User login
Dr. Hospitalist
I recently became chief medical officer (CMO) of our hospital. When a hospitalist’s case comes to our patient-care committee, is it appropriate to inform the patient’s primary-care physician (PCP) of the quality issues? Our hospitalists are independent. There are questions of HIPAA. However, several committee members feel that the PCP, who does not come to the hospital, should be informed. Thank you.
K.A., M.D.
Dr. Hospitalist responds:
Good question. While I’ve participated in similar scenarios, keep in mind that I’m a hospitalist like you, not a lawyer. So, with that rejoinder in mind, let’s take this discussion a few steps further and see what happens.
You state: “when a hospitalist’s case comes to our patient-care committee.” Does that mean peer review? If it does, and what you are describing is a committee that handles privileged and confidential information, then you cannot inform the PCP because you would be violating the basic tenets of peer review.
The principle behind peer review is that it allows physicians to confidentially review the cases of their peers. This is to prevent the information contained in peer review from becoming available to a lawyer by subpoena or by discovery in the courts. The Joint Commission has mandated hospital peer review committees since 1952, and the federal government included language regarding peer-review protection in the Health Care Quality Improvement Act of 1986.
Every state has a law on the books, but the specifics and effectiveness of peer review will vary from state to state (see Florida’s Amendment 7, Kentucky, and Massachusetts). The whole idea is to allow for a process to evaluate physician practice or quality concerns without the fear of discovery or subsequent lawsuit. Even the act of referring a case to peer review is considered a confidential action in my state, so just the referral itself may not be discussed. So if you are referring to peer review, the answer is no, you cannot inform the patient’s PCP. HIPAA does not come into the picture here.
On the other hand, let’s assume, for sake of discussion, that you’ve heard a complaint (or several) about a certain hospitalist, Dr. Nogood. You could, if you desired, refer these complaints to peer review.
If so, then you are immediately bound by those rules of confidentiality. If you don’t refer the case, then you could inform the PCP that you have heard a complaint involving Dr. Nogood and that PCP’s patient.
I can’t see how that would violate HIPAA, because the PCP has an established relationship with that patient, and you might be only reporting facts (the complaint), not passing judgment on the quality of care. And I would not even go that far.
Why stop there? Why not tell that PCP exactly what you think of Dr. Nogood and his clinical practice, the details of the complaints against him, and how you think maybe that PCP should send his patients to someone else for better care? Well, you’re the CMO for the hospital. If you go beyond reporting facts and start reporting opinions, then you’ve just opened yourself up to accusations of restraint of trade by Dr. Nogood.
No matter what you may think of Dr. Nogood’s patient care, unless it falls outside the boundaries of acceptable practice (which can only be determined by a peer review committee), then you should not say anything.
Unless, of course, you want to be accused of spreading rumors, hearsay, and innuendo. Remember, we are talking about an independent practitioner, not a hospital employee.
Overall, it’s a bit of a sticky wicket. If you think the complaint has merit, then it should be sent to peer review—and you may speak no more of it. If you think the complaint is baseless, then why sustain it and tell the PCP?
Peer review is an exceptional process, and the physicians who serve on such committees perform a difficult and selfless service. We should all do our best to uphold its integrity.
I recently became chief medical officer (CMO) of our hospital. When a hospitalist’s case comes to our patient-care committee, is it appropriate to inform the patient’s primary-care physician (PCP) of the quality issues? Our hospitalists are independent. There are questions of HIPAA. However, several committee members feel that the PCP, who does not come to the hospital, should be informed. Thank you.
K.A., M.D.
Dr. Hospitalist responds:
Good question. While I’ve participated in similar scenarios, keep in mind that I’m a hospitalist like you, not a lawyer. So, with that rejoinder in mind, let’s take this discussion a few steps further and see what happens.
You state: “when a hospitalist’s case comes to our patient-care committee.” Does that mean peer review? If it does, and what you are describing is a committee that handles privileged and confidential information, then you cannot inform the PCP because you would be violating the basic tenets of peer review.
The principle behind peer review is that it allows physicians to confidentially review the cases of their peers. This is to prevent the information contained in peer review from becoming available to a lawyer by subpoena or by discovery in the courts. The Joint Commission has mandated hospital peer review committees since 1952, and the federal government included language regarding peer-review protection in the Health Care Quality Improvement Act of 1986.
Every state has a law on the books, but the specifics and effectiveness of peer review will vary from state to state (see Florida’s Amendment 7, Kentucky, and Massachusetts). The whole idea is to allow for a process to evaluate physician practice or quality concerns without the fear of discovery or subsequent lawsuit. Even the act of referring a case to peer review is considered a confidential action in my state, so just the referral itself may not be discussed. So if you are referring to peer review, the answer is no, you cannot inform the patient’s PCP. HIPAA does not come into the picture here.
On the other hand, let’s assume, for sake of discussion, that you’ve heard a complaint (or several) about a certain hospitalist, Dr. Nogood. You could, if you desired, refer these complaints to peer review.
If so, then you are immediately bound by those rules of confidentiality. If you don’t refer the case, then you could inform the PCP that you have heard a complaint involving Dr. Nogood and that PCP’s patient.
I can’t see how that would violate HIPAA, because the PCP has an established relationship with that patient, and you might be only reporting facts (the complaint), not passing judgment on the quality of care. And I would not even go that far.
Why stop there? Why not tell that PCP exactly what you think of Dr. Nogood and his clinical practice, the details of the complaints against him, and how you think maybe that PCP should send his patients to someone else for better care? Well, you’re the CMO for the hospital. If you go beyond reporting facts and start reporting opinions, then you’ve just opened yourself up to accusations of restraint of trade by Dr. Nogood.
No matter what you may think of Dr. Nogood’s patient care, unless it falls outside the boundaries of acceptable practice (which can only be determined by a peer review committee), then you should not say anything.
Unless, of course, you want to be accused of spreading rumors, hearsay, and innuendo. Remember, we are talking about an independent practitioner, not a hospital employee.
Overall, it’s a bit of a sticky wicket. If you think the complaint has merit, then it should be sent to peer review—and you may speak no more of it. If you think the complaint is baseless, then why sustain it and tell the PCP?
Peer review is an exceptional process, and the physicians who serve on such committees perform a difficult and selfless service. We should all do our best to uphold its integrity.
I recently became chief medical officer (CMO) of our hospital. When a hospitalist’s case comes to our patient-care committee, is it appropriate to inform the patient’s primary-care physician (PCP) of the quality issues? Our hospitalists are independent. There are questions of HIPAA. However, several committee members feel that the PCP, who does not come to the hospital, should be informed. Thank you.
K.A., M.D.
Dr. Hospitalist responds:
Good question. While I’ve participated in similar scenarios, keep in mind that I’m a hospitalist like you, not a lawyer. So, with that rejoinder in mind, let’s take this discussion a few steps further and see what happens.
You state: “when a hospitalist’s case comes to our patient-care committee.” Does that mean peer review? If it does, and what you are describing is a committee that handles privileged and confidential information, then you cannot inform the PCP because you would be violating the basic tenets of peer review.
The principle behind peer review is that it allows physicians to confidentially review the cases of their peers. This is to prevent the information contained in peer review from becoming available to a lawyer by subpoena or by discovery in the courts. The Joint Commission has mandated hospital peer review committees since 1952, and the federal government included language regarding peer-review protection in the Health Care Quality Improvement Act of 1986.
Every state has a law on the books, but the specifics and effectiveness of peer review will vary from state to state (see Florida’s Amendment 7, Kentucky, and Massachusetts). The whole idea is to allow for a process to evaluate physician practice or quality concerns without the fear of discovery or subsequent lawsuit. Even the act of referring a case to peer review is considered a confidential action in my state, so just the referral itself may not be discussed. So if you are referring to peer review, the answer is no, you cannot inform the patient’s PCP. HIPAA does not come into the picture here.
On the other hand, let’s assume, for sake of discussion, that you’ve heard a complaint (or several) about a certain hospitalist, Dr. Nogood. You could, if you desired, refer these complaints to peer review.
If so, then you are immediately bound by those rules of confidentiality. If you don’t refer the case, then you could inform the PCP that you have heard a complaint involving Dr. Nogood and that PCP’s patient.
I can’t see how that would violate HIPAA, because the PCP has an established relationship with that patient, and you might be only reporting facts (the complaint), not passing judgment on the quality of care. And I would not even go that far.
Why stop there? Why not tell that PCP exactly what you think of Dr. Nogood and his clinical practice, the details of the complaints against him, and how you think maybe that PCP should send his patients to someone else for better care? Well, you’re the CMO for the hospital. If you go beyond reporting facts and start reporting opinions, then you’ve just opened yourself up to accusations of restraint of trade by Dr. Nogood.
No matter what you may think of Dr. Nogood’s patient care, unless it falls outside the boundaries of acceptable practice (which can only be determined by a peer review committee), then you should not say anything.
Unless, of course, you want to be accused of spreading rumors, hearsay, and innuendo. Remember, we are talking about an independent practitioner, not a hospital employee.
Overall, it’s a bit of a sticky wicket. If you think the complaint has merit, then it should be sent to peer review—and you may speak no more of it. If you think the complaint is baseless, then why sustain it and tell the PCP?
Peer review is an exceptional process, and the physicians who serve on such committees perform a difficult and selfless service. We should all do our best to uphold its integrity.
ONLINE EXCLUSIVE TK
Enter text here
Enter text here
Enter text here
ONLINE EXCLUSIVE TK
Enter text here
Enter text here
Enter text here
ONLINE EXCLUSIVE TK
Enter text here
Enter text here
Enter text here
Making Inroads in Treatment of Adult ALL
SAN FRANCISCO – Several areas of active research are improving the outlook for adults with acute lymphoblastic leukemia, Dr. Partow Kebriaei told attendees of the annual Oncology Congress here.
Investigators are exploring the impact of treatment intensification, stem cell transplantation, use of minimal residual disease to guide therapy, and a host of new agents, according to Dr. Kebriaei of the department of stem cell transplantation and cellular therapy at the University of Texas M.D. Anderson Cancer Center, Houston.
More effective and less toxic treatments are especially needed in this age group, she explained at the congress, which is presented by Reed Medical Education. "We have had great success in eradicating acute lymphoblastic leukemia (ALL) in children but still have a ways to go in adults," Dr. Kebraiei said.
In particular, although both incidence and mortality increase sharply over the age of 50 years, the median age of enrollees in major ALL adult trials has been 30-40 years. "So one thing that we need to think about as we devise more new therapies is how to make them more tolerable or relevant to the older patient," she commented.
Intensified Treatment for Young Adults
The observation that younger adults with ALL, up to the age of 40, have better long-term remission when treated with the more intensive pediatric regimens vs. adult regimens has raised interest in this approach for adults generally, Dr. Kebriaei noted.
A trial of intensified chemotherapy in adults found a significantly better response rate, event-free survival, and overall survival compared with outcomes seen historically with standard-intensity chemotherapy (J. Clin. Oncol. 2009;27:911-8).
But in age-stratified analyses, any survival benefit among patients older than 45 was offset by higher treatment-related mortality. "So, for that older subgroup, treatment intensification still does not really impact outcome favorably," she said.
Additionally, a caveat for the younger adults was that the trial allowed crossover to transplantation for patients having a donor. "So it’s a little bit difficult to ascertain whether these improved results are from the availability of transplant or the intensification of treatment," Dr. Kebriaei commented. "But, I think in general, one can conclude that treatment intensification is effective up to a certain age."
Stem Cell Transplantation
The International ALL Trial assessed the role of stem cell transplantation in adults with ALL in first complete remission. Patients younger than 55 years of age having a sibling donor were allocated to allogeneic transplantation, whereas older patients or those without a donor were randomized to autologous transplantation or chemotherapy.
Among patients not having the Philadelphia chromosome, which confers poorer prognosis, those with a donor were less likely to have a relapse than were those without a donor, whether they had standard- or high-risk disease (Blood 2008;111:1827-33). But treatment-related mortality was increased; it canceled out the relapse benefit in the high-risk group, so that in contrast to the standard-risk group, there was no net improvement in survival.
The higher treatment-related mortality was mainly due to higher rates of infection and graft-vs.-host disease. "So if we want transplant to afford a better outcome to all patients, we are going to have to impact these complications," Dr. Kebriaei maintained.
Of note, in additional trial analyses, chemotherapy was associated with significantly better event-free and overall survival than autologous transplantation.
Efforts to reduce the treatment-related mortality of transplantation include reduced-intensity conditioning regimens that, for example, omit total-body irradiation. Studies of this approach have indeed found that compared with the standard one including total-body irradiation, it achieves a lower rate of deaths due to treatment, and among patients transplanted in first remission, similar overall survival.
"But the most important thing is that if you look at the median age of patients [in these studies], we are now approaching 55, which is more reflective of what we see in the clinic," she noted.
Use of MRD in Risk-Oriented Therapy
"Minimal residual disease [MRD] really defines a submicroscopic ALL and in patients that we would normally term as remission patients," Dr. Kebriaei explained. "It is evaluated by multichannel flow cytometry or PCR [polymerase chain reaction], and it’s really becoming one of the most significant prognostic markers that we have."
For example, in the International ALL Trial, persistent MRD after induction or early consolidation was significantly associated with an increased risk of relapse in patients receiving chemotherapy alone (Br. J. Haematol. 2010;148:80-9). Yet, that was not the whole story.
"Interestingly, here, when they looked at MRD in patients prior to going forward on allogeneic stem cell transplant, they did not see any impact of MRD," she noted. "They also didn’t see an impact of MRD in helping to predict which patients would develop CNS relapse."
Targeted Therapies
Several therapies that target tumors’ molecular vulnerabilities are being incorporated into the treatment of adult ALL to clinical benefit. "I think the most dramatic improvement has been seen with the use of tyrosine kinase inhibitors (TKIs) for the Philadelphia chromosome–positive subset," Dr. Kebriaei commented.
In trials, use of TKIs in these patients has led to higher rates of complete remission, transplantation eligibility, and survival without transplantation. "Now all of these trials allowed transplant as well, so it’s hard to ascertain how much of this impact is coming from more transplant eligibility and how much of it is coming from the impact of the TKIs," she cautioned.
The SWOG S0805 Intergroup trial, open to patients up 50 years old with newly diagnosed Philadelphia chromosome–positive ALL, is looking more closely at the issue, as well as the issue of using TKIs as maintenance therapy. Patients receive dasatinib (Sprycel)-containing induction therapy and, if they undergo transplantation, dasatinib thereafter as well.
In clinical practice, "there is great variation in practice patterns, ranging from providing no TKI in maintenance all the way up to providing 2 years of TKI," Dr. Kebriaei observed. "And unfortunately, there isn’t good data yet published to determine what the best approach will be."
A second targeted therapy being used is rituximab (Rituxan), for ALL expressing CD20, another poor prognostic marker. Adding rituximab to the hyper-CVAD regimen significantly improves survival for patients younger than 60 years (J. Clin. Oncol. 2010;28:3880-9). But in older patients, there was no survival benefit, in part because of increased induction-related mortality.
Novel Agents and Cellular Therapies
The Food and Drug Administration has approved three novel agents for ALL treatment: pegylated asparaginase (Oncaspar), clofarabine (Clolar), and nelarabine (Arranon), and has received a new drug application for liposomal vincristine (Marqibo).
Nelarabine, for example, is a prodrug of ara-G that achieves good response and survival rates in patients with relapsed T-cell ALL, with a dose-limiting toxicity of neurotoxicity. It is now being evaluated when added to hyper-CVAD up front for patients with T-cell ALL, according to Dr. Kebriaei.
The investigational agent inotuzumab ozogamicin, an anti-CD22 antibody conjugated to calicheamicin, achieves an overall response rate of 61% when used as monotherapy in a trial among patients with refractory ALL (Jabbour et al. ASCO 2011 meeting. Abstract 6507).
"Interestingly, almost half of these patients were then able to go on to transplant in complete remission," she noted. Adverse effects included hepatotoxicity and veno-occlusive disease.
Another investigational antibody, blinatumomab, redirects T cells toward lysis of CD19-expressing cells and has been found to achieve complete remission in 13 of 16 patients with precursor B-ALL having persistent MRD (Topp et al. ASH 2009 meeting. Abstract 840).
A final novel strategy being tested is cellular therapy using chimeric antigen receptors (CARs), which are produced by fusing an extracellular single-chain antibody to an intracellular signaling domain. When expressed in T cells, these receptors redirect the cells’ antigen recognition toward a desired target, such as CD19.
"What’s very effective and interesting about this CAR strategy is that it doesn’t rely on preexisting antitumor immunity to generate an antitumor effector response," Dr. Kebriaei noted. "This is particularly important in the setting of ALL, where you have immune dysfunction."
Trials are assessing the use of CARs in the setting of stem cell transplantation, whereby donor T cells are transduced with anti-CD19 CARs and given as a targeted donor lymphocyte infusion.
"Perhaps by incorporating these targeted therapies and cellular therapies with the traditional cytotoxic therapies, we may be able to improve treatment outcomes without adding toxicity," concluded Dr. Kebriaei, who reported having no conflicts of interest related to her presentation.
The Oncology Congress is presented by Reed Medical Education. Reed Medical Education and this news organization are owned by Reed Elsevier Inc.
SAN FRANCISCO – Several areas of active research are improving the outlook for adults with acute lymphoblastic leukemia, Dr. Partow Kebriaei told attendees of the annual Oncology Congress here.
Investigators are exploring the impact of treatment intensification, stem cell transplantation, use of minimal residual disease to guide therapy, and a host of new agents, according to Dr. Kebriaei of the department of stem cell transplantation and cellular therapy at the University of Texas M.D. Anderson Cancer Center, Houston.
More effective and less toxic treatments are especially needed in this age group, she explained at the congress, which is presented by Reed Medical Education. "We have had great success in eradicating acute lymphoblastic leukemia (ALL) in children but still have a ways to go in adults," Dr. Kebraiei said.
In particular, although both incidence and mortality increase sharply over the age of 50 years, the median age of enrollees in major ALL adult trials has been 30-40 years. "So one thing that we need to think about as we devise more new therapies is how to make them more tolerable or relevant to the older patient," she commented.
Intensified Treatment for Young Adults
The observation that younger adults with ALL, up to the age of 40, have better long-term remission when treated with the more intensive pediatric regimens vs. adult regimens has raised interest in this approach for adults generally, Dr. Kebriaei noted.
A trial of intensified chemotherapy in adults found a significantly better response rate, event-free survival, and overall survival compared with outcomes seen historically with standard-intensity chemotherapy (J. Clin. Oncol. 2009;27:911-8).
But in age-stratified analyses, any survival benefit among patients older than 45 was offset by higher treatment-related mortality. "So, for that older subgroup, treatment intensification still does not really impact outcome favorably," she said.
Additionally, a caveat for the younger adults was that the trial allowed crossover to transplantation for patients having a donor. "So it’s a little bit difficult to ascertain whether these improved results are from the availability of transplant or the intensification of treatment," Dr. Kebriaei commented. "But, I think in general, one can conclude that treatment intensification is effective up to a certain age."
Stem Cell Transplantation
The International ALL Trial assessed the role of stem cell transplantation in adults with ALL in first complete remission. Patients younger than 55 years of age having a sibling donor were allocated to allogeneic transplantation, whereas older patients or those without a donor were randomized to autologous transplantation or chemotherapy.
Among patients not having the Philadelphia chromosome, which confers poorer prognosis, those with a donor were less likely to have a relapse than were those without a donor, whether they had standard- or high-risk disease (Blood 2008;111:1827-33). But treatment-related mortality was increased; it canceled out the relapse benefit in the high-risk group, so that in contrast to the standard-risk group, there was no net improvement in survival.
The higher treatment-related mortality was mainly due to higher rates of infection and graft-vs.-host disease. "So if we want transplant to afford a better outcome to all patients, we are going to have to impact these complications," Dr. Kebriaei maintained.
Of note, in additional trial analyses, chemotherapy was associated with significantly better event-free and overall survival than autologous transplantation.
Efforts to reduce the treatment-related mortality of transplantation include reduced-intensity conditioning regimens that, for example, omit total-body irradiation. Studies of this approach have indeed found that compared with the standard one including total-body irradiation, it achieves a lower rate of deaths due to treatment, and among patients transplanted in first remission, similar overall survival.
"But the most important thing is that if you look at the median age of patients [in these studies], we are now approaching 55, which is more reflective of what we see in the clinic," she noted.
