intern Med.2006;166(17):1822–1828.
- ,,, et al.Effects of a multidisciplinary, post‐discharge continuance of care intervention on quality of life, discharge satisfaction, and hospital length of stay: a randomized controlled trial.Int J Qual Health Care.2005;17(1):43–51.
- ,,,.Discharge planning from hospital to home.Cochrane Database Syst Rev.2004(1):CD000313.
- ,.A systematic review of interventions to improve outcomes for elders discharged from the emergency department.Acad Emerg Med.2005;12(10):978–986.
- .Transitional care for older adults: a cost‐effective model.LDI Issue Brief.2004;9(6):1–4.
- ,,, et al.Comprehensive discharge planning and home follow‐up of hospitalized elders: a randomized clinical trial.JAMA.1999;281(7):613–620.
- ,,,,,.A multidisciplinary intervention to prevent the readmission of elderly patients with congestive heart failure.N Engl J Med.1995;333(18):1190–1195.
- ,.Home‐based intervention in congestive heart failure: long‐term implications on readmission and survival.Circulation.2002;105(24):2861–2866.
- ,,, et al.Effectiveness of team‐managed home‐based primary care: a randomized multicenter trial.JAMA.2000;284(22):2877–2885.
- ,,,.Home‐based medication review in older people: is it cost effective?Pharmacoeconomics.2007;25(2):171–180.
- ,,,,.The value of inpatient pharmaceutical counselling to elderly patients prior to discharge.Br J Clin Pharmacol.2002;54(6):657–664.
- ,,,,.Does the addition of a pharmacist transition coordinator improve evidence‐based medication management and health outcomes in older adults moving from the hospital to a long‐term care facility? Results of a randomized, controlled trial.Am J Geriatr Pharmacother.2004;2(4):257–264.
- ,,, et al.Role of pharmacist counseling in preventing adverse drug events after hospitalization.Arch Intern Med.2006;166(5):565–571.
- ,,,,,.An investigation of hospital generated pharmaceutical care when patients are discharged home from hospital.Br J Clin Pharmacol.1997;44(2):163–165.
- ,,.The community assessment risk screen (CARS): identifying elderly persons at risk for hospitalization or emergency department visit.Am J Manag Care.2000;6(8):925–933.
- ,,.“Risk” factors affecting readmission of the elderly into the health care system.Med Care.1986;24(5):429–437.
- ,,.Re‐admission to intensive care: identification of risk factors.Physiother Res Int.2005;10(3):154–163.
- ,,,,,.Preparing patients and caregivers to participate in care delivered across settings: the Care Transitions Intervention.J Am Geriatr Soc.2004;52(11):1817–1825.
- ,,,,.Impact of the rapid diagnosis of influenza on physician decision‐making and patient management in the pediatric emergency department: results of a randomized, prospective, controlled trial.Pediatrics.2003;112(2):363–367.
- ,,,,.A survey on hospitalised community‐acquired pneumonia in Italy.Monaldi Arch Chest Dis.2006;65(2):82–88.
- ,,,,.Determinants of the length of stay in intensive care and in hospital after coronary artery surgery.Br Heart J.1995;73(1):92–98.
- ,,.Variation in duration of hospital stay between hospitals and between doctors within hospitals.Soc Sci Med.1993;37(6):833–839.
- ,,, et al.The impact of standardized order sets and intensive clinical case management on outcomes in community‐acquired pneumonia.Arch Intern Med.2007;167(15):1664–1669.
- ,,.Compliance with medication orders among the elderly after hospital discharge.Hosp Formul.1992;27(7):720–724.
- ,,,.Clinical pharmacists and inpatient medical care: a systematic review.Arch Intern Med.2006;166(9):955–964.
- .Quality improvement and ethical oversight.Ann Intern Med.2007;146(9):680–681.
- ,,, et al.The ethics of using quality improvement methods in health care.Ann Intern Med.2007;146(9):666–673.
- ,,.Enrollment of elderly patients in clinical trials for cancer drug registration: a 7‐year experience by the US Food and Drug Administration.J Clin Oncol.2004;22(22):4626–4631.
- ,,,.Striving to recruit: the difficulties of conducting clinical research on elderly care home residents.J R Soc Med.2007;100(6):258–261.
- ,.Quality‐improvement research and informed consent.N Engl J Med.2008;358(8):765–767.
- ,,,.An evaluation of the impact of the ventilator care bundle.Nurs Crit Care.2005;10(5):242–246.
Elderly patients (aged 65 years and older) consume a disproportionate amount of acute health care resources, composing up to 20% of emergency department (ED) visits,1, 2 having a 2‐fold to 5‐fold increase in likelihood of hospital admission,1 and frequently incurring lengths of hospital stay (LOS) approximately 15% higher than the national averages.3 In addition, they are at increased risk for hospital readmission in the 90‐day interval following hospital discharge.1, 4, 5 Specific risk factors for readmission include age above 80 years, discharge within the previous 30 days, the presence of 3 or more comorbid diagnoses, use of 5 or more prescription medications, difficulty with at least 1 activity of daily living (ADL), and lack of discharge education.6 These risk factors can translate into adverse drug events,79 exacerbations of chronic diseases,10 or functional decline4, 5 that can trigger ED visits or hospital readmission.
Hospital‐based care coordinationdefined as a multidisciplinary interaction between inpatients and providers that focuses on education, communication, and discharge planning with the primary aim of improving outcomeshas demonstrated inconsistent results as a mechanism to reduce LOS, postdischarge ED visits, or hospital readmission rates. While disease‐specific care coordination programs for congestive heart failure and chronic obstructive pulmonary disease have been effective in reducing rehospitalization rates,1015 the benefits of comprehensive care coordination for elderly general medical inpatients with a broader range of diagnoses are less clear. In a group of 750 elderly patients with 1 of 11 common inpatient diagnoses (such as stroke or hip fracture) likely to ultimately require a high level of home support, Coleman et al.16 found that a structured transitional care program centered on a personal coach decreased rehospitalization rates at 30 and 90 days. Preen et al.17 found improved patient involvement and perceived quality of life with care coordination focused on discharge planning, but no impact on LOS. Likewise, a recent meta‐analysis18 failed to demonstrate statistically significant differences in mortality, LOS, or readmission rates in hospitalized patients who received intensive care coordination versus usual care; however, variation in the components of the care coordination intervention and reported outcomes restricted the ability to pool data in this study.
Care coordination programs demonstrating efficacy in reducing health care utilization in elderly medical patients have generally included an outpatient transitional component with out‐of‐hospital postacute care visits by health care personnel such as a nurse, pharmacist, or physician.1923 These offsite interventions generate additional expenses and resource demands that may not be practical for smaller hospitals to implement.24, 25 In contrast, hospital‐based care coordination programs have clear ownership and thus may be more practical to disseminate. Individual elements of hospital‐based care coordination such as pharmacist counseling, discharge education, and telephone follow‐up have been shown to reduce ED visitation and readmission rates in high‐risk elderly patients. Less information is available regarding the impact of these interventions delivered in an aggregate bundle by hospital staff in the absence of bridging transitional visits.2629
The objective of this pilot study was to determine whether a supplemental elderly care bundle, targeted to high‐risk inpatients by hospital staff as an enhancement to existing care coordination, would affect postdischarge readmission and ED visit rates. The intervention was designed to capitalize on existing resources, and focused specifically on elderly inpatients who were hospitalized with diagnoses commonly encountered in a general medical unit and predisposed to recidivism.
Patients and Methods
Patient Selection and Enrollment
The screening population consisted of elderly patients admitted to 1 of 2 hospital‐medicine groups (MedProvider Inpatient Care Unit or Texas Primary Care) at the 900‐bed Baylor University Medical Center (BUMC, Dallas, TX) between March and June 2007 with a diagnosis likely to fall within 1 of 20 frequent Medicare medical diagnosis reimbursement groups (DRGs) at BUMC, as listed in Table 1. Study personnel performed daily chart review to establish eligibility criteria, which included age 70 years, use of 5 medications regularly, 3 chronic comorbid conditions, requirement for assistance with 1 ADL, and preadmission residence at home or assisted living with a reasonable expectation of disposition back to that domicile. These criteria were based on factors found in the literature to be associated with extended LOS and postdischarge readmission/ED visit events.5, 6, 3032 Potential enrollees needed to be conversant in English (a multilingual staff was not feasible due to limited resources for this pilot project) and have reliable phone contact, or have a proxy caregiver who could speak English and be reached by phone. Predefined exclusion criteria were admission primarily for a surgical procedure, terminal diagnosis with life expectancy 6 months, residence in a long‐term care facility (long‐term acute care [LTAC], skilled nursing facility [SNF], or nursing home) prior to hospitalization with anticipated discharge back to that facility, and patient/family refusal to participate. Additionally, with an average LOS between 5 and 6 days in BUMC's Medicare population for the DRGs of interest, it was felt that the effects of the care bundle intervention would be obscured unless initiated early in the hospitalization. Thus, patients who could not be enrolled within 72 hours following admission were subsequently excluded. The Baylor Health Care System (BHCS) Institutional Review Board (IRB) approved this study, and written informed consent was obtained from all patients or their surrogates.
| DRG | DRG Name |
|---|---|
| |
| 127 | Heart failure and shock |
| 14 | Intracranial hemorrhage or cerebral infarction |
| 89 | Simple pneumonia/pleurisy |
| 416 | Septicemia |
| 316 | Renal failure |
| 182 | Esophagitis/gastroenterological/miscellaneous digestive disorders with complications |
| 174 | Gastrointestinal hemorrhage with complications |
| 88 | Chronic obstructive pulmonary disease |
| 320 | Kidney/urinary tract infection with complications |
| 144 | Other circulatory diagnoses with complications |
| 138 | Arrhythmia/conduction disorders with complications |
| 277 | Cellulitis with complications |
| 124 | Circulatory disorders except acute myocardial infarction with cardiac catheterization and complex diagnosis |
| 430 | Psychoses |
| 188 | Other digestive diagnoses with complications |
| 395 | Red blood cell disorders |
| 79 | Respiratory infections and inflammations with complications |
| 524 | Transient ischemia |
| 143 | Chest pain |
| 141 | Syncope and collapse with complications |
Patients meeting eligibility criteria were approached within 72 hours of admission for study participation. After consent and enrollment, patients were randomized to intervention or usual care arms in permuted blocks of 8 via a random number generator and sealed opaque envelopes. Nursing and care coordination staff providing usual care to patients (independent of the research team) were blinded to the treatment group status of enrollees; trial design precluded blinding of study personnel and patients.
Delivery of the Supplemental Care Bundle
Starting no later than 24 hours after enrollment and continuing up to 1 week following hospital discharge, intervention group patients received a targeted care bundle provided by 1 of 3 care coordinators (CCs) and 1 of 4 clinical pharmacists (CPs) working with the study team. The care bundle was designed as an intensive patient‐centered educational program that would augment BUMC's existing care coordination processes (delivered to all patients regardless of study participation); specific elements are displayed in Figure 1. Study CCs saw patients daily throughout their hospital stay, and instructed patients on specific health conditions, with an emphasis on optimizing home self‐care and contingency plans if problems arose. CP visits focused on medication reconciliation and education regarding any new agents started during the hospitalization. The personal health record (PHR) provided a tool to engage patients in self‐care, and as discussed by Coleman et al.,7, 16, 33 promoted information transfer from the hospital to outpatient settings. During the postdischarge phone call, CCs followed a basic script to confirm receipt of medical equipment, medications, home health arrangements, and scheduling of follow‐up appointments. They also used this contact as an opportunity to reinforce patient education on managing their conditions. CPs reviewed medication use (type, schedule, dose), and spoke with patients about any symptoms they may have experienced as medication side effects. If indicated based on their phone discussions, both CCs and CPs could recommend an action plan to the patient.

The study CCs and CPs were existing hospital staff and performed their research activities in addition to their usual duties. Study CCs were highly experienced (averaging 8 years of inpatient floor nursing plus 10 years as CCs) and all had advanced nursing certifications (ACM, BSN, or MSN). The CPs were upper‐level pharmacy residents completing their inpatient clinical rotations. Additional training for both study CCs and CPs was limited to a series of 3 meetings (each 45 minutes in duration) regarding the intent and delivery of the supplemental care bundle, including use of study forms.
At the time of the trial, the particular CCs and CPs chosen to deliver the supplemental care bundle had work assignments ensuring that crossover between intervention and usual care groups would not occur. For example, 1 of the study CCs normally covered a surgical floor such that her normal scope of responsibilities would not influence the medical patients in the study (their baseline care coordination was provided by nonstudy personnel). Medication reconciliation and medication education is generally performed by floor nursing staff rather than CPs at BUMC.
Data Collection and Outcomes Measurement
Following enrollment, demographic information and a basic medical history were documented by research staff. Inaccuracies in medication lists discovered by pharmacists during the medication reconciliation process were entered directly into the universal medication list on the hospital chart. CPs also kept a log of the medication education given to patients (and recommendations for changes to patients' regimens given to physicians) throughout their hospital stay. Study CCs recorded their assessments of patient needs and associated responses. Furthermore, the research team CC prepared an enhanced discharge form that was given to intervention patients in addition to BUMC's standard form. Data on LOS, illness severity (APR‐DRGs), and unplanned hospital readmission or ED visitation at 30 and 60 days postdischarge were collected via BUMC's electronic reporting systems. All patient follow‐up was completed as of September 1, 2007.
Statistical Analyses
Resource and time constraints necessitated a sample size that would allow implementation of the intervention despite a limited number of study CCs and pharmacists. To accommodate these conditions while still generating pilot data, an a priori decision was made to enroll up to 80 patients. Continuous data variables were normally distributed. Differences between groups for continuous variables were assessed with the Student t‐test; differences in proportions between groups were compared with Fisher's exact tests. Time to readmission events between the groups were evaluated in a post hoc manner using the log‐rank test. Data were analyzed using Prism version 5 for Windows (GraphPad Software, Inc., San Diego, CA) and SPSS version 15 for Windows (SPSS Inc., Chicago, IL). P values < 0.05 were considered statistically significant.
Results
The final sample size for this pilot was small, with 41 total patients (21 controls, 20 interventions). The main reason for enrollment failure of patients meeting study criteria was an inability to obtain informed consent. Sixty patients declined participation after being approached, and another 56 patients were unable to give their informed consent due to impairments (poor cognition, medication induced sedation, severity of illness) with lack of an available proxy to give written consent during the 72‐hour postadmission recruitment window. There were no statistically significant differences in the baseline characteristics of the intervention and control groups (Table 2). A similar proportion of patients (23% in the intervention, 15% in controls; P = 0.70) had preexisting diagnoses of dementia or depression. However, on APR‐DRG measures relating to acuity of illness and mortality risk, patients in the intervention group trended toward higher severity (Table 2). Likewise, although it was not a statistically significant difference, 13 of 20 patients in the intervention group were taking medications from 2 drug classes commonly implicated in adverse drug events (warfarin, insulin, diuretics, sedating agents) as part of their discharge medication regimen compared to 10 of 21 patients in the control group.
| Control (n = 21) | Intervention (n = 20) | P Value | |
|---|---|---|---|
| Age in years (mean SD) | 79.8 5.6 | 77.2 5.3 | 0.14 |
| Males, n (%) | 8 (38) | 3 (15) | 0.10 |
| Females, n (%) | 13 (62) | 17 (85) | 0.10 |
| Race, n (%) | |||
| African‐American | 3 (14) | 5 (25) | 0.45 |
| Asian | 0 (0) | 1 (5) | 0.49 |
| Caucasian | 17 (81) | 14 (70) | 0.48 |
| Hispanic | 1 (5) | 0 | 1.0 |
| Preadmission living status, n (%) | |||
| Alone | 6 (29) | 4 (20) | 0.72 |
| With spouse or other family | 11 (52) | 15 (75) | 0.20 |
| Assisted living | 4 (19) | 1 (5) | 0.34 |
| Inpatient medications (mean SD) | 11 3 | 12 5 | 0.18 |
| Charlson score (mean, SD) | 3.2 1.3 | 3.7 1.1 | 0.21 |
| % with APR DRG severity rating 3 | 57.5 | 83.3 | 0.12 |
| % with APR DRG mortality rating 3 | 20.0 | 55.6 | 0.07 |
| Primary admission diagnoses (n cases, in order of frequency) | 3 pneumonia | 3 pneumonia | |
| 3 CHF | 3 syncope | ||
| 2 syncope | 2 CHF | ||
| 2 COPD | 2 COPD | ||
| 2 cellulitis | 2 cellulitis | ||
| 2 GI disorder (nonbleed) | 2 GI disorder (nonbleed) | ||
| 2 GI bleed | 1 GI bleed | ||
| 2 UTI | 1 atrial fibrillation | ||
| 1 atrial fibrillation | 1 encephalopathy | ||
| 1 stroke | 1 TIA | ||
| 1 renal failure | 1 renal failure | ||
| 1 volume depletion |
Study outcomes are displayed in Table 3. Mean LOS is reported as a descriptive finding; there was insufficient power to compare this outcome statistically between groups. The majority of patients were discharged to home. A similar proportion of patients in the intervention (20%) and control groups (22%) who had lived at home immediately prior to admission were discharged from the hospital to skilled care facilities (P = 0.87). The number of readmissions/ED visits (taken as a composite measure of unplanned healthcare utilization) within 30 days of discharge was lower in the intervention group; by 60 days, there was no longer a statistically significant difference in readmission/ED visit rates between groups. For those patients who had a readmission or ED visit following hospital discharge, the intervention group had a longer time interval to first event compared to controls (36.2 versus 15.7 days, P = 0.05). Of the patients discharged to skilled care, 1 in the intervention group (at 53 days) and 1 in the control group (at 16 days) had a readmission/ED visit event. Figure 2 shows time‐to‐first readmission or ED visit event curves at 30 and 60 days for both intervention and control groups. For patients who had a readmission/ED visit event, LOS for this episode was 2.2 2.1 days in controls and 3.7 2.1 days in the intervention group (insufficient power for statistical comparison). The study's small sample size prevented development of a meaningful regression model.

| Outcome Measure | Control (n = 21) | Intervention (n = 20) | P Value |
|---|---|---|---|
| |||
| Length of stay for index hospitalization (days)* | 4.7 3.7 | 6.2 4.1 | |
| 0‐30 day postdischarge readmissions/ED visits | 8 (38%) | 2 (10%) | 0.03 |
| 31‐60 day postdischarge readmissions/ED visits | 1 (5%) | 4 (20%) | 0.18 |
| Total postdischarge readmissions/ED visits at 60 days | 9 | 6 | 0.52 |
Resource utilization and the specifics of patient‐study personnel interaction associated with the intervention were tracked. Research assistants spent an average of 50 minutes daily screening charts for potential candidates. For the 20 patients who received the supplemental elderly care bundle, study CCs averaged 20 to 25 minutes per patient daily of additional time counseling patients and families, identifying and attending to discharge barriers, filling out documentation, and faxing the supplemental study discharge form to the patient's primary care physician. Any residual home care needs or issues unresolved at discharge were addressed with the patient in the 5 to 7 day follow‐up phone call. Similarly, study CPs expended approximately 20 minutes daily per patient providing medication education, reconciliation, and optimization of drug therapy. Study pharmacists recommended a change to the medication regimens of 10 patients in the intervention group; physicians acted upon these recommendations for 7 of the patients. The changes included dosage adjustment, discontinuation of medications due to possible drug interaction or duplication of drugs with the same pharmacologic effect, and addition of medications as indicated by patient condition or to reconcile with patients' at‐home medication regimens. Patients contacted via phone by the study pharmacist within 1 week after discharge were able to describe proper use of new medications started in the hospital and confirm that they obtained or had the means to obtain the prescribed drugs.
Discussion
This pilot study examined the effects of a supplemental care bundle involving patient education and discharge planning delivered by hospital‐based CCs and CPs on the rate of readmission/ED visitation in 41 elderly (70 years of age) patients. The study was not adequately powered to detect an impact of the intervention on index LOS. The care bundle did lead to significantly fewer readmissions or ED visits 30 days postdischarge and appeared to increase the time interval to first unplanned readmission or ED visit compared to usual care. This effect was no longer present at 60 days postdischarge. Resource allocations and scope of duties for CCs and CPs (an average of 20 minutes per patient per day) related to delivering the intervention were realistic for broader implementation in the hospitalized elderly population at high risk for readmission or ED visitation following discharge.
Length of stay for the initial hospitalization associated with the care bundle was an original outcome of interest to the study team. However, with the final enrollment of 41 patients and a power of 0.8, the between group difference would have needed to be 2.6 days to be statistically significant. It is likely that any change in LOS related to the care bundle would be much smaller, particularly since 2 key determinants of LOS, severity of illness and physician behavior, were beyond this patient education‐oriented intervention's scope of influence.3437 Furthermore, the diverse range of eligible diagnoses limited the study CCs' ability to reduce variability through use of clinical care pathways. One approach in leveraging an elderly care bundle to reduce LOS may be to focus on a specific disease that has well‐established inpatient benchmarks and treatment algorithms. For example, in patients with community‐acquired pneumonia, the use of care coordination in combination with standardized order sets decreased LOS without compromising safety, mainly by shortening the time from clinical stability to discharge.38
On separation of the readmission/ED visit outcome into 30 and 60 day postdischarge time frames, the intervention group had a lower rate of unplanned acute health care use within 30 days postdischarge; the difference between groups had dissipated by 60 days postdischarge. This convergence suggests that a hospital‐based intervention's influence is strongest closer to the time of the initial hospital stay, and wanes as more time has elapsed. Indeed, interventions that have successfully maintained lower readmission rates beyond 60 and 90 days postdischarge in a high‐risk elderly population (such as the program advocated by Coleman et al.16) have included a transitional care provider engaging patients during the hospitalization and performing subsequent visits to the home or nursing facility.33 An optimal intervention would capitalize on the hospital‐based staff's ability to improve short‐term readmission/ED visit rates while linking patients to longer‐term transitional care to extend these outcomes. Electronic health records could potentially facilitate these care transitions, beginning with an automated screening process for identification of high‐risk inpatients and continuing through postdischarge follow‐up. How to develop these resources in settings where outpatient practices are independent or only loosely affiliated with hospitals is an area for continued investigation.
In a group of elderly patients with multiple comorbidities and complex pharmacotherapy regimens, the study bundle component targeting medication management appears to be a high‐yield intervention to reduce unplanned health care utilization following hospital discharge. These patients are more susceptible to nonadherence and drug‐related adverse events, which may contribute to hospital readmission or ED visitation.7, 9, 39 Consistent with findings at other sites,28, 40 a heightened level of CP involvement in the care of high‐risk elderly patients may have helped reduce these undesirable outcomes. Of the 9 readmission/ED visit events in the control group, 3 were attributable to medication related complications (2 from sedatives, 1 from a diuretic). None of the readmission/ED visit events in intervention group patients stemmed from medication effects.
Correspondingly, the research CCs' provision of daily condition‐specific education, additional time to more thoroughly investigate discharge needs, engagement of patients' families as active partners in self‐care, and the use of a structured discharge form along with follow‐up phone calls may have better prepared patients to manage their health problems once released from the hospital.26, 28, 29 For example, 1 patient in the control group was readmitted less than 24 hours after initial discharge due to inability to perform self‐care at home. Given the study power issues described previously, data on LOS for the second hospitalization for patients who had a readmission event are difficult to interpret, but could suggest the occurrence of some shorter, preventable readmissions in the control group. Conversely, the readmission/ED visit events in intervention patients appeared to be associated with a specific medical condition (eg, failure of diabetic cellulitis to respond to appropriate outpatient treatment) rather than problems that would have been corrected with an educational/self‐management program such as this targeted care bundle.
This pilot study had several limitations. The main issue was a small patient sample size that was primarily due to an inability to obtain informed consent. Design of the study as a randomized controlled trial and plans to disseminate study findings beyond BHCS necessitated IRB approval rather than delivery of the supplemental care bundle as a quality improvement (QI) project. Placing QI initiatives under research regulations can lead to project delays, higher costs, and patient frustrations with the process.41, 42 This tension was evident during study screening and enrollment, as many patients who otherwise met criteria and would potentially benefit from the intervention were hesitant to participate in a research study or refused to sign a multipage consent document. The difficulties of enrolling elderly patients in clinical trials have been well‐described.43, 44 Further research involving a minimal‐risk, educational intervention such as this elderly care‐bundle would likely better fit under the category of expedited IRB review with waiver or modification of the informed consent process.45
Incomplete blinding could have potentially affected our results. At the study site, the team members delivering the care bundle were a regular part of the hospital staff (as opposed to external researchers), and it is not unusual for a CC or a pharmacist to enter a patient's room (eg, to confirm a drug allergy history). In view of this, the impact of imperfect blinding on 30‐day outcomes would likely be minimal. Furthermore, a floor staff perception that a specific patient was being taken care of by the study team resulting in a lower than usual level of care, would tend to bias the result of the intervention toward the null effect.
vThe study cohort did not have enough subjects to perform analyses (ie, modeling or examination of subgroups) beyond basic comparative findings. Issues such as preadmission living situation and the presence of depression or cognitive impairment (Mini‐Mental Status Exams were not performed on these patients) may potentially influence postdischarge recidivism; their effects can not be reliably ascertained from these data. Additionally, to prevent study personnel from engaging patients who would soon be going home, it was felt that the benefits from the care bundle would be recognized only if the intervention could be initiated within 72 hours of admission and delivered in full, a requirement that further reduced the enrollment pool. The intent of this pilot work was to guide future investigations surrounding hospital‐to‐home transitional care. The next phase of research in this area will need an enhanced sample size with more extensive baseline data collection so that potential confounding factors or outcomes in specific populations can be explored.
Another problem restricting applicability of study findings was the use of only 3 different CCs and 3 pharmacists on the research team to deliver the components of patient education, discharge planning, and medication counseling in the elderly care bundle. Personnel for the trial were chosen for their experience and interest in the area of care transitions. To distinguish the benefit of the elderly care bundle in general versus the expertise of these particular CCs and study pharmacists, a larger‐scale, multisite trial would be necessary. Lastly, due to resource constraints, patients who resided in long‐term care (either LTAC, SNFs, or nursing homes) prior to admission with anticipated return to those sites were not eligible for the study. Similar to the patients whose comorbidities or acute severity of illness prevented informed consent, this segment of the elderly population may have derived even more benefit from receipt of the elderly care bundle.10, 15, 46 Despite exclusion of this group (which would be expected to lessen the impact of the intervention), a difference in readmission/ED visits rates at 30 days following discharge was observed.
