User login
Coding for Biopsies, Shave Removals, and Excisions
In dermatology, samples of skin and subcutaneous tissue are routinely removed to establish a diagnosis, treat symptomatic lesions, or remove potential tumors. The Current Procedural Terminology (CPT) codes used in billing for these procedures typically are generic, but it is important to differentiate between 3 degrees of tissue removal—biopsy, shave removal, and excision—when billing for these services since different codes may be appropriate in each of these circumstances.
Biopsy
Specifically, biopsy (CPT codes 11100/11101) is described as an “independent…procedure to obtain tissue for pathologic examination.”1 The method of biopsy is not specified by CPT and can include any of the following, as long as the primary purpose of the procedure is to remove tissue for analysis: removal by scissors, shaving with a blade or specialized instrument to any level including the subcutaneous fat, extraction using a punch, and excision down to the subcutaneous fat with a scalpel. The feature that differentiates biopsy from shave removal or excision is not depth or extent of tissue mobilization but the intent “to remove a portion of skin, suspect lesion, or entire lesion so that it can be examined histologically.”2 The underlying assumption is that neither definitive clinical nor histologic diagnosis exists prior to biopsy, the purpose of which is to help establish the identity of the lesion.
If the tissue within a large, single lesion is sampled at several separate locations at the same visit, then only a single unit of a single biopsy code (eg, either 11100, 11101, or some site-specific code) should be reported.In contrast, if a number of discrete lesions in the same approximate anatomic area were sampled for diagnoses, each sample taken from separate lesions would constitute a distinct biopsy and would be billed as a separate unit of service.
Shave Removals and Excisions
Shave removal of skin lesions (CPT codes 11300–11313) includes the removal of tangential or saucerized skin lesions to a level no deeper than the base of the dermis. The CPT provides no detailed guidance regarding differentiation of codes for shave removal versus biopsy when a specimen is submitted for histopathologic examination other than the definition of biopsy that was discussed previously. If the tissue is removed specifically for establishing diagnosis, then by definition the procedure should be coded as a biopsy. On the other hand, shave removal implies the intent to completely remove a lesion that already has a presumptive clinical or histologic diagnosis or is being removed for some purpose other than diagnosis (eg, symptomatic relief).
Shave removals are, however, clearly different than excisions (CPT codes 11400–11646), which must proceed through the entire dermis to the subcutis. Additionally, skin lesion excisions include margins, as the intent of an excision procedure is to remove the entire lesion along with a margin of normal skin around it.2
Specialized Biopsy and Excision Codes
While most biopsies, shave removals, and excisions are performed using generic codes, there are specialized circumstances when more specific codes may be preferable. For instance, there are site-specific skin biopsy codes for the nail unit (11755), vermilion and mucosal lip (40490), penis (54100), vulva (56605), and external ear (69100) that take into account the additional complexity of biopsy at these anatomic locations. There also is a site-specific code for eyelid biopsy (67810), which was redefined in 2013 as an “incisional biopsy of eyelid skin including lid margin.”1 Therefore, biopsies of eyelid skin that do not remove the eyelid margin must be coded as 11100/11101, or if the entire cutaneous lesion was removed, can be reclassified as shave removals, which would be coded in the 11310 to 11313 range.
Specialized excision codes include those of the soft tissue. Soft tissue excision codes typically used by dermatologists are not numbered consecutively, are site-specific, and are typically used for resection of benign tumors confined to the subcutaneous tissue below the skin but above the deep fascia. Cysts of all types, including epidermoid and pilar cysts, are specifically excluded from this code set regardless of how large or complex they may be, as they protrude into the dermis or above and are not exclusively in the subcutis. However, lipomas meet the definition for soft-tissue excision, and therefore site-specific soft tissue excision codes can be used in lieu of traditional skin excision codes. The soft-tissue excision codes are distributed throughout the CPT manual, with distinct codes for the abdominal wall (22902, 22903); leg or ankle (27618, 27632); back or flank (21930, 21931); external auditory canal (69145); upper arm or elbow (24075, 24071); face or scalp (21011, 21012); hand or finger (26115, 26111); foot or toe (28043, 28039); forearm or wrist (25075, 25071); hip or pelvis (27047, 27043); thigh or knee (27327, 27337); neck or anterior thorax (21555, 21552); and shoulder (23075, 23071). In general, there are 2 codes for each area—one for smaller and one for larger excisions—but they frequently are out of order (ie, the code associated with a higher numerical value may correspond with the smaller excision). Care should be taken in selecting the correct code. The specific size cutoffs for the various soft tissue excision code sets are different, so it is important to be familiar with the particular CPT descriptions for each.
Final Thoughts
In summary, biopsies, shave removals, and excisions are different procedures and therefore should be coded differently. Although the distinction between biopsies and shave removals is ill defined, remember that biopsies are intended to establish a diagnosis and shave removals are intended to remove the entire lesion. By definition, excisions must include margins and proceed through the dermis to the subcutis. In particular circumstances, site-specific biopsy codes may be appropriate and can be used to code for lipoma excisions.
1. Current Procedural Terminology 2015, Professional Edition. Chicago, Illinois: American Medical Association; 2014.
2. American Medical Association. Biopsy. CPT Assistant. Chicago, IL: American Medical Association: October 2004:4.
In dermatology, samples of skin and subcutaneous tissue are routinely removed to establish a diagnosis, treat symptomatic lesions, or remove potential tumors. The Current Procedural Terminology (CPT) codes used in billing for these procedures typically are generic, but it is important to differentiate between 3 degrees of tissue removal—biopsy, shave removal, and excision—when billing for these services since different codes may be appropriate in each of these circumstances.
Biopsy
Specifically, biopsy (CPT codes 11100/11101) is described as an “independent…procedure to obtain tissue for pathologic examination.”1 The method of biopsy is not specified by CPT and can include any of the following, as long as the primary purpose of the procedure is to remove tissue for analysis: removal by scissors, shaving with a blade or specialized instrument to any level including the subcutaneous fat, extraction using a punch, and excision down to the subcutaneous fat with a scalpel. The feature that differentiates biopsy from shave removal or excision is not depth or extent of tissue mobilization but the intent “to remove a portion of skin, suspect lesion, or entire lesion so that it can be examined histologically.”2 The underlying assumption is that neither definitive clinical nor histologic diagnosis exists prior to biopsy, the purpose of which is to help establish the identity of the lesion.
If the tissue within a large, single lesion is sampled at several separate locations at the same visit, then only a single unit of a single biopsy code (eg, either 11100, 11101, or some site-specific code) should be reported.In contrast, if a number of discrete lesions in the same approximate anatomic area were sampled for diagnoses, each sample taken from separate lesions would constitute a distinct biopsy and would be billed as a separate unit of service.
Shave Removals and Excisions
Shave removal of skin lesions (CPT codes 11300–11313) includes the removal of tangential or saucerized skin lesions to a level no deeper than the base of the dermis. The CPT provides no detailed guidance regarding differentiation of codes for shave removal versus biopsy when a specimen is submitted for histopathologic examination other than the definition of biopsy that was discussed previously. If the tissue is removed specifically for establishing diagnosis, then by definition the procedure should be coded as a biopsy. On the other hand, shave removal implies the intent to completely remove a lesion that already has a presumptive clinical or histologic diagnosis or is being removed for some purpose other than diagnosis (eg, symptomatic relief).
Shave removals are, however, clearly different than excisions (CPT codes 11400–11646), which must proceed through the entire dermis to the subcutis. Additionally, skin lesion excisions include margins, as the intent of an excision procedure is to remove the entire lesion along with a margin of normal skin around it.2
Specialized Biopsy and Excision Codes
While most biopsies, shave removals, and excisions are performed using generic codes, there are specialized circumstances when more specific codes may be preferable. For instance, there are site-specific skin biopsy codes for the nail unit (11755), vermilion and mucosal lip (40490), penis (54100), vulva (56605), and external ear (69100) that take into account the additional complexity of biopsy at these anatomic locations. There also is a site-specific code for eyelid biopsy (67810), which was redefined in 2013 as an “incisional biopsy of eyelid skin including lid margin.”1 Therefore, biopsies of eyelid skin that do not remove the eyelid margin must be coded as 11100/11101, or if the entire cutaneous lesion was removed, can be reclassified as shave removals, which would be coded in the 11310 to 11313 range.
Specialized excision codes include those of the soft tissue. Soft tissue excision codes typically used by dermatologists are not numbered consecutively, are site-specific, and are typically used for resection of benign tumors confined to the subcutaneous tissue below the skin but above the deep fascia. Cysts of all types, including epidermoid and pilar cysts, are specifically excluded from this code set regardless of how large or complex they may be, as they protrude into the dermis or above and are not exclusively in the subcutis. However, lipomas meet the definition for soft-tissue excision, and therefore site-specific soft tissue excision codes can be used in lieu of traditional skin excision codes. The soft-tissue excision codes are distributed throughout the CPT manual, with distinct codes for the abdominal wall (22902, 22903); leg or ankle (27618, 27632); back or flank (21930, 21931); external auditory canal (69145); upper arm or elbow (24075, 24071); face or scalp (21011, 21012); hand or finger (26115, 26111); foot or toe (28043, 28039); forearm or wrist (25075, 25071); hip or pelvis (27047, 27043); thigh or knee (27327, 27337); neck or anterior thorax (21555, 21552); and shoulder (23075, 23071). In general, there are 2 codes for each area—one for smaller and one for larger excisions—but they frequently are out of order (ie, the code associated with a higher numerical value may correspond with the smaller excision). Care should be taken in selecting the correct code. The specific size cutoffs for the various soft tissue excision code sets are different, so it is important to be familiar with the particular CPT descriptions for each.
Final Thoughts
In summary, biopsies, shave removals, and excisions are different procedures and therefore should be coded differently. Although the distinction between biopsies and shave removals is ill defined, remember that biopsies are intended to establish a diagnosis and shave removals are intended to remove the entire lesion. By definition, excisions must include margins and proceed through the dermis to the subcutis. In particular circumstances, site-specific biopsy codes may be appropriate and can be used to code for lipoma excisions.
In dermatology, samples of skin and subcutaneous tissue are routinely removed to establish a diagnosis, treat symptomatic lesions, or remove potential tumors. The Current Procedural Terminology (CPT) codes used in billing for these procedures typically are generic, but it is important to differentiate between 3 degrees of tissue removal—biopsy, shave removal, and excision—when billing for these services since different codes may be appropriate in each of these circumstances.
Biopsy
Specifically, biopsy (CPT codes 11100/11101) is described as an “independent…procedure to obtain tissue for pathologic examination.”1 The method of biopsy is not specified by CPT and can include any of the following, as long as the primary purpose of the procedure is to remove tissue for analysis: removal by scissors, shaving with a blade or specialized instrument to any level including the subcutaneous fat, extraction using a punch, and excision down to the subcutaneous fat with a scalpel. The feature that differentiates biopsy from shave removal or excision is not depth or extent of tissue mobilization but the intent “to remove a portion of skin, suspect lesion, or entire lesion so that it can be examined histologically.”2 The underlying assumption is that neither definitive clinical nor histologic diagnosis exists prior to biopsy, the purpose of which is to help establish the identity of the lesion.
If the tissue within a large, single lesion is sampled at several separate locations at the same visit, then only a single unit of a single biopsy code (eg, either 11100, 11101, or some site-specific code) should be reported.In contrast, if a number of discrete lesions in the same approximate anatomic area were sampled for diagnoses, each sample taken from separate lesions would constitute a distinct biopsy and would be billed as a separate unit of service.
Shave Removals and Excisions
Shave removal of skin lesions (CPT codes 11300–11313) includes the removal of tangential or saucerized skin lesions to a level no deeper than the base of the dermis. The CPT provides no detailed guidance regarding differentiation of codes for shave removal versus biopsy when a specimen is submitted for histopathologic examination other than the definition of biopsy that was discussed previously. If the tissue is removed specifically for establishing diagnosis, then by definition the procedure should be coded as a biopsy. On the other hand, shave removal implies the intent to completely remove a lesion that already has a presumptive clinical or histologic diagnosis or is being removed for some purpose other than diagnosis (eg, symptomatic relief).
Shave removals are, however, clearly different than excisions (CPT codes 11400–11646), which must proceed through the entire dermis to the subcutis. Additionally, skin lesion excisions include margins, as the intent of an excision procedure is to remove the entire lesion along with a margin of normal skin around it.2
Specialized Biopsy and Excision Codes
While most biopsies, shave removals, and excisions are performed using generic codes, there are specialized circumstances when more specific codes may be preferable. For instance, there are site-specific skin biopsy codes for the nail unit (11755), vermilion and mucosal lip (40490), penis (54100), vulva (56605), and external ear (69100) that take into account the additional complexity of biopsy at these anatomic locations. There also is a site-specific code for eyelid biopsy (67810), which was redefined in 2013 as an “incisional biopsy of eyelid skin including lid margin.”1 Therefore, biopsies of eyelid skin that do not remove the eyelid margin must be coded as 11100/11101, or if the entire cutaneous lesion was removed, can be reclassified as shave removals, which would be coded in the 11310 to 11313 range.
Specialized excision codes include those of the soft tissue. Soft tissue excision codes typically used by dermatologists are not numbered consecutively, are site-specific, and are typically used for resection of benign tumors confined to the subcutaneous tissue below the skin but above the deep fascia. Cysts of all types, including epidermoid and pilar cysts, are specifically excluded from this code set regardless of how large or complex they may be, as they protrude into the dermis or above and are not exclusively in the subcutis. However, lipomas meet the definition for soft-tissue excision, and therefore site-specific soft tissue excision codes can be used in lieu of traditional skin excision codes. The soft-tissue excision codes are distributed throughout the CPT manual, with distinct codes for the abdominal wall (22902, 22903); leg or ankle (27618, 27632); back or flank (21930, 21931); external auditory canal (69145); upper arm or elbow (24075, 24071); face or scalp (21011, 21012); hand or finger (26115, 26111); foot or toe (28043, 28039); forearm or wrist (25075, 25071); hip or pelvis (27047, 27043); thigh or knee (27327, 27337); neck or anterior thorax (21555, 21552); and shoulder (23075, 23071). In general, there are 2 codes for each area—one for smaller and one for larger excisions—but they frequently are out of order (ie, the code associated with a higher numerical value may correspond with the smaller excision). Care should be taken in selecting the correct code. The specific size cutoffs for the various soft tissue excision code sets are different, so it is important to be familiar with the particular CPT descriptions for each.
