User login
Sharon Worcester is an award-winning medical journalist for MDedge News. She has been with the company since 1996, first as the Southeast Bureau Chief (1996-2009) when the company was known as International Medical News Group, then as a freelance writer (2010-2015) before returning as a reporter in 2015. She previously worked as a daily newspaper reporter covering health and local government. Sharon currently reports primarily on oncology and hematology. She has a BA from Eckerd College and an MA in Mass Communication/Print Journalism from the University of Florida. Connect with her via LinkedIn and follow her on twitter @SW_MedReporter.
Labor Pattern During TOLAC May Signal Uterine Rupture Risk
DALLAS – Slow progression of labor beyond 7 cm of dilation in women attempting a trial of labor after cesarean section may signal risk for uterine rupture, findings from a case-control study suggest.
In 99 women who experienced uterine rupture while attempting a trial of labor after cesarean section (TOLAC) and 309 controls who did not experience uterine rupture during TOLAC, the time to progress 1 cm of dilation – after adjustment for prior vaginal delivery – was similar until 7 cm of dilation. Once the women reached 7 cm of dilation, however, a 1 cm progression took significantly longer in those who experienced rupture.
For example, progression from 7 cm to 8 cm took a median of 0.33 vs. 0.15 hours in the uterine rupture patients and the controls, respectively, and the progression from 8 cm to 9 cm took a median of 0.24 vs. 0.1 hours in the groups, respectively, Dr. Lorie Harper of Washington University in St. Louis reported at the annual meeting of the Society for Maternal-Fetal Medicine.
"This works out to approx 10-13 minutes longer for the median time to progress 1 cm in the uterine rupture group," she said, noting that the differences were particularly striking at the 95th percentile of time per 1 cm of dilation; for women with a successful trial of labor, each 1 cm of dilation after 7 cm took less than 1 hour, while at the 95th percentile, progression of each 1 cm of dilation after 7 cm took at least 1 hour.
The findings are from a secondary analysis of data from a nested case-control study of women attempting TOLAC within a 17-center retrospective cohort study of women with a prior low transverse cesarean section. Cases included women who experienced uterine rupture, and controls included women attempting TOLAC who reached 10 cm dilation. An additional reference group included 110 women with a failed TOLAC who ultimately underwent repeat cesarean section, and no significant difference was seen between this group and the cases in terms of time to progress after 7 cm. All subjects had only one prior cesarean section.
Uterine rupture for this study was explicitly defined, a priori, as a full-thickness disruption of the uterine wall accompanied by clinical signs, Dr. Harper said.
The cases and controls from both reference groups were similar with respect to age, gravidity, diabetes, hypertension, and type of hospital, although the rate of prior vaginal delivery and black race both were more common in the reference groups. The three groups also were comparable with respect to intrapartum characteristics such as epidural use and gestational age at delivery, although those who experienced uterine rupture were more likely to have been induced and to have received Pitocin, she noted.
Although the case-control design of this study has inherent limitations such as possible selection bias, the study also has strengths, including the large study population of nearly 14,000 women in the original retrospective cohort, she said.
The findings suggest that a protracted labor prior to 7 cm of dilation does not necessarily signify uterine rupture in women attempting a TOLAC, as it was not uncommon during this period for the women to require 2 hours to progress 1 cm, and some still reached 10 cm, Dr. Harper said.
After 7 cm, however, labor dystocia should raise suspicion for uterine rupture in this population, she said.
Although the findings don’t necessarily suggest that intervention such as cesarean delivery is indicated in those with slow progression after 7 cm, they do underscore the need for more careful and frequent monitoring for signs of uterine rupture during active labor in women attempting a TOLAC.
"Instead of waiting 2 hours to check them, maybe they should be checked in an hour to make sure they’re progressing," she said.
This study was supported by the Eunice Kennedy Shriver National Institute of Child Health and Human Development. Dr. Harper said she had no relevant financial disclosures.
DALLAS – Slow progression of labor beyond 7 cm of dilation in women attempting a trial of labor after cesarean section may signal risk for uterine rupture, findings from a case-control study suggest.
In 99 women who experienced uterine rupture while attempting a trial of labor after cesarean section (TOLAC) and 309 controls who did not experience uterine rupture during TOLAC, the time to progress 1 cm of dilation – after adjustment for prior vaginal delivery – was similar until 7 cm of dilation. Once the women reached 7 cm of dilation, however, a 1 cm progression took significantly longer in those who experienced rupture.
For example, progression from 7 cm to 8 cm took a median of 0.33 vs. 0.15 hours in the uterine rupture patients and the controls, respectively, and the progression from 8 cm to 9 cm took a median of 0.24 vs. 0.1 hours in the groups, respectively, Dr. Lorie Harper of Washington University in St. Louis reported at the annual meeting of the Society for Maternal-Fetal Medicine.
"This works out to approx 10-13 minutes longer for the median time to progress 1 cm in the uterine rupture group," she said, noting that the differences were particularly striking at the 95th percentile of time per 1 cm of dilation; for women with a successful trial of labor, each 1 cm of dilation after 7 cm took less than 1 hour, while at the 95th percentile, progression of each 1 cm of dilation after 7 cm took at least 1 hour.
The findings are from a secondary analysis of data from a nested case-control study of women attempting TOLAC within a 17-center retrospective cohort study of women with a prior low transverse cesarean section. Cases included women who experienced uterine rupture, and controls included women attempting TOLAC who reached 10 cm dilation. An additional reference group included 110 women with a failed TOLAC who ultimately underwent repeat cesarean section, and no significant difference was seen between this group and the cases in terms of time to progress after 7 cm. All subjects had only one prior cesarean section.
Uterine rupture for this study was explicitly defined, a priori, as a full-thickness disruption of the uterine wall accompanied by clinical signs, Dr. Harper said.
The cases and controls from both reference groups were similar with respect to age, gravidity, diabetes, hypertension, and type of hospital, although the rate of prior vaginal delivery and black race both were more common in the reference groups. The three groups also were comparable with respect to intrapartum characteristics such as epidural use and gestational age at delivery, although those who experienced uterine rupture were more likely to have been induced and to have received Pitocin, she noted.
Although the case-control design of this study has inherent limitations such as possible selection bias, the study also has strengths, including the large study population of nearly 14,000 women in the original retrospective cohort, she said.
The findings suggest that a protracted labor prior to 7 cm of dilation does not necessarily signify uterine rupture in women attempting a TOLAC, as it was not uncommon during this period for the women to require 2 hours to progress 1 cm, and some still reached 10 cm, Dr. Harper said.
After 7 cm, however, labor dystocia should raise suspicion for uterine rupture in this population, she said.
Although the findings don’t necessarily suggest that intervention such as cesarean delivery is indicated in those with slow progression after 7 cm, they do underscore the need for more careful and frequent monitoring for signs of uterine rupture during active labor in women attempting a TOLAC.
"Instead of waiting 2 hours to check them, maybe they should be checked in an hour to make sure they’re progressing," she said.
This study was supported by the Eunice Kennedy Shriver National Institute of Child Health and Human Development. Dr. Harper said she had no relevant financial disclosures.
DALLAS – Slow progression of labor beyond 7 cm of dilation in women attempting a trial of labor after cesarean section may signal risk for uterine rupture, findings from a case-control study suggest.
In 99 women who experienced uterine rupture while attempting a trial of labor after cesarean section (TOLAC) and 309 controls who did not experience uterine rupture during TOLAC, the time to progress 1 cm of dilation – after adjustment for prior vaginal delivery – was similar until 7 cm of dilation. Once the women reached 7 cm of dilation, however, a 1 cm progression took significantly longer in those who experienced rupture.
For example, progression from 7 cm to 8 cm took a median of 0.33 vs. 0.15 hours in the uterine rupture patients and the controls, respectively, and the progression from 8 cm to 9 cm took a median of 0.24 vs. 0.1 hours in the groups, respectively, Dr. Lorie Harper of Washington University in St. Louis reported at the annual meeting of the Society for Maternal-Fetal Medicine.
"This works out to approx 10-13 minutes longer for the median time to progress 1 cm in the uterine rupture group," she said, noting that the differences were particularly striking at the 95th percentile of time per 1 cm of dilation; for women with a successful trial of labor, each 1 cm of dilation after 7 cm took less than 1 hour, while at the 95th percentile, progression of each 1 cm of dilation after 7 cm took at least 1 hour.
The findings are from a secondary analysis of data from a nested case-control study of women attempting TOLAC within a 17-center retrospective cohort study of women with a prior low transverse cesarean section. Cases included women who experienced uterine rupture, and controls included women attempting TOLAC who reached 10 cm dilation. An additional reference group included 110 women with a failed TOLAC who ultimately underwent repeat cesarean section, and no significant difference was seen between this group and the cases in terms of time to progress after 7 cm. All subjects had only one prior cesarean section.
Uterine rupture for this study was explicitly defined, a priori, as a full-thickness disruption of the uterine wall accompanied by clinical signs, Dr. Harper said.
The cases and controls from both reference groups were similar with respect to age, gravidity, diabetes, hypertension, and type of hospital, although the rate of prior vaginal delivery and black race both were more common in the reference groups. The three groups also were comparable with respect to intrapartum characteristics such as epidural use and gestational age at delivery, although those who experienced uterine rupture were more likely to have been induced and to have received Pitocin, she noted.
Although the case-control design of this study has inherent limitations such as possible selection bias, the study also has strengths, including the large study population of nearly 14,000 women in the original retrospective cohort, she said.
The findings suggest that a protracted labor prior to 7 cm of dilation does not necessarily signify uterine rupture in women attempting a TOLAC, as it was not uncommon during this period for the women to require 2 hours to progress 1 cm, and some still reached 10 cm, Dr. Harper said.
After 7 cm, however, labor dystocia should raise suspicion for uterine rupture in this population, she said.
Although the findings don’t necessarily suggest that intervention such as cesarean delivery is indicated in those with slow progression after 7 cm, they do underscore the need for more careful and frequent monitoring for signs of uterine rupture during active labor in women attempting a TOLAC.
"Instead of waiting 2 hours to check them, maybe they should be checked in an hour to make sure they’re progressing," she said.
This study was supported by the Eunice Kennedy Shriver National Institute of Child Health and Human Development. Dr. Harper said she had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE SOCIETY FOR MATERNAL-FETAL MEDICINE
Major Finding: In 99 women who experienced uterine rupture while attempting a trial of labor after cesarean section (TOLAC) and 309 controls who did not experience uterine rupture during TOLAC, the time to progress 1 cm of dilation – after adjusting for prior vaginal delivery – was similar until 7 cm of dilation. Progression from 7 cm to 8 cm took a median of 0.33 vs. 0.15 hours in the uterine rupture patients and the controls, respectively, and the progression from 8 cm to 9 cm took a median of 0.24 vs. 0.1 hours in the groups, respectively.
Data Source: A nested case-control study of women attempting TOLAC within a 17-center retrospective cohort study of women with a prior low transverse cesarean section.
Disclosures: The study was supported by the Eunice Kennedy Shriver National Institute for Child Health and Human Development. Dr. Harper said she had no relevant financial disclosures.
17P Failed to Help Women With 'Longer Short Cervix'
DALLAS – The drug 17-hydroxyprogesterone caproate, or 17P, is not effective for reducing the risk of preterm delivery in nulliparous women with a cervix length less than the 10th percentile, findings from a randomized placebo-controlled study involving 657 women have shown.
Based on findings from prior studies, 17P is indicated in women with a cervical length of 10-20 mm, which represents only a very small proportion of patients. The objective of the current study was to determine if the benefits of 17P might extend to those with a "longer short cervix," Dr. William Grobman said at the annual meeting of the Society for Maternal-Fetal Medicine.
"Using a cervical length cutoff of the 10th percentile potentially expands the benefits of progesterone to a larger proportion of the population," said Dr. Grobman of the department of obstetrics and gynecology at Northwestern University, Chicago, who was speaking on behalf of the National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network.
Between 16 and 22 weeks’ gestation, when routine anatomic surveys are performed, the 10th percentile for cervical length is 30 mm, he explained.
Of 15,436 women screened at the 14 centers that are part of the Maternal-Fetal Medicine Units Network, 1,588 had a cervical length of less than 30 mm, and 657 consented to randomization. The frequency of preterm birth, defined as delivery prior to 37 weeks’ gestation, was 25.1% in 327 women randomized to receive 17P, and 24.5% in the 330 who received placebo.
There also were no differences in the rates of preterm birth at less than 32 weeks and less than 28 weeks, and no difference in the survival curve – defined as the number of days the women remained pregnant following 17P injection, Dr. Grobman said.
Based on these findings, enrollment in the study was stopped at the third interim analysis, he noted.
As for neonatal outcomes, no difference was seen between the treatment and placebo groups in regard to a composite outcome including, but not limited to, respiratory distress syndrome, bronchopulmonary dysplasia, necrotizing enterocolitis, sepsis, retinopathy of prematurity, and perinatal death.
When neonatal outcomes were analyzed individually, a significant difference was seen between the treatment and placebo groups with regard to sepsis; those in the 17P group had a lower risk of developing sepsis, Dr. Grobman noted.
