User login
Children frequently bullied due to food allergies
One in three children treated at a food allergy clinic reported being bullied specifically because of food allergies, suggesting higher rates of bullying than the approximately 17% previously reported in the U.S. general population.
Although bullying was significantly associated with a lower quality of life and higher distress levels in the children and in the parents of bullied children, parental knowledge of the bullying mediated these measures in both parents and children, according to a study published Dec. 24 in Pediatrics.
Parents were aware of only 52% of their children’s reports of bullying in this sample, but "when parents knew that their children [were] being bullied for any reason, the parents’ quality of life was significantly lower, and the child’s quality of life was significantly better," reported Dr. Eyal Shemesh at New York’s Mount Sinai Medical Center and his associates (Pediatrics 2012 Dec. 24 [doi:10.1542/peds.2012-1180]).
The data come from 251 predominantly white, affluent families who visited Mount Sinai’s Elliot and Roslyn Jaffe Food Allergy Institute between April 2011 and November 2011. All the children participating, aged 8-17 years, had at least one diagnosed food allergy and completed modified versions of the Revised Olweus Bully/Victim Questionnaire. Their parents filled out separate surveys about their children’s experiences of being bullied.
Quality of life and distress were assessed using the Multidimensional Anxiety Scale for Children10 items and the Pediatric Quality of Life Inventory 4.0 in children and the Impact of Events Scale and 17-item Food Allergy Quality of Life Parental Burden in the parents.
The researchers attempted to control for the burden of the food allergy’s severity as a possible confounder in the relationship among bullying, quality of life, and distress by including in the analysis the number of allergies each child had and whether the parents had ever had to use epinephrine.
Nearly half of the children (45%) reported being bullied for any reason (compared with 36% of parents who reported knowing their child had been bullied), and 32% reported being bullied specifically because of their food allergy (compared with 25% of parents reporting knowledge of food allergy–specific bullying).
Although being teased was the most common form of bullying (42% of children), 30% reported having food waved at them, 12% had been forced to touch food, and 10% had had food thrown at them.
Most of the bullying (60%) occurred at school, and classmates were the most common perpetrators, reported by 80% of the bullied children. The children also reported being bullied about food allergies by other students at the school (34%), teachers or staff (11%), and siblings (13%).
Meanwhile, 87% of the children said they told someone about the bullying, usually their parents (71%), a teacher (35%), or a friend (32%). Since children’s quality of life was better and anxiety was lower when their parents knew about the bullying, the researchers suggested that helping children identify and report bullying appears to lessen its impact.
Children reporting frequent bullying had significantly worse quality of life scores compared with children bullied less, but there were no significant differences in anxiety levels between children bullied more or less often.
Limitations of the study included self-reporting and the possibility that children’s reports of bullying due to food allergy and bullying for any reason were conflated. The primarily white, affluent children are also not representative of the general population, and the study lacked a control group of children without food allergies.
Funding for the study came from the Jaffe Family Foundation, the National Institute of Allergy and Infectious Diseases, the Food Allergy Initiative, and and the National Institute of Diabetes and Digestive and Kidney Diseases. One of Dr. Shemesh’s associates in the study, Dr. Scott H. Sicherer, consults for the Food Allergy Initiative and is an adviser for the Food Allergy and Anaphylaxis Network.
Bullies are familiar as the characters we have always loved to hate in television, films, and books, but bullies have recently become something more, said Dr. Mark Schuster and Dr. Laura Bogart. "The bully is no longer simply a representation of a moral lesson or a source of humor."
The bully is now also recognized as a source of long-term health issues, including depression, anxiety, posttraumatic stress, and suicidal ideation. But bullies can be motivated by others’ health conditions, too. Dr. Shemesh’s article about high rates of bullying related to children’s food allergies "underscores the importance of addressing food allergies in a way that protects but does not stigmatize children who have them."
Clinicians should watch for signs a child is being bullied – including emotional symptoms and chronic physical symptoms, as well as physical bruises and scratches – paying particular attention to children with "stigmatizing characteristics that could lead to bullying," such as obesity, disabilities, or gender nonconformity. Providers must also involve parents in recognizing bullying and its harmful long-term effects and making sure they are neither ignoring nor engaging in bullying themselves. "We need a cultural evolution in awareness and repudiation of bullying."
Dr. Schuster is at Boston Children’s Hospital and Dr. Bogart is at Harvard Medical School, Boston. Their comments were taken from an editorial accompanying Dr. Shemesh’s study (Pediatrics 2012 Dec. 24 [doi:10.1542/peds.2012-3253]).
Bullies are familiar as the characters we have always loved to hate in television, films, and books, but bullies have recently become something more, said Dr. Mark Schuster and Dr. Laura Bogart. "The bully is no longer simply a representation of a moral lesson or a source of humor."
The bully is now also recognized as a source of long-term health issues, including depression, anxiety, posttraumatic stress, and suicidal ideation. But bullies can be motivated by others’ health conditions, too. Dr. Shemesh’s article about high rates of bullying related to children’s food allergies "underscores the importance of addressing food allergies in a way that protects but does not stigmatize children who have them."
Clinicians should watch for signs a child is being bullied – including emotional symptoms and chronic physical symptoms, as well as physical bruises and scratches – paying particular attention to children with "stigmatizing characteristics that could lead to bullying," such as obesity, disabilities, or gender nonconformity. Providers must also involve parents in recognizing bullying and its harmful long-term effects and making sure they are neither ignoring nor engaging in bullying themselves. "We need a cultural evolution in awareness and repudiation of bullying."
Dr. Schuster is at Boston Children’s Hospital and Dr. Bogart is at Harvard Medical School, Boston. Their comments were taken from an editorial accompanying Dr. Shemesh’s study (Pediatrics 2012 Dec. 24 [doi:10.1542/peds.2012-3253]).
Bullies are familiar as the characters we have always loved to hate in television, films, and books, but bullies have recently become something more, said Dr. Mark Schuster and Dr. Laura Bogart. "The bully is no longer simply a representation of a moral lesson or a source of humor."
The bully is now also recognized as a source of long-term health issues, including depression, anxiety, posttraumatic stress, and suicidal ideation. But bullies can be motivated by others’ health conditions, too. Dr. Shemesh’s article about high rates of bullying related to children’s food allergies "underscores the importance of addressing food allergies in a way that protects but does not stigmatize children who have them."
Clinicians should watch for signs a child is being bullied – including emotional symptoms and chronic physical symptoms, as well as physical bruises and scratches – paying particular attention to children with "stigmatizing characteristics that could lead to bullying," such as obesity, disabilities, or gender nonconformity. Providers must also involve parents in recognizing bullying and its harmful long-term effects and making sure they are neither ignoring nor engaging in bullying themselves. "We need a cultural evolution in awareness and repudiation of bullying."
Dr. Schuster is at Boston Children’s Hospital and Dr. Bogart is at Harvard Medical School, Boston. Their comments were taken from an editorial accompanying Dr. Shemesh’s study (Pediatrics 2012 Dec. 24 [doi:10.1542/peds.2012-3253]).
One in three children treated at a food allergy clinic reported being bullied specifically because of food allergies, suggesting higher rates of bullying than the approximately 17% previously reported in the U.S. general population.
Although bullying was significantly associated with a lower quality of life and higher distress levels in the children and in the parents of bullied children, parental knowledge of the bullying mediated these measures in both parents and children, according to a study published Dec. 24 in Pediatrics.
Parents were aware of only 52% of their children’s reports of bullying in this sample, but "when parents knew that their children [were] being bullied for any reason, the parents’ quality of life was significantly lower, and the child’s quality of life was significantly better," reported Dr. Eyal Shemesh at New York’s Mount Sinai Medical Center and his associates (Pediatrics 2012 Dec. 24 [doi:10.1542/peds.2012-1180]).
The data come from 251 predominantly white, affluent families who visited Mount Sinai’s Elliot and Roslyn Jaffe Food Allergy Institute between April 2011 and November 2011. All the children participating, aged 8-17 years, had at least one diagnosed food allergy and completed modified versions of the Revised Olweus Bully/Victim Questionnaire. Their parents filled out separate surveys about their children’s experiences of being bullied.
Quality of life and distress were assessed using the Multidimensional Anxiety Scale for Children10 items and the Pediatric Quality of Life Inventory 4.0 in children and the Impact of Events Scale and 17-item Food Allergy Quality of Life Parental Burden in the parents.
The researchers attempted to control for the burden of the food allergy’s severity as a possible confounder in the relationship among bullying, quality of life, and distress by including in the analysis the number of allergies each child had and whether the parents had ever had to use epinephrine.
Nearly half of the children (45%) reported being bullied for any reason (compared with 36% of parents who reported knowing their child had been bullied), and 32% reported being bullied specifically because of their food allergy (compared with 25% of parents reporting knowledge of food allergy–specific bullying).
Although being teased was the most common form of bullying (42% of children), 30% reported having food waved at them, 12% had been forced to touch food, and 10% had had food thrown at them.
Most of the bullying (60%) occurred at school, and classmates were the most common perpetrators, reported by 80% of the bullied children. The children also reported being bullied about food allergies by other students at the school (34%), teachers or staff (11%), and siblings (13%).
Meanwhile, 87% of the children said they told someone about the bullying, usually their parents (71%), a teacher (35%), or a friend (32%). Since children’s quality of life was better and anxiety was lower when their parents knew about the bullying, the researchers suggested that helping children identify and report bullying appears to lessen its impact.
Children reporting frequent bullying had significantly worse quality of life scores compared with children bullied less, but there were no significant differences in anxiety levels between children bullied more or less often.
Limitations of the study included self-reporting and the possibility that children’s reports of bullying due to food allergy and bullying for any reason were conflated. The primarily white, affluent children are also not representative of the general population, and the study lacked a control group of children without food allergies.
Funding for the study came from the Jaffe Family Foundation, the National Institute of Allergy and Infectious Diseases, the Food Allergy Initiative, and and the National Institute of Diabetes and Digestive and Kidney Diseases. One of Dr. Shemesh’s associates in the study, Dr. Scott H. Sicherer, consults for the Food Allergy Initiative and is an adviser for the Food Allergy and Anaphylaxis Network.
One in three children treated at a food allergy clinic reported being bullied specifically because of food allergies, suggesting higher rates of bullying than the approximately 17% previously reported in the U.S. general population.
Although bullying was significantly associated with a lower quality of life and higher distress levels in the children and in the parents of bullied children, parental knowledge of the bullying mediated these measures in both parents and children, according to a study published Dec. 24 in Pediatrics.
Parents were aware of only 52% of their children’s reports of bullying in this sample, but "when parents knew that their children [were] being bullied for any reason, the parents’ quality of life was significantly lower, and the child’s quality of life was significantly better," reported Dr. Eyal Shemesh at New York’s Mount Sinai Medical Center and his associates (Pediatrics 2012 Dec. 24 [doi:10.1542/peds.2012-1180]).
The data come from 251 predominantly white, affluent families who visited Mount Sinai’s Elliot and Roslyn Jaffe Food Allergy Institute between April 2011 and November 2011. All the children participating, aged 8-17 years, had at least one diagnosed food allergy and completed modified versions of the Revised Olweus Bully/Victim Questionnaire. Their parents filled out separate surveys about their children’s experiences of being bullied.
Quality of life and distress were assessed using the Multidimensional Anxiety Scale for Children10 items and the Pediatric Quality of Life Inventory 4.0 in children and the Impact of Events Scale and 17-item Food Allergy Quality of Life Parental Burden in the parents.
The researchers attempted to control for the burden of the food allergy’s severity as a possible confounder in the relationship among bullying, quality of life, and distress by including in the analysis the number of allergies each child had and whether the parents had ever had to use epinephrine.
Nearly half of the children (45%) reported being bullied for any reason (compared with 36% of parents who reported knowing their child had been bullied), and 32% reported being bullied specifically because of their food allergy (compared with 25% of parents reporting knowledge of food allergy–specific bullying).
Although being teased was the most common form of bullying (42% of children), 30% reported having food waved at them, 12% had been forced to touch food, and 10% had had food thrown at them.
Most of the bullying (60%) occurred at school, and classmates were the most common perpetrators, reported by 80% of the bullied children. The children also reported being bullied about food allergies by other students at the school (34%), teachers or staff (11%), and siblings (13%).
Meanwhile, 87% of the children said they told someone about the bullying, usually their parents (71%), a teacher (35%), or a friend (32%). Since children’s quality of life was better and anxiety was lower when their parents knew about the bullying, the researchers suggested that helping children identify and report bullying appears to lessen its impact.
Children reporting frequent bullying had significantly worse quality of life scores compared with children bullied less, but there were no significant differences in anxiety levels between children bullied more or less often.
Limitations of the study included self-reporting and the possibility that children’s reports of bullying due to food allergy and bullying for any reason were conflated. The primarily white, affluent children are also not representative of the general population, and the study lacked a control group of children without food allergies.
Funding for the study came from the Jaffe Family Foundation, the National Institute of Allergy and Infectious Diseases, the Food Allergy Initiative, and and the National Institute of Diabetes and Digestive and Kidney Diseases. One of Dr. Shemesh’s associates in the study, Dr. Scott H. Sicherer, consults for the Food Allergy Initiative and is an adviser for the Food Allergy and Anaphylaxis Network.
FROM PEDIATRICS
Major Finding: A third (32%) of children reported being bullied because of a food allergy; 25% of parents reported knowing their child was bullied for the same reason.
Data Source: Child and parent surveys from 251 families visiting Jaffe Food Allergy Institute at Mount Sinai Medical Center, New York.
Disclosures: Funding was provided by the Jaffe Family Foundation and several of the National Institutes of Health. One of Dr. Shemesh’s associates in the study, Dr. Scott H. Sicherer, consults for the Food Allergy Initiative and the Food Allergy and Anaphylaxis Network.
Acetazolamide and CPAP combined improve OSA at high altitude
Using a combination treatment of acetazolamide and auto-CPAP therapy in patients with obstructive sleep apnea traveling to high altitudes was more effective than CPAP use alone, according to a study published in JAMA.
