User login
Sunless Tanners
Coloring the skin with dihydroxyacetone to create an artificial tan was discovered serendipitously in the 1950s by Eva Wittgenstein, whose patients were taking DHA orally. She observed that when patients regurgitated the DHA, pigmented spots remained on the skin (Science 1960;132:894-5).
The change in pigmentation results from the interaction of DHA with amino acids in the stratum corneum (Br. J. Dermatol. 2003;149:332-40).
Although the first product brought to market to exploit this new knowledge in 1959 met with initial success, it fell into disuse because of the poor cosmetic results (J. Am. Acad. Dermatol. 2003;49:1096-106; South. Med. J. 2005;98:1192-5).
Public awareness of sunless tanning has grown in recent years, however, and has been met with formulations that afford a much improved cosmetic performance, with DHA remaining as the main active ingredient in sunless-tanning agents (South. Med. J. 2005;98:1192-5; Am. J. Clin. Dermatol. 2002;3:317-8).
This column will briefly review the role of sunless-tanning lotions and sprays in dermatology, and will try to place recommendations to patients about sunless tanners in the context of sunscreens and tanning attitudes.
Sunless tanners have been used, with varying degrees of popularity, for 50 years; recent evidence suggests that the use of these products has increased in recent years. A long track record of usage and research indicates that sunless-tanning compounds are safe (J. Environ. Pathol. Toxicol. Oncol. 1984;5:349-51; Am. J. Clin. Dermatol. 2002;3:317-8; South. Med. J. 2005;98:1192-5; J. Am. Acad. Dermatol. 2007;56:387-90.) However, there is some debate as to whether the use of these products renders users more inclined to stay in the sun longer. Also, ongoing research has raised some safety issues regarding DHA.
Chemical Protection
In 2004, Petersen et al. investigated the effects of DHA on cell survival and proliferation of a human keratinocyte cell line, HaCaT. Significant genotoxic activity was identified in these cultured cells, as researchers noted dose- and time-dependent morphologic alterations as well as cytoplasmic budding and cell detachment in DHA-treated cells, and apoptosis and marked declines in proliferation 1 day after DHA exposure. Interestingly, the development of DNA strand breaks was prevented via preincubation with antioxidants. The authors suggested that their findings raised concerns about the long-term use of treating the skin with DHA-containing formulations (Mutat. Res. 2004;560:173-86).
A small study by Faurschou et al. showed that DHA provided human skin with modest UVB protection, with a 5% DHA cream applied three times or a 20% DHA cream applied once yielding an effect similar to an SPF 1.6. They acknowledged that most commercial DHA products contain 3%-5% DHA and offer scant protection. A potential advantage of sunless tanners, if they offer protection, suggested the authors, would be that no spots would be left unattended since such gaps would be conspicuous for lack of browning (Arch. Dermatol. 2004;140:886-7).
Howe, Reed, and Dellavalle contended that DHA in self-tanning agents provided enough UVA protection to warrant use as an adjunct to daily sunscreen use for broad-band protection (J. Am. Acad. Dermatol. 2008;58:894). The researchers referenced a 1975 study in which 3% DHA augmented sunlight tolerance among five patients with UVA-sensitive dermatoses (Dermatologica 1975;150:346-51; J. Am. Acad. Dermatol. 2008;58:894).
In 2009, Choquenet et al. assessed the sun protection potency of self-tanners and foundations using an in vitro method to identify indicators such as sun protection factor (SPF), UVA protection factor (PF-UVA), and UVB/UVA ratio. Using seven amino acids in the corneal cells of the epidermis, the investigators identified SPFs virtually equivalent to zero (approximately SPF 2). Conversely, they found foundations to exhibit satisfactory photostability and a non-negligible SPF, noting that such products are safe given their typically once-daily application (J. Dermatol. 2009;36:587-91).
Attitudes and Behavior
Users of sunless-tanning products were found, in a survey of 2,005 randomly selected South Australian adults published in 2001, to be more likely to use sunscreen but less likely to wear a hat or other sun-protective clothing. Sunburns were also linked to the use of sunless tanners in this study (Med. J. Aust. 2001;174:75-8; J. Am. Acad. Dermatol. 2007;56:387-90).
In 2005, Mahler et al. conducted a randomized, controlled trial with 1-month follow-up of 146 Southern California college students to study the impact of UV photoaging photographs and data on the sun protection plans and behaviors of young adults, and whether sunless-tanning lotion might play a role in sun-protective behavior. Of the 146 volunteers, 91.1% completed the "surprise" 1-month follow-up. The intervention consisted of volunteers being shown a UV facial photo and short video illustrating the etiology and results of photoaging. The investigators found that the UV photographic intervention was successful insofar as significantly better sun protection strategies and behaviors were employed by the test group, compared with controls. In addition, they noted that those who used sunless-tanning lotion were more likely to exhibit extensive sun-protective behavior, compared with individuals who received the intervention alone. The authors suggested that such interventions represented a cost-effective approach that might yield behaviors with long-term health benefits in the form of a lower incidence of skin cancer (Arch. Dermatol. 2005;141:373-80).
Later that year, Sheehan and Lesher reported on their anonymous survey of 121 adults (107 women and 14 men) who received spray-on sunless-tanning treatments between February and May 2004. Most reported that sunless tanning had not or would not affect their use of sunscreen or time spent outdoors. Interestingly, though, 73% of the respondents who had used tanning beds indicated that they had reduced or would reduce their use of indoor tanning. The researchers concluded that practitioners should recommend sunless tanning to their patients who use conventional tanning beds as a way to lower their solar exposure and risk of skin cancer (South. Med. J. 2005;98:1192-5).
In 2006, Brooks et al. reported on their July 2004, greater Boston, cross-sectional survey of 448 nonrandomly selected people aged 18-30 years on the subjects of artificial tanning products, recent history of sunburns, and tanning-bed use. During the preceding year, 22% of respondents had used sunless-tanning products and the same percentage hadn’t but would consider using them in the next year. Users of these lotions were more likely to have been severe burners and, after controlling for skin type, the investigators found that previous and potential users were more likely to have experienced sunburns during the summer and to have used tanning beds than were respondents who had neither used nor planned to use sunless tanners. The researchers concluded that the option of sunless tanning did not seem to lower the incidence of sunburn or the use of tanning beds. Further, they urged caution in offering broad support for artificial tanning products, even though looking for alternatives to UV exposure is to be encouraged (J. Am. Acad. Dermatol. 2006;54:1060-6).
A 2007 study using data from 5,491 completed interviews as part of the National Cancer Institute’s HINTS (Health Information National Trends Survey) 2005 set out to determine the prevalence of sunless-tanning formulation use and to understand the relationship between sunless tanning, indoor tanning, and sun-protective behavior. In so doing, the investigators found that the use of sunless-tanning products was relatively rare, with an estimated 11% of U.S. adults claiming to have used such products in the previous year. Of this group, 13% used sunless tanners more than 25 times; 12% used them 11-24 times; 35% used them 3-10 times; and 40% used them just once or twice. Users and exclusive users were more likely to be women, well educated, and living in the West (J. Am. Acad. Dermatol. 2007;56:387-90).
Recent Cause for Pause
In 2008, Jung et al. used the electron spin resonance spectroscopy–based radical sun protection factor, which measures free-radical reactions in skin biopsies during UV exposure and can determine the protective effect of UV filters and sunscreens, to analyze three different self-tanning agents, including DHA. Noting that the reaction of the reducing sugars in such products and amino acids (Maillard reaction) in the skin layer engendered Amadori products that created free radicals during UV irradiation, the investigators reported that in DHA-treated skin, more than 180% additional radicals were produced during sun exposure, compared with untreated skin. They concluded that the use of self-tanners necessitated reducing solar exposure duration (Spectrochim. Acta A. Mol. Biomol Spectrosc. 2008;69:1423-8). Consequently, DHA users would be well advised to wait at least 24 hours before solar exposure following application of sunless lotion or spray (Dermatol. Clin. 2009;27:149-54).
Conclusion
In addition to the need to continually persuade patients to engage in skin-protective behavior – namely, limiting sun exposure, avoiding peak-time exposures, wearing wide-brimmed hats and clothing with SPF value, and using sunscreens (preferably those containing avobenzone, Mexoryl, zinc oxide, or titanium dioxide) every day – it is incumbent upon dermatologists to disabuse our patients of the idea that untanned skin is less attractive or, conversely, that tans should be equated with attractive skin. Although healthy messages (that there is no such thing as a healthy tan, and that a tan indicates skin damage) are slowly spreading, sunless tanners appear to be a medically and cosmetically acceptable intermediary step, far surpassing the patently detrimental effects of indoor tanning. That said, patients should be advised to refrain from solar exposure for a full 24 hours after applying sunless tanners. Furthermore, much more research is necessary to truly establish that DHA delivers even modest protection from UVA or UVB. Accordingly, patients should be counseled that sunless tanners do not suffice as a base, nor do they justify extended solar exposure, and that sunscreens should also be applied.
Coloring the skin with dihydroxyacetone to create an artificial tan was discovered serendipitously in the 1950s by Eva Wittgenstein, whose patients were taking DHA orally. She observed that when patients regurgitated the DHA, pigmented spots remained on the skin (Science 1960;132:894-5).
The change in pigmentation results from the interaction of DHA with amino acids in the stratum corneum (Br. J. Dermatol. 2003;149:332-40).
Although the first product brought to market to exploit this new knowledge in 1959 met with initial success, it fell into disuse because of the poor cosmetic results (J. Am. Acad. Dermatol. 2003;49:1096-106; South. Med. J. 2005;98:1192-5).
Public awareness of sunless tanning has grown in recent years, however, and has been met with formulations that afford a much improved cosmetic performance, with DHA remaining as the main active ingredient in sunless-tanning agents (South. Med. J. 2005;98:1192-5; Am. J. Clin. Dermatol. 2002;3:317-8).
This column will briefly review the role of sunless-tanning lotions and sprays in dermatology, and will try to place recommendations to patients about sunless tanners in the context of sunscreens and tanning attitudes.
Sunless tanners have been used, with varying degrees of popularity, for 50 years; recent evidence suggests that the use of these products has increased in recent years. A long track record of usage and research indicates that sunless-tanning compounds are safe (J. Environ. Pathol. Toxicol. Oncol. 1984;5:349-51; Am. J. Clin. Dermatol. 2002;3:317-8; South. Med. J. 2005;98:1192-5; J. Am. Acad. Dermatol. 2007;56:387-90.) However, there is some debate as to whether the use of these products renders users more inclined to stay in the sun longer. Also, ongoing research has raised some safety issues regarding DHA.
Chemical Protection
In 2004, Petersen et al. investigated the effects of DHA on cell survival and proliferation of a human keratinocyte cell line, HaCaT. Significant genotoxic activity was identified in these cultured cells, as researchers noted dose- and time-dependent morphologic alterations as well as cytoplasmic budding and cell detachment in DHA-treated cells, and apoptosis and marked declines in proliferation 1 day after DHA exposure. Interestingly, the development of DNA strand breaks was prevented via preincubation with antioxidants. The authors suggested that their findings raised concerns about the long-term use of treating the skin with DHA-containing formulations (Mutat. Res. 2004;560:173-86).
A small study by Faurschou et al. showed that DHA provided human skin with modest UVB protection, with a 5% DHA cream applied three times or a 20% DHA cream applied once yielding an effect similar to an SPF 1.6. They acknowledged that most commercial DHA products contain 3%-5% DHA and offer scant protection. A potential advantage of sunless tanners, if they offer protection, suggested the authors, would be that no spots would be left unattended since such gaps would be conspicuous for lack of browning (Arch. Dermatol. 2004;140:886-7).
Howe, Reed, and Dellavalle contended that DHA in self-tanning agents provided enough UVA protection to warrant use as an adjunct to daily sunscreen use for broad-band protection (J. Am. Acad. Dermatol. 2008;58:894). The researchers referenced a 1975 study in which 3% DHA augmented sunlight tolerance among five patients with UVA-sensitive dermatoses (Dermatologica 1975;150:346-51; J. Am. Acad. Dermatol. 2008;58:894).
In 2009, Choquenet et al. assessed the sun protection potency of self-tanners and foundations using an in vitro method to identify indicators such as sun protection factor (SPF), UVA protection factor (PF-UVA), and UVB/UVA ratio. Using seven amino acids in the corneal cells of the epidermis, the investigators identified SPFs virtually equivalent to zero (approximately SPF 2). Conversely, they found foundations to exhibit satisfactory photostability and a non-negligible SPF, noting that such products are safe given their typically once-daily application (J. Dermatol. 2009;36:587-91).
