User login
Insurer disputes fueling more lawsuits by doctors
Fed up with unfair practices by some insurance companies, more physicians are heading to the courtroom to resolve conflicts with insurers, litigation experts say. In the last year, doctors in various states took legal action against insurers for such allegations as claim denials, underpayments, and network exclusions.
"Providers are becoming increasingly frustrated [with insurers] on a number of different areas," said David Doyle, founder and CEO of CRT Medical Systems, a medical billing and practice-management company based in Novi, Mich. "Physicians are saying, ‘Enough.’ They’re taking the offensive position and going after the payers."
Recent lawsuits highlight this growing trend. In Connecticut, the medical associations of Fairfield and Hartford counties in November issued a legal challenge against UnitedHealthcare for terminating more than 2,000 doctors from its Medicare Advantage plan network. Physicians claim the terminations were made without cause and will severely harm patient care. UnitedHealthcare has said the restructuring was made to encourage higher quality health care coverage. A district court on Dec. 5 temporarily halted the terminations after the medical associations sought emergency relief.
In the fall, the U.S. District Court for the Northern District of Illinois said a lawsuit brought by an Illinois dermatologist could stand against Humana Insurance Co. The doctor claims the insurer informed his patients falsely that he was no longer in the insurer’s network and to find another doctor. The district court found the doctor had alleged sufficient facts to support his claim of tortious contract interference.
Meanwhile, a Los Angeles Superior Court judge ruled on Dec. 9 that a suit by the California Medical Association and several dozen doctors to move forward against Aetna. The CMA sued Aetna in 2012 for allegedly underpaying out-of-network physicians and failing to approve some out-of-network services.
Aetna moved to dismiss the suit, but the court ruled the doctors pled valid claims under the state’s unfair business practice law. A similar lawsuit over payment denials by the Los Angeles County Medical Association is pending against insurer Health Net.
One reason for the increase in lawsuits is that physicians are better at recognizing insurers’ errors than they were in the past, according to Elizabeth Woodcock, founder of Woodcock & Assoc., a medical practice consulting firm in Atlanta.
"As we’ve gotten more electronic systems, [payment issues] become more identified," she said. "We’ve become better at picking these things up."
Historically, doctors primary struggles with insurance companies consisted of late payments and retroactive denials related to eligibility issues, according to Mark *S. Kopson, a Michigan health law attorney and vice chair of membership for the American Health Lawyers Association’s Payers, Plans and Managed Care Practice Group. Today, insurance battles more often stem from disputes over medically necessary treatment and disagreements over pay for performance measures, he said.
"Those are becoming more prevalent and that’s largely due to the change in reimbursement methods," he said. "The Affordable Care Act has had an impact on the issue. There’s a significant increase in performance-based reimbursement."
Network exclusions and terminations are also a growing catalyst for litigation by doctors, legal experts said. Plans are moving to more restrictive networks to leverage physicians into accepting lower contract rates, and to maintain profits and price competitiveness in the market, said Dr. Myles Riner, a managed care consultant and past president of the American College of Emergency Physicians California chapter.
In addition, insurers often attempt to boot physicians who are viewed as "complainers," said Andrew H. Selesnick, a partner at Los Angeles-based Michelman & Robinson, and chair of the firm’s Healthcare Law Department. Mr. Selesnick recently represented a client who received a network termination letter after the doctor successfully advocated for a Medicare patient to receive coverage for a treatment. The insurer withdrew the termination after Mr. Selesnick argued the move appeared retaliatory and warned of pursuing an injunction.
"For the most part, [network] terminations are profit or retaliation motivated," he said. "You really need to fight those bogus terminations."
Physicians’ success suing over insurer conduct has been mixed. For example, In April, jurors awarded Dr. Jeffrey B. Nordella, a California family physician, $3.8 million in damages after Anthem Blue Cross excluded him from its network. Dr. Nordella claimed the insurer was retaliating against him for his advocacy of patients who were denied coverage.
But in May, a Washington state appeals court threw out a lawsuit by the Washington State Medical Association over fair payments for out-of-network emergency services. The WSMA had sued state Insurance Commissioner Mike Kreidler for allegedly failing to enforce a state law compelling insurers to pay the cost of patients’ out-of-network emergency treatment. The court said the association had no grounds to sue Mr. Kreidler.
"In the major litigation, we’ve seen victories both on the provider and on the plan side," Mr. Kopson said. "One thing that is abundantly clear: This type of litigation is extremely complex and it is extremely expensive."
For this reason, it helps to have multiple health providers involved in a class action against insurers or a medical organization that supports the plaintiff physician, he said. Considering the value of the claim is also important before suing, Ms. Woodcock said. In some cases, the cost of attorney and legal expenses far exceed the disputed payment amount, she noted.
Legal standing is another major consideration, Mr. Selesnick said. Doctors should determine whether they have grounds to sue insurers, with an eye toward legal rules and contract terms. Legal counsel is key, Mr. Selesnick said.
Of course, resolving questions and conflicts with insurers early can prevent lawsuits all together and save both sides significant time and expense, Mr. Kopson said.
"Health plans and providers are undeniably in a symbiotic relationship," he said. "It means you have to pursue a collaborative – as opposed to an adversarial – posture. The best way to avoid litigation is to engage in vigorous discussion and negotiation up front before the contract is signed."
*Correction 2/26/14: A previous version of this story gave the incorrect middle initial of Mr. Mark S. Kopson. This version has been updated.
Fed up with unfair practices by some insurance companies, more physicians are heading to the courtroom to resolve conflicts with insurers, litigation experts say. In the last year, doctors in various states took legal action against insurers for such allegations as claim denials, underpayments, and network exclusions.
"Providers are becoming increasingly frustrated [with insurers] on a number of different areas," said David Doyle, founder and CEO of CRT Medical Systems, a medical billing and practice-management company based in Novi, Mich. "Physicians are saying, ‘Enough.’ They’re taking the offensive position and going after the payers."
Recent lawsuits highlight this growing trend. In Connecticut, the medical associations of Fairfield and Hartford counties in November issued a legal challenge against UnitedHealthcare for terminating more than 2,000 doctors from its Medicare Advantage plan network. Physicians claim the terminations were made without cause and will severely harm patient care. UnitedHealthcare has said the restructuring was made to encourage higher quality health care coverage. A district court on Dec. 5 temporarily halted the terminations after the medical associations sought emergency relief.
In the fall, the U.S. District Court for the Northern District of Illinois said a lawsuit brought by an Illinois dermatologist could stand against Humana Insurance Co. The doctor claims the insurer informed his patients falsely that he was no longer in the insurer’s network and to find another doctor. The district court found the doctor had alleged sufficient facts to support his claim of tortious contract interference.
Meanwhile, a Los Angeles Superior Court judge ruled on Dec. 9 that a suit by the California Medical Association and several dozen doctors to move forward against Aetna. The CMA sued Aetna in 2012 for allegedly underpaying out-of-network physicians and failing to approve some out-of-network services.
Aetna moved to dismiss the suit, but the court ruled the doctors pled valid claims under the state’s unfair business practice law. A similar lawsuit over payment denials by the Los Angeles County Medical Association is pending against insurer Health Net.
One reason for the increase in lawsuits is that physicians are better at recognizing insurers’ errors than they were in the past, according to Elizabeth Woodcock, founder of Woodcock & Assoc., a medical practice consulting firm in Atlanta.
"As we’ve gotten more electronic systems, [payment issues] become more identified," she said. "We’ve become better at picking these things up."
Historically, doctors primary struggles with insurance companies consisted of late payments and retroactive denials related to eligibility issues, according to Mark *S. Kopson, a Michigan health law attorney and vice chair of membership for the American Health Lawyers Association’s Payers, Plans and Managed Care Practice Group. Today, insurance battles more often stem from disputes over medically necessary treatment and disagreements over pay for performance measures, he said.
"Those are becoming more prevalent and that’s largely due to the change in reimbursement methods," he said. "The Affordable Care Act has had an impact on the issue. There’s a significant increase in performance-based reimbursement."
Network exclusions and terminations are also a growing catalyst for litigation by doctors, legal experts said. Plans are moving to more restrictive networks to leverage physicians into accepting lower contract rates, and to maintain profits and price competitiveness in the market, said Dr. Myles Riner, a managed care consultant and past president of the American College of Emergency Physicians California chapter.
In addition, insurers often attempt to boot physicians who are viewed as "complainers," said Andrew H. Selesnick, a partner at Los Angeles-based Michelman & Robinson, and chair of the firm’s Healthcare Law Department. Mr. Selesnick recently represented a client who received a network termination letter after the doctor successfully advocated for a Medicare patient to receive coverage for a treatment. The insurer withdrew the termination after Mr. Selesnick argued the move appeared retaliatory and warned of pursuing an injunction.
"For the most part, [network] terminations are profit or retaliation motivated," he said. "You really need to fight those bogus terminations."
Physicians’ success suing over insurer conduct has been mixed. For example, In April, jurors awarded Dr. Jeffrey B. Nordella, a California family physician, $3.8 million in damages after Anthem Blue Cross excluded him from its network. Dr. Nordella claimed the insurer was retaliating against him for his advocacy of patients who were denied coverage.
But in May, a Washington state appeals court threw out a lawsuit by the Washington State Medical Association over fair payments for out-of-network emergency services. The WSMA had sued state Insurance Commissioner Mike Kreidler for allegedly failing to enforce a state law compelling insurers to pay the cost of patients’ out-of-network emergency treatment. The court said the association had no grounds to sue Mr. Kreidler.
"In the major litigation, we’ve seen victories both on the provider and on the plan side," Mr. Kopson said. "One thing that is abundantly clear: This type of litigation is extremely complex and it is extremely expensive."
For this reason, it helps to have multiple health providers involved in a class action against insurers or a medical organization that supports the plaintiff physician, he said. Considering the value of the claim is also important before suing, Ms. Woodcock said. In some cases, the cost of attorney and legal expenses far exceed the disputed payment amount, she noted.
Legal standing is another major consideration, Mr. Selesnick said. Doctors should determine whether they have grounds to sue insurers, with an eye toward legal rules and contract terms. Legal counsel is key, Mr. Selesnick said.
Of course, resolving questions and conflicts with insurers early can prevent lawsuits all together and save both sides significant time and expense, Mr. Kopson said.
"Health plans and providers are undeniably in a symbiotic relationship," he said. "It means you have to pursue a collaborative – as opposed to an adversarial – posture. The best way to avoid litigation is to engage in vigorous discussion and negotiation up front before the contract is signed."
*Correction 2/26/14: A previous version of this story gave the incorrect middle initial of Mr. Mark S. Kopson. This version has been updated.
Fed up with unfair practices by some insurance companies, more physicians are heading to the courtroom to resolve conflicts with insurers, litigation experts say. In the last year, doctors in various states took legal action against insurers for such allegations as claim denials, underpayments, and network exclusions.
"Providers are becoming increasingly frustrated [with insurers] on a number of different areas," said David Doyle, founder and CEO of CRT Medical Systems, a medical billing and practice-management company based in Novi, Mich. "Physicians are saying, ‘Enough.’ They’re taking the offensive position and going after the payers."
Recent lawsuits highlight this growing trend. In Connecticut, the medical associations of Fairfield and Hartford counties in November issued a legal challenge against UnitedHealthcare for terminating more than 2,000 doctors from its Medicare Advantage plan network. Physicians claim the terminations were made without cause and will severely harm patient care. UnitedHealthcare has said the restructuring was made to encourage higher quality health care coverage. A district court on Dec. 5 temporarily halted the terminations after the medical associations sought emergency relief.
In the fall, the U.S. District Court for the Northern District of Illinois said a lawsuit brought by an Illinois dermatologist could stand against Humana Insurance Co. The doctor claims the insurer informed his patients falsely that he was no longer in the insurer’s network and to find another doctor. The district court found the doctor had alleged sufficient facts to support his claim of tortious contract interference.
Meanwhile, a Los Angeles Superior Court judge ruled on Dec. 9 that a suit by the California Medical Association and several dozen doctors to move forward against Aetna. The CMA sued Aetna in 2012 for allegedly underpaying out-of-network physicians and failing to approve some out-of-network services.
Aetna moved to dismiss the suit, but the court ruled the doctors pled valid claims under the state’s unfair business practice law. A similar lawsuit over payment denials by the Los Angeles County Medical Association is pending against insurer Health Net.
One reason for the increase in lawsuits is that physicians are better at recognizing insurers’ errors than they were in the past, according to Elizabeth Woodcock, founder of Woodcock & Assoc., a medical practice consulting firm in Atlanta.
"As we’ve gotten more electronic systems, [payment issues] become more identified," she said. "We’ve become better at picking these things up."
