User login
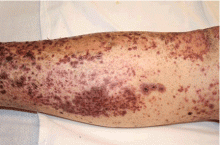
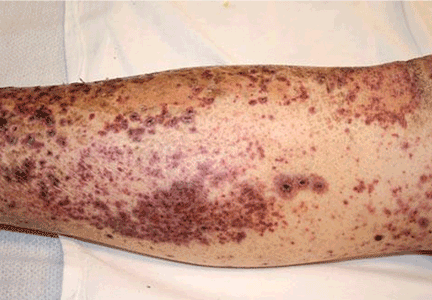
A 72-year-old man with a purpuric rash
A 72-year-old man whose medical history includes diabetes mellitus, hypertension, coronary artery disease, aortic valve replacement, atrial fibrillation, and chronic obstructive pulmonary disease was in his usual state of health until 2 weeks ago, when he developed a purpuric rash on his legs. His physician started him on prednisone 40 mg daily for the rash; however, 1 week later he presented to a hospital emergency room when his family found him confused and diaphoretic.
In the emergency room, he was found to be hypoglycemic, with a serum glucose level of 40 mg/dL, which was promptly treated. His mental status improved partially. In the hospital, the rash worsened and progressed upwards to his trunk and upper extremities. He was transferred to our institution for further workup and management.
A review of systems reveals occasional epistaxis in the summer, recent fatigue, cough, and shortness of breath on exertion. His medications at the time of transfer include warfarin (Coumadin), amlodipine (Norvasc), insulin, ipratropium and albuterol (Combivent) inhalers, and prednisone 40 mg daily. He has not undergone surgery recently.
PHYSICAL EXAMINATION
He is alert and oriented to person but not to time and place.
Vital signs. Oral temperature 101.1°F (38.4°C), pulse rate 108, blood pressure 108/79 mm/Hg, respiratory rate 22, oxygen saturation 93% by pulse oximetry on room air, weight 94 kg (207 lb).
Head, eyes, ears, nose, and throat. No pallor or icterus, pupils are equally reactive, nasal mucosa not inflamed or ulcerated, mucous membranes moist, no sinus tenderness.
Neck. No jugular venous distention and no cervical lymphadenopathy.
Cardiovascular. Tachycardia, irregularly irregular rhythm, prosthetic valve sounds, no murmurs, rubs, or gallops.
Respiratory. Bibasal crackles (right side more than the left). No wheezing.
Abdomen. Soft, nontender, nondistended, no palpable organomegaly, bowel sounds normal.
Extremities. No edema, good peripheral pulses.
Neurologic. No focal deficits noted.
Lymphatic. No enlarged lymph nodes.
Musculoskeletal. Traumatic right second distal interphalangeal amputation. Otherwise, no joint abnormality or restriction of movement.
Initial laboratory values:
- White blood cell count 15.78 × 109/L (normal 4.5–11.0)
- Absolute neutrophil count 13.3 × 109/L (4.0–11.0)
- Hemoglobin 13.3 g/dL (13.5–17.5)
- Platelet count 133 × 109/L (150–400)
- International normalized ratio (INR) 1.8
- Sodium 136 mmol/L (135–146)
- Potassium 4.6 mmol/L (3.5–5.0)
- Blood urea nitrogen 31 mg/dL (10–25)
- Creatinine 1.6 mg/dL (0.70–1.40)
- Glucose 62 mg/dL (65–100)
- Bicarbonate 23 mmol/L (23–32)
- Albumin 2.5 g/dL (3.5–5.0)
- Total protein 4.6 g/dL (6.0–8.4)
- Bilirubin 1.2 mg/dL (0.0–1.5)
- Aspartate aminotransferase 41 U/L (7–40)
- Alanine aminotransferase 74 U/L (5–50)
- Alkaline phosphatase 55 U/L (40–150)
- C-reactive protein 9.9 mg/dL (0.0–1.0).
Other studies
Electrocardiography shows atrial fibrillation and left ventricular hypertrophy, but no acute changes.
Computed tomography (CT) of the head shows no evidence of hemorrhage or infarction.
Blood cultures are sent at the time of hospital admission.
WHICH TEST IS NEXT?
1. Which is the most appropriate next step for this patient?
- Urinalysis
- CT of the chest
- Echocardiography
- Skin biopsy
The rash in Figure 1 is palpable purpura, which strongly suggests small-vessel cutaneous vasculitis, a condition that can occur in a broad range of settings. An underlying cause is identified in over 70% of cases. Cutaneous vasculitis may herald a primary small-vessel systemic vasculitis such as Wegener granulomatosis, microscopic polyangiitis, or Henoch-Schönlein purpura. It can also be secondary to a spectrum of underlying triggers or diseases that include medications, infections, malignancies such as lymphoproliferative disorders, cryoglobulinemia secondary to hepatitis C viral infection, and connective tissue diseases such as rheumatoid arthritis and systemic lupus erythematosus.
Infective endocarditis is associated with a secondary form of vasculitis and is a strong possibility in this patient, who has a prosthetic aortic valve, fever, and a high white blood cell count.
Thrombocytopenia should also prompt an assessment for any drugs the patient is taking that affect platelet function. However, thrombocytopenia typically results in nonpalpable purpura.
Idiopathic isolated cutaneous vasculitis, in which no underlying cause for the cutaneous vasculitis can be identified, is the diagnosis in less than 30% of cases.
A vasculitic disease process can involve multiple sites, which may be asymptomatic on presentation. Identifying these sites is important, not only to establish the diagnosis, but also to detect potentially life-threatening complications early.
Thus, in this patient, urinalysis should be done promptly to check for active sediment consisting of red cell casts, which would suggest renal involvement (glomerulonephritis). Also, a rising blood pressure and creatinine would point to renal involvement and warrant more aggressive initial therapy.
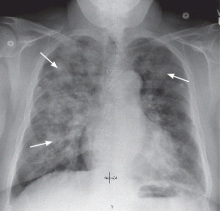
Chest radiography should be done to rule out pulmonary infiltrates, septic emboli, nodules, or cavities that could represent vasculitic or infectious involvement of the lungs. CT of the chest may be needed to further characterize abnormalities on chest radiography.
Echocardiography should certainly be pursued as part of the workup for endocarditis, but urinalysis is of the utmost importance in this patient at this point.
More diagnostic information is needed before considering skin biopsy.
Clues from the urinalysis and chest radiography
Our patient’s sedimentation rate is 24 mm/hour. The urinalysis is strongly positive for blood and a moderate amount of protein but negative for leukocyte esterase and nitrite. The urine sediment contains numerous red blood cell casts and 6 to 10 white blood cells per high-power field.
Pending return of blood cultures, ceftriaxone (Rocephin) and azithromycin (Zithromax) are started to treat possible community-acquired pneumonia. Vancomycin (Vancocin) is empirically added, given the possibility of prosthetic valve endocarditis. Gram stain on blood cultures shows gram-positive cocci.
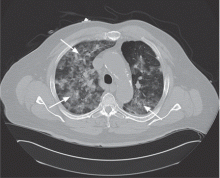
Ground-glass attenuation implies focal or diffuse opacification of the lung that does not obscure the vascular structures, is not associated with air bronchograms, and appears as a “veil” across the lung parenchyma.1 It can be seen in acute diseases such as infection (including pneumonia from atypical bacteria, viruses, acid-fast bacilli, and Pneumocystis jiroveci), pulmonary hemorrhage of any cause, acute viral, eosinophilic, and interstitial pneumonias, and hypersensitivity pneumonitis. It can also be seen in chronic disease states such as interstitial lung disease, bronchoalveolar carcinoma, alveolar proteinosis, and sarcoidosis.
WHICH TEST WOULD NOT HELP?
2. Which of the following tests is least likely to help in the diagnostic evaluation at this point?
- Transthoracic echocardiography
- Transesophageal echocardiography
- Bronchoscopy
- Cystoscopy
In this case, the least likely to help is cystoscopy.
This patient’s vasculitic-appearing rash, ground-glass pulmonary infiltrates, and impaired renal function with red cell casts suggest a pulmonary-renal syndrome, and with this constellation of features, a systemic vasculitis is very likely. Therefore, the focus of the evaluation should be on any evidence to support a diagnosis of vasculitis, as well as other possible causes.
In a patient with diabetes, an artificial heart valve, and fever, the possibility of infection, especially endocarditis, remains high. Transthoracic echocardiography is warranted, and if it is negative for vegetations, transesophageal echocardiography would be a reasonable next option.
Bronchoscopy is warranted to determine if the infiltrates represent pulmonary hemorrhage, which can be seen in certain types of vasculitic and systemic disorders.
The finding of red cell casts in the urine indicates glomerulonephritis, and therefore the kidneys are the likely source of the urinary red blood cells, making cystoscopy of no utility in this current, acute setting.
Case continued: His condition worsens
Transthoracic echocardiography reveals a well-seated mechanical prosthetic aortic valve, trivial aortic regurgitation, a peak gradient of 23 mm Hg and a mean gradient of 12 mm Hg (normal values for his prosthetic valve), and no valvular vegetations. Transesophageal echocardiography confirms the absence of vegetations.
His oxygen requirement increases, and analysis of arterial blood gases reveals a pH of 7.37, Pco2 49 mm Hg (normal range 35–45), Po2 102 mm Hg (normal 80–100), and bicarbonate 28 mmol/L while breathing 100% supplemental oxygen by a nonrebreather face mask. He is taken to the medical intensive care unit for intubation and mechanical ventilation. Bronchoscopy performed while he is intubated confirms diffuse alveolar hemorrhage. Pulse intravenous methylprednisolone (Solu-Medrol) therapy is started.
DIFFUSE ALVEOLAR HEMORRHAGE
3. Which of the following is not true about diffuse alveolar hemorrhage?
- Its onset is usually abrupt or of short duration
- It is always associated with hemoptysis
- Radiography most commonly shows new patchy or diffuse alveolar opacities
- Pulmonary function testing shows increased diffusing capacity of the lung for carbon monoxide (Dlco)
Hemoptysis is absent at presentation in as many as 33% of patients.
The onset of diffuse alveolar hemorrhage is usually abrupt or of short duration, with initial symptoms of cough, fever, and dyspnea. Some patients, such as ours, can present with severe acute respiratory distress syndrome requiring mechanical ventilation. Radiography most often shows new patchy alveolar opacities, and CT may reveal a ground-glass appearance. On pulmonary function testing, the Dlco is high, owing to the hemoglobin within the alveoli.
ACUTE GLOMERULONEPHRITIS PLUS PULMONARY HEMORRHAGE EQUALS…?
4. Which disease could have manifestations consistent with acute glomerulonephritis and pulmonary hemorrhage?
- Antiglomerular basement membrane disease
- Wegener granulomatosis
- Microscopic polyangiitis
- Systemic lupus erythematosus
All of these are possible.
The combined presentation of acute glomerulonephritis and pulmonary hemorrhage (also called pulmonary-renal syndrome) is usually seen in antiglomerular basement membrane disease (Goodpasture syndrome) and small-vessel systemic vasculitides such as Wegener granulomatosis and microscopic polyangiitis.2,3 It can also be seen in patients with systemic lupus erythematosus.
Antiglomerular basement membrane disease
In antiglomerular basement membrane disease, circulating antibodies are directed towards an antigen intrinsic to the glomerular basement membrane, typically leading to acute glomerulonephritis associated with crescent formation. It may present as acute renal failure in which urinalysis shows proteinuria with sediment characterized by red cell casts. Pulmonary involvement, usually alveolar hemorrhage, is present in approximately 60% to 70% of cases.
The diagnosis requires demonstration of antiglomerular basement membrane antibodies in either the serum or the kidney. Renal biopsy is usually recommended because the accuracy of serum assays is variable.
A key histologic feature of the renal lesion in antiglomerular basement membrane disease is crescentic glomerulonephritis in which immunofluorescence microscopy demonstrates the virtually pathognomonic finding of linear deposition of immunoglobulin G along the glomerular capillaries.
The treatment of choice for antiglomerular basement membrane disease is plasmapheresis and immunosuppression with a combination of glucocorticoids and cyclophosphamide (Cytoxan). If the disease is high on the differential diagnosis, empiric plasmapheresis should be started while waiting for diagnostic studies, because the prognosis of untreated glomerulonephritis is poor.
Wegener granulomatosis
Wegener granulomatosis is a systemic vasculitis of the medium and small arteries, arterioles, and venules that classically involves the upper and lower respiratory tracts and the kidneys. Patients may present with persistent rhinorrhea and epistaxis, cough with chest radiographs showing nodules, fixed infiltrates, or cavities, and abnormal urinary sediment with microscopic hematuria with or without red cell casts.
From 75% to 90% of patients with active Wegener granulomatosis are positive for antineutrophil cytoplasmic antibody (ANCA). In 60% to 80% of cases, ANCA is directed against proteinase 3 (PR3), which produces a cytoplasmic standing pattern by immunofluorescence (cANCA), while 5% to 20% have ANCA directed against myeloper-oxidase, which produces a perinuclear staining pattern (pANCA). A small number of patients with Wegener granulomatosis are ANCA-negative.
The diagnosis is usually confirmed by tissue biopsy at the site of active disease, which shows necrotizing vasculitis with granulomatous inflammation. The renal lesion is typically that of a focal, segmental, necrotizing glomerulonephritis that has few to no immune complexes (pauci-immune glomerulonephritis).
The treatment of severe disease involves a combination of cyclophosphamide and glucocorticoids initially to achieve remission followed by maintenance therapy with methotrexate or azathioprine (Imuran).
Microscopic polyangiitis
Microscopic polyangiitis is a systemic vasculitis of the capillaries, venules, and arterioles, with little or no immune complex deposition. Nearly all patients have renal involvement, and 10% to 30% have lung involvement. In those with lung involvement, diffuse alveolar hemorrhage is the most common manifestation.
On histopathologic study, microscopic polyangiitis differs from Wegener granulomatosis in that it does not have granuloma formation. However, the renal lesion is that of a pauci-immune glomerulonephritis and is identical to that seen in Wegener granulomatosis. From 70% to 85% of patients with microscopic polyangiitis are ANCA-positive, and most of these have pANCA.
The management of active severe microscopic polyangiitis is identical to that of Wegener granulomatosis.
Systemic lupus erythematosus
Systemic lupus erythematosus is an autoimmune disease characterized by tissue-binding autoantibody and immune-complex-mediated organ damage. It can involve multiple organ systems, and the diagnosis is based on characteristic clinical features and autoantibodies. The sensitivity of antinuclear antibody for lupus is close to 100%, which makes it a good screening tool. Antibodies to dsDNA and Smith antigen have high specificity for lupus.
About 75% of patients have renal involvement at some point in their disease course. The different types of renal disease in systemic lupus are usually differentiated with a renal biopsy, with immune-complex-mediated glomerular diseases being the most common.
The most common pulmonary manifestation is pleuritis with or without pleural effusion. Life-threatening pulmonary manifestations include pulmonary hemorrhage and interstitial inflammation leading to fibrosis.
Lupus has great clinical variability and the treatment approach is based on the organ manifestations, disease activity, and severity.
CASE CONTINUED: ARRIVING AT THE DIAGNOSIS
We start our patient on cyclophosphamide 175 mg daily in view of possible Wegener granulomatosis.
Even though purpura is extremely rare in primary antiglomerular basement membrane disease, this patient has life-threatening pulmonary hemorrhage, a complication seen in over 50% of these patients. Therefore, plasmapheresis is started empirically.
On the second day of cyclophosphamide treatment, tests for ANCA, glomerular basement membrane antibody, and antinuclear antibody are reported as negative, and complement levels are normal. Bronchoalveolar lavage shows no infection. Follow-up blood cultures are negative.
To summarize the findings so far, this patient has a purpuric skin rash, active urine sediment with red cell casts indicating glomerulonephritis, acute renal failure, and severe pulmonary hemorrhage requiring mechanical ventilation. Although one set of blood cultures showed gram-positive cocci, no source of infection, particularly endocarditis, could be identified.
Antiglomerular basement membrane disease would still be high on the list of suspected diagnoses, given his diffuse alveolar hemorrhage. As mentioned earlier, renal biopsy is imperative to making a diagnosis, because serologic tests have variable accuracy. And making the correct diagnosis has therapeutic implications.
Renal biopsy is performed and shows immune-complex mesangiopathic glomerulonephritis with positive immunofluorescent staining in the mesangium for IgA. Only one glomerulus shows fibrinoid necrosis.
Skin biopsy results obtained earlier showed positive direct immunofluorescence for IgA. Both renal and skin biopsies suggested Henoch-Schönlein purpura.
IgA deposition in the kidney and skin has been associated with liver cirrhosis, celiac disease, and infections with agents such as human immunodeficiency virus, cytomegalovirus, Haemophilus parainfluenzae, and Staphylococcus aureus. In a Japanese study,4 renal biopsy specimens from 116 patients with IgA nephropathy and from 122 patients with other types of kidney disease were examined for the presence of S aureus antigen in the glomeruli. Although antigen was not detected in non-IgA disease, 68% of specimens from patients with IgA nephropathy had S aureus cell envelope antigen together with IgA antibody in the glomeruli. However, no single antigen has been consistently identified, so it seems more probable that the development of IgA deposition in kidneys is a consequence of aberrant IgA immune response rather than the antigen itself.
HENOCH-SCHÖNLEIN PURPURA
Henoch-Schönlein purpura is a systemic vasculitis with a prominent cutaneous component. It is characterized by the tissue deposition of IgA-containing immune complexes. It is predominantly a disease of children but it can be seen in adults. A UK study found the prevalence to be 20 per 100,000 children, with the highest prevalence between ages 4 and 7 (70 per 100,000).5
The four cardinal clinical features of Henoch-Schönlein purpura are purpuric rash, abdominal pain, arthralgia, and renal involvement. Almost all patients have purpuric rash at some point in their disease course. Arthralgia with or without arthritis is typically migratory, oligoarticular, and nondeforming, usually affecting the large joints of the lower extremities; involvement of the upper extremities is less common.
Skin biopsy typically shows leukocytoclastic vasculitis in postcapillary venules with IgA deposition, and these findings are pathognomonic of Henoch-Schönlein purpura.
Gastrointestinal involvement can range from mild symptoms such as nausea, vomiting, abdominal pain, and paralytic ileus to severe disease such as gastrointestinal hemorrhage, bowel infarction, bowel perforation, and intussusception.
Renal involvement is common and is important, as it can in rare cases progress to end-stage renal disease. The urinalysis usually shows mild proteinuria with active sediment with red cell casts. Most patients have relatively mild disease, characterized by asymptomatic hematuria with a normal or slightly elevated creatinine. However, severe involvement may occur, with nephrotic syndrome, hypertension, and acute renal failure.
Different presentation in adults vs children
Adults with Henoch-Schönlein purpura only rarely present with bowel intussusception, whereas some studies have found that adults are more likely than children to develop significant renal involvement, including end-stage renal disease.6,7
There is a general but not absolute correlation between the severity of clinical manifestations and the findings on renal biopsy. A poor prognosis (significant proteinuria, hypertension, renal insufficiency, or end-stage renal disease) is associated with crescent formation involving more than 50% of the glomeruli.8
Our current understanding of the longterm outcome of the renal disease in Henoch-Schönlein purpura is primarily derived from studies in children. In one study, complete recovery occurred in 94% of children and 89% of adults.7 A long-term study of 250 adults with Henoch-Schönlein purpura and renal involvement of sufficient severity to require biopsy reported that, at a median follow up of 15 years, 11% had become dialysis-dependent and 13% had severe renal failure (creatinine clearance < 30 mL/min).6 Recurrence is common, occurring in approximately one-third of patients, more likely in those with nephritis.8
The diagnosis of Henoch-Schönlein purpura is typically made on the basis of key clinical features. In patients such as ours who have an atypical presentation, biopsy of affected skin and renal biopsy can be essential in the diagnosis. Diffuse alveolar hemorrhage is exceedingly rare in Henoch-Schönlein purpura but can be seen, as in our patient.9,10 In this setting, the findings of IgA deposits in skin and renal biopsy specimens, together with the absence of other clinical, serologic, or histologic features of other more-common potential causes, secured the diagnosis in this patient.
Henoch-Schönlein purpura is usually self-limited and requires no specific therapy. Evidence suggests that glucocorticoids enhance the rate of resolution of the arthritis and abdominal pain but do not appear to prevent recurrent disease or lessen the likelihood of progression of renal disease.8 Patients with severe renal involvement with renal function impairment may benefit from pulse intravenous corticosteroid therapy (methylprednisolone 250–1,000 mg per day for 3 days), followed by oral steroids for 3 months.11
In anecdotal reports, renal function improved in 19 of 21 children with Henoch-Schönlein purpura and severe crescentic nephritis.12 Studies have evaluated cyclophosphamide13 and plasmapheresis,14 but their role remains uncertain. Renal transplantation is an option in patients who progress to end-stage renal disease.
OUR CASE CONTINUED
In our patient, plasmapheresis was discontinued. As the pulmonary hemorrhage had developed during treatment with prednisone, we decided to continue cyclophosphamide, given the life-threatening nature of his disease. His pulmonary status improved and he was extubated.
During his initial hospital stay, he was taking heparin for anticoagulation therapy. However, given the life-threatening diffuse alveolar hemorrhage, heparin was stopped during the course of his stay in the intensive care unit. Once he was stable and was transferred out of the intensive care unit, heparin was resumed, and his anticoagulation therapy was bridged to warfarin just before discharge. He was eventually discharged on a tapering dose of oral prednisone and cyclophosphamide for 3 months, after which he was switched to azathioprine for maintenance therapy. He was doing well 6 months later, with a serum creatinine level of 1.6 mg/dL, no red cell casts in the urine, and no rash.
TAKE-HOME POINT
In any case of suspected vasculitis that presents with skin disease, it is essential to look for other sites with potentially life-threatening involvement. Henoch-Schönlein purpura is a systemic vasculitis with a prominent cutaneous component. It is not always benign and can be associated with serious complications such as renal failure, gastrointestinal events, and, very rarely, diffuse alveolar hemorrhage.
- Collins J, Stern EJ. Ground-glass opacity at CT: the ABCs. AJR Am J Roentgenol 1997; 169:355–367.
- Boyce NW, Holdsworth SR. Pulmonary manifestations of the clinical syndrome of acute glomerulonephritis and lung hemorrhage. Am J Kidney Dis 1986; 8:31–36.
- Gallagher H, Kwan JT, Jayne DR. Pulmonary renal syndrome: a 4-year, single-center experience. Am J Kidney Dis 2002; 39:42–47.
- Koyama A, Sharmin S, Sakurai H, et al. Staphylococcus aureus cell envelope antigen is a new candidate for the induction of IgA nephropathy. Kidney Int 2004; 66:121–132.
- Gardner-Medwin JM, Dolezalova P, Cummins C, Southwood TR. Incidence of Henoch-Schönlein purpura, Kawasaki disease, and rare vasculitides in children of different ethnic origins. Lancet 2002; 360:1197–1202.
- Pillebout E, Thervet E, Hill G, Alberti C, Vanhille P, Nochy D. Henoch-Schönlein purpura in adults: outcome and prognostic factors. J Am Soc Nephrol 2002; 13:1271–1278.
- Blanco R, Martinez-Taboada VM, Rodriguez-Valverde V, Garcia-Fuentes M, Gonzalez-Gay MA. Henoch-Schönlein purpura in adulthood and childhood: two different expressions of the same syndrome. Arthritis Rheum 1997; 40:859–864.
- Saulsbury FT. Henoch-Schönlein purpura in children. Report of 100 patients and review of the literature. Medicine (Baltimore) 1999; 78:395–409.
- Nadrous HF, Yu AC, Specks U, Ryu JH. Pulmonary involvement in Henoch-Schönlein purpura. Mayo Clin Proc 2004; 79:1151–1157.
- Vats KR, Vats A, Kim Y, Dassenko D, Sinaiko AR. Henoch-Schönlein purpura and pulmonary hemorrhage: a report and literature review. Pediatr Nephrol 1999; 13:530–534.
- Niaudet P, Habib R. Methylprednisolone pulse therapy in the treatment of severe forms of Schönlein-Henoch purpura nephritis. Pediatr Nephrol 1998; 12:238–243.
- Bergstein J, Leiser J, Andreoli SP. Response of crescentic Henoch-Schöenlein purpura nephritis to corticosteroid and azathioprine therapy. Clin Nephrol 1998; 49:9–14.
- Tarshish P, Bernstein J, Edelmann CM. Henoch-Schönlein purpura nephritis: course of disease and efficacy of cyclophosphamide. Pediatr Nephrol 2004; 19:51–56.
- Hattori M, Ito K, Konomoto T, Kawaguchi H, Yoshioka T, Khono M. Plasmapheresis as the sole therapy for rapidly progressive Henoch-Schönlein purpura nephritis in children. Am J Kidney Dis 1999; 33:427–433.
A 72-year-old man whose medical history includes diabetes mellitus, hypertension, coronary artery disease, aortic valve replacement, atrial fibrillation, and chronic obstructive pulmonary disease was in his usual state of health until 2 weeks ago, when he developed a purpuric rash on his legs. His physician started him on prednisone 40 mg daily for the rash; however, 1 week later he presented to a hospital emergency room when his family found him confused and diaphoretic.
In the emergency room, he was found to be hypoglycemic, with a serum glucose level of 40 mg/dL, which was promptly treated. His mental status improved partially. In the hospital, the rash worsened and progressed upwards to his trunk and upper extremities. He was transferred to our institution for further workup and management.
A review of systems reveals occasional epistaxis in the summer, recent fatigue, cough, and shortness of breath on exertion. His medications at the time of transfer include warfarin (Coumadin), amlodipine (Norvasc), insulin, ipratropium and albuterol (Combivent) inhalers, and prednisone 40 mg daily. He has not undergone surgery recently.
PHYSICAL EXAMINATION
He is alert and oriented to person but not to time and place.
Vital signs. Oral temperature 101.1°F (38.4°C), pulse rate 108, blood pressure 108/79 mm/Hg, respiratory rate 22, oxygen saturation 93% by pulse oximetry on room air, weight 94 kg (207 lb).
Head, eyes, ears, nose, and throat. No pallor or icterus, pupils are equally reactive, nasal mucosa not inflamed or ulcerated, mucous membranes moist, no sinus tenderness.
Neck. No jugular venous distention and no cervical lymphadenopathy.
Cardiovascular. Tachycardia, irregularly irregular rhythm, prosthetic valve sounds, no murmurs, rubs, or gallops.
Respiratory. Bibasal crackles (right side more than the left). No wheezing.
Abdomen. Soft, nontender, nondistended, no palpable organomegaly, bowel sounds normal.
Extremities. No edema, good peripheral pulses.
Neurologic. No focal deficits noted.
Lymphatic. No enlarged lymph nodes.
Musculoskeletal. Traumatic right second distal interphalangeal amputation. Otherwise, no joint abnormality or restriction of movement.
Initial laboratory values:
- White blood cell count 15.78 × 109/L (normal 4.5–11.0)
- Absolute neutrophil count 13.3 × 109/L (4.0–11.0)
- Hemoglobin 13.3 g/dL (13.5–17.5)
- Platelet count 133 × 109/L (150–400)
- International normalized ratio (INR) 1.8
- Sodium 136 mmol/L (135–146)
- Potassium 4.6 mmol/L (3.5–5.0)
- Blood urea nitrogen 31 mg/dL (10–25)
- Creatinine 1.6 mg/dL (0.70–1.40)
- Glucose 62 mg/dL (65–100)
- Bicarbonate 23 mmol/L (23–32)
- Albumin 2.5 g/dL (3.5–5.0)
- Total protein 4.6 g/dL (6.0–8.4)
- Bilirubin 1.2 mg/dL (0.0–1.5)
- Aspartate aminotransferase 41 U/L (7–40)
- Alanine aminotransferase 74 U/L (5–50)
- Alkaline phosphatase 55 U/L (40–150)
- C-reactive protein 9.9 mg/dL (0.0–1.0).
Other studies
Electrocardiography shows atrial fibrillation and left ventricular hypertrophy, but no acute changes.
Computed tomography (CT) of the head shows no evidence of hemorrhage or infarction.
Blood cultures are sent at the time of hospital admission.
WHICH TEST IS NEXT?
1. Which is the most appropriate next step for this patient?
- Urinalysis
- CT of the chest
- Echocardiography
- Skin biopsy
The rash in Figure 1 is palpable purpura, which strongly suggests small-vessel cutaneous vasculitis, a condition that can occur in a broad range of settings. An underlying cause is identified in over 70% of cases. Cutaneous vasculitis may herald a primary small-vessel systemic vasculitis such as Wegener granulomatosis, microscopic polyangiitis, or Henoch-Schönlein purpura. It can also be secondary to a spectrum of underlying triggers or diseases that include medications, infections, malignancies such as lymphoproliferative disorders, cryoglobulinemia secondary to hepatitis C viral infection, and connective tissue diseases such as rheumatoid arthritis and systemic lupus erythematosus.
Infective endocarditis is associated with a secondary form of vasculitis and is a strong possibility in this patient, who has a prosthetic aortic valve, fever, and a high white blood cell count.
Thrombocytopenia should also prompt an assessment for any drugs the patient is taking that affect platelet function. However, thrombocytopenia typically results in nonpalpable purpura.
Idiopathic isolated cutaneous vasculitis, in which no underlying cause for the cutaneous vasculitis can be identified, is the diagnosis in less than 30% of cases.
A vasculitic disease process can involve multiple sites, which may be asymptomatic on presentation. Identifying these sites is important, not only to establish the diagnosis, but also to detect potentially life-threatening complications early.
Thus, in this patient, urinalysis should be done promptly to check for active sediment consisting of red cell casts, which would suggest renal involvement (glomerulonephritis). Also, a rising blood pressure and creatinine would point to renal involvement and warrant more aggressive initial therapy.
Chest radiography should be done to rule out pulmonary infiltrates, septic emboli, nodules, or cavities that could represent vasculitic or infectious involvement of the lungs. CT of the chest may be needed to further characterize abnormalities on chest radiography.
Echocardiography should certainly be pursued as part of the workup for endocarditis, but urinalysis is of the utmost importance in this patient at this point.
More diagnostic information is needed before considering skin biopsy.
Clues from the urinalysis and chest radiography
Our patient’s sedimentation rate is 24 mm/hour. The urinalysis is strongly positive for blood and a moderate amount of protein but negative for leukocyte esterase and nitrite. The urine sediment contains numerous red blood cell casts and 6 to 10 white blood cells per high-power field.
Pending return of blood cultures, ceftriaxone (Rocephin) and azithromycin (Zithromax) are started to treat possible community-acquired pneumonia. Vancomycin (Vancocin) is empirically added, given the possibility of prosthetic valve endocarditis. Gram stain on blood cultures shows gram-positive cocci.
Ground-glass attenuation implies focal or diffuse opacification of the lung that does not obscure the vascular structures, is not associated with air bronchograms, and appears as a “veil” across the lung parenchyma.1 It can be seen in acute diseases such as infection (including pneumonia from atypical bacteria, viruses, acid-fast bacilli, and Pneumocystis jiroveci), pulmonary hemorrhage of any cause, acute viral, eosinophilic, and interstitial pneumonias, and hypersensitivity pneumonitis. It can also be seen in chronic disease states such as interstitial lung disease, bronchoalveolar carcinoma, alveolar proteinosis, and sarcoidosis.
WHICH TEST WOULD NOT HELP?
2. Which of the following tests is least likely to help in the diagnostic evaluation at this point?
- Transthoracic echocardiography
- Transesophageal echocardiography
- Bronchoscopy
- Cystoscopy
In this case, the least likely to help is cystoscopy.
This patient’s vasculitic-appearing rash, ground-glass pulmonary infiltrates, and impaired renal function with red cell casts suggest a pulmonary-renal syndrome, and with this constellation of features, a systemic vasculitis is very likely. Therefore, the focus of the evaluation should be on any evidence to support a diagnosis of vasculitis, as well as other possible causes.
In a patient with diabetes, an artificial heart valve, and fever, the possibility of infection, especially endocarditis, remains high. Transthoracic echocardiography is warranted, and if it is negative for vegetations, transesophageal echocardiography would be a reasonable next option.
Bronchoscopy is warranted to determine if the infiltrates represent pulmonary hemorrhage, which can be seen in certain types of vasculitic and systemic disorders.
The finding of red cell casts in the urine indicates glomerulonephritis, and therefore the kidneys are the likely source of the urinary red blood cells, making cystoscopy of no utility in this current, acute setting.
Case continued: His condition worsens
Transthoracic echocardiography reveals a well-seated mechanical prosthetic aortic valve, trivial aortic regurgitation, a peak gradient of 23 mm Hg and a mean gradient of 12 mm Hg (normal values for his prosthetic valve), and no valvular vegetations. Transesophageal echocardiography confirms the absence of vegetations.
His oxygen requirement increases, and analysis of arterial blood gases reveals a pH of 7.37, Pco2 49 mm Hg (normal range 35–45), Po2 102 mm Hg (normal 80–100), and bicarbonate 28 mmol/L while breathing 100% supplemental oxygen by a nonrebreather face mask. He is taken to the medical intensive care unit for intubation and mechanical ventilation. Bronchoscopy performed while he is intubated confirms diffuse alveolar hemorrhage. Pulse intravenous methylprednisolone (Solu-Medrol) therapy is started.
DIFFUSE ALVEOLAR HEMORRHAGE
3. Which of the following is not true about diffuse alveolar hemorrhage?
- Its onset is usually abrupt or of short duration
- It is always associated with hemoptysis
- Radiography most commonly shows new patchy or diffuse alveolar opacities
- Pulmonary function testing shows increased diffusing capacity of the lung for carbon monoxide (Dlco)
Hemoptysis is absent at presentation in as many as 33% of patients.
