User login
Elderly inpatient care model delivered mixed results
A mobile version of the Acute Care for Elderly inpatient care model reduced the rate of adverse events and shortened hospital stays, but it didn’t reduce 30-day readmission rates or improve patients’ functional status more than standard care did, according to a single-center cohort study.
The Mobile Acute Care for the Elderly (MACE) program at Mount Sinai Medical Center, New York, thus appears to promote better outcomes in some key areas "for this vulnerable older adult population," said Dr. William W. Hung of the department of geriatrics and palliative medicine at Mount Sinai and his associates in a study published online April 22 in JAMA Internal Medicine (2013 April 22 [doi:10.1001/jamainternmed.2013.478]).
However, compared with usual care, the MACE program did not improve patients’ functional status, reduce 30-day readmission rates, decrease visits to the emergency department within 30 days of hospital discharge, or decrease rates of discharge to a skilled nursing facility, the investigators noted.
Introduced in the 1990s, the Acute Care for Elderly unit is "widely accepted as a prototype model to provide inpatient care for older adults," the study authors noted. The model includes a designated hospital unit with a specially designed environment, interdisciplinary caregivers including geriatricians, and particular attention to discharge planning and the avoidance of adverse events.
However, such units "have not been widely disseminated across institutions, particularly because of barriers to initial setup, including costs, staffing, and space needs," the investigators added.
The MACE model delivers care without requiring a dedicated, physical ACE unit.
This mobile approach allows an interdisciplinary team of geriatricians, social workers, and clinical nurse specialists to care for elderly patients admitted to any unit in the hospital. As with the ACE model, the MACE model focuses on reducing the risks of hospitalization, improving coordination with outpatient practice, and discharge planning.
Dr. Hung and his colleagues conducted a 3-year prospective cohort study to determine whether MACE was associated with improved outcomes. They assessed 173 patients aged 75 years and older who received MACE service when they were admitted to the medical center, and 173 control subjects admitted to the general inpatient medical service during the same period.
The two groups were matched for age, primary diagnosis, and ability to ambulate independently. The mean age of both groups was approximately 85 years; approximately 76% of patients were women, 56% were white, and 35% were Medicaid beneficiaries. Fewer than one-third of both groups were able to ambulate independently.
The primary outcome measure was readmission within 30 days of hospital discharge. On that measure, there was no significant difference between the two groups: 15.4% of the patients in the MACE service required readmission, as did 22.4% of the usual-care group, the researchers said.
Similarly, combined rates of readmission plus emergency department visits within 30 days did not differ significantly, at 20.8% for the MACE service and 25.6% for usual care.
Functional status at 30 days also did not differ. Mean scores were similar between the MACE patients and the usual-care patients on two separate measures of the ability to perform basic activities of daily living.
Similarly, overall health status at 30 days, as measured using the Patient Reported Outcomes Measurement Information Systems (PROMIS) 10-item instrument, was not significantly different between the two study groups.
However, the rate of in-hospital adverse events such as falls, bed sores, the need for restraints, and catheter-associated urinary tract infections was significantly lower in the MACE group (9.5%) than in the usual-care group (17.0%).
The adjusted mean length of stay was 0.8 days shorter for the MACE group than for the usual-care group. But discharge destination was similar between the two groups, with 24.9% of the MACE group and 22.5% of the usual-care group requiring discharge to a skilled nursing facility.
Patients in the MACE service were much more likely to report that their caregivers discussed post-discharge care with them (92.2%), compared with those in the usual-care group (67.6%).
Patient satisfaction with care was greater with the MACE service than with usual care on one instrument, the three-item Care Transition Measure. But it was no different on another instrument, the Hospital Consumer Assessment of Healthcare Providers and Systems survey (HCAHPS).
The study may have been subject to selection bias, the investigators noted, because the patients in the MACE service were also receiving their primary care at a geriatric-based practice rather than in a general practice. Also, the investigator who reviewed the medical records for adverse events was not blinded to the patients’ group assignment.
Given the constraints that limit hospitals’ adoption of the ACE unit model, the MACE model "may be a viable alternative, because it can be seamlessly integrated in a hospital’s work flow without the requirement for a dedicated unit," the investigators concluded.
This study was supported by the John A. Hartford Center of Excellence and the Claude D. Pepper Older Americans Independence Center at Mount Sinai. Dr. Hung reported no financial conflicts of interest; one of his associates reported ties to the American Federation for Aging Research, FAIR Health, the U.S. Food and Drug Administration, Medtronic, the National Institute on Aging, and the Pew Charitable Trusts.
The most important barrier to adopting coordinated models of geriatric care such as the MACE model is that it demands change from physicians who "are used to taking responsibility for only a subset of a patient’s health issues, and then only in specific settings," said Dr. Lisa M. Walke and Dr. Mary E. Tinetti.
Other obstacles include the paucity of geriatric specialists to provide this type of care, the lack of data infrastructure for sharing information across inpatient and outpatient sites of care, and the lack of a financial incentive to create such a fully integrated model. "In fact, the current disease-based fee-for-service payment structure creates a disincentive for streamlining care," they said.
Fortunately, health care reform should "encourage a shift from episodic, segmented care toward integrated patient-centered care ... even for our most complex older patients," they said.
Dr. Walke and Dr. Tinetti are in the division of geriatrics at Yale University, New Haven, Conn. Dr. Tinetti is also in the department of chronic disease epidemiology at Yale. They reported no financial conflicts of interest. These remarks were taken from their invited commentary accompanying Dr. Hung’s report (JAMA Intern. Med. 2013 April 22 [doi:10.1001/jamainternmed.2013.493]).
The most important barrier to adopting coordinated models of geriatric care such as the MACE model is that it demands change from physicians who "are used to taking responsibility for only a subset of a patient’s health issues, and then only in specific settings," said Dr. Lisa M. Walke and Dr. Mary E. Tinetti.
Other obstacles include the paucity of geriatric specialists to provide this type of care, the lack of data infrastructure for sharing information across inpatient and outpatient sites of care, and the lack of a financial incentive to create such a fully integrated model. "In fact, the current disease-based fee-for-service payment structure creates a disincentive for streamlining care," they said.
Fortunately, health care reform should "encourage a shift from episodic, segmented care toward integrated patient-centered care ... even for our most complex older patients," they said.
Dr. Walke and Dr. Tinetti are in the division of geriatrics at Yale University, New Haven, Conn. Dr. Tinetti is also in the department of chronic disease epidemiology at Yale. They reported no financial conflicts of interest. These remarks were taken from their invited commentary accompanying Dr. Hung’s report (JAMA Intern. Med. 2013 April 22 [doi:10.1001/jamainternmed.2013.493]).
The most important barrier to adopting coordinated models of geriatric care such as the MACE model is that it demands change from physicians who "are used to taking responsibility for only a subset of a patient’s health issues, and then only in specific settings," said Dr. Lisa M. Walke and Dr. Mary E. Tinetti.
Other obstacles include the paucity of geriatric specialists to provide this type of care, the lack of data infrastructure for sharing information across inpatient and outpatient sites of care, and the lack of a financial incentive to create such a fully integrated model. "In fact, the current disease-based fee-for-service payment structure creates a disincentive for streamlining care," they said.
Fortunately, health care reform should "encourage a shift from episodic, segmented care toward integrated patient-centered care ... even for our most complex older patients," they said.
Dr. Walke and Dr. Tinetti are in the division of geriatrics at Yale University, New Haven, Conn. Dr. Tinetti is also in the department of chronic disease epidemiology at Yale. They reported no financial conflicts of interest. These remarks were taken from their invited commentary accompanying Dr. Hung’s report (JAMA Intern. Med. 2013 April 22 [doi:10.1001/jamainternmed.2013.493]).
A mobile version of the Acute Care for Elderly inpatient care model reduced the rate of adverse events and shortened hospital stays, but it didn’t reduce 30-day readmission rates or improve patients’ functional status more than standard care did, according to a single-center cohort study.
The Mobile Acute Care for the Elderly (MACE) program at Mount Sinai Medical Center, New York, thus appears to promote better outcomes in some key areas "for this vulnerable older adult population," said Dr. William W. Hung of the department of geriatrics and palliative medicine at Mount Sinai and his associates in a study published online April 22 in JAMA Internal Medicine (2013 April 22 [doi:10.1001/jamainternmed.2013.478]).
However, compared with usual care, the MACE program did not improve patients’ functional status, reduce 30-day readmission rates, decrease visits to the emergency department within 30 days of hospital discharge, or decrease rates of discharge to a skilled nursing facility, the investigators noted.
Introduced in the 1990s, the Acute Care for Elderly unit is "widely accepted as a prototype model to provide inpatient care for older adults," the study authors noted. The model includes a designated hospital unit with a specially designed environment, interdisciplinary caregivers including geriatricians, and particular attention to discharge planning and the avoidance of adverse events.
However, such units "have not been widely disseminated across institutions, particularly because of barriers to initial setup, including costs, staffing, and space needs," the investigators added.
The MACE model delivers care without requiring a dedicated, physical ACE unit.
This mobile approach allows an interdisciplinary team of geriatricians, social workers, and clinical nurse specialists to care for elderly patients admitted to any unit in the hospital. As with the ACE model, the MACE model focuses on reducing the risks of hospitalization, improving coordination with outpatient practice, and discharge planning.
Dr. Hung and his colleagues conducted a 3-year prospective cohort study to determine whether MACE was associated with improved outcomes. They assessed 173 patients aged 75 years and older who received MACE service when they were admitted to the medical center, and 173 control subjects admitted to the general inpatient medical service during the same period.
The two groups were matched for age, primary diagnosis, and ability to ambulate independently. The mean age of both groups was approximately 85 years; approximately 76% of patients were women, 56% were white, and 35% were Medicaid beneficiaries. Fewer than one-third of both groups were able to ambulate independently.
The primary outcome measure was readmission within 30 days of hospital discharge. On that measure, there was no significant difference between the two groups: 15.4% of the patients in the MACE service required readmission, as did 22.4% of the usual-care group, the researchers said.
Similarly, combined rates of readmission plus emergency department visits within 30 days did not differ significantly, at 20.8% for the MACE service and 25.6% for usual care.
Functional status at 30 days also did not differ. Mean scores were similar between the MACE patients and the usual-care patients on two separate measures of the ability to perform basic activities of daily living.
Similarly, overall health status at 30 days, as measured using the Patient Reported Outcomes Measurement Information Systems (PROMIS) 10-item instrument, was not significantly different between the two study groups.
However, the rate of in-hospital adverse events such as falls, bed sores, the need for restraints, and catheter-associated urinary tract infections was significantly lower in the MACE group (9.5%) than in the usual-care group (17.0%).
The adjusted mean length of stay was 0.8 days shorter for the MACE group than for the usual-care group. But discharge destination was similar between the two groups, with 24.9% of the MACE group and 22.5% of the usual-care group requiring discharge to a skilled nursing facility.
Patients in the MACE service were much more likely to report that their caregivers discussed post-discharge care with them (92.2%), compared with those in the usual-care group (67.6%).
Patient satisfaction with care was greater with the MACE service than with usual care on one instrument, the three-item Care Transition Measure. But it was no different on another instrument, the Hospital Consumer Assessment of Healthcare Providers and Systems survey (HCAHPS).
The study may have been subject to selection bias, the investigators noted, because the patients in the MACE service were also receiving their primary care at a geriatric-based practice rather than in a general practice. Also, the investigator who reviewed the medical records for adverse events was not blinded to the patients’ group assignment.
Given the constraints that limit hospitals’ adoption of the ACE unit model, the MACE model "may be a viable alternative, because it can be seamlessly integrated in a hospital’s work flow without the requirement for a dedicated unit," the investigators concluded.
This study was supported by the John A. Hartford Center of Excellence and the Claude D. Pepper Older Americans Independence Center at Mount Sinai. Dr. Hung reported no financial conflicts of interest; one of his associates reported ties to the American Federation for Aging Research, FAIR Health, the U.S. Food and Drug Administration, Medtronic, the National Institute on Aging, and the Pew Charitable Trusts.
A mobile version of the Acute Care for Elderly inpatient care model reduced the rate of adverse events and shortened hospital stays, but it didn’t reduce 30-day readmission rates or improve patients’ functional status more than standard care did, according to a single-center cohort study.
The Mobile Acute Care for the Elderly (MACE) program at Mount Sinai Medical Center, New York, thus appears to promote better outcomes in some key areas "for this vulnerable older adult population," said Dr. William W. Hung of the department of geriatrics and palliative medicine at Mount Sinai and his associates in a study published online April 22 in JAMA Internal Medicine (2013 April 22 [doi:10.1001/jamainternmed.2013.478]).
However, compared with usual care, the MACE program did not improve patients’ functional status, reduce 30-day readmission rates, decrease visits to the emergency department within 30 days of hospital discharge, or decrease rates of discharge to a skilled nursing facility, the investigators noted.
Introduced in the 1990s, the Acute Care for Elderly unit is "widely accepted as a prototype model to provide inpatient care for older adults," the study authors noted. The model includes a designated hospital unit with a specially designed environment, interdisciplinary caregivers including geriatricians, and particular attention to discharge planning and the avoidance of adverse events.
However, such units "have not been widely disseminated across institutions, particularly because of barriers to initial setup, including costs, staffing, and space needs," the investigators added.
The MACE model delivers care without requiring a dedicated, physical ACE unit.
This mobile approach allows an interdisciplinary team of geriatricians, social workers, and clinical nurse specialists to care for elderly patients admitted to any unit in the hospital. As with the ACE model, the MACE model focuses on reducing the risks of hospitalization, improving coordination with outpatient practice, and discharge planning.
Dr. Hung and his colleagues conducted a 3-year prospective cohort study to determine whether MACE was associated with improved outcomes. They assessed 173 patients aged 75 years and older who received MACE service when they were admitted to the medical center, and 173 control subjects admitted to the general inpatient medical service during the same period.
The two groups were matched for age, primary diagnosis, and ability to ambulate independently. The mean age of both groups was approximately 85 years; approximately 76% of patients were women, 56% were white, and 35% were Medicaid beneficiaries. Fewer than one-third of both groups were able to ambulate independently.
The primary outcome measure was readmission within 30 days of hospital discharge. On that measure, there was no significant difference between the two groups: 15.4% of the patients in the MACE service required readmission, as did 22.4% of the usual-care group, the researchers said.
Similarly, combined rates of readmission plus emergency department visits within 30 days did not differ significantly, at 20.8% for the MACE service and 25.6% for usual care.
Functional status at 30 days also did not differ. Mean scores were similar between the MACE patients and the usual-care patients on two separate measures of the ability to perform basic activities of daily living.
Similarly, overall health status at 30 days, as measured using the Patient Reported Outcomes Measurement Information Systems (PROMIS) 10-item instrument, was not significantly different between the two study groups.
However, the rate of in-hospital adverse events such as falls, bed sores, the need for restraints, and catheter-associated urinary tract infections was significantly lower in the MACE group (9.5%) than in the usual-care group (17.0%).
The adjusted mean length of stay was 0.8 days shorter for the MACE group than for the usual-care group. But discharge destination was similar between the two groups, with 24.9% of the MACE group and 22.5% of the usual-care group requiring discharge to a skilled nursing facility.
Patients in the MACE service were much more likely to report that their caregivers discussed post-discharge care with them (92.2%), compared with those in the usual-care group (67.6%).
Patient satisfaction with care was greater with the MACE service than with usual care on one instrument, the three-item Care Transition Measure. But it was no different on another instrument, the Hospital Consumer Assessment of Healthcare Providers and Systems survey (HCAHPS).
The study may have been subject to selection bias, the investigators noted, because the patients in the MACE service were also receiving their primary care at a geriatric-based practice rather than in a general practice. Also, the investigator who reviewed the medical records for adverse events was not blinded to the patients’ group assignment.
Given the constraints that limit hospitals’ adoption of the ACE unit model, the MACE model "may be a viable alternative, because it can be seamlessly integrated in a hospital’s work flow without the requirement for a dedicated unit," the investigators concluded.
This study was supported by the John A. Hartford Center of Excellence and the Claude D. Pepper Older Americans Independence Center at Mount Sinai. Dr. Hung reported no financial conflicts of interest; one of his associates reported ties to the American Federation for Aging Research, FAIR Health, the U.S. Food and Drug Administration, Medtronic, the National Institute on Aging, and the Pew Charitable Trusts.
FROM JAMA INTERNAL MEDICINE
Major Finding: Compared with patients who received usual inpatient care, elderly patients cared for by the MACE model had a lower rate of adverse events, shorter hospital stays, and better patient satisfaction; but they had the same 30-day readmission rates, functional status, rates of emergency department visits, and rates of discharge to a skilled nursing facility.
Data Source: A 3-year prospective cohort study involving 173 elderly inpatients cared for by the MACE service and 173 control subjects matched for age, primary diagnosis, and ability to ambulate.
