User login
Consider small-fiber neuropathies in systemic lupus erythematosus
Small-fiber neuropathy is one of the most common types of peripheral neuropathy affecting patients with systemic lupus erythematosus, but it isn’t even mentioned in the American College of Rheumatology neuropsychiatric case definitions of manifestations of the disorder, according to a retrospective analysis of cohort of 2,097 patients with SLE.
Other types of peripheral neuropathy, such as acute inflammatory demyelinating neuropathies (for example, Guillain-Barré syndrome), plexopathies, and mononeuritis multiplex, are well described in the ACR-NPSLE case definitions but occur much less frequently. This, combined with the fact that small-fiber neuropathies often present as "unorthodox" pain patterns, indicates that they are underdiagnosed, said Dr. Amin Oomatia of the University of Cambridge, England, and his coinvestigators at John Hopkins University, Baltimore.
Small-fiber neuropathies arise through mechanisms that are distinct from those of other neuropathies and require different diagnostic strategies to be properly identified. In particular, small-fiber neuropathies do not always conform to the "stocking-and-glove" pattern of pain that is typical of other neuropathies in SLE, so it is likely that many affected patients "may be regarded in routine clinical care as having a ‘nonorganic’ pain disorder.
"Our findings suggest that rheumatologists and other clinicians who confront SLE patients with seemingly improbable pain patterns should consider the diagnosis of a small-fiber neuropathy," the investigators wrote, especially since it may occur in the face of normal electrodiagnostic studies.
Dr. Oomatia and his colleagues based these conclusions on their retrospective study of one medical center’s 25-year experience treating 2,097 SLE patients – the Johns Hopkins Lupus Cohort. Using details in a database of patients’ electronic medical records, they identified 82 patients who had peripheral neuropathies related to SLE.
Only one patient had peripheral neuropathy attributable to Guillain-Barré syndrome, only one patient had a plexopathy, and only six patients had mononeuritis multiplex, demonstrating that these are very infrequent complications of SLE even though they are included in ACR case definitions.
In contrast, 14 patients (17% of those with peripheral neuropathy) had biopsy-proven small-fiber neuropathies, and most of them presented with "an entirely different and unorthodox pain distribution" characterized as patchy, asymmetric, or proximal.
In particular, nine patients had pain affecting the face, torso, and/or proximal extremities. Three had burning pain over their entire bodies, the investigators said (Arthritis Rheum. 2013 Dec. 10 [doi:10.1002/art.38302]).
In these cases, punch skin biopsy showed abnormalities that disproportionately affected the proximal thigh, "which is considered a surrogate indicator of proximal-most dorsal root ganglia neuronal cell loss," they wrote. In contrast, other patients who had the typical distal pattern of neuropathic pain showed decreased intraepidermal nerve-fiber densities in the distal leg, a surrogate indicator of distal-most axonal degeneration.
Another distinguishing feature of small-fiber neuropathy was its association with a history of herpes zoster virus, opportunistic infections, and osteoporotic fractures, all unrelated to corticosteroid dose, Dr. Oomatia and his associates said.
This study was supported in part by the National Institutes of Health and the National Center for Research Resources. No potential financial conflicts of interest were reported.
Small-fiber neuropathy is one of the most common types of peripheral neuropathy affecting patients with systemic lupus erythematosus, but it isn’t even mentioned in the American College of Rheumatology neuropsychiatric case definitions of manifestations of the disorder, according to a retrospective analysis of cohort of 2,097 patients with SLE.
Other types of peripheral neuropathy, such as acute inflammatory demyelinating neuropathies (for example, Guillain-Barré syndrome), plexopathies, and mononeuritis multiplex, are well described in the ACR-NPSLE case definitions but occur much less frequently. This, combined with the fact that small-fiber neuropathies often present as "unorthodox" pain patterns, indicates that they are underdiagnosed, said Dr. Amin Oomatia of the University of Cambridge, England, and his coinvestigators at John Hopkins University, Baltimore.
Small-fiber neuropathies arise through mechanisms that are distinct from those of other neuropathies and require different diagnostic strategies to be properly identified. In particular, small-fiber neuropathies do not always conform to the "stocking-and-glove" pattern of pain that is typical of other neuropathies in SLE, so it is likely that many affected patients "may be regarded in routine clinical care as having a ‘nonorganic’ pain disorder.
"Our findings suggest that rheumatologists and other clinicians who confront SLE patients with seemingly improbable pain patterns should consider the diagnosis of a small-fiber neuropathy," the investigators wrote, especially since it may occur in the face of normal electrodiagnostic studies.
Dr. Oomatia and his colleagues based these conclusions on their retrospective study of one medical center’s 25-year experience treating 2,097 SLE patients – the Johns Hopkins Lupus Cohort. Using details in a database of patients’ electronic medical records, they identified 82 patients who had peripheral neuropathies related to SLE.
Only one patient had peripheral neuropathy attributable to Guillain-Barré syndrome, only one patient had a plexopathy, and only six patients had mononeuritis multiplex, demonstrating that these are very infrequent complications of SLE even though they are included in ACR case definitions.
In contrast, 14 patients (17% of those with peripheral neuropathy) had biopsy-proven small-fiber neuropathies, and most of them presented with "an entirely different and unorthodox pain distribution" characterized as patchy, asymmetric, or proximal.
In particular, nine patients had pain affecting the face, torso, and/or proximal extremities. Three had burning pain over their entire bodies, the investigators said (Arthritis Rheum. 2013 Dec. 10 [doi:10.1002/art.38302]).
In these cases, punch skin biopsy showed abnormalities that disproportionately affected the proximal thigh, "which is considered a surrogate indicator of proximal-most dorsal root ganglia neuronal cell loss," they wrote. In contrast, other patients who had the typical distal pattern of neuropathic pain showed decreased intraepidermal nerve-fiber densities in the distal leg, a surrogate indicator of distal-most axonal degeneration.
Another distinguishing feature of small-fiber neuropathy was its association with a history of herpes zoster virus, opportunistic infections, and osteoporotic fractures, all unrelated to corticosteroid dose, Dr. Oomatia and his associates said.
This study was supported in part by the National Institutes of Health and the National Center for Research Resources. No potential financial conflicts of interest were reported.
Small-fiber neuropathy is one of the most common types of peripheral neuropathy affecting patients with systemic lupus erythematosus, but it isn’t even mentioned in the American College of Rheumatology neuropsychiatric case definitions of manifestations of the disorder, according to a retrospective analysis of cohort of 2,097 patients with SLE.
Other types of peripheral neuropathy, such as acute inflammatory demyelinating neuropathies (for example, Guillain-Barré syndrome), plexopathies, and mononeuritis multiplex, are well described in the ACR-NPSLE case definitions but occur much less frequently. This, combined with the fact that small-fiber neuropathies often present as "unorthodox" pain patterns, indicates that they are underdiagnosed, said Dr. Amin Oomatia of the University of Cambridge, England, and his coinvestigators at John Hopkins University, Baltimore.
Small-fiber neuropathies arise through mechanisms that are distinct from those of other neuropathies and require different diagnostic strategies to be properly identified. In particular, small-fiber neuropathies do not always conform to the "stocking-and-glove" pattern of pain that is typical of other neuropathies in SLE, so it is likely that many affected patients "may be regarded in routine clinical care as having a ‘nonorganic’ pain disorder.
"Our findings suggest that rheumatologists and other clinicians who confront SLE patients with seemingly improbable pain patterns should consider the diagnosis of a small-fiber neuropathy," the investigators wrote, especially since it may occur in the face of normal electrodiagnostic studies.
Dr. Oomatia and his colleagues based these conclusions on their retrospective study of one medical center’s 25-year experience treating 2,097 SLE patients – the Johns Hopkins Lupus Cohort. Using details in a database of patients’ electronic medical records, they identified 82 patients who had peripheral neuropathies related to SLE.
Only one patient had peripheral neuropathy attributable to Guillain-Barré syndrome, only one patient had a plexopathy, and only six patients had mononeuritis multiplex, demonstrating that these are very infrequent complications of SLE even though they are included in ACR case definitions.
In contrast, 14 patients (17% of those with peripheral neuropathy) had biopsy-proven small-fiber neuropathies, and most of them presented with "an entirely different and unorthodox pain distribution" characterized as patchy, asymmetric, or proximal.
In particular, nine patients had pain affecting the face, torso, and/or proximal extremities. Three had burning pain over their entire bodies, the investigators said (Arthritis Rheum. 2013 Dec. 10 [doi:10.1002/art.38302]).
In these cases, punch skin biopsy showed abnormalities that disproportionately affected the proximal thigh, "which is considered a surrogate indicator of proximal-most dorsal root ganglia neuronal cell loss," they wrote. In contrast, other patients who had the typical distal pattern of neuropathic pain showed decreased intraepidermal nerve-fiber densities in the distal leg, a surrogate indicator of distal-most axonal degeneration.
Another distinguishing feature of small-fiber neuropathy was its association with a history of herpes zoster virus, opportunistic infections, and osteoporotic fractures, all unrelated to corticosteroid dose, Dr. Oomatia and his associates said.
This study was supported in part by the National Institutes of Health and the National Center for Research Resources. No potential financial conflicts of interest were reported.
FROM ARTHRITIS AND RHEUMATISM
Major finding: A total of 14 patients, or 17% of 82 with peripheral neuropathies, had biopsy-proven small-fiber neuropathies and often presented with unorthodox patterns of pain.
Data source: A retrospective analysis of data regarding 2,097 consecutive patients with SLE registered in the Johns Hopkins Lupus Cohort during a 25-year period, including 82 who developed peripheral neuropathies related to the disease.
Disclosures: This study was supported in part by the National Institutes of Health and the National Center for Research Resources. No potential financial conflicts of interest were reported.
Psychiatrists least likely specialists to accept insurance
Psychiatrists are markedly less likely than are office-based physicians in other specialties to accept insurance, according to a report published online Dec. 11 in JAMA Psychiatry.
Moreover, psychiatrists’ rates of insurance acceptance are plummeting over time, compared with those of other physicians. In 2009-2010, almost half of all psychiatrists in the United States did not accept private non–capitated insurance, and more than half did not accept Medicare or Medicaid, said Dr. Tara F. Bishop of the departments of public health and medicine, Cornell University, New York, and her associates.
This can adversely affect access to mental health services for patients who are unable to pay for psychiatric care out of their own pockets.
"To our knowledge, no prior studies have documented such a striking difference in insurance acceptance rates between psychiatrists and physicians in other specialties. These low rates of acceptance may affect recent calls for increased access to mental health services, and if the trend of declining acceptance rates continues then the impact may be even more significant," the investigators noted.
Recent reports suggested that nonacceptance of insurance might be particularly high among psychiatrists. Dr. Bishop and her colleagues examined the issue using data from the National Ambulatory Medical Care Survey (NAMCS), a physician survey administered by the Centers for Disease Control and Prevention’s National Center for Health Statistics.
The NAMCS includes data on a nationally representative sample of office-based physicians who account for 90% of outpatient visits across the country each year. The researchers restricted their analysis to study participants who reported that they accepted new patients and whether they accepted those patients’ insurance coverage, for each year between 2005 and 2010. The mean number of physicians surveyed each of these years was 1,250, and approximately 5.5% of them were psychiatrists.
The other specialties covered by NAMCS include internal medicine, general/family practice, obstetrics and gynecology, pediatrics, cardiology, oncology, general surgery, orthopedic surgery, ophthalmology, neurology, urology, dermatology, otolaryngology, and others.
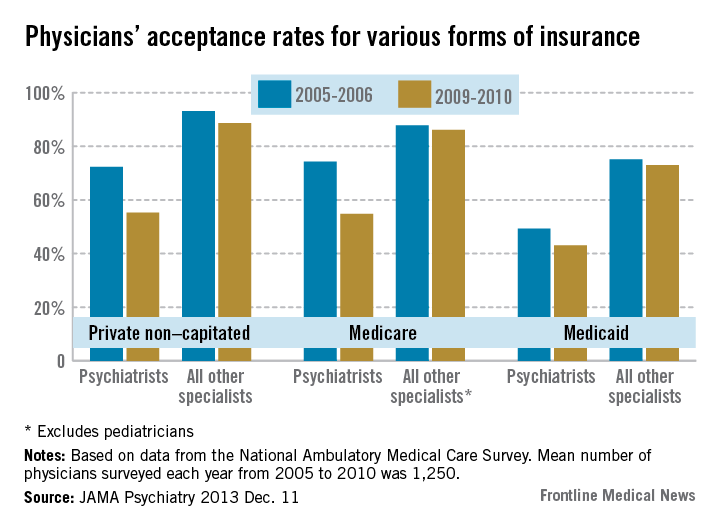
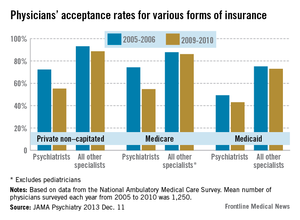
The percentage of psychiatrists who accepted private non–capitated insurance was lower than for all other specialties every year assessed, and it declined by 17% during the study period, from 72.3% in 2005-2006 to 55.3% in 2009-2010. In contrast, the percentage of physicians in other specialties who accepted private non–capitated insurance was 93.1% in 2005-2006 and declined only 4.4%, to 88.7%, in 2009-2010, the researchers said (JAMA Psychiatry 2013 Dec. 11 [doi:10.1001/jamapsychiatry.2013.2862]).
