User login
Long detection cuts inappropriate shocks from ICDs
For patients receiving implantable cardioverter-defibrillators, programming the devices to have prolonged rather than standard-length arrhythmia detection intervals lowers the rate of antitachycardia pacing and shocks delivered, as well as the number of inappropriate shocks, according to the results of ADVANCE III, published in the May 8 issue of JAMA.
In a 2-year clinical trial conducted at 94 medical centers in Europe, the Middle East, Russia, and Africa, 1,902 patients who received single-, dual-, or triple-chamber ICDs for either primary or secondary prevention were randomly assigned to have the devices programmed to deliver therapies at standard detection intervals (954 subjects) or at prolonged detection interval (948 subjects). "The delay allowed nonsustained events to self-terminate, thus avoiding unnecessary therapies," without excessively delaying therapies if they were still needed, said Dr. Maurizio Gasparini of Humanitas Clinical and Research Center, Rozzano (Italy), and his associates in the ADVANCE III (Avoid Delivering Therapies for Nonsustained Arrhythmias in ICD Patients III) study. As this news organization reported, Dr. Gasparini first presented these results last May at the annual meeting of the Heart Rhythm Society in Boston.
During a median follow-up of 1 year, the long-detection–interval group had a significantly lower rate of therapies delivered and a significantly lower rate of inappropriate shocks delivered. They also had a significantly lower rate of hospitalizations (42 vs. 52/100 person-years). But these benefits did not come at the cost of more episodes of syncope, since those rates did not differ significantly between the two study groups (3.1 vs. 1.9/100 person-years, respectively), the investigators said (JAMA 2013;309:1903-11).
"At present, the ‘out of the box’ settings used by some ICD manufacturers may be too conservative, with nominal treatment delays as short as 1-3 seconds. On the basis of previous evidence and the current findings, it seems reasonable that a long-detection interval may be preferable in the majority of patients," they noted.
In an editorial accompanying this report, Dr. Merritt H. Raitt of Portland Veterans Administration Medical Center and Oregon Health and Science University said, "This trial is important in that it extends the study population to include patients with both primary and secondary indications for ICD implants as well as to those with single-chamber ICDs."
Moreover, the findings add "important new information to the evidence base of ICD programming," he said (JAMA 2013;309:1937-8).
"Regardless of whether these programming intervals lead to reduced mortality, the unequivocal reduction in ICD shocks and the reduction in hospitalization without an increase in adverse events such as syncope suggests that this programming approach should be considered for adoption in the care of patients with ICDs and clinical characteristics similar to those enrolled in these studies," Dr. Raitt said.
ADVANCE III was funded by Medtronic. Dr. Gasparini reported ties to Medtronic and Boston Scientific, and his associates reported ties to Medtronic, Sorin, Boston Scientific, St. Jude Medical, Boehringer-Ingelheim, Biotronik, and Biosense-Webster.
For patients receiving implantable cardioverter-defibrillators, programming the devices to have prolonged rather than standard-length arrhythmia detection intervals lowers the rate of antitachycardia pacing and shocks delivered, as well as the number of inappropriate shocks, according to the results of ADVANCE III, published in the May 8 issue of JAMA.
In a 2-year clinical trial conducted at 94 medical centers in Europe, the Middle East, Russia, and Africa, 1,902 patients who received single-, dual-, or triple-chamber ICDs for either primary or secondary prevention were randomly assigned to have the devices programmed to deliver therapies at standard detection intervals (954 subjects) or at prolonged detection interval (948 subjects). "The delay allowed nonsustained events to self-terminate, thus avoiding unnecessary therapies," without excessively delaying therapies if they were still needed, said Dr. Maurizio Gasparini of Humanitas Clinical and Research Center, Rozzano (Italy), and his associates in the ADVANCE III (Avoid Delivering Therapies for Nonsustained Arrhythmias in ICD Patients III) study. As this news organization reported, Dr. Gasparini first presented these results last May at the annual meeting of the Heart Rhythm Society in Boston.
During a median follow-up of 1 year, the long-detection–interval group had a significantly lower rate of therapies delivered and a significantly lower rate of inappropriate shocks delivered. They also had a significantly lower rate of hospitalizations (42 vs. 52/100 person-years). But these benefits did not come at the cost of more episodes of syncope, since those rates did not differ significantly between the two study groups (3.1 vs. 1.9/100 person-years, respectively), the investigators said (JAMA 2013;309:1903-11).
"At present, the ‘out of the box’ settings used by some ICD manufacturers may be too conservative, with nominal treatment delays as short as 1-3 seconds. On the basis of previous evidence and the current findings, it seems reasonable that a long-detection interval may be preferable in the majority of patients," they noted.
In an editorial accompanying this report, Dr. Merritt H. Raitt of Portland Veterans Administration Medical Center and Oregon Health and Science University said, "This trial is important in that it extends the study population to include patients with both primary and secondary indications for ICD implants as well as to those with single-chamber ICDs."
Moreover, the findings add "important new information to the evidence base of ICD programming," he said (JAMA 2013;309:1937-8).
"Regardless of whether these programming intervals lead to reduced mortality, the unequivocal reduction in ICD shocks and the reduction in hospitalization without an increase in adverse events such as syncope suggests that this programming approach should be considered for adoption in the care of patients with ICDs and clinical characteristics similar to those enrolled in these studies," Dr. Raitt said.
ADVANCE III was funded by Medtronic. Dr. Gasparini reported ties to Medtronic and Boston Scientific, and his associates reported ties to Medtronic, Sorin, Boston Scientific, St. Jude Medical, Boehringer-Ingelheim, Biotronik, and Biosense-Webster.
For patients receiving implantable cardioverter-defibrillators, programming the devices to have prolonged rather than standard-length arrhythmia detection intervals lowers the rate of antitachycardia pacing and shocks delivered, as well as the number of inappropriate shocks, according to the results of ADVANCE III, published in the May 8 issue of JAMA.
In a 2-year clinical trial conducted at 94 medical centers in Europe, the Middle East, Russia, and Africa, 1,902 patients who received single-, dual-, or triple-chamber ICDs for either primary or secondary prevention were randomly assigned to have the devices programmed to deliver therapies at standard detection intervals (954 subjects) or at prolonged detection interval (948 subjects). "The delay allowed nonsustained events to self-terminate, thus avoiding unnecessary therapies," without excessively delaying therapies if they were still needed, said Dr. Maurizio Gasparini of Humanitas Clinical and Research Center, Rozzano (Italy), and his associates in the ADVANCE III (Avoid Delivering Therapies for Nonsustained Arrhythmias in ICD Patients III) study. As this news organization reported, Dr. Gasparini first presented these results last May at the annual meeting of the Heart Rhythm Society in Boston.
During a median follow-up of 1 year, the long-detection–interval group had a significantly lower rate of therapies delivered and a significantly lower rate of inappropriate shocks delivered. They also had a significantly lower rate of hospitalizations (42 vs. 52/100 person-years). But these benefits did not come at the cost of more episodes of syncope, since those rates did not differ significantly between the two study groups (3.1 vs. 1.9/100 person-years, respectively), the investigators said (JAMA 2013;309:1903-11).
"At present, the ‘out of the box’ settings used by some ICD manufacturers may be too conservative, with nominal treatment delays as short as 1-3 seconds. On the basis of previous evidence and the current findings, it seems reasonable that a long-detection interval may be preferable in the majority of patients," they noted.
In an editorial accompanying this report, Dr. Merritt H. Raitt of Portland Veterans Administration Medical Center and Oregon Health and Science University said, "This trial is important in that it extends the study population to include patients with both primary and secondary indications for ICD implants as well as to those with single-chamber ICDs."
Moreover, the findings add "important new information to the evidence base of ICD programming," he said (JAMA 2013;309:1937-8).
"Regardless of whether these programming intervals lead to reduced mortality, the unequivocal reduction in ICD shocks and the reduction in hospitalization without an increase in adverse events such as syncope suggests that this programming approach should be considered for adoption in the care of patients with ICDs and clinical characteristics similar to those enrolled in these studies," Dr. Raitt said.
ADVANCE III was funded by Medtronic. Dr. Gasparini reported ties to Medtronic and Boston Scientific, and his associates reported ties to Medtronic, Sorin, Boston Scientific, St. Jude Medical, Boehringer-Ingelheim, Biotronik, and Biosense-Webster.
FROM JAMA
Major Finding: The long-detection–interval group had a significantly lower rate of therapies delivered, a significantly lower rate of inappropriate shocks delivered, and a significantly lower rate of hospitalizations.
Data Source: A prospective randomized international clinical trial involving 954 ICD recipients with standard detection intervals and 948 with prolonged detection intervals, who were followed for 1 year.
Disclosures: ADVANCE III was funded by Medtronic. Dr. Gasparini reported ties to Medtronic and Boston Scientific, and his associates reported ties to Medtronic, Sorin, Boston Scientific, St. Jude Medical, Boehringer-Ingelheim, Biotronik, and Biosense-Webster.
Ambrisentan doesn't help, may worsen pulmonary fibrosis
The endothelin-receptor antagonist ambrisentan not only failed to benefit patients with idiopathic pulmonary fibrosis, it also may have facilitated disease progression in an international phase III clinical trial reported May 7 in Annals of Internal Medicine.
The trial was terminated early when an interim analysis of the data showed that patients treated with ambrisentan were more likely than were control subjects receiving placebo to show progression of idiopathic pulmonary fibrosis (IPF) and to require more hospitalizations for respiratory indications, including acute IPF exacerbations and pneumonia. The findings were the same whether the study subjects had concomitant pulmonary hypertension.
"The observations in this study provide compelling evidence for ambrisentan as an ineffective treatment for patients with IPF and preclude further clinical evaluation of the drug as therapy for the disease. The data provide a basis for explicit guidance to clinicians not to use ambrisentan to treat patients with IPF, regardless of the presence of pulmonary hypertension," said Dr. Ganesh Raghu of the division of pulmonary and critical care medicine, University of Washington Medical Center, Seattle, and his associates.
The researchers undertook this large phase III study because preclinical data suggested that antagonism of endothelin receptors could lessen the severity of pulmonary fibrosis. And in a phase II study involving patients with a variety of interstitial lung diseases, a related endothelin antagonist, bosentan, had improved survival in the subgroup of patients with IPF.
Ambrisentan is a more selective endothelin A-receptor antagonist than bosentan and is currently approved for the treatment of pulmonary arterial hypertension. Dr. Raghu and his colleagues compared it against a matched placebo in 492 IPF patients treated at 136 clinical sites in North America, South America, Europe, Asia, New Zealand, and Australia.
When approximately 75% of the intended total enrollment of 660 patients was reached, an interim safety and efficacy analysis showed that the drug did not improve the primary endpoint, which was a composite of the time to disease progression, death from any cause, hospitalization for respiratory events, or a decrease in lung function. The trial sponsor, Gilead Sciences, terminated the study, and the findings were analyzed on the subjects enrolled up until that point.
The mean interval of exposure to ambrisentan (329 subjects) or placebo (163 subjects) was approximately 35 weeks. At baseline, patients in the active-treatment group and control group were similar regarding demographic traits, pulmonary hemodynamics, lung function, 6-minute walk distance, and quality of life.
Significantly more patients in the ambrisentan group (27.4%) than in the placebo group (17.2%) showed IPF progression. The active-treatment group also had significantly more respiratory hospitalizations (13.4% vs. 5.5%) and deaths (7.9% vs 3.7%) than did the control group, Dr. Raghu and his associates wrote (Ann. Intern. Med. 2013; 158:641-90).
However, there were no significant differences between the two study groups in the secondary endpoints of diffusion capacity for carbon monoxide; forced vital capacity; 6-minute walk distance; scores on the SF-36, which measures quality of life; or scores on the Transitional Dyspnea Index.
These findings were essentially the same when the data were analyzed according to whether or not patients had concomitant pulmonary hypertension at baseline. However, the subset of patients with pulmonary hypertension was small and not adequately powered to demonstrate a significant difference, so this finding should be interpreted with caution, the investigators said.
Regarding adverse events, significantly more patients taking ambrisentan than placebo reported dyspnea, worsening IPF, dizziness, and peripheral edema. Three times as many patients receiving ambrisentan (3%) dropped out of the study because of safety and tolerability issues, compared with those receiving placebo (1%).
This trial was supported by Gilead Sciences, which was involved in all aspects of the study.
