User login
Sharon Worcester is an award-winning medical journalist for MDedge News. She has been with the company since 1996, first as the Southeast Bureau Chief (1996-2009) when the company was known as International Medical News Group, then as a freelance writer (2010-2015) before returning as a reporter in 2015. She previously worked as a daily newspaper reporter covering health and local government. Sharon currently reports primarily on oncology and hematology. She has a BA from Eckerd College and an MA in Mass Communication/Print Journalism from the University of Florida. Connect with her via LinkedIn and follow her on twitter @SW_MedReporter.
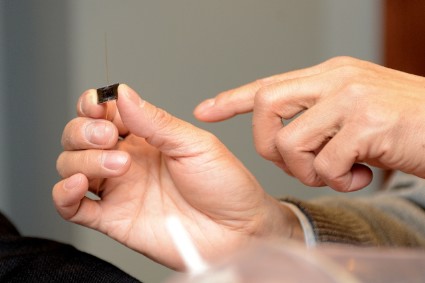
Breath test could improve lung cancer screening
ORLANDO – The presence of certain carbonyl volatile organic compounds in exhaled breath can aid in the detection of early lung cancer, according to Dr. Michael Bousamra.
An analysis of volatile organic compounds (VOCs) in the exhaled breath of 10 lung cancer patients and 88 controls, including 45 who were smokers and 43 who were nonsmokers, identified four carbonyl VOCs that occurred significantly more often in the lung cancer patients’ breath samples than in the control samples: 2-butanone, 3-hydroxy-2-butanone, hydroxylacetaldehyde, and 4-hydroxyhexenal.
Further study of 151 patients with suspicious lung nodules found no single VOC marker that was independently predictive of lung cancer, but when the levels of three or more were elevated in a single patient, the sensitivity and specificity for lung cancer were 60% and 95.2%, respectively. When the levels of at least two of the VOCs were elevated, the sensitivity and specificity were 84.7% and 81%, respectively, and when at least one was elevated, the sensitivity and specificity were 93.8% and 45.2%, respectively.
The absence of VOC elevation was predictive of benign disease in 80% of cases, Dr. Bousamra of the University of Louisville, Ky., reported at the annual meeting of the Society of Thoracic Surgeons.
Notably, the concentrations of three of four VOCs in samples from lung cancer patients decreased to the level found in healthy controls after resection, he explained.
This finding "lends credence to the notion that these carbonyl markers really aren’t indicators of something other than cancer," Dr. Bousamra said.
Of the 151 patients in the study, 109 were diagnosed with lung cancer and 42 with benign nodules. Of those who had lung cancer, 1 had stage 0 disease, 47 had stage I, 18 had stage II, 26 had stage III, and 17 had stage IV.
The exhaled breath samples were collected using a 1-L Tedlar bag and were analyzed by investigators who were blinded to the preoperative diagnosis and pathology, he said.
The findings suggest that these specific VOCs in exhaled breath could be used as an adjunct to computed tomography (CT) for the diagnosis of early lung cancer. In this study, the VOCs were also useful for distinguishing benign from malignant nodules, Dr. Bousamra noted at the meeting.
"When three or four carbonyl markers were elevated, the probability of cancer was very high; when no carbonyl markers – or even one – was elevated, associated pulmonary disease was likely benign. I think that clinical decision making could be assisted in these instances," he said.
Carbonyl VOC testing, however, is not quite ready for prime time, he noted.
Exhaled breath has long been considered a promising noninvasive tool for the diagnosis of early lung cancer, but the studies conducted to date have failed to achieve clinical significance because of a lack of specificity and challenges associated with complex volatile mixtures.
Although the findings of the current study advance the possibility of using exhaled breath in lung cancer diagnosis and clinical decision making, the study was limited by an inadequate control group. In addition, further study is needed in patients who have pulmonary nodules and benign pulmonary disease, as well as in patients following resection, Dr. Bousamra said.
The study also lacked a specific look at patients with chronic obstructive pulmonary disease and other interstitial lung disease common in patients with lung cancer, he noted.
He estimated, however, that VOC testing could be in place to help with the diagnosis of lung cancer within 2 years.
The possibilities for this type of testing are exciting, and the work of Dr. Bousamra and his colleagues represents a window into the future of lung cancer screening and diagnosis, according to the invited discussant, Dr. Tom Varghese Jr., who is with the University of Washington in Seattle.
Lung cancer is the leading cause of cancer deaths worldwide, with higher mortality than the next three leading causes of cancer death combined, Dr. Varghese said.
A large screening trial showed that using low-dose CT for screening could reduce mortality by 20% – a finding that led to the recent endorsement by the U.S. Preventive Services Task Force of low-dose screening CTs for patients who are at high risk.
Such a screening program, if it were applied using strict criteria, "would avert 12,000 lung cancer deaths today," he asserted.
Adding measurement of VOCs in exhaled breath to the screening protocol could result in fewer invasive procedures for abnormal screening results, and VOC measurement could thus prove to be a simple, straight-forward cost-saving measure, Dr. Varghese added.
Dr. Eric Gartman, FCCP, comments: Current lung cancer screening recommendations remain quite controversial, and no matter one’s stance on the data, it would have to be agreed upon that further guidance on the appropriate screening population and further reduction in CT false positives are needed. In the near future, biomarker and exhaled breath phenotypes will dramatically change our screening for lung cancer and lead to earlier diagnoses.
ORLANDO – The presence of certain carbonyl volatile organic compounds in exhaled breath can aid in the detection of early lung cancer, according to Dr. Michael Bousamra.
An analysis of volatile organic compounds (VOCs) in the exhaled breath of 10 lung cancer patients and 88 controls, including 45 who were smokers and 43 who were nonsmokers, identified four carbonyl VOCs that occurred significantly more often in the lung cancer patients’ breath samples than in the control samples: 2-butanone, 3-hydroxy-2-butanone, hydroxylacetaldehyde, and 4-hydroxyhexenal.
Further study of 151 patients with suspicious lung nodules found no single VOC marker that was independently predictive of lung cancer, but when the levels of three or more were elevated in a single patient, the sensitivity and specificity for lung cancer were 60% and 95.2%, respectively. When the levels of at least two of the VOCs were elevated, the sensitivity and specificity were 84.7% and 81%, respectively, and when at least one was elevated, the sensitivity and specificity were 93.8% and 45.2%, respectively.
The absence of VOC elevation was predictive of benign disease in 80% of cases, Dr. Bousamra of the University of Louisville, Ky., reported at the annual meeting of the Society of Thoracic Surgeons.
Notably, the concentrations of three of four VOCs in samples from lung cancer patients decreased to the level found in healthy controls after resection, he explained.
This finding "lends credence to the notion that these carbonyl markers really aren’t indicators of something other than cancer," Dr. Bousamra said.
Of the 151 patients in the study, 109 were diagnosed with lung cancer and 42 with benign nodules. Of those who had lung cancer, 1 had stage 0 disease, 47 had stage I, 18 had stage II, 26 had stage III, and 17 had stage IV.
The exhaled breath samples were collected using a 1-L Tedlar bag and were analyzed by investigators who were blinded to the preoperative diagnosis and pathology, he said.
The findings suggest that these specific VOCs in exhaled breath could be used as an adjunct to computed tomography (CT) for the diagnosis of early lung cancer. In this study, the VOCs were also useful for distinguishing benign from malignant nodules, Dr. Bousamra noted at the meeting.
"When three or four carbonyl markers were elevated, the probability of cancer was very high; when no carbonyl markers – or even one – was elevated, associated pulmonary disease was likely benign. I think that clinical decision making could be assisted in these instances," he said.
Carbonyl VOC testing, however, is not quite ready for prime time, he noted.
Exhaled breath has long been considered a promising noninvasive tool for the diagnosis of early lung cancer, but the studies conducted to date have failed to achieve clinical significance because of a lack of specificity and challenges associated with complex volatile mixtures.
Although the findings of the current study advance the possibility of using exhaled breath in lung cancer diagnosis and clinical decision making, the study was limited by an inadequate control group. In addition, further study is needed in patients who have pulmonary nodules and benign pulmonary disease, as well as in patients following resection, Dr. Bousamra said.
The study also lacked a specific look at patients with chronic obstructive pulmonary disease and other interstitial lung disease common in patients with lung cancer, he noted.
He estimated, however, that VOC testing could be in place to help with the diagnosis of lung cancer within 2 years.
The possibilities for this type of testing are exciting, and the work of Dr. Bousamra and his colleagues represents a window into the future of lung cancer screening and diagnosis, according to the invited discussant, Dr. Tom Varghese Jr., who is with the University of Washington in Seattle.
Lung cancer is the leading cause of cancer deaths worldwide, with higher mortality than the next three leading causes of cancer death combined, Dr. Varghese said.
A large screening trial showed that using low-dose CT for screening could reduce mortality by 20% – a finding that led to the recent endorsement by the U.S. Preventive Services Task Force of low-dose screening CTs for patients who are at high risk.
Such a screening program, if it were applied using strict criteria, "would avert 12,000 lung cancer deaths today," he asserted.
Adding measurement of VOCs in exhaled breath to the screening protocol could result in fewer invasive procedures for abnormal screening results, and VOC measurement could thus prove to be a simple, straight-forward cost-saving measure, Dr. Varghese added.
Dr. Eric Gartman, FCCP, comments: Current lung cancer screening recommendations remain quite controversial, and no matter one’s stance on the data, it would have to be agreed upon that further guidance on the appropriate screening population and further reduction in CT false positives are needed. In the near future, biomarker and exhaled breath phenotypes will dramatically change our screening for lung cancer and lead to earlier diagnoses.
ORLANDO – The presence of certain carbonyl volatile organic compounds in exhaled breath can aid in the detection of early lung cancer, according to Dr. Michael Bousamra.
An analysis of volatile organic compounds (VOCs) in the exhaled breath of 10 lung cancer patients and 88 controls, including 45 who were smokers and 43 who were nonsmokers, identified four carbonyl VOCs that occurred significantly more often in the lung cancer patients’ breath samples than in the control samples: 2-butanone, 3-hydroxy-2-butanone, hydroxylacetaldehyde, and 4-hydroxyhexenal.
Further study of 151 patients with suspicious lung nodules found no single VOC marker that was independently predictive of lung cancer, but when the levels of three or more were elevated in a single patient, the sensitivity and specificity for lung cancer were 60% and 95.2%, respectively. When the levels of at least two of the VOCs were elevated, the sensitivity and specificity were 84.7% and 81%, respectively, and when at least one was elevated, the sensitivity and specificity were 93.8% and 45.2%, respectively.
The absence of VOC elevation was predictive of benign disease in 80% of cases, Dr. Bousamra of the University of Louisville, Ky., reported at the annual meeting of the Society of Thoracic Surgeons.
Notably, the concentrations of three of four VOCs in samples from lung cancer patients decreased to the level found in healthy controls after resection, he explained.
This finding "lends credence to the notion that these carbonyl markers really aren’t indicators of something other than cancer," Dr. Bousamra said.
Of the 151 patients in the study, 109 were diagnosed with lung cancer and 42 with benign nodules. Of those who had lung cancer, 1 had stage 0 disease, 47 had stage I, 18 had stage II, 26 had stage III, and 17 had stage IV.
The exhaled breath samples were collected using a 1-L Tedlar bag and were analyzed by investigators who were blinded to the preoperative diagnosis and pathology, he said.
The findings suggest that these specific VOCs in exhaled breath could be used as an adjunct to computed tomography (CT) for the diagnosis of early lung cancer. In this study, the VOCs were also useful for distinguishing benign from malignant nodules, Dr. Bousamra noted at the meeting.
"When three or four carbonyl markers were elevated, the probability of cancer was very high; when no carbonyl markers – or even one – was elevated, associated pulmonary disease was likely benign. I think that clinical decision making could be assisted in these instances," he said.
Carbonyl VOC testing, however, is not quite ready for prime time, he noted.
Exhaled breath has long been considered a promising noninvasive tool for the diagnosis of early lung cancer, but the studies conducted to date have failed to achieve clinical significance because of a lack of specificity and challenges associated with complex volatile mixtures.
Although the findings of the current study advance the possibility of using exhaled breath in lung cancer diagnosis and clinical decision making, the study was limited by an inadequate control group. In addition, further study is needed in patients who have pulmonary nodules and benign pulmonary disease, as well as in patients following resection, Dr. Bousamra said.
The study also lacked a specific look at patients with chronic obstructive pulmonary disease and other interstitial lung disease common in patients with lung cancer, he noted.
He estimated, however, that VOC testing could be in place to help with the diagnosis of lung cancer within 2 years.
The possibilities for this type of testing are exciting, and the work of Dr. Bousamra and his colleagues represents a window into the future of lung cancer screening and diagnosis, according to the invited discussant, Dr. Tom Varghese Jr., who is with the University of Washington in Seattle.
Lung cancer is the leading cause of cancer deaths worldwide, with higher mortality than the next three leading causes of cancer death combined, Dr. Varghese said.
A large screening trial showed that using low-dose CT for screening could reduce mortality by 20% – a finding that led to the recent endorsement by the U.S. Preventive Services Task Force of low-dose screening CTs for patients who are at high risk.
Such a screening program, if it were applied using strict criteria, "would avert 12,000 lung cancer deaths today," he asserted.
Adding measurement of VOCs in exhaled breath to the screening protocol could result in fewer invasive procedures for abnormal screening results, and VOC measurement could thus prove to be a simple, straight-forward cost-saving measure, Dr. Varghese added.
Dr. Eric Gartman, FCCP, comments: Current lung cancer screening recommendations remain quite controversial, and no matter one’s stance on the data, it would have to be agreed upon that further guidance on the appropriate screening population and further reduction in CT false positives are needed. In the near future, biomarker and exhaled breath phenotypes will dramatically change our screening for lung cancer and lead to earlier diagnoses.
Major finding: Finding three or more specific carbonyl VOCs in exhaled breath was 95% predictive of lung cancer, while no elevation was 80% predictive of benign nodules.
Data source: An analysis of VOCs in the exhaled breath of 151 patients with suspicious lung lesions.
Disclosures: Dr. Bousamra reported having no disclosures.
Trailblazer in psychiatry shares lessons
SAN ANTONIO – Dr. Carolyn B. Robinowitz knows a thing or two about creativity in leadership.
As one of very few female medical students at Washington University School of Medicine in St. Louis in the 1960s (women comprised only 8% of her graduating class), Dr. Robinowitz learned quickly that it would take a creative approach to successfully navigate a career in what was then the male-dominated world of medicine.
She became the first female psychiatrist elected to the American Board of Psychiatry and Neurology and the first female president of that organization, the first woman to serve as president of the Council of Medical Specialty Societies, and the first female psychiatrist to be named dean of a U.S. medical school (at Georgetown University School of Medicine) – just to name a few of her accomplishments. Dr. Robinowitz also holds the mantle as the 134th president of the American Psychiatric Association.
During a session on creativity in leadership at the annual meeting of the American College of Psychiatrists, she shared a bit about her experiences, including a not-so-traditional (at the time) dual medical career marriage, and a rather traditional habit of moving to where there was work – for her husband. She talked about the creative ways she made those moves work in her favor and how she found ways to fit in with her male colleagues – and to make a name for herself in medicine.
After a move to Miami, for example, she had to work hard to gain the respect of her colleagues, and in addition to making sure to demonstrate her medical expertise, she also became an expert on something else of great importance there that helped her to be part of the conversation: the Miami Dolphins.
An important lesson she learned – which is something that is true with patients, as well – is that to work with people, you have to be where they are, she said.
She quickly moved up the career ladder.
Along the way she encountered covert – and sometime overt – gender bias and cultural expectations that conflicted with her goals, she said, adding that women have come a long way since then.
When she first began her work as dean at Georgetown, women comprised 32% of medical students. When she left the position 6 years later, that figure had risen to 47%.
"A lot of that was what was going on nationally," she said.
But she did work to play a part – in her own way – in making a difference.
"Just being visible" was something she found to be important. When young women visited for admissions committee interviews, she would make it a point to be visible, even if just to walk past.
