User login
University of Chicago Hospitalist Scholars Program Wins Award
Under the leadership of David Meltzer, MD, PhD, MHM, the University of Chicago Hospitalist Scholars Program is one of 13 organizations to earn the prestigious Association of American Medical Colleges’ Learning Health System Challenge and Planning Awards.
The program provides training in research, medical education, and quality improvement to help young physicians develop into successful academic hospitalists who can become leaders in these domains. Required resources include mentorship and opportunities for formal didactic instruction for the scholars and a functioning clinical research environment.
The AAMC Learning Health System Challenge and Planning Awards recognize innovations in medical education, care delivery, research, and diversity and inclusion.
Under the leadership of David Meltzer, MD, PhD, MHM, the University of Chicago Hospitalist Scholars Program is one of 13 organizations to earn the prestigious Association of American Medical Colleges’ Learning Health System Challenge and Planning Awards.
The program provides training in research, medical education, and quality improvement to help young physicians develop into successful academic hospitalists who can become leaders in these domains. Required resources include mentorship and opportunities for formal didactic instruction for the scholars and a functioning clinical research environment.
The AAMC Learning Health System Challenge and Planning Awards recognize innovations in medical education, care delivery, research, and diversity and inclusion.
Under the leadership of David Meltzer, MD, PhD, MHM, the University of Chicago Hospitalist Scholars Program is one of 13 organizations to earn the prestigious Association of American Medical Colleges’ Learning Health System Challenge and Planning Awards.
The program provides training in research, medical education, and quality improvement to help young physicians develop into successful academic hospitalists who can become leaders in these domains. Required resources include mentorship and opportunities for formal didactic instruction for the scholars and a functioning clinical research environment.
The AAMC Learning Health System Challenge and Planning Awards recognize innovations in medical education, care delivery, research, and diversity and inclusion.
Physician Value-Based Payment Modifier To Make Changes for Hospitalists
“No man is an island.” Many of the reforms included in the Affordable Care Act (ACA) and other major healthcare legislation in the past decade put that sentiment into practice. This is a seismic shift in medicine and one that will reshape the way consumers and providers understand and relate to the healthcare system.
For consumers, the mandate to maintain health insurance coverage suggests the existence of a shared responsibility around health and wellness. This idea of community is central to many of the reforms for providers, as well. Value-based payment programs for both physicians and hospitals suggest that, given a scarce set of healthcare resources, we should be making sure that what Medicare is purchasing is of value. Even more telling, value is increasingly considered within a context of team-based and coordinated care. The future of healthcare, it seems, is pinned squarely on working together toward a common good.
The Physician Value-Based Payment Modifier (VBPM) is complementary to hospital value-based purchasing, moving the basis of physician payment toward the quality of care delivered, not simply the quantity of services rendered. The cost measures in the VBPM are unambiguously aligned with this ethos of community. Resource use per beneficiary is evaluated as an expression of the total costs borne by the healthcare system annually or within the context of an episode of care. So, in the value modifier, hospitalist groups can expect to see not just the costs that they charge, but also the costs of other physicians and other groups caring for the same Medicare patients. This is an explicit recognition of the myriad of providers engaged with each patient and their collective impact on the healthcare system.
At the same time, the VBPM strives to compare physicians by specialty, acknowledging that these separate communities within the healthcare system have different costs, patterns, and norms. For hospitalists, this comparison highlights some of the complexities of professional identity in what is still a relatively new field. For the measures to be meaningful and actionable, it is critical that comparisons be made amongst like providers.
SHM, through its Public Policy Committee and Performance Measurement and Reporting Committee, is diligently working to ensure that hospitalists are able to report on quality measures that make sense for their practices and that assessments are based on applicable and useful data for quality improvement. At the same time, these committees are working to ensure that hospitalists are evaluated using fair comparisons. In other words, hospitalists should be compared with other hospitalists.
At SHM’s annual meeting next month in Las Vegas (www.hospitalmedicine2014.org), healthcare reform will be discussed in greater detail during two sessions. One will focus on the current state of the ACA and reform efforts in general, and the other will be a workshop focusing specifically on participation in the VBPM. It is imperative that hospitalists are prepared to be successful as many of these changes unfold.
Joshua Lapps is SHM’s government relations specialist.
“No man is an island.” Many of the reforms included in the Affordable Care Act (ACA) and other major healthcare legislation in the past decade put that sentiment into practice. This is a seismic shift in medicine and one that will reshape the way consumers and providers understand and relate to the healthcare system.
For consumers, the mandate to maintain health insurance coverage suggests the existence of a shared responsibility around health and wellness. This idea of community is central to many of the reforms for providers, as well. Value-based payment programs for both physicians and hospitals suggest that, given a scarce set of healthcare resources, we should be making sure that what Medicare is purchasing is of value. Even more telling, value is increasingly considered within a context of team-based and coordinated care. The future of healthcare, it seems, is pinned squarely on working together toward a common good.
The Physician Value-Based Payment Modifier (VBPM) is complementary to hospital value-based purchasing, moving the basis of physician payment toward the quality of care delivered, not simply the quantity of services rendered. The cost measures in the VBPM are unambiguously aligned with this ethos of community. Resource use per beneficiary is evaluated as an expression of the total costs borne by the healthcare system annually or within the context of an episode of care. So, in the value modifier, hospitalist groups can expect to see not just the costs that they charge, but also the costs of other physicians and other groups caring for the same Medicare patients. This is an explicit recognition of the myriad of providers engaged with each patient and their collective impact on the healthcare system.
At the same time, the VBPM strives to compare physicians by specialty, acknowledging that these separate communities within the healthcare system have different costs, patterns, and norms. For hospitalists, this comparison highlights some of the complexities of professional identity in what is still a relatively new field. For the measures to be meaningful and actionable, it is critical that comparisons be made amongst like providers.
SHM, through its Public Policy Committee and Performance Measurement and Reporting Committee, is diligently working to ensure that hospitalists are able to report on quality measures that make sense for their practices and that assessments are based on applicable and useful data for quality improvement. At the same time, these committees are working to ensure that hospitalists are evaluated using fair comparisons. In other words, hospitalists should be compared with other hospitalists.
At SHM’s annual meeting next month in Las Vegas (www.hospitalmedicine2014.org), healthcare reform will be discussed in greater detail during two sessions. One will focus on the current state of the ACA and reform efforts in general, and the other will be a workshop focusing specifically on participation in the VBPM. It is imperative that hospitalists are prepared to be successful as many of these changes unfold.
Joshua Lapps is SHM’s government relations specialist.
“No man is an island.” Many of the reforms included in the Affordable Care Act (ACA) and other major healthcare legislation in the past decade put that sentiment into practice. This is a seismic shift in medicine and one that will reshape the way consumers and providers understand and relate to the healthcare system.
For consumers, the mandate to maintain health insurance coverage suggests the existence of a shared responsibility around health and wellness. This idea of community is central to many of the reforms for providers, as well. Value-based payment programs for both physicians and hospitals suggest that, given a scarce set of healthcare resources, we should be making sure that what Medicare is purchasing is of value. Even more telling, value is increasingly considered within a context of team-based and coordinated care. The future of healthcare, it seems, is pinned squarely on working together toward a common good.
The Physician Value-Based Payment Modifier (VBPM) is complementary to hospital value-based purchasing, moving the basis of physician payment toward the quality of care delivered, not simply the quantity of services rendered. The cost measures in the VBPM are unambiguously aligned with this ethos of community. Resource use per beneficiary is evaluated as an expression of the total costs borne by the healthcare system annually or within the context of an episode of care. So, in the value modifier, hospitalist groups can expect to see not just the costs that they charge, but also the costs of other physicians and other groups caring for the same Medicare patients. This is an explicit recognition of the myriad of providers engaged with each patient and their collective impact on the healthcare system.
At the same time, the VBPM strives to compare physicians by specialty, acknowledging that these separate communities within the healthcare system have different costs, patterns, and norms. For hospitalists, this comparison highlights some of the complexities of professional identity in what is still a relatively new field. For the measures to be meaningful and actionable, it is critical that comparisons be made amongst like providers.
SHM, through its Public Policy Committee and Performance Measurement and Reporting Committee, is diligently working to ensure that hospitalists are able to report on quality measures that make sense for their practices and that assessments are based on applicable and useful data for quality improvement. At the same time, these committees are working to ensure that hospitalists are evaluated using fair comparisons. In other words, hospitalists should be compared with other hospitalists.
At SHM’s annual meeting next month in Las Vegas (www.hospitalmedicine2014.org), healthcare reform will be discussed in greater detail during two sessions. One will focus on the current state of the ACA and reform efforts in general, and the other will be a workshop focusing specifically on participation in the VBPM. It is imperative that hospitalists are prepared to be successful as many of these changes unfold.
Joshua Lapps is SHM’s government relations specialist.
HM14 At Hand Mobile App Enhanced Functionality Helps Hospitalists Plan For Annual Meeting

With its added functionality, the HM14 at Hand app is likely to be even more popular. This year, the HM14 at Hand includes:
- Full program schedule, with the ability to schedule and set reminders for selected sessions;
- Options for presenters and conference-goers to provide contact information to other attendees;
- Presentation notes from speakers;
- The “Scan-to-Win” game, with even more locations to scan in 2014;
- Real-time program alerts for breaking news about the conference;
- Links to other resources for hospitalists;
- NEW: Integration with social media to help you connect with other conference bloggers, tweeters, and posters; and
- NEW: A section for job seekers and career networkers to connect with recruiters.
But don’t wait until you get to the meeting to download the app. HM14 at Hand helps hospitalists plan for the meeting ahead of time by highlighting and saving sessions to attend, lists contact information for other attendees who’ve opted to network via the app, and provides conference updates before and during the meeting.