Final Thoughts
In summary, biopsies, shave removals, and excisions are different procedures and therefore should be coded differently. Although the distinction between biopsies and shave removals is ill defined, remember that biopsies are intended to establish a diagnosis and shave removals are intended to remove the entire lesion. By definition, excisions must include margins and proceed through the dermis to the subcutis. In particular circumstances, site-specific biopsy codes may be appropriate and can be used to code for lipoma excisions.
1. Current Procedural Terminology 2015, Professional Edition. Chicago, Illinois: American Medical Association; 2014.
2. American Medical Association. Biopsy. CPT Assistant. Chicago, IL: American Medical Association: October 2004:4.
1. Current Procedural Terminology 2015, Professional Edition. Chicago, Illinois: American Medical Association; 2014.
2. American Medical Association. Biopsy. CPT Assistant. Chicago, IL: American Medical Association: October 2004:4.
Practice Points
- Biopsies are coded when there is an independent procedure to remove skin for histologic analysis to help establish a definitive histologic diagnosis.
- Coding for shave removals and excisions requires the intent to remove the entire lesion.
- Unlike shave removals, excisions can be coded only if the lesion is removed to the level of the subcutaneous fat.
- When available, site-specific biopsy or soft tissue excision codes may better describe a procedure than standard biopsy or excision codes.
Cosmetic Corner: Dermatologists Weigh in on Men’s Shaving Products
To improve patient care and outcomes, leading dermatologists offered their recommendations on top men's shaving products. Consideration must be given to:
- Alpha Fit by Clarisonic
Pacific Bioscience Laboratories Inc
“Men’s skin is unique, and I like this brush because it is engineered to get men’s skin cleaner and healthier-looking by clearing away dirt, sweat, and oil. It cleanses 6 times better than the hands alone while prepping the face and neck for a closer, smoother shave.”
—Wm. Phillip Werschler, MD, Seattle, Washington
- Aveeno Daily Moisturizing Lotion
Johnson & Johnson Consumer Companies, Inc
“For men who develop irritation from shaving or suffer from pseudofolliculitis barbae, I recommend applying [this product] to damp skin, preferably after showering.”
—Adam J. Friedman, MD, Washington, DC
- Beard Lube Conditioning Shave
Jack Black
“It has jojoba and other oils to soften the beard and prevent drying out the skin.”—Anthony M. Rossi, MD, New York, New York
- CeraVe Facial Moisturizing Lotion AM
Valeant Pharmaceuticals North America LLC
“Patients should use a blade razor (not electric) with a cooling foam or gel and wash with hot water before and cold water right after shaving. I recommend a moisturizer with sunscreen for use every morning instead of an aftershave, and I encourage patients to apply it on the entire face, not just the beard area. [This product] is a good option because it is well tolerated and affordable.”
—Gary Goldenberg, MD, New York, New York
- Gillette Fusion Proglide Clear Shave Gel
Procter & Gamble
—Recommended by Adam J. Friedman, MD, Washington, DC
- PRESCRIBEDsolutions Surface Improvement Exfoliating Polish
Biopelle, Inc
“This cleanser really helps make my skin feel soft after shaving. It is a nice blend of jojoba beads and grittiness for exfoliation and also has a pleasant smell.”
—Joel L. Cohen, MD, Englewood, Colorado
Cutis invites readers to send us their recommendations. Skin care products for babies will be featured in an upcoming edition of Cosmetic Corner. Please e-mail your recommendation(s) to the Editorial Office.
Disclaimer: Opinions expressed herein do not necessarily reflect those of Cutis or Frontline Medical Communications Inc. and shall not be used for product endorsement purposes. Any reference made to a specific commercial product does not indicate or imply that Cutis or Frontline Medical Communications Inc. endorses, recommends, or favors the product mentioned. No guarantee is given to the effects of recommended products.
To improve patient care and outcomes, leading dermatologists offered their recommendations on top men's shaving products. Consideration must be given to:
- Alpha Fit by Clarisonic
Pacific Bioscience Laboratories Inc
“Men’s skin is unique, and I like this brush because it is engineered to get men’s skin cleaner and healthier-looking by clearing away dirt, sweat, and oil. It cleanses 6 times better than the hands alone while prepping the face and neck for a closer, smoother shave.”
—Wm. Phillip Werschler, MD, Seattle, Washington
- Aveeno Daily Moisturizing Lotion
Johnson & Johnson Consumer Companies, Inc
“For men who develop irritation from shaving or suffer from pseudofolliculitis barbae, I recommend applying [this product] to damp skin, preferably after showering.”
—Adam J. Friedman, MD, Washington, DC
- Beard Lube Conditioning Shave
Jack Black
“It has jojoba and other oils to soften the beard and prevent drying out the skin.”—Anthony M. Rossi, MD, New York, New York
- CeraVe Facial Moisturizing Lotion AM
Valeant Pharmaceuticals North America LLC
“Patients should use a blade razor (not electric) with a cooling foam or gel and wash with hot water before and cold water right after shaving. I recommend a moisturizer with sunscreen for use every morning instead of an aftershave, and I encourage patients to apply it on the entire face, not just the beard area. [This product] is a good option because it is well tolerated and affordable.”
—Gary Goldenberg, MD, New York, New York
- Gillette Fusion Proglide Clear Shave Gel
Procter & Gamble
—Recommended by Adam J. Friedman, MD, Washington, DC
- PRESCRIBEDsolutions Surface Improvement Exfoliating Polish
Biopelle, Inc
“This cleanser really helps make my skin feel soft after shaving. It is a nice blend of jojoba beads and grittiness for exfoliation and also has a pleasant smell.”
—Joel L. Cohen, MD, Englewood, Colorado
Cutis invites readers to send us their recommendations. Skin care products for babies will be featured in an upcoming edition of Cosmetic Corner. Please e-mail your recommendation(s) to the Editorial Office.
Disclaimer: Opinions expressed herein do not necessarily reflect those of Cutis or Frontline Medical Communications Inc. and shall not be used for product endorsement purposes. Any reference made to a specific commercial product does not indicate or imply that Cutis or Frontline Medical Communications Inc. endorses, recommends, or favors the product mentioned. No guarantee is given to the effects of recommended products.
To improve patient care and outcomes, leading dermatologists offered their recommendations on top men's shaving products. Consideration must be given to:
- Alpha Fit by Clarisonic
Pacific Bioscience Laboratories Inc
“Men’s skin is unique, and I like this brush because it is engineered to get men’s skin cleaner and healthier-looking by clearing away dirt, sweat, and oil. It cleanses 6 times better than the hands alone while prepping the face and neck for a closer, smoother shave.”
—Wm. Phillip Werschler, MD, Seattle, Washington
- Aveeno Daily Moisturizing Lotion
Johnson & Johnson Consumer Companies, Inc
“For men who develop irritation from shaving or suffer from pseudofolliculitis barbae, I recommend applying [this product] to damp skin, preferably after showering.”
—Adam J. Friedman, MD, Washington, DC
- Beard Lube Conditioning Shave
Jack Black
“It has jojoba and other oils to soften the beard and prevent drying out the skin.”—Anthony M. Rossi, MD, New York, New York
- CeraVe Facial Moisturizing Lotion AM
Valeant Pharmaceuticals North America LLC
“Patients should use a blade razor (not electric) with a cooling foam or gel and wash with hot water before and cold water right after shaving. I recommend a moisturizer with sunscreen for use every morning instead of an aftershave, and I encourage patients to apply it on the entire face, not just the beard area. [This product] is a good option because it is well tolerated and affordable.”
—Gary Goldenberg, MD, New York, New York
- Gillette Fusion Proglide Clear Shave Gel
Procter & Gamble
—Recommended by Adam J. Friedman, MD, Washington, DC
- PRESCRIBEDsolutions Surface Improvement Exfoliating Polish
Biopelle, Inc
“This cleanser really helps make my skin feel soft after shaving. It is a nice blend of jojoba beads and grittiness for exfoliation and also has a pleasant smell.”
—Joel L. Cohen, MD, Englewood, Colorado
Cutis invites readers to send us their recommendations. Skin care products for babies will be featured in an upcoming edition of Cosmetic Corner. Please e-mail your recommendation(s) to the Editorial Office.
Disclaimer: Opinions expressed herein do not necessarily reflect those of Cutis or Frontline Medical Communications Inc. and shall not be used for product endorsement purposes. Any reference made to a specific commercial product does not indicate or imply that Cutis or Frontline Medical Communications Inc. endorses, recommends, or favors the product mentioned. No guarantee is given to the effects of recommended products.
EADV: Intralesional therapy for scleroderma dystrophic calcifications
COPENHAGEN – Intralesional sodium thiosulfate injections are an effective treatment for the painful and disabling dystrophic calcifications associated with systemic sclerosis, lupus, and other autoimmune diseases, as well as with nephrogenic systemic fibrosis, Dr. Jane Baumgartner-Nielsen said at the annual congress of the European Academy of Dermatology and Venereology.
“We suggest that intralesional injections of sodium thiosulfate may be considered in severe or ulcerated lesions before surgery or amputation,” said Dr. Baumgartner-Nielsen of Aarhus (Denmark) University.
Treatment of these often ulcerated cutaneous lesions has traditionally been challenging. While surgery is common, it’s problematic because wound healing is often prolonged in patients with autoimmune disease, she observed.
She presented a case series of six patients who underwent interlesional injections of sodium thiosulfate for painful and disabling dystrophic calcifications. The lesions were located on extensor surfaces or the fingertips. They were extremely painful: patients rated their pain as 9 on a 10-point scale. All six patients were women. Five had anticentromere antibody–positive systemic sclerosis; other investigators have reported that dystrophic calcifications occur in roughly 70% of such patients. The sixth patient had nephrogenic systemic fibrosis.
The six patients underwent a total of 21 injections of eight lesions. The injections were placed at the base of the calcifications. The concentration of sodium thiosulfate employed was 150 mg/mL. Dystrophic calcifications less than 5 mm in diameter on the fingertips received a single injection. Larger lesions complicated by ulceration got four injections at 4-week intervals.
The lesions decreased in size by an average of 67% at 4 weeks and 90% at 12 weeks. Complete remission was achieved by week 12 in half of patients; the other half had 80% reduction of their lesions. All patients reported dramatically less pain and improved physical function, compared with baseline. There were no serious side effects.
Audience member Dr. Alice B. Gottlieb inquired as to how painful the injections are.
“About 9 or 10 on a 10-point scale, but the pain disappears very quickly. In 30 seconds the patient is smiling again,” Dr. Baumgartner-Nielsen replied.
Dr. Gottlieb said she was interested in the intralesional therapy for her pediatric lupus patients with dystrophic calcifications. “But if there’s that much injection site pain, you might have to put the kid out,” noted Dr. Gottlieb, professor and dermatologist-in-chief at Tufts Medical Center, Boston.
Dr. Baumgartner-Nielsen reported having no financial conflicts regarding her study.
COPENHAGEN – Intralesional sodium thiosulfate injections are an effective treatment for the painful and disabling dystrophic calcifications associated with systemic sclerosis, lupus, and other autoimmune diseases, as well as with nephrogenic systemic fibrosis, Dr. Jane Baumgartner-Nielsen said at the annual congress of the European Academy of Dermatology and Venereology.
“We suggest that intralesional injections of sodium thiosulfate may be considered in severe or ulcerated lesions before surgery or amputation,” said Dr. Baumgartner-Nielsen of Aarhus (Denmark) University.
Treatment of these often ulcerated cutaneous lesions has traditionally been challenging. While surgery is common, it’s problematic because wound healing is often prolonged in patients with autoimmune disease, she observed.
She presented a case series of six patients who underwent interlesional injections of sodium thiosulfate for painful and disabling dystrophic calcifications. The lesions were located on extensor surfaces or the fingertips. They were extremely painful: patients rated their pain as 9 on a 10-point scale. All six patients were women. Five had anticentromere antibody–positive systemic sclerosis; other investigators have reported that dystrophic calcifications occur in roughly 70% of such patients. The sixth patient had nephrogenic systemic fibrosis.
The six patients underwent a total of 21 injections of eight lesions. The injections were placed at the base of the calcifications. The concentration of sodium thiosulfate employed was 150 mg/mL. Dystrophic calcifications less than 5 mm in diameter on the fingertips received a single injection. Larger lesions complicated by ulceration got four injections at 4-week intervals.
The lesions decreased in size by an average of 67% at 4 weeks and 90% at 12 weeks. Complete remission was achieved by week 12 in half of patients; the other half had 80% reduction of their lesions. All patients reported dramatically less pain and improved physical function, compared with baseline. There were no serious side effects.
Audience member Dr. Alice B. Gottlieb inquired as to how painful the injections are.
“About 9 or 10 on a 10-point scale, but the pain disappears very quickly. In 30 seconds the patient is smiling again,” Dr. Baumgartner-Nielsen replied.
Dr. Gottlieb said she was interested in the intralesional therapy for her pediatric lupus patients with dystrophic calcifications. “But if there’s that much injection site pain, you might have to put the kid out,” noted Dr. Gottlieb, professor and dermatologist-in-chief at Tufts Medical Center, Boston.
Dr. Baumgartner-Nielsen reported having no financial conflicts regarding her study.
COPENHAGEN – Intralesional sodium thiosulfate injections are an effective treatment for the painful and disabling dystrophic calcifications associated with systemic sclerosis, lupus, and other autoimmune diseases, as well as with nephrogenic systemic fibrosis, Dr. Jane Baumgartner-Nielsen said at the annual congress of the European Academy of Dermatology and Venereology.
“We suggest that intralesional injections of sodium thiosulfate may be considered in severe or ulcerated lesions before surgery or amputation,” said Dr. Baumgartner-Nielsen of Aarhus (Denmark) University.
Treatment of these often ulcerated cutaneous lesions has traditionally been challenging. While surgery is common, it’s problematic because wound healing is often prolonged in patients with autoimmune disease, she observed.
She presented a case series of six patients who underwent interlesional injections of sodium thiosulfate for painful and disabling dystrophic calcifications. The lesions were located on extensor surfaces or the fingertips. They were extremely painful: patients rated their pain as 9 on a 10-point scale. All six patients were women. Five had anticentromere antibody–positive systemic sclerosis; other investigators have reported that dystrophic calcifications occur in roughly 70% of such patients. The sixth patient had nephrogenic systemic fibrosis.
