User login
Psoriasis and acne worse in winter, milder in summer
Psoriasis and acne appear to be susceptible to seasonal variations of clearing and worsening, with an analysis revealing both conditions maintained a significant trend of summer clearing and winter worsening, according to a research letter published in the Journal of the American Academy of Dermatology.
Using Physician’s Global Assessment scales for psoriasis and acne, Dr. Vanessa Lindsay Pascoe and Dr. Alexandra Boer Kimball, both of Massachusetts General Hospital, Boston, collected data from 5,468 psoriasis patients and 9,301 acne patients between June 2011 and May 2014 in the New England area. Among the psoriasis patient group, 16% were seen in the summer, 25% in the fall, 31% in the winter, and 28% in the spring. The trend was similar for acne patients, with 18% seen in the summer, 25% in the fall, 28% in the winter, and 29% in the spring. There were no significant seasonal differences in age or sex for either group.
The percentage of psoriasis patients with clear/almost clear disease was highest in the summer at 20.4%, while the percentage of patients with moderate/severe disease was highest in the winter at 40.5%. For acne, the percentage of patients with clear/almost clear disease was highest in the fall at 17.5%, and the percentage of patients with moderate/severe disease was highest in the winter at 45.9%. Fewer psoriasis and acne patients presented to the clinic in the summer, which the researchers suggested could be due to disease improvement.
“Although the climate of the Northeastern United States may not generalize to regions with less seasonal variation, providers may consider seasonal adjustment of acne plans as they have traditionally done for psoriasis,” the authors wrote. “For example, they may wait until after winter to taper a systemic antibiotic for acne, just as some providers may wait until spring to change systemic psoriasis treatments.”
Read the full article in the Journal of the American Academy of Dermatology.
Psoriasis and acne appear to be susceptible to seasonal variations of clearing and worsening, with an analysis revealing both conditions maintained a significant trend of summer clearing and winter worsening, according to a research letter published in the Journal of the American Academy of Dermatology.
Using Physician’s Global Assessment scales for psoriasis and acne, Dr. Vanessa Lindsay Pascoe and Dr. Alexandra Boer Kimball, both of Massachusetts General Hospital, Boston, collected data from 5,468 psoriasis patients and 9,301 acne patients between June 2011 and May 2014 in the New England area. Among the psoriasis patient group, 16% were seen in the summer, 25% in the fall, 31% in the winter, and 28% in the spring. The trend was similar for acne patients, with 18% seen in the summer, 25% in the fall, 28% in the winter, and 29% in the spring. There were no significant seasonal differences in age or sex for either group.
The percentage of psoriasis patients with clear/almost clear disease was highest in the summer at 20.4%, while the percentage of patients with moderate/severe disease was highest in the winter at 40.5%. For acne, the percentage of patients with clear/almost clear disease was highest in the fall at 17.5%, and the percentage of patients with moderate/severe disease was highest in the winter at 45.9%. Fewer psoriasis and acne patients presented to the clinic in the summer, which the researchers suggested could be due to disease improvement.
“Although the climate of the Northeastern United States may not generalize to regions with less seasonal variation, providers may consider seasonal adjustment of acne plans as they have traditionally done for psoriasis,” the authors wrote. “For example, they may wait until after winter to taper a systemic antibiotic for acne, just as some providers may wait until spring to change systemic psoriasis treatments.”
Read the full article in the Journal of the American Academy of Dermatology.
Psoriasis and acne appear to be susceptible to seasonal variations of clearing and worsening, with an analysis revealing both conditions maintained a significant trend of summer clearing and winter worsening, according to a research letter published in the Journal of the American Academy of Dermatology.
Using Physician’s Global Assessment scales for psoriasis and acne, Dr. Vanessa Lindsay Pascoe and Dr. Alexandra Boer Kimball, both of Massachusetts General Hospital, Boston, collected data from 5,468 psoriasis patients and 9,301 acne patients between June 2011 and May 2014 in the New England area. Among the psoriasis patient group, 16% were seen in the summer, 25% in the fall, 31% in the winter, and 28% in the spring. The trend was similar for acne patients, with 18% seen in the summer, 25% in the fall, 28% in the winter, and 29% in the spring. There were no significant seasonal differences in age or sex for either group.
The percentage of psoriasis patients with clear/almost clear disease was highest in the summer at 20.4%, while the percentage of patients with moderate/severe disease was highest in the winter at 40.5%. For acne, the percentage of patients with clear/almost clear disease was highest in the fall at 17.5%, and the percentage of patients with moderate/severe disease was highest in the winter at 45.9%. Fewer psoriasis and acne patients presented to the clinic in the summer, which the researchers suggested could be due to disease improvement.
“Although the climate of the Northeastern United States may not generalize to regions with less seasonal variation, providers may consider seasonal adjustment of acne plans as they have traditionally done for psoriasis,” the authors wrote. “For example, they may wait until after winter to taper a systemic antibiotic for acne, just as some providers may wait until spring to change systemic psoriasis treatments.”
Read the full article in the Journal of the American Academy of Dermatology.
Interviews with psoriasis patients reveal disease hardships
Interviewing patients who live with psoriasis can reveal important information not included in psoriasis severity measures, according to Dr. David Pariser of Eastern Virginia Medical School, Norfolk, and his associates.
More than 90% of 101 patients with moderate to severe plaque psoriasis, with and without psoriatic arthritis, reported emotional and social impacts to their lives. Social impacts included avoiding/changing activities, relationships, or trying new things. Emotional impacts included a sense of anger, frustration, embarrassment, and self-consciousness; a lowered sense of self-esteem was common. Patients reported impacts in family, professional, social, and educational areas.
Patients with psoriasis and psoriatic arthritis tended to report both symptoms and well-being complications more often, with 77% reporting physical impacts and 34% reporting educational impacts, compared with 38% and 17%, respectively, for those with psoriasis only.
The study data “provide practitioners with deep insight into how patients with moderate to severe psoriasis are suffering, regardless of whether the concerns are elucidated during patient visits. The burdens in patients’ lives support the use of effective treatment; indeed, patients expressed how they value physicians who are knowledgeable about psoriasis and who will try various therapies,” the investigators concluded.
Find the full study in the Journal of Dermatological Treatment (doi: 10.3109/09546634.2015.1044492).
Interviewing patients who live with psoriasis can reveal important information not included in psoriasis severity measures, according to Dr. David Pariser of Eastern Virginia Medical School, Norfolk, and his associates.
More than 90% of 101 patients with moderate to severe plaque psoriasis, with and without psoriatic arthritis, reported emotional and social impacts to their lives. Social impacts included avoiding/changing activities, relationships, or trying new things. Emotional impacts included a sense of anger, frustration, embarrassment, and self-consciousness; a lowered sense of self-esteem was common. Patients reported impacts in family, professional, social, and educational areas.
Patients with psoriasis and psoriatic arthritis tended to report both symptoms and well-being complications more often, with 77% reporting physical impacts and 34% reporting educational impacts, compared with 38% and 17%, respectively, for those with psoriasis only.
The study data “provide practitioners with deep insight into how patients with moderate to severe psoriasis are suffering, regardless of whether the concerns are elucidated during patient visits. The burdens in patients’ lives support the use of effective treatment; indeed, patients expressed how they value physicians who are knowledgeable about psoriasis and who will try various therapies,” the investigators concluded.
Find the full study in the Journal of Dermatological Treatment (doi: 10.3109/09546634.2015.1044492).
Interviewing patients who live with psoriasis can reveal important information not included in psoriasis severity measures, according to Dr. David Pariser of Eastern Virginia Medical School, Norfolk, and his associates.
More than 90% of 101 patients with moderate to severe plaque psoriasis, with and without psoriatic arthritis, reported emotional and social impacts to their lives. Social impacts included avoiding/changing activities, relationships, or trying new things. Emotional impacts included a sense of anger, frustration, embarrassment, and self-consciousness; a lowered sense of self-esteem was common. Patients reported impacts in family, professional, social, and educational areas.
Patients with psoriasis and psoriatic arthritis tended to report both symptoms and well-being complications more often, with 77% reporting physical impacts and 34% reporting educational impacts, compared with 38% and 17%, respectively, for those with psoriasis only.
The study data “provide practitioners with deep insight into how patients with moderate to severe psoriasis are suffering, regardless of whether the concerns are elucidated during patient visits. The burdens in patients’ lives support the use of effective treatment; indeed, patients expressed how they value physicians who are knowledgeable about psoriasis and who will try various therapies,” the investigators concluded.
Find the full study in the Journal of Dermatological Treatment (doi: 10.3109/09546634.2015.1044492).
Psoriasis and herpes are most stigmatized dermatologic conditions
Attitudes toward psoriasis and herpes are significantly more stigmatizing than are perceptions of other dermatologic conditions, reported Dr. Jessica M. Donigan and her associates from Massachusetts General Hospital in Boston.
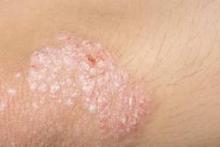
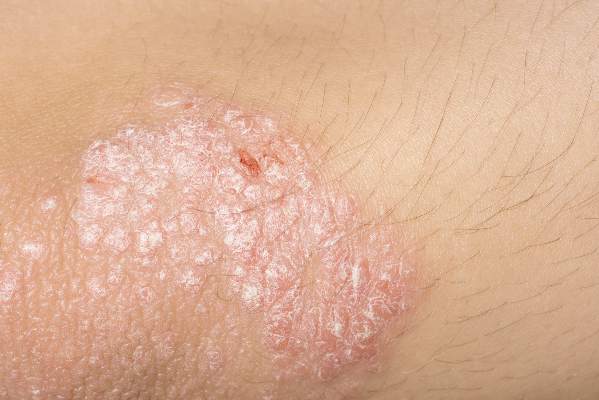
In a survey of 56 adults without any skin conditions aside from typical teenage acne, investigators used an image-based questionnaire to assess attitudes toward psoriasis, compared with other skin conditions such as atopic dermatitis, acne, vitiligo, rosacea, herpes labialis, warts, and tinea versicolor. At least 48% of respondents reported feeling upset by images of psoriasis, although significantly more were upset by images of herpes. Additionally, about 61% believed psoriasis had an infectious cause, with 41% of participants thinking psoriasis lesions looked contagious because of scale, color, and size, the authors reported.