Use of MRD in Risk-Oriented Therapy
"Minimal residual disease [MRD] really defines a submicroscopic ALL and in patients that we would normally term as remission patients," Dr. Kebriaei explained. "It is evaluated by multichannel flow cytometry or PCR [polymerase chain reaction], and it’s really becoming one of the most significant prognostic markers that we have."
For example, in the International ALL Trial, persistent MRD after induction or early consolidation was significantly associated with an increased risk of relapse in patients receiving chemotherapy alone (Br. J. Haematol. 2010;148:80-9). Yet, that was not the whole story.
"Interestingly, here, when they looked at MRD in patients prior to going forward on allogeneic stem cell transplant, they did not see any impact of MRD," she noted. "They also didn’t see an impact of MRD in helping to predict which patients would develop CNS relapse."
Targeted Therapies
Several therapies that target tumors’ molecular vulnerabilities are being incorporated into the treatment of adult ALL to clinical benefit. "I think the most dramatic improvement has been seen with the use of tyrosine kinase inhibitors (TKIs) for the Philadelphia chromosome–positive subset," Dr. Kebriaei commented.
In trials, use of TKIs in these patients has led to higher rates of complete remission, transplantation eligibility, and survival without transplantation. "Now all of these trials allowed transplant as well, so it’s hard to ascertain how much of this impact is coming from more transplant eligibility and how much of it is coming from the impact of the TKIs," she cautioned.
The SWOG S0805 Intergroup trial, open to patients up 50 years old with newly diagnosed Philadelphia chromosome–positive ALL, is looking more closely at the issue, as well as the issue of using TKIs as maintenance therapy. Patients receive dasatinib (Sprycel)-containing induction therapy and, if they undergo transplantation, dasatinib thereafter as well.
In clinical practice, "there is great variation in practice patterns, ranging from providing no TKI in maintenance all the way up to providing 2 years of TKI," Dr. Kebriaei observed. "And unfortunately, there isn’t good data yet published to determine what the best approach will be."
A second targeted therapy being used is rituximab (Rituxan), for ALL expressing CD20, another poor prognostic marker. Adding rituximab to the hyper-CVAD regimen significantly improves survival for patients younger than 60 years (J. Clin. Oncol. 2010;28:3880-9). But in older patients, there was no survival benefit, in part because of increased induction-related mortality.
Novel Agents and Cellular Therapies
The Food and Drug Administration has approved three novel agents for ALL treatment: pegylated asparaginase (Oncaspar), clofarabine (Clolar), and nelarabine (Arranon), and has received a new drug application for liposomal vincristine (Marqibo).
Nelarabine, for example, is a prodrug of ara-G that achieves good response and survival rates in patients with relapsed T-cell ALL, with a dose-limiting toxicity of neurotoxicity. It is now being evaluated when added to hyper-CVAD up front for patients with T-cell ALL, according to Dr. Kebriaei.
The investigational agent inotuzumab ozogamicin, an anti-CD22 antibody conjugated to calicheamicin, achieves an overall response rate of 61% when used as monotherapy in a trial among patients with refractory ALL (Jabbour et al. ASCO 2011 meeting. Abstract 6507).
"Interestingly, almost half of these patients were then able to go on to transplant in complete remission," she noted. Adverse effects included hepatotoxicity and veno-occlusive disease.
Another investigational antibody, blinatumomab, redirects T cells toward lysis of CD19-expressing cells and has been found to achieve complete remission in 13 of 16 patients with precursor B-ALL having persistent MRD (Topp et al. ASH 2009 meeting. Abstract 840).
A final novel strategy being tested is cellular therapy using chimeric antigen receptors (CARs), which are produced by fusing an extracellular single-chain antibody to an intracellular signaling domain. When expressed in T cells, these receptors redirect the cells’ antigen recognition toward a desired target, such as CD19.
"What’s very effective and interesting about this CAR strategy is that it doesn’t rely on preexisting antitumor immunity to generate an antitumor effector response," Dr. Kebriaei noted. "This is particularly important in the setting of ALL, where you have immune dysfunction."
Trials are assessing the use of CARs in the setting of stem cell transplantation, whereby donor T cells are transduced with anti-CD19 CARs and given as a targeted donor lymphocyte infusion.
"Perhaps by incorporating these targeted therapies and cellular therapies with the traditional cytotoxic therapies, we may be able to improve treatment outcomes without adding toxicity," concluded Dr. Kebriaei, who reported having no conflicts of interest related to her presentation.
The Oncology Congress is presented by Reed Medical Education. Reed Medical Education and this news organization are owned by Reed Elsevier Inc.
SAN FRANCISCO – Several areas of active research are improving the outlook for adults with acute lymphoblastic leukemia, Dr. Partow Kebriaei told attendees of the annual Oncology Congress here.
Investigators are exploring the impact of treatment intensification, stem cell transplantation, use of minimal residual disease to guide therapy, and a host of new agents, according to Dr. Kebriaei of the department of stem cell transplantation and cellular therapy at the University of Texas M.D. Anderson Cancer Center, Houston.
More effective and less toxic treatments are especially needed in this age group, she explained at the congress, which is presented by Reed Medical Education. "We have had great success in eradicating acute lymphoblastic leukemia (ALL) in children but still have a ways to go in adults," Dr. Kebraiei said.
In particular, although both incidence and mortality increase sharply over the age of 50 years, the median age of enrollees in major ALL adult trials has been 30-40 years. "So one thing that we need to think about as we devise more new therapies is how to make them more tolerable or relevant to the older patient," she commented.
Intensified Treatment for Young Adults
The observation that younger adults with ALL, up to the age of 40, have better long-term remission when treated with the more intensive pediatric regimens vs. adult regimens has raised interest in this approach for adults generally, Dr. Kebriaei noted.
A trial of intensified chemotherapy in adults found a significantly better response rate, event-free survival, and overall survival compared with outcomes seen historically with standard-intensity chemotherapy (J. Clin. Oncol. 2009;27:911-8).
But in age-stratified analyses, any survival benefit among patients older than 45 was offset by higher treatment-related mortality. "So, for that older subgroup, treatment intensification still does not really impact outcome favorably," she said.
Additionally, a caveat for the younger adults was that the trial allowed crossover to transplantation for patients having a donor. "So it’s a little bit difficult to ascertain whether these improved results are from the availability of transplant or the intensification of treatment," Dr. Kebriaei commented. "But, I think in general, one can conclude that treatment intensification is effective up to a certain age."
Stem Cell Transplantation
The International ALL Trial assessed the role of stem cell transplantation in adults with ALL in first complete remission. Patients younger than 55 years of age having a sibling donor were allocated to allogeneic transplantation, whereas older patients or those without a donor were randomized to autologous transplantation or chemotherapy.
Among patients not having the Philadelphia chromosome, which confers poorer prognosis, those with a donor were less likely to have a relapse than were those without a donor, whether they had standard- or high-risk disease (Blood 2008;111:1827-33). But treatment-related mortality was increased; it canceled out the relapse benefit in the high-risk group, so that in contrast to the standard-risk group, there was no net improvement in survival.
The higher treatment-related mortality was mainly due to higher rates of infection and graft-vs.-host disease. "So if we want transplant to afford a better outcome to all patients, we are going to have to impact these complications," Dr. Kebriaei maintained.
Of note, in additional trial analyses, chemotherapy was associated with significantly better event-free and overall survival than autologous transplantation.
Efforts to reduce the treatment-related mortality of transplantation include reduced-intensity conditioning regimens that, for example, omit total-body irradiation. Studies of this approach have indeed found that compared with the standard one including total-body irradiation, it achieves a lower rate of deaths due to treatment, and among patients transplanted in first remission, similar overall survival.
"But the most important thing is that if you look at the median age of patients [in these studies], we are now approaching 55, which is more reflective of what we see in the clinic," she noted.
Use of MRD in Risk-Oriented Therapy
"Minimal residual disease [MRD] really defines a submicroscopic ALL and in patients that we would normally term as remission patients," Dr. Kebriaei explained. "It is evaluated by multichannel flow cytometry or PCR [polymerase chain reaction], and it’s really becoming one of the most significant prognostic markers that we have."
For example, in the International ALL Trial, persistent MRD after induction or early consolidation was significantly associated with an increased risk of relapse in patients receiving chemotherapy alone (Br. J. Haematol. 2010;148:80-9). Yet, that was not the whole story.
"Interestingly, here, when they looked at MRD in patients prior to going forward on allogeneic stem cell transplant, they did not see any impact of MRD," she noted. "They also didn’t see an impact of MRD in helping to predict which patients would develop CNS relapse."
Targeted Therapies
Several therapies that target tumors’ molecular vulnerabilities are being incorporated into the treatment of adult ALL to clinical benefit. "I think the most dramatic improvement has been seen with the use of tyrosine kinase inhibitors (TKIs) for the Philadelphia chromosome–positive subset," Dr. Kebriaei commented.
In trials, use of TKIs in these patients has led to higher rates of complete remission, transplantation eligibility, and survival without transplantation. "Now all of these trials allowed transplant as well, so it’s hard to ascertain how much of this impact is coming from more transplant eligibility and how much of it is coming from the impact of the TKIs," she cautioned.
The SWOG S0805 Intergroup trial, open to patients up 50 years old with newly diagnosed Philadelphia chromosome–positive ALL, is looking more closely at the issue, as well as the issue of using TKIs as maintenance therapy. Patients receive dasatinib (Sprycel)-containing induction therapy and, if they undergo transplantation, dasatinib thereafter as well.
In clinical practice, "there is great variation in practice patterns, ranging from providing no TKI in maintenance all the way up to providing 2 years of TKI," Dr. Kebriaei observed. "And unfortunately, there isn’t good data yet published to determine what the best approach will be."
A second targeted therapy being used is rituximab (Rituxan), for ALL expressing CD20, another poor prognostic marker. Adding rituximab to the hyper-CVAD regimen significantly improves survival for patients younger than 60 years (J. Clin. Oncol. 2010;28:3880-9). But in older patients, there was no survival benefit, in part because of increased induction-related mortality.
Novel Agents and Cellular Therapies
The Food and Drug Administration has approved three novel agents for ALL treatment: pegylated asparaginase (Oncaspar), clofarabine (Clolar), and nelarabine (Arranon), and has received a new drug application for liposomal vincristine (Marqibo).
Nelarabine, for example, is a prodrug of ara-G that achieves good response and survival rates in patients with relapsed T-cell ALL, with a dose-limiting toxicity of neurotoxicity. It is now being evaluated when added to hyper-CVAD up front for patients with T-cell ALL, according to Dr. Kebriaei.
The investigational agent inotuzumab ozogamicin, an anti-CD22 antibody conjugated to calicheamicin, achieves an overall response rate of 61% when used as monotherapy in a trial among patients with refractory ALL (Jabbour et al. ASCO 2011 meeting. Abstract 6507).
"Interestingly, almost half of these patients were then able to go on to transplant in complete remission," she noted. Adverse effects included hepatotoxicity and veno-occlusive disease.
Another investigational antibody, blinatumomab, redirects T cells toward lysis of CD19-expressing cells and has been found to achieve complete remission in 13 of 16 patients with precursor B-ALL having persistent MRD (Topp et al. ASH 2009 meeting. Abstract 840).
A final novel strategy being tested is cellular therapy using chimeric antigen receptors (CARs), which are produced by fusing an extracellular single-chain antibody to an intracellular signaling domain. When expressed in T cells, these receptors redirect the cells’ antigen recognition toward a desired target, such as CD19.
"What’s very effective and interesting about this CAR strategy is that it doesn’t rely on preexisting antitumor immunity to generate an antitumor effector response," Dr. Kebriaei noted. "This is particularly important in the setting of ALL, where you have immune dysfunction."
Trials are assessing the use of CARs in the setting of stem cell transplantation, whereby donor T cells are transduced with anti-CD19 CARs and given as a targeted donor lymphocyte infusion.
"Perhaps by incorporating these targeted therapies and cellular therapies with the traditional cytotoxic therapies, we may be able to improve treatment outcomes without adding toxicity," concluded Dr. Kebriaei, who reported having no conflicts of interest related to her presentation.
The Oncology Congress is presented by Reed Medical Education. Reed Medical Education and this news organization are owned by Reed Elsevier Inc.
EXPERT ANALYSIS FROM THE ANNUAL ONCOLOGY CONGRESS
Transplant Protocol Benefits Elderly With Hematologic Cancers
An analysis of long-term outcomes for elderly patients with advanced hematologic malignancies suggests they do as well as younger patients when treated with allogeneic hematopoietic cell transplantation following nonmyeloablative conditioning.
In patients aged 60-75 years, the protocol yielded a 5-year overall survival rate of 35% and a progression-free survival rate of 32%, according to a report in the Nov. 2 issue of JAMA. The overall 5-year survival rate was as high as 69% among the patients who had the lowest comorbidity scores and lowest disease risk.
Half of these older patients never required hospitalization either during or after treatment, and two-thirds of the survivors returned to normal or near-normal physical functioning, said Dr. Mohamed L. Sorror of the transplantation biology program at the Fred Hutchinson Cancer Research Center, Seattle, and his associates.
"These results are encouraging given the poor outcomes with nontransplantation treatments, especially for patients with high-risk acute myeloid leukemia, fludarabine-refractory chronic lymphocytic leukemia, or progressive lymphoma," the investigators noted. They assessed outcomes in 372 patients aged 60-75 years who were enrolled in prospective clinical trials of the therapy at 18 medical centers in 1998-2008. The study subjects were being treated for hematologic malignancies including leukemia, myelodysplastic syndromes, myeloproliferative diseases, multiple myeloma, and lymphoma.
Since older patients are not eligible for the intense cytotoxic conditioning regimens that precede high-dose allogeneic hematopoietic cell transplantation, these patients instead underwent nonmyeloablative conditioning that relies on graft-versus-tumor effects to cure the cancer. This included fludarabine and a low dose of total-body irradiation before transplantation and a course of immunosuppression with mycophenolate mofetil and a calcineurin inhibitor (cyclosporine or tacrolimus) afterward.
"These findings should help allay reluctance in entering older patients with hematologic cancers in non- myeloablative [transplant] protocols."
After a median follow-up of 55 months (range, 12-133 months), 133 patients were still alive. Overall 5-year survival was 35%, and 5-year progression-free survival was 32%.
When the data were analyzed by patient age, 5-year overall survival was 38% for those aged 60-64 years, 33% for those aged 65-69, and 25% for those aged 70 and older. "Regardless of age, 5-year survivals ranged from 23% in patients with high comorbidity scores and high disease risk to 69% in patients with low comorbidity scores and low disease risk," Dr. Sorror and his colleagues said (JAMA 2011;306:1874-83).
Approximately two-thirds of the survivors at 5 years had complete resolution of their graft-versus-host disease (GVHD) symptoms and were able to discontinue immunosuppressive medications after a median of 2.5 years. Both the incidence and the resolution of GVHD in these older study subjects were comparable to those reported in the literature for younger patients treated with high-dose hematopoietic cell transplantation.
"These findings, together with the normal to near-normal performance status of surviving patients, should help allay reluctance in entering older patients with hematologic cancers in nonmyeloablative [transplant] protocols," the researchers noted.
Disease progression and relapse accounted for most (135) of the 239 deaths. Relapse rates were 33% at 1 year and 41% at 5 years. Most nonrelapse deaths were attributed to multiple organ failure, GVHD, and infections.
Dr. Sorror and his associates noted that hematologic malignancies are predominantly diseases of the elderly, and the incidence is expected to increase up to 77% during the next 20 years, due in part to the aging of the general population. Yet the latest figures show that only 12% of patients treated with hematopoietic cell transplantation in recent years were older than 60 years.
"This clearly highlights the reluctance of physicians to offer allogeneic hematopoietic cell transplantation to elderly patients," they said.
The investigators are now starting a multicenter longitudinal study to follow such patients from diagnosis onward, in the hope of elucidating "the reasons behind the low rate of referral of older patients to transplantation, [as well as] how nonmyeloablative [transplantation] outcomes compare with those after conventional therapies."
This study was supported by the National Institutes of Health and the Leukemia & Lymphoma Society. Dr. Sorror’s associates reported numerous ties to industry sources.
The promising findings reported by Dr. Sorror and colleagues may have substantial implications for clinical decision making and for health care policies, particularly in view of the aging of the U.S. population, said Dr. Shin Mineishi.
Overall survival, progression-free survival, and other outcomes now appear almost comparable in older patients to those in younger patients. Yet physicians are still reluctant to refer older patients for the procedure. "Without a significant effort to promote the use of allogeneic HSCT [hematopoietic stem cell transplantation] in older patients, only a small fraction will receive the benefit of this new treatment option," he said.
Randomized studies comparing nonmyeloablative vs. reduced intensity allogeneic HSCT are needed, he said. In addition, older patients have different problems from younger patients; among these is that while older patients will require more resources to recover, Medicare provides insufficient coverage for many patients.
"Although age alone should no longer be considered a limiting factor for allogeneic HSCT, more questions have been raised, and more problems need to be resolved for achieving optimal outcomes for older patients receiving allogeneic HSCT."
Dr. Mineishi is in the blood and marrow transplant program at the University of Michigan, Ann Arbor. He reported ties to Genzyme. These remarks were adapted from his editorial accompanying Dr. Sorror’s report (JAMA 2011;306:1918-9).
The promising findings reported by Dr. Sorror and colleagues may have substantial implications for clinical decision making and for health care policies, particularly in view of the aging of the U.S. population, said Dr. Shin Mineishi.
Overall survival, progression-free survival, and other outcomes now appear almost comparable in older patients to those in younger patients. Yet physicians are still reluctant to refer older patients for the procedure. "Without a significant effort to promote the use of allogeneic HSCT [hematopoietic stem cell transplantation] in older patients, only a small fraction will receive the benefit of this new treatment option," he said.
Randomized studies comparing nonmyeloablative vs. reduced intensity allogeneic HSCT are needed, he said. In addition, older patients have different problems from younger patients; among these is that while older patients will require more resources to recover, Medicare provides insufficient coverage for many patients.
"Although age alone should no longer be considered a limiting factor for allogeneic HSCT, more questions have been raised, and more problems need to be resolved for achieving optimal outcomes for older patients receiving allogeneic HSCT."
Dr. Mineishi is in the blood and marrow transplant program at the University of Michigan, Ann Arbor. He reported ties to Genzyme. These remarks were adapted from his editorial accompanying Dr. Sorror’s report (JAMA 2011;306:1918-9).
The promising findings reported by Dr. Sorror and colleagues may have substantial implications for clinical decision making and for health care policies, particularly in view of the aging of the U.S. population, said Dr. Shin Mineishi.
Overall survival, progression-free survival, and other outcomes now appear almost comparable in older patients to those in younger patients. Yet physicians are still reluctant to refer older patients for the procedure. "Without a significant effort to promote the use of allogeneic HSCT [hematopoietic stem cell transplantation] in older patients, only a small fraction will receive the benefit of this new treatment option," he said.
Randomized studies comparing nonmyeloablative vs. reduced intensity allogeneic HSCT are needed, he said. In addition, older patients have different problems from younger patients; among these is that while older patients will require more resources to recover, Medicare provides insufficient coverage for many patients.
"Although age alone should no longer be considered a limiting factor for allogeneic HSCT, more questions have been raised, and more problems need to be resolved for achieving optimal outcomes for older patients receiving allogeneic HSCT."
Dr. Mineishi is in the blood and marrow transplant program at the University of Michigan, Ann Arbor. He reported ties to Genzyme. These remarks were adapted from his editorial accompanying Dr. Sorror’s report (JAMA 2011;306:1918-9).
An analysis of long-term outcomes for elderly patients with advanced hematologic malignancies suggests they do as well as younger patients when treated with allogeneic hematopoietic cell transplantation following nonmyeloablative conditioning.
In patients aged 60-75 years, the protocol yielded a 5-year overall survival rate of 35% and a progression-free survival rate of 32%, according to a report in the Nov. 2 issue of JAMA. The overall 5-year survival rate was as high as 69% among the patients who had the lowest comorbidity scores and lowest disease risk.
Half of these older patients never required hospitalization either during or after treatment, and two-thirds of the survivors returned to normal or near-normal physical functioning, said Dr. Mohamed L. Sorror of the transplantation biology program at the Fred Hutchinson Cancer Research Center, Seattle, and his associates.
"These results are encouraging given the poor outcomes with nontransplantation treatments, especially for patients with high-risk acute myeloid leukemia, fludarabine-refractory chronic lymphocytic leukemia, or progressive lymphoma," the investigators noted. They assessed outcomes in 372 patients aged 60-75 years who were enrolled in prospective clinical trials of the therapy at 18 medical centers in 1998-2008. The study subjects were being treated for hematologic malignancies including leukemia, myelodysplastic syndromes, myeloproliferative diseases, multiple myeloma, and lymphoma.