Attitudes and Behavior
Users of sunless-tanning products were found, in a survey of 2,005 randomly selected South Australian adults published in 2001, to be more likely to use sunscreen but less likely to wear a hat or other sun-protective clothing. Sunburns were also linked to the use of sunless tanners in this study (Med. J. Aust. 2001;174:75-8; J. Am. Acad. Dermatol. 2007;56:387-90).
In 2005, Mahler et al. conducted a randomized, controlled trial with 1-month follow-up of 146 Southern California college students to study the impact of UV photoaging photographs and data on the sun protection plans and behaviors of young adults, and whether sunless-tanning lotion might play a role in sun-protective behavior. Of the 146 volunteers, 91.1% completed the "surprise" 1-month follow-up. The intervention consisted of volunteers being shown a UV facial photo and short video illustrating the etiology and results of photoaging. The investigators found that the UV photographic intervention was successful insofar as significantly better sun protection strategies and behaviors were employed by the test group, compared with controls. In addition, they noted that those who used sunless-tanning lotion were more likely to exhibit extensive sun-protective behavior, compared with individuals who received the intervention alone. The authors suggested that such interventions represented a cost-effective approach that might yield behaviors with long-term health benefits in the form of a lower incidence of skin cancer (Arch. Dermatol. 2005;141:373-80).
Later that year, Sheehan and Lesher reported on their anonymous survey of 121 adults (107 women and 14 men) who received spray-on sunless-tanning treatments between February and May 2004. Most reported that sunless tanning had not or would not affect their use of sunscreen or time spent outdoors. Interestingly, though, 73% of the respondents who had used tanning beds indicated that they had reduced or would reduce their use of indoor tanning. The researchers concluded that practitioners should recommend sunless tanning to their patients who use conventional tanning beds as a way to lower their solar exposure and risk of skin cancer (South. Med. J. 2005;98:1192-5).
In 2006, Brooks et al. reported on their July 2004, greater Boston, cross-sectional survey of 448 nonrandomly selected people aged 18-30 years on the subjects of artificial tanning products, recent history of sunburns, and tanning-bed use. During the preceding year, 22% of respondents had used sunless-tanning products and the same percentage hadn’t but would consider using them in the next year. Users of these lotions were more likely to have been severe burners and, after controlling for skin type, the investigators found that previous and potential users were more likely to have experienced sunburns during the summer and to have used tanning beds than were respondents who had neither used nor planned to use sunless tanners. The researchers concluded that the option of sunless tanning did not seem to lower the incidence of sunburn or the use of tanning beds. Further, they urged caution in offering broad support for artificial tanning products, even though looking for alternatives to UV exposure is to be encouraged (J. Am. Acad. Dermatol. 2006;54:1060-6).
A 2007 study using data from 5,491 completed interviews as part of the National Cancer Institute’s HINTS (Health Information National Trends Survey) 2005 set out to determine the prevalence of sunless-tanning formulation use and to understand the relationship between sunless tanning, indoor tanning, and sun-protective behavior. In so doing, the investigators found that the use of sunless-tanning products was relatively rare, with an estimated 11% of U.S. adults claiming to have used such products in the previous year. Of this group, 13% used sunless tanners more than 25 times; 12% used them 11-24 times; 35% used them 3-10 times; and 40% used them just once or twice. Users and exclusive users were more likely to be women, well educated, and living in the West (J. Am. Acad. Dermatol. 2007;56:387-90).
Recent Cause for Pause
In 2008, Jung et al. used the electron spin resonance spectroscopy–based radical sun protection factor, which measures free-radical reactions in skin biopsies during UV exposure and can determine the protective effect of UV filters and sunscreens, to analyze three different self-tanning agents, including DHA. Noting that the reaction of the reducing sugars in such products and amino acids (Maillard reaction) in the skin layer engendered Amadori products that created free radicals during UV irradiation, the investigators reported that in DHA-treated skin, more than 180% additional radicals were produced during sun exposure, compared with untreated skin. They concluded that the use of self-tanners necessitated reducing solar exposure duration (Spectrochim. Acta A. Mol. Biomol Spectrosc. 2008;69:1423-8). Consequently, DHA users would be well advised to wait at least 24 hours before solar exposure following application of sunless lotion or spray (Dermatol. Clin. 2009;27:149-54).
Conclusion
In addition to the need to continually persuade patients to engage in skin-protective behavior – namely, limiting sun exposure, avoiding peak-time exposures, wearing wide-brimmed hats and clothing with SPF value, and using sunscreens (preferably those containing avobenzone, Mexoryl, zinc oxide, or titanium dioxide) every day – it is incumbent upon dermatologists to disabuse our patients of the idea that untanned skin is less attractive or, conversely, that tans should be equated with attractive skin. Although healthy messages (that there is no such thing as a healthy tan, and that a tan indicates skin damage) are slowly spreading, sunless tanners appear to be a medically and cosmetically acceptable intermediary step, far surpassing the patently detrimental effects of indoor tanning. That said, patients should be advised to refrain from solar exposure for a full 24 hours after applying sunless tanners. Furthermore, much more research is necessary to truly establish that DHA delivers even modest protection from UVA or UVB. Accordingly, patients should be counseled that sunless tanners do not suffice as a base, nor do they justify extended solar exposure, and that sunscreens should also be applied.
Coloring the skin with dihydroxyacetone to create an artificial tan was discovered serendipitously in the 1950s by Eva Wittgenstein, whose patients were taking DHA orally. She observed that when patients regurgitated the DHA, pigmented spots remained on the skin (Science 1960;132:894-5).
The change in pigmentation results from the interaction of DHA with amino acids in the stratum corneum (Br. J. Dermatol. 2003;149:332-40).
Although the first product brought to market to exploit this new knowledge in 1959 met with initial success, it fell into disuse because of the poor cosmetic results (J. Am. Acad. Dermatol. 2003;49:1096-106; South. Med. J. 2005;98:1192-5).
Public awareness of sunless tanning has grown in recent years, however, and has been met with formulations that afford a much improved cosmetic performance, with DHA remaining as the main active ingredient in sunless-tanning agents (South. Med. J. 2005;98:1192-5; Am. J. Clin. Dermatol. 2002;3:317-8).
This column will briefly review the role of sunless-tanning lotions and sprays in dermatology, and will try to place recommendations to patients about sunless tanners in the context of sunscreens and tanning attitudes.
Sunless tanners have been used, with varying degrees of popularity, for 50 years; recent evidence suggests that the use of these products has increased in recent years. A long track record of usage and research indicates that sunless-tanning compounds are safe (J. Environ. Pathol. Toxicol. Oncol. 1984;5:349-51; Am. J. Clin. Dermatol. 2002;3:317-8; South. Med. J. 2005;98:1192-5; J. Am. Acad. Dermatol. 2007;56:387-90.) However, there is some debate as to whether the use of these products renders users more inclined to stay in the sun longer. Also, ongoing research has raised some safety issues regarding DHA.
Chemical Protection
In 2004, Petersen et al. investigated the effects of DHA on cell survival and proliferation of a human keratinocyte cell line, HaCaT. Significant genotoxic activity was identified in these cultured cells, as researchers noted dose- and time-dependent morphologic alterations as well as cytoplasmic budding and cell detachment in DHA-treated cells, and apoptosis and marked declines in proliferation 1 day after DHA exposure. Interestingly, the development of DNA strand breaks was prevented via preincubation with antioxidants. The authors suggested that their findings raised concerns about the long-term use of treating the skin with DHA-containing formulations (Mutat. Res. 2004;560:173-86).
A small study by Faurschou et al. showed that DHA provided human skin with modest UVB protection, with a 5% DHA cream applied three times or a 20% DHA cream applied once yielding an effect similar to an SPF 1.6. They acknowledged that most commercial DHA products contain 3%-5% DHA and offer scant protection. A potential advantage of sunless tanners, if they offer protection, suggested the authors, would be that no spots would be left unattended since such gaps would be conspicuous for lack of browning (Arch. Dermatol. 2004;140:886-7).
Howe, Reed, and Dellavalle contended that DHA in self-tanning agents provided enough UVA protection to warrant use as an adjunct to daily sunscreen use for broad-band protection (J. Am. Acad. Dermatol. 2008;58:894). The researchers referenced a 1975 study in which 3% DHA augmented sunlight tolerance among five patients with UVA-sensitive dermatoses (Dermatologica 1975;150:346-51; J. Am. Acad. Dermatol. 2008;58:894).
In 2009, Choquenet et al. assessed the sun protection potency of self-tanners and foundations using an in vitro method to identify indicators such as sun protection factor (SPF), UVA protection factor (PF-UVA), and UVB/UVA ratio. Using seven amino acids in the corneal cells of the epidermis, the investigators identified SPFs virtually equivalent to zero (approximately SPF 2). Conversely, they found foundations to exhibit satisfactory photostability and a non-negligible SPF, noting that such products are safe given their typically once-daily application (J. Dermatol. 2009;36:587-91).
Attitudes and Behavior
Users of sunless-tanning products were found, in a survey of 2,005 randomly selected South Australian adults published in 2001, to be more likely to use sunscreen but less likely to wear a hat or other sun-protective clothing. Sunburns were also linked to the use of sunless tanners in this study (Med. J. Aust. 2001;174:75-8; J. Am. Acad. Dermatol. 2007;56:387-90).
In 2005, Mahler et al. conducted a randomized, controlled trial with 1-month follow-up of 146 Southern California college students to study the impact of UV photoaging photographs and data on the sun protection plans and behaviors of young adults, and whether sunless-tanning lotion might play a role in sun-protective behavior. Of the 146 volunteers, 91.1% completed the "surprise" 1-month follow-up. The intervention consisted of volunteers being shown a UV facial photo and short video illustrating the etiology and results of photoaging. The investigators found that the UV photographic intervention was successful insofar as significantly better sun protection strategies and behaviors were employed by the test group, compared with controls. In addition, they noted that those who used sunless-tanning lotion were more likely to exhibit extensive sun-protective behavior, compared with individuals who received the intervention alone. The authors suggested that such interventions represented a cost-effective approach that might yield behaviors with long-term health benefits in the form of a lower incidence of skin cancer (Arch. Dermatol. 2005;141:373-80).
Later that year, Sheehan and Lesher reported on their anonymous survey of 121 adults (107 women and 14 men) who received spray-on sunless-tanning treatments between February and May 2004. Most reported that sunless tanning had not or would not affect their use of sunscreen or time spent outdoors. Interestingly, though, 73% of the respondents who had used tanning beds indicated that they had reduced or would reduce their use of indoor tanning. The researchers concluded that practitioners should recommend sunless tanning to their patients who use conventional tanning beds as a way to lower their solar exposure and risk of skin cancer (South. Med. J. 2005;98:1192-5).
In 2006, Brooks et al. reported on their July 2004, greater Boston, cross-sectional survey of 448 nonrandomly selected people aged 18-30 years on the subjects of artificial tanning products, recent history of sunburns, and tanning-bed use. During the preceding year, 22% of respondents had used sunless-tanning products and the same percentage hadn’t but would consider using them in the next year. Users of these lotions were more likely to have been severe burners and, after controlling for skin type, the investigators found that previous and potential users were more likely to have experienced sunburns during the summer and to have used tanning beds than were respondents who had neither used nor planned to use sunless tanners. The researchers concluded that the option of sunless tanning did not seem to lower the incidence of sunburn or the use of tanning beds. Further, they urged caution in offering broad support for artificial tanning products, even though looking for alternatives to UV exposure is to be encouraged (J. Am. Acad. Dermatol. 2006;54:1060-6).
A 2007 study using data from 5,491 completed interviews as part of the National Cancer Institute’s HINTS (Health Information National Trends Survey) 2005 set out to determine the prevalence of sunless-tanning formulation use and to understand the relationship between sunless tanning, indoor tanning, and sun-protective behavior. In so doing, the investigators found that the use of sunless-tanning products was relatively rare, with an estimated 11% of U.S. adults claiming to have used such products in the previous year. Of this group, 13% used sunless tanners more than 25 times; 12% used them 11-24 times; 35% used them 3-10 times; and 40% used them just once or twice. Users and exclusive users were more likely to be women, well educated, and living in the West (J. Am. Acad. Dermatol. 2007;56:387-90).
Recent Cause for Pause
In 2008, Jung et al. used the electron spin resonance spectroscopy–based radical sun protection factor, which measures free-radical reactions in skin biopsies during UV exposure and can determine the protective effect of UV filters and sunscreens, to analyze three different self-tanning agents, including DHA. Noting that the reaction of the reducing sugars in such products and amino acids (Maillard reaction) in the skin layer engendered Amadori products that created free radicals during UV irradiation, the investigators reported that in DHA-treated skin, more than 180% additional radicals were produced during sun exposure, compared with untreated skin. They concluded that the use of self-tanners necessitated reducing solar exposure duration (Spectrochim. Acta A. Mol. Biomol Spectrosc. 2008;69:1423-8). Consequently, DHA users would be well advised to wait at least 24 hours before solar exposure following application of sunless lotion or spray (Dermatol. Clin. 2009;27:149-54).
