User login
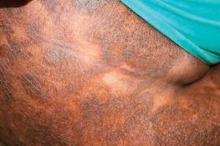
What Is Your Diagnosis? Folliculocentric Tinea Versicolor
Sleep Quality May Impact Skin Health
A recent article in the New York Times ("How Well you Sleep May Hinge on Race," Aug. 20, 2012), discussed a link between ethnicity and quality of sleep. According to the story, non-Hispanic white patients sleep longer with less interruption than people of other ethnicities. Black patients are also most likely to get shorter, more restless sleep, according to the article.
Poor sleep quality has been associated with high blood pressure, obesity, and insulin resistance, which might help explain why people in some minority groups experience higher rates of chronic health conditions.
The article highlighted racial disparity evidence presented at the annual Associated Professional Sleep Societies meeting in Boston in June. White patients from the Chicago area were found to get an average of 7.4 hours of sleep per night; Hispanic and Asian patients averaged 6.9 hours; and black patients averaged 6.8 hours. Sleep quality – defined as ease in falling asleep and length of uninterrupted sleep – was also higher for white patients than for black patients. Even after adjusting for cardiovascular disease, sleep apnea, and obesity, black patients and other ethnic minorities still got less, and more disruptive, sleep than white patients.
Could differences in quality of sleep also be associated with dermatologic conditions that occur at a higher rate in certain ethnic groups?
A study, published earlier this year, found that sleep disturbance correlated with immune system dysregulation (Am. J. Geriatr. Psychiatry 2012 Feb. 10 [epub ahead of print]), which could help explain why atopic dermatitis is seem more frequently in children of Asian and African-American descent?
Interestingly, there have been reports of sleep disturbances in both infants and older children with atopic dermatitis (Asian Pac. J. Allergy Immunol. 2012;30:26-31). But is it the atopic dermatitis that causes poor sleep or the poor sleep that exacerbates the atopic dermatitis?
I think there is probably a relationship in both directions. It would be interesting to study whether socioeconomic and living conditions, regardless of race and ethnicity, are contributing factors. Insights into sleep quality and ethnic disparities may also offer further information on the same disparities seen in skin conditions.
- Naissan Wesley, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
A recent article in the New York Times ("How Well you Sleep May Hinge on Race," Aug. 20, 2012), discussed a link between ethnicity and quality of sleep. According to the story, non-Hispanic white patients sleep longer with less interruption than people of other ethnicities. Black patients are also most likely to get shorter, more restless sleep, according to the article.
Poor sleep quality has been associated with high blood pressure, obesity, and insulin resistance, which might help explain why people in some minority groups experience higher rates of chronic health conditions.
The article highlighted racial disparity evidence presented at the annual Associated Professional Sleep Societies meeting in Boston in June. White patients from the Chicago area were found to get an average of 7.4 hours of sleep per night; Hispanic and Asian patients averaged 6.9 hours; and black patients averaged 6.8 hours. Sleep quality – defined as ease in falling asleep and length of uninterrupted sleep – was also higher for white patients than for black patients. Even after adjusting for cardiovascular disease, sleep apnea, and obesity, black patients and other ethnic minorities still got less, and more disruptive, sleep than white patients.
Could differences in quality of sleep also be associated with dermatologic conditions that occur at a higher rate in certain ethnic groups?
A study, published earlier this year, found that sleep disturbance correlated with immune system dysregulation (Am. J. Geriatr. Psychiatry 2012 Feb. 10 [epub ahead of print]), which could help explain why atopic dermatitis is seem more frequently in children of Asian and African-American descent?
Interestingly, there have been reports of sleep disturbances in both infants and older children with atopic dermatitis (Asian Pac. J. Allergy Immunol. 2012;30:26-31). But is it the atopic dermatitis that causes poor sleep or the poor sleep that exacerbates the atopic dermatitis?
I think there is probably a relationship in both directions. It would be interesting to study whether socioeconomic and living conditions, regardless of race and ethnicity, are contributing factors. Insights into sleep quality and ethnic disparities may also offer further information on the same disparities seen in skin conditions.
- Naissan Wesley, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
A recent article in the New York Times ("How Well you Sleep May Hinge on Race," Aug. 20, 2012), discussed a link between ethnicity and quality of sleep. According to the story, non-Hispanic white patients sleep longer with less interruption than people of other ethnicities. Black patients are also most likely to get shorter, more restless sleep, according to the article.
Poor sleep quality has been associated with high blood pressure, obesity, and insulin resistance, which might help explain why people in some minority groups experience higher rates of chronic health conditions.
The article highlighted racial disparity evidence presented at the annual Associated Professional Sleep Societies meeting in Boston in June. White patients from the Chicago area were found to get an average of 7.4 hours of sleep per night; Hispanic and Asian patients averaged 6.9 hours; and black patients averaged 6.8 hours. Sleep quality – defined as ease in falling asleep and length of uninterrupted sleep – was also higher for white patients than for black patients. Even after adjusting for cardiovascular disease, sleep apnea, and obesity, black patients and other ethnic minorities still got less, and more disruptive, sleep than white patients.
Could differences in quality of sleep also be associated with dermatologic conditions that occur at a higher rate in certain ethnic groups?
A study, published earlier this year, found that sleep disturbance correlated with immune system dysregulation (Am. J. Geriatr. Psychiatry 2012 Feb. 10 [epub ahead of print]), which could help explain why atopic dermatitis is seem more frequently in children of Asian and African-American descent?
Interestingly, there have been reports of sleep disturbances in both infants and older children with atopic dermatitis (Asian Pac. J. Allergy Immunol. 2012;30:26-31). But is it the atopic dermatitis that causes poor sleep or the poor sleep that exacerbates the atopic dermatitis?