The endothelin-receptor antagonist ambrisentan not only failed to benefit patients with idiopathic pulmonary fibrosis, it also may have facilitated disease progression in an international phase III clinical trial reported May 7 in Annals of Internal Medicine.
The trial was terminated early when an interim analysis of the data showed that patients treated with ambrisentan were more likely than were control subjects receiving placebo to show progression of idiopathic pulmonary fibrosis (IPF) and to require more hospitalizations for respiratory indications, including acute IPF exacerbations and pneumonia. The findings were the same whether the study subjects had concomitant pulmonary hypertension.
"The observations in this study provide compelling evidence for ambrisentan as an ineffective treatment for patients with IPF and preclude further clinical evaluation of the drug as therapy for the disease. The data provide a basis for explicit guidance to clinicians not to use ambrisentan to treat patients with IPF, regardless of the presence of pulmonary hypertension," said Dr. Ganesh Raghu of the division of pulmonary and critical care medicine, University of Washington Medical Center, Seattle, and his associates.
The researchers undertook this large phase III study because preclinical data suggested that antagonism of endothelin receptors could lessen the severity of pulmonary fibrosis. And in a phase II study involving patients with a variety of interstitial lung diseases, a related endothelin antagonist, bosentan, had improved survival in the subgroup of patients with IPF.
Ambrisentan is a more selective endothelin A-receptor antagonist than bosentan and is currently approved for the treatment of pulmonary arterial hypertension. Dr. Raghu and his colleagues compared it against a matched placebo in 492 IPF patients treated at 136 clinical sites in North America, South America, Europe, Asia, New Zealand, and Australia.
When approximately 75% of the intended total enrollment of 660 patients was reached, an interim safety and efficacy analysis showed that the drug did not improve the primary endpoint, which was a composite of the time to disease progression, death from any cause, hospitalization for respiratory events, or a decrease in lung function. The trial sponsor, Gilead Sciences, terminated the study, and the findings were analyzed on the subjects enrolled up until that point.
The mean interval of exposure to ambrisentan (329 subjects) or placebo (163 subjects) was approximately 35 weeks. At baseline, patients in the active-treatment group and control group were similar regarding demographic traits, pulmonary hemodynamics, lung function, 6-minute walk distance, and quality of life.
Significantly more patients in the ambrisentan group (27.4%) than in the placebo group (17.2%) showed IPF progression. The active-treatment group also had significantly more respiratory hospitalizations (13.4% vs. 5.5%) and deaths (7.9% vs 3.7%) than did the control group, Dr. Raghu and his associates wrote (Ann. Intern. Med. 2013; 158:641-90).
However, there were no significant differences between the two study groups in the secondary endpoints of diffusion capacity for carbon monoxide; forced vital capacity; 6-minute walk distance; scores on the SF-36, which measures quality of life; or scores on the Transitional Dyspnea Index.
These findings were essentially the same when the data were analyzed according to whether or not patients had concomitant pulmonary hypertension at baseline. However, the subset of patients with pulmonary hypertension was small and not adequately powered to demonstrate a significant difference, so this finding should be interpreted with caution, the investigators said.
Regarding adverse events, significantly more patients taking ambrisentan than placebo reported dyspnea, worsening IPF, dizziness, and peripheral edema. Three times as many patients receiving ambrisentan (3%) dropped out of the study because of safety and tolerability issues, compared with those receiving placebo (1%).
This trial was supported by Gilead Sciences, which was involved in all aspects of the study.
The endothelin-receptor antagonist ambrisentan not only failed to benefit patients with idiopathic pulmonary fibrosis, it also may have facilitated disease progression in an international phase III clinical trial reported May 7 in Annals of Internal Medicine.
The trial was terminated early when an interim analysis of the data showed that patients treated with ambrisentan were more likely than were control subjects receiving placebo to show progression of idiopathic pulmonary fibrosis (IPF) and to require more hospitalizations for respiratory indications, including acute IPF exacerbations and pneumonia. The findings were the same whether the study subjects had concomitant pulmonary hypertension.
"The observations in this study provide compelling evidence for ambrisentan as an ineffective treatment for patients with IPF and preclude further clinical evaluation of the drug as therapy for the disease. The data provide a basis for explicit guidance to clinicians not to use ambrisentan to treat patients with IPF, regardless of the presence of pulmonary hypertension," said Dr. Ganesh Raghu of the division of pulmonary and critical care medicine, University of Washington Medical Center, Seattle, and his associates.
The researchers undertook this large phase III study because preclinical data suggested that antagonism of endothelin receptors could lessen the severity of pulmonary fibrosis. And in a phase II study involving patients with a variety of interstitial lung diseases, a related endothelin antagonist, bosentan, had improved survival in the subgroup of patients with IPF.
Ambrisentan is a more selective endothelin A-receptor antagonist than bosentan and is currently approved for the treatment of pulmonary arterial hypertension. Dr. Raghu and his colleagues compared it against a matched placebo in 492 IPF patients treated at 136 clinical sites in North America, South America, Europe, Asia, New Zealand, and Australia.
When approximately 75% of the intended total enrollment of 660 patients was reached, an interim safety and efficacy analysis showed that the drug did not improve the primary endpoint, which was a composite of the time to disease progression, death from any cause, hospitalization for respiratory events, or a decrease in lung function. The trial sponsor, Gilead Sciences, terminated the study, and the findings were analyzed on the subjects enrolled up until that point.
The mean interval of exposure to ambrisentan (329 subjects) or placebo (163 subjects) was approximately 35 weeks. At baseline, patients in the active-treatment group and control group were similar regarding demographic traits, pulmonary hemodynamics, lung function, 6-minute walk distance, and quality of life.
Significantly more patients in the ambrisentan group (27.4%) than in the placebo group (17.2%) showed IPF progression. The active-treatment group also had significantly more respiratory hospitalizations (13.4% vs. 5.5%) and deaths (7.9% vs 3.7%) than did the control group, Dr. Raghu and his associates wrote (Ann. Intern. Med. 2013; 158:641-90).
However, there were no significant differences between the two study groups in the secondary endpoints of diffusion capacity for carbon monoxide; forced vital capacity; 6-minute walk distance; scores on the SF-36, which measures quality of life; or scores on the Transitional Dyspnea Index.
These findings were essentially the same when the data were analyzed according to whether or not patients had concomitant pulmonary hypertension at baseline. However, the subset of patients with pulmonary hypertension was small and not adequately powered to demonstrate a significant difference, so this finding should be interpreted with caution, the investigators said.
Regarding adverse events, significantly more patients taking ambrisentan than placebo reported dyspnea, worsening IPF, dizziness, and peripheral edema. Three times as many patients receiving ambrisentan (3%) dropped out of the study because of safety and tolerability issues, compared with those receiving placebo (1%).
This trial was supported by Gilead Sciences, which was involved in all aspects of the study.
FROM ANNALS OF INTERNAL MEDICINE
Major Finding: Significantly more patients taking ambrisentan (27.4%) than taking placebo (17.2%) showed IPF progression.
Data Source: A phase III randomized, double-blind clinical trial involving 329 patients with idiopathic pulmonary fibrosis who received ambrisentan and 163 who received a matching placebo for approximately 9 months before the study was terminated.
Disclosures: This trial was supported by ambrisentan-maker Gilead Sciences, which was involved in all aspects of the study.
Depression in adolescence linked to adverse outcomes 10 years later
People who have depression during adolescence are approximately two to three times more likely than others to experience a range of adverse outcomes during the following decade, including poor overall health, migraine headaches, psychological distress, poor social support, heavy drinking, and smoking, according to a report in the May issue of the Journal of Adolescent Health.
However, at the age of 26-27 years, they were no different from people who did not have depression during adolescence in unemployment status, personal income, marital status, or educational attainment, said Kiyuri Naicker of the department of epidemiology and community medicine, University of Ottawa, and her associates.
The findings of this population-based study indicate that "the onset of depression during adolescence may forecast problems in adapting during this key transitional phase leading into adulthood. At this stage, where individuals are setting themselves up for their adult lives, the consequences may be long term and have far-reaching implications; although we might not find immediate effects on employment or relationships, an increased propensity to drink heavily, smoke, feel less healthy, and live a stressful life is likely to impact the capacity of the individual to successfully navigate work and family challenges farther down the road," the investigators reported.
They assessed a variety of health outcomes using information from the National Population Health Survey, a prospective cohort study involving a nationally representative sample of 17,276 Canadians who were aged 12 and older at baseline in 1994. For this study, Ms. Naicker and her colleagues reviewed detailed data collected every 2 years over the course of a decade for 1,027 participants who were aged 26-27 years at the most recent follow-up.
People who had depression during adolescence were 4.91 times more likely than those who did not to experience depression during follow-up and 3.74 times more likely to be taking antidepressants. They also were more likely to be experiencing psychological distress (OR, 3.02); abusing alcohol (OR, 1.78); and smoking at least once a day (OR, 2.89) in early adulthood.
Depression during adolescence also was strongly predictive of migraine headaches (OR, 2.76) during young adulthood. And compared with their nondepressed peers, those who had been depressed during adolescence were much more likely to report 10 years later that they had low levels of social support, high levels of stress, and poor overall health, the investigators said (J. Adolesc. Health 2013;52:533-8).
In contrast, adolescent depression did not correlate with later unemployment, low income, or educational attainment, and was not significantly related to marital status. These outcomes "may be more meaningfully measured in individuals in their thirties," since marriage and career milestones are frequently delayed until that time in the current economic and social environment.
This study was limited in that it included few nonwhite participants. This means that the findings might not be generalizable to other, more diverse populations, and that the researchers were not able to examine the effect of race on the outcomes they assessed.
The study was funded by the M.S.I. Foundation, a health research funding organization based in Alberta, Edmonton. No financial conflicts of interest were reported.
People who have depression during adolescence are approximately two to three times more likely than others to experience a range of adverse outcomes during the following decade, including poor overall health, migraine headaches, psychological distress, poor social support, heavy drinking, and smoking, according to a report in the May issue of the Journal of Adolescent Health.
However, at the age of 26-27 years, they were no different from people who did not have depression during adolescence in unemployment status, personal income, marital status, or educational attainment, said Kiyuri Naicker of the department of epidemiology and community medicine, University of Ottawa, and her associates.
The findings of this population-based study indicate that "the onset of depression during adolescence may forecast problems in adapting during this key transitional phase leading into adulthood. At this stage, where individuals are setting themselves up for their adult lives, the consequences may be long term and have far-reaching implications; although we might not find immediate effects on employment or relationships, an increased propensity to drink heavily, smoke, feel less healthy, and live a stressful life is likely to impact the capacity of the individual to successfully navigate work and family challenges farther down the road," the investigators reported.
They assessed a variety of health outcomes using information from the National Population Health Survey, a prospective cohort study involving a nationally representative sample of 17,276 Canadians who were aged 12 and older at baseline in 1994. For this study, Ms. Naicker and her colleagues reviewed detailed data collected every 2 years over the course of a decade for 1,027 participants who were aged 26-27 years at the most recent follow-up.
People who had depression during adolescence were 4.91 times more likely than those who did not to experience depression during follow-up and 3.74 times more likely to be taking antidepressants. They also were more likely to be experiencing psychological distress (OR, 3.02); abusing alcohol (OR, 1.78); and smoking at least once a day (OR, 2.89) in early adulthood.
Depression during adolescence also was strongly predictive of migraine headaches (OR, 2.76) during young adulthood. And compared with their nondepressed peers, those who had been depressed during adolescence were much more likely to report 10 years later that they had low levels of social support, high levels of stress, and poor overall health, the investigators said (J. Adolesc. Health 2013;52:533-8).
In contrast, adolescent depression did not correlate with later unemployment, low income, or educational attainment, and was not significantly related to marital status. These outcomes "may be more meaningfully measured in individuals in their thirties," since marriage and career milestones are frequently delayed until that time in the current economic and social environment.
This study was limited in that it included few nonwhite participants. This means that the findings might not be generalizable to other, more diverse populations, and that the researchers were not able to examine the effect of race on the outcomes they assessed.
The study was funded by the M.S.I. Foundation, a health research funding organization based in Alberta, Edmonton. No financial conflicts of interest were reported.
People who have depression during adolescence are approximately two to three times more likely than others to experience a range of adverse outcomes during the following decade, including poor overall health, migraine headaches, psychological distress, poor social support, heavy drinking, and smoking, according to a report in the May issue of the Journal of Adolescent Health.