Conclusion
In addition to the need to continually persuade patients to engage in skin-protective behavior – namely, limiting sun exposure, avoiding peak-time exposures, wearing wide-brimmed hats and clothing with SPF value, and using sunscreens (preferably those containing avobenzone, Mexoryl, zinc oxide, or titanium dioxide) every day – it is incumbent upon dermatologists to disabuse our patients of the idea that untanned skin is less attractive or, conversely, that tans should be equated with attractive skin. Although healthy messages (that there is no such thing as a healthy tan, and that a tan indicates skin damage) are slowly spreading, sunless tanners appear to be a medically and cosmetically acceptable intermediary step, far surpassing the patently detrimental effects of indoor tanning. That said, patients should be advised to refrain from solar exposure for a full 24 hours after applying sunless tanners. Furthermore, much more research is necessary to truly establish that DHA delivers even modest protection from UVA or UVB. Accordingly, patients should be counseled that sunless tanners do not suffice as a base, nor do they justify extended solar exposure, and that sunscreens should also be applied.
Scalp, Temple, and Eyelids Present Challenges for Mohs
SAN DIEGO - From messy hair to uncooperative bleeders and pesky nerves, Mohs surgery on the scalp and other difficult locations can try the patience and boost stress hormones.
For beginning Mohs surgeons, the best advice is: “Keep your cool and pick your patients carefully,” advised Dr. Carlos Garcia. “There are certain patients you don’t want to have for your first cases, so choose carefully, and save those until you are more experienced.”
Dr. Garcia, director of surgical dermatology at the University of Oklahoma, Norman, dropped another valuable pearl to novice Mohs practitioners: Know when to call in reinforcements. For example, with primary tumors near the lacrimal system or recurrences in the acral area, “be sure to include a plastic surgeon in your plan, because these are not usually going to be beautiful when you finish.”
The scalp is a very common location for skin cancers and presents a unique set of challenges, Dr. Garcia said. As every parent with a rock-throwing child knows, any scalp wound bleeds in apparent excess of its size.
“No matter what you do, the scalp is going to bleed, and you have to be prepared,” he said. “Most of the small vessels are in the dermis, but the bigger ones are in the deeper layers, and you may be getting into those with Mohs.”
Tumescent anesthesia is a fine approach to hemostasis. “Injected into the dermis, it produces a hard surface and after 15 or 20 minutes you can do surgery with minimal bleeding. The other advantage is that it’s going to give more prolonged hemostasis as well as pain control.”
Locking sutures are another good hemostatic technique, he said. “You can use Prolene or nylon and a running or interrupted suture, but you need to lock in the suture, and you’ll get much better hemostasis from the dermal vessels.”
Hair can also increase the risk for complications. “It’s stressful enough with the bleeding on the scalp, but on top of that you have the hair to deal with,” Dr. Garcia said. “Make sure you have lots of things to take care of that – trimmers, hair clips, mousse, and gel. Do whatever you have to do to get it out of the way.”
Elastic bandages are a must for scalp surgery. “Your patient will need to keep these on during the first 24 hours after surgery when bleeding is the greatest. If you don’t have good compression and warn your patients to maintain it, you’re going to get a lot of phone calls.”
It’s not uncommon for a patient to have multiple cancers or precancerous lesions on the scalp. “My rule of thumb is to get rid of the basic component, and then if I get three epidermal layers with actinic keratosis components but no deep component, I stop the Mohs. Note in the chart that there is a small in situ that will be treated during follow-up,” he said.
Some Mohs surgeons will persist with layers even into the periosteum or bone. “I don’t do bone chiseling because technically I’m not trained to do it, and also because I’m very hesitant because there have been reports of air embolism,” Dr. Garcia said. “The veins from the surface connect very easily with the deeper sinusoidal vessels, and if you have the patient waiting for another layer and not positioned correctly, they can get changing pressure. Air can get in and they can get an embolism in the waiting room. So if you ever delve into this area, be aware of this possibility.” (Dermatol. Surg. 2009;35:1414-21).
Because scalp skin is not very pliable, repair can be a challenge. “Many times I leave these to heal by secondary intention.” It’s not a quick process, though. “If the defect goes to the bone, it’s going to take 3-4 weeks for every centimeter of the wound to completely heal.”
Dr Garcia also passed on some tips about other areas that might challenge the Mohs surgeon:
P Temple: In the temple area, hair and bleeders are the biggest issue. “Get the hair out of the way first and have a couple of mosquito clamps loaded with 4-0 or 5-0 Vicryl to tie off vessels. As a general rule, ligate any blood vessel that’s thicker than a 30-gauge needle.”
The temporal branch of the facial nerve may be at risk if the surgery is near its most superficial area – just over the malar arc. “If you transect any of the branches of the nerve ahead or in front of the external canthus, it will regenerate 100% of the time, and the patient will get full movement back. The closer you get to the preauricular area, the less likely regeneration becomes. If transection happens – and it does – the ear, nose, and throat [specialists] usually will wait 3-4 months before trying to do something about it, to see if there is any spontaneous regeneration.”
P Recurrence in grafted skin or previously irradiated areas: Resist the desire to undertake repeated Mohs, he advised. “These can be bad. They can be too extensive, and you will invest some time and money and some very stressful moments if you get into this.”
P Ear: For tumors in the concha, “Pay attention to the size, type, and proximity to the external canal. It’s really hard to do Mohs excisions in the ear canal.”
P Eyelid: The thinnest skin on the body, the eyelid is even more fragile on elderly people. “This is a very difficult area for me to cut in Mohs. Instead of applying a lot of pressure, I use a number 11 or 15 blade and do several rounds. Use light pressure because the epidermis has a tendency to fold and pull, making it hard to cut.” Bevelling is not as important here because the skin is so friable that the technician can easily flatten it on the slide.
Topical anesthetic ocular drops help the patient tolerate the surgery much better, and allow the placement of a plastic eye shield anchored with a couple of small sutures. “The eye shield and sutures are left in place while the patient is waiting – I just cover it with a full eye patch.”
P Nose: For lesions on the ala or alar arch, cotton swabs, dental rolls, or even a finger push the tissue outward and give good support for excision. “Notching of ala before surgery is a bad prognosis,” Dr. Garcia said. “It means advanced cancer, and this may not be something you want to get into.”
Dr. Garcia said he had no financial disclosures.
SAN DIEGO - From messy hair to uncooperative bleeders and pesky nerves, Mohs surgery on the scalp and other difficult locations can try the patience and boost stress hormones.
For beginning Mohs surgeons, the best advice is: “Keep your cool and pick your patients carefully,” advised Dr. Carlos Garcia. “There are certain patients you don’t want to have for your first cases, so choose carefully, and save those until you are more experienced.”
Dr. Garcia, director of surgical dermatology at the University of Oklahoma, Norman, dropped another valuable pearl to novice Mohs practitioners: Know when to call in reinforcements. For example, with primary tumors near the lacrimal system or recurrences in the acral area, “be sure to include a plastic surgeon in your plan, because these are not usually going to be beautiful when you finish.”
The scalp is a very common location for skin cancers and presents a unique set of challenges, Dr. Garcia said. As every parent with a rock-throwing child knows, any scalp wound bleeds in apparent excess of its size.
“No matter what you do, the scalp is going to bleed, and you have to be prepared,” he said. “Most of the small vessels are in the dermis, but the bigger ones are in the deeper layers, and you may be getting into those with Mohs.”
Tumescent anesthesia is a fine approach to hemostasis. “Injected into the dermis, it produces a hard surface and after 15 or 20 minutes you can do surgery with minimal bleeding. The other advantage is that it’s going to give more prolonged hemostasis as well as pain control.”
Locking sutures are another good hemostatic technique, he said. “You can use Prolene or nylon and a running or interrupted suture, but you need to lock in the suture, and you’ll get much better hemostasis from the dermal vessels.”
Hair can also increase the risk for complications. “It’s stressful enough with the bleeding on the scalp, but on top of that you have the hair to deal with,” Dr. Garcia said. “Make sure you have lots of things to take care of that – trimmers, hair clips, mousse, and gel. Do whatever you have to do to get it out of the way.”
Elastic bandages are a must for scalp surgery. “Your patient will need to keep these on during the first 24 hours after surgery when bleeding is the greatest. If you don’t have good compression and warn your patients to maintain it, you’re going to get a lot of phone calls.”
It’s not uncommon for a patient to have multiple cancers or precancerous lesions on the scalp. “My rule of thumb is to get rid of the basic component, and then if I get three epidermal layers with actinic keratosis components but no deep component, I stop the Mohs. Note in the chart that there is a small in situ that will be treated during follow-up,” he said.
Some Mohs surgeons will persist with layers even into the periosteum or bone. “I don’t do bone chiseling because technically I’m not trained to do it, and also because I’m very hesitant because there have been reports of air embolism,” Dr. Garcia said. “The veins from the surface connect very easily with the deeper sinusoidal vessels, and if you have the patient waiting for another layer and not positioned correctly, they can get changing pressure. Air can get in and they can get an embolism in the waiting room. So if you ever delve into this area, be aware of this possibility.” (Dermatol. Surg. 2009;35:1414-21).
Because scalp skin is not very pliable, repair can be a challenge. “Many times I leave these to heal by secondary intention.” It’s not a quick process, though. “If the defect goes to the bone, it’s going to take 3-4 weeks for every centimeter of the wound to completely heal.”
Dr Garcia also passed on some tips about other areas that might challenge the Mohs surgeon:
P Temple: In the temple area, hair and bleeders are the biggest issue. “Get the hair out of the way first and have a couple of mosquito clamps loaded with 4-0 or 5-0 Vicryl to tie off vessels. As a general rule, ligate any blood vessel that’s thicker than a 30-gauge needle.”
The temporal branch of the facial nerve may be at risk if the surgery is near its most superficial area – just over the malar arc. “If you transect any of the branches of the nerve ahead or in front of the external canthus, it will regenerate 100% of the time, and the patient will get full movement back. The closer you get to the preauricular area, the less likely regeneration becomes. If transection happens – and it does – the ear, nose, and throat [specialists] usually will wait 3-4 months before trying to do something about it, to see if there is any spontaneous regeneration.”
P Recurrence in grafted skin or previously irradiated areas: Resist the desire to undertake repeated Mohs, he advised. “These can be bad. They can be too extensive, and you will invest some time and money and some very stressful moments if you get into this.”
P Ear: For tumors in the concha, “Pay attention to the size, type, and proximity to the external canal. It’s really hard to do Mohs excisions in the ear canal.”
P Eyelid: The thinnest skin on the body, the eyelid is even more fragile on elderly people. “This is a very difficult area for me to cut in Mohs. Instead of applying a lot of pressure, I use a number 11 or 15 blade and do several rounds. Use light pressure because the epidermis has a tendency to fold and pull, making it hard to cut.” Bevelling is not as important here because the skin is so friable that the technician can easily flatten it on the slide.
Topical anesthetic ocular drops help the patient tolerate the surgery much better, and allow the placement of a plastic eye shield anchored with a couple of small sutures. “The eye shield and sutures are left in place while the patient is waiting – I just cover it with a full eye patch.”
P Nose: For lesions on the ala or alar arch, cotton swabs, dental rolls, or even a finger push the tissue outward and give good support for excision. “Notching of ala before surgery is a bad prognosis,” Dr. Garcia said. “It means advanced cancer, and this may not be something you want to get into.”
Dr. Garcia said he had no financial disclosures.
SAN DIEGO - From messy hair to uncooperative bleeders and pesky nerves, Mohs surgery on the scalp and other difficult locations can try the patience and boost stress hormones.
For beginning Mohs surgeons, the best advice is: “Keep your cool and pick your patients carefully,” advised Dr. Carlos Garcia. “There are certain patients you don’t want to have for your first cases, so choose carefully, and save those until you are more experienced.”
Dr. Garcia, director of surgical dermatology at the University of Oklahoma, Norman, dropped another valuable pearl to novice Mohs practitioners: Know when to call in reinforcements. For example, with primary tumors near the lacrimal system or recurrences in the acral area, “be sure to include a plastic surgeon in your plan, because these are not usually going to be beautiful when you finish.”
The scalp is a very common location for skin cancers and presents a unique set of challenges, Dr. Garcia said. As every parent with a rock-throwing child knows, any scalp wound bleeds in apparent excess of its size.
“No matter what you do, the scalp is going to bleed, and you have to be prepared,” he said. “Most of the small vessels are in the dermis, but the bigger ones are in the deeper layers, and you may be getting into those with Mohs.”