I think there is probably a relationship in both directions. It would be interesting to study whether socioeconomic and living conditions, regardless of race and ethnicity, are contributing factors. Insights into sleep quality and ethnic disparities may also offer further information on the same disparities seen in skin conditions.
- Naissan Wesley, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Acanthosis Nigricans Severity Helps Predict Diabetes Risk
BOSTON – Patients with a high grade of acanthosis nigricans should be screened for insulin resistance, according to Dr. Sandhya Venkatswami.
His cross-sectional study found that 47 of 150 acanthosis nigricans patients (31%) were insulin resistant, with an acanthosis nigricans grade of 3 or 4 being more predictive of the condition.
"We suggest that all patients with severe AN [acanthosis nigricans] grades should be evaluated for IR [insulin resistance] and thereby prevent further complications," wrote Dr. Venkatswami, who presented his findings during a poster session at the American Academy of Dermatology’s Summer Academy Meeting.
While previous studies have found acanthosis nigricans to be a marker for prediabetes, Dr. Venkatswami’s study found that taking severity into account helps to further identify patients who may be at risk.
He and his fellow investigators enrolled 150 consecutive patients with acanthosis nigricans of the neck (25 males), aged 18-64 years. The patients were graded according to acanthosis nigricans severity on a scale of I-IV.
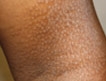
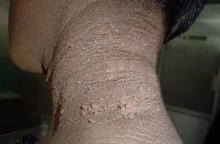
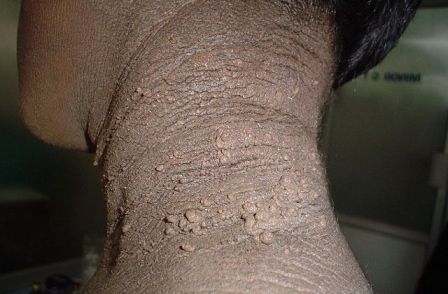
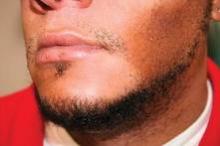
Grade I was defined as acanthosis nigricans that was only visible on close inspection (21 patients); grade II was defined as acanthosis nigricans confined to the base of the skull (58 patients); grade III was defined as acanthosis nigricans that extended laterally to the posterior border of the sternocleidomastoid but was not visible when the patient was facing forward (48 patients); and grade IV was defined as acanthosis nigricans that was visible when the patient was facing forward, as the acanthosis nigricans encircled the neck (23 patients), said Dr. Venkatswami of the department of dermatology, Sri Ramachandra University, Chennai, India.
One patient with grade I acanthosis nigricans was found to be insulin resistant; 10 patients with grade II acanthosis nigricans were found to be insulin resistance; 20 patients with grade III acanthosis nigricans were insulin resistant; and 16 patients with grade IV showed a resistance to insulin.
Secondary study findings showed that patients with higher grades of texture of acanthosis nigricans were also more likely to be insulin resistant. That is, those with visible and extremely coarse "hills and valleys."
"AN lesions are asymptomatic and usually ignored by the patients unless they are of cosmetic concern. However, this is of clinical importance in diagnosing prediabetes," he noted in his poster.
Further studies will look to see if behavior modifications will help lower the risk for diabetes in patients with the condition.
Dr. Venkatswami did not disclose having any conflicts of interest.
BOSTON – Patients with a high grade of acanthosis nigricans should be screened for insulin resistance, according to Dr. Sandhya Venkatswami.
His cross-sectional study found that 47 of 150 acanthosis nigricans patients (31%) were insulin resistant, with an acanthosis nigricans grade of 3 or 4 being more predictive of the condition.
"We suggest that all patients with severe AN [acanthosis nigricans] grades should be evaluated for IR [insulin resistance] and thereby prevent further complications," wrote Dr. Venkatswami, who presented his findings during a poster session at the American Academy of Dermatology’s Summer Academy Meeting.
While previous studies have found acanthosis nigricans to be a marker for prediabetes, Dr. Venkatswami’s study found that taking severity into account helps to further identify patients who may be at risk.
He and his fellow investigators enrolled 150 consecutive patients with acanthosis nigricans of the neck (25 males), aged 18-64 years. The patients were graded according to acanthosis nigricans severity on a scale of I-IV.
Grade I was defined as acanthosis nigricans that was only visible on close inspection (21 patients); grade II was defined as acanthosis nigricans confined to the base of the skull (58 patients); grade III was defined as acanthosis nigricans that extended laterally to the posterior border of the sternocleidomastoid but was not visible when the patient was facing forward (48 patients); and grade IV was defined as acanthosis nigricans that was visible when the patient was facing forward, as the acanthosis nigricans encircled the neck (23 patients), said Dr. Venkatswami of the department of dermatology, Sri Ramachandra University, Chennai, India.
One patient with grade I acanthosis nigricans was found to be insulin resistant; 10 patients with grade II acanthosis nigricans were found to be insulin resistance; 20 patients with grade III acanthosis nigricans were insulin resistant; and 16 patients with grade IV showed a resistance to insulin.
Secondary study findings showed that patients with higher grades of texture of acanthosis nigricans were also more likely to be insulin resistant. That is, those with visible and extremely coarse "hills and valleys."
"AN lesions are asymptomatic and usually ignored by the patients unless they are of cosmetic concern. However, this is of clinical importance in diagnosing prediabetes," he noted in his poster.
Further studies will look to see if behavior modifications will help lower the risk for diabetes in patients with the condition.
Dr. Venkatswami did not disclose having any conflicts of interest.