Women in this study had a singleton pregnancy, and were screened between 16 and 223/7 weeks by a certified sonographer. They had no major fetal anomalies, no increased probability of indicated preterm birth, and no prior loop electrosurgical excision procedure or müllerian anomalies.
Those who consented to participate received an injection of 1 mL of placebo, and those who returned at least 3 days later but before 23 weeks’ gestation were randomized to receive 250 mg of intramuscular 17P weekly, or identically appearing placebo. All received weekly injections until delivery or 37 weeks.
Those in the treatment group were slightly, but significantly older. All other characteristics, including body mass index, race/ethnicity, and estimated gestational age at randomization were similar in the treatment and placebo groups.
The mean cervical length was 24 mm in both groups; less than 10% had a cervical length less than 15 mm, and less than 20% of those had the cervical funnel visualized, Dr. Grobman said.
"Based on these data, we do conclude that weekly intramuscular 17P does not reduce the frequency of preterm birth in nulliparous women with a cervix less than 30 mm," he concluded.
"This is really a study more than anything of women with a longer short cervix," he added, explaining during a question and answer session that the study isn’t powered to look at outcomes for those with other cervical lengths, for example, less than 20 mm or less than 15 mm. About 85% of women in this study had a cervical length between 25 and 30 mm.
Dr. Grobman said he had no relevant financial disclosures.
DALLAS – The drug 17-hydroxyprogesterone caproate, or 17P, is not effective for reducing the risk of preterm delivery in nulliparous women with a cervix length less than the 10th percentile, findings from a randomized placebo-controlled study involving 657 women have shown.
Based on findings from prior studies, 17P is indicated in women with a cervical length of 10-20 mm, which represents only a very small proportion of patients. The objective of the current study was to determine if the benefits of 17P might extend to those with a "longer short cervix," Dr. William Grobman said at the annual meeting of the Society for Maternal-Fetal Medicine.
"Using a cervical length cutoff of the 10th percentile potentially expands the benefits of progesterone to a larger proportion of the population," said Dr. Grobman of the department of obstetrics and gynecology at Northwestern University, Chicago, who was speaking on behalf of the National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network.
Between 16 and 22 weeks’ gestation, when routine anatomic surveys are performed, the 10th percentile for cervical length is 30 mm, he explained.
Of 15,436 women screened at the 14 centers that are part of the Maternal-Fetal Medicine Units Network, 1,588 had a cervical length of less than 30 mm, and 657 consented to randomization. The frequency of preterm birth, defined as delivery prior to 37 weeks’ gestation, was 25.1% in 327 women randomized to receive 17P, and 24.5% in the 330 who received placebo.
There also were no differences in the rates of preterm birth at less than 32 weeks and less than 28 weeks, and no difference in the survival curve – defined as the number of days the women remained pregnant following 17P injection, Dr. Grobman said.
Based on these findings, enrollment in the study was stopped at the third interim analysis, he noted.
As for neonatal outcomes, no difference was seen between the treatment and placebo groups in regard to a composite outcome including, but not limited to, respiratory distress syndrome, bronchopulmonary dysplasia, necrotizing enterocolitis, sepsis, retinopathy of prematurity, and perinatal death.
When neonatal outcomes were analyzed individually, a significant difference was seen between the treatment and placebo groups with regard to sepsis; those in the 17P group had a lower risk of developing sepsis, Dr. Grobman noted.
Women in this study had a singleton pregnancy, and were screened between 16 and 223/7 weeks by a certified sonographer. They had no major fetal anomalies, no increased probability of indicated preterm birth, and no prior loop electrosurgical excision procedure or müllerian anomalies.
Those who consented to participate received an injection of 1 mL of placebo, and those who returned at least 3 days later but before 23 weeks’ gestation were randomized to receive 250 mg of intramuscular 17P weekly, or identically appearing placebo. All received weekly injections until delivery or 37 weeks.
Those in the treatment group were slightly, but significantly older. All other characteristics, including body mass index, race/ethnicity, and estimated gestational age at randomization were similar in the treatment and placebo groups.
The mean cervical length was 24 mm in both groups; less than 10% had a cervical length less than 15 mm, and less than 20% of those had the cervical funnel visualized, Dr. Grobman said.
"Based on these data, we do conclude that weekly intramuscular 17P does not reduce the frequency of preterm birth in nulliparous women with a cervix less than 30 mm," he concluded.
"This is really a study more than anything of women with a longer short cervix," he added, explaining during a question and answer session that the study isn’t powered to look at outcomes for those with other cervical lengths, for example, less than 20 mm or less than 15 mm. About 85% of women in this study had a cervical length between 25 and 30 mm.
Dr. Grobman said he had no relevant financial disclosures.
DALLAS – The drug 17-hydroxyprogesterone caproate, or 17P, is not effective for reducing the risk of preterm delivery in nulliparous women with a cervix length less than the 10th percentile, findings from a randomized placebo-controlled study involving 657 women have shown.
Based on findings from prior studies, 17P is indicated in women with a cervical length of 10-20 mm, which represents only a very small proportion of patients. The objective of the current study was to determine if the benefits of 17P might extend to those with a "longer short cervix," Dr. William Grobman said at the annual meeting of the Society for Maternal-Fetal Medicine.
"Using a cervical length cutoff of the 10th percentile potentially expands the benefits of progesterone to a larger proportion of the population," said Dr. Grobman of the department of obstetrics and gynecology at Northwestern University, Chicago, who was speaking on behalf of the National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network.
Between 16 and 22 weeks’ gestation, when routine anatomic surveys are performed, the 10th percentile for cervical length is 30 mm, he explained.
Of 15,436 women screened at the 14 centers that are part of the Maternal-Fetal Medicine Units Network, 1,588 had a cervical length of less than 30 mm, and 657 consented to randomization. The frequency of preterm birth, defined as delivery prior to 37 weeks’ gestation, was 25.1% in 327 women randomized to receive 17P, and 24.5% in the 330 who received placebo.
There also were no differences in the rates of preterm birth at less than 32 weeks and less than 28 weeks, and no difference in the survival curve – defined as the number of days the women remained pregnant following 17P injection, Dr. Grobman said.
Based on these findings, enrollment in the study was stopped at the third interim analysis, he noted.
As for neonatal outcomes, no difference was seen between the treatment and placebo groups in regard to a composite outcome including, but not limited to, respiratory distress syndrome, bronchopulmonary dysplasia, necrotizing enterocolitis, sepsis, retinopathy of prematurity, and perinatal death.
When neonatal outcomes were analyzed individually, a significant difference was seen between the treatment and placebo groups with regard to sepsis; those in the 17P group had a lower risk of developing sepsis, Dr. Grobman noted.
Women in this study had a singleton pregnancy, and were screened between 16 and 223/7 weeks by a certified sonographer. They had no major fetal anomalies, no increased probability of indicated preterm birth, and no prior loop electrosurgical excision procedure or müllerian anomalies.
Those who consented to participate received an injection of 1 mL of placebo, and those who returned at least 3 days later but before 23 weeks’ gestation were randomized to receive 250 mg of intramuscular 17P weekly, or identically appearing placebo. All received weekly injections until delivery or 37 weeks.
Those in the treatment group were slightly, but significantly older. All other characteristics, including body mass index, race/ethnicity, and estimated gestational age at randomization were similar in the treatment and placebo groups.
The mean cervical length was 24 mm in both groups; less than 10% had a cervical length less than 15 mm, and less than 20% of those had the cervical funnel visualized, Dr. Grobman said.
"Based on these data, we do conclude that weekly intramuscular 17P does not reduce the frequency of preterm birth in nulliparous women with a cervix less than 30 mm," he concluded.
"This is really a study more than anything of women with a longer short cervix," he added, explaining during a question and answer session that the study isn’t powered to look at outcomes for those with other cervical lengths, for example, less than 20 mm or less than 15 mm. About 85% of women in this study had a cervical length between 25 and 30 mm.
Dr. Grobman said he had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE SOCIETY FOR MATERNAL-FETAL MEDICINE
Major Finding: The frequency of preterm birth, defined as delivery prior to 37 weeks’ gestation, was 25.1% in 327 women randomized to receive 17P, and 24.5% in the 330 who received placebo. The mean cervical length was 24 mm in both groups.
Data Source: This was a randomized placebo-controlled trial of 657 pregnant women who were part of the NICHD Maternal-Fetal Medicine Units Network.
Disclosures: Dr. Grobman said he had no relevant financial disclosures.
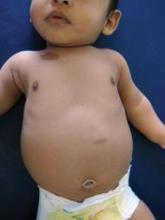
Multiple CALMs in Infancy May Signal NF1
Single café au lait macules are found in about 2.5% of infants and typically are of little concern, but certain syndromes should be suspected in children with multiple lesions or in those who develop new lesions after the first 5-6 years of life, according to Dr. Wynnis L. Tom.
For example, multiple café au lait macules (CALMs) could be a sign of neurofibromatosis type I (NF1), Dr. Tom of the University of California, San Diego, said during a presentation at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Diagnosis of the autosomal dominant syndrome – which results from a neurofibromin defect and occurs in 1 of 2,000-4,500 individuals – requires the presence of two or more of the following diagnostic criteria: six or more CALMs greater than 0.5 cm in diameter in prepubertal children, or greater than 1.5 cm in those postpubertal; two or more neurofibromas of any type, or one plexiform neurofibroma; axillary and/or inguinal freckling (Crowe’s sign); optic glioma; two or more Lisch nodules; a bony lesion (such as sphenoid dysplasia or long bone dysplasia); and a first-degree relative with NF1.
After CALMs, the most common finding in patients with NF1 is axillary and/or inguinal freckling, which occurs in 75%-90% of cases.
"Recognizing NF1 is important, because the syndrome is associated with multiple complications. For example, ocular disease is common in these patients, and can include eye displacement, glaucoma, and visual impairment if the optical nerve is involved," Dr. Tom said.
Also, about 50% of patients have learning disabilities, and 5% have more severe developmental delay. Other complications include hypertension due to renal artery stenosis or (rarely) pheochromocytoma, and an increased risk of malignancy (particularly astrocytomas and malignant peripheral nerve sheath tumors).
The work-up for patients who meet the criteria for NF1 should include referrals for genetic evaluation and counseling, ophthalmological care, and neurologic and developmental services. Also, watch for scoliosis and consider imaging and performing biopsies for lesions with pain or sudden growth, Dr. Tom advised.
Legius syndrome is a more-recently defined NF1-like syndrome, which also is characterized by multiple CALMs with or without intertriginous freckling, although both are often fewer than in patients with true NF1.
This autosomal dominant, gene-related syndrome can be associated with macrocephaly; attention-deficit/hyperactivity disorder and/or other learning disabilities; lipomas; or vascular anomalies, but they do not have the neurofibromas or tumors of NF1. Thus, they likely have a better prognosis.
Other possible diagnoses in patients with multiple CALMs include familial CALMs (without any other findings) and other neuro-cardio-facial-cutaneous syndromes involving the ras/mitogen-activated protein kinase (ras/MAPK) signaling pathway.
Such syndromes may be associated with pigmentary anomalies, facial dysmorphism, short stature, congenital heart defects, neurocognitive defects, and predisposition to malignancy, Dr. Tom said. "Thus, advances in genetic analysis and diagnosis have expanded the number of disorders in which multiple CALMs can be seen. Children with multiple CALMs should, therefore, have thorough physical exams, regular monitoring for additional skin lesions, and appropriate other specialty evaluation," she concluded.
Dr. Tom reported having no disclosures. SDEF and this news organization are owned by Elsevier.
Single café au lait macules are found in about 2.5% of infants and typically are of little concern, but certain syndromes should be suspected in children with multiple lesions or in those who develop new lesions after the first 5-6 years of life, according to Dr. Wynnis L. Tom.
For example, multiple café au lait macules (CALMs) could be a sign of neurofibromatosis type I (NF1), Dr. Tom of the University of California, San Diego, said during a presentation at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Diagnosis of the autosomal dominant syndrome – which results from a neurofibromin defect and occurs in 1 of 2,000-4,500 individuals – requires the presence of two or more of the following diagnostic criteria: six or more CALMs greater than 0.5 cm in diameter in prepubertal children, or greater than 1.5 cm in those postpubertal; two or more neurofibromas of any type, or one plexiform neurofibroma; axillary and/or inguinal freckling (Crowe’s sign); optic glioma; two or more Lisch nodules; a bony lesion (such as sphenoid dysplasia or long bone dysplasia); and a first-degree relative with NF1.
After CALMs, the most common finding in patients with NF1 is axillary and/or inguinal freckling, which occurs in 75%-90% of cases.
"Recognizing NF1 is important, because the syndrome is associated with multiple complications. For example, ocular disease is common in these patients, and can include eye displacement, glaucoma, and visual impairment if the optical nerve is involved," Dr. Tom said.
Also, about 50% of patients have learning disabilities, and 5% have more severe developmental delay. Other complications include hypertension due to renal artery stenosis or (rarely) pheochromocytoma, and an increased risk of malignancy (particularly astrocytomas and malignant peripheral nerve sheath tumors).
The work-up for patients who meet the criteria for NF1 should include referrals for genetic evaluation and counseling, ophthalmological care, and neurologic and developmental services. Also, watch for scoliosis and consider imaging and performing biopsies for lesions with pain or sudden growth, Dr. Tom advised.