"The person with the applicants would say, ‘Oh, that’s our dean,’ " she explained, noting that she felt her presence provided encouragement to those young women, and reinforced the fact that women could – and did –have a place at the head of the table.
Dr. Robinowitz said that during the times when women were such a small minority in leadership roles, there was a sense that the problem would "fix itself when the pipeline got more full," and that female physicians just needed to act more like male physicians if they wanted to succeed.
Research – and her own personal experience – show that is not the case; women and men sometimes have very different styles of leadership.
For example, men might tend to be results oriented, while women tend to be more concerned with the process.
In the past decade, a great deal of research from the fields of neuroscience, psychology, and business has looked at the behaviors of men and women in the workplace; some of that research shows that many of the attributes of women leaders are more conducive to success, she noted.
One survey of CEOs, for example, showed that women are particularly adept at skills such as team building and participatory decision making – important for working successfully with the "new millennial workforce" – and that women are equally as effective as are men when it comes to efficient communication and intellectual stimulation.
"We also know that there is different communication – that women tend to have ‘rapport’ communication (building relationships), while male communication is more ‘report’ communication. We also know that men are more unilaterally focused, more results focused, and less concerned with how to get there," she said.
Regardless of gender-based differences in leadership style (and there are many exceptions when it comes to these generalities), there are certain individual strategies that all leaders, male or female, should keep in mind to attain success and happiness in the work environment, Dr. Robinowitz said.
First, it is important realize that it’s not all about being number one, Dr. Robinowitz said.
Sometimes there is more fulfillment – more of an ability to make a difference – at a different level.
Her other take-home messages are as follows:
• Don’t underestimate your skills, the transferability of your experience, or how you can benefit from continuing professional development (formal or informal).
• Find a mentor, and be a mentor – and remember mentoring is not about age (a person can mentor someone older), it’s about mutual interest and the ability to communicate effectively.
• Work hard.
• Don’t be afraid to speak up.
• Don’t be afraid to be wrong – that’s where learning occurs.
• Have fun; organizational work (with specialty groups such as the American College of Psychiatrists) is different from clinical work and has important value – and it can be fun and fulfilling.
• Lead; don’t treat. As a psychiatrist in a leadership position, it can be tempting to treat, but your coworkers are not your patients," she said.
• Know the 10% rule – 10% of the people do 90% of the work, but don’t discount the other 90% as they have something to contribute, and should be encouraged to do so.
• Give positive reinforcement.
• Know that money has limitations; people really want to be seen as successful and to be part of a successful mission.
• Understand that a win-win approach involving compromise is valuable.
• Recognize your limits and support fresh ideas, energy, resources, and new leaders.
Most importantly, according to Dr. Robinowitz: Enjoy yourself.
Dr. Robinowitz reported having no disclosures.
SAN ANTONIO – Dr. Carolyn B. Robinowitz knows a thing or two about creativity in leadership.
As one of very few female medical students at Washington University School of Medicine in St. Louis in the 1960s (women comprised only 8% of her graduating class), Dr. Robinowitz learned quickly that it would take a creative approach to successfully navigate a career in what was then the male-dominated world of medicine.
She became the first female psychiatrist elected to the American Board of Psychiatry and Neurology and the first female president of that organization, the first woman to serve as president of the Council of Medical Specialty Societies, and the first female psychiatrist to be named dean of a U.S. medical school (at Georgetown University School of Medicine) – just to name a few of her accomplishments. Dr. Robinowitz also holds the mantle as the 134th president of the American Psychiatric Association.
During a session on creativity in leadership at the annual meeting of the American College of Psychiatrists, she shared a bit about her experiences, including a not-so-traditional (at the time) dual medical career marriage, and a rather traditional habit of moving to where there was work – for her husband. She talked about the creative ways she made those moves work in her favor and how she found ways to fit in with her male colleagues – and to make a name for herself in medicine.
After a move to Miami, for example, she had to work hard to gain the respect of her colleagues, and in addition to making sure to demonstrate her medical expertise, she also became an expert on something else of great importance there that helped her to be part of the conversation: the Miami Dolphins.
An important lesson she learned – which is something that is true with patients, as well – is that to work with people, you have to be where they are, she said.
She quickly moved up the career ladder.
Along the way she encountered covert – and sometime overt – gender bias and cultural expectations that conflicted with her goals, she said, adding that women have come a long way since then.
When she first began her work as dean at Georgetown, women comprised 32% of medical students. When she left the position 6 years later, that figure had risen to 47%.
"A lot of that was what was going on nationally," she said.
But she did work to play a part – in her own way – in making a difference.
"Just being visible" was something she found to be important. When young women visited for admissions committee interviews, she would make it a point to be visible, even if just to walk past.
"The person with the applicants would say, ‘Oh, that’s our dean,’ " she explained, noting that she felt her presence provided encouragement to those young women, and reinforced the fact that women could – and did –have a place at the head of the table.
Dr. Robinowitz said that during the times when women were such a small minority in leadership roles, there was a sense that the problem would "fix itself when the pipeline got more full," and that female physicians just needed to act more like male physicians if they wanted to succeed.
Research – and her own personal experience – show that is not the case; women and men sometimes have very different styles of leadership.
For example, men might tend to be results oriented, while women tend to be more concerned with the process.
In the past decade, a great deal of research from the fields of neuroscience, psychology, and business has looked at the behaviors of men and women in the workplace; some of that research shows that many of the attributes of women leaders are more conducive to success, she noted.
One survey of CEOs, for example, showed that women are particularly adept at skills such as team building and participatory decision making – important for working successfully with the "new millennial workforce" – and that women are equally as effective as are men when it comes to efficient communication and intellectual stimulation.
"We also know that there is different communication – that women tend to have ‘rapport’ communication (building relationships), while male communication is more ‘report’ communication. We also know that men are more unilaterally focused, more results focused, and less concerned with how to get there," she said.
Regardless of gender-based differences in leadership style (and there are many exceptions when it comes to these generalities), there are certain individual strategies that all leaders, male or female, should keep in mind to attain success and happiness in the work environment, Dr. Robinowitz said.
First, it is important realize that it’s not all about being number one, Dr. Robinowitz said.
Sometimes there is more fulfillment – more of an ability to make a difference – at a different level.
Her other take-home messages are as follows:
• Don’t underestimate your skills, the transferability of your experience, or how you can benefit from continuing professional development (formal or informal).
• Find a mentor, and be a mentor – and remember mentoring is not about age (a person can mentor someone older), it’s about mutual interest and the ability to communicate effectively.
• Work hard.
• Don’t be afraid to speak up.
• Don’t be afraid to be wrong – that’s where learning occurs.
• Have fun; organizational work (with specialty groups such as the American College of Psychiatrists) is different from clinical work and has important value – and it can be fun and fulfilling.
• Lead; don’t treat. As a psychiatrist in a leadership position, it can be tempting to treat, but your coworkers are not your patients," she said.
• Know the 10% rule – 10% of the people do 90% of the work, but don’t discount the other 90% as they have something to contribute, and should be encouraged to do so.
• Give positive reinforcement.
• Know that money has limitations; people really want to be seen as successful and to be part of a successful mission.
• Understand that a win-win approach involving compromise is valuable.
• Recognize your limits and support fresh ideas, energy, resources, and new leaders.
Most importantly, according to Dr. Robinowitz: Enjoy yourself.
Dr. Robinowitz reported having no disclosures.
SAN ANTONIO – Dr. Carolyn B. Robinowitz knows a thing or two about creativity in leadership.
As one of very few female medical students at Washington University School of Medicine in St. Louis in the 1960s (women comprised only 8% of her graduating class), Dr. Robinowitz learned quickly that it would take a creative approach to successfully navigate a career in what was then the male-dominated world of medicine.
She became the first female psychiatrist elected to the American Board of Psychiatry and Neurology and the first female president of that organization, the first woman to serve as president of the Council of Medical Specialty Societies, and the first female psychiatrist to be named dean of a U.S. medical school (at Georgetown University School of Medicine) – just to name a few of her accomplishments. Dr. Robinowitz also holds the mantle as the 134th president of the American Psychiatric Association.
During a session on creativity in leadership at the annual meeting of the American College of Psychiatrists, she shared a bit about her experiences, including a not-so-traditional (at the time) dual medical career marriage, and a rather traditional habit of moving to where there was work – for her husband. She talked about the creative ways she made those moves work in her favor and how she found ways to fit in with her male colleagues – and to make a name for herself in medicine.
After a move to Miami, for example, she had to work hard to gain the respect of her colleagues, and in addition to making sure to demonstrate her medical expertise, she also became an expert on something else of great importance there that helped her to be part of the conversation: the Miami Dolphins.
An important lesson she learned – which is something that is true with patients, as well – is that to work with people, you have to be where they are, she said.
She quickly moved up the career ladder.
Along the way she encountered covert – and sometime overt – gender bias and cultural expectations that conflicted with her goals, she said, adding that women have come a long way since then.
When she first began her work as dean at Georgetown, women comprised 32% of medical students. When she left the position 6 years later, that figure had risen to 47%.
"A lot of that was what was going on nationally," she said.
But she did work to play a part – in her own way – in making a difference.
"Just being visible" was something she found to be important. When young women visited for admissions committee interviews, she would make it a point to be visible, even if just to walk past.
"The person with the applicants would say, ‘Oh, that’s our dean,’ " she explained, noting that she felt her presence provided encouragement to those young women, and reinforced the fact that women could – and did –have a place at the head of the table.
Dr. Robinowitz said that during the times when women were such a small minority in leadership roles, there was a sense that the problem would "fix itself when the pipeline got more full," and that female physicians just needed to act more like male physicians if they wanted to succeed.
Research – and her own personal experience – show that is not the case; women and men sometimes have very different styles of leadership.
For example, men might tend to be results oriented, while women tend to be more concerned with the process.
In the past decade, a great deal of research from the fields of neuroscience, psychology, and business has looked at the behaviors of men and women in the workplace; some of that research shows that many of the attributes of women leaders are more conducive to success, she noted.
One survey of CEOs, for example, showed that women are particularly adept at skills such as team building and participatory decision making – important for working successfully with the "new millennial workforce" – and that women are equally as effective as are men when it comes to efficient communication and intellectual stimulation.
"We also know that there is different communication – that women tend to have ‘rapport’ communication (building relationships), while male communication is more ‘report’ communication. We also know that men are more unilaterally focused, more results focused, and less concerned with how to get there," she said.
Regardless of gender-based differences in leadership style (and there are many exceptions when it comes to these generalities), there are certain individual strategies that all leaders, male or female, should keep in mind to attain success and happiness in the work environment, Dr. Robinowitz said.
First, it is important realize that it’s not all about being number one, Dr. Robinowitz said.
Sometimes there is more fulfillment – more of an ability to make a difference – at a different level.
Her other take-home messages are as follows:
• Don’t underestimate your skills, the transferability of your experience, or how you can benefit from continuing professional development (formal or informal).
• Find a mentor, and be a mentor – and remember mentoring is not about age (a person can mentor someone older), it’s about mutual interest and the ability to communicate effectively.
• Work hard.
• Don’t be afraid to speak up.
• Don’t be afraid to be wrong – that’s where learning occurs.
• Have fun; organizational work (with specialty groups such as the American College of Psychiatrists) is different from clinical work and has important value – and it can be fun and fulfilling.
• Lead; don’t treat. As a psychiatrist in a leadership position, it can be tempting to treat, but your coworkers are not your patients," she said.
• Know the 10% rule – 10% of the people do 90% of the work, but don’t discount the other 90% as they have something to contribute, and should be encouraged to do so.
• Give positive reinforcement.
• Know that money has limitations; people really want to be seen as successful and to be part of a successful mission.
• Understand that a win-win approach involving compromise is valuable.
• Recognize your limits and support fresh ideas, energy, resources, and new leaders.
Most importantly, according to Dr. Robinowitz: Enjoy yourself.
Dr. Robinowitz reported having no disclosures.
AT THE AMERICAN COLLEGE OF PSYCHIATRISTS MEETING
The future of psychiatry may depend on integrated care
SAN ANTONIO – Questions about how health care reform will affect the practice of medicine are nothing new, but there is particular uncertainty for the field of psychiatry, according to the president-elect of the American Psychiatric Association.
One reason for the uncertainty is that payment streams for psychiatric and substance use care are distinctive and poorly understood, and the scope of the relative sectors – including public, commercial, state, and self-pay – are unique in the field of psychiatry, Dr. Paul Summergrad explained at the annual meeting of the American College of Psychiatrists.
According to a 2011 article in the New England Journal of Medicine, the greatest percentages of U.S. medical spending overall were from "private insurance" and "Medicare, out-of-pocket, and other private spending" (37% and 35%, respectively), but for mental health, Medicaid spending exceeded both of these (28% vs. 27% and 22%, respectively), and "other state and local spending" was also higher (18% vs. 6% for medicine overall).
For substance abuse, other state and local spending dominated at 36%, followed by Medicaid spending at 21% (N. Engl. J. Med. 2011;365:973-5).
"If you look at the total dollars that come into our world, they look different from the outset than they do for anyone else in medicine," Dr. Summergrad said, noting that patients with substance abuse, for example, fall mainly outside of the commercial insurance system.
Also, within Medicaid – the largest payer, the percentage spent on mental health services is about three times higher than for commercial insurance.
The impact of the Affordable Care Act through mandated parity rules for coverage of mental health and substance abuse services could provide for tremendous expansion of services within the insurance realm, he said.
Another reason for the uncertainty is a lack of understanding about the substantial extent and effects of medical and psychiatric comorbidities on the total cost of medical care, and the fact that most ambulatory psychiatric care is provided by physicians other than psychiatrists, said Dr. Summergrad, Dr. Frances S. Arkin Professor and chairman of psychiatry at Tufts Medical Center in Boston.
"This is both a challenge and an opportunity; it’s an opportunity to really improve the care of the patients, and not just individuals who have severe psychiatric illness," he said, noting that those improvements could come not only in terms of the quality of care, but in terms of the cost effectiveness of care – a factor that could benefit both patients and the care system, including psychiatrists.
"The care of our patients is deeply embedded in the general health care system, so for us, the payer environment is problematic, and we know that payment differentials have been deeply discriminatory. It’s part of the reason why, along with intrusive utilization review, many psychiatrists don’t take insurance," he said.
The impact of fourth-party carve-out models on both payment and models of care have had a very problematic impact on both the public and commercial sector – in particular because they don’t take into account the extent of medical-psychiatric comorbidity, he added, noting that "the impact of this commoditization really depends in large measure on stigma associated with mental health and substance abuse care."
Many patients in need can’t get adequate care, and the stigma associated with mental illness keeps them from addressing the problems with insurers or benefits managers.
"The insurance industry has relied, in my view, on that stigma to allow [psychiatric] care to be marginalized," he said.
However, studies consistently show that patients with mental illness and substance abuse issues have higher rates of medical comorbidities, and that patients with chronic medical conditions have higher rates of mental health issues. These interactions result in poorer outcomes and higher costs.
In many studies, the costs associated with treating patients with a psychiatric and/or substance use disorder are two to three times greater when accounting for a patient’s total medical costs, compared with the costs for patients without a behavioral condition, Dr. Summergrad said.
One way that health care reform can benefit patients and potentially psychiatry is through medical and psychiatric care integration. One collaborative team approach involves a behavioral health or chronic disease care manager in a primary care office working with a consulting psychiatrist. In a multisite randomized trial (the Improving Mood: Promoting Access to Collaborative Treatment, or IMPACT study) involving more than 1,800 patients, this collaborative care approach was associated with a 50% or greater reduction in depressive symptoms in 45% of intervention patients, compared with only 19% of usual care patients (Am. J. Manag. Care 2008;14:95-100).
The approach also was associated with decreased costs over a period of 4 years.
Barriers to adoption of such integrated care models include a shrinking proportion of psychiatrists compared with the growing mental health workforce; financing (the disconnected medical and psychiatric payment systems for psychiatrists and other specialists); the fact that electronic medical records systems are not well established in psychiatry, which raises operational and confidentiality issues; and the discrimination against psychiatric care in many insurance plans.
