User login
Emerging Treatment Options for Postinflammatory Hyperpigmentation
A supplement to Skin & Allergy News. This supplement is jointly sponsored by Skin & Allergy News and the Elsevier Office of Continuing Medical Education and supported by Barrier Therapeutics. The supplement is based on a faculty interview.


To view the supplement, click the image above. To take the CME Posttest, download and print out the CME Posttest PDF file, and follow the test instructions.
FACULTY
Susan Taylor, MD
Director, The Skin of Color Center
St. Luke's-Roosevelt Hospital
Columbia University
New York, N.Y.
TARGET AUDIENCE
This activity has been designed to meet the educational needs of Dermatologists and other clinicians.
EDUCATIONAL NEEDS
Disorders of skin pigmentation account for a substantial proportion of many dermatologists' practices. Abnormalities characterized by hyperpigmentation are especially prominent among African-Americans and other darker-skinned individuals. Postinflammatory hyperpigmentation (PIH), an acquired increase in pigmentation secondary to an inflammatory process, is one of the common pigmentation disorders among people of color. PIH poses a therapeutic challenge to the clinician, and many patients find the condition more troubling than its inflammatory precursor. PIH can have a devastating psychological impact and substantially mar an individual's self-esteem.
LEARNING OBJECTIVES
Upon completion of this educational activity, participants should be able to:
• Understand the basic pathophysiology of PIH
• State the principal types of conditions that result in PIH
• Appreciate the impact of PIH and its effects on people of color
• Appreciate the impact of PIH and its effects on people of color
ACCREDITATION STATEMENT
This activity has been planned and implemented in accordance with the Essential Areas and Policies of the Accreditation Council for Continuing Medical Education (ACCME) through the joint sponsorship of the Elsevier Office of ContinuingMedical Education (EOCME) and Skin & Allergy News. The EOCME is accredited by the ACCME to provide continuing medical education (CME) for physicians.
CREDIT DESIGNATION
The EOCME designates this educational activity for a maximum of 0.5 AMA PRA Category 1 Credits. Physicians should only claim credit commensurate with the extent of their participation in the activity.
Term of Approval: October 2007 - October 31, 2008.
*Full faculty disclosures available online.
A supplement to Skin & Allergy News. This supplement is jointly sponsored by Skin & Allergy News and the Elsevier Office of Continuing Medical Education and supported by Barrier Therapeutics. The supplement is based on a faculty interview.


To view the supplement, click the image above. To take the CME Posttest, download and print out the CME Posttest PDF file, and follow the test instructions.
FACULTY
Susan Taylor, MD
Director, The Skin of Color Center
St. Luke's-Roosevelt Hospital
Columbia University
New York, N.Y.
TARGET AUDIENCE
This activity has been designed to meet the educational needs of Dermatologists and other clinicians.
EDUCATIONAL NEEDS
Disorders of skin pigmentation account for a substantial proportion of many dermatologists' practices. Abnormalities characterized by hyperpigmentation are especially prominent among African-Americans and other darker-skinned individuals. Postinflammatory hyperpigmentation (PIH), an acquired increase in pigmentation secondary to an inflammatory process, is one of the common pigmentation disorders among people of color. PIH poses a therapeutic challenge to the clinician, and many patients find the condition more troubling than its inflammatory precursor. PIH can have a devastating psychological impact and substantially mar an individual's self-esteem.
LEARNING OBJECTIVES
Upon completion of this educational activity, participants should be able to:
• Understand the basic pathophysiology of PIH
• State the principal types of conditions that result in PIH
• Appreciate the impact of PIH and its effects on people of color
• Appreciate the impact of PIH and its effects on people of color
ACCREDITATION STATEMENT
This activity has been planned and implemented in accordance with the Essential Areas and Policies of the Accreditation Council for Continuing Medical Education (ACCME) through the joint sponsorship of the Elsevier Office of ContinuingMedical Education (EOCME) and Skin & Allergy News. The EOCME is accredited by the ACCME to provide continuing medical education (CME) for physicians.
CREDIT DESIGNATION
The EOCME designates this educational activity for a maximum of 0.5 AMA PRA Category 1 Credits. Physicians should only claim credit commensurate with the extent of their participation in the activity.
Term of Approval: October 2007 - October 31, 2008.
*Full faculty disclosures available online.
A supplement to Skin & Allergy News. This supplement is jointly sponsored by Skin & Allergy News and the Elsevier Office of Continuing Medical Education and supported by Barrier Therapeutics. The supplement is based on a faculty interview.


To view the supplement, click the image above. To take the CME Posttest, download and print out the CME Posttest PDF file, and follow the test instructions.
FACULTY
Susan Taylor, MD
Director, The Skin of Color Center
St. Luke's-Roosevelt Hospital
Columbia University
New York, N.Y.
TARGET AUDIENCE
This activity has been designed to meet the educational needs of Dermatologists and other clinicians.
EDUCATIONAL NEEDS
Disorders of skin pigmentation account for a substantial proportion of many dermatologists' practices. Abnormalities characterized by hyperpigmentation are especially prominent among African-Americans and other darker-skinned individuals. Postinflammatory hyperpigmentation (PIH), an acquired increase in pigmentation secondary to an inflammatory process, is one of the common pigmentation disorders among people of color. PIH poses a therapeutic challenge to the clinician, and many patients find the condition more troubling than its inflammatory precursor. PIH can have a devastating psychological impact and substantially mar an individual's self-esteem.
