User login
Lucas Franki is an associate editor for MDedge News, and has been with the company since 2014. He has a BA in English from Penn State University and is an Eagle Scout.
Mental health care becoming more accessible to teens
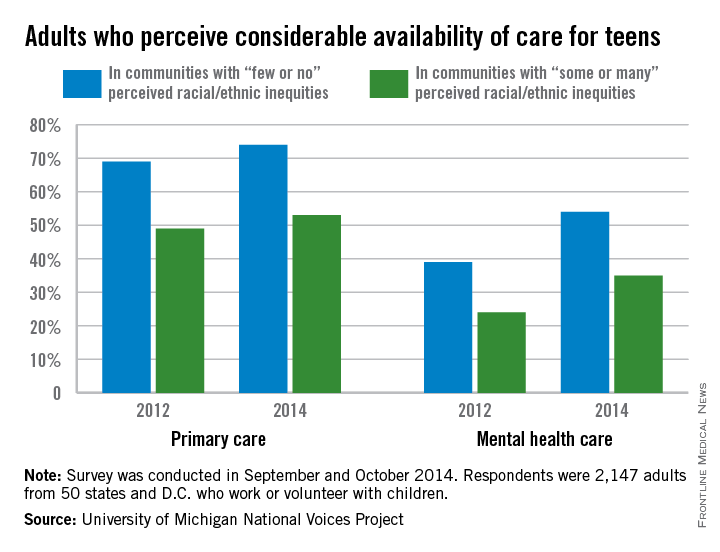
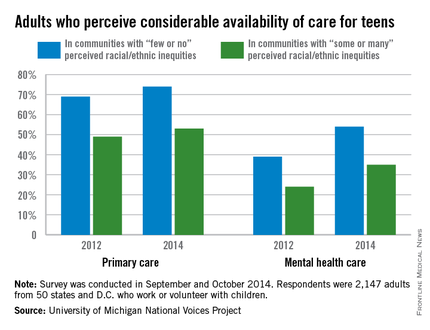
Although adult perception of the availability of mental health care for teenagers has increased significantly since 2012, availability was much lower in communities with perceived inequities, according to a report from the National Voices Project.
In communities where adults felt there were few or no racial/ethnic inequities, 54% believed there to be a considerable amount of mental health care available to teens in 2014, up from 39% in 2012. However, if adults felt their community had some or many racial/ethnic inequities, only 35% believed teens had a considerable amount of available mental health care in 2014, up from 24% in 2012.
Overall, 40% of American adults in 2014 felt there were many mental health care options available for teens, compared with 30% in 2012.
The number of adults who believed teens had many primary care options grew slightly from 2012 to 2014, but just as with mental health, there was a big difference between communities with little or no racial/ethnic inequity and those with some or many inequities. In communities with little or no inequity, 74% said there were many primary care options in 2014, compared with only 53% in communities with inequities.
“Mental health services are perceived as much less available than primary health care services for teens,” Dr. Matthew M. Davis, director of the National Voices Project, said in a written statement. “Given how common mental health concerns are among adolescents, improving access to behavioral services is as important as enhancing access to primary care.”
The data were collected by the University of Michigan 2014 National Voices Project Survey, commissioned by the W.K. Kellogg Foundation.
Although adult perception of the availability of mental health care for teenagers has increased significantly since 2012, availability was much lower in communities with perceived inequities, according to a report from the National Voices Project.
In communities where adults felt there were few or no racial/ethnic inequities, 54% believed there to be a considerable amount of mental health care available to teens in 2014, up from 39% in 2012. However, if adults felt their community had some or many racial/ethnic inequities, only 35% believed teens had a considerable amount of available mental health care in 2014, up from 24% in 2012.

Overall, 40% of American adults in 2014 felt there were many mental health care options available for teens, compared with 30% in 2012.
The number of adults who believed teens had many primary care options grew slightly from 2012 to 2014, but just as with mental health, there was a big difference between communities with little or no racial/ethnic inequity and those with some or many inequities. In communities with little or no inequity, 74% said there were many primary care options in 2014, compared with only 53% in communities with inequities.
“Mental health services are perceived as much less available than primary health care services for teens,” Dr. Matthew M. Davis, director of the National Voices Project, said in a written statement. “Given how common mental health concerns are among adolescents, improving access to behavioral services is as important as enhancing access to primary care.”
The data were collected by the University of Michigan 2014 National Voices Project Survey, commissioned by the W.K. Kellogg Foundation.
Although adult perception of the availability of mental health care for teenagers has increased significantly since 2012, availability was much lower in communities with perceived inequities, according to a report from the National Voices Project.
In communities where adults felt there were few or no racial/ethnic inequities, 54% believed there to be a considerable amount of mental health care available to teens in 2014, up from 39% in 2012. However, if adults felt their community had some or many racial/ethnic inequities, only 35% believed teens had a considerable amount of available mental health care in 2014, up from 24% in 2012.

Overall, 40% of American adults in 2014 felt there were many mental health care options available for teens, compared with 30% in 2012.