Disclosures: This study was supported by the John A. Hartford Center of Excellence and the Claude D. Pepper Older Americans Independence Center at Mount Sinai. Dr. Hung reported no financial conflicts of interest; one of his associates reported ties to the American Federation for Aging Research, FAIR Health, the U.S. Food and Drug Administration, Medtronic, the National Institute on Aging, and the Pew Charitable Trusts.
Supplemental glutamine may harm critically ill patients
Early supplemental glutamine appears to harm rather than benefit critically ill patients who have multiorgan failure, according to a report published online April 18 in the New England Journal of Medicine.
In an international randomized controlled trial, in-hospital mortality and 6-month mortality were significantly increased in patients given intravenous glutamine within 24 hours of presentation to the ICU, compared with those given placebo, said Dr. Daren Heyland of Kingston (Ont.) General Hospital and his associates. A nonsignificant increase was seen in 28-day mortality.
Most of the patients in this study showed no glutamine deficiency at study entry. This observation, together with the primary finding that glutamine therapy may actually be harmful in this setting, "challenges the prevailing concept that glutamine is an essential nutrient that is deficient in critically ill patients and requires immediate supplementation," Dr. Heyland and his colleagues said.
The researchers also assessed whether supplemental antioxidants improved mortality or other outcomes in this study population and found that they did not.
Dr. Heyland and his associates performed this study because glutamine is thought to be rapidly depleted in critical illness and low levels of glutamine have been linked to increased mortality in ICU patients. Metaanalyses of small randomized trials suggested that both glutamine and antioxidant supplementation might improve survival in critically ill patients, but more recent and larger studies failed to confirm such a benefit.
This study included 1,223 consecutive adults who presented to 40 ICUs in the United States, Canada, and Europe during a 6-year period and required mechanical ventilation and had two or more organ failures related to their acute illness. The average patient age was 63 years. Primary diagnoses included cardiovascular, respiratory, gastrointestinal, neurologic, metabolic, and gynecologic disorders as well as sepsis and trauma.
The patients were randomly assigned in a double-blind fashion to receive daily intravenous glutamine, intravenous plus enteral antioxidants, glutamine plus antioxidants, or placebo fluids. The antioxidants included selenium, zinc, beta carotene, vitamin E, and vitamin C.
The primary outcome measure was 28-day mortality. There was a nonsignificant trend toward higher mortality in the patients given glutamine (32.4%) compared with those not given glutamine (27.2%). However, two secondary outcomes – in-hospital mortality and 6-month mortality – both were significantly higher in patients given glutamine than in those not given glutamine. In hospital mortality was 37.2% vs. 31%, respectively; 6-month mortality was 43.7% vs. 37.2%, respectively.
Other secondary outcomes – median time from randomization to ICU discharge and median time to hospital discharge – also were significantly longer for patients who received glutamine (17.1 vs. 13.1 days and 51.1 vs. 40.1 days, respectively), the investigators said (N. Engl. J. Med. 2013 April 18 [doi:10.1056/NEJMoa1212722]).
These results were confirmed in a sensitivity analysis that included only patients who received their assigned intervention for a minimum of 5 days. They also remained the same in several subgroup analyses and in an intention-to-treat analysis.
Glutamine showed no effect on the secondary outcomes of organ failure or infections.
Antioxidants had no significant effect on any outcome, either in the study population as a whole or in any subgroups of patients. "This finding may reflect the true lack of usefulness of antioxidants; alternatively, it may be due to the characteristics of the study population or to the dose and method of administration in this trial," Dr. Heyland and his associates said.
Rates of serious adverse events were similar across all the study groups, but the frequency of excessively high urea levels was greater in patients who received glutamine (13.4%) than in those who did not (4.0%).
There may be several reasons why the findings of this clinical trial are so different from those of previous trials.
The earlier trials were smaller and less methodologically robust, and their results had to be pooled in metaanalyses. Patients in this trial received the highest dose of glutamine currently prescribed for critically ill patients, which is higher than the maximal doses used in previous studies. The agents were administered through both intravenous and enteral routes in this study, while in previous studies the subjects received either exclusively intravenous or exclusively enteral administration.
In addition, "we targeted critically ill patients with multiorgan failure, the majority of whom were in shock, whereas previous studies typically excluded such patients," Dr. Heyland and his colleagues said.
Treatment was initiated within 24 hours of admission to the ICU in this study, but in earlier studies it was given later in the course of critical illness. And finally, most of the patients in this study received enteral nutrition, while those in previous trials received parenteral nutrition.
This study was supported by the Canadian Institutes of Health Research. Fresenius Kabi provided the glutamine supplements and Biosyn provided the selenium to the participating European sites. Dr. Heyland and his associates reported ties to numerous industry sources.
With its exceptionally good design, execution, and analysis, this study "ticks all the boxes for quality," said Dr. Greet Van den Berghe.
The findings allow clinicians "to reject with confidence the hypothesis that glutamine supplementation in very ill patients in the ICU improves outcome," she said.
"Probably the most important contribution of the present trial is that it provides firm support for the need for large, adequately powered, randomized, controlled trials in critical care medicine to investigate whether what we intuitively consider to be the best treatment for our patients also is truly effective and without harm," she wrote.
Dr. Van den Berghe is with the department of cellular and molecular medicine at Leuven (Belgium) Catholic University. She reported receiving a research grant from Baxter Healthcare. These remarks were taken from her editorial accompanying Dr. Heyland’s report (N. Engl. J. Med. 2013 April 18 [doi:10.1056/NEJMe1302301]).
With its exceptionally good design, execution, and analysis, this study "ticks all the boxes for quality," said Dr. Greet Van den Berghe.
The findings allow clinicians "to reject with confidence the hypothesis that glutamine supplementation in very ill patients in the ICU improves outcome," she said.
"Probably the most important contribution of the present trial is that it provides firm support for the need for large, adequately powered, randomized, controlled trials in critical care medicine to investigate whether what we intuitively consider to be the best treatment for our patients also is truly effective and without harm," she wrote.
Dr. Van den Berghe is with the department of cellular and molecular medicine at Leuven (Belgium) Catholic University. She reported receiving a research grant from Baxter Healthcare. These remarks were taken from her editorial accompanying Dr. Heyland’s report (N. Engl. J. Med. 2013 April 18 [doi:10.1056/NEJMe1302301]).
With its exceptionally good design, execution, and analysis, this study "ticks all the boxes for quality," said Dr. Greet Van den Berghe.
The findings allow clinicians "to reject with confidence the hypothesis that glutamine supplementation in very ill patients in the ICU improves outcome," she said.
"Probably the most important contribution of the present trial is that it provides firm support for the need for large, adequately powered, randomized, controlled trials in critical care medicine to investigate whether what we intuitively consider to be the best treatment for our patients also is truly effective and without harm," she wrote.
Dr. Van den Berghe is with the department of cellular and molecular medicine at Leuven (Belgium) Catholic University. She reported receiving a research grant from Baxter Healthcare. These remarks were taken from her editorial accompanying Dr. Heyland’s report (N. Engl. J. Med. 2013 April 18 [doi:10.1056/NEJMe1302301]).
Early supplemental glutamine appears to harm rather than benefit critically ill patients who have multiorgan failure, according to a report published online April 18 in the New England Journal of Medicine.
In an international randomized controlled trial, in-hospital mortality and 6-month mortality were significantly increased in patients given intravenous glutamine within 24 hours of presentation to the ICU, compared with those given placebo, said Dr. Daren Heyland of Kingston (Ont.) General Hospital and his associates. A nonsignificant increase was seen in 28-day mortality.
Most of the patients in this study showed no glutamine deficiency at study entry. This observation, together with the primary finding that glutamine therapy may actually be harmful in this setting, "challenges the prevailing concept that glutamine is an essential nutrient that is deficient in critically ill patients and requires immediate supplementation," Dr. Heyland and his colleagues said.
The researchers also assessed whether supplemental antioxidants improved mortality or other outcomes in this study population and found that they did not.
Dr. Heyland and his associates performed this study because glutamine is thought to be rapidly depleted in critical illness and low levels of glutamine have been linked to increased mortality in ICU patients. Metaanalyses of small randomized trials suggested that both glutamine and antioxidant supplementation might improve survival in critically ill patients, but more recent and larger studies failed to confirm such a benefit.
This study included 1,223 consecutive adults who presented to 40 ICUs in the United States, Canada, and Europe during a 6-year period and required mechanical ventilation and had two or more organ failures related to their acute illness. The average patient age was 63 years. Primary diagnoses included cardiovascular, respiratory, gastrointestinal, neurologic, metabolic, and gynecologic disorders as well as sepsis and trauma.
The patients were randomly assigned in a double-blind fashion to receive daily intravenous glutamine, intravenous plus enteral antioxidants, glutamine plus antioxidants, or placebo fluids. The antioxidants included selenium, zinc, beta carotene, vitamin E, and vitamin C.
The primary outcome measure was 28-day mortality. There was a nonsignificant trend toward higher mortality in the patients given glutamine (32.4%) compared with those not given glutamine (27.2%). However, two secondary outcomes – in-hospital mortality and 6-month mortality – both were significantly higher in patients given glutamine than in those not given glutamine. In hospital mortality was 37.2% vs. 31%, respectively; 6-month mortality was 43.7% vs. 37.2%, respectively.
Other secondary outcomes – median time from randomization to ICU discharge and median time to hospital discharge – also were significantly longer for patients who received glutamine (17.1 vs. 13.1 days and 51.1 vs. 40.1 days, respectively), the investigators said (N. Engl. J. Med. 2013 April 18 [doi:10.1056/NEJMoa1212722]).
These results were confirmed in a sensitivity analysis that included only patients who received their assigned intervention for a minimum of 5 days. They also remained the same in several subgroup analyses and in an intention-to-treat analysis.
Glutamine showed no effect on the secondary outcomes of organ failure or infections.
Antioxidants had no significant effect on any outcome, either in the study population as a whole or in any subgroups of patients. "This finding may reflect the true lack of usefulness of antioxidants; alternatively, it may be due to the characteristics of the study population or to the dose and method of administration in this trial," Dr. Heyland and his associates said.
Rates of serious adverse events were similar across all the study groups, but the frequency of excessively high urea levels was greater in patients who received glutamine (13.4%) than in those who did not (4.0%).
There may be several reasons why the findings of this clinical trial are so different from those of previous trials.
The earlier trials were smaller and less methodologically robust, and their results had to be pooled in metaanalyses. Patients in this trial received the highest dose of glutamine currently prescribed for critically ill patients, which is higher than the maximal doses used in previous studies. The agents were administered through both intravenous and enteral routes in this study, while in previous studies the subjects received either exclusively intravenous or exclusively enteral administration.
In addition, "we targeted critically ill patients with multiorgan failure, the majority of whom were in shock, whereas previous studies typically excluded such patients," Dr. Heyland and his colleagues said.
Treatment was initiated within 24 hours of admission to the ICU in this study, but in earlier studies it was given later in the course of critical illness. And finally, most of the patients in this study received enteral nutrition, while those in previous trials received parenteral nutrition.
This study was supported by the Canadian Institutes of Health Research. Fresenius Kabi provided the glutamine supplements and Biosyn provided the selenium to the participating European sites. Dr. Heyland and his associates reported ties to numerous industry sources.
Early supplemental glutamine appears to harm rather than benefit critically ill patients who have multiorgan failure, according to a report published online April 18 in the New England Journal of Medicine.
In an international randomized controlled trial, in-hospital mortality and 6-month mortality were significantly increased in patients given intravenous glutamine within 24 hours of presentation to the ICU, compared with those given placebo, said Dr. Daren Heyland of Kingston (Ont.) General Hospital and his associates. A nonsignificant increase was seen in 28-day mortality.
Most of the patients in this study showed no glutamine deficiency at study entry. This observation, together with the primary finding that glutamine therapy may actually be harmful in this setting, "challenges the prevailing concept that glutamine is an essential nutrient that is deficient in critically ill patients and requires immediate supplementation," Dr. Heyland and his colleagues said.
The researchers also assessed whether supplemental antioxidants improved mortality or other outcomes in this study population and found that they did not.
Dr. Heyland and his associates performed this study because glutamine is thought to be rapidly depleted in critical illness and low levels of glutamine have been linked to increased mortality in ICU patients. Metaanalyses of small randomized trials suggested that both glutamine and antioxidant supplementation might improve survival in critically ill patients, but more recent and larger studies failed to confirm such a benefit.
This study included 1,223 consecutive adults who presented to 40 ICUs in the United States, Canada, and Europe during a 6-year period and required mechanical ventilation and had two or more organ failures related to their acute illness. The average patient age was 63 years. Primary diagnoses included cardiovascular, respiratory, gastrointestinal, neurologic, metabolic, and gynecologic disorders as well as sepsis and trauma.
The patients were randomly assigned in a double-blind fashion to receive daily intravenous glutamine, intravenous plus enteral antioxidants, glutamine plus antioxidants, or placebo fluids. The antioxidants included selenium, zinc, beta carotene, vitamin E, and vitamin C.
The primary outcome measure was 28-day mortality. There was a nonsignificant trend toward higher mortality in the patients given glutamine (32.4%) compared with those not given glutamine (27.2%). However, two secondary outcomes – in-hospital mortality and 6-month mortality – both were significantly higher in patients given glutamine than in those not given glutamine. In hospital mortality was 37.2% vs. 31%, respectively; 6-month mortality was 43.7% vs. 37.2%, respectively.
Other secondary outcomes – median time from randomization to ICU discharge and median time to hospital discharge – also were significantly longer for patients who received glutamine (17.1 vs. 13.1 days and 51.1 vs. 40.1 days, respectively), the investigators said (N. Engl. J. Med. 2013 April 18 [doi:10.1056/NEJMoa1212722]).
These results were confirmed in a sensitivity analysis that included only patients who received their assigned intervention for a minimum of 5 days. They also remained the same in several subgroup analyses and in an intention-to-treat analysis.
Glutamine showed no effect on the secondary outcomes of organ failure or infections.
Antioxidants had no significant effect on any outcome, either in the study population as a whole or in any subgroups of patients. "This finding may reflect the true lack of usefulness of antioxidants; alternatively, it may be due to the characteristics of the study population or to the dose and method of administration in this trial," Dr. Heyland and his associates said.
Rates of serious adverse events were similar across all the study groups, but the frequency of excessively high urea levels was greater in patients who received glutamine (13.4%) than in those who did not (4.0%).
There may be several reasons why the findings of this clinical trial are so different from those of previous trials.
The earlier trials were smaller and less methodologically robust, and their results had to be pooled in metaanalyses. Patients in this trial received the highest dose of glutamine currently prescribed for critically ill patients, which is higher than the maximal doses used in previous studies. The agents were administered through both intravenous and enteral routes in this study, while in previous studies the subjects received either exclusively intravenous or exclusively enteral administration.
In addition, "we targeted critically ill patients with multiorgan failure, the majority of whom were in shock, whereas previous studies typically excluded such patients," Dr. Heyland and his colleagues said.
Treatment was initiated within 24 hours of admission to the ICU in this study, but in earlier studies it was given later in the course of critical illness. And finally, most of the patients in this study received enteral nutrition, while those in previous trials received parenteral nutrition.
This study was supported by the Canadian Institutes of Health Research. Fresenius Kabi provided the glutamine supplements and Biosyn provided the selenium to the participating European sites. Dr. Heyland and his associates reported ties to numerous industry sources.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: In-hospital mortality was higher (37.2% vs. 31%) in patients receiving glutamine therapy compared with placebo, as was 6-month mortality (43.7% vs. 37.2%).
Data source: An international randomized, double-blind, placebo-controlled trial involving 1,223 critically ill adults in 40 ICUs who were followed for 6 months.
Disclosures: This study was supported by the Canadian Institutes of Health Research. Dr. Heyland and his associates reported ties to numerous industry sources.
Childhood migraine tied to history of infantile colic
Children and adolescents who presented to the emergency department with migraine headache were 6 times more likely to have a history of colic during infancy than were those who presented for other reasons, according to a report in the April 17 issue of JAMA.
In contrast, children and adolescents who presented to the ED with tension-type headache showed no increase in the likelihood that they had experienced infantile colic. This confirms the specificity of the association between migraine – not other types of headache – and colic, said Dr. Silvia Romanello of the department of pediatric emergency care and the pediatric migraine and neurovascular diseases unit, Robert Debré Hospital, Paris, and her associates.
Researchers and clinicians have long suspected an association between the two pain syndromes of colic and migraine, but such a link has not been well studied. Dr. Romanello and her colleagues at three tertiary-care hospitals in France and Italy examined the association in a case-control study involving 328 pediatric patients and 471 controls.
Subjects were aged 6-18 years and presented to EDs with primary headaches during a 3-month study period. A total of 208 were diagnosed by a pediatric neurologist as having primary migraine (142 without aura and 66 with aura), and 120 were diagnosed as having tension-type headache. The control subjects were patients of the same age who presented during the same period with minor trauma.
