User login
Frontline Supervisor Perspectives on Enabling High Reliability and Fostering a Just Culture at the VHA
Frontline Supervisor Perspectives on Enabling High Reliability and Fostering a Just Culture at the VHA
The Veterans Health Administration (VHA) is now in the sixth year of its enterprise-wide transformation into a high reliability organization (HRO). This effort began with a 2016 pilot project and is now implemented in 170 VHA medical centers.1-4 This transformation reflects a commitment to implementing standardized and reliable health care practices.
The VHA HRO implementation strategy includes a multifaceted approach to engage leadership through education, training, leader coaching, and change management initiatives.2 Despite the diversity of facilities in terms of cultures, geographies, and complexities, US Department of Veterans Affairs (VA) medical centers (VAMCs) have increasingly embraced standardized HRO practices. These changes are evident in improvements in VHA All Employee Survey scores, which assess 4 key patient safety culture dimensions: risk identification and just culture, error transparency and mitigation, supervisor communication and trust, and team cohesion and engagement.5 Positive trends in these dimensions highlight a cultural shift toward greater reliability, even amid challenges introduced by the COVID-19 pandemic.
However, this progress has encountered some challenges. Leadership turnover, budgetary constraints, and extensive educational demands for implementing and sustaining HRO practices have created obstacles, particularly for frontline health care practitioners.6 Additionally, there are pockets of resistance similar to what the airline industry faced when implementing crew resource management (CRM). Specifically, senior pilots and legacy leaders were reluctant to abandon their high-status, autocratic management styles and embrace CRM, despite its proven benefits for enhancing commercial airline safety.7 Similarly, some VHA staff have expressed resistance to foundational HRO practices, which include safety huddles, safety forums, leader rounding, and visual management systems.6,8
The training requirements for HRO practices range from a 25-minute introductory course (HRO 101) to a 7.5-hour team training session facilitated by the VHA National Center for Patient Safety (NCPS).9 While some supervisors view these requirements as burdensome, others have demonstrated strong enthusiasm for the process.6 Understanding the perspectives of unit and departmental managers regarding factors that enhance or hinder the adoption of HRO practices is critical for continuous improvement.10-12 Research has suggested that fostering psychological safety can create an environment where new ideas are shared openly, helping organizations navigate resistance to change.13-16
A 2024 quality improvement study, drawing on the perceptions of HRO leads, identified key facilitators, including training, coaching, leader approachability, and psychological safety, as well as barriers such as inadequate training and lack of accountability among managers.17 Building on this work, the current study focused on frontline supervisors, who are directly involved in integrating HRO practices into patient care activities. By addressing both barriers and facilitators, this expanded approach aims to provide a more comprehensive understanding of the challenges influencing HRO implementation in day-to-day operations.
Methods
This quality improvement initiative examined facilitators and barriers to establishing just culture and implementing high reliability practices, focusing on frontline supervisors overseeing clinical care teams (eg, emergency department, critical care) or patient-support functions (eg, dietary services). A questionnaire was sent to a randomized sample of VHA facility supervisors.
A qualitative grounded theory approach was employed to provide a deeper understanding of nuanced phenomena that cannot be captured through numerical data alone. This method enables systematic analysis using open, axial, and thematic coding, ensuring that emerging themes achieve saturation.18,19 It is particularly suited for this study, given the limited prior data on frontline supervisors. Additionally, qualitative methods help mitigate biases common in Likert-style scales, where respondents may lean toward agreement, potentially skewing results.20
Inclusion Criteria
Participants were required to have served as a frontline supervisor for ≥ 6 months. Frontline supervisors are assigned responsibility for supporting staff who deliver services to VHA patients, including clinical care, dietary support, and other functions. These staff must complete baseline HRO cultural training as well as NCPS team training and are responsible for supporting quality, safety, and patient experience. Potential participants were identified from a list of frontline supervisors provided by VHA management. A subset was chosen through random sampling across geographically distributed VHA hospital facilities that vary in size and complexity. Invitations to participate in completing the questionnaire were sent via email, explaining the quality improvement initiative’s purpose, and encouraging voluntary participation. Of 2000 frontline supervisors invited to participate in the initiative, 97 completed the questionnaire. Participants represented a mix of VHA sites in terms of geography, size, and complexity.
Procedures
The authors used a qualitative approach and administered a confidential online survey. Demographic data were collected within the survey to understand characteristics of the participant population, including length of time as a frontline supervisor, facility complexity level, and professional background (clinical vs nonclinical). Survey questions were developed to elicit responses to specific areas of interest based on existing literature related to HRO and just culture.
Facilitators were defined as factors that increase the likelihood of establishing or sustaining high reliability practices and/or culture. Barriers were defined as factors that decrease or inhibit the likelihood of establishing or sustaining high reliability practices and/or culture. The questionnaire consisted of open-ended questions asking frontline supervisors to describe HRO practices and just culture at their individual facility and within their role. Participants also were asked to identify facilitators and barriers that helped or hindered their efforts to establish and maintain high reliability practices and just culture. The questionnaire solicited recommendations for additional support, training, resources, or leadership interventions to strengthen high reliability practices and just culture from each participant.
Analysis
Participant characteristics were analyzed using descriptive statistics. Responses to the 7 open-ended questions were coded and analyzed using ATLAS.ti v.24 qualitative data analysis software by an experienced researcher and coauthor. Grounded theory methodology allowed themes to emerge from the data and although the response rate was limited, the themes reached a saturation point.18,19
Ethical Considerations
Institutional review board (IRB) review and approval were not required for this quality improvement initiative. Formal IRB review and approval of a quality improvement initiative are not required by VHA. Participation was confidential and voluntary, and participants could withdraw at any time without consequences. Completion of the survey indicated consent, and facility names and participant identifiers were not used. Unique numbers were assigned to each participant and all responses were kept confidential and nonattributional. Frequency coding was used to identify the facilitators and barriers to high reliability practices implementation and just culture among frontline supervisors until thematic saturation was obtained.
Results
A total of 2000 frontline supervisors were invited to participate, of whom 97 completed the questionnaire (response rate, 4.9%). Participants were first asked to describe just culture and high reliability practices in their own words. The consensus was that a just culture emphasizes a nonpunitive environment where employees can report errors or incidents without fear of retaliation. It encourages accountability at the systems level, focusing on learning from mistakes to improve processes. In response to a question asking respondents to describe HRO practices and just culture in their own words, participants noted that organizations with a just culture promote open communication, allowing staff to discuss safety issues and concerns without fear of personal blame. Additionally, participants agreed that HRO practices were defined as a set of principles and practices aimed at minimizing errors and promoting safety, especially within complex and high-risk environments. Participants responded that key characteristics include a preoccupation with failure, sensitivity to operations, reluctance to simplify, and a commitment to resilience. HRO practices entail proactively identifying and mitigating risks through open communication and collaboration among team members, they added.
Overall, participants were aligned with their view of the role a frontline supervisor plays in supporting just culture and HRO principles at their facility by fostering open communication and psychological safety, encouraging continuous learning and improvement, and promoting team collaboration and shared accountability. Among frontline supervisors, 93 (96%) identified their role as being critical to creating a safe space and reinforcing just culture and HRO principles at their facility, while 4 (4%) failed to identify a single duty.
Identified Themes
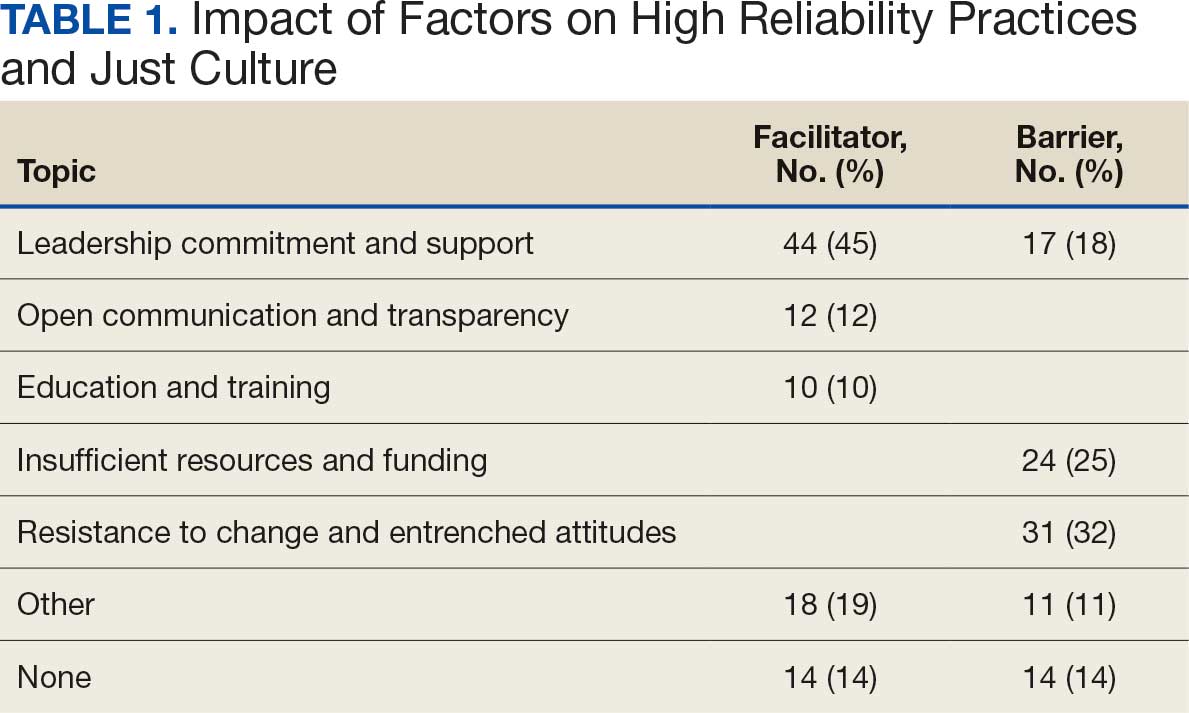
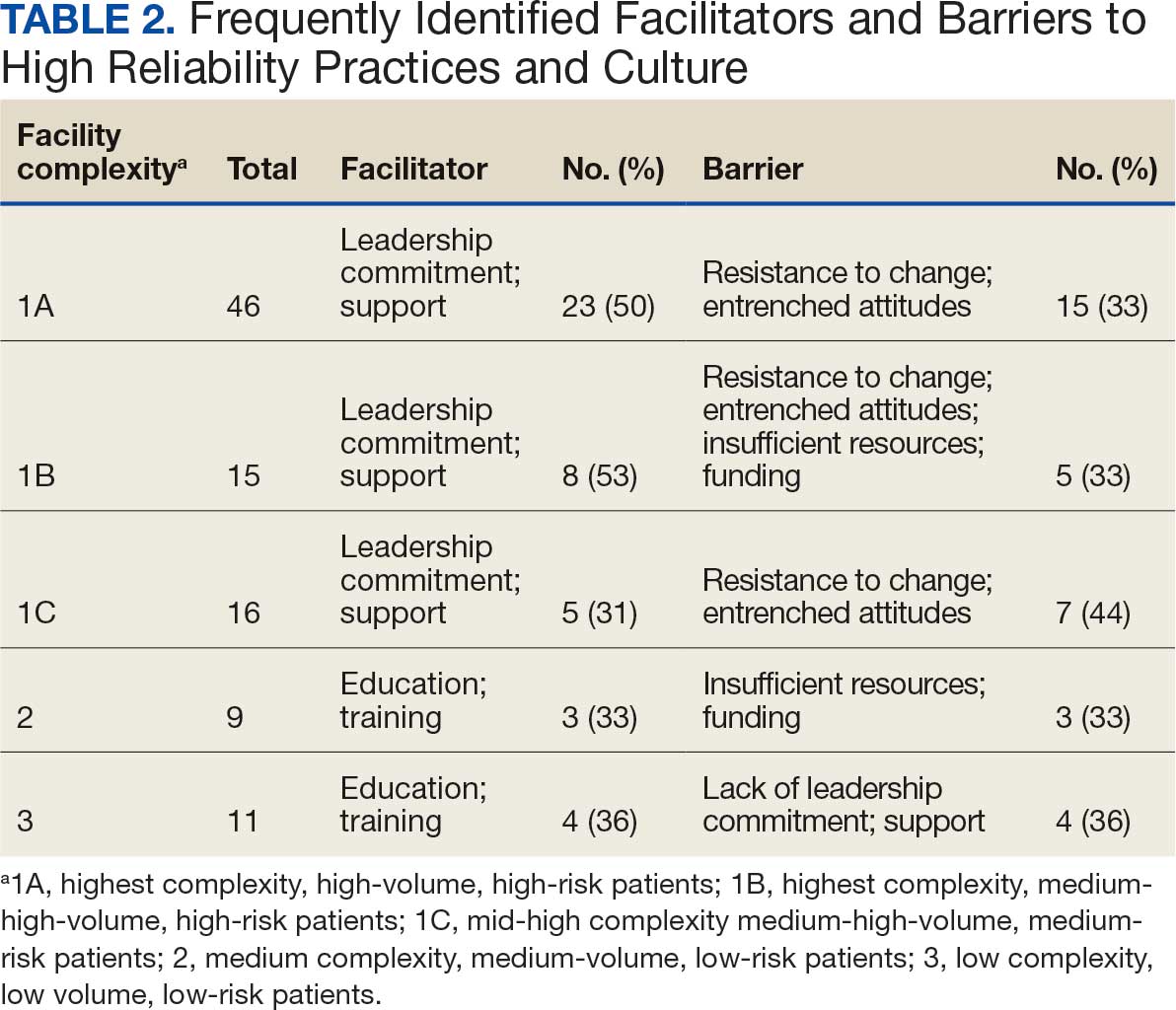
Table 1 summarizes 6 key themes identified from participants’ responses, highlighting the most frequently cited facilitators and barriers to implementing and sustaining high reliability practices and a just culture. Table 2 shows the classification of several themes in relation to facility complexity, emphasizing leadership commitment and support as a pivotal facilitator, while listing resistance to change and entrenched attitudes as a prominent barrier.
Role of Leadership
Facilitators. Leadership commitment and support were the most frequently identified facilitator, accounting for 44 mentions (45%). This aligns with participants’ descriptions of leadership involvement as crucial, particularly in setting standards and fostering accountability throughout the organization. For example, a frontline supervisor with < 5 years of experience from a nonclinical background at a 1B facility remarked, “Facility leadership are involved, which trickles down to lower-level leads and supervisors, which keeps everyone accountable and holds everyone to the same standards.” Participants frequently identified that leaders setting the standard and communicating expectations as paramount facilitators for strengthening high reliability practices and just culture at their facility.
Barriers. A lack of leadership commitment and support was a significant barrier, cited in 17 responses (18%). Participants described this barrier as a deficiency in follow-through, transparency, and presence, which undermines efforts to sustain just culture and high reliability principles. Notably, the lack of leadership commitment and support stood out as a distinct and recurring theme, underscoring its critical role as an independent challenge to achieving organizational goals. “Many leaders are not yet fully bought in,” a respondent explained. “They take the training and pass it off and go right back to their units and focus on blaming or chastis[ing] people for speaking up.” This theme frequently intersected with mentions of insufficient resources and entrenched attitudes, amplifying other challenges.
Open Communication and Transparency
Facilitators. Open communication and transparency were identified as facilitators in 12 responses (12%). Participants emphasized the importance of mechanisms such as HRO meetings and the sharing of “real” examples of positive outcomes from applying HRO principles. Transparent communication fosters psychological safety, allowing staff to report concerns without fear of reprisal. One participant with < 5 years of experience from a clinical background at a 1A facility encapsulated this theme by saying, “Quarterly ‘fireside chats’ are helpful, [this] creates open dialogue about where the next safety issue may occur, what staff need to do their job safely, while also imparting more of the philosophy of HRO that staff may not be aware of.”
Barriers. While communication serves as a facilitator, participants also highlighted barriers such as siloed communication and fear of reprisal. These reflect challenges in creating open and transparent feedback loops essential to high reliability. For example, a participant concluded, “Leadership does not communicate problem-solving efforts and resolution down the chain, they do not see the problems.” Another participant added, “[HRO principles] are not discussed that much.” While this theme presented as a barrier, it was noted less frequently.
Education and Training
Facilitators. Education and training were noted as facilitators in 10 responses (10%), underscoring their role in establishing high reliability practices. Participants suggested tailored training, simulation-based exercises, and mentorship to enhance practical application. However, they noted the importance of linking training to real change and ensuring leadership enforcement of learned behaviors. This theme is best represented by a participant who concluded, “Trainings have helped, but I think as a supervisor, being involved and interacting with your staff, observing, doing the work they do to help identify potential problems areas, especially when new systems are introduced are key. Being hands-on is the only way to successfully manage your team.”
Barriers. Insufficient resources, including time and staffing constraints, were identified as barriers to education and training, accounting for 24 responses (25%). Participants observed that mandatory training without mentorship or application diminishes its effectiveness.
Insufficient Resources and Funding
Barriers. Resource constraints, including low staffing levels and budget cuts, accounted for 24 responses (25%). Participants reported these limitations prevented staff from attending training and affected the overall implementation of just culture and HRO principles. “Low staffing in supporting services as well as in my own service line have created barriers,” a participant reported. Another participant responded that barriers to HRO were primarily “…financial, as the focus is how to curb costs and bring in more funding rather than taking the time to review and apply the concepts of high reliability.”
Resistance to Change and Entrenched Attitudes
Barriers. Resistance to change was the most frequently identified barrier, with 31 responses (32%). One participant described a persistent “gotcha” culture, where blame and punishment hinder progress toward just culture. This entrenched mindset creates significant obstacles to adopting HRO practices and requires active leadership and supervisor intervention to overcome. This theme is best captured by a respondent who noted that “culture change is difficult, especially among staff with such long tenure. It’s a long game.”
Synthesis and Integration of Findings
The data in Table 1 and Table 2 reinforce the themes identified in the qualitative analysis. Leadership commitment and support are pivotal, both as a facilitator and barrier. Open communication and education and training, while recognized as facilitators, were less frequently mentioned, but still critical. Resistance to change and insufficient resources were the most prominent barriers, indicating where organizational efforts should focus to further foster a culture of high reliability.
By addressing these barriers, particularly resistance to change and resource constraints, and leveraging facilitators like leadership engagement and transparent communication, organizations can enhance their implementation of just culture and high reliability practices. These efforts require deliberate strategies, including effective training, mentorship, and the active presence of leadership.
Discussion
This quality improvement initiative builds on prior research by examining the implementation of HRO practices from the perspective of frontline supervisors. Unlike earlier research focused on HRO leads, this study explores the critical role of supervisors who integrate HRO principles into clinical and administrative operations.17 By analyzing their experiences, this study offers practical insights into facilitating HRO implementation across organizational levels.
The findings highlight broad agreement on the value of just culture and HRO principles in fostering safe, accountable health care environments. Participants described just culture as promoting system—level accountability rather than individual blame, encouraging error reporting and learning for continuous improvement. Similarly, HRO practices—emphasizing a preoccupation with failure, operational sensitivity, and resilience— were seen as vital for patient safety in complex settings.
Frontline supervisors play a pivotal role, with 96% of respondents identifying their influence on fostering open communication, psychological safety, and shared accountability. Key facilitators included leadership commitment, open communication, and mentorship. Active leadership involvement was particularly valued, as it trickles down to reinforce standards across all organizational levels. HRO meetings using real-world examples were seen as instrumental in demonstrating the tangible benefits of these principles, helping embed them into daily practices.
Despite these facilitators, several barriers to implementation were noted. Resistance to change and entrenched attitudes, and a persistent gotcha culture undermined efforts to establish just culture. Resource constraints, including staffing shortages and budget limitations, further hindered the adoption of HRO practices. The lack of consistent leadership engagement, marked by limited visibility, follow-through, and transparency, exacerbated these challenges.
HRO leads are important for promoting education and embedding HRO principles into daily operations. These individuals provide vital support to frontline supervisors, translating HRO concepts into actionable practices. However, organizational challenges such as staff turnover and redirected funding have weakened the infrastructure supporting HRO initiatives. The elimination of HRO lead roles due to budgetary pressures at several facilities reflects a short-term focus on operational demands at the expense of long-term cultural transformation.
Additional barriers included siloed communication, fear of reprisal, bureaucratic obstacles, and outdated technology. These challenges limit progress toward high reliability and diminish the effectiveness of HRO principles.
Participants proposed strategies focused on education, training, and leadership engagement. Simulation-based training tailored to specific roles was identified as an effective tool for preparing staff to apply HRO principles in real-world scenarios. Enhanced communication, such as regular leadership rounding and transparent updates on safety concerns, was also emphasized. Participants stressed the importance of showing staff how their feedback influences organizational decisions to build trust and accountability. Finally, standardizing procedures and protocols across facilities was seen as critical for aligning practices and reducing variability in safety processes.
This study underscores the need for sustained leadership commitment and infrastructure to ensure the long-term success of HRO implementation. Addressing the identified barriers and leveraging the proposed mitigation strategies can foster a culture of safety and reliability across the organization.
Limitations
This quality improvement initiative used qualitative grounded theory methods and sampled a relatively small group of experienced leaders specifically involved in implementing HRO within the VHA. In addition, while saturation of themes was reached, the number of responses represents a small sample of VHA frontline supervisors. As such, the findings may not be fully representative of the perspectives of all unit and departmental leaders across the VHA or other health care systems. A previous qualitative quality improvement initiative focused on the perceptions of HRO leads regarding facilitators and barriers to just culture.17 This quality improvement initiative broadened that focus by examining the perspectives of frontline supervisors in the operational environment, who may not be HRO experts but work to implement HRO principles with the guidance of HRO leads (HRO subject matter experts).
There remains an opportunity to address a critical gap by assessing facilitators and barriers beyond the facility level, incorporating both the Veterans Integrated Service Networks (VISN) and VHA Central Office (VHACO). While qualitative methods, such as those used in this study, provide deep insights and detailed understanding, they are limited in their ability to identify system-wide trends and variations at a more strategic VISN and VHACO level. Addressing this could enhance the broader applicability of HRO principles across the VHA.
Conclusions
Successful implementation of the recommendations reported in this study will require sustained focus and continued commitment from all stakeholders across the VHA. As the VHA enters its seventh year on the HRO journey, the risk of organizational drift remains an ongoing concern. Progress has been made, as evidenced by incremental improvements in All Employee Survey scores and increased reporting of adverse events and near misses, but the challenge will be to maintain focus and continue to build upon progress amid the current climate of budgetary constraints.
This study builds on previous quality improvement efforts and provides valuable insights into the barriers and facilitators that can either hinder or support the VHA’s ongoing pursuit of high reliability. The findings offer a model for understanding the complexities of this journey—one that requires continuous effort and adaptation, as there is no definitive endpoint in the quest for high reliability.
Since completion of this study in 2024, the VHA has entered a period of organizational transition and restructuring. Such transitions are often accompanied by increased operational demands and organizational strain. These include realignments, personnel changes, staffing adjustments, workforce reductions, and continued implementation of a new electronic health record system. In this context, maintaining attention to culture, communication, frontline engagement, and mechanisms that provide visibility into organizational climate is essential to sustain momentum in high-reliability efforts.
- Cox GR, Starr LM. VHA’s movement for change: implementing high-reliability principles and practices. J Healthc Manag. 2023;68:151-157. doi:10.1097/jhm-D-23-00056
- Sculli GL, Pendley-Louis R, Neily J, et al. A high-reliability organization framework for health care: A multiyear implementation strategy and associated outcomes. J Patient Saf. 2022;18:64-70. doi:10.1097/pts.0000000000000788
- Murray JS, Clifford J, Larson S, Lee JK, Sculli GL. Implementing just culture to improve patient safety. Mil Med. 2023;188:usac115. doi:10.1093/milmed/usac115
- Merchant NB, O’Neal J, Montoya A, Cox GR, Murray JS. Creating a process for the implementation of tiered huddles in a Veterans Affairs Medical Center. Mil Med. 2023;188:901-906. doi:10.1093/milmed/usac073
- Mohr DC, Chen C, Sullivan J, et al. Development and validation of the Veterans Health Administration Patient Safety Culture Survey. J Patient Saf. 2022;18:539-545. doi:10.1097/PTS.0000000000001027
- Leonard C, Gilmartin H, Starr L, Anderson T. Leadership and the high reliability transformation: a qualitative study at Truman VA medical center. J Healthc Risk Manag. 2024;44:17-23. doi:10.1002/jhrm.21580
- Sculli G, Essen K. Soaring to Success: The Path to Developing High-Reliability Teams. HCPro; 2021.
- Gupta JI, Sivils S, Reppert J, Paulot W, Houchens N, Hummel S. Visual management board implementation to enhance high reliability at a large VA health care system. Fed Pract. 2024;41:242-246. doi:10.12788/fp.0507
- Veterans Health Administration. High Reliability Organization Learning Catalog. US Dept of Veterans Affairs; 2024. Internal document.
- Jahn JLS, Black AE. A model of communicative and hierarchical foundations of high reliability organizing in wildland firefighting teams. Manag Commun Q. 2017;31:356-379. doi:10.1177/0893318917691358
- Myers CG, Sutcliffe KM. High reliability organising in healthcare: still a long way left to go. BMJ Qual Saf. 2022;31:845-848. doi:10.1136/bmjqs-2021-014141
- Abrams J. Model the way to navigate difficult topics. The Learning Professional. 2022;43:14-18.
- McCausland T. Creating psychological safety in the workplace. Research-Technology Management. 2023;66:56-58. doi:10.1080/08956308.2023.2164439
- Murray JS, Kelly S, Hanover C. Promoting psychological safety in healthcare organizations. Mil Med. 2022;187:808- 810. doi:10.1093/milmed/usac041
- Sutton RI, Rao H. The friction project: how smart leaders make the right things easier and the wrong things harder. St. Martin’s Press; 2024.
- Clark TR. The 4 stages of psychological safety: defining the path to inclusion and innovation. Berrett-Koehler Publishers, Inc.; 2020.
- Essen K, Villalobos C, Sculli G, Steinbach L. Establishing a just culture: implications for the Veterans Health Administration journey to high reliability. Fed Pract. 2024;41:290- 297. doi:10.12788/fp.0512
- Creswell JW. Research design: qualitative, quantitative, and mixed methods approaches. 4th ed. SAGE Publications; 2014.
- Patton MQ. Qualitative research & evaluation methods: integrating theory and practice. 4th ed. SAGE Publications, Inc.; 2015.
- Krumpal I. Determinants of social desirability bias in sensitive surveys: a literature review. Qual Quant. 2013;47:2025- 2047. doi:10.1007/s11135-011-9640-9
The Veterans Health Administration (VHA) is now in the sixth year of its enterprise-wide transformation into a high reliability organization (HRO). This effort began with a 2016 pilot project and is now implemented in 170 VHA medical centers.1-4 This transformation reflects a commitment to implementing standardized and reliable health care practices.
The VHA HRO implementation strategy includes a multifaceted approach to engage leadership through education, training, leader coaching, and change management initiatives.2 Despite the diversity of facilities in terms of cultures, geographies, and complexities, US Department of Veterans Affairs (VA) medical centers (VAMCs) have increasingly embraced standardized HRO practices. These changes are evident in improvements in VHA All Employee Survey scores, which assess 4 key patient safety culture dimensions: risk identification and just culture, error transparency and mitigation, supervisor communication and trust, and team cohesion and engagement.5 Positive trends in these dimensions highlight a cultural shift toward greater reliability, even amid challenges introduced by the COVID-19 pandemic.
However, this progress has encountered some challenges. Leadership turnover, budgetary constraints, and extensive educational demands for implementing and sustaining HRO practices have created obstacles, particularly for frontline health care practitioners.6 Additionally, there are pockets of resistance similar to what the airline industry faced when implementing crew resource management (CRM). Specifically, senior pilots and legacy leaders were reluctant to abandon their high-status, autocratic management styles and embrace CRM, despite its proven benefits for enhancing commercial airline safety.7 Similarly, some VHA staff have expressed resistance to foundational HRO practices, which include safety huddles, safety forums, leader rounding, and visual management systems.6,8
The training requirements for HRO practices range from a 25-minute introductory course (HRO 101) to a 7.5-hour team training session facilitated by the VHA National Center for Patient Safety (NCPS).9 While some supervisors view these requirements as burdensome, others have demonstrated strong enthusiasm for the process.6 Understanding the perspectives of unit and departmental managers regarding factors that enhance or hinder the adoption of HRO practices is critical for continuous improvement.10-12 Research has suggested that fostering psychological safety can create an environment where new ideas are shared openly, helping organizations navigate resistance to change.13-16
A 2024 quality improvement study, drawing on the perceptions of HRO leads, identified key facilitators, including training, coaching, leader approachability, and psychological safety, as well as barriers such as inadequate training and lack of accountability among managers.17 Building on this work, the current study focused on frontline supervisors, who are directly involved in integrating HRO practices into patient care activities. By addressing both barriers and facilitators, this expanded approach aims to provide a more comprehensive understanding of the challenges influencing HRO implementation in day-to-day operations.
Methods
This quality improvement initiative examined facilitators and barriers to establishing just culture and implementing high reliability practices, focusing on frontline supervisors overseeing clinical care teams (eg, emergency department, critical care) or patient-support functions (eg, dietary services). A questionnaire was sent to a randomized sample of VHA facility supervisors.
A qualitative grounded theory approach was employed to provide a deeper understanding of nuanced phenomena that cannot be captured through numerical data alone. This method enables systematic analysis using open, axial, and thematic coding, ensuring that emerging themes achieve saturation.18,19 It is particularly suited for this study, given the limited prior data on frontline supervisors. Additionally, qualitative methods help mitigate biases common in Likert-style scales, where respondents may lean toward agreement, potentially skewing results.20
Inclusion Criteria
Participants were required to have served as a frontline supervisor for ≥ 6 months. Frontline supervisors are assigned responsibility for supporting staff who deliver services to VHA patients, including clinical care, dietary support, and other functions. These staff must complete baseline HRO cultural training as well as NCPS team training and are responsible for supporting quality, safety, and patient experience. Potential participants were identified from a list of frontline supervisors provided by VHA management. A subset was chosen through random sampling across geographically distributed VHA hospital facilities that vary in size and complexity. Invitations to participate in completing the questionnaire were sent via email, explaining the quality improvement initiative’s purpose, and encouraging voluntary participation. Of 2000 frontline supervisors invited to participate in the initiative, 97 completed the questionnaire. Participants represented a mix of VHA sites in terms of geography, size, and complexity.
Procedures
The authors used a qualitative approach and administered a confidential online survey. Demographic data were collected within the survey to understand characteristics of the participant population, including length of time as a frontline supervisor, facility complexity level, and professional background (clinical vs nonclinical). Survey questions were developed to elicit responses to specific areas of interest based on existing literature related to HRO and just culture.
Facilitators were defined as factors that increase the likelihood of establishing or sustaining high reliability practices and/or culture. Barriers were defined as factors that decrease or inhibit the likelihood of establishing or sustaining high reliability practices and/or culture. The questionnaire consisted of open-ended questions asking frontline supervisors to describe HRO practices and just culture at their individual facility and within their role. Participants also were asked to identify facilitators and barriers that helped or hindered their efforts to establish and maintain high reliability practices and just culture. The questionnaire solicited recommendations for additional support, training, resources, or leadership interventions to strengthen high reliability practices and just culture from each participant.