Legius syndrome is a more-recently defined NF1-like syndrome, which also is characterized by multiple CALMs with or without intertriginous freckling, although both are often fewer than in patients with true NF1.
This autosomal dominant, gene-related syndrome can be associated with macrocephaly; attention-deficit/hyperactivity disorder and/or other learning disabilities; lipomas; or vascular anomalies, but they do not have the neurofibromas or tumors of NF1. Thus, they likely have a better prognosis.
Other possible diagnoses in patients with multiple CALMs include familial CALMs (without any other findings) and other neuro-cardio-facial-cutaneous syndromes involving the ras/mitogen-activated protein kinase (ras/MAPK) signaling pathway.
Such syndromes may be associated with pigmentary anomalies, facial dysmorphism, short stature, congenital heart defects, neurocognitive defects, and predisposition to malignancy, Dr. Tom said. "Thus, advances in genetic analysis and diagnosis have expanded the number of disorders in which multiple CALMs can be seen. Children with multiple CALMs should, therefore, have thorough physical exams, regular monitoring for additional skin lesions, and appropriate other specialty evaluation," she concluded.
Dr. Tom reported having no disclosures. SDEF and this news organization are owned by Elsevier.
Single café au lait macules are found in about 2.5% of infants and typically are of little concern, but certain syndromes should be suspected in children with multiple lesions or in those who develop new lesions after the first 5-6 years of life, according to Dr. Wynnis L. Tom.
For example, multiple café au lait macules (CALMs) could be a sign of neurofibromatosis type I (NF1), Dr. Tom of the University of California, San Diego, said during a presentation at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Diagnosis of the autosomal dominant syndrome – which results from a neurofibromin defect and occurs in 1 of 2,000-4,500 individuals – requires the presence of two or more of the following diagnostic criteria: six or more CALMs greater than 0.5 cm in diameter in prepubertal children, or greater than 1.5 cm in those postpubertal; two or more neurofibromas of any type, or one plexiform neurofibroma; axillary and/or inguinal freckling (Crowe’s sign); optic glioma; two or more Lisch nodules; a bony lesion (such as sphenoid dysplasia or long bone dysplasia); and a first-degree relative with NF1.
After CALMs, the most common finding in patients with NF1 is axillary and/or inguinal freckling, which occurs in 75%-90% of cases.
"Recognizing NF1 is important, because the syndrome is associated with multiple complications. For example, ocular disease is common in these patients, and can include eye displacement, glaucoma, and visual impairment if the optical nerve is involved," Dr. Tom said.
Also, about 50% of patients have learning disabilities, and 5% have more severe developmental delay. Other complications include hypertension due to renal artery stenosis or (rarely) pheochromocytoma, and an increased risk of malignancy (particularly astrocytomas and malignant peripheral nerve sheath tumors).
The work-up for patients who meet the criteria for NF1 should include referrals for genetic evaluation and counseling, ophthalmological care, and neurologic and developmental services. Also, watch for scoliosis and consider imaging and performing biopsies for lesions with pain or sudden growth, Dr. Tom advised.
Legius syndrome is a more-recently defined NF1-like syndrome, which also is characterized by multiple CALMs with or without intertriginous freckling, although both are often fewer than in patients with true NF1.
This autosomal dominant, gene-related syndrome can be associated with macrocephaly; attention-deficit/hyperactivity disorder and/or other learning disabilities; lipomas; or vascular anomalies, but they do not have the neurofibromas or tumors of NF1. Thus, they likely have a better prognosis.
Other possible diagnoses in patients with multiple CALMs include familial CALMs (without any other findings) and other neuro-cardio-facial-cutaneous syndromes involving the ras/mitogen-activated protein kinase (ras/MAPK) signaling pathway.
Such syndromes may be associated with pigmentary anomalies, facial dysmorphism, short stature, congenital heart defects, neurocognitive defects, and predisposition to malignancy, Dr. Tom said. "Thus, advances in genetic analysis and diagnosis have expanded the number of disorders in which multiple CALMs can be seen. Children with multiple CALMs should, therefore, have thorough physical exams, regular monitoring for additional skin lesions, and appropriate other specialty evaluation," she concluded.
Dr. Tom reported having no disclosures. SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM THE SDEF HAWAII DERMATOLOGY SEMINAR
Let Balance, Aesthetics Guide Volume Replacement
Volume replacement can give an aging face some lift, but it’s not for everyone, according to Dr. Mark G. Rubin.
In a woman with a round face, for example, adding volume to the lower half of the face can create a fuller, heavier appearance rather than a more youthful appearance, he said at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
"We all agree that volume loss is a significant part of aging, but without attention to facial balance and aesthetics, the results of volume replacement can be less than satisfactory," he added, noting that when it comes to facial contouring, an understanding of balance and aesthetics becomes more important than technique.
One important concept to keep in mind is the "triangle of youth," said Dr. Rubin who practices dermatology in Beverly Hills, Calif. He explained that a triangular face is more youthful, which is why volume that promotes roundness can have the opposite effect, even if the volume tends to smooth wrinkles.
Creating a triangular shape by providing fullness and prominence of the cheekbone – as long as it isn’t overdone – can create a youthful, attractive look, he said.
The aging lower half of the face has volume loss in several areas, including the medial cheek/nasojugal groove, the central cheek, the nasolabial folds, the marionette lines, and the prejowl area.
Volume replacement in the marionette lines and at the jaw line can be particularly effective.
In the marionette fold, one technique that can be useful is building a layer of support to push up on the descending cheek, thereby camouflaging its leading edge.
"Sometime you need to add a little support into the lateral lower lip, as well as the horseshoe of the modiolus," he said. "Remember, as you push up on the corner of the lip, that you can accidentally create or aggravate fullness laterally."
Adding filler to the upper vermilion border can also support this approach by tightening the lip and providing some lift to the corner, thereby helping reduce the puffiness created by treating the upper marionette area.
Volume at the jawline can also provide a more youthful look, but keep in mind that the two areas of apparent volume loss – the pre- and postjowl – are actually normal areas, whereas the skin in between has descended, Dr. Rubin explained. Filling these pre- and postjowl pseudodepressions will provide something of an optical illusion, making the jowl look less prominent. Similarly, adding volume at the prejowl sulcus can reduce the sagging appearance of the jowl.
However, a patient with a round face may not be a good candidate for this approach. "Too much volume at the prejowl sulcus in a patient with a round face will make the face look fat," he explained.
Also, in some patients the smoothing of the jaw line may look good on profile, but it can have a masculinizing effect by widening the lateral face when viewed head on.
As for the cheeks, not all "deflate" in the same way, and thus not all will benefit from volume replacement. In those with central cheek hollowing, volume can be very effective in creating a more youthful appearance, as well as in tightening loose skin.
A number of filler options can be considered, including hyaluronic acid (HA) fillers, poly-L-lactic acid, calcium hydroxylapatite, and polymethyl methacrylate (PMMA).
"But for first-time patients, or if you are learning your way, don’t underestimate the value of a reversible filler," he said.
As with the use of neurotoxins, the approach to using fillers can vary without necessarily affecting the outcome. Various physicians have their own preferences for products and injection techniques, yet almost everyone seems to be able to achieve the intended aesthetic goal, he explained.
"So I don’t think the ‘what’ is that important. It’s knowing the ‘where’ and the mastering of an injection technique that means more," he said.
In fact, Food and Drug Administration trial data for most fillers suggest that they are more similar than dissimilar in terms of efficacy, longevity, and adverse effects. Still, although conventional wisdom suggests that particle size, concentration, or lift should affect the final result, and thus in theory there should be one product that is best for each location, there is a lack of agreement.
In Dr. Rubin’s experience, however, HA, PMMA, and calcium hydroxylapatite fillers can have a slight rippling effect when they are injected in areas of soft tissue, such as the central cheek.
"It’s hard to make a smooth contour across 6-8 cm when you are injecting droplets or linear filaments of a filler," he said, noting that poly-L-lactic acid seems to create a smoother contour in that area.
When injecting over bony areas, HA products and calcium hydroxylapatite are acceptable, because the defects are generally smaller and there is less surface area on which to see ripples.
Dr. Rubin is a consultant for Medicis. He also has been involved in FDA clinical trials for Restylane, Perlane, and Artefill. SDEF and this news organization are owned by Elsevier.
Volume replacement can give an aging face some lift, but it’s not for everyone, according to Dr. Mark G. Rubin.
In a woman with a round face, for example, adding volume to the lower half of the face can create a fuller, heavier appearance rather than a more youthful appearance, he said at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
"We all agree that volume loss is a significant part of aging, but without attention to facial balance and aesthetics, the results of volume replacement can be less than satisfactory," he added, noting that when it comes to facial contouring, an understanding of balance and aesthetics becomes more important than technique.
One important concept to keep in mind is the "triangle of youth," said Dr. Rubin who practices dermatology in Beverly Hills, Calif. He explained that a triangular face is more youthful, which is why volume that promotes roundness can have the opposite effect, even if the volume tends to smooth wrinkles.
Creating a triangular shape by providing fullness and prominence of the cheekbone – as long as it isn’t overdone – can create a youthful, attractive look, he said.
The aging lower half of the face has volume loss in several areas, including the medial cheek/nasojugal groove, the central cheek, the nasolabial folds, the marionette lines, and the prejowl area.
Volume replacement in the marionette lines and at the jaw line can be particularly effective.
In the marionette fold, one technique that can be useful is building a layer of support to push up on the descending cheek, thereby camouflaging its leading edge.
"Sometime you need to add a little support into the lateral lower lip, as well as the horseshoe of the modiolus," he said. "Remember, as you push up on the corner of the lip, that you can accidentally create or aggravate fullness laterally."
Adding filler to the upper vermilion border can also support this approach by tightening the lip and providing some lift to the corner, thereby helping reduce the puffiness created by treating the upper marionette area.
Volume at the jawline can also provide a more youthful look, but keep in mind that the two areas of apparent volume loss – the pre- and postjowl – are actually normal areas, whereas the skin in between has descended, Dr. Rubin explained. Filling these pre- and postjowl pseudodepressions will provide something of an optical illusion, making the jowl look less prominent. Similarly, adding volume at the prejowl sulcus can reduce the sagging appearance of the jowl.
However, a patient with a round face may not be a good candidate for this approach. "Too much volume at the prejowl sulcus in a patient with a round face will make the face look fat," he explained.
Also, in some patients the smoothing of the jaw line may look good on profile, but it can have a masculinizing effect by widening the lateral face when viewed head on.
As for the cheeks, not all "deflate" in the same way, and thus not all will benefit from volume replacement. In those with central cheek hollowing, volume can be very effective in creating a more youthful appearance, as well as in tightening loose skin.
A number of filler options can be considered, including hyaluronic acid (HA) fillers, poly-L-lactic acid, calcium hydroxylapatite, and polymethyl methacrylate (PMMA).
"But for first-time patients, or if you are learning your way, don’t underestimate the value of a reversible filler," he said.
As with the use of neurotoxins, the approach to using fillers can vary without necessarily affecting the outcome. Various physicians have their own preferences for products and injection techniques, yet almost everyone seems to be able to achieve the intended aesthetic goal, he explained.
"So I don’t think the ‘what’ is that important. It’s knowing the ‘where’ and the mastering of an injection technique that means more," he said.
In fact, Food and Drug Administration trial data for most fillers suggest that they are more similar than dissimilar in terms of efficacy, longevity, and adverse effects. Still, although conventional wisdom suggests that particle size, concentration, or lift should affect the final result, and thus in theory there should be one product that is best for each location, there is a lack of agreement.
In Dr. Rubin’s experience, however, HA, PMMA, and calcium hydroxylapatite fillers can have a slight rippling effect when they are injected in areas of soft tissue, such as the central cheek.
"It’s hard to make a smooth contour across 6-8 cm when you are injecting droplets or linear filaments of a filler," he said, noting that poly-L-lactic acid seems to create a smoother contour in that area.
When injecting over bony areas, HA products and calcium hydroxylapatite are acceptable, because the defects are generally smaller and there is less surface area on which to see ripples.
Dr. Rubin is a consultant for Medicis. He also has been involved in FDA clinical trials for Restylane, Perlane, and Artefill. SDEF and this news organization are owned by Elsevier.
Volume replacement can give an aging face some lift, but it’s not for everyone, according to Dr. Mark G. Rubin.
In a woman with a round face, for example, adding volume to the lower half of the face can create a fuller, heavier appearance rather than a more youthful appearance, he said at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
"We all agree that volume loss is a significant part of aging, but without attention to facial balance and aesthetics, the results of volume replacement can be less than satisfactory," he added, noting that when it comes to facial contouring, an understanding of balance and aesthetics becomes more important than technique.
One important concept to keep in mind is the "triangle of youth," said Dr. Rubin who practices dermatology in Beverly Hills, Calif. He explained that a triangular face is more youthful, which is why volume that promotes roundness can have the opposite effect, even if the volume tends to smooth wrinkles.
Creating a triangular shape by providing fullness and prominence of the cheekbone – as long as it isn’t overdone – can create a youthful, attractive look, he said.