Patients with recurrent headaches were excluded from the study.
The medical records of all the study subjects were reviewed for a diagnosis of infantile colic. Parent questionnaires confirmed this history in every case.
A total of 72.6% of the patients with primary migraine had a history of infantile colic. The prevalence of colic was similarly high between those who had migraine with aura (69.7%) and those who had migraine without aura (73.9%).
In contrast, only 35% of the patients with tension-type headache had a history of infantile colic. This prevalence was similar to that in the control group (26.5%), the investigators said (JAMA 2013;309:1607-12).
In a further statistical analysis of the data, the association between infantile colic and migraine was highly significant, with an odds ratio of 6.61. No association was seen between infantile colic and tension-type headache or infantile colic and minor trauma.
A subgroup analysis showed that the association between infantile colic and migraine with aura was highly significant, with an OR of 5.73, as was the association between infantile colic and migraine without aura, which had an OR of 7.01. This finding indicates that the two pain disorders, colic and migraine, share a common pathophysiology, Dr. Romanello and her associates said.
Given that diagnosing headache in children can be challenging, another subgroup analysis was performed to explore any possible age-related bias in diagnosis. The results confirmed those of the main study: The association between migraine and infantile colic remained highly significant in both children aged 6-12 years and adolescents aged 13-18 years.
This study was not designed to explore the possible reasons for the strong association between migraine and colic. However, the investigators noted that colic might result from a sensitization of the perivascular nerve terminals in the gut, much as migraine results from a similar process in the brain.
Another possibility is that "molecules known to be involved in the modulation of sensory activity, such as calcitonin-gene-related peptide (CGRP)," which is released during migraine episodes, also may be involved in modulation of abdominal pain "by inducing the neurogenic inflammation of sensory neurons in the gut." If so, drugs that are CGRP antagonists, which are effective in pain management, may be found helpful for both colic and migraine.
In addition, triptans have proved extremely effective against acute attacks of both migraine and abdominal migraine, and eventually may be found useful for infantile colic. However, much more study is needed before such treatment can be considered. "It is currently difficult to imagine that clinical trials will be conducted with such off-label drugs for the treatment of a benign condition such as infantile colic," even though the condition clearly causes pain in infants and significant stress in parents, Dr. Romanello and her associates said.
No financial conflicts of interest were reported.
The report by Romanello and colleagues answers a long-standing question and shows a definite link between pediatric migraine and infantile colic, with an odds ratio of 6.61, said Dr. Leon G. Epstein and Dr. Phyllis C. Zee.
If colic proves to be an early manifestation of migraine, it would explain why most treatments for colic, which have been directed at a gastrointestinal etiology, have consistently been ineffective, they noted.
Dr. Epstein is in the departments of pediatrics and neurology at Northwestern University, Chicago, and the Ann & Robert H. Lurie Children’s Hospital of Chicago. Dr. Zee is in the department of neurology at Northwestern University. Dr. Zee reported numerous ties to industry sources. These remarks were taken from their editorial accompanying Dr. Romanello’s report (JAMA 2013;309:1636-7).
The report by Romanello and colleagues answers a long-standing question and shows a definite link between pediatric migraine and infantile colic, with an odds ratio of 6.61, said Dr. Leon G. Epstein and Dr. Phyllis C. Zee.
If colic proves to be an early manifestation of migraine, it would explain why most treatments for colic, which have been directed at a gastrointestinal etiology, have consistently been ineffective, they noted.
Dr. Epstein is in the departments of pediatrics and neurology at Northwestern University, Chicago, and the Ann & Robert H. Lurie Children’s Hospital of Chicago. Dr. Zee is in the department of neurology at Northwestern University. Dr. Zee reported numerous ties to industry sources. These remarks were taken from their editorial accompanying Dr. Romanello’s report (JAMA 2013;309:1636-7).
The report by Romanello and colleagues answers a long-standing question and shows a definite link between pediatric migraine and infantile colic, with an odds ratio of 6.61, said Dr. Leon G. Epstein and Dr. Phyllis C. Zee.
If colic proves to be an early manifestation of migraine, it would explain why most treatments for colic, which have been directed at a gastrointestinal etiology, have consistently been ineffective, they noted.
Dr. Epstein is in the departments of pediatrics and neurology at Northwestern University, Chicago, and the Ann & Robert H. Lurie Children’s Hospital of Chicago. Dr. Zee is in the department of neurology at Northwestern University. Dr. Zee reported numerous ties to industry sources. These remarks were taken from their editorial accompanying Dr. Romanello’s report (JAMA 2013;309:1636-7).
Children and adolescents who presented to the emergency department with migraine headache were 6 times more likely to have a history of colic during infancy than were those who presented for other reasons, according to a report in the April 17 issue of JAMA.
In contrast, children and adolescents who presented to the ED with tension-type headache showed no increase in the likelihood that they had experienced infantile colic. This confirms the specificity of the association between migraine – not other types of headache – and colic, said Dr. Silvia Romanello of the department of pediatric emergency care and the pediatric migraine and neurovascular diseases unit, Robert Debré Hospital, Paris, and her associates.
Researchers and clinicians have long suspected an association between the two pain syndromes of colic and migraine, but such a link has not been well studied. Dr. Romanello and her colleagues at three tertiary-care hospitals in France and Italy examined the association in a case-control study involving 328 pediatric patients and 471 controls.
Subjects were aged 6-18 years and presented to EDs with primary headaches during a 3-month study period. A total of 208 were diagnosed by a pediatric neurologist as having primary migraine (142 without aura and 66 with aura), and 120 were diagnosed as having tension-type headache. The control subjects were patients of the same age who presented during the same period with minor trauma.
Patients with recurrent headaches were excluded from the study.
The medical records of all the study subjects were reviewed for a diagnosis of infantile colic. Parent questionnaires confirmed this history in every case.
A total of 72.6% of the patients with primary migraine had a history of infantile colic. The prevalence of colic was similarly high between those who had migraine with aura (69.7%) and those who had migraine without aura (73.9%).
In contrast, only 35% of the patients with tension-type headache had a history of infantile colic. This prevalence was similar to that in the control group (26.5%), the investigators said (JAMA 2013;309:1607-12).
In a further statistical analysis of the data, the association between infantile colic and migraine was highly significant, with an odds ratio of 6.61. No association was seen between infantile colic and tension-type headache or infantile colic and minor trauma.
A subgroup analysis showed that the association between infantile colic and migraine with aura was highly significant, with an OR of 5.73, as was the association between infantile colic and migraine without aura, which had an OR of 7.01. This finding indicates that the two pain disorders, colic and migraine, share a common pathophysiology, Dr. Romanello and her associates said.
Given that diagnosing headache in children can be challenging, another subgroup analysis was performed to explore any possible age-related bias in diagnosis. The results confirmed those of the main study: The association between migraine and infantile colic remained highly significant in both children aged 6-12 years and adolescents aged 13-18 years.
This study was not designed to explore the possible reasons for the strong association between migraine and colic. However, the investigators noted that colic might result from a sensitization of the perivascular nerve terminals in the gut, much as migraine results from a similar process in the brain.
Another possibility is that "molecules known to be involved in the modulation of sensory activity, such as calcitonin-gene-related peptide (CGRP)," which is released during migraine episodes, also may be involved in modulation of abdominal pain "by inducing the neurogenic inflammation of sensory neurons in the gut." If so, drugs that are CGRP antagonists, which are effective in pain management, may be found helpful for both colic and migraine.
In addition, triptans have proved extremely effective against acute attacks of both migraine and abdominal migraine, and eventually may be found useful for infantile colic. However, much more study is needed before such treatment can be considered. "It is currently difficult to imagine that clinical trials will be conducted with such off-label drugs for the treatment of a benign condition such as infantile colic," even though the condition clearly causes pain in infants and significant stress in parents, Dr. Romanello and her associates said.
No financial conflicts of interest were reported.
Children and adolescents who presented to the emergency department with migraine headache were 6 times more likely to have a history of colic during infancy than were those who presented for other reasons, according to a report in the April 17 issue of JAMA.
In contrast, children and adolescents who presented to the ED with tension-type headache showed no increase in the likelihood that they had experienced infantile colic. This confirms the specificity of the association between migraine – not other types of headache – and colic, said Dr. Silvia Romanello of the department of pediatric emergency care and the pediatric migraine and neurovascular diseases unit, Robert Debré Hospital, Paris, and her associates.
Researchers and clinicians have long suspected an association between the two pain syndromes of colic and migraine, but such a link has not been well studied. Dr. Romanello and her colleagues at three tertiary-care hospitals in France and Italy examined the association in a case-control study involving 328 pediatric patients and 471 controls.
Subjects were aged 6-18 years and presented to EDs with primary headaches during a 3-month study period. A total of 208 were diagnosed by a pediatric neurologist as having primary migraine (142 without aura and 66 with aura), and 120 were diagnosed as having tension-type headache. The control subjects were patients of the same age who presented during the same period with minor trauma.
Patients with recurrent headaches were excluded from the study.
The medical records of all the study subjects were reviewed for a diagnosis of infantile colic. Parent questionnaires confirmed this history in every case.
A total of 72.6% of the patients with primary migraine had a history of infantile colic. The prevalence of colic was similarly high between those who had migraine with aura (69.7%) and those who had migraine without aura (73.9%).
In contrast, only 35% of the patients with tension-type headache had a history of infantile colic. This prevalence was similar to that in the control group (26.5%), the investigators said (JAMA 2013;309:1607-12).
In a further statistical analysis of the data, the association between infantile colic and migraine was highly significant, with an odds ratio of 6.61. No association was seen between infantile colic and tension-type headache or infantile colic and minor trauma.
A subgroup analysis showed that the association between infantile colic and migraine with aura was highly significant, with an OR of 5.73, as was the association between infantile colic and migraine without aura, which had an OR of 7.01. This finding indicates that the two pain disorders, colic and migraine, share a common pathophysiology, Dr. Romanello and her associates said.
Given that diagnosing headache in children can be challenging, another subgroup analysis was performed to explore any possible age-related bias in diagnosis. The results confirmed those of the main study: The association between migraine and infantile colic remained highly significant in both children aged 6-12 years and adolescents aged 13-18 years.
This study was not designed to explore the possible reasons for the strong association between migraine and colic. However, the investigators noted that colic might result from a sensitization of the perivascular nerve terminals in the gut, much as migraine results from a similar process in the brain.
Another possibility is that "molecules known to be involved in the modulation of sensory activity, such as calcitonin-gene-related peptide (CGRP)," which is released during migraine episodes, also may be involved in modulation of abdominal pain "by inducing the neurogenic inflammation of sensory neurons in the gut." If so, drugs that are CGRP antagonists, which are effective in pain management, may be found helpful for both colic and migraine.
In addition, triptans have proved extremely effective against acute attacks of both migraine and abdominal migraine, and eventually may be found useful for infantile colic. However, much more study is needed before such treatment can be considered. "It is currently difficult to imagine that clinical trials will be conducted with such off-label drugs for the treatment of a benign condition such as infantile colic," even though the condition clearly causes pain in infants and significant stress in parents, Dr. Romanello and her associates said.
No financial conflicts of interest were reported.
FROM JAMA
Major Finding: Almost three-quarters of pediatric patients with primary migraine had a history of infantile colic, compared with 35% of patients with tension-type headache and 26.5% of control subjects.
Data Source: A case-control study involving 208 pediatric patients with primary migraine, 120 with tension-type headache, and 471 with minor trauma (controls) who presented to three European EDs during a 3-month period.
Disclosures: No financial conflicts of interest were reported.
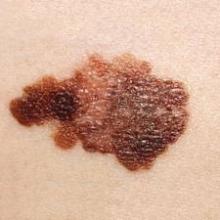
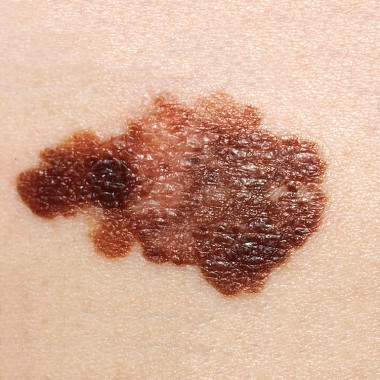
Melanoma increases in adolescents
Since the 1970s, the incidence of melanoma has been rising about 2% per year in adolescents, the same as it has in adults, according to an epidemiologic study published online April 16 in Pediatrics.
The reasons for this increase are not yet clear. Individual-level studies rather than population-level studies are needed to find the explanation for this trend, said Jeannette R. Wong of the division of cancer epidemiology and genetics at the National Cancer Institute, Rockville, Md., and her associates.
Recent studies have documented the increase in adult melanoma cases and "illuminated likely contributing factors," but none have assessed childhood and adolescent melanoma, the researchers noted. They analyzed data from the Surveillance, Epidemiology, and End Results (SEER) database for nine U.S. geographic regions from 1973 through 2009. They identified all first melanomas diagnosed among patients aged 19 years and younger.
A total of 1,317 cases of melanoma were identified during the study period. Because few of the malignancies developed in nonwhite patients or in patients of unknown race/ethnicity, only the 1,230 cases that developed in white patients were included in the analysis.
The overall incidence of melanoma rose by an average of 2% per year for both boys and girls (Pediatrics 2013 April 16 [doi: 10.1542/peds.2012-2520]).
Melanoma was nearly twice as common in girls compared to boys overall (61% vs. 39%) with similar percentages within each age group (0-9 years, 10-14 years, and 15-19 years).
The incidence increased with age. The majority of melanomas – 77% – were diagnosed in adolescents aged 15-19 years. Only 8% of melanomas were diagnosed in children aged 9 years and younger, and 15% were diagnosed in those aged 10-14 years.
The incidence of localized melanoma was much higher (77%) than that of regional (13%), distant (2%), or unstaged disease (8%).
The most frequent melanoma sites in girls were the lower limbs and hips, on which melanomas increased by a significant annual percentage change of 3% over the study period. Among boys, melanomas were most common on the skin of the face and trunk, with annual percentage increase of 5% over the study period.
UVB exposure did not appear to be the primary factor contributing to the increase in melanoma, the researchers noted. In fact, melanoma rates were slightly higher in geographic areas that had low UVB exposure (such as Connecticut and Washington state) than in areas with high UVB exposure (such as Hawaii and California). "However, all significantly increasing trends for melanoma over our study period occurred in sun-exposed areas of the body," they said.
This finding suggests that tanning facilities may instead be a major source of the increase in incidence, because there are many more such facilities in low-UV regions, the researchers said.
Increased use of tanning facilities also may explain why the rate of melanoma is higher in girls than in boys, since girls are much more likely than boys to use such facilities, they added.
It is also possible that heightened awareness of melanoma in recent years has improved detection rates in the pediatric population, the researchers said.
These data are consistent with those of previous studies that have reported increasing rates of melanoma in the pediatric populations of Australia, Sweden, and England.
Although this study included more than 30 years of data on melanoma incidence, it was limited in that it did not include individual-level data on outdoor UV exposure, use of tanning facilities, or familial factors related to melanoma risk, the researchers said.
Since the 1970s, the incidence of melanoma has been rising about 2% per year in adolescents, the same as it has in adults, according to an epidemiologic study published online April 16 in Pediatrics.
The reasons for this increase are not yet clear. Individual-level studies rather than population-level studies are needed to find the explanation for this trend, said Jeannette R. Wong of the division of cancer epidemiology and genetics at the National Cancer Institute, Rockville, Md., and her associates.
Recent studies have documented the increase in adult melanoma cases and "illuminated likely contributing factors," but none have assessed childhood and adolescent melanoma, the researchers noted. They analyzed data from the Surveillance, Epidemiology, and End Results (SEER) database for nine U.S. geographic regions from 1973 through 2009. They identified all first melanomas diagnosed among patients aged 19 years and younger.
A total of 1,317 cases of melanoma were identified during the study period. Because few of the malignancies developed in nonwhite patients or in patients of unknown race/ethnicity, only the 1,230 cases that developed in white patients were included in the analysis.
The overall incidence of melanoma rose by an average of 2% per year for both boys and girls (Pediatrics 2013 April 16 [doi: 10.1542/peds.2012-2520]).
Melanoma was nearly twice as common in girls compared to boys overall (61% vs. 39%) with similar percentages within each age group (0-9 years, 10-14 years, and 15-19 years).
The incidence increased with age. The majority of melanomas – 77% – were diagnosed in adolescents aged 15-19 years. Only 8% of melanomas were diagnosed in children aged 9 years and younger, and 15% were diagnosed in those aged 10-14 years.
The incidence of localized melanoma was much higher (77%) than that of regional (13%), distant (2%), or unstaged disease (8%).
The most frequent melanoma sites in girls were the lower limbs and hips, on which melanomas increased by a significant annual percentage change of 3% over the study period. Among boys, melanomas were most common on the skin of the face and trunk, with annual percentage increase of 5% over the study period.