BOSTON – Patients with a high grade of acanthosis nigricans should be screened for insulin resistance, according to Dr. Sandhya Venkatswami.
His cross-sectional study found that 47 of 150 acanthosis nigricans patients (31%) were insulin resistant, with an acanthosis nigricans grade of 3 or 4 being more predictive of the condition.
"We suggest that all patients with severe AN [acanthosis nigricans] grades should be evaluated for IR [insulin resistance] and thereby prevent further complications," wrote Dr. Venkatswami, who presented his findings during a poster session at the American Academy of Dermatology’s Summer Academy Meeting.
While previous studies have found acanthosis nigricans to be a marker for prediabetes, Dr. Venkatswami’s study found that taking severity into account helps to further identify patients who may be at risk.
He and his fellow investigators enrolled 150 consecutive patients with acanthosis nigricans of the neck (25 males), aged 18-64 years. The patients were graded according to acanthosis nigricans severity on a scale of I-IV.
Grade I was defined as acanthosis nigricans that was only visible on close inspection (21 patients); grade II was defined as acanthosis nigricans confined to the base of the skull (58 patients); grade III was defined as acanthosis nigricans that extended laterally to the posterior border of the sternocleidomastoid but was not visible when the patient was facing forward (48 patients); and grade IV was defined as acanthosis nigricans that was visible when the patient was facing forward, as the acanthosis nigricans encircled the neck (23 patients), said Dr. Venkatswami of the department of dermatology, Sri Ramachandra University, Chennai, India.
One patient with grade I acanthosis nigricans was found to be insulin resistant; 10 patients with grade II acanthosis nigricans were found to be insulin resistance; 20 patients with grade III acanthosis nigricans were insulin resistant; and 16 patients with grade IV showed a resistance to insulin.
Secondary study findings showed that patients with higher grades of texture of acanthosis nigricans were also more likely to be insulin resistant. That is, those with visible and extremely coarse "hills and valleys."
"AN lesions are asymptomatic and usually ignored by the patients unless they are of cosmetic concern. However, this is of clinical importance in diagnosing prediabetes," he noted in his poster.
Further studies will look to see if behavior modifications will help lower the risk for diabetes in patients with the condition.
Dr. Venkatswami did not disclose having any conflicts of interest.
AT THE AMERICAN ACADEMY OF DERMATOLOGY'S SUMMER ACADEMY MEETING
Major Finding: Of 150 patients with acanthosis nigricans, 47 (31%) were insulin resistant.
Data Source: A cross-sectional study of 150 consecutive patients with acanthosis nigricans of the neck who presented to a dermatology practice.
Disclosures: Dr. Venkatswami did not disclose having any conflicts of interest.
Argan Oil for Dry Hair
We were recently asked by a reader if there is any scientific evidence on the benefits of using argan oil to treat dry hair and scalp.
Argan oil is native to Morocco and has been used for centuries in foods and topical preparations. It is a plant oil produced from the argan tree (Argania Spinosa L). Studies have found that the oil has cardioprotective and anti-thrombotic effects when ingested.
Over the past several years, it has become popular in hair care products. While the benefits of consumption of argan oil have been well-studied, its use for hair has not been documented in peer-reviewed literature.
Argan oil may be used on any hair type. It is available in shampoos, conditioners, and leave-in products. I have found that argan oil is beneficial for patients with curly hair, particularly those of African or African-American descent, because it helps to reduce frizz and adds shine. A small amount may be applied to the scalp if dry.
In patients with fine hair, too much oil can be greasy and may weigh curls down. In those cases, small amounts of the oil may be more beneficial. If too much product is used, clarifying shampoos may help remove excess oil.
The number of personal care products on the U.S. market with argan oil as an ingredient increased from just 2 in 2007 to over 100 in 2011. There are many hair care brands that contain argan oil including Moroccanoil, DermOrganic, Josie Maran, One 'N Only, and Organix, among others.
There has been one report of anaphylaxis to argan oil in the literature (Allergy 2010;65:662–3). Studies must be done to assess its actual efficacy for dermatologic scalp conditions and use for ethnic hair.
- Naissan Wesley, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
We were recently asked by a reader if there is any scientific evidence on the benefits of using argan oil to treat dry hair and scalp.
Argan oil is native to Morocco and has been used for centuries in foods and topical preparations. It is a plant oil produced from the argan tree (Argania Spinosa L). Studies have found that the oil has cardioprotective and anti-thrombotic effects when ingested.
Over the past several years, it has become popular in hair care products. While the benefits of consumption of argan oil have been well-studied, its use for hair has not been documented in peer-reviewed literature.
Argan oil may be used on any hair type. It is available in shampoos, conditioners, and leave-in products. I have found that argan oil is beneficial for patients with curly hair, particularly those of African or African-American descent, because it helps to reduce frizz and adds shine. A small amount may be applied to the scalp if dry.
In patients with fine hair, too much oil can be greasy and may weigh curls down. In those cases, small amounts of the oil may be more beneficial. If too much product is used, clarifying shampoos may help remove excess oil.
The number of personal care products on the U.S. market with argan oil as an ingredient increased from just 2 in 2007 to over 100 in 2011. There are many hair care brands that contain argan oil including Moroccanoil, DermOrganic, Josie Maran, One 'N Only, and Organix, among others.
There has been one report of anaphylaxis to argan oil in the literature (Allergy 2010;65:662–3). Studies must be done to assess its actual efficacy for dermatologic scalp conditions and use for ethnic hair.
- Naissan Wesley, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
We were recently asked by a reader if there is any scientific evidence on the benefits of using argan oil to treat dry hair and scalp.