Historically, doctors primary struggles with insurance companies consisted of late payments and retroactive denials related to eligibility issues, according to Mark *S. Kopson, a Michigan health law attorney and vice chair of membership for the American Health Lawyers Association’s Payers, Plans and Managed Care Practice Group. Today, insurance battles more often stem from disputes over medically necessary treatment and disagreements over pay for performance measures, he said.
"Those are becoming more prevalent and that’s largely due to the change in reimbursement methods," he said. "The Affordable Care Act has had an impact on the issue. There’s a significant increase in performance-based reimbursement."
Network exclusions and terminations are also a growing catalyst for litigation by doctors, legal experts said. Plans are moving to more restrictive networks to leverage physicians into accepting lower contract rates, and to maintain profits and price competitiveness in the market, said Dr. Myles Riner, a managed care consultant and past president of the American College of Emergency Physicians California chapter.
In addition, insurers often attempt to boot physicians who are viewed as "complainers," said Andrew H. Selesnick, a partner at Los Angeles-based Michelman & Robinson, and chair of the firm’s Healthcare Law Department. Mr. Selesnick recently represented a client who received a network termination letter after the doctor successfully advocated for a Medicare patient to receive coverage for a treatment. The insurer withdrew the termination after Mr. Selesnick argued the move appeared retaliatory and warned of pursuing an injunction.
"For the most part, [network] terminations are profit or retaliation motivated," he said. "You really need to fight those bogus terminations."
Physicians’ success suing over insurer conduct has been mixed. For example, In April, jurors awarded Dr. Jeffrey B. Nordella, a California family physician, $3.8 million in damages after Anthem Blue Cross excluded him from its network. Dr. Nordella claimed the insurer was retaliating against him for his advocacy of patients who were denied coverage.
But in May, a Washington state appeals court threw out a lawsuit by the Washington State Medical Association over fair payments for out-of-network emergency services. The WSMA had sued state Insurance Commissioner Mike Kreidler for allegedly failing to enforce a state law compelling insurers to pay the cost of patients’ out-of-network emergency treatment. The court said the association had no grounds to sue Mr. Kreidler.
"In the major litigation, we’ve seen victories both on the provider and on the plan side," Mr. Kopson said. "One thing that is abundantly clear: This type of litigation is extremely complex and it is extremely expensive."
For this reason, it helps to have multiple health providers involved in a class action against insurers or a medical organization that supports the plaintiff physician, he said. Considering the value of the claim is also important before suing, Ms. Woodcock said. In some cases, the cost of attorney and legal expenses far exceed the disputed payment amount, she noted.
Legal standing is another major consideration, Mr. Selesnick said. Doctors should determine whether they have grounds to sue insurers, with an eye toward legal rules and contract terms. Legal counsel is key, Mr. Selesnick said.
Of course, resolving questions and conflicts with insurers early can prevent lawsuits all together and save both sides significant time and expense, Mr. Kopson said.
"Health plans and providers are undeniably in a symbiotic relationship," he said. "It means you have to pursue a collaborative – as opposed to an adversarial – posture. The best way to avoid litigation is to engage in vigorous discussion and negotiation up front before the contract is signed."
*Correction 2/26/14: A previous version of this story gave the incorrect middle initial of Mr. Mark S. Kopson. This version has been updated.
New health IT czar takes over in January
Dr. Karen B. DeSalvo has been tapped to become the federal government’s next national coordinator for health information technology, the Health and Human Services Department announced.
Dr. DeSalvo, who helped modernize the New Orleans health care infrastructure after Hurricane Katrina, will play a central role in setting policy around the Medicare and Medicaid Electronic Health Record Incentive Programs, which include "meaningful use" requirements for the use of health IT.
Her first day in the new post will be Jan. 13.
"Dr. DeSalvo’s hands-on experience with health delivery system reform and HIT and its potential to improve health care and public health will be invaluable assets to the Office of the National Coordinator and the [Health and Human Services] department," HHS Secretary Kathleen Sebelius said in an e-mail to ONC staff on Dec. 19.
Dr. DeSalvo, an internist, also currently serves as a senior health policy adviser to New Orleans Mayor Mitch Landrieu. Over the course of her career, she has been an advocate for increasing the use of health IT in primary care and public health, and as part of emergency preparedness efforts. She has also led the planning of the city’s new public hospital, which includes a fully integrated health IT network.
The Healthcare Information and Management Systems Society praised Dr. DeSalvo for her "deep understanding of the value of informatics, as well as the challenges and promise of interoperability."
Dr. DeSalvo replaces Dr. Jacob Reider, the acting national coordinator, who will return to his former role as chief medical officer at the Office of the National Coordinator for Health IT. Dr. Reider took over the top job in the fall, after the departure of Dr. Farzad Mostashari.
mschneider@frontlinemedcom.com
On Twitter @MaryEllenNY
Dr. Karen B. DeSalvo has been tapped to become the federal government’s next national coordinator for health information technology, the Health and Human Services Department announced.
Dr. DeSalvo, who helped modernize the New Orleans health care infrastructure after Hurricane Katrina, will play a central role in setting policy around the Medicare and Medicaid Electronic Health Record Incentive Programs, which include "meaningful use" requirements for the use of health IT.
Her first day in the new post will be Jan. 13.
"Dr. DeSalvo’s hands-on experience with health delivery system reform and HIT and its potential to improve health care and public health will be invaluable assets to the Office of the National Coordinator and the [Health and Human Services] department," HHS Secretary Kathleen Sebelius said in an e-mail to ONC staff on Dec. 19.
Dr. DeSalvo, an internist, also currently serves as a senior health policy adviser to New Orleans Mayor Mitch Landrieu. Over the course of her career, she has been an advocate for increasing the use of health IT in primary care and public health, and as part of emergency preparedness efforts. She has also led the planning of the city’s new public hospital, which includes a fully integrated health IT network.
The Healthcare Information and Management Systems Society praised Dr. DeSalvo for her "deep understanding of the value of informatics, as well as the challenges and promise of interoperability."
Dr. DeSalvo replaces Dr. Jacob Reider, the acting national coordinator, who will return to his former role as chief medical officer at the Office of the National Coordinator for Health IT. Dr. Reider took over the top job in the fall, after the departure of Dr. Farzad Mostashari.
mschneider@frontlinemedcom.com
On Twitter @MaryEllenNY
Dr. Karen B. DeSalvo has been tapped to become the federal government’s next national coordinator for health information technology, the Health and Human Services Department announced.
Dr. DeSalvo, who helped modernize the New Orleans health care infrastructure after Hurricane Katrina, will play a central role in setting policy around the Medicare and Medicaid Electronic Health Record Incentive Programs, which include "meaningful use" requirements for the use of health IT.
Her first day in the new post will be Jan. 13.
"Dr. DeSalvo’s hands-on experience with health delivery system reform and HIT and its potential to improve health care and public health will be invaluable assets to the Office of the National Coordinator and the [Health and Human Services] department," HHS Secretary Kathleen Sebelius said in an e-mail to ONC staff on Dec. 19.
Dr. DeSalvo, an internist, also currently serves as a senior health policy adviser to New Orleans Mayor Mitch Landrieu. Over the course of her career, she has been an advocate for increasing the use of health IT in primary care and public health, and as part of emergency preparedness efforts. She has also led the planning of the city’s new public hospital, which includes a fully integrated health IT network.
The Healthcare Information and Management Systems Society praised Dr. DeSalvo for her "deep understanding of the value of informatics, as well as the challenges and promise of interoperability."
Dr. DeSalvo replaces Dr. Jacob Reider, the acting national coordinator, who will return to his former role as chief medical officer at the Office of the National Coordinator for Health IT. Dr. Reider took over the top job in the fall, after the departure of Dr. Farzad Mostashari.
mschneider@frontlinemedcom.com
On Twitter @MaryEllenNY
Senate passes SGR and budget bill; White House next
The Senate has passed a budget package that includes a 3-month delay in physician pay cuts mandated by the Medicare Sustainable Growth Rate formula but also extends other overall Medicare budget cuts for 2 years.
The Senate voted 64-36 on Dec. 18 to approve the Bipartisan Budget Act of 2013 crafted by Senate Budget Committee Chairman Patty Murray (D-Wash.) and House Budget Committee Chairman Paul Ryan (R-Wisc.). Nine Republican senators voted in favor of the deal, joining 55 Democrats.
The 3-month reprieve from the SGR cuts was added to the budget deal by the House before it voted to approve the package on Dec. 12.
Now, if President Obama signs the budget bill, which is expected, physicians will see 0.5% a month pay increase through Mar. 31.
The Congressional Budget Office estimated that the temporary fix would cost $3.3 billion in 2014 and a total of $7.3 billion through 2023. It would be paid for by cutting Medicaid payments for hospital-based charity care and to long-term care hospitals.
The bill also would extend the 2% sequestration cut to Medicare payments by 2 years, to 2023.
The House has recessed and is not due back until Jan. 7. The Senate has not set its adjournment date yet, but is expected to reconvene on Jan. 6.
Congress is expected to start consideration again of a permanent replacement for the SGR when it returns.
On Twitter @aliciaault
The Senate has passed a budget package that includes a 3-month delay in physician pay cuts mandated by the Medicare Sustainable Growth Rate formula but also extends other overall Medicare budget cuts for 2 years.
The Senate voted 64-36 on Dec. 18 to approve the Bipartisan Budget Act of 2013 crafted by Senate Budget Committee Chairman Patty Murray (D-Wash.) and House Budget Committee Chairman Paul Ryan (R-Wisc.). Nine Republican senators voted in favor of the deal, joining 55 Democrats.
The 3-month reprieve from the SGR cuts was added to the budget deal by the House before it voted to approve the package on Dec. 12.
Now, if President Obama signs the budget bill, which is expected, physicians will see 0.5% a month pay increase through Mar. 31.
The Congressional Budget Office estimated that the temporary fix would cost $3.3 billion in 2014 and a total of $7.3 billion through 2023. It would be paid for by cutting Medicaid payments for hospital-based charity care and to long-term care hospitals.
The bill also would extend the 2% sequestration cut to Medicare payments by 2 years, to 2023.
The House has recessed and is not due back until Jan. 7. The Senate has not set its adjournment date yet, but is expected to reconvene on Jan. 6.
Congress is expected to start consideration again of a permanent replacement for the SGR when it returns.
On Twitter @aliciaault
The Senate has passed a budget package that includes a 3-month delay in physician pay cuts mandated by the Medicare Sustainable Growth Rate formula but also extends other overall Medicare budget cuts for 2 years.
The Senate voted 64-36 on Dec. 18 to approve the Bipartisan Budget Act of 2013 crafted by Senate Budget Committee Chairman Patty Murray (D-Wash.) and House Budget Committee Chairman Paul Ryan (R-Wisc.). Nine Republican senators voted in favor of the deal, joining 55 Democrats.
The 3-month reprieve from the SGR cuts was added to the budget deal by the House before it voted to approve the package on Dec. 12.
Now, if President Obama signs the budget bill, which is expected, physicians will see 0.5% a month pay increase through Mar. 31.
The Congressional Budget Office estimated that the temporary fix would cost $3.3 billion in 2014 and a total of $7.3 billion through 2023. It would be paid for by cutting Medicaid payments for hospital-based charity care and to long-term care hospitals.
The bill also would extend the 2% sequestration cut to Medicare payments by 2 years, to 2023.
The House has recessed and is not due back until Jan. 7. The Senate has not set its adjournment date yet, but is expected to reconvene on Jan. 6.
Congress is expected to start consideration again of a permanent replacement for the SGR when it returns.
On Twitter @aliciaault
Physicians, vendors behind schedule on ICD-10
Physicians, vendors, and health insurance plans are moving forward with their preparations for the ICD-10 coding set, but they aren’t moving fast enough, a survey has shown.
Unless the industry speeds up its work in early 2014, there won’t be adequate time for end-to-end testing and payments could be disrupted when the new code set – formally known as the International Statistical Classification of Diseases and Related Health Problems, 10th Revision – takes effect on Oct. 1, 2014, according to the survey from the Workgroup for Electronic Data Interchange (WEDI).
"Based on the survey results, it is clear the industry continues to make slow progress, but not the amount of progress that is needed for a smooth transition," Jim Daley, chairman of the WEDI, a public-private health information technology group that advises the Health and Human Services department, wrote in a letter to the agency.
The WEDI has been surveying the industry since 2009 to gauge progress toward ICD-10 implementation. The latest results come from an October 2013 survey of providers, vendors, and health plans.
Nearly a quarter of 196 physician practices, hospitals, and health systems surveyed planned to begin their own internal testing of business processes and systems changes by the end of 2013, and just under half said they would conduct internal testing in the first half of 2014. The remaining providers surveyed planned to begin internal testing later in 2014 or did not know when it would occur.