The six patients underwent a total of 21 injections of eight lesions. The injections were placed at the base of the calcifications. The concentration of sodium thiosulfate employed was 150 mg/mL. Dystrophic calcifications less than 5 mm in diameter on the fingertips received a single injection. Larger lesions complicated by ulceration got four injections at 4-week intervals.
The lesions decreased in size by an average of 67% at 4 weeks and 90% at 12 weeks. Complete remission was achieved by week 12 in half of patients; the other half had 80% reduction of their lesions. All patients reported dramatically less pain and improved physical function, compared with baseline. There were no serious side effects.
Audience member Dr. Alice B. Gottlieb inquired as to how painful the injections are.
“About 9 or 10 on a 10-point scale, but the pain disappears very quickly. In 30 seconds the patient is smiling again,” Dr. Baumgartner-Nielsen replied.
Dr. Gottlieb said she was interested in the intralesional therapy for her pediatric lupus patients with dystrophic calcifications. “But if there’s that much injection site pain, you might have to put the kid out,” noted Dr. Gottlieb, professor and dermatologist-in-chief at Tufts Medical Center, Boston.
Dr. Baumgartner-Nielsen reported having no financial conflicts regarding her study.
AT THE EADV CONGRESS
Key clinical point: Intralesional sodium thiosulfate is an effective alternative to surgery for disabling dystrophic calcifications in patients with systemic sclerosis or other autoimmune diseases.
Major finding: Fifty percent of patients with severely painful dystrophic calcifications experienced complete remission 12 weeks after their first intralesional injection of sodium thiosulfate; the remaining lesions were 80% smaller, compared with baseline.
Data source: This was a case series involving six patients with eight treated dystrophic calcifications secondary to systemic sclerosis of nephrogenic systemic fibrosis.
Disclosures: The study presenter reported having no financial conflicts of interest regarding her case series.
EADV: Fractional CO2 laser called ‘unmatched’ for hypertrophic burn scars
COPENHAGEN – The fractional CO2 laser at 10,600 nm has emerged as the premier tool for improving the texture and elasticity of hypertrophic burn scars, Dr. Gerd G. Gauglitz asserted at the annual congress of the European Academy of Dermatology and Venereology.
“When it comes to improving the smoothness and the little elevations that are so bothersome to the burn patient, and especially when it comes to the stiffness of the scar, I think the fractional CO2 laser is the approach that has no competition. There might be other devices to come in the future, but I think the results we now see with the fractional CO2 laser are amazing,” said Dr. Gauglitz of Ludwig-Maximilian University, Munich.
It’s an opinion shared by other experts, he noted. For example, last year a panel of eight prominent American academic and military dermatologists and plastic surgeons with extensive experience in laser therapy of traumatic scars – including Dr. R. Rox Anderson of the Wellman Center for Photomedicine in Boston – published a consensus report that concluded “laser scar therapy, particularly fractional ablative laser resurfacing, represents a promising and vastly underused tool in the multidisciplinary treatment of traumatic scars” (JAMA Dermatol. 2014 Feb;150[2]:187-93).
Moreover, an international expert panel that issued updated clinical recommendations on scar management in 2014 declared that broader application of laser therapy constitutes “one of the most significant advances in scar management over the last 10 years.” The panel, which included Dr. Gauglitz, noted that “positive data for fractional lasers support their use for burn scar treatment” (Dermatol Surg. 2014 Aug;40[8]:817-24).
That being said, the current level of evidence supporting the use of fractional CO2 laser therapy for hypertrophic burn scars is poor, Dr. Gauglitz pointed out. No clear data-driven recommendations exist as to the optimal number of laser sessions, between-treatment intervals, or device settings. This was the impetus for his ongoing prospective, controlled study, evaluating a specific treatment protocol in 20 patients with severe, mature hypertrophic burn scars of an average 12.7 years duration.
For purposes of the study, as well as in his own clinical practice, Dr. Gauglitz utilizes the UltraPulse fractional CO2 laser to improve hypertrophic burn scars. He believes it offers compelling advantages over the alternative SuperPulse and continuous wave fractional CO2 laser technologies. The UltraPulse features the narrowest zone of thermal damage, meaning greater precision, less pain and down time; and a favorable safety profile. Most importantly, it has greater penetration capacity, causing microscopic thermal wounds to a depth of 4 mm below the skin surface, which is important for purposes of collagen remodeling, he explained.
When using CO2 lasers for burn scars, “clinically, we see completed reepithelialization after the procedure and then an ongoing collagen-remodeling phase lasting for up to 9 months. We see improvements in dermal architecture and creation of a collagen subtype profile that’s closer to nonwounded healthy skin,” according to the dermatologist.
Because other studies have relied heavily upon nonstandardized before and after photos and the Vancouver Scar Scale, with relatively short-term follow-up, Dr. Gauglitz and coinvestigators sought to advance the field by incorporating a variety of more objective measures, including the PRIMOS (Phaseshift Rapid in Vivo Measurement of the Skin) three-dimensional device widely utilized for wrinkle measurement, as well as the Cutometer, which evaluates skin elasticity. The investigators are also formally measuring the quality of life impact of their laser regimen.
The study consists of two parts. At the EADV congress, Dr. Gauglitz presented the results of the first part, which involved a single treatment of a 12-by-8 cm2 area, with a comparable untreated control area, and a 6-month follow-up. In the ongoing second part of the study, the same patients are undergoing three treatment sessions on a larger scarred area, with 3-month intervals between sessions. Again, a comparable untreated area of the body serves as the control.
Each treatment session involves three passes with the UltraPulse laser. The first is done at the most intense setting, known by the proprietary name of SCAAR FX (Synergistic Coagulation and Ablation for Advanced Resurfacing). This is aimed at inducing the collagen-remodeling process. The setting is 70-140 mJ/cm2, 250 Hz, with a density of 1%. The second pass utilizes the small-spot ACTIVE FX setting, designed to provide superficial ablative therapy to remove fine elevated scars. This involves 40-90 mJ/cm2 at high density and 300 Hz. The final pass is set at large-spot Active FX and employs 125 mJ/cm2 at low density and 125 Hz; the purpose is to smooth the scar and make the skin surface more homogeneous.
The most interesting aspect about the results, Dr. Gauglitz observed, is that 1 month after treatment, across-the-board improvements were documented, but then continued to grow in magnitude through the final 6-month follow-up – despite no further treatment. This was presumably the consequence of the collagen-remodeling process.
For example, scores on the Vancouver Scar Scale – still the most widely used scoring tool in the burn field – improved from roughly 7 at baseline to 2 at 6 months, compared with no change in the control area. Similarly, scores on the POSAS (Patient and Observer Scar Assessment Scale) showed highly significant and steadily growing improvement over 6 months of follow-up in most domains, including scar pigmentation, thickness, surface area, and flexibility.
Skin elasticity as measured by the Cutometer improved steadily by 28% at the 6-month mark. Likewise, evaluation with the PRIMOS device showed a steadily smoother scar surface over time.
Final results on the Dermatology Life Quality Index (DLQI) are still being tabulated, but there clearly is a strong improvement on this score – much of it attributed to the improved function resulting from greater flexibility.
“The results of fractional CO2 laser therapy are actually difficult to visualize, but patients are incredibly happy. For us, it might not be a big difference, but if you smoothen the scar surface and the patient is suddenly able to apply makeup without making the scar too visible, for those patients it’s a big thing,” Dr. Gauglitz said.
It’s clear from the ongoing multitreatment stage of the study that a single laser session is not optimal. “I think it’s going to be three, at least, for maximum benefit,” the dermatologist commented.
Asked if he thinks the fractional CO2 laser is the most effective tool for all aspects of scar treatment, Dr. Gauglitz was quick to say no.
“It depends, really, on the indication you want to treat. When it comes to erythema, a pulsed dye laser is much more effective than a fractional CO2 laser. For hyperpigmentation, a Q-switched ruby laser or the new picosecond laser might be a more interesting approach,” he replied.
Dr. Gauglitz reported serving on advisory boards and speakers’ bureaus for laser manufacturers Lumenis and Candela as well as for Merz Pharmaceuticals and Sinclair Pharma.
COPENHAGEN – The fractional CO2 laser at 10,600 nm has emerged as the premier tool for improving the texture and elasticity of hypertrophic burn scars, Dr. Gerd G. Gauglitz asserted at the annual congress of the European Academy of Dermatology and Venereology.
“When it comes to improving the smoothness and the little elevations that are so bothersome to the burn patient, and especially when it comes to the stiffness of the scar, I think the fractional CO2 laser is the approach that has no competition. There might be other devices to come in the future, but I think the results we now see with the fractional CO2 laser are amazing,” said Dr. Gauglitz of Ludwig-Maximilian University, Munich.
It’s an opinion shared by other experts, he noted. For example, last year a panel of eight prominent American academic and military dermatologists and plastic surgeons with extensive experience in laser therapy of traumatic scars – including Dr. R. Rox Anderson of the Wellman Center for Photomedicine in Boston – published a consensus report that concluded “laser scar therapy, particularly fractional ablative laser resurfacing, represents a promising and vastly underused tool in the multidisciplinary treatment of traumatic scars” (JAMA Dermatol. 2014 Feb;150[2]:187-93).
Moreover, an international expert panel that issued updated clinical recommendations on scar management in 2014 declared that broader application of laser therapy constitutes “one of the most significant advances in scar management over the last 10 years.” The panel, which included Dr. Gauglitz, noted that “positive data for fractional lasers support their use for burn scar treatment” (Dermatol Surg. 2014 Aug;40[8]:817-24).
That being said, the current level of evidence supporting the use of fractional CO2 laser therapy for hypertrophic burn scars is poor, Dr. Gauglitz pointed out. No clear data-driven recommendations exist as to the optimal number of laser sessions, between-treatment intervals, or device settings. This was the impetus for his ongoing prospective, controlled study, evaluating a specific treatment protocol in 20 patients with severe, mature hypertrophic burn scars of an average 12.7 years duration.
For purposes of the study, as well as in his own clinical practice, Dr. Gauglitz utilizes the UltraPulse fractional CO2 laser to improve hypertrophic burn scars. He believes it offers compelling advantages over the alternative SuperPulse and continuous wave fractional CO2 laser technologies. The UltraPulse features the narrowest zone of thermal damage, meaning greater precision, less pain and down time; and a favorable safety profile. Most importantly, it has greater penetration capacity, causing microscopic thermal wounds to a depth of 4 mm below the skin surface, which is important for purposes of collagen remodeling, he explained.
When using CO2 lasers for burn scars, “clinically, we see completed reepithelialization after the procedure and then an ongoing collagen-remodeling phase lasting for up to 9 months. We see improvements in dermal architecture and creation of a collagen subtype profile that’s closer to nonwounded healthy skin,” according to the dermatologist.
Because other studies have relied heavily upon nonstandardized before and after photos and the Vancouver Scar Scale, with relatively short-term follow-up, Dr. Gauglitz and coinvestigators sought to advance the field by incorporating a variety of more objective measures, including the PRIMOS (Phaseshift Rapid in Vivo Measurement of the Skin) three-dimensional device widely utilized for wrinkle measurement, as well as the Cutometer, which evaluates skin elasticity. The investigators are also formally measuring the quality of life impact of their laser regimen.
The study consists of two parts. At the EADV congress, Dr. Gauglitz presented the results of the first part, which involved a single treatment of a 12-by-8 cm2 area, with a comparable untreated control area, and a 6-month follow-up. In the ongoing second part of the study, the same patients are undergoing three treatment sessions on a larger scarred area, with 3-month intervals between sessions. Again, a comparable untreated area of the body serves as the control.
Each treatment session involves three passes with the UltraPulse laser. The first is done at the most intense setting, known by the proprietary name of SCAAR FX (Synergistic Coagulation and Ablation for Advanced Resurfacing). This is aimed at inducing the collagen-remodeling process. The setting is 70-140 mJ/cm2, 250 Hz, with a density of 1%. The second pass utilizes the small-spot ACTIVE FX setting, designed to provide superficial ablative therapy to remove fine elevated scars. This involves 40-90 mJ/cm2 at high density and 300 Hz. The final pass is set at large-spot Active FX and employs 125 mJ/cm2 at low density and 125 Hz; the purpose is to smooth the scar and make the skin surface more homogeneous.
The most interesting aspect about the results, Dr. Gauglitz observed, is that 1 month after treatment, across-the-board improvements were documented, but then continued to grow in magnitude through the final 6-month follow-up – despite no further treatment. This was presumably the consequence of the collagen-remodeling process.
For example, scores on the Vancouver Scar Scale – still the most widely used scoring tool in the burn field – improved from roughly 7 at baseline to 2 at 6 months, compared with no change in the control area. Similarly, scores on the POSAS (Patient and Observer Scar Assessment Scale) showed highly significant and steadily growing improvement over 6 months of follow-up in most domains, including scar pigmentation, thickness, surface area, and flexibility.
Skin elasticity as measured by the Cutometer improved steadily by 28% at the 6-month mark. Likewise, evaluation with the PRIMOS device showed a steadily smoother scar surface over time.
Final results on the Dermatology Life Quality Index (DLQI) are still being tabulated, but there clearly is a strong improvement on this score – much of it attributed to the improved function resulting from greater flexibility.
“The results of fractional CO2 laser therapy are actually difficult to visualize, but patients are incredibly happy. For us, it might not be a big difference, but if you smoothen the scar surface and the patient is suddenly able to apply makeup without making the scar too visible, for those patients it’s a big thing,” Dr. Gauglitz said.
It’s clear from the ongoing multitreatment stage of the study that a single laser session is not optimal. “I think it’s going to be three, at least, for maximum benefit,” the dermatologist commented.
Asked if he thinks the fractional CO2 laser is the most effective tool for all aspects of scar treatment, Dr. Gauglitz was quick to say no.
“It depends, really, on the indication you want to treat. When it comes to erythema, a pulsed dye laser is much more effective than a fractional CO2 laser. For hyperpigmentation, a Q-switched ruby laser or the new picosecond laser might be a more interesting approach,” he replied.
Dr. Gauglitz reported serving on advisory boards and speakers’ bureaus for laser manufacturers Lumenis and Candela as well as for Merz Pharmaceuticals and Sinclair Pharma.
COPENHAGEN – The fractional CO2 laser at 10,600 nm has emerged as the premier tool for improving the texture and elasticity of hypertrophic burn scars, Dr. Gerd G. Gauglitz asserted at the annual congress of the European Academy of Dermatology and Venereology.