The number of adults who believed teens had many primary care options grew slightly from 2012 to 2014, but just as with mental health, there was a big difference between communities with little or no racial/ethnic inequity and those with some or many inequities. In communities with little or no inequity, 74% said there were many primary care options in 2014, compared with only 53% in communities with inequities.
“Mental health services are perceived as much less available than primary health care services for teens,” Dr. Matthew M. Davis, director of the National Voices Project, said in a written statement. “Given how common mental health concerns are among adolescents, improving access to behavioral services is as important as enhancing access to primary care.”
The data were collected by the University of Michigan 2014 National Voices Project Survey, commissioned by the W.K. Kellogg Foundation.
MDD, schizophrenia neurocognition dysfunction patterns differ
Distinctly different patterns of cognitive deficits are found between schizophrenia and nonpsychotic major depressive disorder, Dr. Shuo-En Hsu and associates reported.
They compared 30 drug-naive participants with schizophrenia, 30 with drug-naive nonpsychotic major depressive disorder (MDD), and 30 matched controls. People with schizophrenia scored significantly worse on the Wisconsin Card Sorting Test than those from the MDD group or the controls, making an average of 17 perseveration errors, about 50% more than the other groups, whose WCST scores were comparable. Patients in both the schizophrenia and MDD groups scored significantly worse than the control group on the Continuous Performance Test, said Dr. Hsu of the department of psychiatry at National Cheng Kung University Hospital in Tainan, Taiwan, and associates.
In contrast to the WCST, patients with MDD performed significantly worse on the Finger Tapping Test than did the schizophrenia or the control-group patients. Schizophrenia patients scored slightly worse than those in the control group, with an average score of about 43, compared with 47 in the control group and 38 in the MDD group.
“Further studies may focus on the qualitative differences between less heterogeneous patient groups; for example, drug-naive patients with schizophrenia and psychotic depression,” the investigators concluded.
Find the full study in the Journal of Affective Disorders (2015;175:133-8 doi:10.1016/j.jad.2014.12.059).
Distinctly different patterns of cognitive deficits are found between schizophrenia and nonpsychotic major depressive disorder, Dr. Shuo-En Hsu and associates reported.
They compared 30 drug-naive participants with schizophrenia, 30 with drug-naive nonpsychotic major depressive disorder (MDD), and 30 matched controls. People with schizophrenia scored significantly worse on the Wisconsin Card Sorting Test than those from the MDD group or the controls, making an average of 17 perseveration errors, about 50% more than the other groups, whose WCST scores were comparable. Patients in both the schizophrenia and MDD groups scored significantly worse than the control group on the Continuous Performance Test, said Dr. Hsu of the department of psychiatry at National Cheng Kung University Hospital in Tainan, Taiwan, and associates.
In contrast to the WCST, patients with MDD performed significantly worse on the Finger Tapping Test than did the schizophrenia or the control-group patients. Schizophrenia patients scored slightly worse than those in the control group, with an average score of about 43, compared with 47 in the control group and 38 in the MDD group.
“Further studies may focus on the qualitative differences between less heterogeneous patient groups; for example, drug-naive patients with schizophrenia and psychotic depression,” the investigators concluded.
Find the full study in the Journal of Affective Disorders (2015;175:133-8 doi:10.1016/j.jad.2014.12.059).
Distinctly different patterns of cognitive deficits are found between schizophrenia and nonpsychotic major depressive disorder, Dr. Shuo-En Hsu and associates reported.
They compared 30 drug-naive participants with schizophrenia, 30 with drug-naive nonpsychotic major depressive disorder (MDD), and 30 matched controls. People with schizophrenia scored significantly worse on the Wisconsin Card Sorting Test than those from the MDD group or the controls, making an average of 17 perseveration errors, about 50% more than the other groups, whose WCST scores were comparable. Patients in both the schizophrenia and MDD groups scored significantly worse than the control group on the Continuous Performance Test, said Dr. Hsu of the department of psychiatry at National Cheng Kung University Hospital in Tainan, Taiwan, and associates.
In contrast to the WCST, patients with MDD performed significantly worse on the Finger Tapping Test than did the schizophrenia or the control-group patients. Schizophrenia patients scored slightly worse than those in the control group, with an average score of about 43, compared with 47 in the control group and 38 in the MDD group.
“Further studies may focus on the qualitative differences between less heterogeneous patient groups; for example, drug-naive patients with schizophrenia and psychotic depression,” the investigators concluded.
Find the full study in the Journal of Affective Disorders (2015;175:133-8 doi:10.1016/j.jad.2014.12.059).
Chromosome deletion linked to PsA risk
A deletion between the ADAMTS9 and MAGI1 genes was associated with psoriatic arthritis and is unrelated to purely cutaneous psoriasis, according to Dr. Antonio Juliá of Vall d’Hebron Research Institute, Barcelona, and his associates.
Of 165 common copy number variants found in both the psoriatic arthritis (PsA) group and control group, only the ADAMTS9-MAGI1 deletion showed a significant association, with an odds ratio of 1.94. A deletion between the HLA-C and HLA-B genes was initially significant, but the association disappeared after correcting for alleles located at those genes already associated with PsA.
The ADAMTS9-MAGI1 deletion occurred significantly less often in patients with cutaneous psoriasis (PsC) than in PsA patients, and there was no significant difference in deletion frequency between the control group and the PsC group.