Tumescent anesthesia is a fine approach to hemostasis. “Injected into the dermis, it produces a hard surface and after 15 or 20 minutes you can do surgery with minimal bleeding. The other advantage is that it’s going to give more prolonged hemostasis as well as pain control.”
Locking sutures are another good hemostatic technique, he said. “You can use Prolene or nylon and a running or interrupted suture, but you need to lock in the suture, and you’ll get much better hemostasis from the dermal vessels.”
Hair can also increase the risk for complications. “It’s stressful enough with the bleeding on the scalp, but on top of that you have the hair to deal with,” Dr. Garcia said. “Make sure you have lots of things to take care of that – trimmers, hair clips, mousse, and gel. Do whatever you have to do to get it out of the way.”
Elastic bandages are a must for scalp surgery. “Your patient will need to keep these on during the first 24 hours after surgery when bleeding is the greatest. If you don’t have good compression and warn your patients to maintain it, you’re going to get a lot of phone calls.”
It’s not uncommon for a patient to have multiple cancers or precancerous lesions on the scalp. “My rule of thumb is to get rid of the basic component, and then if I get three epidermal layers with actinic keratosis components but no deep component, I stop the Mohs. Note in the chart that there is a small in situ that will be treated during follow-up,” he said.
Some Mohs surgeons will persist with layers even into the periosteum or bone. “I don’t do bone chiseling because technically I’m not trained to do it, and also because I’m very hesitant because there have been reports of air embolism,” Dr. Garcia said. “The veins from the surface connect very easily with the deeper sinusoidal vessels, and if you have the patient waiting for another layer and not positioned correctly, they can get changing pressure. Air can get in and they can get an embolism in the waiting room. So if you ever delve into this area, be aware of this possibility.” (Dermatol. Surg. 2009;35:1414-21).
Because scalp skin is not very pliable, repair can be a challenge. “Many times I leave these to heal by secondary intention.” It’s not a quick process, though. “If the defect goes to the bone, it’s going to take 3-4 weeks for every centimeter of the wound to completely heal.”
Dr Garcia also passed on some tips about other areas that might challenge the Mohs surgeon:
P Temple: In the temple area, hair and bleeders are the biggest issue. “Get the hair out of the way first and have a couple of mosquito clamps loaded with 4-0 or 5-0 Vicryl to tie off vessels. As a general rule, ligate any blood vessel that’s thicker than a 30-gauge needle.”
The temporal branch of the facial nerve may be at risk if the surgery is near its most superficial area – just over the malar arc. “If you transect any of the branches of the nerve ahead or in front of the external canthus, it will regenerate 100% of the time, and the patient will get full movement back. The closer you get to the preauricular area, the less likely regeneration becomes. If transection happens – and it does – the ear, nose, and throat [specialists] usually will wait 3-4 months before trying to do something about it, to see if there is any spontaneous regeneration.”
P Recurrence in grafted skin or previously irradiated areas: Resist the desire to undertake repeated Mohs, he advised. “These can be bad. They can be too extensive, and you will invest some time and money and some very stressful moments if you get into this.”
P Ear: For tumors in the concha, “Pay attention to the size, type, and proximity to the external canal. It’s really hard to do Mohs excisions in the ear canal.”
P Eyelid: The thinnest skin on the body, the eyelid is even more fragile on elderly people. “This is a very difficult area for me to cut in Mohs. Instead of applying a lot of pressure, I use a number 11 or 15 blade and do several rounds. Use light pressure because the epidermis has a tendency to fold and pull, making it hard to cut.” Bevelling is not as important here because the skin is so friable that the technician can easily flatten it on the slide.
Topical anesthetic ocular drops help the patient tolerate the surgery much better, and allow the placement of a plastic eye shield anchored with a couple of small sutures. “The eye shield and sutures are left in place while the patient is waiting – I just cover it with a full eye patch.”
P Nose: For lesions on the ala or alar arch, cotton swabs, dental rolls, or even a finger push the tissue outward and give good support for excision. “Notching of ala before surgery is a bad prognosis,” Dr. Garcia said. “It means advanced cancer, and this may not be something you want to get into.”
Dr. Garcia said he had no financial disclosures.
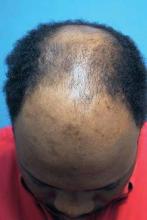
Future Technologies Hold Promise for Hair Restoration
ORLANDO - Expect clinical options for hair restoration to grow in the future, said Dr. Ricardo Mejia.
Robotic hair transfer, multiple technologies to optimize new growth, and even hair cloning could help overcome current limitations in hair transplantation, Dr. Mejia said. Promising technologies could someday supplant donor strip and follicular unit extraction techniques. "We are getting to the age of robotics," Dr. Mejia said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Historically, hair transplantation meant 4-mm plugs transferred at a rate of 10-200 grafts per session over a total of three to eight treatments. Because plugs were placed in a regular pattern, initial results appeared unnatural and very obvious. For some patients, a perception persists that this is still state-of-the-art for hair transplantation, Dr. Mejia said.
A natural, irregular hairline and greater hair density in fewer treatment sessions are now commonplace. "The average session these days of 2,500 grafts is not a big deal," Dr. Mejia said at the meeting.
"Restoring youthful hairlines can be done in single sessions. ... You can get a nice, age-appropriate appearance for an individual," said Dr. Mejia, a hair transplant surgeon in private practice in Jupiter, Fla. Even with recent advances, full growth of hair grafts still takes 6 months to a year, so realistic patient expectations are important.
A new device, NeoGraft Automated Hair Transplant System (NeoGraft), was cleared for marketing by the Food and Drug Administration in March 2009. After a rotating sharp punch scores the skin, a pneumatic suction device extracts the follicles. This technique minimizes injury to the lower half of hair follicles during follicular unit extraction, Dr. Mejia said. The device also implants grafts to a uniform depth.
Researchers are working on a variety of other means to protect grafts during the transfer process. For example, some are developing solutions to protect grafts that contain allopurinol, nitric oxide inhibitors, vitamins, and other components. Also, "we are starting to look at solutions used in organ transplantation." Small studies have shown increased hair survival and growth with these solutions used to optimize protection of organs during transfer, Dr. Mejia said.
Bathing follicular units in autologous platelet-rich plasma to promote healing angiogenesis is another approach. Growth factor components also could be beneficial, Dr. Mejia said. More studies are needed to determine the efficacy of injections of autologous platelet-rich plasma into both the donor area and the recipient areas in clinical practice.
Matching the size of the incision blade to the graft size can also help improve graft survival, Dr. Mejia said. Less trauma, less ischemia, and decreased overall bleeding are associated with finer blades. Although finer blades allow higher-density graft packing, he advised caution because some studies have shown more graft death with higher densities.
Investigators also are looking at technology to optimize new hair growth once the grafts are in place.
"Low-level lasers are getting a lot of attention," Dr. Mejia said. Wavelengths are in the range of 630-670 nm, power densities are between 5-50 mW/cm2, and fluences are 2-20 J/cm2.
The Food and Drug Administration cleared two devices that use low-level light therapy for hair growth: HairMax LaserComb (Lexington International) for men and the MPE-90 Hair Growth Stimulation System (Salon Lasers) for women.
"How good is the HairMax comb?" a meeting attendee asked. Dr. Mejia replied that reviews are mixed: "Hair restoration surgeons are on the fence – some believe in it, some don’t. Some patients are happy with it, some are not."
A lot of research also is underway to refine auto cloning and hair multiplication technologies, Dr. Mejia said.
Dermal papilla cells or fibroblasts are the starting point, because they stimulate formation of new hairs. Multiple companies are working on proprietary processes to spur these fibroblasts to produce enough follicles in culture to replace an entire scalp. This is where they hope "to make their windfall," he said. Research includes fibroblasts grown in subatmospheric oxygen tension, addition of wound-healing factors, and injections of a "hair-stimulating complex" to promote greater hair growth.
TrichoCyte is an example of a cell-based hair regeneration technology in phase II trials based on a proprietary dermal papilla cell process (Intercytex, Manchester, England). "The technique does work but [it is] not completely satisfactory at this point," Dr. Mejia said.
More than half of participants in one protocol for another proprietary cell treatment process showed significant hair growth 1 year later, according to a release announcing phase II study results for Aderans Research Institute.
Considerable work remains to be done before regenerative medical hair cloning becomes a clinically viable option, Dr. Mejia said. "How far out are we? I say 5-10 years."
Dr. Mejia said he had no relevant disclosures.
ORLANDO - Expect clinical options for hair restoration to grow in the future, said Dr. Ricardo Mejia.
Robotic hair transfer, multiple technologies to optimize new growth, and even hair cloning could help overcome current limitations in hair transplantation, Dr. Mejia said. Promising technologies could someday supplant donor strip and follicular unit extraction techniques. "We are getting to the age of robotics," Dr. Mejia said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Historically, hair transplantation meant 4-mm plugs transferred at a rate of 10-200 grafts per session over a total of three to eight treatments. Because plugs were placed in a regular pattern, initial results appeared unnatural and very obvious. For some patients, a perception persists that this is still state-of-the-art for hair transplantation, Dr. Mejia said.
A natural, irregular hairline and greater hair density in fewer treatment sessions are now commonplace. "The average session these days of 2,500 grafts is not a big deal," Dr. Mejia said at the meeting.
"Restoring youthful hairlines can be done in single sessions. ... You can get a nice, age-appropriate appearance for an individual," said Dr. Mejia, a hair transplant surgeon in private practice in Jupiter, Fla. Even with recent advances, full growth of hair grafts still takes 6 months to a year, so realistic patient expectations are important.
A new device, NeoGraft Automated Hair Transplant System (NeoGraft), was cleared for marketing by the Food and Drug Administration in March 2009. After a rotating sharp punch scores the skin, a pneumatic suction device extracts the follicles. This technique minimizes injury to the lower half of hair follicles during follicular unit extraction, Dr. Mejia said. The device also implants grafts to a uniform depth.
Researchers are working on a variety of other means to protect grafts during the transfer process. For example, some are developing solutions to protect grafts that contain allopurinol, nitric oxide inhibitors, vitamins, and other components. Also, "we are starting to look at solutions used in organ transplantation." Small studies have shown increased hair survival and growth with these solutions used to optimize protection of organs during transfer, Dr. Mejia said.
Bathing follicular units in autologous platelet-rich plasma to promote healing angiogenesis is another approach. Growth factor components also could be beneficial, Dr. Mejia said. More studies are needed to determine the efficacy of injections of autologous platelet-rich plasma into both the donor area and the recipient areas in clinical practice.
Matching the size of the incision blade to the graft size can also help improve graft survival, Dr. Mejia said. Less trauma, less ischemia, and decreased overall bleeding are associated with finer blades. Although finer blades allow higher-density graft packing, he advised caution because some studies have shown more graft death with higher densities.
Investigators also are looking at technology to optimize new hair growth once the grafts are in place.
"Low-level lasers are getting a lot of attention," Dr. Mejia said. Wavelengths are in the range of 630-670 nm, power densities are between 5-50 mW/cm2, and fluences are 2-20 J/cm2.
The Food and Drug Administration cleared two devices that use low-level light therapy for hair growth: HairMax LaserComb (Lexington International) for men and the MPE-90 Hair Growth Stimulation System (Salon Lasers) for women.
"How good is the HairMax comb?" a meeting attendee asked. Dr. Mejia replied that reviews are mixed: "Hair restoration surgeons are on the fence – some believe in it, some don’t. Some patients are happy with it, some are not."
A lot of research also is underway to refine auto cloning and hair multiplication technologies, Dr. Mejia said.
Dermal papilla cells or fibroblasts are the starting point, because they stimulate formation of new hairs. Multiple companies are working on proprietary processes to spur these fibroblasts to produce enough follicles in culture to replace an entire scalp. This is where they hope "to make their windfall," he said. Research includes fibroblasts grown in subatmospheric oxygen tension, addition of wound-healing factors, and injections of a "hair-stimulating complex" to promote greater hair growth.
TrichoCyte is an example of a cell-based hair regeneration technology in phase II trials based on a proprietary dermal papilla cell process (Intercytex, Manchester, England). "The technique does work but [it is] not completely satisfactory at this point," Dr. Mejia said.
More than half of participants in one protocol for another proprietary cell treatment process showed significant hair growth 1 year later, according to a release announcing phase II study results for Aderans Research Institute.
Considerable work remains to be done before regenerative medical hair cloning becomes a clinically viable option, Dr. Mejia said. "How far out are we? I say 5-10 years."
Dr. Mejia said he had no relevant disclosures.
ORLANDO - Expect clinical options for hair restoration to grow in the future, said Dr. Ricardo Mejia.