With its added functionality, the HM14 at Hand app is likely to be even more popular. This year, the HM14 at Hand includes:
- Full program schedule, with the ability to schedule and set reminders for selected sessions;
- Options for presenters and conference-goers to provide contact information to other attendees;
- Presentation notes from speakers;
- The “Scan-to-Win” game, with even more locations to scan in 2014;
- Real-time program alerts for breaking news about the conference;
- Links to other resources for hospitalists;
- NEW: Integration with social media to help you connect with other conference bloggers, tweeters, and posters; and
- NEW: A section for job seekers and career networkers to connect with recruiters.
But don’t wait until you get to the meeting to download the app. HM14 at Hand helps hospitalists plan for the meeting ahead of time by highlighting and saving sessions to attend, lists contact information for other attendees who’ve opted to network via the app, and provides conference updates before and during the meeting.

With its added functionality, the HM14 at Hand app is likely to be even more popular. This year, the HM14 at Hand includes:
- Full program schedule, with the ability to schedule and set reminders for selected sessions;
- Options for presenters and conference-goers to provide contact information to other attendees;
- Presentation notes from speakers;
- The “Scan-to-Win” game, with even more locations to scan in 2014;
- Real-time program alerts for breaking news about the conference;
- Links to other resources for hospitalists;
- NEW: Integration with social media to help you connect with other conference bloggers, tweeters, and posters; and
- NEW: A section for job seekers and career networkers to connect with recruiters.
But don’t wait until you get to the meeting to download the app. HM14 at Hand helps hospitalists plan for the meeting ahead of time by highlighting and saving sessions to attend, lists contact information for other attendees who’ve opted to network via the app, and provides conference updates before and during the meeting.
Movers and Shakers in Hospital Medicine
HM MOVERS AND SHAKERS





Business Moves
Sound Physicians, based in Tacoma, Wash., is now providing hospitalist services at both Christus Santa Rosa Health System in San Antonio, Texas, and John Peter Smith Hospital in Fort Worth, Texas. Christus Santa Rosa consists of four acute care hospitals, the Children’s Hospital of San Antonio, and several outpatient clinics and emergency centers in the greater San Antonio area. John Peter Smith Hospital is a 537-bed trauma center serving the central Fort Worth area.
IPC The Hospitalist Company, based in North Hollywood, Calif., has acquired the practice groups of Bruce G. Johnson, DO, PC, in Roseville, Mich.; Allen Trager, DO, PC, in Flint, Mich.; and Victor Toledano, MD, PA, in Ft. Lauderdale, Fla. IPC also completed its acquisition of Park Avenue Health Care Management, LLC; Park Avenue Medical Associates, PC; Park Avenue Medical Associates, LLC; and Geriatric Services, PC, (collectively, “Park Avenue”), all based in White Plains, N.Y. IPC now provides hospitalist services in 28 states.
Heart of Lancaster Regional Medical Center in Lititz, Pa., is now providing pediatric hospitalist services. Initially, the program will staff six pediatric hospitalists at the 148-bed facility. The facility joins Lancaster General Hospital as the second in the county to provide pediatric hospital medicine services.
Morthland College Health Services (MCHS) in West Frankfort, Ill., has assumed coverage of hospitalist services at Harrisburg Medical Center (HMC) in Harrisburg, Ill. MCHS already provides hospital medicine services at Franklin Hospital in Benton, Ill. Morthland College is a small liberal arts college founded in 2009. Harrisburg Medical Center is a 98-bed acute care hospital serving greater Saline County, Ill.
The Ob Hospitalist Group (OBHG), based in Mauldin, S.C., is providing services to Bayhealth Milford Memorial Hospital in Milford, Del. Milford Memorial has served communities in the Milford area since 1938. OBHG provides inpatient OB/GYN services to nearly 50 hospitals and clinics nationwide.
St. Alexius Medical Center in Bismarck, N.D., has partnered with the University of North Dakota to institute a new hospitalist fellowship program in North Dakota. The one-year program is the first of its kind in North Dakota.
HM MOVERS AND SHAKERS





Business Moves
Sound Physicians, based in Tacoma, Wash., is now providing hospitalist services at both Christus Santa Rosa Health System in San Antonio, Texas, and John Peter Smith Hospital in Fort Worth, Texas. Christus Santa Rosa consists of four acute care hospitals, the Children’s Hospital of San Antonio, and several outpatient clinics and emergency centers in the greater San Antonio area. John Peter Smith Hospital is a 537-bed trauma center serving the central Fort Worth area.
IPC The Hospitalist Company, based in North Hollywood, Calif., has acquired the practice groups of Bruce G. Johnson, DO, PC, in Roseville, Mich.; Allen Trager, DO, PC, in Flint, Mich.; and Victor Toledano, MD, PA, in Ft. Lauderdale, Fla. IPC also completed its acquisition of Park Avenue Health Care Management, LLC; Park Avenue Medical Associates, PC; Park Avenue Medical Associates, LLC; and Geriatric Services, PC, (collectively, “Park Avenue”), all based in White Plains, N.Y. IPC now provides hospitalist services in 28 states.
Heart of Lancaster Regional Medical Center in Lititz, Pa., is now providing pediatric hospitalist services. Initially, the program will staff six pediatric hospitalists at the 148-bed facility. The facility joins Lancaster General Hospital as the second in the county to provide pediatric hospital medicine services.
Morthland College Health Services (MCHS) in West Frankfort, Ill., has assumed coverage of hospitalist services at Harrisburg Medical Center (HMC) in Harrisburg, Ill. MCHS already provides hospital medicine services at Franklin Hospital in Benton, Ill. Morthland College is a small liberal arts college founded in 2009. Harrisburg Medical Center is a 98-bed acute care hospital serving greater Saline County, Ill.
The Ob Hospitalist Group (OBHG), based in Mauldin, S.C., is providing services to Bayhealth Milford Memorial Hospital in Milford, Del. Milford Memorial has served communities in the Milford area since 1938. OBHG provides inpatient OB/GYN services to nearly 50 hospitals and clinics nationwide.
St. Alexius Medical Center in Bismarck, N.D., has partnered with the University of North Dakota to institute a new hospitalist fellowship program in North Dakota. The one-year program is the first of its kind in North Dakota.
HM MOVERS AND SHAKERS





Business Moves
Sound Physicians, based in Tacoma, Wash., is now providing hospitalist services at both Christus Santa Rosa Health System in San Antonio, Texas, and John Peter Smith Hospital in Fort Worth, Texas. Christus Santa Rosa consists of four acute care hospitals, the Children’s Hospital of San Antonio, and several outpatient clinics and emergency centers in the greater San Antonio area. John Peter Smith Hospital is a 537-bed trauma center serving the central Fort Worth area.
IPC The Hospitalist Company, based in North Hollywood, Calif., has acquired the practice groups of Bruce G. Johnson, DO, PC, in Roseville, Mich.; Allen Trager, DO, PC, in Flint, Mich.; and Victor Toledano, MD, PA, in Ft. Lauderdale, Fla. IPC also completed its acquisition of Park Avenue Health Care Management, LLC; Park Avenue Medical Associates, PC; Park Avenue Medical Associates, LLC; and Geriatric Services, PC, (collectively, “Park Avenue”), all based in White Plains, N.Y. IPC now provides hospitalist services in 28 states.
Heart of Lancaster Regional Medical Center in Lititz, Pa., is now providing pediatric hospitalist services. Initially, the program will staff six pediatric hospitalists at the 148-bed facility. The facility joins Lancaster General Hospital as the second in the county to provide pediatric hospital medicine services.
Morthland College Health Services (MCHS) in West Frankfort, Ill., has assumed coverage of hospitalist services at Harrisburg Medical Center (HMC) in Harrisburg, Ill. MCHS already provides hospital medicine services at Franklin Hospital in Benton, Ill. Morthland College is a small liberal arts college founded in 2009. Harrisburg Medical Center is a 98-bed acute care hospital serving greater Saline County, Ill.
The Ob Hospitalist Group (OBHG), based in Mauldin, S.C., is providing services to Bayhealth Milford Memorial Hospital in Milford, Del. Milford Memorial has served communities in the Milford area since 1938. OBHG provides inpatient OB/GYN services to nearly 50 hospitals and clinics nationwide.
St. Alexius Medical Center in Bismarck, N.D., has partnered with the University of North Dakota to institute a new hospitalist fellowship program in North Dakota. The one-year program is the first of its kind in North Dakota.
Society of Hospital Medicine’s Project BOOST Reduces Medicare Penalties and Readmissions
SHM’s Project BOOST is accepting applications for its 2014 cohort, giving hospitalists and hospital-based team members time to complete the application and receive buy-in from hospital executives to participate in the program.
And this year is the best year yet to make the case to hospital leadership for using Project BOOST to reduce hospital readmissions. More than 180 hospitals throughout the U.S. have used Project BOOST to systematically tackle readmissions.
Last year, the first peer-reviewed research on Project BOOST, published in the Journal of Hospital Medicine, showed that the program reduced 30-day readmissions to 12.7% from 14.7% among 11 hospitals participating in the study. In addition, media and government agencies taking a hard look at readmissions rates have also used Project BOOST as an example of programs that can reduce readmissions and avoid Medicare penalties.1
Accepted Project BOOST sites begin the yearlong program with an in-person training conference with other BOOST sites. After the training, participants utilize a comprehensive toolkit to begin implementing their own programs, followed by ongoing mentoring with national experts in reducing readmissions and collaboration with other hospitals tackling similar challenges.
Details, educational resources, and free on-demand webinars are available at www.hospitalmedicine.org/projectboost.
Brendon Shank is SHM’s associate vice president of communications.
Reference
SHM’s Project BOOST is accepting applications for its 2014 cohort, giving hospitalists and hospital-based team members time to complete the application and receive buy-in from hospital executives to participate in the program.