Conclusions
This pilot randomized clinical trial (RCT) evaluated the effects of a supplemental, aggregate care bundle centered on patient education, discharge planning, and medication counseling and reconciliation compared to usual care in a group of elderly patients at high risk of readmission or ED visitation following an index hospitalization. The intervention was designed to be reproducible and make use of existing hospital resources. Probably through facilitation of patient self‐care and home management, the elderly care bundle reduced the composite outcome of readmission/ED visits at 30 days postdischarge. By 60 days, this effect had waned, demonstrating the short‐term benefit of a hospital‐based educational intervention and stressing the need to incorporate additional outpatient transitional care support to sustain favorable outcomes. The study was not powered to detect small differences (which would be more likely than a change of multiple days) in length of index hospital stay related to the care bundle. There were important study limitations (primarily associated with small sample size), and this work should be viewed as hypothesis‐generating. Future trials should assess the impact of a standardized targeted care bundle delivered across multiple healthcare systems on a larger cohort of high‐risk elderly patients, including analysis of financial and personnel allocations relative to the benefits of the intervention.
Acknowledgements
The authors thank study pharmacists Kristen Hesch (PharmD), Renee Danysh (PharmD), Rema Thyagarajan (PharmD), and Betina Thomas (PharmD) for providing patients with medication education and conducting medication reconciliation. They also thank Jeanne Bradbury (RN, ACM), Diana Davis (RN, BSN), and Gail McVea (RN, MSN) for their involvement as care coordinators; Veronica Odom (RN) for her contributions as a research nurse; and Marilyn Callies (RN, MBA) for her role as project advisor.
Elderly patients (aged 65 years and older) consume a disproportionate amount of acute health care resources, composing up to 20% of emergency department (ED) visits,1, 2 having a 2‐fold to 5‐fold increase in likelihood of hospital admission,1 and frequently incurring lengths of hospital stay (LOS) approximately 15% higher than the national averages.3 In addition, they are at increased risk for hospital readmission in the 90‐day interval following hospital discharge.1, 4, 5 Specific risk factors for readmission include age above 80 years, discharge within the previous 30 days, the presence of 3 or more comorbid diagnoses, use of 5 or more prescription medications, difficulty with at least 1 activity of daily living (ADL), and lack of discharge education.6 These risk factors can translate into adverse drug events,79 exacerbations of chronic diseases,10 or functional decline4, 5 that can trigger ED visits or hospital readmission.
Hospital‐based care coordinationdefined as a multidisciplinary interaction between inpatients and providers that focuses on education, communication, and discharge planning with the primary aim of improving outcomeshas demonstrated inconsistent results as a mechanism to reduce LOS, postdischarge ED visits, or hospital readmission rates. While disease‐specific care coordination programs for congestive heart failure and chronic obstructive pulmonary disease have been effective in reducing rehospitalization rates,1015 the benefits of comprehensive care coordination for elderly general medical inpatients with a broader range of diagnoses are less clear. In a group of 750 elderly patients with 1 of 11 common inpatient diagnoses (such as stroke or hip fracture) likely to ultimately require a high level of home support, Coleman et al.16 found that a structured transitional care program centered on a personal coach decreased rehospitalization rates at 30 and 90 days. Preen et al.17 found improved patient involvement and perceived quality of life with care coordination focused on discharge planning, but no impact on LOS. Likewise, a recent meta‐analysis18 failed to demonstrate statistically significant differences in mortality, LOS, or readmission rates in hospitalized patients who received intensive care coordination versus usual care; however, variation in the components of the care coordination intervention and reported outcomes restricted the ability to pool data in this study.
Care coordination programs demonstrating efficacy in reducing health care utilization in elderly medical patients have generally included an outpatient transitional component with out‐of‐hospital postacute care visits by health care personnel such as a nurse, pharmacist, or physician.1923 These offsite interventions generate additional expenses and resource demands that may not be practical for smaller hospitals to implement.24, 25 In contrast, hospital‐based care coordination programs have clear ownership and thus may be more practical to disseminate. Individual elements of hospital‐based care coordination such as pharmacist counseling, discharge education, and telephone follow‐up have been shown to reduce ED visitation and readmission rates in high‐risk elderly patients. Less information is available regarding the impact of these interventions delivered in an aggregate bundle by hospital staff in the absence of bridging transitional visits.2629
The objective of this pilot study was to determine whether a supplemental elderly care bundle, targeted to high‐risk inpatients by hospital staff as an enhancement to existing care coordination, would affect postdischarge readmission and ED visit rates. The intervention was designed to capitalize on existing resources, and focused specifically on elderly inpatients who were hospitalized with diagnoses commonly encountered in a general medical unit and predisposed to recidivism.
Patients and Methods
Patient Selection and Enrollment
The screening population consisted of elderly patients admitted to 1 of 2 hospital‐medicine groups (MedProvider Inpatient Care Unit or Texas Primary Care) at the 900‐bed Baylor University Medical Center (BUMC, Dallas, TX) between March and June 2007 with a diagnosis likely to fall within 1 of 20 frequent Medicare medical diagnosis reimbursement groups (DRGs) at BUMC, as listed in Table 1. Study personnel performed daily chart review to establish eligibility criteria, which included age 70 years, use of 5 medications regularly, 3 chronic comorbid conditions, requirement for assistance with 1 ADL, and preadmission residence at home or assisted living with a reasonable expectation of disposition back to that domicile. These criteria were based on factors found in the literature to be associated with extended LOS and postdischarge readmission/ED visit events.5, 6, 3032 Potential enrollees needed to be conversant in English (a multilingual staff was not feasible due to limited resources for this pilot project) and have reliable phone contact, or have a proxy caregiver who could speak English and be reached by phone. Predefined exclusion criteria were admission primarily for a surgical procedure, terminal diagnosis with life expectancy 6 months, residence in a long‐term care facility (long‐term acute care [LTAC], skilled nursing facility [SNF], or nursing home) prior to hospitalization with anticipated discharge back to that facility, and patient/family refusal to participate. Additionally, with an average LOS between 5 and 6 days in BUMC's Medicare population for the DRGs of interest, it was felt that the effects of the care bundle intervention would be obscured unless initiated early in the hospitalization. Thus, patients who could not be enrolled within 72 hours following admission were subsequently excluded. The Baylor Health Care System (BHCS) Institutional Review Board (IRB) approved this study, and written informed consent was obtained from all patients or their surrogates.
| DRG | DRG Name |
|---|---|
| |
| 127 | Heart failure and shock |
| 14 | Intracranial hemorrhage or cerebral infarction |
| 89 | Simple pneumonia/pleurisy |
| 416 | Septicemia |
| 316 | Renal failure |
| 182 | Esophagitis/gastroenterological/miscellaneous digestive disorders with complications |
| 174 | Gastrointestinal hemorrhage with complications |
| 88 | Chronic obstructive pulmonary disease |
| 320 | Kidney/urinary tract infection with complications |
| 144 | Other circulatory diagnoses with complications |
| 138 | Arrhythmia/conduction disorders with complications |
| 277 | Cellulitis with complications |
| 124 | Circulatory disorders except acute myocardial infarction with cardiac catheterization and complex diagnosis |
| 430 | Psychoses |
| 188 | Other digestive diagnoses with complications |
| 395 | Red blood cell disorders |
| 79 | Respiratory infections and inflammations with complications |
| 524 | Transient ischemia |
| 143 | Chest pain |
| 141 | Syncope and collapse with complications |
Patients meeting eligibility criteria were approached within 72 hours of admission for study participation. After consent and enrollment, patients were randomized to intervention or usual care arms in permuted blocks of 8 via a random number generator and sealed opaque envelopes. Nursing and care coordination staff providing usual care to patients (independent of the research team) were blinded to the treatment group status of enrollees; trial design precluded blinding of study personnel and patients.
Delivery of the Supplemental Care Bundle
Starting no later than 24 hours after enrollment and continuing up to 1 week following hospital discharge, intervention group patients received a targeted care bundle provided by 1 of 3 care coordinators (CCs) and 1 of 4 clinical pharmacists (CPs) working with the study team. The care bundle was designed as an intensive patient‐centered educational program that would augment BUMC's existing care coordination processes (delivered to all patients regardless of study participation); specific elements are displayed in Figure 1. Study CCs saw patients daily throughout their hospital stay, and instructed patients on specific health conditions, with an emphasis on optimizing home self‐care and contingency plans if problems arose. CP visits focused on medication reconciliation and education regarding any new agents started during the hospitalization. The personal health record (PHR) provided a tool to engage patients in self‐care, and as discussed by Coleman et al.,7, 16, 33 promoted information transfer from the hospital to outpatient settings. During the postdischarge phone call, CCs followed a basic script to confirm receipt of medical equipment, medications, home health arrangements, and scheduling of follow‐up appointments. They also used this contact as an opportunity to reinforce patient education on managing their conditions. CPs reviewed medication use (type, schedule, dose), and spoke with patients about any symptoms they may have experienced as medication side effects. If indicated based on their phone discussions, both CCs and CPs could recommend an action plan to the patient.

The study CCs and CPs were existing hospital staff and performed their research activities in addition to their usual duties. Study CCs were highly experienced (averaging 8 years of inpatient floor nursing plus 10 years as CCs) and all had advanced nursing certifications (ACM, BSN, or MSN). The CPs were upper‐level pharmacy residents completing their inpatient clinical rotations. Additional training for both study CCs and CPs was limited to a series of 3 meetings (each 45 minutes in duration) regarding the intent and delivery of the supplemental care bundle, including use of study forms.
At the time of the trial, the particular CCs and CPs chosen to deliver the supplemental care bundle had work assignments ensuring that crossover between intervention and usual care groups would not occur. For example, 1 of the study CCs normally covered a surgical floor such that her normal scope of responsibilities would not influence the medical patients in the study (their baseline care coordination was provided by nonstudy personnel). Medication reconciliation and medication education is generally performed by floor nursing staff rather than CPs at BUMC.
Data Collection and Outcomes Measurement
Following enrollment, demographic information and a basic medical history were documented by research staff. Inaccuracies in medication lists discovered by pharmacists during the medication reconciliation process were entered directly into the universal medication list on the hospital chart. CPs also kept a log of the medication education given to patients (and recommendations for changes to patients' regimens given to physicians) throughout their hospital stay. Study CCs recorded their assessments of patient needs and associated responses. Furthermore, the research team CC prepared an enhanced discharge form that was given to intervention patients in addition to BUMC's standard form. Data on LOS, illness severity (APR‐DRGs), and unplanned hospital readmission or ED visitation at 30 and 60 days postdischarge were collected via BUMC's electronic reporting systems. All patient follow‐up was completed as of September 1, 2007.
Statistical Analyses
Resource and time constraints necessitated a sample size that would allow implementation of the intervention despite a limited number of study CCs and pharmacists. To accommodate these conditions while still generating pilot data, an a priori decision was made to enroll up to 80 patients. Continuous data variables were normally distributed. Differences between groups for continuous variables were assessed with the Student t‐test; differences in proportions between groups were compared with Fisher's exact tests. Time to readmission events between the groups were evaluated in a post hoc manner using the log‐rank test. Data were analyzed using Prism version 5 for Windows (GraphPad Software, Inc., San Diego, CA) and SPSS version 15 for Windows (SPSS Inc., Chicago, IL). P values < 0.05 were considered statistically significant.
Results
The final sample size for this pilot was small, with 41 total patients (21 controls, 20 interventions). The main reason for enrollment failure of patients meeting study criteria was an inability to obtain informed consent. Sixty patients declined participation after being approached, and another 56 patients were unable to give their informed consent due to impairments (poor cognition, medication induced sedation, severity of illness) with lack of an available proxy to give written consent during the 72‐hour postadmission recruitment window. There were no statistically significant differences in the baseline characteristics of the intervention and control groups (Table 2). A similar proportion of patients (23% in the intervention, 15% in controls; P = 0.70) had preexisting diagnoses of dementia or depression. However, on APR‐DRG measures relating to acuity of illness and mortality risk, patients in the intervention group trended toward higher severity (Table 2). Likewise, although it was not a statistically significant difference, 13 of 20 patients in the intervention group were taking medications from 2 drug classes commonly implicated in adverse drug events (warfarin, insulin, diuretics, sedating agents) as part of their discharge medication regimen compared to 10 of 21 patients in the control group.
| Control (n = 21) | Intervention (n = 20) | P Value | |
|---|---|---|---|
| Age in years (mean SD) | 79.8 5.6 | 77.2 5.3 | 0.14 |
| Males, n (%) | 8 (38) | 3 (15) | 0.10 |
| Females, n (%) | 13 (62) | 17 (85) | 0.10 |
| Race, n (%) | |||
| African‐American | 3 (14) | 5 (25) | 0.45 |
| Asian | 0 (0) | 1 (5) | 0.49 |
| Caucasian | 17 (81) | 14 (70) | 0.48 |
| Hispanic | 1 (5) | 0 | 1.0 |
| Preadmission living status, n (%) | |||
| Alone | 6 (29) | 4 (20) | 0.72 |
| With spouse or other family | 11 (52) | 15 (75) | 0.20 |
| Assisted living | 4 (19) | 1 (5) | 0.34 |
| Inpatient medications (mean SD) | 11 3 | 12 5 | 0.18 |
| Charlson score (mean, SD) | 3.2 1.3 | 3.7 1.1 | 0.21 |
| % with APR DRG severity rating 3 | 57.5 | 83.3 | 0.12 |
| % with APR DRG mortality rating 3 | 20.0 | 55.6 | 0.07 |
| Primary admission diagnoses (n cases, in order of frequency) | 3 pneumonia | 3 pneumonia | |
| 3 CHF | 3 syncope | ||
| 2 syncope | 2 CHF | ||
| 2 COPD | 2 COPD | ||
| 2 cellulitis | 2 cellulitis | ||
| 2 GI disorder (nonbleed) | 2 GI disorder (nonbleed) | ||
| 2 GI bleed | 1 GI bleed | ||
| 2 UTI | 1 atrial fibrillation | ||
| 1 atrial fibrillation | 1 encephalopathy | ||
| 1 stroke | 1 TIA | ||
| 1 renal failure | 1 renal failure | ||
| 1 volume depletion |
Study outcomes are displayed in Table 3. Mean LOS is reported as a descriptive finding; there was insufficient power to compare this outcome statistically between groups. The majority of patients were discharged to home. A similar proportion of patients in the intervention (20%) and control groups (22%) who had lived at home immediately prior to admission were discharged from the hospital to skilled care facilities (P = 0.87). The number of readmissions/ED visits (taken as a composite measure of unplanned healthcare utilization) within 30 days of discharge was lower in the intervention group; by 60 days, there was no longer a statistically significant difference in readmission/ED visit rates between groups. For those patients who had a readmission or ED visit following hospital discharge, the intervention group had a longer time interval to first event compared to controls (36.2 versus 15.7 days, P = 0.05). Of the patients discharged to skilled care, 1 in the intervention group (at 53 days) and 1 in the control group (at 16 days) had a readmission/ED visit event. Figure 2 shows time‐to‐first readmission or ED visit event curves at 30 and 60 days for both intervention and control groups. For patients who had a readmission/ED visit event, LOS for this episode was 2.2 2.1 days in controls and 3.7 2.1 days in the intervention group (insufficient power for statistical comparison). The study's small sample size prevented development of a meaningful regression model.

| Outcome Measure | Control (n = 21) | Intervention (n = 20) | P Value |
|---|---|---|---|
| |||
| Length of stay for index hospitalization (days)* | 4.7 3.7 | 6.2 4.1 | |
| 0‐30 day postdischarge readmissions/ED visits | 8 (38%) | 2 (10%) | 0.03 |
| 31‐60 day postdischarge readmissions/ED visits | 1 (5%) | 4 (20%) | 0.18 |
| Total postdischarge readmissions/ED visits at 60 days | 9 | 6 | 0.52 |
Resource utilization and the specifics of patient‐study personnel interaction associated with the intervention were tracked. Research assistants spent an average of 50 minutes daily screening charts for potential candidates. For the 20 patients who received the supplemental elderly care bundle, study CCs averaged 20 to 25 minutes per patient daily of additional time counseling patients and families, identifying and attending to discharge barriers, filling out documentation, and faxing the supplemental study discharge form to the patient's primary care physician. Any residual home care needs or issues unresolved at discharge were addressed with the patient in the 5 to 7 day follow‐up phone call. Similarly, study CPs expended approximately 20 minutes daily per patient providing medication education, reconciliation, and optimization of drug therapy. Study pharmacists recommended a change to the medication regimens of 10 patients in the intervention group; physicians acted upon these recommendations for 7 of the patients. The changes included dosage adjustment, discontinuation of medications due to possible drug interaction or duplication of drugs with the same pharmacologic effect, and addition of medications as indicated by patient condition or to reconcile with patients' at‐home medication regimens. Patients contacted via phone by the study pharmacist within 1 week after discharge were able to describe proper use of new medications started in the hospital and confirm that they obtained or had the means to obtain the prescribed drugs.
Discussion
This pilot study examined the effects of a supplemental care bundle involving patient education and discharge planning delivered by hospital‐based CCs and CPs on the rate of readmission/ED visitation in 41 elderly (70 years of age) patients. The study was not adequately powered to detect an impact of the intervention on index LOS. The care bundle did lead to significantly fewer readmissions or ED visits 30 days postdischarge and appeared to increase the time interval to first unplanned readmission or ED visit compared to usual care. This effect was no longer present at 60 days postdischarge. Resource allocations and scope of duties for CCs and CPs (an average of 20 minutes per patient per day) related to delivering the intervention were realistic for broader implementation in the hospitalized elderly population at high risk for readmission or ED visitation following discharge.
Length of stay for the initial hospitalization associated with the care bundle was an original outcome of interest to the study team. However, with the final enrollment of 41 patients and a power of 0.8, the between group difference would have needed to be 2.6 days to be statistically significant. It is likely that any change in LOS related to the care bundle would be much smaller, particularly since 2 key determinants of LOS, severity of illness and physician behavior, were beyond this patient education‐oriented intervention's scope of influence.3437 Furthermore, the diverse range of eligible diagnoses limited the study CCs' ability to reduce variability through use of clinical care pathways. One approach in leveraging an elderly care bundle to reduce LOS may be to focus on a specific disease that has well‐established inpatient benchmarks and treatment algorithms. For example, in patients with community‐acquired pneumonia, the use of care coordination in combination with standardized order sets decreased LOS without compromising safety, mainly by shortening the time from clinical stability to discharge.38
On separation of the readmission/ED visit outcome into 30 and 60 day postdischarge time frames, the intervention group had a lower rate of unplanned acute health care use within 30 days postdischarge; the difference between groups had dissipated by 60 days postdischarge. This convergence suggests that a hospital‐based intervention's influence is strongest closer to the time of the initial hospital stay, and wanes as more time has elapsed. Indeed, interventions that have successfully maintained lower readmission rates beyond 60 and 90 days postdischarge in a high‐risk elderly population (such as the program advocated by Coleman et al.16) have included a transitional care provider engaging patients during the hospitalization and performing subsequent visits to the home or nursing facility.33 An optimal intervention would capitalize on the hospital‐based staff's ability to improve short‐term readmission/ED visit rates while linking patients to longer‐term transitional care to extend these outcomes. Electronic health records could potentially facilitate these care transitions, beginning with an automated screening process for identification of high‐risk inpatients and continuing through postdischarge follow‐up. How to develop these resources in settings where outpatient practices are independent or only loosely affiliated with hospitals is an area for continued investigation.
In a group of elderly patients with multiple comorbidities and complex pharmacotherapy regimens, the study bundle component targeting medication management appears to be a high‐yield intervention to reduce unplanned health care utilization following hospital discharge. These patients are more susceptible to nonadherence and drug‐related adverse events, which may contribute to hospital readmission or ED visitation.7, 9, 39 Consistent with findings at other sites,28, 40 a heightened level of CP involvement in the care of high‐risk elderly patients may have helped reduce these undesirable outcomes. Of the 9 readmission/ED visit events in the control group, 3 were attributable to medication related complications (2 from sedatives, 1 from a diuretic). None of the readmission/ED visit events in intervention group patients stemmed from medication effects.
Correspondingly, the research CCs' provision of daily condition‐specific education, additional time to more thoroughly investigate discharge needs, engagement of patients' families as active partners in self‐care, and the use of a structured discharge form along with follow‐up phone calls may have better prepared patients to manage their health problems once released from the hospital.26, 28, 29 For example, 1 patient in the control group was readmitted less than 24 hours after initial discharge due to inability to perform self‐care at home. Given the study power issues described previously, data on LOS for the second hospitalization for patients who had a readmission event are difficult to interpret, but could suggest the occurrence of some shorter, preventable readmissions in the control group. Conversely, the readmission/ED visit events in intervention patients appeared to be associated with a specific medical condition (eg, failure of diabetic cellulitis to respond to appropriate outpatient treatment) rather than problems that would have been corrected with an educational/self‐management program such as this targeted care bundle.
This pilot study had several limitations. The main issue was a small patient sample size that was primarily due to an inability to obtain informed consent. Design of the study as a randomized controlled trial and plans to disseminate study findings beyond BHCS necessitated IRB approval rather than delivery of the supplemental care bundle as a quality improvement (QI) project. Placing QI initiatives under research regulations can lead to project delays, higher costs, and patient frustrations with the process.41, 42 This tension was evident during study screening and enrollment, as many patients who otherwise met criteria and would potentially benefit from the intervention were hesitant to participate in a research study or refused to sign a multipage consent document. The difficulties of enrolling elderly patients in clinical trials have been well‐described.43, 44 Further research involving a minimal‐risk, educational intervention such as this elderly care‐bundle would likely better fit under the category of expedited IRB review with waiver or modification of the informed consent process.45
Incomplete blinding could have potentially affected our results. At the study site, the team members delivering the care bundle were a regular part of the hospital staff (as opposed to external researchers), and it is not unusual for a CC or a pharmacist to enter a patient's room (eg, to confirm a drug allergy history). In view of this, the impact of imperfect blinding on 30‐day outcomes would likely be minimal. Furthermore, a floor staff perception that a specific patient was being taken care of by the study team resulting in a lower than usual level of care, would tend to bias the result of the intervention toward the null effect.
vThe study cohort did not have enough subjects to perform analyses (ie, modeling or examination of subgroups) beyond basic comparative findings. Issues such as preadmission living situation and the presence of depression or cognitive impairment (Mini‐Mental Status Exams were not performed on these patients) may potentially influence postdischarge recidivism; their effects can not be reliably ascertained from these data. Additionally, to prevent study personnel from engaging patients who would soon be going home, it was felt that the benefits from the care bundle would be recognized only if the intervention could be initiated within 72 hours of admission and delivered in full, a requirement that further reduced the enrollment pool. The intent of this pilot work was to guide future investigations surrounding hospital‐to‐home transitional care. The next phase of research in this area will need an enhanced sample size with more extensive baseline data collection so that potential confounding factors or outcomes in specific populations can be explored.
Another problem restricting applicability of study findings was the use of only 3 different CCs and 3 pharmacists on the research team to deliver the components of patient education, discharge planning, and medication counseling in the elderly care bundle. Personnel for the trial were chosen for their experience and interest in the area of care transitions. To distinguish the benefit of the elderly care bundle in general versus the expertise of these particular CCs and study pharmacists, a larger‐scale, multisite trial would be necessary. Lastly, due to resource constraints, patients who resided in long‐term care (either LTAC, SNFs, or nursing homes) prior to admission with anticipated return to those sites were not eligible for the study. Similar to the patients whose comorbidities or acute severity of illness prevented informed consent, this segment of the elderly population may have derived even more benefit from receipt of the elderly care bundle.10, 15, 46 Despite exclusion of this group (which would be expected to lessen the impact of the intervention), a difference in readmission/ED visits rates at 30 days following discharge was observed.
Conclusions
This pilot randomized clinical trial (RCT) evaluated the effects of a supplemental, aggregate care bundle centered on patient education, discharge planning, and medication counseling and reconciliation compared to usual care in a group of elderly patients at high risk of readmission or ED visitation following an index hospitalization. The intervention was designed to be reproducible and make use of existing hospital resources. Probably through facilitation of patient self‐care and home management, the elderly care bundle reduced the composite outcome of readmission/ED visits at 30 days postdischarge. By 60 days, this effect had waned, demonstrating the short‐term benefit of a hospital‐based educational intervention and stressing the need to incorporate additional outpatient transitional care support to sustain favorable outcomes. The study was not powered to detect small differences (which would be more likely than a change of multiple days) in length of index hospital stay related to the care bundle. There were important study limitations (primarily associated with small sample size), and this work should be viewed as hypothesis‐generating. Future trials should assess the impact of a standardized targeted care bundle delivered across multiple healthcare systems on a larger cohort of high‐risk elderly patients, including analysis of financial and personnel allocations relative to the benefits of the intervention.
Acknowledgements
The authors thank study pharmacists Kristen Hesch (PharmD), Renee Danysh (PharmD), Rema Thyagarajan (PharmD), and Betina Thomas (PharmD) for providing patients with medication education and conducting medication reconciliation. They also thank Jeanne Bradbury (RN, ACM), Diana Davis (RN, BSN), and Gail McVea (RN, MSN) for their involvement as care coordinators; Veronica Odom (RN) for her contributions as a research nurse; and Marilyn Callies (RN, MBA) for her role as project advisor.
- ,.Older adults in the emergency department: a systematic review of patterns of use, adverse outcomes, and effectiveness of interventions.Ann Emerg Med.2002;39(3):238–247.
- ,,,,,.Emergency department utilization by the elderly: analysis of the National Hospital Ambulatory Medical Care Survey.Acad Emerg Med.1996;3(7):694–699.
- ,.2005 National Hospital Discharge Survey.Adv Data.2007(385):1–19.
- ,,,,.Short‐term outcomes of elderly patients discharged from an emergency department.J Am Geriatr Soc.1989;37(10):937–943.
- ,,,,.The discharge of elderly patients from an accident and emergency department: functional changes and risk of readmission.Age Ageing.1990;19(6):415–418.
- ,,,,,.Factors associated with unplanned hospital readmission among patients 65 years of age and older in a Medicare managed care plan.Am J Med.1999;107(1):13–17.
- ,,,.Posthospital medication discrepancies: prevalence and contributing factors.Arch Intern Med.2005;165(16):1842–1847.
- ,.From the emergency department to home.J Clin Nurs.2005;14(6):776–785.