Since older patients are not eligible for the intense cytotoxic conditioning regimens that precede high-dose allogeneic hematopoietic cell transplantation, these patients instead underwent nonmyeloablative conditioning that relies on graft-versus-tumor effects to cure the cancer. This included fludarabine and a low dose of total-body irradiation before transplantation and a course of immunosuppression with mycophenolate mofetil and a calcineurin inhibitor (cyclosporine or tacrolimus) afterward.
"These findings should help allay reluctance in entering older patients with hematologic cancers in non- myeloablative [transplant] protocols."
After a median follow-up of 55 months (range, 12-133 months), 133 patients were still alive. Overall 5-year survival was 35%, and 5-year progression-free survival was 32%.
When the data were analyzed by patient age, 5-year overall survival was 38% for those aged 60-64 years, 33% for those aged 65-69, and 25% for those aged 70 and older. "Regardless of age, 5-year survivals ranged from 23% in patients with high comorbidity scores and high disease risk to 69% in patients with low comorbidity scores and low disease risk," Dr. Sorror and his colleagues said (JAMA 2011;306:1874-83).
Approximately two-thirds of the survivors at 5 years had complete resolution of their graft-versus-host disease (GVHD) symptoms and were able to discontinue immunosuppressive medications after a median of 2.5 years. Both the incidence and the resolution of GVHD in these older study subjects were comparable to those reported in the literature for younger patients treated with high-dose hematopoietic cell transplantation.
"These findings, together with the normal to near-normal performance status of surviving patients, should help allay reluctance in entering older patients with hematologic cancers in nonmyeloablative [transplant] protocols," the researchers noted.
Disease progression and relapse accounted for most (135) of the 239 deaths. Relapse rates were 33% at 1 year and 41% at 5 years. Most nonrelapse deaths were attributed to multiple organ failure, GVHD, and infections.
Dr. Sorror and his associates noted that hematologic malignancies are predominantly diseases of the elderly, and the incidence is expected to increase up to 77% during the next 20 years, due in part to the aging of the general population. Yet the latest figures show that only 12% of patients treated with hematopoietic cell transplantation in recent years were older than 60 years.
"This clearly highlights the reluctance of physicians to offer allogeneic hematopoietic cell transplantation to elderly patients," they said.
The investigators are now starting a multicenter longitudinal study to follow such patients from diagnosis onward, in the hope of elucidating "the reasons behind the low rate of referral of older patients to transplantation, [as well as] how nonmyeloablative [transplantation] outcomes compare with those after conventional therapies."
This study was supported by the National Institutes of Health and the Leukemia & Lymphoma Society. Dr. Sorror’s associates reported numerous ties to industry sources.
An analysis of long-term outcomes for elderly patients with advanced hematologic malignancies suggests they do as well as younger patients when treated with allogeneic hematopoietic cell transplantation following nonmyeloablative conditioning.
In patients aged 60-75 years, the protocol yielded a 5-year overall survival rate of 35% and a progression-free survival rate of 32%, according to a report in the Nov. 2 issue of JAMA. The overall 5-year survival rate was as high as 69% among the patients who had the lowest comorbidity scores and lowest disease risk.
Half of these older patients never required hospitalization either during or after treatment, and two-thirds of the survivors returned to normal or near-normal physical functioning, said Dr. Mohamed L. Sorror of the transplantation biology program at the Fred Hutchinson Cancer Research Center, Seattle, and his associates.
"These results are encouraging given the poor outcomes with nontransplantation treatments, especially for patients with high-risk acute myeloid leukemia, fludarabine-refractory chronic lymphocytic leukemia, or progressive lymphoma," the investigators noted. They assessed outcomes in 372 patients aged 60-75 years who were enrolled in prospective clinical trials of the therapy at 18 medical centers in 1998-2008. The study subjects were being treated for hematologic malignancies including leukemia, myelodysplastic syndromes, myeloproliferative diseases, multiple myeloma, and lymphoma.
Since older patients are not eligible for the intense cytotoxic conditioning regimens that precede high-dose allogeneic hematopoietic cell transplantation, these patients instead underwent nonmyeloablative conditioning that relies on graft-versus-tumor effects to cure the cancer. This included fludarabine and a low dose of total-body irradiation before transplantation and a course of immunosuppression with mycophenolate mofetil and a calcineurin inhibitor (cyclosporine or tacrolimus) afterward.
"These findings should help allay reluctance in entering older patients with hematologic cancers in non- myeloablative [transplant] protocols."
After a median follow-up of 55 months (range, 12-133 months), 133 patients were still alive. Overall 5-year survival was 35%, and 5-year progression-free survival was 32%.
When the data were analyzed by patient age, 5-year overall survival was 38% for those aged 60-64 years, 33% for those aged 65-69, and 25% for those aged 70 and older. "Regardless of age, 5-year survivals ranged from 23% in patients with high comorbidity scores and high disease risk to 69% in patients with low comorbidity scores and low disease risk," Dr. Sorror and his colleagues said (JAMA 2011;306:1874-83).
Approximately two-thirds of the survivors at 5 years had complete resolution of their graft-versus-host disease (GVHD) symptoms and were able to discontinue immunosuppressive medications after a median of 2.5 years. Both the incidence and the resolution of GVHD in these older study subjects were comparable to those reported in the literature for younger patients treated with high-dose hematopoietic cell transplantation.
"These findings, together with the normal to near-normal performance status of surviving patients, should help allay reluctance in entering older patients with hematologic cancers in nonmyeloablative [transplant] protocols," the researchers noted.
Disease progression and relapse accounted for most (135) of the 239 deaths. Relapse rates were 33% at 1 year and 41% at 5 years. Most nonrelapse deaths were attributed to multiple organ failure, GVHD, and infections.
Dr. Sorror and his associates noted that hematologic malignancies are predominantly diseases of the elderly, and the incidence is expected to increase up to 77% during the next 20 years, due in part to the aging of the general population. Yet the latest figures show that only 12% of patients treated with hematopoietic cell transplantation in recent years were older than 60 years.
"This clearly highlights the reluctance of physicians to offer allogeneic hematopoietic cell transplantation to elderly patients," they said.
The investigators are now starting a multicenter longitudinal study to follow such patients from diagnosis onward, in the hope of elucidating "the reasons behind the low rate of referral of older patients to transplantation, [as well as] how nonmyeloablative [transplantation] outcomes compare with those after conventional therapies."
This study was supported by the National Institutes of Health and the Leukemia & Lymphoma Society. Dr. Sorror’s associates reported numerous ties to industry sources.
FROM JAMA
Major Finding: The 5-year survival was 35% overall and as high as 69% in the lowest-risk patients among those aged 60-75 years whose advanced hematologic malignancies were treated using hematopoietic cell transplantation following nonmyeloablative conditioning.
Data Source: An analysis of outcomes among 372 older patients enrolled in prospective clinical trials of transplant therapy at 18 medical centers in 1998-2008.
Disclosures: This study was supported by the National Institutes of Health and the Leukemia & Lymphoma Society. Dr. Sorror's associates reported numerous ties to industry sources.
Diagnostic dilemmas with OCD and other anxiety disorders
Progressive Multifocal Leukoencephalopathy in the Biologic Era: Implications for Practice
Supplement Editor:
Leonard Calabrese, DO
Contents
Introduction: Progressive multifocal leukoencephalopathy in the biologic era
Leonard Calabrese, DO
History and current concepts in the pathogenesis of PML
Eugene O. Major, PhD
The clinical features of PML
Joseph R. Berger, MD
Pharmacovigilance and PML in the oncology setting
Charles L. Bennett, MD, PhD, MPP
Multiple sclerosis, natalizumab, and PML: Helping patients decide
Richard R. Rudick, MD
HIV-associated PML: Changing epidemiology and clinical approach
David M. Simpson, MD, FRCP, MRCPI
PML and rheumatology: The contribution of disease and drugs
Eamonn S. Molloy, MD, MS, MRCPI
Advances in the management of PML: Focus on natalizumab
Robert Fox, MD
A rational approach to PML for the clinician
Leonard Calabrese, DO
Supplement Editor:
Leonard Calabrese, DO
Contents
Introduction: Progressive multifocal leukoencephalopathy in the biologic era
Leonard Calabrese, DO
History and current concepts in the pathogenesis of PML
Eugene O. Major, PhD
The clinical features of PML
Joseph R. Berger, MD
Pharmacovigilance and PML in the oncology setting
Charles L. Bennett, MD, PhD, MPP
Multiple sclerosis, natalizumab, and PML: Helping patients decide
Richard R. Rudick, MD
HIV-associated PML: Changing epidemiology and clinical approach
David M. Simpson, MD, FRCP, MRCPI
PML and rheumatology: The contribution of disease and drugs
Eamonn S. Molloy, MD, MS, MRCPI
Advances in the management of PML: Focus on natalizumab
Robert Fox, MD
A rational approach to PML for the clinician
Leonard Calabrese, DO
Supplement Editor:
Leonard Calabrese, DO
Contents
Introduction: Progressive multifocal leukoencephalopathy in the biologic era
Leonard Calabrese, DO
History and current concepts in the pathogenesis of PML
Eugene O. Major, PhD
The clinical features of PML
Joseph R. Berger, MD
Pharmacovigilance and PML in the oncology setting
Charles L. Bennett, MD, PhD, MPP
Multiple sclerosis, natalizumab, and PML: Helping patients decide
Richard R. Rudick, MD
HIV-associated PML: Changing epidemiology and clinical approach
David M. Simpson, MD, FRCP, MRCPI
PML and rheumatology: The contribution of disease and drugs
Eamonn S. Molloy, MD, MS, MRCPI
Advances in the management of PML: Focus on natalizumab
Robert Fox, MD
A rational approach to PML for the clinician
Leonard Calabrese, DO
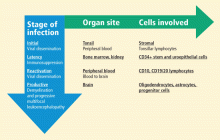
History and current concepts in the pathogenesis of PML
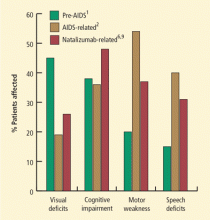
The neuropathology of progressive multifocal leukoencephalopathy (PML) was first reported in 1958 following examination of brain tissue from two cases of chronic lymphocytic leukemia and one case of Hodgkin lymphoma.1 The classic triad of symptoms of PML—cognitive impairment, visual deficits, and motor dysfunction—had been observed previously but had not been formally described.2
Until PML was discovered in patients with autoimmune diseases treated with biologic therapies that do not directly suppress immunity, PML had been considered a very rare, virus-induced demyelinating disease of the white matter that occurred in immune-compromised patients. The incidence of PML rose sharply in the mid-1980s with the pandemic of human immunodeficiency virus (HIV)-1 infection and continues as an acquired immunodeficiency syndrome–defining illness at a rate of approximately 1% to 3% of HIV-1 seropositive individuals; more recently, it has been seen in approximately 1 in 850 natalizumab-treated individuals who have multiple sclerosis (MS). The incidence of PML in natalizumab-treated MS patients increases with dosing; among those who receive 24 or more doses, the incidence is 1 in 400.
The cause of PML was unknown until 1971, when viral particles were observed by electron microscopy in PML brain lesions and subsequently isolated at the University of Wisconsin, Madison, in cultures of human fetal brain tissue.3 The designation of JC virus (JCV) was derived from the initials of the patient whose brain tissue was used for culture and isolation. Variants in the noncoding region of the genome were then serially identified as Mad 1, Mad 2, and so on, representing the geographic location, Madison, Wisconsin, where the virus was identified.
The JCV, a polyomavirus, is a nonenveloped DNA virus with icosahedral structure containing double-stranded DNA genomes. The circular genome of JCV contains early and late transcription units, the latter of which encodes three virion structural proteins—VPl, VP2, and VP3. Humans generate antibodies directed against the amino terminal end of VP1 and perhaps VP2 and VP3.
JC VIRUS PATHOGENESIS
JCV pathogenesis is studied in cell cultures derived from human fetal brain tissue. In vitro, JCV robustly infects astrocytes, making it important to identify the culture’s cellular phenotypes. A cell line was developed that allows multiplication of JCV and, more recently, human multipotential progenitor cells were isolated and are being grown from the human developing brain at various gestational stages. The lineage pathways of these cells can be differentiated into astrocytes, oligodendrocytes, and neurons. Initiating infection in progenitor cells with JC virions made it possible to determine which cells were susceptible to infection. JCV susceptibility is evident in progenitor-derived astrocytes and glial cells, which reflects the pathologic process in PML brain tissue. Neuronal cells, by contrast, are not susceptible to infection.4
JC VIRUS CHARACTERISTICS: GLOBAL DISTRIBUTION, TRIAD OF SYMPTOMS
Subcortical multifocal white matter lesions are the classic feature of PML on neuroimaging. Seroepidemiology of JCV has revealed ubiquitous distribution, with 50% to 60% of adults aged 20 to 50 years demonstrating antibody to JCV.5 The percentage of the population with antibody increases with age, but may vary among geographic regions. Prevalence is lower among remote populations.
Although the initial site of JCV infection is not well characterized, we know that the primary infection is not in the brain. The JCV has a selective tropism for replication in glial cells in the human brain, but the absence of an animal model for PML has hindered our understanding of the JCV migration to the brain and the initiation and development of central nervous system infection.
Although humans carry JCV-specific antibodies, the clinical significance of these antibodies is unknown. Antibody levels rise during active infection, at times to very high titers, but offer no protection. T-cell–mediated immune responses directed to structural and nonstructural proteins are important in controlling infection.
A high index of suspicion for PML is warranted in individuals who demonstrate the classic triad of symptoms (cognitive impairment, visual deficits, and motor dysfunction) and in whom magnetic resonance imaging shows evidence of demyelinated plaque lesions; however, evidence of the presence of JCV DNA in pathologic tissue is necessary to confirm a diagnosis of PML.
The development of an in situ DNA hybridization assay using a biotinylated probe has facilitated identification of JCV DNA in the infected nuclei of the pathologic tissue. The presence of JCV DNA in cerebrospinal fluid (CSF) samples can be detected using a quantitative polymerase chain reaction assay, targeting the viral genome in the amino terminal end of the viral T protein.6 This T protein coding region was targeted because it does not crossreact, even with other human polyomaviruses, and it is intolerant of mutations. This assay is certified by the Clinical Laboratory Improvement Amendments, licensed by the National Institutes of Health; it is the most sensitive (to levels of 10 copies/mL sample) assay available.
JC VIRUS SUSCEPTIBILITY FACTORS
Despite the high prevalence of JCV infection, PML is rare, suggesting important barriers to its development. Although the receptor for JCV has been identified as alpha 2,6-linked sialic acid, the host range for productive infection is controlled by factors within the cell nucleus that bind to the viral promoter; this process initiates transcription of mRNA for the coordinated synthesis of viral proteins. Only certain cells have the necessary DNA binding proteins in high enough concentrations to allow lytic infection to take place, spreading by cell-to-cell contact. These cells include oligodendrocytes, the primary target for JCV, whose destruction leads to PML; astrocytes; and the CD34+ and CD19+ cells of the immune system. JCV can also be found in urine, at times in very high concentrations. It is present in the uroepithelial cells and multiplies without apparent pathologic consequences. Virus isolated from the urine has not been grown in cell culture systems in the laboratory setting.
Bone marrow CD34+ hematopoietic progenitor cells represent a potential pathway of JCV pathogenesis: in six people with PML, latent JCV DNA was demonstrated in pathologic tissue from lymph, spleen, or bone marrow biopsies taken months to years before the patient developed neurologic disease.7
Upon immunosuppression, reactivation of the virus occurs, with evidence of the virus found in CD10 and CD19/20 lymphocytes in the peripheral blood of some individuals. Blood-to-brain viral dissemination results in infection of oligodendrocytes, astrocytes, and progenitor cells.
Susceptibility is related to nucleotide sequences
Susceptibility to PML is associated with promoter/enhancer nucleotide sequences. The tandem repeat nucleotide structure has been found in the peripheral blood leukocytes and the CSF of patients with PML. Although the arrangement of nucleotide sequences in the viral regulatory region is highly variable among patients with PML, there are no alterations in the sequence within the origin of DNA replication. These highly conserved sequences contain regions for DNA-binding proteins that drive transcription, initiating the life cycle of the virus.
The nuclear transcription factor NF-1 is a cell-specific regulator of JCV promoter/enhancer activity. In humans, the NF-1 family of DNA-binding proteins is encoded by four discrete genes, one of which is NF-1 class X (NF-1X), a critical transcription factor that affects JCV cells. The human brain makes NF-1X in concentrations greater than the concentrations of other NF-1 transcription family members of DNA-binding proteins. NF-1X is located adjacent to and interacts with another family of transcription factors, activator protein-1, which has also been associated with JC viral activity.
Spi-B expression a factor in natalizumab-treated patients
Another transcription factor, Spi-B, binds to sequences present in the JCV promoter/enhancer. Spi-B is a regulator of JCV gene expression in susceptible cells and appears to play an important role in JCV activity. The expression of Spi-B is upregulated in patients with MS who are treated with the monoclonal antibody natalizumab, a population of patients in whom PML has been recently described.11–15
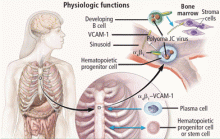
Natalizumab binds to the alpha-4 integrin molecule, preventing hematopoietic stem cells and developing B cells from attaching to a vascular-cell adhesion molecule and forcing them to migrate from the bone marrow (Figure 2).16 An ideal environment is created for JCV when the natalizumab-induced increase in CD34+ cells in the circulation is combined with upregulation of gene cells involved in B-cell maturation. JCV can reside in the bone marrow in a latent state and can use B cells and their DNA-binding proteins to initiate viral multiplication, eventually gaining entry into the brain to cause PML.
In addition to natalizumab, PML has been described in patients treated with efalizumab, another biologic agent that binds alpha-4 integrin molecules on the surface of T and B cells, preventing their entry into the brain, gut, and skin, and forcing migration of bone marrow CD34+ into peripheral circulation for long periods.9,17,18 Rituximab, another monoclonal antibody, binds the CD20 surface molecule on B cells, causing their depletion from the peripheral circulation through complement-mediated cytolysis.7
Risk factors for development of PML
Measurable risk factors for PML include:
- Rising antibody titers
- Evidence of viremia, especially persistent viremia associated with repeat sequences in the regulatory region of the viral genome
- Ineffective T-cell (CD4 and CD8) responses
- Molecular host factors (ie, Spi-B expression in B cells) that support JCV infection in potentially susceptible cells.
The presence of more than one of these risk factors is necessary for development of PML.
VIRAL LATENCY IN B LYMPHOCYTES IN BONE MARROW
A strong link between JCV infection in cells of the immune system and those of the nervous system points to the importance of the tissue origin of JCV latency. Bone marrow harbors CD34+ cells that migrate into the peripheral circulation and undergo differentiation to pre-B and mature B cells, augmenting JCV growth. The emergence of PML in patients treated with natalizumab, rituximab, efalizumab, and other immune-altering drugs underscores this observation.
As noted, the incidence of PML in natalizumab-treated patients with MS and Crohn disease rises as the number of doses increases. Analysis of blood samples collected from patients treated with natalizumab at baseline and again during treatment at months 1 to 12 and beyond 24 months demonstrates that the frequency of CD34+ cells in the peripheral circulation increases with the duration of therapy, adding credence to the theory that CD34+ cells act as a reservoir for latent virus. A higher frequency of CD34+ cells is associated with viremia.
The role of Spi-B in JC virus latency
Understanding the role of Spi-B during JCV latency and reactivation is increasingly important as the number of patients treated with immunomodulatory agents that can develop PML continues to rise. Spi-B is highly represented in the B cell and CD34+ cell fractions. Spi-B expression in B cells correlates with reactivation of JCV in immune cells in natalizumab-treated patients. In a sample of four patients with MS treated with natalizumab who developed PML, T-cell responses have been ineffective (absent or aberrant). Two patients had no detectable T-cell response to JCV; the other two demonstrated response, but their CD4 T-cell responses were dominated by interleukin-10–producing cells.