This is far behind the goals set in the WEDI/NCHICA timeline, which call for completing internal testing in July 2013 to leave time for external testing with payers throughout 2014.
Health plans and vendors also have some catching up to do, according to the survey results. Of the 59 vendors surveyed, about one-fifth said they were halfway or less than halfway complete with product development, a task that was supposed to be done by the end of 2011, according to the suggested timeline. And about one-third of the 98 health insurance plans that responded said they have already begun or expect to begin external testing by the end of 2013, leaving most health plans less than 9 months to complete external testing.
mschneider@frontlinemedcom.com
On Twitter @MaryEllenNY
Physicians, vendors, and health insurance plans are moving forward with their preparations for the ICD-10 coding set, but they aren’t moving fast enough, a survey has shown.
Unless the industry speeds up its work in early 2014, there won’t be adequate time for end-to-end testing and payments could be disrupted when the new code set – formally known as the International Statistical Classification of Diseases and Related Health Problems, 10th Revision – takes effect on Oct. 1, 2014, according to the survey from the Workgroup for Electronic Data Interchange (WEDI).
"Based on the survey results, it is clear the industry continues to make slow progress, but not the amount of progress that is needed for a smooth transition," Jim Daley, chairman of the WEDI, a public-private health information technology group that advises the Health and Human Services department, wrote in a letter to the agency.
The WEDI has been surveying the industry since 2009 to gauge progress toward ICD-10 implementation. The latest results come from an October 2013 survey of providers, vendors, and health plans.
Nearly a quarter of 196 physician practices, hospitals, and health systems surveyed planned to begin their own internal testing of business processes and systems changes by the end of 2013, and just under half said they would conduct internal testing in the first half of 2014. The remaining providers surveyed planned to begin internal testing later in 2014 or did not know when it would occur.
This is far behind the goals set in the WEDI/NCHICA timeline, which call for completing internal testing in July 2013 to leave time for external testing with payers throughout 2014.
Health plans and vendors also have some catching up to do, according to the survey results. Of the 59 vendors surveyed, about one-fifth said they were halfway or less than halfway complete with product development, a task that was supposed to be done by the end of 2011, according to the suggested timeline. And about one-third of the 98 health insurance plans that responded said they have already begun or expect to begin external testing by the end of 2013, leaving most health plans less than 9 months to complete external testing.
mschneider@frontlinemedcom.com
On Twitter @MaryEllenNY
Physicians, vendors, and health insurance plans are moving forward with their preparations for the ICD-10 coding set, but they aren’t moving fast enough, a survey has shown.
Unless the industry speeds up its work in early 2014, there won’t be adequate time for end-to-end testing and payments could be disrupted when the new code set – formally known as the International Statistical Classification of Diseases and Related Health Problems, 10th Revision – takes effect on Oct. 1, 2014, according to the survey from the Workgroup for Electronic Data Interchange (WEDI).
"Based on the survey results, it is clear the industry continues to make slow progress, but not the amount of progress that is needed for a smooth transition," Jim Daley, chairman of the WEDI, a public-private health information technology group that advises the Health and Human Services department, wrote in a letter to the agency.
The WEDI has been surveying the industry since 2009 to gauge progress toward ICD-10 implementation. The latest results come from an October 2013 survey of providers, vendors, and health plans.
Nearly a quarter of 196 physician practices, hospitals, and health systems surveyed planned to begin their own internal testing of business processes and systems changes by the end of 2013, and just under half said they would conduct internal testing in the first half of 2014. The remaining providers surveyed planned to begin internal testing later in 2014 or did not know when it would occur.
This is far behind the goals set in the WEDI/NCHICA timeline, which call for completing internal testing in July 2013 to leave time for external testing with payers throughout 2014.
Health plans and vendors also have some catching up to do, according to the survey results. Of the 59 vendors surveyed, about one-fifth said they were halfway or less than halfway complete with product development, a task that was supposed to be done by the end of 2011, according to the suggested timeline. And about one-third of the 98 health insurance plans that responded said they have already begun or expect to begin external testing by the end of 2013, leaving most health plans less than 9 months to complete external testing.
mschneider@frontlinemedcom.com
On Twitter @MaryEllenNY
HHS call for insurer flexibility meets some doctors’ concerns
Changes designed to make it easier for consumers to buy insurance through the health insurance exchanges address some concerns raised by physicians.
In a rule issued Dec. 12, the Health and Human Services department formalized a requirement that insurers give consumers until Dec. 23 to choose a health insurance plan and until midnight Dec. 31 to pay for it, in order to be considered covered on Jan. 1. State exchanges can set their own rules about Jan. 1 coverage dates, and in some cases, already have, Chiquita Brooks-Lasure, policy director for the HHS center for consumer information and insurance oversight, said during a press briefing.
Some states may elect to allow payment later than Dec. 31, she said. The HHS is asking insurers to consider accepting payment after Jan. 1 and retroactively cover services. Ms. Brooks-Lasure said that Aetna has already said it will accept payment until Jan. 8.
Insurers are also being asked to accept partial payment for the first month’s premium. Payment flexibility "will reduce the risk that patients will start the year without coverage," said Bob Doherty, senior vice president for governmental affairs and public policy at the American College of Physicians.
The agency is also "strongly encouraging" insurers to consider out-of-network providers as in network and to pay for prescription refills even if the drug is not covered under its plan – at least for the month of January.
The request has precedents, Michael Hash, director of the HHS office of health reform, said during the briefing. "This transition opportunity is quite common in the insurance world."
Mr. Doherty said the ACP hopes that "the insurance industry does its part to help ease the transition, especially by allowing patients who are in a course of treatment to keep seeing their doctors even when they are not in the plan’s network and to continue to get the drugs prescribed for them if not on the plan’s formulary."
Physician groups have asked that such a transition period be considered. At a White House meeting on Nov. 26, they expressed concern that patients in the midst of expensive or specialized treatment might experience a major disruption in care if forced to give up a particular physician or therapy when switching to a new plan.
Mr. Hash said insurers were open to accommodating new enrollees. He said the HHS and insurance companies are working together to "make sure that everyone seeking coverage effective Jan. 1 gets coverage."
The HHS also announced on Dec. 12 that the almost 86,000 individuals in the federal high-risk pool, known as the Pre-Existing Condition Insurance Plan (PCIP), have had their coverage extended to Jan. 31. Those policies had been set to expire Dec. 31.
The program has had its share of financial troubles, and in February, the HHS temporarily stopped enrolling new patients. House Republicans charged that the PCIP had been mismanaged and sought to give it more money. That never happened. On the call with reporters, Ms. Brooks Lasure said the program had spent only $4.74 billion of the $5 billion allotted to it under the Affordable Care Act (ACA), and thus, could afford to pay for the additional month.
The American Cancer Society Cancer Action Network (ACSCAN) applauded the PCIP extension. "Extending coverage under PCIP gives patients valuable additional time to select the marketplace plan that best meets their unique needs," ACSCAN president Chris Hansen said in a statement.
House Republicans, however, portrayed the PCIP policy change as "another delay" in ACA implementation. "The administration has known for many months that this law was not ready for prime time, and Americans who depend on high-risk pools would have been better served by the administration admitting their failures sooner and working with the Congress to protect these and other Americans being harmed by the health care law," House Energy and Commerce Committee Chairman Fred Upton (R-Mich.) said in a statement.
On Twitter @aliciaault
Changes designed to make it easier for consumers to buy insurance through the health insurance exchanges address some concerns raised by physicians.
In a rule issued Dec. 12, the Health and Human Services department formalized a requirement that insurers give consumers until Dec. 23 to choose a health insurance plan and until midnight Dec. 31 to pay for it, in order to be considered covered on Jan. 1. State exchanges can set their own rules about Jan. 1 coverage dates, and in some cases, already have, Chiquita Brooks-Lasure, policy director for the HHS center for consumer information and insurance oversight, said during a press briefing.
Some states may elect to allow payment later than Dec. 31, she said. The HHS is asking insurers to consider accepting payment after Jan. 1 and retroactively cover services. Ms. Brooks-Lasure said that Aetna has already said it will accept payment until Jan. 8.
Insurers are also being asked to accept partial payment for the first month’s premium. Payment flexibility "will reduce the risk that patients will start the year without coverage," said Bob Doherty, senior vice president for governmental affairs and public policy at the American College of Physicians.
The agency is also "strongly encouraging" insurers to consider out-of-network providers as in network and to pay for prescription refills even if the drug is not covered under its plan – at least for the month of January.
The request has precedents, Michael Hash, director of the HHS office of health reform, said during the briefing. "This transition opportunity is quite common in the insurance world."
Mr. Doherty said the ACP hopes that "the insurance industry does its part to help ease the transition, especially by allowing patients who are in a course of treatment to keep seeing their doctors even when they are not in the plan’s network and to continue to get the drugs prescribed for them if not on the plan’s formulary."
Physician groups have asked that such a transition period be considered. At a White House meeting on Nov. 26, they expressed concern that patients in the midst of expensive or specialized treatment might experience a major disruption in care if forced to give up a particular physician or therapy when switching to a new plan.
Mr. Hash said insurers were open to accommodating new enrollees. He said the HHS and insurance companies are working together to "make sure that everyone seeking coverage effective Jan. 1 gets coverage."
The HHS also announced on Dec. 12 that the almost 86,000 individuals in the federal high-risk pool, known as the Pre-Existing Condition Insurance Plan (PCIP), have had their coverage extended to Jan. 31. Those policies had been set to expire Dec. 31.
The program has had its share of financial troubles, and in February, the HHS temporarily stopped enrolling new patients. House Republicans charged that the PCIP had been mismanaged and sought to give it more money. That never happened. On the call with reporters, Ms. Brooks Lasure said the program had spent only $4.74 billion of the $5 billion allotted to it under the Affordable Care Act (ACA), and thus, could afford to pay for the additional month.
The American Cancer Society Cancer Action Network (ACSCAN) applauded the PCIP extension. "Extending coverage under PCIP gives patients valuable additional time to select the marketplace plan that best meets their unique needs," ACSCAN president Chris Hansen said in a statement.
House Republicans, however, portrayed the PCIP policy change as "another delay" in ACA implementation. "The administration has known for many months that this law was not ready for prime time, and Americans who depend on high-risk pools would have been better served by the administration admitting their failures sooner and working with the Congress to protect these and other Americans being harmed by the health care law," House Energy and Commerce Committee Chairman Fred Upton (R-Mich.) said in a statement.
On Twitter @aliciaault
Changes designed to make it easier for consumers to buy insurance through the health insurance exchanges address some concerns raised by physicians.
In a rule issued Dec. 12, the Health and Human Services department formalized a requirement that insurers give consumers until Dec. 23 to choose a health insurance plan and until midnight Dec. 31 to pay for it, in order to be considered covered on Jan. 1. State exchanges can set their own rules about Jan. 1 coverage dates, and in some cases, already have, Chiquita Brooks-Lasure, policy director for the HHS center for consumer information and insurance oversight, said during a press briefing.
Some states may elect to allow payment later than Dec. 31, she said. The HHS is asking insurers to consider accepting payment after Jan. 1 and retroactively cover services. Ms. Brooks-Lasure said that Aetna has already said it will accept payment until Jan. 8.
Insurers are also being asked to accept partial payment for the first month’s premium. Payment flexibility "will reduce the risk that patients will start the year without coverage," said Bob Doherty, senior vice president for governmental affairs and public policy at the American College of Physicians.
The agency is also "strongly encouraging" insurers to consider out-of-network providers as in network and to pay for prescription refills even if the drug is not covered under its plan – at least for the month of January.
The request has precedents, Michael Hash, director of the HHS office of health reform, said during the briefing. "This transition opportunity is quite common in the insurance world."
Mr. Doherty said the ACP hopes that "the insurance industry does its part to help ease the transition, especially by allowing patients who are in a course of treatment to keep seeing their doctors even when they are not in the plan’s network and to continue to get the drugs prescribed for them if not on the plan’s formulary."
Physician groups have asked that such a transition period be considered. At a White House meeting on Nov. 26, they expressed concern that patients in the midst of expensive or specialized treatment might experience a major disruption in care if forced to give up a particular physician or therapy when switching to a new plan.
Mr. Hash said insurers were open to accommodating new enrollees. He said the HHS and insurance companies are working together to "make sure that everyone seeking coverage effective Jan. 1 gets coverage."
The HHS also announced on Dec. 12 that the almost 86,000 individuals in the federal high-risk pool, known as the Pre-Existing Condition Insurance Plan (PCIP), have had their coverage extended to Jan. 31. Those policies had been set to expire Dec. 31.