Robotic hair transfer, multiple technologies to optimize new growth, and even hair cloning could help overcome current limitations in hair transplantation, Dr. Mejia said. Promising technologies could someday supplant donor strip and follicular unit extraction techniques. "We are getting to the age of robotics," Dr. Mejia said at the annual meeting of the Florida Society of Dermatologic Surgeons.
Historically, hair transplantation meant 4-mm plugs transferred at a rate of 10-200 grafts per session over a total of three to eight treatments. Because plugs were placed in a regular pattern, initial results appeared unnatural and very obvious. For some patients, a perception persists that this is still state-of-the-art for hair transplantation, Dr. Mejia said.
A natural, irregular hairline and greater hair density in fewer treatment sessions are now commonplace. "The average session these days of 2,500 grafts is not a big deal," Dr. Mejia said at the meeting.
"Restoring youthful hairlines can be done in single sessions. ... You can get a nice, age-appropriate appearance for an individual," said Dr. Mejia, a hair transplant surgeon in private practice in Jupiter, Fla. Even with recent advances, full growth of hair grafts still takes 6 months to a year, so realistic patient expectations are important.
A new device, NeoGraft Automated Hair Transplant System (NeoGraft), was cleared for marketing by the Food and Drug Administration in March 2009. After a rotating sharp punch scores the skin, a pneumatic suction device extracts the follicles. This technique minimizes injury to the lower half of hair follicles during follicular unit extraction, Dr. Mejia said. The device also implants grafts to a uniform depth.
Researchers are working on a variety of other means to protect grafts during the transfer process. For example, some are developing solutions to protect grafts that contain allopurinol, nitric oxide inhibitors, vitamins, and other components. Also, "we are starting to look at solutions used in organ transplantation." Small studies have shown increased hair survival and growth with these solutions used to optimize protection of organs during transfer, Dr. Mejia said.
Bathing follicular units in autologous platelet-rich plasma to promote healing angiogenesis is another approach. Growth factor components also could be beneficial, Dr. Mejia said. More studies are needed to determine the efficacy of injections of autologous platelet-rich plasma into both the donor area and the recipient areas in clinical practice.
Matching the size of the incision blade to the graft size can also help improve graft survival, Dr. Mejia said. Less trauma, less ischemia, and decreased overall bleeding are associated with finer blades. Although finer blades allow higher-density graft packing, he advised caution because some studies have shown more graft death with higher densities.
Investigators also are looking at technology to optimize new hair growth once the grafts are in place.
"Low-level lasers are getting a lot of attention," Dr. Mejia said. Wavelengths are in the range of 630-670 nm, power densities are between 5-50 mW/cm2, and fluences are 2-20 J/cm2.
The Food and Drug Administration cleared two devices that use low-level light therapy for hair growth: HairMax LaserComb (Lexington International) for men and the MPE-90 Hair Growth Stimulation System (Salon Lasers) for women.
"How good is the HairMax comb?" a meeting attendee asked. Dr. Mejia replied that reviews are mixed: "Hair restoration surgeons are on the fence – some believe in it, some don’t. Some patients are happy with it, some are not."
A lot of research also is underway to refine auto cloning and hair multiplication technologies, Dr. Mejia said.
Dermal papilla cells or fibroblasts are the starting point, because they stimulate formation of new hairs. Multiple companies are working on proprietary processes to spur these fibroblasts to produce enough follicles in culture to replace an entire scalp. This is where they hope "to make their windfall," he said. Research includes fibroblasts grown in subatmospheric oxygen tension, addition of wound-healing factors, and injections of a "hair-stimulating complex" to promote greater hair growth.
TrichoCyte is an example of a cell-based hair regeneration technology in phase II trials based on a proprietary dermal papilla cell process (Intercytex, Manchester, England). "The technique does work but [it is] not completely satisfactory at this point," Dr. Mejia said.
More than half of participants in one protocol for another proprietary cell treatment process showed significant hair growth 1 year later, according to a release announcing phase II study results for Aderans Research Institute.
Considerable work remains to be done before regenerative medical hair cloning becomes a clinically viable option, Dr. Mejia said. "How far out are we? I say 5-10 years."
Dr. Mejia said he had no relevant disclosures.
EXPERT ANALYSIS FROM THE ANNUAL MEETING OF THE FLORIDA SOCIETY OF DERMATOLOGIC SURGEONS
Skin of Color: Weighing Risks of Treating Dark Skinned Patients With Isotretinoin
Severe acne has become increasingly common in adult men and women. In skin of color, severe acne results in postinflammatory hyperpigmentation and hyperpigmented scars that are difficult to treat and often cause more distress to the patient than does the acne itself.
Scarring, refractory acne, or nodulo-cystic acne may not respond to traditional therapies and thus may require isotretinoin therapy.
However, many clinicians are rightfully concerned about the legal implications of isotretinoin, particularly the potential for suicide in patients with a history of depression. Clinicians will often not prescribe isotretinoin given these risks, even though their patients may have failed a myriad of topical and oral treatments.
In our clinical experience, severe depression is an underrecognized yet prevalent finding in patients with severe acne. The hyperpigmented scarring is difficult to cover with make-up, particularly for patients with skin types IV-VI. Other cosmetic options are limited.
Patients can develop depression and a lack of self-confidence, particularly if they have been dealing with acne and acne scarring without much relief. It is important to treat these patients aggressively to prevent severe scarring. Often the most effective medication is isotretinoin.
In two well-designed retrospective studies, depression was found to be linked to severe acne, and not to isotretinoin therapy.
In the most recent study, researchers evaluated data from 5,756 patients aged 15-49 years who were prescribed isotretinoin for severe acne between 1980 and 1989. The data were interpreted along with data from hospital discharge and cause-of-death registers from 1980 to 2001 (BMJ 2010;341:c5812).
In this study, 128 patients were admitted to the hospital for attempted suicide. During the year before treatment with isotretinoin, the incidence ratio for attempted suicide was increased 1.57 (95% confidence interval [CI], 0.86–2.63) for all suicide attempts, including repeat attempts, and 1.36 for first attempts only (95% CI, 0.65–2.50), compared to the general population.
The incidence ratio during and up to 6 months after treatment was 1.78 (95% CI, 1.04–2.85) for all attempts and 1.93 (95% CI, 1.08–3.18) for first attempts. Finally, 3 years after treatment the standardized incidence ratio declined to the expected level, 1.04, and remained the same throughout the 15 years of follow-up (95% CI, 0.74–1.43) for all attempts. The ratio for first attempts declined to 0.97 (95% CI, 0.64–1.40).
The authors concluded that suicidal ideation reflects the burden of the disease, rather than treatment with isotretinoin. They suggest that physicians know the psychiatric history of each patient they want to begin on isotretinoin therapy, and follow them closely both throughout the treatment and for up to 1 year after. However, in many patients, the psychiatric morbidity may be related to the acne itself.
Dark-skinned patients develop severe dyschromia from acne lesions which are often difficult to treat. Given the pigmentation of their skin, the severe dyschromia associated with acne, and the lack of cosmetic options for camouflage, these patients may present with signs and symptoms of depression related to their underlying disease. It is imperative that the treating clinician understand each patient's concerns because NOT treating the patient appropriately can be more detrimental to their psychiatric health than treating them with isotretinoin.
Severe acne has become increasingly common in adult men and women. In skin of color, severe acne results in postinflammatory hyperpigmentation and hyperpigmented scars that are difficult to treat and often cause more distress to the patient than does the acne itself.
Scarring, refractory acne, or nodulo-cystic acne may not respond to traditional therapies and thus may require isotretinoin therapy.
However, many clinicians are rightfully concerned about the legal implications of isotretinoin, particularly the potential for suicide in patients with a history of depression. Clinicians will often not prescribe isotretinoin given these risks, even though their patients may have failed a myriad of topical and oral treatments.
In our clinical experience, severe depression is an underrecognized yet prevalent finding in patients with severe acne. The hyperpigmented scarring is difficult to cover with make-up, particularly for patients with skin types IV-VI. Other cosmetic options are limited.
Patients can develop depression and a lack of self-confidence, particularly if they have been dealing with acne and acne scarring without much relief. It is important to treat these patients aggressively to prevent severe scarring. Often the most effective medication is isotretinoin.
In two well-designed retrospective studies, depression was found to be linked to severe acne, and not to isotretinoin therapy.
In the most recent study, researchers evaluated data from 5,756 patients aged 15-49 years who were prescribed isotretinoin for severe acne between 1980 and 1989. The data were interpreted along with data from hospital discharge and cause-of-death registers from 1980 to 2001 (BMJ 2010;341:c5812).
In this study, 128 patients were admitted to the hospital for attempted suicide. During the year before treatment with isotretinoin, the incidence ratio for attempted suicide was increased 1.57 (95% confidence interval [CI], 0.86–2.63) for all suicide attempts, including repeat attempts, and 1.36 for first attempts only (95% CI, 0.65–2.50), compared to the general population.
The incidence ratio during and up to 6 months after treatment was 1.78 (95% CI, 1.04–2.85) for all attempts and 1.93 (95% CI, 1.08–3.18) for first attempts. Finally, 3 years after treatment the standardized incidence ratio declined to the expected level, 1.04, and remained the same throughout the 15 years of follow-up (95% CI, 0.74–1.43) for all attempts. The ratio for first attempts declined to 0.97 (95% CI, 0.64–1.40).
The authors concluded that suicidal ideation reflects the burden of the disease, rather than treatment with isotretinoin. They suggest that physicians know the psychiatric history of each patient they want to begin on isotretinoin therapy, and follow them closely both throughout the treatment and for up to 1 year after. However, in many patients, the psychiatric morbidity may be related to the acne itself.
Dark-skinned patients develop severe dyschromia from acne lesions which are often difficult to treat. Given the pigmentation of their skin, the severe dyschromia associated with acne, and the lack of cosmetic options for camouflage, these patients may present with signs and symptoms of depression related to their underlying disease. It is imperative that the treating clinician understand each patient's concerns because NOT treating the patient appropriately can be more detrimental to their psychiatric health than treating them with isotretinoin.
Severe acne has become increasingly common in adult men and women. In skin of color, severe acne results in postinflammatory hyperpigmentation and hyperpigmented scars that are difficult to treat and often cause more distress to the patient than does the acne itself.
Scarring, refractory acne, or nodulo-cystic acne may not respond to traditional therapies and thus may require isotretinoin therapy.
However, many clinicians are rightfully concerned about the legal implications of isotretinoin, particularly the potential for suicide in patients with a history of depression. Clinicians will often not prescribe isotretinoin given these risks, even though their patients may have failed a myriad of topical and oral treatments.
In our clinical experience, severe depression is an underrecognized yet prevalent finding in patients with severe acne. The hyperpigmented scarring is difficult to cover with make-up, particularly for patients with skin types IV-VI. Other cosmetic options are limited.
Patients can develop depression and a lack of self-confidence, particularly if they have been dealing with acne and acne scarring without much relief. It is important to treat these patients aggressively to prevent severe scarring. Often the most effective medication is isotretinoin.
In two well-designed retrospective studies, depression was found to be linked to severe acne, and not to isotretinoin therapy.
In the most recent study, researchers evaluated data from 5,756 patients aged 15-49 years who were prescribed isotretinoin for severe acne between 1980 and 1989. The data were interpreted along with data from hospital discharge and cause-of-death registers from 1980 to 2001 (BMJ 2010;341:c5812).
In this study, 128 patients were admitted to the hospital for attempted suicide. During the year before treatment with isotretinoin, the incidence ratio for attempted suicide was increased 1.57 (95% confidence interval [CI], 0.86–2.63) for all suicide attempts, including repeat attempts, and 1.36 for first attempts only (95% CI, 0.65–2.50), compared to the general population.
The incidence ratio during and up to 6 months after treatment was 1.78 (95% CI, 1.04–2.85) for all attempts and 1.93 (95% CI, 1.08–3.18) for first attempts. Finally, 3 years after treatment the standardized incidence ratio declined to the expected level, 1.04, and remained the same throughout the 15 years of follow-up (95% CI, 0.74–1.43) for all attempts. The ratio for first attempts declined to 0.97 (95% CI, 0.64–1.40).
The authors concluded that suicidal ideation reflects the burden of the disease, rather than treatment with isotretinoin. They suggest that physicians know the psychiatric history of each patient they want to begin on isotretinoin therapy, and follow them closely both throughout the treatment and for up to 1 year after. However, in many patients, the psychiatric morbidity may be related to the acne itself.
Dark-skinned patients develop severe dyschromia from acne lesions which are often difficult to treat. Given the pigmentation of their skin, the severe dyschromia associated with acne, and the lack of cosmetic options for camouflage, these patients may present with signs and symptoms of depression related to their underlying disease. It is imperative that the treating clinician understand each patient's concerns because NOT treating the patient appropriately can be more detrimental to their psychiatric health than treating them with isotretinoin.