The onset of diffuse alveolar hemorrhage is usually abrupt or of short duration, with initial symptoms of cough, fever, and dyspnea. Some patients, such as ours, can present with severe acute respiratory distress syndrome requiring mechanical ventilation. Radiography most often shows new patchy alveolar opacities, and CT may reveal a ground-glass appearance. On pulmonary function testing, the Dlco is high, owing to the hemoglobin within the alveoli.
ACUTE GLOMERULONEPHRITIS PLUS PULMONARY HEMORRHAGE EQUALS…?
4. Which disease could have manifestations consistent with acute glomerulonephritis and pulmonary hemorrhage?
- Antiglomerular basement membrane disease
- Wegener granulomatosis
- Microscopic polyangiitis
- Systemic lupus erythematosus
All of these are possible.
The combined presentation of acute glomerulonephritis and pulmonary hemorrhage (also called pulmonary-renal syndrome) is usually seen in antiglomerular basement membrane disease (Goodpasture syndrome) and small-vessel systemic vasculitides such as Wegener granulomatosis and microscopic polyangiitis.2,3 It can also be seen in patients with systemic lupus erythematosus.
Antiglomerular basement membrane disease
In antiglomerular basement membrane disease, circulating antibodies are directed towards an antigen intrinsic to the glomerular basement membrane, typically leading to acute glomerulonephritis associated with crescent formation. It may present as acute renal failure in which urinalysis shows proteinuria with sediment characterized by red cell casts. Pulmonary involvement, usually alveolar hemorrhage, is present in approximately 60% to 70% of cases.
The diagnosis requires demonstration of antiglomerular basement membrane antibodies in either the serum or the kidney. Renal biopsy is usually recommended because the accuracy of serum assays is variable.
A key histologic feature of the renal lesion in antiglomerular basement membrane disease is crescentic glomerulonephritis in which immunofluorescence microscopy demonstrates the virtually pathognomonic finding of linear deposition of immunoglobulin G along the glomerular capillaries.
The treatment of choice for antiglomerular basement membrane disease is plasmapheresis and immunosuppression with a combination of glucocorticoids and cyclophosphamide (Cytoxan). If the disease is high on the differential diagnosis, empiric plasmapheresis should be started while waiting for diagnostic studies, because the prognosis of untreated glomerulonephritis is poor.
Wegener granulomatosis
Wegener granulomatosis is a systemic vasculitis of the medium and small arteries, arterioles, and venules that classically involves the upper and lower respiratory tracts and the kidneys. Patients may present with persistent rhinorrhea and epistaxis, cough with chest radiographs showing nodules, fixed infiltrates, or cavities, and abnormal urinary sediment with microscopic hematuria with or without red cell casts.
From 75% to 90% of patients with active Wegener granulomatosis are positive for antineutrophil cytoplasmic antibody (ANCA). In 60% to 80% of cases, ANCA is directed against proteinase 3 (PR3), which produces a cytoplasmic standing pattern by immunofluorescence (cANCA), while 5% to 20% have ANCA directed against myeloper-oxidase, which produces a perinuclear staining pattern (pANCA). A small number of patients with Wegener granulomatosis are ANCA-negative.
The diagnosis is usually confirmed by tissue biopsy at the site of active disease, which shows necrotizing vasculitis with granulomatous inflammation. The renal lesion is typically that of a focal, segmental, necrotizing glomerulonephritis that has few to no immune complexes (pauci-immune glomerulonephritis).
The treatment of severe disease involves a combination of cyclophosphamide and glucocorticoids initially to achieve remission followed by maintenance therapy with methotrexate or azathioprine (Imuran).
Microscopic polyangiitis
Microscopic polyangiitis is a systemic vasculitis of the capillaries, venules, and arterioles, with little or no immune complex deposition. Nearly all patients have renal involvement, and 10% to 30% have lung involvement. In those with lung involvement, diffuse alveolar hemorrhage is the most common manifestation.
On histopathologic study, microscopic polyangiitis differs from Wegener granulomatosis in that it does not have granuloma formation. However, the renal lesion is that of a pauci-immune glomerulonephritis and is identical to that seen in Wegener granulomatosis. From 70% to 85% of patients with microscopic polyangiitis are ANCA-positive, and most of these have pANCA.
The management of active severe microscopic polyangiitis is identical to that of Wegener granulomatosis.
Systemic lupus erythematosus
Systemic lupus erythematosus is an autoimmune disease characterized by tissue-binding autoantibody and immune-complex-mediated organ damage. It can involve multiple organ systems, and the diagnosis is based on characteristic clinical features and autoantibodies. The sensitivity of antinuclear antibody for lupus is close to 100%, which makes it a good screening tool. Antibodies to dsDNA and Smith antigen have high specificity for lupus.
About 75% of patients have renal involvement at some point in their disease course. The different types of renal disease in systemic lupus are usually differentiated with a renal biopsy, with immune-complex-mediated glomerular diseases being the most common.
The most common pulmonary manifestation is pleuritis with or without pleural effusion. Life-threatening pulmonary manifestations include pulmonary hemorrhage and interstitial inflammation leading to fibrosis.
Lupus has great clinical variability and the treatment approach is based on the organ manifestations, disease activity, and severity.
CASE CONTINUED: ARRIVING AT THE DIAGNOSIS
We start our patient on cyclophosphamide 175 mg daily in view of possible Wegener granulomatosis.
Even though purpura is extremely rare in primary antiglomerular basement membrane disease, this patient has life-threatening pulmonary hemorrhage, a complication seen in over 50% of these patients. Therefore, plasmapheresis is started empirically.
On the second day of cyclophosphamide treatment, tests for ANCA, glomerular basement membrane antibody, and antinuclear antibody are reported as negative, and complement levels are normal. Bronchoalveolar lavage shows no infection. Follow-up blood cultures are negative.
To summarize the findings so far, this patient has a purpuric skin rash, active urine sediment with red cell casts indicating glomerulonephritis, acute renal failure, and severe pulmonary hemorrhage requiring mechanical ventilation. Although one set of blood cultures showed gram-positive cocci, no source of infection, particularly endocarditis, could be identified.
Antiglomerular basement membrane disease would still be high on the list of suspected diagnoses, given his diffuse alveolar hemorrhage. As mentioned earlier, renal biopsy is imperative to making a diagnosis, because serologic tests have variable accuracy. And making the correct diagnosis has therapeutic implications.
Renal biopsy is performed and shows immune-complex mesangiopathic glomerulonephritis with positive immunofluorescent staining in the mesangium for IgA. Only one glomerulus shows fibrinoid necrosis.
Skin biopsy results obtained earlier showed positive direct immunofluorescence for IgA. Both renal and skin biopsies suggested Henoch-Schönlein purpura.
IgA deposition in the kidney and skin has been associated with liver cirrhosis, celiac disease, and infections with agents such as human immunodeficiency virus, cytomegalovirus, Haemophilus parainfluenzae, and Staphylococcus aureus. In a Japanese study,4 renal biopsy specimens from 116 patients with IgA nephropathy and from 122 patients with other types of kidney disease were examined for the presence of S aureus antigen in the glomeruli. Although antigen was not detected in non-IgA disease, 68% of specimens from patients with IgA nephropathy had S aureus cell envelope antigen together with IgA antibody in the glomeruli. However, no single antigen has been consistently identified, so it seems more probable that the development of IgA deposition in kidneys is a consequence of aberrant IgA immune response rather than the antigen itself.
HENOCH-SCHÖNLEIN PURPURA
Henoch-Schönlein purpura is a systemic vasculitis with a prominent cutaneous component. It is characterized by the tissue deposition of IgA-containing immune complexes. It is predominantly a disease of children but it can be seen in adults. A UK study found the prevalence to be 20 per 100,000 children, with the highest prevalence between ages 4 and 7 (70 per 100,000).5
The four cardinal clinical features of Henoch-Schönlein purpura are purpuric rash, abdominal pain, arthralgia, and renal involvement. Almost all patients have purpuric rash at some point in their disease course. Arthralgia with or without arthritis is typically migratory, oligoarticular, and nondeforming, usually affecting the large joints of the lower extremities; involvement of the upper extremities is less common.
Skin biopsy typically shows leukocytoclastic vasculitis in postcapillary venules with IgA deposition, and these findings are pathognomonic of Henoch-Schönlein purpura.
Gastrointestinal involvement can range from mild symptoms such as nausea, vomiting, abdominal pain, and paralytic ileus to severe disease such as gastrointestinal hemorrhage, bowel infarction, bowel perforation, and intussusception.
Renal involvement is common and is important, as it can in rare cases progress to end-stage renal disease. The urinalysis usually shows mild proteinuria with active sediment with red cell casts. Most patients have relatively mild disease, characterized by asymptomatic hematuria with a normal or slightly elevated creatinine. However, severe involvement may occur, with nephrotic syndrome, hypertension, and acute renal failure.
Different presentation in adults vs children
Adults with Henoch-Schönlein purpura only rarely present with bowel intussusception, whereas some studies have found that adults are more likely than children to develop significant renal involvement, including end-stage renal disease.6,7
There is a general but not absolute correlation between the severity of clinical manifestations and the findings on renal biopsy. A poor prognosis (significant proteinuria, hypertension, renal insufficiency, or end-stage renal disease) is associated with crescent formation involving more than 50% of the glomeruli.8
Our current understanding of the longterm outcome of the renal disease in Henoch-Schönlein purpura is primarily derived from studies in children. In one study, complete recovery occurred in 94% of children and 89% of adults.7 A long-term study of 250 adults with Henoch-Schönlein purpura and renal involvement of sufficient severity to require biopsy reported that, at a median follow up of 15 years, 11% had become dialysis-dependent and 13% had severe renal failure (creatinine clearance < 30 mL/min).6 Recurrence is common, occurring in approximately one-third of patients, more likely in those with nephritis.8
The diagnosis of Henoch-Schönlein purpura is typically made on the basis of key clinical features. In patients such as ours who have an atypical presentation, biopsy of affected skin and renal biopsy can be essential in the diagnosis. Diffuse alveolar hemorrhage is exceedingly rare in Henoch-Schönlein purpura but can be seen, as in our patient.9,10 In this setting, the findings of IgA deposits in skin and renal biopsy specimens, together with the absence of other clinical, serologic, or histologic features of other more-common potential causes, secured the diagnosis in this patient.
Henoch-Schönlein purpura is usually self-limited and requires no specific therapy. Evidence suggests that glucocorticoids enhance the rate of resolution of the arthritis and abdominal pain but do not appear to prevent recurrent disease or lessen the likelihood of progression of renal disease.8 Patients with severe renal involvement with renal function impairment may benefit from pulse intravenous corticosteroid therapy (methylprednisolone 250–1,000 mg per day for 3 days), followed by oral steroids for 3 months.11
In anecdotal reports, renal function improved in 19 of 21 children with Henoch-Schönlein purpura and severe crescentic nephritis.12 Studies have evaluated cyclophosphamide13 and plasmapheresis,14 but their role remains uncertain. Renal transplantation is an option in patients who progress to end-stage renal disease.
OUR CASE CONTINUED
In our patient, plasmapheresis was discontinued. As the pulmonary hemorrhage had developed during treatment with prednisone, we decided to continue cyclophosphamide, given the life-threatening nature of his disease. His pulmonary status improved and he was extubated.
During his initial hospital stay, he was taking heparin for anticoagulation therapy. However, given the life-threatening diffuse alveolar hemorrhage, heparin was stopped during the course of his stay in the intensive care unit. Once he was stable and was transferred out of the intensive care unit, heparin was resumed, and his anticoagulation therapy was bridged to warfarin just before discharge. He was eventually discharged on a tapering dose of oral prednisone and cyclophosphamide for 3 months, after which he was switched to azathioprine for maintenance therapy. He was doing well 6 months later, with a serum creatinine level of 1.6 mg/dL, no red cell casts in the urine, and no rash.
TAKE-HOME POINT
In any case of suspected vasculitis that presents with skin disease, it is essential to look for other sites with potentially life-threatening involvement. Henoch-Schönlein purpura is a systemic vasculitis with a prominent cutaneous component. It is not always benign and can be associated with serious complications such as renal failure, gastrointestinal events, and, very rarely, diffuse alveolar hemorrhage.
A 72-year-old man whose medical history includes diabetes mellitus, hypertension, coronary artery disease, aortic valve replacement, atrial fibrillation, and chronic obstructive pulmonary disease was in his usual state of health until 2 weeks ago, when he developed a purpuric rash on his legs. His physician started him on prednisone 40 mg daily for the rash; however, 1 week later he presented to a hospital emergency room when his family found him confused and diaphoretic.
In the emergency room, he was found to be hypoglycemic, with a serum glucose level of 40 mg/dL, which was promptly treated. His mental status improved partially. In the hospital, the rash worsened and progressed upwards to his trunk and upper extremities. He was transferred to our institution for further workup and management.
A review of systems reveals occasional epistaxis in the summer, recent fatigue, cough, and shortness of breath on exertion. His medications at the time of transfer include warfarin (Coumadin), amlodipine (Norvasc), insulin, ipratropium and albuterol (Combivent) inhalers, and prednisone 40 mg daily. He has not undergone surgery recently.
PHYSICAL EXAMINATION
He is alert and oriented to person but not to time and place.
Vital signs. Oral temperature 101.1°F (38.4°C), pulse rate 108, blood pressure 108/79 mm/Hg, respiratory rate 22, oxygen saturation 93% by pulse oximetry on room air, weight 94 kg (207 lb).
Head, eyes, ears, nose, and throat. No pallor or icterus, pupils are equally reactive, nasal mucosa not inflamed or ulcerated, mucous membranes moist, no sinus tenderness.
Neck. No jugular venous distention and no cervical lymphadenopathy.
Cardiovascular. Tachycardia, irregularly irregular rhythm, prosthetic valve sounds, no murmurs, rubs, or gallops.
Respiratory. Bibasal crackles (right side more than the left). No wheezing.
Abdomen. Soft, nontender, nondistended, no palpable organomegaly, bowel sounds normal.
Extremities. No edema, good peripheral pulses.
Neurologic. No focal deficits noted.
Lymphatic. No enlarged lymph nodes.
Musculoskeletal. Traumatic right second distal interphalangeal amputation. Otherwise, no joint abnormality or restriction of movement.
Initial laboratory values:
- White blood cell count 15.78 × 109/L (normal 4.5–11.0)
- Absolute neutrophil count 13.3 × 109/L (4.0–11.0)
- Hemoglobin 13.3 g/dL (13.5–17.5)
- Platelet count 133 × 109/L (150–400)
- International normalized ratio (INR) 1.8
- Sodium 136 mmol/L (135–146)
- Potassium 4.6 mmol/L (3.5–5.0)
- Blood urea nitrogen 31 mg/dL (10–25)
- Creatinine 1.6 mg/dL (0.70–1.40)
- Glucose 62 mg/dL (65–100)
- Bicarbonate 23 mmol/L (23–32)
- Albumin 2.5 g/dL (3.5–5.0)
- Total protein 4.6 g/dL (6.0–8.4)
- Bilirubin 1.2 mg/dL (0.0–1.5)
- Aspartate aminotransferase 41 U/L (7–40)
- Alanine aminotransferase 74 U/L (5–50)
- Alkaline phosphatase 55 U/L (40–150)
- C-reactive protein 9.9 mg/dL (0.0–1.0).
Other studies
Electrocardiography shows atrial fibrillation and left ventricular hypertrophy, but no acute changes.
Computed tomography (CT) of the head shows no evidence of hemorrhage or infarction.
Blood cultures are sent at the time of hospital admission.
WHICH TEST IS NEXT?
1. Which is the most appropriate next step for this patient?
- Urinalysis
- CT of the chest
- Echocardiography
- Skin biopsy
The rash in Figure 1 is palpable purpura, which strongly suggests small-vessel cutaneous vasculitis, a condition that can occur in a broad range of settings. An underlying cause is identified in over 70% of cases. Cutaneous vasculitis may herald a primary small-vessel systemic vasculitis such as Wegener granulomatosis, microscopic polyangiitis, or Henoch-Schönlein purpura. It can also be secondary to a spectrum of underlying triggers or diseases that include medications, infections, malignancies such as lymphoproliferative disorders, cryoglobulinemia secondary to hepatitis C viral infection, and connective tissue diseases such as rheumatoid arthritis and systemic lupus erythematosus.
Infective endocarditis is associated with a secondary form of vasculitis and is a strong possibility in this patient, who has a prosthetic aortic valve, fever, and a high white blood cell count.
Thrombocytopenia should also prompt an assessment for any drugs the patient is taking that affect platelet function. However, thrombocytopenia typically results in nonpalpable purpura.
Idiopathic isolated cutaneous vasculitis, in which no underlying cause for the cutaneous vasculitis can be identified, is the diagnosis in less than 30% of cases.
A vasculitic disease process can involve multiple sites, which may be asymptomatic on presentation. Identifying these sites is important, not only to establish the diagnosis, but also to detect potentially life-threatening complications early.
Thus, in this patient, urinalysis should be done promptly to check for active sediment consisting of red cell casts, which would suggest renal involvement (glomerulonephritis). Also, a rising blood pressure and creatinine would point to renal involvement and warrant more aggressive initial therapy.
Chest radiography should be done to rule out pulmonary infiltrates, septic emboli, nodules, or cavities that could represent vasculitic or infectious involvement of the lungs. CT of the chest may be needed to further characterize abnormalities on chest radiography.
Echocardiography should certainly be pursued as part of the workup for endocarditis, but urinalysis is of the utmost importance in this patient at this point.
More diagnostic information is needed before considering skin biopsy.
Clues from the urinalysis and chest radiography
Our patient’s sedimentation rate is 24 mm/hour. The urinalysis is strongly positive for blood and a moderate amount of protein but negative for leukocyte esterase and nitrite. The urine sediment contains numerous red blood cell casts and 6 to 10 white blood cells per high-power field.
Pending return of blood cultures, ceftriaxone (Rocephin) and azithromycin (Zithromax) are started to treat possible community-acquired pneumonia. Vancomycin (Vancocin) is empirically added, given the possibility of prosthetic valve endocarditis. Gram stain on blood cultures shows gram-positive cocci.
Ground-glass attenuation implies focal or diffuse opacification of the lung that does not obscure the vascular structures, is not associated with air bronchograms, and appears as a “veil” across the lung parenchyma.1 It can be seen in acute diseases such as infection (including pneumonia from atypical bacteria, viruses, acid-fast bacilli, and Pneumocystis jiroveci), pulmonary hemorrhage of any cause, acute viral, eosinophilic, and interstitial pneumonias, and hypersensitivity pneumonitis. It can also be seen in chronic disease states such as interstitial lung disease, bronchoalveolar carcinoma, alveolar proteinosis, and sarcoidosis.
WHICH TEST WOULD NOT HELP?
2. Which of the following tests is least likely to help in the diagnostic evaluation at this point?
- Transthoracic echocardiography
- Transesophageal echocardiography
- Bronchoscopy
- Cystoscopy
In this case, the least likely to help is cystoscopy.
This patient’s vasculitic-appearing rash, ground-glass pulmonary infiltrates, and impaired renal function with red cell casts suggest a pulmonary-renal syndrome, and with this constellation of features, a systemic vasculitis is very likely. Therefore, the focus of the evaluation should be on any evidence to support a diagnosis of vasculitis, as well as other possible causes.
In a patient with diabetes, an artificial heart valve, and fever, the possibility of infection, especially endocarditis, remains high. Transthoracic echocardiography is warranted, and if it is negative for vegetations, transesophageal echocardiography would be a reasonable next option.
Bronchoscopy is warranted to determine if the infiltrates represent pulmonary hemorrhage, which can be seen in certain types of vasculitic and systemic disorders.
The finding of red cell casts in the urine indicates glomerulonephritis, and therefore the kidneys are the likely source of the urinary red blood cells, making cystoscopy of no utility in this current, acute setting.
Case continued: His condition worsens
Transthoracic echocardiography reveals a well-seated mechanical prosthetic aortic valve, trivial aortic regurgitation, a peak gradient of 23 mm Hg and a mean gradient of 12 mm Hg (normal values for his prosthetic valve), and no valvular vegetations. Transesophageal echocardiography confirms the absence of vegetations.
His oxygen requirement increases, and analysis of arterial blood gases reveals a pH of 7.37, Pco2 49 mm Hg (normal range 35–45), Po2 102 mm Hg (normal 80–100), and bicarbonate 28 mmol/L while breathing 100% supplemental oxygen by a nonrebreather face mask. He is taken to the medical intensive care unit for intubation and mechanical ventilation. Bronchoscopy performed while he is intubated confirms diffuse alveolar hemorrhage. Pulse intravenous methylprednisolone (Solu-Medrol) therapy is started.
DIFFUSE ALVEOLAR HEMORRHAGE
3. Which of the following is not true about diffuse alveolar hemorrhage?
- Its onset is usually abrupt or of short duration
- It is always associated with hemoptysis
- Radiography most commonly shows new patchy or diffuse alveolar opacities
- Pulmonary function testing shows increased diffusing capacity of the lung for carbon monoxide (Dlco)
Hemoptysis is absent at presentation in as many as 33% of patients.
The onset of diffuse alveolar hemorrhage is usually abrupt or of short duration, with initial symptoms of cough, fever, and dyspnea. Some patients, such as ours, can present with severe acute respiratory distress syndrome requiring mechanical ventilation. Radiography most often shows new patchy alveolar opacities, and CT may reveal a ground-glass appearance. On pulmonary function testing, the Dlco is high, owing to the hemoglobin within the alveoli.
ACUTE GLOMERULONEPHRITIS PLUS PULMONARY HEMORRHAGE EQUALS…?
4. Which disease could have manifestations consistent with acute glomerulonephritis and pulmonary hemorrhage?
- Antiglomerular basement membrane disease
- Wegener granulomatosis
- Microscopic polyangiitis
- Systemic lupus erythematosus
All of these are possible.
The combined presentation of acute glomerulonephritis and pulmonary hemorrhage (also called pulmonary-renal syndrome) is usually seen in antiglomerular basement membrane disease (Goodpasture syndrome) and small-vessel systemic vasculitides such as Wegener granulomatosis and microscopic polyangiitis.2,3 It can also be seen in patients with systemic lupus erythematosus.
Antiglomerular basement membrane disease
In antiglomerular basement membrane disease, circulating antibodies are directed towards an antigen intrinsic to the glomerular basement membrane, typically leading to acute glomerulonephritis associated with crescent formation. It may present as acute renal failure in which urinalysis shows proteinuria with sediment characterized by red cell casts. Pulmonary involvement, usually alveolar hemorrhage, is present in approximately 60% to 70% of cases.
The diagnosis requires demonstration of antiglomerular basement membrane antibodies in either the serum or the kidney. Renal biopsy is usually recommended because the accuracy of serum assays is variable.
A key histologic feature of the renal lesion in antiglomerular basement membrane disease is crescentic glomerulonephritis in which immunofluorescence microscopy demonstrates the virtually pathognomonic finding of linear deposition of immunoglobulin G along the glomerular capillaries.
The treatment of choice for antiglomerular basement membrane disease is plasmapheresis and immunosuppression with a combination of glucocorticoids and cyclophosphamide (Cytoxan). If the disease is high on the differential diagnosis, empiric plasmapheresis should be started while waiting for diagnostic studies, because the prognosis of untreated glomerulonephritis is poor.
Wegener granulomatosis
Wegener granulomatosis is a systemic vasculitis of the medium and small arteries, arterioles, and venules that classically involves the upper and lower respiratory tracts and the kidneys. Patients may present with persistent rhinorrhea and epistaxis, cough with chest radiographs showing nodules, fixed infiltrates, or cavities, and abnormal urinary sediment with microscopic hematuria with or without red cell casts.
From 75% to 90% of patients with active Wegener granulomatosis are positive for antineutrophil cytoplasmic antibody (ANCA). In 60% to 80% of cases, ANCA is directed against proteinase 3 (PR3), which produces a cytoplasmic standing pattern by immunofluorescence (cANCA), while 5% to 20% have ANCA directed against myeloper-oxidase, which produces a perinuclear staining pattern (pANCA). A small number of patients with Wegener granulomatosis are ANCA-negative.
The diagnosis is usually confirmed by tissue biopsy at the site of active disease, which shows necrotizing vasculitis with granulomatous inflammation. The renal lesion is typically that of a focal, segmental, necrotizing glomerulonephritis that has few to no immune complexes (pauci-immune glomerulonephritis).
The treatment of severe disease involves a combination of cyclophosphamide and glucocorticoids initially to achieve remission followed by maintenance therapy with methotrexate or azathioprine (Imuran).
Microscopic polyangiitis
Microscopic polyangiitis is a systemic vasculitis of the capillaries, venules, and arterioles, with little or no immune complex deposition. Nearly all patients have renal involvement, and 10% to 30% have lung involvement. In those with lung involvement, diffuse alveolar hemorrhage is the most common manifestation.
On histopathologic study, microscopic polyangiitis differs from Wegener granulomatosis in that it does not have granuloma formation. However, the renal lesion is that of a pauci-immune glomerulonephritis and is identical to that seen in Wegener granulomatosis. From 70% to 85% of patients with microscopic polyangiitis are ANCA-positive, and most of these have pANCA.
The management of active severe microscopic polyangiitis is identical to that of Wegener granulomatosis.
Systemic lupus erythematosus
Systemic lupus erythematosus is an autoimmune disease characterized by tissue-binding autoantibody and immune-complex-mediated organ damage. It can involve multiple organ systems, and the diagnosis is based on characteristic clinical features and autoantibodies. The sensitivity of antinuclear antibody for lupus is close to 100%, which makes it a good screening tool. Antibodies to dsDNA and Smith antigen have high specificity for lupus.
About 75% of patients have renal involvement at some point in their disease course. The different types of renal disease in systemic lupus are usually differentiated with a renal biopsy, with immune-complex-mediated glomerular diseases being the most common.
The most common pulmonary manifestation is pleuritis with or without pleural effusion. Life-threatening pulmonary manifestations include pulmonary hemorrhage and interstitial inflammation leading to fibrosis.
Lupus has great clinical variability and the treatment approach is based on the organ manifestations, disease activity, and severity.
CASE CONTINUED: ARRIVING AT THE DIAGNOSIS
We start our patient on cyclophosphamide 175 mg daily in view of possible Wegener granulomatosis.
Even though purpura is extremely rare in primary antiglomerular basement membrane disease, this patient has life-threatening pulmonary hemorrhage, a complication seen in over 50% of these patients. Therefore, plasmapheresis is started empirically.
On the second day of cyclophosphamide treatment, tests for ANCA, glomerular basement membrane antibody, and antinuclear antibody are reported as negative, and complement levels are normal. Bronchoalveolar lavage shows no infection. Follow-up blood cultures are negative.
To summarize the findings so far, this patient has a purpuric skin rash, active urine sediment with red cell casts indicating glomerulonephritis, acute renal failure, and severe pulmonary hemorrhage requiring mechanical ventilation. Although one set of blood cultures showed gram-positive cocci, no source of infection, particularly endocarditis, could be identified.
Antiglomerular basement membrane disease would still be high on the list of suspected diagnoses, given his diffuse alveolar hemorrhage. As mentioned earlier, renal biopsy is imperative to making a diagnosis, because serologic tests have variable accuracy. And making the correct diagnosis has therapeutic implications.
Renal biopsy is performed and shows immune-complex mesangiopathic glomerulonephritis with positive immunofluorescent staining in the mesangium for IgA. Only one glomerulus shows fibrinoid necrosis.
Skin biopsy results obtained earlier showed positive direct immunofluorescence for IgA. Both renal and skin biopsies suggested Henoch-Schönlein purpura.
IgA deposition in the kidney and skin has been associated with liver cirrhosis, celiac disease, and infections with agents such as human immunodeficiency virus, cytomegalovirus, Haemophilus parainfluenzae, and Staphylococcus aureus. In a Japanese study,4 renal biopsy specimens from 116 patients with IgA nephropathy and from 122 patients with other types of kidney disease were examined for the presence of S aureus antigen in the glomeruli. Although antigen was not detected in non-IgA disease, 68% of specimens from patients with IgA nephropathy had S aureus cell envelope antigen together with IgA antibody in the glomeruli. However, no single antigen has been consistently identified, so it seems more probable that the development of IgA deposition in kidneys is a consequence of aberrant IgA immune response rather than the antigen itself.
HENOCH-SCHÖNLEIN PURPURA
Henoch-Schönlein purpura is a systemic vasculitis with a prominent cutaneous component. It is characterized by the tissue deposition of IgA-containing immune complexes. It is predominantly a disease of children but it can be seen in adults. A UK study found the prevalence to be 20 per 100,000 children, with the highest prevalence between ages 4 and 7 (70 per 100,000).5
The four cardinal clinical features of Henoch-Schönlein purpura are purpuric rash, abdominal pain, arthralgia, and renal involvement. Almost all patients have purpuric rash at some point in their disease course. Arthralgia with or without arthritis is typically migratory, oligoarticular, and nondeforming, usually affecting the large joints of the lower extremities; involvement of the upper extremities is less common.
Skin biopsy typically shows leukocytoclastic vasculitis in postcapillary venules with IgA deposition, and these findings are pathognomonic of Henoch-Schönlein purpura.
Gastrointestinal involvement can range from mild symptoms such as nausea, vomiting, abdominal pain, and paralytic ileus to severe disease such as gastrointestinal hemorrhage, bowel infarction, bowel perforation, and intussusception.
Renal involvement is common and is important, as it can in rare cases progress to end-stage renal disease. The urinalysis usually shows mild proteinuria with active sediment with red cell casts. Most patients have relatively mild disease, characterized by asymptomatic hematuria with a normal or slightly elevated creatinine. However, severe involvement may occur, with nephrotic syndrome, hypertension, and acute renal failure.
Different presentation in adults vs children
Adults with Henoch-Schönlein purpura only rarely present with bowel intussusception, whereas some studies have found that adults are more likely than children to develop significant renal involvement, including end-stage renal disease.6,7
There is a general but not absolute correlation between the severity of clinical manifestations and the findings on renal biopsy. A poor prognosis (significant proteinuria, hypertension, renal insufficiency, or end-stage renal disease) is associated with crescent formation involving more than 50% of the glomeruli.8
Our current understanding of the longterm outcome of the renal disease in Henoch-Schönlein purpura is primarily derived from studies in children. In one study, complete recovery occurred in 94% of children and 89% of adults.7 A long-term study of 250 adults with Henoch-Schönlein purpura and renal involvement of sufficient severity to require biopsy reported that, at a median follow up of 15 years, 11% had become dialysis-dependent and 13% had severe renal failure (creatinine clearance < 30 mL/min).6 Recurrence is common, occurring in approximately one-third of patients, more likely in those with nephritis.8
The diagnosis of Henoch-Schönlein purpura is typically made on the basis of key clinical features. In patients such as ours who have an atypical presentation, biopsy of affected skin and renal biopsy can be essential in the diagnosis. Diffuse alveolar hemorrhage is exceedingly rare in Henoch-Schönlein purpura but can be seen, as in our patient.9,10 In this setting, the findings of IgA deposits in skin and renal biopsy specimens, together with the absence of other clinical, serologic, or histologic features of other more-common potential causes, secured the diagnosis in this patient.
Henoch-Schönlein purpura is usually self-limited and requires no specific therapy. Evidence suggests that glucocorticoids enhance the rate of resolution of the arthritis and abdominal pain but do not appear to prevent recurrent disease or lessen the likelihood of progression of renal disease.8 Patients with severe renal involvement with renal function impairment may benefit from pulse intravenous corticosteroid therapy (methylprednisolone 250–1,000 mg per day for 3 days), followed by oral steroids for 3 months.11
In anecdotal reports, renal function improved in 19 of 21 children with Henoch-Schönlein purpura and severe crescentic nephritis.12 Studies have evaluated cyclophosphamide13 and plasmapheresis,14 but their role remains uncertain. Renal transplantation is an option in patients who progress to end-stage renal disease.
OUR CASE CONTINUED
In our patient, plasmapheresis was discontinued. As the pulmonary hemorrhage had developed during treatment with prednisone, we decided to continue cyclophosphamide, given the life-threatening nature of his disease. His pulmonary status improved and he was extubated.
During his initial hospital stay, he was taking heparin for anticoagulation therapy. However, given the life-threatening diffuse alveolar hemorrhage, heparin was stopped during the course of his stay in the intensive care unit. Once he was stable and was transferred out of the intensive care unit, heparin was resumed, and his anticoagulation therapy was bridged to warfarin just before discharge. He was eventually discharged on a tapering dose of oral prednisone and cyclophosphamide for 3 months, after which he was switched to azathioprine for maintenance therapy. He was doing well 6 months later, with a serum creatinine level of 1.6 mg/dL, no red cell casts in the urine, and no rash.
TAKE-HOME POINT
In any case of suspected vasculitis that presents with skin disease, it is essential to look for other sites with potentially life-threatening involvement. Henoch-Schönlein purpura is a systemic vasculitis with a prominent cutaneous component. It is not always benign and can be associated with serious complications such as renal failure, gastrointestinal events, and, very rarely, diffuse alveolar hemorrhage.
- Collins J, Stern EJ. Ground-glass opacity at CT: the ABCs. AJR Am J Roentgenol 1997; 169:355–367.
- Boyce NW, Holdsworth SR. Pulmonary manifestations of the clinical syndrome of acute glomerulonephritis and lung hemorrhage. Am J Kidney Dis 1986; 8:31–36.
- Gallagher H, Kwan JT, Jayne DR. Pulmonary renal syndrome: a 4-year, single-center experience. Am J Kidney Dis 2002; 39:42–47.
- Koyama A, Sharmin S, Sakurai H, et al. Staphylococcus aureus cell envelope antigen is a new candidate for the induction of IgA nephropathy. Kidney Int 2004; 66:121–132.