LEARNING OBJECTIVES
Upon completion of this educational activity, participants should be able to:
• Understand the basic pathophysiology of PIH
• State the principal types of conditions that result in PIH
• Appreciate the impact of PIH and its effects on people of color
• Appreciate the impact of PIH and its effects on people of color
ACCREDITATION STATEMENT
This activity has been planned and implemented in accordance with the Essential Areas and Policies of the Accreditation Council for Continuing Medical Education (ACCME) through the joint sponsorship of the Elsevier Office of ContinuingMedical Education (EOCME) and Skin & Allergy News. The EOCME is accredited by the ACCME to provide continuing medical education (CME) for physicians.
CREDIT DESIGNATION
The EOCME designates this educational activity for a maximum of 0.5 AMA PRA Category 1 Credits. Physicians should only claim credit commensurate with the extent of their participation in the activity.
Term of Approval: October 2007 - October 31, 2008.
*Full faculty disclosures available online.
Tort Reform Makes a Comeback
After being relegated to the back burner for months, tort reform has begun bubbling to the surface in editorials, polls, and at last month's televised healthcare summit. The focus has largely remained on how states can rein in unnecessary and expensive medical malpractice lawsuits. But a recent court case in Illinois, a new poll suggesting a high prevalence of "defensive medicine", and the glimmer of a bipartisan proposal for special "health courts" might provide the impetus for reform at the federal level.
According to the Agency for Healthcare Research and Quality (AHRQ), about half of the states have some form of medical liability caps on noneconomic damages or total damages, though the courts haven't always gone along with the limits. Last month, the Illinois Supreme Court ruled that the state's 2005 medical liability cap of $500,000 for doctors and $1 million for hospitals was unconstitutional. In a March 1 editorial, the AMA vowed to fight on, highlighting the positive experiences of tort reform in Texas.
As the "Public Policy" column in the March issue of The Hospitalist suggests, the liability caps approved by Texas voters in 2003 have led to decreases in liability insurance premiums and helped mitigate the state's physician shortage. But the jury is still out on whether the reforms have helped to improve quality and patient access.
Despite the reluctance of many Democrats to pursue liability caps, the concept of health courts has attracted some bipartisan support and the backing of President Obama. As proposed, such courts would consider only medical malpractice cases, similar to the workers' compensation system. A March 2 editorial in Roll Call by analysts at Washington, D.C., think tank Third Way asserts that health courts "can serve as the backbone for fundamental malpractice reform." Whether legislators will support a strong, single spine or more fragmented, state-based systems, however, remains to be seen.
After being relegated to the back burner for months, tort reform has begun bubbling to the surface in editorials, polls, and at last month's televised healthcare summit. The focus has largely remained on how states can rein in unnecessary and expensive medical malpractice lawsuits. But a recent court case in Illinois, a new poll suggesting a high prevalence of "defensive medicine", and the glimmer of a bipartisan proposal for special "health courts" might provide the impetus for reform at the federal level.
According to the Agency for Healthcare Research and Quality (AHRQ), about half of the states have some form of medical liability caps on noneconomic damages or total damages, though the courts haven't always gone along with the limits. Last month, the Illinois Supreme Court ruled that the state's 2005 medical liability cap of $500,000 for doctors and $1 million for hospitals was unconstitutional. In a March 1 editorial, the AMA vowed to fight on, highlighting the positive experiences of tort reform in Texas.
As the "Public Policy" column in the March issue of The Hospitalist suggests, the liability caps approved by Texas voters in 2003 have led to decreases in liability insurance premiums and helped mitigate the state's physician shortage. But the jury is still out on whether the reforms have helped to improve quality and patient access.
Despite the reluctance of many Democrats to pursue liability caps, the concept of health courts has attracted some bipartisan support and the backing of President Obama. As proposed, such courts would consider only medical malpractice cases, similar to the workers' compensation system. A March 2 editorial in Roll Call by analysts at Washington, D.C., think tank Third Way asserts that health courts "can serve as the backbone for fundamental malpractice reform." Whether legislators will support a strong, single spine or more fragmented, state-based systems, however, remains to be seen.
After being relegated to the back burner for months, tort reform has begun bubbling to the surface in editorials, polls, and at last month's televised healthcare summit. The focus has largely remained on how states can rein in unnecessary and expensive medical malpractice lawsuits. But a recent court case in Illinois, a new poll suggesting a high prevalence of "defensive medicine", and the glimmer of a bipartisan proposal for special "health courts" might provide the impetus for reform at the federal level.
According to the Agency for Healthcare Research and Quality (AHRQ), about half of the states have some form of medical liability caps on noneconomic damages or total damages, though the courts haven't always gone along with the limits. Last month, the Illinois Supreme Court ruled that the state's 2005 medical liability cap of $500,000 for doctors and $1 million for hospitals was unconstitutional. In a March 1 editorial, the AMA vowed to fight on, highlighting the positive experiences of tort reform in Texas.
As the "Public Policy" column in the March issue of The Hospitalist suggests, the liability caps approved by Texas voters in 2003 have led to decreases in liability insurance premiums and helped mitigate the state's physician shortage. But the jury is still out on whether the reforms have helped to improve quality and patient access.