And this year is the best year yet to make the case to hospital leadership for using Project BOOST to reduce hospital readmissions. More than 180 hospitals throughout the U.S. have used Project BOOST to systematically tackle readmissions.
Last year, the first peer-reviewed research on Project BOOST, published in the Journal of Hospital Medicine, showed that the program reduced 30-day readmissions to 12.7% from 14.7% among 11 hospitals participating in the study. In addition, media and government agencies taking a hard look at readmissions rates have also used Project BOOST as an example of programs that can reduce readmissions and avoid Medicare penalties.1
Accepted Project BOOST sites begin the yearlong program with an in-person training conference with other BOOST sites. After the training, participants utilize a comprehensive toolkit to begin implementing their own programs, followed by ongoing mentoring with national experts in reducing readmissions and collaboration with other hospitals tackling similar challenges.
Details, educational resources, and free on-demand webinars are available at www.hospitalmedicine.org/projectboost.
Brendon Shank is SHM’s associate vice president of communications.
Reference
SHM’s Project BOOST is accepting applications for its 2014 cohort, giving hospitalists and hospital-based team members time to complete the application and receive buy-in from hospital executives to participate in the program.
And this year is the best year yet to make the case to hospital leadership for using Project BOOST to reduce hospital readmissions. More than 180 hospitals throughout the U.S. have used Project BOOST to systematically tackle readmissions.
Last year, the first peer-reviewed research on Project BOOST, published in the Journal of Hospital Medicine, showed that the program reduced 30-day readmissions to 12.7% from 14.7% among 11 hospitals participating in the study. In addition, media and government agencies taking a hard look at readmissions rates have also used Project BOOST as an example of programs that can reduce readmissions and avoid Medicare penalties.1
Accepted Project BOOST sites begin the yearlong program with an in-person training conference with other BOOST sites. After the training, participants utilize a comprehensive toolkit to begin implementing their own programs, followed by ongoing mentoring with national experts in reducing readmissions and collaboration with other hospitals tackling similar challenges.
Details, educational resources, and free on-demand webinars are available at www.hospitalmedicine.org/projectboost.
Brendon Shank is SHM’s associate vice president of communications.
Reference
Centers for Medicare & Medicaid Services Modify Physician Quality Reporting System
Only 27% of eligible providers participated in the Physician Quality Reporting System (PQRS) in 2011—roughly 26,500 medical practices and 266,500 medical professionals, according to the Centers for Medicare & Medicaid Services (CMS).
“A lot of physicians have walked away [from PQRS] feeling like there are not sufficient measures for them to be measured against,” says Cheryl Damberg, senior principal researcher at RAND corporation and professor at the Pardee RAND Graduate School in Santa Monica, Calif.
Encouraging more participation from hospitalists has been the goal of the Society of Hospital Medicine (SHM) for the last several years, says Gregory Seymann, MD, SFHM, clinical professor and chief in the division of hospital medicine at University of California San Diego Health Sciences and chair of SHM’s Performance Measurement and Reporting Committee (PMRC).
“The committee has tried to champion it the best we can, making sure the measures that are there and in development meet the needs of the specialty,” Dr. Seymann says.
In just one year, the SHM committee managed to increase hospitalist reportable measures in PQRS from a paltry 11—half of which were only for stroke patients—to 21, which now includes things like diabetes exams, osteoporosis management, documentation of current medications, and community-acquired pneumonia treatment.
For Comparison’s Sake
For the first couple of phases of PQRS reporting, very few measures were relevant to hospitalists, Dr. Seymann says. The committee worked to ensure that more measures were added and billing codes modified to include those used by the specialty. Hospital medicine is relatively new, not officially recognized by the American Board of Medical Specialties (ABMS), and hospitalists serve a unique role. Most hospitalists are in internal medicine, family medicine, or pediatrics, but they aren’t doing what the average primary care doctor does, like referral for breast cancer or colon cancer screening, Dr. Seymann adds. Additionally, they aren’t always the provider performing specific cardiac or neurological care.
Hospitalists’ patients usually are in the hospital because they are sick. They may have chronic disease or more complex medical needs (e.g. osteoporosis-related hip fracture) than the average population seen by a non-hospitalist PCP.
If hospitalists are compared to other PCPs, as is the plan in the Physician Value-Based Payment Modifier, it “looks like our patients are dying a lot more frequently, we’re spending a lot of money, and we’re not doing primary care,” Dr. Seymann explains.
New Brand, New Push
PQRS is not new; it is the rebranding of CMS’ Physician Quality Reporting Initiative (PQRI), launched in 2006. But changes to the program are part of a national push to improve healthcare quality and patient care while reimbursing for performance on outcome- and process-based measures instead of simply for the volume of services provided. Each year, CMS updates PQRS rules.
This year is the last one in which providers will receive a bonus for reporting through PQRS. Beginning next year, practitioners that don’t meet the reporting requirements for 2013 will incur a 1.5% penalty—with additional penalties for physicians in groups of 100 or more from the value-based payment modifier. This year also serves as the performance year for 2016, when a 2% penalty for insufficient reporting will be assessed.
In early December 2013, the Centers for Medicare & Medicaid Services (CMS) published the 2014 Physician Fee Schedule and, with it, the final rules for the PQRS. Although many physicians and specialist groups believed the measures included in PQRS in previous years were too limited, CMS has added the additional reporting methodology of qualified clinical data registries (QCDR), which can include measures outside of the PQRS—a marked shift from previous policies.
The rule change, Damberg says, should take some energy out of the discussion surrounding the program and allow more physicians to participate.
“From CMS’ perspective, they want doctors delivering the recommended care and they want doctors to be able to report it out easily,” Damberg says.
Moving Forward
In 2014, providers can submit measures through the new QCDR option, or submit PQRS-identified measures through a Medicare qualified registry, through electronic health records, through the group practice reporting option (GPRO), and through claims-based reporting (though this last option is expected to be phased out over time).
Registries themselves are not new, but they can cost millions of dollars to establish and as much as a million a year to maintain. They typically contain more clinical depth and specificity than claims data, and numerous studies show the use of registries leads to improved patient outcomes.
“We don’t know how many [existing] registries are going to qualify to become these qualified clinical data registries,” says Tom Granatir, senior vice president for health policy and external relations at ABMS. “It’s going to take some time for these registries to evolve.”
Qualified clinical data registries must be in operation for at least one year to be eligible for certification by Medicare. They must include performance data from other payers beyond Medicare. Not only must QCDRs be capable of capturing and sending data, they must also provide national benchmarks to those who submit and must report back at least four times per year.
Granatir believes the QCDR rule, which allows QCDR’s to report measures beyond those included in the PQRS program, will help increase participation and will lead to more practice-based measures, but he fears it may exclude some important nuances of day-to-day patient care.
“The whole point [of quality measure reporting] is to create more public transparency…but if you have measures that are not relevant to what is actually done in practices, then it’s not a useful dataset,” he says.
Ideally, Damberg says, PQRS and other performance measures should enable physicians to do what they do better.
“I think this is really going to raise the stakes for [hospitalists] if they want to control their destiny,” Damberg says. “I think they have to get really engaged in this game and take a pro-active role in looking at where the quality gaps are and how can they better benefit patients. That’s the ultimate goal.”
Kelly April Tyrrell is a freelance writer in Wilmington, Del.
Only 27% of eligible providers participated in the Physician Quality Reporting System (PQRS) in 2011—roughly 26,500 medical practices and 266,500 medical professionals, according to the Centers for Medicare & Medicaid Services (CMS).
“A lot of physicians have walked away [from PQRS] feeling like there are not sufficient measures for them to be measured against,” says Cheryl Damberg, senior principal researcher at RAND corporation and professor at the Pardee RAND Graduate School in Santa Monica, Calif.
Encouraging more participation from hospitalists has been the goal of the Society of Hospital Medicine (SHM) for the last several years, says Gregory Seymann, MD, SFHM, clinical professor and chief in the division of hospital medicine at University of California San Diego Health Sciences and chair of SHM’s Performance Measurement and Reporting Committee (PMRC).
“The committee has tried to champion it the best we can, making sure the measures that are there and in development meet the needs of the specialty,” Dr. Seymann says.
In just one year, the SHM committee managed to increase hospitalist reportable measures in PQRS from a paltry 11—half of which were only for stroke patients—to 21, which now includes things like diabetes exams, osteoporosis management, documentation of current medications, and community-acquired pneumonia treatment.
For Comparison’s Sake
For the first couple of phases of PQRS reporting, very few measures were relevant to hospitalists, Dr. Seymann says. The committee worked to ensure that more measures were added and billing codes modified to include those used by the specialty. Hospital medicine is relatively new, not officially recognized by the American Board of Medical Specialties (ABMS), and hospitalists serve a unique role. Most hospitalists are in internal medicine, family medicine, or pediatrics, but they aren’t doing what the average primary care doctor does, like referral for breast cancer or colon cancer screening, Dr. Seymann adds. Additionally, they aren’t always the provider performing specific cardiac or neurological care.
Hospitalists’ patients usually are in the hospital because they are sick. They may have chronic disease or more complex medical needs (e.g. osteoporosis-related hip fracture) than the average population seen by a non-hospitalist PCP.
If hospitalists are compared to other PCPs, as is the plan in the Physician Value-Based Payment Modifier, it “looks like our patients are dying a lot more frequently, we’re spending a lot of money, and we’re not doing primary care,” Dr. Seymann explains.
New Brand, New Push
PQRS is not new; it is the rebranding of CMS’ Physician Quality Reporting Initiative (PQRI), launched in 2006. But changes to the program are part of a national push to improve healthcare quality and patient care while reimbursing for performance on outcome- and process-based measures instead of simply for the volume of services provided. Each year, CMS updates PQRS rules.