- ,,.Adverse drug events in elderly patients receiving home health services following hospital discharge.Ann Pharmacother.1999;33(11):1147–1153.
- ,,, et al.A randomized trial of the efficacy of multidisciplinary care in heart failure outpatients at high risk of hospital readmission.J Am Coll Cardiol.2002;39(3):471–480.
- ,,,.A systematic review of randomized trials of disease management programs in heart failure.Am J Med.2001;110(5):378–384.
- ,,,,,.Comprehensive discharge planning with postdischarge support for older patients with congestive heart failure: a meta‐analysis.JAMA.2004;291(11):1358–1367.
- ,,,.Case management may reduce length of hospital stay in patients with recurrent admissions for chronic obstructive pulmonary disease.Respirology.2001;6(1):37–42.
- ,,,,,.A chronic disease management programme can reduce days in hospital for patients with chronic obstructive pulmonary disease.Intern Med J.2004;34(11):608–614.
- ,,.Disease management programmes for older people with heart failure: crucial characteristics which improve post‐discharge outcomes.Eur Heart J.2006;27(5):596–612.
- ,,,.The care transitions intervention: results of a randomized controlled trial.Arch Intern Med.2006;166(17):1822–1828.
- ,,, et al.Effects of a multidisciplinary, post‐discharge continuance of care intervention on quality of life, discharge satisfaction, and hospital length of stay: a randomized controlled trial.Int J Qual Health Care.2005;17(1):43–51.
- ,,,.Discharge planning from hospital to home.Cochrane Database Syst Rev.2004(1):CD000313.
- ,.A systematic review of interventions to improve outcomes for elders discharged from the emergency department.Acad Emerg Med.2005;12(10):978–986.
- .Transitional care for older adults: a cost‐effective model.LDI Issue Brief.2004;9(6):1–4.
- ,,, et al.Comprehensive discharge planning and home follow‐up of hospitalized elders: a randomized clinical trial.JAMA.1999;281(7):613–620.
- ,,,,,.A multidisciplinary intervention to prevent the readmission of elderly patients with congestive heart failure.N Engl J Med.1995;333(18):1190–1195.
- ,.Home‐based intervention in congestive heart failure: long‐term implications on readmission and survival.Circulation.2002;105(24):2861–2866.
- ,,, et al.Effectiveness of team‐managed home‐based primary care: a randomized multicenter trial.JAMA.2000;284(22):2877–2885.
- ,,,.Home‐based medication review in older people: is it cost effective?Pharmacoeconomics.2007;25(2):171–180.
- ,,,,.The value of inpatient pharmaceutical counselling to elderly patients prior to discharge.Br J Clin Pharmacol.2002;54(6):657–664.
- ,,,,.Does the addition of a pharmacist transition coordinator improve evidence‐based medication management and health outcomes in older adults moving from the hospital to a long‐term care facility? Results of a randomized, controlled trial.Am J Geriatr Pharmacother.2004;2(4):257–264.
- ,,, et al.Role of pharmacist counseling in preventing adverse drug events after hospitalization.Arch Intern Med.2006;166(5):565–571.
- ,,,,,.An investigation of hospital generated pharmaceutical care when patients are discharged home from hospital.Br J Clin Pharmacol.1997;44(2):163–165.
- ,,.The community assessment risk screen (CARS): identifying elderly persons at risk for hospitalization or emergency department visit.Am J Manag Care.2000;6(8):925–933.
- ,,.“Risk” factors affecting readmission of the elderly into the health care system.Med Care.1986;24(5):429–437.
- ,,.Re‐admission to intensive care: identification of risk factors.Physiother Res Int.2005;10(3):154–163.
- ,,,,,.Preparing patients and caregivers to participate in care delivered across settings: the Care Transitions Intervention.J Am Geriatr Soc.2004;52(11):1817–1825.
- ,,,,.Impact of the rapid diagnosis of influenza on physician decision‐making and patient management in the pediatric emergency department: results of a randomized, prospective, controlled trial.Pediatrics.2003;112(2):363–367.
- ,,,,.A survey on hospitalised community‐acquired pneumonia in Italy.Monaldi Arch Chest Dis.2006;65(2):82–88.
- ,,,,.Determinants of the length of stay in intensive care and in hospital after coronary artery surgery.Br Heart J.1995;73(1):92–98.
- ,,.Variation in duration of hospital stay between hospitals and between doctors within hospitals.Soc Sci Med.1993;37(6):833–839.
- ,,, et al.The impact of standardized order sets and intensive clinical case management on outcomes in community‐acquired pneumonia.Arch Intern Med.2007;167(15):1664–1669.
- ,,.Compliance with medication orders among the elderly after hospital discharge.Hosp Formul.1992;27(7):720–724.
- ,,,.Clinical pharmacists and inpatient medical care: a systematic review.Arch Intern Med.2006;166(9):955–964.
- .Quality improvement and ethical oversight.Ann Intern Med.2007;146(9):680–681.
- ,,, et al.The ethics of using quality improvement methods in health care.Ann Intern Med.2007;146(9):666–673.
- ,,.Enrollment of elderly patients in clinical trials for cancer drug registration: a 7‐year experience by the US Food and Drug Administration.J Clin Oncol.2004;22(22):4626–4631.
- ,,,.Striving to recruit: the difficulties of conducting clinical research on elderly care home residents.J R Soc Med.2007;100(6):258–261.
- ,.Quality‐improvement research and informed consent.N Engl J Med.2008;358(8):765–767.
- ,,,.An evaluation of the impact of the ventilator care bundle.Nurs Crit Care.2005;10(5):242–246.
- ,.Older adults in the emergency department: a systematic review of patterns of use, adverse outcomes, and effectiveness of interventions.Ann Emerg Med.2002;39(3):238–247.
- ,,,,,.Emergency department utilization by the elderly: analysis of the National Hospital Ambulatory Medical Care Survey.Acad Emerg Med.1996;3(7):694–699.
- ,.2005 National Hospital Discharge Survey.Adv Data.2007(385):1–19.
- ,,,,.Short‐term outcomes of elderly patients discharged from an emergency department.J Am Geriatr Soc.1989;37(10):937–943.
- ,,,,.The discharge of elderly patients from an accident and emergency department: functional changes and risk of readmission.Age Ageing.1990;19(6):415–418.
- ,,,,,.Factors associated with unplanned hospital readmission among patients 65 years of age and older in a Medicare managed care plan.Am J Med.1999;107(1):13–17.
- ,,,.Posthospital medication discrepancies: prevalence and contributing factors.Arch Intern Med.2005;165(16):1842–1847.
- ,.From the emergency department to home.J Clin Nurs.2005;14(6):776–785.
- ,,.Adverse drug events in elderly patients receiving home health services following hospital discharge.Ann Pharmacother.1999;33(11):1147–1153.
- ,,, et al.A randomized trial of the efficacy of multidisciplinary care in heart failure outpatients at high risk of hospital readmission.J Am Coll Cardiol.2002;39(3):471–480.
- ,,,.A systematic review of randomized trials of disease management programs in heart failure.Am J Med.2001;110(5):378–384.
- ,,,,,.Comprehensive discharge planning with postdischarge support for older patients with congestive heart failure: a meta‐analysis.JAMA.2004;291(11):1358–1367.
- ,,,.Case management may reduce length of hospital stay in patients with recurrent admissions for chronic obstructive pulmonary disease.Respirology.2001;6(1):37–42.
- ,,,,,.A chronic disease management programme can reduce days in hospital for patients with chronic obstructive pulmonary disease.Intern Med J.2004;34(11):608–614.
- ,,.Disease management programmes for older people with heart failure: crucial characteristics which improve post‐discharge outcomes.Eur Heart J.2006;27(5):596–612.
- ,,,.The care transitions intervention: results of a randomized controlled trial.Arch Intern Med.2006;166(17):1822–1828.
- ,,, et al.Effects of a multidisciplinary, post‐discharge continuance of care intervention on quality of life, discharge satisfaction, and hospital length of stay: a randomized controlled trial.Int J Qual Health Care.2005;17(1):43–51.
- ,,,.Discharge planning from hospital to home.Cochrane Database Syst Rev.2004(1):CD000313.
- ,.A systematic review of interventions to improve outcomes for elders discharged from the emergency department.Acad Emerg Med.2005;12(10):978–986.
- .Transitional care for older adults: a cost‐effective model.LDI Issue Brief.2004;9(6):1–4.
- ,,, et al.Comprehensive discharge planning and home follow‐up of hospitalized elders: a randomized clinical trial.JAMA.1999;281(7):613–620.
- ,,,,,.A multidisciplinary intervention to prevent the readmission of elderly patients with congestive heart failure.N Engl J Med.1995;333(18):1190–1195.
- ,.Home‐based intervention in congestive heart failure: long‐term implications on readmission and survival.Circulation.2002;105(24):2861–2866.
- ,,, et al.Effectiveness of team‐managed home‐based primary care: a randomized multicenter trial.JAMA.2000;284(22):2877–2885.
- ,,,.Home‐based medication review in older people: is it cost effective?Pharmacoeconomics.2007;25(2):171–180.
- ,,,,.The value of inpatient pharmaceutical counselling to elderly patients prior to discharge.Br J Clin Pharmacol.2002;54(6):657–664.
- ,,,,.Does the addition of a pharmacist transition coordinator improve evidence‐based medication management and health outcomes in older adults moving from the hospital to a long‐term care facility? Results of a randomized, controlled trial.Am J Geriatr Pharmacother.2004;2(4):257–264.
- ,,, et al.Role of pharmacist counseling in preventing adverse drug events after hospitalization.Arch Intern Med.2006;166(5):565–571.
- ,,,,,.An investigation of hospital generated pharmaceutical care when patients are discharged home from hospital.Br J Clin Pharmacol.1997;44(2):163–165.
- ,,.The community assessment risk screen (CARS): identifying elderly persons at risk for hospitalization or emergency department visit.Am J Manag Care.2000;6(8):925–933.
- ,,.“Risk” factors affecting readmission of the elderly into the health care system.Med Care.1986;24(5):429–437.
- ,,.Re‐admission to intensive care: identification of risk factors.Physiother Res Int.2005;10(3):154–163.
- ,,,,,.Preparing patients and caregivers to participate in care delivered across settings: the Care Transitions Intervention.J Am Geriatr Soc.2004;52(11):1817–1825.
- ,,,,.Impact of the rapid diagnosis of influenza on physician decision‐making and patient management in the pediatric emergency department: results of a randomized, prospective, controlled trial.Pediatrics.2003;112(2):363–367.
- ,,,,.A survey on hospitalised community‐acquired pneumonia in Italy.Monaldi Arch Chest Dis.2006;65(2):82–88.
- ,,,,.Determinants of the length of stay in intensive care and in hospital after coronary artery surgery.Br Heart J.1995;73(1):92–98.
- ,,.Variation in duration of hospital stay between hospitals and between doctors within hospitals.Soc Sci Med.1993;37(6):833–839.
- ,,, et al.The impact of standardized order sets and intensive clinical case management on outcomes in community‐acquired pneumonia.Arch Intern Med.2007;167(15):1664–1669.
- ,,.Compliance with medication orders among the elderly after hospital discharge.Hosp Formul.1992;27(7):720–724.
- ,,,.Clinical pharmacists and inpatient medical care: a systematic review.Arch Intern Med.2006;166(9):955–964.
- .Quality improvement and ethical oversight.Ann Intern Med.2007;146(9):680–681.
- ,,, et al.The ethics of using quality improvement methods in health care.Ann Intern Med.2007;146(9):666–673.
- ,,.Enrollment of elderly patients in clinical trials for cancer drug registration: a 7‐year experience by the US Food and Drug Administration.J Clin Oncol.2004;22(22):4626–4631.
- ,,,.Striving to recruit: the difficulties of conducting clinical research on elderly care home residents.J R Soc Med.2007;100(6):258–261.
- ,.Quality‐improvement research and informed consent.N Engl J Med.2008;358(8):765–767.
- ,,,.An evaluation of the impact of the ventilator care bundle.Nurs Crit Care.2005;10(5):242–246.
Copyright © 2009 Society of Hospital Medicine
Late Discharges from a Medical Ward
In the past 2 decades, emergency department (ED) overcrowding has become an issue large enough to receive coverage in the popular press, and to spawn research around its causes and effects.116 At the same time, nurses and physicians on the inpatient wards have been urged to shorten the length of stay for patients as health system leaders face an aging population but limited capital to build new beds or hire additional clinical staff. Capacity managementencompassing the flow of patients from ED triage to inpatient dischargehas become a shared concern of clinicians and hospital administrators alike.
How to achieve the goals of diagnosing and healing while ushering patients ever more quickly through the modern hospital is not yet entirely clear. Past research and work by business groups suggests that demand for inpatient beds starts early in the day, but discharges typically occur in the late afternoon.17 This creates a potential bottleneck in patient flow. Many hospitals have implemented measures to improve patient throughput.1821 However, formal research has focused on factors leading to an additional inpatient day.2226 We have found no peer‐reviewed publications that address the problem of same‐day delays by describing hour of day for each step in the discharge process and variables associated with late‐day discharges. To fill this gap, we conducted a prospective cohort study of 209 consecutive discharges from a general medical ward to: (1) describe the natural history of hospital discharge, (2) measure time of day and duration for each step, and (3) identify factors associated with discharges that occur later in the day. We hypothesized that time and duration of discharge would be associated with 5 factors: patient demographics and clinical characteristics, departmental occupancy, type of inpatient testing done immediately prior to discharge, and discharge characteristics such as discharge to a location other than home.
Patients and Methods
Setting
The setting was the Hospitalist Unit of a single teaching hospital in Baltimore (The Johns Hopkins Hospital) from January 1, 2005 to April 30, 2005. Patients entered the cohort upon initiation of the discharge process by the hospitalist team on the Hospitalist Unit, and were followed until they were discharged alive from the hospital.
There were no published data on which to base firm a priori sample size calculations. Based on pilot data, we estimated that a sample size of about 170 would yield precise estimates for means and standard deviations, giving us 80% to 90% power to determine differences in time intervals across categories, with alpha set to 0.05. We estimated that we would need 4 months of data collection to achieve this sample size.
During the period of study, the 16‐bed unit was staffed with in‐house hospitalist attending physicians without house‐staff, from 7 AM (weekdays) or 8 AM (weekends) to 10 PM (Monday to Thursday) or 8 PM (Friday to Sunday). The hospitalist unit had 24‐hour physician coverage, but attending physicians provided overnight coverage from home (backed up by in‐house residents for patient care emergencies). Handoffs of patient care from one attending physician to another typically occurred on Friday afternoon or Monday morning. The unit had 1 dedicated social worker and a nurse clinician who provided part‐time assistance with discharge planning.
Outcome Measurements
We defined the start of the discharge process as the time the patient's last medically necessary test was needed by his or her attending physician. Specifically, physicians were asked when the results of this test first would have been useful in clearing the patient for discharge. In the remainder of this work, we will refer to the start of the discharge process as time decisive test needed.
The end of the discharge process was called the discharge time, and defined as the time the unit clerk saw the patient leave the unit. We defined early discharges as those occurring before the median hour of discharge (3:00 PM), and late discharges as those occurring at or after this hour.
A focus group composed of nurses, physicians, social worker, unit clerks, and support associates (group responsible for cleaning patient rooms) volunteered to map out the discharge process. Based on these discussions, durations in the discharge process were defined as follows: (1) duration 1: time decisive test needed, until time the attending physician was aware of test results; (2) duration 2: time the physician was aware of test results until discharge paperwork was complete; (3) duration 3: time discharge paperwork complete until patient leaves unit; and (4) total discharge duration: time decisive test needed until patient leaves unit.
Exposure Measurements
We categorized exposures into 5 groups: (1) demographics (age, gender, race, source of patient such as outside hospital versus emergency department versus other, and payer on discharge); (2) clinical characteristics (length of stay, any psychiatric diagnosis, any substance abuse diagnosis, and severity of illness); (3) system characteristics (departmental occupancy defined as proportion of hospital beds designated for Department of Medicine patients that were occupied on the day of discharge); (4) last test characteristics (physical exam, laboratory test, procedure, and consult); and (5) discharge characteristics (discharged to home versus not discharged to home, prescriptions filled in hospital pharmacy prior to discharge, and ambulance required for transport).
Psychiatric diagnosis was defined as the presence of any of the following International Classification of Diseases, Ninth Revision, Clinical Modification (ICD‐9‐CM) codes: 290319 (any fourth or fifth digits).27 Substance abuse diagnosis was defined as the presence of any of the following ICD‐9‐CM codes: 303305 (any fourth or fifth digits). Substance abuse codes encompassed drug dependence and abuse, including alcohol dependence and abuse.
The all patient refined diagnosis related group relative weight (APRDRGwt) is a unitless number that estimates the total cost of care for inpatients, based on clinical and demographic characteristics.28 A patient with a relative APRDRGwt of 1 is predicted to have the same cost of care as the national average for inpatients. A patient with a score of 2 is predicted to be twice as costly as the average. In this study, we used APRDRGwt as a gross proxy for severity of illness.
Adjusted length of stay was measured as length of stay minus discharge duration. This adjustment was made to avoid including the exposure (length of stay) in the outcome (discharge duration). Unadjusted length of stay was used when the outcome was discharge time.
Data Sources
We created a separate 4‐item to 9‐item paper questionnaire (included in the Appendix) for each of 4 functional groups participating directly in the discharge process: nurses, physicians, social worker, and unit clerks. Questions were based on staff feedback about the sequence of steps in the discharge process, and potential reasons for delay. The surveys were piloted for several weeks to further refine the wording of questions, and to ensure that the length and location of the surveys minimized workflow interruptions. The questionnaires captured information about the timing of routine events not recorded in existing databases.
Physicians were asked to identify the last test/procedure/consult needed prior to the patient being medically ready for discharge. They were asked when the test results first could have cleared the patient for discharge (time decisive test needed), and when they actually received the test results (time test results back). Nursing and social work surveys provided information on whether or not prescriptions were filled prior to discharge, and the type of transportation used on discharge. Unit clerks documented when the patient left the unit.
Response rates were: nurses (97%), physicians (97%), social worker (99%), and unit clerks (94%). All 4 surveys were completed for 88% of the 209 included patients (prior to 8 exclusions for missing data or extreme outlier observations). Group response rates were tallied at the end of each month and posted on the unit. We did not track how soon after discharge the surveys were completed. However, we reviewed survey responses frequently (often daily, at most every 4 days) and if surveys were incomplete we personally approached staff members to complete the survey.
We supplemented and cross‐checked data from the questionnaire with information from existing hospital databases. These databases were: (1) the patient's medical record for time patient arrived on the floor, and completion time for consults/procedures; (2) the Electronic Bedboard (EBB) for time patient left the unit (as recorded by unit clerk); (3) the Patient Order Entry System for time discharge papers were completed by the physician, and ordering time for select tests; (4) the Electronic Patient Record for demographic information and completion time for select tests; and (5) Datamart, the hospital's administrative/billing database, for information such as length of stay, diagnosis, patient demographics, and insurance status.
Cross‐checking of data and calculation of durations 1, 2, and 3 identified areas of disagreement that were addressed in the following way. Discharge time was provided by 3 sources: social worker and nurses as an ad hoc addition to each of their surveys, unit clerks as a mandatory question on their survey, and unit clerks as entered in the EBB. We used EBB data for discharge time, as this was the most complete and accurate single source of data. However, survey results and knowledge about the sequential process for discharge, suggested that in 20 cases EBB data did not provide the most accurate time. In these cases, discharge time was provided by the unit clerk survey (16 cases), the social work survey (3 cases), and the nursing survey (1 case).
In 28 cases (14%), discharge paperwork was completed before decisive test results were back. And in 8 cases (4%) test results were received earlier than needed. As these were a minority of cases, these negative durations were converted to zero for analysis.
Statistical Analysis
The unit of analysis was the unique hospital discharge. For patients who were discharged from the Hospitalist Unit more than once during the 4‐month study period, each discharge was treated as a separate unit of analysis.
We defined patients discharged before the median discharge time as early discharges, and all others as late discharges. We then categorized patients with discharge durations less than 24 hours as short discharges, and all others as long discharges.
We described the characteristics of 2 groups of patients: early and short discharges versus all others. We used the chi square statistic and Fisher's exact test (when frequency 5 in 1 or both groups) to test the null hypothesis that there was no association between the 2 groups and select patient characteristics. When comparing medians, we used the nonparametric equality of medians test.
For each step in the discharge process, we identified a median time of occurrence. For the first point in the processtime decisive test neededwe also used 1‐way analysis of variance and the F‐test to assess whether or not timing varied significantly by physician.
Because our primary goal was to quantify in hours the association between various factors and discharge time or duration, we used bivariate linear regression models to identify factors associated with time of discharge (primary analysis) and total duration of the discharge process (secondary analysis). We then used multivariate linear regression to identify factors associated with both outcomes. We used forward and backward selection methods to choose the final models for the multivariate analyses, after forcing in the variables for race, sex, and age. Both methods of selection produced identical results. We assessed for colinearity using variance inflation factors.29
Sensitivity Analyses
For both discharge time and discharge duration, we performed regression diagnostics including leverage, Studentized residuals, and influence. Excluding outliers for influence slightly altered the results of our multivariate analyses. However, all variables that were significant at the P < 0.05 level remained significant in the models without outliers.
We chose to include outliers for influence in our final data set after verifying the data as accurate. For discharge time, the number of outliers (3; 1.5%) for influence was in the range expected for a normally distributed data set.
We also tested for normality of the 2 outcome variables. Discharge time was normally distributed, but discharge duration was not. Because of this, we used 2 additional methods to assess the robustness of our results for discharge duration.
First, we log‐transformed the outcome and repeated the analysis. Variables significant in the non‐log‐transformed model remained significant after log‐transformation. Second, we applied bootstrapping30 with 1,000 repetitions for the bivariate and multivariate analyses. The 95% confidence intervals (CIs) (using the bias‐corrected confidence intervals) were modestly altered (some narrowed, some widened), but our conclusions remained the same except for a single variable with borderline significance (payer on discharge) in bivariate analysis. The final reported confidence intervals for discharge duration are based on our analysis without bootstrapping.
Results
Data were collected on 216 patients. Seven patients were excluded from the study, because they were discharged against medical advice. Since these patients left before their decisive test was completed, there was no way to assess duration of the discharge process. Of the remaining 209 patients, 6 patients lacked necessary data to complete analysis (5 without survey data; 1 without administrative data). Two additional patients were eliminated from the final analysis because they bypassed the normal discharge process and were extreme outliers in either discharge time (1 discharged at 1 AM), or discharge duration (1 with discharge duration of 400+ hours). A total of 201 patients were included in the final analyses.
The hospitalist program primarily serves an indigent, local adult population with general medical problems, and this is reflected in the patient characteristics (Table 1). We compared the characteristics of patients discharged early and quickly (discharged prior to median hour of 3:00 PM, and discharge process lasting less than 24 hours) to all other discharges, to identify factors associated with later and longer discharges.
| Early and Short Discharges (n = 75)* | All Other Discharges (n = 126) | P Value | |
|---|---|---|---|
| |||
| Demographics | |||
| Age (years) | |||
| Median | 55 | 55 | 0.73 |
| Range | (19, 94) | (20, 90) | |
| Gender (%) | |||
| Female | 61.3 | 61.1 | 0.98 |
| Race (%) | 0.08 | ||
| African American | 76.0 | 60.3 | |
| Caucasian | 21.3 | 34.9 | |
| Other | 2.7 | 4.8 | |
| Payor on discharge (%) | 0.29 | ||
| Medicaid | 32.0 | 20.6 | |
| Medicare | 32.0 | 38.9 | |
| Self‐pay | 12.0 | 16.7 | |
| Other | 24.0 | 23.8 | |
| Clinical characteristics | |||
| Adjusted length of stay (days) | |||
| Median | 3 | 3 | 0.19 |
| Range | (<1, 20) | (<1, 138) | |
| Substance abuse (%) | 41.3 | 37.3 | 0.57 |
| Psychiatric diagnosis (%) | 20.0 | 25.4 | 0.38 |
| Last test characteristics | |||
| Test type (%) | <0.001 | ||
| Exam | 42.7 | 26.2 | |
| Laboratory test | 38.7 | 13.5 | |
| Procedure | 10.7 | 35.7 | |
| Consult | 8.0 | 24.6 | |
| Discharge characteristics | |||
| Discharged to home (%) | 93.3 | 71.4 | <0.001 |
| Prescriptions filled prior to discharge (%) | 10.7 | 19.8 | 0.09 |
| Ambulance required for transport (%) | 8.0 | 21.4 | 0.01 |
Overall, 81% of patients were admitted from the ED, and 40% of all patients were insured by Medicaid or were self‐pay at time of discharge. Median expected charges were similar to the national average, as demonstrated by the median APRDRGwt of 1.0. Patients stayed an average of 6 days (median = 3 days). Patients with the longest adjusted lengths of stay (>20 days) were never early and short discharges. The most common discharge diagnoses were: congestive heart failure, chest pain or myocardial infarction, pneumonia, asthma/chronic obstructive pulmonary disease, and sickle‐cell disease. Thirty‐nine percent of all patients carried the diagnosis of alcohol or drug dependence or abuse, although for most this was not their discharge diagnosis. None of these demographic or clinical factors were associated with a late or long discharge.
The types of tests patients required on discharge were categorized into 4 groups: consults (18.4%), laboratory tests (22.9%), procedures (26.4%), and physical exam (32.3%). Distribution differed significantly between early and short discharges, and all other discharges (P < 0.001). Procedures and consults were less frequent among early and short discharges (procedures: 10.7% versus 35.7%; consults: 8.0% versus 24.6%).
For all patients, there was fragmentation within the consult and procedure categories. Within the consult group, there were 12 different types of consults ordered, with the dominant category (35.1%) being other. The next highest volume consult was physical/occupational therapy (27.0%). Within the procedure group, there were 11 different types of procedures, with the most common being stress echocardiograms (28.3%). Non‐MRI radiology procedures made up the next largest category (20.8%) and the third was other (18.9%).
Many patients had immediate postdischarge needs, as demonstrated by the 20% of patients not discharged home. The majority (66%) of those who were discharged to a facility required an ambulance. Early and short discharges were less likely to use an ambulance to leave the hospital (8.0% versus 21.4%; P = 0.01), and more likely to be discharged directly to home (99.3% versus 71.4%; P < 0.001).