Analysis
Participant characteristics were analyzed using descriptive statistics. Responses to the 7 open-ended questions were coded and analyzed using ATLAS.ti v.24 qualitative data analysis software by an experienced researcher and coauthor. Grounded theory methodology allowed themes to emerge from the data and although the response rate was limited, the themes reached a saturation point.18,19
Ethical Considerations
Institutional review board (IRB) review and approval were not required for this quality improvement initiative. Formal IRB review and approval of a quality improvement initiative are not required by VHA. Participation was confidential and voluntary, and participants could withdraw at any time without consequences. Completion of the survey indicated consent, and facility names and participant identifiers were not used. Unique numbers were assigned to each participant and all responses were kept confidential and nonattributional. Frequency coding was used to identify the facilitators and barriers to high reliability practices implementation and just culture among frontline supervisors until thematic saturation was obtained.
Results
A total of 2000 frontline supervisors were invited to participate, of whom 97 completed the questionnaire (response rate, 4.9%). Participants were first asked to describe just culture and high reliability practices in their own words. The consensus was that a just culture emphasizes a nonpunitive environment where employees can report errors or incidents without fear of retaliation. It encourages accountability at the systems level, focusing on learning from mistakes to improve processes. In response to a question asking respondents to describe HRO practices and just culture in their own words, participants noted that organizations with a just culture promote open communication, allowing staff to discuss safety issues and concerns without fear of personal blame. Additionally, participants agreed that HRO practices were defined as a set of principles and practices aimed at minimizing errors and promoting safety, especially within complex and high-risk environments. Participants responded that key characteristics include a preoccupation with failure, sensitivity to operations, reluctance to simplify, and a commitment to resilience. HRO practices entail proactively identifying and mitigating risks through open communication and collaboration among team members, they added.
Overall, participants were aligned with their view of the role a frontline supervisor plays in supporting just culture and HRO principles at their facility by fostering open communication and psychological safety, encouraging continuous learning and improvement, and promoting team collaboration and shared accountability. Among frontline supervisors, 93 (96%) identified their role as being critical to creating a safe space and reinforcing just culture and HRO principles at their facility, while 4 (4%) failed to identify a single duty.
Identified Themes
Table 1 summarizes 6 key themes identified from participants’ responses, highlighting the most frequently cited facilitators and barriers to implementing and sustaining high reliability practices and a just culture. Table 2 shows the classification of several themes in relation to facility complexity, emphasizing leadership commitment and support as a pivotal facilitator, while listing resistance to change and entrenched attitudes as a prominent barrier.


Role of Leadership
Facilitators. Leadership commitment and support were the most frequently identified facilitator, accounting for 44 mentions (45%). This aligns with participants’ descriptions of leadership involvement as crucial, particularly in setting standards and fostering accountability throughout the organization. For example, a frontline supervisor with < 5 years of experience from a nonclinical background at a 1B facility remarked, “Facility leadership are involved, which trickles down to lower-level leads and supervisors, which keeps everyone accountable and holds everyone to the same standards.” Participants frequently identified that leaders setting the standard and communicating expectations as paramount facilitators for strengthening high reliability practices and just culture at their facility.
Barriers. A lack of leadership commitment and support was a significant barrier, cited in 17 responses (18%). Participants described this barrier as a deficiency in follow-through, transparency, and presence, which undermines efforts to sustain just culture and high reliability principles. Notably, the lack of leadership commitment and support stood out as a distinct and recurring theme, underscoring its critical role as an independent challenge to achieving organizational goals. “Many leaders are not yet fully bought in,” a respondent explained. “They take the training and pass it off and go right back to their units and focus on blaming or chastis[ing] people for speaking up.” This theme frequently intersected with mentions of insufficient resources and entrenched attitudes, amplifying other challenges.
Open Communication and Transparency
Facilitators. Open communication and transparency were identified as facilitators in 12 responses (12%). Participants emphasized the importance of mechanisms such as HRO meetings and the sharing of “real” examples of positive outcomes from applying HRO principles. Transparent communication fosters psychological safety, allowing staff to report concerns without fear of reprisal. One participant with < 5 years of experience from a clinical background at a 1A facility encapsulated this theme by saying, “Quarterly ‘fireside chats’ are helpful, [this] creates open dialogue about where the next safety issue may occur, what staff need to do their job safely, while also imparting more of the philosophy of HRO that staff may not be aware of.”
Barriers. While communication serves as a facilitator, participants also highlighted barriers such as siloed communication and fear of reprisal. These reflect challenges in creating open and transparent feedback loops essential to high reliability. For example, a participant concluded, “Leadership does not communicate problem-solving efforts and resolution down the chain, they do not see the problems.” Another participant added, “[HRO principles] are not discussed that much.” While this theme presented as a barrier, it was noted less frequently.
Education and Training
Facilitators. Education and training were noted as facilitators in 10 responses (10%), underscoring their role in establishing high reliability practices. Participants suggested tailored training, simulation-based exercises, and mentorship to enhance practical application. However, they noted the importance of linking training to real change and ensuring leadership enforcement of learned behaviors. This theme is best represented by a participant who concluded, “Trainings have helped, but I think as a supervisor, being involved and interacting with your staff, observing, doing the work they do to help identify potential problems areas, especially when new systems are introduced are key. Being hands-on is the only way to successfully manage your team.”
Barriers. Insufficient resources, including time and staffing constraints, were identified as barriers to education and training, accounting for 24 responses (25%). Participants observed that mandatory training without mentorship or application diminishes its effectiveness.
Insufficient Resources and Funding
Barriers. Resource constraints, including low staffing levels and budget cuts, accounted for 24 responses (25%). Participants reported these limitations prevented staff from attending training and affected the overall implementation of just culture and HRO principles. “Low staffing in supporting services as well as in my own service line have created barriers,” a participant reported. Another participant responded that barriers to HRO were primarily “…financial, as the focus is how to curb costs and bring in more funding rather than taking the time to review and apply the concepts of high reliability.”
Resistance to Change and Entrenched Attitudes
Barriers. Resistance to change was the most frequently identified barrier, with 31 responses (32%). One participant described a persistent “gotcha” culture, where blame and punishment hinder progress toward just culture. This entrenched mindset creates significant obstacles to adopting HRO practices and requires active leadership and supervisor intervention to overcome. This theme is best captured by a respondent who noted that “culture change is difficult, especially among staff with such long tenure. It’s a long game.”
Synthesis and Integration of Findings
The data in Table 1 and Table 2 reinforce the themes identified in the qualitative analysis. Leadership commitment and support are pivotal, both as a facilitator and barrier. Open communication and education and training, while recognized as facilitators, were less frequently mentioned, but still critical. Resistance to change and insufficient resources were the most prominent barriers, indicating where organizational efforts should focus to further foster a culture of high reliability.
By addressing these barriers, particularly resistance to change and resource constraints, and leveraging facilitators like leadership engagement and transparent communication, organizations can enhance their implementation of just culture and high reliability practices. These efforts require deliberate strategies, including effective training, mentorship, and the active presence of leadership.
Discussion
This quality improvement initiative builds on prior research by examining the implementation of HRO practices from the perspective of frontline supervisors. Unlike earlier research focused on HRO leads, this study explores the critical role of supervisors who integrate HRO principles into clinical and administrative operations.17 By analyzing their experiences, this study offers practical insights into facilitating HRO implementation across organizational levels.
The findings highlight broad agreement on the value of just culture and HRO principles in fostering safe, accountable health care environments. Participants described just culture as promoting system—level accountability rather than individual blame, encouraging error reporting and learning for continuous improvement. Similarly, HRO practices—emphasizing a preoccupation with failure, operational sensitivity, and resilience— were seen as vital for patient safety in complex settings.
Frontline supervisors play a pivotal role, with 96% of respondents identifying their influence on fostering open communication, psychological safety, and shared accountability. Key facilitators included leadership commitment, open communication, and mentorship. Active leadership involvement was particularly valued, as it trickles down to reinforce standards across all organizational levels. HRO meetings using real-world examples were seen as instrumental in demonstrating the tangible benefits of these principles, helping embed them into daily practices.
Despite these facilitators, several barriers to implementation were noted. Resistance to change and entrenched attitudes, and a persistent gotcha culture undermined efforts to establish just culture. Resource constraints, including staffing shortages and budget limitations, further hindered the adoption of HRO practices. The lack of consistent leadership engagement, marked by limited visibility, follow-through, and transparency, exacerbated these challenges.
HRO leads are important for promoting education and embedding HRO principles into daily operations. These individuals provide vital support to frontline supervisors, translating HRO concepts into actionable practices. However, organizational challenges such as staff turnover and redirected funding have weakened the infrastructure supporting HRO initiatives. The elimination of HRO lead roles due to budgetary pressures at several facilities reflects a short-term focus on operational demands at the expense of long-term cultural transformation.
Additional barriers included siloed communication, fear of reprisal, bureaucratic obstacles, and outdated technology. These challenges limit progress toward high reliability and diminish the effectiveness of HRO principles.
Participants proposed strategies focused on education, training, and leadership engagement. Simulation-based training tailored to specific roles was identified as an effective tool for preparing staff to apply HRO principles in real-world scenarios. Enhanced communication, such as regular leadership rounding and transparent updates on safety concerns, was also emphasized. Participants stressed the importance of showing staff how their feedback influences organizational decisions to build trust and accountability. Finally, standardizing procedures and protocols across facilities was seen as critical for aligning practices and reducing variability in safety processes.
This study underscores the need for sustained leadership commitment and infrastructure to ensure the long-term success of HRO implementation. Addressing the identified barriers and leveraging the proposed mitigation strategies can foster a culture of safety and reliability across the organization.
Limitations
This quality improvement initiative used qualitative grounded theory methods and sampled a relatively small group of experienced leaders specifically involved in implementing HRO within the VHA. In addition, while saturation of themes was reached, the number of responses represents a small sample of VHA frontline supervisors. As such, the findings may not be fully representative of the perspectives of all unit and departmental leaders across the VHA or other health care systems. A previous qualitative quality improvement initiative focused on the perceptions of HRO leads regarding facilitators and barriers to just culture.17 This quality improvement initiative broadened that focus by examining the perspectives of frontline supervisors in the operational environment, who may not be HRO experts but work to implement HRO principles with the guidance of HRO leads (HRO subject matter experts).
There remains an opportunity to address a critical gap by assessing facilitators and barriers beyond the facility level, incorporating both the Veterans Integrated Service Networks (VISN) and VHA Central Office (VHACO). While qualitative methods, such as those used in this study, provide deep insights and detailed understanding, they are limited in their ability to identify system-wide trends and variations at a more strategic VISN and VHACO level. Addressing this could enhance the broader applicability of HRO principles across the VHA.
Conclusions
Successful implementation of the recommendations reported in this study will require sustained focus and continued commitment from all stakeholders across the VHA. As the VHA enters its seventh year on the HRO journey, the risk of organizational drift remains an ongoing concern. Progress has been made, as evidenced by incremental improvements in All Employee Survey scores and increased reporting of adverse events and near misses, but the challenge will be to maintain focus and continue to build upon progress amid the current climate of budgetary constraints.
This study builds on previous quality improvement efforts and provides valuable insights into the barriers and facilitators that can either hinder or support the VHA’s ongoing pursuit of high reliability. The findings offer a model for understanding the complexities of this journey—one that requires continuous effort and adaptation, as there is no definitive endpoint in the quest for high reliability.
Since completion of this study in 2024, the VHA has entered a period of organizational transition and restructuring. Such transitions are often accompanied by increased operational demands and organizational strain. These include realignments, personnel changes, staffing adjustments, workforce reductions, and continued implementation of a new electronic health record system. In this context, maintaining attention to culture, communication, frontline engagement, and mechanisms that provide visibility into organizational climate is essential to sustain momentum in high-reliability efforts.
The Veterans Health Administration (VHA) is now in the sixth year of its enterprise-wide transformation into a high reliability organization (HRO). This effort began with a 2016 pilot project and is now implemented in 170 VHA medical centers.1-4 This transformation reflects a commitment to implementing standardized and reliable health care practices.
The VHA HRO implementation strategy includes a multifaceted approach to engage leadership through education, training, leader coaching, and change management initiatives.2 Despite the diversity of facilities in terms of cultures, geographies, and complexities, US Department of Veterans Affairs (VA) medical centers (VAMCs) have increasingly embraced standardized HRO practices. These changes are evident in improvements in VHA All Employee Survey scores, which assess 4 key patient safety culture dimensions: risk identification and just culture, error transparency and mitigation, supervisor communication and trust, and team cohesion and engagement.5 Positive trends in these dimensions highlight a cultural shift toward greater reliability, even amid challenges introduced by the COVID-19 pandemic.
However, this progress has encountered some challenges. Leadership turnover, budgetary constraints, and extensive educational demands for implementing and sustaining HRO practices have created obstacles, particularly for frontline health care practitioners.6 Additionally, there are pockets of resistance similar to what the airline industry faced when implementing crew resource management (CRM). Specifically, senior pilots and legacy leaders were reluctant to abandon their high-status, autocratic management styles and embrace CRM, despite its proven benefits for enhancing commercial airline safety.7 Similarly, some VHA staff have expressed resistance to foundational HRO practices, which include safety huddles, safety forums, leader rounding, and visual management systems.6,8
The training requirements for HRO practices range from a 25-minute introductory course (HRO 101) to a 7.5-hour team training session facilitated by the VHA National Center for Patient Safety (NCPS).9 While some supervisors view these requirements as burdensome, others have demonstrated strong enthusiasm for the process.6 Understanding the perspectives of unit and departmental managers regarding factors that enhance or hinder the adoption of HRO practices is critical for continuous improvement.10-12 Research has suggested that fostering psychological safety can create an environment where new ideas are shared openly, helping organizations navigate resistance to change.13-16
A 2024 quality improvement study, drawing on the perceptions of HRO leads, identified key facilitators, including training, coaching, leader approachability, and psychological safety, as well as barriers such as inadequate training and lack of accountability among managers.17 Building on this work, the current study focused on frontline supervisors, who are directly involved in integrating HRO practices into patient care activities. By addressing both barriers and facilitators, this expanded approach aims to provide a more comprehensive understanding of the challenges influencing HRO implementation in day-to-day operations.
Methods
This quality improvement initiative examined facilitators and barriers to establishing just culture and implementing high reliability practices, focusing on frontline supervisors overseeing clinical care teams (eg, emergency department, critical care) or patient-support functions (eg, dietary services). A questionnaire was sent to a randomized sample of VHA facility supervisors.
A qualitative grounded theory approach was employed to provide a deeper understanding of nuanced phenomena that cannot be captured through numerical data alone. This method enables systematic analysis using open, axial, and thematic coding, ensuring that emerging themes achieve saturation.18,19 It is particularly suited for this study, given the limited prior data on frontline supervisors. Additionally, qualitative methods help mitigate biases common in Likert-style scales, where respondents may lean toward agreement, potentially skewing results.20
Inclusion Criteria
Participants were required to have served as a frontline supervisor for ≥ 6 months. Frontline supervisors are assigned responsibility for supporting staff who deliver services to VHA patients, including clinical care, dietary support, and other functions. These staff must complete baseline HRO cultural training as well as NCPS team training and are responsible for supporting quality, safety, and patient experience. Potential participants were identified from a list of frontline supervisors provided by VHA management. A subset was chosen through random sampling across geographically distributed VHA hospital facilities that vary in size and complexity. Invitations to participate in completing the questionnaire were sent via email, explaining the quality improvement initiative’s purpose, and encouraging voluntary participation. Of 2000 frontline supervisors invited to participate in the initiative, 97 completed the questionnaire. Participants represented a mix of VHA sites in terms of geography, size, and complexity.
Procedures
The authors used a qualitative approach and administered a confidential online survey. Demographic data were collected within the survey to understand characteristics of the participant population, including length of time as a frontline supervisor, facility complexity level, and professional background (clinical vs nonclinical). Survey questions were developed to elicit responses to specific areas of interest based on existing literature related to HRO and just culture.
Facilitators were defined as factors that increase the likelihood of establishing or sustaining high reliability practices and/or culture. Barriers were defined as factors that decrease or inhibit the likelihood of establishing or sustaining high reliability practices and/or culture. The questionnaire consisted of open-ended questions asking frontline supervisors to describe HRO practices and just culture at their individual facility and within their role. Participants also were asked to identify facilitators and barriers that helped or hindered their efforts to establish and maintain high reliability practices and just culture. The questionnaire solicited recommendations for additional support, training, resources, or leadership interventions to strengthen high reliability practices and just culture from each participant.
Analysis
Participant characteristics were analyzed using descriptive statistics. Responses to the 7 open-ended questions were coded and analyzed using ATLAS.ti v.24 qualitative data analysis software by an experienced researcher and coauthor. Grounded theory methodology allowed themes to emerge from the data and although the response rate was limited, the themes reached a saturation point.18,19
Ethical Considerations
Institutional review board (IRB) review and approval were not required for this quality improvement initiative. Formal IRB review and approval of a quality improvement initiative are not required by VHA. Participation was confidential and voluntary, and participants could withdraw at any time without consequences. Completion of the survey indicated consent, and facility names and participant identifiers were not used. Unique numbers were assigned to each participant and all responses were kept confidential and nonattributional. Frequency coding was used to identify the facilitators and barriers to high reliability practices implementation and just culture among frontline supervisors until thematic saturation was obtained.
Results
A total of 2000 frontline supervisors were invited to participate, of whom 97 completed the questionnaire (response rate, 4.9%). Participants were first asked to describe just culture and high reliability practices in their own words. The consensus was that a just culture emphasizes a nonpunitive environment where employees can report errors or incidents without fear of retaliation. It encourages accountability at the systems level, focusing on learning from mistakes to improve processes. In response to a question asking respondents to describe HRO practices and just culture in their own words, participants noted that organizations with a just culture promote open communication, allowing staff to discuss safety issues and concerns without fear of personal blame. Additionally, participants agreed that HRO practices were defined as a set of principles and practices aimed at minimizing errors and promoting safety, especially within complex and high-risk environments. Participants responded that key characteristics include a preoccupation with failure, sensitivity to operations, reluctance to simplify, and a commitment to resilience. HRO practices entail proactively identifying and mitigating risks through open communication and collaboration among team members, they added.
Overall, participants were aligned with their view of the role a frontline supervisor plays in supporting just culture and HRO principles at their facility by fostering open communication and psychological safety, encouraging continuous learning and improvement, and promoting team collaboration and shared accountability. Among frontline supervisors, 93 (96%) identified their role as being critical to creating a safe space and reinforcing just culture and HRO principles at their facility, while 4 (4%) failed to identify a single duty.
Identified Themes
Table 1 summarizes 6 key themes identified from participants’ responses, highlighting the most frequently cited facilitators and barriers to implementing and sustaining high reliability practices and a just culture. Table 2 shows the classification of several themes in relation to facility complexity, emphasizing leadership commitment and support as a pivotal facilitator, while listing resistance to change and entrenched attitudes as a prominent barrier.


Role of Leadership
Facilitators. Leadership commitment and support were the most frequently identified facilitator, accounting for 44 mentions (45%). This aligns with participants’ descriptions of leadership involvement as crucial, particularly in setting standards and fostering accountability throughout the organization. For example, a frontline supervisor with < 5 years of experience from a nonclinical background at a 1B facility remarked, “Facility leadership are involved, which trickles down to lower-level leads and supervisors, which keeps everyone accountable and holds everyone to the same standards.” Participants frequently identified that leaders setting the standard and communicating expectations as paramount facilitators for strengthening high reliability practices and just culture at their facility.
Barriers. A lack of leadership commitment and support was a significant barrier, cited in 17 responses (18%). Participants described this barrier as a deficiency in follow-through, transparency, and presence, which undermines efforts to sustain just culture and high reliability principles. Notably, the lack of leadership commitment and support stood out as a distinct and recurring theme, underscoring its critical role as an independent challenge to achieving organizational goals. “Many leaders are not yet fully bought in,” a respondent explained. “They take the training and pass it off and go right back to their units and focus on blaming or chastis[ing] people for speaking up.” This theme frequently intersected with mentions of insufficient resources and entrenched attitudes, amplifying other challenges.
Open Communication and Transparency
Facilitators. Open communication and transparency were identified as facilitators in 12 responses (12%). Participants emphasized the importance of mechanisms such as HRO meetings and the sharing of “real” examples of positive outcomes from applying HRO principles. Transparent communication fosters psychological safety, allowing staff to report concerns without fear of reprisal. One participant with < 5 years of experience from a clinical background at a 1A facility encapsulated this theme by saying, “Quarterly ‘fireside chats’ are helpful, [this] creates open dialogue about where the next safety issue may occur, what staff need to do their job safely, while also imparting more of the philosophy of HRO that staff may not be aware of.”
Barriers. While communication serves as a facilitator, participants also highlighted barriers such as siloed communication and fear of reprisal. These reflect challenges in creating open and transparent feedback loops essential to high reliability. For example, a participant concluded, “Leadership does not communicate problem-solving efforts and resolution down the chain, they do not see the problems.” Another participant added, “[HRO principles] are not discussed that much.” While this theme presented as a barrier, it was noted less frequently.
Education and Training
Facilitators. Education and training were noted as facilitators in 10 responses (10%), underscoring their role in establishing high reliability practices. Participants suggested tailored training, simulation-based exercises, and mentorship to enhance practical application. However, they noted the importance of linking training to real change and ensuring leadership enforcement of learned behaviors. This theme is best represented by a participant who concluded, “Trainings have helped, but I think as a supervisor, being involved and interacting with your staff, observing, doing the work they do to help identify potential problems areas, especially when new systems are introduced are key. Being hands-on is the only way to successfully manage your team.”
Barriers. Insufficient resources, including time and staffing constraints, were identified as barriers to education and training, accounting for 24 responses (25%). Participants observed that mandatory training without mentorship or application diminishes its effectiveness.
Insufficient Resources and Funding
Barriers. Resource constraints, including low staffing levels and budget cuts, accounted for 24 responses (25%). Participants reported these limitations prevented staff from attending training and affected the overall implementation of just culture and HRO principles. “Low staffing in supporting services as well as in my own service line have created barriers,” a participant reported. Another participant responded that barriers to HRO were primarily “…financial, as the focus is how to curb costs and bring in more funding rather than taking the time to review and apply the concepts of high reliability.”
Resistance to Change and Entrenched Attitudes
Barriers. Resistance to change was the most frequently identified barrier, with 31 responses (32%). One participant described a persistent “gotcha” culture, where blame and punishment hinder progress toward just culture. This entrenched mindset creates significant obstacles to adopting HRO practices and requires active leadership and supervisor intervention to overcome. This theme is best captured by a respondent who noted that “culture change is difficult, especially among staff with such long tenure. It’s a long game.”
Synthesis and Integration of Findings
The data in Table 1 and Table 2 reinforce the themes identified in the qualitative analysis. Leadership commitment and support are pivotal, both as a facilitator and barrier. Open communication and education and training, while recognized as facilitators, were less frequently mentioned, but still critical. Resistance to change and insufficient resources were the most prominent barriers, indicating where organizational efforts should focus to further foster a culture of high reliability.
By addressing these barriers, particularly resistance to change and resource constraints, and leveraging facilitators like leadership engagement and transparent communication, organizations can enhance their implementation of just culture and high reliability practices. These efforts require deliberate strategies, including effective training, mentorship, and the active presence of leadership.
Discussion
This quality improvement initiative builds on prior research by examining the implementation of HRO practices from the perspective of frontline supervisors. Unlike earlier research focused on HRO leads, this study explores the critical role of supervisors who integrate HRO principles into clinical and administrative operations.17 By analyzing their experiences, this study offers practical insights into facilitating HRO implementation across organizational levels.
The findings highlight broad agreement on the value of just culture and HRO principles in fostering safe, accountable health care environments. Participants described just culture as promoting system—level accountability rather than individual blame, encouraging error reporting and learning for continuous improvement. Similarly, HRO practices—emphasizing a preoccupation with failure, operational sensitivity, and resilience— were seen as vital for patient safety in complex settings.
Frontline supervisors play a pivotal role, with 96% of respondents identifying their influence on fostering open communication, psychological safety, and shared accountability. Key facilitators included leadership commitment, open communication, and mentorship. Active leadership involvement was particularly valued, as it trickles down to reinforce standards across all organizational levels. HRO meetings using real-world examples were seen as instrumental in demonstrating the tangible benefits of these principles, helping embed them into daily practices.
Despite these facilitators, several barriers to implementation were noted. Resistance to change and entrenched attitudes, and a persistent gotcha culture undermined efforts to establish just culture. Resource constraints, including staffing shortages and budget limitations, further hindered the adoption of HRO practices. The lack of consistent leadership engagement, marked by limited visibility, follow-through, and transparency, exacerbated these challenges.
HRO leads are important for promoting education and embedding HRO principles into daily operations. These individuals provide vital support to frontline supervisors, translating HRO concepts into actionable practices. However, organizational challenges such as staff turnover and redirected funding have weakened the infrastructure supporting HRO initiatives. The elimination of HRO lead roles due to budgetary pressures at several facilities reflects a short-term focus on operational demands at the expense of long-term cultural transformation.
Additional barriers included siloed communication, fear of reprisal, bureaucratic obstacles, and outdated technology. These challenges limit progress toward high reliability and diminish the effectiveness of HRO principles.
Participants proposed strategies focused on education, training, and leadership engagement. Simulation-based training tailored to specific roles was identified as an effective tool for preparing staff to apply HRO principles in real-world scenarios. Enhanced communication, such as regular leadership rounding and transparent updates on safety concerns, was also emphasized. Participants stressed the importance of showing staff how their feedback influences organizational decisions to build trust and accountability. Finally, standardizing procedures and protocols across facilities was seen as critical for aligning practices and reducing variability in safety processes.
This study underscores the need for sustained leadership commitment and infrastructure to ensure the long-term success of HRO implementation. Addressing the identified barriers and leveraging the proposed mitigation strategies can foster a culture of safety and reliability across the organization.
Limitations
This quality improvement initiative used qualitative grounded theory methods and sampled a relatively small group of experienced leaders specifically involved in implementing HRO within the VHA. In addition, while saturation of themes was reached, the number of responses represents a small sample of VHA frontline supervisors. As such, the findings may not be fully representative of the perspectives of all unit and departmental leaders across the VHA or other health care systems. A previous qualitative quality improvement initiative focused on the perceptions of HRO leads regarding facilitators and barriers to just culture.17 This quality improvement initiative broadened that focus by examining the perspectives of frontline supervisors in the operational environment, who may not be HRO experts but work to implement HRO principles with the guidance of HRO leads (HRO subject matter experts).
There remains an opportunity to address a critical gap by assessing facilitators and barriers beyond the facility level, incorporating both the Veterans Integrated Service Networks (VISN) and VHA Central Office (VHACO). While qualitative methods, such as those used in this study, provide deep insights and detailed understanding, they are limited in their ability to identify system-wide trends and variations at a more strategic VISN and VHACO level. Addressing this could enhance the broader applicability of HRO principles across the VHA.
Conclusions
Successful implementation of the recommendations reported in this study will require sustained focus and continued commitment from all stakeholders across the VHA. As the VHA enters its seventh year on the HRO journey, the risk of organizational drift remains an ongoing concern. Progress has been made, as evidenced by incremental improvements in All Employee Survey scores and increased reporting of adverse events and near misses, but the challenge will be to maintain focus and continue to build upon progress amid the current climate of budgetary constraints.
This study builds on previous quality improvement efforts and provides valuable insights into the barriers and facilitators that can either hinder or support the VHA’s ongoing pursuit of high reliability. The findings offer a model for understanding the complexities of this journey—one that requires continuous effort and adaptation, as there is no definitive endpoint in the quest for high reliability.
Since completion of this study in 2024, the VHA has entered a period of organizational transition and restructuring. Such transitions are often accompanied by increased operational demands and organizational strain. These include realignments, personnel changes, staffing adjustments, workforce reductions, and continued implementation of a new electronic health record system. In this context, maintaining attention to culture, communication, frontline engagement, and mechanisms that provide visibility into organizational climate is essential to sustain momentum in high-reliability efforts.
- Cox GR, Starr LM. VHA’s movement for change: implementing high-reliability principles and practices. J Healthc Manag. 2023;68:151-157. doi:10.1097/jhm-D-23-00056
- Sculli GL, Pendley-Louis R, Neily J, et al. A high-reliability organization framework for health care: A multiyear implementation strategy and associated outcomes. J Patient Saf. 2022;18:64-70. doi:10.1097/pts.0000000000000788
- Murray JS, Clifford J, Larson S, Lee JK, Sculli GL. Implementing just culture to improve patient safety. Mil Med. 2023;188:usac115. doi:10.1093/milmed/usac115
- Merchant NB, O’Neal J, Montoya A, Cox GR, Murray JS. Creating a process for the implementation of tiered huddles in a Veterans Affairs Medical Center. Mil Med. 2023;188:901-906. doi:10.1093/milmed/usac073
- Mohr DC, Chen C, Sullivan J, et al. Development and validation of the Veterans Health Administration Patient Safety Culture Survey. J Patient Saf. 2022;18:539-545. doi:10.1097/PTS.0000000000001027
- Leonard C, Gilmartin H, Starr L, Anderson T. Leadership and the high reliability transformation: a qualitative study at Truman VA medical center. J Healthc Risk Manag. 2024;44:17-23. doi:10.1002/jhrm.21580
- Sculli G, Essen K. Soaring to Success: The Path to Developing High-Reliability Teams. HCPro; 2021.
- Gupta JI, Sivils S, Reppert J, Paulot W, Houchens N, Hummel S. Visual management board implementation to enhance high reliability at a large VA health care system. Fed Pract. 2024;41:242-246. doi:10.12788/fp.0507
- Veterans Health Administration. High Reliability Organization Learning Catalog. US Dept of Veterans Affairs; 2024. Internal document.
- Jahn JLS, Black AE. A model of communicative and hierarchical foundations of high reliability organizing in wildland firefighting teams. Manag Commun Q. 2017;31:356-379. doi:10.1177/0893318917691358
- Myers CG, Sutcliffe KM. High reliability organising in healthcare: still a long way left to go. BMJ Qual Saf. 2022;31:845-848. doi:10.1136/bmjqs-2021-014141
- Abrams J. Model the way to navigate difficult topics. The Learning Professional. 2022;43:14-18.
- McCausland T. Creating psychological safety in the workplace. Research-Technology Management. 2023;66:56-58. doi:10.1080/08956308.2023.2164439
- Murray JS, Kelly S, Hanover C. Promoting psychological safety in healthcare organizations. Mil Med. 2022;187:808- 810. doi:10.1093/milmed/usac041
- Sutton RI, Rao H. The friction project: how smart leaders make the right things easier and the wrong things harder. St. Martin’s Press; 2024.
- Clark TR. The 4 stages of psychological safety: defining the path to inclusion and innovation. Berrett-Koehler Publishers, Inc.; 2020.
- Essen K, Villalobos C, Sculli G, Steinbach L. Establishing a just culture: implications for the Veterans Health Administration journey to high reliability. Fed Pract. 2024;41:290- 297. doi:10.12788/fp.0512
- Creswell JW. Research design: qualitative, quantitative, and mixed methods approaches. 4th ed. SAGE Publications; 2014.