Similarly, the percentage of psychiatrists who accepted Medicare was lower than that for all other specialists in every year assessed, and it decreased by nearly 20%, from 74.3% at the beginning of the study period to 54.8% at the end. In contrast, the percentage of physicians in other specialties who accepted Medicare did not change over time.
Psychiatrists’ Medicaid acceptance rates also were lower than those of all other specialties each year, but did not decline significantly over time. In 2009-2010, only 49.3% of psychiatrists accepted Medicaid, compared with 75.1% of physicians in other specialties.
This study was unable to assess why psychiatrists are so unlikely to accept insurance, but Dr. Bishop and her associates offered several potential reasons.
First, the time it takes to provide counseling and therapy might be uniquely long for psychiatrists, compared with other physicians. If psychiatrists cannot see as many patients in a day as other physicians, they might opt out of accepting insurance.
Second, psychiatrists might have such a demand for their services that they don’t need to accept insurance. This might stem in part from a shortage of psychiatrists: The number of graduates from psychiatry training programs has declined, while the current workforce is aging rapidly.
Third, the data indicated that solo practitioners were more likely than those in group practice to decline to accept insurance, and psychiatrists are more likely to be in solo practice than physicians in other specialties. "Solo practices often can function with much less infrastructure than larger single-specialty or multispecialty group practices. As a result, they may have little incentive to hire staff to interact with insurance companies," the investigators said.
Dr. Bishop and her colleagues cited several limitations. For example, physicians are not asked by the NAMCS why they opt not to accept insurance. Also, information about insurance acceptance on the part of physicians who practice in hospital outpatient departments is not collected by the NAMCS.
Still, the researchers’ findings suggest that policies aimed at improving access to timely psychiatric care might be limited by the fact that so many psychiatrists don’t accept insurance.
"More research is needed to understand whether low rates of insurance acceptance are a barrier that patients face when trying to seek psychiatric care and a barrier that physicians face when trying to refer their patients for psychiatric care," Dr. Bishop and her associates added.
This study was supported by the National Institute on Aging, Cornell University, the Department of Veterans Affairs, and the National Institutes of Health. No potential financial conflicts of interest were disclosed.
Psychiatrists are markedly less likely than are office-based physicians in other specialties to accept insurance, according to a report published online Dec. 11 in JAMA Psychiatry.
Moreover, psychiatrists’ rates of insurance acceptance are plummeting over time, compared with those of other physicians. In 2009-2010, almost half of all psychiatrists in the United States did not accept private non–capitated insurance, and more than half did not accept Medicare or Medicaid, said Dr. Tara F. Bishop of the departments of public health and medicine, Cornell University, New York, and her associates.

This can adversely affect access to mental health services for patients who are unable to pay for psychiatric care out of their own pockets.
"To our knowledge, no prior studies have documented such a striking difference in insurance acceptance rates between psychiatrists and physicians in other specialties. These low rates of acceptance may affect recent calls for increased access to mental health services, and if the trend of declining acceptance rates continues then the impact may be even more significant," the investigators noted.
Recent reports suggested that nonacceptance of insurance might be particularly high among psychiatrists. Dr. Bishop and her colleagues examined the issue using data from the National Ambulatory Medical Care Survey (NAMCS), a physician survey administered by the Centers for Disease Control and Prevention’s National Center for Health Statistics.
The NAMCS includes data on a nationally representative sample of office-based physicians who account for 90% of outpatient visits across the country each year. The researchers restricted their analysis to study participants who reported that they accepted new patients and whether they accepted those patients’ insurance coverage, for each year between 2005 and 2010. The mean number of physicians surveyed each of these years was 1,250, and approximately 5.5% of them were psychiatrists.
The other specialties covered by NAMCS include internal medicine, general/family practice, obstetrics and gynecology, pediatrics, cardiology, oncology, general surgery, orthopedic surgery, ophthalmology, neurology, urology, dermatology, otolaryngology, and others.
The percentage of psychiatrists who accepted private non–capitated insurance was lower than for all other specialties every year assessed, and it declined by 17% during the study period, from 72.3% in 2005-2006 to 55.3% in 2009-2010. In contrast, the percentage of physicians in other specialties who accepted private non–capitated insurance was 93.1% in 2005-2006 and declined only 4.4%, to 88.7%, in 2009-2010, the researchers said (JAMA Psychiatry 2013 Dec. 11 [doi:10.1001/jamapsychiatry.2013.2862]).
Similarly, the percentage of psychiatrists who accepted Medicare was lower than that for all other specialists in every year assessed, and it decreased by nearly 20%, from 74.3% at the beginning of the study period to 54.8% at the end. In contrast, the percentage of physicians in other specialties who accepted Medicare did not change over time.
Psychiatrists’ Medicaid acceptance rates also were lower than those of all other specialties each year, but did not decline significantly over time. In 2009-2010, only 49.3% of psychiatrists accepted Medicaid, compared with 75.1% of physicians in other specialties.
This study was unable to assess why psychiatrists are so unlikely to accept insurance, but Dr. Bishop and her associates offered several potential reasons.
First, the time it takes to provide counseling and therapy might be uniquely long for psychiatrists, compared with other physicians. If psychiatrists cannot see as many patients in a day as other physicians, they might opt out of accepting insurance.
Second, psychiatrists might have such a demand for their services that they don’t need to accept insurance. This might stem in part from a shortage of psychiatrists: The number of graduates from psychiatry training programs has declined, while the current workforce is aging rapidly.
Third, the data indicated that solo practitioners were more likely than those in group practice to decline to accept insurance, and psychiatrists are more likely to be in solo practice than physicians in other specialties. "Solo practices often can function with much less infrastructure than larger single-specialty or multispecialty group practices. As a result, they may have little incentive to hire staff to interact with insurance companies," the investigators said.
Dr. Bishop and her colleagues cited several limitations. For example, physicians are not asked by the NAMCS why they opt not to accept insurance. Also, information about insurance acceptance on the part of physicians who practice in hospital outpatient departments is not collected by the NAMCS.
Still, the researchers’ findings suggest that policies aimed at improving access to timely psychiatric care might be limited by the fact that so many psychiatrists don’t accept insurance.
"More research is needed to understand whether low rates of insurance acceptance are a barrier that patients face when trying to seek psychiatric care and a barrier that physicians face when trying to refer their patients for psychiatric care," Dr. Bishop and her associates added.
This study was supported by the National Institute on Aging, Cornell University, the Department of Veterans Affairs, and the National Institutes of Health. No potential financial conflicts of interest were disclosed.
Psychiatrists are markedly less likely than are office-based physicians in other specialties to accept insurance, according to a report published online Dec. 11 in JAMA Psychiatry.
Moreover, psychiatrists’ rates of insurance acceptance are plummeting over time, compared with those of other physicians. In 2009-2010, almost half of all psychiatrists in the United States did not accept private non–capitated insurance, and more than half did not accept Medicare or Medicaid, said Dr. Tara F. Bishop of the departments of public health and medicine, Cornell University, New York, and her associates.

This can adversely affect access to mental health services for patients who are unable to pay for psychiatric care out of their own pockets.
"To our knowledge, no prior studies have documented such a striking difference in insurance acceptance rates between psychiatrists and physicians in other specialties. These low rates of acceptance may affect recent calls for increased access to mental health services, and if the trend of declining acceptance rates continues then the impact may be even more significant," the investigators noted.
Recent reports suggested that nonacceptance of insurance might be particularly high among psychiatrists. Dr. Bishop and her colleagues examined the issue using data from the National Ambulatory Medical Care Survey (NAMCS), a physician survey administered by the Centers for Disease Control and Prevention’s National Center for Health Statistics.
The NAMCS includes data on a nationally representative sample of office-based physicians who account for 90% of outpatient visits across the country each year. The researchers restricted their analysis to study participants who reported that they accepted new patients and whether they accepted those patients’ insurance coverage, for each year between 2005 and 2010. The mean number of physicians surveyed each of these years was 1,250, and approximately 5.5% of them were psychiatrists.
The other specialties covered by NAMCS include internal medicine, general/family practice, obstetrics and gynecology, pediatrics, cardiology, oncology, general surgery, orthopedic surgery, ophthalmology, neurology, urology, dermatology, otolaryngology, and others.
The percentage of psychiatrists who accepted private non–capitated insurance was lower than for all other specialties every year assessed, and it declined by 17% during the study period, from 72.3% in 2005-2006 to 55.3% in 2009-2010. In contrast, the percentage of physicians in other specialties who accepted private non–capitated insurance was 93.1% in 2005-2006 and declined only 4.4%, to 88.7%, in 2009-2010, the researchers said (JAMA Psychiatry 2013 Dec. 11 [doi:10.1001/jamapsychiatry.2013.2862]).
Similarly, the percentage of psychiatrists who accepted Medicare was lower than that for all other specialists in every year assessed, and it decreased by nearly 20%, from 74.3% at the beginning of the study period to 54.8% at the end. In contrast, the percentage of physicians in other specialties who accepted Medicare did not change over time.
Psychiatrists’ Medicaid acceptance rates also were lower than those of all other specialties each year, but did not decline significantly over time. In 2009-2010, only 49.3% of psychiatrists accepted Medicaid, compared with 75.1% of physicians in other specialties.
This study was unable to assess why psychiatrists are so unlikely to accept insurance, but Dr. Bishop and her associates offered several potential reasons.
First, the time it takes to provide counseling and therapy might be uniquely long for psychiatrists, compared with other physicians. If psychiatrists cannot see as many patients in a day as other physicians, they might opt out of accepting insurance.
Second, psychiatrists might have such a demand for their services that they don’t need to accept insurance. This might stem in part from a shortage of psychiatrists: The number of graduates from psychiatry training programs has declined, while the current workforce is aging rapidly.
Third, the data indicated that solo practitioners were more likely than those in group practice to decline to accept insurance, and psychiatrists are more likely to be in solo practice than physicians in other specialties. "Solo practices often can function with much less infrastructure than larger single-specialty or multispecialty group practices. As a result, they may have little incentive to hire staff to interact with insurance companies," the investigators said.
Dr. Bishop and her colleagues cited several limitations. For example, physicians are not asked by the NAMCS why they opt not to accept insurance. Also, information about insurance acceptance on the part of physicians who practice in hospital outpatient departments is not collected by the NAMCS.
Still, the researchers’ findings suggest that policies aimed at improving access to timely psychiatric care might be limited by the fact that so many psychiatrists don’t accept insurance.
"More research is needed to understand whether low rates of insurance acceptance are a barrier that patients face when trying to seek psychiatric care and a barrier that physicians face when trying to refer their patients for psychiatric care," Dr. Bishop and her associates added.
This study was supported by the National Institute on Aging, Cornell University, the Department of Veterans Affairs, and the National Institutes of Health. No potential financial conflicts of interest were disclosed.
FROM JAMA PSYCHIATRY
Major finding: Only 72.3% of psychiatrists accepted private, non–capitated insurance in 2005-2006, and that declined to 55.3% in 2009-2010; in contrast, 93.1% of physicians in other specialties accepted private, non–capitated insurance in 2005-2006 and that declined to only 88.7% in 2009-2010.
Data source: An analysis of National Ambulatory Medical Care Survey data concerning insurance acceptance in a nationally representative sample of office-based physicians who provided 90% of outpatient care in the United State in 2005-2010.
Disclosures: This study was supported by the National Institute on Aging, Cornell University, the U.S. Department of Veterans Affairs, and the National Institutes of Health. No potential financial conflicts of interest were disclosed.
Quadrivalent flu vaccine effective in 3- to 8-year-olds
An inactivated quadrivalent influenza vaccine showed an overall efficacy of 55% against influenza A or B of any severity in an industry-sponsored phase III clinical trial involving children aged 3-8 years, which was reported online Dec. 11 in the New England Journal of Medicine.
The vaccine was most useful, with an efficacy of approximately 70%, against moderate to severe influenza. This is "a potentially important endpoint associated with the highest clinical, social, and economic burden" of disease, said Dr. Varsha K. Jain of GlaxoSmithKline Vaccines, King of Prussia, Pa., and his associates.
Participants in the randomized controlled trial were healthy children treated at 15 medical centers in Bangladesh, the Dominican Republic, Honduras, Lebanon, Panama, the Philippines, Thailand, and Turkey. The mean age was 5.4 years, and there were approximately equal numbers of boys and girls.
The 5,168 participants were randomly assigned to receive either the quadrivalent flu vaccine (2,584 children) or the hepatitis A vaccine as a control condition (2,584 children), and were followed for 6-8 months for the development of influenza-like illness. Influenza A or B was confirmed by polymerase chain reaction (PCR) assay of nasal or throat swabs.
The primary endpoint of the study was the development of influenza A or B of any severity during follow-up. A total of 62 children (2.4%) in the vaccine group and 148 (5.7%) in the control group developed influenza, a significant difference.
In a per-protocol analysis involving a subset of 768 children, 58 participants (2.4%) in the flu vaccine group and 128 (5.3%) in the control group developed influenza, also a significant difference.
"The study met its primary objective by showing that the efficacy of the quadrivalent influenza vaccine against any case of PCR-confirmed influenza was 59.3% in the total vaccinated cohort and 55.4% in the per-protocol cohort," Dr. Jain and his associates reported (N. Engl. J. Med. 2013 Dec. 11 [doi: 10.1056/NEJMoa1215817]).
In a further analysis of the data, cases of influenza were categorized as either mild or moderate to severe. The vaccine showed an efficacy of 74.2% against moderate to severe disease among children in the total study cohort, and an efficacy of 73.1% against moderate to severe disease among children in the per-protocol subset.