However, at the age of 26-27 years, they were no different from people who did not have depression during adolescence in unemployment status, personal income, marital status, or educational attainment, said Kiyuri Naicker of the department of epidemiology and community medicine, University of Ottawa, and her associates.
The findings of this population-based study indicate that "the onset of depression during adolescence may forecast problems in adapting during this key transitional phase leading into adulthood. At this stage, where individuals are setting themselves up for their adult lives, the consequences may be long term and have far-reaching implications; although we might not find immediate effects on employment or relationships, an increased propensity to drink heavily, smoke, feel less healthy, and live a stressful life is likely to impact the capacity of the individual to successfully navigate work and family challenges farther down the road," the investigators reported.
They assessed a variety of health outcomes using information from the National Population Health Survey, a prospective cohort study involving a nationally representative sample of 17,276 Canadians who were aged 12 and older at baseline in 1994. For this study, Ms. Naicker and her colleagues reviewed detailed data collected every 2 years over the course of a decade for 1,027 participants who were aged 26-27 years at the most recent follow-up.
People who had depression during adolescence were 4.91 times more likely than those who did not to experience depression during follow-up and 3.74 times more likely to be taking antidepressants. They also were more likely to be experiencing psychological distress (OR, 3.02); abusing alcohol (OR, 1.78); and smoking at least once a day (OR, 2.89) in early adulthood.
Depression during adolescence also was strongly predictive of migraine headaches (OR, 2.76) during young adulthood. And compared with their nondepressed peers, those who had been depressed during adolescence were much more likely to report 10 years later that they had low levels of social support, high levels of stress, and poor overall health, the investigators said (J. Adolesc. Health 2013;52:533-8).
In contrast, adolescent depression did not correlate with later unemployment, low income, or educational attainment, and was not significantly related to marital status. These outcomes "may be more meaningfully measured in individuals in their thirties," since marriage and career milestones are frequently delayed until that time in the current economic and social environment.
This study was limited in that it included few nonwhite participants. This means that the findings might not be generalizable to other, more diverse populations, and that the researchers were not able to examine the effect of race on the outcomes they assessed.
The study was funded by the M.S.I. Foundation, a health research funding organization based in Alberta, Edmonton. No financial conflicts of interest were reported.
FROM THE JOURNAL OF ADOLESCENT HEALTH
Major Finding: People who had depression during adolescence were 4.91 times more likely than those who did not to experience depression during follow-up. They also were more likely to be experiencing psychological distress (OR, 3.02); abusing alcohol (OR, 1.78); and smoking at least once a day (OR, 2.89) in early adulthood.
Data Source: An analysis of data from a prospective cohort study in which 1,027 participants aged 16-17 at baseline were followed every 2 years for a decade.
Disclosures: This study was funded by the M.S.I. Foundation, a health research funding organization based in Alberta, Edmonton. No financial conflicts of interest were reported.
No or mild developmental disability in 73% of extremely preterm
Almost three-quarters of children born extremely preterm showed mild or no neurodevelopmental disability at age 2.5 years, according to a population-based study published in the May 1 issue of JAMA.
In comparison, 78% of control subjects born at term showed no neurodevelopmental disability.
"Improved survival did not translate into increasing disability rates, and we, like others, believe that the neurodevelopmental outcome for extremely preterm children born in the 2000s will be better than for those born in the 1990s," said Dr. Fredrik Serenius of the department of women’s and children’s health, Uppsala University, and his associates in the Extremely Preterm Infants Study in Sweden (EXPRESS).
The investigators noted that their results may not be generalizable to other countries. Sweden has "a rather uniform society without extreme poverty. Antenatal care is easily accessible and utilized by close to 100% of mothers. All citizens are covered by general health insurance including a total of 480 days of parental leave after the child’s birth and additional benefits for severely sick children," they said.
EXPRESS is a national prospective study of all infants born in Sweden before 27 weeks’ gestation during 2004-2007. For this study, Dr. Serenius and his colleagues assessed neurological and developmental outcomes in 456 of these children who survived to 2.5 years of corrected age, as well as in 701 control children matched for residence, sex, day of birth, and mother’s country of origin.
Certified psychologists assessed the children’s cognitive, language, and motor development using the Bayley Scales of Infant and Toddler Development. In addition, specialists in pediatrics or pediatric neurology examined the preterm group for neuromotor function. Parents of children in both study groups were interviewed to ascertain parental education level and overall child health and development.
Among the preterm infants, 42% were neurodevelopmentally normal and 31% were mildly disabled. The remaining 27% were moderately or severely disabled, including four children who were blind and one who was blind and deaf. Seven percent of the preterm group had cerebral palsy – 13 with mild CP, 13 with moderate CP, and 6 with severe CP, the investigators said (JAMA 2013;309:1810-20).
In comparison, 78% of children in the control group were neurodevelopmentally normal and another 19% were mildly disabled. The remaining 3% were moderately or severely disabled, including one with severe CP.
The mean composite cognitive score for children in the preterm group was 94, compared with 104 for the control group. The mean composite language scores were 98 and 109, respectively, and the mean composite motor scores were 94 and 107, respectively.
In the preterm group, these scores rose with increasing gestational age at birth, so that cognitive scores were 2.5 points higher for every additional week of gestational age, language scores were 3.6 points higher for every additional week, and motor scores were 2.5 points higher for every additional week.
Overall, even though prematurity had a "large" impact on neurodevelopmental outcomes, most extremely preterm children emerged with no or only mild disability.
"These results are relevant for clinicians counseling families facing extremely preterm birth," Dr. Serenius and his associates said.
This study was supported in part by the Swedish Research Council. No financial conflicts of interest were reported.
Almost three-quarters of children born extremely preterm showed mild or no neurodevelopmental disability at age 2.5 years, according to a population-based study published in the May 1 issue of JAMA.
In comparison, 78% of control subjects born at term showed no neurodevelopmental disability.
"Improved survival did not translate into increasing disability rates, and we, like others, believe that the neurodevelopmental outcome for extremely preterm children born in the 2000s will be better than for those born in the 1990s," said Dr. Fredrik Serenius of the department of women’s and children’s health, Uppsala University, and his associates in the Extremely Preterm Infants Study in Sweden (EXPRESS).
The investigators noted that their results may not be generalizable to other countries. Sweden has "a rather uniform society without extreme poverty. Antenatal care is easily accessible and utilized by close to 100% of mothers. All citizens are covered by general health insurance including a total of 480 days of parental leave after the child’s birth and additional benefits for severely sick children," they said.
EXPRESS is a national prospective study of all infants born in Sweden before 27 weeks’ gestation during 2004-2007. For this study, Dr. Serenius and his colleagues assessed neurological and developmental outcomes in 456 of these children who survived to 2.5 years of corrected age, as well as in 701 control children matched for residence, sex, day of birth, and mother’s country of origin.
Certified psychologists assessed the children’s cognitive, language, and motor development using the Bayley Scales of Infant and Toddler Development. In addition, specialists in pediatrics or pediatric neurology examined the preterm group for neuromotor function. Parents of children in both study groups were interviewed to ascertain parental education level and overall child health and development.
Among the preterm infants, 42% were neurodevelopmentally normal and 31% were mildly disabled. The remaining 27% were moderately or severely disabled, including four children who were blind and one who was blind and deaf. Seven percent of the preterm group had cerebral palsy – 13 with mild CP, 13 with moderate CP, and 6 with severe CP, the investigators said (JAMA 2013;309:1810-20).
In comparison, 78% of children in the control group were neurodevelopmentally normal and another 19% were mildly disabled. The remaining 3% were moderately or severely disabled, including one with severe CP.
The mean composite cognitive score for children in the preterm group was 94, compared with 104 for the control group. The mean composite language scores were 98 and 109, respectively, and the mean composite motor scores were 94 and 107, respectively.
In the preterm group, these scores rose with increasing gestational age at birth, so that cognitive scores were 2.5 points higher for every additional week of gestational age, language scores were 3.6 points higher for every additional week, and motor scores were 2.5 points higher for every additional week.
Overall, even though prematurity had a "large" impact on neurodevelopmental outcomes, most extremely preterm children emerged with no or only mild disability.
"These results are relevant for clinicians counseling families facing extremely preterm birth," Dr. Serenius and his associates said.
This study was supported in part by the Swedish Research Council. No financial conflicts of interest were reported.
Almost three-quarters of children born extremely preterm showed mild or no neurodevelopmental disability at age 2.5 years, according to a population-based study published in the May 1 issue of JAMA.
In comparison, 78% of control subjects born at term showed no neurodevelopmental disability.
"Improved survival did not translate into increasing disability rates, and we, like others, believe that the neurodevelopmental outcome for extremely preterm children born in the 2000s will be better than for those born in the 1990s," said Dr. Fredrik Serenius of the department of women’s and children’s health, Uppsala University, and his associates in the Extremely Preterm Infants Study in Sweden (EXPRESS).
The investigators noted that their results may not be generalizable to other countries. Sweden has "a rather uniform society without extreme poverty. Antenatal care is easily accessible and utilized by close to 100% of mothers. All citizens are covered by general health insurance including a total of 480 days of parental leave after the child’s birth and additional benefits for severely sick children," they said.
EXPRESS is a national prospective study of all infants born in Sweden before 27 weeks’ gestation during 2004-2007. For this study, Dr. Serenius and his colleagues assessed neurological and developmental outcomes in 456 of these children who survived to 2.5 years of corrected age, as well as in 701 control children matched for residence, sex, day of birth, and mother’s country of origin.
Certified psychologists assessed the children’s cognitive, language, and motor development using the Bayley Scales of Infant and Toddler Development. In addition, specialists in pediatrics or pediatric neurology examined the preterm group for neuromotor function. Parents of children in both study groups were interviewed to ascertain parental education level and overall child health and development.
Among the preterm infants, 42% were neurodevelopmentally normal and 31% were mildly disabled. The remaining 27% were moderately or severely disabled, including four children who were blind and one who was blind and deaf. Seven percent of the preterm group had cerebral palsy – 13 with mild CP, 13 with moderate CP, and 6 with severe CP, the investigators said (JAMA 2013;309:1810-20).
In comparison, 78% of children in the control group were neurodevelopmentally normal and another 19% were mildly disabled. The remaining 3% were moderately or severely disabled, including one with severe CP.
The mean composite cognitive score for children in the preterm group was 94, compared with 104 for the control group. The mean composite language scores were 98 and 109, respectively, and the mean composite motor scores were 94 and 107, respectively.
In the preterm group, these scores rose with increasing gestational age at birth, so that cognitive scores were 2.5 points higher for every additional week of gestational age, language scores were 3.6 points higher for every additional week, and motor scores were 2.5 points higher for every additional week.
Overall, even though prematurity had a "large" impact on neurodevelopmental outcomes, most extremely preterm children emerged with no or only mild disability.
"These results are relevant for clinicians counseling families facing extremely preterm birth," Dr. Serenius and his associates said.
This study was supported in part by the Swedish Research Council. No financial conflicts of interest were reported.
FROM JAMA
Major Finding: Forty-two percent of extremely preterm infants showed no neurodevelopmental disability as toddlers, and another 31% showed mild disability.
Data Source: A population-based prospective cohort study of neurodevelopmental disability in 2- to 3-year-olds in Sweden, including 456 who had been born extremely preterm and 701 who had been born at term.
Disclosures: This study was supported in part by the Swedish Research Council. No financial conflicts of interest were reported.
No correlation found between autism and Lyme disease
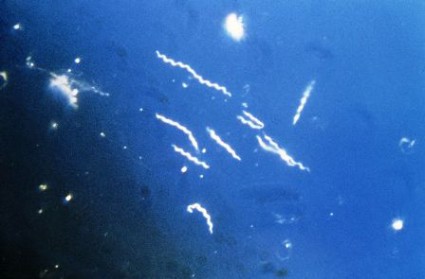
Neither children with autism nor unaffected control subjects showed serologic evidence of Lyme disease in a case-control study published May 1 in JAMA.
This finding refutes the idea proposed in 2008 linking Lyme disease with autism spectrum disorders. That theory "has garnered considerable attention," with researchers reporting that some autistic populations showed seropositivity rates of greater than 20% for the tick-borne disease.
The results of this case-control study involving 70 children with autism and 50 unaffected controls should lay that theory to rest. "[Our] study’s sample size was large enough to effectively rule out the suggested high rates of Lyme disease ... among [autistic] children," said Mary Ajamian of the department of medicine, Columbia University, New York, and her associates.