A total of 39% of respondents thought herpes was the most-bothersome skin disease, compared with 30% for psoriasis, although this difference was not significant (P = .42). As many as 86% said they would feel pity if they saw a person with psoriasis, which was significantly greater for any of the other dermatologic conditions except acne, the investigators said.
The findings suggest that “misconceptions of infection and contagion, and feelings of pity cause psoriasis to be as bothersome as herpes labialis,” Dr. Donigan and her colleagues said.
Additionally, despite participants perceiving the two conditions as similarly bothersome, psoriasis may “have a greater overall impact on quality of life because of its continuity and chronicity,” they said. “Because of its potential lifelong impact, it is important to familiarize the public with psoriasis to aid in destigmatization.”
Read the full report in the Journal of the American Academy of Dermatology.
Attitudes toward psoriasis and herpes are significantly more stigmatizing than are perceptions of other dermatologic conditions, reported Dr. Jessica M. Donigan and her associates from Massachusetts General Hospital in Boston.
In a survey of 56 adults without any skin conditions aside from typical teenage acne, investigators used an image-based questionnaire to assess attitudes toward psoriasis, compared with other skin conditions such as atopic dermatitis, acne, vitiligo, rosacea, herpes labialis, warts, and tinea versicolor. At least 48% of respondents reported feeling upset by images of psoriasis, although significantly more were upset by images of herpes. Additionally, about 61% believed psoriasis had an infectious cause, with 41% of participants thinking psoriasis lesions looked contagious because of scale, color, and size, the authors reported.
A total of 39% of respondents thought herpes was the most-bothersome skin disease, compared with 30% for psoriasis, although this difference was not significant (P = .42). As many as 86% said they would feel pity if they saw a person with psoriasis, which was significantly greater for any of the other dermatologic conditions except acne, the investigators said.
The findings suggest that “misconceptions of infection and contagion, and feelings of pity cause psoriasis to be as bothersome as herpes labialis,” Dr. Donigan and her colleagues said.
Additionally, despite participants perceiving the two conditions as similarly bothersome, psoriasis may “have a greater overall impact on quality of life because of its continuity and chronicity,” they said. “Because of its potential lifelong impact, it is important to familiarize the public with psoriasis to aid in destigmatization.”
Read the full report in the Journal of the American Academy of Dermatology.
Attitudes toward psoriasis and herpes are significantly more stigmatizing than are perceptions of other dermatologic conditions, reported Dr. Jessica M. Donigan and her associates from Massachusetts General Hospital in Boston.
In a survey of 56 adults without any skin conditions aside from typical teenage acne, investigators used an image-based questionnaire to assess attitudes toward psoriasis, compared with other skin conditions such as atopic dermatitis, acne, vitiligo, rosacea, herpes labialis, warts, and tinea versicolor. At least 48% of respondents reported feeling upset by images of psoriasis, although significantly more were upset by images of herpes. Additionally, about 61% believed psoriasis had an infectious cause, with 41% of participants thinking psoriasis lesions looked contagious because of scale, color, and size, the authors reported.
A total of 39% of respondents thought herpes was the most-bothersome skin disease, compared with 30% for psoriasis, although this difference was not significant (P = .42). As many as 86% said they would feel pity if they saw a person with psoriasis, which was significantly greater for any of the other dermatologic conditions except acne, the investigators said.
The findings suggest that “misconceptions of infection and contagion, and feelings of pity cause psoriasis to be as bothersome as herpes labialis,” Dr. Donigan and her colleagues said.
Additionally, despite participants perceiving the two conditions as similarly bothersome, psoriasis may “have a greater overall impact on quality of life because of its continuity and chronicity,” they said. “Because of its potential lifelong impact, it is important to familiarize the public with psoriasis to aid in destigmatization.”
Read the full report in the Journal of the American Academy of Dermatology.
Higher risk of arrhythmia in psoriasis patients
Patients with psoriasis are at increased risk of arrhythmia, with the risk even greater for younger patients and those with psoriatic arthritis, according to a population-based cohort study conducted in Taiwan.
Dr. Hsien-Yi Chiu of National Taiwan University and Wei-Lun Chang of National Yang-Ming University, both in Taipei, and their colleagues, looked at records from 40,637 patients diagnosed with psoriasis and 162,548 age- and sex-matched controls without psoriasis, over a mean follow-up of about 6 years, for the incidence of arrhythmias over a mean of 6 years.
In an article published in the September issue of the Journal of the American Academy of Dermatology, the investigators reported that those patients with psoriasis were at a significantly higher risk of developing arrhythmia, independent of traditional cardiovascular risk factors (adjusted hazard ratio, 1.34; 95% confidence interval, 1.29-1.39). Increased risk for patients with mild disease (aHR,1.35; 95% CI, 1.30-1.41) was comparable to that of patients with severe disease (aHR, 1.25; 95% CI 1.12-1.39) and more pronounced in the subgroup of patients with psoriatic arthritis (aHR, 1.46; 95% CI, 1.22-1.74). Younger patients, between aged 20 and 39 years, were at a higher risk (aHR, 1.39; 95% CI, 1.26-1.54) than older patients in the cohort (J Am Acad Dermatol. 2015 Sep;73:429-38).
Although previous studies have shown severe psoriasis to be associated with a nearly 60% increase in cardiovascular morbidity and mortality beyond traditional risk factors, less is known about arrhythmias specifically. “Inflammation may contribute to the alteration of cardiomyocyte electrophysiology, such as dysregulation of ion channel function, leading to increased risk of arrhythmia,” the investigators wrote.
The authors noted that limitations of their study were the potential surveillance bias for psoriasis patients due to increased hospital visits, and the fact that alcohol and tobacco use was not captured in the patient data. Treatment with systemic therapies may lower cardiovascular risk in psoriasis patients, they added, which may have explained why the arrhythmia risk among patients with severe disease was similar to those with mild disease.
The findings indicate “that psoriasis can be added to future risk-stratification scores for arrhythmia,” the investigators wrote, adding that patients with psoriasis, “especially young patients and those with PsA [psoriatic arthritis] , should be more closely screened for various types of arrhythmia,” with the hope of earlier intervention leading to reduction of cardiovascular morbidity and mortality.
Patients with psoriasis are at increased risk of arrhythmia, with the risk even greater for younger patients and those with psoriatic arthritis, according to a population-based cohort study conducted in Taiwan.
Dr. Hsien-Yi Chiu of National Taiwan University and Wei-Lun Chang of National Yang-Ming University, both in Taipei, and their colleagues, looked at records from 40,637 patients diagnosed with psoriasis and 162,548 age- and sex-matched controls without psoriasis, over a mean follow-up of about 6 years, for the incidence of arrhythmias over a mean of 6 years.
In an article published in the September issue of the Journal of the American Academy of Dermatology, the investigators reported that those patients with psoriasis were at a significantly higher risk of developing arrhythmia, independent of traditional cardiovascular risk factors (adjusted hazard ratio, 1.34; 95% confidence interval, 1.29-1.39). Increased risk for patients with mild disease (aHR,1.35; 95% CI, 1.30-1.41) was comparable to that of patients with severe disease (aHR, 1.25; 95% CI 1.12-1.39) and more pronounced in the subgroup of patients with psoriatic arthritis (aHR, 1.46; 95% CI, 1.22-1.74). Younger patients, between aged 20 and 39 years, were at a higher risk (aHR, 1.39; 95% CI, 1.26-1.54) than older patients in the cohort (J Am Acad Dermatol. 2015 Sep;73:429-38).
Although previous studies have shown severe psoriasis to be associated with a nearly 60% increase in cardiovascular morbidity and mortality beyond traditional risk factors, less is known about arrhythmias specifically. “Inflammation may contribute to the alteration of cardiomyocyte electrophysiology, such as dysregulation of ion channel function, leading to increased risk of arrhythmia,” the investigators wrote.
The authors noted that limitations of their study were the potential surveillance bias for psoriasis patients due to increased hospital visits, and the fact that alcohol and tobacco use was not captured in the patient data. Treatment with systemic therapies may lower cardiovascular risk in psoriasis patients, they added, which may have explained why the arrhythmia risk among patients with severe disease was similar to those with mild disease.
The findings indicate “that psoriasis can be added to future risk-stratification scores for arrhythmia,” the investigators wrote, adding that patients with psoriasis, “especially young patients and those with PsA [psoriatic arthritis] , should be more closely screened for various types of arrhythmia,” with the hope of earlier intervention leading to reduction of cardiovascular morbidity and mortality.
Patients with psoriasis are at increased risk of arrhythmia, with the risk even greater for younger patients and those with psoriatic arthritis, according to a population-based cohort study conducted in Taiwan.
Dr. Hsien-Yi Chiu of National Taiwan University and Wei-Lun Chang of National Yang-Ming University, both in Taipei, and their colleagues, looked at records from 40,637 patients diagnosed with psoriasis and 162,548 age- and sex-matched controls without psoriasis, over a mean follow-up of about 6 years, for the incidence of arrhythmias over a mean of 6 years.
In an article published in the September issue of the Journal of the American Academy of Dermatology, the investigators reported that those patients with psoriasis were at a significantly higher risk of developing arrhythmia, independent of traditional cardiovascular risk factors (adjusted hazard ratio, 1.34; 95% confidence interval, 1.29-1.39). Increased risk for patients with mild disease (aHR,1.35; 95% CI, 1.30-1.41) was comparable to that of patients with severe disease (aHR, 1.25; 95% CI 1.12-1.39) and more pronounced in the subgroup of patients with psoriatic arthritis (aHR, 1.46; 95% CI, 1.22-1.74). Younger patients, between aged 20 and 39 years, were at a higher risk (aHR, 1.39; 95% CI, 1.26-1.54) than older patients in the cohort (J Am Acad Dermatol. 2015 Sep;73:429-38).