"We need to have systems that are much more granular, but the reality is that the data that drive payment systems, and the data that are going to be associated with quality metrics for both individual physicians and systems as a whole, will come out of these systems. If we remain on the outside of them, it will marginalize and put the patients we care for at serious risk," Dr. Summergrad said.
Overcoming the barriers will require research regarding medically comorbid illness and models of care. In addition, increased training and education for all physicians, including those currently in practice and those in training, and electronic medical records that are well adapted for psychiatric practice are needed, he said.
Dr. Summergrad reported having done nonpromotional speaking for CME Outfitters.
SAN ANTONIO – Questions about how health care reform will affect the practice of medicine are nothing new, but there is particular uncertainty for the field of psychiatry, according to the president-elect of the American Psychiatric Association.
One reason for the uncertainty is that payment streams for psychiatric and substance use care are distinctive and poorly understood, and the scope of the relative sectors – including public, commercial, state, and self-pay – are unique in the field of psychiatry, Dr. Paul Summergrad explained at the annual meeting of the American College of Psychiatrists.
According to a 2011 article in the New England Journal of Medicine, the greatest percentages of U.S. medical spending overall were from "private insurance" and "Medicare, out-of-pocket, and other private spending" (37% and 35%, respectively), but for mental health, Medicaid spending exceeded both of these (28% vs. 27% and 22%, respectively), and "other state and local spending" was also higher (18% vs. 6% for medicine overall).
For substance abuse, other state and local spending dominated at 36%, followed by Medicaid spending at 21% (N. Engl. J. Med. 2011;365:973-5).
"If you look at the total dollars that come into our world, they look different from the outset than they do for anyone else in medicine," Dr. Summergrad said, noting that patients with substance abuse, for example, fall mainly outside of the commercial insurance system.
Also, within Medicaid – the largest payer, the percentage spent on mental health services is about three times higher than for commercial insurance.
The impact of the Affordable Care Act through mandated parity rules for coverage of mental health and substance abuse services could provide for tremendous expansion of services within the insurance realm, he said.
Another reason for the uncertainty is a lack of understanding about the substantial extent and effects of medical and psychiatric comorbidities on the total cost of medical care, and the fact that most ambulatory psychiatric care is provided by physicians other than psychiatrists, said Dr. Summergrad, Dr. Frances S. Arkin Professor and chairman of psychiatry at Tufts Medical Center in Boston.
"This is both a challenge and an opportunity; it’s an opportunity to really improve the care of the patients, and not just individuals who have severe psychiatric illness," he said, noting that those improvements could come not only in terms of the quality of care, but in terms of the cost effectiveness of care – a factor that could benefit both patients and the care system, including psychiatrists.
"The care of our patients is deeply embedded in the general health care system, so for us, the payer environment is problematic, and we know that payment differentials have been deeply discriminatory. It’s part of the reason why, along with intrusive utilization review, many psychiatrists don’t take insurance," he said.
The impact of fourth-party carve-out models on both payment and models of care have had a very problematic impact on both the public and commercial sector – in particular because they don’t take into account the extent of medical-psychiatric comorbidity, he added, noting that "the impact of this commoditization really depends in large measure on stigma associated with mental health and substance abuse care."
Many patients in need can’t get adequate care, and the stigma associated with mental illness keeps them from addressing the problems with insurers or benefits managers.
"The insurance industry has relied, in my view, on that stigma to allow [psychiatric] care to be marginalized," he said.
However, studies consistently show that patients with mental illness and substance abuse issues have higher rates of medical comorbidities, and that patients with chronic medical conditions have higher rates of mental health issues. These interactions result in poorer outcomes and higher costs.
In many studies, the costs associated with treating patients with a psychiatric and/or substance use disorder are two to three times greater when accounting for a patient’s total medical costs, compared with the costs for patients without a behavioral condition, Dr. Summergrad said.
One way that health care reform can benefit patients and potentially psychiatry is through medical and psychiatric care integration. One collaborative team approach involves a behavioral health or chronic disease care manager in a primary care office working with a consulting psychiatrist. In a multisite randomized trial (the Improving Mood: Promoting Access to Collaborative Treatment, or IMPACT study) involving more than 1,800 patients, this collaborative care approach was associated with a 50% or greater reduction in depressive symptoms in 45% of intervention patients, compared with only 19% of usual care patients (Am. J. Manag. Care 2008;14:95-100).
The approach also was associated with decreased costs over a period of 4 years.
Barriers to adoption of such integrated care models include a shrinking proportion of psychiatrists compared with the growing mental health workforce; financing (the disconnected medical and psychiatric payment systems for psychiatrists and other specialists); the fact that electronic medical records systems are not well established in psychiatry, which raises operational and confidentiality issues; and the discrimination against psychiatric care in many insurance plans.
"We need to have systems that are much more granular, but the reality is that the data that drive payment systems, and the data that are going to be associated with quality metrics for both individual physicians and systems as a whole, will come out of these systems. If we remain on the outside of them, it will marginalize and put the patients we care for at serious risk," Dr. Summergrad said.
Overcoming the barriers will require research regarding medically comorbid illness and models of care. In addition, increased training and education for all physicians, including those currently in practice and those in training, and electronic medical records that are well adapted for psychiatric practice are needed, he said.
Dr. Summergrad reported having done nonpromotional speaking for CME Outfitters.
SAN ANTONIO – Questions about how health care reform will affect the practice of medicine are nothing new, but there is particular uncertainty for the field of psychiatry, according to the president-elect of the American Psychiatric Association.
One reason for the uncertainty is that payment streams for psychiatric and substance use care are distinctive and poorly understood, and the scope of the relative sectors – including public, commercial, state, and self-pay – are unique in the field of psychiatry, Dr. Paul Summergrad explained at the annual meeting of the American College of Psychiatrists.
According to a 2011 article in the New England Journal of Medicine, the greatest percentages of U.S. medical spending overall were from "private insurance" and "Medicare, out-of-pocket, and other private spending" (37% and 35%, respectively), but for mental health, Medicaid spending exceeded both of these (28% vs. 27% and 22%, respectively), and "other state and local spending" was also higher (18% vs. 6% for medicine overall).
For substance abuse, other state and local spending dominated at 36%, followed by Medicaid spending at 21% (N. Engl. J. Med. 2011;365:973-5).
"If you look at the total dollars that come into our world, they look different from the outset than they do for anyone else in medicine," Dr. Summergrad said, noting that patients with substance abuse, for example, fall mainly outside of the commercial insurance system.
Also, within Medicaid – the largest payer, the percentage spent on mental health services is about three times higher than for commercial insurance.
The impact of the Affordable Care Act through mandated parity rules for coverage of mental health and substance abuse services could provide for tremendous expansion of services within the insurance realm, he said.
Another reason for the uncertainty is a lack of understanding about the substantial extent and effects of medical and psychiatric comorbidities on the total cost of medical care, and the fact that most ambulatory psychiatric care is provided by physicians other than psychiatrists, said Dr. Summergrad, Dr. Frances S. Arkin Professor and chairman of psychiatry at Tufts Medical Center in Boston.
"This is both a challenge and an opportunity; it’s an opportunity to really improve the care of the patients, and not just individuals who have severe psychiatric illness," he said, noting that those improvements could come not only in terms of the quality of care, but in terms of the cost effectiveness of care – a factor that could benefit both patients and the care system, including psychiatrists.
"The care of our patients is deeply embedded in the general health care system, so for us, the payer environment is problematic, and we know that payment differentials have been deeply discriminatory. It’s part of the reason why, along with intrusive utilization review, many psychiatrists don’t take insurance," he said.
The impact of fourth-party carve-out models on both payment and models of care have had a very problematic impact on both the public and commercial sector – in particular because they don’t take into account the extent of medical-psychiatric comorbidity, he added, noting that "the impact of this commoditization really depends in large measure on stigma associated with mental health and substance abuse care."
Many patients in need can’t get adequate care, and the stigma associated with mental illness keeps them from addressing the problems with insurers or benefits managers.
"The insurance industry has relied, in my view, on that stigma to allow [psychiatric] care to be marginalized," he said.
However, studies consistently show that patients with mental illness and substance abuse issues have higher rates of medical comorbidities, and that patients with chronic medical conditions have higher rates of mental health issues. These interactions result in poorer outcomes and higher costs.
In many studies, the costs associated with treating patients with a psychiatric and/or substance use disorder are two to three times greater when accounting for a patient’s total medical costs, compared with the costs for patients without a behavioral condition, Dr. Summergrad said.
One way that health care reform can benefit patients and potentially psychiatry is through medical and psychiatric care integration. One collaborative team approach involves a behavioral health or chronic disease care manager in a primary care office working with a consulting psychiatrist. In a multisite randomized trial (the Improving Mood: Promoting Access to Collaborative Treatment, or IMPACT study) involving more than 1,800 patients, this collaborative care approach was associated with a 50% or greater reduction in depressive symptoms in 45% of intervention patients, compared with only 19% of usual care patients (Am. J. Manag. Care 2008;14:95-100).
The approach also was associated with decreased costs over a period of 4 years.
Barriers to adoption of such integrated care models include a shrinking proportion of psychiatrists compared with the growing mental health workforce; financing (the disconnected medical and psychiatric payment systems for psychiatrists and other specialists); the fact that electronic medical records systems are not well established in psychiatry, which raises operational and confidentiality issues; and the discrimination against psychiatric care in many insurance plans.
"We need to have systems that are much more granular, but the reality is that the data that drive payment systems, and the data that are going to be associated with quality metrics for both individual physicians and systems as a whole, will come out of these systems. If we remain on the outside of them, it will marginalize and put the patients we care for at serious risk," Dr. Summergrad said.
Overcoming the barriers will require research regarding medically comorbid illness and models of care. In addition, increased training and education for all physicians, including those currently in practice and those in training, and electronic medical records that are well adapted for psychiatric practice are needed, he said.
Dr. Summergrad reported having done nonpromotional speaking for CME Outfitters.
EXPERT ANALYSIS AT THE AMERICAN COLLEGE OF PSYCHIATRISTS MEETING
Patient-targeted Googling: Consider patients’ best interests
SAN ANTONIO – Your patients are likely "Googling" you; is turnabout fair play?
The question is a popular one these days. A quick Internet search reveals numerous articles, editorials, and blog posts on the topic. Some authors focus on potential positive aspects of the practice, while others decry it as unethical.
Attendees at an interactive session on "Professionalism and Psychiatry in the Online and Digital Age" held during the annual meeting of the American College of Psychiatrists were similarly divided. One admitted to Googling a patient to verify whether stories the patient told were true or were evidence of grandiosity. Others said they could see value in learning information about a patient that they might not otherwise know.
Another knew of a program where routine Googling of patients was expected.
Some said it’s best to avoid the temptation altogether – that obtaining information online about a patient can be harmful to the therapeutic relationship.
Most agreed there are important ethical implications to consider.
It will take some time before the ethical – and legal – implications of Googling and other online and digital activities are defined and standards established, but one of the session leaders, Dr. Sandra M. DeJong of Cambridge (Mass.) Health Alliance recommended an article from Harvard Review of Psychiatry as an excellent resource for decision-making about Googling patients.
In the article, entitled "Patient-Targeted Googling: The Ethics of Searching Online for Patient Information," Dr. Brian K. Clinton of McLean Hospital, Belmont, Mass., and his colleagues acknowledge that "the Internet has changed the way that medicine and psychiatry are practiced, as patients and physicians now routinely search online for medical and personal information," and they believe that patient-targeted "Googling" – a term they consider to be synonymous with "Internet searching" – is "widespread and deserving of professional and ethical consideration."
While the practice occurs among all types of physicians, it is "especially complicated in a relationship between a patient and a psychiatrist (or other mental health clinician)," they wrote, explaining that what they referred to as patient-targeted Googling, or PTG, has the potential to enhance or interfere with processes inherent in therapeutic relationship (Harv. Rev. Psychiatry 2010;18:103-12).
In some cases, a search can garner useful information. An example involves a case in which collateral information obtained aided in the safety assessment of a suicidal patient in an emergency room. Conversely, ethically problematic motivations for PTG might include curiosity, voyeurism, and habit – and these motivations can result in behaviors that would be considered boundary violations in another setting (for example, Googling a patient’s address and viewing a photograph of her home, which might be analogous to driving by her house).
"Before searching online for patients, psychiatrists should consider the intention of the search, its potential value or risk to the patient, and the anticipated effect of gaining previously unknown information. The psychiatrist is obligated to act in a way that will respect the patient’s best interests and that adheres to professional ethics. However, the results and the potential danger of PTG are not always intuitive or consciously available prior to searches," they wrote.
To aid in the decision making, they propose a pragmatic model for "considering PTG that focuses on practical results of searches and that aims to minimize the risk of exploiting patients."
The model, which provides an approach to clinical ethics that specifies core values that should be balanced in patient care – specifically, the psychiatrist should focus ethical deliberations on the results of the decision both for the patient in question and on general moral principles.
"The psychiatrist must consider how PTG would affect the treatment relationship and the progress toward treatment goals – a thought process that may involve discussions with the patient, the patient’s family, and a clinician’s community of supervisors, colleagues, and consultants," they said.
The model urges clinicians to – at the very least – consider the following six questions on a case-by-case basis before searching online for a patient:
• Why do I want to conduct this search?
• Would my search advance or compromise the treatment?
• Should I obtain informed consent from the patient prior to searching?
• Should I share the results of the search with the patient?
• Should I document the findings of the search in the medical record?
• How do I monitor my motivations and the ongoing risk-benefit profile of searching?
If the answers to these questions suggest that patient-targeted Googling would not serve a particular patient’s best interest or that PTG would not promote the therapeutic process, the psychiatrist should not go forward with the search, the authors said.
Dr. DeJong reported having no disclosures. Dr. Clinton and his colleagues also reported having no disclosures.
SAN ANTONIO – Your patients are likely "Googling" you; is turnabout fair play?
The question is a popular one these days. A quick Internet search reveals numerous articles, editorials, and blog posts on the topic. Some authors focus on potential positive aspects of the practice, while others decry it as unethical.
Attendees at an interactive session on "Professionalism and Psychiatry in the Online and Digital Age" held during the annual meeting of the American College of Psychiatrists were similarly divided. One admitted to Googling a patient to verify whether stories the patient told were true or were evidence of grandiosity. Others said they could see value in learning information about a patient that they might not otherwise know.
Another knew of a program where routine Googling of patients was expected.
Some said it’s best to avoid the temptation altogether – that obtaining information online about a patient can be harmful to the therapeutic relationship.
Most agreed there are important ethical implications to consider.
It will take some time before the ethical – and legal – implications of Googling and other online and digital activities are defined and standards established, but one of the session leaders, Dr. Sandra M. DeJong of Cambridge (Mass.) Health Alliance recommended an article from Harvard Review of Psychiatry as an excellent resource for decision-making about Googling patients.
In the article, entitled "Patient-Targeted Googling: The Ethics of Searching Online for Patient Information," Dr. Brian K. Clinton of McLean Hospital, Belmont, Mass., and his colleagues acknowledge that "the Internet has changed the way that medicine and psychiatry are practiced, as patients and physicians now routinely search online for medical and personal information," and they believe that patient-targeted "Googling" – a term they consider to be synonymous with "Internet searching" – is "widespread and deserving of professional and ethical consideration."
While the practice occurs among all types of physicians, it is "especially complicated in a relationship between a patient and a psychiatrist (or other mental health clinician)," they wrote, explaining that what they referred to as patient-targeted Googling, or PTG, has the potential to enhance or interfere with processes inherent in therapeutic relationship (Harv. Rev. Psychiatry 2010;18:103-12).
In some cases, a search can garner useful information. An example involves a case in which collateral information obtained aided in the safety assessment of a suicidal patient in an emergency room. Conversely, ethically problematic motivations for PTG might include curiosity, voyeurism, and habit – and these motivations can result in behaviors that would be considered boundary violations in another setting (for example, Googling a patient’s address and viewing a photograph of her home, which might be analogous to driving by her house).