Despite the reluctance of many Democrats to pursue liability caps, the concept of health courts has attracted some bipartisan support and the backing of President Obama. As proposed, such courts would consider only medical malpractice cases, similar to the workers' compensation system. A March 2 editorial in Roll Call by analysts at Washington, D.C., think tank Third Way asserts that health courts "can serve as the backbone for fundamental malpractice reform." Whether legislators will support a strong, single spine or more fragmented, state-based systems, however, remains to be seen.
In the Literature: The Latest Research You Need to Know
Clinical question: Does darbepoetin alfa use in patients with diabetes and chronic kidney disease (CKD) who do not require dialysis decrease the risk of death and cardiovascular or renal events?
Background: Anemia is a risk factor for cardiovascular and renal outcomes. The use of erythropoiesis-stimulating agents (ESAs) to increase hemoglobin reduces the need for transfusions and moderately improves quality of life. A placebo-controlled trial to determine if correction of anemia with ESAs improves clinical outcomes has not been conducted.
Study design: Randomized, double-blind, placebo-controlled trial.
Setting: 623 sites in 24 countries.
Synopsis: The study team randomized 4,038 patients to receive either dose-adjusted darbepoetin alfa (goal hemoglobin of 13) or placebo, with rescue doses of darbepoetin for hemoglobin below 9g/dL. The primary endpoints were a composite outcome of death, a cardiovascular event and death, or end-stage renal disease.
The median hemoglobin achieved in the darbepoetin and placebo groups were 12.5g/dL and 10.6g/dL, respectively. The primary cardiovascular endpoint occurred in 31.4% of patients receiving darbepoetin and 29.7% of patients receiving placebo (HR 1.05; 95% CI, 0.94-1.17). The primary renal endpoint occurred in 32.4% of patients assigned to darbepoetin and 30.5% of patients assigned to placebo (HR 1.06; 95% CI 0.95-1.19). Significantly more patients assigned to darbepoetin experienced stroke and VTE, and significantly fewer patients required red-cell transfusions.
Bottom line: Darbepoetin use in patients with diabetes and CKD who do not require dialysis for correction of anemia does not improve clinical outcomes, and carries an increased risk of stroke and VTE.
Citation: Pfeffer MA, Burdmann EA, Chen CY, et al. A trial of darbepoetin alfa in type 2 diabetes and chronic kidney disease. N Engl J Med. 2009;361(21):2019-2032.
Reviewed for TH eWire Charles Baillie, MD, Elizabeth Marandola, MSN, ARNP, Janelle Ocampo, PharmD, BCPS, Craig A. Umscheid, MD, MSCE, Section of Hospital Medicine, Hospital of the University of Pennsylvania, Philadelphia.
For more HM-related research reviews, visit the "In the Literature" section of our Web site.
Clinical question: Does darbepoetin alfa use in patients with diabetes and chronic kidney disease (CKD) who do not require dialysis decrease the risk of death and cardiovascular or renal events?
Background: Anemia is a risk factor for cardiovascular and renal outcomes. The use of erythropoiesis-stimulating agents (ESAs) to increase hemoglobin reduces the need for transfusions and moderately improves quality of life. A placebo-controlled trial to determine if correction of anemia with ESAs improves clinical outcomes has not been conducted.
Study design: Randomized, double-blind, placebo-controlled trial.
Setting: 623 sites in 24 countries.
Synopsis: The study team randomized 4,038 patients to receive either dose-adjusted darbepoetin alfa (goal hemoglobin of 13) or placebo, with rescue doses of darbepoetin for hemoglobin below 9g/dL. The primary endpoints were a composite outcome of death, a cardiovascular event and death, or end-stage renal disease.
The median hemoglobin achieved in the darbepoetin and placebo groups were 12.5g/dL and 10.6g/dL, respectively. The primary cardiovascular endpoint occurred in 31.4% of patients receiving darbepoetin and 29.7% of patients receiving placebo (HR 1.05; 95% CI, 0.94-1.17). The primary renal endpoint occurred in 32.4% of patients assigned to darbepoetin and 30.5% of patients assigned to placebo (HR 1.06; 95% CI 0.95-1.19). Significantly more patients assigned to darbepoetin experienced stroke and VTE, and significantly fewer patients required red-cell transfusions.
Bottom line: Darbepoetin use in patients with diabetes and CKD who do not require dialysis for correction of anemia does not improve clinical outcomes, and carries an increased risk of stroke and VTE.
Citation: Pfeffer MA, Burdmann EA, Chen CY, et al. A trial of darbepoetin alfa in type 2 diabetes and chronic kidney disease. N Engl J Med. 2009;361(21):2019-2032.
Reviewed for TH eWire Charles Baillie, MD, Elizabeth Marandola, MSN, ARNP, Janelle Ocampo, PharmD, BCPS, Craig A. Umscheid, MD, MSCE, Section of Hospital Medicine, Hospital of the University of Pennsylvania, Philadelphia.
For more HM-related research reviews, visit the "In the Literature" section of our Web site.
Clinical question: Does darbepoetin alfa use in patients with diabetes and chronic kidney disease (CKD) who do not require dialysis decrease the risk of death and cardiovascular or renal events?