Treat Your Mohs Tech Well - And Prosper
SAN DIEGO - Train them well, pay them well, appreciate them well – and they will provide years of reliable service.
Those are the simple secrets that allow Mohs surgeons to retain their right-hand man or woman: the Mohs technician, Alexander Lutz said at a meeting sponsored by the American Society of Mohs Surgeons.
Paying careful attention to the details that keep a Mohs technician professionally satisfied and secure will pay off in a big way, said Mr. Lutz, the owner of Travel Tech Mohs Services, Carson, Calif. "It’s important to hold on to your technician – because once they get trained, once they get good – they are going to be in high demand. There is always a need for good Mohs techs."
The Mohs surgeon–technician relationship is a unique one in medicine – a symbiotic relationship not seen in other areas. "It’s a rare relationship between and physician and nonphysician, even more so than a surgeon with his surgical nurse or tech," said Mr. Lutz. "The nurse might be helping the surgeon, but you aren’t depending on them to complete the surgery. With a Mohs technician, you are."
No Mohs surgeon, however talented, can perform good Mohs surgery without precise slides as a guide. The technician brings the key element to the table for success in every case. "What happens if you lose your tech to a competitor? Not only are you not doing any Mohs, your competitor is doing more," he said.
Hiring
There are three ways to hire a technician, Mr. Lutz said: Hire and train an in-house full- or part-time person; borrow a technician from a nearby lab or hospital and either pay that person or pay the lab for that person’s time; or use a travelling service to hire a tech for only the days Mohs occurs at the office.
"Probably the most popular way is to hire and train the person in your office," Mr Lutz said. In every state except New York and Rhode Island, the trainee does not have to be a certified histotechnician. "It can be someone you already have on staff – even your office manager."
The "borrowing" technique only works well if the physician is located near a lab or is already affiliated with a hospital. The "mobile tech" option works for physicians who do the surgery occasionally, but this service isn’t available in all states – California and Florida are probably the best-supplied, he said.
The hiring process should be exacting and include several interviews. "One consideration – though it’s not necessary – is whether they already have Mohs experience. Even if you are considering an experienced histotechnician, they might not be familiar with Mohs. They might be more used to bread-loafing a specimen and looking for tumor, rather than the concept of slicing horizontally and getting underneath it."
Interviewing
Key points to consider when interviewing are whether the individual has good manual dexterity, good communication skills, and "a perfectionist personality," he said. "In my experience, good Mohs techs have a couple of things in common. They are all manually dextrous and perfectionists. I always ask if they have a hobby that shows dexterity, like knitting, musical instruments, or even juggling."
It’s hard to overstate the importance of good communication skills, Mr. Lutz stressed. "This is critical. And it’s one reason why I suggest that you do the interviewing yourself. Don’t delegate it to your practice manager. This person will be working with you every day, and it helps unbelievably if you have good communication, if you like the person, if you believe them to be ethical."
Communication is also important because, as a Mohs surgeon, you will be liable for the technician’s errors. "The Clinical Laboratory Improvement Amendments see you as the lab director, so you are inheriting [the technician’s] mistakes, and their liability is your liability.’
If the interviewee is experienced in Mohs, find out what cryostat he or she is most familiar with, or if the person is cross-trained on several." You want someone who is competent on your cryostat or can learn it quickly."
Physical limitations must be taken into account, even though interviewers are not allowed to ask about them on an application. "The way to deal with this is to put it in the job description," Mr. Lutz said. "They need to be able to lift 30 pounds. They need to be able to stand for at least 30 minutes at a time and to do repetitive tasks. If they sign off on all these things, they’re telling you they are able to do them. Then, if it turns out they can’t, this makes it easier to let them go."
Don’t forget the background check, he added. "I’m always amazed at how many people will hire without doing a background check."
Wage and Benefits
To attract and maintain the best person, the physician has to be prepared to offer a competitive wage, an attractive benefits package with health care and retirement, and the promise of continuous training. "An intensive 4-day course is fine, but even the best is not enough to go back and start cutting good slides. Find somewhere to get hold of pig skin – a pig’s foot from a market is fine and will last a whole day – and let the person practice cutting and sectioning 40 hours a week for a couple of weeks. If you let them take one course and expect to start surgery the next week, I can tell you the stress on both of you is going to be unimaginable."
Communication
Good communication is the foundation of success, he said. "This bears repeating. You want to speak diligently to the tech about what’s happening in surgery, and have that person in the surgical suite with you if possible. If you’re doing anything out of the norm of what they usually see – eyelid with a conjunctival margin, ear wedge with cartilage – you have to let them know, or they can mess up the slides."
Don’t expect a tech to make a silk purse out of a sow’s ear, he said. "They need good sections to make the kind of slides you need for diagnosis. Give them sections with complete margins, with beveled edges and clean cuts and at least 1-2 mm of epidermal rim. Specimens with jagged epidermal edges are difficult to lay flat and tend to pull out of the medium much more than a nice circular or oval cut with a 30- to 45-degree bevel."
Training
Pay a lot of attention to training. "Send them to courses as much as possible so they can hone their skills." Included in training should be courses on cryostat maintenance and adjustment. "Let your techs adjust the cryostat themselves. Don’t be afraid to let the tech learn to do that, to recondition the microtome. That way if there’s a maintenance issue, you won’t be dead in the water. Get them the education they need so if there is a problem, they know what to do to solve it."
Finally, he said, as soon as the new tech is competent, have him or her train another person in the office. This might make some people nervous about job security, but it’s a matter of practicality for everyone. "If that person ever wants to go on vacation, he’ll need someone good to cover for him."
SAN DIEGO - Train them well, pay them well, appreciate them well – and they will provide years of reliable service.
Those are the simple secrets that allow Mohs surgeons to retain their right-hand man or woman: the Mohs technician, Alexander Lutz said at a meeting sponsored by the American Society of Mohs Surgeons.
Paying careful attention to the details that keep a Mohs technician professionally satisfied and secure will pay off in a big way, said Mr. Lutz, the owner of Travel Tech Mohs Services, Carson, Calif. "It’s important to hold on to your technician – because once they get trained, once they get good – they are going to be in high demand. There is always a need for good Mohs techs."
The Mohs surgeon–technician relationship is a unique one in medicine – a symbiotic relationship not seen in other areas. "It’s a rare relationship between and physician and nonphysician, even more so than a surgeon with his surgical nurse or tech," said Mr. Lutz. "The nurse might be helping the surgeon, but you aren’t depending on them to complete the surgery. With a Mohs technician, you are."
No Mohs surgeon, however talented, can perform good Mohs surgery without precise slides as a guide. The technician brings the key element to the table for success in every case. "What happens if you lose your tech to a competitor? Not only are you not doing any Mohs, your competitor is doing more," he said.
Hiring
There are three ways to hire a technician, Mr. Lutz said: Hire and train an in-house full- or part-time person; borrow a technician from a nearby lab or hospital and either pay that person or pay the lab for that person’s time; or use a travelling service to hire a tech for only the days Mohs occurs at the office.
"Probably the most popular way is to hire and train the person in your office," Mr Lutz said. In every state except New York and Rhode Island, the trainee does not have to be a certified histotechnician. "It can be someone you already have on staff – even your office manager."
The "borrowing" technique only works well if the physician is located near a lab or is already affiliated with a hospital. The "mobile tech" option works for physicians who do the surgery occasionally, but this service isn’t available in all states – California and Florida are probably the best-supplied, he said.
The hiring process should be exacting and include several interviews. "One consideration – though it’s not necessary – is whether they already have Mohs experience. Even if you are considering an experienced histotechnician, they might not be familiar with Mohs. They might be more used to bread-loafing a specimen and looking for tumor, rather than the concept of slicing horizontally and getting underneath it."
Interviewing
Key points to consider when interviewing are whether the individual has good manual dexterity, good communication skills, and "a perfectionist personality," he said. "In my experience, good Mohs techs have a couple of things in common. They are all manually dextrous and perfectionists. I always ask if they have a hobby that shows dexterity, like knitting, musical instruments, or even juggling."
It’s hard to overstate the importance of good communication skills, Mr. Lutz stressed. "This is critical. And it’s one reason why I suggest that you do the interviewing yourself. Don’t delegate it to your practice manager. This person will be working with you every day, and it helps unbelievably if you have good communication, if you like the person, if you believe them to be ethical."
Communication is also important because, as a Mohs surgeon, you will be liable for the technician’s errors. "The Clinical Laboratory Improvement Amendments see you as the lab director, so you are inheriting [the technician’s] mistakes, and their liability is your liability.’
If the interviewee is experienced in Mohs, find out what cryostat he or she is most familiar with, or if the person is cross-trained on several." You want someone who is competent on your cryostat or can learn it quickly."
Physical limitations must be taken into account, even though interviewers are not allowed to ask about them on an application. "The way to deal with this is to put it in the job description," Mr. Lutz said. "They need to be able to lift 30 pounds. They need to be able to stand for at least 30 minutes at a time and to do repetitive tasks. If they sign off on all these things, they’re telling you they are able to do them. Then, if it turns out they can’t, this makes it easier to let them go."
Don’t forget the background check, he added. "I’m always amazed at how many people will hire without doing a background check."
Wage and Benefits
To attract and maintain the best person, the physician has to be prepared to offer a competitive wage, an attractive benefits package with health care and retirement, and the promise of continuous training. "An intensive 4-day course is fine, but even the best is not enough to go back and start cutting good slides. Find somewhere to get hold of pig skin – a pig’s foot from a market is fine and will last a whole day – and let the person practice cutting and sectioning 40 hours a week for a couple of weeks. If you let them take one course and expect to start surgery the next week, I can tell you the stress on both of you is going to be unimaginable."
Communication
Good communication is the foundation of success, he said. "This bears repeating. You want to speak diligently to the tech about what’s happening in surgery, and have that person in the surgical suite with you if possible. If you’re doing anything out of the norm of what they usually see – eyelid with a conjunctival margin, ear wedge with cartilage – you have to let them know, or they can mess up the slides."
Don’t expect a tech to make a silk purse out of a sow’s ear, he said. "They need good sections to make the kind of slides you need for diagnosis. Give them sections with complete margins, with beveled edges and clean cuts and at least 1-2 mm of epidermal rim. Specimens with jagged epidermal edges are difficult to lay flat and tend to pull out of the medium much more than a nice circular or oval cut with a 30- to 45-degree bevel."
Training
Pay a lot of attention to training. "Send them to courses as much as possible so they can hone their skills." Included in training should be courses on cryostat maintenance and adjustment. "Let your techs adjust the cryostat themselves. Don’t be afraid to let the tech learn to do that, to recondition the microtome. That way if there’s a maintenance issue, you won’t be dead in the water. Get them the education they need so if there is a problem, they know what to do to solve it."
Finally, he said, as soon as the new tech is competent, have him or her train another person in the office. This might make some people nervous about job security, but it’s a matter of practicality for everyone. "If that person ever wants to go on vacation, he’ll need someone good to cover for him."
SAN DIEGO - Train them well, pay them well, appreciate them well – and they will provide years of reliable service.
Those are the simple secrets that allow Mohs surgeons to retain their right-hand man or woman: the Mohs technician, Alexander Lutz said at a meeting sponsored by the American Society of Mohs Surgeons.
Paying careful attention to the details that keep a Mohs technician professionally satisfied and secure will pay off in a big way, said Mr. Lutz, the owner of Travel Tech Mohs Services, Carson, Calif. "It’s important to hold on to your technician – because once they get trained, once they get good – they are going to be in high demand. There is always a need for good Mohs techs."
The Mohs surgeon–technician relationship is a unique one in medicine – a symbiotic relationship not seen in other areas. "It’s a rare relationship between and physician and nonphysician, even more so than a surgeon with his surgical nurse or tech," said Mr. Lutz. "The nurse might be helping the surgeon, but you aren’t depending on them to complete the surgery. With a Mohs technician, you are."
No Mohs surgeon, however talented, can perform good Mohs surgery without precise slides as a guide. The technician brings the key element to the table for success in every case. "What happens if you lose your tech to a competitor? Not only are you not doing any Mohs, your competitor is doing more," he said.
Hiring
There are three ways to hire a technician, Mr. Lutz said: Hire and train an in-house full- or part-time person; borrow a technician from a nearby lab or hospital and either pay that person or pay the lab for that person’s time; or use a travelling service to hire a tech for only the days Mohs occurs at the office.
"Probably the most popular way is to hire and train the person in your office," Mr Lutz said. In every state except New York and Rhode Island, the trainee does not have to be a certified histotechnician. "It can be someone you already have on staff – even your office manager."
The "borrowing" technique only works well if the physician is located near a lab or is already affiliated with a hospital. The "mobile tech" option works for physicians who do the surgery occasionally, but this service isn’t available in all states – California and Florida are probably the best-supplied, he said.