The program has had its share of financial troubles, and in February, the HHS temporarily stopped enrolling new patients. House Republicans charged that the PCIP had been mismanaged and sought to give it more money. That never happened. On the call with reporters, Ms. Brooks Lasure said the program had spent only $4.74 billion of the $5 billion allotted to it under the Affordable Care Act (ACA), and thus, could afford to pay for the additional month.
The American Cancer Society Cancer Action Network (ACSCAN) applauded the PCIP extension. "Extending coverage under PCIP gives patients valuable additional time to select the marketplace plan that best meets their unique needs," ACSCAN president Chris Hansen said in a statement.
House Republicans, however, portrayed the PCIP policy change as "another delay" in ACA implementation. "The administration has known for many months that this law was not ready for prime time, and Americans who depend on high-risk pools would have been better served by the administration admitting their failures sooner and working with the Congress to protect these and other Americans being harmed by the health care law," House Energy and Commerce Committee Chairman Fred Upton (R-Mich.) said in a statement.
On Twitter @aliciaault
House budget includes SGR patch; permanent fix sails through committees
WASHINGTON – Congress has moved the ball forward on permanently replacing the Medicare Sustainable Growth Rate formula, but with time short for a fix by year’s end the House has voted to approve a temporary 3-month reprieve from the 20% cut due to take effect Jan. 1.
In a 332-94 vote, with eight abstentions, the House on Dec. 12 approved the Bipartisan Budget Act of 2013, a wide-ranging budget agreement that includes the 3-month patch. The bill also would increase physician pay by 0.5% through March.
The Congressional Budget Office estimated that the temporary fix would cost $3.3 billion in 2014 and a total of $7.3 billion through 2023. The fix would be paid for by cutting Medicaid payments for hospital-based charity care and to long-term care hospitals.
It also would extend the 2% sequestration cuts for Medicare providers by 2 years, from 2021 to 2023.
The Senate has yet to consider the budget package including the SGR patch; it is expected to do so before its holiday recess. President Obama has said that he supports the deal.
The agreement, brokered by House Budget Committee Chairman Paul Ryan (R-Wisc.) and Senate Budget Committee Chairman Patty Murray (D-Wash.), adds about $63 billion in discretionary federal spending over 2 years and makes targeted cuts and fee hikes to bring about overall deficit reduction of about $23 billion.
Although physician groups aren’t thrilled about the continuation of the Medicare cuts under sequestration, most favor the temporary SGR reprieve and the restoration of some funding to federal health programs.
Dr. Ardis Dee Hoven, president of the American Medical Association, said that the continuation of the sequester cuts in Medicare is "frustrating" and poses the risk of destabilizing physician practices. "The concept of the sequester is probably not the best way to rein in spending," she said.
Dr. Clifford A. Hudis, president of the American Society of Clinical Oncology, praised the agreement for providing funds that could restore cuts in medical research and cancer care at the National Institutes of Health. He expressed disappointment, however, that the bill does not reverse cuts to Medicare, including reductions in the payments for physician-administered drugs under Medicare Part B.
"Oncologists are doing everything possible to continue providing care for Medicare patients, but this reduction has forced many in private practice to send patients to hospitals for chemotherapy because they cannot afford to administer these drugs in their office," Dr. Hudis said in a statement.
Physician organizations viewed the patch as necessary while Congress continues to work on a permanent SGR fix. Both the House and Senate took steps toward that goal on Dec. 12.
The House Ways and Means Committee voted 39-0 to approve its replacement proposal, which essentially adds on to the bill approved by the House Energy and Commerce Committee in July.
"This may not be the final step, it’s a very important step forward," said Rep. Kevin Brady (R-Tex.), chairman of the Ways and Means Health Subcommittee.
The House did not address how to pay for the permanent replacement. House Ways and Means Chairman Dave Camp (R-Mich.) noted that the Congressional Budget Office has estimated that it will cost $116 billion over 10 years to repeal the SGR, which is "more than half the cost 2 years ago." Even though that is the lowest estimate ever, "I am of no illusion that finding pay-fors will be an easy task," he said.
The Senate Finance Committee also did not include a way to pay for repeal in its proposal.
The bill had widespread bipartisan support in the committee, but some Senators raised concerns about the lack of a funding mechanism. Sen. Pat Roberts (R-Kan.) said that he wouldn’t support the bill until he could see how it would be funded.
Sen. Orrin Hatch (R- Utah), the committee’s top-ranking Republican, said that the offsets would be worked out once the bill had cleared the initial policymaking phase.
"This bill will be offset, period, or it’s not going to go through both houses," he said. "This bill will be paid for."
The panel agreed to add a provision aimed at expanding access to community mental health services. The amendment, offered by Sen. Debbie Stabenow (D-Mich.) and Sen. Roy Blunt (R-Mo.), would create pilot programs in 10 states to ensure that community behavioral health clinics offer a full range of mental health services, including 24-hour crisis care, substance abuse treatment, and expanded support for families.
Physician groups praised the continued congressional action.
The AMA "strongly commends members of the House Ways and Means Committee and the Senate Finance Committee for the tremendous progress they have made toward repealing Medicare’s failed Sustainable Growth Rate (SGR) formula and creating a stronger Medicare program," Dr. Hoven said in a statement. "The AMA will continue to work collaboratively with Congress so that a bipartisan agreement can be signed into law early next year to repeal the failed SGR payment formula."
The American College of Physicians said that it, too, would work to ensure that a bill moves through Congress and gets to the White House for approval soon.
"The bills reported today ... will help ensure that Medicare patients continue to have access to their physicians," said Dr. Charles Cutler, chairman of the ACP Board of Regents. "Their efforts will work to stabilize payments, provide multiple pathways for physicians to qualify for positive updates and to participate in alternative payment models, create positive incentives for patient-centered medical homes, provide assistance to small practices, and needed funding for development of quality measures."
The American College of Cardiology said in a statement that the proposals accomplished two of its highest priorities: eliminating the SGR and including provisions that will emphasize quality of care, including "provisions that emphasize the importance of clinical data registries, quality measure development, and appropriate use criteria to promote evidence-based care."
"We caution that our final support rests upon the caveat that paying for this legislation must not cause harm to patients and the physicians who care for them," Dr. John Gordon Harold, ACC president, said in the statement.
Legislators from the Finance Committee and the Ways and Means Committee celebrated their votes in a joint statement. In the statement, Sen. Hatch also issued a word of caution.
"Now that this legislation moves out of Committee and onto the floor, we need to continue to work together to ensure that this smart policy becomes law and ensure that it doesn’t add one dime to our nation’s debt."
WASHINGTON – Congress has moved the ball forward on permanently replacing the Medicare Sustainable Growth Rate formula, but with time short for a fix by year’s end the House has voted to approve a temporary 3-month reprieve from the 20% cut due to take effect Jan. 1.
In a 332-94 vote, with eight abstentions, the House on Dec. 12 approved the Bipartisan Budget Act of 2013, a wide-ranging budget agreement that includes the 3-month patch. The bill also would increase physician pay by 0.5% through March.
The Congressional Budget Office estimated that the temporary fix would cost $3.3 billion in 2014 and a total of $7.3 billion through 2023. The fix would be paid for by cutting Medicaid payments for hospital-based charity care and to long-term care hospitals.
It also would extend the 2% sequestration cuts for Medicare providers by 2 years, from 2021 to 2023.
The Senate has yet to consider the budget package including the SGR patch; it is expected to do so before its holiday recess. President Obama has said that he supports the deal.
The agreement, brokered by House Budget Committee Chairman Paul Ryan (R-Wisc.) and Senate Budget Committee Chairman Patty Murray (D-Wash.), adds about $63 billion in discretionary federal spending over 2 years and makes targeted cuts and fee hikes to bring about overall deficit reduction of about $23 billion.
Although physician groups aren’t thrilled about the continuation of the Medicare cuts under sequestration, most favor the temporary SGR reprieve and the restoration of some funding to federal health programs.
Dr. Ardis Dee Hoven, president of the American Medical Association, said that the continuation of the sequester cuts in Medicare is "frustrating" and poses the risk of destabilizing physician practices. "The concept of the sequester is probably not the best way to rein in spending," she said.
Dr. Clifford A. Hudis, president of the American Society of Clinical Oncology, praised the agreement for providing funds that could restore cuts in medical research and cancer care at the National Institutes of Health. He expressed disappointment, however, that the bill does not reverse cuts to Medicare, including reductions in the payments for physician-administered drugs under Medicare Part B.
"Oncologists are doing everything possible to continue providing care for Medicare patients, but this reduction has forced many in private practice to send patients to hospitals for chemotherapy because they cannot afford to administer these drugs in their office," Dr. Hudis said in a statement.
Physician organizations viewed the patch as necessary while Congress continues to work on a permanent SGR fix. Both the House and Senate took steps toward that goal on Dec. 12.
The House Ways and Means Committee voted 39-0 to approve its replacement proposal, which essentially adds on to the bill approved by the House Energy and Commerce Committee in July.
"This may not be the final step, it’s a very important step forward," said Rep. Kevin Brady (R-Tex.), chairman of the Ways and Means Health Subcommittee.
The House did not address how to pay for the permanent replacement. House Ways and Means Chairman Dave Camp (R-Mich.) noted that the Congressional Budget Office has estimated that it will cost $116 billion over 10 years to repeal the SGR, which is "more than half the cost 2 years ago." Even though that is the lowest estimate ever, "I am of no illusion that finding pay-fors will be an easy task," he said.
The Senate Finance Committee also did not include a way to pay for repeal in its proposal.
The bill had widespread bipartisan support in the committee, but some Senators raised concerns about the lack of a funding mechanism. Sen. Pat Roberts (R-Kan.) said that he wouldn’t support the bill until he could see how it would be funded.
Sen. Orrin Hatch (R- Utah), the committee’s top-ranking Republican, said that the offsets would be worked out once the bill had cleared the initial policymaking phase.
"This bill will be offset, period, or it’s not going to go through both houses," he said. "This bill will be paid for."
The panel agreed to add a provision aimed at expanding access to community mental health services. The amendment, offered by Sen. Debbie Stabenow (D-Mich.) and Sen. Roy Blunt (R-Mo.), would create pilot programs in 10 states to ensure that community behavioral health clinics offer a full range of mental health services, including 24-hour crisis care, substance abuse treatment, and expanded support for families.
Physician groups praised the continued congressional action.
The AMA "strongly commends members of the House Ways and Means Committee and the Senate Finance Committee for the tremendous progress they have made toward repealing Medicare’s failed Sustainable Growth Rate (SGR) formula and creating a stronger Medicare program," Dr. Hoven said in a statement. "The AMA will continue to work collaboratively with Congress so that a bipartisan agreement can be signed into law early next year to repeal the failed SGR payment formula."
The American College of Physicians said that it, too, would work to ensure that a bill moves through Congress and gets to the White House for approval soon.
"The bills reported today ... will help ensure that Medicare patients continue to have access to their physicians," said Dr. Charles Cutler, chairman of the ACP Board of Regents. "Their efforts will work to stabilize payments, provide multiple pathways for physicians to qualify for positive updates and to participate in alternative payment models, create positive incentives for patient-centered medical homes, provide assistance to small practices, and needed funding for development of quality measures."
The American College of Cardiology said in a statement that the proposals accomplished two of its highest priorities: eliminating the SGR and including provisions that will emphasize quality of care, including "provisions that emphasize the importance of clinical data registries, quality measure development, and appropriate use criteria to promote evidence-based care."
"We caution that our final support rests upon the caveat that paying for this legislation must not cause harm to patients and the physicians who care for them," Dr. John Gordon Harold, ACC president, said in the statement.
Legislators from the Finance Committee and the Ways and Means Committee celebrated their votes in a joint statement. In the statement, Sen. Hatch also issued a word of caution.
"Now that this legislation moves out of Committee and onto the floor, we need to continue to work together to ensure that this smart policy becomes law and ensure that it doesn’t add one dime to our nation’s debt."
WASHINGTON – Congress has moved the ball forward on permanently replacing the Medicare Sustainable Growth Rate formula, but with time short for a fix by year’s end the House has voted to approve a temporary 3-month reprieve from the 20% cut due to take effect Jan. 1.
In a 332-94 vote, with eight abstentions, the House on Dec. 12 approved the Bipartisan Budget Act of 2013, a wide-ranging budget agreement that includes the 3-month patch. The bill also would increase physician pay by 0.5% through March.
The Congressional Budget Office estimated that the temporary fix would cost $3.3 billion in 2014 and a total of $7.3 billion through 2023. The fix would be paid for by cutting Medicaid payments for hospital-based charity care and to long-term care hospitals.