Patients with obstructive sleep apnea (OSA) who took acetazolamide and used CPAP at two different altitudes higher than baseline had lower apnea/hypopnea index scores and higher nighttime oxygen saturation percentages than patients who took a placebo and used CPAP.
Dr. Tsogyal Latshang and associates at the University Hospital Zurich reported the results of their randomized, placebo-controlled, double-blind crossover study with 51 OSA patients in JAMA Dec. 12 (2012 [doi:10.1001/jama.2012.94847]).
All the patients, who normally live below 800 meters altitude and use CPAP regularly, underwent sleep studies during the summer of 2009, first at the University Hospital Zurich (490 m) and then at two Swiss mountain resorts, one at 1,630 m and one at 2,590 m, during two 3-day trips.
The patients took either acetazolamide or a placebo while spending 2 days at 1,630 m and 1 day at 2,590 m. The acetazolamide was dispensed as one 250-mg dose each morning and two 250-mg doses each evening before meals; the placebo looked identical.
After 2 weeks spent below 800 m following the first 3-day trip, the patients then spent another 3 days at the high-altitude resorts to take the other intervention (acetazolamide or placebo). During the sleep studies, instead of using their own CPAP devices, the patients all used the same type of autoadjusting CPAP machine with their own masks.
The combination therapy of acetazolamide and CPAP increased the patients’ median nighttime oxygen saturation at 1,630 meters by 1%, from 93% with placebo to 94% with combination therapy. At 2,590 meters, the increase was 2%, from 89% with placebo to 91% with combination therapy. At the higher altitude, patients receiving combination therapy spent a median 13% of nighttime sleep with oxygen saturation below 90%, compared to a median of 57% (P less than .001) below 90% oxygen saturation with placebo.
Patients receiving combination therapy also had lower apnea/hypopnea index scores at both altitudes, compared with placebo. The median at baseline, in the hospital at 490 meters with CPAP only, was 6.6 events/hour. At 1,630 meters, patients with placebo had a median 10.7 events/h, compared with 5.8 when taking acetazolamide. At 2,590 m, patients’ median apnea/hypopnea index improved from 19.3 events/h with placebo to 6.8 with acetazolamide. (All P values under .001)
"The reduction in the apnea/hypopnea index was mainly related to a lower number of central apneas/hypopneas, particularly during nonrapid eye movement sleep, but obstructive apneas/hypopneas were slightly reduced as well (at 2,590 m)," the researchers reported.
Secondary outcomes measured included sleep time, exercise performance, vigilance symptoms, and adverse effects. Patients taking acetazolamide slept a median 24 minutes more (451 minutes, compared with 427) at 1,630 m and 34 minutes more (446 minutes, compared with 412) at 2,590 m (P less than .001). Sleep efficiency and nonrapid eye movement sleep were also higher with combination therapy than placebo, although self-reported daytime sleepiness was not significantly different.
Patients’ heart rate was slightly lower with combination therapy (59 beats per minute, compared with 60 at 1,630 m; and 61 bmp, compared with 64 at 2,590 m), and patients taking acetazolamide had lower blood pressure at altitude than with placebo (96 mm HG, compared with 101 mm HG at 1,630 m; and 99 mm HG, compared with 104 mm HG at 2,590 m; P < .05)
The most common adverse effects reported with acetazolamide were an unpleasant taste in the mouth and mild to moderate paresthesias, but no patients discontinued therapy. Primary study limitations include the limited ability to generalize beyond short high-altitude duration and beyond the predominantly middle-aged male cohort, who were moderately obese and had only stable comorbidities.
The study was funded by grants from the Swiss National Science Foundation, Lung Leagues of Zurich and Schaffhausen, Center for Clinical Research, University of Zurich, University Hospital Zurich, and Philips Respironics (unconditional grant) in Switzerland. The only disclosure reported was Dr. Bloch’s consultancy for IMT Medical and his receipt of unconditional institutional grants from Philips Respironics and ResMed.
Dr. Paul A. Selecky comments: Very interesting findings that will be useful to physicians with OSA patients who want to go to higher altitudes.
Dr. Paul A. Selecky |
Dr. Paul A. Selecky comments: Very interesting findings that will be useful to physicians with OSA patients who want to go to higher altitudes.
Dr. Paul A. Selecky |
Dr. Paul A. Selecky comments: Very interesting findings that will be useful to physicians with OSA patients who want to go to higher altitudes.
Dr. Paul A. Selecky |
Using a combination treatment of acetazolamide and auto-CPAP therapy in patients with obstructive sleep apnea traveling to high altitudes was more effective than CPAP use alone, according to a study published in JAMA.
Patients with obstructive sleep apnea (OSA) who took acetazolamide and used CPAP at two different altitudes higher than baseline had lower apnea/hypopnea index scores and higher nighttime oxygen saturation percentages than patients who took a placebo and used CPAP.
Dr. Tsogyal Latshang and associates at the University Hospital Zurich reported the results of their randomized, placebo-controlled, double-blind crossover study with 51 OSA patients in JAMA Dec. 12 (2012 [doi:10.1001/jama.2012.94847]).
All the patients, who normally live below 800 meters altitude and use CPAP regularly, underwent sleep studies during the summer of 2009, first at the University Hospital Zurich (490 m) and then at two Swiss mountain resorts, one at 1,630 m and one at 2,590 m, during two 3-day trips.
The patients took either acetazolamide or a placebo while spending 2 days at 1,630 m and 1 day at 2,590 m. The acetazolamide was dispensed as one 250-mg dose each morning and two 250-mg doses each evening before meals; the placebo looked identical.
After 2 weeks spent below 800 m following the first 3-day trip, the patients then spent another 3 days at the high-altitude resorts to take the other intervention (acetazolamide or placebo). During the sleep studies, instead of using their own CPAP devices, the patients all used the same type of autoadjusting CPAP machine with their own masks.
The combination therapy of acetazolamide and CPAP increased the patients’ median nighttime oxygen saturation at 1,630 meters by 1%, from 93% with placebo to 94% with combination therapy. At 2,590 meters, the increase was 2%, from 89% with placebo to 91% with combination therapy. At the higher altitude, patients receiving combination therapy spent a median 13% of nighttime sleep with oxygen saturation below 90%, compared to a median of 57% (P less than .001) below 90% oxygen saturation with placebo.
Patients receiving combination therapy also had lower apnea/hypopnea index scores at both altitudes, compared with placebo. The median at baseline, in the hospital at 490 meters with CPAP only, was 6.6 events/hour. At 1,630 meters, patients with placebo had a median 10.7 events/h, compared with 5.8 when taking acetazolamide. At 2,590 m, patients’ median apnea/hypopnea index improved from 19.3 events/h with placebo to 6.8 with acetazolamide. (All P values under .001)
"The reduction in the apnea/hypopnea index was mainly related to a lower number of central apneas/hypopneas, particularly during nonrapid eye movement sleep, but obstructive apneas/hypopneas were slightly reduced as well (at 2,590 m)," the researchers reported.
Secondary outcomes measured included sleep time, exercise performance, vigilance symptoms, and adverse effects. Patients taking acetazolamide slept a median 24 minutes more (451 minutes, compared with 427) at 1,630 m and 34 minutes more (446 minutes, compared with 412) at 2,590 m (P less than .001). Sleep efficiency and nonrapid eye movement sleep were also higher with combination therapy than placebo, although self-reported daytime sleepiness was not significantly different.
Patients’ heart rate was slightly lower with combination therapy (59 beats per minute, compared with 60 at 1,630 m; and 61 bmp, compared with 64 at 2,590 m), and patients taking acetazolamide had lower blood pressure at altitude than with placebo (96 mm HG, compared with 101 mm HG at 1,630 m; and 99 mm HG, compared with 104 mm HG at 2,590 m; P < .05)
The most common adverse effects reported with acetazolamide were an unpleasant taste in the mouth and mild to moderate paresthesias, but no patients discontinued therapy. Primary study limitations include the limited ability to generalize beyond short high-altitude duration and beyond the predominantly middle-aged male cohort, who were moderately obese and had only stable comorbidities.
The study was funded by grants from the Swiss National Science Foundation, Lung Leagues of Zurich and Schaffhausen, Center for Clinical Research, University of Zurich, University Hospital Zurich, and Philips Respironics (unconditional grant) in Switzerland. The only disclosure reported was Dr. Bloch’s consultancy for IMT Medical and his receipt of unconditional institutional grants from Philips Respironics and ResMed.
Using a combination treatment of acetazolamide and auto-CPAP therapy in patients with obstructive sleep apnea traveling to high altitudes was more effective than CPAP use alone, according to a study published in JAMA.
Patients with obstructive sleep apnea (OSA) who took acetazolamide and used CPAP at two different altitudes higher than baseline had lower apnea/hypopnea index scores and higher nighttime oxygen saturation percentages than patients who took a placebo and used CPAP.
Dr. Tsogyal Latshang and associates at the University Hospital Zurich reported the results of their randomized, placebo-controlled, double-blind crossover study with 51 OSA patients in JAMA Dec. 12 (2012 [doi:10.1001/jama.2012.94847]).
All the patients, who normally live below 800 meters altitude and use CPAP regularly, underwent sleep studies during the summer of 2009, first at the University Hospital Zurich (490 m) and then at two Swiss mountain resorts, one at 1,630 m and one at 2,590 m, during two 3-day trips.
The patients took either acetazolamide or a placebo while spending 2 days at 1,630 m and 1 day at 2,590 m. The acetazolamide was dispensed as one 250-mg dose each morning and two 250-mg doses each evening before meals; the placebo looked identical.
After 2 weeks spent below 800 m following the first 3-day trip, the patients then spent another 3 days at the high-altitude resorts to take the other intervention (acetazolamide or placebo). During the sleep studies, instead of using their own CPAP devices, the patients all used the same type of autoadjusting CPAP machine with their own masks.
The combination therapy of acetazolamide and CPAP increased the patients’ median nighttime oxygen saturation at 1,630 meters by 1%, from 93% with placebo to 94% with combination therapy. At 2,590 meters, the increase was 2%, from 89% with placebo to 91% with combination therapy. At the higher altitude, patients receiving combination therapy spent a median 13% of nighttime sleep with oxygen saturation below 90%, compared to a median of 57% (P less than .001) below 90% oxygen saturation with placebo.
Patients receiving combination therapy also had lower apnea/hypopnea index scores at both altitudes, compared with placebo. The median at baseline, in the hospital at 490 meters with CPAP only, was 6.6 events/hour. At 1,630 meters, patients with placebo had a median 10.7 events/h, compared with 5.8 when taking acetazolamide. At 2,590 m, patients’ median apnea/hypopnea index improved from 19.3 events/h with placebo to 6.8 with acetazolamide. (All P values under .001)
"The reduction in the apnea/hypopnea index was mainly related to a lower number of central apneas/hypopneas, particularly during nonrapid eye movement sleep, but obstructive apneas/hypopneas were slightly reduced as well (at 2,590 m)," the researchers reported.
Secondary outcomes measured included sleep time, exercise performance, vigilance symptoms, and adverse effects. Patients taking acetazolamide slept a median 24 minutes more (451 minutes, compared with 427) at 1,630 m and 34 minutes more (446 minutes, compared with 412) at 2,590 m (P less than .001). Sleep efficiency and nonrapid eye movement sleep were also higher with combination therapy than placebo, although self-reported daytime sleepiness was not significantly different.
Patients’ heart rate was slightly lower with combination therapy (59 beats per minute, compared with 60 at 1,630 m; and 61 bmp, compared with 64 at 2,590 m), and patients taking acetazolamide had lower blood pressure at altitude than with placebo (96 mm HG, compared with 101 mm HG at 1,630 m; and 99 mm HG, compared with 104 mm HG at 2,590 m; P < .05)
The most common adverse effects reported with acetazolamide were an unpleasant taste in the mouth and mild to moderate paresthesias, but no patients discontinued therapy. Primary study limitations include the limited ability to generalize beyond short high-altitude duration and beyond the predominantly middle-aged male cohort, who were moderately obese and had only stable comorbidities.
The study was funded by grants from the Swiss National Science Foundation, Lung Leagues of Zurich and Schaffhausen, Center for Clinical Research, University of Zurich, University Hospital Zurich, and Philips Respironics (unconditional grant) in Switzerland. The only disclosure reported was Dr. Bloch’s consultancy for IMT Medical and his receipt of unconditional institutional grants from Philips Respironics and ResMed.
FROM JAMA
Major Finding: The combined use of acetazolamide (750 mg/day) and auto-CPAP therapy for obstructive sleep apnea at high altitudes resulted in higher nighttime oxygen saturation (94% at 1,630 meters and 91% at 2,590 m), compared with placebo (93% and 89%, respectively).
Data Source: A randomized, placebo-controlled, double-blind, crossover trial with 51 obstructive sleep apnea patients.
Disclosures: The study was funded by grants from the Swiss National Science Foundation, Lung Leagues of Zurich and Schaffhausen, Center for Clinical Research, University of Zurich, University Hospital Zurich, and Philips Respironics (unconditional grant) in Switzerland. The only disclosure reported was Dr. Bloch’s consultancy for IMT Medical and his receipt of unconditional institutional grants from Philips Respironics and ResMed.
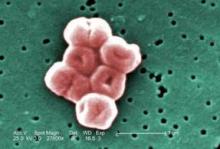
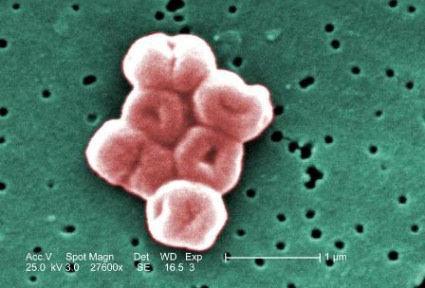
Even after room cleaning, Acinetobacter baumannii persists
After terminal cleaning of ICU rooms that were contaminated with the multidrug-resistant Acinetobacter baumannii, half the rooms still contained the pathogen, primarily on the floor, bedside tables, call buttons, door handles, and a supply cart, according to a study published in the December issue of American Journal of Infection Control.