The aging lower half of the face has volume loss in several areas, including the medial cheek/nasojugal groove, the central cheek, the nasolabial folds, the marionette lines, and the prejowl area.
Volume replacement in the marionette lines and at the jaw line can be particularly effective.
In the marionette fold, one technique that can be useful is building a layer of support to push up on the descending cheek, thereby camouflaging its leading edge.
"Sometime you need to add a little support into the lateral lower lip, as well as the horseshoe of the modiolus," he said. "Remember, as you push up on the corner of the lip, that you can accidentally create or aggravate fullness laterally."
Adding filler to the upper vermilion border can also support this approach by tightening the lip and providing some lift to the corner, thereby helping reduce the puffiness created by treating the upper marionette area.
Volume at the jawline can also provide a more youthful look, but keep in mind that the two areas of apparent volume loss – the pre- and postjowl – are actually normal areas, whereas the skin in between has descended, Dr. Rubin explained. Filling these pre- and postjowl pseudodepressions will provide something of an optical illusion, making the jowl look less prominent. Similarly, adding volume at the prejowl sulcus can reduce the sagging appearance of the jowl.
However, a patient with a round face may not be a good candidate for this approach. "Too much volume at the prejowl sulcus in a patient with a round face will make the face look fat," he explained.
Also, in some patients the smoothing of the jaw line may look good on profile, but it can have a masculinizing effect by widening the lateral face when viewed head on.
As for the cheeks, not all "deflate" in the same way, and thus not all will benefit from volume replacement. In those with central cheek hollowing, volume can be very effective in creating a more youthful appearance, as well as in tightening loose skin.
A number of filler options can be considered, including hyaluronic acid (HA) fillers, poly-L-lactic acid, calcium hydroxylapatite, and polymethyl methacrylate (PMMA).
"But for first-time patients, or if you are learning your way, don’t underestimate the value of a reversible filler," he said.
As with the use of neurotoxins, the approach to using fillers can vary without necessarily affecting the outcome. Various physicians have their own preferences for products and injection techniques, yet almost everyone seems to be able to achieve the intended aesthetic goal, he explained.
"So I don’t think the ‘what’ is that important. It’s knowing the ‘where’ and the mastering of an injection technique that means more," he said.
In fact, Food and Drug Administration trial data for most fillers suggest that they are more similar than dissimilar in terms of efficacy, longevity, and adverse effects. Still, although conventional wisdom suggests that particle size, concentration, or lift should affect the final result, and thus in theory there should be one product that is best for each location, there is a lack of agreement.
In Dr. Rubin’s experience, however, HA, PMMA, and calcium hydroxylapatite fillers can have a slight rippling effect when they are injected in areas of soft tissue, such as the central cheek.
"It’s hard to make a smooth contour across 6-8 cm when you are injecting droplets or linear filaments of a filler," he said, noting that poly-L-lactic acid seems to create a smoother contour in that area.
When injecting over bony areas, HA products and calcium hydroxylapatite are acceptable, because the defects are generally smaller and there is less surface area on which to see ripples.
Dr. Rubin is a consultant for Medicis. He also has been involved in FDA clinical trials for Restylane, Perlane, and Artefill. SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM THE SDEF HAWAII DERMATOLOGY SEMINAR
Preterm Birth Risk Linked to Longer Residence in U.S.
DALLAS – Preterm birth may be related in part to potentially preventable environmental factors, data from the National Health and Nutrition Examination Survey (NHANES) from 1999 through 2006 suggest.
Survey responses from 2,441 Hispanic women with a prior live birth show that the rate of births prior to 36 weeks’ gestation in Hispanic immigrants who resided in the United States for less than 10 years was 3.1%, which was significantly lower than the 7.4% rate among those who lived in the United States for more than 10 years, and the 10.1% rate among Hispanic women born in the United States (age adjusted odds ratios, 2.1 and 3.1, respectively), Dr. Radek Bukowski reported at the annual meeting of the Society for Maternal-Fetal Medicine.
The findings were similar after further adjustment for numerous factors that might affect preterm birth risk, such as age, body mass index, education, nutrition, marital status, sexual behaviors, toxic exposures, income, smoking status, diabetes, and hypertension (fully adjusted odds ratios, 2.1 and 3.5), said Dr. Bukowski of the University of Texas Medical Branch at Galveston.
One factor – language spoken at home – did appear to have a modifying effect on the association between length of residence in the United States and the risk of preterm birth, however.
"Compared with women who lived in the United States less than 10 years, those who lived here 10 years or longer and those who were born in the United States had the highest risk if they predominantly or exclusively spoke Spanish at home," Dr. Bukowski said.
Also, body mass index was negatively associated with preterm birth, and hypertension was positively associated with preterm birth, but these were not found to be independent risk factors in the fully adjusted model, he said.
Although nongenetic environmental factors have been thought to play a role in preterm birth risk, it has not been clear whether risk is predominantly related to genetic or environmental factors. However, many immigrants are known to have a lower risk, which could be related to better diet and health status, he said.
Although limited by the study’s cross-sectional design, the current findings suggest that risk is acquired with residence in the United States. Given this, as well as the fact that preterm birth was not associated with a number of other risk factors in this study, it is possible that the level of risk is modifiable, Dr. Bukowski concluded.
Dr. Bukowski said he had no relevant financial disclosures.
DALLAS – Preterm birth may be related in part to potentially preventable environmental factors, data from the National Health and Nutrition Examination Survey (NHANES) from 1999 through 2006 suggest.
Survey responses from 2,441 Hispanic women with a prior live birth show that the rate of births prior to 36 weeks’ gestation in Hispanic immigrants who resided in the United States for less than 10 years was 3.1%, which was significantly lower than the 7.4% rate among those who lived in the United States for more than 10 years, and the 10.1% rate among Hispanic women born in the United States (age adjusted odds ratios, 2.1 and 3.1, respectively), Dr. Radek Bukowski reported at the annual meeting of the Society for Maternal-Fetal Medicine.
The findings were similar after further adjustment for numerous factors that might affect preterm birth risk, such as age, body mass index, education, nutrition, marital status, sexual behaviors, toxic exposures, income, smoking status, diabetes, and hypertension (fully adjusted odds ratios, 2.1 and 3.5), said Dr. Bukowski of the University of Texas Medical Branch at Galveston.
One factor – language spoken at home – did appear to have a modifying effect on the association between length of residence in the United States and the risk of preterm birth, however.
"Compared with women who lived in the United States less than 10 years, those who lived here 10 years or longer and those who were born in the United States had the highest risk if they predominantly or exclusively spoke Spanish at home," Dr. Bukowski said.
Also, body mass index was negatively associated with preterm birth, and hypertension was positively associated with preterm birth, but these were not found to be independent risk factors in the fully adjusted model, he said.
Although nongenetic environmental factors have been thought to play a role in preterm birth risk, it has not been clear whether risk is predominantly related to genetic or environmental factors. However, many immigrants are known to have a lower risk, which could be related to better diet and health status, he said.
Although limited by the study’s cross-sectional design, the current findings suggest that risk is acquired with residence in the United States. Given this, as well as the fact that preterm birth was not associated with a number of other risk factors in this study, it is possible that the level of risk is modifiable, Dr. Bukowski concluded.
Dr. Bukowski said he had no relevant financial disclosures.
DALLAS – Preterm birth may be related in part to potentially preventable environmental factors, data from the National Health and Nutrition Examination Survey (NHANES) from 1999 through 2006 suggest.
Survey responses from 2,441 Hispanic women with a prior live birth show that the rate of births prior to 36 weeks’ gestation in Hispanic immigrants who resided in the United States for less than 10 years was 3.1%, which was significantly lower than the 7.4% rate among those who lived in the United States for more than 10 years, and the 10.1% rate among Hispanic women born in the United States (age adjusted odds ratios, 2.1 and 3.1, respectively), Dr. Radek Bukowski reported at the annual meeting of the Society for Maternal-Fetal Medicine.
The findings were similar after further adjustment for numerous factors that might affect preterm birth risk, such as age, body mass index, education, nutrition, marital status, sexual behaviors, toxic exposures, income, smoking status, diabetes, and hypertension (fully adjusted odds ratios, 2.1 and 3.5), said Dr. Bukowski of the University of Texas Medical Branch at Galveston.
One factor – language spoken at home – did appear to have a modifying effect on the association between length of residence in the United States and the risk of preterm birth, however.
"Compared with women who lived in the United States less than 10 years, those who lived here 10 years or longer and those who were born in the United States had the highest risk if they predominantly or exclusively spoke Spanish at home," Dr. Bukowski said.
Also, body mass index was negatively associated with preterm birth, and hypertension was positively associated with preterm birth, but these were not found to be independent risk factors in the fully adjusted model, he said.
Although nongenetic environmental factors have been thought to play a role in preterm birth risk, it has not been clear whether risk is predominantly related to genetic or environmental factors. However, many immigrants are known to have a lower risk, which could be related to better diet and health status, he said.
Although limited by the study’s cross-sectional design, the current findings suggest that risk is acquired with residence in the United States. Given this, as well as the fact that preterm birth was not associated with a number of other risk factors in this study, it is possible that the level of risk is modifiable, Dr. Bukowski concluded.
Dr. Bukowski said he had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE SOCIETY FOR MATERNAL-FETAL MEDICINE
Major Finding: Survey responses from 2,441 Hispanic women with a prior live birth show that the rate of births prior to 36 weeks’ gestation in Hispanic immigrants who resided in the United States for less than 10 years was 3.1%, significantly lower than the 7.4% rate among those who lived in the United States for more than 10 years, and the 10.1% rate among Hispanic women born in the United States (age adjusted odds ratios, 2.1 and 3.1, respectively).
Data Source: The study involved NHANES data from 1999-2006.
Disclosures: Dr. Bukowski said he had no relevant financial disclosures.
Extremes of SGA, LGA Linked With Autism Risk
DALLAS – The risk of autism is significantly increased in both very small and very large for gestational age infants, compared with average for gestational age infants, according to findings from a large retrospective population-based cohort study.
The findings, which indicate that the risk for autism is increased by 10% for very small for gestational age (SGA) and 12% for very large for gestational age (LGA) infants confirm similar findings from prior smaller studies, and also provide new information about the influence of birth weight on the risk, Dr. Gaea Moore reported at the annual meeting of the Society for Maternal-Fetal Medicine.
Of the nearly 6 million infants from the 1991-2001 California birth cohort, 21,717 who were eventually diagnosed with autism were included in the study. When stratified based on birth weight, the likelihood of autism in the SGA group was significant only in the preterm very SGA infants (those above the 95th percentile), said Dr. Moore of the University of Colorado at Denver, Aurora.
In the LGA group, the pattern was more complex. A significantly increased risk for autism was found only in very LGA infants (above the 95th percentile) born at term (greater than 39 weeks’ gestation).
"Interestingly, we found a protective effect in the LGA birth weight group, which was significant in the preterm period at less than 32 weeks," Dr. Moore said, noting that the finding was significant for both LGA and very LGA infants.
The findings confirm the results of multiple smaller analyses, but also provide a "new piece of the puzzle," she said.
"That is the finding that very SGA children born in the preterm setting have an increased risk of autism," she said, adding, "We suspect that the association might be the result of a combination of neurologic insults at a key window of development – likely, whatever contributed to the restricted growth in the intrauterine environment, combined with the typical neurological insults of prematurity."
As for the dichotomous pattern of risk in the LGA infants, the finding may explain why LGA birth weight has not been associated with autism in the past, she said, explaining that the protection afforded in the preterm period likely cancelled out the increased risk at term.
The increased risk in the term setting may reflect maternal abnormalities such as obesity and diabetes, which are risk factors both for delivery of an LGA child, and for delivery of a child with autism, she noted.
"The decreased risk in the preterm period (for LGA infants), is interesting. We know that LGA preterm infants have a higher rate of survival and a higher rate of survival without major morbidity. Thus, these larger preterm infants may simply survive prematurity with a lesser degree of neurologic insult," she suggested.
Alternately, the finding may reflect incorrect dating, which would explain both larger infants and infants less likely to sustain perinatal or neurological injury, she said.
The findings have implications for heightened screening for SGA and LGA during pregnancy, as well as for encouraging appropriate weight gain during pregnancy, she concluded.
Dr. Moore said she had no relevant financial disclosures.
DALLAS – The risk of autism is significantly increased in both very small and very large for gestational age infants, compared with average for gestational age infants, according to findings from a large retrospective population-based cohort study.
The findings, which indicate that the risk for autism is increased by 10% for very small for gestational age (SGA) and 12% for very large for gestational age (LGA) infants confirm similar findings from prior smaller studies, and also provide new information about the influence of birth weight on the risk, Dr. Gaea Moore reported at the annual meeting of the Society for Maternal-Fetal Medicine.
Of the nearly 6 million infants from the 1991-2001 California birth cohort, 21,717 who were eventually diagnosed with autism were included in the study. When stratified based on birth weight, the likelihood of autism in the SGA group was significant only in the preterm very SGA infants (those above the 95th percentile), said Dr. Moore of the University of Colorado at Denver, Aurora.
In the LGA group, the pattern was more complex. A significantly increased risk for autism was found only in very LGA infants (above the 95th percentile) born at term (greater than 39 weeks’ gestation).