Background: Anemia is a risk factor for cardiovascular and renal outcomes. The use of erythropoiesis-stimulating agents (ESAs) to increase hemoglobin reduces the need for transfusions and moderately improves quality of life. A placebo-controlled trial to determine if correction of anemia with ESAs improves clinical outcomes has not been conducted.
Study design: Randomized, double-blind, placebo-controlled trial.
Setting: 623 sites in 24 countries.
Synopsis: The study team randomized 4,038 patients to receive either dose-adjusted darbepoetin alfa (goal hemoglobin of 13) or placebo, with rescue doses of darbepoetin for hemoglobin below 9g/dL. The primary endpoints were a composite outcome of death, a cardiovascular event and death, or end-stage renal disease.
The median hemoglobin achieved in the darbepoetin and placebo groups were 12.5g/dL and 10.6g/dL, respectively. The primary cardiovascular endpoint occurred in 31.4% of patients receiving darbepoetin and 29.7% of patients receiving placebo (HR 1.05; 95% CI, 0.94-1.17). The primary renal endpoint occurred in 32.4% of patients assigned to darbepoetin and 30.5% of patients assigned to placebo (HR 1.06; 95% CI 0.95-1.19). Significantly more patients assigned to darbepoetin experienced stroke and VTE, and significantly fewer patients required red-cell transfusions.
Bottom line: Darbepoetin use in patients with diabetes and CKD who do not require dialysis for correction of anemia does not improve clinical outcomes, and carries an increased risk of stroke and VTE.
Citation: Pfeffer MA, Burdmann EA, Chen CY, et al. A trial of darbepoetin alfa in type 2 diabetes and chronic kidney disease. N Engl J Med. 2009;361(21):2019-2032.
Reviewed for TH eWire Charles Baillie, MD, Elizabeth Marandola, MSN, ARNP, Janelle Ocampo, PharmD, BCPS, Craig A. Umscheid, MD, MSCE, Section of Hospital Medicine, Hospital of the University of Pennsylvania, Philadelphia.
For more HM-related research reviews, visit the "In the Literature" section of our Web site.
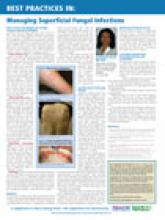
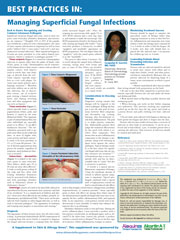
BEST PRACTICES IN: Managing Superficial Fungal Infections
A supplement to Skin & Allergy News. This supplement was sponsored by Ferndale Laboratories Inc. and Primus Pharmaceuticals, makers of Aloquin Gel and Alcortin A Gel.
- Back to Basics: Recognizing and Treating Common Cutaneous Pathogens
- Diagnosis
- Considerations in Choosing Therapy
- Maximizing Treatment Success
- Counseling Patients About Preventing Infection and Transmission
Faculty/Faculty Disclosure
Jacquelyn B. Garrett, MD, FAAD
Diplomate, American Board of Dermatology,
Dermatology private practice at Christian Hospital,
St. Louis, MO
Dr. Garrett has nothing to disclose.
Copyright (C) 2009 Elsevier Inc.
A supplement to Skin & Allergy News. This supplement was sponsored by Ferndale Laboratories Inc. and Primus Pharmaceuticals, makers of Aloquin Gel and Alcortin A Gel.
- Back to Basics: Recognizing and Treating Common Cutaneous Pathogens
- Diagnosis
- Considerations in Choosing Therapy
- Maximizing Treatment Success
- Counseling Patients About Preventing Infection and Transmission
Faculty/Faculty Disclosure
Jacquelyn B. Garrett, MD, FAAD
Diplomate, American Board of Dermatology,
Dermatology private practice at Christian Hospital,
St. Louis, MO
Dr. Garrett has nothing to disclose.
Copyright (C) 2009 Elsevier Inc.
A supplement to Skin & Allergy News. This supplement was sponsored by Ferndale Laboratories Inc. and Primus Pharmaceuticals, makers of Aloquin Gel and Alcortin A Gel.
- Back to Basics: Recognizing and Treating Common Cutaneous Pathogens
- Diagnosis
- Considerations in Choosing Therapy
- Maximizing Treatment Success
- Counseling Patients About Preventing Infection and Transmission
Faculty/Faculty Disclosure
Jacquelyn B. Garrett, MD, FAAD
Diplomate, American Board of Dermatology,
Dermatology private practice at Christian Hospital,
St. Louis, MO
Dr. Garrett has nothing to disclose.
Copyright (C) 2009 Elsevier Inc.
Wired to Lead
With prods from technological advancement and political pressure, the use of digital medicine is expected to take another leap forward this year—and hospitalists can be among those who benefit most, according to a presentation at an American College of Physicians meeting last month.
The workshop, "Wired and Wireless Health," held as part of the New Jersey Chapter regional meeting in Woodbridge, N.J., focused on three areas of health information technology (IT): social networking, applications and devices, and infrastructure. Steven Peskin, MD, MBA, FACP, says social networking Web sites like Sermo and Medscape Physician Connect offer portals for the "sharing of clinical insights and solutions to practical clinical problems in a way that promises to hone best practices."