“When it comes to improving the smoothness and the little elevations that are so bothersome to the burn patient, and especially when it comes to the stiffness of the scar, I think the fractional CO2 laser is the approach that has no competition. There might be other devices to come in the future, but I think the results we now see with the fractional CO2 laser are amazing,” said Dr. Gauglitz of Ludwig-Maximilian University, Munich.
It’s an opinion shared by other experts, he noted. For example, last year a panel of eight prominent American academic and military dermatologists and plastic surgeons with extensive experience in laser therapy of traumatic scars – including Dr. R. Rox Anderson of the Wellman Center for Photomedicine in Boston – published a consensus report that concluded “laser scar therapy, particularly fractional ablative laser resurfacing, represents a promising and vastly underused tool in the multidisciplinary treatment of traumatic scars” (JAMA Dermatol. 2014 Feb;150[2]:187-93).
Moreover, an international expert panel that issued updated clinical recommendations on scar management in 2014 declared that broader application of laser therapy constitutes “one of the most significant advances in scar management over the last 10 years.” The panel, which included Dr. Gauglitz, noted that “positive data for fractional lasers support their use for burn scar treatment” (Dermatol Surg. 2014 Aug;40[8]:817-24).
That being said, the current level of evidence supporting the use of fractional CO2 laser therapy for hypertrophic burn scars is poor, Dr. Gauglitz pointed out. No clear data-driven recommendations exist as to the optimal number of laser sessions, between-treatment intervals, or device settings. This was the impetus for his ongoing prospective, controlled study, evaluating a specific treatment protocol in 20 patients with severe, mature hypertrophic burn scars of an average 12.7 years duration.
For purposes of the study, as well as in his own clinical practice, Dr. Gauglitz utilizes the UltraPulse fractional CO2 laser to improve hypertrophic burn scars. He believes it offers compelling advantages over the alternative SuperPulse and continuous wave fractional CO2 laser technologies. The UltraPulse features the narrowest zone of thermal damage, meaning greater precision, less pain and down time; and a favorable safety profile. Most importantly, it has greater penetration capacity, causing microscopic thermal wounds to a depth of 4 mm below the skin surface, which is important for purposes of collagen remodeling, he explained.
When using CO2 lasers for burn scars, “clinically, we see completed reepithelialization after the procedure and then an ongoing collagen-remodeling phase lasting for up to 9 months. We see improvements in dermal architecture and creation of a collagen subtype profile that’s closer to nonwounded healthy skin,” according to the dermatologist.
Because other studies have relied heavily upon nonstandardized before and after photos and the Vancouver Scar Scale, with relatively short-term follow-up, Dr. Gauglitz and coinvestigators sought to advance the field by incorporating a variety of more objective measures, including the PRIMOS (Phaseshift Rapid in Vivo Measurement of the Skin) three-dimensional device widely utilized for wrinkle measurement, as well as the Cutometer, which evaluates skin elasticity. The investigators are also formally measuring the quality of life impact of their laser regimen.
The study consists of two parts. At the EADV congress, Dr. Gauglitz presented the results of the first part, which involved a single treatment of a 12-by-8 cm2 area, with a comparable untreated control area, and a 6-month follow-up. In the ongoing second part of the study, the same patients are undergoing three treatment sessions on a larger scarred area, with 3-month intervals between sessions. Again, a comparable untreated area of the body serves as the control.
Each treatment session involves three passes with the UltraPulse laser. The first is done at the most intense setting, known by the proprietary name of SCAAR FX (Synergistic Coagulation and Ablation for Advanced Resurfacing). This is aimed at inducing the collagen-remodeling process. The setting is 70-140 mJ/cm2, 250 Hz, with a density of 1%. The second pass utilizes the small-spot ACTIVE FX setting, designed to provide superficial ablative therapy to remove fine elevated scars. This involves 40-90 mJ/cm2 at high density and 300 Hz. The final pass is set at large-spot Active FX and employs 125 mJ/cm2 at low density and 125 Hz; the purpose is to smooth the scar and make the skin surface more homogeneous.
The most interesting aspect about the results, Dr. Gauglitz observed, is that 1 month after treatment, across-the-board improvements were documented, but then continued to grow in magnitude through the final 6-month follow-up – despite no further treatment. This was presumably the consequence of the collagen-remodeling process.
For example, scores on the Vancouver Scar Scale – still the most widely used scoring tool in the burn field – improved from roughly 7 at baseline to 2 at 6 months, compared with no change in the control area. Similarly, scores on the POSAS (Patient and Observer Scar Assessment Scale) showed highly significant and steadily growing improvement over 6 months of follow-up in most domains, including scar pigmentation, thickness, surface area, and flexibility.
Skin elasticity as measured by the Cutometer improved steadily by 28% at the 6-month mark. Likewise, evaluation with the PRIMOS device showed a steadily smoother scar surface over time.
Final results on the Dermatology Life Quality Index (DLQI) are still being tabulated, but there clearly is a strong improvement on this score – much of it attributed to the improved function resulting from greater flexibility.
“The results of fractional CO2 laser therapy are actually difficult to visualize, but patients are incredibly happy. For us, it might not be a big difference, but if you smoothen the scar surface and the patient is suddenly able to apply makeup without making the scar too visible, for those patients it’s a big thing,” Dr. Gauglitz said.
It’s clear from the ongoing multitreatment stage of the study that a single laser session is not optimal. “I think it’s going to be three, at least, for maximum benefit,” the dermatologist commented.
Asked if he thinks the fractional CO2 laser is the most effective tool for all aspects of scar treatment, Dr. Gauglitz was quick to say no.
“It depends, really, on the indication you want to treat. When it comes to erythema, a pulsed dye laser is much more effective than a fractional CO2 laser. For hyperpigmentation, a Q-switched ruby laser or the new picosecond laser might be a more interesting approach,” he replied.
Dr. Gauglitz reported serving on advisory boards and speakers’ bureaus for laser manufacturers Lumenis and Candela as well as for Merz Pharmaceuticals and Sinclair Pharma.
AT THE EADV CONGRESS
Key clinical point: Fractional CO2 laser therapy for hypertrophic burn scars provides unequaled improvements in skin softness and elasticity, as well as surface smoothness and relief.
Major finding: Scores on the Vancouver Scar Scale progressively dropped from roughly 7 to 2, with a 28% increase in scar elasticity as measured by the Cutometer, in the 6 months following one fractional CO2 laser treatment session in patients with severe hypertrophic burn scars.
Data source: This ongoing prospective study involves 20 patients with mature hypertrophic burn scars, treated with a fractional CO2 laser once or every 3 months, with untreated skin areas serving as the control.
Disclosures: Dr. Gauglitz reported serving on advisory boards and speakers’ bureaus for laser manufacturers Lumenis and Candela, as well as Merz Pharmaceuticals and Sinclair Pharma.
Hyaluronidase eases post-Mohs periorbital swelling
CHICAGO – Hyaluronidase can speed the resolution of postoperative periorbital lymphedema in patients undergoing Mohs micrographic surgery and flap repair, a prospective case series suggests.
Lymphedema resolved in all seven cases treated with hyaluronidase (Hyalase) injections in 4-6 weeks, compared with 3 months as would be expected, Dr. Sweta Rai, of St John’s Institute of Dermatology, King’s College London, said at the annual meeting of the American Society for Dermatologic Surgery.
“In the periorbital area where the skin is very thin and therefore even small amounts of lymphovascular fluid is visible, postoperative lymphedema is a cosmetic concern, especially as patients want to resume their daily activities as soon as possible postoperatively,” she said in an interview.
Hyaluronidase is widely used in cosmetic surgery in the breakdown of hyaluronic acid fillers, where the mucolytic enzyme splits and lowers the viscosity of hyaluronic acid in the extracellular matrix.
Dr. Rai and her coauthor Dr. Hooman Khorasani, chief of Mohs, reconstructive, and cosmetic surgery at Mount Sinai School of Medicine in New York, turned to hyaluronidase because it’s well documented that hyaluronic acid is produced by the body as an automatic response to promote wound healing
Patients undergoing Mohs surgery for large eye tumors often require complex flap repairs that cross the lower eyelid and cheek junction, which results in greater lymphedema. Hyaluronic acid produces a scaffolding effect at the wound site that, in combination with periorbital lymphedema when the vascular channels are cut, is thought to lead to fluid stasis. Hyaluronidase breaks down this scaffolding, allowing the lymphovascular fluid to drain into the subcutaneous tissue, Dr. Rai explained.
The investigators use a 1,500-unit vial of generic hyaluronidase diluted with 1.5 mL of normal saline and inject 100-150 units subcutaneously starting 2 weeks postoperatively at the time of suture removal and repeat the injections every 2 weeks until the swelling resolves.
Patients should undergo an intradermal prick test prior to injections to exclude the risk of type I hypersensitivity anaphylaxis previously reported with human hyaluronidase injections, Dr. Rai cautioned.
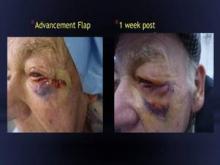
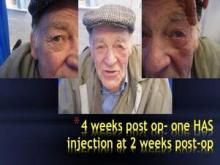
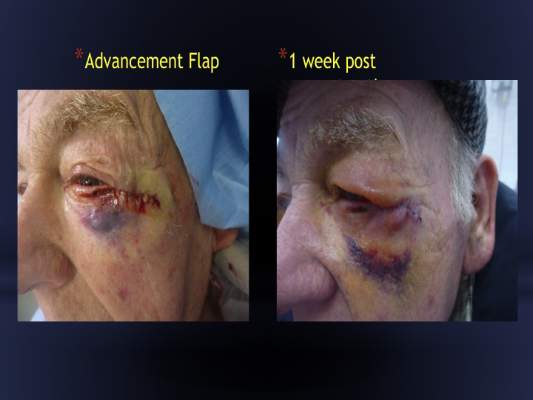
In all seven patients, aged 42-80 years, periorbital lymphedema resolved with 150-450 units of hyaluronidase. The patients included a women referred for treatment 2 months after Mohs surgery. The index case, involving a man with a periorbital defect and a medially based advancement flap, resolved with only a single 150-unit injection given 2 weeks after surgery, Dr. Rai said.
“Most of my patients are working and lead busy work and social lives, and they’ve all commented on how pleased they are with the results and on how quickly they are able to resume their normal lives,” she said.
The maximum number of injections needed in the cohort was three. No adverse events have been reported.
Session comoderator Dr. Seemal Desai, a dermatologist in private practice near Dallas, said the technique is very practical, hits an unmet need, and could potentially prevent tropia when used around the eye.
“My only comment is that if you’re using human hyaluronidase, the skin testing to make sure there is no anaphylaxis is important,” he said. “But if you’re using synthetic or recombinant hyaluronidase, which is really what we use here more, I don’t think that would be an issue. I think this was a great idea to do this, especially for advancement flaps.”
Fellow comoderator and Mohs surgeon Dr. Ramona Behshad, in private practice in St. Louis, Mo., said the case series provides a novel and practical use for hyaluronidase, which is “very underused” in dermatology practices and often goes to waste because it expires.
Dr. Rai and her maxillofacial surgery colleagues at King’s College are performing a randomized controlled trial using hyaluronidase on all head and neck postoperative wounds to assess its effect on postoperative lymphedema and recovery times with and without the agent. “Hopefully, this will provide further information on its efficacy including other sites on the head and neck,” she said.
CHICAGO – Hyaluronidase can speed the resolution of postoperative periorbital lymphedema in patients undergoing Mohs micrographic surgery and flap repair, a prospective case series suggests.
Lymphedema resolved in all seven cases treated with hyaluronidase (Hyalase) injections in 4-6 weeks, compared with 3 months as would be expected, Dr. Sweta Rai, of St John’s Institute of Dermatology, King’s College London, said at the annual meeting of the American Society for Dermatologic Surgery.
“In the periorbital area where the skin is very thin and therefore even small amounts of lymphovascular fluid is visible, postoperative lymphedema is a cosmetic concern, especially as patients want to resume their daily activities as soon as possible postoperatively,” she said in an interview.
Hyaluronidase is widely used in cosmetic surgery in the breakdown of hyaluronic acid fillers, where the mucolytic enzyme splits and lowers the viscosity of hyaluronic acid in the extracellular matrix.
Dr. Rai and her coauthor Dr. Hooman Khorasani, chief of Mohs, reconstructive, and cosmetic surgery at Mount Sinai School of Medicine in New York, turned to hyaluronidase because it’s well documented that hyaluronic acid is produced by the body as an automatic response to promote wound healing
Patients undergoing Mohs surgery for large eye tumors often require complex flap repairs that cross the lower eyelid and cheek junction, which results in greater lymphedema. Hyaluronic acid produces a scaffolding effect at the wound site that, in combination with periorbital lymphedema when the vascular channels are cut, is thought to lead to fluid stasis. Hyaluronidase breaks down this scaffolding, allowing the lymphovascular fluid to drain into the subcutaneous tissue, Dr. Rai explained.
The investigators use a 1,500-unit vial of generic hyaluronidase diluted with 1.5 mL of normal saline and inject 100-150 units subcutaneously starting 2 weeks postoperatively at the time of suture removal and repeat the injections every 2 weeks until the swelling resolves.
Patients should undergo an intradermal prick test prior to injections to exclude the risk of type I hypersensitivity anaphylaxis previously reported with human hyaluronidase injections, Dr. Rai cautioned.
In all seven patients, aged 42-80 years, periorbital lymphedema resolved with 150-450 units of hyaluronidase. The patients included a women referred for treatment 2 months after Mohs surgery. The index case, involving a man with a periorbital defect and a medially based advancement flap, resolved with only a single 150-unit injection given 2 weeks after surgery, Dr. Rai said.
“Most of my patients are working and lead busy work and social lives, and they’ve all commented on how pleased they are with the results and on how quickly they are able to resume their normal lives,” she said.
The maximum number of injections needed in the cohort was three. No adverse events have been reported.
Session comoderator Dr. Seemal Desai, a dermatologist in private practice near Dallas, said the technique is very practical, hits an unmet need, and could potentially prevent tropia when used around the eye.
“My only comment is that if you’re using human hyaluronidase, the skin testing to make sure there is no anaphylaxis is important,” he said. “But if you’re using synthetic or recombinant hyaluronidase, which is really what we use here more, I don’t think that would be an issue. I think this was a great idea to do this, especially for advancement flaps.”