Although previous studies have shown severe psoriasis to be associated with a nearly 60% increase in cardiovascular morbidity and mortality beyond traditional risk factors, less is known about arrhythmias specifically. “Inflammation may contribute to the alteration of cardiomyocyte electrophysiology, such as dysregulation of ion channel function, leading to increased risk of arrhythmia,” the investigators wrote.
The authors noted that limitations of their study were the potential surveillance bias for psoriasis patients due to increased hospital visits, and the fact that alcohol and tobacco use was not captured in the patient data. Treatment with systemic therapies may lower cardiovascular risk in psoriasis patients, they added, which may have explained why the arrhythmia risk among patients with severe disease was similar to those with mild disease.
The findings indicate “that psoriasis can be added to future risk-stratification scores for arrhythmia,” the investigators wrote, adding that patients with psoriasis, “especially young patients and those with PsA [psoriatic arthritis] , should be more closely screened for various types of arrhythmia,” with the hope of earlier intervention leading to reduction of cardiovascular morbidity and mortality.
FROM THE JOURNAL OF THE AMERICAN ACADEMY OF DERMATOLOGY
Key clinical point: Patients with psoriasis are at an increased risk of developing arrhythmias compared to those without psoriasis.
Major finding: After researchers adjusted for medical history and medication use, patients with psoriasis were at increased risk of overall arrhythmia (adjusted hazard ratio, 1.34; 95% confidence interval, 1.29-1.39).
Data source: A retrospective cohort study using data from almost 41,000 psoriasis patients identified from the Taiwan National Health Insurance Research Database, and almost 163,000 age and sex-matched cohorts from the same database
Disclosures: Study was institutionally funded. Dr. Chiu, Ms. Chang, and three other authors had no disclosures; one author disclosed having conducted clinical trials, or having received honoraria from several companies, including Pfizer and Novartis, and having received speaking fees from AbbVie.
Celiac disease ‘as common as psoriasis’
PARK CITY, UTAH – Dr. John J. Zone first began to study gluten sensitivity in 1977, an interest that left some of his clinician colleagues wondering why.
“Everybody told me I was crazy – that this was extremely rare. So I always say I was gluten when gluten wasn’t cool,” Dr. Zone, professor and chairman of dermatology at the University of Utah, Salt Lake City, told attendees at the annual meeting of the Pacific Dermatologic Association.
These days, it’s hard to shop in a food market without noticing all the gluten-free foods available, from pizza dough to beer. Many restaurants also serve gluten-free dishes. But is it hype, or is gluten sensitivity that common? Five percent of people in the United States “will say they are gluten sensitive,” he said. “In fact, 1% of Caucasians actually have celiac disease and 1% of Caucasians have gluten sensitivity that can be documented by challenge but don’t have celiac disease, while 3% have nothing.”
Gluten is a group of proteins contained in wheat, barley, and rye that is insoluble in water. Dr. Zone described celiac disease as a “spectrum of disease” characterized by inflammation of the small intestinal mucosa that occurs with the ingestion of gluten. The condition improves when gluten is removed from the diet. From a genetic standpoint, having a predisposition to express human leukocyte antigen-DQ2 or HLA-DQ8 is required for a diagnosis of celiac disease (CD). An estimated 20%-25% of whites “have that HLA background, but it is rare in Asians,” he said. “The receptors coded by HLA genes are essential for the processing of the gliadin antigen in CD.”
The hallmark for CD is a blood test for immunoglobulin A (IgA) anti-tissue transglutaminase antibodies, which are detectable in patients with untreated disease. “You should be able to get that test for $50 or $60 in any laboratory in the country,” Dr. Zone said. “It’s about 98% reliable. You also want to do a total serum IgA to rule out IgA-deficiency.”
CD clusters with other autoimmune disorders such as Addison’s disease, autoimmune thyroiditis, atrophic gastritis, systemic lupus erythematosus, rheumatoid arthritis, myasthenia gravis, and vitiligo. It’s also common in Down syndrome. “Many patients with histological inflammation have atypical intestinal symptoms or none at all,” he said. “Clinical studies have shown that only 15%-20% of CD patients identified by serology and confirmed by biopsy have classical symptoms of diarrhea and malabsorption.” The presenting symptom in patients with celiac disease may be limited to only aphthous stomatitis, eczema, alopecia areata, psoriasis, or diabetes, along with fatigue or anemia.
Researchers who analyzed the prevalence of CD in the United States estimated the risk to be 1:133 among individuals deemed not to be at risk, 1:56 in symptomatic patients, 1:39 in second-degree relatives, and 1:22 in first-degree relatives (Arch Intern Med. 2003;163[3]:286-92.). “We tested 2,100 people in Utah and found the prevalence among first-degree relatives was 1:12,” Dr. Zone said. “The point is that CD is common, not rare. It’s as common as psoriasis. It profoundly affects the immune system, which is the modulator of inflammatory skin disease.”
Dr. Zone reported having no financial disclosures.
PARK CITY, UTAH – Dr. John J. Zone first began to study gluten sensitivity in 1977, an interest that left some of his clinician colleagues wondering why.
“Everybody told me I was crazy – that this was extremely rare. So I always say I was gluten when gluten wasn’t cool,” Dr. Zone, professor and chairman of dermatology at the University of Utah, Salt Lake City, told attendees at the annual meeting of the Pacific Dermatologic Association.
These days, it’s hard to shop in a food market without noticing all the gluten-free foods available, from pizza dough to beer. Many restaurants also serve gluten-free dishes. But is it hype, or is gluten sensitivity that common? Five percent of people in the United States “will say they are gluten sensitive,” he said. “In fact, 1% of Caucasians actually have celiac disease and 1% of Caucasians have gluten sensitivity that can be documented by challenge but don’t have celiac disease, while 3% have nothing.”
Gluten is a group of proteins contained in wheat, barley, and rye that is insoluble in water. Dr. Zone described celiac disease as a “spectrum of disease” characterized by inflammation of the small intestinal mucosa that occurs with the ingestion of gluten. The condition improves when gluten is removed from the diet. From a genetic standpoint, having a predisposition to express human leukocyte antigen-DQ2 or HLA-DQ8 is required for a diagnosis of celiac disease (CD). An estimated 20%-25% of whites “have that HLA background, but it is rare in Asians,” he said. “The receptors coded by HLA genes are essential for the processing of the gliadin antigen in CD.”
The hallmark for CD is a blood test for immunoglobulin A (IgA) anti-tissue transglutaminase antibodies, which are detectable in patients with untreated disease. “You should be able to get that test for $50 or $60 in any laboratory in the country,” Dr. Zone said. “It’s about 98% reliable. You also want to do a total serum IgA to rule out IgA-deficiency.”
CD clusters with other autoimmune disorders such as Addison’s disease, autoimmune thyroiditis, atrophic gastritis, systemic lupus erythematosus, rheumatoid arthritis, myasthenia gravis, and vitiligo. It’s also common in Down syndrome. “Many patients with histological inflammation have atypical intestinal symptoms or none at all,” he said. “Clinical studies have shown that only 15%-20% of CD patients identified by serology and confirmed by biopsy have classical symptoms of diarrhea and malabsorption.” The presenting symptom in patients with celiac disease may be limited to only aphthous stomatitis, eczema, alopecia areata, psoriasis, or diabetes, along with fatigue or anemia.
Researchers who analyzed the prevalence of CD in the United States estimated the risk to be 1:133 among individuals deemed not to be at risk, 1:56 in symptomatic patients, 1:39 in second-degree relatives, and 1:22 in first-degree relatives (Arch Intern Med. 2003;163[3]:286-92.). “We tested 2,100 people in Utah and found the prevalence among first-degree relatives was 1:12,” Dr. Zone said. “The point is that CD is common, not rare. It’s as common as psoriasis. It profoundly affects the immune system, which is the modulator of inflammatory skin disease.”
Dr. Zone reported having no financial disclosures.
PARK CITY, UTAH – Dr. John J. Zone first began to study gluten sensitivity in 1977, an interest that left some of his clinician colleagues wondering why.
“Everybody told me I was crazy – that this was extremely rare. So I always say I was gluten when gluten wasn’t cool,” Dr. Zone, professor and chairman of dermatology at the University of Utah, Salt Lake City, told attendees at the annual meeting of the Pacific Dermatologic Association.
These days, it’s hard to shop in a food market without noticing all the gluten-free foods available, from pizza dough to beer. Many restaurants also serve gluten-free dishes. But is it hype, or is gluten sensitivity that common? Five percent of people in the United States “will say they are gluten sensitive,” he said. “In fact, 1% of Caucasians actually have celiac disease and 1% of Caucasians have gluten sensitivity that can be documented by challenge but don’t have celiac disease, while 3% have nothing.”
Gluten is a group of proteins contained in wheat, barley, and rye that is insoluble in water. Dr. Zone described celiac disease as a “spectrum of disease” characterized by inflammation of the small intestinal mucosa that occurs with the ingestion of gluten. The condition improves when gluten is removed from the diet. From a genetic standpoint, having a predisposition to express human leukocyte antigen-DQ2 or HLA-DQ8 is required for a diagnosis of celiac disease (CD). An estimated 20%-25% of whites “have that HLA background, but it is rare in Asians,” he said. “The receptors coded by HLA genes are essential for the processing of the gliadin antigen in CD.”
The hallmark for CD is a blood test for immunoglobulin A (IgA) anti-tissue transglutaminase antibodies, which are detectable in patients with untreated disease. “You should be able to get that test for $50 or $60 in any laboratory in the country,” Dr. Zone said. “It’s about 98% reliable. You also want to do a total serum IgA to rule out IgA-deficiency.”
CD clusters with other autoimmune disorders such as Addison’s disease, autoimmune thyroiditis, atrophic gastritis, systemic lupus erythematosus, rheumatoid arthritis, myasthenia gravis, and vitiligo. It’s also common in Down syndrome. “Many patients with histological inflammation have atypical intestinal symptoms or none at all,” he said. “Clinical studies have shown that only 15%-20% of CD patients identified by serology and confirmed by biopsy have classical symptoms of diarrhea and malabsorption.” The presenting symptom in patients with celiac disease may be limited to only aphthous stomatitis, eczema, alopecia areata, psoriasis, or diabetes, along with fatigue or anemia.