In a post hoc exploratory analysis, the quadrivalent flu vaccine "was associated with an 80% reduction in the rate of lower respiratory tract illness (the most common serious outcome of influenza) and a 70% reduction in the rate of body temperature above 39 C, as compared with the control vaccine," the investigators said.
Serious adverse events occurred in 1.4% of the flu vaccine group and 0.9% of the control group, a nonsignificant difference. "There were no notable differences between the flu vaccine group and the control group with respect to safety endpoints, except that pain at the injection site was reported more frequently in the flu vaccine group," Dr. Jain and his associates said.
Until now, the evidence from randomized trials in support of the use of inactivated influenza vaccines among healthy children has been limited. This study provides evidence of the quadrivalent vaccine’s efficacy and safety, they added.
The quadrivalent vaccine contained strains of influenza A/California/7/2009 (H1N1), A/Victoria/210/2009 (H3N2), B/Brisbane/60/2008 (Victoria), and B/Florida/4/2006 (Yamagata).
This trial was funded by the vaccine manufacturer, GlaxoSmithKline. Dr. Jain and some of his associates are employed by GlaxoSmithKline. Dr. Jain’s associates also reported ties to Sanofi Pasteur, Novartis, and other companies.
An inactivated quadrivalent influenza vaccine showed an overall efficacy of 55% against influenza A or B of any severity in an industry-sponsored phase III clinical trial involving children aged 3-8 years, which was reported online Dec. 11 in the New England Journal of Medicine.
The vaccine was most useful, with an efficacy of approximately 70%, against moderate to severe influenza. This is "a potentially important endpoint associated with the highest clinical, social, and economic burden" of disease, said Dr. Varsha K. Jain of GlaxoSmithKline Vaccines, King of Prussia, Pa., and his associates.
Participants in the randomized controlled trial were healthy children treated at 15 medical centers in Bangladesh, the Dominican Republic, Honduras, Lebanon, Panama, the Philippines, Thailand, and Turkey. The mean age was 5.4 years, and there were approximately equal numbers of boys and girls.
The 5,168 participants were randomly assigned to receive either the quadrivalent flu vaccine (2,584 children) or the hepatitis A vaccine as a control condition (2,584 children), and were followed for 6-8 months for the development of influenza-like illness. Influenza A or B was confirmed by polymerase chain reaction (PCR) assay of nasal or throat swabs.
The primary endpoint of the study was the development of influenza A or B of any severity during follow-up. A total of 62 children (2.4%) in the vaccine group and 148 (5.7%) in the control group developed influenza, a significant difference.
In a per-protocol analysis involving a subset of 768 children, 58 participants (2.4%) in the flu vaccine group and 128 (5.3%) in the control group developed influenza, also a significant difference.
"The study met its primary objective by showing that the efficacy of the quadrivalent influenza vaccine against any case of PCR-confirmed influenza was 59.3% in the total vaccinated cohort and 55.4% in the per-protocol cohort," Dr. Jain and his associates reported (N. Engl. J. Med. 2013 Dec. 11 [doi: 10.1056/NEJMoa1215817]).
In a further analysis of the data, cases of influenza were categorized as either mild or moderate to severe. The vaccine showed an efficacy of 74.2% against moderate to severe disease among children in the total study cohort, and an efficacy of 73.1% against moderate to severe disease among children in the per-protocol subset.
In a post hoc exploratory analysis, the quadrivalent flu vaccine "was associated with an 80% reduction in the rate of lower respiratory tract illness (the most common serious outcome of influenza) and a 70% reduction in the rate of body temperature above 39 C, as compared with the control vaccine," the investigators said.
Serious adverse events occurred in 1.4% of the flu vaccine group and 0.9% of the control group, a nonsignificant difference. "There were no notable differences between the flu vaccine group and the control group with respect to safety endpoints, except that pain at the injection site was reported more frequently in the flu vaccine group," Dr. Jain and his associates said.
Until now, the evidence from randomized trials in support of the use of inactivated influenza vaccines among healthy children has been limited. This study provides evidence of the quadrivalent vaccine’s efficacy and safety, they added.
The quadrivalent vaccine contained strains of influenza A/California/7/2009 (H1N1), A/Victoria/210/2009 (H3N2), B/Brisbane/60/2008 (Victoria), and B/Florida/4/2006 (Yamagata).
This trial was funded by the vaccine manufacturer, GlaxoSmithKline. Dr. Jain and some of his associates are employed by GlaxoSmithKline. Dr. Jain’s associates also reported ties to Sanofi Pasteur, Novartis, and other companies.
An inactivated quadrivalent influenza vaccine showed an overall efficacy of 55% against influenza A or B of any severity in an industry-sponsored phase III clinical trial involving children aged 3-8 years, which was reported online Dec. 11 in the New England Journal of Medicine.
The vaccine was most useful, with an efficacy of approximately 70%, against moderate to severe influenza. This is "a potentially important endpoint associated with the highest clinical, social, and economic burden" of disease, said Dr. Varsha K. Jain of GlaxoSmithKline Vaccines, King of Prussia, Pa., and his associates.
Participants in the randomized controlled trial were healthy children treated at 15 medical centers in Bangladesh, the Dominican Republic, Honduras, Lebanon, Panama, the Philippines, Thailand, and Turkey. The mean age was 5.4 years, and there were approximately equal numbers of boys and girls.
The 5,168 participants were randomly assigned to receive either the quadrivalent flu vaccine (2,584 children) or the hepatitis A vaccine as a control condition (2,584 children), and were followed for 6-8 months for the development of influenza-like illness. Influenza A or B was confirmed by polymerase chain reaction (PCR) assay of nasal or throat swabs.
The primary endpoint of the study was the development of influenza A or B of any severity during follow-up. A total of 62 children (2.4%) in the vaccine group and 148 (5.7%) in the control group developed influenza, a significant difference.
In a per-protocol analysis involving a subset of 768 children, 58 participants (2.4%) in the flu vaccine group and 128 (5.3%) in the control group developed influenza, also a significant difference.
"The study met its primary objective by showing that the efficacy of the quadrivalent influenza vaccine against any case of PCR-confirmed influenza was 59.3% in the total vaccinated cohort and 55.4% in the per-protocol cohort," Dr. Jain and his associates reported (N. Engl. J. Med. 2013 Dec. 11 [doi: 10.1056/NEJMoa1215817]).
In a further analysis of the data, cases of influenza were categorized as either mild or moderate to severe. The vaccine showed an efficacy of 74.2% against moderate to severe disease among children in the total study cohort, and an efficacy of 73.1% against moderate to severe disease among children in the per-protocol subset.
In a post hoc exploratory analysis, the quadrivalent flu vaccine "was associated with an 80% reduction in the rate of lower respiratory tract illness (the most common serious outcome of influenza) and a 70% reduction in the rate of body temperature above 39 C, as compared with the control vaccine," the investigators said.
Serious adverse events occurred in 1.4% of the flu vaccine group and 0.9% of the control group, a nonsignificant difference. "There were no notable differences between the flu vaccine group and the control group with respect to safety endpoints, except that pain at the injection site was reported more frequently in the flu vaccine group," Dr. Jain and his associates said.
Until now, the evidence from randomized trials in support of the use of inactivated influenza vaccines among healthy children has been limited. This study provides evidence of the quadrivalent vaccine’s efficacy and safety, they added.
The quadrivalent vaccine contained strains of influenza A/California/7/2009 (H1N1), A/Victoria/210/2009 (H3N2), B/Brisbane/60/2008 (Victoria), and B/Florida/4/2006 (Yamagata).
This trial was funded by the vaccine manufacturer, GlaxoSmithKline. Dr. Jain and some of his associates are employed by GlaxoSmithKline. Dr. Jain’s associates also reported ties to Sanofi Pasteur, Novartis, and other companies.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: A total of 2.4% of the flu vaccine group developed influenza A or B, compared with 5.7% of the control group.
Data source: An international, randomized controlled phase III study involving 5,168 children aged 3-8 years who received either a quadrivalent flu vaccine or a control vaccine and were followed for 6-8 months.
Disclosures: This trial was funded by the vaccine manufacturer, GlaxoSmithKline. Dr. Jain and some of his associates are employed by GlaxoSmithKline. Dr. Jain’s associates also reported ties to Sanofi Pasteur, Novartis, and other companies.
CPAP improves resistant hypertension in patients with obstructive sleep apnea
For patients who have resistant hypertension and obstructive sleep apnea, 3 months of treatment with continuous positive airway pressure significantly reduces mean and diastolic blood pressure and improves the nocturnal blood pressure pattern, according to a report published online Dec. 10 in JAMA.
These improvements are dose related, with mean blood pressure decreasing 1.3 mm Hg, systolic blood pressure decreasing 1.9 mm Hg, and diastolic blood pressure decreasing 1.0 mm Hg for every additional hour of CPAP use, said Dr. Miguel-Angel Martinez-Garcia of the respiratory department at Hospital Universitario y Politecnico La Fe, Valencia (Spain), and his associates.
"Obstructive sleep apnea is highly prevalent in patients with resistant hypertension, regardless of other confounding variables such as the presence of obesity, thus suggesting this subgroup of hypertensive patients is a potential worthwhile population for CPAP treatment," they said.
"International guidelines have pointed out that even minimal reductions in blood pressure levels (to the order of 2-3 mm Hg of systolic pressure) could have a clinically significant effect by greatly reducing subsequent cardiovascular mortality (between 6% and 8% for stroke and 4% and 5% for coronary heart disease)," Dr. Martinez-Garcia and his colleagues noted.
Previous studies have shown that CPAP produces clinically significant decreases in blood pressure levels, but all have had "significant methodological limitations such as small cohorts or lack of randomization." So Dr. Martinez-Garcia and his associates performed a large randomized multicenter clinical trial to assess the issue.
They identified 194 adults treated at 24 teaching hospitals across Spain who had resistant hypertension unrelated to known causes such as primary aldosteronism, renal artery stenosis, or renal insufficiency. Resistant hypertension was confirmed via 24-hour ambulatory blood pressure monitoring. The study subjects also had obstructive sleep apnea, which was confirmed by standard sleep studies.
These subjects were randomly assigned to receive CPAP (98 patients) or no intervention (96 patients who served as controls) while continuing their usual regimens of antihypertensive treatment. Approximately 69% of the subjects were men; the mean age was 56 years, the mean body mass index was 34.1, the mean number of antihypertensive drugs taken was 3.8, and the mean apnea-hypopnea index was 40.4 events per hour.
In the intention-to-treat analysis, after 3 months, the CPAP group achieved significantly greater decreases in 24-hour mean blood pressure and 24-hour mean diastolic blood pressure, and showed greater improvements during the night than during daytime. They also converted to more favorable nocturnal "dipper" and "riser" patterns in blood pressure, indicating decreased cardiovascular risk.
In the per-protocol analysis involving the 71 CPAP patients and 87 controls who adhered to the study protocol, these improvements were even more pronounced: The CPAP group showed a significant 4.4–mm HG decrease in 24-hour mean blood pressure, a 4.9–mm Hg decrease in systolic blood pressure, and a 4.1–mm Hg decrease in diastolic blood pressure (JAMA 2013 Dec. 10 [doi:10.1001/jama.2012.281250]).
At night, these figures were even better, with a 7.1–mm Hg decrease in systolic blood pressure and 4.1–mm Hg decrease in diastolic blood pressure. And again, the CPAP patients were more likely to convert to more favorable nocturnal "dipper" and "riser" patters in blood pressure.
There also was a positive linear correlation between the number of hours of CPAP use per night and the decrease in 24-hour mean blood pressure and diastolic blood pressure.
"Our results confirm that there is a clinically and statistically significant reduction in both 24-hour mean and diastolic blood pressure levels, especially during the night and in those patients with acceptable CPAP adherence," Dr. Martinez-Garcia and his associates said.
Further research is warranted to assess whether these benefits translate into better health outcomes in the long term, they added.
This study was supported by Philips Respironics, Sociedad Espanola de Neumologia, Instituto de Salud Carlos III, and Sociedad Valencia de Neumologia. No conflicts of interest were reported.
For patients who have resistant hypertension and obstructive sleep apnea, 3 months of treatment with continuous positive airway pressure significantly reduces mean and diastolic blood pressure and improves the nocturnal blood pressure pattern, according to a report published online Dec. 10 in JAMA.
These improvements are dose related, with mean blood pressure decreasing 1.3 mm Hg, systolic blood pressure decreasing 1.9 mm Hg, and diastolic blood pressure decreasing 1.0 mm Hg for every additional hour of CPAP use, said Dr. Miguel-Angel Martinez-Garcia of the respiratory department at Hospital Universitario y Politecnico La Fe, Valencia (Spain), and his associates.
"Obstructive sleep apnea is highly prevalent in patients with resistant hypertension, regardless of other confounding variables such as the presence of obesity, thus suggesting this subgroup of hypertensive patients is a potential worthwhile population for CPAP treatment," they said.
"International guidelines have pointed out that even minimal reductions in blood pressure levels (to the order of 2-3 mm Hg of systolic pressure) could have a clinically significant effect by greatly reducing subsequent cardiovascular mortality (between 6% and 8% for stroke and 4% and 5% for coronary heart disease)," Dr. Martinez-Garcia and his colleagues noted.
Previous studies have shown that CPAP produces clinically significant decreases in blood pressure levels, but all have had "significant methodological limitations such as small cohorts or lack of randomization." So Dr. Martinez-Garcia and his associates performed a large randomized multicenter clinical trial to assess the issue.