This year is the last one in which providers will receive a bonus for reporting through PQRS. Beginning next year, practitioners that don’t meet the reporting requirements for 2013 will incur a 1.5% penalty—with additional penalties for physicians in groups of 100 or more from the value-based payment modifier. This year also serves as the performance year for 2016, when a 2% penalty for insufficient reporting will be assessed.
In early December 2013, the Centers for Medicare & Medicaid Services (CMS) published the 2014 Physician Fee Schedule and, with it, the final rules for the PQRS. Although many physicians and specialist groups believed the measures included in PQRS in previous years were too limited, CMS has added the additional reporting methodology of qualified clinical data registries (QCDR), which can include measures outside of the PQRS—a marked shift from previous policies.
The rule change, Damberg says, should take some energy out of the discussion surrounding the program and allow more physicians to participate.
“From CMS’ perspective, they want doctors delivering the recommended care and they want doctors to be able to report it out easily,” Damberg says.
Moving Forward
In 2014, providers can submit measures through the new QCDR option, or submit PQRS-identified measures through a Medicare qualified registry, through electronic health records, through the group practice reporting option (GPRO), and through claims-based reporting (though this last option is expected to be phased out over time).
Registries themselves are not new, but they can cost millions of dollars to establish and as much as a million a year to maintain. They typically contain more clinical depth and specificity than claims data, and numerous studies show the use of registries leads to improved patient outcomes.
“We don’t know how many [existing] registries are going to qualify to become these qualified clinical data registries,” says Tom Granatir, senior vice president for health policy and external relations at ABMS. “It’s going to take some time for these registries to evolve.”
Qualified clinical data registries must be in operation for at least one year to be eligible for certification by Medicare. They must include performance data from other payers beyond Medicare. Not only must QCDRs be capable of capturing and sending data, they must also provide national benchmarks to those who submit and must report back at least four times per year.
Granatir believes the QCDR rule, which allows QCDR’s to report measures beyond those included in the PQRS program, will help increase participation and will lead to more practice-based measures, but he fears it may exclude some important nuances of day-to-day patient care.
“The whole point [of quality measure reporting] is to create more public transparency…but if you have measures that are not relevant to what is actually done in practices, then it’s not a useful dataset,” he says.
Ideally, Damberg says, PQRS and other performance measures should enable physicians to do what they do better.
“I think this is really going to raise the stakes for [hospitalists] if they want to control their destiny,” Damberg says. “I think they have to get really engaged in this game and take a pro-active role in looking at where the quality gaps are and how can they better benefit patients. That’s the ultimate goal.”
Kelly April Tyrrell is a freelance writer in Wilmington, Del.
Only 27% of eligible providers participated in the Physician Quality Reporting System (PQRS) in 2011—roughly 26,500 medical practices and 266,500 medical professionals, according to the Centers for Medicare & Medicaid Services (CMS).
“A lot of physicians have walked away [from PQRS] feeling like there are not sufficient measures for them to be measured against,” says Cheryl Damberg, senior principal researcher at RAND corporation and professor at the Pardee RAND Graduate School in Santa Monica, Calif.
Encouraging more participation from hospitalists has been the goal of the Society of Hospital Medicine (SHM) for the last several years, says Gregory Seymann, MD, SFHM, clinical professor and chief in the division of hospital medicine at University of California San Diego Health Sciences and chair of SHM’s Performance Measurement and Reporting Committee (PMRC).
“The committee has tried to champion it the best we can, making sure the measures that are there and in development meet the needs of the specialty,” Dr. Seymann says.
In just one year, the SHM committee managed to increase hospitalist reportable measures in PQRS from a paltry 11—half of which were only for stroke patients—to 21, which now includes things like diabetes exams, osteoporosis management, documentation of current medications, and community-acquired pneumonia treatment.
For Comparison’s Sake
For the first couple of phases of PQRS reporting, very few measures were relevant to hospitalists, Dr. Seymann says. The committee worked to ensure that more measures were added and billing codes modified to include those used by the specialty. Hospital medicine is relatively new, not officially recognized by the American Board of Medical Specialties (ABMS), and hospitalists serve a unique role. Most hospitalists are in internal medicine, family medicine, or pediatrics, but they aren’t doing what the average primary care doctor does, like referral for breast cancer or colon cancer screening, Dr. Seymann adds. Additionally, they aren’t always the provider performing specific cardiac or neurological care.
Hospitalists’ patients usually are in the hospital because they are sick. They may have chronic disease or more complex medical needs (e.g. osteoporosis-related hip fracture) than the average population seen by a non-hospitalist PCP.
If hospitalists are compared to other PCPs, as is the plan in the Physician Value-Based Payment Modifier, it “looks like our patients are dying a lot more frequently, we’re spending a lot of money, and we’re not doing primary care,” Dr. Seymann explains.
New Brand, New Push
PQRS is not new; it is the rebranding of CMS’ Physician Quality Reporting Initiative (PQRI), launched in 2006. But changes to the program are part of a national push to improve healthcare quality and patient care while reimbursing for performance on outcome- and process-based measures instead of simply for the volume of services provided. Each year, CMS updates PQRS rules.
This year is the last one in which providers will receive a bonus for reporting through PQRS. Beginning next year, practitioners that don’t meet the reporting requirements for 2013 will incur a 1.5% penalty—with additional penalties for physicians in groups of 100 or more from the value-based payment modifier. This year also serves as the performance year for 2016, when a 2% penalty for insufficient reporting will be assessed.
In early December 2013, the Centers for Medicare & Medicaid Services (CMS) published the 2014 Physician Fee Schedule and, with it, the final rules for the PQRS. Although many physicians and specialist groups believed the measures included in PQRS in previous years were too limited, CMS has added the additional reporting methodology of qualified clinical data registries (QCDR), which can include measures outside of the PQRS—a marked shift from previous policies.
The rule change, Damberg says, should take some energy out of the discussion surrounding the program and allow more physicians to participate.
“From CMS’ perspective, they want doctors delivering the recommended care and they want doctors to be able to report it out easily,” Damberg says.
Moving Forward
In 2014, providers can submit measures through the new QCDR option, or submit PQRS-identified measures through a Medicare qualified registry, through electronic health records, through the group practice reporting option (GPRO), and through claims-based reporting (though this last option is expected to be phased out over time).
Registries themselves are not new, but they can cost millions of dollars to establish and as much as a million a year to maintain. They typically contain more clinical depth and specificity than claims data, and numerous studies show the use of registries leads to improved patient outcomes.
“We don’t know how many [existing] registries are going to qualify to become these qualified clinical data registries,” says Tom Granatir, senior vice president for health policy and external relations at ABMS. “It’s going to take some time for these registries to evolve.”
Qualified clinical data registries must be in operation for at least one year to be eligible for certification by Medicare. They must include performance data from other payers beyond Medicare. Not only must QCDRs be capable of capturing and sending data, they must also provide national benchmarks to those who submit and must report back at least four times per year.
Granatir believes the QCDR rule, which allows QCDR’s to report measures beyond those included in the PQRS program, will help increase participation and will lead to more practice-based measures, but he fears it may exclude some important nuances of day-to-day patient care.
“The whole point [of quality measure reporting] is to create more public transparency…but if you have measures that are not relevant to what is actually done in practices, then it’s not a useful dataset,” he says.
Ideally, Damberg says, PQRS and other performance measures should enable physicians to do what they do better.
“I think this is really going to raise the stakes for [hospitalists] if they want to control their destiny,” Damberg says. “I think they have to get really engaged in this game and take a pro-active role in looking at where the quality gaps are and how can they better benefit patients. That’s the ultimate goal.”
Kelly April Tyrrell is a freelance writer in Wilmington, Del.
Aggregate Early Warning Score Results Mixed for High-Risk Pediatric Patients
Clinical question: Do rapid response systems (RRS) reduce the rate of critical deterioration (CD) in hospitalized children?
Background: Over the past decade, a majority of pediatric inpatient units and freestanding children’s hospitals have instituted RRSs that utilize medical emergency teams (MET) to rapidly evaluate clinically deteriorating patients. Pediatric RRSs manifest variability between institutions in MET composition and RRS triggers. Prior studies of RRSs in the pediatric population have been mixed, with a lack of robust evidence that RRSs reduce hospital mortality and cardiopulmonary arrest rates. Evaluation of the effect of RRSs in pediatric units and hospitals is complicated by the heterogeneity of pediatric RRS implementation and the overall low rate of in-hospital cardiopulmonary arrest and death. In a 2012 study, the authors defined CD events as those leading to ICU transfer and subsequent mechanical ventilation (noninvasive or invasive) or vasopressor infusion within 12 hours. CD event rates, quantified as an event rate per 1,000 non-ICU patient-days, were found to be associated with a >13-fold increase in risk of in-hospital death and were believed to be a valid proximate outcome for in-hospital mortality.
Study design: Single-center interrupted time series analysis
Setting: 516-bed urban, tertiary care, freestanding children’s hospital.
Synopsis: The RRS at this institution consisted of an aggregate early warning score (EWS), which triggered the response of a MET (within 30 minutes) 24 hours a day, seven days a week. Distinct from the code-blue team, the MET comprised PICU staff, including: (1) a fellow, attending, or nurse practitioner; (2) a nurse; and (3) a respiratory therapist. Researchers compared the 32 months prior to implementation to the 27 months after implementation. An interrupted time series analysis was performed using advanced statistical modeling with adjustments for season, ward, and case-mix index.
Although there were no significant differences in rates of cardiopulmonary arrest or mortality, adjusted analysis revealed a net 62% reduction in CD event rate (IRR=0.38) after initiation of the RRS. Adjusted analysis also found a net 83% reduction in mechanical ventilation events (IRR=0.17) and a net 80% reduction in vasopressor use (IRR=0.20). Of note, these reductions were not significant in the unadjusted analyses. After transfer to the ICU, time elapsed until initiation of either mechanical ventilation or vasopressor use was longer.