Fellow comoderator and Mohs surgeon Dr. Ramona Behshad, in private practice in St. Louis, Mo., said the case series provides a novel and practical use for hyaluronidase, which is “very underused” in dermatology practices and often goes to waste because it expires.
Dr. Rai and her maxillofacial surgery colleagues at King’s College are performing a randomized controlled trial using hyaluronidase on all head and neck postoperative wounds to assess its effect on postoperative lymphedema and recovery times with and without the agent. “Hopefully, this will provide further information on its efficacy including other sites on the head and neck,” she said.
CHICAGO – Hyaluronidase can speed the resolution of postoperative periorbital lymphedema in patients undergoing Mohs micrographic surgery and flap repair, a prospective case series suggests.
Lymphedema resolved in all seven cases treated with hyaluronidase (Hyalase) injections in 4-6 weeks, compared with 3 months as would be expected, Dr. Sweta Rai, of St John’s Institute of Dermatology, King’s College London, said at the annual meeting of the American Society for Dermatologic Surgery.
“In the periorbital area where the skin is very thin and therefore even small amounts of lymphovascular fluid is visible, postoperative lymphedema is a cosmetic concern, especially as patients want to resume their daily activities as soon as possible postoperatively,” she said in an interview.
Hyaluronidase is widely used in cosmetic surgery in the breakdown of hyaluronic acid fillers, where the mucolytic enzyme splits and lowers the viscosity of hyaluronic acid in the extracellular matrix.
Dr. Rai and her coauthor Dr. Hooman Khorasani, chief of Mohs, reconstructive, and cosmetic surgery at Mount Sinai School of Medicine in New York, turned to hyaluronidase because it’s well documented that hyaluronic acid is produced by the body as an automatic response to promote wound healing
Patients undergoing Mohs surgery for large eye tumors often require complex flap repairs that cross the lower eyelid and cheek junction, which results in greater lymphedema. Hyaluronic acid produces a scaffolding effect at the wound site that, in combination with periorbital lymphedema when the vascular channels are cut, is thought to lead to fluid stasis. Hyaluronidase breaks down this scaffolding, allowing the lymphovascular fluid to drain into the subcutaneous tissue, Dr. Rai explained.
The investigators use a 1,500-unit vial of generic hyaluronidase diluted with 1.5 mL of normal saline and inject 100-150 units subcutaneously starting 2 weeks postoperatively at the time of suture removal and repeat the injections every 2 weeks until the swelling resolves.
Patients should undergo an intradermal prick test prior to injections to exclude the risk of type I hypersensitivity anaphylaxis previously reported with human hyaluronidase injections, Dr. Rai cautioned.
In all seven patients, aged 42-80 years, periorbital lymphedema resolved with 150-450 units of hyaluronidase. The patients included a women referred for treatment 2 months after Mohs surgery. The index case, involving a man with a periorbital defect and a medially based advancement flap, resolved with only a single 150-unit injection given 2 weeks after surgery, Dr. Rai said.
“Most of my patients are working and lead busy work and social lives, and they’ve all commented on how pleased they are with the results and on how quickly they are able to resume their normal lives,” she said.
The maximum number of injections needed in the cohort was three. No adverse events have been reported.
Session comoderator Dr. Seemal Desai, a dermatologist in private practice near Dallas, said the technique is very practical, hits an unmet need, and could potentially prevent tropia when used around the eye.
“My only comment is that if you’re using human hyaluronidase, the skin testing to make sure there is no anaphylaxis is important,” he said. “But if you’re using synthetic or recombinant hyaluronidase, which is really what we use here more, I don’t think that would be an issue. I think this was a great idea to do this, especially for advancement flaps.”
Fellow comoderator and Mohs surgeon Dr. Ramona Behshad, in private practice in St. Louis, Mo., said the case series provides a novel and practical use for hyaluronidase, which is “very underused” in dermatology practices and often goes to waste because it expires.
Dr. Rai and her maxillofacial surgery colleagues at King’s College are performing a randomized controlled trial using hyaluronidase on all head and neck postoperative wounds to assess its effect on postoperative lymphedema and recovery times with and without the agent. “Hopefully, this will provide further information on its efficacy including other sites on the head and neck,” she said.
AT THE ASDS ANNUAL MEETING
Key clinical point: Hyaluronidase injections speed resolution of periorbital postoperative lymphedema in patients undergoing Mohs surgery and flap repair.
Major finding: Lymphedema resolved in all seven cases within 4-6 weeks of hyaluronidase administration.
Data source: The study was a prospective case series of seven patients.
Disclosures: The authors reported having no financial disclosures.
Biopsy-site photography an easy winner on all counts
CHICAGO – Biopsy-site photography appears to reduce the risk of potential wrong-site surgery and can easily be incorporated into dermatology practice, according to Dr. Jeremy Etzkorn.
When Dr. Etzkorn took on this quality improvement initiative on his own, only 5 of 239 routine biopsy-site photographs evaluated were inadequate. The biopsy site was not clearly marked in two photos with multiple suspicious lesions, and anatomic landmarks were absent in three.
“Almost 98% of the time, the photograph was adequate, which just shows it doesn’t require much training or time to get images of the skin,” the Mohs surgeon said at the annual meeting of the American Society for Dermatologic Surgery.
Biopsy-site photos were taken primarily by medical assistants, as well as nurses, who received minimal, informal training on digital photography and were guided to take at least one photograph with anatomic landmarks present.
Dr. Etzkorn of the University of Pennsylvania Health System, Philadelphia, conducted a prospective, observational cohort study of 329 patients/tumors referred for Mohs micrographic surgery or standard excision to the dermatologic surgery unit at Penn Dermatology. Patients were asked to identify their biopsy site, indicate whether they remembered a photo being taken, and quantify on a 10-point scale their level of confidence that the originally biopsied site was treated on the day of surgery.
Dr. Etzkorn identified the biopsy site before consulting the medical record for a biopsy-site photograph. If the photo was absent and he and the patient agreed on the biopsy site, they proceeded to surgery. If there was any disagreement, surgery was postponed and the referring physician consulted.
Overall, 239 patients (73%) had biopsy-site photographs, and 90 patients (27%), referred to the practice before photography was implemented, did not.
In 12.5% of cases, the patient misidentified the biopsy site, and in 6.7% of cases the physician did, which is similar to what has been reported in the literature, Dr. Etzkorn said.
Biopsy-site photography prevented wrong-site surgery in 3 of the 239 cases (1.25%) where these photographs were available. “Without the photo I would normally have done surgery on that site because the patient was confident it was the right site; I was confident it was the right site,” he said.
Importantly, all three lesions were biopsied, and all were squamous cell carcinoma in situ. So while it was the wrong site, the surgery would not have been inappropriate, Dr. Etzkorn noted.
Surgery was postponed to consult the referring physician in 3% of cases (10/329).
Complete patient confidence (10 of 10 points) that the correct site was treated was achieved in 95% of cases, with most of the remaining patients at 9 of 10 points, he said.
Risk factors for patient biopsy-site misidentification were the inability to see the site without a mirror (odds ratio, 3.95; P = .002) and time between the biopsy and surgery (OR, 2.19; P = .028). Prior studies have also shown that difficult-to-visualize sites are associated with biopsy-site misidentification, he noted.
For Dr. Etzkorn, the risk of biopsy-site misidentification quadrupled if there were multiple simultaneous biopsies from different locations (OR, 4.39; P = .003) and tripled with longer time, defined as longer than a 6-week delay vs. a delay of less than 6 weeks between biopsy and surgery (OR, 3.68; P = .007).
A biopsy-site photograph significantly increased the odds that a patient was completely confident the correct site was treated (OR, 5.48; P = .001), as did the use of Mohs surgery vs. excision (OR, 4.87; P = .017).
Once again, time between the biopsy and surgery was a significant risk factor for postponing surgery (OR, 3.52; P = .035), whereas the presence of a biopsy-site photograph cut that risk by almost 13-fold (OR, 12.5: P less than .001), Dr. Etzkorn reported.
“Biopsy-site photography is associated with increased patient confidence that the correct site is treated, decreases in surgical postponement, and the ability to identify wrong-site surgery and prevent it,” he concluded.
Dr. Etzkorn and his coauthor reported having no relevant financial disclosures.
CHICAGO – Biopsy-site photography appears to reduce the risk of potential wrong-site surgery and can easily be incorporated into dermatology practice, according to Dr. Jeremy Etzkorn.
When Dr. Etzkorn took on this quality improvement initiative on his own, only 5 of 239 routine biopsy-site photographs evaluated were inadequate. The biopsy site was not clearly marked in two photos with multiple suspicious lesions, and anatomic landmarks were absent in three.
“Almost 98% of the time, the photograph was adequate, which just shows it doesn’t require much training or time to get images of the skin,” the Mohs surgeon said at the annual meeting of the American Society for Dermatologic Surgery.
Biopsy-site photos were taken primarily by medical assistants, as well as nurses, who received minimal, informal training on digital photography and were guided to take at least one photograph with anatomic landmarks present.
Dr. Etzkorn of the University of Pennsylvania Health System, Philadelphia, conducted a prospective, observational cohort study of 329 patients/tumors referred for Mohs micrographic surgery or standard excision to the dermatologic surgery unit at Penn Dermatology. Patients were asked to identify their biopsy site, indicate whether they remembered a photo being taken, and quantify on a 10-point scale their level of confidence that the originally biopsied site was treated on the day of surgery.
Dr. Etzkorn identified the biopsy site before consulting the medical record for a biopsy-site photograph. If the photo was absent and he and the patient agreed on the biopsy site, they proceeded to surgery. If there was any disagreement, surgery was postponed and the referring physician consulted.
Overall, 239 patients (73%) had biopsy-site photographs, and 90 patients (27%), referred to the practice before photography was implemented, did not.
In 12.5% of cases, the patient misidentified the biopsy site, and in 6.7% of cases the physician did, which is similar to what has been reported in the literature, Dr. Etzkorn said.
Biopsy-site photography prevented wrong-site surgery in 3 of the 239 cases (1.25%) where these photographs were available. “Without the photo I would normally have done surgery on that site because the patient was confident it was the right site; I was confident it was the right site,” he said.
Importantly, all three lesions were biopsied, and all were squamous cell carcinoma in situ. So while it was the wrong site, the surgery would not have been inappropriate, Dr. Etzkorn noted.
Surgery was postponed to consult the referring physician in 3% of cases (10/329).
Complete patient confidence (10 of 10 points) that the correct site was treated was achieved in 95% of cases, with most of the remaining patients at 9 of 10 points, he said.
Risk factors for patient biopsy-site misidentification were the inability to see the site without a mirror (odds ratio, 3.95; P = .002) and time between the biopsy and surgery (OR, 2.19; P = .028). Prior studies have also shown that difficult-to-visualize sites are associated with biopsy-site misidentification, he noted.
For Dr. Etzkorn, the risk of biopsy-site misidentification quadrupled if there were multiple simultaneous biopsies from different locations (OR, 4.39; P = .003) and tripled with longer time, defined as longer than a 6-week delay vs. a delay of less than 6 weeks between biopsy and surgery (OR, 3.68; P = .007).
A biopsy-site photograph significantly increased the odds that a patient was completely confident the correct site was treated (OR, 5.48; P = .001), as did the use of Mohs surgery vs. excision (OR, 4.87; P = .017).
Once again, time between the biopsy and surgery was a significant risk factor for postponing surgery (OR, 3.52; P = .035), whereas the presence of a biopsy-site photograph cut that risk by almost 13-fold (OR, 12.5: P less than .001), Dr. Etzkorn reported.
“Biopsy-site photography is associated with increased patient confidence that the correct site is treated, decreases in surgical postponement, and the ability to identify wrong-site surgery and prevent it,” he concluded.
Dr. Etzkorn and his coauthor reported having no relevant financial disclosures.
CHICAGO – Biopsy-site photography appears to reduce the risk of potential wrong-site surgery and can easily be incorporated into dermatology practice, according to Dr. Jeremy Etzkorn.
When Dr. Etzkorn took on this quality improvement initiative on his own, only 5 of 239 routine biopsy-site photographs evaluated were inadequate. The biopsy site was not clearly marked in two photos with multiple suspicious lesions, and anatomic landmarks were absent in three.
“Almost 98% of the time, the photograph was adequate, which just shows it doesn’t require much training or time to get images of the skin,” the Mohs surgeon said at the annual meeting of the American Society for Dermatologic Surgery.
Biopsy-site photos were taken primarily by medical assistants, as well as nurses, who received minimal, informal training on digital photography and were guided to take at least one photograph with anatomic landmarks present.
Dr. Etzkorn of the University of Pennsylvania Health System, Philadelphia, conducted a prospective, observational cohort study of 329 patients/tumors referred for Mohs micrographic surgery or standard excision to the dermatologic surgery unit at Penn Dermatology. Patients were asked to identify their biopsy site, indicate whether they remembered a photo being taken, and quantify on a 10-point scale their level of confidence that the originally biopsied site was treated on the day of surgery.
Dr. Etzkorn identified the biopsy site before consulting the medical record for a biopsy-site photograph. If the photo was absent and he and the patient agreed on the biopsy site, they proceeded to surgery. If there was any disagreement, surgery was postponed and the referring physician consulted.
Overall, 239 patients (73%) had biopsy-site photographs, and 90 patients (27%), referred to the practice before photography was implemented, did not.
In 12.5% of cases, the patient misidentified the biopsy site, and in 6.7% of cases the physician did, which is similar to what has been reported in the literature, Dr. Etzkorn said.
Biopsy-site photography prevented wrong-site surgery in 3 of the 239 cases (1.25%) where these photographs were available. “Without the photo I would normally have done surgery on that site because the patient was confident it was the right site; I was confident it was the right site,” he said.
Importantly, all three lesions were biopsied, and all were squamous cell carcinoma in situ. So while it was the wrong site, the surgery would not have been inappropriate, Dr. Etzkorn noted.
Surgery was postponed to consult the referring physician in 3% of cases (10/329).
Complete patient confidence (10 of 10 points) that the correct site was treated was achieved in 95% of cases, with most of the remaining patients at 9 of 10 points, he said.
Risk factors for patient biopsy-site misidentification were the inability to see the site without a mirror (odds ratio, 3.95; P = .002) and time between the biopsy and surgery (OR, 2.19; P = .028). Prior studies have also shown that difficult-to-visualize sites are associated with biopsy-site misidentification, he noted.
For Dr. Etzkorn, the risk of biopsy-site misidentification quadrupled if there were multiple simultaneous biopsies from different locations (OR, 4.39; P = .003) and tripled with longer time, defined as longer than a 6-week delay vs. a delay of less than 6 weeks between biopsy and surgery (OR, 3.68; P = .007).