UVB exposure did not appear to be the primary factor contributing to the increase in melanoma, the researchers noted. In fact, melanoma rates were slightly higher in geographic areas that had low UVB exposure (such as Connecticut and Washington state) than in areas with high UVB exposure (such as Hawaii and California). "However, all significantly increasing trends for melanoma over our study period occurred in sun-exposed areas of the body," they said.
This finding suggests that tanning facilities may instead be a major source of the increase in incidence, because there are many more such facilities in low-UV regions, the researchers said.
Increased use of tanning facilities also may explain why the rate of melanoma is higher in girls than in boys, since girls are much more likely than boys to use such facilities, they added.
It is also possible that heightened awareness of melanoma in recent years has improved detection rates in the pediatric population, the researchers said.
These data are consistent with those of previous studies that have reported increasing rates of melanoma in the pediatric populations of Australia, Sweden, and England.
Although this study included more than 30 years of data on melanoma incidence, it was limited in that it did not include individual-level data on outdoor UV exposure, use of tanning facilities, or familial factors related to melanoma risk, the researchers said.
Since the 1970s, the incidence of melanoma has been rising about 2% per year in adolescents, the same as it has in adults, according to an epidemiologic study published online April 16 in Pediatrics.
The reasons for this increase are not yet clear. Individual-level studies rather than population-level studies are needed to find the explanation for this trend, said Jeannette R. Wong of the division of cancer epidemiology and genetics at the National Cancer Institute, Rockville, Md., and her associates.
Recent studies have documented the increase in adult melanoma cases and "illuminated likely contributing factors," but none have assessed childhood and adolescent melanoma, the researchers noted. They analyzed data from the Surveillance, Epidemiology, and End Results (SEER) database for nine U.S. geographic regions from 1973 through 2009. They identified all first melanomas diagnosed among patients aged 19 years and younger.
A total of 1,317 cases of melanoma were identified during the study period. Because few of the malignancies developed in nonwhite patients or in patients of unknown race/ethnicity, only the 1,230 cases that developed in white patients were included in the analysis.
The overall incidence of melanoma rose by an average of 2% per year for both boys and girls (Pediatrics 2013 April 16 [doi: 10.1542/peds.2012-2520]).
Melanoma was nearly twice as common in girls compared to boys overall (61% vs. 39%) with similar percentages within each age group (0-9 years, 10-14 years, and 15-19 years).
The incidence increased with age. The majority of melanomas – 77% – were diagnosed in adolescents aged 15-19 years. Only 8% of melanomas were diagnosed in children aged 9 years and younger, and 15% were diagnosed in those aged 10-14 years.
The incidence of localized melanoma was much higher (77%) than that of regional (13%), distant (2%), or unstaged disease (8%).
The most frequent melanoma sites in girls were the lower limbs and hips, on which melanomas increased by a significant annual percentage change of 3% over the study period. Among boys, melanomas were most common on the skin of the face and trunk, with annual percentage increase of 5% over the study period.
UVB exposure did not appear to be the primary factor contributing to the increase in melanoma, the researchers noted. In fact, melanoma rates were slightly higher in geographic areas that had low UVB exposure (such as Connecticut and Washington state) than in areas with high UVB exposure (such as Hawaii and California). "However, all significantly increasing trends for melanoma over our study period occurred in sun-exposed areas of the body," they said.
This finding suggests that tanning facilities may instead be a major source of the increase in incidence, because there are many more such facilities in low-UV regions, the researchers said.
Increased use of tanning facilities also may explain why the rate of melanoma is higher in girls than in boys, since girls are much more likely than boys to use such facilities, they added.
It is also possible that heightened awareness of melanoma in recent years has improved detection rates in the pediatric population, the researchers said.
These data are consistent with those of previous studies that have reported increasing rates of melanoma in the pediatric populations of Australia, Sweden, and England.
Although this study included more than 30 years of data on melanoma incidence, it was limited in that it did not include individual-level data on outdoor UV exposure, use of tanning facilities, or familial factors related to melanoma risk, the researchers said.
FROM PEDIATRICS
Major finding: The incidence of melanoma has increased by an average of 2% per year for both boys and girls in the past 30 years.
Data source: An analysis from the SEER database of 1,317 cases of melanoma arising in patients younger than 19 years from the period 1973-2009.
Disclosures: This study was supported in part by the National Institutes of Health and the National Cancer Institute. No financial conflicts of interest were reported.
Abdominal, thoracic CT scans reliably detect incidental low lumbar BMD
Abdominal and thoracic CT scans obtained for a variety of reasons, such as to assess pain, GI symptoms, or urinary tract complaints, also can be used "opportunistically" to examine lumbar bone mineral density and screen for occult osteoporosis, according to a report in the April 16 issue of the Annals of Internal Medicine.
Abdominal and thoracic CT scans done in routine practice happen to include imaging of the L1 level, which can easily be identified because it is the first non–rib-bearing vertebra. Such scans readily yield data on lumbar bone mineral density (BMD), which is a clinically useful way to diagnose or rule out osteoporosis, said Dr. Perry J. Pickhardt of the department of radiology and his associates at the University of Wisconsin, Madison.
It is important not to confuse this standard CT scanning with quantitative CT (QCT) scanning. QCT "is more labor-intensive; requires an imaging phantom or angle-corrected [region-of-interest] measurement of bone, muscle, and fat at multiple levels; and involves additional money, time, and radiation exposure," they explained.
Unlike dual-energy x-ray absorptiometry (DXA) screening or QCT assessment, "the method that we used requires a negligible amount of training and time; could be applied prospectively by the interpreting radiologist or retrospectively by a radiologist or even nonradiologist; adds no cost; and requires no additional patient time, equipment, software, or radiation exposure," the investigators wrote.
Such incidental CT scans can be assessed retrospectively because they are almost always stored indefinitely in electronic medical records, they noted.
Dr. Pickhardt and his colleagues evaluated CT-derived BMD assessment and compared it against DXA scanning of the hips and spine by identifying 1,867 adults who had undergone the two types of scanning within a 6-month period during the 10-year study interval. They retrieved and reviewed the images, paying particular attention to obvious moderate or severe compression deformities on the CT images, rather than to milder ones, "to avoid ambiguity related to more subjective borderline or mild compression deformities."
The study subjects had a total of 2,063 pairs of CT and DXA assessments that had been performed a median of 67 days apart. A total of 81% of these subjects were women, and the mean age was 59 years.
These patients had undergone abdominal or thoracic CT for a variety of clinical indications, most often for a suspected mass or an oncologic work-up (414 subjects), genitourinary problems (402 subjects), gastrointestinal symptoms (398 subjects), and/or unexplained abdominal pain or symptoms (374 subjects).
Approximately 55% of the CT scans involved intravenous contrast. The use of contrast had no effect on the interpretation of lumbar data on the scans.
The DXA screening identified 22.9% of the study subjects as osteoporotic, 44.8% as osteopenic, and 32.3% as having normal BMD. The CT scans were significantly more sensitive than DXA at distinguishing these three states.
In particular, CT scans identified 119 patients as having osteoporosis, with readily identifiable moderate or severe vertebral fractures, when DXA had classified 62 of these patients as having normal BMD (12 subjects) or only osteopenia (50 subjects).
"Our observations are consistent with prior studies documenting that many patients without osteoporosis diagnosed by DXA will sustain fragility fractures, and suggest that CT attenuation may be a more accurate risk predictor," Dr. Pickhardt and his associates wrote (Ann. Intern. Med. 2013:158:588-95).
If their findings are confirmed in other studies, it may become routine for all abdominal and thoracic CT scans performed for any reason to be used for lumbar BMD assessment as well. "In the future, it may even be possible to incorporate CT ... data into fracture risk assessment tools," they added.
This should result in substantial savings in health care costs since osteoporosis will be diagnosed and treated earlier, before fractures occur, and since it also will reduce the number of costly DXA studies performed.
More than 80 million CT scans were performed in the United States in 2011, "most of which carry potentially useful information about BMD," the researchers noted.
The investigators are now turning their attention to using pelvic CT scans that were obtained for various clinical indications to assess hip BMD. "We are currently investigating the potential for deriving a DXA-equivalent T-score for the hips from standard pelvic CT scans by using a dedicated software tool," Dr. Pickhardt and his associates said.
This study was funded by the National Institutes of Health. None of the investigators reported having any financial conflicts of interest.
Dr. Pickhardt and his associates "have laid all the groundwork needed to justify using conventional CT imaging to detect incidental osteoporosis," said Dr. Sumit R. Majumdar and Dr. William D. Leslie.
Given the large number of such CT scans performed every year, "the idea of extracting more information from imaging data collected for other purposes holds merit," they said.
"It is now up to the rest of us to safely and cost-effectively translate this new knowledge into everyday clinical practice," Dr. Majumdar and Dr. Leslie said.
Dr. Majumdar is with the University of Alberta, Edmonton. Dr. Leslie is with the University of Manitoba, Winnipeg. Neither reported any financial conflicts of interest. These remarks were taken from their editorial, which accompanied Dr. Pickhardt’s report (Ann. Intern. Med. 2013;158:630-1).
Dr. Pickhardt and his associates "have laid all the groundwork needed to justify using conventional CT imaging to detect incidental osteoporosis," said Dr. Sumit R. Majumdar and Dr. William D. Leslie.
Given the large number of such CT scans performed every year, "the idea of extracting more information from imaging data collected for other purposes holds merit," they said.
"It is now up to the rest of us to safely and cost-effectively translate this new knowledge into everyday clinical practice," Dr. Majumdar and Dr. Leslie said.
Dr. Majumdar is with the University of Alberta, Edmonton. Dr. Leslie is with the University of Manitoba, Winnipeg. Neither reported any financial conflicts of interest. These remarks were taken from their editorial, which accompanied Dr. Pickhardt’s report (Ann. Intern. Med. 2013;158:630-1).
Dr. Pickhardt and his associates "have laid all the groundwork needed to justify using conventional CT imaging to detect incidental osteoporosis," said Dr. Sumit R. Majumdar and Dr. William D. Leslie.
Given the large number of such CT scans performed every year, "the idea of extracting more information from imaging data collected for other purposes holds merit," they said.
"It is now up to the rest of us to safely and cost-effectively translate this new knowledge into everyday clinical practice," Dr. Majumdar and Dr. Leslie said.
Dr. Majumdar is with the University of Alberta, Edmonton. Dr. Leslie is with the University of Manitoba, Winnipeg. Neither reported any financial conflicts of interest. These remarks were taken from their editorial, which accompanied Dr. Pickhardt’s report (Ann. Intern. Med. 2013;158:630-1).
Abdominal and thoracic CT scans obtained for a variety of reasons, such as to assess pain, GI symptoms, or urinary tract complaints, also can be used "opportunistically" to examine lumbar bone mineral density and screen for occult osteoporosis, according to a report in the April 16 issue of the Annals of Internal Medicine.
Abdominal and thoracic CT scans done in routine practice happen to include imaging of the L1 level, which can easily be identified because it is the first non–rib-bearing vertebra. Such scans readily yield data on lumbar bone mineral density (BMD), which is a clinically useful way to diagnose or rule out osteoporosis, said Dr. Perry J. Pickhardt of the department of radiology and his associates at the University of Wisconsin, Madison.
It is important not to confuse this standard CT scanning with quantitative CT (QCT) scanning. QCT "is more labor-intensive; requires an imaging phantom or angle-corrected [region-of-interest] measurement of bone, muscle, and fat at multiple levels; and involves additional money, time, and radiation exposure," they explained.
Unlike dual-energy x-ray absorptiometry (DXA) screening or QCT assessment, "the method that we used requires a negligible amount of training and time; could be applied prospectively by the interpreting radiologist or retrospectively by a radiologist or even nonradiologist; adds no cost; and requires no additional patient time, equipment, software, or radiation exposure," the investigators wrote.
Such incidental CT scans can be assessed retrospectively because they are almost always stored indefinitely in electronic medical records, they noted.
Dr. Pickhardt and his colleagues evaluated CT-derived BMD assessment and compared it against DXA scanning of the hips and spine by identifying 1,867 adults who had undergone the two types of scanning within a 6-month period during the 10-year study interval. They retrieved and reviewed the images, paying particular attention to obvious moderate or severe compression deformities on the CT images, rather than to milder ones, "to avoid ambiguity related to more subjective borderline or mild compression deformities."
The study subjects had a total of 2,063 pairs of CT and DXA assessments that had been performed a median of 67 days apart. A total of 81% of these subjects were women, and the mean age was 59 years.
These patients had undergone abdominal or thoracic CT for a variety of clinical indications, most often for a suspected mass or an oncologic work-up (414 subjects), genitourinary problems (402 subjects), gastrointestinal symptoms (398 subjects), and/or unexplained abdominal pain or symptoms (374 subjects).
Approximately 55% of the CT scans involved intravenous contrast. The use of contrast had no effect on the interpretation of lumbar data on the scans.
The DXA screening identified 22.9% of the study subjects as osteoporotic, 44.8% as osteopenic, and 32.3% as having normal BMD. The CT scans were significantly more sensitive than DXA at distinguishing these three states.
In particular, CT scans identified 119 patients as having osteoporosis, with readily identifiable moderate or severe vertebral fractures, when DXA had classified 62 of these patients as having normal BMD (12 subjects) or only osteopenia (50 subjects).
"Our observations are consistent with prior studies documenting that many patients without osteoporosis diagnosed by DXA will sustain fragility fractures, and suggest that CT attenuation may be a more accurate risk predictor," Dr. Pickhardt and his associates wrote (Ann. Intern. Med. 2013:158:588-95).
If their findings are confirmed in other studies, it may become routine for all abdominal and thoracic CT scans performed for any reason to be used for lumbar BMD assessment as well. "In the future, it may even be possible to incorporate CT ... data into fracture risk assessment tools," they added.
This should result in substantial savings in health care costs since osteoporosis will be diagnosed and treated earlier, before fractures occur, and since it also will reduce the number of costly DXA studies performed.
More than 80 million CT scans were performed in the United States in 2011, "most of which carry potentially useful information about BMD," the researchers noted.
The investigators are now turning their attention to using pelvic CT scans that were obtained for various clinical indications to assess hip BMD. "We are currently investigating the potential for deriving a DXA-equivalent T-score for the hips from standard pelvic CT scans by using a dedicated software tool," Dr. Pickhardt and his associates said.
This study was funded by the National Institutes of Health. None of the investigators reported having any financial conflicts of interest.
Abdominal and thoracic CT scans obtained for a variety of reasons, such as to assess pain, GI symptoms, or urinary tract complaints, also can be used "opportunistically" to examine lumbar bone mineral density and screen for occult osteoporosis, according to a report in the April 16 issue of the Annals of Internal Medicine.
Abdominal and thoracic CT scans done in routine practice happen to include imaging of the L1 level, which can easily be identified because it is the first non–rib-bearing vertebra. Such scans readily yield data on lumbar bone mineral density (BMD), which is a clinically useful way to diagnose or rule out osteoporosis, said Dr. Perry J. Pickhardt of the department of radiology and his associates at the University of Wisconsin, Madison.
It is important not to confuse this standard CT scanning with quantitative CT (QCT) scanning. QCT "is more labor-intensive; requires an imaging phantom or angle-corrected [region-of-interest] measurement of bone, muscle, and fat at multiple levels; and involves additional money, time, and radiation exposure," they explained.
Unlike dual-energy x-ray absorptiometry (DXA) screening or QCT assessment, "the method that we used requires a negligible amount of training and time; could be applied prospectively by the interpreting radiologist or retrospectively by a radiologist or even nonradiologist; adds no cost; and requires no additional patient time, equipment, software, or radiation exposure," the investigators wrote.
Such incidental CT scans can be assessed retrospectively because they are almost always stored indefinitely in electronic medical records, they noted.
Dr. Pickhardt and his colleagues evaluated CT-derived BMD assessment and compared it against DXA scanning of the hips and spine by identifying 1,867 adults who had undergone the two types of scanning within a 6-month period during the 10-year study interval. They retrieved and reviewed the images, paying particular attention to obvious moderate or severe compression deformities on the CT images, rather than to milder ones, "to avoid ambiguity related to more subjective borderline or mild compression deformities."
The study subjects had a total of 2,063 pairs of CT and DXA assessments that had been performed a median of 67 days apart. A total of 81% of these subjects were women, and the mean age was 59 years.
These patients had undergone abdominal or thoracic CT for a variety of clinical indications, most often for a suspected mass or an oncologic work-up (414 subjects), genitourinary problems (402 subjects), gastrointestinal symptoms (398 subjects), and/or unexplained abdominal pain or symptoms (374 subjects).
Approximately 55% of the CT scans involved intravenous contrast. The use of contrast had no effect on the interpretation of lumbar data on the scans.