Longitudinal examination of CSF samples from 13 MS patients who were treated with natalizumab and subsequently developed PML revealed persistence of viral load even though all patients experienced immune reconstitution inflammatory syndrome and most had high levels of anti-JCV antibodies.19
SUMMARY
Despite the prevalence of JCV in the population, the development of PML is rare. Levels of JCV antibody rise during the course of active JCV infection, but they do not protect against infection. T-cell responses directed to structural and nonstructural proteins play a role in controlling infection. Latency of JCV is associated with specific cells of the immune system, and its reactivation can follow alteration of normal immune cell function—either immunosuppression or immunomodulation. Risk factors for the development of PML include rising antibody titers and ineffective T-cell (CD4 and CD8) responses.
DISCUSSION
Dr. Berger: Does natalizumab upregulate Spi-B in glial cells?
Dr. Major: We never tested this directly. From human brain cultures, we know that Spi-B is made in glial cells, not in neurons. We are considering the idea that wherever JCV binds, it takes advantage of certain types of DNA-binding proteins in the molecular regulation. If the binding takes place in an immune system cell, for example, Spi-B plays an important role.
Dr. Berger: Koralnik et al demonstrated JCV excretion in urine in MS patients after 12 months of treatment with natalizumab, and at 18 months, viremia in 60% of the patients.20 Yet, repeated studies of patients taking natalizumab have failed to demonstrate viremia or conversion of virus in the archetype. How do these findings correlate with your thoughts on the action of natalizumab in the pathogenesis of PML?
Dr. Major: We certainly know that natalizumab forces migration of hematopoietic stem cells and pre-B cells out of the marrow, but our findings have differed somewhat from those of Koralnik’s laboratory. For example, in the several hundred nucleotide sequences we have looked at in PML brain tissue, we have found the Mad 1 genotype once. We consider Mad 1 to be a potential laboratory contamination, so if we find Mad 1 we resequence the sample. We never clone because cloning can introduce alterations; we sequence directly from the clinical tissue. We can identify Mad 1 because our assay is very sensitive. In normal individuals, CD34+ cells compose approximately 0.01% of the peripheral circulation; in individuals treated with natalizumab, however, their composition is 0.1% to 0.3%. So if there is a potential for latent infection, we have an opportunity to find it in those cells. Its presence does not necessarily mean that the individual is going to develop PML, however; there are other controlling factors.
Dr. Rudick: Have you found the virus in B cells in healthy people?
Dr. Major: Yes we have, in about one-third. It is higher than what we would expect to see in the normal population.
Dr. Rudick: How can that finding be turned into something that’s clinically useful?
Dr. Major: If you’re trying to identify persons who are more susceptible to PML given underlying risk factors—treatment with natalizumab or rituximab, presence of HIV infection, or some other immune-altering condition—looking at one parameter isn’t going to help. Based on the available data, rising antibody titers signals an active infection, and viremia of any kind means probable latent infection. Because this is a small event in very few cells, you will not have the numbers of cells needed to identify susceptibility in a normal population. For now, we monitor patients at risk and, if we find viremia, we assess the cell population to determine whether a molecular factor like Spi-B is upregulated. We hope to develop an assay in which we can obtain one test tube of blood and report T-cell responses, molecular factors, antibody titer, and presence or absence of viremia. Such an assay would provide the data necessary to make a clinical decision.
- Astrom KE, Mancall EL, Richardson EP. Progressive multifocal leukoencephalopathy; a hitherto unrecognized complication of chronic lymphatic leukaemia and Hodgkin’s disease. Brain 1958; 81:93–111.
- Hallervorden J. Eigennartige und nicht rubriziebare Prozesse. In:Bumke O, ed. Handbuch der Geiteskranheiten. Vol. 2. Die Anatomie der Psychosen. Berlin: Springer; 1930:1063–1107.
- Padgett BL, Walker DL, ZuRhein GM, Eckroade RJ, Dessel BH. Cultivation of a papova-like virus from human brain with progressive multifocal leucoencephalopathy. Lancet 1971; 1:1257–1260.
- Major EO, Amemiya K, Tornatore CS, Houff SA, Berger JR. Pathogenesis and molecular biology of progressive multifocal leukoencephalopathy, the JC virus-induced demyelinating disease of the human brain. Clin Microbiol Rev 1992; 5:49–73.
- Walker D, Padgett B. The epidemiology of human polyomaviruses. In:Sever J, Madden D, eds. Polyomaviruses and Human Neurological Disease. New York, NY: Alan R. Liss, Inc.; 1983:99–106.
- Ryschkewitsch C, Jensen P, Hou J, Fahle G, Fischer S, Major EO. Comparison of PCR-southern hybridization and quantitative realtime PCR for the detection of JC and BK viral nucleotide sequences in urine and cerebrospinal fluid. J Virol Methods 2004; 121:217–221.
- Monaco MC, Jensen PN, Hou J, Durham LC, Major EO. Detection of JC virus DNA in human tonsil tissue: evidence for site of initial viral infection. J Virol 1998; 72:9918–9923.
- Major EO. Progressive multifocal leukoencephalopathy in patients on immunomodulatory therapies. Annu Rev Med 2010; 61:35–47.
- Imperiale M, Major E. Polyomavirus. In:Knipe D, Howley P, eds. Field Virology. 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2007:2263–2298.
- Langer-Gould A, Atlas SW, Green AJ, Bollen AW, Pelletier D. Progressive multifocal leukoencephalopathy in a patient treated with natalizumab. N Engl J Med 2005; 353:375–381.
- Van Assche G, Van Ranst M, Sciot R, et al. Progressive multifocal leukoencephalopathy after natalizumab therapy for Crohn’s disease. N Engl J Med 2005; 353:362–368.
- Kleinschmidt-DeMasters BK, Tyler KL. Progressive multifocal leukoencephalopathy complicating treatment with natalizumab and interferon beta-1a for multiple sclerosis. N Engl J Med 2005; 353:369–374.
- Bozic C, Belcher G, Kooijmans-Coutinho M, et al. Natalizumab utilization and safety in patients with relapsing multiple sclerosis: updated results from TOUCH™ and TYGRIS. Paper presented at: 60th Annual Meeting of the American Academy of Neurology; April 15, 2008; Chicago, IL.
- Kappos L, Bates D, Hartung HP, et al. Natalizumab treatment for multiple sclerosis: recommendations for patient selection and monitoring. Lancet Neurol 2007; 6:431–441.
- Major EO. Reemergence of PML in natalizumab-treated patients—new cases, same concerns. N Engl J Med 2009; 361:1041–1043.
- Vugmeyster Y, Kikuchi T, Lowes MA, et al. Efalizumab (anti-CD11a)-induced increase in peripheral blood leukocytes in psoriasis patients is preferentially mediated by altered trafficking of memory CD8+ T cells into lesional skin. Clin Immunol 2004; 113:38–46.
- Guttman-Yassky E, Vugmeyster Y, Lowes MA, et al. Blockade of CD11a by efalizumab in psoriasis patients induces a unique state of T-cell hyporesponsiveness. J Invest Dermatol 2008; 128:1182–1191.
- Carson KR, Evens AM, Richey EA, et al. Progressive multifocal leukoencephalopathy after rituximab therapy in HIV-negative patients: a report of 57 cases from the Research on Adverse Drug Events and Reports project. Blood 2009; 113:4834–4840.
- Ryschkewitsch CF, Jensen PN, Monaco MC, Major EO. JC virus persistence following progressive multifocal leukoencephalopathy in multiple sclerosis patients treated with natalizumab. Ann Neurol 2010; 68:384–391.
- Koralnik IJ, Du Pasquier RA, Kuroda MJ, et al. Association of prolonged survival in HLA-A2+ progressive multifocal leuko encephalopathy patients with a CTL response specific for a commonly recognized JC virus epitope. J Immunol 2002; 168:499–504.
The neuropathology of progressive multifocal leukoencephalopathy (PML) was first reported in 1958 following examination of brain tissue from two cases of chronic lymphocytic leukemia and one case of Hodgkin lymphoma.1 The classic triad of symptoms of PML—cognitive impairment, visual deficits, and motor dysfunction—had been observed previously but had not been formally described.2
Until PML was discovered in patients with autoimmune diseases treated with biologic therapies that do not directly suppress immunity, PML had been considered a very rare, virus-induced demyelinating disease of the white matter that occurred in immune-compromised patients. The incidence of PML rose sharply in the mid-1980s with the pandemic of human immunodeficiency virus (HIV)-1 infection and continues as an acquired immunodeficiency syndrome–defining illness at a rate of approximately 1% to 3% of HIV-1 seropositive individuals; more recently, it has been seen in approximately 1 in 850 natalizumab-treated individuals who have multiple sclerosis (MS). The incidence of PML in natalizumab-treated MS patients increases with dosing; among those who receive 24 or more doses, the incidence is 1 in 400.
The cause of PML was unknown until 1971, when viral particles were observed by electron microscopy in PML brain lesions and subsequently isolated at the University of Wisconsin, Madison, in cultures of human fetal brain tissue.3 The designation of JC virus (JCV) was derived from the initials of the patient whose brain tissue was used for culture and isolation. Variants in the noncoding region of the genome were then serially identified as Mad 1, Mad 2, and so on, representing the geographic location, Madison, Wisconsin, where the virus was identified.
The JCV, a polyomavirus, is a nonenveloped DNA virus with icosahedral structure containing double-stranded DNA genomes. The circular genome of JCV contains early and late transcription units, the latter of which encodes three virion structural proteins—VPl, VP2, and VP3. Humans generate antibodies directed against the amino terminal end of VP1 and perhaps VP2 and VP3.
JC VIRUS PATHOGENESIS
JCV pathogenesis is studied in cell cultures derived from human fetal brain tissue. In vitro, JCV robustly infects astrocytes, making it important to identify the culture’s cellular phenotypes. A cell line was developed that allows multiplication of JCV and, more recently, human multipotential progenitor cells were isolated and are being grown from the human developing brain at various gestational stages. The lineage pathways of these cells can be differentiated into astrocytes, oligodendrocytes, and neurons. Initiating infection in progenitor cells with JC virions made it possible to determine which cells were susceptible to infection. JCV susceptibility is evident in progenitor-derived astrocytes and glial cells, which reflects the pathologic process in PML brain tissue. Neuronal cells, by contrast, are not susceptible to infection.4
JC VIRUS CHARACTERISTICS: GLOBAL DISTRIBUTION, TRIAD OF SYMPTOMS
Subcortical multifocal white matter lesions are the classic feature of PML on neuroimaging. Seroepidemiology of JCV has revealed ubiquitous distribution, with 50% to 60% of adults aged 20 to 50 years demonstrating antibody to JCV.5 The percentage of the population with antibody increases with age, but may vary among geographic regions. Prevalence is lower among remote populations.
Although the initial site of JCV infection is not well characterized, we know that the primary infection is not in the brain. The JCV has a selective tropism for replication in glial cells in the human brain, but the absence of an animal model for PML has hindered our understanding of the JCV migration to the brain and the initiation and development of central nervous system infection.
Although humans carry JCV-specific antibodies, the clinical significance of these antibodies is unknown. Antibody levels rise during active infection, at times to very high titers, but offer no protection. T-cell–mediated immune responses directed to structural and nonstructural proteins are important in controlling infection.
A high index of suspicion for PML is warranted in individuals who demonstrate the classic triad of symptoms (cognitive impairment, visual deficits, and motor dysfunction) and in whom magnetic resonance imaging shows evidence of demyelinated plaque lesions; however, evidence of the presence of JCV DNA in pathologic tissue is necessary to confirm a diagnosis of PML.
The development of an in situ DNA hybridization assay using a biotinylated probe has facilitated identification of JCV DNA in the infected nuclei of the pathologic tissue. The presence of JCV DNA in cerebrospinal fluid (CSF) samples can be detected using a quantitative polymerase chain reaction assay, targeting the viral genome in the amino terminal end of the viral T protein.6 This T protein coding region was targeted because it does not crossreact, even with other human polyomaviruses, and it is intolerant of mutations. This assay is certified by the Clinical Laboratory Improvement Amendments, licensed by the National Institutes of Health; it is the most sensitive (to levels of 10 copies/mL sample) assay available.
JC VIRUS SUSCEPTIBILITY FACTORS
Despite the high prevalence of JCV infection, PML is rare, suggesting important barriers to its development. Although the receptor for JCV has been identified as alpha 2,6-linked sialic acid, the host range for productive infection is controlled by factors within the cell nucleus that bind to the viral promoter; this process initiates transcription of mRNA for the coordinated synthesis of viral proteins. Only certain cells have the necessary DNA binding proteins in high enough concentrations to allow lytic infection to take place, spreading by cell-to-cell contact. These cells include oligodendrocytes, the primary target for JCV, whose destruction leads to PML; astrocytes; and the CD34+ and CD19+ cells of the immune system. JCV can also be found in urine, at times in very high concentrations. It is present in the uroepithelial cells and multiplies without apparent pathologic consequences. Virus isolated from the urine has not been grown in cell culture systems in the laboratory setting.
Bone marrow CD34+ hematopoietic progenitor cells represent a potential pathway of JCV pathogenesis: in six people with PML, latent JCV DNA was demonstrated in pathologic tissue from lymph, spleen, or bone marrow biopsies taken months to years before the patient developed neurologic disease.7
Upon immunosuppression, reactivation of the virus occurs, with evidence of the virus found in CD10 and CD19/20 lymphocytes in the peripheral blood of some individuals. Blood-to-brain viral dissemination results in infection of oligodendrocytes, astrocytes, and progenitor cells.
Susceptibility is related to nucleotide sequences
Susceptibility to PML is associated with promoter/enhancer nucleotide sequences. The tandem repeat nucleotide structure has been found in the peripheral blood leukocytes and the CSF of patients with PML. Although the arrangement of nucleotide sequences in the viral regulatory region is highly variable among patients with PML, there are no alterations in the sequence within the origin of DNA replication. These highly conserved sequences contain regions for DNA-binding proteins that drive transcription, initiating the life cycle of the virus.
The nuclear transcription factor NF-1 is a cell-specific regulator of JCV promoter/enhancer activity. In humans, the NF-1 family of DNA-binding proteins is encoded by four discrete genes, one of which is NF-1 class X (NF-1X), a critical transcription factor that affects JCV cells. The human brain makes NF-1X in concentrations greater than the concentrations of other NF-1 transcription family members of DNA-binding proteins. NF-1X is located adjacent to and interacts with another family of transcription factors, activator protein-1, which has also been associated with JC viral activity.
Spi-B expression a factor in natalizumab-treated patients
Another transcription factor, Spi-B, binds to sequences present in the JCV promoter/enhancer. Spi-B is a regulator of JCV gene expression in susceptible cells and appears to play an important role in JCV activity. The expression of Spi-B is upregulated in patients with MS who are treated with the monoclonal antibody natalizumab, a population of patients in whom PML has been recently described.11–15
Natalizumab binds to the alpha-4 integrin molecule, preventing hematopoietic stem cells and developing B cells from attaching to a vascular-cell adhesion molecule and forcing them to migrate from the bone marrow (Figure 2).16 An ideal environment is created for JCV when the natalizumab-induced increase in CD34+ cells in the circulation is combined with upregulation of gene cells involved in B-cell maturation. JCV can reside in the bone marrow in a latent state and can use B cells and their DNA-binding proteins to initiate viral multiplication, eventually gaining entry into the brain to cause PML.
In addition to natalizumab, PML has been described in patients treated with efalizumab, another biologic agent that binds alpha-4 integrin molecules on the surface of T and B cells, preventing their entry into the brain, gut, and skin, and forcing migration of bone marrow CD34+ into peripheral circulation for long periods.9,17,18 Rituximab, another monoclonal antibody, binds the CD20 surface molecule on B cells, causing their depletion from the peripheral circulation through complement-mediated cytolysis.7
Risk factors for development of PML
Measurable risk factors for PML include:
- Rising antibody titers
- Evidence of viremia, especially persistent viremia associated with repeat sequences in the regulatory region of the viral genome
- Ineffective T-cell (CD4 and CD8) responses
- Molecular host factors (ie, Spi-B expression in B cells) that support JCV infection in potentially susceptible cells.
The presence of more than one of these risk factors is necessary for development of PML.
VIRAL LATENCY IN B LYMPHOCYTES IN BONE MARROW
A strong link between JCV infection in cells of the immune system and those of the nervous system points to the importance of the tissue origin of JCV latency. Bone marrow harbors CD34+ cells that migrate into the peripheral circulation and undergo differentiation to pre-B and mature B cells, augmenting JCV growth. The emergence of PML in patients treated with natalizumab, rituximab, efalizumab, and other immune-altering drugs underscores this observation.
As noted, the incidence of PML in natalizumab-treated patients with MS and Crohn disease rises as the number of doses increases. Analysis of blood samples collected from patients treated with natalizumab at baseline and again during treatment at months 1 to 12 and beyond 24 months demonstrates that the frequency of CD34+ cells in the peripheral circulation increases with the duration of therapy, adding credence to the theory that CD34+ cells act as a reservoir for latent virus. A higher frequency of CD34+ cells is associated with viremia.
The role of Spi-B in JC virus latency
Understanding the role of Spi-B during JCV latency and reactivation is increasingly important as the number of patients treated with immunomodulatory agents that can develop PML continues to rise. Spi-B is highly represented in the B cell and CD34+ cell fractions. Spi-B expression in B cells correlates with reactivation of JCV in immune cells in natalizumab-treated patients. In a sample of four patients with MS treated with natalizumab who developed PML, T-cell responses have been ineffective (absent or aberrant). Two patients had no detectable T-cell response to JCV; the other two demonstrated response, but their CD4 T-cell responses were dominated by interleukin-10–producing cells.
Longitudinal examination of CSF samples from 13 MS patients who were treated with natalizumab and subsequently developed PML revealed persistence of viral load even though all patients experienced immune reconstitution inflammatory syndrome and most had high levels of anti-JCV antibodies.19
SUMMARY
Despite the prevalence of JCV in the population, the development of PML is rare. Levels of JCV antibody rise during the course of active JCV infection, but they do not protect against infection. T-cell responses directed to structural and nonstructural proteins play a role in controlling infection. Latency of JCV is associated with specific cells of the immune system, and its reactivation can follow alteration of normal immune cell function—either immunosuppression or immunomodulation. Risk factors for the development of PML include rising antibody titers and ineffective T-cell (CD4 and CD8) responses.
DISCUSSION
Dr. Berger: Does natalizumab upregulate Spi-B in glial cells?
Dr. Major: We never tested this directly. From human brain cultures, we know that Spi-B is made in glial cells, not in neurons. We are considering the idea that wherever JCV binds, it takes advantage of certain types of DNA-binding proteins in the molecular regulation. If the binding takes place in an immune system cell, for example, Spi-B plays an important role.
Dr. Berger: Koralnik et al demonstrated JCV excretion in urine in MS patients after 12 months of treatment with natalizumab, and at 18 months, viremia in 60% of the patients.20 Yet, repeated studies of patients taking natalizumab have failed to demonstrate viremia or conversion of virus in the archetype. How do these findings correlate with your thoughts on the action of natalizumab in the pathogenesis of PML?
Dr. Major: We certainly know that natalizumab forces migration of hematopoietic stem cells and pre-B cells out of the marrow, but our findings have differed somewhat from those of Koralnik’s laboratory. For example, in the several hundred nucleotide sequences we have looked at in PML brain tissue, we have found the Mad 1 genotype once. We consider Mad 1 to be a potential laboratory contamination, so if we find Mad 1 we resequence the sample. We never clone because cloning can introduce alterations; we sequence directly from the clinical tissue. We can identify Mad 1 because our assay is very sensitive. In normal individuals, CD34+ cells compose approximately 0.01% of the peripheral circulation; in individuals treated with natalizumab, however, their composition is 0.1% to 0.3%. So if there is a potential for latent infection, we have an opportunity to find it in those cells. Its presence does not necessarily mean that the individual is going to develop PML, however; there are other controlling factors.
Dr. Rudick: Have you found the virus in B cells in healthy people?
Dr. Major: Yes we have, in about one-third. It is higher than what we would expect to see in the normal population.
Dr. Rudick: How can that finding be turned into something that’s clinically useful?
Dr. Major: If you’re trying to identify persons who are more susceptible to PML given underlying risk factors—treatment with natalizumab or rituximab, presence of HIV infection, or some other immune-altering condition—looking at one parameter isn’t going to help. Based on the available data, rising antibody titers signals an active infection, and viremia of any kind means probable latent infection. Because this is a small event in very few cells, you will not have the numbers of cells needed to identify susceptibility in a normal population. For now, we monitor patients at risk and, if we find viremia, we assess the cell population to determine whether a molecular factor like Spi-B is upregulated. We hope to develop an assay in which we can obtain one test tube of blood and report T-cell responses, molecular factors, antibody titer, and presence or absence of viremia. Such an assay would provide the data necessary to make a clinical decision.