Even rooms of patients who had not had a culture test positive for A. baumannii in more than a month had samples test positive for the bacterium, "suggesting a potential longevity of contamination on surfaces in patient rooms," Paula Strassle and her associates at the University of Maryland, Baltimore, reported (Am. J. Infect. Control 2012;40:1005-7).
At the University of Maryland Medical Center, investigators collected 487 cultures from 32 medical, surgery, and cardiac surgery ICU rooms of patients who had a known infection or history of colonization with strains of A. baumannii that are resistant to at least two classes of antibiotics. Between March 2009 and April 2011, the samples were collected when a patient was scheduled to be discharged and then after terminal cleaning by hospital environmental services staff before a new patient was admitted.
The cleaning staff, who were not aware of the study, removed curtains, infusion pumps, and respiratory equipment from the rooms and cleaned rooms from the top down using Virex II 256 wipes and mopping from back to front with an 8- to 10-minute dwell time.
The team collected samples from the rooms’ sink drains, edges of basins, bed rail buttons, bedside table handles, vital sign monitor buttons, call buttons/remotes, supply cart drawer handles, door handles (interior and exterior), infusion pump buttons, ventilator machine buttons, and floor around the beds.
Before cleaning, 15 of the 32 rooms (46.9%) and 41 of the 268 swabbed sites (15.3%) were found positive for the pathogen. The sites with the highest rates of contamination before cleaning included the floor (12/32, 37.5%); supply carts (7/30, 23.3%); bed rails (5/24, 20.8%); and ventilators (3/15, 20%).
After cleaning, 8 of the 32 rooms (25%, all of which had been contaminated before cleaning) and 12 of the 219 swabbed sites (5.5%) tested positive for A. baumannii. The contaminated sites included the floor (4/32, 12.5%); the bedside table (2/27, 7.4%); the call buttons (2/20, 10%); the door handles (3/32, 9.4%); and a supply cart (1/26, 3.8%).
The fact that half of the originally contaminated rooms had persistent contamination after cleaning led the researchers to conclude that current cleaning techniques may be inadequate to fully remove this pathogen. Noting the stronger effectiveness of methods such as hydrogen peroxide vapor and ultraviolet light, the authors acknowledged these methods may be difficult to implement because of the extra time involved with their use.
The authors also acknowledged that their study was limited because the cleaning staff were not observed, which meant that possibly poor cleaning techniques that could be improved with better communication with and training of cleaning staffs were not observed. The A. baumannii samples were not compared using molecular typing, so the researchers also could not unequivocally state that the post- and precleaning contamination was with identical strains within each room.
The study was funded by the National Institutes of Health. The authors said they had no relevant financial disclosures.
After terminal cleaning of ICU rooms that were contaminated with the multidrug-resistant Acinetobacter baumannii, half the rooms still contained the pathogen, primarily on the floor, bedside tables, call buttons, door handles, and a supply cart, according to a study published in the December issue of American Journal of Infection Control.
Even rooms of patients who had not had a culture test positive for A. baumannii in more than a month had samples test positive for the bacterium, "suggesting a potential longevity of contamination on surfaces in patient rooms," Paula Strassle and her associates at the University of Maryland, Baltimore, reported (Am. J. Infect. Control 2012;40:1005-7).
At the University of Maryland Medical Center, investigators collected 487 cultures from 32 medical, surgery, and cardiac surgery ICU rooms of patients who had a known infection or history of colonization with strains of A. baumannii that are resistant to at least two classes of antibiotics. Between March 2009 and April 2011, the samples were collected when a patient was scheduled to be discharged and then after terminal cleaning by hospital environmental services staff before a new patient was admitted.
The cleaning staff, who were not aware of the study, removed curtains, infusion pumps, and respiratory equipment from the rooms and cleaned rooms from the top down using Virex II 256 wipes and mopping from back to front with an 8- to 10-minute dwell time.
The team collected samples from the rooms’ sink drains, edges of basins, bed rail buttons, bedside table handles, vital sign monitor buttons, call buttons/remotes, supply cart drawer handles, door handles (interior and exterior), infusion pump buttons, ventilator machine buttons, and floor around the beds.
Before cleaning, 15 of the 32 rooms (46.9%) and 41 of the 268 swabbed sites (15.3%) were found positive for the pathogen. The sites with the highest rates of contamination before cleaning included the floor (12/32, 37.5%); supply carts (7/30, 23.3%); bed rails (5/24, 20.8%); and ventilators (3/15, 20%).
After cleaning, 8 of the 32 rooms (25%, all of which had been contaminated before cleaning) and 12 of the 219 swabbed sites (5.5%) tested positive for A. baumannii. The contaminated sites included the floor (4/32, 12.5%); the bedside table (2/27, 7.4%); the call buttons (2/20, 10%); the door handles (3/32, 9.4%); and a supply cart (1/26, 3.8%).
The fact that half of the originally contaminated rooms had persistent contamination after cleaning led the researchers to conclude that current cleaning techniques may be inadequate to fully remove this pathogen. Noting the stronger effectiveness of methods such as hydrogen peroxide vapor and ultraviolet light, the authors acknowledged these methods may be difficult to implement because of the extra time involved with their use.
The authors also acknowledged that their study was limited because the cleaning staff were not observed, which meant that possibly poor cleaning techniques that could be improved with better communication with and training of cleaning staffs were not observed. The A. baumannii samples were not compared using molecular typing, so the researchers also could not unequivocally state that the post- and precleaning contamination was with identical strains within each room.
The study was funded by the National Institutes of Health. The authors said they had no relevant financial disclosures.
After terminal cleaning of ICU rooms that were contaminated with the multidrug-resistant Acinetobacter baumannii, half the rooms still contained the pathogen, primarily on the floor, bedside tables, call buttons, door handles, and a supply cart, according to a study published in the December issue of American Journal of Infection Control.
Even rooms of patients who had not had a culture test positive for A. baumannii in more than a month had samples test positive for the bacterium, "suggesting a potential longevity of contamination on surfaces in patient rooms," Paula Strassle and her associates at the University of Maryland, Baltimore, reported (Am. J. Infect. Control 2012;40:1005-7).
At the University of Maryland Medical Center, investigators collected 487 cultures from 32 medical, surgery, and cardiac surgery ICU rooms of patients who had a known infection or history of colonization with strains of A. baumannii that are resistant to at least two classes of antibiotics. Between March 2009 and April 2011, the samples were collected when a patient was scheduled to be discharged and then after terminal cleaning by hospital environmental services staff before a new patient was admitted.
The cleaning staff, who were not aware of the study, removed curtains, infusion pumps, and respiratory equipment from the rooms and cleaned rooms from the top down using Virex II 256 wipes and mopping from back to front with an 8- to 10-minute dwell time.
The team collected samples from the rooms’ sink drains, edges of basins, bed rail buttons, bedside table handles, vital sign monitor buttons, call buttons/remotes, supply cart drawer handles, door handles (interior and exterior), infusion pump buttons, ventilator machine buttons, and floor around the beds.
Before cleaning, 15 of the 32 rooms (46.9%) and 41 of the 268 swabbed sites (15.3%) were found positive for the pathogen. The sites with the highest rates of contamination before cleaning included the floor (12/32, 37.5%); supply carts (7/30, 23.3%); bed rails (5/24, 20.8%); and ventilators (3/15, 20%).
After cleaning, 8 of the 32 rooms (25%, all of which had been contaminated before cleaning) and 12 of the 219 swabbed sites (5.5%) tested positive for A. baumannii. The contaminated sites included the floor (4/32, 12.5%); the bedside table (2/27, 7.4%); the call buttons (2/20, 10%); the door handles (3/32, 9.4%); and a supply cart (1/26, 3.8%).
The fact that half of the originally contaminated rooms had persistent contamination after cleaning led the researchers to conclude that current cleaning techniques may be inadequate to fully remove this pathogen. Noting the stronger effectiveness of methods such as hydrogen peroxide vapor and ultraviolet light, the authors acknowledged these methods may be difficult to implement because of the extra time involved with their use.
The authors also acknowledged that their study was limited because the cleaning staff were not observed, which meant that possibly poor cleaning techniques that could be improved with better communication with and training of cleaning staffs were not observed. The A. baumannii samples were not compared using molecular typing, so the researchers also could not unequivocally state that the post- and precleaning contamination was with identical strains within each room.
The study was funded by the National Institutes of Health. The authors said they had no relevant financial disclosures.
FROM AMERICAN JOURNAL OF INFECTION CONTROL
Major Finding: In hospital rooms whose last discharged patient had an Acinetobacter baumannii infection, 25% of the rooms were still contaminated after terminal cleaning, compared with 46.9% of the rooms tested before cleaning.
Data Source: A study of 487 cultures were collected before and after cleaning from 32 medical, surgical, and cardiac surgery ICU rooms of discharged patients who had a known A. baumannii colonization or infection.
Disclosures: The study was funded by a National Institutes of Health grant. The authors reported having no relevant financial conflicts.
Tdap Vaccine Safety Comparable to Td for Seniors
The tetanus-diphtheria-acellular pertussis vaccine was as safe in seniors as the tetanus-diphtheria vaccine, a finding that supports a federal recommendation to reduce pertussis risk among the elderly via Tdap vaccination.
The findings offer "empirical safety data to suggest that [the Advisory Committee on Immunization Practices’] recommendation for immunizing adults 65 years and older with Tdap to reduce the risk of pertussis in the elderly and their contacts should not have untoward safety consequences," noted Hung Fu Tseng, Ph.D., of Kaiser Permanente Southern California and his associates (Clin. Infect. Dis. 2012 Nov. 29 [doi:10.1093/cid/cis871]).
A total of 36,078 pertussis cases have been reported this year through mid-November in the United States – the highest rate in 5 decades (MMWR 2012;61:ND637-47).
The Centers for Disease Control and Prevention recommends that the pertussis vaccine be administered to babies over 2 months, children, adolescents, and adults, including pregnant women and seniors. In 2010, ACIP recommended a single dose of Tdap for seniors instead of Td, if they had not already received Tdap.
But with limited safety data on Tdap’s use among adults 65 years and older, "evaluation of the safety of the vaccine in this population becomes essential," the study authors noted.
Dr. Tseng’s study used data from seven HMOs participating in the Vaccine Safety Datalink Project. The investigators first used a matched-cohort design to compare safety.
A total of 119,573 adults 65 years and older received the Tdap vaccine between Jan. 1, 2006, and Dec. 31, 2010. All participants had been continuously enrolled in their HMO for a year before vaccination and until at least 84 days afterward.
The adverse events in the Tdap group were compared with those of 119,573 seniors in the same HMOs who received the Td vaccine during the same period. Patients were matched based on sex, site, season (April-October, November-March) and age group (65-69 years, 70-74 years, 75 years and older).
The researchers examined seven categories of adverse events: Guillain-Barré syndrome (GBS); brachial neuritis; paralytic syndromes; medically attended inflammatory or allergic events; cranial nerve disorders (including Bell’s palsy); "anaphylaxis and generalized reaction"; and meningitis, encephalitis, and encephalopathy.
The incidence of these adverse events was comparable between the Tdap and Td cohorts, after medical records reviews confirmed diagnosis.
The researchers also assessed safety with a self-controlled case series. Time periods in which adverse events occurred in Tdap-vaccinated patients were compared with subsequent periods of the same length, starting the day after each adverse event’s risk window ended.
All adverse events except "medically attended inflammatory or allergic events" were similar in the compared time periods. During the risk window, 612 patients experienced an inflammatory or allergic event, compared with 385 in the comparison time frame, for an incidence risk ratio of 1.59 (95% confidence interval, 1.40-1.81). This elevated risk matches past clinical trials data and VAERS reports, and is comparable to the risk profile of inflammatory or allergic events following Td vaccination.
Overall, "the risk of the prespecified events following Tdap is comparable to that following Td vaccination in the elderly population," the authors noted.
Limitations of this study include the exclusion of nonprespecified adverse events and the potential for misclassification of exposure and/or event status (such as false negatives) in the electronic medical records used.
The study was funded through a subcontract from the Centers for Disease Control and Prevention with America’s Health Insurance Plans. Dr. Tseng reported receiving support from Novartis Vaccine, and several of the study’s other authors reported receiving research support from pharmaceutical companies.
The tetanus-diphtheria-acellular pertussis vaccine was as safe in seniors as the tetanus-diphtheria vaccine, a finding that supports a federal recommendation to reduce pertussis risk among the elderly via Tdap vaccination.
The findings offer "empirical safety data to suggest that [the Advisory Committee on Immunization Practices’] recommendation for immunizing adults 65 years and older with Tdap to reduce the risk of pertussis in the elderly and their contacts should not have untoward safety consequences," noted Hung Fu Tseng, Ph.D., of Kaiser Permanente Southern California and his associates (Clin. Infect. Dis. 2012 Nov. 29 [doi:10.1093/cid/cis871]).
A total of 36,078 pertussis cases have been reported this year through mid-November in the United States – the highest rate in 5 decades (MMWR 2012;61:ND637-47).
The Centers for Disease Control and Prevention recommends that the pertussis vaccine be administered to babies over 2 months, children, adolescents, and adults, including pregnant women and seniors. In 2010, ACIP recommended a single dose of Tdap for seniors instead of Td, if they had not already received Tdap.
But with limited safety data on Tdap’s use among adults 65 years and older, "evaluation of the safety of the vaccine in this population becomes essential," the study authors noted.
Dr. Tseng’s study used data from seven HMOs participating in the Vaccine Safety Datalink Project. The investigators first used a matched-cohort design to compare safety.
A total of 119,573 adults 65 years and older received the Tdap vaccine between Jan. 1, 2006, and Dec. 31, 2010. All participants had been continuously enrolled in their HMO for a year before vaccination and until at least 84 days afterward.
The adverse events in the Tdap group were compared with those of 119,573 seniors in the same HMOs who received the Td vaccine during the same period. Patients were matched based on sex, site, season (April-October, November-March) and age group (65-69 years, 70-74 years, 75 years and older).
The researchers examined seven categories of adverse events: Guillain-Barré syndrome (GBS); brachial neuritis; paralytic syndromes; medically attended inflammatory or allergic events; cranial nerve disorders (including Bell’s palsy); "anaphylaxis and generalized reaction"; and meningitis, encephalitis, and encephalopathy.