- Patton MQ. Qualitative research & evaluation methods: integrating theory and practice. 4th ed. SAGE Publications, Inc.; 2015.
- Krumpal I. Determinants of social desirability bias in sensitive surveys: a literature review. Qual Quant. 2013;47:2025- 2047. doi:10.1007/s11135-011-9640-9
- Cox GR, Starr LM. VHA’s movement for change: implementing high-reliability principles and practices. J Healthc Manag. 2023;68:151-157. doi:10.1097/jhm-D-23-00056
- Sculli GL, Pendley-Louis R, Neily J, et al. A high-reliability organization framework for health care: A multiyear implementation strategy and associated outcomes. J Patient Saf. 2022;18:64-70. doi:10.1097/pts.0000000000000788
- Murray JS, Clifford J, Larson S, Lee JK, Sculli GL. Implementing just culture to improve patient safety. Mil Med. 2023;188:usac115. doi:10.1093/milmed/usac115
- Merchant NB, O’Neal J, Montoya A, Cox GR, Murray JS. Creating a process for the implementation of tiered huddles in a Veterans Affairs Medical Center. Mil Med. 2023;188:901-906. doi:10.1093/milmed/usac073
- Mohr DC, Chen C, Sullivan J, et al. Development and validation of the Veterans Health Administration Patient Safety Culture Survey. J Patient Saf. 2022;18:539-545. doi:10.1097/PTS.0000000000001027
- Leonard C, Gilmartin H, Starr L, Anderson T. Leadership and the high reliability transformation: a qualitative study at Truman VA medical center. J Healthc Risk Manag. 2024;44:17-23. doi:10.1002/jhrm.21580
- Sculli G, Essen K. Soaring to Success: The Path to Developing High-Reliability Teams. HCPro; 2021.
- Gupta JI, Sivils S, Reppert J, Paulot W, Houchens N, Hummel S. Visual management board implementation to enhance high reliability at a large VA health care system. Fed Pract. 2024;41:242-246. doi:10.12788/fp.0507
- Veterans Health Administration. High Reliability Organization Learning Catalog. US Dept of Veterans Affairs; 2024. Internal document.
- Jahn JLS, Black AE. A model of communicative and hierarchical foundations of high reliability organizing in wildland firefighting teams. Manag Commun Q. 2017;31:356-379. doi:10.1177/0893318917691358
- Myers CG, Sutcliffe KM. High reliability organising in healthcare: still a long way left to go. BMJ Qual Saf. 2022;31:845-848. doi:10.1136/bmjqs-2021-014141
- Abrams J. Model the way to navigate difficult topics. The Learning Professional. 2022;43:14-18.
- McCausland T. Creating psychological safety in the workplace. Research-Technology Management. 2023;66:56-58. doi:10.1080/08956308.2023.2164439
- Murray JS, Kelly S, Hanover C. Promoting psychological safety in healthcare organizations. Mil Med. 2022;187:808- 810. doi:10.1093/milmed/usac041
- Sutton RI, Rao H. The friction project: how smart leaders make the right things easier and the wrong things harder. St. Martin’s Press; 2024.
- Clark TR. The 4 stages of psychological safety: defining the path to inclusion and innovation. Berrett-Koehler Publishers, Inc.; 2020.
- Essen K, Villalobos C, Sculli G, Steinbach L. Establishing a just culture: implications for the Veterans Health Administration journey to high reliability. Fed Pract. 2024;41:290- 297. doi:10.12788/fp.0512
- Creswell JW. Research design: qualitative, quantitative, and mixed methods approaches. 4th ed. SAGE Publications; 2014.
- Patton MQ. Qualitative research & evaluation methods: integrating theory and practice. 4th ed. SAGE Publications, Inc.; 2015.
- Krumpal I. Determinants of social desirability bias in sensitive surveys: a literature review. Qual Quant. 2013;47:2025- 2047. doi:10.1007/s11135-011-9640-9
Frontline Supervisor Perspectives on Enabling High Reliability and Fostering a Just Culture at the VHA
Frontline Supervisor Perspectives on Enabling High Reliability and Fostering a Just Culture at the VHA
A case-based framework for de-escalating conflict
Hospital medicine can be a demanding and fast-paced environment where resources are stretched thin, with both clinicians and patients stressed. A hospitalist’s role is dynamic, serving as an advocate, leader, or role model while working with interdisciplinary and diverse teams for the welfare of the patient. This constellation of pressures makes a degree of conflict inevitable.
Often, an unexpected scenario can render the hospitalist uncertain and yet the hospitalist’s response can escalate or deescalate conflict. The multiple roles that a hospitalist represents may buckle to the single role of advocating for themselves, a colleague, or a patient in a tense scenario. When this happens, many hospitalists feel disempowered to respond.
De-escalation is a practical skill that involves being calm, respectful, and open minded toward the other person, while also maintaining boundaries. Here we provide case-based tips and skills that highlight the role for de-escalation.
Questions to ask yourself in midst of conflict:
- How did the problematic behavior make you feel?
- What will be your approach in handling this?
- When should you address this?
- What is the outcome you are hoping to achieve?
- What is the outcome the other person is hoping to achieve?
Case 1
There is a female physician rounding with your team. Introductions were made at the start of a patient encounter. The patient repeatedly calls the female physician by her first name and refers to a male colleague as “doctor.”
Commentary: This scenario is commonly encountered by women who are physicians. They may be mistaken for the nurse, a technician, or a housekeeper. This exacerbates inequality and impostor syndrome as women can feel unheard, undervalued, and not recognized for their expertise and achievements. It can be challenging for a woman to reaffirm herself as she worries that the patient will not respect her or will think that she is being aggressive.
Approach: It is vital to interject by firmly reintroducing the female physician by her correct title. If you are the subject of this scenario, you may interject by firmly reintroducing yourself. If the patient or a colleague continues to refer to her by her first name, it is appropriate to say, “Please call her Dr. XYZ.” There is likely another female colleague or trainee nearby that will view this scenario as a model for setting boundaries.
To prevent similar future situations, consistently refer to all peers by their title in front of patients and peers in all professional settings (such as lectures, luncheons, etc.) to establish this as a cultural norm. Also, utilize hospital badges that clearly display roles in large letters.
Case 2
During sign out from a colleague, the colleague repeatedly refers to a patient hospitalized with sickle cell disease as a “frequent flyer” and “drug seeker,” and then remarks, “you know how these patients are.”
Commentary: A situation like this raises concerns about bias and stereotyping. Everyone has implicit bias. Recognizing and acknowledging when implicit bias affects objectivity in patient care is vital to providing appropriate care. It can be intimidating to broach this subject with a colleague as it may cause the colleague to become defensive and uncomfortable as revealing another person’s bias can be difficult. But physicians owe it to a patient’s wellbeing to remain objective and to prevent future colleagues from providing subpar care as a result.
Approach: In this case, saying, “Sometimes my previous experiences can affect my thinking. Will you explain what behaviors the patient has shown this admission that are concerning to you? This will allow me to grasp the complexity of the situation.” Another strategy is to share that there are new recommendations for how to use language about patients with sickle cell disease and patients who require opioids as a part of their treatment plan. Your hospitalist group could have a journal club on how bias affects patients and about the best practices in the care of people with sickle cell disease. A next step could be to build a quality improvement project to review the care of patients hospitalized for sickle cell disease or opioid use.
Case 3
You are conducting bedside rounds with your team. Your intern, a person of color, begins to present. The patient interjects by requesting that the intern leave as he “does not want a foreigner taking care” of him.
Commentary: Requests like this can be shocking. The team leader has a responsibility to immediately act to ensure the psychological safety of the team. Ideally, your response should set firm boundaries and expectations that support the learner as a valued and respected clinician and allow the intern to complete the presentation. In this scenario, regardless of the response the patient takes, it is vital to maintain a safe environment for the trainee. It is crucial to debrief with the team immediately after as an exchange of thoughts and emotions in a safe space can allow for everyone to feel welcome. Additionally, this debrief can provide insights to the team leader of how to address similar situations in the future. The opportunity to allow the intern to no longer follow the patient should be offered, and if the intern opts to no longer follow the patient, accommodations should be made.
Approach: “This physician is a member of the medical team, and we are all working together to provide you with the best care. Everyone on this team is an equal. We value diversity of our team members as it allows us to take care of all our patients. We respect you and expect respect for each member of the team. If you feel that you are unable to respect our team members right now, we will leave for now and return later.” To ensure the patient is provided with appropriate care, be sure to debrief with the patient’s nurse.
Conclusion
These scenarios represent some of the many complex interpersonal challenges hospitalists encounter. These approaches are suggestions that are open to improvement as de-escalation of a conflict is a critical and evolving skill and practice.
For more tips on managing conflict, consider reading “Crucial Conversations” by Kerry Patterson and colleagues. These skills can provide the tools we need to recenter ourselves when we are in the midst of these challenging situations.
Dr. Rawal is clinical assistant professor of medicine at the University of Pittsburgh Medical Center. Dr. Ashford is assistant professor and program director in the department of internal medicine/pediatrics at the University of Nebraska Medical Center, Omaha. Dr. Lee and Dr. Barrett are based in the department of internal medicine, University of New Mexico School of Medicine, Albuquerque. This article is sponsored by the SHM Physicians in Training (PIT) committee, which submits quarterly content to The Hospitalist on topics relevant to trainees and early career hospitalists.
Hospital medicine can be a demanding and fast-paced environment where resources are stretched thin, with both clinicians and patients stressed. A hospitalist’s role is dynamic, serving as an advocate, leader, or role model while working with interdisciplinary and diverse teams for the welfare of the patient. This constellation of pressures makes a degree of conflict inevitable.
Often, an unexpected scenario can render the hospitalist uncertain and yet the hospitalist’s response can escalate or deescalate conflict. The multiple roles that a hospitalist represents may buckle to the single role of advocating for themselves, a colleague, or a patient in a tense scenario. When this happens, many hospitalists feel disempowered to respond.
De-escalation is a practical skill that involves being calm, respectful, and open minded toward the other person, while also maintaining boundaries. Here we provide case-based tips and skills that highlight the role for de-escalation.
Questions to ask yourself in midst of conflict:
- How did the problematic behavior make you feel?
- What will be your approach in handling this?
- When should you address this?
- What is the outcome you are hoping to achieve?
- What is the outcome the other person is hoping to achieve?
Case 1
There is a female physician rounding with your team. Introductions were made at the start of a patient encounter. The patient repeatedly calls the female physician by her first name and refers to a male colleague as “doctor.”
Commentary: This scenario is commonly encountered by women who are physicians. They may be mistaken for the nurse, a technician, or a housekeeper. This exacerbates inequality and impostor syndrome as women can feel unheard, undervalued, and not recognized for their expertise and achievements. It can be challenging for a woman to reaffirm herself as she worries that the patient will not respect her or will think that she is being aggressive.
Approach: It is vital to interject by firmly reintroducing the female physician by her correct title. If you are the subject of this scenario, you may interject by firmly reintroducing yourself. If the patient or a colleague continues to refer to her by her first name, it is appropriate to say, “Please call her Dr. XYZ.” There is likely another female colleague or trainee nearby that will view this scenario as a model for setting boundaries.
To prevent similar future situations, consistently refer to all peers by their title in front of patients and peers in all professional settings (such as lectures, luncheons, etc.) to establish this as a cultural norm. Also, utilize hospital badges that clearly display roles in large letters.
Case 2
During sign out from a colleague, the colleague repeatedly refers to a patient hospitalized with sickle cell disease as a “frequent flyer” and “drug seeker,” and then remarks, “you know how these patients are.”
Commentary: A situation like this raises concerns about bias and stereotyping. Everyone has implicit bias. Recognizing and acknowledging when implicit bias affects objectivity in patient care is vital to providing appropriate care. It can be intimidating to broach this subject with a colleague as it may cause the colleague to become defensive and uncomfortable as revealing another person’s bias can be difficult. But physicians owe it to a patient’s wellbeing to remain objective and to prevent future colleagues from providing subpar care as a result.
Approach: In this case, saying, “Sometimes my previous experiences can affect my thinking. Will you explain what behaviors the patient has shown this admission that are concerning to you? This will allow me to grasp the complexity of the situation.” Another strategy is to share that there are new recommendations for how to use language about patients with sickle cell disease and patients who require opioids as a part of their treatment plan. Your hospitalist group could have a journal club on how bias affects patients and about the best practices in the care of people with sickle cell disease. A next step could be to build a quality improvement project to review the care of patients hospitalized for sickle cell disease or opioid use.
Case 3
You are conducting bedside rounds with your team. Your intern, a person of color, begins to present. The patient interjects by requesting that the intern leave as he “does not want a foreigner taking care” of him.
Commentary: Requests like this can be shocking. The team leader has a responsibility to immediately act to ensure the psychological safety of the team. Ideally, your response should set firm boundaries and expectations that support the learner as a valued and respected clinician and allow the intern to complete the presentation. In this scenario, regardless of the response the patient takes, it is vital to maintain a safe environment for the trainee. It is crucial to debrief with the team immediately after as an exchange of thoughts and emotions in a safe space can allow for everyone to feel welcome. Additionally, this debrief can provide insights to the team leader of how to address similar situations in the future. The opportunity to allow the intern to no longer follow the patient should be offered, and if the intern opts to no longer follow the patient, accommodations should be made.
Approach: “This physician is a member of the medical team, and we are all working together to provide you with the best care. Everyone on this team is an equal. We value diversity of our team members as it allows us to take care of all our patients. We respect you and expect respect for each member of the team. If you feel that you are unable to respect our team members right now, we will leave for now and return later.” To ensure the patient is provided with appropriate care, be sure to debrief with the patient’s nurse.
Conclusion
These scenarios represent some of the many complex interpersonal challenges hospitalists encounter. These approaches are suggestions that are open to improvement as de-escalation of a conflict is a critical and evolving skill and practice.
For more tips on managing conflict, consider reading “Crucial Conversations” by Kerry Patterson and colleagues. These skills can provide the tools we need to recenter ourselves when we are in the midst of these challenging situations.
Dr. Rawal is clinical assistant professor of medicine at the University of Pittsburgh Medical Center. Dr. Ashford is assistant professor and program director in the department of internal medicine/pediatrics at the University of Nebraska Medical Center, Omaha. Dr. Lee and Dr. Barrett are based in the department of internal medicine, University of New Mexico School of Medicine, Albuquerque. This article is sponsored by the SHM Physicians in Training (PIT) committee, which submits quarterly content to The Hospitalist on topics relevant to trainees and early career hospitalists.
Hospital medicine can be a demanding and fast-paced environment where resources are stretched thin, with both clinicians and patients stressed. A hospitalist’s role is dynamic, serving as an advocate, leader, or role model while working with interdisciplinary and diverse teams for the welfare of the patient. This constellation of pressures makes a degree of conflict inevitable.
Often, an unexpected scenario can render the hospitalist uncertain and yet the hospitalist’s response can escalate or deescalate conflict. The multiple roles that a hospitalist represents may buckle to the single role of advocating for themselves, a colleague, or a patient in a tense scenario. When this happens, many hospitalists feel disempowered to respond.
De-escalation is a practical skill that involves being calm, respectful, and open minded toward the other person, while also maintaining boundaries. Here we provide case-based tips and skills that highlight the role for de-escalation.
Questions to ask yourself in midst of conflict:
- How did the problematic behavior make you feel?
- What will be your approach in handling this?
- When should you address this?
- What is the outcome you are hoping to achieve?
- What is the outcome the other person is hoping to achieve?
Case 1
There is a female physician rounding with your team. Introductions were made at the start of a patient encounter. The patient repeatedly calls the female physician by her first name and refers to a male colleague as “doctor.”
Commentary: This scenario is commonly encountered by women who are physicians. They may be mistaken for the nurse, a technician, or a housekeeper. This exacerbates inequality and impostor syndrome as women can feel unheard, undervalued, and not recognized for their expertise and achievements. It can be challenging for a woman to reaffirm herself as she worries that the patient will not respect her or will think that she is being aggressive.
Approach: It is vital to interject by firmly reintroducing the female physician by her correct title. If you are the subject of this scenario, you may interject by firmly reintroducing yourself. If the patient or a colleague continues to refer to her by her first name, it is appropriate to say, “Please call her Dr. XYZ.” There is likely another female colleague or trainee nearby that will view this scenario as a model for setting boundaries.
To prevent similar future situations, consistently refer to all peers by their title in front of patients and peers in all professional settings (such as lectures, luncheons, etc.) to establish this as a cultural norm. Also, utilize hospital badges that clearly display roles in large letters.
Case 2
During sign out from a colleague, the colleague repeatedly refers to a patient hospitalized with sickle cell disease as a “frequent flyer” and “drug seeker,” and then remarks, “you know how these patients are.”
Commentary: A situation like this raises concerns about bias and stereotyping. Everyone has implicit bias. Recognizing and acknowledging when implicit bias affects objectivity in patient care is vital to providing appropriate care. It can be intimidating to broach this subject with a colleague as it may cause the colleague to become defensive and uncomfortable as revealing another person’s bias can be difficult. But physicians owe it to a patient’s wellbeing to remain objective and to prevent future colleagues from providing subpar care as a result.
Approach: In this case, saying, “Sometimes my previous experiences can affect my thinking. Will you explain what behaviors the patient has shown this admission that are concerning to you? This will allow me to grasp the complexity of the situation.” Another strategy is to share that there are new recommendations for how to use language about patients with sickle cell disease and patients who require opioids as a part of their treatment plan. Your hospitalist group could have a journal club on how bias affects patients and about the best practices in the care of people with sickle cell disease. A next step could be to build a quality improvement project to review the care of patients hospitalized for sickle cell disease or opioid use.
Case 3
You are conducting bedside rounds with your team. Your intern, a person of color, begins to present. The patient interjects by requesting that the intern leave as he “does not want a foreigner taking care” of him.
Commentary: Requests like this can be shocking. The team leader has a responsibility to immediately act to ensure the psychological safety of the team. Ideally, your response should set firm boundaries and expectations that support the learner as a valued and respected clinician and allow the intern to complete the presentation. In this scenario, regardless of the response the patient takes, it is vital to maintain a safe environment for the trainee. It is crucial to debrief with the team immediately after as an exchange of thoughts and emotions in a safe space can allow for everyone to feel welcome. Additionally, this debrief can provide insights to the team leader of how to address similar situations in the future. The opportunity to allow the intern to no longer follow the patient should be offered, and if the intern opts to no longer follow the patient, accommodations should be made.
Approach: “This physician is a member of the medical team, and we are all working together to provide you with the best care. Everyone on this team is an equal. We value diversity of our team members as it allows us to take care of all our patients. We respect you and expect respect for each member of the team. If you feel that you are unable to respect our team members right now, we will leave for now and return later.” To ensure the patient is provided with appropriate care, be sure to debrief with the patient’s nurse.
Conclusion
These scenarios represent some of the many complex interpersonal challenges hospitalists encounter. These approaches are suggestions that are open to improvement as de-escalation of a conflict is a critical and evolving skill and practice.
For more tips on managing conflict, consider reading “Crucial Conversations” by Kerry Patterson and colleagues. These skills can provide the tools we need to recenter ourselves when we are in the midst of these challenging situations.
Dr. Rawal is clinical assistant professor of medicine at the University of Pittsburgh Medical Center. Dr. Ashford is assistant professor and program director in the department of internal medicine/pediatrics at the University of Nebraska Medical Center, Omaha. Dr. Lee and Dr. Barrett are based in the department of internal medicine, University of New Mexico School of Medicine, Albuquerque. This article is sponsored by the SHM Physicians in Training (PIT) committee, which submits quarterly content to The Hospitalist on topics relevant to trainees and early career hospitalists.
Reflecting on 2021, looking forward to 2022
This month marks the end of my first full calendar year as SHM CEO. Over the years, I have made it a habit to take time to reflect during the month of December, assessing the previous year by reviewing what went well and what could have gone better, and how I can grow and change to meet the needs of future challenges. This reflection sets the stage for my personal and professional “New Year” goals.
This year, 2021, is certainly a year deserving of reflection, and I believe 2022 (and beyond) will need ambitious goals made by dedicated leaders, hospitalists included. Here are my thoughts on what went well in 2021 and what I wish went better – from our greater society to our specialty, to SHM.
Society (as in the larger society)
What went well: Vaccines
There is a lot to be impressed with in 2021, and for me, at the top of that list are the COVID-19 vaccines. I realize the research for mRNA vaccines started more than 20 years ago, and the most successful mRNA vaccine companies have been around for more than a decade, but to roll out a COVID-19 vaccine in less than a year is still just incredible. To take a disease with a 2% mortality rate for someone like myself and effectively reduce that to near zero is something historians will be writing about for years to come.
What I wish went better: Open dialogue
I can’t remember when we stopped listening to each other, and by that, I mean listening to those who do not think exactly like ourselves. As a kid, I was taught to be careful about discussing topics at social events that could go sideways. That usually involved politics, money, or strong beliefs, but wow – now, that list is much longer. Talking about the weather used to be safe, but not anymore. If I were to show pictures of the recent flooding in Annapolis? There would almost certainly be a debate about climate change. At least we can agree on Ted Lasso as a safe topic.
Our specialty
What went well: Hospitalists are vital
There are many, many professions that deserve “hero” status for their part in taming this pandemic: nurses, doctors, emergency medical services, physical therapists, physician assistants, nurse practitioners, administrators, and more. But in the doctor category, hospitalists are at the top. Along with our emergency department and intensivist colleagues, hospitalists are one of the pillars of the inpatient response to COVID. More than 3.2 million COVID-19 hospitalizations have occurred, according to the Centers for Disease Control and Prevention, with numerous state dashboards showing three-quarters of those are cared for on general medical wards, the domain of hospitalists (for example, see my own state of Maryland’s COVID-19 dashboard: https://coronavirus.maryland.gov).
We’ve always had “two patients” – the patient in the bed and the health care system. Many hospitalists have helped their institutions by building COVID care teams, COVID wards, or in the case of Dr. Mindy Kantsiper, building an entire COVID field hospital in a convention center. Without hospitalists, both patients and the system that serves them would have fared much worse in this pandemic. Hospitalists are vital to patients and the health care system. The end. Period. End of story.
What I wish went better: Getting credit
As a profession, we need to be more deliberate about getting credit for the fantastic work we have done to care for COVID-19 patients, as well as inpatients in general. SHM can and must focus more on how to highlight the great work hospitalists have done and will continue to do. A greater understanding by the health care industry – as well as the general public – regarding the important role we play for patient care will help add autonomy in our profession, which in turn adds to resilience during these challenging times.
SHM
What went well: Membership grew
This is the one thing that we at SHM – and I personally – are most proud of. SHM is a membership society; it is the single most important metric for me personally. If physicians aren’t joining, then we are not meeting our core mission to provide value to hospitalists. My sense is the services SHM provides to hospitalists continue to be of value – even during these strenuous times of the pandemic when we had to be physically distant.
Whether it’s our Government Relations Department advocating for hospitalists in Washington, or the Journal of Hospital Medicine, or this very magazine, The Hospitalist, or SHM’s numerous educational offerings, chapter events, and SHM national meetings (Converge, Pediatric Hospital Medicine, Leadership Academies, Academic Hospitalist Academy, and more), SHM continues to provide hospitalists with vital tools to help you in your career.
This is also very much a two-way street. If you are reading this, know that without you, our members, our success would not be possible. Your passion and partnership drive us to innovate to meet your needs and those of the patients you serve every day. Thank you for your continued support and inspiration.
What could have gone better: Seeing more of you, in person
This is a tough one for me. Everything I worried about going wrong for SHM in 2021 never materialized. A year ago, my fears for SHM were that membership would shrink, finances would dry up, and the SHM staff would leave (by furlough or by choice). Thankfully, membership grew, our finances are in very good shape for any year, let alone a pandemic year, and the staff have remained at SHM and are engaged and dedicated! SHM even received a “Best Place to Work” award from the Philadelphia Business Journal.
Maybe the one regret I have is that we could not do more in-person events. But even there, I think we did better than most. We had some chapter meetings in person, and the October 2021 Leadership Academy hosted 110 hospitalist leaders, in person, at Amelia Island, Fla. That Leadership Academy went off without a hitch, and the early reviews are superb. I am very optimistic about 2022 in-person events!
Looking forward: 2022 and beyond
I have no illusions that 2022 is going to be easy. I know that the pandemic will not be gone (even though cases are falling nationwide as of this writing), that our nation will struggle with how to deal with polarization, and the workplace will continue to be redefined. Yet, I can’t help but be optimistic.
The pandemic will end eventually; all pandemics do. My hope is that young leaders will step forward to help our nation work through the divisive challenges, and some of those leaders will even be hospitalists! I also know that our profession is more vital than ever, for both patients and the health care system. We’re even getting ready to celebrate SHM’s 25th anniversary, and we can’t wait to revisit our humble beginnings while looking at the bright future of our society and our field.
I am working on my 2022 “New Year” goals, but you can be pretty sure they will revolve around making the world a better place, investing in people, and being ethical and transparent.
Dr. Howell is the CEO of the Society of Hospital Medicine.
This month marks the end of my first full calendar year as SHM CEO. Over the years, I have made it a habit to take time to reflect during the month of December, assessing the previous year by reviewing what went well and what could have gone better, and how I can grow and change to meet the needs of future challenges. This reflection sets the stage for my personal and professional “New Year” goals.
This year, 2021, is certainly a year deserving of reflection, and I believe 2022 (and beyond) will need ambitious goals made by dedicated leaders, hospitalists included. Here are my thoughts on what went well in 2021 and what I wish went better – from our greater society to our specialty, to SHM.
Society (as in the larger society)
What went well: Vaccines
There is a lot to be impressed with in 2021, and for me, at the top of that list are the COVID-19 vaccines. I realize the research for mRNA vaccines started more than 20 years ago, and the most successful mRNA vaccine companies have been around for more than a decade, but to roll out a COVID-19 vaccine in less than a year is still just incredible. To take a disease with a 2% mortality rate for someone like myself and effectively reduce that to near zero is something historians will be writing about for years to come.
What I wish went better: Open dialogue
I can’t remember when we stopped listening to each other, and by that, I mean listening to those who do not think exactly like ourselves. As a kid, I was taught to be careful about discussing topics at social events that could go sideways. That usually involved politics, money, or strong beliefs, but wow – now, that list is much longer. Talking about the weather used to be safe, but not anymore. If I were to show pictures of the recent flooding in Annapolis? There would almost certainly be a debate about climate change. At least we can agree on Ted Lasso as a safe topic.
Our specialty
What went well: Hospitalists are vital
There are many, many professions that deserve “hero” status for their part in taming this pandemic: nurses, doctors, emergency medical services, physical therapists, physician assistants, nurse practitioners, administrators, and more. But in the doctor category, hospitalists are at the top. Along with our emergency department and intensivist colleagues, hospitalists are one of the pillars of the inpatient response to COVID. More than 3.2 million COVID-19 hospitalizations have occurred, according to the Centers for Disease Control and Prevention, with numerous state dashboards showing three-quarters of those are cared for on general medical wards, the domain of hospitalists (for example, see my own state of Maryland’s COVID-19 dashboard: https://coronavirus.maryland.gov).
We’ve always had “two patients” – the patient in the bed and the health care system. Many hospitalists have helped their institutions by building COVID care teams, COVID wards, or in the case of Dr. Mindy Kantsiper, building an entire COVID field hospital in a convention center. Without hospitalists, both patients and the system that serves them would have fared much worse in this pandemic. Hospitalists are vital to patients and the health care system. The end. Period. End of story.
What I wish went better: Getting credit
As a profession, we need to be more deliberate about getting credit for the fantastic work we have done to care for COVID-19 patients, as well as inpatients in general. SHM can and must focus more on how to highlight the great work hospitalists have done and will continue to do. A greater understanding by the health care industry – as well as the general public – regarding the important role we play for patient care will help add autonomy in our profession, which in turn adds to resilience during these challenging times.
SHM
What went well: Membership grew
This is the one thing that we at SHM – and I personally – are most proud of. SHM is a membership society; it is the single most important metric for me personally. If physicians aren’t joining, then we are not meeting our core mission to provide value to hospitalists. My sense is the services SHM provides to hospitalists continue to be of value – even during these strenuous times of the pandemic when we had to be physically distant.
Whether it’s our Government Relations Department advocating for hospitalists in Washington, or the Journal of Hospital Medicine, or this very magazine, The Hospitalist, or SHM’s numerous educational offerings, chapter events, and SHM national meetings (Converge, Pediatric Hospital Medicine, Leadership Academies, Academic Hospitalist Academy, and more), SHM continues to provide hospitalists with vital tools to help you in your career.
This is also very much a two-way street. If you are reading this, know that without you, our members, our success would not be possible. Your passion and partnership drive us to innovate to meet your needs and those of the patients you serve every day. Thank you for your continued support and inspiration.
What could have gone better: Seeing more of you, in person
This is a tough one for me. Everything I worried about going wrong for SHM in 2021 never materialized. A year ago, my fears for SHM were that membership would shrink, finances would dry up, and the SHM staff would leave (by furlough or by choice). Thankfully, membership grew, our finances are in very good shape for any year, let alone a pandemic year, and the staff have remained at SHM and are engaged and dedicated! SHM even received a “Best Place to Work” award from the Philadelphia Business Journal.
Maybe the one regret I have is that we could not do more in-person events. But even there, I think we did better than most. We had some chapter meetings in person, and the October 2021 Leadership Academy hosted 110 hospitalist leaders, in person, at Amelia Island, Fla. That Leadership Academy went off without a hitch, and the early reviews are superb. I am very optimistic about 2022 in-person events!
Looking forward: 2022 and beyond
I have no illusions that 2022 is going to be easy. I know that the pandemic will not be gone (even though cases are falling nationwide as of this writing), that our nation will struggle with how to deal with polarization, and the workplace will continue to be redefined. Yet, I can’t help but be optimistic.
The pandemic will end eventually; all pandemics do. My hope is that young leaders will step forward to help our nation work through the divisive challenges, and some of those leaders will even be hospitalists! I also know that our profession is more vital than ever, for both patients and the health care system. We’re even getting ready to celebrate SHM’s 25th anniversary, and we can’t wait to revisit our humble beginnings while looking at the bright future of our society and our field.
I am working on my 2022 “New Year” goals, but you can be pretty sure they will revolve around making the world a better place, investing in people, and being ethical and transparent.
Dr. Howell is the CEO of the Society of Hospital Medicine.
This month marks the end of my first full calendar year as SHM CEO. Over the years, I have made it a habit to take time to reflect during the month of December, assessing the previous year by reviewing what went well and what could have gone better, and how I can grow and change to meet the needs of future challenges. This reflection sets the stage for my personal and professional “New Year” goals.
This year, 2021, is certainly a year deserving of reflection, and I believe 2022 (and beyond) will need ambitious goals made by dedicated leaders, hospitalists included. Here are my thoughts on what went well in 2021 and what I wish went better – from our greater society to our specialty, to SHM.
Society (as in the larger society)
What went well: Vaccines
There is a lot to be impressed with in 2021, and for me, at the top of that list are the COVID-19 vaccines. I realize the research for mRNA vaccines started more than 20 years ago, and the most successful mRNA vaccine companies have been around for more than a decade, but to roll out a COVID-19 vaccine in less than a year is still just incredible. To take a disease with a 2% mortality rate for someone like myself and effectively reduce that to near zero is something historians will be writing about for years to come.