The neuropathology of progressive multifocal leukoencephalopathy (PML) was first reported in 1958 following examination of brain tissue from two cases of chronic lymphocytic leukemia and one case of Hodgkin lymphoma.1 The classic triad of symptoms of PML—cognitive impairment, visual deficits, and motor dysfunction—had been observed previously but had not been formally described.2
Until PML was discovered in patients with autoimmune diseases treated with biologic therapies that do not directly suppress immunity, PML had been considered a very rare, virus-induced demyelinating disease of the white matter that occurred in immune-compromised patients. The incidence of PML rose sharply in the mid-1980s with the pandemic of human immunodeficiency virus (HIV)-1 infection and continues as an acquired immunodeficiency syndrome–defining illness at a rate of approximately 1% to 3% of HIV-1 seropositive individuals; more recently, it has been seen in approximately 1 in 850 natalizumab-treated individuals who have multiple sclerosis (MS). The incidence of PML in natalizumab-treated MS patients increases with dosing; among those who receive 24 or more doses, the incidence is 1 in 400.
The cause of PML was unknown until 1971, when viral particles were observed by electron microscopy in PML brain lesions and subsequently isolated at the University of Wisconsin, Madison, in cultures of human fetal brain tissue.3 The designation of JC virus (JCV) was derived from the initials of the patient whose brain tissue was used for culture and isolation. Variants in the noncoding region of the genome were then serially identified as Mad 1, Mad 2, and so on, representing the geographic location, Madison, Wisconsin, where the virus was identified.
The JCV, a polyomavirus, is a nonenveloped DNA virus with icosahedral structure containing double-stranded DNA genomes. The circular genome of JCV contains early and late transcription units, the latter of which encodes three virion structural proteins—VPl, VP2, and VP3. Humans generate antibodies directed against the amino terminal end of VP1 and perhaps VP2 and VP3.
JC VIRUS PATHOGENESIS
JCV pathogenesis is studied in cell cultures derived from human fetal brain tissue. In vitro, JCV robustly infects astrocytes, making it important to identify the culture’s cellular phenotypes. A cell line was developed that allows multiplication of JCV and, more recently, human multipotential progenitor cells were isolated and are being grown from the human developing brain at various gestational stages. The lineage pathways of these cells can be differentiated into astrocytes, oligodendrocytes, and neurons. Initiating infection in progenitor cells with JC virions made it possible to determine which cells were susceptible to infection. JCV susceptibility is evident in progenitor-derived astrocytes and glial cells, which reflects the pathologic process in PML brain tissue. Neuronal cells, by contrast, are not susceptible to infection.4
JC VIRUS CHARACTERISTICS: GLOBAL DISTRIBUTION, TRIAD OF SYMPTOMS
Subcortical multifocal white matter lesions are the classic feature of PML on neuroimaging. Seroepidemiology of JCV has revealed ubiquitous distribution, with 50% to 60% of adults aged 20 to 50 years demonstrating antibody to JCV.5 The percentage of the population with antibody increases with age, but may vary among geographic regions. Prevalence is lower among remote populations.
Although the initial site of JCV infection is not well characterized, we know that the primary infection is not in the brain. The JCV has a selective tropism for replication in glial cells in the human brain, but the absence of an animal model for PML has hindered our understanding of the JCV migration to the brain and the initiation and development of central nervous system infection.
Although humans carry JCV-specific antibodies, the clinical significance of these antibodies is unknown. Antibody levels rise during active infection, at times to very high titers, but offer no protection. T-cell–mediated immune responses directed to structural and nonstructural proteins are important in controlling infection.
A high index of suspicion for PML is warranted in individuals who demonstrate the classic triad of symptoms (cognitive impairment, visual deficits, and motor dysfunction) and in whom magnetic resonance imaging shows evidence of demyelinated plaque lesions; however, evidence of the presence of JCV DNA in pathologic tissue is necessary to confirm a diagnosis of PML.
The development of an in situ DNA hybridization assay using a biotinylated probe has facilitated identification of JCV DNA in the infected nuclei of the pathologic tissue. The presence of JCV DNA in cerebrospinal fluid (CSF) samples can be detected using a quantitative polymerase chain reaction assay, targeting the viral genome in the amino terminal end of the viral T protein.6 This T protein coding region was targeted because it does not crossreact, even with other human polyomaviruses, and it is intolerant of mutations. This assay is certified by the Clinical Laboratory Improvement Amendments, licensed by the National Institutes of Health; it is the most sensitive (to levels of 10 copies/mL sample) assay available.
JC VIRUS SUSCEPTIBILITY FACTORS
Despite the high prevalence of JCV infection, PML is rare, suggesting important barriers to its development. Although the receptor for JCV has been identified as alpha 2,6-linked sialic acid, the host range for productive infection is controlled by factors within the cell nucleus that bind to the viral promoter; this process initiates transcription of mRNA for the coordinated synthesis of viral proteins. Only certain cells have the necessary DNA binding proteins in high enough concentrations to allow lytic infection to take place, spreading by cell-to-cell contact. These cells include oligodendrocytes, the primary target for JCV, whose destruction leads to PML; astrocytes; and the CD34+ and CD19+ cells of the immune system. JCV can also be found in urine, at times in very high concentrations. It is present in the uroepithelial cells and multiplies without apparent pathologic consequences. Virus isolated from the urine has not been grown in cell culture systems in the laboratory setting.
Bone marrow CD34+ hematopoietic progenitor cells represent a potential pathway of JCV pathogenesis: in six people with PML, latent JCV DNA was demonstrated in pathologic tissue from lymph, spleen, or bone marrow biopsies taken months to years before the patient developed neurologic disease.7
Upon immunosuppression, reactivation of the virus occurs, with evidence of the virus found in CD10 and CD19/20 lymphocytes in the peripheral blood of some individuals. Blood-to-brain viral dissemination results in infection of oligodendrocytes, astrocytes, and progenitor cells.
Susceptibility is related to nucleotide sequences
Susceptibility to PML is associated with promoter/enhancer nucleotide sequences. The tandem repeat nucleotide structure has been found in the peripheral blood leukocytes and the CSF of patients with PML. Although the arrangement of nucleotide sequences in the viral regulatory region is highly variable among patients with PML, there are no alterations in the sequence within the origin of DNA replication. These highly conserved sequences contain regions for DNA-binding proteins that drive transcription, initiating the life cycle of the virus.
The nuclear transcription factor NF-1 is a cell-specific regulator of JCV promoter/enhancer activity. In humans, the NF-1 family of DNA-binding proteins is encoded by four discrete genes, one of which is NF-1 class X (NF-1X), a critical transcription factor that affects JCV cells. The human brain makes NF-1X in concentrations greater than the concentrations of other NF-1 transcription family members of DNA-binding proteins. NF-1X is located adjacent to and interacts with another family of transcription factors, activator protein-1, which has also been associated with JC viral activity.
Spi-B expression a factor in natalizumab-treated patients
Another transcription factor, Spi-B, binds to sequences present in the JCV promoter/enhancer. Spi-B is a regulator of JCV gene expression in susceptible cells and appears to play an important role in JCV activity. The expression of Spi-B is upregulated in patients with MS who are treated with the monoclonal antibody natalizumab, a population of patients in whom PML has been recently described.11–15
Natalizumab binds to the alpha-4 integrin molecule, preventing hematopoietic stem cells and developing B cells from attaching to a vascular-cell adhesion molecule and forcing them to migrate from the bone marrow (Figure 2).16 An ideal environment is created for JCV when the natalizumab-induced increase in CD34+ cells in the circulation is combined with upregulation of gene cells involved in B-cell maturation. JCV can reside in the bone marrow in a latent state and can use B cells and their DNA-binding proteins to initiate viral multiplication, eventually gaining entry into the brain to cause PML.
In addition to natalizumab, PML has been described in patients treated with efalizumab, another biologic agent that binds alpha-4 integrin molecules on the surface of T and B cells, preventing their entry into the brain, gut, and skin, and forcing migration of bone marrow CD34+ into peripheral circulation for long periods.9,17,18 Rituximab, another monoclonal antibody, binds the CD20 surface molecule on B cells, causing their depletion from the peripheral circulation through complement-mediated cytolysis.7
Risk factors for development of PML
Measurable risk factors for PML include:
- Rising antibody titers
- Evidence of viremia, especially persistent viremia associated with repeat sequences in the regulatory region of the viral genome
- Ineffective T-cell (CD4 and CD8) responses
- Molecular host factors (ie, Spi-B expression in B cells) that support JCV infection in potentially susceptible cells.
The presence of more than one of these risk factors is necessary for development of PML.
VIRAL LATENCY IN B LYMPHOCYTES IN BONE MARROW
A strong link between JCV infection in cells of the immune system and those of the nervous system points to the importance of the tissue origin of JCV latency. Bone marrow harbors CD34+ cells that migrate into the peripheral circulation and undergo differentiation to pre-B and mature B cells, augmenting JCV growth. The emergence of PML in patients treated with natalizumab, rituximab, efalizumab, and other immune-altering drugs underscores this observation.
As noted, the incidence of PML in natalizumab-treated patients with MS and Crohn disease rises as the number of doses increases. Analysis of blood samples collected from patients treated with natalizumab at baseline and again during treatment at months 1 to 12 and beyond 24 months demonstrates that the frequency of CD34+ cells in the peripheral circulation increases with the duration of therapy, adding credence to the theory that CD34+ cells act as a reservoir for latent virus. A higher frequency of CD34+ cells is associated with viremia.
The role of Spi-B in JC virus latency
Understanding the role of Spi-B during JCV latency and reactivation is increasingly important as the number of patients treated with immunomodulatory agents that can develop PML continues to rise. Spi-B is highly represented in the B cell and CD34+ cell fractions. Spi-B expression in B cells correlates with reactivation of JCV in immune cells in natalizumab-treated patients. In a sample of four patients with MS treated with natalizumab who developed PML, T-cell responses have been ineffective (absent or aberrant). Two patients had no detectable T-cell response to JCV; the other two demonstrated response, but their CD4 T-cell responses were dominated by interleukin-10–producing cells.
Longitudinal examination of CSF samples from 13 MS patients who were treated with natalizumab and subsequently developed PML revealed persistence of viral load even though all patients experienced immune reconstitution inflammatory syndrome and most had high levels of anti-JCV antibodies.19
SUMMARY
Despite the prevalence of JCV in the population, the development of PML is rare. Levels of JCV antibody rise during the course of active JCV infection, but they do not protect against infection. T-cell responses directed to structural and nonstructural proteins play a role in controlling infection. Latency of JCV is associated with specific cells of the immune system, and its reactivation can follow alteration of normal immune cell function—either immunosuppression or immunomodulation. Risk factors for the development of PML include rising antibody titers and ineffective T-cell (CD4 and CD8) responses.
DISCUSSION
Dr. Berger: Does natalizumab upregulate Spi-B in glial cells?
Dr. Major: We never tested this directly. From human brain cultures, we know that Spi-B is made in glial cells, not in neurons. We are considering the idea that wherever JCV binds, it takes advantage of certain types of DNA-binding proteins in the molecular regulation. If the binding takes place in an immune system cell, for example, Spi-B plays an important role.
Dr. Berger: Koralnik et al demonstrated JCV excretion in urine in MS patients after 12 months of treatment with natalizumab, and at 18 months, viremia in 60% of the patients.20 Yet, repeated studies of patients taking natalizumab have failed to demonstrate viremia or conversion of virus in the archetype. How do these findings correlate with your thoughts on the action of natalizumab in the pathogenesis of PML?
Dr. Major: We certainly know that natalizumab forces migration of hematopoietic stem cells and pre-B cells out of the marrow, but our findings have differed somewhat from those of Koralnik’s laboratory. For example, in the several hundred nucleotide sequences we have looked at in PML brain tissue, we have found the Mad 1 genotype once. We consider Mad 1 to be a potential laboratory contamination, so if we find Mad 1 we resequence the sample. We never clone because cloning can introduce alterations; we sequence directly from the clinical tissue. We can identify Mad 1 because our assay is very sensitive. In normal individuals, CD34+ cells compose approximately 0.01% of the peripheral circulation; in individuals treated with natalizumab, however, their composition is 0.1% to 0.3%. So if there is a potential for latent infection, we have an opportunity to find it in those cells. Its presence does not necessarily mean that the individual is going to develop PML, however; there are other controlling factors.
Dr. Rudick: Have you found the virus in B cells in healthy people?
Dr. Major: Yes we have, in about one-third. It is higher than what we would expect to see in the normal population.
Dr. Rudick: How can that finding be turned into something that’s clinically useful?
Dr. Major: If you’re trying to identify persons who are more susceptible to PML given underlying risk factors—treatment with natalizumab or rituximab, presence of HIV infection, or some other immune-altering condition—looking at one parameter isn’t going to help. Based on the available data, rising antibody titers signals an active infection, and viremia of any kind means probable latent infection. Because this is a small event in very few cells, you will not have the numbers of cells needed to identify susceptibility in a normal population. For now, we monitor patients at risk and, if we find viremia, we assess the cell population to determine whether a molecular factor like Spi-B is upregulated. We hope to develop an assay in which we can obtain one test tube of blood and report T-cell responses, molecular factors, antibody titer, and presence or absence of viremia. Such an assay would provide the data necessary to make a clinical decision.
- Astrom KE, Mancall EL, Richardson EP. Progressive multifocal leukoencephalopathy; a hitherto unrecognized complication of chronic lymphatic leukaemia and Hodgkin’s disease. Brain 1958; 81:93–111.
- Hallervorden J. Eigennartige und nicht rubriziebare Prozesse. In:Bumke O, ed. Handbuch der Geiteskranheiten. Vol. 2. Die Anatomie der Psychosen. Berlin: Springer; 1930:1063–1107.
- Padgett BL, Walker DL, ZuRhein GM, Eckroade RJ, Dessel BH. Cultivation of a papova-like virus from human brain with progressive multifocal leucoencephalopathy. Lancet 1971; 1:1257–1260.
- Major EO, Amemiya K, Tornatore CS, Houff SA, Berger JR. Pathogenesis and molecular biology of progressive multifocal leukoencephalopathy, the JC virus-induced demyelinating disease of the human brain. Clin Microbiol Rev 1992; 5:49–73.
- Walker D, Padgett B. The epidemiology of human polyomaviruses. In:Sever J, Madden D, eds. Polyomaviruses and Human Neurological Disease. New York, NY: Alan R. Liss, Inc.; 1983:99–106.
- Ryschkewitsch C, Jensen P, Hou J, Fahle G, Fischer S, Major EO. Comparison of PCR-southern hybridization and quantitative realtime PCR for the detection of JC and BK viral nucleotide sequences in urine and cerebrospinal fluid. J Virol Methods 2004; 121:217–221.
- Monaco MC, Jensen PN, Hou J, Durham LC, Major EO. Detection of JC virus DNA in human tonsil tissue: evidence for site of initial viral infection. J Virol 1998; 72:9918–9923.
- Major EO. Progressive multifocal leukoencephalopathy in patients on immunomodulatory therapies. Annu Rev Med 2010; 61:35–47.
- Imperiale M, Major E. Polyomavirus. In:Knipe D, Howley P, eds. Field Virology. 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2007:2263–2298.
- Langer-Gould A, Atlas SW, Green AJ, Bollen AW, Pelletier D. Progressive multifocal leukoencephalopathy in a patient treated with natalizumab. N Engl J Med 2005; 353:375–381.
- Van Assche G, Van Ranst M, Sciot R, et al. Progressive multifocal leukoencephalopathy after natalizumab therapy for Crohn’s disease. N Engl J Med 2005; 353:362–368.
- Kleinschmidt-DeMasters BK, Tyler KL. Progressive multifocal leukoencephalopathy complicating treatment with natalizumab and interferon beta-1a for multiple sclerosis. N Engl J Med 2005; 353:369–374.
- Bozic C, Belcher G, Kooijmans-Coutinho M, et al. Natalizumab utilization and safety in patients with relapsing multiple sclerosis: updated results from TOUCH™ and TYGRIS. Paper presented at: 60th Annual Meeting of the American Academy of Neurology; April 15, 2008; Chicago, IL.
- Kappos L, Bates D, Hartung HP, et al. Natalizumab treatment for multiple sclerosis: recommendations for patient selection and monitoring. Lancet Neurol 2007; 6:431–441.
- Major EO. Reemergence of PML in natalizumab-treated patients—new cases, same concerns. N Engl J Med 2009; 361:1041–1043.
- Vugmeyster Y, Kikuchi T, Lowes MA, et al. Efalizumab (anti-CD11a)-induced increase in peripheral blood leukocytes in psoriasis patients is preferentially mediated by altered trafficking of memory CD8+ T cells into lesional skin. Clin Immunol 2004; 113:38–46.
- Guttman-Yassky E, Vugmeyster Y, Lowes MA, et al. Blockade of CD11a by efalizumab in psoriasis patients induces a unique state of T-cell hyporesponsiveness. J Invest Dermatol 2008; 128:1182–1191.
- Carson KR, Evens AM, Richey EA, et al. Progressive multifocal leukoencephalopathy after rituximab therapy in HIV-negative patients: a report of 57 cases from the Research on Adverse Drug Events and Reports project. Blood 2009; 113:4834–4840.
- Ryschkewitsch CF, Jensen PN, Monaco MC, Major EO. JC virus persistence following progressive multifocal leukoencephalopathy in multiple sclerosis patients treated with natalizumab. Ann Neurol 2010; 68:384–391.
- Koralnik IJ, Du Pasquier RA, Kuroda MJ, et al. Association of prolonged survival in HLA-A2+ progressive multifocal leuko encephalopathy patients with a CTL response specific for a commonly recognized JC virus epitope. J Immunol 2002; 168:499–504.
- Astrom KE, Mancall EL, Richardson EP. Progressive multifocal leukoencephalopathy; a hitherto unrecognized complication of chronic lymphatic leukaemia and Hodgkin’s disease. Brain 1958; 81:93–111.
- Hallervorden J. Eigennartige und nicht rubriziebare Prozesse. In:Bumke O, ed. Handbuch der Geiteskranheiten. Vol. 2. Die Anatomie der Psychosen. Berlin: Springer; 1930:1063–1107.
- Padgett BL, Walker DL, ZuRhein GM, Eckroade RJ, Dessel BH. Cultivation of a papova-like virus from human brain with progressive multifocal leucoencephalopathy. Lancet 1971; 1:1257–1260.
- Major EO, Amemiya K, Tornatore CS, Houff SA, Berger JR. Pathogenesis and molecular biology of progressive multifocal leukoencephalopathy, the JC virus-induced demyelinating disease of the human brain. Clin Microbiol Rev 1992; 5:49–73.
- Walker D, Padgett B. The epidemiology of human polyomaviruses. In:Sever J, Madden D, eds. Polyomaviruses and Human Neurological Disease. New York, NY: Alan R. Liss, Inc.; 1983:99–106.
- Ryschkewitsch C, Jensen P, Hou J, Fahle G, Fischer S, Major EO. Comparison of PCR-southern hybridization and quantitative realtime PCR for the detection of JC and BK viral nucleotide sequences in urine and cerebrospinal fluid. J Virol Methods 2004; 121:217–221.
- Monaco MC, Jensen PN, Hou J, Durham LC, Major EO. Detection of JC virus DNA in human tonsil tissue: evidence for site of initial viral infection. J Virol 1998; 72:9918–9923.
- Major EO. Progressive multifocal leukoencephalopathy in patients on immunomodulatory therapies. Annu Rev Med 2010; 61:35–47.
- Imperiale M, Major E. Polyomavirus. In:Knipe D, Howley P, eds. Field Virology. 5th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2007:2263–2298.
- Langer-Gould A, Atlas SW, Green AJ, Bollen AW, Pelletier D. Progressive multifocal leukoencephalopathy in a patient treated with natalizumab. N Engl J Med 2005; 353:375–381.
- Van Assche G, Van Ranst M, Sciot R, et al. Progressive multifocal leukoencephalopathy after natalizumab therapy for Crohn’s disease. N Engl J Med 2005; 353:362–368.
- Kleinschmidt-DeMasters BK, Tyler KL. Progressive multifocal leukoencephalopathy complicating treatment with natalizumab and interferon beta-1a for multiple sclerosis. N Engl J Med 2005; 353:369–374.