The DXA screening identified 22.9% of the study subjects as osteoporotic, 44.8% as osteopenic, and 32.3% as having normal BMD. The CT scans were significantly more sensitive than DXA at distinguishing these three states.
In particular, CT scans identified 119 patients as having osteoporosis, with readily identifiable moderate or severe vertebral fractures, when DXA had classified 62 of these patients as having normal BMD (12 subjects) or only osteopenia (50 subjects).
"Our observations are consistent with prior studies documenting that many patients without osteoporosis diagnosed by DXA will sustain fragility fractures, and suggest that CT attenuation may be a more accurate risk predictor," Dr. Pickhardt and his associates wrote (Ann. Intern. Med. 2013:158:588-95).
If their findings are confirmed in other studies, it may become routine for all abdominal and thoracic CT scans performed for any reason to be used for lumbar BMD assessment as well. "In the future, it may even be possible to incorporate CT ... data into fracture risk assessment tools," they added.
This should result in substantial savings in health care costs since osteoporosis will be diagnosed and treated earlier, before fractures occur, and since it also will reduce the number of costly DXA studies performed.
More than 80 million CT scans were performed in the United States in 2011, "most of which carry potentially useful information about BMD," the researchers noted.
The investigators are now turning their attention to using pelvic CT scans that were obtained for various clinical indications to assess hip BMD. "We are currently investigating the potential for deriving a DXA-equivalent T-score for the hips from standard pelvic CT scans by using a dedicated software tool," Dr. Pickhardt and his associates said.
This study was funded by the National Institutes of Health. None of the investigators reported having any financial conflicts of interest.
FROM ANNALS OF INTERNAL MEDICINE
Major Finding: Conventional abdominal and CT scans performed for various indications were more accurate than DXA at assessing lumbar BMD and identifying occult osteoporosis.
Data Source: A 10-year cross-sectional study comparing incidental spine imaging on conventional CT scans against DXA screening in 1,867 adults from the general population.
Disclosures: This study was funded by the National Institutes of Health. None of the investigators reported having any financial conflicts of interest.
Cancer patients embrace pioneer assisted-suicide program
The Death with Dignity program, a pioneering program that includes medically assisted suicide for competent, terminally ill adults treated at a comprehensive cancer center in Seattle, has been well accepted by patients, families, and clinicians, according to a report published online April 11 in the New England Journal of Medicine.
The report details the experience in 2009-2011 with the Death with Dignity program at the Seattle Cancer Care Alliance, which serves all of the Pacific Northwest. The program, "designed to adhere to legal regulations, maintain safety, and ensure the quality of patient care," allows patients with a life expectancy of 6 months or less because of a diagnosed medical condition (usually cancer) to request and self-administer lethal medication prescribed by a physician.
This experience may help to inform efforts to introduce similar programs in other states. At present, Hawaii, Pennsylvania, and Vermont are all considering pertinent legislation, said Dr. Elizabeth Trice Loggers of the Fred Hutchinson Cancer Research Center, Seattle, and her associates.
The program’s policy – written by the Seattle Cancer Care Alliance’s medical director and approved by a majority of the medical executive committee members, as with any clinical policy – requires that patients request information about medically assisted suicide from their physicians, or that these clinicians raise the topic, to be considered for referral. Participation is entirely voluntary for medical staff and faculty members.
Every patient who is a potential participant is first assigned an advocate, a licensed social worker employed by the Alliance, who assists patients, family members, pharmacists, and physicians throughout a multistep process of participating. This advocate also tracks compliance with required documentation for the state Department of Health.
The advocate, as well as the attending physician, ensures that all potential participants are aware of alternatives to medically assisted suicide, such as palliative care and hospice care. The patient’s terminal status is verified, and if the attending physician doesn’t wish to participate, a prescribing physician and a consulting physician are chosen from a group of willing providers.
Psychosocial and psychological assessments are required to ensure the patient’s competence to make the choice of assisted suicide and to identify any depression, which would make the patient ineligible to participate. The patient’s preferences for interventions and health-care directives are documented. Grief support, legacy support, and bereavement support are offered through periodic calls and visits.
The patient and his or her family meet with the prescribing clinician and the consulting clinician to review the diagnosis, prognosis, treatment alternatives, and end-of-life issues. After a mandatory waiting period of 15 days, a written prescription is then sent to the pharmacy, and the pharmacist schedules another appointment with the patient and family to discuss preparation of the drug(s), potential side effects, and the concomitant use of prescription antiemetics.
Patients are then free to fill the prescription or not and to take the drug(s) or not, as they wish.
To date, 114 patients have inquired about the Death with Dignity program, and 44 (38%) either did not pursue the matter further or were deemed ineligible to participate.
Thirty patients (26%) have made a first oral request to initiate the process but either decided not to participate or died before completing the process. Forty patients (35% of those who made an initial inquiry) received prescriptions for lethal medication, and all 40 have died. Twenty-four chose to die by ingesting the medication (secobarbital).
Thus, only 21% of the participants actually used assisted suicide. Death with Dignity participants accounted for 2.4% of all annual deaths among patients at the Seattle Cancer Center Alliance.*
The reasons patients gave most often for participating in the assisted-suicide program were loss of autonomy (97%), inability to engage in enjoyable activities (89%), and loss of dignity (75%).
"We have not received any complaints from family members or caregivers regarding our process or the manner of death. Anecdotally, families describe the death as peaceful (even when death has taken longer than the average of approximately 35 minutes)," Dr. Loggers and her associates wrote physician (N. Engl. J. Med. 2013 April 11;368:1417-24 [doi:10.1056/NEJMsa1213398]).
"Both patients and families frequently express gratitude after the patient received the prescription, regardless of whether it is ever filled or ingested, typically referencing an important sense of control in an uncertain situation," they noted.
Opponents of medically assisted suicide have argued that legislation would disproportionately affect vulnerable populations, such as racial or ethnic minorities, low-income groups, or cognitively impaired patients. The Death with Dignity experience refutes this argument, as most participants were white, male, and well educated, the investigators said.
There have been no unexpected complications among patients who chose assisted suicide, but one patient remained alive for a day after taking the medication. This protracted dying process caused distress to both the family members and the clinicians involved. Similar cases have been reported previously, they added.
*Correction, 4/12/13: An earlier version of this story described findings from a study (citation) in the New England Journal of Medicine. That study misstated the percentage of Death with Dignity patients among all annual patient deaths reported at the Seattle Cancer Center Alliance.
The Death with Dignity program, a pioneering program that includes medically assisted suicide for competent, terminally ill adults treated at a comprehensive cancer center in Seattle, has been well accepted by patients, families, and clinicians, according to a report published online April 11 in the New England Journal of Medicine.
The report details the experience in 2009-2011 with the Death with Dignity program at the Seattle Cancer Care Alliance, which serves all of the Pacific Northwest. The program, "designed to adhere to legal regulations, maintain safety, and ensure the quality of patient care," allows patients with a life expectancy of 6 months or less because of a diagnosed medical condition (usually cancer) to request and self-administer lethal medication prescribed by a physician.
This experience may help to inform efforts to introduce similar programs in other states. At present, Hawaii, Pennsylvania, and Vermont are all considering pertinent legislation, said Dr. Elizabeth Trice Loggers of the Fred Hutchinson Cancer Research Center, Seattle, and her associates.
The program’s policy – written by the Seattle Cancer Care Alliance’s medical director and approved by a majority of the medical executive committee members, as with any clinical policy – requires that patients request information about medically assisted suicide from their physicians, or that these clinicians raise the topic, to be considered for referral. Participation is entirely voluntary for medical staff and faculty members.
Every patient who is a potential participant is first assigned an advocate, a licensed social worker employed by the Alliance, who assists patients, family members, pharmacists, and physicians throughout a multistep process of participating. This advocate also tracks compliance with required documentation for the state Department of Health.
The advocate, as well as the attending physician, ensures that all potential participants are aware of alternatives to medically assisted suicide, such as palliative care and hospice care. The patient’s terminal status is verified, and if the attending physician doesn’t wish to participate, a prescribing physician and a consulting physician are chosen from a group of willing providers.
Psychosocial and psychological assessments are required to ensure the patient’s competence to make the choice of assisted suicide and to identify any depression, which would make the patient ineligible to participate. The patient’s preferences for interventions and health-care directives are documented. Grief support, legacy support, and bereavement support are offered through periodic calls and visits.
The patient and his or her family meet with the prescribing clinician and the consulting clinician to review the diagnosis, prognosis, treatment alternatives, and end-of-life issues. After a mandatory waiting period of 15 days, a written prescription is then sent to the pharmacy, and the pharmacist schedules another appointment with the patient and family to discuss preparation of the drug(s), potential side effects, and the concomitant use of prescription antiemetics.
Patients are then free to fill the prescription or not and to take the drug(s) or not, as they wish.
To date, 114 patients have inquired about the Death with Dignity program, and 44 (38%) either did not pursue the matter further or were deemed ineligible to participate.
Thirty patients (26%) have made a first oral request to initiate the process but either decided not to participate or died before completing the process. Forty patients (35% of those who made an initial inquiry) received prescriptions for lethal medication, and all 40 have died. Twenty-four chose to die by ingesting the medication (secobarbital).
Thus, only 21% of the participants actually used assisted suicide. Death with Dignity participants accounted for 2.4% of all annual deaths among patients at the Seattle Cancer Center Alliance.*
The reasons patients gave most often for participating in the assisted-suicide program were loss of autonomy (97%), inability to engage in enjoyable activities (89%), and loss of dignity (75%).
"We have not received any complaints from family members or caregivers regarding our process or the manner of death. Anecdotally, families describe the death as peaceful (even when death has taken longer than the average of approximately 35 minutes)," Dr. Loggers and her associates wrote physician (N. Engl. J. Med. 2013 April 11;368:1417-24 [doi:10.1056/NEJMsa1213398]).
"Both patients and families frequently express gratitude after the patient received the prescription, regardless of whether it is ever filled or ingested, typically referencing an important sense of control in an uncertain situation," they noted.
Opponents of medically assisted suicide have argued that legislation would disproportionately affect vulnerable populations, such as racial or ethnic minorities, low-income groups, or cognitively impaired patients. The Death with Dignity experience refutes this argument, as most participants were white, male, and well educated, the investigators said.
There have been no unexpected complications among patients who chose assisted suicide, but one patient remained alive for a day after taking the medication. This protracted dying process caused distress to both the family members and the clinicians involved. Similar cases have been reported previously, they added.
*Correction, 4/12/13: An earlier version of this story described findings from a study (citation) in the New England Journal of Medicine. That study misstated the percentage of Death with Dignity patients among all annual patient deaths reported at the Seattle Cancer Center Alliance.
The Death with Dignity program, a pioneering program that includes medically assisted suicide for competent, terminally ill adults treated at a comprehensive cancer center in Seattle, has been well accepted by patients, families, and clinicians, according to a report published online April 11 in the New England Journal of Medicine.
The report details the experience in 2009-2011 with the Death with Dignity program at the Seattle Cancer Care Alliance, which serves all of the Pacific Northwest. The program, "designed to adhere to legal regulations, maintain safety, and ensure the quality of patient care," allows patients with a life expectancy of 6 months or less because of a diagnosed medical condition (usually cancer) to request and self-administer lethal medication prescribed by a physician.
This experience may help to inform efforts to introduce similar programs in other states. At present, Hawaii, Pennsylvania, and Vermont are all considering pertinent legislation, said Dr. Elizabeth Trice Loggers of the Fred Hutchinson Cancer Research Center, Seattle, and her associates.
The program’s policy – written by the Seattle Cancer Care Alliance’s medical director and approved by a majority of the medical executive committee members, as with any clinical policy – requires that patients request information about medically assisted suicide from their physicians, or that these clinicians raise the topic, to be considered for referral. Participation is entirely voluntary for medical staff and faculty members.
Every patient who is a potential participant is first assigned an advocate, a licensed social worker employed by the Alliance, who assists patients, family members, pharmacists, and physicians throughout a multistep process of participating. This advocate also tracks compliance with required documentation for the state Department of Health.
The advocate, as well as the attending physician, ensures that all potential participants are aware of alternatives to medically assisted suicide, such as palliative care and hospice care. The patient’s terminal status is verified, and if the attending physician doesn’t wish to participate, a prescribing physician and a consulting physician are chosen from a group of willing providers.
Psychosocial and psychological assessments are required to ensure the patient’s competence to make the choice of assisted suicide and to identify any depression, which would make the patient ineligible to participate. The patient’s preferences for interventions and health-care directives are documented. Grief support, legacy support, and bereavement support are offered through periodic calls and visits.
The patient and his or her family meet with the prescribing clinician and the consulting clinician to review the diagnosis, prognosis, treatment alternatives, and end-of-life issues. After a mandatory waiting period of 15 days, a written prescription is then sent to the pharmacy, and the pharmacist schedules another appointment with the patient and family to discuss preparation of the drug(s), potential side effects, and the concomitant use of prescription antiemetics.
Patients are then free to fill the prescription or not and to take the drug(s) or not, as they wish.
To date, 114 patients have inquired about the Death with Dignity program, and 44 (38%) either did not pursue the matter further or were deemed ineligible to participate.
Thirty patients (26%) have made a first oral request to initiate the process but either decided not to participate or died before completing the process. Forty patients (35% of those who made an initial inquiry) received prescriptions for lethal medication, and all 40 have died. Twenty-four chose to die by ingesting the medication (secobarbital).
Thus, only 21% of the participants actually used assisted suicide. Death with Dignity participants accounted for 2.4% of all annual deaths among patients at the Seattle Cancer Center Alliance.*
The reasons patients gave most often for participating in the assisted-suicide program were loss of autonomy (97%), inability to engage in enjoyable activities (89%), and loss of dignity (75%).
"We have not received any complaints from family members or caregivers regarding our process or the manner of death. Anecdotally, families describe the death as peaceful (even when death has taken longer than the average of approximately 35 minutes)," Dr. Loggers and her associates wrote physician (N. Engl. J. Med. 2013 April 11;368:1417-24 [doi:10.1056/NEJMsa1213398]).
"Both patients and families frequently express gratitude after the patient received the prescription, regardless of whether it is ever filled or ingested, typically referencing an important sense of control in an uncertain situation," they noted.
Opponents of medically assisted suicide have argued that legislation would disproportionately affect vulnerable populations, such as racial or ethnic minorities, low-income groups, or cognitively impaired patients. The Death with Dignity experience refutes this argument, as most participants were white, male, and well educated, the investigators said.
There have been no unexpected complications among patients who chose assisted suicide, but one patient remained alive for a day after taking the medication. This protracted dying process caused distress to both the family members and the clinicians involved. Similar cases have been reported previously, they added.
*Correction, 4/12/13: An earlier version of this story described findings from a study (citation) in the New England Journal of Medicine. That study misstated the percentage of Death with Dignity patients among all annual patient deaths reported at the Seattle Cancer Center Alliance.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: None of the 114 patients who participated in the Death with Dignity (assisted-suicide) program during a 2-year period, nor their family members and caregivers, have complained about the process or manner of death.
Data source: A descriptive study of the experience to date concerning the Death with Dignity program serving patients throughout the Pacific Northwest at a comprehensive cancer center.
Disclosures: No financial conflicts of interest were reported.
Rituximab may obviate radiation in mediastinal B-cell lymphoma
Adding rituximab to combination chemotherapy for primary mediastinal B-cell lymphoma yields a high cure rate and may obviate the need for thoracic radiation therapy, a study has shown.
Patients in a single-group, prospective phase II study were treated with dose-adjusted etoposide, doxorubicin, cyclophosphamide with vincristine, prednisone, and rituximab (DA-EPOCH-R). All but 2 of the 51 adults with lymphoma in the study were able to forgo radiotherapy, and there were no recurrences during a median follow-up of 5 years, reported Dr. Kieron Dunleavy of the National Cancer Institute and his colleagues.
"These findings suggest that DA-EPOCH-R is a therapeutic advance for this type of lymphoma," they wrote (N. Engl. J. Med. 2013;368:1408-16 [doi:10.1056/NEJMoa1214561]).
In a previous study, Dr. Dunleavy and his colleagues found that DA-EPOCH yielded an overall survival of 79%. To examine whether the addition of rituximab would further improve outcomes, they enrolled treatment-naive patients who had masses of at least 5 cm and presented over a 13-year period.
The study patients’ median age was 30 years (range, 19-52 years), and 59% were women. Mediastinal B-cell lymphoma was advanced, with a median tumor diameter of 11 cm. Approximately 30% of patients had stage IV disease.
All 51 patients received six to eight cycles of DA-EPOCH-R. Two patients showed persistent focal disease after therapy, and one patient showed disease progression. Two of the patients then underwent mediastinal radiotherapy, and one underwent excisional biopsy. All three were disease free thereafter.
After follow-up, ranging from 3 to 156 months, overall survival was 97% and event-free survival was 93%, with no recurrences of the cancer, the investigators reported.