Ms. Ajamian and her colleagues reported their findings in a Research Letter to the Editor. They performed serologic testing for Lyme disease on two populations: 37 children aged 2-18 years who had autism and 27 unaffected siblings, all from the Autism Genetic Resource Exchange (AGRE); and 33 children with autism, 8 unaffected siblings, and 15 unrelated healthy control subjects from the Weill Cornell Autism Research Program (WCARP).
Subjects in the AGRE program resided chiefly in the northeastern and western United States, and their serum samples had been collected during 1999-2001 and stored. The WCARP subjects lived primarily in Connecticut, New Jersey, and New York, and their serum samples had been collected during 2010-2012 and stored.
Two serum samples from patients with culture-confirmed Lyme disease were used as positive controls.
The size of this study population would provide greater than 90% power to detect an association between Lyme disease and autism, based on the assumption that controls would have a prevalence of 1% or less of the infection and that cases would have the suggested prevalence of 20%.
None of the children with autism and none of the unaffected controls showed serologic evidence of Lyme disease by two-tier testing, Ms. Ajamian and her associates said (JAMA 2013;309:1771-3).
On ELISA testing, one child with autism tested positive for anti–Borrelia burgdorferi IgG, and four had borderline positive results for IgM. However, all were found to be negative on confirmatory Western blot testing.
Similarly, four of the control subjects tested positive for anti–B. burgdorferi IgG, one had borderline positive results for IgG, and one was positive for IgM. However, all were found to be negative on confirmatory Western blot testing.
Ms. Ajamian and her colleagues said one possible limitation of the study is the absence of information about the lifestyles of the patients and controls, including the amount of time they spent outdoors. The researchers also pointed out that their analysis did not address the question of whether Lyme disease might cause autism-like behavioral deficits.
This study was supported in part by the Department of Defense and the National Institutes of Health. Ms. Ajamian reported no financial conflicts of interest; her associates reported ties to Immunetics, Bio-Rad, DiaSorin, BioMerieux, Abbott, and Baxter.
Neither children with autism nor unaffected control subjects showed serologic evidence of Lyme disease in a case-control study published May 1 in JAMA.
This finding refutes the idea proposed in 2008 linking Lyme disease with autism spectrum disorders. That theory "has garnered considerable attention," with researchers reporting that some autistic populations showed seropositivity rates of greater than 20% for the tick-borne disease.
The results of this case-control study involving 70 children with autism and 50 unaffected controls should lay that theory to rest. "[Our] study’s sample size was large enough to effectively rule out the suggested high rates of Lyme disease ... among [autistic] children," said Mary Ajamian of the department of medicine, Columbia University, New York, and her associates.
Ms. Ajamian and her colleagues reported their findings in a Research Letter to the Editor. They performed serologic testing for Lyme disease on two populations: 37 children aged 2-18 years who had autism and 27 unaffected siblings, all from the Autism Genetic Resource Exchange (AGRE); and 33 children with autism, 8 unaffected siblings, and 15 unrelated healthy control subjects from the Weill Cornell Autism Research Program (WCARP).
Subjects in the AGRE program resided chiefly in the northeastern and western United States, and their serum samples had been collected during 1999-2001 and stored. The WCARP subjects lived primarily in Connecticut, New Jersey, and New York, and their serum samples had been collected during 2010-2012 and stored.
Two serum samples from patients with culture-confirmed Lyme disease were used as positive controls.
The size of this study population would provide greater than 90% power to detect an association between Lyme disease and autism, based on the assumption that controls would have a prevalence of 1% or less of the infection and that cases would have the suggested prevalence of 20%.
None of the children with autism and none of the unaffected controls showed serologic evidence of Lyme disease by two-tier testing, Ms. Ajamian and her associates said (JAMA 2013;309:1771-3).
On ELISA testing, one child with autism tested positive for anti–Borrelia burgdorferi IgG, and four had borderline positive results for IgM. However, all were found to be negative on confirmatory Western blot testing.
Similarly, four of the control subjects tested positive for anti–B. burgdorferi IgG, one had borderline positive results for IgG, and one was positive for IgM. However, all were found to be negative on confirmatory Western blot testing.
Ms. Ajamian and her colleagues said one possible limitation of the study is the absence of information about the lifestyles of the patients and controls, including the amount of time they spent outdoors. The researchers also pointed out that their analysis did not address the question of whether Lyme disease might cause autism-like behavioral deficits.
This study was supported in part by the Department of Defense and the National Institutes of Health. Ms. Ajamian reported no financial conflicts of interest; her associates reported ties to Immunetics, Bio-Rad, DiaSorin, BioMerieux, Abbott, and Baxter.
Neither children with autism nor unaffected control subjects showed serologic evidence of Lyme disease in a case-control study published May 1 in JAMA.
This finding refutes the idea proposed in 2008 linking Lyme disease with autism spectrum disorders. That theory "has garnered considerable attention," with researchers reporting that some autistic populations showed seropositivity rates of greater than 20% for the tick-borne disease.
The results of this case-control study involving 70 children with autism and 50 unaffected controls should lay that theory to rest. "[Our] study’s sample size was large enough to effectively rule out the suggested high rates of Lyme disease ... among [autistic] children," said Mary Ajamian of the department of medicine, Columbia University, New York, and her associates.
Ms. Ajamian and her colleagues reported their findings in a Research Letter to the Editor. They performed serologic testing for Lyme disease on two populations: 37 children aged 2-18 years who had autism and 27 unaffected siblings, all from the Autism Genetic Resource Exchange (AGRE); and 33 children with autism, 8 unaffected siblings, and 15 unrelated healthy control subjects from the Weill Cornell Autism Research Program (WCARP).
Subjects in the AGRE program resided chiefly in the northeastern and western United States, and their serum samples had been collected during 1999-2001 and stored. The WCARP subjects lived primarily in Connecticut, New Jersey, and New York, and their serum samples had been collected during 2010-2012 and stored.
Two serum samples from patients with culture-confirmed Lyme disease were used as positive controls.
The size of this study population would provide greater than 90% power to detect an association between Lyme disease and autism, based on the assumption that controls would have a prevalence of 1% or less of the infection and that cases would have the suggested prevalence of 20%.
None of the children with autism and none of the unaffected controls showed serologic evidence of Lyme disease by two-tier testing, Ms. Ajamian and her associates said (JAMA 2013;309:1771-3).
On ELISA testing, one child with autism tested positive for anti–Borrelia burgdorferi IgG, and four had borderline positive results for IgM. However, all were found to be negative on confirmatory Western blot testing.
Similarly, four of the control subjects tested positive for anti–B. burgdorferi IgG, one had borderline positive results for IgG, and one was positive for IgM. However, all were found to be negative on confirmatory Western blot testing.
Ms. Ajamian and her colleagues said one possible limitation of the study is the absence of information about the lifestyles of the patients and controls, including the amount of time they spent outdoors. The researchers also pointed out that their analysis did not address the question of whether Lyme disease might cause autism-like behavioral deficits.
This study was supported in part by the Department of Defense and the National Institutes of Health. Ms. Ajamian reported no financial conflicts of interest; her associates reported ties to Immunetics, Bio-Rad, DiaSorin, BioMerieux, Abbott, and Baxter.
FROM JAMA
Major Finding: The rate of seropositivity for Lyme disease was 0% in children with autism and 0% in unaffected controls.
Data Source: A case-control study involving two-tiered serologic testing of samples from 70 children with autism and 50 unaffected control subjects.
Disclosures: This study was supported in part by the Department of Defense and the National Institutes of Health. Ms. Ajamian reported no financial conflicts of interest. Her associates reported ties to Immunetics, Bio-Rad, DiaSorin, BioMerieux, Abbott, and Baxter.
USPSTF: Screen All Patients Aged 15-65 for HIV
All patients aged 15-65 years should be screened for HIV, regardless of their risk level, according to updated recommendations of the U.S. Preventive Services Task Force published online April 30 in the Annals of Internal Medicine.
The new strategy will substantially decrease the HIV disease burden across the country, dramatically reduce transmission of the virus, and markedly curtail infected patients’ progression to AIDS and death, said Dr. Virginia A. Moyer, chair of the USPSTF and professor of pediatrics at Baylor University and Texas Children’s Hospital, Houston, and her associates.
In its last set of HIV screening recommendations, issued in 2005, the USPSTF advised screening only at-risk patients. At that time, the task force cautioned that testing of the general population would cause undue psychological harm and that treatment before symptom onset would expose patients to serious adverse effects without exerting enough benefit to outweigh that disadvantage.
But 8 years later, new, convincing evidence shows "with high certainty" that identifying and treating HIV infection in asymptomatic people will substantially benefit public health as well as the health of those individual patients.
This change in screening recommendations is "of critical significance," because it brings the USPSTF into line with the Centers for Disease Control and Prevention on the issue of HIV screening, Dr. Moupali Das and Dr. Paul Volberding said in an editorial accompanying the new recommendations.
"Now, with an increasing consensus on population-wide screening, a growing belief in universal treatment, and the goal of near-universal access to medical care under the Affordable Care Act, we may ultimately awaken from the nightmare of the HIV/AIDS epidemic," Dr. Das and Dr. Volberding noted.
Three key research findings drove the task force to update HIV screening guidelines.
First, it is now known that 20% of people infected with HIV are not aware that they are infected. That means an estimated 236,400 people in the United States don’t know that they should take precautions against transmitting the virus and begin treatment to limit HIV-related illness and end-organ damage, Dr. Moyer and her colleagues said (Ann. Intern. Med. 2013 [doi:10.7326/0003-4819-159-1-201307020-00645]).
Second, it has been proved that initiation of antiretroviral therapy before carriers become symptomatic – when CD4 counts are between 0.200 and 0.500 x 109 cells/L – markedly reduces progression to AIDS and death.
"Hesitation in screening diminishes with the acceptance of HIV infection as a chronic disease that can be controlled by increasingly potent, convenient, and safe drugs," Dr. Das and Dr. Volberding said in their editorial (Ann. Intern. Med. 2013 [doi:10.7326/0003-4819-159-1-201307020-00643]).
And third, the overall harms of screening the general population and treating those who are found to be HIV-positive are now considered "small." Both conventional and rapid screening tests are highly accurate, with sensitivities and specificities topping 99.5% – so the potential harms of false-negative and false-positive results are minimal. And treatment is highly effective, with benefits clearly outweighing adverse effects, Dr. Moyer and her associates said.
Accordingly, the USPSTF now recommends HIV screening for adolescents as young as 15 years and adults as old as 65 years, regardless of their risk status. And HIV screening remains advisable for patients of any age who are at risk.
The USPSTF also renewed its recommendation that all pregnant women should be screened for HIV, because identification and treatment "dramatically reduces the rate of mother-to-child transmission." Women screened during a previous pregnancy should be rescreened with every subsequent pregnancy.
"Both of these major U.S. treatment guidelines [the USPSTF’s and the CDC’s] now agree that all infected persons should be offered antiretroviral therapy ... to enable a more complete immune reconstitution with the goal of achieving a near-normal lifespan," said Dr. Das of the University of San Francisco and Dr. Volberding of the University of California San Francisco AIDS Research Institute. "Making an early diagnosis by screening asymptomatic persons is thus a vitally important entry into life-extending management."
The evidence is insufficient to establish what the optimal interval should be between screenings. However, it is "reasonable" to rescreen at-risk people at 1-year intervals. This includes patients who engage in high-risk behaviors and those who live in or receive medical care in high-prevalence settings such as correctional facilities, homeless shelters, TB clinics, sexually transmitted infection clinics, and clinics that serve men who have sex with men.
In addition, "the USPSTF concurs with the CDC’s recommendation that HIV screening should be voluntary and done only with the patient’s knowledge and understanding." Both organizations recommend that patients be fully informed about HIV infection and the meaning of test results and that they be screened unless they specifically decline (opt out of) HIV testing.
Although funded by the Agency for Healthcare Research and Quality under a congressional mandate, the USPSTF is a voluntary group of clinicians and public health experts that is independent of the federal government and compiles recommendations about preventive care for a range of health conditions.
Dr. Moyer and her associates reported no financial conflicts of interest. Dr. Das and Dr. Volberding also reported no financial conflicts of interest.
All patients aged 15-65 years should be screened for HIV, regardless of their risk level, according to updated recommendations of the U.S. Preventive Services Task Force published online April 30 in the Annals of Internal Medicine.