“It is possible, however, that once the specific biological mechanisms influenced by this genetic variation are identified, more targeted analysis will reveal association to other PsA phenotypes,” the investigators noted.
Find the full study in Annals of the Rheumatic Diseases (doi:10.1136/annrheumdis-2014-207190)
A deletion between the ADAMTS9 and MAGI1 genes was associated with psoriatic arthritis and is unrelated to purely cutaneous psoriasis, according to Dr. Antonio Juliá of Vall d’Hebron Research Institute, Barcelona, and his associates.
Of 165 common copy number variants found in both the psoriatic arthritis (PsA) group and control group, only the ADAMTS9-MAGI1 deletion showed a significant association, with an odds ratio of 1.94. A deletion between the HLA-C and HLA-B genes was initially significant, but the association disappeared after correcting for alleles located at those genes already associated with PsA.
The ADAMTS9-MAGI1 deletion occurred significantly less often in patients with cutaneous psoriasis (PsC) than in PsA patients, and there was no significant difference in deletion frequency between the control group and the PsC group.
“It is possible, however, that once the specific biological mechanisms influenced by this genetic variation are identified, more targeted analysis will reveal association to other PsA phenotypes,” the investigators noted.
Find the full study in Annals of the Rheumatic Diseases (doi:10.1136/annrheumdis-2014-207190)
A deletion between the ADAMTS9 and MAGI1 genes was associated with psoriatic arthritis and is unrelated to purely cutaneous psoriasis, according to Dr. Antonio Juliá of Vall d’Hebron Research Institute, Barcelona, and his associates.
Of 165 common copy number variants found in both the psoriatic arthritis (PsA) group and control group, only the ADAMTS9-MAGI1 deletion showed a significant association, with an odds ratio of 1.94. A deletion between the HLA-C and HLA-B genes was initially significant, but the association disappeared after correcting for alleles located at those genes already associated with PsA.
The ADAMTS9-MAGI1 deletion occurred significantly less often in patients with cutaneous psoriasis (PsC) than in PsA patients, and there was no significant difference in deletion frequency between the control group and the PsC group.
“It is possible, however, that once the specific biological mechanisms influenced by this genetic variation are identified, more targeted analysis will reveal association to other PsA phenotypes,” the investigators noted.
Find the full study in Annals of the Rheumatic Diseases (doi:10.1136/annrheumdis-2014-207190)
Slow spindle assembly in human oocyte meiosis leads to frequent aneuploidy
The high rate of aneuploidy in human eggs could be explained by an unusually long meiotic spindle assembly period which favors chromosome segregation errors, according to a new study published in Science.
Dr. Zuzana Holubcova and her colleagues established an experimental system for ex vivo high-resolution fluorescence microscopy of human oocytes that allowed them to observe the major stages of meiosis in the laboratory.
Human oocyte spindle assembly was controlled primarily by chromosomes and the small guanosine triphosphatase Ran and was independent of centrosomes or other microtubule organization. This process took about 16 hours to complete, considerably longer than 30 minutes needed for spindle assembly in cells undergoing mitosis or the 3-5 hours required for mouse oocyte meiosis.
While nearly all oocytes progressed into anaphase with bipolar spindles, over the course of spindle assembly, 44% of spindles showed moderate instability with an apolar phase, and 38% of spindles showed severe instability with a multipolar phase. Oocytes with abnormal spindles were more likely to have persistent lagging chromosomes during anaphase, which were associated with abnormal kinetochore-microtubule attachments.
“Spindle instability may reflect attempts of the chromosomes to establish stable bipolar microtubule attachments, which could be more challenging in human oocytes, possibly due to structural features of their chromosomes abnormal attachments,” the researchers wrote. “Progression into anaphase with these abnormal attachments would put the oocyte at risk of chromosome segregation errors, providing at least one mechanism for the relatively frequent aneuploidy of eggs, even in young women.”
Find the full study in Science (doi: 10.1126/science.aaa9529).
Watch a video of spindle assembly here.
This video shows 3D volume reconstructions of kinetochores, chromosomes, and microtubules in cold-treated human oocytes fixed during early (left) or late (right) spindle assembly.
Credit: Zuzana Holubcova and Melina Schuh, MRC Laboratory of Molecular Biology
The high rate of aneuploidy in human eggs could be explained by an unusually long meiotic spindle assembly period which favors chromosome segregation errors, according to a new study published in Science.
Dr. Zuzana Holubcova and her colleagues established an experimental system for ex vivo high-resolution fluorescence microscopy of human oocytes that allowed them to observe the major stages of meiosis in the laboratory.
Human oocyte spindle assembly was controlled primarily by chromosomes and the small guanosine triphosphatase Ran and was independent of centrosomes or other microtubule organization. This process took about 16 hours to complete, considerably longer than 30 minutes needed for spindle assembly in cells undergoing mitosis or the 3-5 hours required for mouse oocyte meiosis.
While nearly all oocytes progressed into anaphase with bipolar spindles, over the course of spindle assembly, 44% of spindles showed moderate instability with an apolar phase, and 38% of spindles showed severe instability with a multipolar phase. Oocytes with abnormal spindles were more likely to have persistent lagging chromosomes during anaphase, which were associated with abnormal kinetochore-microtubule attachments.