Primary mediastinal B-cell lymphoma develops in the thymus, "predominantly affects young women, is aggressive, and typically is manifested by a localized, bulky mediastinal mass, often with pleural and pericardial effusions," they noted. There have been few prospective studies of the disease; and the findings have been conflicting, so at present there are no treatment standards. Immunochemotherapy usually does not achieve tumor control. Mediastinal radiotherapy (associated with severe late adverse effects) after aggressive chemotherapy is the current regimen.
The toxic effects of the chemotherapy regimen were similar to other previously reported events. Neutropenia occurred during half of the chemotherapy cycles overall, thrombocytopenia occurred in 6%, and hospitalization was required for fever and neutropenia in 13% of the cycles. There were no significant cardiac toxic effects.
Dr. Dunleavy and his associates also reported the results of DA-EPOCH-R therapy in an independent retrospective cohort of 16 patients treated at Stanford (Calif.) University Medical Center during the past 5 years. All of the Stanford patients were able to forgo radiation therapy, and event-free survival was 100%.
An international trial of DA-EPOCH-R for treating children or adolescents with primary mediastinal B-cell lymphoma is currently underway (clinical trial number NCT01516567).
The study was supported by the National Cancer Institute. Amgen provided filgrastim for the study but had no involvement with study design or with data collection or analysis. The investigators reported having no relevant financial conflicts.
Adding rituximab to combination chemotherapy for primary mediastinal B-cell lymphoma yields a high cure rate and may obviate the need for thoracic radiation therapy, a study has shown.
Patients in a single-group, prospective phase II study were treated with dose-adjusted etoposide, doxorubicin, cyclophosphamide with vincristine, prednisone, and rituximab (DA-EPOCH-R). All but 2 of the 51 adults with lymphoma in the study were able to forgo radiotherapy, and there were no recurrences during a median follow-up of 5 years, reported Dr. Kieron Dunleavy of the National Cancer Institute and his colleagues.
"These findings suggest that DA-EPOCH-R is a therapeutic advance for this type of lymphoma," they wrote (N. Engl. J. Med. 2013;368:1408-16 [doi:10.1056/NEJMoa1214561]).
In a previous study, Dr. Dunleavy and his colleagues found that DA-EPOCH yielded an overall survival of 79%. To examine whether the addition of rituximab would further improve outcomes, they enrolled treatment-naive patients who had masses of at least 5 cm and presented over a 13-year period.
The study patients’ median age was 30 years (range, 19-52 years), and 59% were women. Mediastinal B-cell lymphoma was advanced, with a median tumor diameter of 11 cm. Approximately 30% of patients had stage IV disease.
All 51 patients received six to eight cycles of DA-EPOCH-R. Two patients showed persistent focal disease after therapy, and one patient showed disease progression. Two of the patients then underwent mediastinal radiotherapy, and one underwent excisional biopsy. All three were disease free thereafter.
After follow-up, ranging from 3 to 156 months, overall survival was 97% and event-free survival was 93%, with no recurrences of the cancer, the investigators reported.
Primary mediastinal B-cell lymphoma develops in the thymus, "predominantly affects young women, is aggressive, and typically is manifested by a localized, bulky mediastinal mass, often with pleural and pericardial effusions," they noted. There have been few prospective studies of the disease; and the findings have been conflicting, so at present there are no treatment standards. Immunochemotherapy usually does not achieve tumor control. Mediastinal radiotherapy (associated with severe late adverse effects) after aggressive chemotherapy is the current regimen.
The toxic effects of the chemotherapy regimen were similar to other previously reported events. Neutropenia occurred during half of the chemotherapy cycles overall, thrombocytopenia occurred in 6%, and hospitalization was required for fever and neutropenia in 13% of the cycles. There were no significant cardiac toxic effects.
Dr. Dunleavy and his associates also reported the results of DA-EPOCH-R therapy in an independent retrospective cohort of 16 patients treated at Stanford (Calif.) University Medical Center during the past 5 years. All of the Stanford patients were able to forgo radiation therapy, and event-free survival was 100%.
An international trial of DA-EPOCH-R for treating children or adolescents with primary mediastinal B-cell lymphoma is currently underway (clinical trial number NCT01516567).
The study was supported by the National Cancer Institute. Amgen provided filgrastim for the study but had no involvement with study design or with data collection or analysis. The investigators reported having no relevant financial conflicts.
Adding rituximab to combination chemotherapy for primary mediastinal B-cell lymphoma yields a high cure rate and may obviate the need for thoracic radiation therapy, a study has shown.
Patients in a single-group, prospective phase II study were treated with dose-adjusted etoposide, doxorubicin, cyclophosphamide with vincristine, prednisone, and rituximab (DA-EPOCH-R). All but 2 of the 51 adults with lymphoma in the study were able to forgo radiotherapy, and there were no recurrences during a median follow-up of 5 years, reported Dr. Kieron Dunleavy of the National Cancer Institute and his colleagues.
"These findings suggest that DA-EPOCH-R is a therapeutic advance for this type of lymphoma," they wrote (N. Engl. J. Med. 2013;368:1408-16 [doi:10.1056/NEJMoa1214561]).
In a previous study, Dr. Dunleavy and his colleagues found that DA-EPOCH yielded an overall survival of 79%. To examine whether the addition of rituximab would further improve outcomes, they enrolled treatment-naive patients who had masses of at least 5 cm and presented over a 13-year period.
The study patients’ median age was 30 years (range, 19-52 years), and 59% were women. Mediastinal B-cell lymphoma was advanced, with a median tumor diameter of 11 cm. Approximately 30% of patients had stage IV disease.
All 51 patients received six to eight cycles of DA-EPOCH-R. Two patients showed persistent focal disease after therapy, and one patient showed disease progression. Two of the patients then underwent mediastinal radiotherapy, and one underwent excisional biopsy. All three were disease free thereafter.
After follow-up, ranging from 3 to 156 months, overall survival was 97% and event-free survival was 93%, with no recurrences of the cancer, the investigators reported.
Primary mediastinal B-cell lymphoma develops in the thymus, "predominantly affects young women, is aggressive, and typically is manifested by a localized, bulky mediastinal mass, often with pleural and pericardial effusions," they noted. There have been few prospective studies of the disease; and the findings have been conflicting, so at present there are no treatment standards. Immunochemotherapy usually does not achieve tumor control. Mediastinal radiotherapy (associated with severe late adverse effects) after aggressive chemotherapy is the current regimen.
The toxic effects of the chemotherapy regimen were similar to other previously reported events. Neutropenia occurred during half of the chemotherapy cycles overall, thrombocytopenia occurred in 6%, and hospitalization was required for fever and neutropenia in 13% of the cycles. There were no significant cardiac toxic effects.
Dr. Dunleavy and his associates also reported the results of DA-EPOCH-R therapy in an independent retrospective cohort of 16 patients treated at Stanford (Calif.) University Medical Center during the past 5 years. All of the Stanford patients were able to forgo radiation therapy, and event-free survival was 100%.
An international trial of DA-EPOCH-R for treating children or adolescents with primary mediastinal B-cell lymphoma is currently underway (clinical trial number NCT01516567).
The study was supported by the National Cancer Institute. Amgen provided filgrastim for the study but had no involvement with study design or with data collection or analysis. The investigators reported having no relevant financial conflicts.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major finding: Overall survival was 97% in adults treated with DA-EPOCH-R, and event-free survival was 93%.
Data source: A phase II, prospective clinical trial of 51 adults with primary mediastinal B-cell lymphoma who were followed for a median of 5 years.
Disclosures: The study was supported by the National Cancer Institute. Amgen provided filgrastim for the study but had no involvement with study design or with data collection or analysis. The investigators reported having no relevant financial conflicts.
Cuba's economic crisis yielded reduced diabetes, CVD, death
A severe economic crisis in Cuba in 1991-1995 that caused extreme food and fuel shortages was associated with a population-wide loss of 4-5 kg in weight, accompanied by dramatic reductions in diabetes and cardiovascular mortality, according to a report published online April 9 in the BMJ.
As the crisis resolved, the population’s rebound in body weight was associated with a rise in diabetes incidence and mortality, and a leveling off of the decline in CV mortality, said Dr. Manuel Franco of the social and cardiovascular epidemiology research group, University of Alcala, Madrid, and his associates.
"The Cuban experience shows that within a relatively short period, modest weight loss in the whole population can have a profound effect on the overall burden of diabetes," as well as CV disease and all-cause mortality." These data are a notable illustration of the potential health benefits of reversing the global obesity epidemic," the investigators said.
Dr. Franco and his colleagues studied population-wide changes in body weight over time using data from several annual cross-sectional health surveys performed in the province of Cienfuegos, Cuba, from 1980 to 2010. Each year’s surveys involved 1,000-2,000 respondents aged 15 years and older who self-reported their physical activity levels. Population data regarding energy intake, smoking, diabetes, and mortality were derived from other surveys.
During the economic crisis, food was scarce and motorized transportation came to a virtual standstill in Cuba. The consequent increase in walking and biking, together with reduced caloric intake, "put the entire population in a negative energy balance," they said.
Urban agriculture was encouraged, giving more people access to fresh produce. Public health campaigns emphasized community gardening and improved nutrition, and more than 1 million bicycles were distributed to the population.
The Cuban economy began recovering in 1996 and has shown sustained growth since 2000.
Several health issues reflected this time trend.
The average daily intake of energy per capita decreased to a nadir in the mid-1990s, then rebounded to pre-crisis levels in the mid-2000s and has since increased further. There was a concomitant population-wide decrease of 5.5 kg across all categories of body mass index in the mid-1990s, a rebound to pre-crisis levels in the mid-2000s, and a striking rise in more recent years.
The proportion of the population who were at normal weight was highest, at 56%, in 1995, the final year of the economic crisis. This decreased to 42% in 2010. Concomitantly, the proportion of the population who were overweight or obese rose from a low of 33% to a high of 53%.
Similarly, the incidence of diabetes was stable at roughly 1.5-1.8/1,000 population before the economic crisis. It fell to 1.2/1,000 during the crisis and remained low for a few years, then sharply increased beginning in the year 2000. The incidence of diabetes exceeded pre-crisis levels, at 2.2/1,000, in 2002, and rose again to 2.4/1,000 in 2009.
Thus, the overall incidence of diabetes decreased by 53% during and immediately after the economic crisis, then rose by 140% during the subsequent economic recovery, the researchers wrote (BMJ 2013;346:f1515[doi:10.1136/bmj.f1515]).
Diabetes mortality followed a similar pattern, decreasing by 50% during and immediately after the crisis, rebounding by 49% by 2002, and returning to pre-crisis levels by 2010.
Trends in mortality from coronary heart disease also followed suit, falling markedly by 34% during and immediately following the economic crisis, then rebounding to pre-crisis levels. Stroke mortality also followed this pattern. Cancer mortality did not.
"Our study presents the first observation of a population-wide event of this magnitude and its subsequent effects on public health," said Dr. Franco, who is also in the department of epidemiology, Johns Hopkins Bloomberg School of Public Health, Baltimore, and his associates.
In contrast, studies of the effectiveness of preventive lifestyle strategies "have either not produced a beneficial effect on cardiovascular mortality or diabetes control and mortality, or have been unsuccessful in reducing risk to a sufficient degree to warrant a conclusion," the investigators said.
This study was limited in that it could not account for the effects of a concomitant decrease in both the prevalence and the amount of cigarette smoking in Cuba during the economic crisis, they added.
No financial conflicts of interest were reported.
The findings of Franco and colleagues "add powerful evidence that a reduction in overweight and obesity would have major population-wide benefits," said Dr. Walter C. Willett.
"To achieve this is perhaps the major public health and societal challenge of the century," he noted.
Potential strategies to achieve this include "educational efforts, redesign of built environments to promote physical activity, changes in food systems, restrictions on aggressive promotion of unhealthy drinks and foods to children, and economic strategies such as taxation." Independent of these measures, "physicians can help by monitoring weight and counseling patients who gain weight before they become overweight. Recent evidence indicates that clinic based weight loss programs can be effective. Physicians can help promote healthy social norms by visibly engaging in healthy behaviors."
Dr. Willett is professor and chair of the department of nutrition at Harvard School of Public Health, Boston. He reported no financial conflicts of interest. These remarks were taken from his editorial comment accompanying Dr. Franco’s report (BMJ 2013;346:f1777 [doi:10.1136/bmj.f1777]).
The findings of Franco and colleagues "add powerful evidence that a reduction in overweight and obesity would have major population-wide benefits," said Dr. Walter C. Willett.
"To achieve this is perhaps the major public health and societal challenge of the century," he noted.
Potential strategies to achieve this include "educational efforts, redesign of built environments to promote physical activity, changes in food systems, restrictions on aggressive promotion of unhealthy drinks and foods to children, and economic strategies such as taxation." Independent of these measures, "physicians can help by monitoring weight and counseling patients who gain weight before they become overweight. Recent evidence indicates that clinic based weight loss programs can be effective. Physicians can help promote healthy social norms by visibly engaging in healthy behaviors."
Dr. Willett is professor and chair of the department of nutrition at Harvard School of Public Health, Boston. He reported no financial conflicts of interest. These remarks were taken from his editorial comment accompanying Dr. Franco’s report (BMJ 2013;346:f1777 [doi:10.1136/bmj.f1777]).
The findings of Franco and colleagues "add powerful evidence that a reduction in overweight and obesity would have major population-wide benefits," said Dr. Walter C. Willett.
"To achieve this is perhaps the major public health and societal challenge of the century," he noted.
Potential strategies to achieve this include "educational efforts, redesign of built environments to promote physical activity, changes in food systems, restrictions on aggressive promotion of unhealthy drinks and foods to children, and economic strategies such as taxation." Independent of these measures, "physicians can help by monitoring weight and counseling patients who gain weight before they become overweight. Recent evidence indicates that clinic based weight loss programs can be effective. Physicians can help promote healthy social norms by visibly engaging in healthy behaviors."
Dr. Willett is professor and chair of the department of nutrition at Harvard School of Public Health, Boston. He reported no financial conflicts of interest. These remarks were taken from his editorial comment accompanying Dr. Franco’s report (BMJ 2013;346:f1777 [doi:10.1136/bmj.f1777]).
A severe economic crisis in Cuba in 1991-1995 that caused extreme food and fuel shortages was associated with a population-wide loss of 4-5 kg in weight, accompanied by dramatic reductions in diabetes and cardiovascular mortality, according to a report published online April 9 in the BMJ.
As the crisis resolved, the population’s rebound in body weight was associated with a rise in diabetes incidence and mortality, and a leveling off of the decline in CV mortality, said Dr. Manuel Franco of the social and cardiovascular epidemiology research group, University of Alcala, Madrid, and his associates.
"The Cuban experience shows that within a relatively short period, modest weight loss in the whole population can have a profound effect on the overall burden of diabetes," as well as CV disease and all-cause mortality." These data are a notable illustration of the potential health benefits of reversing the global obesity epidemic," the investigators said.
Dr. Franco and his colleagues studied population-wide changes in body weight over time using data from several annual cross-sectional health surveys performed in the province of Cienfuegos, Cuba, from 1980 to 2010. Each year’s surveys involved 1,000-2,000 respondents aged 15 years and older who self-reported their physical activity levels. Population data regarding energy intake, smoking, diabetes, and mortality were derived from other surveys.
During the economic crisis, food was scarce and motorized transportation came to a virtual standstill in Cuba. The consequent increase in walking and biking, together with reduced caloric intake, "put the entire population in a negative energy balance," they said.
Urban agriculture was encouraged, giving more people access to fresh produce. Public health campaigns emphasized community gardening and improved nutrition, and more than 1 million bicycles were distributed to the population.
The Cuban economy began recovering in 1996 and has shown sustained growth since 2000.
Several health issues reflected this time trend.
The average daily intake of energy per capita decreased to a nadir in the mid-1990s, then rebounded to pre-crisis levels in the mid-2000s and has since increased further. There was a concomitant population-wide decrease of 5.5 kg across all categories of body mass index in the mid-1990s, a rebound to pre-crisis levels in the mid-2000s, and a striking rise in more recent years.
The proportion of the population who were at normal weight was highest, at 56%, in 1995, the final year of the economic crisis. This decreased to 42% in 2010. Concomitantly, the proportion of the population who were overweight or obese rose from a low of 33% to a high of 53%.
Similarly, the incidence of diabetes was stable at roughly 1.5-1.8/1,000 population before the economic crisis. It fell to 1.2/1,000 during the crisis and remained low for a few years, then sharply increased beginning in the year 2000. The incidence of diabetes exceeded pre-crisis levels, at 2.2/1,000, in 2002, and rose again to 2.4/1,000 in 2009.
Thus, the overall incidence of diabetes decreased by 53% during and immediately after the economic crisis, then rose by 140% during the subsequent economic recovery, the researchers wrote (BMJ 2013;346:f1515[doi:10.1136/bmj.f1515]).