"Before searching online for patients, psychiatrists should consider the intention of the search, its potential value or risk to the patient, and the anticipated effect of gaining previously unknown information. The psychiatrist is obligated to act in a way that will respect the patient’s best interests and that adheres to professional ethics. However, the results and the potential danger of PTG are not always intuitive or consciously available prior to searches," they wrote.
To aid in the decision making, they propose a pragmatic model for "considering PTG that focuses on practical results of searches and that aims to minimize the risk of exploiting patients."
The model, which provides an approach to clinical ethics that specifies core values that should be balanced in patient care – specifically, the psychiatrist should focus ethical deliberations on the results of the decision both for the patient in question and on general moral principles.
"The psychiatrist must consider how PTG would affect the treatment relationship and the progress toward treatment goals – a thought process that may involve discussions with the patient, the patient’s family, and a clinician’s community of supervisors, colleagues, and consultants," they said.
The model urges clinicians to – at the very least – consider the following six questions on a case-by-case basis before searching online for a patient:
• Why do I want to conduct this search?
• Would my search advance or compromise the treatment?
• Should I obtain informed consent from the patient prior to searching?
• Should I share the results of the search with the patient?
• Should I document the findings of the search in the medical record?
• How do I monitor my motivations and the ongoing risk-benefit profile of searching?
If the answers to these questions suggest that patient-targeted Googling would not serve a particular patient’s best interest or that PTG would not promote the therapeutic process, the psychiatrist should not go forward with the search, the authors said.
Dr. DeJong reported having no disclosures. Dr. Clinton and his colleagues also reported having no disclosures.
SAN ANTONIO – Your patients are likely "Googling" you; is turnabout fair play?
The question is a popular one these days. A quick Internet search reveals numerous articles, editorials, and blog posts on the topic. Some authors focus on potential positive aspects of the practice, while others decry it as unethical.
Attendees at an interactive session on "Professionalism and Psychiatry in the Online and Digital Age" held during the annual meeting of the American College of Psychiatrists were similarly divided. One admitted to Googling a patient to verify whether stories the patient told were true or were evidence of grandiosity. Others said they could see value in learning information about a patient that they might not otherwise know.
Another knew of a program where routine Googling of patients was expected.
Some said it’s best to avoid the temptation altogether – that obtaining information online about a patient can be harmful to the therapeutic relationship.
Most agreed there are important ethical implications to consider.
It will take some time before the ethical – and legal – implications of Googling and other online and digital activities are defined and standards established, but one of the session leaders, Dr. Sandra M. DeJong of Cambridge (Mass.) Health Alliance recommended an article from Harvard Review of Psychiatry as an excellent resource for decision-making about Googling patients.
In the article, entitled "Patient-Targeted Googling: The Ethics of Searching Online for Patient Information," Dr. Brian K. Clinton of McLean Hospital, Belmont, Mass., and his colleagues acknowledge that "the Internet has changed the way that medicine and psychiatry are practiced, as patients and physicians now routinely search online for medical and personal information," and they believe that patient-targeted "Googling" – a term they consider to be synonymous with "Internet searching" – is "widespread and deserving of professional and ethical consideration."
While the practice occurs among all types of physicians, it is "especially complicated in a relationship between a patient and a psychiatrist (or other mental health clinician)," they wrote, explaining that what they referred to as patient-targeted Googling, or PTG, has the potential to enhance or interfere with processes inherent in therapeutic relationship (Harv. Rev. Psychiatry 2010;18:103-12).
In some cases, a search can garner useful information. An example involves a case in which collateral information obtained aided in the safety assessment of a suicidal patient in an emergency room. Conversely, ethically problematic motivations for PTG might include curiosity, voyeurism, and habit – and these motivations can result in behaviors that would be considered boundary violations in another setting (for example, Googling a patient’s address and viewing a photograph of her home, which might be analogous to driving by her house).
"Before searching online for patients, psychiatrists should consider the intention of the search, its potential value or risk to the patient, and the anticipated effect of gaining previously unknown information. The psychiatrist is obligated to act in a way that will respect the patient’s best interests and that adheres to professional ethics. However, the results and the potential danger of PTG are not always intuitive or consciously available prior to searches," they wrote.
To aid in the decision making, they propose a pragmatic model for "considering PTG that focuses on practical results of searches and that aims to minimize the risk of exploiting patients."
The model, which provides an approach to clinical ethics that specifies core values that should be balanced in patient care – specifically, the psychiatrist should focus ethical deliberations on the results of the decision both for the patient in question and on general moral principles.
"The psychiatrist must consider how PTG would affect the treatment relationship and the progress toward treatment goals – a thought process that may involve discussions with the patient, the patient’s family, and a clinician’s community of supervisors, colleagues, and consultants," they said.
The model urges clinicians to – at the very least – consider the following six questions on a case-by-case basis before searching online for a patient:
• Why do I want to conduct this search?
• Would my search advance or compromise the treatment?
• Should I obtain informed consent from the patient prior to searching?
• Should I share the results of the search with the patient?
• Should I document the findings of the search in the medical record?
• How do I monitor my motivations and the ongoing risk-benefit profile of searching?
If the answers to these questions suggest that patient-targeted Googling would not serve a particular patient’s best interest or that PTG would not promote the therapeutic process, the psychiatrist should not go forward with the search, the authors said.
Dr. DeJong reported having no disclosures. Dr. Clinton and his colleagues also reported having no disclosures.
EXPERT ANALYSIS AT THE AMERICAN COLLEGE OF PSYCHIATRISTS MEETING
Prior resection poses certain risks in lung transplantation
ORLANDO – Prior lung resection is associated with increased early mortality and with a more than twofold increased risk of renal failure requiring dialysis in lung transplant recipients, data from the United Network for Organ Sharing suggest.
Prior resection is not, however, associated with increased long-term mortality, prolonged hospital length of stay, or airway dehiscence, Dr. Asvin M. Ganapathi reported at the annual meeting of the Society of Thoracic Surgeons.
Of 15,300 adult lung transplant recipients in the UNOS database who received lungs between October 1999 and December 2011, 80 had a prior lobectomy and 22 had a prior pneumonectomy. After 3:1 propensity matching based on 17 recipient variables known to affect perioperative morbidity and mortality, 90-day mortality in 306 nonresection patients was 5.8%, compared with 13.9% in the 102 with prior resection. Renal failure requiring dialysis occurred in 6.6% and 13.9% of patients in the groups, respectively, said Dr. Ganapathi of the anesthesiology division of Duke University, Durham, N.C.
Hospital length of stay longer than 25 days was required in 36.9% and 36.4% of the nonresection and resection groups, respectively, and airway dehiscence occurred in 1.3% and 2%, he said.
Survival at 1 and 5 years was 83.6% and 48.4% in the nonresection group, and 78.9% and 45.6% in the prior-resection group.
A subanalysis comparing the prior-lobectomy patients with patients with no prior resection revealed no differences between the two groups in any of the examined outcomes, although there was a trend toward increased 90-day mortality in the lobectomy patient, and a more than twofold increase in renal failure requiring dialysis. A subanalysis comparing those with prior pneumonectomy with those with no prior resection showed a significantly greater need for dialysis in the pneumonectomy patients (8.9% vs. 3.8%), and a trend toward increased 90-day mortality in the pneumonectomy patients, but no differences in the other examined outcomes.
The propensity-matched groups were similar with respect to recipient, donor, and operative characteristics. There were 10 double and 12 single lung transplants after pneumonectomy, and 51 double and 29 single transplants after lobectomy.
Lung transplantation provides a durable, efficacious treatment for end-stage lung disease, but indications for transplant can vary, and as a result, a select group of patients may have had prior lung resection for treatment of their underlying disease, Dr. Ganapathi said.
Both lobectomy and pneumonectomy are known to cause anatomic changes such as mediastinal shift and vascular abnormalities.
"As such, a history of previous lung resection may affect selection of donor organs and increase the difficulty of transplantation," he said.
In fact, historically, prior thoracic surgery was considered a relative contraindication to lung transplantation because of increased risk of poor outcomes, but recent case reports and single-institution case series – though limited by small patient numbers and the inclusion of both major and minor thoracic procedures ranging from chest tube insertion to pneumonectomy – have suggested that transplantation is feasible in these patients, he said.
Studies specifically looking at lung transplant after resection are lacking; the largest series involved pneumonectomy and included only 14 patients, he said.
The current findings suggest that prior resection should not preclude lung transplantation.
Notable limits of the study include its retrospective design, which may have introduced unexpected bias into the analysis; the fact that the analysis is limited to the variable collected for the UNOS database; and the number of patients with prior resection, although this may be secondary to underreporting of prior thoracic procedures in the UNOS candidate registration form or a result of data being collected only from 1999 onward.
Other variables that may have been of interest for the current analysis were knowledge of laterality of prior resection, time from resection to treatment, days of postoperative ventilator use, and operative time, Dr. Ganapathi noted. Specifically, in cases of single lung transplant, the issue of laterality would be of great interest, he said.
"In conclusion, lung transplantation subsequent to previous major lung resection is associated with an increased risk of early mortality, but did not demonstrate any significant long-term survival differences. Additionally, prior major lung resection predisposes to increased morbidity in the form of renal failure requiring dialysis," he said. The increased rate of dialysis may be secondary to longer operative time, the need for cardiopulmonary bypass, or other unquantified factors, he added.
Careful, individualized preoperative recipient evaluation and technical planning are necessary to minimize these risks in the patients, he concluded.
Dr. Ganapathi reported having no relevant disclosures.
ORLANDO – Prior lung resection is associated with increased early mortality and with a more than twofold increased risk of renal failure requiring dialysis in lung transplant recipients, data from the United Network for Organ Sharing suggest.
Prior resection is not, however, associated with increased long-term mortality, prolonged hospital length of stay, or airway dehiscence, Dr. Asvin M. Ganapathi reported at the annual meeting of the Society of Thoracic Surgeons.
Of 15,300 adult lung transplant recipients in the UNOS database who received lungs between October 1999 and December 2011, 80 had a prior lobectomy and 22 had a prior pneumonectomy. After 3:1 propensity matching based on 17 recipient variables known to affect perioperative morbidity and mortality, 90-day mortality in 306 nonresection patients was 5.8%, compared with 13.9% in the 102 with prior resection. Renal failure requiring dialysis occurred in 6.6% and 13.9% of patients in the groups, respectively, said Dr. Ganapathi of the anesthesiology division of Duke University, Durham, N.C.
Hospital length of stay longer than 25 days was required in 36.9% and 36.4% of the nonresection and resection groups, respectively, and airway dehiscence occurred in 1.3% and 2%, he said.
Survival at 1 and 5 years was 83.6% and 48.4% in the nonresection group, and 78.9% and 45.6% in the prior-resection group.
A subanalysis comparing the prior-lobectomy patients with patients with no prior resection revealed no differences between the two groups in any of the examined outcomes, although there was a trend toward increased 90-day mortality in the lobectomy patient, and a more than twofold increase in renal failure requiring dialysis. A subanalysis comparing those with prior pneumonectomy with those with no prior resection showed a significantly greater need for dialysis in the pneumonectomy patients (8.9% vs. 3.8%), and a trend toward increased 90-day mortality in the pneumonectomy patients, but no differences in the other examined outcomes.
The propensity-matched groups were similar with respect to recipient, donor, and operative characteristics. There were 10 double and 12 single lung transplants after pneumonectomy, and 51 double and 29 single transplants after lobectomy.
Lung transplantation provides a durable, efficacious treatment for end-stage lung disease, but indications for transplant can vary, and as a result, a select group of patients may have had prior lung resection for treatment of their underlying disease, Dr. Ganapathi said.
Both lobectomy and pneumonectomy are known to cause anatomic changes such as mediastinal shift and vascular abnormalities.
"As such, a history of previous lung resection may affect selection of donor organs and increase the difficulty of transplantation," he said.
In fact, historically, prior thoracic surgery was considered a relative contraindication to lung transplantation because of increased risk of poor outcomes, but recent case reports and single-institution case series – though limited by small patient numbers and the inclusion of both major and minor thoracic procedures ranging from chest tube insertion to pneumonectomy – have suggested that transplantation is feasible in these patients, he said.
Studies specifically looking at lung transplant after resection are lacking; the largest series involved pneumonectomy and included only 14 patients, he said.
The current findings suggest that prior resection should not preclude lung transplantation.
Notable limits of the study include its retrospective design, which may have introduced unexpected bias into the analysis; the fact that the analysis is limited to the variable collected for the UNOS database; and the number of patients with prior resection, although this may be secondary to underreporting of prior thoracic procedures in the UNOS candidate registration form or a result of data being collected only from 1999 onward.
Other variables that may have been of interest for the current analysis were knowledge of laterality of prior resection, time from resection to treatment, days of postoperative ventilator use, and operative time, Dr. Ganapathi noted. Specifically, in cases of single lung transplant, the issue of laterality would be of great interest, he said.
"In conclusion, lung transplantation subsequent to previous major lung resection is associated with an increased risk of early mortality, but did not demonstrate any significant long-term survival differences. Additionally, prior major lung resection predisposes to increased morbidity in the form of renal failure requiring dialysis," he said. The increased rate of dialysis may be secondary to longer operative time, the need for cardiopulmonary bypass, or other unquantified factors, he added.
Careful, individualized preoperative recipient evaluation and technical planning are necessary to minimize these risks in the patients, he concluded.
Dr. Ganapathi reported having no relevant disclosures.
ORLANDO – Prior lung resection is associated with increased early mortality and with a more than twofold increased risk of renal failure requiring dialysis in lung transplant recipients, data from the United Network for Organ Sharing suggest.
Prior resection is not, however, associated with increased long-term mortality, prolonged hospital length of stay, or airway dehiscence, Dr. Asvin M. Ganapathi reported at the annual meeting of the Society of Thoracic Surgeons.
Of 15,300 adult lung transplant recipients in the UNOS database who received lungs between October 1999 and December 2011, 80 had a prior lobectomy and 22 had a prior pneumonectomy. After 3:1 propensity matching based on 17 recipient variables known to affect perioperative morbidity and mortality, 90-day mortality in 306 nonresection patients was 5.8%, compared with 13.9% in the 102 with prior resection. Renal failure requiring dialysis occurred in 6.6% and 13.9% of patients in the groups, respectively, said Dr. Ganapathi of the anesthesiology division of Duke University, Durham, N.C.
Hospital length of stay longer than 25 days was required in 36.9% and 36.4% of the nonresection and resection groups, respectively, and airway dehiscence occurred in 1.3% and 2%, he said.
Survival at 1 and 5 years was 83.6% and 48.4% in the nonresection group, and 78.9% and 45.6% in the prior-resection group.
A subanalysis comparing the prior-lobectomy patients with patients with no prior resection revealed no differences between the two groups in any of the examined outcomes, although there was a trend toward increased 90-day mortality in the lobectomy patient, and a more than twofold increase in renal failure requiring dialysis. A subanalysis comparing those with prior pneumonectomy with those with no prior resection showed a significantly greater need for dialysis in the pneumonectomy patients (8.9% vs. 3.8%), and a trend toward increased 90-day mortality in the pneumonectomy patients, but no differences in the other examined outcomes.
The propensity-matched groups were similar with respect to recipient, donor, and operative characteristics. There were 10 double and 12 single lung transplants after pneumonectomy, and 51 double and 29 single transplants after lobectomy.
Lung transplantation provides a durable, efficacious treatment for end-stage lung disease, but indications for transplant can vary, and as a result, a select group of patients may have had prior lung resection for treatment of their underlying disease, Dr. Ganapathi said.
Both lobectomy and pneumonectomy are known to cause anatomic changes such as mediastinal shift and vascular abnormalities.
"As such, a history of previous lung resection may affect selection of donor organs and increase the difficulty of transplantation," he said.