Argan oil is native to Morocco and has been used for centuries in foods and topical preparations. It is a plant oil produced from the argan tree (Argania Spinosa L). Studies have found that the oil has cardioprotective and anti-thrombotic effects when ingested.
Over the past several years, it has become popular in hair care products. While the benefits of consumption of argan oil have been well-studied, its use for hair has not been documented in peer-reviewed literature.
Argan oil may be used on any hair type. It is available in shampoos, conditioners, and leave-in products. I have found that argan oil is beneficial for patients with curly hair, particularly those of African or African-American descent, because it helps to reduce frizz and adds shine. A small amount may be applied to the scalp if dry.
In patients with fine hair, too much oil can be greasy and may weigh curls down. In those cases, small amounts of the oil may be more beneficial. If too much product is used, clarifying shampoos may help remove excess oil.
The number of personal care products on the U.S. market with argan oil as an ingredient increased from just 2 in 2007 to over 100 in 2011. There are many hair care brands that contain argan oil including Moroccanoil, DermOrganic, Josie Maran, One 'N Only, and Organix, among others.
There has been one report of anaphylaxis to argan oil in the literature (Allergy 2010;65:662–3). Studies must be done to assess its actual efficacy for dermatologic scalp conditions and use for ethnic hair.
- Naissan Wesley, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Skin of Color: Barriers to Melanoma Detection
Melanoma accounts for 75% of all skin cancer deaths. Ultraviolet exposure is still targeted as the major etiologic factor, but for black patients, skin erythema has been estimated to occur at a UV radiation dose 6-to-33 times greater than that experienced by white patients. Many have concluded that this is why black patients experience lower rates of melanoma than white patients.
Black patients, however, present at a later stage and have a higher melanoma-specific mortality, both of which have been linked to time of diagnosis and the ability to seek care at the onset of localized disease. Thus, there still exists a barrier to the detection and treatment of melanoma in black patients.
In the July issue of Archives of Dermatology (2012;148:797-801), an article highlighted the anatomic distribution of malignant melanoma in the non-Hispanic black patient in an effort to explore how distribution of melanoma relates to UV exposure.
Data from 46 population-based cancer registries were analyzed. The most frequent site of melanoma in non-Hispanic black patients – both male and female, between the years 1998 and 2007 – was found to be the lower limbs and hip (58.9%). Of those, 27% were of the acral lentiginous type, which is not associated with exposure to UV rays.
The second most common location was the trunk (16.5%), which affected patients at a younger age; 46% of females and 31% of males were less than 44 years of age. The median age was 56 years for males and 48 years for females at presentation.
This study reiterates the burden of melanoma in the black community. It also highlights gaps in the detection of melanoma, which may be because of site of diagnosis – such as those of the acral lentiginous types – and unclear risk factors, the general underestimation of risk, and access to care.
- Lily Talakoub, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Melanoma accounts for 75% of all skin cancer deaths. Ultraviolet exposure is still targeted as the major etiologic factor, but for black patients, skin erythema has been estimated to occur at a UV radiation dose 6-to-33 times greater than that experienced by white patients. Many have concluded that this is why black patients experience lower rates of melanoma than white patients.
Black patients, however, present at a later stage and have a higher melanoma-specific mortality, both of which have been linked to time of diagnosis and the ability to seek care at the onset of localized disease. Thus, there still exists a barrier to the detection and treatment of melanoma in black patients.
In the July issue of Archives of Dermatology (2012;148:797-801), an article highlighted the anatomic distribution of malignant melanoma in the non-Hispanic black patient in an effort to explore how distribution of melanoma relates to UV exposure.
Data from 46 population-based cancer registries were analyzed. The most frequent site of melanoma in non-Hispanic black patients – both male and female, between the years 1998 and 2007 – was found to be the lower limbs and hip (58.9%). Of those, 27% were of the acral lentiginous type, which is not associated with exposure to UV rays.
The second most common location was the trunk (16.5%), which affected patients at a younger age; 46% of females and 31% of males were less than 44 years of age. The median age was 56 years for males and 48 years for females at presentation.
This study reiterates the burden of melanoma in the black community. It also highlights gaps in the detection of melanoma, which may be because of site of diagnosis – such as those of the acral lentiginous types – and unclear risk factors, the general underestimation of risk, and access to care.
- Lily Talakoub, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Melanoma accounts for 75% of all skin cancer deaths. Ultraviolet exposure is still targeted as the major etiologic factor, but for black patients, skin erythema has been estimated to occur at a UV radiation dose 6-to-33 times greater than that experienced by white patients. Many have concluded that this is why black patients experience lower rates of melanoma than white patients.
Black patients, however, present at a later stage and have a higher melanoma-specific mortality, both of which have been linked to time of diagnosis and the ability to seek care at the onset of localized disease. Thus, there still exists a barrier to the detection and treatment of melanoma in black patients.
In the July issue of Archives of Dermatology (2012;148:797-801), an article highlighted the anatomic distribution of malignant melanoma in the non-Hispanic black patient in an effort to explore how distribution of melanoma relates to UV exposure.
Data from 46 population-based cancer registries were analyzed. The most frequent site of melanoma in non-Hispanic black patients – both male and female, between the years 1998 and 2007 – was found to be the lower limbs and hip (58.9%). Of those, 27% were of the acral lentiginous type, which is not associated with exposure to UV rays.
The second most common location was the trunk (16.5%), which affected patients at a younger age; 46% of females and 31% of males were less than 44 years of age. The median age was 56 years for males and 48 years for females at presentation.