- Bozic C, Belcher G, Kooijmans-Coutinho M, et al. Natalizumab utilization and safety in patients with relapsing multiple sclerosis: updated results from TOUCH™ and TYGRIS. Paper presented at: 60th Annual Meeting of the American Academy of Neurology; April 15, 2008; Chicago, IL.
- Kappos L, Bates D, Hartung HP, et al. Natalizumab treatment for multiple sclerosis: recommendations for patient selection and monitoring. Lancet Neurol 2007; 6:431–441.
- Major EO. Reemergence of PML in natalizumab-treated patients—new cases, same concerns. N Engl J Med 2009; 361:1041–1043.
- Vugmeyster Y, Kikuchi T, Lowes MA, et al. Efalizumab (anti-CD11a)-induced increase in peripheral blood leukocytes in psoriasis patients is preferentially mediated by altered trafficking of memory CD8+ T cells into lesional skin. Clin Immunol 2004; 113:38–46.
- Guttman-Yassky E, Vugmeyster Y, Lowes MA, et al. Blockade of CD11a by efalizumab in psoriasis patients induces a unique state of T-cell hyporesponsiveness. J Invest Dermatol 2008; 128:1182–1191.
- Carson KR, Evens AM, Richey EA, et al. Progressive multifocal leukoencephalopathy after rituximab therapy in HIV-negative patients: a report of 57 cases from the Research on Adverse Drug Events and Reports project. Blood 2009; 113:4834–4840.
- Ryschkewitsch CF, Jensen PN, Monaco MC, Major EO. JC virus persistence following progressive multifocal leukoencephalopathy in multiple sclerosis patients treated with natalizumab. Ann Neurol 2010; 68:384–391.
- Koralnik IJ, Du Pasquier RA, Kuroda MJ, et al. Association of prolonged survival in HLA-A2+ progressive multifocal leuko encephalopathy patients with a CTL response specific for a commonly recognized JC virus epitope. J Immunol 2002; 168:499–504.
The clinical features of PML
Progressive multifocal leukoencephalopathy (PML) was a rare disease until the era of human immunodeficiency virus (HIV) infection, when the number of cases of PML markedly increased. We are now entering a new era in which PML is being observed in patients treated with biologic agents for diseases not associated with development of PML.
This article reviews the epidemiology and symptoms that characterize PML, the identification of lesions on radiographic imaging that support the diagnosis, the value of laboratory studies and immunocytochemistry in the diagnosis, and clinical outcomes.
CHANGING EPIDEMIOLOGY OF PML
The pre-AIDS era
Lesions of subcortical white matter characterize PML and the patient’s clinical manifestations reflect their location. Brooks and Walker1 reviewed 69 pathologically confirmed and 40 virologically and pathologically confirmed cases of PML in the era before AIDS, and categorized the neurologic signs and symptoms at onset and during disease progression; the clinical picture had three significant findings:
- Impaired vision: Defective vision, most commonly homonymous hemianopsia, was the most frequent presenting sign, present in 35% to 45% of cases. At the time of diagnosis, 6% to 8% of the patients were cortically blind because of bioccipital pathology.
- Motor weakness: Motor weakness was the initial sign in 25% to 33% of patients. At the time of diagnosis, hemiparesis or hemiplegia was present in nearly all patients.
- Changes in mentation: A change in mentation, including personality change, difficulty with memory, emotional lability, and frank dementia, was the presenting sign in approximately one-third of cases and eventually involved most patients.
AIDS-related PML
The epidemiology of PML changed with the AIDS pandemic. From 1958 to 1984, Brooks and Walker1 identified 230 cases of PML; in the period from 1981 to 1994, Berger and colleagues2 described 154 cases of AIDS-related PML that had been identified by the University of Miami Medical Center and the Broward County medical examiner’s office. The frequency of PML from 1991 through 1994 was 12-fold greater than the frequency 10 years earlier, from 1981 through 1984. Among the patients with AIDS-related PML, the most common initial symptoms were weakness (42%), speech abnormalities (40%), cognitive abnormalities (36%), gait abnormalities (29%), sensory loss (19%), and visual impairment (19%), followed by seizures, diplopia, and limb incoordination. The most common findings at the time of initial physical examination were weakness (54%), followed by gait abnormalities (20%), cognitive abnormalities (20%), dysarthria (24%), aphasia (19%), sensory loss (19%), visual impairment (17%), and oculomotor palsy (6%). For about 5% of patients with PML, it is the heralding manifestation of AIDS.
Although clinical features consistent with cerebral hemisphere lesions are most common, brainstem and cerebellar findings are also observed. Among these are ataxia, dysmetria, dysarthria, and oculomotor nerve palsies.2–4 Other signs and symptoms associated with PML include headache, vertigo, seizures, sensory deficits, parkinsonism, 5 aphasia, and neglect syndromes.1–4 In some cases, the coexistence of encephalitis with HIV infection could have accounted for some of the symptoms.
PML associated with monoclonal antibody therapy
Natalizumab is an alpha-4-beta-1 integrin inhibitor approved for the treatment of relapsing-remitting multiple sclerosis (MS); patients taking natalizumab represent the second largest group with PML (the largest group is patients with AIDS). Natalizumab-associated PML has some noteworthy features. The most common clinical presentations are cognitive disorders (48%), motor abnormalities (37%), language disturbances (31%), and visual defects (26%). Lesions are often monofocal rather than multifocal and the most common site of involvement is the frontal lobe.6 Among MS patients with natalizumab-associated PML, 30% to 40% have gadolinium-enhancing lesions on magnetic resonance imaging (MRI) at the time of diagnosis.
IMMUNE RECONSTITUTION INFLAMMATORY SYNDROME
Among patients with HIV, predictors for the development of IRIS include antiretroviral naiveté, profoundly low CD4 lymphocyte counts (< 50 cells/mm3), a rapid decrease in HIV load, and the presence of active or subclinical opportunistic infections at the time of initiation of combined antiretroviral therapy. Tan and colleagues8 have reported the largest series to date. Of the 54 patients in their series, 36 developed PML and IRIS simultaneously, and 18 had worsening of preexisting PML. Although some investigators have recommended corticosteroid therapy for PML-IRIS, no controlled trials have been conducted and caution has been advised, particularly in patients without contrast enhancement on MRI or mass effect.
DIAGNOSTIC TESTING: NEUROIMAGING, CEREBROSPINAL FLUID ANALYSIS
Neuroimaging, including computed tomography (CT) and MRI, is a useful diagnostic tool for investigating a patient with PML. Cerebrospinal fluid (CSF) analysis for the presence of JC virus (JCV) may play a significant role, but it primarily serves to rule out other illnesses.
Computed tomography: lesion size may not reflect clinical status
On CT, demyelinating lesions appear as subcortical hypodensities, often with a propensity for parietooccipital areas that are confined to the white matter at the junction interface of the gray-white junction of the cortex.9–11 Lesions may be seen in the corpus callosum, thalamus, and basal ganglia,9 but changes in the size of lesions observed on CT do not necessarily reflect clinical progression.12 Prior to the availability of highly active antiretroviral therapy (HAART) for the treatment of AIDS, mass effect was exceptionally rare. However, the development of IRIS with PML, typically in AIDS patients following the use of HAART, may be associated with edema.13 Single-dose intravenous contrast and delayed, double-dose contrast CT scanning enhancement is observed in a minority of patients, typically fewer than 10%.8 This enhancement is generally faint and peripherally located.
Magnetic resonance imaging may show lesions before clinical disease
MRI is vastly more sensitive than CT in detecting the demyelinating lesions of PML.9,14 On rare occasions, MRI will clearly demonstrate pathology when CT is normal. In fact, MRI may show lesions in advance of clinically apparent disease.15 The characteristics of these lesions are hyperintensity on T2-weighted imaging, fluid-attenuated inversion recovery sequences, and hypointensity on T1-weighted image. Apparent diffusion coefficients (ADC) on MRI are typically normal to low in new lesions and at the advancing edge of lesions; the ADC was typically higher in the center of lesions.16
As observed on CT, approximately 10% of patients exhibit a faint rim of gadolinium enhancement.2,9 Enhancement is more common with PML-IRIS, and the distribution of lesions parallels what is seen pathologically. Enhancement PML lesions have altered signal characteristics compared with the surrounding white matter.9,17–19 In contrast, 15% of HIV-associated PML showed gadolinium enhancement on MRI at the time of diagnosis.6,9
Cerebrospinal fluid analysis
With the exception of polymerase chain reaction (PCR) for JCV, the primary utility of lumbar puncture in the setting of possible PML is to exclude the presence of other illnesses, including treatable infections.
CSF findings in patients with PML are nonspecific, with most patients demon strating a normal profile. A mild lymphocytic pleocytosis, which is rarely (if ever) more than 25 leukocytes/mL, occurs in 15% of patients. Total protein level is mildly elevated in approximately 20% to 30% of patients.
The CSF examination in HIV-infected patients with PML may reflect changes associated with HIV: low-grade lymphocytic pleocytosis (< 20 cells/mm3), mildly elevated protein (< 65 mg/dL), and elevated immunoglobulin G and oligoclonal bands. These abnormalities should not be attributed to PML.
DIAGNOSIS
The most reliable and accurate method for the diagnosis of PML remains brain biopsy that demonstrates the characteristic triad of histopathologic findings (demyelination, bizarre astrocytes, and enlarged oligodendrocyte nuclei) coupled with evidence of JCV infection. With respect to the latter, in situ hybridization or immunocytochemistry can be employed. In situ DNADNA hybridization is a method of annealing JCV DNA to complementary strands either in paraffin-embedded tissue or in frozen sections from biopsy samples.
In immunocytochemistry, antibodies to both T antigen and the common polyomavirus capsid antigen are used to detect cells undergoing productive viral infection. Cells that are positive by in situ hybridization are in a stage of active viral replication. Cells positive by immunocytochemistry that are expressing viral capsid antigens are in a stage of viral transcription and translation (ie, undergoing productive infection). In addition to their utility in confirming a diagnosis of PML, these techniques have demonstrated the presence of JCV in perivascular locations and at sites distant from foci of demyelination. Alternatively, PCR may be used to demonstrate JCV in brain tissue.
In the absence of biopsy, which few deem necessary today, a widely employed approach to diagnosis requires the demonstration of:
- JCV in the CSF by PCR
- Compatible clinical presentation
- An MRI finding consistent with PML
- No other alternative diagnosis.
With an ultrasensitive PCR technique, sensitivities should approach or may exceed 95%, but PCR sensitivity remains at 75% in some laboratories. Because the viral copy numbers in the CSF may be low, particularly in a patient treated with a monoclonal antibody such as natalizumab, the CSF PCR may be falsely negative.
If clinical suspicion of the disease remains high in the face of an initially negative CSF JCV, the CSF analysis should be repeated. CSF analysis for JCV is approximately 99% specific, but recent studies demonstrating low copy numbers of JCV in the CSF of patients with MS have raised concerns about potential pitfalls of this assay.20
PROGNOSIS
Until recently, PML was regarded as virtually universally fatal. The mean survival in the pre-AIDS era was approximately 6 months, and mortality was 80% within 9 months of disease onset. Rarely, patients had long survivals that ranged from 5 years to 19 years.
In the early years of the AIDS era, survival with PML did not appear to differ significantly from that observed in the pre-AIDS years. In the largest study of HIV-associated PML in the era prior to HAART, the median survival was 183 days.2 However, the majority of individuals were dead within 3 months of diagnosis. Only 8% to 10% of patients survived longer than 12 months, which has been regarded as “prolonged survival.” This long survival skewed the mean and median survival rates in this population.
Several factors have since been identified that correlate with prolonged survival in HIV-associated PML, including PML as the heralding manifestation of HIV, CD4 counts exceeding 300 cells per mm3, contrast enhancement of the lesions on radiographic imaging, low copy number or decreasing JCV titers in CSF,21–24 and the presence of JCV-specific cytotoxic T cells.25 A better prognosis has also been postulated for higher CSF levels of macrophage chemoattractant protein-126 and PML associated with JCV VP1 loop-specific polymorphisms.27
Prognosis of HIV-associated PML improves with immune system restoration
In the era of HAART, not only has the incidence of HIV-associated PML declined, but the prognosis of affected patients has improved as well. This development highlights the importance of restoration of the immune system in both disease prevention and survival. Some estimate that as many as 50% of HAART-treated patients with PML exhibit prolonged survival. In one study of 25 patients, the median survival was more than 46 weeks.28
Nonetheless, PML continues to have the worst prognosis of any AIDS-related cerebral disorder, with those having advanced immunosuppression being most susceptible to the disorder. For AIDS patients with PML, those who were HAART-naïve at the time of diagnosis appear to have better survival than treatment-experienced patients.29 Survival also correlates with reduced JCV load in the CSF30 and improved CD4 lymphocyte counts (CD4 counts > 100 cells/mm3).31
Prognosis of natalizumab-associated PML is different
The prognosis of natalizumab-associated PML differs from that of HIV-associated PML. In a series of 35 patients, 25 (71%) patients were alive on average 6 months after diagnosis.32 Prognosis was worse with a longer time to diagnosis and the presence of widespread disease.
Most deaths in patients taking natalizumab who developed PML have occurred during IRIS. Steroid treatment of IRIS appears to improve prognosis,8 but no scientifically rigorous study has been undertaken to demonstrate this recommendation.7 Among the survivors, neurologic deficit was mild in one-third, moderate in one-third, and severe in one-third of patients.
CONCLUSION: DISPELLING SOME MYTHS
Several assumptions about PML are not necessarily true. For example, although PML implies the presence of multifocal lesions as a characteristic of the disease, the lesions may be monofocal, especially with natalizumab-associated PML. The lesions of PML may show early gadolinium enhancement on neuroimaging. Although lesions typically are seen in subcortical white matter, cortical involvement also may be observed. Cerebellar granular cell degeneration may occur in association with PML or in isolation. Disease progression and death are not inevitable, even in the absence of treatment. The most important determinant for survival is restoration of the immune system.
DISCUSSION
Dr. Calabrese: Why are sensory deficits so common?
Dr. Berger: We don’t know. Because we see involvement in the parietal lobe, we would anticipate observing sensory deficits. I think that a lot of sensation occurs deep in the thalamic area, which is not often involved in PML. Also, we often don’t test for some of the deficits that may occur.
Dr. Rudick: Do you know of any cases of natalizumab-associated PML detected as an incidental finding on MRI, making a case for screening MRI in patients without clinical symptoms?
Dr. Berger: There have been a handful of cases, including one of the seminal cases of natalizumab-associated PML, in which MRI abnormalities were observed in advance of clinically recognized symptomatology.
Dr. Calabrese: The correlate question is, if a patient with a risk factor—be it HIV or treatment with a biologic agent—has a common neurocognitive sign or perhaps some subtle motor findings, does a normal MRI have 100% negative predictive value?
Dr. Berger: I have yet to see somebody with PML who has a normal MRI.
Dr. Simpson: What you may see are lesions that are not typical MRI lesions of white matter hypointensity. In some cases, as Dr. Berger mentioned in his summary, we’ll see cerebellar degeneration—atrophy—but not necessarily white matter lesions.
- Brooks BR, Walker DL. Progressive multifocal leukoencephalopathy. Neurol Clin 1984; 2:299–313.
- Berger JR, Pall L, Lanska D, Whiteman M. Progressive multifocal leukoencephalopathy in patients with HIV infection. J Neurovirol 1998; 4:59–68.
- Parr J, Horoupian DS, Winkelman AC. Cerebellar form of progressive multifocal leukoencephalopathy (PML). Can J Neurol Sci 1979; 6:123–128.
- Jones HR, Hedley-Whyte ET, Freidberg SR, Kelleher JE, Krolikowski J. Primary cerebellopontine progressive multifocal leukoencephalopathy diagnosed premortem by cerebellar biopsy. Ann Neurol 1982; 11:199–202.
- O’Riordan S, McGuigan C, Farrell M, Hutchinson M. Progressive multifocal leucoencephalopathy presenting with parkinsonism. J Neurol 2003; 250:1379–1381.
- Clifford DB, De Luca A, Simpson DM, Arendt G, Giovannoni G, Nath A. Natalizumab-associated progressive multifocal leukoencephalopathy in patients with multiple sclerosis: lessons from 28 cases. Lancet Neurol 2010; 9:438–446.
- Berger JR. Steroids for PML-IRIS. A double-edged sword? Neurology 2009; 72:1454–1455.
- Tan K, Roda R, Ostrow L, McArthur J, Nath A. PML-IRIS in patients with HIV infection: clinical manifestations and treatment with steroids. Neurology 2009; 72:1458–1464.
- Whiteman ML, Post MJ, Berger JR, Tate LG, Bell MD, Limonte LP. Progressive multifocal leukoencephalopathy in 47 HIV-seropositive patients: neuroimaging with clinical and pathologic correlation. Radiology 1993; 187:233–240.
- Conomy JP, Weinstein MA, Agamanolis D, Holt WS. Computed tomography in progressive multifocal leukoencephalopathy. AJR Am J Roentgenol 1976; 127:663–665.
- Huckman MS. Computed tomography in the diagnosis of degenerative brain disease. Radiol Clin North Am 1982; 20:169–183.
- Krupp LB, Lipton RB, Swerdlow ML, Leeds NE, Llena J. Progressive multifocal leukoencephalopathy: clinical and radiographic features. Ann Neurol 1985; 17:344–349.
- Rushing EJ, Liappis A, Smirniotopoulos JD, et al. Immune reconstitution inflammatory syndrome of the brain: case illustrations of a challenging entity. J Neuropathol Exp Neurol 2008; 67:819–827.
- Post MJ, Sheldon JJ, Hensley GT, et al. Central nervous system disease in acquired immunodeficiency syndrome: prospective correlation using CT, MR imaging, and pathologic studies. Radiology 1986; 158:141–148.
- Langer-Gould A, Atlas SW, Green AJ, Bollen AW, Pelletier D. Progressive multifocal leukoencephalopathy in a patient treated with natalizumab. N Engl J Med 2005; 353:375–381.
- Bergui M, Bradac GB, Oguz KK, et al. Progressive multifocal leukoencephalopathy: diffusion-weighted imaging and pathological correlations. Neuroradiology 2004; 46:22–25.
- Guilleux MH, Steiner RE, Young IR. MR imaging in progressive multifocal leukoencephalopathy. AJNR Am J Neuroradiol 1986; 7:1033–1035.
- Levy JD, Cottingham KL, Campbell RJ, et al. Progressive multifocal leukoencephalopathy and magnetic resonance imaging. Ann Neurol 1986; 19:399–401.
- Mark AS, Atlas SW. Progressive multifocal leukoencephalopathy in patients with AIDS: appearance on MR images. Radiology 1989; 173:517–520.
- Iacobaeus E, Ryschkewitsch C, Gravell M, et al. Analysis of cerebrospinal fluid and cerebrospinal fluid cells from patients with multiple sclerosis for detection of JC virus DNA. Mult Scler 2009; 15:28–35.
- Berger JR, Levy RM, Flomenhoft D, Dobbs M. Predictive factors for prolonged survival in acquired immunodeficiency syndrome-associated progressive multifocal leukoencephalopathy. Ann Neurol 1998; 44:341–349.
- Taoufik Y, Gasnault J, Karaterki A, et al. Prognostic value of JC virus load in cerebrospinal fluid of patients with progressive multifocal leukoencephalopathy. J Infect Dis 1998; 178:1816–1820.
- Yiannoutsos CT, Major EO, Curfman B, et al. Relation of JC virus DNA in the cerebrospinal fluid to survival in acquired immunodeficiency syndrome patients with biopsy-proven progressive multifocal leukoencephalopathy. Ann Neurol 1999; 45:816–821.
- Bossolasco S, Calori G, Moretti F, et al. Prognostic significance of JC virus DNA levels in cerebrospinal fluid of patients with HIV-associated progressive multifocal leukoencephalopathy. Clin Infect Dis 2005; 40:738–744.
- Du Pasquier RA, Clark KW, Smith PS, et al. JCV-specific cellular immune response correlates with a favorable clinical outcome in HIV-infected individuals with progressive multifocal leukoencephalopathy. J Neurovirol 2001; 7:318–322.
- Marzocchetti A, Cingolani A, Giambenedetto SD, et al. Macrophage chemoattractant protein-1 levels in cerebrospinal fluid correlate with containment of JC virus and prognosis of acquired immunodeficiency syndrome-associated progressive multifocal leukoencephalopathy. J Neurovirol 2005; 11:219–224.