They identified 194 adults treated at 24 teaching hospitals across Spain who had resistant hypertension unrelated to known causes such as primary aldosteronism, renal artery stenosis, or renal insufficiency. Resistant hypertension was confirmed via 24-hour ambulatory blood pressure monitoring. The study subjects also had obstructive sleep apnea, which was confirmed by standard sleep studies.
These subjects were randomly assigned to receive CPAP (98 patients) or no intervention (96 patients who served as controls) while continuing their usual regimens of antihypertensive treatment. Approximately 69% of the subjects were men; the mean age was 56 years, the mean body mass index was 34.1, the mean number of antihypertensive drugs taken was 3.8, and the mean apnea-hypopnea index was 40.4 events per hour.
In the intention-to-treat analysis, after 3 months, the CPAP group achieved significantly greater decreases in 24-hour mean blood pressure and 24-hour mean diastolic blood pressure, and showed greater improvements during the night than during daytime. They also converted to more favorable nocturnal "dipper" and "riser" patterns in blood pressure, indicating decreased cardiovascular risk.
In the per-protocol analysis involving the 71 CPAP patients and 87 controls who adhered to the study protocol, these improvements were even more pronounced: The CPAP group showed a significant 4.4–mm HG decrease in 24-hour mean blood pressure, a 4.9–mm Hg decrease in systolic blood pressure, and a 4.1–mm Hg decrease in diastolic blood pressure (JAMA 2013 Dec. 10 [doi:10.1001/jama.2012.281250]).
At night, these figures were even better, with a 7.1–mm Hg decrease in systolic blood pressure and 4.1–mm Hg decrease in diastolic blood pressure. And again, the CPAP patients were more likely to convert to more favorable nocturnal "dipper" and "riser" patters in blood pressure.
There also was a positive linear correlation between the number of hours of CPAP use per night and the decrease in 24-hour mean blood pressure and diastolic blood pressure.
"Our results confirm that there is a clinically and statistically significant reduction in both 24-hour mean and diastolic blood pressure levels, especially during the night and in those patients with acceptable CPAP adherence," Dr. Martinez-Garcia and his associates said.
Further research is warranted to assess whether these benefits translate into better health outcomes in the long term, they added.
This study was supported by Philips Respironics, Sociedad Espanola de Neumologia, Instituto de Salud Carlos III, and Sociedad Valencia de Neumologia. No conflicts of interest were reported.
For patients who have resistant hypertension and obstructive sleep apnea, 3 months of treatment with continuous positive airway pressure significantly reduces mean and diastolic blood pressure and improves the nocturnal blood pressure pattern, according to a report published online Dec. 10 in JAMA.
These improvements are dose related, with mean blood pressure decreasing 1.3 mm Hg, systolic blood pressure decreasing 1.9 mm Hg, and diastolic blood pressure decreasing 1.0 mm Hg for every additional hour of CPAP use, said Dr. Miguel-Angel Martinez-Garcia of the respiratory department at Hospital Universitario y Politecnico La Fe, Valencia (Spain), and his associates.
"Obstructive sleep apnea is highly prevalent in patients with resistant hypertension, regardless of other confounding variables such as the presence of obesity, thus suggesting this subgroup of hypertensive patients is a potential worthwhile population for CPAP treatment," they said.
"International guidelines have pointed out that even minimal reductions in blood pressure levels (to the order of 2-3 mm Hg of systolic pressure) could have a clinically significant effect by greatly reducing subsequent cardiovascular mortality (between 6% and 8% for stroke and 4% and 5% for coronary heart disease)," Dr. Martinez-Garcia and his colleagues noted.
Previous studies have shown that CPAP produces clinically significant decreases in blood pressure levels, but all have had "significant methodological limitations such as small cohorts or lack of randomization." So Dr. Martinez-Garcia and his associates performed a large randomized multicenter clinical trial to assess the issue.
They identified 194 adults treated at 24 teaching hospitals across Spain who had resistant hypertension unrelated to known causes such as primary aldosteronism, renal artery stenosis, or renal insufficiency. Resistant hypertension was confirmed via 24-hour ambulatory blood pressure monitoring. The study subjects also had obstructive sleep apnea, which was confirmed by standard sleep studies.
These subjects were randomly assigned to receive CPAP (98 patients) or no intervention (96 patients who served as controls) while continuing their usual regimens of antihypertensive treatment. Approximately 69% of the subjects were men; the mean age was 56 years, the mean body mass index was 34.1, the mean number of antihypertensive drugs taken was 3.8, and the mean apnea-hypopnea index was 40.4 events per hour.
In the intention-to-treat analysis, after 3 months, the CPAP group achieved significantly greater decreases in 24-hour mean blood pressure and 24-hour mean diastolic blood pressure, and showed greater improvements during the night than during daytime. They also converted to more favorable nocturnal "dipper" and "riser" patterns in blood pressure, indicating decreased cardiovascular risk.
In the per-protocol analysis involving the 71 CPAP patients and 87 controls who adhered to the study protocol, these improvements were even more pronounced: The CPAP group showed a significant 4.4–mm HG decrease in 24-hour mean blood pressure, a 4.9–mm Hg decrease in systolic blood pressure, and a 4.1–mm Hg decrease in diastolic blood pressure (JAMA 2013 Dec. 10 [doi:10.1001/jama.2012.281250]).
At night, these figures were even better, with a 7.1–mm Hg decrease in systolic blood pressure and 4.1–mm Hg decrease in diastolic blood pressure. And again, the CPAP patients were more likely to convert to more favorable nocturnal "dipper" and "riser" patters in blood pressure.
There also was a positive linear correlation between the number of hours of CPAP use per night and the decrease in 24-hour mean blood pressure and diastolic blood pressure.
"Our results confirm that there is a clinically and statistically significant reduction in both 24-hour mean and diastolic blood pressure levels, especially during the night and in those patients with acceptable CPAP adherence," Dr. Martinez-Garcia and his associates said.
Further research is warranted to assess whether these benefits translate into better health outcomes in the long term, they added.
This study was supported by Philips Respironics, Sociedad Espanola de Neumologia, Instituto de Salud Carlos III, and Sociedad Valencia de Neumologia. No conflicts of interest were reported.
FROM JAMA
Major finding: In the per-protocol analysis involving the 71 CPAP patients and 87 controls who adhered to the study protocol, the CPAP group showed a significant 4.4–mm HG decrease in 24-hour mean blood pressure, a 4.9–mm Hg decrease in systolic blood pressure, and a 4.1–mm Hg decrease in diastolic blood pressure.
Data source: An open-label multicenter randomized clinical trial involving 194 patients with concomitant resistant hypertension and obstructive sleep apnea who received either CPAP or no intervention for 3 months.
Disclosures: This study was supported by Philips Respironics, Sociedad Espanola de Neumologia, Instituto de Salud Carlos III, and Sociedad Valencia de Neumologia. No conflicts of interest were reported.
Gastric acid inhibitors linked to vitamin B12 deficiency
The use of gastric acid inhibitors for 2 or more years is strongly associated with symptomatic vitamin B12 deficiency, according to a report published online Dec. 10 in JAMA.
This association with proton pump inhibitors (PPIs) and histamine H2 receptor antagonists (H2RA) was stronger than that for other conditions known to be associated with vitamin B12 deficiency, such as thyroid disease, diabetes, and atrophic gastritis, said Jameson R. Lam of the division of research, Kaiser Permanente, Oakland, Calif., and his associates.
"These findings do not recommend against acid suppression for persons with clear indications for treatment, but clinicians should exercise appropriate vigilance when prescribing these medications and use the lowest possible effective dose," the investigators said.
Previous studies of the relationship between these drugs and vitamin B12 deficiency have produced conflicting results, and there haven’t been any large population-based studies to date. Mr. Lam and his colleagues examined this issue by performing a case-control study within a large, community-based population that was ethnically diverse and had equal access to health care.
The case subjects were adults within the Kaiser Northern California health care system who had a new diagnosis of vitamin B12 deficiency between 1997 and 2011. People who had conditions known to cause vitamin B12 deficiency directly were excluded from the study.
Control subjects for each case subject were up to 10 adults who did not have vitamin B12 deficiency and who were matched for sex, area of residence, race/ethnicity, year of birth, and membership duration.
Only people who had taken PPIs or H2RAs for 2 years or more were included. This yielded 25,956 cases and 184,199 matched controls for the analysis.
In the primary analyses, a new diagnosis of vitamin B12 deficiency was more common in PPI users than in nonusers, with an odds ratio of 1.65. It also was more common in H2RA users than in nonusers, with an OR of 1.25, the investigators said (JAMA 2013;310:2435-42).
Using a higher mean daily dose of PPIs (1.5 or more PPI pills per day) was more strongly associated with vitamin B12 deficiency, with an OR of 1.95, than was a lower mean daily dose (less than 0.75 PPI pills per day), which had an OR of 1.63. This same pattern was seen with higher vs lower H2RA doses.
Similarly, vitamin B12 deficiency was more strongly associated with longer durations of PPI use than with shorter durations. However, no such trend was noted with the duration of H2RA use.
The strength of the association between vitamin B12 deficiency and PPI use diminished after the medication was discontinued. The link was strongest among current users (OR, 1.80), weaker among patients whose most recent use was 2-3 years previously (OR, 1.43), and weakest among those whose most recent use was 3 or more years previously (OR, 1.38).
The association between vitamin B12 deficiency and the use of acid inhibitors was strongest among patients younger than 30 years of age and diminished with increasing age. It also was stronger among women than among men. However, the strength of the association did not differ across racial/ethnic categories, or between patients who had a GERD diagnosis and those who did not.
The strength of the association also did not change over time; it was similar between cases diagnosed in 1997-2003, before PPIs were made available as over-the-counter medications, as among cases diagnosed afterward.
"At a minimum, the use of these medications identifies a population at higher risk of B12 deficiency, independent of additional risk factors," Dr. Lam and his associates said.
This study was supported by Kaiser Permanente. Dr. Lam reported no conflicts of interest; one of his associates reported receiving grants from Wyeth/Pfizer.
The use of gastric acid inhibitors for 2 or more years is strongly associated with symptomatic vitamin B12 deficiency, according to a report published online Dec. 10 in JAMA.
This association with proton pump inhibitors (PPIs) and histamine H2 receptor antagonists (H2RA) was stronger than that for other conditions known to be associated with vitamin B12 deficiency, such as thyroid disease, diabetes, and atrophic gastritis, said Jameson R. Lam of the division of research, Kaiser Permanente, Oakland, Calif., and his associates.
"These findings do not recommend against acid suppression for persons with clear indications for treatment, but clinicians should exercise appropriate vigilance when prescribing these medications and use the lowest possible effective dose," the investigators said.
Previous studies of the relationship between these drugs and vitamin B12 deficiency have produced conflicting results, and there haven’t been any large population-based studies to date. Mr. Lam and his colleagues examined this issue by performing a case-control study within a large, community-based population that was ethnically diverse and had equal access to health care.
The case subjects were adults within the Kaiser Northern California health care system who had a new diagnosis of vitamin B12 deficiency between 1997 and 2011. People who had conditions known to cause vitamin B12 deficiency directly were excluded from the study.
Control subjects for each case subject were up to 10 adults who did not have vitamin B12 deficiency and who were matched for sex, area of residence, race/ethnicity, year of birth, and membership duration.
Only people who had taken PPIs or H2RAs for 2 years or more were included. This yielded 25,956 cases and 184,199 matched controls for the analysis.
In the primary analyses, a new diagnosis of vitamin B12 deficiency was more common in PPI users than in nonusers, with an odds ratio of 1.65. It also was more common in H2RA users than in nonusers, with an OR of 1.25, the investigators said (JAMA 2013;310:2435-42).
Using a higher mean daily dose of PPIs (1.5 or more PPI pills per day) was more strongly associated with vitamin B12 deficiency, with an OR of 1.95, than was a lower mean daily dose (less than 0.75 PPI pills per day), which had an OR of 1.63. This same pattern was seen with higher vs lower H2RA doses.
Similarly, vitamin B12 deficiency was more strongly associated with longer durations of PPI use than with shorter durations. However, no such trend was noted with the duration of H2RA use.
The strength of the association between vitamin B12 deficiency and PPI use diminished after the medication was discontinued. The link was strongest among current users (OR, 1.80), weaker among patients whose most recent use was 2-3 years previously (OR, 1.43), and weakest among those whose most recent use was 3 or more years previously (OR, 1.38).
The association between vitamin B12 deficiency and the use of acid inhibitors was strongest among patients younger than 30 years of age and diminished with increasing age. It also was stronger among women than among men. However, the strength of the association did not differ across racial/ethnic categories, or between patients who had a GERD diagnosis and those who did not.
The strength of the association also did not change over time; it was similar between cases diagnosed in 1997-2003, before PPIs were made available as over-the-counter medications, as among cases diagnosed afterward.
"At a minimum, the use of these medications identifies a population at higher risk of B12 deficiency, independent of additional risk factors," Dr. Lam and his associates said.
This study was supported by Kaiser Permanente. Dr. Lam reported no conflicts of interest; one of his associates reported receiving grants from Wyeth/Pfizer.
The use of gastric acid inhibitors for 2 or more years is strongly associated with symptomatic vitamin B12 deficiency, according to a report published online Dec. 10 in JAMA.
This association with proton pump inhibitors (PPIs) and histamine H2 receptor antagonists (H2RA) was stronger than that for other conditions known to be associated with vitamin B12 deficiency, such as thyroid disease, diabetes, and atrophic gastritis, said Jameson R. Lam of the division of research, Kaiser Permanente, Oakland, Calif., and his associates.