As executive vice president and chief medical officer of Yardley, Pa.-based MediMedia USA, Dr. Peskin preaches the value of digital technology for inpatient care. Hospitalists, in particular, can use handheld devices and applications to deliver faster care and receive test results more quickly.
“There’s an app for that,” he quips, noting Modality and MedCalc. SHM is nearing launch of its new mobile resource center, which is supported by Epocrates and offers hospitalists exclusive commentary on the latest news and research in HM and hospitalist practice management.
Dr. Peskin, while an ardent supporter of the use of digital technology to improve patient care, is quick to caution that technology has its place. Privacy concerns, which are often associated with electronic health records (EHR), are a major consideration physicians should keep in mind when incorporating advances in iPhones, BlackBerrys, or other smartphones, he says.
"Digital medicine is not a substitute for clinical experience," Dr. Peskin says. "But it can improve clinical judgment and better clinical judgment. I like to say, 'Use computers for what they do well and use your brain for what it does well.'"
With prods from technological advancement and political pressure, the use of digital medicine is expected to take another leap forward this year—and hospitalists can be among those who benefit most, according to a presentation at an American College of Physicians meeting last month.
The workshop, "Wired and Wireless Health," held as part of the New Jersey Chapter regional meeting in Woodbridge, N.J., focused on three areas of health information technology (IT): social networking, applications and devices, and infrastructure. Steven Peskin, MD, MBA, FACP, says social networking Web sites like Sermo and Medscape Physician Connect offer portals for the "sharing of clinical insights and solutions to practical clinical problems in a way that promises to hone best practices."
As executive vice president and chief medical officer of Yardley, Pa.-based MediMedia USA, Dr. Peskin preaches the value of digital technology for inpatient care. Hospitalists, in particular, can use handheld devices and applications to deliver faster care and receive test results more quickly.
“There’s an app for that,” he quips, noting Modality and MedCalc. SHM is nearing launch of its new mobile resource center, which is supported by Epocrates and offers hospitalists exclusive commentary on the latest news and research in HM and hospitalist practice management.
Dr. Peskin, while an ardent supporter of the use of digital technology to improve patient care, is quick to caution that technology has its place. Privacy concerns, which are often associated with electronic health records (EHR), are a major consideration physicians should keep in mind when incorporating advances in iPhones, BlackBerrys, or other smartphones, he says.
"Digital medicine is not a substitute for clinical experience," Dr. Peskin says. "But it can improve clinical judgment and better clinical judgment. I like to say, 'Use computers for what they do well and use your brain for what it does well.'"
With prods from technological advancement and political pressure, the use of digital medicine is expected to take another leap forward this year—and hospitalists can be among those who benefit most, according to a presentation at an American College of Physicians meeting last month.
The workshop, "Wired and Wireless Health," held as part of the New Jersey Chapter regional meeting in Woodbridge, N.J., focused on three areas of health information technology (IT): social networking, applications and devices, and infrastructure. Steven Peskin, MD, MBA, FACP, says social networking Web sites like Sermo and Medscape Physician Connect offer portals for the "sharing of clinical insights and solutions to practical clinical problems in a way that promises to hone best practices."
As executive vice president and chief medical officer of Yardley, Pa.-based MediMedia USA, Dr. Peskin preaches the value of digital technology for inpatient care. Hospitalists, in particular, can use handheld devices and applications to deliver faster care and receive test results more quickly.
“There’s an app for that,” he quips, noting Modality and MedCalc. SHM is nearing launch of its new mobile resource center, which is supported by Epocrates and offers hospitalists exclusive commentary on the latest news and research in HM and hospitalist practice management.
Dr. Peskin, while an ardent supporter of the use of digital technology to improve patient care, is quick to caution that technology has its place. Privacy concerns, which are often associated with electronic health records (EHR), are a major consideration physicians should keep in mind when incorporating advances in iPhones, BlackBerrys, or other smartphones, he says.
"Digital medicine is not a substitute for clinical experience," Dr. Peskin says. "But it can improve clinical judgment and better clinical judgment. I like to say, 'Use computers for what they do well and use your brain for what it does well.'"
Dress for Success
The oft-quoted Hippocrates once stated that physicians should be “clean in person, well-dressed, and anointed with sweet-smelling unguents.” So are hospitalists heeding the father of modern medicine’s counsel about physician appearance in the 21st century?
According to an informal survey about workplace attire conducted recently at the-hospitalist.org, a majority of hospitalists are wearing professional apparel while on the job.
In response to the question "What do you typically wear to work?" more than half (54%) of voters said they dress business casual, commonly defined as a dress shirt, slacks, belt, shoes, and socks for men, and a dress shirt, reasonable-length skirt or full-length trousers, shoes, and hosiery for women. Another 13% stated they wear a suit to work. Meanwhile, the other third of respondents said they dress in scrubs (22%), khakis and polo shirts (10%), and jeans and T-shirts (2%).
Most hospitalists at IPC: The Hospitalist Co., a national physician group practice based in North Hollywood, Calif., opt for business-casual dress, says Rafael Barretto, DO, the company's associate medical director for the Michigan region. While IPC does not have a strict dress code, it does give guidelines to its hospitalists and encourages them to avoid wearing sandals, tennis shoes, and jeans to work.