The hiring process should be exacting and include several interviews. "One consideration – though it’s not necessary – is whether they already have Mohs experience. Even if you are considering an experienced histotechnician, they might not be familiar with Mohs. They might be more used to bread-loafing a specimen and looking for tumor, rather than the concept of slicing horizontally and getting underneath it."
Interviewing
Key points to consider when interviewing are whether the individual has good manual dexterity, good communication skills, and "a perfectionist personality," he said. "In my experience, good Mohs techs have a couple of things in common. They are all manually dextrous and perfectionists. I always ask if they have a hobby that shows dexterity, like knitting, musical instruments, or even juggling."
It’s hard to overstate the importance of good communication skills, Mr. Lutz stressed. "This is critical. And it’s one reason why I suggest that you do the interviewing yourself. Don’t delegate it to your practice manager. This person will be working with you every day, and it helps unbelievably if you have good communication, if you like the person, if you believe them to be ethical."
Communication is also important because, as a Mohs surgeon, you will be liable for the technician’s errors. "The Clinical Laboratory Improvement Amendments see you as the lab director, so you are inheriting [the technician’s] mistakes, and their liability is your liability.’
If the interviewee is experienced in Mohs, find out what cryostat he or she is most familiar with, or if the person is cross-trained on several." You want someone who is competent on your cryostat or can learn it quickly."
Physical limitations must be taken into account, even though interviewers are not allowed to ask about them on an application. "The way to deal with this is to put it in the job description," Mr. Lutz said. "They need to be able to lift 30 pounds. They need to be able to stand for at least 30 minutes at a time and to do repetitive tasks. If they sign off on all these things, they’re telling you they are able to do them. Then, if it turns out they can’t, this makes it easier to let them go."
Don’t forget the background check, he added. "I’m always amazed at how many people will hire without doing a background check."
Wage and Benefits
To attract and maintain the best person, the physician has to be prepared to offer a competitive wage, an attractive benefits package with health care and retirement, and the promise of continuous training. "An intensive 4-day course is fine, but even the best is not enough to go back and start cutting good slides. Find somewhere to get hold of pig skin – a pig’s foot from a market is fine and will last a whole day – and let the person practice cutting and sectioning 40 hours a week for a couple of weeks. If you let them take one course and expect to start surgery the next week, I can tell you the stress on both of you is going to be unimaginable."
Communication
Good communication is the foundation of success, he said. "This bears repeating. You want to speak diligently to the tech about what’s happening in surgery, and have that person in the surgical suite with you if possible. If you’re doing anything out of the norm of what they usually see – eyelid with a conjunctival margin, ear wedge with cartilage – you have to let them know, or they can mess up the slides."
Don’t expect a tech to make a silk purse out of a sow’s ear, he said. "They need good sections to make the kind of slides you need for diagnosis. Give them sections with complete margins, with beveled edges and clean cuts and at least 1-2 mm of epidermal rim. Specimens with jagged epidermal edges are difficult to lay flat and tend to pull out of the medium much more than a nice circular or oval cut with a 30- to 45-degree bevel."
Training
Pay a lot of attention to training. "Send them to courses as much as possible so they can hone their skills." Included in training should be courses on cryostat maintenance and adjustment. "Let your techs adjust the cryostat themselves. Don’t be afraid to let the tech learn to do that, to recondition the microtome. That way if there’s a maintenance issue, you won’t be dead in the water. Get them the education they need so if there is a problem, they know what to do to solve it."
Finally, he said, as soon as the new tech is competent, have him or her train another person in the office. This might make some people nervous about job security, but it’s a matter of practicality for everyone. "If that person ever wants to go on vacation, he’ll need someone good to cover for him."
EXPERT ANALYSIS FROM A MEETING SPONSORED BY THE AMERICAN SOCIETY OF MOHS SURGERY
Expert: Cellulite Treatment Effectiveness Unproven, Studies Flawed
LAS VEGAS – Treatment for cellulite is a multibillion dollar industry of unproved therapies, according to Dr. Mathew M. Avram.
Some treatments that claim to lessen cellulite may have produced minor, temporary improvements in flawed studies, but none has been proven to be truly effective, said Dr. Avram of Harvard University and director of Massachusetts General Hospital’s Dermatology Laser and Cosmetic Center, Boston.
There is no medical reason to treat cellulite, which is normal in the female dermis and is not associated with morbidity or mortality. Many women care about it anyway "because every tabloid likes to show celebrities and their cellulite running around in Hawaii," he said at the seminar sponsored by Skin Disease Education Foundation (SDEF).
Many physicians and patients misunderstand cellulite, which is simply gender-related differences in the structure of subcutaneous fat lobules and the connective tissue septae that divide them, usually in the thigh area, Dr. Avram said. The treatment industry capitalizes on this ignorance.
"We need to educate our patients that cellulite is a totally normal condition" and treatments are at best mildly helpful for a short period of time, he said. "We need to be skeptical as well. There is a consistent history of inflated and unsubstantiated claims of success."
Fat removal technologies have no effect on cellulite because fat and cellulite are distinct. Weight and cellulite are unrelated. Cellulite is nearly universal in postpubertal females even if they are lean, but most obese males do not have cellulite unless they have androgen deficiency. "Exercise doesn’t really help it," he explained.
There is no good evidence for invasive treatments such as liposuction, subcision, mesotherapy, or carboxytherapy. Most data on noninvasive treatments measure results by body circumference, "which isn’t relevant to cellulite, so it’s hard to know whether or not there is improvement," he noted.
Flawed studies of treatments such as noninvasive Endermologie (mechanical cell stimulation), unipolar and bipolar radiofrequency, devices combining lasers and light sources, and topical treatments show modest, temporary benefit, he said.
Nearly 2 decades ago, a study of topical retinoids for cellulite showed some improvements, but this may have just been temporary improvements in inflammation, Dr. Avram said. Multiple expensive topical formulations have shown no significant efficacy, including xanthines, lactic acid, and aminophylline.
At least three laser devices that are cleared by the Food and Drug Administration are used to treat cellulite, but these devices only needed to prove safety, not efficacy, to achieve clearance, noted Dr. Avram, who is a lawyer as well as a physician. Studies of two of the laser devices suggested that they may produce temporary and limited decreases in limb circumference, which is a poor measure of cellulite.
A study of the third device treated 17 patients twice weekly for 4 weeks with a dual wavelength laser system with vacuum suction and mechanical massage (Plast. Reconstr. Surg. 2010;125:1788-96). The study suggested that 14 patients (82%) showed "improvement" at 1 month as measured by VECTRA 3-D photographs, but initial cellulite irregularities and any possible improvements were more difficult to see by conventional digital photography. The study did not define "improvement" and included no control sites or histology to assess improvement, noted Dr. Avram.
"This is really a flawed study," he said.
A separate study of a unipolar radiofrequency device for treating cellulite in 30 patients reported a mean 2.45-cm improvement in thigh circumference in 27 patients at 6 months with changes in upper dermis fibrosis on histology (Dermatol. Surg. 2008;34:204-9). However, circumference is an inherently imprecise measure that is irrelevant to cellulite, Dr. Avram noted.
"We need a set of criteria by which we can assess the efficacy of these technologies," he said. Photography is difficult and easily manipulated to exaggerate results. Ultrasound is imprecise and user dependent. MRI is expensive and requires specific coils for fat and 3-D imaging systems.
"At a minimum we need to have untreated controls, weight maintenance during studies, and laboratory data to confirm safety," Dr. Avram said. "We must hold our industry and our colleagues to high standards" and demand proof of scientifically important efficacy.
Physicians also should question whether the postulated mechanisms of action for these new technologies make sense with regard to cellulite. Any study without a histology report, for example, has no basis for a claim of efficacy in treating cellulite, he said.
Dr. Avram holds stock options in Zeltiq Aesthetics. SDEF and this news organization are owned by Elsevier.
LAS VEGAS – Treatment for cellulite is a multibillion dollar industry of unproved therapies, according to Dr. Mathew M. Avram.
Some treatments that claim to lessen cellulite may have produced minor, temporary improvements in flawed studies, but none has been proven to be truly effective, said Dr. Avram of Harvard University and director of Massachusetts General Hospital’s Dermatology Laser and Cosmetic Center, Boston.
There is no medical reason to treat cellulite, which is normal in the female dermis and is not associated with morbidity or mortality. Many women care about it anyway "because every tabloid likes to show celebrities and their cellulite running around in Hawaii," he said at the seminar sponsored by Skin Disease Education Foundation (SDEF).
Many physicians and patients misunderstand cellulite, which is simply gender-related differences in the structure of subcutaneous fat lobules and the connective tissue septae that divide them, usually in the thigh area, Dr. Avram said. The treatment industry capitalizes on this ignorance.
"We need to educate our patients that cellulite is a totally normal condition" and treatments are at best mildly helpful for a short period of time, he said. "We need to be skeptical as well. There is a consistent history of inflated and unsubstantiated claims of success."
Fat removal technologies have no effect on cellulite because fat and cellulite are distinct. Weight and cellulite are unrelated. Cellulite is nearly universal in postpubertal females even if they are lean, but most obese males do not have cellulite unless they have androgen deficiency. "Exercise doesn’t really help it," he explained.
There is no good evidence for invasive treatments such as liposuction, subcision, mesotherapy, or carboxytherapy. Most data on noninvasive treatments measure results by body circumference, "which isn’t relevant to cellulite, so it’s hard to know whether or not there is improvement," he noted.
Flawed studies of treatments such as noninvasive Endermologie (mechanical cell stimulation), unipolar and bipolar radiofrequency, devices combining lasers and light sources, and topical treatments show modest, temporary benefit, he said.
Nearly 2 decades ago, a study of topical retinoids for cellulite showed some improvements, but this may have just been temporary improvements in inflammation, Dr. Avram said. Multiple expensive topical formulations have shown no significant efficacy, including xanthines, lactic acid, and aminophylline.
At least three laser devices that are cleared by the Food and Drug Administration are used to treat cellulite, but these devices only needed to prove safety, not efficacy, to achieve clearance, noted Dr. Avram, who is a lawyer as well as a physician. Studies of two of the laser devices suggested that they may produce temporary and limited decreases in limb circumference, which is a poor measure of cellulite.
A study of the third device treated 17 patients twice weekly for 4 weeks with a dual wavelength laser system with vacuum suction and mechanical massage (Plast. Reconstr. Surg. 2010;125:1788-96). The study suggested that 14 patients (82%) showed "improvement" at 1 month as measured by VECTRA 3-D photographs, but initial cellulite irregularities and any possible improvements were more difficult to see by conventional digital photography. The study did not define "improvement" and included no control sites or histology to assess improvement, noted Dr. Avram.
"This is really a flawed study," he said.
A separate study of a unipolar radiofrequency device for treating cellulite in 30 patients reported a mean 2.45-cm improvement in thigh circumference in 27 patients at 6 months with changes in upper dermis fibrosis on histology (Dermatol. Surg. 2008;34:204-9). However, circumference is an inherently imprecise measure that is irrelevant to cellulite, Dr. Avram noted.
"We need a set of criteria by which we can assess the efficacy of these technologies," he said. Photography is difficult and easily manipulated to exaggerate results. Ultrasound is imprecise and user dependent. MRI is expensive and requires specific coils for fat and 3-D imaging systems.
"At a minimum we need to have untreated controls, weight maintenance during studies, and laboratory data to confirm safety," Dr. Avram said. "We must hold our industry and our colleagues to high standards" and demand proof of scientifically important efficacy.
Physicians also should question whether the postulated mechanisms of action for these new technologies make sense with regard to cellulite. Any study without a histology report, for example, has no basis for a claim of efficacy in treating cellulite, he said.
Dr. Avram holds stock options in Zeltiq Aesthetics. SDEF and this news organization are owned by Elsevier.
LAS VEGAS – Treatment for cellulite is a multibillion dollar industry of unproved therapies, according to Dr. Mathew M. Avram.
Some treatments that claim to lessen cellulite may have produced minor, temporary improvements in flawed studies, but none has been proven to be truly effective, said Dr. Avram of Harvard University and director of Massachusetts General Hospital’s Dermatology Laser and Cosmetic Center, Boston.
There is no medical reason to treat cellulite, which is normal in the female dermis and is not associated with morbidity or mortality. Many women care about it anyway "because every tabloid likes to show celebrities and their cellulite running around in Hawaii," he said at the seminar sponsored by Skin Disease Education Foundation (SDEF).
Many physicians and patients misunderstand cellulite, which is simply gender-related differences in the structure of subcutaneous fat lobules and the connective tissue septae that divide them, usually in the thigh area, Dr. Avram said. The treatment industry capitalizes on this ignorance.