- Gardner-Medwin JM, Dolezalova P, Cummins C, Southwood TR. Incidence of Henoch-Schönlein purpura, Kawasaki disease, and rare vasculitides in children of different ethnic origins. Lancet 2002; 360:1197–1202.
- Pillebout E, Thervet E, Hill G, Alberti C, Vanhille P, Nochy D. Henoch-Schönlein purpura in adults: outcome and prognostic factors. J Am Soc Nephrol 2002; 13:1271–1278.
- Blanco R, Martinez-Taboada VM, Rodriguez-Valverde V, Garcia-Fuentes M, Gonzalez-Gay MA. Henoch-Schönlein purpura in adulthood and childhood: two different expressions of the same syndrome. Arthritis Rheum 1997; 40:859–864.
- Saulsbury FT. Henoch-Schönlein purpura in children. Report of 100 patients and review of the literature. Medicine (Baltimore) 1999; 78:395–409.
- Nadrous HF, Yu AC, Specks U, Ryu JH. Pulmonary involvement in Henoch-Schönlein purpura. Mayo Clin Proc 2004; 79:1151–1157.
- Vats KR, Vats A, Kim Y, Dassenko D, Sinaiko AR. Henoch-Schönlein purpura and pulmonary hemorrhage: a report and literature review. Pediatr Nephrol 1999; 13:530–534.
- Niaudet P, Habib R. Methylprednisolone pulse therapy in the treatment of severe forms of Schönlein-Henoch purpura nephritis. Pediatr Nephrol 1998; 12:238–243.
- Bergstein J, Leiser J, Andreoli SP. Response of crescentic Henoch-Schöenlein purpura nephritis to corticosteroid and azathioprine therapy. Clin Nephrol 1998; 49:9–14.
- Tarshish P, Bernstein J, Edelmann CM. Henoch-Schönlein purpura nephritis: course of disease and efficacy of cyclophosphamide. Pediatr Nephrol 2004; 19:51–56.
- Hattori M, Ito K, Konomoto T, Kawaguchi H, Yoshioka T, Khono M. Plasmapheresis as the sole therapy for rapidly progressive Henoch-Schönlein purpura nephritis in children. Am J Kidney Dis 1999; 33:427–433.
- Collins J, Stern EJ. Ground-glass opacity at CT: the ABCs. AJR Am J Roentgenol 1997; 169:355–367.
- Boyce NW, Holdsworth SR. Pulmonary manifestations of the clinical syndrome of acute glomerulonephritis and lung hemorrhage. Am J Kidney Dis 1986; 8:31–36.
- Gallagher H, Kwan JT, Jayne DR. Pulmonary renal syndrome: a 4-year, single-center experience. Am J Kidney Dis 2002; 39:42–47.
- Koyama A, Sharmin S, Sakurai H, et al. Staphylococcus aureus cell envelope antigen is a new candidate for the induction of IgA nephropathy. Kidney Int 2004; 66:121–132.
- Gardner-Medwin JM, Dolezalova P, Cummins C, Southwood TR. Incidence of Henoch-Schönlein purpura, Kawasaki disease, and rare vasculitides in children of different ethnic origins. Lancet 2002; 360:1197–1202.
- Pillebout E, Thervet E, Hill G, Alberti C, Vanhille P, Nochy D. Henoch-Schönlein purpura in adults: outcome and prognostic factors. J Am Soc Nephrol 2002; 13:1271–1278.
- Blanco R, Martinez-Taboada VM, Rodriguez-Valverde V, Garcia-Fuentes M, Gonzalez-Gay MA. Henoch-Schönlein purpura in adulthood and childhood: two different expressions of the same syndrome. Arthritis Rheum 1997; 40:859–864.
- Saulsbury FT. Henoch-Schönlein purpura in children. Report of 100 patients and review of the literature. Medicine (Baltimore) 1999; 78:395–409.
- Nadrous HF, Yu AC, Specks U, Ryu JH. Pulmonary involvement in Henoch-Schönlein purpura. Mayo Clin Proc 2004; 79:1151–1157.
- Vats KR, Vats A, Kim Y, Dassenko D, Sinaiko AR. Henoch-Schönlein purpura and pulmonary hemorrhage: a report and literature review. Pediatr Nephrol 1999; 13:530–534.
- Niaudet P, Habib R. Methylprednisolone pulse therapy in the treatment of severe forms of Schönlein-Henoch purpura nephritis. Pediatr Nephrol 1998; 12:238–243.
- Bergstein J, Leiser J, Andreoli SP. Response of crescentic Henoch-Schöenlein purpura nephritis to corticosteroid and azathioprine therapy. Clin Nephrol 1998; 49:9–14.
- Tarshish P, Bernstein J, Edelmann CM. Henoch-Schönlein purpura nephritis: course of disease and efficacy of cyclophosphamide. Pediatr Nephrol 2004; 19:51–56.
- Hattori M, Ito K, Konomoto T, Kawaguchi H, Yoshioka T, Khono M. Plasmapheresis as the sole therapy for rapidly progressive Henoch-Schönlein purpura nephritis in children. Am J Kidney Dis 1999; 33:427–433.
New developments in the diagnosis of fibromyalgia syndrome: Say goodbye to tender points?
A relatively new diagnostic tool, the Symptom Intensity Scale, is an easy, quick way to assess both regional pain and fatigue in a patient. It can be used to establish the diagnosis of fibromyalgia syndrome and measure its severity in daily clinical practice without the need to count tender points. It can also be used to detect fibromyalgia as a comorbidity in other clinical illnesses; by uncovering fibromyalgia, the questionnaire serves as a surrogate measure of depression, anxiety, other serious personality disorders, previous or ongoing abuse, and, when fatigue is the dominant symptom, a consideration of obstructive sleep apnea—all part of the pathoetiology of fibromyalgia in that individual.
This manuscript reviews previous criteria and definitions by which fibromyalgia syndrome was recognized, describes how the new questionnaire was developed, and discusses its implications. It is not meant as a review of the pathogenesis or treatment of fibromyalgia or when to send the patient to the rheumatologist. Each of those topics requires lengthy and complex discussions, which are beyond the scope of this paper.
A COMMON, MULTIFACTORIAL DISEASE
The pathoetiology of fibromyalgia syndrome is rooted in disordered sleep, increased stress, and abnormal neurosensory processing, with secondary endocrine and autonomic dysfunction in those who are genetically predisposed.1–4 Because fibromyalgia is multifactorial, it is best understood from the perspective of an inclusive biopsychosocial model rather than a limited biomedical model.5 Its characteristic signs and symptoms are best understood as emanating from a physiologic state, called central sensitization syndrome, in which the nervous system overresponds to stimuli.1,3 This anomalous state of heightened nervous system response is not confined to the peripheral nervous system, but is also present in the autonomic and central nervous systems.3,4
Fibromyalgia syndrome is common, affecting 0.5% to 5% of the general population,6 and is either the second or third most common diagnosis in a rheumatology practice. Importantly for internists, a diagnosis of fibromyalgia syndrome should be made in 10% to 15% of primary care patients.7 The high prevalence alone demands diagnostic recognition.
KNOWN IN HISTORY AND LITERATURE
Although the designation fibromyalgia syndrome is new, the illness has been with us for as long as we’ve been us. In fact, the word rheumatology may have its origin in fibromyalgia syndrome. Galen (about 180 ad) blamed the symptoms of diffuse pain on the “rheuma,” which has been interpreted as “a great fluxion which races [from the center?] to various parts of the body, and goes from one to another.”8 (Is this the origin of blood-letting as a treatment for diseases?) In 1592, the French physician Guillaume de Baillou introduced the term rheumatism to describe both muscle and joint pain.9
Literature also knows fibromyalgia syndrome. Hans Christian Andersen described a supersensitive princess for whom a pea beneath many mattresses was sufficient to ruin her sleep. In The Fall of the House of Usher, Edgar Allan Poe described Roderick Usher as having an “acute bodily illness and mental disorder that oppressed him.” Usher would wear garments of only soft texture because rough cloth was painful. Light hurt his eyes, forcing him to keep the curtains drawn. Although he had previously played and enjoyed violin music, he could no longer tolerate the sound of the violin. In fact, he suffered such hyperacusis that he could hear his sister moving in her grave many floors below. Other stories by Poe such as Rats in the Wall and The Tell-Tale Heart give more evidence that he was well acquainted with the symptoms of central sensitization syndrome.
HOW THE DEFINITION HAS EVOLVED
To recognize fibromyalgia we need an accurate definition, which has evolved over the years. If we don’t know where we’ve been, it is difficult to understand where we are now or how we got here.
Gowers,10 in 1904, was the first to describe diffuse pain as “fibrositis.” He believed that the pain was due to proliferation or inflammation (or both) of subcutaneous and fibrous tissue, a histopathology that has not been satisfactorily demonstrated to this date. Unfortunately for our purposes, his paper was a descriptive essay that made no attempt at codification. In fact, attempts to clinically define and classify fibromyalgia syndrome have been relatively recent.
Hench11 proposed the first clinical definition in 1976, and it probably did more harm than good. His criteria were two: pain, and no physiologic explanation. The diagnosis was therefore made by ruling out everything else rather than by ruling it in by clinical criteria. Consequently, the diagnosing physician had to investigate the symptom or symptoms by ordering potentially limitless testing, which all had to be normal before the diagnosis could be entertained. I continue to see this phenomenon today as new patients with classic fibromyalgia syndrome arrive carrying reports of normal magnetic imaging of the entire body and serologic testing—a “connective tissue disease workup.”
Counting tender points
Smythe (1979)12 was the first to define and classify fibromyalgia syndrome as a rule-in diagnosis. Smythe’s criteria included tender points in at least 12 of 14 anatomic locations using 4 kg of pressure. In practice, the pressure is approximate—the nail bed blanches in a normotensive examiner with a force of 4 kg. He also described four necessary signs and symptoms: diffuse pain of at least 3 months’ duration, disturbed sleep, skin-roll tenderness at the upper trapezius border, and normal results on laboratory tests. He and Moldofsky13 also found a relationship between disordered slow-wave sleep and the symptoms of fibromyalgia syndrome.
Yunus et al (1981)14 compared signs and symptoms in 50 patients with fibromyalgia syndrome and 50 healthy controls to develop criteria for the disease. Of the resulting criteria, two were mandatory: diffuse pain of at least 3 months’ duration and lack of other obvious causes. The definition also required tenderness in at least 5 of 40 tender points and outlined 10 minor criteria.
Signs and factors that modulate fibromyalgia syndrome and that were derived from these minor criteria are still clinically important today. Factors that aggravate pain include cold or humid weather, fatigue, sedentary state, anxiety, and overactivity. Relieving factors include a hot shower, physical activity, warm dry weather, and massage.
The American College of Rheumatology (1990). Understanding that at any one time approximately 15% of the general population experiences widespread pain,15 a committee of the American College of Rheumatology (ACR) set out to differentiate patients with fibromyalgia syndrome from those with less severe widespread pain. The committee compared signs and symptoms in 293 patients deemed by experts to have fibromyalgia syndrome and 265 control patients matched for age, sex, and concomitant rheumatic disorders. 16
The symptom of widespread pain of at least 3 months’ duration and tenderness in at least 11 of 18 points became the ACR’s diagnostic criteria and provided a sensitivity of 88% and a specificity of 81% compared with the experts’ opinion as the gold standard test.
Low specificity is one of the recognized problems with the ACR criteria: 19% of patients with at least 11 tender points did not have fibromyalgia syndrome. In addition, tender points don’t correlate well with some measures of illness activity, such as the Fibromyalgia Impact Questionnaire.17
Is the tender-point count a good measure?
The best argument for continuing to count tender points as part of the clinical evaluation is that it is a measure of severity. Higher numbers of tender points indicate greater psychological distress and greater severity and frequency of other, closely related fibromyalgia symptoms.18,19 Nearly everyone in the general population has at least a few tender points.16 In fibromyalgia syndrome, the tender-point count is a good status surrogate, a measure of the state of the illness.
But should a state/status measure be used as an illness trait and a criterion for diagnosis? I believe not. Consider, as an analogy, the use of the erythrocyte sedimentation rate in patients with rheumatoid arthritis. An elevated sedimentation rate may indicate increased systemic inflammation, but it is a measure of the status of rheumatoid arthritis, not a trait of this disease. This is why I believe that most rheumatologists would disagree with using some value of the erythrocyte sedimentation rate as a criterion for the diagnosis of rheumatoid arthritis and, by analogy, the tender-point count as a criterion for the diagnosis of fibromyalgia syndrome. Also, the number of tender points, a surrogate for diffuse pain, does not fully capture the essence of the illness, in which accompanying fatigue is often severe and nearly always present.20
A CONTEMPORARY DEFINITION AND ITS VALIDATION
As the concept of fibromyalgia syndrome evolved, a movement away from tender points took hold.21
The Manchester criteria22 used a pain diagram to establish the diagnosis, in which the patient indicated the areas of pain on a simple drawing, obviating the need for tender points. It showed good agreement with the ACR criteria, and in fact identified patients with more severe symptoms.
The London Fibromyalgia Epidemiology Study Screening Questionnaire,23 designed as an epidemiologic tool to estimate the prevalence of the syndrome, was the first test to specifically include both pain and fatigue.
White et al,24 in a very important subsequent study, showed that higher fatigue scores differentiated patients with widespread pain and only a few tender points (7–10) from those with more tender points. This report helped to set the stage for the Symptom Intensity Scale.
What the Symptom Intensity Scale measures
- The Regional Pain Scale score, which is the number of anatomic areas—out of a possible 19—in which the patient feels pain
- A fatigue visual analogue scale score, in which the patient makes a mark somewhere along a 10-cm line to indicate how tired he or she feels. Subsequently, the clinician measures the position of the mark from the left end of the line with a ruler.
How the Symptom Intensity Scale was developed
Wolfe (2003)25 mailed a survey to 12,799 patients who had rheumatoid arthritis, osteoarthritis, or fibromyalgia syndrome. The questionnaire asked respondents if they had pain in 38 articular and nonarticular anatomic regions and to complete a 10-cm fatigue visual analogue scale. He observed that pain in a subset of 19 primarily nonarticular sites differentiated fibromyalgia syndrome from the other two diseases. Calling the number of painful areas of these 19 sites the Regional Pain Scale, he analyzed this measure using Mokken analysis and Rasch analysis to ensure that the questionnaire was statistically valid.
Wolfe also showed that a score of at least 8 points on the Regional Pain Scale, combined with a score of at least 6 cm on the fatigue visual analogue scale, provided the best diagnostic precision consistent with a diagnosis of fibromyalgia syndrome. The combination of these two measures became known as the Survey Criteria.
Katz, Wolfe, and Michaud (2006)26 next compared the diagnostic precision of the Survey Criteria, the ACR criteria, and a physician’s clinical diagnosis. The clinicians made their clinical diagnosis by “considering the long-term patient-clinician experience [including] factors related to pain, tenderness, fatigue, sleep disturbance, comorbidity, and psychosocial variables,” or as I call it, the company fibromyalgia syndrome keeps (Table 2).7,14,16,20 The Survey Criteria (8 points or higher on the Regional Pain Scale plus 6 cm or higher on the fatigue visual analogue scale) showed a roughly 75% concordance among all three definitions in 206 patients with fibromyalgia syndrome. In a cohort with clinically diagnosed fibromyalgia syndrome, a Regional Pain Scale score of 8 or more had a sensitivity of 83.2%, a specificity of 87.6%, and a percent correct of 85.4%. The authors reported that a score of 6 cm or more on the fatigue visual analogue scale “was also at the optimum level” for diagnosing fibromyalgia, but they did not provide more information.
Wolfe and Rasker (2006),27 using these data, devised the Symptom Intensity Scale, the score of which is calculated as the fatigue visual analogue scale score plus half the Regional Pain Scale score, all divided by 2. The scale is therefore a continuous variable rather than a categorical one, and scores can range from 0 to 9.75.
The authors gave the questionnaire to 25,417 patients who had various rheumatic diseases and found that a score of 5.75 or higher differentiated fibromyalgia syndrome from other rheumatic diseases, identifying 95% of patients who would satisfy the Survey Criteria for fibromyalgia.
In addition, they found a linear relationship between the Symptom Intensity Scale score and key symptoms of fibromyalgia syndrome. Of even greater importance, the Symptom Intensity Scale score showed closer association with general health than scores on the Health Assessment Questionnaire, a 27-question patient activity scale, the Arthritis Impact Measurement Scale, or the Short Form-36. It also proved to correlate with mood, probability of having diabetes, need for hospitalization, history of or relative time to myocardial infarction, number of comorbidities, rate of disability, and risk of early death (relative risk 1.12, 95% confidence interval 1.10–1.14). The Symptom Intensity Scale is therefore a diagnostic tool as well as a simple measure of general health among all rheumatic disease patients.
IMPLICATIONS OF THE SYMPTOM INTENSITY SCALE
Three arguments provide a strong rationale for using the Symptom Intensity Scale in the outpatient clinic to investigate the biopsychosocial aspects of illness in our patients:
- It is a simple way to measure overall health
- It can uncover comorbid depression
- It can detect fibromyalgia syndrome in patients who have other diseases.
It measures overall health
Unlike instruments intended for a particular disease such as the Disease Activity Score, which measures disease severity only in rheumatoid arthritis, the Symptom Intensity Scale score can also be used as a measure of global health (or disease severity), and the Survey Criteria (8 or more on the Regional Pain Score and 6 or more on the fatigue visual analogue scale) can be used to establish diagnosis. In fact, instruments like the Disease Activity Score essentially ignore biopsychosocial issues that are captured by the Symptom Intensity Scale.27
By detecting fibromyalgia syndrome in our patients, we identify people with symptoms of pain and distress that do not easily fit the prevalent model of organic disease. Measures like the Disease Activity Score are specifically suited as end points in controlled efficacy trials, but if these are the only measures physicians use to estimate a patient’s health in the clinic, they do so at their own and their patient’s peril.27
Because the continuous Symptom Intensity Scale score strongly correlates with patient-perceived pain, depression, and general health, it is an ideal instrument for outpatient evaluation. It complements a complete patient history and physical examination by measuring biopsychosocial factors.
It uncovers comorbid depression
Rheumatologists do a woeful job of recognizing and diagnosing depression in patients with rheumatoid arthritis. Sleath et al28 found that patients with rheumatoid arthritis who were diagnosed with depression in the office were always the ones who initiated the discussion of that diagnosis. Their doctors did not elicit it.
Middleton et al29 found that patients with concomitant fibromyalgia syndrome and systemic lupus erythematosus (SLE) had higher depression scores than did SLE patients without fibromyalgia syndrome. Moussavi et al,30 writing for the World Health Organization about the findings of a 60-country survey, concluded: “The comorbid state of depression incrementally worsens health compared with depression alone, with any of the chronic diseases alone, and with any combination of chronic diseases without depression.”30
Worse health implies earlier death. Ang et al31 reported that a higher average 4-year depression scale score conferred a hazard ratio of 1.35 (P < .001) for earlier death among 1,290 rheumatoid arthritis patients followed for 12 years.
By using a test like the Symptom Intensity Scale to detect fibromyalgia syndrome alone or to detect it in patients with other diseases, we implicitly recognize the high likelihood of simultaneous depression. Recognition and treatment of depression will improve overall health.
It can detect fibromyalgia syndrome in patients with other diseases
Not surprisingly, distress-related fibromyalgia syndrome is more common in patients with chronic rheumatic or arthritic diseases, with a frequency ranging from 5% in osteoarthritis to 47% in Sjögren syndrome.1 When present, fibromyalgia syndrome changes the features of the other disease.
Wolfe and Michaud32 used the Survey Criteria to evaluate 11,866 rheumatoid arthritis patients and found that 17.1% of them also had fibromyalgia syndrome, and those that did had higher levels of pain, greater global severity, higher scores on the Health Assessment Questionnaire and Short Form-36 mental component, and more disability than those without fibromyalgia syndrome.
Urrows et al33 found that the mean tender-joint count correlated with the mean tenderpoint count in 67 patients with rheumatoid arthritis followed for 75 days. Comorbid fibromyalgia syndrome rendered joints more tender, so that an examiner using the tender-joint count as a major indicator of disease severity might overestimate severity and excessively treat a rheumatoid arthritis patient with unrecognized concurrent fibromyalgia syndrome. Because comorbid fibromyalgia syndrome can inflate Health Assessment Questionnaire scores and subjective pain scale scores in rheumatoid arthritis, more appropriate investigation and management decisions should follow recognition.
Concurrent fibromyalgia syndrome can also be troublesome in SLE. Patients with fibromyalgia syndrome had greater disability than patients without fibromyalgia syndrome despite having no worse SLE damage scores.29 Comorbid fibromyalgia syndrome in SLE has also been shown to diminish quality of life as measured by the Short Form-36.34
Fibromyalgia syndrome also has the potential to confound the diagnosis of concomitant diseases. Wolfe et al35 found that 22.1% of 458 patients with SLE also had fibromyalgia syndrome using the Symptom Intensity Scale criteria. At the time of referral to a rheumatologist, patients who met the criteria for fibromyalgia syndrome were more likely to have self-reported a diagnosis of SLE than were patients for whom SLE had been previously physician-confirmed. The authors warned that fibromyalgia syndrome could intrude into the precision of the diagnosis if only a positive antinuclear antibody test and “soft” SLE criteria were used for diagnosis. If we are unaware of fibromyalgia syndrome, spurious diagnoses may ensue.
BOTTOM LINE
I use the Symptom Intensity Scale as part of routine evaluation in my office. Most patients can complete it with no instruction in 2 minutes or less. I believe it should be used in the clinic to confirm a diagnosis of fibromyalgia syndrome in patients with chronic diffuse pain at rest and to identify comorbid distress in patients with other diseases. This test complements a careful patient history and physical examination, and through its symptom and general health correlations facilitates characterization of our patients’ illnesses in line with the biopsychosocial model.
Since the Symptom Intensity Scale has been shown to be an accurate surrogate measure for general health, depression, disability, and death, fibromyalgia syndrome diagnosed using this instrument implies that this illness is not just centrally mediated pain, but that it carries increased medical risk. It can also be used as a research tool to measure the prevalence of fibromyalgia syndrome in other diseases.
Although the Symptom Intensity Scale is not yet recognized by the ACR as part (or the whole) of the classification criteria for fibromyalgia syndrome, it has already been shown in published studies to be a valid research tool, and it will very likely be the cornerstone of the new criteria.
Goodbye to tender points? Get used to it.
- Wilke WS. The clinical utility of fibromyalgia. J Clin Rheumatol 1999; 5:97–103.
- Cohen H, Buskila D, Neumann L, Ebstein RP. Confirmation of an association between fibromyalgia and serotonin transporter region (5-HTTLPR) polymorphism, and relationship to anxiety-related personality traits. Arthritis Rheum 2002; 46:845–847.
- Geisser ME, Glass JM, Rajcevska LD, et al. A psychophysical study of auditory and pressure sensitivity in patients with fibromyalgia and healthy controls. J Pain 2008; 9:417–422.
- Katz DL, Greene L, Ali A, Faridi Z. The pain of fibromyalgia syndrome is due to muscle hypoperfusion induced by regional vasomotor dysregulation. Med Hypotheses 2007; 69:517–525.
- Engel GL. The need for a new medical model: a challenge for biomedicine. Science 1977; 196:129–136.
- Gran JT. The epidemiology of chronic generalized musculoskeletal pain. Best Pract Res Clin Rheumatol 2003; 17:547–561.
- Wolfe F, Ross K, Anderson J, Russell IJ, Hebert L. The prevalence and characteristics of fibromyalgia in the general population. Arthritis Rheum 1995; 38:19–28.
- Lagier R. Nosology versus pathology, two approaches to rheumatic diseases illustrated by Alfred Baring Garrod and Jean-Martin Charcot. Rheumatology (Oxford) 2001; 40:467–471.
- Ruhman W. The earliest book on rheumatism. Br J Rheumatol 1940; 2:140–162.
- Gowers WR. A lecture on lumbago: its lessons and analogues. Br Med J 1904; 1:117–121.
- Hench PK. Nonarticular rheumatism. Arthritis Rheum 1976; 19(suppl):1081–1088.
- Smythe HA. “Fibrositis” as a disorder of pain modulation. Clin Rheum Dis 1979; 5:823–832.
- Smythe HA, Moldofsky H. Two contributions to understanding of the “fibrositis” syndrome. Bull Rheum Dis 1977–1978; 28:928–931.
- Yunus M, Masi AT, Calabro JJ, Miller KA, Feigenbaum SL. Primary fibromyalgia (fibrositis): clinical study of 50 patients with matched controls. Semin Arthritis Rheum 1981; 11:151–171.
- Croft P, Rigby AS, Boswell R, Schollum J, Silman A. The prevalence of chronic widespread pain in the general population. J Rheumatol 1993; 20:710–713.
- Wolfe F, Smythe HA, Yunus MB, et al. The American College of Rheumatology 1990 Criteria for Classification of Fibromyalgia. Report of the Multicenter Criteria Committee. Arthritis Rheum 1990; 33:160–172.
- McVeigh JG, Finch MB, Hurley DA, Basford JR, Sim J, Baxter GD. Tender point count and total myalgic score in fibromyalgia: changes over a 28-day period. Rheumatol Int 2007; 27:1011–1018.
- Croft P, Schollum J, Silman A. Population study of tender point counts and pain as evidence of fibromyalgia. BMJ 1994; 309:696–699.
- Wolfe F. The relation between tender points and fibromyalgia symptom variables: evidence that fibromyalgia is not a discrete disorder in the clinic. Ann Rheum Dis 1997; 56:268–271.
- Mease PJ, Arnold LM, Crofford LJ, et al. Identifying the clinical domains of fibromyalgia: contributions from clinician and patient Delphi exercises. Arthritis Rheum 2008; 59:952–960.
- Harth M, Nielson WR. The fibromyalgia tender points: use them or lose them? A brief review of the controversy. J Rheumatol 2007; 34:914–922.
- Macfarlane GJ, Croft PR, Schollum J, Silman AJ. Widespread pain: is an improved classification possible? J Rheumatol 1996; 23:1628–1632.
- White KP, Harth M, Speechley M, Ostbye T. Testing an instrument to screen for fibromyalgia syndrome in general population studies: the London Fibromyalgia Epidemiology Study Screening Questionnaire. J Rheumatol 1999; 26:880–884.
- White KP, Speechly M, Harth M, Osbye T. The London Fibromyalgia Epidemiology Study: comparing the demographic and clinical characteristics in 100 random community cases of fibromyalgia versus controls. J Rheumatol 1999; 26:1577–1585.
- Wolfe F. Pain extent and diagnosis: development and validation of the regional pain scale in 12,799 patients with rheumatic disease. J Rheumatolol 2003; 30:369–378.
- Katz RS, Wolfe F, Michaud K. Fibromyalgia diagnosis. a comparison of clinical, survey, and American College of Rheumatology criteria. Arthritis Rheum 2006; 54:169–176.
- Wolfe F, Rasker JJ. The Symptom Intensity Scale, fibromyalgia, and the meaning of fibromyalgia-like symptoms. J Rheumatol 2006; 33:2291–2299.
- Sleath B, Chewning B, De Vellis BM, et al. Communication about depression during rheumatoid arthritis patient visits. Arthritis Rheum 2008; 59:186–191.
- Middleton GD, McFarlin JE, Lippski PE. The prevalence and clinical impact of fibromyalgia in systemic lupus erythematosus. Arthritis Rheum 1994; 37:1181–1188.
- Moussavi S, Chatterji S, Verdes E, Tandon A, Patel V, Ustun B. Depression, chronic diseases, and decrements in health: results from the World Health Surveys. Lancet 2007; 370:851–858.
- Ang DC, Choi H, Kroenke K, Wolfe F. Comorbid depression is an independent risk factor for mortality in patients with rheumatoid arthritis. J Rheumatol 2005; 32:1013–1019.
- Wolfe F, Michaud K. Severe rheumatoid arthritis (RA), worse outcomes, comorbid illness, and sociodemograghic disadvantage characterize RA patients with fibromyalgia. J Rheumatol 2004; 31:695–700.
- Urrows S, Affleck G, Tennen H, Higgins P. Unique clinical and psychological correlates of fibromyalgia tender points and joint tenderness in rheumatoid arthritis. Arthritis Rheum 1994; 37:1513–1520.
- Gladman DD, Urowitz MB, Gough J, MacKinnon A. Fibromyalgia is a major contributor to quality of life in lupus. J Rheumatol 1997; 24:2145–2148.
- Wolfe F, Petri M, Alarcon GS, et al. Fibromyalgia, systemic lupus erythematosus (SLE) and evaluation of SLE activity. J Rheumatol 2009; 36:.27–33.
A relatively new diagnostic tool, the Symptom Intensity Scale, is an easy, quick way to assess both regional pain and fatigue in a patient. It can be used to establish the diagnosis of fibromyalgia syndrome and measure its severity in daily clinical practice without the need to count tender points. It can also be used to detect fibromyalgia as a comorbidity in other clinical illnesses; by uncovering fibromyalgia, the questionnaire serves as a surrogate measure of depression, anxiety, other serious personality disorders, previous or ongoing abuse, and, when fatigue is the dominant symptom, a consideration of obstructive sleep apnea—all part of the pathoetiology of fibromyalgia in that individual.
This manuscript reviews previous criteria and definitions by which fibromyalgia syndrome was recognized, describes how the new questionnaire was developed, and discusses its implications. It is not meant as a review of the pathogenesis or treatment of fibromyalgia or when to send the patient to the rheumatologist. Each of those topics requires lengthy and complex discussions, which are beyond the scope of this paper.
A COMMON, MULTIFACTORIAL DISEASE
The pathoetiology of fibromyalgia syndrome is rooted in disordered sleep, increased stress, and abnormal neurosensory processing, with secondary endocrine and autonomic dysfunction in those who are genetically predisposed.1–4 Because fibromyalgia is multifactorial, it is best understood from the perspective of an inclusive biopsychosocial model rather than a limited biomedical model.5 Its characteristic signs and symptoms are best understood as emanating from a physiologic state, called central sensitization syndrome, in which the nervous system overresponds to stimuli.1,3 This anomalous state of heightened nervous system response is not confined to the peripheral nervous system, but is also present in the autonomic and central nervous systems.3,4
Fibromyalgia syndrome is common, affecting 0.5% to 5% of the general population,6 and is either the second or third most common diagnosis in a rheumatology practice. Importantly for internists, a diagnosis of fibromyalgia syndrome should be made in 10% to 15% of primary care patients.7 The high prevalence alone demands diagnostic recognition.
KNOWN IN HISTORY AND LITERATURE
Although the designation fibromyalgia syndrome is new, the illness has been with us for as long as we’ve been us. In fact, the word rheumatology may have its origin in fibromyalgia syndrome. Galen (about 180 ad) blamed the symptoms of diffuse pain on the “rheuma,” which has been interpreted as “a great fluxion which races [from the center?] to various parts of the body, and goes from one to another.”8 (Is this the origin of blood-letting as a treatment for diseases?) In 1592, the French physician Guillaume de Baillou introduced the term rheumatism to describe both muscle and joint pain.9
Literature also knows fibromyalgia syndrome. Hans Christian Andersen described a supersensitive princess for whom a pea beneath many mattresses was sufficient to ruin her sleep. In The Fall of the House of Usher, Edgar Allan Poe described Roderick Usher as having an “acute bodily illness and mental disorder that oppressed him.” Usher would wear garments of only soft texture because rough cloth was painful. Light hurt his eyes, forcing him to keep the curtains drawn. Although he had previously played and enjoyed violin music, he could no longer tolerate the sound of the violin. In fact, he suffered such hyperacusis that he could hear his sister moving in her grave many floors below. Other stories by Poe such as Rats in the Wall and The Tell-Tale Heart give more evidence that he was well acquainted with the symptoms of central sensitization syndrome.
HOW THE DEFINITION HAS EVOLVED
To recognize fibromyalgia we need an accurate definition, which has evolved over the years. If we don’t know where we’ve been, it is difficult to understand where we are now or how we got here.
Gowers,10 in 1904, was the first to describe diffuse pain as “fibrositis.” He believed that the pain was due to proliferation or inflammation (or both) of subcutaneous and fibrous tissue, a histopathology that has not been satisfactorily demonstrated to this date. Unfortunately for our purposes, his paper was a descriptive essay that made no attempt at codification. In fact, attempts to clinically define and classify fibromyalgia syndrome have been relatively recent.
Hench11 proposed the first clinical definition in 1976, and it probably did more harm than good. His criteria were two: pain, and no physiologic explanation. The diagnosis was therefore made by ruling out everything else rather than by ruling it in by clinical criteria. Consequently, the diagnosing physician had to investigate the symptom or symptoms by ordering potentially limitless testing, which all had to be normal before the diagnosis could be entertained. I continue to see this phenomenon today as new patients with classic fibromyalgia syndrome arrive carrying reports of normal magnetic imaging of the entire body and serologic testing—a “connective tissue disease workup.”
Counting tender points
Smythe (1979)12 was the first to define and classify fibromyalgia syndrome as a rule-in diagnosis. Smythe’s criteria included tender points in at least 12 of 14 anatomic locations using 4 kg of pressure. In practice, the pressure is approximate—the nail bed blanches in a normotensive examiner with a force of 4 kg. He also described four necessary signs and symptoms: diffuse pain of at least 3 months’ duration, disturbed sleep, skin-roll tenderness at the upper trapezius border, and normal results on laboratory tests. He and Moldofsky13 also found a relationship between disordered slow-wave sleep and the symptoms of fibromyalgia syndrome.
Yunus et al (1981)14 compared signs and symptoms in 50 patients with fibromyalgia syndrome and 50 healthy controls to develop criteria for the disease. Of the resulting criteria, two were mandatory: diffuse pain of at least 3 months’ duration and lack of other obvious causes. The definition also required tenderness in at least 5 of 40 tender points and outlined 10 minor criteria.