The incidence of these adverse events was comparable between the Tdap and Td cohorts, after medical records reviews confirmed diagnosis.
The researchers also assessed safety with a self-controlled case series. Time periods in which adverse events occurred in Tdap-vaccinated patients were compared with subsequent periods of the same length, starting the day after each adverse event’s risk window ended.
All adverse events except "medically attended inflammatory or allergic events" were similar in the compared time periods. During the risk window, 612 patients experienced an inflammatory or allergic event, compared with 385 in the comparison time frame, for an incidence risk ratio of 1.59 (95% confidence interval, 1.40-1.81). This elevated risk matches past clinical trials data and VAERS reports, and is comparable to the risk profile of inflammatory or allergic events following Td vaccination.
Overall, "the risk of the prespecified events following Tdap is comparable to that following Td vaccination in the elderly population," the authors noted.
Limitations of this study include the exclusion of nonprespecified adverse events and the potential for misclassification of exposure and/or event status (such as false negatives) in the electronic medical records used.
The study was funded through a subcontract from the Centers for Disease Control and Prevention with America’s Health Insurance Plans. Dr. Tseng reported receiving support from Novartis Vaccine, and several of the study’s other authors reported receiving research support from pharmaceutical companies.
The tetanus-diphtheria-acellular pertussis vaccine was as safe in seniors as the tetanus-diphtheria vaccine, a finding that supports a federal recommendation to reduce pertussis risk among the elderly via Tdap vaccination.
The findings offer "empirical safety data to suggest that [the Advisory Committee on Immunization Practices’] recommendation for immunizing adults 65 years and older with Tdap to reduce the risk of pertussis in the elderly and their contacts should not have untoward safety consequences," noted Hung Fu Tseng, Ph.D., of Kaiser Permanente Southern California and his associates (Clin. Infect. Dis. 2012 Nov. 29 [doi:10.1093/cid/cis871]).
A total of 36,078 pertussis cases have been reported this year through mid-November in the United States – the highest rate in 5 decades (MMWR 2012;61:ND637-47).
The Centers for Disease Control and Prevention recommends that the pertussis vaccine be administered to babies over 2 months, children, adolescents, and adults, including pregnant women and seniors. In 2010, ACIP recommended a single dose of Tdap for seniors instead of Td, if they had not already received Tdap.
But with limited safety data on Tdap’s use among adults 65 years and older, "evaluation of the safety of the vaccine in this population becomes essential," the study authors noted.
Dr. Tseng’s study used data from seven HMOs participating in the Vaccine Safety Datalink Project. The investigators first used a matched-cohort design to compare safety.
A total of 119,573 adults 65 years and older received the Tdap vaccine between Jan. 1, 2006, and Dec. 31, 2010. All participants had been continuously enrolled in their HMO for a year before vaccination and until at least 84 days afterward.
The adverse events in the Tdap group were compared with those of 119,573 seniors in the same HMOs who received the Td vaccine during the same period. Patients were matched based on sex, site, season (April-October, November-March) and age group (65-69 years, 70-74 years, 75 years and older).
The researchers examined seven categories of adverse events: Guillain-Barré syndrome (GBS); brachial neuritis; paralytic syndromes; medically attended inflammatory or allergic events; cranial nerve disorders (including Bell’s palsy); "anaphylaxis and generalized reaction"; and meningitis, encephalitis, and encephalopathy.
The incidence of these adverse events was comparable between the Tdap and Td cohorts, after medical records reviews confirmed diagnosis.
The researchers also assessed safety with a self-controlled case series. Time periods in which adverse events occurred in Tdap-vaccinated patients were compared with subsequent periods of the same length, starting the day after each adverse event’s risk window ended.
All adverse events except "medically attended inflammatory or allergic events" were similar in the compared time periods. During the risk window, 612 patients experienced an inflammatory or allergic event, compared with 385 in the comparison time frame, for an incidence risk ratio of 1.59 (95% confidence interval, 1.40-1.81). This elevated risk matches past clinical trials data and VAERS reports, and is comparable to the risk profile of inflammatory or allergic events following Td vaccination.
Overall, "the risk of the prespecified events following Tdap is comparable to that following Td vaccination in the elderly population," the authors noted.
Limitations of this study include the exclusion of nonprespecified adverse events and the potential for misclassification of exposure and/or event status (such as false negatives) in the electronic medical records used.
The study was funded through a subcontract from the Centers for Disease Control and Prevention with America’s Health Insurance Plans. Dr. Tseng reported receiving support from Novartis Vaccine, and several of the study’s other authors reported receiving research support from pharmaceutical companies.
FROM THE JOURNAL OF CLINICAL INFECTIOUS DISEASES
Major Finding: The risk of adverse events with the Tdap vaccine in the elderly was comparable to that of the standard Td vaccine when administered to seniors over 65 years, including a slight increase in inflammatory or allergic events in the week after Tdap (IRR, 1.59; 95% CI, 1.40-1.81) which is similar to Td reactions.
Data Source: The findings are based on a study with both matched cohort and self-controlled case series designs that involved 119,573 seniors who received the Tdap vaccine and 119,573 seniors who received the standard Td vaccine between January 2006 and December 2010, using data drawn from seven U.S. health maintenance organizations.
Disclosures: The study was funded through a subcontract from the Centers for Disease Control and Prevention with America’s Health Insurance Plans. Dr. Tseng reported receiving support from Novartis Vaccine, and several of the study’s other authors reported receiving research support from pharmaceutical companies.
Marijuana Use Linked to Better Adherence in Psychosis
First-episode psychosis patients who continue to use marijuana after beginning treatment are more likely to adhere to their medication regimen than are cannabis users who quit. But continued users also are more likely to have increased levels of symptoms after adjustment for this adherence, according to a small prospective 1-year study published in Schizophrenia Research.
The study found no significant differences between continued marijuana users and those who quit after beginning treatment in terms of the patients’ depression severity, time to remission, risk of relapse in the first year of treatment, or scores on the Positive and Negative Syndrome Scale (PANSS).
Previous research has shown that 18%-30% of first-episode psychosis (FEP) patients regularly use marijuana and 40%-60% meet the criteria for lifetime diagnosis of cannabis abuse or dependence. Dr. Kia Faridi at the Prevention and Early Intervention Program for Psychosis (PEPP-Montreal) and his associates set out to determine whether a link exists between medication adherence and continuation of marijuana use, and whether this interaction affect symptom levels a year later (Schizophr. Res. 2012;141:78-82 [doi:10.1016/j.schres.2012.07.023])
From 192 FEP patients consecutively admitted to PEPP, the authors identified 62 who met the DSM-IV criteria at baseline for active cannabis use disorder or polysubstance disorder with cannabis. The authors were able to collect sufficient data for 48 of these patients for the full year of the study.
All 48, like the others admitted to PEPP, were aged 14-30, met the DSM-IV criteria for psychotic symptoms for at least a week, and had less than a month of past treatment with antipsychotics. The population was predominately male, and more than half came from lower-middle or lower socioeconomic class.
Once entering treatment, 20 of them (41.2%) stopped using marijuana and 28 patients (58.7%) continued. Researchers interviewed the patients every 3 months to determine medication adherence, defined as taking medications more than 75% of the time. At the 6-month follow-up, adherence dropped for both groups. However, it picked back up for the marijuana users by the 12-month follow-up, when 92% of them were regularly taking their antipsychotics, compared with adherence among only 40% of the patients no longer using marijuana (P less than .01).
This finding surprised the researchers, since it conflicts with past research. But they noted the small sample size and hypothesized that those who quit using marijuana may be attributing their psychosis symptoms to the THC and therefore neglecting to continue with medication after having ceased using marijuana. Meanwhile, those who continue to use marijuana may be deciding to stick with their medications to treat ongoing psychosis symptoms.
Cannabis use was significantly associated with higher levels of symptoms – but only after researchers controlled for medication adherence (P = .03). Secondarily, the study revealed that a good number of patients using marijuana can stop using it after entering treatment despite the link between quitting marijuana and lower medication adherence. "Unsurprisingly, patients with more severe substance use disorder at baseline were more likely to persist in using cannabis," the authors wrote.
The authors said their findings point out the value of helping patients stop (or reduce) marijuana use because of the drug’s apparent negative influence on their psychotic symptoms.
Dr. Faridi’s fellowship is partly funded by Pfizer Canada. The other authors cited funding from Pfizer Canada, the Canada Research Chairs Program, and multiple pharmaceutical companies.
First-episode psychosis patients who continue to use marijuana after beginning treatment are more likely to adhere to their medication regimen than are cannabis users who quit. But continued users also are more likely to have increased levels of symptoms after adjustment for this adherence, according to a small prospective 1-year study published in Schizophrenia Research.
The study found no significant differences between continued marijuana users and those who quit after beginning treatment in terms of the patients’ depression severity, time to remission, risk of relapse in the first year of treatment, or scores on the Positive and Negative Syndrome Scale (PANSS).
Previous research has shown that 18%-30% of first-episode psychosis (FEP) patients regularly use marijuana and 40%-60% meet the criteria for lifetime diagnosis of cannabis abuse or dependence. Dr. Kia Faridi at the Prevention and Early Intervention Program for Psychosis (PEPP-Montreal) and his associates set out to determine whether a link exists between medication adherence and continuation of marijuana use, and whether this interaction affect symptom levels a year later (Schizophr. Res. 2012;141:78-82 [doi:10.1016/j.schres.2012.07.023])
From 192 FEP patients consecutively admitted to PEPP, the authors identified 62 who met the DSM-IV criteria at baseline for active cannabis use disorder or polysubstance disorder with cannabis. The authors were able to collect sufficient data for 48 of these patients for the full year of the study.
All 48, like the others admitted to PEPP, were aged 14-30, met the DSM-IV criteria for psychotic symptoms for at least a week, and had less than a month of past treatment with antipsychotics. The population was predominately male, and more than half came from lower-middle or lower socioeconomic class.
Once entering treatment, 20 of them (41.2%) stopped using marijuana and 28 patients (58.7%) continued. Researchers interviewed the patients every 3 months to determine medication adherence, defined as taking medications more than 75% of the time. At the 6-month follow-up, adherence dropped for both groups. However, it picked back up for the marijuana users by the 12-month follow-up, when 92% of them were regularly taking their antipsychotics, compared with adherence among only 40% of the patients no longer using marijuana (P less than .01).
This finding surprised the researchers, since it conflicts with past research. But they noted the small sample size and hypothesized that those who quit using marijuana may be attributing their psychosis symptoms to the THC and therefore neglecting to continue with medication after having ceased using marijuana. Meanwhile, those who continue to use marijuana may be deciding to stick with their medications to treat ongoing psychosis symptoms.
Cannabis use was significantly associated with higher levels of symptoms – but only after researchers controlled for medication adherence (P = .03). Secondarily, the study revealed that a good number of patients using marijuana can stop using it after entering treatment despite the link between quitting marijuana and lower medication adherence. "Unsurprisingly, patients with more severe substance use disorder at baseline were more likely to persist in using cannabis," the authors wrote.
The authors said their findings point out the value of helping patients stop (or reduce) marijuana use because of the drug’s apparent negative influence on their psychotic symptoms.
Dr. Faridi’s fellowship is partly funded by Pfizer Canada. The other authors cited funding from Pfizer Canada, the Canada Research Chairs Program, and multiple pharmaceutical companies.
First-episode psychosis patients who continue to use marijuana after beginning treatment are more likely to adhere to their medication regimen than are cannabis users who quit. But continued users also are more likely to have increased levels of symptoms after adjustment for this adherence, according to a small prospective 1-year study published in Schizophrenia Research.
The study found no significant differences between continued marijuana users and those who quit after beginning treatment in terms of the patients’ depression severity, time to remission, risk of relapse in the first year of treatment, or scores on the Positive and Negative Syndrome Scale (PANSS).
Previous research has shown that 18%-30% of first-episode psychosis (FEP) patients regularly use marijuana and 40%-60% meet the criteria for lifetime diagnosis of cannabis abuse or dependence. Dr. Kia Faridi at the Prevention and Early Intervention Program for Psychosis (PEPP-Montreal) and his associates set out to determine whether a link exists between medication adherence and continuation of marijuana use, and whether this interaction affect symptom levels a year later (Schizophr. Res. 2012;141:78-82 [doi:10.1016/j.schres.2012.07.023])
From 192 FEP patients consecutively admitted to PEPP, the authors identified 62 who met the DSM-IV criteria at baseline for active cannabis use disorder or polysubstance disorder with cannabis. The authors were able to collect sufficient data for 48 of these patients for the full year of the study.
All 48, like the others admitted to PEPP, were aged 14-30, met the DSM-IV criteria for psychotic symptoms for at least a week, and had less than a month of past treatment with antipsychotics. The population was predominately male, and more than half came from lower-middle or lower socioeconomic class.
Once entering treatment, 20 of them (41.2%) stopped using marijuana and 28 patients (58.7%) continued. Researchers interviewed the patients every 3 months to determine medication adherence, defined as taking medications more than 75% of the time. At the 6-month follow-up, adherence dropped for both groups. However, it picked back up for the marijuana users by the 12-month follow-up, when 92% of them were regularly taking their antipsychotics, compared with adherence among only 40% of the patients no longer using marijuana (P less than .01).
This finding surprised the researchers, since it conflicts with past research. But they noted the small sample size and hypothesized that those who quit using marijuana may be attributing their psychosis symptoms to the THC and therefore neglecting to continue with medication after having ceased using marijuana. Meanwhile, those who continue to use marijuana may be deciding to stick with their medications to treat ongoing psychosis symptoms.
Cannabis use was significantly associated with higher levels of symptoms – but only after researchers controlled for medication adherence (P = .03). Secondarily, the study revealed that a good number of patients using marijuana can stop using it after entering treatment despite the link between quitting marijuana and lower medication adherence. "Unsurprisingly, patients with more severe substance use disorder at baseline were more likely to persist in using cannabis," the authors wrote.
The authors said their findings point out the value of helping patients stop (or reduce) marijuana use because of the drug’s apparent negative influence on their psychotic symptoms.