Researchers who analyzed the prevalence of CD in the United States estimated the risk to be 1:133 among individuals deemed not to be at risk, 1:56 in symptomatic patients, 1:39 in second-degree relatives, and 1:22 in first-degree relatives (Arch Intern Med. 2003;163[3]:286-92.). “We tested 2,100 people in Utah and found the prevalence among first-degree relatives was 1:12,” Dr. Zone said. “The point is that CD is common, not rare. It’s as common as psoriasis. It profoundly affects the immune system, which is the modulator of inflammatory skin disease.”
Dr. Zone reported having no financial disclosures.
EXPERT ANALYSIS FROM PDA 2015
Simple screening tool can help detect psoriatic arthritis
PARK CITY, UTAH – Since most people with psoriatic arthritis (PsA) develop psoriasis before joint symptoms, it’s helpful to have a simple screening test for the condition.
One of Dr. Philip Mease’s favorite PsA screening tools is the Psoriasis Epidemiology Screening Test (PEST), which was first described at the 2009 annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis (GRAPPA) and consists of five simple questions. They are: Have you ever had a swollen joint (or joints)? Has a doctor ever told you that you have arthritis? Do your fingernails or toes have holes or pits? Have you had pain in your heel? Have you had a finger or toe that was completely swollen and painful for no apparent reason? (Clin Exp Rheumatol. 2009;27:469-74).
“Just these five simple questions, or trying to remember a few of them, can help you in your review of systems,” Dr. Mease, director of arthritis research at Swedish Medical Center, Seattle, said at the annual meeting of the Pacific Dermatologic Association. “I think patients appreciate it when you look beyond the skin in your questioning. These can pick up [PsA] with a high sensitivity and specificity” of 0.92 and 0.78, respectively.
He went on to discuss current PsA treatment approaches. According to an evidence review that he and his associates in GRAPPA published in 2009, biologics (anti–tumor necrosis factor inhibitors) as a group were found to be effective in all five domains of the disease: peripheral arthritis, skin and nail disease, axial disease, dactylitis, and enthesitis, while the oral disease-modifying antirheumatic drugs (DMARDs) were effective for peripheral arthritis and skin and nail disease.
Other treatments that were found effective are: psoralen and UVA/UVB for skin and nail disease, physiotherapy for axial disease, intra-articular steroids for peripheral arthritis, and NSAIDs for peripheral arthritis and axial disease (J Rheum. 2009;33:1417-21). “Patients with mild disease can be tried on NSAIDs, especially in a patient with monoarticular disease, but for the most part we need to move on to using systemic medication,” he said. Updated recommendations from GRAPPA include new data regarding ustekinumab, apremilast, and secukinumab, as well as data on comorbidities (J Rheumatol. 2015;42[6]:1052-5).
According to Dr. Mease, controlled trials of DMARDs in PsA patients have yielded treatment effects that range from marginal in the joints to marginal or none at all in the skin. Data from the Methotrexate in Psoriatic Arthritis trial conducted in the United Kingdom and published in 2012 showed no evidence that methotrexate improves inflammatory synovitis in active PsA (Rheumatol. 2012;51:1368-77).
“There were issues with this trial, including the fact that it took 5 years to enroll patients, and many dropped out, so I don’t think it’s a very reliable study,” said Dr. Mease, who is also a professor of medicine in the division of rheumatology at the University of Washington, Seattle. “Currently, Amgen is in the process of starting a trial in which the goal is to enroll 840 subjects with early PsA who are being randomized to methotrexate alone, Enbrel alone, or Enbrel plus methotrexate. This, I think, is going to give us a better answer about the effectiveness of methotrexate. It will also teach us about whether there’s a value in combining an anti-TNF inhibitor with methotrexate. We still don’t know the answer to that question.”
The most recent data on methotrexate come from an open-label trial known as TICOPA, which used a tight control treatment paradigm through 48 weeks of treatment. A subanalysis of 188 patients treated with methotrexate through 12 weeks was presented at the 2015 meeting of the European League Against Rheumatism. It revealed that 41% of patients achieved an ACR 20, 22% achieved minimal disease activity, 62% experienced an improvement in dactylitis, and 25% experienced an improvement in enthesitis.
“So we have a few data suggesting that methotrexate may be modestly effective in treating PsA,” Dr. Mease said. “We often will start with methotrexate unless the patient has really aggressive disease activity. If they get some effect from the drug but not enough, we’ll often add a biologic agent but often keep some methotrexate in the background, even at 10 mg per week, in order to reduce immunogenicity from a biologic.”
Dr. Mease disclosed that he has received research grants, consultation fees, and/or speaker honoraria from AbbVie, Amgen, Bristol-Myers Squibb, Celgene, Crescendo Bioscience, Genentech, GlaxoSmithKline, Janssen, Eli Lilly, Merck, Novartis, Pfizer, and UCB.
PARK CITY, UTAH – Since most people with psoriatic arthritis (PsA) develop psoriasis before joint symptoms, it’s helpful to have a simple screening test for the condition.
One of Dr. Philip Mease’s favorite PsA screening tools is the Psoriasis Epidemiology Screening Test (PEST), which was first described at the 2009 annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis (GRAPPA) and consists of five simple questions. They are: Have you ever had a swollen joint (or joints)? Has a doctor ever told you that you have arthritis? Do your fingernails or toes have holes or pits? Have you had pain in your heel? Have you had a finger or toe that was completely swollen and painful for no apparent reason? (Clin Exp Rheumatol. 2009;27:469-74).
“Just these five simple questions, or trying to remember a few of them, can help you in your review of systems,” Dr. Mease, director of arthritis research at Swedish Medical Center, Seattle, said at the annual meeting of the Pacific Dermatologic Association. “I think patients appreciate it when you look beyond the skin in your questioning. These can pick up [PsA] with a high sensitivity and specificity” of 0.92 and 0.78, respectively.
He went on to discuss current PsA treatment approaches. According to an evidence review that he and his associates in GRAPPA published in 2009, biologics (anti–tumor necrosis factor inhibitors) as a group were found to be effective in all five domains of the disease: peripheral arthritis, skin and nail disease, axial disease, dactylitis, and enthesitis, while the oral disease-modifying antirheumatic drugs (DMARDs) were effective for peripheral arthritis and skin and nail disease.
Other treatments that were found effective are: psoralen and UVA/UVB for skin and nail disease, physiotherapy for axial disease, intra-articular steroids for peripheral arthritis, and NSAIDs for peripheral arthritis and axial disease (J Rheum. 2009;33:1417-21). “Patients with mild disease can be tried on NSAIDs, especially in a patient with monoarticular disease, but for the most part we need to move on to using systemic medication,” he said. Updated recommendations from GRAPPA include new data regarding ustekinumab, apremilast, and secukinumab, as well as data on comorbidities (J Rheumatol. 2015;42[6]:1052-5).
According to Dr. Mease, controlled trials of DMARDs in PsA patients have yielded treatment effects that range from marginal in the joints to marginal or none at all in the skin. Data from the Methotrexate in Psoriatic Arthritis trial conducted in the United Kingdom and published in 2012 showed no evidence that methotrexate improves inflammatory synovitis in active PsA (Rheumatol. 2012;51:1368-77).
“There were issues with this trial, including the fact that it took 5 years to enroll patients, and many dropped out, so I don’t think it’s a very reliable study,” said Dr. Mease, who is also a professor of medicine in the division of rheumatology at the University of Washington, Seattle. “Currently, Amgen is in the process of starting a trial in which the goal is to enroll 840 subjects with early PsA who are being randomized to methotrexate alone, Enbrel alone, or Enbrel plus methotrexate. This, I think, is going to give us a better answer about the effectiveness of methotrexate. It will also teach us about whether there’s a value in combining an anti-TNF inhibitor with methotrexate. We still don’t know the answer to that question.”
The most recent data on methotrexate come from an open-label trial known as TICOPA, which used a tight control treatment paradigm through 48 weeks of treatment. A subanalysis of 188 patients treated with methotrexate through 12 weeks was presented at the 2015 meeting of the European League Against Rheumatism. It revealed that 41% of patients achieved an ACR 20, 22% achieved minimal disease activity, 62% experienced an improvement in dactylitis, and 25% experienced an improvement in enthesitis.
“So we have a few data suggesting that methotrexate may be modestly effective in treating PsA,” Dr. Mease said. “We often will start with methotrexate unless the patient has really aggressive disease activity. If they get some effect from the drug but not enough, we’ll often add a biologic agent but often keep some methotrexate in the background, even at 10 mg per week, in order to reduce immunogenicity from a biologic.”
Dr. Mease disclosed that he has received research grants, consultation fees, and/or speaker honoraria from AbbVie, Amgen, Bristol-Myers Squibb, Celgene, Crescendo Bioscience, Genentech, GlaxoSmithKline, Janssen, Eli Lilly, Merck, Novartis, Pfizer, and UCB.
PARK CITY, UTAH – Since most people with psoriatic arthritis (PsA) develop psoriasis before joint symptoms, it’s helpful to have a simple screening test for the condition.
One of Dr. Philip Mease’s favorite PsA screening tools is the Psoriasis Epidemiology Screening Test (PEST), which was first described at the 2009 annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis (GRAPPA) and consists of five simple questions. They are: Have you ever had a swollen joint (or joints)? Has a doctor ever told you that you have arthritis? Do your fingernails or toes have holes or pits? Have you had pain in your heel? Have you had a finger or toe that was completely swollen and painful for no apparent reason? (Clin Exp Rheumatol. 2009;27:469-74).
“Just these five simple questions, or trying to remember a few of them, can help you in your review of systems,” Dr. Mease, director of arthritis research at Swedish Medical Center, Seattle, said at the annual meeting of the Pacific Dermatologic Association. “I think patients appreciate it when you look beyond the skin in your questioning. These can pick up [PsA] with a high sensitivity and specificity” of 0.92 and 0.78, respectively.
He went on to discuss current PsA treatment approaches. According to an evidence review that he and his associates in GRAPPA published in 2009, biologics (anti–tumor necrosis factor inhibitors) as a group were found to be effective in all five domains of the disease: peripheral arthritis, skin and nail disease, axial disease, dactylitis, and enthesitis, while the oral disease-modifying antirheumatic drugs (DMARDs) were effective for peripheral arthritis and skin and nail disease.