Based on process mapping, we defined a 4‐step sequential discharge process for all patients (Figure 1). The first step was: decisive test needed by physician to discharge patient. Subgroup analysis demonstrated no significant difference in the timing of this step by individual physician (P = 0.44). The remaining 3 steps were as follows: physician aware of test results, discharge paperwork complete by physician, and patient leaves the unit. Each of the 4 steps showed wide variability in hour of occurrence.
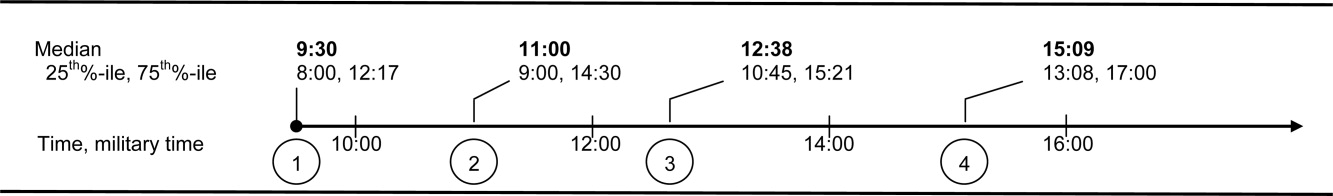
Total discharge duration showed even more variability than the time of day when steps were likely to occur (Figure 2). Median duration of the discharge process was 7.6 hours (25th% to 75th%: 4 to 22 hours). Median duration from decisive test needed until resulted (duration 1) was 2 hours (25th% to 75th%: 0 to 8 hours); between test resulted until discharge paperwork complete (duration 2) was 1.4 hours (25th% to 75th%: 0.3 to 4.2 hours); and between discharge paperwork complete and patient leaving the unit (duration 3) was 2.0 hours (25th% to 75th%: 1.1 to 3.1 hours). All durations were skewed to the right, with durations 1 and 2 each taking at least 24 hours to occur in 10% of patients.
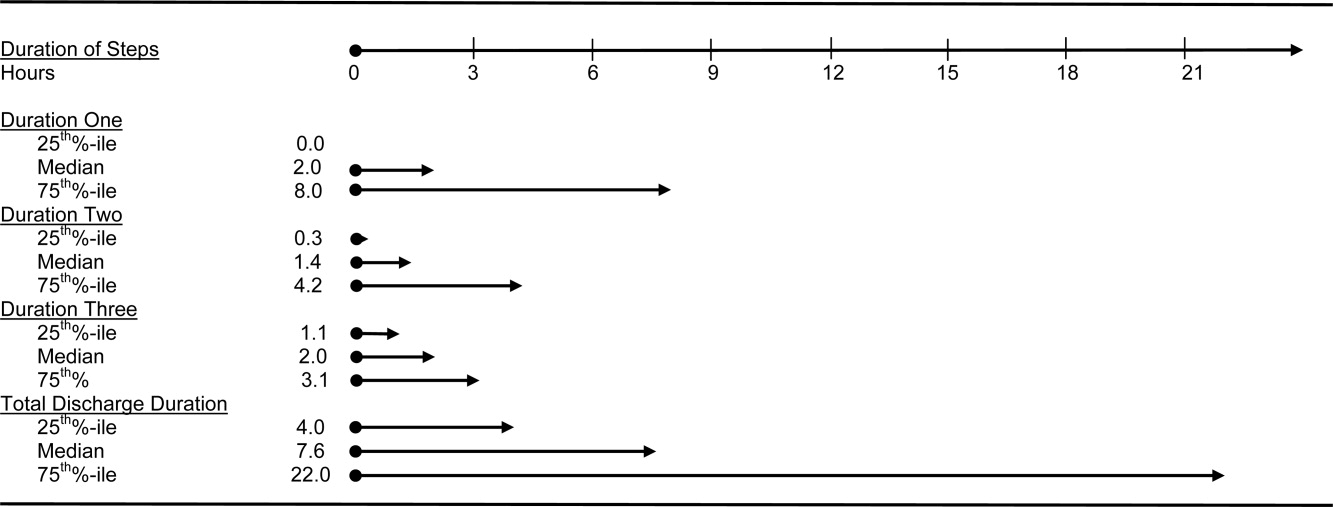
The final multivariate model for time of discharge contained 6 covariates: age, sex, race, test type, prescriptions filled prior to discharge, and need for an ambulance on discharge (Table 2). Special discharge needs continued to be associated with later discharges. Those patients who required an ambulance for transport had mean discharge times that were later by 1.5 hours (95% CI, 0.42.5). If staff obtained discharge medications for patients, these patients left 1.4 hours later than those patients who filled their prescriptions on their own (95% CI, 0.32.4). Patients requiring a consult or procedure also had significantly later discharges (1.2 hours for consults, 95% CI, 0.12.4; 1.1 hours for procedures, 95% CI, 0.12.1) than those needing a bedside exam. Age, sex, and race remained insignificant at the P 0.05 level in the final multivariate model. Length of stay was significantly associated with discharge time in crude analysis, but this variable dropped out of the final multivariate model.
| Adjusted Coefficient, Discharge Time as Outcome in Hours (95% CI)* | P Value | Adjusted Coefficient, Discharge Duration as Outcome in Hours (95% CI) | P Value | |
|---|---|---|---|---|
| ||||
| Demographics | ||||
| Age in quartiles (years) | ||||
| 7294 | 0.5 (0.5, 1.6) | 0.33 | 0.6 (8.3, 7.2) | 0.88 |
| 5671 | 0.5 (0.6, 1.6) | 0.41 | 1.3 (9.2, 6.6) | 0.75 |
| 4455 | 0.2 (0.9, 1.3) | 0.74 | 1.2 (9.0, 6.5) | 0.76 |
| Male gender | 0.0 (0.8, 0.8) | 0.97 | 1.2 (6.8, 4.5) | 0.69 |
| African American race | 0.1 (0.7, 0.9) | 0.80 | 0.3 (5.6, 6.1) | 0.93 |
| Last test characteristics | ||||
| Test type | ||||
| Consult | 1.2 (0.1, 2.4) | 0.04 | 14.8 (6.5, 23.1) | 0.001 |
| Procedure | 1.1 (0.1, 2.1) | 0.03 | 13.4 (6.0, 20.7) | <0.001 |
| Laboratory test | 0.8 (1.8, 0.3) | 0.14 | 0.9 (8.4, 6.6) | 0.82 |
| Exam (reference) | ||||
| Discharge needs | ||||
| Prescriptions filled prior to discharge | 1.4 (0.3, 2.4) | 0.02 | ||
| Not discharged to home | 28.9 (21.9, 35.9) | <0.001 | ||
| Ambulance required for transport | 1.5 (0.4, 2.5) | 0.007 | ||
We used duration of discharge as a secondary outcome measure. The final multivariate model for discharge duration included: age, sex, race, test type, and discharge to a facility (Table 2). Those who went to a facility on average left 28.9 hours (95% CI, 21.935.9) later than those who went home. Test type continued to show a significant association with discharge duration, although the estimates were slightly lower in the adjusted model. Need for a consult was associated with a discharge that was on average 14.8 hours (95% CI, 6.523.1) longer than discharges contingent on a physical exam. Similarly, those patients who had procedures had discharges that were on average 13.4 hours (95% CI, 6.020.7) longer than those whose last test was an exam. Several factors that were significantly associated with discharge duration in unadjusted analyses dropped out of the final multivariate model. These included: need for an ambulance, length of stay, insurance status, and medical complexity as estimated by APRDRGwt.
Conclusions
We found that discharge time and duration had wide variability and that certain factors were associated with only one outcome variabledischarge time or duration. Two factorsneed for an ambulance and filling of prescriptions prior to dischargewere associated with later hour of discharge. Discharge to a location other than home was associated with prolonged discharge duration. Test characteristicsin particular need for a procedure and consultwere significantly associated with both longer and later discharges.
In bivariate analysis, several factors were not associated with discharge time or duration. These were: African‐American race, sex, age, Department of Medicine occupancy on day of discharge, source of admission, psychiatric comorbidity, and substance abuse comorbidity. We had expected higher occupancy to delay discharge as demand exceeded capacity for tests, consults, etc. Our findings suggest that even though our study was conducted during the winter months when hospital occupancy is typically at its peak, supply of staff was still adequate enough to meet high demand. We had also expected that psychiatric and substance abuse comorbidities would prolong discharge as prior studies have found some of these diagnoses to be associated with longer lengths of stay.3134 However, our results do not support such an association, and may reflect our decision to group all psychiatric diagnoses together due to limited sample size.
The main strength of our study is the use of 2 outcome variablestime and durationto define delayed discharges. Our findings demonstrate that few factors are associated with both later and longer discharges. In an era when avoiding emergency room walkouts through early morning hospital discharges can be as important as managing overall length of stay, identifying factors associated with both duration and timing of discharges addresses actual challenges faced by hospitals with limited resources. Prior studies have rarely addressed both outcomes. An additional strength of our study is our use of an interdisciplinary survey. The discharge process is a key component of the inpatient stay, but it is also one for which no group is entirely responsible. Through the development and administration of an interdisciplinary survey, our study adds detail to existing descriptions of this fragmented process, and identifies potential areas for improvement.
Several limitations of our study deserve comment. First, we examined patients discharged from a hospitalist unit without house‐staff at an urban tertiary care hospital. Our findings may need additional interpretation prior to their application in dissimilar settings such as: (1) resident‐covered units in which workflow is shaped by teaching rounds, and (2) nonacademic hospitals in which incentives to provide rapid consults and procedures may be different. Second, we relied on self‐reporting for certain variables such as time decisive test needed. This may be subject to recall bias, as we did not have staff to independently verify recalled times. However, since the discharge process is generally a linear one, we were able to verify the general scope of recalled times with times date‐stamped by the computer during the discharge process (eg, checking that time decisive test needed did not occur after the discharge worksheet had been finalized in the electronic order‐entry system). Third, our sample size was not large enough to control for disease‐specific quality measures. Of note, prior studies have not identified a consistently positive or negative relationship between quality of care and efficiency.3538
Past work has used administrative and survey data to analyze the effect of discharge planning interventions on financial or quality outcomes. Outcomes have included readmissions, mortality, patient satisfaction, length of stay, and inappropriate bed days.22, 3845 However, as capacity management has become a more pressing issue for hospitals, greater focus is being placed on the mismatch between supply and demand of patients at each hour of the day. The relevant unit of measure for efficient discharges has become hour of day, in addition to total length of stay. Some hospital improvement projects have already addressed this shift in thinking.20, 21 Our study adds to this work by formally describing the precise timing and duration of steps in the discharge process, and identifying factors associated with both time and duration.
We believe the results of our study have several implications for hospital administrators and patients interested in more timely care. First, the methods used provide a tangible framework for addressing problems that cross disciplines (eg, nursing, physician, social work) and departments (eg, medicine and radiology), and have a multitude of potential causes and confounders. The survey results offer guidance on where to focus resources, provide a shared baseline metric for improvement, and suggest the cross‐functional team that should be involved in change efforts. Such an approach may be useful for addressing common system‐based challenges in inpatient quality and safety.
Second, with specific regard to discharge planning, our study supports the notion that modifiable factors are associated with discharge time and duration. However, we also describe a fragmented discharge process, with no single bottleneck or department responsible for the majority of late and long discharges. Although procedures and consults were both associated with longer and later discharges, only 26% of patients required a procedure prior to discharge, and 18% required a consult. Moreover, among procedures, different people and events are needed to carry out the 2 most popular procedures: stress echocardiograms, and non‐MRI radiology procedures. Hospital leadership at the highest levels will be required to improve efficiency based on local usage patterns, and to increase coordination among the multiple interdepartmental processes that make up the more general categories of procedure and consult.
Acknowledgements
The authors thank the patients and staff of the Hospitalist Unit for their participation in this study. In addition, they sincerely thank Paul X. Allen, Richard O. Davis, Ronald R. Peterson, and Shuai Shao. They also thank the anonymous reviewers for their thoughtful comments.
- ,,,,.Emergency departments and crowding in United States teaching hospitals.Ann Emerg Med.1991;20:980–986.
- ,,,,,.A conceptual model of emergency department crowding.Ann Emerg Med.2003;42:173–180.
- ,,.Frequent overcrowding in U.S. emergency departments.Acad Emerg Med.2001;8:151–155.
- ,,,,.The effect of hospital occupancy on emergency department length of stay and patient disposition.Acad Emerg Med.2003;10:127–133.
- .Calculus, chaos, and other models of emergency department crowding.Ann Emerg Med.2003;42:181–184.
- ,.Increased health care costs associated with ED overcrowding.Am J Emerg Med.1994;12:265–266.
- ,,, et al.Decreased health care quality associated with emergency department overcrowding.Eur J Emerg Med.1999;6:105–107.
- ,,.Can good bed management solve the overcrowding in accident and emergency departments?Emerg Med J.2003;20:149–155.
- ,.Emergency department overcrowding in the United States: an emerging threat to patient safety and public health.Emerg Med J.2003;20:402–405.
- General Accounting Office. Hospital emergency departments: crowded conditions vary among hospitals and communities. 2003:GAO‐03–460. Available at: http://www.gao.gov/new.items/d03460.pdf. Accessed October.
- ,.Do you want to die?Time.1990;135:58–60+
- .The ER crisis.Ladies Home J.2001;118:70–79.
- .Placing emergency department crowding on the decision agenda.Nurs Econ.2005;23:14–24.
- .Crisis seen in nation's ER care. Washington Post. June 15,2006;A01.
- Committee on the Future of Emergency Care in the United States Health System.Hospital‐based Emergency Care: at the Breaking Point.Washington DC:National Academies Press;2006.
- ,,, et al.Waits to see an emergency department physician: U.S. trends and predictors, 1997–2004.Health Aff.2008;27:w84–w95.
- Advisory Board.Maximizing Hospital Capacity: Expediting Throughput in an Era of Shortage. Health Care Advisory Board research study.Washington DC:Advisory Board; September 12,2002.
- ,,,.Does U.S. hospital capacity need to be expanded?Health Aff.2003;22:40–54.
- Institute for Healthcare Improvement.Optimizing Patient Flow: Moving Patients Smoothly Through Acute Care Settings.Cambridge, MA:Institute for Healthcare Improvement;2003.
- ,. Leveraging six sigma to improve hospital bed availability. Available at: http://healthcare.isixsigma.com/library/content/c030708a.asp. Accessed October2008.
- University Health System Consortium. Managing patient flow implementation: 2005 benchmarking project field brief. Available at: http://www.musc.edu/medcenter/UHC‐CCP/PFMgmtFldBk.pdf.
- ,,,.Discharge planning from hospital to home.Cochrane Database Syst Rev.2004;1:CD000313.
- ,,, et al.Predictors of inappropriate hospital days in a department of internal medicine.Int J Epidemiol.1998;27:513–519.
- ,,.Utilisation of hospital beds by the elderly—a cohort study of admissions to a teaching hospital.Ir Med J.1995;88:124–126.
- ,,,,,.Demographic and clinical characteristics as predictors of length of hospitalization and readmission.J Clin Psychol.1977;33:1093–1099.
- ,,,.The epidemiology of delays in a teaching hospital: the development and use of a tool that detects unnecessary hospital days.Med Care.1989;27:112–129.
- American Medical Association.AMA Physician ICD‐9‐CM 2004, Vols 1 and 2.Eden Prairie, MN:Ingenix;2003.
- 3M Health Information Systems and the Maryland Health Care Payment System: frequently asked questions.2004. Available at: http://multimedia.mmm.com/mws/mediawebserver.dyn?6666660Zjcf6lVs6EVs66S7wwCOrrrrQ‐.
- .Statistics with STATA.Belmont, CA:Duxbury Press;2004.
- ,.Statistical data analysis in the computer age.Science.1991;253:390–395.
- ,,,,.Psychological comorbidity and length of stay in the general hospital.Am J Psychiatry.1991;148(3):324–329.
- ,,,,,.Psychiatric comorbidity and greater hospitalization risk, longer length of stay, and higher hospitalization costs in older adults with heart failure.J Am Geriatr Soc.2007;55:1585–1591.
- ,,,.Does psychiatric comorbidity increase the length of stay in general hospitals?Gen Hosp Psychiatry.2001;23:8–14.
- ,,.The impact of psychiatric comorbidity on length of stay of medical inpatients.Gen Hosp Psychiatry.2003;25:14–19.
- ,,,,,.The implications of regional variations in Medicare spending. Part 1: The content, quality, and accessibility of care.Ann Intern Med.2003;138:273–287.
- ,,,,,.The implications of regional variations in Medicare spending. Part 2: Health outcomes and satisfaction with care.Ann Intern Med.2003;138:288–298.
- ,,, et al.Is early too early? Effect of shorter stays after bypass surgery.Ann Thorac Surg.2007;83:100–107.
- ,.Excess length of stay, charges, and mortality attributable to medical injuries during hospitalization.JAMA.2003;290:1868–1874.
- ,,, et al.Comprehensive discharge planning and home follow‐up of hospitalized elders, a randomized clinical trial.JAMA.1999;281:613–620.
- ,,,,,.Comprehensive discharge planning for the hospitalized elderly, a randomized clinical trial.Ann Intern Med.1994;120:999–1006.
- ,.Evaluating hospital discharge planning: a randomized clinical trial.Med Care.1993;31:358–370.
- ,,,,.Does a dedicated discharge coordinator improve the quality of hospital discharge?Qual Health Care.1996;5:89–96.
- ,,, et al.The effect of a hospitalist service with nurse discharge planner on patient care in an academic teaching hospital.Am J Med.2001;111:627–632.
- ,,,,,.Comprehensive discharge planning with postdischarge support for older patients with congestive heart failure: a meta‐analysis.JAMA.2004;291:1358–1367.
- ,,.Does increased access to primary care reduce hospital readmissions?N Engl J Med.1996;334:1441–1447.
In the past 2 decades, emergency department (ED) overcrowding has become an issue large enough to receive coverage in the popular press, and to spawn research around its causes and effects.116 At the same time, nurses and physicians on the inpatient wards have been urged to shorten the length of stay for patients as health system leaders face an aging population but limited capital to build new beds or hire additional clinical staff. Capacity managementencompassing the flow of patients from ED triage to inpatient dischargehas become a shared concern of clinicians and hospital administrators alike.
How to achieve the goals of diagnosing and healing while ushering patients ever more quickly through the modern hospital is not yet entirely clear. Past research and work by business groups suggests that demand for inpatient beds starts early in the day, but discharges typically occur in the late afternoon.17 This creates a potential bottleneck in patient flow. Many hospitals have implemented measures to improve patient throughput.1821 However, formal research has focused on factors leading to an additional inpatient day.2226 We have found no peer‐reviewed publications that address the problem of same‐day delays by describing hour of day for each step in the discharge process and variables associated with late‐day discharges. To fill this gap, we conducted a prospective cohort study of 209 consecutive discharges from a general medical ward to: (1) describe the natural history of hospital discharge, (2) measure time of day and duration for each step, and (3) identify factors associated with discharges that occur later in the day. We hypothesized that time and duration of discharge would be associated with 5 factors: patient demographics and clinical characteristics, departmental occupancy, type of inpatient testing done immediately prior to discharge, and discharge characteristics such as discharge to a location other than home.
Patients and Methods
Setting
The setting was the Hospitalist Unit of a single teaching hospital in Baltimore (The Johns Hopkins Hospital) from January 1, 2005 to April 30, 2005. Patients entered the cohort upon initiation of the discharge process by the hospitalist team on the Hospitalist Unit, and were followed until they were discharged alive from the hospital.
There were no published data on which to base firm a priori sample size calculations. Based on pilot data, we estimated that a sample size of about 170 would yield precise estimates for means and standard deviations, giving us 80% to 90% power to determine differences in time intervals across categories, with alpha set to 0.05. We estimated that we would need 4 months of data collection to achieve this sample size.
During the period of study, the 16‐bed unit was staffed with in‐house hospitalist attending physicians without house‐staff, from 7 AM (weekdays) or 8 AM (weekends) to 10 PM (Monday to Thursday) or 8 PM (Friday to Sunday). The hospitalist unit had 24‐hour physician coverage, but attending physicians provided overnight coverage from home (backed up by in‐house residents for patient care emergencies). Handoffs of patient care from one attending physician to another typically occurred on Friday afternoon or Monday morning. The unit had 1 dedicated social worker and a nurse clinician who provided part‐time assistance with discharge planning.
Outcome Measurements
We defined the start of the discharge process as the time the patient's last medically necessary test was needed by his or her attending physician. Specifically, physicians were asked when the results of this test first would have been useful in clearing the patient for discharge. In the remainder of this work, we will refer to the start of the discharge process as time decisive test needed.
The end of the discharge process was called the discharge time, and defined as the time the unit clerk saw the patient leave the unit. We defined early discharges as those occurring before the median hour of discharge (3:00 PM), and late discharges as those occurring at or after this hour.
A focus group composed of nurses, physicians, social worker, unit clerks, and support associates (group responsible for cleaning patient rooms) volunteered to map out the discharge process. Based on these discussions, durations in the discharge process were defined as follows: (1) duration 1: time decisive test needed, until time the attending physician was aware of test results; (2) duration 2: time the physician was aware of test results until discharge paperwork was complete; (3) duration 3: time discharge paperwork complete until patient leaves unit; and (4) total discharge duration: time decisive test needed until patient leaves unit.
Exposure Measurements
We categorized exposures into 5 groups: (1) demographics (age, gender, race, source of patient such as outside hospital versus emergency department versus other, and payer on discharge); (2) clinical characteristics (length of stay, any psychiatric diagnosis, any substance abuse diagnosis, and severity of illness); (3) system characteristics (departmental occupancy defined as proportion of hospital beds designated for Department of Medicine patients that were occupied on the day of discharge); (4) last test characteristics (physical exam, laboratory test, procedure, and consult); and (5) discharge characteristics (discharged to home versus not discharged to home, prescriptions filled in hospital pharmacy prior to discharge, and ambulance required for transport).
Psychiatric diagnosis was defined as the presence of any of the following International Classification of Diseases, Ninth Revision, Clinical Modification (ICD‐9‐CM) codes: 290319 (any fourth or fifth digits).27 Substance abuse diagnosis was defined as the presence of any of the following ICD‐9‐CM codes: 303305 (any fourth or fifth digits). Substance abuse codes encompassed drug dependence and abuse, including alcohol dependence and abuse.
The all patient refined diagnosis related group relative weight (APRDRGwt) is a unitless number that estimates the total cost of care for inpatients, based on clinical and demographic characteristics.28 A patient with a relative APRDRGwt of 1 is predicted to have the same cost of care as the national average for inpatients. A patient with a score of 2 is predicted to be twice as costly as the average. In this study, we used APRDRGwt as a gross proxy for severity of illness.
Adjusted length of stay was measured as length of stay minus discharge duration. This adjustment was made to avoid including the exposure (length of stay) in the outcome (discharge duration). Unadjusted length of stay was used when the outcome was discharge time.
Data Sources
We created a separate 4‐item to 9‐item paper questionnaire (included in the Appendix) for each of 4 functional groups participating directly in the discharge process: nurses, physicians, social worker, and unit clerks. Questions were based on staff feedback about the sequence of steps in the discharge process, and potential reasons for delay. The surveys were piloted for several weeks to further refine the wording of questions, and to ensure that the length and location of the surveys minimized workflow interruptions. The questionnaires captured information about the timing of routine events not recorded in existing databases.
Physicians were asked to identify the last test/procedure/consult needed prior to the patient being medically ready for discharge. They were asked when the test results first could have cleared the patient for discharge (time decisive test needed), and when they actually received the test results (time test results back). Nursing and social work surveys provided information on whether or not prescriptions were filled prior to discharge, and the type of transportation used on discharge. Unit clerks documented when the patient left the unit.
Response rates were: nurses (97%), physicians (97%), social worker (99%), and unit clerks (94%). All 4 surveys were completed for 88% of the 209 included patients (prior to 8 exclusions for missing data or extreme outlier observations). Group response rates were tallied at the end of each month and posted on the unit. We did not track how soon after discharge the surveys were completed. However, we reviewed survey responses frequently (often daily, at most every 4 days) and if surveys were incomplete we personally approached staff members to complete the survey.
We supplemented and cross‐checked data from the questionnaire with information from existing hospital databases. These databases were: (1) the patient's medical record for time patient arrived on the floor, and completion time for consults/procedures; (2) the Electronic Bedboard (EBB) for time patient left the unit (as recorded by unit clerk); (3) the Patient Order Entry System for time discharge papers were completed by the physician, and ordering time for select tests; (4) the Electronic Patient Record for demographic information and completion time for select tests; and (5) Datamart, the hospital's administrative/billing database, for information such as length of stay, diagnosis, patient demographics, and insurance status.
Cross‐checking of data and calculation of durations 1, 2, and 3 identified areas of disagreement that were addressed in the following way. Discharge time was provided by 3 sources: social worker and nurses as an ad hoc addition to each of their surveys, unit clerks as a mandatory question on their survey, and unit clerks as entered in the EBB. We used EBB data for discharge time, as this was the most complete and accurate single source of data. However, survey results and knowledge about the sequential process for discharge, suggested that in 20 cases EBB data did not provide the most accurate time. In these cases, discharge time was provided by the unit clerk survey (16 cases), the social work survey (3 cases), and the nursing survey (1 case).
In 28 cases (14%), discharge paperwork was completed before decisive test results were back. And in 8 cases (4%) test results were received earlier than needed. As these were a minority of cases, these negative durations were converted to zero for analysis.
Statistical Analysis
The unit of analysis was the unique hospital discharge. For patients who were discharged from the Hospitalist Unit more than once during the 4‐month study period, each discharge was treated as a separate unit of analysis.
We defined patients discharged before the median discharge time as early discharges, and all others as late discharges. We then categorized patients with discharge durations less than 24 hours as short discharges, and all others as long discharges.
We described the characteristics of 2 groups of patients: early and short discharges versus all others. We used the chi square statistic and Fisher's exact test (when frequency 5 in 1 or both groups) to test the null hypothesis that there was no association between the 2 groups and select patient characteristics. When comparing medians, we used the nonparametric equality of medians test.
For each step in the discharge process, we identified a median time of occurrence. For the first point in the processtime decisive test neededwe also used 1‐way analysis of variance and the F‐test to assess whether or not timing varied significantly by physician.