It also would extend the 2% sequestration cuts for Medicare providers by 2 years, from 2021 to 2023.
The Senate has yet to consider the budget package including the SGR patch; it is expected to do so before its holiday recess. President Obama has said that he supports the deal.
The agreement, brokered by House Budget Committee Chairman Paul Ryan (R-Wisc.) and Senate Budget Committee Chairman Patty Murray (D-Wash.), adds about $63 billion in discretionary federal spending over 2 years and makes targeted cuts and fee hikes to bring about overall deficit reduction of about $23 billion.
Although physician groups aren’t thrilled about the continuation of the Medicare cuts under sequestration, most favor the temporary SGR reprieve and the restoration of some funding to federal health programs.
Dr. Ardis Dee Hoven, president of the American Medical Association, said that the continuation of the sequester cuts in Medicare is "frustrating" and poses the risk of destabilizing physician practices. "The concept of the sequester is probably not the best way to rein in spending," she said.
Dr. Clifford A. Hudis, president of the American Society of Clinical Oncology, praised the agreement for providing funds that could restore cuts in medical research and cancer care at the National Institutes of Health. He expressed disappointment, however, that the bill does not reverse cuts to Medicare, including reductions in the payments for physician-administered drugs under Medicare Part B.
"Oncologists are doing everything possible to continue providing care for Medicare patients, but this reduction has forced many in private practice to send patients to hospitals for chemotherapy because they cannot afford to administer these drugs in their office," Dr. Hudis said in a statement.
Physician organizations viewed the patch as necessary while Congress continues to work on a permanent SGR fix. Both the House and Senate took steps toward that goal on Dec. 12.
The House Ways and Means Committee voted 39-0 to approve its replacement proposal, which essentially adds on to the bill approved by the House Energy and Commerce Committee in July.
"This may not be the final step, it’s a very important step forward," said Rep. Kevin Brady (R-Tex.), chairman of the Ways and Means Health Subcommittee.
The House did not address how to pay for the permanent replacement. House Ways and Means Chairman Dave Camp (R-Mich.) noted that the Congressional Budget Office has estimated that it will cost $116 billion over 10 years to repeal the SGR, which is "more than half the cost 2 years ago." Even though that is the lowest estimate ever, "I am of no illusion that finding pay-fors will be an easy task," he said.
The Senate Finance Committee also did not include a way to pay for repeal in its proposal.
The bill had widespread bipartisan support in the committee, but some Senators raised concerns about the lack of a funding mechanism. Sen. Pat Roberts (R-Kan.) said that he wouldn’t support the bill until he could see how it would be funded.
Sen. Orrin Hatch (R- Utah), the committee’s top-ranking Republican, said that the offsets would be worked out once the bill had cleared the initial policymaking phase.
"This bill will be offset, period, or it’s not going to go through both houses," he said. "This bill will be paid for."
The panel agreed to add a provision aimed at expanding access to community mental health services. The amendment, offered by Sen. Debbie Stabenow (D-Mich.) and Sen. Roy Blunt (R-Mo.), would create pilot programs in 10 states to ensure that community behavioral health clinics offer a full range of mental health services, including 24-hour crisis care, substance abuse treatment, and expanded support for families.
Physician groups praised the continued congressional action.
The AMA "strongly commends members of the House Ways and Means Committee and the Senate Finance Committee for the tremendous progress they have made toward repealing Medicare’s failed Sustainable Growth Rate (SGR) formula and creating a stronger Medicare program," Dr. Hoven said in a statement. "The AMA will continue to work collaboratively with Congress so that a bipartisan agreement can be signed into law early next year to repeal the failed SGR payment formula."
The American College of Physicians said that it, too, would work to ensure that a bill moves through Congress and gets to the White House for approval soon.
"The bills reported today ... will help ensure that Medicare patients continue to have access to their physicians," said Dr. Charles Cutler, chairman of the ACP Board of Regents. "Their efforts will work to stabilize payments, provide multiple pathways for physicians to qualify for positive updates and to participate in alternative payment models, create positive incentives for patient-centered medical homes, provide assistance to small practices, and needed funding for development of quality measures."
The American College of Cardiology said in a statement that the proposals accomplished two of its highest priorities: eliminating the SGR and including provisions that will emphasize quality of care, including "provisions that emphasize the importance of clinical data registries, quality measure development, and appropriate use criteria to promote evidence-based care."
"We caution that our final support rests upon the caveat that paying for this legislation must not cause harm to patients and the physicians who care for them," Dr. John Gordon Harold, ACC president, said in the statement.
Legislators from the Finance Committee and the Ways and Means Committee celebrated their votes in a joint statement. In the statement, Sen. Hatch also issued a word of caution.
"Now that this legislation moves out of Committee and onto the floor, we need to continue to work together to ensure that this smart policy becomes law and ensure that it doesn’t add one dime to our nation’s debt."
Congress poised to vote on 3-month SGR patch
WASHINGTON – Congress is preparing to vote on a proposal that would give physicians a temporary 3-month reprieve from the 20% Medicare pay cut that’s due to take effect on Jan. 1.
The proposal was quickly attached to legislation federal budget legislation that would also ameliorate some of the automatic, across-the-board spending cuts known as sequestration.
The House is scheduled to vote on the budget measure before it leaves for a month-long recess on Dec. 13. It is expected that the "doc fix" proposal could be voted on within the same time frame; however, it may not get support of the full House, even though there is bipartisan consensus to replace the Sustainable Growth Rate formula.
At a House Rules Committee hearing on Dec. 11, Democratic leaders said that they would not support the temporary SGR patch unless Republicans agreed to also vote on restoring unemployment compensation benefits for 3 months. Those benefits are due to expire at the end of December for 1.3 million Americans.
"I’m not sure that Democrats can vote for a package that adds SGR, which we support, but does not allow us to address long-term unemployment," said Rep. Nita Lowey (D-N.Y.).
The SGR amendment would increase physician fees by 0.5% for January-March 2014 and encourage Congress to keep working on a new, permanent Medicare fee system teamed with reduced administrative burdens and timely feedback on performance and to develop new payment models.
The temporary fix would be paid for by adjusting disproportionate share payments for hospitals, according to Rep. Michael Burgess (R-Tex.), an ob.gyn. who serves on the Rules Committee. The payment mechanism is noncontroversial, he said in an interview.
Physician groups have said that they would support a short-term fix, provided lawmakers continue working on a permanent repeal of the SGR.
"This is simply a pathway," Dr. Ardis Dee Hoven, president of the American Medical Association, said in an interview. "We want to keep up the momentum to get the SGR repealed. We recognize that it’s going to take a little more time."
Dr. Molly Cooke, president of the American College of Physicians, agreed. "This measure will allow Congress time to complete work early next year on comprehensive legislation to repeal the Medicare SGR formula," she said in a statement.
The Senate Finance Committee and the House Ways and Means Committee are both meeting to vote on proposals to permanently replace the SGR on Dec. 12.
On Twitter @aliciaault
WASHINGTON – Congress is preparing to vote on a proposal that would give physicians a temporary 3-month reprieve from the 20% Medicare pay cut that’s due to take effect on Jan. 1.
The proposal was quickly attached to legislation federal budget legislation that would also ameliorate some of the automatic, across-the-board spending cuts known as sequestration.
The House is scheduled to vote on the budget measure before it leaves for a month-long recess on Dec. 13. It is expected that the "doc fix" proposal could be voted on within the same time frame; however, it may not get support of the full House, even though there is bipartisan consensus to replace the Sustainable Growth Rate formula.
At a House Rules Committee hearing on Dec. 11, Democratic leaders said that they would not support the temporary SGR patch unless Republicans agreed to also vote on restoring unemployment compensation benefits for 3 months. Those benefits are due to expire at the end of December for 1.3 million Americans.
"I’m not sure that Democrats can vote for a package that adds SGR, which we support, but does not allow us to address long-term unemployment," said Rep. Nita Lowey (D-N.Y.).
The SGR amendment would increase physician fees by 0.5% for January-March 2014 and encourage Congress to keep working on a new, permanent Medicare fee system teamed with reduced administrative burdens and timely feedback on performance and to develop new payment models.
The temporary fix would be paid for by adjusting disproportionate share payments for hospitals, according to Rep. Michael Burgess (R-Tex.), an ob.gyn. who serves on the Rules Committee. The payment mechanism is noncontroversial, he said in an interview.
Physician groups have said that they would support a short-term fix, provided lawmakers continue working on a permanent repeal of the SGR.
"This is simply a pathway," Dr. Ardis Dee Hoven, president of the American Medical Association, said in an interview. "We want to keep up the momentum to get the SGR repealed. We recognize that it’s going to take a little more time."
Dr. Molly Cooke, president of the American College of Physicians, agreed. "This measure will allow Congress time to complete work early next year on comprehensive legislation to repeal the Medicare SGR formula," she said in a statement.
The Senate Finance Committee and the House Ways and Means Committee are both meeting to vote on proposals to permanently replace the SGR on Dec. 12.
On Twitter @aliciaault
WASHINGTON – Congress is preparing to vote on a proposal that would give physicians a temporary 3-month reprieve from the 20% Medicare pay cut that’s due to take effect on Jan. 1.
The proposal was quickly attached to legislation federal budget legislation that would also ameliorate some of the automatic, across-the-board spending cuts known as sequestration.
The House is scheduled to vote on the budget measure before it leaves for a month-long recess on Dec. 13. It is expected that the "doc fix" proposal could be voted on within the same time frame; however, it may not get support of the full House, even though there is bipartisan consensus to replace the Sustainable Growth Rate formula.
At a House Rules Committee hearing on Dec. 11, Democratic leaders said that they would not support the temporary SGR patch unless Republicans agreed to also vote on restoring unemployment compensation benefits for 3 months. Those benefits are due to expire at the end of December for 1.3 million Americans.
"I’m not sure that Democrats can vote for a package that adds SGR, which we support, but does not allow us to address long-term unemployment," said Rep. Nita Lowey (D-N.Y.).
The SGR amendment would increase physician fees by 0.5% for January-March 2014 and encourage Congress to keep working on a new, permanent Medicare fee system teamed with reduced administrative burdens and timely feedback on performance and to develop new payment models.
The temporary fix would be paid for by adjusting disproportionate share payments for hospitals, according to Rep. Michael Burgess (R-Tex.), an ob.gyn. who serves on the Rules Committee. The payment mechanism is noncontroversial, he said in an interview.
Physician groups have said that they would support a short-term fix, provided lawmakers continue working on a permanent repeal of the SGR.
"This is simply a pathway," Dr. Ardis Dee Hoven, president of the American Medical Association, said in an interview. "We want to keep up the momentum to get the SGR repealed. We recognize that it’s going to take a little more time."
Dr. Molly Cooke, president of the American College of Physicians, agreed. "This measure will allow Congress time to complete work early next year on comprehensive legislation to repeal the Medicare SGR formula," she said in a statement.
The Senate Finance Committee and the House Ways and Means Committee are both meeting to vote on proposals to permanently replace the SGR on Dec. 12.
On Twitter @aliciaault
AT A HOUSE RULES COMMITTEE HEARING
ACA enrollment grows, but still less than expected
Even with a burst of activity on the state and federal health insurance exchanges during November, numbers released Dec. 11 by the Health and Human Services department indicate that the Obama administration may not be on track to meet the goal set by the Congressional Budget Office – insuring 7 million individuals by Mar. 31, 2014, the end of the current open enrollment for health insurance under the Affordable Care Act.
But Michael Hash, director of the HHS Office of Health Reform, said in a briefing with reporters, "We’re on track." Americans still have 6 months to enroll, he noted, and the expectation is that most people will sign up towards the end of that period.
According to HHS’s mid-December enrollment report, 364,682 individuals selected a health insurance plan from a state or federal exchange in October and November. The bulk of those (227,478) used a state-based exchange, while 137,204 signed up via the federal exchange, which operates in 36 states. The biggest proportion of overall sign-ups came in November, with 258,497 selecting a plan in the state or federal exchanges.
The numbers include consumers who have paid their first health insurance premium as well as those who have not.
About 2.3 million Americans have been determined to be eligible to enroll in a marketplace plan, but only 364,000 have actually selected a plan. Of the 2.3 million, 41% (944,531) are eligible for financial assistance. That number includes people who didn’t apply for financial assistance, who applied for financial assistance and were found ineligible, or those whose applications for financial assistance are pending, according to the HHS report.
Further, just over 803,000 consumers have been determined to be eligible for coverage from Medicaid or the Children’s Health Insurance Program (CHIP).
Enrollment has increased in part because of improvements to the federal exchange website, healthcare.gov. Mr. Hash said. "Healthcare.gov is night and day from where it was on October the first," he said in comments made in advance of testimony by HHS Secretary Kathleen Sebelius at a hearing called by the House Energy and Commerce Committee’s Health Subcommittee.