The new strategy will substantially decrease the HIV disease burden across the country, dramatically reduce transmission of the virus, and markedly curtail infected patients’ progression to AIDS and death, said Dr. Virginia A. Moyer, chair of the USPSTF and professor of pediatrics at Baylor University and Texas Children’s Hospital, Houston, and her associates.
In its last set of HIV screening recommendations, issued in 2005, the USPSTF advised screening only at-risk patients. At that time, the task force cautioned that testing of the general population would cause undue psychological harm and that treatment before symptom onset would expose patients to serious adverse effects without exerting enough benefit to outweigh that disadvantage.
But 8 years later, new, convincing evidence shows "with high certainty" that identifying and treating HIV infection in asymptomatic people will substantially benefit public health as well as the health of those individual patients.
This change in screening recommendations is "of critical significance," because it brings the USPSTF into line with the Centers for Disease Control and Prevention on the issue of HIV screening, Dr. Moupali Das and Dr. Paul Volberding said in an editorial accompanying the new recommendations.
"Now, with an increasing consensus on population-wide screening, a growing belief in universal treatment, and the goal of near-universal access to medical care under the Affordable Care Act, we may ultimately awaken from the nightmare of the HIV/AIDS epidemic," Dr. Das and Dr. Volberding noted.
Three key research findings drove the task force to update HIV screening guidelines.
First, it is now known that 20% of people infected with HIV are not aware that they are infected. That means an estimated 236,400 people in the United States don’t know that they should take precautions against transmitting the virus and begin treatment to limit HIV-related illness and end-organ damage, Dr. Moyer and her colleagues said (Ann. Intern. Med. 2013 [doi:10.7326/0003-4819-159-1-201307020-00645]).
Second, it has been proved that initiation of antiretroviral therapy before carriers become symptomatic – when CD4 counts are between 0.200 and 0.500 x 109 cells/L – markedly reduces progression to AIDS and death.
"Hesitation in screening diminishes with the acceptance of HIV infection as a chronic disease that can be controlled by increasingly potent, convenient, and safe drugs," Dr. Das and Dr. Volberding said in their editorial (Ann. Intern. Med. 2013 [doi:10.7326/0003-4819-159-1-201307020-00643]).
And third, the overall harms of screening the general population and treating those who are found to be HIV-positive are now considered "small." Both conventional and rapid screening tests are highly accurate, with sensitivities and specificities topping 99.5% – so the potential harms of false-negative and false-positive results are minimal. And treatment is highly effective, with benefits clearly outweighing adverse effects, Dr. Moyer and her associates said.
Accordingly, the USPSTF now recommends HIV screening for adolescents as young as 15 years and adults as old as 65 years, regardless of their risk status. And HIV screening remains advisable for patients of any age who are at risk.
The USPSTF also renewed its recommendation that all pregnant women should be screened for HIV, because identification and treatment "dramatically reduces the rate of mother-to-child transmission." Women screened during a previous pregnancy should be rescreened with every subsequent pregnancy.
"Both of these major U.S. treatment guidelines [the USPSTF’s and the CDC’s] now agree that all infected persons should be offered antiretroviral therapy ... to enable a more complete immune reconstitution with the goal of achieving a near-normal lifespan," said Dr. Das of the University of San Francisco and Dr. Volberding of the University of California San Francisco AIDS Research Institute. "Making an early diagnosis by screening asymptomatic persons is thus a vitally important entry into life-extending management."
The evidence is insufficient to establish what the optimal interval should be between screenings. However, it is "reasonable" to rescreen at-risk people at 1-year intervals. This includes patients who engage in high-risk behaviors and those who live in or receive medical care in high-prevalence settings such as correctional facilities, homeless shelters, TB clinics, sexually transmitted infection clinics, and clinics that serve men who have sex with men.
In addition, "the USPSTF concurs with the CDC’s recommendation that HIV screening should be voluntary and done only with the patient’s knowledge and understanding." Both organizations recommend that patients be fully informed about HIV infection and the meaning of test results and that they be screened unless they specifically decline (opt out of) HIV testing.
Although funded by the Agency for Healthcare Research and Quality under a congressional mandate, the USPSTF is a voluntary group of clinicians and public health experts that is independent of the federal government and compiles recommendations about preventive care for a range of health conditions.
Dr. Moyer and her associates reported no financial conflicts of interest. Dr. Das and Dr. Volberding also reported no financial conflicts of interest.
All patients aged 15-65 years should be screened for HIV, regardless of their risk level, according to updated recommendations of the U.S. Preventive Services Task Force published online April 30 in the Annals of Internal Medicine.
The new strategy will substantially decrease the HIV disease burden across the country, dramatically reduce transmission of the virus, and markedly curtail infected patients’ progression to AIDS and death, said Dr. Virginia A. Moyer, chair of the USPSTF and professor of pediatrics at Baylor University and Texas Children’s Hospital, Houston, and her associates.
In its last set of HIV screening recommendations, issued in 2005, the USPSTF advised screening only at-risk patients. At that time, the task force cautioned that testing of the general population would cause undue psychological harm and that treatment before symptom onset would expose patients to serious adverse effects without exerting enough benefit to outweigh that disadvantage.
But 8 years later, new, convincing evidence shows "with high certainty" that identifying and treating HIV infection in asymptomatic people will substantially benefit public health as well as the health of those individual patients.
This change in screening recommendations is "of critical significance," because it brings the USPSTF into line with the Centers for Disease Control and Prevention on the issue of HIV screening, Dr. Moupali Das and Dr. Paul Volberding said in an editorial accompanying the new recommendations.
"Now, with an increasing consensus on population-wide screening, a growing belief in universal treatment, and the goal of near-universal access to medical care under the Affordable Care Act, we may ultimately awaken from the nightmare of the HIV/AIDS epidemic," Dr. Das and Dr. Volberding noted.
Three key research findings drove the task force to update HIV screening guidelines.
First, it is now known that 20% of people infected with HIV are not aware that they are infected. That means an estimated 236,400 people in the United States don’t know that they should take precautions against transmitting the virus and begin treatment to limit HIV-related illness and end-organ damage, Dr. Moyer and her colleagues said (Ann. Intern. Med. 2013 [doi:10.7326/0003-4819-159-1-201307020-00645]).
Second, it has been proved that initiation of antiretroviral therapy before carriers become symptomatic – when CD4 counts are between 0.200 and 0.500 x 109 cells/L – markedly reduces progression to AIDS and death.
"Hesitation in screening diminishes with the acceptance of HIV infection as a chronic disease that can be controlled by increasingly potent, convenient, and safe drugs," Dr. Das and Dr. Volberding said in their editorial (Ann. Intern. Med. 2013 [doi:10.7326/0003-4819-159-1-201307020-00643]).
And third, the overall harms of screening the general population and treating those who are found to be HIV-positive are now considered "small." Both conventional and rapid screening tests are highly accurate, with sensitivities and specificities topping 99.5% – so the potential harms of false-negative and false-positive results are minimal. And treatment is highly effective, with benefits clearly outweighing adverse effects, Dr. Moyer and her associates said.
Accordingly, the USPSTF now recommends HIV screening for adolescents as young as 15 years and adults as old as 65 years, regardless of their risk status. And HIV screening remains advisable for patients of any age who are at risk.
The USPSTF also renewed its recommendation that all pregnant women should be screened for HIV, because identification and treatment "dramatically reduces the rate of mother-to-child transmission." Women screened during a previous pregnancy should be rescreened with every subsequent pregnancy.
"Both of these major U.S. treatment guidelines [the USPSTF’s and the CDC’s] now agree that all infected persons should be offered antiretroviral therapy ... to enable a more complete immune reconstitution with the goal of achieving a near-normal lifespan," said Dr. Das of the University of San Francisco and Dr. Volberding of the University of California San Francisco AIDS Research Institute. "Making an early diagnosis by screening asymptomatic persons is thus a vitally important entry into life-extending management."
The evidence is insufficient to establish what the optimal interval should be between screenings. However, it is "reasonable" to rescreen at-risk people at 1-year intervals. This includes patients who engage in high-risk behaviors and those who live in or receive medical care in high-prevalence settings such as correctional facilities, homeless shelters, TB clinics, sexually transmitted infection clinics, and clinics that serve men who have sex with men.
In addition, "the USPSTF concurs with the CDC’s recommendation that HIV screening should be voluntary and done only with the patient’s knowledge and understanding." Both organizations recommend that patients be fully informed about HIV infection and the meaning of test results and that they be screened unless they specifically decline (opt out of) HIV testing.
Although funded by the Agency for Healthcare Research and Quality under a congressional mandate, the USPSTF is a voluntary group of clinicians and public health experts that is independent of the federal government and compiles recommendations about preventive care for a range of health conditions.
Dr. Moyer and her associates reported no financial conflicts of interest. Dr. Das and Dr. Volberding also reported no financial conflicts of interest.
FROM THE ANNALS OF INTERNAL MEDICINE
Diabetes care has improved but still falls short
Adults with diabetes made substantial gains since 1999 in adherence to preventive practices and in control of risk factors for diabetic complications, according to a report published online April 25 in the New England Journal of Medicine.
However, up to half of these patients still failed to meet targets for glycemic control, blood pressure, and lipid control, and approximately half reported that they never received diabetes education, usually neglected getting the recommended yearly vaccinations, and failed to get the recommended annual dental and eye examinations, said Dr. Mohammed K. Ali of the Centers for Disease Control and Prevention, Atlanta, and his associates (N. Engl. J. Med. 2013;368:1613-24).
The investigators examined changes over time in diabetes care by analyzing data from a series of National Health and Nutrition Examination Surveys (NHANES 1999-2002, 2003-2006, and 2007-2010) and Behavioral Risk Factor Surveillance System surveys (2000, 2004, and 2008). Both sets of surveys include nationally representative samples of the population, and both also rely on self-reports of health-related behavior.
For this study, Dr. Ali and his colleagues included data from 3,355 NHANES participants and 97,310 BRFSS participants who reported having diabetes.
Between the earliest (1999-2002) and the most recent (2007-2010) survey, the proportion of patients with poor glycemic control decreased by 5.8 percentage points, while the proportion who met recommended targets for glycated hemoglobin level, blood pressure, and LDL cholesterol levels rose substantially (by 7.9, 11.7, and 20.8 percentage points, respectively).
Similarly, the population distributions of glycated hemoglobin levels, LDL cholesterol levels, and blood pressure levels all improved significantly over time. The mean glycated hemoglobin levels dropped by 0.4 percentage points, and the mean LDL cholesterol level declined by 17.7 mg/dL, to 99.5 mg/dL. The mean blood pressure decreased by 4/2 mm Hg, to 130/68 mm Hg.
At the same time, the proportion of adults with diabetes who were free of microalbuminuria rose by 4.0 percentage points, and the 10-year risk of coronary heart disease dropped significantly by 2.8 percentage points.
However, up to half of the diabetes patients in the most recent surveys still failed to meet targets for glycated hemoglobin level, blood pressure, or LDL cholesterol levels, and more than 22% still smoked. Only 14.3% of the survey participants met the targets for all four risk factors, the investigators said.
Only 22.4% of the respondents got their annual flu vaccines, annual eye exams, and annual foot exams as recommended.
When the data were analyzed by patient age, younger adults with diabetes (those aged 44 years and younger) showed no improvements in meeting their treatment goals or in following preventive recommendations. The reason for this lack of improvement isn’t clear, but the finding "suggests that younger adults with diabetes need further attention," Dr. Ali and his associates said.
Respondents with limited access to health care and those of lower socioeconomic status were more likely than others to have suboptimal control of risk factors throughout the study period.
"Our findings concur with previous reports: Health insurance coverage was significantly and consistently associated with better, more improved risk-factor profiles and preventive practices during the 12 years examined in our study," the investigators noted.
"Unfortunately, the proportion of persons with diabetes who do not have health insurance has remained the same, despite increases in mean income and educational level over the study period," they concluded.
No financial conflicts of interest were reported.
There is reason to celebrate the improvements in achieving glycemic, blood-pressure, and lipid targets documented in the study by Dr. Ali and his colleagues, but the data also show "there’s a long way to go to deliver the quality of diabetes care that truly meets our patients’ needs," according to Dr. Graham T. McMahon and Dr. Robert G. Dluhy.
"The next wave of improvement in the delivery of diabetes care will probably come through intensive quality improvement and a movement away from episodic care toward the chronic care model and panel management," they predicted.