Bottom line: With an aggregate EWS identifying high-risk patients requiring rapid evaluation by a MET, a pediatric RRS reduces adjusted rates of CD events but might not yield significant reductions in unadjusted rates of mortality, cardiopulmonary arrest, or CD events.
Citation: Bonafide CP, Localio AR, Roberts KE, Nadkarni VM, Weirich CM, Keren R. Impact of rapid response system imple-mentation on critical deterioration events in children. JAMA Pediatr. 2014;168(1):25-33.
Reviewed by Pediatric Editor Weijen Chang, MD, SFHM, FAAP, associate clinical professor of medicine and pediatrics at the University of California at San Diego School of Medicine, and a hospitalist at both UCSD Medical Center and Rady Children’s Hospital.
Clinical question: Do rapid response systems (RRS) reduce the rate of critical deterioration (CD) in hospitalized children?
Background: Over the past decade, a majority of pediatric inpatient units and freestanding children’s hospitals have instituted RRSs that utilize medical emergency teams (MET) to rapidly evaluate clinically deteriorating patients. Pediatric RRSs manifest variability between institutions in MET composition and RRS triggers. Prior studies of RRSs in the pediatric population have been mixed, with a lack of robust evidence that RRSs reduce hospital mortality and cardiopulmonary arrest rates. Evaluation of the effect of RRSs in pediatric units and hospitals is complicated by the heterogeneity of pediatric RRS implementation and the overall low rate of in-hospital cardiopulmonary arrest and death. In a 2012 study, the authors defined CD events as those leading to ICU transfer and subsequent mechanical ventilation (noninvasive or invasive) or vasopressor infusion within 12 hours. CD event rates, quantified as an event rate per 1,000 non-ICU patient-days, were found to be associated with a >13-fold increase in risk of in-hospital death and were believed to be a valid proximate outcome for in-hospital mortality.
Study design: Single-center interrupted time series analysis
Setting: 516-bed urban, tertiary care, freestanding children’s hospital.
Synopsis: The RRS at this institution consisted of an aggregate early warning score (EWS), which triggered the response of a MET (within 30 minutes) 24 hours a day, seven days a week. Distinct from the code-blue team, the MET comprised PICU staff, including: (1) a fellow, attending, or nurse practitioner; (2) a nurse; and (3) a respiratory therapist. Researchers compared the 32 months prior to implementation to the 27 months after implementation. An interrupted time series analysis was performed using advanced statistical modeling with adjustments for season, ward, and case-mix index.
Although there were no significant differences in rates of cardiopulmonary arrest or mortality, adjusted analysis revealed a net 62% reduction in CD event rate (IRR=0.38) after initiation of the RRS. Adjusted analysis also found a net 83% reduction in mechanical ventilation events (IRR=0.17) and a net 80% reduction in vasopressor use (IRR=0.20). Of note, these reductions were not significant in the unadjusted analyses. After transfer to the ICU, time elapsed until initiation of either mechanical ventilation or vasopressor use was longer.
Bottom line: With an aggregate EWS identifying high-risk patients requiring rapid evaluation by a MET, a pediatric RRS reduces adjusted rates of CD events but might not yield significant reductions in unadjusted rates of mortality, cardiopulmonary arrest, or CD events.
Citation: Bonafide CP, Localio AR, Roberts KE, Nadkarni VM, Weirich CM, Keren R. Impact of rapid response system imple-mentation on critical deterioration events in children. JAMA Pediatr. 2014;168(1):25-33.
Reviewed by Pediatric Editor Weijen Chang, MD, SFHM, FAAP, associate clinical professor of medicine and pediatrics at the University of California at San Diego School of Medicine, and a hospitalist at both UCSD Medical Center and Rady Children’s Hospital.
Clinical question: Do rapid response systems (RRS) reduce the rate of critical deterioration (CD) in hospitalized children?
Background: Over the past decade, a majority of pediatric inpatient units and freestanding children’s hospitals have instituted RRSs that utilize medical emergency teams (MET) to rapidly evaluate clinically deteriorating patients. Pediatric RRSs manifest variability between institutions in MET composition and RRS triggers. Prior studies of RRSs in the pediatric population have been mixed, with a lack of robust evidence that RRSs reduce hospital mortality and cardiopulmonary arrest rates. Evaluation of the effect of RRSs in pediatric units and hospitals is complicated by the heterogeneity of pediatric RRS implementation and the overall low rate of in-hospital cardiopulmonary arrest and death. In a 2012 study, the authors defined CD events as those leading to ICU transfer and subsequent mechanical ventilation (noninvasive or invasive) or vasopressor infusion within 12 hours. CD event rates, quantified as an event rate per 1,000 non-ICU patient-days, were found to be associated with a >13-fold increase in risk of in-hospital death and were believed to be a valid proximate outcome for in-hospital mortality.
Study design: Single-center interrupted time series analysis
Setting: 516-bed urban, tertiary care, freestanding children’s hospital.
Synopsis: The RRS at this institution consisted of an aggregate early warning score (EWS), which triggered the response of a MET (within 30 minutes) 24 hours a day, seven days a week. Distinct from the code-blue team, the MET comprised PICU staff, including: (1) a fellow, attending, or nurse practitioner; (2) a nurse; and (3) a respiratory therapist. Researchers compared the 32 months prior to implementation to the 27 months after implementation. An interrupted time series analysis was performed using advanced statistical modeling with adjustments for season, ward, and case-mix index.
Although there were no significant differences in rates of cardiopulmonary arrest or mortality, adjusted analysis revealed a net 62% reduction in CD event rate (IRR=0.38) after initiation of the RRS. Adjusted analysis also found a net 83% reduction in mechanical ventilation events (IRR=0.17) and a net 80% reduction in vasopressor use (IRR=0.20). Of note, these reductions were not significant in the unadjusted analyses. After transfer to the ICU, time elapsed until initiation of either mechanical ventilation or vasopressor use was longer.
Bottom line: With an aggregate EWS identifying high-risk patients requiring rapid evaluation by a MET, a pediatric RRS reduces adjusted rates of CD events but might not yield significant reductions in unadjusted rates of mortality, cardiopulmonary arrest, or CD events.
Citation: Bonafide CP, Localio AR, Roberts KE, Nadkarni VM, Weirich CM, Keren R. Impact of rapid response system imple-mentation on critical deterioration events in children. JAMA Pediatr. 2014;168(1):25-33.
Reviewed by Pediatric Editor Weijen Chang, MD, SFHM, FAAP, associate clinical professor of medicine and pediatrics at the University of California at San Diego School of Medicine, and a hospitalist at both UCSD Medical Center and Rady Children’s Hospital.
Benefits of Membership in Society of Hospital Medicine Plentiful
Hospital medicine has always been more than a medical specialty; it is a movement to improve healthcare delivered in the hospital and to make the hospital a vital part of the healthcare system in every community served.
SHM’s members have always been at the forefront of that movement. The benefits of SHM membership now keep more than 12,000 SHM members ahead of the curve in a rapidly growing and evolving medical specialty. Although SHM membership offers numerous benefits, many SHM members tell others that simply being part of the movement to transform healthcare and revolutionize patient care is the main reason they joined SHM and renew every year.
Exclusive member benefits include:
- Access to the Hospital Medicine Exchange, an exclusive online member community for networking and collaboration;
- Opportunities to make your voice heard on important policy and regulatory issues affecting hospitalists and their patients;
- Enhanced professional satisfaction gained through networking with hospitalists on a local and national level;
- Complimentary subscription to The Hospitalist news magazine and to the Journal of Hospital Medicine, the first peer-reviewed journal in hospital medicine;
- Member discounts on educational events, including our annual meeting, and select resources available in our online store;
- Access to SHM’s Career Center, with hundreds of positions and top-of-the-line functionality;
- Fellowship in Hospital Medicine designation opportunities (FHM, SFHM, MHM);
- Program discounts on medical liability insurance through The Doctors Company;
- Member discounts on Wiley educational products; and
- NEW: Free and discounted coding services from The Coding Network.
To become a member, visit www.hospitalmedicine.org/membership.
Hospital medicine has always been more than a medical specialty; it is a movement to improve healthcare delivered in the hospital and to make the hospital a vital part of the healthcare system in every community served.
SHM’s members have always been at the forefront of that movement. The benefits of SHM membership now keep more than 12,000 SHM members ahead of the curve in a rapidly growing and evolving medical specialty. Although SHM membership offers numerous benefits, many SHM members tell others that simply being part of the movement to transform healthcare and revolutionize patient care is the main reason they joined SHM and renew every year.
Exclusive member benefits include:
- Access to the Hospital Medicine Exchange, an exclusive online member community for networking and collaboration;
- Opportunities to make your voice heard on important policy and regulatory issues affecting hospitalists and their patients;
- Enhanced professional satisfaction gained through networking with hospitalists on a local and national level;
- Complimentary subscription to The Hospitalist news magazine and to the Journal of Hospital Medicine, the first peer-reviewed journal in hospital medicine;
- Member discounts on educational events, including our annual meeting, and select resources available in our online store;
- Access to SHM’s Career Center, with hundreds of positions and top-of-the-line functionality;
- Fellowship in Hospital Medicine designation opportunities (FHM, SFHM, MHM);
- Program discounts on medical liability insurance through The Doctors Company;
- Member discounts on Wiley educational products; and
- NEW: Free and discounted coding services from The Coding Network.
To become a member, visit www.hospitalmedicine.org/membership.
Hospital medicine has always been more than a medical specialty; it is a movement to improve healthcare delivered in the hospital and to make the hospital a vital part of the healthcare system in every community served.