This study reiterates the burden of melanoma in the black community. It also highlights gaps in the detection of melanoma, which may be because of site of diagnosis – such as those of the acral lentiginous types – and unclear risk factors, the general underestimation of risk, and access to care.
- Lily Talakoub, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Melanoma in the Skin of Color Population
Dr. Rossi discusses melanoma in the skin of color population including the incidence and presentation of melanoma as well as factors contributing to delayed diagnosis in these patients. He also gives recommendations to physicians to help educate their patients. For more information, read Dr. Rossi's article in the May 2012 issue, "Melanoma in Skin of Color."
Dr. Rossi discusses melanoma in the skin of color population including the incidence and presentation of melanoma as well as factors contributing to delayed diagnosis in these patients. He also gives recommendations to physicians to help educate their patients. For more information, read Dr. Rossi's article in the May 2012 issue, "Melanoma in Skin of Color."
Dr. Rossi discusses melanoma in the skin of color population including the incidence and presentation of melanoma as well as factors contributing to delayed diagnosis in these patients. He also gives recommendations to physicians to help educate their patients. For more information, read Dr. Rossi's article in the May 2012 issue, "Melanoma in Skin of Color."
Treatments for Skin of Color [book review]
Skin of Color: Dry Shampoo
Ethnic hair can become dry, brittle, and fractured when exposed to harsh solvents, heat, and repeat chemical treatments. To combat these issues, consider discussing the use of dry shampoo with your patients.
Dry shampoo is a powdered substance used to absorb oil in hair when traditional shampoo is not available, or for use with hair that dries out after repeat washings.
The ingredients in dry shampoo are called "absorbing agents," which soak up excess oil and dirt on the scalp. The most common absorbing agents are Oryza sativa starch, aluminum starch octenylsuccinate, zea mays starch, and silica.
There are two types of dry shampoo: those that come in a loose powder form and those that come in an aerosol form.
Powder dry shampoo can be applied directly to the scalp from the bottle and either brushed through or massaged in. Dry shampoo aerosol can be sprayed directly onto the scalp from a few inches away.
Recent advances in dry shampoos have instituted different coloring agents to help match the hair, as well as fragrances to mask any odor.
Many of these products can be found on www.dryshampoo.com.
- Lily Talakoub, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Ethnic hair can become dry, brittle, and fractured when exposed to harsh solvents, heat, and repeat chemical treatments. To combat these issues, consider discussing the use of dry shampoo with your patients.
Dry shampoo is a powdered substance used to absorb oil in hair when traditional shampoo is not available, or for use with hair that dries out after repeat washings.
The ingredients in dry shampoo are called "absorbing agents," which soak up excess oil and dirt on the scalp. The most common absorbing agents are Oryza sativa starch, aluminum starch octenylsuccinate, zea mays starch, and silica.
There are two types of dry shampoo: those that come in a loose powder form and those that come in an aerosol form.
Powder dry shampoo can be applied directly to the scalp from the bottle and either brushed through or massaged in. Dry shampoo aerosol can be sprayed directly onto the scalp from a few inches away.
Recent advances in dry shampoos have instituted different coloring agents to help match the hair, as well as fragrances to mask any odor.
Many of these products can be found on www.dryshampoo.com.
- Lily Talakoub, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Ethnic hair can become dry, brittle, and fractured when exposed to harsh solvents, heat, and repeat chemical treatments. To combat these issues, consider discussing the use of dry shampoo with your patients.
Dry shampoo is a powdered substance used to absorb oil in hair when traditional shampoo is not available, or for use with hair that dries out after repeat washings.
The ingredients in dry shampoo are called "absorbing agents," which soak up excess oil and dirt on the scalp. The most common absorbing agents are Oryza sativa starch, aluminum starch octenylsuccinate, zea mays starch, and silica.
There are two types of dry shampoo: those that come in a loose powder form and those that come in an aerosol form.
Powder dry shampoo can be applied directly to the scalp from the bottle and either brushed through or massaged in. Dry shampoo aerosol can be sprayed directly onto the scalp from a few inches away.
Recent advances in dry shampoos have instituted different coloring agents to help match the hair, as well as fragrances to mask any odor.
Many of these products can be found on www.dryshampoo.com.
- Lily Talakoub, M.D.
Do you have questions about treating patients with darker skin? If so, send them to sknews@elsevier.com.
Skin Risks of Alternative Medicine Explored
NEW YORK – Much of the complementary and alternative medicine that is practiced by Asian and Hispanic cultures can actually do more harm than good, according to Dr. Roopal V. Kundu.
In these cultures, patients often view illness as having strong spiritual origins and consequences, she said at the seminar. Illness "can have a dramatic effect on psyche."
In the traditional Hispanic community, many individuals have seen or are concurrently seeing a local healer, said Dr. Kundu, director of the Northwestern Center for Ethnic Skin at Northwestern University, Chicago. These healers might be practitioners of curanderismo, in which they believe they are healing as a "gift from a higher power," while employing prayers, baths, and botanicals to combat illness. Another practice is espiritismo, which is a belief that good and evil spirits affect health.
Asian patients, meanwhile, have their own set of healers and practices. For example, patients may practice "cupping" for chronic pain and respiratory disease, whereby a glass or plastic cup is placed over the back to create a local vacuum, in the hopes of relieving congestion and increasing circulation.
"Wet cupping" is similar, except that a small scratch or incision is made prior to the cupping procedure.
Both cupping practices leave behind circular patterns of erythema, edema, and ecchymosis, and could be mistaken for child abuse or another skin disorder, said Dr. Kundu, who recently published a paper on this and other Asian dermatoses (Int. J. Dermatol. 2012;51:372-82).