In fact, historically, prior thoracic surgery was considered a relative contraindication to lung transplantation because of increased risk of poor outcomes, but recent case reports and single-institution case series – though limited by small patient numbers and the inclusion of both major and minor thoracic procedures ranging from chest tube insertion to pneumonectomy – have suggested that transplantation is feasible in these patients, he said.
Studies specifically looking at lung transplant after resection are lacking; the largest series involved pneumonectomy and included only 14 patients, he said.
The current findings suggest that prior resection should not preclude lung transplantation.
Notable limits of the study include its retrospective design, which may have introduced unexpected bias into the analysis; the fact that the analysis is limited to the variable collected for the UNOS database; and the number of patients with prior resection, although this may be secondary to underreporting of prior thoracic procedures in the UNOS candidate registration form or a result of data being collected only from 1999 onward.
Other variables that may have been of interest for the current analysis were knowledge of laterality of prior resection, time from resection to treatment, days of postoperative ventilator use, and operative time, Dr. Ganapathi noted. Specifically, in cases of single lung transplant, the issue of laterality would be of great interest, he said.
"In conclusion, lung transplantation subsequent to previous major lung resection is associated with an increased risk of early mortality, but did not demonstrate any significant long-term survival differences. Additionally, prior major lung resection predisposes to increased morbidity in the form of renal failure requiring dialysis," he said. The increased rate of dialysis may be secondary to longer operative time, the need for cardiopulmonary bypass, or other unquantified factors, he added.
Careful, individualized preoperative recipient evaluation and technical planning are necessary to minimize these risks in the patients, he concluded.
Dr. Ganapathi reported having no relevant disclosures.
AT THE STS ANNUAL MEETING
Major finding: Survival at 1 and 5 years was 83.6% and 48.4%, respectively, in the nonresection group, and 78.9% and 45.6% in the prior-resection group.
Data source: An analysis of data from more than 15,000 patients in the United Network of Organ Sharing database.
Disclosures: Dr. Ganapathi reported having no relevant disclosures.
High-yield techniques in brief CBT sessions can promote adherence
SAN ANTONIO – Treatment adherence is a problem for about half of all psychiatric patients, but certain high-yield techniques for enhancing adherence can be used effectively during brief cognitive-behavioral therapy sessions, according to Dr. Donna M. Sudak and Dr. Jesse H. Wright.
Maximizing the collaborative therapeutic relationship is particularly important, as this can facilitate open discussion about adherence, Dr. Sudak, professor and director of the psychotherapy training program at Drexel University, Philadelphia, and Dr. Wright, professor and director of the depression center at the University of Louisville (Ky.), said in a joint presentation at the annual meeting of the American College of Psychiatrists.
"No electronic reminder is as helpful for adherence as having a good relationship with the patient and asking regularly [about adherence]," Dr. Sudak said.
It is important, however, to ask in a way that helps patients tell you about any difficulties they are having.
Asking a patient, "You’re taking your medicine every day, right?" will typically elicit an affirmative response, in part because people just want to be good patients, Dr. Sudak said.
Encouraging open dialogue about how hard it can be to remember to take medication every day, and explaining to patients that the goal is to have them take their medication as often as possible – and discussing ways to reach that goal – will likely do more to encourage patients to discuss adherence problems, she said.
In addition to normalizing the illness and adherence problems through such dialogue, providing patients with printed educational materials about the importance of adherence – and repeating these efforts at intervals to reinforce the message – is also important, Dr. Sudak said, noting that this is particularly important for patients who have just been discharged from the hospital, because these patients might have particular difficulty remembering instructions.
Asking first about the benefits of medication, rather than about side effects, also is an important strategy; this puts the focus on the positive aspects of treatment, instead of reminding the patient about the potential negative aspects, she said.
And remember that adherence issues change across the life cycle. For example, when a patient transitions from home to a college dorm or to independent living, adherence issues can arise. Thus, adherence should be routinely monitored.
Collaboration, a nonjudgmental approach, and realistic expectations are important throughout treatment.
Other strategies for promoting adherence include involving the patient’s family if possible and if helpful; linking adherence to the patient’s goals and most distressing symptoms; and simplifying medication regimens when possible.
Jointly and relentlessly pursuing solutions to side effects also is imperative; pointing out that medication has effects that are desired, as well as effects that are not – and working to minimize the undesirable effects – will encourage persistence on the part of the patient, Dr. Sudak said.
She and Dr. Wright provided numerous specific behavioral and cognitive methods for improving adherence.
Behavioral methods that might help patients with adherence include storing medication in a place where it will be seen each day, pairing medication taking with routine activities, and using a reminder system, such as a 7-day pill container.
"These are very commonsense kinds of approaches ... but they can really be very helpful," Dr. Wright said.
Behavioral contracts and written adherence plans also can prove helpful, he said, adding that it also is important to analyze barriers to adherence and to devise written methods for overcoming those barriers.
An example of a barrier might be running out of samples of medication before a scheduled doctor visit; a potential solution would be to have the patient count pills carefully, call the nurse a week before more samples will be needed, and make a plan to pick them up during a weekday while the nurse is available.
Another barrier might be a voice telling a patient that the medication is causing harm; a possible solution would be to remind the patient that the voices are a symptom of the patient’s illness, and that it is not necessary to do what the voices say. The patient also could be instructed to review a list of positive reasons to take the medication.
These and other behavioral techniques and barriers/solutions can be written on 3-by-5 "coping cards" that capture the key points of the session. The patient can take these cards home to serve as reminders.
As for cognitive methods, Dr. Sudak and Dr. Wright recommended eliciting cognitions about taking medication, and about the illness, to identify and modify dysfunctional family beliefs about medication, and to write down the old belief and the new more-functional belief.
Cognitions that can interfere with adherence include:
• Specific ideas about the illness or medication – such as a belief that antidepressant medications are addictive. Education should be provided to counter these beliefs.
• More general beliefs (family or cultural beliefs/values) about physicians or medication – such as beliefs that individuals should be able to handle medical problems on their own. These beliefs should be examined, and logical analysis should be employed to explore and correct them.
• Beliefs about medication that echo beliefs about the self. For example, a patient might believe he is vulnerable in general, and thus believe he is prone to side effects. Belief work can help in these cases.
• Basic mistrust and interpersonal beliefs that interfere more globally. More specific trust work can help in these cases.
Additional cognitive strategies that can help with adherence are pro/con lists, evaluating thoughts for accuracy, developing new rules and beliefs about medication, problem solving and planning, and cognitive rehearsal, they said.
Dr. Sudak and Dr. Wright are two of four coauthors of the book, "High-Yield Cognitive-Behavior Therapy for Brief Sessions: An Illustrated Guide (Washington: American Psychiatric Publishing, 2010). They both receive book royalties from American Psychiatric Publishing; Lippincott, Williams & Wilkins; and John Wiley & Sons. Dr. Sudak also serves on an editorial board, receives honoraria from Elsevier, and is a consultant for Takeda Pharmaceuticals. Dr. Wright also receives royalties for the development of software (Empower Interactive, Mindstreet).
SAN ANTONIO – Treatment adherence is a problem for about half of all psychiatric patients, but certain high-yield techniques for enhancing adherence can be used effectively during brief cognitive-behavioral therapy sessions, according to Dr. Donna M. Sudak and Dr. Jesse H. Wright.
Maximizing the collaborative therapeutic relationship is particularly important, as this can facilitate open discussion about adherence, Dr. Sudak, professor and director of the psychotherapy training program at Drexel University, Philadelphia, and Dr. Wright, professor and director of the depression center at the University of Louisville (Ky.), said in a joint presentation at the annual meeting of the American College of Psychiatrists.
"No electronic reminder is as helpful for adherence as having a good relationship with the patient and asking regularly [about adherence]," Dr. Sudak said.
It is important, however, to ask in a way that helps patients tell you about any difficulties they are having.
Asking a patient, "You’re taking your medicine every day, right?" will typically elicit an affirmative response, in part because people just want to be good patients, Dr. Sudak said.
Encouraging open dialogue about how hard it can be to remember to take medication every day, and explaining to patients that the goal is to have them take their medication as often as possible – and discussing ways to reach that goal – will likely do more to encourage patients to discuss adherence problems, she said.
In addition to normalizing the illness and adherence problems through such dialogue, providing patients with printed educational materials about the importance of adherence – and repeating these efforts at intervals to reinforce the message – is also important, Dr. Sudak said, noting that this is particularly important for patients who have just been discharged from the hospital, because these patients might have particular difficulty remembering instructions.
Asking first about the benefits of medication, rather than about side effects, also is an important strategy; this puts the focus on the positive aspects of treatment, instead of reminding the patient about the potential negative aspects, she said.
And remember that adherence issues change across the life cycle. For example, when a patient transitions from home to a college dorm or to independent living, adherence issues can arise. Thus, adherence should be routinely monitored.
Collaboration, a nonjudgmental approach, and realistic expectations are important throughout treatment.
Other strategies for promoting adherence include involving the patient’s family if possible and if helpful; linking adherence to the patient’s goals and most distressing symptoms; and simplifying medication regimens when possible.
Jointly and relentlessly pursuing solutions to side effects also is imperative; pointing out that medication has effects that are desired, as well as effects that are not – and working to minimize the undesirable effects – will encourage persistence on the part of the patient, Dr. Sudak said.
She and Dr. Wright provided numerous specific behavioral and cognitive methods for improving adherence.
Behavioral methods that might help patients with adherence include storing medication in a place where it will be seen each day, pairing medication taking with routine activities, and using a reminder system, such as a 7-day pill container.
"These are very commonsense kinds of approaches ... but they can really be very helpful," Dr. Wright said.
Behavioral contracts and written adherence plans also can prove helpful, he said, adding that it also is important to analyze barriers to adherence and to devise written methods for overcoming those barriers.
An example of a barrier might be running out of samples of medication before a scheduled doctor visit; a potential solution would be to have the patient count pills carefully, call the nurse a week before more samples will be needed, and make a plan to pick them up during a weekday while the nurse is available.
Another barrier might be a voice telling a patient that the medication is causing harm; a possible solution would be to remind the patient that the voices are a symptom of the patient’s illness, and that it is not necessary to do what the voices say. The patient also could be instructed to review a list of positive reasons to take the medication.
These and other behavioral techniques and barriers/solutions can be written on 3-by-5 "coping cards" that capture the key points of the session. The patient can take these cards home to serve as reminders.
As for cognitive methods, Dr. Sudak and Dr. Wright recommended eliciting cognitions about taking medication, and about the illness, to identify and modify dysfunctional family beliefs about medication, and to write down the old belief and the new more-functional belief.
Cognitions that can interfere with adherence include:
• Specific ideas about the illness or medication – such as a belief that antidepressant medications are addictive. Education should be provided to counter these beliefs.
• More general beliefs (family or cultural beliefs/values) about physicians or medication – such as beliefs that individuals should be able to handle medical problems on their own. These beliefs should be examined, and logical analysis should be employed to explore and correct them.
• Beliefs about medication that echo beliefs about the self. For example, a patient might believe he is vulnerable in general, and thus believe he is prone to side effects. Belief work can help in these cases.
• Basic mistrust and interpersonal beliefs that interfere more globally. More specific trust work can help in these cases.
Additional cognitive strategies that can help with adherence are pro/con lists, evaluating thoughts for accuracy, developing new rules and beliefs about medication, problem solving and planning, and cognitive rehearsal, they said.
Dr. Sudak and Dr. Wright are two of four coauthors of the book, "High-Yield Cognitive-Behavior Therapy for Brief Sessions: An Illustrated Guide (Washington: American Psychiatric Publishing, 2010). They both receive book royalties from American Psychiatric Publishing; Lippincott, Williams & Wilkins; and John Wiley & Sons. Dr. Sudak also serves on an editorial board, receives honoraria from Elsevier, and is a consultant for Takeda Pharmaceuticals. Dr. Wright also receives royalties for the development of software (Empower Interactive, Mindstreet).
SAN ANTONIO – Treatment adherence is a problem for about half of all psychiatric patients, but certain high-yield techniques for enhancing adherence can be used effectively during brief cognitive-behavioral therapy sessions, according to Dr. Donna M. Sudak and Dr. Jesse H. Wright.
Maximizing the collaborative therapeutic relationship is particularly important, as this can facilitate open discussion about adherence, Dr. Sudak, professor and director of the psychotherapy training program at Drexel University, Philadelphia, and Dr. Wright, professor and director of the depression center at the University of Louisville (Ky.), said in a joint presentation at the annual meeting of the American College of Psychiatrists.
"No electronic reminder is as helpful for adherence as having a good relationship with the patient and asking regularly [about adherence]," Dr. Sudak said.
It is important, however, to ask in a way that helps patients tell you about any difficulties they are having.
Asking a patient, "You’re taking your medicine every day, right?" will typically elicit an affirmative response, in part because people just want to be good patients, Dr. Sudak said.
Encouraging open dialogue about how hard it can be to remember to take medication every day, and explaining to patients that the goal is to have them take their medication as often as possible – and discussing ways to reach that goal – will likely do more to encourage patients to discuss adherence problems, she said.
In addition to normalizing the illness and adherence problems through such dialogue, providing patients with printed educational materials about the importance of adherence – and repeating these efforts at intervals to reinforce the message – is also important, Dr. Sudak said, noting that this is particularly important for patients who have just been discharged from the hospital, because these patients might have particular difficulty remembering instructions.
Asking first about the benefits of medication, rather than about side effects, also is an important strategy; this puts the focus on the positive aspects of treatment, instead of reminding the patient about the potential negative aspects, she said.
And remember that adherence issues change across the life cycle. For example, when a patient transitions from home to a college dorm or to independent living, adherence issues can arise. Thus, adherence should be routinely monitored.
Collaboration, a nonjudgmental approach, and realistic expectations are important throughout treatment.
Other strategies for promoting adherence include involving the patient’s family if possible and if helpful; linking adherence to the patient’s goals and most distressing symptoms; and simplifying medication regimens when possible.
Jointly and relentlessly pursuing solutions to side effects also is imperative; pointing out that medication has effects that are desired, as well as effects that are not – and working to minimize the undesirable effects – will encourage persistence on the part of the patient, Dr. Sudak said.
She and Dr. Wright provided numerous specific behavioral and cognitive methods for improving adherence.
Behavioral methods that might help patients with adherence include storing medication in a place where it will be seen each day, pairing medication taking with routine activities, and using a reminder system, such as a 7-day pill container.
"These are very commonsense kinds of approaches ... but they can really be very helpful," Dr. Wright said.
Behavioral contracts and written adherence plans also can prove helpful, he said, adding that it also is important to analyze barriers to adherence and to devise written methods for overcoming those barriers.
An example of a barrier might be running out of samples of medication before a scheduled doctor visit; a potential solution would be to have the patient count pills carefully, call the nurse a week before more samples will be needed, and make a plan to pick them up during a weekday while the nurse is available.
Another barrier might be a voice telling a patient that the medication is causing harm; a possible solution would be to remind the patient that the voices are a symptom of the patient’s illness, and that it is not necessary to do what the voices say. The patient also could be instructed to review a list of positive reasons to take the medication.
These and other behavioral techniques and barriers/solutions can be written on 3-by-5 "coping cards" that capture the key points of the session. The patient can take these cards home to serve as reminders.
As for cognitive methods, Dr. Sudak and Dr. Wright recommended eliciting cognitions about taking medication, and about the illness, to identify and modify dysfunctional family beliefs about medication, and to write down the old belief and the new more-functional belief.
Cognitions that can interfere with adherence include:
• Specific ideas about the illness or medication – such as a belief that antidepressant medications are addictive. Education should be provided to counter these beliefs.
• More general beliefs (family or cultural beliefs/values) about physicians or medication – such as beliefs that individuals should be able to handle medical problems on their own. These beliefs should be examined, and logical analysis should be employed to explore and correct them.
• Beliefs about medication that echo beliefs about the self. For example, a patient might believe he is vulnerable in general, and thus believe he is prone to side effects. Belief work can help in these cases.
• Basic mistrust and interpersonal beliefs that interfere more globally. More specific trust work can help in these cases.