Incentive systems for clinicians that reward incremental improvement, not just the achievement of target goals, would be helpful. Such incentives may be financial, but others, such as public profiling "or the provision of credits in a program that allows continuous maintenance of certification, may also be motivational," they added.
Dr. McMahon and Dr. Dluhy are in the division of endocrinology, diabetes, and hypertension at Brigham and Women’s Hospital, Boston. Dr. McMahon is the medical education editor at the New England Journal of Medicine, and Dr. Dluhy is an associate editor at the journal. They reported no other financial conflicts of interest. These remarks were taken from their editorial accompanying Dr. Ali’s report (N. Engl. J. Med. 2013;368:1650-1).
There is reason to celebrate the improvements in achieving glycemic, blood-pressure, and lipid targets documented in the study by Dr. Ali and his colleagues, but the data also show "there’s a long way to go to deliver the quality of diabetes care that truly meets our patients’ needs," according to Dr. Graham T. McMahon and Dr. Robert G. Dluhy.
"The next wave of improvement in the delivery of diabetes care will probably come through intensive quality improvement and a movement away from episodic care toward the chronic care model and panel management," they predicted.
Incentive systems for clinicians that reward incremental improvement, not just the achievement of target goals, would be helpful. Such incentives may be financial, but others, such as public profiling "or the provision of credits in a program that allows continuous maintenance of certification, may also be motivational," they added.
Dr. McMahon and Dr. Dluhy are in the division of endocrinology, diabetes, and hypertension at Brigham and Women’s Hospital, Boston. Dr. McMahon is the medical education editor at the New England Journal of Medicine, and Dr. Dluhy is an associate editor at the journal. They reported no other financial conflicts of interest. These remarks were taken from their editorial accompanying Dr. Ali’s report (N. Engl. J. Med. 2013;368:1650-1).
There is reason to celebrate the improvements in achieving glycemic, blood-pressure, and lipid targets documented in the study by Dr. Ali and his colleagues, but the data also show "there’s a long way to go to deliver the quality of diabetes care that truly meets our patients’ needs," according to Dr. Graham T. McMahon and Dr. Robert G. Dluhy.
"The next wave of improvement in the delivery of diabetes care will probably come through intensive quality improvement and a movement away from episodic care toward the chronic care model and panel management," they predicted.
Incentive systems for clinicians that reward incremental improvement, not just the achievement of target goals, would be helpful. Such incentives may be financial, but others, such as public profiling "or the provision of credits in a program that allows continuous maintenance of certification, may also be motivational," they added.
Dr. McMahon and Dr. Dluhy are in the division of endocrinology, diabetes, and hypertension at Brigham and Women’s Hospital, Boston. Dr. McMahon is the medical education editor at the New England Journal of Medicine, and Dr. Dluhy is an associate editor at the journal. They reported no other financial conflicts of interest. These remarks were taken from their editorial accompanying Dr. Ali’s report (N. Engl. J. Med. 2013;368:1650-1).
Adults with diabetes made substantial gains since 1999 in adherence to preventive practices and in control of risk factors for diabetic complications, according to a report published online April 25 in the New England Journal of Medicine.
However, up to half of these patients still failed to meet targets for glycemic control, blood pressure, and lipid control, and approximately half reported that they never received diabetes education, usually neglected getting the recommended yearly vaccinations, and failed to get the recommended annual dental and eye examinations, said Dr. Mohammed K. Ali of the Centers for Disease Control and Prevention, Atlanta, and his associates (N. Engl. J. Med. 2013;368:1613-24).
The investigators examined changes over time in diabetes care by analyzing data from a series of National Health and Nutrition Examination Surveys (NHANES 1999-2002, 2003-2006, and 2007-2010) and Behavioral Risk Factor Surveillance System surveys (2000, 2004, and 2008). Both sets of surveys include nationally representative samples of the population, and both also rely on self-reports of health-related behavior.
For this study, Dr. Ali and his colleagues included data from 3,355 NHANES participants and 97,310 BRFSS participants who reported having diabetes.
Between the earliest (1999-2002) and the most recent (2007-2010) survey, the proportion of patients with poor glycemic control decreased by 5.8 percentage points, while the proportion who met recommended targets for glycated hemoglobin level, blood pressure, and LDL cholesterol levels rose substantially (by 7.9, 11.7, and 20.8 percentage points, respectively).
Similarly, the population distributions of glycated hemoglobin levels, LDL cholesterol levels, and blood pressure levels all improved significantly over time. The mean glycated hemoglobin levels dropped by 0.4 percentage points, and the mean LDL cholesterol level declined by 17.7 mg/dL, to 99.5 mg/dL. The mean blood pressure decreased by 4/2 mm Hg, to 130/68 mm Hg.
At the same time, the proportion of adults with diabetes who were free of microalbuminuria rose by 4.0 percentage points, and the 10-year risk of coronary heart disease dropped significantly by 2.8 percentage points.
However, up to half of the diabetes patients in the most recent surveys still failed to meet targets for glycated hemoglobin level, blood pressure, or LDL cholesterol levels, and more than 22% still smoked. Only 14.3% of the survey participants met the targets for all four risk factors, the investigators said.
Only 22.4% of the respondents got their annual flu vaccines, annual eye exams, and annual foot exams as recommended.
When the data were analyzed by patient age, younger adults with diabetes (those aged 44 years and younger) showed no improvements in meeting their treatment goals or in following preventive recommendations. The reason for this lack of improvement isn’t clear, but the finding "suggests that younger adults with diabetes need further attention," Dr. Ali and his associates said.
Respondents with limited access to health care and those of lower socioeconomic status were more likely than others to have suboptimal control of risk factors throughout the study period.
"Our findings concur with previous reports: Health insurance coverage was significantly and consistently associated with better, more improved risk-factor profiles and preventive practices during the 12 years examined in our study," the investigators noted.
"Unfortunately, the proportion of persons with diabetes who do not have health insurance has remained the same, despite increases in mean income and educational level over the study period," they concluded.
No financial conflicts of interest were reported.
Adults with diabetes made substantial gains since 1999 in adherence to preventive practices and in control of risk factors for diabetic complications, according to a report published online April 25 in the New England Journal of Medicine.
However, up to half of these patients still failed to meet targets for glycemic control, blood pressure, and lipid control, and approximately half reported that they never received diabetes education, usually neglected getting the recommended yearly vaccinations, and failed to get the recommended annual dental and eye examinations, said Dr. Mohammed K. Ali of the Centers for Disease Control and Prevention, Atlanta, and his associates (N. Engl. J. Med. 2013;368:1613-24).
The investigators examined changes over time in diabetes care by analyzing data from a series of National Health and Nutrition Examination Surveys (NHANES 1999-2002, 2003-2006, and 2007-2010) and Behavioral Risk Factor Surveillance System surveys (2000, 2004, and 2008). Both sets of surveys include nationally representative samples of the population, and both also rely on self-reports of health-related behavior.
For this study, Dr. Ali and his colleagues included data from 3,355 NHANES participants and 97,310 BRFSS participants who reported having diabetes.
Between the earliest (1999-2002) and the most recent (2007-2010) survey, the proportion of patients with poor glycemic control decreased by 5.8 percentage points, while the proportion who met recommended targets for glycated hemoglobin level, blood pressure, and LDL cholesterol levels rose substantially (by 7.9, 11.7, and 20.8 percentage points, respectively).
Similarly, the population distributions of glycated hemoglobin levels, LDL cholesterol levels, and blood pressure levels all improved significantly over time. The mean glycated hemoglobin levels dropped by 0.4 percentage points, and the mean LDL cholesterol level declined by 17.7 mg/dL, to 99.5 mg/dL. The mean blood pressure decreased by 4/2 mm Hg, to 130/68 mm Hg.
At the same time, the proportion of adults with diabetes who were free of microalbuminuria rose by 4.0 percentage points, and the 10-year risk of coronary heart disease dropped significantly by 2.8 percentage points.
However, up to half of the diabetes patients in the most recent surveys still failed to meet targets for glycated hemoglobin level, blood pressure, or LDL cholesterol levels, and more than 22% still smoked. Only 14.3% of the survey participants met the targets for all four risk factors, the investigators said.
Only 22.4% of the respondents got their annual flu vaccines, annual eye exams, and annual foot exams as recommended.
When the data were analyzed by patient age, younger adults with diabetes (those aged 44 years and younger) showed no improvements in meeting their treatment goals or in following preventive recommendations. The reason for this lack of improvement isn’t clear, but the finding "suggests that younger adults with diabetes need further attention," Dr. Ali and his associates said.
Respondents with limited access to health care and those of lower socioeconomic status were more likely than others to have suboptimal control of risk factors throughout the study period.
"Our findings concur with previous reports: Health insurance coverage was significantly and consistently associated with better, more improved risk-factor profiles and preventive practices during the 12 years examined in our study," the investigators noted.
"Unfortunately, the proportion of persons with diabetes who do not have health insurance has remained the same, despite increases in mean income and educational level over the study period," they concluded.
No financial conflicts of interest were reported.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: The proportion of adults with diabetes who met recommended targets for glycated hemoglobin levels, blood pressure, and LDL cholesterol levels rose substantially (by 7.9, 11.7, and 20.8 percentage points, respectively) between 1999 and 2010.
Data Source: An analysis of cross-sectional data on 3,355 NHANES and 97,310 BRFSS participants with diabetes who were surveyed between 1999 and 2010.
Disclosures: No financial conflicts of interest were reported.
BLOCK-HF published: Biventricular pacing aids certain heart failure patients
Biventricular pacing is superior to conventional right ventricular pacing in patients who have atrioventricular block and left ventricular systolic dysfunction with mild to moderate heart failure, according to a study that was presented at the American Heart Association meeting last November and has now been published online April 24 in the New England Journal of Medicine.
In the industry-sponsored prospective randomized clinical trial, 691 patients at 58 medical centers in the United States and Canada were randomly assigned to receive right ventricular or biventricular pacing using a pacemaker or implantable cardioverter defibrillator (ICD), during an 8-year period, said Dr. Anne B. Curtis, professor and chair of the department of medicine at the University of Buffalo (N.Y.), and her associates.
After a mean follow-up of 37 months, the primary outcome – a composite of death from any cause, an urgent care visit for HF, or an increase of 15% or more in LV end-systolic volume index – occurred in 53.3% of the biventricular group, which was significantly lower than the 64.3% rate in the right ventricular group. This benefit was seen both in patients given a pacemaker and in those given an ICD, with the two devices exerting "a remarkably similar clinical effect" even though there was a marked difference in mean ejection fraction between pacemaker recipients and ICD recipients. This suggests that the benefit of biventricular pacing is not likely to be strongly related to EF, the investigators said (N. Engl. J. Med. 2013 April 24 [doi:10.1056/NEJMoa1210356]).
At the AHA meeting, study discussant Dr. Gerasimos S. Filippatos of the University of Athens said that the BLOCK-HF results would certainly lead to a reconsideration of current European Society of Cardiology and joint American College of Cardiology/AHA/Heart Rhythm Society guidelines for heart failure patients with heart block.
The authors noted that BLOCK-HF adds to the body of evidence suggesting that biventricular pacing in patients with AV block preserves systolic function." Dr. Curtis said while presenting the results in November that one of the key points of BLOCK-HF "was to look at whether or not putting patients through the added difficulty of implanting a biventricular pacing device has clear benefits – and the answer is yes."
This study was funded by Medtronic, which also provided the data collection and analysis. Dr. Curtis and her associates reported numerous ties to industry sources.
Biventricular pacing is superior to conventional right ventricular pacing in patients who have atrioventricular block and left ventricular systolic dysfunction with mild to moderate heart failure, according to a study that was presented at the American Heart Association meeting last November and has now been published online April 24 in the New England Journal of Medicine.
In the industry-sponsored prospective randomized clinical trial, 691 patients at 58 medical centers in the United States and Canada were randomly assigned to receive right ventricular or biventricular pacing using a pacemaker or implantable cardioverter defibrillator (ICD), during an 8-year period, said Dr. Anne B. Curtis, professor and chair of the department of medicine at the University of Buffalo (N.Y.), and her associates.