Similarly, "coining," "spooning," or "cao gio" is a Vietnamese dermabrasion therapy, whereby skin is lubricated with oils and then rubbed firmly using the edge of a spoon or coin.
The result will be parallel lines of ecchymoses on the chest and back in a "pine tree" pattern, said Dr. Kundu.
Another Asian practice, moxibustion, or moxa, involves burning materials on the skin to combat atopic dermatitis, postherpetic neuralgia, and tinea pedis. The small, circular scars left behind approximate cigarette burns.
She also advised questioning the use of hair oils in Southeast Asian and black patients. Mustard, coconut, and amla oil are supposed to be toxic to certain dermatophytes, said Dr. Kundu. However, she warned, the theory might backfire in practice. "Are the different oils perpetuating different organisms and allowing [tinea capitas]?"
Finally, Dr. Kundu noted that among Asian and Hispanic populations, decision making by family consensus is the norm. "With almost all of my ethnic patients, I almost always have someone else in the room – a sister, brother, parent, child, uncle," she said. "You’re kind of engaging both of them in the dialogue and [the patient is] often looking toward that person for help in navigating the health care system."
Dr. Kundu stated that she had no relevant relationships with industry to disclose.
NEW YORK – Much of the complementary and alternative medicine that is practiced by Asian and Hispanic cultures can actually do more harm than good, according to Dr. Roopal V. Kundu.
In these cultures, patients often view illness as having strong spiritual origins and consequences, she said at the seminar. Illness "can have a dramatic effect on psyche."
In the traditional Hispanic community, many individuals have seen or are concurrently seeing a local healer, said Dr. Kundu, director of the Northwestern Center for Ethnic Skin at Northwestern University, Chicago. These healers might be practitioners of curanderismo, in which they believe they are healing as a "gift from a higher power," while employing prayers, baths, and botanicals to combat illness. Another practice is espiritismo, which is a belief that good and evil spirits affect health.
Asian patients, meanwhile, have their own set of healers and practices. For example, patients may practice "cupping" for chronic pain and respiratory disease, whereby a glass or plastic cup is placed over the back to create a local vacuum, in the hopes of relieving congestion and increasing circulation.
"Wet cupping" is similar, except that a small scratch or incision is made prior to the cupping procedure.
Both cupping practices leave behind circular patterns of erythema, edema, and ecchymosis, and could be mistaken for child abuse or another skin disorder, said Dr. Kundu, who recently published a paper on this and other Asian dermatoses (Int. J. Dermatol. 2012;51:372-82).
Similarly, "coining," "spooning," or "cao gio" is a Vietnamese dermabrasion therapy, whereby skin is lubricated with oils and then rubbed firmly using the edge of a spoon or coin.
The result will be parallel lines of ecchymoses on the chest and back in a "pine tree" pattern, said Dr. Kundu.
Another Asian practice, moxibustion, or moxa, involves burning materials on the skin to combat atopic dermatitis, postherpetic neuralgia, and tinea pedis. The small, circular scars left behind approximate cigarette burns.
She also advised questioning the use of hair oils in Southeast Asian and black patients. Mustard, coconut, and amla oil are supposed to be toxic to certain dermatophytes, said Dr. Kundu. However, she warned, the theory might backfire in practice. "Are the different oils perpetuating different organisms and allowing [tinea capitas]?"
Finally, Dr. Kundu noted that among Asian and Hispanic populations, decision making by family consensus is the norm. "With almost all of my ethnic patients, I almost always have someone else in the room – a sister, brother, parent, child, uncle," she said. "You’re kind of engaging both of them in the dialogue and [the patient is] often looking toward that person for help in navigating the health care system."
Dr. Kundu stated that she had no relevant relationships with industry to disclose.
NEW YORK – Much of the complementary and alternative medicine that is practiced by Asian and Hispanic cultures can actually do more harm than good, according to Dr. Roopal V. Kundu.
In these cultures, patients often view illness as having strong spiritual origins and consequences, she said at the seminar. Illness "can have a dramatic effect on psyche."
In the traditional Hispanic community, many individuals have seen or are concurrently seeing a local healer, said Dr. Kundu, director of the Northwestern Center for Ethnic Skin at Northwestern University, Chicago. These healers might be practitioners of curanderismo, in which they believe they are healing as a "gift from a higher power," while employing prayers, baths, and botanicals to combat illness. Another practice is espiritismo, which is a belief that good and evil spirits affect health.
Asian patients, meanwhile, have their own set of healers and practices. For example, patients may practice "cupping" for chronic pain and respiratory disease, whereby a glass or plastic cup is placed over the back to create a local vacuum, in the hopes of relieving congestion and increasing circulation.
"Wet cupping" is similar, except that a small scratch or incision is made prior to the cupping procedure.
Both cupping practices leave behind circular patterns of erythema, edema, and ecchymosis, and could be mistaken for child abuse or another skin disorder, said Dr. Kundu, who recently published a paper on this and other Asian dermatoses (Int. J. Dermatol. 2012;51:372-82).
Similarly, "coining," "spooning," or "cao gio" is a Vietnamese dermabrasion therapy, whereby skin is lubricated with oils and then rubbed firmly using the edge of a spoon or coin.
The result will be parallel lines of ecchymoses on the chest and back in a "pine tree" pattern, said Dr. Kundu.
Another Asian practice, moxibustion, or moxa, involves burning materials on the skin to combat atopic dermatitis, postherpetic neuralgia, and tinea pedis. The small, circular scars left behind approximate cigarette burns.
She also advised questioning the use of hair oils in Southeast Asian and black patients. Mustard, coconut, and amla oil are supposed to be toxic to certain dermatophytes, said Dr. Kundu. However, she warned, the theory might backfire in practice. "Are the different oils perpetuating different organisms and allowing [tinea capitas]?"