Dr. Faridi’s fellowship is partly funded by Pfizer Canada. The other authors cited funding from Pfizer Canada, the Canada Research Chairs Program, and multiple pharmaceutical companies.
FROM SCHIZOPHRENIA RESEARCH
Major Finding: Of 48 first-episode psychosis patients who used cannabis at baseline, the 28 who continued to use after entering treatment had higher rates of medication adherence (25 patients, 92%), compared with the 20 who ceased use (8 patients adherent, 40%). But cannabis use was associated with increased symptom levels after adjustment for medication adherence (P = .03).
Data Source: The findings are based on a prospective cohort study of 48 patients pulled from 192 consecutive admissions to the Prevention and Early Intervention Program for Psychoses in Montreal.
Disclosures: Dr. Faridi’s fellowship was partly funded by Pfizer Canada. The other authors cited funding from Pfizer Canada, the Canada Research Chairs Program, and multiple pharmaceutical companies.
Patients at Risk for Psychosis Show Gradual Decrease in Hippocampal Volume
Patients with an at-risk mental state for psychosis gradually lost hippocampal volume as analyzed with MRI even though only about half of them progressed to full psychosis, according to a longitudinal study published in Schizophrenia Research.
Among the 18 patients who were prospectively followed, no significant differences in hippocampal volume loss were noted between those who transitioned and those who did not, reported Dr. Anna Walter and her associates at University of Basel and University Hospital Basel in Switzerland (Schizophr. Res. 2012 Nov. 5 [doi: 10.1016/j.schres.2012.10.013]).
The longitudinal study examined the extent to which hippocampal volume changes in antipsychotic-naive individuals with an at-risk mental state at the early stages of psychosis. The researchers expected to find decreases in hippocampal volume because past research has shown gray matter volume reductions in first-episode and chronic schizophrenia patients, but findings in patients with an at-risk mental state have been contradictory.
The 18 patients’ at-risk states were defined using Personal Assessment and Crisis Evaluation (PACE) by meeting at least one of three criteria: attenuated psychotic symptoms, brief limited intermittent psychotic symptoms, or a first-degree relative with a psychotic disorder, as well as two indicators in the patient of a clinical change. None had a previous psychotic disorder, borderline personality disorder, or a substance abuse problem, and none had symptoms that clearly derived from an organic disorder. Though none had taken antipsychotics, some had taken antidepressants.
The patients received MRI head scans at intake that included measurement of whole brain volume to allow for correction of head size differences. They were assessed with the Brief Psychiatric Rating Scale (BPRS) each month during the first year of the study, and every 3 months in the second and third years. They were assessed annually in subsequent years until the end of May 2007 or until they transitioned to psychosis, defined with ICD-10 research criteria and confirmed 1 year later. Average follow-up time was 5 years.
Patients were scanned a second time after transitioning to psychosis or at the end of follow-up (1,178 ± 501 days for transitioning patients; 1,541 ± 224 days for nontransitioning). To analyze hippocampal volume, the researchers used a "linear mixed effects model that included a random intercept factor for the subjects and fixed effects for time, hemisphere, age, medication, [whole brain volume] (at baseline) and time by hemisphere interaction."
Although no significant differences existed between those who transitioned to psychosis and those who did not in terms of age, sex, baseline education, and interscan-interval, those who transitioned did trend toward comparatively higher scores at baseline on BPRS and the Scale for the Assessment of Negative Symptoms (SANS).
By the time of follow-up scans, five patients had begun taking antipsychotics; the others were all still antipsychotic naive. The scan analyses revealed a significant reduction in hippocampal volume over time in all the patients, but no statistical difference was found in the hippocampal changes across hemispheres despite a trend for smaller volume on the left side. Also, no statistically significant differences were found in the hippocampal volume reductions between the patients who transitioned and those who did not, showing no "progressive disease-stage related decrease of [hippocampal volume]."
In the second scans of the transitioned patients who had begun taking antipsychotics, the researchers found the drugs were associated with increased hippocampal volume. However, no links between hippocampal volume changes and symptoms (compared to baseline symptoms on BPRS and SANS) appeared, even after accounting for whole brain volume.
The study was funded by a Swiss National Science Foundation grant, and the authors declared no conflicts of interest.
Patients with an at-risk mental state for psychosis gradually lost hippocampal volume as analyzed with MRI even though only about half of them progressed to full psychosis, according to a longitudinal study published in Schizophrenia Research.
Among the 18 patients who were prospectively followed, no significant differences in hippocampal volume loss were noted between those who transitioned and those who did not, reported Dr. Anna Walter and her associates at University of Basel and University Hospital Basel in Switzerland (Schizophr. Res. 2012 Nov. 5 [doi: 10.1016/j.schres.2012.10.013]).
The longitudinal study examined the extent to which hippocampal volume changes in antipsychotic-naive individuals with an at-risk mental state at the early stages of psychosis. The researchers expected to find decreases in hippocampal volume because past research has shown gray matter volume reductions in first-episode and chronic schizophrenia patients, but findings in patients with an at-risk mental state have been contradictory.
The 18 patients’ at-risk states were defined using Personal Assessment and Crisis Evaluation (PACE) by meeting at least one of three criteria: attenuated psychotic symptoms, brief limited intermittent psychotic symptoms, or a first-degree relative with a psychotic disorder, as well as two indicators in the patient of a clinical change. None had a previous psychotic disorder, borderline personality disorder, or a substance abuse problem, and none had symptoms that clearly derived from an organic disorder. Though none had taken antipsychotics, some had taken antidepressants.
The patients received MRI head scans at intake that included measurement of whole brain volume to allow for correction of head size differences. They were assessed with the Brief Psychiatric Rating Scale (BPRS) each month during the first year of the study, and every 3 months in the second and third years. They were assessed annually in subsequent years until the end of May 2007 or until they transitioned to psychosis, defined with ICD-10 research criteria and confirmed 1 year later. Average follow-up time was 5 years.
Patients were scanned a second time after transitioning to psychosis or at the end of follow-up (1,178 ± 501 days for transitioning patients; 1,541 ± 224 days for nontransitioning). To analyze hippocampal volume, the researchers used a "linear mixed effects model that included a random intercept factor for the subjects and fixed effects for time, hemisphere, age, medication, [whole brain volume] (at baseline) and time by hemisphere interaction."
Although no significant differences existed between those who transitioned to psychosis and those who did not in terms of age, sex, baseline education, and interscan-interval, those who transitioned did trend toward comparatively higher scores at baseline on BPRS and the Scale for the Assessment of Negative Symptoms (SANS).
By the time of follow-up scans, five patients had begun taking antipsychotics; the others were all still antipsychotic naive. The scan analyses revealed a significant reduction in hippocampal volume over time in all the patients, but no statistical difference was found in the hippocampal changes across hemispheres despite a trend for smaller volume on the left side. Also, no statistically significant differences were found in the hippocampal volume reductions between the patients who transitioned and those who did not, showing no "progressive disease-stage related decrease of [hippocampal volume]."
In the second scans of the transitioned patients who had begun taking antipsychotics, the researchers found the drugs were associated with increased hippocampal volume. However, no links between hippocampal volume changes and symptoms (compared to baseline symptoms on BPRS and SANS) appeared, even after accounting for whole brain volume.
The study was funded by a Swiss National Science Foundation grant, and the authors declared no conflicts of interest.
Patients with an at-risk mental state for psychosis gradually lost hippocampal volume as analyzed with MRI even though only about half of them progressed to full psychosis, according to a longitudinal study published in Schizophrenia Research.
Among the 18 patients who were prospectively followed, no significant differences in hippocampal volume loss were noted between those who transitioned and those who did not, reported Dr. Anna Walter and her associates at University of Basel and University Hospital Basel in Switzerland (Schizophr. Res. 2012 Nov. 5 [doi: 10.1016/j.schres.2012.10.013]).
The longitudinal study examined the extent to which hippocampal volume changes in antipsychotic-naive individuals with an at-risk mental state at the early stages of psychosis. The researchers expected to find decreases in hippocampal volume because past research has shown gray matter volume reductions in first-episode and chronic schizophrenia patients, but findings in patients with an at-risk mental state have been contradictory.
The 18 patients’ at-risk states were defined using Personal Assessment and Crisis Evaluation (PACE) by meeting at least one of three criteria: attenuated psychotic symptoms, brief limited intermittent psychotic symptoms, or a first-degree relative with a psychotic disorder, as well as two indicators in the patient of a clinical change. None had a previous psychotic disorder, borderline personality disorder, or a substance abuse problem, and none had symptoms that clearly derived from an organic disorder. Though none had taken antipsychotics, some had taken antidepressants.
The patients received MRI head scans at intake that included measurement of whole brain volume to allow for correction of head size differences. They were assessed with the Brief Psychiatric Rating Scale (BPRS) each month during the first year of the study, and every 3 months in the second and third years. They were assessed annually in subsequent years until the end of May 2007 or until they transitioned to psychosis, defined with ICD-10 research criteria and confirmed 1 year later. Average follow-up time was 5 years.
Patients were scanned a second time after transitioning to psychosis or at the end of follow-up (1,178 ± 501 days for transitioning patients; 1,541 ± 224 days for nontransitioning). To analyze hippocampal volume, the researchers used a "linear mixed effects model that included a random intercept factor for the subjects and fixed effects for time, hemisphere, age, medication, [whole brain volume] (at baseline) and time by hemisphere interaction."
Although no significant differences existed between those who transitioned to psychosis and those who did not in terms of age, sex, baseline education, and interscan-interval, those who transitioned did trend toward comparatively higher scores at baseline on BPRS and the Scale for the Assessment of Negative Symptoms (SANS).
By the time of follow-up scans, five patients had begun taking antipsychotics; the others were all still antipsychotic naive. The scan analyses revealed a significant reduction in hippocampal volume over time in all the patients, but no statistical difference was found in the hippocampal changes across hemispheres despite a trend for smaller volume on the left side. Also, no statistically significant differences were found in the hippocampal volume reductions between the patients who transitioned and those who did not, showing no "progressive disease-stage related decrease of [hippocampal volume]."
In the second scans of the transitioned patients who had begun taking antipsychotics, the researchers found the drugs were associated with increased hippocampal volume. However, no links between hippocampal volume changes and symptoms (compared to baseline symptoms on BPRS and SANS) appeared, even after accounting for whole brain volume.
The study was funded by a Swiss National Science Foundation grant, and the authors declared no conflicts of interest.
FROM SCHIZOPHRENIA RESEARCH
Major Finding: Of 18 patients with an at-risk mental state prospectively followed over several years, all showed a gradual significant decrease in hippocampal volume on MRI (P less than .05), even though 8 transitioned to psychosis while 10 did not; increased hippocampal volume was associated with antipsychotic medication use (P less than .05) at follow-up.
Data Source: The findings are based on a prospective cohort study of 18 patients recruited between March 2000 and February 2003 at a specialized clinic for the early detection of psychosis within University Hospital in Basel, Switzerland, and followed through the end of May 2007 or until they transitioned to frank psychosis.
Disclosures: The study was funded with a Swiss National Science Foundation grant. The authors had no disclosures.
Zolpidem Linked to Higher Inpatient Fall Rates
Administration of zolpidem in hospital patients is associated with a significantly higher risk of falls according to a Mayo Clinic study published Nov. 19 in the Journal of Hospital Medicine.
After accounting for a large range of confounders, the researchers found that one additional fall could be expected for every 55 inpatients who received zolpidem. Patients receiving zolpidem were more than three times more likely to fall compared with those who were prescribed it but did not receive it.
Dr. Bhanu Prakash Kolla at the Mayo Clinic’s Center for Sleep Medicine in Rochester, Minn., and his associates, analyzed the fall rate among 16,320 patients admitted to Mayo Clinic hospitals in 2010. All patients over age 18 who had been prescribed zolpidem but were neither pregnant nor ICU patients were included in the analysis (J. Hosp. Med. 2012 Nov. 19 [doi: 10.1002/jhm.1985]).
Using the inpatients pharmacy electronic database and patient records, the authors compared the rate of falls among patients who were actually administered zolpidem to the rate among those who did not receive the medication despite being prescribed it on an "as-needed" basis.
Among the 4,962 patients who received zolpidem, their 151 falls resulted in a fall rate of 3.04%, compared to a fall rate of 0.71% (81 falls) in the 11,358 patients who were prescribed but not administered zolpidem during their hospital stay.
Incidentally, patients not prescribed zolpidem (n = 25,627) had a fall rate of 1.42%, just slightly lower than the overall fall rate of 1.47% among all patients prescribed zolpidem, whether they received it or not. But when all patients who did not receive zolpidem were combined independent of whether they were prescribed it, their 1.24% fall rate was a significant 1.8% higher than that of patients receiving the drug.
The authors recommended that, given the current absence of evidence for other safer hypnotic alternatives for inpatients, "nonpharmacological measures to improve the sleep of hospitalized patients should be investigated as preferred methods to provide safe relief from complaints of disturbed sleep."
The researchers controlled for confounders that may increase fall risk, including age, length of hospital stay, being on a surgical floor, zolpidem dose, visual impairment, gait abnormalities, cognitive impairment/dementia, insomnia, delirium, comorbidities (measured with the Charlson comorbidity index) and patient’s Hendrich’s fall risk score.
The analysis also controlled for medications that patients received in the 24 hours before the fall that are already associated with an increased fall risk, including antidepressants, antipsychotics, antihistamines, sedative antidepressants including trazodone and mirtazapine, benzodiazepines, and opioids.
A univariate analysis revealed that all factors significantly associated with a higher fall rate included zolpidem use (OR = 4.37), being male (OR = 1.36) and having insomnia (OR = 2.37) or delirium (OR = 4.96) as well as increasing age, zolpidem dose, comorbidity scores and fall risk scores.
When the researchers accounted for all statistically significant additional fall risk factors, the association between zolpidem use and fall risk was still significant with an OR of 6.39. There was no statistically significant association identified for the other medications accounted for in the analysis.
The study was funded through the Mayo Clinic’s fellowship training program, and the authors had no disclosures.