After a mean follow-up of 37 months, the primary outcome – a composite of death from any cause, an urgent care visit for HF, or an increase of 15% or more in LV end-systolic volume index – occurred in 53.3% of the biventricular group, which was significantly lower than the 64.3% rate in the right ventricular group. This benefit was seen both in patients given a pacemaker and in those given an ICD, with the two devices exerting "a remarkably similar clinical effect" even though there was a marked difference in mean ejection fraction between pacemaker recipients and ICD recipients. This suggests that the benefit of biventricular pacing is not likely to be strongly related to EF, the investigators said (N. Engl. J. Med. 2013 April 24 [doi:10.1056/NEJMoa1210356]).
At the AHA meeting, study discussant Dr. Gerasimos S. Filippatos of the University of Athens said that the BLOCK-HF results would certainly lead to a reconsideration of current European Society of Cardiology and joint American College of Cardiology/AHA/Heart Rhythm Society guidelines for heart failure patients with heart block.
The authors noted that BLOCK-HF adds to the body of evidence suggesting that biventricular pacing in patients with AV block preserves systolic function." Dr. Curtis said while presenting the results in November that one of the key points of BLOCK-HF "was to look at whether or not putting patients through the added difficulty of implanting a biventricular pacing device has clear benefits – and the answer is yes."
This study was funded by Medtronic, which also provided the data collection and analysis. Dr. Curtis and her associates reported numerous ties to industry sources.
Biventricular pacing is superior to conventional right ventricular pacing in patients who have atrioventricular block and left ventricular systolic dysfunction with mild to moderate heart failure, according to a study that was presented at the American Heart Association meeting last November and has now been published online April 24 in the New England Journal of Medicine.
In the industry-sponsored prospective randomized clinical trial, 691 patients at 58 medical centers in the United States and Canada were randomly assigned to receive right ventricular or biventricular pacing using a pacemaker or implantable cardioverter defibrillator (ICD), during an 8-year period, said Dr. Anne B. Curtis, professor and chair of the department of medicine at the University of Buffalo (N.Y.), and her associates.
After a mean follow-up of 37 months, the primary outcome – a composite of death from any cause, an urgent care visit for HF, or an increase of 15% or more in LV end-systolic volume index – occurred in 53.3% of the biventricular group, which was significantly lower than the 64.3% rate in the right ventricular group. This benefit was seen both in patients given a pacemaker and in those given an ICD, with the two devices exerting "a remarkably similar clinical effect" even though there was a marked difference in mean ejection fraction between pacemaker recipients and ICD recipients. This suggests that the benefit of biventricular pacing is not likely to be strongly related to EF, the investigators said (N. Engl. J. Med. 2013 April 24 [doi:10.1056/NEJMoa1210356]).
At the AHA meeting, study discussant Dr. Gerasimos S. Filippatos of the University of Athens said that the BLOCK-HF results would certainly lead to a reconsideration of current European Society of Cardiology and joint American College of Cardiology/AHA/Heart Rhythm Society guidelines for heart failure patients with heart block.
The authors noted that BLOCK-HF adds to the body of evidence suggesting that biventricular pacing in patients with AV block preserves systolic function." Dr. Curtis said while presenting the results in November that one of the key points of BLOCK-HF "was to look at whether or not putting patients through the added difficulty of implanting a biventricular pacing device has clear benefits – and the answer is yes."
This study was funded by Medtronic, which also provided the data collection and analysis. Dr. Curtis and her associates reported numerous ties to industry sources.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: The rate of death from any cause, an urgent care visit for HF, or an increase of 15% or more in LV end-systolic volume index occurred in 53.3% of the biventricular-pacing group, compared with 64.3% of the right ventricular–pacing group.
Data Source: A prospective multicenter randomized trial involving 349 patients assigned to biventricular and 342 assigned to conventional right ventricular pacing who were followed for a mean of 37 months.
Disclosures: This study was funded by Medtronic, which also provided the data collection and analysis. Dr. Curtis and her associates reported numerous ties to industry sources.
Perioperative beta-blockers cut 30-day mortality, cardiac morbidity
For patients at elevated cardiac risk who are undergoing major noncardiac surgery, early perioperative use of beta-blockers is associated with significantly lower 30-day all-cause mortality and cardiac morbidity, according to a report in the April 24 issue of JAMA.
In a retrospective cohort study, this association was strongest in the patients at highest cardiac risk – those with two or more factors on the six-item Cardiac Risk Index, said Dr. Martin J. London of the department of anesthesia and perioperative care, U.S. Department of Veterans Affairs Medical Center, San Francisco, and his associates.
Beta-blocker use in this setting remains controversial, and the use of perioperative beta-blockers has been declining, because of safety concerns. To examine whether high-risk patients are helped or harmed by the treatment, Dr. London and his colleagues analyzed data from the VA Surgical Quality Improvement Program database, a VA pharmacy database, and a VA administrative database.
They assessed the records of 136,745 patients who had vascular, general, neurologic, orthopedic, thoracic, urologic, or otolaryngologic surgery at 104 VA medical centers in 2005-2010.
A total of 40.3% of these subjects had received beta-blockers on the day of or the day after surgery, and 33.2% were given outpatient prescriptions for beta-blockers within 7 days of surgery.
There was a modest but significant decline in beta-blocker use during the 5-year study period, from 43.5% in the first year to 36.2% in the last. A similar national trend has been reported in previous studies. "This may be related to the findings of the POISE trial of increased stroke and death in treated patients, leading to more conservative guideline recommendations within this period," the investigators said.
They performed 1:1 propensity matching and identified 37,805 matched pairs of exposed and nonexposed patients for the primary outcome analysis. The primary outcome measure – all-cause mortality at 30 days – was significantly lower (relative risk 0.73) among patients who used beta-blockers than among those who did not, with a number needed to treat of 241 (JAMA 2013;309:1704-13).
The study subjects were categorized according to their scores on the revised Cardiac Risk Index, which includes six variables: high-risk surgery, cerebrovascular disease, ischemic heart disease, heart failure, diabetes, and renal insufficiency. Patients who had two or more of these CRI risk factors showed the greatest mortality benefit from perioperative beta-blocker therapy, with an relative risk of 0.63.
When the data were broken down by type of surgery, mortality remained significantly lower in beta-blocker users, compared with nonusers for every category except vascular surgery. In previous studies, beta-blockers have shown equivocal benefit in this same subgroup of surgery patients, Dr. London and his associates noted.
The secondary outcome measure of the study was a composite of Q-wave myocardial infarction or nonfatal cardiac arrest at 30 days. These may be rare complications but they are highly predictive of subsequent mortality, the researchers said.
Again, patients who took beta-blockers showed significantly less cardiac morbidity than those who did not, with a relative risk of 0.67 and a number needed to treat of 339.
The study results remained robust in a sensitivity analysis that categorized patients according to whether they had been taking beta-blockers before hospitalization, as well as in a sensitivity analysis that categorized patients as either acute or chronic users of beta-blockers.
This study confirmed the previous finding that withdrawal of beta-blockers within 30 days of surgery is associated with increased mortality. In this study, the risk of death was approximately doubled if beta-blockers were withdrawn perioperatively.
In a post hoc analysis, "we were unable to demonstrate significant associations of perioperative beta-blockade with the risk of postoperative stroke." There was no significant difference in stroke rates between patients who received beta-blockers and those who did not, Dr. London and his colleagues said.
This study was supported by a grant from the Anesthesia Patient Safety Foundation. Dr. London reported no financial conflicts of interest. An associate reported ties to Roche, Resverlogie, Anthera, and Sanofi.
For patients at elevated cardiac risk who are undergoing major noncardiac surgery, early perioperative use of beta-blockers is associated with significantly lower 30-day all-cause mortality and cardiac morbidity, according to a report in the April 24 issue of JAMA.
In a retrospective cohort study, this association was strongest in the patients at highest cardiac risk – those with two or more factors on the six-item Cardiac Risk Index, said Dr. Martin J. London of the department of anesthesia and perioperative care, U.S. Department of Veterans Affairs Medical Center, San Francisco, and his associates.
Beta-blocker use in this setting remains controversial, and the use of perioperative beta-blockers has been declining, because of safety concerns. To examine whether high-risk patients are helped or harmed by the treatment, Dr. London and his colleagues analyzed data from the VA Surgical Quality Improvement Program database, a VA pharmacy database, and a VA administrative database.
They assessed the records of 136,745 patients who had vascular, general, neurologic, orthopedic, thoracic, urologic, or otolaryngologic surgery at 104 VA medical centers in 2005-2010.
A total of 40.3% of these subjects had received beta-blockers on the day of or the day after surgery, and 33.2% were given outpatient prescriptions for beta-blockers within 7 days of surgery.
There was a modest but significant decline in beta-blocker use during the 5-year study period, from 43.5% in the first year to 36.2% in the last. A similar national trend has been reported in previous studies. "This may be related to the findings of the POISE trial of increased stroke and death in treated patients, leading to more conservative guideline recommendations within this period," the investigators said.
They performed 1:1 propensity matching and identified 37,805 matched pairs of exposed and nonexposed patients for the primary outcome analysis. The primary outcome measure – all-cause mortality at 30 days – was significantly lower (relative risk 0.73) among patients who used beta-blockers than among those who did not, with a number needed to treat of 241 (JAMA 2013;309:1704-13).
The study subjects were categorized according to their scores on the revised Cardiac Risk Index, which includes six variables: high-risk surgery, cerebrovascular disease, ischemic heart disease, heart failure, diabetes, and renal insufficiency. Patients who had two or more of these CRI risk factors showed the greatest mortality benefit from perioperative beta-blocker therapy, with an relative risk of 0.63.
When the data were broken down by type of surgery, mortality remained significantly lower in beta-blocker users, compared with nonusers for every category except vascular surgery. In previous studies, beta-blockers have shown equivocal benefit in this same subgroup of surgery patients, Dr. London and his associates noted.
The secondary outcome measure of the study was a composite of Q-wave myocardial infarction or nonfatal cardiac arrest at 30 days. These may be rare complications but they are highly predictive of subsequent mortality, the researchers said.
Again, patients who took beta-blockers showed significantly less cardiac morbidity than those who did not, with a relative risk of 0.67 and a number needed to treat of 339.
The study results remained robust in a sensitivity analysis that categorized patients according to whether they had been taking beta-blockers before hospitalization, as well as in a sensitivity analysis that categorized patients as either acute or chronic users of beta-blockers.
This study confirmed the previous finding that withdrawal of beta-blockers within 30 days of surgery is associated with increased mortality. In this study, the risk of death was approximately doubled if beta-blockers were withdrawn perioperatively.
In a post hoc analysis, "we were unable to demonstrate significant associations of perioperative beta-blockade with the risk of postoperative stroke." There was no significant difference in stroke rates between patients who received beta-blockers and those who did not, Dr. London and his colleagues said.
This study was supported by a grant from the Anesthesia Patient Safety Foundation. Dr. London reported no financial conflicts of interest. An associate reported ties to Roche, Resverlogie, Anthera, and Sanofi.
For patients at elevated cardiac risk who are undergoing major noncardiac surgery, early perioperative use of beta-blockers is associated with significantly lower 30-day all-cause mortality and cardiac morbidity, according to a report in the April 24 issue of JAMA.
In a retrospective cohort study, this association was strongest in the patients at highest cardiac risk – those with two or more factors on the six-item Cardiac Risk Index, said Dr. Martin J. London of the department of anesthesia and perioperative care, U.S. Department of Veterans Affairs Medical Center, San Francisco, and his associates.
Beta-blocker use in this setting remains controversial, and the use of perioperative beta-blockers has been declining, because of safety concerns. To examine whether high-risk patients are helped or harmed by the treatment, Dr. London and his colleagues analyzed data from the VA Surgical Quality Improvement Program database, a VA pharmacy database, and a VA administrative database.
They assessed the records of 136,745 patients who had vascular, general, neurologic, orthopedic, thoracic, urologic, or otolaryngologic surgery at 104 VA medical centers in 2005-2010.
A total of 40.3% of these subjects had received beta-blockers on the day of or the day after surgery, and 33.2% were given outpatient prescriptions for beta-blockers within 7 days of surgery.
There was a modest but significant decline in beta-blocker use during the 5-year study period, from 43.5% in the first year to 36.2% in the last. A similar national trend has been reported in previous studies. "This may be related to the findings of the POISE trial of increased stroke and death in treated patients, leading to more conservative guideline recommendations within this period," the investigators said.
They performed 1:1 propensity matching and identified 37,805 matched pairs of exposed and nonexposed patients for the primary outcome analysis. The primary outcome measure – all-cause mortality at 30 days – was significantly lower (relative risk 0.73) among patients who used beta-blockers than among those who did not, with a number needed to treat of 241 (JAMA 2013;309:1704-13).