Finally, Dr. Kundu noted that among Asian and Hispanic populations, decision making by family consensus is the norm. "With almost all of my ethnic patients, I almost always have someone else in the room – a sister, brother, parent, child, uncle," she said. "You’re kind of engaging both of them in the dialogue and [the patient is] often looking toward that person for help in navigating the health care system."
Dr. Kundu stated that she had no relevant relationships with industry to disclose.
EXPERT ANALYSIS FROM THE SKIN OF COLOR SEMINAR SERIES
CTCL Proves Challenging in Skin of Color Patients
Over the past 4 decades, cutaneous T-cell lymphoma diagnoses have been on the rise, especially among black and other skin of color patients. Unfortunately, this form of skin cancer can be a diagnostic challenge.
Regarding diagnosis, cutaneous T-cell lymphoma (CTCL) is the wild card of dermatology; it is a great mimicker of many skin disorders, and can look like almost anything. However, the most striking feature of the condition – and the key to diagnosis in ethnic skin – is its polymorphous pigmentation that is unique to skin of color.
CTCL lesions may be flat or raised, and may mimic other skin disorders associated with pigment change. These can include tinea versicolor, vitiligo, pityriasis rosea, and psoriasis. Lichen planus pigmentosus and progressive macular hypomelanosis are other important CTCL mimickers. Consider all of these conditions in the differential diagnosis.
An excellent resource for photos and descriptions of CTCL, as well as CTCL look-alikes, is an article by Dr. Ginette A. Hinds and Dr. Peter Heald (J. Am. Acad. Dermatol. 2009;60:359-75). The article also highlights the clinical variants within the mycosis fungoides subtype, the most common form of CTCL among blacks.
For example, look out for the "herald patch" of unilesional mycosis fungoides, which takes the form of a single large, dyspigmented patch. According to the authors, this variant has an excellent prognosis, possibly because of an active immune response that limits the initial spread of disease and contributes to preventing relapse.
Another variant is pigmented purpuric mycosis fungoides, which can often be confused with the benign pigmented purpura syndromes of Schamberg’s disease (progressive pigmented purpuric dermatitis), Gougerot-Blum syndrome (pigmented purpuric lichenoid dermatitis), Majocchi’s disease (purpura annularis telangiectodes), Doucas and Kapetanakis (lymphocytic capillaritis of unknown cause), and lichen aureus. The key to diagnosis in this case is recalling that "the lesions of the benign syndromes rarely assume the morphology and distribution found with mycosis fungoides," Dr. Hinds and Dr. Heald wrote.
Not only is mycosis fungoides difficult to diagnose, but it is especially prevalent among black patients. For instance, a 1988 study looking at Surveillance, Epidemiology, and End Results (SEER) data from 1973 through 1984 found that the incidence among black patients was twice that of white patients: 0.52/100,000 vs. 0.26 (JAMA 1988;260:42-46).
Similarly, in another study of 132 black patients with skin cancer, mycosis fungoides represented 12.1% of all skin neoplasms (Dermatol. Clin. 1988;6:397-405).
Mycosis fungoides is the fourth most common skin cancer among Japanese patients, representing approximately 5% of all skin malignancies in the population.
The incidence of CTCL and its subtypes is only increasing. A 2007 study that extended the SEER data mentioned above from 1973 to 2002 and included all CTCL cases found an incidence rate of 9.0 for black patients, per 1 million person-years, compared with 6.1 for white patients (Arch. Dermatol. 2007;143:854-9).
As in many skin cancers, early diagnosis can make the difference in successful outcomes. So add CTCL, and especially the mycosis fungoides subtype, to your differential when confronting pigmentation disorders in skin of color patients.
Dr. Roberts is past president of the Women’s Dermatologic Society (WDS) as well as past president of the California Society of Dermatology and Dermatologic Surgery (Calderm). She was a founding director of dermatopathology at the Loma Linda University Medical Center (Calif.). She currently runs a private practice in Rancho Mirage, Calif.
She disclosed financial relationships with Allergan, L’Oréal/La Roche Posay, Skin Medica, and Valeant Pharmaceuticals.
Over the past 4 decades, cutaneous T-cell lymphoma diagnoses have been on the rise, especially among black and other skin of color patients. Unfortunately, this form of skin cancer can be a diagnostic challenge.
Regarding diagnosis, cutaneous T-cell lymphoma (CTCL) is the wild card of dermatology; it is a great mimicker of many skin disorders, and can look like almost anything. However, the most striking feature of the condition – and the key to diagnosis in ethnic skin – is its polymorphous pigmentation that is unique to skin of color.
CTCL lesions may be flat or raised, and may mimic other skin disorders associated with pigment change. These can include tinea versicolor, vitiligo, pityriasis rosea, and psoriasis. Lichen planus pigmentosus and progressive macular hypomelanosis are other important CTCL mimickers. Consider all of these conditions in the differential diagnosis.
An excellent resource for photos and descriptions of CTCL, as well as CTCL look-alikes, is an article by Dr. Ginette A. Hinds and Dr. Peter Heald (J. Am. Acad. Dermatol. 2009;60:359-75). The article also highlights the clinical variants within the mycosis fungoides subtype, the most common form of CTCL among blacks.
For example, look out for the "herald patch" of unilesional mycosis fungoides, which takes the form of a single large, dyspigmented patch. According to the authors, this variant has an excellent prognosis, possibly because of an active immune response that limits the initial spread of disease and contributes to preventing relapse.