Additional cognitive strategies that can help with adherence are pro/con lists, evaluating thoughts for accuracy, developing new rules and beliefs about medication, problem solving and planning, and cognitive rehearsal, they said.
Dr. Sudak and Dr. Wright are two of four coauthors of the book, "High-Yield Cognitive-Behavior Therapy for Brief Sessions: An Illustrated Guide (Washington: American Psychiatric Publishing, 2010). They both receive book royalties from American Psychiatric Publishing; Lippincott, Williams & Wilkins; and John Wiley & Sons. Dr. Sudak also serves on an editorial board, receives honoraria from Elsevier, and is a consultant for Takeda Pharmaceuticals. Dr. Wright also receives royalties for the development of software (Empower Interactive, Mindstreet).
AT THE AMERICAN COLLEGE OF PSYCHIATRISTS MEETING
New guidelines issued for geriatric care in the ED
New consensus-based guidelines aim to provide a standardized approach to improving the care of patients in geriatric emergency departments.
The Geriatric Emergency Department Guidelines are the result of a 2-year effort by representatives from the American College of Emergency Physicians, the American Geriatrics Society, the Society for Academic Emergency Medicine, and the Emergency Nurses Association. According to 2010 Census data, more than 40 million Americans are now over the age of 65 years. Further, the populations of adults aged 65 years and older and those aged 85 years and older are increasing at rates substantially greater than those of the general population.
"The subsequent increased need for health care for this burgeoning geriatric population represents an unprecedented and overwhelming challenge to the American health care system as a whole and to emergency departments [EDs] specifically," the authors state.
In response to this challenge, geriatric EDs are becoming increasingly common. The new guidelines address the special needs of the geriatric population, and propose methods for ensuring that those needs are met, as "the contemporary emergency medicine management model may not be adequate for geriatric adults."
"Similar programs designed for other age groups (pediatric) or directed toward specific diseases (STEMI [ST segment elevation myocardial infarction], stroke, and trauma) have improved care both in individual EDs and system wide, resulting in better, more cost-effective care and ultimately, better patient outcomes," the guideline writers note.
Among the topics addressed in detail in the guidelines are geriatric ED staffing, equipment, education, policies and procedures, follow-up care, and performance improvement measures.
According to the guidelines, an effective program will:
• Involve hospital site-specific staff and overall local coordination resources.
The guidelines spell out qualifications and responsibilities for the geriatric ED medical director, nurse manager, and staff physicians, nurses, specialists, and ancillary service providers.
• Decrease hospital admissions through effective follow-up and care transition plans.
The guidelines state that clinical patient information should be provided in a format best suited for elder adults and that department leaders should maintain relationships and resources in the community that can be used by patients to facilitate care following discharge.
• Include specialty-specific education and training of a multidisciplinary staff, with assessment for interdisciplinary core competencies.
Education should include "go-live" implementation sessions, as well as community awareness, involvement, and outreach, and regular educational assessment and implementation of site-specific educational needs.
• Assess quality, and implement an effective quality improvement program that involves collection and monitoring of relevant data.
The guidelines provide an explicit geriatric program quality-improvement plan designed to be conducive to staff education and program success.
• Utilize equipment designed for a patient population with specific needs.
For example, effective and comfortable evaluation requires equipment that takes into consideration issues of mobility, incontinence, and behavioral needs while minimizing iatrogenic complications. The physical plant of a geriatric ED should similarly promote safety, comfort, mobility, memory cues, and sensorial perception for elders, according to the guidelines.
• Put in place readily available and easily accessed policies, procedures, and protocols that address the challenges involved in caring for geriatric patients in the ED.
These might address screening for risk of added needs assessment, consultation, and intervention, for example. The guidelines offer specific recommendations and tools for medication management, fall assessment, use of urinary catheters, addressing delirium and dementia, and providing palliative care.
The detailed recommendations provided for each of these topics represent research- and consensus-based best practices from the perspectives of the agencies involved in their development, the authors note.
"Improved attention to the needs of this challenging population has the opportunity to more effectively allocate health care resources, optimize admission and readmission rates, while simultaneously decreasing iatrogenic complications and the resultant increased length-of-stay and decreased reimbursement," they wrote, concluding that with implementation of the recommendations, "hospitals, regardless of size, will positively impact the care of the geriatric emergency patients."
New consensus-based guidelines aim to provide a standardized approach to improving the care of patients in geriatric emergency departments.
The Geriatric Emergency Department Guidelines are the result of a 2-year effort by representatives from the American College of Emergency Physicians, the American Geriatrics Society, the Society for Academic Emergency Medicine, and the Emergency Nurses Association. According to 2010 Census data, more than 40 million Americans are now over the age of 65 years. Further, the populations of adults aged 65 years and older and those aged 85 years and older are increasing at rates substantially greater than those of the general population.
"The subsequent increased need for health care for this burgeoning geriatric population represents an unprecedented and overwhelming challenge to the American health care system as a whole and to emergency departments [EDs] specifically," the authors state.
In response to this challenge, geriatric EDs are becoming increasingly common. The new guidelines address the special needs of the geriatric population, and propose methods for ensuring that those needs are met, as "the contemporary emergency medicine management model may not be adequate for geriatric adults."
"Similar programs designed for other age groups (pediatric) or directed toward specific diseases (STEMI [ST segment elevation myocardial infarction], stroke, and trauma) have improved care both in individual EDs and system wide, resulting in better, more cost-effective care and ultimately, better patient outcomes," the guideline writers note.
Among the topics addressed in detail in the guidelines are geriatric ED staffing, equipment, education, policies and procedures, follow-up care, and performance improvement measures.
According to the guidelines, an effective program will:
• Involve hospital site-specific staff and overall local coordination resources.
The guidelines spell out qualifications and responsibilities for the geriatric ED medical director, nurse manager, and staff physicians, nurses, specialists, and ancillary service providers.
• Decrease hospital admissions through effective follow-up and care transition plans.
The guidelines state that clinical patient information should be provided in a format best suited for elder adults and that department leaders should maintain relationships and resources in the community that can be used by patients to facilitate care following discharge.
• Include specialty-specific education and training of a multidisciplinary staff, with assessment for interdisciplinary core competencies.
Education should include "go-live" implementation sessions, as well as community awareness, involvement, and outreach, and regular educational assessment and implementation of site-specific educational needs.
• Assess quality, and implement an effective quality improvement program that involves collection and monitoring of relevant data.
The guidelines provide an explicit geriatric program quality-improvement plan designed to be conducive to staff education and program success.
• Utilize equipment designed for a patient population with specific needs.
For example, effective and comfortable evaluation requires equipment that takes into consideration issues of mobility, incontinence, and behavioral needs while minimizing iatrogenic complications. The physical plant of a geriatric ED should similarly promote safety, comfort, mobility, memory cues, and sensorial perception for elders, according to the guidelines.
• Put in place readily available and easily accessed policies, procedures, and protocols that address the challenges involved in caring for geriatric patients in the ED.
These might address screening for risk of added needs assessment, consultation, and intervention, for example. The guidelines offer specific recommendations and tools for medication management, fall assessment, use of urinary catheters, addressing delirium and dementia, and providing palliative care.
The detailed recommendations provided for each of these topics represent research- and consensus-based best practices from the perspectives of the agencies involved in their development, the authors note.
"Improved attention to the needs of this challenging population has the opportunity to more effectively allocate health care resources, optimize admission and readmission rates, while simultaneously decreasing iatrogenic complications and the resultant increased length-of-stay and decreased reimbursement," they wrote, concluding that with implementation of the recommendations, "hospitals, regardless of size, will positively impact the care of the geriatric emergency patients."
New consensus-based guidelines aim to provide a standardized approach to improving the care of patients in geriatric emergency departments.
The Geriatric Emergency Department Guidelines are the result of a 2-year effort by representatives from the American College of Emergency Physicians, the American Geriatrics Society, the Society for Academic Emergency Medicine, and the Emergency Nurses Association. According to 2010 Census data, more than 40 million Americans are now over the age of 65 years. Further, the populations of adults aged 65 years and older and those aged 85 years and older are increasing at rates substantially greater than those of the general population.
"The subsequent increased need for health care for this burgeoning geriatric population represents an unprecedented and overwhelming challenge to the American health care system as a whole and to emergency departments [EDs] specifically," the authors state.
In response to this challenge, geriatric EDs are becoming increasingly common. The new guidelines address the special needs of the geriatric population, and propose methods for ensuring that those needs are met, as "the contemporary emergency medicine management model may not be adequate for geriatric adults."
"Similar programs designed for other age groups (pediatric) or directed toward specific diseases (STEMI [ST segment elevation myocardial infarction], stroke, and trauma) have improved care both in individual EDs and system wide, resulting in better, more cost-effective care and ultimately, better patient outcomes," the guideline writers note.
Among the topics addressed in detail in the guidelines are geriatric ED staffing, equipment, education, policies and procedures, follow-up care, and performance improvement measures.
According to the guidelines, an effective program will:
• Involve hospital site-specific staff and overall local coordination resources.
The guidelines spell out qualifications and responsibilities for the geriatric ED medical director, nurse manager, and staff physicians, nurses, specialists, and ancillary service providers.
• Decrease hospital admissions through effective follow-up and care transition plans.
The guidelines state that clinical patient information should be provided in a format best suited for elder adults and that department leaders should maintain relationships and resources in the community that can be used by patients to facilitate care following discharge.
• Include specialty-specific education and training of a multidisciplinary staff, with assessment for interdisciplinary core competencies.
Education should include "go-live" implementation sessions, as well as community awareness, involvement, and outreach, and regular educational assessment and implementation of site-specific educational needs.
• Assess quality, and implement an effective quality improvement program that involves collection and monitoring of relevant data.
The guidelines provide an explicit geriatric program quality-improvement plan designed to be conducive to staff education and program success.
• Utilize equipment designed for a patient population with specific needs.
For example, effective and comfortable evaluation requires equipment that takes into consideration issues of mobility, incontinence, and behavioral needs while minimizing iatrogenic complications. The physical plant of a geriatric ED should similarly promote safety, comfort, mobility, memory cues, and sensorial perception for elders, according to the guidelines.
• Put in place readily available and easily accessed policies, procedures, and protocols that address the challenges involved in caring for geriatric patients in the ED.
These might address screening for risk of added needs assessment, consultation, and intervention, for example. The guidelines offer specific recommendations and tools for medication management, fall assessment, use of urinary catheters, addressing delirium and dementia, and providing palliative care.
The detailed recommendations provided for each of these topics represent research- and consensus-based best practices from the perspectives of the agencies involved in their development, the authors note.
"Improved attention to the needs of this challenging population has the opportunity to more effectively allocate health care resources, optimize admission and readmission rates, while simultaneously decreasing iatrogenic complications and the resultant increased length-of-stay and decreased reimbursement," they wrote, concluding that with implementation of the recommendations, "hospitals, regardless of size, will positively impact the care of the geriatric emergency patients."
Meaningful use criteria bolster lung cancer screening program
ORLANDO – A novel lung cancer screening program based in part on smoking-related meaningful use criteria proved feasible and was successful for identifying patients at a National Comprehensive Cancer Network cancer center who were eligible for screening.
The program, which was launched in January 2013, led to the screening of 110 patients and the detection and treatment of three stage I lung cancers during the first 7 months, Dr. Dan J. Raz of the City of Hope Medical Center in Duarte, Calif., reported at the annual meeting of the Society of Thoracic Surgeons.
During the first 3 months of the program, before the tobacco screen was developed, only four patients were enrolled – two by physician referral and two by self-referral. At that point, the tobacco screen was implemented, and 418 patients potentially eligible for screening were identified, Dr. Raz said.
The tobacco screen, which contained smoking-related meaningful use criteria established by the Centers for Medicare & Medicaid Services as part of the standards for electronic health records (EHRs), was easily implemented and took an average of less than 2 minutes to complete and enter into the EHR, he noted.
Pack-year calculations and quit dates for former smokers also were included in the tobacco screen.
The lung cancer screening program – known as the tobacco exposure program – was run by a nurse practitioner who also was a licensed tobacco dependency counselor. The tobacco screen was administered to all ambulatory adult patients every 6 months. Weekly electronic reports were generated to identify patients who met criteria for lung cancer screening eligibility.
Those who met the criteria, and who hadn’t undergone a chest or head computed tomography (CT) scan in the prior 12 months and who weren’t undergoing cancer treatment, were contacted to review the information. The primary treating physician also was contacted regarding the plan for lung cancer screening.
"Disappointingly, only 14% of those [identified as potentially eligible] enrolled," he said.
Of the 110 patients ultimately screened, 53% were identified using the tobacco screen, 29% were self-referred, and 18% were physician-referred.
About half of the 418 patients identified as potentially eligible couldn’t be reached by phone, and another third didn’t meet eligibility criteria or didn’t participate for another reason, but only 10 (2%) refused because of cost. The hospital discounted the cost of the CT to $150 for those without insurance coverage.
A comparison of the groups of patients who were self-referred, physician-referred, and identified using the tobacco screen showed that Asian patients, who made up 25% of the total patient population at the hospital, were underrepresented in the tobacco screen group, and those with a history of cancer comprised 82% of the group identified by the tobacco screen, Dr. Raz said. The former finding could be attributed to a language barrier, and the latter finding is not surprising given that the study hospital is a cancer center, Dr. Raz said.
"Lung cancer screening with low-dose radiation CT scans saves lives, it’s safe, and it’s cost effective. The U.S. Preventive Services Task Force recommends lung cancer screening, as do a number of other professional organizations, including the STS [Society of Thoracic Surgeons]," he said.
Still, it is believed that only a minority of those eligible undergo screening, he added, noting that a 2013 survey suggested that the median number of patients screened per year per lung cancer screening program is only 10.
The current findings suggest that augmenting meaningful use tobacco questions as part of a lung cancer screening program is feasible. This approach increased participation in the City of Hope Medical Center screening program.
"We think it’s a method that other centers can use or that primary care physicians can use to identify patients within their programs or within their systems," he said, noting that use of the tobacco screen also provides clinicians with an opportunity for smoking cessation intervention. In addition, the tobacco screen represents a useful research tool in that it systematically collects data on tobacco history.
As the "resource-consuming" nature of the program might be considered a limitation, efforts are underway to implement an automatic alert system based on the EHR to flag patients who meet lung cancer screening criteria and to automatically book a consultation. The program might also be improved by better outreach to non-English-speaking patients, and through systematic referral of high-risk patients, Dr. Raz said.
Dr. Raz reported having no disclosures.
ORLANDO – A novel lung cancer screening program based in part on smoking-related meaningful use criteria proved feasible and was successful for identifying patients at a National Comprehensive Cancer Network cancer center who were eligible for screening.
The program, which was launched in January 2013, led to the screening of 110 patients and the detection and treatment of three stage I lung cancers during the first 7 months, Dr. Dan J. Raz of the City of Hope Medical Center in Duarte, Calif., reported at the annual meeting of the Society of Thoracic Surgeons.
During the first 3 months of the program, before the tobacco screen was developed, only four patients were enrolled – two by physician referral and two by self-referral. At that point, the tobacco screen was implemented, and 418 patients potentially eligible for screening were identified, Dr. Raz said.
The tobacco screen, which contained smoking-related meaningful use criteria established by the Centers for Medicare & Medicaid Services as part of the standards for electronic health records (EHRs), was easily implemented and took an average of less than 2 minutes to complete and enter into the EHR, he noted.
Pack-year calculations and quit dates for former smokers also were included in the tobacco screen.
The lung cancer screening program – known as the tobacco exposure program – was run by a nurse practitioner who also was a licensed tobacco dependency counselor. The tobacco screen was administered to all ambulatory adult patients every 6 months. Weekly electronic reports were generated to identify patients who met criteria for lung cancer screening eligibility.
Those who met the criteria, and who hadn’t undergone a chest or head computed tomography (CT) scan in the prior 12 months and who weren’t undergoing cancer treatment, were contacted to review the information. The primary treating physician also was contacted regarding the plan for lung cancer screening.