"These findings do not recommend against acid suppression for persons with clear indications for treatment, but clinicians should exercise appropriate vigilance when prescribing these medications and use the lowest possible effective dose," the investigators said.
Previous studies of the relationship between these drugs and vitamin B12 deficiency have produced conflicting results, and there haven’t been any large population-based studies to date. Mr. Lam and his colleagues examined this issue by performing a case-control study within a large, community-based population that was ethnically diverse and had equal access to health care.
The case subjects were adults within the Kaiser Northern California health care system who had a new diagnosis of vitamin B12 deficiency between 1997 and 2011. People who had conditions known to cause vitamin B12 deficiency directly were excluded from the study.
Control subjects for each case subject were up to 10 adults who did not have vitamin B12 deficiency and who were matched for sex, area of residence, race/ethnicity, year of birth, and membership duration.
Only people who had taken PPIs or H2RAs for 2 years or more were included. This yielded 25,956 cases and 184,199 matched controls for the analysis.
In the primary analyses, a new diagnosis of vitamin B12 deficiency was more common in PPI users than in nonusers, with an odds ratio of 1.65. It also was more common in H2RA users than in nonusers, with an OR of 1.25, the investigators said (JAMA 2013;310:2435-42).
Using a higher mean daily dose of PPIs (1.5 or more PPI pills per day) was more strongly associated with vitamin B12 deficiency, with an OR of 1.95, than was a lower mean daily dose (less than 0.75 PPI pills per day), which had an OR of 1.63. This same pattern was seen with higher vs lower H2RA doses.
Similarly, vitamin B12 deficiency was more strongly associated with longer durations of PPI use than with shorter durations. However, no such trend was noted with the duration of H2RA use.
The strength of the association between vitamin B12 deficiency and PPI use diminished after the medication was discontinued. The link was strongest among current users (OR, 1.80), weaker among patients whose most recent use was 2-3 years previously (OR, 1.43), and weakest among those whose most recent use was 3 or more years previously (OR, 1.38).
The association between vitamin B12 deficiency and the use of acid inhibitors was strongest among patients younger than 30 years of age and diminished with increasing age. It also was stronger among women than among men. However, the strength of the association did not differ across racial/ethnic categories, or between patients who had a GERD diagnosis and those who did not.
The strength of the association also did not change over time; it was similar between cases diagnosed in 1997-2003, before PPIs were made available as over-the-counter medications, as among cases diagnosed afterward.
"At a minimum, the use of these medications identifies a population at higher risk of B12 deficiency, independent of additional risk factors," Dr. Lam and his associates said.
This study was supported by Kaiser Permanente. Dr. Lam reported no conflicts of interest; one of his associates reported receiving grants from Wyeth/Pfizer.
FROM JAMA
Major finding: A new diagnosis of vitamin B12 deficiency was more common in PPI users than in nonusers (odds ratio, 1.65), and more common in H2RA users than in nonusers (OR, 1.25).
Data source: A case-control study comparing the use of gastric acid inhibitors among 25,956 patients newly diagnosed with vitamin B12 deficiency in 1997-2011 and 184,199 matched controls without such deficiency.
Disclosures: This study was supported by Kaiser Permanente. Dr. Lam reported no conflicts of interest; one of his associates reported receiving grants from Wyeth/Pfizer.
18% of lung cancers caught by CT screening were indolent
An estimated 18% of the early lung cancers detected by low-dose CT screening in the National Lung Screening Trial were likely indolent and probably represent overdiagnosis, according to a report published online Dec. 9 in JAMA Internal Medicine.
The National Lung Screening Trial (NLST) found "an encouraging" 20% relative reduction in lung cancer–specific mortality among high-risk patients who were screened using low-dose CT, compared with chest radiography. "These findings were met with enthusiasm, but before a widespread public health screening program is implemented, risks of screening also need to be considered," said Dr. Edward F. Patz Jr. of the department of radiology, Duke University Medical Center, Durham, N.C., and his associates in the NLST.
The chief risk in this case is overdiagnosis: identifying an early-stage lesion in an asymptomatic patient that would not progress or affect that patient’s long-term health. It is likely that some of the tumors detected on low-dose CT were just such indolent cancers, and that those patients unnecessarily underwent invasive diagnostic procedures, surgical resection, and multiple follow-up studies.
To estimate how many of the detected cancers in the NLST were indolent – and thus overdiagnosed – Dr. Patz and his colleagues used statistical probability methods to analyze extended follow-up data from the study.
The NLST involved 53,452 men and women aged 55-74 years who were enrolled during 2002-2004 and who had at least a 30-pack-year history of cigarette smoking. The patients were randomly assigned to undergo lung cancer screening using either three annual low-dose CT exams or three annual single-view chest radiographs.
Mean follow-up was approximately 6 years. "At the end of the entire trial, there were 1,089 total lung cancer cases in the low-dose CT arm (649 detected by low-dose CT screening) and 969 cases in the [radiology] arm, for an excess of 120 cases. This gives [an] excess cancer rate of 18.5%," the investigators said (JAMA Intern. Med. 2013 Dec. 9 [doi:10.1001/jamainternmed.2013.12738]).
"The data from this study suggest that ... 18% of persons in the low-dose CT arm with screen-detected lung cancer and 22% of those in the low-dose CT arm with screen-detected NSCLC [non–small cell lung cancer] may be cases of overdiagnosis," Dr. Patz and his associates said. "In other words, if these individuals had not entered the NLST, they would not have received a lung cancer diagnosis or treatment, at least for the next 5 years."
In the future, the study authors noted, "once there are better biomarkers and imaging techniques to predict which individuals with a diagnosis of lung cancer will have more or less aggressive disease, treatment options can be optimized, and a mass screening program can become more valuable."
The National Institutes of Health supported the NSLT. No financial conflicts of interest were reported.
An estimated 18% of the early lung cancers detected by low-dose CT screening in the National Lung Screening Trial were likely indolent and probably represent overdiagnosis, according to a report published online Dec. 9 in JAMA Internal Medicine.
The National Lung Screening Trial (NLST) found "an encouraging" 20% relative reduction in lung cancer–specific mortality among high-risk patients who were screened using low-dose CT, compared with chest radiography. "These findings were met with enthusiasm, but before a widespread public health screening program is implemented, risks of screening also need to be considered," said Dr. Edward F. Patz Jr. of the department of radiology, Duke University Medical Center, Durham, N.C., and his associates in the NLST.
The chief risk in this case is overdiagnosis: identifying an early-stage lesion in an asymptomatic patient that would not progress or affect that patient’s long-term health. It is likely that some of the tumors detected on low-dose CT were just such indolent cancers, and that those patients unnecessarily underwent invasive diagnostic procedures, surgical resection, and multiple follow-up studies.
To estimate how many of the detected cancers in the NLST were indolent – and thus overdiagnosed – Dr. Patz and his colleagues used statistical probability methods to analyze extended follow-up data from the study.
The NLST involved 53,452 men and women aged 55-74 years who were enrolled during 2002-2004 and who had at least a 30-pack-year history of cigarette smoking. The patients were randomly assigned to undergo lung cancer screening using either three annual low-dose CT exams or three annual single-view chest radiographs.
Mean follow-up was approximately 6 years. "At the end of the entire trial, there were 1,089 total lung cancer cases in the low-dose CT arm (649 detected by low-dose CT screening) and 969 cases in the [radiology] arm, for an excess of 120 cases. This gives [an] excess cancer rate of 18.5%," the investigators said (JAMA Intern. Med. 2013 Dec. 9 [doi:10.1001/jamainternmed.2013.12738]).
"The data from this study suggest that ... 18% of persons in the low-dose CT arm with screen-detected lung cancer and 22% of those in the low-dose CT arm with screen-detected NSCLC [non–small cell lung cancer] may be cases of overdiagnosis," Dr. Patz and his associates said. "In other words, if these individuals had not entered the NLST, they would not have received a lung cancer diagnosis or treatment, at least for the next 5 years."
In the future, the study authors noted, "once there are better biomarkers and imaging techniques to predict which individuals with a diagnosis of lung cancer will have more or less aggressive disease, treatment options can be optimized, and a mass screening program can become more valuable."
The National Institutes of Health supported the NSLT. No financial conflicts of interest were reported.
An estimated 18% of the early lung cancers detected by low-dose CT screening in the National Lung Screening Trial were likely indolent and probably represent overdiagnosis, according to a report published online Dec. 9 in JAMA Internal Medicine.
The National Lung Screening Trial (NLST) found "an encouraging" 20% relative reduction in lung cancer–specific mortality among high-risk patients who were screened using low-dose CT, compared with chest radiography. "These findings were met with enthusiasm, but before a widespread public health screening program is implemented, risks of screening also need to be considered," said Dr. Edward F. Patz Jr. of the department of radiology, Duke University Medical Center, Durham, N.C., and his associates in the NLST.
The chief risk in this case is overdiagnosis: identifying an early-stage lesion in an asymptomatic patient that would not progress or affect that patient’s long-term health. It is likely that some of the tumors detected on low-dose CT were just such indolent cancers, and that those patients unnecessarily underwent invasive diagnostic procedures, surgical resection, and multiple follow-up studies.
To estimate how many of the detected cancers in the NLST were indolent – and thus overdiagnosed – Dr. Patz and his colleagues used statistical probability methods to analyze extended follow-up data from the study.
The NLST involved 53,452 men and women aged 55-74 years who were enrolled during 2002-2004 and who had at least a 30-pack-year history of cigarette smoking. The patients were randomly assigned to undergo lung cancer screening using either three annual low-dose CT exams or three annual single-view chest radiographs.
Mean follow-up was approximately 6 years. "At the end of the entire trial, there were 1,089 total lung cancer cases in the low-dose CT arm (649 detected by low-dose CT screening) and 969 cases in the [radiology] arm, for an excess of 120 cases. This gives [an] excess cancer rate of 18.5%," the investigators said (JAMA Intern. Med. 2013 Dec. 9 [doi:10.1001/jamainternmed.2013.12738]).
"The data from this study suggest that ... 18% of persons in the low-dose CT arm with screen-detected lung cancer and 22% of those in the low-dose CT arm with screen-detected NSCLC [non–small cell lung cancer] may be cases of overdiagnosis," Dr. Patz and his associates said. "In other words, if these individuals had not entered the NLST, they would not have received a lung cancer diagnosis or treatment, at least for the next 5 years."
In the future, the study authors noted, "once there are better biomarkers and imaging techniques to predict which individuals with a diagnosis of lung cancer will have more or less aggressive disease, treatment options can be optimized, and a mass screening program can become more valuable."
The National Institutes of Health supported the NSLT. No financial conflicts of interest were reported.
FROM JAMA INTERNAL MEDICINE
Major Finding: An estimated 18% of lung cancers detected by low-dose CT screening in the National Lung Screening Trial were likely indolent and may represent cases of overdiagnosis.
Data Source: A secondary analysis of data from the NLST which involved 53,452 patients aged 55-74 years who were at high risk for lung cancer because of their history of heavy smoking.
Disclosures: The National Institutes of Health supported the NSLT. No financial conflicts of interest were reported.
Smoking cessation agents don’t raise serious CVD risks
The three smoking cessation agents bupropion, varenicline, and nicotine replacement therapy did not raise the risk of serious adverse cardiovascular events in a network meta-analysis of 63 randomized clinical trials reported online Dec. 9 in Circulation.
This finding held true in the main analysis that included 30,508 patients attempting to quit smoking, in a subgroup analysis of the highest-risk patients who had a history of conditions predisposing them to cardiovascular events, and in a sensitivity analysis that broke down cardiovascular events by type and seriousness.
"Given the current findings of low risk of serious CVD events attributed to smoking cessation pharmacotherapies, combined with the well-established CVD and mortality risks of continued smoking, the benefits of use would seem to outweigh the risks," said Edward J. Mills, Ph.D., of the Stanford (Calif.) Prevention Research Center, and his associates.
The investigators performed the meta-analysis because recent reports have raised concerns that these agents may raise cardiovascular risks. They used a statistical technique known as network meta-analysis to examine both direct, head-to-head comparison studies and indirect evidence, "thus increasing the power and interpretability of a comparative analysis."
They included any randomized clinical trial of any of the three pharmacotherapies that were of any duration and that reported on any cardiovascular events. Dr. Mills and his colleagues then considered two separate definitions of cardiovascular events: the first was any such event, including minor occurrences such as palpitations, and the second was only major adverse cardiovascular events as defined by the Food and Drug Administration, which is "considered to be a more stringent definition of important patient outcomes."
A total of 19 of the randomized clinical trials assessed nicotine replacement therapy against placebo, 27 assessed bupropion against placebo, 18 assessed varenicline against placebo, 1 assessed high-dose nicotine replacement therapy against placebo, 1 assessed combination nicotine replacement therapy against a control condition, 2 assessed bupropion against varenicline, 3 assessed bupropion against nicotine replacement therapy, and 1 assessed varenicline against nicotine replacement therapy.
Both a pairwise meta-analysis and the network meta-analysis demonstrated that none of the three pharmacotherapies raised the risk of major adverse cardiovascular events. Bupropion appeared to exert a protective effect against both minor and major events, while varenicline showed no harmful or beneficial effect at all concerning minor or major cardiovascular events.
"Nicotine replacement therapy, the most widely used pharmacotherapy for smoking cessation, was associated with an increase in cardiovascular events that was driven by lower-risk events" such as palpitations and tachycardia, which are "well known and largely benign" effects of nicotine replacement, Dr. Mills and his associates said (Circulation 2013 Dec. 9 [doi:10.1161/circulationaha.113.003961]).