“Spindle instability may reflect attempts of the chromosomes to establish stable bipolar microtubule attachments, which could be more challenging in human oocytes, possibly due to structural features of their chromosomes abnormal attachments,” the researchers wrote. “Progression into anaphase with these abnormal attachments would put the oocyte at risk of chromosome segregation errors, providing at least one mechanism for the relatively frequent aneuploidy of eggs, even in young women.”
Find the full study in Science (doi: 10.1126/science.aaa9529).
Watch a video of spindle assembly here.
This video shows 3D volume reconstructions of kinetochores, chromosomes, and microtubules in cold-treated human oocytes fixed during early (left) or late (right) spindle assembly.
Credit: Zuzana Holubcova and Melina Schuh, MRC Laboratory of Molecular Biology
The high rate of aneuploidy in human eggs could be explained by an unusually long meiotic spindle assembly period which favors chromosome segregation errors, according to a new study published in Science.
Dr. Zuzana Holubcova and her colleagues established an experimental system for ex vivo high-resolution fluorescence microscopy of human oocytes that allowed them to observe the major stages of meiosis in the laboratory.
Human oocyte spindle assembly was controlled primarily by chromosomes and the small guanosine triphosphatase Ran and was independent of centrosomes or other microtubule organization. This process took about 16 hours to complete, considerably longer than 30 minutes needed for spindle assembly in cells undergoing mitosis or the 3-5 hours required for mouse oocyte meiosis.
While nearly all oocytes progressed into anaphase with bipolar spindles, over the course of spindle assembly, 44% of spindles showed moderate instability with an apolar phase, and 38% of spindles showed severe instability with a multipolar phase. Oocytes with abnormal spindles were more likely to have persistent lagging chromosomes during anaphase, which were associated with abnormal kinetochore-microtubule attachments.
“Spindle instability may reflect attempts of the chromosomes to establish stable bipolar microtubule attachments, which could be more challenging in human oocytes, possibly due to structural features of their chromosomes abnormal attachments,” the researchers wrote. “Progression into anaphase with these abnormal attachments would put the oocyte at risk of chromosome segregation errors, providing at least one mechanism for the relatively frequent aneuploidy of eggs, even in young women.”
Find the full study in Science (doi: 10.1126/science.aaa9529).
Watch a video of spindle assembly here.
This video shows 3D volume reconstructions of kinetochores, chromosomes, and microtubules in cold-treated human oocytes fixed during early (left) or late (right) spindle assembly.
Credit: Zuzana Holubcova and Melina Schuh, MRC Laboratory of Molecular Biology
Creativity important to the identity of bipolar patients
In a small study, five themes were identified with regard to creativity and how it is influenced by bipolar disorder, according to Sheri L. Johnson, Ph.D., and her associates.
Study participants took three tests: the Seven-up Seven-down scale, the Brief Quality of Life in Bipolar Disorder scale, and the Creative Achievement Questionnaire. After qualitative analysis, several themes emerged: the pros and cons of manic energy, benefits of altered thinking, finding a balance of medication that promotes creativity, the idea of creativity as central to the identity of a person with BD, and the importance of creativity in reducing stigma and improving treatment.
“Participants were eager to see their creativity taken into account within treatment as a way to help foster more positive communication and to combat the stigma that they all too often experience. As such, creativity appears to be a positive focus for promoting growth and wellness, and for reducing stigma,” the investigators said.
Find the full study in Qualitative Health Research (doi: 10.1177/1049732315578403).
In a small study, five themes were identified with regard to creativity and how it is influenced by bipolar disorder, according to Sheri L. Johnson, Ph.D., and her associates.
Study participants took three tests: the Seven-up Seven-down scale, the Brief Quality of Life in Bipolar Disorder scale, and the Creative Achievement Questionnaire. After qualitative analysis, several themes emerged: the pros and cons of manic energy, benefits of altered thinking, finding a balance of medication that promotes creativity, the idea of creativity as central to the identity of a person with BD, and the importance of creativity in reducing stigma and improving treatment.
“Participants were eager to see their creativity taken into account within treatment as a way to help foster more positive communication and to combat the stigma that they all too often experience. As such, creativity appears to be a positive focus for promoting growth and wellness, and for reducing stigma,” the investigators said.
Find the full study in Qualitative Health Research (doi: 10.1177/1049732315578403).
In a small study, five themes were identified with regard to creativity and how it is influenced by bipolar disorder, according to Sheri L. Johnson, Ph.D., and her associates.
Study participants took three tests: the Seven-up Seven-down scale, the Brief Quality of Life in Bipolar Disorder scale, and the Creative Achievement Questionnaire. After qualitative analysis, several themes emerged: the pros and cons of manic energy, benefits of altered thinking, finding a balance of medication that promotes creativity, the idea of creativity as central to the identity of a person with BD, and the importance of creativity in reducing stigma and improving treatment.
“Participants were eager to see their creativity taken into account within treatment as a way to help foster more positive communication and to combat the stigma that they all too often experience. As such, creativity appears to be a positive focus for promoting growth and wellness, and for reducing stigma,” the investigators said.