Because our primary goal was to quantify in hours the association between various factors and discharge time or duration, we used bivariate linear regression models to identify factors associated with time of discharge (primary analysis) and total duration of the discharge process (secondary analysis). We then used multivariate linear regression to identify factors associated with both outcomes. We used forward and backward selection methods to choose the final models for the multivariate analyses, after forcing in the variables for race, sex, and age. Both methods of selection produced identical results. We assessed for colinearity using variance inflation factors.29
Sensitivity Analyses
For both discharge time and discharge duration, we performed regression diagnostics including leverage, Studentized residuals, and influence. Excluding outliers for influence slightly altered the results of our multivariate analyses. However, all variables that were significant at the P < 0.05 level remained significant in the models without outliers.
We chose to include outliers for influence in our final data set after verifying the data as accurate. For discharge time, the number of outliers (3; 1.5%) for influence was in the range expected for a normally distributed data set.
We also tested for normality of the 2 outcome variables. Discharge time was normally distributed, but discharge duration was not. Because of this, we used 2 additional methods to assess the robustness of our results for discharge duration.
First, we log‐transformed the outcome and repeated the analysis. Variables significant in the non‐log‐transformed model remained significant after log‐transformation. Second, we applied bootstrapping30 with 1,000 repetitions for the bivariate and multivariate analyses. The 95% confidence intervals (CIs) (using the bias‐corrected confidence intervals) were modestly altered (some narrowed, some widened), but our conclusions remained the same except for a single variable with borderline significance (payer on discharge) in bivariate analysis. The final reported confidence intervals for discharge duration are based on our analysis without bootstrapping.
Results
Data were collected on 216 patients. Seven patients were excluded from the study, because they were discharged against medical advice. Since these patients left before their decisive test was completed, there was no way to assess duration of the discharge process. Of the remaining 209 patients, 6 patients lacked necessary data to complete analysis (5 without survey data; 1 without administrative data). Two additional patients were eliminated from the final analysis because they bypassed the normal discharge process and were extreme outliers in either discharge time (1 discharged at 1 AM), or discharge duration (1 with discharge duration of 400+ hours). A total of 201 patients were included in the final analyses.
The hospitalist program primarily serves an indigent, local adult population with general medical problems, and this is reflected in the patient characteristics (Table 1). We compared the characteristics of patients discharged early and quickly (discharged prior to median hour of 3:00 PM, and discharge process lasting less than 24 hours) to all other discharges, to identify factors associated with later and longer discharges.
| Early and Short Discharges (n = 75)* | All Other Discharges (n = 126) | P Value | |
|---|---|---|---|
| |||
| Demographics | |||
| Age (years) | |||
| Median | 55 | 55 | 0.73 |
| Range | (19, 94) | (20, 90) | |
| Gender (%) | |||
| Female | 61.3 | 61.1 | 0.98 |
| Race (%) | 0.08 | ||
| African American | 76.0 | 60.3 | |
| Caucasian | 21.3 | 34.9 | |
| Other | 2.7 | 4.8 | |
| Payor on discharge (%) | 0.29 | ||
| Medicaid | 32.0 | 20.6 | |
| Medicare | 32.0 | 38.9 | |
| Self‐pay | 12.0 | 16.7 | |
| Other | 24.0 | 23.8 | |
| Clinical characteristics | |||
| Adjusted length of stay (days) | |||
| Median | 3 | 3 | 0.19 |
| Range | (<1, 20) | (<1, 138) | |
| Substance abuse (%) | 41.3 | 37.3 | 0.57 |
| Psychiatric diagnosis (%) | 20.0 | 25.4 | 0.38 |
| Last test characteristics | |||
| Test type (%) | <0.001 | ||
| Exam | 42.7 | 26.2 | |
| Laboratory test | 38.7 | 13.5 | |
| Procedure | 10.7 | 35.7 | |
| Consult | 8.0 | 24.6 | |
| Discharge characteristics | |||
| Discharged to home (%) | 93.3 | 71.4 | <0.001 |
| Prescriptions filled prior to discharge (%) | 10.7 | 19.8 | 0.09 |
| Ambulance required for transport (%) | 8.0 | 21.4 | 0.01 |
Overall, 81% of patients were admitted from the ED, and 40% of all patients were insured by Medicaid or were self‐pay at time of discharge. Median expected charges were similar to the national average, as demonstrated by the median APRDRGwt of 1.0. Patients stayed an average of 6 days (median = 3 days). Patients with the longest adjusted lengths of stay (>20 days) were never early and short discharges. The most common discharge diagnoses were: congestive heart failure, chest pain or myocardial infarction, pneumonia, asthma/chronic obstructive pulmonary disease, and sickle‐cell disease. Thirty‐nine percent of all patients carried the diagnosis of alcohol or drug dependence or abuse, although for most this was not their discharge diagnosis. None of these demographic or clinical factors were associated with a late or long discharge.
The types of tests patients required on discharge were categorized into 4 groups: consults (18.4%), laboratory tests (22.9%), procedures (26.4%), and physical exam (32.3%). Distribution differed significantly between early and short discharges, and all other discharges (P < 0.001). Procedures and consults were less frequent among early and short discharges (procedures: 10.7% versus 35.7%; consults: 8.0% versus 24.6%).
For all patients, there was fragmentation within the consult and procedure categories. Within the consult group, there were 12 different types of consults ordered, with the dominant category (35.1%) being other. The next highest volume consult was physical/occupational therapy (27.0%). Within the procedure group, there were 11 different types of procedures, with the most common being stress echocardiograms (28.3%). Non‐MRI radiology procedures made up the next largest category (20.8%) and the third was other (18.9%).
Many patients had immediate postdischarge needs, as demonstrated by the 20% of patients not discharged home. The majority (66%) of those who were discharged to a facility required an ambulance. Early and short discharges were less likely to use an ambulance to leave the hospital (8.0% versus 21.4%; P = 0.01), and more likely to be discharged directly to home (99.3% versus 71.4%; P < 0.001).
Based on process mapping, we defined a 4‐step sequential discharge process for all patients (Figure 1). The first step was: decisive test needed by physician to discharge patient. Subgroup analysis demonstrated no significant difference in the timing of this step by individual physician (P = 0.44). The remaining 3 steps were as follows: physician aware of test results, discharge paperwork complete by physician, and patient leaves the unit. Each of the 4 steps showed wide variability in hour of occurrence.

Total discharge duration showed even more variability than the time of day when steps were likely to occur (Figure 2). Median duration of the discharge process was 7.6 hours (25th% to 75th%: 4 to 22 hours). Median duration from decisive test needed until resulted (duration 1) was 2 hours (25th% to 75th%: 0 to 8 hours); between test resulted until discharge paperwork complete (duration 2) was 1.4 hours (25th% to 75th%: 0.3 to 4.2 hours); and between discharge paperwork complete and patient leaving the unit (duration 3) was 2.0 hours (25th% to 75th%: 1.1 to 3.1 hours). All durations were skewed to the right, with durations 1 and 2 each taking at least 24 hours to occur in 10% of patients.

The final multivariate model for time of discharge contained 6 covariates: age, sex, race, test type, prescriptions filled prior to discharge, and need for an ambulance on discharge (Table 2). Special discharge needs continued to be associated with later discharges. Those patients who required an ambulance for transport had mean discharge times that were later by 1.5 hours (95% CI, 0.42.5). If staff obtained discharge medications for patients, these patients left 1.4 hours later than those patients who filled their prescriptions on their own (95% CI, 0.32.4). Patients requiring a consult or procedure also had significantly later discharges (1.2 hours for consults, 95% CI, 0.12.4; 1.1 hours for procedures, 95% CI, 0.12.1) than those needing a bedside exam. Age, sex, and race remained insignificant at the P 0.05 level in the final multivariate model. Length of stay was significantly associated with discharge time in crude analysis, but this variable dropped out of the final multivariate model.
| Adjusted Coefficient, Discharge Time as Outcome in Hours (95% CI)* | P Value | Adjusted Coefficient, Discharge Duration as Outcome in Hours (95% CI) | P Value | |
|---|---|---|---|---|
| ||||
| Demographics | ||||
| Age in quartiles (years) | ||||
| 7294 | 0.5 (0.5, 1.6) | 0.33 | 0.6 (8.3, 7.2) | 0.88 |
| 5671 | 0.5 (0.6, 1.6) | 0.41 | 1.3 (9.2, 6.6) | 0.75 |
| 4455 | 0.2 (0.9, 1.3) | 0.74 | 1.2 (9.0, 6.5) | 0.76 |
| Male gender | 0.0 (0.8, 0.8) | 0.97 | 1.2 (6.8, 4.5) | 0.69 |
| African American race | 0.1 (0.7, 0.9) | 0.80 | 0.3 (5.6, 6.1) | 0.93 |
| Last test characteristics | ||||
| Test type | ||||
| Consult | 1.2 (0.1, 2.4) | 0.04 | 14.8 (6.5, 23.1) | 0.001 |
| Procedure | 1.1 (0.1, 2.1) | 0.03 | 13.4 (6.0, 20.7) | <0.001 |
| Laboratory test | 0.8 (1.8, 0.3) | 0.14 | 0.9 (8.4, 6.6) | 0.82 |
| Exam (reference) | ||||
| Discharge needs | ||||
| Prescriptions filled prior to discharge | 1.4 (0.3, 2.4) | 0.02 | ||
| Not discharged to home | 28.9 (21.9, 35.9) | <0.001 | ||
| Ambulance required for transport | 1.5 (0.4, 2.5) | 0.007 | ||
We used duration of discharge as a secondary outcome measure. The final multivariate model for discharge duration included: age, sex, race, test type, and discharge to a facility (Table 2). Those who went to a facility on average left 28.9 hours (95% CI, 21.935.9) later than those who went home. Test type continued to show a significant association with discharge duration, although the estimates were slightly lower in the adjusted model. Need for a consult was associated with a discharge that was on average 14.8 hours (95% CI, 6.523.1) longer than discharges contingent on a physical exam. Similarly, those patients who had procedures had discharges that were on average 13.4 hours (95% CI, 6.020.7) longer than those whose last test was an exam. Several factors that were significantly associated with discharge duration in unadjusted analyses dropped out of the final multivariate model. These included: need for an ambulance, length of stay, insurance status, and medical complexity as estimated by APRDRGwt.
Conclusions
We found that discharge time and duration had wide variability and that certain factors were associated with only one outcome variabledischarge time or duration. Two factorsneed for an ambulance and filling of prescriptions prior to dischargewere associated with later hour of discharge. Discharge to a location other than home was associated with prolonged discharge duration. Test characteristicsin particular need for a procedure and consultwere significantly associated with both longer and later discharges.
In bivariate analysis, several factors were not associated with discharge time or duration. These were: African‐American race, sex, age, Department of Medicine occupancy on day of discharge, source of admission, psychiatric comorbidity, and substance abuse comorbidity. We had expected higher occupancy to delay discharge as demand exceeded capacity for tests, consults, etc. Our findings suggest that even though our study was conducted during the winter months when hospital occupancy is typically at its peak, supply of staff was still adequate enough to meet high demand. We had also expected that psychiatric and substance abuse comorbidities would prolong discharge as prior studies have found some of these diagnoses to be associated with longer lengths of stay.3134 However, our results do not support such an association, and may reflect our decision to group all psychiatric diagnoses together due to limited sample size.
The main strength of our study is the use of 2 outcome variablestime and durationto define delayed discharges. Our findings demonstrate that few factors are associated with both later and longer discharges. In an era when avoiding emergency room walkouts through early morning hospital discharges can be as important as managing overall length of stay, identifying factors associated with both duration and timing of discharges addresses actual challenges faced by hospitals with limited resources. Prior studies have rarely addressed both outcomes. An additional strength of our study is our use of an interdisciplinary survey. The discharge process is a key component of the inpatient stay, but it is also one for which no group is entirely responsible. Through the development and administration of an interdisciplinary survey, our study adds detail to existing descriptions of this fragmented process, and identifies potential areas for improvement.
Several limitations of our study deserve comment. First, we examined patients discharged from a hospitalist unit without house‐staff at an urban tertiary care hospital. Our findings may need additional interpretation prior to their application in dissimilar settings such as: (1) resident‐covered units in which workflow is shaped by teaching rounds, and (2) nonacademic hospitals in which incentives to provide rapid consults and procedures may be different. Second, we relied on self‐reporting for certain variables such as time decisive test needed. This may be subject to recall bias, as we did not have staff to independently verify recalled times. However, since the discharge process is generally a linear one, we were able to verify the general scope of recalled times with times date‐stamped by the computer during the discharge process (eg, checking that time decisive test needed did not occur after the discharge worksheet had been finalized in the electronic order‐entry system). Third, our sample size was not large enough to control for disease‐specific quality measures. Of note, prior studies have not identified a consistently positive or negative relationship between quality of care and efficiency.3538
Past work has used administrative and survey data to analyze the effect of discharge planning interventions on financial or quality outcomes. Outcomes have included readmissions, mortality, patient satisfaction, length of stay, and inappropriate bed days.22, 3845 However, as capacity management has become a more pressing issue for hospitals, greater focus is being placed on the mismatch between supply and demand of patients at each hour of the day. The relevant unit of measure for efficient discharges has become hour of day, in addition to total length of stay. Some hospital improvement projects have already addressed this shift in thinking.20, 21 Our study adds to this work by formally describing the precise timing and duration of steps in the discharge process, and identifying factors associated with both time and duration.
We believe the results of our study have several implications for hospital administrators and patients interested in more timely care. First, the methods used provide a tangible framework for addressing problems that cross disciplines (eg, nursing, physician, social work) and departments (eg, medicine and radiology), and have a multitude of potential causes and confounders. The survey results offer guidance on where to focus resources, provide a shared baseline metric for improvement, and suggest the cross‐functional team that should be involved in change efforts. Such an approach may be useful for addressing common system‐based challenges in inpatient quality and safety.
Second, with specific regard to discharge planning, our study supports the notion that modifiable factors are associated with discharge time and duration. However, we also describe a fragmented discharge process, with no single bottleneck or department responsible for the majority of late and long discharges. Although procedures and consults were both associated with longer and later discharges, only 26% of patients required a procedure prior to discharge, and 18% required a consult. Moreover, among procedures, different people and events are needed to carry out the 2 most popular procedures: stress echocardiograms, and non‐MRI radiology procedures. Hospital leadership at the highest levels will be required to improve efficiency based on local usage patterns, and to increase coordination among the multiple interdepartmental processes that make up the more general categories of procedure and consult.
Acknowledgements
The authors thank the patients and staff of the Hospitalist Unit for their participation in this study. In addition, they sincerely thank Paul X. Allen, Richard O. Davis, Ronald R. Peterson, and Shuai Shao. They also thank the anonymous reviewers for their thoughtful comments.
In the past 2 decades, emergency department (ED) overcrowding has become an issue large enough to receive coverage in the popular press, and to spawn research around its causes and effects.116 At the same time, nurses and physicians on the inpatient wards have been urged to shorten the length of stay for patients as health system leaders face an aging population but limited capital to build new beds or hire additional clinical staff. Capacity managementencompassing the flow of patients from ED triage to inpatient dischargehas become a shared concern of clinicians and hospital administrators alike.
How to achieve the goals of diagnosing and healing while ushering patients ever more quickly through the modern hospital is not yet entirely clear. Past research and work by business groups suggests that demand for inpatient beds starts early in the day, but discharges typically occur in the late afternoon.17 This creates a potential bottleneck in patient flow. Many hospitals have implemented measures to improve patient throughput.1821 However, formal research has focused on factors leading to an additional inpatient day.2226 We have found no peer‐reviewed publications that address the problem of same‐day delays by describing hour of day for each step in the discharge process and variables associated with late‐day discharges. To fill this gap, we conducted a prospective cohort study of 209 consecutive discharges from a general medical ward to: (1) describe the natural history of hospital discharge, (2) measure time of day and duration for each step, and (3) identify factors associated with discharges that occur later in the day. We hypothesized that time and duration of discharge would be associated with 5 factors: patient demographics and clinical characteristics, departmental occupancy, type of inpatient testing done immediately prior to discharge, and discharge characteristics such as discharge to a location other than home.
Patients and Methods
Setting
The setting was the Hospitalist Unit of a single teaching hospital in Baltimore (The Johns Hopkins Hospital) from January 1, 2005 to April 30, 2005. Patients entered the cohort upon initiation of the discharge process by the hospitalist team on the Hospitalist Unit, and were followed until they were discharged alive from the hospital.
There were no published data on which to base firm a priori sample size calculations. Based on pilot data, we estimated that a sample size of about 170 would yield precise estimates for means and standard deviations, giving us 80% to 90% power to determine differences in time intervals across categories, with alpha set to 0.05. We estimated that we would need 4 months of data collection to achieve this sample size.
During the period of study, the 16‐bed unit was staffed with in‐house hospitalist attending physicians without house‐staff, from 7 AM (weekdays) or 8 AM (weekends) to 10 PM (Monday to Thursday) or 8 PM (Friday to Sunday). The hospitalist unit had 24‐hour physician coverage, but attending physicians provided overnight coverage from home (backed up by in‐house residents for patient care emergencies). Handoffs of patient care from one attending physician to another typically occurred on Friday afternoon or Monday morning. The unit had 1 dedicated social worker and a nurse clinician who provided part‐time assistance with discharge planning.
Outcome Measurements
We defined the start of the discharge process as the time the patient's last medically necessary test was needed by his or her attending physician. Specifically, physicians were asked when the results of this test first would have been useful in clearing the patient for discharge. In the remainder of this work, we will refer to the start of the discharge process as time decisive test needed.
The end of the discharge process was called the discharge time, and defined as the time the unit clerk saw the patient leave the unit. We defined early discharges as those occurring before the median hour of discharge (3:00 PM), and late discharges as those occurring at or after this hour.
A focus group composed of nurses, physicians, social worker, unit clerks, and support associates (group responsible for cleaning patient rooms) volunteered to map out the discharge process. Based on these discussions, durations in the discharge process were defined as follows: (1) duration 1: time decisive test needed, until time the attending physician was aware of test results; (2) duration 2: time the physician was aware of test results until discharge paperwork was complete; (3) duration 3: time discharge paperwork complete until patient leaves unit; and (4) total discharge duration: time decisive test needed until patient leaves unit.
Exposure Measurements
We categorized exposures into 5 groups: (1) demographics (age, gender, race, source of patient such as outside hospital versus emergency department versus other, and payer on discharge); (2) clinical characteristics (length of stay, any psychiatric diagnosis, any substance abuse diagnosis, and severity of illness); (3) system characteristics (departmental occupancy defined as proportion of hospital beds designated for Department of Medicine patients that were occupied on the day of discharge); (4) last test characteristics (physical exam, laboratory test, procedure, and consult); and (5) discharge characteristics (discharged to home versus not discharged to home, prescriptions filled in hospital pharmacy prior to discharge, and ambulance required for transport).
Psychiatric diagnosis was defined as the presence of any of the following International Classification of Diseases, Ninth Revision, Clinical Modification (ICD‐9‐CM) codes: 290319 (any fourth or fifth digits).27 Substance abuse diagnosis was defined as the presence of any of the following ICD‐9‐CM codes: 303305 (any fourth or fifth digits). Substance abuse codes encompassed drug dependence and abuse, including alcohol dependence and abuse.
The all patient refined diagnosis related group relative weight (APRDRGwt) is a unitless number that estimates the total cost of care for inpatients, based on clinical and demographic characteristics.28 A patient with a relative APRDRGwt of 1 is predicted to have the same cost of care as the national average for inpatients. A patient with a score of 2 is predicted to be twice as costly as the average. In this study, we used APRDRGwt as a gross proxy for severity of illness.
Adjusted length of stay was measured as length of stay minus discharge duration. This adjustment was made to avoid including the exposure (length of stay) in the outcome (discharge duration). Unadjusted length of stay was used when the outcome was discharge time.
Data Sources
We created a separate 4‐item to 9‐item paper questionnaire (included in the Appendix) for each of 4 functional groups participating directly in the discharge process: nurses, physicians, social worker, and unit clerks. Questions were based on staff feedback about the sequence of steps in the discharge process, and potential reasons for delay. The surveys were piloted for several weeks to further refine the wording of questions, and to ensure that the length and location of the surveys minimized workflow interruptions. The questionnaires captured information about the timing of routine events not recorded in existing databases.
Physicians were asked to identify the last test/procedure/consult needed prior to the patient being medically ready for discharge. They were asked when the test results first could have cleared the patient for discharge (time decisive test needed), and when they actually received the test results (time test results back). Nursing and social work surveys provided information on whether or not prescriptions were filled prior to discharge, and the type of transportation used on discharge. Unit clerks documented when the patient left the unit.
Response rates were: nurses (97%), physicians (97%), social worker (99%), and unit clerks (94%). All 4 surveys were completed for 88% of the 209 included patients (prior to 8 exclusions for missing data or extreme outlier observations). Group response rates were tallied at the end of each month and posted on the unit. We did not track how soon after discharge the surveys were completed. However, we reviewed survey responses frequently (often daily, at most every 4 days) and if surveys were incomplete we personally approached staff members to complete the survey.
We supplemented and cross‐checked data from the questionnaire with information from existing hospital databases. These databases were: (1) the patient's medical record for time patient arrived on the floor, and completion time for consults/procedures; (2) the Electronic Bedboard (EBB) for time patient left the unit (as recorded by unit clerk); (3) the Patient Order Entry System for time discharge papers were completed by the physician, and ordering time for select tests; (4) the Electronic Patient Record for demographic information and completion time for select tests; and (5) Datamart, the hospital's administrative/billing database, for information such as length of stay, diagnosis, patient demographics, and insurance status.
Cross‐checking of data and calculation of durations 1, 2, and 3 identified areas of disagreement that were addressed in the following way. Discharge time was provided by 3 sources: social worker and nurses as an ad hoc addition to each of their surveys, unit clerks as a mandatory question on their survey, and unit clerks as entered in the EBB. We used EBB data for discharge time, as this was the most complete and accurate single source of data. However, survey results and knowledge about the sequential process for discharge, suggested that in 20 cases EBB data did not provide the most accurate time. In these cases, discharge time was provided by the unit clerk survey (16 cases), the social work survey (3 cases), and the nursing survey (1 case).
In 28 cases (14%), discharge paperwork was completed before decisive test results were back. And in 8 cases (4%) test results were received earlier than needed. As these were a minority of cases, these negative durations were converted to zero for analysis.
Statistical Analysis
The unit of analysis was the unique hospital discharge. For patients who were discharged from the Hospitalist Unit more than once during the 4‐month study period, each discharge was treated as a separate unit of analysis.
We defined patients discharged before the median discharge time as early discharges, and all others as late discharges. We then categorized patients with discharge durations less than 24 hours as short discharges, and all others as long discharges.
We described the characteristics of 2 groups of patients: early and short discharges versus all others. We used the chi square statistic and Fisher's exact test (when frequency 5 in 1 or both groups) to test the null hypothesis that there was no association between the 2 groups and select patient characteristics. When comparing medians, we used the nonparametric equality of medians test.
For each step in the discharge process, we identified a median time of occurrence. For the first point in the processtime decisive test neededwe also used 1‐way analysis of variance and the F‐test to assess whether or not timing varied significantly by physician.
Because our primary goal was to quantify in hours the association between various factors and discharge time or duration, we used bivariate linear regression models to identify factors associated with time of discharge (primary analysis) and total duration of the discharge process (secondary analysis). We then used multivariate linear regression to identify factors associated with both outcomes. We used forward and backward selection methods to choose the final models for the multivariate analyses, after forcing in the variables for race, sex, and age. Both methods of selection produced identical results. We assessed for colinearity using variance inflation factors.29
Sensitivity Analyses
For both discharge time and discharge duration, we performed regression diagnostics including leverage, Studentized residuals, and influence. Excluding outliers for influence slightly altered the results of our multivariate analyses. However, all variables that were significant at the P < 0.05 level remained significant in the models without outliers.
We chose to include outliers for influence in our final data set after verifying the data as accurate. For discharge time, the number of outliers (3; 1.5%) for influence was in the range expected for a normally distributed data set.
We also tested for normality of the 2 outcome variables. Discharge time was normally distributed, but discharge duration was not. Because of this, we used 2 additional methods to assess the robustness of our results for discharge duration.
First, we log‐transformed the outcome and repeated the analysis. Variables significant in the non‐log‐transformed model remained significant after log‐transformation. Second, we applied bootstrapping30 with 1,000 repetitions for the bivariate and multivariate analyses. The 95% confidence intervals (CIs) (using the bias‐corrected confidence intervals) were modestly altered (some narrowed, some widened), but our conclusions remained the same except for a single variable with borderline significance (payer on discharge) in bivariate analysis. The final reported confidence intervals for discharge duration are based on our analysis without bootstrapping.
Results
Data were collected on 216 patients. Seven patients were excluded from the study, because they were discharged against medical advice. Since these patients left before their decisive test was completed, there was no way to assess duration of the discharge process. Of the remaining 209 patients, 6 patients lacked necessary data to complete analysis (5 without survey data; 1 without administrative data). Two additional patients were eliminated from the final analysis because they bypassed the normal discharge process and were extreme outliers in either discharge time (1 discharged at 1 AM), or discharge duration (1 with discharge duration of 400+ hours). A total of 201 patients were included in the final analyses.
The hospitalist program primarily serves an indigent, local adult population with general medical problems, and this is reflected in the patient characteristics (Table 1). We compared the characteristics of patients discharged early and quickly (discharged prior to median hour of 3:00 PM, and discharge process lasting less than 24 hours) to all other discharges, to identify factors associated with later and longer discharges.
| Early and Short Discharges (n = 75)* | All Other Discharges (n = 126) | P Value | |
|---|---|---|---|
| |||
| Demographics | |||
| Age (years) | |||
| Median | 55 | 55 | 0.73 |
| Range | (19, 94) | (20, 90) | |
| Gender (%) | |||
| Female | 61.3 | 61.1 | 0.98 |
| Race (%) | 0.08 | ||
| African American | 76.0 | 60.3 | |
| Caucasian | 21.3 | 34.9 | |
| Other | 2.7 | 4.8 | |
| Payor on discharge (%) | 0.29 | ||
| Medicaid | 32.0 | 20.6 | |
| Medicare | 32.0 | 38.9 | |
| Self‐pay | 12.0 | 16.7 | |
| Other | 24.0 | 23.8 | |
| Clinical characteristics | |||
| Adjusted length of stay (days) | |||
| Median | 3 | 3 | 0.19 |
| Range | (<1, 20) | (<1, 138) | |
| Substance abuse (%) | 41.3 | 37.3 | 0.57 |
| Psychiatric diagnosis (%) | 20.0 | 25.4 | 0.38 |
| Last test characteristics | |||
| Test type (%) | <0.001 | ||
| Exam | 42.7 | 26.2 | |
| Laboratory test | 38.7 | 13.5 | |
| Procedure | 10.7 | 35.7 | |
| Consult | 8.0 | 24.6 | |
| Discharge characteristics | |||
| Discharged to home (%) | 93.3 | 71.4 | <0.001 |
| Prescriptions filled prior to discharge (%) | 10.7 | 19.8 | 0.09 |
| Ambulance required for transport (%) | 8.0 | 21.4 | 0.01 |
Overall, 81% of patients were admitted from the ED, and 40% of all patients were insured by Medicaid or were self‐pay at time of discharge. Median expected charges were similar to the national average, as demonstrated by the median APRDRGwt of 1.0. Patients stayed an average of 6 days (median = 3 days). Patients with the longest adjusted lengths of stay (>20 days) were never early and short discharges. The most common discharge diagnoses were: congestive heart failure, chest pain or myocardial infarction, pneumonia, asthma/chronic obstructive pulmonary disease, and sickle‐cell disease. Thirty‐nine percent of all patients carried the diagnosis of alcohol or drug dependence or abuse, although for most this was not their discharge diagnosis. None of these demographic or clinical factors were associated with a late or long discharge.