"Interestingly, we found a protective effect in the LGA birth weight group, which was significant in the preterm period at less than 32 weeks," Dr. Moore said, noting that the finding was significant for both LGA and very LGA infants.
The findings confirm the results of multiple smaller analyses, but also provide a "new piece of the puzzle," she said.
"That is the finding that very SGA children born in the preterm setting have an increased risk of autism," she said, adding, "We suspect that the association might be the result of a combination of neurologic insults at a key window of development – likely, whatever contributed to the restricted growth in the intrauterine environment, combined with the typical neurological insults of prematurity."
As for the dichotomous pattern of risk in the LGA infants, the finding may explain why LGA birth weight has not been associated with autism in the past, she said, explaining that the protection afforded in the preterm period likely cancelled out the increased risk at term.
The increased risk in the term setting may reflect maternal abnormalities such as obesity and diabetes, which are risk factors both for delivery of an LGA child, and for delivery of a child with autism, she noted.
"The decreased risk in the preterm period (for LGA infants), is interesting. We know that LGA preterm infants have a higher rate of survival and a higher rate of survival without major morbidity. Thus, these larger preterm infants may simply survive prematurity with a lesser degree of neurologic insult," she suggested.
Alternately, the finding may reflect incorrect dating, which would explain both larger infants and infants less likely to sustain perinatal or neurological injury, she said.
The findings have implications for heightened screening for SGA and LGA during pregnancy, as well as for encouraging appropriate weight gain during pregnancy, she concluded.
Dr. Moore said she had no relevant financial disclosures.
DALLAS – The risk of autism is significantly increased in both very small and very large for gestational age infants, compared with average for gestational age infants, according to findings from a large retrospective population-based cohort study.
The findings, which indicate that the risk for autism is increased by 10% for very small for gestational age (SGA) and 12% for very large for gestational age (LGA) infants confirm similar findings from prior smaller studies, and also provide new information about the influence of birth weight on the risk, Dr. Gaea Moore reported at the annual meeting of the Society for Maternal-Fetal Medicine.
Of the nearly 6 million infants from the 1991-2001 California birth cohort, 21,717 who were eventually diagnosed with autism were included in the study. When stratified based on birth weight, the likelihood of autism in the SGA group was significant only in the preterm very SGA infants (those above the 95th percentile), said Dr. Moore of the University of Colorado at Denver, Aurora.
In the LGA group, the pattern was more complex. A significantly increased risk for autism was found only in very LGA infants (above the 95th percentile) born at term (greater than 39 weeks’ gestation).
"Interestingly, we found a protective effect in the LGA birth weight group, which was significant in the preterm period at less than 32 weeks," Dr. Moore said, noting that the finding was significant for both LGA and very LGA infants.
The findings confirm the results of multiple smaller analyses, but also provide a "new piece of the puzzle," she said.
"That is the finding that very SGA children born in the preterm setting have an increased risk of autism," she said, adding, "We suspect that the association might be the result of a combination of neurologic insults at a key window of development – likely, whatever contributed to the restricted growth in the intrauterine environment, combined with the typical neurological insults of prematurity."
As for the dichotomous pattern of risk in the LGA infants, the finding may explain why LGA birth weight has not been associated with autism in the past, she said, explaining that the protection afforded in the preterm period likely cancelled out the increased risk at term.
The increased risk in the term setting may reflect maternal abnormalities such as obesity and diabetes, which are risk factors both for delivery of an LGA child, and for delivery of a child with autism, she noted.
"The decreased risk in the preterm period (for LGA infants), is interesting. We know that LGA preterm infants have a higher rate of survival and a higher rate of survival without major morbidity. Thus, these larger preterm infants may simply survive prematurity with a lesser degree of neurologic insult," she suggested.
Alternately, the finding may reflect incorrect dating, which would explain both larger infants and infants less likely to sustain perinatal or neurological injury, she said.
The findings have implications for heightened screening for SGA and LGA during pregnancy, as well as for encouraging appropriate weight gain during pregnancy, she concluded.
Dr. Moore said she had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE SOCIETY FOR MATERNAL-FETAL MEDICINE
Major Finding: The risk for autism is increased by 10% and 12% for very small for gestational age and very large for gestational age infants.
Data Source: A retrospective population-based study of nearly 6 million infants from 1991-2001 California birth cohort, including 21,717 who were eventually diagnosed with autism.
Disclosures: Dr. Moore said she had no relevant financial disclosures.
Microarray Testing Bests Karyotyping for Prenatal Cytogenetic Diagnoses
DALLAS – Chromosomal microarray, or CMA, is as effective as karyotyping for identifying common aneuploidies during routine and high-risk prenatal screening, and it also provides clinically significant and relevant information in patients with a normal karyotype, according to findings from a prospective study involving more than 4,400 women.
The findings support a transition from the use of karyotyping to the use of CMA as the first tier test for invasive cytogenetic testing, Dr. Ronald Wapner said at the annual meeting of the Society for Maternal-Fetal Medicine.
Reporting on behalf of the Prenatal Microarray Study Group of the Eunice Kennedy Shriver National Institute of Child Health and Human Development, Dr. Wapner noted that the analyses were performed on 4,391 samples, of which about half were obtained by chorionic villus sampling and about half by amniocentesis. DNA extraction or microarray failed in 51 samples, for a CMA success rate of nearly 99%.
He reported the findings from 4,282 samples with nonmosaic karyotype results.
Indications for enrollment among the 4,401 women who participated in the study included advanced maternal age in about half of the patients, a positive first or second trimester screen in about 20%, and an abnormal ultrasound in about 25%, with "other" indications accounting for the remaining participants.
Of all cases with common autosomal or sex chromosome aneuploidy identified by karyotyping, 100% were confirmed by microarray testing, said Dr. Wapner, chief of maternal fetal medicine at Columbia University Medical Center, New York.
Eight of the samples were identified as mosaic by microarray testing, but none of those led to an incorrect diagnosis; interestingly, all eight were from chorionic villus samples, Dr. Wapner noted. "Therefore, we can say very comfortably that CMA is a 100% comparison with karyotyping for common autosomal and sex chromosome aneuploidies."
Consistent with what is known about the technique of microarray testing; however, none of the triploidy pregnancies were identified, but 15 of 17 were correctly called using maternal cell contamination results, he noted.
Among participants with normal karyotypes, 35 (0.9%) had a CMA finding included on a predetermined pathogenic list. Of 94 (2.5%) with another finding not on the list, about two-thirds were determined by a clinical advisory committee to be clinically relevant. Thus, 96 samples (2.5%) were found to have clinically relevant material beyond what was seen on the karyotype, Dr. Wapner said.
A break-down based on participant’s indication for testing showed that of cases with an ultrasound abnormality, 6% had additional clinically significant results on CMA despite a normal karyotype, and of those with advanced maternal age or a positive screen, 1.6%-1.7% had additional clinically significant results on CMA despite a normal karyotype.
The findings indicate that a transition from karyotyping to CMA for prenatal cytogenetic diagnosis is warranted, Dr. Wapner said. "But if we are going to use CMA in prenatal care, particularly, we will have to have an additional approach that will allow the detection of triploidy pregnancy, and there are many that are available," he added.
Also, the transition will require a very methodical, well-thought-out approach including development of standardized pre- and post-test counseling, and discussion of how to manage some of the unusual findings identified using CMA, he noted.
Dr. Wapner said he had no relevant financial disclosures.
DALLAS – Chromosomal microarray, or CMA, is as effective as karyotyping for identifying common aneuploidies during routine and high-risk prenatal screening, and it also provides clinically significant and relevant information in patients with a normal karyotype, according to findings from a prospective study involving more than 4,400 women.
The findings support a transition from the use of karyotyping to the use of CMA as the first tier test for invasive cytogenetic testing, Dr. Ronald Wapner said at the annual meeting of the Society for Maternal-Fetal Medicine.
Reporting on behalf of the Prenatal Microarray Study Group of the Eunice Kennedy Shriver National Institute of Child Health and Human Development, Dr. Wapner noted that the analyses were performed on 4,391 samples, of which about half were obtained by chorionic villus sampling and about half by amniocentesis. DNA extraction or microarray failed in 51 samples, for a CMA success rate of nearly 99%.
He reported the findings from 4,282 samples with nonmosaic karyotype results.
Indications for enrollment among the 4,401 women who participated in the study included advanced maternal age in about half of the patients, a positive first or second trimester screen in about 20%, and an abnormal ultrasound in about 25%, with "other" indications accounting for the remaining participants.
Of all cases with common autosomal or sex chromosome aneuploidy identified by karyotyping, 100% were confirmed by microarray testing, said Dr. Wapner, chief of maternal fetal medicine at Columbia University Medical Center, New York.
Eight of the samples were identified as mosaic by microarray testing, but none of those led to an incorrect diagnosis; interestingly, all eight were from chorionic villus samples, Dr. Wapner noted. "Therefore, we can say very comfortably that CMA is a 100% comparison with karyotyping for common autosomal and sex chromosome aneuploidies."
Consistent with what is known about the technique of microarray testing; however, none of the triploidy pregnancies were identified, but 15 of 17 were correctly called using maternal cell contamination results, he noted.
Among participants with normal karyotypes, 35 (0.9%) had a CMA finding included on a predetermined pathogenic list. Of 94 (2.5%) with another finding not on the list, about two-thirds were determined by a clinical advisory committee to be clinically relevant. Thus, 96 samples (2.5%) were found to have clinically relevant material beyond what was seen on the karyotype, Dr. Wapner said.
A break-down based on participant’s indication for testing showed that of cases with an ultrasound abnormality, 6% had additional clinically significant results on CMA despite a normal karyotype, and of those with advanced maternal age or a positive screen, 1.6%-1.7% had additional clinically significant results on CMA despite a normal karyotype.
The findings indicate that a transition from karyotyping to CMA for prenatal cytogenetic diagnosis is warranted, Dr. Wapner said. "But if we are going to use CMA in prenatal care, particularly, we will have to have an additional approach that will allow the detection of triploidy pregnancy, and there are many that are available," he added.
Also, the transition will require a very methodical, well-thought-out approach including development of standardized pre- and post-test counseling, and discussion of how to manage some of the unusual findings identified using CMA, he noted.
Dr. Wapner said he had no relevant financial disclosures.
DALLAS – Chromosomal microarray, or CMA, is as effective as karyotyping for identifying common aneuploidies during routine and high-risk prenatal screening, and it also provides clinically significant and relevant information in patients with a normal karyotype, according to findings from a prospective study involving more than 4,400 women.
The findings support a transition from the use of karyotyping to the use of CMA as the first tier test for invasive cytogenetic testing, Dr. Ronald Wapner said at the annual meeting of the Society for Maternal-Fetal Medicine.
Reporting on behalf of the Prenatal Microarray Study Group of the Eunice Kennedy Shriver National Institute of Child Health and Human Development, Dr. Wapner noted that the analyses were performed on 4,391 samples, of which about half were obtained by chorionic villus sampling and about half by amniocentesis. DNA extraction or microarray failed in 51 samples, for a CMA success rate of nearly 99%.
He reported the findings from 4,282 samples with nonmosaic karyotype results.
Indications for enrollment among the 4,401 women who participated in the study included advanced maternal age in about half of the patients, a positive first or second trimester screen in about 20%, and an abnormal ultrasound in about 25%, with "other" indications accounting for the remaining participants.
Of all cases with common autosomal or sex chromosome aneuploidy identified by karyotyping, 100% were confirmed by microarray testing, said Dr. Wapner, chief of maternal fetal medicine at Columbia University Medical Center, New York.
Eight of the samples were identified as mosaic by microarray testing, but none of those led to an incorrect diagnosis; interestingly, all eight were from chorionic villus samples, Dr. Wapner noted. "Therefore, we can say very comfortably that CMA is a 100% comparison with karyotyping for common autosomal and sex chromosome aneuploidies."
Consistent with what is known about the technique of microarray testing; however, none of the triploidy pregnancies were identified, but 15 of 17 were correctly called using maternal cell contamination results, he noted.
Among participants with normal karyotypes, 35 (0.9%) had a CMA finding included on a predetermined pathogenic list. Of 94 (2.5%) with another finding not on the list, about two-thirds were determined by a clinical advisory committee to be clinically relevant. Thus, 96 samples (2.5%) were found to have clinically relevant material beyond what was seen on the karyotype, Dr. Wapner said.
A break-down based on participant’s indication for testing showed that of cases with an ultrasound abnormality, 6% had additional clinically significant results on CMA despite a normal karyotype, and of those with advanced maternal age or a positive screen, 1.6%-1.7% had additional clinically significant results on CMA despite a normal karyotype.
The findings indicate that a transition from karyotyping to CMA for prenatal cytogenetic diagnosis is warranted, Dr. Wapner said. "But if we are going to use CMA in prenatal care, particularly, we will have to have an additional approach that will allow the detection of triploidy pregnancy, and there are many that are available," he added.
Also, the transition will require a very methodical, well-thought-out approach including development of standardized pre- and post-test counseling, and discussion of how to manage some of the unusual findings identified using CMA, he noted.