What I wish went better: Open dialogue
I can’t remember when we stopped listening to each other, and by that, I mean listening to those who do not think exactly like ourselves. As a kid, I was taught to be careful about discussing topics at social events that could go sideways. That usually involved politics, money, or strong beliefs, but wow – now, that list is much longer. Talking about the weather used to be safe, but not anymore. If I were to show pictures of the recent flooding in Annapolis? There would almost certainly be a debate about climate change. At least we can agree on Ted Lasso as a safe topic.
Our specialty
What went well: Hospitalists are vital
There are many, many professions that deserve “hero” status for their part in taming this pandemic: nurses, doctors, emergency medical services, physical therapists, physician assistants, nurse practitioners, administrators, and more. But in the doctor category, hospitalists are at the top. Along with our emergency department and intensivist colleagues, hospitalists are one of the pillars of the inpatient response to COVID. More than 3.2 million COVID-19 hospitalizations have occurred, according to the Centers for Disease Control and Prevention, with numerous state dashboards showing three-quarters of those are cared for on general medical wards, the domain of hospitalists (for example, see my own state of Maryland’s COVID-19 dashboard: https://coronavirus.maryland.gov).
We’ve always had “two patients” – the patient in the bed and the health care system. Many hospitalists have helped their institutions by building COVID care teams, COVID wards, or in the case of Dr. Mindy Kantsiper, building an entire COVID field hospital in a convention center. Without hospitalists, both patients and the system that serves them would have fared much worse in this pandemic. Hospitalists are vital to patients and the health care system. The end. Period. End of story.
What I wish went better: Getting credit
As a profession, we need to be more deliberate about getting credit for the fantastic work we have done to care for COVID-19 patients, as well as inpatients in general. SHM can and must focus more on how to highlight the great work hospitalists have done and will continue to do. A greater understanding by the health care industry – as well as the general public – regarding the important role we play for patient care will help add autonomy in our profession, which in turn adds to resilience during these challenging times.
SHM
What went well: Membership grew
This is the one thing that we at SHM – and I personally – are most proud of. SHM is a membership society; it is the single most important metric for me personally. If physicians aren’t joining, then we are not meeting our core mission to provide value to hospitalists. My sense is the services SHM provides to hospitalists continue to be of value – even during these strenuous times of the pandemic when we had to be physically distant.
Whether it’s our Government Relations Department advocating for hospitalists in Washington, or the Journal of Hospital Medicine, or this very magazine, The Hospitalist, or SHM’s numerous educational offerings, chapter events, and SHM national meetings (Converge, Pediatric Hospital Medicine, Leadership Academies, Academic Hospitalist Academy, and more), SHM continues to provide hospitalists with vital tools to help you in your career.
This is also very much a two-way street. If you are reading this, know that without you, our members, our success would not be possible. Your passion and partnership drive us to innovate to meet your needs and those of the patients you serve every day. Thank you for your continued support and inspiration.
What could have gone better: Seeing more of you, in person
This is a tough one for me. Everything I worried about going wrong for SHM in 2021 never materialized. A year ago, my fears for SHM were that membership would shrink, finances would dry up, and the SHM staff would leave (by furlough or by choice). Thankfully, membership grew, our finances are in very good shape for any year, let alone a pandemic year, and the staff have remained at SHM and are engaged and dedicated! SHM even received a “Best Place to Work” award from the Philadelphia Business Journal.
Maybe the one regret I have is that we could not do more in-person events. But even there, I think we did better than most. We had some chapter meetings in person, and the October 2021 Leadership Academy hosted 110 hospitalist leaders, in person, at Amelia Island, Fla. That Leadership Academy went off without a hitch, and the early reviews are superb. I am very optimistic about 2022 in-person events!
Looking forward: 2022 and beyond
I have no illusions that 2022 is going to be easy. I know that the pandemic will not be gone (even though cases are falling nationwide as of this writing), that our nation will struggle with how to deal with polarization, and the workplace will continue to be redefined. Yet, I can’t help but be optimistic.
The pandemic will end eventually; all pandemics do. My hope is that young leaders will step forward to help our nation work through the divisive challenges, and some of those leaders will even be hospitalists! I also know that our profession is more vital than ever, for both patients and the health care system. We’re even getting ready to celebrate SHM’s 25th anniversary, and we can’t wait to revisit our humble beginnings while looking at the bright future of our society and our field.
I am working on my 2022 “New Year” goals, but you can be pretty sure they will revolve around making the world a better place, investing in people, and being ethical and transparent.
Dr. Howell is the CEO of the Society of Hospital Medicine.
Residency programs readjust during COVID
Hospitalist-honed agility proves invaluable
It could be argued that hospital medicine in the United States was made vital by a major infectious disease epidemic – the HIV/AIDS crisis – said Emily Gottenborg, MD, a hospitalist and program director of hospitalist training at the University of Colorado at Denver, Aurora. Certainly, it was born out of the need for change, for physicians who could coordinate complex patient care plans and serve as the “quarterbacks” of the hospital. “As a result, we have always been very nimble and ready to embrace change,” said Dr. Gottenborg.
That hospitalist-honed agility and penchant for innovation has proven to be invaluable during the current COVID-19 pandemic as hospital medicine–focused residency programs have been forced to pivot quickly and modify their agendas. From managing the pandemic’s impact on residents’ day-to-day experiences, to carefully balancing educational needs and goals, program leaders have worked tirelessly to ensure that residents continue to receive excellent training.
The overarching theme across U.S.-based residency programs is that the educational changes and challenges during the COVID-19 pandemic have often been one and the same.
Service versus education
At the beginning of the pandemic, trainees at the University of Pittsburgh Medical Center were limited in seeing COVID patients in order to curb exposure. But now that COVID appears to be the new normal, “I think the question becomes: ‘How do we incorporate our trainees to take care of COVID patients since it seems it will be staying around for a while?’ ” said Rachna Rawal, MD, a hospitalist and clinical assistant professor of medicine at UPMC.
This dilemma highlights the conflict between service and education. Residents have been motivated and eager to help, which has been beneficial whenever there is a surge. “At the same time, you want to preserve their education, and it’s a very difficult balance at times,” said Dr. Rawal. It’s also challenging to figure out the safest way for residents to see patients, as well as how to include medical students, since interns and residents serve as important educational resources for them.
Keeping trainees involved with daily virtual conferences rather than in-person interactions raises the question of whether or not the engagement is equivalent. “It’s harder to keep them accountable when they’re not in person, but it’s also not worth the risk given the COVID numbers at times,” Dr. Rawal said. The goal has become to make sure residents stay safe while still feeling that they are getting a good education.
A balancing act
“I think early on, there was a lot of pride in what we were doing, that we were on the front line managing this thing that was emerging,” said Daniel Ricotta, MD, a hospitalist and associate program director of the internal medicine residency at Beth Israel Deaconess Medical Center and assistant professor of medicine at Harvard Medical School, both in Boston. “And now I think people are starting to feel a little bit weary.”
It has been demanding trying to manage ongoing educational needs through this time. “At the end of the day, residents are still trainees and have to be trained and educated. They’re not just worker bees taking care of patients,” Dr. Ricotta said. Residents need a well-rounded clinical experience – “they can’t just take care of COVID patients and then be able to graduate as general internists,” he said – but that becomes onerous when the hospital is full of patients with COVID.
Along with balancing residents’ clinical immersion, Dr. Ricotta said there has been the challenge of doing “the content-based teaching from didactics that occur in the context of clinical work, but are somewhat separated when you need to limit the number of people in the rooms and try to keep as many people at home as possible when they’re not taking care of patients in order to limit their level of risk.” Adjusting and readjusting both of these aspects has had a major impact on residents’ day-to-day education.
“A big part of residency is community,” noted Dr. Ricotta, but the sense of community has been disrupted because some of the bonding experiences residents used to do outside the hospital to build that community have necessarily gone by the wayside. This particularly affects interns from around the country who are meeting each other for the first time. “We actually had a normal intern orientation this year, but last year, when everything was virtual, we were trying to find ways to bridge relationships in a way that was safe and socially distanced,” he said.
Improving quality
UC Denver is unique in that they have a 3-year program specifically for hospital medicine residents, said Dr. Gottenborg. Right away, “our residents rose to the challenge and wanted to be part of the workforce that helps care for this critical population of [COVID] patients.” The residents were able to run the ICUs and take care of COVID patients, but in exchange, they had to give up some of their elective rotation time.
One aspect of the UC Denver hospital medicine residency program is participation in projects that focus on how to improve the health care system. Over the past year, the residents worked on one project in particular that focused on restructuring the guidelines for consulting physical therapists. Since many patients end up needing a physical therapist for a variety of reasons, a full hospital puts increased strain on their workload, making their time more precious.
“[The project] forced us to think about the right criteria to consult them,” explained Dr. Gottenborg. “We cut down essentially all the inappropriate consults to PT, opening their time. That project was driven by how the residents were experiencing the pandemic in the hospital.”
Learning to adapt
“The training environment during this pandemic has been tumultuous for both our residents and medical students,” said Alan M. Hall, MD, associate professor of internal medicine and pediatrics and assistant dean of curriculum integration at the University of Kentucky, Lexington. Along with treating patients with COVID-19, he said trainees have also had to cope with anxiety about getting the virus themselves or inadvertently bringing it home to their families.
Like most medical schools, University of Kentucky students were shifted away from clinical rotations and into alternative and online education for a time. When they returned to in-person education, the students were initially restricted from seeing patients with confirmed or suspected COVID-19 in order to reduce their personal risk and to conserve personal protective equipment.
This especially impacted certain rotations, such as pediatrics. Because respiratory symptoms are common in this population, students were greatly limited in the number of new patients they could see. Now they are given the option to see patients with COVID-19 if they want to.
“Our residents have had to adapt to seemingly endless changes during this pandemic,” Dr. Hall said. For example, at the beginning of the surge, the internal medicine residents trained for a completely new clinical model, though this ultimately never needed to be implemented. Then they had to adjust to extremely high census numbers that continue to have an effect on almost all of their rotations.
Conversely, the pediatrics residents saw far fewer inpatients last winter than they typically would. This made it more difficult for them to feel comfortable when census numbers increased with common diagnoses like bronchiolitis. “However, those respiratory viruses that were hibernating last winter caused an unusual and challenging summer surge,” Dr. Hall said.
The biggest challenge though “is knowing that there is not a perfect solution for this global pandemic’s effect on medical education,” said Dr. Hall. “We can’t possibly perfectly balance the safety of our learners and their families with the dangers of COVID-19.”
Leadership discussions
As a residency program leader, Dr. Ricotta said there are conversations about multiple topics, including maintaining a safe learning environment; providing important aspects of residency training; whether to go back to full in-person teaching, keep doing virtual teaching, or implement a hybrid model; and how to help residents understand the balance between their personal and professional lives, especially in terms of safety.
“They have to their lives outside of the hospital, but we also are trying to instill ... what their responsibility is to society, to their patients, and to each other,” said Dr. Ricotta.
A more recent discussion has been about how to manage the COVID vaccine boosters. “We can’t have everyone getting vaccines at the same time because they might have symptoms afterward, and then be out sick – you’re missing half your workforce,” Dr. Ricotta said. But staggering residents’ booster shots created yet another dilemma around deciding who received the booster sooner rather than later.
The biggest consideration for Dr. Gottenborg’s leadership team was deciding whether to use their residents to help with the COVID surges or keep them in a traditional residency experience. While the residents wanted to be part of the pandemic response, there were many factors to consider. Ultimately, they came up with a balance between the amount of time residents should spend taking care of COVID patients while also assuring that they leave the program with all the skills and experiences they need.
Though Dr. Hall works more closely with medical students than residents, he sees the challenges and effects as being similar. Creating harmony between a safe learning environment and students’ educational goals has been the topic of endless discussions. This includes decisions as to whether or not students should be involved in person in certain activities such as large classroom didactics, written exams, seeing patients in clinical settings, and small group discussions.
Recruitment effects
When it comes to recruiting during a global pandemic, the experiences and predictions are mixed. Dr. Hall believes virtual interviews are making recruitment easier, but in turn, the fact that they are virtual also makes it harder for the applicant to get a good feel for the program and the people involved in it.
Dr. Ricotta reported that recruitment numbers have been fairly steady at Beth Israel Deaconess over the last few years. “In addition to the critical care physicians, hospital medicine was really the front line of this pandemic and so in some ways, we gained some recognition that we may not have had otherwise,” said Dr. Ricotta. He believes this has the benefit of attracting some residents, but at the same time, it could potentially scare others away from what they perceive as a demanding, grueling job. “I think it has been mixed. It’s dependent on the person.”
At UC Denver, Dr. Gottenborg said they are seeing a rapid rise in the number of applications and interest in their programs. Still, “I think this could go both ways,” she acknowledged. With the focus on hospital medicine in the media, medical students are more aware of the specialty and what it involves. “I think the sense of mission is really exemplified and everyone is talking about it,” she said. This is evident in the arrival this summer of the first new class of interns since the pandemic. “They’re incredibly passionate about the work,” said Dr. Gottenborg.
However, there is also the notable increase in physician burnout since the pandemic started. That this has been regularly featured in the media leaves Dr. Gottenborg to wonder if prospective residents will shy away from hospital medicine because they believe it is an area that leads to burnout. “I hope that’s not the case,” she said.
“I would actually argue [recruitment] is easier,” said Dr. Rawal. Like Dr. Hall, she sees virtual interviews as a big benefit to prospective trainees because they don’t have to spend a large amount of money on travel, food, and other expenses like they did before, a welcome relief for residents with significant debt. “I think that is one very big positive from the pandemic,” she said. Her trainees were advised to make a final list and consider going to see the top two or three in person, but “at this point, there’s really no expectation to go see all 15 places that you look into.”
Dr. Rawal also pointed out that recruitment is affected by whether or not trainees are expected to see COVID patients. “I know in some places they aren’t and in some places they are, so it just depends on where you are and what you’re looking for,” she said.
Shifts in education
It remains to be seen if all the educational changes will be permanent, though it appears that many will remain. Dr. Hall hopes that virtual visits to provide care to patients who have difficulty getting to physical clinics will continue to be a focus for hospital medicine trainees. “For medical students, I think this will allow us to better assess what content can best be delivered in person, synchronously online, or asynchronously through recorded content,” he said.
Dr. Ricotta predicts that virtual conferences will become more pervasive as academic hospitals continue to acquire more community hospitals, especially for grand rounds. “The virtual teaching that occurred in the residency program because it’s required by the [Accreditation Council for Graduate Medical Education] has, I think, informed how academic centers do ongoing faculty development, professional development, and obviously education for the residents,” Dr. Ricotta said. “I think virtual teaching is here to stay.” This includes telehealth training, which had not been a widespread part of residency education before now.
Trainees have been given tools to handle high patient censuses and learned a whole new set of communication skills, thanks to the pandemic, said Dr. Rawal. There has been a focus on learning how to advocate for the vaccine, along with education on situations like how to have conversations with patients who don’t believe they have COVID, even when their tests are positive. “Learning to handle these situations and still be a physician and provide appropriate care regardless of the patient’s views is very important. This is not something I learned in my training because it never came up,” she said.
Dr. Gottenborg has been impressed by the resident workforce’s response across all specialties throughout these difficult days. “They were universally ready to dive in and work long hours and care for these very sick patients and ultimately share their experiences so that we could do it better as these patients continue to flow through our systems,” she said. “It has been very invigorating.”
The pandemic has also put a spotlight on the importance of being flexible, as well as various problems with how health care systems operate, “which, for people in our field, gets us both excited and gives us a lot of work to do,” said Dr. Gottenborg. “Our residents see that and feel that and will hopefully continue to hold that torch in hospital medicine.”
In spite of everything, Dr. Rawal believes this is an exhilarating time to be a trainee. “They’re getting an opportunity that none of us got. Usually, when policies are made, we really don’t see the immediate impact.” But with recent mandates like masks and social distancing, “the rate of change that they get to see things happen is exciting. They’re going to be a very exciting group of physicians.”
Hospitalist-honed agility proves invaluable
Hospitalist-honed agility proves invaluable
It could be argued that hospital medicine in the United States was made vital by a major infectious disease epidemic – the HIV/AIDS crisis – said Emily Gottenborg, MD, a hospitalist and program director of hospitalist training at the University of Colorado at Denver, Aurora. Certainly, it was born out of the need for change, for physicians who could coordinate complex patient care plans and serve as the “quarterbacks” of the hospital. “As a result, we have always been very nimble and ready to embrace change,” said Dr. Gottenborg.
That hospitalist-honed agility and penchant for innovation has proven to be invaluable during the current COVID-19 pandemic as hospital medicine–focused residency programs have been forced to pivot quickly and modify their agendas. From managing the pandemic’s impact on residents’ day-to-day experiences, to carefully balancing educational needs and goals, program leaders have worked tirelessly to ensure that residents continue to receive excellent training.
The overarching theme across U.S.-based residency programs is that the educational changes and challenges during the COVID-19 pandemic have often been one and the same.
Service versus education
At the beginning of the pandemic, trainees at the University of Pittsburgh Medical Center were limited in seeing COVID patients in order to curb exposure. But now that COVID appears to be the new normal, “I think the question becomes: ‘How do we incorporate our trainees to take care of COVID patients since it seems it will be staying around for a while?’ ” said Rachna Rawal, MD, a hospitalist and clinical assistant professor of medicine at UPMC.
This dilemma highlights the conflict between service and education. Residents have been motivated and eager to help, which has been beneficial whenever there is a surge. “At the same time, you want to preserve their education, and it’s a very difficult balance at times,” said Dr. Rawal. It’s also challenging to figure out the safest way for residents to see patients, as well as how to include medical students, since interns and residents serve as important educational resources for them.
Keeping trainees involved with daily virtual conferences rather than in-person interactions raises the question of whether or not the engagement is equivalent. “It’s harder to keep them accountable when they’re not in person, but it’s also not worth the risk given the COVID numbers at times,” Dr. Rawal said. The goal has become to make sure residents stay safe while still feeling that they are getting a good education.
A balancing act
“I think early on, there was a lot of pride in what we were doing, that we were on the front line managing this thing that was emerging,” said Daniel Ricotta, MD, a hospitalist and associate program director of the internal medicine residency at Beth Israel Deaconess Medical Center and assistant professor of medicine at Harvard Medical School, both in Boston. “And now I think people are starting to feel a little bit weary.”
It has been demanding trying to manage ongoing educational needs through this time. “At the end of the day, residents are still trainees and have to be trained and educated. They’re not just worker bees taking care of patients,” Dr. Ricotta said. Residents need a well-rounded clinical experience – “they can’t just take care of COVID patients and then be able to graduate as general internists,” he said – but that becomes onerous when the hospital is full of patients with COVID.
Along with balancing residents’ clinical immersion, Dr. Ricotta said there has been the challenge of doing “the content-based teaching from didactics that occur in the context of clinical work, but are somewhat separated when you need to limit the number of people in the rooms and try to keep as many people at home as possible when they’re not taking care of patients in order to limit their level of risk.” Adjusting and readjusting both of these aspects has had a major impact on residents’ day-to-day education.
“A big part of residency is community,” noted Dr. Ricotta, but the sense of community has been disrupted because some of the bonding experiences residents used to do outside the hospital to build that community have necessarily gone by the wayside. This particularly affects interns from around the country who are meeting each other for the first time. “We actually had a normal intern orientation this year, but last year, when everything was virtual, we were trying to find ways to bridge relationships in a way that was safe and socially distanced,” he said.
Improving quality
UC Denver is unique in that they have a 3-year program specifically for hospital medicine residents, said Dr. Gottenborg. Right away, “our residents rose to the challenge and wanted to be part of the workforce that helps care for this critical population of [COVID] patients.” The residents were able to run the ICUs and take care of COVID patients, but in exchange, they had to give up some of their elective rotation time.
One aspect of the UC Denver hospital medicine residency program is participation in projects that focus on how to improve the health care system. Over the past year, the residents worked on one project in particular that focused on restructuring the guidelines for consulting physical therapists. Since many patients end up needing a physical therapist for a variety of reasons, a full hospital puts increased strain on their workload, making their time more precious.
“[The project] forced us to think about the right criteria to consult them,” explained Dr. Gottenborg. “We cut down essentially all the inappropriate consults to PT, opening their time. That project was driven by how the residents were experiencing the pandemic in the hospital.”
Learning to adapt
“The training environment during this pandemic has been tumultuous for both our residents and medical students,” said Alan M. Hall, MD, associate professor of internal medicine and pediatrics and assistant dean of curriculum integration at the University of Kentucky, Lexington. Along with treating patients with COVID-19, he said trainees have also had to cope with anxiety about getting the virus themselves or inadvertently bringing it home to their families.
Like most medical schools, University of Kentucky students were shifted away from clinical rotations and into alternative and online education for a time. When they returned to in-person education, the students were initially restricted from seeing patients with confirmed or suspected COVID-19 in order to reduce their personal risk and to conserve personal protective equipment.
This especially impacted certain rotations, such as pediatrics. Because respiratory symptoms are common in this population, students were greatly limited in the number of new patients they could see. Now they are given the option to see patients with COVID-19 if they want to.
“Our residents have had to adapt to seemingly endless changes during this pandemic,” Dr. Hall said. For example, at the beginning of the surge, the internal medicine residents trained for a completely new clinical model, though this ultimately never needed to be implemented. Then they had to adjust to extremely high census numbers that continue to have an effect on almost all of their rotations.
Conversely, the pediatrics residents saw far fewer inpatients last winter than they typically would. This made it more difficult for them to feel comfortable when census numbers increased with common diagnoses like bronchiolitis. “However, those respiratory viruses that were hibernating last winter caused an unusual and challenging summer surge,” Dr. Hall said.
The biggest challenge though “is knowing that there is not a perfect solution for this global pandemic’s effect on medical education,” said Dr. Hall. “We can’t possibly perfectly balance the safety of our learners and their families with the dangers of COVID-19.”
Leadership discussions
As a residency program leader, Dr. Ricotta said there are conversations about multiple topics, including maintaining a safe learning environment; providing important aspects of residency training; whether to go back to full in-person teaching, keep doing virtual teaching, or implement a hybrid model; and how to help residents understand the balance between their personal and professional lives, especially in terms of safety.
“They have to their lives outside of the hospital, but we also are trying to instill ... what their responsibility is to society, to their patients, and to each other,” said Dr. Ricotta.
A more recent discussion has been about how to manage the COVID vaccine boosters. “We can’t have everyone getting vaccines at the same time because they might have symptoms afterward, and then be out sick – you’re missing half your workforce,” Dr. Ricotta said. But staggering residents’ booster shots created yet another dilemma around deciding who received the booster sooner rather than later.
The biggest consideration for Dr. Gottenborg’s leadership team was deciding whether to use their residents to help with the COVID surges or keep them in a traditional residency experience. While the residents wanted to be part of the pandemic response, there were many factors to consider. Ultimately, they came up with a balance between the amount of time residents should spend taking care of COVID patients while also assuring that they leave the program with all the skills and experiences they need.
Though Dr. Hall works more closely with medical students than residents, he sees the challenges and effects as being similar. Creating harmony between a safe learning environment and students’ educational goals has been the topic of endless discussions. This includes decisions as to whether or not students should be involved in person in certain activities such as large classroom didactics, written exams, seeing patients in clinical settings, and small group discussions.
Recruitment effects
When it comes to recruiting during a global pandemic, the experiences and predictions are mixed. Dr. Hall believes virtual interviews are making recruitment easier, but in turn, the fact that they are virtual also makes it harder for the applicant to get a good feel for the program and the people involved in it.
Dr. Ricotta reported that recruitment numbers have been fairly steady at Beth Israel Deaconess over the last few years. “In addition to the critical care physicians, hospital medicine was really the front line of this pandemic and so in some ways, we gained some recognition that we may not have had otherwise,” said Dr. Ricotta. He believes this has the benefit of attracting some residents, but at the same time, it could potentially scare others away from what they perceive as a demanding, grueling job. “I think it has been mixed. It’s dependent on the person.”
At UC Denver, Dr. Gottenborg said they are seeing a rapid rise in the number of applications and interest in their programs. Still, “I think this could go both ways,” she acknowledged. With the focus on hospital medicine in the media, medical students are more aware of the specialty and what it involves. “I think the sense of mission is really exemplified and everyone is talking about it,” she said. This is evident in the arrival this summer of the first new class of interns since the pandemic. “They’re incredibly passionate about the work,” said Dr. Gottenborg.
However, there is also the notable increase in physician burnout since the pandemic started. That this has been regularly featured in the media leaves Dr. Gottenborg to wonder if prospective residents will shy away from hospital medicine because they believe it is an area that leads to burnout. “I hope that’s not the case,” she said.
“I would actually argue [recruitment] is easier,” said Dr. Rawal. Like Dr. Hall, she sees virtual interviews as a big benefit to prospective trainees because they don’t have to spend a large amount of money on travel, food, and other expenses like they did before, a welcome relief for residents with significant debt. “I think that is one very big positive from the pandemic,” she said. Her trainees were advised to make a final list and consider going to see the top two or three in person, but “at this point, there’s really no expectation to go see all 15 places that you look into.”
Dr. Rawal also pointed out that recruitment is affected by whether or not trainees are expected to see COVID patients. “I know in some places they aren’t and in some places they are, so it just depends on where you are and what you’re looking for,” she said.
Shifts in education
It remains to be seen if all the educational changes will be permanent, though it appears that many will remain. Dr. Hall hopes that virtual visits to provide care to patients who have difficulty getting to physical clinics will continue to be a focus for hospital medicine trainees. “For medical students, I think this will allow us to better assess what content can best be delivered in person, synchronously online, or asynchronously through recorded content,” he said.
Dr. Ricotta predicts that virtual conferences will become more pervasive as academic hospitals continue to acquire more community hospitals, especially for grand rounds. “The virtual teaching that occurred in the residency program because it’s required by the [Accreditation Council for Graduate Medical Education] has, I think, informed how academic centers do ongoing faculty development, professional development, and obviously education for the residents,” Dr. Ricotta said. “I think virtual teaching is here to stay.” This includes telehealth training, which had not been a widespread part of residency education before now.
Trainees have been given tools to handle high patient censuses and learned a whole new set of communication skills, thanks to the pandemic, said Dr. Rawal. There has been a focus on learning how to advocate for the vaccine, along with education on situations like how to have conversations with patients who don’t believe they have COVID, even when their tests are positive. “Learning to handle these situations and still be a physician and provide appropriate care regardless of the patient’s views is very important. This is not something I learned in my training because it never came up,” she said.
Dr. Gottenborg has been impressed by the resident workforce’s response across all specialties throughout these difficult days. “They were universally ready to dive in and work long hours and care for these very sick patients and ultimately share their experiences so that we could do it better as these patients continue to flow through our systems,” she said. “It has been very invigorating.”
The pandemic has also put a spotlight on the importance of being flexible, as well as various problems with how health care systems operate, “which, for people in our field, gets us both excited and gives us a lot of work to do,” said Dr. Gottenborg. “Our residents see that and feel that and will hopefully continue to hold that torch in hospital medicine.”
In spite of everything, Dr. Rawal believes this is an exhilarating time to be a trainee. “They’re getting an opportunity that none of us got. Usually, when policies are made, we really don’t see the immediate impact.” But with recent mandates like masks and social distancing, “the rate of change that they get to see things happen is exciting. They’re going to be a very exciting group of physicians.”
It could be argued that hospital medicine in the United States was made vital by a major infectious disease epidemic – the HIV/AIDS crisis – said Emily Gottenborg, MD, a hospitalist and program director of hospitalist training at the University of Colorado at Denver, Aurora. Certainly, it was born out of the need for change, for physicians who could coordinate complex patient care plans and serve as the “quarterbacks” of the hospital. “As a result, we have always been very nimble and ready to embrace change,” said Dr. Gottenborg.
That hospitalist-honed agility and penchant for innovation has proven to be invaluable during the current COVID-19 pandemic as hospital medicine–focused residency programs have been forced to pivot quickly and modify their agendas. From managing the pandemic’s impact on residents’ day-to-day experiences, to carefully balancing educational needs and goals, program leaders have worked tirelessly to ensure that residents continue to receive excellent training.
The overarching theme across U.S.-based residency programs is that the educational changes and challenges during the COVID-19 pandemic have often been one and the same.
Service versus education
At the beginning of the pandemic, trainees at the University of Pittsburgh Medical Center were limited in seeing COVID patients in order to curb exposure. But now that COVID appears to be the new normal, “I think the question becomes: ‘How do we incorporate our trainees to take care of COVID patients since it seems it will be staying around for a while?’ ” said Rachna Rawal, MD, a hospitalist and clinical assistant professor of medicine at UPMC.
This dilemma highlights the conflict between service and education. Residents have been motivated and eager to help, which has been beneficial whenever there is a surge. “At the same time, you want to preserve their education, and it’s a very difficult balance at times,” said Dr. Rawal. It’s also challenging to figure out the safest way for residents to see patients, as well as how to include medical students, since interns and residents serve as important educational resources for them.
Keeping trainees involved with daily virtual conferences rather than in-person interactions raises the question of whether or not the engagement is equivalent. “It’s harder to keep them accountable when they’re not in person, but it’s also not worth the risk given the COVID numbers at times,” Dr. Rawal said. The goal has become to make sure residents stay safe while still feeling that they are getting a good education.
A balancing act
“I think early on, there was a lot of pride in what we were doing, that we were on the front line managing this thing that was emerging,” said Daniel Ricotta, MD, a hospitalist and associate program director of the internal medicine residency at Beth Israel Deaconess Medical Center and assistant professor of medicine at Harvard Medical School, both in Boston. “And now I think people are starting to feel a little bit weary.”
It has been demanding trying to manage ongoing educational needs through this time. “At the end of the day, residents are still trainees and have to be trained and educated. They’re not just worker bees taking care of patients,” Dr. Ricotta said. Residents need a well-rounded clinical experience – “they can’t just take care of COVID patients and then be able to graduate as general internists,” he said – but that becomes onerous when the hospital is full of patients with COVID.
Along with balancing residents’ clinical immersion, Dr. Ricotta said there has been the challenge of doing “the content-based teaching from didactics that occur in the context of clinical work, but are somewhat separated when you need to limit the number of people in the rooms and try to keep as many people at home as possible when they’re not taking care of patients in order to limit their level of risk.” Adjusting and readjusting both of these aspects has had a major impact on residents’ day-to-day education.
“A big part of residency is community,” noted Dr. Ricotta, but the sense of community has been disrupted because some of the bonding experiences residents used to do outside the hospital to build that community have necessarily gone by the wayside. This particularly affects interns from around the country who are meeting each other for the first time. “We actually had a normal intern orientation this year, but last year, when everything was virtual, we were trying to find ways to bridge relationships in a way that was safe and socially distanced,” he said.
Improving quality
UC Denver is unique in that they have a 3-year program specifically for hospital medicine residents, said Dr. Gottenborg. Right away, “our residents rose to the challenge and wanted to be part of the workforce that helps care for this critical population of [COVID] patients.” The residents were able to run the ICUs and take care of COVID patients, but in exchange, they had to give up some of their elective rotation time.