The types of tests patients required on discharge were categorized into 4 groups: consults (18.4%), laboratory tests (22.9%), procedures (26.4%), and physical exam (32.3%). Distribution differed significantly between early and short discharges, and all other discharges (P < 0.001). Procedures and consults were less frequent among early and short discharges (procedures: 10.7% versus 35.7%; consults: 8.0% versus 24.6%).
For all patients, there was fragmentation within the consult and procedure categories. Within the consult group, there were 12 different types of consults ordered, with the dominant category (35.1%) being other. The next highest volume consult was physical/occupational therapy (27.0%). Within the procedure group, there were 11 different types of procedures, with the most common being stress echocardiograms (28.3%). Non‐MRI radiology procedures made up the next largest category (20.8%) and the third was other (18.9%).
Many patients had immediate postdischarge needs, as demonstrated by the 20% of patients not discharged home. The majority (66%) of those who were discharged to a facility required an ambulance. Early and short discharges were less likely to use an ambulance to leave the hospital (8.0% versus 21.4%; P = 0.01), and more likely to be discharged directly to home (99.3% versus 71.4%; P < 0.001).
Based on process mapping, we defined a 4‐step sequential discharge process for all patients (Figure 1). The first step was: decisive test needed by physician to discharge patient. Subgroup analysis demonstrated no significant difference in the timing of this step by individual physician (P = 0.44). The remaining 3 steps were as follows: physician aware of test results, discharge paperwork complete by physician, and patient leaves the unit. Each of the 4 steps showed wide variability in hour of occurrence.

Total discharge duration showed even more variability than the time of day when steps were likely to occur (Figure 2). Median duration of the discharge process was 7.6 hours (25th% to 75th%: 4 to 22 hours). Median duration from decisive test needed until resulted (duration 1) was 2 hours (25th% to 75th%: 0 to 8 hours); between test resulted until discharge paperwork complete (duration 2) was 1.4 hours (25th% to 75th%: 0.3 to 4.2 hours); and between discharge paperwork complete and patient leaving the unit (duration 3) was 2.0 hours (25th% to 75th%: 1.1 to 3.1 hours). All durations were skewed to the right, with durations 1 and 2 each taking at least 24 hours to occur in 10% of patients.

The final multivariate model for time of discharge contained 6 covariates: age, sex, race, test type, prescriptions filled prior to discharge, and need for an ambulance on discharge (Table 2). Special discharge needs continued to be associated with later discharges. Those patients who required an ambulance for transport had mean discharge times that were later by 1.5 hours (95% CI, 0.42.5). If staff obtained discharge medications for patients, these patients left 1.4 hours later than those patients who filled their prescriptions on their own (95% CI, 0.32.4). Patients requiring a consult or procedure also had significantly later discharges (1.2 hours for consults, 95% CI, 0.12.4; 1.1 hours for procedures, 95% CI, 0.12.1) than those needing a bedside exam. Age, sex, and race remained insignificant at the P 0.05 level in the final multivariate model. Length of stay was significantly associated with discharge time in crude analysis, but this variable dropped out of the final multivariate model.
| Adjusted Coefficient, Discharge Time as Outcome in Hours (95% CI)* | P Value | Adjusted Coefficient, Discharge Duration as Outcome in Hours (95% CI) | P Value | |
|---|---|---|---|---|
| ||||
| Demographics | ||||
| Age in quartiles (years) | ||||
| 7294 | 0.5 (0.5, 1.6) | 0.33 | 0.6 (8.3, 7.2) | 0.88 |
| 5671 | 0.5 (0.6, 1.6) | 0.41 | 1.3 (9.2, 6.6) | 0.75 |
| 4455 | 0.2 (0.9, 1.3) | 0.74 | 1.2 (9.0, 6.5) | 0.76 |
| Male gender | 0.0 (0.8, 0.8) | 0.97 | 1.2 (6.8, 4.5) | 0.69 |
| African American race | 0.1 (0.7, 0.9) | 0.80 | 0.3 (5.6, 6.1) | 0.93 |
| Last test characteristics | ||||
| Test type | ||||
| Consult | 1.2 (0.1, 2.4) | 0.04 | 14.8 (6.5, 23.1) | 0.001 |
| Procedure | 1.1 (0.1, 2.1) | 0.03 | 13.4 (6.0, 20.7) | <0.001 |
| Laboratory test | 0.8 (1.8, 0.3) | 0.14 | 0.9 (8.4, 6.6) | 0.82 |
| Exam (reference) | ||||
| Discharge needs | ||||
| Prescriptions filled prior to discharge | 1.4 (0.3, 2.4) | 0.02 | ||
| Not discharged to home | 28.9 (21.9, 35.9) | <0.001 | ||
| Ambulance required for transport | 1.5 (0.4, 2.5) | 0.007 | ||
We used duration of discharge as a secondary outcome measure. The final multivariate model for discharge duration included: age, sex, race, test type, and discharge to a facility (Table 2). Those who went to a facility on average left 28.9 hours (95% CI, 21.935.9) later than those who went home. Test type continued to show a significant association with discharge duration, although the estimates were slightly lower in the adjusted model. Need for a consult was associated with a discharge that was on average 14.8 hours (95% CI, 6.523.1) longer than discharges contingent on a physical exam. Similarly, those patients who had procedures had discharges that were on average 13.4 hours (95% CI, 6.020.7) longer than those whose last test was an exam. Several factors that were significantly associated with discharge duration in unadjusted analyses dropped out of the final multivariate model. These included: need for an ambulance, length of stay, insurance status, and medical complexity as estimated by APRDRGwt.
Conclusions
We found that discharge time and duration had wide variability and that certain factors were associated with only one outcome variabledischarge time or duration. Two factorsneed for an ambulance and filling of prescriptions prior to dischargewere associated with later hour of discharge. Discharge to a location other than home was associated with prolonged discharge duration. Test characteristicsin particular need for a procedure and consultwere significantly associated with both longer and later discharges.
In bivariate analysis, several factors were not associated with discharge time or duration. These were: African‐American race, sex, age, Department of Medicine occupancy on day of discharge, source of admission, psychiatric comorbidity, and substance abuse comorbidity. We had expected higher occupancy to delay discharge as demand exceeded capacity for tests, consults, etc. Our findings suggest that even though our study was conducted during the winter months when hospital occupancy is typically at its peak, supply of staff was still adequate enough to meet high demand. We had also expected that psychiatric and substance abuse comorbidities would prolong discharge as prior studies have found some of these diagnoses to be associated with longer lengths of stay.3134 However, our results do not support such an association, and may reflect our decision to group all psychiatric diagnoses together due to limited sample size.
The main strength of our study is the use of 2 outcome variablestime and durationto define delayed discharges. Our findings demonstrate that few factors are associated with both later and longer discharges. In an era when avoiding emergency room walkouts through early morning hospital discharges can be as important as managing overall length of stay, identifying factors associated with both duration and timing of discharges addresses actual challenges faced by hospitals with limited resources. Prior studies have rarely addressed both outcomes. An additional strength of our study is our use of an interdisciplinary survey. The discharge process is a key component of the inpatient stay, but it is also one for which no group is entirely responsible. Through the development and administration of an interdisciplinary survey, our study adds detail to existing descriptions of this fragmented process, and identifies potential areas for improvement.
Several limitations of our study deserve comment. First, we examined patients discharged from a hospitalist unit without house‐staff at an urban tertiary care hospital. Our findings may need additional interpretation prior to their application in dissimilar settings such as: (1) resident‐covered units in which workflow is shaped by teaching rounds, and (2) nonacademic hospitals in which incentives to provide rapid consults and procedures may be different. Second, we relied on self‐reporting for certain variables such as time decisive test needed. This may be subject to recall bias, as we did not have staff to independently verify recalled times. However, since the discharge process is generally a linear one, we were able to verify the general scope of recalled times with times date‐stamped by the computer during the discharge process (eg, checking that time decisive test needed did not occur after the discharge worksheet had been finalized in the electronic order‐entry system). Third, our sample size was not large enough to control for disease‐specific quality measures. Of note, prior studies have not identified a consistently positive or negative relationship between quality of care and efficiency.3538
Past work has used administrative and survey data to analyze the effect of discharge planning interventions on financial or quality outcomes. Outcomes have included readmissions, mortality, patient satisfaction, length of stay, and inappropriate bed days.22, 3845 However, as capacity management has become a more pressing issue for hospitals, greater focus is being placed on the mismatch between supply and demand of patients at each hour of the day. The relevant unit of measure for efficient discharges has become hour of day, in addition to total length of stay. Some hospital improvement projects have already addressed this shift in thinking.20, 21 Our study adds to this work by formally describing the precise timing and duration of steps in the discharge process, and identifying factors associated with both time and duration.
We believe the results of our study have several implications for hospital administrators and patients interested in more timely care. First, the methods used provide a tangible framework for addressing problems that cross disciplines (eg, nursing, physician, social work) and departments (eg, medicine and radiology), and have a multitude of potential causes and confounders. The survey results offer guidance on where to focus resources, provide a shared baseline metric for improvement, and suggest the cross‐functional team that should be involved in change efforts. Such an approach may be useful for addressing common system‐based challenges in inpatient quality and safety.
Second, with specific regard to discharge planning, our study supports the notion that modifiable factors are associated with discharge time and duration. However, we also describe a fragmented discharge process, with no single bottleneck or department responsible for the majority of late and long discharges. Although procedures and consults were both associated with longer and later discharges, only 26% of patients required a procedure prior to discharge, and 18% required a consult. Moreover, among procedures, different people and events are needed to carry out the 2 most popular procedures: stress echocardiograms, and non‐MRI radiology procedures. Hospital leadership at the highest levels will be required to improve efficiency based on local usage patterns, and to increase coordination among the multiple interdepartmental processes that make up the more general categories of procedure and consult.
Acknowledgements
The authors thank the patients and staff of the Hospitalist Unit for their participation in this study. In addition, they sincerely thank Paul X. Allen, Richard O. Davis, Ronald R. Peterson, and Shuai Shao. They also thank the anonymous reviewers for their thoughtful comments.
- ,,,,.Emergency departments and crowding in United States teaching hospitals.Ann Emerg Med.1991;20:980–986.
- ,,,,,.A conceptual model of emergency department crowding.Ann Emerg Med.2003;42:173–180.
- ,,.Frequent overcrowding in U.S. emergency departments.Acad Emerg Med.2001;8:151–155.
- ,,,,.The effect of hospital occupancy on emergency department length of stay and patient disposition.Acad Emerg Med.2003;10:127–133.
- .Calculus, chaos, and other models of emergency department crowding.Ann Emerg Med.2003;42:181–184.
- ,.Increased health care costs associated with ED overcrowding.Am J Emerg Med.1994;12:265–266.
- ,,, et al.Decreased health care quality associated with emergency department overcrowding.Eur J Emerg Med.1999;6:105–107.
- ,,.Can good bed management solve the overcrowding in accident and emergency departments?Emerg Med J.2003;20:149–155.
- ,.Emergency department overcrowding in the United States: an emerging threat to patient safety and public health.Emerg Med J.2003;20:402–405.
- General Accounting Office. Hospital emergency departments: crowded conditions vary among hospitals and communities. 2003:GAO‐03–460. Available at: http://www.gao.gov/new.items/d03460.pdf. Accessed October.
- ,.Do you want to die?Time.1990;135:58–60+
- .The ER crisis.Ladies Home J.2001;118:70–79.
- .Placing emergency department crowding on the decision agenda.Nurs Econ.2005;23:14–24.
- .Crisis seen in nation's ER care. Washington Post. June 15,2006;A01.
- Committee on the Future of Emergency Care in the United States Health System.Hospital‐based Emergency Care: at the Breaking Point.Washington DC:National Academies Press;2006.
- ,,, et al.Waits to see an emergency department physician: U.S. trends and predictors, 1997–2004.Health Aff.2008;27:w84–w95.
- Advisory Board.Maximizing Hospital Capacity: Expediting Throughput in an Era of Shortage. Health Care Advisory Board research study.Washington DC:Advisory Board; September 12,2002.
- ,,,.Does U.S. hospital capacity need to be expanded?Health Aff.2003;22:40–54.
- Institute for Healthcare Improvement.Optimizing Patient Flow: Moving Patients Smoothly Through Acute Care Settings.Cambridge, MA:Institute for Healthcare Improvement;2003.
- ,. Leveraging six sigma to improve hospital bed availability. Available at: http://healthcare.isixsigma.com/library/content/c030708a.asp. Accessed October2008.
- University Health System Consortium. Managing patient flow implementation: 2005 benchmarking project field brief. Available at: http://www.musc.edu/medcenter/UHC‐CCP/PFMgmtFldBk.pdf.
- ,,,.Discharge planning from hospital to home.Cochrane Database Syst Rev.2004;1:CD000313.
- ,,, et al.Predictors of inappropriate hospital days in a department of internal medicine.Int J Epidemiol.1998;27:513–519.
- ,,.Utilisation of hospital beds by the elderly—a cohort study of admissions to a teaching hospital.Ir Med J.1995;88:124–126.
- ,,,,,.Demographic and clinical characteristics as predictors of length of hospitalization and readmission.J Clin Psychol.1977;33:1093–1099.
- ,,,.The epidemiology of delays in a teaching hospital: the development and use of a tool that detects unnecessary hospital days.Med Care.1989;27:112–129.
- American Medical Association.AMA Physician ICD‐9‐CM 2004, Vols 1 and 2.Eden Prairie, MN:Ingenix;2003.
- 3M Health Information Systems and the Maryland Health Care Payment System: frequently asked questions.2004. Available at: http://multimedia.mmm.com/mws/mediawebserver.dyn?6666660Zjcf6lVs6EVs66S7wwCOrrrrQ‐.
- .Statistics with STATA.Belmont, CA:Duxbury Press;2004.
- ,.Statistical data analysis in the computer age.Science.1991;253:390–395.
- ,,,,.Psychological comorbidity and length of stay in the general hospital.Am J Psychiatry.1991;148(3):324–329.
- ,,,,,.Psychiatric comorbidity and greater hospitalization risk, longer length of stay, and higher hospitalization costs in older adults with heart failure.J Am Geriatr Soc.2007;55:1585–1591.
- ,,,.Does psychiatric comorbidity increase the length of stay in general hospitals?Gen Hosp Psychiatry.2001;23:8–14.
- ,,.The impact of psychiatric comorbidity on length of stay of medical inpatients.Gen Hosp Psychiatry.2003;25:14–19.
- ,,,,,.The implications of regional variations in Medicare spending. Part 1: The content, quality, and accessibility of care.Ann Intern Med.2003;138:273–287.
- ,,,,,.The implications of regional variations in Medicare spending. Part 2: Health outcomes and satisfaction with care.Ann Intern Med.2003;138:288–298.
- ,,, et al.Is early too early? Effect of shorter stays after bypass surgery.Ann Thorac Surg.2007;83:100–107.
- ,.Excess length of stay, charges, and mortality attributable to medical injuries during hospitalization.JAMA.2003;290:1868–1874.
- ,,, et al.Comprehensive discharge planning and home follow‐up of hospitalized elders, a randomized clinical trial.JAMA.1999;281:613–620.
- ,,,,,.Comprehensive discharge planning for the hospitalized elderly, a randomized clinical trial.Ann Intern Med.1994;120:999–1006.
- ,.Evaluating hospital discharge planning: a randomized clinical trial.Med Care.1993;31:358–370.
- ,,,,.Does a dedicated discharge coordinator improve the quality of hospital discharge?Qual Health Care.1996;5:89–96.
- ,,, et al.The effect of a hospitalist service with nurse discharge planner on patient care in an academic teaching hospital.Am J Med.2001;111:627–632.
- ,,,,,.Comprehensive discharge planning with postdischarge support for older patients with congestive heart failure: a meta‐analysis.JAMA.2004;291:1358–1367.
- ,,.Does increased access to primary care reduce hospital readmissions?N Engl J Med.1996;334:1441–1447.
- ,,,,.Emergency departments and crowding in United States teaching hospitals.Ann Emerg Med.1991;20:980–986.
- ,,,,,.A conceptual model of emergency department crowding.Ann Emerg Med.2003;42:173–180.
- ,,.Frequent overcrowding in U.S. emergency departments.Acad Emerg Med.2001;8:151–155.
- ,,,,.The effect of hospital occupancy on emergency department length of stay and patient disposition.Acad Emerg Med.2003;10:127–133.
- .Calculus, chaos, and other models of emergency department crowding.Ann Emerg Med.2003;42:181–184.
- ,.Increased health care costs associated with ED overcrowding.Am J Emerg Med.1994;12:265–266.
- ,,, et al.Decreased health care quality associated with emergency department overcrowding.Eur J Emerg Med.1999;6:105–107.
- ,,.Can good bed management solve the overcrowding in accident and emergency departments?Emerg Med J.2003;20:149–155.
- ,.Emergency department overcrowding in the United States: an emerging threat to patient safety and public health.Emerg Med J.2003;20:402–405.
- General Accounting Office. Hospital emergency departments: crowded conditions vary among hospitals and communities. 2003:GAO‐03–460. Available at: http://www.gao.gov/new.items/d03460.pdf. Accessed October.
- ,.Do you want to die?Time.1990;135:58–60+
- .The ER crisis.Ladies Home J.2001;118:70–79.
- .Placing emergency department crowding on the decision agenda.Nurs Econ.2005;23:14–24.
- .Crisis seen in nation's ER care. Washington Post. June 15,2006;A01.
- Committee on the Future of Emergency Care in the United States Health System.Hospital‐based Emergency Care: at the Breaking Point.Washington DC:National Academies Press;2006.
- ,,, et al.Waits to see an emergency department physician: U.S. trends and predictors, 1997–2004.Health Aff.2008;27:w84–w95.
- Advisory Board.Maximizing Hospital Capacity: Expediting Throughput in an Era of Shortage. Health Care Advisory Board research study.Washington DC:Advisory Board; September 12,2002.
- ,,,.Does U.S. hospital capacity need to be expanded?Health Aff.2003;22:40–54.
- Institute for Healthcare Improvement.Optimizing Patient Flow: Moving Patients Smoothly Through Acute Care Settings.Cambridge, MA:Institute for Healthcare Improvement;2003.
- ,. Leveraging six sigma to improve hospital bed availability. Available at: http://healthcare.isixsigma.com/library/content/c030708a.asp. Accessed October2008.
- University Health System Consortium. Managing patient flow implementation: 2005 benchmarking project field brief. Available at: http://www.musc.edu/medcenter/UHC‐CCP/PFMgmtFldBk.pdf.
- ,,,.Discharge planning from hospital to home.Cochrane Database Syst Rev.2004;1:CD000313.
- ,,, et al.Predictors of inappropriate hospital days in a department of internal medicine.Int J Epidemiol.1998;27:513–519.
- ,,.Utilisation of hospital beds by the elderly—a cohort study of admissions to a teaching hospital.Ir Med J.1995;88:124–126.
- ,,,,,.Demographic and clinical characteristics as predictors of length of hospitalization and readmission.J Clin Psychol.1977;33:1093–1099.
- ,,,.The epidemiology of delays in a teaching hospital: the development and use of a tool that detects unnecessary hospital days.Med Care.1989;27:112–129.
- American Medical Association.AMA Physician ICD‐9‐CM 2004, Vols 1 and 2.Eden Prairie, MN:Ingenix;2003.
- 3M Health Information Systems and the Maryland Health Care Payment System: frequently asked questions.2004. Available at: http://multimedia.mmm.com/mws/mediawebserver.dyn?6666660Zjcf6lVs6EVs66S7wwCOrrrrQ‐.
- .Statistics with STATA.Belmont, CA:Duxbury Press;2004.
- ,.Statistical data analysis in the computer age.Science.1991;253:390–395.
- ,,,,.Psychological comorbidity and length of stay in the general hospital.Am J Psychiatry.1991;148(3):324–329.
- ,,,,,.Psychiatric comorbidity and greater hospitalization risk, longer length of stay, and higher hospitalization costs in older adults with heart failure.J Am Geriatr Soc.2007;55:1585–1591.
- ,,,.Does psychiatric comorbidity increase the length of stay in general hospitals?Gen Hosp Psychiatry.2001;23:8–14.
- ,,.The impact of psychiatric comorbidity on length of stay of medical inpatients.Gen Hosp Psychiatry.2003;25:14–19.
- ,,,,,.The implications of regional variations in Medicare spending. Part 1: The content, quality, and accessibility of care.Ann Intern Med.2003;138:273–287.
- ,,,,,.The implications of regional variations in Medicare spending. Part 2: Health outcomes and satisfaction with care.Ann Intern Med.2003;138:288–298.
- ,,, et al.Is early too early? Effect of shorter stays after bypass surgery.Ann Thorac Surg.2007;83:100–107.
- ,.Excess length of stay, charges, and mortality attributable to medical injuries during hospitalization.JAMA.2003;290:1868–1874.
- ,,, et al.Comprehensive discharge planning and home follow‐up of hospitalized elders, a randomized clinical trial.JAMA.1999;281:613–620.
- ,,,,,.Comprehensive discharge planning for the hospitalized elderly, a randomized clinical trial.Ann Intern Med.1994;120:999–1006.
- ,.Evaluating hospital discharge planning: a randomized clinical trial.Med Care.1993;31:358–370.
- ,,,,.Does a dedicated discharge coordinator improve the quality of hospital discharge?Qual Health Care.1996;5:89–96.
- ,,, et al.The effect of a hospitalist service with nurse discharge planner on patient care in an academic teaching hospital.Am J Med.2001;111:627–632.
- ,,,,,.Comprehensive discharge planning with postdischarge support for older patients with congestive heart failure: a meta‐analysis.JAMA.2004;291:1358–1367.
- ,,.Does increased access to primary care reduce hospital readmissions?N Engl J Med.1996;334:1441–1447.
Copyright © 2009 Society of Hospital Medicine
Caught in the Web: e‐Diagnosis
The approach to clinical conundrums by an expert clinician is revealed through the presentation of an actual patient's case in an approach typical of a morning report. Similarly to patient care, sequential pieces of information are provided to the clinician, who is unfamiliar with the case. The focus is on the thought processes of both the clinical team caring for the patient and the discussant.
A 52‐year‐old woman presented with a 3‐month history of progressive bilateral leg edema and dyspnea while climbing a flight of stairs or while walking up a steep slope. She also complained of a tingling sensation in both hands and fingers, which started about 2 months prior to the onset of edema. She did not describe sensory problems in the lower extremities and did not have any other neurological complaints. She denied fever, cough, chest pain, palpitations, orthopnea, paroxysmal nocturnal dyspnea, and dark stools. She had no history of hypertension, diabetes, dyslipidemia, or asthma and had never been hospitalized. She did not smoke or consume alcohol and used no medications, including over‐the‐counter drugs or dietary supplements. The patient was born in Japan and had not traveled outside the country since her birth. She was a homemaker and had worked occasionally as a manual laborer in sugar cane agriculture. A review of systems revealed no history of polydipsia, polyuria, or cold or heat intolerance but did identify new hair growth, especially on the extremities.
This middle‐aged woman shows progressive changes in her general health status that are characterized by edema and dyspnea on effort. The differential diagnosis of edema includes a broad spectrum of illnesses, such as cardiac, lung, renal, endocrine, and hepatic diseases. Because of the life‐threatening potential, my first concern is cardiac disease, although the patient is not experiencing typical symptoms of ischemic heart disease or congestive failure. Bilateral and distal distribution of neuropathic symptoms is likely due to diseases of peripheral nerves rather than those of the central nervous system. Her complaint of a bilateral tingling sensation in the hands may suggest carpal tunnel syndrome as a result of her long‐term agricultural work. Other possible causes include radiculopathy of the cervical spine or polyneuropathy. Clues in the physical examination may help narrow the differential diagnosis to a cardiac, hepatic, or endocrine disorder.
The patient appeared ill. Her weight had increased from 48 to 61 kg since she was last weighed 6 months previously. Her blood pressure was 140/78 mm Hg, her heart rate was 72 beats/minute with a regular rhythm, her respiratory rate was 18/minute, and her temperature was 37.5C. The jugular venous pressure was elevated at 10 cm above the sternal angle. A grade III/VI systolic ejection murmur was evident at the second interspace along the left sternal border. The second heart sound was fixed and split. There were decreased breath sounds and complete dullness to percussion over both lower lung fields. Shifting dullness was noted on abdominal examination. There was pitting edema from the feet to the thighs, with slow pit‐recovery time in both legs, and she exhibited generalized hirsutism on the face, body, and extremities. There was no lymphadenopathy. On neurological examination, her mental status was normal. The cranial nerves were normal, as was coordination. There was mild generalized distal‐dominant motor weakness with generalized hyporeflexia. Sensory testing demonstrated glove‐and‐stocking type loss of sensation to pinpricks as well as dysesthesia in all extremities. Phalen and Tinel tests were negative.