"IPC considers patients' attitudes on physician appearance to be very important. We want our patients to trust that we're going to do the best we can to take care of them," says Dr. Barretto, who cites several research studies, including a report published in the November 2005 issue of The American Journal of Medicine, that found patients favor physicians in professional attire.
"Fortunately or unfortunately, perception is reality and hospitalists need to be concerned with how a patient or a patient's family perceives them," says Chris Frost, MD, senior vice president of hospital medicine for TeamHealth Hospital Medicine, a national hospitalist management company in Knoxville, Tenn. TeamHealth has a company-wide policy that discourages its physicians from engaging in unprofessional dress.
"Hospitalists only have one chance to make a first impression. If a hospitalist is dressed poorly, that could overshadow any good patient care he or she provides," Dr. Frost says.
The oft-quoted Hippocrates once stated that physicians should be “clean in person, well-dressed, and anointed with sweet-smelling unguents.” So are hospitalists heeding the father of modern medicine’s counsel about physician appearance in the 21st century?
According to an informal survey about workplace attire conducted recently at the-hospitalist.org, a majority of hospitalists are wearing professional apparel while on the job.
In response to the question "What do you typically wear to work?" more than half (54%) of voters said they dress business casual, commonly defined as a dress shirt, slacks, belt, shoes, and socks for men, and a dress shirt, reasonable-length skirt or full-length trousers, shoes, and hosiery for women. Another 13% stated they wear a suit to work. Meanwhile, the other third of respondents said they dress in scrubs (22%), khakis and polo shirts (10%), and jeans and T-shirts (2%).
Most hospitalists at IPC: The Hospitalist Co., a national physician group practice based in North Hollywood, Calif., opt for business-casual dress, says Rafael Barretto, DO, the company's associate medical director for the Michigan region. While IPC does not have a strict dress code, it does give guidelines to its hospitalists and encourages them to avoid wearing sandals, tennis shoes, and jeans to work.
"IPC considers patients' attitudes on physician appearance to be very important. We want our patients to trust that we're going to do the best we can to take care of them," says Dr. Barretto, who cites several research studies, including a report published in the November 2005 issue of The American Journal of Medicine, that found patients favor physicians in professional attire.
"Fortunately or unfortunately, perception is reality and hospitalists need to be concerned with how a patient or a patient's family perceives them," says Chris Frost, MD, senior vice president of hospital medicine for TeamHealth Hospital Medicine, a national hospitalist management company in Knoxville, Tenn. TeamHealth has a company-wide policy that discourages its physicians from engaging in unprofessional dress.
"Hospitalists only have one chance to make a first impression. If a hospitalist is dressed poorly, that could overshadow any good patient care he or she provides," Dr. Frost says.
The oft-quoted Hippocrates once stated that physicians should be “clean in person, well-dressed, and anointed with sweet-smelling unguents.” So are hospitalists heeding the father of modern medicine’s counsel about physician appearance in the 21st century?
According to an informal survey about workplace attire conducted recently at the-hospitalist.org, a majority of hospitalists are wearing professional apparel while on the job.
In response to the question "What do you typically wear to work?" more than half (54%) of voters said they dress business casual, commonly defined as a dress shirt, slacks, belt, shoes, and socks for men, and a dress shirt, reasonable-length skirt or full-length trousers, shoes, and hosiery for women. Another 13% stated they wear a suit to work. Meanwhile, the other third of respondents said they dress in scrubs (22%), khakis and polo shirts (10%), and jeans and T-shirts (2%).
Most hospitalists at IPC: The Hospitalist Co., a national physician group practice based in North Hollywood, Calif., opt for business-casual dress, says Rafael Barretto, DO, the company's associate medical director for the Michigan region. While IPC does not have a strict dress code, it does give guidelines to its hospitalists and encourages them to avoid wearing sandals, tennis shoes, and jeans to work.
"IPC considers patients' attitudes on physician appearance to be very important. We want our patients to trust that we're going to do the best we can to take care of them," says Dr. Barretto, who cites several research studies, including a report published in the November 2005 issue of The American Journal of Medicine, that found patients favor physicians in professional attire.
"Fortunately or unfortunately, perception is reality and hospitalists need to be concerned with how a patient or a patient's family perceives them," says Chris Frost, MD, senior vice president of hospital medicine for TeamHealth Hospital Medicine, a national hospitalist management company in Knoxville, Tenn. TeamHealth has a company-wide policy that discourages its physicians from engaging in unprofessional dress.
"Hospitalists only have one chance to make a first impression. If a hospitalist is dressed poorly, that could overshadow any good patient care he or she provides," Dr. Frost says.
ONLINE EXCLUSIVE: Audio interview with HM director Greg Maynard
ONLINE EXCLUSIVE: Audio interview with Washington, D.C., hospitalist Patrick Conway
ONLINE EXCLUSIVE: Audio interview with HM10 Course Director Amir Jaffer, MD, FHM
Dr. Jaffer discusses HM10 keynote speakers Paul Levy and Bob Wachter
Click here to listen to the audio.
Dr. Jaffer explains what the average hospitalist should expect at HM10 in Washington, D.C.
Click here to listen to the audio.
Dr. Jaffer discusses how the national healthcare reform debate will backdrop HM10, and how new peer-reviewed, seat-limited workshops will enhance the HM10 experience.
Click here to listen to the audio.