Other treatments that were found effective are: psoralen and UVA/UVB for skin and nail disease, physiotherapy for axial disease, intra-articular steroids for peripheral arthritis, and NSAIDs for peripheral arthritis and axial disease (J Rheum. 2009;33:1417-21). “Patients with mild disease can be tried on NSAIDs, especially in a patient with monoarticular disease, but for the most part we need to move on to using systemic medication,” he said. Updated recommendations from GRAPPA include new data regarding ustekinumab, apremilast, and secukinumab, as well as data on comorbidities (J Rheumatol. 2015;42[6]:1052-5).
According to Dr. Mease, controlled trials of DMARDs in PsA patients have yielded treatment effects that range from marginal in the joints to marginal or none at all in the skin. Data from the Methotrexate in Psoriatic Arthritis trial conducted in the United Kingdom and published in 2012 showed no evidence that methotrexate improves inflammatory synovitis in active PsA (Rheumatol. 2012;51:1368-77).
“There were issues with this trial, including the fact that it took 5 years to enroll patients, and many dropped out, so I don’t think it’s a very reliable study,” said Dr. Mease, who is also a professor of medicine in the division of rheumatology at the University of Washington, Seattle. “Currently, Amgen is in the process of starting a trial in which the goal is to enroll 840 subjects with early PsA who are being randomized to methotrexate alone, Enbrel alone, or Enbrel plus methotrexate. This, I think, is going to give us a better answer about the effectiveness of methotrexate. It will also teach us about whether there’s a value in combining an anti-TNF inhibitor with methotrexate. We still don’t know the answer to that question.”
The most recent data on methotrexate come from an open-label trial known as TICOPA, which used a tight control treatment paradigm through 48 weeks of treatment. A subanalysis of 188 patients treated with methotrexate through 12 weeks was presented at the 2015 meeting of the European League Against Rheumatism. It revealed that 41% of patients achieved an ACR 20, 22% achieved minimal disease activity, 62% experienced an improvement in dactylitis, and 25% experienced an improvement in enthesitis.
“So we have a few data suggesting that methotrexate may be modestly effective in treating PsA,” Dr. Mease said. “We often will start with methotrexate unless the patient has really aggressive disease activity. If they get some effect from the drug but not enough, we’ll often add a biologic agent but often keep some methotrexate in the background, even at 10 mg per week, in order to reduce immunogenicity from a biologic.”
Dr. Mease disclosed that he has received research grants, consultation fees, and/or speaker honoraria from AbbVie, Amgen, Bristol-Myers Squibb, Celgene, Crescendo Bioscience, Genentech, GlaxoSmithKline, Janssen, Eli Lilly, Merck, Novartis, Pfizer, and UCB.
EXPERT ANALYSIS AT PDA 2015
Maintaining Adherence to Psoriasis Treatments
Adherence to psoriasis therapies, especially topical therapy, is remarkably poor. Dr. Steven Feldman discusses the patient-physician relationship and ways that physicians can help patients so they're not fearful of taking their medications. He discusses follow-up with patients and special considerations for patients with scalp psoriasis.
The psoriasis audiocast series is created in collaboration with Cutis® and the National Psoriasis Foundation®.
Adherence to psoriasis therapies, especially topical therapy, is remarkably poor. Dr. Steven Feldman discusses the patient-physician relationship and ways that physicians can help patients so they're not fearful of taking their medications. He discusses follow-up with patients and special considerations for patients with scalp psoriasis.
The psoriasis audiocast series is created in collaboration with Cutis® and the National Psoriasis Foundation®.
Adherence to psoriasis therapies, especially topical therapy, is remarkably poor. Dr. Steven Feldman discusses the patient-physician relationship and ways that physicians can help patients so they're not fearful of taking their medications. He discusses follow-up with patients and special considerations for patients with scalp psoriasis.
The psoriasis audiocast series is created in collaboration with Cutis® and the National Psoriasis Foundation®.
As psoriasis maintenance therapy, step-down matched full-dose etanercept for quality of life measures
At 6 months, quality of life is largely the same whether psoriasis patients stay on their initial etanercept (Enbrel) dose of 50 mg twice weekly or step down to 50 mg once weekly with topical corticosteroids, according to a Canadian trial published in the Journal of The European Academy of Dermatology and Venereology.
“The opportunity to use a topical agent seemed to improve [patients’] overall satisfaction,” and weekly “etanercept and topical may be a less costly option compared with” etanercept twice weekly, said the investigators, led by Dr. Kim Papp, of Probity Medical Research in Waterloo, Ont.
Previously, the investigators showed that the step-down strategy works as well as full-dose maintenance in clearing the skin. They wanted to check if that also held true for quality of life, as assessed by the Dermatology Life Quality Index (DLQI) and the Treatment Satisfaction Questionnaire for Medication (TSQM). (J Eur Acad Dermatol Venereol. 2015 Aug;29(8):1555-61).
The 287 patients, all with moderate-to-severe plaque psoriasis for at least half a year, received etanercept 50 mg twice weekly for 12 weeks; 144 were then randomized to stay on that dose, and 143 others to drop to 50 mg weekly with the addition of topicals as required through week 24. The mean age of patients in the trial was 45 years; 88% of the subjects were white and 65% were men.
Topicals included hydrocortisone 2.5%, beta methasone valerate 0.1%, betamethasone dipropionate 0.05%, clobetasol 0.05%, calcitriol, or calcipotriol plus betamethasone dipropionate 0.05%; the topicals were selected by the researchers, who were allowed to change them as needed.
The mean change in DLQI from baseline to week 24 was 10.7 points in the etanercept group and 9.9 points in the etanercept-plus-topical group. Mean change in TSQM effectiveness, convenience, side-effects, and global satisfaction was 27.1, 14.8, -0.7 and 26.7 points in the etanercept group, and 32.5, 18.5, 1.3, and 28.4 points in the etanercept-plus-topical group. Healthcare visits, employment status, work productivity, and ability to perform daily activities were similar between the treatment arms.
The study was descriptive; the investigators didn’t run statistical analyses. Even so, measures of quality of life “were numerically similar in patients who stayed on etanercept 50 mg [twice weekly] and patients who received etanercept 50 mg [weekly] plus topical therapies. No notable differences between treatment arms ... were observed. Additionally, improvements in [Psoriasis Area and Severity Index] scores appeared to correlate with improvements in patient reported outcomes,” the investigators said.
“The duration of treatment with topical therapies was only 12 weeks; a longer duration may result in loss of efficacy as adherence to topical therapies may decrease with time,” they noted.
The work was funded by etanercept’s maker, Amgen. Dr. Papp reported consulting for the company. Two other investigators have been Amgen advisors and reported research grants, speakers fees, or other payments.
At 6 months, quality of life is largely the same whether psoriasis patients stay on their initial etanercept (Enbrel) dose of 50 mg twice weekly or step down to 50 mg once weekly with topical corticosteroids, according to a Canadian trial published in the Journal of The European Academy of Dermatology and Venereology.
“The opportunity to use a topical agent seemed to improve [patients’] overall satisfaction,” and weekly “etanercept and topical may be a less costly option compared with” etanercept twice weekly, said the investigators, led by Dr. Kim Papp, of Probity Medical Research in Waterloo, Ont.
Previously, the investigators showed that the step-down strategy works as well as full-dose maintenance in clearing the skin. They wanted to check if that also held true for quality of life, as assessed by the Dermatology Life Quality Index (DLQI) and the Treatment Satisfaction Questionnaire for Medication (TSQM). (J Eur Acad Dermatol Venereol. 2015 Aug;29(8):1555-61).
The 287 patients, all with moderate-to-severe plaque psoriasis for at least half a year, received etanercept 50 mg twice weekly for 12 weeks; 144 were then randomized to stay on that dose, and 143 others to drop to 50 mg weekly with the addition of topicals as required through week 24. The mean age of patients in the trial was 45 years; 88% of the subjects were white and 65% were men.
Topicals included hydrocortisone 2.5%, beta methasone valerate 0.1%, betamethasone dipropionate 0.05%, clobetasol 0.05%, calcitriol, or calcipotriol plus betamethasone dipropionate 0.05%; the topicals were selected by the researchers, who were allowed to change them as needed.
The mean change in DLQI from baseline to week 24 was 10.7 points in the etanercept group and 9.9 points in the etanercept-plus-topical group. Mean change in TSQM effectiveness, convenience, side-effects, and global satisfaction was 27.1, 14.8, -0.7 and 26.7 points in the etanercept group, and 32.5, 18.5, 1.3, and 28.4 points in the etanercept-plus-topical group. Healthcare visits, employment status, work productivity, and ability to perform daily activities were similar between the treatment arms.
The study was descriptive; the investigators didn’t run statistical analyses. Even so, measures of quality of life “were numerically similar in patients who stayed on etanercept 50 mg [twice weekly] and patients who received etanercept 50 mg [weekly] plus topical therapies. No notable differences between treatment arms ... were observed. Additionally, improvements in [Psoriasis Area and Severity Index] scores appeared to correlate with improvements in patient reported outcomes,” the investigators said.
“The duration of treatment with topical therapies was only 12 weeks; a longer duration may result in loss of efficacy as adherence to topical therapies may decrease with time,” they noted.
The work was funded by etanercept’s maker, Amgen. Dr. Papp reported consulting for the company. Two other investigators have been Amgen advisors and reported research grants, speakers fees, or other payments.
At 6 months, quality of life is largely the same whether psoriasis patients stay on their initial etanercept (Enbrel) dose of 50 mg twice weekly or step down to 50 mg once weekly with topical corticosteroids, according to a Canadian trial published in the Journal of The European Academy of Dermatology and Venereology.
“The opportunity to use a topical agent seemed to improve [patients’] overall satisfaction,” and weekly “etanercept and topical may be a less costly option compared with” etanercept twice weekly, said the investigators, led by Dr. Kim Papp, of Probity Medical Research in Waterloo, Ont.