- Delbue S, Branchetti E, Bertolacci S, et al. JC virus VP1 loop-specific polymorphisms are associated with favorable prognosis for progressive multifocal leukoencephalopathy. J Neurovirol 2009; 15:51–56.
- Clifford DB, Yiannoutsos C, Glicksman M, et al. HAART improves prognosis in HIV-associated progressive multifocal leukoencephalopathy. Neurology 1999; 52:623–625.
- Wyen C, Hoffmann C, Schmeisser N, et al. Progressive multi focal leukoencephalopathy in patients on highly active antiretroviral therapy: survival and risk factors of death. J Acquir Immune Defic Syndr 2004; 37:1263–1268.
- De Luca A, Giancola ML, Ammassari A, et al. The effect of potent antiretroviral therapy and JC virus load in cerebrospinal fluid on clinical outcome of patients with AIDS-associated progressive multifocal leukoencephalopathy. J Infect Dis 2000; 182:1077–1083.
- Berenguer J, Miralles P, Arrizabalaga J, et al. Clinical course and prognostic factors of progressive multifocal leukoencephalopathy in patients treated with highly active antiretroviral therapy. Clin Infect Dis 2003; 36:1047–1052.
- Vermersch P, Kappos L, Gold R, et al. Clinical outcomes of natalizumab associated progressive multifocal leukoencephalopathy. Neurology 2011; 76:1697–1704.
Progressive multifocal leukoencephalopathy (PML) was a rare disease until the era of human immunodeficiency virus (HIV) infection, when the number of cases of PML markedly increased. We are now entering a new era in which PML is being observed in patients treated with biologic agents for diseases not associated with development of PML.
This article reviews the epidemiology and symptoms that characterize PML, the identification of lesions on radiographic imaging that support the diagnosis, the value of laboratory studies and immunocytochemistry in the diagnosis, and clinical outcomes.
CHANGING EPIDEMIOLOGY OF PML
The pre-AIDS era
Lesions of subcortical white matter characterize PML and the patient’s clinical manifestations reflect their location. Brooks and Walker1 reviewed 69 pathologically confirmed and 40 virologically and pathologically confirmed cases of PML in the era before AIDS, and categorized the neurologic signs and symptoms at onset and during disease progression; the clinical picture had three significant findings:
- Impaired vision: Defective vision, most commonly homonymous hemianopsia, was the most frequent presenting sign, present in 35% to 45% of cases. At the time of diagnosis, 6% to 8% of the patients were cortically blind because of bioccipital pathology.
- Motor weakness: Motor weakness was the initial sign in 25% to 33% of patients. At the time of diagnosis, hemiparesis or hemiplegia was present in nearly all patients.
- Changes in mentation: A change in mentation, including personality change, difficulty with memory, emotional lability, and frank dementia, was the presenting sign in approximately one-third of cases and eventually involved most patients.
AIDS-related PML
The epidemiology of PML changed with the AIDS pandemic. From 1958 to 1984, Brooks and Walker1 identified 230 cases of PML; in the period from 1981 to 1994, Berger and colleagues2 described 154 cases of AIDS-related PML that had been identified by the University of Miami Medical Center and the Broward County medical examiner’s office. The frequency of PML from 1991 through 1994 was 12-fold greater than the frequency 10 years earlier, from 1981 through 1984. Among the patients with AIDS-related PML, the most common initial symptoms were weakness (42%), speech abnormalities (40%), cognitive abnormalities (36%), gait abnormalities (29%), sensory loss (19%), and visual impairment (19%), followed by seizures, diplopia, and limb incoordination. The most common findings at the time of initial physical examination were weakness (54%), followed by gait abnormalities (20%), cognitive abnormalities (20%), dysarthria (24%), aphasia (19%), sensory loss (19%), visual impairment (17%), and oculomotor palsy (6%). For about 5% of patients with PML, it is the heralding manifestation of AIDS.
Although clinical features consistent with cerebral hemisphere lesions are most common, brainstem and cerebellar findings are also observed. Among these are ataxia, dysmetria, dysarthria, and oculomotor nerve palsies.2–4 Other signs and symptoms associated with PML include headache, vertigo, seizures, sensory deficits, parkinsonism, 5 aphasia, and neglect syndromes.1–4 In some cases, the coexistence of encephalitis with HIV infection could have accounted for some of the symptoms.
PML associated with monoclonal antibody therapy
Natalizumab is an alpha-4-beta-1 integrin inhibitor approved for the treatment of relapsing-remitting multiple sclerosis (MS); patients taking natalizumab represent the second largest group with PML (the largest group is patients with AIDS). Natalizumab-associated PML has some noteworthy features. The most common clinical presentations are cognitive disorders (48%), motor abnormalities (37%), language disturbances (31%), and visual defects (26%). Lesions are often monofocal rather than multifocal and the most common site of involvement is the frontal lobe.6 Among MS patients with natalizumab-associated PML, 30% to 40% have gadolinium-enhancing lesions on magnetic resonance imaging (MRI) at the time of diagnosis.
IMMUNE RECONSTITUTION INFLAMMATORY SYNDROME
Among patients with HIV, predictors for the development of IRIS include antiretroviral naiveté, profoundly low CD4 lymphocyte counts (< 50 cells/mm3), a rapid decrease in HIV load, and the presence of active or subclinical opportunistic infections at the time of initiation of combined antiretroviral therapy. Tan and colleagues8 have reported the largest series to date. Of the 54 patients in their series, 36 developed PML and IRIS simultaneously, and 18 had worsening of preexisting PML. Although some investigators have recommended corticosteroid therapy for PML-IRIS, no controlled trials have been conducted and caution has been advised, particularly in patients without contrast enhancement on MRI or mass effect.
DIAGNOSTIC TESTING: NEUROIMAGING, CEREBROSPINAL FLUID ANALYSIS
Neuroimaging, including computed tomography (CT) and MRI, is a useful diagnostic tool for investigating a patient with PML. Cerebrospinal fluid (CSF) analysis for the presence of JC virus (JCV) may play a significant role, but it primarily serves to rule out other illnesses.
Computed tomography: lesion size may not reflect clinical status
On CT, demyelinating lesions appear as subcortical hypodensities, often with a propensity for parietooccipital areas that are confined to the white matter at the junction interface of the gray-white junction of the cortex.9–11 Lesions may be seen in the corpus callosum, thalamus, and basal ganglia,9 but changes in the size of lesions observed on CT do not necessarily reflect clinical progression.12 Prior to the availability of highly active antiretroviral therapy (HAART) for the treatment of AIDS, mass effect was exceptionally rare. However, the development of IRIS with PML, typically in AIDS patients following the use of HAART, may be associated with edema.13 Single-dose intravenous contrast and delayed, double-dose contrast CT scanning enhancement is observed in a minority of patients, typically fewer than 10%.8 This enhancement is generally faint and peripherally located.
Magnetic resonance imaging may show lesions before clinical disease
MRI is vastly more sensitive than CT in detecting the demyelinating lesions of PML.9,14 On rare occasions, MRI will clearly demonstrate pathology when CT is normal. In fact, MRI may show lesions in advance of clinically apparent disease.15 The characteristics of these lesions are hyperintensity on T2-weighted imaging, fluid-attenuated inversion recovery sequences, and hypointensity on T1-weighted image. Apparent diffusion coefficients (ADC) on MRI are typically normal to low in new lesions and at the advancing edge of lesions; the ADC was typically higher in the center of lesions.16
As observed on CT, approximately 10% of patients exhibit a faint rim of gadolinium enhancement.2,9 Enhancement is more common with PML-IRIS, and the distribution of lesions parallels what is seen pathologically. Enhancement PML lesions have altered signal characteristics compared with the surrounding white matter.9,17–19 In contrast, 15% of HIV-associated PML showed gadolinium enhancement on MRI at the time of diagnosis.6,9
Cerebrospinal fluid analysis
With the exception of polymerase chain reaction (PCR) for JCV, the primary utility of lumbar puncture in the setting of possible PML is to exclude the presence of other illnesses, including treatable infections.
CSF findings in patients with PML are nonspecific, with most patients demon strating a normal profile. A mild lymphocytic pleocytosis, which is rarely (if ever) more than 25 leukocytes/mL, occurs in 15% of patients. Total protein level is mildly elevated in approximately 20% to 30% of patients.
The CSF examination in HIV-infected patients with PML may reflect changes associated with HIV: low-grade lymphocytic pleocytosis (< 20 cells/mm3), mildly elevated protein (< 65 mg/dL), and elevated immunoglobulin G and oligoclonal bands. These abnormalities should not be attributed to PML.
DIAGNOSIS
The most reliable and accurate method for the diagnosis of PML remains brain biopsy that demonstrates the characteristic triad of histopathologic findings (demyelination, bizarre astrocytes, and enlarged oligodendrocyte nuclei) coupled with evidence of JCV infection. With respect to the latter, in situ hybridization or immunocytochemistry can be employed. In situ DNADNA hybridization is a method of annealing JCV DNA to complementary strands either in paraffin-embedded tissue or in frozen sections from biopsy samples.
In immunocytochemistry, antibodies to both T antigen and the common polyomavirus capsid antigen are used to detect cells undergoing productive viral infection. Cells that are positive by in situ hybridization are in a stage of active viral replication. Cells positive by immunocytochemistry that are expressing viral capsid antigens are in a stage of viral transcription and translation (ie, undergoing productive infection). In addition to their utility in confirming a diagnosis of PML, these techniques have demonstrated the presence of JCV in perivascular locations and at sites distant from foci of demyelination. Alternatively, PCR may be used to demonstrate JCV in brain tissue.
In the absence of biopsy, which few deem necessary today, a widely employed approach to diagnosis requires the demonstration of:
- JCV in the CSF by PCR
- Compatible clinical presentation
- An MRI finding consistent with PML
- No other alternative diagnosis.
With an ultrasensitive PCR technique, sensitivities should approach or may exceed 95%, but PCR sensitivity remains at 75% in some laboratories. Because the viral copy numbers in the CSF may be low, particularly in a patient treated with a monoclonal antibody such as natalizumab, the CSF PCR may be falsely negative.
If clinical suspicion of the disease remains high in the face of an initially negative CSF JCV, the CSF analysis should be repeated. CSF analysis for JCV is approximately 99% specific, but recent studies demonstrating low copy numbers of JCV in the CSF of patients with MS have raised concerns about potential pitfalls of this assay.20
PROGNOSIS
Until recently, PML was regarded as virtually universally fatal. The mean survival in the pre-AIDS era was approximately 6 months, and mortality was 80% within 9 months of disease onset. Rarely, patients had long survivals that ranged from 5 years to 19 years.
In the early years of the AIDS era, survival with PML did not appear to differ significantly from that observed in the pre-AIDS years. In the largest study of HIV-associated PML in the era prior to HAART, the median survival was 183 days.2 However, the majority of individuals were dead within 3 months of diagnosis. Only 8% to 10% of patients survived longer than 12 months, which has been regarded as “prolonged survival.” This long survival skewed the mean and median survival rates in this population.
Several factors have since been identified that correlate with prolonged survival in HIV-associated PML, including PML as the heralding manifestation of HIV, CD4 counts exceeding 300 cells per mm3, contrast enhancement of the lesions on radiographic imaging, low copy number or decreasing JCV titers in CSF,21–24 and the presence of JCV-specific cytotoxic T cells.25 A better prognosis has also been postulated for higher CSF levels of macrophage chemoattractant protein-126 and PML associated with JCV VP1 loop-specific polymorphisms.27
Prognosis of HIV-associated PML improves with immune system restoration
In the era of HAART, not only has the incidence of HIV-associated PML declined, but the prognosis of affected patients has improved as well. This development highlights the importance of restoration of the immune system in both disease prevention and survival. Some estimate that as many as 50% of HAART-treated patients with PML exhibit prolonged survival. In one study of 25 patients, the median survival was more than 46 weeks.28
Nonetheless, PML continues to have the worst prognosis of any AIDS-related cerebral disorder, with those having advanced immunosuppression being most susceptible to the disorder. For AIDS patients with PML, those who were HAART-naïve at the time of diagnosis appear to have better survival than treatment-experienced patients.29 Survival also correlates with reduced JCV load in the CSF30 and improved CD4 lymphocyte counts (CD4 counts > 100 cells/mm3).31
Prognosis of natalizumab-associated PML is different
The prognosis of natalizumab-associated PML differs from that of HIV-associated PML. In a series of 35 patients, 25 (71%) patients were alive on average 6 months after diagnosis.32 Prognosis was worse with a longer time to diagnosis and the presence of widespread disease.
Most deaths in patients taking natalizumab who developed PML have occurred during IRIS. Steroid treatment of IRIS appears to improve prognosis,8 but no scientifically rigorous study has been undertaken to demonstrate this recommendation.7 Among the survivors, neurologic deficit was mild in one-third, moderate in one-third, and severe in one-third of patients.
CONCLUSION: DISPELLING SOME MYTHS
Several assumptions about PML are not necessarily true. For example, although PML implies the presence of multifocal lesions as a characteristic of the disease, the lesions may be monofocal, especially with natalizumab-associated PML. The lesions of PML may show early gadolinium enhancement on neuroimaging. Although lesions typically are seen in subcortical white matter, cortical involvement also may be observed. Cerebellar granular cell degeneration may occur in association with PML or in isolation. Disease progression and death are not inevitable, even in the absence of treatment. The most important determinant for survival is restoration of the immune system.
DISCUSSION
Dr. Calabrese: Why are sensory deficits so common?
Dr. Berger: We don’t know. Because we see involvement in the parietal lobe, we would anticipate observing sensory deficits. I think that a lot of sensation occurs deep in the thalamic area, which is not often involved in PML. Also, we often don’t test for some of the deficits that may occur.
Dr. Rudick: Do you know of any cases of natalizumab-associated PML detected as an incidental finding on MRI, making a case for screening MRI in patients without clinical symptoms?
Dr. Berger: There have been a handful of cases, including one of the seminal cases of natalizumab-associated PML, in which MRI abnormalities were observed in advance of clinically recognized symptomatology.
Dr. Calabrese: The correlate question is, if a patient with a risk factor—be it HIV or treatment with a biologic agent—has a common neurocognitive sign or perhaps some subtle motor findings, does a normal MRI have 100% negative predictive value?
Dr. Berger: I have yet to see somebody with PML who has a normal MRI.
Dr. Simpson: What you may see are lesions that are not typical MRI lesions of white matter hypointensity. In some cases, as Dr. Berger mentioned in his summary, we’ll see cerebellar degeneration—atrophy—but not necessarily white matter lesions.
Progressive multifocal leukoencephalopathy (PML) was a rare disease until the era of human immunodeficiency virus (HIV) infection, when the number of cases of PML markedly increased. We are now entering a new era in which PML is being observed in patients treated with biologic agents for diseases not associated with development of PML.
This article reviews the epidemiology and symptoms that characterize PML, the identification of lesions on radiographic imaging that support the diagnosis, the value of laboratory studies and immunocytochemistry in the diagnosis, and clinical outcomes.
CHANGING EPIDEMIOLOGY OF PML
The pre-AIDS era
Lesions of subcortical white matter characterize PML and the patient’s clinical manifestations reflect their location. Brooks and Walker1 reviewed 69 pathologically confirmed and 40 virologically and pathologically confirmed cases of PML in the era before AIDS, and categorized the neurologic signs and symptoms at onset and during disease progression; the clinical picture had three significant findings:
- Impaired vision: Defective vision, most commonly homonymous hemianopsia, was the most frequent presenting sign, present in 35% to 45% of cases. At the time of diagnosis, 6% to 8% of the patients were cortically blind because of bioccipital pathology.
- Motor weakness: Motor weakness was the initial sign in 25% to 33% of patients. At the time of diagnosis, hemiparesis or hemiplegia was present in nearly all patients.
- Changes in mentation: A change in mentation, including personality change, difficulty with memory, emotional lability, and frank dementia, was the presenting sign in approximately one-third of cases and eventually involved most patients.
AIDS-related PML
The epidemiology of PML changed with the AIDS pandemic. From 1958 to 1984, Brooks and Walker1 identified 230 cases of PML; in the period from 1981 to 1994, Berger and colleagues2 described 154 cases of AIDS-related PML that had been identified by the University of Miami Medical Center and the Broward County medical examiner’s office. The frequency of PML from 1991 through 1994 was 12-fold greater than the frequency 10 years earlier, from 1981 through 1984. Among the patients with AIDS-related PML, the most common initial symptoms were weakness (42%), speech abnormalities (40%), cognitive abnormalities (36%), gait abnormalities (29%), sensory loss (19%), and visual impairment (19%), followed by seizures, diplopia, and limb incoordination. The most common findings at the time of initial physical examination were weakness (54%), followed by gait abnormalities (20%), cognitive abnormalities (20%), dysarthria (24%), aphasia (19%), sensory loss (19%), visual impairment (17%), and oculomotor palsy (6%). For about 5% of patients with PML, it is the heralding manifestation of AIDS.
Although clinical features consistent with cerebral hemisphere lesions are most common, brainstem and cerebellar findings are also observed. Among these are ataxia, dysmetria, dysarthria, and oculomotor nerve palsies.2–4 Other signs and symptoms associated with PML include headache, vertigo, seizures, sensory deficits, parkinsonism, 5 aphasia, and neglect syndromes.1–4 In some cases, the coexistence of encephalitis with HIV infection could have accounted for some of the symptoms.
PML associated with monoclonal antibody therapy
Natalizumab is an alpha-4-beta-1 integrin inhibitor approved for the treatment of relapsing-remitting multiple sclerosis (MS); patients taking natalizumab represent the second largest group with PML (the largest group is patients with AIDS). Natalizumab-associated PML has some noteworthy features. The most common clinical presentations are cognitive disorders (48%), motor abnormalities (37%), language disturbances (31%), and visual defects (26%). Lesions are often monofocal rather than multifocal and the most common site of involvement is the frontal lobe.6 Among MS patients with natalizumab-associated PML, 30% to 40% have gadolinium-enhancing lesions on magnetic resonance imaging (MRI) at the time of diagnosis.
IMMUNE RECONSTITUTION INFLAMMATORY SYNDROME
Among patients with HIV, predictors for the development of IRIS include antiretroviral naiveté, profoundly low CD4 lymphocyte counts (< 50 cells/mm3), a rapid decrease in HIV load, and the presence of active or subclinical opportunistic infections at the time of initiation of combined antiretroviral therapy. Tan and colleagues8 have reported the largest series to date. Of the 54 patients in their series, 36 developed PML and IRIS simultaneously, and 18 had worsening of preexisting PML. Although some investigators have recommended corticosteroid therapy for PML-IRIS, no controlled trials have been conducted and caution has been advised, particularly in patients without contrast enhancement on MRI or mass effect.
DIAGNOSTIC TESTING: NEUROIMAGING, CEREBROSPINAL FLUID ANALYSIS
Neuroimaging, including computed tomography (CT) and MRI, is a useful diagnostic tool for investigating a patient with PML. Cerebrospinal fluid (CSF) analysis for the presence of JC virus (JCV) may play a significant role, but it primarily serves to rule out other illnesses.
Computed tomography: lesion size may not reflect clinical status
On CT, demyelinating lesions appear as subcortical hypodensities, often with a propensity for parietooccipital areas that are confined to the white matter at the junction interface of the gray-white junction of the cortex.9–11 Lesions may be seen in the corpus callosum, thalamus, and basal ganglia,9 but changes in the size of lesions observed on CT do not necessarily reflect clinical progression.12 Prior to the availability of highly active antiretroviral therapy (HAART) for the treatment of AIDS, mass effect was exceptionally rare. However, the development of IRIS with PML, typically in AIDS patients following the use of HAART, may be associated with edema.13 Single-dose intravenous contrast and delayed, double-dose contrast CT scanning enhancement is observed in a minority of patients, typically fewer than 10%.8 This enhancement is generally faint and peripherally located.
Magnetic resonance imaging may show lesions before clinical disease
MRI is vastly more sensitive than CT in detecting the demyelinating lesions of PML.9,14 On rare occasions, MRI will clearly demonstrate pathology when CT is normal. In fact, MRI may show lesions in advance of clinically apparent disease.15 The characteristics of these lesions are hyperintensity on T2-weighted imaging, fluid-attenuated inversion recovery sequences, and hypointensity on T1-weighted image. Apparent diffusion coefficients (ADC) on MRI are typically normal to low in new lesions and at the advancing edge of lesions; the ADC was typically higher in the center of lesions.16
As observed on CT, approximately 10% of patients exhibit a faint rim of gadolinium enhancement.2,9 Enhancement is more common with PML-IRIS, and the distribution of lesions parallels what is seen pathologically. Enhancement PML lesions have altered signal characteristics compared with the surrounding white matter.9,17–19 In contrast, 15% of HIV-associated PML showed gadolinium enhancement on MRI at the time of diagnosis.6,9
Cerebrospinal fluid analysis
With the exception of polymerase chain reaction (PCR) for JCV, the primary utility of lumbar puncture in the setting of possible PML is to exclude the presence of other illnesses, including treatable infections.