"We need to educate our patients that cellulite is a totally normal condition" and treatments are at best mildly helpful for a short period of time, he said. "We need to be skeptical as well. There is a consistent history of inflated and unsubstantiated claims of success."
Fat removal technologies have no effect on cellulite because fat and cellulite are distinct. Weight and cellulite are unrelated. Cellulite is nearly universal in postpubertal females even if they are lean, but most obese males do not have cellulite unless they have androgen deficiency. "Exercise doesn’t really help it," he explained.
There is no good evidence for invasive treatments such as liposuction, subcision, mesotherapy, or carboxytherapy. Most data on noninvasive treatments measure results by body circumference, "which isn’t relevant to cellulite, so it’s hard to know whether or not there is improvement," he noted.
Flawed studies of treatments such as noninvasive Endermologie (mechanical cell stimulation), unipolar and bipolar radiofrequency, devices combining lasers and light sources, and topical treatments show modest, temporary benefit, he said.
Nearly 2 decades ago, a study of topical retinoids for cellulite showed some improvements, but this may have just been temporary improvements in inflammation, Dr. Avram said. Multiple expensive topical formulations have shown no significant efficacy, including xanthines, lactic acid, and aminophylline.
At least three laser devices that are cleared by the Food and Drug Administration are used to treat cellulite, but these devices only needed to prove safety, not efficacy, to achieve clearance, noted Dr. Avram, who is a lawyer as well as a physician. Studies of two of the laser devices suggested that they may produce temporary and limited decreases in limb circumference, which is a poor measure of cellulite.
A study of the third device treated 17 patients twice weekly for 4 weeks with a dual wavelength laser system with vacuum suction and mechanical massage (Plast. Reconstr. Surg. 2010;125:1788-96). The study suggested that 14 patients (82%) showed "improvement" at 1 month as measured by VECTRA 3-D photographs, but initial cellulite irregularities and any possible improvements were more difficult to see by conventional digital photography. The study did not define "improvement" and included no control sites or histology to assess improvement, noted Dr. Avram.
"This is really a flawed study," he said.
A separate study of a unipolar radiofrequency device for treating cellulite in 30 patients reported a mean 2.45-cm improvement in thigh circumference in 27 patients at 6 months with changes in upper dermis fibrosis on histology (Dermatol. Surg. 2008;34:204-9). However, circumference is an inherently imprecise measure that is irrelevant to cellulite, Dr. Avram noted.
"We need a set of criteria by which we can assess the efficacy of these technologies," he said. Photography is difficult and easily manipulated to exaggerate results. Ultrasound is imprecise and user dependent. MRI is expensive and requires specific coils for fat and 3-D imaging systems.
"At a minimum we need to have untreated controls, weight maintenance during studies, and laboratory data to confirm safety," Dr. Avram said. "We must hold our industry and our colleagues to high standards" and demand proof of scientifically important efficacy.
Physicians also should question whether the postulated mechanisms of action for these new technologies make sense with regard to cellulite. Any study without a histology report, for example, has no basis for a claim of efficacy in treating cellulite, he said.
Dr. Avram holds stock options in Zeltiq Aesthetics. SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM A DERMATOLOGY SEMINAR
Propranolol Plus Laser Equals New Option for Infantile Hemangiomas
LONDON - The combined use of propranolol and laser therapy has positive, additive effects on infantile hemangiomas, according to the results of a prospective, observational study.
While the beta-blocker appears to stop proliferation, laser therapy seems to induce the early shrinkage of these common childhood benign vascular tumors.
This offers a new option for treating infants with problematic, proliferating hemangiomas, Dr. Margitta Poetke of the Elisabeth Klinik in Berlin said at the Excellence in Paediatrics meeting.
Since 2008, when the use of propranolol was first proposed for the treatment for infantile hemangiomas (N. Engl. J. Med. 2008;358:2649-51), there have been several studies investigating its potential use. Dr. Poetke and her team reported their first experience of using propranolol in combination with laser therapy.
Hemangiomas are abnormal buildups of blood vessels in the skin or internal organs. They typically occur after the age of 3 months, rapidly proliferate and mature between 6 months and 1 year, and then regress until they partially or fully resolve by the age of 5-7 years.
The small study involved 23 infants with hemangiomas and other benign large vessel tumors who were between ages 2 months and 3.5 years. All infants had facial hemangiomas that were causing severe functional impairment, such as occlusion of the eye or destruction of the lip.
Nine infants were treated with propranolol (2 mg/kg per day) alone, and 14 received the beta-blocker in combination with laser therapy; 7 had received prior oral corticosteroid therapy. Treatment was for 6-8 months, with 2-18 months’ follow-up. The effects of treatment were assessed using color-coded duplex sonography, with photographs taken at 1, 3, and 6 months, and after the end of therapy.
Of the nine infants treated with propranolol only, those with cutaneous hemangiomas responded better than those with subcutaneous hemangiomas, and treatment appeared to be more effective in the younger children (less than 6 months) than in older children. Full regression of the hemangiomas was not always achieved on treatment, however, and rebound growth was seen after treatment was halted in six children – two with subcutaneous hemangiomas and four with cutaneous/subcutaneous hemangiomas.
Propranolol plus laser therapy appeared to be more effective, with only one rebound hemangioma occurring in a child with a cutaneous/subcutaneous hemangioma out of 14 children treated with the combination. The reason for this rebound may be that the child received only one treatment, Dr. Poetke said.
"Laser treatment in combination with propranolol seems to have an additive, positive effect," said Dr. Poetke. She noted that the combination lightened the skin and flattened lesions, and "the risk of a rebound growth seems to be much lower."
Side effects included nocturnal restlessness, listlessness, reduced hair growth, and diarrhea, which affected one child each, and bradycardia in two children. Treatment was stopped because of suckling weakness in one child, and because of no effect in another.
These data suggest that propranolol plus laser therapy may be an alternative approach to corticosteroids in the first-line medical treatment of infant hemangiomas, Dr. Poetke said. With potentially fewer side effects and less chance of rebound hemangioma than corticosteroids, propranolol may be safer and more effective, particularly when combined with laser treatment.
Treatment with propranolol needs to start early, however, be given for at least 6 months, and, ideally, be combined with laser therapy to optimize the regression of the hemangioma and to avoid regrowth, she said.
Dr. Poetke said she had no relevant financial disclosures.
LONDON - The combined use of propranolol and laser therapy has positive, additive effects on infantile hemangiomas, according to the results of a prospective, observational study.
While the beta-blocker appears to stop proliferation, laser therapy seems to induce the early shrinkage of these common childhood benign vascular tumors.
This offers a new option for treating infants with problematic, proliferating hemangiomas, Dr. Margitta Poetke of the Elisabeth Klinik in Berlin said at the Excellence in Paediatrics meeting.
Since 2008, when the use of propranolol was first proposed for the treatment for infantile hemangiomas (N. Engl. J. Med. 2008;358:2649-51), there have been several studies investigating its potential use. Dr. Poetke and her team reported their first experience of using propranolol in combination with laser therapy.
Hemangiomas are abnormal buildups of blood vessels in the skin or internal organs. They typically occur after the age of 3 months, rapidly proliferate and mature between 6 months and 1 year, and then regress until they partially or fully resolve by the age of 5-7 years.
The small study involved 23 infants with hemangiomas and other benign large vessel tumors who were between ages 2 months and 3.5 years. All infants had facial hemangiomas that were causing severe functional impairment, such as occlusion of the eye or destruction of the lip.
Nine infants were treated with propranolol (2 mg/kg per day) alone, and 14 received the beta-blocker in combination with laser therapy; 7 had received prior oral corticosteroid therapy. Treatment was for 6-8 months, with 2-18 months’ follow-up. The effects of treatment were assessed using color-coded duplex sonography, with photographs taken at 1, 3, and 6 months, and after the end of therapy.
Of the nine infants treated with propranolol only, those with cutaneous hemangiomas responded better than those with subcutaneous hemangiomas, and treatment appeared to be more effective in the younger children (less than 6 months) than in older children. Full regression of the hemangiomas was not always achieved on treatment, however, and rebound growth was seen after treatment was halted in six children – two with subcutaneous hemangiomas and four with cutaneous/subcutaneous hemangiomas.
Propranolol plus laser therapy appeared to be more effective, with only one rebound hemangioma occurring in a child with a cutaneous/subcutaneous hemangioma out of 14 children treated with the combination. The reason for this rebound may be that the child received only one treatment, Dr. Poetke said.
"Laser treatment in combination with propranolol seems to have an additive, positive effect," said Dr. Poetke. She noted that the combination lightened the skin and flattened lesions, and "the risk of a rebound growth seems to be much lower."
Side effects included nocturnal restlessness, listlessness, reduced hair growth, and diarrhea, which affected one child each, and bradycardia in two children. Treatment was stopped because of suckling weakness in one child, and because of no effect in another.
These data suggest that propranolol plus laser therapy may be an alternative approach to corticosteroids in the first-line medical treatment of infant hemangiomas, Dr. Poetke said. With potentially fewer side effects and less chance of rebound hemangioma than corticosteroids, propranolol may be safer and more effective, particularly when combined with laser treatment.
Treatment with propranolol needs to start early, however, be given for at least 6 months, and, ideally, be combined with laser therapy to optimize the regression of the hemangioma and to avoid regrowth, she said.
Dr. Poetke said she had no relevant financial disclosures.
LONDON - The combined use of propranolol and laser therapy has positive, additive effects on infantile hemangiomas, according to the results of a prospective, observational study.
While the beta-blocker appears to stop proliferation, laser therapy seems to induce the early shrinkage of these common childhood benign vascular tumors.
This offers a new option for treating infants with problematic, proliferating hemangiomas, Dr. Margitta Poetke of the Elisabeth Klinik in Berlin said at the Excellence in Paediatrics meeting.
Since 2008, when the use of propranolol was first proposed for the treatment for infantile hemangiomas (N. Engl. J. Med. 2008;358:2649-51), there have been several studies investigating its potential use. Dr. Poetke and her team reported their first experience of using propranolol in combination with laser therapy.
Hemangiomas are abnormal buildups of blood vessels in the skin or internal organs. They typically occur after the age of 3 months, rapidly proliferate and mature between 6 months and 1 year, and then regress until they partially or fully resolve by the age of 5-7 years.
The small study involved 23 infants with hemangiomas and other benign large vessel tumors who were between ages 2 months and 3.5 years. All infants had facial hemangiomas that were causing severe functional impairment, such as occlusion of the eye or destruction of the lip.
Nine infants were treated with propranolol (2 mg/kg per day) alone, and 14 received the beta-blocker in combination with laser therapy; 7 had received prior oral corticosteroid therapy. Treatment was for 6-8 months, with 2-18 months’ follow-up. The effects of treatment were assessed using color-coded duplex sonography, with photographs taken at 1, 3, and 6 months, and after the end of therapy.
Of the nine infants treated with propranolol only, those with cutaneous hemangiomas responded better than those with subcutaneous hemangiomas, and treatment appeared to be more effective in the younger children (less than 6 months) than in older children. Full regression of the hemangiomas was not always achieved on treatment, however, and rebound growth was seen after treatment was halted in six children – two with subcutaneous hemangiomas and four with cutaneous/subcutaneous hemangiomas.
Propranolol plus laser therapy appeared to be more effective, with only one rebound hemangioma occurring in a child with a cutaneous/subcutaneous hemangioma out of 14 children treated with the combination. The reason for this rebound may be that the child received only one treatment, Dr. Poetke said.
"Laser treatment in combination with propranolol seems to have an additive, positive effect," said Dr. Poetke. She noted that the combination lightened the skin and flattened lesions, and "the risk of a rebound growth seems to be much lower."
Side effects included nocturnal restlessness, listlessness, reduced hair growth, and diarrhea, which affected one child each, and bradycardia in two children. Treatment was stopped because of suckling weakness in one child, and because of no effect in another.
These data suggest that propranolol plus laser therapy may be an alternative approach to corticosteroids in the first-line medical treatment of infant hemangiomas, Dr. Poetke said. With potentially fewer side effects and less chance of rebound hemangioma than corticosteroids, propranolol may be safer and more effective, particularly when combined with laser treatment.
Treatment with propranolol needs to start early, however, be given for at least 6 months, and, ideally, be combined with laser therapy to optimize the regression of the hemangioma and to avoid regrowth, she said.
Dr. Poetke said she had no relevant financial disclosures.
FROM THE EXCELLENCE IN PAEDIATRICS ANNUAL MEETING
Major Finding: Of 14 infants given propranolol in combination with laser therapy, only 1 child experienced a rebound of their hemangioma.
Data Source: Prospective, observational study of 23 infants with large facial hemangiomas that were causing severe functional impairment.
Disclosures: Dr. Poetke said she had no relevant financial disclosures.