The elevated venous pressure and pitting edema with slow recovery suggest high venous pressure edema rather than hypoproteinemic edema. Complete bilateral dullness of the chest and shifting dullness of the abdomen indicate the presence of bilateral pleural effusion and ascites. Edema from high venous pressure is usually caused by right, left, or biventricular cardiac failure. A fixed splitting of the second heart sound suggests an atrial septal defect, which is a rare cause of progressive right heart failure in adults. I recommend checking the patient's thyroid function to investigate the possibility of hypothyroidism, which is a common illness among middle‐aged women and could contribute to her edema as well as hirsutism. The neurological findings suggest a generalized polyneuropathy. The unusual combination of high venous pressure edema and polyneuropathy may indicate a rare multisystem disorder such as amyloidosis. Alternatively, the patient might have developed multiple diseases during the same time period. For instance, diabetic polyneuropathy is the most common cause of polyneuropathy among the middle‐aged. Finally, the differential diagnosis of hirsutism includes ovarian, adrenal, or pituitary sources of hyperandrogenism in addition to hypothyroidism. I would first evaluate for diabetes, thyroid disease, and cardiac disease and would like to see the results of laboratory tests for thyrotropin and plasma glucose as well as chest radiography and electrocardiography.
The white‐cell count was 5400/mm3 with a normal differential. Hemoglobin was 10.7 g/dL with normal red‐cell indices, and the platelet count was 276,000/mm3. The erythrocyte sedimentation rate was 29 mm/hour. Other laboratory tests revealed the following values: total protein, 6.2 g/dL; albumin, 3.3 g/dL; blood urea nitrogen, 12 mg/dL; creatinine, 0.7 mg/dL; aspartate aminotransferase, 6 U/L; alanine aminotransferase, 2 U/L; lactate dehydrogenase, 96 U/L; alkaline phosphatase, 115 U/L; creatine phosphokinase, 60 U/L; total bilirubin, 0.9 mg/dL; glucose, 96 mg/dL; hemoglobin A1c, 4.6%; total cholesterol, 111 mg/dL; and thyrotropin, 6.32 mIU/mL (normal range, 0.50‐5.00 mIU/mL). Serum free thyroxine, triiodothyronine, and urine testosterone were normal. Serum dehydroepiandrosterone sulfate was mildly elevated for her age (864 ng/mL: normal range, 180‐750 ng/mL). Serological studies for human immunodeficiency virus, human T‐lymphotrophic virus type 1, and syphilis were negative. Urinalysis was weakly positive for protein but negative for casts and occult blood. The stool was negative for occult blood.
A chest radiograph showed bilateral pleural effusions. Computed tomography demonstrated bilateral pleural effusions, ascites, mild hepatomegaly, and small, multiple, mediastinal lymph nodes. Her electrocardiogram was normal. A transesophageal echocardiogram with agitated saline contrast demonstrated normal ventricular systolic and diastolic function and no atrial septal defect. The inferior vena cava did not collapse with inspiration, and there was no evidence of infiltrative cardiomyopathy.
These laboratory results rule out diabetes as the cause of the polyneuropathy. The subclinical hypothyroidism would not explain profound edema and hirsutism. A serum albumin level of 3.3 g/dL confirms high venous pressure edema rather than hypoproteinemic edema. Normochromic, normocytic anemia and a mildly elevated sedimentation rate point to a chronic illness or inflammatory state. The mediastinal lymphadenopathy may reflect congestion as a result of the high venous pressure or reflect a systemic disease involving lymph nodes. Normal ventricular function with high venous pressure is suggestive of heart failure from diastolic dysfunction, although the patient does not have risk factors for diastolic dysfunction, such as hypertension, and has no other echocardiographic features of diastolic impairment. The combination of hyperandrogenism and neuropathy points to a systemic process, such as a paraneoplastic syndrome. I would next investigate the source of the excess androgens.
Because serum dehydroepiandrosterone sulfate was mildly elevated, I‐131 aldosterol scintigraphy was performed, and it was negative. Electromyography showed a pattern of generalized sensorimotor polyneuropathy.
At this point, it appears that cardiac, endocrine, hepatic, and renal diseases have been largely ruled out as a cause of her symptoms. Reframing and unifying the important clinical problems for this patient may be useful in resolving this diagnostic puzzle. They include (1) systemic high venous pressure edema; (2) generalized sensorimotor polyneuropathy; (3) hirsutism; (4) normocytic, normochromic anemia; (5) an elevated erythrocyte sedimentation rate; (6) mediastinal lymphadenopathy; and (7) subclinical hypothyroidism. At this point, I cannot unify these pieces of information into a single diagnosis. I would search the medical literature, focusing on these terms.
A general internist consultant performed MEDLINE and Google Scholar searches using the key words edema, polyneuropathy, and hirsutism. This search suggested the diagnosis of Crow‐Fukase syndrome, also known as POEMS (polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes) syndrome. Subsequent evaluations were performed. First, serum protein electrophoresis revealed the presence of monoclonal proteins, although hypergammaglobulinemia was not present. Second, a bone marrow examination demonstrated increased abnormal plasma cell proliferation (7%), although a radiographic skeletal survey found no lesions suggestive of plasmacytoma. Third, cerebrospinal fluid analysis showed normal cell counts but increased protein concentration (202 mg/dL). Fourth, a blood sample referred to an outside laboratory demonstrated elevated levels of vascular endothelial growth factor (3902 pg/mL: normal range, 150‐500 pg/mL). On the basis of these findings, the diagnosis of POEMS syndrome was made. After oral prednisolone (40 mg/day) was initiated, the systemic edema improved gradually, and she did well during the 2‐year follow‐up period.
Commentary
POEMS syndrome, also known as Crow‐Fukase syndrome, is a rare multisystem disorder first described by Crow in 1956.1, 2 It is characterized by polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes, as indicated by the acronym. The diagnosis of POEMS syndrome is difficult as this syndrome is rare and requires high clinical suspicion. According to a nationwide cross‐sectional survey in Japan, the prevalence of POEMS syndrome is very low (about 3 patients per 1,000,000 persons),3 and its prevalence in Western countries is considered even lower than that in Japan. The average age at onset is around 45 to 50 years old, and men are twice as likely to have this syndrome as women.46 Table 1 shows the diagnostic criteria of POEMS syndrome, based on research by Dispenzieri and others at the Mayo Clinic, and Table 2 presents the relative frequency of these clinical features.6, 7 The initial symptomatology generally includes polyneuropathy, skin changes, and generalized edema, which are nonspecific symptoms, as are other well‐recognized associated conditions such as clubbing, weight loss, thrombocytosis, polycythemia, and hyperhidrosis. Thus, it is important to consider this syndrome when one is facing an undiagnosed illness involving multiple organ systems and to distinguish it from other conditions such as multiple myeloma, amyloidosis, and monoclonal gammopathy of undetermined significance. Vascular endothelial growth factor is thought to be involved in the edema of POEMS syndrome, as massive release from aggregated platelets increases vascular permeability and venous pressure.710
| |
| Major criteria | Polyneuropathy |
| Monoclonal plasma cell‐proliferative disorder | |
| Minor criteria | Sclerotic bone lesions |
| Castleman disease | |
| Organomegaly (splenomegaly, hepatomegaly, or lymphadenopathy) | |
| Edema (peripheral edema, pleural effusion, or ascites) | |
| Endocrinopathy (adrenal, thyroid, pituitary, gonadal, parathyroid, or pancreatic) | |
| Skin changes (hyperpigmentation, hirsutism, plethora, hemangiomata, and white nails) | |
| Papilledema | |
| Characteristic | % |
|---|---|
| |
| Peripheral neuropathy | 100 |
| Monoclonal plasma cell dyscrasia | 100 |
| Sclerotic bone lesions | 97 |
| Endocrinopathy | 71 |
| Skin changes | 68 |
| Organomegaly | 46 |
| Extravascular volume overload | 39 |
| Papilledema | 29 |
| Castleman disease | 11 |
Data regarding treatment and survival are largely observational. Overall mean survival from diagnosis in the 2003 Dispenzieri cohort was 13.7 years, with death often due to infection or cardiorespiratory failure.6 When a solitary plasmacytoma or osteosclerotic myeloma is present, radiation to the lesion can often lead to clinical remission. Other treatment options include alkylating agents and/or high‐dose chemotherapy with peripheral stem‐cell transplantation, corticosteroids, and supportive care.7
Clinicians frequently use the internet to aid in the clinical decision process. In a survey of the Royal New Zealand College of General Practitioners,11 half reported that they used the Internet to search for clinical information. Two well‐known resources are MEDLINE, which contains over 11 million references dating back to the 1960s, and internet search engines such as Google (and a more recent product, Google Scholar, which attempts to sort search results by including factors such as the author, the publication in which the article appears, and how often the article has been cited).
MEDLINE searches a well‐defined set of journals and uses the Medical Subject Headings (MeSH) vocabulary, which consists of sets of descriptive terms organized in a hierarchical structure to allow searching with various levels of specificity. For instance, entering the term heart attack will map to the MeSH term myocardial infarction and will also include more specific terms such as myocardial stunning and cardiogenic shock.
Google, in comparison, explores resources beyond journals without any clear boundary to its scope, and its advanced search functions can be occasionally unreliable. For instance, search results are occasionally marred by outdated citation information and may include materials that are not truly scholarly. However, search engines can search through the actual text of manuscripts and access the gray literature, which includes open‐source material that is usually original but not widely distributed or often easily available, such as technical reports and dissertations. A direct study comparing the results of searches in PubMed (one of the MEDLINE search engines) and Google Scholar is difficult, but the critical characteristics of each can be compared and contrasted (Table 3).
| Google Scholar | PubMed |
|---|---|
| 1. Database selection is clumped under subject areas, and it cannot be searched with unique identifiers: Con | 1. It allows one to choose a database at the outset and can search with a unique identifier (PubMed identifier): Pro |
| 2. Results cannot be filtered (ie, it does not allow multiple article selection): Con | 2. The single citation matcher allows retrieval of articles with pieces of information: Pro |
| 3. A search for related articles or similar pages is not available: Con | 3. It allows article selection by checkbox to reduce the number of articles relevant to the search query and to append the filter to search box: Pro |
| 4. It allows one to search by without words to exclude unwanted and confusing retrieved data: Pro | 4. It provides unique identifier (PubMed identifier) for each retrieved article for easy communicability: Pro |
| 5. It allows one to search a single journal/publication of interest: Pro | 5. Search are limited to journals only; it does not include the grey area of literature: Con |
| 6. Initial search results are those articles that are most cited by journals that themselves are the most cited: Pro | 6. It lists search results in chronological order and not by relevance: Con |
Internet searches may also suggest diagnoses from a compilation of clinical features, such as in this case. To be successful, such a search must complement the cognitive process; a search engine cannot completely replace clinical judgment. Clinicians must be able to identify salient clinical features and generate high‐yield search terms and then exercise skill in sifting through the citations to arrive at the appropriate diagnosis. A recent study found that Google searches revealed the correct diagnosis in 58% of the case records of the New England Journal of Medicine,12 although each search query resulted in many results, which then had to be manually reviewed for appropriateness within the case's context.
Like a traditional diagnostic test, a search can be described by sensitivity, specificity, and the number of articles needed to read.13 For example, in a study comparing the performance of search strategies to identify clinical practice guidelines in Google Scholar and SUMSearch (another freely accessible search engine), using the term guideline yielded the highest sensitivity, and using the term practice guideline generated the highest specificity and the lowest number of articles needed to read (Table 4).14
| Search Strategy | Sensitivity (%) | Specificity (%) | NNR |
|---|---|---|---|
| |||
| SUMSearch | |||
| Guideline* | 81.51 (74.5388.49) | 74.29 (72.6475.94) | 8.18 (6.9010.05) |
| Recommendation* | 60.50 (51.7269.28) | 76.28 (74.6777.89) | 9.93 (8.1412.72) |
| Practice guideline* | 40.34 (31.5249.16) | 89.45 (88.2990.61) | 6.96 (5.529.43) |
| Google Scholar | |||
| Guideline/s | 31.93 (23.5640.30) | 78.05 (76.5079.60) | 16.67 (12.7624.04) |
| Recommendation/s | 8.40 (3.4213.38) | 92.11 (91.0993.13) | 22.42 (13.9756.82) |
| Practice guideline/s | 11.76 (5.9817.54) | 95.72 (94.9696.48) | 9.29 (6.2118.38) |
Although there are several other popular hosts of web‐based search engines, a more robust decision‐support program may help physicians more efficiently consider relevant diagnoses. One program, named Isabel, has been developed through the indexing of a database of more than 11,000 diseases according to word patterns in journal articles associated with each disease, and it is updated as new and relevant articles emerge. One recent study demonstrated that the correct diagnosis was made in 48 of 50 cases (96%) with specific, key findings as search terms but in only 37 of the same 50 cases (74%) if the entire case history was simply pasted in, again emphasizing the importance of specific search terms.15
POEMS syndrome is a rare entity occasionally seen in middle‐aged individuals and marked by a multitude of nonspecific findings, particularly polyneuropathy and plasma cell dyscrasia. In this case, the diagnostic test was an internet search based on the most prominent clinical symptoms. Such a strategy can provide a powerful addition to traditional literature and MEDLINE resources. However, the efficiency of this process is heavily dependent on the quality of the search strategy and, therefore, the cognitive faculties of the treating physician to avoid the predictable shortcoming of low specificity. Garbage in, garbage out still applies whether the computer in question is the human mind or the desktop PC.
Teaching Points
-
POEMS syndrome, also known as Crow‐Fukase syndrome, is a rare multisystem disorder characterized by polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes.
-
Internet‐based searches, including Google and MEDLINE, are being used more frequently because they are widely available, quick, and freely accessed.
-
Internet searches appear most useful as adjuncts to PubMed and clinical reasoning in identifying case reports when a well‐constructed collection of symptoms and signs is used for searches.
- .Peripheral neuritis in myelomatosis.Br Med J.1956;2(4996):802–804.
- ,,,,,.Plasma cell dyscrasia with polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes: the POEMS syndrome. Report on two cases and a review of the literature.Medicine (Baltimore).1980;59(4):311–322.
- .Nationwide Epidemiologic Survey of Crow‐Fukase Syndrome in 2004.Tokyo, Japan:Japanese Ministry of Health and Welfare Government Report, 2004.
- ,,, et al.The Crow‐Fukase syndrome: a study of 102 cases in Japan.Neurology.1984;34(6):712–720.
- ,,.POEMS syndrome: a study of 25 cases and a review of the literature. French Study Group on POEMS Syndrome.Am J Med.1994;97(6):543–553.
- ,,, et al.POEMS syndrome: definitions and long‐term outcome.Blood.2003;101(7):2496–2506.
- .POEMS syndrome.Hematology.2005;1(1):360–367.
- ,,,,.Greatly raised vascular endothelial growth factor (VEGF) in POEMS syndrome.Lancet.1996;347(9002):702.
- ,.Assessment of hypoproteinaemic oedema: a simple physical sign.Br Med J.1978;1(6117):890–891.
- ,,, et al.Ratio of serum vascular endothelial growth factor to platelet count correlates with disease activity in a patient with POEMS syndrome.Eur J Intern Med.2002;13(1):70–74.
- .In search of evidence: family practitioners' use of the Internet for clinical information.J Med Libr Assoc.2002;90(4):370–379.
- ,.Googling for a diagnosis—use of Google as a diagnostic aid: internet based study.BMJ.2006;333(7579):1143–5114.
- ,,.The number needed to read—a new measure of journal value.Health Info Libr J.2005;22(2):81–82.
- ,,,.Developing search strategies for clinical practice guidelines in SUMSearch and Google Scholar and assessing their retrieval performance.BMC Med Res Methodol.2007;7:28.
- ,.Performance of a web‐based clinical diagnosis support system for internists.J Gen Intern Med.2008;23(suppl 1):37–40.
The approach to clinical conundrums by an expert clinician is revealed through the presentation of an actual patient's case in an approach typical of a morning report. Similarly to patient care, sequential pieces of information are provided to the clinician, who is unfamiliar with the case. The focus is on the thought processes of both the clinical team caring for the patient and the discussant.
A 52‐year‐old woman presented with a 3‐month history of progressive bilateral leg edema and dyspnea while climbing a flight of stairs or while walking up a steep slope. She also complained of a tingling sensation in both hands and fingers, which started about 2 months prior to the onset of edema. She did not describe sensory problems in the lower extremities and did not have any other neurological complaints. She denied fever, cough, chest pain, palpitations, orthopnea, paroxysmal nocturnal dyspnea, and dark stools. She had no history of hypertension, diabetes, dyslipidemia, or asthma and had never been hospitalized. She did not smoke or consume alcohol and used no medications, including over‐the‐counter drugs or dietary supplements. The patient was born in Japan and had not traveled outside the country since her birth. She was a homemaker and had worked occasionally as a manual laborer in sugar cane agriculture. A review of systems revealed no history of polydipsia, polyuria, or cold or heat intolerance but did identify new hair growth, especially on the extremities.
This middle‐aged woman shows progressive changes in her general health status that are characterized by edema and dyspnea on effort. The differential diagnosis of edema includes a broad spectrum of illnesses, such as cardiac, lung, renal, endocrine, and hepatic diseases. Because of the life‐threatening potential, my first concern is cardiac disease, although the patient is not experiencing typical symptoms of ischemic heart disease or congestive failure. Bilateral and distal distribution of neuropathic symptoms is likely due to diseases of peripheral nerves rather than those of the central nervous system. Her complaint of a bilateral tingling sensation in the hands may suggest carpal tunnel syndrome as a result of her long‐term agricultural work. Other possible causes include radiculopathy of the cervical spine or polyneuropathy. Clues in the physical examination may help narrow the differential diagnosis to a cardiac, hepatic, or endocrine disorder.
The patient appeared ill. Her weight had increased from 48 to 61 kg since she was last weighed 6 months previously. Her blood pressure was 140/78 mm Hg, her heart rate was 72 beats/minute with a regular rhythm, her respiratory rate was 18/minute, and her temperature was 37.5C. The jugular venous pressure was elevated at 10 cm above the sternal angle. A grade III/VI systolic ejection murmur was evident at the second interspace along the left sternal border. The second heart sound was fixed and split. There were decreased breath sounds and complete dullness to percussion over both lower lung fields. Shifting dullness was noted on abdominal examination. There was pitting edema from the feet to the thighs, with slow pit‐recovery time in both legs, and she exhibited generalized hirsutism on the face, body, and extremities. There was no lymphadenopathy. On neurological examination, her mental status was normal. The cranial nerves were normal, as was coordination. There was mild generalized distal‐dominant motor weakness with generalized hyporeflexia. Sensory testing demonstrated glove‐and‐stocking type loss of sensation to pinpricks as well as dysesthesia in all extremities. Phalen and Tinel tests were negative.
The elevated venous pressure and pitting edema with slow recovery suggest high venous pressure edema rather than hypoproteinemic edema. Complete bilateral dullness of the chest and shifting dullness of the abdomen indicate the presence of bilateral pleural effusion and ascites. Edema from high venous pressure is usually caused by right, left, or biventricular cardiac failure. A fixed splitting of the second heart sound suggests an atrial septal defect, which is a rare cause of progressive right heart failure in adults. I recommend checking the patient's thyroid function to investigate the possibility of hypothyroidism, which is a common illness among middle‐aged women and could contribute to her edema as well as hirsutism. The neurological findings suggest a generalized polyneuropathy. The unusual combination of high venous pressure edema and polyneuropathy may indicate a rare multisystem disorder such as amyloidosis. Alternatively, the patient might have developed multiple diseases during the same time period. For instance, diabetic polyneuropathy is the most common cause of polyneuropathy among the middle‐aged. Finally, the differential diagnosis of hirsutism includes ovarian, adrenal, or pituitary sources of hyperandrogenism in addition to hypothyroidism. I would first evaluate for diabetes, thyroid disease, and cardiac disease and would like to see the results of laboratory tests for thyrotropin and plasma glucose as well as chest radiography and electrocardiography.
The white‐cell count was 5400/mm3 with a normal differential. Hemoglobin was 10.7 g/dL with normal red‐cell indices, and the platelet count was 276,000/mm3. The erythrocyte sedimentation rate was 29 mm/hour. Other laboratory tests revealed the following values: total protein, 6.2 g/dL; albumin, 3.3 g/dL; blood urea nitrogen, 12 mg/dL; creatinine, 0.7 mg/dL; aspartate aminotransferase, 6 U/L; alanine aminotransferase, 2 U/L; lactate dehydrogenase, 96 U/L; alkaline phosphatase, 115 U/L; creatine phosphokinase, 60 U/L; total bilirubin, 0.9 mg/dL; glucose, 96 mg/dL; hemoglobin A1c, 4.6%; total cholesterol, 111 mg/dL; and thyrotropin, 6.32 mIU/mL (normal range, 0.50‐5.00 mIU/mL). Serum free thyroxine, triiodothyronine, and urine testosterone were normal. Serum dehydroepiandrosterone sulfate was mildly elevated for her age (864 ng/mL: normal range, 180‐750 ng/mL). Serological studies for human immunodeficiency virus, human T‐lymphotrophic virus type 1, and syphilis were negative. Urinalysis was weakly positive for protein but negative for casts and occult blood. The stool was negative for occult blood.
A chest radiograph showed bilateral pleural effusions. Computed tomography demonstrated bilateral pleural effusions, ascites, mild hepatomegaly, and small, multiple, mediastinal lymph nodes. Her electrocardiogram was normal. A transesophageal echocardiogram with agitated saline contrast demonstrated normal ventricular systolic and diastolic function and no atrial septal defect. The inferior vena cava did not collapse with inspiration, and there was no evidence of infiltrative cardiomyopathy.
These laboratory results rule out diabetes as the cause of the polyneuropathy. The subclinical hypothyroidism would not explain profound edema and hirsutism. A serum albumin level of 3.3 g/dL confirms high venous pressure edema rather than hypoproteinemic edema. Normochromic, normocytic anemia and a mildly elevated sedimentation rate point to a chronic illness or inflammatory state. The mediastinal lymphadenopathy may reflect congestion as a result of the high venous pressure or reflect a systemic disease involving lymph nodes. Normal ventricular function with high venous pressure is suggestive of heart failure from diastolic dysfunction, although the patient does not have risk factors for diastolic dysfunction, such as hypertension, and has no other echocardiographic features of diastolic impairment. The combination of hyperandrogenism and neuropathy points to a systemic process, such as a paraneoplastic syndrome. I would next investigate the source of the excess androgens.
Because serum dehydroepiandrosterone sulfate was mildly elevated, I‐131 aldosterol scintigraphy was performed, and it was negative. Electromyography showed a pattern of generalized sensorimotor polyneuropathy.
At this point, it appears that cardiac, endocrine, hepatic, and renal diseases have been largely ruled out as a cause of her symptoms. Reframing and unifying the important clinical problems for this patient may be useful in resolving this diagnostic puzzle. They include (1) systemic high venous pressure edema; (2) generalized sensorimotor polyneuropathy; (3) hirsutism; (4) normocytic, normochromic anemia; (5) an elevated erythrocyte sedimentation rate; (6) mediastinal lymphadenopathy; and (7) subclinical hypothyroidism. At this point, I cannot unify these pieces of information into a single diagnosis. I would search the medical literature, focusing on these terms.
A general internist consultant performed MEDLINE and Google Scholar searches using the key words edema, polyneuropathy, and hirsutism. This search suggested the diagnosis of Crow‐Fukase syndrome, also known as POEMS (polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes) syndrome. Subsequent evaluations were performed. First, serum protein electrophoresis revealed the presence of monoclonal proteins, although hypergammaglobulinemia was not present. Second, a bone marrow examination demonstrated increased abnormal plasma cell proliferation (7%), although a radiographic skeletal survey found no lesions suggestive of plasmacytoma. Third, cerebrospinal fluid analysis showed normal cell counts but increased protein concentration (202 mg/dL). Fourth, a blood sample referred to an outside laboratory demonstrated elevated levels of vascular endothelial growth factor (3902 pg/mL: normal range, 150‐500 pg/mL). On the basis of these findings, the diagnosis of POEMS syndrome was made. After oral prednisolone (40 mg/day) was initiated, the systemic edema improved gradually, and she did well during the 2‐year follow‐up period.
Commentary
POEMS syndrome, also known as Crow‐Fukase syndrome, is a rare multisystem disorder first described by Crow in 1956.1, 2 It is characterized by polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes, as indicated by the acronym. The diagnosis of POEMS syndrome is difficult as this syndrome is rare and requires high clinical suspicion. According to a nationwide cross‐sectional survey in Japan, the prevalence of POEMS syndrome is very low (about 3 patients per 1,000,000 persons),3 and its prevalence in Western countries is considered even lower than that in Japan. The average age at onset is around 45 to 50 years old, and men are twice as likely to have this syndrome as women.46 Table 1 shows the diagnostic criteria of POEMS syndrome, based on research by Dispenzieri and others at the Mayo Clinic, and Table 2 presents the relative frequency of these clinical features.6, 7 The initial symptomatology generally includes polyneuropathy, skin changes, and generalized edema, which are nonspecific symptoms, as are other well‐recognized associated conditions such as clubbing, weight loss, thrombocytosis, polycythemia, and hyperhidrosis. Thus, it is important to consider this syndrome when one is facing an undiagnosed illness involving multiple organ systems and to distinguish it from other conditions such as multiple myeloma, amyloidosis, and monoclonal gammopathy of undetermined significance. Vascular endothelial growth factor is thought to be involved in the edema of POEMS syndrome, as massive release from aggregated platelets increases vascular permeability and venous pressure.710
| |
| Major criteria | Polyneuropathy |
| Monoclonal plasma cell‐proliferative disorder | |
| Minor criteria | Sclerotic bone lesions |
| Castleman disease | |
| Organomegaly (splenomegaly, hepatomegaly, or lymphadenopathy) | |
| Edema (peripheral edema, pleural effusion, or ascites) | |
| Endocrinopathy (adrenal, thyroid, pituitary, gonadal, parathyroid, or pancreatic) | |
| Skin changes (hyperpigmentation, hirsutism, plethora, hemangiomata, and white nails) | |
| Papilledema | |
| Characteristic | % |
|---|---|
| |
| Peripheral neuropathy | 100 |
| Monoclonal plasma cell dyscrasia | 100 |
| Sclerotic bone lesions | 97 |
| Endocrinopathy | 71 |
| Skin changes | 68 |
| Organomegaly | 46 |
| Extravascular volume overload | 39 |
| Papilledema | 29 |
| Castleman disease | 11 |
Data regarding treatment and survival are largely observational. Overall mean survival from diagnosis in the 2003 Dispenzieri cohort was 13.7 years, with death often due to infection or cardiorespiratory failure.6 When a solitary plasmacytoma or osteosclerotic myeloma is present, radiation to the lesion can often lead to clinical remission. Other treatment options include alkylating agents and/or high‐dose chemotherapy with peripheral stem‐cell transplantation, corticosteroids, and supportive care.7
Clinicians frequently use the internet to aid in the clinical decision process. In a survey of the Royal New Zealand College of General Practitioners,11 half reported that they used the Internet to search for clinical information. Two well‐known resources are MEDLINE, which contains over 11 million references dating back to the 1960s, and internet search engines such as Google (and a more recent product, Google Scholar, which attempts to sort search results by including factors such as the author, the publication in which the article appears, and how often the article has been cited).