Previously, the investigators showed that the step-down strategy works as well as full-dose maintenance in clearing the skin. They wanted to check if that also held true for quality of life, as assessed by the Dermatology Life Quality Index (DLQI) and the Treatment Satisfaction Questionnaire for Medication (TSQM). (J Eur Acad Dermatol Venereol. 2015 Aug;29(8):1555-61).
The 287 patients, all with moderate-to-severe plaque psoriasis for at least half a year, received etanercept 50 mg twice weekly for 12 weeks; 144 were then randomized to stay on that dose, and 143 others to drop to 50 mg weekly with the addition of topicals as required through week 24. The mean age of patients in the trial was 45 years; 88% of the subjects were white and 65% were men.
Topicals included hydrocortisone 2.5%, beta methasone valerate 0.1%, betamethasone dipropionate 0.05%, clobetasol 0.05%, calcitriol, or calcipotriol plus betamethasone dipropionate 0.05%; the topicals were selected by the researchers, who were allowed to change them as needed.
The mean change in DLQI from baseline to week 24 was 10.7 points in the etanercept group and 9.9 points in the etanercept-plus-topical group. Mean change in TSQM effectiveness, convenience, side-effects, and global satisfaction was 27.1, 14.8, -0.7 and 26.7 points in the etanercept group, and 32.5, 18.5, 1.3, and 28.4 points in the etanercept-plus-topical group. Healthcare visits, employment status, work productivity, and ability to perform daily activities were similar between the treatment arms.
The study was descriptive; the investigators didn’t run statistical analyses. Even so, measures of quality of life “were numerically similar in patients who stayed on etanercept 50 mg [twice weekly] and patients who received etanercept 50 mg [weekly] plus topical therapies. No notable differences between treatment arms ... were observed. Additionally, improvements in [Psoriasis Area and Severity Index] scores appeared to correlate with improvements in patient reported outcomes,” the investigators said.
“The duration of treatment with topical therapies was only 12 weeks; a longer duration may result in loss of efficacy as adherence to topical therapies may decrease with time,” they noted.
The work was funded by etanercept’s maker, Amgen. Dr. Papp reported consulting for the company. Two other investigators have been Amgen advisors and reported research grants, speakers fees, or other payments.
FROM THE JOURNAL OF THE EUROPEAN ACADEMY OF DERMATOLOGY AND VENEROLOGY
Biologic treatment for psoriasis found to have CVD benefits
PARK CITY, UTAH – Evidence is mounting that the use of biologic therapies is associated with certain cardiovascular benefits in patients with psoriasis.
However, until the strength of the evidence becomes more robust, Dr. Jashin J. Wu does not recommend that patients are prescribed tumor necrosis factor (TNF) inhibitors specifically to reduce the risk of cardiovascular disease. “If systemic therapy is a consideration in the setting of CVD [cardiovascular disease] risk, it would appear that TNF inhibitors and methotrexate offer the best evidence of benefit,” Dr. Wu, director of the psoriasis clinic and director of dermatology research in the department of dermatology at Kaiser Permanente Los Angeles Medical Center, said at the annual meeting of the Pacific Dermatologic Association.
The National Psoriasis Foundation recently published a consensus statement about the potential impact of current therapies on cardiovascular disease, including the risk of diabetes (J Am Acad Dermatol. 2014;70[1]:168-77). In a retrospective study of 121,280 patients with rheumatoid arthritis (RA) or psoriasis, drug regimens were categorized into four mutually exclusive groups: TNF inhibitors with or without other disease-modifying antirheumatic drugs (DMARDs), methotrexate without TNF inhibitors or hydroxychloroquine, hydroxychloroquine without TNF inhibitors or methotrexate; and other nonbiologic DMARDs without TNF inhibitors, methotrexate or hydroxychloroquine (referent group). The researchers found that adjusted Cox proportional hazards for the risk of diabetes were lower among those on TNF inhibitors (hazard ratio, 0.62; 95% confidence interval, 0.42-0.91) and hydroxychloroquine (HR, 0.54; 95% CI, 0.36-0.80), compared with those on methotrexate (HR, 0.77, 95% CI, 0.53-1.13) (JAMA. 2011 Jun 22;305[24]:2525-31).
Increased carotid intimal media thickness (IMT) is also an independent predictor of CVD. In a prospective, observational study, 20 psoriasis patients received a 12-week treatment of TNF inhibitors (Ann Rheum Dis. 2011 Apr;70[4]:705-6). After 12 weeks, 9 patients continued on their TNF-inhibitor regimen (group 1), while 11 discontinued treatment because of financial constraints (group 2). Another 20 psoriasis patients who did not receive biologic therapy served as controls (group 3). The researchers measured IMT by carotid ultrasound at baseline, week 12 and at 2 years. They found that between baseline and 2 years, IMT decreased from 0.70 mm to 0.63 mm in group 1, from 0.71 to 0.67 in group 2, and increased from 0.79 to 0.82 in group 3. “This seems to suggest that the use of TNF inhibitors may improve atherosclerosis,” said Dr. Wu, who is currently running seven clinical trials of psoriasis patients. Similar findings were seen in a larger study that examined 224 patients with psoriatic arthritis and followed them for a mean of 55 months: 124 on TNF inhibitors, 104 on DMARDs, and 305 matched controls (Arterioscler Thromb Vasc Biol. 2011 Mar;31[3]:705-120).
In a separate study of 16 psoriasis patients treated with TNF inhibitors, researchers used ultrasound to measure IMT of carotid and brachial arteries after 6 months of therapy (J Am Acad Dermatol. 2013 Oct;69[4]:523-9). At baseline, all 16 patients had an IMT greater than normal. In those without initial calcified atherosclerotic plaques, 13 of 16 had a significant decrease of IMT (P = .0002). In those with initial calcified atherosclerotic plaques, 3 of 16 patients had a nonsignificant increase in IMT.
Increased arterial stiffness is another independent predictor of CVD. In a controlled study of 55 patients with psoriatic arthritis, RA, or ankylosing spondylitis, researchers used aortic pulse-wave velocity to measure aortic stiffness. Almost 35% of the patients (36) received TNF inhibitors while the remaining 19 did not receive treatment (Am J Hypertens. 2012 Jun;25[6]:644-50). After 1 year of follow-up, use of TNF inhibitors was associated with a significant improvement in aortic pulse-wave velocity (P = .02) and reduced carotid IMT progression (P = .04).
Other evidence suggests that systemic therapy with TNF inhibitors is associated with the reduction of cardiovascular events, including myocardial infarction. In a study led by Dr. Wu, 8,845 Kaiser Permanente patients with psoriasis were evaluated between Jan. 1, 2004, and Nov. 30, 2010, and placed into one of three groups: treatment with a TNF inhibitor, treatment with oral therapy or phototherapy, or treatment with a topical agent (referent group) (Arch Dermatol. 2012 Nov;148[11]:1244-50). On multivariate analysis, the investigators found that the use of TNF inhibitors was associated with a significant reduction in the rate of incident MI (HR, 0.50; P = .003), compared with the use of topical agents.
Dr. Wu went on to note that C-reactive protein (CRP) is a predictor of CVD such as MI, peripheral arterial disease, and sudden cardiac death. In a retrospective cohort study, Dr. Wu and his associates evaluated Kaiser Permanente patients with psoriasis, psoriatic arthritis, or RA who were treated with a combination of TNF plus methotrexate, or with methotrexate alone from Jan. 1, 2002, to July 31, 2011 (J. Am. Acad. Dermatol. 2015;72[5]:917-9). Only patients in the combination therapy group had a clinically and statistically significant decrease in CRP, compared with baseline (a mean decrease of 5.18 mg/dL). No significant changes between the two groups were observed in terms of BMI, blood pressure, fasting glucose, hemoglobin A1C, total cholesterol, LDL cholesterol, HDL cholesterol, triglycerides, or alanine aminotransferase.
HDL cholesterol composition and function have also been studied in psoriasis patients. In one trial, HDL cholesterol was isolated from 15 psoriasis patients at baseline and after effective topical and/or systemic psoriasis therapy, and from 15 healthy controls matched for age and sex (J. Invest. Dermatol. 2014;134[3]:635-42). The researchers found that HDL cholesterol from psoriasis patients showed a significantly impaired capability to mobilize cholesterol from macrophages. However, psoriasis therapy recovered HDL cholesterol composition and function, but had no effect on serum HDL cholesterol levels.
A better understanding of the cardiovascular effects of biologic therapy should be gleaned from the Vascular Inflammation in Psoriasis Trial, which includes $3.8 million in funding from the National Institutes of Health, to prospectively study the effect of therapy on biomarkers and on positron emission tomography with 18fluorodeoxyglucose (FDG-PET)/CT scan. The 1-year study just completed enrolling patients into one of three treatment groups: adalimumab, UVB phototherapy, or placebo. Biomarkers such as CRP, lipids, and imaging will be assessed at baseline, weeks 4, 8, 12, and then every 12 weeks. “The theory is that adalimumab, but not UVB phototherapy, will improve biomarkers and reduce vascular inflammation as measured by FDG-PET/CT scan,” Dr. Wu said. “Aggressive systemic therapy may alter the natural history of cardiovascular disease.”
Current recommendations from the National Psoriasis Foundation call for an assessment of blood pressure, pulse, and body mass index every 2 years, and an assessment of fasting blood glucose and lipid levels every 5 years, or every 2 years if the patient has additional risk factors.
Dr. Wu reported that he has received research and consulting fees from numerous pharmaceutical companies, including AbbVie and Amgen. These go to his employer.
PARK CITY, UTAH – Evidence is mounting that the use of biologic therapies is associated with certain cardiovascular benefits in patients with psoriasis.
However, until the strength of the evidence becomes more robust, Dr. Jashin J. Wu does not recommend that patients are prescribed tumor necrosis factor (TNF) inhibitors specifically to reduce the risk of cardiovascular disease. “If systemic therapy is a consideration in the setting of CVD [cardiovascular disease] risk, it would appear that TNF inhibitors and methotrexate offer the best evidence of benefit,” Dr. Wu, director of the psoriasis clinic and director of dermatology research in the department of dermatology at Kaiser Permanente Los Angeles Medical Center, said at the annual meeting of the Pacific Dermatologic Association.