CSF findings in patients with PML are nonspecific, with most patients demon strating a normal profile. A mild lymphocytic pleocytosis, which is rarely (if ever) more than 25 leukocytes/mL, occurs in 15% of patients. Total protein level is mildly elevated in approximately 20% to 30% of patients.
The CSF examination in HIV-infected patients with PML may reflect changes associated with HIV: low-grade lymphocytic pleocytosis (< 20 cells/mm3), mildly elevated protein (< 65 mg/dL), and elevated immunoglobulin G and oligoclonal bands. These abnormalities should not be attributed to PML.
DIAGNOSIS
The most reliable and accurate method for the diagnosis of PML remains brain biopsy that demonstrates the characteristic triad of histopathologic findings (demyelination, bizarre astrocytes, and enlarged oligodendrocyte nuclei) coupled with evidence of JCV infection. With respect to the latter, in situ hybridization or immunocytochemistry can be employed. In situ DNADNA hybridization is a method of annealing JCV DNA to complementary strands either in paraffin-embedded tissue or in frozen sections from biopsy samples.
In immunocytochemistry, antibodies to both T antigen and the common polyomavirus capsid antigen are used to detect cells undergoing productive viral infection. Cells that are positive by in situ hybridization are in a stage of active viral replication. Cells positive by immunocytochemistry that are expressing viral capsid antigens are in a stage of viral transcription and translation (ie, undergoing productive infection). In addition to their utility in confirming a diagnosis of PML, these techniques have demonstrated the presence of JCV in perivascular locations and at sites distant from foci of demyelination. Alternatively, PCR may be used to demonstrate JCV in brain tissue.
In the absence of biopsy, which few deem necessary today, a widely employed approach to diagnosis requires the demonstration of:
- JCV in the CSF by PCR
- Compatible clinical presentation
- An MRI finding consistent with PML
- No other alternative diagnosis.
With an ultrasensitive PCR technique, sensitivities should approach or may exceed 95%, but PCR sensitivity remains at 75% in some laboratories. Because the viral copy numbers in the CSF may be low, particularly in a patient treated with a monoclonal antibody such as natalizumab, the CSF PCR may be falsely negative.
If clinical suspicion of the disease remains high in the face of an initially negative CSF JCV, the CSF analysis should be repeated. CSF analysis for JCV is approximately 99% specific, but recent studies demonstrating low copy numbers of JCV in the CSF of patients with MS have raised concerns about potential pitfalls of this assay.20
PROGNOSIS
Until recently, PML was regarded as virtually universally fatal. The mean survival in the pre-AIDS era was approximately 6 months, and mortality was 80% within 9 months of disease onset. Rarely, patients had long survivals that ranged from 5 years to 19 years.
In the early years of the AIDS era, survival with PML did not appear to differ significantly from that observed in the pre-AIDS years. In the largest study of HIV-associated PML in the era prior to HAART, the median survival was 183 days.2 However, the majority of individuals were dead within 3 months of diagnosis. Only 8% to 10% of patients survived longer than 12 months, which has been regarded as “prolonged survival.” This long survival skewed the mean and median survival rates in this population.
Several factors have since been identified that correlate with prolonged survival in HIV-associated PML, including PML as the heralding manifestation of HIV, CD4 counts exceeding 300 cells per mm3, contrast enhancement of the lesions on radiographic imaging, low copy number or decreasing JCV titers in CSF,21–24 and the presence of JCV-specific cytotoxic T cells.25 A better prognosis has also been postulated for higher CSF levels of macrophage chemoattractant protein-126 and PML associated with JCV VP1 loop-specific polymorphisms.27
Prognosis of HIV-associated PML improves with immune system restoration
In the era of HAART, not only has the incidence of HIV-associated PML declined, but the prognosis of affected patients has improved as well. This development highlights the importance of restoration of the immune system in both disease prevention and survival. Some estimate that as many as 50% of HAART-treated patients with PML exhibit prolonged survival. In one study of 25 patients, the median survival was more than 46 weeks.28
Nonetheless, PML continues to have the worst prognosis of any AIDS-related cerebral disorder, with those having advanced immunosuppression being most susceptible to the disorder. For AIDS patients with PML, those who were HAART-naïve at the time of diagnosis appear to have better survival than treatment-experienced patients.29 Survival also correlates with reduced JCV load in the CSF30 and improved CD4 lymphocyte counts (CD4 counts > 100 cells/mm3).31
Prognosis of natalizumab-associated PML is different
The prognosis of natalizumab-associated PML differs from that of HIV-associated PML. In a series of 35 patients, 25 (71%) patients were alive on average 6 months after diagnosis.32 Prognosis was worse with a longer time to diagnosis and the presence of widespread disease.
Most deaths in patients taking natalizumab who developed PML have occurred during IRIS. Steroid treatment of IRIS appears to improve prognosis,8 but no scientifically rigorous study has been undertaken to demonstrate this recommendation.7 Among the survivors, neurologic deficit was mild in one-third, moderate in one-third, and severe in one-third of patients.
CONCLUSION: DISPELLING SOME MYTHS
Several assumptions about PML are not necessarily true. For example, although PML implies the presence of multifocal lesions as a characteristic of the disease, the lesions may be monofocal, especially with natalizumab-associated PML. The lesions of PML may show early gadolinium enhancement on neuroimaging. Although lesions typically are seen in subcortical white matter, cortical involvement also may be observed. Cerebellar granular cell degeneration may occur in association with PML or in isolation. Disease progression and death are not inevitable, even in the absence of treatment. The most important determinant for survival is restoration of the immune system.
DISCUSSION
Dr. Calabrese: Why are sensory deficits so common?
Dr. Berger: We don’t know. Because we see involvement in the parietal lobe, we would anticipate observing sensory deficits. I think that a lot of sensation occurs deep in the thalamic area, which is not often involved in PML. Also, we often don’t test for some of the deficits that may occur.
Dr. Rudick: Do you know of any cases of natalizumab-associated PML detected as an incidental finding on MRI, making a case for screening MRI in patients without clinical symptoms?
Dr. Berger: There have been a handful of cases, including one of the seminal cases of natalizumab-associated PML, in which MRI abnormalities were observed in advance of clinically recognized symptomatology.
Dr. Calabrese: The correlate question is, if a patient with a risk factor—be it HIV or treatment with a biologic agent—has a common neurocognitive sign or perhaps some subtle motor findings, does a normal MRI have 100% negative predictive value?
Dr. Berger: I have yet to see somebody with PML who has a normal MRI.
Dr. Simpson: What you may see are lesions that are not typical MRI lesions of white matter hypointensity. In some cases, as Dr. Berger mentioned in his summary, we’ll see cerebellar degeneration—atrophy—but not necessarily white matter lesions.
- Brooks BR, Walker DL. Progressive multifocal leukoencephalopathy. Neurol Clin 1984; 2:299–313.
- Berger JR, Pall L, Lanska D, Whiteman M. Progressive multifocal leukoencephalopathy in patients with HIV infection. J Neurovirol 1998; 4:59–68.
- Parr J, Horoupian DS, Winkelman AC. Cerebellar form of progressive multifocal leukoencephalopathy (PML). Can J Neurol Sci 1979; 6:123–128.
- Jones HR, Hedley-Whyte ET, Freidberg SR, Kelleher JE, Krolikowski J. Primary cerebellopontine progressive multifocal leukoencephalopathy diagnosed premortem by cerebellar biopsy. Ann Neurol 1982; 11:199–202.
- O’Riordan S, McGuigan C, Farrell M, Hutchinson M. Progressive multifocal leucoencephalopathy presenting with parkinsonism. J Neurol 2003; 250:1379–1381.
- Clifford DB, De Luca A, Simpson DM, Arendt G, Giovannoni G, Nath A. Natalizumab-associated progressive multifocal leukoencephalopathy in patients with multiple sclerosis: lessons from 28 cases. Lancet Neurol 2010; 9:438–446.
- Berger JR. Steroids for PML-IRIS. A double-edged sword? Neurology 2009; 72:1454–1455.
- Tan K, Roda R, Ostrow L, McArthur J, Nath A. PML-IRIS in patients with HIV infection: clinical manifestations and treatment with steroids. Neurology 2009; 72:1458–1464.
- Whiteman ML, Post MJ, Berger JR, Tate LG, Bell MD, Limonte LP. Progressive multifocal leukoencephalopathy in 47 HIV-seropositive patients: neuroimaging with clinical and pathologic correlation. Radiology 1993; 187:233–240.
- Conomy JP, Weinstein MA, Agamanolis D, Holt WS. Computed tomography in progressive multifocal leukoencephalopathy. AJR Am J Roentgenol 1976; 127:663–665.
- Huckman MS. Computed tomography in the diagnosis of degenerative brain disease. Radiol Clin North Am 1982; 20:169–183.
- Krupp LB, Lipton RB, Swerdlow ML, Leeds NE, Llena J. Progressive multifocal leukoencephalopathy: clinical and radiographic features. Ann Neurol 1985; 17:344–349.
- Rushing EJ, Liappis A, Smirniotopoulos JD, et al. Immune reconstitution inflammatory syndrome of the brain: case illustrations of a challenging entity. J Neuropathol Exp Neurol 2008; 67:819–827.
- Post MJ, Sheldon JJ, Hensley GT, et al. Central nervous system disease in acquired immunodeficiency syndrome: prospective correlation using CT, MR imaging, and pathologic studies. Radiology 1986; 158:141–148.
- Langer-Gould A, Atlas SW, Green AJ, Bollen AW, Pelletier D. Progressive multifocal leukoencephalopathy in a patient treated with natalizumab. N Engl J Med 2005; 353:375–381.
- Bergui M, Bradac GB, Oguz KK, et al. Progressive multifocal leukoencephalopathy: diffusion-weighted imaging and pathological correlations. Neuroradiology 2004; 46:22–25.
- Guilleux MH, Steiner RE, Young IR. MR imaging in progressive multifocal leukoencephalopathy. AJNR Am J Neuroradiol 1986; 7:1033–1035.
- Levy JD, Cottingham KL, Campbell RJ, et al. Progressive multifocal leukoencephalopathy and magnetic resonance imaging. Ann Neurol 1986; 19:399–401.
- Mark AS, Atlas SW. Progressive multifocal leukoencephalopathy in patients with AIDS: appearance on MR images. Radiology 1989; 173:517–520.
- Iacobaeus E, Ryschkewitsch C, Gravell M, et al. Analysis of cerebrospinal fluid and cerebrospinal fluid cells from patients with multiple sclerosis for detection of JC virus DNA. Mult Scler 2009; 15:28–35.
- Berger JR, Levy RM, Flomenhoft D, Dobbs M. Predictive factors for prolonged survival in acquired immunodeficiency syndrome-associated progressive multifocal leukoencephalopathy. Ann Neurol 1998; 44:341–349.
- Taoufik Y, Gasnault J, Karaterki A, et al. Prognostic value of JC virus load in cerebrospinal fluid of patients with progressive multifocal leukoencephalopathy. J Infect Dis 1998; 178:1816–1820.
- Yiannoutsos CT, Major EO, Curfman B, et al. Relation of JC virus DNA in the cerebrospinal fluid to survival in acquired immunodeficiency syndrome patients with biopsy-proven progressive multifocal leukoencephalopathy. Ann Neurol 1999; 45:816–821.
- Bossolasco S, Calori G, Moretti F, et al. Prognostic significance of JC virus DNA levels in cerebrospinal fluid of patients with HIV-associated progressive multifocal leukoencephalopathy. Clin Infect Dis 2005; 40:738–744.
- Du Pasquier RA, Clark KW, Smith PS, et al. JCV-specific cellular immune response correlates with a favorable clinical outcome in HIV-infected individuals with progressive multifocal leukoencephalopathy. J Neurovirol 2001; 7:318–322.
- Marzocchetti A, Cingolani A, Giambenedetto SD, et al. Macrophage chemoattractant protein-1 levels in cerebrospinal fluid correlate with containment of JC virus and prognosis of acquired immunodeficiency syndrome-associated progressive multifocal leukoencephalopathy. J Neurovirol 2005; 11:219–224.
- Delbue S, Branchetti E, Bertolacci S, et al. JC virus VP1 loop-specific polymorphisms are associated with favorable prognosis for progressive multifocal leukoencephalopathy. J Neurovirol 2009; 15:51–56.
- Clifford DB, Yiannoutsos C, Glicksman M, et al. HAART improves prognosis in HIV-associated progressive multifocal leukoencephalopathy. Neurology 1999; 52:623–625.
- Wyen C, Hoffmann C, Schmeisser N, et al. Progressive multi focal leukoencephalopathy in patients on highly active antiretroviral therapy: survival and risk factors of death. J Acquir Immune Defic Syndr 2004; 37:1263–1268.
- De Luca A, Giancola ML, Ammassari A, et al. The effect of potent antiretroviral therapy and JC virus load in cerebrospinal fluid on clinical outcome of patients with AIDS-associated progressive multifocal leukoencephalopathy. J Infect Dis 2000; 182:1077–1083.
- Berenguer J, Miralles P, Arrizabalaga J, et al. Clinical course and prognostic factors of progressive multifocal leukoencephalopathy in patients treated with highly active antiretroviral therapy. Clin Infect Dis 2003; 36:1047–1052.
- Vermersch P, Kappos L, Gold R, et al. Clinical outcomes of natalizumab associated progressive multifocal leukoencephalopathy. Neurology 2011; 76:1697–1704.
- Brooks BR, Walker DL. Progressive multifocal leukoencephalopathy. Neurol Clin 1984; 2:299–313.
- Berger JR, Pall L, Lanska D, Whiteman M. Progressive multifocal leukoencephalopathy in patients with HIV infection. J Neurovirol 1998; 4:59–68.
- Parr J, Horoupian DS, Winkelman AC. Cerebellar form of progressive multifocal leukoencephalopathy (PML). Can J Neurol Sci 1979; 6:123–128.
- Jones HR, Hedley-Whyte ET, Freidberg SR, Kelleher JE, Krolikowski J. Primary cerebellopontine progressive multifocal leukoencephalopathy diagnosed premortem by cerebellar biopsy. Ann Neurol 1982; 11:199–202.
- O’Riordan S, McGuigan C, Farrell M, Hutchinson M. Progressive multifocal leucoencephalopathy presenting with parkinsonism. J Neurol 2003; 250:1379–1381.
- Clifford DB, De Luca A, Simpson DM, Arendt G, Giovannoni G, Nath A. Natalizumab-associated progressive multifocal leukoencephalopathy in patients with multiple sclerosis: lessons from 28 cases. Lancet Neurol 2010; 9:438–446.
- Berger JR. Steroids for PML-IRIS. A double-edged sword? Neurology 2009; 72:1454–1455.
- Tan K, Roda R, Ostrow L, McArthur J, Nath A. PML-IRIS in patients with HIV infection: clinical manifestations and treatment with steroids. Neurology 2009; 72:1458–1464.
- Whiteman ML, Post MJ, Berger JR, Tate LG, Bell MD, Limonte LP. Progressive multifocal leukoencephalopathy in 47 HIV-seropositive patients: neuroimaging with clinical and pathologic correlation. Radiology 1993; 187:233–240.
- Conomy JP, Weinstein MA, Agamanolis D, Holt WS. Computed tomography in progressive multifocal leukoencephalopathy. AJR Am J Roentgenol 1976; 127:663–665.
- Huckman MS. Computed tomography in the diagnosis of degenerative brain disease. Radiol Clin North Am 1982; 20:169–183.
- Krupp LB, Lipton RB, Swerdlow ML, Leeds NE, Llena J. Progressive multifocal leukoencephalopathy: clinical and radiographic features. Ann Neurol 1985; 17:344–349.
- Rushing EJ, Liappis A, Smirniotopoulos JD, et al. Immune reconstitution inflammatory syndrome of the brain: case illustrations of a challenging entity. J Neuropathol Exp Neurol 2008; 67:819–827.
- Post MJ, Sheldon JJ, Hensley GT, et al. Central nervous system disease in acquired immunodeficiency syndrome: prospective correlation using CT, MR imaging, and pathologic studies. Radiology 1986; 158:141–148.
- Langer-Gould A, Atlas SW, Green AJ, Bollen AW, Pelletier D. Progressive multifocal leukoencephalopathy in a patient treated with natalizumab. N Engl J Med 2005; 353:375–381.
- Bergui M, Bradac GB, Oguz KK, et al. Progressive multifocal leukoencephalopathy: diffusion-weighted imaging and pathological correlations. Neuroradiology 2004; 46:22–25.
- Guilleux MH, Steiner RE, Young IR. MR imaging in progressive multifocal leukoencephalopathy. AJNR Am J Neuroradiol 1986; 7:1033–1035.
- Levy JD, Cottingham KL, Campbell RJ, et al. Progressive multifocal leukoencephalopathy and magnetic resonance imaging. Ann Neurol 1986; 19:399–401.
- Mark AS, Atlas SW. Progressive multifocal leukoencephalopathy in patients with AIDS: appearance on MR images. Radiology 1989; 173:517–520.
- Iacobaeus E, Ryschkewitsch C, Gravell M, et al. Analysis of cerebrospinal fluid and cerebrospinal fluid cells from patients with multiple sclerosis for detection of JC virus DNA. Mult Scler 2009; 15:28–35.
- Berger JR, Levy RM, Flomenhoft D, Dobbs M. Predictive factors for prolonged survival in acquired immunodeficiency syndrome-associated progressive multifocal leukoencephalopathy. Ann Neurol 1998; 44:341–349.
- Taoufik Y, Gasnault J, Karaterki A, et al. Prognostic value of JC virus load in cerebrospinal fluid of patients with progressive multifocal leukoencephalopathy. J Infect Dis 1998; 178:1816–1820.
- Yiannoutsos CT, Major EO, Curfman B, et al. Relation of JC virus DNA in the cerebrospinal fluid to survival in acquired immunodeficiency syndrome patients with biopsy-proven progressive multifocal leukoencephalopathy. Ann Neurol 1999; 45:816–821.
- Bossolasco S, Calori G, Moretti F, et al. Prognostic significance of JC virus DNA levels in cerebrospinal fluid of patients with HIV-associated progressive multifocal leukoencephalopathy. Clin Infect Dis 2005; 40:738–744.
- Du Pasquier RA, Clark KW, Smith PS, et al. JCV-specific cellular immune response correlates with a favorable clinical outcome in HIV-infected individuals with progressive multifocal leukoencephalopathy. J Neurovirol 2001; 7:318–322.
- Marzocchetti A, Cingolani A, Giambenedetto SD, et al. Macrophage chemoattractant protein-1 levels in cerebrospinal fluid correlate with containment of JC virus and prognosis of acquired immunodeficiency syndrome-associated progressive multifocal leukoencephalopathy. J Neurovirol 2005; 11:219–224.
- Delbue S, Branchetti E, Bertolacci S, et al. JC virus VP1 loop-specific polymorphisms are associated with favorable prognosis for progressive multifocal leukoencephalopathy. J Neurovirol 2009; 15:51–56.
- Clifford DB, Yiannoutsos C, Glicksman M, et al. HAART improves prognosis in HIV-associated progressive multifocal leukoencephalopathy. Neurology 1999; 52:623–625.
- Wyen C, Hoffmann C, Schmeisser N, et al. Progressive multi focal leukoencephalopathy in patients on highly active antiretroviral therapy: survival and risk factors of death. J Acquir Immune Defic Syndr 2004; 37:1263–1268.
- De Luca A, Giancola ML, Ammassari A, et al. The effect of potent antiretroviral therapy and JC virus load in cerebrospinal fluid on clinical outcome of patients with AIDS-associated progressive multifocal leukoencephalopathy. J Infect Dis 2000; 182:1077–1083.
- Berenguer J, Miralles P, Arrizabalaga J, et al. Clinical course and prognostic factors of progressive multifocal leukoencephalopathy in patients treated with highly active antiretroviral therapy. Clin Infect Dis 2003; 36:1047–1052.
- Vermersch P, Kappos L, Gold R, et al. Clinical outcomes of natalizumab associated progressive multifocal leukoencephalopathy. Neurology 2011; 76:1697–1704.