Signs and factors that modulate fibromyalgia syndrome and that were derived from these minor criteria are still clinically important today. Factors that aggravate pain include cold or humid weather, fatigue, sedentary state, anxiety, and overactivity. Relieving factors include a hot shower, physical activity, warm dry weather, and massage.
The American College of Rheumatology (1990). Understanding that at any one time approximately 15% of the general population experiences widespread pain,15 a committee of the American College of Rheumatology (ACR) set out to differentiate patients with fibromyalgia syndrome from those with less severe widespread pain. The committee compared signs and symptoms in 293 patients deemed by experts to have fibromyalgia syndrome and 265 control patients matched for age, sex, and concomitant rheumatic disorders. 16
The symptom of widespread pain of at least 3 months’ duration and tenderness in at least 11 of 18 points became the ACR’s diagnostic criteria and provided a sensitivity of 88% and a specificity of 81% compared with the experts’ opinion as the gold standard test.
Low specificity is one of the recognized problems with the ACR criteria: 19% of patients with at least 11 tender points did not have fibromyalgia syndrome. In addition, tender points don’t correlate well with some measures of illness activity, such as the Fibromyalgia Impact Questionnaire.17
Is the tender-point count a good measure?
The best argument for continuing to count tender points as part of the clinical evaluation is that it is a measure of severity. Higher numbers of tender points indicate greater psychological distress and greater severity and frequency of other, closely related fibromyalgia symptoms.18,19 Nearly everyone in the general population has at least a few tender points.16 In fibromyalgia syndrome, the tender-point count is a good status surrogate, a measure of the state of the illness.
But should a state/status measure be used as an illness trait and a criterion for diagnosis? I believe not. Consider, as an analogy, the use of the erythrocyte sedimentation rate in patients with rheumatoid arthritis. An elevated sedimentation rate may indicate increased systemic inflammation, but it is a measure of the status of rheumatoid arthritis, not a trait of this disease. This is why I believe that most rheumatologists would disagree with using some value of the erythrocyte sedimentation rate as a criterion for the diagnosis of rheumatoid arthritis and, by analogy, the tender-point count as a criterion for the diagnosis of fibromyalgia syndrome. Also, the number of tender points, a surrogate for diffuse pain, does not fully capture the essence of the illness, in which accompanying fatigue is often severe and nearly always present.20
A CONTEMPORARY DEFINITION AND ITS VALIDATION
As the concept of fibromyalgia syndrome evolved, a movement away from tender points took hold.21
The Manchester criteria22 used a pain diagram to establish the diagnosis, in which the patient indicated the areas of pain on a simple drawing, obviating the need for tender points. It showed good agreement with the ACR criteria, and in fact identified patients with more severe symptoms.
The London Fibromyalgia Epidemiology Study Screening Questionnaire,23 designed as an epidemiologic tool to estimate the prevalence of the syndrome, was the first test to specifically include both pain and fatigue.
White et al,24 in a very important subsequent study, showed that higher fatigue scores differentiated patients with widespread pain and only a few tender points (7–10) from those with more tender points. This report helped to set the stage for the Symptom Intensity Scale.
What the Symptom Intensity Scale measures
- The Regional Pain Scale score, which is the number of anatomic areas—out of a possible 19—in which the patient feels pain
- A fatigue visual analogue scale score, in which the patient makes a mark somewhere along a 10-cm line to indicate how tired he or she feels. Subsequently, the clinician measures the position of the mark from the left end of the line with a ruler.
How the Symptom Intensity Scale was developed
Wolfe (2003)25 mailed a survey to 12,799 patients who had rheumatoid arthritis, osteoarthritis, or fibromyalgia syndrome. The questionnaire asked respondents if they had pain in 38 articular and nonarticular anatomic regions and to complete a 10-cm fatigue visual analogue scale. He observed that pain in a subset of 19 primarily nonarticular sites differentiated fibromyalgia syndrome from the other two diseases. Calling the number of painful areas of these 19 sites the Regional Pain Scale, he analyzed this measure using Mokken analysis and Rasch analysis to ensure that the questionnaire was statistically valid.
Wolfe also showed that a score of at least 8 points on the Regional Pain Scale, combined with a score of at least 6 cm on the fatigue visual analogue scale, provided the best diagnostic precision consistent with a diagnosis of fibromyalgia syndrome. The combination of these two measures became known as the Survey Criteria.
Katz, Wolfe, and Michaud (2006)26 next compared the diagnostic precision of the Survey Criteria, the ACR criteria, and a physician’s clinical diagnosis. The clinicians made their clinical diagnosis by “considering the long-term patient-clinician experience [including] factors related to pain, tenderness, fatigue, sleep disturbance, comorbidity, and psychosocial variables,” or as I call it, the company fibromyalgia syndrome keeps (Table 2).7,14,16,20 The Survey Criteria (8 points or higher on the Regional Pain Scale plus 6 cm or higher on the fatigue visual analogue scale) showed a roughly 75% concordance among all three definitions in 206 patients with fibromyalgia syndrome. In a cohort with clinically diagnosed fibromyalgia syndrome, a Regional Pain Scale score of 8 or more had a sensitivity of 83.2%, a specificity of 87.6%, and a percent correct of 85.4%. The authors reported that a score of 6 cm or more on the fatigue visual analogue scale “was also at the optimum level” for diagnosing fibromyalgia, but they did not provide more information.
Wolfe and Rasker (2006),27 using these data, devised the Symptom Intensity Scale, the score of which is calculated as the fatigue visual analogue scale score plus half the Regional Pain Scale score, all divided by 2. The scale is therefore a continuous variable rather than a categorical one, and scores can range from 0 to 9.75.
The authors gave the questionnaire to 25,417 patients who had various rheumatic diseases and found that a score of 5.75 or higher differentiated fibromyalgia syndrome from other rheumatic diseases, identifying 95% of patients who would satisfy the Survey Criteria for fibromyalgia.
In addition, they found a linear relationship between the Symptom Intensity Scale score and key symptoms of fibromyalgia syndrome. Of even greater importance, the Symptom Intensity Scale score showed closer association with general health than scores on the Health Assessment Questionnaire, a 27-question patient activity scale, the Arthritis Impact Measurement Scale, or the Short Form-36. It also proved to correlate with mood, probability of having diabetes, need for hospitalization, history of or relative time to myocardial infarction, number of comorbidities, rate of disability, and risk of early death (relative risk 1.12, 95% confidence interval 1.10–1.14). The Symptom Intensity Scale is therefore a diagnostic tool as well as a simple measure of general health among all rheumatic disease patients.
IMPLICATIONS OF THE SYMPTOM INTENSITY SCALE
Three arguments provide a strong rationale for using the Symptom Intensity Scale in the outpatient clinic to investigate the biopsychosocial aspects of illness in our patients:
- It is a simple way to measure overall health
- It can uncover comorbid depression
- It can detect fibromyalgia syndrome in patients who have other diseases.
It measures overall health
Unlike instruments intended for a particular disease such as the Disease Activity Score, which measures disease severity only in rheumatoid arthritis, the Symptom Intensity Scale score can also be used as a measure of global health (or disease severity), and the Survey Criteria (8 or more on the Regional Pain Score and 6 or more on the fatigue visual analogue scale) can be used to establish diagnosis. In fact, instruments like the Disease Activity Score essentially ignore biopsychosocial issues that are captured by the Symptom Intensity Scale.27
By detecting fibromyalgia syndrome in our patients, we identify people with symptoms of pain and distress that do not easily fit the prevalent model of organic disease. Measures like the Disease Activity Score are specifically suited as end points in controlled efficacy trials, but if these are the only measures physicians use to estimate a patient’s health in the clinic, they do so at their own and their patient’s peril.27
Because the continuous Symptom Intensity Scale score strongly correlates with patient-perceived pain, depression, and general health, it is an ideal instrument for outpatient evaluation. It complements a complete patient history and physical examination by measuring biopsychosocial factors.
It uncovers comorbid depression
Rheumatologists do a woeful job of recognizing and diagnosing depression in patients with rheumatoid arthritis. Sleath et al28 found that patients with rheumatoid arthritis who were diagnosed with depression in the office were always the ones who initiated the discussion of that diagnosis. Their doctors did not elicit it.
Middleton et al29 found that patients with concomitant fibromyalgia syndrome and systemic lupus erythematosus (SLE) had higher depression scores than did SLE patients without fibromyalgia syndrome. Moussavi et al,30 writing for the World Health Organization about the findings of a 60-country survey, concluded: “The comorbid state of depression incrementally worsens health compared with depression alone, with any of the chronic diseases alone, and with any combination of chronic diseases without depression.”30
Worse health implies earlier death. Ang et al31 reported that a higher average 4-year depression scale score conferred a hazard ratio of 1.35 (P < .001) for earlier death among 1,290 rheumatoid arthritis patients followed for 12 years.
By using a test like the Symptom Intensity Scale to detect fibromyalgia syndrome alone or to detect it in patients with other diseases, we implicitly recognize the high likelihood of simultaneous depression. Recognition and treatment of depression will improve overall health.
It can detect fibromyalgia syndrome in patients with other diseases
Not surprisingly, distress-related fibromyalgia syndrome is more common in patients with chronic rheumatic or arthritic diseases, with a frequency ranging from 5% in osteoarthritis to 47% in Sjögren syndrome.1 When present, fibromyalgia syndrome changes the features of the other disease.
Wolfe and Michaud32 used the Survey Criteria to evaluate 11,866 rheumatoid arthritis patients and found that 17.1% of them also had fibromyalgia syndrome, and those that did had higher levels of pain, greater global severity, higher scores on the Health Assessment Questionnaire and Short Form-36 mental component, and more disability than those without fibromyalgia syndrome.
Urrows et al33 found that the mean tender-joint count correlated with the mean tenderpoint count in 67 patients with rheumatoid arthritis followed for 75 days. Comorbid fibromyalgia syndrome rendered joints more tender, so that an examiner using the tender-joint count as a major indicator of disease severity might overestimate severity and excessively treat a rheumatoid arthritis patient with unrecognized concurrent fibromyalgia syndrome. Because comorbid fibromyalgia syndrome can inflate Health Assessment Questionnaire scores and subjective pain scale scores in rheumatoid arthritis, more appropriate investigation and management decisions should follow recognition.
Concurrent fibromyalgia syndrome can also be troublesome in SLE. Patients with fibromyalgia syndrome had greater disability than patients without fibromyalgia syndrome despite having no worse SLE damage scores.29 Comorbid fibromyalgia syndrome in SLE has also been shown to diminish quality of life as measured by the Short Form-36.34
Fibromyalgia syndrome also has the potential to confound the diagnosis of concomitant diseases. Wolfe et al35 found that 22.1% of 458 patients with SLE also had fibromyalgia syndrome using the Symptom Intensity Scale criteria. At the time of referral to a rheumatologist, patients who met the criteria for fibromyalgia syndrome were more likely to have self-reported a diagnosis of SLE than were patients for whom SLE had been previously physician-confirmed. The authors warned that fibromyalgia syndrome could intrude into the precision of the diagnosis if only a positive antinuclear antibody test and “soft” SLE criteria were used for diagnosis. If we are unaware of fibromyalgia syndrome, spurious diagnoses may ensue.
BOTTOM LINE
I use the Symptom Intensity Scale as part of routine evaluation in my office. Most patients can complete it with no instruction in 2 minutes or less. I believe it should be used in the clinic to confirm a diagnosis of fibromyalgia syndrome in patients with chronic diffuse pain at rest and to identify comorbid distress in patients with other diseases. This test complements a careful patient history and physical examination, and through its symptom and general health correlations facilitates characterization of our patients’ illnesses in line with the biopsychosocial model.
Since the Symptom Intensity Scale has been shown to be an accurate surrogate measure for general health, depression, disability, and death, fibromyalgia syndrome diagnosed using this instrument implies that this illness is not just centrally mediated pain, but that it carries increased medical risk. It can also be used as a research tool to measure the prevalence of fibromyalgia syndrome in other diseases.
Although the Symptom Intensity Scale is not yet recognized by the ACR as part (or the whole) of the classification criteria for fibromyalgia syndrome, it has already been shown in published studies to be a valid research tool, and it will very likely be the cornerstone of the new criteria.
Goodbye to tender points? Get used to it.
A relatively new diagnostic tool, the Symptom Intensity Scale, is an easy, quick way to assess both regional pain and fatigue in a patient. It can be used to establish the diagnosis of fibromyalgia syndrome and measure its severity in daily clinical practice without the need to count tender points. It can also be used to detect fibromyalgia as a comorbidity in other clinical illnesses; by uncovering fibromyalgia, the questionnaire serves as a surrogate measure of depression, anxiety, other serious personality disorders, previous or ongoing abuse, and, when fatigue is the dominant symptom, a consideration of obstructive sleep apnea—all part of the pathoetiology of fibromyalgia in that individual.
This manuscript reviews previous criteria and definitions by which fibromyalgia syndrome was recognized, describes how the new questionnaire was developed, and discusses its implications. It is not meant as a review of the pathogenesis or treatment of fibromyalgia or when to send the patient to the rheumatologist. Each of those topics requires lengthy and complex discussions, which are beyond the scope of this paper.
A COMMON, MULTIFACTORIAL DISEASE
The pathoetiology of fibromyalgia syndrome is rooted in disordered sleep, increased stress, and abnormal neurosensory processing, with secondary endocrine and autonomic dysfunction in those who are genetically predisposed.1–4 Because fibromyalgia is multifactorial, it is best understood from the perspective of an inclusive biopsychosocial model rather than a limited biomedical model.5 Its characteristic signs and symptoms are best understood as emanating from a physiologic state, called central sensitization syndrome, in which the nervous system overresponds to stimuli.1,3 This anomalous state of heightened nervous system response is not confined to the peripheral nervous system, but is also present in the autonomic and central nervous systems.3,4
Fibromyalgia syndrome is common, affecting 0.5% to 5% of the general population,6 and is either the second or third most common diagnosis in a rheumatology practice. Importantly for internists, a diagnosis of fibromyalgia syndrome should be made in 10% to 15% of primary care patients.7 The high prevalence alone demands diagnostic recognition.
KNOWN IN HISTORY AND LITERATURE
Although the designation fibromyalgia syndrome is new, the illness has been with us for as long as we’ve been us. In fact, the word rheumatology may have its origin in fibromyalgia syndrome. Galen (about 180 ad) blamed the symptoms of diffuse pain on the “rheuma,” which has been interpreted as “a great fluxion which races [from the center?] to various parts of the body, and goes from one to another.”8 (Is this the origin of blood-letting as a treatment for diseases?) In 1592, the French physician Guillaume de Baillou introduced the term rheumatism to describe both muscle and joint pain.9
Literature also knows fibromyalgia syndrome. Hans Christian Andersen described a supersensitive princess for whom a pea beneath many mattresses was sufficient to ruin her sleep. In The Fall of the House of Usher, Edgar Allan Poe described Roderick Usher as having an “acute bodily illness and mental disorder that oppressed him.” Usher would wear garments of only soft texture because rough cloth was painful. Light hurt his eyes, forcing him to keep the curtains drawn. Although he had previously played and enjoyed violin music, he could no longer tolerate the sound of the violin. In fact, he suffered such hyperacusis that he could hear his sister moving in her grave many floors below. Other stories by Poe such as Rats in the Wall and The Tell-Tale Heart give more evidence that he was well acquainted with the symptoms of central sensitization syndrome.
HOW THE DEFINITION HAS EVOLVED
To recognize fibromyalgia we need an accurate definition, which has evolved over the years. If we don’t know where we’ve been, it is difficult to understand where we are now or how we got here.
Gowers,10 in 1904, was the first to describe diffuse pain as “fibrositis.” He believed that the pain was due to proliferation or inflammation (or both) of subcutaneous and fibrous tissue, a histopathology that has not been satisfactorily demonstrated to this date. Unfortunately for our purposes, his paper was a descriptive essay that made no attempt at codification. In fact, attempts to clinically define and classify fibromyalgia syndrome have been relatively recent.
Hench11 proposed the first clinical definition in 1976, and it probably did more harm than good. His criteria were two: pain, and no physiologic explanation. The diagnosis was therefore made by ruling out everything else rather than by ruling it in by clinical criteria. Consequently, the diagnosing physician had to investigate the symptom or symptoms by ordering potentially limitless testing, which all had to be normal before the diagnosis could be entertained. I continue to see this phenomenon today as new patients with classic fibromyalgia syndrome arrive carrying reports of normal magnetic imaging of the entire body and serologic testing—a “connective tissue disease workup.”
Counting tender points
Smythe (1979)12 was the first to define and classify fibromyalgia syndrome as a rule-in diagnosis. Smythe’s criteria included tender points in at least 12 of 14 anatomic locations using 4 kg of pressure. In practice, the pressure is approximate—the nail bed blanches in a normotensive examiner with a force of 4 kg. He also described four necessary signs and symptoms: diffuse pain of at least 3 months’ duration, disturbed sleep, skin-roll tenderness at the upper trapezius border, and normal results on laboratory tests. He and Moldofsky13 also found a relationship between disordered slow-wave sleep and the symptoms of fibromyalgia syndrome.
Yunus et al (1981)14 compared signs and symptoms in 50 patients with fibromyalgia syndrome and 50 healthy controls to develop criteria for the disease. Of the resulting criteria, two were mandatory: diffuse pain of at least 3 months’ duration and lack of other obvious causes. The definition also required tenderness in at least 5 of 40 tender points and outlined 10 minor criteria.
Signs and factors that modulate fibromyalgia syndrome and that were derived from these minor criteria are still clinically important today. Factors that aggravate pain include cold or humid weather, fatigue, sedentary state, anxiety, and overactivity. Relieving factors include a hot shower, physical activity, warm dry weather, and massage.
The American College of Rheumatology (1990). Understanding that at any one time approximately 15% of the general population experiences widespread pain,15 a committee of the American College of Rheumatology (ACR) set out to differentiate patients with fibromyalgia syndrome from those with less severe widespread pain. The committee compared signs and symptoms in 293 patients deemed by experts to have fibromyalgia syndrome and 265 control patients matched for age, sex, and concomitant rheumatic disorders. 16
The symptom of widespread pain of at least 3 months’ duration and tenderness in at least 11 of 18 points became the ACR’s diagnostic criteria and provided a sensitivity of 88% and a specificity of 81% compared with the experts’ opinion as the gold standard test.
Low specificity is one of the recognized problems with the ACR criteria: 19% of patients with at least 11 tender points did not have fibromyalgia syndrome. In addition, tender points don’t correlate well with some measures of illness activity, such as the Fibromyalgia Impact Questionnaire.17
Is the tender-point count a good measure?
The best argument for continuing to count tender points as part of the clinical evaluation is that it is a measure of severity. Higher numbers of tender points indicate greater psychological distress and greater severity and frequency of other, closely related fibromyalgia symptoms.18,19 Nearly everyone in the general population has at least a few tender points.16 In fibromyalgia syndrome, the tender-point count is a good status surrogate, a measure of the state of the illness.
But should a state/status measure be used as an illness trait and a criterion for diagnosis? I believe not. Consider, as an analogy, the use of the erythrocyte sedimentation rate in patients with rheumatoid arthritis. An elevated sedimentation rate may indicate increased systemic inflammation, but it is a measure of the status of rheumatoid arthritis, not a trait of this disease. This is why I believe that most rheumatologists would disagree with using some value of the erythrocyte sedimentation rate as a criterion for the diagnosis of rheumatoid arthritis and, by analogy, the tender-point count as a criterion for the diagnosis of fibromyalgia syndrome. Also, the number of tender points, a surrogate for diffuse pain, does not fully capture the essence of the illness, in which accompanying fatigue is often severe and nearly always present.20
A CONTEMPORARY DEFINITION AND ITS VALIDATION
As the concept of fibromyalgia syndrome evolved, a movement away from tender points took hold.21
The Manchester criteria22 used a pain diagram to establish the diagnosis, in which the patient indicated the areas of pain on a simple drawing, obviating the need for tender points. It showed good agreement with the ACR criteria, and in fact identified patients with more severe symptoms.
The London Fibromyalgia Epidemiology Study Screening Questionnaire,23 designed as an epidemiologic tool to estimate the prevalence of the syndrome, was the first test to specifically include both pain and fatigue.
White et al,24 in a very important subsequent study, showed that higher fatigue scores differentiated patients with widespread pain and only a few tender points (7–10) from those with more tender points. This report helped to set the stage for the Symptom Intensity Scale.
What the Symptom Intensity Scale measures
- The Regional Pain Scale score, which is the number of anatomic areas—out of a possible 19—in which the patient feels pain
- A fatigue visual analogue scale score, in which the patient makes a mark somewhere along a 10-cm line to indicate how tired he or she feels. Subsequently, the clinician measures the position of the mark from the left end of the line with a ruler.
How the Symptom Intensity Scale was developed
Wolfe (2003)25 mailed a survey to 12,799 patients who had rheumatoid arthritis, osteoarthritis, or fibromyalgia syndrome. The questionnaire asked respondents if they had pain in 38 articular and nonarticular anatomic regions and to complete a 10-cm fatigue visual analogue scale. He observed that pain in a subset of 19 primarily nonarticular sites differentiated fibromyalgia syndrome from the other two diseases. Calling the number of painful areas of these 19 sites the Regional Pain Scale, he analyzed this measure using Mokken analysis and Rasch analysis to ensure that the questionnaire was statistically valid.
Wolfe also showed that a score of at least 8 points on the Regional Pain Scale, combined with a score of at least 6 cm on the fatigue visual analogue scale, provided the best diagnostic precision consistent with a diagnosis of fibromyalgia syndrome. The combination of these two measures became known as the Survey Criteria.
Katz, Wolfe, and Michaud (2006)26 next compared the diagnostic precision of the Survey Criteria, the ACR criteria, and a physician’s clinical diagnosis. The clinicians made their clinical diagnosis by “considering the long-term patient-clinician experience [including] factors related to pain, tenderness, fatigue, sleep disturbance, comorbidity, and psychosocial variables,” or as I call it, the company fibromyalgia syndrome keeps (Table 2).7,14,16,20 The Survey Criteria (8 points or higher on the Regional Pain Scale plus 6 cm or higher on the fatigue visual analogue scale) showed a roughly 75% concordance among all three definitions in 206 patients with fibromyalgia syndrome. In a cohort with clinically diagnosed fibromyalgia syndrome, a Regional Pain Scale score of 8 or more had a sensitivity of 83.2%, a specificity of 87.6%, and a percent correct of 85.4%. The authors reported that a score of 6 cm or more on the fatigue visual analogue scale “was also at the optimum level” for diagnosing fibromyalgia, but they did not provide more information.
Wolfe and Rasker (2006),27 using these data, devised the Symptom Intensity Scale, the score of which is calculated as the fatigue visual analogue scale score plus half the Regional Pain Scale score, all divided by 2. The scale is therefore a continuous variable rather than a categorical one, and scores can range from 0 to 9.75.
The authors gave the questionnaire to 25,417 patients who had various rheumatic diseases and found that a score of 5.75 or higher differentiated fibromyalgia syndrome from other rheumatic diseases, identifying 95% of patients who would satisfy the Survey Criteria for fibromyalgia.
In addition, they found a linear relationship between the Symptom Intensity Scale score and key symptoms of fibromyalgia syndrome. Of even greater importance, the Symptom Intensity Scale score showed closer association with general health than scores on the Health Assessment Questionnaire, a 27-question patient activity scale, the Arthritis Impact Measurement Scale, or the Short Form-36. It also proved to correlate with mood, probability of having diabetes, need for hospitalization, history of or relative time to myocardial infarction, number of comorbidities, rate of disability, and risk of early death (relative risk 1.12, 95% confidence interval 1.10–1.14). The Symptom Intensity Scale is therefore a diagnostic tool as well as a simple measure of general health among all rheumatic disease patients.
IMPLICATIONS OF THE SYMPTOM INTENSITY SCALE
Three arguments provide a strong rationale for using the Symptom Intensity Scale in the outpatient clinic to investigate the biopsychosocial aspects of illness in our patients:
- It is a simple way to measure overall health
- It can uncover comorbid depression
- It can detect fibromyalgia syndrome in patients who have other diseases.
It measures overall health
Unlike instruments intended for a particular disease such as the Disease Activity Score, which measures disease severity only in rheumatoid arthritis, the Symptom Intensity Scale score can also be used as a measure of global health (or disease severity), and the Survey Criteria (8 or more on the Regional Pain Score and 6 or more on the fatigue visual analogue scale) can be used to establish diagnosis. In fact, instruments like the Disease Activity Score essentially ignore biopsychosocial issues that are captured by the Symptom Intensity Scale.27
By detecting fibromyalgia syndrome in our patients, we identify people with symptoms of pain and distress that do not easily fit the prevalent model of organic disease. Measures like the Disease Activity Score are specifically suited as end points in controlled efficacy trials, but if these are the only measures physicians use to estimate a patient’s health in the clinic, they do so at their own and their patient’s peril.27
Because the continuous Symptom Intensity Scale score strongly correlates with patient-perceived pain, depression, and general health, it is an ideal instrument for outpatient evaluation. It complements a complete patient history and physical examination by measuring biopsychosocial factors.
It uncovers comorbid depression
Rheumatologists do a woeful job of recognizing and diagnosing depression in patients with rheumatoid arthritis. Sleath et al28 found that patients with rheumatoid arthritis who were diagnosed with depression in the office were always the ones who initiated the discussion of that diagnosis. Their doctors did not elicit it.
Middleton et al29 found that patients with concomitant fibromyalgia syndrome and systemic lupus erythematosus (SLE) had higher depression scores than did SLE patients without fibromyalgia syndrome. Moussavi et al,30 writing for the World Health Organization about the findings of a 60-country survey, concluded: “The comorbid state of depression incrementally worsens health compared with depression alone, with any of the chronic diseases alone, and with any combination of chronic diseases without depression.”30
Worse health implies earlier death. Ang et al31 reported that a higher average 4-year depression scale score conferred a hazard ratio of 1.35 (P < .001) for earlier death among 1,290 rheumatoid arthritis patients followed for 12 years.
By using a test like the Symptom Intensity Scale to detect fibromyalgia syndrome alone or to detect it in patients with other diseases, we implicitly recognize the high likelihood of simultaneous depression. Recognition and treatment of depression will improve overall health.
It can detect fibromyalgia syndrome in patients with other diseases
Not surprisingly, distress-related fibromyalgia syndrome is more common in patients with chronic rheumatic or arthritic diseases, with a frequency ranging from 5% in osteoarthritis to 47% in Sjögren syndrome.1 When present, fibromyalgia syndrome changes the features of the other disease.
Wolfe and Michaud32 used the Survey Criteria to evaluate 11,866 rheumatoid arthritis patients and found that 17.1% of them also had fibromyalgia syndrome, and those that did had higher levels of pain, greater global severity, higher scores on the Health Assessment Questionnaire and Short Form-36 mental component, and more disability than those without fibromyalgia syndrome.
Urrows et al33 found that the mean tender-joint count correlated with the mean tenderpoint count in 67 patients with rheumatoid arthritis followed for 75 days. Comorbid fibromyalgia syndrome rendered joints more tender, so that an examiner using the tender-joint count as a major indicator of disease severity might overestimate severity and excessively treat a rheumatoid arthritis patient with unrecognized concurrent fibromyalgia syndrome. Because comorbid fibromyalgia syndrome can inflate Health Assessment Questionnaire scores and subjective pain scale scores in rheumatoid arthritis, more appropriate investigation and management decisions should follow recognition.
Concurrent fibromyalgia syndrome can also be troublesome in SLE. Patients with fibromyalgia syndrome had greater disability than patients without fibromyalgia syndrome despite having no worse SLE damage scores.29 Comorbid fibromyalgia syndrome in SLE has also been shown to diminish quality of life as measured by the Short Form-36.34
Fibromyalgia syndrome also has the potential to confound the diagnosis of concomitant diseases. Wolfe et al35 found that 22.1% of 458 patients with SLE also had fibromyalgia syndrome using the Symptom Intensity Scale criteria. At the time of referral to a rheumatologist, patients who met the criteria for fibromyalgia syndrome were more likely to have self-reported a diagnosis of SLE than were patients for whom SLE had been previously physician-confirmed. The authors warned that fibromyalgia syndrome could intrude into the precision of the diagnosis if only a positive antinuclear antibody test and “soft” SLE criteria were used for diagnosis. If we are unaware of fibromyalgia syndrome, spurious diagnoses may ensue.
BOTTOM LINE
I use the Symptom Intensity Scale as part of routine evaluation in my office. Most patients can complete it with no instruction in 2 minutes or less. I believe it should be used in the clinic to confirm a diagnosis of fibromyalgia syndrome in patients with chronic diffuse pain at rest and to identify comorbid distress in patients with other diseases. This test complements a careful patient history and physical examination, and through its symptom and general health correlations facilitates characterization of our patients’ illnesses in line with the biopsychosocial model.
Since the Symptom Intensity Scale has been shown to be an accurate surrogate measure for general health, depression, disability, and death, fibromyalgia syndrome diagnosed using this instrument implies that this illness is not just centrally mediated pain, but that it carries increased medical risk. It can also be used as a research tool to measure the prevalence of fibromyalgia syndrome in other diseases.
Although the Symptom Intensity Scale is not yet recognized by the ACR as part (or the whole) of the classification criteria for fibromyalgia syndrome, it has already been shown in published studies to be a valid research tool, and it will very likely be the cornerstone of the new criteria.
Goodbye to tender points? Get used to it.
- Wilke WS. The clinical utility of fibromyalgia. J Clin Rheumatol 1999; 5:97–103.
- Cohen H, Buskila D, Neumann L, Ebstein RP. Confirmation of an association between fibromyalgia and serotonin transporter region (5-HTTLPR) polymorphism, and relationship to anxiety-related personality traits. Arthritis Rheum 2002; 46:845–847.
- Geisser ME, Glass JM, Rajcevska LD, et al. A psychophysical study of auditory and pressure sensitivity in patients with fibromyalgia and healthy controls. J Pain 2008; 9:417–422.
- Katz DL, Greene L, Ali A, Faridi Z. The pain of fibromyalgia syndrome is due to muscle hypoperfusion induced by regional vasomotor dysregulation. Med Hypotheses 2007; 69:517–525.
- Engel GL. The need for a new medical model: a challenge for biomedicine. Science 1977; 196:129–136.
- Gran JT. The epidemiology of chronic generalized musculoskeletal pain. Best Pract Res Clin Rheumatol 2003; 17:547–561.
- Wolfe F, Ross K, Anderson J, Russell IJ, Hebert L. The prevalence and characteristics of fibromyalgia in the general population. Arthritis Rheum 1995; 38:19–28.
- Lagier R. Nosology versus pathology, two approaches to rheumatic diseases illustrated by Alfred Baring Garrod and Jean-Martin Charcot. Rheumatology (Oxford) 2001; 40:467–471.
- Ruhman W. The earliest book on rheumatism. Br J Rheumatol 1940; 2:140–162.
- Gowers WR. A lecture on lumbago: its lessons and analogues. Br Med J 1904; 1:117–121.
- Hench PK. Nonarticular rheumatism. Arthritis Rheum 1976; 19(suppl):1081–1088.
- Smythe HA. “Fibrositis” as a disorder of pain modulation. Clin Rheum Dis 1979; 5:823–832.
- Smythe HA, Moldofsky H. Two contributions to understanding of the “fibrositis” syndrome. Bull Rheum Dis 1977–1978; 28:928–931.
- Yunus M, Masi AT, Calabro JJ, Miller KA, Feigenbaum SL. Primary fibromyalgia (fibrositis): clinical study of 50 patients with matched controls. Semin Arthritis Rheum 1981; 11:151–171.
- Croft P, Rigby AS, Boswell R, Schollum J, Silman A. The prevalence of chronic widespread pain in the general population. J Rheumatol 1993; 20:710–713.
- Wolfe F, Smythe HA, Yunus MB, et al. The American College of Rheumatology 1990 Criteria for Classification of Fibromyalgia. Report of the Multicenter Criteria Committee. Arthritis Rheum 1990; 33:160–172.
- McVeigh JG, Finch MB, Hurley DA, Basford JR, Sim J, Baxter GD. Tender point count and total myalgic score in fibromyalgia: changes over a 28-day period. Rheumatol Int 2007; 27:1011–1018.
- Croft P, Schollum J, Silman A. Population study of tender point counts and pain as evidence of fibromyalgia. BMJ 1994; 309:696–699.
- Wolfe F. The relation between tender points and fibromyalgia symptom variables: evidence that fibromyalgia is not a discrete disorder in the clinic. Ann Rheum Dis 1997; 56:268–271.
- Mease PJ, Arnold LM, Crofford LJ, et al. Identifying the clinical domains of fibromyalgia: contributions from clinician and patient Delphi exercises. Arthritis Rheum 2008; 59:952–960.
- Harth M, Nielson WR. The fibromyalgia tender points: use them or lose them? A brief review of the controversy. J Rheumatol 2007; 34:914–922.
- Macfarlane GJ, Croft PR, Schollum J, Silman AJ. Widespread pain: is an improved classification possible? J Rheumatol 1996; 23:1628–1632.
- White KP, Harth M, Speechley M, Ostbye T. Testing an instrument to screen for fibromyalgia syndrome in general population studies: the London Fibromyalgia Epidemiology Study Screening Questionnaire. J Rheumatol 1999; 26:880–884.
- White KP, Speechly M, Harth M, Osbye T. The London Fibromyalgia Epidemiology Study: comparing the demographic and clinical characteristics in 100 random community cases of fibromyalgia versus controls. J Rheumatol 1999; 26:1577–1585.
- Wolfe F. Pain extent and diagnosis: development and validation of the regional pain scale in 12,799 patients with rheumatic disease. J Rheumatolol 2003; 30:369–378.