One aspect of the UC Denver hospital medicine residency program is participation in projects that focus on how to improve the health care system. Over the past year, the residents worked on one project in particular that focused on restructuring the guidelines for consulting physical therapists. Since many patients end up needing a physical therapist for a variety of reasons, a full hospital puts increased strain on their workload, making their time more precious.
“[The project] forced us to think about the right criteria to consult them,” explained Dr. Gottenborg. “We cut down essentially all the inappropriate consults to PT, opening their time. That project was driven by how the residents were experiencing the pandemic in the hospital.”
Learning to adapt
“The training environment during this pandemic has been tumultuous for both our residents and medical students,” said Alan M. Hall, MD, associate professor of internal medicine and pediatrics and assistant dean of curriculum integration at the University of Kentucky, Lexington. Along with treating patients with COVID-19, he said trainees have also had to cope with anxiety about getting the virus themselves or inadvertently bringing it home to their families.
Like most medical schools, University of Kentucky students were shifted away from clinical rotations and into alternative and online education for a time. When they returned to in-person education, the students were initially restricted from seeing patients with confirmed or suspected COVID-19 in order to reduce their personal risk and to conserve personal protective equipment.
This especially impacted certain rotations, such as pediatrics. Because respiratory symptoms are common in this population, students were greatly limited in the number of new patients they could see. Now they are given the option to see patients with COVID-19 if they want to.
“Our residents have had to adapt to seemingly endless changes during this pandemic,” Dr. Hall said. For example, at the beginning of the surge, the internal medicine residents trained for a completely new clinical model, though this ultimately never needed to be implemented. Then they had to adjust to extremely high census numbers that continue to have an effect on almost all of their rotations.
Conversely, the pediatrics residents saw far fewer inpatients last winter than they typically would. This made it more difficult for them to feel comfortable when census numbers increased with common diagnoses like bronchiolitis. “However, those respiratory viruses that were hibernating last winter caused an unusual and challenging summer surge,” Dr. Hall said.
The biggest challenge though “is knowing that there is not a perfect solution for this global pandemic’s effect on medical education,” said Dr. Hall. “We can’t possibly perfectly balance the safety of our learners and their families with the dangers of COVID-19.”
Leadership discussions
As a residency program leader, Dr. Ricotta said there are conversations about multiple topics, including maintaining a safe learning environment; providing important aspects of residency training; whether to go back to full in-person teaching, keep doing virtual teaching, or implement a hybrid model; and how to help residents understand the balance between their personal and professional lives, especially in terms of safety.
“They have to their lives outside of the hospital, but we also are trying to instill ... what their responsibility is to society, to their patients, and to each other,” said Dr. Ricotta.
A more recent discussion has been about how to manage the COVID vaccine boosters. “We can’t have everyone getting vaccines at the same time because they might have symptoms afterward, and then be out sick – you’re missing half your workforce,” Dr. Ricotta said. But staggering residents’ booster shots created yet another dilemma around deciding who received the booster sooner rather than later.
The biggest consideration for Dr. Gottenborg’s leadership team was deciding whether to use their residents to help with the COVID surges or keep them in a traditional residency experience. While the residents wanted to be part of the pandemic response, there were many factors to consider. Ultimately, they came up with a balance between the amount of time residents should spend taking care of COVID patients while also assuring that they leave the program with all the skills and experiences they need.
Though Dr. Hall works more closely with medical students than residents, he sees the challenges and effects as being similar. Creating harmony between a safe learning environment and students’ educational goals has been the topic of endless discussions. This includes decisions as to whether or not students should be involved in person in certain activities such as large classroom didactics, written exams, seeing patients in clinical settings, and small group discussions.
Recruitment effects
When it comes to recruiting during a global pandemic, the experiences and predictions are mixed. Dr. Hall believes virtual interviews are making recruitment easier, but in turn, the fact that they are virtual also makes it harder for the applicant to get a good feel for the program and the people involved in it.
Dr. Ricotta reported that recruitment numbers have been fairly steady at Beth Israel Deaconess over the last few years. “In addition to the critical care physicians, hospital medicine was really the front line of this pandemic and so in some ways, we gained some recognition that we may not have had otherwise,” said Dr. Ricotta. He believes this has the benefit of attracting some residents, but at the same time, it could potentially scare others away from what they perceive as a demanding, grueling job. “I think it has been mixed. It’s dependent on the person.”
At UC Denver, Dr. Gottenborg said they are seeing a rapid rise in the number of applications and interest in their programs. Still, “I think this could go both ways,” she acknowledged. With the focus on hospital medicine in the media, medical students are more aware of the specialty and what it involves. “I think the sense of mission is really exemplified and everyone is talking about it,” she said. This is evident in the arrival this summer of the first new class of interns since the pandemic. “They’re incredibly passionate about the work,” said Dr. Gottenborg.
However, there is also the notable increase in physician burnout since the pandemic started. That this has been regularly featured in the media leaves Dr. Gottenborg to wonder if prospective residents will shy away from hospital medicine because they believe it is an area that leads to burnout. “I hope that’s not the case,” she said.
“I would actually argue [recruitment] is easier,” said Dr. Rawal. Like Dr. Hall, she sees virtual interviews as a big benefit to prospective trainees because they don’t have to spend a large amount of money on travel, food, and other expenses like they did before, a welcome relief for residents with significant debt. “I think that is one very big positive from the pandemic,” she said. Her trainees were advised to make a final list and consider going to see the top two or three in person, but “at this point, there’s really no expectation to go see all 15 places that you look into.”
Dr. Rawal also pointed out that recruitment is affected by whether or not trainees are expected to see COVID patients. “I know in some places they aren’t and in some places they are, so it just depends on where you are and what you’re looking for,” she said.
Shifts in education
It remains to be seen if all the educational changes will be permanent, though it appears that many will remain. Dr. Hall hopes that virtual visits to provide care to patients who have difficulty getting to physical clinics will continue to be a focus for hospital medicine trainees. “For medical students, I think this will allow us to better assess what content can best be delivered in person, synchronously online, or asynchronously through recorded content,” he said.
Dr. Ricotta predicts that virtual conferences will become more pervasive as academic hospitals continue to acquire more community hospitals, especially for grand rounds. “The virtual teaching that occurred in the residency program because it’s required by the [Accreditation Council for Graduate Medical Education] has, I think, informed how academic centers do ongoing faculty development, professional development, and obviously education for the residents,” Dr. Ricotta said. “I think virtual teaching is here to stay.” This includes telehealth training, which had not been a widespread part of residency education before now.
Trainees have been given tools to handle high patient censuses and learned a whole new set of communication skills, thanks to the pandemic, said Dr. Rawal. There has been a focus on learning how to advocate for the vaccine, along with education on situations like how to have conversations with patients who don’t believe they have COVID, even when their tests are positive. “Learning to handle these situations and still be a physician and provide appropriate care regardless of the patient’s views is very important. This is not something I learned in my training because it never came up,” she said.
Dr. Gottenborg has been impressed by the resident workforce’s response across all specialties throughout these difficult days. “They were universally ready to dive in and work long hours and care for these very sick patients and ultimately share their experiences so that we could do it better as these patients continue to flow through our systems,” she said. “It has been very invigorating.”
The pandemic has also put a spotlight on the importance of being flexible, as well as various problems with how health care systems operate, “which, for people in our field, gets us both excited and gives us a lot of work to do,” said Dr. Gottenborg. “Our residents see that and feel that and will hopefully continue to hold that torch in hospital medicine.”
In spite of everything, Dr. Rawal believes this is an exhilarating time to be a trainee. “They’re getting an opportunity that none of us got. Usually, when policies are made, we really don’t see the immediate impact.” But with recent mandates like masks and social distancing, “the rate of change that they get to see things happen is exciting. They’re going to be a very exciting group of physicians.”
Hospitalist movers and shakers – December 2021
Narine Sargsyan, MD, recently was named the 2021 Alton Memorial Hospital (Alton, Ill.) Chairman’s Award winner. Serving as BJC Medical Group’s hospitalist medical director and hospital department chief of medicine, Dr. Sargsyan won the award based on the nominations of her fellow physicians.
The Chairman’s Award goes to an Alton Memorial staff member acknowledged for contributions to the facility and the community, including promotion and execution of outstanding customer service. Dr. Sargsyan has been a point person for Alton’s treatment of patients during the COVID-19 pandemic, recruiting new hospitalists to treat hospital inpatients. She also served on a committee selecting the inaugural resident class for the Southern Illinois University School of Medicine’s Family Residency program.
Alice Tang, DO, recently was named chief medical officer at Sentara Northern Virginia Medical Center (Woodbridge, Va.). The former medical director at Sentara Lake Ridge Hospital also directed the stroke program at Sentara Northern Virginia Medical Center, so she is familiar with her new facility.
The hospital medicine veteran specialized in emergency medicine and earned her health care MBA from George Washington University. Dr. Tang said her goal as CMO is to enhance the care environment while simultaneously raising the level of the care given by Sentara providers.
Faisal Keen, MD, has been named 2021 Physician of the Year at Sarasota Memorial Hospital’s Sarasota (Fla.) campus. The award winner was selected by a panel of SMH physician leaders.
Dr. Keen has been a hospitalist at SMH Sarasota for the past 6 years.
In presenting Dr. Keen with the award, the staff paid particular compliment to the care he provided to the facility’s hundreds of COVID-19 patients throughout the pandemic. At one point during the surge, Dr. Keen worked 30 shifts during a single month. Among the praises he received during the award presentation were those for his efforts in hurricane preparedness and helping physicians at SMH utilize technology in their patient care.
Jeffrey Crowder, MSPA, PA-C, recently became the first physician assistant to be named chief of hospitalist service at Maine Veterans Affairs Medical Center (Augusta, Me.). He is the first PA to hold the position at any Maine VA hospital. Mr. Crowder held the role in an acting position for the previous year, helping Maine VA Augusta navigate the COVID-19 pandemic.
Mr. Crowder will oversee 13 physicians and 9 PAs in providing care to Maine’s veterans. Included in the facility are intensive care and medical surgery units. Mr. Crowder’s group is responsible for part-time coverage at the 60-bed Togus Community Living Center.
Southeast Iowa Regional Medical Center (West Burlington, Iowa) has expanded its hospitalist program, adding the service to its Fort Madison campus. The health system’s hospitalist program was initiated at SEIRMC’s West Burlington campus back in 2010. That facility now includes 12 full-time and five part-time hospitalist physicians.
OB Hospitalist Group (Greenville, S.C.) has been acquired by Kohlberg & Company LLC (Mount Kisco, N.Y.), giving the nation’s largest dedicated obstetric hospitalist provider a new stakeholder. OBHG hopes to expand its services, which already include 200 hospital partners across 34 states.
OBHG’s network of providers includes more than 1,100 clinicians, with sites normally featuring an OB emergency department with a practicing ob.gyn. on site around the clock. Kohlberg & Company was founded in 1987 and has organized nine private equity funds, raising $12 billion of equity capital.
Narine Sargsyan, MD, recently was named the 2021 Alton Memorial Hospital (Alton, Ill.) Chairman’s Award winner. Serving as BJC Medical Group’s hospitalist medical director and hospital department chief of medicine, Dr. Sargsyan won the award based on the nominations of her fellow physicians.
The Chairman’s Award goes to an Alton Memorial staff member acknowledged for contributions to the facility and the community, including promotion and execution of outstanding customer service. Dr. Sargsyan has been a point person for Alton’s treatment of patients during the COVID-19 pandemic, recruiting new hospitalists to treat hospital inpatients. She also served on a committee selecting the inaugural resident class for the Southern Illinois University School of Medicine’s Family Residency program.
Alice Tang, DO, recently was named chief medical officer at Sentara Northern Virginia Medical Center (Woodbridge, Va.). The former medical director at Sentara Lake Ridge Hospital also directed the stroke program at Sentara Northern Virginia Medical Center, so she is familiar with her new facility.
The hospital medicine veteran specialized in emergency medicine and earned her health care MBA from George Washington University. Dr. Tang said her goal as CMO is to enhance the care environment while simultaneously raising the level of the care given by Sentara providers.
Faisal Keen, MD, has been named 2021 Physician of the Year at Sarasota Memorial Hospital’s Sarasota (Fla.) campus. The award winner was selected by a panel of SMH physician leaders.
Dr. Keen has been a hospitalist at SMH Sarasota for the past 6 years.
In presenting Dr. Keen with the award, the staff paid particular compliment to the care he provided to the facility’s hundreds of COVID-19 patients throughout the pandemic. At one point during the surge, Dr. Keen worked 30 shifts during a single month. Among the praises he received during the award presentation were those for his efforts in hurricane preparedness and helping physicians at SMH utilize technology in their patient care.
Jeffrey Crowder, MSPA, PA-C, recently became the first physician assistant to be named chief of hospitalist service at Maine Veterans Affairs Medical Center (Augusta, Me.). He is the first PA to hold the position at any Maine VA hospital. Mr. Crowder held the role in an acting position for the previous year, helping Maine VA Augusta navigate the COVID-19 pandemic.
Mr. Crowder will oversee 13 physicians and 9 PAs in providing care to Maine’s veterans. Included in the facility are intensive care and medical surgery units. Mr. Crowder’s group is responsible for part-time coverage at the 60-bed Togus Community Living Center.
Southeast Iowa Regional Medical Center (West Burlington, Iowa) has expanded its hospitalist program, adding the service to its Fort Madison campus. The health system’s hospitalist program was initiated at SEIRMC’s West Burlington campus back in 2010. That facility now includes 12 full-time and five part-time hospitalist physicians.
OB Hospitalist Group (Greenville, S.C.) has been acquired by Kohlberg & Company LLC (Mount Kisco, N.Y.), giving the nation’s largest dedicated obstetric hospitalist provider a new stakeholder. OBHG hopes to expand its services, which already include 200 hospital partners across 34 states.
OBHG’s network of providers includes more than 1,100 clinicians, with sites normally featuring an OB emergency department with a practicing ob.gyn. on site around the clock. Kohlberg & Company was founded in 1987 and has organized nine private equity funds, raising $12 billion of equity capital.
Narine Sargsyan, MD, recently was named the 2021 Alton Memorial Hospital (Alton, Ill.) Chairman’s Award winner. Serving as BJC Medical Group’s hospitalist medical director and hospital department chief of medicine, Dr. Sargsyan won the award based on the nominations of her fellow physicians.
The Chairman’s Award goes to an Alton Memorial staff member acknowledged for contributions to the facility and the community, including promotion and execution of outstanding customer service. Dr. Sargsyan has been a point person for Alton’s treatment of patients during the COVID-19 pandemic, recruiting new hospitalists to treat hospital inpatients. She also served on a committee selecting the inaugural resident class for the Southern Illinois University School of Medicine’s Family Residency program.
Alice Tang, DO, recently was named chief medical officer at Sentara Northern Virginia Medical Center (Woodbridge, Va.). The former medical director at Sentara Lake Ridge Hospital also directed the stroke program at Sentara Northern Virginia Medical Center, so she is familiar with her new facility.
The hospital medicine veteran specialized in emergency medicine and earned her health care MBA from George Washington University. Dr. Tang said her goal as CMO is to enhance the care environment while simultaneously raising the level of the care given by Sentara providers.
Faisal Keen, MD, has been named 2021 Physician of the Year at Sarasota Memorial Hospital’s Sarasota (Fla.) campus. The award winner was selected by a panel of SMH physician leaders.
Dr. Keen has been a hospitalist at SMH Sarasota for the past 6 years.
In presenting Dr. Keen with the award, the staff paid particular compliment to the care he provided to the facility’s hundreds of COVID-19 patients throughout the pandemic. At one point during the surge, Dr. Keen worked 30 shifts during a single month. Among the praises he received during the award presentation were those for his efforts in hurricane preparedness and helping physicians at SMH utilize technology in their patient care.
Jeffrey Crowder, MSPA, PA-C, recently became the first physician assistant to be named chief of hospitalist service at Maine Veterans Affairs Medical Center (Augusta, Me.). He is the first PA to hold the position at any Maine VA hospital. Mr. Crowder held the role in an acting position for the previous year, helping Maine VA Augusta navigate the COVID-19 pandemic.
Mr. Crowder will oversee 13 physicians and 9 PAs in providing care to Maine’s veterans. Included in the facility are intensive care and medical surgery units. Mr. Crowder’s group is responsible for part-time coverage at the 60-bed Togus Community Living Center.
Southeast Iowa Regional Medical Center (West Burlington, Iowa) has expanded its hospitalist program, adding the service to its Fort Madison campus. The health system’s hospitalist program was initiated at SEIRMC’s West Burlington campus back in 2010. That facility now includes 12 full-time and five part-time hospitalist physicians.
OB Hospitalist Group (Greenville, S.C.) has been acquired by Kohlberg & Company LLC (Mount Kisco, N.Y.), giving the nation’s largest dedicated obstetric hospitalist provider a new stakeholder. OBHG hopes to expand its services, which already include 200 hospital partners across 34 states.
OBHG’s network of providers includes more than 1,100 clinicians, with sites normally featuring an OB emergency department with a practicing ob.gyn. on site around the clock. Kohlberg & Company was founded in 1987 and has organized nine private equity funds, raising $12 billion of equity capital.
Hospitalists helped plan COVID-19 field hospitals
‘It’s a great thing to be overprepared’
At the height of the COVID-19 pandemic’s terrifying first wave in the spring of 2020, dozens of hospitals in high-incidence areas either planned or opened temporary, emergency field hospitals to cover anticipated demand for beds beyond the capacity of local permanent hospitals.
Chastened by images of overwhelmed health care systems in Northern Italy and other hard-hit areas,1 the planners used available modeling tools and estimates for projecting maximum potential need in worst-case scenarios. Some of these temporary hospitals never opened. Others opened in convention centers, parking garages, or parking lot tents, and ended up being used to a lesser degree than the worst-case scenarios.
But those who participated in the planning – including, in many cases, hospitalists – believe they created alternate care site manuals that could be quickly revived in the event of future COVID surges or other, similar crises. Better to plan for too much, they say, than not plan for enough.
Field hospitals or alternate care sites are defined in a recent journal article in Prehospital Disaster Medicine as “locations that can be converted to provide either inpatient and/or outpatient health services when existing facilities are compromised by a hazard impact or the volume of patients exceeds available capacity and/or capabilities.”2
The lead author of that report, Sue Anne Bell, PhD, FNP-BC, a disaster expert and assistant professor of nursing at the University of Michigan (UM), was one of five members of the leadership team for planning UM’s field hospital. They used an organizational unit structure based on the U.S. military’s staffing structure, with their work organized around six units of planning: personnel and labor, security, clinical operations, logistics and supply, planning and training, and communications. This team planned a 519-bed step-down care facility, the Michigan Medicine Field Hospital, for a 73,000-foot indoor track and performance facility at the university, three miles from UM’s main hospital. The aim was to provide safe care in a resource-limited environment.
“We were prepared, but the need never materialized as the peak of COVID cases started to subside,” Dr. Bell said. The team was ready to open within days using a “T-Minus” framework of days remaining on an official countdown clock. But when the need and deadlines kept getting pushed back, that gave them more time to develop clearer procedures.
Two Michigan Medicine hospitalists, Christopher Smith, MD, and David Paje, MD, MPH, both professors at UM’s medical school, were intimately involved in the process. “I was the medical director for the respiratory care unit that was opened for COVID patients, so I was pulled in to assist in the field hospital planning,” said Dr. Smith.
Dr. Paje was director of the short-stay unit and had been a medical officer in the U.S. Army, with training in how to set up military field hospitals. He credits that background as helpful for UM’s COVID field hospital planning, along with his experience in hospital medicine operations.
“We expected that these patients would need the expertise of hospitalists, who had quickly become familiar with the peculiarities of the new disease. That played a role in the decisions we made. Hospitalists were at the front lines of COVID care and had unique clinical insights about managing those with severe disease,” Dr. Paje added.
“When we started, the projections were dire. You don’t want to believe something like that is going to happen. When COVID started to cool off, it was more of a relief to us than anything else,” Dr. Smith said. “Still, it was a very worthwhile exercise. At the end of the day, we put together a comprehensive guide, which is ready for the next crisis.”
Baltimore builds a convention center hospital
A COVID-19 field hospital was planned and executed at an exhibit hall in the Baltimore Convention Center, starting in March 2020 under the leadership of Johns Hopkins Bayview hospitalist Eric Howell, MD, MHM, who eventually handed over responsibilities as chief medical officer when he assumed the position of CEO for the Society of Hospital Medicine in July of that year.
Hopkins collaborated with the University of Maryland health system and state leaders, including the Secretary of Health, to open a 252-bed temporary facility, which at its peak carried a census of 48 patients, with no on-site mortality or cardiac arrests, before it was closed in June 2021 – ready to reopen if necessary. It also served as Baltimore’s major site for polymerase chain reaction COVID-19 testing, vaccinations, and monoclonal antibody infusions, along with medical research.
“My belief at the time we started was that my entire 20-year career as a hospitalist had prepared me for the challenge of opening a COVID field hospital,” Dr. Howell said. “I had learned how to build clinical programs. The difference was that instead of months and years to build a program, we only had a few weeks.”
His first request was to bring on an associate medical director for the field hospital, Melinda E. Kantsiper, MD, a hospitalist and director of clinical operations in the Division of Hospital Medicine at Johns Hopkins Bayview. She became the field hospital’s CMO when Dr. Howell moved to SHM. “As hospitalists, we are trained to care for the patient in front of us while at the same time creating systems that can adjust to rapidly changing circumstances,” Dr. Kantsiper said. “We did what was asked and set up a field hospital that cared for a total of 1,500 COVID patients.”
Hospitalists have the tools that are needed for this work, and shouldn’t be reluctant to contribute to field hospital planning, she said. “This was a real eye-opener for me. Eric explained to me that hospitalists really practice acute care medicine, which doesn’t have to be within the four walls of a hospital.”
The Baltimore field hospital has been a fantastic experience, Dr. Kantsiper added. “But it’s not a building designed for health care delivery.” For the right group of providers, the experience of working in a temporary facility such as this can be positive and exhilarating. “But we need to make sure we take care of our staff. It takes a toll. How we keep them safe – physically and emotionally – has to be top of mind,” she said.
The leaders at Hopkins Medicine and their collaborators truly engaged with the field hospital’s mission, Dr. Howell added.
“They gave us a lot of autonomy and helped us break down barriers. They gave us the political capital to say proper PPE was absolutely essential. As hard and devastating as the pandemic has been, one take-away is that we showed that we can be more flexible and elastic in response to actual needs than we used to think.”
Range of challenges
Among the questions that need to be answered by a field hospital’s planners, the first is ‘where to put it?’ The answer is, hopefully, someplace not too far away, large enough, with ready access to supplies and intake. The next question is ‘who is the patient?’ Clinicians must determine who goes to the field hospital versus who stays at the standing hospital. How sick should these patients be? And when do they need to go back to the permanent hospital? Can staff be trained to recognize when patients in the field hospital are starting to decompensate? The EPIC Deterioration Index3 is a proprietary prediction model that was used by more than a hundred hospitals during the pandemic.
The hospitalist team may develop specific inclusion and exclusion criteria – for example, don’t admit patients who are receiving oxygen therapy above a certain threshold or who are hemodynamically unstable. These criteria should reflect the capacity of the field hospital and the needs of the permanent hospital. At Michigan, as at other field hospital sites, the goal was to offer a step-down or postacute setting for patients with COVID-19 who were too sick to return home but didn’t need acute or ICU-level care, thereby freeing up beds at the permanent hospital for patients who were sicker.
Other questions: What is the process for admissions and discharges? How will patients be transported? What kind of staffing is needed, and what levels of care will be provided? What about rehabilitation services, or palliative care? What about patients with substance abuse or psychiatric comorbidities?
“Are we going to do paper charting? How will that work out for long-term documentation and billing?” Dr. Bell said. A clear reporting structure and communication pathways are essential. Among the other operational processes to address, outlined in Dr. Bell’s article, are orientation and training, PPE donning and doffing procedures, the code or rapid response team, patient and staff food and nutrition, infection control protocols, pharmacy services, access to radiology, rounding procedures, staff support, and the morgue.
One other issue that shouldn’t be overlooked is health equity in the field hospital. “Providing safe and equitable care should be the focus. Thinking who goes to the field hospital should be done within a health equity framework,” Dr. Bell said.4 She also wonders if field hospital planners are sharing their experience with colleagues across the country and developing more collaborative relationships with other hospitals in their communities.
“Field hospitals can be different things,” Dr. Bell said. “The important take-home is it doesn’t have to be in a tent or a parking garage, which can be suboptimal.” In many cases, it may be better to focus on finding unused space within the hospital – whether a lobby, staff lounge, or unoccupied unit – closer to personnel, supplies, pharmacy, and the like. “I think the pandemic showed us how unprepared we were as a health care system, and how much more we need to do in preparation for future crises.”
Limits to the temporary hospital
In New York City, which had the country’s worst COVID-19 outbreak during the first surge in the spring of 2020, a 1,000-bed field hospital was opened at the Jacob Javits Center in March 2020 and closed that June. “I was in the field hospital early, in March and April, when our hospitals were temporarily overrun,” said hospitalist Mona Krouss, MD, FACP, CPPS, NYC Health + Hospitals’ director of patient safety. “My role was to figure out how to get patients on our medical floors into these field hospitals, with responsibility for helping to revise admission criteria,” she said.
“No one knew how horrible it would become. This was so unanticipated, so difficult to operationalize. What they were able to create was amazing, but there were just too many barriers to have it work smoothly,” Dr. Krouss said.
“The military stepped in, and they helped us so much. We wouldn’t have been able to survive without their help.” But there is only so much a field hospital can do to provide acute medical care. Later, military medical teams shifted to roles in temporary units inside the permanent hospitals. “They came to the hospital wanting to be deployed,” she said.
“We could only send patients [to the field hospital] who were fairly stable, and choosing the right ones was difficult.” Dr. Krouss said. In the end, not a lot of COVID-19 patients from NYC Health + Hospitals ended up going to the Javits Center, in part because the paperwork and logistics of getting someone in was a barrier, Dr. Krouss said. A process was established for referring doctors to call a phone number and speak with a New York City Department of Health employee to go through the criteria for admission to the field hospital.
“That could take up to 30 minutes before getting approval. Then you had to go through the same process all over again for sign-out to another physician, and then register the patient with a special bar code. Then you had to arrange ambulance transfer. Doctors didn’t want to go through all of that – everybody was too busy,” she explained. Hospitalists have since worked on streamlining the criteria. “Now we have a good process for the future. We made it more seamless,” she noted.
Susan Lee, DO, MBA, hospitalist and chief medical officer for Renown Regional Medical Center in Reno, Nev., helped to plan an alternate care site in anticipation of up to a thousand COVID patients in her community – far beyond the scope of the existing hospitals. Hospitalists were involved the entire time in planning, design of the unit, design of staffing models, care protocols, and the like, working through an evidence-based medical committee and a COVID-19 provider task force for the Renown Health System.
“Because of a history of fires and earthquakes in this region, we had an emergency planning infrastructure in place. We put the field hospital on the first and second floors of a parking garage, with built-in negative pressure capacity. We also built space for staff break rooms and desk space. It took 10 days to build the hospital, thanks to some very talented people in management and facility design,” Dr. Lee said.
Then, the hospital was locked up and sat empty for 7 months, until the surge in December 2020, when Reno was hit by a bigger wave – this time exceeding the hospitals’ capacity. Through mid-January of 2021, clinicians cared for approximately 240 COVID-19 patients, up to 47 at a time, in the field hospital. A third wave in the autumn of 2021 plateaued at a level lower than the previous fall, so the field hospital is not currently needed.
Replicating hospital work flows
“We ensured that everybody who needed to be within the walls of the permanent hospitals was able to stay there,” said Dr. Lee’s colleague, hospitalist Adnan (Eddy) Akbar, MD. “The postacute system we ordinarily rely on was no longer accepting patients. Other hospitals in the area were able to manage within their capacity because Renown’s field hospital could admit excess patients. We tried to replicate in the field hospital, as much as possible, the work flows and systems of our main hospital.”
When the field hospital finally opened, Dr. Akbar said, “we had a good feeling. We were ready. If something more catastrophic had come down, we were ready to care for more patients. In the field hospital you have to keep monitoring your work flow – almost on a daily basis. But we felt privileged to be working for a system where you knew you can go and care for everyone who needed care.”
One upside of the field hospital experience for participating clinicians, Dr. Lee added, is the opportunity to practice creatively. “The downside is it’s extremely expensive, and has consequences for the mental health of staff. Like so many of these things, it wore on people over time – such as all the time spent donning and doffing protective equipment. And recently the patients have become a lot less gracious.”
Amy Baughman, MD, a hospitalist at Massachusetts General Hospital in Boston, was co-medical director of the postacute care section of a 1,000-bed field hospital, Boston Hope Medical Center, opened in April 2020 at the Boston Convention and Exhibition Center. The other half of the facility was dedicated to undomiciled COVID-19 patients who had no place else to go. Peak census was around 100 patients, housed on four units, each with a clinical team led by a physician.
Dr. Baughman’s field hospital experience has taught her the importance of “staying within your domain of expertise. Physicians are attracted to difficult problems and want to do everything themselves. Next time I won’t be the one installing hand sanitizer dispensers.” A big part of running a field hospital is logistics, she said, and physicians are trained clinicians, not necessarily logistics engineers.
“So it’s important to partner with logistics experts. A huge part of our success in building a facility in 9 days of almost continuous construction was the involvement of the National Guard,” she said. An incident command system was led by an experienced military general incident commander, with two clinical codirectors. The army also sent in full teams of health professionals.
The facility admitted a lot fewer patients than the worst-case projections before it closed in June 2020. “But at the end of the day, we provided a lot of excellent care,” Dr. Baughman said. “This was about preparing for a disaster. It was all hands on deck, and the hands were health professionals. We spent a lot of money for the patients we took care of, but we had no choice, based on what we believed could happen. At that time, so many nursing facilities and homeless shelters were closed to us. It was impossible to predict what utilization would be.”
Subsequent experience has taught that a lot of even seriously ill COVID-19 patients can be managed safely at home, for example, using accelerated home oxygen monitoring with telelinked pulse oximeters. But in the beginning, Dr. Baughman said, “it was a new situation for us. We had seen what happened in Europe and China. It’s a great thing to be overprepared.”
References
1. Horowitz J. Italy’s health care system groans under coronavirus – a warning to the world. New York Times. 2020 Mar 12.
2. Bell SA et al. T-Minus 10 days: The role of an academic medical institution in field hospital planning. Prehosp Disaster Med. 2021 Feb 18:1-6. doi: 10.1017/S1049023X21000224.
3. Singh K et al. Evaluating a widely implemented proprietary deterioration index model among hospitalized patients with COVID-19. Ann Am Thorac Soc. 2021 Jul;18(7):1129-37. doi: 10.1513/AnnalsATS.202006-698OC.
4. Bell SA et al. Alternate care sites during COVID-19 pandemic: Policy implications for pandemic surge planning. Disaster Med Public Health Prep. 2021 Jul 23;1-3. doi: 10.1017/dmp.2021.241.
‘It’s a great thing to be overprepared’
‘It’s a great thing to be overprepared’
At the height of the COVID-19 pandemic’s terrifying first wave in the spring of 2020, dozens of hospitals in high-incidence areas either planned or opened temporary, emergency field hospitals to cover anticipated demand for beds beyond the capacity of local permanent hospitals.