The National Psoriasis Foundation recently published a consensus statement about the potential impact of current therapies on cardiovascular disease, including the risk of diabetes (J Am Acad Dermatol. 2014;70[1]:168-77). In a retrospective study of 121,280 patients with rheumatoid arthritis (RA) or psoriasis, drug regimens were categorized into four mutually exclusive groups: TNF inhibitors with or without other disease-modifying antirheumatic drugs (DMARDs), methotrexate without TNF inhibitors or hydroxychloroquine, hydroxychloroquine without TNF inhibitors or methotrexate; and other nonbiologic DMARDs without TNF inhibitors, methotrexate or hydroxychloroquine (referent group). The researchers found that adjusted Cox proportional hazards for the risk of diabetes were lower among those on TNF inhibitors (hazard ratio, 0.62; 95% confidence interval, 0.42-0.91) and hydroxychloroquine (HR, 0.54; 95% CI, 0.36-0.80), compared with those on methotrexate (HR, 0.77, 95% CI, 0.53-1.13) (JAMA. 2011 Jun 22;305[24]:2525-31).
Increased carotid intimal media thickness (IMT) is also an independent predictor of CVD. In a prospective, observational study, 20 psoriasis patients received a 12-week treatment of TNF inhibitors (Ann Rheum Dis. 2011 Apr;70[4]:705-6). After 12 weeks, 9 patients continued on their TNF-inhibitor regimen (group 1), while 11 discontinued treatment because of financial constraints (group 2). Another 20 psoriasis patients who did not receive biologic therapy served as controls (group 3). The researchers measured IMT by carotid ultrasound at baseline, week 12 and at 2 years. They found that between baseline and 2 years, IMT decreased from 0.70 mm to 0.63 mm in group 1, from 0.71 to 0.67 in group 2, and increased from 0.79 to 0.82 in group 3. “This seems to suggest that the use of TNF inhibitors may improve atherosclerosis,” said Dr. Wu, who is currently running seven clinical trials of psoriasis patients. Similar findings were seen in a larger study that examined 224 patients with psoriatic arthritis and followed them for a mean of 55 months: 124 on TNF inhibitors, 104 on DMARDs, and 305 matched controls (Arterioscler Thromb Vasc Biol. 2011 Mar;31[3]:705-120).
In a separate study of 16 psoriasis patients treated with TNF inhibitors, researchers used ultrasound to measure IMT of carotid and brachial arteries after 6 months of therapy (J Am Acad Dermatol. 2013 Oct;69[4]:523-9). At baseline, all 16 patients had an IMT greater than normal. In those without initial calcified atherosclerotic plaques, 13 of 16 had a significant decrease of IMT (P = .0002). In those with initial calcified atherosclerotic plaques, 3 of 16 patients had a nonsignificant increase in IMT.
Increased arterial stiffness is another independent predictor of CVD. In a controlled study of 55 patients with psoriatic arthritis, RA, or ankylosing spondylitis, researchers used aortic pulse-wave velocity to measure aortic stiffness. Almost 35% of the patients (36) received TNF inhibitors while the remaining 19 did not receive treatment (Am J Hypertens. 2012 Jun;25[6]:644-50). After 1 year of follow-up, use of TNF inhibitors was associated with a significant improvement in aortic pulse-wave velocity (P = .02) and reduced carotid IMT progression (P = .04).
Other evidence suggests that systemic therapy with TNF inhibitors is associated with the reduction of cardiovascular events, including myocardial infarction. In a study led by Dr. Wu, 8,845 Kaiser Permanente patients with psoriasis were evaluated between Jan. 1, 2004, and Nov. 30, 2010, and placed into one of three groups: treatment with a TNF inhibitor, treatment with oral therapy or phototherapy, or treatment with a topical agent (referent group) (Arch Dermatol. 2012 Nov;148[11]:1244-50). On multivariate analysis, the investigators found that the use of TNF inhibitors was associated with a significant reduction in the rate of incident MI (HR, 0.50; P = .003), compared with the use of topical agents.
Dr. Wu went on to note that C-reactive protein (CRP) is a predictor of CVD such as MI, peripheral arterial disease, and sudden cardiac death. In a retrospective cohort study, Dr. Wu and his associates evaluated Kaiser Permanente patients with psoriasis, psoriatic arthritis, or RA who were treated with a combination of TNF plus methotrexate, or with methotrexate alone from Jan. 1, 2002, to July 31, 2011 (J. Am. Acad. Dermatol. 2015;72[5]:917-9). Only patients in the combination therapy group had a clinically and statistically significant decrease in CRP, compared with baseline (a mean decrease of 5.18 mg/dL). No significant changes between the two groups were observed in terms of BMI, blood pressure, fasting glucose, hemoglobin A1C, total cholesterol, LDL cholesterol, HDL cholesterol, triglycerides, or alanine aminotransferase.
HDL cholesterol composition and function have also been studied in psoriasis patients. In one trial, HDL cholesterol was isolated from 15 psoriasis patients at baseline and after effective topical and/or systemic psoriasis therapy, and from 15 healthy controls matched for age and sex (J. Invest. Dermatol. 2014;134[3]:635-42). The researchers found that HDL cholesterol from psoriasis patients showed a significantly impaired capability to mobilize cholesterol from macrophages. However, psoriasis therapy recovered HDL cholesterol composition and function, but had no effect on serum HDL cholesterol levels.
A better understanding of the cardiovascular effects of biologic therapy should be gleaned from the Vascular Inflammation in Psoriasis Trial, which includes $3.8 million in funding from the National Institutes of Health, to prospectively study the effect of therapy on biomarkers and on positron emission tomography with 18fluorodeoxyglucose (FDG-PET)/CT scan. The 1-year study just completed enrolling patients into one of three treatment groups: adalimumab, UVB phototherapy, or placebo. Biomarkers such as CRP, lipids, and imaging will be assessed at baseline, weeks 4, 8, 12, and then every 12 weeks. “The theory is that adalimumab, but not UVB phototherapy, will improve biomarkers and reduce vascular inflammation as measured by FDG-PET/CT scan,” Dr. Wu said. “Aggressive systemic therapy may alter the natural history of cardiovascular disease.”
Current recommendations from the National Psoriasis Foundation call for an assessment of blood pressure, pulse, and body mass index every 2 years, and an assessment of fasting blood glucose and lipid levels every 5 years, or every 2 years if the patient has additional risk factors.
Dr. Wu reported that he has received research and consulting fees from numerous pharmaceutical companies, including AbbVie and Amgen. These go to his employer.
PARK CITY, UTAH – Evidence is mounting that the use of biologic therapies is associated with certain cardiovascular benefits in patients with psoriasis.
However, until the strength of the evidence becomes more robust, Dr. Jashin J. Wu does not recommend that patients are prescribed tumor necrosis factor (TNF) inhibitors specifically to reduce the risk of cardiovascular disease. “If systemic therapy is a consideration in the setting of CVD [cardiovascular disease] risk, it would appear that TNF inhibitors and methotrexate offer the best evidence of benefit,” Dr. Wu, director of the psoriasis clinic and director of dermatology research in the department of dermatology at Kaiser Permanente Los Angeles Medical Center, said at the annual meeting of the Pacific Dermatologic Association.
The National Psoriasis Foundation recently published a consensus statement about the potential impact of current therapies on cardiovascular disease, including the risk of diabetes (J Am Acad Dermatol. 2014;70[1]:168-77). In a retrospective study of 121,280 patients with rheumatoid arthritis (RA) or psoriasis, drug regimens were categorized into four mutually exclusive groups: TNF inhibitors with or without other disease-modifying antirheumatic drugs (DMARDs), methotrexate without TNF inhibitors or hydroxychloroquine, hydroxychloroquine without TNF inhibitors or methotrexate; and other nonbiologic DMARDs without TNF inhibitors, methotrexate or hydroxychloroquine (referent group). The researchers found that adjusted Cox proportional hazards for the risk of diabetes were lower among those on TNF inhibitors (hazard ratio, 0.62; 95% confidence interval, 0.42-0.91) and hydroxychloroquine (HR, 0.54; 95% CI, 0.36-0.80), compared with those on methotrexate (HR, 0.77, 95% CI, 0.53-1.13) (JAMA. 2011 Jun 22;305[24]:2525-31).
Increased carotid intimal media thickness (IMT) is also an independent predictor of CVD. In a prospective, observational study, 20 psoriasis patients received a 12-week treatment of TNF inhibitors (Ann Rheum Dis. 2011 Apr;70[4]:705-6). After 12 weeks, 9 patients continued on their TNF-inhibitor regimen (group 1), while 11 discontinued treatment because of financial constraints (group 2). Another 20 psoriasis patients who did not receive biologic therapy served as controls (group 3). The researchers measured IMT by carotid ultrasound at baseline, week 12 and at 2 years. They found that between baseline and 2 years, IMT decreased from 0.70 mm to 0.63 mm in group 1, from 0.71 to 0.67 in group 2, and increased from 0.79 to 0.82 in group 3. “This seems to suggest that the use of TNF inhibitors may improve atherosclerosis,” said Dr. Wu, who is currently running seven clinical trials of psoriasis patients. Similar findings were seen in a larger study that examined 224 patients with psoriatic arthritis and followed them for a mean of 55 months: 124 on TNF inhibitors, 104 on DMARDs, and 305 matched controls (Arterioscler Thromb Vasc Biol. 2011 Mar;31[3]:705-120).
In a separate study of 16 psoriasis patients treated with TNF inhibitors, researchers used ultrasound to measure IMT of carotid and brachial arteries after 6 months of therapy (J Am Acad Dermatol. 2013 Oct;69[4]:523-9). At baseline, all 16 patients had an IMT greater than normal. In those without initial calcified atherosclerotic plaques, 13 of 16 had a significant decrease of IMT (P = .0002). In those with initial calcified atherosclerotic plaques, 3 of 16 patients had a nonsignificant increase in IMT.