A biopsy-site photograph significantly increased the odds that a patient was completely confident the correct site was treated (OR, 5.48; P = .001), as did the use of Mohs surgery vs. excision (OR, 4.87; P = .017).
Once again, time between the biopsy and surgery was a significant risk factor for postponing surgery (OR, 3.52; P = .035), whereas the presence of a biopsy-site photograph cut that risk by almost 13-fold (OR, 12.5: P less than .001), Dr. Etzkorn reported.
“Biopsy-site photography is associated with increased patient confidence that the correct site is treated, decreases in surgical postponement, and the ability to identify wrong-site surgery and prevent it,” he concluded.
Dr. Etzkorn and his coauthor reported having no relevant financial disclosures.
AT THE ASDS ANNUAL MEETING
Key clinical point: Biopsy-site photography reduces surgical delays, identifies potential wrong-site surgery, and increases patient confidence.
Major finding: Having biopsy-site photos can help prevent wrong-site surgery.
Data source: A prospective, observational cohort study of 329 patients referred for Mohs surgery or standard excision.
Disclosures: Dr. Etzkorn and his coauthor reported having no relevant financial disclosures.
Pearls from the ASDS meeting
The annual American Society for Dermatologic Surgery conference in Chicago Oct. 15-18 was one of the best attended meeting in years. From injectables to lasers to reconstruction, the newest information was distributed among the members.
Here are pearls gained from the ASDS conference that every dermatologist should know:
There are reports of temporary alopecia of the beard area in men after deoxycholic acid (Kybella) injections in the submentum. Patients should be counseled prior to injection. Deeper injections in males, pinching up the skin, and penetrating the needle to the hub are measures that have been suggested to help minimize the risk of this potential side effect.
More than 60 cases of blindness secondary to filler injections have been reported, but such cases are likely underreported. The majority of reports were from South Korea and most cases were due to autologous fat transfer. High risk areas include the glabella, nasal dorsum, and anteromedial cheek/tear trough due to retrograde flow of a filler embolus to the ophthalmic artery from anastomoses with the angular, dorsal nasal, and supratrochlear arteries. Cannulas are recommended as they are considered safer than needles, particularly when injecting either fat or fillers in the mid face area.
However, even cannulas are not foolproof. There are some areas where periosteal placement of filler is important and therefore the use of needles is required, such as the anterosuperior temple, zygomaticomalar cheek, and central chin. Expert knowledge of the vascular anatomy of the face, including location and depth of important vessels, is a must.
If a vascular occlusion occurs – particularly to the ophthalmic artery that can result in blindness – symptoms may include pain, visual disturbances, vomiting, and blanching/reticulation of blood vessels on the skin surface. Time is of the essence in preventing or reversing vision loss. If a hyaluronic acid filler was used, retrobulbar injection of at least 1,000 units of hyaluronidase and referral to an ophthalmologist should be done within minutes.
For body contouring and skin tightening, cryolipolysis and high-intensity focused ultrasound have shown results over the past several years. However, newer technologies including nonthermal focused ultrasound, multipolar radiofrequency, and fractional radiofrequency with microneedling, and a 1064 nm diode laser also show some promise.
The ablative fractional CO2 laser was shown to be helpful for hypopigmented scars.
Malpractice lawsuits against cosmetic procedures are highest among physician extenders (physician assistants, nurses, assistants, etc).
Dr. Wesley and Dr. Talakoub are co-contributors to a monthly Aesthetic Dermatology column in Dermatology News. Dr. Talakoub is in private practice in McLean, Va. Dr. Wesley practices dermatology in Beverly Hills, Calif. This month’s column is by Dr. Wesley.
This article was updated Nov. 16, 2015.
The annual American Society for Dermatologic Surgery conference in Chicago Oct. 15-18 was one of the best attended meeting in years. From injectables to lasers to reconstruction, the newest information was distributed among the members.
Here are pearls gained from the ASDS conference that every dermatologist should know:
There are reports of temporary alopecia of the beard area in men after deoxycholic acid (Kybella) injections in the submentum. Patients should be counseled prior to injection. Deeper injections in males, pinching up the skin, and penetrating the needle to the hub are measures that have been suggested to help minimize the risk of this potential side effect.
More than 60 cases of blindness secondary to filler injections have been reported, but such cases are likely underreported. The majority of reports were from South Korea and most cases were due to autologous fat transfer. High risk areas include the glabella, nasal dorsum, and anteromedial cheek/tear trough due to retrograde flow of a filler embolus to the ophthalmic artery from anastomoses with the angular, dorsal nasal, and supratrochlear arteries. Cannulas are recommended as they are considered safer than needles, particularly when injecting either fat or fillers in the mid face area.
However, even cannulas are not foolproof. There are some areas where periosteal placement of filler is important and therefore the use of needles is required, such as the anterosuperior temple, zygomaticomalar cheek, and central chin. Expert knowledge of the vascular anatomy of the face, including location and depth of important vessels, is a must.
If a vascular occlusion occurs – particularly to the ophthalmic artery that can result in blindness – symptoms may include pain, visual disturbances, vomiting, and blanching/reticulation of blood vessels on the skin surface. Time is of the essence in preventing or reversing vision loss. If a hyaluronic acid filler was used, retrobulbar injection of at least 1,000 units of hyaluronidase and referral to an ophthalmologist should be done within minutes.
For body contouring and skin tightening, cryolipolysis and high-intensity focused ultrasound have shown results over the past several years. However, newer technologies including nonthermal focused ultrasound, multipolar radiofrequency, and fractional radiofrequency with microneedling, and a 1064 nm diode laser also show some promise.
The ablative fractional CO2 laser was shown to be helpful for hypopigmented scars.
Malpractice lawsuits against cosmetic procedures are highest among physician extenders (physician assistants, nurses, assistants, etc).
Dr. Wesley and Dr. Talakoub are co-contributors to a monthly Aesthetic Dermatology column in Dermatology News. Dr. Talakoub is in private practice in McLean, Va. Dr. Wesley practices dermatology in Beverly Hills, Calif. This month’s column is by Dr. Wesley.
This article was updated Nov. 16, 2015.
The annual American Society for Dermatologic Surgery conference in Chicago Oct. 15-18 was one of the best attended meeting in years. From injectables to lasers to reconstruction, the newest information was distributed among the members.
Here are pearls gained from the ASDS conference that every dermatologist should know:
There are reports of temporary alopecia of the beard area in men after deoxycholic acid (Kybella) injections in the submentum. Patients should be counseled prior to injection. Deeper injections in males, pinching up the skin, and penetrating the needle to the hub are measures that have been suggested to help minimize the risk of this potential side effect.
More than 60 cases of blindness secondary to filler injections have been reported, but such cases are likely underreported. The majority of reports were from South Korea and most cases were due to autologous fat transfer. High risk areas include the glabella, nasal dorsum, and anteromedial cheek/tear trough due to retrograde flow of a filler embolus to the ophthalmic artery from anastomoses with the angular, dorsal nasal, and supratrochlear arteries. Cannulas are recommended as they are considered safer than needles, particularly when injecting either fat or fillers in the mid face area.
However, even cannulas are not foolproof. There are some areas where periosteal placement of filler is important and therefore the use of needles is required, such as the anterosuperior temple, zygomaticomalar cheek, and central chin. Expert knowledge of the vascular anatomy of the face, including location and depth of important vessels, is a must.
If a vascular occlusion occurs – particularly to the ophthalmic artery that can result in blindness – symptoms may include pain, visual disturbances, vomiting, and blanching/reticulation of blood vessels on the skin surface. Time is of the essence in preventing or reversing vision loss. If a hyaluronic acid filler was used, retrobulbar injection of at least 1,000 units of hyaluronidase and referral to an ophthalmologist should be done within minutes.
For body contouring and skin tightening, cryolipolysis and high-intensity focused ultrasound have shown results over the past several years. However, newer technologies including nonthermal focused ultrasound, multipolar radiofrequency, and fractional radiofrequency with microneedling, and a 1064 nm diode laser also show some promise.
The ablative fractional CO2 laser was shown to be helpful for hypopigmented scars.
Malpractice lawsuits against cosmetic procedures are highest among physician extenders (physician assistants, nurses, assistants, etc).
Dr. Wesley and Dr. Talakoub are co-contributors to a monthly Aesthetic Dermatology column in Dermatology News. Dr. Talakoub is in private practice in McLean, Va. Dr. Wesley practices dermatology in Beverly Hills, Calif. This month’s column is by Dr. Wesley.
This article was updated Nov. 16, 2015.
EADV: Best treatments for great saphenous vein reflux
COPENHAGEN – Superior 5-year outcomes for great saphenous vein reflux were achieved with conventional surgery and endovenous laser ablation as compared with ultrasound-guided foam sclerotherapy in a randomized trial, Dr. Simone van der Velden reported at the annual congress of the European Academy of Dermatology and Venereology.
The multicenter study included 224 randomized legs belonging to symptomatic patients with a target great saphenous vein diameter of at least 5 mm. If deemed necessary, patients could undergo one re-treatment at 3 or 12 months after their initial procedure. At 5 years of follow-up, 86% of the treated legs were available for long-term evaluation, noted Dr. van der Velden of Erasmus University Medical Center in Rotterdam, the Netherlands.
The primary endpoint was obliteration or absence of the treated great saphenous vein segment. This was achieved with conventional surgery in 85% of treated cases, in 77% of legs treated with endovenous laser ablation (EVLA), and in 23% with ultrasound-guided foam sclerotherapy (UGFS).
Absence of above-the-knee greater saphenous vein reflux – a secondary endpoint – was achieved in 85% of the conventional surgery group and in 82% of the EVLA group, both of which were significantly better results than the 41% response with UGFS.
Another secondary endpoint was grade II neovascularization. Here again, both conventional surgery and EVLA outperformed UGFS, with rates of 17%, 13%, and 4%, respectively. In contrast, there was no significant difference between the three treatment groups in terms of the presence of refluxing tributaries above or below knee level, she continued.
Scores on the disease-specific Chronic Venous Insufficiency quality of life Questionnaire (CIVIQ) deteriorated over time in the UGFS group, improved in the EVLA-treated patients, and remained stable in the conventional surgery group.
Conventional surgery was performed under general anesthesia and entailed high ligation of the saphenofemoral junction and phlebectomy of tributaries. In contrast, EVLA was done under local tumescent anesthesia using a 940-nm laser. The laser fiber was introduced at knee level, positioned 1-2 cm below the saphenofemoral junction, and delivered an energy of roughly 60 Joules/cm2.
For UGFS, operators utilized a foam comprising 1 mL of sodium tetradecyl sulfate per 3 mL of air. A maximum of 10 mL of foam could be injected per treatment session, depending upon the diameter of the great saphenous vein and length of the refluxing trunk. Phlebectomies in this group were performed only in the event of patient complaints.
Of note, patients in the minimally invasive UGFS group required re-treatment three times more often than did those in the other two study arms.
Dr. van der Velden said she has heard from some UGFS partisans that she and her coinvestigators may have undertreated patients in that study arm because they didn’t routinely perform phlebectomies of the tributaries, and the average amount of foam they injected, about 4.5 mL, was on the low side.
The study was sponsored by Erasmus University. Dr. van der Velden reported having no financial conflicts of interest.
COPENHAGEN – Superior 5-year outcomes for great saphenous vein reflux were achieved with conventional surgery and endovenous laser ablation as compared with ultrasound-guided foam sclerotherapy in a randomized trial, Dr. Simone van der Velden reported at the annual congress of the European Academy of Dermatology and Venereology.
The multicenter study included 224 randomized legs belonging to symptomatic patients with a target great saphenous vein diameter of at least 5 mm. If deemed necessary, patients could undergo one re-treatment at 3 or 12 months after their initial procedure. At 5 years of follow-up, 86% of the treated legs were available for long-term evaluation, noted Dr. van der Velden of Erasmus University Medical Center in Rotterdam, the Netherlands.
The primary endpoint was obliteration or absence of the treated great saphenous vein segment. This was achieved with conventional surgery in 85% of treated cases, in 77% of legs treated with endovenous laser ablation (EVLA), and in 23% with ultrasound-guided foam sclerotherapy (UGFS).
Absence of above-the-knee greater saphenous vein reflux – a secondary endpoint – was achieved in 85% of the conventional surgery group and in 82% of the EVLA group, both of which were significantly better results than the 41% response with UGFS.
Another secondary endpoint was grade II neovascularization. Here again, both conventional surgery and EVLA outperformed UGFS, with rates of 17%, 13%, and 4%, respectively. In contrast, there was no significant difference between the three treatment groups in terms of the presence of refluxing tributaries above or below knee level, she continued.
Scores on the disease-specific Chronic Venous Insufficiency quality of life Questionnaire (CIVIQ) deteriorated over time in the UGFS group, improved in the EVLA-treated patients, and remained stable in the conventional surgery group.
Conventional surgery was performed under general anesthesia and entailed high ligation of the saphenofemoral junction and phlebectomy of tributaries. In contrast, EVLA was done under local tumescent anesthesia using a 940-nm laser. The laser fiber was introduced at knee level, positioned 1-2 cm below the saphenofemoral junction, and delivered an energy of roughly 60 Joules/cm2.
For UGFS, operators utilized a foam comprising 1 mL of sodium tetradecyl sulfate per 3 mL of air. A maximum of 10 mL of foam could be injected per treatment session, depending upon the diameter of the great saphenous vein and length of the refluxing trunk. Phlebectomies in this group were performed only in the event of patient complaints.
Of note, patients in the minimally invasive UGFS group required re-treatment three times more often than did those in the other two study arms.
Dr. van der Velden said she has heard from some UGFS partisans that she and her coinvestigators may have undertreated patients in that study arm because they didn’t routinely perform phlebectomies of the tributaries, and the average amount of foam they injected, about 4.5 mL, was on the low side.
The study was sponsored by Erasmus University. Dr. van der Velden reported having no financial conflicts of interest.
COPENHAGEN – Superior 5-year outcomes for great saphenous vein reflux were achieved with conventional surgery and endovenous laser ablation as compared with ultrasound-guided foam sclerotherapy in a randomized trial, Dr. Simone van der Velden reported at the annual congress of the European Academy of Dermatology and Venereology.