Chastened by images of overwhelmed health care systems in Northern Italy and other hard-hit areas,1 the planners used available modeling tools and estimates for projecting maximum potential need in worst-case scenarios. Some of these temporary hospitals never opened. Others opened in convention centers, parking garages, or parking lot tents, and ended up being used to a lesser degree than the worst-case scenarios.
But those who participated in the planning – including, in many cases, hospitalists – believe they created alternate care site manuals that could be quickly revived in the event of future COVID surges or other, similar crises. Better to plan for too much, they say, than not plan for enough.
Field hospitals or alternate care sites are defined in a recent journal article in Prehospital Disaster Medicine as “locations that can be converted to provide either inpatient and/or outpatient health services when existing facilities are compromised by a hazard impact or the volume of patients exceeds available capacity and/or capabilities.”2
The lead author of that report, Sue Anne Bell, PhD, FNP-BC, a disaster expert and assistant professor of nursing at the University of Michigan (UM), was one of five members of the leadership team for planning UM’s field hospital. They used an organizational unit structure based on the U.S. military’s staffing structure, with their work organized around six units of planning: personnel and labor, security, clinical operations, logistics and supply, planning and training, and communications. This team planned a 519-bed step-down care facility, the Michigan Medicine Field Hospital, for a 73,000-foot indoor track and performance facility at the university, three miles from UM’s main hospital. The aim was to provide safe care in a resource-limited environment.
“We were prepared, but the need never materialized as the peak of COVID cases started to subside,” Dr. Bell said. The team was ready to open within days using a “T-Minus” framework of days remaining on an official countdown clock. But when the need and deadlines kept getting pushed back, that gave them more time to develop clearer procedures.
Two Michigan Medicine hospitalists, Christopher Smith, MD, and David Paje, MD, MPH, both professors at UM’s medical school, were intimately involved in the process. “I was the medical director for the respiratory care unit that was opened for COVID patients, so I was pulled in to assist in the field hospital planning,” said Dr. Smith.
Dr. Paje was director of the short-stay unit and had been a medical officer in the U.S. Army, with training in how to set up military field hospitals. He credits that background as helpful for UM’s COVID field hospital planning, along with his experience in hospital medicine operations.
“We expected that these patients would need the expertise of hospitalists, who had quickly become familiar with the peculiarities of the new disease. That played a role in the decisions we made. Hospitalists were at the front lines of COVID care and had unique clinical insights about managing those with severe disease,” Dr. Paje added.
“When we started, the projections were dire. You don’t want to believe something like that is going to happen. When COVID started to cool off, it was more of a relief to us than anything else,” Dr. Smith said. “Still, it was a very worthwhile exercise. At the end of the day, we put together a comprehensive guide, which is ready for the next crisis.”
Baltimore builds a convention center hospital
A COVID-19 field hospital was planned and executed at an exhibit hall in the Baltimore Convention Center, starting in March 2020 under the leadership of Johns Hopkins Bayview hospitalist Eric Howell, MD, MHM, who eventually handed over responsibilities as chief medical officer when he assumed the position of CEO for the Society of Hospital Medicine in July of that year.
Hopkins collaborated with the University of Maryland health system and state leaders, including the Secretary of Health, to open a 252-bed temporary facility, which at its peak carried a census of 48 patients, with no on-site mortality or cardiac arrests, before it was closed in June 2021 – ready to reopen if necessary. It also served as Baltimore’s major site for polymerase chain reaction COVID-19 testing, vaccinations, and monoclonal antibody infusions, along with medical research.
“My belief at the time we started was that my entire 20-year career as a hospitalist had prepared me for the challenge of opening a COVID field hospital,” Dr. Howell said. “I had learned how to build clinical programs. The difference was that instead of months and years to build a program, we only had a few weeks.”
His first request was to bring on an associate medical director for the field hospital, Melinda E. Kantsiper, MD, a hospitalist and director of clinical operations in the Division of Hospital Medicine at Johns Hopkins Bayview. She became the field hospital’s CMO when Dr. Howell moved to SHM. “As hospitalists, we are trained to care for the patient in front of us while at the same time creating systems that can adjust to rapidly changing circumstances,” Dr. Kantsiper said. “We did what was asked and set up a field hospital that cared for a total of 1,500 COVID patients.”
Hospitalists have the tools that are needed for this work, and shouldn’t be reluctant to contribute to field hospital planning, she said. “This was a real eye-opener for me. Eric explained to me that hospitalists really practice acute care medicine, which doesn’t have to be within the four walls of a hospital.”
The Baltimore field hospital has been a fantastic experience, Dr. Kantsiper added. “But it’s not a building designed for health care delivery.” For the right group of providers, the experience of working in a temporary facility such as this can be positive and exhilarating. “But we need to make sure we take care of our staff. It takes a toll. How we keep them safe – physically and emotionally – has to be top of mind,” she said.
The leaders at Hopkins Medicine and their collaborators truly engaged with the field hospital’s mission, Dr. Howell added.
“They gave us a lot of autonomy and helped us break down barriers. They gave us the political capital to say proper PPE was absolutely essential. As hard and devastating as the pandemic has been, one take-away is that we showed that we can be more flexible and elastic in response to actual needs than we used to think.”
Range of challenges
Among the questions that need to be answered by a field hospital’s planners, the first is ‘where to put it?’ The answer is, hopefully, someplace not too far away, large enough, with ready access to supplies and intake. The next question is ‘who is the patient?’ Clinicians must determine who goes to the field hospital versus who stays at the standing hospital. How sick should these patients be? And when do they need to go back to the permanent hospital? Can staff be trained to recognize when patients in the field hospital are starting to decompensate? The EPIC Deterioration Index3 is a proprietary prediction model that was used by more than a hundred hospitals during the pandemic.
The hospitalist team may develop specific inclusion and exclusion criteria – for example, don’t admit patients who are receiving oxygen therapy above a certain threshold or who are hemodynamically unstable. These criteria should reflect the capacity of the field hospital and the needs of the permanent hospital. At Michigan, as at other field hospital sites, the goal was to offer a step-down or postacute setting for patients with COVID-19 who were too sick to return home but didn’t need acute or ICU-level care, thereby freeing up beds at the permanent hospital for patients who were sicker.
Other questions: What is the process for admissions and discharges? How will patients be transported? What kind of staffing is needed, and what levels of care will be provided? What about rehabilitation services, or palliative care? What about patients with substance abuse or psychiatric comorbidities?
“Are we going to do paper charting? How will that work out for long-term documentation and billing?” Dr. Bell said. A clear reporting structure and communication pathways are essential. Among the other operational processes to address, outlined in Dr. Bell’s article, are orientation and training, PPE donning and doffing procedures, the code or rapid response team, patient and staff food and nutrition, infection control protocols, pharmacy services, access to radiology, rounding procedures, staff support, and the morgue.
One other issue that shouldn’t be overlooked is health equity in the field hospital. “Providing safe and equitable care should be the focus. Thinking who goes to the field hospital should be done within a health equity framework,” Dr. Bell said.4 She also wonders if field hospital planners are sharing their experience with colleagues across the country and developing more collaborative relationships with other hospitals in their communities.
“Field hospitals can be different things,” Dr. Bell said. “The important take-home is it doesn’t have to be in a tent or a parking garage, which can be suboptimal.” In many cases, it may be better to focus on finding unused space within the hospital – whether a lobby, staff lounge, or unoccupied unit – closer to personnel, supplies, pharmacy, and the like. “I think the pandemic showed us how unprepared we were as a health care system, and how much more we need to do in preparation for future crises.”
Limits to the temporary hospital
In New York City, which had the country’s worst COVID-19 outbreak during the first surge in the spring of 2020, a 1,000-bed field hospital was opened at the Jacob Javits Center in March 2020 and closed that June. “I was in the field hospital early, in March and April, when our hospitals were temporarily overrun,” said hospitalist Mona Krouss, MD, FACP, CPPS, NYC Health + Hospitals’ director of patient safety. “My role was to figure out how to get patients on our medical floors into these field hospitals, with responsibility for helping to revise admission criteria,” she said.
“No one knew how horrible it would become. This was so unanticipated, so difficult to operationalize. What they were able to create was amazing, but there were just too many barriers to have it work smoothly,” Dr. Krouss said.
“The military stepped in, and they helped us so much. We wouldn’t have been able to survive without their help.” But there is only so much a field hospital can do to provide acute medical care. Later, military medical teams shifted to roles in temporary units inside the permanent hospitals. “They came to the hospital wanting to be deployed,” she said.
“We could only send patients [to the field hospital] who were fairly stable, and choosing the right ones was difficult.” Dr. Krouss said. In the end, not a lot of COVID-19 patients from NYC Health + Hospitals ended up going to the Javits Center, in part because the paperwork and logistics of getting someone in was a barrier, Dr. Krouss said. A process was established for referring doctors to call a phone number and speak with a New York City Department of Health employee to go through the criteria for admission to the field hospital.
“That could take up to 30 minutes before getting approval. Then you had to go through the same process all over again for sign-out to another physician, and then register the patient with a special bar code. Then you had to arrange ambulance transfer. Doctors didn’t want to go through all of that – everybody was too busy,” she explained. Hospitalists have since worked on streamlining the criteria. “Now we have a good process for the future. We made it more seamless,” she noted.
Susan Lee, DO, MBA, hospitalist and chief medical officer for Renown Regional Medical Center in Reno, Nev., helped to plan an alternate care site in anticipation of up to a thousand COVID patients in her community – far beyond the scope of the existing hospitals. Hospitalists were involved the entire time in planning, design of the unit, design of staffing models, care protocols, and the like, working through an evidence-based medical committee and a COVID-19 provider task force for the Renown Health System.
“Because of a history of fires and earthquakes in this region, we had an emergency planning infrastructure in place. We put the field hospital on the first and second floors of a parking garage, with built-in negative pressure capacity. We also built space for staff break rooms and desk space. It took 10 days to build the hospital, thanks to some very talented people in management and facility design,” Dr. Lee said.
Then, the hospital was locked up and sat empty for 7 months, until the surge in December 2020, when Reno was hit by a bigger wave – this time exceeding the hospitals’ capacity. Through mid-January of 2021, clinicians cared for approximately 240 COVID-19 patients, up to 47 at a time, in the field hospital. A third wave in the autumn of 2021 plateaued at a level lower than the previous fall, so the field hospital is not currently needed.
Replicating hospital work flows
“We ensured that everybody who needed to be within the walls of the permanent hospitals was able to stay there,” said Dr. Lee’s colleague, hospitalist Adnan (Eddy) Akbar, MD. “The postacute system we ordinarily rely on was no longer accepting patients. Other hospitals in the area were able to manage within their capacity because Renown’s field hospital could admit excess patients. We tried to replicate in the field hospital, as much as possible, the work flows and systems of our main hospital.”
When the field hospital finally opened, Dr. Akbar said, “we had a good feeling. We were ready. If something more catastrophic had come down, we were ready to care for more patients. In the field hospital you have to keep monitoring your work flow – almost on a daily basis. But we felt privileged to be working for a system where you knew you can go and care for everyone who needed care.”
One upside of the field hospital experience for participating clinicians, Dr. Lee added, is the opportunity to practice creatively. “The downside is it’s extremely expensive, and has consequences for the mental health of staff. Like so many of these things, it wore on people over time – such as all the time spent donning and doffing protective equipment. And recently the patients have become a lot less gracious.”
Amy Baughman, MD, a hospitalist at Massachusetts General Hospital in Boston, was co-medical director of the postacute care section of a 1,000-bed field hospital, Boston Hope Medical Center, opened in April 2020 at the Boston Convention and Exhibition Center. The other half of the facility was dedicated to undomiciled COVID-19 patients who had no place else to go. Peak census was around 100 patients, housed on four units, each with a clinical team led by a physician.
Dr. Baughman’s field hospital experience has taught her the importance of “staying within your domain of expertise. Physicians are attracted to difficult problems and want to do everything themselves. Next time I won’t be the one installing hand sanitizer dispensers.” A big part of running a field hospital is logistics, she said, and physicians are trained clinicians, not necessarily logistics engineers.
“So it’s important to partner with logistics experts. A huge part of our success in building a facility in 9 days of almost continuous construction was the involvement of the National Guard,” she said. An incident command system was led by an experienced military general incident commander, with two clinical codirectors. The army also sent in full teams of health professionals.
The facility admitted a lot fewer patients than the worst-case projections before it closed in June 2020. “But at the end of the day, we provided a lot of excellent care,” Dr. Baughman said. “This was about preparing for a disaster. It was all hands on deck, and the hands were health professionals. We spent a lot of money for the patients we took care of, but we had no choice, based on what we believed could happen. At that time, so many nursing facilities and homeless shelters were closed to us. It was impossible to predict what utilization would be.”
Subsequent experience has taught that a lot of even seriously ill COVID-19 patients can be managed safely at home, for example, using accelerated home oxygen monitoring with telelinked pulse oximeters. But in the beginning, Dr. Baughman said, “it was a new situation for us. We had seen what happened in Europe and China. It’s a great thing to be overprepared.”
References
1. Horowitz J. Italy’s health care system groans under coronavirus – a warning to the world. New York Times. 2020 Mar 12.
2. Bell SA et al. T-Minus 10 days: The role of an academic medical institution in field hospital planning. Prehosp Disaster Med. 2021 Feb 18:1-6. doi: 10.1017/S1049023X21000224.
3. Singh K et al. Evaluating a widely implemented proprietary deterioration index model among hospitalized patients with COVID-19. Ann Am Thorac Soc. 2021 Jul;18(7):1129-37. doi: 10.1513/AnnalsATS.202006-698OC.
4. Bell SA et al. Alternate care sites during COVID-19 pandemic: Policy implications for pandemic surge planning. Disaster Med Public Health Prep. 2021 Jul 23;1-3. doi: 10.1017/dmp.2021.241.
At the height of the COVID-19 pandemic’s terrifying first wave in the spring of 2020, dozens of hospitals in high-incidence areas either planned or opened temporary, emergency field hospitals to cover anticipated demand for beds beyond the capacity of local permanent hospitals.
Chastened by images of overwhelmed health care systems in Northern Italy and other hard-hit areas,1 the planners used available modeling tools and estimates for projecting maximum potential need in worst-case scenarios. Some of these temporary hospitals never opened. Others opened in convention centers, parking garages, or parking lot tents, and ended up being used to a lesser degree than the worst-case scenarios.
But those who participated in the planning – including, in many cases, hospitalists – believe they created alternate care site manuals that could be quickly revived in the event of future COVID surges or other, similar crises. Better to plan for too much, they say, than not plan for enough.
Field hospitals or alternate care sites are defined in a recent journal article in Prehospital Disaster Medicine as “locations that can be converted to provide either inpatient and/or outpatient health services when existing facilities are compromised by a hazard impact or the volume of patients exceeds available capacity and/or capabilities.”2
The lead author of that report, Sue Anne Bell, PhD, FNP-BC, a disaster expert and assistant professor of nursing at the University of Michigan (UM), was one of five members of the leadership team for planning UM’s field hospital. They used an organizational unit structure based on the U.S. military’s staffing structure, with their work organized around six units of planning: personnel and labor, security, clinical operations, logistics and supply, planning and training, and communications. This team planned a 519-bed step-down care facility, the Michigan Medicine Field Hospital, for a 73,000-foot indoor track and performance facility at the university, three miles from UM’s main hospital. The aim was to provide safe care in a resource-limited environment.
“We were prepared, but the need never materialized as the peak of COVID cases started to subside,” Dr. Bell said. The team was ready to open within days using a “T-Minus” framework of days remaining on an official countdown clock. But when the need and deadlines kept getting pushed back, that gave them more time to develop clearer procedures.
Two Michigan Medicine hospitalists, Christopher Smith, MD, and David Paje, MD, MPH, both professors at UM’s medical school, were intimately involved in the process. “I was the medical director for the respiratory care unit that was opened for COVID patients, so I was pulled in to assist in the field hospital planning,” said Dr. Smith.
Dr. Paje was director of the short-stay unit and had been a medical officer in the U.S. Army, with training in how to set up military field hospitals. He credits that background as helpful for UM’s COVID field hospital planning, along with his experience in hospital medicine operations.
“We expected that these patients would need the expertise of hospitalists, who had quickly become familiar with the peculiarities of the new disease. That played a role in the decisions we made. Hospitalists were at the front lines of COVID care and had unique clinical insights about managing those with severe disease,” Dr. Paje added.
“When we started, the projections were dire. You don’t want to believe something like that is going to happen. When COVID started to cool off, it was more of a relief to us than anything else,” Dr. Smith said. “Still, it was a very worthwhile exercise. At the end of the day, we put together a comprehensive guide, which is ready for the next crisis.”
Baltimore builds a convention center hospital
A COVID-19 field hospital was planned and executed at an exhibit hall in the Baltimore Convention Center, starting in March 2020 under the leadership of Johns Hopkins Bayview hospitalist Eric Howell, MD, MHM, who eventually handed over responsibilities as chief medical officer when he assumed the position of CEO for the Society of Hospital Medicine in July of that year.
Hopkins collaborated with the University of Maryland health system and state leaders, including the Secretary of Health, to open a 252-bed temporary facility, which at its peak carried a census of 48 patients, with no on-site mortality or cardiac arrests, before it was closed in June 2021 – ready to reopen if necessary. It also served as Baltimore’s major site for polymerase chain reaction COVID-19 testing, vaccinations, and monoclonal antibody infusions, along with medical research.
“My belief at the time we started was that my entire 20-year career as a hospitalist had prepared me for the challenge of opening a COVID field hospital,” Dr. Howell said. “I had learned how to build clinical programs. The difference was that instead of months and years to build a program, we only had a few weeks.”
His first request was to bring on an associate medical director for the field hospital, Melinda E. Kantsiper, MD, a hospitalist and director of clinical operations in the Division of Hospital Medicine at Johns Hopkins Bayview. She became the field hospital’s CMO when Dr. Howell moved to SHM. “As hospitalists, we are trained to care for the patient in front of us while at the same time creating systems that can adjust to rapidly changing circumstances,” Dr. Kantsiper said. “We did what was asked and set up a field hospital that cared for a total of 1,500 COVID patients.”
Hospitalists have the tools that are needed for this work, and shouldn’t be reluctant to contribute to field hospital planning, she said. “This was a real eye-opener for me. Eric explained to me that hospitalists really practice acute care medicine, which doesn’t have to be within the four walls of a hospital.”
The Baltimore field hospital has been a fantastic experience, Dr. Kantsiper added. “But it’s not a building designed for health care delivery.” For the right group of providers, the experience of working in a temporary facility such as this can be positive and exhilarating. “But we need to make sure we take care of our staff. It takes a toll. How we keep them safe – physically and emotionally – has to be top of mind,” she said.
The leaders at Hopkins Medicine and their collaborators truly engaged with the field hospital’s mission, Dr. Howell added.
“They gave us a lot of autonomy and helped us break down barriers. They gave us the political capital to say proper PPE was absolutely essential. As hard and devastating as the pandemic has been, one take-away is that we showed that we can be more flexible and elastic in response to actual needs than we used to think.”
Range of challenges
Among the questions that need to be answered by a field hospital’s planners, the first is ‘where to put it?’ The answer is, hopefully, someplace not too far away, large enough, with ready access to supplies and intake. The next question is ‘who is the patient?’ Clinicians must determine who goes to the field hospital versus who stays at the standing hospital. How sick should these patients be? And when do they need to go back to the permanent hospital? Can staff be trained to recognize when patients in the field hospital are starting to decompensate? The EPIC Deterioration Index3 is a proprietary prediction model that was used by more than a hundred hospitals during the pandemic.
The hospitalist team may develop specific inclusion and exclusion criteria – for example, don’t admit patients who are receiving oxygen therapy above a certain threshold or who are hemodynamically unstable. These criteria should reflect the capacity of the field hospital and the needs of the permanent hospital. At Michigan, as at other field hospital sites, the goal was to offer a step-down or postacute setting for patients with COVID-19 who were too sick to return home but didn’t need acute or ICU-level care, thereby freeing up beds at the permanent hospital for patients who were sicker.
Other questions: What is the process for admissions and discharges? How will patients be transported? What kind of staffing is needed, and what levels of care will be provided? What about rehabilitation services, or palliative care? What about patients with substance abuse or psychiatric comorbidities?
“Are we going to do paper charting? How will that work out for long-term documentation and billing?” Dr. Bell said. A clear reporting structure and communication pathways are essential. Among the other operational processes to address, outlined in Dr. Bell’s article, are orientation and training, PPE donning and doffing procedures, the code or rapid response team, patient and staff food and nutrition, infection control protocols, pharmacy services, access to radiology, rounding procedures, staff support, and the morgue.
One other issue that shouldn’t be overlooked is health equity in the field hospital. “Providing safe and equitable care should be the focus. Thinking who goes to the field hospital should be done within a health equity framework,” Dr. Bell said.4 She also wonders if field hospital planners are sharing their experience with colleagues across the country and developing more collaborative relationships with other hospitals in their communities.
“Field hospitals can be different things,” Dr. Bell said. “The important take-home is it doesn’t have to be in a tent or a parking garage, which can be suboptimal.” In many cases, it may be better to focus on finding unused space within the hospital – whether a lobby, staff lounge, or unoccupied unit – closer to personnel, supplies, pharmacy, and the like. “I think the pandemic showed us how unprepared we were as a health care system, and how much more we need to do in preparation for future crises.”
Limits to the temporary hospital
In New York City, which had the country’s worst COVID-19 outbreak during the first surge in the spring of 2020, a 1,000-bed field hospital was opened at the Jacob Javits Center in March 2020 and closed that June. “I was in the field hospital early, in March and April, when our hospitals were temporarily overrun,” said hospitalist Mona Krouss, MD, FACP, CPPS, NYC Health + Hospitals’ director of patient safety. “My role was to figure out how to get patients on our medical floors into these field hospitals, with responsibility for helping to revise admission criteria,” she said.
“No one knew how horrible it would become. This was so unanticipated, so difficult to operationalize. What they were able to create was amazing, but there were just too many barriers to have it work smoothly,” Dr. Krouss said.
“The military stepped in, and they helped us so much. We wouldn’t have been able to survive without their help.” But there is only so much a field hospital can do to provide acute medical care. Later, military medical teams shifted to roles in temporary units inside the permanent hospitals. “They came to the hospital wanting to be deployed,” she said.
“We could only send patients [to the field hospital] who were fairly stable, and choosing the right ones was difficult.” Dr. Krouss said. In the end, not a lot of COVID-19 patients from NYC Health + Hospitals ended up going to the Javits Center, in part because the paperwork and logistics of getting someone in was a barrier, Dr. Krouss said. A process was established for referring doctors to call a phone number and speak with a New York City Department of Health employee to go through the criteria for admission to the field hospital.
“That could take up to 30 minutes before getting approval. Then you had to go through the same process all over again for sign-out to another physician, and then register the patient with a special bar code. Then you had to arrange ambulance transfer. Doctors didn’t want to go through all of that – everybody was too busy,” she explained. Hospitalists have since worked on streamlining the criteria. “Now we have a good process for the future. We made it more seamless,” she noted.
Susan Lee, DO, MBA, hospitalist and chief medical officer for Renown Regional Medical Center in Reno, Nev., helped to plan an alternate care site in anticipation of up to a thousand COVID patients in her community – far beyond the scope of the existing hospitals. Hospitalists were involved the entire time in planning, design of the unit, design of staffing models, care protocols, and the like, working through an evidence-based medical committee and a COVID-19 provider task force for the Renown Health System.
“Because of a history of fires and earthquakes in this region, we had an emergency planning infrastructure in place. We put the field hospital on the first and second floors of a parking garage, with built-in negative pressure capacity. We also built space for staff break rooms and desk space. It took 10 days to build the hospital, thanks to some very talented people in management and facility design,” Dr. Lee said.
Then, the hospital was locked up and sat empty for 7 months, until the surge in December 2020, when Reno was hit by a bigger wave – this time exceeding the hospitals’ capacity. Through mid-January of 2021, clinicians cared for approximately 240 COVID-19 patients, up to 47 at a time, in the field hospital. A third wave in the autumn of 2021 plateaued at a level lower than the previous fall, so the field hospital is not currently needed.
Replicating hospital work flows
“We ensured that everybody who needed to be within the walls of the permanent hospitals was able to stay there,” said Dr. Lee’s colleague, hospitalist Adnan (Eddy) Akbar, MD. “The postacute system we ordinarily rely on was no longer accepting patients. Other hospitals in the area were able to manage within their capacity because Renown’s field hospital could admit excess patients. We tried to replicate in the field hospital, as much as possible, the work flows and systems of our main hospital.”
When the field hospital finally opened, Dr. Akbar said, “we had a good feeling. We were ready. If something more catastrophic had come down, we were ready to care for more patients. In the field hospital you have to keep monitoring your work flow – almost on a daily basis. But we felt privileged to be working for a system where you knew you can go and care for everyone who needed care.”
One upside of the field hospital experience for participating clinicians, Dr. Lee added, is the opportunity to practice creatively. “The downside is it’s extremely expensive, and has consequences for the mental health of staff. Like so many of these things, it wore on people over time – such as all the time spent donning and doffing protective equipment. And recently the patients have become a lot less gracious.”
Amy Baughman, MD, a hospitalist at Massachusetts General Hospital in Boston, was co-medical director of the postacute care section of a 1,000-bed field hospital, Boston Hope Medical Center, opened in April 2020 at the Boston Convention and Exhibition Center. The other half of the facility was dedicated to undomiciled COVID-19 patients who had no place else to go. Peak census was around 100 patients, housed on four units, each with a clinical team led by a physician.
Dr. Baughman’s field hospital experience has taught her the importance of “staying within your domain of expertise. Physicians are attracted to difficult problems and want to do everything themselves. Next time I won’t be the one installing hand sanitizer dispensers.” A big part of running a field hospital is logistics, she said, and physicians are trained clinicians, not necessarily logistics engineers.
“So it’s important to partner with logistics experts. A huge part of our success in building a facility in 9 days of almost continuous construction was the involvement of the National Guard,” she said. An incident command system was led by an experienced military general incident commander, with two clinical codirectors. The army also sent in full teams of health professionals.
The facility admitted a lot fewer patients than the worst-case projections before it closed in June 2020. “But at the end of the day, we provided a lot of excellent care,” Dr. Baughman said. “This was about preparing for a disaster. It was all hands on deck, and the hands were health professionals. We spent a lot of money for the patients we took care of, but we had no choice, based on what we believed could happen. At that time, so many nursing facilities and homeless shelters were closed to us. It was impossible to predict what utilization would be.”
Subsequent experience has taught that a lot of even seriously ill COVID-19 patients can be managed safely at home, for example, using accelerated home oxygen monitoring with telelinked pulse oximeters. But in the beginning, Dr. Baughman said, “it was a new situation for us. We had seen what happened in Europe and China. It’s a great thing to be overprepared.”
References
1. Horowitz J. Italy’s health care system groans under coronavirus – a warning to the world. New York Times. 2020 Mar 12.
2. Bell SA et al. T-Minus 10 days: The role of an academic medical institution in field hospital planning. Prehosp Disaster Med. 2021 Feb 18:1-6. doi: 10.1017/S1049023X21000224.
3. Singh K et al. Evaluating a widely implemented proprietary deterioration index model among hospitalized patients with COVID-19. Ann Am Thorac Soc. 2021 Jul;18(7):1129-37. doi: 10.1513/AnnalsATS.202006-698OC.
4. Bell SA et al. Alternate care sites during COVID-19 pandemic: Policy implications for pandemic surge planning. Disaster Med Public Health Prep. 2021 Jul 23;1-3. doi: 10.1017/dmp.2021.241.
What does it mean to be a trustworthy male ally?
“If you want to be trusted, be trustworthy” – Stephen Covey
A few years ago, while working in my office, a female colleague stopped by for a casual chat. During the course of the conversation, she noticed that I did not have any diplomas or certificates hanging on my office walls. Instead, there were clusters of pictures drawn by my children, family photos, and a white board with my “to-do” list. The only wall art was a print of Banksy’s “The Thinker Monkey,” which depicts a monkey with its fist to its chin similar to Rodin’s famous sculpture, “Le Penseur.”
When asked why I didn’t hang any diplomas or awards, I replied that I preferred to keep my office atmosphere light and fun, and to focus on future goals rather than past accomplishments. I could see her jaw tense. Her frustration appeared deep, but it was for reasons beyond just my self-righteous tone. She said, “You know, I appreciate your focus on future goals, but it’s a pretty privileged position to not have to worry about sharing your accomplishments publicly.”
What followed was a discussion that was generative, enlightening, uncomfortable, and necessary. I had never considered what I chose to hang (or not hang) on my office walls as a privilege, and that was exactly the point. She described numerous episodes when her accomplishments were overlooked or (worse) attributed to a male colleague because she was a woman. I began to understand that graceful self-promotion is not optional for many women in medicine, it is a necessary skill.
This is just one example of how my privilege as a male in medicine contributed to my ignorance of the gender inequities that my female coworkers have faced throughout their careers. My colleague showed a lot of grace by taking the time to help me navigate my male privilege in a constructive manner. I decided to learn more about gender inequities, and eventually determined that I was woefully inadequate as a male ally, not by refusal but by ignorance. I wanted to start earning my colleague’s trust that I would be an ally that she could count on.
Trustworthiness
I wanted to be a trustworthy ally, but what does that entail? Perhaps we can learn from medical education. Trust is a complex construct that is increasingly used as a framework for assessing medical students and residents, such as with entrustable professional activities (EPAs).1,2 Multiple studies have examined the characteristics that make a learner “trustworthy” when determining how much supervision is required.3-8 Ten Cate and Chen performed an interpretivist, narrative review to synthesize the medical education literature on learner trustworthiness in the past 15 years,9 developing five major themes that contribute to trustworthiness: Humility, Capability, Agency, Reliability, and Integrity. Let’s examine each of these through the lens of male allyship.
Humility
Humility involves knowing one’s limits, asking for help, and being receptive to feedback.9 The first thing men need to do is to put their egos in check and recognize that women do not need rescuing; they need partnership. Systemic inequities have led to men holding the majority of leadership positions and significant sociopolitical capital, and correcting these inequities is more feasible when those in leadership and positions of power contribute. Women don’t need knights in shining armor, they need collaborative activism.
Humility also means a willingness to admit fallibility and to ask for help. Men often don’t know what they don’t know (see my foibles in the opening). As David G. Smith, PhD, and W. Brad Johnson, PhD, write in their book, “Good Guys,” “There are no perfect allies. As you work to become a better ally for the women around you, you will undoubtedly make a mistake.”10 Men must accept feedback on their shortcomings as allies without feeling as though they are losing their sociopolitical standing. Allyship for women does not mean there is a devaluing of men. We must escape a “zero-sum” mindset. Mistakes are where growth happens, but only if we approach our missteps with humility.
Capability
Capability entails having the necessary knowledge, skills, and attitudes to be a strong ally. Allyship is not intuitive for most men for several reasons. Many men do not experience the same biases or systemic inequities that women do, and therefore perceive them less frequently. I want to acknowledge that men can be victims of other systemic biases such as those against one’s race, ethnicity, gender identity, sexual orientation, religion, or any number of factors. Men who face inequities for these other reasons may be more cognizant of the biases women face. Even so, allyship is a skill that few men have been explicitly taught. Even if taught, few standard or organized mechanisms for feedback on allyship capability exist. How, then, can men become capable allies?