MEDLINE searches a well‐defined set of journals and uses the Medical Subject Headings (MeSH) vocabulary, which consists of sets of descriptive terms organized in a hierarchical structure to allow searching with various levels of specificity. For instance, entering the term heart attack will map to the MeSH term myocardial infarction and will also include more specific terms such as myocardial stunning and cardiogenic shock.
Google, in comparison, explores resources beyond journals without any clear boundary to its scope, and its advanced search functions can be occasionally unreliable. For instance, search results are occasionally marred by outdated citation information and may include materials that are not truly scholarly. However, search engines can search through the actual text of manuscripts and access the gray literature, which includes open‐source material that is usually original but not widely distributed or often easily available, such as technical reports and dissertations. A direct study comparing the results of searches in PubMed (one of the MEDLINE search engines) and Google Scholar is difficult, but the critical characteristics of each can be compared and contrasted (Table 3).
| Google Scholar | PubMed |
|---|---|
| 1. Database selection is clumped under subject areas, and it cannot be searched with unique identifiers: Con | 1. It allows one to choose a database at the outset and can search with a unique identifier (PubMed identifier): Pro |
| 2. Results cannot be filtered (ie, it does not allow multiple article selection): Con | 2. The single citation matcher allows retrieval of articles with pieces of information: Pro |
| 3. A search for related articles or similar pages is not available: Con | 3. It allows article selection by checkbox to reduce the number of articles relevant to the search query and to append the filter to search box: Pro |
| 4. It allows one to search by without words to exclude unwanted and confusing retrieved data: Pro | 4. It provides unique identifier (PubMed identifier) for each retrieved article for easy communicability: Pro |
| 5. It allows one to search a single journal/publication of interest: Pro | 5. Search are limited to journals only; it does not include the grey area of literature: Con |
| 6. Initial search results are those articles that are most cited by journals that themselves are the most cited: Pro | 6. It lists search results in chronological order and not by relevance: Con |
Internet searches may also suggest diagnoses from a compilation of clinical features, such as in this case. To be successful, such a search must complement the cognitive process; a search engine cannot completely replace clinical judgment. Clinicians must be able to identify salient clinical features and generate high‐yield search terms and then exercise skill in sifting through the citations to arrive at the appropriate diagnosis. A recent study found that Google searches revealed the correct diagnosis in 58% of the case records of the New England Journal of Medicine,12 although each search query resulted in many results, which then had to be manually reviewed for appropriateness within the case's context.
Like a traditional diagnostic test, a search can be described by sensitivity, specificity, and the number of articles needed to read.13 For example, in a study comparing the performance of search strategies to identify clinical practice guidelines in Google Scholar and SUMSearch (another freely accessible search engine), using the term guideline yielded the highest sensitivity, and using the term practice guideline generated the highest specificity and the lowest number of articles needed to read (Table 4).14
| Search Strategy | Sensitivity (%) | Specificity (%) | NNR |
|---|---|---|---|
| |||
| SUMSearch | |||
| Guideline* | 81.51 (74.5388.49) | 74.29 (72.6475.94) | 8.18 (6.9010.05) |
| Recommendation* | 60.50 (51.7269.28) | 76.28 (74.6777.89) | 9.93 (8.1412.72) |
| Practice guideline* | 40.34 (31.5249.16) | 89.45 (88.2990.61) | 6.96 (5.529.43) |
| Google Scholar | |||
| Guideline/s | 31.93 (23.5640.30) | 78.05 (76.5079.60) | 16.67 (12.7624.04) |
| Recommendation/s | 8.40 (3.4213.38) | 92.11 (91.0993.13) | 22.42 (13.9756.82) |
| Practice guideline/s | 11.76 (5.9817.54) | 95.72 (94.9696.48) | 9.29 (6.2118.38) |
Although there are several other popular hosts of web‐based search engines, a more robust decision‐support program may help physicians more efficiently consider relevant diagnoses. One program, named Isabel, has been developed through the indexing of a database of more than 11,000 diseases according to word patterns in journal articles associated with each disease, and it is updated as new and relevant articles emerge. One recent study demonstrated that the correct diagnosis was made in 48 of 50 cases (96%) with specific, key findings as search terms but in only 37 of the same 50 cases (74%) if the entire case history was simply pasted in, again emphasizing the importance of specific search terms.15
POEMS syndrome is a rare entity occasionally seen in middle‐aged individuals and marked by a multitude of nonspecific findings, particularly polyneuropathy and plasma cell dyscrasia. In this case, the diagnostic test was an internet search based on the most prominent clinical symptoms. Such a strategy can provide a powerful addition to traditional literature and MEDLINE resources. However, the efficiency of this process is heavily dependent on the quality of the search strategy and, therefore, the cognitive faculties of the treating physician to avoid the predictable shortcoming of low specificity. Garbage in, garbage out still applies whether the computer in question is the human mind or the desktop PC.
Teaching Points
-
POEMS syndrome, also known as Crow‐Fukase syndrome, is a rare multisystem disorder characterized by polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes.
-
Internet‐based searches, including Google and MEDLINE, are being used more frequently because they are widely available, quick, and freely accessed.
-
Internet searches appear most useful as adjuncts to PubMed and clinical reasoning in identifying case reports when a well‐constructed collection of symptoms and signs is used for searches.
The approach to clinical conundrums by an expert clinician is revealed through the presentation of an actual patient's case in an approach typical of a morning report. Similarly to patient care, sequential pieces of information are provided to the clinician, who is unfamiliar with the case. The focus is on the thought processes of both the clinical team caring for the patient and the discussant.
A 52‐year‐old woman presented with a 3‐month history of progressive bilateral leg edema and dyspnea while climbing a flight of stairs or while walking up a steep slope. She also complained of a tingling sensation in both hands and fingers, which started about 2 months prior to the onset of edema. She did not describe sensory problems in the lower extremities and did not have any other neurological complaints. She denied fever, cough, chest pain, palpitations, orthopnea, paroxysmal nocturnal dyspnea, and dark stools. She had no history of hypertension, diabetes, dyslipidemia, or asthma and had never been hospitalized. She did not smoke or consume alcohol and used no medications, including over‐the‐counter drugs or dietary supplements. The patient was born in Japan and had not traveled outside the country since her birth. She was a homemaker and had worked occasionally as a manual laborer in sugar cane agriculture. A review of systems revealed no history of polydipsia, polyuria, or cold or heat intolerance but did identify new hair growth, especially on the extremities.
This middle‐aged woman shows progressive changes in her general health status that are characterized by edema and dyspnea on effort. The differential diagnosis of edema includes a broad spectrum of illnesses, such as cardiac, lung, renal, endocrine, and hepatic diseases. Because of the life‐threatening potential, my first concern is cardiac disease, although the patient is not experiencing typical symptoms of ischemic heart disease or congestive failure. Bilateral and distal distribution of neuropathic symptoms is likely due to diseases of peripheral nerves rather than those of the central nervous system. Her complaint of a bilateral tingling sensation in the hands may suggest carpal tunnel syndrome as a result of her long‐term agricultural work. Other possible causes include radiculopathy of the cervical spine or polyneuropathy. Clues in the physical examination may help narrow the differential diagnosis to a cardiac, hepatic, or endocrine disorder.
The patient appeared ill. Her weight had increased from 48 to 61 kg since she was last weighed 6 months previously. Her blood pressure was 140/78 mm Hg, her heart rate was 72 beats/minute with a regular rhythm, her respiratory rate was 18/minute, and her temperature was 37.5C. The jugular venous pressure was elevated at 10 cm above the sternal angle. A grade III/VI systolic ejection murmur was evident at the second interspace along the left sternal border. The second heart sound was fixed and split. There were decreased breath sounds and complete dullness to percussion over both lower lung fields. Shifting dullness was noted on abdominal examination. There was pitting edema from the feet to the thighs, with slow pit‐recovery time in both legs, and she exhibited generalized hirsutism on the face, body, and extremities. There was no lymphadenopathy. On neurological examination, her mental status was normal. The cranial nerves were normal, as was coordination. There was mild generalized distal‐dominant motor weakness with generalized hyporeflexia. Sensory testing demonstrated glove‐and‐stocking type loss of sensation to pinpricks as well as dysesthesia in all extremities. Phalen and Tinel tests were negative.
The elevated venous pressure and pitting edema with slow recovery suggest high venous pressure edema rather than hypoproteinemic edema. Complete bilateral dullness of the chest and shifting dullness of the abdomen indicate the presence of bilateral pleural effusion and ascites. Edema from high venous pressure is usually caused by right, left, or biventricular cardiac failure. A fixed splitting of the second heart sound suggests an atrial septal defect, which is a rare cause of progressive right heart failure in adults. I recommend checking the patient's thyroid function to investigate the possibility of hypothyroidism, which is a common illness among middle‐aged women and could contribute to her edema as well as hirsutism. The neurological findings suggest a generalized polyneuropathy. The unusual combination of high venous pressure edema and polyneuropathy may indicate a rare multisystem disorder such as amyloidosis. Alternatively, the patient might have developed multiple diseases during the same time period. For instance, diabetic polyneuropathy is the most common cause of polyneuropathy among the middle‐aged. Finally, the differential diagnosis of hirsutism includes ovarian, adrenal, or pituitary sources of hyperandrogenism in addition to hypothyroidism. I would first evaluate for diabetes, thyroid disease, and cardiac disease and would like to see the results of laboratory tests for thyrotropin and plasma glucose as well as chest radiography and electrocardiography.
The white‐cell count was 5400/mm3 with a normal differential. Hemoglobin was 10.7 g/dL with normal red‐cell indices, and the platelet count was 276,000/mm3. The erythrocyte sedimentation rate was 29 mm/hour. Other laboratory tests revealed the following values: total protein, 6.2 g/dL; albumin, 3.3 g/dL; blood urea nitrogen, 12 mg/dL; creatinine, 0.7 mg/dL; aspartate aminotransferase, 6 U/L; alanine aminotransferase, 2 U/L; lactate dehydrogenase, 96 U/L; alkaline phosphatase, 115 U/L; creatine phosphokinase, 60 U/L; total bilirubin, 0.9 mg/dL; glucose, 96 mg/dL; hemoglobin A1c, 4.6%; total cholesterol, 111 mg/dL; and thyrotropin, 6.32 mIU/mL (normal range, 0.50‐5.00 mIU/mL). Serum free thyroxine, triiodothyronine, and urine testosterone were normal. Serum dehydroepiandrosterone sulfate was mildly elevated for her age (864 ng/mL: normal range, 180‐750 ng/mL). Serological studies for human immunodeficiency virus, human T‐lymphotrophic virus type 1, and syphilis were negative. Urinalysis was weakly positive for protein but negative for casts and occult blood. The stool was negative for occult blood.
A chest radiograph showed bilateral pleural effusions. Computed tomography demonstrated bilateral pleural effusions, ascites, mild hepatomegaly, and small, multiple, mediastinal lymph nodes. Her electrocardiogram was normal. A transesophageal echocardiogram with agitated saline contrast demonstrated normal ventricular systolic and diastolic function and no atrial septal defect. The inferior vena cava did not collapse with inspiration, and there was no evidence of infiltrative cardiomyopathy.
These laboratory results rule out diabetes as the cause of the polyneuropathy. The subclinical hypothyroidism would not explain profound edema and hirsutism. A serum albumin level of 3.3 g/dL confirms high venous pressure edema rather than hypoproteinemic edema. Normochromic, normocytic anemia and a mildly elevated sedimentation rate point to a chronic illness or inflammatory state. The mediastinal lymphadenopathy may reflect congestion as a result of the high venous pressure or reflect a systemic disease involving lymph nodes. Normal ventricular function with high venous pressure is suggestive of heart failure from diastolic dysfunction, although the patient does not have risk factors for diastolic dysfunction, such as hypertension, and has no other echocardiographic features of diastolic impairment. The combination of hyperandrogenism and neuropathy points to a systemic process, such as a paraneoplastic syndrome. I would next investigate the source of the excess androgens.
Because serum dehydroepiandrosterone sulfate was mildly elevated, I‐131 aldosterol scintigraphy was performed, and it was negative. Electromyography showed a pattern of generalized sensorimotor polyneuropathy.
At this point, it appears that cardiac, endocrine, hepatic, and renal diseases have been largely ruled out as a cause of her symptoms. Reframing and unifying the important clinical problems for this patient may be useful in resolving this diagnostic puzzle. They include (1) systemic high venous pressure edema; (2) generalized sensorimotor polyneuropathy; (3) hirsutism; (4) normocytic, normochromic anemia; (5) an elevated erythrocyte sedimentation rate; (6) mediastinal lymphadenopathy; and (7) subclinical hypothyroidism. At this point, I cannot unify these pieces of information into a single diagnosis. I would search the medical literature, focusing on these terms.
A general internist consultant performed MEDLINE and Google Scholar searches using the key words edema, polyneuropathy, and hirsutism. This search suggested the diagnosis of Crow‐Fukase syndrome, also known as POEMS (polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes) syndrome. Subsequent evaluations were performed. First, serum protein electrophoresis revealed the presence of monoclonal proteins, although hypergammaglobulinemia was not present. Second, a bone marrow examination demonstrated increased abnormal plasma cell proliferation (7%), although a radiographic skeletal survey found no lesions suggestive of plasmacytoma. Third, cerebrospinal fluid analysis showed normal cell counts but increased protein concentration (202 mg/dL). Fourth, a blood sample referred to an outside laboratory demonstrated elevated levels of vascular endothelial growth factor (3902 pg/mL: normal range, 150‐500 pg/mL). On the basis of these findings, the diagnosis of POEMS syndrome was made. After oral prednisolone (40 mg/day) was initiated, the systemic edema improved gradually, and she did well during the 2‐year follow‐up period.
Commentary
POEMS syndrome, also known as Crow‐Fukase syndrome, is a rare multisystem disorder first described by Crow in 1956.1, 2 It is characterized by polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes, as indicated by the acronym. The diagnosis of POEMS syndrome is difficult as this syndrome is rare and requires high clinical suspicion. According to a nationwide cross‐sectional survey in Japan, the prevalence of POEMS syndrome is very low (about 3 patients per 1,000,000 persons),3 and its prevalence in Western countries is considered even lower than that in Japan. The average age at onset is around 45 to 50 years old, and men are twice as likely to have this syndrome as women.46 Table 1 shows the diagnostic criteria of POEMS syndrome, based on research by Dispenzieri and others at the Mayo Clinic, and Table 2 presents the relative frequency of these clinical features.6, 7 The initial symptomatology generally includes polyneuropathy, skin changes, and generalized edema, which are nonspecific symptoms, as are other well‐recognized associated conditions such as clubbing, weight loss, thrombocytosis, polycythemia, and hyperhidrosis. Thus, it is important to consider this syndrome when one is facing an undiagnosed illness involving multiple organ systems and to distinguish it from other conditions such as multiple myeloma, amyloidosis, and monoclonal gammopathy of undetermined significance. Vascular endothelial growth factor is thought to be involved in the edema of POEMS syndrome, as massive release from aggregated platelets increases vascular permeability and venous pressure.710
| |
| Major criteria | Polyneuropathy |
| Monoclonal plasma cell‐proliferative disorder | |
| Minor criteria | Sclerotic bone lesions |
| Castleman disease | |
| Organomegaly (splenomegaly, hepatomegaly, or lymphadenopathy) | |
| Edema (peripheral edema, pleural effusion, or ascites) | |
| Endocrinopathy (adrenal, thyroid, pituitary, gonadal, parathyroid, or pancreatic) | |
| Skin changes (hyperpigmentation, hirsutism, plethora, hemangiomata, and white nails) | |
| Papilledema | |
| Characteristic | % |
|---|---|
| |
| Peripheral neuropathy | 100 |
| Monoclonal plasma cell dyscrasia | 100 |
| Sclerotic bone lesions | 97 |
| Endocrinopathy | 71 |
| Skin changes | 68 |
| Organomegaly | 46 |
| Extravascular volume overload | 39 |
| Papilledema | 29 |
| Castleman disease | 11 |
Data regarding treatment and survival are largely observational. Overall mean survival from diagnosis in the 2003 Dispenzieri cohort was 13.7 years, with death often due to infection or cardiorespiratory failure.6 When a solitary plasmacytoma or osteosclerotic myeloma is present, radiation to the lesion can often lead to clinical remission. Other treatment options include alkylating agents and/or high‐dose chemotherapy with peripheral stem‐cell transplantation, corticosteroids, and supportive care.7
Clinicians frequently use the internet to aid in the clinical decision process. In a survey of the Royal New Zealand College of General Practitioners,11 half reported that they used the Internet to search for clinical information. Two well‐known resources are MEDLINE, which contains over 11 million references dating back to the 1960s, and internet search engines such as Google (and a more recent product, Google Scholar, which attempts to sort search results by including factors such as the author, the publication in which the article appears, and how often the article has been cited).
MEDLINE searches a well‐defined set of journals and uses the Medical Subject Headings (MeSH) vocabulary, which consists of sets of descriptive terms organized in a hierarchical structure to allow searching with various levels of specificity. For instance, entering the term heart attack will map to the MeSH term myocardial infarction and will also include more specific terms such as myocardial stunning and cardiogenic shock.
Google, in comparison, explores resources beyond journals without any clear boundary to its scope, and its advanced search functions can be occasionally unreliable. For instance, search results are occasionally marred by outdated citation information and may include materials that are not truly scholarly. However, search engines can search through the actual text of manuscripts and access the gray literature, which includes open‐source material that is usually original but not widely distributed or often easily available, such as technical reports and dissertations. A direct study comparing the results of searches in PubMed (one of the MEDLINE search engines) and Google Scholar is difficult, but the critical characteristics of each can be compared and contrasted (Table 3).
| Google Scholar | PubMed |
|---|---|
| 1. Database selection is clumped under subject areas, and it cannot be searched with unique identifiers: Con | 1. It allows one to choose a database at the outset and can search with a unique identifier (PubMed identifier): Pro |
| 2. Results cannot be filtered (ie, it does not allow multiple article selection): Con | 2. The single citation matcher allows retrieval of articles with pieces of information: Pro |
| 3. A search for related articles or similar pages is not available: Con | 3. It allows article selection by checkbox to reduce the number of articles relevant to the search query and to append the filter to search box: Pro |
| 4. It allows one to search by without words to exclude unwanted and confusing retrieved data: Pro | 4. It provides unique identifier (PubMed identifier) for each retrieved article for easy communicability: Pro |
| 5. It allows one to search a single journal/publication of interest: Pro | 5. Search are limited to journals only; it does not include the grey area of literature: Con |
| 6. Initial search results are those articles that are most cited by journals that themselves are the most cited: Pro | 6. It lists search results in chronological order and not by relevance: Con |
Internet searches may also suggest diagnoses from a compilation of clinical features, such as in this case. To be successful, such a search must complement the cognitive process; a search engine cannot completely replace clinical judgment. Clinicians must be able to identify salient clinical features and generate high‐yield search terms and then exercise skill in sifting through the citations to arrive at the appropriate diagnosis. A recent study found that Google searches revealed the correct diagnosis in 58% of the case records of the New England Journal of Medicine,12 although each search query resulted in many results, which then had to be manually reviewed for appropriateness within the case's context.
Like a traditional diagnostic test, a search can be described by sensitivity, specificity, and the number of articles needed to read.13 For example, in a study comparing the performance of search strategies to identify clinical practice guidelines in Google Scholar and SUMSearch (another freely accessible search engine), using the term guideline yielded the highest sensitivity, and using the term practice guideline generated the highest specificity and the lowest number of articles needed to read (Table 4).14
| Search Strategy | Sensitivity (%) | Specificity (%) | NNR |
|---|---|---|---|
| |||
| SUMSearch | |||
| Guideline* | 81.51 (74.5388.49) | 74.29 (72.6475.94) | 8.18 (6.9010.05) |
| Recommendation* | 60.50 (51.7269.28) | 76.28 (74.6777.89) | 9.93 (8.1412.72) |
| Practice guideline* | 40.34 (31.5249.16) | 89.45 (88.2990.61) | 6.96 (5.529.43) |
| Google Scholar | |||
| Guideline/s | 31.93 (23.5640.30) | 78.05 (76.5079.60) | 16.67 (12.7624.04) |
| Recommendation/s | 8.40 (3.4213.38) | 92.11 (91.0993.13) | 22.42 (13.9756.82) |
| Practice guideline/s | 11.76 (5.9817.54) | 95.72 (94.9696.48) | 9.29 (6.2118.38) |
Although there are several other popular hosts of web‐based search engines, a more robust decision‐support program may help physicians more efficiently consider relevant diagnoses. One program, named Isabel, has been developed through the indexing of a database of more than 11,000 diseases according to word patterns in journal articles associated with each disease, and it is updated as new and relevant articles emerge. One recent study demonstrated that the correct diagnosis was made in 48 of 50 cases (96%) with specific, key findings as search terms but in only 37 of the same 50 cases (74%) if the entire case history was simply pasted in, again emphasizing the importance of specific search terms.15
POEMS syndrome is a rare entity occasionally seen in middle‐aged individuals and marked by a multitude of nonspecific findings, particularly polyneuropathy and plasma cell dyscrasia. In this case, the diagnostic test was an internet search based on the most prominent clinical symptoms. Such a strategy can provide a powerful addition to traditional literature and MEDLINE resources. However, the efficiency of this process is heavily dependent on the quality of the search strategy and, therefore, the cognitive faculties of the treating physician to avoid the predictable shortcoming of low specificity. Garbage in, garbage out still applies whether the computer in question is the human mind or the desktop PC.
Teaching Points
-
POEMS syndrome, also known as Crow‐Fukase syndrome, is a rare multisystem disorder characterized by polyneuropathy, organomegaly, endocrinopathy, monoclonal gammopathy, and skin changes.
-
Internet‐based searches, including Google and MEDLINE, are being used more frequently because they are widely available, quick, and freely accessed.
-
Internet searches appear most useful as adjuncts to PubMed and clinical reasoning in identifying case reports when a well‐constructed collection of symptoms and signs is used for searches.
- .Peripheral neuritis in myelomatosis.Br Med J.1956;2(4996):802–804.
- ,,,,,.Plasma cell dyscrasia with polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes: the POEMS syndrome. Report on two cases and a review of the literature.Medicine (Baltimore).1980;59(4):311–322.
- .Nationwide Epidemiologic Survey of Crow‐Fukase Syndrome in 2004.Tokyo, Japan:Japanese Ministry of Health and Welfare Government Report, 2004.
- ,,, et al.The Crow‐Fukase syndrome: a study of 102 cases in Japan.Neurology.1984;34(6):712–720.
- ,,.POEMS syndrome: a study of 25 cases and a review of the literature. French Study Group on POEMS Syndrome.Am J Med.1994;97(6):543–553.
- ,,, et al.POEMS syndrome: definitions and long‐term outcome.Blood.2003;101(7):2496–2506.
- .POEMS syndrome.Hematology.2005;1(1):360–367.
- ,,,,.Greatly raised vascular endothelial growth factor (VEGF) in POEMS syndrome.Lancet.1996;347(9002):702.
- ,.Assessment of hypoproteinaemic oedema: a simple physical sign.Br Med J.1978;1(6117):890–891.
- ,,, et al.Ratio of serum vascular endothelial growth factor to platelet count correlates with disease activity in a patient with POEMS syndrome.Eur J Intern Med.2002;13(1):70–74.
- .In search of evidence: family practitioners' use of the Internet for clinical information.J Med Libr Assoc.2002;90(4):370–379.
- ,.Googling for a diagnosis—use of Google as a diagnostic aid: internet based study.BMJ.2006;333(7579):1143–5114.
- ,,.The number needed to read—a new measure of journal value.Health Info Libr J.2005;22(2):81–82.
- ,,,.Developing search strategies for clinical practice guidelines in SUMSearch and Google Scholar and assessing their retrieval performance.BMC Med Res Methodol.2007;7:28.
- ,.Performance of a web‐based clinical diagnosis support system for internists.J Gen Intern Med.2008;23(suppl 1):37–40.
- .Peripheral neuritis in myelomatosis.Br Med J.1956;2(4996):802–804.
- ,,,,,.Plasma cell dyscrasia with polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes: the POEMS syndrome. Report on two cases and a review of the literature.Medicine (Baltimore).1980;59(4):311–322.
- .Nationwide Epidemiologic Survey of Crow‐Fukase Syndrome in 2004.Tokyo, Japan:Japanese Ministry of Health and Welfare Government Report, 2004.
- ,,, et al.The Crow‐Fukase syndrome: a study of 102 cases in Japan.Neurology.1984;34(6):712–720.
- ,,.POEMS syndrome: a study of 25 cases and a review of the literature. French Study Group on POEMS Syndrome.Am J Med.1994;97(6):543–553.
- ,,, et al.POEMS syndrome: definitions and long‐term outcome.Blood.2003;101(7):2496–2506.
- .POEMS syndrome.Hematology.2005;1(1):360–367.
- ,,,,.Greatly raised vascular endothelial growth factor (VEGF) in POEMS syndrome.Lancet.1996;347(9002):702.
- ,.Assessment of hypoproteinaemic oedema: a simple physical sign.Br Med J.1978;1(6117):890–891.
- ,,, et al.Ratio of serum vascular endothelial growth factor to platelet count correlates with disease activity in a patient with POEMS syndrome.Eur J Intern Med.2002;13(1):70–74.
- .In search of evidence: family practitioners' use of the Internet for clinical information.J Med Libr Assoc.2002;90(4):370–379.
- ,.Googling for a diagnosis—use of Google as a diagnostic aid: internet based study.BMJ.2006;333(7579):1143–5114.
- ,,.The number needed to read—a new measure of journal value.Health Info Libr J.2005;22(2):81–82.
- ,,,.Developing search strategies for clinical practice guidelines in SUMSearch and Google Scholar and assessing their retrieval performance.BMC Med Res Methodol.2007;7:28.
- ,.Performance of a web‐based clinical diagnosis support system for internists.J Gen Intern Med.2008;23(suppl 1):37–40.