"Disappointingly, only 14% of those [identified as potentially eligible] enrolled," he said.
Of the 110 patients ultimately screened, 53% were identified using the tobacco screen, 29% were self-referred, and 18% were physician-referred.
About half of the 418 patients identified as potentially eligible couldn’t be reached by phone, and another third didn’t meet eligibility criteria or didn’t participate for another reason, but only 10 (2%) refused because of cost. The hospital discounted the cost of the CT to $150 for those without insurance coverage.
A comparison of the groups of patients who were self-referred, physician-referred, and identified using the tobacco screen showed that Asian patients, who made up 25% of the total patient population at the hospital, were underrepresented in the tobacco screen group, and those with a history of cancer comprised 82% of the group identified by the tobacco screen, Dr. Raz said. The former finding could be attributed to a language barrier, and the latter finding is not surprising given that the study hospital is a cancer center, Dr. Raz said.
"Lung cancer screening with low-dose radiation CT scans saves lives, it’s safe, and it’s cost effective. The U.S. Preventive Services Task Force recommends lung cancer screening, as do a number of other professional organizations, including the STS [Society of Thoracic Surgeons]," he said.
Still, it is believed that only a minority of those eligible undergo screening, he added, noting that a 2013 survey suggested that the median number of patients screened per year per lung cancer screening program is only 10.
The current findings suggest that augmenting meaningful use tobacco questions as part of a lung cancer screening program is feasible. This approach increased participation in the City of Hope Medical Center screening program.
"We think it’s a method that other centers can use or that primary care physicians can use to identify patients within their programs or within their systems," he said, noting that use of the tobacco screen also provides clinicians with an opportunity for smoking cessation intervention. In addition, the tobacco screen represents a useful research tool in that it systematically collects data on tobacco history.
As the "resource-consuming" nature of the program might be considered a limitation, efforts are underway to implement an automatic alert system based on the EHR to flag patients who meet lung cancer screening criteria and to automatically book a consultation. The program might also be improved by better outreach to non-English-speaking patients, and through systematic referral of high-risk patients, Dr. Raz said.
Dr. Raz reported having no disclosures.
ORLANDO – A novel lung cancer screening program based in part on smoking-related meaningful use criteria proved feasible and was successful for identifying patients at a National Comprehensive Cancer Network cancer center who were eligible for screening.
The program, which was launched in January 2013, led to the screening of 110 patients and the detection and treatment of three stage I lung cancers during the first 7 months, Dr. Dan J. Raz of the City of Hope Medical Center in Duarte, Calif., reported at the annual meeting of the Society of Thoracic Surgeons.
During the first 3 months of the program, before the tobacco screen was developed, only four patients were enrolled – two by physician referral and two by self-referral. At that point, the tobacco screen was implemented, and 418 patients potentially eligible for screening were identified, Dr. Raz said.
The tobacco screen, which contained smoking-related meaningful use criteria established by the Centers for Medicare & Medicaid Services as part of the standards for electronic health records (EHRs), was easily implemented and took an average of less than 2 minutes to complete and enter into the EHR, he noted.
Pack-year calculations and quit dates for former smokers also were included in the tobacco screen.
The lung cancer screening program – known as the tobacco exposure program – was run by a nurse practitioner who also was a licensed tobacco dependency counselor. The tobacco screen was administered to all ambulatory adult patients every 6 months. Weekly electronic reports were generated to identify patients who met criteria for lung cancer screening eligibility.
Those who met the criteria, and who hadn’t undergone a chest or head computed tomography (CT) scan in the prior 12 months and who weren’t undergoing cancer treatment, were contacted to review the information. The primary treating physician also was contacted regarding the plan for lung cancer screening.
"Disappointingly, only 14% of those [identified as potentially eligible] enrolled," he said.
Of the 110 patients ultimately screened, 53% were identified using the tobacco screen, 29% were self-referred, and 18% were physician-referred.
About half of the 418 patients identified as potentially eligible couldn’t be reached by phone, and another third didn’t meet eligibility criteria or didn’t participate for another reason, but only 10 (2%) refused because of cost. The hospital discounted the cost of the CT to $150 for those without insurance coverage.
A comparison of the groups of patients who were self-referred, physician-referred, and identified using the tobacco screen showed that Asian patients, who made up 25% of the total patient population at the hospital, were underrepresented in the tobacco screen group, and those with a history of cancer comprised 82% of the group identified by the tobacco screen, Dr. Raz said. The former finding could be attributed to a language barrier, and the latter finding is not surprising given that the study hospital is a cancer center, Dr. Raz said.
"Lung cancer screening with low-dose radiation CT scans saves lives, it’s safe, and it’s cost effective. The U.S. Preventive Services Task Force recommends lung cancer screening, as do a number of other professional organizations, including the STS [Society of Thoracic Surgeons]," he said.
Still, it is believed that only a minority of those eligible undergo screening, he added, noting that a 2013 survey suggested that the median number of patients screened per year per lung cancer screening program is only 10.
The current findings suggest that augmenting meaningful use tobacco questions as part of a lung cancer screening program is feasible. This approach increased participation in the City of Hope Medical Center screening program.
"We think it’s a method that other centers can use or that primary care physicians can use to identify patients within their programs or within their systems," he said, noting that use of the tobacco screen also provides clinicians with an opportunity for smoking cessation intervention. In addition, the tobacco screen represents a useful research tool in that it systematically collects data on tobacco history.
As the "resource-consuming" nature of the program might be considered a limitation, efforts are underway to implement an automatic alert system based on the EHR to flag patients who meet lung cancer screening criteria and to automatically book a consultation. The program might also be improved by better outreach to non-English-speaking patients, and through systematic referral of high-risk patients, Dr. Raz said.
Dr. Raz reported having no disclosures.
AT THE STS ANNUAL MEETING
Major finding: A total of 110 patients were screened, and three stage I lung cancers were detected and treated during the first 7 months of the screening program.
Data source: A novel lung cancer screening program.
Disclosures: Dr. Raz reported having no disclosures.
CBT: Making the most of a brief session
SAN ANTONIO – Cognitive-behavioral therapy, or CBT, can be effectively used during brief sessions in certain cases.
For example, brief CBT sessions can be useful in patients with Axis I disorders for which pharmacotherapy is being used effectively, and in patients in whom symptom complexity does not appear to require longer sessions, Dr. Donna M. Sudak and Dr. Jesse H. Wright said during a premeeting workshop at the annual meeting of the American College of Psychiatrists.
Other patients for whom brief CBT sessions might be indicated include inpatients; those with a preference for shorter sessions; those on long-term pharmacotherapy; and those with illnesses for which brief treatment may be advantageous, including psychosis, bipolar disorder, obsessive-compulsive disorder, uncomplicated anxiety disorders, and substance abuse requiring frequent visits, according to Dr. Sudak, professor and director of the psychotherapy training program at Drexel University, Philadelphia, and Dr. Wright, professor and director of the Depression Center at the University of Louisville (Ky.).
The format for providing brief CBT sessions can vary. For some patients, an initial evaluation followed by brief sessions might be appropriate. Other patients might be best served with several 50-minute sessions, followed by a transition to brief sessions later in treatment. Some patients might require a mixture of 50-minute and brief sessions, and some might do well with a team approach in which a psychiatrist provides brief sessions and a nonphysician CBT-trained therapist provides longer sessions or a nonphysician therapist provides therapy from a different orientation.
The selected format should be based on the patient’s need and preference, and can change over time, Dr. Wright said, noting that many patients prefer brief sessions because of time constraints.
Numerous high-yield interventions can be used in brief CBT sessions. Some examples include adherence enhancement; behavioral activation, which is particularly potent for treating depression; breathing retraining; CBT for insomnia, which is an area of increasing interest; cognitive-behavioral rehearsal; collaborative empiricism; collaborative goal setting; computer-assisted CBT; eliciting of and modification of automatic thoughts; exposure; cognitive error identification; motivational interviewing; psychoeducation; and relapse prevention.
Dr. Sudak and Dr. Wright shared several strategies aimed at enhancing the effect of brief CBT sessions.
Improving each session
First, make certain to have a clear formulation of the patient, they said.
Key elements of the formulation include diagnosis and symptoms; formative influences; situational issues and biological factors; strengths and assets; cross-sectional and longitudinal formulation; and a working hypothesis and treatment plan that is developed based on how all of these factors "pull together to influence the way this person thinks about the world, and [her] skill set in terms of working with other people and managing [her] own emotions."
Miniformulations developed during the course of care also can be helpful. These formulations address a specific issue that needs to be addressed "right now." Such formulations are collaboratively developed, simple and easily understood, and provide targeted direction for therapy interventions.
Dr. Sudak said she will sometimes draw a miniformulation on a whiteboard during a session, and will have the patient draw the same on a piece of paper to take home. She gave an example involving a "feedback loop" in a patient who hears teenage girls laughing while he is walking to the store. He experiences the thought that they are laughing at him, and that they therefore must think he is "a loser." This causes feelings of fear and sadness, leading him to keep his eyes down and return home without going to the store.
The miniformulation in this case involved drawing a circular graphic to outline the feedback loop and work on strategies for developing more realistic, healthier thoughts about being out in public, and for working on becoming more comfortable around other people, gradually increasing the ability to be in public settings.
A specific treatment plan should be developed for each session based on these formulations.
Techniques used in the course of treatment should include those that are most likely to be effective in briefer formats. Particularly high-yield techniques for brief CBT sessions include adherence enhancement, behavioral activation, and thought change records.
Also, special attention should be paid to the relationship and to pacing.
Enhancing the therapeutic relationship is important regardless of session length, but is particularly important for brief sessions, Dr. Wright said.
Helpful techniques for relationship building include emphasizing a team approach with shared responsibility; staying tuned to the patient’s emotion – and responding with accurate empathy; giving the patient your full attention and avoiding digressions; choosing targets for change with high relevance and opportunities for success; and building communication skills. In addition, listening carefully, giving clear explanations, summarizing key points, and asking for and giving feedback help build relationships.
As for pacing, Dr. Sudak advised thinking of CBT as a learning model; if too much material is given too quickly it won’t be absorbed.
Session notes help focus time
The use of therapy notes can help with maintaining the focus on session goals. Providing and requesting feedback also can help keep the session on target, and can provide a summary with take-home points.
Handouts and homework assignments are important for brief CBT sessions, and should be readily available; in the brief session setting, there is little time for searching and downloading. Keep handouts and/or an Internet resource list readily accessible. It might be helpful to have a library of handouts or self-help materials set up in your office, Dr. Sudak noted.
Homework assignments such as thought records and activity schedules can be useful but should be developed collaboratively and rehearsed in advance to allow for troubleshooting when obstacles arise. Always be sure to follow up on assignments from the last session, Dr. Sudak said.
Difficulties with homework completion occur and should be normalized. When such difficulties occur, the assignments should be evaluated to determine whether they were appropriate and relevant to the session or problem, and it should be determined whether the patient was adequately prepared. Starting or completing assignments during the session can help, and it is important to check for negative thoughts about the homework, and to identify barriers and find solutions, she said.
"When the homework doesn’t go so well, part of what we have to do is not give up on it. One of the things that happens a lot, I think ... is that it’s easier to jettison that plan than to figure out why it didn’t work," Dr. Sudak said.
Figuring out what the barriers are can be a learning experience for both patient and therapist.
Brief CBT sessions have a great deal of potential for helping many patients, but in Dr. Sudak’s and Dr. Wright’s experiences, brief CBT sessions should be avoided in:
• Those with a diagnosis and complexity that suggest a need for full-course, standard CBT. They might include patients with personality disorders, history of trauma, family conflict, resistant depression, or acute crisis.
• Patients in whom brief CBT sessions have been tried but did not appear to meet their needs.
Dr. Sudak and Dr. Wright are two of four coauthors of the book "High-Yield Cognitive-Behavior Therapy for Brief Sessions: An Illustrated Guide" (Washington: American Psychiatric Association, 2010). They receive book royalties from American Psychiatric Publishing; Lippincott Williams & Wilkins; and John Wiley & Sons. Dr. Sudak is also on the editorial board of, and receives honoraria from, Elsevier, and is a consultant for Takeda Pharmaceuticals. Dr. Wright also receives royalties for the development of software (Empower Interactive, Mindstreet).
SAN ANTONIO – Cognitive-behavioral therapy, or CBT, can be effectively used during brief sessions in certain cases.
For example, brief CBT sessions can be useful in patients with Axis I disorders for which pharmacotherapy is being used effectively, and in patients in whom symptom complexity does not appear to require longer sessions, Dr. Donna M. Sudak and Dr. Jesse H. Wright said during a premeeting workshop at the annual meeting of the American College of Psychiatrists.
Other patients for whom brief CBT sessions might be indicated include inpatients; those with a preference for shorter sessions; those on long-term pharmacotherapy; and those with illnesses for which brief treatment may be advantageous, including psychosis, bipolar disorder, obsessive-compulsive disorder, uncomplicated anxiety disorders, and substance abuse requiring frequent visits, according to Dr. Sudak, professor and director of the psychotherapy training program at Drexel University, Philadelphia, and Dr. Wright, professor and director of the Depression Center at the University of Louisville (Ky.).
The format for providing brief CBT sessions can vary. For some patients, an initial evaluation followed by brief sessions might be appropriate. Other patients might be best served with several 50-minute sessions, followed by a transition to brief sessions later in treatment. Some patients might require a mixture of 50-minute and brief sessions, and some might do well with a team approach in which a psychiatrist provides brief sessions and a nonphysician CBT-trained therapist provides longer sessions or a nonphysician therapist provides therapy from a different orientation.
The selected format should be based on the patient’s need and preference, and can change over time, Dr. Wright said, noting that many patients prefer brief sessions because of time constraints.
Numerous high-yield interventions can be used in brief CBT sessions. Some examples include adherence enhancement; behavioral activation, which is particularly potent for treating depression; breathing retraining; CBT for insomnia, which is an area of increasing interest; cognitive-behavioral rehearsal; collaborative empiricism; collaborative goal setting; computer-assisted CBT; eliciting of and modification of automatic thoughts; exposure; cognitive error identification; motivational interviewing; psychoeducation; and relapse prevention.
Dr. Sudak and Dr. Wright shared several strategies aimed at enhancing the effect of brief CBT sessions.
Improving each session
First, make certain to have a clear formulation of the patient, they said.
Key elements of the formulation include diagnosis and symptoms; formative influences; situational issues and biological factors; strengths and assets; cross-sectional and longitudinal formulation; and a working hypothesis and treatment plan that is developed based on how all of these factors "pull together to influence the way this person thinks about the world, and [her] skill set in terms of working with other people and managing [her] own emotions."
Miniformulations developed during the course of care also can be helpful. These formulations address a specific issue that needs to be addressed "right now." Such formulations are collaboratively developed, simple and easily understood, and provide targeted direction for therapy interventions.
Dr. Sudak said she will sometimes draw a miniformulation on a whiteboard during a session, and will have the patient draw the same on a piece of paper to take home. She gave an example involving a "feedback loop" in a patient who hears teenage girls laughing while he is walking to the store. He experiences the thought that they are laughing at him, and that they therefore must think he is "a loser." This causes feelings of fear and sadness, leading him to keep his eyes down and return home without going to the store.
The miniformulation in this case involved drawing a circular graphic to outline the feedback loop and work on strategies for developing more realistic, healthier thoughts about being out in public, and for working on becoming more comfortable around other people, gradually increasing the ability to be in public settings.
A specific treatment plan should be developed for each session based on these formulations.
Techniques used in the course of treatment should include those that are most likely to be effective in briefer formats. Particularly high-yield techniques for brief CBT sessions include adherence enhancement, behavioral activation, and thought change records.
Also, special attention should be paid to the relationship and to pacing.
Enhancing the therapeutic relationship is important regardless of session length, but is particularly important for brief sessions, Dr. Wright said.