Overall, 83% of completed applications were done electronically, either through healthcare.gov or a state exchange website, or online when individuals applied at a community center or some other assistance location.
Mr. Hash also said that demand for exchange plans continues to grow, citing increasing visits to the federal and state websites and calls to the call centers.
Since Oct. 1, there have been 10.6 million visits to state exchanges and 1.7 million calls to state call centers. There have been 28.4 million visits to healthcare.gov and 3.4 million calls.
On Twitter @aliciaault
Even with a burst of activity on the state and federal health insurance exchanges during November, numbers released Dec. 11 by the Health and Human Services department indicate that the Obama administration may not be on track to meet the goal set by the Congressional Budget Office – insuring 7 million individuals by Mar. 31, 2014, the end of the current open enrollment for health insurance under the Affordable Care Act.
But Michael Hash, director of the HHS Office of Health Reform, said in a briefing with reporters, "We’re on track." Americans still have 6 months to enroll, he noted, and the expectation is that most people will sign up towards the end of that period.
According to HHS’s mid-December enrollment report, 364,682 individuals selected a health insurance plan from a state or federal exchange in October and November. The bulk of those (227,478) used a state-based exchange, while 137,204 signed up via the federal exchange, which operates in 36 states. The biggest proportion of overall sign-ups came in November, with 258,497 selecting a plan in the state or federal exchanges.
The numbers include consumers who have paid their first health insurance premium as well as those who have not.
About 2.3 million Americans have been determined to be eligible to enroll in a marketplace plan, but only 364,000 have actually selected a plan. Of the 2.3 million, 41% (944,531) are eligible for financial assistance. That number includes people who didn’t apply for financial assistance, who applied for financial assistance and were found ineligible, or those whose applications for financial assistance are pending, according to the HHS report.
Further, just over 803,000 consumers have been determined to be eligible for coverage from Medicaid or the Children’s Health Insurance Program (CHIP).
Enrollment has increased in part because of improvements to the federal exchange website, healthcare.gov. Mr. Hash said. "Healthcare.gov is night and day from where it was on October the first," he said in comments made in advance of testimony by HHS Secretary Kathleen Sebelius at a hearing called by the House Energy and Commerce Committee’s Health Subcommittee.
Overall, 83% of completed applications were done electronically, either through healthcare.gov or a state exchange website, or online when individuals applied at a community center or some other assistance location.
Mr. Hash also said that demand for exchange plans continues to grow, citing increasing visits to the federal and state websites and calls to the call centers.
Since Oct. 1, there have been 10.6 million visits to state exchanges and 1.7 million calls to state call centers. There have been 28.4 million visits to healthcare.gov and 3.4 million calls.
On Twitter @aliciaault
Even with a burst of activity on the state and federal health insurance exchanges during November, numbers released Dec. 11 by the Health and Human Services department indicate that the Obama administration may not be on track to meet the goal set by the Congressional Budget Office – insuring 7 million individuals by Mar. 31, 2014, the end of the current open enrollment for health insurance under the Affordable Care Act.
But Michael Hash, director of the HHS Office of Health Reform, said in a briefing with reporters, "We’re on track." Americans still have 6 months to enroll, he noted, and the expectation is that most people will sign up towards the end of that period.
According to HHS’s mid-December enrollment report, 364,682 individuals selected a health insurance plan from a state or federal exchange in October and November. The bulk of those (227,478) used a state-based exchange, while 137,204 signed up via the federal exchange, which operates in 36 states. The biggest proportion of overall sign-ups came in November, with 258,497 selecting a plan in the state or federal exchanges.
The numbers include consumers who have paid their first health insurance premium as well as those who have not.
About 2.3 million Americans have been determined to be eligible to enroll in a marketplace plan, but only 364,000 have actually selected a plan. Of the 2.3 million, 41% (944,531) are eligible for financial assistance. That number includes people who didn’t apply for financial assistance, who applied for financial assistance and were found ineligible, or those whose applications for financial assistance are pending, according to the HHS report.
Further, just over 803,000 consumers have been determined to be eligible for coverage from Medicaid or the Children’s Health Insurance Program (CHIP).
Enrollment has increased in part because of improvements to the federal exchange website, healthcare.gov. Mr. Hash said. "Healthcare.gov is night and day from where it was on October the first," he said in comments made in advance of testimony by HHS Secretary Kathleen Sebelius at a hearing called by the House Energy and Commerce Committee’s Health Subcommittee.
Overall, 83% of completed applications were done electronically, either through healthcare.gov or a state exchange website, or online when individuals applied at a community center or some other assistance location.
Mr. Hash also said that demand for exchange plans continues to grow, citing increasing visits to the federal and state websites and calls to the call centers.
Since Oct. 1, there have been 10.6 million visits to state exchanges and 1.7 million calls to state call centers. There have been 28.4 million visits to healthcare.gov and 3.4 million calls.
On Twitter @aliciaault
CMS extends Stage 2 ‘meaningful use’ reporting through 2016
Medicare officials have extended Stage 2 of the "meaningful use" Electronic Health Record Incentive Program through the end of 2016.
The change, announced on Dec. 6, means that the earliest that physicians will progress to Stage 3 of the meaningful use requirements will be in January 2017. Officials at the Centers for Medicare and Medicaid Services are still developing the Stage 3 requirements and expect to issue a proposed rule sometime in the fall of 2014.
The extension primarily affects physicians who began attesting to meaningful EHR use in 2011 and 2012. Those physicians were scheduled to advance to Stage 3 in 2016, after 2 years of working on Stage 2. The change means that they will have an additional year at Stage 2.
"The goal of this change is twofold: First, to allow CMS and [the Office of the National Coordinator for Health Information Technology] to focus efforts on the successful implementation of the enhanced patient engagement, interoperability, and health information exchange requirements in Stage 2; and second, to utilize data from Stage 2 participation to inform policy decisions for Stage 3," Robert Tagalicod, director of the office of e-Health Standards and Services at the CMS, and Dr. Jacob Reider, acting National Coordinator for Health Information Technology, wrote in a blog post announcing the change.
Over the last several months, a growing number of physician organizations and some lawmakers have called on the government to give physicians more time to meet Stage 2 requirements, saying that pushing forward with the aggressive timetable would leave many rural physicians behind.
"This new proposed timeline tracks ongoing conversations we at CMS and [the Office of the National Coordinator] have had with providers, consumers, health care associations, EHR developers, and other stakeholders in the health care industry," Mr. Tagalicod and Dr. Reider wrote. "This timeline allows for enhanced program analysis of Stage 2 data to inform the improvements in care delivery outcomes in Stage 3."
But Thomas A. Leary, vice president for government relations at HIMSS, said that while the extension of Stage 2 meaningful use is a positive step, his organization still wants to see Medicare officials give physicians a few more months to report on their first year of Stage 2 implementation. The extra time would help physicians, hospitals, and vendors who are having difficulty upgrading to the 2014 EHR certification requirements, according to HIMSS.
mschneider@frontlinemedcom.com
On Twitter @MaryEllenNY
Medicare officials have extended Stage 2 of the "meaningful use" Electronic Health Record Incentive Program through the end of 2016.
The change, announced on Dec. 6, means that the earliest that physicians will progress to Stage 3 of the meaningful use requirements will be in January 2017. Officials at the Centers for Medicare and Medicaid Services are still developing the Stage 3 requirements and expect to issue a proposed rule sometime in the fall of 2014.
The extension primarily affects physicians who began attesting to meaningful EHR use in 2011 and 2012. Those physicians were scheduled to advance to Stage 3 in 2016, after 2 years of working on Stage 2. The change means that they will have an additional year at Stage 2.
"The goal of this change is twofold: First, to allow CMS and [the Office of the National Coordinator for Health Information Technology] to focus efforts on the successful implementation of the enhanced patient engagement, interoperability, and health information exchange requirements in Stage 2; and second, to utilize data from Stage 2 participation to inform policy decisions for Stage 3," Robert Tagalicod, director of the office of e-Health Standards and Services at the CMS, and Dr. Jacob Reider, acting National Coordinator for Health Information Technology, wrote in a blog post announcing the change.
Over the last several months, a growing number of physician organizations and some lawmakers have called on the government to give physicians more time to meet Stage 2 requirements, saying that pushing forward with the aggressive timetable would leave many rural physicians behind.
"This new proposed timeline tracks ongoing conversations we at CMS and [the Office of the National Coordinator] have had with providers, consumers, health care associations, EHR developers, and other stakeholders in the health care industry," Mr. Tagalicod and Dr. Reider wrote. "This timeline allows for enhanced program analysis of Stage 2 data to inform the improvements in care delivery outcomes in Stage 3."
But Thomas A. Leary, vice president for government relations at HIMSS, said that while the extension of Stage 2 meaningful use is a positive step, his organization still wants to see Medicare officials give physicians a few more months to report on their first year of Stage 2 implementation. The extra time would help physicians, hospitals, and vendors who are having difficulty upgrading to the 2014 EHR certification requirements, according to HIMSS.
mschneider@frontlinemedcom.com
On Twitter @MaryEllenNY
Medicare officials have extended Stage 2 of the "meaningful use" Electronic Health Record Incentive Program through the end of 2016.
The change, announced on Dec. 6, means that the earliest that physicians will progress to Stage 3 of the meaningful use requirements will be in January 2017. Officials at the Centers for Medicare and Medicaid Services are still developing the Stage 3 requirements and expect to issue a proposed rule sometime in the fall of 2014.
The extension primarily affects physicians who began attesting to meaningful EHR use in 2011 and 2012. Those physicians were scheduled to advance to Stage 3 in 2016, after 2 years of working on Stage 2. The change means that they will have an additional year at Stage 2.
"The goal of this change is twofold: First, to allow CMS and [the Office of the National Coordinator for Health Information Technology] to focus efforts on the successful implementation of the enhanced patient engagement, interoperability, and health information exchange requirements in Stage 2; and second, to utilize data from Stage 2 participation to inform policy decisions for Stage 3," Robert Tagalicod, director of the office of e-Health Standards and Services at the CMS, and Dr. Jacob Reider, acting National Coordinator for Health Information Technology, wrote in a blog post announcing the change.
Over the last several months, a growing number of physician organizations and some lawmakers have called on the government to give physicians more time to meet Stage 2 requirements, saying that pushing forward with the aggressive timetable would leave many rural physicians behind.
"This new proposed timeline tracks ongoing conversations we at CMS and [the Office of the National Coordinator] have had with providers, consumers, health care associations, EHR developers, and other stakeholders in the health care industry," Mr. Tagalicod and Dr. Reider wrote. "This timeline allows for enhanced program analysis of Stage 2 data to inform the improvements in care delivery outcomes in Stage 3."
But Thomas A. Leary, vice president for government relations at HIMSS, said that while the extension of Stage 2 meaningful use is a positive step, his organization still wants to see Medicare officials give physicians a few more months to report on their first year of Stage 2 implementation. The extra time would help physicians, hospitals, and vendors who are having difficulty upgrading to the 2014 EHR certification requirements, according to HIMSS.
mschneider@frontlinemedcom.com
On Twitter @MaryEllenNY
States take different paths in Medicaid expansion
When the Supreme Court upheld the constitutionality of the Affordable Care Act in 2012, it also ruled that states could choose whether to substantially expand their Medicaid programs. That decision has created a split across the country, with about half of the states choosing to take federal dollars to expand their programs and the others opting out.
There’s no deadline on Medicaid expansion, so those states that have opted out so far can always choose to expand at a later date.

Here’s a look at two bellwether states: California, which has accepted federal money to expand its Medi-Cal program, and Texas, which has opted out of the expansion.
California Gov. Jerry Brown (D), a strong supporter of the ACA, announced that his state would expand Medicaid to include low-income individuals up to 138% of the federal poverty level starting on Jan. 1, 2014. All of the new enrollees – likely 1 million Californians – will be added to the state’s growing Medicaid managed care program.
Conversely, Texas Gov. Rick Perry (R) deemed Medicaid expansion "a misguided, and ultimately doomed, attempt to mask the shortcomings of Obamacare."
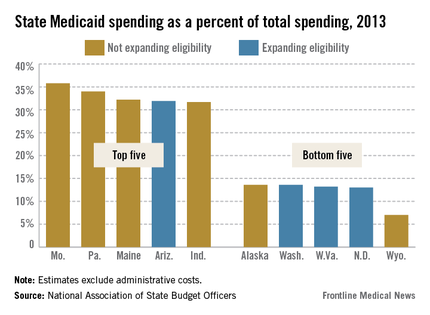
California: Pay cuts complicate expansion
Physicians in California are bracing for a significant Medicaid pay cut at the same time as about a million residents are set to join the program.