Administration of zolpidem in hospital patients is associated with a significantly higher risk of falls according to a Mayo Clinic study published Nov. 19 in the Journal of Hospital Medicine.
After accounting for a large range of confounders, the researchers found that one additional fall could be expected for every 55 inpatients who received zolpidem. Patients receiving zolpidem were more than three times more likely to fall compared with those who were prescribed it but did not receive it.
Dr. Bhanu Prakash Kolla at the Mayo Clinic’s Center for Sleep Medicine in Rochester, Minn., and his associates, analyzed the fall rate among 16,320 patients admitted to Mayo Clinic hospitals in 2010. All patients over age 18 who had been prescribed zolpidem but were neither pregnant nor ICU patients were included in the analysis (J. Hosp. Med. 2012 Nov. 19 [doi: 10.1002/jhm.1985]).
Using the inpatients pharmacy electronic database and patient records, the authors compared the rate of falls among patients who were actually administered zolpidem to the rate among those who did not receive the medication despite being prescribed it on an "as-needed" basis.
Among the 4,962 patients who received zolpidem, their 151 falls resulted in a fall rate of 3.04%, compared to a fall rate of 0.71% (81 falls) in the 11,358 patients who were prescribed but not administered zolpidem during their hospital stay.
Incidentally, patients not prescribed zolpidem (n = 25,627) had a fall rate of 1.42%, just slightly lower than the overall fall rate of 1.47% among all patients prescribed zolpidem, whether they received it or not. But when all patients who did not receive zolpidem were combined independent of whether they were prescribed it, their 1.24% fall rate was a significant 1.8% higher than that of patients receiving the drug.
The authors recommended that, given the current absence of evidence for other safer hypnotic alternatives for inpatients, "nonpharmacological measures to improve the sleep of hospitalized patients should be investigated as preferred methods to provide safe relief from complaints of disturbed sleep."
The researchers controlled for confounders that may increase fall risk, including age, length of hospital stay, being on a surgical floor, zolpidem dose, visual impairment, gait abnormalities, cognitive impairment/dementia, insomnia, delirium, comorbidities (measured with the Charlson comorbidity index) and patient’s Hendrich’s fall risk score.
The analysis also controlled for medications that patients received in the 24 hours before the fall that are already associated with an increased fall risk, including antidepressants, antipsychotics, antihistamines, sedative antidepressants including trazodone and mirtazapine, benzodiazepines, and opioids.
A univariate analysis revealed that all factors significantly associated with a higher fall rate included zolpidem use (OR = 4.37), being male (OR = 1.36) and having insomnia (OR = 2.37) or delirium (OR = 4.96) as well as increasing age, zolpidem dose, comorbidity scores and fall risk scores.
When the researchers accounted for all statistically significant additional fall risk factors, the association between zolpidem use and fall risk was still significant with an OR of 6.39. There was no statistically significant association identified for the other medications accounted for in the analysis.
The study was funded through the Mayo Clinic’s fellowship training program, and the authors had no disclosures.
Administration of zolpidem in hospital patients is associated with a significantly higher risk of falls according to a Mayo Clinic study published Nov. 19 in the Journal of Hospital Medicine.
After accounting for a large range of confounders, the researchers found that one additional fall could be expected for every 55 inpatients who received zolpidem. Patients receiving zolpidem were more than three times more likely to fall compared with those who were prescribed it but did not receive it.
Dr. Bhanu Prakash Kolla at the Mayo Clinic’s Center for Sleep Medicine in Rochester, Minn., and his associates, analyzed the fall rate among 16,320 patients admitted to Mayo Clinic hospitals in 2010. All patients over age 18 who had been prescribed zolpidem but were neither pregnant nor ICU patients were included in the analysis (J. Hosp. Med. 2012 Nov. 19 [doi: 10.1002/jhm.1985]).
Using the inpatients pharmacy electronic database and patient records, the authors compared the rate of falls among patients who were actually administered zolpidem to the rate among those who did not receive the medication despite being prescribed it on an "as-needed" basis.
Among the 4,962 patients who received zolpidem, their 151 falls resulted in a fall rate of 3.04%, compared to a fall rate of 0.71% (81 falls) in the 11,358 patients who were prescribed but not administered zolpidem during their hospital stay.
Incidentally, patients not prescribed zolpidem (n = 25,627) had a fall rate of 1.42%, just slightly lower than the overall fall rate of 1.47% among all patients prescribed zolpidem, whether they received it or not. But when all patients who did not receive zolpidem were combined independent of whether they were prescribed it, their 1.24% fall rate was a significant 1.8% higher than that of patients receiving the drug.
The authors recommended that, given the current absence of evidence for other safer hypnotic alternatives for inpatients, "nonpharmacological measures to improve the sleep of hospitalized patients should be investigated as preferred methods to provide safe relief from complaints of disturbed sleep."
The researchers controlled for confounders that may increase fall risk, including age, length of hospital stay, being on a surgical floor, zolpidem dose, visual impairment, gait abnormalities, cognitive impairment/dementia, insomnia, delirium, comorbidities (measured with the Charlson comorbidity index) and patient’s Hendrich’s fall risk score.
The analysis also controlled for medications that patients received in the 24 hours before the fall that are already associated with an increased fall risk, including antidepressants, antipsychotics, antihistamines, sedative antidepressants including trazodone and mirtazapine, benzodiazepines, and opioids.
A univariate analysis revealed that all factors significantly associated with a higher fall rate included zolpidem use (OR = 4.37), being male (OR = 1.36) and having insomnia (OR = 2.37) or delirium (OR = 4.96) as well as increasing age, zolpidem dose, comorbidity scores and fall risk scores.
When the researchers accounted for all statistically significant additional fall risk factors, the association between zolpidem use and fall risk was still significant with an OR of 6.39. There was no statistically significant association identified for the other medications accounted for in the analysis.
The study was funded through the Mayo Clinic’s fellowship training program, and the authors had no disclosures.
FROM THE JOURNAL OF HOSPITAL MEDICINE
Major Finding: The fall risk in 4,962 hospital inpatients who received zolpidem was 3.04% vs. 0.71% in 11,358 inpatients who were prescribed but not administered the drug.
Data Source: The findings are based on a retrospective cohort study of 16,320 adult patients admitted in 2010 to Mayo Clinic hospitals who were prescribed zolpidem, excluding ICU and pregnant patients.
Disclosures: The study was funded through the Mayo Clinic’s fellowship training program, and the authors had no disclosures.
Doctors Need More Resources to Manage Pediatric Concussion
Pediatric primary care and emergency providers often feel ill prepared or lacking in resources, time, or training to effectively manage concussion in children and educate families about the condition and recovery, according to a survey published in the November 2012 issue of Pediatrics.
The findings come from a survey assessing what practicing physicians, nurse practitioners, and physician assistants know about concussion as well as their treatment practices and any perceived obstacles to managing the condition, reported by Dr. Mark R. Zonfrillo of the center for injury research and prevention at Children’s Hospital of Philadelphia and the University of Pennsylvania and his associates (Pediatrics 2012;130:1-6).
An online survey using multiple-choice, Likert scale, and open-ended questions was sent to 276 providers in the Children’s Hospital of Philadelphia Care Network and Emergency Department e-mail lists. The 53% response rate included 145 responding providers with a diverse range of experience. Sixty-one percent were pediatric primary care providers, and 39% were pediatric emergency care providers.
A total of 91% of respondents reported having cared for at least one patient with concussion in the past 3 months. Most of these providers (134, or 92%) referred at least one patient to a concussion specialist after the first exam, usually either because they were uncomfortable with managing the concussion (49%) or because they did not have the necessary resources to manage it (47%). In addition, 30% of primary care providers and 68% of emergency providers said their "setting is not always appropriate for management," the investigators said.
Both primary care providers and emergency providers were highly likely to refer concussion patients to sports medicine doctors or clinics (67% vs. 75%, respectively); primary care respondents were twice as likely as emergency providers to refer patients to neurologists (46% vs. 22%). Emergency providers also were likely to refer to a trauma surgeon or clinic (83%), while primary care providers rarely did (13%).
Past studies have found that approximately 100,000-140,000 U.S. children go to the emergency department each year for concussion, but parents and children may underreport concussion symptoms, and many youth sports coaches have misconceptions about them.
In the two scenarios presented in the survey – one of a patient with a subtle concussion and the other of a patient with more obvious symptoms – almost all respondents determined that both hypothetical patients had a concussion. However, some respondents did not recognize some of the symptoms of concussion, including abnormal eye tracking (17%), difficulty concentrating (11%), vestibular disturbance (9%), worsening school performance (6%), and sensitivity to light or noise (6%). "These more subtle signs of concussion may present in isolation and thus may be the only indication that a child has sustained the injury," the authors wrote.
A total of 104 providers reported they did not have access to a provider decision support tool relating to concussion, and 96% of these believed one would be helpful. All 57 respondents who said they didn’t have discharge instructions related to concussion said support tools would be helpful.
Doctors cited a lack of training most often when it came to obstacles to educating families about the diagnosis and recommending time off before returning to school or sports. Further, 69% of primary care providers and 77% of emergency providers said they don’t have enough time to complete formal neurocognitive testing for concussed patients.
The study was funded by the Children’s Hospital of Philadelphia Department of Pediatrics Chair’s Initiative. The authors said they had no relevant financial disclosures.
Concussion is an injury doctors will see in their practice regularly because it is happening more frequently. There is increased awareness about concussion, doctors are picking up previously unreported concussions, and more state laws require medical clearance after a concussion before a return to play. There also are more children participating in contact sports year-round and at younger ages, so there is more exposure for injury. Pediatricians need to feel confident that they can provide adequate frontline care, according to Dr. Kevin Walter.
Dr. Zonfrillo’s findings indicate there is still a lot of confusion about what a concussion is, most likely because medical education about concussion is lacking. Also, kids often lie to get back to playing. As with everything in medicine, providers are being asked to do more with less time. Although there are resources like the Centers for Disease Control and Prevention’s Heads-Up tool kit and the American Academy of Pediatrics 2010 clinical report (Pediatrics 2010;126:597-615), what would be most helpful is for health systems to have a protocol or best practice guideline for providers in that system.
With concussions, everyone is different, and the cookie cutter approach used for other conditions doesn’t work with concussion. Concussion is broader and more general, so providers have to individualize care management to each patient according to the patient’s injury and situation.
Dr. Walter is with the department of orthopedic surgery and the department of pediatrics at the Medical College of Wisconsin, Milwaukee, and was lead author of the AAP’s clinical report "Sport-Related Concussion in Children and Adolescents." He made these comments during an interview.
Concussion is an injury doctors will see in their practice regularly because it is happening more frequently. There is increased awareness about concussion, doctors are picking up previously unreported concussions, and more state laws require medical clearance after a concussion before a return to play. There also are more children participating in contact sports year-round and at younger ages, so there is more exposure for injury. Pediatricians need to feel confident that they can provide adequate frontline care, according to Dr. Kevin Walter.
Dr. Zonfrillo’s findings indicate there is still a lot of confusion about what a concussion is, most likely because medical education about concussion is lacking. Also, kids often lie to get back to playing. As with everything in medicine, providers are being asked to do more with less time. Although there are resources like the Centers for Disease Control and Prevention’s Heads-Up tool kit and the American Academy of Pediatrics 2010 clinical report (Pediatrics 2010;126:597-615), what would be most helpful is for health systems to have a protocol or best practice guideline for providers in that system.
With concussions, everyone is different, and the cookie cutter approach used for other conditions doesn’t work with concussion. Concussion is broader and more general, so providers have to individualize care management to each patient according to the patient’s injury and situation.
Dr. Walter is with the department of orthopedic surgery and the department of pediatrics at the Medical College of Wisconsin, Milwaukee, and was lead author of the AAP’s clinical report "Sport-Related Concussion in Children and Adolescents." He made these comments during an interview.
Concussion is an injury doctors will see in their practice regularly because it is happening more frequently. There is increased awareness about concussion, doctors are picking up previously unreported concussions, and more state laws require medical clearance after a concussion before a return to play. There also are more children participating in contact sports year-round and at younger ages, so there is more exposure for injury. Pediatricians need to feel confident that they can provide adequate frontline care, according to Dr. Kevin Walter.
Dr. Zonfrillo’s findings indicate there is still a lot of confusion about what a concussion is, most likely because medical education about concussion is lacking. Also, kids often lie to get back to playing. As with everything in medicine, providers are being asked to do more with less time. Although there are resources like the Centers for Disease Control and Prevention’s Heads-Up tool kit and the American Academy of Pediatrics 2010 clinical report (Pediatrics 2010;126:597-615), what would be most helpful is for health systems to have a protocol or best practice guideline for providers in that system.
With concussions, everyone is different, and the cookie cutter approach used for other conditions doesn’t work with concussion. Concussion is broader and more general, so providers have to individualize care management to each patient according to the patient’s injury and situation.
Dr. Walter is with the department of orthopedic surgery and the department of pediatrics at the Medical College of Wisconsin, Milwaukee, and was lead author of the AAP’s clinical report "Sport-Related Concussion in Children and Adolescents." He made these comments during an interview.
Pediatric primary care and emergency providers often feel ill prepared or lacking in resources, time, or training to effectively manage concussion in children and educate families about the condition and recovery, according to a survey published in the November 2012 issue of Pediatrics.
The findings come from a survey assessing what practicing physicians, nurse practitioners, and physician assistants know about concussion as well as their treatment practices and any perceived obstacles to managing the condition, reported by Dr. Mark R. Zonfrillo of the center for injury research and prevention at Children’s Hospital of Philadelphia and the University of Pennsylvania and his associates (Pediatrics 2012;130:1-6).
An online survey using multiple-choice, Likert scale, and open-ended questions was sent to 276 providers in the Children’s Hospital of Philadelphia Care Network and Emergency Department e-mail lists. The 53% response rate included 145 responding providers with a diverse range of experience. Sixty-one percent were pediatric primary care providers, and 39% were pediatric emergency care providers.