Dr. Jaffer explains how first-time HM10 attendees can maximize their time in D.C.
Click here to listen to the audio.
Dr. Jaffer discusses HM10 keynote speakers Paul Levy and Bob Wachter
Click here to listen to the audio.
Dr. Jaffer explains what the average hospitalist should expect at HM10 in Washington, D.C.
Click here to listen to the audio.
Dr. Jaffer discusses how the national healthcare reform debate will backdrop HM10, and how new peer-reviewed, seat-limited workshops will enhance the HM10 experience.
Click here to listen to the audio.
Dr. Jaffer explains how first-time HM10 attendees can maximize their time in D.C.
Click here to listen to the audio.
Dr. Jaffer discusses HM10 keynote speakers Paul Levy and Bob Wachter
Click here to listen to the audio.
Dr. Jaffer explains what the average hospitalist should expect at HM10 in Washington, D.C.
Click here to listen to the audio.
Dr. Jaffer discusses how the national healthcare reform debate will backdrop HM10, and how new peer-reviewed, seat-limited workshops will enhance the HM10 experience.
Click here to listen to the audio.
Dr. Jaffer explains how first-time HM10 attendees can maximize their time in D.C.
Click here to listen to the audio.
Massachusetts Update
Massachusetts Update
With the ongoing debate about healthcare reform, I’m curious to know how it worked out in Massachusetts. Didn’t they give everyone health insurance several years ago?
R. McCoy, MD
Birmingham, Ala.
Dr. Hospitalist responds: In 2006, Massachusetts legislators took the same approach to healthcare insurance as they do to auto insurance: require everyone to purchase a plan. If you can’t afford to purchase health insurance, the state provides you insurance through a state-subsidized plan. The state covers individuals earning up to 100% of the federal poverty level (FPL) and partially subsidizes coverage for those earning up to 300% of the FPL.
So how did Massachusetts come up with the money to pay for healthcare insurance for all of its residents? The state traditionally utilized money from a “free-care pool” to partially reimburse hospitals and community health centers for the care provided to indigents. The money in the free-care pool was generated from state and federal taxes, and from assessments on hospitals and healthcare insurance providers. With expanded insurance coverage, Massachusetts estimated that the cost of healthcare delivered to the uninsured would decrease, and the free-care pool could offset the remaining costs of insuring those below the FPL.
Starting in 2007, residents of Massachusetts were required to demonstrate proof of health insurance on their state income tax returns. The state levied penalties on those who failed to obtain coverage. The legislation also required insurers’ family plans to cover young adults up to age 25 or at least two years after they were no longer dependent on their parents. Additionally, businesses with 10 or more employees had to contribute a reasonable amount to their employees’ health insurance premiums or risk a financial penalty.
The Massachusetts health plan has produced both intended and unintended consequences. The plan was successful in its primary goal of insuring its citizens. By the end of 2008, 97% of Massachusetts’ residents were covered. But the system has not increased access to providers because of a shortage of primary-care physicians (PCPs). (Critics also point out that the plan has done nothing to increase the numbers of PCPs in the state.)
Another unexpected outcome is that healthcare costs have increased. The initial expectation was that increasing the percentage of insured individuals would lower overall costs. However, this has not been realized. In fact, the reallocation of funds from the free-care pool has birthed other problems. The state’s “safety net” hospitals—which traditionally have served urban, low-income populations—have experienced financial hardships.
These unexpected findings have not deterred Massachusetts from further efforts to address healthcare reform. In 2008, a special commission was charged with recommendations for a “common payment methodology” that would apply to both public and private payors. The goal is to slow the growth of healthcare costs without adversely affecting the quality of care.
The commission issued its recommendations in July 2009 (www.mass.gov). It suggested “Massachusetts has among the highest healthcare costs in the U.S. … and based on recent history, are projected to grow faster than for the U.S. as a whole.” In its report, the commission was critical of the present fee-for-service reimbursement model and stated that the model was the primary reason for escalating healthcare costs.
The commission noted the fee-for-service model rewards providers for providing more, but not better, care and also encourages providers to provide more-costly services without regard to evidence-based guidelines or a patient’s need. The commission recommended that “global payments with adjustments to reward provision of accessible and high-quality care become the predominant form of payment to providers in Massachusetts.” For the record, the legislature has not acted on the commission recommendations. TH
IMAGE SOURCE: AMANE KANEKO
Massachusetts Update
With the ongoing debate about healthcare reform, I’m curious to know how it worked out in Massachusetts. Didn’t they give everyone health insurance several years ago?
R. McCoy, MD
Birmingham, Ala.
Dr. Hospitalist responds: In 2006, Massachusetts legislators took the same approach to healthcare insurance as they do to auto insurance: require everyone to purchase a plan. If you can’t afford to purchase health insurance, the state provides you insurance through a state-subsidized plan. The state covers individuals earning up to 100% of the federal poverty level (FPL) and partially subsidizes coverage for those earning up to 300% of the FPL.
So how did Massachusetts come up with the money to pay for healthcare insurance for all of its residents? The state traditionally utilized money from a “free-care pool” to partially reimburse hospitals and community health centers for the care provided to indigents. The money in the free-care pool was generated from state and federal taxes, and from assessments on hospitals and healthcare insurance providers. With expanded insurance coverage, Massachusetts estimated that the cost of healthcare delivered to the uninsured would decrease, and the free-care pool could offset the remaining costs of insuring those below the FPL.