Just like in medical education, men must become self-directed learners who seek to build capability and receive feedback on their performance as allies. Men should seek allyship training through local women-in-medicine programs or organizations, or through the increasing number of national education options such as the recent ADVANCE PHM Gender Equity Symposium. As with learning any skill, men should go to the literature, seeking knowledge from experts in the field. I recommend starting with “Good Guys: How Men Can Be Better Allies for Women in the Workplace10 or “Athena Rising: How and Why Men Should Mentor Women.”11 Both books, by Dr. Smith and Dr. Johnson, are great entry points into the gender allyship literature. Seek out other resources from local experts on gender equity and allyship. Both aforementioned books were recommended to me by a friend and gender equity expert; without her guidance I would not have known where to start.
Agency
Agency involves being proactive and engaged rather than passive or apathetic. Men must be enthusiastic allies who seek out opportunities to mentor and sponsor women rather than waiting for others to ask. Agency requires being curious and passionate about improving. Most men in medicine are not openly and explicitly misogynistic or sexist, but many are only passive when it comes to gender equity and allyship. Trustworthy allyship entails turning passive support into active change. Not sure how to start? A good first step is to ask female colleagues questions such as, “What can I do to be a better ally for you in the workplace?” or “What are some things at work that are most challenging to you, but I might not notice because I’m a man?” Curiosity is the springboard toward agency.
Reliability
Reliability means being conscientious, accountable, and doing what we say we will do. Nothing undermines trustworthiness faster than making a commitment and not following through. Allyship cannot be a show or an attempt to get public plaudits. It is a longitudinal commitment to supporting women through individual mentorship and sponsorship, and to work toward institutional and systems change.
Reliability also means taking an equitable approach to what Dr. Smith and Dr. Johnson call “office housework.” They define this as “administrative work that is necessary but undervalued, unlikely to lead to promotion, and disproportionately assigned to women.”10 In medicine, these tasks include organizing meetings, taking notes, planning social events, and remembering to celebrate colleagues’ achievements and milestones. Men should take on more of these tasks and advocate for change when the distribution of office housework in their workplace is inequitably directed toward women.
Integrity
Integrity involves honesty, professionalism, and benevolence. It is about making the morally correct choice even if there is potential risk. When men see gender inequity, they have an obligation to speak up. Whether it is overtly misogynistic behavior, subtle sexism, use of gendered language, inequitable distribution of office housework, lack of inclusivity and recognition for women, or another form of inequity, men must act with integrity and make it clear that they are partnering with women for change. Integrity means being an ally even when women are not present, and advocating that women be “at the table” for important conversations.
Beyond the individual
Allyship cannot end with individual actions; systems changes that build trustworthy institutions are necessary. Organizational leaders must approach gender conversations with humility to critically examine inequities and agency to implement meaningful changes. Workplace cultures and institutional policies should be reviewed with an eye toward system-level integrity and reliability for promoting and supporting women. Ongoing faculty and staff development programs must provide men with the knowledge, skills, and attitudes (capability) to be strong allies. We have a long history of male-dominated institutions that are unfair or (worse) unsafe for women. Many systems are designed in a way that disadvantages women. These systems must be redesigned through an equity lens to start building trust with women in medicine.
Becoming trustworthy is a process
Even the best male allies have room to improve their trustworthiness. Many men (myself included) have a LOT of room to improve, but they should not get discouraged by the amount of ground to be gained. Steady, deliberate improvement in men’s humility, capability, agency, reliability, and integrity can build the foundation of trust with female colleagues. Trust takes time. It takes effort. It takes vulnerability. It is an ongoing, developmental process that requires deliberate practice, frequent reflection, and feedback from our female colleagues.
Dr. Kinnear is associate professor of internal medicine and pediatrics in the Division of Hospital Medicine at Cincinnati Children’s Hospital Medical Center and University of Cincinnati Medical Center. He is associate program director for the Med-Peds and Internal Medicine residency programs.
References
1. Ten Cate O. Nuts and bolts of entrustable professional activities. J Grad Med Educ. 2013 Mar;5(1):157-8. doi: 10.4300/JGME-D-12-00380.1.
2. Ten Cate O. Entrustment decisions: Bringing the patient into the assessment equation. Acad Med. 2017 Jun;92(6):736-8. doi: 10.1097/ACM.0000000000001623.
3. Kennedy TJT et al. Point-of-care assessment of medical trainee competence for independent clinical work. Acad Med. 2008 Oct;83(10 Suppl):S89-92. doi: 10.1097/ACM.0b013e318183c8b7.
4. Choo KJ et al. How do supervising physicians decide to entrust residents with unsupervised tasks? A qualitative analysis. J Hosp Med. 2014 Mar;9(3):169-75. doi: 10.1002/jhm.2150.
5. Hauer KE et al. How clinical supervisors develop trust in their trainees: A qualitative study. Med Educ. 2015 Aug;49(8):783-95. doi: 10.1111/medu.12745.
6. Sterkenburg A et al. When do supervising physicians decide to entrust residents with unsupervised tasks? Acad Med. 2010 Sep;85(9):1408-17. doi: 10.1097/ACM.0b013e3181eab0ec.
7. Sheu L et al. How supervisor experience influences trust, supervision, and trainee learning: A qualitative study. Acad Med. 2017 Sep;92(9):1320-7. doi: 10.1097/ACM.0000000000001560.
8. Pingree EW et al. Encouraging entrustment: A qualitative study of resident behaviors that promote entrustment. Acad Med. 2020 Nov;95(11):1718-25. doi: 10.1097/ACM.0000000000003487.
9. Ten Cate O, Chen HC. The ingredients of a rich entrustment decision. Med Teach. 2020 Dec;42(12):1413-20. doi: 10.1080/0142159X.2020.1817348.
10. Smith DG, Johnson WB. Good guys: How men can be better allies for women in the workplace: Harvard Business School Publishing Corporation 2020.
11. Johnson WB, Smith D. Athena rising: How and why men should mentor women: Routledge 2016.
“If you want to be trusted, be trustworthy” – Stephen Covey
A few years ago, while working in my office, a female colleague stopped by for a casual chat. During the course of the conversation, she noticed that I did not have any diplomas or certificates hanging on my office walls. Instead, there were clusters of pictures drawn by my children, family photos, and a white board with my “to-do” list. The only wall art was a print of Banksy’s “The Thinker Monkey,” which depicts a monkey with its fist to its chin similar to Rodin’s famous sculpture, “Le Penseur.”
When asked why I didn’t hang any diplomas or awards, I replied that I preferred to keep my office atmosphere light and fun, and to focus on future goals rather than past accomplishments. I could see her jaw tense. Her frustration appeared deep, but it was for reasons beyond just my self-righteous tone. She said, “You know, I appreciate your focus on future goals, but it’s a pretty privileged position to not have to worry about sharing your accomplishments publicly.”
What followed was a discussion that was generative, enlightening, uncomfortable, and necessary. I had never considered what I chose to hang (or not hang) on my office walls as a privilege, and that was exactly the point. She described numerous episodes when her accomplishments were overlooked or (worse) attributed to a male colleague because she was a woman. I began to understand that graceful self-promotion is not optional for many women in medicine, it is a necessary skill.
This is just one example of how my privilege as a male in medicine contributed to my ignorance of the gender inequities that my female coworkers have faced throughout their careers. My colleague showed a lot of grace by taking the time to help me navigate my male privilege in a constructive manner. I decided to learn more about gender inequities, and eventually determined that I was woefully inadequate as a male ally, not by refusal but by ignorance. I wanted to start earning my colleague’s trust that I would be an ally that she could count on.
Trustworthiness
I wanted to be a trustworthy ally, but what does that entail? Perhaps we can learn from medical education. Trust is a complex construct that is increasingly used as a framework for assessing medical students and residents, such as with entrustable professional activities (EPAs).1,2 Multiple studies have examined the characteristics that make a learner “trustworthy” when determining how much supervision is required.3-8 Ten Cate and Chen performed an interpretivist, narrative review to synthesize the medical education literature on learner trustworthiness in the past 15 years,9 developing five major themes that contribute to trustworthiness: Humility, Capability, Agency, Reliability, and Integrity. Let’s examine each of these through the lens of male allyship.
Humility
Humility involves knowing one’s limits, asking for help, and being receptive to feedback.9 The first thing men need to do is to put their egos in check and recognize that women do not need rescuing; they need partnership. Systemic inequities have led to men holding the majority of leadership positions and significant sociopolitical capital, and correcting these inequities is more feasible when those in leadership and positions of power contribute. Women don’t need knights in shining armor, they need collaborative activism.
Humility also means a willingness to admit fallibility and to ask for help. Men often don’t know what they don’t know (see my foibles in the opening). As David G. Smith, PhD, and W. Brad Johnson, PhD, write in their book, “Good Guys,” “There are no perfect allies. As you work to become a better ally for the women around you, you will undoubtedly make a mistake.”10 Men must accept feedback on their shortcomings as allies without feeling as though they are losing their sociopolitical standing. Allyship for women does not mean there is a devaluing of men. We must escape a “zero-sum” mindset. Mistakes are where growth happens, but only if we approach our missteps with humility.
Capability
Capability entails having the necessary knowledge, skills, and attitudes to be a strong ally. Allyship is not intuitive for most men for several reasons. Many men do not experience the same biases or systemic inequities that women do, and therefore perceive them less frequently. I want to acknowledge that men can be victims of other systemic biases such as those against one’s race, ethnicity, gender identity, sexual orientation, religion, or any number of factors. Men who face inequities for these other reasons may be more cognizant of the biases women face. Even so, allyship is a skill that few men have been explicitly taught. Even if taught, few standard or organized mechanisms for feedback on allyship capability exist. How, then, can men become capable allies?
Just like in medical education, men must become self-directed learners who seek to build capability and receive feedback on their performance as allies. Men should seek allyship training through local women-in-medicine programs or organizations, or through the increasing number of national education options such as the recent ADVANCE PHM Gender Equity Symposium. As with learning any skill, men should go to the literature, seeking knowledge from experts in the field. I recommend starting with “Good Guys: How Men Can Be Better Allies for Women in the Workplace10 or “Athena Rising: How and Why Men Should Mentor Women.”11 Both books, by Dr. Smith and Dr. Johnson, are great entry points into the gender allyship literature. Seek out other resources from local experts on gender equity and allyship. Both aforementioned books were recommended to me by a friend and gender equity expert; without her guidance I would not have known where to start.
Agency
Agency involves being proactive and engaged rather than passive or apathetic. Men must be enthusiastic allies who seek out opportunities to mentor and sponsor women rather than waiting for others to ask. Agency requires being curious and passionate about improving. Most men in medicine are not openly and explicitly misogynistic or sexist, but many are only passive when it comes to gender equity and allyship. Trustworthy allyship entails turning passive support into active change. Not sure how to start? A good first step is to ask female colleagues questions such as, “What can I do to be a better ally for you in the workplace?” or “What are some things at work that are most challenging to you, but I might not notice because I’m a man?” Curiosity is the springboard toward agency.
Reliability
Reliability means being conscientious, accountable, and doing what we say we will do. Nothing undermines trustworthiness faster than making a commitment and not following through. Allyship cannot be a show or an attempt to get public plaudits. It is a longitudinal commitment to supporting women through individual mentorship and sponsorship, and to work toward institutional and systems change.
Reliability also means taking an equitable approach to what Dr. Smith and Dr. Johnson call “office housework.” They define this as “administrative work that is necessary but undervalued, unlikely to lead to promotion, and disproportionately assigned to women.”10 In medicine, these tasks include organizing meetings, taking notes, planning social events, and remembering to celebrate colleagues’ achievements and milestones. Men should take on more of these tasks and advocate for change when the distribution of office housework in their workplace is inequitably directed toward women.
Integrity
Integrity involves honesty, professionalism, and benevolence. It is about making the morally correct choice even if there is potential risk. When men see gender inequity, they have an obligation to speak up. Whether it is overtly misogynistic behavior, subtle sexism, use of gendered language, inequitable distribution of office housework, lack of inclusivity and recognition for women, or another form of inequity, men must act with integrity and make it clear that they are partnering with women for change. Integrity means being an ally even when women are not present, and advocating that women be “at the table” for important conversations.
Beyond the individual
Allyship cannot end with individual actions; systems changes that build trustworthy institutions are necessary. Organizational leaders must approach gender conversations with humility to critically examine inequities and agency to implement meaningful changes. Workplace cultures and institutional policies should be reviewed with an eye toward system-level integrity and reliability for promoting and supporting women. Ongoing faculty and staff development programs must provide men with the knowledge, skills, and attitudes (capability) to be strong allies. We have a long history of male-dominated institutions that are unfair or (worse) unsafe for women. Many systems are designed in a way that disadvantages women. These systems must be redesigned through an equity lens to start building trust with women in medicine.
Becoming trustworthy is a process
Even the best male allies have room to improve their trustworthiness. Many men (myself included) have a LOT of room to improve, but they should not get discouraged by the amount of ground to be gained. Steady, deliberate improvement in men’s humility, capability, agency, reliability, and integrity can build the foundation of trust with female colleagues. Trust takes time. It takes effort. It takes vulnerability. It is an ongoing, developmental process that requires deliberate practice, frequent reflection, and feedback from our female colleagues.
Dr. Kinnear is associate professor of internal medicine and pediatrics in the Division of Hospital Medicine at Cincinnati Children’s Hospital Medical Center and University of Cincinnati Medical Center. He is associate program director for the Med-Peds and Internal Medicine residency programs.
References
1. Ten Cate O. Nuts and bolts of entrustable professional activities. J Grad Med Educ. 2013 Mar;5(1):157-8. doi: 10.4300/JGME-D-12-00380.1.
2. Ten Cate O. Entrustment decisions: Bringing the patient into the assessment equation. Acad Med. 2017 Jun;92(6):736-8. doi: 10.1097/ACM.0000000000001623.
3. Kennedy TJT et al. Point-of-care assessment of medical trainee competence for independent clinical work. Acad Med. 2008 Oct;83(10 Suppl):S89-92. doi: 10.1097/ACM.0b013e318183c8b7.
4. Choo KJ et al. How do supervising physicians decide to entrust residents with unsupervised tasks? A qualitative analysis. J Hosp Med. 2014 Mar;9(3):169-75. doi: 10.1002/jhm.2150.
5. Hauer KE et al. How clinical supervisors develop trust in their trainees: A qualitative study. Med Educ. 2015 Aug;49(8):783-95. doi: 10.1111/medu.12745.
6. Sterkenburg A et al. When do supervising physicians decide to entrust residents with unsupervised tasks? Acad Med. 2010 Sep;85(9):1408-17. doi: 10.1097/ACM.0b013e3181eab0ec.
7. Sheu L et al. How supervisor experience influences trust, supervision, and trainee learning: A qualitative study. Acad Med. 2017 Sep;92(9):1320-7. doi: 10.1097/ACM.0000000000001560.
8. Pingree EW et al. Encouraging entrustment: A qualitative study of resident behaviors that promote entrustment. Acad Med. 2020 Nov;95(11):1718-25. doi: 10.1097/ACM.0000000000003487.
9. Ten Cate O, Chen HC. The ingredients of a rich entrustment decision. Med Teach. 2020 Dec;42(12):1413-20. doi: 10.1080/0142159X.2020.1817348.
10. Smith DG, Johnson WB. Good guys: How men can be better allies for women in the workplace: Harvard Business School Publishing Corporation 2020.
11. Johnson WB, Smith D. Athena rising: How and why men should mentor women: Routledge 2016.
“If you want to be trusted, be trustworthy” – Stephen Covey
A few years ago, while working in my office, a female colleague stopped by for a casual chat. During the course of the conversation, she noticed that I did not have any diplomas or certificates hanging on my office walls. Instead, there were clusters of pictures drawn by my children, family photos, and a white board with my “to-do” list. The only wall art was a print of Banksy’s “The Thinker Monkey,” which depicts a monkey with its fist to its chin similar to Rodin’s famous sculpture, “Le Penseur.”
When asked why I didn’t hang any diplomas or awards, I replied that I preferred to keep my office atmosphere light and fun, and to focus on future goals rather than past accomplishments. I could see her jaw tense. Her frustration appeared deep, but it was for reasons beyond just my self-righteous tone. She said, “You know, I appreciate your focus on future goals, but it’s a pretty privileged position to not have to worry about sharing your accomplishments publicly.”
What followed was a discussion that was generative, enlightening, uncomfortable, and necessary. I had never considered what I chose to hang (or not hang) on my office walls as a privilege, and that was exactly the point. She described numerous episodes when her accomplishments were overlooked or (worse) attributed to a male colleague because she was a woman. I began to understand that graceful self-promotion is not optional for many women in medicine, it is a necessary skill.
This is just one example of how my privilege as a male in medicine contributed to my ignorance of the gender inequities that my female coworkers have faced throughout their careers. My colleague showed a lot of grace by taking the time to help me navigate my male privilege in a constructive manner. I decided to learn more about gender inequities, and eventually determined that I was woefully inadequate as a male ally, not by refusal but by ignorance. I wanted to start earning my colleague’s trust that I would be an ally that she could count on.
Trustworthiness
I wanted to be a trustworthy ally, but what does that entail? Perhaps we can learn from medical education. Trust is a complex construct that is increasingly used as a framework for assessing medical students and residents, such as with entrustable professional activities (EPAs).1,2 Multiple studies have examined the characteristics that make a learner “trustworthy” when determining how much supervision is required.3-8 Ten Cate and Chen performed an interpretivist, narrative review to synthesize the medical education literature on learner trustworthiness in the past 15 years,9 developing five major themes that contribute to trustworthiness: Humility, Capability, Agency, Reliability, and Integrity. Let’s examine each of these through the lens of male allyship.
Humility
Humility involves knowing one’s limits, asking for help, and being receptive to feedback.9 The first thing men need to do is to put their egos in check and recognize that women do not need rescuing; they need partnership. Systemic inequities have led to men holding the majority of leadership positions and significant sociopolitical capital, and correcting these inequities is more feasible when those in leadership and positions of power contribute. Women don’t need knights in shining armor, they need collaborative activism.
Humility also means a willingness to admit fallibility and to ask for help. Men often don’t know what they don’t know (see my foibles in the opening). As David G. Smith, PhD, and W. Brad Johnson, PhD, write in their book, “Good Guys,” “There are no perfect allies. As you work to become a better ally for the women around you, you will undoubtedly make a mistake.”10 Men must accept feedback on their shortcomings as allies without feeling as though they are losing their sociopolitical standing. Allyship for women does not mean there is a devaluing of men. We must escape a “zero-sum” mindset. Mistakes are where growth happens, but only if we approach our missteps with humility.
Capability
Capability entails having the necessary knowledge, skills, and attitudes to be a strong ally. Allyship is not intuitive for most men for several reasons. Many men do not experience the same biases or systemic inequities that women do, and therefore perceive them less frequently. I want to acknowledge that men can be victims of other systemic biases such as those against one’s race, ethnicity, gender identity, sexual orientation, religion, or any number of factors. Men who face inequities for these other reasons may be more cognizant of the biases women face. Even so, allyship is a skill that few men have been explicitly taught. Even if taught, few standard or organized mechanisms for feedback on allyship capability exist. How, then, can men become capable allies?
Just like in medical education, men must become self-directed learners who seek to build capability and receive feedback on their performance as allies. Men should seek allyship training through local women-in-medicine programs or organizations, or through the increasing number of national education options such as the recent ADVANCE PHM Gender Equity Symposium. As with learning any skill, men should go to the literature, seeking knowledge from experts in the field. I recommend starting with “Good Guys: How Men Can Be Better Allies for Women in the Workplace10 or “Athena Rising: How and Why Men Should Mentor Women.”11 Both books, by Dr. Smith and Dr. Johnson, are great entry points into the gender allyship literature. Seek out other resources from local experts on gender equity and allyship. Both aforementioned books were recommended to me by a friend and gender equity expert; without her guidance I would not have known where to start.
Agency
Agency involves being proactive and engaged rather than passive or apathetic. Men must be enthusiastic allies who seek out opportunities to mentor and sponsor women rather than waiting for others to ask. Agency requires being curious and passionate about improving. Most men in medicine are not openly and explicitly misogynistic or sexist, but many are only passive when it comes to gender equity and allyship. Trustworthy allyship entails turning passive support into active change. Not sure how to start? A good first step is to ask female colleagues questions such as, “What can I do to be a better ally for you in the workplace?” or “What are some things at work that are most challenging to you, but I might not notice because I’m a man?” Curiosity is the springboard toward agency.
Reliability
Reliability means being conscientious, accountable, and doing what we say we will do. Nothing undermines trustworthiness faster than making a commitment and not following through. Allyship cannot be a show or an attempt to get public plaudits. It is a longitudinal commitment to supporting women through individual mentorship and sponsorship, and to work toward institutional and systems change.
Reliability also means taking an equitable approach to what Dr. Smith and Dr. Johnson call “office housework.” They define this as “administrative work that is necessary but undervalued, unlikely to lead to promotion, and disproportionately assigned to women.”10 In medicine, these tasks include organizing meetings, taking notes, planning social events, and remembering to celebrate colleagues’ achievements and milestones. Men should take on more of these tasks and advocate for change when the distribution of office housework in their workplace is inequitably directed toward women.
Integrity
Integrity involves honesty, professionalism, and benevolence. It is about making the morally correct choice even if there is potential risk. When men see gender inequity, they have an obligation to speak up. Whether it is overtly misogynistic behavior, subtle sexism, use of gendered language, inequitable distribution of office housework, lack of inclusivity and recognition for women, or another form of inequity, men must act with integrity and make it clear that they are partnering with women for change. Integrity means being an ally even when women are not present, and advocating that women be “at the table” for important conversations.
Beyond the individual
Allyship cannot end with individual actions; systems changes that build trustworthy institutions are necessary. Organizational leaders must approach gender conversations with humility to critically examine inequities and agency to implement meaningful changes. Workplace cultures and institutional policies should be reviewed with an eye toward system-level integrity and reliability for promoting and supporting women. Ongoing faculty and staff development programs must provide men with the knowledge, skills, and attitudes (capability) to be strong allies. We have a long history of male-dominated institutions that are unfair or (worse) unsafe for women. Many systems are designed in a way that disadvantages women. These systems must be redesigned through an equity lens to start building trust with women in medicine.
Becoming trustworthy is a process
Even the best male allies have room to improve their trustworthiness. Many men (myself included) have a LOT of room to improve, but they should not get discouraged by the amount of ground to be gained. Steady, deliberate improvement in men’s humility, capability, agency, reliability, and integrity can build the foundation of trust with female colleagues. Trust takes time. It takes effort. It takes vulnerability. It is an ongoing, developmental process that requires deliberate practice, frequent reflection, and feedback from our female colleagues.
Dr. Kinnear is associate professor of internal medicine and pediatrics in the Division of Hospital Medicine at Cincinnati Children’s Hospital Medical Center and University of Cincinnati Medical Center. He is associate program director for the Med-Peds and Internal Medicine residency programs.
References
1. Ten Cate O. Nuts and bolts of entrustable professional activities. J Grad Med Educ. 2013 Mar;5(1):157-8. doi: 10.4300/JGME-D-12-00380.1.
2. Ten Cate O. Entrustment decisions: Bringing the patient into the assessment equation. Acad Med. 2017 Jun;92(6):736-8. doi: 10.1097/ACM.0000000000001623.
3. Kennedy TJT et al. Point-of-care assessment of medical trainee competence for independent clinical work. Acad Med. 2008 Oct;83(10 Suppl):S89-92. doi: 10.1097/ACM.0b013e318183c8b7.
4. Choo KJ et al. How do supervising physicians decide to entrust residents with unsupervised tasks? A qualitative analysis. J Hosp Med. 2014 Mar;9(3):169-75. doi: 10.1002/jhm.2150.
5. Hauer KE et al. How clinical supervisors develop trust in their trainees: A qualitative study. Med Educ. 2015 Aug;49(8):783-95. doi: 10.1111/medu.12745.
6. Sterkenburg A et al. When do supervising physicians decide to entrust residents with unsupervised tasks? Acad Med. 2010 Sep;85(9):1408-17. doi: 10.1097/ACM.0b013e3181eab0ec.
7. Sheu L et al. How supervisor experience influences trust, supervision, and trainee learning: A qualitative study. Acad Med. 2017 Sep;92(9):1320-7. doi: 10.1097/ACM.0000000000001560.
8. Pingree EW et al. Encouraging entrustment: A qualitative study of resident behaviors that promote entrustment. Acad Med. 2020 Nov;95(11):1718-25. doi: 10.1097/ACM.0000000000003487.
9. Ten Cate O, Chen HC. The ingredients of a rich entrustment decision. Med Teach. 2020 Dec;42(12):1413-20. doi: 10.1080/0142159X.2020.1817348.
10. Smith DG, Johnson WB. Good guys: How men can be better allies for women in the workplace: Harvard Business School Publishing Corporation 2020.
11. Johnson WB, Smith D. Athena rising: How and why men should mentor women: Routledge 2016.
Hospitalist movers and shakers - November 2021
Vineet Chopra, MD, MSc, FHM, recently became chair of the Department of Medicine at the University of Colorado School of Medicine, Aurora. He had previously been the chief of the Division of Hospital Medicine at the University of Michigan Health system. He assumed his new role in October 2021.
Dr. Chopra, who specializes in research and mentorship in patient safety, helped create innovations in care delivery at the University of Michigan, including direct care hospitalist services at VA Ann Arbor Health Care and two other community hospitals.
In his safety-conscious research, Dr. Chopra focuses on preventing complications created within the hospital environment. He also is the first hospitalist to be named deputy editor of the Annals of Internal Medicine. He has written more than 250 peer-reviewed articles. Among the myriad awards he has received, Dr. Chopra recently earned the Kaiser Permanente Award for Clinical Teaching at the UM School of Medicine.
Steve Phillipson, MD, FHM, has been named regional director of hospital medicine at Aspirus Health (Wausau, Wisc.). Dr. Phillipson will oversee the hospitalist programs at 17 Aspirus hospitals in Wisconsin and Michigan.
Dr. Phillipson has worked with Aspirus since 2009, with stints in the emergency department and as a hospitalist. As Aspirus Wausau Hospital director of medicine, he chaired the facility’s COVID-19 treatment team.
Hackensack (N.J.) Meridian University Medical Center has hired Patricia (Patti) L. Fisher, MD, MHA, to be the institution’s chief medical officer. Dr. Fisher joined the medical center from Central Vermont Medical Center where she served as chief medical officer and chief safety officer, with direct oversight of hospital risk management, operations of all hospital-based services, IS services and quality including patient safety and regulatory compliance.
As a board-certified hospitalist, Dr. Fisher also served as clinical assistant professor in the Department of Family Medicine at the University of Vermont, Burlington. Dr. Fisher earned her medical degree from The University of Texas in Houston and completed residency through Forbes Family Practice Residency in Pittsburgh.
Martin Chaney, MD, has been chosen by the Maury Regional Health Board of Trustees to serve as interim chief executive officer. He was formerly the chief medical officer at MRH, which is based in Columbia, Tenn. Dr. Chaney began his new role in October, replacing Alan Watson, the CEO since 2012.
Dr. Chaney has spent 18 of his 25 years in medicine with MRH, where most recently he has focused on clinical quality, physician recruitment, and establishing and expanding the hospital medicine program.
Hyung (Harry) Cho, MD, SFHM, has been placed on Modern Healthcare’s Top 25 Innovators list for 2021, getting recognized for innovation and leadership in creating value and safety initiatives in New York City’s public health system. Dr. Cho became NYC Health + Hospitals’ first chief value officer in 2019, and his programs have created an estimated $11 million in savings per year by preventing unnecessary testing and treatment that can lead to patient harm.
A member of the Society of Hospital Medicine’s editorial advisory board, Dr. Cho is also SHM’s hospitalist liaison with the COVID-19 Real-Time Learning Network, which collaborates with the Centers for Disease Control and Prevention and the Infectious Diseases Society of America.
Raymond Kiser, MD, a hospitalist and nephrologist at Columbus (Ind.) Regional Health, has been named the Douglas J. Leonard Caregiver of the Year. The award is given by the Indiana Hospital Association to health care workers whose care is considered exemplary by both peers and patients.
Dr. Kiser has been with CRH for 7 years, including stints as associate chief medical officer and chief of staff.
Justin Buchholz, DO, has been elevated to medical director of the hospitalist teams at Regional Medical Center (Alamosa, Colo.) and Conejos County Hospital (La Jara, Colo.). Dr. Buchholz has been a full-time hospitalist and assistant medical director at Parkview Medical Center (Pueblo, Colo.) for the past 3 years. He also worked on a part-time basis seeing patients at the Regional Medical Center.
Dr. Buchholz completed his residency at Parkview Medical Center and was named Resident of the Year in his final year with the internal medicine program.
Kenneth Mishark, MD, SFHM, a hospitalist with the Mayo Clinic Hospital (Tucson, Ariz.), will serve on the board of directors for Anigent, a drug diversion-prevention company based in Chesterfield, Mo. He will be charged with helping Anigent better serve health systems with its drug-diversion software.
Dr. Mishark is vice-chair of diversion prevention across the whole Mayo Clinic. A one-time physician in the United States Air Force, Dr. Mishark previously has been the Mayo Clinic’s Healthcare Information Coordination Committee chair.
Core Clinical Partners (Tulsa, Okla.) has announced it will join with Hillcrest HealthCare System (Tulsa, Okla.) to provide hospitalist services to Hillcrest’s eight sites across Oklahoma. The partnership will begin at four locations in December 2021, and four others in March 2022.
In expanding its services, Core Clinical Partners will create 70 new physician positions, as well as a systemwide medical director. Core will manage hospitalist operations at Hillcrest Medical Center, Hillcrest Hospital South, Hillcrest Hospital Pryor, Hillcrest Hospital Claremore, Bailey Medical Center, Hillcrest Hospital Cushing, Hillcrest Hospital Henryetta, and Tulsa Spine and Specialty Hospital.
Vineet Chopra, MD, MSc, FHM, recently became chair of the Department of Medicine at the University of Colorado School of Medicine, Aurora. He had previously been the chief of the Division of Hospital Medicine at the University of Michigan Health system. He assumed his new role in October 2021.
Dr. Chopra, who specializes in research and mentorship in patient safety, helped create innovations in care delivery at the University of Michigan, including direct care hospitalist services at VA Ann Arbor Health Care and two other community hospitals.
In his safety-conscious research, Dr. Chopra focuses on preventing complications created within the hospital environment. He also is the first hospitalist to be named deputy editor of the Annals of Internal Medicine. He has written more than 250 peer-reviewed articles. Among the myriad awards he has received, Dr. Chopra recently earned the Kaiser Permanente Award for Clinical Teaching at the UM School of Medicine.
Steve Phillipson, MD, FHM, has been named regional director of hospital medicine at Aspirus Health (Wausau, Wisc.). Dr. Phillipson will oversee the hospitalist programs at 17 Aspirus hospitals in Wisconsin and Michigan.
Dr. Phillipson has worked with Aspirus since 2009, with stints in the emergency department and as a hospitalist. As Aspirus Wausau Hospital director of medicine, he chaired the facility’s COVID-19 treatment team.