- Katz RS, Wolfe F, Michaud K. Fibromyalgia diagnosis. a comparison of clinical, survey, and American College of Rheumatology criteria. Arthritis Rheum 2006; 54:169–176.
- Wolfe F, Rasker JJ. The Symptom Intensity Scale, fibromyalgia, and the meaning of fibromyalgia-like symptoms. J Rheumatol 2006; 33:2291–2299.
- Sleath B, Chewning B, De Vellis BM, et al. Communication about depression during rheumatoid arthritis patient visits. Arthritis Rheum 2008; 59:186–191.
- Middleton GD, McFarlin JE, Lippski PE. The prevalence and clinical impact of fibromyalgia in systemic lupus erythematosus. Arthritis Rheum 1994; 37:1181–1188.
- Moussavi S, Chatterji S, Verdes E, Tandon A, Patel V, Ustun B. Depression, chronic diseases, and decrements in health: results from the World Health Surveys. Lancet 2007; 370:851–858.
- Ang DC, Choi H, Kroenke K, Wolfe F. Comorbid depression is an independent risk factor for mortality in patients with rheumatoid arthritis. J Rheumatol 2005; 32:1013–1019.
- Wolfe F, Michaud K. Severe rheumatoid arthritis (RA), worse outcomes, comorbid illness, and sociodemograghic disadvantage characterize RA patients with fibromyalgia. J Rheumatol 2004; 31:695–700.
- Urrows S, Affleck G, Tennen H, Higgins P. Unique clinical and psychological correlates of fibromyalgia tender points and joint tenderness in rheumatoid arthritis. Arthritis Rheum 1994; 37:1513–1520.
- Gladman DD, Urowitz MB, Gough J, MacKinnon A. Fibromyalgia is a major contributor to quality of life in lupus. J Rheumatol 1997; 24:2145–2148.
- Wolfe F, Petri M, Alarcon GS, et al. Fibromyalgia, systemic lupus erythematosus (SLE) and evaluation of SLE activity. J Rheumatol 2009; 36:.27–33.
- Wilke WS. The clinical utility of fibromyalgia. J Clin Rheumatol 1999; 5:97–103.
- Cohen H, Buskila D, Neumann L, Ebstein RP. Confirmation of an association between fibromyalgia and serotonin transporter region (5-HTTLPR) polymorphism, and relationship to anxiety-related personality traits. Arthritis Rheum 2002; 46:845–847.
- Geisser ME, Glass JM, Rajcevska LD, et al. A psychophysical study of auditory and pressure sensitivity in patients with fibromyalgia and healthy controls. J Pain 2008; 9:417–422.
- Katz DL, Greene L, Ali A, Faridi Z. The pain of fibromyalgia syndrome is due to muscle hypoperfusion induced by regional vasomotor dysregulation. Med Hypotheses 2007; 69:517–525.
- Engel GL. The need for a new medical model: a challenge for biomedicine. Science 1977; 196:129–136.
- Gran JT. The epidemiology of chronic generalized musculoskeletal pain. Best Pract Res Clin Rheumatol 2003; 17:547–561.
- Wolfe F, Ross K, Anderson J, Russell IJ, Hebert L. The prevalence and characteristics of fibromyalgia in the general population. Arthritis Rheum 1995; 38:19–28.
- Lagier R. Nosology versus pathology, two approaches to rheumatic diseases illustrated by Alfred Baring Garrod and Jean-Martin Charcot. Rheumatology (Oxford) 2001; 40:467–471.
- Ruhman W. The earliest book on rheumatism. Br J Rheumatol 1940; 2:140–162.
- Gowers WR. A lecture on lumbago: its lessons and analogues. Br Med J 1904; 1:117–121.
- Hench PK. Nonarticular rheumatism. Arthritis Rheum 1976; 19(suppl):1081–1088.
- Smythe HA. “Fibrositis” as a disorder of pain modulation. Clin Rheum Dis 1979; 5:823–832.
- Smythe HA, Moldofsky H. Two contributions to understanding of the “fibrositis” syndrome. Bull Rheum Dis 1977–1978; 28:928–931.
- Yunus M, Masi AT, Calabro JJ, Miller KA, Feigenbaum SL. Primary fibromyalgia (fibrositis): clinical study of 50 patients with matched controls. Semin Arthritis Rheum 1981; 11:151–171.
- Croft P, Rigby AS, Boswell R, Schollum J, Silman A. The prevalence of chronic widespread pain in the general population. J Rheumatol 1993; 20:710–713.
- Wolfe F, Smythe HA, Yunus MB, et al. The American College of Rheumatology 1990 Criteria for Classification of Fibromyalgia. Report of the Multicenter Criteria Committee. Arthritis Rheum 1990; 33:160–172.
- McVeigh JG, Finch MB, Hurley DA, Basford JR, Sim J, Baxter GD. Tender point count and total myalgic score in fibromyalgia: changes over a 28-day period. Rheumatol Int 2007; 27:1011–1018.
- Croft P, Schollum J, Silman A. Population study of tender point counts and pain as evidence of fibromyalgia. BMJ 1994; 309:696–699.
- Wolfe F. The relation between tender points and fibromyalgia symptom variables: evidence that fibromyalgia is not a discrete disorder in the clinic. Ann Rheum Dis 1997; 56:268–271.
- Mease PJ, Arnold LM, Crofford LJ, et al. Identifying the clinical domains of fibromyalgia: contributions from clinician and patient Delphi exercises. Arthritis Rheum 2008; 59:952–960.
- Harth M, Nielson WR. The fibromyalgia tender points: use them or lose them? A brief review of the controversy. J Rheumatol 2007; 34:914–922.
- Macfarlane GJ, Croft PR, Schollum J, Silman AJ. Widespread pain: is an improved classification possible? J Rheumatol 1996; 23:1628–1632.
- White KP, Harth M, Speechley M, Ostbye T. Testing an instrument to screen for fibromyalgia syndrome in general population studies: the London Fibromyalgia Epidemiology Study Screening Questionnaire. J Rheumatol 1999; 26:880–884.
- White KP, Speechly M, Harth M, Osbye T. The London Fibromyalgia Epidemiology Study: comparing the demographic and clinical characteristics in 100 random community cases of fibromyalgia versus controls. J Rheumatol 1999; 26:1577–1585.
- Wolfe F. Pain extent and diagnosis: development and validation of the regional pain scale in 12,799 patients with rheumatic disease. J Rheumatolol 2003; 30:369–378.
- Katz RS, Wolfe F, Michaud K. Fibromyalgia diagnosis. a comparison of clinical, survey, and American College of Rheumatology criteria. Arthritis Rheum 2006; 54:169–176.
- Wolfe F, Rasker JJ. The Symptom Intensity Scale, fibromyalgia, and the meaning of fibromyalgia-like symptoms. J Rheumatol 2006; 33:2291–2299.
- Sleath B, Chewning B, De Vellis BM, et al. Communication about depression during rheumatoid arthritis patient visits. Arthritis Rheum 2008; 59:186–191.
- Middleton GD, McFarlin JE, Lippski PE. The prevalence and clinical impact of fibromyalgia in systemic lupus erythematosus. Arthritis Rheum 1994; 37:1181–1188.
- Moussavi S, Chatterji S, Verdes E, Tandon A, Patel V, Ustun B. Depression, chronic diseases, and decrements in health: results from the World Health Surveys. Lancet 2007; 370:851–858.
- Ang DC, Choi H, Kroenke K, Wolfe F. Comorbid depression is an independent risk factor for mortality in patients with rheumatoid arthritis. J Rheumatol 2005; 32:1013–1019.
- Wolfe F, Michaud K. Severe rheumatoid arthritis (RA), worse outcomes, comorbid illness, and sociodemograghic disadvantage characterize RA patients with fibromyalgia. J Rheumatol 2004; 31:695–700.
- Urrows S, Affleck G, Tennen H, Higgins P. Unique clinical and psychological correlates of fibromyalgia tender points and joint tenderness in rheumatoid arthritis. Arthritis Rheum 1994; 37:1513–1520.
- Gladman DD, Urowitz MB, Gough J, MacKinnon A. Fibromyalgia is a major contributor to quality of life in lupus. J Rheumatol 1997; 24:2145–2148.
- Wolfe F, Petri M, Alarcon GS, et al. Fibromyalgia, systemic lupus erythematosus (SLE) and evaluation of SLE activity. J Rheumatol 2009; 36:.27–33.
KEY POINTS
- The Symptom Intensity Scale questionnaire consists of two parts: a list of 19 anatomic areas in which the patient is asked if he or she feels pain (the total number of yes answers being the Regional Pain Scale score), and a visual analogue scale for fatigue.
- According to the Survey Criteria, a diagnosis of fibromyalgia can be entertained if the Regional Pain Scale score is 8 points or higher and the fatigue visual analogue scale score is 6 cm or higher.
- The number of tender points, a surrogate for diffuse pain, does not fully capture the essence of fibromyalgia syndrome, in which accompanying fatigue is often severe and nearly always present.
- The Symptom Intensity Scale is an accurate surrogate measure for general health, depression, disability, and death. Fibromyalgia syndrome diagnosed with this instrument implies that this illness carries increased medical risk.
Problems with Using Women's Cancer Screening Rates to Measure Performance
Grand Rounds: Boy, 10, With Knee Pain
A 10-year-old boy first complained of right knee pain two months prior to presentation. There was no traumatic event to explain the pain and no prior viral or bacterial illness. Radiographs taken earlier at another facility were initially pronounced normal. One month later, repeat x-rays showed a possible hairline fracture, and MRI was ordered. MRI documented a destructive lesion in the right distal femur with a soft-tissue mass that was worrisome for primary bone malignancy.
The boy was placed on weight-bearing restrictions and was given a wheelchair. Unfortunately, he fell from the wheelchair and sustained a pathologic fracture through the lesion (see Figure 1). He was transported to the hospital and admitted. A biopsy was performed with a closed reduction, as the fracture was maligned. The patient was placed in a long leg cast with a pelvic band.
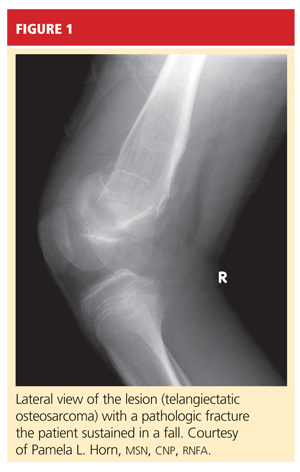
His history was previously unremarkable. He was taking no medications and had experienced no recent illnesses. His surgical/medical history was positive for a tonsillectomy at an early age and a fracture of the right proximal femur at age 2. On examination, he was noted to be talkative with his family but guarded during conversations with staff.
His physical exam was positive for pain at the right distal femur and knee with palpation; otherwise, all other systems were unremarkable. The patient was in too much pain to range the knee and had been placed in a long posterior leg splint (prior to surgery and application of the cast). Distally, his right lower extremity motor and sensory function were intact.
The patient’s vital signs were within normal limits, and results from his blood chemistries and alkaline phosphatase and C-reactive protein levels were unremarkable. Findings on the complete blood cell count were slightly abnormal: Hemoglobin was 11 g and the hematocrit, 33% (both within normal limits); however, in the differential there was an elevation in segmented neutrophils (72%, compared with a reference range of 31% to 61%), with Döhle bodies present—possibly signifying acute and/or chronic systemic infection or malignancy. The lymphocyte count represented 11% of the total white blood cell count (range, 28% to 48%), and platelets were 82 x 103/mL (normal range, 150 to 350 x 103/mL). The patient’s erythrocyte sedimentation rate was 44 mm/h (normal range, 0 to 20).
Result from pathology were positive for osteosarcoma, telangiectatic type. The patient underwent a nuclear medicine bone scan that showed no metastases, and chest CT was negative for pulmonary lesions as well. After a psychology consult, the boy was gently told about his condition.
Treatment then proceeded, including surgical placement of a double-lumen chest catheter for delivery of neoadjuvant and adjuvant chemotherapy. Doxorubicin, cisplatin, and methotrexate were used because the boy was enrolled in an international cooperative trial through the Children’s Oncology Group for treatment of localized osteosarcoma.
Discussion
Osteosarcoma (OS) is the most common primary bone malignancy.1,2 Approximately 5% of all pediatric patients with tumors present with this diagnosis, and about 400 new cases are diagnosed in the United States each year.1 Most osteosarcomas develop in the bones of the lower extremities and in the humerus, affecting males more often than females.1-3 This kind of malignancy is frequently seen during the adolescent growth spurt, but it can affect patients of any age.1,2 Patients usually present with pain or functional limitation in gait or daily activities or both.1-3
The telangiectatic subtype of OS is a rare, aggressive variant that represents 2% to 12% of all cases of OS.4-6 Telangiectatic OS (TOS) is characterized by multiple aneurysmally dilated, blood-filled cavities with high-grade sarcomatous cells seen in the peripheral rim and septae.3,7,8 This process can cause the lesion to resemble an aneurysmal bone cyst, explaining why some cases of TOS are misdiagnosed—with delayed time to treatment and increased morbidity and mortality.3,5 Generally, TOS patients are more likely than other OS patients to have tumors of femoral location, larger lesions, and normal alkaline phosphatase values. Many have pathologic fractures on presentation.7
The medical literature chronicles a long debate regarding the difference in mortality between patients with OS and those with TOS. It was once believed that patients with TOS were at higher risk for recurrence (especially those with a pathologic fracture) and mortality. However, in recent studies examining newer neoadjuvant and adjuvant chemotherapies, mortality rates for the two conditions are similar and certainly lower than they were many years ago.7,8 In one study, a better histologic response was reported to neoadjuvant chemotherapy in patients with TOS than with OS.7
Diagnosis
The first diagnostic tool used for patients with suspected OS or TOS is a plain radiographic film. A TOS lesion is lytic, with no areas of sclerosis, and almost always involves the long bones. It is poorly defined, destroying the cortex with formation of periosteal bone and invading the soft tissue. An initial pattern of parallel striations is highly suggestive of TOS.5
MRI and CT often reveal thick nodular tissue in a largely hemorrhagic and/or necrotic osseous lesion, with an associated soft-tissue mass that allows distinction from an aneurysmal bone cyst.3 Next, patients generally undergo a nuclear medicine bone scan and CT of the chest to observe for signs of metastases. Chest CT is commonly repeated on a regular basis during and after treatment.9
Pathologic evaluation, the final step to diagnosis, is very important, especially in the effort to differentiate TOS from an aneurysmal bone cyst. The typical gross findings for a TOS tumor include a dominant cystic cavity–like architecture, with a pushing peripheral margin that frequently expands and erodes the adjacent cortex and extends into the surrounding tissue. There is usually no area of intramural bone tissue.
Microscopically, the cystic areas contain clots and fragments of tumor that are often lined with a layer of neoplasm. The blood-filled telangiectatic spaces form in these areas. The spaces are irregularly shaped and typically traversed by septae composed in part of neoplastic cells. Osteoid formation through these cells can appear as a fine, ice-like material between tumor cells.4,7
Treatment
The main goals of treatment are to limit the anatomical extent of the disease, decrease the possibility of recurrence, and restore the highest possible level of function.2 Initial treatment of any OS or TOS consists of aggressive, immediate chemotherapy prior to and after any surgical intervention.1 (Chemotherapy will not be discussed in further detail here.) Surgical treatments for patients younger than 14 include amputation (above the lesion with wide margins), an expanding prosthesis, or rotationplasty. The location and extent of the tumor, the patient’s age, and his or her desired lifestyle will all have an impact on the choice of surgery.10
Historic data demonstrate that patients who undergo amputation alone almost always develop metastatic disease.1 Other data show that only 10% of patients with OS have been cured by chemotherapy alone. Yet when medical treatment is combined with surgical treatment, the overall expected cure rate can be as high as 65%.2
Discussing amputation with a young patient and the family can be emotionally difficult. If functional levels are to be restored, above-knee amputation (AKA) is the least favored surgical method. Compared with healthy individuals, patients who undergo AKA will walk 43% less quickly and will expend much more energy. These patients frequently have an inefficient gait and, given their limited reserve, they may lose the ability to walk altogether.2
Reconstructive surgical options include limb-salvage procedures; since the late 1980s, these have become the standard of care for OS at all sites.11 One such option includes removal of the lesion (eg, a distal femoral or proximal tibial lesion) with acceptable margins and replacement of the lost bone with an allograft or with a metallic prosthesis and knee joint (called arthroplasty). This endoprosthesis expands as the child grows (by way of a minor surgical procedure or a magnetic spring) so there is no apparent discrepancy between limb lengths, and the patient’s appearance is as normal and socially acceptable as possible.1,2
Because the case patient developed a pathologic fracture through his TOS tumor, he was not a candidate for endoprosthesis. His options were AKA or rotationplasty.
This procedure was first described in 195012 for treatment of proximal focal femoral deficiency. It is considered an alternative for skeletally immature individuals for whom the goal is to preserve function.
When AKA is indicated, the lower limb can be salvaged to allow functioning similar to that of a patient with a below-knee amputation (BKA). During rotationplasty, all but the most proximal aspect of the femur is resected. The tibia is externally rotated on the axis of the neurovascular bundle, then an arthrodesis of the proximal portion of the femur and the tibial plateau is performed (see Figure 2).
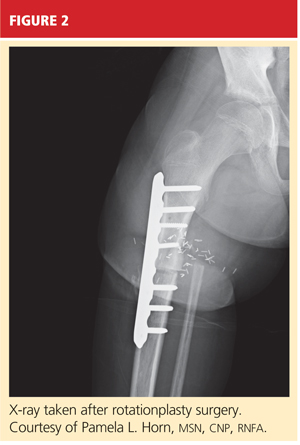
The end result is an extremity with the appearance, dimensions, and functional potential of a BKA. The ankle is rotated 180° so that it can serve as the new knee joint, and the attached foot, now pointing in the opposite direction, acts as the residual limb for fitting a prosthesis.2 This procedure is favored in patients with an extensive soft-tissue mass, intra-articular extension of the tumor, and/or pathologic fractures. It can also help prevent phantom pain.13
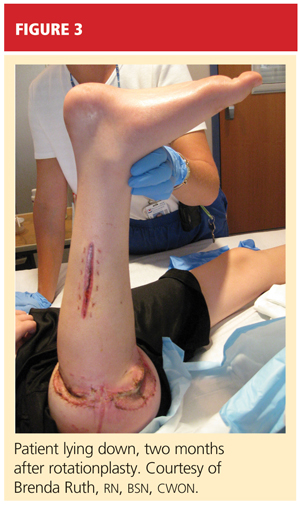
The Case Patient
After psychological evaluation of the patient and extensive family discussion, he underwent successful rotationplasty. The day after his surgery, however, he developed compartment syndrome and was required to undergo fasciotomies of the calf and proximal thigh. His wounds were treated, a skin graft was performed to close the proximal thigh wound, and his calf wounds were sutured closed (see Figures 3 and 4). His hip range of motion is excellent, and his ankle range of motion continues to improve with physical therapy.
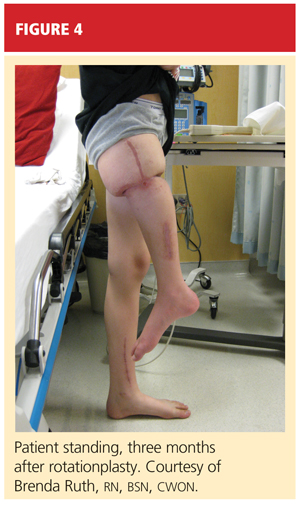
At this writing, the patient was scheduled for his first prosthetic fitting, and he had nearly completed his chemotherapy. His outlook is very promising.
Conclusion
TOS is a rare, aggressive subtype of OS but the most common primary malignant bone tumor of childhood. In the past, outcomes in patients treated with surgery alone were poor. With the advent of chemotherapy and the combination of medical and surgical treatment, TOS-associated mortality has continued to decline. There is no significant difference in outcomes among the available surgical options, but limb-salvage surgical procedures usually offer patients much better function and quality of life. The most important consideration is early diagnosis followed by immediate treatment.
1. Siegel HJ, Pressey JG. Current concepts on the surgical and medical management of osteosarcoma. Expert Rev Anticancer Ther. 2008;8(8):1257-1269.
2. Marulanda GA, Henderson ER, Johnson DA, et al. Orthopedic surgery options for the treatment of primary osteosarcoma. Cancer Control. 2008;15(1):13-20.
3. Murphey MD, wan Jaovisidha S, Temple HT, et al. Telangiectatic osteosarcoma: radiologic-pathologic comparison. Radiology. 2003;229(2):545-553.
4. Mervak TR, Unni KK, Pritchard DJ, McLeod RA. Telangiectatic osteosarcoma. Clin Orthop Relat Res. 1991 Sep;270:135-139.
5. Vanel D, Tcheng S, Contesso G, et al. The radiological appearances of telangiectatic osteosarcoma: a study of 14 cases. Skeletal Radiol. 1987;16(3):196-200.
6. Ferrari S, Smeland S, Mercuri M, et al. Neoadjuvant chemotherapy with high-dose ifosfamide, high-dose methotrexate, cisplatin, and doxorubicin for patients with localized osteosarcoma of the extremity: a joint study by the Italian and Scandinavian Sarcoma Groups. J Clin Oncol. 2005;23(34):8845-8852.
7. Bacci G, Ferrari S, Ruggieri P, et al. Telangiectatic osteosarcoma of the extremity: neoadjuvant chemotherapy in 24 cases. Acta Orthop Scand. 2001;72(2):167-172.
8. Weiss A, Khoury JD, Hoffer FA, et al. Telangiectatic osteosarcoma: the St. Jude Children’s Research Hospital’s experience. Cancer. 2007;109(8):1627-1637.
9. Agarwal M, Anchan C, Shah M, et al. Limb salvage surgery for osteosarcoma: effective low-cost treatment. Clin Orthop Relat Res. 2007;459:82-91.
10. Bacci G, Ferrari S, Lari S, et al. Osteosarcoma of the limb: amputation or limb salvage in patients treated by neoadjuvant chemotherapy. J Bone Joint Surg Br. 2002;84(1):88-92.
11. Simon MA, Aschliman MA, Thomas N, Mankin HJ. Limb-salvage treatment versus amputation for osteosarcoma of the distal end of the femur. J Bone Joint Surg Am. 1986;68(9):1331-1337.
12. Van Nes CP. Rotation-plasty for congenital defects of the femur: making use of the shortened limb to control the knee joint of a prosthesis. J Bone Joint Surg. 1950;32B:12-16.
13. Sawamura C, Hornicek FJ, Gebhardt MC. Complications and risk factors for failure of rotationplasty: review of 25 patients. Clin Orthop Relat Res. 2008;466(6):1302-1308.
A 10-year-old boy first complained of right knee pain two months prior to presentation. There was no traumatic event to explain the pain and no prior viral or bacterial illness. Radiographs taken earlier at another facility were initially pronounced normal. One month later, repeat x-rays showed a possible hairline fracture, and MRI was ordered. MRI documented a destructive lesion in the right distal femur with a soft-tissue mass that was worrisome for primary bone malignancy.
The boy was placed on weight-bearing restrictions and was given a wheelchair. Unfortunately, he fell from the wheelchair and sustained a pathologic fracture through the lesion (see Figure 1). He was transported to the hospital and admitted. A biopsy was performed with a closed reduction, as the fracture was maligned. The patient was placed in a long leg cast with a pelvic band.

His history was previously unremarkable. He was taking no medications and had experienced no recent illnesses. His surgical/medical history was positive for a tonsillectomy at an early age and a fracture of the right proximal femur at age 2. On examination, he was noted to be talkative with his family but guarded during conversations with staff.
His physical exam was positive for pain at the right distal femur and knee with palpation; otherwise, all other systems were unremarkable. The patient was in too much pain to range the knee and had been placed in a long posterior leg splint (prior to surgery and application of the cast). Distally, his right lower extremity motor and sensory function were intact.
The patient’s vital signs were within normal limits, and results from his blood chemistries and alkaline phosphatase and C-reactive protein levels were unremarkable. Findings on the complete blood cell count were slightly abnormal: Hemoglobin was 11 g and the hematocrit, 33% (both within normal limits); however, in the differential there was an elevation in segmented neutrophils (72%, compared with a reference range of 31% to 61%), with Döhle bodies present—possibly signifying acute and/or chronic systemic infection or malignancy. The lymphocyte count represented 11% of the total white blood cell count (range, 28% to 48%), and platelets were 82 x 103/mL (normal range, 150 to 350 x 103/mL). The patient’s erythrocyte sedimentation rate was 44 mm/h (normal range, 0 to 20).
Result from pathology were positive for osteosarcoma, telangiectatic type. The patient underwent a nuclear medicine bone scan that showed no metastases, and chest CT was negative for pulmonary lesions as well. After a psychology consult, the boy was gently told about his condition.
Treatment then proceeded, including surgical placement of a double-lumen chest catheter for delivery of neoadjuvant and adjuvant chemotherapy. Doxorubicin, cisplatin, and methotrexate were used because the boy was enrolled in an international cooperative trial through the Children’s Oncology Group for treatment of localized osteosarcoma.
Discussion
Osteosarcoma (OS) is the most common primary bone malignancy.1,2 Approximately 5% of all pediatric patients with tumors present with this diagnosis, and about 400 new cases are diagnosed in the United States each year.1 Most osteosarcomas develop in the bones of the lower extremities and in the humerus, affecting males more often than females.1-3 This kind of malignancy is frequently seen during the adolescent growth spurt, but it can affect patients of any age.1,2 Patients usually present with pain or functional limitation in gait or daily activities or both.1-3
The telangiectatic subtype of OS is a rare, aggressive variant that represents 2% to 12% of all cases of OS.4-6 Telangiectatic OS (TOS) is characterized by multiple aneurysmally dilated, blood-filled cavities with high-grade sarcomatous cells seen in the peripheral rim and septae.3,7,8 This process can cause the lesion to resemble an aneurysmal bone cyst, explaining why some cases of TOS are misdiagnosed—with delayed time to treatment and increased morbidity and mortality.3,5 Generally, TOS patients are more likely than other OS patients to have tumors of femoral location, larger lesions, and normal alkaline phosphatase values. Many have pathologic fractures on presentation.7
The medical literature chronicles a long debate regarding the difference in mortality between patients with OS and those with TOS. It was once believed that patients with TOS were at higher risk for recurrence (especially those with a pathologic fracture) and mortality. However, in recent studies examining newer neoadjuvant and adjuvant chemotherapies, mortality rates for the two conditions are similar and certainly lower than they were many years ago.7,8 In one study, a better histologic response was reported to neoadjuvant chemotherapy in patients with TOS than with OS.7
Diagnosis
The first diagnostic tool used for patients with suspected OS or TOS is a plain radiographic film. A TOS lesion is lytic, with no areas of sclerosis, and almost always involves the long bones. It is poorly defined, destroying the cortex with formation of periosteal bone and invading the soft tissue. An initial pattern of parallel striations is highly suggestive of TOS.5
MRI and CT often reveal thick nodular tissue in a largely hemorrhagic and/or necrotic osseous lesion, with an associated soft-tissue mass that allows distinction from an aneurysmal bone cyst.3 Next, patients generally undergo a nuclear medicine bone scan and CT of the chest to observe for signs of metastases. Chest CT is commonly repeated on a regular basis during and after treatment.9
Pathologic evaluation, the final step to diagnosis, is very important, especially in the effort to differentiate TOS from an aneurysmal bone cyst. The typical gross findings for a TOS tumor include a dominant cystic cavity–like architecture, with a pushing peripheral margin that frequently expands and erodes the adjacent cortex and extends into the surrounding tissue. There is usually no area of intramural bone tissue.
Microscopically, the cystic areas contain clots and fragments of tumor that are often lined with a layer of neoplasm. The blood-filled telangiectatic spaces form in these areas. The spaces are irregularly shaped and typically traversed by septae composed in part of neoplastic cells. Osteoid formation through these cells can appear as a fine, ice-like material between tumor cells.4,7
Treatment
The main goals of treatment are to limit the anatomical extent of the disease, decrease the possibility of recurrence, and restore the highest possible level of function.2 Initial treatment of any OS or TOS consists of aggressive, immediate chemotherapy prior to and after any surgical intervention.1 (Chemotherapy will not be discussed in further detail here.) Surgical treatments for patients younger than 14 include amputation (above the lesion with wide margins), an expanding prosthesis, or rotationplasty. The location and extent of the tumor, the patient’s age, and his or her desired lifestyle will all have an impact on the choice of surgery.10
Historic data demonstrate that patients who undergo amputation alone almost always develop metastatic disease.1 Other data show that only 10% of patients with OS have been cured by chemotherapy alone. Yet when medical treatment is combined with surgical treatment, the overall expected cure rate can be as high as 65%.2
Discussing amputation with a young patient and the family can be emotionally difficult. If functional levels are to be restored, above-knee amputation (AKA) is the least favored surgical method. Compared with healthy individuals, patients who undergo AKA will walk 43% less quickly and will expend much more energy. These patients frequently have an inefficient gait and, given their limited reserve, they may lose the ability to walk altogether.2
Reconstructive surgical options include limb-salvage procedures; since the late 1980s, these have become the standard of care for OS at all sites.11 One such option includes removal of the lesion (eg, a distal femoral or proximal tibial lesion) with acceptable margins and replacement of the lost bone with an allograft or with a metallic prosthesis and knee joint (called arthroplasty). This endoprosthesis expands as the child grows (by way of a minor surgical procedure or a magnetic spring) so there is no apparent discrepancy between limb lengths, and the patient’s appearance is as normal and socially acceptable as possible.1,2
Because the case patient developed a pathologic fracture through his TOS tumor, he was not a candidate for endoprosthesis. His options were AKA or rotationplasty.
This procedure was first described in 195012 for treatment of proximal focal femoral deficiency. It is considered an alternative for skeletally immature individuals for whom the goal is to preserve function.
When AKA is indicated, the lower limb can be salvaged to allow functioning similar to that of a patient with a below-knee amputation (BKA). During rotationplasty, all but the most proximal aspect of the femur is resected. The tibia is externally rotated on the axis of the neurovascular bundle, then an arthrodesis of the proximal portion of the femur and the tibial plateau is performed (see Figure 2).

The end result is an extremity with the appearance, dimensions, and functional potential of a BKA. The ankle is rotated 180° so that it can serve as the new knee joint, and the attached foot, now pointing in the opposite direction, acts as the residual limb for fitting a prosthesis.2 This procedure is favored in patients with an extensive soft-tissue mass, intra-articular extension of the tumor, and/or pathologic fractures. It can also help prevent phantom pain.13

The Case Patient
After psychological evaluation of the patient and extensive family discussion, he underwent successful rotationplasty. The day after his surgery, however, he developed compartment syndrome and was required to undergo fasciotomies of the calf and proximal thigh. His wounds were treated, a skin graft was performed to close the proximal thigh wound, and his calf wounds were sutured closed (see Figures 3 and 4). His hip range of motion is excellent, and his ankle range of motion continues to improve with physical therapy.

At this writing, the patient was scheduled for his first prosthetic fitting, and he had nearly completed his chemotherapy. His outlook is very promising.
Conclusion
TOS is a rare, aggressive subtype of OS but the most common primary malignant bone tumor of childhood. In the past, outcomes in patients treated with surgery alone were poor. With the advent of chemotherapy and the combination of medical and surgical treatment, TOS-associated mortality has continued to decline. There is no significant difference in outcomes among the available surgical options, but limb-salvage surgical procedures usually offer patients much better function and quality of life. The most important consideration is early diagnosis followed by immediate treatment.
A 10-year-old boy first complained of right knee pain two months prior to presentation. There was no traumatic event to explain the pain and no prior viral or bacterial illness. Radiographs taken earlier at another facility were initially pronounced normal. One month later, repeat x-rays showed a possible hairline fracture, and MRI was ordered. MRI documented a destructive lesion in the right distal femur with a soft-tissue mass that was worrisome for primary bone malignancy.
The boy was placed on weight-bearing restrictions and was given a wheelchair. Unfortunately, he fell from the wheelchair and sustained a pathologic fracture through the lesion (see Figure 1). He was transported to the hospital and admitted. A biopsy was performed with a closed reduction, as the fracture was maligned. The patient was placed in a long leg cast with a pelvic band.

His history was previously unremarkable. He was taking no medications and had experienced no recent illnesses. His surgical/medical history was positive for a tonsillectomy at an early age and a fracture of the right proximal femur at age 2. On examination, he was noted to be talkative with his family but guarded during conversations with staff.
His physical exam was positive for pain at the right distal femur and knee with palpation; otherwise, all other systems were unremarkable. The patient was in too much pain to range the knee and had been placed in a long posterior leg splint (prior to surgery and application of the cast). Distally, his right lower extremity motor and sensory function were intact.
The patient’s vital signs were within normal limits, and results from his blood chemistries and alkaline phosphatase and C-reactive protein levels were unremarkable. Findings on the complete blood cell count were slightly abnormal: Hemoglobin was 11 g and the hematocrit, 33% (both within normal limits); however, in the differential there was an elevation in segmented neutrophils (72%, compared with a reference range of 31% to 61%), with Döhle bodies present—possibly signifying acute and/or chronic systemic infection or malignancy. The lymphocyte count represented 11% of the total white blood cell count (range, 28% to 48%), and platelets were 82 x 103/mL (normal range, 150 to 350 x 103/mL). The patient’s erythrocyte sedimentation rate was 44 mm/h (normal range, 0 to 20).
Result from pathology were positive for osteosarcoma, telangiectatic type. The patient underwent a nuclear medicine bone scan that showed no metastases, and chest CT was negative for pulmonary lesions as well. After a psychology consult, the boy was gently told about his condition.