"Concerns about adverse cardiovascular events need to be balanced with the consistent evidence for the benefit of smoking cessation, and patients should be counseled about what adverse events may be associated with smoking cessation therapies, the symptoms associated with the withdrawal period from cigarettes, and symptoms that may be due to existing cardiovascular diseases," the investigators added.
This study was supported by the Canadian Institutes of Health Research, the U.S. National Institutes of Health, and the California Tobacco-Related Disease Research Program. Dr. Mills reported ties to Merck; Pfizer, maker of Chantix (varenicline); Novartis; Takeda; and GlaxoSmithKline, maker of Zyban (bupropion); and his associates reported ties to Pfizer.
Smoking cessation has benefits that extend well beyond cardiovascular disease, both for the individual patient and for the general public, said Dr. Jonathan M. Samet.
Any increased risk for minor cardiovascular events associated with nicotine replacement therapy must be viewed against "the declines in risk for CVD and other diseases that follow successful cessation," he said.
"Even with the assumption of [an excess CVD] risk associated with nicotine replacement therapy, the population-level benefits far exceed the estimated increase."
Dr. Samet is in the department of preventive medicine and the Institute for Global Health at the University of Southern California, Los Angeles. His work is supported by the National Cancer Institute and the FDA Center for Tobacco Products. These remarks were taken from his editorial accompanying Dr. Mills’ report (Circulation 2013 Dec. 9 [doi:10.1161/circulationaha.113.006928]).
Smoking cessation has benefits that extend well beyond cardiovascular disease, both for the individual patient and for the general public, said Dr. Jonathan M. Samet.
Any increased risk for minor cardiovascular events associated with nicotine replacement therapy must be viewed against "the declines in risk for CVD and other diseases that follow successful cessation," he said.
"Even with the assumption of [an excess CVD] risk associated with nicotine replacement therapy, the population-level benefits far exceed the estimated increase."
Dr. Samet is in the department of preventive medicine and the Institute for Global Health at the University of Southern California, Los Angeles. His work is supported by the National Cancer Institute and the FDA Center for Tobacco Products. These remarks were taken from his editorial accompanying Dr. Mills’ report (Circulation 2013 Dec. 9 [doi:10.1161/circulationaha.113.006928]).
Smoking cessation has benefits that extend well beyond cardiovascular disease, both for the individual patient and for the general public, said Dr. Jonathan M. Samet.
Any increased risk for minor cardiovascular events associated with nicotine replacement therapy must be viewed against "the declines in risk for CVD and other diseases that follow successful cessation," he said.
"Even with the assumption of [an excess CVD] risk associated with nicotine replacement therapy, the population-level benefits far exceed the estimated increase."
Dr. Samet is in the department of preventive medicine and the Institute for Global Health at the University of Southern California, Los Angeles. His work is supported by the National Cancer Institute and the FDA Center for Tobacco Products. These remarks were taken from his editorial accompanying Dr. Mills’ report (Circulation 2013 Dec. 9 [doi:10.1161/circulationaha.113.006928]).
The three smoking cessation agents bupropion, varenicline, and nicotine replacement therapy did not raise the risk of serious adverse cardiovascular events in a network meta-analysis of 63 randomized clinical trials reported online Dec. 9 in Circulation.
This finding held true in the main analysis that included 30,508 patients attempting to quit smoking, in a subgroup analysis of the highest-risk patients who had a history of conditions predisposing them to cardiovascular events, and in a sensitivity analysis that broke down cardiovascular events by type and seriousness.
"Given the current findings of low risk of serious CVD events attributed to smoking cessation pharmacotherapies, combined with the well-established CVD and mortality risks of continued smoking, the benefits of use would seem to outweigh the risks," said Edward J. Mills, Ph.D., of the Stanford (Calif.) Prevention Research Center, and his associates.
The investigators performed the meta-analysis because recent reports have raised concerns that these agents may raise cardiovascular risks. They used a statistical technique known as network meta-analysis to examine both direct, head-to-head comparison studies and indirect evidence, "thus increasing the power and interpretability of a comparative analysis."
They included any randomized clinical trial of any of the three pharmacotherapies that were of any duration and that reported on any cardiovascular events. Dr. Mills and his colleagues then considered two separate definitions of cardiovascular events: the first was any such event, including minor occurrences such as palpitations, and the second was only major adverse cardiovascular events as defined by the Food and Drug Administration, which is "considered to be a more stringent definition of important patient outcomes."
A total of 19 of the randomized clinical trials assessed nicotine replacement therapy against placebo, 27 assessed bupropion against placebo, 18 assessed varenicline against placebo, 1 assessed high-dose nicotine replacement therapy against placebo, 1 assessed combination nicotine replacement therapy against a control condition, 2 assessed bupropion against varenicline, 3 assessed bupropion against nicotine replacement therapy, and 1 assessed varenicline against nicotine replacement therapy.
Both a pairwise meta-analysis and the network meta-analysis demonstrated that none of the three pharmacotherapies raised the risk of major adverse cardiovascular events. Bupropion appeared to exert a protective effect against both minor and major events, while varenicline showed no harmful or beneficial effect at all concerning minor or major cardiovascular events.
"Nicotine replacement therapy, the most widely used pharmacotherapy for smoking cessation, was associated with an increase in cardiovascular events that was driven by lower-risk events" such as palpitations and tachycardia, which are "well known and largely benign" effects of nicotine replacement, Dr. Mills and his associates said (Circulation 2013 Dec. 9 [doi:10.1161/circulationaha.113.003961]).
"Concerns about adverse cardiovascular events need to be balanced with the consistent evidence for the benefit of smoking cessation, and patients should be counseled about what adverse events may be associated with smoking cessation therapies, the symptoms associated with the withdrawal period from cigarettes, and symptoms that may be due to existing cardiovascular diseases," the investigators added.
This study was supported by the Canadian Institutes of Health Research, the U.S. National Institutes of Health, and the California Tobacco-Related Disease Research Program. Dr. Mills reported ties to Merck; Pfizer, maker of Chantix (varenicline); Novartis; Takeda; and GlaxoSmithKline, maker of Zyban (bupropion); and his associates reported ties to Pfizer.
The three smoking cessation agents bupropion, varenicline, and nicotine replacement therapy did not raise the risk of serious adverse cardiovascular events in a network meta-analysis of 63 randomized clinical trials reported online Dec. 9 in Circulation.
This finding held true in the main analysis that included 30,508 patients attempting to quit smoking, in a subgroup analysis of the highest-risk patients who had a history of conditions predisposing them to cardiovascular events, and in a sensitivity analysis that broke down cardiovascular events by type and seriousness.
"Given the current findings of low risk of serious CVD events attributed to smoking cessation pharmacotherapies, combined with the well-established CVD and mortality risks of continued smoking, the benefits of use would seem to outweigh the risks," said Edward J. Mills, Ph.D., of the Stanford (Calif.) Prevention Research Center, and his associates.
The investigators performed the meta-analysis because recent reports have raised concerns that these agents may raise cardiovascular risks. They used a statistical technique known as network meta-analysis to examine both direct, head-to-head comparison studies and indirect evidence, "thus increasing the power and interpretability of a comparative analysis."
They included any randomized clinical trial of any of the three pharmacotherapies that were of any duration and that reported on any cardiovascular events. Dr. Mills and his colleagues then considered two separate definitions of cardiovascular events: the first was any such event, including minor occurrences such as palpitations, and the second was only major adverse cardiovascular events as defined by the Food and Drug Administration, which is "considered to be a more stringent definition of important patient outcomes."
A total of 19 of the randomized clinical trials assessed nicotine replacement therapy against placebo, 27 assessed bupropion against placebo, 18 assessed varenicline against placebo, 1 assessed high-dose nicotine replacement therapy against placebo, 1 assessed combination nicotine replacement therapy against a control condition, 2 assessed bupropion against varenicline, 3 assessed bupropion against nicotine replacement therapy, and 1 assessed varenicline against nicotine replacement therapy.
Both a pairwise meta-analysis and the network meta-analysis demonstrated that none of the three pharmacotherapies raised the risk of major adverse cardiovascular events. Bupropion appeared to exert a protective effect against both minor and major events, while varenicline showed no harmful or beneficial effect at all concerning minor or major cardiovascular events.
"Nicotine replacement therapy, the most widely used pharmacotherapy for smoking cessation, was associated with an increase in cardiovascular events that was driven by lower-risk events" such as palpitations and tachycardia, which are "well known and largely benign" effects of nicotine replacement, Dr. Mills and his associates said (Circulation 2013 Dec. 9 [doi:10.1161/circulationaha.113.003961]).
"Concerns about adverse cardiovascular events need to be balanced with the consistent evidence for the benefit of smoking cessation, and patients should be counseled about what adverse events may be associated with smoking cessation therapies, the symptoms associated with the withdrawal period from cigarettes, and symptoms that may be due to existing cardiovascular diseases," the investigators added.
This study was supported by the Canadian Institutes of Health Research, the U.S. National Institutes of Health, and the California Tobacco-Related Disease Research Program. Dr. Mills reported ties to Merck; Pfizer, maker of Chantix (varenicline); Novartis; Takeda; and GlaxoSmithKline, maker of Zyban (bupropion); and his associates reported ties to Pfizer.
FROM CIRCULATION
Major Finding: Bupropion appeared to protect against minor or serious CVD events, varenicline showed no harmful or beneficial effect on minor or serious CVD events, and nicotine replacement therapy showed no effect on serious CVD events but raised the risk of minor events such as palpitations and tachycardia.
Data Source: A network meta-analysis of 63 randomized clinical trials involving 30,508 patients attempting to quit smoking in which cardiovascular events were tracked.
Disclosures: This study was supported by the Canadian Institutes of Health Research, the U.S. National Institutes of Health, and the California Tobacco-Related Disease Research Program. Dr. Mills reported ties to Merck; Pfizer, maker of Chantix (varenicline); Novartis; Takeda; and GlaxoSmithKline, maker of Zyban (bupropion); and his associates reported ties to Pfizer.
Diabetes morbidity varies with patient age, disease duration
Both patient age and the duration of type 2 diabetes independently determine the clinical course of the disease among adults aged 60 to 80-plus years, according to a report published online Dec. 9 in JAMA Internal Medicine.
The cardiovascular complications of diabetes are considered the most common as well as the most serious complications in patients of all ages, and preventing them by concentrating on glycemic control has been the mainstay of diabetes management. But this large cohort study showed that among older patients and those with longer disease duration, hypoglycemia rates approached those of coronary artery disease, said Dr. Elbert S. Huang of the University of Chicago and his associates in the Diabetes and Aging Study.
This means that the core focus on glycemic control is inappropriate for a substantial number of older diabetes patients. "To the extent that hypoglycemia is an adverse effect of treatment, its emergence as a dominant ‘complication’ raises serious concerns about the acceptable limits of iatrogenesis," they noted.
Dr. Huang and his colleagues examined the clinical course of type 2 diabetes in older adults because "most of our current understanding" is based on studies from the 1990s," and diabetes care has evolved since that time.
They analyzed data from the Kaiser Permanente Northern California Diabetes Registry concerning 72,310 diabetes patients aged 60 years and older at baseline in 2004. These study participants were followed for up to 7 years (mean follow-up, 5.4 years) for acute hyperglycemic events requiring hospitalization; acute hypoglycemic events requiring emergency department visits or hospitalization; microvascular complications such as severe eye disease, incident end-stage renal disease, peripheral vascular disease, and amputation; nonfatal cardiovascular complications such as myocardial infarction, coronary artery bypass graft surgery, angioplasty, ischemic or hemorrhagic stroke, carotid endarterectomy, and congestive heart failure; and fatal complications of any kind.
The mean patient age was 71 years, and about 15% of the study population was aged 80 years and older. The cohort was ethnically diverse and had equal access to health care, and most patients were receiving statins and angiotensin-converting enzyme (ACE) inhibitors appropriately.
Both patient age and duration of type 2 diabetes had a significant, independent effect on which complications were likely to arise. "Most notably, the risk of hypoglycemia rose markedly" with increasing age and duration of disease, so that it outpaced both coronary and cerebrovascular events as the most common serious complication in this subset of the population, the investigators reported (JAMA Intern. Med. 2013 Dec. 9 [doi: 10.1001/jamainternmed.2013.12956]).
Hypoglycemia was even fairly frequent among younger patients: It was the fourth most common complication among patients in their 60s and the third most common among patients in their 70s.
The rate of hypoglycemic events ranged from a low of 3.0 per 1,000 person-years among the youngest patients with the shortest duration of disease to a high of 19.6 per 1,000 person-years among the oldest patients with the longest duration of disease. (The corresponding rates of coronary artery disease events were 8.5 and 24.1 per 1,000 person-years.) This suggests that intensive glycemic control may not be a helpful treatment goal and may even be harmful to the latter group.
In addition, among the oldest patients who had a long duration of diabetes (more than 10 years), the rate of acute hyperglycemic events was only 2.35 per 1,000 person-years. This also suggests that intensive glycemic control to guard against hyperglycemic events may not be helpful in such patients.
"Our observations ... provide additional support for the reorientation of care of older patients with diabetes away from intensive glycemic control as the core focus of management. The distinctive clinical course of different patient strata supports recommendations to individualize glycemic targets among older people," Dr. Huang and his associates said.
The Diabetes and Aging Study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases and the University of Chicago. No financial conflicts of interest were reported.