Hackensack (N.J.) Meridian University Medical Center has hired Patricia (Patti) L. Fisher, MD, MHA, to be the institution’s chief medical officer. Dr. Fisher joined the medical center from Central Vermont Medical Center where she served as chief medical officer and chief safety officer, with direct oversight of hospital risk management, operations of all hospital-based services, IS services and quality including patient safety and regulatory compliance.
As a board-certified hospitalist, Dr. Fisher also served as clinical assistant professor in the Department of Family Medicine at the University of Vermont, Burlington. Dr. Fisher earned her medical degree from The University of Texas in Houston and completed residency through Forbes Family Practice Residency in Pittsburgh.
Martin Chaney, MD, has been chosen by the Maury Regional Health Board of Trustees to serve as interim chief executive officer. He was formerly the chief medical officer at MRH, which is based in Columbia, Tenn. Dr. Chaney began his new role in October, replacing Alan Watson, the CEO since 2012.
Dr. Chaney has spent 18 of his 25 years in medicine with MRH, where most recently he has focused on clinical quality, physician recruitment, and establishing and expanding the hospital medicine program.
Hyung (Harry) Cho, MD, SFHM, has been placed on Modern Healthcare’s Top 25 Innovators list for 2021, getting recognized for innovation and leadership in creating value and safety initiatives in New York City’s public health system. Dr. Cho became NYC Health + Hospitals’ first chief value officer in 2019, and his programs have created an estimated $11 million in savings per year by preventing unnecessary testing and treatment that can lead to patient harm.
A member of the Society of Hospital Medicine’s editorial advisory board, Dr. Cho is also SHM’s hospitalist liaison with the COVID-19 Real-Time Learning Network, which collaborates with the Centers for Disease Control and Prevention and the Infectious Diseases Society of America.
Raymond Kiser, MD, a hospitalist and nephrologist at Columbus (Ind.) Regional Health, has been named the Douglas J. Leonard Caregiver of the Year. The award is given by the Indiana Hospital Association to health care workers whose care is considered exemplary by both peers and patients.
Dr. Kiser has been with CRH for 7 years, including stints as associate chief medical officer and chief of staff.
Justin Buchholz, DO, has been elevated to medical director of the hospitalist teams at Regional Medical Center (Alamosa, Colo.) and Conejos County Hospital (La Jara, Colo.). Dr. Buchholz has been a full-time hospitalist and assistant medical director at Parkview Medical Center (Pueblo, Colo.) for the past 3 years. He also worked on a part-time basis seeing patients at the Regional Medical Center.
Dr. Buchholz completed his residency at Parkview Medical Center and was named Resident of the Year in his final year with the internal medicine program.
Kenneth Mishark, MD, SFHM, a hospitalist with the Mayo Clinic Hospital (Tucson, Ariz.), will serve on the board of directors for Anigent, a drug diversion-prevention company based in Chesterfield, Mo. He will be charged with helping Anigent better serve health systems with its drug-diversion software.
Dr. Mishark is vice-chair of diversion prevention across the whole Mayo Clinic. A one-time physician in the United States Air Force, Dr. Mishark previously has been the Mayo Clinic’s Healthcare Information Coordination Committee chair.
Core Clinical Partners (Tulsa, Okla.) has announced it will join with Hillcrest HealthCare System (Tulsa, Okla.) to provide hospitalist services to Hillcrest’s eight sites across Oklahoma. The partnership will begin at four locations in December 2021, and four others in March 2022.
In expanding its services, Core Clinical Partners will create 70 new physician positions, as well as a systemwide medical director. Core will manage hospitalist operations at Hillcrest Medical Center, Hillcrest Hospital South, Hillcrest Hospital Pryor, Hillcrest Hospital Claremore, Bailey Medical Center, Hillcrest Hospital Cushing, Hillcrest Hospital Henryetta, and Tulsa Spine and Specialty Hospital.
Vineet Chopra, MD, MSc, FHM, recently became chair of the Department of Medicine at the University of Colorado School of Medicine, Aurora. He had previously been the chief of the Division of Hospital Medicine at the University of Michigan Health system. He assumed his new role in October 2021.
Dr. Chopra, who specializes in research and mentorship in patient safety, helped create innovations in care delivery at the University of Michigan, including direct care hospitalist services at VA Ann Arbor Health Care and two other community hospitals.
In his safety-conscious research, Dr. Chopra focuses on preventing complications created within the hospital environment. He also is the first hospitalist to be named deputy editor of the Annals of Internal Medicine. He has written more than 250 peer-reviewed articles. Among the myriad awards he has received, Dr. Chopra recently earned the Kaiser Permanente Award for Clinical Teaching at the UM School of Medicine.
Steve Phillipson, MD, FHM, has been named regional director of hospital medicine at Aspirus Health (Wausau, Wisc.). Dr. Phillipson will oversee the hospitalist programs at 17 Aspirus hospitals in Wisconsin and Michigan.
Dr. Phillipson has worked with Aspirus since 2009, with stints in the emergency department and as a hospitalist. As Aspirus Wausau Hospital director of medicine, he chaired the facility’s COVID-19 treatment team.
Hackensack (N.J.) Meridian University Medical Center has hired Patricia (Patti) L. Fisher, MD, MHA, to be the institution’s chief medical officer. Dr. Fisher joined the medical center from Central Vermont Medical Center where she served as chief medical officer and chief safety officer, with direct oversight of hospital risk management, operations of all hospital-based services, IS services and quality including patient safety and regulatory compliance.
As a board-certified hospitalist, Dr. Fisher also served as clinical assistant professor in the Department of Family Medicine at the University of Vermont, Burlington. Dr. Fisher earned her medical degree from The University of Texas in Houston and completed residency through Forbes Family Practice Residency in Pittsburgh.
Martin Chaney, MD, has been chosen by the Maury Regional Health Board of Trustees to serve as interim chief executive officer. He was formerly the chief medical officer at MRH, which is based in Columbia, Tenn. Dr. Chaney began his new role in October, replacing Alan Watson, the CEO since 2012.
Dr. Chaney has spent 18 of his 25 years in medicine with MRH, where most recently he has focused on clinical quality, physician recruitment, and establishing and expanding the hospital medicine program.
Hyung (Harry) Cho, MD, SFHM, has been placed on Modern Healthcare’s Top 25 Innovators list for 2021, getting recognized for innovation and leadership in creating value and safety initiatives in New York City’s public health system. Dr. Cho became NYC Health + Hospitals’ first chief value officer in 2019, and his programs have created an estimated $11 million in savings per year by preventing unnecessary testing and treatment that can lead to patient harm.
A member of the Society of Hospital Medicine’s editorial advisory board, Dr. Cho is also SHM’s hospitalist liaison with the COVID-19 Real-Time Learning Network, which collaborates with the Centers for Disease Control and Prevention and the Infectious Diseases Society of America.
Raymond Kiser, MD, a hospitalist and nephrologist at Columbus (Ind.) Regional Health, has been named the Douglas J. Leonard Caregiver of the Year. The award is given by the Indiana Hospital Association to health care workers whose care is considered exemplary by both peers and patients.
Dr. Kiser has been with CRH for 7 years, including stints as associate chief medical officer and chief of staff.
Justin Buchholz, DO, has been elevated to medical director of the hospitalist teams at Regional Medical Center (Alamosa, Colo.) and Conejos County Hospital (La Jara, Colo.). Dr. Buchholz has been a full-time hospitalist and assistant medical director at Parkview Medical Center (Pueblo, Colo.) for the past 3 years. He also worked on a part-time basis seeing patients at the Regional Medical Center.
Dr. Buchholz completed his residency at Parkview Medical Center and was named Resident of the Year in his final year with the internal medicine program.
Kenneth Mishark, MD, SFHM, a hospitalist with the Mayo Clinic Hospital (Tucson, Ariz.), will serve on the board of directors for Anigent, a drug diversion-prevention company based in Chesterfield, Mo. He will be charged with helping Anigent better serve health systems with its drug-diversion software.
Dr. Mishark is vice-chair of diversion prevention across the whole Mayo Clinic. A one-time physician in the United States Air Force, Dr. Mishark previously has been the Mayo Clinic’s Healthcare Information Coordination Committee chair.
Core Clinical Partners (Tulsa, Okla.) has announced it will join with Hillcrest HealthCare System (Tulsa, Okla.) to provide hospitalist services to Hillcrest’s eight sites across Oklahoma. The partnership will begin at four locations in December 2021, and four others in March 2022.
In expanding its services, Core Clinical Partners will create 70 new physician positions, as well as a systemwide medical director. Core will manage hospitalist operations at Hillcrest Medical Center, Hillcrest Hospital South, Hillcrest Hospital Pryor, Hillcrest Hospital Claremore, Bailey Medical Center, Hillcrest Hospital Cushing, Hillcrest Hospital Henryetta, and Tulsa Spine and Specialty Hospital.
Mentoring is key to growing women’s leadership in medicine
Men may think they are supportive of women in the workplace, but if you ask women, they say there is a discrepancy, according to W. Brad Johnson, PhD, a clinical psychologist and professor at the United States Naval Academy in Annapolis, Md.
“We may think we are acting as allies to women because we believe in it, but it may not be showing up in the execution,” he said in a presentation at the virtual Advance PHM Gender Equity Conference.
Although women currently account for the majority of medical school students, they make up only 16% of the population of medical school deans, 18% of department chairs, and 25% of full professors, according to 2019 data from the Association of American Medical Colleges, Dr. Johnson said.
The “missing ingredient” in increasing the number of women in medical faculty positions is that women are less mentored. Some barriers to mentorship include men’s concerns that women will take offers of mentorship the wrong way, but “it is incredibly rare for women to make a false accusation” of harassment in a mentorship situation, said Dr. Johnson.
Dr. Johnson offered some guidance for how men can become better allies for women in the workplace through interpersonal allyship, public allyship, and systemic allyship.
Interpersonal allyship and opportunities for mentoring women in medicine start by building trust, friendship, and collegiality between men and women colleagues, Dr. Johnson explained.
He provided some guidance for men to “sharpen their gender intelligence,” which starts with listening. Surveys of women show that they would like male colleagues to be a sounding board, rather than simply offering to jump in with a fix for a problem. “Show humility,” he said, don’t be afraid to ask questions, and don’t assume that a colleague wants something in particular because she is a woman.
“A lot of men get stuck on breaking the ice and getting started with a mentoring conversation,” Dr. Johnson said. One way to is by telling a female colleague who gave an outstanding presentation, or has conducted outstanding research, that you want to keep her in your organization and that she is welcome to talk about her goals. Women appreciate mentoring as “a constellation” and a way to build support, and have one person introduce them to others who can build a network and promote opportunities for leadership. Also, he encouraged men to be open to feedback from female colleagues on how they can be more supportive in the workplace. Sincerity and genuine effort go a long way towards improving gender equity.
Public allyship can take many forms, including putting women center stage to share their own ideas, Dr. Johnson said. Surveys of women show that they often feel dismissed or slighted and not given credit for an idea that was ultimately presented by a male colleague, he noted. Instead, be a female colleague’s biggest fan, and put her in the spotlight if she is truly the expert on the topic at hand.
Women also may be hamstrung in acceding to leadership positions by the use of subjective evaluations, said Dr. Johnson. He cited a 2018 analysis of 81,000 performance evaluations by the Harvard Business Review in which the top positive term used to describe men was analytical, while the top positive term used to describe women was compassionate. “All these things go with pay and promotions, and they tend to disadvantage women,” he said.
Dr. Johnson provided two avenues for how men can effectively show up as allies for women in the workplace.
First, start at the top. CEOs and senior men in an organization have a unique opportunity to set an example and talk publicly about supporting and promoting women, said Dr. Johnson.
Second, work at the grassroots level. He encouraged men to educate themselves with gender equity workshops, and act as collaborators. “Don’t tell women how to do gender equity,” he said, but show up, be present, be mindful, and be patient if someone seems not to respond immediately to opportunities for mentoring or sponsorship.
“Claiming ally or mentor status with someone from a nondominant group may invoke power, privilege, or even ownership” without intention, he said. Instead, “Always let others label you and the nature of the relationship [such as ally or mentor].”
For more information about allyship, visit Dr. Johnson’s website, workplaceallies.com.
Men may think they are supportive of women in the workplace, but if you ask women, they say there is a discrepancy, according to W. Brad Johnson, PhD, a clinical psychologist and professor at the United States Naval Academy in Annapolis, Md.
“We may think we are acting as allies to women because we believe in it, but it may not be showing up in the execution,” he said in a presentation at the virtual Advance PHM Gender Equity Conference.
Although women currently account for the majority of medical school students, they make up only 16% of the population of medical school deans, 18% of department chairs, and 25% of full professors, according to 2019 data from the Association of American Medical Colleges, Dr. Johnson said.
The “missing ingredient” in increasing the number of women in medical faculty positions is that women are less mentored. Some barriers to mentorship include men’s concerns that women will take offers of mentorship the wrong way, but “it is incredibly rare for women to make a false accusation” of harassment in a mentorship situation, said Dr. Johnson.
Dr. Johnson offered some guidance for how men can become better allies for women in the workplace through interpersonal allyship, public allyship, and systemic allyship.
Interpersonal allyship and opportunities for mentoring women in medicine start by building trust, friendship, and collegiality between men and women colleagues, Dr. Johnson explained.
He provided some guidance for men to “sharpen their gender intelligence,” which starts with listening. Surveys of women show that they would like male colleagues to be a sounding board, rather than simply offering to jump in with a fix for a problem. “Show humility,” he said, don’t be afraid to ask questions, and don’t assume that a colleague wants something in particular because she is a woman.
“A lot of men get stuck on breaking the ice and getting started with a mentoring conversation,” Dr. Johnson said. One way to is by telling a female colleague who gave an outstanding presentation, or has conducted outstanding research, that you want to keep her in your organization and that she is welcome to talk about her goals. Women appreciate mentoring as “a constellation” and a way to build support, and have one person introduce them to others who can build a network and promote opportunities for leadership. Also, he encouraged men to be open to feedback from female colleagues on how they can be more supportive in the workplace. Sincerity and genuine effort go a long way towards improving gender equity.
Public allyship can take many forms, including putting women center stage to share their own ideas, Dr. Johnson said. Surveys of women show that they often feel dismissed or slighted and not given credit for an idea that was ultimately presented by a male colleague, he noted. Instead, be a female colleague’s biggest fan, and put her in the spotlight if she is truly the expert on the topic at hand.
Women also may be hamstrung in acceding to leadership positions by the use of subjective evaluations, said Dr. Johnson. He cited a 2018 analysis of 81,000 performance evaluations by the Harvard Business Review in which the top positive term used to describe men was analytical, while the top positive term used to describe women was compassionate. “All these things go with pay and promotions, and they tend to disadvantage women,” he said.
Dr. Johnson provided two avenues for how men can effectively show up as allies for women in the workplace.
First, start at the top. CEOs and senior men in an organization have a unique opportunity to set an example and talk publicly about supporting and promoting women, said Dr. Johnson.
Second, work at the grassroots level. He encouraged men to educate themselves with gender equity workshops, and act as collaborators. “Don’t tell women how to do gender equity,” he said, but show up, be present, be mindful, and be patient if someone seems not to respond immediately to opportunities for mentoring or sponsorship.
“Claiming ally or mentor status with someone from a nondominant group may invoke power, privilege, or even ownership” without intention, he said. Instead, “Always let others label you and the nature of the relationship [such as ally or mentor].”
For more information about allyship, visit Dr. Johnson’s website, workplaceallies.com.
Men may think they are supportive of women in the workplace, but if you ask women, they say there is a discrepancy, according to W. Brad Johnson, PhD, a clinical psychologist and professor at the United States Naval Academy in Annapolis, Md.
“We may think we are acting as allies to women because we believe in it, but it may not be showing up in the execution,” he said in a presentation at the virtual Advance PHM Gender Equity Conference.
Although women currently account for the majority of medical school students, they make up only 16% of the population of medical school deans, 18% of department chairs, and 25% of full professors, according to 2019 data from the Association of American Medical Colleges, Dr. Johnson said.
The “missing ingredient” in increasing the number of women in medical faculty positions is that women are less mentored. Some barriers to mentorship include men’s concerns that women will take offers of mentorship the wrong way, but “it is incredibly rare for women to make a false accusation” of harassment in a mentorship situation, said Dr. Johnson.
Dr. Johnson offered some guidance for how men can become better allies for women in the workplace through interpersonal allyship, public allyship, and systemic allyship.
Interpersonal allyship and opportunities for mentoring women in medicine start by building trust, friendship, and collegiality between men and women colleagues, Dr. Johnson explained.
He provided some guidance for men to “sharpen their gender intelligence,” which starts with listening. Surveys of women show that they would like male colleagues to be a sounding board, rather than simply offering to jump in with a fix for a problem. “Show humility,” he said, don’t be afraid to ask questions, and don’t assume that a colleague wants something in particular because she is a woman.
“A lot of men get stuck on breaking the ice and getting started with a mentoring conversation,” Dr. Johnson said. One way to is by telling a female colleague who gave an outstanding presentation, or has conducted outstanding research, that you want to keep her in your organization and that she is welcome to talk about her goals. Women appreciate mentoring as “a constellation” and a way to build support, and have one person introduce them to others who can build a network and promote opportunities for leadership. Also, he encouraged men to be open to feedback from female colleagues on how they can be more supportive in the workplace. Sincerity and genuine effort go a long way towards improving gender equity.
Public allyship can take many forms, including putting women center stage to share their own ideas, Dr. Johnson said. Surveys of women show that they often feel dismissed or slighted and not given credit for an idea that was ultimately presented by a male colleague, he noted. Instead, be a female colleague’s biggest fan, and put her in the spotlight if she is truly the expert on the topic at hand.
Women also may be hamstrung in acceding to leadership positions by the use of subjective evaluations, said Dr. Johnson. He cited a 2018 analysis of 81,000 performance evaluations by the Harvard Business Review in which the top positive term used to describe men was analytical, while the top positive term used to describe women was compassionate. “All these things go with pay and promotions, and they tend to disadvantage women,” he said.
Dr. Johnson provided two avenues for how men can effectively show up as allies for women in the workplace.
First, start at the top. CEOs and senior men in an organization have a unique opportunity to set an example and talk publicly about supporting and promoting women, said Dr. Johnson.
Second, work at the grassroots level. He encouraged men to educate themselves with gender equity workshops, and act as collaborators. “Don’t tell women how to do gender equity,” he said, but show up, be present, be mindful, and be patient if someone seems not to respond immediately to opportunities for mentoring or sponsorship.
“Claiming ally or mentor status with someone from a nondominant group may invoke power, privilege, or even ownership” without intention, he said. Instead, “Always let others label you and the nature of the relationship [such as ally or mentor].”
For more information about allyship, visit Dr. Johnson’s website, workplaceallies.com.
FROM THE ADVANCE PHM GENDER EQUITY CONFERENCE
Hospitals must identify and empower women leaders
Many potential leaders in academic medicine go unidentified, and finding those leaders is key to improving gender equity in academic medicine, said Nancy Spector, MD, in a presentation at the virtual Advance PHM Gender Equity Conference.
“I think it is important to reframe what it means to be a leader, and to empower yourself to think of yourself as a leader,” said Dr. Spector, executive director for executive leadership in academic medicine program at Drexel University, Philadelphia.
“Some of the best leaders I know do not have titles,” she emphasized.
Steps to stimulate the system changes needed to promote gender equity include building policies around the life cycle, revising departmental and division governance, and tracking metrics at the individual, departmental, and organizational level, Dr. Spector said.
Aligning gender-equity efforts with institutional priorities and navigating politics to effect changes in the gender equity landscape are ongoing objectives, she said.
Dr. Spector offered advice to men and women looking to shift the system and promote gender equity. She emphasized the challenge of overcoming psychological associations of men and women in leadership roles. “Men are more often associated with agentic qualities, which convey assertion and control,” she said. Men in leadership are more often described as aggressive, ambitious, dominant, self-confident, forceful, self-reliant, and individualistic.
By contrast, “women are associated with communal qualities, which convey a concern for compassionate treatment of others,” and are more often described as affectionate, helpful, kind, sympathetic, sensitive, gentle, and well spoken, she noted.
Although agentic traits are most often associated with effective leadership, in fact, “the most effective contemporary leaders have both agentic and communal traits,” said Dr. Spector.
However, “if a woman leader is very communal, she may be viewed as not assertive enough, and it she is highly agentic, she is criticized for being too domineering or controlling,” she said.
To help get past these associations, changes are needed at the individual level, leader level, and institutional level, Dr. Spector said.
On the individual level, women seeking to improve the situation for gender equity should engage with male allies and build a pipeline of mentorship and sponsorship to help identify future leaders, she said.
Women and men should obtain leadership training, and “become a student of leadership,” she advised. “Be in a learning mode,” and then think how to apply what you have learned, which may include setting challenging learning goals, experimenting with alternative strategies, learning about different leadership styles, and learning about differences in leaders’ values and attitudes.
For women, being pulled in many directions is the norm. “Are you being strategic with how you serve on committees?” Dr. Spector asked.
Make the most of how you choose to share your time, and “garner the skill of graceful self-promotion, which is often a hard skill for women,” she noted. She also urged women to make the most of professional networking and social capital.
At the leader level, the advice Dr. Spector offered to leaders on building gender equity in their institutions include ensuring a critical mass of women in leadership track positions. “Avoid having a sole woman member of a team,” she said.
Dr. Spector also emphasized the importance of giving employees with family responsibilities more time for promotion, and welcoming back women who step away from the workforce and choose to return. Encourage men to participate in family-friendly benefits. “Standardize processes that support the life cycle of a faculty member or the person you’re hiring,” and ensure inclusive times and venues for major meetings, committee work, and social events, she added.
Dr. Spector’s strategies for institutions include quantifying disparities by using real time dashboards to show both leading and lagging indicators, setting goals, and measuring achievements.
“Create an infrastructure to support women’s leadership,” she said. Such an infrastructure could include not only robust committees for women in science and medicine, but also supporting women to attend leadership training both inside and outside their institutions.
Dr. Spector noted that professional organizations also have a role to play in support of women’s leadership.
“Make a public pledge to gender equity,” she said. She encouraged professional organizations to tie diversity and inclusion metrics to performance reviews, and to prioritize the examination and mitigation of disparities, and report challenges and successes.
When creating policies to promote gender equity, “get out of your silo,” Dr. Spector emphasized. Understand the drivers rather than simply judging the behaviors.
“Even if we disagree on something, we need to work together, and empower everyone to be thoughtful drivers of change,” she concluded.
Dr. Spector disclosed grant funding from the Department of Health & Human Services, the Agency for Healthcare Research and Quality, and the Patient-Centered Outcomes Research Institute. She also disclosed receiving monetary awards, honoraria, and travel reimbursement from multiple academic and professional organization for teaching and consulting programs. Dr. Spector also cofunded and holds equity interest in the I-PASS Patient Safety Institute, a company created to assist institutions in implementing the I-PASS Handoff Program.
Many potential leaders in academic medicine go unidentified, and finding those leaders is key to improving gender equity in academic medicine, said Nancy Spector, MD, in a presentation at the virtual Advance PHM Gender Equity Conference.
“I think it is important to reframe what it means to be a leader, and to empower yourself to think of yourself as a leader,” said Dr. Spector, executive director for executive leadership in academic medicine program at Drexel University, Philadelphia.
“Some of the best leaders I know do not have titles,” she emphasized.
Steps to stimulate the system changes needed to promote gender equity include building policies around the life cycle, revising departmental and division governance, and tracking metrics at the individual, departmental, and organizational level, Dr. Spector said.
Aligning gender-equity efforts with institutional priorities and navigating politics to effect changes in the gender equity landscape are ongoing objectives, she said.
Dr. Spector offered advice to men and women looking to shift the system and promote gender equity. She emphasized the challenge of overcoming psychological associations of men and women in leadership roles. “Men are more often associated with agentic qualities, which convey assertion and control,” she said. Men in leadership are more often described as aggressive, ambitious, dominant, self-confident, forceful, self-reliant, and individualistic.
By contrast, “women are associated with communal qualities, which convey a concern for compassionate treatment of others,” and are more often described as affectionate, helpful, kind, sympathetic, sensitive, gentle, and well spoken, she noted.
Although agentic traits are most often associated with effective leadership, in fact, “the most effective contemporary leaders have both agentic and communal traits,” said Dr. Spector.
However, “if a woman leader is very communal, she may be viewed as not assertive enough, and it she is highly agentic, she is criticized for being too domineering or controlling,” she said.
To help get past these associations, changes are needed at the individual level, leader level, and institutional level, Dr. Spector said.
On the individual level, women seeking to improve the situation for gender equity should engage with male allies and build a pipeline of mentorship and sponsorship to help identify future leaders, she said.
Women and men should obtain leadership training, and “become a student of leadership,” she advised. “Be in a learning mode,” and then think how to apply what you have learned, which may include setting challenging learning goals, experimenting with alternative strategies, learning about different leadership styles, and learning about differences in leaders’ values and attitudes.
For women, being pulled in many directions is the norm. “Are you being strategic with how you serve on committees?” Dr. Spector asked.
Make the most of how you choose to share your time, and “garner the skill of graceful self-promotion, which is often a hard skill for women,” she noted. She also urged women to make the most of professional networking and social capital.
At the leader level, the advice Dr. Spector offered to leaders on building gender equity in their institutions include ensuring a critical mass of women in leadership track positions. “Avoid having a sole woman member of a team,” she said.
Dr. Spector also emphasized the importance of giving employees with family responsibilities more time for promotion, and welcoming back women who step away from the workforce and choose to return. Encourage men to participate in family-friendly benefits. “Standardize processes that support the life cycle of a faculty member or the person you’re hiring,” and ensure inclusive times and venues for major meetings, committee work, and social events, she added.
Dr. Spector’s strategies for institutions include quantifying disparities by using real time dashboards to show both leading and lagging indicators, setting goals, and measuring achievements.
“Create an infrastructure to support women’s leadership,” she said. Such an infrastructure could include not only robust committees for women in science and medicine, but also supporting women to attend leadership training both inside and outside their institutions.
Dr. Spector noted that professional organizations also have a role to play in support of women’s leadership.
“Make a public pledge to gender equity,” she said. She encouraged professional organizations to tie diversity and inclusion metrics to performance reviews, and to prioritize the examination and mitigation of disparities, and report challenges and successes.
When creating policies to promote gender equity, “get out of your silo,” Dr. Spector emphasized. Understand the drivers rather than simply judging the behaviors.
“Even if we disagree on something, we need to work together, and empower everyone to be thoughtful drivers of change,” she concluded.
Dr. Spector disclosed grant funding from the Department of Health & Human Services, the Agency for Healthcare Research and Quality, and the Patient-Centered Outcomes Research Institute. She also disclosed receiving monetary awards, honoraria, and travel reimbursement from multiple academic and professional organization for teaching and consulting programs. Dr. Spector also cofunded and holds equity interest in the I-PASS Patient Safety Institute, a company created to assist institutions in implementing the I-PASS Handoff Program.
Many potential leaders in academic medicine go unidentified, and finding those leaders is key to improving gender equity in academic medicine, said Nancy Spector, MD, in a presentation at the virtual Advance PHM Gender Equity Conference.
“I think it is important to reframe what it means to be a leader, and to empower yourself to think of yourself as a leader,” said Dr. Spector, executive director for executive leadership in academic medicine program at Drexel University, Philadelphia.
“Some of the best leaders I know do not have titles,” she emphasized.
Steps to stimulate the system changes needed to promote gender equity include building policies around the life cycle, revising departmental and division governance, and tracking metrics at the individual, departmental, and organizational level, Dr. Spector said.
Aligning gender-equity efforts with institutional priorities and navigating politics to effect changes in the gender equity landscape are ongoing objectives, she said.
Dr. Spector offered advice to men and women looking to shift the system and promote gender equity. She emphasized the challenge of overcoming psychological associations of men and women in leadership roles. “Men are more often associated with agentic qualities, which convey assertion and control,” she said. Men in leadership are more often described as aggressive, ambitious, dominant, self-confident, forceful, self-reliant, and individualistic.
By contrast, “women are associated with communal qualities, which convey a concern for compassionate treatment of others,” and are more often described as affectionate, helpful, kind, sympathetic, sensitive, gentle, and well spoken, she noted.
Although agentic traits are most often associated with effective leadership, in fact, “the most effective contemporary leaders have both agentic and communal traits,” said Dr. Spector.
However, “if a woman leader is very communal, she may be viewed as not assertive enough, and it she is highly agentic, she is criticized for being too domineering or controlling,” she said.
To help get past these associations, changes are needed at the individual level, leader level, and institutional level, Dr. Spector said.
On the individual level, women seeking to improve the situation for gender equity should engage with male allies and build a pipeline of mentorship and sponsorship to help identify future leaders, she said.
Women and men should obtain leadership training, and “become a student of leadership,” she advised. “Be in a learning mode,” and then think how to apply what you have learned, which may include setting challenging learning goals, experimenting with alternative strategies, learning about different leadership styles, and learning about differences in leaders’ values and attitudes.
For women, being pulled in many directions is the norm. “Are you being strategic with how you serve on committees?” Dr. Spector asked.
Make the most of how you choose to share your time, and “garner the skill of graceful self-promotion, which is often a hard skill for women,” she noted. She also urged women to make the most of professional networking and social capital.
At the leader level, the advice Dr. Spector offered to leaders on building gender equity in their institutions include ensuring a critical mass of women in leadership track positions. “Avoid having a sole woman member of a team,” she said.
Dr. Spector also emphasized the importance of giving employees with family responsibilities more time for promotion, and welcoming back women who step away from the workforce and choose to return. Encourage men to participate in family-friendly benefits. “Standardize processes that support the life cycle of a faculty member or the person you’re hiring,” and ensure inclusive times and venues for major meetings, committee work, and social events, she added.
Dr. Spector’s strategies for institutions include quantifying disparities by using real time dashboards to show both leading and lagging indicators, setting goals, and measuring achievements.
“Create an infrastructure to support women’s leadership,” she said. Such an infrastructure could include not only robust committees for women in science and medicine, but also supporting women to attend leadership training both inside and outside their institutions.
Dr. Spector noted that professional organizations also have a role to play in support of women’s leadership.
“Make a public pledge to gender equity,” she said. She encouraged professional organizations to tie diversity and inclusion metrics to performance reviews, and to prioritize the examination and mitigation of disparities, and report challenges and successes.
When creating policies to promote gender equity, “get out of your silo,” Dr. Spector emphasized. Understand the drivers rather than simply judging the behaviors.
“Even if we disagree on something, we need to work together, and empower everyone to be thoughtful drivers of change,” she concluded.
Dr. Spector disclosed grant funding from the Department of Health & Human Services, the Agency for Healthcare Research and Quality, and the Patient-Centered Outcomes Research Institute. She also disclosed receiving monetary awards, honoraria, and travel reimbursement from multiple academic and professional organization for teaching and consulting programs. Dr. Spector also cofunded and holds equity interest in the I-PASS Patient Safety Institute, a company created to assist institutions in implementing the I-PASS Handoff Program.
FROM THE ADVANCE PHM GENDER EQUITY CONFERENCE




