Treatment then proceeded, including surgical placement of a double-lumen chest catheter for delivery of neoadjuvant and adjuvant chemotherapy. Doxorubicin, cisplatin, and methotrexate were used because the boy was enrolled in an international cooperative trial through the Children’s Oncology Group for treatment of localized osteosarcoma.
Discussion
Osteosarcoma (OS) is the most common primary bone malignancy.1,2 Approximately 5% of all pediatric patients with tumors present with this diagnosis, and about 400 new cases are diagnosed in the United States each year.1 Most osteosarcomas develop in the bones of the lower extremities and in the humerus, affecting males more often than females.1-3 This kind of malignancy is frequently seen during the adolescent growth spurt, but it can affect patients of any age.1,2 Patients usually present with pain or functional limitation in gait or daily activities or both.1-3
The telangiectatic subtype of OS is a rare, aggressive variant that represents 2% to 12% of all cases of OS.4-6 Telangiectatic OS (TOS) is characterized by multiple aneurysmally dilated, blood-filled cavities with high-grade sarcomatous cells seen in the peripheral rim and septae.3,7,8 This process can cause the lesion to resemble an aneurysmal bone cyst, explaining why some cases of TOS are misdiagnosed—with delayed time to treatment and increased morbidity and mortality.3,5 Generally, TOS patients are more likely than other OS patients to have tumors of femoral location, larger lesions, and normal alkaline phosphatase values. Many have pathologic fractures on presentation.7
The medical literature chronicles a long debate regarding the difference in mortality between patients with OS and those with TOS. It was once believed that patients with TOS were at higher risk for recurrence (especially those with a pathologic fracture) and mortality. However, in recent studies examining newer neoadjuvant and adjuvant chemotherapies, mortality rates for the two conditions are similar and certainly lower than they were many years ago.7,8 In one study, a better histologic response was reported to neoadjuvant chemotherapy in patients with TOS than with OS.7
Diagnosis
The first diagnostic tool used for patients with suspected OS or TOS is a plain radiographic film. A TOS lesion is lytic, with no areas of sclerosis, and almost always involves the long bones. It is poorly defined, destroying the cortex with formation of periosteal bone and invading the soft tissue. An initial pattern of parallel striations is highly suggestive of TOS.5
MRI and CT often reveal thick nodular tissue in a largely hemorrhagic and/or necrotic osseous lesion, with an associated soft-tissue mass that allows distinction from an aneurysmal bone cyst.3 Next, patients generally undergo a nuclear medicine bone scan and CT of the chest to observe for signs of metastases. Chest CT is commonly repeated on a regular basis during and after treatment.9
Pathologic evaluation, the final step to diagnosis, is very important, especially in the effort to differentiate TOS from an aneurysmal bone cyst. The typical gross findings for a TOS tumor include a dominant cystic cavity–like architecture, with a pushing peripheral margin that frequently expands and erodes the adjacent cortex and extends into the surrounding tissue. There is usually no area of intramural bone tissue.
Microscopically, the cystic areas contain clots and fragments of tumor that are often lined with a layer of neoplasm. The blood-filled telangiectatic spaces form in these areas. The spaces are irregularly shaped and typically traversed by septae composed in part of neoplastic cells. Osteoid formation through these cells can appear as a fine, ice-like material between tumor cells.4,7
Treatment
The main goals of treatment are to limit the anatomical extent of the disease, decrease the possibility of recurrence, and restore the highest possible level of function.2 Initial treatment of any OS or TOS consists of aggressive, immediate chemotherapy prior to and after any surgical intervention.1 (Chemotherapy will not be discussed in further detail here.) Surgical treatments for patients younger than 14 include amputation (above the lesion with wide margins), an expanding prosthesis, or rotationplasty. The location and extent of the tumor, the patient’s age, and his or her desired lifestyle will all have an impact on the choice of surgery.10
Historic data demonstrate that patients who undergo amputation alone almost always develop metastatic disease.1 Other data show that only 10% of patients with OS have been cured by chemotherapy alone. Yet when medical treatment is combined with surgical treatment, the overall expected cure rate can be as high as 65%.2
Discussing amputation with a young patient and the family can be emotionally difficult. If functional levels are to be restored, above-knee amputation (AKA) is the least favored surgical method. Compared with healthy individuals, patients who undergo AKA will walk 43% less quickly and will expend much more energy. These patients frequently have an inefficient gait and, given their limited reserve, they may lose the ability to walk altogether.2
Reconstructive surgical options include limb-salvage procedures; since the late 1980s, these have become the standard of care for OS at all sites.11 One such option includes removal of the lesion (eg, a distal femoral or proximal tibial lesion) with acceptable margins and replacement of the lost bone with an allograft or with a metallic prosthesis and knee joint (called arthroplasty). This endoprosthesis expands as the child grows (by way of a minor surgical procedure or a magnetic spring) so there is no apparent discrepancy between limb lengths, and the patient’s appearance is as normal and socially acceptable as possible.1,2
Because the case patient developed a pathologic fracture through his TOS tumor, he was not a candidate for endoprosthesis. His options were AKA or rotationplasty.
This procedure was first described in 195012 for treatment of proximal focal femoral deficiency. It is considered an alternative for skeletally immature individuals for whom the goal is to preserve function.
When AKA is indicated, the lower limb can be salvaged to allow functioning similar to that of a patient with a below-knee amputation (BKA). During rotationplasty, all but the most proximal aspect of the femur is resected. The tibia is externally rotated on the axis of the neurovascular bundle, then an arthrodesis of the proximal portion of the femur and the tibial plateau is performed (see Figure 2).

The end result is an extremity with the appearance, dimensions, and functional potential of a BKA. The ankle is rotated 180° so that it can serve as the new knee joint, and the attached foot, now pointing in the opposite direction, acts as the residual limb for fitting a prosthesis.2 This procedure is favored in patients with an extensive soft-tissue mass, intra-articular extension of the tumor, and/or pathologic fractures. It can also help prevent phantom pain.13

The Case Patient
After psychological evaluation of the patient and extensive family discussion, he underwent successful rotationplasty. The day after his surgery, however, he developed compartment syndrome and was required to undergo fasciotomies of the calf and proximal thigh. His wounds were treated, a skin graft was performed to close the proximal thigh wound, and his calf wounds were sutured closed (see Figures 3 and 4). His hip range of motion is excellent, and his ankle range of motion continues to improve with physical therapy.

At this writing, the patient was scheduled for his first prosthetic fitting, and he had nearly completed his chemotherapy. His outlook is very promising.
Conclusion
TOS is a rare, aggressive subtype of OS but the most common primary malignant bone tumor of childhood. In the past, outcomes in patients treated with surgery alone were poor. With the advent of chemotherapy and the combination of medical and surgical treatment, TOS-associated mortality has continued to decline. There is no significant difference in outcomes among the available surgical options, but limb-salvage surgical procedures usually offer patients much better function and quality of life. The most important consideration is early diagnosis followed by immediate treatment.
1. Siegel HJ, Pressey JG. Current concepts on the surgical and medical management of osteosarcoma. Expert Rev Anticancer Ther. 2008;8(8):1257-1269.
2. Marulanda GA, Henderson ER, Johnson DA, et al. Orthopedic surgery options for the treatment of primary osteosarcoma. Cancer Control. 2008;15(1):13-20.
3. Murphey MD, wan Jaovisidha S, Temple HT, et al. Telangiectatic osteosarcoma: radiologic-pathologic comparison. Radiology. 2003;229(2):545-553.
4. Mervak TR, Unni KK, Pritchard DJ, McLeod RA. Telangiectatic osteosarcoma. Clin Orthop Relat Res. 1991 Sep;270:135-139.
5. Vanel D, Tcheng S, Contesso G, et al. The radiological appearances of telangiectatic osteosarcoma: a study of 14 cases. Skeletal Radiol. 1987;16(3):196-200.
6. Ferrari S, Smeland S, Mercuri M, et al. Neoadjuvant chemotherapy with high-dose ifosfamide, high-dose methotrexate, cisplatin, and doxorubicin for patients with localized osteosarcoma of the extremity: a joint study by the Italian and Scandinavian Sarcoma Groups. J Clin Oncol. 2005;23(34):8845-8852.
7. Bacci G, Ferrari S, Ruggieri P, et al. Telangiectatic osteosarcoma of the extremity: neoadjuvant chemotherapy in 24 cases. Acta Orthop Scand. 2001;72(2):167-172.
8. Weiss A, Khoury JD, Hoffer FA, et al. Telangiectatic osteosarcoma: the St. Jude Children’s Research Hospital’s experience. Cancer. 2007;109(8):1627-1637.
9. Agarwal M, Anchan C, Shah M, et al. Limb salvage surgery for osteosarcoma: effective low-cost treatment. Clin Orthop Relat Res. 2007;459:82-91.
10. Bacci G, Ferrari S, Lari S, et al. Osteosarcoma of the limb: amputation or limb salvage in patients treated by neoadjuvant chemotherapy. J Bone Joint Surg Br. 2002;84(1):88-92.
11. Simon MA, Aschliman MA, Thomas N, Mankin HJ. Limb-salvage treatment versus amputation for osteosarcoma of the distal end of the femur. J Bone Joint Surg Am. 1986;68(9):1331-1337.
12. Van Nes CP. Rotation-plasty for congenital defects of the femur: making use of the shortened limb to control the knee joint of a prosthesis. J Bone Joint Surg. 1950;32B:12-16.
13. Sawamura C, Hornicek FJ, Gebhardt MC. Complications and risk factors for failure of rotationplasty: review of 25 patients. Clin Orthop Relat Res. 2008;466(6):1302-1308.
1. Siegel HJ, Pressey JG. Current concepts on the surgical and medical management of osteosarcoma. Expert Rev Anticancer Ther. 2008;8(8):1257-1269.
2. Marulanda GA, Henderson ER, Johnson DA, et al. Orthopedic surgery options for the treatment of primary osteosarcoma. Cancer Control. 2008;15(1):13-20.
3. Murphey MD, wan Jaovisidha S, Temple HT, et al. Telangiectatic osteosarcoma: radiologic-pathologic comparison. Radiology. 2003;229(2):545-553.
4. Mervak TR, Unni KK, Pritchard DJ, McLeod RA. Telangiectatic osteosarcoma. Clin Orthop Relat Res. 1991 Sep;270:135-139.
5. Vanel D, Tcheng S, Contesso G, et al. The radiological appearances of telangiectatic osteosarcoma: a study of 14 cases. Skeletal Radiol. 1987;16(3):196-200.
6. Ferrari S, Smeland S, Mercuri M, et al. Neoadjuvant chemotherapy with high-dose ifosfamide, high-dose methotrexate, cisplatin, and doxorubicin for patients with localized osteosarcoma of the extremity: a joint study by the Italian and Scandinavian Sarcoma Groups. J Clin Oncol. 2005;23(34):8845-8852.
7. Bacci G, Ferrari S, Ruggieri P, et al. Telangiectatic osteosarcoma of the extremity: neoadjuvant chemotherapy in 24 cases. Acta Orthop Scand. 2001;72(2):167-172.
8. Weiss A, Khoury JD, Hoffer FA, et al. Telangiectatic osteosarcoma: the St. Jude Children’s Research Hospital’s experience. Cancer. 2007;109(8):1627-1637.
9. Agarwal M, Anchan C, Shah M, et al. Limb salvage surgery for osteosarcoma: effective low-cost treatment. Clin Orthop Relat Res. 2007;459:82-91.
10. Bacci G, Ferrari S, Lari S, et al. Osteosarcoma of the limb: amputation or limb salvage in patients treated by neoadjuvant chemotherapy. J Bone Joint Surg Br. 2002;84(1):88-92.
11. Simon MA, Aschliman MA, Thomas N, Mankin HJ. Limb-salvage treatment versus amputation for osteosarcoma of the distal end of the femur. J Bone Joint Surg Am. 1986;68(9):1331-1337.
12. Van Nes CP. Rotation-plasty for congenital defects of the femur: making use of the shortened limb to control the knee joint of a prosthesis. J Bone Joint Surg. 1950;32B:12-16.
13. Sawamura C, Hornicek FJ, Gebhardt MC. Complications and risk factors for failure of rotationplasty: review of 25 patients. Clin Orthop Relat Res. 2008;466(6):1302-1308.
Ellis-van Creveld Syndrome: Case Report and Review of the Literature
A Comparative Split-Face Study of Cryosurgery and Trichloroacetic Acid 100% Peels in the Treatment of HIV-Associated Disseminated Facial Molluscum Contagiosum
Acute Generalized Exanthematous Pustulosis: An Enigmatic Drug-Induced Reaction
Mobbing is not PTSD
Giving all due respect to James Randolph Hillard, MD, I cannot agree with his posttraumatic stress disorder (PTSD) diagnosis, given the information he provided in “Workplace mobbing: Are they really out to get your patient?” (Current Psychiatry). He does not make a case for DSM-IV-TR Criterion A (the person has been exposed to a traumatic event in which both of the following were present: the event involved actual or threatened death or serious injury, or a threat to the physical integrity of self or others [A1] and the person’s response involved intense fear, helplessness, or horror [A2]),1 despite what other “stress” symptoms the patient experienced.
If data exist that correspond with Criterion A, let us know. Criterion A exists for a purpose, and unless it’s changed in DSM-V clinicians should stick to what’s defined and not make up their own diagnosis.
Melvyn Nizny, MD, DLF
Cincinnati, OH
Reference
1. Diagnostic and statistical manual of mental disorders, 4th ed, text rev. Washington DC: American Psychiatric Association; 2000.
Dr. Hillard responds
Dr. Nizny makes a very interesting point. DSM-IV-TR requires that a patient must meet 6 sets of criteria for a PTSD diagnosis. The patient described in my article convincingly met Criterion A2 and Criteria B, C, D, E, and F. In terms of Criterion A1, DSM-IV-TR states: “Traumatic events that are experienced directly include, but are not limited to, military combat, violent physical assault (sexual assault, physical attack, robbery, mugging), being kidnapped, being taken hostage, terrorist attack, torture, incarcerations as a prisoner of war or in a concentration camp, natural or manmade disasters, severe automobile accidents, or being diagnosed with a life-threatening illness.”
I think I can make the case that the patient described in my article meets the “letter” of Criterion A1 by arguing that he experienced threat of “serious injury.” He faced loss of livelihood, loss of much of his core identity, and loss of nearly his whole social network, which consisted mostly of people at his place of employment.
I am fairly sure, however, that such an argument does not follow the spirit of Criterion A1, which seems to imply that PTSD should be diagnosed only if there has been a physical threat. On the other hand, I do not have much sympathy with that concept. Why should threats of physical harm be more likely to produce symptoms than other types of threats? Recent empirical studies1 do not support the existence of a posttraumatic stress syndrome uniquely associated with physical threats, as opposed to all other threats.
Dr. Nizny notes that Criterion A exists for a purpose, but for what purpose? Michael First, MD, co-chair and editor of DSM-IV-TR, was quoted as giving a partial answer: “The litigation about PTSD when we were working on DSM-IV was going crazy, so we thought it would be wise to limit it to high-magnitude events…there was a huge debate over how broad versus how narrow Criterion A should be.”2 In the same article, Dr. First is quoted as stating that the definition “should change with the next revision of the Diagnostic and Statistical Manual.” The committee that designed the criteria for PTSD in DSM-IV in 1994 would probably have preferred to have seen this patient diagnosed as “adjustment disorder with mixed anxiety and depressed mood,” probably to make it less likely that he could successfully sue for damages.
I am convinced that workplace mobbing can present a pathogenic stress to victims that is as severe as that caused by physical injuries or threats. Furthermore, I am convinced that mobbing victims are entitled to have their day in court, as are victims of physical injuries in the workplace. Finally, I am convinced that when psychiatrists underestimate the severity of stress involved in workplace mobbing, they are at risk of failing to treat their patients appropriately. For these reasons, I have not chosen to use a “strict constructionist” approach to diagnosis in this case.
James Randolph Hillard, MD
Associate provost for human health affairs
Michigan State University
East Lansing, MI
Giving all due respect to James Randolph Hillard, MD, I cannot agree with his posttraumatic stress disorder (PTSD) diagnosis, given the information he provided in “Workplace mobbing: Are they really out to get your patient?” (Current Psychiatry). He does not make a case for DSM-IV-TR Criterion A (the person has been exposed to a traumatic event in which both of the following were present: the event involved actual or threatened death or serious injury, or a threat to the physical integrity of self or others [A1] and the person’s response involved intense fear, helplessness, or horror [A2]),1 despite what other “stress” symptoms the patient experienced.
If data exist that correspond with Criterion A, let us know. Criterion A exists for a purpose, and unless it’s changed in DSM-V clinicians should stick to what’s defined and not make up their own diagnosis.
Melvyn Nizny, MD, DLF
Cincinnati, OH
Reference
1. Diagnostic and statistical manual of mental disorders, 4th ed, text rev. Washington DC: American Psychiatric Association; 2000.
Dr. Hillard responds
Dr. Nizny makes a very interesting point. DSM-IV-TR requires that a patient must meet 6 sets of criteria for a PTSD diagnosis. The patient described in my article convincingly met Criterion A2 and Criteria B, C, D, E, and F. In terms of Criterion A1, DSM-IV-TR states: “Traumatic events that are experienced directly include, but are not limited to, military combat, violent physical assault (sexual assault, physical attack, robbery, mugging), being kidnapped, being taken hostage, terrorist attack, torture, incarcerations as a prisoner of war or in a concentration camp, natural or manmade disasters, severe automobile accidents, or being diagnosed with a life-threatening illness.”
I think I can make the case that the patient described in my article meets the “letter” of Criterion A1 by arguing that he experienced threat of “serious injury.” He faced loss of livelihood, loss of much of his core identity, and loss of nearly his whole social network, which consisted mostly of people at his place of employment.
I am fairly sure, however, that such an argument does not follow the spirit of Criterion A1, which seems to imply that PTSD should be diagnosed only if there has been a physical threat. On the other hand, I do not have much sympathy with that concept. Why should threats of physical harm be more likely to produce symptoms than other types of threats? Recent empirical studies1 do not support the existence of a posttraumatic stress syndrome uniquely associated with physical threats, as opposed to all other threats.
Dr. Nizny notes that Criterion A exists for a purpose, but for what purpose? Michael First, MD, co-chair and editor of DSM-IV-TR, was quoted as giving a partial answer: “The litigation about PTSD when we were working on DSM-IV was going crazy, so we thought it would be wise to limit it to high-magnitude events…there was a huge debate over how broad versus how narrow Criterion A should be.”2 In the same article, Dr. First is quoted as stating that the definition “should change with the next revision of the Diagnostic and Statistical Manual.” The committee that designed the criteria for PTSD in DSM-IV in 1994 would probably have preferred to have seen this patient diagnosed as “adjustment disorder with mixed anxiety and depressed mood,” probably to make it less likely that he could successfully sue for damages.
I am convinced that workplace mobbing can present a pathogenic stress to victims that is as severe as that caused by physical injuries or threats. Furthermore, I am convinced that mobbing victims are entitled to have their day in court, as are victims of physical injuries in the workplace. Finally, I am convinced that when psychiatrists underestimate the severity of stress involved in workplace mobbing, they are at risk of failing to treat their patients appropriately. For these reasons, I have not chosen to use a “strict constructionist” approach to diagnosis in this case.
James Randolph Hillard, MD
Associate provost for human health affairs
Michigan State University
East Lansing, MI
Giving all due respect to James Randolph Hillard, MD, I cannot agree with his posttraumatic stress disorder (PTSD) diagnosis, given the information he provided in “Workplace mobbing: Are they really out to get your patient?” (Current Psychiatry). He does not make a case for DSM-IV-TR Criterion A (the person has been exposed to a traumatic event in which both of the following were present: the event involved actual or threatened death or serious injury, or a threat to the physical integrity of self or others [A1] and the person’s response involved intense fear, helplessness, or horror [A2]),1 despite what other “stress” symptoms the patient experienced.
If data exist that correspond with Criterion A, let us know. Criterion A exists for a purpose, and unless it’s changed in DSM-V clinicians should stick to what’s defined and not make up their own diagnosis.
Melvyn Nizny, MD, DLF
Cincinnati, OH
Reference
1. Diagnostic and statistical manual of mental disorders, 4th ed, text rev. Washington DC: American Psychiatric Association; 2000.
Dr. Hillard responds
Dr. Nizny makes a very interesting point. DSM-IV-TR requires that a patient must meet 6 sets of criteria for a PTSD diagnosis. The patient described in my article convincingly met Criterion A2 and Criteria B, C, D, E, and F. In terms of Criterion A1, DSM-IV-TR states: “Traumatic events that are experienced directly include, but are not limited to, military combat, violent physical assault (sexual assault, physical attack, robbery, mugging), being kidnapped, being taken hostage, terrorist attack, torture, incarcerations as a prisoner of war or in a concentration camp, natural or manmade disasters, severe automobile accidents, or being diagnosed with a life-threatening illness.”
I think I can make the case that the patient described in my article meets the “letter” of Criterion A1 by arguing that he experienced threat of “serious injury.” He faced loss of livelihood, loss of much of his core identity, and loss of nearly his whole social network, which consisted mostly of people at his place of employment.
I am fairly sure, however, that such an argument does not follow the spirit of Criterion A1, which seems to imply that PTSD should be diagnosed only if there has been a physical threat. On the other hand, I do not have much sympathy with that concept. Why should threats of physical harm be more likely to produce symptoms than other types of threats? Recent empirical studies1 do not support the existence of a posttraumatic stress syndrome uniquely associated with physical threats, as opposed to all other threats.
Dr. Nizny notes that Criterion A exists for a purpose, but for what purpose? Michael First, MD, co-chair and editor of DSM-IV-TR, was quoted as giving a partial answer: “The litigation about PTSD when we were working on DSM-IV was going crazy, so we thought it would be wise to limit it to high-magnitude events…there was a huge debate over how broad versus how narrow Criterion A should be.”2 In the same article, Dr. First is quoted as stating that the definition “should change with the next revision of the Diagnostic and Statistical Manual.” The committee that designed the criteria for PTSD in DSM-IV in 1994 would probably have preferred to have seen this patient diagnosed as “adjustment disorder with mixed anxiety and depressed mood,” probably to make it less likely that he could successfully sue for damages.
I am convinced that workplace mobbing can present a pathogenic stress to victims that is as severe as that caused by physical injuries or threats. Furthermore, I am convinced that mobbing victims are entitled to have their day in court, as are victims of physical injuries in the workplace. Finally, I am convinced that when psychiatrists underestimate the severity of stress involved in workplace mobbing, they are at risk of failing to treat their patients appropriately. For these reasons, I have not chosen to use a “strict constructionist” approach to diagnosis in this case.
James Randolph Hillard, MD
Associate provost for human health affairs
Michigan State University
East Lansing, MI
SJS is diagnosed, but not quickly...Lithium unmonitored, kidney failure followed...more...
SJS is diagnosed, but not quickly
AFTER MULTIPLE HOSPITAL VISITS FOR A RASH, a 34-year-old man was sent to a regional medical center for treatment. The rash was eventually diagnosed as a reaction to allopurinol, a potential side effect that was prominently noted in the drug warnings.
The patient developed Stevens-Johnson syndrome. He recovered after several days in the intensive care unit and was discharged with mild scarring over 80% of his body.
PLAINTIFF’S CLAIM The defendants negligently failed to diagnose a drug reaction after multiple reports of a known side effect.
DOCTORS’ DEFENSE Rashes are a common complaint in an emergency room; delayed withdrawal of the drug caused no additional harm.
VERDICT $72,500 South Carolina settlement.
COMMENT Although instances are rare, failure to diagnose and treat a dermatologic problem promptly can have catastrophic results. Stevens-Johnson syndrome needs to be included in the differential diagnosis of drug reactions and must be handled promptly. (See “Derm diagnoses you can’t afford to miss”.)
Lithium unmonitored, kidney failure followed
A WOMAN WAS STARTED ON LITHIUM, but the doctor who wrote the prescription never ordered follow-up blood tests for creatinine levels. When her blood was tested 7 years later by another physician for another medical problem, her creatinine levels were high.
The physician sent the woman to a nephrologist, who discontinued the lithium. Three years later the patient went into renal failure. She received a kidney transplant from her sister. The patient, 39 years of age, will have to take antirejection medication for the rest of her life. The plaintiff sued the doctor who wrote the original prescription as well as 2 other physicians who treated her.
PLAINTIFF’S CLAIM The 2 physicians who treated her saw blood test results showing a rise in creatinine, which should have prompted them to act.
DOCTORS’ DEFENSE No information about the doctors’ defense is available.
VERDICT $2 million New Jersey settlement.
COMMENT Certain medications, such as lithium, require careful and frequent monitoring. Although such surveillance is seldom evidence-based, this is probably one of those times when covering yourself is a guiding precept.
One more drug leads to one big problem
A 56-YEAR-OLD MAN WAS HOSPITALIZED WITH PNEUMONIA, for which his physician prescribed fluconazole (supplied by the hospital pharmacy). The patient was taking cyclosporine, prescribed after a kidney transplant 20 years earlier, and atorvastatin. Lab work performed a week later revealed renal function problems. The patient’s medications weren’t adjusted.
The patient’s wife had him transferred to another facility, where he was diagnosed with rhabdomyolysis resulting from the multiple medications. After extensive hospitalization and rehabilitation, the patient was left with debilitating muscle weakness, especially in his legs.
PLAINTIFF’S CLAIM The hospital and doctor were negligent in failing to recognize the potential for adverse interaction among atorvastatin, cyclosporine, and fluconazole, and in failing to discontinue the atorvastatin.
THE DEFENSE No information about the nature of the defense is available.
VERDICT $1.63 million gross verdict in West Virginia.
COMMENT Can you remember all those CYP450 drug-drug interactions? Neither can I. So when a patient is on an unfamiliar medication (cyclosporine isn’t a regular in my practice), it’s worth looking up the drug and exploring potential problems.
Necrotizing fasciitis leads to lost use of arm
REDNESS AND SWELLING OF THE RIGHT ARM, vomiting, and dehydration brought a 30-year-old woman to the family practice clinic at an Air Force base. The patient’s medical history included endometriosis, hypothyroidism, insomnia, headaches, anxiety, and diffuse cellulitis. She took many drugs for pain associated with the endometriosis and cellulitis, including opioids such as hydromorphone. She also took lorazepam for anxiety.
About 2 weeks later she was seen by an endocrinologist at a hospital for testing related to hypothyroidism. She had a fever and skin lesions, which prompted the endocrinologist to refer her to the Air Force base emergency room for treatment of an infection.
A month later, the patient returned to the endocrinologist, who placed a peripherally inserted catheter on the inside of her right arm near the elbow to facilitate blood drawing for endocrine tests. After 10 days, the patient experienced redness, pain, and swelling in her right arm. A few days later, she saw a family practitioner at the Air Force family practice clinic, who told her to go home, take ibuprofen, and come back if the symptoms didn’t improve.
Four days later, the patient was brought to the Air Force base emergency room and diagnosed with necrotizing fasciitis. After immediate aggressive debridement, she was transferred to another hospital, where she underwent 5 surgeries, including skin grafts. As a result, her right arm is withered and scarred and lacks the muscles and tendons necessary to sustain meaningful activity. The patient has to wear a prosthetic device over her forearm and wrist to provide support and compression, and she suffers continuous, debilitating pain, for which she wears a fentanyl transdermal patch. She is unable to work.
PLAINTIFF’S CLAIM Her arm was not properly examined when the redness and swelling developed; cellulitis should have been diagnosed during that first visit.
DOCTOR’S DEFENSE The patient didn’t complain about her right arm during the initial visit to the family practice clinic, and neither the doctor nor his assistant noted any problems, as evidenced by the lack of mention of the arm in the chart notes. The chart recorded complaints of vomiting, dehydration, and “the same symptoms I always have” and noted that the patient had come to the clinic to refill a lorazepam/hydromorphone prescription to replace a lost bottle of pills. The infection occurred after the visit; once the process began, nothing could be done to alter the outcome.
VERDICT $8.6 million Illinois bench verdict.
COMMENT It is crucial to recognize aggressive skin infections, including necrotizing fasciitis, and to initiate prompt treatment.
SJS is diagnosed, but not quickly
AFTER MULTIPLE HOSPITAL VISITS FOR A RASH, a 34-year-old man was sent to a regional medical center for treatment. The rash was eventually diagnosed as a reaction to allopurinol, a potential side effect that was prominently noted in the drug warnings.
The patient developed Stevens-Johnson syndrome. He recovered after several days in the intensive care unit and was discharged with mild scarring over 80% of his body.
PLAINTIFF’S CLAIM The defendants negligently failed to diagnose a drug reaction after multiple reports of a known side effect.
DOCTORS’ DEFENSE Rashes are a common complaint in an emergency room; delayed withdrawal of the drug caused no additional harm.
VERDICT $72,500 South Carolina settlement.
COMMENT Although instances are rare, failure to diagnose and treat a dermatologic problem promptly can have catastrophic results. Stevens-Johnson syndrome needs to be included in the differential diagnosis of drug reactions and must be handled promptly. (See “Derm diagnoses you can’t afford to miss”.)
Lithium unmonitored, kidney failure followed
A WOMAN WAS STARTED ON LITHIUM, but the doctor who wrote the prescription never ordered follow-up blood tests for creatinine levels. When her blood was tested 7 years later by another physician for another medical problem, her creatinine levels were high.
The physician sent the woman to a nephrologist, who discontinued the lithium. Three years later the patient went into renal failure. She received a kidney transplant from her sister. The patient, 39 years of age, will have to take antirejection medication for the rest of her life. The plaintiff sued the doctor who wrote the original prescription as well as 2 other physicians who treated her.
PLAINTIFF’S CLAIM The 2 physicians who treated her saw blood test results showing a rise in creatinine, which should have prompted them to act.
DOCTORS’ DEFENSE No information about the doctors’ defense is available.
VERDICT $2 million New Jersey settlement.
COMMENT Certain medications, such as lithium, require careful and frequent monitoring. Although such surveillance is seldom evidence-based, this is probably one of those times when covering yourself is a guiding precept.
One more drug leads to one big problem
A 56-YEAR-OLD MAN WAS HOSPITALIZED WITH PNEUMONIA, for which his physician prescribed fluconazole (supplied by the hospital pharmacy). The patient was taking cyclosporine, prescribed after a kidney transplant 20 years earlier, and atorvastatin. Lab work performed a week later revealed renal function problems. The patient’s medications weren’t adjusted.
The patient’s wife had him transferred to another facility, where he was diagnosed with rhabdomyolysis resulting from the multiple medications. After extensive hospitalization and rehabilitation, the patient was left with debilitating muscle weakness, especially in his legs.
PLAINTIFF’S CLAIM The hospital and doctor were negligent in failing to recognize the potential for adverse interaction among atorvastatin, cyclosporine, and fluconazole, and in failing to discontinue the atorvastatin.
THE DEFENSE No information about the nature of the defense is available.
VERDICT $1.63 million gross verdict in West Virginia.
COMMENT Can you remember all those CYP450 drug-drug interactions? Neither can I. So when a patient is on an unfamiliar medication (cyclosporine isn’t a regular in my practice), it’s worth looking up the drug and exploring potential problems.
Necrotizing fasciitis leads to lost use of arm
REDNESS AND SWELLING OF THE RIGHT ARM, vomiting, and dehydration brought a 30-year-old woman to the family practice clinic at an Air Force base. The patient’s medical history included endometriosis, hypothyroidism, insomnia, headaches, anxiety, and diffuse cellulitis. She took many drugs for pain associated with the endometriosis and cellulitis, including opioids such as hydromorphone. She also took lorazepam for anxiety.
About 2 weeks later she was seen by an endocrinologist at a hospital for testing related to hypothyroidism. She had a fever and skin lesions, which prompted the endocrinologist to refer her to the Air Force base emergency room for treatment of an infection.
A month later, the patient returned to the endocrinologist, who placed a peripherally inserted catheter on the inside of her right arm near the elbow to facilitate blood drawing for endocrine tests. After 10 days, the patient experienced redness, pain, and swelling in her right arm. A few days later, she saw a family practitioner at the Air Force family practice clinic, who told her to go home, take ibuprofen, and come back if the symptoms didn’t improve.
Four days later, the patient was brought to the Air Force base emergency room and diagnosed with necrotizing fasciitis. After immediate aggressive debridement, she was transferred to another hospital, where she underwent 5 surgeries, including skin grafts. As a result, her right arm is withered and scarred and lacks the muscles and tendons necessary to sustain meaningful activity. The patient has to wear a prosthetic device over her forearm and wrist to provide support and compression, and she suffers continuous, debilitating pain, for which she wears a fentanyl transdermal patch. She is unable to work.
PLAINTIFF’S CLAIM Her arm was not properly examined when the redness and swelling developed; cellulitis should have been diagnosed during that first visit.
DOCTOR’S DEFENSE The patient didn’t complain about her right arm during the initial visit to the family practice clinic, and neither the doctor nor his assistant noted any problems, as evidenced by the lack of mention of the arm in the chart notes. The chart recorded complaints of vomiting, dehydration, and “the same symptoms I always have” and noted that the patient had come to the clinic to refill a lorazepam/hydromorphone prescription to replace a lost bottle of pills. The infection occurred after the visit; once the process began, nothing could be done to alter the outcome.
VERDICT $8.6 million Illinois bench verdict.
COMMENT It is crucial to recognize aggressive skin infections, including necrotizing fasciitis, and to initiate prompt treatment.
SJS is diagnosed, but not quickly
AFTER MULTIPLE HOSPITAL VISITS FOR A RASH, a 34-year-old man was sent to a regional medical center for treatment. The rash was eventually diagnosed as a reaction to allopurinol, a potential side effect that was prominently noted in the drug warnings.
The patient developed Stevens-Johnson syndrome. He recovered after several days in the intensive care unit and was discharged with mild scarring over 80% of his body.