Dr. Wapner said he had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE SOCIETY FOR MATERNAL-FETAL MEDICINE
Major Finding: Of all cases with common autosomal or sex chromosome aneuploidy identified by karyotyping, 100% were confirmed by microarray testing.
Data Source: This was a prospective, multicenter, masked comparison of chromosomal microarray and karyotyping for cytogenetic prenatal diagnoses in a study enrolling of 4,401 women, in which 4,391 samples were studied.
Disclosures: Dr. Wapner said he had no relevant financial disclosures.
Intra-Articular Glucocorticoids Controlled Early RA
Unguided intra-articular betamethasone injections provide rapid and enduring control of inflammation in both small and large peripheral joints when used as a component of a treat-to-target strategy in patients with early rheumatoid arthritis, according to findings from the randomized, placebo-controlled trial.
The findings are among the first to systematically demonstrate efficacy and feasibility of intra-articular glucocorticoid injections when used in combination with disease-modifying antirheumatic drugs (DMARDs) in the setting of early rheumatoid arthritis (RA), Dr. Merete Lund Hetland of Copenhagen University Hospital and her colleagues wrote in a report published online in the Feb. 1 issue of Annals of Rheumatic Diseases.
The 160 DMARD-naive patients who participated in the CIMESTRA (Ciclosporin, Methotrexate, Steroid in RA) study had early active RA of less than 6 months duration. They were randomized to receive either 7.5 mg-20 mg of methotrexate weekly plus 2.5 mg/kg per day of ciclosporin or methotrexate plus placebo-ciclosporin. Both groups were given intra-articular injections of 7 mg/mL of betamethasone in up to four swollen joints at baseline and at weeks 2, 4, 6, and 8, and then every 4 weeks thereafter for up to 2 years. Since the combination and monotherapy groups had similar clinical and radiographic outcomes, as well as a similar number of injections and cumulative betamethasone dose after 5 years, data from both treatment arms were pooled for the current analysis.
A total of 2,166 injections were given, including 1,373 first injections, 531 second injections, and 262 third injections. The median dose of betamethasone decreased from 28 mg at baseline to 0 mg at the following visits, and the cumulative dose after 2 years was 77 mg, which corresponds to less than 1 mg prednisolone daily. The median cumulative number of injections per patient was 13.
Within 2 weeks of the initial joint injections, the median 28-joint count Disease Activity Score (DAS28) had decreased from 5.5 to 3. By 6 weeks, the DAS28 had decreased to 2.6, the investigators wrote (Ann. Rheum. Dis. 2012 Feb. 1[doi:10.1136/annrheumdis-2011-200632]).
"Thus, the median number of swollen and tender joints had decreased sharply to 0 and 3, respectively, and remained low. By weeks 2, 4, and 6, respectively, 50%, 58.1%, and 61.7% of patients had achieved a good EULAR response, and 39%, 42%, and 47% were in DAS28 remission," they said.
The injections also provided good long-term efficacy. After 1 and 2 years, 62.3% and 55.5%, respectively, of the swollen joints injected at baseline had not relapsed.
An analysis by joint area showed that benefits of joint injection persisted at 2 years was 51.2% for elbows, 60.1% for ankles, 54.8% for wrists, 55.3% for knees, 52.3% for metacarpophalangeal (MCP) joints, 53.6% for metatarsophalangeal (MTP) joints, 49.5% for shoulders, and 73.7% for proximal interphalangeal (PIP) joints. Persistence of join injection benefits was significantly higher for first-time injections.
For example, the 1-year survival was 63.6% for first-time injections, compared with 48.7% and 32.4% for second and third injections, respectively. The 2-year survival for first-time injections was 56.6%, compared with 43.4% and 31.3% for second and third injections, respectively.
Both the magnetic resonance imaging synovitis score of MCP joints and anticyclic citrullinated peptide (anti-CCP) positivity each were significantly associated with persistence of joint injection benefits (hazard ratios, 1.078 per synovitis score unit, and 0.661, respectively). The anti-CCP finding "may reflect the emerging pattern of different pathogenesis and treatment responses in anti-CCP–positive and –negative disease," the investigators noted, adding: "The increased joint injection survival in our anti-CCP–positive patients with RA may indicate that the local immunosuppressive effect of joint injections targets specific processes in these patients. To this end, it is of particular interest that antibodies against citrullinated proteins seem locally to enhance the inflammatory process in experimental murine autoimmune arthritis."
In contract, serum C-reactive protein and immunoglobulin M–rheumatoid factor (IgM-RF) were not associated with persistence of joint injection benefits in this study, they noted.
Patients in CIMESTRA had at least two swollen joints at baseline and had not received glucocorticoid treatment within 4 weeks prior to enrollment. All patients received calcium and vitamin D supplementation, and those with a Z score of less than 0 in the femoral neck or lumbar spine also received 10 mg/day of alendronate.
Treatment was well tolerated. No cases of septic arthritis or aseptic necrosis occurred. One patient had a spontaneous spinal fracture, but other adverse events occurred only rarely and were mild and transient.
The findings indicate that unguided intra-articular injections of betamethasone in patients with early RA result in rapid, effective, and long-lasting inflammatory control in both small and large peripheral joints and that these injections are a well tolerated component in a treatment strategy aimed at remission, the investigators said.
Rheumatologists should consider including such injections in combination with aggressive DMARD treatment as part of a treat to target strategy in patients with early RA, they concluded.
The CIMESTRA study was supported by a grant from the Danish Rheumatism Association. Novartis Healthcare Denmark A/S provided ciclosporin and placebo-ciclosporin and sponsored an independent good clinical practice monitor. Nycomed provided methotrexate, folic acid and calcium/vitamin D. Schering-Plough provided injectable betamethasone. Merck Sharp and Dohme provided alendronate. The authors had no individual disclosures to report.
Unguided intra-articular betamethasone injections provide rapid and enduring control of inflammation in both small and large peripheral joints when used as a component of a treat-to-target strategy in patients with early rheumatoid arthritis, according to findings from the randomized, placebo-controlled trial.
The findings are among the first to systematically demonstrate efficacy and feasibility of intra-articular glucocorticoid injections when used in combination with disease-modifying antirheumatic drugs (DMARDs) in the setting of early rheumatoid arthritis (RA), Dr. Merete Lund Hetland of Copenhagen University Hospital and her colleagues wrote in a report published online in the Feb. 1 issue of Annals of Rheumatic Diseases.
The 160 DMARD-naive patients who participated in the CIMESTRA (Ciclosporin, Methotrexate, Steroid in RA) study had early active RA of less than 6 months duration. They were randomized to receive either 7.5 mg-20 mg of methotrexate weekly plus 2.5 mg/kg per day of ciclosporin or methotrexate plus placebo-ciclosporin. Both groups were given intra-articular injections of 7 mg/mL of betamethasone in up to four swollen joints at baseline and at weeks 2, 4, 6, and 8, and then every 4 weeks thereafter for up to 2 years. Since the combination and monotherapy groups had similar clinical and radiographic outcomes, as well as a similar number of injections and cumulative betamethasone dose after 5 years, data from both treatment arms were pooled for the current analysis.
A total of 2,166 injections were given, including 1,373 first injections, 531 second injections, and 262 third injections. The median dose of betamethasone decreased from 28 mg at baseline to 0 mg at the following visits, and the cumulative dose after 2 years was 77 mg, which corresponds to less than 1 mg prednisolone daily. The median cumulative number of injections per patient was 13.
Within 2 weeks of the initial joint injections, the median 28-joint count Disease Activity Score (DAS28) had decreased from 5.5 to 3. By 6 weeks, the DAS28 had decreased to 2.6, the investigators wrote (Ann. Rheum. Dis. 2012 Feb. 1[doi:10.1136/annrheumdis-2011-200632]).
"Thus, the median number of swollen and tender joints had decreased sharply to 0 and 3, respectively, and remained low. By weeks 2, 4, and 6, respectively, 50%, 58.1%, and 61.7% of patients had achieved a good EULAR response, and 39%, 42%, and 47% were in DAS28 remission," they said.
The injections also provided good long-term efficacy. After 1 and 2 years, 62.3% and 55.5%, respectively, of the swollen joints injected at baseline had not relapsed.
An analysis by joint area showed that benefits of joint injection persisted at 2 years was 51.2% for elbows, 60.1% for ankles, 54.8% for wrists, 55.3% for knees, 52.3% for metacarpophalangeal (MCP) joints, 53.6% for metatarsophalangeal (MTP) joints, 49.5% for shoulders, and 73.7% for proximal interphalangeal (PIP) joints. Persistence of join injection benefits was significantly higher for first-time injections.
For example, the 1-year survival was 63.6% for first-time injections, compared with 48.7% and 32.4% for second and third injections, respectively. The 2-year survival for first-time injections was 56.6%, compared with 43.4% and 31.3% for second and third injections, respectively.
Both the magnetic resonance imaging synovitis score of MCP joints and anticyclic citrullinated peptide (anti-CCP) positivity each were significantly associated with persistence of joint injection benefits (hazard ratios, 1.078 per synovitis score unit, and 0.661, respectively). The anti-CCP finding "may reflect the emerging pattern of different pathogenesis and treatment responses in anti-CCP–positive and –negative disease," the investigators noted, adding: "The increased joint injection survival in our anti-CCP–positive patients with RA may indicate that the local immunosuppressive effect of joint injections targets specific processes in these patients. To this end, it is of particular interest that antibodies against citrullinated proteins seem locally to enhance the inflammatory process in experimental murine autoimmune arthritis."
In contract, serum C-reactive protein and immunoglobulin M–rheumatoid factor (IgM-RF) were not associated with persistence of joint injection benefits in this study, they noted.
Patients in CIMESTRA had at least two swollen joints at baseline and had not received glucocorticoid treatment within 4 weeks prior to enrollment. All patients received calcium and vitamin D supplementation, and those with a Z score of less than 0 in the femoral neck or lumbar spine also received 10 mg/day of alendronate.
Treatment was well tolerated. No cases of septic arthritis or aseptic necrosis occurred. One patient had a spontaneous spinal fracture, but other adverse events occurred only rarely and were mild and transient.
The findings indicate that unguided intra-articular injections of betamethasone in patients with early RA result in rapid, effective, and long-lasting inflammatory control in both small and large peripheral joints and that these injections are a well tolerated component in a treatment strategy aimed at remission, the investigators said.
Rheumatologists should consider including such injections in combination with aggressive DMARD treatment as part of a treat to target strategy in patients with early RA, they concluded.
The CIMESTRA study was supported by a grant from the Danish Rheumatism Association. Novartis Healthcare Denmark A/S provided ciclosporin and placebo-ciclosporin and sponsored an independent good clinical practice monitor. Nycomed provided methotrexate, folic acid and calcium/vitamin D. Schering-Plough provided injectable betamethasone. Merck Sharp and Dohme provided alendronate. The authors had no individual disclosures to report.
Unguided intra-articular betamethasone injections provide rapid and enduring control of inflammation in both small and large peripheral joints when used as a component of a treat-to-target strategy in patients with early rheumatoid arthritis, according to findings from the randomized, placebo-controlled trial.
The findings are among the first to systematically demonstrate efficacy and feasibility of intra-articular glucocorticoid injections when used in combination with disease-modifying antirheumatic drugs (DMARDs) in the setting of early rheumatoid arthritis (RA), Dr. Merete Lund Hetland of Copenhagen University Hospital and her colleagues wrote in a report published online in the Feb. 1 issue of Annals of Rheumatic Diseases.
The 160 DMARD-naive patients who participated in the CIMESTRA (Ciclosporin, Methotrexate, Steroid in RA) study had early active RA of less than 6 months duration. They were randomized to receive either 7.5 mg-20 mg of methotrexate weekly plus 2.5 mg/kg per day of ciclosporin or methotrexate plus placebo-ciclosporin. Both groups were given intra-articular injections of 7 mg/mL of betamethasone in up to four swollen joints at baseline and at weeks 2, 4, 6, and 8, and then every 4 weeks thereafter for up to 2 years. Since the combination and monotherapy groups had similar clinical and radiographic outcomes, as well as a similar number of injections and cumulative betamethasone dose after 5 years, data from both treatment arms were pooled for the current analysis.
A total of 2,166 injections were given, including 1,373 first injections, 531 second injections, and 262 third injections. The median dose of betamethasone decreased from 28 mg at baseline to 0 mg at the following visits, and the cumulative dose after 2 years was 77 mg, which corresponds to less than 1 mg prednisolone daily. The median cumulative number of injections per patient was 13.
Within 2 weeks of the initial joint injections, the median 28-joint count Disease Activity Score (DAS28) had decreased from 5.5 to 3. By 6 weeks, the DAS28 had decreased to 2.6, the investigators wrote (Ann. Rheum. Dis. 2012 Feb. 1[doi:10.1136/annrheumdis-2011-200632]).
"Thus, the median number of swollen and tender joints had decreased sharply to 0 and 3, respectively, and remained low. By weeks 2, 4, and 6, respectively, 50%, 58.1%, and 61.7% of patients had achieved a good EULAR response, and 39%, 42%, and 47% were in DAS28 remission," they said.
The injections also provided good long-term efficacy. After 1 and 2 years, 62.3% and 55.5%, respectively, of the swollen joints injected at baseline had not relapsed.