SHM’s members have always been at the forefront of that movement. The benefits of SHM membership now keep more than 12,000 SHM members ahead of the curve in a rapidly growing and evolving medical specialty. Although SHM membership offers numerous benefits, many SHM members tell others that simply being part of the movement to transform healthcare and revolutionize patient care is the main reason they joined SHM and renew every year.
Exclusive member benefits include:
- Access to the Hospital Medicine Exchange, an exclusive online member community for networking and collaboration;
- Opportunities to make your voice heard on important policy and regulatory issues affecting hospitalists and their patients;
- Enhanced professional satisfaction gained through networking with hospitalists on a local and national level;
- Complimentary subscription to The Hospitalist news magazine and to the Journal of Hospital Medicine, the first peer-reviewed journal in hospital medicine;
- Member discounts on educational events, including our annual meeting, and select resources available in our online store;
- Access to SHM’s Career Center, with hundreds of positions and top-of-the-line functionality;
- Fellowship in Hospital Medicine designation opportunities (FHM, SFHM, MHM);
- Program discounts on medical liability insurance through The Doctors Company;
- Member discounts on Wiley educational products; and
- NEW: Free and discounted coding services from The Coding Network.
To become a member, visit www.hospitalmedicine.org/membership.
Society of Hospital Medicine Uses Social Media to Connect Members
Now more than ever, social media and SHM are connecting hospitalists with peers and experts in healthcare. Last year, SHM launched a new blog, The Hospital Leader (http://blogs.hospitalmedicine.org/Blog), and introduced hospitalists to eight prominent voices in the HM movement. In January, SHM used Twitter (http://www.twitter.com/shmlive) to educate hospitalists and others on CMS’ changes to the “two-midnight rule” through a live tweet of a free webinar.
Since its inception in October 2012, nearly 3,000 hospitalists have logged into HMX more than 72,000 times to ask questions, share experiences, and learn from other hospitalists across the country.
Want to connect with the other hospitalists and experts in healthcare? Here’s how:
- Ask questions and get real-world answers at Hospital Medicine Exchange (HMX): http://connect.hospitalmedicine.org/home.
- Join SHM’s 2,200-plus followers on Twitter for quick news and information about the hospital medicine movement: https://twitter.com/shmlive.
- For new research in hospital medicine, follow the Journal of Hospital Medicine on Twitter: https://twitter.com/JHospMedicine.
- Get regular insight from leaders and experts in the movement at SHM’s blog, The Hospital Leader: http://blogs.hospitalmedicine.org/Blog.
- “Like” and “share” away with SHM on Facebook: www.facebook.com/Hospitalists.
Tweeting at HM14? Use #HospMed14
Last year, tweets about SHM’s annual meeting reached thousands, creating more than two million impressions. This year will be even bigger. Join the conversation with leaders in the specialty, using #hospmed14 whenever you do.
Now more than ever, social media and SHM are connecting hospitalists with peers and experts in healthcare. Last year, SHM launched a new blog, The Hospital Leader (http://blogs.hospitalmedicine.org/Blog), and introduced hospitalists to eight prominent voices in the HM movement. In January, SHM used Twitter (http://www.twitter.com/shmlive) to educate hospitalists and others on CMS’ changes to the “two-midnight rule” through a live tweet of a free webinar.
Since its inception in October 2012, nearly 3,000 hospitalists have logged into HMX more than 72,000 times to ask questions, share experiences, and learn from other hospitalists across the country.
Want to connect with the other hospitalists and experts in healthcare? Here’s how:
- Ask questions and get real-world answers at Hospital Medicine Exchange (HMX): http://connect.hospitalmedicine.org/home.
- Join SHM’s 2,200-plus followers on Twitter for quick news and information about the hospital medicine movement: https://twitter.com/shmlive.
- For new research in hospital medicine, follow the Journal of Hospital Medicine on Twitter: https://twitter.com/JHospMedicine.
- Get regular insight from leaders and experts in the movement at SHM’s blog, The Hospital Leader: http://blogs.hospitalmedicine.org/Blog.
- “Like” and “share” away with SHM on Facebook: www.facebook.com/Hospitalists.
Tweeting at HM14? Use #HospMed14
Last year, tweets about SHM’s annual meeting reached thousands, creating more than two million impressions. This year will be even bigger. Join the conversation with leaders in the specialty, using #hospmed14 whenever you do.
Now more than ever, social media and SHM are connecting hospitalists with peers and experts in healthcare. Last year, SHM launched a new blog, The Hospital Leader (http://blogs.hospitalmedicine.org/Blog), and introduced hospitalists to eight prominent voices in the HM movement. In January, SHM used Twitter (http://www.twitter.com/shmlive) to educate hospitalists and others on CMS’ changes to the “two-midnight rule” through a live tweet of a free webinar.
Since its inception in October 2012, nearly 3,000 hospitalists have logged into HMX more than 72,000 times to ask questions, share experiences, and learn from other hospitalists across the country.
Want to connect with the other hospitalists and experts in healthcare? Here’s how:
- Ask questions and get real-world answers at Hospital Medicine Exchange (HMX): http://connect.hospitalmedicine.org/home.
- Join SHM’s 2,200-plus followers on Twitter for quick news and information about the hospital medicine movement: https://twitter.com/shmlive.
- For new research in hospital medicine, follow the Journal of Hospital Medicine on Twitter: https://twitter.com/JHospMedicine.
- Get regular insight from leaders and experts in the movement at SHM’s blog, The Hospital Leader: http://blogs.hospitalmedicine.org/Blog.
- “Like” and “share” away with SHM on Facebook: www.facebook.com/Hospitalists.
Tweeting at HM14? Use #HospMed14
Last year, tweets about SHM’s annual meeting reached thousands, creating more than two million impressions. This year will be even bigger. Join the conversation with leaders in the specialty, using #hospmed14 whenever you do.
The Costs of Quality Care in Pediatric Hospital Medicine
“Dr. Chang? Oh my, it’s Dr. Chang! And his little son!” I called them “mall moments.” I would be at the local shopping mall with my father, picking up new clothes for the upcoming school year, when suddenly an elderly woman would approach. My father, despite his inability to remember my own birthday, would warmly grasp the woman’s hands, gaze into her eyes, ask about her family, then reminisce about her late husband and his last days in the hospital. After a few minutes, she would say something like, “Well, your father is the best doctor in Bakersfield, and you’ll be lucky to grow up to be just like him.”
And this would be fine, except the same scene would replay at the supermarket, the dry cleaners, and the local Chinese restaurant (the only place my father would eat out until he discovered the exotic pleasures of sushi). I wondered how my father ever got any errands done, with all his patients chatting with him along the way. Looking back on these “moments,” it is clear to me that this was my father’s measure of quality—his patients loved him. Other doctors loved him. The nurses—well, maybe not so much. He was a doctor’s doctor.
Quality measures? After working in his office, I only knew of two: The waiting room must be empty before the doors are closed and locked, and no patient ever gets turned away, for any reason. By seven o’clock in the evening, these measures got pretty old. But simple credos made him one of the most beloved physicians in Kern County, Calif.
Quality, in whatever form it takes, has a cost, however. My father divorced twice. My own “quality” time with him was spent making weekend rounds at the seemingly innumerable nursing homes around Bakersfield, Calif., although this was great olfactory training for my future career as a hospitalist. Many a parent’s day was spent with only my mother present, and I would be lying if I said I didn’t envy the other children with both parents doting over their science projects.
As we in pediatric hospital medicine (PHM) embark on a journey to define and promote quality in our care of children, we are well aware that adhering to our defined standards of quality will have a cost. What has been discussed less, but is perhaps even more elementary, is the cost of simply endeavoring to define and measure quality itself. This has not slowed down the onslaught of newly defined quality measures in PHM. Quality measures from the adult HM world, such as readmission rates, adherence to national guidelines, and communication with primary care providers, have been extracted and repurposed.
Attempts to extrapolate these measures to PHM have been less than successful. Alverson and O’Callaghan recently made a compelling case debunking readmission rates as a valid quality measure in PHM.1 Compliance with Children’s Asthma Care (CAC) measures was not found to decrease asthma-related readmissions or subsequent ED visits in a 2011 study, although a study published in 2012 showed an association between compliance with asthma action plans at discharge and lower readmission rates.2,3 Documentation of primary care follow-up for patients discharged from a free-standing children’s hospital actually increased the readmission rate (if that is believed to be a quality measure).4
Yet quality measures continue to be created, espoused, and studied. Payments to accountable care organizations (ACO), hospitals, and individual providers are being tied to performance on quality measures. Medicare is considering quality measures that can be applied to PHM, which might affect future payments to children’s hospitals. Paciorkowski and colleagues recently described the development of 87 performance indicators specific to PHM that could be used to track quality of care on a division level, 79 of which were provider specific.5 A committee of pediatric hospitalists led by Paul Hain, MD, recently proposed a “dashboard” of metrics pertaining to descriptive, quality, productivity, and other data that could be used to compare PHM groups across the country.6 Many hospitalist groups already have instituted financial incentives tied to provider or group-specific quality measures.7 Pay-for-performance has arrived in adult HM and is now pulling out of the station: next stop, PHM.
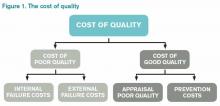
Source: From Crosby P. B. Quality Is Free: The Art of Making Quality Certain. New York: McGraw-Hill; 1979.
The Rest of the Cost Story
Like any labor-intensive process in medicine, defining, measuring, and improving quality has a cost. A 2007 survey of four urban teaching hospitals found that core QI activities required 1%-2% of the total operating revenue.8 The QI activity costs fall into the category of the “cost of good quality,” as defined by Philip Crosby in his book, Quality is Free (see Figure 1).9 Although hospital operations with better process “sigma” will have lower prevention and appraisal costs, these can never be fully eliminated.