Diabetes mortality followed a similar pattern, decreasing by 50% during and immediately after the crisis, rebounding by 49% by 2002, and returning to pre-crisis levels by 2010.
Trends in mortality from coronary heart disease also followed suit, falling markedly by 34% during and immediately following the economic crisis, then rebounding to pre-crisis levels. Stroke mortality also followed this pattern. Cancer mortality did not.
"Our study presents the first observation of a population-wide event of this magnitude and its subsequent effects on public health," said Dr. Franco, who is also in the department of epidemiology, Johns Hopkins Bloomberg School of Public Health, Baltimore, and his associates.
In contrast, studies of the effectiveness of preventive lifestyle strategies "have either not produced a beneficial effect on cardiovascular mortality or diabetes control and mortality, or have been unsuccessful in reducing risk to a sufficient degree to warrant a conclusion," the investigators said.
This study was limited in that it could not account for the effects of a concomitant decrease in both the prevalence and the amount of cigarette smoking in Cuba during the economic crisis, they added.
No financial conflicts of interest were reported.
A severe economic crisis in Cuba in 1991-1995 that caused extreme food and fuel shortages was associated with a population-wide loss of 4-5 kg in weight, accompanied by dramatic reductions in diabetes and cardiovascular mortality, according to a report published online April 9 in the BMJ.
As the crisis resolved, the population’s rebound in body weight was associated with a rise in diabetes incidence and mortality, and a leveling off of the decline in CV mortality, said Dr. Manuel Franco of the social and cardiovascular epidemiology research group, University of Alcala, Madrid, and his associates.
"The Cuban experience shows that within a relatively short period, modest weight loss in the whole population can have a profound effect on the overall burden of diabetes," as well as CV disease and all-cause mortality." These data are a notable illustration of the potential health benefits of reversing the global obesity epidemic," the investigators said.
Dr. Franco and his colleagues studied population-wide changes in body weight over time using data from several annual cross-sectional health surveys performed in the province of Cienfuegos, Cuba, from 1980 to 2010. Each year’s surveys involved 1,000-2,000 respondents aged 15 years and older who self-reported their physical activity levels. Population data regarding energy intake, smoking, diabetes, and mortality were derived from other surveys.
During the economic crisis, food was scarce and motorized transportation came to a virtual standstill in Cuba. The consequent increase in walking and biking, together with reduced caloric intake, "put the entire population in a negative energy balance," they said.
Urban agriculture was encouraged, giving more people access to fresh produce. Public health campaigns emphasized community gardening and improved nutrition, and more than 1 million bicycles were distributed to the population.
The Cuban economy began recovering in 1996 and has shown sustained growth since 2000.
Several health issues reflected this time trend.
The average daily intake of energy per capita decreased to a nadir in the mid-1990s, then rebounded to pre-crisis levels in the mid-2000s and has since increased further. There was a concomitant population-wide decrease of 5.5 kg across all categories of body mass index in the mid-1990s, a rebound to pre-crisis levels in the mid-2000s, and a striking rise in more recent years.
The proportion of the population who were at normal weight was highest, at 56%, in 1995, the final year of the economic crisis. This decreased to 42% in 2010. Concomitantly, the proportion of the population who were overweight or obese rose from a low of 33% to a high of 53%.
Similarly, the incidence of diabetes was stable at roughly 1.5-1.8/1,000 population before the economic crisis. It fell to 1.2/1,000 during the crisis and remained low for a few years, then sharply increased beginning in the year 2000. The incidence of diabetes exceeded pre-crisis levels, at 2.2/1,000, in 2002, and rose again to 2.4/1,000 in 2009.
Thus, the overall incidence of diabetes decreased by 53% during and immediately after the economic crisis, then rose by 140% during the subsequent economic recovery, the researchers wrote (BMJ 2013;346:f1515[doi:10.1136/bmj.f1515]).
Diabetes mortality followed a similar pattern, decreasing by 50% during and immediately after the crisis, rebounding by 49% by 2002, and returning to pre-crisis levels by 2010.
Trends in mortality from coronary heart disease also followed suit, falling markedly by 34% during and immediately following the economic crisis, then rebounding to pre-crisis levels. Stroke mortality also followed this pattern. Cancer mortality did not.
"Our study presents the first observation of a population-wide event of this magnitude and its subsequent effects on public health," said Dr. Franco, who is also in the department of epidemiology, Johns Hopkins Bloomberg School of Public Health, Baltimore, and his associates.
In contrast, studies of the effectiveness of preventive lifestyle strategies "have either not produced a beneficial effect on cardiovascular mortality or diabetes control and mortality, or have been unsuccessful in reducing risk to a sufficient degree to warrant a conclusion," the investigators said.
This study was limited in that it could not account for the effects of a concomitant decrease in both the prevalence and the amount of cigarette smoking in Cuba during the economic crisis, they added.
No financial conflicts of interest were reported.
FROM BMJ
Major finding: The overall diabetes incidence decreased by 53% during and immediately after the economic crisis, then rebounded, rising by 140% during the subsequent economic recovery.
Data source: An analysis of cross-sectional population surveys in Cienfuegos, Cuba, from 1980 to 2010.
Disclosures: No financial conflicts of interest were reported.
New guideline tries to rein in neurocysticercosis treatment controversy
A new evidence-based guideline for both adults and children who have neurocysticercosis – tapeworm larvae seeded in the brain parenchyma – suggests that clinicians should consider treating with albendazole plus either dexamethasone or prednisolone.
It is hoped that the combination of the cysticidal drug albendazole and a corticosteroid will reduce both the number of active brain lesions and the frequency of the seizures they cause, according to lead author Dr. Ruth Ann Baird and her associates on the American Academy of Neurology’s guideline development subcommittee.
The optimal treatment for neurocysticercosis has been controversial, with experts debating the usefulness and potential dangers of cysticidal therapy, steroid therapy, and antiepileptic therapy. Dr. Baird of the department of clinical neurology at Indiana University, Indianapolis, and her colleagues performed a systematic review of the English- and Spanish-language medical literature to clarify the issue (Neurology 2013;80:1424-9).
Unfortunately, even a close review of the best 123 articles available did little to resolve the controversy. The studies used widely varying methodologies and different criteria for judging improvement on brain imaging, making comparisons and pooling of the data difficult. Also, the quality of the data in most of the available studies was suboptimal.
The committee, however, was able to reach some conclusions.
"Based on imaging findings in four Class I studies (three concordant, one underpowered study failing to show an effect) and a meta-analysis of two Class I and four Class II studies, albendazole (400 mg b.i.d. for adults or weight-based dosing for either adults or children) is probably safe and effective in reducing both the number of cysts and long-term seizure frequency," they said.
"In most studies, corticosteroids were coadministered, in varying dosages, and this combination appears effective [but] the evidence is insufficient to support or refute the use of steroid treatment alone in patients with intraparenchymal neurocysticercosis," the committee noted.
There also was no evidence on which to base a recommendation regarding optimal timing of steroid therapy, the committee added.
The AAN-sponsored guideline is also endorsed by the American Epilepsy Society.
Historically, the side effect of greatest concern in such cases has been large-scale parasite death induced by antihelminthic agents like albendazole, but this danger was emphasized in only a single study, in which the data are now considered to be only of class-IV quality.
Smaller but better-quality studies have since shown no increase in seizure frequency or other adverse effects with use of albendazole. All such studies, however, excluded patients who had massive cerebral edema or "innumerable" brain lesions, Dr. Baird and her associates noted.
The guideline also stated that, "given the well-established efficacy and safety of a broad range of AEDs [antiepileptic drugs] and the frequency with which neurocysticercosis causes seizures, it is reasonable to treat these patients with AEDs at least until the active lesions have subsided."
The authors concluded the guideline with a call for future researchers to definitively establish whether combination cysticidal and steroid therapy is beneficial, to determine the appropriate use and timing of adjuvant corticosteroids, to address HIV coinfection that can alter the efficacy of antihelminthic drugs or induce significant drug-drug interactions, and to focus on clinical outcomes rather than just brain imaging studies.
The guideline was developed with financial support from the American Academy of Neurology. Dr. Baird reported no financial conflicts of interest. One coauthor reported receiving honoraria from UCB Pharma and another reported formerly serving on a speakers’ bureau for Boehringer Ingelheim.
A new evidence-based guideline for both adults and children who have neurocysticercosis – tapeworm larvae seeded in the brain parenchyma – suggests that clinicians should consider treating with albendazole plus either dexamethasone or prednisolone.
It is hoped that the combination of the cysticidal drug albendazole and a corticosteroid will reduce both the number of active brain lesions and the frequency of the seizures they cause, according to lead author Dr. Ruth Ann Baird and her associates on the American Academy of Neurology’s guideline development subcommittee.
The optimal treatment for neurocysticercosis has been controversial, with experts debating the usefulness and potential dangers of cysticidal therapy, steroid therapy, and antiepileptic therapy. Dr. Baird of the department of clinical neurology at Indiana University, Indianapolis, and her colleagues performed a systematic review of the English- and Spanish-language medical literature to clarify the issue (Neurology 2013;80:1424-9).
Unfortunately, even a close review of the best 123 articles available did little to resolve the controversy. The studies used widely varying methodologies and different criteria for judging improvement on brain imaging, making comparisons and pooling of the data difficult. Also, the quality of the data in most of the available studies was suboptimal.
The committee, however, was able to reach some conclusions.
"Based on imaging findings in four Class I studies (three concordant, one underpowered study failing to show an effect) and a meta-analysis of two Class I and four Class II studies, albendazole (400 mg b.i.d. for adults or weight-based dosing for either adults or children) is probably safe and effective in reducing both the number of cysts and long-term seizure frequency," they said.
"In most studies, corticosteroids were coadministered, in varying dosages, and this combination appears effective [but] the evidence is insufficient to support or refute the use of steroid treatment alone in patients with intraparenchymal neurocysticercosis," the committee noted.
There also was no evidence on which to base a recommendation regarding optimal timing of steroid therapy, the committee added.
The AAN-sponsored guideline is also endorsed by the American Epilepsy Society.
Historically, the side effect of greatest concern in such cases has been large-scale parasite death induced by antihelminthic agents like albendazole, but this danger was emphasized in only a single study, in which the data are now considered to be only of class-IV quality.
Smaller but better-quality studies have since shown no increase in seizure frequency or other adverse effects with use of albendazole. All such studies, however, excluded patients who had massive cerebral edema or "innumerable" brain lesions, Dr. Baird and her associates noted.
The guideline also stated that, "given the well-established efficacy and safety of a broad range of AEDs [antiepileptic drugs] and the frequency with which neurocysticercosis causes seizures, it is reasonable to treat these patients with AEDs at least until the active lesions have subsided."
The authors concluded the guideline with a call for future researchers to definitively establish whether combination cysticidal and steroid therapy is beneficial, to determine the appropriate use and timing of adjuvant corticosteroids, to address HIV coinfection that can alter the efficacy of antihelminthic drugs or induce significant drug-drug interactions, and to focus on clinical outcomes rather than just brain imaging studies.
The guideline was developed with financial support from the American Academy of Neurology. Dr. Baird reported no financial conflicts of interest. One coauthor reported receiving honoraria from UCB Pharma and another reported formerly serving on a speakers’ bureau for Boehringer Ingelheim.
A new evidence-based guideline for both adults and children who have neurocysticercosis – tapeworm larvae seeded in the brain parenchyma – suggests that clinicians should consider treating with albendazole plus either dexamethasone or prednisolone.
It is hoped that the combination of the cysticidal drug albendazole and a corticosteroid will reduce both the number of active brain lesions and the frequency of the seizures they cause, according to lead author Dr. Ruth Ann Baird and her associates on the American Academy of Neurology’s guideline development subcommittee.
The optimal treatment for neurocysticercosis has been controversial, with experts debating the usefulness and potential dangers of cysticidal therapy, steroid therapy, and antiepileptic therapy. Dr. Baird of the department of clinical neurology at Indiana University, Indianapolis, and her colleagues performed a systematic review of the English- and Spanish-language medical literature to clarify the issue (Neurology 2013;80:1424-9).
Unfortunately, even a close review of the best 123 articles available did little to resolve the controversy. The studies used widely varying methodologies and different criteria for judging improvement on brain imaging, making comparisons and pooling of the data difficult. Also, the quality of the data in most of the available studies was suboptimal.
The committee, however, was able to reach some conclusions.
"Based on imaging findings in four Class I studies (three concordant, one underpowered study failing to show an effect) and a meta-analysis of two Class I and four Class II studies, albendazole (400 mg b.i.d. for adults or weight-based dosing for either adults or children) is probably safe and effective in reducing both the number of cysts and long-term seizure frequency," they said.
"In most studies, corticosteroids were coadministered, in varying dosages, and this combination appears effective [but] the evidence is insufficient to support or refute the use of steroid treatment alone in patients with intraparenchymal neurocysticercosis," the committee noted.
There also was no evidence on which to base a recommendation regarding optimal timing of steroid therapy, the committee added.
The AAN-sponsored guideline is also endorsed by the American Epilepsy Society.
Historically, the side effect of greatest concern in such cases has been large-scale parasite death induced by antihelminthic agents like albendazole, but this danger was emphasized in only a single study, in which the data are now considered to be only of class-IV quality.
Smaller but better-quality studies have since shown no increase in seizure frequency or other adverse effects with use of albendazole. All such studies, however, excluded patients who had massive cerebral edema or "innumerable" brain lesions, Dr. Baird and her associates noted.
The guideline also stated that, "given the well-established efficacy and safety of a broad range of AEDs [antiepileptic drugs] and the frequency with which neurocysticercosis causes seizures, it is reasonable to treat these patients with AEDs at least until the active lesions have subsided."
The authors concluded the guideline with a call for future researchers to definitively establish whether combination cysticidal and steroid therapy is beneficial, to determine the appropriate use and timing of adjuvant corticosteroids, to address HIV coinfection that can alter the efficacy of antihelminthic drugs or induce significant drug-drug interactions, and to focus on clinical outcomes rather than just brain imaging studies.
The guideline was developed with financial support from the American Academy of Neurology. Dr. Baird reported no financial conflicts of interest. One coauthor reported receiving honoraria from UCB Pharma and another reported formerly serving on a speakers’ bureau for Boehringer Ingelheim.
FROM NEUROLOGY
Mortality after surgery for radiation-related cardiac problems unexpectedly high
Mortality is twice as high for cancer survivors undergoing cardiac surgery to correct damage done by thoracic radiation therapy as it is among matched patients who are undergoing the same procedures but who haven’t been exposed to radiotherapy, according to a report published online April 8 in Circulation.
In what they described as "the largest study to assess long-term survival in this population undergoing complex cardiac surgery and compare them to a well-matched comparison population," investigators found that mortality was 55% in the patients who had received radiation therapy, compared with 28% in the nonexposed controls. At least half of the deaths among the cancer survivors were attributed to cardiopulmonary disease, while only 5% were due to recurrent malignancy.
"Surgical intervention should be applied cautiously to patients who have had significant thoracic radiation previously," including survivors of breast, lung, hematologic, thyroid, and other cancers.
Trying to gauge mortality risk in such patients solely by using their preoperative scores on standard risk-prediction measures is inaccurate at best. In this study population, the survivors of breast, lung, hematologic, thyroid, and other cancers would have been deemed at intermediate risk for undergoing cardiac surgery, with an expected mortality of only 3%-5% based on their preoperative assessments – 10 times lower than their actual postoperative mortality, said Dr. Willis Wu and his associates at the Heart and Vascular Institute at the Cleveland Clinic.
"Our findings suggest that surgical intervention should be applied cautiously to patients who have had significant thoracic radiation previously," they wrote. Cardiac surgery that is considered conventional or even routine in most patients – including coronary artery bypass graft, valve repair, valve replacement, vascular surgery, pericardiectomy, left ventricular assist device implantation, and myectomy – may actually worsen the condition of radiation-exposed patients.
"It seems appropriate to examine other types of treatment options in patients with radiation heart disease who have significant valvular, coronary, or myocardial disease," the researchers noted.
Dr. Wu and his associates performed their retrospective observational study because of the dearth of information regarding long-term outcomes in cancer survivors who were exposed to chest irradiation. This knowledge gap makes treatment decisions "especially difficult" once radiation-related heart disease is discovered.
Such patients are known to have high rates of coronary artery, valvular, pericardial, myocardial, and conduction disease that progresses over time and may not become evident until decades after cancer treatment was completed.
Surgery is often thought necessary to effectively address these cardiac complications of prior radiation therapy. "These patients have multiple cardiac lesions and [often] have comorbidities such as pulmonary or vascular disease related to radiation," the investigators said.
They analyzed the medical records of 478 patients undergoing cardiac surgery at their tertiary care center in 2000-2003. A total of 173 had a prior history of malignancy treated with chest irradiation; the remaining 305 patients had no such history and were matched to the radiation group for age, sex, type of surgery, and date of surgery.