An analysis by joint area showed that benefits of joint injection persisted at 2 years was 51.2% for elbows, 60.1% for ankles, 54.8% for wrists, 55.3% for knees, 52.3% for metacarpophalangeal (MCP) joints, 53.6% for metatarsophalangeal (MTP) joints, 49.5% for shoulders, and 73.7% for proximal interphalangeal (PIP) joints. Persistence of join injection benefits was significantly higher for first-time injections.
For example, the 1-year survival was 63.6% for first-time injections, compared with 48.7% and 32.4% for second and third injections, respectively. The 2-year survival for first-time injections was 56.6%, compared with 43.4% and 31.3% for second and third injections, respectively.
Both the magnetic resonance imaging synovitis score of MCP joints and anticyclic citrullinated peptide (anti-CCP) positivity each were significantly associated with persistence of joint injection benefits (hazard ratios, 1.078 per synovitis score unit, and 0.661, respectively). The anti-CCP finding "may reflect the emerging pattern of different pathogenesis and treatment responses in anti-CCP–positive and –negative disease," the investigators noted, adding: "The increased joint injection survival in our anti-CCP–positive patients with RA may indicate that the local immunosuppressive effect of joint injections targets specific processes in these patients. To this end, it is of particular interest that antibodies against citrullinated proteins seem locally to enhance the inflammatory process in experimental murine autoimmune arthritis."
In contract, serum C-reactive protein and immunoglobulin M–rheumatoid factor (IgM-RF) were not associated with persistence of joint injection benefits in this study, they noted.
Patients in CIMESTRA had at least two swollen joints at baseline and had not received glucocorticoid treatment within 4 weeks prior to enrollment. All patients received calcium and vitamin D supplementation, and those with a Z score of less than 0 in the femoral neck or lumbar spine also received 10 mg/day of alendronate.
Treatment was well tolerated. No cases of septic arthritis or aseptic necrosis occurred. One patient had a spontaneous spinal fracture, but other adverse events occurred only rarely and were mild and transient.
The findings indicate that unguided intra-articular injections of betamethasone in patients with early RA result in rapid, effective, and long-lasting inflammatory control in both small and large peripheral joints and that these injections are a well tolerated component in a treatment strategy aimed at remission, the investigators said.
Rheumatologists should consider including such injections in combination with aggressive DMARD treatment as part of a treat to target strategy in patients with early RA, they concluded.
The CIMESTRA study was supported by a grant from the Danish Rheumatism Association. Novartis Healthcare Denmark A/S provided ciclosporin and placebo-ciclosporin and sponsored an independent good clinical practice monitor. Nycomed provided methotrexate, folic acid and calcium/vitamin D. Schering-Plough provided injectable betamethasone. Merck Sharp and Dohme provided alendronate. The authors had no individual disclosures to report.
FROM ANNALS OF THE RHEUMATIC DISEASES
Major Finding: By weeks 2, 4, and 6, respectively, 50.0%, 58.1%, and 61.7% of patients had achieved a good EULAR response, and 39%, 42%, and 47% were in DAS28 remission. After 1 and 2 years, remission was persistent in 62.3% and 55.5%, respectively, of the swollen joints injected at baseline.
Data Source: The randomized, double-blind, placebo controlled CIMESTRA study.
Disclosures: The CIMESTRA study was supported by a grant from the Danish Rheumatism Association. Novartis Healthcare Denmark A/S provided ciclosporin and placebo-ciclosporin and sponsored an independent good clinical practice monitor. Nycomed provided methotrexate, folic acid, and calcium/vitamin D. Schering-Plough provided injectable betamethasone. Merck Sharp and Dohme provided alendronate. The authors had no individual disclosures to report.
JSLE Imparts Severe Organ Involvement
Children with juvenile-onset systemic lupus erythematosus tend to have significant disease activity and high rates of organ involvement with damage accumulation, according to findings from the UK JSLE Cohort Study.
The findings underscore the complex and severe nature of JSLE and the need for pediatric multidisciplinary management that "considers carefully issues related to disease activity and damage and medications, along with growth, puberty, educational development and psychosocial well being," Dr. Louise Watson of the University of Liverpool, England, and her colleagues from the UK JSLE Study Group said online in the Jan. 31 issue of Arthritis & Rheumatism.
In the 198 patients from the cohort who fulfilled four or more American College of Rheumatology SLE criteria and who were followed for 4.5 years, disease progression was evident in multiple organ systems, based on assessment using a pediatric adaptation of the British Isles Lupus Assessment Group (pBILAG2004) disease activity index. For example, renal involvement was present in 47% of the patients at baseline and had progressed to 80% at the time of the latest analysis, the investigators said (Arthritis Rheum. 2012 Jan. 31 [doi:10.1002/art.34410]).
At the last analysis, 82% of patients had musculoskeletal involvement, 91% had hematologic involvement, 54% had immunologic involvement, and 26% had neurologic involvement, as measured by pBILAG2004.
Of note, pBILAG2004, which collects more detailed information about organ-related disease activity than do the ACR criteria, demonstrated markedly greater actual organ involvement than indicated by the respective ACR criteria for various organ systems, they said.
The median pBILAG2004 score decreased from 8.5 at baseline to 2 at 12 months’ follow-up, representing a statistically significant improvement, and the systemic lupus erythematosus disease activity index (SLEDAI) score decreased significantly over 12 months from 12 points to 4 points. Although disease activity improved over time, disease damage accrual secondary to JSLE was notable. Even after only 4.5 years of follow-up, 28% of patients demonstrated disease-associated damage at the time of data analysis.
"There is a predominance of neurological disease damage involving 15 patients, of whom 6 have experienced one or more cerebrovascular accidents," Dr. Watson and her associates wrote, noting that severe scarring alopecia occurred in 20 patients and that 7 had renal damage, including 1 child with renal failure.
The investigators also found that steroid use among the cohort was high at 93%, and that 24% required cyclophosphamide – a finding that underlines the burden of disease in pediatric patients and the importance of developing steroid-sparing regimens following robust randomized controlled trials for new interventions in JSLE. "Alternative therapies to relieve the burden of corticosteroids on this population are urgently required," they added.
The UK JSLE cohort is a multidisciplinary, multicenter collaborative network established in 2006 to determine the clinical characteristics of JSLE and to support clinical translational research. Patients include children with symptom onset prior to age 17 years. The median age at diagnosis was 12.6 years, and the median time from symptom onset to diagnosis was 3.2 months.
There were other findings of note from this analysis of cohort data:
–Important gender differences in disease prevalence and characteristics. A sex distribution of 5.6 females to every male (but only 2.7 females to every male among those under age 10 years) "is typical of childhood-onset disease where a female predominance is less striking than in adult-onset disease," the investigators said.
Males in this cohort also were more likely to present at a younger age than females, and they had a greater likelihood of having a discoid rash and a reduced likelihood of having had arthritis.
–A high incidence (38%) of family history of autoimmune disease. This finding, in the context of the generally more severe JSLE phenotype compared with adult SLE, a very early age of onset, short time exposure to potential environmental triggers of lupus, and the relatively high male-to-female sex ratio compared with adult disease, points to "probable genetic factors being important in the pathogenesis of JSLE compared to later-onset disease," Dr. Watson and her associates noted.
–Important ethnic differences in regard to disease incidence. There was a significantly higher standardized incidence among nonwhites than among whites. This finding underscores the need for ensuring availability and provision of specialty care in affected ethnic communities and for recognizing the effects of ethnicity in future interventional trials, they said.
–Diagnosis during the teenage years in about half of the patients in the cohort. This finding of diagnosis during a critical time for adolescent growth, puberty, education, and emotional maturation emphasizes the importance of access to specialty, multidisciplinary, pediatric, and adolescent holistic care for patients with JSLE, the investigators said.
The findings illustrate a similar pattern of predominant clinical manifestations and severe disease phenotype as reported from other JSLE cohorts, and the disease-related damage over a relatively short follow-up period is "likely to have significant long-lasting physical and or psychosocial impact and consequences," the investigators wrote.
"Determining the effect of lupus-associated damage on the developing child requires large, prospective long-term studies, together with improved disease biomarkers, to assess the true physical and psychosocial impact of this condition," Dr. Watson and her associates said.
This study was supported by Lupus UK, private benefactors, and the Alder Hey Children’s Kidney Fund. The investigators had no conflicts of interest to declare.
Children with juvenile-onset systemic lupus erythematosus tend to have significant disease activity and high rates of organ involvement with damage accumulation, according to findings from the UK JSLE Cohort Study.
The findings underscore the complex and severe nature of JSLE and the need for pediatric multidisciplinary management that "considers carefully issues related to disease activity and damage and medications, along with growth, puberty, educational development and psychosocial well being," Dr. Louise Watson of the University of Liverpool, England, and her colleagues from the UK JSLE Study Group said online in the Jan. 31 issue of Arthritis & Rheumatism.
In the 198 patients from the cohort who fulfilled four or more American College of Rheumatology SLE criteria and who were followed for 4.5 years, disease progression was evident in multiple organ systems, based on assessment using a pediatric adaptation of the British Isles Lupus Assessment Group (pBILAG2004) disease activity index. For example, renal involvement was present in 47% of the patients at baseline and had progressed to 80% at the time of the latest analysis, the investigators said (Arthritis Rheum. 2012 Jan. 31 [doi:10.1002/art.34410]).
At the last analysis, 82% of patients had musculoskeletal involvement, 91% had hematologic involvement, 54% had immunologic involvement, and 26% had neurologic involvement, as measured by pBILAG2004.
Of note, pBILAG2004, which collects more detailed information about organ-related disease activity than do the ACR criteria, demonstrated markedly greater actual organ involvement than indicated by the respective ACR criteria for various organ systems, they said.
The median pBILAG2004 score decreased from 8.5 at baseline to 2 at 12 months’ follow-up, representing a statistically significant improvement, and the systemic lupus erythematosus disease activity index (SLEDAI) score decreased significantly over 12 months from 12 points to 4 points. Although disease activity improved over time, disease damage accrual secondary to JSLE was notable. Even after only 4.5 years of follow-up, 28% of patients demonstrated disease-associated damage at the time of data analysis.
"There is a predominance of neurological disease damage involving 15 patients, of whom 6 have experienced one or more cerebrovascular accidents," Dr. Watson and her associates wrote, noting that severe scarring alopecia occurred in 20 patients and that 7 had renal damage, including 1 child with renal failure.
The investigators also found that steroid use among the cohort was high at 93%, and that 24% required cyclophosphamide – a finding that underlines the burden of disease in pediatric patients and the importance of developing steroid-sparing regimens following robust randomized controlled trials for new interventions in JSLE. "Alternative therapies to relieve the burden of corticosteroids on this population are urgently required," they added.
The UK JSLE cohort is a multidisciplinary, multicenter collaborative network established in 2006 to determine the clinical characteristics of JSLE and to support clinical translational research. Patients include children with symptom onset prior to age 17 years. The median age at diagnosis was 12.6 years, and the median time from symptom onset to diagnosis was 3.2 months.
There were other findings of note from this analysis of cohort data:
–Important gender differences in disease prevalence and characteristics. A sex distribution of 5.6 females to every male (but only 2.7 females to every male among those under age 10 years) "is typical of childhood-onset disease where a female predominance is less striking than in adult-onset disease," the investigators said.
Males in this cohort also were more likely to present at a younger age than females, and they had a greater likelihood of having a discoid rash and a reduced likelihood of having had arthritis.
–A high incidence (38%) of family history of autoimmune disease. This finding, in the context of the generally more severe JSLE phenotype compared with adult SLE, a very early age of onset, short time exposure to potential environmental triggers of lupus, and the relatively high male-to-female sex ratio compared with adult disease, points to "probable genetic factors being important in the pathogenesis of JSLE compared to later-onset disease," Dr. Watson and her associates noted.
–Important ethnic differences in regard to disease incidence. There was a significantly higher standardized incidence among nonwhites than among whites. This finding underscores the need for ensuring availability and provision of specialty care in affected ethnic communities and for recognizing the effects of ethnicity in future interventional trials, they said.
–Diagnosis during the teenage years in about half of the patients in the cohort. This finding of diagnosis during a critical time for adolescent growth, puberty, education, and emotional maturation emphasizes the importance of access to specialty, multidisciplinary, pediatric, and adolescent holistic care for patients with JSLE, the investigators said.
The findings illustrate a similar pattern of predominant clinical manifestations and severe disease phenotype as reported from other JSLE cohorts, and the disease-related damage over a relatively short follow-up period is "likely to have significant long-lasting physical and or psychosocial impact and consequences," the investigators wrote.
"Determining the effect of lupus-associated damage on the developing child requires large, prospective long-term studies, together with improved disease biomarkers, to assess the true physical and psychosocial impact of this condition," Dr. Watson and her associates said.
This study was supported by Lupus UK, private benefactors, and the Alder Hey Children’s Kidney Fund. The investigators had no conflicts of interest to declare.
Children with juvenile-onset systemic lupus erythematosus tend to have significant disease activity and high rates of organ involvement with damage accumulation, according to findings from the UK JSLE Cohort Study.