Despite our attempts at controlling costs, most ongoing QI efforts focused on improving clinical quality alone are doomed to fail with regard to providing bottom-line cost reductions.10 QI efforts that focus on decreasing variability in the use of best practices, such as the National Surgical Quality Improvement Program (NSQIP), have brought improvements in both outcomes and reduced costs of complications.11 Not only do these QI efforts lower the “cost of poor quality,” but they may provide less measurable benefits, such as reduced opportunity costs. Whether these efforts can compensate by reducing the cost of poor quality can be speculative. Some HM authorities, such as Duke University Health CMO Thomas Owens, have made the case, especially to hospital administrators, for espousing a more formulaic return on investment (ROI) calculation for HM QI efforts, taking into account reduced opportunity costs.12
But measured costs tell only part of the story. For every new quality measure that is defined, there are also unmeasured costs to measuring and collecting evidence of quality. Being constantly measured and assessed often leads to a perceived loss of autonomy, and this can lead to burnout; more than 40% of respondents from local hospitalist groups in the most recent SHM Career Satisfaction Survey indicated that optimal autonomy was among the four most important factors for job satisfaction.13 The same survey found that hospitalists were least satisfied with organizational climate, autonomy, and availability of personal time.14
As many a hospitalist can relate, although involvement in QI processes is considered a cornerstone of hospitalist practice, increased time spent in a given QI activity rarely translates to increased compensation. Fourteen percent of hospitalists in a recent SHM Focused Survey reported not even having dedicated time for or being compensated for QI.
Which is not to say, of course, that defining and measuring quality is not a worthy pursuit. On the contrary, QI is a pillar of hospital medicine practice. A recent survey showed that 84% of pediatric hospitalists participated in QI initiatives, and 72% considered the variety of pursuits inherent in a PHM career as a factor influencing career choice.15 But just as we are now focused on choosing wisely in diagnosing and treating our patients, we should also be choosing wisely in diagnosing and treating our systems. What is true for our patients is true for our system of care—simply ordering the test can lead to a cascade of interventions that can be not only costly but also potentially dangerous for the patient.
Physician-defined quality measures in adult HM have now been adopted as yardsticks with which to measure all hospitals—and with which to punish those who do not measure up. In 1984, Dr. Earl Steinberg, then a professor of medicine at Johns Hopkins, published a seminal article in the New England Journal of Medicine describing potential cost savings to the Medicare program from reductions in hospital readmissions.16 This was the match that lit the fuse to what is now the Affordable Care Act Hospital Readmissions Reduction Program. Yet, this quality measure might not even be a quality measure of…quality. A 2013 JAMA study showed that readmission rates for acute myocardial infarction and pneumonia were not correlated with mortality, the time-tested gold standard for quality in medicine.17 That has not stopped Medicare from levying $227 million in fines on 2,225 hospitals across the country beginning Oct. 1, 2013 for excess readmissions in Year 2 of the Hospital Readmissions Reduction Program.18 It seems that we have built it, and they have come, and now they won’t leave.
In Sum
What is the lesson for PHM? Assessing and improving quality of care remains a necessary cornerstone of PHM, but choosing meaningful quality measures is difficult and can have long-term consequences. The choices we make with regard to the direction of QI will, however, define the future of pediatric healthcare for decades to come. As such, we cannot waste both financial and human resources on defining and assessing quality measures that may sound superficially important but, in the end, are not reflective of the real quality of care provided to our patients.
My father, in his adherence to his own ideal of quality medical care, reaped the unintended consequences of his pursuit of quality medical care. Sometimes, though just sometimes, there are unintended consequences to the unintended consequences. I learned, and was perhaps inspired, just by watching him interact with patients and their families. Somehow I don’t think my own children will learn much by watching me interact with my computer.
Dr. Chang is pediatric editor of The Hospitalist. He is associate clinical professor of medicine and pediatrics at the University of California at San Diego (UCSD) School of Medicine, and a hospitalist at both UCSD Medical Center and Rady Children’s Hospital. Send comments and questions to wwch@ucsd.edu.
“Dr. Chang? Oh my, it’s Dr. Chang! And his little son!” I called them “mall moments.” I would be at the local shopping mall with my father, picking up new clothes for the upcoming school year, when suddenly an elderly woman would approach. My father, despite his inability to remember my own birthday, would warmly grasp the woman’s hands, gaze into her eyes, ask about her family, then reminisce about her late husband and his last days in the hospital. After a few minutes, she would say something like, “Well, your father is the best doctor in Bakersfield, and you’ll be lucky to grow up to be just like him.”
And this would be fine, except the same scene would replay at the supermarket, the dry cleaners, and the local Chinese restaurant (the only place my father would eat out until he discovered the exotic pleasures of sushi). I wondered how my father ever got any errands done, with all his patients chatting with him along the way. Looking back on these “moments,” it is clear to me that this was my father’s measure of quality—his patients loved him. Other doctors loved him. The nurses—well, maybe not so much. He was a doctor’s doctor.
Quality measures? After working in his office, I only knew of two: The waiting room must be empty before the doors are closed and locked, and no patient ever gets turned away, for any reason. By seven o’clock in the evening, these measures got pretty old. But simple credos made him one of the most beloved physicians in Kern County, Calif.
Quality, in whatever form it takes, has a cost, however. My father divorced twice. My own “quality” time with him was spent making weekend rounds at the seemingly innumerable nursing homes around Bakersfield, Calif., although this was great olfactory training for my future career as a hospitalist. Many a parent’s day was spent with only my mother present, and I would be lying if I said I didn’t envy the other children with both parents doting over their science projects.
As we in pediatric hospital medicine (PHM) embark on a journey to define and promote quality in our care of children, we are well aware that adhering to our defined standards of quality will have a cost. What has been discussed less, but is perhaps even more elementary, is the cost of simply endeavoring to define and measure quality itself. This has not slowed down the onslaught of newly defined quality measures in PHM. Quality measures from the adult HM world, such as readmission rates, adherence to national guidelines, and communication with primary care providers, have been extracted and repurposed.
Attempts to extrapolate these measures to PHM have been less than successful. Alverson and O’Callaghan recently made a compelling case debunking readmission rates as a valid quality measure in PHM.1 Compliance with Children’s Asthma Care (CAC) measures was not found to decrease asthma-related readmissions or subsequent ED visits in a 2011 study, although a study published in 2012 showed an association between compliance with asthma action plans at discharge and lower readmission rates.2,3 Documentation of primary care follow-up for patients discharged from a free-standing children’s hospital actually increased the readmission rate (if that is believed to be a quality measure).4
Yet quality measures continue to be created, espoused, and studied. Payments to accountable care organizations (ACO), hospitals, and individual providers are being tied to performance on quality measures. Medicare is considering quality measures that can be applied to PHM, which might affect future payments to children’s hospitals. Paciorkowski and colleagues recently described the development of 87 performance indicators specific to PHM that could be used to track quality of care on a division level, 79 of which were provider specific.5 A committee of pediatric hospitalists led by Paul Hain, MD, recently proposed a “dashboard” of metrics pertaining to descriptive, quality, productivity, and other data that could be used to compare PHM groups across the country.6 Many hospitalist groups already have instituted financial incentives tied to provider or group-specific quality measures.7 Pay-for-performance has arrived in adult HM and is now pulling out of the station: next stop, PHM.
Source: From Crosby P. B. Quality Is Free: The Art of Making Quality Certain. New York: McGraw-Hill; 1979.
The Rest of the Cost Story
Like any labor-intensive process in medicine, defining, measuring, and improving quality has a cost. A 2007 survey of four urban teaching hospitals found that core QI activities required 1%-2% of the total operating revenue.8 The QI activity costs fall into the category of the “cost of good quality,” as defined by Philip Crosby in his book, Quality is Free (see Figure 1).9 Although hospital operations with better process “sigma” will have lower prevention and appraisal costs, these can never be fully eliminated.
Despite our attempts at controlling costs, most ongoing QI efforts focused on improving clinical quality alone are doomed to fail with regard to providing bottom-line cost reductions.10 QI efforts that focus on decreasing variability in the use of best practices, such as the National Surgical Quality Improvement Program (NSQIP), have brought improvements in both outcomes and reduced costs of complications.11 Not only do these QI efforts lower the “cost of poor quality,” but they may provide less measurable benefits, such as reduced opportunity costs. Whether these efforts can compensate by reducing the cost of poor quality can be speculative. Some HM authorities, such as Duke University Health CMO Thomas Owens, have made the case, especially to hospital administrators, for espousing a more formulaic return on investment (ROI) calculation for HM QI efforts, taking into account reduced opportunity costs.12
But measured costs tell only part of the story. For every new quality measure that is defined, there are also unmeasured costs to measuring and collecting evidence of quality. Being constantly measured and assessed often leads to a perceived loss of autonomy, and this can lead to burnout; more than 40% of respondents from local hospitalist groups in the most recent SHM Career Satisfaction Survey indicated that optimal autonomy was among the four most important factors for job satisfaction.13 The same survey found that hospitalists were least satisfied with organizational climate, autonomy, and availability of personal time.14
As many a hospitalist can relate, although involvement in QI processes is considered a cornerstone of hospitalist practice, increased time spent in a given QI activity rarely translates to increased compensation. Fourteen percent of hospitalists in a recent SHM Focused Survey reported not even having dedicated time for or being compensated for QI.
Which is not to say, of course, that defining and measuring quality is not a worthy pursuit. On the contrary, QI is a pillar of hospital medicine practice. A recent survey showed that 84% of pediatric hospitalists participated in QI initiatives, and 72% considered the variety of pursuits inherent in a PHM career as a factor influencing career choice.15 But just as we are now focused on choosing wisely in diagnosing and treating our patients, we should also be choosing wisely in diagnosing and treating our systems. What is true for our patients is true for our system of care—simply ordering the test can lead to a cascade of interventions that can be not only costly but also potentially dangerous for the patient.