Find the full study in Qualitative Health Research (doi: 10.1177/1049732315578403).
Stroke, blindness are risks of unintended injection of fillers into blood vessels
Rare but serious side effects can result when soft tissue fillers are unintentionally injected into blood vessels in the face, according to a press release from the Food and Drug Administration.
Blood vessels can be blocked and blood flow restricted following unintentional soft tissue filler injection. The injection material can also migrate and embolization may cause vision impairment, blindness, stroke, and skin necrosis. Some injection sites result in blood vessel blockage more often, including the glabella and the periorbital region, though blockage can occur at any site on the face.
The FDA recommends that only people with appropriate training and knowledge of injection areas deliver injections, and that patients understand the risk beforehand and potential symptoms afterwards. A full list of recommendations can be found on the FDA website.
“FDA is working with manufacturers to update their labeling. The request asks that the labeling include additional warnings, precautions, and other statements about the risk of unintentional injection into blood vessels, consistent with the recommendations in this communication, so that both health care providers and patients would have a better understanding of the risks,” the FDA said.
Find the full press release on the FDA website.
Rare but serious side effects can result when soft tissue fillers are unintentionally injected into blood vessels in the face, according to a press release from the Food and Drug Administration.
Blood vessels can be blocked and blood flow restricted following unintentional soft tissue filler injection. The injection material can also migrate and embolization may cause vision impairment, blindness, stroke, and skin necrosis. Some injection sites result in blood vessel blockage more often, including the glabella and the periorbital region, though blockage can occur at any site on the face.
The FDA recommends that only people with appropriate training and knowledge of injection areas deliver injections, and that patients understand the risk beforehand and potential symptoms afterwards. A full list of recommendations can be found on the FDA website.
“FDA is working with manufacturers to update their labeling. The request asks that the labeling include additional warnings, precautions, and other statements about the risk of unintentional injection into blood vessels, consistent with the recommendations in this communication, so that both health care providers and patients would have a better understanding of the risks,” the FDA said.
Find the full press release on the FDA website.
Rare but serious side effects can result when soft tissue fillers are unintentionally injected into blood vessels in the face, according to a press release from the Food and Drug Administration.
Blood vessels can be blocked and blood flow restricted following unintentional soft tissue filler injection. The injection material can also migrate and embolization may cause vision impairment, blindness, stroke, and skin necrosis. Some injection sites result in blood vessel blockage more often, including the glabella and the periorbital region, though blockage can occur at any site on the face.
The FDA recommends that only people with appropriate training and knowledge of injection areas deliver injections, and that patients understand the risk beforehand and potential symptoms afterwards. A full list of recommendations can be found on the FDA website.
“FDA is working with manufacturers to update their labeling. The request asks that the labeling include additional warnings, precautions, and other statements about the risk of unintentional injection into blood vessels, consistent with the recommendations in this communication, so that both health care providers and patients would have a better understanding of the risks,” the FDA said.
Find the full press release on the FDA website.
Slower teen reaction times may increase anxiety and depression risk later in life
Adolescents with slower processing speeds and longer reaction times were at a greater risk of anxiety and depression later in life, according to Catharine R. Gale, Ph.D., of the University of Southampton (England) and her associates.
In this 20-year study of 705 males and females, longer reaction time at 16 years indicated a small but significant association with poorer mental health at age 36.
Adjusting for sex, parental social class, General Health Questionnaire (GHQ) score at age 16 years, health behaviors at age 36 years, and allostatic load had little effect on the association between reaction time and the GHQ score, but the association was weakened with Hospital Anxiety and Depression Scale (HADS) scores for both anxiety and depression. Smoking had a mediating effect on the HADS anxiety score, but not on the depression subscale.
“Further prospective studies of the relation between reaction time and mental health outcomes in other samples are needed to gauge whether reaction time is a true risk factor for mental disorders and to confirm the mediating roles played by smoking and allostatic load,” the investigators noted.
Find the full study in Psychosomatic Medicine (doi:10.1097/PSY.0000000000000189).
Adolescents with slower processing speeds and longer reaction times were at a greater risk of anxiety and depression later in life, according to Catharine R. Gale, Ph.D., of the University of Southampton (England) and her associates.
In this 20-year study of 705 males and females, longer reaction time at 16 years indicated a small but significant association with poorer mental health at age 36.
Adjusting for sex, parental social class, General Health Questionnaire (GHQ) score at age 16 years, health behaviors at age 36 years, and allostatic load had little effect on the association between reaction time and the GHQ score, but the association was weakened with Hospital Anxiety and Depression Scale (HADS) scores for both anxiety and depression. Smoking had a mediating effect on the HADS anxiety score, but not on the depression subscale.
“Further prospective studies of the relation between reaction time and mental health outcomes in other samples are needed to gauge whether reaction time is a true risk factor for mental disorders and to confirm the mediating roles played by smoking and allostatic load,” the investigators noted.
Find the full study in Psychosomatic Medicine (doi:10.1097/PSY.0000000000000189).
Adolescents with slower processing speeds and longer reaction times were at a greater risk of anxiety and depression later in life, according to Catharine R. Gale, Ph.D., of the University of Southampton (England) and her associates.