The findings underscore the complex and severe nature of JSLE and the need for pediatric multidisciplinary management that "considers carefully issues related to disease activity and damage and medications, along with growth, puberty, educational development and psychosocial well being," Dr. Louise Watson of the University of Liverpool, England, and her colleagues from the UK JSLE Study Group said online in the Jan. 31 issue of Arthritis & Rheumatism.
In the 198 patients from the cohort who fulfilled four or more American College of Rheumatology SLE criteria and who were followed for 4.5 years, disease progression was evident in multiple organ systems, based on assessment using a pediatric adaptation of the British Isles Lupus Assessment Group (pBILAG2004) disease activity index. For example, renal involvement was present in 47% of the patients at baseline and had progressed to 80% at the time of the latest analysis, the investigators said (Arthritis Rheum. 2012 Jan. 31 [doi:10.1002/art.34410]).
At the last analysis, 82% of patients had musculoskeletal involvement, 91% had hematologic involvement, 54% had immunologic involvement, and 26% had neurologic involvement, as measured by pBILAG2004.
Of note, pBILAG2004, which collects more detailed information about organ-related disease activity than do the ACR criteria, demonstrated markedly greater actual organ involvement than indicated by the respective ACR criteria for various organ systems, they said.
The median pBILAG2004 score decreased from 8.5 at baseline to 2 at 12 months’ follow-up, representing a statistically significant improvement, and the systemic lupus erythematosus disease activity index (SLEDAI) score decreased significantly over 12 months from 12 points to 4 points. Although disease activity improved over time, disease damage accrual secondary to JSLE was notable. Even after only 4.5 years of follow-up, 28% of patients demonstrated disease-associated damage at the time of data analysis.
"There is a predominance of neurological disease damage involving 15 patients, of whom 6 have experienced one or more cerebrovascular accidents," Dr. Watson and her associates wrote, noting that severe scarring alopecia occurred in 20 patients and that 7 had renal damage, including 1 child with renal failure.
The investigators also found that steroid use among the cohort was high at 93%, and that 24% required cyclophosphamide – a finding that underlines the burden of disease in pediatric patients and the importance of developing steroid-sparing regimens following robust randomized controlled trials for new interventions in JSLE. "Alternative therapies to relieve the burden of corticosteroids on this population are urgently required," they added.
The UK JSLE cohort is a multidisciplinary, multicenter collaborative network established in 2006 to determine the clinical characteristics of JSLE and to support clinical translational research. Patients include children with symptom onset prior to age 17 years. The median age at diagnosis was 12.6 years, and the median time from symptom onset to diagnosis was 3.2 months.
There were other findings of note from this analysis of cohort data:
–Important gender differences in disease prevalence and characteristics. A sex distribution of 5.6 females to every male (but only 2.7 females to every male among those under age 10 years) "is typical of childhood-onset disease where a female predominance is less striking than in adult-onset disease," the investigators said.
Males in this cohort also were more likely to present at a younger age than females, and they had a greater likelihood of having a discoid rash and a reduced likelihood of having had arthritis.
–A high incidence (38%) of family history of autoimmune disease. This finding, in the context of the generally more severe JSLE phenotype compared with adult SLE, a very early age of onset, short time exposure to potential environmental triggers of lupus, and the relatively high male-to-female sex ratio compared with adult disease, points to "probable genetic factors being important in the pathogenesis of JSLE compared to later-onset disease," Dr. Watson and her associates noted.
–Important ethnic differences in regard to disease incidence. There was a significantly higher standardized incidence among nonwhites than among whites. This finding underscores the need for ensuring availability and provision of specialty care in affected ethnic communities and for recognizing the effects of ethnicity in future interventional trials, they said.
–Diagnosis during the teenage years in about half of the patients in the cohort. This finding of diagnosis during a critical time for adolescent growth, puberty, education, and emotional maturation emphasizes the importance of access to specialty, multidisciplinary, pediatric, and adolescent holistic care for patients with JSLE, the investigators said.
The findings illustrate a similar pattern of predominant clinical manifestations and severe disease phenotype as reported from other JSLE cohorts, and the disease-related damage over a relatively short follow-up period is "likely to have significant long-lasting physical and or psychosocial impact and consequences," the investigators wrote.
"Determining the effect of lupus-associated damage on the developing child requires large, prospective long-term studies, together with improved disease biomarkers, to assess the true physical and psychosocial impact of this condition," Dr. Watson and her associates said.
This study was supported by Lupus UK, private benefactors, and the Alder Hey Children’s Kidney Fund. The investigators had no conflicts of interest to declare.
FROM ARTHRITIS & RHEUMATISM
Major Finding: In the 198 patients from the cohort who fulfilled four or more American College of Rheumatology SLE criteria and who were followed for 4.5 years, disease progression was evident in multiple organ systems. Renal involvement was present in 47% of the patients at baseline and had progressed to 80% at the time of the latest analysis, at which time 82% of patients had musculoskeletal involvement, 91% had hematologic involvement, 54% had immunologic involvement, and 26% had neurologic involvement.
Data Source: The UK JSLE Cohort Study.
Disclosures: This study was supported by Lupus UK, private benefactors, and the Alder Hey Children’s Kidney Fund. The investigators had no conflicts of interest to disclose.
Obesity Prevalence Appears to Be Leveling Off
The prevalence of obesity in the United States appears to have plateaued, according to data from the 2009–2010 National Health and Nutrition Examination Survey (NHANES) conducted by the U.S. Centers for Disease Control and Prevention.
Following dramatic increases in the prevalence of obesity in adults, children, and adolescents in the 1980s and 1990s, as well as changes in the distribution of body mass index, no significant changes were seen in 2009–2010, compared with 2003–2008 figures in adults, and compared with 2007–2008 prevalence rates in children and adolescents.
For example, based on data from the 5,926 men and women with measured weight and height who participated in the 2009–2010 NHANES, the age-adjusted prevalence of obesity was roughly 35% for both men and women, which was not significantly different overall compared with the prevalence from 2003–2008, Katherine M. Flegal, Ph.D., and her colleagues from the National Center for Health Statistics, CDC, Hyattsville, Md., reported.
Despite the lack of change overall, the analysis of adult data did indicate, however, that obesity increased in certain segments of the population. While no significant increase was seen among women overall (age- and race-adjusted annual change in odds ratio from 1999 to 2010, 1.01), statistically significant increases were seen among non-Hispanic black women (OR, 1.03) and Mexican American women (1.03), the investigators noted (JAMA 2012 Jan. 17 [doi:10.1001/jama.2012.39]).
A significant linear trend was also seen in men over the 12-year period (annual change in OR, 1.04).
As for BMI, the age-adjusted mean in both men and women was 28.7, and the trends over time in this study were similar to those seen with obesity, with a significant increase seen in men, but not in women, over the 12 years, the investigators said.
In a separate cross-sectional analysis of data from 4,111 children and adolescents who participated in NHANES, the 2009–2010 obesity prevalence of 9.7% in infants and toddlers up to age 2 years, and 16.9% for those aged 2–19 years, did not differ significantly from the 2007–2008 prevalence, and no difference was seen between males and females in regard to obesity prevalence, Cynthia L. Ogden, Ph.D., and her colleagues, also from the National Center for Health Statistics, CDC, reported in the same issue of JAMA.
A trend analysis over the 12-year study period did indicate, however, that the obesity prevalence among males aged 2–19 years increased significantly between 1999–2000 and 2009–2010 (OR, 1.05) per 2-year survey cycle, and that there was a significant increasing trend for non-Hispanic black males (OR, 1.10). Also, BMI increased significantly in males aged 12 through 19 years (JAMA 2012 Jan. 17 [doi:10.1001/jama.2012.40]).
Investigators for both analyses noted that it is important to keep in mind that BMI is an “imperfect measure of body fat.”
None of the authors indicated having relevant conflicts of interest.
Obesity prevalence plateaued overall, but continued to climb in men.
Source ©okeyphotos/iStockphoto.com
The prevalence of obesity in the United States appears to have plateaued, according to data from the 2009–2010 National Health and Nutrition Examination Survey (NHANES) conducted by the U.S. Centers for Disease Control and Prevention.
Following dramatic increases in the prevalence of obesity in adults, children, and adolescents in the 1980s and 1990s, as well as changes in the distribution of body mass index, no significant changes were seen in 2009–2010, compared with 2003–2008 figures in adults, and compared with 2007–2008 prevalence rates in children and adolescents.
For example, based on data from the 5,926 men and women with measured weight and height who participated in the 2009–2010 NHANES, the age-adjusted prevalence of obesity was roughly 35% for both men and women, which was not significantly different overall compared with the prevalence from 2003–2008, Katherine M. Flegal, Ph.D., and her colleagues from the National Center for Health Statistics, CDC, Hyattsville, Md., reported.
Despite the lack of change overall, the analysis of adult data did indicate, however, that obesity increased in certain segments of the population. While no significant increase was seen among women overall (age- and race-adjusted annual change in odds ratio from 1999 to 2010, 1.01), statistically significant increases were seen among non-Hispanic black women (OR, 1.03) and Mexican American women (1.03), the investigators noted (JAMA 2012 Jan. 17 [doi:10.1001/jama.2012.39]).
A significant linear trend was also seen in men over the 12-year period (annual change in OR, 1.04).
As for BMI, the age-adjusted mean in both men and women was 28.7, and the trends over time in this study were similar to those seen with obesity, with a significant increase seen in men, but not in women, over the 12 years, the investigators said.
In a separate cross-sectional analysis of data from 4,111 children and adolescents who participated in NHANES, the 2009–2010 obesity prevalence of 9.7% in infants and toddlers up to age 2 years, and 16.9% for those aged 2–19 years, did not differ significantly from the 2007–2008 prevalence, and no difference was seen between males and females in regard to obesity prevalence, Cynthia L. Ogden, Ph.D., and her colleagues, also from the National Center for Health Statistics, CDC, reported in the same issue of JAMA.
A trend analysis over the 12-year study period did indicate, however, that the obesity prevalence among males aged 2–19 years increased significantly between 1999–2000 and 2009–2010 (OR, 1.05) per 2-year survey cycle, and that there was a significant increasing trend for non-Hispanic black males (OR, 1.10). Also, BMI increased significantly in males aged 12 through 19 years (JAMA 2012 Jan. 17 [doi:10.1001/jama.2012.40]).
Investigators for both analyses noted that it is important to keep in mind that BMI is an “imperfect measure of body fat.”
None of the authors indicated having relevant conflicts of interest.
Obesity prevalence plateaued overall, but continued to climb in men.
Source ©okeyphotos/iStockphoto.com
The prevalence of obesity in the United States appears to have plateaued, according to data from the 2009–2010 National Health and Nutrition Examination Survey (NHANES) conducted by the U.S. Centers for Disease Control and Prevention.
Following dramatic increases in the prevalence of obesity in adults, children, and adolescents in the 1980s and 1990s, as well as changes in the distribution of body mass index, no significant changes were seen in 2009–2010, compared with 2003–2008 figures in adults, and compared with 2007–2008 prevalence rates in children and adolescents.
For example, based on data from the 5,926 men and women with measured weight and height who participated in the 2009–2010 NHANES, the age-adjusted prevalence of obesity was roughly 35% for both men and women, which was not significantly different overall compared with the prevalence from 2003–2008, Katherine M. Flegal, Ph.D., and her colleagues from the National Center for Health Statistics, CDC, Hyattsville, Md., reported.
Despite the lack of change overall, the analysis of adult data did indicate, however, that obesity increased in certain segments of the population. While no significant increase was seen among women overall (age- and race-adjusted annual change in odds ratio from 1999 to 2010, 1.01), statistically significant increases were seen among non-Hispanic black women (OR, 1.03) and Mexican American women (1.03), the investigators noted (JAMA 2012 Jan. 17 [doi:10.1001/jama.2012.39]).
A significant linear trend was also seen in men over the 12-year period (annual change in OR, 1.04).
As for BMI, the age-adjusted mean in both men and women was 28.7, and the trends over time in this study were similar to those seen with obesity, with a significant increase seen in men, but not in women, over the 12 years, the investigators said.
In a separate cross-sectional analysis of data from 4,111 children and adolescents who participated in NHANES, the 2009–2010 obesity prevalence of 9.7% in infants and toddlers up to age 2 years, and 16.9% for those aged 2–19 years, did not differ significantly from the 2007–2008 prevalence, and no difference was seen between males and females in regard to obesity prevalence, Cynthia L. Ogden, Ph.D., and her colleagues, also from the National Center for Health Statistics, CDC, reported in the same issue of JAMA.
A trend analysis over the 12-year study period did indicate, however, that the obesity prevalence among males aged 2–19 years increased significantly between 1999–2000 and 2009–2010 (OR, 1.05) per 2-year survey cycle, and that there was a significant increasing trend for non-Hispanic black males (OR, 1.10). Also, BMI increased significantly in males aged 12 through 19 years (JAMA 2012 Jan. 17 [doi:10.1001/jama.2012.40]).
Investigators for both analyses noted that it is important to keep in mind that BMI is an “imperfect measure of body fat.”
None of the authors indicated having relevant conflicts of interest.
Obesity prevalence plateaued overall, but continued to climb in men.
Source ©okeyphotos/iStockphoto.com
From JAMA