The multicenter study included 224 randomized legs belonging to symptomatic patients with a target great saphenous vein diameter of at least 5 mm. If deemed necessary, patients could undergo one re-treatment at 3 or 12 months after their initial procedure. At 5 years of follow-up, 86% of the treated legs were available for long-term evaluation, noted Dr. van der Velden of Erasmus University Medical Center in Rotterdam, the Netherlands.
The primary endpoint was obliteration or absence of the treated great saphenous vein segment. This was achieved with conventional surgery in 85% of treated cases, in 77% of legs treated with endovenous laser ablation (EVLA), and in 23% with ultrasound-guided foam sclerotherapy (UGFS).
Absence of above-the-knee greater saphenous vein reflux – a secondary endpoint – was achieved in 85% of the conventional surgery group and in 82% of the EVLA group, both of which were significantly better results than the 41% response with UGFS.
Another secondary endpoint was grade II neovascularization. Here again, both conventional surgery and EVLA outperformed UGFS, with rates of 17%, 13%, and 4%, respectively. In contrast, there was no significant difference between the three treatment groups in terms of the presence of refluxing tributaries above or below knee level, she continued.
Scores on the disease-specific Chronic Venous Insufficiency quality of life Questionnaire (CIVIQ) deteriorated over time in the UGFS group, improved in the EVLA-treated patients, and remained stable in the conventional surgery group.
Conventional surgery was performed under general anesthesia and entailed high ligation of the saphenofemoral junction and phlebectomy of tributaries. In contrast, EVLA was done under local tumescent anesthesia using a 940-nm laser. The laser fiber was introduced at knee level, positioned 1-2 cm below the saphenofemoral junction, and delivered an energy of roughly 60 Joules/cm2.
For UGFS, operators utilized a foam comprising 1 mL of sodium tetradecyl sulfate per 3 mL of air. A maximum of 10 mL of foam could be injected per treatment session, depending upon the diameter of the great saphenous vein and length of the refluxing trunk. Phlebectomies in this group were performed only in the event of patient complaints.
Of note, patients in the minimally invasive UGFS group required re-treatment three times more often than did those in the other two study arms.
Dr. van der Velden said she has heard from some UGFS partisans that she and her coinvestigators may have undertreated patients in that study arm because they didn’t routinely perform phlebectomies of the tributaries, and the average amount of foam they injected, about 4.5 mL, was on the low side.
The study was sponsored by Erasmus University. Dr. van der Velden reported having no financial conflicts of interest.
AT THE EADV CONGRESS
Key clinical point: Long-term outcomes for treatment of great saphenous vein reflux were significantly better with conventional surgery or endovenous laser ablation than with ultrasound-guided foam sclerotherapy.
Major finding: Obliteration or absence of the treated great saphenous vein segment was achieved with conventional surgery in 85% of treated cases, with endovenous laser ablation (EVLA) in 77% of legs treated, and with ultrasound-guided foam sclerotherapy (UGFS) in 23%.
Data source: This multicenter clinical trial with 5-year follow-up included 224 legs randomized to one of three popular treatments for great saphenous varicose veins.
Disclosures: The study was sponsored by Erasmus University. The presenter reported having no financial conflicts of interest.
Deoxycholic acid effective in trimming extreme and very mild chin fat
CHICAGO – Deoxycholic acid injections benefit patients on either end of the spectrum with mild or extreme submental fat, a phase III safety study shows.
“What this study shows is that the applicability of the product is wider than what’s represented in the registration trials because they looked at a very narrow band and this includes people with very mild and extreme [submental fat],” Dr. Richard G. Glogau of San Francisco Dermatology and the University of California, San Francisco, said in an interview. He presented the results of the study at the annual meeting of the American Society for Dermatologic Surgery.
Deoxycholic acid gained U.S. approval in April 2015 as the first injectable cytolytic drug to treat moderate to severe convexity or fullness associated with submental fat (SMF) in adults. It is marketed as Kybella.
Because treatment can be tailored based on the amount and thickness of SMF, the study sought to evaluate deoxycholic acid 2 mg/cm2 or placebo for up to six treatments 1 month apart in 47 patients with mild SMF and 46 patients with extreme SMF based on Clinician-Reported Submental Fat Rating Scale (CR-SMFRS) scores of 1 (mild) or 4 (extreme).
The predominantly female cohort had an average age of 48 years in the mild SMF group and 51 years in the extreme SMF group and a mean body mass index of 25 kg/m2 and 32.5 kg/m2, respectively. About 30% of patients in the extreme SMF group had moderate to severe skin laxity compared with about 15% in the mild SMF group.
The mean number of treatment sessions was 4.9 for placebo and 4.2 for deoxycholic acid in the mild SMF group, and 5.6 for placebo and 4.9 for deoxycholic acid in the extreme SMF group.
“I don’t think in the real world that’s our experience,” Dr. Glogau said at the meeting. “People in the mild group get by with much less and, conversely, people at the extreme end would be happy to go on higher than four or five treatments, depending on what size they started with.”
The mean total injection volume across all treatments was 17.2 mL, 13.9 mL, 38.4 mL, and 31.6 mL, respectively, which is consistent with the need for less product in mild SMF.
In the mild SMF group, SMF was reduced by one grade in significantly more patients following deoxycholic acid treatment than placebo as measured with the CR-SMFRS (74.2% vs. 20%), the Patient-Rated SMFRS (67.7% vs. 33.3%), or a composite of the two scales (61.3% vs. 6.7%).
The percentages of patients with extreme SMF achieving a one-grade improvement with deoxycholic acid were even higher: CR-SMFRS (96.4% vs. 26.7%), PR-SMFRS (89.3% vs. 46.7%), or the composite (89.3% vs. 13.3%), said Dr. Glogau.
Moreover, SMF improved by two grades on the composite endpoint in 43% of extreme SMF patients treated with deoxycholic acid vs. 0% given placebo. P values for all comparisons were less than .05.
“To reach a two-grade change in virtually anything you want to study is difficult to achieve, so I think this is a significant landmark that came out of this study,” Dr. Glogau said.
Significantly more deoxycholic acid–treated patients also reported being satisfied with the appearance of their face and chin compared with those given placebo in the mild SMF (80% vs. 46.7%; P less than .05) and extreme SMF (71.4% vs. 0%; P less than .05) groups.
Despite reductions in SMF, skin laxity was unchanged or got only slightly better from baseline in all patients on deoxycholic acid. This is not surprising, because deoxycholic acid exerts its killing effect on fat cells only, not on fibrous septae or the dermis, and skin laxity is a reflection of inherent elasticity in the dermis, together with the fibrous septae in the fat running between skin and muscle, Dr. Glogau explained.
Most adverse events were mild or moderate in severity and transient in nature, he said. Among mild SMF patients, pain was reported in 74% treated with deoxycholic acid vs. 50% with placebo, bruising in 48% vs. 50%, edema in 42% vs. 25%, numbness in 48% vs. 6%, and swelling in 42% vs. 13%. The percentages were generally similar in the extreme SMF group.
“I think the incidence of hematoma and bruising is actually a function of injection technique and numbers out in clinical practice are somewhat lower,” Dr. Glogau observed.
No drug-related serious adverse events were reported. Nerve paresis was reported in two deoxycholic acid–treated patients with mild SMF and resolved without sequelae after 4 days and after 52 days.
Dysphagia was reported in one deoxycholic acid–treated patient with extreme SMF and resolved without sequelae after 2 days.
None of the events precluded patients from receiving additional treatment, even within the 30-day interval, he said, adding that in practice most clinicians are using longer breaks between treatments.
During a discussion of the study, Dr. Glogau said he uses lidocaine to reduce pain and that local anesthesia should be standard with deoxycholic acid injections.
Fellow presenter Dr. Brian Biesman, director of the Nashville (Tenn.) Centre for Laser and Facial Surgery, said that he was injected with deoxycholic acid both with and without local anesthesia and that they’ve used local anesthesia ever since.
“It makes a huge difference from a patient experience standpoint, of being extraordinarily unpleasant without it – and I have a pretty good pain tolerance – to being extraordinarily unremarkable,” Dr. Biesman said.
Session moderator Dr. Wendy Roberts of Dermatology Rancho Mirage (Calif.), said that Dr. Glogau’s study provides clinicians with data to support deoxycholic acid use in a broader range of patients.
“Now we have a real resource that we can reference and say as a matter of fact, for mild submental fullness you will get a result and this is the study. So you’re not wasting your money, you’re not wasting your time,” she said in an interview. “I think it’s extremely important. In Southern California where I practice, people don’t want to get to be moderate to severe.”
The oral abstract session included several other deoxycholic acid presentations including long-term follow-up from phase II/III trials showing that improvements in SMF severity are maintained for up to 4 years after treatment. The improvements were due to deoxycholic acid treatment, as body weight did not significantly change throughout the follow-up period, said study author Dr. Ashish Bhatia of the DuPage Medical Group, in Naperville, Ill.
Dr. Kenneth Beer of Palm Beach (Fla.) Cosmetic, provided details on the ongoing Kythera-sponsored CONTOUR: Condition of Submental Fullness and Treatment Outcomes Registry study looking at how SMF is treated in clinical practice and the risks and benefits associated with treatment.
Kythera Biopharmaceuticals markets Kybella, which is also known as ATX-101. Dr. Glogau, Dr. Roberts, Dr. Bhatia, and Dr. Beer reported ties to Kythera. Several coauthors also disclosed ties to the company.
CHICAGO – Deoxycholic acid injections benefit patients on either end of the spectrum with mild or extreme submental fat, a phase III safety study shows.
“What this study shows is that the applicability of the product is wider than what’s represented in the registration trials because they looked at a very narrow band and this includes people with very mild and extreme [submental fat],” Dr. Richard G. Glogau of San Francisco Dermatology and the University of California, San Francisco, said in an interview. He presented the results of the study at the annual meeting of the American Society for Dermatologic Surgery.
Deoxycholic acid gained U.S. approval in April 2015 as the first injectable cytolytic drug to treat moderate to severe convexity or fullness associated with submental fat (SMF) in adults. It is marketed as Kybella.
Because treatment can be tailored based on the amount and thickness of SMF, the study sought to evaluate deoxycholic acid 2 mg/cm2 or placebo for up to six treatments 1 month apart in 47 patients with mild SMF and 46 patients with extreme SMF based on Clinician-Reported Submental Fat Rating Scale (CR-SMFRS) scores of 1 (mild) or 4 (extreme).
The predominantly female cohort had an average age of 48 years in the mild SMF group and 51 years in the extreme SMF group and a mean body mass index of 25 kg/m2 and 32.5 kg/m2, respectively. About 30% of patients in the extreme SMF group had moderate to severe skin laxity compared with about 15% in the mild SMF group.
The mean number of treatment sessions was 4.9 for placebo and 4.2 for deoxycholic acid in the mild SMF group, and 5.6 for placebo and 4.9 for deoxycholic acid in the extreme SMF group.
“I don’t think in the real world that’s our experience,” Dr. Glogau said at the meeting. “People in the mild group get by with much less and, conversely, people at the extreme end would be happy to go on higher than four or five treatments, depending on what size they started with.”
The mean total injection volume across all treatments was 17.2 mL, 13.9 mL, 38.4 mL, and 31.6 mL, respectively, which is consistent with the need for less product in mild SMF.
In the mild SMF group, SMF was reduced by one grade in significantly more patients following deoxycholic acid treatment than placebo as measured with the CR-SMFRS (74.2% vs. 20%), the Patient-Rated SMFRS (67.7% vs. 33.3%), or a composite of the two scales (61.3% vs. 6.7%).
The percentages of patients with extreme SMF achieving a one-grade improvement with deoxycholic acid were even higher: CR-SMFRS (96.4% vs. 26.7%), PR-SMFRS (89.3% vs. 46.7%), or the composite (89.3% vs. 13.3%), said Dr. Glogau.
Moreover, SMF improved by two grades on the composite endpoint in 43% of extreme SMF patients treated with deoxycholic acid vs. 0% given placebo. P values for all comparisons were less than .05.
“To reach a two-grade change in virtually anything you want to study is difficult to achieve, so I think this is a significant landmark that came out of this study,” Dr. Glogau said.
Significantly more deoxycholic acid–treated patients also reported being satisfied with the appearance of their face and chin compared with those given placebo in the mild SMF (80% vs. 46.7%; P less than .05) and extreme SMF (71.4% vs. 0%; P less than .05) groups.
Despite reductions in SMF, skin laxity was unchanged or got only slightly better from baseline in all patients on deoxycholic acid. This is not surprising, because deoxycholic acid exerts its killing effect on fat cells only, not on fibrous septae or the dermis, and skin laxity is a reflection of inherent elasticity in the dermis, together with the fibrous septae in the fat running between skin and muscle, Dr. Glogau explained.
Most adverse events were mild or moderate in severity and transient in nature, he said. Among mild SMF patients, pain was reported in 74% treated with deoxycholic acid vs. 50% with placebo, bruising in 48% vs. 50%, edema in 42% vs. 25%, numbness in 48% vs. 6%, and swelling in 42% vs. 13%. The percentages were generally similar in the extreme SMF group.
“I think the incidence of hematoma and bruising is actually a function of injection technique and numbers out in clinical practice are somewhat lower,” Dr. Glogau observed.
No drug-related serious adverse events were reported. Nerve paresis was reported in two deoxycholic acid–treated patients with mild SMF and resolved without sequelae after 4 days and after 52 days.
Dysphagia was reported in one deoxycholic acid–treated patient with extreme SMF and resolved without sequelae after 2 days.
None of the events precluded patients from receiving additional treatment, even within the 30-day interval, he said, adding that in practice most clinicians are using longer breaks between treatments.
During a discussion of the study, Dr. Glogau said he uses lidocaine to reduce pain and that local anesthesia should be standard with deoxycholic acid injections.
Fellow presenter Dr. Brian Biesman, director of the Nashville (Tenn.) Centre for Laser and Facial Surgery, said that he was injected with deoxycholic acid both with and without local anesthesia and that they’ve used local anesthesia ever since.
“It makes a huge difference from a patient experience standpoint, of being extraordinarily unpleasant without it – and I have a pretty good pain tolerance – to being extraordinarily unremarkable,” Dr. Biesman said.
Session moderator Dr. Wendy Roberts of Dermatology Rancho Mirage (Calif.), said that Dr. Glogau’s study provides clinicians with data to support deoxycholic acid use in a broader range of patients.