Physician-defined quality measures in adult HM have now been adopted as yardsticks with which to measure all hospitals—and with which to punish those who do not measure up. In 1984, Dr. Earl Steinberg, then a professor of medicine at Johns Hopkins, published a seminal article in the New England Journal of Medicine describing potential cost savings to the Medicare program from reductions in hospital readmissions.16 This was the match that lit the fuse to what is now the Affordable Care Act Hospital Readmissions Reduction Program. Yet, this quality measure might not even be a quality measure of…quality. A 2013 JAMA study showed that readmission rates for acute myocardial infarction and pneumonia were not correlated with mortality, the time-tested gold standard for quality in medicine.17 That has not stopped Medicare from levying $227 million in fines on 2,225 hospitals across the country beginning Oct. 1, 2013 for excess readmissions in Year 2 of the Hospital Readmissions Reduction Program.18 It seems that we have built it, and they have come, and now they won’t leave.
In Sum
What is the lesson for PHM? Assessing and improving quality of care remains a necessary cornerstone of PHM, but choosing meaningful quality measures is difficult and can have long-term consequences. The choices we make with regard to the direction of QI will, however, define the future of pediatric healthcare for decades to come. As such, we cannot waste both financial and human resources on defining and assessing quality measures that may sound superficially important but, in the end, are not reflective of the real quality of care provided to our patients.
My father, in his adherence to his own ideal of quality medical care, reaped the unintended consequences of his pursuit of quality medical care. Sometimes, though just sometimes, there are unintended consequences to the unintended consequences. I learned, and was perhaps inspired, just by watching him interact with patients and their families. Somehow I don’t think my own children will learn much by watching me interact with my computer.
Dr. Chang is pediatric editor of The Hospitalist. He is associate clinical professor of medicine and pediatrics at the University of California at San Diego (UCSD) School of Medicine, and a hospitalist at both UCSD Medical Center and Rady Children’s Hospital. Send comments and questions to wwch@ucsd.edu.
“Dr. Chang? Oh my, it’s Dr. Chang! And his little son!” I called them “mall moments.” I would be at the local shopping mall with my father, picking up new clothes for the upcoming school year, when suddenly an elderly woman would approach. My father, despite his inability to remember my own birthday, would warmly grasp the woman’s hands, gaze into her eyes, ask about her family, then reminisce about her late husband and his last days in the hospital. After a few minutes, she would say something like, “Well, your father is the best doctor in Bakersfield, and you’ll be lucky to grow up to be just like him.”
And this would be fine, except the same scene would replay at the supermarket, the dry cleaners, and the local Chinese restaurant (the only place my father would eat out until he discovered the exotic pleasures of sushi). I wondered how my father ever got any errands done, with all his patients chatting with him along the way. Looking back on these “moments,” it is clear to me that this was my father’s measure of quality—his patients loved him. Other doctors loved him. The nurses—well, maybe not so much. He was a doctor’s doctor.
Quality measures? After working in his office, I only knew of two: The waiting room must be empty before the doors are closed and locked, and no patient ever gets turned away, for any reason. By seven o’clock in the evening, these measures got pretty old. But simple credos made him one of the most beloved physicians in Kern County, Calif.
Quality, in whatever form it takes, has a cost, however. My father divorced twice. My own “quality” time with him was spent making weekend rounds at the seemingly innumerable nursing homes around Bakersfield, Calif., although this was great olfactory training for my future career as a hospitalist. Many a parent’s day was spent with only my mother present, and I would be lying if I said I didn’t envy the other children with both parents doting over their science projects.
As we in pediatric hospital medicine (PHM) embark on a journey to define and promote quality in our care of children, we are well aware that adhering to our defined standards of quality will have a cost. What has been discussed less, but is perhaps even more elementary, is the cost of simply endeavoring to define and measure quality itself. This has not slowed down the onslaught of newly defined quality measures in PHM. Quality measures from the adult HM world, such as readmission rates, adherence to national guidelines, and communication with primary care providers, have been extracted and repurposed.
Attempts to extrapolate these measures to PHM have been less than successful. Alverson and O’Callaghan recently made a compelling case debunking readmission rates as a valid quality measure in PHM.1 Compliance with Children’s Asthma Care (CAC) measures was not found to decrease asthma-related readmissions or subsequent ED visits in a 2011 study, although a study published in 2012 showed an association between compliance with asthma action plans at discharge and lower readmission rates.2,3 Documentation of primary care follow-up for patients discharged from a free-standing children’s hospital actually increased the readmission rate (if that is believed to be a quality measure).4
Yet quality measures continue to be created, espoused, and studied. Payments to accountable care organizations (ACO), hospitals, and individual providers are being tied to performance on quality measures. Medicare is considering quality measures that can be applied to PHM, which might affect future payments to children’s hospitals. Paciorkowski and colleagues recently described the development of 87 performance indicators specific to PHM that could be used to track quality of care on a division level, 79 of which were provider specific.5 A committee of pediatric hospitalists led by Paul Hain, MD, recently proposed a “dashboard” of metrics pertaining to descriptive, quality, productivity, and other data that could be used to compare PHM groups across the country.6 Many hospitalist groups already have instituted financial incentives tied to provider or group-specific quality measures.7 Pay-for-performance has arrived in adult HM and is now pulling out of the station: next stop, PHM.
Source: From Crosby P. B. Quality Is Free: The Art of Making Quality Certain. New York: McGraw-Hill; 1979.
The Rest of the Cost Story
Like any labor-intensive process in medicine, defining, measuring, and improving quality has a cost. A 2007 survey of four urban teaching hospitals found that core QI activities required 1%-2% of the total operating revenue.8 The QI activity costs fall into the category of the “cost of good quality,” as defined by Philip Crosby in his book, Quality is Free (see Figure 1).9 Although hospital operations with better process “sigma” will have lower prevention and appraisal costs, these can never be fully eliminated.
Despite our attempts at controlling costs, most ongoing QI efforts focused on improving clinical quality alone are doomed to fail with regard to providing bottom-line cost reductions.10 QI efforts that focus on decreasing variability in the use of best practices, such as the National Surgical Quality Improvement Program (NSQIP), have brought improvements in both outcomes and reduced costs of complications.11 Not only do these QI efforts lower the “cost of poor quality,” but they may provide less measurable benefits, such as reduced opportunity costs. Whether these efforts can compensate by reducing the cost of poor quality can be speculative. Some HM authorities, such as Duke University Health CMO Thomas Owens, have made the case, especially to hospital administrators, for espousing a more formulaic return on investment (ROI) calculation for HM QI efforts, taking into account reduced opportunity costs.12
But measured costs tell only part of the story. For every new quality measure that is defined, there are also unmeasured costs to measuring and collecting evidence of quality. Being constantly measured and assessed often leads to a perceived loss of autonomy, and this can lead to burnout; more than 40% of respondents from local hospitalist groups in the most recent SHM Career Satisfaction Survey indicated that optimal autonomy was among the four most important factors for job satisfaction.13 The same survey found that hospitalists were least satisfied with organizational climate, autonomy, and availability of personal time.14
As many a hospitalist can relate, although involvement in QI processes is considered a cornerstone of hospitalist practice, increased time spent in a given QI activity rarely translates to increased compensation. Fourteen percent of hospitalists in a recent SHM Focused Survey reported not even having dedicated time for or being compensated for QI.
Which is not to say, of course, that defining and measuring quality is not a worthy pursuit. On the contrary, QI is a pillar of hospital medicine practice. A recent survey showed that 84% of pediatric hospitalists participated in QI initiatives, and 72% considered the variety of pursuits inherent in a PHM career as a factor influencing career choice.15 But just as we are now focused on choosing wisely in diagnosing and treating our patients, we should also be choosing wisely in diagnosing and treating our systems. What is true for our patients is true for our system of care—simply ordering the test can lead to a cascade of interventions that can be not only costly but also potentially dangerous for the patient.
Physician-defined quality measures in adult HM have now been adopted as yardsticks with which to measure all hospitals—and with which to punish those who do not measure up. In 1984, Dr. Earl Steinberg, then a professor of medicine at Johns Hopkins, published a seminal article in the New England Journal of Medicine describing potential cost savings to the Medicare program from reductions in hospital readmissions.16 This was the match that lit the fuse to what is now the Affordable Care Act Hospital Readmissions Reduction Program. Yet, this quality measure might not even be a quality measure of…quality. A 2013 JAMA study showed that readmission rates for acute myocardial infarction and pneumonia were not correlated with mortality, the time-tested gold standard for quality in medicine.17 That has not stopped Medicare from levying $227 million in fines on 2,225 hospitals across the country beginning Oct. 1, 2013 for excess readmissions in Year 2 of the Hospital Readmissions Reduction Program.18 It seems that we have built it, and they have come, and now they won’t leave.
In Sum
What is the lesson for PHM? Assessing and improving quality of care remains a necessary cornerstone of PHM, but choosing meaningful quality measures is difficult and can have long-term consequences. The choices we make with regard to the direction of QI will, however, define the future of pediatric healthcare for decades to come. As such, we cannot waste both financial and human resources on defining and assessing quality measures that may sound superficially important but, in the end, are not reflective of the real quality of care provided to our patients.
My father, in his adherence to his own ideal of quality medical care, reaped the unintended consequences of his pursuit of quality medical care. Sometimes, though just sometimes, there are unintended consequences to the unintended consequences. I learned, and was perhaps inspired, just by watching him interact with patients and their families. Somehow I don’t think my own children will learn much by watching me interact with my computer.
Dr. Chang is pediatric editor of The Hospitalist. He is associate clinical professor of medicine and pediatrics at the University of California at San Diego (UCSD) School of Medicine, and a hospitalist at both UCSD Medical Center and Rady Children’s Hospital. Send comments and questions to wwch@ucsd.edu.