Increased arterial stiffness is another independent predictor of CVD. In a controlled study of 55 patients with psoriatic arthritis, RA, or ankylosing spondylitis, researchers used aortic pulse-wave velocity to measure aortic stiffness. Almost 35% of the patients (36) received TNF inhibitors while the remaining 19 did not receive treatment (Am J Hypertens. 2012 Jun;25[6]:644-50). After 1 year of follow-up, use of TNF inhibitors was associated with a significant improvement in aortic pulse-wave velocity (P = .02) and reduced carotid IMT progression (P = .04).
Other evidence suggests that systemic therapy with TNF inhibitors is associated with the reduction of cardiovascular events, including myocardial infarction. In a study led by Dr. Wu, 8,845 Kaiser Permanente patients with psoriasis were evaluated between Jan. 1, 2004, and Nov. 30, 2010, and placed into one of three groups: treatment with a TNF inhibitor, treatment with oral therapy or phototherapy, or treatment with a topical agent (referent group) (Arch Dermatol. 2012 Nov;148[11]:1244-50). On multivariate analysis, the investigators found that the use of TNF inhibitors was associated with a significant reduction in the rate of incident MI (HR, 0.50; P = .003), compared with the use of topical agents.
Dr. Wu went on to note that C-reactive protein (CRP) is a predictor of CVD such as MI, peripheral arterial disease, and sudden cardiac death. In a retrospective cohort study, Dr. Wu and his associates evaluated Kaiser Permanente patients with psoriasis, psoriatic arthritis, or RA who were treated with a combination of TNF plus methotrexate, or with methotrexate alone from Jan. 1, 2002, to July 31, 2011 (J. Am. Acad. Dermatol. 2015;72[5]:917-9). Only patients in the combination therapy group had a clinically and statistically significant decrease in CRP, compared with baseline (a mean decrease of 5.18 mg/dL). No significant changes between the two groups were observed in terms of BMI, blood pressure, fasting glucose, hemoglobin A1C, total cholesterol, LDL cholesterol, HDL cholesterol, triglycerides, or alanine aminotransferase.
HDL cholesterol composition and function have also been studied in psoriasis patients. In one trial, HDL cholesterol was isolated from 15 psoriasis patients at baseline and after effective topical and/or systemic psoriasis therapy, and from 15 healthy controls matched for age and sex (J. Invest. Dermatol. 2014;134[3]:635-42). The researchers found that HDL cholesterol from psoriasis patients showed a significantly impaired capability to mobilize cholesterol from macrophages. However, psoriasis therapy recovered HDL cholesterol composition and function, but had no effect on serum HDL cholesterol levels.
A better understanding of the cardiovascular effects of biologic therapy should be gleaned from the Vascular Inflammation in Psoriasis Trial, which includes $3.8 million in funding from the National Institutes of Health, to prospectively study the effect of therapy on biomarkers and on positron emission tomography with 18fluorodeoxyglucose (FDG-PET)/CT scan. The 1-year study just completed enrolling patients into one of three treatment groups: adalimumab, UVB phototherapy, or placebo. Biomarkers such as CRP, lipids, and imaging will be assessed at baseline, weeks 4, 8, 12, and then every 12 weeks. “The theory is that adalimumab, but not UVB phototherapy, will improve biomarkers and reduce vascular inflammation as measured by FDG-PET/CT scan,” Dr. Wu said. “Aggressive systemic therapy may alter the natural history of cardiovascular disease.”
Current recommendations from the National Psoriasis Foundation call for an assessment of blood pressure, pulse, and body mass index every 2 years, and an assessment of fasting blood glucose and lipid levels every 5 years, or every 2 years if the patient has additional risk factors.
Dr. Wu reported that he has received research and consulting fees from numerous pharmaceutical companies, including AbbVie and Amgen. These go to his employer.
EXPERT ANALYSIS AT PDA 2015
Uveitis and Psoriasis
We are all aware of the association of psoriasis with systemic comorbidities. Psoriasis, psoriatic arthritis (PsA), and uveitis are inflammatory disorders that have notable overlap in their inflammatory pathways. In an article published online on July 29 in JAMA Dermatology, Egeberg et al investigated the potential bidirectional relationship between psoriatic disease and uveitis.
The researchers conducted a study (1997-2011) of 74,129 patients aged 18 years and older with incident psoriasis who were identified through administrative registries. There also were 13,114 patients with uveitis identified from the study cohort.
Incidence rates for uveitis per 10,000 person-years were 2.02 (95% CI [confidence interval], 1.99-2.06) for the reference population, 2.88 (95% CI, 2.33-3.56) for patients with mild psoriasis, 4.23 (2.40-7.45) for severe psoriasis, and 5.49 (95% CI, 3.36-8.96) for PsA. Incidence rate ratios per 10,000 person-years for the reference population, which included participants without uveitis, were 9.37 (95% CI, 9.30-9.45) for patients with mild psoriasis, 1.12 (95% CI, 1.10-1.15) for severe psoriasis, and 1.04 (95% CI, 1.01-1.06) for PsA. Patients with uveitis had corresponding incidence rates of 15.51 (95% CI, 12.92-18.62) for mild psoriasis, 2.66 (95% CI, 1.72-4.13) for severe psoriasis, and 4.25 (95% CI, 3.00-6.01) for PsA. Incidence rate ratios per 10,000 person-years for patients with uveitis were 1.59 (95% CI, 1.32-1.91) for mild psoriasis, 2.17 (95% CI, 1.40-3.38) for severe psoriasis, and 3.77 (95% CI, 2.66-5.34) for PsA.
The authors concluded that there is a bidirectional association between psoriatic disease and uveitis. They noted that increased focus on ocular symptoms in patients with psoriasis and PsA and on cutaneous and joint symptoms in patients with prior or current uveitis may be appropriate.
What’s the issue?
This research adds to the potential comorbidities of psoriasis and also adds a potential comorbidity of uveitis itself. Therefore, it would be helpful to add ocular symptoms to our review of systems in those with psoriatic disease. How will this information affect your workup of psoriasis patients?
We are all aware of the association of psoriasis with systemic comorbidities. Psoriasis, psoriatic arthritis (PsA), and uveitis are inflammatory disorders that have notable overlap in their inflammatory pathways. In an article published online on July 29 in JAMA Dermatology, Egeberg et al investigated the potential bidirectional relationship between psoriatic disease and uveitis.
The researchers conducted a study (1997-2011) of 74,129 patients aged 18 years and older with incident psoriasis who were identified through administrative registries. There also were 13,114 patients with uveitis identified from the study cohort.
Incidence rates for uveitis per 10,000 person-years were 2.02 (95% CI [confidence interval], 1.99-2.06) for the reference population, 2.88 (95% CI, 2.33-3.56) for patients with mild psoriasis, 4.23 (2.40-7.45) for severe psoriasis, and 5.49 (95% CI, 3.36-8.96) for PsA. Incidence rate ratios per 10,000 person-years for the reference population, which included participants without uveitis, were 9.37 (95% CI, 9.30-9.45) for patients with mild psoriasis, 1.12 (95% CI, 1.10-1.15) for severe psoriasis, and 1.04 (95% CI, 1.01-1.06) for PsA. Patients with uveitis had corresponding incidence rates of 15.51 (95% CI, 12.92-18.62) for mild psoriasis, 2.66 (95% CI, 1.72-4.13) for severe psoriasis, and 4.25 (95% CI, 3.00-6.01) for PsA. Incidence rate ratios per 10,000 person-years for patients with uveitis were 1.59 (95% CI, 1.32-1.91) for mild psoriasis, 2.17 (95% CI, 1.40-3.38) for severe psoriasis, and 3.77 (95% CI, 2.66-5.34) for PsA.
The authors concluded that there is a bidirectional association between psoriatic disease and uveitis. They noted that increased focus on ocular symptoms in patients with psoriasis and PsA and on cutaneous and joint symptoms in patients with prior or current uveitis may be appropriate.
What’s the issue?
This research adds to the potential comorbidities of psoriasis and also adds a potential comorbidity of uveitis itself. Therefore, it would be helpful to add ocular symptoms to our review of systems in those with psoriatic disease. How will this information affect your workup of psoriasis patients?
We are all aware of the association of psoriasis with systemic comorbidities. Psoriasis, psoriatic arthritis (PsA), and uveitis are inflammatory disorders that have notable overlap in their inflammatory pathways. In an article published online on July 29 in JAMA Dermatology, Egeberg et al investigated the potential bidirectional relationship between psoriatic disease and uveitis.
The researchers conducted a study (1997-2011) of 74,129 patients aged 18 years and older with incident psoriasis who were identified through administrative registries. There also were 13,114 patients with uveitis identified from the study cohort.
Incidence rates for uveitis per 10,000 person-years were 2.02 (95% CI [confidence interval], 1.99-2.06) for the reference population, 2.88 (95% CI, 2.33-3.56) for patients with mild psoriasis, 4.23 (2.40-7.45) for severe psoriasis, and 5.49 (95% CI, 3.36-8.96) for PsA. Incidence rate ratios per 10,000 person-years for the reference population, which included participants without uveitis, were 9.37 (95% CI, 9.30-9.45) for patients with mild psoriasis, 1.12 (95% CI, 1.10-1.15) for severe psoriasis, and 1.04 (95% CI, 1.01-1.06) for PsA. Patients with uveitis had corresponding incidence rates of 15.51 (95% CI, 12.92-18.62) for mild psoriasis, 2.66 (95% CI, 1.72-4.13) for severe psoriasis, and 4.25 (95% CI, 3.00-6.01) for PsA. Incidence rate ratios per 10,000 person-years for patients with uveitis were 1.59 (95% CI, 1.32-1.91) for mild psoriasis, 2.17 (95% CI, 1.40-3.38) for severe psoriasis, and 3.77 (95% CI, 2.66-5.34) for PsA.
The authors concluded that there is a bidirectional association between psoriatic disease and uveitis. They noted that increased focus on ocular symptoms in patients with psoriasis and PsA and on cutaneous and joint symptoms in patients with prior or current uveitis may be appropriate.
What’s the issue?
This research adds to the potential comorbidities of psoriasis and also adds a potential comorbidity of uveitis itself. Therefore, it would be helpful to add ocular symptoms to our review of systems in those with psoriatic disease. How will this information affect your workup of psoriasis patients?