“Now we have a real resource that we can reference and say as a matter of fact, for mild submental fullness you will get a result and this is the study. So you’re not wasting your money, you’re not wasting your time,” she said in an interview. “I think it’s extremely important. In Southern California where I practice, people don’t want to get to be moderate to severe.”
The oral abstract session included several other deoxycholic acid presentations including long-term follow-up from phase II/III trials showing that improvements in SMF severity are maintained for up to 4 years after treatment. The improvements were due to deoxycholic acid treatment, as body weight did not significantly change throughout the follow-up period, said study author Dr. Ashish Bhatia of the DuPage Medical Group, in Naperville, Ill.
Dr. Kenneth Beer of Palm Beach (Fla.) Cosmetic, provided details on the ongoing Kythera-sponsored CONTOUR: Condition of Submental Fullness and Treatment Outcomes Registry study looking at how SMF is treated in clinical practice and the risks and benefits associated with treatment.
Kythera Biopharmaceuticals markets Kybella, which is also known as ATX-101. Dr. Glogau, Dr. Roberts, Dr. Bhatia, and Dr. Beer reported ties to Kythera. Several coauthors also disclosed ties to the company.
CHICAGO – Deoxycholic acid injections benefit patients on either end of the spectrum with mild or extreme submental fat, a phase III safety study shows.
“What this study shows is that the applicability of the product is wider than what’s represented in the registration trials because they looked at a very narrow band and this includes people with very mild and extreme [submental fat],” Dr. Richard G. Glogau of San Francisco Dermatology and the University of California, San Francisco, said in an interview. He presented the results of the study at the annual meeting of the American Society for Dermatologic Surgery.
Deoxycholic acid gained U.S. approval in April 2015 as the first injectable cytolytic drug to treat moderate to severe convexity or fullness associated with submental fat (SMF) in adults. It is marketed as Kybella.
Because treatment can be tailored based on the amount and thickness of SMF, the study sought to evaluate deoxycholic acid 2 mg/cm2 or placebo for up to six treatments 1 month apart in 47 patients with mild SMF and 46 patients with extreme SMF based on Clinician-Reported Submental Fat Rating Scale (CR-SMFRS) scores of 1 (mild) or 4 (extreme).
The predominantly female cohort had an average age of 48 years in the mild SMF group and 51 years in the extreme SMF group and a mean body mass index of 25 kg/m2 and 32.5 kg/m2, respectively. About 30% of patients in the extreme SMF group had moderate to severe skin laxity compared with about 15% in the mild SMF group.
The mean number of treatment sessions was 4.9 for placebo and 4.2 for deoxycholic acid in the mild SMF group, and 5.6 for placebo and 4.9 for deoxycholic acid in the extreme SMF group.
“I don’t think in the real world that’s our experience,” Dr. Glogau said at the meeting. “People in the mild group get by with much less and, conversely, people at the extreme end would be happy to go on higher than four or five treatments, depending on what size they started with.”
The mean total injection volume across all treatments was 17.2 mL, 13.9 mL, 38.4 mL, and 31.6 mL, respectively, which is consistent with the need for less product in mild SMF.
In the mild SMF group, SMF was reduced by one grade in significantly more patients following deoxycholic acid treatment than placebo as measured with the CR-SMFRS (74.2% vs. 20%), the Patient-Rated SMFRS (67.7% vs. 33.3%), or a composite of the two scales (61.3% vs. 6.7%).
The percentages of patients with extreme SMF achieving a one-grade improvement with deoxycholic acid were even higher: CR-SMFRS (96.4% vs. 26.7%), PR-SMFRS (89.3% vs. 46.7%), or the composite (89.3% vs. 13.3%), said Dr. Glogau.
Moreover, SMF improved by two grades on the composite endpoint in 43% of extreme SMF patients treated with deoxycholic acid vs. 0% given placebo. P values for all comparisons were less than .05.
“To reach a two-grade change in virtually anything you want to study is difficult to achieve, so I think this is a significant landmark that came out of this study,” Dr. Glogau said.
Significantly more deoxycholic acid–treated patients also reported being satisfied with the appearance of their face and chin compared with those given placebo in the mild SMF (80% vs. 46.7%; P less than .05) and extreme SMF (71.4% vs. 0%; P less than .05) groups.
Despite reductions in SMF, skin laxity was unchanged or got only slightly better from baseline in all patients on deoxycholic acid. This is not surprising, because deoxycholic acid exerts its killing effect on fat cells only, not on fibrous septae or the dermis, and skin laxity is a reflection of inherent elasticity in the dermis, together with the fibrous septae in the fat running between skin and muscle, Dr. Glogau explained.
Most adverse events were mild or moderate in severity and transient in nature, he said. Among mild SMF patients, pain was reported in 74% treated with deoxycholic acid vs. 50% with placebo, bruising in 48% vs. 50%, edema in 42% vs. 25%, numbness in 48% vs. 6%, and swelling in 42% vs. 13%. The percentages were generally similar in the extreme SMF group.
“I think the incidence of hematoma and bruising is actually a function of injection technique and numbers out in clinical practice are somewhat lower,” Dr. Glogau observed.
No drug-related serious adverse events were reported. Nerve paresis was reported in two deoxycholic acid–treated patients with mild SMF and resolved without sequelae after 4 days and after 52 days.
Dysphagia was reported in one deoxycholic acid–treated patient with extreme SMF and resolved without sequelae after 2 days.
None of the events precluded patients from receiving additional treatment, even within the 30-day interval, he said, adding that in practice most clinicians are using longer breaks between treatments.
During a discussion of the study, Dr. Glogau said he uses lidocaine to reduce pain and that local anesthesia should be standard with deoxycholic acid injections.
Fellow presenter Dr. Brian Biesman, director of the Nashville (Tenn.) Centre for Laser and Facial Surgery, said that he was injected with deoxycholic acid both with and without local anesthesia and that they’ve used local anesthesia ever since.
“It makes a huge difference from a patient experience standpoint, of being extraordinarily unpleasant without it – and I have a pretty good pain tolerance – to being extraordinarily unremarkable,” Dr. Biesman said.
Session moderator Dr. Wendy Roberts of Dermatology Rancho Mirage (Calif.), said that Dr. Glogau’s study provides clinicians with data to support deoxycholic acid use in a broader range of patients.
“Now we have a real resource that we can reference and say as a matter of fact, for mild submental fullness you will get a result and this is the study. So you’re not wasting your money, you’re not wasting your time,” she said in an interview. “I think it’s extremely important. In Southern California where I practice, people don’t want to get to be moderate to severe.”
The oral abstract session included several other deoxycholic acid presentations including long-term follow-up from phase II/III trials showing that improvements in SMF severity are maintained for up to 4 years after treatment. The improvements were due to deoxycholic acid treatment, as body weight did not significantly change throughout the follow-up period, said study author Dr. Ashish Bhatia of the DuPage Medical Group, in Naperville, Ill.
Dr. Kenneth Beer of Palm Beach (Fla.) Cosmetic, provided details on the ongoing Kythera-sponsored CONTOUR: Condition of Submental Fullness and Treatment Outcomes Registry study looking at how SMF is treated in clinical practice and the risks and benefits associated with treatment.
Kythera Biopharmaceuticals markets Kybella, which is also known as ATX-101. Dr. Glogau, Dr. Roberts, Dr. Bhatia, and Dr. Beer reported ties to Kythera. Several coauthors also disclosed ties to the company.
AT THE ASDS ANNUAL MEETING
Key clinical point: Deoxycholic acid injection reduces submental fat in patients with mild or extreme submental fullness.
Major finding: Submental fat improved by two grades in 43% of patients treated with deoxycholic acid vs. 0% given placebo.
Data source: A double-blind, phase III safety study comparing Kybella to placebo in 93 patients with mild or extreme submental fat.
Disclosures: Dr. Glogau, Dr. Roberts, Dr. Bhatia, and Dr. Beer reported ties to Kythera Biopharmaceuticals. Several coauthors also disclosed ties to Kythera.
OnabotulinumtoxinA associated with reduced severity of PAH
The severity of primary axillary hyperhidrosis (PAH) decreased in more than half of patients who received onabotulinumtoxinA injections, in a nonrandomized, open-label study.
The researchers gave 144 adolescents with PAH up to six treatments with the drug, with retreatment occurring no sooner than 8 weeks after a prior treatment and no later than 44 weeks after the initial treatment.
Patients were retreated if they had 50 mg or more of spontaneous resting axillary sweat production in each axilla, following injections to each axilla. Fifty-six patients received one treatment, 59 patients received two treatments, 20 received three treatments, 6 received four treatments, and 3 received five treatments. Patients’ scores on the 4-point Hyperhidrosis Disease Severity Scale (HDSS) were among the measures used to evaluate responses to the onabotulinumtoxinA injections.
Results showed that 72.3% of patients experienced at least a 2-point improvement in their HDSS score at 4 weeks after their first treatment, and 56.6% of patients experienced a 2-point or greater improvement at 8 weeks following their second round of injections.
Mean sweat production declined by an average of 83.9% 4 weeks after treatment, and by an average of 78.1% 8 weeks after treatment. More than 50% of patients experienced at least a 90% reduction in sweat production at the 4th week following one of their injections (either the first, second, or third treatment).
Ninety-two patients (63.9%) reported experiencing adverse events (AEs), with upper respiratory tract infections having occurred the most frequently. While most of such adverse events “were mild or moderate in severity,” three patients experienced serious AEs and an additional three experienced severe AEs. Eight patients (5.6%) had 10 treatment-related AEs, including hyperhidrosis (back and palms), injection-site pain, lymphadenopathy, nausea, injection-site irritation, self-reported compensatory sweating (palms), dizziness, and pruritus.
“This study demonstrated that the efficacy and safety of onabotulinumtoxinA in treating PAH reported in previous registration clinical trials in adults can be extended to adolescents,” wrote Dr. Dee Anna Glaser of Saint Louis University and her colleagues.
Dr. Glaser is a paid consultant and investigator for Allergan, Dermira, and Miramar Labs. She has received research grants and honoraria from these companies and is an investigator for Ulthera. Her coauthors disclosed ties to Allergan.
Read the study in Pediatric Dermatology (doi: 10.1111/pde.12620).
The severity of primary axillary hyperhidrosis (PAH) decreased in more than half of patients who received onabotulinumtoxinA injections, in a nonrandomized, open-label study.
The researchers gave 144 adolescents with PAH up to six treatments with the drug, with retreatment occurring no sooner than 8 weeks after a prior treatment and no later than 44 weeks after the initial treatment.
Patients were retreated if they had 50 mg or more of spontaneous resting axillary sweat production in each axilla, following injections to each axilla. Fifty-six patients received one treatment, 59 patients received two treatments, 20 received three treatments, 6 received four treatments, and 3 received five treatments. Patients’ scores on the 4-point Hyperhidrosis Disease Severity Scale (HDSS) were among the measures used to evaluate responses to the onabotulinumtoxinA injections.
Results showed that 72.3% of patients experienced at least a 2-point improvement in their HDSS score at 4 weeks after their first treatment, and 56.6% of patients experienced a 2-point or greater improvement at 8 weeks following their second round of injections.
Mean sweat production declined by an average of 83.9% 4 weeks after treatment, and by an average of 78.1% 8 weeks after treatment. More than 50% of patients experienced at least a 90% reduction in sweat production at the 4th week following one of their injections (either the first, second, or third treatment).
Ninety-two patients (63.9%) reported experiencing adverse events (AEs), with upper respiratory tract infections having occurred the most frequently. While most of such adverse events “were mild or moderate in severity,” three patients experienced serious AEs and an additional three experienced severe AEs. Eight patients (5.6%) had 10 treatment-related AEs, including hyperhidrosis (back and palms), injection-site pain, lymphadenopathy, nausea, injection-site irritation, self-reported compensatory sweating (palms), dizziness, and pruritus.
“This study demonstrated that the efficacy and safety of onabotulinumtoxinA in treating PAH reported in previous registration clinical trials in adults can be extended to adolescents,” wrote Dr. Dee Anna Glaser of Saint Louis University and her colleagues.
Dr. Glaser is a paid consultant and investigator for Allergan, Dermira, and Miramar Labs. She has received research grants and honoraria from these companies and is an investigator for Ulthera. Her coauthors disclosed ties to Allergan.
Read the study in Pediatric Dermatology (doi: 10.1111/pde.12620).
The severity of primary axillary hyperhidrosis (PAH) decreased in more than half of patients who received onabotulinumtoxinA injections, in a nonrandomized, open-label study.
The researchers gave 144 adolescents with PAH up to six treatments with the drug, with retreatment occurring no sooner than 8 weeks after a prior treatment and no later than 44 weeks after the initial treatment.
Patients were retreated if they had 50 mg or more of spontaneous resting axillary sweat production in each axilla, following injections to each axilla. Fifty-six patients received one treatment, 59 patients received two treatments, 20 received three treatments, 6 received four treatments, and 3 received five treatments. Patients’ scores on the 4-point Hyperhidrosis Disease Severity Scale (HDSS) were among the measures used to evaluate responses to the onabotulinumtoxinA injections.
Results showed that 72.3% of patients experienced at least a 2-point improvement in their HDSS score at 4 weeks after their first treatment, and 56.6% of patients experienced a 2-point or greater improvement at 8 weeks following their second round of injections.
Mean sweat production declined by an average of 83.9% 4 weeks after treatment, and by an average of 78.1% 8 weeks after treatment. More than 50% of patients experienced at least a 90% reduction in sweat production at the 4th week following one of their injections (either the first, second, or third treatment).
Ninety-two patients (63.9%) reported experiencing adverse events (AEs), with upper respiratory tract infections having occurred the most frequently. While most of such adverse events “were mild or moderate in severity,” three patients experienced serious AEs and an additional three experienced severe AEs. Eight patients (5.6%) had 10 treatment-related AEs, including hyperhidrosis (back and palms), injection-site pain, lymphadenopathy, nausea, injection-site irritation, self-reported compensatory sweating (palms), dizziness, and pruritus.
“This study demonstrated that the efficacy and safety of onabotulinumtoxinA in treating PAH reported in previous registration clinical trials in adults can be extended to adolescents,” wrote Dr. Dee Anna Glaser of Saint Louis University and her colleagues.
Dr. Glaser is a paid consultant and investigator for Allergan, Dermira, and Miramar Labs. She has received research grants and honoraria from these companies and is an investigator for Ulthera. Her coauthors disclosed ties to Allergan.
Read the study in Pediatric Dermatology (doi: 10.1111/pde.12620).
FROM PEDIATRIC DERMATOLOGY