Another variant is pigmented purpuric mycosis fungoides, which can often be confused with the benign pigmented purpura syndromes of Schamberg’s disease (progressive pigmented purpuric dermatitis), Gougerot-Blum syndrome (pigmented purpuric lichenoid dermatitis), Majocchi’s disease (purpura annularis telangiectodes), Doucas and Kapetanakis (lymphocytic capillaritis of unknown cause), and lichen aureus. The key to diagnosis in this case is recalling that "the lesions of the benign syndromes rarely assume the morphology and distribution found with mycosis fungoides," Dr. Hinds and Dr. Heald wrote.
Not only is mycosis fungoides difficult to diagnose, but it is especially prevalent among black patients. For instance, a 1988 study looking at Surveillance, Epidemiology, and End Results (SEER) data from 1973 through 1984 found that the incidence among black patients was twice that of white patients: 0.52/100,000 vs. 0.26 (JAMA 1988;260:42-46).
Similarly, in another study of 132 black patients with skin cancer, mycosis fungoides represented 12.1% of all skin neoplasms (Dermatol. Clin. 1988;6:397-405).
Mycosis fungoides is the fourth most common skin cancer among Japanese patients, representing approximately 5% of all skin malignancies in the population.
The incidence of CTCL and its subtypes is only increasing. A 2007 study that extended the SEER data mentioned above from 1973 to 2002 and included all CTCL cases found an incidence rate of 9.0 for black patients, per 1 million person-years, compared with 6.1 for white patients (Arch. Dermatol. 2007;143:854-9).
As in many skin cancers, early diagnosis can make the difference in successful outcomes. So add CTCL, and especially the mycosis fungoides subtype, to your differential when confronting pigmentation disorders in skin of color patients.
Dr. Roberts is past president of the Women’s Dermatologic Society (WDS) as well as past president of the California Society of Dermatology and Dermatologic Surgery (Calderm). She was a founding director of dermatopathology at the Loma Linda University Medical Center (Calif.). She currently runs a private practice in Rancho Mirage, Calif.
She disclosed financial relationships with Allergan, L’Oréal/La Roche Posay, Skin Medica, and Valeant Pharmaceuticals.
Over the past 4 decades, cutaneous T-cell lymphoma diagnoses have been on the rise, especially among black and other skin of color patients. Unfortunately, this form of skin cancer can be a diagnostic challenge.
Regarding diagnosis, cutaneous T-cell lymphoma (CTCL) is the wild card of dermatology; it is a great mimicker of many skin disorders, and can look like almost anything. However, the most striking feature of the condition – and the key to diagnosis in ethnic skin – is its polymorphous pigmentation that is unique to skin of color.
CTCL lesions may be flat or raised, and may mimic other skin disorders associated with pigment change. These can include tinea versicolor, vitiligo, pityriasis rosea, and psoriasis. Lichen planus pigmentosus and progressive macular hypomelanosis are other important CTCL mimickers. Consider all of these conditions in the differential diagnosis.
An excellent resource for photos and descriptions of CTCL, as well as CTCL look-alikes, is an article by Dr. Ginette A. Hinds and Dr. Peter Heald (J. Am. Acad. Dermatol. 2009;60:359-75). The article also highlights the clinical variants within the mycosis fungoides subtype, the most common form of CTCL among blacks.
For example, look out for the "herald patch" of unilesional mycosis fungoides, which takes the form of a single large, dyspigmented patch. According to the authors, this variant has an excellent prognosis, possibly because of an active immune response that limits the initial spread of disease and contributes to preventing relapse.
Another variant is pigmented purpuric mycosis fungoides, which can often be confused with the benign pigmented purpura syndromes of Schamberg’s disease (progressive pigmented purpuric dermatitis), Gougerot-Blum syndrome (pigmented purpuric lichenoid dermatitis), Majocchi’s disease (purpura annularis telangiectodes), Doucas and Kapetanakis (lymphocytic capillaritis of unknown cause), and lichen aureus. The key to diagnosis in this case is recalling that "the lesions of the benign syndromes rarely assume the morphology and distribution found with mycosis fungoides," Dr. Hinds and Dr. Heald wrote.
Not only is mycosis fungoides difficult to diagnose, but it is especially prevalent among black patients. For instance, a 1988 study looking at Surveillance, Epidemiology, and End Results (SEER) data from 1973 through 1984 found that the incidence among black patients was twice that of white patients: 0.52/100,000 vs. 0.26 (JAMA 1988;260:42-46).
Similarly, in another study of 132 black patients with skin cancer, mycosis fungoides represented 12.1% of all skin neoplasms (Dermatol. Clin. 1988;6:397-405).
Mycosis fungoides is the fourth most common skin cancer among Japanese patients, representing approximately 5% of all skin malignancies in the population.
The incidence of CTCL and its subtypes is only increasing. A 2007 study that extended the SEER data mentioned above from 1973 to 2002 and included all CTCL cases found an incidence rate of 9.0 for black patients, per 1 million person-years, compared with 6.1 for white patients (Arch. Dermatol. 2007;143:854-9).
As in many skin cancers, early diagnosis can make the difference in successful outcomes. So add CTCL, and especially the mycosis fungoides subtype, to your differential when confronting pigmentation disorders in skin of color patients.
Dr. Roberts is past president of the Women’s Dermatologic Society (WDS) as well as past president of the California Society of Dermatology and Dermatologic Surgery (Calderm). She was a founding director of dermatopathology at the Loma Linda University Medical Center (Calif.). She currently runs a private practice in Rancho Mirage, Calif.
She disclosed financial relationships with Allergan, L’Oréal/La Roche Posay, Skin Medica, and Valeant Pharmaceuticals.