In this 20-year study of 705 males and females, longer reaction time at 16 years indicated a small but significant association with poorer mental health at age 36.
Adjusting for sex, parental social class, General Health Questionnaire (GHQ) score at age 16 years, health behaviors at age 36 years, and allostatic load had little effect on the association between reaction time and the GHQ score, but the association was weakened with Hospital Anxiety and Depression Scale (HADS) scores for both anxiety and depression. Smoking had a mediating effect on the HADS anxiety score, but not on the depression subscale.
“Further prospective studies of the relation between reaction time and mental health outcomes in other samples are needed to gauge whether reaction time is a true risk factor for mental disorders and to confirm the mediating roles played by smoking and allostatic load,” the investigators noted.
Find the full study in Psychosomatic Medicine (doi:10.1097/PSY.0000000000000189).
ADHD diagnosis less common in Hispanics
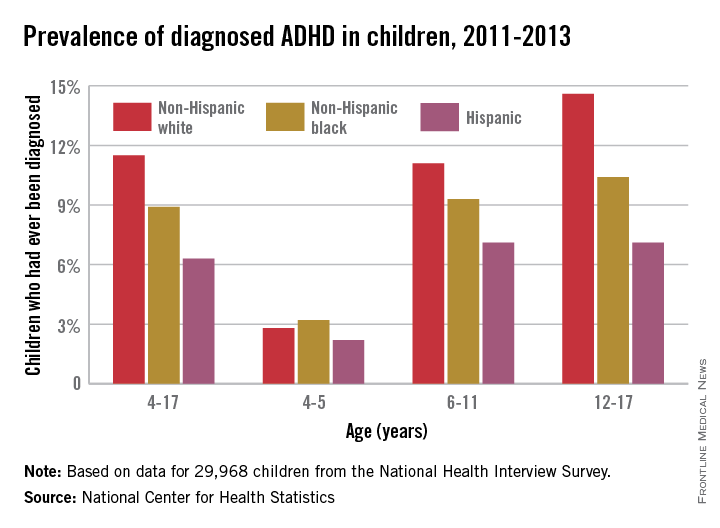
Hispanic children aged 6-17 years were significantly less likely to have ever been diagnosed with attention-deficit/hyperactivity disorder than were non-Hispanic white or non-Hispanic black children in 2011-2013, according to a report from the National Center for Health Statistics.
In children aged 6-11 years, the prevalence of a lifetime ADHD diagnosis was 11.1% for non-Hispanic whites, 9.3% for non-Hispanic blacks, and 7.1% for Hispanic children in 2011-2013. For children aged 12-17 years, Hispanic diagnosis remained at 7.1%, while the rate increased to 14.6% for whites and 10.4% for blacks.
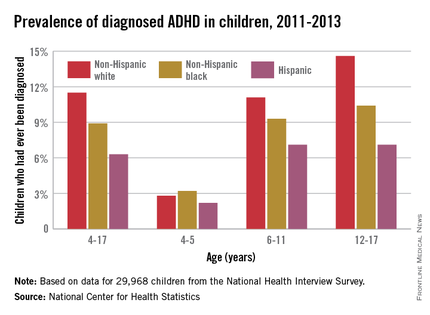
There were no significant differences in diagnosis between ethnicities for children aged 4-5, with ADHD rates ranging from 2.2% to 3.2%. Overall, 11.5% of white children aged 4-17 had ever been diagnosed with ADHD, compared with 8.9% of black children and 6.3% of Hispanic children, the NCHS reported.
Boys of all ages were much more likely to have a diagnosis of ADHD than were girls in 2011-2013, with 4.3% of boys aged 4-5 years receiving a diagnosis, compared with 1.2% of girls. This gap widened to 13.2% and 5.6% for those aged 6-11 years and to 16.3% and 7.1% for those aged 12-17 years.
Children with public insurance were more likely to be diagnosed with ADHD compared with those who had private insurance and those who were uninsured, with an overall rate of 11.7% for publicly insured children, 8.6% for the privately insured, and 5.7% for the uninsured. Living in a household making less than 200% of the federal poverty threshold increased ADHD diagnosis in children aged 4-11 years, but this effect disappeared in children aged 12-17 years, according to the NCHS report.
“In view of the economic and social costs associated with ADHD and the potential benefits of treatment, the continued surveillance of diagnosed ADHD is warranted,” said Patricia N. Pastor, Ph.D., and her associates at the NCHS, Hyattsville, Md.
The NCHS report used data for 29,968 children from the National Health Interview Survey.
Hispanic children aged 6-17 years were significantly less likely to have ever been diagnosed with attention-deficit/hyperactivity disorder than were non-Hispanic white or non-Hispanic black children in 2011-2013, according to a report from the National Center for Health Statistics.
In children aged 6-11 years, the prevalence of a lifetime ADHD diagnosis was 11.1% for non-Hispanic whites, 9.3% for non-Hispanic blacks, and 7.1% for Hispanic children in 2011-2013. For children aged 12-17 years, Hispanic diagnosis remained at 7.1%, while the rate increased to 14.6% for whites and 10.4% for blacks.