The patients exposed to radiation were relatively young but had advanced symptoms. Forty-five percent had obstructive proximal coronary artery disease; one-fourth had already undergone open heart surgery, including 16% who had prior coronary artery bypass graft surgery. There also was a high prevalence of valvular disease, with 51% of patients showing at least moderate mitral regurgitation, 6% showing severe mitral stenosis, 29% showing at least moderate aortic regurgitation, 23% showing severe aortic stenosis, and 34% showing at least moderate tricuspid regurgitation.
The mean interval between the current cardiac surgery and the last thoracic radiation treatment was 18 years. Approximately 53% of the study patients had survived breast cancer, 27% had survived Hodgkin’s lymphoma, 7% had survived lung cancer, 6% had survived non-Hodgkin’s lymphoma, and 8% had survived other malignancies including thyroid and testicular cancers.
Approximately 75% of both study groups were women.
During a mean follow-up of 7.6 years, overall mortality was 37%. Despite the success of the cardiac procedures, a significantly higher proportion of radiation-exposed patients died (55%), compared with the unexposed patients (28%), for a hazard ratio of 2.54, Dr. Wu and his colleagues said (Circulation 2013 April 8; doi:10.1161/CIRCULATIONAHA.13.001435).
Mortality was significantly higher across all subgroups of patients exposed to radiation. In particular, it was high among patients expected to have low mortality: 43% in patients aged younger than 65 years and 45% in those with lower preoperative risk scores. In fact, the youngest patients in the radiation group fared worse than the oldest patients in the comparison group.
Mortality also was significantly higher for the radiation-exposed patients than for controls across all types of cardiac surgery.
The cause of death was not known for a substantial proportion of subjects in this study, but cardiopulmonary causes were implicated in at least half of the deaths among radiation-exposed patients. "Why this should be the case in a group of patients who received potentially life-preserving revascularization, valve, and other procedures is unknown at present," Dr. Wu and his associates said.
In addition, patients with radiation-related heart disease had longer hospital stays, were more likely to develop atrial fibrillation after surgery, were more likely to require pacemaker implantation after surgery, had higher rates of ventricular dysfunction and of valvular regurgitation following surgery, and had higher 30-day mortality.
The finding that radiation-exposed patients "remained in hospital for a considerable period after their surgery" suggests that the procedures and postoperative courses were complicated.
"Radiation patients frequently develop pulmonary complications as a result of open heart surgery, not the least of which are recurrent pleural effusions and severe restrictive lung disease. It is our experience that respiratory complications may significantly compromise function and survival in patients with extensive prior radiation," the researchers said.
"Additionally, the presence of myocardial disease either as a result of the underlying cardiac condition (potentially exacerbated by prior chemotherapy) or as a consequence of a restrictive-type cardiomyopathy produced by the effects of radiation may play a role in impaired survival and is not necessarily improved by valvular or revascularization surgery," they said.
The radiation-exposed patients’ poor long-term survival after conventional cardiac surgery indicates that other, nonsurgical treatments may be necessary for this complex patient population, they added.
No relevant financial conflicts were reported.
There is little doubt that prior radiotherapy complicates surgery. Specifically, standard radiation used with curative intent for breast cancer, lymphoma, and a few other mediastinal/thorax malignancies, has important long-term effects.
Dr. Murthy |
These authors report on the increased complications and mortality of open heart operation following chest radiation given on average, some 20 years before. What is left out is that it is the radiotherapy itself that may be responsible for the current pathology for which many of the patients are requiring their heart operations. So you have the classic "insult-to-injury" of radiation being both the cause as well as the impediment to cure, in many of these circumstances. The caveat, of course, is that without their index radiotherapy, these patients would not have survived to now be burdened by the latent effects of ionizing radiation on the thorax.
Sudish Murthy, MD, FACS, is surgical director, Center of Major Airway Disease, The Cleveland Clinic.
There is little doubt that prior radiotherapy complicates surgery. Specifically, standard radiation used with curative intent for breast cancer, lymphoma, and a few other mediastinal/thorax malignancies, has important long-term effects.
Dr. Murthy |
These authors report on the increased complications and mortality of open heart operation following chest radiation given on average, some 20 years before. What is left out is that it is the radiotherapy itself that may be responsible for the current pathology for which many of the patients are requiring their heart operations. So you have the classic "insult-to-injury" of radiation being both the cause as well as the impediment to cure, in many of these circumstances. The caveat, of course, is that without their index radiotherapy, these patients would not have survived to now be burdened by the latent effects of ionizing radiation on the thorax.
Sudish Murthy, MD, FACS, is surgical director, Center of Major Airway Disease, The Cleveland Clinic.
There is little doubt that prior radiotherapy complicates surgery. Specifically, standard radiation used with curative intent for breast cancer, lymphoma, and a few other mediastinal/thorax malignancies, has important long-term effects.
Dr. Murthy |
These authors report on the increased complications and mortality of open heart operation following chest radiation given on average, some 20 years before. What is left out is that it is the radiotherapy itself that may be responsible for the current pathology for which many of the patients are requiring their heart operations. So you have the classic "insult-to-injury" of radiation being both the cause as well as the impediment to cure, in many of these circumstances. The caveat, of course, is that without their index radiotherapy, these patients would not have survived to now be burdened by the latent effects of ionizing radiation on the thorax.
Sudish Murthy, MD, FACS, is surgical director, Center of Major Airway Disease, The Cleveland Clinic.
Mortality is twice as high for cancer survivors undergoing cardiac surgery to correct damage done by thoracic radiation therapy as it is among matched patients who are undergoing the same procedures but who haven’t been exposed to radiotherapy, according to a report published online April 8 in Circulation.
In what they described as "the largest study to assess long-term survival in this population undergoing complex cardiac surgery and compare them to a well-matched comparison population," investigators found that mortality was 55% in the patients who had received radiation therapy, compared with 28% in the nonexposed controls. At least half of the deaths among the cancer survivors were attributed to cardiopulmonary disease, while only 5% were due to recurrent malignancy.
"Surgical intervention should be applied cautiously to patients who have had significant thoracic radiation previously," including survivors of breast, lung, hematologic, thyroid, and other cancers.
Trying to gauge mortality risk in such patients solely by using their preoperative scores on standard risk-prediction measures is inaccurate at best. In this study population, the survivors of breast, lung, hematologic, thyroid, and other cancers would have been deemed at intermediate risk for undergoing cardiac surgery, with an expected mortality of only 3%-5% based on their preoperative assessments – 10 times lower than their actual postoperative mortality, said Dr. Willis Wu and his associates at the Heart and Vascular Institute at the Cleveland Clinic.
"Our findings suggest that surgical intervention should be applied cautiously to patients who have had significant thoracic radiation previously," they wrote. Cardiac surgery that is considered conventional or even routine in most patients – including coronary artery bypass graft, valve repair, valve replacement, vascular surgery, pericardiectomy, left ventricular assist device implantation, and myectomy – may actually worsen the condition of radiation-exposed patients.
"It seems appropriate to examine other types of treatment options in patients with radiation heart disease who have significant valvular, coronary, or myocardial disease," the researchers noted.
Dr. Wu and his associates performed their retrospective observational study because of the dearth of information regarding long-term outcomes in cancer survivors who were exposed to chest irradiation. This knowledge gap makes treatment decisions "especially difficult" once radiation-related heart disease is discovered.
Such patients are known to have high rates of coronary artery, valvular, pericardial, myocardial, and conduction disease that progresses over time and may not become evident until decades after cancer treatment was completed.
Surgery is often thought necessary to effectively address these cardiac complications of prior radiation therapy. "These patients have multiple cardiac lesions and [often] have comorbidities such as pulmonary or vascular disease related to radiation," the investigators said.
They analyzed the medical records of 478 patients undergoing cardiac surgery at their tertiary care center in 2000-2003. A total of 173 had a prior history of malignancy treated with chest irradiation; the remaining 305 patients had no such history and were matched to the radiation group for age, sex, type of surgery, and date of surgery.
The patients exposed to radiation were relatively young but had advanced symptoms. Forty-five percent had obstructive proximal coronary artery disease; one-fourth had already undergone open heart surgery, including 16% who had prior coronary artery bypass graft surgery. There also was a high prevalence of valvular disease, with 51% of patients showing at least moderate mitral regurgitation, 6% showing severe mitral stenosis, 29% showing at least moderate aortic regurgitation, 23% showing severe aortic stenosis, and 34% showing at least moderate tricuspid regurgitation.
The mean interval between the current cardiac surgery and the last thoracic radiation treatment was 18 years. Approximately 53% of the study patients had survived breast cancer, 27% had survived Hodgkin’s lymphoma, 7% had survived lung cancer, 6% had survived non-Hodgkin’s lymphoma, and 8% had survived other malignancies including thyroid and testicular cancers.
Approximately 75% of both study groups were women.
During a mean follow-up of 7.6 years, overall mortality was 37%. Despite the success of the cardiac procedures, a significantly higher proportion of radiation-exposed patients died (55%), compared with the unexposed patients (28%), for a hazard ratio of 2.54, Dr. Wu and his colleagues said (Circulation 2013 April 8; doi:10.1161/CIRCULATIONAHA.13.001435).
Mortality was significantly higher across all subgroups of patients exposed to radiation. In particular, it was high among patients expected to have low mortality: 43% in patients aged younger than 65 years and 45% in those with lower preoperative risk scores. In fact, the youngest patients in the radiation group fared worse than the oldest patients in the comparison group.
Mortality also was significantly higher for the radiation-exposed patients than for controls across all types of cardiac surgery.
The cause of death was not known for a substantial proportion of subjects in this study, but cardiopulmonary causes were implicated in at least half of the deaths among radiation-exposed patients. "Why this should be the case in a group of patients who received potentially life-preserving revascularization, valve, and other procedures is unknown at present," Dr. Wu and his associates said.
In addition, patients with radiation-related heart disease had longer hospital stays, were more likely to develop atrial fibrillation after surgery, were more likely to require pacemaker implantation after surgery, had higher rates of ventricular dysfunction and of valvular regurgitation following surgery, and had higher 30-day mortality.
The finding that radiation-exposed patients "remained in hospital for a considerable period after their surgery" suggests that the procedures and postoperative courses were complicated.
"Radiation patients frequently develop pulmonary complications as a result of open heart surgery, not the least of which are recurrent pleural effusions and severe restrictive lung disease. It is our experience that respiratory complications may significantly compromise function and survival in patients with extensive prior radiation," the researchers said.
"Additionally, the presence of myocardial disease either as a result of the underlying cardiac condition (potentially exacerbated by prior chemotherapy) or as a consequence of a restrictive-type cardiomyopathy produced by the effects of radiation may play a role in impaired survival and is not necessarily improved by valvular or revascularization surgery," they said.
The radiation-exposed patients’ poor long-term survival after conventional cardiac surgery indicates that other, nonsurgical treatments may be necessary for this complex patient population, they added.
No relevant financial conflicts were reported.
Mortality is twice as high for cancer survivors undergoing cardiac surgery to correct damage done by thoracic radiation therapy as it is among matched patients who are undergoing the same procedures but who haven’t been exposed to radiotherapy, according to a report published online April 8 in Circulation.
In what they described as "the largest study to assess long-term survival in this population undergoing complex cardiac surgery and compare them to a well-matched comparison population," investigators found that mortality was 55% in the patients who had received radiation therapy, compared with 28% in the nonexposed controls. At least half of the deaths among the cancer survivors were attributed to cardiopulmonary disease, while only 5% were due to recurrent malignancy.
"Surgical intervention should be applied cautiously to patients who have had significant thoracic radiation previously," including survivors of breast, lung, hematologic, thyroid, and other cancers.
Trying to gauge mortality risk in such patients solely by using their preoperative scores on standard risk-prediction measures is inaccurate at best. In this study population, the survivors of breast, lung, hematologic, thyroid, and other cancers would have been deemed at intermediate risk for undergoing cardiac surgery, with an expected mortality of only 3%-5% based on their preoperative assessments – 10 times lower than their actual postoperative mortality, said Dr. Willis Wu and his associates at the Heart and Vascular Institute at the Cleveland Clinic.
"Our findings suggest that surgical intervention should be applied cautiously to patients who have had significant thoracic radiation previously," they wrote. Cardiac surgery that is considered conventional or even routine in most patients – including coronary artery bypass graft, valve repair, valve replacement, vascular surgery, pericardiectomy, left ventricular assist device implantation, and myectomy – may actually worsen the condition of radiation-exposed patients.
"It seems appropriate to examine other types of treatment options in patients with radiation heart disease who have significant valvular, coronary, or myocardial disease," the researchers noted.
Dr. Wu and his associates performed their retrospective observational study because of the dearth of information regarding long-term outcomes in cancer survivors who were exposed to chest irradiation. This knowledge gap makes treatment decisions "especially difficult" once radiation-related heart disease is discovered.
Such patients are known to have high rates of coronary artery, valvular, pericardial, myocardial, and conduction disease that progresses over time and may not become evident until decades after cancer treatment was completed.
Surgery is often thought necessary to effectively address these cardiac complications of prior radiation therapy. "These patients have multiple cardiac lesions and [often] have comorbidities such as pulmonary or vascular disease related to radiation," the investigators said.
They analyzed the medical records of 478 patients undergoing cardiac surgery at their tertiary care center in 2000-2003. A total of 173 had a prior history of malignancy treated with chest irradiation; the remaining 305 patients had no such history and were matched to the radiation group for age, sex, type of surgery, and date of surgery.
The patients exposed to radiation were relatively young but had advanced symptoms. Forty-five percent had obstructive proximal coronary artery disease; one-fourth had already undergone open heart surgery, including 16% who had prior coronary artery bypass graft surgery. There also was a high prevalence of valvular disease, with 51% of patients showing at least moderate mitral regurgitation, 6% showing severe mitral stenosis, 29% showing at least moderate aortic regurgitation, 23% showing severe aortic stenosis, and 34% showing at least moderate tricuspid regurgitation.
The mean interval between the current cardiac surgery and the last thoracic radiation treatment was 18 years. Approximately 53% of the study patients had survived breast cancer, 27% had survived Hodgkin’s lymphoma, 7% had survived lung cancer, 6% had survived non-Hodgkin’s lymphoma, and 8% had survived other malignancies including thyroid and testicular cancers.
Approximately 75% of both study groups were women.
During a mean follow-up of 7.6 years, overall mortality was 37%. Despite the success of the cardiac procedures, a significantly higher proportion of radiation-exposed patients died (55%), compared with the unexposed patients (28%), for a hazard ratio of 2.54, Dr. Wu and his colleagues said (Circulation 2013 April 8; doi:10.1161/CIRCULATIONAHA.13.001435).
Mortality was significantly higher across all subgroups of patients exposed to radiation. In particular, it was high among patients expected to have low mortality: 43% in patients aged younger than 65 years and 45% in those with lower preoperative risk scores. In fact, the youngest patients in the radiation group fared worse than the oldest patients in the comparison group.
Mortality also was significantly higher for the radiation-exposed patients than for controls across all types of cardiac surgery.
The cause of death was not known for a substantial proportion of subjects in this study, but cardiopulmonary causes were implicated in at least half of the deaths among radiation-exposed patients. "Why this should be the case in a group of patients who received potentially life-preserving revascularization, valve, and other procedures is unknown at present," Dr. Wu and his associates said.
In addition, patients with radiation-related heart disease had longer hospital stays, were more likely to develop atrial fibrillation after surgery, were more likely to require pacemaker implantation after surgery, had higher rates of ventricular dysfunction and of valvular regurgitation following surgery, and had higher 30-day mortality.
The finding that radiation-exposed patients "remained in hospital for a considerable period after their surgery" suggests that the procedures and postoperative courses were complicated.
"Radiation patients frequently develop pulmonary complications as a result of open heart surgery, not the least of which are recurrent pleural effusions and severe restrictive lung disease. It is our experience that respiratory complications may significantly compromise function and survival in patients with extensive prior radiation," the researchers said.
"Additionally, the presence of myocardial disease either as a result of the underlying cardiac condition (potentially exacerbated by prior chemotherapy) or as a consequence of a restrictive-type cardiomyopathy produced by the effects of radiation may play a role in impaired survival and is not necessarily improved by valvular or revascularization surgery," they said.
The radiation-exposed patients’ poor long-term survival after conventional cardiac surgery indicates that other, nonsurgical treatments may be necessary for this complex patient population, they added.
No relevant financial conflicts were reported.
FROM CIRCULATION
Major Finding: Despite the success of the cardiac procedures, a significantly higher proportion of radiation-exposed patients died during follow-up (55%), compared with the unexposed patients (28%).
Data Source: A retrospective, single-center, observational study involving 173 cancer survivors who were previously exposed to thoracic radiotherapy and 305 matched controls who underwent cardiac surgery in 2000-2003 and were followed for approximately 7 years.
Disclosures: No relevant financial conflicts were reported.