Helpful techniques for relationship building include emphasizing a team approach with shared responsibility; staying tuned to the patient’s emotion – and responding with accurate empathy; giving the patient your full attention and avoiding digressions; choosing targets for change with high relevance and opportunities for success; and building communication skills. In addition, listening carefully, giving clear explanations, summarizing key points, and asking for and giving feedback help build relationships.
As for pacing, Dr. Sudak advised thinking of CBT as a learning model; if too much material is given too quickly it won’t be absorbed.
Session notes help focus time
The use of therapy notes can help with maintaining the focus on session goals. Providing and requesting feedback also can help keep the session on target, and can provide a summary with take-home points.
Handouts and homework assignments are important for brief CBT sessions, and should be readily available; in the brief session setting, there is little time for searching and downloading. Keep handouts and/or an Internet resource list readily accessible. It might be helpful to have a library of handouts or self-help materials set up in your office, Dr. Sudak noted.
Homework assignments such as thought records and activity schedules can be useful but should be developed collaboratively and rehearsed in advance to allow for troubleshooting when obstacles arise. Always be sure to follow up on assignments from the last session, Dr. Sudak said.
Difficulties with homework completion occur and should be normalized. When such difficulties occur, the assignments should be evaluated to determine whether they were appropriate and relevant to the session or problem, and it should be determined whether the patient was adequately prepared. Starting or completing assignments during the session can help, and it is important to check for negative thoughts about the homework, and to identify barriers and find solutions, she said.
"When the homework doesn’t go so well, part of what we have to do is not give up on it. One of the things that happens a lot, I think ... is that it’s easier to jettison that plan than to figure out why it didn’t work," Dr. Sudak said.
Figuring out what the barriers are can be a learning experience for both patient and therapist.
Brief CBT sessions have a great deal of potential for helping many patients, but in Dr. Sudak’s and Dr. Wright’s experiences, brief CBT sessions should be avoided in:
• Those with a diagnosis and complexity that suggest a need for full-course, standard CBT. They might include patients with personality disorders, history of trauma, family conflict, resistant depression, or acute crisis.
• Patients in whom brief CBT sessions have been tried but did not appear to meet their needs.
Dr. Sudak and Dr. Wright are two of four coauthors of the book "High-Yield Cognitive-Behavior Therapy for Brief Sessions: An Illustrated Guide" (Washington: American Psychiatric Association, 2010). They receive book royalties from American Psychiatric Publishing; Lippincott Williams & Wilkins; and John Wiley & Sons. Dr. Sudak is also on the editorial board of, and receives honoraria from, Elsevier, and is a consultant for Takeda Pharmaceuticals. Dr. Wright also receives royalties for the development of software (Empower Interactive, Mindstreet).
SAN ANTONIO – Cognitive-behavioral therapy, or CBT, can be effectively used during brief sessions in certain cases.
For example, brief CBT sessions can be useful in patients with Axis I disorders for which pharmacotherapy is being used effectively, and in patients in whom symptom complexity does not appear to require longer sessions, Dr. Donna M. Sudak and Dr. Jesse H. Wright said during a premeeting workshop at the annual meeting of the American College of Psychiatrists.
Other patients for whom brief CBT sessions might be indicated include inpatients; those with a preference for shorter sessions; those on long-term pharmacotherapy; and those with illnesses for which brief treatment may be advantageous, including psychosis, bipolar disorder, obsessive-compulsive disorder, uncomplicated anxiety disorders, and substance abuse requiring frequent visits, according to Dr. Sudak, professor and director of the psychotherapy training program at Drexel University, Philadelphia, and Dr. Wright, professor and director of the Depression Center at the University of Louisville (Ky.).
The format for providing brief CBT sessions can vary. For some patients, an initial evaluation followed by brief sessions might be appropriate. Other patients might be best served with several 50-minute sessions, followed by a transition to brief sessions later in treatment. Some patients might require a mixture of 50-minute and brief sessions, and some might do well with a team approach in which a psychiatrist provides brief sessions and a nonphysician CBT-trained therapist provides longer sessions or a nonphysician therapist provides therapy from a different orientation.
The selected format should be based on the patient’s need and preference, and can change over time, Dr. Wright said, noting that many patients prefer brief sessions because of time constraints.
Numerous high-yield interventions can be used in brief CBT sessions. Some examples include adherence enhancement; behavioral activation, which is particularly potent for treating depression; breathing retraining; CBT for insomnia, which is an area of increasing interest; cognitive-behavioral rehearsal; collaborative empiricism; collaborative goal setting; computer-assisted CBT; eliciting of and modification of automatic thoughts; exposure; cognitive error identification; motivational interviewing; psychoeducation; and relapse prevention.
Dr. Sudak and Dr. Wright shared several strategies aimed at enhancing the effect of brief CBT sessions.
Improving each session
First, make certain to have a clear formulation of the patient, they said.
Key elements of the formulation include diagnosis and symptoms; formative influences; situational issues and biological factors; strengths and assets; cross-sectional and longitudinal formulation; and a working hypothesis and treatment plan that is developed based on how all of these factors "pull together to influence the way this person thinks about the world, and [her] skill set in terms of working with other people and managing [her] own emotions."
Miniformulations developed during the course of care also can be helpful. These formulations address a specific issue that needs to be addressed "right now." Such formulations are collaboratively developed, simple and easily understood, and provide targeted direction for therapy interventions.
Dr. Sudak said she will sometimes draw a miniformulation on a whiteboard during a session, and will have the patient draw the same on a piece of paper to take home. She gave an example involving a "feedback loop" in a patient who hears teenage girls laughing while he is walking to the store. He experiences the thought that they are laughing at him, and that they therefore must think he is "a loser." This causes feelings of fear and sadness, leading him to keep his eyes down and return home without going to the store.
The miniformulation in this case involved drawing a circular graphic to outline the feedback loop and work on strategies for developing more realistic, healthier thoughts about being out in public, and for working on becoming more comfortable around other people, gradually increasing the ability to be in public settings.
A specific treatment plan should be developed for each session based on these formulations.
Techniques used in the course of treatment should include those that are most likely to be effective in briefer formats. Particularly high-yield techniques for brief CBT sessions include adherence enhancement, behavioral activation, and thought change records.
Also, special attention should be paid to the relationship and to pacing.
Enhancing the therapeutic relationship is important regardless of session length, but is particularly important for brief sessions, Dr. Wright said.
Helpful techniques for relationship building include emphasizing a team approach with shared responsibility; staying tuned to the patient’s emotion – and responding with accurate empathy; giving the patient your full attention and avoiding digressions; choosing targets for change with high relevance and opportunities for success; and building communication skills. In addition, listening carefully, giving clear explanations, summarizing key points, and asking for and giving feedback help build relationships.
As for pacing, Dr. Sudak advised thinking of CBT as a learning model; if too much material is given too quickly it won’t be absorbed.
Session notes help focus time
The use of therapy notes can help with maintaining the focus on session goals. Providing and requesting feedback also can help keep the session on target, and can provide a summary with take-home points.
Handouts and homework assignments are important for brief CBT sessions, and should be readily available; in the brief session setting, there is little time for searching and downloading. Keep handouts and/or an Internet resource list readily accessible. It might be helpful to have a library of handouts or self-help materials set up in your office, Dr. Sudak noted.
Homework assignments such as thought records and activity schedules can be useful but should be developed collaboratively and rehearsed in advance to allow for troubleshooting when obstacles arise. Always be sure to follow up on assignments from the last session, Dr. Sudak said.
Difficulties with homework completion occur and should be normalized. When such difficulties occur, the assignments should be evaluated to determine whether they were appropriate and relevant to the session or problem, and it should be determined whether the patient was adequately prepared. Starting or completing assignments during the session can help, and it is important to check for negative thoughts about the homework, and to identify barriers and find solutions, she said.
"When the homework doesn’t go so well, part of what we have to do is not give up on it. One of the things that happens a lot, I think ... is that it’s easier to jettison that plan than to figure out why it didn’t work," Dr. Sudak said.
Figuring out what the barriers are can be a learning experience for both patient and therapist.
Brief CBT sessions have a great deal of potential for helping many patients, but in Dr. Sudak’s and Dr. Wright’s experiences, brief CBT sessions should be avoided in:
• Those with a diagnosis and complexity that suggest a need for full-course, standard CBT. They might include patients with personality disorders, history of trauma, family conflict, resistant depression, or acute crisis.
• Patients in whom brief CBT sessions have been tried but did not appear to meet their needs.
Dr. Sudak and Dr. Wright are two of four coauthors of the book "High-Yield Cognitive-Behavior Therapy for Brief Sessions: An Illustrated Guide" (Washington: American Psychiatric Association, 2010). They receive book royalties from American Psychiatric Publishing; Lippincott Williams & Wilkins; and John Wiley & Sons. Dr. Sudak is also on the editorial board of, and receives honoraria from, Elsevier, and is a consultant for Takeda Pharmaceuticals. Dr. Wright also receives royalties for the development of software (Empower Interactive, Mindstreet).
EXPERT ANALYSIS FROM THE AMERICAN COLLEGE OF PSYCHIATRISTS MEETING
Symptom summary worksheets alert patients to signs of mania, depression
SAN ANTONIO – Don’t underestimate the value of a symptom summary worksheet when it comes to working with patients with bipolar disorder, Dr. Jesse H. Wright advised.
The symptom summary worksheet is a powerful tool for helping a patient learn to recognize the signs of an impending shift toward hypomania or depression, Dr. Wright said at the annual meeting of the American College of Psychiatrists.
The purpose of the worksheet is to help the patient and/or family members develop a customized list of early signs that such a shift is occurring, said Dr. Wright, professor and director of the depression center at the University of Louisville (Ky.).
The idea is to help the patient become more attuned to those signs, and to develop cognitive-behavioral or medication strategies that might interrupt the escalation into full-blown mania or very deep depression, he said during a workshop on cognitive-behavioral therapy for brief sessions.
Brief-session CBT can be useful in patients with bipolar disorder, and a review of the symptom summary worksheet can be incorporated into the session, he said.
"We want them to develop a skill set so that when they start to see something happening, they have something to do for it," he added.
Dr. Donna M. Sudak, who conducted the CBT workshop along with Dr. Wright, cautioned that symptom summary worksheets won’t necessarily have an immediate impact.
"It may not work the first time, but over time, as people really begin to develop the capacity to look at the onset of symptoms and catch it earlier, it’s really pretty remarkable. ... I call it an ‘early warning system,’ " said Dr. Sudak, professor and director of the psychotherapy training program at Drexel University, Philadelphia.
A simple example provided by Dr. Wright involved a patient who starts going to bed an hour later than usual and who spends that time surfing the Web, which gets her "worked up about new business ideas." This leads to sleep disruption, and she begins to escalate.
Monitoring this behavior allows for a plan to be put into place to address sleep hygiene issues when they arise.
"If she’s willing to do that, it might interrupt full-blown mania," Dr. Wright said.
Dr. Sudak and Dr. Wright are two of four coauthors of the book, "High-Yield Cognitive-Behavior Therapy for Brief Sessions: An Illustrated Guide (Washington: American Psychiatric Publishing, 2010). They both receive book royalties from American Psychiatric Publishing; Lippincott, Williams & Wilkins; and John Wiley & Sons. Dr. Sudak also serves on an editorial board, receives honoraria from Elsevier, and is a consultant for Takeda Pharmaceuticals. Dr. Wright also receives royalties for the development of software (Empower Interactive, Mindstreet).
SAN ANTONIO – Don’t underestimate the value of a symptom summary worksheet when it comes to working with patients with bipolar disorder, Dr. Jesse H. Wright advised.
The symptom summary worksheet is a powerful tool for helping a patient learn to recognize the signs of an impending shift toward hypomania or depression, Dr. Wright said at the annual meeting of the American College of Psychiatrists.
The purpose of the worksheet is to help the patient and/or family members develop a customized list of early signs that such a shift is occurring, said Dr. Wright, professor and director of the depression center at the University of Louisville (Ky.).
The idea is to help the patient become more attuned to those signs, and to develop cognitive-behavioral or medication strategies that might interrupt the escalation into full-blown mania or very deep depression, he said during a workshop on cognitive-behavioral therapy for brief sessions.
Brief-session CBT can be useful in patients with bipolar disorder, and a review of the symptom summary worksheet can be incorporated into the session, he said.
"We want them to develop a skill set so that when they start to see something happening, they have something to do for it," he added.
Dr. Donna M. Sudak, who conducted the CBT workshop along with Dr. Wright, cautioned that symptom summary worksheets won’t necessarily have an immediate impact.
"It may not work the first time, but over time, as people really begin to develop the capacity to look at the onset of symptoms and catch it earlier, it’s really pretty remarkable. ... I call it an ‘early warning system,’ " said Dr. Sudak, professor and director of the psychotherapy training program at Drexel University, Philadelphia.
A simple example provided by Dr. Wright involved a patient who starts going to bed an hour later than usual and who spends that time surfing the Web, which gets her "worked up about new business ideas." This leads to sleep disruption, and she begins to escalate.
Monitoring this behavior allows for a plan to be put into place to address sleep hygiene issues when they arise.
"If she’s willing to do that, it might interrupt full-blown mania," Dr. Wright said.
Dr. Sudak and Dr. Wright are two of four coauthors of the book, "High-Yield Cognitive-Behavior Therapy for Brief Sessions: An Illustrated Guide (Washington: American Psychiatric Publishing, 2010). They both receive book royalties from American Psychiatric Publishing; Lippincott, Williams & Wilkins; and John Wiley & Sons. Dr. Sudak also serves on an editorial board, receives honoraria from Elsevier, and is a consultant for Takeda Pharmaceuticals. Dr. Wright also receives royalties for the development of software (Empower Interactive, Mindstreet).
SAN ANTONIO – Don’t underestimate the value of a symptom summary worksheet when it comes to working with patients with bipolar disorder, Dr. Jesse H. Wright advised.
The symptom summary worksheet is a powerful tool for helping a patient learn to recognize the signs of an impending shift toward hypomania or depression, Dr. Wright said at the annual meeting of the American College of Psychiatrists.
The purpose of the worksheet is to help the patient and/or family members develop a customized list of early signs that such a shift is occurring, said Dr. Wright, professor and director of the depression center at the University of Louisville (Ky.).
The idea is to help the patient become more attuned to those signs, and to develop cognitive-behavioral or medication strategies that might interrupt the escalation into full-blown mania or very deep depression, he said during a workshop on cognitive-behavioral therapy for brief sessions.
Brief-session CBT can be useful in patients with bipolar disorder, and a review of the symptom summary worksheet can be incorporated into the session, he said.
"We want them to develop a skill set so that when they start to see something happening, they have something to do for it," he added.
Dr. Donna M. Sudak, who conducted the CBT workshop along with Dr. Wright, cautioned that symptom summary worksheets won’t necessarily have an immediate impact.
"It may not work the first time, but over time, as people really begin to develop the capacity to look at the onset of symptoms and catch it earlier, it’s really pretty remarkable. ... I call it an ‘early warning system,’ " said Dr. Sudak, professor and director of the psychotherapy training program at Drexel University, Philadelphia.
A simple example provided by Dr. Wright involved a patient who starts going to bed an hour later than usual and who spends that time surfing the Web, which gets her "worked up about new business ideas." This leads to sleep disruption, and she begins to escalate.
Monitoring this behavior allows for a plan to be put into place to address sleep hygiene issues when they arise.
"If she’s willing to do that, it might interrupt full-blown mania," Dr. Wright said.
Dr. Sudak and Dr. Wright are two of four coauthors of the book, "High-Yield Cognitive-Behavior Therapy for Brief Sessions: An Illustrated Guide (Washington: American Psychiatric Publishing, 2010). They both receive book royalties from American Psychiatric Publishing; Lippincott, Williams & Wilkins; and John Wiley & Sons. Dr. Sudak also serves on an editorial board, receives honoraria from Elsevier, and is a consultant for Takeda Pharmaceuticals. Dr. Wright also receives royalties for the development of software (Empower Interactive, Mindstreet).
EXPERT ANALYSIS FROM THE AMERICAN COLLEGE OF PSYCHIATRISTS MEETING