The pending cuts are just one part of a complex health care picture in California, where experts are far from certain about what the expansion of Medi-Cal will mean for physicians and patients.
"I think we’re going to have a real problem in California with all the new Medi-Cal patients," said Dr. Mark Dressner, who works at a federally qualified health center in Long Beach and is the president of the California Academy of Family Physicians. "Who is going to see them when there’s going to be so many other people in the system?"
The Kaiser Family Foundation estimates that between 990,000 and 1.4 million individuals, mostly single adults, will enter Medi-Cal by 2019 because of the ACA-permitted expansion. Currently, about 8.5 million residents are enrolled. Newly eligible individuals will be enrolled in the program’s managed care health plans.
These new patients could have a hard time finding a doctor. Medi-Cal is one of the lowest payers in the nation, paying between $18 and $24 for an office visit, according to the California Medical Association.
That’s about to be compounded by a pay cut approved by the state and the Centers for Medicare and Medicaid Services in 2011. Physicians tried unsuccessfully to fight the cut in court. Now the state is implementing it retroactively, which means that Medi-Cal payments could be cut 15%-20% over the next few years.
"It really undermines efforts to successfully implement the Affordable Care Act in California," said Lisa Folberg, vice president of medical and regulatory policy at the California Medical Association.
There are broad exceptions to the cut. It does not apply to most primary care services in either managed care plans or fee-for-service Medi-Cal, or to specialty services provided through managed care plans, Ms. Folberg said. And some managed care companies have announced that they will use their discretion in setting payment rates to shield their contracted physicians from the cuts.
"Unfortunately, that doesn’t help the cancer patient on Medi-Cal in Bakersfield who has fee-for-service Medi-Cal and can’t find an oncologist," Ms. Folberg said.
Dr. Darin Latimore, president of the California chapter of the American College of Physicians, said large health systems likely will be able to work around the cuts, using group visits and physician extenders. But small physician practices in rural areas aren’t equipped to make those changes, he said.
"They are not in a position to move work on to others in order to be more efficient and see more Medi-Cal patients," said Dr. Latimore, associate dean of medicine at the University of California Davis.
The result will be that physicians who work outside of the state’s safety net system will be less likely to participate in the Medi-Cal program or will strictly limit the number of patients they see. That will translate to longer waits to get an appointment and shorter visits for Medi-Cal patients.
Another concern: Patients entering Medi-Cal managed care plans might not have access to a broad network of physicians. While California has network adequacy laws, state oversight is inadequate, according to Ms. Folberg. For the most part, the plans are on an honor system.
There are some bright spots for the Medi-Cal expansion. The ACA includes an increase in Medicaid payments to physicians for 146 primary care services provided in 2013 and 2014. The provision temporarily raises payments up to Medicare rates, which for California physicians means a 136% hike on average, according to an analysis from the Kaiser Family Foundation.
But those payments were delayed, with the first checks going out to physicians in November 2013. That delay could cost the state in physician participation.
"I think the longer it takes to implement that, the less likely it is that it will affect any decisions about whether to participate more fully in the program than you would have otherwise," said Christopher Perrone, deputy director of the health reform and public programs initiative at the California HealthCare Foundation.
And the temporary nature of the pay increase adds to the problem, Mr. Perrone said. "I don’t see California sustaining that increase on its own and I haven’t heard anyone suggest that the federal government would sustain it after the 2 years."
Mr. Perrone said it’s more likely that physicians who are already committed to participating in Medi-Cal will use the money to invest in electronic health records and other telemedicine features, and hire medical assistants.
But with so many small and solo physicians shying away from Medi-Cal because of low payments, community clinics and health centers will have to pick up the slack.
"All these issues together really point to the importance of the community health centers and the role we are going to be playing in ensuring access," said Carmela Castellano-Garcia, president and CEO of the California Primary Care Association.
Federally qualified health centers are in a better position financially because they are paid an enhanced Medicaid rate and won’t be subject to the coming Medi-Cal cuts, Ms. Castellano-Garcia said. And the ACA has directed an influx of cash to these centers as well – more than $500 million in California alone to establish new sites, expand services, and support major capital improvement projects, according to the Health and Human Services department.
Texas: No expansion means doctors will keep feeling pressure
Texas has the highest number of uninsured residents in the United States – a quarter of its 26 million residents lacking coverage – but Gov. Rick Perry (R) refused to expand Medicaid, which could cover as many as 500,000 to 1 million Texans.
The governor’s decision will stay in place at least until 2015, when the state legislature reconvenes.
Some physicians in Texas are not upset by the decision – they consider Medicaid to be low-paying program and full of bureaucratic hassles.
Others – including many of the primary care organizations – disagree.
The Texas Medical Association, the Texas Academy of Family Physicians, and the Texas chapter of the American Congress of Obstetricians and Gynecologists all support the expansion of Medicaid allowed by the ACA.
In April, Gov. Perry reiterated his position. "Medicaid expansion is a misguided, and ultimately doomed, attempt to mask the shortcomings of Obamacare," he said in a statement. Instead of expansion, he favors flexibility for the state to manage its Medicaid program.
State Rep. John Zerwas (R-Simonton), an anesthesiologist, introduced H.B. 3791 that would give that flexibility, but it did not get consideration by the full House before the legislature adjourned in May.
The TMA supported Dr. Zerwas’ proposal, but also is in favor of expanding Medicaid, said Dr. Stephen L. Brotherton, TMA president. More people would have some type of insurance, but they might not necessarily have good access to care, he said.
That’s because Texas has a shortage of primary care physicians. The number of primary care physicians per capita is lower than the national average – at about 70/100,000 in 2011, compared with 80/100,000 nationally, according to the Texas Department of State Health Services, in the publication "Supply Trends Among Licensed Health Professions, Texas, 1980-2011. In rural areas, it’s even lower – about 50/100,000.
Then there’s the question of just how many physicians will take Medicaid. A 2012 TMA survey found that only 31% of doctors in the state were accepting new Medicaid patients.
Medicaid payment rates are so low that Dr. Brotherton, who practices in Ft. Worth, said that he treats Medicaid patients as charity care. "It’s much less expensive for me to do it for nothing as donated time," he said.
Dr. Moss Hampton, chairman of District XI of ACOG, added, "Medicaid doesn’t cover the cost of taking care of the patient."
For Medicaid expansion to eventually be successful, "there would have to be a better payment rate and less of a hassle factor," said Dr. Hampton, chairman of the obstetrics and gynecology department at Texas Tech Health Sciences Center at the Permian Basin in Odessa.
"It’s hard to get doctors to accept Medicaid because of the rates they pay," agreed Dr. Clare Hawkins, TAFP president, who added that Texas physicians also feel that it’s hard to comply with differing rules among various Medicaid managed care programs.
Even so, expansion will mean getting more patients into preventive care, and a reduction in emergency department visits and more expensive hospital care – costs that are being borne by all Texans, including physicians, said Dr. Hawkins, who is program director of the San Jacinto Methodist Hospital Family Medicine Residency Program in Baytown, Texas.
Although uninsured Texas residents are already receiving care – in emergency departments and at clinics – Medicaid expansion could bring a big uptick in office visits, especially to ob.gyn. practices, Dr. Hampton said. The need for those services is growing with a state law that went into effect on Oct. 29 that makes it prohibitive for most Planned Parenthood clinics and other community clinics that provide abortion services to stay open.
"What that’s done is cut out a very large group of providers, and now we’re trying to find providers to help take care of those folks," who normally use those clinics, she said.
In the absence of Medicaid expansion, Texas physicians are hoping to start receiving higher Medicaid payments that were due to start in Jan. 2013. An estimated 25,000 Texas doctors are eligible for Medicaid pay that will be on par with Medicare. But Texas has not begun to distribute that money and will not likely do so until March, according to the TMA.
When the Supreme Court upheld the constitutionality of the Affordable Care Act in 2012, it also ruled that states could choose whether to substantially expand their Medicaid programs. That decision has created a split across the country, with about half of the states choosing to take federal dollars to expand their programs and the others opting out.
There’s no deadline on Medicaid expansion, so those states that have opted out so far can always choose to expand at a later date.

Here’s a look at two bellwether states: California, which has accepted federal money to expand its Medi-Cal program, and Texas, which has opted out of the expansion.
California Gov. Jerry Brown (D), a strong supporter of the ACA, announced that his state would expand Medicaid to include low-income individuals up to 138% of the federal poverty level starting on Jan. 1, 2014. All of the new enrollees – likely 1 million Californians – will be added to the state’s growing Medicaid managed care program.
Conversely, Texas Gov. Rick Perry (R) deemed Medicaid expansion "a misguided, and ultimately doomed, attempt to mask the shortcomings of Obamacare."

California: Pay cuts complicate expansion
Physicians in California are bracing for a significant Medicaid pay cut at the same time as about a million residents are set to join the program.
The pending cuts are just one part of a complex health care picture in California, where experts are far from certain about what the expansion of Medi-Cal will mean for physicians and patients.
"I think we’re going to have a real problem in California with all the new Medi-Cal patients," said Dr. Mark Dressner, who works at a federally qualified health center in Long Beach and is the president of the California Academy of Family Physicians. "Who is going to see them when there’s going to be so many other people in the system?"
The Kaiser Family Foundation estimates that between 990,000 and 1.4 million individuals, mostly single adults, will enter Medi-Cal by 2019 because of the ACA-permitted expansion. Currently, about 8.5 million residents are enrolled. Newly eligible individuals will be enrolled in the program’s managed care health plans.
These new patients could have a hard time finding a doctor. Medi-Cal is one of the lowest payers in the nation, paying between $18 and $24 for an office visit, according to the California Medical Association.
That’s about to be compounded by a pay cut approved by the state and the Centers for Medicare and Medicaid Services in 2011. Physicians tried unsuccessfully to fight the cut in court. Now the state is implementing it retroactively, which means that Medi-Cal payments could be cut 15%-20% over the next few years.
"It really undermines efforts to successfully implement the Affordable Care Act in California," said Lisa Folberg, vice president of medical and regulatory policy at the California Medical Association.
There are broad exceptions to the cut. It does not apply to most primary care services in either managed care plans or fee-for-service Medi-Cal, or to specialty services provided through managed care plans, Ms. Folberg said. And some managed care companies have announced that they will use their discretion in setting payment rates to shield their contracted physicians from the cuts.
"Unfortunately, that doesn’t help the cancer patient on Medi-Cal in Bakersfield who has fee-for-service Medi-Cal and can’t find an oncologist," Ms. Folberg said.
Dr. Darin Latimore, president of the California chapter of the American College of Physicians, said large health systems likely will be able to work around the cuts, using group visits and physician extenders. But small physician practices in rural areas aren’t equipped to make those changes, he said.
"They are not in a position to move work on to others in order to be more efficient and see more Medi-Cal patients," said Dr. Latimore, associate dean of medicine at the University of California Davis.
The result will be that physicians who work outside of the state’s safety net system will be less likely to participate in the Medi-Cal program or will strictly limit the number of patients they see. That will translate to longer waits to get an appointment and shorter visits for Medi-Cal patients.
Another concern: Patients entering Medi-Cal managed care plans might not have access to a broad network of physicians. While California has network adequacy laws, state oversight is inadequate, according to Ms. Folberg. For the most part, the plans are on an honor system.
There are some bright spots for the Medi-Cal expansion. The ACA includes an increase in Medicaid payments to physicians for 146 primary care services provided in 2013 and 2014. The provision temporarily raises payments up to Medicare rates, which for California physicians means a 136% hike on average, according to an analysis from the Kaiser Family Foundation.
But those payments were delayed, with the first checks going out to physicians in November 2013. That delay could cost the state in physician participation.
"I think the longer it takes to implement that, the less likely it is that it will affect any decisions about whether to participate more fully in the program than you would have otherwise," said Christopher Perrone, deputy director of the health reform and public programs initiative at the California HealthCare Foundation.
And the temporary nature of the pay increase adds to the problem, Mr. Perrone said. "I don’t see California sustaining that increase on its own and I haven’t heard anyone suggest that the federal government would sustain it after the 2 years."
Mr. Perrone said it’s more likely that physicians who are already committed to participating in Medi-Cal will use the money to invest in electronic health records and other telemedicine features, and hire medical assistants.
But with so many small and solo physicians shying away from Medi-Cal because of low payments, community clinics and health centers will have to pick up the slack.
"All these issues together really point to the importance of the community health centers and the role we are going to be playing in ensuring access," said Carmela Castellano-Garcia, president and CEO of the California Primary Care Association.