PLAINTIFF’S CLAIM The defendants negligently failed to diagnose a drug reaction after multiple reports of a known side effect.
DOCTORS’ DEFENSE Rashes are a common complaint in an emergency room; delayed withdrawal of the drug caused no additional harm.
VERDICT $72,500 South Carolina settlement.
COMMENT Although instances are rare, failure to diagnose and treat a dermatologic problem promptly can have catastrophic results. Stevens-Johnson syndrome needs to be included in the differential diagnosis of drug reactions and must be handled promptly. (See “Derm diagnoses you can’t afford to miss”.)
Lithium unmonitored, kidney failure followed
A WOMAN WAS STARTED ON LITHIUM, but the doctor who wrote the prescription never ordered follow-up blood tests for creatinine levels. When her blood was tested 7 years later by another physician for another medical problem, her creatinine levels were high.
The physician sent the woman to a nephrologist, who discontinued the lithium. Three years later the patient went into renal failure. She received a kidney transplant from her sister. The patient, 39 years of age, will have to take antirejection medication for the rest of her life. The plaintiff sued the doctor who wrote the original prescription as well as 2 other physicians who treated her.
PLAINTIFF’S CLAIM The 2 physicians who treated her saw blood test results showing a rise in creatinine, which should have prompted them to act.
DOCTORS’ DEFENSE No information about the doctors’ defense is available.
VERDICT $2 million New Jersey settlement.
COMMENT Certain medications, such as lithium, require careful and frequent monitoring. Although such surveillance is seldom evidence-based, this is probably one of those times when covering yourself is a guiding precept.
One more drug leads to one big problem
A 56-YEAR-OLD MAN WAS HOSPITALIZED WITH PNEUMONIA, for which his physician prescribed fluconazole (supplied by the hospital pharmacy). The patient was taking cyclosporine, prescribed after a kidney transplant 20 years earlier, and atorvastatin. Lab work performed a week later revealed renal function problems. The patient’s medications weren’t adjusted.
The patient’s wife had him transferred to another facility, where he was diagnosed with rhabdomyolysis resulting from the multiple medications. After extensive hospitalization and rehabilitation, the patient was left with debilitating muscle weakness, especially in his legs.
PLAINTIFF’S CLAIM The hospital and doctor were negligent in failing to recognize the potential for adverse interaction among atorvastatin, cyclosporine, and fluconazole, and in failing to discontinue the atorvastatin.
THE DEFENSE No information about the nature of the defense is available.
VERDICT $1.63 million gross verdict in West Virginia.
COMMENT Can you remember all those CYP450 drug-drug interactions? Neither can I. So when a patient is on an unfamiliar medication (cyclosporine isn’t a regular in my practice), it’s worth looking up the drug and exploring potential problems.
Necrotizing fasciitis leads to lost use of arm
REDNESS AND SWELLING OF THE RIGHT ARM, vomiting, and dehydration brought a 30-year-old woman to the family practice clinic at an Air Force base. The patient’s medical history included endometriosis, hypothyroidism, insomnia, headaches, anxiety, and diffuse cellulitis. She took many drugs for pain associated with the endometriosis and cellulitis, including opioids such as hydromorphone. She also took lorazepam for anxiety.
About 2 weeks later she was seen by an endocrinologist at a hospital for testing related to hypothyroidism. She had a fever and skin lesions, which prompted the endocrinologist to refer her to the Air Force base emergency room for treatment of an infection.
A month later, the patient returned to the endocrinologist, who placed a peripherally inserted catheter on the inside of her right arm near the elbow to facilitate blood drawing for endocrine tests. After 10 days, the patient experienced redness, pain, and swelling in her right arm. A few days later, she saw a family practitioner at the Air Force family practice clinic, who told her to go home, take ibuprofen, and come back if the symptoms didn’t improve.
Four days later, the patient was brought to the Air Force base emergency room and diagnosed with necrotizing fasciitis. After immediate aggressive debridement, she was transferred to another hospital, where she underwent 5 surgeries, including skin grafts. As a result, her right arm is withered and scarred and lacks the muscles and tendons necessary to sustain meaningful activity. The patient has to wear a prosthetic device over her forearm and wrist to provide support and compression, and she suffers continuous, debilitating pain, for which she wears a fentanyl transdermal patch. She is unable to work.
PLAINTIFF’S CLAIM Her arm was not properly examined when the redness and swelling developed; cellulitis should have been diagnosed during that first visit.
DOCTOR’S DEFENSE The patient didn’t complain about her right arm during the initial visit to the family practice clinic, and neither the doctor nor his assistant noted any problems, as evidenced by the lack of mention of the arm in the chart notes. The chart recorded complaints of vomiting, dehydration, and “the same symptoms I always have” and noted that the patient had come to the clinic to refill a lorazepam/hydromorphone prescription to replace a lost bottle of pills. The infection occurred after the visit; once the process began, nothing could be done to alter the outcome.
VERDICT $8.6 million Illinois bench verdict.
COMMENT It is crucial to recognize aggressive skin infections, including necrotizing fasciitis, and to initiate prompt treatment.
Colpocleisis: A simple, effective, and underutilized procedure
CASE 1: Problematic prolapse, but no incontinence
An 81-year-old multiparous woman, who has a history of recurrent stage-III pelvic organ prolapse (POP), reports worsening discomfort that makes it difficult for her to care for her ailing husband. She also has “trouble” with bladder emptying and constipation, but denies any loss of urine. She has not had vaginal intercourse in more than a decade because of her husband’s medical condition.
Aside from health issues—she suffers from obesity, coronary artery disease, hypertension, and diabetes—the patient is content with her marriage of 58 years.
Urodynamic testing fails to demonstrate detrusor overactivity, stress urinary incontinence, or intrinsic sphincteric deficiency. A cough stress test is repeated after reduction of her prolapse using a large cotton swab, and confirms the findings of the urodynamic tests.
Is reconstructive surgery appropriate for this patient?
Traditional reconstructive surgical procedures for treating POP fail in as many as 30% of patients, and new approaches—some involving grafts—are proposed every day, often without much data behind them.1
Regardless of the approach, reconstructive surgery is a lengthy procedure that subjects patients who are already medically compromised to significant risk, including bleeding, infection, and fluid shifts. Delayed return to normal activity may be especially costly among elderly women because of the risk of venous thromboembolism.
Because of the high failure rate, slow recovery, and risk of complications, reconstructive surgery may not be as appropriate as colpocleisis for the woman described above. Colpocleisis—suturing the inside walls of the vagina together—has an efficacy rate exceeding 90%.2 This relatively simple operation has been around for almost two centuries and has a good track record, but is often overlooked when counseling a patient about her options.
Any frail, elderly woman who has stage-III or -IV POP who does not desire to preserve coital ability is a candidate for colpocleisis (TABLE). Advantages include:
- a short operating time
- few complications
- amenability of local anesthesia
- short hospitalization
- speedy recovery
- high success rate
- low rate of regret.2-5
Because it precludes coital activity, however, colpocleisis may cause problems with self-image. It also may lead to de novo or worsening urinary incontinence and complicate or delay the diagnosis of cervical and endometrial pathology.
This article explores these issues through a case-based discussion of colpocleisis, including a detailed description of surgical technique.
TABLE
Requirements for colpocleisis
Both of the following must be present
|
Plus at least one of the following
|
Colpocleisis, as noted, entails suturing the inside walls of the vagina together. It is controversial because of its impact on coital activity. With careful patient selection, however, colpocleisis is considered a valid option for frail and elderly women who have POP and do not desire or foresee the possibility of future vaginal intercourse. Such women may represent a surprising percentage of the elderly population. A community-based survey found that 78% of married women 70 to 79 years old are not sexually active,6 and a study from The Netherlands found a prevalence of symptomatic POP of 11.4% among white women 45 to 85 years old.7
The fundamental reason for choosing an obliterative procedure such as colpocleisis over total pelvic reconstruction is to treat the prolapse with the least invasive technique in the shortest time. Hysterectomy, which often adds 30 to 80 minutes to the procedure, should therefore be performed only in patients who have a suspicious finding upon initial evaluation. For the same reason, partial colpocleisis—performed using the LeFort technique with limited dissection—has become the most popular obliterative approach. We try to avoid a total colpocleisis procedure—also known as colpectomy—in which the entire vaginal epithelium is stripped, because it is feasible only when the uterus is already absent or scheduled to be removed concomitantly.
(Note: The term vaginectomy should be reserved for gynecologic oncology procedures performed to remove vaginal cancer. Vaginectomy entails full-thickness excision of the vaginal walls, including the fibromuscular layer, as opposed to excision of the epithelial layer only, as in colpocleisis. In this article, we present the LeFort method, a partial colpocleisis technique, because we believe it is more easily adapted by the general gynecologist.8)
CASE 1 RESOLVED
After detailed counseling, which includes family members, the patient opts to undergo colpocleisis. The procedure takes 45 minutes. She is discharged on postoperative Day 1, and reports substantially improved quality of life.
CASE 2: Recurrent prolapse and problems with a pessary
A 72-year-old multiparous, widowed woman experiences recurrent stage-III isolated apical prolapse. She has already undergone two reconstructive procedures, and was discouraged from undergoing a third because of her chronic obstructive lung disease. She tried to use a Gellhorn-type pessary, which required a doctor’s intervention to insert and remove. Frustrated by the many office visits involved in having the pessary checked, she now demands surgical therapy. Another gynecologist has offered to repair the prolapse using mesh, but the patient has concerns about the safety and efficacy of the procedure because it is a relatively new approach.
In addition to the recurrent prolapse, she loses urine with stress and urge. She often has a postvoid residual volume >100 cc; urodynamic assessment confirms mixed urinary incontinence. The patient does not foresee any change in her social status (unmarried, sexually inactive).
Is colpocleisis a reasonable option?
Although the pessary is a helpful conservative alternative for women who are either unable or unwilling to undergo complex surgical pelvic repair and is considered first-line treatment by a majority of urogynecologists, it sometimes becomes more difficult to maintain than the patient is willing to tolerate.9 When a woman cannot remove and reinsert the device herself, the pessary requires a lifelong commitment to doctor’s visits every 2 or 3 months. This commitment is especially problematic for patients who become unable to drive or who lack social support.
Maintenance of the pessary becomes more frustrating as the patient becomes more dependent. Many gynecologists have seen a patient who developed a serious complication such as vesicovaginal or rectovaginal fistula because of a neglected pessary.10
In Case 2, the patient appears to be a potential candidate for colpocleisis, given her age and single status. Although pelvic floor repair appears to be safe in older women, any perioperative complication in a patient 70 years of age or older doubles the risk of discharge to a care facility.11,12 Women who have already undergone several surgeries or who have advanced medical problems such as coronary artery disease or cancer should be counseled thoroughly about the safety and efficacy of colpocleisis.
As for self-image, colpocleisis eliminates prolapse and reduces the genital hiatus. If the patient understands that colpocleisis is obliterative for the vagina but may improve the external appearance of the genital area, she may be more accepting of the procedure. One recent prospective, multicenter study found that only 2% of women thought their body looked worse 1 year after colpocleisis; 60% thought their body looked better.5
When reviewing treatment options, inform the patient that the pessary is a palliative option, whereas surgical therapy aims to be definitive.
CASE 2 RESOLVED
After comprehensive counseling, the patient elects to undergo colpocleisis, along with placement of a midurethral sling. She is discharged 1 day after surgery, and reports substantially improved urinary function, including bladder emptying, and quality of life. She says she would recommend the procedure to any woman who has a similar condition.
CASE 3: Pessary-related complications, incontinence, and underlying medical conditions
A 92-year-old multiparous widow, whose stage-IV uterovaginal prolapse has been managed by a pessary, develops vaginal ulcers in both anterior and posterior walls. After removal of the pessary and 4 weeks of treatment with vaginal estrogen, a smaller pessary is inserted, but she again develops ulcers and bleeding.
The patient’s medical condition is complicated by hypertension and generalized arthritis. She has urodynamically confirmed mixed urinary incontinence. She lives with her daughter and does not want to be placed in a nursing home.
What treatment options should you offer to her?
Because of this patient’s advanced age, poor health, and pessary-related problems, she is an ideal candidate for colpocleisis, provided she consents to the procedure after thorough counseling about its benefits and limitations.
Preoperative concerns
A thorough history, physical examination, and normal Pap test are necessary. If a suspicious pelvic mass or uterine bleeding is present, transvaginal ultrasonography (US) is crucial. In-office endometrial sampling also is necessary in any woman who has unexplained vaginal bleeding. More invasive procedures such as dilatation and curettage and hysteroscopy are needed only when the biopsy is inadequate or endometrial thickness exceeds 4 mm on transvaginal US.13
All elderly women who have high-risk medical problems must be cleared for surgery, with the necessary cardiac and pulmonary workup completed before the procedure.
Because colpocleisis is an extraperitoneal procedure, we have adapted use of over-the-counter enema products on the day before surgery in lieu of mechanical bowel preparation, which may lead to dehydration in very elderly women.
Coordinated consultation between the surgeon and anesthesiologist is necessary to determine the type of anesthesia to be used. Sedation and local anesthesia can be adequate for extremely high-risk women.14,15 Antibiotic prophylaxis is conventional for all patients.
Surgical technique
The LeFort method involves denudation and approximation of the midportions of the anterior and posterior vaginal walls.8 This operation creates a longitudinal vaginal septum with bilateral channels on each side, which serve as conduits for any secretion or bleeding from the apical vagina (FIGURE 1A AND B). Aggressive perineorraphy is also needed to shorten the genital hiatus. The following description incorporates perineorraphy into the LeFort technique.
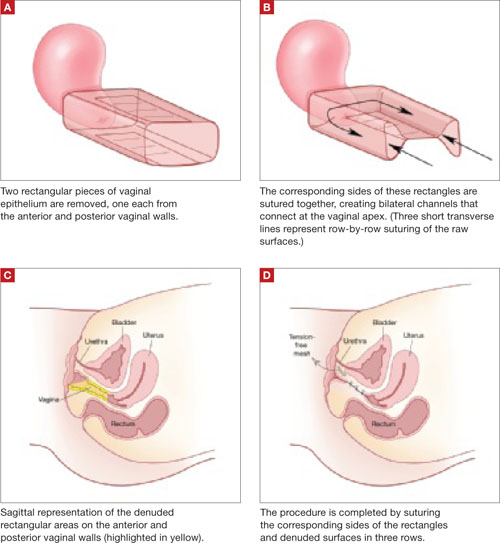
FIGURE 1 Principles of LeFort colpocleisis
The depiction here is not anatomically precise: The vagina is illustrated as a rectangular prism to clarify the relationship between tissues.
Patient positioning
Place the patient in the dorsal lithotomy position, using stirrups to support the entire leg up to the knee. Let the patient’s buttocks overhang the edge of the table by 1 to 2 inches. A slight Trendelenburg position is imperative, especially when operating on the anterior compartment of the vagina. The bladder should be only partially emptied because the leakage of urine from the bladder makes it easier to identify inadvertent cystotomy. Infiltration of local anesthetic solution to develop the surgical planes is acceptable.
Initiating the procedure
Remove a rectangular piece of vaginal epithelium from the anterior vaginal wall, beginning 2 to 3 cm distal to the vaginal apex (or cervix, if the uterus is present) and ending immediately proximal to the urethrovesical junction to leave space for midurethral sling placement. Remove a similarly sized piece of epithelium from the posterior vaginal wall. This posterior rectangle is an almost geometric projection of the anterior rectangle, but is somewhat longer (2 to 3 cm) (FIGURE 1).
When removing the vaginal epithelium, it may be helpful to use the skills developed for anterior and posterior colporraphy. Our operation begins with a 5- to 6-cm transverse incision at the anterior vaginal apex, which creates the proximal side of the anterior rectangle described above (FIGURE 2A).
As you develop the plane between the epithelium and fibromuscular layer, make a midline sagittal incision and extend it to the urethrovesical junction (FIGURE 2B). Dissect the epithelium off the fibromuscular layer approximately 3 cm bilaterally, then make a transverse incision at the urethrovesical junction. Finally, remove the anterior rectangle in two pieces by cutting along the lateral sides (FIGURE 2C AND D). Remove the posterior rectangle using the same technique, but also excise a triangular piece of skin from the posterior fourchette for the perineorraphy portion of the procedure (FIGURE 2E).
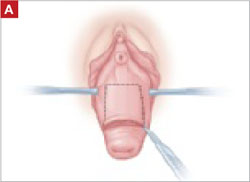
FIGURE 2 LeFort technique, step by step
Begin with a 5–6 cm transverse incision at the anterior vaginal apex.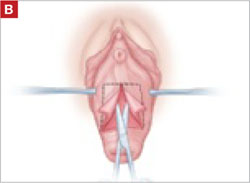
Dissect the epithelium off the fibromuscular layer, with a midline sagittal incision extending to the urethrovesical junction.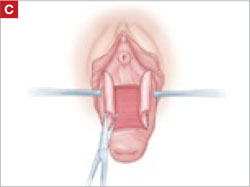
After dissection is completed, make a transverse incision at the urethrovesical junction, and remove the anterior rectangle in two pieces by cutting along the lateral sides.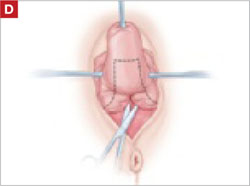
Denude the posterior rectangle using the same technique. In addition, excise a triangular piece of skin from the perineum.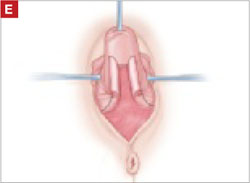
The posterior rectangle is ready for removal.
Suturing
Suture the apical sides of the anterior and posterior rectangles together using a continuous running technique (FIGURE 2F). Then approximate the lateral sides bilaterally using continuous sutures.
To ensure adherence of the anterior and posterior rectangles, stitch the raw surfaces together in three rows (FIGURE 2G). Do not include the distal 2 cm of the posterior vagina because you will need to leave room for perineorraphy.
Using several sutures, reapproximate the torn perineal fibromuscular structures in the midline to perform perineorraphy (FIGURE 2H). Close the distal vagina, beginning at the midpoint of the anterior transverse side, which lies at the urethrovesical junction (FIGURE 2I). Continue this suture on the posterior vagina and then the perineal body, sagittally, creating a small invagination in the distal vagina (FIGURE 2J).
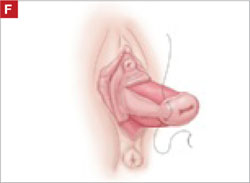
FIGURE 2 LeFort technique, step by step
Suture all but the distal sides of the rectangles between the anterior and posterior vaginal walls.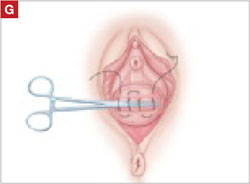
Also stitch together the raw surfaces in three rows in an imbricating fashion.
Perform perineorraphy.
Close the distal vagina, starting at the midpoint of the anterior transverse side. If indicated, place a midurethral sling.
Final appearance.
Sling procedure
We place a midurethral sling as part of most colpocleisis operations. It is best to do this after the colpocleisis but before the perineorraphy.
In our cases, cystoscopy with simultaneous intravenous indigo carmine injection is standard before perineorraphy, even when a sling procedure is not planned. This safeguard ensures ureteral patency, which can be compromised (although rarely) in these procedures. Cutting and replacement of one of the sutures that approximate the raw tissues typically resolve the problem.16
Special considerations
Here are additional key points about colpocleisis, based on our experience:
- If an ulcer lies within the area designated to be denuded, some debridement to freshen up the surface will suffice. An ulcer is not an indication to deviate from the standard procedure.
- A modification developed by Goodall and Power may allow coitus by removing only a triangular piece of epithelium from each wall, leaving more room for the channels.17
- We have been unable to find any report of uterine or cervical cancer after colpocleisis, despite a MEDLINE search of the literature in English. Even so, the lateral channels created by the LeFort procedure allow any bleeding to escape the vagina, and may therefore enable recognition of malignancy. When noninvasive imaging techniques such as US or magnetic resonance are inadequate, vaginoscopy and hysteroscopy may be accomplished via these channels.
- When colpocleisis is performed in a hysterectomized woman, no lateral channel is necessary. Therefore, it is appropriate to do total colpocleisis.18,19
- When a patient with POP has a rectovaginal or vesicovaginal fistula caused by a neglected pessary, the addition of LeFort colpocleisis to the fistula repair may provide an effective treatment for both problems.10
Surgical outcomes
Success rate
Evidence concerning colpocleisis comes from case series, some of which are more than 30 years old. Although the definition of success is not clear in some series, the reported success rate has always exceeded 90% over the past three decades.2,18-22 Moreover, some of these reports involve as many as 30 years of follow-up.
Perioperative complication
In a recent review of the literature, the procedure-related mortality rate was 0.025%.2 When the authors focused only on studies published since 1980, major complications due to the patient’s underlying cardiovascular and pulmonary condition were seen in 2% of cases. Major surgical complications such as pyelonephritis and bleeding requiring transfusion occurred in 4% of cases, and less severe complications occurred in 15%.
In a study that included women who underwent concomitant vaginal hysterectomy, hysterectomy prolonged the surgery by 52 minutes, with a 5% rate of laparotomy as a result of intraoperative bleeding.22
In our series of 40 colpocleisis cases, we noted no instance in which a patient regretted the procedure.18 Others have also reported a low rate of regret—the highest being 9%.3-5,19-21
Using validated questionnaires, FitzGerald and colleagues found significant improvement in mental and physical quality of life, as well as urinary, colorectal, and bulge-related pelvic floor symptoms, 1 year after colpocleisis.5
De novo or worsening urinary incontinence is one of the drawbacks of colpocleisis. However, the same risk is present in approximately 40% of women who undergo surgical reconstructive procedures for POP without a continence operation.23 Because preoperative urinary retention is common in women who have POP, the decision to add a potentially harmful continence procedure is complicated in colpocleisis candidates. A small case series reported that the success rate ranged from 90% to 94% in women who underwent a midurethral tension-free sling procedure for the treatment of urinary incontinence at the time of colpocleisis.5
Preoperative urodynamic studies to detect urethral intrinsic deficiency and detrusor dysfunction are prudent, and detailed counseling of the patient about urinary control is vital. We perform a midurethral sling procedure in most of our colpocleisis cases, and have had pleasing results.
CASE 3 RESOLVED
The patient decides to undergo partial colpocleisis using the LeFort procedure, along with placement of a midurethral sling, for a total operative time of 75 minutes. She is discharged 1 day later and reports substantial improvement in urinary function and quality of life.
1. Luber KM, Boero S, Choe JY. The demographics of pelvic floor disorders: current observations and future projections. Am J Obstet Gynecol. 2001;184:1496-1503.
2. FitzGerald MP, Richter HE, Siddique S, Thompson P, Zyczynski H, Weber A. For the Pelvic Floor Disorders Network. Colpocleisis: a review. Int Urogynecol J Pelvic Floor Dysfunct. 2006;17:261-271.
3. Wheeler TL, Jr, Richter HE, Burgio KL, et al. Regret, satisfaction, and symptom improvement: analysis of the impact of partial colpocleisis for the management of severe pelvic organ prolapse. Am J Obstet Gynecol. 2005;193:2067-2070.
4. Hullfish KL, Bovbjerg VE, Steers WD. Colpocleisis for pelvic organ prolapse: patient goals, quality of life, and satisfaction. Obstet Gynecol. 2007;110(2 Pt 1):341-345.
5. FitzGerald MP, Richter HE, Bradley CS, et al. For the Pelvic Floor Disorders Network. Pelvic support, pelvic symptoms, and patient satisfaction after colpocleisis. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19:1603-1609.
6. Patel D, Gillespie B, Foxman B. Sexual behavior of older women: results of a random-digit-dialing survey of 2,000 women in the United States. Sex Transm Dis. 2003;30:216-220.
7. Slieker-ten Hove MC, Pool-Goudzwaard AL, Eijkemans MJ, Steegers-Theunissen RP, Burger CW, Vierhout ME. Symptomatic pelvic organ prolapse and possible risk factors in a general population. Am J Obstet Gynecol. 2009;200:184.e1-184.e7.
8. Berlin F. Three cases of complete prolapsus uteri operated upon according to the method of Leon LeFort. Am J Obstet Gynecol. 1881;14:866-868.
9. Cundiff GW, Weidner AC, Visco AG, Bump RC, Addison WA. A survey of pessary use by members of the American Urogynecologic Society. Obstet Gynecol. 2000;95(6 Pt 1):931-935.
10. Esin S, Harmanli OH. Large vesicovaginal fistula in women with pelvic organ prolapse: the role of colpocleisis revisited. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19:1711-1713.
11. Gerten KA, Markland AD, Lloyd LK, Richter HE. Prolapse and incontinence surgery in older women. J Urol. 2008;179:2111-2118.
12. Manku K, Bacchetti P, Leung JM. Prognostic significance of postoperative in-hospital complications in elderly patients. I. Long-term survival. Anesth Analg. 2003;96:583-589.
13. American College of Obstetricians and Gynecologists. ACOG Committee Opinion No. 426: The role of transvaginal ultrasonography in the evaluation of postmenopausal bleeding. Obstet Gynecol. 2009;113(2 Pt 1):462-464.
14. Moore RD, Miklos JR. Colpocleisis and tension-free vaginal tape sling for severe uterine and vaginal prolapse and stress urinary incontinence under local anesthesia. J Am Assoc Gynecol Laparosc. 2003;10:276-280.
15. Buchsbaum GM, Albushies DT, Schoenecker E, Duecy EE, Glantz JC. Local anesthesia with sedation for vaginal reconstructive surgery. Int Urogynecol J Pelvic Floor Dysfunct. 2006;17:211-214.
16. Gustilo-Ashby AM, Jelovsek JE, Barber MD, Yoo EH, Paraiso MF, Walters MD. The incidence of ureteral obstruction and the value of intraoperative cystoscopy during vaginal surgery for pelvic organ prolapse. Am J Obstet Gynecol. 2006;194:1478-1485.
17. Goodall JR, Power RMH. A modification of the Le Fort operation for increasing its scope. Am J Obstet Gynecol. 1937;34:968-976.
18. Harmanli OH, Dandolu V, Chatwani AJ, Grody MT. Total colpocleisis for severe pelvic organ prolapse. J Reprod Med. 2003;48:703-706.
19. DeLancey JOL, Morley GW. Total colpocleisis for vaginal eversion. Am J Obstet Gynecol. 1997;176:1228-1232.
20. Goldman J, Ovadia J, Feldberg D. The Neugebauer-Le Fort operation: a review of 118 partial colpocleises. Eur J Obstet Gynecol Reprod Biol. 1981;12:31-35.
21. Ubachs JM, van Sante TJ, Schellekens LA. Partial colpocleisis by a modification of Le Fort’s operation. Obstet Gynecol. 1973;42:415-420.
22. Von Pechmann WS, Mutone MD, Fyffe J, Hale DS. Total colpocleisis with high levator plication for the treatment of advanced pelvic organ prolapse. Am J Obstet Gynecol. 2003;189:121-126.
23. Albo ME, Richter HE, Brubaker L, et al. For Urinary Incontinence Treatment Network. Burch colposuspension versus fascial sling to reduce urinary stress incontinence. N Engl J Med. 2007;356:2143-2155.
CASE 1: Problematic prolapse, but no incontinence
An 81-year-old multiparous woman, who has a history of recurrent stage-III pelvic organ prolapse (POP), reports worsening discomfort that makes it difficult for her to care for her ailing husband. She also has “trouble” with bladder emptying and constipation, but denies any loss of urine. She has not had vaginal intercourse in more than a decade because of her husband’s medical condition.
Aside from health issues—she suffers from obesity, coronary artery disease, hypertension, and diabetes—the patient is content with her marriage of 58 years.
Urodynamic testing fails to demonstrate detrusor overactivity, stress urinary incontinence, or intrinsic sphincteric deficiency. A cough stress test is repeated after reduction of her prolapse using a large cotton swab, and confirms the findings of the urodynamic tests.
Is reconstructive surgery appropriate for this patient?
Traditional reconstructive surgical procedures for treating POP fail in as many as 30% of patients, and new approaches—some involving grafts—are proposed every day, often without much data behind them.1
Regardless of the approach, reconstructive surgery is a lengthy procedure that subjects patients who are already medically compromised to significant risk, including bleeding, infection, and fluid shifts. Delayed return to normal activity may be especially costly among elderly women because of the risk of venous thromboembolism.
Because of the high failure rate, slow recovery, and risk of complications, reconstructive surgery may not be as appropriate as colpocleisis for the woman described above. Colpocleisis—suturing the inside walls of the vagina together—has an efficacy rate exceeding 90%.2 This relatively simple operation has been around for almost two centuries and has a good track record, but is often overlooked when counseling a patient about her options.
Any frail, elderly woman who has stage-III or -IV POP who does not desire to preserve coital ability is a candidate for colpocleisis (TABLE). Advantages include:
- a short operating time
- few complications
- amenability of local anesthesia
- short hospitalization
- speedy recovery
- high success rate
- low rate of regret.2-5
Because it precludes coital activity, however, colpocleisis may cause problems with self-image. It also may lead to de novo or worsening urinary incontinence and complicate or delay the diagnosis of cervical and endometrial pathology.
This article explores these issues through a case-based discussion of colpocleisis, including a detailed description of surgical technique.
TABLE
Requirements for colpocleisis
Both of the following must be present
|
Plus at least one of the following
|
Colpocleisis, as noted, entails suturing the inside walls of the vagina together. It is controversial because of its impact on coital activity. With careful patient selection, however, colpocleisis is considered a valid option for frail and elderly women who have POP and do not desire or foresee the possibility of future vaginal intercourse. Such women may represent a surprising percentage of the elderly population. A community-based survey found that 78% of married women 70 to 79 years old are not sexually active,6 and a study from The Netherlands found a prevalence of symptomatic POP of 11.4% among white women 45 to 85 years old.7
The fundamental reason for choosing an obliterative procedure such as colpocleisis over total pelvic reconstruction is to treat the prolapse with the least invasive technique in the shortest time. Hysterectomy, which often adds 30 to 80 minutes to the procedure, should therefore be performed only in patients who have a suspicious finding upon initial evaluation. For the same reason, partial colpocleisis—performed using the LeFort technique with limited dissection—has become the most popular obliterative approach. We try to avoid a total colpocleisis procedure—also known as colpectomy—in which the entire vaginal epithelium is stripped, because it is feasible only when the uterus is already absent or scheduled to be removed concomitantly.
(Note: The term vaginectomy should be reserved for gynecologic oncology procedures performed to remove vaginal cancer. Vaginectomy entails full-thickness excision of the vaginal walls, including the fibromuscular layer, as opposed to excision of the epithelial layer only, as in colpocleisis. In this article, we present the LeFort method, a partial colpocleisis technique, because we believe it is more easily adapted by the general gynecologist.8)
CASE 1 RESOLVED
After detailed counseling, which includes family members, the patient opts to undergo colpocleisis. The procedure takes 45 minutes. She is discharged on postoperative Day 1, and reports substantially improved quality of life.
CASE 2: Recurrent prolapse and problems with a pessary
A 72-year-old multiparous, widowed woman experiences recurrent stage-III isolated apical prolapse. She has already undergone two reconstructive procedures, and was discouraged from undergoing a third because of her chronic obstructive lung disease. She tried to use a Gellhorn-type pessary, which required a doctor’s intervention to insert and remove. Frustrated by the many office visits involved in having the pessary checked, she now demands surgical therapy. Another gynecologist has offered to repair the prolapse using mesh, but the patient has concerns about the safety and efficacy of the procedure because it is a relatively new approach.
In addition to the recurrent prolapse, she loses urine with stress and urge. She often has a postvoid residual volume >100 cc; urodynamic assessment confirms mixed urinary incontinence. The patient does not foresee any change in her social status (unmarried, sexually inactive).
Is colpocleisis a reasonable option?
Although the pessary is a helpful conservative alternative for women who are either unable or unwilling to undergo complex surgical pelvic repair and is considered first-line treatment by a majority of urogynecologists, it sometimes becomes more difficult to maintain than the patient is willing to tolerate.9 When a woman cannot remove and reinsert the device herself, the pessary requires a lifelong commitment to doctor’s visits every 2 or 3 months. This commitment is especially problematic for patients who become unable to drive or who lack social support.
Maintenance of the pessary becomes more frustrating as the patient becomes more dependent. Many gynecologists have seen a patient who developed a serious complication such as vesicovaginal or rectovaginal fistula because of a neglected pessary.10
In Case 2, the patient appears to be a potential candidate for colpocleisis, given her age and single status. Although pelvic floor repair appears to be safe in older women, any perioperative complication in a patient 70 years of age or older doubles the risk of discharge to a care facility.11,12 Women who have already undergone several surgeries or who have advanced medical problems such as coronary artery disease or cancer should be counseled thoroughly about the safety and efficacy of colpocleisis.
As for self-image, colpocleisis eliminates prolapse and reduces the genital hiatus. If the patient understands that colpocleisis is obliterative for the vagina but may improve the external appearance of the genital area, she may be more accepting of the procedure. One recent prospective, multicenter study found that only 2% of women thought their body looked worse 1 year after colpocleisis; 60% thought their body looked better.5
When reviewing treatment options, inform the patient that the pessary is a palliative option, whereas surgical therapy aims to be definitive.
CASE 2 RESOLVED
After comprehensive counseling, the patient elects to undergo colpocleisis, along with placement of a midurethral sling. She is discharged 1 day after surgery, and reports substantially improved urinary function, including bladder emptying, and quality of life. She says she would recommend the procedure to any woman who has a similar condition.
CASE 3: Pessary-related complications, incontinence, and underlying medical conditions
A 92-year-old multiparous widow, whose stage-IV uterovaginal prolapse has been managed by a pessary, develops vaginal ulcers in both anterior and posterior walls. After removal of the pessary and 4 weeks of treatment with vaginal estrogen, a smaller pessary is inserted, but she again develops ulcers and bleeding.