There were no significant differences in diagnosis between ethnicities for children aged 4-5, with ADHD rates ranging from 2.2% to 3.2%. Overall, 11.5% of white children aged 4-17 had ever been diagnosed with ADHD, compared with 8.9% of black children and 6.3% of Hispanic children, the NCHS reported.
Boys of all ages were much more likely to have a diagnosis of ADHD than were girls in 2011-2013, with 4.3% of boys aged 4-5 years receiving a diagnosis, compared with 1.2% of girls. This gap widened to 13.2% and 5.6% for those aged 6-11 years and to 16.3% and 7.1% for those aged 12-17 years.
Children with public insurance were more likely to be diagnosed with ADHD compared with those who had private insurance and those who were uninsured, with an overall rate of 11.7% for publicly insured children, 8.6% for the privately insured, and 5.7% for the uninsured. Living in a household making less than 200% of the federal poverty threshold increased ADHD diagnosis in children aged 4-11 years, but this effect disappeared in children aged 12-17 years, according to the NCHS report.
“In view of the economic and social costs associated with ADHD and the potential benefits of treatment, the continued surveillance of diagnosed ADHD is warranted,” said Patricia N. Pastor, Ph.D., and her associates at the NCHS, Hyattsville, Md.
The NCHS report used data for 29,968 children from the National Health Interview Survey.
Hispanic children aged 6-17 years were significantly less likely to have ever been diagnosed with attention-deficit/hyperactivity disorder than were non-Hispanic white or non-Hispanic black children in 2011-2013, according to a report from the National Center for Health Statistics.
In children aged 6-11 years, the prevalence of a lifetime ADHD diagnosis was 11.1% for non-Hispanic whites, 9.3% for non-Hispanic blacks, and 7.1% for Hispanic children in 2011-2013. For children aged 12-17 years, Hispanic diagnosis remained at 7.1%, while the rate increased to 14.6% for whites and 10.4% for blacks.

There were no significant differences in diagnosis between ethnicities for children aged 4-5, with ADHD rates ranging from 2.2% to 3.2%. Overall, 11.5% of white children aged 4-17 had ever been diagnosed with ADHD, compared with 8.9% of black children and 6.3% of Hispanic children, the NCHS reported.
Boys of all ages were much more likely to have a diagnosis of ADHD than were girls in 2011-2013, with 4.3% of boys aged 4-5 years receiving a diagnosis, compared with 1.2% of girls. This gap widened to 13.2% and 5.6% for those aged 6-11 years and to 16.3% and 7.1% for those aged 12-17 years.
Children with public insurance were more likely to be diagnosed with ADHD compared with those who had private insurance and those who were uninsured, with an overall rate of 11.7% for publicly insured children, 8.6% for the privately insured, and 5.7% for the uninsured. Living in a household making less than 200% of the federal poverty threshold increased ADHD diagnosis in children aged 4-11 years, but this effect disappeared in children aged 12-17 years, according to the NCHS report.
“In view of the economic and social costs associated with ADHD and the potential benefits of treatment, the continued surveillance of diagnosed ADHD is warranted,” said Patricia N. Pastor, Ph.D., and her associates at the NCHS, Hyattsville, Md.
The NCHS report used data for 29,968 children from the National Health Interview Survey.
Community-level interventions increase HPV immunization rates
Interventions at the practice and community level appear to be an effective way to boost human papillomavirus immunization rates, according to a systematic review by Linda Niccolai, Ph.D., of the Yale School of Public Health, and Dr. Caitlin Hansen of the Yale School of Medicine, both in New Haven, Conn.
The authors looked at 14 studies in the review with approaches including reminder and recall, physician-focused intervention, school-based programs, and social marketing. Of the included studies, 12 showed a significant increase in HPV immunization rates after the intervention, 1 showed a nonsignificant increase, and 1 showed mixed results.
“The choice of a particular strategy may depend on considerations, such as financial and logistical challenges. Future research should explore how best to widely disseminate and sustain programs that work and evaluate the effectiveness of alternative untested strategies using rigorous and high-quality research methods,” the investigators concluded.
Find the full study in JAMA Pediatrics (doi:10.1001/jamapediatrics.2015.0310).
Interventions at the practice and community level appear to be an effective way to boost human papillomavirus immunization rates, according to a systematic review by Linda Niccolai, Ph.D., of the Yale School of Public Health, and Dr. Caitlin Hansen of the Yale School of Medicine, both in New Haven, Conn.
The authors looked at 14 studies in the review with approaches including reminder and recall, physician-focused intervention, school-based programs, and social marketing. Of the included studies, 12 showed a significant increase in HPV immunization rates after the intervention, 1 showed a nonsignificant increase, and 1 showed mixed results.
“The choice of a particular strategy may depend on considerations, such as financial and logistical challenges. Future research should explore how best to widely disseminate and sustain programs that work and evaluate the effectiveness of alternative untested strategies using rigorous and high-quality research methods,” the investigators concluded.
Find the full study in JAMA Pediatrics (doi:10.1001/jamapediatrics.2015.0310).