Starting in 2007, residents of Massachusetts were required to demonstrate proof of health insurance on their state income tax returns. The state levied penalties on those who failed to obtain coverage. The legislation also required insurers’ family plans to cover young adults up to age 25 or at least two years after they were no longer dependent on their parents. Additionally, businesses with 10 or more employees had to contribute a reasonable amount to their employees’ health insurance premiums or risk a financial penalty.
The Massachusetts health plan has produced both intended and unintended consequences. The plan was successful in its primary goal of insuring its citizens. By the end of 2008, 97% of Massachusetts’ residents were covered. But the system has not increased access to providers because of a shortage of primary-care physicians (PCPs). (Critics also point out that the plan has done nothing to increase the numbers of PCPs in the state.)
Another unexpected outcome is that healthcare costs have increased. The initial expectation was that increasing the percentage of insured individuals would lower overall costs. However, this has not been realized. In fact, the reallocation of funds from the free-care pool has birthed other problems. The state’s “safety net” hospitals—which traditionally have served urban, low-income populations—have experienced financial hardships.
These unexpected findings have not deterred Massachusetts from further efforts to address healthcare reform. In 2008, a special commission was charged with recommendations for a “common payment methodology” that would apply to both public and private payors. The goal is to slow the growth of healthcare costs without adversely affecting the quality of care.
The commission issued its recommendations in July 2009 (www.mass.gov). It suggested “Massachusetts has among the highest healthcare costs in the U.S. … and based on recent history, are projected to grow faster than for the U.S. as a whole.” In its report, the commission was critical of the present fee-for-service reimbursement model and stated that the model was the primary reason for escalating healthcare costs.
The commission noted the fee-for-service model rewards providers for providing more, but not better, care and also encourages providers to provide more-costly services without regard to evidence-based guidelines or a patient’s need. The commission recommended that “global payments with adjustments to reward provision of accessible and high-quality care become the predominant form of payment to providers in Massachusetts.” For the record, the legislature has not acted on the commission recommendations. TH
IMAGE SOURCE: AMANE KANEKO
Massachusetts Update
With the ongoing debate about healthcare reform, I’m curious to know how it worked out in Massachusetts. Didn’t they give everyone health insurance several years ago?
R. McCoy, MD
Birmingham, Ala.
Dr. Hospitalist responds: In 2006, Massachusetts legislators took the same approach to healthcare insurance as they do to auto insurance: require everyone to purchase a plan. If you can’t afford to purchase health insurance, the state provides you insurance through a state-subsidized plan. The state covers individuals earning up to 100% of the federal poverty level (FPL) and partially subsidizes coverage for those earning up to 300% of the FPL.
So how did Massachusetts come up with the money to pay for healthcare insurance for all of its residents? The state traditionally utilized money from a “free-care pool” to partially reimburse hospitals and community health centers for the care provided to indigents. The money in the free-care pool was generated from state and federal taxes, and from assessments on hospitals and healthcare insurance providers. With expanded insurance coverage, Massachusetts estimated that the cost of healthcare delivered to the uninsured would decrease, and the free-care pool could offset the remaining costs of insuring those below the FPL.
Starting in 2007, residents of Massachusetts were required to demonstrate proof of health insurance on their state income tax returns. The state levied penalties on those who failed to obtain coverage. The legislation also required insurers’ family plans to cover young adults up to age 25 or at least two years after they were no longer dependent on their parents. Additionally, businesses with 10 or more employees had to contribute a reasonable amount to their employees’ health insurance premiums or risk a financial penalty.
The Massachusetts health plan has produced both intended and unintended consequences. The plan was successful in its primary goal of insuring its citizens. By the end of 2008, 97% of Massachusetts’ residents were covered. But the system has not increased access to providers because of a shortage of primary-care physicians (PCPs). (Critics also point out that the plan has done nothing to increase the numbers of PCPs in the state.)
Another unexpected outcome is that healthcare costs have increased. The initial expectation was that increasing the percentage of insured individuals would lower overall costs. However, this has not been realized. In fact, the reallocation of funds from the free-care pool has birthed other problems. The state’s “safety net” hospitals—which traditionally have served urban, low-income populations—have experienced financial hardships.
These unexpected findings have not deterred Massachusetts from further efforts to address healthcare reform. In 2008, a special commission was charged with recommendations for a “common payment methodology” that would apply to both public and private payors. The goal is to slow the growth of healthcare costs without adversely affecting the quality of care.
The commission issued its recommendations in July 2009 (www.mass.gov). It suggested “Massachusetts has among the highest healthcare costs in the U.S. … and based on recent history, are projected to grow faster than for the U.S. as a whole.” In its report, the commission was critical of the present fee-for-service reimbursement model and stated that the model was the primary reason for escalating healthcare costs.
The commission noted the fee-for-service model rewards providers for providing more, but not better, care and also encourages providers to provide more-costly services without regard to evidence-based guidelines or a patient’s need. The commission recommended that “global payments with adjustments to reward provision of accessible and high-quality care become the predominant form of payment to providers in Massachusetts.” For the record, the legislature has not acted on the commission recommendations. TH
IMAGE SOURCE: AMANE KANEKO