Both patient age and the duration of type 2 diabetes independently determine the clinical course of the disease among adults aged 60 to 80-plus years, according to a report published online Dec. 9 in JAMA Internal Medicine.
The cardiovascular complications of diabetes are considered the most common as well as the most serious complications in patients of all ages, and preventing them by concentrating on glycemic control has been the mainstay of diabetes management. But this large cohort study showed that among older patients and those with longer disease duration, hypoglycemia rates approached those of coronary artery disease, said Dr. Elbert S. Huang of the University of Chicago and his associates in the Diabetes and Aging Study.
This means that the core focus on glycemic control is inappropriate for a substantial number of older diabetes patients. "To the extent that hypoglycemia is an adverse effect of treatment, its emergence as a dominant ‘complication’ raises serious concerns about the acceptable limits of iatrogenesis," they noted.
Dr. Huang and his colleagues examined the clinical course of type 2 diabetes in older adults because "most of our current understanding" is based on studies from the 1990s," and diabetes care has evolved since that time.
They analyzed data from the Kaiser Permanente Northern California Diabetes Registry concerning 72,310 diabetes patients aged 60 years and older at baseline in 2004. These study participants were followed for up to 7 years (mean follow-up, 5.4 years) for acute hyperglycemic events requiring hospitalization; acute hypoglycemic events requiring emergency department visits or hospitalization; microvascular complications such as severe eye disease, incident end-stage renal disease, peripheral vascular disease, and amputation; nonfatal cardiovascular complications such as myocardial infarction, coronary artery bypass graft surgery, angioplasty, ischemic or hemorrhagic stroke, carotid endarterectomy, and congestive heart failure; and fatal complications of any kind.
The mean patient age was 71 years, and about 15% of the study population was aged 80 years and older. The cohort was ethnically diverse and had equal access to health care, and most patients were receiving statins and angiotensin-converting enzyme (ACE) inhibitors appropriately.
Both patient age and duration of type 2 diabetes had a significant, independent effect on which complications were likely to arise. "Most notably, the risk of hypoglycemia rose markedly" with increasing age and duration of disease, so that it outpaced both coronary and cerebrovascular events as the most common serious complication in this subset of the population, the investigators reported (JAMA Intern. Med. 2013 Dec. 9 [doi: 10.1001/jamainternmed.2013.12956]).
Hypoglycemia was even fairly frequent among younger patients: It was the fourth most common complication among patients in their 60s and the third most common among patients in their 70s.
The rate of hypoglycemic events ranged from a low of 3.0 per 1,000 person-years among the youngest patients with the shortest duration of disease to a high of 19.6 per 1,000 person-years among the oldest patients with the longest duration of disease. (The corresponding rates of coronary artery disease events were 8.5 and 24.1 per 1,000 person-years.) This suggests that intensive glycemic control may not be a helpful treatment goal and may even be harmful to the latter group.
In addition, among the oldest patients who had a long duration of diabetes (more than 10 years), the rate of acute hyperglycemic events was only 2.35 per 1,000 person-years. This also suggests that intensive glycemic control to guard against hyperglycemic events may not be helpful in such patients.
"Our observations ... provide additional support for the reorientation of care of older patients with diabetes away from intensive glycemic control as the core focus of management. The distinctive clinical course of different patient strata supports recommendations to individualize glycemic targets among older people," Dr. Huang and his associates said.
The Diabetes and Aging Study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases and the University of Chicago. No financial conflicts of interest were reported.
Both patient age and the duration of type 2 diabetes independently determine the clinical course of the disease among adults aged 60 to 80-plus years, according to a report published online Dec. 9 in JAMA Internal Medicine.
The cardiovascular complications of diabetes are considered the most common as well as the most serious complications in patients of all ages, and preventing them by concentrating on glycemic control has been the mainstay of diabetes management. But this large cohort study showed that among older patients and those with longer disease duration, hypoglycemia rates approached those of coronary artery disease, said Dr. Elbert S. Huang of the University of Chicago and his associates in the Diabetes and Aging Study.
This means that the core focus on glycemic control is inappropriate for a substantial number of older diabetes patients. "To the extent that hypoglycemia is an adverse effect of treatment, its emergence as a dominant ‘complication’ raises serious concerns about the acceptable limits of iatrogenesis," they noted.
Dr. Huang and his colleagues examined the clinical course of type 2 diabetes in older adults because "most of our current understanding" is based on studies from the 1990s," and diabetes care has evolved since that time.
They analyzed data from the Kaiser Permanente Northern California Diabetes Registry concerning 72,310 diabetes patients aged 60 years and older at baseline in 2004. These study participants were followed for up to 7 years (mean follow-up, 5.4 years) for acute hyperglycemic events requiring hospitalization; acute hypoglycemic events requiring emergency department visits or hospitalization; microvascular complications such as severe eye disease, incident end-stage renal disease, peripheral vascular disease, and amputation; nonfatal cardiovascular complications such as myocardial infarction, coronary artery bypass graft surgery, angioplasty, ischemic or hemorrhagic stroke, carotid endarterectomy, and congestive heart failure; and fatal complications of any kind.
The mean patient age was 71 years, and about 15% of the study population was aged 80 years and older. The cohort was ethnically diverse and had equal access to health care, and most patients were receiving statins and angiotensin-converting enzyme (ACE) inhibitors appropriately.
Both patient age and duration of type 2 diabetes had a significant, independent effect on which complications were likely to arise. "Most notably, the risk of hypoglycemia rose markedly" with increasing age and duration of disease, so that it outpaced both coronary and cerebrovascular events as the most common serious complication in this subset of the population, the investigators reported (JAMA Intern. Med. 2013 Dec. 9 [doi: 10.1001/jamainternmed.2013.12956]).
Hypoglycemia was even fairly frequent among younger patients: It was the fourth most common complication among patients in their 60s and the third most common among patients in their 70s.
The rate of hypoglycemic events ranged from a low of 3.0 per 1,000 person-years among the youngest patients with the shortest duration of disease to a high of 19.6 per 1,000 person-years among the oldest patients with the longest duration of disease. (The corresponding rates of coronary artery disease events were 8.5 and 24.1 per 1,000 person-years.) This suggests that intensive glycemic control may not be a helpful treatment goal and may even be harmful to the latter group.
In addition, among the oldest patients who had a long duration of diabetes (more than 10 years), the rate of acute hyperglycemic events was only 2.35 per 1,000 person-years. This also suggests that intensive glycemic control to guard against hyperglycemic events may not be helpful in such patients.
"Our observations ... provide additional support for the reorientation of care of older patients with diabetes away from intensive glycemic control as the core focus of management. The distinctive clinical course of different patient strata supports recommendations to individualize glycemic targets among older people," Dr. Huang and his associates said.
The Diabetes and Aging Study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases and the University of Chicago. No financial conflicts of interest were reported.
FROM JAMA INTERNAL MEDICINE
Major finding: The rate of serious hypoglycemic events per 1,000 person-years rose from 3.0 in the youngest patients with the shortest duration of disease to a high of 19.6 in the oldest patients with the longest duration of disease.
Data source: A cohort study involving 72,310 patients aged 60 years and older with type 2 diabetes who were enrolled in a northern California health care system and were followed for a mean of 5 years for the development of serious complications of the disease.
Disclosures: The Diabetes and Aging Study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases and the University of Chicago. No financial conflicts of interest were reported.
Multiple births declined in tandem with IVF reforms
The rate of triplet and higher-order births in the United States has declined since 1998, coincident with efforts to limit the number of embryos transferred during IVF procedures, according to a report published online Dec. 4 in the New England Journal of Medicine.
A similar effort to reduce multiple births resulting from non-IVF fertility treatments would decrease the rate even further, bringing it more into line with the "natural" rate of multiple births that occurred before fertility treatments became available in 1971, said Dr. Aniket D. Kulkarni of the women’s health and fertility branch at the Centers for Disease Control and Prevention, Atlanta, and her associates.
The investigators wanted to examine time trends in multiple births across the country, in particular the contribution that fertility treatments make to multiple births, but statistics regarding births that result from non-IVF fertility treatments are "not directly ascertainable" because there is no legal mandate to report those births, they noted. In contrast, multiple births resulting from IVF can be ascertained from a national registry of those births.
Dr. Kulkarni and her colleagues analyzed data on all live births that occurred from 1971 to 2011, then used statistical methods to estimate the proportion that occurred from natural conception, IVF, and non-IVF fertility treatments. They also used statistical methods to account for the effect of maternal age on multiple births.
The overall proportion of national births that were multiple births rose from 1.8% in 1971 to 3.5% in 2011.
This rate, however, did not show a continuous increase over the 4-decade study period, but rather showed a rise until approximately the last decade, followed by a steady decline.
By 2011, they estimated, 36% of twin births and 77% of triplet and higher-order births in the United States resulted from fertility treatments.
The rate of triplet and higher-order births increased from 1971 and reached its peak in 1998, the year that the Society for Assisted Reproductive Technology first issued practice guidelines designed to limit the number of embryos transferred during IVF cycles. The national rate of triplet and higher-order births then began to decline, going from 1.94 per 1,000 live births in 1998 to 1.37 per 1,000 in 2011.
This represents a 29% reduction, Dr. Kulkarni and her associates said (N. Engl. J. Med. 2013 [doi:10.1056/NEJMoa1301467]). The decline coincided with a 70% reduction in transfers of three or more embryos during IVF.
The trends for non-IVF fertility treatments were "less favorable," the researchers noted. In particular, ovulation induction and ovarian stimulation continue to contribute heavily to the national rate of triplet and higher-order multiple births.
Adherence to more prudent practice patterns, such as the use of low-dose gonadotropins, could reduce the rate of multiple births "while maintaining acceptable per-cycle pregnancy rates," they said, adding that mandating the public reporting of births resulting from non-IVF fertility treatments also would help by facilitating data analysis.
This study was supported by the U.S. Centers for Disease Control and Prevention. Dr. Kulkarni reported no financial conflicts of interest; an associate reported ties to Alere.
The rate of triplet and higher-order births in the United States has declined since 1998, coincident with efforts to limit the number of embryos transferred during IVF procedures, according to a report published online Dec. 4 in the New England Journal of Medicine.
A similar effort to reduce multiple births resulting from non-IVF fertility treatments would decrease the rate even further, bringing it more into line with the "natural" rate of multiple births that occurred before fertility treatments became available in 1971, said Dr. Aniket D. Kulkarni of the women’s health and fertility branch at the Centers for Disease Control and Prevention, Atlanta, and her associates.
The investigators wanted to examine time trends in multiple births across the country, in particular the contribution that fertility treatments make to multiple births, but statistics regarding births that result from non-IVF fertility treatments are "not directly ascertainable" because there is no legal mandate to report those births, they noted. In contrast, multiple births resulting from IVF can be ascertained from a national registry of those births.
Dr. Kulkarni and her colleagues analyzed data on all live births that occurred from 1971 to 2011, then used statistical methods to estimate the proportion that occurred from natural conception, IVF, and non-IVF fertility treatments. They also used statistical methods to account for the effect of maternal age on multiple births.
The overall proportion of national births that were multiple births rose from 1.8% in 1971 to 3.5% in 2011.
This rate, however, did not show a continuous increase over the 4-decade study period, but rather showed a rise until approximately the last decade, followed by a steady decline.
By 2011, they estimated, 36% of twin births and 77% of triplet and higher-order births in the United States resulted from fertility treatments.
The rate of triplet and higher-order births increased from 1971 and reached its peak in 1998, the year that the Society for Assisted Reproductive Technology first issued practice guidelines designed to limit the number of embryos transferred during IVF cycles. The national rate of triplet and higher-order births then began to decline, going from 1.94 per 1,000 live births in 1998 to 1.37 per 1,000 in 2011.
This represents a 29% reduction, Dr. Kulkarni and her associates said (N. Engl. J. Med. 2013 [doi:10.1056/NEJMoa1301467]). The decline coincided with a 70% reduction in transfers of three or more embryos during IVF.
The trends for non-IVF fertility treatments were "less favorable," the researchers noted. In particular, ovulation induction and ovarian stimulation continue to contribute heavily to the national rate of triplet and higher-order multiple births.
Adherence to more prudent practice patterns, such as the use of low-dose gonadotropins, could reduce the rate of multiple births "while maintaining acceptable per-cycle pregnancy rates," they said, adding that mandating the public reporting of births resulting from non-IVF fertility treatments also would help by facilitating data analysis.
This study was supported by the U.S. Centers for Disease Control and Prevention. Dr. Kulkarni reported no financial conflicts of interest; an associate reported ties to Alere.
The rate of triplet and higher-order births in the United States has declined since 1998, coincident with efforts to limit the number of embryos transferred during IVF procedures, according to a report published online Dec. 4 in the New England Journal of Medicine.
A similar effort to reduce multiple births resulting from non-IVF fertility treatments would decrease the rate even further, bringing it more into line with the "natural" rate of multiple births that occurred before fertility treatments became available in 1971, said Dr. Aniket D. Kulkarni of the women’s health and fertility branch at the Centers for Disease Control and Prevention, Atlanta, and her associates.
The investigators wanted to examine time trends in multiple births across the country, in particular the contribution that fertility treatments make to multiple births, but statistics regarding births that result from non-IVF fertility treatments are "not directly ascertainable" because there is no legal mandate to report those births, they noted. In contrast, multiple births resulting from IVF can be ascertained from a national registry of those births.