Interventions at the practice and community level appear to be an effective way to boost human papillomavirus immunization rates, according to a systematic review by Linda Niccolai, Ph.D., of the Yale School of Public Health, and Dr. Caitlin Hansen of the Yale School of Medicine, both in New Haven, Conn.
The authors looked at 14 studies in the review with approaches including reminder and recall, physician-focused intervention, school-based programs, and social marketing. Of the included studies, 12 showed a significant increase in HPV immunization rates after the intervention, 1 showed a nonsignificant increase, and 1 showed mixed results.
“The choice of a particular strategy may depend on considerations, such as financial and logistical challenges. Future research should explore how best to widely disseminate and sustain programs that work and evaluate the effectiveness of alternative untested strategies using rigorous and high-quality research methods,” the investigators concluded.
Find the full study in JAMA Pediatrics (doi:10.1001/jamapediatrics.2015.0310).
Larger-gauge PICCs, VTE history increase PICC-DVT risk
Risk factors of upper-extremity deep vein thrombosis associated with peripherally inserted central catheters include a history of venous thromboembolism and a larger-gauge catheter, according to Dr. Vineet Chopra and his associates at the University of Michigan Health System, Ann Arbor.
Compared to 4-Fr gauge PICCs, 5-Fr and 6-Fr PICCs significantly increased PICC-DVT risk, with odds ratios of 2.7 and 7.4, respectively. The OR for patients with a prior history of VTE was 1.7. While any surgery with a PICC in place increased risk, the OR was higher in surgery lasting less than 2 hours (2.75 vs. 2.17). PICCs inserted into the brachial or cephalic vein also increased PICC-DVT risk, compared with the basilic vein, with ORs of 6.8 and 5.8, respectively.
Patients who received both aspirin and statins were at a significantly lower risk of PICC-DVT than those who received only one drug or neither, with an OR of 0.31 for those who got both, compared with 0.77 for aspirin and 0.61 for statins. Pharmacologic VTE prophylaxis also benefited patients with an OR of DVT at 0.72.
“Given the existence of other supportive data regarding the influence of VTE prophylaxis on PICC-DVT and a potentially protective role of statins on thrombosis, further controlled studies of VTE prophylaxis, antiplatelet treatment, and statins to prevent PICC-DVT appear warranted,” the investigators recommended.
Find the full study in Thrombosis Research (doi:10.1016/j.thromres.2015.02.0120).
Risk factors of upper-extremity deep vein thrombosis associated with peripherally inserted central catheters include a history of venous thromboembolism and a larger-gauge catheter, according to Dr. Vineet Chopra and his associates at the University of Michigan Health System, Ann Arbor.
Compared to 4-Fr gauge PICCs, 5-Fr and 6-Fr PICCs significantly increased PICC-DVT risk, with odds ratios of 2.7 and 7.4, respectively. The OR for patients with a prior history of VTE was 1.7. While any surgery with a PICC in place increased risk, the OR was higher in surgery lasting less than 2 hours (2.75 vs. 2.17). PICCs inserted into the brachial or cephalic vein also increased PICC-DVT risk, compared with the basilic vein, with ORs of 6.8 and 5.8, respectively.
Patients who received both aspirin and statins were at a significantly lower risk of PICC-DVT than those who received only one drug or neither, with an OR of 0.31 for those who got both, compared with 0.77 for aspirin and 0.61 for statins. Pharmacologic VTE prophylaxis also benefited patients with an OR of DVT at 0.72.
“Given the existence of other supportive data regarding the influence of VTE prophylaxis on PICC-DVT and a potentially protective role of statins on thrombosis, further controlled studies of VTE prophylaxis, antiplatelet treatment, and statins to prevent PICC-DVT appear warranted,” the investigators recommended.
Find the full study in Thrombosis Research (doi:10.1016/j.thromres.2015.02.0120).
Risk factors of upper-extremity deep vein thrombosis associated with peripherally inserted central catheters include a history of venous thromboembolism and a larger-gauge catheter, according to Dr. Vineet Chopra and his associates at the University of Michigan Health System, Ann Arbor.
Compared to 4-Fr gauge PICCs, 5-Fr and 6-Fr PICCs significantly increased PICC-DVT risk, with odds ratios of 2.7 and 7.4, respectively. The OR for patients with a prior history of VTE was 1.7. While any surgery with a PICC in place increased risk, the OR was higher in surgery lasting less than 2 hours (2.75 vs. 2.17). PICCs inserted into the brachial or cephalic vein also increased PICC-DVT risk, compared with the basilic vein, with ORs of 6.8 and 5.8, respectively.
Patients who received both aspirin and statins were at a significantly lower risk of PICC-DVT than those who received only one drug or neither, with an OR of 0.31 for those who got both, compared with 0.77 for aspirin and 0.61 for statins. Pharmacologic VTE prophylaxis also benefited patients with an OR of DVT at 0.72.
“Given the existence of other supportive data regarding the influence of VTE prophylaxis on PICC-DVT and a potentially protective role of statins on thrombosis, further controlled studies of VTE prophylaxis, antiplatelet treatment, and statins to prevent PICC-DVT appear warranted,” the investigators recommended.
Find the full study in Thrombosis Research (doi:10.1016/j.thromres.2015.02.0120).