A total of 91% of respondents reported having cared for at least one patient with concussion in the past 3 months. Most of these providers (134, or 92%) referred at least one patient to a concussion specialist after the first exam, usually either because they were uncomfortable with managing the concussion (49%) or because they did not have the necessary resources to manage it (47%). In addition, 30% of primary care providers and 68% of emergency providers said their "setting is not always appropriate for management," the investigators said.
Both primary care providers and emergency providers were highly likely to refer concussion patients to sports medicine doctors or clinics (67% vs. 75%, respectively); primary care respondents were twice as likely as emergency providers to refer patients to neurologists (46% vs. 22%). Emergency providers also were likely to refer to a trauma surgeon or clinic (83%), while primary care providers rarely did (13%).
Past studies have found that approximately 100,000-140,000 U.S. children go to the emergency department each year for concussion, but parents and children may underreport concussion symptoms, and many youth sports coaches have misconceptions about them.
In the two scenarios presented in the survey – one of a patient with a subtle concussion and the other of a patient with more obvious symptoms – almost all respondents determined that both hypothetical patients had a concussion. However, some respondents did not recognize some of the symptoms of concussion, including abnormal eye tracking (17%), difficulty concentrating (11%), vestibular disturbance (9%), worsening school performance (6%), and sensitivity to light or noise (6%). "These more subtle signs of concussion may present in isolation and thus may be the only indication that a child has sustained the injury," the authors wrote.
A total of 104 providers reported they did not have access to a provider decision support tool relating to concussion, and 96% of these believed one would be helpful. All 57 respondents who said they didn’t have discharge instructions related to concussion said support tools would be helpful.
Doctors cited a lack of training most often when it came to obstacles to educating families about the diagnosis and recommending time off before returning to school or sports. Further, 69% of primary care providers and 77% of emergency providers said they don’t have enough time to complete formal neurocognitive testing for concussed patients.
The study was funded by the Children’s Hospital of Philadelphia Department of Pediatrics Chair’s Initiative. The authors said they had no relevant financial disclosures.
Pediatric primary care and emergency providers often feel ill prepared or lacking in resources, time, or training to effectively manage concussion in children and educate families about the condition and recovery, according to a survey published in the November 2012 issue of Pediatrics.
The findings come from a survey assessing what practicing physicians, nurse practitioners, and physician assistants know about concussion as well as their treatment practices and any perceived obstacles to managing the condition, reported by Dr. Mark R. Zonfrillo of the center for injury research and prevention at Children’s Hospital of Philadelphia and the University of Pennsylvania and his associates (Pediatrics 2012;130:1-6).
An online survey using multiple-choice, Likert scale, and open-ended questions was sent to 276 providers in the Children’s Hospital of Philadelphia Care Network and Emergency Department e-mail lists. The 53% response rate included 145 responding providers with a diverse range of experience. Sixty-one percent were pediatric primary care providers, and 39% were pediatric emergency care providers.
A total of 91% of respondents reported having cared for at least one patient with concussion in the past 3 months. Most of these providers (134, or 92%) referred at least one patient to a concussion specialist after the first exam, usually either because they were uncomfortable with managing the concussion (49%) or because they did not have the necessary resources to manage it (47%). In addition, 30% of primary care providers and 68% of emergency providers said their "setting is not always appropriate for management," the investigators said.
Both primary care providers and emergency providers were highly likely to refer concussion patients to sports medicine doctors or clinics (67% vs. 75%, respectively); primary care respondents were twice as likely as emergency providers to refer patients to neurologists (46% vs. 22%). Emergency providers also were likely to refer to a trauma surgeon or clinic (83%), while primary care providers rarely did (13%).
Past studies have found that approximately 100,000-140,000 U.S. children go to the emergency department each year for concussion, but parents and children may underreport concussion symptoms, and many youth sports coaches have misconceptions about them.
In the two scenarios presented in the survey – one of a patient with a subtle concussion and the other of a patient with more obvious symptoms – almost all respondents determined that both hypothetical patients had a concussion. However, some respondents did not recognize some of the symptoms of concussion, including abnormal eye tracking (17%), difficulty concentrating (11%), vestibular disturbance (9%), worsening school performance (6%), and sensitivity to light or noise (6%). "These more subtle signs of concussion may present in isolation and thus may be the only indication that a child has sustained the injury," the authors wrote.
A total of 104 providers reported they did not have access to a provider decision support tool relating to concussion, and 96% of these believed one would be helpful. All 57 respondents who said they didn’t have discharge instructions related to concussion said support tools would be helpful.
Doctors cited a lack of training most often when it came to obstacles to educating families about the diagnosis and recommending time off before returning to school or sports. Further, 69% of primary care providers and 77% of emergency providers said they don’t have enough time to complete formal neurocognitive testing for concussed patients.
The study was funded by the Children’s Hospital of Philadelphia Department of Pediatrics Chair’s Initiative. The authors said they had no relevant financial disclosures.
FROM PEDIATRICS
Major Finding: Although 91% of pediatric and emergency providers reported caring for at least one concussed patient in the past 3 months, pediatric providers reported referring patients to specialists because they did not feel comfortable with management (49%) or lacked adequate resources for management (47%).
Data Source: Results are from a survey of 145 providers that included physicians, nurse practitioners, and physician assistants in the emergency department and primary care network of the Children’s Hospital of Philadelphia Care Network and Emergency Department.
Disclosures: The research was funded by the Children’s Hospital of Philadelphia Department of Pediatrics Chair’s Initiative. The authors said they had no relevant financial disclosures.
ASCO Update Keeps Breast Cancer Survivor Guidelines Intact
The American Society of Clinical Oncology has issued updated recommendations for the follow-up care of breast cancer survivors, but made no changes from guidelines released in 2006.
The current guidelines include recommendations for all oncologists, primary care providers, and nurses who treat asymptomatic breast cancer survivors. They emphasize physical exams, patient history, and mammography, but discourage routine blood tests, biomarker studies, and other imaging in the absence of symptoms.
An American Society of Clinical Oncology (ASCO) panel reviewed the literature for studies that specifically focused on patient management for patients who had finished their primary therapy to cure breast cancer. The updated recommendations were published online Nov. 5 in the Journal of Clinical Oncology (doi: 10.1200/JCO.2012.45.9859).
Dr. James L. Khatcheressian, from the Virginia Cancer Institute in Richmond, and his associates on the ASCO Clinical Practice Guidelines Committee searched Medline and the Cochrane Library for all systematic reviews, clinical practice guidelines, and randomized controlled trials published between March 2006 and March 2012.
The committee primarily sought outcomes data on "disease-free survival, overall survival, health-related quality of life, reduced toxicity, and cost effectiveness." Its analysis of nine systematic reviews (including three meta-analyses) and five randomized controlled trials led the committee to conclude that no modifications to the clinical practice guidelines from 6 years ago were necessary.
The recommendations are as follows:
• Providers should give women a physical exam and history every 3-6 months for the first 3 years after they receive primary therapy. Then, a history and physical exam should be conducted every 6-12 months for the next 2 years, followed by annual ones.
• Women who had breast-conserving surgery should receive their first mammogram at least 6 months after completing radiation therapy, followed by a mammogram every 6-12 months. Once they achieve "stability of mammographic findings" after completing locoregional therapy, mammography can be done yearly.
• Women should be advised to do monthly breast self-exams and be educated about symptoms indicating possible cancer recurrence, such as lumps, bone pain, chest pain, dyspnea, abdominal pain, or persistent headaches.
• Those who meet the criteria for high risk of family breast cancer should be referred to genetic counseling. These criteria include "Ashkenazi Jewish heritage; history of ovarian cancer at any age in the patient or any first- or second-degree relatives; any first-degree relative with a history of breast cancer diagnosed before the age of 50 years; two or more first- or second-degree relatives diagnosed with breast cancer at any age; patient or relative with diagnosis of bilateral breast cancer; and history of breast cancer in a male relative."
• Women should also receive regular annual gynecologic care, except those who had a total hysterectomy or oophorectomy, who can have less frequent checkups. Women who take tamoxifen should be instructed to tell their doctor about any vaginal bleeding since they are at a higher risk for endometrial cancer.
Although the committee recommends continuous care by a doctor with experience in breast exams and cancer survivors, they note that "follow-up by a primary care provider seems to lead to the same health outcomes as specialist follow-up, with good patient satisfaction." Women with early-stage breast cancer wishing to be treated by their primary care provider may be transferred a year after diagnosis.
The clinical practice guidelines note that routine blood tests (CBC testing and chemistry panels), breast cancer tumor marker testing, and imaging studies besides mammograms are not recommended if patients have no symptoms. Chest x-rays, bone scans, liver ultrasounds, CT scans, 18F-deoxyglucose (FDG)–PET scans, and breast MRIs also are not recommended for standard follow-up care.
However, the committee stated that the practice guidelines are voluntary, and "do not account for individual variation among patients and may not reflect the most recent evidence." Therefore, management of each patient should depend on her case history and circumstances, and rely on the professional judgment of her doctor.
While the committee concluded that no new evidence warrants changes to the guidelines, it said that research is needed (in particular, randomized controlled trials) on comparative effectiveness of different surveillance strategies and duration of follow-up. It also called for more research into tumor marker testing and identification of patient subsets that would benefit from various models of care.
The article received no external funding. Lead author Dr. N. Lynn Henry has been paid for consultancy or advisory work for GE Healthcare. No other disclosures were reported.
The American Society of Clinical Oncology has issued updated recommendations for the follow-up care of breast cancer survivors, but made no changes from guidelines released in 2006.
The current guidelines include recommendations for all oncologists, primary care providers, and nurses who treat asymptomatic breast cancer survivors. They emphasize physical exams, patient history, and mammography, but discourage routine blood tests, biomarker studies, and other imaging in the absence of symptoms.
An American Society of Clinical Oncology (ASCO) panel reviewed the literature for studies that specifically focused on patient management for patients who had finished their primary therapy to cure breast cancer. The updated recommendations were published online Nov. 5 in the Journal of Clinical Oncology (doi: 10.1200/JCO.2012.45.9859).
Dr. James L. Khatcheressian, from the Virginia Cancer Institute in Richmond, and his associates on the ASCO Clinical Practice Guidelines Committee searched Medline and the Cochrane Library for all systematic reviews, clinical practice guidelines, and randomized controlled trials published between March 2006 and March 2012.
The committee primarily sought outcomes data on "disease-free survival, overall survival, health-related quality of life, reduced toxicity, and cost effectiveness." Its analysis of nine systematic reviews (including three meta-analyses) and five randomized controlled trials led the committee to conclude that no modifications to the clinical practice guidelines from 6 years ago were necessary.
The recommendations are as follows:
• Providers should give women a physical exam and history every 3-6 months for the first 3 years after they receive primary therapy. Then, a history and physical exam should be conducted every 6-12 months for the next 2 years, followed by annual ones.
• Women who had breast-conserving surgery should receive their first mammogram at least 6 months after completing radiation therapy, followed by a mammogram every 6-12 months. Once they achieve "stability of mammographic findings" after completing locoregional therapy, mammography can be done yearly.
• Women should be advised to do monthly breast self-exams and be educated about symptoms indicating possible cancer recurrence, such as lumps, bone pain, chest pain, dyspnea, abdominal pain, or persistent headaches.
• Those who meet the criteria for high risk of family breast cancer should be referred to genetic counseling. These criteria include "Ashkenazi Jewish heritage; history of ovarian cancer at any age in the patient or any first- or second-degree relatives; any first-degree relative with a history of breast cancer diagnosed before the age of 50 years; two or more first- or second-degree relatives diagnosed with breast cancer at any age; patient or relative with diagnosis of bilateral breast cancer; and history of breast cancer in a male relative."
• Women should also receive regular annual gynecologic care, except those who had a total hysterectomy or oophorectomy, who can have less frequent checkups. Women who take tamoxifen should be instructed to tell their doctor about any vaginal bleeding since they are at a higher risk for endometrial cancer.
Although the committee recommends continuous care by a doctor with experience in breast exams and cancer survivors, they note that "follow-up by a primary care provider seems to lead to the same health outcomes as specialist follow-up, with good patient satisfaction." Women with early-stage breast cancer wishing to be treated by their primary care provider may be transferred a year after diagnosis.
The clinical practice guidelines note that routine blood tests (CBC testing and chemistry panels), breast cancer tumor marker testing, and imaging studies besides mammograms are not recommended if patients have no symptoms. Chest x-rays, bone scans, liver ultrasounds, CT scans, 18F-deoxyglucose (FDG)–PET scans, and breast MRIs also are not recommended for standard follow-up care.
However, the committee stated that the practice guidelines are voluntary, and "do not account for individual variation among patients and may not reflect the most recent evidence." Therefore, management of each patient should depend on her case history and circumstances, and rely on the professional judgment of her doctor.
While the committee concluded that no new evidence warrants changes to the guidelines, it said that research is needed (in particular, randomized controlled trials) on comparative effectiveness of different surveillance strategies and duration of follow-up. It also called for more research into tumor marker testing and identification of patient subsets that would benefit from various models of care.
The article received no external funding. Lead author Dr. N. Lynn Henry has been paid for consultancy or advisory work for GE Healthcare. No other disclosures were reported.
The American Society of Clinical Oncology has issued updated recommendations for the follow-up care of breast cancer survivors, but made no changes from guidelines released in 2006.
The current guidelines include recommendations for all oncologists, primary care providers, and nurses who treat asymptomatic breast cancer survivors. They emphasize physical exams, patient history, and mammography, but discourage routine blood tests, biomarker studies, and other imaging in the absence of symptoms.
An American Society of Clinical Oncology (ASCO) panel reviewed the literature for studies that specifically focused on patient management for patients who had finished their primary therapy to cure breast cancer. The updated recommendations were published online Nov. 5 in the Journal of Clinical Oncology (doi: 10.1200/JCO.2012.45.9859).
Dr. James L. Khatcheressian, from the Virginia Cancer Institute in Richmond, and his associates on the ASCO Clinical Practice Guidelines Committee searched Medline and the Cochrane Library for all systematic reviews, clinical practice guidelines, and randomized controlled trials published between March 2006 and March 2012.