The patient’s medical condition is complicated by hypertension and generalized arthritis. She has urodynamically confirmed mixed urinary incontinence. She lives with her daughter and does not want to be placed in a nursing home.
What treatment options should you offer to her?
Because of this patient’s advanced age, poor health, and pessary-related problems, she is an ideal candidate for colpocleisis, provided she consents to the procedure after thorough counseling about its benefits and limitations.
Preoperative concerns
A thorough history, physical examination, and normal Pap test are necessary. If a suspicious pelvic mass or uterine bleeding is present, transvaginal ultrasonography (US) is crucial. In-office endometrial sampling also is necessary in any woman who has unexplained vaginal bleeding. More invasive procedures such as dilatation and curettage and hysteroscopy are needed only when the biopsy is inadequate or endometrial thickness exceeds 4 mm on transvaginal US.13
All elderly women who have high-risk medical problems must be cleared for surgery, with the necessary cardiac and pulmonary workup completed before the procedure.
Because colpocleisis is an extraperitoneal procedure, we have adapted use of over-the-counter enema products on the day before surgery in lieu of mechanical bowel preparation, which may lead to dehydration in very elderly women.
Coordinated consultation between the surgeon and anesthesiologist is necessary to determine the type of anesthesia to be used. Sedation and local anesthesia can be adequate for extremely high-risk women.14,15 Antibiotic prophylaxis is conventional for all patients.
Surgical technique
The LeFort method involves denudation and approximation of the midportions of the anterior and posterior vaginal walls.8 This operation creates a longitudinal vaginal septum with bilateral channels on each side, which serve as conduits for any secretion or bleeding from the apical vagina (FIGURE 1A AND B). Aggressive perineorraphy is also needed to shorten the genital hiatus. The following description incorporates perineorraphy into the LeFort technique.

FIGURE 1 Principles of LeFort colpocleisis
The depiction here is not anatomically precise: The vagina is illustrated as a rectangular prism to clarify the relationship between tissues.
Patient positioning
Place the patient in the dorsal lithotomy position, using stirrups to support the entire leg up to the knee. Let the patient’s buttocks overhang the edge of the table by 1 to 2 inches. A slight Trendelenburg position is imperative, especially when operating on the anterior compartment of the vagina. The bladder should be only partially emptied because the leakage of urine from the bladder makes it easier to identify inadvertent cystotomy. Infiltration of local anesthetic solution to develop the surgical planes is acceptable.
Initiating the procedure
Remove a rectangular piece of vaginal epithelium from the anterior vaginal wall, beginning 2 to 3 cm distal to the vaginal apex (or cervix, if the uterus is present) and ending immediately proximal to the urethrovesical junction to leave space for midurethral sling placement. Remove a similarly sized piece of epithelium from the posterior vaginal wall. This posterior rectangle is an almost geometric projection of the anterior rectangle, but is somewhat longer (2 to 3 cm) (FIGURE 1).
When removing the vaginal epithelium, it may be helpful to use the skills developed for anterior and posterior colporraphy. Our operation begins with a 5- to 6-cm transverse incision at the anterior vaginal apex, which creates the proximal side of the anterior rectangle described above (FIGURE 2A).
As you develop the plane between the epithelium and fibromuscular layer, make a midline sagittal incision and extend it to the urethrovesical junction (FIGURE 2B). Dissect the epithelium off the fibromuscular layer approximately 3 cm bilaterally, then make a transverse incision at the urethrovesical junction. Finally, remove the anterior rectangle in two pieces by cutting along the lateral sides (FIGURE 2C AND D). Remove the posterior rectangle using the same technique, but also excise a triangular piece of skin from the posterior fourchette for the perineorraphy portion of the procedure (FIGURE 2E).

FIGURE 2 LeFort technique, step by step
Begin with a 5–6 cm transverse incision at the anterior vaginal apex.
Dissect the epithelium off the fibromuscular layer, with a midline sagittal incision extending to the urethrovesical junction.
After dissection is completed, make a transverse incision at the urethrovesical junction, and remove the anterior rectangle in two pieces by cutting along the lateral sides.
Denude the posterior rectangle using the same technique. In addition, excise a triangular piece of skin from the perineum.
The posterior rectangle is ready for removal.
Suturing
Suture the apical sides of the anterior and posterior rectangles together using a continuous running technique (FIGURE 2F). Then approximate the lateral sides bilaterally using continuous sutures.
To ensure adherence of the anterior and posterior rectangles, stitch the raw surfaces together in three rows (FIGURE 2G). Do not include the distal 2 cm of the posterior vagina because you will need to leave room for perineorraphy.
Using several sutures, reapproximate the torn perineal fibromuscular structures in the midline to perform perineorraphy (FIGURE 2H). Close the distal vagina, beginning at the midpoint of the anterior transverse side, which lies at the urethrovesical junction (FIGURE 2I). Continue this suture on the posterior vagina and then the perineal body, sagittally, creating a small invagination in the distal vagina (FIGURE 2J).

FIGURE 2 LeFort technique, step by step
Suture all but the distal sides of the rectangles between the anterior and posterior vaginal walls.
Also stitch together the raw surfaces in three rows in an imbricating fashion.
Perform perineorraphy.
Close the distal vagina, starting at the midpoint of the anterior transverse side. If indicated, place a midurethral sling.
Final appearance.
Sling procedure
We place a midurethral sling as part of most colpocleisis operations. It is best to do this after the colpocleisis but before the perineorraphy.
In our cases, cystoscopy with simultaneous intravenous indigo carmine injection is standard before perineorraphy, even when a sling procedure is not planned. This safeguard ensures ureteral patency, which can be compromised (although rarely) in these procedures. Cutting and replacement of one of the sutures that approximate the raw tissues typically resolve the problem.16
Special considerations
Here are additional key points about colpocleisis, based on our experience:
- If an ulcer lies within the area designated to be denuded, some debridement to freshen up the surface will suffice. An ulcer is not an indication to deviate from the standard procedure.
- A modification developed by Goodall and Power may allow coitus by removing only a triangular piece of epithelium from each wall, leaving more room for the channels.17
- We have been unable to find any report of uterine or cervical cancer after colpocleisis, despite a MEDLINE search of the literature in English. Even so, the lateral channels created by the LeFort procedure allow any bleeding to escape the vagina, and may therefore enable recognition of malignancy. When noninvasive imaging techniques such as US or magnetic resonance are inadequate, vaginoscopy and hysteroscopy may be accomplished via these channels.
- When colpocleisis is performed in a hysterectomized woman, no lateral channel is necessary. Therefore, it is appropriate to do total colpocleisis.18,19
- When a patient with POP has a rectovaginal or vesicovaginal fistula caused by a neglected pessary, the addition of LeFort colpocleisis to the fistula repair may provide an effective treatment for both problems.10
Surgical outcomes
Success rate
Evidence concerning colpocleisis comes from case series, some of which are more than 30 years old. Although the definition of success is not clear in some series, the reported success rate has always exceeded 90% over the past three decades.2,18-22 Moreover, some of these reports involve as many as 30 years of follow-up.
Perioperative complication
In a recent review of the literature, the procedure-related mortality rate was 0.025%.2 When the authors focused only on studies published since 1980, major complications due to the patient’s underlying cardiovascular and pulmonary condition were seen in 2% of cases. Major surgical complications such as pyelonephritis and bleeding requiring transfusion occurred in 4% of cases, and less severe complications occurred in 15%.
In a study that included women who underwent concomitant vaginal hysterectomy, hysterectomy prolonged the surgery by 52 minutes, with a 5% rate of laparotomy as a result of intraoperative bleeding.22
In our series of 40 colpocleisis cases, we noted no instance in which a patient regretted the procedure.18 Others have also reported a low rate of regret—the highest being 9%.3-5,19-21
Using validated questionnaires, FitzGerald and colleagues found significant improvement in mental and physical quality of life, as well as urinary, colorectal, and bulge-related pelvic floor symptoms, 1 year after colpocleisis.5
De novo or worsening urinary incontinence is one of the drawbacks of colpocleisis. However, the same risk is present in approximately 40% of women who undergo surgical reconstructive procedures for POP without a continence operation.23 Because preoperative urinary retention is common in women who have POP, the decision to add a potentially harmful continence procedure is complicated in colpocleisis candidates. A small case series reported that the success rate ranged from 90% to 94% in women who underwent a midurethral tension-free sling procedure for the treatment of urinary incontinence at the time of colpocleisis.5
Preoperative urodynamic studies to detect urethral intrinsic deficiency and detrusor dysfunction are prudent, and detailed counseling of the patient about urinary control is vital. We perform a midurethral sling procedure in most of our colpocleisis cases, and have had pleasing results.
CASE 3 RESOLVED
The patient decides to undergo partial colpocleisis using the LeFort procedure, along with placement of a midurethral sling, for a total operative time of 75 minutes. She is discharged 1 day later and reports substantial improvement in urinary function and quality of life.
CASE 1: Problematic prolapse, but no incontinence
An 81-year-old multiparous woman, who has a history of recurrent stage-III pelvic organ prolapse (POP), reports worsening discomfort that makes it difficult for her to care for her ailing husband. She also has “trouble” with bladder emptying and constipation, but denies any loss of urine. She has not had vaginal intercourse in more than a decade because of her husband’s medical condition.
Aside from health issues—she suffers from obesity, coronary artery disease, hypertension, and diabetes—the patient is content with her marriage of 58 years.
Urodynamic testing fails to demonstrate detrusor overactivity, stress urinary incontinence, or intrinsic sphincteric deficiency. A cough stress test is repeated after reduction of her prolapse using a large cotton swab, and confirms the findings of the urodynamic tests.
Is reconstructive surgery appropriate for this patient?
Traditional reconstructive surgical procedures for treating POP fail in as many as 30% of patients, and new approaches—some involving grafts—are proposed every day, often without much data behind them.1
Regardless of the approach, reconstructive surgery is a lengthy procedure that subjects patients who are already medically compromised to significant risk, including bleeding, infection, and fluid shifts. Delayed return to normal activity may be especially costly among elderly women because of the risk of venous thromboembolism.
Because of the high failure rate, slow recovery, and risk of complications, reconstructive surgery may not be as appropriate as colpocleisis for the woman described above. Colpocleisis—suturing the inside walls of the vagina together—has an efficacy rate exceeding 90%.2 This relatively simple operation has been around for almost two centuries and has a good track record, but is often overlooked when counseling a patient about her options.
Any frail, elderly woman who has stage-III or -IV POP who does not desire to preserve coital ability is a candidate for colpocleisis (TABLE). Advantages include:
- a short operating time
- few complications
- amenability of local anesthesia
- short hospitalization
- speedy recovery
- high success rate
- low rate of regret.2-5
Because it precludes coital activity, however, colpocleisis may cause problems with self-image. It also may lead to de novo or worsening urinary incontinence and complicate or delay the diagnosis of cervical and endometrial pathology.
This article explores these issues through a case-based discussion of colpocleisis, including a detailed description of surgical technique.
TABLE
Requirements for colpocleisis
Both of the following must be present
|
Plus at least one of the following
|
Colpocleisis, as noted, entails suturing the inside walls of the vagina together. It is controversial because of its impact on coital activity. With careful patient selection, however, colpocleisis is considered a valid option for frail and elderly women who have POP and do not desire or foresee the possibility of future vaginal intercourse. Such women may represent a surprising percentage of the elderly population. A community-based survey found that 78% of married women 70 to 79 years old are not sexually active,6 and a study from The Netherlands found a prevalence of symptomatic POP of 11.4% among white women 45 to 85 years old.7
The fundamental reason for choosing an obliterative procedure such as colpocleisis over total pelvic reconstruction is to treat the prolapse with the least invasive technique in the shortest time. Hysterectomy, which often adds 30 to 80 minutes to the procedure, should therefore be performed only in patients who have a suspicious finding upon initial evaluation. For the same reason, partial colpocleisis—performed using the LeFort technique with limited dissection—has become the most popular obliterative approach. We try to avoid a total colpocleisis procedure—also known as colpectomy—in which the entire vaginal epithelium is stripped, because it is feasible only when the uterus is already absent or scheduled to be removed concomitantly.
(Note: The term vaginectomy should be reserved for gynecologic oncology procedures performed to remove vaginal cancer. Vaginectomy entails full-thickness excision of the vaginal walls, including the fibromuscular layer, as opposed to excision of the epithelial layer only, as in colpocleisis. In this article, we present the LeFort method, a partial colpocleisis technique, because we believe it is more easily adapted by the general gynecologist.8)
CASE 1 RESOLVED
After detailed counseling, which includes family members, the patient opts to undergo colpocleisis. The procedure takes 45 minutes. She is discharged on postoperative Day 1, and reports substantially improved quality of life.
CASE 2: Recurrent prolapse and problems with a pessary
A 72-year-old multiparous, widowed woman experiences recurrent stage-III isolated apical prolapse. She has already undergone two reconstructive procedures, and was discouraged from undergoing a third because of her chronic obstructive lung disease. She tried to use a Gellhorn-type pessary, which required a doctor’s intervention to insert and remove. Frustrated by the many office visits involved in having the pessary checked, she now demands surgical therapy. Another gynecologist has offered to repair the prolapse using mesh, but the patient has concerns about the safety and efficacy of the procedure because it is a relatively new approach.
In addition to the recurrent prolapse, she loses urine with stress and urge. She often has a postvoid residual volume >100 cc; urodynamic assessment confirms mixed urinary incontinence. The patient does not foresee any change in her social status (unmarried, sexually inactive).
Is colpocleisis a reasonable option?
Although the pessary is a helpful conservative alternative for women who are either unable or unwilling to undergo complex surgical pelvic repair and is considered first-line treatment by a majority of urogynecologists, it sometimes becomes more difficult to maintain than the patient is willing to tolerate.9 When a woman cannot remove and reinsert the device herself, the pessary requires a lifelong commitment to doctor’s visits every 2 or 3 months. This commitment is especially problematic for patients who become unable to drive or who lack social support.
Maintenance of the pessary becomes more frustrating as the patient becomes more dependent. Many gynecologists have seen a patient who developed a serious complication such as vesicovaginal or rectovaginal fistula because of a neglected pessary.10
In Case 2, the patient appears to be a potential candidate for colpocleisis, given her age and single status. Although pelvic floor repair appears to be safe in older women, any perioperative complication in a patient 70 years of age or older doubles the risk of discharge to a care facility.11,12 Women who have already undergone several surgeries or who have advanced medical problems such as coronary artery disease or cancer should be counseled thoroughly about the safety and efficacy of colpocleisis.
As for self-image, colpocleisis eliminates prolapse and reduces the genital hiatus. If the patient understands that colpocleisis is obliterative for the vagina but may improve the external appearance of the genital area, she may be more accepting of the procedure. One recent prospective, multicenter study found that only 2% of women thought their body looked worse 1 year after colpocleisis; 60% thought their body looked better.5
When reviewing treatment options, inform the patient that the pessary is a palliative option, whereas surgical therapy aims to be definitive.
CASE 2 RESOLVED
After comprehensive counseling, the patient elects to undergo colpocleisis, along with placement of a midurethral sling. She is discharged 1 day after surgery, and reports substantially improved urinary function, including bladder emptying, and quality of life. She says she would recommend the procedure to any woman who has a similar condition.
CASE 3: Pessary-related complications, incontinence, and underlying medical conditions
A 92-year-old multiparous widow, whose stage-IV uterovaginal prolapse has been managed by a pessary, develops vaginal ulcers in both anterior and posterior walls. After removal of the pessary and 4 weeks of treatment with vaginal estrogen, a smaller pessary is inserted, but she again develops ulcers and bleeding.
The patient’s medical condition is complicated by hypertension and generalized arthritis. She has urodynamically confirmed mixed urinary incontinence. She lives with her daughter and does not want to be placed in a nursing home.
What treatment options should you offer to her?
Because of this patient’s advanced age, poor health, and pessary-related problems, she is an ideal candidate for colpocleisis, provided she consents to the procedure after thorough counseling about its benefits and limitations.
Preoperative concerns
A thorough history, physical examination, and normal Pap test are necessary. If a suspicious pelvic mass or uterine bleeding is present, transvaginal ultrasonography (US) is crucial. In-office endometrial sampling also is necessary in any woman who has unexplained vaginal bleeding. More invasive procedures such as dilatation and curettage and hysteroscopy are needed only when the biopsy is inadequate or endometrial thickness exceeds 4 mm on transvaginal US.13
All elderly women who have high-risk medical problems must be cleared for surgery, with the necessary cardiac and pulmonary workup completed before the procedure.
Because colpocleisis is an extraperitoneal procedure, we have adapted use of over-the-counter enema products on the day before surgery in lieu of mechanical bowel preparation, which may lead to dehydration in very elderly women.
Coordinated consultation between the surgeon and anesthesiologist is necessary to determine the type of anesthesia to be used. Sedation and local anesthesia can be adequate for extremely high-risk women.14,15 Antibiotic prophylaxis is conventional for all patients.
Surgical technique
The LeFort method involves denudation and approximation of the midportions of the anterior and posterior vaginal walls.8 This operation creates a longitudinal vaginal septum with bilateral channels on each side, which serve as conduits for any secretion or bleeding from the apical vagina (FIGURE 1A AND B). Aggressive perineorraphy is also needed to shorten the genital hiatus. The following description incorporates perineorraphy into the LeFort technique.

FIGURE 1 Principles of LeFort colpocleisis
The depiction here is not anatomically precise: The vagina is illustrated as a rectangular prism to clarify the relationship between tissues.
Patient positioning
Place the patient in the dorsal lithotomy position, using stirrups to support the entire leg up to the knee. Let the patient’s buttocks overhang the edge of the table by 1 to 2 inches. A slight Trendelenburg position is imperative, especially when operating on the anterior compartment of the vagina. The bladder should be only partially emptied because the leakage of urine from the bladder makes it easier to identify inadvertent cystotomy. Infiltration of local anesthetic solution to develop the surgical planes is acceptable.
Initiating the procedure
Remove a rectangular piece of vaginal epithelium from the anterior vaginal wall, beginning 2 to 3 cm distal to the vaginal apex (or cervix, if the uterus is present) and ending immediately proximal to the urethrovesical junction to leave space for midurethral sling placement. Remove a similarly sized piece of epithelium from the posterior vaginal wall. This posterior rectangle is an almost geometric projection of the anterior rectangle, but is somewhat longer (2 to 3 cm) (FIGURE 1).
When removing the vaginal epithelium, it may be helpful to use the skills developed for anterior and posterior colporraphy. Our operation begins with a 5- to 6-cm transverse incision at the anterior vaginal apex, which creates the proximal side of the anterior rectangle described above (FIGURE 2A).
As you develop the plane between the epithelium and fibromuscular layer, make a midline sagittal incision and extend it to the urethrovesical junction (FIGURE 2B). Dissect the epithelium off the fibromuscular layer approximately 3 cm bilaterally, then make a transverse incision at the urethrovesical junction. Finally, remove the anterior rectangle in two pieces by cutting along the lateral sides (FIGURE 2C AND D). Remove the posterior rectangle using the same technique, but also excise a triangular piece of skin from the posterior fourchette for the perineorraphy portion of the procedure (FIGURE 2E).

FIGURE 2 LeFort technique, step by step
Begin with a 5–6 cm transverse incision at the anterior vaginal apex.
Dissect the epithelium off the fibromuscular layer, with a midline sagittal incision extending to the urethrovesical junction.
After dissection is completed, make a transverse incision at the urethrovesical junction, and remove the anterior rectangle in two pieces by cutting along the lateral sides.
Denude the posterior rectangle using the same technique. In addition, excise a triangular piece of skin from the perineum.
The posterior rectangle is ready for removal.
Suturing
Suture the apical sides of the anterior and posterior rectangles together using a continuous running technique (FIGURE 2F). Then approximate the lateral sides bilaterally using continuous sutures.
To ensure adherence of the anterior and posterior rectangles, stitch the raw surfaces together in three rows (FIGURE 2G). Do not include the distal 2 cm of the posterior vagina because you will need to leave room for perineorraphy.
Using several sutures, reapproximate the torn perineal fibromuscular structures in the midline to perform perineorraphy (FIGURE 2H). Close the distal vagina, beginning at the midpoint of the anterior transverse side, which lies at the urethrovesical junction (FIGURE 2I). Continue this suture on the posterior vagina and then the perineal body, sagittally, creating a small invagination in the distal vagina (FIGURE 2J).

FIGURE 2 LeFort technique, step by step
Suture all but the distal sides of the rectangles between the anterior and posterior vaginal walls.
Also stitch together the raw surfaces in three rows in an imbricating fashion.
Perform perineorraphy.
Close the distal vagina, starting at the midpoint of the anterior transverse side. If indicated, place a midurethral sling.
Final appearance.
Sling procedure
We place a midurethral sling as part of most colpocleisis operations. It is best to do this after the colpocleisis but before the perineorraphy.
In our cases, cystoscopy with simultaneous intravenous indigo carmine injection is standard before perineorraphy, even when a sling procedure is not planned. This safeguard ensures ureteral patency, which can be compromised (although rarely) in these procedures. Cutting and replacement of one of the sutures that approximate the raw tissues typically resolve the problem.16
Special considerations
Here are additional key points about colpocleisis, based on our experience:
- If an ulcer lies within the area designated to be denuded, some debridement to freshen up the surface will suffice. An ulcer is not an indication to deviate from the standard procedure.
- A modification developed by Goodall and Power may allow coitus by removing only a triangular piece of epithelium from each wall, leaving more room for the channels.17
- We have been unable to find any report of uterine or cervical cancer after colpocleisis, despite a MEDLINE search of the literature in English. Even so, the lateral channels created by the LeFort procedure allow any bleeding to escape the vagina, and may therefore enable recognition of malignancy. When noninvasive imaging techniques such as US or magnetic resonance are inadequate, vaginoscopy and hysteroscopy may be accomplished via these channels.
- When colpocleisis is performed in a hysterectomized woman, no lateral channel is necessary. Therefore, it is appropriate to do total colpocleisis.18,19
- When a patient with POP has a rectovaginal or vesicovaginal fistula caused by a neglected pessary, the addition of LeFort colpocleisis to the fistula repair may provide an effective treatment for both problems.10
Surgical outcomes
Success rate
Evidence concerning colpocleisis comes from case series, some of which are more than 30 years old. Although the definition of success is not clear in some series, the reported success rate has always exceeded 90% over the past three decades.2,18-22 Moreover, some of these reports involve as many as 30 years of follow-up.
Perioperative complication
In a recent review of the literature, the procedure-related mortality rate was 0.025%.2 When the authors focused only on studies published since 1980, major complications due to the patient’s underlying cardiovascular and pulmonary condition were seen in 2% of cases. Major surgical complications such as pyelonephritis and bleeding requiring transfusion occurred in 4% of cases, and less severe complications occurred in 15%.
In a study that included women who underwent concomitant vaginal hysterectomy, hysterectomy prolonged the surgery by 52 minutes, with a 5% rate of laparotomy as a result of intraoperative bleeding.22
In our series of 40 colpocleisis cases, we noted no instance in which a patient regretted the procedure.18 Others have also reported a low rate of regret—the highest being 9%.3-5,19-21
Using validated questionnaires, FitzGerald and colleagues found significant improvement in mental and physical quality of life, as well as urinary, colorectal, and bulge-related pelvic floor symptoms, 1 year after colpocleisis.5
De novo or worsening urinary incontinence is one of the drawbacks of colpocleisis. However, the same risk is present in approximately 40% of women who undergo surgical reconstructive procedures for POP without a continence operation.23 Because preoperative urinary retention is common in women who have POP, the decision to add a potentially harmful continence procedure is complicated in colpocleisis candidates. A small case series reported that the success rate ranged from 90% to 94% in women who underwent a midurethral tension-free sling procedure for the treatment of urinary incontinence at the time of colpocleisis.5
Preoperative urodynamic studies to detect urethral intrinsic deficiency and detrusor dysfunction are prudent, and detailed counseling of the patient about urinary control is vital. We perform a midurethral sling procedure in most of our colpocleisis cases, and have had pleasing results.
CASE 3 RESOLVED
The patient decides to undergo partial colpocleisis using the LeFort procedure, along with placement of a midurethral sling, for a total operative time of 75 minutes. She is discharged 1 day later and reports substantial improvement in urinary function and quality of life.
1. Luber KM, Boero S, Choe JY. The demographics of pelvic floor disorders: current observations and future projections. Am J Obstet Gynecol. 2001;184:1496-1503.
2. FitzGerald MP, Richter HE, Siddique S, Thompson P, Zyczynski H, Weber A. For the Pelvic Floor Disorders Network. Colpocleisis: a review. Int Urogynecol J Pelvic Floor Dysfunct. 2006;17:261-271.
3. Wheeler TL, Jr, Richter HE, Burgio KL, et al. Regret, satisfaction, and symptom improvement: analysis of the impact of partial colpocleisis for the management of severe pelvic organ prolapse. Am J Obstet Gynecol. 2005;193:2067-2070.
4. Hullfish KL, Bovbjerg VE, Steers WD. Colpocleisis for pelvic organ prolapse: patient goals, quality of life, and satisfaction. Obstet Gynecol. 2007;110(2 Pt 1):341-345.
5. FitzGerald MP, Richter HE, Bradley CS, et al. For the Pelvic Floor Disorders Network. Pelvic support, pelvic symptoms, and patient satisfaction after colpocleisis. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19:1603-1609.
6. Patel D, Gillespie B, Foxman B. Sexual behavior of older women: results of a random-digit-dialing survey of 2,000 women in the United States. Sex Transm Dis. 2003;30:216-220.
7. Slieker-ten Hove MC, Pool-Goudzwaard AL, Eijkemans MJ, Steegers-Theunissen RP, Burger CW, Vierhout ME. Symptomatic pelvic organ prolapse and possible risk factors in a general population. Am J Obstet Gynecol. 2009;200:184.e1-184.e7.
8. Berlin F. Three cases of complete prolapsus uteri operated upon according to the method of Leon LeFort. Am J Obstet Gynecol. 1881;14:866-868.
9. Cundiff GW, Weidner AC, Visco AG, Bump RC, Addison WA. A survey of pessary use by members of the American Urogynecologic Society. Obstet Gynecol. 2000;95(6 Pt 1):931-935.
10. Esin S, Harmanli OH. Large vesicovaginal fistula in women with pelvic organ prolapse: the role of colpocleisis revisited. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19:1711-1713.
11. Gerten KA, Markland AD, Lloyd LK, Richter HE. Prolapse and incontinence surgery in older women. J Urol. 2008;179:2111-2118.
12. Manku K, Bacchetti P, Leung JM. Prognostic significance of postoperative in-hospital complications in elderly patients. I. Long-term survival. Anesth Analg. 2003;96:583-589.
13. American College of Obstetricians and Gynecologists. ACOG Committee Opinion No. 426: The role of transvaginal ultrasonography in the evaluation of postmenopausal bleeding. Obstet Gynecol. 2009;113(2 Pt 1):462-464.
14. Moore RD, Miklos JR. Colpocleisis and tension-free vaginal tape sling for severe uterine and vaginal prolapse and stress urinary incontinence under local anesthesia. J Am Assoc Gynecol Laparosc. 2003;10:276-280.
15. Buchsbaum GM, Albushies DT, Schoenecker E, Duecy EE, Glantz JC. Local anesthesia with sedation for vaginal reconstructive surgery. Int Urogynecol J Pelvic Floor Dysfunct. 2006;17:211-214.
16. Gustilo-Ashby AM, Jelovsek JE, Barber MD, Yoo EH, Paraiso MF, Walters MD. The incidence of ureteral obstruction and the value of intraoperative cystoscopy during vaginal surgery for pelvic organ prolapse. Am J Obstet Gynecol. 2006;194:1478-1485.
17. Goodall JR, Power RMH. A modification of the Le Fort operation for increasing its scope. Am J Obstet Gynecol. 1937;34:968-976.
18. Harmanli OH, Dandolu V, Chatwani AJ, Grody MT. Total colpocleisis for severe pelvic organ prolapse. J Reprod Med. 2003;48:703-706.
19. DeLancey JOL, Morley GW. Total colpocleisis for vaginal eversion. Am J Obstet Gynecol. 1997;176:1228-1232.
20. Goldman J, Ovadia J, Feldberg D. The Neugebauer-Le Fort operation: a review of 118 partial colpocleises. Eur J Obstet Gynecol Reprod Biol. 1981;12:31-35.
21. Ubachs JM, van Sante TJ, Schellekens LA. Partial colpocleisis by a modification of Le Fort’s operation. Obstet Gynecol. 1973;42:415-420.
22. Von Pechmann WS, Mutone MD, Fyffe J, Hale DS. Total colpocleisis with high levator plication for the treatment of advanced pelvic organ prolapse. Am J Obstet Gynecol. 2003;189:121-126.
23. Albo ME, Richter HE, Brubaker L, et al. For Urinary Incontinence Treatment Network. Burch colposuspension versus fascial sling to reduce urinary stress incontinence. N Engl J Med. 2007;356:2143-2155.
1. Luber KM, Boero S, Choe JY. The demographics of pelvic floor disorders: current observations and future projections. Am J Obstet Gynecol. 2001;184:1496-1503.
2. FitzGerald MP, Richter HE, Siddique S, Thompson P, Zyczynski H, Weber A. For the Pelvic Floor Disorders Network. Colpocleisis: a review. Int Urogynecol J Pelvic Floor Dysfunct. 2006;17:261-271.
3. Wheeler TL, Jr, Richter HE, Burgio KL, et al. Regret, satisfaction, and symptom improvement: analysis of the impact of partial colpocleisis for the management of severe pelvic organ prolapse. Am J Obstet Gynecol. 2005;193:2067-2070.
4. Hullfish KL, Bovbjerg VE, Steers WD. Colpocleisis for pelvic organ prolapse: patient goals, quality of life, and satisfaction. Obstet Gynecol. 2007;110(2 Pt 1):341-345.
5. FitzGerald MP, Richter HE, Bradley CS, et al. For the Pelvic Floor Disorders Network. Pelvic support, pelvic symptoms, and patient satisfaction after colpocleisis. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19:1603-1609.
6. Patel D, Gillespie B, Foxman B. Sexual behavior of older women: results of a random-digit-dialing survey of 2,000 women in the United States. Sex Transm Dis. 2003;30:216-220.
7. Slieker-ten Hove MC, Pool-Goudzwaard AL, Eijkemans MJ, Steegers-Theunissen RP, Burger CW, Vierhout ME. Symptomatic pelvic organ prolapse and possible risk factors in a general population. Am J Obstet Gynecol. 2009;200:184.e1-184.e7.
8. Berlin F. Three cases of complete prolapsus uteri operated upon according to the method of Leon LeFort. Am J Obstet Gynecol. 1881;14:866-868.
9. Cundiff GW, Weidner AC, Visco AG, Bump RC, Addison WA. A survey of pessary use by members of the American Urogynecologic Society. Obstet Gynecol. 2000;95(6 Pt 1):931-935.
10. Esin S, Harmanli OH. Large vesicovaginal fistula in women with pelvic organ prolapse: the role of colpocleisis revisited. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19:1711-1713.
11. Gerten KA, Markland AD, Lloyd LK, Richter HE. Prolapse and incontinence surgery in older women. J Urol. 2008;179:2111-2118.
12. Manku K, Bacchetti P, Leung JM. Prognostic significance of postoperative in-hospital complications in elderly patients. I. Long-term survival. Anesth Analg. 2003;96:583-589.
13. American College of Obstetricians and Gynecologists. ACOG Committee Opinion No. 426: The role of transvaginal ultrasonography in the evaluation of postmenopausal bleeding. Obstet Gynecol. 2009;113(2 Pt 1):462-464.
14. Moore RD, Miklos JR. Colpocleisis and tension-free vaginal tape sling for severe uterine and vaginal prolapse and stress urinary incontinence under local anesthesia. J Am Assoc Gynecol Laparosc. 2003;10:276-280.
15. Buchsbaum GM, Albushies DT, Schoenecker E, Duecy EE, Glantz JC. Local anesthesia with sedation for vaginal reconstructive surgery. Int Urogynecol J Pelvic Floor Dysfunct. 2006;17:211-214.
16. Gustilo-Ashby AM, Jelovsek JE, Barber MD, Yoo EH, Paraiso MF, Walters MD. The incidence of ureteral obstruction and the value of intraoperative cystoscopy during vaginal surgery for pelvic organ prolapse. Am J Obstet Gynecol. 2006;194:1478-1485.
17. Goodall JR, Power RMH. A modification of the Le Fort operation for increasing its scope. Am J Obstet Gynecol. 1937;34:968-976.
18. Harmanli OH, Dandolu V, Chatwani AJ, Grody MT. Total colpocleisis for severe pelvic organ prolapse. J Reprod Med. 2003;48:703-706.
19. DeLancey JOL, Morley GW. Total colpocleisis for vaginal eversion. Am J Obstet Gynecol. 1997;176:1228-1232.
20. Goldman J, Ovadia J, Feldberg D. The Neugebauer-Le Fort operation: a review of 118 partial colpocleises. Eur J Obstet Gynecol Reprod Biol. 1981;12:31-35.
21. Ubachs JM, van Sante TJ, Schellekens LA. Partial colpocleisis by a modification of Le Fort’s operation. Obstet Gynecol. 1973;42:415-420.
22. Von Pechmann WS, Mutone MD, Fyffe J, Hale DS. Total colpocleisis with high levator plication for the treatment of advanced pelvic organ prolapse. Am J Obstet Gynecol. 2003;189:121-126.
23. Albo ME, Richter HE, Brubaker L, et al. For Urinary Incontinence Treatment Network. Burch colposuspension versus fascial sling to reduce urinary stress incontinence. N Engl J Med. 2007;356:2143-2155.