The study subjects were categorized according to their scores on the revised Cardiac Risk Index, which includes six variables: high-risk surgery, cerebrovascular disease, ischemic heart disease, heart failure, diabetes, and renal insufficiency. Patients who had two or more of these CRI risk factors showed the greatest mortality benefit from perioperative beta-blocker therapy, with an relative risk of 0.63.
When the data were broken down by type of surgery, mortality remained significantly lower in beta-blocker users, compared with nonusers for every category except vascular surgery. In previous studies, beta-blockers have shown equivocal benefit in this same subgroup of surgery patients, Dr. London and his associates noted.
The secondary outcome measure of the study was a composite of Q-wave myocardial infarction or nonfatal cardiac arrest at 30 days. These may be rare complications but they are highly predictive of subsequent mortality, the researchers said.
Again, patients who took beta-blockers showed significantly less cardiac morbidity than those who did not, with a relative risk of 0.67 and a number needed to treat of 339.
The study results remained robust in a sensitivity analysis that categorized patients according to whether they had been taking beta-blockers before hospitalization, as well as in a sensitivity analysis that categorized patients as either acute or chronic users of beta-blockers.
This study confirmed the previous finding that withdrawal of beta-blockers within 30 days of surgery is associated with increased mortality. In this study, the risk of death was approximately doubled if beta-blockers were withdrawn perioperatively.
In a post hoc analysis, "we were unable to demonstrate significant associations of perioperative beta-blockade with the risk of postoperative stroke." There was no significant difference in stroke rates between patients who received beta-blockers and those who did not, Dr. London and his colleagues said.
This study was supported by a grant from the Anesthesia Patient Safety Foundation. Dr. London reported no financial conflicts of interest. An associate reported ties to Roche, Resverlogie, Anthera, and Sanofi.
FROM JAMA
Major finding: All-cause mortality at 30 days was significantly lower in high-risk patients who received perioperative beta-blockers than in those who did not, with an RR of 0.73.
Data source: A retrospective cohort study involving 136,745 VA patients undergoing noncardiac surgery during a 5-year period.
Disclosures: This study was supported by a grant from the Anesthesia Patient Safety Foundation. Dr. London reported no financial conflicts of interest. An associate reported ties to Roche, Resverlogie, Anthera, and Sanofi.
Alternative therapies may help lower blood pressure
Certain alternative approaches – notably aerobic exercise and resistance training – reduce blood pressure and can be considered adjunctive to standard dietary and medical therapies for hypertension, according to an American Heart Association scientific statement published April 22 in Hypertension.
The evidence supporting biofeedback techniques, isometric handgrip exercise, and device-guided slow breathing is not as strong, but these approaches also are likely effective at reducing blood pressure by a small amount. For other alternative therapies such as meditation, yoga, relaxation therapy, stress-reduction techniques, and acupuncture, the evidence to date is insufficient to support their use as adjunctive treatments for HT.
These are the main conclusions of the AHA scientific statement that aims to "provide an up-to-date assessment of the evidence supporting the blood pressure lowering efficacy of several alternative approaches." The statement also provides practical recommendations for clinicians to incorporate these alternative approaches into their practices, said Dr. Robert D. Brook, chair of the writing committee, and his associates.
They reviewed the literature published during the past 6 years and identified 124 studies of behavioral therapies, 105 of noninvasive procedures and devices, and 773 of exercise-based regimens for reducing blood pressure.
The overall quality of these studies was not good. Most were observational, and even the randomized clinical trials often were flawed by inadequate randomization methods, the use of suboptimal control groups, small sample sizes, and short follow-ups. Many of the reviewed studies also had selection, compliance, and other biases.
Overall, the committee found that "it is reasonable for all patients with BP levels higher than 120/80 mm Hg to consider a trial of alternative approaches as adjuvant methods to help lower BP." However, since no alternative modality can reliably decrease BP by 20/10 mm Hg or more, patients "who require this magnitude of BP reduction should employ alternative approaches only after they are first treated with appropriate pharmacologic strategies," according to the statement.
"It should also be emphasized that most alternative approaches reduce systolic BP only by 2-10 mm Hg. Hence, only a minority of patients will be successful in reaching goals using these treatment modalities alone when BP is 10/5 mm Hg above target."
Of all the alternative therapies, dynamic aerobic exercise was found to have the highest level of evidence that it decreases blood pressure, along with the greatest potential for improving other cardiovascular health factors such as lipid levels and glucose levels. "Numerous observational cohorts also suggest that aerobic exercise may reduce CV risk in a dose-dependent manner," Dr. Brook and his associates noted.
Therefore aerobic exercise "should be considered the primary alternative modality to help reduce BP," according to the statement.
Resistance training also had a high level of evidence that it lowers blood pressure, and also was associated with additional cardiovascular benefits, so it also is "highly recommended by our review." Most patients "should start with aerobic or resistance exercise (alone or together) as the first alternative approach unless contraindicated or they are unwilling or unable to exercise."
If this isn’t sufficiently effective, clinicians should next consider recommending device-guided deep breathing or isometric handgrip exercise. These two approaches had a greater weight of evidence supporting their efficacy and were more practical to use in a real-world setting than were the remaining alternative therapies, said Dr. Brook, associate professor of medicine at the University of Michigan, Ann Arbor, and his colleagues.
Biofeedback also is supported by a moderate level of evidence.
It is not yet established how long trials of various alternative therapies should be given before the clinician can decide whether they have been effective. "However, 3 months is a reasonable time frame given that most of the approaches reduced BP among the studies within this period, when they were effective," the investigators said.
Certain alternative approaches – notably aerobic exercise and resistance training – reduce blood pressure and can be considered adjunctive to standard dietary and medical therapies for hypertension, according to an American Heart Association scientific statement published April 22 in Hypertension.
The evidence supporting biofeedback techniques, isometric handgrip exercise, and device-guided slow breathing is not as strong, but these approaches also are likely effective at reducing blood pressure by a small amount. For other alternative therapies such as meditation, yoga, relaxation therapy, stress-reduction techniques, and acupuncture, the evidence to date is insufficient to support their use as adjunctive treatments for HT.
These are the main conclusions of the AHA scientific statement that aims to "provide an up-to-date assessment of the evidence supporting the blood pressure lowering efficacy of several alternative approaches." The statement also provides practical recommendations for clinicians to incorporate these alternative approaches into their practices, said Dr. Robert D. Brook, chair of the writing committee, and his associates.
They reviewed the literature published during the past 6 years and identified 124 studies of behavioral therapies, 105 of noninvasive procedures and devices, and 773 of exercise-based regimens for reducing blood pressure.
The overall quality of these studies was not good. Most were observational, and even the randomized clinical trials often were flawed by inadequate randomization methods, the use of suboptimal control groups, small sample sizes, and short follow-ups. Many of the reviewed studies also had selection, compliance, and other biases.
Overall, the committee found that "it is reasonable for all patients with BP levels higher than 120/80 mm Hg to consider a trial of alternative approaches as adjuvant methods to help lower BP." However, since no alternative modality can reliably decrease BP by 20/10 mm Hg or more, patients "who require this magnitude of BP reduction should employ alternative approaches only after they are first treated with appropriate pharmacologic strategies," according to the statement.
"It should also be emphasized that most alternative approaches reduce systolic BP only by 2-10 mm Hg. Hence, only a minority of patients will be successful in reaching goals using these treatment modalities alone when BP is 10/5 mm Hg above target."
Of all the alternative therapies, dynamic aerobic exercise was found to have the highest level of evidence that it decreases blood pressure, along with the greatest potential for improving other cardiovascular health factors such as lipid levels and glucose levels. "Numerous observational cohorts also suggest that aerobic exercise may reduce CV risk in a dose-dependent manner," Dr. Brook and his associates noted.
Therefore aerobic exercise "should be considered the primary alternative modality to help reduce BP," according to the statement.
Resistance training also had a high level of evidence that it lowers blood pressure, and also was associated with additional cardiovascular benefits, so it also is "highly recommended by our review." Most patients "should start with aerobic or resistance exercise (alone or together) as the first alternative approach unless contraindicated or they are unwilling or unable to exercise."
If this isn’t sufficiently effective, clinicians should next consider recommending device-guided deep breathing or isometric handgrip exercise. These two approaches had a greater weight of evidence supporting their efficacy and were more practical to use in a real-world setting than were the remaining alternative therapies, said Dr. Brook, associate professor of medicine at the University of Michigan, Ann Arbor, and his colleagues.
Biofeedback also is supported by a moderate level of evidence.
It is not yet established how long trials of various alternative therapies should be given before the clinician can decide whether they have been effective. "However, 3 months is a reasonable time frame given that most of the approaches reduced BP among the studies within this period, when they were effective," the investigators said.
Certain alternative approaches – notably aerobic exercise and resistance training – reduce blood pressure and can be considered adjunctive to standard dietary and medical therapies for hypertension, according to an American Heart Association scientific statement published April 22 in Hypertension.
The evidence supporting biofeedback techniques, isometric handgrip exercise, and device-guided slow breathing is not as strong, but these approaches also are likely effective at reducing blood pressure by a small amount. For other alternative therapies such as meditation, yoga, relaxation therapy, stress-reduction techniques, and acupuncture, the evidence to date is insufficient to support their use as adjunctive treatments for HT.
These are the main conclusions of the AHA scientific statement that aims to "provide an up-to-date assessment of the evidence supporting the blood pressure lowering efficacy of several alternative approaches." The statement also provides practical recommendations for clinicians to incorporate these alternative approaches into their practices, said Dr. Robert D. Brook, chair of the writing committee, and his associates.
They reviewed the literature published during the past 6 years and identified 124 studies of behavioral therapies, 105 of noninvasive procedures and devices, and 773 of exercise-based regimens for reducing blood pressure.
The overall quality of these studies was not good. Most were observational, and even the randomized clinical trials often were flawed by inadequate randomization methods, the use of suboptimal control groups, small sample sizes, and short follow-ups. Many of the reviewed studies also had selection, compliance, and other biases.
Overall, the committee found that "it is reasonable for all patients with BP levels higher than 120/80 mm Hg to consider a trial of alternative approaches as adjuvant methods to help lower BP." However, since no alternative modality can reliably decrease BP by 20/10 mm Hg or more, patients "who require this magnitude of BP reduction should employ alternative approaches only after they are first treated with appropriate pharmacologic strategies," according to the statement.
"It should also be emphasized that most alternative approaches reduce systolic BP only by 2-10 mm Hg. Hence, only a minority of patients will be successful in reaching goals using these treatment modalities alone when BP is 10/5 mm Hg above target."
Of all the alternative therapies, dynamic aerobic exercise was found to have the highest level of evidence that it decreases blood pressure, along with the greatest potential for improving other cardiovascular health factors such as lipid levels and glucose levels. "Numerous observational cohorts also suggest that aerobic exercise may reduce CV risk in a dose-dependent manner," Dr. Brook and his associates noted.
Therefore aerobic exercise "should be considered the primary alternative modality to help reduce BP," according to the statement.
Resistance training also had a high level of evidence that it lowers blood pressure, and also was associated with additional cardiovascular benefits, so it also is "highly recommended by our review." Most patients "should start with aerobic or resistance exercise (alone or together) as the first alternative approach unless contraindicated or they are unwilling or unable to exercise."
If this isn’t sufficiently effective, clinicians should next consider recommending device-guided deep breathing or isometric handgrip exercise. These two approaches had a greater weight of evidence supporting their efficacy and were more practical to use in a real-world setting than were the remaining alternative therapies, said Dr. Brook, associate professor of medicine at the University of Michigan, Ann Arbor, and his colleagues.
Biofeedback also is supported by a moderate level of evidence.
It is not yet established how long trials of various alternative therapies should be given before the clinician can decide whether they have been effective. "However, 3 months is a reasonable time frame given that most of the approaches reduced BP among the studies within this period, when they were effective," the investigators said.
FROM HYPERTENSION
Major Finding: Among several alternative therapies for decreasing blood pressure, aerobic exercise and resistance training are the two with the strongest evidence supporting their effectiveness.
Data Source: A review of the medical literature during the past 6 years regarding behavioral regimens (124 studies), noninvasive procedures and devices (105 studies), and exercise-based regimens (773 studies) for reducing blood pressure.
Disclosures: Funding sources and conflict-of-interest disclosures were not available.