The committee primarily sought outcomes data on "disease-free survival, overall survival, health-related quality of life, reduced toxicity, and cost effectiveness." Its analysis of nine systematic reviews (including three meta-analyses) and five randomized controlled trials led the committee to conclude that no modifications to the clinical practice guidelines from 6 years ago were necessary.
The recommendations are as follows:
• Providers should give women a physical exam and history every 3-6 months for the first 3 years after they receive primary therapy. Then, a history and physical exam should be conducted every 6-12 months for the next 2 years, followed by annual ones.
• Women who had breast-conserving surgery should receive their first mammogram at least 6 months after completing radiation therapy, followed by a mammogram every 6-12 months. Once they achieve "stability of mammographic findings" after completing locoregional therapy, mammography can be done yearly.
• Women should be advised to do monthly breast self-exams and be educated about symptoms indicating possible cancer recurrence, such as lumps, bone pain, chest pain, dyspnea, abdominal pain, or persistent headaches.
• Those who meet the criteria for high risk of family breast cancer should be referred to genetic counseling. These criteria include "Ashkenazi Jewish heritage; history of ovarian cancer at any age in the patient or any first- or second-degree relatives; any first-degree relative with a history of breast cancer diagnosed before the age of 50 years; two or more first- or second-degree relatives diagnosed with breast cancer at any age; patient or relative with diagnosis of bilateral breast cancer; and history of breast cancer in a male relative."
• Women should also receive regular annual gynecologic care, except those who had a total hysterectomy or oophorectomy, who can have less frequent checkups. Women who take tamoxifen should be instructed to tell their doctor about any vaginal bleeding since they are at a higher risk for endometrial cancer.
Although the committee recommends continuous care by a doctor with experience in breast exams and cancer survivors, they note that "follow-up by a primary care provider seems to lead to the same health outcomes as specialist follow-up, with good patient satisfaction." Women with early-stage breast cancer wishing to be treated by their primary care provider may be transferred a year after diagnosis.
The clinical practice guidelines note that routine blood tests (CBC testing and chemistry panels), breast cancer tumor marker testing, and imaging studies besides mammograms are not recommended if patients have no symptoms. Chest x-rays, bone scans, liver ultrasounds, CT scans, 18F-deoxyglucose (FDG)–PET scans, and breast MRIs also are not recommended for standard follow-up care.
However, the committee stated that the practice guidelines are voluntary, and "do not account for individual variation among patients and may not reflect the most recent evidence." Therefore, management of each patient should depend on her case history and circumstances, and rely on the professional judgment of her doctor.
While the committee concluded that no new evidence warrants changes to the guidelines, it said that research is needed (in particular, randomized controlled trials) on comparative effectiveness of different surveillance strategies and duration of follow-up. It also called for more research into tumor marker testing and identification of patient subsets that would benefit from various models of care.
The article received no external funding. Lead author Dr. N. Lynn Henry has been paid for consultancy or advisory work for GE Healthcare. No other disclosures were reported.
FROM THE JOURNAL OF CLINICAL ONCOLOGY
Major Finding: Updated recommendations from the American Society of Clinical Oncology’s guidelines on follow-up care for breast cancer survivors remain unchanged from 2006 guidelines, and include regular physical exams and mammography.
Data Source: The updated review of the literature consisted of 14 studies, including 9 systematic reviews and 5 randomized controlled trials.
Disclosures: The article received no external funding. Lead author Dr. N. Lynn Henry has been paid for consultancy or advisory work for GE Healthcare. No other disclosures were reported.
Third MMR Dose Helps Control Mumps Outbreak
Administering a third booster dose of the MMR vaccine during a mumps outbreak has been shown to decrease the spread of the disease in an already highly vaccinated population, according to a study published online in Pediatrics.
The vaccination intervention in one community led to a 96% drop (from 4.93% to 0.13%) in mumps attack rates among 11- to 17-year-olds, the population targeted in the intervention, reported Dr. Ikechukwu U. Ogbuanu of the epidemic intelligence center at the Centers for Disease Control and Prevention and his associates (Pediatrics 2012 Nov. 5 [doi:10.1542/peds.2012.0177]). The communitywide rate decreased by 75.6% (from a 0.86% attack ratio preintervention to 0.21% in the 3-week postintervention period).
A mumps outbreak involving 3,502 cases in the Northeastern United States from June 1, 2009, to June 30, 2010, included 790 cases in a close-knit Orthodox Jewish community in Orange County, N.Y. Officials selected that community, which represented 22.6% of the outbreak’s cases, to initiate a third-dose MMR vaccination intervention in three schools when standard outbreak control measures failed to slow the disease spread.
The outbreak had been traced to an 11-year-old U.S. resident who had received two doses of the MMR vaccine but had just returned from the United Kingdom where a mumps outbreak was ongoing. After he attended an Orthodox Jewish boys’ camp in New York, 25 cases were reported among campers. The disease then spread to families in the community when these boys returned home, reaching 392 cases in Orange County by Dec. 31, 2009. Among those who contracted the disease, 74% (290 patients) had received both MMR vaccine doses.
A third dose of the MMR was offered to 6th-12th graders at three of four schools in Orange County. Schools eligible for the intervention were required to have high two-dose MMR coverage and to have ongoing mumps transmission for the 2 weeks leading up to the intervention. Students who had not gotten mumps during the outbreak and had already had two doses of the MMR vaccine were eligible to receive the third dose from Jan. 19 to Feb. 2, 2010. Of 2,178 eligible students, 1,755 (80.6%) received the third dose.
Researchers then calculated mumps attack rates three times: in the 3 weeks before and after the vaccination intervention, and at 3 weeks following the second 3-week report. The average mumps incubation period is 16-18 days. Researchers divided the new mumps cases in each data collection period by the number of students who did not have mumps at the start of the period, to get the attack ratios.
The mumps attack rate among all students at the three schools dropped from 4.9% in the 3 weeks before the third dose was administered to 1.55% in the 3 weeks afterward (P value less than .001). During this second phase, rates were similar among vaccinated (1.60%) and unvaccinated (1.67%) students, but cases among vaccinated students were eight times lower (P = .097)* in the third phase of data collection, when the overall attack rate among all the students at the intervention schools dropped to 0.13%.
Follow-up data from 1,597 students who received the third dose (91% response rate) revealed adverse events occurring in 115 students (7.2%), primarily "pain, redness, or swelling at the injection site" and "joint or muscle aches." No students reported serious adverse events.
One study limitation was that the intervention occurred after the outbreak’s peak, so "it is not possible to exclude the possibility that the rapid decline in incidence after the intervention was entirely unrelated to our intervention," the authors wrote. The authors also noted their results mean a third MMR dose might be effective in outbreak control only in "highly vaccinated populations in certain settings" but do "not support the routine use of a third dose of mumps vaccine in national vaccination programs."
The investigators reported no external funding and no financial disclosures.
*Correction, 11/06/2012: An earlier version of this article misstated the p value.
Administering a third booster dose of the MMR vaccine during a mumps outbreak has been shown to decrease the spread of the disease in an already highly vaccinated population, according to a study published online in Pediatrics.
The vaccination intervention in one community led to a 96% drop (from 4.93% to 0.13%) in mumps attack rates among 11- to 17-year-olds, the population targeted in the intervention, reported Dr. Ikechukwu U. Ogbuanu of the epidemic intelligence center at the Centers for Disease Control and Prevention and his associates (Pediatrics 2012 Nov. 5 [doi:10.1542/peds.2012.0177]). The communitywide rate decreased by 75.6% (from a 0.86% attack ratio preintervention to 0.21% in the 3-week postintervention period).
A mumps outbreak involving 3,502 cases in the Northeastern United States from June 1, 2009, to June 30, 2010, included 790 cases in a close-knit Orthodox Jewish community in Orange County, N.Y. Officials selected that community, which represented 22.6% of the outbreak’s cases, to initiate a third-dose MMR vaccination intervention in three schools when standard outbreak control measures failed to slow the disease spread.
The outbreak had been traced to an 11-year-old U.S. resident who had received two doses of the MMR vaccine but had just returned from the United Kingdom where a mumps outbreak was ongoing. After he attended an Orthodox Jewish boys’ camp in New York, 25 cases were reported among campers. The disease then spread to families in the community when these boys returned home, reaching 392 cases in Orange County by Dec. 31, 2009. Among those who contracted the disease, 74% (290 patients) had received both MMR vaccine doses.
A third dose of the MMR was offered to 6th-12th graders at three of four schools in Orange County. Schools eligible for the intervention were required to have high two-dose MMR coverage and to have ongoing mumps transmission for the 2 weeks leading up to the intervention. Students who had not gotten mumps during the outbreak and had already had two doses of the MMR vaccine were eligible to receive the third dose from Jan. 19 to Feb. 2, 2010. Of 2,178 eligible students, 1,755 (80.6%) received the third dose.
Researchers then calculated mumps attack rates three times: in the 3 weeks before and after the vaccination intervention, and at 3 weeks following the second 3-week report. The average mumps incubation period is 16-18 days. Researchers divided the new mumps cases in each data collection period by the number of students who did not have mumps at the start of the period, to get the attack ratios.
The mumps attack rate among all students at the three schools dropped from 4.9% in the 3 weeks before the third dose was administered to 1.55% in the 3 weeks afterward (P value less than .001). During this second phase, rates were similar among vaccinated (1.60%) and unvaccinated (1.67%) students, but cases among vaccinated students were eight times lower (P = .097)* in the third phase of data collection, when the overall attack rate among all the students at the intervention schools dropped to 0.13%.
Follow-up data from 1,597 students who received the third dose (91% response rate) revealed adverse events occurring in 115 students (7.2%), primarily "pain, redness, or swelling at the injection site" and "joint or muscle aches." No students reported serious adverse events.
One study limitation was that the intervention occurred after the outbreak’s peak, so "it is not possible to exclude the possibility that the rapid decline in incidence after the intervention was entirely unrelated to our intervention," the authors wrote. The authors also noted their results mean a third MMR dose might be effective in outbreak control only in "highly vaccinated populations in certain settings" but do "not support the routine use of a third dose of mumps vaccine in national vaccination programs."
The investigators reported no external funding and no financial disclosures.
*Correction, 11/06/2012: An earlier version of this article misstated the p value.
Administering a third booster dose of the MMR vaccine during a mumps outbreak has been shown to decrease the spread of the disease in an already highly vaccinated population, according to a study published online in Pediatrics.
The vaccination intervention in one community led to a 96% drop (from 4.93% to 0.13%) in mumps attack rates among 11- to 17-year-olds, the population targeted in the intervention, reported Dr. Ikechukwu U. Ogbuanu of the epidemic intelligence center at the Centers for Disease Control and Prevention and his associates (Pediatrics 2012 Nov. 5 [doi:10.1542/peds.2012.0177]). The communitywide rate decreased by 75.6% (from a 0.86% attack ratio preintervention to 0.21% in the 3-week postintervention period).
A mumps outbreak involving 3,502 cases in the Northeastern United States from June 1, 2009, to June 30, 2010, included 790 cases in a close-knit Orthodox Jewish community in Orange County, N.Y. Officials selected that community, which represented 22.6% of the outbreak’s cases, to initiate a third-dose MMR vaccination intervention in three schools when standard outbreak control measures failed to slow the disease spread.
The outbreak had been traced to an 11-year-old U.S. resident who had received two doses of the MMR vaccine but had just returned from the United Kingdom where a mumps outbreak was ongoing. After he attended an Orthodox Jewish boys’ camp in New York, 25 cases were reported among campers. The disease then spread to families in the community when these boys returned home, reaching 392 cases in Orange County by Dec. 31, 2009. Among those who contracted the disease, 74% (290 patients) had received both MMR vaccine doses.
A third dose of the MMR was offered to 6th-12th graders at three of four schools in Orange County. Schools eligible for the intervention were required to have high two-dose MMR coverage and to have ongoing mumps transmission for the 2 weeks leading up to the intervention. Students who had not gotten mumps during the outbreak and had already had two doses of the MMR vaccine were eligible to receive the third dose from Jan. 19 to Feb. 2, 2010. Of 2,178 eligible students, 1,755 (80.6%) received the third dose.
Researchers then calculated mumps attack rates three times: in the 3 weeks before and after the vaccination intervention, and at 3 weeks following the second 3-week report. The average mumps incubation period is 16-18 days. Researchers divided the new mumps cases in each data collection period by the number of students who did not have mumps at the start of the period, to get the attack ratios.
The mumps attack rate among all students at the three schools dropped from 4.9% in the 3 weeks before the third dose was administered to 1.55% in the 3 weeks afterward (P value less than .001). During this second phase, rates were similar among vaccinated (1.60%) and unvaccinated (1.67%) students, but cases among vaccinated students were eight times lower (P = .097)* in the third phase of data collection, when the overall attack rate among all the students at the intervention schools dropped to 0.13%.
Follow-up data from 1,597 students who received the third dose (91% response rate) revealed adverse events occurring in 115 students (7.2%), primarily "pain, redness, or swelling at the injection site" and "joint or muscle aches." No students reported serious adverse events.
One study limitation was that the intervention occurred after the outbreak’s peak, so "it is not possible to exclude the possibility that the rapid decline in incidence after the intervention was entirely unrelated to our intervention," the authors wrote. The authors also noted their results mean a third MMR dose might be effective in outbreak control only in "highly vaccinated populations in certain settings" but do "not support the routine use of a third dose of mumps vaccine in national vaccination programs."
The investigators reported no external funding and no financial disclosures.
*Correction, 11/06/2012: An earlier version of this article misstated the p value.
FROM PEDIATRICS
Major Finding: Administration of a third MMR vaccine dose among two-dose vaccinated 11- to 17-year-olds during a mumps outbreak led to a 96% drop in cases (from 4.93% to 0.13%) among that population and a 75.6% drop among the larger community (from 0.86% to 0.21%) (P value less than .005 only among the 11- to 17-year-old group).
Data Source: The data are from a nonrandomized trial with an interrupted time series design involving 2,178 eligible students in three schools in Orange County, N.Y., from Jan. 19 to Feb. 2, 2010; 1, 755 of the students (80.6%) received the third dose of MMR vaccine.
Disclosures: The study received no external funding, and the authors said they had no disclosures to report.