Dr. Kulkarni and her colleagues analyzed data on all live births that occurred from 1971 to 2011, then used statistical methods to estimate the proportion that occurred from natural conception, IVF, and non-IVF fertility treatments. They also used statistical methods to account for the effect of maternal age on multiple births.
The overall proportion of national births that were multiple births rose from 1.8% in 1971 to 3.5% in 2011.
This rate, however, did not show a continuous increase over the 4-decade study period, but rather showed a rise until approximately the last decade, followed by a steady decline.
By 2011, they estimated, 36% of twin births and 77% of triplet and higher-order births in the United States resulted from fertility treatments.
The rate of triplet and higher-order births increased from 1971 and reached its peak in 1998, the year that the Society for Assisted Reproductive Technology first issued practice guidelines designed to limit the number of embryos transferred during IVF cycles. The national rate of triplet and higher-order births then began to decline, going from 1.94 per 1,000 live births in 1998 to 1.37 per 1,000 in 2011.
This represents a 29% reduction, Dr. Kulkarni and her associates said (N. Engl. J. Med. 2013 [doi:10.1056/NEJMoa1301467]). The decline coincided with a 70% reduction in transfers of three or more embryos during IVF.
The trends for non-IVF fertility treatments were "less favorable," the researchers noted. In particular, ovulation induction and ovarian stimulation continue to contribute heavily to the national rate of triplet and higher-order multiple births.
Adherence to more prudent practice patterns, such as the use of low-dose gonadotropins, could reduce the rate of multiple births "while maintaining acceptable per-cycle pregnancy rates," they said, adding that mandating the public reporting of births resulting from non-IVF fertility treatments also would help by facilitating data analysis.
This study was supported by the U.S. Centers for Disease Control and Prevention. Dr. Kulkarni reported no financial conflicts of interest; an associate reported ties to Alere.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: The rate of triplet and higher-order births reached its peak in 1998 – the year that the Society for Assisted Reproductive Technology first issued practice guidelines designed to limit the number of embryos transferred during IVF cycles – and then began to decline, from 1.94 per 1,000 live births in 1998 to 1.37 per 1,000 in 2011.
Data Source: An analysis of national data on multiple births from 1971, when fertility treatments were first introduced, through 2011.
Disclosures: This study was supported by the U.S. Centers for Disease Control and Prevention. Ms. Kulkarni reported no financial conflicts of interest; an associate reported ties to Alere.
Handoff intervention cuts medical errors in hospitalized children
An intervention to improve communication and provide more structure to patient "handoffs" among residents dramatically reduced medical errors and preventable adverse events in hospitalized children, according to a report published online Dec. 3 in JAMA.
In a single-center study comparing patient handoffs during the 3-month period before the intervention was implemented against the 3-month period afterward, the rate of medical errors dropped by 46%, from 33.8/100 admissions to 18.3/100. Preventable adverse events similarly decreased, from 3.3/100 admissions to 1.5/100, said Dr. Amy J. Starmer of Boston Children’s Hospital and Harvard Medical School, Boston, and her associates.
"Given the increasing frequency of handoffs in hospitals following resident work-hour reductions and the high frequency with which miscommunications lead to serious medical errors," widespread use of such handoff interventions could have a substantial impact on patient health, they noted.
The investigators performed the before-and-after comparison on two inpatient pediatric units within the same hospital, which included 1,255 children requiring general, subspecialty, and complex-care services during the study period. A total of 42 first-year and third-year residents cared for these patients and participated in the intervention.
Before the intervention, patient handoffs had no standardized structure and involved the use of a printed document that included basic patient information but was not integrated into the electronic health record system.
For the intervention, the residents attended a 2-hour training session in which they discussed best practices for verbal and written handoffs. Handoff procedures were structured to occur on a team basis rather than individually, in a dedicated physical space that was private and quiet, and which were periodically overseen by a chief resident or attending physician.
One of the pediatric units also began using a computerized rather than printed handoff document that was integrated into the electronic health record system and included much more detailed, and regularly updated, patient information.
Overall, 350 medical errors and adverse events were tabulated during the study period, including 77% related to medications, 8.3% related to medical procedures, 4.3% related to diagnostic tests, 3.4% related to other therapies, and 3.7% related to falls.
In particular, the rate of errors that could have had important clinical consequences dropped from 7.3/100 to 3.3/100 admissions, and the rate of errors that could have had such consequences but were prevented decreased from 15/100 to 8.3/100 admissions.
As expected, the rate of nonpreventable errors remained constant (JAMA 2013 Dec. 3 [doi:10.1001/jama.2013.281961]).
Forty of the written handoff documents were reviewed for the presence of 14 important items of patient information. After the intervention, the number of key data omissions was significantly reduced.
"Written handoffs were more comprehensive after the interventions, and verbal handoffs were more likely to occur in a quiet, private location," Dr. Starmer and her associates said.
This study was supported by the Controlled Risk Insurance Company Risk Management Foundation, Boston Children’s Hospital Program for Patient Safety and Quality Research, the Agency for Healthcare Research and Quality, the Child Health Corporation of America, and the National Institutes of Health. No financial conflicts of interest were reported.
Although this study had numerous strengths, its results should be considered preliminary until they can be replicated; further study is still needed to confirm the findings, better characterize and refine the key elements of the handoff intervention, and establish whether the benefits are sustained beyond 3 months, said Dr. Leora I. Horwitz.
Meanwhile, other methods of improving safety at patient handoffs should be considered. "There is now promising work in automatically aggregating data to characterize patients’ clinical condition, identify early deterioration, or prospectively identify patients who have not yet received standard of care, potentially enabling clinicians to convert the existing static handoff process to a real-time dynamic reassessment of clinical condition and patient care," she said.
Dr. Leora I. Horwitz is in the department of internal medicine at Yale University and at the Center for Outcomes Research and Evaluation at Yale–New Haven (Conn.) Hospital. She reported no financial conflicts of interest. These remarks were taken from her editorial accompanying Dr. Starmer’s report (JAMA 2013;310:2255-6).
Although this study had numerous strengths, its results should be considered preliminary until they can be replicated; further study is still needed to confirm the findings, better characterize and refine the key elements of the handoff intervention, and establish whether the benefits are sustained beyond 3 months, said Dr. Leora I. Horwitz.
Meanwhile, other methods of improving safety at patient handoffs should be considered. "There is now promising work in automatically aggregating data to characterize patients’ clinical condition, identify early deterioration, or prospectively identify patients who have not yet received standard of care, potentially enabling clinicians to convert the existing static handoff process to a real-time dynamic reassessment of clinical condition and patient care," she said.
Dr. Leora I. Horwitz is in the department of internal medicine at Yale University and at the Center for Outcomes Research and Evaluation at Yale–New Haven (Conn.) Hospital. She reported no financial conflicts of interest. These remarks were taken from her editorial accompanying Dr. Starmer’s report (JAMA 2013;310:2255-6).
Although this study had numerous strengths, its results should be considered preliminary until they can be replicated; further study is still needed to confirm the findings, better characterize and refine the key elements of the handoff intervention, and establish whether the benefits are sustained beyond 3 months, said Dr. Leora I. Horwitz.
Meanwhile, other methods of improving safety at patient handoffs should be considered. "There is now promising work in automatically aggregating data to characterize patients’ clinical condition, identify early deterioration, or prospectively identify patients who have not yet received standard of care, potentially enabling clinicians to convert the existing static handoff process to a real-time dynamic reassessment of clinical condition and patient care," she said.
Dr. Leora I. Horwitz is in the department of internal medicine at Yale University and at the Center for Outcomes Research and Evaluation at Yale–New Haven (Conn.) Hospital. She reported no financial conflicts of interest. These remarks were taken from her editorial accompanying Dr. Starmer’s report (JAMA 2013;310:2255-6).
An intervention to improve communication and provide more structure to patient "handoffs" among residents dramatically reduced medical errors and preventable adverse events in hospitalized children, according to a report published online Dec. 3 in JAMA.
In a single-center study comparing patient handoffs during the 3-month period before the intervention was implemented against the 3-month period afterward, the rate of medical errors dropped by 46%, from 33.8/100 admissions to 18.3/100. Preventable adverse events similarly decreased, from 3.3/100 admissions to 1.5/100, said Dr. Amy J. Starmer of Boston Children’s Hospital and Harvard Medical School, Boston, and her associates.
"Given the increasing frequency of handoffs in hospitals following resident work-hour reductions and the high frequency with which miscommunications lead to serious medical errors," widespread use of such handoff interventions could have a substantial impact on patient health, they noted.
The investigators performed the before-and-after comparison on two inpatient pediatric units within the same hospital, which included 1,255 children requiring general, subspecialty, and complex-care services during the study period. A total of 42 first-year and third-year residents cared for these patients and participated in the intervention.
Before the intervention, patient handoffs had no standardized structure and involved the use of a printed document that included basic patient information but was not integrated into the electronic health record system.
For the intervention, the residents attended a 2-hour training session in which they discussed best practices for verbal and written handoffs. Handoff procedures were structured to occur on a team basis rather than individually, in a dedicated physical space that was private and quiet, and which were periodically overseen by a chief resident or attending physician.
One of the pediatric units also began using a computerized rather than printed handoff document that was integrated into the electronic health record system and included much more detailed, and regularly updated, patient information.
Overall, 350 medical errors and adverse events were tabulated during the study period, including 77% related to medications, 8.3% related to medical procedures, 4.3% related to diagnostic tests, 3.4% related to other therapies, and 3.7% related to falls.
In particular, the rate of errors that could have had important clinical consequences dropped from 7.3/100 to 3.3/100 admissions, and the rate of errors that could have had such consequences but were prevented decreased from 15/100 to 8.3/100 admissions.
As expected, the rate of nonpreventable errors remained constant (JAMA 2013 Dec. 3 [doi:10.1001/jama.2013.281961]).
Forty of the written handoff documents were reviewed for the presence of 14 important items of patient information. After the intervention, the number of key data omissions was significantly reduced.
"Written handoffs were more comprehensive after the interventions, and verbal handoffs were more likely to occur in a quiet, private location," Dr. Starmer and her associates said.
This study was supported by the Controlled Risk Insurance Company Risk Management Foundation, Boston Children’s Hospital Program for Patient Safety and Quality Research, the Agency for Healthcare Research and Quality, the Child Health Corporation of America, and the National Institutes of Health. No financial conflicts of interest were reported.
An intervention to improve communication and provide more structure to patient "handoffs" among residents dramatically reduced medical errors and preventable adverse events in hospitalized children, according to a report published online Dec. 3 in JAMA.
In a single-center study comparing patient handoffs during the 3-month period before the intervention was implemented against the 3-month period afterward, the rate of medical errors dropped by 46%, from 33.8/100 admissions to 18.3/100. Preventable adverse events similarly decreased, from 3.3/100 admissions to 1.5/100, said Dr. Amy J. Starmer of Boston Children’s Hospital and Harvard Medical School, Boston, and her associates.
"Given the increasing frequency of handoffs in hospitals following resident work-hour reductions and the high frequency with which miscommunications lead to serious medical errors," widespread use of such handoff interventions could have a substantial impact on patient health, they noted.
The investigators performed the before-and-after comparison on two inpatient pediatric units within the same hospital, which included 1,255 children requiring general, subspecialty, and complex-care services during the study period. A total of 42 first-year and third-year residents cared for these patients and participated in the intervention.
Before the intervention, patient handoffs had no standardized structure and involved the use of a printed document that included basic patient information but was not integrated into the electronic health record system.
For the intervention, the residents attended a 2-hour training session in which they discussed best practices for verbal and written handoffs. Handoff procedures were structured to occur on a team basis rather than individually, in a dedicated physical space that was private and quiet, and which were periodically overseen by a chief resident or attending physician.
One of the pediatric units also began using a computerized rather than printed handoff document that was integrated into the electronic health record system and included much more detailed, and regularly updated, patient information.
Overall, 350 medical errors and adverse events were tabulated during the study period, including 77% related to medications, 8.3% related to medical procedures, 4.3% related to diagnostic tests, 3.4% related to other therapies, and 3.7% related to falls.
In particular, the rate of errors that could have had important clinical consequences dropped from 7.3/100 to 3.3/100 admissions, and the rate of errors that could have had such consequences but were prevented decreased from 15/100 to 8.3/100 admissions.
As expected, the rate of nonpreventable errors remained constant (JAMA 2013 Dec. 3 [doi:10.1001/jama.2013.281961]).
Forty of the written handoff documents were reviewed for the presence of 14 important items of patient information. After the intervention, the number of key data omissions was significantly reduced.
"Written handoffs were more comprehensive after the interventions, and verbal handoffs were more likely to occur in a quiet, private location," Dr. Starmer and her associates said.
This study was supported by the Controlled Risk Insurance Company Risk Management Foundation, Boston Children’s Hospital Program for Patient Safety and Quality Research, the Agency for Healthcare Research and Quality, the Child Health Corporation of America, and the National Institutes of Health. No financial conflicts of interest were reported.
FROM JAMA
Major finding: The rate of medical errors decreased from 33.8/100 to 18.3/100 admissions after the handoff intervention was implemented, and the rate of preventable adverse events decreased from 3.3/100 to 1.5/100 admissions.
Data source: A prospective intervention study comparing medical errors during the 3 months before and after implementation of an intervention to standardize patient handoffs between resident physicians.
Disclosures: This study was supported by the Controlled Risk Insurance Company Risk Management Foundation, Boston Children’s Hospital Program for Patient Safety and Quality Research, the Agency for Healthcare Research and Quality, the Child Health Corporation of America, and the National Institutes of Health. No financial conflicts of interest were reported.