Federally qualified health centers are in a better position financially because they are paid an enhanced Medicaid rate and won’t be subject to the coming Medi-Cal cuts, Ms. Castellano-Garcia said. And the ACA has directed an influx of cash to these centers as well – more than $500 million in California alone to establish new sites, expand services, and support major capital improvement projects, according to the Health and Human Services department.
Texas: No expansion means doctors will keep feeling pressure
Texas has the highest number of uninsured residents in the United States – a quarter of its 26 million residents lacking coverage – but Gov. Rick Perry (R) refused to expand Medicaid, which could cover as many as 500,000 to 1 million Texans.
The governor’s decision will stay in place at least until 2015, when the state legislature reconvenes.
Some physicians in Texas are not upset by the decision – they consider Medicaid to be low-paying program and full of bureaucratic hassles.
Others – including many of the primary care organizations – disagree.
The Texas Medical Association, the Texas Academy of Family Physicians, and the Texas chapter of the American Congress of Obstetricians and Gynecologists all support the expansion of Medicaid allowed by the ACA.
In April, Gov. Perry reiterated his position. "Medicaid expansion is a misguided, and ultimately doomed, attempt to mask the shortcomings of Obamacare," he said in a statement. Instead of expansion, he favors flexibility for the state to manage its Medicaid program.
State Rep. John Zerwas (R-Simonton), an anesthesiologist, introduced H.B. 3791 that would give that flexibility, but it did not get consideration by the full House before the legislature adjourned in May.
The TMA supported Dr. Zerwas’ proposal, but also is in favor of expanding Medicaid, said Dr. Stephen L. Brotherton, TMA president. More people would have some type of insurance, but they might not necessarily have good access to care, he said.
That’s because Texas has a shortage of primary care physicians. The number of primary care physicians per capita is lower than the national average – at about 70/100,000 in 2011, compared with 80/100,000 nationally, according to the Texas Department of State Health Services, in the publication "Supply Trends Among Licensed Health Professions, Texas, 1980-2011. In rural areas, it’s even lower – about 50/100,000.
Then there’s the question of just how many physicians will take Medicaid. A 2012 TMA survey found that only 31% of doctors in the state were accepting new Medicaid patients.
Medicaid payment rates are so low that Dr. Brotherton, who practices in Ft. Worth, said that he treats Medicaid patients as charity care. "It’s much less expensive for me to do it for nothing as donated time," he said.
Dr. Moss Hampton, chairman of District XI of ACOG, added, "Medicaid doesn’t cover the cost of taking care of the patient."
For Medicaid expansion to eventually be successful, "there would have to be a better payment rate and less of a hassle factor," said Dr. Hampton, chairman of the obstetrics and gynecology department at Texas Tech Health Sciences Center at the Permian Basin in Odessa.
"It’s hard to get doctors to accept Medicaid because of the rates they pay," agreed Dr. Clare Hawkins, TAFP president, who added that Texas physicians also feel that it’s hard to comply with differing rules among various Medicaid managed care programs.
Even so, expansion will mean getting more patients into preventive care, and a reduction in emergency department visits and more expensive hospital care – costs that are being borne by all Texans, including physicians, said Dr. Hawkins, who is program director of the San Jacinto Methodist Hospital Family Medicine Residency Program in Baytown, Texas.
Although uninsured Texas residents are already receiving care – in emergency departments and at clinics – Medicaid expansion could bring a big uptick in office visits, especially to ob.gyn. practices, Dr. Hampton said. The need for those services is growing with a state law that went into effect on Oct. 29 that makes it prohibitive for most Planned Parenthood clinics and other community clinics that provide abortion services to stay open.
"What that’s done is cut out a very large group of providers, and now we’re trying to find providers to help take care of those folks," who normally use those clinics, she said.
In the absence of Medicaid expansion, Texas physicians are hoping to start receiving higher Medicaid payments that were due to start in Jan. 2013. An estimated 25,000 Texas doctors are eligible for Medicaid pay that will be on par with Medicare. But Texas has not begun to distribute that money and will not likely do so until March, according to the TMA.
When the Supreme Court upheld the constitutionality of the Affordable Care Act in 2012, it also ruled that states could choose whether to substantially expand their Medicaid programs. That decision has created a split across the country, with about half of the states choosing to take federal dollars to expand their programs and the others opting out.
There’s no deadline on Medicaid expansion, so those states that have opted out so far can always choose to expand at a later date.

Here’s a look at two bellwether states: California, which has accepted federal money to expand its Medi-Cal program, and Texas, which has opted out of the expansion.
California Gov. Jerry Brown (D), a strong supporter of the ACA, announced that his state would expand Medicaid to include low-income individuals up to 138% of the federal poverty level starting on Jan. 1, 2014. All of the new enrollees – likely 1 million Californians – will be added to the state’s growing Medicaid managed care program.
Conversely, Texas Gov. Rick Perry (R) deemed Medicaid expansion "a misguided, and ultimately doomed, attempt to mask the shortcomings of Obamacare."

California: Pay cuts complicate expansion
Physicians in California are bracing for a significant Medicaid pay cut at the same time as about a million residents are set to join the program.
The pending cuts are just one part of a complex health care picture in California, where experts are far from certain about what the expansion of Medi-Cal will mean for physicians and patients.
"I think we’re going to have a real problem in California with all the new Medi-Cal patients," said Dr. Mark Dressner, who works at a federally qualified health center in Long Beach and is the president of the California Academy of Family Physicians. "Who is going to see them when there’s going to be so many other people in the system?"
The Kaiser Family Foundation estimates that between 990,000 and 1.4 million individuals, mostly single adults, will enter Medi-Cal by 2019 because of the ACA-permitted expansion. Currently, about 8.5 million residents are enrolled. Newly eligible individuals will be enrolled in the program’s managed care health plans.
These new patients could have a hard time finding a doctor. Medi-Cal is one of the lowest payers in the nation, paying between $18 and $24 for an office visit, according to the California Medical Association.
That’s about to be compounded by a pay cut approved by the state and the Centers for Medicare and Medicaid Services in 2011. Physicians tried unsuccessfully to fight the cut in court. Now the state is implementing it retroactively, which means that Medi-Cal payments could be cut 15%-20% over the next few years.
"It really undermines efforts to successfully implement the Affordable Care Act in California," said Lisa Folberg, vice president of medical and regulatory policy at the California Medical Association.
There are broad exceptions to the cut. It does not apply to most primary care services in either managed care plans or fee-for-service Medi-Cal, or to specialty services provided through managed care plans, Ms. Folberg said. And some managed care companies have announced that they will use their discretion in setting payment rates to shield their contracted physicians from the cuts.
"Unfortunately, that doesn’t help the cancer patient on Medi-Cal in Bakersfield who has fee-for-service Medi-Cal and can’t find an oncologist," Ms. Folberg said.
Dr. Darin Latimore, president of the California chapter of the American College of Physicians, said large health systems likely will be able to work around the cuts, using group visits and physician extenders. But small physician practices in rural areas aren’t equipped to make those changes, he said.
"They are not in a position to move work on to others in order to be more efficient and see more Medi-Cal patients," said Dr. Latimore, associate dean of medicine at the University of California Davis.
The result will be that physicians who work outside of the state’s safety net system will be less likely to participate in the Medi-Cal program or will strictly limit the number of patients they see. That will translate to longer waits to get an appointment and shorter visits for Medi-Cal patients.
Another concern: Patients entering Medi-Cal managed care plans might not have access to a broad network of physicians. While California has network adequacy laws, state oversight is inadequate, according to Ms. Folberg. For the most part, the plans are on an honor system.
There are some bright spots for the Medi-Cal expansion. The ACA includes an increase in Medicaid payments to physicians for 146 primary care services provided in 2013 and 2014. The provision temporarily raises payments up to Medicare rates, which for California physicians means a 136% hike on average, according to an analysis from the Kaiser Family Foundation.
But those payments were delayed, with the first checks going out to physicians in November 2013. That delay could cost the state in physician participation.
"I think the longer it takes to implement that, the less likely it is that it will affect any decisions about whether to participate more fully in the program than you would have otherwise," said Christopher Perrone, deputy director of the health reform and public programs initiative at the California HealthCare Foundation.
And the temporary nature of the pay increase adds to the problem, Mr. Perrone said. "I don’t see California sustaining that increase on its own and I haven’t heard anyone suggest that the federal government would sustain it after the 2 years."
Mr. Perrone said it’s more likely that physicians who are already committed to participating in Medi-Cal will use the money to invest in electronic health records and other telemedicine features, and hire medical assistants.
But with so many small and solo physicians shying away from Medi-Cal because of low payments, community clinics and health centers will have to pick up the slack.
"All these issues together really point to the importance of the community health centers and the role we are going to be playing in ensuring access," said Carmela Castellano-Garcia, president and CEO of the California Primary Care Association.
Federally qualified health centers are in a better position financially because they are paid an enhanced Medicaid rate and won’t be subject to the coming Medi-Cal cuts, Ms. Castellano-Garcia said. And the ACA has directed an influx of cash to these centers as well – more than $500 million in California alone to establish new sites, expand services, and support major capital improvement projects, according to the Health and Human Services department.
Texas: No expansion means doctors will keep feeling pressure
Texas has the highest number of uninsured residents in the United States – a quarter of its 26 million residents lacking coverage – but Gov. Rick Perry (R) refused to expand Medicaid, which could cover as many as 500,000 to 1 million Texans.
The governor’s decision will stay in place at least until 2015, when the state legislature reconvenes.
Some physicians in Texas are not upset by the decision – they consider Medicaid to be low-paying program and full of bureaucratic hassles.
Others – including many of the primary care organizations – disagree.
The Texas Medical Association, the Texas Academy of Family Physicians, and the Texas chapter of the American Congress of Obstetricians and Gynecologists all support the expansion of Medicaid allowed by the ACA.
In April, Gov. Perry reiterated his position. "Medicaid expansion is a misguided, and ultimately doomed, attempt to mask the shortcomings of Obamacare," he said in a statement. Instead of expansion, he favors flexibility for the state to manage its Medicaid program.
State Rep. John Zerwas (R-Simonton), an anesthesiologist, introduced H.B. 3791 that would give that flexibility, but it did not get consideration by the full House before the legislature adjourned in May.
The TMA supported Dr. Zerwas’ proposal, but also is in favor of expanding Medicaid, said Dr. Stephen L. Brotherton, TMA president. More people would have some type of insurance, but they might not necessarily have good access to care, he said.
That’s because Texas has a shortage of primary care physicians. The number of primary care physicians per capita is lower than the national average – at about 70/100,000 in 2011, compared with 80/100,000 nationally, according to the Texas Department of State Health Services, in the publication "Supply Trends Among Licensed Health Professions, Texas, 1980-2011. In rural areas, it’s even lower – about 50/100,000.
Then there’s the question of just how many physicians will take Medicaid. A 2012 TMA survey found that only 31% of doctors in the state were accepting new Medicaid patients.
Medicaid payment rates are so low that Dr. Brotherton, who practices in Ft. Worth, said that he treats Medicaid patients as charity care. "It’s much less expensive for me to do it for nothing as donated time," he said.
Dr. Moss Hampton, chairman of District XI of ACOG, added, "Medicaid doesn’t cover the cost of taking care of the patient."
For Medicaid expansion to eventually be successful, "there would have to be a better payment rate and less of a hassle factor," said Dr. Hampton, chairman of the obstetrics and gynecology department at Texas Tech Health Sciences Center at the Permian Basin in Odessa.
"It’s hard to get doctors to accept Medicaid because of the rates they pay," agreed Dr. Clare Hawkins, TAFP president, who added that Texas physicians also feel that it’s hard to comply with differing rules among various Medicaid managed care programs.
Even so, expansion will mean getting more patients into preventive care, and a reduction in emergency department visits and more expensive hospital care – costs that are being borne by all Texans, including physicians, said Dr. Hawkins, who is program director of the San Jacinto Methodist Hospital Family Medicine Residency Program in Baytown, Texas.
Although uninsured Texas residents are already receiving care – in emergency departments and at clinics – Medicaid expansion could bring a big uptick in office visits, especially to ob.gyn. practices, Dr. Hampton said. The need for those services is growing with a state law that went into effect on Oct. 29 that makes it prohibitive for most Planned Parenthood clinics and other community clinics that provide abortion services to stay open.
"What that’s done is cut out a very large group of providers, and now we’re trying to find providers to help take care of those folks," who normally use those clinics, she said.
In the absence of Medicaid expansion, Texas physicians are hoping to start receiving higher Medicaid payments that were due to start in Jan. 2013. An estimated 25,000 Texas doctors are eligible for Medicaid pay that will be on par with Medicare. But Texas has not begun to distribute that money and will not likely do so until March, according to the TMA.